Laparoscopic Whipple procedure: review of the literature
|
|
|
- Melvyn Reeves
- 5 years ago
- Views:
Transcription
1 J Hepatobiliary Pancreat Surg (2009) 16: DOI /s TOPICS Evolution and challenge in endoscopic HBP surgery Laparoscopic Whipple procedure: review of the literature Michel Gagner Æ Mariano Palermo Received: 1 March 2009 / Accepted: 31 March 2009 / Published online: 28 July 2009 Ó Springer 2009 Abstract Introduction Laparoscopic pancreatic surgery represents one of the most advanced applications for laparoscopic surgery currently in use. In the past, minimally invasive techniques were only used for diagnostic laparoscopy, staging of pancreatic cancer, and palliative procedures for unresectable pancreatic cancer. With new advances in technology and instrumentation, some sophisticated procedures are currently available, such as the Whipple procedure, one of the most sophisticated applications of minimally invasive surgery. Materials and methods A review of the literature shows that 146 laparoscopic Whipple procedures have been published worldwide since The authors analyzed blood loss, mean operating time, hospital stay, conversion rate, mean age, mortality rate, lymph nodes in the pathologic findings, follow up, and complications. Results Mean age was 59.1 years; mean operating time was 439 min. The average blood loss for the reviewed literature was 143 ml; median hospital stay was 18 days; conversion rate was 46%; number of lymph nodes in the pathologic findings was 19; and mortalities related to the procedure was low, 2 patients (1.3%) and the complication rate was 16% (23/46 patients). Complications included 2 hemorrhages, 4 bowel obstructions, 1 stress ulcer, 1 delay of gastric emptying, 4 pneumonias, and 11 leaks. M. Gagner (&) Department of Surgery, Mount Sinai Medical Center, 4300 Alton Road, Miami Beach, FL 33140, USA gagner.michel@gmail.com M. Palermo Department of Surgery, Hospital Nacional Prof. A. Posadas. Haedo, Buenos Aires, Argentina Conclusion This review demonstrates that the laparoscopic Whipple procedure is not only feasible but also safe, with low mortality and acceptable rates of complications. Introduction The laparoscopic approach for tumors located in the head of the pancreas is not universally accepted, because of its technical difficulties and highly trained surgeons required to perform this operation [1]. Laparoscopic pancreatic surgery represents one of the most advanced applications for laparoscopic surgery currently in use. These advances in technology and techniques have widely opened new gates to a wide range of applications in patients with pancreatic disease [1 5]. The first successful pancreatoduodenectomies were performed by Walter Kausch in 1912 and Allan Whipple in The first laparoscopic pancreatoduodenectomy was described in 1994 [6 10]. Laparoscopic pancreatic surgery uses a relatively new approach. In the past, the minimally invasive techniques were only used for diagnostic laparoscopy to evaluate periampullary malignancies, staging of pancreatic cancer, and palliative procedures for unresectable pancreatic cancer. With new advances in technology and instrumentation during the past decade, use of laparoscopic procedures for pancreatic disease has expanded to necrosectomy for necrotizing pancreatitis, drainage procedures for pancreatic pseudocysts, and distal resections of pancreatic tumors [11 14]. Currently, it is feasible to perform some sophisticated procedures such as the Whipple procedure, one of the most sophisticated applications of minimally invasive surgery.
2 J Hepatobiliary Pancreat Surg (2009) 16: This article reviews the literature regarding laparoscopy in the management of benign and malignant pancreatic disease that were treated by a Whipple procedure. Whipple procedure: surgical technique The laparoscopic technique for a Whipple procedure is a modification of Longmire and Traverso and pylorus-preserving pancreatoduodenectomy. Under general anesthesia, the patient is placed in a supine position with the legs abducted. Carbon dioxide pneumoperitoneum is established using an open technique through a 10-mm trocar over the umbilicus. A 30 telescope is inserted to examine the peritoneal cavity, liver, stomach, and mesentery vessels. Then 4 to 6 more trocars are inserted under direct vision in the epigastrium and upper quadrants. The peritoneum covering the common bile duct (CBD) is opened anteriorly and laterally, and is then dissected free posteromedially from the portal vein and the right hepatic artery. Using a 2-0 nylon suture passed through the abdominal wall in the right subcostal area and passed under the CBD, creating a suspension with minimum retraction. The CBD is then transected at least 2 cm above the pancreatic cystic duct junction using an endoscopic linear stapler. The first portion of the duodenum is then divided 1 cm distal to the pylorus, can be easily identified by looking inferiorly for the veins of Mayo and by palpating a slight induration in the area. After dissection of the gastrocolic ligament is completed, gastroepiploic vessels derived from the gastroduodenal vessels are double clipped with titanium clips. Using a right-angled dissector under the pylorus, a window of 1 cm 2 is created that allows passage of an endoscopic linear 12-mm stapler. Similarly, the duodenojejunal junction is transected as close to the proximal jejunum as possible, with the sample stapler to the right of the mesenteric vessels. The proximal jejunum retracts in the retroperitoneum and is freed at the ligament of Treitz. After transection, the gastroduodenal artery is exposed as the antrum of the stomach is pushed toward the left upper quadrant. The artery is dissected from the pancreatic neck and more so superiorly near its origin. From the hepatic artery, it is double-clipped with titanium clips and divided. The pancreas above the mesenteric vein and the portal vein is then transected using scissors. This sections the inferior and superior pancreatic vessel arcades controlled with a combination of metallic clips and cautery. A 10-mm, ultrasonic dissector can be used. The pancreatic duct is easily seen because of the magnification. It is left open and can be cannulated with a 5-Fr pediatric feeding tube. The uncinate process is resected from the mesenteric vessels by using an endoscopic linear stapler with two cartridges 60 mm long or using the ultrasonic dissector. The resected specimen is then inserted into a bag and left in the lower quadrant of the abdomen for later extraction. At this time, 3 anastomoses need to be created, and a good 2-handed technique with fast intracorporeal knot tying is necessary. The proximal jejunal loop is prepared for this task by further mobilizing the Treitz ligament, and several vessels are taken with the hook cautery and metallic clips. The loop is passed and advanced behind the mesenteric vessels through the ligament of Treitz. The pancreas to jejunum anastomosis is created first because of its need for precision and delicate sutures, and it is easier to perform with the free jejunal loop. The anastomosis is created in 2 layers: an outer layer with interrupted 3-0 silk and an inner layer with 4-0 absorbable sutures placed with a semi-curved needle, taking the duct to the antimesenteric side of the jejunum through the whole wall. Then 4 to 6 interrupted sutures are positioned beginning posteriorly. The hepaticojejunostomy is created in a similar fashion with intracorporeal sutures starting posteriorly, using 6 to 10 sutures. The distance between each anastomosis is 10 cm. The pylorojejunostomy is created using a 3-0 absorbable monofilament suture. The gallbladder can be removed after the sutures are placed. The specimen is extracted through the 18-mm umbilical trocar, the largest. Drains are positioned below and above the anastomosis and passed through the trocar sites in the right subcostal and right paramedian areas. A feeding jejunostomy is needed and a nasogastric tube is placed and its position verified. The fascial wounds are closed with 2-0 absorbable sutures [9]. Methods The following variables of each article: blood loss, mean operating time, hospital stay, conversion rate, mean age, mortality, lymph nodes in the pathology, follow up, and complications. Complications were determined to be bleeding, bowel obstruction, stress ulcer, delay gastric emptying, leak, and pneumonia. Results A review of the literature shows that 146 laparoscopic Whipple procedures have been published since The 14 publications with 146 Whipple procedures are listed in Table 1. Mean age was 59 (43 71) years. Mean operating time was min. Range was 284 min [1] to 660 min [19] (Table 2).
3 728 J Hepatobiliary Pancreat Surg (2009) 16: Table 1 Publications of laparoscopic Whipple reviewed Author Year of publication Number of procedures Gagner Gagner Gentileschi/Gagner Masson Milone/Gagner Amori Dulucq Staudacher Dulucq Lu Zheng Palanivelu Pugliese Sa Cunha Total 146 Table 2 Blood loss, operation time and hospital stay References Blood loss (ml) Operating time (min) Hospital stay (days) Dulucq et al. [1] Assalia and Gagner [25] Dulucq et al. [11] 107 ± ± ± 2.7 Staudacher et al. [14] 325 ± ± ± 2 Lu et al. [15] Zheng et al. [16] Ammori [19] Range Blood loss average for the reviewed literature was ml, with a range of 50 ml [16] to 770 ml [15] (see Table 2). The average number of hospital-stay days was 18, 7 days [18] to39[15] (see Table 2). Conversion rates were 46% (12 to 100%). Mean number of lymph nodes in the pathology was 19 (13 26). Mortality rates related with the procedure were low, only 2 (1.3%) patients died during the peri operative period. Follow up was an average of 11 months (2 32). Complication rates were 16% of patients (23/146). Complications were 2 hemorrhages, 4 bowel obstructions, 1 stress ulcer, 1 delay of gastric emptying, 4 pneumonias, and 11 leaks (Fig. 1) [16 20]. Histopathological findings were: Ampulloma (n = 62) Pancreatic adenocarcinoma (n = 45) Chronic pancreatitis (n = 13) Neuroendocrine tumors (n = 5) Fig. 1 Complications Cystadenocarcinoma (n = 5) Metastasis (n = 4) Low bile duct carcinoma (n = 3) Pancreatic mixed carcinoma (n = 1) Cholangiocarcinoma (n = 3) Mesenchymal tumor (n = 1) Duodenal adenocarcinoma (n = 2) Serous cystadenoma (n = 1) (Fig. 2) Discussion Some articles in the literature report that performing a Whipple procedure laparoscopically is feasible, but differences with the open technique have not been documented [4, 21, 22]. These authors say that the laparoscopic approach for distal pancreatectomy is easier than the Whipple procedure and is more accepted [4]. The total number of laparoscopic pancreatic resections remain small and many reports are often based on limited experience. In a recent multi-institutional study, 127 pancreatic resections in 27 European centers were described [23]. Most were distal resections. Another study from France, in a single institution, has 48 cases of laparoscopic pancreatic surgery, and only one was a Whipple procedure and one total pancreatectomy, the rest were distal resections or enucleations [24]. As stated previously,
4 J Hepatobiliary Pancreat Surg (2009) 16: also similar. The difference was that we noted more wound infections in the open group (16%). Also, the pancreatic fistula, which was 18% for the laparoscopic procedure, compared with the literature of open techniques increased from 2% to 30% [10]. Therefore, when techniques were compared for all the items reviewed, no large differences were noted between them. The principle disadvantage of the laparoscopic approach is the difficult and lengthy learning curve required. The principle advantage of the laparoscopic Whipple procedure is that it is a minimally invasive with all the advantages that that offers. However, although no benefit seemed to be derived from use of a laparoscopic approach, randomized controlled trials must be performed to achieve strong conclusions. One major concern always raised in cases of malignant disease treated by laparoscopy is whether this surgery is an adequate cancer operation, allowing tumor-free margins and sufficiently extensive lymph node dissection while being minimally invasive [16]. In review of the literature, the authors observed that extended lymphadenectomy is not necessary, because it does not prolong patient survival. Laparoscopic surgery causes less immunodeficiency with the open approach, which seems to be an important advantage for cancer patients. Conclusion Fig. 2 Summary of histopathologic findings laparoscopic pancreatectomy series remain small, particularly those on Whipple procedures. A retrospective review from Italy, a study of 19 patients with cephalic pancreatic cancer, was published in 2008, and 13 cases could be finished laparoscopically with good results [10]. In the review of the literature, we found good results, but the laparoscopic approach is not universally accepted as the best one because of long operating time, technically difficult procedure, and a lack of reduction in length of hospital stay. When the results from this review were compared with those of a meta-analysis with regard to comparison between two open techniques, published by Diener and colleagues [21], the operating time was determined to be similar (mean of laparoscopic vs. 401 open); blood loss was higher in the open technique (819.6 open vs laparoscopic); hospital stay was similar in comparing both techniques (20.9 days for the open group vs for the laparoscopic group); and mortality rate was also similar (1.54 open vs. 1.3 laparoscopic). The complications were This review demonstrates that the laparoscopic Whipple procedure is not only feasible but safe, with low mortality and acceptable complication rates. However, the laparoscopic Whipple procedure should be performed in selected cases by a highly skilled laparoscopic surgeon to be feasible, safe, and achieve good results. In case of doubt or difficulties in the dissection, an open resection should be performed. References 1. Dulucq JL, Wintringer P, Stabilini C, Feryn T, Perissat J, Mahajna A. Are major laparoscopic pancreatic resections worthwhile? A prospective study of 32 patients in a single institution. Surg Endosc. 2005;19(8): Olivié D, Lepanto L, Billiard JS, Audet P, Lavallée JM. Predicting resectability of pancreatic head cáncer with multi-detector CT. Surgical and pathologic correlation. JOP. 2007;8(6): Mori T, Abe N, Sugiyama M, Atomi Y. Laparoscopic pancreatic surgery. J Hepatobiliary Pancreat Surg. 2005;12(6): Masson B, Sa-Cunha A, Laurent C, Rault A, Collet D. Laparoscopic pancreatectomy: report of 22 cases. Ann Chir. 2003; 128(7): Spanknebel K, Conlon KC. Advances in the surgical management of pancreatic cancer. Cancer J. 2001;7(4):
5 730 J Hepatobiliary Pancreat Surg (2009) 16: Strasberg SM, Drebin JA, Soper NJ. Evolution and current status of the Whipple procedure: an update for gastroenterologists. Gastroenterology. 1997;113(3): Schäfer M, Müllhaupt B, Clavien PA. Evidence based pancreatic head resection for pancreatic cancer and chronic pancreatitis. Ann Surg. 2002;236(2): Gagner M, Pomp A. Laparoscopic pancreatic resection: is it a worthwhile? J Gastrointest Surg. 1997;1(1):20 5. (discussion 25-6). 9. Gagner M, Pomp A. Laparoscopic pylorus preserving pancreatoduodenectomy. Surg Endosc. 1994;8(5): Pugliese R, Scandroglio I, Sansonna F, Maggioni D, Costanzi A, Citterio D, et al. Laparoscopic pancreaticoduodenectomy: a retrospective review of 19 cases. Surg Laparosc Endosc Percutan Tech. 2008;18(1): Dulucq JL, Wintringer P, Mahajna A. Laparoscopic pancreaticoduodenectomy for benign and malignant diseases. Surg Endosc. 2006;20(7): Palanivelu C, Jani K, Senthilnathan P, Parthasarathi R, Rajapandian S, Madhankumar MV. Laparoscopic pancreaticoduodenectomy: technique and outcomes. J Am Coll Surg. 2007; 205(2): Milone L, Turner P, Gagner M. Laparoscopic surgery for pancreatic tumors, an uptake. Minerva Chir. 2004;59(2): Staudacher C, Orsenigo E, Baccari P, Di Palo S, Crippa S. Laparoscopic assisted duodenopancreatectomy. Surg Endosc. 2005;19(3): Lu B, Cai X, Lu W, Huang Y, Jin X. Laparoscopic pancreaticoduodenectomy to treat cancer of the ampulla the Vater. JSLS. 2006;10(1): Zheng MH, Feng B, Lu AG, Li JW, Hu WG, Wang ML, et al. Laparoscopic pancreaticoduodenectomy for ductal adenocarcinoma of common bile duct: a case report and literature review. Med Sci Monit. 2006;12(6):CS Sa Cunha A, Rault A, Beau C, Laurent C, Collet D, Masson B. A single institution prospective study of laparoscopic pancreatic resection. Arch Surg. 2008;143(3): (discussion 295). 18. Gentileschi P, Gagner M. Laparoscopic pancreatic resection. Chir Ital. 2001;53(3): Ammori BJ. Laparoscopic hand assisted pancreaticoduodenectomy: initial UK experience. Surg Endosc. 2004;18(4): Huang J, Yeo C, Sohn T, Lillemoe KD, Sauter PK, Coleman J, et al. Quality of life and outcomes after pancreaticoduodenectomy. Ann Surg. 2000;231(6): Diener M, Knaebel P, Heukaufer C, Antes G, Buchler M, Seiler C. A systematic review and meta-analysis of pylorus preserving versus classical pancreaticoduodenectomy for surgical treatment of periampullary and pancreatic carcinoma. Ann Surg. 2007;245(2): Raut C, Tseng J, Sun C, Wang H, Wolff RA, Crane CH, et al. Impact of resection status on pattern failure and survival after pancreaticoduodenectomy for pancreatic adenocarcinoma. Ann Surg. 2007;246(1): Eubanks S, Swanstron L, Soper N. Mastery of endoscopic and laparoscopic surgery. Lippincott Williams & Wilkins 2000, Chapter 32. Laparoscopic Pancreatic Surgery. Michel Gagner Pappas T, Pryor A, Harnisch M. Atlas of laparoscopic surgery. 3rd ed. New York: Springer; Assalia A, Gagner M. Laparoscopic pancreatic surgery for islet cell tumors of the pancreas. World J Surg. 2004; 28(12): 9 47.
Pylorus Preserving Pancreaticoduodenectomy
 REVIEW Pylorus Preserving Pancreaticoduodenectomy Jacqueline M. Garonzik-Wang, M. B. Majella Doyle Pancreaticoduodenectomy (PD) has become the standard of care for resectable pancreatic cancer and premalignant
REVIEW Pylorus Preserving Pancreaticoduodenectomy Jacqueline M. Garonzik-Wang, M. B. Majella Doyle Pancreaticoduodenectomy (PD) has become the standard of care for resectable pancreatic cancer and premalignant
The first total laparoscopic pancreatoduodenectomy in Poland
 Case report Videosurgery Andrzej Budzyński 1, Anna Zub-Pokrowiecka 1, Anna Zychowicz 1, Michał Pędziwiatr 1, Mateusz Wierdak 2, Maciej Matłok 1, Małgorzata Zając 1 12 nd Department of General Surgery,
Case report Videosurgery Andrzej Budzyński 1, Anna Zub-Pokrowiecka 1, Anna Zychowicz 1, Michał Pędziwiatr 1, Mateusz Wierdak 2, Maciej Matłok 1, Małgorzata Zając 1 12 nd Department of General Surgery,
The Whipple Operation Illustrations
 The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
Yoshitsugu; Kanematsu, Takashi; Kur
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Laparoscopic Middle Pancreatectomy Surgery Kitasato, Amane; Adachi, Tomohiko; Yoshitsugu; Kanematsu, Takashi; Kur Hepato-Gastroenterology, 59(120),
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Laparoscopic Middle Pancreatectomy Surgery Kitasato, Amane; Adachi, Tomohiko; Yoshitsugu; Kanematsu, Takashi; Kur Hepato-Gastroenterology, 59(120),
Pancreaticoduodenectomy the anatomy and the surgical approaches
 Pancreaticoduodenectomy the anatomy and the surgical approaches Paul BS LAI Division of Hepato biliary and Pancreatic Surgery Department of Surgery The Chinese Univesity of Hong Kong Whipple s operation
Pancreaticoduodenectomy the anatomy and the surgical approaches Paul BS LAI Division of Hepato biliary and Pancreatic Surgery Department of Surgery The Chinese Univesity of Hong Kong Whipple s operation
Citation Hepato-Gastroenterology, 55(86-87),
 NAOSITE: Nagasaki University's Ac Title Author(s) Combined pancreatic resection and p multiple lesions of the pancreas: i of the pancreas concomitant with du Kuroki, Tamotsu; Tajima, Yoshitsugu Tomohiko;
NAOSITE: Nagasaki University's Ac Title Author(s) Combined pancreatic resection and p multiple lesions of the pancreas: i of the pancreas concomitant with du Kuroki, Tamotsu; Tajima, Yoshitsugu Tomohiko;
Anatomy of the SMALL INTESTINE. Dr. Noman Ullah Wazir PMC
 Anatomy of the SMALL INTESTINE Dr. Noman Ullah Wazir PMC SMALL INTESTINE The small intestine, consists of the duodenum, jejunum, and illium. It extends from the pylorus to the ileocecal junction were the
Anatomy of the SMALL INTESTINE Dr. Noman Ullah Wazir PMC SMALL INTESTINE The small intestine, consists of the duodenum, jejunum, and illium. It extends from the pylorus to the ileocecal junction were the
Total laparoscopic pancreaticoduodenectomy: a retrospective study of 27 cases treated in a single institution
 Original Article Total laparoscopic pancreaticoduodenectomy: a retrospective study of 27 cases treated in a single institution Hong Li 1, Jie Zhu 2, Bin Zhang 1, Gencong Li 1, Xinhua Zhou 3, Dansong Yu
Original Article Total laparoscopic pancreaticoduodenectomy: a retrospective study of 27 cases treated in a single institution Hong Li 1, Jie Zhu 2, Bin Zhang 1, Gencong Li 1, Xinhua Zhou 3, Dansong Yu
The abdominal Esophagus, Stomach and the Duodenum. Prof. Oluwadiya KS
 The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
LAPAROSCOPIC WHIPPLE' S PROCEDURE PRESENT PAST AND FUTURE
 LAPAROSCOPIC WHIPPLE' S PROCEDURE PRESENT PAST AND FUTURE Dr. VINOD KUMAR SINGH, M.S, D.MAS CONSULTANT GENERAL SURGEON Member of world association of laparoscopic surgeons Project submitted toward completion
LAPAROSCOPIC WHIPPLE' S PROCEDURE PRESENT PAST AND FUTURE Dr. VINOD KUMAR SINGH, M.S, D.MAS CONSULTANT GENERAL SURGEON Member of world association of laparoscopic surgeons Project submitted toward completion
Pancreas-Preserving Total Duodenectomy
 How I do it Dig Surg 1998;15:398 403 Gregory G. Tsiotos Michael G. Sarr Division of Gastroenterologic and General Surgery, Department of Surgery, Mayo Clinic, Rochester, Minn., USA Pancreas-Preserving
How I do it Dig Surg 1998;15:398 403 Gregory G. Tsiotos Michael G. Sarr Division of Gastroenterologic and General Surgery, Department of Surgery, Mayo Clinic, Rochester, Minn., USA Pancreas-Preserving
Laparoscopy-assisted D2 radical distal subtotal gastrectomy
 Masters of Gastrointestinal Surgery Laparoscopy-assisted D2 radical distal subtotal gastrectomy Xiaogeng Chen, Weihua Li, Jinsi Wang, Changshun Yang Department of Tumor Surgery, Fujian Provincial Hospital,
Masters of Gastrointestinal Surgery Laparoscopy-assisted D2 radical distal subtotal gastrectomy Xiaogeng Chen, Weihua Li, Jinsi Wang, Changshun Yang Department of Tumor Surgery, Fujian Provincial Hospital,
JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES
 JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES THE PROBLEM DUODENAL / PANCREATIC INJURIES Difficult to diagnose Not very common Anatomic and physiologic challenges 90% rate of associated
JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES THE PROBLEM DUODENAL / PANCREATIC INJURIES Difficult to diagnose Not very common Anatomic and physiologic challenges 90% rate of associated
د. عصام طارق. Objectives:
 GI anatomy Lecture: 5 د. عصام طارق Objectives: To describe anatomy of stomach, duodenum & pancreas. To list their main relations. To define their blood & nerve supply. To list their lymph drainage. To
GI anatomy Lecture: 5 د. عصام طارق Objectives: To describe anatomy of stomach, duodenum & pancreas. To list their main relations. To define their blood & nerve supply. To list their lymph drainage. To
Dr. Zahiri. In the name of God
 Dr. Zahiri In the name of God small intestine = small bowel is the part of the gastrointestinal tract Boundaries: Pylorus Ileosecal junction Function: digestion and absorption of food It receives bile
Dr. Zahiri In the name of God small intestine = small bowel is the part of the gastrointestinal tract Boundaries: Pylorus Ileosecal junction Function: digestion and absorption of food It receives bile
Pancreas Quizzes c. Both A and B a. Directly into the blood stream (not using ducts)
 Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
Technical considerations for the fully robotic pancreaticoduodenectomy
 Surgical Techniques on Pancreatic Surgery Technical considerations for the fully robotic pancreaticoduodenectomy Daniel Galvez, Rebecca Sorber, Ammar A. Javed, Jin He Department of Surgery, The Johns Hopkins
Surgical Techniques on Pancreatic Surgery Technical considerations for the fully robotic pancreaticoduodenectomy Daniel Galvez, Rebecca Sorber, Ammar A. Javed, Jin He Department of Surgery, The Johns Hopkins
ADVANCED LAPAROSCOPIC PANCREAS SURGERY A HANDS-ON WORKSHOP
 ADVANCED LAPAROSCOPIC PANCREAS SURGERY A HANDS-ON WORKSHOP 3-4 November 2017 at the AMC in Amsterdam Organizing committee: Mo Abu Hilal, Professor of Surgery at Southampton University Marc Besselink, Professor
ADVANCED LAPAROSCOPIC PANCREAS SURGERY A HANDS-ON WORKSHOP 3-4 November 2017 at the AMC in Amsterdam Organizing committee: Mo Abu Hilal, Professor of Surgery at Southampton University Marc Besselink, Professor
Prevention Of Pancreaticojejunal Fistula After Whipple Procedure
 ISPUB.COM The Internet Journal of Surgery Volume 4 Number 2 Prevention Of Pancreaticojejunal Fistula After Whipple Procedure N Barbetakis, K Setsiz Citation N Barbetakis, K Setsiz. Prevention Of Pancreaticojejunal
ISPUB.COM The Internet Journal of Surgery Volume 4 Number 2 Prevention Of Pancreaticojejunal Fistula After Whipple Procedure N Barbetakis, K Setsiz Citation N Barbetakis, K Setsiz. Prevention Of Pancreaticojejunal
Original Article Difficulties and countermeasures of laparoscopic pancreaticoduodenectomy: report of 18 cases
 Int J Clin Exp Med 2016;9(2):2451-2457 www.ijcem.com /ISSN:1940-5901/IJCEM0016024 Original Article Difficulties and countermeasures of laparoscopic pancreaticoduodenectomy: report of 18 cases Xiaoming
Int J Clin Exp Med 2016;9(2):2451-2457 www.ijcem.com /ISSN:1940-5901/IJCEM0016024 Original Article Difficulties and countermeasures of laparoscopic pancreaticoduodenectomy: report of 18 cases Xiaoming
An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein
 J Gastrointest Surg (2007) 11:425 431 DOI 10.1007/s11605-007-0131-1 An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein Rory L. Smoot & John D. Christein &
J Gastrointest Surg (2007) 11:425 431 DOI 10.1007/s11605-007-0131-1 An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein Rory L. Smoot & John D. Christein &
Feasibility of Laparoscopic Distal Spleno-Pancreatectomy Following Previous Necrosectomy. A Case Report
 CASE REPORT Feasibility of Laparoscopic Distal Spleno-Pancreatectomy Following Previous Necrosectomy. A Case Report Anil K Hemandas 1, Gaurav Jain 1, Farina Fong 1, Brian Stedman 2, Eleanor Jaynes 3, Mohammad
CASE REPORT Feasibility of Laparoscopic Distal Spleno-Pancreatectomy Following Previous Necrosectomy. A Case Report Anil K Hemandas 1, Gaurav Jain 1, Farina Fong 1, Brian Stedman 2, Eleanor Jaynes 3, Mohammad
THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY 2013/12/21
 THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY Tsann-Long Hwang, MD, FACS Department of Surgery Chang Gung Memorial Hospital Chang Gung University Taipei, TAIWAN 2013/12/21 THE DIFFICULTY
THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY Tsann-Long Hwang, MD, FACS Department of Surgery Chang Gung Memorial Hospital Chang Gung University Taipei, TAIWAN 2013/12/21 THE DIFFICULTY
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Outcomes associated with robotic approach to pancreatic resections
 Short Communication (Management of Foregut Malignancies and Hepatobiliary Tract and Pancreas Malignancies) Outcomes associated with robotic approach to pancreatic resections Caitlin Takahashi 1, Ravi Shridhar
Short Communication (Management of Foregut Malignancies and Hepatobiliary Tract and Pancreas Malignancies) Outcomes associated with robotic approach to pancreatic resections Caitlin Takahashi 1, Ravi Shridhar
Totally laparoscopic total gastrectomy for locally advanced middle-upper-third gastric cancer
 Original Article on Gastrointestinal Surgery Totally laparoscopic total gastrectomy for locally advanced middle-upper-third gastric cancer Mi Lin, Chang-Ming Huang, Chao-Hui Zheng, Ping Li, Jian-Wei Xie,
Original Article on Gastrointestinal Surgery Totally laparoscopic total gastrectomy for locally advanced middle-upper-third gastric cancer Mi Lin, Chang-Ming Huang, Chao-Hui Zheng, Ping Li, Jian-Wei Xie,
General Surgery PURPLE SERVICE MUHC-RVH Site
 Preamble HPB is a clinical teaching unit with several different vocations: It regroups all solid organ Transplantation as well as most advanced Hepatobiliary and Pancreatic clinical activities performed
Preamble HPB is a clinical teaching unit with several different vocations: It regroups all solid organ Transplantation as well as most advanced Hepatobiliary and Pancreatic clinical activities performed
Block 3: DISSECTION 2 CELIAC TRUNK, JEJUNUM/ILEUM, LARGE INTESTINE, DUODENUM, PANCREAS, PORTAL VEIN; MOBILIZATION OF THE LIVER
 1 Block 3: DISSECTION 2 CELIAC TRUNK, JEJUNUM/ILEUM, LARGE INTESTINE, DUODENUM, PANCREAS, PORTAL VEIN; MOBILIZATION OF THE LIVER Attempt to complete as much as you can of the dissection explained in the
1 Block 3: DISSECTION 2 CELIAC TRUNK, JEJUNUM/ILEUM, LARGE INTESTINE, DUODENUM, PANCREAS, PORTAL VEIN; MOBILIZATION OF THE LIVER Attempt to complete as much as you can of the dissection explained in the
Laparoscopic Subtotal Gastrectomy for Gastric Cancer
 SCIENTIFIC PAPER Laparoscopic Subtotal Gastrectomy for Gastric Cancer Danny Rosin, MD, Yuri Goldes, MD, Barak Bar Zakai, MD, Moshe Shabtai, MD, Amram Ayalon, MD, Oded Zmora, MD ABSTRACT Background: The
SCIENTIFIC PAPER Laparoscopic Subtotal Gastrectomy for Gastric Cancer Danny Rosin, MD, Yuri Goldes, MD, Barak Bar Zakai, MD, Moshe Shabtai, MD, Amram Ayalon, MD, Oded Zmora, MD ABSTRACT Background: The
Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 14
 Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 14 Contents 14. Neuroendocrine Tumours 161 14.1. Diagnostic algorithm
Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 14 Contents 14. Neuroendocrine Tumours 161 14.1. Diagnostic algorithm
Surgical Management of CBD Injury Jin Seok Heo
 Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
Laparoscopic extended right hemicolectomy with D3
 Surgical Technique Page 1 of 11 Laparoscopic extended right hemicolectomy with D3 lymphadenectomy Weixian Hu, Jiabin Zheng, Yong Li Department of General Surgery, Guangdong General Hospital, Guangdong
Surgical Technique Page 1 of 11 Laparoscopic extended right hemicolectomy with D3 lymphadenectomy Weixian Hu, Jiabin Zheng, Yong Li Department of General Surgery, Guangdong General Hospital, Guangdong
Objectives. Intraoperative Consultation of the Whipple Resection Specimen. Pancreas Anatomy. Pancreatic ductal carcinoma 11/10/2014
 Intraoperative Consultation of the Whipple Resection Specimen Pathology Update Faculty of Medicine, University of Toronto November 15, 2014 John W. Wong, MD, FRCPC Department of Anatomical Pathology Sunnybrook
Intraoperative Consultation of the Whipple Resection Specimen Pathology Update Faculty of Medicine, University of Toronto November 15, 2014 John W. Wong, MD, FRCPC Department of Anatomical Pathology Sunnybrook
5/17/2013. Pancreatic Cancer. Postgraduate Course in General Surgery CASE 1: CASE 1: Overview. Case presentation. Differential diagnosis
 Overview Case presentation Postgraduate Course in General Surgery Differential diagnosis Diagnosis and therapy Eric K. Nakakura Koloa, HI March 26, 2013 Outcomes CASE 1: CASE 1: A 78-year-old man developed
Overview Case presentation Postgraduate Course in General Surgery Differential diagnosis Diagnosis and therapy Eric K. Nakakura Koloa, HI March 26, 2013 Outcomes CASE 1: CASE 1: A 78-year-old man developed
Management of biliary injury after laparoscopic cholecystectomy N. Dayes Kings County Hospital Center & Long Island College Hospital 8/19/2010
 Management of biliary injury after laparoscopic cholecystectomy N. Dayes Kings County Hospital Center & Long Island College Hospital 8/19/2010 Case Presentation 30 y.o. woman with 2 weeks of RUQ abdominal
Management of biliary injury after laparoscopic cholecystectomy N. Dayes Kings County Hospital Center & Long Island College Hospital 8/19/2010 Case Presentation 30 y.o. woman with 2 weeks of RUQ abdominal
Index (SIRS), 158, 173
 Index A Acute pancreatitis surgery abdominal compartment syndrome, 188 adjuvant treatment, 194 anterior approach, 175 antibiotic prophylaxis, 166 167, 197 Atlanta classification, 181 classification of
Index A Acute pancreatitis surgery abdominal compartment syndrome, 188 adjuvant treatment, 194 anterior approach, 175 antibiotic prophylaxis, 166 167, 197 Atlanta classification, 181 classification of
Accessory Glands of Digestive System
 Accessory Glands of Digestive System The liver The liver is soft and pliable and occupies the upper part of the abdominal cavity just beneath the diaphragm. The greater part of the liver is situated under
Accessory Glands of Digestive System The liver The liver is soft and pliable and occupies the upper part of the abdominal cavity just beneath the diaphragm. The greater part of the liver is situated under
3/28/2012. Periampullary Tumors. Postgraduate Course in General Surgery CASE 1: CASE 1: Overview. Eric K. Nakakura Ko Olina, HI
 Overview Postgraduate Course in General Surgery Case presentation Differential diagnosis Diagnosis and therapy Outcomes Principles of palliative care Eric K. Nakakura Ko Olina, HI March 27, 2012 CASE 1:
Overview Postgraduate Course in General Surgery Case presentation Differential diagnosis Diagnosis and therapy Outcomes Principles of palliative care Eric K. Nakakura Ko Olina, HI March 27, 2012 CASE 1:
PANCREAS DUCTAL ADENOCARCINOMA PDAC
 CONTENTS PANCREAS DUCTAL ADENOCARCINOMA PDAC I. What is the pancreas? II. III. IV. What is pancreas cancer? What is the epidemiology of Pancreatic Ductal Adenocarcinoma (PDAC)? What are the risk factors
CONTENTS PANCREAS DUCTAL ADENOCARCINOMA PDAC I. What is the pancreas? II. III. IV. What is pancreas cancer? What is the epidemiology of Pancreatic Ductal Adenocarcinoma (PDAC)? What are the risk factors
Pancreatico-Duodenal Trauma: Drain, Debride, Divert, Despair BACKGROUND EPIDEMIOLOGY 9/11/2018
 Pancreatico-Duodenal Trauma: Drain, Debride, Divert, Despair Rochelle A. Dicker, M.D. Professor of Surgery and Anesthesia UCLA BACKGROUND Lancet 1827: Travers, B Rupture of the Pancreas British Journal
Pancreatico-Duodenal Trauma: Drain, Debride, Divert, Despair Rochelle A. Dicker, M.D. Professor of Surgery and Anesthesia UCLA BACKGROUND Lancet 1827: Travers, B Rupture of the Pancreas British Journal
Palliative Laparoscopic Hepatico- and Gastrojejunostomy for Advanced Pancreatic Cancer
 SCIENTIFIC PAPER Palliative Laparoscopic Hepatico- and Gastrojejunostomy for Advanced Pancreatic Cancer Paolo Gentileschi, MD, Subhash Kini, MD, Michel Gagner, MD, FACS, FRCSC ABSTRACT Only 10% to 20%
SCIENTIFIC PAPER Palliative Laparoscopic Hepatico- and Gastrojejunostomy for Advanced Pancreatic Cancer Paolo Gentileschi, MD, Subhash Kini, MD, Michel Gagner, MD, FACS, FRCSC ABSTRACT Only 10% to 20%
Pathways of Regional Spread in Pancreatic Cancer
 Pathways of Regional Spread in Pancreatic Cancer 12 Chusilp Charnsangavej, M.D. Regional spread of pancreatic ductal adenocarcinoma is common at the time of diagnosis, and it is often associated with poor
Pathways of Regional Spread in Pancreatic Cancer 12 Chusilp Charnsangavej, M.D. Regional spread of pancreatic ductal adenocarcinoma is common at the time of diagnosis, and it is often associated with poor
Duodenum retroperitoneal
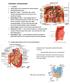 Duodenum retroperitoneal C shaped Initial region out of stomach into small intestine RETROperitoneal viscus Superior 1 st part duodenal cap ; moves upwards and backwards to lie on the R crura medial to
Duodenum retroperitoneal C shaped Initial region out of stomach into small intestine RETROperitoneal viscus Superior 1 st part duodenal cap ; moves upwards and backwards to lie on the R crura medial to
ABDOMEN - GI. Duodenum
 TALA SALEH ABDOMEN - GI Duodenum - Notice the shape of the duodenum, it looks like capital G shape tube which extends from the pyloroduodenal junction to the duodenojejunal junction. - It is 10 inches
TALA SALEH ABDOMEN - GI Duodenum - Notice the shape of the duodenum, it looks like capital G shape tube which extends from the pyloroduodenal junction to the duodenojejunal junction. - It is 10 inches
Laparoscopic Central Pancreatectomy: A Review of 51 Cases
 REVIEW ARTICLE Laparoscopic Central Pancreatectomy: A Review of 51 Cases Marcel Autran C. Machado, MD, Rodrigo Can ada Surjan, MD, Marina G. Epstein, MD, and Fabio Ferrari Makdissi, MD Background: Central
REVIEW ARTICLE Laparoscopic Central Pancreatectomy: A Review of 51 Cases Marcel Autran C. Machado, MD, Rodrigo Can ada Surjan, MD, Marina G. Epstein, MD, and Fabio Ferrari Makdissi, MD Background: Central
INFORMATION ON PANCREATIC HEAD AND PERIAMPULLARY CANCER
 INFORMATION ON PANCREATIC HEAD AND PERIAMPULLARY CANCER What is Pancreas? The pancreas is a gland located in the back of your abdomen behind the stomach. pancreas is divided into four parts: the head,
INFORMATION ON PANCREATIC HEAD AND PERIAMPULLARY CANCER What is Pancreas? The pancreas is a gland located in the back of your abdomen behind the stomach. pancreas is divided into four parts: the head,
Pancreas & Biliary System. Dr. Vohra & Dr. Jamila
 Pancreas & Biliary System Dr. Vohra & Dr. Jamila 1 Objectives At the end of the lecture, the student should be able to describe the: Location, surface anatomy, parts, relations & peritoneal reflection
Pancreas & Biliary System Dr. Vohra & Dr. Jamila 1 Objectives At the end of the lecture, the student should be able to describe the: Location, surface anatomy, parts, relations & peritoneal reflection
Cattell-Braasch maneuver combined with superior mesenteric artery first approach for resection of borderline resectable pancreatic cancer
 Masters of Surgery Page 1 of 5 Cattell-Braasch maneuver combined with superior mesenteric artery first approach for resection of borderline resectable pancreatic cancer Tingsong Yang 1, Fairweather Mark
Masters of Surgery Page 1 of 5 Cattell-Braasch maneuver combined with superior mesenteric artery first approach for resection of borderline resectable pancreatic cancer Tingsong Yang 1, Fairweather Mark
PANCREATODUODENECTOMY VERSUS WHIPPLE HEAD OF THE PANCREAS PYLORUS PRESERVING PROCEDURE FOR ADENOCARCINOMA OF THE INTRODUCTION
 HPB Surgery 1989, Vol. 1, pp. 195-200 Reprints available directly from the publisher Photocopying permitted by license only (C) 1989 Harwood Academic Publishers GmbH Printed in Great Britain PYLORUS PRESERVING
HPB Surgery 1989, Vol. 1, pp. 195-200 Reprints available directly from the publisher Photocopying permitted by license only (C) 1989 Harwood Academic Publishers GmbH Printed in Great Britain PYLORUS PRESERVING
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of laparoscopic distal pancreatectomy Laparoscopic distal pancreatectomy is the
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of laparoscopic distal pancreatectomy Laparoscopic distal pancreatectomy is the
To describe the liver. To list main structures in porta hepatis.
 GI anatomy Lecture: 6 د. عصام طارق Objectives: To describe the liver. To list main structures in porta hepatis. To define portal system & portosystemic anastomosis. To list parts of biliary system. To
GI anatomy Lecture: 6 د. عصام طارق Objectives: To describe the liver. To list main structures in porta hepatis. To define portal system & portosystemic anastomosis. To list parts of biliary system. To
Multiple Primary Quiz
 Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
Local Experience of Laparoscopic Pancreatectomy
 VOL.11 VOL.12NO.5 NO.6 MAY JUNE 20062007 Medical Bulletin Local Experience of Laparoscopic Pancreatectomy Dr. Chung-ngai Tang Consultant Surgeon Chief of Hepatobiliary Surgery Co-director of Minimal Access
VOL.11 VOL.12NO.5 NO.6 MAY JUNE 20062007 Medical Bulletin Local Experience of Laparoscopic Pancreatectomy Dr. Chung-ngai Tang Consultant Surgeon Chief of Hepatobiliary Surgery Co-director of Minimal Access
Totally laparoscopic distal gastrectomy reconstructed by Rouxen-Y with D2 lymphadenectomy and needle catheter jejunostomy for gastric cancer
 Masters of Gastrointestinal Surgery Totally laparoscopic distal gastrectomy reconstructed by Rouxen-Y with D2 lymphadenectomy and needle catheter jejunostomy for gastric cancer Xin Ye, Jian-Chun Yu, Wei-Ming
Masters of Gastrointestinal Surgery Totally laparoscopic distal gastrectomy reconstructed by Rouxen-Y with D2 lymphadenectomy and needle catheter jejunostomy for gastric cancer Xin Ye, Jian-Chun Yu, Wei-Ming
The peritoneum. Prof. Oluwadiya KS, MBBS, FMCS(Orthop) Website:
 The peritoneum Prof. Oluwadiya KS, MBBS, FMCS(Orthop) Website: http://oluwadiya.com The peritoneum Serous membrane that lines the abdominopelvic cavity and invests the viscera The largest serous membrane
The peritoneum Prof. Oluwadiya KS, MBBS, FMCS(Orthop) Website: http://oluwadiya.com The peritoneum Serous membrane that lines the abdominopelvic cavity and invests the viscera The largest serous membrane
Laparoscopic spleen-preserving complete splenic hilum lymphadenectomy for advanced proximal gastric cancer
 Review Article Page 1 of 5 Laparoscopic spleen-preserving complete splenic hilum lymphadenectomy for advanced proximal gastric cancer Wei Wang*, Wejun Xiong*, Qiqi Peng, Shanao Ye, Yansheng Zheng, Lijie
Review Article Page 1 of 5 Laparoscopic spleen-preserving complete splenic hilum lymphadenectomy for advanced proximal gastric cancer Wei Wang*, Wejun Xiong*, Qiqi Peng, Shanao Ye, Yansheng Zheng, Lijie
Li Yang, Diancai Zhang, Fengyuan Li, Xiang Ma. Introduction
 Original Article on Gastrointestinal Surgery Simultaneous laparoscopic distal gastrectomy (uncut Roux-en-Y anastomosis), right hemi-colectomy and radical rectectomy (Dixon) in a synchronous triple primary
Original Article on Gastrointestinal Surgery Simultaneous laparoscopic distal gastrectomy (uncut Roux-en-Y anastomosis), right hemi-colectomy and radical rectectomy (Dixon) in a synchronous triple primary
Endoscopic Ultrasonography Assessment for Ampullary and Bile Duct Malignancy
 Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
PANCREATIC CANCER GUIDELINES
 PANCREATIC CANCER GUIDELINES North-East London Cancer Network & Barts and the London HPB Centre PROTOCOL FOR MANAGEMENT OF PANCREATIC CANCER (SEPTEMBER 2010) I. PRE-REFERRAL GUIDELINES Screening 1. Offer
PANCREATIC CANCER GUIDELINES North-East London Cancer Network & Barts and the London HPB Centre PROTOCOL FOR MANAGEMENT OF PANCREATIC CANCER (SEPTEMBER 2010) I. PRE-REFERRAL GUIDELINES Screening 1. Offer
Clinical benefit of Totally Laparoscopic over Laparoscopically Assisted Distal Gastrectomy with Roux-en-Y Reconstruction for Early Gastric Cancer
 Med. Bull. Fukuoka Univ. 39 3/4 251 256 2012 Clinical benefit of Totally Laparoscopic over Laparoscopically Assisted Distal Gastrectomy with Roux-en-Y Reconstruction for Early Gastric Cancer Tatsuya HASHIMOTO,
Med. Bull. Fukuoka Univ. 39 3/4 251 256 2012 Clinical benefit of Totally Laparoscopic over Laparoscopically Assisted Distal Gastrectomy with Roux-en-Y Reconstruction for Early Gastric Cancer Tatsuya HASHIMOTO,
Laparoscopic Intestinal Derotation. Original Technique
 TECHNICAL REPORT Original Technique Mario Valle, MD, FICS, Orietta Federici, MD, Enrico Tarantino, MD, Francesco Corona, MD, and Alfredo Garofalo, MD Abstract: The intestinal derotation technique, introduced
TECHNICAL REPORT Original Technique Mario Valle, MD, FICS, Orietta Federici, MD, Enrico Tarantino, MD, Francesco Corona, MD, and Alfredo Garofalo, MD Abstract: The intestinal derotation technique, introduced
Laparoscopic extended right hemicolectomy with D3 lymphadenectomy
 Surgical Technique Page 1 of 10 Laparoscopic extended right hemicolectomy with D3 lymphadenectomy Yong Li General Surgery, Guangdong General Hospital and Guangdong Academy of Medical Sciences, Guangzhou
Surgical Technique Page 1 of 10 Laparoscopic extended right hemicolectomy with D3 lymphadenectomy Yong Li General Surgery, Guangdong General Hospital and Guangdong Academy of Medical Sciences, Guangzhou
-Ensherah Mokheemer. -Shatha Al-Jaberi محمد المحتسب- 1 P a g e
 9-9 -Ensherah Mokheemer -Shatha Al-Jaberi محمد المحتسب- 1 P a g e Small intestine has three regions: ( االثني عشر( The duodenum The jejunum The ileum Small intestine Duodenum: -c-shaped -The concavity
9-9 -Ensherah Mokheemer -Shatha Al-Jaberi محمد المحتسب- 1 P a g e Small intestine has three regions: ( االثني عشر( The duodenum The jejunum The ileum Small intestine Duodenum: -c-shaped -The concavity
Small Plicae Circularis. Short Closely packed together. Sparse, completely absent at distal part Lymphoid Nodule
 Intestines Differences Between Jejunum and Ileum Types Jejunum Ileum Color Deeper red Paler pink Calibre Bigger Smaller Thickness of wall Thick and Heavy Thin and Lighter Vascularity Highly vascularised
Intestines Differences Between Jejunum and Ileum Types Jejunum Ileum Color Deeper red Paler pink Calibre Bigger Smaller Thickness of wall Thick and Heavy Thin and Lighter Vascularity Highly vascularised
Cover Page. The following handle holds various files of this Leiden University dissertation:
 Cover Page The following handle holds various files of this Leiden University dissertation: http://hdl.handle.net/1887/6119 Author: Spruit, E.N. Title: Increasing the efficiency of laparoscopic surgical
Cover Page The following handle holds various files of this Leiden University dissertation: http://hdl.handle.net/1887/6119 Author: Spruit, E.N. Title: Increasing the efficiency of laparoscopic surgical
Fat Tissue Infiltration into the Pancreas Parenchyme and Its Effect on the Result of Surgery
 Korean Journal of HBP Surgery Vol. 15,. 2, May 2011 O riginal Article Fat Tissue Infiltration into the Pancreas Parenchyme and Its Effect on the Result of Surgery Purpose: In Korea, there are few reports
Korean Journal of HBP Surgery Vol. 15,. 2, May 2011 O riginal Article Fat Tissue Infiltration into the Pancreas Parenchyme and Its Effect on the Result of Surgery Purpose: In Korea, there are few reports
Minimally Invasive Esophagectomy
 Minimally Invasive Esophagectomy M A R K B E R R Y, M D A S S O C I AT E P R O F E S S O R D E PA R T M E N T OF C A R D I O T H O R A C I C S U R G E R Y S TA N F O R D U N I V E R S I T Y S E P T E M
Minimally Invasive Esophagectomy M A R K B E R R Y, M D A S S O C I AT E P R O F E S S O R D E PA R T M E N T OF C A R D I O T H O R A C I C S U R G E R Y S TA N F O R D U N I V E R S I T Y S E P T E M
Surgical anatomy of the biliary tract
 HPB, 2008; 10: 7276 REVIEW ARTICLE Surgical anatomy of the biliary tract DENIS CASTAING Centre hépato-biliaire, Hôpital Paul Brousse, Assistance Publique- Hôpitaux de Paris, Université Paris XI, Paris,
HPB, 2008; 10: 7276 REVIEW ARTICLE Surgical anatomy of the biliary tract DENIS CASTAING Centre hépato-biliaire, Hôpital Paul Brousse, Assistance Publique- Hôpitaux de Paris, Université Paris XI, Paris,
Pancreatic pseudocysts (PP) are chronic collections of
 JOURNAL OF LAPAROENDOSCOPIC & ADVANCED SURGICAL TECHNIQUES Volume 20, Number 9, 2010 ª Mary Ann Liebert, Inc. DOI: 10.1089/lap.2009.0421 Hand-Sewn Cystogastrostomy Using the Novel Single-Incision Laparoscopy
JOURNAL OF LAPAROENDOSCOPIC & ADVANCED SURGICAL TECHNIQUES Volume 20, Number 9, 2010 ª Mary Ann Liebert, Inc. DOI: 10.1089/lap.2009.0421 Hand-Sewn Cystogastrostomy Using the Novel Single-Incision Laparoscopy
Intraabdominal Roux-en-Y reconstruction with a novel stapling technique after laparoscopic distal gastrectomy
 Gastric Cancer (2009) 12: 164 169 DOI 10.1007/s10120-009-0520-0 Technical note 2009 by International and Japanese Gastric Cancer Associations Intraabdominal Roux-en-Y reconstruction with a novel stapling
Gastric Cancer (2009) 12: 164 169 DOI 10.1007/s10120-009-0520-0 Technical note 2009 by International and Japanese Gastric Cancer Associations Intraabdominal Roux-en-Y reconstruction with a novel stapling
The jejunum and the Ileum. Prof. Oluwadiya KS
 The jejunum and the Ileum Prof. Oluwadiya KS www.oluwadiya.siteled.com Introduction Introduction The small intestine (SI) comprises of the duodenum, jejunum and the ileum The jejunum is the second part
The jejunum and the Ileum Prof. Oluwadiya KS www.oluwadiya.siteled.com Introduction Introduction The small intestine (SI) comprises of the duodenum, jejunum and the ileum The jejunum is the second part
Robotic-Assisted Pancreatoduodenectomy
 Curr Surg Rep (2013) 1:98 105 DOI 10.1007/s40137-013-0017-y MINIMALLY INVASIVE PANCREATIC SURGERY (MG HOUSE, SECTION EDITOR) Robotic-Assisted Pancreatoduodenectomy Mohammad Khreiss Herbert J. Zeh Brian
Curr Surg Rep (2013) 1:98 105 DOI 10.1007/s40137-013-0017-y MINIMALLY INVASIVE PANCREATIC SURGERY (MG HOUSE, SECTION EDITOR) Robotic-Assisted Pancreatoduodenectomy Mohammad Khreiss Herbert J. Zeh Brian
Minimally Invasive Esophagectomy
 American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition
 22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
BILIARY TRACT & PANCREAS, PART II
 CME Pretest BILIARY TRACT & PANCREAS, PART II VOLUME 41 1 2015 A pretest is mandatory to earn CME credit on the posttest. The pretest should be completed BEFORE reading the overview. Both tests must be
CME Pretest BILIARY TRACT & PANCREAS, PART II VOLUME 41 1 2015 A pretest is mandatory to earn CME credit on the posttest. The pretest should be completed BEFORE reading the overview. Both tests must be
Surgical Management of Pancreatic Cancer
 I Congresso de Oncologia D Or July 5-6, 2013 Surgical Management of Pancreatic Cancer Michael A. Choti, MD, MBA, FACS Department of Surgery Johns Hopkins University School of Medicine, Baltimore, MD Estimated
I Congresso de Oncologia D Or July 5-6, 2013 Surgical Management of Pancreatic Cancer Michael A. Choti, MD, MBA, FACS Department of Surgery Johns Hopkins University School of Medicine, Baltimore, MD Estimated
Surgical Treatment for Periampullary Carcinoma A Study of 129 Patients*)
 Hiroshima Journal of Medical Sciences Vol. 33, No. 2, 179,...183, June, 1984 HJM 33-24 179 Surgical Treatment for Periampullary Carcinoma A Study of 129 Patients*) Tsuneo TAN AKA, Motomu KODAMA, Rokuro
Hiroshima Journal of Medical Sciences Vol. 33, No. 2, 179,...183, June, 1984 HJM 33-24 179 Surgical Treatment for Periampullary Carcinoma A Study of 129 Patients*) Tsuneo TAN AKA, Motomu KODAMA, Rokuro
Complex pancreatico- duodenal injuries. Elmin Steyn Head, Division of Surgery Faculty of Health Sciences Stellenbosch University
 Complex pancreatico- duodenal injuries Elmin Steyn Head, Division of Surgery Faculty of Health Sciences Stellenbosch University Pancreatic and duodenal trauma: daunting or simply confusing? 2-4% of abdominal
Complex pancreatico- duodenal injuries Elmin Steyn Head, Division of Surgery Faculty of Health Sciences Stellenbosch University Pancreatic and duodenal trauma: daunting or simply confusing? 2-4% of abdominal
Cholangiocarcinoma (Bile Duct Cancer)
 Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Exploring Anatomy: the Human Abdomen
 Exploring Anatomy: the Human Abdomen PERITONEUM AND PERITONEAL CAVITY PERITONEUM The peritoneum is a thin serous membrane that lines the abdominal cavity and covers, in variable amounts, the viscera within
Exploring Anatomy: the Human Abdomen PERITONEUM AND PERITONEAL CAVITY PERITONEUM The peritoneum is a thin serous membrane that lines the abdominal cavity and covers, in variable amounts, the viscera within
Pancreas Case Scenario #1
 Pancreas Case Scenario #1 An 85 year old white female presented to her primary care physician with increasing abdominal pain. On 8/19 she had a CT scan of the abdomen and pelvis. This showed a 4.6 cm mass
Pancreas Case Scenario #1 An 85 year old white female presented to her primary care physician with increasing abdominal pain. On 8/19 she had a CT scan of the abdomen and pelvis. This showed a 4.6 cm mass
Laparoscopy-assisted radical total gastrectomy plus D2 lymph node dissection
 Masters of Gastrointestinal Surgery Laparoscopy-assisted radical total gastrectomy plus D2 lymph node dissection Chaohui Zheng, Changming Huang, Ping Li, Jianwei Xie, Jiabin Wang, Jianxian Lin, Jun Lu
Masters of Gastrointestinal Surgery Laparoscopy-assisted radical total gastrectomy plus D2 lymph node dissection Chaohui Zheng, Changming Huang, Ping Li, Jianwei Xie, Jiabin Wang, Jianxian Lin, Jun Lu
Pancreas (Exocrine) Protocol applies to all carcinomas of the exocrine pancreas.
 Pancreas (Exocrine) Protocol applies to all carcinomas of the exocrine pancreas. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition Procedures Cytology (No Accompanying Checklist)
Pancreas (Exocrine) Protocol applies to all carcinomas of the exocrine pancreas. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition Procedures Cytology (No Accompanying Checklist)
Laparoscopic and Thoracoscopic Ivor Lewis Esophagectomy With Colonic Interposition
 HOW TO DO IT Laparoscopic and Thoracoscopic Ivor Lewis Esophagectomy With Colonic Interposition Ninh T. Nguyen, MD, FACS, Marcelo Hinojosa, MD, Christine Fayad, BS, James Gray, BS, Zuri Murrell, MD, and
HOW TO DO IT Laparoscopic and Thoracoscopic Ivor Lewis Esophagectomy With Colonic Interposition Ninh T. Nguyen, MD, FACS, Marcelo Hinojosa, MD, Christine Fayad, BS, James Gray, BS, Zuri Murrell, MD, and
Anatomy: Know Your Abdomen
 Anatomy: Know Your Abdomen Glossary Abdomen - part of the body below the thorax (chest cavity); separated by the diaphragm. Anterior - towards the front of the body. For example, the umbilicus is anterior
Anatomy: Know Your Abdomen Glossary Abdomen - part of the body below the thorax (chest cavity); separated by the diaphragm. Anterior - towards the front of the body. For example, the umbilicus is anterior
Lab Monitor Images Dissection of the Abdominal Vasculature + Lower Digestive System
 Lab Monitor Images Dissection of the Abdominal Vasculature + Lower Digestive System Stomach & Duodenum Frontal (AP) View Nasogastric tube 2 1 3 4 Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum
Lab Monitor Images Dissection of the Abdominal Vasculature + Lower Digestive System Stomach & Duodenum Frontal (AP) View Nasogastric tube 2 1 3 4 Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum
AATS Focus on Thoracic Surgery: Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017?
 AATS Focus on Thoracic Surgery: Mastering Surgical Innovation Las Vegas, NV October 28, 2017 Session VIII: Video Session Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017? James D.
AATS Focus on Thoracic Surgery: Mastering Surgical Innovation Las Vegas, NV October 28, 2017 Session VIII: Video Session Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017? James D.
Title total gastrectomy for patients with. Citation Surgical endoscopy (2009), 23(9): 2.
 Title Intracorporeal esophagojejunal anas total gastrectomy for patients with Okabe, Hiroshi; Obama, Kazutaka; Ta Author(s) Akinari; Kawamura, Jun-ichiro; Naga Atsushi; Watanabe, Go; Kanaya, Seii Citation
Title Intracorporeal esophagojejunal anas total gastrectomy for patients with Okabe, Hiroshi; Obama, Kazutaka; Ta Author(s) Akinari; Kawamura, Jun-ichiro; Naga Atsushi; Watanabe, Go; Kanaya, Seii Citation
Management of Pancreatic Fistulae
 Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Outcomes of pancreaticoduodenectomy in patients with metastatic cancer
 Korean J Hepatobiliary Pancreat Surg 2014;18:147-151 http://dx.doi.org/.14701/kjhbps.2014.18.4.147 Original Article Outcomes of pancreaticoduodenectomy in patients with metastatic cancer Joo Hwa Kwak,
Korean J Hepatobiliary Pancreat Surg 2014;18:147-151 http://dx.doi.org/.14701/kjhbps.2014.18.4.147 Original Article Outcomes of pancreaticoduodenectomy in patients with metastatic cancer Joo Hwa Kwak,
Extended Lymph Node Dissection in Pancreaticoduodenenctomy? A Case-control Study
 ORIGINAL ARTICLE Extended Lymph Node Dissection in Pancreaticoduodenenctomy? A Case-control Study Dionysios Dellaportas 1, Nikolaos Arkadopoulos 2, Panagis Michael Lykoudis 3, Despoina Myoteri 4, Amanda
ORIGINAL ARTICLE Extended Lymph Node Dissection in Pancreaticoduodenenctomy? A Case-control Study Dionysios Dellaportas 1, Nikolaos Arkadopoulos 2, Panagis Michael Lykoudis 3, Despoina Myoteri 4, Amanda
P resently, pancreaticoduodenectomy is widely accepted as the standard surgical procedure for patients with
 OPEN SUBJECT AREAS: CANCER THERAPY PANCREATIC CANCER GASTROINTESTINAL CANCER OUTCOMES RESEARCH Received 13 May 2013 Accepted 3 June 2013 Published 25 June 2013 Correspondence and requests for materials
OPEN SUBJECT AREAS: CANCER THERAPY PANCREATIC CANCER GASTROINTESTINAL CANCER OUTCOMES RESEARCH Received 13 May 2013 Accepted 3 June 2013 Published 25 June 2013 Correspondence and requests for materials
Pancreas and Biliary System
 Pancreas and Biliary System Please view our Editing File before studying this lecture to check for any changes. Color Code Important Doctors Notes Notes/Extra explanation Objectives At the end of the lecture,
Pancreas and Biliary System Please view our Editing File before studying this lecture to check for any changes. Color Code Important Doctors Notes Notes/Extra explanation Objectives At the end of the lecture,
Open and minimally invasive pancreatic surgery a review of the literature
 Systematic Review Open and minimally invasive pancreatic surgery a review of the literature Brandon C. Chapman 1, Kristen DeSanto 2, Bulent Salman 3, Barish H. Edil 1 1 Department of Surgery, 2 Health
Systematic Review Open and minimally invasive pancreatic surgery a review of the literature Brandon C. Chapman 1, Kristen DeSanto 2, Bulent Salman 3, Barish H. Edil 1 1 Department of Surgery, 2 Health
Minimally Invasive Esophagectomy- Valuable. Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006
 Minimally Invasive Esophagectomy- Valuable Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006 Overview Esophageal carcinoma What is minimally invasive esophagectomy (MIE)?
Minimally Invasive Esophagectomy- Valuable Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006 Overview Esophageal carcinoma What is minimally invasive esophagectomy (MIE)?
Bile Duct Injury during Lap Chole. Bile Duct Injury during cholecystectomy TOPICS. 1. Prevalence, mechanisms, prevention and diagnosis
 Bile Duct Injury during cholecystectomy Catherine HUBERT Jean-Fran François GIGOT Benoît t NAVEZ Division of Hepato-Biliary Biliary-Pancreatic Surgery Department of Abdominal Surgery and Transplantation
Bile Duct Injury during cholecystectomy Catherine HUBERT Jean-Fran François GIGOT Benoît t NAVEZ Division of Hepato-Biliary Biliary-Pancreatic Surgery Department of Abdominal Surgery and Transplantation
A video demonstration of the Li s anastomosis the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma
 Surgical Technique A video demonstration of the the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma Yan Zheng*, Yin Li*, Zongfei Wang, Haibo Sun, Ruixiang Zhang
Surgical Technique A video demonstration of the the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma Yan Zheng*, Yin Li*, Zongfei Wang, Haibo Sun, Ruixiang Zhang
Robotic distal pancreatectomy: experience in a high-volume center
 Original Article Page 1 of 6 Robotic distal pancreatectomy: experience in a high-volume center Qu Liu, Wenbo Tang, Ruiquan Zhou, Zhiming Zhao, Yuanxing Gao, Minggen Hu, Chenggang Li, Xuan Zhang, Rong Liu
Original Article Page 1 of 6 Robotic distal pancreatectomy: experience in a high-volume center Qu Liu, Wenbo Tang, Ruiquan Zhou, Zhiming Zhao, Yuanxing Gao, Minggen Hu, Chenggang Li, Xuan Zhang, Rong Liu
Case Scenario 1. Discharge Summary
 Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
