Metabolic Studies of Human Bone In Vitro.
|
|
|
- Isabel Cain
- 5 years ago
- Views:
Transcription
1 Journal of Clinical Investigation Vol. 44, No. 11, 1965 Metabolic Studies of Human Bone In Vitro. II. Changes in Hyperparathyroidism * BARRY FLANAGAN t AND GORG NICHOLS, JR. t (From the Department of Medicine, Harvard Medical School and Peter Bent Brigham Hospital, Boston, Mass.) Generalied bone disease has long been recognied as a feature of hyperparathyroidism, but the functional disturbance at the tissue level responsible for its appearance has not been studied extensively. The demonstration that human bone metabolism may be examined directly by incubation of fresh biopsy samples in vitro and the establishment of normal rates for certain metabolic functions in normal adult human bone (1) opened the way to re-examination of this problem. The purpose of this paper is to report the results obtained in bone removed at biopsy from a group of eight surgically proven hyperparathyroid patients. These suggest the existence of two biochemically distinct skeletal metabolic responses to hyperparathyroidism, a view that appears to be supported by prior animal studies (2-6), and the results of some supplementary experiments using the rat as a model. * Submitted for publication May 6, 1965; accepted July 15, Supported largely by the John H. Hartford Foundation of New York and in part by grant AM from the Institute of Arthritis and Metabolic Diseases of the National Institutes of Health and the general research support grant from the National Institutes of Health to the Peter Bent Brigham Hospital. Some of the patients were hospitalied in the Clinical Research Center of the Peter Bent Brigham Hospital supported by grant 8M1-FR of the National Institutes of Health. Presented in part at the national meeting of the American Federation for Clinical Research, Atlantic City, N. J., May 3, 1964, and at the Second Parathyroid Symposium at No6rdwijk, the Netherlands, August t Postdoctoral fellow, Division of Arthritis and Metabolic Diseases, U. S. Public Health Service. : Address requests for reprints to Dr. George Nichols, Jr., Dept. of Medicine, Harvard Medical School, Boston, Mass Methods Bone samples from eight hyperparathyroid patients ranging in age from 32 to 78 years, two males and six females, were used. Four had adenomata proven at operation, two had parathyroid hyperplasia, and one had a parathyroid carcinoma. All were cured of hyperparathyroidism by extirpation of the appropriate parathyroid tissue. Samples of mixed bone (cortical and trabecular) were removed from the iliac crests of these patients by open biopsy for metabolic study either before or at the time of parathyroid exploration. The remaining patient exhibited renal failure, raised serum calcium and alkaline phosphatase levels, and a pathologic fracture of the patella associated with cystic change. After patellectomy, half of the bone was submitted for histologic examination and the remainder used for metabolic studies. This patient died suddenly in renal failure, and permission for post-mortem examination of the parathyroids was not obtained. A summary of the pertinent findings in these patients is presented in Table I. Daily total urinary hydroxyproline output was measured with the subjects on a gelatin-free diet for 48 hours before and during the collections by a modification (7) of the method of Prockop and Udenfriend (8). The mean daily output over a period of at least 4 days was determined. Blood for serum alkaline phosphatase activity was measured by the method of Bessey, Lowry, and Brock (9) at 3-day intervals during a hospital investigation of approximately 2 weeks, and the highest recorded values were utilied in the analysis of the results. ighty- to eighty-five-day-old rats of the Sprague- Dawley strain were divided into five groups. Group 1 served as untreated controls. Groups 2, 3, 4, and 5 received 1, 2, 3, and 4 daily doses of 2 U of parathyroid extract (PT) 1 by subcutaneous injection, the last dose in each case being given 16 to 18 hours before death. The administration of excess hormone in the presence of intact parathyroids was considered to provide the model that most closely approximates the human disease. After death by decapitation animal bone samples were taken from the upper tibial and lower femoral metaphyses as previously described (1). These and the human samples removed at biopsy were similarly collected into chilled (2 to 4 C) Krebs-Ringer medium, buffered with bicarbonate at ph 7.4, and maintained at this temperature 1 li Lilly Co., Indianapolis, Ind.
2 1796 BARRY FLANAGAN AND GORG NICHOLS, JR. TABL I Pertinent clinical data for the patients reported* Serum 24-hour urine output Alkaline phos- Hydroxy- Pathologic Patient Age Sex Complaints Ca P phatase Ca proline X rays diagnosis years mqi my& B-L mg mg L moles/ units L "Continuous" group R. C. 5 F Peptic ulcer Typical changes Parathyroid in skull and carcinoma phalanges. D. 41 F Renal stone Typical changes Parathyroid Weight loss in skull and adenoma Anorexia hands (15 g in wt) Mass in neck D. S. 51 M Peptic ulcer Osteoporosis Generalied para- Polyuria Rarefaction thyroid hyper- Polydipsia Left lower plasia Weight loss femoral Uremia metaphysis Nephrocalcinosis upon biopsy R. W. 36 M Uremia Cyst of right Osteitis fibrosa Pain in knee patella with cystica (no neck fracture exploration) W. M. 32 M Terminal uremia with Rarefaction in Generalied parakidney transplant hands and feet thyroid chief cell Limb pain Metastatic hyperplasia Metastatic calcification calcification in shoulder and hand "Intermittent" group C. M. 5 F Duodenal ulcer Negative Right lower para- Renal stone thyroid adenoma M. C. 45 F Duodenal ulcer Negative Right lower para- Renal stone thyroid adenoma M. N. 78 F Constipation Negative Right lower para- Weight loss thyroid adenoma Confusion * The patients have been divided into a "continuous" and an "intermittent" group (see Results section of text for details). Note that seven of the eight had surgically proven parathyroid disease; one had changes in bone histology characteristic of hyperparathyroidism. Normal ranges for the values cited are as follows: serum calcium, 4.5 to 5.5 mq per L; serum phosphorus,.9 to 1.2 mmoles per L; serum alkaline phosphatase,.6 to 2.3 Bessey-Lowry units per 1 ml (males),.5 to 1.9 Bessey-Lowry units per 1 ml (females). Twenty-four-hour urinary hydroxyproline output in adults on a gelatin-free diet was 24.7 l 2.5 mg. The upper limits of normal 24-hour urinary calcium output after 1 week on a 2-mg calcium intake is 15 mg per day. throughout the preparative procedures. The subsequent handling of the tissue in preparation for incubation, the conditions of incubation, the collection of the various fractions, the analyses, and the calculation of results were carried out as previously described (1, 2, 6, 1). Results The initial assumption was made in these experiments that bone metabolism in hyperparathyroid patients would differ from that of normal adults, but no consistent pattern of change was found upon first examination. Closer scrutiny, however, revealed that patients could be divided into two groups, one characteried by greatly increased bone metabolic activity, and the other by normal or decreased activity. For reasons that will be brought out in the Discussion, we have chosen to regard the former as indicative of continuous hypersecretion, and the latter as indicative of intermittent hypersecretion, of parathyroid hormone. The data are presented in this fashion in Figures 1 through 6, together with the previously established values for normal adult human bone for comparison (1). The changes in bone cell oxygen uptake in the two groups of subjects in this study are presented in Figure 1. The intermittent group showed a mean increase of approximately 8%o above normal. This difference did not quite reach acceptable levels of statistical significance. The continuous group showed an increase of approximately 16%o above the normal level, a difference that was significant at p <.1. The mean rates of lactate production by bone from the two groups are shown in Figure 2. Lactate production in the intermittent group was
3 MTABOLIC STUDIS OF HUMAN BON IN VITRO 1797 Dl U NORMAL HYPRSCRTION - 'INTRMITTNT HYPRSCRTION - CONTINUOUS' _-c CL a, I-j 4,t 5L C, NO. OF (8) (3) 5) SUBJCTS FIG. 1. MAN OXYGN UPTAK OF HUMAN BON FROM NORMAL PATINTS AND TH TWO GROUPS OF PATINTS WITH HYPRPARATHYROIDISM. The magnitude of 1 S of each mean is indicated in this and subsequent Figures by the vertical line extending above each bar. Individual values were calculated from the total 2 uptake of the bone during 2 to 4 hours. See Discussion section of text for details on "intermittent" and "continuous" groups. normal, whereas the continuous group showed a highly significant threefold elevation of lactate production above the normal range (p <.1). Rates of proline incorporation into the cell fraction and collagen of the bone samples are shown in Figure 3. As has been observed previously the labeling in the cells was about 1 times greater than in the collagen' (1). The intermittent group again showed no significant difference from normal with respect to incorporation into the cells, whereas the continuous group showed a marked mean elevation of incorporation. The wide variation in the values in this group (note the large standard error) prevented the difference from reaching an acceptable level of statistical significance; however, it should be noted that all the individual values were at least double the mean normal value. The rate of incorporation of proline into collagen, on the other hand, showed very striking and opposing changes. The intermittent group showed a mean incorporation rate decreased to approximately 4% of the normal value, which was significant at p <.2, whereas the continuous group showed a sevenfold mean increase in incorporation rate over the normal level, which was significant at p <.5. Again it was noteworthy that despite wide variations in the values in hyperparathyroid groups, all were clearly different from the mean normal value. Glucose incorporation rates for bone from the three groups are presented in Figure 4. The changes in incorporation into both cells and collagen generally resembled those found for proline in the corresponding intermittent and continuous groups, although the clear depression of collagen
4 BARRY FLANAGAN AND GORG NICHOLS, JR. T [l NORMAL * HYPRSCRTION - INTRMITTNT' * HYPRSCRTION - 'CONTINUOUS 2. I., 11-J 1. L T o NO. OF (6) (3) (5) SUBJCTS FIG. 2. RATS OF LACTAT PRODUCTION BY BON FROM TH TWO HYPR- PARATHYROID GROUPS COMPARD TO NORMAL SUBJCTS. Individual values were derived from the release of lactate (measured chemically) into the incubation medium during 2 to 4 hours of incubation. ach represents the mean of at least two incubations of bone from the same subject. labeling from proline in this intermittent group was absent when glucose was the labeled substrate. However, none of the changes even in the continuous group reached statistically acceptable levels because of the very wide scatter of the values, a phenomenon perhaps related to varying endogenous glucose stores from sample to sample. The total 24-hour excretion of hydroxyproline in the urine was measured in these patients and compared to that of normal ones. The mean values observed in the two hyperparathyroid groups are compared with the mean values of a group of seven normal adult subjects in Figure 5. The intermittent hypersecretion group showed no significant difference from the normal group, whereas the continuous hypersecretion group showed a fivefold mean increase over the normal value, the difference being significant at p <.1. These changes correlated closely with the alterations in serum alkaline phosphatase levels found in these patients, which are presented in Figure 6. Again the intermittent group showed no deviation from normal, whereas the continuous group showed a mean threefold increase above the normal range. An inhibition of proline incorporation into collagen such as was seen in the intermittent group has been shown to be an early effect of a single dose of parathyroid hormone (6) rather than a stimulation such as appeared in the continuous group. It became of interest, therefore, to determine whether the increases in collagen biosynthesis in bone that had been shown to follow as a secondary phenomenon after a single dose of PT (4, 5) also developed during continuous hormone administration. - The effects of multiple
5 MTABOLIC STUDIS OF HUMAN BON IN VITRO O COLLAGN Dg NORMAL I HYPRSCRTION - INTRMITTNT * HYPRCSCRTION - 'CONTINUOUS 7 I I I m co) 3 N, U) uii -J so 8 u 6 c =r 4 O. 2 NO. OF (6) (3) (5) SUBJCTS (6) (3) (4) FIG. 3. RATS OF PROLIN INCORPORATION INTO TH CLL FRACTION AND COLLAGN OF BON SAMPLS FROM TH THR GROUPS. Data were calculated from the over-all uptake of "C label from the medium over 3 to 4 hours of incubation and have been expressed in terms of millimicromoles of proline in order to eliminate differences due to differences in medium proline specific activity. Note that the ordinate scale on the left is for the cell fraction, whereas the one on the right with units 1 times smaller refers to the collagen. daily doses of PT on these phenomena were therefore investigated in rats. Data from a typical set of experiments are shown in Figure 7, which contrasts the effects of PT treatment on proline incorporation into collagen and lactate production. It can be seen that the depression of collagen synthesis noted in previous experiments was apparent again after 1 and 2 days of treatment. However, by the third and fourth days this inhibition had either disappeared or had been overwhelmed by a secondary stimulation of the synthetic rate. It was particularly interesting to note that the single dose that caused a depression of synthesis on the first day was quite ineffective in suppressing the increased synthesis, which had begun to appear by 3 and 4 days. Although the timing of these effects varied somewhat from experiment to experiment, both the initial inhibition of collagen synthesis and the later stimulation proved statistically significantly different from controls, p <.2 and <.5, respectively, when data from several experiments were pooled. In contrast to these changes in proline incorporation into collagen no depression of lactate production occurred. Instead a continuously increasing rate of production was noted with continuing treatment. This increase had become statistically significant by the third day of treatment. In contrast to the apparent response of human bone that these experiments were designed to duplicate, no consistent changes in bone oxygen consumption and glucose uptake were demonstrable under the dosage schedules used.
6 18 BARRY FLANAGAN AND GORG NICHOLS, JR. 18 r 'CLL FRACTION' COLLAGN,13 16 L : -r 12 C]1 NORMAL HYPRSCRTION - 'INTRMITTNT' * HYPRSCRTION - 'CONTINUOUS' T ' K 1- lo 1 U) Cf) w 8C M 6,. 3 8 %a 6 * 4qC 4 2C,2 NO.OF (4) SUBJCTS (3) (4) -( (5) (3) (4) FIG. 4. INCORPORATION OF GLUCOS INTO CLLS AND COLLAGN IN BON FROM NORMAL SUBJCTS AND TH TWO HYPRPARATHYROID GROUPS. Data have been calculated and expressed as in Figure 3. Note that the scale for cell label is on the left and the one for collagen is on the right. Again the units in the former are 1 times the latter. Both are 1 times those for proline, reflecting the proportionately greater incorporation of glucose into the tissue. Discussion The results presented here indicate that two distinct types of abnormal bone metabolism appear to exist in hyperparathyroidism. Moreover, when patients are separated into two groups on the basis of such in vitro metabolic data alone, the members of each group turn out to have common clinical characteristics as well. Bone metabolism in the continuous group was characteried by increased activity, often very striking, in all the metabolic systems measured. These patients exhibited the majority of the usual clinical signs and symptoms of hyperparathyroidism. Hypercalcemia and elevated serum alkaline phosphatase levels, hypercalciuria and increased total 24-hour urinary hydroxyproline excretion, and some X-ray evidence of bone disease were present in all. Symptoms were more variable, but all gave one or more complaints suggesting hypercalcemia either present at the time of study or troublesome in the recent past. In contrast, bone from the intermittent group was metabolically normal with two exceptions: oxygen consumption tended to be elevated, and the incorporation of proline into collagen was significantly decreased. This pattern was found in bone from those patients who were distinguished by the paucity of their manifestations of parathyroid disturbance. X-ray evidence of bone disease was notably absent, and hypercalciuria was either minimal or only intermittently present. Moreover, serum Ca and P concentrations were borderline or normal, whereas serum alkaline phosphatase activity was not elevated, and urine hydroxyproline excretion was in the normal range. Indeed, the diagnosis had to be made in
7 MTABOLIC STUDIS OF HUMAN BON IN VITRO 181 IR( ovv ( 16C [ NORMAL 14. OM HYPRSCRTION - 'INTRMITTNT' U HYPRSCRTION - CONTINUOUS 12.A- I.' 8.) ) D ' 6.C 4.c NO OF SUBJCTS (3) FIG. 5. MAN TOTAL 24-HouR URIN HYDROXYPROLIN CONTNT IN TH TWO GROUPS OF HYPRPARATHYROID SUBJCTS AND SVN ADULTS WITHOUT BON OR KIDNY DISAS. these patients on the basis of recurrent kidney stone formation, minimal, often intermittent, hypercalcemia or hypercalciuria, and abnormal response to tests of the control of parathyroid function, or all of these symptoms (11, 12). The demonstration of these two distinct patterns of response raises the question of whether the difference between these two groups is a quantitative or a qualitative one, a question made more pertinent by Costello and Dent's recent suggestion that there may exist a separate hormone responsible for the changes of osteitis fibrosa cystica (13). Although the data presented here cannot exclude the existence of two different hormones acting on bone or, indeed, of two differing tissue responses to the same hormone, they do not seem to necessitate such postulates. All of the bone metabolic changes observed in these samples, with the possible exception of the increased oxygen consumption, have now been observed in animals treated with PT under various schedules (4-6). The only question that remained open is, can the increase in collagen biosynthesis that follows secondarily after the initial inhibition caused by PT occur even if repeated doses of hormone are given. It appears to be answered affirmatively by the animal experiments reported above. On the basis of these findings it seems reasonable for the present to regard the two different
8 182 BARRY FLANAGAN AND GORG NICHOLS, JR. 6. [ I HYPRSCRTION - INTRMITTNT' * HYPRSCRTION- 'CONTINUOUS' a T U) C -j m 4. L 2. k NO OF SUBJCTS (3) (5) FIG. 6. MAN PLASMA ALKALIN PHOSPHATAS ACTIVITY MASURD IN BSSY-LOWRY UNITS IN TH TWO GROUPS OF HYPRPARATHYROID PATINTS. The limits of the normal range in this laboratory are shown by the two dotted lines. responses seen in the human subjects as variations in the intensity or degree of disturbance of parathyroid function. As the disease involves not only hypersecretion of the hormone but also loss of secretory control in the abnormal gland or glands (11, 14), this hypothesis may be taken one step further to suggest an explanation for the appearance of two types of bone metabolic response in these patients, an explanation which, incidentally, provided the names "intermittent" and "continuous" used in this work to designate the two groups. One group, according to this view, will contain those patients in whom the sum of the secretion from the normal and abnormal parathyroids only intermittently exceeds normal. This can theoretically occur since the secretory rate of the abnormal gland, while excessive and uncontrolled, also fluctuates, as is attested to by the fluctuating hypercalcemia clinically seen in patients with parathyroid adenomata. Thus total secretion would be excessive at times when the output of the abnormal gland was greater than could be compensated for by reduction of the secretion of the normal glands.2 The animal work implies that bone from such individuals should exhibit only the acute effects of hormone-increased lactate production (2, 3) and an inhibition of proline incorporation (5, 6), whereas clinical considerations suggest that these patients should exhibit minimal symptoms and signs of the disease. The other group will then include all patients with more active abnormal glands in whom the level of hor- 2According to this hypothesis, the intermittent group should theoretically include only patients with adenoma, as is borne out by the surgical findings (Table I).
9 MTABOLIC STUDIS OF HUMAN BON IN VITRO 183 monal secretion is continuously above normal. In such individuals bone metabolic patterns should resemble those seen in the animals who had received the maximal number of doses of PT. Similarly, the clinical manifestations of the disease would be expected to be most florid in this group. The high degree to which the clinical manifestations of the disease in the two groups coincided with these predictions is indicated by the data in Table I. The observations regarding lactate production are in keeping with the findings in all animal studies including the present one. The absence of a significant elevation in the intermittent group would imply that the stimulus was either not sufficiently prolonged or severe to produce it. Similarly, the failure to reproduce the increased oxygen utiliation in the animal model while at the same time producing the other changes found in the human situation suggests that a more chronic degree of stimulation of the bone cells may also be required to produce this phenomenon. The association of the elevation of serum alkaline phosphatase and urinary hydroxyproline I a N -J DAYS OF TRATMNT r I 3 FIG. 7. CHANGS IN RATS OF PROLIN INCORPORATION INTO COLLAGN AND LACTAT PRODUCTION IN BON FROM ANIMALS TRATD FOR INCRASING PRIODS WITH DAILY INJCTIONS OF PARATHYROID XTRACT IN A TYPICAL XPRIMNT. ach bar in the case of proline represents one, or the mean of two or three, separate incubations of samples taken from a single pool of bone derived from two to four rats. In the case of lactate each bar represents the means of three to four samples from the same pool. Note that the scale on the left ordinate is for proline, whereas the one on the right is for lactate. "I I levels in this disease has previously been described. Both are regarded as sensitive clinical indexes of bone involvement; increased alkaline phosphatase is associated with an increase in osteoblastic activity (14), and increased urinary hydroxyproline is associated with an increase in either collagen synthesis or breakdown or both (7, 11).3 The results of the in vitro metabolic bone studies reported here suggest that some abnormality of bone metabolism exists in this disease even in the absence of clinical evidence of bone involvement by these indexes. The fact that the abnormality observed under these conditions did not involve any stimulation of new collagen biosynthesis may be in some way related to this absence of change. The ultimate value of metabolic studies of bone in vitro as a tool in the diagnosis of hyperparathyroidism remains to be proven. At present, the procedure remains too traumatic and the techniques too complex for routine clinical use. However, in two patients (M.C., C.M.) results obtained at biopsy did prove useful in establishing the diagnosis preoperatively. It must be pointed out that the biochemical lesions in bone cannot yet be called pathognomonic of an excess of parathyroid hormone. If and when such lesions can be established as pathognomonic and if, as seems likely from unpublished experiments, the methods can be adapted to studying much smaller fragments of bone, then these measurements may prove to be the most rapid and certain means of diagnosing hyperparathyroidism yet devised. Summary 1) Two types of metabolic change found in vitro in bone from hyperparathyroid patients have been presented. 2) These are interpreted as manifestations of differing degrees of overactivity of the parathyroids, one group reflecting intermittent, and the other continuous, hypersecretion of parathyroid hormone. 3) The intermittent group is characteried by a depression of proline utiliation for collagen 3The findings in patient.d., the most florid case of all, are of interest with regard to the source of the urinary hydroxyproline in this disease. After removal of the adenoma, the 24-hour urinary hydroxyproline output fell from 197 mg in one day to the normal range.
10 184 synthesis occurring with a modest increase in oxygen consumption. 4) The continuous group is characteried by larger increases in oxygen utiliation, increased lactate production, and increased utiliation of proline for collagen synthesis together with raised levels of serum alkaline phosphatase and urinary hydroxyproline. 5) The significance of these changes is discussed in relation to the actions of the hormone and to the clinical presentation and diagnosis of the disease. 6) Some partial support for this hypothesis is provided by animal experiments. Acknowledgments We are greatly indebted to Drs. H. Banks, W. Green, and T. Quigley for supplying the human bone samples. The skilled technical assistance of Mrs. Norma Steinberg, Mrs. Susan Ault, and Miss Hanne Alstrup is gratefully acknowledged. References 1. Flanagan, B., and G. Nichols, Jr. Metabolic studies of human bone in vitro. I. Normal bone. J. dlin. Invest. 1965, 44, Borle, A. B., N. Nichols, and G. Nichols, Jr. Metabolic studies of bone in vitro. II. The metabolic patterns of accretion and resorption. J. biol. Chem. 196, 235, Neuman, W. F., and C. M. Dowse. Possible fundamental action of parathyroid hormone in bone in The Parathyroids, R.. Greep and R. V. Talmage, BARRY FLANAGAN AND GORG NICHOLS, JR. ds. Springfield, Ill., Charles C Thomas, 1961, p Vaes, G. M., and G. Nichols, Jr. ffects of a massive dose of parathyroid extract on bone metabolic pathways. ndocrinology 1962, 7, Johnston, C. C., Jr., W. P. Deiss, Jr., and. B. Miner. Bone matrix biosynthesis in vitro. II. ffects of parathyroid hormone. J. biol. Chem. 1962, 237, Flanagan, B., and G. Nichols, Jr. Parathyroid inhibition of bone collagen synthesis. ndocrinology 1964, 74, Jasin, H.., C. Fink, J. D. Smiley, and M. Ziff. Influence of growth on total urinary hydroxyproline. J. dlin. Invest. 1962, 41, Prockop, D. J., and S. Udenfriend. A specific method for the analysis of hydroxyproline in tissues and urine. Analyt. Biochem. 196, 1, Bessey,. A.,. H. Lowry, and M. J. Brock. A method for the rapid determination of alkaline phosphatase with five cubic millimeters of serum. J. biol. Chem. 1946, 164, Flanagan, B., and G. Nichols, Jr. Metabolic studies of bone in vitro. IV. Collagen biosynthesis by surviving bone fragments in vitro. J. biol. Chem. 1962, 237, Keiser, H. R., J. R. Gill, Jr., A. Sjoerdsma, and F. C. Bartter. Relation between urinary hydroxyproline and parathyroid function. J. dlin. Invest. 1964, 43, Nichols, G., Jr., and B. Flanagan. valuation of parathyroid function by responses to infusions of calcium and DTA. In preparation. 13. Costello, J. M., and C.. Dent. Hypo-hyperparathyroidism. Arch. Dis. Childh. 1963, 38, Albright, F., and. C. Reifenstein. The Parathyroid Glands and Metabolic Bone Disease. Baltimore, Williams & Wilkins, 1948.
Metabolic Studies of Human Bone In Vitro.
 Journal of Clinical Investigation Vol. 44, No. 11, 1965 Metabolic Studies of Human Bone In Vitro. I. Normal Bone * BARRY FLANAGAN t AND GEORGE NICHOLS, JR. t (From the Department of Medicine, Harvard Medical
Journal of Clinical Investigation Vol. 44, No. 11, 1965 Metabolic Studies of Human Bone In Vitro. I. Normal Bone * BARRY FLANAGAN t AND GEORGE NICHOLS, JR. t (From the Department of Medicine, Harvard Medical
HYPERPARATHYROIDIS M FAISAL GHANI SIDDIQUI MBBS; FCPS; PGDIP-BIOMEDICAL ETHICS; MCPS-HPE
 HYPERPARATHYROIDIS M FAISAL GHANI SIDDIQUI MBBS; FCPS; PGDIP-BIOMEDICAL ETHICS; MCPS-HPE PROFESSOR OF SURGERY J I N N A H S I N D H M E D I C A L U N I V E R S I T Y PREAMBLE Anatomy & physiology of the
HYPERPARATHYROIDIS M FAISAL GHANI SIDDIQUI MBBS; FCPS; PGDIP-BIOMEDICAL ETHICS; MCPS-HPE PROFESSOR OF SURGERY J I N N A H S I N D H M E D I C A L U N I V E R S I T Y PREAMBLE Anatomy & physiology of the
Southern Derbyshire Shared Care Pathology Guidelines. Primary Hyperparathyroidism
 Southern Derbyshire Shared Care Pathology Guidelines Primary Hyperparathyroidism Please use this Guideline in Conjunction with the Hypercalcaemia Guideline Definition Driven by hyperfunction of one or
Southern Derbyshire Shared Care Pathology Guidelines Primary Hyperparathyroidism Please use this Guideline in Conjunction with the Hypercalcaemia Guideline Definition Driven by hyperfunction of one or
Awaisheh. Mousa Al-Abbadi. Abdullah Alaraj. 1 Page
 f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
PRIMARY HYPERPARATHYROIDISM
 PRIMARY HYPERPARATHYROIDISM HYPERPARATHYROIDISM Inappropriate excess secretion of Parathyroid Hormone in Primary Hyperparathyroidism Appropriate Hypersecretion in Secondary Hyperparathyroidism PTH and
PRIMARY HYPERPARATHYROIDISM HYPERPARATHYROIDISM Inappropriate excess secretion of Parathyroid Hormone in Primary Hyperparathyroidism Appropriate Hypersecretion in Secondary Hyperparathyroidism PTH and
NEOPLASMS OF THE THYROID PATHOLOGY OF PARATHYROID GLANDS. BY: Shifaa Qa qa
 NEOPLASMS OF THE THYROID PATHOLOGY OF PARATHYROID GLANDS BY: Shifaa Qa qa Neoplasmas of the thyroid thyroid nodules Neoplastic ---- benign, malignant Non neoplastic Solitary nodules ----- neoplastic Nodules
NEOPLASMS OF THE THYROID PATHOLOGY OF PARATHYROID GLANDS BY: Shifaa Qa qa Neoplasmas of the thyroid thyroid nodules Neoplastic ---- benign, malignant Non neoplastic Solitary nodules ----- neoplastic Nodules
CKD: Bone Mineral Metabolism. Peter Birks, Nephrology Fellow
 CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
Calcium Nephrolithiasis and Bone Health. Noah S. Schenkman, MD
 Calcium Nephrolithiasis and Bone Health Noah S. Schenkman, MD Associate Professor of Urology and Residency Program Director, University of Virginia Health System; Charlottesville, Virginia Objectives:
Calcium Nephrolithiasis and Bone Health Noah S. Schenkman, MD Associate Professor of Urology and Residency Program Director, University of Virginia Health System; Charlottesville, Virginia Objectives:
The Skeletal Response to Aging: There s No Bones About It!
 The Skeletal Response to Aging: There s No Bones About It! April 7, 2001 Joseph E. Zerwekh, Ph.D. Interrelationship of Intestinal, Skeletal, and Renal Systems to the Overall Maintenance of Normal Calcium
The Skeletal Response to Aging: There s No Bones About It! April 7, 2001 Joseph E. Zerwekh, Ph.D. Interrelationship of Intestinal, Skeletal, and Renal Systems to the Overall Maintenance of Normal Calcium
Approach to a patient with hypercalcemia
 Approach to a patient with hypercalcemia Ana-Maria Chindris, MD Division of Endocrinology Mayo Clinic Florida 2013 MFMER slide-1 Background Hypercalcemia is a problem frequently encountered in clinical
Approach to a patient with hypercalcemia Ana-Maria Chindris, MD Division of Endocrinology Mayo Clinic Florida 2013 MFMER slide-1 Background Hypercalcemia is a problem frequently encountered in clinical
Calcium metabolism and the Parathyroid Glands. Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands
 Calcium metabolism and the Parathyroid Glands Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands Calcium is an essential element for contraction of voluntary/smooth
Calcium metabolism and the Parathyroid Glands Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands Calcium is an essential element for contraction of voluntary/smooth
Radiographic Appearance Of Primary Hyperparathyroidism With Atypical Parathyroid Adenoma
 ISPUB.COM The Internet Journal of Internal Medicine Volume 6 Number 2 Radiographic Appearance Of Primary Hyperparathyroidism With Atypical Parathyroid Adenoma P George, N Philip, B Pawar Citation P George,
ISPUB.COM The Internet Journal of Internal Medicine Volume 6 Number 2 Radiographic Appearance Of Primary Hyperparathyroidism With Atypical Parathyroid Adenoma P George, N Philip, B Pawar Citation P George,
Case study Group 2 presentation
 Case study Group 2 presentation Patient profile HN 3095-57 Female 60 years old Hometown : Sa Kaeo province Occupation : farmer No drug and food allergy Chief complain Left neck mass 10 years PTA that gradually
Case study Group 2 presentation Patient profile HN 3095-57 Female 60 years old Hometown : Sa Kaeo province Occupation : farmer No drug and food allergy Chief complain Left neck mass 10 years PTA that gradually
4/20/2015. The Neck xt Exploration: Intraoperative Parathyroid Hormone (IOPTH) Testing During Surgical Parathyroidectomy. Learning Objectives
 The Neck xt Exploration: Intraoperative Parathyroid Hormone (IOPTH) Testing During Surgical Parathyroidectomy Nichole Korpi-Steiner, PhD, DABCC, FACB University of North Carolina Chapel Hill, NC Learning
The Neck xt Exploration: Intraoperative Parathyroid Hormone (IOPTH) Testing During Surgical Parathyroidectomy Nichole Korpi-Steiner, PhD, DABCC, FACB University of North Carolina Chapel Hill, NC Learning
II. RELATION TO BONE DISEASE INTRODUCTION. M.M. POPOVTZER, W.E. HUFFER, W.P. GElS, W.S. HAMMOND, T.E. STARZL
 II. RELATION TO BONE DISEASE M.M. POPOVTZER, W.E. HUFFER, W.P. GElS, W.S. HAMMOND, T.E. STARZL INTRODUCTION It has been generally assumed that azotemic osteodystrophy resolves after kidney transplantation
II. RELATION TO BONE DISEASE M.M. POPOVTZER, W.E. HUFFER, W.P. GElS, W.S. HAMMOND, T.E. STARZL INTRODUCTION It has been generally assumed that azotemic osteodystrophy resolves after kidney transplantation
Actions of Parathyroid Hormone in the Vitamin D-deficient
 Journal of Clinical Investigation Vol. 44, No. 12, 1965 Actions of Parathyroid Hormone in the Vitamin D-deficient Dog * ROBERT L. NEY,t WILLIAM Y. W. Au,t GERALD KELLY, I. RADDE, AND FREDERIC C. BARTTER
Journal of Clinical Investigation Vol. 44, No. 12, 1965 Actions of Parathyroid Hormone in the Vitamin D-deficient Dog * ROBERT L. NEY,t WILLIAM Y. W. Au,t GERALD KELLY, I. RADDE, AND FREDERIC C. BARTTER
Magnesium Homeostasis
 ECTS PhD Training Course, Rome 3 rd September 2008 Disorders of Calcium, Phosphate h and Magnesium Homeostasis Richard Eastell Professor of Bone Metabolism Academic Unit of Bone Metabolism University of
ECTS PhD Training Course, Rome 3 rd September 2008 Disorders of Calcium, Phosphate h and Magnesium Homeostasis Richard Eastell Professor of Bone Metabolism Academic Unit of Bone Metabolism University of
"Asymptomatic" Hyperparathyroidism: Reasons for Parathyroidectomy
 "Asymptomatic" Hyperparathyroidism: Reasons for Parathyroidectomy Rebecca S. Sippel, M.D. Assistant Professor Department of Surgery Section of Endocrine Surgery University of Wisconsin Primary Hyperparathyroidism
"Asymptomatic" Hyperparathyroidism: Reasons for Parathyroidectomy Rebecca S. Sippel, M.D. Assistant Professor Department of Surgery Section of Endocrine Surgery University of Wisconsin Primary Hyperparathyroidism
hypercalcemia of malignancy hyperparathyroidism PHPT the most common cause of hypercalcemia in the outpatient setting the second most common cause
 hyperparathyroidism A 68-year-old woman with documented osteoporosis has blood tests showing elevated serum calcium and parathyroid hormone (PTH) levels: 11.2 mg/dl (8.8 10.1 mg/dl) and 88 pg/ml (10-60),
hyperparathyroidism A 68-year-old woman with documented osteoporosis has blood tests showing elevated serum calcium and parathyroid hormone (PTH) levels: 11.2 mg/dl (8.8 10.1 mg/dl) and 88 pg/ml (10-60),
When the level of calcium in the blood falls too low, the parathyroid glands secrete just enough PTH to restore the blood calcium level.
 Hyperparathyroidism Primary hyperparathyroidism is a disorder of the parathyroid glands, also called parathyroids. Primary means this disorder originates in the parathyroids: One or more enlarged, overactive
Hyperparathyroidism Primary hyperparathyroidism is a disorder of the parathyroid glands, also called parathyroids. Primary means this disorder originates in the parathyroids: One or more enlarged, overactive
Primary hyperparathyroidism A clinical study
 Med. J. Malaysia Vol. 43 No. 3 September 1988 Primary hyperparathyroidism A clinical study K. L. Goh, MBBS(Mal), MRCP(UK) Lecturer in Medicine F. Wang, MBBS(Sing), FRCP(Edin), FRACP, FACP Professor ofmedicine
Med. J. Malaysia Vol. 43 No. 3 September 1988 Primary hyperparathyroidism A clinical study K. L. Goh, MBBS(Mal), MRCP(UK) Lecturer in Medicine F. Wang, MBBS(Sing), FRCP(Edin), FRACP, FACP Professor ofmedicine
Thyroid and parathyroid glands
 Thyroid and parathyroid glands Dr. Isabel Hwang Department of Physiology Faculty of Medicine University of Hong Kong May 2007 The thyroid gland straddles the esophagus, just below the larynx, in the neck.
Thyroid and parathyroid glands Dr. Isabel Hwang Department of Physiology Faculty of Medicine University of Hong Kong May 2007 The thyroid gland straddles the esophagus, just below the larynx, in the neck.
Acid-Base Alterations and Renal Gluconeogenesis: Effect
 Journal of Clinical Investigation Vol. 46, No. 7, 1967 Acid-Base Alterations and Renal Gluconeogenesis: Effect of ph, Bicarbonate Concentration, and Pco2 * DONALD E. KAMM,t ROBERT E. Fuisz,4 A. DAVID GOODMAN,
Journal of Clinical Investigation Vol. 46, No. 7, 1967 Acid-Base Alterations and Renal Gluconeogenesis: Effect of ph, Bicarbonate Concentration, and Pco2 * DONALD E. KAMM,t ROBERT E. Fuisz,4 A. DAVID GOODMAN,
Clinical Approach to Hypercalcemia For the Primary Care Provider
 Clinical Approach to Hypercalcemia For the Primary Care Provider Christina Maser, MD FACS UCSF Fresno Department of Surgery, Endocrine Surgery 2/2/19 Objectives Recognition of pitfalls of diagnosis of
Clinical Approach to Hypercalcemia For the Primary Care Provider Christina Maser, MD FACS UCSF Fresno Department of Surgery, Endocrine Surgery 2/2/19 Objectives Recognition of pitfalls of diagnosis of
Bone and Mineral. Comprehensive Menu for the Management of Bone and Mineral Related Diseases
 Bone and Mineral Comprehensive Menu for the Management of Bone and Mineral Related Diseases Innovation to Assist in Clinical Diagnosis and Treatment DiaSorin offers a specialty line of Bone and Mineral
Bone and Mineral Comprehensive Menu for the Management of Bone and Mineral Related Diseases Innovation to Assist in Clinical Diagnosis and Treatment DiaSorin offers a specialty line of Bone and Mineral
during this time he was not allowed to sit up. He maintained his THYROID BODIES. METABOLIC STUDY III
 A CASE OF OSTEITIS FIBROSA CYSTICA (OSTEOMALACIA?) WITH EVIDENCE OF HYPERACTIVITY OF THE PARA- THYROID BODIES. METABOLIC STUDY III By W. S. McCLELLAN' AND R. R. HANNON (From the Russell Sage Institute
A CASE OF OSTEITIS FIBROSA CYSTICA (OSTEOMALACIA?) WITH EVIDENCE OF HYPERACTIVITY OF THE PARA- THYROID BODIES. METABOLIC STUDY III By W. S. McCLELLAN' AND R. R. HANNON (From the Russell Sage Institute
Bone and Renal Stone Disease in Patients Operated for Primary Hyperparathyroidism in Pakistan: Is the Pattern of Disease different from the West?
 ecommons@aku Section of Urology Department of Surgery August 1999 Bone and Renal Stone Disease in Patients Operated for Primary Hyperparathyroidism in Pakistan: Is the Pattern of Disease different from
ecommons@aku Section of Urology Department of Surgery August 1999 Bone and Renal Stone Disease in Patients Operated for Primary Hyperparathyroidism in Pakistan: Is the Pattern of Disease different from
Relation between Urinary Hydroxyproline and Parathyroid
 Journal of Clinical nvestigation Vol. 43, No. 6, 1964 Relation between Urinary Hydroxyproline and Parathyroid Function * HARRY R. KESER, JOHN R. GLL, JR., ALBERT SJOERDSMA, AND FREDERC C. BARTTER (From
Journal of Clinical nvestigation Vol. 43, No. 6, 1964 Relation between Urinary Hydroxyproline and Parathyroid Function * HARRY R. KESER, JOHN R. GLL, JR., ALBERT SJOERDSMA, AND FREDERC C. BARTTER (From
B. Environmental Factors. a. The major risk factor to papillary thyroid cancer is exposure to ionizing radiation, during the first 2 decades of life.
 B. Environmental Factors. a. The major risk factor to papillary thyroid cancer is exposure to ionizing radiation, during the first 2 decades of life. b. Deficiency of dietary iodine: - Is linked with a
B. Environmental Factors. a. The major risk factor to papillary thyroid cancer is exposure to ionizing radiation, during the first 2 decades of life. b. Deficiency of dietary iodine: - Is linked with a
Hyperparathyroidism: Operative Considerations. Financial Disclosures: None. Hyperparathyroidism. Hyperparathyroidism 11/10/2012
 Hyperparathyroidism: Operative Considerations Financial Disclosures: None Steven J Wang, MD FACS Associate Professor Dept of Otolaryngology-Head and Neck Surgery University of California, San Francisco
Hyperparathyroidism: Operative Considerations Financial Disclosures: None Steven J Wang, MD FACS Associate Professor Dept of Otolaryngology-Head and Neck Surgery University of California, San Francisco
PRIMARY HYPERPARATHYROIDISM PRIMARY HYPERPARATHYROIDISM. Hyperparathyroidism Etiology. Common Complex Insidious Chronic Global Only cure is surgery
 ENDOCRINE DISORDER PRIMARY HYPERPARATHYROIDISM Roseann P. Velez, DNP, FNP Francis J. Velez, MD, FACS Common Complex Insidious Chronic Global Only cure is surgery HYPERPARATHYROIDISM PARATHRYOID GLANDS
ENDOCRINE DISORDER PRIMARY HYPERPARATHYROIDISM Roseann P. Velez, DNP, FNP Francis J. Velez, MD, FACS Common Complex Insidious Chronic Global Only cure is surgery HYPERPARATHYROIDISM PARATHRYOID GLANDS
Kobe University Repository : Kernel
 Title Author(s) Citation Issue date 2009-09 Resource Type Resource Version DOI URL Kobe University Repository : Kernel Marked increase in bone formation markers after cinacalcet treatment by mechanisms
Title Author(s) Citation Issue date 2009-09 Resource Type Resource Version DOI URL Kobe University Repository : Kernel Marked increase in bone formation markers after cinacalcet treatment by mechanisms
Thyrocalcitonin and the Response to Parathyroid
 Journal ofclnical Investigation Vol. 46, ao. 1, 1967 Thyrocalcitonin and the Response to Parathyroid Hormone * CONSTANTINE ANAST, CLAUDE D. ARNAUD, HOWARD RASMUSSEN,t AND ALAN TENENHOUSE (From the Department
Journal ofclnical Investigation Vol. 46, ao. 1, 1967 Thyrocalcitonin and the Response to Parathyroid Hormone * CONSTANTINE ANAST, CLAUDE D. ARNAUD, HOWARD RASMUSSEN,t AND ALAN TENENHOUSE (From the Department
Pathologic Fracture of the Femur in Brown Tumor Induced in Parathyroid Carcinoma: A Case Report
 CASE REPORT Hip Pelvis 28(3): 173-177, 2016 http://dx.doi.org/10.5371/hp.2016.28.3.173 Print ISSN 2287-3260 Online ISSN 2287-3279 Pathologic Fracture of the Femur in Brown Tumor Induced in Parathyroid
CASE REPORT Hip Pelvis 28(3): 173-177, 2016 http://dx.doi.org/10.5371/hp.2016.28.3.173 Print ISSN 2287-3260 Online ISSN 2287-3279 Pathologic Fracture of the Femur in Brown Tumor Induced in Parathyroid
The parathyroid glands participate in the regulation
 41 HERNAN I. VARGAS STANLEY R. KLEIN The parathyroid glands participate in the regulation of calcium metabolism. Disorders of the parathyroid gland are most commonly a result of hyperfunction and rarely
41 HERNAN I. VARGAS STANLEY R. KLEIN The parathyroid glands participate in the regulation of calcium metabolism. Disorders of the parathyroid gland are most commonly a result of hyperfunction and rarely
Hyperparathyroidism. When to Suspect, How to Diagnose, When and How to Intervene. Johanna A. Pallotta, MD, FACP, FACE
 Hyperparathyroidism When to Suspect, How to Diagnose, When and How to Intervene Johanna A. Pallotta, MD, FACP, FACE Potential conflicts of interest: None Johanna A. Pallotta, MD Outline Definition of hyperparathyroidism
Hyperparathyroidism When to Suspect, How to Diagnose, When and How to Intervene Johanna A. Pallotta, MD, FACP, FACE Potential conflicts of interest: None Johanna A. Pallotta, MD Outline Definition of hyperparathyroidism
Research Article Primary Hyperparathyroidism: 11-Year Experience in a Single Institute in Thailand
 International Endocrinology Volume 2012, Article ID 952426, 4 pages doi:10.1155/2012/952426 Research Article Primary Hyperparathyroidism: 11-Year Experience in a Single Institute in Thailand Poramaporn
International Endocrinology Volume 2012, Article ID 952426, 4 pages doi:10.1155/2012/952426 Research Article Primary Hyperparathyroidism: 11-Year Experience in a Single Institute in Thailand Poramaporn
EGTA, and Urinary Electrolyte Excretion *
 Journal of Clnical Investigation Vol. 46, No. 5, 1967 Thyrocalcitonin, EGTA, and Urinary Electrolyte Excretion * HOWARD RASMUSSEN,t CONSTANTINE ANAST, AND CLAUDE ARNAUD (From the Department of Biochemistry,
Journal of Clnical Investigation Vol. 46, No. 5, 1967 Thyrocalcitonin, EGTA, and Urinary Electrolyte Excretion * HOWARD RASMUSSEN,t CONSTANTINE ANAST, AND CLAUDE ARNAUD (From the Department of Biochemistry,
Hypo-hyperparathyroidism
 Arch. Dis. Childh., 1968, 43, 295. Hypo-hyperparathyroidism E. H. ALLEN, F. J. C. MILLARD*, and J. R. NASSIM From the Royal National Orthopaedic Hospital and St. George's Hospital, London In 1963 Costello
Arch. Dis. Childh., 1968, 43, 295. Hypo-hyperparathyroidism E. H. ALLEN, F. J. C. MILLARD*, and J. R. NASSIM From the Royal National Orthopaedic Hospital and St. George's Hospital, London In 1963 Costello
Index. B BMC. See Bone mineral content BMD. See Bone mineral density Bone anabolic impact, Bone mass acquisition
 A Acid base balance dietary protein detrimental effects of, 19 Acid base balance bicarbonate effects, 176 in bone human studies, 174 mechanisms, 173 174 in muscle aging, 174 175 alkali supplementation
A Acid base balance dietary protein detrimental effects of, 19 Acid base balance bicarbonate effects, 176 in bone human studies, 174 mechanisms, 173 174 in muscle aging, 174 175 alkali supplementation
Secondary Hyperparathyroidism: Where are we now?
 Secondary Hyperparathyroidism: Where are we now? Dylan M. Barth, Pharm.D. PGY-1 Pharmacy Resident Mayo Clinic 2017 MFMER slide-1 Objectives Identify risk factors for the development of complications caused
Secondary Hyperparathyroidism: Where are we now? Dylan M. Barth, Pharm.D. PGY-1 Pharmacy Resident Mayo Clinic 2017 MFMER slide-1 Objectives Identify risk factors for the development of complications caused
STUDIES ON THE PHYSIOLOGY OF THE PARATHYROID GLANDS
 STUDIES ON THE PHYSIOLOGY OF THE PARATHYROID GLANDS V. ACTION OF PARATHYROID EXTRACT ON THE RENAL THRESHOLD FOR PHOSPHORUS By READ ELLSWORTH (From the Medical Clinic, the School of Medicine, Johns Hopkins
STUDIES ON THE PHYSIOLOGY OF THE PARATHYROID GLANDS V. ACTION OF PARATHYROID EXTRACT ON THE RENAL THRESHOLD FOR PHOSPHORUS By READ ELLSWORTH (From the Medical Clinic, the School of Medicine, Johns Hopkins
Ca, Mg metabolism, bone diseases. Tamás Kőszegi Pécs University, Department of Laboratory Medicine Pécs, Hungary
 Ca, Mg metabolism, bone diseases Tamás Kőszegi Pécs University, Department of Laboratory Medicine Pécs, Hungary Calcium homeostasis Ca 1000g in adults 99% in bones (extracellular with Mg, P) Plasma/intracellular
Ca, Mg metabolism, bone diseases Tamás Kőszegi Pécs University, Department of Laboratory Medicine Pécs, Hungary Calcium homeostasis Ca 1000g in adults 99% in bones (extracellular with Mg, P) Plasma/intracellular
Women s Health in General Practice Symposium 2015 Thyroid & Parathyroid Cases
 Women s Health in General Practice Symposium 2015 Thyroid & Parathyroid Cases Bill Fleming Epworth Freemasons Hospital 1 Common Endocrine Presentations anatomical problems thyroid nodule / goitre embryological
Women s Health in General Practice Symposium 2015 Thyroid & Parathyroid Cases Bill Fleming Epworth Freemasons Hospital 1 Common Endocrine Presentations anatomical problems thyroid nodule / goitre embryological
Primary Hyperparathyroidism
 Primary Hyperparathyroidism Copyright Copyright 2019 2019 American American Associa7on Associa7on of Clinical of Clinical Endocrinologists Endocrinologists 1 Primary Hyperparathyroidism In primary hyperparathyroidism
Primary Hyperparathyroidism Copyright Copyright 2019 2019 American American Associa7on Associa7on of Clinical of Clinical Endocrinologists Endocrinologists 1 Primary Hyperparathyroidism In primary hyperparathyroidism
CKD-Mineral Bone Disorder (MBD) Pathogenesis of Metabolic Bone Disease. Grants: NIH, Abbott, Amgen, OPKO, Shire
 Pathogenesis of Metabolic Bone Disease Stuart M. Sprague, D.O. Chief, Division of Nephrology and Hypertension Professor of Medicine NorthShore University HealthSystem University of Chicago Pritzker School
Pathogenesis of Metabolic Bone Disease Stuart M. Sprague, D.O. Chief, Division of Nephrology and Hypertension Professor of Medicine NorthShore University HealthSystem University of Chicago Pritzker School
The Parathyroid Glands
 The Parathyroid Glands Bởi: OpenStaxCollege The parathyroid glands are tiny, round structures usually found embedded in the posterior surface of the thyroid gland ([link]). A thick connective tissue capsule
The Parathyroid Glands Bởi: OpenStaxCollege The parathyroid glands are tiny, round structures usually found embedded in the posterior surface of the thyroid gland ([link]). A thick connective tissue capsule
Osteoporosis. Treatment of a Silently Developing Disease
 Osteoporosis Treatment of a Silently Developing Disease Marc K. Drezner, MD Senior Associate Dean Emeritus Professor of Medicine Emeritus University of Wisconsin-Madison Auditorium The Forest at Duke October
Osteoporosis Treatment of a Silently Developing Disease Marc K. Drezner, MD Senior Associate Dean Emeritus Professor of Medicine Emeritus University of Wisconsin-Madison Auditorium The Forest at Duke October
PT Final Exam. July 2018 Core Content Review 6 Presented by Mark. Copyright 2018 PT Final Exam
 PT Final Exam July 2018 Core Content Review 6 Presented by Mark A 34 year old male comes to your clinic with reoccurring hamstring tears. Upon examination, the therapist is able to achieve 130 degrees
PT Final Exam July 2018 Core Content Review 6 Presented by Mark A 34 year old male comes to your clinic with reoccurring hamstring tears. Upon examination, the therapist is able to achieve 130 degrees
Persistent post transplant hyperparathyroidism. Shiva Seyrafian IUMS-97/10/18-8/1/2019
 Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital
 Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital E-mail: snigwekar@mgh.harvard.edu March 13, 2017 Disclosures statement: Consultant: Allena, Becker
Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital E-mail: snigwekar@mgh.harvard.edu March 13, 2017 Disclosures statement: Consultant: Allena, Becker
Stromal Fat Content of the Parathyroid Gland
 Stromal Fat Content of the Parathyroid Gland TAKAO OBARA,* YOSHIHIDE FUJIMOTO* AND MOTOHIKO AIBA** *Department of Endocrine Surgery and **Department of Surgical Pathology, Tokyo Women's Medical College,
Stromal Fat Content of the Parathyroid Gland TAKAO OBARA,* YOSHIHIDE FUJIMOTO* AND MOTOHIKO AIBA** *Department of Endocrine Surgery and **Department of Surgical Pathology, Tokyo Women's Medical College,
Parathyroid hormone (serum, plasma)
 Parathyroid hormone (serum, plasma) 1 Name and description of analyte 1.1 Name of analyte Parathyroid hormone (PTH) 1.2 Alternative names Parathormone 1.3 NMLC code 1.4 Description of analyte PTH is an
Parathyroid hormone (serum, plasma) 1 Name and description of analyte 1.1 Name of analyte Parathyroid hormone (PTH) 1.2 Alternative names Parathormone 1.3 NMLC code 1.4 Description of analyte PTH is an
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: testing_serum_vitamin_d_levels 9/2015 2/2017 2/2018 2/2017 Description of Procedure or Service Vitamin D,
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: testing_serum_vitamin_d_levels 9/2015 2/2017 2/2018 2/2017 Description of Procedure or Service Vitamin D,
hyperplastic parathyroid glands
 Journal of Clinical Pathology, 1978, 31, 626-632 A histological comparison of adenomatous and hyperplastic parathyroid glands D. A. S. LAWRENCE From the Department of Histopathology, Royal Free Hospital,
Journal of Clinical Pathology, 1978, 31, 626-632 A histological comparison of adenomatous and hyperplastic parathyroid glands D. A. S. LAWRENCE From the Department of Histopathology, Royal Free Hospital,
PARATHORMONE DOSAGE AND SERUM CALCIUM AND PHOSPHORUS IN EXPERIMENTAL CHRONIC HYPER- PARATHYROIDISM LEADING TO OSTITIS FIBROSA 1
 PARATHORMONE DOSAGE AND SERUM CALCIUM AND PHOSPHORUS IN EXPERIMENTAL CHRONIC HYPER- PARATHYROIDISM LEADING TO OSTITIS FIBROSA 1 By AARON BODANSKY, PH.D., AND HENRY L. JAFFE, M.D. (From the Laboratory Division
PARATHORMONE DOSAGE AND SERUM CALCIUM AND PHOSPHORUS IN EXPERIMENTAL CHRONIC HYPER- PARATHYROIDISM LEADING TO OSTITIS FIBROSA 1 By AARON BODANSKY, PH.D., AND HENRY L. JAFFE, M.D. (From the Laboratory Division
DR. DARWISH H. BADRAN. Parathyroid glands
 Parathyroid glands History 1849 - Sir Richard owen provided 1st accurate description of normal parathyroid glands after examining Indian Rhinoceros 1879 - Anton Wölfer described tetany in a patient
Parathyroid glands History 1849 - Sir Richard owen provided 1st accurate description of normal parathyroid glands after examining Indian Rhinoceros 1879 - Anton Wölfer described tetany in a patient
Parathyroid surgery at Massachusetts General Hospital: Information for patients and families
 Parathyroid surgery at Massachusetts General Hospital: Information for patients and families We are pleased that you have chosen Massachusetts General Hospital to receive treatment for your parathyroid
Parathyroid surgery at Massachusetts General Hospital: Information for patients and families We are pleased that you have chosen Massachusetts General Hospital to receive treatment for your parathyroid
Hypoparathyroid Patients *
 Journal of Clinical Investigation Vol. 44, No. 6, 1965 Effects of Serum Calcium Level and Parathyroid Extracts on Phosphate and Calcium Excretion in Hypoparathyroid Patients * EUGENE EISENBERG t (From
Journal of Clinical Investigation Vol. 44, No. 6, 1965 Effects of Serum Calcium Level and Parathyroid Extracts on Phosphate and Calcium Excretion in Hypoparathyroid Patients * EUGENE EISENBERG t (From
HYPERCALCEMIA. Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences
 HYPERCALCEMIA Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ESSENTIALS OF DIAGNOSIS Serum calcium level > 10.5 mg/dl Serum ionized
HYPERCALCEMIA Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ESSENTIALS OF DIAGNOSIS Serum calcium level > 10.5 mg/dl Serum ionized
Bone strength is proportional to bone mass, measured with DXA. Bone turnover markers indicate the status of bone quality.
 Bone strength is proportional to bone mass, measured with DXA Bone quality depend on bone architecture, rate of bone turnover, quality of bone matrix. Bone turnover markers indicate the status of bone
Bone strength is proportional to bone mass, measured with DXA Bone quality depend on bone architecture, rate of bone turnover, quality of bone matrix. Bone turnover markers indicate the status of bone
Pediatric metabolic bone diseases
 Pediatric metabolic bone diseases Classification and overview of clinical and radiological findings M. Mearadji International Foundation for Pediatric Imaging Aid www.ifpia.com Introduction Metabolic bone
Pediatric metabolic bone diseases Classification and overview of clinical and radiological findings M. Mearadji International Foundation for Pediatric Imaging Aid www.ifpia.com Introduction Metabolic bone
Functions of the Skeletal System. Chapter 6: Osseous Tissue and Bone Structure. Classification of Bones. Bone Shapes
 Chapter 6: Osseous Tissue and Bone Structure Functions of the Skeletal System 1. Support 2. Storage of minerals (calcium) 3. Storage of lipids (yellow marrow) 4. Blood cell production (red marrow) 5. Protection
Chapter 6: Osseous Tissue and Bone Structure Functions of the Skeletal System 1. Support 2. Storage of minerals (calcium) 3. Storage of lipids (yellow marrow) 4. Blood cell production (red marrow) 5. Protection
OGY. IV. THE METABOLISM OF IODINE IN
 RADIOACTIVE IODINE AS AN INDICATOR IN THYROID PHYSIOL- OGY IV THE METABOLISM OF IODINE IN GRAVES' 1 By S HERTZ, A ROBERTS, AND W T SALTER (From the Thyroid Clinic of the Massachusetts General Hospital,
RADIOACTIVE IODINE AS AN INDICATOR IN THYROID PHYSIOL- OGY IV THE METABOLISM OF IODINE IN GRAVES' 1 By S HERTZ, A ROBERTS, AND W T SALTER (From the Thyroid Clinic of the Massachusetts General Hospital,
HORMONE * effects are presented in schematic form in Figure 1. Certain predictions concerning the physiological
 Journal of Clinical Investigation Vol. 42, No. 12, 1963 THE RELATIONSHIP BETWEEN VITAMIN D AND PARATHYROID HORMONE * By HOWARD RASMUSSEN, HECTOR DELUCA, CLAUDE ARNAUD,t CHARLES HAWKER, AND MARIT VON STEDINGK
Journal of Clinical Investigation Vol. 42, No. 12, 1963 THE RELATIONSHIP BETWEEN VITAMIN D AND PARATHYROID HORMONE * By HOWARD RASMUSSEN, HECTOR DELUCA, CLAUDE ARNAUD,t CHARLES HAWKER, AND MARIT VON STEDINGK
The Calcium Conundrum: When, What and How to Give Calcium in Pediatric CKD/ESRD
 The Calcium Conundrum: When, What and How to Give Calcium in Pediatric CKD/ESRD Jess Tower MS RD LD 3/18/19 Children s Mercy Hospital jdtower@cmh.edu 816 460 1067 Disclosures Nothing to disclose 1 How
The Calcium Conundrum: When, What and How to Give Calcium in Pediatric CKD/ESRD Jess Tower MS RD LD 3/18/19 Children s Mercy Hospital jdtower@cmh.edu 816 460 1067 Disclosures Nothing to disclose 1 How
Hypercalcemia. Hypercalcemia: When to Worry, When to Treat! Mineral Metabolism : A Short Course
 Hypercalcemia: When to Worry, When to Treat! Michael A. Levine has no financial relationships to disclose or Conflicts of Interest to resolve. Michael A. Levine, M.D. This presentation will not involve
Hypercalcemia: When to Worry, When to Treat! Michael A. Levine has no financial relationships to disclose or Conflicts of Interest to resolve. Michael A. Levine, M.D. This presentation will not involve
The Parathyroid Glands Secrete Parathyroid Hormone, which Regulates Calcium, Magnesium, and Phosphate Ion Levels
 17.6 The Parathyroid Glands Secrete Parathyroid Hormone, which Regulates Calcium, Magnesium, and Phosphate Ion Levels Partially embedded in the posterior surface of the lateral lobes of the thyroid gland
17.6 The Parathyroid Glands Secrete Parathyroid Hormone, which Regulates Calcium, Magnesium, and Phosphate Ion Levels Partially embedded in the posterior surface of the lateral lobes of the thyroid gland
Figures and tables in this presentation were adopted from various printed and electronic resorces and serve strictly for educational purposes.
 Academic lectures 3rd year of Medical faculty Figures and tables in this presentation were adopted from various printed and electronic resorces and serve strictly for educational purposes. ENDOCRINOLOGY
Academic lectures 3rd year of Medical faculty Figures and tables in this presentation were adopted from various printed and electronic resorces and serve strictly for educational purposes. ENDOCRINOLOGY
Cases in Endocrinology
 Bones, Moans and Groans Diagnosing and Treating Primary Hyperparathyroidism By M. Usman Chaudhry, MD Table 1 Laboratory parameters Her bone density had osteopenic T-Scores of -2.3 at lumbar spine, and
Bones, Moans and Groans Diagnosing and Treating Primary Hyperparathyroidism By M. Usman Chaudhry, MD Table 1 Laboratory parameters Her bone density had osteopenic T-Scores of -2.3 at lumbar spine, and
Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff.
 Hypercalcaemia Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff. Mild (usually no symptoms) 2.6 3.0 mmol/l Moderate (start to develop symptoms) 3.0 3.4
Hypercalcaemia Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff. Mild (usually no symptoms) 2.6 3.0 mmol/l Moderate (start to develop symptoms) 3.0 3.4
ISSN East Cent. Afr. J. s
 56 The Surgical Management of Primary Hyperparathyroidism: The Experience in Tikur Anbessa Specialized Tertiary Referral and Teaching Hospital, Addis Ababa, Ethiopia Sahilu Wondimu 1, Berhanu Nega 2 1
56 The Surgical Management of Primary Hyperparathyroidism: The Experience in Tikur Anbessa Specialized Tertiary Referral and Teaching Hospital, Addis Ababa, Ethiopia Sahilu Wondimu 1, Berhanu Nega 2 1
25/10/56. Hypothyroidism Myxedema in adults Cretinism congenital deficiency of thyroid hormone Hashimoto thyroiditis. Simple goiter (nontoxic goiter)
 THERAPEUTIC USES OF THYROID HORMONE Supeecha Wittayalertpunya Wannarasmi Ketchart Nov 2013 Hyperthyroidism (Thyrotoxicosis) Grave s disease (diffuse toxic goiter) Toxic uninodular & Toxic multinodular
THERAPEUTIC USES OF THYROID HORMONE Supeecha Wittayalertpunya Wannarasmi Ketchart Nov 2013 Hyperthyroidism (Thyrotoxicosis) Grave s disease (diffuse toxic goiter) Toxic uninodular & Toxic multinodular
Metabolic Bone Disease (Past, Present and Future Challenges in the Management)
 Metabolic Bone Disease 871 151 Metabolic Bone Disease (Past, Present and Future Challenges in the Management) SNA RIZVI INTRODUCTION The past 40 years have seen some important historical events leading
Metabolic Bone Disease 871 151 Metabolic Bone Disease (Past, Present and Future Challenges in the Management) SNA RIZVI INTRODUCTION The past 40 years have seen some important historical events leading
ORIGINAL ARTICLE. Persistent Parathyroid Hormone Elevation Following Curative Parathyroidectomy for Primary Hyperparathyroidism
 Persistent Parathyroid Hormone Elevation Following Curative Parathyroidectomy for Primary Hyperparathyroidism Elizabeth A. Mittendorf, MD; Christopher R. McHenry, MD ORIGINAL ARTICLE Background: Persistent
Persistent Parathyroid Hormone Elevation Following Curative Parathyroidectomy for Primary Hyperparathyroidism Elizabeth A. Mittendorf, MD; Christopher R. McHenry, MD ORIGINAL ARTICLE Background: Persistent
Endocrine Regulation of Calcium and Phosphate Metabolism
 Endocrine Regulation of Calcium and Phosphate Metabolism Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C516, Block C, Research Building, School of Medicine Tel: 88208252 Email: wanghuiping@zju.edu.cn
Endocrine Regulation of Calcium and Phosphate Metabolism Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C516, Block C, Research Building, School of Medicine Tel: 88208252 Email: wanghuiping@zju.edu.cn
Case Report A Reference Finding Rarely Seen in Primary Hyperparathyroidism: Brown Tumor
 Case Reports in Medicine Volume 2012, Article ID 432676, 4 pages doi:10.1155/2012/432676 Case Report A Reference Finding Rarely Seen in Primary Hyperparathyroidism: Brown Tumor F. Mantar, 1 S. Gunduz,
Case Reports in Medicine Volume 2012, Article ID 432676, 4 pages doi:10.1155/2012/432676 Case Report A Reference Finding Rarely Seen in Primary Hyperparathyroidism: Brown Tumor F. Mantar, 1 S. Gunduz,
Index. Bacterial infection of joint, immobilization
 Index ADP (Adenosine diphosphate), 65--Q6 Ambulation, early or postoperative, 8 Anemia, pressure sore formation in, 113-114 Antagonist muscles, 72 Arteriovenous shunting, bed rest and, 27-28 ATP (Adenosine
Index ADP (Adenosine diphosphate), 65--Q6 Ambulation, early or postoperative, 8 Anemia, pressure sore formation in, 113-114 Antagonist muscles, 72 Arteriovenous shunting, bed rest and, 27-28 ATP (Adenosine
Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff.
 Authoriser: Fiona Davidson Page 1 of 5 Hypercalcaemia Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff. Mild (usually no symptoms) 2.6 3.0 mmol/l Moderate
Authoriser: Fiona Davidson Page 1 of 5 Hypercalcaemia Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff. Mild (usually no symptoms) 2.6 3.0 mmol/l Moderate
Sensipar. Sensipar (cinacalcet) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.46 Subject: Sensipar Page: 1 of 5 Last Review Date: June 22, 2018 Sensipar Description Sensipar (cinacalcet)
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.46 Subject: Sensipar Page: 1 of 5 Last Review Date: June 22, 2018 Sensipar Description Sensipar (cinacalcet)
GASTRIC FUNCTION IN PRIMARY HYPERPARATHYROIDISM IN MAN. Mary G. McGeown and A. M. Connell
 GASTRIC FUNCTION IN PRIMARY HYPERPARATHYROIDISM IN MAN Mary G. McGeown and A. M. Connell The Renal Unit, Belfast City Hospital, Belfast and Department of Internal Medicine, Cincinnati General Hospital,
GASTRIC FUNCTION IN PRIMARY HYPERPARATHYROIDISM IN MAN Mary G. McGeown and A. M. Connell The Renal Unit, Belfast City Hospital, Belfast and Department of Internal Medicine, Cincinnati General Hospital,
Progressive renal failure in surgically treated hyperparathyroidism
 J Clin Pathol 1981 ;34:730-737 Progressive renal failure in surgically treated hyperparathyroidism JANE DIXON,* JF SMITH From the *Department of Pathology, John Radcliffe Hospital, Headington, Oxford and
J Clin Pathol 1981 ;34:730-737 Progressive renal failure in surgically treated hyperparathyroidism JANE DIXON,* JF SMITH From the *Department of Pathology, John Radcliffe Hospital, Headington, Oxford and
17. CALCIUM AND PHOSPHOROUS METABOLISM. Calcium. Role of calcium ROLE OF CALCIUM STORAGE. Calcium movement
 17. CALCIUM AND PHOSPHOROUS METABOLISM Many physiological processes are regulated directly or indirectly by calcium. Furthermore, the main physical structure of vertebrates and other species depend on
17. CALCIUM AND PHOSPHOROUS METABOLISM Many physiological processes are regulated directly or indirectly by calcium. Furthermore, the main physical structure of vertebrates and other species depend on
The relief of bone pain in primary biliary cirrhosis with calcium infusions
 Gut, 1974, 15, 788-793 The relief of bone pain in primary biliary cirrhosis with calcium infusions A. B. AJDUKIEWICZ, J. E. AGNEW, P. D. BYERS, M. R. WILLS1, AND SHEILA SHERLOCK From the Departments of
Gut, 1974, 15, 788-793 The relief of bone pain in primary biliary cirrhosis with calcium infusions A. B. AJDUKIEWICZ, J. E. AGNEW, P. D. BYERS, M. R. WILLS1, AND SHEILA SHERLOCK From the Departments of
SUMMARY OF PRODUCT CHARACTERISTICS
 SUMMARY OF PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Colecalciferol Meda 800 IU tablet 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Each tablet contains colecalciferol (vitamin D 3 ) 800 IU
SUMMARY OF PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Colecalciferol Meda 800 IU tablet 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Each tablet contains colecalciferol (vitamin D 3 ) 800 IU
Hypocalcemia 6/8/12. Normal value. Physiologic functions. Nephron a functional unit of kidney. Influencing factors in Calcium and Phosphate Balance
 Normal value Hypocalcemia Serum calcium Total mg/dl Ionized mg/dl Cord blood 9.0 ~ 11.5 5.0 ~ 6.o New born (1 st 24 hrs) 9.0 ~ 10.6 4.3 ~ 5.1 24~ 48 hrs 7.0 ~12.0 4.0 ~4.7 Child 8.8 ~10.8 4.8 ~4.92 There
Normal value Hypocalcemia Serum calcium Total mg/dl Ionized mg/dl Cord blood 9.0 ~ 11.5 5.0 ~ 6.o New born (1 st 24 hrs) 9.0 ~ 10.6 4.3 ~ 5.1 24~ 48 hrs 7.0 ~12.0 4.0 ~4.7 Child 8.8 ~10.8 4.8 ~4.92 There
20. CALCIUM AND PHOSPHOROUS METABOLISM
 20. CALCIUM AND PHOSPHOROUS METABOLISM Many physiological processes are regulated directly or indirectly by calcium. Furthermore, the main physical structure of vertebrates and other species depend on
20. CALCIUM AND PHOSPHOROUS METABOLISM Many physiological processes are regulated directly or indirectly by calcium. Furthermore, the main physical structure of vertebrates and other species depend on
THE ASSOCIATION OF PRIMARY HYPERPARATHYROIDISM WITH DISORDERS OF THE THYROID GLAND AND CARPENTRY OUR EXPERIENCE
 24 MEDICINSKI GLASNIK / str. 24-30 Snežana Marinković, Nenad Laketić 1 THE ASSOCIATION OF PRIMARY HYPERPARATHYROIDISM WITH DISORDERS OF THE THYROID GLAND AND CARPENTRY OUR EXPERIENCE Introduction Primary
24 MEDICINSKI GLASNIK / str. 24-30 Snežana Marinković, Nenad Laketić 1 THE ASSOCIATION OF PRIMARY HYPERPARATHYROIDISM WITH DISORDERS OF THE THYROID GLAND AND CARPENTRY OUR EXPERIENCE Introduction Primary
Hths 2231 Laboratory 13 Alterations in Musculoskeletal
 Watch Movie: Osteoporosis Answer the movie questions on the worksheet. Complete activities 1-4. Activity #1: Click on the website link in activity 1 to review the structure and function of bone. Activity
Watch Movie: Osteoporosis Answer the movie questions on the worksheet. Complete activities 1-4. Activity #1: Click on the website link in activity 1 to review the structure and function of bone. Activity
PHOSPHORUS CONTENT OF THE BLOOD IN DIABETES
 10 BLOOD PHOSPHORUS IN HEALTH AND DISEASE: IV-THE PHOSPHORUS CONTENT OF THE BLOOD IN DIABETES MELLITUS F B BYROM From the Dunn Laboratories, London Hospital Received for publication November 24th, 1928
10 BLOOD PHOSPHORUS IN HEALTH AND DISEASE: IV-THE PHOSPHORUS CONTENT OF THE BLOOD IN DIABETES MELLITUS F B BYROM From the Dunn Laboratories, London Hospital Received for publication November 24th, 1928
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: testing_serum_vitamin_d_levels 9/2015 2/2018 2/2019 2/2018 Description of Procedure or Service Vitamin D,
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: testing_serum_vitamin_d_levels 9/2015 2/2018 2/2019 2/2018 Description of Procedure or Service Vitamin D,
Chapter 5: Evaluation and treatment of kidney transplant bone disease Kidney International (2009) 76 (Suppl 113), S100 S110; doi: /ki.2009.
 http://www.kidney-international.org & 2009 KDIGO Chapter 5: Evaluation and treatment of kidney transplant bone disease ; doi:10.1038/ki.2009.193 Grade for strength of recommendation a Strength Wording
http://www.kidney-international.org & 2009 KDIGO Chapter 5: Evaluation and treatment of kidney transplant bone disease ; doi:10.1038/ki.2009.193 Grade for strength of recommendation a Strength Wording
Osteoporosis. When we talk about osteoporosis, we have to be familiar with the constituents of bone and what it is formed of.
 Osteoporosis When we talk about osteoporosis, we have to be familiar with the constituents of bone and what it is formed of. Osteoblasts by definition are those cells present in the bone and are involved
Osteoporosis When we talk about osteoporosis, we have to be familiar with the constituents of bone and what it is formed of. Osteoblasts by definition are those cells present in the bone and are involved
Case Report Rare Skeletal Complications in the Setting of Primary Hyperparathyroidism
 Case Reports in Endocrinology Volume 2015, Article ID 139751, 4 pages http://dx.doi.org/10.1155/2015/139751 Case Report Rare Skeletal Complications in the Setting of Primary Hyperparathyroidism Nikos Sabanis,
Case Reports in Endocrinology Volume 2015, Article ID 139751, 4 pages http://dx.doi.org/10.1155/2015/139751 Case Report Rare Skeletal Complications in the Setting of Primary Hyperparathyroidism Nikos Sabanis,
Case 4 Generalised bone pain
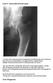 Case 4 Generalised bone pain C A 34- year- old woman presented complaining of multifocal pain in her chest and legs. The pain was intermittent, was aggravated by weight bearing. Initially was alleviated
Case 4 Generalised bone pain C A 34- year- old woman presented complaining of multifocal pain in her chest and legs. The pain was intermittent, was aggravated by weight bearing. Initially was alleviated
Skeletal. Parathyroid hormone-related protein Analyte Information
 Skeletal Parathyroid hormone-related protein Analyte Information 1 2012-04-04 Parathyroid hormone related protein (PTHrP) Introduction Parathyroid hormone-related protein (PTHrP) is actually a family of
Skeletal Parathyroid hormone-related protein Analyte Information 1 2012-04-04 Parathyroid hormone related protein (PTHrP) Introduction Parathyroid hormone-related protein (PTHrP) is actually a family of
PRIMARY HYPERPARATHYROIDISM WITH RICKETS. KRITHIKA.P Dr.L.N.Padmasani Unit 1 Sri Ramachandra Medical College
 PRIMARY HYPERPARATHYROIDISM WITH RICKETS KRITHIKA.P Dr.L.N.Padmasani Unit 1 Sri Ramachandra Medical College Presenting Complaints v 17 year old developmentally normal adolescent boy, first of a twin pregnancy,
PRIMARY HYPERPARATHYROIDISM WITH RICKETS KRITHIKA.P Dr.L.N.Padmasani Unit 1 Sri Ramachandra Medical College Presenting Complaints v 17 year old developmentally normal adolescent boy, first of a twin pregnancy,
(From the Department of Biochemistry, McGill University, Montreal.)
 385 6I2.492.8:6I2.466.6I THE EFFECT OF ANTERIOR PITUITARY EXTRACTS ON ACETONE BODY EXCRETION IN THE RAT. BY PETER T. BLACK, J. B. COLLIP AND D. L. THOMSON. (From the Department of Biochemistry, McGill
385 6I2.492.8:6I2.466.6I THE EFFECT OF ANTERIOR PITUITARY EXTRACTS ON ACETONE BODY EXCRETION IN THE RAT. BY PETER T. BLACK, J. B. COLLIP AND D. L. THOMSON. (From the Department of Biochemistry, McGill
Clodronate BE/H/PSUR/001/001 October 2011 Agreed CSP
 Clodronate BE/H/PSUR/001/001 October 2011 Agreed CSP 4. CLINICAL PARTICULARS 4.1 Therapeutic indications Intravenous use Treatment of hypercalcemia due to malignancy. Oral use Treatment of hypercalcemia
Clodronate BE/H/PSUR/001/001 October 2011 Agreed CSP 4. CLINICAL PARTICULARS 4.1 Therapeutic indications Intravenous use Treatment of hypercalcemia due to malignancy. Oral use Treatment of hypercalcemia
