6. DIABETIC NEPHROPATHY
|
|
|
- Dwight Morrison
- 5 years ago
- Views:
Transcription
1 How to Cite this article: Diabetic Nephropathy - ejifcc 20/ DIABETIC NEPHROPATHY Gábor L. Kovács 6.1 Summary Between 20% and 40% of patients with diabetes ultimately develop diabetic nephropathy, which in the US is the most common cause of endstage renal disease requiring dialysis. Diabetic nephropathy has several distinct phases of development and multiple mechanisms contribute to the development of the disease and its outcomes. This Review provides a summary of the latest published data dealing with these mechanisms; it focuses not only on candidate genes associated with susceptibility to diabetic nephropathy but also on alterations in various cytokines and their interaction with products of advanced glycation and oxidant stress. Additionally, the interactions between fibrotic and hemodynamic cytokines, such as transforming growth factor β1 and angiotensin II, respectively, are discussed in the context of new information concerning nephropathy development. We touch on the expanding clinical data regarding markers of nephropathy, such as microalbuminuria, and put them into context; microalbuminuria reflects cardiovascular and not renal risk. If albuminuria levels continue to increase over time then nephropathy is present. Lastly, we look at advances being made to enable identification of genetically predisposed individuals. 6.2 Introduction Diabetic nephropathy is the most common cause of end-stage renal disease requiring dialysis in the US (1). The incidence of diabetic nephropathy in this country has increased substantially over the past few years. Advanced diabetic nephropathy is also the leading cause of glomerulosclerosis and end-stage renal disease worldwide (2, 3). Between 20% and 40% of patients with diabetes ultimately develop nephropathy, although the reason why not all patients with diabetes develop this complication is unknown. The natural history of diabetic nephropathy differs according to the type of diabetes and whether microalbuminuria (defined as > 30 mg but < 300 mg albumin in the urine per day) is present. If untreated, 80% of people who have type 1 diabetes and microalbuminuria will progress to overt nephropathy (i.e. proteinuria characterized by > 300 mg albumin excreted daily), whereas only 20-40% of those with type 2 diabetes over a period of 15 years will progress. As Nielsen et al. (4) demonstrated 40
2 more than a decade ago, a clear, early predictor of disease progression is increasing systolic blood pressure, even within the prehypertensive range. Among patients who have type 1 diabetes with nephropathy and hypertension, 50% will go on to develop end-stage renal disease within a decade (5). Mortality among dialysis patients with diabetes is 22% higher in the first year following the initiation of dialysis and 15% higher at 5 years than that among dialysis patients without diabetes (6). Diabetic nephropathy has several distinct phases of development. Functional changes occur in the nephron at the level of the glomerulus, including glomerular hyperfiltration and hyperperfusion, before the onset of any measurable clinical changes. Subsequently, thickening of the glomerular basement membrane, glomerular hypertrophy, and mesangial expansion take place. Seminal studies by Mauer and colleagues (3) and Steinke and colleagues (7) demonstrated that individuals with type 1 diabetes and microalbuminuria in whom these histological alterations were detected were destined to progress to overt nephropathy. Microalbuminuria, however, has a variable course; its progression to macroalbuminuria (> 300 mg per day) is unpredictable and does not always lead to development of nephropathy (7). Moreover, the rate of kidney function decline after the development of nephropathy is highly variable between patients and is influenced by additional factors, including blood pressure and glycemic control. Multiple mechanisms contribute to the development and outcomes of diabetic nephropathy, such as an interaction between hyperglycemia-induced metabolic and hemodynamic changes and genetic predisposition, which sets the stage for kidney injury (8). Hemodynamic factors are the activation of various vasoactive systems, such as the renin-angiotensin-aldosterone and endothelin systems. In response, secretion of profibrotic cytokines, such as transforming growth factor β1 (TGF-β1), is increased and further hemodynamic changes occur, such as increased systemic and intraglomerular pressure. Metabolic pathway involvement, among other features, leads to nonenzymatic glycosylation, increased protein kinase C (PKC) activity, and abnormal polyol metabolism. Findings from various studies support an association between increased secretion of inflammatory molecules, such as cytokines, growth factors and metalloproteinases, and development of diabetic nephropathy (9). Oxidative stress also seems to play a central part (11). Studies that have used inhibitors of the pathways involved in genesis of diabetic nephropathy have shed light on the pathogenesis of this condition but have not led to expansion of the therapeutic armamentarium to halt the disease process (10). This Review is intended for a clinical audience and we discuss pathological changes to the glomeruli during the development of diabetic nephropathy. Although many factors have been implicated in the pathogenesis of diabetic nephropathy, we have focused on the particular factors outlined above. 6.3 Hemodynamic pathways The early signs of glomerular hyperperfusion and hyperfiltration result from decreased resistance in both the afferent and efferent arterioles of the glomerulus. The afferent arteriole seems to have a greater decrease in resistance than the efferent. Many factors have been reported to be involved in this defective autoregulation, including prostanoids, nitric oxide, vascular endothelial growth factor (VEGF; now formally known as VEGF-A), TGF-β1, and the renin angiotensin 41
3 system, specifically angiotensin II. These early hemodynamic changes facilitate albumin leakage from the glomerular capillaries and overproduction of mesangial cell matrix, as well as thickening of the glomerular basement membrane and injury to podocytes (12). In addition, increased mechanical strain resulting from these hemodynamic changes can induce localized release of certain cytokines and growth factors (13, 14). The renal hemodynamic changes are mediated partly by the actions of vasoactive hormones, such as angiotensin II and endothelin. Glomerular hypertension and hyperfiltration contribute to the development of diabetic nephropathy because use of renin angiotensin blockers preserves kidney function and morphology. Blockade of the renin angiotensin aldosterone system antagonizes the profibrotic effects of angiotensin II by reducing its stimulation of TGF-β1 (15). Support that such profibrotic effects underlie diabetic nephropathy has also been provided by study of an animal model of diabetic nephropathy (16). Transient blockade of the renin angiotensin system (for 7 weeks) in prediabetic rats reduced proteinuria and improved glomerular structure. Additionally, the administration of an angiotensin-converting-enzyme inhibitor to patients with type 1 diabetes and nephropathy lowered serum concentrations of TGF-β1 (17). A correlation exists between decreased levels of TGF-β1 in serum and urine and renoprotection, as determined by changes in the glomerular filtration rate over time. We discuss this effect further in the Cytokines section. 6.4 Hyperglycemia and advanced glycosylation end products Hyperglycemia is a crucial factor in the development of diabetic nephropathy because of its effects on glomerular and mesangial cells, but alone it is not causative. Mesangial cells are crucial for maintenance of glomerular capillary structure and for the modulation of glomerular filtration via smooth-muscle activity. Hyperglycemia is associated with an increase in mesangial cell proliferation and hypertrophy, as well as increased matrix production and basement membrane thickening. In vitro studies have demonstrated that hyperglycemia is associated with increased mesangial cell matrix production (18, 19) and mesangial cell apoptosis (20, 21). Mesangial cell expansion seems to be mediated in part by an increase in the mesangial cell glucose concentration, since similar changes in mesangial function can be induced in a normal glucose milieu by overexpression of glucose transporters, such as GLUT1 and GLUT4, thereby increasing glucose entry into the cells (19). Hyperglycemia might also upregulate VEGF expression in podocytes (14), which could markedly increases vascular permeability (22, 23). Hyperglycemia, however, does not account fully for the risk of diabetic nephropathy, as shown by studies in which kidneys from nondiabetic donors were transplanted into patients with diabetes and nephropathy developed irrespective of the glucose control (24). Hyperglycemia might, therefore, be necessary for but not sufficient to cause renal damage. Three mechanisms have been postulated that explain how hyperglycemia causes tissue damage: nonenzymatic glycosylation that generates advanced glycosylation end products, activation of PKC, and acceleration of the aldose reductase pathway (25, 26). Oxidative stress seems to be a theme common to all three pathways (27). 42
4 6.5 Glycosylation Glycosylation of tissue proteins contributes to the development of diabetic nephropathy and other microvascular complications. In chronic hyperglycemia, some of the excess glucose combines with free amino acids on circulating or tissue proteins. This nonenzymatic process affects the glomerular basement membrane and other matrix components in the glomerulus and initially leads to formation of reversible early glycosylation end products and, later, irreversible advanced glycosylation end products. These advanced products can be involved in the pathogenesis of diabetic nephropathy by altering signal transduction via alteration in the level of soluble signals, such as cytokines, hormones and free radicals. Circulating levels of advanced glycosylation end products are raised in people with diabetes, particularly those with renal insufficiency, since they are normally excreted in the urine (28). The net effect is tissue accumulation of advanced glycosylation end products (in part by cross-linking with collagen) that contributes to the associated renal and microvascular complications (29). Moreover, advanced glycosylation end products (AGE) interact with the AGE receptor, and nitric oxide concentrations are reduced in a dose-dependent manner (30). 6.6 Protein kinase C Other proposed mechanisms by which hyperglycemia promotes the development of diabetic nephropathy include activation of PKC (31). Specifically, activation of this enzyme leads to increased secretion of vasodilatory prostanoids, which contributes to glomerular hyperfiltration. By activation of TGF-β1, PKC might also increase production of extracellular matrix by mesangial cells (32). The mechanism by which hyperglycemia leads to PKC activation involves de novo formation of diacylglycerol and oxidative stress (33). PKC activation induces the activity of mitogen-activated protein kinases (MAPK) in response to extracellular stimuli through dual phosphorylation at conserved threonine and tyrosine residues. The coactivation of PKC and MAPK in the presence of high glucose concentrations indicates that these two families of enzymes are linked (34). 6.7 Aldose reductase pathway The polyol pathway is implicated in the pathogenesis of diabetic nephropathy. A number of studies have shown a decrease in urinary albumin excretion in animals administered aldose reductase inhibitors (35), but in humans these agents have not been studied widely and the results are inconclusive. 6.8 Prorenin Initial clinical studies in children and adolescents suggest that increased plasma prorenin activity is a risk factor for the development of diabetic nephropathy (36, 37). The prorenin receptor in the kidney is located in the mesangium and podocytes, and its blockade has a beneficial effect on kidneys in animal models of diabetes. This effect is mediated by intracellular signals that are both dependent on and 43
5 independent of the renin angiotensin system. Prorenin binds to a specific tissue receptor that promotes activation of p44/p42 MAPK (38). A possible pathogenic role for prorenin in the development of diabetic nephropathy was noted in an experimental model of diabetes-mice with streptozotocin-induced diabetes. Sustained prorenin-receptor blockade abolished MAPK activation and prevented the development of nephropathy despite an unaltered increase in angiotensin II activity (39). If prorenin is a key player in the pathogenesis of this disease, use of renin inhibitors for hypertension that increase prorenin concentrations should demonstrate a harmful effect. To date, no such adverse effects have been reported. 6.9 Cytokines Activation of cytokines, profibrotic elements, inflammation, and vascular growth factors such as VEGF might be involved in the matrix accumulation that arises in diabetic nephropathy (40-42). Although some evidence suggests that VEGF increases permeability of the glomerular filtration barrier to proteins (22), levels of this growth factor can be low in patients with diabetic nephropathy. Thus, the role of VEGF in the pathophysiology of nephropathy is unclear. Hyperglycemia is thought to stimulate VEGF expression and, therefore, act as a mediator of endothelial injury in human diabetes (40, 41). Studies showed initially that in patients with diabetic nephropathy the degree of neovascularization was increased and correlated with expression of VEGF and angiopoetin (43-45). Later findings, however, showed that levels of VEGF messenger RNA were actually decreased in patients with diabetic nephropathy (46). Evidence against the roles of VEGF and angiopoetin demonstrates promotion of vessel leakage and reduction in transendothelial electrical resistance; these two growth factors have key roles in development of retinopathy and contribute to nephropathy development in animal models. Further evidence to support a pathogenic role for VEGF in diabetic nephropathy is the observation that VEGF blockade improves albuminuria in an experimental model of the disorder (41, 42). Animal studies that used a neutralizing antibody to VEGF demonstrated the involvement of this growth factor in glomerular hypertrophy and mesangial matrix accumulation (41, 47). High glucose levels, TGF-β1, and angiotensin II stimulate VEGF expression, which leads to the synthesis of endothelial nitric oxide. This action promotes vasodilatation and hyperfiltration, which are the early processes in diabetic nephropathy. VEGF also stimulates the production of the α3 chain of collagen IV, an important component of the glomerular basement membrane. Indirect evidence suggests that increased production of this collagen chain contributes to the thickening of the glomerular basement membrane observed in diabetic nephropathy. In animal studies, administration of an antibody to VEGF decreased urinary albumin excretion compared with that in untreated diabetic controls (22). Findings from some studies refute a causative role for high VEGF levels in diabetic nephropathy. Instead, results imply that low levels are harmful. Eremina et al. (48) 44
6 showed in a mouse model that VEGF is produced by podocytes and is necessary for glomerular endothelial cell survival and differentiation as well as for mesangial cell development and differentiation. Gene expression of VEGF is decreased in humans with diabetic nephropathy (49), although whether this effect is due to podocytes loss, leading to reduced production of VEGF, has been questioned. Baelde et al. (46) showed that VEGF messenger RNA concentrations were decreased in the glomeruli of patients with diabetic nephropathy and correlated with reduction in the number of podocytes and progression of renal disease. Hyperglycemia also increases the expression of TGF-β1 in the glomeruli and of matrix proteins specifically stimulated by this cytokine (42). In the glomeruli of rats with streptozotocininduced diabetes, TGF-β1 levels are increased, and use of a neutralizing antibody to TGF-β1 prevents renal changes of diabetic nephropathy in these animals. In addition, connective tissue growth factor and heat shock proteins, which are encoded by TGF-β1-inducible genes, have fibrogenic effects on the kidneys of patients with diabetes. However, diabetes is associated with decreased expression of renal bone morphogenetic protein 7, which in turn seems to counter the profibrogenic actions of TGF-β1 (17). Evidence clearly shows that TGF-β1 contributes to the cellular hypertrophy and increased synthesis of collagen, both of which occur in diabetic nephropathy (17, 42, 50, 51). Further evidence for these actions is provided by studies in which the combination of an antibody to TGF-β1 plus an angiotensin-converting-enzyme inhibitor normalized levels of protein in the urine of rats with diabetic nephropathy; proteinuria was only partly resolved with the use of an angiotensin-converting-enzyme inhibitor alone (52). Glomerulosclerosis and tubulointerstitial injury were also improved by the combined therapy. The administration of hepatocyte growth factor, which specifically blocks the profibrotic actions of TGF-β1, ameliorates diabetic nephropathy in mice (53). Inflammatory cytokines also contribute to the development and progression of diabetic nephropathy, specifically interleukin 1 (IL-1), IL-6 and IL-18 and tumor necrosis factor. Concentrations of all these cytokines were increased in models of diabetic nephropathy and seemed to affect the disease via multiple mechanisms. In addition, raised levels of several of these cytokines in serum and urine correlate with progression of nephropathy, indicated by increased urinary albumin excretion (54). Each cytokines has several different effects. IL-1 alters the expression of chemotactic factors and adhesion molecules, alters intraglomerular hemodynamics (by affecting mesangial cell prostaglandin synthesis), might increase vascular endothelial cell permeability, and increases hyaluron production by renal tubular epithelial cells (which in turn could increase glomerular cellularity) (55). IL-6 has a strong association with the development of glomerular basement membrane thickening as well as possible relationships with increased endothelial permeability and mesangial cell proliferation. IL-18 induces the production of other inflammatory cytokines, such as IL-1, interferon γ and tumor necrosis factor, and might be associated with endothelial cell apoptosis. Tumor necrosis factor has the widest variety of biological activities and effects that contribute to development of diabetic nephropathy - too many to describe here. Importantly, though, it causes direct renal injury as a cytotoxin, as well as affecting apoptosis, glomerular hemodynamics, endothelial 45
7 permeability, and cell-cell adhesion. It also seems to play an important part in the early hypertrophy and hyperfunction of diabetic nephropathy (54, 56, 57) Lipid mediators Small lipids derived from arachidonic acid have been implicated in the pathogenesis of diabetic nephropathy. Cyclo-oxygenase 2 breaks down arachidonic acid into several different prostanoids. In a rat model of streptozotocin-induced diabetes, levels of inflammatory prostanoids, such as prostaglandins E 2 and I 2, were raised (58). Furthermore, increased expression of cyclooxygenase 2 has been reported in animal studies of diabetes and in the macula densa of kidneys from humans with diabetes (59). In diabetic rats, inhibition of cyclo-oxygenase 2 is associated with decreased glomerular hyperfiltration (60). A more detailed characterization of how the production of prostanoids affects the pathogenesis of diabetic nephropathy is needed. Arachidonic acid can also be oxidized by lipoxygenases (61). Evidence is accumulating that some of the products derived from the actions of lipoxygenases contribute to diabetic nephropathy. Specifically, levels of lipoxygenases 12 and 15 are increased in diabetic animals. In addition, high glucose levels increase expression of lipoxygenases 12 and 15 in cultured mesangial cells. To conclude, this pathway has a key mediatory role in the critical processes of mesangial cell hypertrophy and extracellular matrix accumulation mediated by TGF-β1 and angiotensin II (61) Oxidative stress Generally, metabolic activity within the nephron produces a large amount of reactive oxygen species that are counterbalanced by a large number of antioxidant enzymes and free radical scavenging systems. Reactive oxygen species mediate many negative biological effects, including peroxidation of cell membrane lipids, oxidation of proteins, renal vasoconstriction and damage to DNA. Unfortunately, hyperglycemia tips the balance towards production of reactive oxygen species, most of which seem to be generated in the mitochondria (62). The metabolism of glucose through harmful alternate pathways, such as via PKC activation and advanced glycation end-product formation, in the setting of hyperglycemia also seems partly dependent on reactive oxygen species (62-64). Hyperglycemia specifically induces oxidative stress, even before diabetes becomes clinically apparent. Concentrations of markers of DNA damage induced by reactive oxygen species are higher in patients with more-severe nephropathy (i.e. proteinuria versus microalbuminuria). Furthermore, histological analysis of human kidney biopsy specimens has detected products of glyco-oxidation (combined products of glycation and protein oxidation) and lipoxidation in the mesangial matrix and glomeruli, whereas these lesions are much less common in specimens from individuals without diabetes (64, 65). 46
8 6.12 Nephrin Podocytes (specialized visceral epithelial cells) are important for the maintenance of the dynamic functional barrier (66). Nephrin, a protein found in these cells, is crucial for maintaining the integrity of the intact filtration barrier. The renal expression of nephrin might be impaired in diabetic nephropathy.patients with diabetic nephropathy have markedly reduced renal nephrin expression and fewer electron-dense slit diaphragms compared with patients without diabetes and minimal nephropathic changes or controls (67). Furthermore, nephrin excretion is raised 17-30% in patients with diabetes (with and without albuminuria) compared with that in individuals without diabetes. Thus, nephrin excretion could be an early finding of podocyte injury, even before the onset of albuminuria (13, 14). Treatment with blockers of the reninangiotensin-aldosterone system might help protect nephrin expression. In a study of patients with type 2 diabetes, treatment with an angiotensin-converting-enzyme inhibitor for 2 years maintained nephrin expression at control levels compared with that in untreated patients with diabetes (23). By contrast, the expression of two other important podocyte and slit diaphragm proteins, podocin and CD2AP, was similar in the three groups. Comparable decreases in renal nephrin expression were reported in other studies of diabetic nephropathy (68, 69) Genetic susceptibility Genotype seems to be an important determinant of both incidence and severity of diabetic nephropathy (9, 31, 70). The increase in risk cannot be explained by the duration of diabetes or hypertension, or the degree of glycemic control. Environmental and genetic factors must, therefore, have roles in the pathogenesis of diabetic nephropathy. In patients with type 1 or type 2 diabetes, the likelihood of developing diabetic nephropathy is markedly increased in those who have a sibling or parent with diabetic nephropathy (71, 72). One study evaluated Pima Indian families in whom two successive generations had type 2 diabetes (72). The likelihood of the offspring developing overt proteinuria was 14% if neither parent had proteinuria, 23% if one parent had proteinuria and 46% if both parents had proteinuria. Advances in molecular genetics have led to the development of a system for genotyping single-nucleotide polymorphisms and have enabled exploration of loci involved in diabetic nephropathy in genome-wide association studies. In the search for susceptibility genes for microvascular complications of diabetes in Pima Indians, four loci on chromosomes 3, 7, 9 and 20 were identified (73). Additional loci are identified as diabetic nephropathy susceptibility genes areas on chromosomes 7q21.3, 10p15.3, 14q23.1 and 18q22.3 (74, 75). Association studies of candidate genes have been the most common approach to identify genes involved in susceptibility to diabetic nephropathy. The greatest risks seem to be associated with genes encoding angiotensinconverting enzyme, angiotensin II receptor, cytokines, proteins involved in glucose or lipid metabolism, and extracellular matrix proteins. The angiotensin-converting-enzyme gene (ACE) polymorphism has been explored in several studies. The insertion-deletion polymorphism is responsible for the difference 47
9 between individuals in plasma levels of angiotensin-converting enzyme. In patients with type 2 diabetes, the DD polymorphism of the ACE gene has been associated with an increased risk of developing diabetic nephropathy, severe proteinuria, progressive renal failure, and of mortality during dialysis (76-78). In addition, an analysis of more than 1,000 white patients with type 1 diabetes showed a strong correlation between genetic variation in the ACE gene and the development of nephropathy (79). Other studies have, however, produced conflicting data. A critical review of 19 studies that examined a possible link between this gene and diabetic nephropathy failed to confirm an association among white people with either type 1 or type 2 diabetes, although a possible association in Asians could not be excluded (78). Ongoing studies are taking a multigene approach, since the likelihood of diabetic nephropathy being a single-gene disease is low Conclusions While progression to diabetic nephropathy cannot yet be prevented, the pathogenesis is better characterized than a decade ago. The hemodynamic changes of glomerular hyperperfusion and hyperfiltration become evident before the earliest measurable clinical signs of nephropathy but do not predict the demise of kidney function. Various structural changes, including podocyte foot process effacement, decrease in podocyte number, thickening of the glomerular basement membrane and mesangial expansion, all occur with the early changes. These features, when assessed independently, cannot, however, predict disease progression. Hyperglycemia plays a central part in a cascade of damaging effects mediated by cytokines and growth factors that produces oxidative stress, abnormal glycosylation, lipid peroxidation, and the production of further inflammatory elements. With the anticipated completion of current studies that are evaluating the genetics of nephropathy in the next 2-4 years, understanding of how to integrate genetic and environmental susceptibility factors into risk assessment should be improved. This knowledge should give clinicians the ability to predict earlier who will develop nephropathy and, therefore, improve prevention of this devastating disease. Key points Microalbuminuria is not a predictor of nephropathy development in individuals with diabetes Multiple mechanisms are operative in diabetes that are related to injury to the kidney and, in susceptible individuals, contribute to nephropathy development Defects in nephrin and podocin are central to the development of macroalbuminuria and associated with nephropathy progression Abnormally high concentrations of lipids contribute to β-cell injury and development of albuminuria Recommended literature: 1. Held PJ, et al. The United States Renal Data System s 1991 annual data report: an introduction. Am J Kidney Dis 1991;18: Makino H, et al. Phenotypic modulation of the mesangium reflected by contractile proteins in diabetes. Diabetes 1996;45:
10 3. Mauer SM, et al. Structural-functional relationships in diabetic nephropathy. J Clin Invest 1984;74: Nielsen S, et al. The clinical course of renal function in NIDDM patients with normoand microalbuminuria. J Intern Med 1997;241: Raile K, et al. Diabetic nephropathy in 27,805 children, adolescents, and adults with type 1 diabetes: effect of diabetes duration, A1C, hypertension, dyslipidemia, diabetes onset, and sex. Diabetes Care 2007;30: Remuzzi G, et al. Clinical practice. Nephropathy in patients with type 2 diabetes. N Engl J Med 2002;346: Steinke JM, et al. The early natural history of nephropathy in type 1 diabetes: III. Predictors of 5-year urinary albumin excretion rate patterns in initially normoalbuminuric patients. Diabetes 2005;54: Ziyadeh FN Mediators of diabetic renal disease: the case for TGF-â as the major mediator. J Am Soc Nephrol 2004;5(Suppl 1):S55-S Ichinose K, et al. Recent advancement of understanding pathogenesis of type 1 diabetes and potential relevance to diabetic nephropathy. Am J Nephrol 2007;7: Raptis AE, Viberti G. Pathogenesis of diabetic nephropathy. Exp Clin Endocrinol Diabetes 2001;09(Suppl 2):S424-S Singh DK, et al. () Mechanisms of disease: the hypoxic tubular hypothesis of diabetic nephropathy. Nat Clin Pract Nephrol 2008;4: Ziyadeh FN, Wolf G. Pathogenesis of the podocytopathy and proteinuria in diabetic glomerulopathy. Curr Diabetes Rev 2008;4: Wolf G, Ziyadeh FN. Molecular mechanisms of diabetic renal hypertrophy. Kidney Int 1999;56: Wolf G, Ziyadeh FN. Cellular and molecular mechanisms of proteinuria in diabetic nephropathy. Nephron Physiol 2007;106: Hilgers KF, Veelken R. Type 2 diabetic nephropathy: never too early to treat? J Am Soc Nephrol 2005;16: Nagai Y, et al. Temporary angiotensin II blockade at the prediabetic stage attenuates the development of renal injury in type 2 diabetic rats. J Am Soc Nephrol 2005;16: Sharma K, et al. Captopril-induced reduction of serum levels of transforming growth factor-â1 correlates with long-term renoprotection in insulindependent diabetic patients. Am J Kidney Dis 1999;34: Harris RD, et al. Global glomerular sclerosis and glomerular arteriolar hyalinosis in insulin dependent diabetes. Kidney Int 1991;40: Heilig CW, et al. Overexpression of glucose transporters in rat mesangial cells cultured in a normal glucose milieu mimics the diabetic phenotype. J Clin Invest 1995;96: Mishra R, et al. High glucose evokes an intrinsic proapoptotic signaling pathway in mesangial cells. Kidney Int 2005;67: Lin CL, et al. Wnt/â-catenin signaling modulates survival of high glucose-stressed mesangial cells. J Am Soc Nephrol 2006;17: Chen ZJ, et al. Expression of VEGF in kidney of diabetic rats [Chinese]. Sichuan Da Xue Xue Bao Yi Xue Ban 2007;38: Wolf G, et al. From the periphery of the glomerular capillary wall toward the center of disease: podocyte injury comes of age in diabetic nephropathy. Diabetes 2005;54: Mauer SM, et al. The development of lesions in the glomerular basement membrane and mesangium after transplantation of normal kidneys to diabetic patients. Diabetes 1983;32: Friedman EA. Advanced glycation endproducts in diabetic nephropathy. Nephrol Dial Transplant 1999;14(Suppl 3):S1-S9. 49
11 26. Porte D Jr, Schwartz MW. Diabetes complications: why is glucose potentially toxic? Science 1996;272: Brownlee M. Biochemistry and molecular cell biology of diabetic complications. Nature 2001;414: Makita Z, et al. Advanced glycosylation end products in patients with diabetic nephropathy.n Engl J Med 1991;325: Singh AK, et al. Effect of glycated proteins on the matrix of glomerular epithelial cells. J Am Soc Nephrol 1998;9: Hogan M, et al. Advanced glycosylation endproducts block the antiproliferative effect of nitric oxide Role in the vascular and renal complications of diabetes mellitus. J Clin Invest 1992;90: Cooper ME. Pathogenesis prevention and treatment of diabetic nephropathy. Lancet 1998;352: Yamagishi S, et al. Molecular mechanisms of diabetic nephropathy and its therapeutic intervention. Curr Drug Targets 2007;8: Kunisaki M, et al. Normalization of diacylglycerol-protein kinase C activation by vitamin E in aorta of diabetic rats and cultured rat smooth muscle cells exposed to elevated glucose levels. Diabetes 1994;43: Haneda M, et al. Abnormalities in protein kinase C and MAP kinase cascade in mesangial cells cultured under high glucose conditions. J Diabetes Complications 1995;9: Tilton RG, et al. Prevention of hemodynamic and vascular albumin filtration changes in diabetic rats by aldose reductase inhibitors. Diabetes 1989;38: Wilson DM, Luetscher JA. Plasma prorenin activity and complications in children with insulindependent diabetes mellitus. N Engl J Med 1990;323: Daneman D, et al. Plasma prorenin as an early marker of nephropathy in diabetic (IDDM) adolescents. Kidney Int 1994;46: Nguyen G. Renin/prorenin receptors. Kidney Int 2006;69: Ichihara A, et al. Prorenin receptor blockade inhibits development of glomerulosclerosis in diabetic angiotensin II type 1a receptor-deficient mice. J Am Soc Nephrol 2006;17: Hohenstein B, et al. Local VEGF activity but not VEGF expression is tightly regulated during diabetic nephropathy in man. Kidney Int 2006;69: De Vriese AS, et al. Antibodies against vascular endothelial growth factor improve early renal dysfunction in experimental diabetes. J Am Soc Nephrol 2001;12: Sharma K, Ziyadeh FN. Hyperglycemia and diabetic kidney disease. The case for transforming growth factor-beta as a key mediator. Diabetes 1995;44: Kanesaki Y, et al. Vascular endothelial growth factor gene expression is correlated with glomerular neovascularization in human diabetic nephropathy. Am J Kidney Dis 2005;45: Satchell SC, et al. Angiopoietin 1 and vascular endothelial growth factor modulate human glomerular endothelial cell barrier properties. J Am Soc Nephrol 2004;15: Tsilibary EC. Microvascular basement membranes in diabetes mellitus. J Pathol 2003;200: Baelde HJ, et al. Reduction of VEGF-A and CTGF expression in diabetic nephropathy is associated with podocyte loss. Kidney Int 2007;71: Flyvbjerg A, et al. Amelioration of long-term renal changes in obese type 2 diabetic mice by a neutralizing vascular endothelial growth factor antibody. Diabetes 2002;51: Eremina V, et al. Vascular endothelial growth factor a signaling in the podocyteendothelial compartment is required for mesangial cell migration and survival. J Am Soc Nephrol 2006;17:
12 49. Bortoloso E, et al. Quantitave and qualitative changes in vascular endothelial growth factor gene expression in glomeruli of patients with type 2 diabetes. Eur J Endocrinol 2004;150: Janssen B, et al. Carnosine as a protective factor in diabetic nephropathy: association with a leucine repeat of the carnosinase gene CNDP1. Diabetes 2005;54: Isaka Y, et al. Application of gene therapy to diabetic nephropathy. Kidney Int Suppl 1997;60:S100-S Benigni A, et al. Add-on anti-tgf-beta antibody to ACE inhibitor arrests progressive diabetic nephropathy in the rat. J Am Soc Nephrol 2003;14: Dai C, et al. Intravenous administration of hepatocyte growth factor gene ameliorates diabetic nephropathy in mice. J Am Soc Nephrol 2004;15: Navarro-Gonzalez JF, Mora-Fernandez C.The role of inflammatory cytokines in diabetic nephropathy. J Am Soc Nephrol 2008;19: Jones S, et al. Regulation of renal proximal tubular epithelial cell hyaluronan generation: implications for diabetic nephropathy. Kidney Int 2001;59: DiPetrillo K, et al. Urinary tumor necrosis factor contributes to sodium retention and renal hypertrophy during diabetes. Am J Physiol Renal Physiol 2003;284:F113-F DiPetrillo K, Gesek FA Pentoxifylline ameliorates renal tumor necrosis factor expression, sodium retention, and renal hypertrophy in diabetic rats. Am J Nephrol 2004;24: Imig JD. Eicosanoids and renal vascular function in diseases. Clin Sci (Lond) 2006;111: Pope JE, et al. A meta-analysis of the effects of nonsteroidal anti-inflammatory drugs on blood pressure. Arch Intern Med 1993;153: Hao CM, Breyer MD. Physiologic and pathophysiologic roles of lipid mediators in the kidney. Kidney Int 2007;71: Hao CM, Breyer MD. Roles of lipid mediators in kidney injury. Semin Nephrol 2007;27: Nishikawa T, et al. Impact of mitochondrial ROS production on diabetic vascular complications. Diabetes Res Clin Pract 2007;77(Suppl 1):S41-S Kiritoshi S, et al. Reactive oxygen species from mitochondria induce cyclooxygenase-2 gene expression in human mesangial cells potential role in diabetic nephropathy. Diabetes 2003;52: Vasavada N and Agarwal R () Role of oxidative stress in diabetic nephropathy. Adv Chronic Kidney Dis 2005;12: Suzuki D, et al. Immunohistochemical evidence for an increased oxidative stress and carbonyl modification of proteins in diabetic glomerular lesions. J Am Soc Nephrol 10: Mundel P, Shankland SJ. Podocyte biology and response to injury. J Am Soc Nephrol 2002;13: Benigni A, et al. Selective impairment of gene expression and assembly of nephrin in human diabetic nephropathy. Kidney Int 2004;65: Langham RG, et al. Proteinuria and the expression of the podocyte slit diaphragm protein, nephrin, in diabetic nephropathy: effects of angiotensin converting enzyme inhibition. Diabetologia 2002;45: Doublier S, et al. Nephrin expression is reduced in human diabetic nephropathy: evidence for a distinct role for glycated albumin and angiotensin II. Diabetes 2003;52: Adler S. Diabetic nephropathy: Linking histology, cell biology, and genetics. Kidney Int 2004;66: Trevisan R, Viberti G. Genetic factors in the development of diabetic nephropathy. J Lab Clin Med 1995;126: Pettitt DJ, et al. Familial predisposition to renal disease in two generations of Pima Indians with type 2 (non-insulin-dependent) diabetes mellitus. Diabetologia 1990;33:
13 73. Imperatore G, et al. Sib-pair linkage analysis for susceptibility genes for microvascular complications among Pima Indians with type 2 diabetes. Pima Diabetes Genes Group. Diabetes 1998;47: Vardarli I, et al. Gene for susceptibility to diabetic nephropathy in type 2 diabetes maps to 18q Kidney Int 2002;62: Iyengar SK, et al. Genome-wide scans for diabetic nephropathy and albuminuria in multiethnic populations: the family investigation of nephropathy and diabetes (FIND). Diabetes 2007;56: Movva S, et al. Relationship of angiotensinconverting enzyme gene polymorphism with nephropathy associated with type 2 diabetes mellitus in Asian Indians. J Diabetes Complications 2007;21: Jeffers BW, et al. Angiotensin-converting enzyme gene polymorphism in non-insulin dependent diabetes mellitus and its relationship with diabetic nephropathy. Kidney Int 1997;52: Kunz R, et al. Association between the angiotensin-converting enzymeinsertion/deletion polymorphism and diabetic nephropathy: a methodologic appraisal and systematic review. J Am Soc Nephrol 1998;9: Boright AP, et al. Genetic variation at the ACE gene is associated with persistent microalbuminuria and severe nephropathy in type 1 diabetes: the DCCT/ EDIC Genetics Study. Diabetes 2005;54:
Risk Factors for Diabetic Nephropathy
 Risk Factors for Diabetic Nephropathy Amalkumar Bhattacharya Associate Professor in Medicine, Government Medical College, Surat - 395 001. 55 EPIDEMILGY AND DIABETES TYPE Diabetic nephropathy can occur
Risk Factors for Diabetic Nephropathy Amalkumar Bhattacharya Associate Professor in Medicine, Government Medical College, Surat - 395 001. 55 EPIDEMILGY AND DIABETES TYPE Diabetic nephropathy can occur
Diabetic Nephropathy
 Diabetic Nephropathy Objectives: Know what Diabetic Nephropathy means. Know how common is Diabetic nephropathy in Saudi Arabia and to appreciate how bad are this complications. Know the risk factors of
Diabetic Nephropathy Objectives: Know what Diabetic Nephropathy means. Know how common is Diabetic nephropathy in Saudi Arabia and to appreciate how bad are this complications. Know the risk factors of
renoprotection therapy goals 208, 209
 Subject Index Aldosterone, plasminogen activator inhibitor-1 induction 163, 164, 168 Aminopeptidases angiotensin II processing 64 66, 214 diabetic expression 214, 215 Angiotensin I intrarenal compartmentalization
Subject Index Aldosterone, plasminogen activator inhibitor-1 induction 163, 164, 168 Aminopeptidases angiotensin II processing 64 66, 214 diabetic expression 214, 215 Angiotensin I intrarenal compartmentalization
Lecture 19 Summary Gestational Diabetes and Complications of Diabetes. Gestational diabetes;
 Lecture 19 Summary Gestational Diabetes and Complications of Diabetes Gestational diabetes; - Type of diabetes that only develops during pregnancy Usually diagnosed in late pregnancy Causes high blood
Lecture 19 Summary Gestational Diabetes and Complications of Diabetes Gestational diabetes; - Type of diabetes that only develops during pregnancy Usually diagnosed in late pregnancy Causes high blood
Diabetic Nephropathy 2009
 Diabetic Nephropathy 2009 Michael T McDermott MD Director, Endocrinology and Diabetes Practice University of Colorado Hospital Michael.mcdermott@ucdenver.edu Diabetic Nephropathy Clinical Stages Hyperfunction
Diabetic Nephropathy 2009 Michael T McDermott MD Director, Endocrinology and Diabetes Practice University of Colorado Hospital Michael.mcdermott@ucdenver.edu Diabetic Nephropathy Clinical Stages Hyperfunction
Podocyte Biology and clinical applications Dr. F. Ahmadi Professor Of Nephrology TUMS
 Podocyte Biology and clinical applications Dr. F. Ahmadi Professor Of Nephrology TUMS Proteinuria is a major healthcare problem that affects several hundred million people worldwide. Proteinuria is a cardinal
Podocyte Biology and clinical applications Dr. F. Ahmadi Professor Of Nephrology TUMS Proteinuria is a major healthcare problem that affects several hundred million people worldwide. Proteinuria is a cardinal
DIABETIC NEPHROPATHY- PATHOGENESIS AND NEWER TARGETS IN TREATMENT
 Review Article DIABETIC NEPHROPATHY- PATHOGENESIS AND NEWER TARGETS IN TREATMENT Hemanth Kumar. N, Prashanth. S*, Vidya Sagar J Vaagdevi College of Pharmacy, Ramnagar, Warangal, Andhra Pradesh, INDIA.
Review Article DIABETIC NEPHROPATHY- PATHOGENESIS AND NEWER TARGETS IN TREATMENT Hemanth Kumar. N, Prashanth. S*, Vidya Sagar J Vaagdevi College of Pharmacy, Ramnagar, Warangal, Andhra Pradesh, INDIA.
Pathogenesis of diabetic nephropathy
 MINI REVIEW Zemin Cao, Mark E Cooper* ABSTRACT As the increasing prevalence of diabetes reaches epidemic proportions worldwide, diabetic nephropathy and associated end-stage renal failure will be an unavoidable
MINI REVIEW Zemin Cao, Mark E Cooper* ABSTRACT As the increasing prevalence of diabetes reaches epidemic proportions worldwide, diabetic nephropathy and associated end-stage renal failure will be an unavoidable
REVIEW ARTICLE NEWER BIOMARKERS IN EARLY DIABETIC NEPHROPATHY
 JCD REVIEW ARTICLE NEWER BIOMARKERS IN EARLY DIABETIC NEPHROPATHY SAPTARSHI MUKHOPADHYAY* *FACULTY (DEPARTMENT OF MEDICINE), B R SINGH HOSPITAL (EASTERN RAILWAY), KOLKATA. INTRODUCTION renal disease. It
JCD REVIEW ARTICLE NEWER BIOMARKERS IN EARLY DIABETIC NEPHROPATHY SAPTARSHI MUKHOPADHYAY* *FACULTY (DEPARTMENT OF MEDICINE), B R SINGH HOSPITAL (EASTERN RAILWAY), KOLKATA. INTRODUCTION renal disease. It
Ahamed and Banji, IJPSR, 2012; Vol. 3(2): ISSN:
 IJPSR (2012), Vol. 3, Issue 02 (Review Article) Received on 24 September, 2011; received in revised form 09 January, 2012; accepted 29 January, 2012 A REVIEW ON DIABETIC NEUROPATHY AND NEPHROPATHY Mohd.
IJPSR (2012), Vol. 3, Issue 02 (Review Article) Received on 24 September, 2011; received in revised form 09 January, 2012; accepted 29 January, 2012 A REVIEW ON DIABETIC NEUROPATHY AND NEPHROPATHY Mohd.
ROLE OF ANGIOTENSIN CONVERTING ENZYME INHIBITORS AND ANGIOTENSIN RECEPTOR BLOCKERS IN TYPE I DIABETIC NEPHROPATHY DR.NASIM MUSA
 ROLE OF ANGIOTENSIN CONVERTING ENZYME INHIBITORS AND ANGIOTENSIN RECEPTOR BLOCKERS IN TYPE I DIABETIC NEPHROPATHY DR.NASIM MUSA Type I IDDM is characterized by The abrupt onset of symptoms Insulinopenia
ROLE OF ANGIOTENSIN CONVERTING ENZYME INHIBITORS AND ANGIOTENSIN RECEPTOR BLOCKERS IN TYPE I DIABETIC NEPHROPATHY DR.NASIM MUSA Type I IDDM is characterized by The abrupt onset of symptoms Insulinopenia
Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009
 www.ivis.org Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009 São Paulo, Brazil - 2009 Next WSAVA Congress : Reprinted in IVIS with the permission of the Congress Organizers PROTEINURIA
www.ivis.org Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009 São Paulo, Brazil - 2009 Next WSAVA Congress : Reprinted in IVIS with the permission of the Congress Organizers PROTEINURIA
CLINICIAN INTERVIEW A REVIEW OF THE CURRENT TREATMENT MODALITIES FOR DIABETIC NEPHROPATHY. Interview with Ralph Rabkin, MD
 A REVIEW OF THE CURRENT TREATMENT MODALITIES FOR DIABETIC NEPHROPATHY Interview with Ralph Rabkin, MD Dr Rabkin is Professor of Medicine, Emeritus, Active, at Stanford University School of Medicine, Stanford,
A REVIEW OF THE CURRENT TREATMENT MODALITIES FOR DIABETIC NEPHROPATHY Interview with Ralph Rabkin, MD Dr Rabkin is Professor of Medicine, Emeritus, Active, at Stanford University School of Medicine, Stanford,
Diabetic Nephropathy. Introduction/Clinical Setting. Pathologic Findings Light Microscopy. J. Charles Jennette
 12 Diabetic Nephropathy J. Charles Jennette Introduction/Clinical Setting Diabetic nephropathy is a clinical syndrome in a patient with diabetes mellitus that is characterized by persistent albuminuria,
12 Diabetic Nephropathy J. Charles Jennette Introduction/Clinical Setting Diabetic nephropathy is a clinical syndrome in a patient with diabetes mellitus that is characterized by persistent albuminuria,
Diabetic Nephropathy in Spontaneously Diabetic Torii (SDT) Rats
 The Open Diabetes Journal, 2011, 4, 45-49 45 Diabetic Nephropathy in Spontaneously Diabetic Torii (SDT) Rats Takeshi Ohta * and Tomohiko Sasase Open Access Biological/Pharmacological Research Laboratories,
The Open Diabetes Journal, 2011, 4, 45-49 45 Diabetic Nephropathy in Spontaneously Diabetic Torii (SDT) Rats Takeshi Ohta * and Tomohiko Sasase Open Access Biological/Pharmacological Research Laboratories,
The retinal renin-angiotensin system: implications for therapy in diabetic retinopathy
 (2002) 16, S42 S46 2002 Nature Publishing Group All rights reserved 0950-9240/02 $25.00 www.nature.com/jhh : implications for therapy in diabetic retinopathy AK Sjølie 1 and N Chaturvedi 2 1 Department
(2002) 16, S42 S46 2002 Nature Publishing Group All rights reserved 0950-9240/02 $25.00 www.nature.com/jhh : implications for therapy in diabetic retinopathy AK Sjølie 1 and N Chaturvedi 2 1 Department
RENAL HISTOPATHOLOGY
 RENAL HISTOPATHOLOGY Peter McCue, M.D. Department of Pathology, Anatomy & Cell Biology Sidney Kimmel Medical College There are no conflicts of interest. 1 Goals and Objectives! Goals Provide introduction
RENAL HISTOPATHOLOGY Peter McCue, M.D. Department of Pathology, Anatomy & Cell Biology Sidney Kimmel Medical College There are no conflicts of interest. 1 Goals and Objectives! Goals Provide introduction
Effects of beraprost sodium on renal function and inflammatory factors of rats with diabetic nephropathy
 Effects of beraprost sodium on renal function and inflammatory factors of rats with diabetic nephropathy J. Guan 1,2, L. Long 1, Y.-Q. Chen 1, Y. Yin 1, L. Li 1, C.-X. Zhang 1, L. Deng 1 and L.-H. Tian
Effects of beraprost sodium on renal function and inflammatory factors of rats with diabetic nephropathy J. Guan 1,2, L. Long 1, Y.-Q. Chen 1, Y. Yin 1, L. Li 1, C.-X. Zhang 1, L. Deng 1 and L.-H. Tian
Ο ρόλος των τριγλυκεριδίων στην παθογένεια των μικροαγγειοπαθητικών επιπλοκών του σακχαρώδη διαβήτη
 Ο ρόλος των τριγλυκεριδίων στην παθογένεια των μικροαγγειοπαθητικών επιπλοκών του σακχαρώδη διαβήτη Κωνσταντίνος Τζιόμαλος Επίκουρος Καθηγητής Παθολογίας Α Προπαιδευτική Παθολογική Κλινική, Νοσοκομείο
Ο ρόλος των τριγλυκεριδίων στην παθογένεια των μικροαγγειοπαθητικών επιπλοκών του σακχαρώδη διαβήτη Κωνσταντίνος Τζιόμαλος Επίκουρος Καθηγητής Παθολογίας Α Προπαιδευτική Παθολογική Κλινική, Νοσοκομείο
3. PODOCYTE INJURY IN GLOMERULAR DISEASES
 How to Cite this article: Podocyte Injury in Glomerular Diseases - ejifcc 20/01 2009 http://www.ifcc.org 3. PODOCYTE INJURY IN GLOMERULAR DISEASES Mirjana Sabljar Matovinović Podocytes are injured in diabetic
How to Cite this article: Podocyte Injury in Glomerular Diseases - ejifcc 20/01 2009 http://www.ifcc.org 3. PODOCYTE INJURY IN GLOMERULAR DISEASES Mirjana Sabljar Matovinović Podocytes are injured in diabetic
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
SLOWING PROGRESSION OF KIDNEY DISEASE. Mark Rosenberg MD University of Minnesota
 SLOWING PROGRESSION OF KIDNEY DISEASE Mark Rosenberg MD University of Minnesota OUTLINE 1. Epidemiology of progression 2. Therapy to slow progression a. Blood Pressure control b. Renin-angiotensin-aldosterone
SLOWING PROGRESSION OF KIDNEY DISEASE Mark Rosenberg MD University of Minnesota OUTLINE 1. Epidemiology of progression 2. Therapy to slow progression a. Blood Pressure control b. Renin-angiotensin-aldosterone
Index. Note: Page numbers of article titles are in boldface type.
 Heart Failure Clin 2 (2006) 101 105 Index Note: Page numbers of article titles are in boldface type. A ACE inhibitors, in diabetic hypertension, 30 31 Adipokines, cardiovascular events related to, 6 Advanced
Heart Failure Clin 2 (2006) 101 105 Index Note: Page numbers of article titles are in boldface type. A ACE inhibitors, in diabetic hypertension, 30 31 Adipokines, cardiovascular events related to, 6 Advanced
Glomerular filtration rate (GFR)
 LECTURE NO (2) Renal Physiology Glomerular filtration rate (GFR) Faculty Of Medicine Dept.Of Physiology The glomerulus Is a tuft of capillaries enclosed within a Bowman capsule. It is supplied by an afferent
LECTURE NO (2) Renal Physiology Glomerular filtration rate (GFR) Faculty Of Medicine Dept.Of Physiology The glomerulus Is a tuft of capillaries enclosed within a Bowman capsule. It is supplied by an afferent
Dr. Hayam Gad Associate Professor of Physiology College of Medicine King Saud University
 Dr. Hayam Gad Associate Professor of Physiology College of Medicine King Saud University INTRODUCTION Diabetic nephropathy (DN) DN is defined as the appearance of persistent clinical albuminuria in an
Dr. Hayam Gad Associate Professor of Physiology College of Medicine King Saud University INTRODUCTION Diabetic nephropathy (DN) DN is defined as the appearance of persistent clinical albuminuria in an
Kidney disease in people with diabetes. Ian Gallen
 Kidney disease in people with diabetes Ian Gallen Why is it important Major cause of early death in DM Major cause of amputation RRT is arduous for the patient and expensive Nephropathy is largely avoidable
Kidney disease in people with diabetes Ian Gallen Why is it important Major cause of early death in DM Major cause of amputation RRT is arduous for the patient and expensive Nephropathy is largely avoidable
Managing patients with renal disease
 Managing patients with renal disease Hiddo Lambers Heerspink, MD University Medical Centre Groningen, The Netherlands Asian Cardio Diabetes Forum April 23 24, 216 Kuala Lumpur, Malaysia Prevalent cases,
Managing patients with renal disease Hiddo Lambers Heerspink, MD University Medical Centre Groningen, The Netherlands Asian Cardio Diabetes Forum April 23 24, 216 Kuala Lumpur, Malaysia Prevalent cases,
Ανάπτυξη Βιοτράπεζας για την Ανίχνευση Πρώιμων Βιοδεικτών σε Ασθενείς με Χρόνια Νεφρική Νόσο
 Ανάπτυξη Βιοτράπεζας για την Ανίχνευση Πρώιμων Βιοδεικτών σε Ασθενείς με Χρόνια Νεφρική Νόσο ΔΗΜΗΤΡΙΟΣ Σ. ΓΟΥΜΕΝΟΣ Νεφρολογικό και Μεταμοσχευτικό Κέντρο Πανεπιστημιακό Νοσοκομείο Πατρών Causes of chronic
Ανάπτυξη Βιοτράπεζας για την Ανίχνευση Πρώιμων Βιοδεικτών σε Ασθενείς με Χρόνια Νεφρική Νόσο ΔΗΜΗΤΡΙΟΣ Σ. ΓΟΥΜΕΝΟΣ Νεφρολογικό και Μεταμοσχευτικό Κέντρο Πανεπιστημιακό Νοσοκομείο Πατρών Causes of chronic
For more information about how to cite these materials visit
 Author(s): Frank Brosius, M.D, 2011 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Author(s): Frank Brosius, M.D, 2011 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Collin County Community College RENAL PHYSIOLOGY
 Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 RENAL PHYSIOLOGY Glomerular Filtration Filtration process that occurs in Bowman s Capsule Blood is filtered and
Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 RENAL PHYSIOLOGY Glomerular Filtration Filtration process that occurs in Bowman s Capsule Blood is filtered and
The Ebf1 knockout mouse and glomerular maturation
 Repository of the Max Delbrück Center for Molecular Medicine (MDC) Berlin (Germany) http://edoc.mdc-berlin.de/14009/ The Ebf1 knockout mouse and glomerular maturation Schmidt-Ott, K.M. Published in final
Repository of the Max Delbrück Center for Molecular Medicine (MDC) Berlin (Germany) http://edoc.mdc-berlin.de/14009/ The Ebf1 knockout mouse and glomerular maturation Schmidt-Ott, K.M. Published in final
Chapter 1 RENAL HAEMODYNAMICS AND GLOMERULAR FILTRATION
 3 Chapter 1 RENAL HAEMODYNAMICS AND GLOMERULAR FILTRATION David Shirley, Giovambattista Capasso and Robert Unwin The kidney has three homeostatic functions that can broadly be described as excretory, regulatory
3 Chapter 1 RENAL HAEMODYNAMICS AND GLOMERULAR FILTRATION David Shirley, Giovambattista Capasso and Robert Unwin The kidney has three homeostatic functions that can broadly be described as excretory, regulatory
Obesity mediated hypertension and renal dysfunction
 Obesity mediated hypertension and renal dysfunction Gergely Bodor Marion Hervouet Nicky Honnef Mariarosaria Malgadi Julie Robert Tutor: Pr Alina Parvu Objectives 1. Introduction 2. Renal structural and
Obesity mediated hypertension and renal dysfunction Gergely Bodor Marion Hervouet Nicky Honnef Mariarosaria Malgadi Julie Robert Tutor: Pr Alina Parvu Objectives 1. Introduction 2. Renal structural and
RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM
 RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM RENAL PHYSIOLOGY - ANATOMY Glomerulus + renal tubule Each kidney has 1.3 million nephrons Cortical nephrons (85%) have shorter Loop of Henle than Juxtamedullary nephrons
RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM RENAL PHYSIOLOGY - ANATOMY Glomerulus + renal tubule Each kidney has 1.3 million nephrons Cortical nephrons (85%) have shorter Loop of Henle than Juxtamedullary nephrons
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
The interest in microalbuminuria originated. Cardiovascular Implications of Albuminuria. R e v i e w P a p e r.
 R e v i e w P a p e r Cardiovascular Implications of Albuminuria Katherine R. Tuttle, MD Microalbuminuria is a major independent risk factor for cardiovascular disease (CVD) events in persons with diabetes
R e v i e w P a p e r Cardiovascular Implications of Albuminuria Katherine R. Tuttle, MD Microalbuminuria is a major independent risk factor for cardiovascular disease (CVD) events in persons with diabetes
Running head: NEPHRON 1. The nephron the functional unit of the kidney. [Student Name] [Name of Institute] Author Note
![Running head: NEPHRON 1. The nephron the functional unit of the kidney. [Student Name] [Name of Institute] Author Note Running head: NEPHRON 1. The nephron the functional unit of the kidney. [Student Name] [Name of Institute] Author Note](/thumbs/77/75431210.jpg) Running head: NEPHRON 1 The nephron the functional unit of the kidney [Student Name] [Name of Institute] Author Note NEPHRON 2 The nephron the functional unit of the kidney The kidney is an important excretory
Running head: NEPHRON 1 The nephron the functional unit of the kidney [Student Name] [Name of Institute] Author Note NEPHRON 2 The nephron the functional unit of the kidney The kidney is an important excretory
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,350 108,000 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,350 108,000 1.7 M Open access books available International authors and editors Downloads Our
Prof. Andrzej Wiecek Department of Nephrology, Endocrinology and Metabolic Diseases Medical University of Silesia Katowice, Poland.
 What could be the role of renal denervation in chronic kidney disease? Andrzej Wiecek, Katowice, Poland Chairs: Peter J. Blankestijn, Utrecht, The Netherlands Jonathan Moss, Glasgow, UK Prof. Andrzej Wiecek
What could be the role of renal denervation in chronic kidney disease? Andrzej Wiecek, Katowice, Poland Chairs: Peter J. Blankestijn, Utrecht, The Netherlands Jonathan Moss, Glasgow, UK Prof. Andrzej Wiecek
ORIGINAL ARTICLE Urinary type IV collagen levels in diabetes mellitus
 Malaysian J Pathol 21; 32(1) : 43 47 ORIGINAL ARTICLE Urinary type IV collagen levels in diabetes mellitus Pavai STHANESHWAR MBBS, MD and *Siew-Pheng CHAN MBBS, FRCP Departments of Pathology and *Medicine,
Malaysian J Pathol 21; 32(1) : 43 47 ORIGINAL ARTICLE Urinary type IV collagen levels in diabetes mellitus Pavai STHANESHWAR MBBS, MD and *Siew-Pheng CHAN MBBS, FRCP Departments of Pathology and *Medicine,
Reversal of Microalbuminuria A Causative Factor of Diabetic Nephropathy is Achieved with ACE Inhibitors than Strict Glycemic Control
 ISSN 0976 3333 Available Online at www.ijpba.info International Journal of Pharmaceutical & Biological Archives 2013; 4(5): 923-928 ORIGINAL RESEARCH ARTICLE Reversal of Microalbuminuria A Causative Factor
ISSN 0976 3333 Available Online at www.ijpba.info International Journal of Pharmaceutical & Biological Archives 2013; 4(5): 923-928 ORIGINAL RESEARCH ARTICLE Reversal of Microalbuminuria A Causative Factor
Cardiovascular Protection and the RAS
 Cardiovascular Protection and the RAS Katalin Kauser, MD, PhD, DSc Senior Associate Director, Boehringer Ingelheim Pharmaceutical Inc. Micardis Product Pipeline Scientific Support Ridgefield, CT, USA Cardiovascular
Cardiovascular Protection and the RAS Katalin Kauser, MD, PhD, DSc Senior Associate Director, Boehringer Ingelheim Pharmaceutical Inc. Micardis Product Pipeline Scientific Support Ridgefield, CT, USA Cardiovascular
Peggy Roestenberg - The role of CTGF in diabetic nephropathy. Chapter 1. General introduction and outline of the thesis
 Chapter 1 General introduction and outline of the thesis Chapter 1 Peggy Roestenberg - The role of CTGF in diabetic nephropathy DIABETES MELLITUS The number of patients with diabetes mellitus (DM) is rapidly
Chapter 1 General introduction and outline of the thesis Chapter 1 Peggy Roestenberg - The role of CTGF in diabetic nephropathy DIABETES MELLITUS The number of patients with diabetes mellitus (DM) is rapidly
Factors Influencing the Risk of Diabetic Nephropathy
 Factors Influencing the Risk of Diabetic Nephropathy - Analyses of Genes, Smoking and Diet Anna Möllsten Department of Clinical Sciences, Paediatrics Umeå University, Sweden 2006 UMEÅ UNIVERSITY MEDICAL
Factors Influencing the Risk of Diabetic Nephropathy - Analyses of Genes, Smoking and Diet Anna Möllsten Department of Clinical Sciences, Paediatrics Umeå University, Sweden 2006 UMEÅ UNIVERSITY MEDICAL
Renal Physiology - Lectures
 Renal Physiology 2011 Lisa M. Harrison-Bernard, PhD lharris@lsuhsc.edu Renal Physiology - Lectures Physiology of Body Fluids 2. Structure & Function of the Kidneys 3. Renal Clearance & Glomerular Filtration
Renal Physiology 2011 Lisa M. Harrison-Bernard, PhD lharris@lsuhsc.edu Renal Physiology - Lectures Physiology of Body Fluids 2. Structure & Function of the Kidneys 3. Renal Clearance & Glomerular Filtration
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Physiopathologie de la Néphropathie Diabétique
 Physiopathologie de la Néphropathie Diabétique Philippe Rieu Service de Néphrologie et de Transplantation UMR CNRS 6198 Reims Development of diabetic nephropathy 160 14 12 GFR (ml/min) 120 80 40 I II III
Physiopathologie de la Néphropathie Diabétique Philippe Rieu Service de Néphrologie et de Transplantation UMR CNRS 6198 Reims Development of diabetic nephropathy 160 14 12 GFR (ml/min) 120 80 40 I II III
Metabolic syndrome, obesity, diabetes, and theier implications
 Metabolic syndrome, obesity, diabetes, and theier implications jan.krtil@lf1.cuni.cz Institute of Medical Biochemistry and Laboratory Diagnostics &1 st Department of Medicine Diabetes mellitus type 2 (T2DM)
Metabolic syndrome, obesity, diabetes, and theier implications jan.krtil@lf1.cuni.cz Institute of Medical Biochemistry and Laboratory Diagnostics &1 st Department of Medicine Diabetes mellitus type 2 (T2DM)
Week 3, Lecture 5a. Pathophysiology of Diabetes. Simin Liu, MD, ScD
 Week 3, Lecture 5a Pathophysiology of Diabetes Simin Liu, MD, ScD General Model of Peptide Hormone Action Hormone Plasma Membrane Activated Nucleus Cellular Trafficking Enzymes Inhibited Receptor Effector
Week 3, Lecture 5a Pathophysiology of Diabetes Simin Liu, MD, ScD General Model of Peptide Hormone Action Hormone Plasma Membrane Activated Nucleus Cellular Trafficking Enzymes Inhibited Receptor Effector
Prevention And Treatment of Diabetic Nephropathy. MOH Clinical Practice Guidelines 3/2006 Dr Stephen Chew Tec Huan
 Prevention And Treatment of Diabetic Nephropathy MOH Clinical Practice Guidelines 3/2006 Dr Stephen Chew Tec Huan Prevention Tight glucose control reduces the development of diabetic nephropathy Progression
Prevention And Treatment of Diabetic Nephropathy MOH Clinical Practice Guidelines 3/2006 Dr Stephen Chew Tec Huan Prevention Tight glucose control reduces the development of diabetic nephropathy Progression
Renal physiology D.HAMMOUDI.MD
 Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Obesity and Chronic Kidney. The Catholic University of Korea Cheol Whee Park, M.D.
 Obesity and Chronic Kidney Disease The Catholic University of Korea Cheol Whee Park, M.D. Epidemic Obesity and type 2 Diabetes in Asia Yoon KH, et al. Lancet 368:1681-1688, 2006 [1 단계 ] 지방세포가커진다 [2 단계
Obesity and Chronic Kidney Disease The Catholic University of Korea Cheol Whee Park, M.D. Epidemic Obesity and type 2 Diabetes in Asia Yoon KH, et al. Lancet 368:1681-1688, 2006 [1 단계 ] 지방세포가커진다 [2 단계
FAMILIAL FACTORS AND DIABETIC NEPHROPATHY IN TYPE 1 DIABETES
 Department of Medicine Division of Nephrology University of Helsinki Finland FAMILIAL FACTORS AND DIABETIC NEPHROPATHY IN TYPE 1 DIABETES Johan Fagerudd ACADEMIC DISSERTATION To be presented for public
Department of Medicine Division of Nephrology University of Helsinki Finland FAMILIAL FACTORS AND DIABETIC NEPHROPATHY IN TYPE 1 DIABETES Johan Fagerudd ACADEMIC DISSERTATION To be presented for public
Glomerular pathology in systemic disease
 Glomerular pathology in systemic disease Lecture outline Lupus nephritis Diabetic nephropathy Glomerulonephritis Associated with Bacterial Endocarditis and Other Systemic Infections Henoch-Schonlein Purpura
Glomerular pathology in systemic disease Lecture outline Lupus nephritis Diabetic nephropathy Glomerulonephritis Associated with Bacterial Endocarditis and Other Systemic Infections Henoch-Schonlein Purpura
Diabetic Kidney Disease Tripti Singh MD Department of Nephrology University of Wisconsin
 Diabetic Kidney Disease Tripti Singh MD Department of Nephrology University of Wisconsin Disclosures I have no financial relationship with the manufacturers of any commercial product discussed during this
Diabetic Kidney Disease Tripti Singh MD Department of Nephrology University of Wisconsin Disclosures I have no financial relationship with the manufacturers of any commercial product discussed during this
Urinary bladder provides a temporary storage reservoir for urine
 Urinary System Organs Kidney Filters blood, allowing toxins, metabolic wastes, and excess ions to leave the body in urine Urinary bladder provides a temporary storage reservoir for urine Paired ureters
Urinary System Organs Kidney Filters blood, allowing toxins, metabolic wastes, and excess ions to leave the body in urine Urinary bladder provides a temporary storage reservoir for urine Paired ureters
SGLT2 inhibition in diabetes: extending from glycaemic control to renal and cardiovascular protection
 SGLT2 inhibition in diabetes: extending from glycaemic control to renal and cardiovascular protection Hiddo Lambers Heerspink Department of Clinical Pharmacy and Pharmacology University Medical Center
SGLT2 inhibition in diabetes: extending from glycaemic control to renal and cardiovascular protection Hiddo Lambers Heerspink Department of Clinical Pharmacy and Pharmacology University Medical Center
Overview of glomerular diseases
 Overview of glomerular diseases *Endothelial cells are fenestrated each fenestra: 70-100nm in diameter Contractile, capable of proliferation, makes ECM & releases mediators *Glomerular basement membrane
Overview of glomerular diseases *Endothelial cells are fenestrated each fenestra: 70-100nm in diameter Contractile, capable of proliferation, makes ECM & releases mediators *Glomerular basement membrane
BY BERNARD ZINMAN, MD
 Understanding the Relationship Between Hyperglycemia and Microvascular Complications Jointly sponsored by The Dulaney Foundation and DIABETIC MICROVASCULAR COMPLICATIONS TODAY. Release Date: August 2006.
Understanding the Relationship Between Hyperglycemia and Microvascular Complications Jointly sponsored by The Dulaney Foundation and DIABETIC MICROVASCULAR COMPLICATIONS TODAY. Release Date: August 2006.
Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance
 Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance Matthew R. Weir, MD Professor and Director Division of Nephrology University of Maryland School of Medicine Overview Introduction Mechanisms
Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance Matthew R. Weir, MD Professor and Director Division of Nephrology University of Maryland School of Medicine Overview Introduction Mechanisms
CHARLES UNIVERSITY IN PRAGUE THIRD FACULTY OF MEDICINE PHD THESIS MARIANNA ROMŽOVÁ
 CHARLES UNIVERSITY IN PRAGUE THIRD FACULTY OF MEDICINE PHD THESIS MARIANNA ROMŽOVÁ PRAGUE, 2007 THIRD FACULTY OF MEDICINE CHARLES UNIVERSITY IN PRAGUE Division of Cell and Molecular Biology Institute of
CHARLES UNIVERSITY IN PRAGUE THIRD FACULTY OF MEDICINE PHD THESIS MARIANNA ROMŽOVÁ PRAGUE, 2007 THIRD FACULTY OF MEDICINE CHARLES UNIVERSITY IN PRAGUE Division of Cell and Molecular Biology Institute of
ARGININE VASOPRESSIN (AVP)
 ARGININE VASOPRESSIN (AVP) AFFECTS BLOOD PRESSURE AND RENAL WATER REABSORPTION WHAT ELSE DOES IT DO? Michael F. Michelis, M.D., F.A.C.P., F.A.S.N. Director, Division of Nephrology Lenox Hill Hospital,
ARGININE VASOPRESSIN (AVP) AFFECTS BLOOD PRESSURE AND RENAL WATER REABSORPTION WHAT ELSE DOES IT DO? Michael F. Michelis, M.D., F.A.C.P., F.A.S.N. Director, Division of Nephrology Lenox Hill Hospital,
Insulin Resistance. Biol 405 Molecular Medicine
 Insulin Resistance Biol 405 Molecular Medicine Insulin resistance: a subnormal biological response to insulin. Defects of either insulin secretion or insulin action can cause diabetes mellitus. Insulin-dependent
Insulin Resistance Biol 405 Molecular Medicine Insulin resistance: a subnormal biological response to insulin. Defects of either insulin secretion or insulin action can cause diabetes mellitus. Insulin-dependent
Copyright 2009 Pearson Education, Inc. Copyright 2009 Pearson Education, Inc. Figure 19-1c. Efferent arteriole. Juxtaglomerular apparatus
 /6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
/6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
19. RENAL PHYSIOLOGY ROLE OF THE URINARY SYSTEM THE URINARY SYSTEM. Components and function. V BS 122 Physiology II 151 Class of 2011
 19. RENAL PHYSIOLOGY THE URINARY SYSTEM Components and function The urinary system is composed of two kidneys, the functionally filtering apparatus, which connect through two tubular structures called
19. RENAL PHYSIOLOGY THE URINARY SYSTEM Components and function The urinary system is composed of two kidneys, the functionally filtering apparatus, which connect through two tubular structures called
THE RENOPROTECTIVE EFFECT OF FOODS HIGH IN OMEGA-3 FATTY ACIDS IN A RAT MODEL OF TYPE 1 DIABETES
 THE RENOPROTECTIVE EFFECT OF FOODS HIGH IN OMEGA-3 FATTY ACIDS IN A RAT MODEL OF TYPE 1 DIABETES A Dissertation submitted to the Faculty of the Graduate School of Arts and Sciences of Georgetown University
THE RENOPROTECTIVE EFFECT OF FOODS HIGH IN OMEGA-3 FATTY ACIDS IN A RAT MODEL OF TYPE 1 DIABETES A Dissertation submitted to the Faculty of the Graduate School of Arts and Sciences of Georgetown University
Urinary Physiology. Chapter 17 Outline. Kidney Function. Chapter 17
 Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Pathogenesis of IgA Nephropathy. Shokoufeh Savaj MD Associate Professor of Medicine Firoozgar hospital- IUMS
 Pathogenesis of IgA Nephropathy Shokoufeh Savaj MD Associate Professor of Medicine Firoozgar hospital- IUMS History Immunoglobin A nephropathy was first described by Berger and Hinglais in 1968 in Paris
Pathogenesis of IgA Nephropathy Shokoufeh Savaj MD Associate Professor of Medicine Firoozgar hospital- IUMS History Immunoglobin A nephropathy was first described by Berger and Hinglais in 1968 in Paris
JOSHUA K. KAYIMA INTERLINKING CARDIOVASCULAR DISEASE, CHRONIC KIDNEY DISEASE, AND OBESITY
 INTERLINKING CARDIOVASCULAR DISEASE, CHRONIC KIDNEY DISEASE, AND OBESITY JOSHUA K. KAYIMA ASSOCIATE PROFESSOR DEPT. OF CLINICAL MEDICINE AND THERAPEUTICS UNIVERSITY OF NAIROBI Introduction According to
INTERLINKING CARDIOVASCULAR DISEASE, CHRONIC KIDNEY DISEASE, AND OBESITY JOSHUA K. KAYIMA ASSOCIATE PROFESSOR DEPT. OF CLINICAL MEDICINE AND THERAPEUTICS UNIVERSITY OF NAIROBI Introduction According to
ACEIs / ARBs NDHP dihydropyridine ( DHP ) ACEIs ARBs ACEIs ARBs NDHP. ( GFR ) 60 ml/min/1.73m ( chronic kidney disease, CKD )
 005 16 175-180 1 1 ( chronic kidney disease, CKD ) 003 ( end-stage renal disease, ESRD ) Angiotensin-converting enzyme inhibitors ( ) angiotensin receptor blockers ( ) nondihydropyridine ( NDHP ) / NDHP
005 16 175-180 1 1 ( chronic kidney disease, CKD ) 003 ( end-stage renal disease, ESRD ) Angiotensin-converting enzyme inhibitors ( ) angiotensin receptor blockers ( ) nondihydropyridine ( NDHP ) / NDHP
New Perspectives on Diabetic Vascular Complications: The Loss of Endogenous Protective Factors Induced by Hyperglycemia
 New Perspectives on Diabetic Vascular Complications: The Loss of Endogenous Protective Factors Induced by Hyperglycemia The Harvard community has made this article openly available. Please share how this
New Perspectives on Diabetic Vascular Complications: The Loss of Endogenous Protective Factors Induced by Hyperglycemia The Harvard community has made this article openly available. Please share how this
A clinical syndrome, composed mainly of:
 Nephritic syndrome We will discuss: 1)Nephritic syndrome: -Acute postinfectious (poststreptococcal) GN -IgA nephropathy -Hereditary nephritis 2)Rapidly progressive GN (RPGN) A clinical syndrome, composed
Nephritic syndrome We will discuss: 1)Nephritic syndrome: -Acute postinfectious (poststreptococcal) GN -IgA nephropathy -Hereditary nephritis 2)Rapidly progressive GN (RPGN) A clinical syndrome, composed
By: Dr. Foadoddini Department of Physiology & Pharmacology Birjand University of Medical Sciences. Body fluids and.
 By: Dr. Foadoddini Department of Physiology & Pharmacology Birjand University of Medical Sciences Body fluids and Renal physiology 25 Volume and Osmolality of Extracellular and Intracellular Fluids
By: Dr. Foadoddini Department of Physiology & Pharmacology Birjand University of Medical Sciences Body fluids and Renal physiology 25 Volume and Osmolality of Extracellular and Intracellular Fluids
Human Urogenital System 26-1
 Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Cardiovascular Implications of Proteinuria
 Cardiovascular Implications of Proteinuria B. S. Kasinath, MD University of Texas Health Science Center South Texas Veterans Health Care System San Antonio Objectives Mechanisms of albumin handling by
Cardiovascular Implications of Proteinuria B. S. Kasinath, MD University of Texas Health Science Center South Texas Veterans Health Care System San Antonio Objectives Mechanisms of albumin handling by
Mohammad Husain Department of Biotechnology, Jamia Millia Islamia New Delhi
 Role of Vitamin D receptor (VDR) in HIV induced tubular injury Mohammad Husain Department of Biotechnology, Jamia Millia Islamia New Delhi 07/10/2015 INTRODUCTION Vitamin D is technically not a Vitamin;
Role of Vitamin D receptor (VDR) in HIV induced tubular injury Mohammad Husain Department of Biotechnology, Jamia Millia Islamia New Delhi 07/10/2015 INTRODUCTION Vitamin D is technically not a Vitamin;
RENAL GRAND ROUNDS. Vitamin D- Beyond the bone. Dr Krishna Pakkivenkata. 9 th April 2010.
 RENAL GRAND ROUNDS Vitamin D- Beyond the bone Dr Krishna Pakkivenkata. 9 th April 2010. Brief history Secosteroid. 1920 s-exposure to sunlight prevented rickets. 1936- structure of Vit D was discovered.
RENAL GRAND ROUNDS Vitamin D- Beyond the bone Dr Krishna Pakkivenkata. 9 th April 2010. Brief history Secosteroid. 1920 s-exposure to sunlight prevented rickets. 1936- structure of Vit D was discovered.
Hypertension and diabetic nephropathy
 Hypertension and diabetic nephropathy Elisabeth R. Mathiesen Professor, Chief Physician, Dr sci Dep. Of Endocrinology Rigshospitalet, University of Copenhagen Denmark Hypertension Brain Eye Heart Kidney
Hypertension and diabetic nephropathy Elisabeth R. Mathiesen Professor, Chief Physician, Dr sci Dep. Of Endocrinology Rigshospitalet, University of Copenhagen Denmark Hypertension Brain Eye Heart Kidney
Mouse Models of Diabetic Nephropathy. Mount Sinai / Jefferson / Einstein / Minnesota Erwin Böttinger, PI Kumar Sharma, Co-PI
 Mouse Models of Diabetic Nephropathy Mount Sinai / Jefferson / Einstein / Minnesota Erwin Böttinger, PI Kumar Sharma, Co-PI Group Members Mount Sinai: Phenotyping, Molecular Pathology & Validation Erwin
Mouse Models of Diabetic Nephropathy Mount Sinai / Jefferson / Einstein / Minnesota Erwin Böttinger, PI Kumar Sharma, Co-PI Group Members Mount Sinai: Phenotyping, Molecular Pathology & Validation Erwin
LECTURE 25: FILTRATION AND CLEARANCE NEPHRON FILTRATION
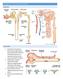 LECTURE 25: FILTRATION AND CLEARANCE NEPHRON FILTRATION 1. Everything in the plasma is filtered except large proteins and red blood cells. The filtrate in Bowman s capsule is an isosmotic fluid that is
LECTURE 25: FILTRATION AND CLEARANCE NEPHRON FILTRATION 1. Everything in the plasma is filtered except large proteins and red blood cells. The filtrate in Bowman s capsule is an isosmotic fluid that is
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
RENAL PHYSIOLOGY DR.CHARUSHILA RUKADIKAR ASSISTANT PROFESSOR PHYSIOLOGY
 RENAL PHYSIOLOGY DR.CHARUSHILA RUKADIKAR ASSISTANT PROFESSOR PHYSIOLOGY GROSS ANATOMY Location *Bean-shaped *Retroperitoneal *At level of T12 L1 vertebrae. *The right kidney lies slightly inferior to left
RENAL PHYSIOLOGY DR.CHARUSHILA RUKADIKAR ASSISTANT PROFESSOR PHYSIOLOGY GROSS ANATOMY Location *Bean-shaped *Retroperitoneal *At level of T12 L1 vertebrae. *The right kidney lies slightly inferior to left
Diabetic nephropathy: Linking histology, cell biology, and genetics
 Kidney International, Vol. 66 (2004), pp. 2095 2106 Diabetic nephropathy: Linking histology, cell biology, and genetics NEPHROLOGY FORUM Principal discussant: SHARON ADLER Harbor-UCLA Medical Center, Division
Kidney International, Vol. 66 (2004), pp. 2095 2106 Diabetic nephropathy: Linking histology, cell biology, and genetics NEPHROLOGY FORUM Principal discussant: SHARON ADLER Harbor-UCLA Medical Center, Division
Diabetes. Albumin. Analyte Information
 Diabetes Albumin Analyte Information -1-2014-05-02 Albumin Introduction Albumin consists of a single polypeptide chain of 585 amino acids with molecular weight of 66.5 kda. The chain is characterized by
Diabetes Albumin Analyte Information -1-2014-05-02 Albumin Introduction Albumin consists of a single polypeptide chain of 585 amino acids with molecular weight of 66.5 kda. The chain is characterized by
Therapeutic approaches to slowing the progression of diabetic nephropathy is less best?
 www.drugsincontext.com The journal of interventions in clinical practice REVIEW Therapeutic approaches to slowing the progression of diabetic nephropathy is less best? FULL TEXT ARTICLE Eva Vivian, 1 Chelsea
www.drugsincontext.com The journal of interventions in clinical practice REVIEW Therapeutic approaches to slowing the progression of diabetic nephropathy is less best? FULL TEXT ARTICLE Eva Vivian, 1 Chelsea
COMPLETE INHIBITION OF RENAL RESERVE IN CHRONIC RENAL FAILURE BY A COMBINATION OF ACEI AND ARB
 COMPLETE INHIBITION OF RENAL RESERVE IN CHRONIC RENAL FAILURE BY A COMBINATION OF ACEI AND ARB CG Musso ¹, J Reynaldi¹, N Imperiali ¹, L Algranati ¹, DG Oreopoulos ² Nephrology Department Hospital Italiano
COMPLETE INHIBITION OF RENAL RESERVE IN CHRONIC RENAL FAILURE BY A COMBINATION OF ACEI AND ARB CG Musso ¹, J Reynaldi¹, N Imperiali ¹, L Algranati ¹, DG Oreopoulos ² Nephrology Department Hospital Italiano
Diabetes and Kidney Disease. Kris Bentley Renal Nurse practitioner 2018
 Diabetes and Kidney Disease Kris Bentley Renal Nurse practitioner 2018 Aims Develop an understanding of Chronic Kidney Disease Understand how diabetes impacts on your kidneys Be able to recognise the risk
Diabetes and Kidney Disease Kris Bentley Renal Nurse practitioner 2018 Aims Develop an understanding of Chronic Kidney Disease Understand how diabetes impacts on your kidneys Be able to recognise the risk
Responding to the challenge of diabetic nephropathy: the historic evolution of detection, prevention and management
 (2000) 14, 667 685 2000 Macmillan Publishers Ltd All rights reserved 0950-9240/00 $15.00 www.nature.com/jhh REVIEW ARTICLE Responding to the challenge of diabetic nephropathy: the historic evolution of
(2000) 14, 667 685 2000 Macmillan Publishers Ltd All rights reserved 0950-9240/00 $15.00 www.nature.com/jhh REVIEW ARTICLE Responding to the challenge of diabetic nephropathy: the historic evolution of
Case # 2 3/27/2017. Disclosure of Relevant Financial Relationships. Clinical history. Clinical history. Laboratory findings
 Case # 2 Christopher Larsen, MD Arkana Laboratories Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to influence or control the content
Case # 2 Christopher Larsen, MD Arkana Laboratories Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to influence or control the content
Dr Ian Roberts Oxford. Oxford Pathology Course 2010 for FRCPath Illustration-Cellular Pathology. Oxford Radcliffe NHS Trust
 Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Present the basic diagnostic features of the commonest conditions causing proteinuria & haematuria Highlight diagnostic pitfalls Nephrotic
Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Present the basic diagnostic features of the commonest conditions causing proteinuria & haematuria Highlight diagnostic pitfalls Nephrotic
Hyperglycemia: Type I Diabetes Mellitus
 296 PHYSIOLOGY CASES AND PROBLEMS Case 53 Hyperglycemia: Type I Diabetes Mellitus David Mandel was diagnosed with type I (insulin-dependent) diabetes mellitus when he was 12 years old (see Cases 30 and
296 PHYSIOLOGY CASES AND PROBLEMS Case 53 Hyperglycemia: Type I Diabetes Mellitus David Mandel was diagnosed with type I (insulin-dependent) diabetes mellitus when he was 12 years old (see Cases 30 and
The topic of normal vascular and glomerular anatomy is introduced
 Normal Vascular and Glomerular Anatomy Arthur H. Cohen Richard J. Glassock The topic of normal vascular and glomerular anatomy is introduced here to serve as a reference point for later illustrations of
Normal Vascular and Glomerular Anatomy Arthur H. Cohen Richard J. Glassock The topic of normal vascular and glomerular anatomy is introduced here to serve as a reference point for later illustrations of
Innate immune system and adiponectin in diabetic nephropathy in type 1 diabetes
 Department of Medicine Division of Nephrology Helsinki University Central Hospital Helsinki, Finland Folkhälsan Research Center Folkhälsan Institue of Genetics University of Helsinki Innate immune system
Department of Medicine Division of Nephrology Helsinki University Central Hospital Helsinki, Finland Folkhälsan Research Center Folkhälsan Institue of Genetics University of Helsinki Innate immune system
Histology Urinary system
 Histology Urinary system Urinary system Composed of two kidneys, two ureters, the urinary bladder, and the urethra, the urinary system plays a critical role in: 1- Blood filtration,(filtration of cellular
Histology Urinary system Urinary system Composed of two kidneys, two ureters, the urinary bladder, and the urethra, the urinary system plays a critical role in: 1- Blood filtration,(filtration of cellular
Section Title. Subject Index
 Section Title Subject Index Acute kidney injury definitions 287 289 hypoxia 287, 290 overview 286, 287 sublethal tubular injury adaptive responses 292, 293 combination of sublethal injuries 291, 292 detection
Section Title Subject Index Acute kidney injury definitions 287 289 hypoxia 287, 290 overview 286, 287 sublethal tubular injury adaptive responses 292, 293 combination of sublethal injuries 291, 292 detection
Pathology of endocrine pancreas. By: Shifaa Alqa qa
 Pathology of endocrine pancreas By: Shifaa Alqa qa major cell types: Beta ----- insulin Alpha ----- glucagon Delta ----- somatostatin PP (pancreatic polypeptide) cells ------ VIP DIABETES MELLITUS Normal
Pathology of endocrine pancreas By: Shifaa Alqa qa major cell types: Beta ----- insulin Alpha ----- glucagon Delta ----- somatostatin PP (pancreatic polypeptide) cells ------ VIP DIABETES MELLITUS Normal
Basic Functions of the Kidneys
 Dr. Adelina Vlad Basic Functions of the Kidneys Eliminate plasma METABOLIC WASTE PRODUCTS and FOREIGN COMPOUNDS The kidney are the primary means for eliminating metabolic waste products (urea, creatinine,
Dr. Adelina Vlad Basic Functions of the Kidneys Eliminate plasma METABOLIC WASTE PRODUCTS and FOREIGN COMPOUNDS The kidney are the primary means for eliminating metabolic waste products (urea, creatinine,
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
