Localized 18 F-fluorodeoxyglucose uptake at the pancreatic head during remission phase of autoimmune pancreatitis: A case report
|
|
|
- Jesse Waters
- 5 years ago
- Views:
Transcription
1 ONOLOGY LETTERS 12: 01-05, 2016 Localized F-fluorodeoxyglucose uptake at the pancreatic head during remission phase of autoimmune pancreatitis: case report YOSHIKUNI YONENG 1,2, FUMIKI KUSHIHT 1, JOT WTNE 1, TIJI TOHYM 1, HITOSHI INOUE 1, TSURO SUGIT 3 and YSUTSUGU TK 1 1 epartment of Hepatobiliary Pancreatic and reast Surgery, Ehime University Graduate School of Medicine, Toon, Ehime ; 2 epartment of Surgery, Nagahama ity Hospital, Nagahama, Shiga ; 3 Pathology ivision, Ehime University Hospital, Toon, Ehime , Japan Received February 4, 2015; ccepted March 15, 2016 OI: /ol bstract. utoimmune pancreatitis (IP) is a unique form of pancreatitis, histopathologically characterized by dense lymphoplasmacytic infiltration and fibrosis of the pancreas with obliterative phlebitis. IP is associated with a good response to steroid therapy. ifferentiation between IP and pancreatic cancer to determine a preoperative diagnosis is often challenging, despite the use of various diagnostic modalities, including computed tomography (T), magnetic resonance imaging and endoscopic retrograde cholangiopancreatography. It has been reported that F fluorodeoxyglucose ( F FG) positron emission tomography (PET)/T may be a useful tool for distinguishing between the two diseases. In the present case report, a 71 year old male patient presented with a well circumscribed, solitary, nodular and homogenous F FG uptake at the pancreatic head, while receiving maintenance steroid therapy in the remission phase of IP; preoperatively, the patient had been strongly suspected of having pancreatic cancer. Pathological examination revealed post treatment relapse of IP. The present case highlights the diagnostic and management difficulties with IP in the remission phase. In certain cases, it remains challenging to differentiate the two diseases, even using the latest modalities. Introduction utoimmune pancreatitis (IP) is a unique form of pancreatitis that is histopathologically characterized by dense lymphoplasmacytic infiltration and fibrosis of the pancreas with obliterative phlebitis (1). Pancreatic cancer is one of the leading causes of mortality in Japan and Western countries (2). This type of tumor orrespondence to: r Yoshikuni Yonenaga, epartment of Surgery, Nagahama ity Hospital, 313 Ooinui cho, Nagahama, Shiga , Japan E mail: yoney@m.ehime u.ac.jp Key words: F fluorodeoxyglucose positron emission tomography, autoimmune pancreatitis, pancreatic cancer, pancreatoduodenectomy is associated with poor prognosis, due to its aggressive biology and the difficulty in making an early diagnosis. Patients with IP share numerous clinical features with pancreatic cancer patients, including advanced age, painless jaundice, weight loss, new onset diabetes mellitus and elevated serum levels of carbohydrate antigen () 19 9 (3). Such factors commonly render the differentiation between IP and pancreatic cancer rather challenging; however, distinguishing between the two diseases is crucial, as their treatments and prognoses are vastly different (4). n accurate preoperative diagnosis of IP is required in order to avoid unnecessary surgery and to achieve clinical remission with steroid therapy. F fluorodeoxyglucose ( F FG) positron emission tomography (PET)/computed tomography (T) has been reported to assist with this differentiation (2,3,5). The current study reports the case of a patient who presented with a new localized F FG uptake at the pancreatic head and normal serum immunoglobulin G4 (IgG4) levels during the remission phase of IP, and had been strongly suspected of having pancreatic cancer preoperatively. Written informed consent to publish was obtained from the patient. ase report 71 year old male patient was admitted to Shiritsu Oozu Hospital (Oozu, Japan) after presenting with worsening diabetes mellitus in pril The patient had a history of two abdominal surgeries: choledochectomy and choledochojejunostomy, due to choledocholithiasis 28 years prior to admission; and a right lateral hepatic sectoriectomy, due to intrahepatic stones 3 years prior to admission. IP was suspected following a workup, which included examining the serum IgG4 levels and an F FG PET/T, and the patient was referred to the Ehime University Hospital (Toon, Japan). bdominal ultrasonography and T imaging (rilliance 64; Philips, Tokyo, Japan) revealed enlargement of the pancreatic head and body (Fig. 1 and ). Endoscopic retrograde cholangiopancreatography (ERP; JF 260V; Olympus orporation, Tokyo, Japan) showed diffuse narrowing of the main pancreatic duct (MP) in the pancreatic head and body (Fig. 1). F FG PET/T (iscovery ST Elite; GE Healthcare Life Sciences, Hino, Japan), which had been performed during the previous hospital stay, revealed a strong and diffuse uptake of
2 02 YONENG et al: LOLIZE F-FG UPTKE T THE PNRETI HE IN THE REMISSION PHSE OF IP Figure 2. Follow up images acquired 3 months after the initiation of steroid therapy. ( and ) omputed tomography showing that the enlargement of the pancreatic head (circle) and body had markedly improved. () Endoscopic retrograde cholangiopancreatography showing that the diffuse narrowing of the main pancreatic duct had fully recovered. Figure 1. Images prior to initiation of steroid therapy. ( and ) T scans showing enlargement of the pancreatic head (circle) and body upon initial diagnosis. () Endoscopic retrograde cholangiopancreatography showing diffuse narrowing of the main pancreatic duct in the pancreatic head and body, upon initial diagnosis. () F FG positron emission tomography/t showing a strong and diffuse uptake of F FG throughout the entire pancreas. T, computed tomography; F FG, F fluorodeoxyglucose. F FG throughout the entire pancreas (Fig. 1). The serum IgG4 level was markedly elevated (158 mg/dl; normal range, mg/dl). diagnosis of IP was thereby established, and steroid therapy was initiated. The initial oral prednisolone dose administered was 30 mg/day. Following the initiation of the steroid therapy, the enlargement of the pancreatic head and body markedly improved, the diffuse narrowing of the MP fully recovered (Fig. 2 ), and the IgG4 level dropped to within normal limits. The oral steroid therapy regimen was as follows: The initial dose was administered daily for 2 weeks, followed by gradual tapering of the dose by 5 mg every 2 weeks, until a daily dose of 5 mg was reached. Subsequently, maintenance steroid therapy (5 mg/day) was administered, based on the Japanese consensus guidelines for the management of IP (6). Follow up examinations were performed on an outpatient basis. t 10 months after the initiation of the steroid therapy, elevated serum levels of amylase (255 IU/l; normal range, IU/l) and lipase (91 IU/l; normal range, IU/l) were detected, and a T scan revealed a 2 cm low attenuation mass at the pancreatic head and dilation of the MP (Fig. 3 and ). The patient was readmitted to the hospital due to a suspected relapse of IP. Magnetic resonance imaging (MRI) revealed tumor like enlargement at the pancreatic head, and obstruction of the MP with dilatation of the upstream MP. ERP showed a ~2 cm long stricture of the MP at the pancreatic head and a dilatation of the body and tail portion of MP that measured 5 mm in diameter (Fig. 3). ased on these radiographic findings, it was difficult to decide between recurrence of IP and pancreatic cancer. The serum levels of 19 9, duke pancreatic monoclonal antigen type 2, and Span 1 were normal. The serum level of carcinoembryonic antigen was slightly elevated (7.1 ng/ml; normal range, <5.0 ng/ml). The serum level of IgG4 was 106 mg/dl, which was below the cutoff value ( 135 mg/dl) of the Japanese clinical diagnostic criteria for IP (1). F FG PET/T
3 ONOLOGY LETTERS 12: 01-05, Figure 3. Follow up images acquired 10 months after the initiation of steroid therapy. ( and ) T scan showing a low attenuation mass measuring 2 cm at the pancreatic head (circle) and dilation of the MP (arrow), which had not been observed in previous T scans (Figs. 1 and 2). () Endoscopic retrograde cholangiopancreatography showing an ~2 cm long stricture of the MP at the pancreatic head and dilatation of the the body and tail portion of MP measuring 5 mm in diameter. () F FG positron emission tomography/t showing a well circumscribed uptake of F FG at the location where the pancreatic head mass was identified by T scan. T, computed tomography; F FG, F fluorodeoxyglucose; MP, main pancreatic duct. (quiduo P 7000; Toshiba Medical Systems, Ootawara, Japan) showed a well circumscribed, solitary, nodular and homogenous F FG uptake, with a maximum standardized uptake value of 7.82 at the location where the pancreatic head mass was identified by T scan (Fig. 3). No abnormal extrapancreatic uptake of F FG was observed. The patient was referred to the epartment of Hepatobiliary Pancreatic and reast Surgery, Ehime University Hospital with a suspected diagnosis of concomitant Figure 4. Pathological examination revealing diffuse lymphoplasmacytic infiltrate with fibrosis, periductal lymphoplasmacytic infiltrate in the pancreatic head mass: () x40 and () x400 magnification. () Elastica Masson staining showing obliterative phlebitis in this specimen. () n abundance of IgG4 positive cells was observed in the lymphoplasmacytic infiltrate (>10 cells/high power field). pancreatic cancer with IP, and pancreatoduodenectomy was performed. The formalin fixed paraffin embedded 4 µm sections were used for hematoxylin and eosin staining, Elastica-Masson staining and IgG4 immunostaining (mouse anti-human IgG4 monoclonal antibody; dilution, 1:400; catalog no., GTX75819; GeneTex, Irvine,, US). Pathological examination revealed diffuse lymphoplasmacytic infiltrate with fibrosis, periductal lymphoplasmacytic infiltrate
4 04 YONENG et al: LOLIZE F-FG UPTKE T THE PNRETI HE IN THE REMISSION PHSE OF IP and obliterative phlebitis (Fig. 4 ). The lymphoplasmacytic infiltrate included an abundance of IgG4 positive cells [>10 cells/high power field (HPF)] (Fig. 4), which forms one of the histological criteria for IP proposed by the Mayo linic (7). No malignant cells were found. Recurrent IP was therefore diagnosed. Maintenance steroid therapy was resumed following surgery, and, at the time of writing the present study, no recurrent IP in the pancreatic remnant has been identified for 4 years after surgery. iscussion IP is a distinct form of pancreatitis characterized by the involvement of autoimmune mechanisms, such as hypergamma globulinemia, increased serum levels of IgG, increased serum levels of IgG4 or the presence of autoantibodies (1). IP has been associated with an effective response to steroid therapy (1). The pathological features of this disorder are characterized by periductal lymphoplasmacytic infiltrate and lymphoplasmacytic infiltrate showing abundant (>10 cells/hpf) IgG4 positive cells (7). This lymphoplasmacytic infiltration is often accompanied by stroriform fibrosis and obliterative phlebitis (7). These characteristic features can distinguish IP from normal chronic pancreatitis (7). The clinical spectrum of IP includes sclerosing cholangitis, retroperitoneal fibrosis, hilar lymphadenopathy, salivary gland swelling and interstitional pneumonia (8). Some of these extrapancreatic lesions show pathological findings similar to those of pancreatic lesions (8). IP and pancreatic cancer share several characteristics; however, the therapeutic methods for each of these diseases are vastly different. Pancreatic cancer requires surgery, while steroid therapy is effective for IP without the need for surgical intervention (4). It is therefore crucial to distinguish IP from pancreatic cancer; however, in certain cases, differential diagnosis is challenging, despite the use of numerous different diagnostic modalities, such as T and MRI scans, and ERP. Nakazawa et al (9) reported that 7/37 (.9%) patients with IP underwent surgical intervention due to having been misdiagnosed with pancreatic or bile duct cancer. Kamisawa et al (4) also reported that 6/17 (35.3%) patients with focal mass forming IP were surgically treated due to the suspicion of pancreatic cancer. Other studies have reported the utility of F FG PET/T for the differentiation of IP from pancreatic cancer (2,3,5). F FG PET/T is a sensitive modality used for the diagnosis of malignancies. Since F FG uptake is caused by increased glucose utilization of tumor cells and is also observed at inflammatory sites, F FG uptake is a shared finding between IP and pancreatic cancer. Kamisawa et al (5) concluded that F FG PET/T can assist in the differentiation between the two diseases by assessing F FG uptake patterns in the pancreas and extrapancreatic lesions. Lee et al (3) indicated that, in severe cases, using PET/T can detect the presence of diffuse F FG uptake by the pancreas, or concomitant extrapancreatic uptake by the salivary glands, which can aid in differentiation. Ozaki et al (2) also reported that the typical F FG PET findings for IP are an irregular contour, longitudinal shape, heterogeneous accumulation and multiple localizations, whereas those for pancreatic cancer are a smooth contour, nodular shape, homogenous accumulation and solitary localization. Shigekawa et al (8) indicated that the accumulation patterns of F FG were nodular and solitary in the majority of cases of pancreatic cancer that they examined, and that the possibility of IP was increased if the F FG accumulation in the pancreas had a longitudinal shape; however, nodular and solitary F FG accumulations were also observed in IP, corresponding with focal changes in the pancreas on T or ERP. It was also reported that F FG uptake in extrapancreatic lesions, including the extra abdominal lymph nodes, salivary glands, eyes and biliary duct, may be helpful in differentiating between pancreatic cancer and IP. Kamisawa et al (4) proposed an algorithm for the clinical management of a mass like lesion on the pancreatic head, with particular emphasis on the differentiation between IP and pancreatic cancer. They identified 6 imaging characteristics, a combination of T and ERP findings, that were highly suggestive of IP. The findings were as follows: i) elayed enhancement of the enlarged pancreas on T scan; ii) a capsule like rim on T scan, iii) the presence of extrapancreatic lesions, such as salivary gland swelling, retroperitoneal mass or stenosis of the upper or intrahepatic bile duct on T scan or ERP; iv) 3 cm long narrowed portion of the MP on ERP; v) skipped lesions of the MP on ERP, and vi) a maximal diameter of <5 mm of the upstream MP on ERP. In the present case, none of these imaging characteristics were observed. ccording to this algorithm, in cases with no positive imaging factors for IP, surgery should be considered under the provisional diagnosis of pancreatic cancer. Several studies have reported cases of pancreatic cancer complicated with IP simultaneously (10 13) or during follow up (14 ). Loos et al (15) reported a case of a patient who developed a metastatic adenocarcinoma of the pancreatobiliary system within a year after the histologically confirmed diagnosis of IP. In addition, among the reports, 3 patients were diagnosed with pancreatic cancer during maintenance steroid therapy (16 ). In general, the risk of pancreatic cancer is markedly increased in patients with chronic pancreatitis (14); however, the association between IP and pancreatic cancer remains unknown. ased on earlier reports of cancer development during the course of maintenance steroid therapy for IP, three key findings of the present study, and the algorithm proposed by Kamisawa et al (4), the patient was diagnosed with pancreatic cancer during the course of maintenance steroid therapy for IP, and pancreatoduodenectomy was performed. The aforementioned key findings of the present study were the following: i) etection by PET/T scan of a well circumscribed, solitary, nodular and homogenous F FG uptake at the same area where a pancreatic head mass was identified; ii) no extrapancreatic uptake; and iii) normal serum IgG4 levels. Pathological examination revealed diffuse lymphoplasmacytic infiltrate with fibrosis, periductal infiltrate, obliterative phlebitis, IgG4 positive cells and absence of malignant cells; therefore, post treatment relapse of IP was eventually diagnosed. t the time of writing the present study, no recurrent IP in the pancreatic remnant of the patient had been identified for 4 years after surgery. Of note, authors from the Mayo linic recently reported that the relapse rate of IP patients who underwent pancreatoduodenectomy as the initial treatment
5 ONOLOGY LETTERS 12: 01-05, was markedly lower than that of patients who had not undergone pancreatoduodenectomy (the corticosteroid treated group) (19). While the underlying mechanisms are unclear, this is a noteworthy observation that requires further study. In summary, the current study reported the case of a patient who presented with a new mass at the pancreatic head and an upstream dilatation of the MP while receiving a maintenance dosage of steroids in the remission phase of IP. The present study highlights the challenges faced by clinicians in the diagnosis and management of IP in remission. In certain cases, the differentiation between pancreatic cancer and IP remains difficult, despite the use of the latest diagnostic modalities. References 1. Okazaki K, Kawa S, Kamisawa T, Naruse S, Tanaka S, Nishimori I, Ohara H, Ito T, Kiriyama S, Inui K, et al: linical diagnostic criteria of autoimmune pancreatitis: Revised proposal. J Gastroenterol 41: , Ozaki Y, Oguchi K, Hamano H, rakura N, Muraki T, Kiyosawa K, Momose M, Kadoya M, Miyata K, izawa T and Kawa S: ifferentiation of autoimmune pancreatitis from suspected pancreatic cancer by fluorine fluorodeoxyglucose positron emission tomography. J Gastroenterol 43: , Lee TY, Kim MH, Park do H, Seo W, Lee SK, Kim JS and Lee KT: Utility of F FG PET/T for differentiation of autoimmune pancreatitis with atypical pancreatic imaging findings from pancreatic cancer. JR m J Roentgenol 193: , Kamisawa T, Imai M, Yui hen P, Tu Y, Egawa N, Tsuruta K, Okamoto, Suzuki M and Kamata N: Strategy for differentiating autoimmune pancreatitis from pancreatic cancer. Pancreas 37: e62 e67, Kamisawa T, Takum K, njiki H, Egawa N, Kurata M, Honda G and Tsuruta K: FG PET/T findings of autoimmune pancreatitis. Hepatogastroenterology 57: , Kamisawa T, Okazaki K, Kawa S, Shimosegawa T and Tanaka M; Research ommittee for Intractable Pancreatic isease and Japan Pancreas Society: Japanese consensus guidelines for management of autoimmune pancreatitis: III. Treatment and prognosis of IP. J Gastroenterol 45: , hari ST, Smyrk T, Levy MJ, Topazian M, Takahashi N, Zhang L, lain JE, Pearson RK, Petersen T, Vege SS and Farnell M: iagnosis of autoimmune pancreatitis: The Mayo linic experience. lin Gastroenterol Hepatol 4: , Shigekawa M, Yamao K, Sawaki, Hara K, Takagi T, hatia V, Nishio M, Tamaki T, El min H, Sayed Zel and Mizuno N: Is ()F fluorodeoxyglucose positron emission tomography meaningful for estimating the efficacy of corticosteroid therapy in patients with autoimmune pancreatitis? J Hepatobiliary Pancreat Sci 17: , Nakazawa T, Ohara H, Sano H, ndo T, Imai H, Takada H, Hayashi K, Kitajima Y and Joh T: ifficulty in diagnosing autoimmune pancreatitis by imaging findings. Gastrointest Endosc 65: , Inoue H, Miyatani H, Sawada Y and Yoshida Y: case of pancreas cancer with autoimmune pancreatitis. Pancreas 33: , Witkiewicz K, Kennedy EP, Kennyon L, Yeo J and Hruban RH: Synchronous autoimmune pancreatitis and infiltrating pancreatic ductal adenocarcinoma: ase report and review of the literature. Hum Pathol 39: , Motosugi U, Ichikawa T, Yamaguchi H, Nakazawa T, Katoh R, Itakura J, Fujii H, Sato T, raki T and Shimizu M: Small invasive ductal adenocarcinoma of the pancreas associated with lymphoplasmacytic sclerosing pancreatitis. Pathol Int 59: , handrasegaram M, hiam S, Nguyen NQ, Ruszkiewicz, hung, Neo EL, hen JW, Worthley S and rooke Smith ME: case of pancreatic cancer in the setting of autoimmune pancreatitis with nondiagnostic serum markers. ase Rep Surg 2013: , Ghazale and hari S: Is autoimmune pancreatitis a risk factor for pancreatic cancer? Pancreas 35: 376, Loos M, Esposito I, Hedderich M, Ludwig L, Fingerle, Friess H, Klöppel G and üchler P: utoimmune pancreatitis complicated by carcinoma of the pancreatobiliary system: case report and review of the literature. Pancreas 40: , Fukui T, Mitsuyama T, Takaoka M, Uchida K, Matsushita M and Okazaki K: Pancreatic cancer associated with autoimmune pancreatitis in remission. Intern Med 47: , Kubota K, Iida H, Fujisawa T, Yoneda M, Inamori M, be Y, Kirikoshi H, Saito S, Ohshiro H, Kakuta Y and Nakajima : linical factors predictive of spontaneous remission or relapse in cases of autoimmune pancreatitis. Gastrointest Endosc 66: , Gupta R, Khosroshahi, Shinagare S, Fernandez, Ferrone, Lauwers GY, Stone JH and eshpande V: oes autoimmune pancreatitis increase the risk of pancreatic carcinoma? retrospective analysis of pancreatic resections. Pancreas 42: , Sah RP, hari ST, Pannala R, Sugumar, lain JE, Levy MJ, Pearson RK, Smyrk T, Petersen T, Topazian M, et al: ifferences in clinical profile and relapse rate of type 1 versus type 2 autoimmune pancreatitis. Gastroenterology 139: ; quiz e12 e13, 2010.
Diagnostic Algorithm for Autoimmune Pancreatitis in Korea
 Review Article The Korean Journal of Pancreas and Biliary Tract 2014;19(1):7-12 pissn 1976-3573 eissn 2288-0941 한국에서자가면역췌장염의진단전략 성균관대학교의과대학삼성서울병원내과학교실 이종균 Diagnostic Algorithm for Autoimmune Pancreatitis
Review Article The Korean Journal of Pancreas and Biliary Tract 2014;19(1):7-12 pissn 1976-3573 eissn 2288-0941 한국에서자가면역췌장염의진단전략 성균관대학교의과대학삼성서울병원내과학교실 이종균 Diagnostic Algorithm for Autoimmune Pancreatitis
IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis?
 CASE REPORT IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis? Keita Saeki 1, Shigenari Hozawa 1, Naoteru Miyata 1,
CASE REPORT IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis? Keita Saeki 1, Shigenari Hozawa 1, Naoteru Miyata 1,
Immunoglobulin G4-Related Disease with Several Inflammatory Foci
 CASE REPORT Immunoglobulin G4-Related Disease with Several Inflammatory Foci Akira Sakamaki 1, Kenya Kamimura 1, Kazuhiko Shioji 1, Junko Sakurada 2, Takeshi Nakatsue 3, Yoko Wada 3, Michitaka Imai 1,
CASE REPORT Immunoglobulin G4-Related Disease with Several Inflammatory Foci Akira Sakamaki 1, Kenya Kamimura 1, Kazuhiko Shioji 1, Junko Sakurada 2, Takeshi Nakatsue 3, Yoko Wada 3, Michitaka Imai 1,
CASE REPORT. Abstract. Introduction. Case Report
 CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
Comparison of multidetector-row computed tomography findings of IgG4-related sclerosing cholangitis and cholangiocarcinoma
 Comparison of multidetector-row computed tomography findings of IgG4-related sclerosing cholangitis and cholangiocarcinoma Poster No.: C-0245 Congress: ECR 2014 Type: Scientific Exhibit Authors: M. Yata,
Comparison of multidetector-row computed tomography findings of IgG4-related sclerosing cholangitis and cholangiocarcinoma Poster No.: C-0245 Congress: ECR 2014 Type: Scientific Exhibit Authors: M. Yata,
The most common presentation of autoimmune pancreatitis. A Diagnostic Strategy to Distinguish Autoimmune Pancreatitis From Pancreatic Cancer
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1097 1103 A Diagnostic Strategy to Distinguish Autoimmune Pancreatitis From Pancreatic Cancer SURESH T. CHARI,* NAOKI TAKAHASHI, MICHAEL J. LEVY,* THOMAS
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1097 1103 A Diagnostic Strategy to Distinguish Autoimmune Pancreatitis From Pancreatic Cancer SURESH T. CHARI,* NAOKI TAKAHASHI, MICHAEL J. LEVY,* THOMAS
Long-term Outcome of Autoimmune Pancreatitis after Oral Prednisolone Therapy
 ORIGINAL ARTICLE Long-term Outcome of Autoimmune Pancreatitis after Oral Prednisolone Therapy Takayoshi Nishino 1, Fumitake Toki 2,HiroyasuOyama 3, Kyoko Shimizu 1 and Keiko Shiratori 1 Abstract Objective
ORIGINAL ARTICLE Long-term Outcome of Autoimmune Pancreatitis after Oral Prednisolone Therapy Takayoshi Nishino 1, Fumitake Toki 2,HiroyasuOyama 3, Kyoko Shimizu 1 and Keiko Shiratori 1 Abstract Objective
IgG4-related sclerosing disease
 IgG4-related sclerosing disease TERUMI KAMISAWA, KENSUKE TAKUMA, NAOTO EGAWA Department of Internal Medicine Tokyo Metropolitan Komagome Hospital 3-18-22 Honkomagome, Bunkyo-ku, Tokyo 113-8677, Japan JAPAN
IgG4-related sclerosing disease TERUMI KAMISAWA, KENSUKE TAKUMA, NAOTO EGAWA Department of Internal Medicine Tokyo Metropolitan Komagome Hospital 3-18-22 Honkomagome, Bunkyo-ku, Tokyo 113-8677, Japan JAPAN
Value of Serum IgG4 in the Diagnosis of Autoimmune Pancreatitis and in Distinguishing it from Acute and Chronic Pancreatitis of Other Etiology
 94 Jul 2017 Vol 10 No.3 North American Journal of Medicine and Science Original Research Value of Serum IgG4 in the Diagnosis of Autoimmune Pancreatitis and in Distinguishing it from Acute and Chronic
94 Jul 2017 Vol 10 No.3 North American Journal of Medicine and Science Original Research Value of Serum IgG4 in the Diagnosis of Autoimmune Pancreatitis and in Distinguishing it from Acute and Chronic
Strategy to differentiate autoimmune pancreatitis from pancreas cancer
 Online Submissions: http://www.wjgnet.com/1007-9327office wjg@wjgnet.com doi:10.3748/wjg.v18.i10.1015 World J Gastroenterol 2012 March 14; 18(10): 1015-1020 ISSN 1007-9327 (print) ISSN 2219-2840 (online)
Online Submissions: http://www.wjgnet.com/1007-9327office wjg@wjgnet.com doi:10.3748/wjg.v18.i10.1015 World J Gastroenterol 2012 March 14; 18(10): 1015-1020 ISSN 1007-9327 (print) ISSN 2219-2840 (online)
Review Article The Utility of Serum IgG4 Concentrations as a Biomarker
 International Rheumatology Volume 2012, Article ID 198314, 4 pages doi:10.1155/2012/198314 Review Article The Utility of Serum IgG4 Concentrations as a Biomarker Shigeyuki Kawa, 1 Tetsuya Ito, 2 Takayuki
International Rheumatology Volume 2012, Article ID 198314, 4 pages doi:10.1155/2012/198314 Review Article The Utility of Serum IgG4 Concentrations as a Biomarker Shigeyuki Kawa, 1 Tetsuya Ito, 2 Takayuki
Autoimmune Pancreatitis: A Great Imitator
 Massachusetts General Hospital Harvard Medical School Autoimmune Pancreatitis: A Great Imitator Dushyant V Sahani MD dsahani@partners.org Autoimmune Pancreatitis: Learning Objectives Clinical manifestations
Massachusetts General Hospital Harvard Medical School Autoimmune Pancreatitis: A Great Imitator Dushyant V Sahani MD dsahani@partners.org Autoimmune Pancreatitis: Learning Objectives Clinical manifestations
Differentiating Immunoglobulin G4-Related Sclerosing Cholangitis from Hilar Cholangiocarcinoma
 Gut and Liver, Vol. 7, No. 2, March 2013, pp. 234-238 ORiginal Article Differentiating Immunoglobulin G4-Related Sclerosing Cholangitis from Hilar Cholangiocarcinoma Taku Tabata*, Terumi Kamisawa*, Seiichi
Gut and Liver, Vol. 7, No. 2, March 2013, pp. 234-238 ORiginal Article Differentiating Immunoglobulin G4-Related Sclerosing Cholangitis from Hilar Cholangiocarcinoma Taku Tabata*, Terumi Kamisawa*, Seiichi
CASE 01 LA Path Slide Seminar 13 March, 08. Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center
 CASE 01 LA Path Slide Seminar 13 March, 08 Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center Clinical History 60 year old male presented with obstructive jaundice
CASE 01 LA Path Slide Seminar 13 March, 08 Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center Clinical History 60 year old male presented with obstructive jaundice
Isolated Mass-Forming IgG4-Related Cholangitis as an Initial Clinical Presentation of Systemic IgG4-Related Disease
 Journal of Pathology and Translational Medicine 2016; 50: 300-305 CASE STUDY Isolated Mass-Forming IgG4-Related Cholangitis as an Initial Clinical Presentation of Systemic IgG4-Related Disease Seokhwi
Journal of Pathology and Translational Medicine 2016; 50: 300-305 CASE STUDY Isolated Mass-Forming IgG4-Related Cholangitis as an Initial Clinical Presentation of Systemic IgG4-Related Disease Seokhwi
A Case of Pancreatic Carcinoma with Bilateral Hilar
 Shinshu Med J, 66⑵:151~155, 2018 A Case of Pancreatic Carcinoma with Bilateral Hilar 18 F-FDG and 67 Ga Hyperaccumulation Satoshi Kawakami 1 )*, Yasunari Fujinaga 1), Shin Yanagisawa 1) Masumi Kadoya 1),
Shinshu Med J, 66⑵:151~155, 2018 A Case of Pancreatic Carcinoma with Bilateral Hilar 18 F-FDG and 67 Ga Hyperaccumulation Satoshi Kawakami 1 )*, Yasunari Fujinaga 1), Shin Yanagisawa 1) Masumi Kadoya 1),
An Autopsy Case of Autoimmune Pancreatitis
 MULTIMEDIA ARTICLE - Clinical Imaging An Autopsy Case of Autoimmune Pancreatitis Yohei Kitano 1, Kakuya Matsumoto 1, Kenji Chisaka 1, Masako Imazawa 1, Kenji Takahashi 1, Yukiomi Nakade 1, Mituyoshi Okada
MULTIMEDIA ARTICLE - Clinical Imaging An Autopsy Case of Autoimmune Pancreatitis Yohei Kitano 1, Kakuya Matsumoto 1, Kenji Chisaka 1, Masako Imazawa 1, Kenji Takahashi 1, Yukiomi Nakade 1, Mituyoshi Okada
Autoimmune pancreatitis (AIP) can be defined as a
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:1010 1016 Diagnosis of Autoimmune Pancreatitis: The Mayo Clinic Experience SURESH T. CHARI,* THOMAS C. SMYRK, MICHAEL J. LEVY,* MARK D. TOPAZIAN,* NAOKI
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:1010 1016 Diagnosis of Autoimmune Pancreatitis: The Mayo Clinic Experience SURESH T. CHARI,* THOMAS C. SMYRK, MICHAEL J. LEVY,* MARK D. TOPAZIAN,* NAOKI
Overview of Diagnostic Criteria for Autoimmune Pancreatitis
 2007 년도대한췌담도학회추계학술대회 Session II: Comparison of Diagnostic Criteria for AIP: Japan, USA & Korea Overview of Diagnostic Criteria for Autoimmune Pancreatitis Department of Internal Medicine, Seoul National
2007 년도대한췌담도학회추계학술대회 Session II: Comparison of Diagnostic Criteria for AIP: Japan, USA & Korea Overview of Diagnostic Criteria for Autoimmune Pancreatitis Department of Internal Medicine, Seoul National
A Case of Autoimmune Pancreatitis Associated with Retroperitoneal Fibrosis
 CASE REPORT A Case of Autoimmune Pancreatitis Associated with Retroperitoneal Fibrosis Koushiro Ohtsubo 1, Hiroyuki Watanabe 1, Tomoya Tsuchiyama 1, Hisatsugu Mouri 1, Yasushi Yamaguchi 1, Yoshiharu Motoo
CASE REPORT A Case of Autoimmune Pancreatitis Associated with Retroperitoneal Fibrosis Koushiro Ohtsubo 1, Hiroyuki Watanabe 1, Tomoya Tsuchiyama 1, Hisatsugu Mouri 1, Yasushi Yamaguchi 1, Yoshiharu Motoo
Multiple Primary Quiz
 Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
Autoimmune pancreatitis (AIP) was described more than a
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:1229 1234 The Use of Immunoglobulin G4 Immunostaining in Diagnosing Pancreatic and Extrapancreatic Involvement in Autoimmune Pancreatitis MAESHA G. DEHERAGODA,*
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:1229 1234 The Use of Immunoglobulin G4 Immunostaining in Diagnosing Pancreatic and Extrapancreatic Involvement in Autoimmune Pancreatitis MAESHA G. DEHERAGODA,*
Incidence of Malignancy in Type 1 Autoimmune Pancreatitis
 ORIGINAL ARTICLE Incidence of Malignancy in Type 1 Autoimmune Pancreatitis Junko Tahara 1, Kyoko Shimizu 1, Junichi Akao 1, Yukiko Takayama 1, Katsutoshi Tokushige 1, Masakazu Yamamoto 2 1 Department of
ORIGINAL ARTICLE Incidence of Malignancy in Type 1 Autoimmune Pancreatitis Junko Tahara 1, Kyoko Shimizu 1, Junichi Akao 1, Yukiko Takayama 1, Katsutoshi Tokushige 1, Masakazu Yamamoto 2 1 Department of
Case Report IgG4-Seronegative Autoimmune Pancreatitis and Sclerosing Cholangitis
 Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 591360, 6 pages http://dx.doi.org/10.1155/2015/591360 Case Report IgG4-Seronegative Autoimmune Pancreatitis and Sclerosing Cholangitis
Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 591360, 6 pages http://dx.doi.org/10.1155/2015/591360 Case Report IgG4-Seronegative Autoimmune Pancreatitis and Sclerosing Cholangitis
A case of retroperitoneal fibrosis responding to steroid therapy
 Challenging Clinical Cases Vol. 43 (6): 1185-1189, November - December, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0520 A case of retroperitoneal fibrosis responding to steroid therapy Ryuta Watanabe 1, Akira
Challenging Clinical Cases Vol. 43 (6): 1185-1189, November - December, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0520 A case of retroperitoneal fibrosis responding to steroid therapy Ryuta Watanabe 1, Akira
Autoimmune pancreatitis
 Review Article Autoimmune pancreatitis Ayodeji Oluwarotimi Omiyale Department of Cellular Pathology, Maidstone Hospital, Maidstone, Kent, UK Correspondence to: Ayodeji Oluwarotimi Omiyale. Department of
Review Article Autoimmune pancreatitis Ayodeji Oluwarotimi Omiyale Department of Cellular Pathology, Maidstone Hospital, Maidstone, Kent, UK Correspondence to: Ayodeji Oluwarotimi Omiyale. Department of
Localized autoimmune pancreatitis mimicking pancreatic cancer: Case report and literature review
 Case Report Localized autoimmune pancreatitis mimicking pancreatic cancer: Case report and literature review Journal of International Medical Research 2018, Vol. 46(4) 1657 1665! The Author(s) 2018 Reprints
Case Report Localized autoimmune pancreatitis mimicking pancreatic cancer: Case report and literature review Journal of International Medical Research 2018, Vol. 46(4) 1657 1665! The Author(s) 2018 Reprints
IgG4-related Sclerosing Disease of the Lung without Pancreas Involvement: Presentation on 18F-FDG PET/CT
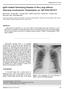 J Radiol Sci 2013; 38: 129-133 IgG4-related Sclerosing Disease of the Lung without Pancreas Involvement: Presentation on 18F-FDG PET/CT Han-Jui Lee 1 Yi-Chen Yeh 2,3 Chun-Ku Chen 1,3 Rheun-Chuan Lee 1,3
J Radiol Sci 2013; 38: 129-133 IgG4-related Sclerosing Disease of the Lung without Pancreas Involvement: Presentation on 18F-FDG PET/CT Han-Jui Lee 1 Yi-Chen Yeh 2,3 Chun-Ku Chen 1,3 Rheun-Chuan Lee 1,3
Hideaki Miura, Yasutaka Miyachi. Department of Internal Medicine, Social Insurance Central General Hospital. Tokyo, Japan
 CASE REPORT IgG4-Related Retroperitoneal Fibrosis and Sclerosing Cholangitis Independent of Autoimmune Pancreatitis. A Recurrent Case after a 5-Year History of Spontaneous Remission Hideaki Miura, Yasutaka
CASE REPORT IgG4-Related Retroperitoneal Fibrosis and Sclerosing Cholangitis Independent of Autoimmune Pancreatitis. A Recurrent Case after a 5-Year History of Spontaneous Remission Hideaki Miura, Yasutaka
Autoimmune Pancreatitis & Cholangiopathy. Goal and Objectives
 Autoimmune Pancreatitis & Cholangiopathy Kaveh Sharzehi, MD, MS Assistant Professor of Medicine Medical Director of Endoscopy Section of Gastroenterology Lewis Katz School of Medicine at Temple University
Autoimmune Pancreatitis & Cholangiopathy Kaveh Sharzehi, MD, MS Assistant Professor of Medicine Medical Director of Endoscopy Section of Gastroenterology Lewis Katz School of Medicine at Temple University
The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
Citation American Journal of Surgery, 196(5)
 NAOSITE: Nagasaki University's Ac Title Author(s) Multifocal branch-duct pancreatic i neoplasms Tajima, Yoshitsugu; Kuroki, Tamotsu Amane; Adachi, Tomohiko; Mishima, T Kanematsu, Takashi Citation American
NAOSITE: Nagasaki University's Ac Title Author(s) Multifocal branch-duct pancreatic i neoplasms Tajima, Yoshitsugu; Kuroki, Tamotsu Amane; Adachi, Tomohiko; Mishima, T Kanematsu, Takashi Citation American
Type 2 Autoimmune Pancreatitis with Crohn s Disease
 doi: 10.2169/internalmedicine.0213-17 Intern Med 57: 2957-2962, 2018 http://internmed.jp CASE REPORT Type 2 Autoimmune Pancreatitis with Crohn s Disease Yoon Suk Lee, Nam-Hoon Kim, Jun Hyuk Son, Jung Wook
doi: 10.2169/internalmedicine.0213-17 Intern Med 57: 2957-2962, 2018 http://internmed.jp CASE REPORT Type 2 Autoimmune Pancreatitis with Crohn s Disease Yoon Suk Lee, Nam-Hoon Kim, Jun Hyuk Son, Jung Wook
autoimmune pancreatitis from pancreatic cancer
 Zhang et al. BMC Cancer (2017) 17:695 DOI 10.1186/s12885-017-3665-y RESEARCH ARTICLE Open Access 18 F- FDG PET/CT helps differentiate autoimmune pancreatitis from pancreatic cancer Jian Zhang 1,2, Guorong
Zhang et al. BMC Cancer (2017) 17:695 DOI 10.1186/s12885-017-3665-y RESEARCH ARTICLE Open Access 18 F- FDG PET/CT helps differentiate autoimmune pancreatitis from pancreatic cancer Jian Zhang 1,2, Guorong
Autoimmune pancreatitis (AIP), a clinical entity originally
 Autoimmune Pancreatitis: A Multiorgan Disease Presenting a Conundrum for Clinicians in the West Eileen Kim, MD, Rebecca Voaklander, MD, Franklin E. Kasmin, MD, William H. Brown, MD, Rifat Mannan, MD, and
Autoimmune Pancreatitis: A Multiorgan Disease Presenting a Conundrum for Clinicians in the West Eileen Kim, MD, Rebecca Voaklander, MD, Franklin E. Kasmin, MD, William H. Brown, MD, Rifat Mannan, MD, and
Usefulness of PET/CT Imaging in Systemic IgG4-related Sclerosing Disease. A Report of Three Cases
 MULTIMEDIA ARTICLE - Clinical Imaging Usefulness of PET/CT Imaging in Systemic IgG4-related Sclerosing Disease. A Report of Three Cases Vien X Nguyen 1, Giovanni De Petris 2, Ba D Nguyen 3 Departments
MULTIMEDIA ARTICLE - Clinical Imaging Usefulness of PET/CT Imaging in Systemic IgG4-related Sclerosing Disease. A Report of Three Cases Vien X Nguyen 1, Giovanni De Petris 2, Ba D Nguyen 3 Departments
FDG-PET Findings of Intraductal Oncocytic Papillary Neoplasms of the Pancreas: Two Case Reports
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
IgG4-Related Sclerosing Cholangitis
 REVIEW IgG4-Related Sclerosing Cholangitis Emma L. Culver, B.Sc., M.B.Ch.B., D.Phil., M.R.C.P.,* and Eleanor Barnes, M.B.B.S., D.Phil., M.R.C.P.*,, BACKGROUND IgG4-related sclerosing cholangitis (IgG4-SC)
REVIEW IgG4-Related Sclerosing Cholangitis Emma L. Culver, B.Sc., M.B.Ch.B., D.Phil., M.R.C.P.,* and Eleanor Barnes, M.B.B.S., D.Phil., M.R.C.P.*,, BACKGROUND IgG4-related sclerosing cholangitis (IgG4-SC)
Autoimmune Pancreatitis: A Succinct Overview
 REVIEW ARTICLE Autoimmune Pancreatitis: A Succinct Overview Juan Putra, Xiaoying Liu Department of Pathology, Dartmouth-Hitchcock Medical Center, One Medical Center Drive Lebanon, NH 03756, USA ABSTRACT
REVIEW ARTICLE Autoimmune Pancreatitis: A Succinct Overview Juan Putra, Xiaoying Liu Department of Pathology, Dartmouth-Hitchcock Medical Center, One Medical Center Drive Lebanon, NH 03756, USA ABSTRACT
Diagnosis of tumor extension in biliary carcinoma has. Differential Diagnosis and Treatment of Biliary Strictures
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
IgG4 Related disease a retrospective descriptive study highlighting Canadian experiences in diagnosis and management
 Patel et al. BMC Gastroenterology 2013, 13:168 RESEARCH ARTICLE Open Access IgG4 Related disease a retrospective descriptive study highlighting Canadian experiences in diagnosis and management Harshna
Patel et al. BMC Gastroenterology 2013, 13:168 RESEARCH ARTICLE Open Access IgG4 Related disease a retrospective descriptive study highlighting Canadian experiences in diagnosis and management Harshna
Autoimmune pancreatitis can transform into chronic features similar to advanced
 Autoimmune pancreatitis can transform into chronic features similar to advanced chronic pancreatitis with functional insufficiency following severe calcification Short Title: AIP can transform into chronic
Autoimmune pancreatitis can transform into chronic features similar to advanced chronic pancreatitis with functional insufficiency following severe calcification Short Title: AIP can transform into chronic
Autoimmune pancreatitis: the classification puzzle
 Advances in Medical Sciences Vol. 52 2007 Autoimmune pancreatitis: the classification puzzle 71 Autoimmune pancreatitis: the classification puzzle Fantini L, Zanini N, Fiscaletti M, Calculli L, Casadei
Advances in Medical Sciences Vol. 52 2007 Autoimmune pancreatitis: the classification puzzle 71 Autoimmune pancreatitis: the classification puzzle Fantini L, Zanini N, Fiscaletti M, Calculli L, Casadei
Endoscopic Ultrasonography Findings in Autoimmune Pancreatitis: Be Aware of the Ambiguous Features and Look for the Pivotal Ones
 MULTIMEDIA ARTICLE - Clinical Imaging Endoscopic Ultrasonography Findings in Autoimmune Pancreatitis: Be Aware of the Ambiguous Features and Look for the Pivotal Ones Stefania De Lisi 1, Elisabetta Buscarini
MULTIMEDIA ARTICLE - Clinical Imaging Endoscopic Ultrasonography Findings in Autoimmune Pancreatitis: Be Aware of the Ambiguous Features and Look for the Pivotal Ones Stefania De Lisi 1, Elisabetta Buscarini
Lymphoplasmacytic sclerosing pancreatitis without IgG4 tissue infiltration or serum IgG4 elevation: IgG4-related disease without IgG4
 238 & 2015 USCAP, Inc All rights reserved 0893-3952/15 $32.00 Lymphoplasmacytic sclerosing pancreatitis without IgG4 tissue infiltration or serum IgG4 elevation: IgG4-related disease without IgG4 Phil
238 & 2015 USCAP, Inc All rights reserved 0893-3952/15 $32.00 Lymphoplasmacytic sclerosing pancreatitis without IgG4 tissue infiltration or serum IgG4 elevation: IgG4-related disease without IgG4 Phil
Clinical profile and treatment outcomes in autoimmune pancreatitis: a report from North India
 ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-7 Clinical profile and treatment outcomes in autoimmune pancreatitis: a report from North India Surinder S. Rana a, Rajesh Gupta b, Ritambhra Nada
ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-7 Clinical profile and treatment outcomes in autoimmune pancreatitis: a report from North India Surinder S. Rana a, Rajesh Gupta b, Ritambhra Nada
Sonographic findings of immunoglobulin G4-related sc. Author(s) Akihiro; Nakamaru, Yuji; Hatanaka, Kanako C.; Shimiz
 Title Sonographic findings of immunoglobulin G4-related sc Omotehara, Satomi; Nishida, Mutsumi; Satoh, Megumi; Author(s) Akihiro; Nakamaru, Yuji; Hatanaka, Kanako C.; Shimiz CitationJournal of medical
Title Sonographic findings of immunoglobulin G4-related sc Omotehara, Satomi; Nishida, Mutsumi; Satoh, Megumi; Author(s) Akihiro; Nakamaru, Yuji; Hatanaka, Kanako C.; Shimiz CitationJournal of medical
Ulcerative Colitis and Immunoglobulin G4
 Gut and Liver, Vol. 8, No. 1, January 2014, pp. 29-4 ORiginal Article Ulcerative Colitis and Immunoglobulin G4 Go Kuwata*, Terumi Kamisawa*, Koichi Koizumi*, Taku Tabata*, Seiichi Hara*, Sawako Kuruma*,
Gut and Liver, Vol. 8, No. 1, January 2014, pp. 29-4 ORiginal Article Ulcerative Colitis and Immunoglobulin G4 Go Kuwata*, Terumi Kamisawa*, Koichi Koizumi*, Taku Tabata*, Seiichi Hara*, Sawako Kuruma*,
How 5 Diseases Became One. Moez Tajdin R3 McGill University
 How 5 Diseases Became One Moez Tajdin R3 McGill University Conflicts of Interest None! Mr. M. ID: 65 M PMH Benign prostatic hyperplasia Prostate cancer Awaiting biopsy Skin rash Dyslipidemia Hypertension
How 5 Diseases Became One Moez Tajdin R3 McGill University Conflicts of Interest None! Mr. M. ID: 65 M PMH Benign prostatic hyperplasia Prostate cancer Awaiting biopsy Skin rash Dyslipidemia Hypertension
Clinical Study Type 1 Autoimmune Pancreatitis Can Transform into Chronic Pancreatitis: A Long-Term Follow-Up Study of 73 Japanese Patients
 International Rheumatology Volume 2013, Article ID 272595, 8 pages http://dx.doi.org/10.1155/2013/272595 Clinical Study Type 1 Autoimmune Pancreatitis Can Transform into Chronic Pancreatitis: A Long-Term
International Rheumatology Volume 2013, Article ID 272595, 8 pages http://dx.doi.org/10.1155/2013/272595 Clinical Study Type 1 Autoimmune Pancreatitis Can Transform into Chronic Pancreatitis: A Long-Term
Case Report An IgG4-Related Salivary Gland Disorder: A Case Series Presenting with a Different Clinical Setting
 Case Reports in Immunology Volume 2011, Article ID 236079, 4 pages doi:10.1155/2011/236079 Case Report An IgG4-Related Salivary Gland Disorder: A Case Series Presenting with a Different Clinical Setting
Case Reports in Immunology Volume 2011, Article ID 236079, 4 pages doi:10.1155/2011/236079 Case Report An IgG4-Related Salivary Gland Disorder: A Case Series Presenting with a Different Clinical Setting
Amendment of the Japanese Consensus Guidelines for Autoimmune Pancreatitis, 2013 III. Treatment and prognosis of autoimmune pancreatitis
 J Gastroenterol (2014) 49:961 970 DOI 10.1007/s00535-014-0945-z SPECIAL ARTICLE Amendment of the Japanese Consensus Guidelines for Autoimmune Pancreatitis, 2013 III. Treatment and prognosis of autoimmune
J Gastroenterol (2014) 49:961 970 DOI 10.1007/s00535-014-0945-z SPECIAL ARTICLE Amendment of the Japanese Consensus Guidelines for Autoimmune Pancreatitis, 2013 III. Treatment and prognosis of autoimmune
Autoimmune Chronic Pancreatitis Relapsing Despite the Maintenance Dose of Steroid
 The Korean Journal of Internal Medicine: 20:163-167, 2005 Autoimmune Chronic Pancreatitis Relapsing Despite the Maintenance Dose of Steroid Dae Keun Pyun, M.D., Won Beom Choi, M.D., Myung Hwan Kim, M.D.,
The Korean Journal of Internal Medicine: 20:163-167, 2005 Autoimmune Chronic Pancreatitis Relapsing Despite the Maintenance Dose of Steroid Dae Keun Pyun, M.D., Won Beom Choi, M.D., Myung Hwan Kim, M.D.,
Overview of the Immunoglobulin G4-related Disease Spectrum
 Review Article The Korean Journal of Pancreas and Biliary Tract 2015;20:124-129 http://dx.doi.org/10.15279/kpba.2015.20.3.124 pissn 1976-3573 eissn 2288-0941 면역글로불린 G4 연관질환의개요 1 한림대학교의과대학한림대학교성심병원내과, 2
Review Article The Korean Journal of Pancreas and Biliary Tract 2015;20:124-129 http://dx.doi.org/10.15279/kpba.2015.20.3.124 pissn 1976-3573 eissn 2288-0941 면역글로불린 G4 연관질환의개요 1 한림대학교의과대학한림대학교성심병원내과, 2
AN UNUSUAL CASE OF OBSTRUCTIVE JAUNDICE- SURGICAL DILEMMA. Dr. Tejaswi Sindhiya Ragni
 AN UNUSUAL CASE OF OBSTRUCTIVE JAUNDICE- SURGICAL DILEMMA Dr. Tejaswi Sindhiya Ragni A 65 year old male from Bangalore, farmer Presented with: Fever - 1 month Yellow discolouration of eyes and urine- 1month
AN UNUSUAL CASE OF OBSTRUCTIVE JAUNDICE- SURGICAL DILEMMA Dr. Tejaswi Sindhiya Ragni A 65 year old male from Bangalore, farmer Presented with: Fever - 1 month Yellow discolouration of eyes and urine- 1month
Primary Sclerosing Cholangitis and Cholestatic liver diseases. Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants
 Primary Sclerosing Cholangitis and Cholestatic liver diseases Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants I have nothing to disclose Educational Objectives What is PSC? Understand the cholestatic
Primary Sclerosing Cholangitis and Cholestatic liver diseases Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants I have nothing to disclose Educational Objectives What is PSC? Understand the cholestatic
An Intraductal Papillary Neoplasm of the Bile Duct at the Duodenal Papilla
 Published online: July 2, 2014 1662 6575/14/0072 0417$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
Published online: July 2, 2014 1662 6575/14/0072 0417$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
Autoimmune Pancreatitis, Pancreatic and Extrapancreatic Imaging Findings
 Autoimmune Pancreatitis, Pancreatic and Extrapancreatic Imaging Findings Poster No.: R-0074 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: J. Stegeman, A. Borsaru; Clayton/AU Keywords: Education
Autoimmune Pancreatitis, Pancreatic and Extrapancreatic Imaging Findings Poster No.: R-0074 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: J. Stegeman, A. Borsaru; Clayton/AU Keywords: Education
Case Report Thoracic Paravertebral Mass as an Infrequent Manifestation of IgG4-Related Disease
 Hindawi Case Reports in Rheumatology Volume 2017, Article ID 4716245, 4 pages https://doi.org/10.1155/2017/4716245 Case Report Thoracic Paravertebral Mass as an Infrequent Manifestation of IgG4-Related
Hindawi Case Reports in Rheumatology Volume 2017, Article ID 4716245, 4 pages https://doi.org/10.1155/2017/4716245 Case Report Thoracic Paravertebral Mass as an Infrequent Manifestation of IgG4-Related
Chronic Pancreatitis
 Falk Symposium 161 October 12, 2007 Chronic Pancreatitis David C Whitcomb MD PhD Giant Eagle Foundation Professor of Cancer Genetics. Professor of Medicine, Cell biology & Physiology, and Human Genetics
Falk Symposium 161 October 12, 2007 Chronic Pancreatitis David C Whitcomb MD PhD Giant Eagle Foundation Professor of Cancer Genetics. Professor of Medicine, Cell biology & Physiology, and Human Genetics
Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma
 Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma Authors: R. Revert Espí, Y. Fernandez Nuñez, I. Carbonell, D. P. Gómez valencia,
Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma Authors: R. Revert Espí, Y. Fernandez Nuñez, I. Carbonell, D. P. Gómez valencia,
Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
 Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
Endoscopic Resection of Ampullary Neuroendocrine Tumor
 CASE REPORT Endoscopic Resection of Ampullary Neuroendocrine Tumor Hiroyuki Fukasawa, Shigetaka Tounou, Masashi Nabetani and Tomoki Michida Abstract We report the case of a 57-year-old man with a 1.0-cm
CASE REPORT Endoscopic Resection of Ampullary Neuroendocrine Tumor Hiroyuki Fukasawa, Shigetaka Tounou, Masashi Nabetani and Tomoki Michida Abstract We report the case of a 57-year-old man with a 1.0-cm
ACUTE CHOLANGITIS AS a result of an occluded
 Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Dilemmas in autoimmune pancreatitis. Surgical resection or not?
 DOI: 10.4149/BLL_2016_090 Bratisl Med J 2016; 117 (8) CLINICAL STUDY Dilemmas in autoimmune pancreatitis. Surgical resection or not? Hoffmanova I 1, Gurlich R 2, Janik V 3, Szabo A 4, Vernerova Z 4 Second
DOI: 10.4149/BLL_2016_090 Bratisl Med J 2016; 117 (8) CLINICAL STUDY Dilemmas in autoimmune pancreatitis. Surgical resection or not? Hoffmanova I 1, Gurlich R 2, Janik V 3, Szabo A 4, Vernerova Z 4 Second
Introduction of GB polyp
 Management of Gallbladder Polyp as Physician's View Sang Hyub Lee, MD, PhD Seoul National University College of Medicine Seoul National University Bundang Hospital Department of Internal Medicine Division
Management of Gallbladder Polyp as Physician's View Sang Hyub Lee, MD, PhD Seoul National University College of Medicine Seoul National University Bundang Hospital Department of Internal Medicine Division
Diagnosis of IgG4-related sclerosing cholangitis
 Online Submissions: http://www.wjgnet.com/esps/ bpgoffice@wjgnet.com doi:10.3748/wjg.v19.i43.7661 World J Gastroenterol 2013 November 21; 19(43): 7661-7670 ISSN 1007-9327 (print) ISSN 2219-2840 (online)
Online Submissions: http://www.wjgnet.com/esps/ bpgoffice@wjgnet.com doi:10.3748/wjg.v19.i43.7661 World J Gastroenterol 2013 November 21; 19(43): 7661-7670 ISSN 1007-9327 (print) ISSN 2219-2840 (online)
Cerebral involvement in IgG4-related disease
 ORIGINAL RESEARCH Clinical Medicine 2015 Vol 15, No 2: 130 4 Cerebral involvement in IgG4-related disease Authors: Deepak Joshi, A Rolf Jager, B Steven Hurel, C Stephen P Pereira, D Gavin J Johnson, E
ORIGINAL RESEARCH Clinical Medicine 2015 Vol 15, No 2: 130 4 Cerebral involvement in IgG4-related disease Authors: Deepak Joshi, A Rolf Jager, B Steven Hurel, C Stephen P Pereira, D Gavin J Johnson, E
Diagnostic And Therapeutic Challenges in IgG4-Related disease in the Sphenoid Sinus
 Diagnostic And Therapeutic Challenges in IgG4-Related disease in the Sphenoid Sinus Omar Abu Suliman, MBBS, SB-ORL Senior Registrar, otolaryngology Head & neck surgery King Abdullah Medical City, Makkah,
Diagnostic And Therapeutic Challenges in IgG4-Related disease in the Sphenoid Sinus Omar Abu Suliman, MBBS, SB-ORL Senior Registrar, otolaryngology Head & neck surgery King Abdullah Medical City, Makkah,
Immunoglobulin G4 Non-Related Sclerosing Disease with Intracardiac Mass Mimicking Mitral Stenosis: Case Report
 SE REPORT ardiovascular isorders J Korean Med Sci 2013; 28: 1830-1834 Immunoglobulin G4 Non-Related Sclerosing isease with Intracardiac Mass Mimicking Mitral Stenosis: ase Report Ji-won Hwang, 1 * Sung-Ji
SE REPORT ardiovascular isorders J Korean Med Sci 2013; 28: 1830-1834 Immunoglobulin G4 Non-Related Sclerosing isease with Intracardiac Mass Mimicking Mitral Stenosis: ase Report Ji-won Hwang, 1 * Sung-Ji
D DAVID PUBLISHING. Groove Pancreatitis: A Case Report. 1. Introduction. 2. Case Report
 Journal of Pharmacy and Pharmacology 6 (2018) 415-419 doi: 10.17265/2328-2150/2018.04.013 D DAVID PUBLISHING Luciana Leony Valente, Mariama Alves Dantas Fagundes, Camila Medrado Pereira Barbosa, Hélio
Journal of Pharmacy and Pharmacology 6 (2018) 415-419 doi: 10.17265/2328-2150/2018.04.013 D DAVID PUBLISHING Luciana Leony Valente, Mariama Alves Dantas Fagundes, Camila Medrado Pereira Barbosa, Hélio
ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1089 1096 ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT Presentation and Management of Post-treatment Relapse in Autoimmune Pancreatitis/Immunoglobulin
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1089 1096 ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT Presentation and Management of Post-treatment Relapse in Autoimmune Pancreatitis/Immunoglobulin
Chronic Sclerosing Dacryoadenitis
 The Korean Journal of Pathology 2008; 42: 118-22 Chronic Sclerosing Dacryoadenitis - Report of 2 Cases - Ji Eun Kwon Sang Kyum Kim Sang-Ryul Lee 1 Woo-Ick Yang Haeryoung Kim 2 Department of Pathology and
The Korean Journal of Pathology 2008; 42: 118-22 Chronic Sclerosing Dacryoadenitis - Report of 2 Cases - Ji Eun Kwon Sang Kyum Kim Sang-Ryul Lee 1 Woo-Ick Yang Haeryoung Kim 2 Department of Pathology and
IgG4 Disease. General Principles of IgG4-related disease. EL Cluvar, AC Bateman
 IgG4 Disease General Principles of IgG4-related disease. EL Cluvar, AC Bateman Diagnostic Guidelines for IgG4-related disease with a focus on histopathological criteria. V Deshpande, A Khosroshahi Diagnostic
IgG4 Disease General Principles of IgG4-related disease. EL Cluvar, AC Bateman Diagnostic Guidelines for IgG4-related disease with a focus on histopathological criteria. V Deshpande, A Khosroshahi Diagnostic
Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review
 Review Article Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review Min-Jie Yang, Su Li, Yong-Guang Liu, Na Jiao, Jing-Shan Gong Department of Radiology, Shenzhen
Review Article Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review Min-Jie Yang, Su Li, Yong-Guang Liu, Na Jiao, Jing-Shan Gong Department of Radiology, Shenzhen
Case Scenario 1. Discharge Summary
 Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Autoimmune Pancreatitis and Retroperitoneal Fibrosis
 Autoimmune Pancreatitis and Retroperitoneal Fibrosis Thomas C. Smyrk, MD Associate Professor of Pathology Mayo Clinic, Rochester MN 55902 smyrk.thomas@mayo.edu Summary Retroperitoneal fibrosis complicated
Autoimmune Pancreatitis and Retroperitoneal Fibrosis Thomas C. Smyrk, MD Associate Professor of Pathology Mayo Clinic, Rochester MN 55902 smyrk.thomas@mayo.edu Summary Retroperitoneal fibrosis complicated
Intrahepatic Sarcomatoid Cholangiocarcinoma with Portal Vein Thrombosis: A Case Report 1
 Intrahepatic Sarcomatoid Cholangiocarcinoma with Portal Vein Thrombosis: A Case Report 1 Jae-Hoon Lim, M.D., Jin Woong Kim, M.D., Suk Hee Heo, M.D., Yong Yeon Jeong, M.D., Heoung Keun Kang, M.D. A 53-year-old
Intrahepatic Sarcomatoid Cholangiocarcinoma with Portal Vein Thrombosis: A Case Report 1 Jae-Hoon Lim, M.D., Jin Woong Kim, M.D., Suk Hee Heo, M.D., Yong Yeon Jeong, M.D., Heoung Keun Kang, M.D. A 53-year-old
IgG4-related systemic disease (ISD) is a multisystem
 Utility of Serum Immunoglobulin G4 in Distinguishing Immunoglobulin G4-Associated Cholangitis from Cholangiocarcinoma Abdul M. Oseini, 1 * Roongruedee Chaiteerakij, 1 * Abdirashid M. Shire, 1 Amaar Ghazale,
Utility of Serum Immunoglobulin G4 in Distinguishing Immunoglobulin G4-Associated Cholangitis from Cholangiocarcinoma Abdul M. Oseini, 1 * Roongruedee Chaiteerakij, 1 * Abdirashid M. Shire, 1 Amaar Ghazale,
Title. CitationHepato-Gastroenterology, 61(135): Issue Date Doc URL. Type. File Information. IgG4-Related Sclerosing Cholangitis
 Title Difference from Bile Duct Cancer and Relationship be IgG4-Related Sclerosing Cholangitis Kuwatani, Masaki; Kawakami, Hiroshi; Zen, Yoh; Kawak Author(s) Sakamoto, Naoya CitationHepato-Gastroenterology,
Title Difference from Bile Duct Cancer and Relationship be IgG4-Related Sclerosing Cholangitis Kuwatani, Masaki; Kawakami, Hiroshi; Zen, Yoh; Kawak Author(s) Sakamoto, Naoya CitationHepato-Gastroenterology,
Biliary tree dilation - and now what?
 Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
Index. Surg Oncol Clin N Am 16 (2007) Note: Page numbers of article titles are in boldface type.
 Surg Oncol Clin N Am 16 (2007) 465 469 Index Note: Page numbers of article titles are in boldface type. A Adjuvant therapy, preoperative for gastric cancer, staging and, 339 B Breast cancer, metabolic
Surg Oncol Clin N Am 16 (2007) 465 469 Index Note: Page numbers of article titles are in boldface type. A Adjuvant therapy, preoperative for gastric cancer, staging and, 339 B Breast cancer, metabolic
Biliary cancers: imaging diagnosis. Study of 30 cases
 Biliary cancers: imaging diagnosis. Study of 30 cases N Hammoune, S Semlali, M Eddarai, T. Amil, M Zentar, S. El Kandri,, M Benameur,, S Chaouir. Radiology Department. Mohamed V Military Hospital. Rabat-
Biliary cancers: imaging diagnosis. Study of 30 cases N Hammoune, S Semlali, M Eddarai, T. Amil, M Zentar, S. El Kandri,, M Benameur,, S Chaouir. Radiology Department. Mohamed V Military Hospital. Rabat-
Sakamoto et al. Journal of Medical Case Reports (2018) 12:136
 Sakamoto et al. Journal of Medical Case Reports (2018) 12:136 https://doi.org/10.1186/s13256-018-1671-6 CASE REPORT Open Access Successful resection of a slow-growing synchronous pulmonary metastasis from
Sakamoto et al. Journal of Medical Case Reports (2018) 12:136 https://doi.org/10.1186/s13256-018-1671-6 CASE REPORT Open Access Successful resection of a slow-growing synchronous pulmonary metastasis from
Clinical Study Evaluation and Clinical Validity of a New Questionnaire for Mikulicz s Disease
 International Rheumatology Volume 2, Article ID 283459, pages doi:1.1155/2/283459 Clinical Study Evaluation and Clinical Validity of a New Questionnaire for Mikulicz s Disease Motohisa Yamamoto, 1 Hiroki
International Rheumatology Volume 2, Article ID 283459, pages doi:1.1155/2/283459 Clinical Study Evaluation and Clinical Validity of a New Questionnaire for Mikulicz s Disease Motohisa Yamamoto, 1 Hiroki
Histological diagnosis of autoimmune pancreatitis using EUSguided trucut biopsy: a comparison study with EUS-FNA
 J Gastroenterol (2009) 44:742 750 DOI 10.1007/s00535-009-0062-6 ORIGINAL ARTICLE LIVER, PANCREAS, AND BILIARY TRACT Histological of autoimmune pancreatitis using EUSguided trucut biopsy: a comparison study
J Gastroenterol (2009) 44:742 750 DOI 10.1007/s00535-009-0062-6 ORIGINAL ARTICLE LIVER, PANCREAS, AND BILIARY TRACT Histological of autoimmune pancreatitis using EUSguided trucut biopsy: a comparison study
Case Report Usefulness of minor salivary gland biopsy in the diagnosis of IgG4-related disease: a case report
 Int J Clin Exp Pathol 2014;7(5):2673-2677 www.ijcep.com /ISSN:1936-2625/IJCEP0000175 Case Report Usefulness of minor salivary gland biopsy in the diagnosis of IgG4-related disease: a case report Kentaro
Int J Clin Exp Pathol 2014;7(5):2673-2677 www.ijcep.com /ISSN:1936-2625/IJCEP0000175 Case Report Usefulness of minor salivary gland biopsy in the diagnosis of IgG4-related disease: a case report Kentaro
IgG4-related Kidney Disease in Which the Urinalysis, Kidney Function and Imaging Findings Were Normal
 CASE REPORT IgG4-related Kidney Disease in Which the Urinalysis, Kidney Function and Imaging Findings Were Normal Miho Otani 1, Masahiro Morinaga 1, Yoshihiko Nakajima 1, Hiromi Tomioka 2, Michiko Nishii
CASE REPORT IgG4-related Kidney Disease in Which the Urinalysis, Kidney Function and Imaging Findings Were Normal Miho Otani 1, Masahiro Morinaga 1, Yoshihiko Nakajima 1, Hiromi Tomioka 2, Michiko Nishii
Endoscopic Ultrasonography Assessment for Ampullary and Bile Duct Malignancy
 Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Autoimmune Pancreatitis: Case Series and Review of the Literature.
 Available online at www.annclinlabsci.org Annals of Clinical & Laboratory Science, vol. 39, no. 2, 2009 167 Autoimmune Pancreatitis: Case Series and Review of the Literature. Rada Shakov, 1 Joseph R. DePasquale,
Available online at www.annclinlabsci.org Annals of Clinical & Laboratory Science, vol. 39, no. 2, 2009 167 Autoimmune Pancreatitis: Case Series and Review of the Literature. Rada Shakov, 1 Joseph R. DePasquale,
Autoimmune Pancreatitis: Instrumental Diagnosis
 AISP - 28th National Congress. Verona (Italy). October 28-30, 2004. Autoimmune Pancreatitis: Instrumental Diagnosis Giovanni Morana 1, Margherita Tapparelli 2, Niccolò Faccioli 2, Mirko D Onofrio 2, Roberto
AISP - 28th National Congress. Verona (Italy). October 28-30, 2004. Autoimmune Pancreatitis: Instrumental Diagnosis Giovanni Morana 1, Margherita Tapparelli 2, Niccolò Faccioli 2, Mirko D Onofrio 2, Roberto
IgG4-Related Disease: Dataset of 235 Consecutive Patients
 IgG-Related Disease: Dataset of 235 Consecutive Patients Dai Inoue, MD, PhD, Kotaro Yoshida, MD, PhD, Norihide Yoneda, MD, PhD, Kumi Ozaki, MD, PhD, Takashi Matsubara, MD, PhD, Keiichi Nagai, MD, PhD,
IgG-Related Disease: Dataset of 235 Consecutive Patients Dai Inoue, MD, PhD, Kotaro Yoshida, MD, PhD, Norihide Yoneda, MD, PhD, Kumi Ozaki, MD, PhD, Takashi Matsubara, MD, PhD, Keiichi Nagai, MD, PhD,
Imaging in gastric cancer
 Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Intraductal Papillary-Mucinous Neoplasm of the Pancreas Penetrating to the Stomach and the Common Bile Duct
 CASE REPORT Intraductal Papillary-Mucinous Neoplasm of the Pancreas Penetrating to the Stomach and the Common Bile Duct Norihiro Goto 1, Masahiro Yoshioka 1, Motohito Hayashi 1, Toshinao Itani 1, Jun Mimura
CASE REPORT Intraductal Papillary-Mucinous Neoplasm of the Pancreas Penetrating to the Stomach and the Common Bile Duct Norihiro Goto 1, Masahiro Yoshioka 1, Motohito Hayashi 1, Toshinao Itani 1, Jun Mimura
State of the Art Imaging for Hepatic Malignancy: My Assignment
 State of the Art Imaging for Hepatic Malignancy: My Assignment CT vs MR vs MRCP Which one to choose for HCC vs Cholangiocarcinoma What special protocols to use for liver tumors Role of PET and Duplex US
State of the Art Imaging for Hepatic Malignancy: My Assignment CT vs MR vs MRCP Which one to choose for HCC vs Cholangiocarcinoma What special protocols to use for liver tumors Role of PET and Duplex US
Endoscopic Management of Biliary Strictures. Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center
 Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
Tratamiento endoscópico de la CEP. En quien como y cuando?
 Tratamiento endoscópico de la CEP. En quien como y cuando? Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques University of Barcelona
Tratamiento endoscópico de la CEP. En quien como y cuando? Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques University of Barcelona
Incidence of Malignancies in Patients with IgG4-related Disease
 ORIGINAL ARTICLE Incidence of Malignancies in Patients with IgG4-related Disease Kenji Hirano 1, Minoru Tada 1, Naoki Sasahira 1, Hiroyuki Isayama 1, Suguru Mizuno 1, Kaoru Takagi 1, Takeo Watanabe 1,
ORIGINAL ARTICLE Incidence of Malignancies in Patients with IgG4-related Disease Kenji Hirano 1, Minoru Tada 1, Naoki Sasahira 1, Hiroyuki Isayama 1, Suguru Mizuno 1, Kaoru Takagi 1, Takeo Watanabe 1,
A Case of IgG4-Related Disease with Bronchial Asthma and Chronic Rhinosinusitis in Korea
 CSE REPORT Immunology, llergic Disorders & Rheumatology http://dx.doi.org/10.3346/jkms.2014.29.4.599 J Korean Med Sci 2014; 29: 599-603 Case of IgG4-Related Disease with ronchial sthma and Chronic Rhinosinusitis
CSE REPORT Immunology, llergic Disorders & Rheumatology http://dx.doi.org/10.3346/jkms.2014.29.4.599 J Korean Med Sci 2014; 29: 599-603 Case of IgG4-Related Disease with ronchial sthma and Chronic Rhinosinusitis
