Living related donor pancreas and pancreas-kidney transplantation
|
|
|
- Harvey Leonard
- 5 years ago
- Views:
Transcription
1 Living related donor pancreas and pancreas-kidney transplantation Abhinav Humar, Rainer W G Gruessner and David E R Sutherland Department of Surgery, University of Minnesota, Minneapolis, Minnesota, USA Correspondence to Dr David E R Sutherland, Department of Surgery, University of Minnesota, Box 280 Mayo, 420 Delaware Street SE, Minneapolis, MN 55455, USA Our experience with living related donor (LRD) pancreas transplants shows that they can be performed with low morbidity and mortality for both donors and recipients.the recipient survival rate is 90% at both 1 and 5 years pott-transplant. Our overall pancreas graft survival rate is comparable to that for cadaver transplants; if only technically successful cases are included, the graft survival rate is significantly better for LRD (versus cadaver) transplants. Advantages for LRD recipients include fewer rejection episodes, less immunosuppression, lower incidence of graft loss from rejection, and elimination of waiting time. Donor mortality in our series was 0%, and the incidence of surgical complications about 10 15%. LRD pancreas transplants are an attractive option for endocrine replacement therapy in certain diabetic patients.optimal candidates are: (i) patients who are highly sensitized and have a low probability of receiving a cadaver graft; (ii) patients who should avoid high-dose immunosuppression; (iii) patients with nondiabetic identical twins; and (iv) uremic patients who want one operation with no waiting in order to remain or become dialysis free as well as insulin-independent.these transplants can be performed safely in all recipient categories pancreas transplant alone, pancreas after kidney or simultaneous pancreas kidney transplant. In all groups, LRD transplants should be done only when the donor, the recipient, and the entire family understands the advantages and disadvantages of LRD versus cadaver transplants. The success with living related donors (LRDs) for kidney transplantation has led to their use for other solid organs. The pancreas was the first extrarenal organ to successfully use LRDs 1. Over the last 5 years, LRDs have been used in liver, lung, and intestinal transplants. LRD transplants offer several advantages (versus cadaver transplants), including elimination of waiting time, decreased cold ischemic injury, improved immunological matching, and overall improved graft survival. Use of LRDs also expands the donor pool, which is important for organs such as kidney and liver, where there is a shortage of cadaver organs. However, the number of pancreas transplants currently being performed is less than the number of cadaver organs available; if matching is ignored, there is no shortage of pancreases at present. The main advantages of LRD pancreas transplants (versus cadaver transplants) are Bnhth Medical Bulltim 1997^3 (No 4) The Britiih Council 1997
2 Transplantation Donor evaluation a lower incidence of rejection episodes, higher graft survival rates 2, and elimination of waiting time. Rejection has been a major problem after cadaver pancreas transplants, particularly when done without a kidney, accounting for up to 30% of graft loss within the first year 3 ; the corresponding number after LRD transplants is significantly lower 4-5. With new immunosuppressants, the cadaver organ rejection rate is now low 3, giving less incentive for a solitary LRD pancreas transplant than before, but a shortage of cadaver pancreases for all who could benefit remains as incentive for the LRD approach. This immunological and logistical advantage must be weighed against the higher technical failure rate seen with LRD (versus cadaver) pancreas transplants. Only a segment of the pancreas is transplanted, and the vessels used for engraftment (splenic artery and vein) are shorter and smaller in diameter. Thus, LRD pancreas grafts are more prone to arterial and venous thrombosis than their cadaver counterparts. Nonetheless, the technical failure rate after LRD pancreas transplants has been lower than the immunological failure rate (i.e. graft loss from rejection) after cadaver solitary pancreas transplants 6. Therefore, for technically successful pancreas transplants, the probability of long-term success is significantly better with an LRD (versus a cadaver) allograft. Another advantage of LRD transplants is that they may be the only option for highly sensitized patients and for those requiring minimal immunosuppression. LRD pancreas transplants may be done either for nonuremic patients (PTA, pancreas transplant alone) or for patients who have received a previous kidney transplant (PAK, pancreas after kidney). Another option for uremic patients with insulin-dependent diabetes mellitus (IDDM) is a simultaneous pancreas-kidney transplant (SPK). Compared with a sequential transplant (PAK), an SPK transplant requires only one procedure, and the physical consequences are no different for the donor. For uremic diabetic patients who want only one operation and want to avoid or minimize time on dialysis, a LRD SPK transplant is particularly attractive. LRD transplants have the potential for harm to the donor. Thus, it is crucial that all potential donors undergo a thorough pre-operative evaluation. The purpose is two-fold: first, to ensure that the donor is healthy enough to undergo the operation safely; and, second, to ensure that the reduced pancreatic mass would be sufficient to maintain a normal metabolic state. 880 Bnhsh MadtcalBulletin 1997,53 (No 4)
3 Living related donor pancreas and pancreas kidney transplantation The general health of the donor is best ascertained by a detailed history and physical examination, looking for evidence of cardiovascular, pulmonary, renal, and major gastrointestinal disease. This part of the workup is no different from the evaluation for any other general surgical patient undergoing a pancreatic resection. Endocrinological evaluation includes family history. Potential donors should be at least 10 years older than the age of onset of diabetes in the recipient (and the onset of diabetes in the recipient must have been at least 10 years pretransplant). In addition, for sibling donors, no family member other than the recipient should be diabetic. When these two criteria are met, donors are at no greater risk for diabetes than the general population, even if they are HLA-identical with the recipient. Potential donors should be asked about their alcohol intake. Female donors who have had previous pregnancies should be asked about gestational diabetes. Metabolic studies must include measurement of the hemoglobin Ale (should be <6%) and an oral glucose tolerance test (OGTT). Plasma glucose is determined in response to a 75 g oral glucose load. Using criteria outlined by the National Diabetes Data Group, potential donors must be excluded if fasting glucose levels are > HOmg/dl (6 mmol/1), if glucose at 2 h post-ingestion measures >140mg/dl (7.7 mmol/1), or if any glucose value between 1 and 120 min is > 200 mg/dl (11 mmol/1) 6. If these studies are normal, insulin secretion should be evaluated in response to an intravenous glucose tolerance test (IVGTT). This test is performed by administering 20 g glucose (as D 50 W) intravenously (i.v.) and obtaining samples for glucose and insulin levels over a 30 min period after the injection of glucose. Only individuals with post-i.v. glucose stimulatory first-phase insulin levels above the 30th percentile of the normal range should be accepted as donors 7. Lastly, some radiological assessment of the vascular anatomy should be done. This step is more important if the kidney is to be procured also, as the vascular anatomy of the splenic artery is fairly constant in comparison to the renal arteries. An aortogram may be done, but more recently, we have been using a noninvasive magnetic resonance angiogram (MRA) study. It will demonstrate any anatomical abnormalities of the pancreas as well as the vascular anatomy of the celiac trunk and renal vessels. In our last 20 SPK donors, MRA has documented normal anatomy of the celiac and superior mesenteric arteries and normal size and location of the splenic artery. At our center, between January 1, 1978 and March 15, 1997, a total of 103 LRD pancreas transplants have been done (51 PTA, 32 PAK, and 20 SPK). Of the 103 donors, only 3 have not remained normoglycemic (2 at 1 year, 1 at 4 years). All 3 had a normal OGTT, but they donated before routine use of IVGTT; in retrospect, all 3 had low insulin Bntiih M+dical Bu/Ufin 1997,53 (No 4) 881
4 Transplantation responses 7. None of the donors meeting the current criteria of the IVGTT insulin response have become significantly hyperglycemic after hemipancreatectomy, though 3 have developed mild elevations of their hemoglobin Ale levels 8. Operative techniques Donor Pancreas procurement may be done through a subcostal or midline abdominal incision. For SPK donors, a midline incision is preferred. If the kidney is to be removed, it is generally removed first. The right or left kidney can be used, depending on the vascular anatomy. Initially our preference was to procure the right kidney (a somewhat easier dissection); we now prefer to use the left kidney (because of concurrent partial mobilization of the pancreas, greater length of the renal vein, and lack of liver mobilization). The colon on the appropriate side is reflected medially; on the left side, the henocolic ligament should be preserved, if possible: it may carry collateral blood vessels to the spleen. The kidney can then be dissected from the surrounding perirenal fat. Once the vessels have been dissected free, hepann (70 units/kg) is given and the kidney removed. The hepann effect can then be reversed with protamine (1 cc/1000 units of heparin) before the pancreas is mobilized. Procurement of the distal pancreas begins with dividing the gastrocolic ligament laterally to the inferior margin of the spleen (Fig. 1A). Care should be taken to preserve the gastroepipiloic artery and the short gastric vessels, to diminish the likelihood of devascularizing of the spleen. The retropentoneal attachments of the spleen are not disturbed, and the spleen is not mobilized. The stomach can then be retracted superiorly, and the inferior margin of the distal pancreas is mobilized. A peritoneal incision is made over the tail of the pancreas at its junction with the spleen. The pancreas is gently dissected off the splenic surface. The splenic vessels are then identified, and the main trunks of both the splenic artery and vein divided proximal to the splenic branches (again, preserving collateral blood vessels supplying the spleen). The superior margin of the pancreas is then mobilized, retaining the splenic artery and vein in continuity with the body and tail of the pancreas. As the pancreas is elevated from its bed and retracted medially, the confluence of the inferior mesentery vein (IMV) as it joins the splenic vein can be seen. The location of this confluence varies; it can be very close to the junction of the superior mesentenc vein (SMV) and the 882 Bnbsh Medical BulUttn 1997^3 (No 4)
5 Living related donor pancreas and pancreas kidney transplantation v,: Spltnic a. & v. ligat«d and divided hort gastric «. troplplolc a. Fig. 1 (A) Technique of distal pancreatectomy in living related donor for segmental transplantation' from Sutherland ef a/. (B) Segmental pancreas removed with preservation of donor spleen: from Sutherland ef af. Bnfuh Medico/ Bu/I.fin 1997,53 (No 4) 883
6 Transplantation Recipient splenic vein. Once the IMV is divided, the pancreas can be mobilized further to the surgical neck. The portal vein is identified at the confluence of the SMV and splenic vein. The avascular plane between the pancreas and portal vein is bluntly dissected to define the narrowest portion of the pancreas (i.e. the neck). At this site, the pancreas is divided. The splenic artery is then isolated at its origin off the celiac trunk. The pancreatic neck can then be divided using multiple 4.0 silk ligatures. Both ends of the pancreatic duct should be identified. The proximal end can be oversewn, and the distal duct tacked with 7.0 Prolene sutures for identification. The cut edge of the proximal pancreas can be oversewn with interrupted sutures in a U-type fashion to 'fishmouth' the proximal cut edge and to decrease the likelihood of pancreatic fluid leaking from the smaller ducts. At this point, the segmental pancreas graft is ready for removal (Fig. IB). The donor is again heparinized (70 units/kg), the splenic artery and vein divided, and the pancreas removed (Fig. IB). Protamine is again given to reverse the hepann effect. The graft is then flushed ex vivo via the splenic artery with University of Wisconsin (UW) solution (about 20 cc) and briefly stored at 4 C in UW before implantation. Before closure, the viability of the spleen must be carefully assessed. If there is bleeding from the spleen, or if it does not appear viable, it should be removed. The recipient operation is not very different from its cadaver counterpart. A lower abdominal midline incision is used. If a kidney graft is to be implanted, it should be placed on the left side. The pancreas graft should be placed on the right side if possible, because of the more superficial location of the vessels on this side. In preparation for the pancreas graft implantation, all branches of the iliac vein, including the hypogastric, should be divided (allowing the vein to he in a more superficial location). To allow for a better alignment, we have often found it useful to divide the internal iliac artery. Doing so gives a better lie to the graft after it is implanted and decreases the chances of the graft artery kinking. The donor splenic artery can then be anastomosed end to side to the external or common iliac artery; the splenic vein is anastomosed end to side to the iliac vein. Pancreatic exocrine secretions can be managed by a number of techniques. If the pancreatic duct is of adequate size, a direct anastomosis between the duct and bladder mucosa can be constructed with interrupted 7.0 absorbable sutures (Fig. 2A,B). If the duct is small 884 Bnhih Medical Bulletin 1997,53 (No 4)
7 Living related donor pancreas and pancreas kidney transplantation Fig. 2 (A,B) Technique of bladder drainage for legmental pancreas graft from Pneto M eta/" Pancreatic Duel Mucosa to Mucoaa Anastomose tntamal fcac- Sptonic Artery Anastomosis External Mac- Splenic Vein Anattomosi* Complatad Pancraattc Cystoctomy and the diameter of the cut edge of the pancreas is small, then an invagination technique can be used. The pancreas graft is invaginated into the bladder using one internal layer of 4.0 absorbable sutures and one external layer of interrupted 4.0 nonabsorbable sutures. Doing so obviates the need for a tedious duct-to-mucosa anastomosis, but it could create problems from exposure of exocrine pancreas tissue to urine. The duct may also be injected with a liquid, such as silicone, that polymerizes rapidly. This obviates the need for, and complications of, an anastomosis to the recipient bladder or bowel. The exocrine pancreas undergoes fibrosis, but the endocrine pancreas remains intact. One drawback with this technique is the inability to monitor exocrine function (through urine amylase levels) as a marker of rejection. The pancreatic duct may also be drained enterally, using a Roux-en-Y limb of distal bowel (Fig. 3). As with duct injection, one drawback is the inability to monitor exocrine function as a marker of rejection. Therefore, our current preference is bladder drainage with a direct anastomosis between the pancreatic duct and the bladder mucosa if British Medical BuH.f/n 1997,53 (No *) 885
8 Transplantation Proximal Jtjunum Roux-en-Y Fig. 3 Technique of enteric drainage for tegmental pancreas graftj. from Prieto M efa/ u. Postoperative care Donor External JUac- Splenc v. Anastomosis IntemaJ Nac-sptontc a Anastomosis Pancreaaco-jejunostomy possible, which allows monitoring of pancreas exocrine secretions in the urine. This is particularly important in solitary pancreas transplants, less so in SPK where the creatinine level can be used as a marker for kidney rejection. Isolated rejection episodes of the pancreas do occur in SPK recipients, but are rare. Postoperative care of donors is not unlike that of any other patient undergoing a major abdominal procedure. A nasograstric tube should be left in place and removed when bowel function returns. Serial hemoglobin determinations are made to monitor for bleeding. Blood sugar and amylase levels are checked routinely. A persistent elevation of the serum amylase level may suggest pancreatitis, a leak, or pseudocyst formation. If pain over the splemc bed persists or is severe, a splenic radionucleotide scan should be obtamed to ensure viability of the spleen. 886 Bnhth MtdKal Bulletin 1997,53 (No 4)
9 Living related donor pancreas and pancreas kidney transplantation If the scan suggests infarction of the spleen, a splenectomy should be done. Donors can usually be discharged home within 1 week. Recipient /mmunosuppress/on The initial care of LRD recipients is similar to that of cadaver recipients. Plasma glucose levels are determined regularly, and insulin is administered as needed to keep blood sugar levels 150mg/dl during the first 14 days post-transplant. Intravenous fluids are given according to the central venous pressure and urine output. A nasograstric tube should be left in place until postoperative ileus resolves, usually between postoperative days (POD) 5 and 7. Given the higher incidence of thrombosis of LRD grafts, some form of coagulation prophylaxis should be instituted. We now systemically hepannize all LRD recipients. Generally, hepann is started intraoperatively at 200 uruts/h, with full heparimzation achieved by 4 6h postoperatively. On POD 5, Coumadin is started and maintained for 6 months (target INR = 2). Thereafter, recipients take low-dose acetylsalicyhc acid (80mg/day) indefinitely. With this aggressive anticoagulation regimen, we have seen a significant decrease in the incidence of graft thrombosis, but no serious bleeding complications. With our current immunosuppressive protocol, all but HLA-identical recipients receive anti-thymocyte globulin (ATG, lomg/kg i.v.) for 5-10 days. Tacrolimus is used as the mainstay immunosuppressive agent. A dose of 2 mg orally twice per day is started on POD 1 or when the serum creatinine level is <3.0mg/dl. The dose is then adjusted to achieve levels of 8-12ng/ml during the first month and 5-10ng/ml thereafter. Prednisone (2mg/kg/day) is started intra-operatively, then tapered to 0.6mg/kg/day by 1 week post-transplant, and 0.1 mg/kg/day by 1 month post-transplant. Once recipients are able to tolerate oral intake, mycophenolate mofetil (MMF) is started at 1.5 g twice per day. Before oral intake, azathioprine is used at 1.25mg/kg i.v. Patients tolerating both MMF and tacrolimus (or cyclosponne) at 6 months are withdrawn from prednisone. Bnhsh M.dtcal Bulletin 1997,53 (No 4) 887
10 Transplantation Complications Donor Potential complications for donors include bleeding, splenic infarct or abscess, pancreatitis, pseudocyst, and intra-abdominal abscess formation. Intra-operative bleeding may be encountered with the dissection of the tail of the pancreas from the hilum of the spleen. Operative trauma to the spleen resulting in capsular tears may result in significant bleeding and require splenectomy. Postoperative bleeding from the cut surface of the pancreas is also a potential hazard. Procurement of the kidney can increase the potential sources of bleeding. Of our 20 SPK donors, 4 (20%) required a blood transfusion peri-operatively. Besides operative trauma, the spleen may also need to be removed if blood supply to it is insufficient after ligation of the splenic vessels. If the spleen infarcts postoperatively, the recipient will have pain over the splenic region, radiating to the left shoulder. Areas of infarct may later develop an abscess. If a radionucleotide spleen scan shows persistent lack of uptake in a recipient with persistent pain, a splenectomy should be done. Pancreatitis of the residual head and body of the gland is generally not a problem. Pancreatic leakage may occur, either from the main duct or, more commonly, from the small pancreatic duct branches. Of our 103 donors, 1 required a relaparatomy to religate the cut surface of the pancreas after a staple closure. Smaller leaks may later form a pseudocyst, which may become infected. Generally, pseudocysts can be treated successfully with CT-guided percutaneous drainage. Of our 103 donors, 8 developed symptomatic peripancreatic fluid collections postoperatively. Of these, 7 were successfully treated with percutaneous drainage, while 1 required an open drainage procedure. As with any abdominal procedure, other complications can occur, such as small bowel obstruction secondary to adhesions. A serious complication for donors is the development of diabetes mellitus. In our series, 3 donors have developed mild diabetes controlled with oral hypoglycemics. Another 3 donors have had elevated postoperative hemoglobin Ale, though none of them have required oral hypoglycemics. Diabetes can be avoided by adhering to the strict preoperative endocrine evaluation outlined previously. Moreover, we now exclude obese (body mass index >27 kg/m 2 ) donors, older (age >45 years) donors, and donors with a history of gestational diabetes or significant alcohol intake. Intra-operatively, we remove no more than half of the gland (i.e. we divide it at the neck, just anterior to the portal vein). Postoperatively, all donors must undergo annual follow-up testing 888 Bntnh M»<JKOI Bullatm 1997;53 (No A)
11 Living related donor pancreas and pancreas kidney transplantation involving OGTT and measurement of hemoglobin Ale levels, to allow long-term assessment of outcome. Recipient Postoperative complications for LRD recipients are similar to those seen for cadaver recipients bleeding, thrombosis, pancreatitis, infections and rejection. The relative frequency of these complications, however, differs. The incidence of thrombosis is significantly higher with the segmental LRD grafts (versus the whole-organ cadaver) 9. Of our 103 LRD pancreas grafts, 19 (18.5%) were lost because of vascular thrombosis. LRD grafts are at higher risk for thrombosis because the splenic artery and vein allow for less flexibility (compared with the Y-graft used for cadaver grafts); also, they are more prone to bending or twisting. With whole-organ cadaver grafts, there is a dual blood supply (splenic and superior mesenteric arteries); segmental grafts depend on a single vessel (splenic artery). Therefore, partial or complete thrombosis would be more detrimental in a segmental graft. Since instituting our aggressive anticoagulation regimen, we have seen a dramatic decline in graft loss secondary to thrombosis. Another important step to prevent thrombosis is proper alignment of the recipient vessels, with the recipient external iliac artery lying lateral to the vein. We frequently divide the internal iliac artery to allow more flexibility and to avoid impingement of the external iliac artery on the splenic vein 10. Other reasons for graft loss at early post-transplant include deep infections and graft pancreatitis. The incidence of infection is generally lower with segmental LRD grafts (versus whole-organ cadaver grafts); perhaps related to the absence of duodenum, with its potential for leakage and contamination with enteric flora. Only 2 LRD recipients in our series have lost their graft because of pancreatitis. Rejection is a less common problem after LRD transplants (versus cadaver transplants). Over an 18 year period, only 13% of our LRD allograft recipients lost their grafts because of chrome rejection versus 41% of our cadaver recipients 11. In our last 20 LRD SPK recipients, only 8 had rejection episodes; only 1 lost the pancreas graft to rejection. All 20 kidneys are functioning and all of the LRD SPK recipients are alive. Even excluding HLA-identical transplants, the incidence of rejection is lower after LRD (versus cadaver) transplants. The newer immunosuppressive drugs (tacrolimus, MMF) may also be contributing to the lower incidence. British Medical Bulletin (No 4) 889
12 Transplantation Results References Our mortality rate for donors has been 0%. Nor have we seen any recipient deaths directly attributable to the operative procedure. Donor outcome, however, must also take into account surgical complications and metabolic changes postdonation. In our series, the overall incidence of serious surgical donor complications requiring re-operation or radiological interventions was 10-15%. If strict selection criteria are met, the complication of insulin insufficiency in donors can be avoided. Only 3 of our donors developed mild diabetes requiring oral hypoglycemics; all 3 donated before routine use of IVGTT in our preoperative evaluation. A quality of life questionnaire was distributed to our 20 SPK donors. Of the 16 who responded, 15 stated they had made the correct decision to donate. Our pancreas graft survival rate at 1 year was 75%; patient survival, 90%. In the subgroup of 20 SPK recipients, patient survival at 1 year was 100%; pancreas graft survival, 78% and kidney graft survival, 100% 12. Currently, all 20 kidney grafts and 15 of the pancreas grafts are functioning. A quality of life survey was also distributed to these 20 recipients. Of the 14 who responded, all 14 stated they made the correct decision to undergo the transplant; all 14 reported an improvement in their health compared with 1 year pretransplant. Sutherland DER, Goetz FC, Na)anan JS. Living related donor segmental pancreatectomy for transplantation. Transplant Proc 1980, 12: Sutherland DER, Goetz FC, Gillingham K et al. Medical risks and benefits of pancreas transplants from living related donors. In: Land W, Dosseter JB eds. Organ Replacement Therapy: Ethics, justice and Commerce. Berlin: Springer, 1991; Gruessner A, Sutherland DER. Pancreas transplantation in the United States (US) and non-us as reported to the United Network for Organ Sharing (UNOS) and the International Pancreas Transplant Registry (IPTR). In Cecka JM, Terasaki PI. eds Clinical Transplants Los Angeles, CA: UCLA Tissue Type Laboratory, 1997, Sutherland DER, Goetz FC, Najanan JS. Pancreas transplants from related donors. Transplantation 1984; Sutherland DER, Gruessner RWG, Moudry-Munns KC, Gruessner A, Na]anan JS. Pancreas transplants from living-related donors. Transplant Proc 1994; National Diabetes Data Group. Classification and diagnosis of diabetes melhtus and other categories of glucose intolerance. Diabetes 1979; Kendall DM, Sutherland DER, Goetz FC, Najanan JS. Metabolic effect of hemipancreatectomy in living related pancreas transplant donors: preoperative prediction of postoperative oral glucose tolerance. Diabetes 1989; 38: Seaquist ER, Robertson RP. Effect of hemipancreatectomy on pancreatic alpha and beta cell function in healthy human donors / Clin Invest 1992, Bnhih Medical Bulletin (No. 4)
13 Living related donor pancreas and pancreas kidney transplantation 9 Sutherland DER, Dunn DL, Goetz FC et al. A 10-year experience with 290 pancreas transplants at a single institution Ann Surg 1989; Gruessner RWG, Sutherland DER. Pancreas transplantation. Part II the recipient operation. Surg Rounds 1994; 17: Gruessner RWG, Najanan JS, Gruessner AC, Sutherland DER. Pancreas transplants from living related donors. In Touraine JL et al. eds. Organ Shortage: The Solutions. The Netherlands- Kluwer, 1995; Gruessner RWG, Kendall DM, Drangsteveit MB et al. Simultaneous pancreas-kidney transplantation from live donors. Ann Surg 1997; 226(4). 13 Sutherland DER, Goetz FC, Ehck BA et al. Pancreas and islet transplantation in diabetic patients with long-term follow-up in selected cases. In: Friedman EA, L'Esperance FA. eds. Diabetic Renal Retinal Syndrome, Prevention and Management. New York: Grune and Stratton, 1982; Pneto M, Sutherland DER, Goetz FC et al. Pancreas transplant results according to the technique of duct management bladder versus enteric drainage. Surgery 1987; 102: Bnhth Medical Bulkhn (No 4) 891
Pancreas Transplantation From Living Donors: A Single Center Experience of 20 Cases
 American Journal of Transplantation 2016; 16: 2413 2420 Wiley Periodicals Inc. Copyright 2016 The American Society of Transplantation and the American Society of Transplant Surgeons doi: 10.1111/ajt.13738
American Journal of Transplantation 2016; 16: 2413 2420 Wiley Periodicals Inc. Copyright 2016 The American Society of Transplantation and the American Society of Transplant Surgeons doi: 10.1111/ajt.13738
Pancreas Transplantation
 5 Pancreas Transplantation Abhinav Humar, Khalid O. Khwaja, and David E.R. Sutherland Standard Procedure a) Pretransplant Evaluation b) Surgical Technique c) Postoperative Care d) Results e) Islet Cell
5 Pancreas Transplantation Abhinav Humar, Khalid O. Khwaja, and David E.R. Sutherland Standard Procedure a) Pretransplant Evaluation b) Surgical Technique c) Postoperative Care d) Results e) Islet Cell
Pancreas Transplantation. Sonia Clarke-Swaby Recipient Kidney/pancreas Transplant Co-ordinator Guy s Hospital
 Pancreas Transplantation Sonia Clarke-Swaby Recipient Kidney/pancreas Transplant Co-ordinator Guy s Hospital Introduction Selection criteria, New innovation Complications, Success rates, Life expectancy
Pancreas Transplantation Sonia Clarke-Swaby Recipient Kidney/pancreas Transplant Co-ordinator Guy s Hospital Introduction Selection criteria, New innovation Complications, Success rates, Life expectancy
Pancreas and Pancreas-Kidney Transplantation By: Kay R. Brown, CLCP
 Pancreas and Pancreas-Kidney Transplantation By: Kay R. Brown, CLCP Pancreas transplant recipients are usually under age 50. The majority of pancreas transplants are performed on diabetics, who are generally
Pancreas and Pancreas-Kidney Transplantation By: Kay R. Brown, CLCP Pancreas transplant recipients are usually under age 50. The majority of pancreas transplants are performed on diabetics, who are generally
Pancreas After Islet Transplantation: A First Report of the International Pancreas Transplant Registry
 American Journal of Transplantation 2016; 16: 688 693 Wiley Periodicals Inc. Brief Communication Copyright 2015 The American Society of Transplantation and the American Society of Transplant Surgeons doi:
American Journal of Transplantation 2016; 16: 688 693 Wiley Periodicals Inc. Brief Communication Copyright 2015 The American Society of Transplantation and the American Society of Transplant Surgeons doi:
The Whipple Operation Illustrations
 The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
PANCREAS TRANSPLANTATION WAS first described
 0163-769X/04/$20.00/0 Endocrine Reviews 25(6):919 946 Printed in U.S.A. Copyright 2004 by The Endocrine Society doi: 10.1210/er.2002-0036 Pancreas Transplantation: Indications and Consequences JENNIFER
0163-769X/04/$20.00/0 Endocrine Reviews 25(6):919 946 Printed in U.S.A. Copyright 2004 by The Endocrine Society doi: 10.1210/er.2002-0036 Pancreas Transplantation: Indications and Consequences JENNIFER
Pancreas after Kidney Transplants in Posturemic Patients with Type I Diabetes Mellitus
 J Am Soc Nephrol 12: 2490 2499, 2001 Pancreas after Kidney Transplants in Posturemic Patients with Type I Diabetes Mellitus ANGELIKA C. GRUESSNER, DAVID E. R. SUTHERLAND, DAVID L. DUNN, JOHN S. NAJARIAN,
J Am Soc Nephrol 12: 2490 2499, 2001 Pancreas after Kidney Transplants in Posturemic Patients with Type I Diabetes Mellitus ANGELIKA C. GRUESSNER, DAVID E. R. SUTHERLAND, DAVID L. DUNN, JOHN S. NAJARIAN,
JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES
 JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES THE PROBLEM DUODENAL / PANCREATIC INJURIES Difficult to diagnose Not very common Anatomic and physiologic challenges 90% rate of associated
JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES THE PROBLEM DUODENAL / PANCREATIC INJURIES Difficult to diagnose Not very common Anatomic and physiologic challenges 90% rate of associated
Pancreas Quizzes c. Both A and B a. Directly into the blood stream (not using ducts)
 Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
Pancreas & Biliary System. Dr. Vohra & Dr. Jamila
 Pancreas & Biliary System Dr. Vohra & Dr. Jamila 1 Objectives At the end of the lecture, the student should be able to describe the: Location, surface anatomy, parts, relations & peritoneal reflection
Pancreas & Biliary System Dr. Vohra & Dr. Jamila 1 Objectives At the end of the lecture, the student should be able to describe the: Location, surface anatomy, parts, relations & peritoneal reflection
Vascular Remodelling in Pancreas Transplantation
 Vascular Remodelling in Pancreas Transplantation Prof Steve White Consultant HPB/Transplant Surgeon The Freeman Hospital Newcastle President Elect EPITA European Pancreas Transplants Pancreas Transplants
Vascular Remodelling in Pancreas Transplantation Prof Steve White Consultant HPB/Transplant Surgeon The Freeman Hospital Newcastle President Elect EPITA European Pancreas Transplants Pancreas Transplants
Accessory Glands of Digestive System
 Accessory Glands of Digestive System The liver The liver is soft and pliable and occupies the upper part of the abdominal cavity just beneath the diaphragm. The greater part of the liver is situated under
Accessory Glands of Digestive System The liver The liver is soft and pliable and occupies the upper part of the abdominal cavity just beneath the diaphragm. The greater part of the liver is situated under
DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis.
 DISCHARGE SUMMARY DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis. OPERATIONS/PROCEDURES: Living related renal transplantation. HISTORY: For full details
DISCHARGE SUMMARY DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis. OPERATIONS/PROCEDURES: Living related renal transplantation. HISTORY: For full details
Renal Transplant Surgery
 Renal Transplant Surgery Mr Somaiah Aroori MS MD EBS in HPB FRCS Consultant HPB & Renal Transplant Surgeon SWTC, Derriford Hospital, Plymouth Over next few minutes Aim to cover Details of Transplant procedure
Renal Transplant Surgery Mr Somaiah Aroori MS MD EBS in HPB FRCS Consultant HPB & Renal Transplant Surgeon SWTC, Derriford Hospital, Plymouth Over next few minutes Aim to cover Details of Transplant procedure
Eilandjes transplantatie. Eelco de Koning, LUMC 14 februari 2008
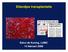 Eilandjes transplantatie Eelco de Koning, LUMC 14 februari 2008 Pancreas or islets? What tissue do we wish to transplant? Is there competition for donor pancreas? How does the islet isolation and transplantation
Eilandjes transplantatie Eelco de Koning, LUMC 14 februari 2008 Pancreas or islets? What tissue do we wish to transplant? Is there competition for donor pancreas? How does the islet isolation and transplantation
Clinical Policy: Pancreas Transplantation Reference Number: PA.CP.MP.102
 Clinical Policy: Reference Number: PA.CP.MP.102 Effective Date: 01/18 Last Review Date: 03/17 Revision Log Coding Implications Description This policy describes the medical necessity requirements for pancreas
Clinical Policy: Reference Number: PA.CP.MP.102 Effective Date: 01/18 Last Review Date: 03/17 Revision Log Coding Implications Description This policy describes the medical necessity requirements for pancreas
Increased Early Rejection Rate after Conversion from Tacrolimus in Kidney and Pancreas Transplantation
 Increased Early Rejection Rate after Conversion from Tacrolimus in Kidney and Pancreas Transplantation Gary W Barone 1, Beverley L Ketel 1, Sameh R Abul-Ezz 2, Meredith L Lightfoot 1 1 Department of Surgery
Increased Early Rejection Rate after Conversion from Tacrolimus in Kidney and Pancreas Transplantation Gary W Barone 1, Beverley L Ketel 1, Sameh R Abul-Ezz 2, Meredith L Lightfoot 1 1 Department of Surgery
Pancreatic Transplantation
 Chapter 73 Pancreatic Transplantation Angelika C. Gruessner, Raja Kandaswamy, Khalid M. Khan, David E. R. Sutherland, and Rainer W. Gruessner Introduction The treatment options for insulin-dependent diabetes
Chapter 73 Pancreatic Transplantation Angelika C. Gruessner, Raja Kandaswamy, Khalid M. Khan, David E. R. Sutherland, and Rainer W. Gruessner Introduction The treatment options for insulin-dependent diabetes
The Spleen. Dr Fahad Ullah
 The Spleen BY Dr Fahad Ullah Spleen The spleen is an largest lymphoid organ shaped like a shoe that lies relative to the 9th and 11th ribs and is located in the left hypochondrium. Thus, the spleen is
The Spleen BY Dr Fahad Ullah Spleen The spleen is an largest lymphoid organ shaped like a shoe that lies relative to the 9th and 11th ribs and is located in the left hypochondrium. Thus, the spleen is
Technique of Split-Liver Transplant for Two Adult Recipients
 F'UJIUWA H.EAL,THCAREi, INC. PRESENTS IMAGES mljk?zr 3TUiVU?MAZ7ON Technique of Split-Liver Transplant for Two Adult Recipients Abhinuv Humur, KhuLid Khwuju> Timothy D. SieLu$'John R. Luke, und WiLLium
F'UJIUWA H.EAL,THCAREi, INC. PRESENTS IMAGES mljk?zr 3TUiVU?MAZ7ON Technique of Split-Liver Transplant for Two Adult Recipients Abhinuv Humur, KhuLid Khwuju> Timothy D. SieLu$'John R. Luke, und WiLLium
Records. Adult Kidney Pancreas Transplant Recipient Registration Worksheet. Recipient Information. Provider Information.
 Records Adult Kidney Pancreas Transplant Recipient Registration Worksheet FORM APPROVED: O.M.B. NO. 0915 0157 Expiration Date: 07/31/2020 Note: These worksheets are provided to function as a guide to what
Records Adult Kidney Pancreas Transplant Recipient Registration Worksheet FORM APPROVED: O.M.B. NO. 0915 0157 Expiration Date: 07/31/2020 Note: These worksheets are provided to function as a guide to what
For more information about how to cite these materials visit
 Author(s): Silas P. Norman, M.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Author(s): Silas P. Norman, M.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
MEDICAL MANAGEMENT POLICY
 PAGE: 1 of 5 MEDICAL MANAGEMENT POLICY This medical policy is not a guarantee of benefits or coverage, nor should it be deemed as medical advice. In the event of any conflict concerning benefit coverage,
PAGE: 1 of 5 MEDICAL MANAGEMENT POLICY This medical policy is not a guarantee of benefits or coverage, nor should it be deemed as medical advice. In the event of any conflict concerning benefit coverage,
Parenchyma-sparing lung resections are a potential therapeutic
 Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
H. Le Dinh, A. DeRoover, C. Coimbra, L. Weekers, J. Léonet, M. Meurisse, and J.P. Squifflet
 Evolution of Native Kidney Function After Pancreas Transplantation Alone H. Le Dinh, A. DeRoover, C. Coimbra, L. Weekers, J. Léonet, M. Meurisse, and J.P. Squifflet ABSTRACT Introduction. This study investigated
Evolution of Native Kidney Function After Pancreas Transplantation Alone H. Le Dinh, A. DeRoover, C. Coimbra, L. Weekers, J. Léonet, M. Meurisse, and J.P. Squifflet ABSTRACT Introduction. This study investigated
SINCE the introduction of Imuran and
 Cadaveric Renal Transplantation With Cyclosporin-A and Steroids T. R. Hakala, T. E. Starzl, J. T. Rosenthal, B. Shaw, and S. watsuki SNCE the introduction of muran and prednisone in 1961, and despite the
Cadaveric Renal Transplantation With Cyclosporin-A and Steroids T. R. Hakala, T. E. Starzl, J. T. Rosenthal, B. Shaw, and S. watsuki SNCE the introduction of muran and prednisone in 1961, and despite the
The abdominal Esophagus, Stomach and the Duodenum. Prof. Oluwadiya KS
 The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
Journal of Medical Imaging and Radiation Oncology
 Journal of Medical Imaging and Radiation Oncology 62 (2018) 504 511 MEDICAL IMAGING PICTORIAL ESSAY Imaging in pancreas transplantation complications: Temporal classification Paula Gallego Ferrero and
Journal of Medical Imaging and Radiation Oncology 62 (2018) 504 511 MEDICAL IMAGING PICTORIAL ESSAY Imaging in pancreas transplantation complications: Temporal classification Paula Gallego Ferrero and
ABDOMEN - GI. Duodenum
 TALA SALEH ABDOMEN - GI Duodenum - Notice the shape of the duodenum, it looks like capital G shape tube which extends from the pyloroduodenal junction to the duodenojejunal junction. - It is 10 inches
TALA SALEH ABDOMEN - GI Duodenum - Notice the shape of the duodenum, it looks like capital G shape tube which extends from the pyloroduodenal junction to the duodenojejunal junction. - It is 10 inches
Visceral aneurysm. Diagnosis and Interventions M.NEDEVSKA
 Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
PENETRATING COLON TRAUMA: THE CURRENT EVIDENCE
 PENETRATING COLON TRAUMA: THE CURRENT EVIDENCE Samuel Hawkins MD CASE PRESENTATION 22M BIBEMS s/p multiple GSW ABCs intact Normotensive, non-tachycardic Secondary Survey: 4 truncal bullet holes L superior
PENETRATING COLON TRAUMA: THE CURRENT EVIDENCE Samuel Hawkins MD CASE PRESENTATION 22M BIBEMS s/p multiple GSW ABCs intact Normotensive, non-tachycardic Secondary Survey: 4 truncal bullet holes L superior
Live Donor Small Bowel Transplantation. Enrico Benedetti, MD, FACS Warren H. Cole Chair in Surgery Professor and Head Department of Surgery
 Live Donor Small Bowel Transplantation Enrico Benedetti, MD, FACS Warren H. Cole Chair in Surgery Professor and Head Department of Surgery INTESTINAL TRANSPLANTATION: A RELATIVE RARE PROCEDURE In 2017
Live Donor Small Bowel Transplantation Enrico Benedetti, MD, FACS Warren H. Cole Chair in Surgery Professor and Head Department of Surgery INTESTINAL TRANSPLANTATION: A RELATIVE RARE PROCEDURE In 2017
Patient Education. Transplant Services. Benefits and. Of a kidney/pancreas transplant
 Patient Education Benefits and Risks Of a kidney/pancreas transplant This chapter discusses the benefits as well as the risks of a kidney and/or pancreas transplant. The complications of transplant and
Patient Education Benefits and Risks Of a kidney/pancreas transplant This chapter discusses the benefits as well as the risks of a kidney and/or pancreas transplant. The complications of transplant and
Case Report Transplantation of Horseshoe Kidney from Living, Genetically Unrelated Donor
 Case Reports in Transplantation Volume 2015, Article ID 390381, 4 pages http://dx.doi.org/10.1155/2015/390381 Case Report Transplantation of Horseshoe Kidney from Living, Genetically Unrelated Donor Kazuro
Case Reports in Transplantation Volume 2015, Article ID 390381, 4 pages http://dx.doi.org/10.1155/2015/390381 Case Report Transplantation of Horseshoe Kidney from Living, Genetically Unrelated Donor Kazuro
Transplant Surgery. Patient Education Guide to Your Kidney/Pancreas Transplant Page 9-1. For a kidney/pancreas transplant. Before Your Surgery
 Patient Education Page 9-1 Transplant Surgery For a kidney/pancreas transplant By the time you have your transplant surgery, you may have been waiting for some time. Reading this chapter before surgery
Patient Education Page 9-1 Transplant Surgery For a kidney/pancreas transplant By the time you have your transplant surgery, you may have been waiting for some time. Reading this chapter before surgery
Pancreas Graft Drainage in Recipient Duodenum: Preliminary Experience
 Pancreas Graft Drainage in Recipient Duodenum: Preliminary Experience Arnaud De Roover, 1 Caria Coimbra, 1 Olivier Detrγ, 1 Catherine Van Kemseke, 2 Jean-Paul Squifflet, 1 Pierre Honoré, 1 and Michel Meurisse
Pancreas Graft Drainage in Recipient Duodenum: Preliminary Experience Arnaud De Roover, 1 Caria Coimbra, 1 Olivier Detrγ, 1 Catherine Van Kemseke, 2 Jean-Paul Squifflet, 1 Pierre Honoré, 1 and Michel Meurisse
د. عصام طارق. Objectives:
 GI anatomy Lecture: 5 د. عصام طارق Objectives: To describe anatomy of stomach, duodenum & pancreas. To list their main relations. To define their blood & nerve supply. To list their lymph drainage. To
GI anatomy Lecture: 5 د. عصام طارق Objectives: To describe anatomy of stomach, duodenum & pancreas. To list their main relations. To define their blood & nerve supply. To list their lymph drainage. To
THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY 2013/12/21
 THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY Tsann-Long Hwang, MD, FACS Department of Surgery Chang Gung Memorial Hospital Chang Gung University Taipei, TAIWAN 2013/12/21 THE DIFFICULTY
THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY Tsann-Long Hwang, MD, FACS Department of Surgery Chang Gung Memorial Hospital Chang Gung University Taipei, TAIWAN 2013/12/21 THE DIFFICULTY
Pancreas Transplantation
 REVIEW ARTICLE Pancreas Transplantation Yi-Ming Shyr* Divisions of General and Transplantation Surgery, Department of Surgery, Taipei Veterans General Hospital and National Yang-Ming University, Taipei,
REVIEW ARTICLE Pancreas Transplantation Yi-Ming Shyr* Divisions of General and Transplantation Surgery, Department of Surgery, Taipei Veterans General Hospital and National Yang-Ming University, Taipei,
-12. -Renad Habahbeh. -Dr Mohammad mohtasib
 -12 -Renad Habahbeh - -Dr Mohammad mohtasib The Gallbladder -The gallbladder has a body, a fundus (a rounded end), a neck, Hartmann s pouch before the neck and a cystic duct that meets the common hepatic
-12 -Renad Habahbeh - -Dr Mohammad mohtasib The Gallbladder -The gallbladder has a body, a fundus (a rounded end), a neck, Hartmann s pouch before the neck and a cystic duct that meets the common hepatic
Chapter 4 Section 24.7
 Surgery Chapter 4 Section 24.7 Simultaneous Pancreas-Kidney (SPK), Pancreas-After-Kidney (PAK), And Pancreas-Transplant-Alone (PTA), And Pancreatic Islet Cell Transplantation Issue Date: February 5, 1996
Surgery Chapter 4 Section 24.7 Simultaneous Pancreas-Kidney (SPK), Pancreas-After-Kidney (PAK), And Pancreas-Transplant-Alone (PTA), And Pancreatic Islet Cell Transplantation Issue Date: February 5, 1996
Biology Human Anatomy Abdominal and Pelvic Cavities
 Biology 351 - Human Anatomy Abdominal and Pelvic Cavities Please place your name and I.D. number on the back of the last page of this exam. You must answer all questions on this exam. Because statistics
Biology 351 - Human Anatomy Abdominal and Pelvic Cavities Please place your name and I.D. number on the back of the last page of this exam. You must answer all questions on this exam. Because statistics
AN EXPERIMENTAL TUBE PEDICLE LINED WITH SMALL BOWEL. By J. H. GOLDIN, F.R.C.S.(Edin.) Plastic Surgery Unit, St Thomas' Hospital, London
 British Journal of Plastic Surgery (I972), 25, 388-39z AN EXPERIMENTAL TUBE PEDICLE LINED WITH SMALL BOWEL By J. H. GOLDIN, F.R.C.S.(Edin.) Plastic Surgery Unit, St Thomas' Hospital, London ONE of the
British Journal of Plastic Surgery (I972), 25, 388-39z AN EXPERIMENTAL TUBE PEDICLE LINED WITH SMALL BOWEL By J. H. GOLDIN, F.R.C.S.(Edin.) Plastic Surgery Unit, St Thomas' Hospital, London ONE of the
Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition
 22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
YOU MUST BRING GLOVES FOR THIS ACTIVITY
 ACTIVITY 10: VESSELS AND CIRCULATION OBJECTIVES: 1) How to get ready: Read Chapter 23, McKinley et al., Human Anatomy, 5e. All text references are for this textbook. 2) Observe and sketch histology slide
ACTIVITY 10: VESSELS AND CIRCULATION OBJECTIVES: 1) How to get ready: Read Chapter 23, McKinley et al., Human Anatomy, 5e. All text references are for this textbook. 2) Observe and sketch histology slide
VESSELS: GROSS ANATOMY
 ACTIVITY 10: VESSELS AND CIRCULATION OBJECTIVES: 1) How to get ready: Read Chapter 23, McKinley et al., Human Anatomy, 4e. All text references are for this textbook. 2) Observe and sketch histology slide
ACTIVITY 10: VESSELS AND CIRCULATION OBJECTIVES: 1) How to get ready: Read Chapter 23, McKinley et al., Human Anatomy, 4e. All text references are for this textbook. 2) Observe and sketch histology slide
Lab Monitor Images Dissection of the Abdominal Vasculature + Lower Digestive System
 Lab Monitor Images Dissection of the Abdominal Vasculature + Lower Digestive System Stomach & Duodenum Frontal (AP) View Nasogastric tube 2 1 3 4 Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum
Lab Monitor Images Dissection of the Abdominal Vasculature + Lower Digestive System Stomach & Duodenum Frontal (AP) View Nasogastric tube 2 1 3 4 Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum
Islet and Pancreas Transplantation
 Islet and Pancreas Transplantation Julie Wardle Specialist Nurse Coordinator Indication for Transplant Treatment option for a select groups of patients with type 1 diabetes Aged 18 years or over Recurrent
Islet and Pancreas Transplantation Julie Wardle Specialist Nurse Coordinator Indication for Transplant Treatment option for a select groups of patients with type 1 diabetes Aged 18 years or over Recurrent
Liver Transplantation
 1 Liver Transplantation Department of Surgery Yonsei University Wonju College of Medicine Kim Myoung Soo M.D. ysms91@wonju.yonsei.ac.kr http://gs.yonsei.ac.kr History Development of Liver transplantation
1 Liver Transplantation Department of Surgery Yonsei University Wonju College of Medicine Kim Myoung Soo M.D. ysms91@wonju.yonsei.ac.kr http://gs.yonsei.ac.kr History Development of Liver transplantation
J Am Soc Nephrol 14: , 2003
 J Am Soc Nephrol 14: 208 213, 2003 Kidney Allograft and Patient Survival in Type I Diabetic Recipients of Cadaveric Kidney Alone Versus Simultaneous Pancreas/Kidney Transplants: A Multivariate Analysis
J Am Soc Nephrol 14: 208 213, 2003 Kidney Allograft and Patient Survival in Type I Diabetic Recipients of Cadaveric Kidney Alone Versus Simultaneous Pancreas/Kidney Transplants: A Multivariate Analysis
Management of Pancreatic Fistulae
 Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
16 April 2010 Resident Teaching Conference. Pancreatitis. W. H. Nealon, M.D., F.A.C.S. J.J. Smith, M.D., D.W.D.
 16 April 2010 Resident Teaching Conference Pancreatitis W. H. Nealon, M.D., F.A.C.S. J.J. Smith, M.D., D.W.D. Santorini Wirsung anatomy.med.umich.edu/.../ duodenum_ans.html Bud and ductology Ventral pancreatic
16 April 2010 Resident Teaching Conference Pancreatitis W. H. Nealon, M.D., F.A.C.S. J.J. Smith, M.D., D.W.D. Santorini Wirsung anatomy.med.umich.edu/.../ duodenum_ans.html Bud and ductology Ventral pancreatic
Pancreatico-Duodenal Trauma: Drain, Debride, Divert, Despair BACKGROUND EPIDEMIOLOGY 9/11/2018
 Pancreatico-Duodenal Trauma: Drain, Debride, Divert, Despair Rochelle A. Dicker, M.D. Professor of Surgery and Anesthesia UCLA BACKGROUND Lancet 1827: Travers, B Rupture of the Pancreas British Journal
Pancreatico-Duodenal Trauma: Drain, Debride, Divert, Despair Rochelle A. Dicker, M.D. Professor of Surgery and Anesthesia UCLA BACKGROUND Lancet 1827: Travers, B Rupture of the Pancreas British Journal
Pancreas and Biliary System
 Pancreas and Biliary System Please view our Editing File before studying this lecture to check for any changes. Color Code Important Doctors Notes Notes/Extra explanation Objectives At the end of the lecture,
Pancreas and Biliary System Please view our Editing File before studying this lecture to check for any changes. Color Code Important Doctors Notes Notes/Extra explanation Objectives At the end of the lecture,
Appendix 5. EFSUMB Newsletter. Gastroenterological Ultrasound
 EFSUMB Newsletter 87 Examinations should encompass the full range of pathological conditions listed below A log book listing the types of examinations undertaken should be kept Training should usually
EFSUMB Newsletter 87 Examinations should encompass the full range of pathological conditions listed below A log book listing the types of examinations undertaken should be kept Training should usually
Information for patients (and their families) waiting for liver transplantation
 Information for patients (and their families) waiting for liver transplantation Waiting list? What is liver transplant? Postoperative conditions? Ver.: 5/2017 1 What is a liver transplant? Liver transplantation
Information for patients (and their families) waiting for liver transplantation Waiting list? What is liver transplant? Postoperative conditions? Ver.: 5/2017 1 What is a liver transplant? Liver transplantation
PANCREAS TRANSPLANTATION: INDICATIONS, CLINICAL MANAGEMENT, AND OUTCOMES
 [Frontiers in Bioscience 2, e34-40, August 1, 1997] PANCREAS TRANSPLANTATION: INDICATIONS, CLINICAL MANAGEMENT, AND OUTCOMES John P. Leone, MD, PhD 1, Abhinav Humar 1, Rainer W. G. Gruessner, MD, PhD 2,
[Frontiers in Bioscience 2, e34-40, August 1, 1997] PANCREAS TRANSPLANTATION: INDICATIONS, CLINICAL MANAGEMENT, AND OUTCOMES John P. Leone, MD, PhD 1, Abhinav Humar 1, Rainer W. G. Gruessner, MD, PhD 2,
Allogeneic Pancreas Transplant
 Protocol Allogeneic Pancreas Transplant (70302) Medical Benefit Effective Date: 07/01/14 Next Review Date: 05/18 Preauthorization Yes Review Dates: 09/09, 09/10, 09/11, 07/12, 05/13, 05/14, 05/15, 05/16,
Protocol Allogeneic Pancreas Transplant (70302) Medical Benefit Effective Date: 07/01/14 Next Review Date: 05/18 Preauthorization Yes Review Dates: 09/09, 09/10, 09/11, 07/12, 05/13, 05/14, 05/15, 05/16,
PANCREAS DUCTAL ADENOCARCINOMA PDAC
 CONTENTS PANCREAS DUCTAL ADENOCARCINOMA PDAC I. What is the pancreas? II. III. IV. What is pancreas cancer? What is the epidemiology of Pancreatic Ductal Adenocarcinoma (PDAC)? What are the risk factors
CONTENTS PANCREAS DUCTAL ADENOCARCINOMA PDAC I. What is the pancreas? II. III. IV. What is pancreas cancer? What is the epidemiology of Pancreatic Ductal Adenocarcinoma (PDAC)? What are the risk factors
Chapter 4 Section Simultaneous Pancreas-Kidney (SPK), Pancreas-After-Kidney (PAK), And Pancreas-Transplant-Alone (PTA)
 Surgery Chapter 4 Section 24.7 Simultaneous Pancreas-Kidney (SPK), Pancreas-After-Kidney (PAK), And Pancreas-Transplant-Alone Issue Date: February 5, 1996 Authority: 32 CFR 199.4(e)(5) 1.0 CPT 1 PROCEDURE
Surgery Chapter 4 Section 24.7 Simultaneous Pancreas-Kidney (SPK), Pancreas-After-Kidney (PAK), And Pancreas-Transplant-Alone Issue Date: February 5, 1996 Authority: 32 CFR 199.4(e)(5) 1.0 CPT 1 PROCEDURE
Allogeneic Pancreas Transplant
 Protocol Allogeneic Pancreas Transplant (70302) Medical Benefit Effective Date: 07/01/14 Next Review Date: 05/15 Preauthorization Yes Review Dates: 09/09, 09/10, 09/11, 07/12, 05/13, 05/14 The following
Protocol Allogeneic Pancreas Transplant (70302) Medical Benefit Effective Date: 07/01/14 Next Review Date: 05/15 Preauthorization Yes Review Dates: 09/09, 09/10, 09/11, 07/12, 05/13, 05/14 The following
Duodenum retroperitoneal
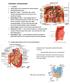 Duodenum retroperitoneal C shaped Initial region out of stomach into small intestine RETROperitoneal viscus Superior 1 st part duodenal cap ; moves upwards and backwards to lie on the R crura medial to
Duodenum retroperitoneal C shaped Initial region out of stomach into small intestine RETROperitoneal viscus Superior 1 st part duodenal cap ; moves upwards and backwards to lie on the R crura medial to
Anatomy of the liver and pancreas
 Anatomy of the liver and pancreas Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk abdulameerh@yahoo.com Liver Aorta Pulm. Trunk Rt. At, Duct. Art. Lt. Ven. Rt. Ven. Internal Posterior
Anatomy of the liver and pancreas Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk abdulameerh@yahoo.com Liver Aorta Pulm. Trunk Rt. At, Duct. Art. Lt. Ven. Rt. Ven. Internal Posterior
Citation Hepato-Gastroenterology, 55(86-87),
 NAOSITE: Nagasaki University's Ac Title Author(s) Combined pancreatic resection and p multiple lesions of the pancreas: i of the pancreas concomitant with du Kuroki, Tamotsu; Tajima, Yoshitsugu Tomohiko;
NAOSITE: Nagasaki University's Ac Title Author(s) Combined pancreatic resection and p multiple lesions of the pancreas: i of the pancreas concomitant with du Kuroki, Tamotsu; Tajima, Yoshitsugu Tomohiko;
Morbidity and Mortality After Living Kidney Donation, : Survey of United States Transplant Centers
 American Journal of Transplantation 2003; 3: 830 834 Copyright # Blackwell Munksgaard 2003 Blackwell Munksgaard ISSN 1600-6135 Morbidity and Mortality After Living Kidney Donation, 1999 2001: Survey of
American Journal of Transplantation 2003; 3: 830 834 Copyright # Blackwell Munksgaard 2003 Blackwell Munksgaard ISSN 1600-6135 Morbidity and Mortality After Living Kidney Donation, 1999 2001: Survey of
Vascular Imaging in the Pediatric Abdomen. Jonathan Swanson, MD
 Vascular Imaging in the Pediatric Abdomen Jonathan Swanson, MD Goals and Objectives To understand the imaging approach, appearance, and clinical manifestations of the common pediatric abdominal vascular
Vascular Imaging in the Pediatric Abdomen Jonathan Swanson, MD Goals and Objectives To understand the imaging approach, appearance, and clinical manifestations of the common pediatric abdominal vascular
Exploring Anatomy: the Human Abdomen
 Exploring Anatomy: the Human Abdomen PERITONEUM AND PERITONEAL CAVITY PERITONEUM The peritoneum is a thin serous membrane that lines the abdominal cavity and covers, in variable amounts, the viscera within
Exploring Anatomy: the Human Abdomen PERITONEUM AND PERITONEAL CAVITY PERITONEUM The peritoneum is a thin serous membrane that lines the abdominal cavity and covers, in variable amounts, the viscera within
Postoperative monitoring after
 Postoperative monitoring after kidney transplantation Bundit sakulchairungrueng,md Vascular and Transplantation Unit Faculty of Medicine Ramathibodi Hospital Mahidol University Reference Introduction A
Postoperative monitoring after kidney transplantation Bundit sakulchairungrueng,md Vascular and Transplantation Unit Faculty of Medicine Ramathibodi Hospital Mahidol University Reference Introduction A
associated with serious complications, but reduce occurrences with preventive measures
 Wk 9. Management of Clients with Diabetes Mellitus 1. Diabetes Mellitus body s inability to metabolize carbohydrates, fats, proteins hyperglycemia associated with serious complications, but reduce occurrences
Wk 9. Management of Clients with Diabetes Mellitus 1. Diabetes Mellitus body s inability to metabolize carbohydrates, fats, proteins hyperglycemia associated with serious complications, but reduce occurrences
Retroperitoneal Systemic-Enteric Dr. International (CC BY-NC-ND 4.0).
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Simultaneous Pancreas and Kidney Co Retroperitoneal Systemic-Enteric Dr Ono, Shinichiro; Kuroki, Tamotsu; K Chen, Yin-Yin; Chen, Shin-Chin; Egu
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Simultaneous Pancreas and Kidney Co Retroperitoneal Systemic-Enteric Dr Ono, Shinichiro; Kuroki, Tamotsu; K Chen, Yin-Yin; Chen, Shin-Chin; Egu
ANATOMY OF PELVICAYCEAL SYSTEM -DR. RAHUL BEVARA
 1 ANATOMY OF PELVICAYCEAL SYSTEM -DR. RAHUL BEVARA 2 KIDNEY:ANATOMY OVERVIEW Kidneys are retroperitoneal, in posterior abdominal region, extending from T12 L3 Bean-shaped Right kidney is lower than left
1 ANATOMY OF PELVICAYCEAL SYSTEM -DR. RAHUL BEVARA 2 KIDNEY:ANATOMY OVERVIEW Kidneys are retroperitoneal, in posterior abdominal region, extending from T12 L3 Bean-shaped Right kidney is lower than left
Anatomy: Know Your Abdomen
 Anatomy: Know Your Abdomen Glossary Abdomen - part of the body below the thorax (chest cavity); separated by the diaphragm. Anterior - towards the front of the body. For example, the umbilicus is anterior
Anatomy: Know Your Abdomen Glossary Abdomen - part of the body below the thorax (chest cavity); separated by the diaphragm. Anterior - towards the front of the body. For example, the umbilicus is anterior
Single Center Analysis of Mortality in 202 Consecutive Pancreas Transplants
 Single Center Analysis of Mortality in 202 Consecutive Pancreas Transplants Robert J. Stratta, MD 1, Alan C. Farney, MD, PhD 1, Giuseppe Orlando, MD, PhD 1, Umar Farooq, MD 1, Yousef Al-Shraideh, MBBCh
Single Center Analysis of Mortality in 202 Consecutive Pancreas Transplants Robert J. Stratta, MD 1, Alan C. Farney, MD, PhD 1, Giuseppe Orlando, MD, PhD 1, Umar Farooq, MD 1, Yousef Al-Shraideh, MBBCh
Surgical anatomy of the biliary tract
 HPB, 2008; 10: 7276 REVIEW ARTICLE Surgical anatomy of the biliary tract DENIS CASTAING Centre hépato-biliaire, Hôpital Paul Brousse, Assistance Publique- Hôpitaux de Paris, Université Paris XI, Paris,
HPB, 2008; 10: 7276 REVIEW ARTICLE Surgical anatomy of the biliary tract DENIS CASTAING Centre hépato-biliaire, Hôpital Paul Brousse, Assistance Publique- Hôpitaux de Paris, Université Paris XI, Paris,
Topic: Pancreas Transplant Date of Origin: January Section: Transplant Last Reviewed Date: August 2013
 Medical Policy Manual Topic: Pancreas Transplant Date of Origin: January 1996 Section: Transplant Last Reviewed Date: August 2013 Policy No: 6 Effective Date: November 1, 2013 IMPORTANT REMINDER Medical
Medical Policy Manual Topic: Pancreas Transplant Date of Origin: January 1996 Section: Transplant Last Reviewed Date: August 2013 Policy No: 6 Effective Date: November 1, 2013 IMPORTANT REMINDER Medical
Upon completion of the transplant rotation, Residents will understand the basic principles of organ transplantation and immunology.
 Transplantation Rotation Length: 1-2 Months, PGY-4 year Location: University of California at San Francisco, Department of Surgery Primary Supervisor: Ryutaro Hirose, M.D., Associate Program Director Contact
Transplantation Rotation Length: 1-2 Months, PGY-4 year Location: University of California at San Francisco, Department of Surgery Primary Supervisor: Ryutaro Hirose, M.D., Associate Program Director Contact
Having an operation on the pancreas
 Having an operation on the pancreas Let us assume you (the reader) are going to have a pancreatic resection. The following section attempts to answer some of the questions you may have in mind, and the
Having an operation on the pancreas Let us assume you (the reader) are going to have a pancreatic resection. The following section attempts to answer some of the questions you may have in mind, and the
Nasogastric tube. Stomach. Pylorus. Duodenum 1. Duodenum 2. Duodenum 3. Duodenum 4
 Esophagus Barium Swallow Stomach and Duodenum 4 year old Upper GI Nasogastric tube Stomach and Duodenum 4 year old Upper GI Nasogastric tube Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum 4
Esophagus Barium Swallow Stomach and Duodenum 4 year old Upper GI Nasogastric tube Stomach and Duodenum 4 year old Upper GI Nasogastric tube Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum 4
An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein
 J Gastrointest Surg (2007) 11:425 431 DOI 10.1007/s11605-007-0131-1 An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein Rory L. Smoot & John D. Christein &
J Gastrointest Surg (2007) 11:425 431 DOI 10.1007/s11605-007-0131-1 An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein Rory L. Smoot & John D. Christein &
FEP Medical Policy Manual
 FEP Medical Policy Manual Effective Date: January 15, 2019 Related Policies: 1.01.30 Artificial Pancreas Device Systems 7.03.12 Autologous Islet transplantation Allogeneic Pancreas Transplant Description
FEP Medical Policy Manual Effective Date: January 15, 2019 Related Policies: 1.01.30 Artificial Pancreas Device Systems 7.03.12 Autologous Islet transplantation Allogeneic Pancreas Transplant Description
Small Plicae Circularis. Short Closely packed together. Sparse, completely absent at distal part Lymphoid Nodule
 Intestines Differences Between Jejunum and Ileum Types Jejunum Ileum Color Deeper red Paler pink Calibre Bigger Smaller Thickness of wall Thick and Heavy Thin and Lighter Vascularity Highly vascularised
Intestines Differences Between Jejunum and Ileum Types Jejunum Ileum Color Deeper red Paler pink Calibre Bigger Smaller Thickness of wall Thick and Heavy Thin and Lighter Vascularity Highly vascularised
Surgical Aspects of Kidney and Pancreas Transplant. Hannah Choate, MD
 Surgical Aspects of Kidney and Pancreas Transplant Hannah Choate, MD I have no financial disclosures or conflicts of interest Kidney transplantation Indications ESRD or advancing CKD with GFR less than
Surgical Aspects of Kidney and Pancreas Transplant Hannah Choate, MD I have no financial disclosures or conflicts of interest Kidney transplantation Indications ESRD or advancing CKD with GFR less than
Total Pancreatectomy and Islet Auto Transplantation (TPIAT)
 Total Pancreatectomy and Islet Auto Transplantation (TPIAT) Dhiraj Yadav, MD MPH Professor of Medicine Division of Gastroenterology & Hepatology University of Pittsburgh Medical Center PSG Meeting Sept
Total Pancreatectomy and Islet Auto Transplantation (TPIAT) Dhiraj Yadav, MD MPH Professor of Medicine Division of Gastroenterology & Hepatology University of Pittsburgh Medical Center PSG Meeting Sept
AFfER THE PIONEER WORK on "cluster" splanchnic
 Gastrie Outlet Obstruction by a Donor Aortic Tube After En Bloc Liver Pancreas Transplantation: A Case Report B. Deylgat, H. Topai, N. Meurisse, 1. Jochmans, R. Aerts, D. Vanbeckevoort, D. Monbaliu, and
Gastrie Outlet Obstruction by a Donor Aortic Tube After En Bloc Liver Pancreas Transplantation: A Case Report B. Deylgat, H. Topai, N. Meurisse, 1. Jochmans, R. Aerts, D. Vanbeckevoort, D. Monbaliu, and
UEMS & EBS: DIVISION OF TRANSPLANT SURGERY
 CURRICULUM AND SYLLABUS TRANSPLANTATION Module 1: Multi-organ retrieval Ability to evaluate donor suitability Ability to retrieve abdominal organs for transplantation Evaluation of donor/ organs suitability
CURRICULUM AND SYLLABUS TRANSPLANTATION Module 1: Multi-organ retrieval Ability to evaluate donor suitability Ability to retrieve abdominal organs for transplantation Evaluation of donor/ organs suitability
Your pancreas transplant
 Renal and transplant service Your pancreas transplant Information for patients, families and carers Introduction What is pancreas transplantation? A pancreas transplant is a major surgical procedure to
Renal and transplant service Your pancreas transplant Information for patients, families and carers Introduction What is pancreas transplantation? A pancreas transplant is a major surgical procedure to
TRANSPLANTATION IN DIABETIC PATIENTS. A.Tarik Kizilisik, MD, MSc, FACS, FICS Director & Primary Transplant Surgeon Lutheran Transplant Center
 TRANSPLANTATION IN DIABETIC PATIENTS A.Tarik Kizilisik, MD, MSc, FACS, FICS Director & Primary Transplant Surgeon Lutheran Transplant Center Diabetes is the pandemic of the new millennium 24 million diabetics
TRANSPLANTATION IN DIABETIC PATIENTS A.Tarik Kizilisik, MD, MSc, FACS, FICS Director & Primary Transplant Surgeon Lutheran Transplant Center Diabetes is the pandemic of the new millennium 24 million diabetics
SURGERY, TRANSPLANTATION AND POLYCYSTIC DISEASE. Mr Nick Inston PhD FRCS Consultant Transplant Surgeon Queen Elizabeth Hospital Birmingham
 SURGERY, TRANSPLANTATION AND POLYCYSTIC DISEASE Mr Nick Inston PhD FRCS Consultant Transplant Surgeon Queen Elizabeth Hospital Birmingham What are polycystic kidneys and livers?! Cystic degenerative condition!
SURGERY, TRANSPLANTATION AND POLYCYSTIC DISEASE Mr Nick Inston PhD FRCS Consultant Transplant Surgeon Queen Elizabeth Hospital Birmingham What are polycystic kidneys and livers?! Cystic degenerative condition!
Reinterventions belong to complications
 Reinterventions belong to complications Pancreatic surgery is the archetypus of complex abdominal surgery Mortality (1-4%) and morbidity (7-60%) rates are relevant even at high volume centres Reinterventions
Reinterventions belong to complications Pancreatic surgery is the archetypus of complex abdominal surgery Mortality (1-4%) and morbidity (7-60%) rates are relevant even at high volume centres Reinterventions
Biology Human Anatomy Abdominal and Pelvic Cavities
 Biology 351 - Human Anatomy Abdominal and Pelvic Cavities You must answer all questions on this exam. Because statistics demonstrate that, on average, between 2-5 questions on every 100-point exam are
Biology 351 - Human Anatomy Abdominal and Pelvic Cavities You must answer all questions on this exam. Because statistics demonstrate that, on average, between 2-5 questions on every 100-point exam are
ACUTE PANCREATITIS: NEW CLASSIFICATION OF AN OLD FOE. T Barrow, A Nasrullah, S Liong, V Rudralingam, S A Sukumar
 ACUTE PANCREATITIS: NEW CLASSIFICATION OF AN OLD FOE T Barrow, A Nasrullah, S Liong, V Rudralingam, S A Sukumar LEARNING OBJECTIVES q Through a series of cases illustrate the updated Atlanta symposium
ACUTE PANCREATITIS: NEW CLASSIFICATION OF AN OLD FOE T Barrow, A Nasrullah, S Liong, V Rudralingam, S A Sukumar LEARNING OBJECTIVES q Through a series of cases illustrate the updated Atlanta symposium
Pancreas Transplantation: A Daring Concept 17 December 1966
 Pancreas Transplantation Pancreas Transplantation: A Daring Concept 17 December 1966 Rutger J. Ploeg, MD PhD Abdominal & Transplant Surgery University Medical Centre Groningen The Netherlands Diabetes
Pancreas Transplantation Pancreas Transplantation: A Daring Concept 17 December 1966 Rutger J. Ploeg, MD PhD Abdominal & Transplant Surgery University Medical Centre Groningen The Netherlands Diabetes
AORTIC GRAFT INFECTION
 NURSING CARE Theresa O Keefe NUM Vascular Unit PAH Vascular infections are serious They are associated with high morbidity and mortality The primary cause of surgical wound infections is contamination
NURSING CARE Theresa O Keefe NUM Vascular Unit PAH Vascular infections are serious They are associated with high morbidity and mortality The primary cause of surgical wound infections is contamination
Case Report Spleen-Preserving Surgery in Splenic Artery Aneurysm
 Hindawi Case Reports in Surgery Volume 2017, Article ID 8716962, 4 pages https://doi.org/10.1155/2017/8716962 Case Report Spleen-Preserving Surgery in Splenic Artery Aneurysm Ulaş Aday,Emre Bozdağ,EbubekirGündeş,Selçuk
Hindawi Case Reports in Surgery Volume 2017, Article ID 8716962, 4 pages https://doi.org/10.1155/2017/8716962 Case Report Spleen-Preserving Surgery in Splenic Artery Aneurysm Ulaş Aday,Emre Bozdağ,EbubekirGündeş,Selçuk
Information for Consent Cholecystectomy (Laparoscopic/Open) 膽囊切除術 ( 腹腔鏡 / 開放性 )
 Version 1.0 Page 1 of 3 Information for Consent Cholecystectomy (Laparoscopic/Open) 膽囊切除術 ( 腹腔鏡 / 開放性 ) Introduction Gallbladder is a sac connected to the biliary tree. It serves the function of concentration
Version 1.0 Page 1 of 3 Information for Consent Cholecystectomy (Laparoscopic/Open) 膽囊切除術 ( 腹腔鏡 / 開放性 ) Introduction Gallbladder is a sac connected to the biliary tree. It serves the function of concentration
SELECTED ABSTRACTS. All (n) % 3-year GS 88% 82% 86% 85% 88% 80% % 3-year DC-GS 95% 87% 94% 89% 96% 80%
 SELECTED ABSTRACTS The following are summaries of selected posters presented at the American Transplant Congress on May 5 9, 2007, in San Humar A, Gillingham KJ, Payne WD, et al. Review of >1000 kidney
SELECTED ABSTRACTS The following are summaries of selected posters presented at the American Transplant Congress on May 5 9, 2007, in San Humar A, Gillingham KJ, Payne WD, et al. Review of >1000 kidney
BK virus infection in renal transplant recipients: single centre experience. Dr Wong Lok Yan Ivy
 BK virus infection in renal transplant recipients: single centre experience Dr Wong Lok Yan Ivy Background BK virus nephropathy (BKVN) has emerged as an important cause of renal graft dysfunction in recent
BK virus infection in renal transplant recipients: single centre experience Dr Wong Lok Yan Ivy Background BK virus nephropathy (BKVN) has emerged as an important cause of renal graft dysfunction in recent
Expanded Criteria Recipients: Are there any Limits
 Expanded Criteria Recipients: Are there any Limits Andreas Paul, MD, MSc, FRCS Department of General-, Visceral- and Transplant Surgery, University Hospital Essen Ruhr Area 5.200 000 inhabitants University
Expanded Criteria Recipients: Are there any Limits Andreas Paul, MD, MSc, FRCS Department of General-, Visceral- and Transplant Surgery, University Hospital Essen Ruhr Area 5.200 000 inhabitants University
