Catastrophic antiphospholipid syndrome: first signs in the neonatal period
|
|
|
- Timothy Page
- 5 years ago
- Views:
Transcription
1 DOI /s SHORT REPORT Catastrophic antiphospholipid syndrome: first signs in the neonatal period Marta Cabral & Clara Abadesso & Marta Conde & Helena Almeida & Helena Carreiro Received: 14 June 2011 /Accepted: 2 August 2011 # Springer-Verlag 2011 Abstract The term catastrophic antiphospholipid syndrome (CAPS) is used to define a subset of the antiphospholipid syndrome (APS) characterized by the clinical evidence of three or more organ involvement by thrombotic events in a short period of time and with laboratory confirmation of the presence of antiphospholipid antibodies. We describe a male infant first admitted at 17 days old for necrotizing enteritis complicated by cardiac and renal failure. Because of progressive renal function deterioration, a renal biopsy was performed at 8 months old, and histopathologic examination was compatible with renal venous thrombosis. Laboratory searching for vascular, prothrombotic, and metabolic disease was M. Conde Pediatric Rheumatology Clinics, Department of Pediatrics, mssr.cabral@gmail.com C. Abadesso : H. Almeida Pediatric Intensive Care Unit, Department of Pediatrics, H. Carreiro Department of Pediatrics, Present Address: M. Cabral (*) Pediatric Rheumatology Clinics, Department of Pediatrics, mssr.cabral@gmail.com negative. Five months later, he developed two different episodes (20-day range) of ischemic stroke. Genetic test for thrombophilic conditions was positive for two different mutations, and repeatedly high titers of lupus anticoagulant, anticardiolipin, and anti-β2glicoprotein I antibodies were found. He was treated successfully with anticoagulants and showed a favorable clinical evolution. To the best of our knowledge, this is the youngest patient reported with probable CAPS. Although rare, APS/CAPS in the neonatal period or in the first year of life must be suspected in infants presenting with thrombotic phenomena. The present case illustrates the importance of an early diagnosis and treatment to enhance possibilities of survival. Keywords Catastrophic. Antiphospholipid. Syndrome. Thrombosis. Infant Introduction The antiphospholipid syndrome (APS) is a noninflammatory autoimmune disorder characterized by the association of thrombotic phenomena and/or recurrent fetal loss, in combination with elevated titers of antiphospholipid (apl) antibodies [11]. The Sapporo criteria are the most acceptable diagnostic criteria for APS, and its last revision (2006) defines one clinical criterion and one laboratory criterion for its definite diagnosis (Table 1). Despite the strong association between apl antibodies and thrombosis, its pathogenic role in the development of thrombosis has not been fully elucidated [9]. These antibodies are not always pathogenic and can be present in several situations, for example, infections, autoimmune diseases, tumors, and even in 3 4% of healthy individuals, without being related to thrombotic phenomena [7]. An unusual
2 Table 1 Revised classification criteria for the antiphospholipid syndrome (2006) Antiphospholipid antibody syndrome (APS) is present if at least one of the clinical criteria and one of the laboratory criteria that follow are met Clinical criteria (1) Vascular thrombosis One or more clinical episodes of arterial, venous, or small vessel thrombosis in any tissue or organ. Thrombosis must be confirmed by objective validated criteria (i.e., unequivocal findings of appropriate imaging studies or histopathology). For histopathologic confirmation, thrombosis should be present without significant evidence of inflammation in the vessel wall. (2) Pregnancy morbidity (a) One or more unexplained deaths of a morphologically normal fetus at or beyond the 10th week of gestation, with normal fetal morphology documented by ultrasound or by direct examination of the fetus, or (b) One or more premature births of a morphologically normal neonate before the 34th week of gestation because of: eclampsia or severe preeclampsia defined according to standard definitions, or recognized features of placental insufficiency, or (c) Three or more unexplained consecutive spontaneous abortions before the 10th week of gestation, with maternal anatomic or hormonal abnormalities and paternal and maternal chromosomal causes excluded Laboratory criteria (1) Lupus anticoagulant (LA) present in plasma, on two or more occasions, at least 12 weeks apart, detected according to the guidelines of the International Society on Thrombosis and Haemostasis (Scientific Subcommittee on Las/phospholipid-dependent antibodies) (2) Anticardiolipin (Acl) antibody of IgG and/or IgM isotype in serum or plasma, present in medium or high titer (> the 99th percentile), on two or more occasions, at least 12 weeks apart, measured by a standardized ELISA (3) Anti-β2 glycoprotein-i antibody of IgG and/or IgM isotype in serum or plasma present in medium or high titer (> the 99th percentile), on two or more occasions, at least 12 weeks apart, measured by a standardized ELISA, according to recommended procedures Classification of APS should be avoided if less than 12 weeks or more than 5 years separate the positive apl test and the clinical manifestation. Coexisting inherited or acquired factors for thrombosis are not reasons for excluding patients from APS trials variant of the APS, termed the catastrophic antiphospholipid syndrome (CAPS), was first described by Asherson in 1992, and represents the extreme end of the APS spectrum, resulting in multiorgan failure [4, 18]. Although CAPS represents 0.8 1% of all patients with APS, it is usually a life-threatening medical situation that requires high clinical awareness [4]. The diagnosis of CAPS is based on the preliminary criteria for its classification, defined by the international consensus statement in 2003 (Table 2) [4]. Thrombotic events may present in patients as a free-standing condition (primary APS) or be associated with other autoimmune diseases, most commonly systemic lupus erythematosus (SLE; secondary APS) [5, 10, 12, 18, 20]. There are no prospective studies because of the rarity of the condition, and CAPS treatment is not currently standardized [4], but anticoagulation, corticosteroids, plasma exchange, intravenous gammaglobulins, and immunosuppressant agents are the most commonly used therapies [7]. Despite adequate therapy, the mortality remains high, approximately 50%, with cardiac problems as the main cause. Once recovery has ensued, patients usually have a stable course, but require continued anticoagulation [2]. A recent study has documented that 66% of CAPS patients who have survived the initial catastrophic event had remained symptom free for an average follow-up of 62.7 months, and 26% developed further APS-related events; however, there were no instances of further catastrophic events [8]. Because of pediatric CAPS rarity, only individual case reports or small case series have been reported in the literature and, therefore, few information exist on the pediatric aspects and long-term outcomeofthisdisorder[6, 10]. Case report We present a male, caucasian neonate from healthy nonconsanguineous parents, labor and delivery at 36th week of pregnancy, 50th percentile for weight and height, and Apgar score of 7/9. He was first admitted to the hospital emergency care at 17 days old with irritability, marked abdominal distension with tenderness, vomiting and bloody stool, and signs of shock (delayed capillary refill, persistent tachycardia, and hypotension). Laboratory findings include hemoglobin (Hgb) 15.6 g/dl, 22,700 leukocytes/mm 3, 500,000 platelets/mm 3, C-reactive protein (CRP) 1.26 mg/dl, and metabolic acidosis (ph, 7.0; HCO3, 12 mmol/l; alkaline excess, 18 mmol/l; lactate, 12.7 mmol/l). The abdominal ultrasonography showed increased amounts of intraperitoneal non-loculated purulent fluid and markedly distended small bowel loops. After stabilization in the intensive care unit, an exploratory laparotomy was performed. Extensive small bowel necrosis was found, and resection was made with ileostomies. The histopathology was compatible with the small bowel s transmural infarction (necrotizing enteritis). After surgery, septic shock evolved to multiorgan failure, with severe hypotension, cardiac dysfunction, and profound laboratory abnormalities (Hgb, 9.3 g/dl; 2,200 leukocytes/mm 3 ; 53,000 platelets/mm 3 ; CRP, 35 mg/dl; and
3 Table 2 Criteria for the classification of catastrophic APS by international consensus statement on classification criteria and treatment guidelines (2003) (1) Evidence of involvement of three or more organs, systems, and/or tissues a (2) Development of manifestations simultaneously or in less than a week (3) Confirmation by histopathology of small vessel occlusion in at least one organ or tissue b (4) Laboratory confirmation of the presence of antiphospholipid antibodies (lupus anticoagulant and/or anticardiolipin antibodies) c Definite catastrophic APS All four criteria Probable catastrophic APS All four criteria, except for only two organs, systems, and/or tissues involvement All four criteria, except for the absence of laboratory confirmation at least 6 weeks apart due to the early death of a patient never tested for apl before the catastrophic APS 1, 2, and 4 1, 3, and 4 and the development of a third event in more than a week but less than a month, despite anticoagulation a Usually, clinical evidence of vessel occlusions, confirmed by imaging techniques when appropriate. Renal involvement is defined by a 50% rise in serum creatinine, severe systemic hypertension (>180/100 mmhg), and/or proteinuria (>500 mg/24 h) b For histopathological confirmation, significant evidence of thrombosis must be present, although vasculitis may coexist occasionally c If the patient had not been previously diagnosed as having an APS, the laboratory confirmation requires that presence of antiphospholipids must be detected on two or more occasions at least 6 weeks apart (not necessarily at the time of the event) disseminated intravascular coagulation with hepatic insufficiency), requiring invasive ventilatory and inotropic support. Blood and intra-abdominal fluid cultures were positive for Escherichia coli. At the fourth day, the patient became stable and 4 weeks later underwent a second surgery to assess for viability of the remaining bowel. Twenty-four hours later, he suddenly developed shock with severe cardiac failure (dilated myocardiopathy with decreased ejection fraction of the left ventricle), with troponin (13.46 ng/ml) and activated partial thromboplastin time (aptt) (>160 s) elevation. After a period of hypotension, he developed severe hypertension and oligoanuric acute renal failure (glomerular filtration rate (GFR), ml/min/1.73 m 2 ) with macroscopic hematuria. The doppler ultrasonography showed an atrophic right kidney with poor corticomedullary differentiation, with its main artery not visualized. The patient required continuous venovenous hemodiafiltration for 20 days. Hypertension (average, 180/110 mmhg) was very difficult to control requiring a combination of eight antihypertensive drugs. The abdominal magnetic resonance (MR) angiography confirmed the right kidney s atrophy with marked hypoperfusion of its main artery, and radionuclide imaging with 99m Tc-MAG3 showed its severe decreased function (7%). Screening for hereditary prothrombotic and metabolic diseases was negative (Table 3). At 6 months old, he was discharged with a delayed growth, controlled hypertension, left ventricle hypertrophy, and mild-to-moderate renal insufficiency (GFR, 32 ml/min/1.73 m 2 ) under conservative treatment. Two months later, right nephrectomy was performed and hypertension stabilized. The histopathology documented a generalized cortical atrophy (Fig. 1), reduction of the main renal vein and its branches lumen by chronic thromboses, with signs of recanalizing thrombi, and histological features of fibrous intimal hyperplasia of the interlobular and small arteries, abnormalities compatible with renal vein thrombosis, thrombotic microangiopathy, and subsequent chronic renal ischemia (Fig. 2). At 13 months old, he presented with focal tonic-clonic seizures and right hemiparesis. Brain CT revealed an acute infarct involving the left frontal, temporal, and parietal lobes, without associated hemorrhage (Fig. 3). He was treated with acetylsalicylic acid 5 mg/kg/day and phenobarbital with improvement, but 20 days later, he developed left hemiparesis de novo accompanied by axial weakness, right eye exophoria, and generalized hyperreflexia. Brain CT and MR angiography showed multiple de novo acute ischemic infarcts in the frontal, right temporal, and parietal lobes (Fig. 3). Intracardiac, carotid, and vertebral arteries thrombus/masses were excluded by doppler ultrasonography. Subcutaneous low-molecular-weight heparin (LMWH) 1 mg/kg/day was added. At that time, genetic test for thrombophilias showed two different mutations: heterozygosity for prothrombin gene mutation (PT 20210G>A) and homozygosity for plasminogen activator inhibitor-1 gene mutation (PAI-1 675G>A). Immunologic studies revealed positive antinuclear antibody (ANA) titer 1/640 and positive anticardiolipin (acl; 1.8 U/mL (<1.1)) and antiβ2glycoprotein I (anti-β2gpi; IgM, 1.0 U/mL; IgG, 25.1 U/mL (<20)) antibodies (Table 3). Erythrocyte sedimentation rate was 22 mm/1sth. At 24 months old, immunologic studies demonstrated persistent positive ANA titer 1/640, mild positive lupus
4 Table 3 Laboratory searching for prothrombotic, autoimmune, and metabolic diseases and its evolution Metabolic disease Ammonia, pyruvate, lactate, carnitine and acylcarnitine, uric acid, purine and pyrimidine blood levels, quantitation of plasma and Normal/negative urinary amino acids, organic acids and mucopolysaccharides, redox potential, genetic test for Williams syndrome, and muscular biopsy Prothrombotic disease Patient s age Units (reference values) (months) PT (max.) s (10 14) aptt (max) > > > seconds ( ) D-dimers (max) μg/l (<190) Protein C % (40 92) Protein S % (33 69) Factor V Leiden % (50 150) PAI U/ml ( ) Antithrombin III % (82 139) Homocysteine 9.88 μmol/l (5 12) Factor VII 70 % (70 130) Factor VIII 113 % (50 150) Lupus anticoagulant s (<45) acp ab total titer 1, U/mL (positive, total titer >1.1, or IgM or IgG >15) IgM IgG Anti-β2GPI ab IgM U/mL (positive, IgM or IgG >10) IgG 25.1 > Autoimmune disease ANA 1/640 1/640 Neg 1/640 Neg 1/320 Neg 1/160 Anti-dsDNA, anti- Neg Neg Neg Neg Neg Neg Neg Neg SM, anti-rnp, anti-ssa, anti- SSB and ANCA antibodies C3, C4, CH50 Normal Normal PT prothrombin time, aptt activated partial thromboplastin time, PAI-1 plasminogen activator inhibitor type 1, acp ab anticardiolipin IgG antibodies, Anti-β2GPI ab anti-β2glicoproteini antibodies, ANA antinuclear antibody, ANCA anti-neutrophil cytoplasm, Neg negative
5 a Fig. 1 Generalized cortical atrophy, with preservation of glomerular structures (fetal isotype) in more than 2/3 of the cortical thickness b anticoagulant (LA) (screening test, 47.3 s (<45); confirmatory test, 32.4 s (<38)), and positive acl (5.4 U/mL) and anti-β2gpi (IgM, 2 U/mL; IgG, >150 U/mL) antibodies. Three months later, LA, acl, and anti-β2gpi antibodies became negative. At that time, the patient s mother, previously healthy and with no previous history of fetal losses or thromboembolic events, was tested negative for immunologic studies, including apl antibodies. Additionally, there was no family history of thrombotic disorders or fetal losses. A retrospective diagnosis of probable CAPS was made. The clinical evolution was favorable, and after 5 years of follow-up, the patient is asymptomatic while anticoagulated (LMWH), despite intermittent laboratory signs of disease s activity (Table 3) and the residual sequelae: developmental delay, systemic hypertension, and mild renal insufficiency. c Discussion In children, the frequency of apl-related thrombotic events is generally lower than in adults, but several common infections are likely responsible for higher percentage of nonpathogenic and transient apl antibodies in childhood [6]. Nevertheless, most of the clinical features that occur in adults with apl antibodies have also been described in children [6]. In pediatrics, the incidence peak for thrombotic events occurs in the neonate. The use of central catheter, asphyxia, septicemia, and dehydration are major risk factors for thrombosis in most studies [19]. We believe that the first thrombotic event, and the first manifestation of APS in this patient, was the small bowel s transmural infarction, which took place during his first month of life. Both thrombosis and APS should be a differential diagnosis Fig. 2 a, b Reduction of the main renal vein and its branches lumen by chronic thromboses, with signs of recanalizing thrombi, c histological features of fibrous intimal hyperplasia of interlobular and small arteries, abnormalities compatible with renal vein thrombosis, thrombotic microangiopathy, and subsequent chronic renal ischemia on necrotizing enterocolitis (NEC) at that time, but it was initially assigned to the prematurity, even being a near-term infant. Although more common in premature infants, NEC
6 Fig. 3 a Acute infarct involving the left frontal, temporal, and parietal lobes, without associated hemorrhage, b multiple de novo acute ischemic infarcts in the frontal, right temporal, and parietal lobes a b can occur in term and near-term babies, being its incidence inversely associated to birth weight and gestational age [21]. Unfortunately, apl antibodies were not performed but, retrospectively, we can reasonably suspect they were already present at that time. Considering this episode as the first manifestation of CAPS in this patient, and to the best of our knowledge, this is the youngest patient (17 days old) with probable CAPS [13, 17]. According to Asherson, precipitant factors for APS have been recognized in 45% of patients, most commonly infections (20%). Other trigger factors that have been reported include trauma and surgical procedures (14%), drugs (5%), or autoimmune diseases flares (3%) [2]. In this patient, possible precipitant factors could have been: (1) infection/septic shock preceding the small bowel s infarction, (2) the last surgery, and therapeutic procedures he was submitted during septic shock preceding right renal vein thrombosis. Both vascular cerebral accidents were not related to an apparent trigger factor. Special concern is needed when dealing with aplpositive children who have other congenital or acquired prothrombotic risks, and APS patients should be stratified according to that [6, 16]. This patient had both central lines and a positive prothrombin gene and PAI-1 mutations, which probably contributed as additional risk factors for thrombosis, as it was seen in another infantile APS published recently [14]. The diagnosis of CAPS is still controversial because of its recent description and the few number of cases reported [4]. Clinically, the patients present predominantly with small vessel occlusions involving parenchymal organs, but large vessel occlusive disease can also occur [2]. In a series of 50 patients with CAPS, Asherson et al. reported that the kidney (78%), lung (66%), and central nervous system (56%) are the most affected organs [1, 18]. In our patient, two of these main groups of organs were affected. Hypertension is a well-documented complication of APS and CAPS. In the series reported by Nochy et al., hypertension was present in 93% of the APS patients; in some of them, it was the only clinical sign of nephropathy, and it can be very difficult to treat [22], as was seen in our patient. In case of kidney involvement, good control of systemic hypertension and adequate anticoagulation may have important prognostic implications in preventing progression to end-stage renal disease [22]. In our patient, nephrectomy of the atrophic kidney was necessary to control hypertension because anticoagulation was postponed until thrombosis has been confirmed by histopathology. Several other clinical features are relatively common in these patients, predominantly during disease s acute phase, such as thrombocytopenia, seizures, mesenteric inflammatory vaso-occlusive disease with secondary small bowel infarctation, intrarenal vascular lesions (thrombotic microangiophaty), livedo reticularis, or hemolytic anemia [3, 11, 15, 20]. The first four of these recognized manifestations associated with CAPS were present in our patient. The clinical features depend on which organs are affected and on the extent of thrombosis [2]. Because of tissue necrosis, excessive cytokine release leads to a systemic inflammatory response accountable for some of the CAPS non-thrombotic manifestations, particularly the acute respiratory distress syndrome (ARDS) and myocardial dysfunction [2]. Our patient never had ARDS, but myocardial dysfunction complicated by acute cardiac collapse was present. The preliminary criteria for CAPS classification define probable and definite CAPS (Table 2) [4]. Definite CAPS is considered when all four criteria are met. Our patient presented as a probable CAPS with three of the four defined criteria: three-organ involvement (small bowel, right kidney, and brain), histopathologic evidence of thrombosis (renal vein thrombosis), and positive acp and anti-β2gpi antibodies on two occasions at least 6 weeks apart. The occurrence of different thrombotic episodes
7 simultaneously or in less than 1 week was not recognized. However, Asherson et al. emphasized that these criteria are mostly empirical, have been accepted for classification purposes, and are not intended to be used as strict diagnostic criteria in a given patient [4]. We believe that our patient s apl antibodies (acl and anti-β2gpi) had been produced de novo by himself instead of transplacental passage of antibodies from his mother [19], who was tested negative for apl antibodies. Additionally, serum patient s determination occurred when a maternal origin for these antibodies would be improbable (14 and 24 months old). Lack of prospective and randomized treatment trials has led to considerable debate on the appropriate management of children with CAPS [6]. It has three clear aims: to treat any identifiable precipitating factor, to prevent and treat the ongoing thrombotic events, and to suppress the excessive cytokine storm [4, 7]. There is a general agreement that long-term anticoagulation is needed in a child who experienced an apl-related thrombosis to prevent recurrences, but there is no consensus about the duration and intensity of this therapy [6]. In regard to this patient, the hypertension and the renal failure were considered a consequence of the unexpected renal vein thrombosis in the first months of life, but his neurologic sequelae could have been avoided with an earlier diagnosis. Nevertheless, after 5 years of follow-up under anticoagulation, he had no more thrombotic events. It is essential to start treatment as soon as this condition is suspected [7], and we think that the non-progressing clinical evolution in this patient was the result of an appropriate treatment initiated as soon as the diagnosis was established. Finally, although rare, CAPS in neonatal period or in the first year of life must be suspected in infants presenting with thrombotic phenomena, even if they have been born from a mother without SLE or APS [19]. Conflict of interest competing interests. References The authors declare that they have no 1. Asherson R (1998) Catastrophic antiphospholipid syndrome. Clinical and laboratory features of 50 patients. Medicine (Balt) 77: Asherson R (2005) The catastrophic antiphospholipid (Asherson s) syndrome in 2004 a review. Autoimmun Rev 4: Asherson R, Cervera R (2003) The antiphospholipid syndrome: multiple faces beyond the classical presentation. Autoimmun Rev 2: Asherson R, Cervera R, Groot P, Erkan D, Boffa M, Piette J et al (2003) Catastrophic antiphospholipid syndrome: international consensus statement on classification criteria and treatment guidelines. Lupus 12: Asherson RA, Khamashta MA, Ordi-Ros J, Derksen RH, Machin SJ, Barquinero J, Outt HH, Harris EN, Vilardell- Torres M, Hughes GR (1989) The primary antiphospholipid syndrome: major clinical and serological features. Medicine (Balt) 68: Avcin T, Cimaz R, Meroni PL (2002) Recent advances in antiphospholipid antibodies and antiphospholipid syndromes in pediatric populations. Lupus 11: Campos L, Kiss M, D Amico E, Silva C (2003) Antiphospholipid antibodies and antiphospholipid syndrome in 57 children and adolescents with systemic lupus erythematosus. Lupus 12: Erkan D, Asherson RA, Espinosa G, Cervera R, Font J, Piette JC, Lockshin MD (2003) Long-term outcome of catastrophic antiphospholipid syndrome survivors. Ann Rheum Dis 62: Espinosa G, Cervera R, Font J, Shoenfeld Y (2003) Antiphospholipid syndrome: pathogenic mechanisms. Autoimmun Rev 2: Gattorno M, Falcini F, Ravelli A, Zulian F, Buoncompagni A, Martini G, Resti M, Picco P, Martini A (2003) Outcome of primary antiphospholipid syndrome in childhood. Lupus 12: Hanly J (2003) Antiphospholipid syndrome: an overview. CMAJ 168: Harris E, Pierangeli S (2004) Primary, secondary, catastrophic antiphospholipid syndrome: is there a difference? Thromb Res 114: Iglesias-Jiménez E, Camacho-Lovillo M, Falcón-Neyra D, Lirola-Cruz J, Neth O (2010) Infant with probable catastrophic antiphospholipid syndrome successfully managed with rituximab. Pediatrics 125: Kim H, Hwang H, Chae J, Kim K, Hwang Y, Lim B (2010) Ischemic stroke in a 7-month old infant with antiphospholipid antibody and homozygous c677t MTHFR polymorphism. Journal Child Neurol 25: Krause I, Blank M, Fraser A, Lorber M, Stojanovich L, Rovensky J, Shoenfeld Y (2005) The association of thrombocytopenia with systemic manifestations in the antiphospholipid syndrome. Immunobiology 210: Miyakis S, Lockshin M, Atsumi T, Branch D, Brey R, Cervera R, Derksen RH, de Groot PG, Koike T, Meroni PL, Reber G, Shoenfeld Y, Tincani A, Vlachoyiannopoulos PG, Krilis SA (2006) International consensus statement on an update of the classification criteria for definite antiphospholipid syndrome (APS). J Thromb Haemost 4: Navarrete N, Macías P, Jaén F, Hidalgo C, Cáliz R, Jiménez- Alonso R (2005) Two cases of catastrophic antiphospholipid syndrome. Lupus 14: Olguin-Ortega L, Jara LJ, Becerra M, Ariza R, Espinoza L, Wilson W, Barile-Fabris L (2003) Neurological involvement as a poor prognostic factor in catastrophic antiphospholipid syndrome: autopsy findings in 12 cases. Lupus 12: Rolim S, Castro M, Santiago M (2006) Neonatal antiphospholipid syndrome. Lupus 15: Soltész P, Veres K, Lakos G, Kiss E, Muszbek L, Szegedi G (2003) Evaluation of clinical and laboratory features of antiphospholipid syndrome: a retrospective study of 637 patients. Lupus 12: Springer S, Annibale D (2011) Title of subordinate document. In: Pediatric necrotizing enterocolitis. Medscape reference. Available via DIALOG overview of subordinate document. Accessed 21 July Uthman I, Khamashta M (2006) Antiphospholipid syndrome and the kidneys. Semin Arthritis Rheum 35:
Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria
 Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria Farjah H AlGahtani Associate professor,md,mph Leukemia,Lymphoma in adolescent,thromboembolic
Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria Farjah H AlGahtani Associate professor,md,mph Leukemia,Lymphoma in adolescent,thromboembolic
Mortality in the Catastrophic Antiphospholipid Syndrome
 ARTHRITIS & RHEUMATISM Vol. 54, No. 8, August 2006, pp 2568 2576 DOI 10.1002/art.22018 2006, American College of Rheumatology Mortality in the Catastrophic Antiphospholipid Syndrome Causes of Death and
ARTHRITIS & RHEUMATISM Vol. 54, No. 8, August 2006, pp 2568 2576 DOI 10.1002/art.22018 2006, American College of Rheumatology Mortality in the Catastrophic Antiphospholipid Syndrome Causes of Death and
Sindrome da anticorpi antifosfolipidi: clinica e terapia. Vittorio Pengo Clinical Cardiology, Padova, Italy
 Sindrome da anticorpi antifosfolipidi: clinica e terapia Vittorio Pengo Clinical Cardiology, Padova, Italy Revised Classification Criteria for the Antiphospholipid Syndrome J Thromb Haemost 2006;4:295-306
Sindrome da anticorpi antifosfolipidi: clinica e terapia Vittorio Pengo Clinical Cardiology, Padova, Italy Revised Classification Criteria for the Antiphospholipid Syndrome J Thromb Haemost 2006;4:295-306
Prevalence of antiphospholipid auto antibodies in patients with thrombosis
 EUROPEAN ACADEMIC RESEARCH Vol. IV, Issue 6/ September 2016 ISSN 2286-4822 www.euacademic.org Impact Factor: 3.4546 (UIF) DRJI Value: 5.9 (B+) Prevalence of antiphospholipid auto antibodies in patients
EUROPEAN ACADEMIC RESEARCH Vol. IV, Issue 6/ September 2016 ISSN 2286-4822 www.euacademic.org Impact Factor: 3.4546 (UIF) DRJI Value: 5.9 (B+) Prevalence of antiphospholipid auto antibodies in patients
SWISS SOCIETY OF NEONATOLOGY. Neonatal cerebral infarction
 SWISS SOCIETY OF NEONATOLOGY Neonatal cerebral infarction May 2002 2 Mann C, Neonatal and Pediatric Intensive Care Unit, Landeskrankenhaus und Akademisches Lehrkrankenhaus Feldkirch, Austria Swiss Society
SWISS SOCIETY OF NEONATOLOGY Neonatal cerebral infarction May 2002 2 Mann C, Neonatal and Pediatric Intensive Care Unit, Landeskrankenhaus und Akademisches Lehrkrankenhaus Feldkirch, Austria Swiss Society
Are there still any valid indications for thrombophilia screening in DVT?
 Carotid artery stenosis and risk of stroke Are there still any valid indications for thrombophilia screening in DVT? Armando Mansilha MD, PhD, FEBVS Faculty of Medicine of University of Porto Munich, 2016
Carotid artery stenosis and risk of stroke Are there still any valid indications for thrombophilia screening in DVT? Armando Mansilha MD, PhD, FEBVS Faculty of Medicine of University of Porto Munich, 2016
ORIGINAL PAPERS. Marek Cieśla 1, B D, Ewa Wypasek 1, 2, B D 1, 2, A, E, F. Abstract
 ORIGINAL PAPERS Adv Clin Exp Med 2014, 23, 5, 729 733 ISSN 1899 5276 Copyright by Wroclaw Medical University Marek Cieśla 1, B D, Ewa Wypasek 1, 2, B D 1, 2, A, E, F, Anetta Undas IgA Antiphospholipid
ORIGINAL PAPERS Adv Clin Exp Med 2014, 23, 5, 729 733 ISSN 1899 5276 Copyright by Wroclaw Medical University Marek Cieśla 1, B D, Ewa Wypasek 1, 2, B D 1, 2, A, E, F, Anetta Undas IgA Antiphospholipid
Thrombophilia: To test or not to test
 Kenneth Bauer, MD Harvard Medical School, Boston, MA Professor of Medicine VA Boston Healthcare System Chief, Hematology Section Beth Israel Deaconess Medical Center, Boston, MA Director, Thrombosis Clinical
Kenneth Bauer, MD Harvard Medical School, Boston, MA Professor of Medicine VA Boston Healthcare System Chief, Hematology Section Beth Israel Deaconess Medical Center, Boston, MA Director, Thrombosis Clinical
Key words: antiphospholipid syndrome, trombosis, pathogenesis
 26. XI,. 4/2011,.,..,..,., -..,,. 2GPI. -,.,,., -,, -, -,,,,, IL-1, IL-2, IL-6, IL-8, IL-12, IL-10, TNF, INF-. :,, N. Stoilov, R. Rashkov and R. Stoilov. ANTIPHOSPHOLIPID SYNDROME HISTORICAL DATA, ETI-
26. XI,. 4/2011,.,..,..,., -..,,. 2GPI. -,.,,., -,, -, -,,,,, IL-1, IL-2, IL-6, IL-8, IL-12, IL-10, TNF, INF-. :,, N. Stoilov, R. Rashkov and R. Stoilov. ANTIPHOSPHOLIPID SYNDROME HISTORICAL DATA, ETI-
Current View of the Treatment of Antiphospholipid Syndrome
 GROUPE HOSPITALIER PITIE SALPETRIERE Current View of the Treatment of Antiphospholipid Syndrome Pr Zahir AMOURA Department of Internal Medicine French National Reference center for SLE and APS Hôpital
GROUPE HOSPITALIER PITIE SALPETRIERE Current View of the Treatment of Antiphospholipid Syndrome Pr Zahir AMOURA Department of Internal Medicine French National Reference center for SLE and APS Hôpital
Antiphospholipid Syndrome Handbook
 Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, Oier Ateka-Barrutia, and Munther A. Khamashta Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, MD, PhD Lupus Research Unit The Rayne
Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, Oier Ateka-Barrutia, and Munther A. Khamashta Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, MD, PhD Lupus Research Unit The Rayne
CASE REPORT. Malgorzata Biernacka-Zielinska, Joanna Lipinska, Joanna Szymanska-Kaluza, Jerzy Stanczyk and Elzbieta Smolewska *
 Biernacka-Zielinska et al. Journal of Medical Case Reports 2013, 7:221 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Recurrent arterial and venous thrombosis in a 16- year-old boy in the course
Biernacka-Zielinska et al. Journal of Medical Case Reports 2013, 7:221 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Recurrent arterial and venous thrombosis in a 16- year-old boy in the course
The Antiphospholipid Syndrome
 The Antiphospholipid Syndrome 1 / 6 2 / 6 3 / 6 The Antiphospholipid Syndrome Antiphospholipid antibody syndrome (commonly called antiphospholipid syndrome or APS) is an autoimmune disease present mostly
The Antiphospholipid Syndrome 1 / 6 2 / 6 3 / 6 The Antiphospholipid Syndrome Antiphospholipid antibody syndrome (commonly called antiphospholipid syndrome or APS) is an autoimmune disease present mostly
Thrombophilia. Stephan Moll, MD Medicine, Heme-Coag UNC Chapel Hill, NC. GASCO Atlanta Sept 8 th, Disclosures. Conflicts of interest: NONE
 LA APLA 1 3 ACA Anti-ß2-GP I 2 45 Thrombophilia Stephan Moll, MD Medicine, Heme-Coag UNC Chapel Hill, NC GASCO Atlanta Sept 8 th, 2017 Disclosures Conflicts of interest: NONE Off-label product use discussion:
LA APLA 1 3 ACA Anti-ß2-GP I 2 45 Thrombophilia Stephan Moll, MD Medicine, Heme-Coag UNC Chapel Hill, NC GASCO Atlanta Sept 8 th, 2017 Disclosures Conflicts of interest: NONE Off-label product use discussion:
Thrombophilia. Diagnosis and Management. Kevin P. Hubbard, DO, FACOI
 Thrombophilia Diagnosis and Management Kevin P. Hubbard, DO, FACOI Clinical Professor of Medicine Kansas City University of Medicine and Biosciences-College of Osteopathic Medicine Kansas City, Missouri
Thrombophilia Diagnosis and Management Kevin P. Hubbard, DO, FACOI Clinical Professor of Medicine Kansas City University of Medicine and Biosciences-College of Osteopathic Medicine Kansas City, Missouri
Should infants with perinatal thrombosis be screened for thrombophilia and treated by anticoagulants?
 Should infants with perinatal thrombosis be screened for thrombophilia and treated by anticoagulants? Shoshana Revel-Vilk, MD MSc Pediatric Hematology Center, Pediatric Hematology/Oncology Department,
Should infants with perinatal thrombosis be screened for thrombophilia and treated by anticoagulants? Shoshana Revel-Vilk, MD MSc Pediatric Hematology Center, Pediatric Hematology/Oncology Department,
AN INTERESTING CASE OF RESPIRATORY DISTRESS. Dr.V.Akila Devi DNB PG Southern Railway Headquarters Hospital Chennai
 AN INTERESTING CASE OF RESPIRATORY DISTRESS Dr.V.Akila Devi DNB PG Southern Railway Headquarters Hospital Chennai 11 month old female infant 1 st born to parents of NC marriage referred from Kolkatta H/O:
AN INTERESTING CASE OF RESPIRATORY DISTRESS Dr.V.Akila Devi DNB PG Southern Railway Headquarters Hospital Chennai 11 month old female infant 1 st born to parents of NC marriage referred from Kolkatta H/O:
Anti β 2. -Glycoprotein I and Antiphosphatidylserine Antibodies Are Predictors of Arterial Thrombosis in Patients With Antiphospholipid Syndrome
 Coagulation and Transfusion Medicine / PREDICTIVE VALUE OF ANTIPHOSPHOLIPID ANTIBODIES Anti β -Glycoprotein I and Antiphosphatidylserine Antibodies Are Predictors of Arterial Thrombosis in Patients With
Coagulation and Transfusion Medicine / PREDICTIVE VALUE OF ANTIPHOSPHOLIPID ANTIBODIES Anti β -Glycoprotein I and Antiphosphatidylserine Antibodies Are Predictors of Arterial Thrombosis in Patients With
A Case of Antiphospholipid Syndrome Refractory to Secondary Anticoagulating Prophylaxis after Deep Vein Thrombosis- Pulmonary Embolism
 CASE REPORT http://dx.doi.org/10.4046/trd.2014.77.6.274 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2014;77:274-278 A Case of Antiphospholipid Syndrome Refractory to Secondary Anticoagulating
CASE REPORT http://dx.doi.org/10.4046/trd.2014.77.6.274 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2014;77:274-278 A Case of Antiphospholipid Syndrome Refractory to Secondary Anticoagulating
THROMBOPHILIA SCREENING
 THROMBOPHILIA SCREENING Introduction The regulation of haemostasis Normally, when a clot occurs, it exactly occurs where it has to be and does not grow more than necessary due to the action of the haemostasis
THROMBOPHILIA SCREENING Introduction The regulation of haemostasis Normally, when a clot occurs, it exactly occurs where it has to be and does not grow more than necessary due to the action of the haemostasis
Review Article. Catastrophic Antiphospholipid Syndrome. Introduction. Etiopathogenesis. Man-Chi Leung and Woon-Leung Ng
 Review Article Catastrophic Antiphospholipid Syndrome Man-Chi Leung and Woon-Leung Ng Abstract: Keywords: The catastrophic antiphospholipid syndrome is a potentially life threatening rheumatological condition
Review Article Catastrophic Antiphospholipid Syndrome Man-Chi Leung and Woon-Leung Ng Abstract: Keywords: The catastrophic antiphospholipid syndrome is a potentially life threatening rheumatological condition
Case Report Lower Limb Ischemia: Aortoiliac Thrombosis Related to Antiphospholipid Syndrome (APS) Case Report and Review of the Literature
 Case Reports in Surgery Volume 2013, Article ID 536971, 4 pages http://dx.doi.org/10.1155/2013/536971 Case Report Lower Limb Ischemia: Aortoiliac Thrombosis Related to Antiphospholipid Syndrome (APS) Case
Case Reports in Surgery Volume 2013, Article ID 536971, 4 pages http://dx.doi.org/10.1155/2013/536971 Case Report Lower Limb Ischemia: Aortoiliac Thrombosis Related to Antiphospholipid Syndrome (APS) Case
Catastrophic antiphospholipid syndrome: A rare but serious complication of antiphospholipid antibody syndrome Sandhu VK*; Singh H
 Open Journal of Clinical & Medical Case Reports Volume 3 (2017) Issue 4 ISSN 2379-1039 Catastrophic antiphospholipid syndrome: A rare but serious complication of antiphospholipid antibody syndrome Sandhu
Open Journal of Clinical & Medical Case Reports Volume 3 (2017) Issue 4 ISSN 2379-1039 Catastrophic antiphospholipid syndrome: A rare but serious complication of antiphospholipid antibody syndrome Sandhu
Some renal vascular disorders
 Some renal vascular disorders Introduction Nearly all diseases of the kidney involve the renal blood vessels secondarily We will discuss: -Hypertension (arterionephrosclerosis in benign HTN & hyperplastic
Some renal vascular disorders Introduction Nearly all diseases of the kidney involve the renal blood vessels secondarily We will discuss: -Hypertension (arterionephrosclerosis in benign HTN & hyperplastic
Thrombophilia. Dr. A Sarrafnejad PhD Dep. Immunology School of public health TUMS
 Autoimmune Thrombophilia Dr. A Sarrafnejad PhD Dep. Immunology School of public health TUMS Saraf@sina.tums.ac.ir Acquired Thrombophilia HIT PNH Cyckle cell Anemia Myeloproliferative lf Diseases Thrombocytosis
Autoimmune Thrombophilia Dr. A Sarrafnejad PhD Dep. Immunology School of public health TUMS Saraf@sina.tums.ac.ir Acquired Thrombophilia HIT PNH Cyckle cell Anemia Myeloproliferative lf Diseases Thrombocytosis
VTE in Children: Practical Issues
 VTE in Children: Practical Issues Wasil Jastaniah MBBS,FAAP,FRCPC Consultant Pediatric Hem/Onc/BMT May 2012 Top 10 Reasons Why Pediatric VTE is Different 1. Social, ethical, and legal implications. 2.
VTE in Children: Practical Issues Wasil Jastaniah MBBS,FAAP,FRCPC Consultant Pediatric Hem/Onc/BMT May 2012 Top 10 Reasons Why Pediatric VTE is Different 1. Social, ethical, and legal implications. 2.
AMPLIADO SÍNDROME ANTIFOSFOLÍPIDO SÍNDROME DE SJÖGREN María José Cuadrado Lozano Clínica Universidad de Navarra-Madrid
 AMPLIADO SÍNDROME ANTIFOSFOLÍPIDO SÍNDROME DE SJÖGREN María José Cuadrado Lozano Clínica Universidad de Navarra-Madrid PLASMABLAST PROLIFERATION IS ASSOCIATED WITH TLR7 POLYMORPHISMS AND UPREGULATION OF
AMPLIADO SÍNDROME ANTIFOSFOLÍPIDO SÍNDROME DE SJÖGREN María José Cuadrado Lozano Clínica Universidad de Navarra-Madrid PLASMABLAST PROLIFERATION IS ASSOCIATED WITH TLR7 POLYMORPHISMS AND UPREGULATION OF
CLINICAL CASE PRESENTATION
 European Winter School of Internal Medicine 2015 Riga, Latvia, 26-30 January CLINICAL CASE PRESENTATION Vasiliy Chulkov South Ural State Medical University (Chelyabinsk, Russia) CHELYABINSK CLINICAL HISTORY
European Winter School of Internal Medicine 2015 Riga, Latvia, 26-30 January CLINICAL CASE PRESENTATION Vasiliy Chulkov South Ural State Medical University (Chelyabinsk, Russia) CHELYABINSK CLINICAL HISTORY
Središnja medicinska knjižnica
 Središnja medicinska knjižnica Jelušić M., Starčević K., Vidović M., Dobrota S., Potočki K., Banfić Lj., Anić B. (2013) Familial antiphospholipid syndrome presenting as bivessel arterial occlusion in a
Središnja medicinska knjižnica Jelušić M., Starčević K., Vidović M., Dobrota S., Potočki K., Banfić Lj., Anić B. (2013) Familial antiphospholipid syndrome presenting as bivessel arterial occlusion in a
Lupus anticoagulant and anticardiolipin antibodies in SLE with secondary Antiphospholipid Antibody Syndrome
 Turk J Hematol 2007; 24:69-74 Turkish Society of Hematology RESEARCH ARTICLE Lupus anticoagulant and anticardiolipin antibodies in SLE with secondary Antiphospholipid Antibody Syndrome Shveta Garg, Annamma
Turk J Hematol 2007; 24:69-74 Turkish Society of Hematology RESEARCH ARTICLE Lupus anticoagulant and anticardiolipin antibodies in SLE with secondary Antiphospholipid Antibody Syndrome Shveta Garg, Annamma
Rituximab. B Cell Inhibition in APS. Methods. B Cell Inhibition in APS. Disclosure 11/6/2011
 Rituximab in Antiphospholipid Syndrome (RITAPS) A Pilot Open-Label Phase II Prospective Trial for Non-Criteria Manifestations of Antiphospholipid Antibodies (NCT: 00537290) Disclosure Research Support:
Rituximab in Antiphospholipid Syndrome (RITAPS) A Pilot Open-Label Phase II Prospective Trial for Non-Criteria Manifestations of Antiphospholipid Antibodies (NCT: 00537290) Disclosure Research Support:
Antiphospholipid Syndrome
 Antiphospholipid Syndrome EliA Cardiolipin and EliA β2-glycoprotein I Fully Automated Testing for Antiphospholipid Syndrome (APS) Testing for APS according to classification criteria determination of anti-β2-glycoprotein
Antiphospholipid Syndrome EliA Cardiolipin and EliA β2-glycoprotein I Fully Automated Testing for Antiphospholipid Syndrome (APS) Testing for APS according to classification criteria determination of anti-β2-glycoprotein
PD Dr. med. habil. Michaela Jaksch, Consultant Laboratory Medicine, Medical Director, Freiburg Medical Laboratory ME LLC, Dubai, UAE
 Autoimmune Disorders in Gynecology/Obstetrics PD Dr. med. habil. Michaela Jaksch, Consultant Laboratory Medicine, Medical Director, Freiburg Medical Laboratory ME LLC, Dubai, UAE Abstract The spectrum
Autoimmune Disorders in Gynecology/Obstetrics PD Dr. med. habil. Michaela Jaksch, Consultant Laboratory Medicine, Medical Director, Freiburg Medical Laboratory ME LLC, Dubai, UAE Abstract The spectrum
Anaesthesiologic management of a parturient with a known antiphospholipid syndrome
 Anaesthesiologic management of a parturient with a known antiphospholipid syndrome Pascal Vuilleumier Universitätsklinik für Anästhesie und Schmerztherapie Case presentation: Mrs A. B. 1975 Early monday
Anaesthesiologic management of a parturient with a known antiphospholipid syndrome Pascal Vuilleumier Universitätsklinik für Anästhesie und Schmerztherapie Case presentation: Mrs A. B. 1975 Early monday
DISCLOSURE. Presented by: Merav Sendowski, MD Oregon Health and Science University
 Thrombophilia! DISCLOSURE Presented by: Merav Sendowski, MD Oregon Health and Science University Created by: Thomas Deloughery, MD Oregon Health and Science University Current Relevant Financial Relationship(s)
Thrombophilia! DISCLOSURE Presented by: Merav Sendowski, MD Oregon Health and Science University Created by: Thomas Deloughery, MD Oregon Health and Science University Current Relevant Financial Relationship(s)
monoclonal gammopathy of undetermin Citation Rheumatology international, 33(1),
 NAOSITE: Nagasaki University's Ac Title Author(s) Renal thrombotic microangiopathies/ in a patient with primary Sjögren's monoclonal gammopathy of undetermin Koga, Tomohiro; Yamasaki, Satoshi; Atsushi;
NAOSITE: Nagasaki University's Ac Title Author(s) Renal thrombotic microangiopathies/ in a patient with primary Sjögren's monoclonal gammopathy of undetermin Koga, Tomohiro; Yamasaki, Satoshi; Atsushi;
A Case of Massive Pulmonary Embolism in Systemic Lupus Erythematosus without Antiphospholipid Antibody
 Journal of Rheumatic Diseases Vol. 22, No. 2, April, 2015 http://dx.doi.org/10.4078/jrd.2015.22.2.106 Case Report A Case of Massive Pulmonary Embolism in Systemic Lupus Erythematosus without Antiphospholipid
Journal of Rheumatic Diseases Vol. 22, No. 2, April, 2015 http://dx.doi.org/10.4078/jrd.2015.22.2.106 Case Report A Case of Massive Pulmonary Embolism in Systemic Lupus Erythematosus without Antiphospholipid
1. INSTRUCTIONS 2. DEFINITION OF HUS
 CQ_IBK_aHUS_01 / version 25/11/09 European Paediatric Research Group for HUS and related disorders Case questionnaire for diarrhoea negative/vtec (STEC) negative cases acute phase 1. INSTRUCTIONS Please
CQ_IBK_aHUS_01 / version 25/11/09 European Paediatric Research Group for HUS and related disorders Case questionnaire for diarrhoea negative/vtec (STEC) negative cases acute phase 1. INSTRUCTIONS Please
February 2016, Volume: 8, Issue: 2, Pages: , DOI:
 Electronic Physician (ISSN: 2008-5842) http://www.ephysician.ir February 2016, Volume: 8, Issue: 2, Pages: 1874-1879, DOI: http://dx.doi.org/10.19082/1874 Pulmonary embolism in an adolescent girl with
Electronic Physician (ISSN: 2008-5842) http://www.ephysician.ir February 2016, Volume: 8, Issue: 2, Pages: 1874-1879, DOI: http://dx.doi.org/10.19082/1874 Pulmonary embolism in an adolescent girl with
Clinical and immunological characteristics of antiphospholipid syndrome in an Asian population: a retrospective study
 Asian Pacific Journal of Allergy and Immunology ORIGINAL ARTICLE Clinical and immunological characteristics of antiphospholipid syndrome in an Asian population: a retrospective study Kanon Jatuworapruk,
Asian Pacific Journal of Allergy and Immunology ORIGINAL ARTICLE Clinical and immunological characteristics of antiphospholipid syndrome in an Asian population: a retrospective study Kanon Jatuworapruk,
Clinical consequences of antiphospholipid antibodies
 Clinical consequences of antiphospholipid antibodies R.H.W.M. Derksen 1*, P.G. de Groot 2,3 1 Department of Rheumatology and Clinical Immunology, Room F02.127, 2 Thrombosis and Haemostasis Laboratory,
Clinical consequences of antiphospholipid antibodies R.H.W.M. Derksen 1*, P.G. de Groot 2,3 1 Department of Rheumatology and Clinical Immunology, Room F02.127, 2 Thrombosis and Haemostasis Laboratory,
Case report 24 th Summer School of Internal Medicine 2015
 Case report 24 th Summer School of Internal Medicine 2015 Goldmannová D., Horák P., Skácelová M. IIIrd Internal Clinic - endocrinology, diabetology, rheumatology, nephrology University hospital Olomouc,
Case report 24 th Summer School of Internal Medicine 2015 Goldmannová D., Horák P., Skácelová M. IIIrd Internal Clinic - endocrinology, diabetology, rheumatology, nephrology University hospital Olomouc,
Arterial Ischemic Stroke with Protein S Deficiency in Pakistan
 Case Reports Arterial Ischemic Stroke with Protein S Deficiency in Pakistan Faika Usman, Ali Hassan, Arsalan Ahmad From Section of Neurology, Department of Medicine, Shifa International Hospitals and College
Case Reports Arterial Ischemic Stroke with Protein S Deficiency in Pakistan Faika Usman, Ali Hassan, Arsalan Ahmad From Section of Neurology, Department of Medicine, Shifa International Hospitals and College
LUPUS CAN DO EVERYTHING, BUT NOT EVERYTHING IS LUPUS LUPUS 101 SLE SUBSETS AUTOIMMUNE DISEASE 11/4/2013 HOWARD HAUPTMAN, MD IDIOPATHIC DISCOID LUPUS
 LUPUS 101 LUPUS CAN DO EVERYTHING, BUT NOT EVERYTHING IS LUPUS HOWARD HAUPTMAN, MD IDIOPATHIC DISCOID LUPUS SLE SUBSETS SUBACUTE CUTANEOUS LUPUS DRUG INDUCED LUPUS NEONATAL LUPUS LATE ONSET LUPUS ANTI-PHOSPHOLIPID
LUPUS 101 LUPUS CAN DO EVERYTHING, BUT NOT EVERYTHING IS LUPUS HOWARD HAUPTMAN, MD IDIOPATHIC DISCOID LUPUS SLE SUBSETS SUBACUTE CUTANEOUS LUPUS DRUG INDUCED LUPUS NEONATAL LUPUS LATE ONSET LUPUS ANTI-PHOSPHOLIPID
HEME 10 Bleeding Disorders
 HEME 10 Bleeding Disorders When injury occurs, three mechanisms occur Blood vessels Primary hemostasis Secondary hemostasis Diseases of the blood vessels Platelet disorders Thrombocytopenia Functional
HEME 10 Bleeding Disorders When injury occurs, three mechanisms occur Blood vessels Primary hemostasis Secondary hemostasis Diseases of the blood vessels Platelet disorders Thrombocytopenia Functional
Antiphospholipid Antibody Syndrome: Management Issues for the Hematologist
 Antiphospholipid Antibody Syndrome: Management Issues for the Hematologist Wisconsin Institute of Discovery Karen Rossi/Bristol-Myers Squibb Morey A. Blinder, MD Washington University, St. Louis, MO March
Antiphospholipid Antibody Syndrome: Management Issues for the Hematologist Wisconsin Institute of Discovery Karen Rossi/Bristol-Myers Squibb Morey A. Blinder, MD Washington University, St. Louis, MO March
Approach to Thrombosis
 Approach to Thrombosis Theera Ruchutrakool, M.D. Division of Hematology Department of Medicine Siriraj Hospital Faculty of Medicine Mahidol University Approach to Thrombosis Thrombosis: thrombus formation
Approach to Thrombosis Theera Ruchutrakool, M.D. Division of Hematology Department of Medicine Siriraj Hospital Faculty of Medicine Mahidol University Approach to Thrombosis Thrombosis: thrombus formation
Case Report Catastrophic Antiphospholipid Syndrome
 Case Reports in Rheumatology Volume 2016, Article ID 4161439, 4 pages http://dx.doi.org/10.1155/2016/4161439 Case Report Catastrophic Antiphospholipid Syndrome Rawhya R. El-Shereef, 1 Zein El-Abedin, 2
Case Reports in Rheumatology Volume 2016, Article ID 4161439, 4 pages http://dx.doi.org/10.1155/2016/4161439 Case Report Catastrophic Antiphospholipid Syndrome Rawhya R. El-Shereef, 1 Zein El-Abedin, 2
Supplemental Figures and Legends
 Supplemental Figures and Legends Online Figure 1. 18 year old female with SLE and acute homonymous hemianopsia, confusional state, and cognitive dysfunction. A. This TEE four chamber view demonstrates
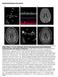
Supplemental Figures and Legends Online Figure 1. 18 year old female with SLE and acute homonymous hemianopsia, confusional state, and cognitive dysfunction. A. This TEE four chamber view demonstrates
Daniel Egan, MD April 13, 2012
 Daniel Egan, MD April 13, 2012 Aug 2006 (at age 15): Acute unprovoked DVT in left common femoral vein Factor V Leiden heterozygous Positive lupus inhibitor Lovenox BID 2 weeks later: increased clot burden,
Daniel Egan, MD April 13, 2012 Aug 2006 (at age 15): Acute unprovoked DVT in left common femoral vein Factor V Leiden heterozygous Positive lupus inhibitor Lovenox BID 2 weeks later: increased clot burden,
Pathophysiology. Tutorial 3 Hemodynamic Disorders
 Pathophysiology Tutorial 3 Hemodynamic Disorders ILOs Recall different causes of thrombosis. Explain different types of embolism and their predisposing factors. Differentiate between hemorrhage types.
Pathophysiology Tutorial 3 Hemodynamic Disorders ILOs Recall different causes of thrombosis. Explain different types of embolism and their predisposing factors. Differentiate between hemorrhage types.
Medical Complications of Pregnancy
 Medical Complications of Pregnancy Systems Cardiovascular Pulmonary Endocrine Gastrointestinal Urologic Neurologic Cardiovascular System Physiologic anemia 3:1 increase of plasma volume:rbc mass Treat
Medical Complications of Pregnancy Systems Cardiovascular Pulmonary Endocrine Gastrointestinal Urologic Neurologic Cardiovascular System Physiologic anemia 3:1 increase of plasma volume:rbc mass Treat
Lupus Anticoagulants (LA), Antiphospholipid (APL) Antibodies & APL Syndrome: Review & Update. Antiphospholipid. Antiphospholipid
 , Antiphospholipid (APL) Antibodies & APL Syndrome: Review & Update William L. Nichols, MD Mayo Clinic College of Medicine Rochester, Minnesota USA Disclosures & Objectives (Nichols) Disclosures Relevant
, Antiphospholipid (APL) Antibodies & APL Syndrome: Review & Update William L. Nichols, MD Mayo Clinic College of Medicine Rochester, Minnesota USA Disclosures & Objectives (Nichols) Disclosures Relevant
Thursday, February 26, :00 am. Regulation of Coagulation/Disseminated Intravascular Coagulation HEMOSTASIS/THROMBOSIS III
 REGULATION OF COAGULATION Introduction HEMOSTASIS/THROMBOSIS III Regulation of Coagulation/Disseminated Coagulation necessary for maintenance of vascular integrity Enough fibrinogen to clot all vessels
REGULATION OF COAGULATION Introduction HEMOSTASIS/THROMBOSIS III Regulation of Coagulation/Disseminated Coagulation necessary for maintenance of vascular integrity Enough fibrinogen to clot all vessels
Acta Medica Okayama. Catastrophic secondary antiphospholipid syndrome with peripheral nervous system involvement: a case report.
 Acta Medica Okayama Volume 58, Issue 2 2004 Article 7 APRIL 2004 Catastrophic secondary antiphospholipid syndrome with peripheral nervous system involvement: a case report. Nilgun Erten Bulent Saka M Akif
Acta Medica Okayama Volume 58, Issue 2 2004 Article 7 APRIL 2004 Catastrophic secondary antiphospholipid syndrome with peripheral nervous system involvement: a case report. Nilgun Erten Bulent Saka M Akif
Genetic Tests for the Better Outcome of VTE? 서울대학교병원혈액종양내과윤성수
 Genetic Tests for the Better Outcome of VTE? 서울대학교병원혈액종양내과윤성수 Thrombophilia A hereditary or acquired disorder predisposing to thrombosis Questions Why should we test? Who should we test For what disorders?
Genetic Tests for the Better Outcome of VTE? 서울대학교병원혈액종양내과윤성수 Thrombophilia A hereditary or acquired disorder predisposing to thrombosis Questions Why should we test? Who should we test For what disorders?
ISTITUTO DI RICERCHE FARMACOLOGICHE MARIO NEGRI CLINICAL RESEARCH CENTER ALDO E FOR CELE RARE DACCO DISEASES ALDO E CELE DACCO
 ISTITUTO DI RICERCHE FARMACOLOGICHE MARIO NEGRI CENTRO MARIO DI NEGRI RICERCHE INSTITUTE CLINICHE FOR PHARMACOLOGICAL PER LE MALATTIE RESEARCH RARE CLINICAL RESEARCH CENTER ALDO E FOR CELE RARE DACCO DISEASES
ISTITUTO DI RICERCHE FARMACOLOGICHE MARIO NEGRI CENTRO MARIO DI NEGRI RICERCHE INSTITUTE CLINICHE FOR PHARMACOLOGICAL PER LE MALATTIE RESEARCH RARE CLINICAL RESEARCH CENTER ALDO E FOR CELE RARE DACCO DISEASES
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Lapeyraque A-L, Malina M, Fremeaux-Bacchi V, et al. Eculizumab
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Lapeyraque A-L, Malina M, Fremeaux-Bacchi V, et al. Eculizumab
EDUCATIONAL COMMENTARY DISSEMINATED INTRAVASCULAR COAGULATION
 EDUCATIONAL COMMENTARY DISSEMINATED INTRAVASCULAR COAGULATION Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE
EDUCATIONAL COMMENTARY DISSEMINATED INTRAVASCULAR COAGULATION Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE
THROMBOSIS RISK FACTOR ASSESSMENT
 Name: Procedure: Doctor: Date: THROMBOSIS RISK FACTOR ASSESSMENT CHOOSE ALL THAT APPLY EACH RISK FACTOR REPRESENTS 1 POINT Age 41 60 years Minor Surgery Planned History of Prior Major Surgery (< 1 month)
Name: Procedure: Doctor: Date: THROMBOSIS RISK FACTOR ASSESSMENT CHOOSE ALL THAT APPLY EACH RISK FACTOR REPRESENTS 1 POINT Age 41 60 years Minor Surgery Planned History of Prior Major Surgery (< 1 month)
THROMBOPHILIA TESTING: PROS AND CONS SHANNON CARPENTER, MD MS CHILDREN S MERCY HOSPITAL KANSAS CITY, MO
 THROMBOPHILIA TESTING: PROS AND CONS SHANNON CARPENTER, MD MS CHILDREN S MERCY HOSPITAL KANSAS CITY, MO DISCLAIMER I m a pediatrician I will be discussing this issue primarily from a pediatric perspective
THROMBOPHILIA TESTING: PROS AND CONS SHANNON CARPENTER, MD MS CHILDREN S MERCY HOSPITAL KANSAS CITY, MO DISCLAIMER I m a pediatrician I will be discussing this issue primarily from a pediatric perspective
PS + MPs PS - MPs 37% 36% 64% 64%
 Supplementary Figure 1. Amount and distribution of phosphatidylserine negative (PS - ) and phosphatidylserine positive (PS + ) MPs in 280 SLE patients and 280 controls. Circles are proportional to the
Supplementary Figure 1. Amount and distribution of phosphatidylserine negative (PS - ) and phosphatidylserine positive (PS + ) MPs in 280 SLE patients and 280 controls. Circles are proportional to the
Anticardiolipin Antibodies in Patients With Type 2 Diabetes Mellitus
 CM&R Rapid Release. Published online ahead of print February 26, 2009 as doi:10.3121/cmr.2008.828 Original Research Anticardiolipin Antibodies in Patients With Type 2 Diabetes Mellitus José María Calvo-Romero,
CM&R Rapid Release. Published online ahead of print February 26, 2009 as doi:10.3121/cmr.2008.828 Original Research Anticardiolipin Antibodies in Patients With Type 2 Diabetes Mellitus José María Calvo-Romero,
THROMBOTIC MICROANGIOPATHY. Jun-Ki Park 7/19/11
 THROMBOTIC MICROANGIOPATHY Jun-Ki Park 7/19/11 TMAs are microvascular occlusive disorders characterized by systemic or intrarenal aggregation of platelets, thrombocytopenia, and mechanical injury to erythrocytes.
THROMBOTIC MICROANGIOPATHY Jun-Ki Park 7/19/11 TMAs are microvascular occlusive disorders characterized by systemic or intrarenal aggregation of platelets, thrombocytopenia, and mechanical injury to erythrocytes.
Clinical features of Antiphospholipid syndrome (APS) Panayiotis G. Vlachoyiannopoulos MD Medical School National University of Athens 2005
 Clinical features of Antiphospholipid syndrome (APS) Panayiotis G. Vlachoyiannopoulos MD Medical School National University of Athens 2005 Antiphospholipid Syndrome: Definition Recurrent arterial and/or
Clinical features of Antiphospholipid syndrome (APS) Panayiotis G. Vlachoyiannopoulos MD Medical School National University of Athens 2005 Antiphospholipid Syndrome: Definition Recurrent arterial and/or
The complex treatment including rituximab in the Management of Catastrophic Antiphospholid Syndrome with renal involvement
 Rymarz and Niemczyk BMC Nephrology (2018) 19:132 https://doi.org/10.1186/s12882-018-0928-z CASE REPORT Open Access The complex treatment including rituximab in the Management of Catastrophic Antiphospholid
Rymarz and Niemczyk BMC Nephrology (2018) 19:132 https://doi.org/10.1186/s12882-018-0928-z CASE REPORT Open Access The complex treatment including rituximab in the Management of Catastrophic Antiphospholid
Lung diseases of Vascular Origin. By: Shefaa Qa qqa
 Lung diseases of Vascular Origin By: Shefaa Qa qqa Pulmonary Hypertension Pulmonary hypertension is defined as a mean pulmonary artery pressure greater than or equal to 25 mm Hg at rest. Based on underlying
Lung diseases of Vascular Origin By: Shefaa Qa qqa Pulmonary Hypertension Pulmonary hypertension is defined as a mean pulmonary artery pressure greater than or equal to 25 mm Hg at rest. Based on underlying
Antiphospholipid antibodies
 CARDIOLOGY PATIENT PAGE CARDIOLOGY PATIENT PAGE Antiphospholipid Antibodies Caron P. Misita, PharmD; Stephan Moll, MD Antiphospholipid antibodies (APLAs) are proteins that may be present in the blood and
CARDIOLOGY PATIENT PAGE CARDIOLOGY PATIENT PAGE Antiphospholipid Antibodies Caron P. Misita, PharmD; Stephan Moll, MD Antiphospholipid antibodies (APLAs) are proteins that may be present in the blood and
SWISS SOCIETY OF NEONATOLOGY. Spontaneous intestinal perforation or necrotizing enterocolitis?
 SWISS SOCIETY OF NEONATOLOGY Spontaneous intestinal perforation or necrotizing enterocolitis? June 2004 2 Stocker M, Berger TM, Neonatal and Pediatric Intensive Care Unit, Children s Hospital of Lucerne,
SWISS SOCIETY OF NEONATOLOGY Spontaneous intestinal perforation or necrotizing enterocolitis? June 2004 2 Stocker M, Berger TM, Neonatal and Pediatric Intensive Care Unit, Children s Hospital of Lucerne,
Case Report Catastrophic Antiphospholipid Syndrome Presenting as Bilateral Central Retinal Artery Occlusions
 Hindawi Publishing Corporation Case Reports in Ophthalmological Medicine Volume 2015, Article ID 206906, 5 pages http://dx.doi.org/10.1155/2015/206906 Case Report Catastrophic Antiphospholipid Syndrome
Hindawi Publishing Corporation Case Reports in Ophthalmological Medicine Volume 2015, Article ID 206906, 5 pages http://dx.doi.org/10.1155/2015/206906 Case Report Catastrophic Antiphospholipid Syndrome
OPEN ACCESS TEXTBOOK OF GENERAL SURGERY
 OPEN ACCESS TEXTBOOK OF GENERAL SURGERY MESENTERIC ISCHAEMIA P Zwanepoel INTRODUCTION Mesenteric ischaemia results from hypoperfusion of the gut, most commonly due to occlusion, thrombosis or vasospasm.
OPEN ACCESS TEXTBOOK OF GENERAL SURGERY MESENTERIC ISCHAEMIA P Zwanepoel INTRODUCTION Mesenteric ischaemia results from hypoperfusion of the gut, most commonly due to occlusion, thrombosis or vasospasm.
PURPOSE SCIENTIFIC QUESTIONS. How the prevalence of the nine different apl varies among the different age groups of patients with SLE?
 Project plan The prevalence of IgG, IgM, and IgA antibodies against cardiolipin, β2-glycoprotein I and domain I of β2-glycoprotein I in a large cohort of patients with Systemic Lupus Erythematosus and
Project plan The prevalence of IgG, IgM, and IgA antibodies against cardiolipin, β2-glycoprotein I and domain I of β2-glycoprotein I in a large cohort of patients with Systemic Lupus Erythematosus and
Guidelines for management of stroke in childhood
 Guidelines for management of stroke in childhood A clinical syndrome typified by rapidly developing signs of focal or global disturbance of cerebral functions, lasting more than 24 hrs or leading to death,
Guidelines for management of stroke in childhood A clinical syndrome typified by rapidly developing signs of focal or global disturbance of cerebral functions, lasting more than 24 hrs or leading to death,
Catastrophic antiphospholipid syndrome: how to diagnose a rare but highly fatal disease
 502919TAB5610.1177/1759720X13502919Therapeutic Advances in Musculoskeletal DiseaseCL Aguiar and D Erkan 2013502919 Therapeutic Advances in Musculoskeletal Disease Review Catastrophic antiphospholipid syndrome:
502919TAB5610.1177/1759720X13502919Therapeutic Advances in Musculoskeletal DiseaseCL Aguiar and D Erkan 2013502919 Therapeutic Advances in Musculoskeletal Disease Review Catastrophic antiphospholipid syndrome:
9/25/2013 SYSTEMIC LUPUS ERYTHEMATOSUS (SLE)
 SYSTEMIC LUPUS ERYTHEMATOSUS (SLE) 1 Other Types of Lupus Discoid Lupus Erythematosus Lupus Pernio --- Sarcoidosis Lupus Vulgaris --- Tuberculosis of the face Manifestations of SLE Fever Rashes Arthritis
SYSTEMIC LUPUS ERYTHEMATOSUS (SLE) 1 Other Types of Lupus Discoid Lupus Erythematosus Lupus Pernio --- Sarcoidosis Lupus Vulgaris --- Tuberculosis of the face Manifestations of SLE Fever Rashes Arthritis
Year 2004 Paper one: Questions supplied by Megan
 QUESTION 53 Endothelial cell pathology on renal biopsy is most characteristic of which one of the following diagnoses? A. Pre-eclampsia B. Haemolytic uraemic syndrome C. Lupus nephritis D. Immunoglobulin
QUESTION 53 Endothelial cell pathology on renal biopsy is most characteristic of which one of the following diagnoses? A. Pre-eclampsia B. Haemolytic uraemic syndrome C. Lupus nephritis D. Immunoglobulin
Evaluation of antiphospholipid antibodies testing for the diagnosis of antiphospholipid syndrome
 Original Article Evaluation of antiphospholipid antibodies testing for the diagnosis of antiphospholipid syndrome Paula Gonçalves Perches¹, Daniela Pezzutti Domingues¹, Andréia Latanza Gomes², Augusta
Original Article Evaluation of antiphospholipid antibodies testing for the diagnosis of antiphospholipid syndrome Paula Gonçalves Perches¹, Daniela Pezzutti Domingues¹, Andréia Latanza Gomes², Augusta
Sinus and Cerebral Vein Thrombosis
 Sinus and Cerebral Vein Thrombosis A Summary Sinus and cerebral vein clots are uncommon. They can lead to severe headaches, confusion, and stroke-like symptoms. They may lead to bleeding into the surrounding
Sinus and Cerebral Vein Thrombosis A Summary Sinus and cerebral vein clots are uncommon. They can lead to severe headaches, confusion, and stroke-like symptoms. They may lead to bleeding into the surrounding
Case Report Antiphospholipid Syndrome: Multiple Manifestations in a Single Patient A High Suspicion Is Still Needed
 Hindawi Case Reports in Medicine Volume 2017, Article ID 5797041, 4 pages https://doi.org/10.1155/2017/5797041 Case Report Antiphospholipid Syndrome: Multiple Manifestations in a Single Patient A High
Hindawi Case Reports in Medicine Volume 2017, Article ID 5797041, 4 pages https://doi.org/10.1155/2017/5797041 Case Report Antiphospholipid Syndrome: Multiple Manifestations in a Single Patient A High
P-RMS: LT/H/PSUR/0004/001
 Core Safety Profile Active substance: Dalteparine Pharmaceutical form(s)/strength: Solution for injection, 2500 I.U./0.2ml, 2500 I.U./ml, 5000 I.U./0.2ml, 7500 I.U./0.3ml, 7500 I.U./0.75ml, 10000 I.U./0.4ml,
Core Safety Profile Active substance: Dalteparine Pharmaceutical form(s)/strength: Solution for injection, 2500 I.U./0.2ml, 2500 I.U./ml, 5000 I.U./0.2ml, 7500 I.U./0.3ml, 7500 I.U./0.75ml, 10000 I.U./0.4ml,
AUTOIMMUNE DISORDERS IN THE ACUTE SETTING
 AUTOIMMUNE DISORDERS IN THE ACUTE SETTING Diagnosis and Treatment Goals Aimee Borazanci, MD BNI Neuroimmunology Objectives Give an update on the causes for admission, clinical features, and outcomes of
AUTOIMMUNE DISORDERS IN THE ACUTE SETTING Diagnosis and Treatment Goals Aimee Borazanci, MD BNI Neuroimmunology Objectives Give an update on the causes for admission, clinical features, and outcomes of
Systemic Lupus Erythematosus among Jordanians: A Single Rheumatology Unit Experience
 Systemic Lupus Erythematosus among Jordanians: A Single Rheumatology Unit Experience Ala M. AlHeresh MD* ABSTRACT Objectives: To study the characteristics of Systemic Lupus Erythematosus in Jordan and
Systemic Lupus Erythematosus among Jordanians: A Single Rheumatology Unit Experience Ala M. AlHeresh MD* ABSTRACT Objectives: To study the characteristics of Systemic Lupus Erythematosus in Jordan and
Keywords: apl, Hughes syndrome, pregnancy loss, prothrombin, thrombosis. Introduction
 Journal of Thrombosis and Haemostasis, 10: 2512 2518 DOI: 10.1111/jth.12014 ORIGINAL ARTICLE Clinical accuracy for diagnosis of antiphospholipid syndrome in systemic lupus erythematosus: evaluation of
Journal of Thrombosis and Haemostasis, 10: 2512 2518 DOI: 10.1111/jth.12014 ORIGINAL ARTICLE Clinical accuracy for diagnosis of antiphospholipid syndrome in systemic lupus erythematosus: evaluation of
Atypical Subacute Recurrence of Catastrophic Antiphospholipid Syndrome in a Japanese Female Patient
 CASE REPORT Atypical Subacute Recurrence of Catastrophic Antiphospholipid Syndrome in a Japanese Female Patient Masanobu Horikoshi 1, Shigeko Inokuma 1, Erika Matsubara 1, Yasunori Honda 1, Rika Okada
CASE REPORT Atypical Subacute Recurrence of Catastrophic Antiphospholipid Syndrome in a Japanese Female Patient Masanobu Horikoshi 1, Shigeko Inokuma 1, Erika Matsubara 1, Yasunori Honda 1, Rika Okada
You admitted a previously healthy nullipara at 36 weeks gestation who presented with new-onset periorbital edema and is found to have blood pressure
 Preeclampsia Case report You admitted a previously healthy nullipara at 36 weeks gestation who presented with new-onset periorbital edema and is found to have blood pressure readings of 150/100 to 155/105
Preeclampsia Case report You admitted a previously healthy nullipara at 36 weeks gestation who presented with new-onset periorbital edema and is found to have blood pressure readings of 150/100 to 155/105
VENOUS THROMBOEMBOLISM AND CORONARY ARTERY DISEASE: IS THERE A LINK?
 VENOUS THROMBOEMBOLISM AND CORONARY ARTERY DISEASE: IS THERE A LINK? Ayman El-Menyar (1), MD, Hassan Al-Thani (2),MD (1)Clinical Research Consultant, (2) Head of Vascular Surgery, Hamad General Hospital
VENOUS THROMBOEMBOLISM AND CORONARY ARTERY DISEASE: IS THERE A LINK? Ayman El-Menyar (1), MD, Hassan Al-Thani (2),MD (1)Clinical Research Consultant, (2) Head of Vascular Surgery, Hamad General Hospital
Antiphospholipid Syndrome ( APS)
 Antiphospholipid Syndrome ( APS) Edward John Walter Bowie, MD Mayo Medical School the first to identify APS as an acquired thrombophilia Graham Robert Vivian Hughes MD FRCP Unit Rayne Institute St Thomas
Antiphospholipid Syndrome ( APS) Edward John Walter Bowie, MD Mayo Medical School the first to identify APS as an acquired thrombophilia Graham Robert Vivian Hughes MD FRCP Unit Rayne Institute St Thomas
Mabel Labrada, MD Miami VA Medical Center
 Mabel Labrada, MD Miami VA Medical Center *1-Treatment for acute DVT with underlying malignancy is for 3 months. *2-Treatment of provoked acute proximal DVT can be stopped after 3months of treatment and
Mabel Labrada, MD Miami VA Medical Center *1-Treatment for acute DVT with underlying malignancy is for 3 months. *2-Treatment of provoked acute proximal DVT can be stopped after 3months of treatment and
DOWNLOAD OR READ : POSITIVE OPTIONS FOR ANTIPHOSPHOLIPID SYNDROME APS SELF HELP AND TREATMENT PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : POSITIVE OPTIONS FOR ANTIPHOSPHOLIPID SYNDROME APS SELF HELP AND TREATMENT PDF EBOOK EPUB MOBI Page 1 Page 2 positive options for antiphospholipid syndrome aps self help and treatment
DOWNLOAD OR READ : POSITIVE OPTIONS FOR ANTIPHOSPHOLIPID SYNDROME APS SELF HELP AND TREATMENT PDF EBOOK EPUB MOBI Page 1 Page 2 positive options for antiphospholipid syndrome aps self help and treatment
Hematologic Disorders. Assistant professor of anesthesia
 Preoperative Evaluation Hematologic Disorders Dr M.Razavi Assistant professor of anesthesia Anemia Evaluation needs to consider the extent and type of surgery, the anticipated blood loss, and the patient's
Preoperative Evaluation Hematologic Disorders Dr M.Razavi Assistant professor of anesthesia Anemia Evaluation needs to consider the extent and type of surgery, the anticipated blood loss, and the patient's
Most Common Hemostasis Consults: Thrombocytopenia
 Most Common Hemostasis Consults: Thrombocytopenia Cindy Neunert, MS MSCS Assistant Professor, Pediatrics CUMC Columbia University TSHNA Meeting, April 15, 2016 Financial Disclosures No relevant financial
Most Common Hemostasis Consults: Thrombocytopenia Cindy Neunert, MS MSCS Assistant Professor, Pediatrics CUMC Columbia University TSHNA Meeting, April 15, 2016 Financial Disclosures No relevant financial
SWISS SOCIETY OF NEONATOLOGY. Classical presentation of a newborn infant with renal vein thrombosis
 SWISS SOCIETY OF NEONATOLOGY Classical presentation of a newborn infant with renal vein thrombosis December 2017 Wendelspiess M, Schifferli A, Rudin C, Kaempfen S, Department of Neonatology (WM, KS), Department
SWISS SOCIETY OF NEONATOLOGY Classical presentation of a newborn infant with renal vein thrombosis December 2017 Wendelspiess M, Schifferli A, Rudin C, Kaempfen S, Department of Neonatology (WM, KS), Department
Thrombophilia due to Activated Protein C Resistance
 CASE REPORT JIACM 2005; 6(3): 244-7 Thrombophilia due to Activated Protein C Resistance Kamal S Saini*, Mrinal M Patnaik*, Vidya S Nagar**, Alaka K Deshpande*** Abstract Thrombophilia is a hereditary or
CASE REPORT JIACM 2005; 6(3): 244-7 Thrombophilia due to Activated Protein C Resistance Kamal S Saini*, Mrinal M Patnaik*, Vidya S Nagar**, Alaka K Deshpande*** Abstract Thrombophilia is a hereditary or
Diagnosis and Treatment of Deep Venous Thrombosis and Pulmonary Embolism
 Agency for Healthcare Research and Quality Evidence Report/Technology Assessment Diagnosis and Treatment of Deep Venous Thrombosis and Pulmonary Embolism Summary Number 68 Overview Venous thromboembolism
Agency for Healthcare Research and Quality Evidence Report/Technology Assessment Diagnosis and Treatment of Deep Venous Thrombosis and Pulmonary Embolism Summary Number 68 Overview Venous thromboembolism
Antiphospholipid antibody syndrome an overview
 Antiphospholipid antibody syndrome an overview C Sridevi, DNB (Medicine) DNB (Cardiology) MNAMS* P Krishnam Raju, MD DM (Cardiology)* INTRODUCTION Antiphospholipid antibody syndrome (APLAS) was first described
Antiphospholipid antibody syndrome an overview C Sridevi, DNB (Medicine) DNB (Cardiology) MNAMS* P Krishnam Raju, MD DM (Cardiology)* INTRODUCTION Antiphospholipid antibody syndrome (APLAS) was first described
Approach to disseminated intravascular coagulation
 Approach to disseminated intravascular coagulation Khaire Ananta Shankarrao 1, Anil Burley 2, Deshmukh 3 1.MD Scholar, [kayachikitsa] 2.Professor,MD kayachikitsa. 3.Professor and HOD,Kayachikitsa. CSMSS
Approach to disseminated intravascular coagulation Khaire Ananta Shankarrao 1, Anil Burley 2, Deshmukh 3 1.MD Scholar, [kayachikitsa] 2.Professor,MD kayachikitsa. 3.Professor and HOD,Kayachikitsa. CSMSS
Close Association between valvular heart disease and central nervous system manifestations in the antiphospholipid syndrome
 ARD Online First, published on March 18, 2005 as 10.1136/ard.2004.032813 1 Close Association between valvular heart disease and central nervous system manifestations in the antiphospholipid syndrome Category:
ARD Online First, published on March 18, 2005 as 10.1136/ard.2004.032813 1 Close Association between valvular heart disease and central nervous system manifestations in the antiphospholipid syndrome Category:
Purpura fulminans: A rare presentation of antiphospholipid syndrome
 www.edoriumjournals.com CLINICAL IMAGE PEER REVIEWED OPEN ACCESS Purpura fulminans: A rare presentation of antiphospholipid syndrome Ahmed S. Mahmood, Noor Q. Omar, Sudheer Chauhan, Jose Cervantes ABSTRACT
www.edoriumjournals.com CLINICAL IMAGE PEER REVIEWED OPEN ACCESS Purpura fulminans: A rare presentation of antiphospholipid syndrome Ahmed S. Mahmood, Noor Q. Omar, Sudheer Chauhan, Jose Cervantes ABSTRACT
Hemostasis. PHYSIOLOGICAL BLOOD CLOTTING IN RESPONSE TO INJURY OR LEAK no disclosures
 Hemostasis PHYSIOLOGICAL BLOOD CLOTTING IN RESPONSE TO INJURY OR LEAK no disclosures Disorders of Hemostasis - Hemophilia - von Willebrand Disease HEMOPHILIA A defect in the thrombin propagation phase
Hemostasis PHYSIOLOGICAL BLOOD CLOTTING IN RESPONSE TO INJURY OR LEAK no disclosures Disorders of Hemostasis - Hemophilia - von Willebrand Disease HEMOPHILIA A defect in the thrombin propagation phase
SWISS SOCIETY OF NEONATOLOGY. Severe apnea and bradycardia in a term infant
 SWISS SOCIETY OF NEONATOLOGY Severe apnea and bradycardia in a term infant October 2014 2 Walker JH, Arlettaz Mieth R, Däster C, Division of Neonatology, University Hospital Zurich, Switzerland Swiss Society
SWISS SOCIETY OF NEONATOLOGY Severe apnea and bradycardia in a term infant October 2014 2 Walker JH, Arlettaz Mieth R, Däster C, Division of Neonatology, University Hospital Zurich, Switzerland Swiss Society
