Treatment of Autoimmune Diabetes by Inhibiting the Initial Event
|
|
|
- Alaina Houston
- 5 years ago
- Views:
Transcription
1 pissn eissn REVIEW ARTICLE Treatment of Autoimmune Diabetes by Inhibiting the Initial Event * Department of Medicine, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul , Korea Recent papers have shown that the initial event in the pathogenesis of autoimmune type 1 diabetes (T1D) comprises sensing of molecular patterns released from apoptotic β-cells by innate immune receptors such as toll-like receptor (TLR). We have reported that apoptotic β-cells undergoing secondary necrosis called late apoptotic β-cells stimulate dendritic cells (DCs) and induce diabetogenic T cell priming through TLR2. The role of other innate immune receptors such as TLR7 or TLR9 in the initiation of T1D has also been suggested. We hypothesized that TLR2 blockade could inhibit T1D at the initial step of T1D. Indeed, when a TLR2 agonist, Pam3CSK 4 was administered chronically, the development of T1D in nonobese diabetic (NOD) mice was inhibited. Diabetogenic T cell priming by DCs was attenuated by chronic treatment with Pam3CSK 4, indicating DC tolerance. For the treatment of established T1D, immune tolerance alone is not enough because β-cell mass is critically reduced. We employed TLR2 tolerance in conjunction with islet transplantation, which led to reversal of newly established T1D. Dipeptidyl peptidase 4 (DPP4) inhibitors are a new class of anti-diabetic agents that have beneficial effects on β-cells. We investigated whether a combination of DPP4 inhibition and TLR2 tolerization could reverse newly established T1D without islet transplantation. We could achieve normoglycemia by TLR2 tolerization in combination with DPP4 inhibition but not by TLR2 tolerization or DPP4 inhibition alone. β-cell mass was significantly increased by combined treatment with TLR2 tolerization and DPP4 inhibition. These results suggest the possibility that a novel strategy of TLR tolerization will be available for the inhibition or treatment of established T1D when combined with measures increasing critically reduced β-cell mass of T1D patients such as DPP4 inhibition or stem cell technology. [Immune Network 2013;13(5): ] INTRODUCTION While the last step in the development of type 1 diabetes (T1D) is death of β-cells producing insulin, the initial step or the initial event of T1D has been unclear. Recent papers have shown the role of β-cell death in the initial course of T1D, suggesting that β-cell death or apoptosis is α and ω in the pathogenesis of T1D. Such findings provide not only innovative scientific clues to the understanding of T1D but also a novel strategy for the inhibition of treatment T1D. In this review, we will summarize recent findings regarding the relationship between β-cell death and autoimmunity, and their application to the prevention or treatment of T1D. β-cell APOPTOSIS AS A MECHANISM OF DIABETOGENIC T CELL SENSITIZATION IN T1D In T1D, apoptosis of pancreatic β-cells appears to be the Received on September 16, Revised on September 27, Accepted on October 4, CC This is an open access article distributed under the terms of the Creative Commons Attribution Non-Commercial License ( which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. *Corresponding Author., Department of Medicine, Samsung Medical Center, Sungkyunkwan University School of Medicine, 50, Irwon-dong Gangnam-gu, Seoul, Korea. Tel: ; Fax: ; mslee0923@ skku.edu Keywords: Type 1 diabetes, Autoimmunity, TLR2, Tolerance, DPP4 Abbreviations: T1D, type 1 diabetes; TLR, toll-like receptor; DC, dendritic cell; NOD, nonobese diabetic; DPP4, dipeptidyl peptidase, Mφ, macrophage; DAMP, death-associated molecular pattern; APC, antigen-presenting cell; CRAMP, cathelicidin-related antimicrobial peptide; GLP-1, glucagon-like peptide 1; ipsc, induced pleuripotent stem cell 194
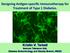
2 last step in the development of diabetes. After a long sequence of autoimmune processes, finally β-cell apoptosis occurs and clinically overt diabetes ensues when β-cell mass is lowered below a certain threshold (1,2). In contrast, the initial event in the development of T1D has been unclear, while the initial event could be more important both scientifically and clinically compared to the last event. Clues to the initial event came after the elucidation of the cell death mechanism and cloning of innate immune receptors. Suggestion that cell death and the initiation of autoimmunity are interrelated was from the observation that there is a transient wave of physiological β-cell apoptosis peaking at 2 3 weeks of age during the pancreas organogenesis (3,4), which coincides with the onset of autoimmunity to β-cell autoantigens in nonobese diabetic (NOD) mice developing classical T1D. Apoptotic cells are rapidly engulfed by macrophages (Mφs), thus no inflammation ensues after apoptosis. In contrast, necrotic cells release death-associated molecular pattern (DAMP) and can stimulate antigen-presenting cells (APCs) such as Mφs or dendritic cells (DCs), which acts as an alarm signal for immune stimulation. Mφs of NOD mice have been reported to have defect in their phagocytic capability, which may allow apoptotic cells to undergo secondary necrosis. Such secondary necrotic β-cells can induce inflammation or immunity through innate immune receptors. Indeed, we observed that insulinoma cells undergoing secondary necrosis can stimulate Mφs in a TLR2-dependent pathway, inducing inflammatory cytokine release from Mφs (5). We also found that and priming of diabetogenic T cells by DCs in vivo that occurs selectively in pancreatic lymph nodes due to β-cell death is also dependent on TLR2. In vivo role of TLR2 in the development of T1D was further supported by a marked decrease in the incidence of diabetes in two types of T1D animal models multiple low-dose streptozotocin model and spontaneous T1D model of NOD mice (5). Role of TLRs other than TLR2 in T1D has also been suggested in a recent paper reporting that activation of TLR9 of plasmacytoid DCs by a complex of self DNA, anti-double-strand DNA antibody released from B-1a lymphocytes in response to β-cell apoptosis and DNAbinding cathelicidin-related antimicrobial peptide (CRAMP) released from neutrophils in the initiation of T1D (6). INHIBITION OF T1D BY TLR2 TOLERANCE These results showing the sensing of DAMP from β-cells by TLR2 on DCs in the initial step of the development of T1D Figure 1. TLR2 tolerance induced by prolonged treatment with Pam3CSK 4 in vivo. (A) When CD4 + diabetogenic T cells from BDC2.5/NOD mice were labeled with carboxyfluorescein succinimidyl ester (CFSE) and transferred into control recipient NOD mice, CD4 + T cell proliferation measured by analyzing CFSE dilution by FACS analysis gated on CD4 + and Vβ4 + cells was observed specifically in the pancreatic lymph nodes but not in the mesenteric lymph nodes, as previously reported (16). In NOD mice treated with Pam3CSK 4 in vivo for 3 weeks, CD4 + diabetogenic T cell proliferation was significantly attenuated, indicating DC tolerance. Pooled results (right). A representative histogram (left). (B) Splenocytes prepared from NOD mice to which Pam3CSK 4 was administered for 3 weeks, were further treated with Pam3CSK 4 (black line) or PBS (gray filled histogram) in vitro for 1 day. The induction of costimulatory molecules on DCs by in vitro treatment with Pam3CSK 4 that was determined by FACS analysis gated on CD11c + cells was significantly lower compared to control NOD mice, suggesting DC tolerance. Fold changes of mean fluorescent intensities (MFI) (lower). (C) No significant difference in the expression of costimulatory molecules on splenic DCs between NOD mice that were treated with Pam3CSK 4 in vivo (black line) and control NOD mice (gray line), suggests that in vivo Pam3CSK 4 treatment for 3 weeks does not activate DCs. (***p<0.005; *p<0.05; ns, not significant) (Originally published in The Journal of Immunology. Kim D. H., J-C. Lee, S. Kim S, S. H. Oh, M.-K. Lee, K.-W. Kim, M.-S. Lee Inhibition of autoimmune diabetes by TLR2 tolerance. J. Immunol.187: Copyright c [2011] The American Association of Immunologists, Inc.) 195
3 imply that TLR2 blockade could be employed to inhibit autoimmune diabetes. Thus, we employed the strategy of TLR2 tolerance induction which is similar to the well-known LPS tolerance (7). Indeed, when we administered a TLR2 agonist, Pam3CSK 4 to NOD mice since 3 weeks of age, the incidence of diabetes was significantly suppressed, suggesting that TLR2 tolerance can inhibit the development of T1D (8). The inhibition of T1D by chronic treatment with Pam3CSK 4 could be attributed to TLR2 tolerance of DCs since diabetogenic T cell proliferation in pancreatic lymph nodes by DCs was significantly suppressed after prolonged treatment with Pam3CSK 4 (Fig. 1A). Induction of costimulatory signals on DCs by in vitro incubation with Pam3CSK 4 was also attenuated by chronic administration of Pam3CSK 4 in vivo for 3 weeks, again attesting the induction of DC tolerance (8) (Fig. 1B). On the other hand, the expression of costimulatory molecules on DCs was not changed by in vivo treatment with Pam3CSK 4 alone, suggesting that prolonged Pam3CSK 4 administration itself does not activate DCs (Fig. 1C). When we studied the molecular mechanism of TLR2 tolerance by chronic treatment with TLR2 agonist, decreased expression of IRAK-1 and -4, positive regulator of TLR signaling, and increased expression of IRAK-M, a negative regulator of TLR signaling were noted. Downregulation of IRAK-1 and -4 protein levels was due to proteasomal degradation as the reduced IRAK-1 and -4 protein levels were restored by proteasomal inhibitors. In this regard, a recent paper showed contribution of IRAK-4 to TLR2 tolerance but not to endotoxin tolerance (9), which can explain the selective TLR2 tolerance after treatment with Pam3CSK 4 without heterotolerance to endotoxin (8). Besides DC tolerance, other immune mechanisms such as changes in Th1/Th2 polarization or Treg cells can play a role in the inhibition of T1D after chronic treatment with Pam3CSK 4. However, we observed no changes in the Th1/Th2 polarity and the number or activity Treg cells after Pam3CSK 4 treatment, while we cannot totally eliminate the role of Th1/Th2 polarization or Treg cells in the inhibition of T1D by Pam3CSK 4 (8). reduced below a certain threshold in clinically overt T1D. Immune tolerance in established T1D is also different from that in prediabetic animal models in that immune tolerization should be targeted to sensitized T cells rather than naïve T cells. To confirm that TLR2 tolerance could be induced in sensitized T cells, adoptive transfer experiment was conducted in which transfer of sensitized T cells from diabetic NOD mice rapidly induces diabetes in nondiabetic NOD mice. When we administered Pam3CSK 4 to recipient mice since just before adoptive transfer of T cells from diabetic mice, the development of diabetes in the recipient mice was significantly suppressed (Fig. 2), suggesting that TLR2 tolerization can block activity of sensitized T cells as well. Sustained interaction between DCs and diabetogenic T cells may be necessary for full in vivo activity of effector T cells. To attain another goal for the treatment of established T1D-replenishment of critically reduced β-cell mass, we employed a well-known strategy of islet transplantation. When islets were grafted under the kidney capsule of newly diabetic NOD mice, blood glucose was normalized immediately. However, diabetes recurred in 10 days because already established autoimmunity destroys islet graft. In contrast, when we administered Pam3CSK 4 since just before islet transplantation, blood glucose was maintained below diabetic level in most mice as long as Pam3CSK 4 was administered (8), suggesting TREATMENT OF ESTABLISHED T1D BY TLR2 TOLERANCE IN CONJUNCTION WITH MEASURES INCREASING β-cell MASS While T1D of NOD mice could be inhibited by TLR2 tolerization, immune tolerance alone is not enough for the treatment of established T1D because β-cell mass is already critically Figure 2. Effect of in vivo treatment with Pam3CSK 4 on diabetes transfer by sensitized diabetogenic T cells. The incidence of diabetes after adoptive transfer (AT) of splenocytes from diabetic NOD mice to irradiated nondiabetic recipient NOD mice was significantly reduced by treatment of the recipient NOD mice with Pam3CSK 4 for 2 weeks before AT (p<0.005). (Originally published in The Journal of Immunology. Kim D. H., J-C. Lee, S. Kim S, S. H. Oh, M.-K. Lee, K.-W. Kim, M.-S. Lee Inhibition of autoimmune diabetes by TLR2 tolerance. J. Immunol.187: Copyright c [2011] The American Association of Immunologists, Inc.) 196
4 successful treatment of newly established T1D by a combination of TLR2 tolerance and islet transplantation. While established T1D could be treated by a combination of TLR2 tolerization and islet transplantation, supply of islets is too limited to cover clinical demand, which preclude the clinical application of islet transplantation for the treatment of established T1D. We thus employed another strategy of increasing reduced β-cell mass. Recently, glucagon-like peptide 1 (GLP-1) mimetics or dipeptidyl peptidase 4 (DPP4) inhibitors that inhibit degradation of GLP-1 by DPP4 in vivo, are being used as new classes of anti-hyperglycemic agents with β-cell trophic action not only in animal model of diabetes (10,11) but also in humans (12). We investigated whether a combination of DPP4 inhibition by DA1229, a novel inhibitor of DPP4 (13) and TLR2 tolerance could treat established T1D. Indeed, euglycemia was achieved in more than 80% of newly diabetic NOD mice after chronic treatment with Pam3CSK 4 in combination with DA1229, while treatment with Pam3CSK 4 or DA1229 alone was without effect (14). Consistent with the improved blood glucose level, β-cell mass was significantly increased after combined treatment with Pam3CSK 4 and DA1229 but not after treatment with Pam3CSK 4 or DA1229 alone. The increase in β-cell mass could be attributed to the enhanced proliferation of β-cells as evidenced by increased number of bromodeoxyuridine-incorporating β-cells and an increased number of small β-cell units that comprise less than four β-cells and represent β -cell neogenesis, which was observed in diabetic NOD mice treated with Pam3CSK 4 in combination with DA1229 but not in those treated with Pam3CSK 4 or DA1229 alone (14). These data suggest the possibility that a combination of TLR2 tolerization and DPP4 inhibition could employed as a new method for the treatment of established T1D without islet transplantation. CONCLUSION While it has been elusive for a long time, the real identity of the initial event of T1D is finally emerging, which was owing to the elucidation of the relationship between cell death and innate immune responses and characterization of innate immune receptors. Such a revelation is likely, to lead to the development of novel strategies for the prevention or treatment of T1D. Methods increasing β-cell mass is already available such as DPP4 inhibitors or GLP-1 mimetics. Better methods to increase β-cell mass will be available in the future since the discovery of inducible pleuripotent stem cell (ipsc) technology (15). By combining such methods of increasing β-cell mass and inhibition of the initial event of T1D, clinically applicable methods of treating established T1D patients will be finally available. ACKNOWLEDGEMENTS We thank Dr. H-J Kim (Dong-A Pharmaceutical) for kind provision of DA1229. This study was supported by the Bio Research & Development Program ( ) and the Korea Healthcare Technology Research & Development Project, Ministry for Health, Welfare & Family Affairs, Korea. (A080967). Lee M-S is the recipient of a Global Research Laboratory Grant (K A ) and Bio & Medical Technology Development Program ( ) of the National Research Foundation of Korea. CONFLICTS OF INTEREST The author has no financial conflict of interest. REFERENCES 1. Kim, Y.-H., S. Kim, K.-A. Kim, H. Yagita, N. Kayagaki, K.-W. Kim, and M.-S. Lee Apoptosis of pancreatic β-cells detected in accelerated diabetes of NOD mice:no role of Fas-Fas ligand interaction in autoimmune diabetes. Eur. J. Immunol. 29: O Brien, B. A., B. V. Harmon, D. P. Cameron, and D. J. Allan Apoptosis is the mode of β-cell death responsible for the development of IDDM in the nonobese diabetic (NOD) mouse. Diabetes 46: Finegood, D. T., M. D. MaArthur, D. Kojwang, M. J. Thomas, B. G. Topp, T. Leonard, and R. E. Buckingham β-cell mass dynamics in Zucker Diabetic Fatty rats. Diabetes 50: Trudeau, J. D., J. P. Dutz, E. Arany, D. J. Hill, W. E. Fieldus, and D. T. Finegood Neonatal beta-cell apoptosis: a trigger for autoimmune diabetes? Diabetes 49: Kim, H. S., M. S. Han, K. W. Chung, S. Kim, E. Kim, M. J. Kim, E. Jang, H. A. Lee, J. Youn, S. Akira, and M.-S. Lee Toll-like receptor 2 senses beta-cell death and contributes to the initiation of autoimmune diabetes. Immunity 27: Diana, J., Y. Simoni, L. Furio, L. Beaudoin, B. Agerberth, F. Barrat, and A. Lehuen Crosstalk between neutrophils, B-1a cells and plasmacytoid dendritic cells initiates autoimmune diabetes. Nat. Med. 19: Cavaillon, J. M., C. Adrie, C. Fitting, and M. Adib-Conquy Endotoxin tolerance: is there a clinical relevance? J. Endotoxin Res. 9:
5 8. Kim, D. H., J.-C. Lee, S. Kim, S. H. Oh, M.-K. Lee, K.-W. Kim, and M.-S. Lee Inhibition of autoimmune diabetes by TLR2 tolerance. J. Immunol. 187: Xiong, Y., M. Pennini, S. N. Vogel, and A. E. Medvedev IRAK4 kinase activity is not required for induction of endotoxin tolerance but contributes to TLR2-mediated tolerance. J. Leukocyte Biol. 94: Mu, J., J. Woods, Y. P. Zhou, R. S. Roy, Z. Li, E. Zycband, Y. Feng, L. Zhu, L. C., A. D. Howard, D. E. Moller, N. A. Thonberry, and B. B. Zhang Chronic inhibition of dipeptidyl peptidase-4 with a sitagliptin analog preserves pancreatic beta-cell mass and function in a rodent model of type 2 diabetes. Diabetes 55: Xu, G., D. A. Stoffers, J. F. Habener, and S. Bonner-Weir Exendin-4 stimulates both beta-cell replication and neogenesis, resulting in increased beta-cell mass and improved glucose tolerance in diabetic rats. Diabetes 48: Butler, A. E., M. Campbell-Thompson, T. Gurlo, D. W. Dawson, M. Atkinson, and P. C. Butler Marked expansion of exocrine and endocrine pancreas with incretin therapy in humans with increased exocrine pancreas dysplasia and the potential for glucagon-producing neuroendocrine tumors. Diabetes 62: Cho, J. M., H. W. Jang, H. Cheon, Y. T. Jeong, D.-H. Kim, Y.-M. Lim, S.-h. Choi, E.-K. Yang, C.-Y. Shin, M.-H. Son, S. H. Kim, H.-J. Kim, and M.-S. Lee A novel dipeptidyl peptidase IV inhibitor DA-1229 ameliorates streptozotocin-induced diabetes by increasing β-cell replication and neogenesis. Diabetes Res. Clin. Pract. 91: Kim, D. H., J.-C. Lee, M.-K. Lee, K.-W. Kim, and M.-S. Lee Treatment of autoimmune diabetes by toll-like receptor 2 tolerance in conjunction with dipeptidyl peptidase 4 inhibition. Diabetologia 55: Jeon, K., H. Lim, J. H. Kim, N. V. Thuan, S. H. Park, Y. M. Lim, H. Y. Choi, E. R. Lee, J. H. Kim, M. S. Lee, and S.-G. Cho Differentiation and Transplantation of functional pancreatic beta cells generated from induced pluripotent stem cells derived from a type 1 diabetes mouse model. Stem Cells Dev. 21: Turley, S., L. Poirot, M. Hattori, C. Benoist, and D. Mathis Physiological beta cell death triggers priming of self-reactive T cells by dendritic cells in a type-1 diabetes model. J. Exp. Med. 198:
β-cell Preservation and Regeneration After Islet Transplantation
 β-cell Preservation and Regeneration After Islet Transplantation Jyuhn-Huarng Juang, MD Division of Endocrinology and Metabolism, Department of Internal Medicine, Chang Gung University and Memorial Hospital,
β-cell Preservation and Regeneration After Islet Transplantation Jyuhn-Huarng Juang, MD Division of Endocrinology and Metabolism, Department of Internal Medicine, Chang Gung University and Memorial Hospital,
The Effects of Exenatide on the Autoimmune Development of Diabetes. A Senior Honors Thesis
 The Effects of Exenatide on the Autoimmune Development of Diabetes A Senior Honors Thesis Presented in Partial Fulfillment of the Requirements for Graduation with Distinction in Microbiology in the Undergraduate
The Effects of Exenatide on the Autoimmune Development of Diabetes A Senior Honors Thesis Presented in Partial Fulfillment of the Requirements for Graduation with Distinction in Microbiology in the Undergraduate
T-cell activation T cells migrate to secondary lymphoid tissues where they interact with antigen, antigen-presenting cells, and other lymphocytes:
 Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
T-cell activation T cells migrate to secondary lymphoid tissues where they interact with antigen, antigen-presenting cells, and other lymphocytes:
 Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
NIH Public Access Author Manuscript Diabetologia. Author manuscript; available in PMC 2014 February 01.
 NIH Public Access Author Manuscript Published in final edited form as: Diabetologia. 2013 February ; 56(2): 231 233. doi:10.1007/s00125-012-2788-6. Lipotoxicity impairs incretin signalling V. Poitout 1,2
NIH Public Access Author Manuscript Published in final edited form as: Diabetologia. 2013 February ; 56(2): 231 233. doi:10.1007/s00125-012-2788-6. Lipotoxicity impairs incretin signalling V. Poitout 1,2
Tolerance 2. Regulatory T cells; why tolerance fails. Abul K. Abbas UCSF. FOCiS
 1 Tolerance 2. Regulatory T cells; why tolerance fails Abul K. Abbas UCSF FOCiS 2 Lecture outline Regulatory T cells: functions and clinical relevance Pathogenesis of autoimmunity: why selftolerance fails
1 Tolerance 2. Regulatory T cells; why tolerance fails Abul K. Abbas UCSF FOCiS 2 Lecture outline Regulatory T cells: functions and clinical relevance Pathogenesis of autoimmunity: why selftolerance fails
Antigen Presentation and T Lymphocyte Activation. Abul K. Abbas UCSF. FOCiS
 1 Antigen Presentation and T Lymphocyte Activation Abul K. Abbas UCSF FOCiS 2 Lecture outline Dendritic cells and antigen presentation The role of the MHC T cell activation Costimulation, the B7:CD28 family
1 Antigen Presentation and T Lymphocyte Activation Abul K. Abbas UCSF FOCiS 2 Lecture outline Dendritic cells and antigen presentation The role of the MHC T cell activation Costimulation, the B7:CD28 family
IMO-8400, a novel TLR7, TLR8 and TLR9 antagonist, psoriasis
 IMO-8400, a novel TLR7, TLR8 and TLR9 antagonist, inhibits disease development in mouse models of psoriasis Weiwen e Ja Jiang, Fu-Gang Zhu, Dong Yu, Ekambar R. Kandimalla, a a, Nicola La Monica, and Sudhir
IMO-8400, a novel TLR7, TLR8 and TLR9 antagonist, inhibits disease development in mouse models of psoriasis Weiwen e Ja Jiang, Fu-Gang Zhu, Dong Yu, Ekambar R. Kandimalla, a a, Nicola La Monica, and Sudhir
What is Autoimmunity?
 Autoimmunity What is Autoimmunity? Robert Beatty MCB150 Autoimmunity is an immune response to self antigens that results in disease. The immune response to self is a result of a breakdown in immune tolerance.
Autoimmunity What is Autoimmunity? Robert Beatty MCB150 Autoimmunity is an immune response to self antigens that results in disease. The immune response to self is a result of a breakdown in immune tolerance.
What is Autoimmunity?
 Autoimmunity What is Autoimmunity? Robert Beatty MCB150 Autoimmunity is an immune response to self antigens that results in disease. The immune response to self is a result of a breakdown in immune tolerance.
Autoimmunity What is Autoimmunity? Robert Beatty MCB150 Autoimmunity is an immune response to self antigens that results in disease. The immune response to self is a result of a breakdown in immune tolerance.
Designing An)gen- specific Immunotherapy for Treatment of Type 1 Diabetes.
 Designing An)gen- specific Immunotherapy for Treatment of Type 1 Diabetes. Kristin V. Tarbell Immune Tolerance Unit, Diabetes Endocrinology and Obesity Branch, NIDDK Outline Background on type 1 diabetes
Designing An)gen- specific Immunotherapy for Treatment of Type 1 Diabetes. Kristin V. Tarbell Immune Tolerance Unit, Diabetes Endocrinology and Obesity Branch, NIDDK Outline Background on type 1 diabetes
TCR, MHC and coreceptors
 Cooperation In Immune Responses Antigen processing how peptides get into MHC Antigen processing involves the intracellular proteolytic generation of MHC binding proteins Protein antigens may be processed
Cooperation In Immune Responses Antigen processing how peptides get into MHC Antigen processing involves the intracellular proteolytic generation of MHC binding proteins Protein antigens may be processed
Determinants of Immunogenicity and Tolerance. Abul K. Abbas, MD Department of Pathology University of California San Francisco
 Determinants of Immunogenicity and Tolerance Abul K. Abbas, MD Department of Pathology University of California San Francisco EIP Symposium Feb 2016 Why do some people respond to therapeutic proteins?
Determinants of Immunogenicity and Tolerance Abul K. Abbas, MD Department of Pathology University of California San Francisco EIP Symposium Feb 2016 Why do some people respond to therapeutic proteins?
Combined Rho-kinase inhibition and immunogenic cell death triggers and propagates immunity against cancer
 Supplementary Information Combined Rho-kinase inhibition and immunogenic cell death triggers and propagates immunity against cancer Gi-Hoon Nam, Eun-Jung Lee, Yoon Kyoung Kim, Yeonsun Hong, Yoonjeong Choi,
Supplementary Information Combined Rho-kinase inhibition and immunogenic cell death triggers and propagates immunity against cancer Gi-Hoon Nam, Eun-Jung Lee, Yoon Kyoung Kim, Yeonsun Hong, Yoonjeong Choi,
Adaptive immune responses: T cell-mediated immunity
 MICR2209 Adaptive immune responses: T cell-mediated immunity Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will discuss the T-cell mediated immune response, how it is activated,
MICR2209 Adaptive immune responses: T cell-mediated immunity Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will discuss the T-cell mediated immune response, how it is activated,
T Cell Development II: Positive and Negative Selection
 T Cell Development II: Positive and Negative Selection 8 88 The two phases of thymic development: - production of T cell receptors for antigen, by rearrangement of the TCR genes CD4 - selection of T cells
T Cell Development II: Positive and Negative Selection 8 88 The two phases of thymic development: - production of T cell receptors for antigen, by rearrangement of the TCR genes CD4 - selection of T cells
The Diabetes Epidemic in Korea
 Review Article Endocrinol Metab 2016;31:349-33 http://dx.doi.org/.3803/enm.2016.31.3.349 pissn 2093-96X eissn 2093-978 The Diabetes Epidemic in Korea Junghyun Noh Department of Internal Medicine, Inje
Review Article Endocrinol Metab 2016;31:349-33 http://dx.doi.org/.3803/enm.2016.31.3.349 pissn 2093-96X eissn 2093-978 The Diabetes Epidemic in Korea Junghyun Noh Department of Internal Medicine, Inje
Exploiting antigen specific approaches to induce tolerance in Type 1 Diabetes
 Exploiting antigen specific approaches to induce tolerance in Type 1 Diabetes A THESIS SUBMITTED TO THE FACULTY OF THE GRADUATE SCHOOL OF THE UNIVERSITY OF MINNESOTA BY Caitlin A. Heiderscheidt IN PARTIAL
Exploiting antigen specific approaches to induce tolerance in Type 1 Diabetes A THESIS SUBMITTED TO THE FACULTY OF THE GRADUATE SCHOOL OF THE UNIVERSITY OF MINNESOTA BY Caitlin A. Heiderscheidt IN PARTIAL
Immunological alterations in mice irradiated with low doses
 Immunological alterations in mice irradiated with low doses "Frédéric Joliot-Curie" National Research Institute for Radiobiology and Radiohygiene, Budapest, Hungary The structure of the immune system INNATE
Immunological alterations in mice irradiated with low doses "Frédéric Joliot-Curie" National Research Institute for Radiobiology and Radiohygiene, Budapest, Hungary The structure of the immune system INNATE
Immune response to infection
 Immune response to infection Dr. Sandra Nitsche (Sandra.Nitsche@rub.de ) 20.06.2018 1 Course of acute infection Typical acute infection that is cleared by an adaptive immune reaction 1. invasion of pathogen
Immune response to infection Dr. Sandra Nitsche (Sandra.Nitsche@rub.de ) 20.06.2018 1 Course of acute infection Typical acute infection that is cleared by an adaptive immune reaction 1. invasion of pathogen
News Release. Title Transfusion of immunoregulatory M2 macrophages derived from bone marrow or ips cells ameliorates crescentic glomerulonephritis
 News Release Title Transfusion of immunoregulatory M2 macrophages derived from bone marrow or ips cells ameliorates crescentic glomerulonephritis Key Points Administration of CD206 + M2 macrophages artificially
News Release Title Transfusion of immunoregulatory M2 macrophages derived from bone marrow or ips cells ameliorates crescentic glomerulonephritis Key Points Administration of CD206 + M2 macrophages artificially
Intracellular MHC class II molecules promote TLR-triggered innate. immune responses by maintaining Btk activation
 Intracellular MHC class II molecules promote TLR-triggered innate immune responses by maintaining Btk activation Xingguang Liu, Zhenzhen Zhan, Dong Li, Li Xu, Feng Ma, Peng Zhang, Hangping Yao and Xuetao
Intracellular MHC class II molecules promote TLR-triggered innate immune responses by maintaining Btk activation Xingguang Liu, Zhenzhen Zhan, Dong Li, Li Xu, Feng Ma, Peng Zhang, Hangping Yao and Xuetao
Gamma-aminobutyric acid (GABA) treatment blocks inflammatory pathways and promotes survival and proliferation of pancreatic beta cells
 Gamma-aminobutyric acid (GABA) treatment blocks inflammatory pathways and promotes survival and proliferation of pancreatic beta cells Gérald J. Prud homme, MD, FRCPC Keenan Research Centre for Biomedical
Gamma-aminobutyric acid (GABA) treatment blocks inflammatory pathways and promotes survival and proliferation of pancreatic beta cells Gérald J. Prud homme, MD, FRCPC Keenan Research Centre for Biomedical
Evgenija Homšak,M.Ph., M.Sc., EuSpLM. Department for laboratory diagnostics University Clinical Centre Maribor Slovenia
 Evgenija Homšak,M.Ph., M.Sc., EuSpLM. Department for laboratory diagnostics University Clinical Centre Maribor Slovenia 14th EFLM Continuing Postgraduate Course in Clinical Chemistry and Laboratory Medicine
Evgenija Homšak,M.Ph., M.Sc., EuSpLM. Department for laboratory diagnostics University Clinical Centre Maribor Slovenia 14th EFLM Continuing Postgraduate Course in Clinical Chemistry and Laboratory Medicine
T cell maturation. T-cell Maturation. What allows T cell maturation?
 T-cell Maturation What allows T cell maturation? Direct contact with thymic epithelial cells Influence of thymic hormones Growth factors (cytokines, CSF) T cell maturation T cell progenitor DN DP SP 2ry
T-cell Maturation What allows T cell maturation? Direct contact with thymic epithelial cells Influence of thymic hormones Growth factors (cytokines, CSF) T cell maturation T cell progenitor DN DP SP 2ry
MOLECULAR IMMUNOLOGY Manipulation of immune response Autoimmune diseases & the pathogenic mechanism
 MOLECULAR IMMUNOLOGY Manipulation of immune response Autoimmune diseases & the pathogenic mechanism SCHMAIEL SHIRDEL CONTENT 2 Introduction Autoimmune diseases Classification Involved components Autoimmune
MOLECULAR IMMUNOLOGY Manipulation of immune response Autoimmune diseases & the pathogenic mechanism SCHMAIEL SHIRDEL CONTENT 2 Introduction Autoimmune diseases Classification Involved components Autoimmune
Immunological Tolerance
 Immunological Tolerance Introduction Definition: Unresponsiveness to an antigen that is induced by exposure to that antigen Tolerogen = tolerogenic antigen = antigen that induces tolerance Important for
Immunological Tolerance Introduction Definition: Unresponsiveness to an antigen that is induced by exposure to that antigen Tolerogen = tolerogenic antigen = antigen that induces tolerance Important for
1. Overview of Adaptive Immunity
 Chapter 17A: Adaptive Immunity Part I 1. Overview of Adaptive Immunity 2. T and B Cell Production 3. Antigens & Antigen Presentation 4. Helper T cells 1. Overview of Adaptive Immunity The Nature of Adaptive
Chapter 17A: Adaptive Immunity Part I 1. Overview of Adaptive Immunity 2. T and B Cell Production 3. Antigens & Antigen Presentation 4. Helper T cells 1. Overview of Adaptive Immunity The Nature of Adaptive
Principles of Adaptive Immunity
 Principles of Adaptive Immunity Chapter 3 Parham Hans de Haard 17 th of May 2010 Agenda Recognition molecules of adaptive immune system Features adaptive immune system Immunoglobulins and T-cell receptors
Principles of Adaptive Immunity Chapter 3 Parham Hans de Haard 17 th of May 2010 Agenda Recognition molecules of adaptive immune system Features adaptive immune system Immunoglobulins and T-cell receptors
SUPPLEMENTARY INFORMATION
 doi:10.1038/nature10134 Supplementary Figure 1. Anti-inflammatory activity of sfc. a, Autoantibody immune complexes crosslink activating Fc receptors, promoting activation of macrophages, and WWW.NATURE.COM/NATURE
doi:10.1038/nature10134 Supplementary Figure 1. Anti-inflammatory activity of sfc. a, Autoantibody immune complexes crosslink activating Fc receptors, promoting activation of macrophages, and WWW.NATURE.COM/NATURE
Innate immunity. Abul K. Abbas University of California San Francisco. FOCiS
 1 Innate immunity Abul K. Abbas University of California San Francisco FOCiS 2 Lecture outline Components of innate immunity Recognition of microbes and dead cells Toll Like Receptors NOD Like Receptors/Inflammasome
1 Innate immunity Abul K. Abbas University of California San Francisco FOCiS 2 Lecture outline Components of innate immunity Recognition of microbes and dead cells Toll Like Receptors NOD Like Receptors/Inflammasome
Autoimmunity. Autoimmunity arises because of defects in central or peripheral tolerance of lymphocytes to selfantigens
 Autoimmunity Autoimmunity arises because of defects in central or peripheral tolerance of lymphocytes to selfantigens Autoimmune disease can be caused to primary defects in B cells, T cells and possibly
Autoimmunity Autoimmunity arises because of defects in central or peripheral tolerance of lymphocytes to selfantigens Autoimmune disease can be caused to primary defects in B cells, T cells and possibly
Attribution: University of Michigan Medical School, Department of Microbiology and Immunology
 Attribution: University of Michigan Medical School, Department of Microbiology and Immunology License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution
Attribution: University of Michigan Medical School, Department of Microbiology and Immunology License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution
CD90 + Human Dermal Stromal Cells Are Potent Inducers of FoxP3 + Regulatory T Cells
 CD90 + Human Dermal Stromal Cells Are Potent Inducers of FoxP3 + Regulatory T Cells Karin Pfisterer, Karoline M Lipnik, Erhard Hofer and Adelheid Elbe-Bürger Journal of Investigative Dermatology (2015)
CD90 + Human Dermal Stromal Cells Are Potent Inducers of FoxP3 + Regulatory T Cells Karin Pfisterer, Karoline M Lipnik, Erhard Hofer and Adelheid Elbe-Bürger Journal of Investigative Dermatology (2015)
Discussion & Conclusion
 Discussion & Conclusion 7. Discussion DPP-4 inhibitors augment the effects of incretin hormones by prolonging their half-life and represent a new therapeutic approach for the treatment of type 2 diabetes
Discussion & Conclusion 7. Discussion DPP-4 inhibitors augment the effects of incretin hormones by prolonging their half-life and represent a new therapeutic approach for the treatment of type 2 diabetes
Type 1 Diabetes: Islet expressing GAD65 (green) with DAPI (Blue) Islet expressing Insulin (red) in 3D confocal imaging
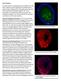 Type 1 Diabetes: Our group has been studying autoimmune diabetes for many years. Recently, we have developed a humanized mouse model of Type 1 Diabetes (T1D). We believe this model will help understand
Type 1 Diabetes: Our group has been studying autoimmune diabetes for many years. Recently, we have developed a humanized mouse model of Type 1 Diabetes (T1D). We believe this model will help understand
T Lymphocyte Activation and Costimulation. FOCiS. Lecture outline
 1 T Lymphocyte Activation and Costimulation Abul K. Abbas, MD UCSF FOCiS 2 Lecture outline T cell activation Costimulation, the B7:CD28 family Inhibitory receptors of T cells Targeting costimulators for
1 T Lymphocyte Activation and Costimulation Abul K. Abbas, MD UCSF FOCiS 2 Lecture outline T cell activation Costimulation, the B7:CD28 family Inhibitory receptors of T cells Targeting costimulators for
IMIDIA IMPROVING BETA-CELL FUNCTION AND IDENTIFICATION OF DIAGNOSTIC BIOMARKERS FOR TREATMENT MONITORING IN DIABETES. A. Ktorza, B.
 IMIDIA IMPROVING BETA-CELL FUNCTION AND IDENTIFICATION OF DIAGNOSTIC BIOMARKERS FOR TREATMENT MONITORING IN DIABETES A. Ktorza, B. Thorens DIABETES Definition Diabetes is a metabolic disease characterized
IMIDIA IMPROVING BETA-CELL FUNCTION AND IDENTIFICATION OF DIAGNOSTIC BIOMARKERS FOR TREATMENT MONITORING IN DIABETES A. Ktorza, B. Thorens DIABETES Definition Diabetes is a metabolic disease characterized
Effector mechanisms of cell-mediated immunity: Properties of effector, memory and regulatory T cells
 ICI Basic Immunology course Effector mechanisms of cell-mediated immunity: Properties of effector, memory and regulatory T cells Abul K. Abbas, MD UCSF Stages in the development of T cell responses: induction
ICI Basic Immunology course Effector mechanisms of cell-mediated immunity: Properties of effector, memory and regulatory T cells Abul K. Abbas, MD UCSF Stages in the development of T cell responses: induction
SEVENTH EDITION CHAPTER
 Judy Owen Jenni Punt Sharon Stranford Kuby Immunology SEVENTH EDITION CHAPTER 16 Tolerance, Autoimmunity, and Transplantation Copyright 2013 by W. H. Freeman and Company Immune tolerance: history * Some
Judy Owen Jenni Punt Sharon Stranford Kuby Immunology SEVENTH EDITION CHAPTER 16 Tolerance, Autoimmunity, and Transplantation Copyright 2013 by W. H. Freeman and Company Immune tolerance: history * Some
TLR2- and Dectin 1 Associated Innate Immune Response Modulates T-Cell Response to Pancreatic b-cell Antigen and Prevents Type 1 Diabetes
 Diabetes Volume 64, April 2015 1341 Subha Karumuthil-Melethil, 1 M. Hanief Sofi, 2 Radhika Gudi, 3 Benjamin M. Johnson, 2 Nicolas Perez, 1 and Chenthamarakshan Vasu 2,3 TLR2- and Dectin 1 Associated Innate
Diabetes Volume 64, April 2015 1341 Subha Karumuthil-Melethil, 1 M. Hanief Sofi, 2 Radhika Gudi, 3 Benjamin M. Johnson, 2 Nicolas Perez, 1 and Chenthamarakshan Vasu 2,3 TLR2- and Dectin 1 Associated Innate
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,100 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,100 116,000 120M Open access books available International authors and editors Downloads Our
Effector T Cells and
 1 Effector T Cells and Cytokines Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School 2 Lecture outline Cytokines Subsets of CD4+ T cells: definitions, functions, development New
1 Effector T Cells and Cytokines Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School 2 Lecture outline Cytokines Subsets of CD4+ T cells: definitions, functions, development New
Cellular Immune response. Jianzhong Chen, Ph.D Institute of immunology, ZJU
 Cellular Immune response Jianzhong Chen, Ph.D Institute of immunology, ZJU Concept of adaptive immune response T cell-mediated adaptive immune response I. Concept of immune response A collective and coordinated
Cellular Immune response Jianzhong Chen, Ph.D Institute of immunology, ZJU Concept of adaptive immune response T cell-mediated adaptive immune response I. Concept of immune response A collective and coordinated
Tolerance 2. Regulatory T cells; why tolerance fails. FOCiS. Lecture outline. Regulatory T cells. Regulatory T cells: functions and clinical relevance
 1 Tolerance 2. Regulatory T cells; why tolerance fails Abul K. Abbas UCSF FOCiS 2 Lecture outline Regulatory T cells: functions and clinical relevance Pathogenesis of autoimmunity: why selftolerance fails
1 Tolerance 2. Regulatory T cells; why tolerance fails Abul K. Abbas UCSF FOCiS 2 Lecture outline Regulatory T cells: functions and clinical relevance Pathogenesis of autoimmunity: why selftolerance fails
CELL BIOLOGY - CLUTCH CH THE IMMUNE SYSTEM.
 !! www.clutchprep.com CONCEPT: OVERVIEW OF HOST DEFENSES The human body contains three lines of against infectious agents (pathogens) 1. Mechanical and chemical boundaries (part of the innate immune system)
!! www.clutchprep.com CONCEPT: OVERVIEW OF HOST DEFENSES The human body contains three lines of against infectious agents (pathogens) 1. Mechanical and chemical boundaries (part of the innate immune system)
Cell-mediated Immunity
 Cellular & Molecular Immunology Cell-mediated Immunity Nicholas M. Ponzio, Ph.D. Department of Pathology & Laboratory Medicine April 6, 2009 Today s Presentation: Overview Cellular Interactions In Humoral
Cellular & Molecular Immunology Cell-mediated Immunity Nicholas M. Ponzio, Ph.D. Department of Pathology & Laboratory Medicine April 6, 2009 Today s Presentation: Overview Cellular Interactions In Humoral
Self-tolerance. Lack of immune responsiveness to an individual s own tissue antigens. Central Tolerance. Peripheral tolerance
 Autoimmunity Self-tolerance Lack of immune responsiveness to an individual s own tissue antigens Central Tolerance Peripheral tolerance Factors Regulating Immune Response Antigen availability Properties
Autoimmunity Self-tolerance Lack of immune responsiveness to an individual s own tissue antigens Central Tolerance Peripheral tolerance Factors Regulating Immune Response Antigen availability Properties
General Biology. A summary of innate and acquired immunity. 11. The Immune System. Repetition. The Lymphatic System. Course No: BNG2003 Credits: 3.
 A summary of innate and acquired immunity General iology INNATE IMMUNITY Rapid responses to a broad range of microbes Course No: NG00 Credits:.00 External defenses Invading microbes (pathogens). The Immune
A summary of innate and acquired immunity General iology INNATE IMMUNITY Rapid responses to a broad range of microbes Course No: NG00 Credits:.00 External defenses Invading microbes (pathogens). The Immune
Natural Killer Cells: Development, Diversity, and Applications to Human Disease Dr. Michael A. Caligiuri
 Natural Killer Cells: Development, Diversity, November 26, 2008 The Ohio State University Comprehensive Cancer Center The James Cancer Hospital and Solove Research Institute Columbus, Ohio, USA 1 Human
Natural Killer Cells: Development, Diversity, November 26, 2008 The Ohio State University Comprehensive Cancer Center The James Cancer Hospital and Solove Research Institute Columbus, Ohio, USA 1 Human
Advancing Opportunities To Prevent Type 1 Diabetes
 Advancing Opportunities To Prevent Type 1 Diabetes Dr. Allison Green Centre for Immunology and Infection Hull York Medical School York University Type 1 Diabetes Insulin deficiency destabilizes regulation
Advancing Opportunities To Prevent Type 1 Diabetes Dr. Allison Green Centre for Immunology and Infection Hull York Medical School York University Type 1 Diabetes Insulin deficiency destabilizes regulation
IMMUNOBIOLOGY OF TRANSPLANTATION. Wasim Dar
 IMMUNOBIOLOGY OF TRANSPLANTATION Wasim Dar Immunobiology of Transplantation Overview Transplantation: A complex immunologic process Contributions Innate Immunity Adaptive immunity T Cells B Cells HLA Consequences
IMMUNOBIOLOGY OF TRANSPLANTATION Wasim Dar Immunobiology of Transplantation Overview Transplantation: A complex immunologic process Contributions Innate Immunity Adaptive immunity T Cells B Cells HLA Consequences
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS. Choompone Sakonwasun, MD (Hons), FRCPT
 ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
Immunology for the Rheumatologist
 Immunology for the Rheumatologist Rheumatologists frequently deal with the immune system gone awry, rarely studying normal immunology. This program is an overview and discussion of the function of the
Immunology for the Rheumatologist Rheumatologists frequently deal with the immune system gone awry, rarely studying normal immunology. This program is an overview and discussion of the function of the
Supplemental Table I.
 Supplemental Table I Male / Mean ± SEM n Mean ± SEM n Body weight, g 29.2±0.4 17 29.7±0.5 17 Total cholesterol, mg/dl 534.0±30.8 17 561.6±26.1 17 HDL-cholesterol, mg/dl 9.6±0.8 17 10.1±0.7 17 Triglycerides,
Supplemental Table I Male / Mean ± SEM n Mean ± SEM n Body weight, g 29.2±0.4 17 29.7±0.5 17 Total cholesterol, mg/dl 534.0±30.8 17 561.6±26.1 17 HDL-cholesterol, mg/dl 9.6±0.8 17 10.1±0.7 17 Triglycerides,
T Cell Activation, Costimulation and Regulation
 1 T Cell Activation, Costimulation and Regulation Abul K. Abbas, MD University of California San Francisco 2 Lecture outline T cell antigen recognition and activation Costimulation, the B7:CD28 family
1 T Cell Activation, Costimulation and Regulation Abul K. Abbas, MD University of California San Francisco 2 Lecture outline T cell antigen recognition and activation Costimulation, the B7:CD28 family
Immunology Lecture 4. Clinical Relevance of the Immune System
 Immunology Lecture 4 The Well Patient: How innate and adaptive immune responses maintain health - 13, pg 169-181, 191-195. Immune Deficiency - 15 Autoimmunity - 16 Transplantation - 17, pg 260-270 Tumor
Immunology Lecture 4 The Well Patient: How innate and adaptive immune responses maintain health - 13, pg 169-181, 191-195. Immune Deficiency - 15 Autoimmunity - 16 Transplantation - 17, pg 260-270 Tumor
Practical Strategies for the Clinical Use of Incretin Mimetics CME/CE. CME/CE Released: 09/15/2009; Valid for credit through 09/15/2010
 Practical Strategies for the Clinical Use of Incretin Mimetics CME/CE Robert R. Henry, MD Authors and Disclosures CME/CE Released: 09/15/2009; Valid for credit through 09/15/2010 Introduction Type 2 diabetes
Practical Strategies for the Clinical Use of Incretin Mimetics CME/CE Robert R. Henry, MD Authors and Disclosures CME/CE Released: 09/15/2009; Valid for credit through 09/15/2010 Introduction Type 2 diabetes
2. Innate immunity 2013
 1 Innate Immune Responses 3 Innate immunity Abul K. Abbas University of California San Francisco The initial responses to: 1. Microbes: essential early mechanisms to prevent, control, or eliminate infection;
1 Innate Immune Responses 3 Innate immunity Abul K. Abbas University of California San Francisco The initial responses to: 1. Microbes: essential early mechanisms to prevent, control, or eliminate infection;
Immunology and Immunotherapy 101 for the Non-Immunologist
 Immunology and Immunotherapy 101 for the Non-Immunologist Stephen P. Schoenberger, Ph.D La Jolla Institute for Allergy and Immunology & UCSD Moores Cancer Center Disclosures Human Longevity Inc: Salary
Immunology and Immunotherapy 101 for the Non-Immunologist Stephen P. Schoenberger, Ph.D La Jolla Institute for Allergy and Immunology & UCSD Moores Cancer Center Disclosures Human Longevity Inc: Salary
B6/COLODR/SPL/11C/83/LAP/#2.006 B6/COLODR/SPL/11C/86/LAP/#2.016 CD11C B6/COLODR/SPL/11C/80/LAP/#2.011 CD11C
 CD3-specific antibody-induced immune tolerance and suppression of autoimmune encephalomyelitis involves TGF-β production through phagocytes digesting apoptotic T cells Sylvain Perruche 1,3, Pin Zhang 1,
CD3-specific antibody-induced immune tolerance and suppression of autoimmune encephalomyelitis involves TGF-β production through phagocytes digesting apoptotic T cells Sylvain Perruche 1,3, Pin Zhang 1,
Structure and Function of Antigen Recognition Molecules
 MICR2209 Structure and Function of Antigen Recognition Molecules Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will examine the major receptors used by cells of the innate and
MICR2209 Structure and Function of Antigen Recognition Molecules Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will examine the major receptors used by cells of the innate and
SUPPLEMENTARY INFORMATION
 doi:1.138/nature1554 a TNF-α + in CD4 + cells [%] 1 GF SPF 6 b IL-1 + in CD4 + cells [%] 5 4 3 2 1 Supplementary Figure 1. Effect of microbiota on cytokine profiles of T cells in GALT. Frequencies of TNF-α
doi:1.138/nature1554 a TNF-α + in CD4 + cells [%] 1 GF SPF 6 b IL-1 + in CD4 + cells [%] 5 4 3 2 1 Supplementary Figure 1. Effect of microbiota on cytokine profiles of T cells in GALT. Frequencies of TNF-α
Lecture outline. Immunological tolerance and immune regulation. Central and peripheral tolerance. Inhibitory receptors of T cells. Regulatory T cells
 1 Immunological tolerance and immune regulation Abul K. Abbas UCSF 2 Lecture outline Central and peripheral tolerance Inhibitory receptors of T cells Regulatory T cells 1 The immunological equilibrium:
1 Immunological tolerance and immune regulation Abul K. Abbas UCSF 2 Lecture outline Central and peripheral tolerance Inhibitory receptors of T cells Regulatory T cells 1 The immunological equilibrium:
Immunology 2011 Lecture 11 Innate Immunity & Genetics of Inbreeding. 6 October
 Immunology 2011 Lecture 11 Innate Immunity & Genetics of Inbreeding 6 October HANDOUT #6, Problem Set 3 TODAY Innate Immunity no core notes Genetics of Inbreeding - Appendix 10 MHC & Transplantation, Chapter
Immunology 2011 Lecture 11 Innate Immunity & Genetics of Inbreeding 6 October HANDOUT #6, Problem Set 3 TODAY Innate Immunity no core notes Genetics of Inbreeding - Appendix 10 MHC & Transplantation, Chapter
Scope. History. History. Incretins. Incretin-based Therapy and DPP-4 Inhibitors
 Plasma Glucose (mg/dl) Plasma Insulin (pmol/l) Incretin-based Therapy and Inhibitors Scope Mechanism of action ผศ.ดร.นพ.ว ระเดช พ ศประเสร ฐ สาขาว ชาโภชนว ทยาคล น ก ภาคว ชาอาย รศาสตร คณะแพทยศาสตร มหาว ทยาล
Plasma Glucose (mg/dl) Plasma Insulin (pmol/l) Incretin-based Therapy and Inhibitors Scope Mechanism of action ผศ.ดร.นพ.ว ระเดช พ ศประเสร ฐ สาขาว ชาโภชนว ทยาคล น ก ภาคว ชาอาย รศาสตร คณะแพทยศาสตร มหาว ทยาล
The development of T cells in the thymus
 T cells rearrange their receptors in the thymus whereas B cells do so in the bone marrow. The development of T cells in the thymus The lobular/cellular organization of the thymus Immature cells are called
T cells rearrange their receptors in the thymus whereas B cells do so in the bone marrow. The development of T cells in the thymus The lobular/cellular organization of the thymus Immature cells are called
Autoimmune Diseases. Betsy Kirchner CNP The Cleveland Clinic
 Autoimmune Diseases Betsy Kirchner CNP The Cleveland Clinic Disclosures (financial) No relevant disclosures Learning Objectives Explain the pathophysiology of autoimmune disease Discuss safe administration
Autoimmune Diseases Betsy Kirchner CNP The Cleveland Clinic Disclosures (financial) No relevant disclosures Learning Objectives Explain the pathophysiology of autoimmune disease Discuss safe administration
ACTIVATION OF T LYMPHOCYTES AND CELL MEDIATED IMMUNITY
 ACTIVATION OF T LYMPHOCYTES AND CELL MEDIATED IMMUNITY The recognition of specific antigen by naïve T cell induces its own activation and effector phases. T helper cells recognize peptide antigens through
ACTIVATION OF T LYMPHOCYTES AND CELL MEDIATED IMMUNITY The recognition of specific antigen by naïve T cell induces its own activation and effector phases. T helper cells recognize peptide antigens through
Hepatitis C Virus and Cytokine Responses
 Hepatitis C Virus and Cytokine Responses Eui-Cheol Shin, M.D., Ph.D. Laboratory of Immunology & Infectious Diseases (LIID), Graduate School of Medical Science & Engineering (GSMSE), KAIST Daejeon, Korea
Hepatitis C Virus and Cytokine Responses Eui-Cheol Shin, M.D., Ph.D. Laboratory of Immunology & Infectious Diseases (LIID), Graduate School of Medical Science & Engineering (GSMSE), KAIST Daejeon, Korea
Antiangiogenesis - Immune Therapy Combinations. George Coukos, MD, PhD Heinz Zwierzina, MD
 Antiangiogenesis - Immune Therapy Combinations George Coukos, MD, PhD Heinz Zwierzina, MD Overview Effect of VEGF on antitumor immune response Antigen presentation Effector mechanisms Ying and yang and
Antiangiogenesis - Immune Therapy Combinations George Coukos, MD, PhD Heinz Zwierzina, MD Overview Effect of VEGF on antitumor immune response Antigen presentation Effector mechanisms Ying and yang and
Tolerance, autoimmunity and the pathogenesis of immunemediated inflammatory diseases. Abul K. Abbas UCSF
 Tolerance, autoimmunity and the pathogenesis of immunemediated inflammatory diseases Abul K. Abbas UCSF Balancing lymphocyte activation and control Activation Effector T cells Tolerance Regulatory T cells
Tolerance, autoimmunity and the pathogenesis of immunemediated inflammatory diseases Abul K. Abbas UCSF Balancing lymphocyte activation and control Activation Effector T cells Tolerance Regulatory T cells
Innate immune regulation of T-helper (Th) cell homeostasis in the intestine
 Innate immune regulation of T-helper (Th) cell homeostasis in the intestine Masayuki Fukata, MD, Ph.D. Research Scientist II Division of Gastroenterology, Department of Medicine, F. Widjaja Foundation,
Innate immune regulation of T-helper (Th) cell homeostasis in the intestine Masayuki Fukata, MD, Ph.D. Research Scientist II Division of Gastroenterology, Department of Medicine, F. Widjaja Foundation,
CD4 + T cells recovered in Rag2 / recipient ( 10 5 ) Heart Lung Pancreas
 a CD4 + T cells recovered in Rag2 / recipient ( 1 5 ) Heart Lung Pancreas.5 1 2 4 6 2 4 6 Ctla4 +/+ Ctla4 / Ctla4 / Lung Ctla4 / Pancreas b Heart Lung Pancreas Ctla4 +/+ Ctla4 / Ctla4 / Lung Ctla4 / Pancreas
a CD4 + T cells recovered in Rag2 / recipient ( 1 5 ) Heart Lung Pancreas.5 1 2 4 6 2 4 6 Ctla4 +/+ Ctla4 / Ctla4 / Lung Ctla4 / Pancreas b Heart Lung Pancreas Ctla4 +/+ Ctla4 / Ctla4 / Lung Ctla4 / Pancreas
Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD-
 Supplementary Methods Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD- L1 (10F.9G2, rat IgG2b, k), and PD-L2 (3.2, mouse IgG1) have been described (24). Anti-CTLA-4 (clone
Supplementary Methods Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD- L1 (10F.9G2, rat IgG2b, k), and PD-L2 (3.2, mouse IgG1) have been described (24). Anti-CTLA-4 (clone
Micr-6005, Current Concepts of Immunology (Rutgers course number: 16:681:543) Spring 2009 Semester
 Micr-6005, Current Concepts of Immunology (Rutgers course number: 16:681:543) (3 Credits) Spring 2009 Semester Course Director: (732-235-4501, ) Please note that this course is offered once every 2 years.
Micr-6005, Current Concepts of Immunology (Rutgers course number: 16:681:543) (3 Credits) Spring 2009 Semester Course Director: (732-235-4501, ) Please note that this course is offered once every 2 years.
NKTR-255: Accessing IL-15 Therapeutic Potential through Robust and Sustained Engagement of Innate and Adaptive Immunity
 NKTR-255: Accessing IL-15 Therapeutic Potential through Robust and Sustained Engagement of Innate and Adaptive Immunity Peiwen Kuo Scientist, Research Biology Nektar Therapeutics August 31 st, 2018 Emerging
NKTR-255: Accessing IL-15 Therapeutic Potential through Robust and Sustained Engagement of Innate and Adaptive Immunity Peiwen Kuo Scientist, Research Biology Nektar Therapeutics August 31 st, 2018 Emerging
Supplementary Figure Legends. group) and analyzed for Siglec-G expression utilizing a monoclonal antibody to Siglec-G (clone SH2.1).
 Supplementary Figure Legends Supplemental Figure : Naïve T cells express Siglec-G. Splenocytes were isolated from WT B or Siglec-G -/- animals that have not been transplanted (n= per group) and analyzed
Supplementary Figure Legends Supplemental Figure : Naïve T cells express Siglec-G. Splenocytes were isolated from WT B or Siglec-G -/- animals that have not been transplanted (n= per group) and analyzed
Immunology Basics Relevant to Cancer Immunotherapy: T Cell Activation, Costimulation, and Effector T Cells
 Immunology Basics Relevant to Cancer Immunotherapy: T Cell Activation, Costimulation, and Effector T Cells Andrew H. Lichtman, M.D. Ph.D. Department of Pathology Brigham and Women s Hospital and Harvard
Immunology Basics Relevant to Cancer Immunotherapy: T Cell Activation, Costimulation, and Effector T Cells Andrew H. Lichtman, M.D. Ph.D. Department of Pathology Brigham and Women s Hospital and Harvard
The toll-like receptor 4 ligands Mrp8 and Mrp14 play a critical role in the development of autoreactive CD8 + T cells
 1 SUPPLEMENTARY INFORMATION The toll-like receptor 4 ligands Mrp8 and Mrp14 play a critical role in the development of autoreactive CD8 + T cells Karin Loser 1,2,6, Thomas Vogl 2,3, Maik Voskort 1, Aloys
1 SUPPLEMENTARY INFORMATION The toll-like receptor 4 ligands Mrp8 and Mrp14 play a critical role in the development of autoreactive CD8 + T cells Karin Loser 1,2,6, Thomas Vogl 2,3, Maik Voskort 1, Aloys
Immune responses in autoimmune diseases
 Immune responses in autoimmune diseases Erika Jensen-Jarolim Dept. of Pathophysiology Medical University Vienna CCHD Lecture January 24, 2007 Primary immune organs: Bone marrow Thymus Secondary: Lymph
Immune responses in autoimmune diseases Erika Jensen-Jarolim Dept. of Pathophysiology Medical University Vienna CCHD Lecture January 24, 2007 Primary immune organs: Bone marrow Thymus Secondary: Lymph
Scott Abrams, Ph.D. Professor of Oncology, x4375 Kuby Immunology SEVENTH EDITION
 Scott Abrams, Ph.D. Professor of Oncology, x4375 scott.abrams@roswellpark.org Kuby Immunology SEVENTH EDITION CHAPTER 13 Effector Responses: Cell- and Antibody-Mediated Immunity Copyright 2013 by W. H.
Scott Abrams, Ph.D. Professor of Oncology, x4375 scott.abrams@roswellpark.org Kuby Immunology SEVENTH EDITION CHAPTER 13 Effector Responses: Cell- and Antibody-Mediated Immunity Copyright 2013 by W. H.
11/25/2017. THE IMMUNE SYSTEM Chapter 43 IMMUNITY INNATE IMMUNITY EXAMPLE IN INSECTS BARRIER DEFENSES INNATE IMMUNITY OF VERTEBRATES
 THE IMMUNE SYSTEM Chapter 43 IMMUNITY INNATE IMMUNITY EXAMPLE IN INSECTS Exoskeleton made of chitin forms the first barrier to pathogens Digestive system is protected by a chitin-based barrier and lysozyme,
THE IMMUNE SYSTEM Chapter 43 IMMUNITY INNATE IMMUNITY EXAMPLE IN INSECTS Exoskeleton made of chitin forms the first barrier to pathogens Digestive system is protected by a chitin-based barrier and lysozyme,
The Adaptive Immune Response: T lymphocytes and Their Functional Types *
 OpenStax-CNX module: m46560 1 The Adaptive Immune Response: T lymphocytes and Their Functional Types * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution
OpenStax-CNX module: m46560 1 The Adaptive Immune Response: T lymphocytes and Their Functional Types * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution
Cutaneous Immunology: Innate Immune Responses. Skin Biology Lecture Series
 Cutaneous Immunology: Innate Immune Responses Skin Biology Lecture Series The Immune Response: Innate and Adaptive Components Source: Wolff, Goldsmith, Katz, Gilchrest, Paller, Leffell. Fitzpatrick s Dermatology
Cutaneous Immunology: Innate Immune Responses Skin Biology Lecture Series The Immune Response: Innate and Adaptive Components Source: Wolff, Goldsmith, Katz, Gilchrest, Paller, Leffell. Fitzpatrick s Dermatology
Animal Models to Understand Immunity
 Animal Models to Understand Immunity Hussein El Saghire hesaghir@sckcen.be Innate Adaptive immunity Immunity MAPK and NF-kB TLR pathways receptors Fast Slow Non-specific Specific NOD-like receptors T-cell
Animal Models to Understand Immunity Hussein El Saghire hesaghir@sckcen.be Innate Adaptive immunity Immunity MAPK and NF-kB TLR pathways receptors Fast Slow Non-specific Specific NOD-like receptors T-cell
Advances in Cancer Immunotherapy
 Advances in Cancer Immunotherapy Immunology 101 for the Non-Immunologist Arnold H. Zea, PhD azea@lsuhsc.edu Disclosures No relevant financial relationships to disclose This presentation does not contain
Advances in Cancer Immunotherapy Immunology 101 for the Non-Immunologist Arnold H. Zea, PhD azea@lsuhsc.edu Disclosures No relevant financial relationships to disclose This presentation does not contain
Pathogenesis of lupus apoptosis clearance and regulation of self tolerance. Durga Prasanna Misra
 Pathogenesis of lupus apoptosis clearance and regulation of self tolerance Durga Prasanna Misra Format Apoptosis Apoptosis in SLE Decreased apoptosis of autoreactive cells Increased apoptosis Defective
Pathogenesis of lupus apoptosis clearance and regulation of self tolerance Durga Prasanna Misra Format Apoptosis Apoptosis in SLE Decreased apoptosis of autoreactive cells Increased apoptosis Defective
The Immune System: Innate and Adaptive Body Defenses Outline PART 1: INNATE DEFENSES 21.1 Surface barriers act as the first line of defense to keep
 The Immune System: Innate and Adaptive Body Defenses Outline PART 1: INNATE DEFENSES 21.1 Surface barriers act as the first line of defense to keep invaders out of the body (pp. 772 773; Fig. 21.1; Table
The Immune System: Innate and Adaptive Body Defenses Outline PART 1: INNATE DEFENSES 21.1 Surface barriers act as the first line of defense to keep invaders out of the body (pp. 772 773; Fig. 21.1; Table
% of live splenocytes. STAT5 deletion. (open shapes) % ROSA + % floxed
 Supp. Figure 1. a 14 1 1 8 6 spleen cells (x1 6 ) 16 % of live splenocytes 5 4 3 1 % of live splenocytes 8 6 4 b 1 1 c % of CD11c + splenocytes (closed shapes) 8 6 4 8 6 4 % ROSA + (open shapes) % floxed
Supp. Figure 1. a 14 1 1 8 6 spleen cells (x1 6 ) 16 % of live splenocytes 5 4 3 1 % of live splenocytes 8 6 4 b 1 1 c % of CD11c + splenocytes (closed shapes) 8 6 4 8 6 4 % ROSA + (open shapes) % floxed
Type 1 diabetes (T1D) is a T cell-mediated autoimmune
 Interferon- initiates type 1 diabetes in nonobese diabetic mice Qing Li*, Baohui Xu, Sara A. Michie, Kathleen H. Rubins*, Robert D. Schreriber, and Hugh O. McDevitt* *Departments of Microbiology and Immunology
Interferon- initiates type 1 diabetes in nonobese diabetic mice Qing Li*, Baohui Xu, Sara A. Michie, Kathleen H. Rubins*, Robert D. Schreriber, and Hugh O. McDevitt* *Departments of Microbiology and Immunology
Secondary Negative Effects of Isolation Enzyme (s) On Human Islets. A.N.Balamurugan
 Secondary Negative Effects of Isolation Enzyme (s) On Human Islets A.N.Balamurugan Human Islets Functional Mass Preservation 18-25 min 10 min 8-12 min 10-15 min 45-60 min pancreas in chamber 37º Sub-Optimal
Secondary Negative Effects of Isolation Enzyme (s) On Human Islets A.N.Balamurugan Human Islets Functional Mass Preservation 18-25 min 10 min 8-12 min 10-15 min 45-60 min pancreas in chamber 37º Sub-Optimal
1. The scavenger receptor, CD36, functions as a coreceptor for which TLR? a. TLR ½ b. TLR 3 c. TLR 4 d. TLR 2/6
 Allergy and Immunology Review Corner: Cellular and Molecular Immunology, 8th Edition By Abul K. Abbas, MBBS, Andrew H. H. Lichtman, MD, PhD and Shiv Pillai, MBBS, PhD. Chapter 4 (pages 62-74): Innate Immunity
Allergy and Immunology Review Corner: Cellular and Molecular Immunology, 8th Edition By Abul K. Abbas, MBBS, Andrew H. H. Lichtman, MD, PhD and Shiv Pillai, MBBS, PhD. Chapter 4 (pages 62-74): Innate Immunity
Mechanisms of allergen-specific immunotherapy
 2012 KAAACI/EAAS Spring Mechanisms of allergen-specific immunotherapy Woo-Jung Song, MD Division of Allergy and Clinical Immunology Department of Internal Medicine Seoul National University Hospital, Seoul,
2012 KAAACI/EAAS Spring Mechanisms of allergen-specific immunotherapy Woo-Jung Song, MD Division of Allergy and Clinical Immunology Department of Internal Medicine Seoul National University Hospital, Seoul,
DNA vaccine, peripheral T-cell tolerance modulation 185
 Subject Index Airway hyperresponsiveness (AHR) animal models 41 43 asthma inhibition 45 overview 41 mast cell modulation of T-cells 62 64 respiratory tolerance 40, 41 Tregs inhibition role 44 respiratory
Subject Index Airway hyperresponsiveness (AHR) animal models 41 43 asthma inhibition 45 overview 41 mast cell modulation of T-cells 62 64 respiratory tolerance 40, 41 Tregs inhibition role 44 respiratory
Lecture 9: T-cell Mediated Immunity
 Lecture 9: T-cell Mediated Immunity Questions to Consider How do T cells know where to go? Questions to Consider How do T cells know where to go? How does antigen get targeted to a T cell expressing the
Lecture 9: T-cell Mediated Immunity Questions to Consider How do T cells know where to go? Questions to Consider How do T cells know where to go? How does antigen get targeted to a T cell expressing the
2/16/2018. The Immune System and Cancer. Fatal Melanoma Transferred in a Donated Kidney 16 years after Melanoma Surgery
 C007: Immunology of Melanoma: Mechanisms of Immune Therapies Delphine J. Lee, MD, PhD Chief and Program Director, Dermatology, Harbor UCLA Medical Center Principal Investigator, Los Angeles Biomedical
C007: Immunology of Melanoma: Mechanisms of Immune Therapies Delphine J. Lee, MD, PhD Chief and Program Director, Dermatology, Harbor UCLA Medical Center Principal Investigator, Los Angeles Biomedical
Discover the PD-1 pathway and its role in cancer 105/15 -ONCO- 07/15
 Discover the PD-1 pathway and its role in cancer 105/15 -ONCO- 07/15 Immunology in cancer The role of immunology in cancer Evolving knowledge of the immune system has provided a better understanding of
Discover the PD-1 pathway and its role in cancer 105/15 -ONCO- 07/15 Immunology in cancer The role of immunology in cancer Evolving knowledge of the immune system has provided a better understanding of
Role of Th17 cells in the immunopathogenesis of dry eye disease
 Role of Th17 cells in the immunopathogenesis of dry eye disease The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters Citation Chauhan,
Role of Th17 cells in the immunopathogenesis of dry eye disease The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters Citation Chauhan,
FOR OPTIMAL GUT HEALTH KEMIN.COM/GUTHEALTH
 FOR OPTIMAL GUT HEALTH KEMIN.COM/GUTHEALTH ALETA A SOURCE OF 1,3-BETA GLUCANS Aleta is highly bioavailable, offering a concentration greater than 5% of 1,3-beta glucans. Aleta provides a consistent response
FOR OPTIMAL GUT HEALTH KEMIN.COM/GUTHEALTH ALETA A SOURCE OF 1,3-BETA GLUCANS Aleta is highly bioavailable, offering a concentration greater than 5% of 1,3-beta glucans. Aleta provides a consistent response
