Faculty Affiliation. Faculty Disclosures. Learning Objectives. Macrovascular and Microvascular Complications
|
|
|
- Pamela O’Brien’
- 5 years ago
- Views:
Transcription
1 Faculty Affiliation Combined Targeted Approaches for the Treatment of Type 2 Diabetes: The Role of the Kidney Mark Stolar, MD Associate Professor of Clinical Medicine Division of General Internal Medicine and Geriatrics Northwestern University Feinberg School of Medicine Chicago, Illinois Sponsored by Integrity Continuing Education, Inc. Supported by an educational grant from AstraZeneca. 1 2 Faculty Disclosures Consultant: AstraZeneca, Takeda Speakers bureau: AstraZeneca, Takeda Learning Objectives Implement current evidence-based guidelines for the detection and diagnosis of prediabetes and diabetes Describe the role of the kidney and sodiumglucose co-transporter 2 (SGLT2) inhibitionbased therapeutic strategies Apply evidence-based and individualized management strategies to ensure appropriate and effective management of type 2 diabetes mellitus (T2DM) 3 4 Prevalence and Burden of Diabetes in the United States Macrovascular and Microvascular Complications Affects ~26 million individuals Estimated that ~3% of adults will have diabetes by 25 7th leading cause of death in 212 Disease sequelae include: Kidney failure, lower-limb amputations, blindness, neuropathy, cardiovascular disease (CVD), and stroke Diabetes diagnosis continues to increase because of obesity epidemic Macrovascular Coronary artery disease 5% of people with T2DM die of coronary artery disease Peripheral arterial disease 2-fold increase in lowerlimb amputations Cerebrovascular disease 15%-4% increased risk of stroke Microvascular Neuropathy Affects up to 5% of patients with diabetes Retinopathy After 15 years, ~1% of patients with diabetes develop severe visual impairment Nephropathy 1%-2% of people with T2DM die of kidney failure Centers for Disease Control and Prevention. Diabetes Report Card 212. American Diabetes Association. Diabetes Care. 213;36: American Diabetes Association. Diabetes Care. 214;37(suppl 1):S14-S8. 5 Fowler MJ. Clin Diabetes. 28;26(2):
2 CVD in T2DM The Natural History of T2DM Major cause of morbidity and mortality for individuals with diabetes Largest contributor to diabetes-associated direct and indirect costs Common T2DM comorbidities (eg, hypertension and dyslipidemia) are clear risk factors for CVD Diabetes confers independent risk for CVD Years from diagnosis Incretin effect -Cell function Insulin resistance Insulin secretion Postprandial glucose Fasting glucose Prediabetes Onset Diagnosis Microvascular complications Macrovascular complications Type 2 diabetes ADA 215 Guidelines. Diabetes Care. 215;38(suppl 1):S49 S57. 7 Defronzo RA. Diabetes. 29;58: ; Holman RR. Diabetes Res Clin Pract. 1998;4(suppl):S21-S25; U.K. Prospective Diabetes Study Group. Diabetes. 1995;44: ; Ramlo-Halsted BA, Edelman SV. Prim Care. 1999;26: ; Nathan DM. N Engl J Med. 22;347: Progressive β-cell Dysfunction Is a Key Driver of Progressive Dysglycemia in T2DM ADA Guideline Recommendations for Prevention or Delay of Diabetes Onset Deteriorating β-cell function is partially driven by the incretin defect By the time of diabetes onset, up to 8% of β-cell function may be lost 1,2 PPG FPG β-cell Function Normal Impaired Glucose Glucose Tolerance Tolerance Insulin Resistance Insulin Secretion Diagnosis Severity of Glucose Intolerance Time in Years PPG, postprandial plasma glucose; FPG, fasting plasma glucose. 1. Defronzo RA. Diabetes. 29;58: ; 2. Fehse F, et al. J Clin Endocrinol Metab. 25;9: ; Figure adapted from Kendall DM, et al. Am J Med.29;122(6, suppl):s37-s5. 9 Recommendations Patients with impaired glucose tolerance (IGT) A, impaired fasting glucose (IFG) E, or an A1c 5.7% 6.4% E should be referred to an intensive diet and physical activity behavioral counseling program targeting loss of 7% of body weight and increasing moderate-intensity physical activity (such as brisk walking) to at least 15 min/week. Follow-up counseling may be important for success. B Based on the cost-effectiveness of diabetes prevention, such programs should be covered by third-party payers. B Metformin therapy for prevention of type 2 diabetes may be considered in those with IGT A, IFG E, or an A1c 5.7% 6.4% E, especially for those with BMI >35 kg/m 2, aged <6 years, and women with prior gestational diabetes mellitus. A At least annual monitoring for the development of diabetes in those with prediabetes is suggested. E Screening for and treatment of modifiable risk factors for CVD is suggested. B Diabetes self-management education and support programs are appropriate venues for people with prediabetes to receive education and support to develop and maintain behaviors that can prevent or delay the onset of diabetes. C ADA, American Diabetes Association; BMI, body mass index. ADA 215 Guidelines. Diabetes Care 215;38(suppl 1):S a 1 Risk Prevention Trials: Lifestyle Modification Risk Prevention Trials: Medication Study Da Qing Finnish Diabetes Prevention Study Groups Control, diet, exercise, diet & exercise Control, lifestyle Average Follow-up (Years) Incidence of Diabetes* Relative Risk Reduction (%) P Value 31% (control vs diet); 46% (control vs exercise); all <.5 42% (control vs diet and exercise) % <.1 US DPP PBO, lifestyle % <.1 Indian DPP Control, lifestyle *Per 1 person-years. DPP, Diabetes Prevention Program; PBO, placebo. Reviewed in Kahn SE, et al. Lancet. 214;383(9922): % Study Groups Average Follow-up (Years) Incidence of Diabetes* Relative Risk Reduction (%) P Value US DPP PBO, metformin % <.1 Indian DPP Control, metformin %.29 Nepi Antidiabetes Study PBO, glimepiride %.72 STOP-NIDDM PBO, acarbose %.15 XENDOS PBO, orlistat %.24 NAVIGATOR PBO, nateglinide % NS ORIGIN Control, insulin glargine %.6 TRIPOD PBO, troglitazone % <.1 US DPP PBO, troglitazone % <.1 DREAM PBO, rosiglitazone % <.1 ACT NOW PBO, pioglitazone % <.1 *Per 1 person-years. NS, not significant. Reviewed in Kahn SE, et al. Lancet. 214;383(9922):
3 Hazard Ratio Hazard Ratio Hazard Ratio Hazard Ratio 1-year Follow-up of Intensive Glucose Control in T2DM: Myocardial Infarction United Kingdom Prospective Diabetes Study Survivor Cohort 1-year Follow-up of Intensive Glucose Control in T2DM: Death From Any Cause United Kingdom Prospective Diabetes Study Survivor Cohort SU-INS SU-INS P=.52 P= P=.1 P= P=.44 P= P=.1 P= Risk of myocardial infarction was reduced in patients treated with SU-INS (15%) or (33%) vs conventional therapy.* Risk of death from any cause was reduced in patients treated with SU-INS (13%) or (27%) vs conventional therapy.* *Conventional therapy was dietary restriction alone. SU, sulfonylurea; INS, insulin;, metformin. Holman RR, et al. N Engl J Med. 28;359(15): *Conventional therapy was dietary restriction alone. Holman RR, et al. N Engl J Med. 28;359(15): ADA Guidelines for Diabetes Screening Guideline Recommendations for Screening and Diagnosis Adults BMI >25 kg/m 2 * with additional risk factors >45 years of age without risk factors Children and adolescents Overweight with 2 risk factors Individuals with normal test results should follow up every 3 years *BMI >23 kg/m 2 for Asian Americans. ADA 215 Guidelines. Diabetes Care. 215;38(suppl 1):S8-S General Risk Factors for Diabetes Metabolic Risk Factors for Diabetes Physical inactivity Increased caloric intake (obesity) First-degree relative with diabetes Race/ethnicity Delivery of a baby weighing >9 lb or diagnosed with gestational diabetes mellitus Clinical conditions associated with insulin resistance (eg, severe obesity, metabolic syndrome, acanthosis nigricans) Polycystic ovarian syndrome A1c >5.7%, IGT, or IFG on previous testing Hypertension (>14/9 mm Hg or on therapy for hypertension) HDL-C level 35 mg/dl (.9 mmol/l) and/or a triglyceride level 25 mg/dl (2.82 mmol/l) History of CVD American Diabetes Association. Diabetes Care. 214;37(suppl 1):S14-S8. 18 HDL-C, high-density lipoprotein cholesterol. American Diabetes Association. Diabetes Care. 214;37(suppl 1):S14-S
4 Individualization of Care: ADA/EASD Position Statement Approach to management of hyperglycemia: More stringent Less stringent Patient attitude and expected treatment efforts Highly motivated, adherent, excellent self-care capacities Less motivated, nonadherent, poor self-care capacities Guideline Recommendations for Management of T2DM Risks potentially associated with hypoglycemia, other adverse events Disease duration Low Newly diagnosed High Long-standing Life expectancy Long Short Important comorbidities Absent Few/mild Severe Established vascular complications Absent Few/mild Severe Resources, support system Readily available Limited Management of hyperglycemia in type 2 diabetes: a patient-centered approach. Position statement of the ADA and the European Association for the Study of Diabetes (EASD). Diabetologia. February Goals of Therapy in T2DM Management Recommendations for Dietary Modifications Glycemic Control Decreases onset and progression of T2DM-related microvascular complications Impact on cardiovascular complications remains uncertain Modest long-term benefit to achievement of good glycemic control early in disease course Aggressive control in older patients with advanced disease may present some risk without significant benefit Comprehensive Cardiovascular Risk Reduction Reduces CVD risk in T2DM Significant benefits of globally addressing multiple risk factors Strategies Smoking cessation Blood pressure (BP) control Lipid management (statins) Antiplatelet therapy in some circumstances Reduce total daily calorie intake Reduce sodium intake: <23 mg/day; lower for patients with hypertension Reduce simple carbohydrates, sugars, and high-fat foods (eliminate trans fats) Limit saturated fat: <7% of calories, <2-3 g/day Limit cholesterol: <2 mg/day Increase water-soluble fiber: 1-25 g/day Increase unsaturated fat and marine-based omega-3s Limit alcohol consumption: <1 drink day for adult women and 2 drinks per day for adult men Inzucchi SE, et al. Diabetes Care. 215;38(1): ADA 215 Guidelines. Diabetes Care. 215;38(suppl 1):S2-S3. 23 ADA 215 Guidelines. Diabetes Care. 215;38(suppl 1):S2-S3. Evert AB, et al. Diabetes Care. 214;37(suppl 1):S12 S Recommendations for Physical Activity Psychosocial Assessment and Care Children 6 minutes of physical activity each day (Grade B) Adults 15 minutes/week of moderate-intensity aerobic physical activity (5%-7% of maximum heart rate), spread over at least 3 days/week with no more than 2 consecutive days without exercise (Grade A) Reduce sedentary time, particularly by breaking up extended amounts of time (>9 min) spent sitting (Grade B) In the absence of contraindications, resistance training at least twice per week (Grade A) Assessment of patient s psychological and social situation Psychosocial screening and follow-up: Attitudes about illness Expectations for medical management and outcomes Affect/mood Quality of life Financial, social, and emotional resources Psychiatric history Routinely screen for psychosocial problems: depression, diabetes-related distress, anxiety, eating disorders, and cognitive impairment Patients 65 years of age should be screened and treated for depression Patients with comorbid depression should receive a stepwise collaborative care approach for depression management ADA 215 Guidelines. Diabetes Care. 215;38(suppl 1):S2-S3. 27 ADA 215 Guidelines. Diabetes Care. 215;38(suppl 1):S2-S
5 Negative Reactions to Initial Diagnosis of Diabetes Are Common Guilty Type 1 Type 2 Angry Depressed Pharmacologic Treatment of T2DM Anxious Agreeing (%) Base: all patients Peyrot M, et al. Diabetes Care. 25;28(11): Pharmacologic Targeting of Pathophysiological Disturbances in T2DM Pharmacologic Targeting of Pathophysiological Disturbances in T2DM (cont d) Decreased INS secretion Decreased incretin effect Increased lipolysis GLP-1 RAs DPP-4 inhibitors TZDs SUs Meglitinides GLP-1 RAs DPP-4 inhibitors Bile acid sequestrants α-glucosidase inhibitors TZDs Increased glucagon secretion HYPERGLYCEMIA Increased glucose reabsorption GLP-1 RAs DPP-4 inhibitors Amylin analogs SGLT2 inhibitors Increased HGP Neurotransmitter dysfunction Decreased glucose uptake GLP-1 RAs TZDs HGP, hepatic glucose production. DeFronzo RA. Diabetes. 29;58: GLP-1, glucagon-like peptide 1; RA, receptor agonist; DPP-4, dipeptidyl peptidase-4; TZDs, thiazolidinediones. DeFronzo RA. Diabetes. 29;58: The Role of the Kidney in Glucose Homeostasis Targeting the Kidney for the Treatment of T2DM: SGLT2 Inhibition Under normal conditions, the kidney is involved in maintaining glucose homeostasis via 3 different mechanisms: Release of glucose into circulation via gluconeogenesis Uptake of glucose to meet its own energy needs Reabsorption of glucose from the glomerular filtrate Abdul-Ghani MA, et al. Endocr Rev. 211;32(4): Gerich JE. Diabet Med. 21;27: Stumvoll M, et al. J Clin Invest. 1995;96:
6 Altered Renal Glucose Control in Diabetes Glucose Reabsorption in the Kidney by SGLT2 Gluconeogenesis is increased in postprandial and postabsorptive states in patients with T2DM Renal contribution to hyperglycemia postprandially is significant 3-fold increase in glucose output relative to patients without diabetes In renal insufficiency renal glucose output is decreased increasing risk of hypoglycemia Glucose reabsorption Increased SGLT2 expression and activity in renal epithelial cells from patients with diabetes vs normoglycemic individuals GLUT, glucose transporter; ATP, adenosine triphosphate; ATPase, adenosine triphosphatase; S1, segment 1; S2, segment 2; S3, segment 3. Marsenic O. Am J Kidney Dis. 29;53: Bakris GL, et al. Kidney Int. 29;75(12): Rahmoune H, et al. Diabetes. 25;54(12): Gerich JE. Diabet Med. 21;27: Whaley JM, et al. Diabetes Metab Syndr Obes. 212;5: Rosenwasser RF, et al. Diabetes Metab Syndr Obes. 213;6: Rationale for SGLT2 Inhibitors Therapeutic Benefits Associated with SGLT2 Inhibition SGLT2 is a low-affinity, high-capacity glucose transporter located in the proximal tubule and is responsible for 9% of glucose reabsorption Mutation in SGLT2 transporter is linked to hereditary renal glycosuria, a relatively benign condition in humans Selective SGLT2 inhibitors have a novel and unique mechanism of action reducing blood glucose levels by increasing renal excretion of glucose Insulin-independent glucose lowering poses little risk of hypoglycemia Selective SGLT2 inhibition would also cause urine loss of the calories from glucose, potentially leading to weight loss Reduces A1c, FPG, and PPG by an INS-independent mechanism Weight loss due to renal glucosuria/negative caloric balance Reduces BP Improves INS sensitivity and INS secretion (ie, correction of glucotoxicity) Gerich JE. Diabet Med. 21;27: Plosker GL. Drugs. 212;72: Whaley JM, et al. Diabetes Metab Syndr Obes. 212;5: Mudaliar S, et al. Diabetes Technol Ther. 214;16: Brooks AM, Thacker SM. Ann Pharmacother. 29;42(7): Merovci A, et al. J Clin Invest. 214;124(2): Case Study: A 65-year-old Female Current Exam Case Study: 65-year-old Female Physical exam (BP higher vs last visit): Height: 5 5 Weight: 195 lb BMI: 31 kg/m 2 BP: 15/81 Current medications: extended release 15 mg/day with evening meal Dietary review: Consumes mostly high-fat and high-carbohydrate diet Activity review: Limited physical activity due to arthritis of the knees 41 6
7 LS Mean Change (±SE) in HbA1c From Baseline (%) C-Pep (-12) / G (-12) 1/TGD Change in Baseline A1c (%) Case Study: A 65-year-old Female Current Laboratory Results Diabetes Panel Today 3 Months Ago 6 Months Ago A1c 8.2% 7.8% 7.6% FPG 155 mg/dl 142 mg/dl 138 mg/dl Lipid Panel Today 3 Months Ago 6 Months Ago Total Cholesterol 24 mg/dl 245 mg/dl 25 mg/dl LDL-C 13 mg/dl 144 mg/dl 15 mg/dl HDL-C 39 mg/dl 37 mg/dl 36 mg/dl Triglycerides 25 mg/dl 28 mg/dl 21 mg/dl Case Study: Discussion What are your primary goals for treatment of this patient? What is more important in this patient: glycemic control or disease progression? What adjustments would you make to the patient s treatment plan? Increase dose to maximum daily dose? Add a second medication? If so, what medication would you recommend? What is the most important determinant of your choice in this patient? How can you ensure that needed lifestyle modifications are successful? (Success brings success) Currently Approved SGLT2 Inhibitors Overview of SGLT2 Inhibitor Glycemic Efficacy: Changes in Baseline A1c Level SGLT2 Inhibitor Initial Dose Max Dose* Renal Dose Adjustment Canagliflozin (CANA) Dapagliflozin (DAPA) Empagliflozin (EMPA) 1 mg qd 3 mg qd 5 mg qd 1 mg qd 1 mg qd 25 mg qd egfr 45 <6 ml/min/1.73 m 2 : 1 mg CANA qd egfr <45 ml/min/1.73 m 2 : Not recommended egfr <3 ml/min/1.73 m 2 : egfr <6 ml/min/1.73 m 2 : Not recommended egfr <3 ml/min/1.73 m 2 : egfr <45 ml/min/1.73 m 2 : Not recommended egfr <3 ml/min/1.73 m 2 : CANA DAPA EMPA PBO SGLT2 inhibitor (low dose)* SGLT2 inhibitor (high dose)* *May be prescribed for patients requiring better glycemic control if agent is well tolerated. qd, once per day; egfr, estimated glomerular filtration rate. Med Lett Drugs Ther. 214;56(1457): *Doses evaluated in studies cited: CANA=1 or 3 mg, DAPA=5 or 1 mg, EMPA=1 or 25 mg. MONO, monotherapy; PIO, pioglitazone; GLIM, glimepiride; SITA, sitagliptin. 45 CANA Treatment Improves Glycemic Levels Independent of Disease Duration Effects of DAPA Treatment on β-cell Function N Baseline (%) T2DM Duration <5 Years % (95% CI: -.84, -.56) -.96% (95% CI: -1.1, -.82) T2DM Duration 5-<1 Years % (95% CI: -.9, -.59) -.91% (95% CI: -1.6, -.75) T2DM Duration 1 Years % (95% CI: -.89, -.58) -.85% (95% CI: -1., -.7) C-Pep (-12) / G (-12) DAPA PBO Baseline * DAPA PBO Treatment DAPA PBO Baseline Two weeks of DAPA treatment was associated with increased C-Pep ( 12) /G ( 12) IR, suggesting an improvement in β-cell function. * DAPA PBO Treatment LS, least squares; SE, standard error; CI, confidence interval. Wilding JP, et al. J Diabetes Complications. 215;29(3): Placebo CANA 1 mg CANA 3 mg 46 *P <.5 vs baseline and vs placebo. ΔC-Pep (-12), incremental area under the plasma C-peptide concentration curve; ΔG (-12), incremental area under the plasma glucose concentration curve; TGD, total body glucose disposal; IR, insulin resistance Merovci A, et al. J Clin Endocrinol Metab. 215;1(5):
8 Mean (SE) HbA1c, % Change in Total Body Weight From BL (kg) Change in HbA1c From BL (%) Change in Baseline Body Weight (kg) Change in Adipose Tissue Volume (cm 3 ) Overview of Changes in Body Weight Associated with SGLT2 Inhibition Effects of Dapagliflozin on Regional Adipose Tissue Distribution CANA DAPA EMPA Mean change from baseline in VAT and SAT volume with treatment at 24 weeks 2 PBO + n=42; n=37 DAPA 1 mg + n=37; n= * *Doses evaluated in studies cited: CANA=1 or 3 mg, DAPA=5 or 1 mg, EMPA=1 or 25 mg. PBO SGLT2 inhibitor (low dose)* SGLT2 inhibitor (high dose)* VAT SAT -8 Dapagliflozin reduces total body weight predominantly by reducing fat mass, visceral adipose tissue (VAT), and subcutaneous adipose tissue (SAT) volume. *VAT, cm 3 (95 CI = to -68.6; nominal P =.84). SAT, cm 3 (95% CI = -359 to -1.1; nominal P =.385). Bolinder J, et al. J Clin Endocrinol Metab (3): DAPA Added on to Metformin Durably Reduces A1c Levels & Body Weight at 4 Years Combination Therapy with SGLT2 Inhibitors.6.4.2% (95% CI:.5.36) Diff..3% (95% CI:.51 to.9).1% (95% CI:.25 to.5) SGLT2 Inhibitor Previously Studied Therapeutic Combinations Dual Therapy Triple Therapy Study Week Sample size per time point (excluding data after rescue), n DAPA GLIP DAPA + GLIP + CANA Sulfonylurea and sulfonylurea and PIO INS ± other AHAs N 4 41 BL (%) kg (95% CI:.6 1.4) Diff kg (95% CI: 5.31 to 3.46) 3.65 kg (95% CI: 4.3 to 3.1) DAPA EMPA Sulfonylurea PIO Sulfonylurea and sulfonylurea and DPP-4 inhibitor INS ± other AHAs and sulfonylurea PIO ± Study Week Sample size (including data after rescue), n DAPA GLIP DAPA + GLIP + N 4 41 BL, baseline; GLIP, glipizide. BL (kg) Del Prato S, et al. Diabetes Obes Metab. 215; AHAs, antihyperglycemic agents. Peene B, et al. Ther Adv Endocrinol Metab. 214;5(5): Wilding JP. Metabolism. 214;63(1): Add-on Therapy with DAPA and SAXA for Patients Inadequately Controlled With Currently Approved Fixed-dose SGLT2 Inhibitor Combination Therapies SAXA+DAPA+ SAXA+ DAPA+ Combination CANA/ Initial Dose 5/5-15/5 mg bid with meals Maximum Daily Dose 3/2 mg Renal Dose Adjustment egfr 45-<6 ml/min/1.73 m 2 : Adjust to 5 mg CANA bid egfr <45 ml/min/1.73 m 2 : 8. DAPA/ 5/5-1/1 mg qd in the morning 1/2 mg egfr <6 ml/min/1.73 m 2 : Weeks EMPA/ linagliptin 1/5 mg qd in the morning, with or without food 25/5 mg egfr <45 ml/min/1.73 m 2 : Not recommended egfr <3 ml/min/1.73 m 2 : SAXA, saxagliptin. Rosenstock J, et al. Diabetes Care. 215;38(3): bid, twice a day. Med Lett Drugs Ther. 214;56(1457):
9 LS Mean % Change (±SE) in Systolic BP From Baseline (mm Hg) LS Mean % Change (±SE) in Body Weight From Baseline HbA1c (%) Adjusted Mean Change From Baseline HbA1c (%) INS Dose (U/day) Change From Baseline HbA1c (%) Fixed-dose Combination Therapy: EMPA and Linagliptin Mean baseline 7.99% 8.4% 7.99% 8.5% 8.5% (64 mmol/mol) (64 mmol/mol) (64 mmol/mol) (64 mmol/mol) (64 mmol/mol).. EMPA 25 mg/linagliptin 5 mg (n=134) EMPA 1 mg/linagliptin 5 mg (n=135) EMPA 25 mg (n=133) EMPA 1 mg (n=132) Linagliptin 5 mg (n=133) -.51% % % % -1.22% (95% CI: -.39,.7) P= (95% CI: -.9,.43) P< (95% CI: -.94,.48) P< (95% CI: -.94,.48) P<.1 Change From Baseline HbA1c (mmol/mol) Long-term Treatment with SGLT2 Inhibitors Special Populations: Obesity, Hypertension, CVD Reductions from baseline HbA1c with EMPA/linagliptin were greater vs linagliptin and EMPA 1 mg, but not vs EMPA 25 mg. Lewin A, et al. Diabetes Care. 215;38(3): EMPA in Obese Patients Inadequately Controlled with INS at 1 Year Effects of SGLT2 Inhibitors on BP INS Dose HbA1c Week 11.2 ± 2.1 MDI INS + placebo 92.9 ± ± % ±.7% (6 ±.8 mmol/mol) 7.24% ±.7% (58 ±.8 mmol/mol) 7.8% ±.7% (54 ±.8 mmol/mol) MDI INS + EMPA 1 mg MDI INS + EMPA 25 mg 52 weeks of EMPA treatment was associated with reduced A1c levels, INS requirements, and body weight in obese patients with T2DM. SGLT2 inhibition is associated with reductions in BP presumably due to chronic natriuresis although changes in insulin sensitivity cannot be excluded Decreases in systolic BP have consistently been observed with CANA, DAPA, and EMPA treatment (up to 5 mm Hg with DAPA) Reports of changes in diastolic BP have been smaller and inconsistent May afford vascular protection, particularly against the risks of stroke and heart failure. These benefits not yet demonstrated in clinical trials MDI, multiple daily injection. Rosenstock J, et al. Diabetes Care. 214;37(7): Foote C, et al. Diab Vasc Dis Res. 212;9(2): Haring HU, et al. Diabetes Care. 214;37(6): CANA Improves Weight and Systolic BP in Older* Patients with T2DM at 2 Years Add-on DAPA Improves Glycemic Control in Older Patients with Advanced T2DM and Preexisting CVD Baseline (kg) Weight LS mean % change -.6% (-.6 kg) -3.% (-2.7 kg) -3.8% (-3.5 kg) -2.3% (95% CI: -3.1, -1.6) (-2.1 kg) -3.2% (95% CI: -4., -2.4) (-2.9 kg) Placebo CANA 1 mg CANA 3 mg Efficacy endpoint evaluation period Placebo; HbA1c baseline 8.% DAPA; HbA1c baseline 8.% Time Point (Weeks) -.4 Baseline (mm Hg) LS mean % change -.6 Systolic BP Time Point (Weeks) *55-8 years of age. Bode B, et al. Diabetes Obes Metab. 215;17(3): mm Hg -1.2 mm Hg -3. mm Hg -5.8 mm Hg (95% CI: -8., -3.5) -7.5 mm Hg (95% CI: -9.8, -5.2) DAPA added on to background therapy improved A1c levels without increasing hypoglycemic risk, promoted weight loss, and was well tolerated in patients >65 years old. Leiter LA, et al. J Am Geriatr Soc. 214;62(7): Time (Weeks) 59 9
10 CANA Monotherapy Improves Cardiovascular Risk Factors Safety and Tolerability Outcome Measure CANA 1 mg CANA 3 mg Difference versus placebo Systolic BP -3.7* -5.4* Diastolic BP Triglycerides (mg/dl) LDL-C (mg/dl) HDL-C (mg/dl) 6.8* 6.1 LDL-C/HDL-C Non HDL-C (mg/dl) *P<.1; P<.1. Stenlof K, et al. Diabetes Obes Metab. 213;15: Adverse Events Associated with SGLT2 Inhibitor Treatment Patients for Whom SGLT2 Inhibitors Are Not Recommended Most common adverse events (AEs): Genital mycotic infections (GMIs) Lower urinary tract infections (UTIs) Usually mild in intensity and respond to standard over-the-counter treatment More often observed in women than in men Risk higher for women prone to fungal infection and uncircumcised men Meta-analysis of 8 studies found GMIs and UTIs to be more common with SGLT2 inhibitor treatment* vs other antidiabetics AE Odds Ratio 95% CI UTI , 1.9 GMI , 7.45 Patients with chronic kidney disease Increased risk of SGLT2 inhibitor-associated hypoglycemia when combined with other background therapies Decreased or lack of efficacy Particularly susceptible to nephrotoxic effects of SGLT2 inhibitors Patients with history of bladder cancer Possible increased risk of bladder cancer was observed in DAPA trials DAPA should not be used in patients with history of bladder cancer *CANA or DAPA. Nauck MA. Drug Des Devel Ther. 214;8: Vasilakou D, et al. Ann Intern Med. 213;159(4): Yale JF, et al. Diabetes Obes Metab. 213;15(5): Mikhail N. World J Diabetes. 214;5(6): Peene B, et al. Ther Adv Endocrinol Metab. 214;5(5): Summary Prompt diagnosis of diabetes and achievement of glycemic control is necessary to reduce the risk of microvascular and possibly cardiovascular complications T2DM management requires individualized treatment, patient education, and support to empower patients to manage their disease SGLT2 inhibitors: Target hyperglycemia through prevention of renal glucose reabsorption Are effective alone and with oral therapies or INS Are associated with a low risk for hypoglycemia and other side effects Thank You! 64 1
Faculty Affiliation. Faculty Disclosures. Learning Objectives. Prevalence and Burden of Diabetes in the United States
 Faculty Affiliation Combined Targeted Approaches for the Treatment of Type 2 Diabetes: The Role of the Kidney Mark Stolar, MD Associate Professor of Clinical Medicine Division of General Internal Medicine
Faculty Affiliation Combined Targeted Approaches for the Treatment of Type 2 Diabetes: The Role of the Kidney Mark Stolar, MD Associate Professor of Clinical Medicine Division of General Internal Medicine
CANA DAPA EMPA. Change in Baseline Body Weight (kg) *Doses evaluated in studies cited: CANA=100 or 300 mg, DAPA=5 or 10 mg, EMPA=10 or 25 mg.
 CANA DAPA EMPA Change in Baseline Body Weight (kg) 2 1 0-1 -2-3 -4-5 PBO SGLT2 inhibitor (low dose)* SGLT2 inhibitor (high dose)* *Doses evaluated in studies cited: CANA=100 or 300 mg, DAPA=5 or 10 mg,
CANA DAPA EMPA Change in Baseline Body Weight (kg) 2 1 0-1 -2-3 -4-5 PBO SGLT2 inhibitor (low dose)* SGLT2 inhibitor (high dose)* *Doses evaluated in studies cited: CANA=100 or 300 mg, DAPA=5 or 10 mg,
SESSION 4 12:30pm 1:45pm
 SESSION 4 12:30pm 1:45pm Addressing Renal-Mediated Glucose Homeostasis: Diabetes and the Kidney SPEAKER Davida Kruger, MSN, BC-ADM, APRN Presenter Disclosure Information The following relationships exist
SESSION 4 12:30pm 1:45pm Addressing Renal-Mediated Glucose Homeostasis: Diabetes and the Kidney SPEAKER Davida Kruger, MSN, BC-ADM, APRN Presenter Disclosure Information The following relationships exist
The Emerging Role of the Kidney and SGLT2 Inhibition for Patients with Type 2 Diabetes
 Silvio E. Inzucchi, MD The Emerging Role of the Kidney and SGLT2 Inhibition for Patients with Type 2 Diabetes Professor of Medicine Clinical Director Section of Endocrinology Yale University New Haven,
Silvio E. Inzucchi, MD The Emerging Role of the Kidney and SGLT2 Inhibition for Patients with Type 2 Diabetes Professor of Medicine Clinical Director Section of Endocrinology Yale University New Haven,
Oral Hypoglycemics and Risk of Adverse Cardiac Events: A Summary of the Controversy
 Oral Hypoglycemics and Risk of Adverse Cardiac Events: A Summary of the Controversy Jeffrey Boord, MD, MPH Advances in Cardiovascular Medicine Kingston, Jamaica December 7, 2012 VanderbiltHeart.com Outline
Oral Hypoglycemics and Risk of Adverse Cardiac Events: A Summary of the Controversy Jeffrey Boord, MD, MPH Advances in Cardiovascular Medicine Kingston, Jamaica December 7, 2012 VanderbiltHeart.com Outline
Multiple Factors Should Be Considered When Setting a Glycemic Goal
 Multiple Facts Should Be Considered When Setting a Glycemic Goal Patient attitude and expected treatment effts Risks potentially associated with hypoglycemia, other adverse events Disease duration Me stringent
Multiple Facts Should Be Considered When Setting a Glycemic Goal Patient attitude and expected treatment effts Risks potentially associated with hypoglycemia, other adverse events Disease duration Me stringent
Obesity, Insulin Resistance, Metabolic Syndrome, and the Natural History of Type 2 Diabetes
 Obesity, Insulin Resistance, Metabolic Syndrome, and the Natural History of Type 2 Diabetes Genetics, environment, and lifestyle (obesity, inactivity, poor diet) Impaired fasting glucose Decreased β-cell
Obesity, Insulin Resistance, Metabolic Syndrome, and the Natural History of Type 2 Diabetes Genetics, environment, and lifestyle (obesity, inactivity, poor diet) Impaired fasting glucose Decreased β-cell
IDF Regions and global projections of the number of people with diabetes (20-79 years), 2013 and Diabetes Atlas -sixth Edition: IDF 2013
 IDF Regions and global projections of the number of people with diabetes (20-79 years), 2013 and 2035 Diabetes Atlas -sixth Edition: IDF 2013 Diabetes Atlas -sixth Edition: IDF 2013 Chronic complications
IDF Regions and global projections of the number of people with diabetes (20-79 years), 2013 and 2035 Diabetes Atlas -sixth Edition: IDF 2013 Diabetes Atlas -sixth Edition: IDF 2013 Chronic complications
Standards of Medical Care in Diabetes 2016
 Standards of Medical Care in Diabetes 2016 Care Delivery Systems 33-49% of patients still do not meet targets for A1C, blood pressure, or lipids. 14% meet targets for all A1C, BP, lipids, and nonsmoking
Standards of Medical Care in Diabetes 2016 Care Delivery Systems 33-49% of patients still do not meet targets for A1C, blood pressure, or lipids. 14% meet targets for all A1C, BP, lipids, and nonsmoking
Pre-diabetes. Pharmacological Approaches to Delay Progression to Diabetes
 Pre-diabetes Pharmacological Approaches to Delay Progression to Diabetes Overview Definition of Pre-diabetes Risk Factors for Pre-diabetes Clinical practice guidelines for diabetes Management, including
Pre-diabetes Pharmacological Approaches to Delay Progression to Diabetes Overview Definition of Pre-diabetes Risk Factors for Pre-diabetes Clinical practice guidelines for diabetes Management, including
SGLT2 Inhibition in the Management of T2DM: Potential Impact on CVD Risk
 Managing Diabetes & CVD: Expling New Evidence & Opptunities ESC Congress, London, UK 30 August, 2015 SGLT2 Inhibition in the Management of T2DM: Potential Impact on CVD Risk Silvio E. Inzucchi MD Yale
Managing Diabetes & CVD: Expling New Evidence & Opptunities ESC Congress, London, UK 30 August, 2015 SGLT2 Inhibition in the Management of T2DM: Potential Impact on CVD Risk Silvio E. Inzucchi MD Yale
Newer Drugs in the Management of Type 2 Diabetes Mellitus
 Newer Drugs in the Management of Type 2 Diabetes Mellitus Dr. C. Dinesh M. Naidu Professor of Pharmacology, Kamineni Institute of Medical Sciences, Narketpally. 1 Presentation Outline Introduction Pathogenesis
Newer Drugs in the Management of Type 2 Diabetes Mellitus Dr. C. Dinesh M. Naidu Professor of Pharmacology, Kamineni Institute of Medical Sciences, Narketpally. 1 Presentation Outline Introduction Pathogenesis
Non-insulin treatment in Type 1 DM Sang Yong Kim
 Non-insulin treatment in Type 1 DM Sang Yong Kim Chosun University Hospital Conflict of interest disclosure None Committee of Scientific Affairs Committee of Scientific Affairs Insulin therapy is the mainstay
Non-insulin treatment in Type 1 DM Sang Yong Kim Chosun University Hospital Conflict of interest disclosure None Committee of Scientific Affairs Committee of Scientific Affairs Insulin therapy is the mainstay
A Practical Approach to the Use of Diabetes Medications
 A Practical Approach to the Use of Diabetes Medications Juan Pablo Frias, M.D., FACE President, National Research Institute, Los Angles, CA Clinical Faculty, University of California, San Diego, CA OUTLINE
A Practical Approach to the Use of Diabetes Medications Juan Pablo Frias, M.D., FACE President, National Research Institute, Los Angles, CA Clinical Faculty, University of California, San Diego, CA OUTLINE
Diabetes Guidelines in View of Recent Clinical Trials Are They Still Applicable?
 Diabetes Guidelines in View of Recent Clinical Trials Are They Still Applicable? Jay S. Skyler, MD, MACP Division of Endocrinology, Diabetes, and Metabolism and Diabetes Research Institute University of
Diabetes Guidelines in View of Recent Clinical Trials Are They Still Applicable? Jay S. Skyler, MD, MACP Division of Endocrinology, Diabetes, and Metabolism and Diabetes Research Institute University of
GLP-1. GLP-1 is produced by the L-cells of the gut after food intake in two biologically active forms It is rapidly degraded by DPP-4.
 GLP-1 GLP-1 is produced by the L-cells of the gut after food intake in two biologically active forms It is rapidly degraded by DPP-4 Food intake éinsulin Gut églucose uptake Pancreas Beta cells Alpha cells
GLP-1 GLP-1 is produced by the L-cells of the gut after food intake in two biologically active forms It is rapidly degraded by DPP-4 Food intake éinsulin Gut églucose uptake Pancreas Beta cells Alpha cells
Type 2 Diabetes Mellitus 2011
 2011 Michael T. McDermott MD Director, Endocrinology and Diabetes Practice University of Colorado Hospital Michael.mcdermott@ucdenver.edu Diabetes Mellitus Diagnosis 2011 Diabetes Mellitus Fasting Glucose
2011 Michael T. McDermott MD Director, Endocrinology and Diabetes Practice University of Colorado Hospital Michael.mcdermott@ucdenver.edu Diabetes Mellitus Diagnosis 2011 Diabetes Mellitus Fasting Glucose
Wayne Gravois, MD August 6, 2017
 Wayne Gravois, MD August 6, 2017 Americans with Diabetes (Millions) 40 30 Source: National Diabetes Statistics Report, 2011, 2017 Millions 20 10 0 1980 2009 2015 2007 - $174 Billion 2015 - $245 Billion
Wayne Gravois, MD August 6, 2017 Americans with Diabetes (Millions) 40 30 Source: National Diabetes Statistics Report, 2011, 2017 Millions 20 10 0 1980 2009 2015 2007 - $174 Billion 2015 - $245 Billion
Abbreviations DPP-IV dipeptidyl peptidase IV DREAM Diabetes REduction Assessment with ramipril and rosiglitazone
 Index Abbreviations DPP-IV dipeptidyl peptidase IV DREAM Diabetes REduction Assessment with ramipril and rosiglitazone Medication GAD glutamic acid decarboxylase GLP-1 glucagon-like peptide 1 NPH neutral
Index Abbreviations DPP-IV dipeptidyl peptidase IV DREAM Diabetes REduction Assessment with ramipril and rosiglitazone Medication GAD glutamic acid decarboxylase GLP-1 glucagon-like peptide 1 NPH neutral
IMPROVED DIAGNOSIS OF TYPE 2 DIABETES AND TAILORING MEDICATIONS
 IMPROVED DIAGNOSIS OF TYPE 2 DIABETES AND TAILORING MEDICATIONS Dr Bidhu Mohapatra, MBBS, MD, FRACP Consultant Physician Endocrinology and General Medicine Introduction 382 million people affected by diabetes
IMPROVED DIAGNOSIS OF TYPE 2 DIABETES AND TAILORING MEDICATIONS Dr Bidhu Mohapatra, MBBS, MD, FRACP Consultant Physician Endocrinology and General Medicine Introduction 382 million people affected by diabetes
Diabetes Mellitus: Implications of New Clinical Trials and New Medications
 Diabetes Mellitus: Implications of New Clinical Trials and New Medications Estimates of Diagnosed Diabetes in Adults, 2005 Alka M. Kanaya, MD Asst. Professor of Medicine UCSF, Primary Care CME October
Diabetes Mellitus: Implications of New Clinical Trials and New Medications Estimates of Diagnosed Diabetes in Adults, 2005 Alka M. Kanaya, MD Asst. Professor of Medicine UCSF, Primary Care CME October
Vipul Lakhani, MD Oregon Medical Group Endocrinology
 Vipul Lakhani, MD Oregon Medical Group Endocrinology Disclosures None Objectives Be able to diagnose diabetes and assess control Be able to identify appropriate classes of medications for diabetes treatment
Vipul Lakhani, MD Oregon Medical Group Endocrinology Disclosures None Objectives Be able to diagnose diabetes and assess control Be able to identify appropriate classes of medications for diabetes treatment
Application of the Diabetes Algorithm to a Patient
 Application of the Diabetes Algorithm to a Patient Apply knowledge gained from this activity to improve disease management and outcomes for patients with T2DM and obesity Note: The cases in this deck represent
Application of the Diabetes Algorithm to a Patient Apply knowledge gained from this activity to improve disease management and outcomes for patients with T2DM and obesity Note: The cases in this deck represent
Diabetes update - Diagnosis and Treatment
 Diabetes update - Diagnosis and Treatment Eugene J Barrett, MD,PhD Madge Jones Professor of Medicine Director, University of Virginia Diabetes Center Disclosures - None Case 1 - Screening for Diabetes
Diabetes update - Diagnosis and Treatment Eugene J Barrett, MD,PhD Madge Jones Professor of Medicine Director, University of Virginia Diabetes Center Disclosures - None Case 1 - Screening for Diabetes
Standards of Care in Diabetes What's New? Veronica Brady, FNP-BC, PhD, BC-ADM,CDE Karmella Thomas, RD, LD,CDE
 Standards of Care in Diabetes 2016-- What's New? Veronica Brady, FNP-BC, PhD, BC-ADM,CDE Karmella Thomas, RD, LD,CDE Terminology No longer using the term diabetic. Diabetes does not define people. People
Standards of Care in Diabetes 2016-- What's New? Veronica Brady, FNP-BC, PhD, BC-ADM,CDE Karmella Thomas, RD, LD,CDE Terminology No longer using the term diabetic. Diabetes does not define people. People
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE. Single Technology Appraisal. Canagliflozin in combination therapy for treating type 2 diabetes
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Single Technology Appraisal Canagliflozin in combination therapy for Final scope Remit/appraisal objective To appraise the clinical and cost effectiveness
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Single Technology Appraisal Canagliflozin in combination therapy for Final scope Remit/appraisal objective To appraise the clinical and cost effectiveness
Sodium-Glucose Co-Transporter 2 (SGLT-2) Inhibitors Drug Class Prior Authorization Protocol
 Sodium-Glucose Co-Transporter 2 (SGLT-2) Inhibitors Drug Class Prior Authorization Protocol Line of Business: Medicaid P&T Approval Date: February 21, 2018 Effective Date: April 1, 2018 This policy has
Sodium-Glucose Co-Transporter 2 (SGLT-2) Inhibitors Drug Class Prior Authorization Protocol Line of Business: Medicaid P&T Approval Date: February 21, 2018 Effective Date: April 1, 2018 This policy has
Adult Diabetes Clinician Guide NOVEMBER 2017
 Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Adult Diabetes Clinician Guide Introduction NOVEMBER 2017 This evidence-based guideline summary is based on the 2017 KP National Diabetes Guideline.
Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Adult Diabetes Clinician Guide Introduction NOVEMBER 2017 This evidence-based guideline summary is based on the 2017 KP National Diabetes Guideline.
Diabetes mellitus. Treatment
 Diabetes mellitus Treatment Recommended glycemic targets for the clinical management of diabetes(ada) Fasting glycemia: 80-110 mg/dl Postprandial : 100-145 mg/dl HbA1c: < 6,5 % Total cholesterol: < 200
Diabetes mellitus Treatment Recommended glycemic targets for the clinical management of diabetes(ada) Fasting glycemia: 80-110 mg/dl Postprandial : 100-145 mg/dl HbA1c: < 6,5 % Total cholesterol: < 200
Diabetes 2013: Achieving Goals Through Comprehensive Treatment. Session 2: Individualizing Therapy
 Diabetes 2013: Achieving Goals Through Comprehensive Treatment Session 2: Individualizing Therapy Joshua L. Cohen, M.D., F.A.C.P. Professor of Medicine Interim Director, Division of Endocrinology & Metabolism
Diabetes 2013: Achieving Goals Through Comprehensive Treatment Session 2: Individualizing Therapy Joshua L. Cohen, M.D., F.A.C.P. Professor of Medicine Interim Director, Division of Endocrinology & Metabolism
Disclosures. Diabetes and Cardiovascular Risk Management. Learning Objectives. Atherosclerotic Cardiovascular Disease
 Disclosures Diabetes and Cardiovascular Risk Management Tony Hampton, MD, MBA Medical Director Advocate Aurora Operating System Advocate Aurora Healthcare Downers Grove, IL No conflicts or disclosures
Disclosures Diabetes and Cardiovascular Risk Management Tony Hampton, MD, MBA Medical Director Advocate Aurora Operating System Advocate Aurora Healthcare Downers Grove, IL No conflicts or disclosures
Cardiovascular Benefits of Two Classes of Antihyperglycemic Medications
 Cardiovascular Benefits of Two Classes of Antihyperglycemic Medications Nathan Woolever, Pharm.D., Resident Pharmacist Pharmacy Grand Rounds November 6 th, 2018 Franciscan Healthcare La Crosse, WI 2017
Cardiovascular Benefits of Two Classes of Antihyperglycemic Medications Nathan Woolever, Pharm.D., Resident Pharmacist Pharmacy Grand Rounds November 6 th, 2018 Franciscan Healthcare La Crosse, WI 2017
Diabetes and New Meds for Cardiovascular Risk Reduction. F. Dwight Chrisman, MD, FACC. Disclosures: BI Boehringer Ingelheim speaker
 Diabetes and New Meds for Cardiovascular Risk Reduction F. Dwight Chrisman, MD, FACC Disclosures: BI Boehringer Ingelheim speaker 1 Prevalence of DM DM state specific prevalence 2006 4%-6% 6-8% 8-10% 10-12%
Diabetes and New Meds for Cardiovascular Risk Reduction F. Dwight Chrisman, MD, FACC Disclosures: BI Boehringer Ingelheim speaker 1 Prevalence of DM DM state specific prevalence 2006 4%-6% 6-8% 8-10% 10-12%
Early treatment for patients with Type 2 Diabetes
 Israel Society of Internal Medicine Kibutz Hagoshrim, June 22, 2012 Early treatment for patients with Type 2 Diabetes Eduard Montanya Hospital Universitari Bellvitge-IDIBELL CIBERDEM University of Barcelona
Israel Society of Internal Medicine Kibutz Hagoshrim, June 22, 2012 Early treatment for patients with Type 2 Diabetes Eduard Montanya Hospital Universitari Bellvitge-IDIBELL CIBERDEM University of Barcelona
Diabetes Mellitus II CPG
 1 Diabetes Mellitus II CPG Candidates for Screening Integrated Complex Care Patients: Check Yearly Prediabetes: Check Yearly No Diabetes Mellitus (DM) Risk Factors: Check at Age 45, Repeat Every 3 Years
1 Diabetes Mellitus II CPG Candidates for Screening Integrated Complex Care Patients: Check Yearly Prediabetes: Check Yearly No Diabetes Mellitus (DM) Risk Factors: Check at Age 45, Repeat Every 3 Years
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE. Proposed Health Technology Appraisal
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Proposed Health Technology Appraisal Dapagliflozin in combination therapy for the Final scope Remit/appraisal objective To appraise the clinical and
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Proposed Health Technology Appraisal Dapagliflozin in combination therapy for the Final scope Remit/appraisal objective To appraise the clinical and
What s New in Diabetes Treatment. Disclosures
 What s New in Diabetes Treatment Shiri Levy M.D. Henry Ford Hospital Senior Staff Physician Service Chief, West Bloomfield Hospital Endocrinology, Metabolism, Bone and Mineral Disorders Disclosures None
What s New in Diabetes Treatment Shiri Levy M.D. Henry Ford Hospital Senior Staff Physician Service Chief, West Bloomfield Hospital Endocrinology, Metabolism, Bone and Mineral Disorders Disclosures None
The ABCs (A1C, BP and Cholesterol) of Diabetes
 The ABCs (A1C, BP and Cholesterol) of Diabetes Gregg Simonson, PhD Director, Professional Training and Consulting International Diabetes Center; Adjunct Assistant Professor, University of Minnesota Department
The ABCs (A1C, BP and Cholesterol) of Diabetes Gregg Simonson, PhD Director, Professional Training and Consulting International Diabetes Center; Adjunct Assistant Professor, University of Minnesota Department
Joslin Diabetes Center Joslin Diabetes Forum 2013: The Impact of Comorbidities on Glucose Control Scenario 2: Reduced Renal Function
 Scenario 2: Reduced Renal Function 62 y.o. white man with type 2 diabetes for 18 years Hypertension and hypercholesterolemia Known proliferative retinopathy Current medications: Metformin 1000 mg bid Glyburide
Scenario 2: Reduced Renal Function 62 y.o. white man with type 2 diabetes for 18 years Hypertension and hypercholesterolemia Known proliferative retinopathy Current medications: Metformin 1000 mg bid Glyburide
Diabete: terapia nei pazienti a rischio cardiovascolare
 Diabete: terapia nei pazienti a rischio cardiovascolare Giorgio Sesti Università Magna Graecia di Catanzaro Cardiovascular mortality in relation to diabetes mellitus and a prior MI: A Danish Population
Diabete: terapia nei pazienti a rischio cardiovascolare Giorgio Sesti Università Magna Graecia di Catanzaro Cardiovascular mortality in relation to diabetes mellitus and a prior MI: A Danish Population
Case Studies in Type 2 Diabetes Mellitus: Focus on Cardiovascular Outcomes Trials
 Case Studies in Type 2 Diabetes Mellitus: Focus on Cardiovascular Outcomes Trials Louis Kuritzky MD Clinical Assistant Professor Emeritus Department of Community Health and Family Medicine College of Medicine
Case Studies in Type 2 Diabetes Mellitus: Focus on Cardiovascular Outcomes Trials Louis Kuritzky MD Clinical Assistant Professor Emeritus Department of Community Health and Family Medicine College of Medicine
Chief of Endocrinology East Orange General Hospital
 Targeting the Incretins System: Can it Improve Our Ability to Treat Type 2 Diabetes? Darshi Sunderam, MD Darshi Sunderam, MD Chief of Endocrinology East Orange General Hospital Age-adjusted Percentage
Targeting the Incretins System: Can it Improve Our Ability to Treat Type 2 Diabetes? Darshi Sunderam, MD Darshi Sunderam, MD Chief of Endocrinology East Orange General Hospital Age-adjusted Percentage
Diabesity. Metabolic dysfunction that ranges from mild blood glucose imbalance to full fledged Type 2 DM Signs
 Diabesity Metabolic dysfunction that ranges from mild blood glucose imbalance to full fledged Type 2 DM Signs Abdominal obesity Low HDL, high LDL, and high triglycerides HTN High blood glucose (F>100l,
Diabesity Metabolic dysfunction that ranges from mild blood glucose imbalance to full fledged Type 2 DM Signs Abdominal obesity Low HDL, high LDL, and high triglycerides HTN High blood glucose (F>100l,
DIABETES DEBATE - IS NEW BETTER?
 DIABETES DEBATE - IS NEW BETTER? WHAT MEDICATION CLASS AFTER METFORMIN TO CONTROL BLOOD SUGAR Dr. Lydia Hatcher, MD, CCFP, FCFP, CHE, D-CAPM Associate Clinical Professor of Family Medicine, McMaster Chief
DIABETES DEBATE - IS NEW BETTER? WHAT MEDICATION CLASS AFTER METFORMIN TO CONTROL BLOOD SUGAR Dr. Lydia Hatcher, MD, CCFP, FCFP, CHE, D-CAPM Associate Clinical Professor of Family Medicine, McMaster Chief
Current Diabetes Care for Internists:2011
 Current Diabetes Care for Internists:2011 Petch Rawdaree, DM, MSc, DLSHTM Faculty of Medicine Vajira Hospital University of Bangkok Metropolis 19 th January 2011 ก ก 1. ก ก ก ก 2. ก ก ก ก ก 3. ก ก ก ก
Current Diabetes Care for Internists:2011 Petch Rawdaree, DM, MSc, DLSHTM Faculty of Medicine Vajira Hospital University of Bangkok Metropolis 19 th January 2011 ก ก 1. ก ก ก ก 2. ก ก ก ก ก 3. ก ก ก ก
01/09/2017. Outline. SGLT 2 inhibitor? Diabetes Patients: Complex and Heterogeneous. Association between diabetes and cardiovascular events
 MICROVASCULAR COMPLICATIONS Incidence of outcome g 1 Cardioprotective Effects of SGLT2s Relevant for Which T2 Diabetes Patient? SGLT 2 inhibitor? 58 year old, waist circumference 5 cm, PMH: IHD On statin,
MICROVASCULAR COMPLICATIONS Incidence of outcome g 1 Cardioprotective Effects of SGLT2s Relevant for Which T2 Diabetes Patient? SGLT 2 inhibitor? 58 year old, waist circumference 5 cm, PMH: IHD On statin,
Practical Strategies for the Clinical Use of Incretin Mimetics CME/CE. CME/CE Released: 09/15/2009; Valid for credit through 09/15/2010
 Practical Strategies for the Clinical Use of Incretin Mimetics CME/CE Robert R. Henry, MD Authors and Disclosures CME/CE Released: 09/15/2009; Valid for credit through 09/15/2010 Introduction Type 2 diabetes
Practical Strategies for the Clinical Use of Incretin Mimetics CME/CE Robert R. Henry, MD Authors and Disclosures CME/CE Released: 09/15/2009; Valid for credit through 09/15/2010 Introduction Type 2 diabetes
Beyond Basal Insulin: Intensification of Therapy Jennifer D Souza, PharmD, CDE, BC-ADM
 Beyond Basal Insulin: Intensification of Therapy Jennifer D Souza, PharmD, CDE, BC-ADM Disclosures Jennifer D Souza has no conflicts of interest to disclose. 2 When Basal Insulin Is Not Enough Learning
Beyond Basal Insulin: Intensification of Therapy Jennifer D Souza, PharmD, CDE, BC-ADM Disclosures Jennifer D Souza has no conflicts of interest to disclose. 2 When Basal Insulin Is Not Enough Learning
Medical therapy advances London/Manchester RCP February/June 2016
 Medical therapy advances London/Manchester RCP February/June 2016 Advances in medical therapies for diabetes mellitus Duality of interest: The speaker or institutions with which he is associated has received
Medical therapy advances London/Manchester RCP February/June 2016 Advances in medical therapies for diabetes mellitus Duality of interest: The speaker or institutions with which he is associated has received
Quick Reference Guide
 2013 Clinical Practice Guidelines Quick Reference Guide (Updated November 2016) 416569-16 guidelines.diabetes.ca diabetes.ca 1-800-BANTING (226-8464) Copyright 2016 Canadian Diabetes Association SCREENING
2013 Clinical Practice Guidelines Quick Reference Guide (Updated November 2016) 416569-16 guidelines.diabetes.ca diabetes.ca 1-800-BANTING (226-8464) Copyright 2016 Canadian Diabetes Association SCREENING
Update on Agents for Type 2 Diabetes
 Update on Agents for Type 2 Diabetes This presentation will: Outline the clinical considerations in the selection of pharmacotherapy for type 2 diabetes, including degree of A1C lowering achieved, patient-specific
Update on Agents for Type 2 Diabetes This presentation will: Outline the clinical considerations in the selection of pharmacotherapy for type 2 diabetes, including degree of A1C lowering achieved, patient-specific
Efficacy and Safety of Sitagliptin in Various Clinical Settings of T2DM
 Efficacy and Safety of Sitagliptin in arious Clinical Settings of T2DM Young Min Cho, MD, PhD Division of Endocrinology and Metabolism Department of Internal Medicine Seoul National University College
Efficacy and Safety of Sitagliptin in arious Clinical Settings of T2DM Young Min Cho, MD, PhD Division of Endocrinology and Metabolism Department of Internal Medicine Seoul National University College
The Many Faces of T2DM in Long-term Care Facilities
 The Many Faces of T2DM in Long-term Care Facilities Question #1 Which of the following is a risk factor for increased hypoglycemia in older patients that may suggest the need to relax hyperglycemia treatment
The Many Faces of T2DM in Long-term Care Facilities Question #1 Which of the following is a risk factor for increased hypoglycemia in older patients that may suggest the need to relax hyperglycemia treatment
Metabolic Syndrome. Shon Meek MD, PhD Mayo Clinic Florida Endocrinology
 Metabolic Syndrome Shon Meek MD, PhD Mayo Clinic Florida Endocrinology Disclosure No conflict of interest No financial disclosure Does This Patient Have Metabolic Syndrome? 1. Yes 2. No Does This Patient
Metabolic Syndrome Shon Meek MD, PhD Mayo Clinic Florida Endocrinology Disclosure No conflict of interest No financial disclosure Does This Patient Have Metabolic Syndrome? 1. Yes 2. No Does This Patient
1. Pharmacokinetics. When is steady state achieved? Steady-state was reached after 4 to 5 days of once-daily dosing with Sulisent 100 mg to 300mg.
 1. Pharmacokinetics How is Sulisent metabolized? Sulisent has a novel mechanism of action that targets the kidneys and allows for excess glucose excretion resulting in urinary calorie loss. Sulisent is
1. Pharmacokinetics How is Sulisent metabolized? Sulisent has a novel mechanism of action that targets the kidneys and allows for excess glucose excretion resulting in urinary calorie loss. Sulisent is
Modulating the Incretin System: A New Therapeutic Strategy for Type 2 Diabetes
 Modulating the Incretin System: A New Therapeutic Strategy for Type 2 Diabetes Geneva Clark Briggs, PharmD, BCPS Adjunct Professor at University of Appalachia College of Pharmacy Clinical Associate, Medical
Modulating the Incretin System: A New Therapeutic Strategy for Type 2 Diabetes Geneva Clark Briggs, PharmD, BCPS Adjunct Professor at University of Appalachia College of Pharmacy Clinical Associate, Medical
DPP-4/SGLT2 inhibitor combined therapy for type 2 diabetes
 THERAPY REVIEW DPP-4/SGLT2 inhibitor combined therapy for type 2 diabetes STEVE CHAPLIN SPL DPP-4 inhibitors and SGLT2 inhibitors lower blood glucose by complementary mechanisms of action, and two fixeddose
THERAPY REVIEW DPP-4/SGLT2 inhibitor combined therapy for type 2 diabetes STEVE CHAPLIN SPL DPP-4 inhibitors and SGLT2 inhibitors lower blood glucose by complementary mechanisms of action, and two fixeddose
Evidence-Based Glucose Management in Type 2 Diabetes
 Evidence-Based Glucose Management in Type 2 Diabetes James R. Gavin III, MD, PhD CEO and Chief Medical Officer Healing Our Village, Inc. Clinical Professor of Medicine Emory University School of Medicine
Evidence-Based Glucose Management in Type 2 Diabetes James R. Gavin III, MD, PhD CEO and Chief Medical Officer Healing Our Village, Inc. Clinical Professor of Medicine Emory University School of Medicine
Drug Class Monograph
 Drug Class Monograph Class: Sodium-Glucose Co-Transporter 2 (SGLT-2) Inhibitors Drugs: Farxiga (dapagliflozin), Invokamet (canagliflozin/metformin), Invokana (canagliflozin), Jardiance (empagliflozin),
Drug Class Monograph Class: Sodium-Glucose Co-Transporter 2 (SGLT-2) Inhibitors Drugs: Farxiga (dapagliflozin), Invokamet (canagliflozin/metformin), Invokana (canagliflozin), Jardiance (empagliflozin),
Why Do We Care About Prediabetes?
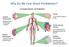 Why Do We Care About Prediabetes? Complications of Diabetes Diabetic Retinopathy Leading cause of blindness in adults 1,2 Diabetic Nephropathy Leading cause of Kidney failure Stroke 2- to 4-fold increase
Why Do We Care About Prediabetes? Complications of Diabetes Diabetic Retinopathy Leading cause of blindness in adults 1,2 Diabetic Nephropathy Leading cause of Kidney failure Stroke 2- to 4-fold increase
Objectives. Objectives. Alejandro J. de la Torre, MD Cook Children s Hospital May 30, 2015
 Alejandro J. de la Torre, MD Cook Children s Hospital May 30, 2015 Presentation downloaded from http://ce.unthsc.edu Objectives Understand that the obesity epidemic is also affecting children and adolescents
Alejandro J. de la Torre, MD Cook Children s Hospital May 30, 2015 Presentation downloaded from http://ce.unthsc.edu Objectives Understand that the obesity epidemic is also affecting children and adolescents
Clinical Overview of Combination Therapy with Sitagliptin and Metformin
 Clinical Overview of Combination Therapy with Sitagliptin and Metformin 1 Contents Pathophysiology of type 2 diabetes and mechanism of action of sitagliptin Clinical data overview of sitagliptin: Monotherapy
Clinical Overview of Combination Therapy with Sitagliptin and Metformin 1 Contents Pathophysiology of type 2 diabetes and mechanism of action of sitagliptin Clinical data overview of sitagliptin: Monotherapy
Drug Class Review Newer Diabetes Medications and Combinations
 Drug Class Review Newer Diabetes Medications and Combinations Final Update 2 Report July 2016 The purpose reports is to make available information regarding the comparative clinical effectiveness and harms
Drug Class Review Newer Diabetes Medications and Combinations Final Update 2 Report July 2016 The purpose reports is to make available information regarding the comparative clinical effectiveness and harms
Presenter Disclosure Information
 Prediabetes & Type 2 Diabetes Prevention Cari Ritter, PA-C Presenter Disclosure Information In compliance with the accrediting board policies, the American Diabetes Association requires the following disclosure
Prediabetes & Type 2 Diabetes Prevention Cari Ritter, PA-C Presenter Disclosure Information In compliance with the accrediting board policies, the American Diabetes Association requires the following disclosure
Diabetes Update: Diabetes Management In Primary Care. Jonathon M. Firnhaber, MD, FAAFP
 Diabetes Update: Diabetes Management In Primary Care Jonathon M. Firnhaber, MD, FAAFP Learning objectives 1. Critically evaluate the evidence emerging within diabetes research as it applies to recommendations
Diabetes Update: Diabetes Management In Primary Care Jonathon M. Firnhaber, MD, FAAFP Learning objectives 1. Critically evaluate the evidence emerging within diabetes research as it applies to recommendations
CURRENT CONTROVERSIES IN DIABETES CARE
 CURRENT CONTROVERSIES IN DIABETES CARE Robert B. Baron MD MS Professor and Associate Dean UCSF School of Medicine Declaration of full disclosure: No conflict of interest Diabetes Mellitus: U.S. Impact
CURRENT CONTROVERSIES IN DIABETES CARE Robert B. Baron MD MS Professor and Associate Dean UCSF School of Medicine Declaration of full disclosure: No conflict of interest Diabetes Mellitus: U.S. Impact
Canadian Society of Internal Medicine Annual Meeting 2016 Montreal, QC
 Canadian Society of Internal Medicine Annual Meeting 2016 Montreal, QC Choosing the Right Agent for your Patient with diabetes: Individualizing type 2 diabetes management in light of the expanding therapies
Canadian Society of Internal Medicine Annual Meeting 2016 Montreal, QC Choosing the Right Agent for your Patient with diabetes: Individualizing type 2 diabetes management in light of the expanding therapies
Standards of Medical Care In Diabetes
 Standards of Medical Care In Diabetes - 2017 Robert E. Ratner, MD, FACP, FACE Professor of Medicine Georgetown University School of Medicine Disclosed no conflict of interest Standards of Care Professional.diabetes.org/SOC
Standards of Medical Care In Diabetes - 2017 Robert E. Ratner, MD, FACP, FACE Professor of Medicine Georgetown University School of Medicine Disclosed no conflict of interest Standards of Care Professional.diabetes.org/SOC
The promise of the thiazolidinediones in the management of type 2 diabetes-associated cardiovascular disease
 The promise of the thiazolidinediones in the management of type 2 diabetes-associated cardiovascular disease Steve Smith, Group Director Scientific Affairs, Diabetes & Metabolism GlaxoSmithKline R & D
The promise of the thiazolidinediones in the management of type 2 diabetes-associated cardiovascular disease Steve Smith, Group Director Scientific Affairs, Diabetes & Metabolism GlaxoSmithKline R & D
Comprehensive Diabetes Treatment
 Comprehensive Diabetes Treatment Joshua L. Cohen, M.D., F.A.C.P. Professor of Medicine Interim Director, Division of Endocrinology & Metabolism The George Washington University School of Medicine Diabetes
Comprehensive Diabetes Treatment Joshua L. Cohen, M.D., F.A.C.P. Professor of Medicine Interim Director, Division of Endocrinology & Metabolism The George Washington University School of Medicine Diabetes
Oral Agents. Ian Gallen Consultant Community Diabetologist Royal Berkshire Hospital Reading UK
 Oral Agents Ian Gallen Consultant Community Diabetologist Royal Berkshire Hospital Reading UK What would your ideal diabetes drug do? Effective in lowering HbA1c No hypoglycaemia No effect on weight/ weight
Oral Agents Ian Gallen Consultant Community Diabetologist Royal Berkshire Hospital Reading UK What would your ideal diabetes drug do? Effective in lowering HbA1c No hypoglycaemia No effect on weight/ weight
Learning and Earning with Gateway Professional Education CME/CEU Webinar Series. Diabetes Update July 6, :00pm 1:00pm
 Learning and Earning with Gateway Professional Education CME/CEU Webinar Series Diabetes Update July 6, 2017 12:00pm 1:00pm Jennifer Pennock Holst, MD Endocrinology, Diabetes & Metabolism AHN Center for
Learning and Earning with Gateway Professional Education CME/CEU Webinar Series Diabetes Update July 6, 2017 12:00pm 1:00pm Jennifer Pennock Holst, MD Endocrinology, Diabetes & Metabolism AHN Center for
1,2,3 1. Diabetes in the Latino Population: A Case-based Approach to Optimal Management. Why Are We Concerned about Diabetes Among Latinos?
 Diabetes in the Latino Population: A Case-based Approach to Optimal Management 1 Learner Objectives Upon completion, attendees should be able to: List the medical, social, and economic ways in which diabetes
Diabetes in the Latino Population: A Case-based Approach to Optimal Management 1 Learner Objectives Upon completion, attendees should be able to: List the medical, social, and economic ways in which diabetes
DM-2 Therapy Update: GLP-1, SGLT-2 Inhibitors, and Inhaled Insulin, Oh My!
 DM-2 Therapy Update: GLP-1, SGLT-2 Inhibitors, and Inhaled Insulin, Oh My! Kevin M. Pantalone, DO, ECNU, CCD Associate Staff Director of Clinical Research Department of Endocrinology Endocrinology and
DM-2 Therapy Update: GLP-1, SGLT-2 Inhibitors, and Inhaled Insulin, Oh My! Kevin M. Pantalone, DO, ECNU, CCD Associate Staff Director of Clinical Research Department of Endocrinology Endocrinology and
Diabetes Mellitus: Overview and Guidelines
 Diabetes Mellitus: Overview and Guidelines Rezvan Salehidoost, M.D., Endocrinologist Abidi Diabetes Master Class IMPORTANCE? Why is it interesting to do research in diabetes J. Olefsky, JAMA 2001:285:628-632
Diabetes Mellitus: Overview and Guidelines Rezvan Salehidoost, M.D., Endocrinologist Abidi Diabetes Master Class IMPORTANCE? Why is it interesting to do research in diabetes J. Olefsky, JAMA 2001:285:628-632
Addressing Addressing Challenges in Type 2 Challenges in Type 2 Diabetes Diabetes Speaker:
 Addressing Challenges in Type 2 Diabetes Geneva Briggs, PharmD,, BCPS Addressing Challenges in Type 2 Diabetes Speaker: Dr. Geneva Clark Briggs, a board-certified Pharmacotherapy Specialist, received her
Addressing Challenges in Type 2 Diabetes Geneva Briggs, PharmD,, BCPS Addressing Challenges in Type 2 Diabetes Speaker: Dr. Geneva Clark Briggs, a board-certified Pharmacotherapy Specialist, received her
GLP 1 agonists Winning the Losing Battle. Dr Bernard SAMIA. KCS Congress: Impact through collaboration
 GLP 1 agonists Winning the Losing Battle Dr Bernard SAMIA KCS Congress: Impact through collaboration CONTACT: Tel. +254 735 833 803 Email: kcardiacs@gmail.com Web: www.kenyacardiacs.org Disclosures I have
GLP 1 agonists Winning the Losing Battle Dr Bernard SAMIA KCS Congress: Impact through collaboration CONTACT: Tel. +254 735 833 803 Email: kcardiacs@gmail.com Web: www.kenyacardiacs.org Disclosures I have
Multi-factor approach to reduce cardiovascular risk in diabetes
 Multi-factor approach to reduce cardiovascular risk in diabetes Prof. Nicola Napoli, MD PhD Division of Endocrinology and Diabetes Università Campus Bio-Medico di Roma Washington University in St Louis
Multi-factor approach to reduce cardiovascular risk in diabetes Prof. Nicola Napoli, MD PhD Division of Endocrinology and Diabetes Università Campus Bio-Medico di Roma Washington University in St Louis
Type 2 Diabetes: Where Do We Start with Treatment? DIABETES EDUCATION. Diabetes Mellitus: Complications and Co-Morbid Conditions
 Diabetes Mellitus: Complications and Co-Morbid Conditions ADA Guidelines for Glycemic Control: 2016 Retinopathy Between 2005-2008, 28.5% of patients with diabetes 40 years and older diagnosed with diabetic
Diabetes Mellitus: Complications and Co-Morbid Conditions ADA Guidelines for Glycemic Control: 2016 Retinopathy Between 2005-2008, 28.5% of patients with diabetes 40 years and older diagnosed with diabetic
Combination treatment for T2DM
 Combination treatment for T2DM Date of approval: December 2016 SAGLB.DIA.16.08.0657 Abbreviations ADA: American Diabetes Association CVD: Cardiovascular disease DPP-4: Dipeptidyl Peptidase-4 EASD: European
Combination treatment for T2DM Date of approval: December 2016 SAGLB.DIA.16.08.0657 Abbreviations ADA: American Diabetes Association CVD: Cardiovascular disease DPP-4: Dipeptidyl Peptidase-4 EASD: European
Management of Diabetes Mellitus: A Primary Care Perspective
 Management of Diabetes Mellitus: A Primary Care Perspective Robert B. Baron MD MS Professor and Associate Dean UCSF School of Medicine Declaration of full disclosure: No conflict of interest Screening
Management of Diabetes Mellitus: A Primary Care Perspective Robert B. Baron MD MS Professor and Associate Dean UCSF School of Medicine Declaration of full disclosure: No conflict of interest Screening
Professor Rudy Bilous James Cook University Hospital
 Professor Rudy Bilous James Cook University Hospital Rate per 100 patient years Rate per 100 patient years 16 Risk of retinopathy progression 16 Risk of developing microalbuminuria 12 12 8 8 4 0 0 5 6
Professor Rudy Bilous James Cook University Hospital Rate per 100 patient years Rate per 100 patient years 16 Risk of retinopathy progression 16 Risk of developing microalbuminuria 12 12 8 8 4 0 0 5 6
Efficacy and Safety of Initial Combination Therapy in Treatment-Naïve Type 2 Diabetes Patients: A Systematic Review and Meta-analysis
 Diabetes Ther (2018) 9:1995 2014 https://doi.org/10.1007/s13300-018-0493-2 ORIGINAL RESEARCH Efficacy and Safety of Initial Combination Therapy in Treatment-Naïve Type 2 Diabetes Patients: A Systematic
Diabetes Ther (2018) 9:1995 2014 https://doi.org/10.1007/s13300-018-0493-2 ORIGINAL RESEARCH Efficacy and Safety of Initial Combination Therapy in Treatment-Naïve Type 2 Diabetes Patients: A Systematic
Type 2 Diabetes Management: Case 1: Reducing Hypoglycemic Risk Case 2: Reducing Cardiovascular Risk
 Type 2 Diabetes Management M. Susan Burke, MD, FACP Clinical Associate Professor of Medicine Sidney Kimmel Medical College at Thomas Jefferson University Senior Advisor, Lankenau Medical Associates Lankenau
Type 2 Diabetes Management M. Susan Burke, MD, FACP Clinical Associate Professor of Medicine Sidney Kimmel Medical College at Thomas Jefferson University Senior Advisor, Lankenau Medical Associates Lankenau
Pharmacology Update for the Adult Patient - Newer Oral Medications for Diabetes
 Pharmacology Update for the Adult Patient - Newer Oral Medications for Diabetes Brooke Hudspeth, PharmD, CDE, MLDE Director of Diabetes Prevention, Kroger Pharmacy Adjunct Assistant Professor, University
Pharmacology Update for the Adult Patient - Newer Oral Medications for Diabetes Brooke Hudspeth, PharmD, CDE, MLDE Director of Diabetes Prevention, Kroger Pharmacy Adjunct Assistant Professor, University
DPP-4 inhibitor. The new class drug for Diabetes
 DPP-4 inhibitor The new class drug for Diabetes 1 Cause of Death in Korea 1 st ; Neoplasm 2 nd ; Cardiovascular Disease 3 rd ; Cerebrovascular Disease Diabetes 2 Incidence of Fatal or Nonfatal MI During
DPP-4 inhibitor The new class drug for Diabetes 1 Cause of Death in Korea 1 st ; Neoplasm 2 nd ; Cardiovascular Disease 3 rd ; Cerebrovascular Disease Diabetes 2 Incidence of Fatal or Nonfatal MI During
Diabetes: Definition Pathophysiology Treatment Goals. By Scott Magee, MD, FACE
 Diabetes: Definition Pathophysiology Treatment Goals By Scott Magee, MD, FACE Disclosures No disclosures to report Definition of Diabetes Mellitus Diabetes Mellitus comprises a group of disorders characterized
Diabetes: Definition Pathophysiology Treatment Goals By Scott Magee, MD, FACE Disclosures No disclosures to report Definition of Diabetes Mellitus Diabetes Mellitus comprises a group of disorders characterized
Peter Stein, MD Janssen Research and Development
 New Agents and Technologies in the Pipeline for the Treatment of Patients with Diabetes Peter Stein, MD Janssen Research and Development Agents in Phase 3 Development for T2DM Long-acting GLP-1 analogues
New Agents and Technologies in the Pipeline for the Treatment of Patients with Diabetes Peter Stein, MD Janssen Research and Development Agents in Phase 3 Development for T2DM Long-acting GLP-1 analogues
Ambrish Mithal MD, DM
 Ambrish Mithal MD, DM Chairman, Division of Endocrinology and Diabetes Medanta The Medicity Padma Bhushan Awardee 2015, Member Governing Council, Indian Council of Medical Research (ICMR) Dr Mithal is
Ambrish Mithal MD, DM Chairman, Division of Endocrinology and Diabetes Medanta The Medicity Padma Bhushan Awardee 2015, Member Governing Council, Indian Council of Medical Research (ICMR) Dr Mithal is
Quick Reference Guide
 2018 Clinical Practice Guidelines Quick Reference Guide 416569-18 guidelines.diabetes.ca diabetes.ca 1-800-BANTING (226-8464) Screening and Diagnosis Assess risk ANNUALLY if: Family history (First-degree
2018 Clinical Practice Guidelines Quick Reference Guide 416569-18 guidelines.diabetes.ca diabetes.ca 1-800-BANTING (226-8464) Screening and Diagnosis Assess risk ANNUALLY if: Family history (First-degree
LATE BREAKING STUDIES IN DM AND CAD. Will this change the guidelines?
 LATE BREAKING STUDIES IN DM AND CAD Will this change the guidelines? Objectives 1. Discuss current guidelines for prevention of CHD in diabetes. 2. Discuss the FDA Guidance for Industry regarding evaluating
LATE BREAKING STUDIES IN DM AND CAD Will this change the guidelines? Objectives 1. Discuss current guidelines for prevention of CHD in diabetes. 2. Discuss the FDA Guidance for Industry regarding evaluating
Janice Lazear, DNP, FNP-C, CDE DIAGNOSIS AND CLASSIFICATION OF DIABETES
 Janice Lazear, DNP, FNP-C, CDE DIAGNOSIS AND CLASSIFICATION OF DIABETES Objectives u At conclusion of the lecture the participant will be able to: 1. Differentiate between the classifications of diabetes
Janice Lazear, DNP, FNP-C, CDE DIAGNOSIS AND CLASSIFICATION OF DIABETES Objectives u At conclusion of the lecture the participant will be able to: 1. Differentiate between the classifications of diabetes
Hanyang University Guri Hospital Chang Beom Lee
 Hanyang University Guri Hospital Chang Beom Lee Meal prayer, Van Brekelenkam 17 th C Introduction 2012 ADA/EASD Position Statement Proper Patients for Pioglitazone β-cell Preservation by Pioglitazone Benefit
Hanyang University Guri Hospital Chang Beom Lee Meal prayer, Van Brekelenkam 17 th C Introduction 2012 ADA/EASD Position Statement Proper Patients for Pioglitazone β-cell Preservation by Pioglitazone Benefit
Management of Diabetes
 Management of Diabetes Mellitus: Which Drugs for Which Patients? Robert B. Baron MD MS Professor and Associate Dean UCSF School of Medicine baron@medicine.ucsf.edu Disclosure No relevant financial relationships
Management of Diabetes Mellitus: Which Drugs for Which Patients? Robert B. Baron MD MS Professor and Associate Dean UCSF School of Medicine baron@medicine.ucsf.edu Disclosure No relevant financial relationships
Multiple Small Feedings of the Mind: Diabetes. Sonja K Fredrickson, MD, BC-ADM March 7, 2014
 Multiple Small Feedings of the Mind: Diabetes Sonja K Fredrickson, MD, BC-ADM March 7, 2014 Question 1: Setting A1c Goals Describe the evidence based approach to determining the target HgbA1c in different
Multiple Small Feedings of the Mind: Diabetes Sonja K Fredrickson, MD, BC-ADM March 7, 2014 Question 1: Setting A1c Goals Describe the evidence based approach to determining the target HgbA1c in different
Management of Diabetes Mellitus: A Primary Care Perspective. Screening for Diabetes Advantages of HbA1c as a Diagnostic Test
 Management of Diabetes Mellitus: A Primary Care Perspective Robert B. Baron MD MS Professor and Associate Dean UCSF School of Medicine Declaration of full disclosure: No conflict of interest Screening
Management of Diabetes Mellitus: A Primary Care Perspective Robert B. Baron MD MS Professor and Associate Dean UCSF School of Medicine Declaration of full disclosure: No conflict of interest Screening
CURRENT ISSUES IN DIABETES MANAGEMENT. Screening for Diabetes Advantages of HbA1c as a Diagnostic Test. Diagnosis of Diabetes 2013
 CURRENT ISSUES IN DIABETES MANAGEMENT Robert B. Baron MD MS Professor and Associate Dean UCSF School of Medicine Declaration of full disclosure: No conflict of interest Screening for Diabetes 2013 BMI
CURRENT ISSUES IN DIABETES MANAGEMENT Robert B. Baron MD MS Professor and Associate Dean UCSF School of Medicine Declaration of full disclosure: No conflict of interest Screening for Diabetes 2013 BMI
What s New on the Horizon: Diabetes Medication Update
 What s New on the Horizon: Diabetes Medication Update Outline of Talk Newly released and upcoming medications: the incretins, DPP-IV inhibitors, and what s coming Revised ADA/EASD and AACE guidelines:
What s New on the Horizon: Diabetes Medication Update Outline of Talk Newly released and upcoming medications: the incretins, DPP-IV inhibitors, and what s coming Revised ADA/EASD and AACE guidelines:
Treating Patients with PRE- DIABETES David Doriguzzi, PA-C First Valley Medical Group. Learning Objectives. Background
 Treating Patients with PRE- DIABETES David Doriguzzi, PA-C First Valley Medical Group Learning Objectives To accurately make the diagnosis of pre-diabetes/metabolic syndrome To understand the prevalence
Treating Patients with PRE- DIABETES David Doriguzzi, PA-C First Valley Medical Group Learning Objectives To accurately make the diagnosis of pre-diabetes/metabolic syndrome To understand the prevalence
ESC GUIDELINES ON DIABETES AND CARDIOVASCULAR DISEASES
 ESC GUIDELINES ON DIABETES AND CARDIOVASCULAR DISEASES Pr. Michel KOMAJDA Institute of Cardiology - IHU ICAN Pitie Salpetriere Hospital - University Pierre and Marie Curie, Paris (France) DEFINITION A
ESC GUIDELINES ON DIABETES AND CARDIOVASCULAR DISEASES Pr. Michel KOMAJDA Institute of Cardiology - IHU ICAN Pitie Salpetriere Hospital - University Pierre and Marie Curie, Paris (France) DEFINITION A
