Is hyperfiltration associated with the future risk of developing diabetic nephropathy? A meta-analysis.
|
|
|
- Melvyn Bishop
- 5 years ago
- Views:
Transcription
1 Is hyperfiltration associated with the future risk of developing diabetic nephropathy? A meta-analysis. Magee, G. M., Bilous, R. W., Cardwell, C., Hunter, S. J., Kee, F., & Fogarty, D. (2009). Is hyperfiltration associated with the future risk of developing diabetic nephropathy? A meta-analysis. Diabetologia, 52(4), DOI: /s Published in: Diabetologia Document Version: Publisher's PDF, also known as Version of record Queen's University Belfast - Research Portal: Link to publication record in Queen's University Belfast Research Portal General rights Copyright for the publications made accessible via the Queen's University Belfast Research Portal is retained by the author(s) and / or other copyright owners and it is a condition of accessing these publications that users recognise and abide by the legal requirements associated with these rights. Take down policy The Research Portal is Queen's institutional repository that provides access to Queen's research output. Every effort has been made to ensure that content in the Research Portal does not infringe any person's rights, or applicable UK laws. If you discover content in the Research Portal that you believe breaches copyright or violates any law, please contact openaccess@qub.ac.uk. Download date:13. Nov. 2018
2 Diabetologia (2009) 52: DOI /s META-ANALYSIS Is hyperfiltration associated with the future risk of developing diabetic nephropathy? A meta-analysis G. M. Magee & R. W. Bilous & C. R. Cardwell & S. J. Hunter & F. Kee & D. G. Fogarty Received: 20 November 2008 / Accepted: 21 December 2008 / Published online: 7 February 2009 # Springer-Verlag 2009 Abstract Aims/hypothesis Glomerular hyperfiltration is a wellestablished phenomenon occurring early in some patients with type 1 diabetes. However, there is no consistent answer regarding whether hyperfiltration predicts later development of nephropathy. We performed a systematic review and meta-analysis of observational studies that compared the risk of developing diabetic nephropathy in patients with and without glomerular hyperfiltration and also explored the impact of baseline GFR. Methods A systematic review and meta-analysis was carried out. Cohort studies in type 1 diabetic participants were included if they contained data on the development of incipient or overt nephropathy with baseline measurement of GFR and presence or absence of hyperfiltration. Results We included ten cohort studies following 780 patients. After a study median follow-up of 11.2 years, 130 patients had developed nephropathy. Using a random G. M. Magee (*) : S. J. Hunter Regional Centre for Diabetes and Endocrinology, Level 1, Royal Victoria Hospital, Grosvenor Road, Belfast BT12 6BA, UK gmagee13@qub.ac.uk R. W. Bilous Newcastle University, Newcastle Upon Tyne, UK R. W. Bilous James Cook University Hospital, Middlesbrough, UK C. R. Cardwell : F. Kee : D. G. Fogarty Department of Epidemiology and Public Health, School of Medicine and Dentistry, Queen s University, Belfast, Northern Ireland, UK effects model, the pooled odds of progression to a minimum of microalbuminuria in patients with hyperfiltration was 2.71 (95% CI ) times that of patients with normofiltration. There was moderate heterogeneity (heterogeneity test p=0.05, measure of degree of inconsistency= 48%) and some evidence of funnel plot asymmetry, possibly due to publication bias. The pooled weighted mean difference in baseline GFR was 13.8 ml min m 2 (95% CI ) greater in the group progressing to nephropathy than in those not progressing (heterogeneity test p<0.01). Conclusions/interpretation In published studies, individuals with glomerular hyperfiltration were at increased risk of progression to diabetic nephropathy using study level data. Further larger studies are required to explore this relationship and the role of potential confounding variables. Keywords Diabetic nephropathy. Glomerular hyperfiltration. Meta-analysis. Observational studies. Progression Abbreviation I 2 Measure of degree of inconsistency Introduction Glomerular hyperfiltration is a phenomenon found early in the clinical course of diabetes and its presence has been suggested to be a risk factor for future diabetic nephropathy [1]. In animal studies, when new-onset diabetes is induced by streptozotocin in Munich Wistar rats, single nephron GFR is increased in animals with moderate hyperglycaemia [2, 3]. Clinically, GFR is increased in newly diagnosed type 1 diabetic patients compared with non diabetic patients of a
3 692 Diabetologia (2009) 52: similar age. Moreover, in approximately 25 40% of patients with type 1 diabetes, GFR can increase to as much as ml/min. This is assumed to be related to metabolic control, as reduction of blood glucose with insulin therapy returns GFR to near normal levels [4, 5]. Glomerular hyperfiltration has been attributed to abnormalities in the glomerulus and glomerular vessels. GFR is determined by renal plasma flow, the transmembrane hydraulic pressure gradients and the ultrafiltration coefficient. Renal plasma flow is reliant on changes between afferent and efferent renal arteriolar resistance; the transmembrane hydraulic pressure gradient is the difference between the mean pressure in the glomerular capillary and the proximal tubule; and the ultrafiltration coefficient is related to the filtration surface area and its permeability. All of these factors are altered in patients with diabetes, although the timing of these dynamic changes is still unclear [6 8]. Uncertainty remains regarding whether glomerular haemodynamic changes similar to those found in patients with type 1 diabetes mellitus are also present in type 2 diabetes. In studies in Pima Indians, GFR was found to be 15% higher in recent-onset type 2 diabetic patients [9]. However, these changes were no longer significant when corrected for body surface area and were not confirmed by another smaller study [10]. Additionally, in longitudinal studies the GFR was found to be elevated at the onset of type 2 diabetes and remained so until the onset of overt nephropathy [11]. Similar changes have been demonstrated in white patients, with hyperfiltration present in 16% of 110 previously untreated type 2 diabetic patients [12]. Further cross-sectional studies measuring GFR isotopically have also demonstrated hyperfiltration in various racial groups [13-17]. Renal haemodynamics are likely to play a crucial role in the progression of diabetic nephropathy and may even contribute to its initiation. The available evidence on hyperfiltration risk in human studies is, however, conflicting, while the power of many studies to determine whether hyperfiltration predicts later development of nephropathy is limited. Therefore we performed a systematic review and meta-analysis of studies that compared the risk of developing diabetic nephropathy in type 1 diabetic patients with and without glomerular hyperfiltration at baseline; we also assessed the effect on progression to nephropathy of baseline GFR measurements as a more continuous variable. Methods Literature search MEDLINE and EMBASE were searched from the start date of each source to March 2008 using the search strategy: (Diabetes mellitus, type 1 or Diabetes complications or Diabetes or Diabetes mellitus, type 2 or Diabetes mellitus) and (Nephropathy or Incipient or Diabetic nephropathies or Overt or Proteinuria or Albuminuria or Microalbuminuria) and (Glomerular filtration rate or Hyperfiltration) and (Cohort studies or Case control studies). There were no limits on language. Abstracts were screened independently by two investigators (G. M. Magee and D. G. Fogarty) and full text articles were retrieved if relevant. Bibliographies of retrieved papers were also searched. Inclusion and exclusion criteria Studies with type 1 diabetes were included if they contained data on the development of incipient or overt nephropathy over time. Development of diabetic nephropathy was defined by the progression from normoalbuminuria to microalbuminuria or macroalbuminuria during the duration of follow-up. Albumin excretion rates categorising incipient or overt nephropathy were taken as stated by the individual papers, as they were dependent on the assay used by each laboratory. Data on patients who developed transient or intermittent microalbuminuria, as defined in the studies, were not included in the analysis. Studies also had to include baseline mean GFR measurements or a baseline determination of the presence or absence of hyperfiltration. The level of hyperfiltration was usually defined by the studies depending upon the method of GFR determination employed. This information enabled us to identify a group of patients who were hyperfiltering at the beginning of the studies and a group with normal GFR, and extract the number of patients in each group who subsequently developed diabetic nephropathy. To enable GFR to be assessed as a continuous measure, the baseline mean (± SD) GFR of those who later developed and did not develop nephropathy was also extracted from the papers where possible. All relevant papers were included and attempts were made to contact original authors if data were missing. Any disagreements in numbers were resolved by consensus between G. M. Magee, C. R. Cardwell and D. G. Fogarty. Studies or cases in studies were excluded if they were not normoalbuminuric at baseline or if follow-up data were missing. Data extraction Eligible studies were assessed independently by two reviewers (G. M. Magee and C. R. Cardwell). Study information on country, year of publication, duration of follow-up, duration of diabetes at baseline, age of diagnosis of diabetes, a measure of glycaemic control and blood pressure was also retrieved. Not all studies defined a level for hyperfiltration. In these cases, a level greater or equal to 140 ml min m 2 was used arbitrarily. Statistical analysis ORs and their SEs were calculated for the association between progression to incipient or overt nephropathy and the baseline presence of hyperfiltration for
4 Diabetologia (2009) 52: each study. A combined pooled OR was then derived using a random effects model, as we had anticipated some between-study heterogeneity, given that observational studies were being reviewed. Mean baseline differences in GFR between patients progressing to nephropathy and those without nephropathy during follow-up were also calculated, enabling a pooled weighted mean difference in GFR to be formulated, again using a random effects model to allow for between-study heterogeneity. Tests for heterogeneity between studies were conducted and the measure of degree of inconsistency (I 2 ) statistic was used to quantify the degree of this heterogeneity [18]. This value describes the total variation across the studies that is due to heterogeneity rather than chance (with I 2 values of 25%, 50% and 75% being tentatively considered low, moderate and high heterogeneity respectively). Publication bias was analysed by examining a funnel plot looking for asymmetry in plotted ORs against the SE of the logarithm of the ORs (a measure of study size). Begg s and Egger s tests for publication bias were also applied [19, 20]. All statistical analyses were performed using Stata 9.0 software (Stata, College Station, TX, USA). Results A total of 23 papers was retrieved for further evaluation, from which three cohort studies were selected for the metaanalysis. A further eight studies with the desired information were retrieved from studying bibliographies. We excluded 77 abstracts, five due to the presence of baseline microalbuminuria or proteinuria, 14 due to study design, four because studies contained participants without diabetes and 15 because other causes of nephropathy were included. Ten excluded studies described the use of novel markers and 29 others were excluded as they did not have any patients with GFR in the hyperfiltration range at baseline or because data were presented in such a way that the baseline GFRs could not be derived. One initially included report was subsequently removed from the analysis because it comprised patients with type 2 diabetes only, and as such was felt to be not comparable to the other studies [21]. In the end, ten cohort studies from six countries following 780 patients were included in this meta-analysis [22 31]. The publication years spanned three decades from 1984 to 2006 and all studies were of type 1 diabetic patients. The mean age at diabetes diagnosis was 12.3 years. The definition of hyperfiltration across the studies ranged from 125 to 140 ml min m 2. Four studies did not define a level of hyperfiltration and in these, this was arbitrarily taken as 140 ml min m 2 (Table 1). At the start of the studies, the mean duration of diabetes was 8.1 years and the mean overall follow-up of the cohorts was 11.2 years (Table 1). No studies had any participants on anti-hypertensive medication at baseline. In the three oldest studies HbA 1c was not available as a measure of glycaemic control, two other studies used HbA 1 measurements (Table 1). An estimate of HbA 1c (%) was established for these older studies using mean plasma glucose results and the reverse of the formula for estimated average glucose [32]: estimated average glucose ðmmol= 1Þ¼ 1:583 HbA 1c 2:52 (Table 1). The mean HbA 1c of Table 1 Characteristics of ten studies included in the meta-analysis First author [reference no.] Year Country Hyperfiltration definition (ml min m 2 ) a Patients included (n) Mean age at diagnosis (years) Mean follow-up (years) Mean baseline diabetes duration (years) Mean baseline HbA 1c (%) Progression No progression Mean baseline blood pressure (mmhg) Progression No progression Mogensen [22] 1984 Denmark ND b 7.4 b 135/89 124/80 Lervang [23] 1988 Denmark ND b 7.2 b 118/76 119/76 Lervang [24] 1992 Denmark ND b /83 115/70 Chiarelli [25] 1995 Italy 140 c d 9.5 d NA NA Yip [26] 1996 England NA NA NA NA Caramori [27] 1999 Brazil 134 c d 9.9 d NA NA Dahlquist [28] 2001 Sweden /74 115/74 Amin [29] 2005 England NA NA Steinke [30] 2005 USA /64 114/64 Zerbini [31] 2006 Italy ND /74 118/74 Total 780 Mean /77 118/73 a Where not defined (ND), arbitrarily set at >140 ml min m 2 b HbA 1c estimated using reverse estimated average glucose formula (these values omitted when calculating mean) c Single compartment GFR estimation technique d HbA 1 measurements (these values omitted when calculating mean) NA, not available
5 694 Diabetologia (2009) 52: Fig. 1 Forest plot of studies investigating the association between hyperfiltration and progression Number of studies, n=10. a Test for heterogeneity χ 2 =17.15, df=9.0, p=0.05; I 2 =48 (95% CI 0 75)%; test patients with progression to nephropathy was 10.5% compared with 9.6% in those not progressing. The association between hyperfiltration and progression to diabetic nephropathy is shown in Fig. 1. Using the random effects model, the pooled odds of progression to a minimum of incipient nephropathy was 2.71 (95% CI ) times those in patients with normofiltration at baseline, but there was evidence of heterogeneity (p=0.05, I 2 = 48%). In addition, the funnel plot shown in Fig. 2 suggests some evidence of asymmetry, although formal tests were not significant (Begg s p=0.2, Egger s p=0.1). Of the ten studies included, nine compared the mean difference in GFR in the groups with and without progression. One study could not be included for analysis on this point, as the relevant data could not be extracted [26]. In the nine studies included, the combined mean baseline GFR was 13.8 ml min m 2 greater in the patient groups progressing to nephropathy than in those not progressing. However, there was marked heterogeneity (I 2 =77% [95% CI 57 88%]) between studies, indicating that it may not be appropriate to produce overall estimates (Fig. 3). The funnel Standard error of logged OR [24] [23] [26] [31] [28] 1.6 [27] [22] OR Fig. 2 Funnel plot of the association between hyperfiltration and diabetic nephropathy. Dashed line, pooled estimate; dots, study as denoted by reference number [30] [25] [29] for overall effect Z=2.39, p=0.02. DN, diabetic nephropathy; HF, baseline hyperfiltration plot (not shown) suggested very little evidence of publication bias (Begg s test p=0.92, Egger s test p=0.99). Analysis excluding the two studies that used an uncorrected single compartment model for GFR calculation did not considerably alter the overall OR or improve heterogeneity. Discussion This meta-analysis indicates that type 1 diabetic patients with hyperfiltration are 2.7 times more likely to progress to incipient nephropathy than those with normofiltration and that patients who progressed had a higher baseline GFR. The strength of this analysis is that it is the first study combining estimates from previous smaller observational studies on the risk of progression in the presence of hyperfiltration and thereby allowing more power to detect any differences as significant. However, these findings should be interpreted cautiously, as for both analyses there was apparent heterogeneity. Furthermore, in the hyperfiltration analysis, although not detected in formal tests, a funnel plot supplied evidence of asymmetry, with small published studies observing more marked increases in the risk of progression to nephropathy after hyperfiltration. This pattern is consistent with publication bias (resulting from small studies observing no associations or inverse associations not being published), which, if present, would result in the combined OR overestimating the increased risk of progression to nephropathy after hyperfiltration. The association between progression and hyperfiltration had an I 2 value of 48%, indicating low to moderate heterogeneity, but this was greater (I 2 =77%) when the mean GFR between patients who progressed and those who did not was compared. There are various explanations for this marked heterogeneity, including differences in the year
6 Diabetologia (2009) 52: Fig. 3 Forest plot of studies investigating the association between baseline GFR and progression. Number of studies, n=9. a Test for heterogeneity χ 2 =35.24, df=8, p<0.001; I 2 =77 (95% CI 57 88)%; test for overall effect Z=3.06, p=0.002 of study, glycaemic control, treatments and improvement in screening for complications. Various techniques were employed throughout the studies to measure the GFR, with some of the studies using a single compartment analysis. This has been shown to overestimate GFR by as much as 25% to 30% in the upper range of clearance values when compared with a two compartment model [33]. The use of this model, if not corrected, would tend to overestimate the numbers of patients with hyperfiltration. When the studies not correcting for this potential weakness were removed from our analysis, heterogeneity did not improve and the combined OR did not markedly change, falling to 2.32 (Fig. 3). Hyperfiltration has been found to be more prevalent in those with recent onset of diabetes and when glycaemic control is poor [1, 4, 5]. It would therefore be essential to compare duration of diabetes at entry into the study, as patients with shorter disease duration are more likely to have hyperfiltration. The mean duration of diabetes at entry into the studies analysed was 8.1 years, but this ranged from 3.4 to 12.6 years [22, 23]. Patients should therefore have been on established glycaemic therapy even in the studies with the shortest disease duration at baseline. Two studies had calculated odds strongly against hyperfiltration as a risk factor for progression [23, 24]. The first of these had the shortest duration of diabetes, but participants were diagnosed at an older mean age of 18.9 years and followed up for the longest period of time (18.5 years). It is therefore surprising that this group, with a 69% prevalence of hyperfiltration, had the lowest risk of progressing to nephropathy. It is generally recognised that younger age of diabetes onset also leads to a younger age of progression [34]; however, these older patients were diagnosed years after exposure to pubertal hormonal changes, which are thought to increase hyperfiltration, and perhaps this plays some part in confounding against their overall risk of progression [29]. In other words, the pathophysiology of increased GFR may differ at different ages and these differences may themselves confer variable nephropathy risk. In one study, the calculated odds of progression at 33.1 was double that of the next nearest (16.4) [22, 29]. There are a number of possible explanations for this disparity of effect, including the fact that this study was the first of its kind, and also the smallest. In addition, progression to microalbuminuria was defined as an increase in urinary albumin excretion (determined by radioimmunoassay) by a factor of more than 3 at follow-up. When compared with all other studies, where microalbuminuria was generally defined as 20 to 200 μg/ min, this approach may lead to overestimation of progression to microalbuminuria based upon lower initial urinary albumin excretion. Also, in this study, patients who progressed had a markedly higher baseline GFR (all >150 ml min m 2 ) than those not progressing compared with some of the later studies. The role of different levels of hyperfiltration could only be assessed in a larger study or with individual patient level data. It has been proposed that high glomerular plasma flow increases intracapillary pressure; there is a relative constriction of the efferent glomerular arteriole resulting in a flux of plasma proteins into the mesangium [2, 35, 36]. This, in turn, leads to proliferation of mesangial cells and matrix, a forerunner of glomerulosclerosis. One potential cellular mechanism whereby these haemodynamic changes may lead to this sclerotic process is the effect of stretch induced by increased intraglomerular pressure on increasing fibronectin levels in mesangial cells via p38 mitogenactivated protein kinase, as has been demonstrated in mouse models [37]. This has been shown to increase podocyte hypertrophy in vitro and leads to local activation of the angiotensin system [38, 39]. Hyperglycaemia can cause an increase in GFR, so the role of glycaemic control and diabetes treatment is important. Comparison of baseline glycaemic control across the studies showed that the mean HbA 1c in patients with
7 696 Diabetologia (2009) 52: progression was 10.5% vs 9.6% in those not progressing. This may be a confounder in the overall calculated odds of progression. Reported baseline blood pressure was also higher, when available, in the progressing patients (123/77 vs 118/73 mmhg). An adjusted OR would be required to correct for the potential confounding factors of glycaemic control, blood pressure and diabetes duration, but in order to achieve this, individual patient level data would be necessary. However, in view of the age of some of the studies involved, the original data are unlikely to be available. The progression to overt nephropathy as an endpoint was also assessed. However, three of the studies were not specifically designed or of long enough duration to look for proteinuria [29-31] and a further study did not discriminate between incipient and overt nephropathy [24], leaving very small numbers for analysis. Hyperfiltration has been associated with a greater rate of decline in GFR [40]. Additionally, there is a normal physiological decline in GFR associated with ageing. Most of the individual studies assessed here were not adjusted for age-related decline as a factor in GFR prediction or for the effects of hyperfiltration on promoting a more rapid decline in GFR rather than nephropathy as such, so we were unable to analyse these effects in the identified studies [41 43]. In conclusion, in the identified studies, individuals with type 1 diabetes who had glomerular hyperfiltration or elevated GFR subsequently had an increased risk of developing diabetic nephropathy. However, additional studies using patient level data are required to examine whether this increased risk would persist after adjustment for the confounding effects of glycaemic control, diabetes duration and blood pressure. Confirmation of hyperfiltration as a risk marker might enable future studies to assess how early GFR reduction using agents that block the renin angiotensin aldosterone system impacts on the development of incipient nephropathy. Ongoing studies are evaluating these drugs, but they are not stratifying treatment based upon baseline GFR [44, 45]. Acknowledgements This study was supported by the Northern Ireland Kidney Research Fund and the Metabolic Unit Research Fund. Duality of interest The authors declare that there is no duality of interest associated with this manuscript. References 1. Mogensen CE, Christensen CK, Pedersen MM et al (1990) Renal and glycemic determinants of glomerular hyperfiltration in normoalbuminuric diabetics. J Diabetes Complications 4: Hostetter TH, Troy JL, Brenner BM (1981) Glomerular haemodynamics in experimental diabetes mellitus. Kidney Int 19: Reubi FC (1953) Glomerular filtration rate, renal blood flow and blood viscosity during and after diabetic coma. Circ Res 1: Mogensen CE (1971) Glomerular filtration rate and renal plasma flow in short-term and long-term juvenile diabetes mellitus. Scand J Clin Lab Invest 28: Wiseman MJ, Viberti GC, Keen H (1984) Threshold effect of plasma glucose in the glomerular hyperfiltration of diabetes. Nephron 38: Steffes M, Bilous R, Sutherland D, Mauer S (1992) Cell and matrix components of the glomerular mesangium in type I diabetes. Diabetes 41: Osterby R, Parving H, Hommel E, Jorgensen H, Lokkegaard H (1990) Glomerular structure and function in diabetic nephropathy. Early to advanced stage. Diabetes 39: Bak M, Thomsen K, Christiansen T, Flyvbjerg A (2000) Renal enlargement precedes renal hyperfiltration in early experimental diabetes in rats. J Am Soc Nephrol 11: Myers BD, Nelson RG, Williams GW et al (1991) Glomerular function in Pima Indians with non insulin-dependent diabetes mellitus of recent onset. J Clin Invest 88: Schmitz A, Christensen T, Jensent FT (1989) Glomerular filtration rate and kidney volume in normoalbuminuric non-insulin-dependent diabetics-lack of glomerular hyperfiltration and renal hypertrophy in uncomplicated NIDDM. Scand J Clin Lab Invest 49: Nelson RG, Bennett PH, Beck GJ et al (1996) Development and progression of renal disease in Pima Indians with non insulin dependent diabetes mellitus. N Engl J Med 335: Vora JP, Dolben J, Dean JD et al (1992) Renal haemodynamics in newly presenting non insulin dependent diabetes mellitus. Kidney Int 41: Taniwaki H, Ishimura E, Emoto M et al (2000) Relationship between urinary albumin excretion and glomerular filtration rate in normotensive, non proteinuric patients with type 2 diabetes mellitus. Nephron 86: Palmisano JJ, Lebovitz HE (1989) Renal function in black Americans with type II diabetes. J Diabetes Complications 3: Bruce R, Rutland M, Cundy T (1994) Glomerular hyperfiltration in young Polynesians with type 2 diabetes. Diabetes Res Clin Pract 25: Lee KU, Park JY, Hwang IR et al (1995) Glomerular hyperfiltration in Koreans with non-insulin-dependent diabetes mellitus. Am J Kidney Dis 26: Vedel P, Obel J, Nielsen FS et al (1996) Glomerular hyperfiltration in microalbuminuric NIDDM patients. Diabetologia 39: Higgins JPT, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327: Begg CB, Mazumdar M (1994) Operating characteristics of a rank correlation test for publication bias. Biometrics 50: Egger M, Davey Smith G, Schneider M, Minder C (1997) Bias in meta-analysis detected by a simple graphical test. BMJ 315: Murussi M, Gross JL, Silveiro SP (2006) Glomerular filtration rate changes in normoalbuminuric and microalbuminuric Type 2 diabetic patients and normal individuals: A 10-year follow-up. J Diabetes Complications 20: Mogensen CE (1986) Early glomerular hyperfiltration in insulindependent diabetics and late nephropathy. Scand J Clin Lab Invest 46: Lervang HH, Jensen S, Brochner-Mortensen J, Ditzel J (1988) Early glomerular hyperfiltration and the development of late nephropathy in type 1 (insulin-dependent) diabetes mellitus. Diabetologia 31:
8 Diabetologia (2009) 52: Lervang HH, Jensen S, Brochner-Mortensen J, Ditzel J (1992) Does increased glomerular filtration rate or disturbed tubular function early in the course of childhood type 1 diabetes predict the development of nephropathy? Diabet Med 9: Chiarelli F, Verrotti A, Morgese G (1995) Glomerular hyperfiltration increases the risk of developing microalbuminuria in diabetic children. Pediatr Nephrol 9: Yip JW, Jones SL, Wiseman MJ, Hill C, Viberti G (1996) Glomerular hyperfiltration in the prediction of nephropathy in IDDM: a 10-year follow-up study. Diabetes 45: Caramori M, Gross J, Pecis M, de Azevedo M (1999) Glomerular filtration rate, urinary albumin excretion rate, and blood pressure changes in normoalbuminuric normotensive type 1 diabetic patients: an 8-year follow-up study. Diabetes Care 22: Dahlquist G, Stattin E, Rudberg S (2001) Urinary albumin excretion rate and glomerular filtration rate in the prediction of diabetic nephropathy; a long-term follow-up study of childhood onset type-1 diabetic patients. Nephrol Dial Transplant 16: Amin R, Turner C, van Aken S et al (2005) The relationship between microalbuminuria and glomerular filtration rate in young type 1 diabetic subjects: The Oxford Regional Prospective Study. Kidney Int 68: Steinke JM, Sinaiko AR, Kramer MS et al (2005) The early natural history of nephropathy in type 1 diabetes: predictors of 5 year urinary albumin excretion rate patterns in initially normoalbuminuric patients. Diabetes 54: Zerbini G, Bonfanti R, Meschi F et al (2006) Persistent renal hypertrophy and faster decline of glomerular filtration rate precede the development of microalbuminuria in type 1 diabetes. Diabetes 55: Manley SE (2008) Estimated average glucose derived from HbA1c (eag): Report from the European Association for the Study of Diabetes (EASD), Amsterdam Diabet Med 25: Brøchner-Mortensen J, Rohbrandt K, Lauritzen RB (1977) Precision of single injection [ 51 Cr]EDTA plasma clearance and endogenous creatinine clearance determinations in children. Scand J Clin Lab Invest 37: Amin R, Widmer B, Prevost AT et al (2008) Risk of microalbuminuria and progression to macroalbuminuria in a cohort with childhood onset type 1 diabetes: prospective observational study. BMJ 336: O'Bryan GT, Hostetter TH (1997) The renal haemodynamic basis of diabetic nephropathy. Semin Nephrol 17: Olson JL, Hostetter TH, Rennke HG, Brenner BM, Venkatachalam MA (1982) Altered glomerular permselectivity and progressive sclerosis following extreme ablation of renal mass. Kidney Int 22: Gruden G, Zonca S, Hayward A et al (2000) Mechanical stretchinduced fibronectin and transforming growth factor-beta1 production in human mesangial cells is p38 mitogen-activated protein kinase-dependent. Diabetes 49: Petermann AT, Pippin J, Durvasula R et al (2005) Mechanical stretch induces podocyte hypertrophy in vitro. Kidney Int 67: Durvasula RV, Petermann AT, Hiromura K et al (2004) Activation of a local tissue angiotensin system in podocytes by mechanical strain. Kidney Int 65: Perkins BA, Ficociello LH, Ostrander BE et al (2007) Microalbuminuria and the risk for early progressive renal function decline in type 1 diabetes. J Am Soc Nephrol 18: Silveiro S, Friedman R, de Azevedo M, Canani L, Gross J (1996) Five-year prospective study of glomerular filtration rate and albumin excretion rate in normofiltering and hyperfiltering normoalbuminuric NIDDM patients. Diabetes Care 19: Premaratne E, Macisaac RJ, Tsalamandris C, Panagiotopoulos S, Smith T, Jerums G (2005) Renal hyperfiltration in type 2 diabetes: effect of age-related decline in glomerular filtration rate. Diabetologia 48: Rius F, Pizarro E, Salinas I, Lucas A, Sanmarti A, Romero R (1995) Age as a determinant of glomerular filtration rate in noninsulin-dependent diabetes mellitus. Nephrol Dial Transplant 10: Klein R, Zinman B, Gardiner R et al (2005) The relationship of diabetic retinopathy to preclinical diabetic glomerulopathy lesions in type 1 diabetic patients: The Renin Angiotensin System Study. Diabetes 54: The DIRECT Programme Study Group (2005) The DIabetic REtinopathy Candesartan Trials (DIRECT) programme: baseline characteristics. J Renin Angiotensin Aldosterone Syst 6:25 32
Renal Hyperfiltration and the Development of Microalbuminuria in Type 1 Diabetes
 Renal Hyperfiltration and the Development of Microalbuminuria in Type 1 Diabetes The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters
Renal Hyperfiltration and the Development of Microalbuminuria in Type 1 Diabetes The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters
Early Glomerular Filtration Rate Loss as a Marker of Diabetic Nephropathy
 Early Glomerular Filtration Rate Loss as a Marker of Diabetic Nephropathy George Jerums, MBBS, MD, FRACP, 1 Elif Ekinci, MBBS, 2 Sianna Panagiotopoulos, PhD 3 and Richard J MacIsaac, MBBS, PhD, FRACP 4
Early Glomerular Filtration Rate Loss as a Marker of Diabetic Nephropathy George Jerums, MBBS, MD, FRACP, 1 Elif Ekinci, MBBS, 2 Sianna Panagiotopoulos, PhD 3 and Richard J MacIsaac, MBBS, PhD, FRACP 4
The clinical significance of hyperfiltration in diabetes
 Diabetologia (2010) 53:2093 2104 DOI 10.1007/s00125-010-1794-9 REVIEW The clinical significance of hyperfiltration in diabetes G. Jerums & E. Premaratne & S. Panagiotopoulos & R. J. MacIsaac Received:
Diabetologia (2010) 53:2093 2104 DOI 10.1007/s00125-010-1794-9 REVIEW The clinical significance of hyperfiltration in diabetes G. Jerums & E. Premaratne & S. Panagiotopoulos & R. J. MacIsaac Received:
Hyperfiltration in type 1 diabetes: does it exist and does it matter for nephropathy?
 Diabetologia (212) 55:155 1513 DOI 1.17/s125-12-2485-5 ARTICLE Hyperfiltration in type 1 diabetes: does it exist and does it matter for nephropathy? M. C. Thomas & J. L. Moran & V. Harjutsalo & L. Thorn
Diabetologia (212) 55:155 1513 DOI 1.17/s125-12-2485-5 ARTICLE Hyperfiltration in type 1 diabetes: does it exist and does it matter for nephropathy? M. C. Thomas & J. L. Moran & V. Harjutsalo & L. Thorn
Renal hyperfiltration in type 2 diabetes: effect of age-related decline in glomerular filtration rate
 Diabetologia (2005) 48: 2486 2493 DOI 10.1007/s00125-005-0002-9 ARTICLE E. Premaratne. R. J. MacIsaac. C. Tsalamandris. S. Panagiotopoulos. T. Smith. G. Jerums Renal hyperfiltration in type 2 diabetes:
Diabetologia (2005) 48: 2486 2493 DOI 10.1007/s00125-005-0002-9 ARTICLE E. Premaratne. R. J. MacIsaac. C. Tsalamandris. S. Panagiotopoulos. T. Smith. G. Jerums Renal hyperfiltration in type 2 diabetes:
Diabetic nephropathy affects 25 30% of type 1
 Low Glomerular Filtration Rate in Normoalbuminuric Type 1 Diabetic Patients An Indicator of More Advanced Glomerular Lesions M. Luiza Caramori, 1 Paola Fioretto, 2 and Michael Mauer 1 Increased urinary
Low Glomerular Filtration Rate in Normoalbuminuric Type 1 Diabetic Patients An Indicator of More Advanced Glomerular Lesions M. Luiza Caramori, 1 Paola Fioretto, 2 and Michael Mauer 1 Increased urinary
Laboratory Assessment of Diabetic Kidney Disease
 Laboratory Assessment of Diabetic Kidney Disease Andrew S. Narva 1 and Rudolf W. Bilous 2 In Brief Regardless of etiology, chronic kidney disease (CKD) is identified by two laboratory tests: 1) estimated
Laboratory Assessment of Diabetic Kidney Disease Andrew S. Narva 1 and Rudolf W. Bilous 2 In Brief Regardless of etiology, chronic kidney disease (CKD) is identified by two laboratory tests: 1) estimated
Prevention And Treatment of Diabetic Nephropathy. MOH Clinical Practice Guidelines 3/2006 Dr Stephen Chew Tec Huan
 Prevention And Treatment of Diabetic Nephropathy MOH Clinical Practice Guidelines 3/2006 Dr Stephen Chew Tec Huan Prevention Tight glucose control reduces the development of diabetic nephropathy Progression
Prevention And Treatment of Diabetic Nephropathy MOH Clinical Practice Guidelines 3/2006 Dr Stephen Chew Tec Huan Prevention Tight glucose control reduces the development of diabetic nephropathy Progression
Risk factors associated with the development of overt nephropathy in type 2 diabetes patients: A 12 years observational study
 Indian J Med Res 136, July 2012, pp 46-53 Risk factors associated with the development of overt nephropathy in type 2 diabetes patients: A 12 years observational study Vijay Viswanathan, Priyanka Tilak
Indian J Med Res 136, July 2012, pp 46-53 Risk factors associated with the development of overt nephropathy in type 2 diabetes patients: A 12 years observational study Vijay Viswanathan, Priyanka Tilak
Diabetologia 9 Springer-Verlag 1994
 Diabetologia (1994) 37:708-712 Diabetologia 9 Springer-Verlag 1994 Monitoring kidney function in diabetic nephropathy P. Rossing, A.-S. Astrup, U. M. Smidt, H.-H. Parving Steno Diabetes Center, Gentofte,
Diabetologia (1994) 37:708-712 Diabetologia 9 Springer-Verlag 1994 Monitoring kidney function in diabetic nephropathy P. Rossing, A.-S. Astrup, U. M. Smidt, H.-H. Parving Steno Diabetes Center, Gentofte,
Diabetologia 9 Springer-Verlag 1993
 Diabetologia (1993) 36:734-740 Diabetologia 9 Springer-Verlag 1993 Impact of initial treatment on renal function in newly-diagnosed Type 2 (non-insulin-dependent) diabetes mellitus J. P. Vora I, J. Dolben
Diabetologia (1993) 36:734-740 Diabetologia 9 Springer-Verlag 1993 Impact of initial treatment on renal function in newly-diagnosed Type 2 (non-insulin-dependent) diabetes mellitus J. P. Vora I, J. Dolben
Diabetologia 9. Impact of metabolic control in progression of clinical diabetic nephropathy
 Diabetologia (1987) 3:82-86 Diabetologia 9 Impact of metabolic control in progression of clinical diabetic nephropathy G. Nyberg a, G. Blohm6 z and G. Nord6n 1 Departments of 1Nephrology and 2Medieine
Diabetologia (1987) 3:82-86 Diabetologia 9 Impact of metabolic control in progression of clinical diabetic nephropathy G. Nyberg a, G. Blohm6 z and G. Nord6n 1 Departments of 1Nephrology and 2Medieine
Functional and Morphological Renal Manifestations in Diabetes Mellitus
 Diabetologia (1981) 21:89-93 Diabetologia 9 Springer-Verlag 1981 Review Articles Functional and Morphological Renal Manifestations in Diabetes Mellitus C. E. Mogensen, M. W. Steffes, T. Deckert and J.
Diabetologia (1981) 21:89-93 Diabetologia 9 Springer-Verlag 1981 Review Articles Functional and Morphological Renal Manifestations in Diabetes Mellitus C. E. Mogensen, M. W. Steffes, T. Deckert and J.
The CARI Guidelines Caring for Australasians with Renal Impairment. ACE Inhibitor and Angiotensin II Antagonist Combination Treatment GUIDELINES
 ACE Inhibitor and Angiotensin II Antagonist Combination Treatment Date written: September 2004 Final submission: September 2005 Author: Kathy Nicholls GUIDELINES No recommendations possible based on Level
ACE Inhibitor and Angiotensin II Antagonist Combination Treatment Date written: September 2004 Final submission: September 2005 Author: Kathy Nicholls GUIDELINES No recommendations possible based on Level
Diabetic Nephropathy
 Diabetic Nephropathy Objectives: Know what Diabetic Nephropathy means. Know how common is Diabetic nephropathy in Saudi Arabia and to appreciate how bad are this complications. Know the risk factors of
Diabetic Nephropathy Objectives: Know what Diabetic Nephropathy means. Know how common is Diabetic nephropathy in Saudi Arabia and to appreciate how bad are this complications. Know the risk factors of
Springer-Verlag 1981
 Diabetologia (1981) 21:178-183 Diabetologia @ Springer-Verlag 1981 Diabetic Nephropathy: Fault or Destiny? T. Deckert and J. E. Poulsen Steno Memorial Hospital, Gentofte, Denmark Summary. Twenty-one young
Diabetologia (1981) 21:178-183 Diabetologia @ Springer-Verlag 1981 Diabetic Nephropathy: Fault or Destiny? T. Deckert and J. E. Poulsen Steno Memorial Hospital, Gentofte, Denmark Summary. Twenty-one young
Arteriolar Hyalinosis Predicts Increase in Albuminuria and GFR Decline in Normo- and Microalbuminuric Japanese Patients With Type 2 Diabetes
 Diabetes Care Volume 40, October 2017 1373 Arteriolar Hyalinosis Predicts Increase in Albuminuria and GFR Decline in Normo- and Microalbuminuric Japanese Patients With Type 2 Diabetes Tatsumi Moriya, 1
Diabetes Care Volume 40, October 2017 1373 Arteriolar Hyalinosis Predicts Increase in Albuminuria and GFR Decline in Normo- and Microalbuminuric Japanese Patients With Type 2 Diabetes Tatsumi Moriya, 1
The retinal renin-angiotensin system: implications for therapy in diabetic retinopathy
 (2002) 16, S42 S46 2002 Nature Publishing Group All rights reserved 0950-9240/02 $25.00 www.nature.com/jhh : implications for therapy in diabetic retinopathy AK Sjølie 1 and N Chaturvedi 2 1 Department
(2002) 16, S42 S46 2002 Nature Publishing Group All rights reserved 0950-9240/02 $25.00 www.nature.com/jhh : implications for therapy in diabetic retinopathy AK Sjølie 1 and N Chaturvedi 2 1 Department
Reversal of Microalbuminuria A Causative Factor of Diabetic Nephropathy is Achieved with ACE Inhibitors than Strict Glycemic Control
 ISSN 0976 3333 Available Online at www.ijpba.info International Journal of Pharmaceutical & Biological Archives 2013; 4(5): 923-928 ORIGINAL RESEARCH ARTICLE Reversal of Microalbuminuria A Causative Factor
ISSN 0976 3333 Available Online at www.ijpba.info International Journal of Pharmaceutical & Biological Archives 2013; 4(5): 923-928 ORIGINAL RESEARCH ARTICLE Reversal of Microalbuminuria A Causative Factor
Is the new Mayo Clinic Quadratic (MCQ) equation useful for the estimation of glomerular filtration rate in type 2 diabetic patients?
 Diabetes Care Publish Ahead of Print, published online October 3, 2008 The MCQ equation in DM2 patients Is the new Mayo Clinic Quadratic (MCQ) equation useful for the estimation of glomerular filtration
Diabetes Care Publish Ahead of Print, published online October 3, 2008 The MCQ equation in DM2 patients Is the new Mayo Clinic Quadratic (MCQ) equation useful for the estimation of glomerular filtration
SGLT2 inhibition in diabetes: extending from glycaemic control to renal and cardiovascular protection
 SGLT2 inhibition in diabetes: extending from glycaemic control to renal and cardiovascular protection Hiddo Lambers Heerspink Department of Clinical Pharmacy and Pharmacology University Medical Center
SGLT2 inhibition in diabetes: extending from glycaemic control to renal and cardiovascular protection Hiddo Lambers Heerspink Department of Clinical Pharmacy and Pharmacology University Medical Center
Hypertension and diabetic nephropathy
 Hypertension and diabetic nephropathy Elisabeth R. Mathiesen Professor, Chief Physician, Dr sci Dep. Of Endocrinology Rigshospitalet, University of Copenhagen Denmark Hypertension Brain Eye Heart Kidney
Hypertension and diabetic nephropathy Elisabeth R. Mathiesen Professor, Chief Physician, Dr sci Dep. Of Endocrinology Rigshospitalet, University of Copenhagen Denmark Hypertension Brain Eye Heart Kidney
The standard structural changes seen in type 1
 Podocyte Number in Normotensive Type 1 Diabetic Patients With Albuminuria Kathryn E. White, 1 Rudolf W. Bilous, 1 Sally M. Marshall, 1 Meguid El Nahas, 2 Giuseppe Remuzzi, 3 Giampiero Piras, 4 Salvatore
Podocyte Number in Normotensive Type 1 Diabetic Patients With Albuminuria Kathryn E. White, 1 Rudolf W. Bilous, 1 Sally M. Marshall, 1 Meguid El Nahas, 2 Giuseppe Remuzzi, 3 Giampiero Piras, 4 Salvatore
The CARI Guidelines Caring for Australasians with Renal Impairment. Antihypertensive therapy in diabetic nephropathy GUIDELINES
 Antihypertensive therapy in diabetic nephropathy Date written: September 2004 Final submission: September 2005 Author: Kathy Nicholls GUIDELINES a. Adequate control of blood pressure (BP) slows progression
Antihypertensive therapy in diabetic nephropathy Date written: September 2004 Final submission: September 2005 Author: Kathy Nicholls GUIDELINES a. Adequate control of blood pressure (BP) slows progression
Supplementary Online Content
 Supplementary Online Content Tsai WC, Wu HY, Peng YS, et al. Association of intensive blood pressure control and kidney disease progression in nondiabetic patients with chronic kidney disease: a systematic
Supplementary Online Content Tsai WC, Wu HY, Peng YS, et al. Association of intensive blood pressure control and kidney disease progression in nondiabetic patients with chronic kidney disease: a systematic
ROLE OF ANGIOTENSIN CONVERTING ENZYME INHIBITORS AND ANGIOTENSIN RECEPTOR BLOCKERS IN TYPE I DIABETIC NEPHROPATHY DR.NASIM MUSA
 ROLE OF ANGIOTENSIN CONVERTING ENZYME INHIBITORS AND ANGIOTENSIN RECEPTOR BLOCKERS IN TYPE I DIABETIC NEPHROPATHY DR.NASIM MUSA Type I IDDM is characterized by The abrupt onset of symptoms Insulinopenia
ROLE OF ANGIOTENSIN CONVERTING ENZYME INHIBITORS AND ANGIOTENSIN RECEPTOR BLOCKERS IN TYPE I DIABETIC NEPHROPATHY DR.NASIM MUSA Type I IDDM is characterized by The abrupt onset of symptoms Insulinopenia
Managing patients with renal disease
 Managing patients with renal disease Hiddo Lambers Heerspink, MD University Medical Centre Groningen, The Netherlands Asian Cardio Diabetes Forum April 23 24, 216 Kuala Lumpur, Malaysia Prevalent cases,
Managing patients with renal disease Hiddo Lambers Heerspink, MD University Medical Centre Groningen, The Netherlands Asian Cardio Diabetes Forum April 23 24, 216 Kuala Lumpur, Malaysia Prevalent cases,
Diabetologia 9 Springer-Verlag 1981
 Diabetologia (1981) 2:451-456 Diabetologia 9 Springer-Verlag 1981 Originals Increased Kidney Size, Glomerular Filtration Rate and Renal Plasma Flow in Short-Term Insulin-Dependent Diabetics J. Sandahl
Diabetologia (1981) 2:451-456 Diabetologia 9 Springer-Verlag 1981 Originals Increased Kidney Size, Glomerular Filtration Rate and Renal Plasma Flow in Short-Term Insulin-Dependent Diabetics J. Sandahl
Diabetic Nephropathy in Spontaneously Diabetic Torii (SDT) Rats
 The Open Diabetes Journal, 2011, 4, 45-49 45 Diabetic Nephropathy in Spontaneously Diabetic Torii (SDT) Rats Takeshi Ohta * and Tomohiko Sasase Open Access Biological/Pharmacological Research Laboratories,
The Open Diabetes Journal, 2011, 4, 45-49 45 Diabetic Nephropathy in Spontaneously Diabetic Torii (SDT) Rats Takeshi Ohta * and Tomohiko Sasase Open Access Biological/Pharmacological Research Laboratories,
REVIEW ARTICLE NEWER BIOMARKERS IN EARLY DIABETIC NEPHROPATHY
 JCD REVIEW ARTICLE NEWER BIOMARKERS IN EARLY DIABETIC NEPHROPATHY SAPTARSHI MUKHOPADHYAY* *FACULTY (DEPARTMENT OF MEDICINE), B R SINGH HOSPITAL (EASTERN RAILWAY), KOLKATA. INTRODUCTION renal disease. It
JCD REVIEW ARTICLE NEWER BIOMARKERS IN EARLY DIABETIC NEPHROPATHY SAPTARSHI MUKHOPADHYAY* *FACULTY (DEPARTMENT OF MEDICINE), B R SINGH HOSPITAL (EASTERN RAILWAY), KOLKATA. INTRODUCTION renal disease. It
Diabetic Nephropathy. Introduction/Clinical Setting. Pathologic Findings Light Microscopy. J. Charles Jennette
 12 Diabetic Nephropathy J. Charles Jennette Introduction/Clinical Setting Diabetic nephropathy is a clinical syndrome in a patient with diabetes mellitus that is characterized by persistent albuminuria,
12 Diabetic Nephropathy J. Charles Jennette Introduction/Clinical Setting Diabetic nephropathy is a clinical syndrome in a patient with diabetes mellitus that is characterized by persistent albuminuria,
Evaluation. Abstract: Introduction: Micro-vascular. ESRD. Due ARTICLE 1,2. treatment for DM Bhubaneswar life span resulting 3 Tutor.
 ORIGINAL RESEARCH ARTICLE http: ://www.eternalpublication.com INTERNATIONAL JOURNAL OF ANATOMY PHYSIOLOGY AND BIOCHEMISTRY IJAPB: Volume: 2; Issue: 6; June 2015 ISSN(Online):2394-3440 Evaluation of Biochemical
ORIGINAL RESEARCH ARTICLE http: ://www.eternalpublication.com INTERNATIONAL JOURNAL OF ANATOMY PHYSIOLOGY AND BIOCHEMISTRY IJAPB: Volume: 2; Issue: 6; June 2015 ISSN(Online):2394-3440 Evaluation of Biochemical
Tubular markers do not predict the decline in glomerular filtration rate in type 1 diabetic patients with overt nephropathy
 http://www.kidney-international.org & 2011 International Society of Nephrology original article see commentary on page 1042 Tubular markers do not predict the decline in glomerular filtration rate in type
http://www.kidney-international.org & 2011 International Society of Nephrology original article see commentary on page 1042 Tubular markers do not predict the decline in glomerular filtration rate in type
Glomerular size- and charge selectivity in Type 2 (non-insulin-dependent) diabetic patients with diabetic nephropathy
 Diabetologia (1994) 37:195-21 Springer-Verlag 1994 Glomerular size- and charge selectivity in Type 2 (non-insulin-dependent) diabetic patients with diabetic nephropathy M.-A. Gall, P. Rossing, A. Kofoed-Enevoldsen,
Diabetologia (1994) 37:195-21 Springer-Verlag 1994 Glomerular size- and charge selectivity in Type 2 (non-insulin-dependent) diabetic patients with diabetic nephropathy M.-A. Gall, P. Rossing, A. Kofoed-Enevoldsen,
Diabetologia 9 Springer-Verlag 1981
 Diabetologia (1981) 20:457-461 Diabetologia 9 Springer-Verlag 1981 A Prospective Study of Glomerular Filtration Rate and Arterial Blood Pressure in Insulin-Dependent Diabetics with Diabetic Nephropathy
Diabetologia (1981) 20:457-461 Diabetologia 9 Springer-Verlag 1981 A Prospective Study of Glomerular Filtration Rate and Arterial Blood Pressure in Insulin-Dependent Diabetics with Diabetic Nephropathy
Diabetes has become the most common
 P O S I T I O N S T A T E M E N T Diabetic Nephropathy AMERICAN DIABETES ASSOCIATION Diabetes has become the most common single cause of end-stage renal disease (ESRD) in the U.S. and Europe; this is due
P O S I T I O N S T A T E M E N T Diabetic Nephropathy AMERICAN DIABETES ASSOCIATION Diabetes has become the most common single cause of end-stage renal disease (ESRD) in the U.S. and Europe; this is due
Risk Factors for Diabetic Nephropathy
 Risk Factors for Diabetic Nephropathy Amalkumar Bhattacharya Associate Professor in Medicine, Government Medical College, Surat - 395 001. 55 EPIDEMILGY AND DIABETES TYPE Diabetic nephropathy can occur
Risk Factors for Diabetic Nephropathy Amalkumar Bhattacharya Associate Professor in Medicine, Government Medical College, Surat - 395 001. 55 EPIDEMILGY AND DIABETES TYPE Diabetic nephropathy can occur
Microvascular Disease in Type 1 Diabetes
 Microvascular Disease in Type 1 Diabetes Jay S. Skyler, MD, MACP Division of Endocrinology, Diabetes, and Metabolism and Diabetes Research Institute University of Miami Miller School of Medicine The Course
Microvascular Disease in Type 1 Diabetes Jay S. Skyler, MD, MACP Division of Endocrinology, Diabetes, and Metabolism and Diabetes Research Institute University of Miami Miller School of Medicine The Course
Renal Protection Staying on Target
 Update Staying on Target James Barton, MD, FRCPC As presented at the University of Saskatchewan's Management of Diabetes & Its Complications (May 2004) Gwen s case Gwen, 49, asks you to take on her primary
Update Staying on Target James Barton, MD, FRCPC As presented at the University of Saskatchewan's Management of Diabetes & Its Complications (May 2004) Gwen s case Gwen, 49, asks you to take on her primary
SHORT COMMUNICATION. G. Joshy & P. Dunn & M. Fisher & R. Lawrenson
 Diabetologia (2009) 52:1474 1478 DOI 10.1007/s00125-009-1380-1 SHORT COMMUNICATION Ethnic differences in the natural progression of nephropathy among diabetes patients in New Zealand: hospital admission
Diabetologia (2009) 52:1474 1478 DOI 10.1007/s00125-009-1380-1 SHORT COMMUNICATION Ethnic differences in the natural progression of nephropathy among diabetes patients in New Zealand: hospital admission
The CARI Guidelines Caring for Australians with Renal Impairment. Specific effects of calcium channel blockers in diabetic nephropathy GUIDELINES
 Specific effects of calcium channel blockers in diabetic nephropathy Date written: September 2004 Final submission: September 2005 Author: Kathy Nicholls GUIDELINES a. Non-dihydropyridine calcium channel
Specific effects of calcium channel blockers in diabetic nephropathy Date written: September 2004 Final submission: September 2005 Author: Kathy Nicholls GUIDELINES a. Non-dihydropyridine calcium channel
Diabetes and Kidney Disease. Kris Bentley Renal Nurse practitioner 2018
 Diabetes and Kidney Disease Kris Bentley Renal Nurse practitioner 2018 Aims Develop an understanding of Chronic Kidney Disease Understand how diabetes impacts on your kidneys Be able to recognise the risk
Diabetes and Kidney Disease Kris Bentley Renal Nurse practitioner 2018 Aims Develop an understanding of Chronic Kidney Disease Understand how diabetes impacts on your kidneys Be able to recognise the risk
For more information about how to cite these materials visit
 Author(s): Frank Brosius, M.D, 2011 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Author(s): Frank Brosius, M.D, 2011 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Impaired protein tolerance test as a marker of early renal dysfunction in type 2 diabetes mellitus
 Original Research Article Impaired protein tolerance test as a marker of early renal dysfunction in type 2 diabetes mellitus Devabhaktuni Siva Sankar 1, Shaik Khaja Rassul 1* 1 Assistant Professor of Medicine,
Original Research Article Impaired protein tolerance test as a marker of early renal dysfunction in type 2 diabetes mellitus Devabhaktuni Siva Sankar 1, Shaik Khaja Rassul 1* 1 Assistant Professor of Medicine,
Diabetic Nephropathy. Objectives:
 There are, in truth, no specialties in medicine, since to know fully many of the most important diseases a man must be familiar with their manifestations in many organs. William Osler 1894. Objectives:
There are, in truth, no specialties in medicine, since to know fully many of the most important diseases a man must be familiar with their manifestations in many organs. William Osler 1894. Objectives:
The increasing prevalence of obesity in children
 IN THE LITERATURE Kidney Disease in Childhood-Onset Diabetes Commentary on Amin R, Widmer B, Prevost AT, et al: Risk of Microalbuminuria and Progression to Macroalbuminuria in a Cohort With Childhood Onset
IN THE LITERATURE Kidney Disease in Childhood-Onset Diabetes Commentary on Amin R, Widmer B, Prevost AT, et al: Risk of Microalbuminuria and Progression to Macroalbuminuria in a Cohort With Childhood Onset
Early-onset microalbuminuria in children with type 1 diabetes in Kuwait.
 Curr Pediatr Res 2017; 21 (2): 254-259 ISSN 0971-9032 www.currentpediatrics.com Early-onset microalbuminuria in children with type 1 diabetes in Kuwait. Amal A Al-Eisa 1, Ayedh Al-Hajri 2, Sulaiman Al-Shuaib
Curr Pediatr Res 2017; 21 (2): 254-259 ISSN 0971-9032 www.currentpediatrics.com Early-onset microalbuminuria in children with type 1 diabetes in Kuwait. Amal A Al-Eisa 1, Ayedh Al-Hajri 2, Sulaiman Al-Shuaib
Diabetologia 9 Springer-Verlag 1995
 Diabetologia (1995) 38:1218-1222 Diabetologia 9 Springer-Verlag 1995 Albumin excretion rate levels in non-diabetic offspring of NIDDM patients and out nephropathy G. Gruden, P. Cavallo-Perin, C. Olivetti,.
Diabetologia (1995) 38:1218-1222 Diabetologia 9 Springer-Verlag 1995 Albumin excretion rate levels in non-diabetic offspring of NIDDM patients and out nephropathy G. Gruden, P. Cavallo-Perin, C. Olivetti,.
Diabetic Nephropathy
 Diabetic Nephropathy Larry Lehrner, Ph.D.,M.D. llehrner@ksosn.com Commercial Support Acknowledgement: There is no outside support for this activity Financial Disclosure: stocks > 50,000 Bayer, J&J, Norvartis,Novo
Diabetic Nephropathy Larry Lehrner, Ph.D.,M.D. llehrner@ksosn.com Commercial Support Acknowledgement: There is no outside support for this activity Financial Disclosure: stocks > 50,000 Bayer, J&J, Norvartis,Novo
SLOWING PROGRESSION OF KIDNEY DISEASE. Mark Rosenberg MD University of Minnesota
 SLOWING PROGRESSION OF KIDNEY DISEASE Mark Rosenberg MD University of Minnesota OUTLINE 1. Epidemiology of progression 2. Therapy to slow progression a. Blood Pressure control b. Renin-angiotensin-aldosterone
SLOWING PROGRESSION OF KIDNEY DISEASE Mark Rosenberg MD University of Minnesota OUTLINE 1. Epidemiology of progression 2. Therapy to slow progression a. Blood Pressure control b. Renin-angiotensin-aldosterone
University of Groningen. C-reactive protein and albuminuria Stuveling, Erik Marcel
 University of Groningen C-reactive protein and albuminuria Stuveling, Erik Marcel IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please
University of Groningen C-reactive protein and albuminuria Stuveling, Erik Marcel IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please
ORIGINAL ARTICLE Urinary type IV collagen levels in diabetes mellitus
 Malaysian J Pathol 21; 32(1) : 43 47 ORIGINAL ARTICLE Urinary type IV collagen levels in diabetes mellitus Pavai STHANESHWAR MBBS, MD and *Siew-Pheng CHAN MBBS, FRCP Departments of Pathology and *Medicine,
Malaysian J Pathol 21; 32(1) : 43 47 ORIGINAL ARTICLE Urinary type IV collagen levels in diabetes mellitus Pavai STHANESHWAR MBBS, MD and *Siew-Pheng CHAN MBBS, FRCP Departments of Pathology and *Medicine,
Does renin angiotensin system blockade deserve preferred status over other anti-hypertensive medications for the treatment of people with diabetes?
 Editorial Page 1 of 6 Does renin angiotensin system blockade deserve preferred status over other anti-hypertensive medications for the treatment of people with diabetes? Joshua I. Barzilay 1, Paul K. Whelton
Editorial Page 1 of 6 Does renin angiotensin system blockade deserve preferred status over other anti-hypertensive medications for the treatment of people with diabetes? Joshua I. Barzilay 1, Paul K. Whelton
The CARI Guidelines Caring for Australasians with Renal Impairment. Protein Restriction to prevent the progression of diabetic nephropathy GUIDELINES
 Protein Restriction to prevent the progression of diabetic nephropathy Date written: September 2004 Final submission: September 2005 Author: Kathy Nicholls GUIDELINES a. A small volume of evidence suggests
Protein Restriction to prevent the progression of diabetic nephropathy Date written: September 2004 Final submission: September 2005 Author: Kathy Nicholls GUIDELINES a. A small volume of evidence suggests
Assessment of glomerular filtration rate in healthy subjects and normoalbuminuric diabetic patients: validity of a new (MDRD) prediction equation
 Nephrol Dial Transplant (2002) 17: 1909 1913 Original Article Assessment of glomerular filtration rate in healthy subjects and normoalbuminuric diabetic patients: validity of a new () prediction equation
Nephrol Dial Transplant (2002) 17: 1909 1913 Original Article Assessment of glomerular filtration rate in healthy subjects and normoalbuminuric diabetic patients: validity of a new () prediction equation
Increased Risk of Renal Deterioration Associated with Low e-gfr in Type 2 Diabetes Mellitus Only in Albuminuric Subjects
 ORIGINAL ARTICLE Increased Risk of Renal Deterioration Associated with Low e-gfr in Type 2 Diabetes Mellitus Only in Albuminuric Subjects Shu Meguro, Toshikatsu Shigihara, Yusuke Kabeya, Masuomi Tomita
ORIGINAL ARTICLE Increased Risk of Renal Deterioration Associated with Low e-gfr in Type 2 Diabetes Mellitus Only in Albuminuric Subjects Shu Meguro, Toshikatsu Shigihara, Yusuke Kabeya, Masuomi Tomita
It is well recognized that persons with non. Microalbuminuria, Blood Pressure, Metabolic Control, and Renal Involvement
 AJH 1997;10:189S 197S Microalbuminuria, Blood Pressure, Metabolic Control, and Renal Involvement Longitudinal Studies in White Non Insulin-Dependent Diabetic Patients Anita Schmitz In the present paper,
AJH 1997;10:189S 197S Microalbuminuria, Blood Pressure, Metabolic Control, and Renal Involvement Longitudinal Studies in White Non Insulin-Dependent Diabetic Patients Anita Schmitz In the present paper,
No significant differences in short-term renal prognosis between living kidney donors with and without diabetes
 Clin Exp Nephrol (218) 22:694 71 https://doi.org/1.17/s1157-17-1487-5 ORIGINAL ARTICLE No significant differences in short-term renal prognosis between living kidney donors with and without diabetes Takahiro
Clin Exp Nephrol (218) 22:694 71 https://doi.org/1.17/s1157-17-1487-5 ORIGINAL ARTICLE No significant differences in short-term renal prognosis between living kidney donors with and without diabetes Takahiro
Determinants of Decline in Glomerular Filtration Rate in Nonproteinuric Subjects with or without Diabetes and Hypertension
 Determinants of Decline in Glomerular Filtration Rate in Nonproteinuric Subjects with or without Diabetes and Hypertension Hiroki Yokoyama,* Sakiko Kanno,* Suguho Takahashi,* Daishiro Yamada,* Hiroshi
Determinants of Decline in Glomerular Filtration Rate in Nonproteinuric Subjects with or without Diabetes and Hypertension Hiroki Yokoyama,* Sakiko Kanno,* Suguho Takahashi,* Daishiro Yamada,* Hiroshi
THE KIDNEY IN DIABETES MELLITUS URINARY TRANSFERRIN EXCRETION, HYPERTENSION, AND THE ROLE OF ANGIOTENSIN CONVERTING ENZYME INHIBITORS IN THERAPY
 THE KIDNEY IN DIABETES MELLITUS URINARY TRANSFERRIN EXCRETION, HYPERTENSION, THE SYSTEM, AND THE ROLE OF ANGIOTENSIN CONVERTING ENZYME INHIBITORS IN THERAPY by MARK JOHN O'DONNELL A thesis submitted to
THE KIDNEY IN DIABETES MELLITUS URINARY TRANSFERRIN EXCRETION, HYPERTENSION, THE SYSTEM, AND THE ROLE OF ANGIOTENSIN CONVERTING ENZYME INHIBITORS IN THERAPY by MARK JOHN O'DONNELL A thesis submitted to
University of Groningen. Evaluation of renal end points in nephrology trials Weldegiorgis, Misghina Tekeste
 University of Groningen Evaluation of renal end points in nephrology trials Weldegiorgis, Misghina Tekeste IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
University of Groningen Evaluation of renal end points in nephrology trials Weldegiorgis, Misghina Tekeste IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
Diabetic Nephropathy 2009
 Diabetic Nephropathy 2009 Michael T McDermott MD Director, Endocrinology and Diabetes Practice University of Colorado Hospital Michael.mcdermott@ucdenver.edu Diabetic Nephropathy Clinical Stages Hyperfunction
Diabetic Nephropathy 2009 Michael T McDermott MD Director, Endocrinology and Diabetes Practice University of Colorado Hospital Michael.mcdermott@ucdenver.edu Diabetic Nephropathy Clinical Stages Hyperfunction
Higher levels of Urinary Albumin Excretion within the Normal Range Predict Faster Decline in Glomerular Filtration Rate in Diabetic Patients
 Diabetes Care Publish Ahead of Print, published online May 12, 2009 Albuminuria and GFR Decline in Diabetes Higher levels of Urinary Albumin Excretion within the Normal Range Predict Faster Decline in
Diabetes Care Publish Ahead of Print, published online May 12, 2009 Albuminuria and GFR Decline in Diabetes Higher levels of Urinary Albumin Excretion within the Normal Range Predict Faster Decline in
Acute Effects of Different Intensities of Exercise in Normoalbuminuric/ Normotensive Patients With Type 1 Diabetes
 Clinical Care/Education/Nutrition O R I G I N A L A R T I C L E Acute Effects of Different Intensities of Exercise in Normoalbuminuric/ Normotensive Patients With Type 1 Diabetes JAMES T. LANE, MD 1 TIMOTHY
Clinical Care/Education/Nutrition O R I G I N A L A R T I C L E Acute Effects of Different Intensities of Exercise in Normoalbuminuric/ Normotensive Patients With Type 1 Diabetes JAMES T. LANE, MD 1 TIMOTHY
CLINICIAN INTERVIEW A REVIEW OF THE CURRENT TREATMENT MODALITIES FOR DIABETIC NEPHROPATHY. Interview with Ralph Rabkin, MD
 A REVIEW OF THE CURRENT TREATMENT MODALITIES FOR DIABETIC NEPHROPATHY Interview with Ralph Rabkin, MD Dr Rabkin is Professor of Medicine, Emeritus, Active, at Stanford University School of Medicine, Stanford,
A REVIEW OF THE CURRENT TREATMENT MODALITIES FOR DIABETIC NEPHROPATHY Interview with Ralph Rabkin, MD Dr Rabkin is Professor of Medicine, Emeritus, Active, at Stanford University School of Medicine, Stanford,
T he classical definition of diabetic nephropathy
 624 REVIEW Recent advances in diabetic nephropathy S M Marshall... Diabetic nephropathy is the leading cause of end stage renal disease worldwide and is associated with increased cardiovascular risk. The
624 REVIEW Recent advances in diabetic nephropathy S M Marshall... Diabetic nephropathy is the leading cause of end stage renal disease worldwide and is associated with increased cardiovascular risk. The
Urine albumin to creatinine ratio-response to exercise in diabetes
 Archives of Disease in Childhood, 1985, 60, 305-310 Urine albumin to creatinine ratio-response to in diabetes I G JEFFERSON, S A GREENE, M A SMITH, R F SMITH, N K G GRIFFIN, AND J D BAUM Children's Diabetes
Archives of Disease in Childhood, 1985, 60, 305-310 Urine albumin to creatinine ratio-response to in diabetes I G JEFFERSON, S A GREENE, M A SMITH, R F SMITH, N K G GRIFFIN, AND J D BAUM Children's Diabetes
Therapeutic approaches to slowing the progression of diabetic nephropathy is less best?
 www.drugsincontext.com The journal of interventions in clinical practice REVIEW Therapeutic approaches to slowing the progression of diabetic nephropathy is less best? FULL TEXT ARTICLE Eva Vivian, 1 Chelsea
www.drugsincontext.com The journal of interventions in clinical practice REVIEW Therapeutic approaches to slowing the progression of diabetic nephropathy is less best? FULL TEXT ARTICLE Eva Vivian, 1 Chelsea
1. Albuminuria an early sign of glomerular damage and renal disease. albuminuria
 1. Albuminuria an early sign of glomerular damage and renal disease albuminuria Cardio-renal continuum REGRESS Target organ damage Asymptomatic CKD New risk factors Atherosclerosis Target organ damage
1. Albuminuria an early sign of glomerular damage and renal disease albuminuria Cardio-renal continuum REGRESS Target organ damage Asymptomatic CKD New risk factors Atherosclerosis Target organ damage
Comparison between the efficacy of double blockade and single blockade of RAAS in diabetic kidney disease
 International Journal of Advances in Medicine Gupta A et al. Int J Adv Med. 2018 Aug;5(4):931-935 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20183122
International Journal of Advances in Medicine Gupta A et al. Int J Adv Med. 2018 Aug;5(4):931-935 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20183122
An acute fall in estimated glomerular filtration rate during treatment with losartan predicts a slower decrease in long-term renal function
 original article http://www.kidney-international.org & 2011 International Society of Nephrology see commentary on page 235 An acute fall in estimated glomerular filtration rate during treatment with losartan
original article http://www.kidney-international.org & 2011 International Society of Nephrology see commentary on page 235 An acute fall in estimated glomerular filtration rate during treatment with losartan
Cardiovascular disease (CVD) is the major cause. Microalbuminuria: Definition, Detection, and Clinical Significance. R e v i e w P a p e r
 R e v i e w P a p e r Microalbuminuria: Definition, Detection, and Clinical Significance Robert D. Toto, MD Proteinuria is a sign of abnormal excretion of protein by the kidney but is a nonspecific term
R e v i e w P a p e r Microalbuminuria: Definition, Detection, and Clinical Significance Robert D. Toto, MD Proteinuria is a sign of abnormal excretion of protein by the kidney but is a nonspecific term
Actualités néphrologiques Jean Hamburger 23 Avril Marie Courbebaisse, Service de Physiologie Hôpital Européen Georges Pompidou, Paris
 Single nephron GFR Actualités néphrologiques Jean Hamburger 23 Avril 2018 Marie Courbebaisse, Service de Physiologie Hôpital Européen Georges Pompidou, Paris Introdution Glomerular filtration and SNGFR
Single nephron GFR Actualités néphrologiques Jean Hamburger 23 Avril 2018 Marie Courbebaisse, Service de Physiologie Hôpital Européen Georges Pompidou, Paris Introdution Glomerular filtration and SNGFR
Responding to the challenge of diabetic nephropathy: the historic evolution of detection, prevention and management
 (2000) 14, 667 685 2000 Macmillan Publishers Ltd All rights reserved 0950-9240/00 $15.00 www.nature.com/jhh REVIEW ARTICLE Responding to the challenge of diabetic nephropathy: the historic evolution of
(2000) 14, 667 685 2000 Macmillan Publishers Ltd All rights reserved 0950-9240/00 $15.00 www.nature.com/jhh REVIEW ARTICLE Responding to the challenge of diabetic nephropathy: the historic evolution of
Diabetes has become the most common
 P O S I T I O N S T A T E M E N T Diabetic Nephropathy AMERICAN DIABETES ASSOCIATION Diabetes has become the most common single cause of end-stage renal disease (ESRD) in the U.S. and Europe; this is due
P O S I T I O N S T A T E M E N T Diabetic Nephropathy AMERICAN DIABETES ASSOCIATION Diabetes has become the most common single cause of end-stage renal disease (ESRD) in the U.S. and Europe; this is due
Diabetic Nephropathy
 Diabetic Nephropathy Outline Introduction of diabetic nephropathy Manifestations of diabetic nephropathy Staging of diabetic nephropathy Microalbuminuria Diagnosis of diabetic nephropathy Treatment of
Diabetic Nephropathy Outline Introduction of diabetic nephropathy Manifestations of diabetic nephropathy Staging of diabetic nephropathy Microalbuminuria Diagnosis of diabetic nephropathy Treatment of
The interest in microalbuminuria originated. Cardiovascular Implications of Albuminuria. R e v i e w P a p e r.
 R e v i e w P a p e r Cardiovascular Implications of Albuminuria Katherine R. Tuttle, MD Microalbuminuria is a major independent risk factor for cardiovascular disease (CVD) events in persons with diabetes
R e v i e w P a p e r Cardiovascular Implications of Albuminuria Katherine R. Tuttle, MD Microalbuminuria is a major independent risk factor for cardiovascular disease (CVD) events in persons with diabetes
Renoprotection in diabetes: genetic and non-genetic risk factors and treatment*
 Diabetologia (1998) 41: 745±759 Ó Springer-Verlag 1998 Review Renoprotection in diabetes: genetic and non-genetic risk factors and treatment* H.-H. Parving Steno Diabetes Center, Gentofte, Denmark Keywords
Diabetologia (1998) 41: 745±759 Ó Springer-Verlag 1998 Review Renoprotection in diabetes: genetic and non-genetic risk factors and treatment* H.-H. Parving Steno Diabetes Center, Gentofte, Denmark Keywords
Diabetologia 9 Springer-Verlag 1981
 Diabetologia (1981) 21 : 368-373 Diabetologia 9 Springer-Verlag 1981 Effect of Intravenous Glucose Infusion on Renal Function in Normal Man and in Insulin-Dependent Diabetics J. Sandahl Christiansen, M.
Diabetologia (1981) 21 : 368-373 Diabetologia 9 Springer-Verlag 1981 Effect of Intravenous Glucose Infusion on Renal Function in Normal Man and in Insulin-Dependent Diabetics J. Sandahl Christiansen, M.
Renal System Physiology
 M58_MARI0000_00_SE_EX09.qxd 7/18/11 2:37 PM Page 399 E X E R C I S E 9 Renal System Physiology Advance Preparation/Comments 1. Prior to the lab, suggest to the students that they become familiar with the
M58_MARI0000_00_SE_EX09.qxd 7/18/11 2:37 PM Page 399 E X E R C I S E 9 Renal System Physiology Advance Preparation/Comments 1. Prior to the lab, suggest to the students that they become familiar with the
Life Science Journal 2014;11(10)
 Performance of CKD-EPI versus MDRD among Diabetic Egyptians Khaled Abou-Seif, Yahya Makkeyah, Maha Behairy and Mohamed Mostafa Ali Internal Medicine & Nephrology Department, Ain Shams University Mahabehairy80@gmail.com
Performance of CKD-EPI versus MDRD among Diabetic Egyptians Khaled Abou-Seif, Yahya Makkeyah, Maha Behairy and Mohamed Mostafa Ali Internal Medicine & Nephrology Department, Ain Shams University Mahabehairy80@gmail.com
Invited Revie W. Diabetic nephropathy: the modulating influence of glucose on transforming factor D production
 Histol Histopathol (1 998) 13: 565-574 Histology and Histopathology Invited Revie W Diabetic nephropathy: the modulating influence of glucose on transforming factor D production A.O. Phillips lnstitute
Histol Histopathol (1 998) 13: 565-574 Histology and Histopathology Invited Revie W Diabetic nephropathy: the modulating influence of glucose on transforming factor D production A.O. Phillips lnstitute
Change in the distribution of albuminuria according to estimated glomerular filtration rate in Pima Indians with type 2 diabetes
 Diabetes Care Publish Ahead of Print, published online July 10, 2009 Change in the distribution of albuminuria according to estimated glomerular filtration rate in Pima Indians with type 2 diabetes MEDA
Diabetes Care Publish Ahead of Print, published online July 10, 2009 Change in the distribution of albuminuria according to estimated glomerular filtration rate in Pima Indians with type 2 diabetes MEDA
Progressive Renal Disease: A Disorder of Adaptation
 Quarterly Journal of Medicine. New Series 70. No. 263, pp. 185-189, March 1989 Editorial Progressive Renal Disease: A Disorder of Adaptation SHARON ANDERSON and BARRY M. BRENNER From the Renal Division
Quarterly Journal of Medicine. New Series 70. No. 263, pp. 185-189, March 1989 Editorial Progressive Renal Disease: A Disorder of Adaptation SHARON ANDERSON and BARRY M. BRENNER From the Renal Division
Natural History of Nephropathy in Type I Diabetes. Relationship to Metabolic Control and Blood Pressure
 Natural History of Nephropathy in Type I Diabetes Relationship to Metabolic Control and Blood Pressure CHRISTOPH HASSLACHER, EBERHARD RITZ, JANKE TERPSTRA, GEBHARD GALLASCH, GABRIELE KUNOWSKI, AND CORNELIA
Natural History of Nephropathy in Type I Diabetes Relationship to Metabolic Control and Blood Pressure CHRISTOPH HASSLACHER, EBERHARD RITZ, JANKE TERPSTRA, GEBHARD GALLASCH, GABRIELE KUNOWSKI, AND CORNELIA
New Treatment Options for Diabetic Nephropathy patients. Prof. M. Burnier, Service of Nephrology and Hypertension CHUV, Lausanne, Switzerland
 New Treatment Options for Diabetic Nephropathy patients Prof. M. Burnier, Service of Nephrology and Hypertension CHUV, Lausanne, Switzerland Diabetes and nephropathy Diabetic nephropathy is the most common
New Treatment Options for Diabetic Nephropathy patients Prof. M. Burnier, Service of Nephrology and Hypertension CHUV, Lausanne, Switzerland Diabetes and nephropathy Diabetic nephropathy is the most common
EARLY DIABETIC NEPHROPATHY. Roger K Ferguson, FACP, FACC, FCCP*
 Bahrain Medical Bulletin, Volume 18, Number 2, June 1996 Editorial EARLY DIABETIC NEPHROPATHY Roger K Ferguson, FACP, FACC, FCCP* Diabetes mellitus is becoming commoner in almost all parts of the world.
Bahrain Medical Bulletin, Volume 18, Number 2, June 1996 Editorial EARLY DIABETIC NEPHROPATHY Roger K Ferguson, FACP, FACC, FCCP* Diabetes mellitus is becoming commoner in almost all parts of the world.
Effect of Long-Term Administration of Prostaglandin I 2 in Incipient Diabetic Nephropathy
 Original Paper Nephron 2002;92:788 796 DOI: 10.1159/000065445 Accepted: April 16, 2002 Effect of Long-Term Administration of Prostaglandin I 2 in Incipient Diabetic Nephropathy Akira Owada Shin Suda Toshihiko
Original Paper Nephron 2002;92:788 796 DOI: 10.1159/000065445 Accepted: April 16, 2002 Effect of Long-Term Administration of Prostaglandin I 2 in Incipient Diabetic Nephropathy Akira Owada Shin Suda Toshihiko
Supplementary Online Content
 Supplementary Online Content Wu HY, Peng YS, Chiang CK, et al. Diagnostic performance of random urine samples using albumin concentration vs ratio of albumin to creatinine for microalbuminuria screening
Supplementary Online Content Wu HY, Peng YS, Chiang CK, et al. Diagnostic performance of random urine samples using albumin concentration vs ratio of albumin to creatinine for microalbuminuria screening
The hypertensive kidney and its Management
 The hypertensive kidney and its Management Dr H0 Chung Ping Hypertension Management Seminar 20061124 Hypertensive kidney Kidney damage asymptomatic till late stage Viscous cycle to augment renal damage
The hypertensive kidney and its Management Dr H0 Chung Ping Hypertension Management Seminar 20061124 Hypertensive kidney Kidney damage asymptomatic till late stage Viscous cycle to augment renal damage
Glomerular filtration rate (GFR)
 LECTURE NO (2) Renal Physiology Glomerular filtration rate (GFR) Faculty Of Medicine Dept.Of Physiology The glomerulus Is a tuft of capillaries enclosed within a Bowman capsule. It is supplied by an afferent
LECTURE NO (2) Renal Physiology Glomerular filtration rate (GFR) Faculty Of Medicine Dept.Of Physiology The glomerulus Is a tuft of capillaries enclosed within a Bowman capsule. It is supplied by an afferent
Measuring urinary tubular biomarkers in type 2 diabetes does not add prognostic value beyond established risk factors
 http://www.kidney-international.org & 2012 International Society of Nephrology Measuring urinary tubular biomarkers in type 2 diabetes does not add prognostic value beyond established risk factors Bryan
http://www.kidney-international.org & 2012 International Society of Nephrology Measuring urinary tubular biomarkers in type 2 diabetes does not add prognostic value beyond established risk factors Bryan
egfr > 50 (n = 13,916)
 Saxagliptin and Cardiovascular Risk in Patients with Type 2 Diabetes Mellitus and Moderate or Severe Renal Impairment: Observations from the SAVOR-TIMI 53 Trial Supplementary Table 1. Characteristics according
Saxagliptin and Cardiovascular Risk in Patients with Type 2 Diabetes Mellitus and Moderate or Severe Renal Impairment: Observations from the SAVOR-TIMI 53 Trial Supplementary Table 1. Characteristics according
LECTURE 25: FILTRATION AND CLEARANCE NEPHRON FILTRATION
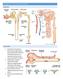 LECTURE 25: FILTRATION AND CLEARANCE NEPHRON FILTRATION 1. Everything in the plasma is filtered except large proteins and red blood cells. The filtrate in Bowman s capsule is an isosmotic fluid that is
LECTURE 25: FILTRATION AND CLEARANCE NEPHRON FILTRATION 1. Everything in the plasma is filtered except large proteins and red blood cells. The filtrate in Bowman s capsule is an isosmotic fluid that is
Pregnancy and progression of diabetic nephropathy
 Diabetologia 2002) 45: 36±41 Ó Springer-Verlag 2002 Articles Pregnancy and progression of diabetic nephropathy K. Rossing, P. Jacobsen, E. Hommel, E. Mathiesen, A. Svenningsen, P. Rossing, H-H. Parving
Diabetologia 2002) 45: 36±41 Ó Springer-Verlag 2002 Articles Pregnancy and progression of diabetic nephropathy K. Rossing, P. Jacobsen, E. Hommel, E. Mathiesen, A. Svenningsen, P. Rossing, H-H. Parving
Glomerular hyperfiltration predicts the development of microalbuminuria in stage 1 hypertension: The HARVEST
 original article http://www.kidney-international.org & 2006 International Society of Nephrology Glomerular hyperfiltration predicts the development of microalbuminuria in stage 1 hypertension: The HARVEST
original article http://www.kidney-international.org & 2006 International Society of Nephrology Glomerular hyperfiltration predicts the development of microalbuminuria in stage 1 hypertension: The HARVEST
DIABETIC NEPHROPATHY; CHANGES IN SERUM URIC ACID WITH ADVANCING STAGES
 The Professional Medical Journal DOI: 10.17957/TPMJ/17.3681 DIABETIC NEPHROPATHY; CHANGES IN SERUM URIC ACID WITH ADVANCING STAGES ORIGINAL PROF-3681 1. MBBS, M.Phil. Physiology, Ph.D. Scholar Continental
The Professional Medical Journal DOI: 10.17957/TPMJ/17.3681 DIABETIC NEPHROPATHY; CHANGES IN SERUM URIC ACID WITH ADVANCING STAGES ORIGINAL PROF-3681 1. MBBS, M.Phil. Physiology, Ph.D. Scholar Continental
The CARI Guidelines Caring for Australians with Renal Impairment. Control of Hypercholesterolaemia and Progression of Diabetic Nephropathy
 Control of Hypercholesterolaemia and Progression of Diabetic Nephropathy Date written: September 2004 Final submission: September 2005 Author: Kathy Nicholls GUIDELINES a. All hypercholesterolaemic diabetics
Control of Hypercholesterolaemia and Progression of Diabetic Nephropathy Date written: September 2004 Final submission: September 2005 Author: Kathy Nicholls GUIDELINES a. All hypercholesterolaemic diabetics
Diabetologia Springer-Verlag 1986
 Diabetologia (1986) 29: 211-215 Diabetologia Springer-Verlag 1986 Acute reduction of arterial blood pressure reduces urinary albumin excretion in Type 1 (insulin-dependent) diabetic patients with incipient
Diabetologia (1986) 29: 211-215 Diabetologia Springer-Verlag 1986 Acute reduction of arterial blood pressure reduces urinary albumin excretion in Type 1 (insulin-dependent) diabetic patients with incipient
6. DIABETIC NEPHROPATHY
 How to Cite this article: Diabetic Nephropathy - ejifcc 20/01 2009 http://www.ifcc.org 6. DIABETIC NEPHROPATHY Gábor L. Kovács 6.1 Summary Between 20% and 40% of patients with diabetes ultimately develop
How to Cite this article: Diabetic Nephropathy - ejifcc 20/01 2009 http://www.ifcc.org 6. DIABETIC NEPHROPATHY Gábor L. Kovács 6.1 Summary Between 20% and 40% of patients with diabetes ultimately develop
