Original Article Difficulties and countermeasures of laparoscopic pancreaticoduodenectomy: report of 18 cases
|
|
|
- Spencer Watkins
- 5 years ago
- Views:
Transcription
1 Int J Clin Exp Med 2016;9(2): /ISSN: /IJCEM Original Article Difficulties and countermeasures of laparoscopic pancreaticoduodenectomy: report of 18 cases Xiaoming Wang, Minghua Hu, Weidong Sun, Weidong Zhang, Yaqi Jiang, Xiaosan Fang, Meng Han Department of Hepatobiliary Surgery, Yijishan Hospital of Wannan Medical College, Wuhu , Anhui, China Received September 11, 2015; Accepted December 17, 2015; Epub February 15, 2016; Published February 29, 2016 Abstract: Objective: In this study, we aimed to investigate the difficulties and countermeasures related to laparoscopic pancreaticoduodenectomy (LP). Methods: A retrospective analysis was performed on the surgical methods and clinical data of 18 LP cases at our hospital between December 2009 and November Results: All 18 surgeries were completed successfully. The operation time was 465 ± 93 min, and the intraoperative blood loss was 380 ± 216 ml. All cases had negative surgical margins, and there were 14.3 ± 6.7 pieces of scavenged lymph nodes. Postoperative complicating pulmonary infection occurred in 1 case that resolved after enhancement of anti-infectious activity. Mal-healing of incisions occurred in 1 case, and a second-stage suture was performed. Seroperitoneum accompanied with infection occurred in 1 case, and reoperative drainage was performed. Bile leakage occurred in 2 cases that resolved after drainage, and pancreatic leakage occurred in 2 cases, presenting as secondary intra-abdominal bleeding in 1 case that was treated with reoperation for hemostasis; in the other case, pancreatic leakage resolved after drainage. Conclusions: Improvements in the surgical approach, uncinate process resection, and pancreaticojejunostomy could improve the feasibility and safety of LP. Keywords: Laparoscopy, pancreaticoduodenectomy, surgical approach, pancreaticojejunostomy Introduction Since Gagner successfully performed laparoscopic pancreaticoduodenectomy (LP) in 1 patient with chronic pancreatitis for the first time in 1994 [1], many hospitals, both domestic and abroad, have performed LP. In most literature reports, the technological aspect was the focus of the study, the cases were few, and some cases were reported independently [2, 3]; moreover, the short-term effects were not ideal, the complication rate was higher than that for open surgery, and the operative time was significantly prolonged, diminishing the advantages of microinvasive surgery [4-9]. Therefore, the use of LP was controversial and developed slowly. In recent years, with the continuous advances in surgical techniques and improvement of surgical instruments, LP has greatly progressed, and recent reports have described encouraging results [10-15]. However, because the pancreas has a deep anatomical location, in addition to its complex structure and close proximity to many major blood vessels, LP remains one of the most challenging endoscopic surgeries. Currently, the major technical problems related to LP are as follows: the surgical approach still follows the traditional model of open surgery and cannot fit the requirements of endoscopic operations; the resection of the pancreatic uncinate process under laparoscope guidance is still associated with some technical difficulty and bleeding risk; and the technique for gastrointestinal reconstruction under endoscopic guidance is difficult, especially for pancreaticojejunostomy. Therefore, the key was determining how to improve laparoscopic techniques and the LP experience, thus ensuring outcomes similar to those of open surgery. Between December 2009 and November 2013, 18 patients underwent LP at our hospital with satisfactory results. These cases are reported below and were investigated in relation to the abovementioned problems. Clinical data and methods General data The 18 LP patients included 10 men and 8 women aged years (Table 1). All patients
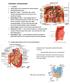
2 Table 1. The general information of the 18 cases No Gender Age BMI TBIL(1) umol/l TBIL(2) umol/l CA19-9 U/ml Pathology Complications 1 M carcinoma of CBD Pulmonary infection and bile leakage 2 M duodenal papilla cancer incision mal-healing 3 F duodenal papilla cancer 4 M pancreatic carcinoma 5 F adenocarcinoma of CBD intra-abdominal infection 6 M pancreatic carcinoma 7 F carcinoma of CBD bile leakage 8 M chronic calcific pancreatitis 9 M pancreatic carcinoma pancreatic leakage 10 M carcinoma of CBD 11 F duodenal papilla cancer pancreatic leakage and intra-abdominal bleeding 12 M duodenal papilla cancer 13 F duodenal papilla cancer 14 M duodenal papilla cancer 15 F pancreatic carcinoma 16 M duodenal papilla cancer 17 F pancreatic solid pseudo-papilloma 18 F duodenal papilla cancer BMI: body mass index, TBIL: total bilirubin, CBD: common bile duct. TBIL(1): TBIL before operation. TBIL(2): TBIL 1 week after operation. were preoperatively confirmed to have ampullary or pancreatic head tumors using B ultrasound, computed tomography, magnetic resonance imaging, or endoscopic retrograde cholangiopancreatography. The case selection criteria were as follows: tumor diameter < 3 cm, no signs of peripheral vascular invasion, no obvious lymphadenectasis, and no distant metastasis. This study was conducted in accordance with the declaration of Helsinki. This study was conducted with approval from the Ethics Committee of Wannan Medical College. Written informed consent was obtained from all participants. Surgical approach Anesthesia and position: The patient was administered general anesthesia in the supinestraddle position. The laparoscope was inserted through a small incision at the lower edge of the umbilical ring (or 3-5 cm below the umbilicus). Then, 4 incisions were made at the lower rib margin of the left and right anterior axillary lines and slightly above the umbilicus level of the left and right clavicular middle lines, as the primary and secondary operating holes. The surgeon stood on the left side of the patient, and the assistant stood on the right side. Exploration: Conventional exploration was performed toward the liver, abdominal cavity, and omentum to investigate whether metastatic lesion(s), cholestatic liver, and bile duct dilatation existed. An ultrasound knife was used to transect the right stomach-colon ligament and flexura hepatica coli. A Kocher incision was then made, the duodenum was lifted with nondamaged grasping forceps, and the tissues were freed from Toldt s gap and leftward until the duodenal horizontal portion to assess for inferior vena cava invasion. The transverse mesocolon was then pulled leftward, and the superior mesenteric vein was exposed at the duodenal horizontal portion (Figure 1). The vascular sheath was opened and freed upward, anatomically transecting branch vessels such as the right gastroepiploic vein. The lower edge of the pancreas was freed and lifted, and the part behind the pancreas was resected until the intersection at the splenic vein. It could then be determined whether the tumor had invaded the superior mesenteric vein and whether LP could be performed. Lymph node dissection of the duodenohepatic ligament: The gastroduodenal artery was anatomically transected at the portal vein triangle after the beginning portion of the portal vein was revealed and freed along its surface toward the porta hepatis. It was then separated from the hepatic artery and bile duct, which are located at its front. The hepatic artery sheath was cut open, and the common hepatic artery 2452 Int J Clin Exp Med 2016;9(2):
3 Figure 1. The superior mesenteric vein was exposed on the duodenal horizontal part. Figure 3. Penetration-suture method was performed to suture the pancreatic broken end and the intestinal wall. Figure 2. Pancreatic suspension method was used to resect the uncinate process. Figure 4. Completed pancreaticojejunostomy. and proper hepatic artery were fully dissected and skeletonized. The lymph nodes in this region were scavenged. Specimen dissection and uncinate process resection (pancreatic head hanging method, Figure 2): The surgeon freed the arcus major ventriculi and arcus minor ventriculi, transected the gastric body, opened/resected the gallbladder, and transected the common hepatic duct. Then, the surgeon transected the jejunum 15 cm to the Treitz ligament and pulled the proximal jejunum to the right through the mesenteric vessels. An electric coagulation hook or ultrasonic knife was used to transect the pancreatic neck. A sling protruded from the pancreatic head and the uncinate process, and was suspended and pulled to the right. The superior mesenteric vein was then pulled to the left, and the vascular branches between the superior mesenteric vein and the pancreatic head were then dissected individually from the bottom to the top. The surgeon identified the superior mesenteric artery and opened the artery sheath, and used an ultrasound knife to dissect the uncinate process from the right wall of the superior mesenteric artery. The larger branch should be dissected after being clipped; meanwhile, the surrounding lymph adipose tissues should be cleaned. Thus, the specimen was completely resected and removed through the small incision on the middle abdomen. Digestive tract reconstruction with the child surgical method: Before the pancreaticojejunostomy, 10 patients underwent traditional pancreatic duct-mucosal side anastomosis, and the remaining 8 patients underwent a selfdesigned single-layer penetrative pancreas intestinal side anastomosis. The specific procedures were as follows (Figures 3 and 4): (i) Penetrative suture-with the pancreatic duct as 2453 Int J Clin Exp Med 2016;9(2):
4 the center, 2-3 sutures were applied at the top and the bottom, with about a 1 cm margin; each suture was inserted with the needle from the anterior wall of the pancreatic broken end and withdrawn from the rear wall, which then penetrated the seromuscular layer of the jejunal mesentery edge from the back to the front and was not tied temporarily. For anastomosis of the pancreatic duct and jejunal mucosa, holes were made in the corresponding lateral intestinal wall of the pancreatic duct and then interruptedly sutured with 0/5 absorbable threads. The frame was placed in the pancreatic duct, and the other end was inserted into the intestine. (ii) The detained suture was tied into a knot, while attention was paid to cover the pancreatic broken end with the jejunal wall. (iii) Strengthening the suture-one suture was strengthened on the corresponding anterior and posterior pancreatic wall of the pancreatic duct. Results Surgical results The operations were successful in all 18 patients. The operation time was 465 ± 93 min, and the intraoperative blood loss was 380 ± 216 ml. Postoperative pathology There were 4 cases of lower adenocarcinoma of the common bile duct, 8 cases of duodenal papilla cancer, 4 cases of pancreatic adenocarcinoma, 1 case of chronic calcific pancreatitis accompanied by cyst formation, and 1 case of pancreatic solid pseudo-papilloma; the tumor diameter was < 3 cm, and the edges of all samples were negative. There were 14.3 ± 6.7 pieces of scavenged lymph nodes. Postoperative complications There was 1 case of postoperative pulmonary Staphylococcus aureus infection, which resolved after enhancement of anti-infection activity; 1 case of incision mal-healing, for which a second-stage suture was performed; 1 case of seroperitoneum, due to poor drainage, accompanied by infection, for which surgical drainage was performed again; and 2 cases of bile leakage that resolved after drainage. There were 2 cases of pancreatic leakage (both were treated with conventional anastomosis), 1 of which was accompanied by secondary intraabdominal bleeding and found to have dehiscence in the anterior wall of the pancreatic anastomosis; the patient in this case underwent resuturing and double-catheter washing after which the condition resolved. In the other case, pancreatic leakage resolved after drainage. Discussion Currently, the surgical approaches of LP mostly follow those of open surgery. However, because of the limits associated with the operating hole and viewing angles, application of the surgical approach followed in laparotomy to laparoscopic surgery is difficult. Therefore, the first challenge while performing the surgery was the method of LP. Recently, some scholars have reported the superior mesenteric artery first approach [16-19]. In this study, we used the superior mesenteric vein-portal vein sequential approach, as we believe that exploration toward the superior mesenteric vein-portal vein caused difficulties in LP, and, to some extent, because the superior mesenteric vein-portal vein would ensure a successful LP. This is because (i) exploration toward the superior mesenteric vein was an important basis in determining whether the lesion could be removed; (ii) the major risk of dangerous triangle resection, namely, the uncinate process resection, was to dissect the uncinate process and anterior mesenteric vessels; and (iii) the scavenging of lymph nodes was expanded with the superior mesenteric vein-portal vein as the axis. The superior mesenteric vein in traditional LP is explored from the uncinate process of the blood vessels, as follows: the lower edge of the pancreas is exposed with the middle colic vein or the right gastroepiploic vein, and then the branch vessels and the superior mesenteric vein are identified. However, the superior mesenteric vein in this section was the shortest and had the most branches; in addition to the right gastroepiploic vein, the anterior pancreaticoduodenal vein and other branches still existed. These vessels were imported into the superior mesenteric vein with different stems and planes; thus, it would be difficult to grasp the anatomical structure during the separation, and, any damage would cause uncontrolled bleeding. Therefore, it was one of the intraop Int J Clin Exp Med 2016;9(2):
5 erative steps with the highest bleeding risk. In this study, according to the segment characteristics of the superior mesenteric vein-portal vein, the exploration of blood vessels began from the horizontal segment of the duodenum. This section was longer and entirely within the mesentery, had no association with the vessels in the horizontal portion of the duodenum, and would be convenient and safe for exposure. The vascular sheath was opened from this site and freed upward along the intrathecal space, and the vascular branches within the uncinate process segment could be quickly located and processed; meanwhile, the posterior pancreatic vascular segment could be explored. This surgical approach progressed sequentially from the bottom up, which not only made the laparoscopic operation convenient but also allowed the exploration and separation to be finished at the same time, shortened the operation time, reduced bleeding, and produced good outcomes. One focus of the LP debate was whether full resection of the uncinate process could be achieved; if the endoscopy could not fully resect the uncinate process, radical effects would result. Anatomically, the pancreatic uncinate process often has partial tissues surrounding the rear of the superior mesenteric vein and is difficult to expose, making resection difficult and increasing the possibility of bleeding; thus, it was called a dangerous triangle. It was once reported that the pancreatic uncinate process was resected with the endoscopic resection closer, which was a simple procedure; however, there might exist pancreatic tissue residue, and lymph node dissection could not be realized. In this study, the pancreatic head suspension method was used to complete the resection of the uncinate process [20, 21] and achieved good results. This method had the following advantages: (i) It exposed the portal vein and superior mesenteric vein during the whole procedure, significantly reducing the chances of injuring the minor vessels, and improving surgical safety. (ii) It increased the distance between the pancreatic head uncinate process with the portal vein and the superior mesenteric vein and obtained the best exposure. (iii) It made the seemingly wide and thick uncinate process mesenterium appear narrow and thin, as indicated in the manner of a complete plane and improved surgical outcomes. (iv) It simplified the operation and ensured appropriate exposure, which originally required multiple equipment, by using a single suspension; meanwhile, the sling position could be adjusted at any time, thus ensuring the tension between the uncinate process and mesenteric vessels. (v) Tightening the sling could play a role in pressure-hemostasis toward the pancreatic broken end, thus reducing bleeding. The laparoscopic technique has been widely used in various fields of abdominal surgeries; however, LP was still in the exploratory stage, and one of the most important reasons is that there is no ideal method for pancreaticojejunostomy. Currently, endoscopic pancreaticojejunostomy can be performed by using various methods [22-26]; however, regardless of endend anastomosis or end-lateral side anastomosis, the pancreas was considered a hollow organ, and the pancreatic broken end was divided into the anterior and posterior walls for ring anastomosis with the jejunum. Therefore, it would inevitably lead to the following issues: (i) The suture levels would be increased, resulting in a time-consuming suture procedure. (ii) Each suture could tie less tissue and be prone to cutting and tearing. (iii) Suturing the posterior wall was difficult and was prone to bleeding. In fact, the pancreaticojejunostomy was the anastomosis of 1 parenchymal organ and a hollow organ. The key factor to ensure the success of pancreaticojejunostomy is that the pancreatic broken ends should be firmly anastomosed to the jejunal wall, allowing the pancreatic juice inside the main pancreatic duct to enter the intestine. According to this concept, we modified the traditional end-lateral anastomosis and designed a new anastomotic approach-single-layer penetrative pancreaticojejunal anastomosis, which greatly simplified the procedures of pancreaticojejunostomy and is especially suitable for endoscopy. This method had the following characteristics: (i) it has a single-layer suture and no requirement for suturing the posterior pancreatic wall separately, making the operation easy; (ii) the penetrative suture ties more tissues, which would not cause pancreatic tearing or anastomotic dehiscence, thus strengthening the suture; (iii) there is no need to excessively free the pancreatic ends, thus reducing the risk of bleeding; and (iv) the pancreatic broken end is closely attached to the intestinal wall after knotting 2455 Int J Clin Exp Med 2016;9(2):
6 the suture, reducing the dead space between them and becoming more conducive to healing with the pancreatic broken end. In this study, this approach significantly shortened the operation time and reduced the incidence of pancreatic fistula. Although LP has some risks, the application of a more appropriate surgical approach-a suspension method of uncinate process resection and single-layer penetrative pancreaticojejunostomy aimed at the difficulties of this surgery-could make the surgery much safer. Acknowledgements The authors thank Dr. Pei Wu for his valuable help in proofreading this article. Disclosure of conflict of interest None. Address correspondence to: Xiaoming Wang, Department of Hepatobiliary Surgery, Yijishan Hospital of Wannan Medical College, Wuhu , Anhui, China. Tel: ; Fax: ; xiaomingwangcn@163.com References [1] Gagner M and Pomp A. Laparoscopic pylorus-preserving pancreatoduodenectomy. Surg Endosc 1994; 8: [2] Zheng MH, Feng B, Lu AG, Li JW, Hu WG, Wang ML, Zang L, Dong F, Mao ZH, Peng YF and Jiang Y. Laparoscopic pancreaticoduodenectomy for ductal adenocarcinoma of common bile duct: a case report and literature review. Med Sci Monit 2006; 12: CS57-CS60. [3] Cai X, Wang Y, Yu H, Liang X, Xu B and Peng S. Completed laparoscopic pancreaticoduodenectomy. Surg Laparosc Endosc Percutan Tech 2008; 18: [4] Dulucq JL, Wintringer P and Mahajna A. Laparoscopic pancreaticoduodenectomy for benign and malignant diseases. Surg Endosc 2006; 20: [5] Palanivelu C, Jani K, Senthilnathan P, Parthasarathi R, Rajapandian S and Madhankumar MV. Laparoscopic pancreaticoduodenectomy: technique and outcomes. J Am Coll Surg 2007; 205: [6] Pugliese R, Scandroglio I, Sansonna F, Maggioni D, Costanzi A, Citterio D, Ferrari GC, Di Lernia S and Magistro C. Laparoscopic pancreaticoduodenectomy: a retrospective review of 19 cases. Surg Laparosc Endosc Percutan Tech 2008; 18: [7] Gagner M and Palermo M. Laparoscopic Whipple procedure: review of the literature. J Hepatobiliary Pancreat Surg 2009; 16: [8] Kendrick ML and Cusati D. Total laparoscopic pancreaticoduodenectomy: feasibility and outcome in an early experience. Arch Surg 2010; 145: [9] Gumbs AA, Rodriguez Rivera AM, Milone L and Hoffman JP. Laparoscopic pancreatoduodenectomy: a review of 285 published cases. Ann Surg Oncol 2011; 18: [10] Asbun HJ and Stauffer JA. Laparoscopic vs open pancreaticoduodenectomy: overall outcomes and severity of complications using the Accordion Severity Grading System. J Am Coll Surg 2012; 215: [11] Kim SC, Song KB, Jung YS, Kim YH, Park do H, Lee SS, Seo DW, Lee SK, Kim MH, Park KM and Lee YJ. Short-term clinical outcomes for 100 consecutive cases of laparoscopic pylorus-preserving pancreatoduodenectomy: improvement with surgical experience. Surg Endosc 2013; 27: [12] Nakamura M and Nakashima H. Laparoscopic distal pancreatectomy and pancreatoduodenectomy: is it worthwhile? A meta-analysis of laparoscopic pancreatectomy. J Hepatobiliary Pancreat Sci 2013; 20: [13] Corcione F, Pirozzi F, Cuccurullo D, Piccolboni D, Caracino V, Galante F, Cusano D and Sciuto A. Laparoscopic pancreaticoduodenectomy: experience of 22 cases. Surg Endosc 2013; 27: [14] Correa-Gallego C, Dinkelspiel HE, Sulimanoff I, Fisher S, Viñuela EF, Kingham TP, Fong Y, DeMatteo RP, D Angelica MI, Jarnagin WR and Allen PJ. Minimally-invasive vs open pancreaticoduodenectomy: systematic review and meta-analysis. J Am Coll Surg 2014; 218: [15] Subar D, Gobardhan PD and Gayet B. Laparoscopic pancreatic surgery: an overview of the literature and experiences of a single center. Best Pract Res Clin Gastroenterol 2014; 28: [16] Cho A, Yamamoto H and Kainuma O. Tips of laparoscopic pancreaticoduodenectomy: superior mesenteric artery first approach (with video). J Hepatobiliary Pancreat Sci 2014; 21: E19-E21. [17] Alvarado-Bachmann R, Choi J, Gananadha S, Hugh TJ and Samra JS. The infracolic approach to pancreatoduodenectomy for large pancreatic head tumours invading the colon. Eur J Surg Oncol 2010; 36: [18] Honda G, Kurata M, Okuda Y, Kobayashi S, Sakamoto K and Takahashi K. Laparoscopic pancreaticoduodenectomy: taking advantage 2456 Int J Clin Exp Med 2016;9(2):
7 of the unique view from the caudal side. J Am Coll Surg 2013; 217: e45-e49. [19] Ogiso S, Conrad C, Araki K, Basso V and Gayet B. Posterior approach for laparoscopic pancreaticoduodenectomy to prevent replaced hepatic artery injury. Ann Surg Oncol 2013; 20: [20] Kuroki T, Tajima Y, Kitasato A, Adachi T and Kanematsu T. Pancreas-hanging maneuver in laparoscopic pancreaticoduodenectomy: a new technique for the safe resection of the pancreas head. Surg Endosc 2010; 24: [21] Addeo P, Marzano E, Rosso E and Pessaux P. Hanging maneuver during pancreaticoduodenectomy: a technique to improve R0 resection. Surg Endosc 2011; 25: [22] Lu B, Huang Y, Cai X, Huang F, Li J, Lu W, Xu J, Liu Z, Yan Y and Li J. A novel method for reconstruction in laparoscopic pancreaticoduodenectomy: an experience of 13 cases. Front Med China 2007; 1: [23] Nakamura Y, Matsumoto S, Matsushita A, Yoshioka M, Shimizu T, Yamahatsu K and Uchida E. Pancreaticojejunostomy with closure of the pancreatic stump by endoscopic linear stapler in laparoscopic pancreaticoduodenectomy: a reliable technique and benefits for pancreatic resection. Asian J Endosc Surg 2012; 5: [24] Lei Z, Zhifei W, Jun X, Chang L, Lishan X, Yinghui G and Bo Z. Pancreaticojejunostomy sleeve reconstruction after pancreaticoduodenectomy in laparoscopic and open surgery. JSLS 2013; 17: [25] Cho A, Yamamoto H, Kainuma O, Muto Y, Park S, Arimitsu H, Sato M, Souda H, Ikeda A, Nabeya Y, Takiguchi N and Nagata M. Performing simple and safe dunking pancreaticojejunostomy using mattress sutures in pure laparoscopic pancreaticoduodenectomy. Surg Endosc 2014; 28: [26] Hughes SJ, Neichoy B and Behrns KE. Laparoscopic intussuscepting pancreaticojejunostomy. J Gastrointest Surg 2014; 18: Int J Clin Exp Med 2016;9(2):
Laparoscopy-assisted D2 radical distal subtotal gastrectomy
 Masters of Gastrointestinal Surgery Laparoscopy-assisted D2 radical distal subtotal gastrectomy Xiaogeng Chen, Weihua Li, Jinsi Wang, Changshun Yang Department of Tumor Surgery, Fujian Provincial Hospital,
Masters of Gastrointestinal Surgery Laparoscopy-assisted D2 radical distal subtotal gastrectomy Xiaogeng Chen, Weihua Li, Jinsi Wang, Changshun Yang Department of Tumor Surgery, Fujian Provincial Hospital,
The Whipple Operation Illustrations
 The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
Yoshitsugu; Kanematsu, Takashi; Kur
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Laparoscopic Middle Pancreatectomy Surgery Kitasato, Amane; Adachi, Tomohiko; Yoshitsugu; Kanematsu, Takashi; Kur Hepato-Gastroenterology, 59(120),
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Laparoscopic Middle Pancreatectomy Surgery Kitasato, Amane; Adachi, Tomohiko; Yoshitsugu; Kanematsu, Takashi; Kur Hepato-Gastroenterology, 59(120),
Citation Hepato-Gastroenterology, 55(86-87),
 NAOSITE: Nagasaki University's Ac Title Author(s) Combined pancreatic resection and p multiple lesions of the pancreas: i of the pancreas concomitant with du Kuroki, Tamotsu; Tajima, Yoshitsugu Tomohiko;
NAOSITE: Nagasaki University's Ac Title Author(s) Combined pancreatic resection and p multiple lesions of the pancreas: i of the pancreas concomitant with du Kuroki, Tamotsu; Tajima, Yoshitsugu Tomohiko;
Anatomy of laparoscopy-assisted distal D2 radical gastrectomy for gastric cancer
 Masters of Gastrointestinal Surgery Anatomy of laparoscopy-assisted distal D2 radical gastrectomy for gastric cancer Da-Guang Wang, Liang He, Yang Zhang, Jing-Hai Yu, Yan Chen, Ming-Jie Xia, Jian Suo Department
Masters of Gastrointestinal Surgery Anatomy of laparoscopy-assisted distal D2 radical gastrectomy for gastric cancer Da-Guang Wang, Liang He, Yang Zhang, Jing-Hai Yu, Yan Chen, Ming-Jie Xia, Jian Suo Department
The first total laparoscopic pancreatoduodenectomy in Poland
 Case report Videosurgery Andrzej Budzyński 1, Anna Zub-Pokrowiecka 1, Anna Zychowicz 1, Michał Pędziwiatr 1, Mateusz Wierdak 2, Maciej Matłok 1, Małgorzata Zając 1 12 nd Department of General Surgery,
Case report Videosurgery Andrzej Budzyński 1, Anna Zub-Pokrowiecka 1, Anna Zychowicz 1, Michał Pędziwiatr 1, Mateusz Wierdak 2, Maciej Matłok 1, Małgorzata Zając 1 12 nd Department of General Surgery,
Pancreaticoduodenectomy the anatomy and the surgical approaches
 Pancreaticoduodenectomy the anatomy and the surgical approaches Paul BS LAI Division of Hepato biliary and Pancreatic Surgery Department of Surgery The Chinese Univesity of Hong Kong Whipple s operation
Pancreaticoduodenectomy the anatomy and the surgical approaches Paul BS LAI Division of Hepato biliary and Pancreatic Surgery Department of Surgery The Chinese Univesity of Hong Kong Whipple s operation
Laparoscopic Whipple procedure: review of the literature
 J Hepatobiliary Pancreat Surg (2009) 16:726 730 DOI 10.1007/s00534-009-0142-2 TOPICS Evolution and challenge in endoscopic HBP surgery Laparoscopic Whipple procedure: review of the literature Michel Gagner
J Hepatobiliary Pancreat Surg (2009) 16:726 730 DOI 10.1007/s00534-009-0142-2 TOPICS Evolution and challenge in endoscopic HBP surgery Laparoscopic Whipple procedure: review of the literature Michel Gagner
Total laparoscopic pancreaticoduodenectomy: a retrospective study of 27 cases treated in a single institution
 Original Article Total laparoscopic pancreaticoduodenectomy: a retrospective study of 27 cases treated in a single institution Hong Li 1, Jie Zhu 2, Bin Zhang 1, Gencong Li 1, Xinhua Zhou 3, Dansong Yu
Original Article Total laparoscopic pancreaticoduodenectomy: a retrospective study of 27 cases treated in a single institution Hong Li 1, Jie Zhu 2, Bin Zhang 1, Gencong Li 1, Xinhua Zhou 3, Dansong Yu
A video demonstration of the Li s anastomosis the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma
 Surgical Technique A video demonstration of the the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma Yan Zheng*, Yin Li*, Zongfei Wang, Haibo Sun, Ruixiang Zhang
Surgical Technique A video demonstration of the the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma Yan Zheng*, Yin Li*, Zongfei Wang, Haibo Sun, Ruixiang Zhang
Prevention Of Pancreaticojejunal Fistula After Whipple Procedure
 ISPUB.COM The Internet Journal of Surgery Volume 4 Number 2 Prevention Of Pancreaticojejunal Fistula After Whipple Procedure N Barbetakis, K Setsiz Citation N Barbetakis, K Setsiz. Prevention Of Pancreaticojejunal
ISPUB.COM The Internet Journal of Surgery Volume 4 Number 2 Prevention Of Pancreaticojejunal Fistula After Whipple Procedure N Barbetakis, K Setsiz Citation N Barbetakis, K Setsiz. Prevention Of Pancreaticojejunal
Laparoscopy-assisted radical total gastrectomy plus D2 lymph node dissection
 Masters of Gastrointestinal Surgery Laparoscopy-assisted radical total gastrectomy plus D2 lymph node dissection Chaohui Zheng, Changming Huang, Ping Li, Jianwei Xie, Jiabin Wang, Jianxian Lin, Jun Lu
Masters of Gastrointestinal Surgery Laparoscopy-assisted radical total gastrectomy plus D2 lymph node dissection Chaohui Zheng, Changming Huang, Ping Li, Jianwei Xie, Jiabin Wang, Jianxian Lin, Jun Lu
The abdominal Esophagus, Stomach and the Duodenum. Prof. Oluwadiya KS
 The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
Duodenum retroperitoneal
 Duodenum retroperitoneal C shaped Initial region out of stomach into small intestine RETROperitoneal viscus Superior 1 st part duodenal cap ; moves upwards and backwards to lie on the R crura medial to
Duodenum retroperitoneal C shaped Initial region out of stomach into small intestine RETROperitoneal viscus Superior 1 st part duodenal cap ; moves upwards and backwards to lie on the R crura medial to
Block 3: DISSECTION 2 CELIAC TRUNK, JEJUNUM/ILEUM, LARGE INTESTINE, DUODENUM, PANCREAS, PORTAL VEIN; MOBILIZATION OF THE LIVER
 1 Block 3: DISSECTION 2 CELIAC TRUNK, JEJUNUM/ILEUM, LARGE INTESTINE, DUODENUM, PANCREAS, PORTAL VEIN; MOBILIZATION OF THE LIVER Attempt to complete as much as you can of the dissection explained in the
1 Block 3: DISSECTION 2 CELIAC TRUNK, JEJUNUM/ILEUM, LARGE INTESTINE, DUODENUM, PANCREAS, PORTAL VEIN; MOBILIZATION OF THE LIVER Attempt to complete as much as you can of the dissection explained in the
Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping
 GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
Accessory Glands of Digestive System
 Accessory Glands of Digestive System The liver The liver is soft and pliable and occupies the upper part of the abdominal cavity just beneath the diaphragm. The greater part of the liver is situated under
Accessory Glands of Digestive System The liver The liver is soft and pliable and occupies the upper part of the abdominal cavity just beneath the diaphragm. The greater part of the liver is situated under
Pylorus Preserving Pancreaticoduodenectomy
 REVIEW Pylorus Preserving Pancreaticoduodenectomy Jacqueline M. Garonzik-Wang, M. B. Majella Doyle Pancreaticoduodenectomy (PD) has become the standard of care for resectable pancreatic cancer and premalignant
REVIEW Pylorus Preserving Pancreaticoduodenectomy Jacqueline M. Garonzik-Wang, M. B. Majella Doyle Pancreaticoduodenectomy (PD) has become the standard of care for resectable pancreatic cancer and premalignant
Endoscopic Ultrasonography Assessment for Ampullary and Bile Duct Malignancy
 Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Totally laparoscopic total gastrectomy for locally advanced middle-upper-third gastric cancer
 Original Article on Gastrointestinal Surgery Totally laparoscopic total gastrectomy for locally advanced middle-upper-third gastric cancer Mi Lin, Chang-Ming Huang, Chao-Hui Zheng, Ping Li, Jian-Wei Xie,
Original Article on Gastrointestinal Surgery Totally laparoscopic total gastrectomy for locally advanced middle-upper-third gastric cancer Mi Lin, Chang-Ming Huang, Chao-Hui Zheng, Ping Li, Jian-Wei Xie,
Therapeutic effect of laparoscopy-assisted D2 radical gastrectomy in 106 patients with advanced gastric cancer
 JBUON 2013; 18(3): 689-694 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Therapeutic effect of laparoscopy-assisted D2 radical gastrectomy in
JBUON 2013; 18(3): 689-694 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Therapeutic effect of laparoscopy-assisted D2 radical gastrectomy in
Laparoscopic extended right hemicolectomy with D3
 Surgical Technique Page 1 of 11 Laparoscopic extended right hemicolectomy with D3 lymphadenectomy Weixian Hu, Jiabin Zheng, Yong Li Department of General Surgery, Guangdong General Hospital, Guangdong
Surgical Technique Page 1 of 11 Laparoscopic extended right hemicolectomy with D3 lymphadenectomy Weixian Hu, Jiabin Zheng, Yong Li Department of General Surgery, Guangdong General Hospital, Guangdong
Anatomy of the SMALL INTESTINE. Dr. Noman Ullah Wazir PMC
 Anatomy of the SMALL INTESTINE Dr. Noman Ullah Wazir PMC SMALL INTESTINE The small intestine, consists of the duodenum, jejunum, and illium. It extends from the pylorus to the ileocecal junction were the
Anatomy of the SMALL INTESTINE Dr. Noman Ullah Wazir PMC SMALL INTESTINE The small intestine, consists of the duodenum, jejunum, and illium. It extends from the pylorus to the ileocecal junction were the
Development of lymph node dissection in laparoscopic gastrectomy: safety and technical tips
 Review Article Development of lymph node dissection in laparoscopic gastrectomy: safety and technical tips Ru-Hong Tu, Ping Li, Jian-Wei Xie, Jia-Bin Wang, Jian-Xian Lin, Jun Lu, Qi-Yue Chen, Long-Long
Review Article Development of lymph node dissection in laparoscopic gastrectomy: safety and technical tips Ru-Hong Tu, Ping Li, Jian-Wei Xie, Jia-Bin Wang, Jian-Xian Lin, Jun Lu, Qi-Yue Chen, Long-Long
Cattell-Braasch maneuver combined with superior mesenteric artery first approach for resection of borderline resectable pancreatic cancer
 Masters of Surgery Page 1 of 5 Cattell-Braasch maneuver combined with superior mesenteric artery first approach for resection of borderline resectable pancreatic cancer Tingsong Yang 1, Fairweather Mark
Masters of Surgery Page 1 of 5 Cattell-Braasch maneuver combined with superior mesenteric artery first approach for resection of borderline resectable pancreatic cancer Tingsong Yang 1, Fairweather Mark
Pancreas & Biliary System. Dr. Vohra & Dr. Jamila
 Pancreas & Biliary System Dr. Vohra & Dr. Jamila 1 Objectives At the end of the lecture, the student should be able to describe the: Location, surface anatomy, parts, relations & peritoneal reflection
Pancreas & Biliary System Dr. Vohra & Dr. Jamila 1 Objectives At the end of the lecture, the student should be able to describe the: Location, surface anatomy, parts, relations & peritoneal reflection
Nasogastric tube. Stomach. Pylorus. Duodenum 1. Duodenum 2. Duodenum 3. Duodenum 4
 Esophagus Barium Swallow Stomach and Duodenum 4 year old Upper GI Nasogastric tube Stomach and Duodenum 4 year old Upper GI Nasogastric tube Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum 4
Esophagus Barium Swallow Stomach and Duodenum 4 year old Upper GI Nasogastric tube Stomach and Duodenum 4 year old Upper GI Nasogastric tube Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum 4
Li Yang, Diancai Zhang, Fengyuan Li, Xiang Ma. Introduction
 Original Article on Gastrointestinal Surgery Simultaneous laparoscopic distal gastrectomy (uncut Roux-en-Y anastomosis), right hemi-colectomy and radical rectectomy (Dixon) in a synchronous triple primary
Original Article on Gastrointestinal Surgery Simultaneous laparoscopic distal gastrectomy (uncut Roux-en-Y anastomosis), right hemi-colectomy and radical rectectomy (Dixon) in a synchronous triple primary
Pancreas Quizzes c. Both A and B a. Directly into the blood stream (not using ducts)
 Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
Totally laparoscopic distal gastrectomy reconstructed by Rouxen-Y with D2 lymphadenectomy and needle catheter jejunostomy for gastric cancer
 Masters of Gastrointestinal Surgery Totally laparoscopic distal gastrectomy reconstructed by Rouxen-Y with D2 lymphadenectomy and needle catheter jejunostomy for gastric cancer Xin Ye, Jian-Chun Yu, Wei-Ming
Masters of Gastrointestinal Surgery Totally laparoscopic distal gastrectomy reconstructed by Rouxen-Y with D2 lymphadenectomy and needle catheter jejunostomy for gastric cancer Xin Ye, Jian-Chun Yu, Wei-Ming
P resently, pancreaticoduodenectomy is widely accepted as the standard surgical procedure for patients with
 OPEN SUBJECT AREAS: CANCER THERAPY PANCREATIC CANCER GASTROINTESTINAL CANCER OUTCOMES RESEARCH Received 13 May 2013 Accepted 3 June 2013 Published 25 June 2013 Correspondence and requests for materials
OPEN SUBJECT AREAS: CANCER THERAPY PANCREATIC CANCER GASTROINTESTINAL CANCER OUTCOMES RESEARCH Received 13 May 2013 Accepted 3 June 2013 Published 25 June 2013 Correspondence and requests for materials
An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein
 J Gastrointest Surg (2007) 11:425 431 DOI 10.1007/s11605-007-0131-1 An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein Rory L. Smoot & John D. Christein &
J Gastrointest Surg (2007) 11:425 431 DOI 10.1007/s11605-007-0131-1 An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein Rory L. Smoot & John D. Christein &
BLOCK IV: OFFICIAL BODY PARTS LIST FOR ANTERIOR ABDOMINAL WALL AND ABDOMINAL CONTENTS
 BLOCK IV: OFFICIAL BODY PARTS LIST FOR ANTERIOR ABDOMINAL WALL AND ABDOMINAL CONTENTS External oblique muscle Muscular portion Aponeurotic portion Superficial inguinal ring Lateral (inferior) crus Medial
BLOCK IV: OFFICIAL BODY PARTS LIST FOR ANTERIOR ABDOMINAL WALL AND ABDOMINAL CONTENTS External oblique muscle Muscular portion Aponeurotic portion Superficial inguinal ring Lateral (inferior) crus Medial
ABDOMEN - GI. Duodenum
 TALA SALEH ABDOMEN - GI Duodenum - Notice the shape of the duodenum, it looks like capital G shape tube which extends from the pyloroduodenal junction to the duodenojejunal junction. - It is 10 inches
TALA SALEH ABDOMEN - GI Duodenum - Notice the shape of the duodenum, it looks like capital G shape tube which extends from the pyloroduodenal junction to the duodenojejunal junction. - It is 10 inches
Laparoscopic extended right hemicolectomy with D3 lymphadenectomy
 Surgical Technique Page 1 of 10 Laparoscopic extended right hemicolectomy with D3 lymphadenectomy Yong Li General Surgery, Guangdong General Hospital and Guangdong Academy of Medical Sciences, Guangzhou
Surgical Technique Page 1 of 10 Laparoscopic extended right hemicolectomy with D3 lymphadenectomy Yong Li General Surgery, Guangdong General Hospital and Guangdong Academy of Medical Sciences, Guangzhou
Outcomes of robotic surgery for pancreatic ductal adenocarcinoma
 Original Article Outcomes of robotic surgery for pancreatic ductal adenocarcinoma Qian Zhan 1,2, Xiaxing Deng 1,2, Yuanchi Weng 1,2, Jiabin Jin 1,2, Zhichong Wu 1,2, Hongwei Li 1,2, Baiyong Shen 1,2, Chenghong
Original Article Outcomes of robotic surgery for pancreatic ductal adenocarcinoma Qian Zhan 1,2, Xiaxing Deng 1,2, Yuanchi Weng 1,2, Jiabin Jin 1,2, Zhichong Wu 1,2, Hongwei Li 1,2, Baiyong Shen 1,2, Chenghong
Prognostic factors for survival of patients with ampullary carcinoma after local resection. Abstract
 UPPER GI ANZJSurg.com Prognostic factors for survival of patients with ampullary carcinoma after local resection Xiangqian Zhao, Jiahong Dong, Xiaoqiang Huang, Wenzhi Zhang and Kai Jiang Hospital and Institute
UPPER GI ANZJSurg.com Prognostic factors for survival of patients with ampullary carcinoma after local resection Xiangqian Zhao, Jiahong Dong, Xiaoqiang Huang, Wenzhi Zhang and Kai Jiang Hospital and Institute
SURGICAL TECHNIQUE. Radical treatment for left upper-lobe cancer via complete VATS. Jun Liu, Fei Cui, Shu-Ben Li. Introduction
 SURGICAL TECHNIQUE Radical treatment for left upper-lobe cancer via complete VATS Jun Liu, Fei Cui, Shu-Ben Li The First Affiliated Hospital of Guangzhou Medical College, Guangzhou, China ABSTRACT KEYWORDS
SURGICAL TECHNIQUE Radical treatment for left upper-lobe cancer via complete VATS Jun Liu, Fei Cui, Shu-Ben Li The First Affiliated Hospital of Guangzhou Medical College, Guangzhou, China ABSTRACT KEYWORDS
Intraabdominal Roux-en-Y reconstruction with a novel stapling technique after laparoscopic distal gastrectomy
 Gastric Cancer (2009) 12: 164 169 DOI 10.1007/s10120-009-0520-0 Technical note 2009 by International and Japanese Gastric Cancer Associations Intraabdominal Roux-en-Y reconstruction with a novel stapling
Gastric Cancer (2009) 12: 164 169 DOI 10.1007/s10120-009-0520-0 Technical note 2009 by International and Japanese Gastric Cancer Associations Intraabdominal Roux-en-Y reconstruction with a novel stapling
Multiple Primary Quiz
 Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
WORLD JOURNAL OF SURGICAL ONCOLOGY
 Wu et al. World Journal of Surgical Oncology 2014, 12:322 WORLD JOURNAL OF SURGICAL ONCOLOGY TECHNICAL INNOVATIONS Open Access Three-step method for systematic lymphadenectomy in gastric cancer surgery
Wu et al. World Journal of Surgical Oncology 2014, 12:322 WORLD JOURNAL OF SURGICAL ONCOLOGY TECHNICAL INNOVATIONS Open Access Three-step method for systematic lymphadenectomy in gastric cancer surgery
Small Plicae Circularis. Short Closely packed together. Sparse, completely absent at distal part Lymphoid Nodule
 Intestines Differences Between Jejunum and Ileum Types Jejunum Ileum Color Deeper red Paler pink Calibre Bigger Smaller Thickness of wall Thick and Heavy Thin and Lighter Vascularity Highly vascularised
Intestines Differences Between Jejunum and Ileum Types Jejunum Ileum Color Deeper red Paler pink Calibre Bigger Smaller Thickness of wall Thick and Heavy Thin and Lighter Vascularity Highly vascularised
Surgical Treatment for Carcinoma of the Ampulla of Vater and Residual Pancreatic Function before and after Pancreaticoduodenectomy*)
 Hiroshima Journal of Medical Sciences Vol. 32, No. 4, 455,-...,460, December, 1983 HIJM 32-68 455 Surgical Treatment for Carcinoma of the Ampulla of Vater and Residual Pancreatic Function before and after
Hiroshima Journal of Medical Sciences Vol. 32, No. 4, 455,-...,460, December, 1983 HIJM 32-68 455 Surgical Treatment for Carcinoma of the Ampulla of Vater and Residual Pancreatic Function before and after
Lab Monitor Images Dissection of the Abdominal Vasculature + Lower Digestive System
 Lab Monitor Images Dissection of the Abdominal Vasculature + Lower Digestive System Stomach & Duodenum Frontal (AP) View Nasogastric tube 2 1 3 4 Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum
Lab Monitor Images Dissection of the Abdominal Vasculature + Lower Digestive System Stomach & Duodenum Frontal (AP) View Nasogastric tube 2 1 3 4 Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum
Laparoscopic spleen-preserving complete splenic hilum lymphadenectomy for advanced proximal gastric cancer
 Review Article Page 1 of 5 Laparoscopic spleen-preserving complete splenic hilum lymphadenectomy for advanced proximal gastric cancer Wei Wang*, Wejun Xiong*, Qiqi Peng, Shanao Ye, Yansheng Zheng, Lijie
Review Article Page 1 of 5 Laparoscopic spleen-preserving complete splenic hilum lymphadenectomy for advanced proximal gastric cancer Wei Wang*, Wejun Xiong*, Qiqi Peng, Shanao Ye, Yansheng Zheng, Lijie
Technical considerations for the fully robotic pancreaticoduodenectomy
 Surgical Techniques on Pancreatic Surgery Technical considerations for the fully robotic pancreaticoduodenectomy Daniel Galvez, Rebecca Sorber, Ammar A. Javed, Jin He Department of Surgery, The Johns Hopkins
Surgical Techniques on Pancreatic Surgery Technical considerations for the fully robotic pancreaticoduodenectomy Daniel Galvez, Rebecca Sorber, Ammar A. Javed, Jin He Department of Surgery, The Johns Hopkins
ADVANCED LAPAROSCOPIC PANCREAS SURGERY A HANDS-ON WORKSHOP
 ADVANCED LAPAROSCOPIC PANCREAS SURGERY A HANDS-ON WORKSHOP 3-4 November 2017 at the AMC in Amsterdam Organizing committee: Mo Abu Hilal, Professor of Surgery at Southampton University Marc Besselink, Professor
ADVANCED LAPAROSCOPIC PANCREAS SURGERY A HANDS-ON WORKSHOP 3-4 November 2017 at the AMC in Amsterdam Organizing committee: Mo Abu Hilal, Professor of Surgery at Southampton University Marc Besselink, Professor
Robotic-assisted right upper lobectomy
 Robotic Thoracic Surgery Column Robotic-assisted right upper lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital, Shenyang 110015,
Robotic Thoracic Surgery Column Robotic-assisted right upper lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital, Shenyang 110015,
To describe the liver. To list main structures in porta hepatis.
 GI anatomy Lecture: 6 د. عصام طارق Objectives: To describe the liver. To list main structures in porta hepatis. To define portal system & portosystemic anastomosis. To list parts of biliary system. To
GI anatomy Lecture: 6 د. عصام طارق Objectives: To describe the liver. To list main structures in porta hepatis. To define portal system & portosystemic anastomosis. To list parts of biliary system. To
Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
 Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
Objectives. Intraoperative Consultation of the Whipple Resection Specimen. Pancreas Anatomy. Pancreatic ductal carcinoma 11/10/2014
 Intraoperative Consultation of the Whipple Resection Specimen Pathology Update Faculty of Medicine, University of Toronto November 15, 2014 John W. Wong, MD, FRCPC Department of Anatomical Pathology Sunnybrook
Intraoperative Consultation of the Whipple Resection Specimen Pathology Update Faculty of Medicine, University of Toronto November 15, 2014 John W. Wong, MD, FRCPC Department of Anatomical Pathology Sunnybrook
Imaging in gastric cancer
 Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
د. عصام طارق. Objectives:
 GI anatomy Lecture: 5 د. عصام طارق Objectives: To describe anatomy of stomach, duodenum & pancreas. To list their main relations. To define their blood & nerve supply. To list their lymph drainage. To
GI anatomy Lecture: 5 د. عصام طارق Objectives: To describe anatomy of stomach, duodenum & pancreas. To list their main relations. To define their blood & nerve supply. To list their lymph drainage. To
Dr. Zahiri. In the name of God
 Dr. Zahiri In the name of God small intestine = small bowel is the part of the gastrointestinal tract Boundaries: Pylorus Ileosecal junction Function: digestion and absorption of food It receives bile
Dr. Zahiri In the name of God small intestine = small bowel is the part of the gastrointestinal tract Boundaries: Pylorus Ileosecal junction Function: digestion and absorption of food It receives bile
Variations in portal and hepatic vein branching of the liver
 Yamagata Med J (ISSN 0288-030X)2015;33(2):115-121 DOI 10.15022/00003476 Variations in portal and hepatic vein branching of the liver Wataru Kimura, Tsuyoshi Fukumoto, Toshihiro Watanabe, Ichiro Hirai First
Yamagata Med J (ISSN 0288-030X)2015;33(2):115-121 DOI 10.15022/00003476 Variations in portal and hepatic vein branching of the liver Wataru Kimura, Tsuyoshi Fukumoto, Toshihiro Watanabe, Ichiro Hirai First
Surgical Treatment for Periampullary Carcinoma A Study of 129 Patients*)
 Hiroshima Journal of Medical Sciences Vol. 33, No. 2, 179,...183, June, 1984 HJM 33-24 179 Surgical Treatment for Periampullary Carcinoma A Study of 129 Patients*) Tsuneo TAN AKA, Motomu KODAMA, Rokuro
Hiroshima Journal of Medical Sciences Vol. 33, No. 2, 179,...183, June, 1984 HJM 33-24 179 Surgical Treatment for Periampullary Carcinoma A Study of 129 Patients*) Tsuneo TAN AKA, Motomu KODAMA, Rokuro
Outcomes associated with robotic approach to pancreatic resections
 Short Communication (Management of Foregut Malignancies and Hepatobiliary Tract and Pancreas Malignancies) Outcomes associated with robotic approach to pancreatic resections Caitlin Takahashi 1, Ravi Shridhar
Short Communication (Management of Foregut Malignancies and Hepatobiliary Tract and Pancreas Malignancies) Outcomes associated with robotic approach to pancreatic resections Caitlin Takahashi 1, Ravi Shridhar
-12. -Renad Habahbeh. -Dr Mohammad mohtasib
 -12 -Renad Habahbeh - -Dr Mohammad mohtasib The Gallbladder -The gallbladder has a body, a fundus (a rounded end), a neck, Hartmann s pouch before the neck and a cystic duct that meets the common hepatic
-12 -Renad Habahbeh - -Dr Mohammad mohtasib The Gallbladder -The gallbladder has a body, a fundus (a rounded end), a neck, Hartmann s pouch before the neck and a cystic duct that meets the common hepatic
Cholangiocarcinoma (Bile Duct Cancer)
 Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Original Article Anatomical characteristics of the fascial space during laparoscopic pancreaticoduodenectomy using cadaveric models
 Int J Clin Exp Med 2018;11(2):1254-1259 www.ijcem.com /ISSN:1940-5901/IJCEM0059780 Original Article Anatomical characteristics of the fascial space during laparoscopic pancreaticoduodenectomy using cadaveric
Int J Clin Exp Med 2018;11(2):1254-1259 www.ijcem.com /ISSN:1940-5901/IJCEM0059780 Original Article Anatomical characteristics of the fascial space during laparoscopic pancreaticoduodenectomy using cadaveric
Lecture 02 Anatomy of the LIVER
 Lecture 02 Anatomy of the LIVER BY Dr Farooq Khan Aurakzai Dated: 02.01.2018 Introduction to Liver Largest gland in the body. 2 nd largest organ of the body. Weight approximately 1500 gm, and is roughly
Lecture 02 Anatomy of the LIVER BY Dr Farooq Khan Aurakzai Dated: 02.01.2018 Introduction to Liver Largest gland in the body. 2 nd largest organ of the body. Weight approximately 1500 gm, and is roughly
Cover Page. The following handle holds various files of this Leiden University dissertation:
 Cover Page The following handle holds various files of this Leiden University dissertation: http://hdl.handle.net/1887/6119 Author: Spruit, E.N. Title: Increasing the efficiency of laparoscopic surgical
Cover Page The following handle holds various files of this Leiden University dissertation: http://hdl.handle.net/1887/6119 Author: Spruit, E.N. Title: Increasing the efficiency of laparoscopic surgical
Anatomy: Know Your Abdomen
 Anatomy: Know Your Abdomen Glossary Abdomen - part of the body below the thorax (chest cavity); separated by the diaphragm. Anterior - towards the front of the body. For example, the umbilicus is anterior
Anatomy: Know Your Abdomen Glossary Abdomen - part of the body below the thorax (chest cavity); separated by the diaphragm. Anterior - towards the front of the body. For example, the umbilicus is anterior
Case Scenario 1. Discharge Summary
 Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Original Article A novel approach to locate renal artery during retroperitoneal laparoendoscopic single-site radical nephrectomy
 Int J Clin Exp Med 2014;7(7):1752-1756 www.ijcem.com /ISSN:1940-5901/IJCEM0000870 Original Article during radical nephrectomy Lixin Shi, Wei Cai, Juan Dong, Jiangping Gao, Hongzhao Li, Shengkun Sun, Qiang
Int J Clin Exp Med 2014;7(7):1752-1756 www.ijcem.com /ISSN:1940-5901/IJCEM0000870 Original Article during radical nephrectomy Lixin Shi, Wei Cai, Juan Dong, Jiangping Gao, Hongzhao Li, Shengkun Sun, Qiang
Fat Tissue Infiltration into the Pancreas Parenchyme and Its Effect on the Result of Surgery
 Korean Journal of HBP Surgery Vol. 15,. 2, May 2011 O riginal Article Fat Tissue Infiltration into the Pancreas Parenchyme and Its Effect on the Result of Surgery Purpose: In Korea, there are few reports
Korean Journal of HBP Surgery Vol. 15,. 2, May 2011 O riginal Article Fat Tissue Infiltration into the Pancreas Parenchyme and Its Effect on the Result of Surgery Purpose: In Korea, there are few reports
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Appendix 5. EFSUMB Newsletter. Gastroenterological Ultrasound
 EFSUMB Newsletter 87 Examinations should encompass the full range of pathological conditions listed below A log book listing the types of examinations undertaken should be kept Training should usually
EFSUMB Newsletter 87 Examinations should encompass the full range of pathological conditions listed below A log book listing the types of examinations undertaken should be kept Training should usually
Laparoscopic total mesorectal excision (TME) with electric hook for rectal cancer
 Technical Note Page 1 of 8 Laparoscopic total mesorectal excision (TME) with electric hook for rectal cancer Gong Chen, Rong-Xin Zhang, Zhi-Tao Xiao Department of Colorectal Surgery, Sun Yat-sen University
Technical Note Page 1 of 8 Laparoscopic total mesorectal excision (TME) with electric hook for rectal cancer Gong Chen, Rong-Xin Zhang, Zhi-Tao Xiao Department of Colorectal Surgery, Sun Yat-sen University
Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition
 22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
Pancreas and Biliary System
 Pancreas and Biliary System Please view our Editing File before studying this lecture to check for any changes. Color Code Important Doctors Notes Notes/Extra explanation Objectives At the end of the lecture,
Pancreas and Biliary System Please view our Editing File before studying this lecture to check for any changes. Color Code Important Doctors Notes Notes/Extra explanation Objectives At the end of the lecture,
Tools of the Gastroenterologist: Introduction to GI Endoscopy
 Tools of the Gastroenterologist: Introduction to GI Endoscopy Objectives Endoscopy Upper endoscopy Colonoscopy Endoscopic retrograde cholangiopancreatography (ERCP) Endoscopic ultrasound (EUS) Endoscopic
Tools of the Gastroenterologist: Introduction to GI Endoscopy Objectives Endoscopy Upper endoscopy Colonoscopy Endoscopic retrograde cholangiopancreatography (ERCP) Endoscopic ultrasound (EUS) Endoscopic
Surface Anatomy. Location Shape Weight Role of Five Surfaces Borders Fissures Lobes Peritoneal Lig
 The Liver Functions Bile production and secretion Detoxification Storage of glycogen Protein synthesis Production of heparin and bile pigments Erythropoiesis (in fetus) Surface Anatomy Location Shape Weight
The Liver Functions Bile production and secretion Detoxification Storage of glycogen Protein synthesis Production of heparin and bile pigments Erythropoiesis (in fetus) Surface Anatomy Location Shape Weight
Robotic-assisted right inferior lobectomy
 Robotic Thoracic Surgery Column Page 1 of 6 Robotic-assisted right inferior lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital,
Robotic Thoracic Surgery Column Page 1 of 6 Robotic-assisted right inferior lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital,
Radical nerve dissection for the carcinoma of head of pancreas: report of 30 cases
 Original Article Radical nerve dissection for the carcinoma of head of pancreas: report of 30 cases Qing Lin, Langping Tan, Yu Zhou, Quanbo Zhou, Rufu Chen Department of Biliary and Pancreatic Surgery,
Original Article Radical nerve dissection for the carcinoma of head of pancreas: report of 30 cases Qing Lin, Langping Tan, Yu Zhou, Quanbo Zhou, Rufu Chen Department of Biliary and Pancreatic Surgery,
Citation American Journal of Surgery, 196(5)
 NAOSITE: Nagasaki University's Ac Title Author(s) Multifocal branch-duct pancreatic i neoplasms Tajima, Yoshitsugu; Kuroki, Tamotsu Amane; Adachi, Tomohiko; Mishima, T Kanematsu, Takashi Citation American
NAOSITE: Nagasaki University's Ac Title Author(s) Multifocal branch-duct pancreatic i neoplasms Tajima, Yoshitsugu; Kuroki, Tamotsu Amane; Adachi, Tomohiko; Mishima, T Kanematsu, Takashi Citation American
Pancreas-Preserving Total Duodenectomy
 How I do it Dig Surg 1998;15:398 403 Gregory G. Tsiotos Michael G. Sarr Division of Gastroenterologic and General Surgery, Department of Surgery, Mayo Clinic, Rochester, Minn., USA Pancreas-Preserving
How I do it Dig Surg 1998;15:398 403 Gregory G. Tsiotos Michael G. Sarr Division of Gastroenterologic and General Surgery, Department of Surgery, Mayo Clinic, Rochester, Minn., USA Pancreas-Preserving
To evaluate 792 patients with malignant biliary obstruction after inner-stents drainage procedure
 To evaluate 792 patients with malignant biliary obstruction after inner-stents drainage procedure Zhu wei, Zhang xiquan, Pan xiaolin, Dong ge, Guo feng. The Cardio-Interventional Center, The 148th PLA
To evaluate 792 patients with malignant biliary obstruction after inner-stents drainage procedure Zhu wei, Zhang xiquan, Pan xiaolin, Dong ge, Guo feng. The Cardio-Interventional Center, The 148th PLA
Left-sided approach for suprapancreatic lymph node dissection in laparoscopy-assisted distal gastrectomy without duodenal transection
 Gastric Cancer (2009) 12: 106 112 DOI 10.1007/s10120-009-0508-9 Technical note 2009 by International and Japanese Gastric Cancer Associations Left-sided approach for suprapancreatic lymph node dissection
Gastric Cancer (2009) 12: 106 112 DOI 10.1007/s10120-009-0508-9 Technical note 2009 by International and Japanese Gastric Cancer Associations Left-sided approach for suprapancreatic lymph node dissection
Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 14
 Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 14 Contents 14. Neuroendocrine Tumours 161 14.1. Diagnostic algorithm
Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 14 Contents 14. Neuroendocrine Tumours 161 14.1. Diagnostic algorithm
pitfall Table 1 4 disorientation pitfall pitfall Table 1 Tel:
 11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
PANCREAS DUCTAL ADENOCARCINOMA PDAC
 CONTENTS PANCREAS DUCTAL ADENOCARCINOMA PDAC I. What is the pancreas? II. III. IV. What is pancreas cancer? What is the epidemiology of Pancreatic Ductal Adenocarcinoma (PDAC)? What are the risk factors
CONTENTS PANCREAS DUCTAL ADENOCARCINOMA PDAC I. What is the pancreas? II. III. IV. What is pancreas cancer? What is the epidemiology of Pancreatic Ductal Adenocarcinoma (PDAC)? What are the risk factors
Original Article Hand-assisted laparoscopic versus open surgery radical gastrectomy for advanced distal gastric cancer: a prospective randomized study
 Int J Clin Exp Med 2017;10(3):5001-5010 www.ijcem.com /ISSN:1940-5901/IJCEM0042542 Original Article Hand-assisted laparoscopic versus open surgery radical gastrectomy for advanced distal gastric cancer:
Int J Clin Exp Med 2017;10(3):5001-5010 www.ijcem.com /ISSN:1940-5901/IJCEM0042542 Original Article Hand-assisted laparoscopic versus open surgery radical gastrectomy for advanced distal gastric cancer:
Surgical Management of CBD Injury Jin Seok Heo
 Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
MATERIALS AND METHODS Patients
 Yonago Acta medica 216;59:232 236 Original Article Usefulness of T-Shaped Gauze for Precise Dissection of Supra-Pancreatic Lymph Nodes and for Reduced Postoperative Pancreatic Fistula in Patients Undergoing
Yonago Acta medica 216;59:232 236 Original Article Usefulness of T-Shaped Gauze for Precise Dissection of Supra-Pancreatic Lymph Nodes and for Reduced Postoperative Pancreatic Fistula in Patients Undergoing
Yurong Liang, Jing Wang, Xianjie Shi, Jiahong Dong, and Wanqing Gu. 1. Introduction. 2. Patients and Methods
 Gastroenterology Research and Practice Volume 2015, Article ID 934565, 4 pages http://dx.doi.org/10.1155/2015/934565 Clinical Study Application of a Gastroduodenal Artery Graft for Reconstruction of the
Gastroenterology Research and Practice Volume 2015, Article ID 934565, 4 pages http://dx.doi.org/10.1155/2015/934565 Clinical Study Application of a Gastroduodenal Artery Graft for Reconstruction of the
Three-dimensional computed tomography simulation for laparoscopic lymph node dissection in the treatment of proximal gastric cancer
 Review Article Three-dimensional computed tomography simulation for laparoscopic lymph node dissection in the treatment of proximal gastric cancer Hideki Sunagawa, Takahiro Kinoshita Gastric Surgery Division,
Review Article Three-dimensional computed tomography simulation for laparoscopic lymph node dissection in the treatment of proximal gastric cancer Hideki Sunagawa, Takahiro Kinoshita Gastric Surgery Division,
Laparoscopic Subtotal Gastrectomy for Gastric Cancer
 SCIENTIFIC PAPER Laparoscopic Subtotal Gastrectomy for Gastric Cancer Danny Rosin, MD, Yuri Goldes, MD, Barak Bar Zakai, MD, Moshe Shabtai, MD, Amram Ayalon, MD, Oded Zmora, MD ABSTRACT Background: The
SCIENTIFIC PAPER Laparoscopic Subtotal Gastrectomy for Gastric Cancer Danny Rosin, MD, Yuri Goldes, MD, Barak Bar Zakai, MD, Moshe Shabtai, MD, Amram Ayalon, MD, Oded Zmora, MD ABSTRACT Background: The
Topics: Staging and treatment for pancreatic cancer. Staging systems for pancreatic cancer: Differences between the Japanese and UICC systems
 M. J Hep Kobari Bil Pancr and S. Surg Matsuno: (1998) Staging 5:121 127 system for pancreatic cancer 121 Topics: Staging and treatment for pancreatic cancer Staging systems for pancreatic cancer: Differences
M. J Hep Kobari Bil Pancr and S. Surg Matsuno: (1998) Staging 5:121 127 system for pancreatic cancer 121 Topics: Staging and treatment for pancreatic cancer Staging systems for pancreatic cancer: Differences
Development of pancreas and Small Intestine. ANATOMY DEPARTMENT DR.SANAA AL-AlSHAARAWY DR.ESSAM Eldin Salama
 Development of pancreas and Small Intestine ANATOMY DEPARTMENT DR.SANAA AL-AlSHAARAWY DR.ESSAM Eldin Salama OBJECTIVES At the end of the lecture, the students should be able to : Describe the development
Development of pancreas and Small Intestine ANATOMY DEPARTMENT DR.SANAA AL-AlSHAARAWY DR.ESSAM Eldin Salama OBJECTIVES At the end of the lecture, the students should be able to : Describe the development
Robotic thoracic surgery: S 1+2 segmentectomy of left upper lobe
 Case Report Page 1 of 5 Robotic thoracic surgery: S 1+2 segmentectomy of left upper lobe Hailei Du, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Han Wu, Dingpei Han, Kai Chen, Jie Xiang, Hecheng
Case Report Page 1 of 5 Robotic thoracic surgery: S 1+2 segmentectomy of left upper lobe Hailei Du, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Han Wu, Dingpei Han, Kai Chen, Jie Xiang, Hecheng
Laparoscopic resection of hilar cholangiocarcinoma
 TECHNICAL ADVANCE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/10.4174/astr.2015.89.4.228 Annals of Surgical Treatment and Research Laparoscopic resection of hilar cholangiocarcinoma Woohyung Lee,
TECHNICAL ADVANCE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/10.4174/astr.2015.89.4.228 Annals of Surgical Treatment and Research Laparoscopic resection of hilar cholangiocarcinoma Woohyung Lee,
The peritoneum. Prof. Oluwadiya KS, MBBS, FMCS(Orthop) Website:
 The peritoneum Prof. Oluwadiya KS, MBBS, FMCS(Orthop) Website: http://oluwadiya.com The peritoneum Serous membrane that lines the abdominopelvic cavity and invests the viscera The largest serous membrane
The peritoneum Prof. Oluwadiya KS, MBBS, FMCS(Orthop) Website: http://oluwadiya.com The peritoneum Serous membrane that lines the abdominopelvic cavity and invests the viscera The largest serous membrane
Single-Incision Laparoscopic Surgery Versus Standard Laparoscopic Surgery for Unroofing of Hepatic Cysts
 SCIENTIFIC PAPER Single-Incision Laparoscopic Surgery Versus Standard Laparoscopic Surgery for of s Shuodong Wu, MD, Yongnan Li, MM, Yu Tian, MD, Min Li, MM ABSTRACT Background and Objectives: The aim
SCIENTIFIC PAPER Single-Incision Laparoscopic Surgery Versus Standard Laparoscopic Surgery for of s Shuodong Wu, MD, Yongnan Li, MM, Yu Tian, MD, Min Li, MM ABSTRACT Background and Objectives: The aim
Classification of nodal stations in gastric cancer
 Review Article Classification of nodal stations in gastric cancer Fausto Rosa 1, Guido Costamagna 2, Giovanni Battista Doglietto 1, Sergio Alfieri 1 1 Department of Digestive Surgery, 2 Department of Digestive
Review Article Classification of nodal stations in gastric cancer Fausto Rosa 1, Guido Costamagna 2, Giovanni Battista Doglietto 1, Sergio Alfieri 1 1 Department of Digestive Surgery, 2 Department of Digestive
Tornado Roux-en-Y anastomosis in laparoscopy-assisted distal gastrectomy
 Gastric Cancer (2008) 11: 181 185 DOI 10.1007/s10120-008-0474-7 Technical note 2008 by International and Japanese Gastric Cancer Associations Tornado Roux-en-Y anastomosis in laparoscopy-assisted distal
Gastric Cancer (2008) 11: 181 185 DOI 10.1007/s10120-008-0474-7 Technical note 2008 by International and Japanese Gastric Cancer Associations Tornado Roux-en-Y anastomosis in laparoscopy-assisted distal
General Surgery PURPLE SERVICE MUHC-RVH Site
 Preamble HPB is a clinical teaching unit with several different vocations: It regroups all solid organ Transplantation as well as most advanced Hepatobiliary and Pancreatic clinical activities performed
Preamble HPB is a clinical teaching unit with several different vocations: It regroups all solid organ Transplantation as well as most advanced Hepatobiliary and Pancreatic clinical activities performed
Pancreas Case Scenario #1
 Pancreas Case Scenario #1 An 85 year old white female presented to her primary care physician with increasing abdominal pain. On 8/19 she had a CT scan of the abdomen and pelvis. This showed a 4.6 cm mass
Pancreas Case Scenario #1 An 85 year old white female presented to her primary care physician with increasing abdominal pain. On 8/19 she had a CT scan of the abdomen and pelvis. This showed a 4.6 cm mass
Robotic-Assisted Pancreatoduodenectomy
 Curr Surg Rep (2013) 1:98 105 DOI 10.1007/s40137-013-0017-y MINIMALLY INVASIVE PANCREATIC SURGERY (MG HOUSE, SECTION EDITOR) Robotic-Assisted Pancreatoduodenectomy Mohammad Khreiss Herbert J. Zeh Brian
Curr Surg Rep (2013) 1:98 105 DOI 10.1007/s40137-013-0017-y MINIMALLY INVASIVE PANCREATIC SURGERY (MG HOUSE, SECTION EDITOR) Robotic-Assisted Pancreatoduodenectomy Mohammad Khreiss Herbert J. Zeh Brian
BY DR NOMAN ULLAH WAZIR
 BY DR NOMAN ULLAH WAZIR The stomach (from ancient Greek word stomachos, stoma means mouth) is a muscular, hollow and the most dilated part of the GIT. It starts from the point where esophagus ends. It
BY DR NOMAN ULLAH WAZIR The stomach (from ancient Greek word stomachos, stoma means mouth) is a muscular, hollow and the most dilated part of the GIT. It starts from the point where esophagus ends. It
