Outcomes of robotic surgery for pancreatic ductal adenocarcinoma
|
|
|
- Charleen Lewis
- 6 years ago
- Views:
Transcription
1 Original Article Outcomes of robotic surgery for pancreatic ductal adenocarcinoma Qian Zhan 1,2, Xiaxing Deng 1,2, Yuanchi Weng 1,2, Jiabin Jin 1,2, Zhichong Wu 1,2, Hongwei Li 1,2, Baiyong Shen 1,2, Chenghong Peng 1,2 1 Department of General Surgery, Ruijin Hospital, Shanghai , China; 2 Research Institute of Pancreatic Diseases, School of medicine, Shanghai Jiaotong University, Shanghai , China Correspondence to: Chenghong Peng, MD, PhD. Department of General Surgery, Ruijin Hospital, Shanghai , China; Research Institute of Pancreatic Diseases, School of Medicine, Shanghai Jiaotong University, 197 Ruijin Er Road, Shanghai , China. chhpeng@yeah.net. Authors introduction: Qian Zhan, female, who was born in Sept, She studied in the Shanghai Second Medical University during 1998 to She majored in Clinical Medicine, and earned her master degree in In 2005, she went to the Beaujon Hospital of Paris 7th University in France, as a foreign intern. Later, she came to postgraduate work and residencies in the general surgery department of Shanghai Ruijin Hospital. Her clinical work is focused on multidisciplinary especially postoperative management for the patients with pancreatic cancer. In addition, she is a lead researcher in the pancreatic cancer group for nano based drug delivery systems. Chenghong Peng, male, who was born in Apr, He worked in the 2nd Affiliated Hospital of Zhejiang University School of Medicine during 1989 to In 2002, Chenghong Peng came to Shanghai Ruijin Hospital and began to take charge of general surgery department. As a pioneer in the hepatobiliopancreatic field, Chenghong Peng devoted himself in the basic and clinical research of pancreatic tumors. He brings forth new ideas by creating Pancreatic multiple treatment collaborating groups, which integrate the advantages of gastroenterology department, endoscopy department, radiology department, pathology department and SICU. He constantly strives for excellence in pancreatic surgery. In the previous five years, he performed more than 300 cases of pancreatectomy each year, and has accomplished more than 2,000 cases of pancreatectomy altogether, among which the resectable rate is 74%. Besides, he is also committed to laparoscopic surgery and robotic surgery. He has achieved more than 200 laparoscopic hepatectomies, 150 laparoscopic pancreatectomies and 500 robotic hepatobiliopancreatic surgeries (350 robotic pancreatic surgeries included), which keeps leading position in China. In 2011, Chenghong Peng has won the first prize in 3rd international congress of CRSA, which marked that our achievement in robotic surgery was recognized by oversea peers. Qian Zhan Chenghong Peng
2 Chinese Journal of Cancer Research, Vol 27, No 6 December Background: To explore the effectiveness, safety, and efficacy of the robot-assisted surgery in the radical resection of pancreatic ductal adenocarcinoma (PDAC). Methods: The clinical data of 72 patients with PDAC who underwent radical resection using the da Vinci Surgical System from April 2010 to December 2014 were retrospectively analyzed. Results: Among these 72 patients, three were converted to conventional laparotomy due to the vascular invasion or due to the difficulties in tissue isolation from the surrounding organs. Among 39 patients who underwent the pancreatoduodenectomy, the average operative time was 395.3±118.8 min, and the mean intra-operative blood loss was 447.3±269.9 ml. Among 31 patients who underwent the distal pancreatectomy (DP), the average operative time was 185.5±74.1 min, and the mean intra-operative blood loss was 267.1±305.3 ml. In two patients who received the middle pancreatectomy (MP), the average operative time was 225 min and mean intra-operative blood loss was 100 ml. Among all the 72 patients, an average of 4.2±2.6 lymph nodes were dissected, with an average hospital stay of 22.6±10.7 days. Complications were observed in 18 patients, which included pancreatic fistula (n=11), bile leak (n=5), anastomotic bleeding (n=2), pancreatic fistula complicated with portal vein thrombosis (n=1), and anastomotic bleeding complicated with acute renal failure (n=1). Except that one patient died due to post-operative bleeding and acute renal failure, all the other patients were cured after conservative treatment. These 72 patients were followed for 1-45 (15.6±5.8) months, during which 10 patients died. Eleven patients suffered from recurrence or metastasis, among which 6 had local recurrence, 4 had liver metastasis, and 1 had ascites accompnaied with incision site tumor metastasis. Conclusions: Radical resection of PDAC by robotic surgical system is safe and feasible. It has less surgical trauma and enables faster post-operative recovery, and therefore can achieve the lymph node dissection scope and tumor resection margin required by the standards of radical resection for pancreatic cancer. Nevertheless, its long-term efficacy requires further validation. Keywords: Robot-assisted surgery; radical resection; pancreatic ductal adenocarcinoma (PDAC) Submitted Jan 13, Accepted for publication May 08, doi: /j.issn View this article at: Introduction Pancreatic ductal adenocarcinoma (PDAC) is one of the most malignant digestive tumors due to its high potentials of local invasion and distant metastasis. Surgical resection is the only hope for achieving long-term survival in PDAC patients. Robot-assisted surgery is a novel minimally invasive technique that has been applied in the radical treatment of pancreatic diseases. For the highly malignant PDAC, few studies have explored its role due to the large surgical challenges, high technical requirements, and difficulties in the radical treatment for this malignancy (1-4). In our center, a total of 72 PDAC patients underwent the radical resection using the robotic surgical system between April 2010 and December 2014, and the related data are summarized as follows. Patients and methods Clinical data Seventy-two patients entered the final analysis, among whom there were 49 men and 23 women, with an average age of 62.3±6.5 years. The clinical manifestations included left upper abdominal pain (n=22), jaundice (n=8), progressive emaciation (n=4), and fatigue and anorexia (n=5). The remaining patients had no obvious symptom. The pre-operative imaging detected lesions in the head (n=39; including 3 in the uncinate process), body (n=13), or tail of the pancreas (n=20). The pre-operative CA199 level increased in 52 patients ( ,065.8 U/L; mean: 2,259.3 U/L). Seventeen patients also had diabetes and 18 were accompanied with hypertension. Two patients had a previous history of pancreatitis, and two patients had
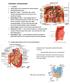
3 606 Zhan et al. Robotic surgery for PDAC heart disease (premature ventricular beat and right bundle branch block, respectively). All patients signed the informed consent before the surgery. The case selection criteria were as follows: the general condition was good and without a history of severe heart and/or lung diseases; could tolerate the general anesthesia; the lesion was solitary and isolated; no local infiltration or distant metastasis was detected on medical imaging; and, there was no history of abdominal operation. Since Buchs et al. (5) had documented that age was not a contraindication of robot-assisted pancreatic surgery, no specific age limits were set in our series. The exclusion criteria were as follows: with any contraindication of open pancreatic surgeries; could not tolerate the pneumoperitoneum; with tight abdominal adhesions; the tumor was too large and had invaded the adjacent organs and large blood vessels, which prevented the laparoscopic operations; and pre-operatively judged as in the American Joint Committee on Cancer (AJCC) stage III or IV. Figure 1 Port set-up for robot-assisted pancreatic resection. C, camera port (12 mm); R1, left robotic instrument port (12 mm); R2, right robotic instrument port (8 mm); R3, third robotic instrument port (8 mm); A, assistant port (12 mm). Surgical techniques The operation was performed using the da Vinci Model S Surgical System (Intuitive Surgical, Sunnyvale, CA, USA). After tracheal intubation under general anesthesia, the robot operating arms were installed over the patient s head. The patient s body position was determined based on the specific surgical procedures. A carbon dioxide (CO 2 ) pneumoperitoneum up to 15 mmhg pressure was established. The laparoscope was inserted to explore the abdominal cavity to further identify whether there was any surgical contraindication. If there was no tight abdominal adhesion or diffuse tumor invasion/metastasis, the surgical instruments were then inserted using the 5-port method (Figure 1). The operating arms were further installed. The intra-operative lymph node dissection was performed according to the 5th criteria published by Japan Pancreas Society in A specimen bag was inserted via the puncture port to harvest the specimen. If the specimen was too large, the puncture port might be properly enlarged. One or two abdominal drainage tubes were placed after the surgery. Pancreatoduodenectomy (PD) Open the gastrocolic ligament to enter the lesser sac. Isolate the hepatic flexure colon to expose the duodenum and superior mesenteric vein (SMV) for establishing the Kocher incision. Thoroughly isolate the duodenum and Figure 2 Dissection of the hepatic hilum. CBD, common bile duct; HA, hepatic artery; PV, portal vein. pancreatic uncinate, and meanwhile dissect the lymph node stations 13 and 17. Dissect the hepatoduodenal ligament and then the gallbladder; then, the common bile duct was transected at the cystic duct level, and the surrounding lymph nodes were dissected. Dissect the hepatic artery, isolate and ligate the gastroduodenal artery, and dissect the lymph nodes around the hepatic artery and near the portal vein (Figure 2). After the pancreas was divided using the ultrasonic scalpel, the uncinate was isolated upwards along the SMV and the jejunum was divided under the Treitz ligament using the Endo-GIA ( mm; Johnson & Johnson, USA) (Figure 3). After the dissection of the lymph node stations 8 and 9, the main pancreatic duct was found at the pancreatic stump and then the supporting tube was placed. Pancreaticojejunostomy, hepaticojejunostomy and gastrojejunostomy were performed using the robotic devices. The specimen was divided and harvested.
4 Chinese Journal of Cancer Research, Vol 27, No 6 December Figure 3 Dissection of the uncinate process. SMV, superior mesenteric vein; SMA, superior mesenteric artery. Figure 5 The residual pancreatic surface after DP. AA, abdominal aorta; HA, hepatic artery; PV, portal vein; SMV, superior mesenteric vein; DP, distal pancreatectomy. stomach using the 4-0 Vicryl sutures (interrupted sutures for gastric mucosa, with interrupted fixation at the outer ring) (Figure 4). Double-channel drainage tubes were placed near the pancreaticogastric anastomosis and pancreatic stump (at the head of pancreas). Figure 4 End-to-side pancreaticogastric anastomosis. Double-channel drainage tubes were placed near the pancreaticoenteric and biliary-enteric anastomoses. Middle pancreatectomy (MP) Open the gastrocolic ligament to expose the middle section of pancreas. After the tumor was localized, a tunnel behind the pancreas was created by dissecting the upper and lower edges of the pancreas. At the head of the pancreas 1cm away from the tumor, the pancreas was transected using the ultrasonic scalpel or Endo-GIA ( mm; Johnson & Johnson, USA). The pancreatic remnant was sutured using the 4-0 Vicryl sutures to prevent any pancreatic fistula. At the tail of the pancreas 2 cm away from the tumor, the pancreas was transected with an ultrasonic scalpel or electrocautery hook. After the main pancreatic duct was found, a proper pancreatic duct-supporting tube was placed. A pancreatic duct-to-gastric mucosa anastomosis was created at the posterior gastric wall near the greater curvature of Distal pancreatectomy (DP) Open the gastrocolic ligament using the ultrasonic scalpel to expose the pancreas. Dissect the upper and lower edges of the normal pancreatic tissue at the right side of the mass to establish a tunnel behind the pancreas. Then, hang upward the pancreatic tissue to expand the postpancreatic tunnel. The pancreas was divided about 2 cm away from the right side of the mass using the Endo-GIA ( mm; Johnson & Johnson, USA), followed by the clamping of the splenic artery and vein using two hem-olok clips. The post-pancreatic gap was dissected leftwards to dissociate the pancreatic tail, splenic artery and vein, and spleen; meanwhile, the lymph node stations 10, 11, and 18 were also dissected. After the specimen was isolated, the lymph node stations 9, 8a, 14, and 16 were dissected; then, the specimen was harvested. After the abdominal cavity was rinsed, the double- and single-channel drainage tubes were placed at the residual pancreas and splenic fossa, respectively (Figure 5). Results There were three patients converted to conventional laparotomy. Of these three patients, two were scheduled for robotic PD. One patient, however, was converted to laparotomy because the tumor was too large and the tissue
5 608 Zhan et al. Robotic surgery for PDAC Table 1 Patient characteristics and surgical data Variables PD (n=39) MP (n=2) DP (n=31) Total (n=72) Age 60.3± ± ±6.5 Gender (male/female) 29/10 1/1 19/12 49/23 Operative time (min) 395.3± ± ±143.8 Intra-operative blood loss (ml) 447.3± ± ±297.5 Blood transfusion rate (%) 38.5 (15/39) 0 (0/2) 3.2 (1/31) 22.2 (16/72) Conversion rate (%) 5.1 (2/39) 0 (0/2) 3.2 (1/31) 4.2 (3/72) Morbidities (%) 20.5 (8/39) 50.0 (1/2) 29.0 (9/31) 25.0 (18/72) Reoperation rate (%) 0 (0/39) 0 (0/2) 6.5 (2/31) 2.8 (2/72) Post-operative hospital stay (days) 23.2± ± ±10.7 Mortality (%) 0 (0/39) 0 (0/2) 3.2 (1/31) 1.4 (1/72) Tumor size (cm) 2.3± ± ±1.4 Lymph nodes resected 4.0± ± ±2.6 PD, pancreatoduodenectomy; MP, middle pancreatectomy; DP, distal pancreatectomy. isolation was extremely difficult. In another patient, PD + SMA reconstruction were performed because the tumor invaded the SMA. In the remaining patient who was scheduled for robotic DP, conversion was performed due to the tumor invasion of the transverse colon, left adrenal gland and stomach wall. Robot-assisted surgery in the radical resection of PDAC was successfully performed in the remaining 69 patients, including 37 cases of PD, 2 cases of MP, and 30 cases of DP. In one patient who received DP, the intra-operative exploration showed that the tumor had invaded the SMV; then, reconstruction of the SMV was performed under the robotic devices. Complications were observed in 18 patients (25.0%), which included pancreatic fistula (n=11), bile leak (n=5), anastomotic bleeding (n=2), pancreatic fistula complicated with portal vein thrombosis (n=1), and anastomotic bleeding complicated with acute renal failure (n=1). Except that one patient was died of postoperative anastomotic bleeding accompanied with acute renal failure and one patient further underwent DSA embolization after anastomotic bleeding, all the remaining patients were smoothly discharged after conservative treatment (Table 1). These 72 patients were followed up for 1-45 months (mean, 15.6±5.8 months), with a median overall survival (OS) of 19.6 months. Nineteen patients received routine chemotherapy after the surgery. Fifty-one of the 72 patients are currently alive and well without recurrence. Ten patients died. Eleven patients suffered from recurrence or metastasis, among which 6 had local recurrence, 4 had liver metastasis, and 1 had ascites accompanied with incision site tumor metastasis. The disease-free survival (DFS) was 3-18 months (median, 9.6 months). Discussion The pancreas has a complex anatomical structure where the organ is located deeply and has tight connections with the surrounding vessels, making the surgery particularly difficult. Even worse, the PDAC has increased local invasion and distant metastasis in its early stages, posing huge challenge to the surgeons. Thus, the minimally invasive surgery for pancreatic cancer develops slowly. There were few reports on the laparoscopic surgery for pancreatic cancer, which were often accompanied with high rate of conversion to open surgery and high incidence of pancreatic fistula (6-8). The past decade has witnessed the increasingly wider application of robot-assisted laparoscopic surgery (9). Along with the technical development, the robot-assisted surgery for pancreatic diseases has attracted more attention (9). In 2003, Giulianotti et al. completed the first robot-assisted laparoscopic pancreatic resection (10). Since then, more investigations have been made on the applications of various surgical resection procedures for pancreas using the robotic surgical systems (11-13). Today, the main controversies on the role of minimally invasive surgery for pancreatic malignancies include the effectiveness of radical resection of tumor and the real benefit of patients from the surgery. Therefore, there are
6 Chinese Journal of Cancer Research, Vol 27, No 6 December even higher requirements on the surgical techniques, which include: (I) the pancreatic cancer is highly malignant and can easily penetrate the pancreatic capsule and thus invade the surrounding tissues/organs, making the resection of the mass particularly difficult; (II) lymphatic metastasis is common in patients with pancreatic cancer, which decides the scope and extent of lymph node dissection and has a fundamental impact on the outcomes of the radical treatment for pancreatic cancer; and (III) for pancreatic cancer patients with portal vein and/or SMV involvement, vascular reconstruction may be required to ensure a good therapeutic effectiveness. Compared with the conventional laparoscopic surgeries, the robot-assisted surgeries have many advantages such as smaller incisions, faster post-operative recovery, and less trauma and stress response; also, the robotic system can display clear 3-D images, provide Endo Wrist TM wristsimulating devices with seven degrees of freedom, and enable tremor filtration, which provides better solutions for the division of pancreas uncinate process, fine separation between pancreatic mass and surrounding tissues, retroperitoneal lymph node dissection, skeletalization of the structures inside the hepatoduodenal ligament, and reconstruction of major vessles (e.g., portal vein). (I) When the robotic surgical system is applied for the radical resection of pancreatic cancer, an upward visual field may be adopted, via which the fine dissection of the tissues at the pancreatic head and neck can be performed at the vessel-free zone among the lower edge of the duodenum, the upper edge of pancreas, the SMV, and the neck of pancreas under direct vision, so as to create a portal veinpancreas tunnel (14). Thus, the resection of the mass at the pancreatic head/neck can achieve the meeting of the upward and downward operations, which is particularly useful in the division of the uncinate process when a tumor in the uncinate process compresses the vessels; (II) when the robotic system is applied for PD, MP, and DP for the patients with pancreatic cancer, the operator can observe upwardly the post-pancreatic tunnel created during mass resection; meanwhile, the lymph nodes behind the pancreas can be clearly visible in the surgical field. Thus, it increases the completeness of lymph node dissection and increases the rate of R0 resection (compared with the laparoscopic surgeries) (15). Compared with the laparoscopic radical resection of pancreatic cancer, the robotic surgical system enables a finer lymph node dissection, which lowers the risk of vascular injury and uncontrollable bleeding; in particular, it improves the safety during the removal of lymph node stations 7, 8, 9, 11, 12, 14, and 16. In our current study, the lymph nodes were dissected according to the standard radical treatment procedure for pancreatic cancer, during which fewer lymph nodes were removed, which might be explained by the fact that lymph node dissection was not performed after the en bloc resection of the specimen; (III) also in our study, intra-operative exploration in one patient with cancer in the pancreatic head and body showed that the SMV had been invaded by the tumor. After the reconstruction of the SMV, the patient recovered well, without obvious complication. No tumor recurrence or metastasis was noted during the 20-month follow-up. These findings demonstrated the feasibility of robotic surgical system in combination with vascular resection & reconstruction in treating pancreatic cancer; (IV) under the help of the upward operation angle and the flexible Endo Wrist TM wrist devices in the da Vinci system, the operator can complete the reconstruction of gastrointestinal tract (e.g., pancreaticojejunostomy, hepaticojejunostomy and gastrojejunostomy), which is particularly useful for the minimally invasive surgery for carcinoma in the head of pancreas that may require PD. Among these 72 patients, three were converted to conventional laparotomy due to the vascular invasion by the surrounding organs and the difficulties in tissue isolation. In two of these three patients, open surgery was performed instead the tumor invasion onto the superior mesenteric artery, adrenal glands, and post-gastric wall. The diseases were then pathologically confirmed to be the AJCC stage III and IV pancreatic cancer, respectively. According to literature and our experiences, the robotic surgical system should be applied for patients with AJCC stage I or II pancreatic cancer without portal system invasion. In our series, the incidence of post-operative complications was 25.0% (18/72), among which the incidence of pancreatic fistula was 15.3% (11/72), the re-operation rate was 2.8% (2/72), and the mortality was 1.4% (1/72). These data were similar to those reported by Giullianotti et al. (16) in 134 patients who had undergone robotic pancreatic surgeries; however, since the sample size was small in our series, and the complications after robot-assisted surgeries for pancreatic cancer await further studies and larger sample sizes. In our current study, the average post-operative hospital stay was 22.6±10.7 days, which was relatively longer than those reported in literature. That may be explained by the differences in health care systems and the lack of homebased nursing in China; as a result, the post-operative
7 610 Zhan et al. Robotic surgery for PDAC recovery was mainly done in hospitals, leading to longer hospital stay. As shown in our clinical experiences, robotic radical resection for PDAC is feasible and safe in well selected patients. Thorough assessment of pre-operative imaging data and surgeons with rich experience in robotic surgeries are key to the success of these procedures. The robotic surgical system has advantages including small trauma and quick postoperative recovery; meanwhile, it breaks through the technical bottlenecks including complicated anastomosis and extensive lymph node dissection that are extremely difficult under the conventional laparoscopic pancreatic surgeries. Thus, the robotic surgery system has expanded the indications in the treatment of pancreatic tumors, with particularly better effectiveness for those still in AJCC stages I and II. However, its further advantages and longterm effectiveness still require validations by comparing with the open surgeries before it can be widely accepted by more clinicians and patients. Acknowledgements None. Footnote Conflicts of Interest: The authors have no conflicts of interest to declare. References 1. Sudan R, Puri V, Sudan D. Robotically assisted biliary pancreatic diversion with a duodenal switch: a new technique. Surg Endosc 2007;21: Kang CM, Kim DH, Lee WJ, et al. Conventional laparoscopic and robot-assisted spleen-preserving pancreatectomy: does da Vinci have clinical advantages? Surg Endosc 2011;25: Ntourakis D, Marzano E, De Blasi V, et al. Robotic left pancreatectomy for pancreatic solid pseudopapillary tumor. Ann Surg Oncol 2011;18: Narula VK, Mikami DJ, Melvin WS. Robotic and laparoscopic pancreaticoduodenectomy: a hybrid approach. Pancreas 2010;39: Buchs NC, Addeo P, Bianco FM, et al. Outcomes of robot-assisted pancreaticoduodenectomy in patients older than 70 years: a comparative study. World J Surg 2010;34: Kooby DA, Gillespie T, Bentrem D, et al. Left-sided pancreatectomy: a multicenter comparison of laparoscopic and open approaches. Ann Surg 2008;248: Jayaraman S, Gonen M, Brennan MF, et al. Laparoscopic distal pancreatectomy: evolution of a technique at a single institution. J Am Coll Surg 2010;211: Vijan SS, Ahmed KA, Harmsen WS, et al. Laparoscopic vs open distal pancreatectomy: a single-institution comparative study. Arch Surg 2010;145: Hanly EJ, Talamini MA. Robotic abdominal surgery. Am J Surg 2004;188:19S-26S. 10. Giulianotti PC, Coratti A, Angelini M, et al. Robotics in general surgery: personal experience in a large community hospital. Arch Surg 2003;138: Giulianotti PC, Sbrana F, Bianco FM, et al. Robot-assisted laparoscopic middle pancreatectomy. J Laparoendosc Adv Surg Tech A 2010;20: Horiguchi A, Uyama I, Miyakawa S. Robot-assisted laparoscopic pancreaticoduodenectomy. J Hepatobiliary Pancreat Sci 2011;18: Kim DH, Kang CM, Lee WJ, et al. The first experience of robot assisted spleen-preserving laparoscopic distal pancreatectomy in Korea. Yonsei Med J 2011;52: Lanfranco AR, Castellanos AE, Desai JP, et al. Robotic surgery: a current perspective. Ann Surg 2004;239: Daouadi M, Zureikat AH, Zenati MS, et al. Robot-assisted minimally invasive distal pancreatectomy is superior to the laparoscopic technique. Ann Surg 2013;257: Giulianotti PC, Sbrana F, Bianco FM, et al. Robot-assisted laparoscopic pancreatic surgery: single-surgeon experience. Surg Endosc 2010;24: Cite this article as: Zhan Q, Deng X, Weng Y, Jin J, Wu Z, Li H, Shen B, Peng C. Outcomes of robotic surgery for pancreatic ductal adenocarcinoma.. doi: /j.issn
Laparoscopy-assisted D2 radical distal subtotal gastrectomy
 Masters of Gastrointestinal Surgery Laparoscopy-assisted D2 radical distal subtotal gastrectomy Xiaogeng Chen, Weihua Li, Jinsi Wang, Changshun Yang Department of Tumor Surgery, Fujian Provincial Hospital,
Masters of Gastrointestinal Surgery Laparoscopy-assisted D2 radical distal subtotal gastrectomy Xiaogeng Chen, Weihua Li, Jinsi Wang, Changshun Yang Department of Tumor Surgery, Fujian Provincial Hospital,
The Whipple Operation Illustrations
 The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Cattell-Braasch maneuver combined with superior mesenteric artery first approach for resection of borderline resectable pancreatic cancer
 Masters of Surgery Page 1 of 5 Cattell-Braasch maneuver combined with superior mesenteric artery first approach for resection of borderline resectable pancreatic cancer Tingsong Yang 1, Fairweather Mark
Masters of Surgery Page 1 of 5 Cattell-Braasch maneuver combined with superior mesenteric artery first approach for resection of borderline resectable pancreatic cancer Tingsong Yang 1, Fairweather Mark
Multiple Primary Quiz
 Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
Totally laparoscopic distal gastrectomy reconstructed by Rouxen-Y with D2 lymphadenectomy and needle catheter jejunostomy for gastric cancer
 Masters of Gastrointestinal Surgery Totally laparoscopic distal gastrectomy reconstructed by Rouxen-Y with D2 lymphadenectomy and needle catheter jejunostomy for gastric cancer Xin Ye, Jian-Chun Yu, Wei-Ming
Masters of Gastrointestinal Surgery Totally laparoscopic distal gastrectomy reconstructed by Rouxen-Y with D2 lymphadenectomy and needle catheter jejunostomy for gastric cancer Xin Ye, Jian-Chun Yu, Wei-Ming
Ruijin robotic thoracic surgery: S segmentectomy of the left upper lobe
 Case Report Page 1 of 5 Ruijin robotic thoracic surgery: S 1+2+3 segmentectomy of the left upper lobe Han Wu, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Hailei Du, Dingpei Han, Kai Chen,
Case Report Page 1 of 5 Ruijin robotic thoracic surgery: S 1+2+3 segmentectomy of the left upper lobe Han Wu, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Hailei Du, Dingpei Han, Kai Chen,
Anatomy of laparoscopy-assisted distal D2 radical gastrectomy for gastric cancer
 Masters of Gastrointestinal Surgery Anatomy of laparoscopy-assisted distal D2 radical gastrectomy for gastric cancer Da-Guang Wang, Liang He, Yang Zhang, Jing-Hai Yu, Yan Chen, Ming-Jie Xia, Jian Suo Department
Masters of Gastrointestinal Surgery Anatomy of laparoscopy-assisted distal D2 radical gastrectomy for gastric cancer Da-Guang Wang, Liang He, Yang Zhang, Jing-Hai Yu, Yan Chen, Ming-Jie Xia, Jian Suo Department
Robotic-assisted right upper lobectomy
 Robotic Thoracic Surgery Column Robotic-assisted right upper lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital, Shenyang 110015,
Robotic Thoracic Surgery Column Robotic-assisted right upper lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital, Shenyang 110015,
Laparoscopy-assisted radical total gastrectomy plus D2 lymph node dissection
 Masters of Gastrointestinal Surgery Laparoscopy-assisted radical total gastrectomy plus D2 lymph node dissection Chaohui Zheng, Changming Huang, Ping Li, Jianwei Xie, Jiabin Wang, Jianxian Lin, Jun Lu
Masters of Gastrointestinal Surgery Laparoscopy-assisted radical total gastrectomy plus D2 lymph node dissection Chaohui Zheng, Changming Huang, Ping Li, Jianwei Xie, Jiabin Wang, Jianxian Lin, Jun Lu
An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein
 J Gastrointest Surg (2007) 11:425 431 DOI 10.1007/s11605-007-0131-1 An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein Rory L. Smoot & John D. Christein &
J Gastrointest Surg (2007) 11:425 431 DOI 10.1007/s11605-007-0131-1 An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein Rory L. Smoot & John D. Christein &
Pylorus Preserving Pancreaticoduodenectomy
 REVIEW Pylorus Preserving Pancreaticoduodenectomy Jacqueline M. Garonzik-Wang, M. B. Majella Doyle Pancreaticoduodenectomy (PD) has become the standard of care for resectable pancreatic cancer and premalignant
REVIEW Pylorus Preserving Pancreaticoduodenectomy Jacqueline M. Garonzik-Wang, M. B. Majella Doyle Pancreaticoduodenectomy (PD) has become the standard of care for resectable pancreatic cancer and premalignant
Objectives. Intraoperative Consultation of the Whipple Resection Specimen. Pancreas Anatomy. Pancreatic ductal carcinoma 11/10/2014
 Intraoperative Consultation of the Whipple Resection Specimen Pathology Update Faculty of Medicine, University of Toronto November 15, 2014 John W. Wong, MD, FRCPC Department of Anatomical Pathology Sunnybrook
Intraoperative Consultation of the Whipple Resection Specimen Pathology Update Faculty of Medicine, University of Toronto November 15, 2014 John W. Wong, MD, FRCPC Department of Anatomical Pathology Sunnybrook
Outcomes associated with robotic approach to pancreatic resections
 Short Communication (Management of Foregut Malignancies and Hepatobiliary Tract and Pancreas Malignancies) Outcomes associated with robotic approach to pancreatic resections Caitlin Takahashi 1, Ravi Shridhar
Short Communication (Management of Foregut Malignancies and Hepatobiliary Tract and Pancreas Malignancies) Outcomes associated with robotic approach to pancreatic resections Caitlin Takahashi 1, Ravi Shridhar
A video demonstration of the Li s anastomosis the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma
 Surgical Technique A video demonstration of the the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma Yan Zheng*, Yin Li*, Zongfei Wang, Haibo Sun, Ruixiang Zhang
Surgical Technique A video demonstration of the the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma Yan Zheng*, Yin Li*, Zongfei Wang, Haibo Sun, Ruixiang Zhang
SURGICAL TECHNIQUE. Radical treatment for left upper-lobe cancer via complete VATS. Jun Liu, Fei Cui, Shu-Ben Li. Introduction
 SURGICAL TECHNIQUE Radical treatment for left upper-lobe cancer via complete VATS Jun Liu, Fei Cui, Shu-Ben Li The First Affiliated Hospital of Guangzhou Medical College, Guangzhou, China ABSTRACT KEYWORDS
SURGICAL TECHNIQUE Radical treatment for left upper-lobe cancer via complete VATS Jun Liu, Fei Cui, Shu-Ben Li The First Affiliated Hospital of Guangzhou Medical College, Guangzhou, China ABSTRACT KEYWORDS
Prevention Of Pancreaticojejunal Fistula After Whipple Procedure
 ISPUB.COM The Internet Journal of Surgery Volume 4 Number 2 Prevention Of Pancreaticojejunal Fistula After Whipple Procedure N Barbetakis, K Setsiz Citation N Barbetakis, K Setsiz. Prevention Of Pancreaticojejunal
ISPUB.COM The Internet Journal of Surgery Volume 4 Number 2 Prevention Of Pancreaticojejunal Fistula After Whipple Procedure N Barbetakis, K Setsiz Citation N Barbetakis, K Setsiz. Prevention Of Pancreaticojejunal
The first total laparoscopic pancreatoduodenectomy in Poland
 Case report Videosurgery Andrzej Budzyński 1, Anna Zub-Pokrowiecka 1, Anna Zychowicz 1, Michał Pędziwiatr 1, Mateusz Wierdak 2, Maciej Matłok 1, Małgorzata Zając 1 12 nd Department of General Surgery,
Case report Videosurgery Andrzej Budzyński 1, Anna Zub-Pokrowiecka 1, Anna Zychowicz 1, Michał Pędziwiatr 1, Mateusz Wierdak 2, Maciej Matłok 1, Małgorzata Zając 1 12 nd Department of General Surgery,
Pancreaticoduodenectomy the anatomy and the surgical approaches
 Pancreaticoduodenectomy the anatomy and the surgical approaches Paul BS LAI Division of Hepato biliary and Pancreatic Surgery Department of Surgery The Chinese Univesity of Hong Kong Whipple s operation
Pancreaticoduodenectomy the anatomy and the surgical approaches Paul BS LAI Division of Hepato biliary and Pancreatic Surgery Department of Surgery The Chinese Univesity of Hong Kong Whipple s operation
Robotic thoracic surgery: S 1+2 segmentectomy of left upper lobe
 Case Report Page 1 of 5 Robotic thoracic surgery: S 1+2 segmentectomy of left upper lobe Hailei Du, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Han Wu, Dingpei Han, Kai Chen, Jie Xiang, Hecheng
Case Report Page 1 of 5 Robotic thoracic surgery: S 1+2 segmentectomy of left upper lobe Hailei Du, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Han Wu, Dingpei Han, Kai Chen, Jie Xiang, Hecheng
Pancreas Quizzes c. Both A and B a. Directly into the blood stream (not using ducts)
 Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
Imaging in gastric cancer
 Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Robotic-assisted right inferior lobectomy
 Robotic Thoracic Surgery Column Page 1 of 6 Robotic-assisted right inferior lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital,
Robotic Thoracic Surgery Column Page 1 of 6 Robotic-assisted right inferior lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital,
Citation Hepato-Gastroenterology, 55(86-87),
 NAOSITE: Nagasaki University's Ac Title Author(s) Combined pancreatic resection and p multiple lesions of the pancreas: i of the pancreas concomitant with du Kuroki, Tamotsu; Tajima, Yoshitsugu Tomohiko;
NAOSITE: Nagasaki University's Ac Title Author(s) Combined pancreatic resection and p multiple lesions of the pancreas: i of the pancreas concomitant with du Kuroki, Tamotsu; Tajima, Yoshitsugu Tomohiko;
Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping
 GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
Robotic distal pancreatectomy: experience in a high-volume center
 Original Article Page 1 of 6 Robotic distal pancreatectomy: experience in a high-volume center Qu Liu, Wenbo Tang, Ruiquan Zhou, Zhiming Zhao, Yuanxing Gao, Minggen Hu, Chenggang Li, Xuan Zhang, Rong Liu
Original Article Page 1 of 6 Robotic distal pancreatectomy: experience in a high-volume center Qu Liu, Wenbo Tang, Ruiquan Zhou, Zhiming Zhao, Yuanxing Gao, Minggen Hu, Chenggang Li, Xuan Zhang, Rong Liu
Radical nerve dissection for the carcinoma of head of pancreas: report of 30 cases
 Original Article Radical nerve dissection for the carcinoma of head of pancreas: report of 30 cases Qing Lin, Langping Tan, Yu Zhou, Quanbo Zhou, Rufu Chen Department of Biliary and Pancreatic Surgery,
Original Article Radical nerve dissection for the carcinoma of head of pancreas: report of 30 cases Qing Lin, Langping Tan, Yu Zhou, Quanbo Zhou, Rufu Chen Department of Biliary and Pancreatic Surgery,
Accessory Glands of Digestive System
 Accessory Glands of Digestive System The liver The liver is soft and pliable and occupies the upper part of the abdominal cavity just beneath the diaphragm. The greater part of the liver is situated under
Accessory Glands of Digestive System The liver The liver is soft and pliable and occupies the upper part of the abdominal cavity just beneath the diaphragm. The greater part of the liver is situated under
The abdominal Esophagus, Stomach and the Duodenum. Prof. Oluwadiya KS
 The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES
 JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES THE PROBLEM DUODENAL / PANCREATIC INJURIES Difficult to diagnose Not very common Anatomic and physiologic challenges 90% rate of associated
JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES THE PROBLEM DUODENAL / PANCREATIC INJURIES Difficult to diagnose Not very common Anatomic and physiologic challenges 90% rate of associated
Robotic-assisted McKeown esophagectomy
 Case Report Page 1 of 8 Robotic-assisted McKeown esophagectomy Dingpei Han, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Han Wu, Hailei Du, Kai Chen, Jie Xiang, Hecheng Li Department of Thoracic
Case Report Page 1 of 8 Robotic-assisted McKeown esophagectomy Dingpei Han, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Han Wu, Hailei Du, Kai Chen, Jie Xiang, Hecheng Li Department of Thoracic
ADVANCED LAPAROSCOPIC PANCREAS SURGERY A HANDS-ON WORKSHOP
 ADVANCED LAPAROSCOPIC PANCREAS SURGERY A HANDS-ON WORKSHOP 3-4 November 2017 at the AMC in Amsterdam Organizing committee: Mo Abu Hilal, Professor of Surgery at Southampton University Marc Besselink, Professor
ADVANCED LAPAROSCOPIC PANCREAS SURGERY A HANDS-ON WORKSHOP 3-4 November 2017 at the AMC in Amsterdam Organizing committee: Mo Abu Hilal, Professor of Surgery at Southampton University Marc Besselink, Professor
Surgical Management of CBD Injury Jin Seok Heo
 Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
د. عصام طارق. Objectives:
 GI anatomy Lecture: 5 د. عصام طارق Objectives: To describe anatomy of stomach, duodenum & pancreas. To list their main relations. To define their blood & nerve supply. To list their lymph drainage. To
GI anatomy Lecture: 5 د. عصام طارق Objectives: To describe anatomy of stomach, duodenum & pancreas. To list their main relations. To define their blood & nerve supply. To list their lymph drainage. To
Technical considerations for the fully robotic pancreaticoduodenectomy
 Surgical Techniques on Pancreatic Surgery Technical considerations for the fully robotic pancreaticoduodenectomy Daniel Galvez, Rebecca Sorber, Ammar A. Javed, Jin He Department of Surgery, The Johns Hopkins
Surgical Techniques on Pancreatic Surgery Technical considerations for the fully robotic pancreaticoduodenectomy Daniel Galvez, Rebecca Sorber, Ammar A. Javed, Jin He Department of Surgery, The Johns Hopkins
General Surgery PURPLE SERVICE MUHC-RVH Site
 Preamble HPB is a clinical teaching unit with several different vocations: It regroups all solid organ Transplantation as well as most advanced Hepatobiliary and Pancreatic clinical activities performed
Preamble HPB is a clinical teaching unit with several different vocations: It regroups all solid organ Transplantation as well as most advanced Hepatobiliary and Pancreatic clinical activities performed
Appendix 5. EFSUMB Newsletter. Gastroenterological Ultrasound
 EFSUMB Newsletter 87 Examinations should encompass the full range of pathological conditions listed below A log book listing the types of examinations undertaken should be kept Training should usually
EFSUMB Newsletter 87 Examinations should encompass the full range of pathological conditions listed below A log book listing the types of examinations undertaken should be kept Training should usually
Pancreas & Biliary System. Dr. Vohra & Dr. Jamila
 Pancreas & Biliary System Dr. Vohra & Dr. Jamila 1 Objectives At the end of the lecture, the student should be able to describe the: Location, surface anatomy, parts, relations & peritoneal reflection
Pancreas & Biliary System Dr. Vohra & Dr. Jamila 1 Objectives At the end of the lecture, the student should be able to describe the: Location, surface anatomy, parts, relations & peritoneal reflection
Robotic-assisted left inferior lobectomy
 Robotic Thoracic Surgery Column Robotic-assisted left inferior lobectomy Shiguang Xu, Hao Meng, Tong Wang, Wei Xu, Xingchi Liu, Shumin Wang Department of Thoracic Surgery, Northern Hospital, Shenyang 110015,
Robotic Thoracic Surgery Column Robotic-assisted left inferior lobectomy Shiguang Xu, Hao Meng, Tong Wang, Wei Xu, Xingchi Liu, Shumin Wang Department of Thoracic Surgery, Northern Hospital, Shenyang 110015,
THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY 2013/12/21
 THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY Tsann-Long Hwang, MD, FACS Department of Surgery Chang Gung Memorial Hospital Chang Gung University Taipei, TAIWAN 2013/12/21 THE DIFFICULTY
THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY Tsann-Long Hwang, MD, FACS Department of Surgery Chang Gung Memorial Hospital Chang Gung University Taipei, TAIWAN 2013/12/21 THE DIFFICULTY
Nasogastric tube. Stomach. Pylorus. Duodenum 1. Duodenum 2. Duodenum 3. Duodenum 4
 Esophagus Barium Swallow Stomach and Duodenum 4 year old Upper GI Nasogastric tube Stomach and Duodenum 4 year old Upper GI Nasogastric tube Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum 4
Esophagus Barium Swallow Stomach and Duodenum 4 year old Upper GI Nasogastric tube Stomach and Duodenum 4 year old Upper GI Nasogastric tube Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum 4
Yoshitsugu; Kanematsu, Takashi; Kur
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Laparoscopic Middle Pancreatectomy Surgery Kitasato, Amane; Adachi, Tomohiko; Yoshitsugu; Kanematsu, Takashi; Kur Hepato-Gastroenterology, 59(120),
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Laparoscopic Middle Pancreatectomy Surgery Kitasato, Amane; Adachi, Tomohiko; Yoshitsugu; Kanematsu, Takashi; Kur Hepato-Gastroenterology, 59(120),
Endoscopic Ultrasonography Assessment for Ampullary and Bile Duct Malignancy
 Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Serous Cystic Neoplasm: Do We Have to Wait Till It Causes Trouble?
 Korean Journal of HBP Surgery Case Report Vol. 15, No. 2, May 2011 Serous Cystic Neoplasm: Do We Have to Wait Till It Causes Trouble? Serous cystic neoplasm (SCN) of the pancreas is considered a benign
Korean Journal of HBP Surgery Case Report Vol. 15, No. 2, May 2011 Serous Cystic Neoplasm: Do We Have to Wait Till It Causes Trouble? Serous cystic neoplasm (SCN) of the pancreas is considered a benign
Surgical Management of Pancreatic Cancer
 I Congresso de Oncologia D Or July 5-6, 2013 Surgical Management of Pancreatic Cancer Michael A. Choti, MD, MBA, FACS Department of Surgery Johns Hopkins University School of Medicine, Baltimore, MD Estimated
I Congresso de Oncologia D Or July 5-6, 2013 Surgical Management of Pancreatic Cancer Michael A. Choti, MD, MBA, FACS Department of Surgery Johns Hopkins University School of Medicine, Baltimore, MD Estimated
Laparoscopic & Robotic Surgery in Pancreas Disease
 2007 년도대한췌담도학회추계학술대회 Session IV: Recent Updates in Pancreatobiliary Diseases Laparoscopic & Robotic Surgery in Pancreas Disease Department of Surgery, Yonsei University College of Medicine, Korea Woo-Jung
2007 년도대한췌담도학회추계학술대회 Session IV: Recent Updates in Pancreatobiliary Diseases Laparoscopic & Robotic Surgery in Pancreas Disease Department of Surgery, Yonsei University College of Medicine, Korea Woo-Jung
ABDOMEN - GI. Duodenum
 TALA SALEH ABDOMEN - GI Duodenum - Notice the shape of the duodenum, it looks like capital G shape tube which extends from the pyloroduodenal junction to the duodenojejunal junction. - It is 10 inches
TALA SALEH ABDOMEN - GI Duodenum - Notice the shape of the duodenum, it looks like capital G shape tube which extends from the pyloroduodenal junction to the duodenojejunal junction. - It is 10 inches
Laparoscopic extended right hemicolectomy with D3
 Surgical Technique Page 1 of 11 Laparoscopic extended right hemicolectomy with D3 lymphadenectomy Weixian Hu, Jiabin Zheng, Yong Li Department of General Surgery, Guangdong General Hospital, Guangdong
Surgical Technique Page 1 of 11 Laparoscopic extended right hemicolectomy with D3 lymphadenectomy Weixian Hu, Jiabin Zheng, Yong Li Department of General Surgery, Guangdong General Hospital, Guangdong
Evaluation of Suspected Pancreatic Cancer
 Evaluation of Suspected Pancreatic Cancer October 15, 2015 If you experience technical difficulty during the presentation: Contact WebEx Technical Support directly at: US Toll Free: 1-866-779-3239 Toll
Evaluation of Suspected Pancreatic Cancer October 15, 2015 If you experience technical difficulty during the presentation: Contact WebEx Technical Support directly at: US Toll Free: 1-866-779-3239 Toll
Small Plicae Circularis. Short Closely packed together. Sparse, completely absent at distal part Lymphoid Nodule
 Intestines Differences Between Jejunum and Ileum Types Jejunum Ileum Color Deeper red Paler pink Calibre Bigger Smaller Thickness of wall Thick and Heavy Thin and Lighter Vascularity Highly vascularised
Intestines Differences Between Jejunum and Ileum Types Jejunum Ileum Color Deeper red Paler pink Calibre Bigger Smaller Thickness of wall Thick and Heavy Thin and Lighter Vascularity Highly vascularised
Trauma. Neck trauma zones. Neck Injuries 1/3/2018. Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure
 Trauma 45 minutes highest points Ahmed Mahmoud, MD Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure Neck trauma zones Airway ;Rapid sequence intubation Breathing ;Needle
Trauma 45 minutes highest points Ahmed Mahmoud, MD Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure Neck trauma zones Airway ;Rapid sequence intubation Breathing ;Needle
Visceral aneurysm. Diagnosis and Interventions M.NEDEVSKA
 Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Left-sided approach for suprapancreatic lymph node dissection in laparoscopy-assisted distal gastrectomy without duodenal transection
 Gastric Cancer (2009) 12: 106 112 DOI 10.1007/s10120-009-0508-9 Technical note 2009 by International and Japanese Gastric Cancer Associations Left-sided approach for suprapancreatic lymph node dissection
Gastric Cancer (2009) 12: 106 112 DOI 10.1007/s10120-009-0508-9 Technical note 2009 by International and Japanese Gastric Cancer Associations Left-sided approach for suprapancreatic lymph node dissection
Dr. Zahiri. In the name of God
 Dr. Zahiri In the name of God small intestine = small bowel is the part of the gastrointestinal tract Boundaries: Pylorus Ileosecal junction Function: digestion and absorption of food It receives bile
Dr. Zahiri In the name of God small intestine = small bowel is the part of the gastrointestinal tract Boundaries: Pylorus Ileosecal junction Function: digestion and absorption of food It receives bile
Radical nerve dissection for the carcinoma of head of pancreas: report of 30 cases
 Review Article Radical nerve dissection for the carcinoma of head of pancreas: report of 30 cases Qing Lin, Langping Tan, Yu Zhou, Quanbo Zhou, Rufu Chen Department of Biliary and Pancreatic Surgery, Sun
Review Article Radical nerve dissection for the carcinoma of head of pancreas: report of 30 cases Qing Lin, Langping Tan, Yu Zhou, Quanbo Zhou, Rufu Chen Department of Biliary and Pancreatic Surgery, Sun
PANCREAS DUCTAL ADENOCARCINOMA PDAC
 CONTENTS PANCREAS DUCTAL ADENOCARCINOMA PDAC I. What is the pancreas? II. III. IV. What is pancreas cancer? What is the epidemiology of Pancreatic Ductal Adenocarcinoma (PDAC)? What are the risk factors
CONTENTS PANCREAS DUCTAL ADENOCARCINOMA PDAC I. What is the pancreas? II. III. IV. What is pancreas cancer? What is the epidemiology of Pancreatic Ductal Adenocarcinoma (PDAC)? What are the risk factors
Li Yang, Diancai Zhang, Fengyuan Li, Xiang Ma. Introduction
 Original Article on Gastrointestinal Surgery Simultaneous laparoscopic distal gastrectomy (uncut Roux-en-Y anastomosis), right hemi-colectomy and radical rectectomy (Dixon) in a synchronous triple primary
Original Article on Gastrointestinal Surgery Simultaneous laparoscopic distal gastrectomy (uncut Roux-en-Y anastomosis), right hemi-colectomy and radical rectectomy (Dixon) in a synchronous triple primary
INNOVATION. Harmonic INSPIRED BY TRADITION. HARMONIC FOCUS + Long Shears with Adaptive Tissue Technology
 INNOVATION INSPIRED BY TRADITION HARMONIC FOCUS + Long Shears with Adaptive Tissue Technology Precise, controlled dissection Consistent, reliable seals* Access and visibility in deep spaces *In a pre-clinical
INNOVATION INSPIRED BY TRADITION HARMONIC FOCUS + Long Shears with Adaptive Tissue Technology Precise, controlled dissection Consistent, reliable seals* Access and visibility in deep spaces *In a pre-clinical
Lab Monitor Images Dissection of the Abdominal Vasculature + Lower Digestive System
 Lab Monitor Images Dissection of the Abdominal Vasculature + Lower Digestive System Stomach & Duodenum Frontal (AP) View Nasogastric tube 2 1 3 4 Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum
Lab Monitor Images Dissection of the Abdominal Vasculature + Lower Digestive System Stomach & Duodenum Frontal (AP) View Nasogastric tube 2 1 3 4 Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum
Surgical management of HCC. Evangelos Prassas Hepatobiliary and Pancreatic Surgery / Liver Transplantation Kings College Hospital / London
 Surgical management of HCC Evangelos Prassas Hepatobiliary and Pancreatic Surgery / Liver Transplantation Kings College Hospital / London Global distribution of HCC and staging systems WEST 1. Italy (Milan,
Surgical management of HCC Evangelos Prassas Hepatobiliary and Pancreatic Surgery / Liver Transplantation Kings College Hospital / London Global distribution of HCC and staging systems WEST 1. Italy (Milan,
Robotic thoracic surgery of total thymectomy
 Robotic Thoracic Surgery Column Page 1 of 5 Robotic thoracic surgery of total thymectomy Shiguang Xu, Xingchi Liu, Bo Li, Renquan Ding, Tong Wang, Shumin Wang Department of Thoracic Surgery, Northern Hospital,
Robotic Thoracic Surgery Column Page 1 of 5 Robotic thoracic surgery of total thymectomy Shiguang Xu, Xingchi Liu, Bo Li, Renquan Ding, Tong Wang, Shumin Wang Department of Thoracic Surgery, Northern Hospital,
Laparoscopic extended right hemicolectomy with D3 lymphadenectomy
 Surgical Technique Page 1 of 10 Laparoscopic extended right hemicolectomy with D3 lymphadenectomy Yong Li General Surgery, Guangdong General Hospital and Guangdong Academy of Medical Sciences, Guangzhou
Surgical Technique Page 1 of 10 Laparoscopic extended right hemicolectomy with D3 lymphadenectomy Yong Li General Surgery, Guangdong General Hospital and Guangdong Academy of Medical Sciences, Guangzhou
Surgical anatomy of the biliary tract
 HPB, 2008; 10: 7276 REVIEW ARTICLE Surgical anatomy of the biliary tract DENIS CASTAING Centre hépato-biliaire, Hôpital Paul Brousse, Assistance Publique- Hôpitaux de Paris, Université Paris XI, Paris,
HPB, 2008; 10: 7276 REVIEW ARTICLE Surgical anatomy of the biliary tract DENIS CASTAING Centre hépato-biliaire, Hôpital Paul Brousse, Assistance Publique- Hôpitaux de Paris, Université Paris XI, Paris,
Totally laparoscopic total gastrectomy for locally advanced middle-upper-third gastric cancer
 Original Article on Gastrointestinal Surgery Totally laparoscopic total gastrectomy for locally advanced middle-upper-third gastric cancer Mi Lin, Chang-Ming Huang, Chao-Hui Zheng, Ping Li, Jian-Wei Xie,
Original Article on Gastrointestinal Surgery Totally laparoscopic total gastrectomy for locally advanced middle-upper-third gastric cancer Mi Lin, Chang-Ming Huang, Chao-Hui Zheng, Ping Li, Jian-Wei Xie,
Case Scenario 1. Discharge Summary
 Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Educational system of laparoscopic gastrectomy for trainee how to teach, how to learn
 Review Article on Gastrointestinal Surgery Educational system of laparoscopic gastrectomy for trainee how to teach, how to learn Akio Kaito, Takahiro Kinoshita Contributions: (I) Conception and design:
Review Article on Gastrointestinal Surgery Educational system of laparoscopic gastrectomy for trainee how to teach, how to learn Akio Kaito, Takahiro Kinoshita Contributions: (I) Conception and design:
Bile Duct Injury during Lap Chole. Bile Duct Injury during cholecystectomy TOPICS. 1. Prevalence, mechanisms, prevention and diagnosis
 Bile Duct Injury during cholecystectomy Catherine HUBERT Jean-Fran François GIGOT Benoît t NAVEZ Division of Hepato-Biliary Biliary-Pancreatic Surgery Department of Abdominal Surgery and Transplantation
Bile Duct Injury during cholecystectomy Catherine HUBERT Jean-Fran François GIGOT Benoît t NAVEZ Division of Hepato-Biliary Biliary-Pancreatic Surgery Department of Abdominal Surgery and Transplantation
Duodenum retroperitoneal
 Duodenum retroperitoneal C shaped Initial region out of stomach into small intestine RETROperitoneal viscus Superior 1 st part duodenal cap ; moves upwards and backwards to lie on the R crura medial to
Duodenum retroperitoneal C shaped Initial region out of stomach into small intestine RETROperitoneal viscus Superior 1 st part duodenal cap ; moves upwards and backwards to lie on the R crura medial to
The Spleen. Dr Fahad Ullah
 The Spleen BY Dr Fahad Ullah Spleen The spleen is an largest lymphoid organ shaped like a shoe that lies relative to the 9th and 11th ribs and is located in the left hypochondrium. Thus, the spleen is
The Spleen BY Dr Fahad Ullah Spleen The spleen is an largest lymphoid organ shaped like a shoe that lies relative to the 9th and 11th ribs and is located in the left hypochondrium. Thus, the spleen is
6 th August 2018 Day 1 - Gallbladder & Bile duct Topic
 Venue: Sterling Hospital Auditorium, Sterling Hospitals, Gurukul Road Ahmedabad, Gujarat 6 th August 2018 Day 1 - Gallbladder & Bile duct Registration(8:00am-8:15am) Inauguration(8:15am-8:30am) Welcome
Venue: Sterling Hospital Auditorium, Sterling Hospitals, Gurukul Road Ahmedabad, Gujarat 6 th August 2018 Day 1 - Gallbladder & Bile duct Registration(8:00am-8:15am) Inauguration(8:15am-8:30am) Welcome
Appendix 9: Endoscopic Ultrasound in Gastroenterology
 Appendix 9: Endoscopic Ultrasound in Gastroenterology This curriculum is intended for clinicians who perform endoscopic ultrasonography (EUS) in gastroenterology. It includes standards for theoretical
Appendix 9: Endoscopic Ultrasound in Gastroenterology This curriculum is intended for clinicians who perform endoscopic ultrasonography (EUS) in gastroenterology. It includes standards for theoretical
Therapeutic effect of laparoscopy-assisted D2 radical gastrectomy in 106 patients with advanced gastric cancer
 JBUON 2013; 18(3): 689-694 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Therapeutic effect of laparoscopy-assisted D2 radical gastrectomy in
JBUON 2013; 18(3): 689-694 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Therapeutic effect of laparoscopy-assisted D2 radical gastrectomy in
To describe the liver. To list main structures in porta hepatis.
 GI anatomy Lecture: 6 د. عصام طارق Objectives: To describe the liver. To list main structures in porta hepatis. To define portal system & portosystemic anastomosis. To list parts of biliary system. To
GI anatomy Lecture: 6 د. عصام طارق Objectives: To describe the liver. To list main structures in porta hepatis. To define portal system & portosystemic anastomosis. To list parts of biliary system. To
Informed Consent Gastrectomy
 Informed Consent Gastrectomy Department of Surgery, Nagasaki University Graduate School of Biomedical Sciences Important things you need to know Patient choice is an important part of your care. You have
Informed Consent Gastrectomy Department of Surgery, Nagasaki University Graduate School of Biomedical Sciences Important things you need to know Patient choice is an important part of your care. You have
Topics: Staging and treatment for pancreatic cancer. Staging systems for pancreatic cancer: Differences between the Japanese and UICC systems
 M. J Hep Kobari Bil Pancr and S. Surg Matsuno: (1998) Staging 5:121 127 system for pancreatic cancer 121 Topics: Staging and treatment for pancreatic cancer Staging systems for pancreatic cancer: Differences
M. J Hep Kobari Bil Pancr and S. Surg Matsuno: (1998) Staging 5:121 127 system for pancreatic cancer 121 Topics: Staging and treatment for pancreatic cancer Staging systems for pancreatic cancer: Differences
Uniportal video-assisted thoracic surgery for complicated pulmonary resections
 Review Article on Thoracic Surgery Uniportal video-assisted thoracic surgery for complicated pulmonary resections Ding-Pei Han, Jie Xiang, Run-Sen Jin, Yan-Xia Hu, He-Cheng Li Jiaotong University School
Review Article on Thoracic Surgery Uniportal video-assisted thoracic surgery for complicated pulmonary resections Ding-Pei Han, Jie Xiang, Run-Sen Jin, Yan-Xia Hu, He-Cheng Li Jiaotong University School
Total laparoscopic pancreaticoduodenectomy: a retrospective study of 27 cases treated in a single institution
 Original Article Total laparoscopic pancreaticoduodenectomy: a retrospective study of 27 cases treated in a single institution Hong Li 1, Jie Zhu 2, Bin Zhang 1, Gencong Li 1, Xinhua Zhou 3, Dansong Yu
Original Article Total laparoscopic pancreaticoduodenectomy: a retrospective study of 27 cases treated in a single institution Hong Li 1, Jie Zhu 2, Bin Zhang 1, Gencong Li 1, Xinhua Zhou 3, Dansong Yu
Surgical Treatment for Carcinoma of the Ampulla of Vater and Residual Pancreatic Function before and after Pancreaticoduodenectomy*)
 Hiroshima Journal of Medical Sciences Vol. 32, No. 4, 455,-...,460, December, 1983 HIJM 32-68 455 Surgical Treatment for Carcinoma of the Ampulla of Vater and Residual Pancreatic Function before and after
Hiroshima Journal of Medical Sciences Vol. 32, No. 4, 455,-...,460, December, 1983 HIJM 32-68 455 Surgical Treatment for Carcinoma of the Ampulla of Vater and Residual Pancreatic Function before and after
GALLBLADDER CANCER. Lidie M. Lajoie MD Downstate Surgery M&M July 21, 2011
 GALLBLADDER CANCER Lidie M. Lajoie MD Downstate Surgery M&M July 21, 2011 Agenda Case Presentation Epidemiology Pathogenesis & Pathology Staging Presentation & Diagnosis Stage-wise Management Outcomes/Prognosis
GALLBLADDER CANCER Lidie M. Lajoie MD Downstate Surgery M&M July 21, 2011 Agenda Case Presentation Epidemiology Pathogenesis & Pathology Staging Presentation & Diagnosis Stage-wise Management Outcomes/Prognosis
Clinical benefit of Totally Laparoscopic over Laparoscopically Assisted Distal Gastrectomy with Roux-en-Y Reconstruction for Early Gastric Cancer
 Med. Bull. Fukuoka Univ. 39 3/4 251 256 2012 Clinical benefit of Totally Laparoscopic over Laparoscopically Assisted Distal Gastrectomy with Roux-en-Y Reconstruction for Early Gastric Cancer Tatsuya HASHIMOTO,
Med. Bull. Fukuoka Univ. 39 3/4 251 256 2012 Clinical benefit of Totally Laparoscopic over Laparoscopically Assisted Distal Gastrectomy with Roux-en-Y Reconstruction for Early Gastric Cancer Tatsuya HASHIMOTO,
Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 14
 Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 14 Contents 14. Neuroendocrine Tumours 161 14.1. Diagnostic algorithm
Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 14 Contents 14. Neuroendocrine Tumours 161 14.1. Diagnostic algorithm
Laparoscopic spleen-preserving complete splenic hilum lymphadenectomy for advanced proximal gastric cancer
 Review Article Page 1 of 5 Laparoscopic spleen-preserving complete splenic hilum lymphadenectomy for advanced proximal gastric cancer Wei Wang*, Wejun Xiong*, Qiqi Peng, Shanao Ye, Yansheng Zheng, Lijie
Review Article Page 1 of 5 Laparoscopic spleen-preserving complete splenic hilum lymphadenectomy for advanced proximal gastric cancer Wei Wang*, Wejun Xiong*, Qiqi Peng, Shanao Ye, Yansheng Zheng, Lijie
Pancreas Case Scenario #1
 Pancreas Case Scenario #1 An 85 year old white female presented to her primary care physician with increasing abdominal pain. On 8/19 she had a CT scan of the abdomen and pelvis. This showed a 4.6 cm mass
Pancreas Case Scenario #1 An 85 year old white female presented to her primary care physician with increasing abdominal pain. On 8/19 she had a CT scan of the abdomen and pelvis. This showed a 4.6 cm mass
Minimally Invasive Esophagectomy
 American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
 Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
Block 3: DISSECTION 2 CELIAC TRUNK, JEJUNUM/ILEUM, LARGE INTESTINE, DUODENUM, PANCREAS, PORTAL VEIN; MOBILIZATION OF THE LIVER
 1 Block 3: DISSECTION 2 CELIAC TRUNK, JEJUNUM/ILEUM, LARGE INTESTINE, DUODENUM, PANCREAS, PORTAL VEIN; MOBILIZATION OF THE LIVER Attempt to complete as much as you can of the dissection explained in the
1 Block 3: DISSECTION 2 CELIAC TRUNK, JEJUNUM/ILEUM, LARGE INTESTINE, DUODENUM, PANCREAS, PORTAL VEIN; MOBILIZATION OF THE LIVER Attempt to complete as much as you can of the dissection explained in the
Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review
 Review Article Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review Min-Jie Yang, Su Li, Yong-Guang Liu, Na Jiao, Jing-Shan Gong Department of Radiology, Shenzhen
Review Article Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review Min-Jie Yang, Su Li, Yong-Guang Liu, Na Jiao, Jing-Shan Gong Department of Radiology, Shenzhen
Intraabdominal Roux-en-Y reconstruction with a novel stapling technique after laparoscopic distal gastrectomy
 Gastric Cancer (2009) 12: 164 169 DOI 10.1007/s10120-009-0520-0 Technical note 2009 by International and Japanese Gastric Cancer Associations Intraabdominal Roux-en-Y reconstruction with a novel stapling
Gastric Cancer (2009) 12: 164 169 DOI 10.1007/s10120-009-0520-0 Technical note 2009 by International and Japanese Gastric Cancer Associations Intraabdominal Roux-en-Y reconstruction with a novel stapling
Pancreas and Biliary System
 Pancreas and Biliary System Please view our Editing File before studying this lecture to check for any changes. Color Code Important Doctors Notes Notes/Extra explanation Objectives At the end of the lecture,
Pancreas and Biliary System Please view our Editing File before studying this lecture to check for any changes. Color Code Important Doctors Notes Notes/Extra explanation Objectives At the end of the lecture,
Surface Anatomy. Location Shape Weight Role of Five Surfaces Borders Fissures Lobes Peritoneal Lig
 The Liver Functions Bile production and secretion Detoxification Storage of glycogen Protein synthesis Production of heparin and bile pigments Erythropoiesis (in fetus) Surface Anatomy Location Shape Weight
The Liver Functions Bile production and secretion Detoxification Storage of glycogen Protein synthesis Production of heparin and bile pigments Erythropoiesis (in fetus) Surface Anatomy Location Shape Weight
Original article: new surgical approaches to the Klatskin tumour
 Alimentary Pharmacology & Therapeutics Original article: new surgical approaches to the Klatskin tumour T. M. VAN GULIK*, S. DINANT*, O. R. C. BUSCH*, E. A. J. RAUWS, H. OBERTOP* & D. J. GOUMA Departments
Alimentary Pharmacology & Therapeutics Original article: new surgical approaches to the Klatskin tumour T. M. VAN GULIK*, S. DINANT*, O. R. C. BUSCH*, E. A. J. RAUWS, H. OBERTOP* & D. J. GOUMA Departments
Complications after laparoscopic gastric bypass for morbid obesity. Background LGBP. Eirik Hornes Halvorsen, MD, PhD Oslo
 Complications after laparoscopic gastric bypass for morbid obesity Eirik Hornes Halvorsen, MD, PhD Oslo 20.05.2015 Background Ca 3000 patients are surgically treated for morbid obesity in Norway each year.
Complications after laparoscopic gastric bypass for morbid obesity Eirik Hornes Halvorsen, MD, PhD Oslo 20.05.2015 Background Ca 3000 patients are surgically treated for morbid obesity in Norway each year.
Mousa Salah. Dr. Mohammad Al. Mohtasib. 1 P a g e
 8 Mousa Salah Dr. Mohammad Al. Mohtasib 1 P a g e In the previous lecture we talked about the peritoneum, and we said that the peritonium is a serous sac, and it consists of two layers, visceral and parietal.
8 Mousa Salah Dr. Mohammad Al. Mohtasib 1 P a g e In the previous lecture we talked about the peritoneum, and we said that the peritonium is a serous sac, and it consists of two layers, visceral and parietal.
SETTING Fudan University Shanghai Cancer Center. RESPONSIBLE PARTY Haiquan Chen MD.
 OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
Pancreatic Adenocarcinoma: Everything You Need to Know From Cross-Sectional Imaging to Treatment
 Pancreatic Adenocarcinoma: Everything You Need to Know From Cross-Sectional Imaging to Treatment Andrew W. Bowman, MD PhD Assistant Professor of Radiology Mayo Clinic Florida SCBT-MR Annual Meeting Nashville,
Pancreatic Adenocarcinoma: Everything You Need to Know From Cross-Sectional Imaging to Treatment Andrew W. Bowman, MD PhD Assistant Professor of Radiology Mayo Clinic Florida SCBT-MR Annual Meeting Nashville,
Robot-Assisted Minimally Invasive Distal Pancreatectomy Is Superior to the Laparoscopic Technique
 ORIGINAL ARTICLE Robot-Assisted Minimally Invasive Distal Pancreatectomy Is Superior to the Laparoscopic Technique Mustapha Daouadi, MD, Amer H. Zureikat, MD, Mazen S. Zenati, MD, MPH, PhD, Haroon Choudry,
ORIGINAL ARTICLE Robot-Assisted Minimally Invasive Distal Pancreatectomy Is Superior to the Laparoscopic Technique Mustapha Daouadi, MD, Amer H. Zureikat, MD, Mazen S. Zenati, MD, MPH, PhD, Haroon Choudry,
Minimally Invasive Esophagectomy
 Minimally Invasive Esophagectomy M A R K B E R R Y, M D A S S O C I AT E P R O F E S S O R D E PA R T M E N T OF C A R D I O T H O R A C I C S U R G E R Y S TA N F O R D U N I V E R S I T Y S E P T E M
Minimally Invasive Esophagectomy M A R K B E R R Y, M D A S S O C I AT E P R O F E S S O R D E PA R T M E N T OF C A R D I O T H O R A C I C S U R G E R Y S TA N F O R D U N I V E R S I T Y S E P T E M
BILIARY TRACT & PANCREAS, PART II
 CME Pretest BILIARY TRACT & PANCREAS, PART II VOLUME 41 1 2015 A pretest is mandatory to earn CME credit on the posttest. The pretest should be completed BEFORE reading the overview. Both tests must be
CME Pretest BILIARY TRACT & PANCREAS, PART II VOLUME 41 1 2015 A pretest is mandatory to earn CME credit on the posttest. The pretest should be completed BEFORE reading the overview. Both tests must be
The Learning Curve for Minimally Invasive Esophagectomy
 The Learning Curve for Minimally Invasive Esophagectomy AATS Focus on Thoracic Surgery Mastering Surgical Innovation Las Vegas Nevada Oct. 27-28 2017 Scott J Swanson, M.D. Professor of Surgery Harvard
The Learning Curve for Minimally Invasive Esophagectomy AATS Focus on Thoracic Surgery Mastering Surgical Innovation Las Vegas Nevada Oct. 27-28 2017 Scott J Swanson, M.D. Professor of Surgery Harvard
