Welcome to Renal- Redwood and Beech Ward! A Junior Doctors Guide
|
|
|
- Lesley Simpson
- 5 years ago
- Views:
Transcription
1 Welcome to Renal- Redwood and Beech Ward! A Junior Doctors Guide
2 Contents Contents E rror! Bookmark not defined. Introduction..3 The Team 3 The Typical Week and investigations. 4 Clinics. 5 Renal investigations. 6
3 Introduction Welcome to the Renal Unit of Darent Valley Hospital! The Unit shares beds on Redwood ward ( mainly AKI, Dialysis and transplant patients) and on Beech ward ( mainly Aki, general medicine patients). We share Redwood with our Urology colleagues and Beech with our Diabetes and Endocrinology colleagues. This guide will hopefully give you all the essential information and tools you need in order for you to have a great time and learning experience with us. The Team Dr Nihil Chitalia - Consultant Nephrologist Dr Andrew Coutinho - Consultant Nephrologist Dr Noshaba Khiljee- Consultant in Acute Medicine and Nephrology Dr Jonathan Kwan - Consultant Nephrologist Dr Nang Aye- Renal specialist CT level doctor Foundation Year doctor x 2
4 The Typical Week It is advisable that when coming in everyday to liaise with the nurse in charge to identify: 1. New patients 2. Patients needing review 3. Patients that could potentially go home Beech Ward rounds Monday am Full Ward round. On rare occasions this may be conducted in the afternoon if the Consultant is in clinic that morning. Tuesday am SHO/HO ward round Wednesday pm SHO/HO ward round Thursday am Full Ward round Friday SHO/HO ward round Redwood Ward Rounds Monday Consultant led round AKI and referral rounds 12:30- Renal debrief and MDT Tuesday :15- Alternate week Radiology MDT Junior led ward rounds AKI and referral rounds 12:00-13:00- Renal Histology MDT with Guys and St.Thomas Hospital and Kings College Hospital Wednesday Consultant Led Ward Rounds AKI and referral rounds Thursday Junior led ward rounds AKI and referral rounds 12:30-14:00 Grand Round
5 Friday Consultant Led Ward Rounds AKI and referral rounds Any day can have procedures performed- temporary line, tunnelled line insertions and renal biopsies. You are encouraged to attend our ward rounds or meetings on the Main dialysis satellite unit as well. Juniors are encouraged to partake in audit and Mortality and Morbidity meetings (every 3 months) Currently the audits running- AKI stage 3 Audit Contrast prophylaxis audit Hyper-kalemia audit IV fluids audit Renal Anaemia audit Renal Clinics Monday Am- DVH Monday PM- Sidcup Tuesday AM- Kings College Hospital alternate week Tuesday PM- DVH and Erith Wednesday AM- Kings College Hospital alternate week and Gravesend weekly Wednesday PM- DVH Thursday AM- Gravesend Thursday PM- Sidcup Friday AM- DVH These clinics are staffed by the Consultants on a rota basis, but we would encourage you to attend and observe or see a few patients if you are interested in Renal Medicine.
6 Teaching You will have Monday afternoon teaching that is conducted jointly with the Respiratory department from 13:00 to 14:00 hrs weekly. You also have your designated FY, CT level teaching and Grand Round, which is counted as an hour of teaching. You are encouraged to attend all these during the week EDNs (Electronic Discharge Notice, aka TTOs/Discharge Summaries) This is a document which is completed electronically which serves as an official discharge letter for the patient. It also serves a few other important purposes: 1. Information for the patient regarding their diagnosis and advice on the future management of their condition i.e. medications, alarm symptoms etc. 2. The GP will usually be sent a copy of the EDN via and so therefore this document serves as an important communication tool between the hospital team and the GP. If any further investigations are required, tests need or follow up appointments etc., it is usually under Instructions for GP within the EDN. To give examples, the most common instructions for the GP would are to arrange repeat U+Es if started on new medications, outpatient referrals and warfarin checks. 3. Pharmacy it important that the medications is filled in correctly specifying which medications are new, which are old and which have been changed. Liaise with the ward pharmacist who would be more than happy to help! 4. Consultant follow up The Renal consultant will usually make a decision on this on the ward round. To summarise if all these main points are implemented on EDNs you find that this document becomes very useful for AE, on call team and importantly your team! Tip: Try and have the patient s medical history in category of diagnosis filled out in the diagnosis section of the EDN and any investigations, ECHOs, CXRs/CTPAs, etc. fill out in the procedure section of the EDN for easy access of the reader.
7 Investigations in Renal Patients Generally these are the same as for any group of patients. However, patients with acute kidney injury should receive a thorough assessment including: 1. Urine dipstick test on arrival on Beech Ward and Urine Microscopy (MSU) 2. Renal tract ultrasound within 24 hours 3. Serum electrophoresis, serum free light chains and urine Bence - Jones protein (urine electrophoresis) on all patients with unexplained AKI or CKD. 4. ANCA, Anti GBM, C3/C4, Immunoglobulins and auto-antibody screen IF urine dipstick is positive for blood and protein 5. Urine for Protein: Creatinine ratio (plain white top container, early morning sample), for quantification of proteinuria if protein on dipstick 6. Renal Unit Profile to be requested rather than Electrolytes as this gives Calcium, phosphate and also bicarbonate 7. Ferritin / B12 and folate in patients with anaemia 8. PTH level in anyone with significant renal impairment (GFR <30) needs doing once during admission 9. Further specific tests e.g. nuclear medicine scans, should only be done after discussion with the consultants
8 Important Contact details Emma Ross (Renal secretary) Laura Jarvis (Renal secretary) King s Dartford satellite dialysis unit 8855/8861 Dr Chitalia/Coutinho/Kwan office 8696 William Harvey Hospital, Ashford Immunology dept (for urgent ANCA, anti-gbm and auto-antibodies) Tacrolimus results (immunosuppressant levels) Here are a few Guidelines that have been attached to assist you, but you will find a lot of information on ADAGIO as well.
9 The linked image cannot be displayed. The file may have been moved, renamed, or deleted. Verify that the link points to the correct file and location. Patient Name: Hospital Number: DOB: NHS Number: AKI Bundle checklist This patient has been identified as having Acute Kidney Injury - AKI Please ensure the following steps have been taken AKI Serum creatinine criteria Urine output criteria STAGE 1 Increase in serum creatinine of 26 mcrmol/l or more within 48 hours OR Less than 0.5 ml/kg/hour for more 1.5 to 2-fold increase from baseline than 6 hours 2 Increase in serum creatinine to more than 2 to 3-fold from baseline Less than 0.5 ml/kg/hour for more than 12 hours 3 Increase in serum creatinine to more than 3-fold from baseline OR Less than 0.3 ml/kg/hour for 24 hours or anuria for 12 hours Serum creatinine more than 354 mcrmol/l with an acute increase of at least 44 mcrmol/ L Actions Required Fluid Balance - Check for signs of dehydration - Prescribe IV fluid if indicated Low Blood - Withhold anti-hypertensive if SBP<110, and monitor Pressure - Bolus 250 ml N/Saline if hypovolemic unless systolic BP evidence of symptomatic heart failure and re-assess (<110 mm of Hg) Urine - Catheterise if: palpable bladder/ urinary retention OR Oliguric AKI stage 2/3 Imaging - Request urgent renal US scan if suspected obstruction/ no clear cause of AKI Drugs - Review Medication - Stop /withhold nephrotoxins Sepsis - Assess for signs of sepsis. Urgent Rx of any infection (Speak with Microbiology if indicated) Tick when done Cause of AKI: Obstructive Uropathy: (document likely cause) yes/ no Refer to Nephrology if indicated (see flowchart) Renal screen * if clinically indicated (active urinary sediment/clinical suspicion) Daily U & E s Relevant investigations Discharge summary to have AKI section filled
10 The linked image cannot be displayed. The file may have been moved, renamed, or deleted. Verify that the link points to the correct file and location. Patient Name: Hospital Number: DOB: NHS Number: New Diagnosis of AKI Stage 1 / Stage 2 / Stage 3 Alert on ipath and telepath system- Look at these systems for AKI stage Ward team to review patient and confirm Alert (Exclude patients on dialysis or stable CKD) Confirmed AKI- Necessary steps to be initiated by parent team o o o o o o Fluid Balance- Check for dehydration and treat, requires frequent assessment, too much fluid can be harmful (IV fluid, Input/output charts) Low BP- withhold anti-hypertensives (If angina present continue beta blockers but consider reduced dose/review) Urine dipstick test and microscopy (urinary catheterisation if obstruction suspected) Imaging- Urgent renal ultrasound if obstruction suspected or AKI has no identifiable cause Drugs and Toxins- Stop NSAIDS, Withhold ACE inhibitors and AR2B s, review use of metformin, trimethoprim and avoid gentamicin / aminoglycosides, Judiciously use radio-contrast agent. See Contrast Induced Nephrotoxicity guidance on ADAGIO Sepsis- Look for sepsis and treat accordingly, see trust sepsis guidelines Diagnose and treat other acute illness contributing to AKI Mandatory review by senior member of team (Registrar/Consultant) Critical care team referral in appropriate cases (i.e. hypotension not responding to fluids, multi organ failure) Daily U&E s Referral to Renal team AKI stage 1, AKI stage 2- if progression, no renal recovery or suspected glomerular cause or vasculitis AKI stage 3- Urgent renal referral Refer urgently if any complications of AKI or, need for RRT (Hyperkalemia, pulmonary oedema, severe metabolic acidosis, ph <7.2, Uraemic pericarditis / encephalopathy) Inform Renal team of all Dialysis and Kidney transplant patients admitted to your ward *Renal Screen: Urine MSSU, Urine Protein:Creatinine ratio, Urine Bence-Jones protein, ANCA, Anti-GBM antibody, ANA, C3, C4, serum electrophoresis, serum free light chains See ADAGIO- AKI link for management of Hyperkalemia, Contrast Induced nephropathy guidance and other advice
11 Fluids Adult Maintenance Fluids Adult Resuscitation or Replacement Fluids Baseline Requirements mmol sodium, 40-80mol potassium and L water per 24 hours Oral, enteral or parenteral route Adjust estimated requirements according to changes in sensible or insensible losses Sensible Losses (measurable) Surgical drains Vomiting Diarrhoea Urine (variable amounts of electrolytes) Insensible Losses Respiration Perspiration Metabolism Increase in pyrexia or tachypnoea (Mainly water) Regular assessment of volume and hydration status Daily weights Fluid charts Measured electrolytes Available parenteral solutions (if required) Hartmans solution/ringer s lactate Normal Saline 5% dextrose 0.4%/0.18% dextrose/saline Potassium usually added additionally Give According to Clinical Scenario General Volume Replacement or Expansion Give balanced crystalloid solutions (Hartman s solution/ringer s lactate) These contain small amounts of potassium. Avoid in hyperkalaemia. If AKI only use these if close (HDU) monitoring of potassium or Colloids Avoid high molecular weight (>200kDa starches in severe sepsis due to risk of AKI Assess vital signs, postural blood pressure, capillary refill, JVP and consider invasive or non-invasive measurement using flow-based technology Haemorrhage Give blood and blood products Balanced crystalloid or colloid may be given while blood awaited Clinical assessment as above Severe Free Water Losses (hypernatraemia) 5% dextrose or 4%/0.18% dextrose/saline Hypochloraemia (vomiting, NG drainage) Give normal saline (Potassium repletion usually also required) website: info@londonaki.net
12 Contrast Induced Nephropathy (CIN) Prophylaxis Assess Risk High volume (>100mls) iodinated contrast procedure and CKD with egfr<60 (particularly diabetic nephropathy) or AKI Other risk factors dehydration, heart failure, severe sepsis, cirrhosis, nephrotoxins (NSAIDS, aminoglycosides). Risk factors are multiplicative. Is Contrast Procedure Necessary? Yes Resuscitate to Euvolaemia Give Prophylaxis if High Risk Volume expansion (unless hypervolaemic) with normal saline or or 1.26% bicarbonate Sample regimens IV Na bicarbonate 1.26% 3mls/Kg/hr for 1 hour pre-procedure and 6 hours post-procedure or IV 0.9% normal saline 1ml/kg/hr 12 hours pre and 12 hours post procedure Minimise contrast, use low or iso-osmolar contrast Monitor Function To 72 Hours in High Risk Cases If oliguria or rising creatinine early referral to local renal team. NB there is no-proven role for N-Acetyl cysteine, post-contrast dialysis/cvvh or routine cessation of metformin or ACE inbitors. website: info@londonaki.net
13
Nephrology. 3 rd Year Revision Session 06/05/17 Cathal Hannan
 Nephrology 3 rd Year Revision Session 06/05/17 Cathal Hannan Aims Acute Kidney Injury-recognition and management Sample OSCE Station Clinically relevant renal physiology Aetiology of Chronic Kidney Disease
Nephrology 3 rd Year Revision Session 06/05/17 Cathal Hannan Aims Acute Kidney Injury-recognition and management Sample OSCE Station Clinically relevant renal physiology Aetiology of Chronic Kidney Disease
Acute Kidney Injury shared guidance
 Acute Kidney Injury shared guidance Acute Kidney Injury (AKI) Fluid balance assessment (NICE CG 169) Assess the patient s likely fluid and electrolyte needs 1.History previous limited intake, thirst, abnormal
Acute Kidney Injury shared guidance Acute Kidney Injury (AKI) Fluid balance assessment (NICE CG 169) Assess the patient s likely fluid and electrolyte needs 1.History previous limited intake, thirst, abnormal
The role of the Nephrologist in Acute Kidney Injury. Rebecca Brown Consultant Nephrologist Royal Liverpool University Hospital
 The role of the Nephrologist in Acute Kidney Injury Rebecca Brown Consultant Nephrologist Royal Liverpool University Hospital Overview Impact of AKI Need for change Who needs a Nephrologist Are we making
The role of the Nephrologist in Acute Kidney Injury Rebecca Brown Consultant Nephrologist Royal Liverpool University Hospital Overview Impact of AKI Need for change Who needs a Nephrologist Are we making
ACUTE KIDNEY INJURY FOCUS ON OBSTETRICS DONNA HIGGINS, CLINICAL NURSE EDUCATOR, NORTHERN LINCOLNSHIRE HOSPITALS NHS FOUNDATION TRUST
 ACUTE KIDNEY INJURY FOCUS ON OBSTETRICS DONNA HIGGINS, CLINICAL NURSE EDUCATOR, NORTHERN LINCOLNSHIRE HOSPITALS NHS FOUNDATION TRUST AIMS & OBJECTIVES Review the functions of the kidney Identify renal
ACUTE KIDNEY INJURY FOCUS ON OBSTETRICS DONNA HIGGINS, CLINICAL NURSE EDUCATOR, NORTHERN LINCOLNSHIRE HOSPITALS NHS FOUNDATION TRUST AIMS & OBJECTIVES Review the functions of the kidney Identify renal
Acute Kidney Injury (AKI) Undergraduate nurse education
 Acute Kidney Injury (AKI) Undergraduate nurse education Year Three Developed Summer 2017 Objectives Understand Acute Kidney Injury and its relevance to patient care. Brief revision of the Anatomy and physiology
Acute Kidney Injury (AKI) Undergraduate nurse education Year Three Developed Summer 2017 Objectives Understand Acute Kidney Injury and its relevance to patient care. Brief revision of the Anatomy and physiology
An Introduction to Acute Kidney Injury (AKI) An Education Package for Healthcare Professionals in Medical Directorates
 An Introduction to Acute Kidney Injury (AKI) An Education Package for Healthcare Professionals in Medical Directorates STH Acute Kidney Injury (AKI) Project 1 What is Acute Kidney Injury (AKI)? AKI is
An Introduction to Acute Kidney Injury (AKI) An Education Package for Healthcare Professionals in Medical Directorates STH Acute Kidney Injury (AKI) Project 1 What is Acute Kidney Injury (AKI)? AKI is
London Strategic Clinical Networks. My AKI. Guidance for patients with, or recovering from, acute kidney injury
 London Strategic Clinical Networks My AKI Guidance for patients with, or recovering from, acute kidney injury Supporting the delivery of equitable, high quality AKI care through collaboration www.londonaki.net
London Strategic Clinical Networks My AKI Guidance for patients with, or recovering from, acute kidney injury Supporting the delivery of equitable, high quality AKI care through collaboration www.londonaki.net
Fluid assessment, monitoring and therapy for the acute nurse
 Fluid assessment, monitoring and therapy for the acute nurse Kelly Wright Lead Nurse for AKI King s College Hospital Aims and objectives Aims and objectives Why do we worry about volume assessment? Completing
Fluid assessment, monitoring and therapy for the acute nurse Kelly Wright Lead Nurse for AKI King s College Hospital Aims and objectives Aims and objectives Why do we worry about volume assessment? Completing
Doncaster & Bassetlaw. AKI guidelines for primary care
 Doncaster & Bassetlaw AKI guidelines for primary care Contents: FLOW DIAGRAM: MANAGEMENT OF PATIENTS WITH AKI DETECTED IN PRIMARY CARE... 2 FLOW DIAGRAM: MANAGEMENT OF HYPERKALAEMIA.... 3 FLOW DIAGRAM:
Doncaster & Bassetlaw AKI guidelines for primary care Contents: FLOW DIAGRAM: MANAGEMENT OF PATIENTS WITH AKI DETECTED IN PRIMARY CARE... 2 FLOW DIAGRAM: MANAGEMENT OF HYPERKALAEMIA.... 3 FLOW DIAGRAM:
Ricky Bell Renal/ICM Registrar
 Ricky Bell Renal/ICM Registrar Objectives When to call renal How to manage the patient with AKI How the manage the patient with CKD (HD/PD) Special AKI situations What do the guidelines say? My referral
Ricky Bell Renal/ICM Registrar Objectives When to call renal How to manage the patient with AKI How the manage the patient with CKD (HD/PD) Special AKI situations What do the guidelines say? My referral
Liverpool experience of Community AKI care
 Liverpool experience of Community AKI care Shahed Ahmed Consultant Nephrologist and Honorary Lecturer Royal Liverpool University Hospital shahed.ahmed@rlbuht.nhs.uk Is AKI really a problem? 100000, deaths
Liverpool experience of Community AKI care Shahed Ahmed Consultant Nephrologist and Honorary Lecturer Royal Liverpool University Hospital shahed.ahmed@rlbuht.nhs.uk Is AKI really a problem? 100000, deaths
Community & In-hospital ACUTE KIDNEY INJURY (AKI) Guidelines
 Community & In-hospital ACUTE KIDNEY INJURY (AKI) Guidelines Aug 2017 Page 1 of 18 Contents Page Primary and community care Prevention of acute kidney injury 3 Community AKI guideline 4 AKI Sick Day Guidance
Community & In-hospital ACUTE KIDNEY INJURY (AKI) Guidelines Aug 2017 Page 1 of 18 Contents Page Primary and community care Prevention of acute kidney injury 3 Community AKI guideline 4 AKI Sick Day Guidance
CKD and risk management : NICE guideline
 CKD and risk management : NICE guideline 2008-2014 Shahed Ahmed Consultant Nephrologist shahed.ahmed@rlbuht.nhs.uk Key points : Changing parameters of CKD and NICE guidance CKD and age related change of
CKD and risk management : NICE guideline 2008-2014 Shahed Ahmed Consultant Nephrologist shahed.ahmed@rlbuht.nhs.uk Key points : Changing parameters of CKD and NICE guidance CKD and age related change of
Professor Suetonia Palmer
 Professor Suetonia Palmer Department of Medicine Nephrologist Christchurch Hospital Christchurch 14:00-14:55 WS #108: The Kidney Test - When To Test and When to Refer ( and When Not To) 15:05-16:00 WS
Professor Suetonia Palmer Department of Medicine Nephrologist Christchurch Hospital Christchurch 14:00-14:55 WS #108: The Kidney Test - When To Test and When to Refer ( and When Not To) 15:05-16:00 WS
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
Southern Derbyshire Shared Care Pathology Guidelines. AKI guidelines for primary care
 Southern Derbyshire Shared Care Pathology Guidelines AKI guidelines for primary care Contents: Flow Diagram: Recommended response time to AKI warning stage test results for adults in primary care 2 Table
Southern Derbyshire Shared Care Pathology Guidelines AKI guidelines for primary care Contents: Flow Diagram: Recommended response time to AKI warning stage test results for adults in primary care 2 Table
Medicine Dr. Dana Lecture 1 Acute Kidney Injury (AKI)
 Medicine Dr. Dana Lecture 1 Acute Kidney Injury (AKI) Renal function Kidney has many roles: 1. Excretory function 2. Osmolality regulation 3. Acid base balance 4. BP regulation through salt and water balance
Medicine Dr. Dana Lecture 1 Acute Kidney Injury (AKI) Renal function Kidney has many roles: 1. Excretory function 2. Osmolality regulation 3. Acid base balance 4. BP regulation through salt and water balance
Acute Kidney Injury 2
 South West Cardiovascular Strategic Clinical Network Acute Kidney Injury 2 Audit review meeting 18/07/2014 Redwood Education Centre Author: Summary of results: Dr Preetham Boddana Consultant Nephrologist
South West Cardiovascular Strategic Clinical Network Acute Kidney Injury 2 Audit review meeting 18/07/2014 Redwood Education Centre Author: Summary of results: Dr Preetham Boddana Consultant Nephrologist
Preventing Acute Kidney Injury
 Preventing Acute Kidney Injury Dr Andy Lewington MSc Clin Ed FRCP Consultant Nephrologist/Honorary Clinical Associate Professor Director of Undergraduate Medical Education Leeds Teaching Hospitals A.J.P.Lewington@leeds.ac.uk
Preventing Acute Kidney Injury Dr Andy Lewington MSc Clin Ed FRCP Consultant Nephrologist/Honorary Clinical Associate Professor Director of Undergraduate Medical Education Leeds Teaching Hospitals A.J.P.Lewington@leeds.ac.uk
Cheshire & Mersey AKI Network Manual. 2 nd Edition, April 2016
 Cheshire & Mersey AKI Network Manual 2 nd Edition, April 2016 Page 1 of 20 Introduction 3 Prevention of acute kidney injury 4 PRIMARY & COMMUNITY CARE Primary Care AKI Management guideline 5 AKI Sick Day
Cheshire & Mersey AKI Network Manual 2 nd Edition, April 2016 Page 1 of 20 Introduction 3 Prevention of acute kidney injury 4 PRIMARY & COMMUNITY CARE Primary Care AKI Management guideline 5 AKI Sick Day
Lower Urinary Tract Infection (UTI) in Males
 Lower Urinary Tract Infection (UTI) in Males Clinical presentation For patients in care homes see UTI in adults where IV Antibiotics in the community may be appropriate (under development) History and
Lower Urinary Tract Infection (UTI) in Males Clinical presentation For patients in care homes see UTI in adults where IV Antibiotics in the community may be appropriate (under development) History and
Chronic Kidney Disease (CKD) and egfr: Decision and Dilemma. Dr Bhavna K Pandya Consultant Nephrologist University Hospital Aintree
 Chronic Kidney Disease (CKD) and egfr: Decision and Dilemma Dr Bhavna K Pandya Consultant Nephrologist University Hospital Aintree Topics CKD background egfr background Patient with egfr Referral Guidelines
Chronic Kidney Disease (CKD) and egfr: Decision and Dilemma Dr Bhavna K Pandya Consultant Nephrologist University Hospital Aintree Topics CKD background egfr background Patient with egfr Referral Guidelines
Guidelines for slow loading of patients on warfarin for Atrial Fibrillation (AF) in the non acute setting
 ANTICOAGULANT SERVICE Guidelines for slow loading of patients on warfarin for Atrial Fibrillation (AF) in the non acute setting Introduction Fast loading of warfarin carries a risk of over anticoagulation
ANTICOAGULANT SERVICE Guidelines for slow loading of patients on warfarin for Atrial Fibrillation (AF) in the non acute setting Introduction Fast loading of warfarin carries a risk of over anticoagulation
Please inform the Diabetes Nurse Specialist that this patient has been admitted within 24hrs of admission.
 Adult Diabetic Ketoacidosis Care Bundle (V1. Issued October 2014 Review October 2015) Improving patient care This pack includes: DKA Management Guideline Name: (Patient Addressograph) DOB: Hospital No:
Adult Diabetic Ketoacidosis Care Bundle (V1. Issued October 2014 Review October 2015) Improving patient care This pack includes: DKA Management Guideline Name: (Patient Addressograph) DOB: Hospital No:
NICE Clinical Guideline 169 Acute Kidney Injury Local Implementation Gap Analysis
 NICE Clinical Guideline 169 Acute Kidney Injury Local Implementation Gap Analysis Please tick appropriate box in response to questions below and return to Michelle Timoney (michelle.timoney@nhs.net) by
NICE Clinical Guideline 169 Acute Kidney Injury Local Implementation Gap Analysis Please tick appropriate box in response to questions below and return to Michelle Timoney (michelle.timoney@nhs.net) by
Chronic kidney disease screening and assessment
 Care map information Information resources for patients and carers Aboriginal and Torres Strait Islanders DEFINITION OF CKD egfr
Care map information Information resources for patients and carers Aboriginal and Torres Strait Islanders DEFINITION OF CKD egfr
WEEK. MPharm Programme. Acute Kidney Injury. Alan M. Green MPHM13: Acute Kidney Injury. Slide 1 of 47
 MPharm Programme Acute Kidney Injury Alan M. Green 2017 Slide 1 of 47 Overview Renal Function What is it? Why does it matter? What causes it? Who is at risk? What can we (Pharmacists) do? How do you recognise
MPharm Programme Acute Kidney Injury Alan M. Green 2017 Slide 1 of 47 Overview Renal Function What is it? Why does it matter? What causes it? Who is at risk? What can we (Pharmacists) do? How do you recognise
CONTROLLED DOCUMENT. Diagnosis and Initial Management of Acute Kidney Injury. Controlled Document Number: CG013. Version Number: 2
 CONTROLLED DOCUMENT Diagnosis and Initial Management of Acute Kidney Injury CATEGORY: CLASSIFICATION: Controlled Document Number: Version Number: 2 Controlled Document Sponsor: Controlled Document Lead
CONTROLLED DOCUMENT Diagnosis and Initial Management of Acute Kidney Injury CATEGORY: CLASSIFICATION: Controlled Document Number: Version Number: 2 Controlled Document Sponsor: Controlled Document Lead
Acute Kidney Injury in The Acute Oncology Patient
 Acute Kidney Injury in The Acute Oncology Patient Dr Andrew Lewington BSc MEd MD FRCP Consultant Renal Physician/Honorary Senior Lecturer Leeds Teaching Hospitals Definition Definitions and terminology
Acute Kidney Injury in The Acute Oncology Patient Dr Andrew Lewington BSc MEd MD FRCP Consultant Renal Physician/Honorary Senior Lecturer Leeds Teaching Hospitals Definition Definitions and terminology
Acute Kidney Injury in the ED
 + Acute Kidney Injury in the ED + Dr Eric Clark, MD FRCPC University of Ottawa Canada Canadian Association of Emergency Physicians + Outline 1. Diagnostic challenges 2. ED treatment 3. Contrast induced
+ Acute Kidney Injury in the ED + Dr Eric Clark, MD FRCPC University of Ottawa Canada Canadian Association of Emergency Physicians + Outline 1. Diagnostic challenges 2. ED treatment 3. Contrast induced
Prevention of Contrast Induced Nephropathy (CIN) Guidelines
 Prevention of Contrast Induced Nephropathy (CIN) Guidelines This procedural document supersedes: PAT/T 48 v.1 - Guidelines for Prevention of Contrast Induced Nephropathy (CIN) Did you print this document
Prevention of Contrast Induced Nephropathy (CIN) Guidelines This procedural document supersedes: PAT/T 48 v.1 - Guidelines for Prevention of Contrast Induced Nephropathy (CIN) Did you print this document
QUICK REFERENCE FOR HEALTHCARE PROVIDERS
 KEY MESSAGES 1 SCREENING CRITERIA Screen: Patients with DM and/or hypertension at least yearly. Consider screening patients with: Age >65 years old Family history of stage 5 CKD or hereditary kidney disease
KEY MESSAGES 1 SCREENING CRITERIA Screen: Patients with DM and/or hypertension at least yearly. Consider screening patients with: Age >65 years old Family history of stage 5 CKD or hereditary kidney disease
Intestinal Failure Referral Form
 Intestinal Failure Referral Form This form must be completed in full and emailed to UCLH.IFReferrals@nhs.net or call 07958 263178. Please complete all sections of the form. Please note that incomplete
Intestinal Failure Referral Form This form must be completed in full and emailed to UCLH.IFReferrals@nhs.net or call 07958 263178. Please complete all sections of the form. Please note that incomplete
Shared Care Guideline Metolazone for fluid management in CKD (Adults)
 Shared Care Guideline Metolazone for fluid management in CKD (Adults) It is vital for safe and appropriate patient care that there is a clear understanding of where clinical and prescribing responsibility
Shared Care Guideline Metolazone for fluid management in CKD (Adults) It is vital for safe and appropriate patient care that there is a clear understanding of where clinical and prescribing responsibility
Acute Kidney Injury (AKI) In Primary Care Supporting early detection and consistent management
 Acute Kidney Injury (AKI) In Primary Care Supporting early detection and consistent management Responding to AKI Warning Stage Test Results for Adults in Primary Care: Best Practice Guidance AKI in Primary
Acute Kidney Injury (AKI) In Primary Care Supporting early detection and consistent management Responding to AKI Warning Stage Test Results for Adults in Primary Care: Best Practice Guidance AKI in Primary
Acute Kidney Injury. I. David Weiner, M.D. Division of Nephrology, Hypertension and Transplantation University of Florida and NF/SGVHS
 Acute Kidney Injury I. David Weiner, M.D. Division of Nephrology, Hypertension and Transplantation University of Florida and NF/SGVHS 374-6102 David.Weiner@medicine.ufl.edu www.renallectures.com Concentration
Acute Kidney Injury I. David Weiner, M.D. Division of Nephrology, Hypertension and Transplantation University of Florida and NF/SGVHS 374-6102 David.Weiner@medicine.ufl.edu www.renallectures.com Concentration
London Strategic Clinical Networks. Quality Standard. Version 1.0 (2015)
 London Strategic Clinical Networks Quality Standard Version 1.0 (2015) Supporting the delivery of equitable, high quality AKI care through collaboration www.londonaki.net @LondonAKI Overview The management
London Strategic Clinical Networks Quality Standard Version 1.0 (2015) Supporting the delivery of equitable, high quality AKI care through collaboration www.londonaki.net @LondonAKI Overview The management
Irish Practice Nurses Association Annual Conference Tullamore Court Hotel OCTOBER 6 th 2012
 Irish Practice Nurses Association Annual Conference Tullamore Court Hotel OCTOBER 6 th 2012 Susan McKenna Renal Clinical Nurse Specialist Cavan General Hospital Renal patient population ACUTE RENAL FAILURE
Irish Practice Nurses Association Annual Conference Tullamore Court Hotel OCTOBER 6 th 2012 Susan McKenna Renal Clinical Nurse Specialist Cavan General Hospital Renal patient population ACUTE RENAL FAILURE
Management of Nephrotic Syndrome
 Management of Nephrotic Syndrome 1. Introduction Incidence 2-4/100,000. Boys > girls 3:2; age of onset 2-6 years 80% of cases in children is due to minimal change (MCD) of which 80% will respond to steroid
Management of Nephrotic Syndrome 1. Introduction Incidence 2-4/100,000. Boys > girls 3:2; age of onset 2-6 years 80% of cases in children is due to minimal change (MCD) of which 80% will respond to steroid
Chronic kidney disease (CKD) (Southampton pathway)
 Background information Patient information Key messages for this pathway Definitions and abbreviations used in this pathway Classification of CKD Diagnosis of CKD Summary of referral criteria Screening
Background information Patient information Key messages for this pathway Definitions and abbreviations used in this pathway Classification of CKD Diagnosis of CKD Summary of referral criteria Screening
LRI Children s Hospital
 LRI Children s Hospital Management of Henoch Schönlein Purpura (HSP) in children Staff relevant to: Clinical staff working within the UHL Children s Hospital. Team approval date: July 2017 Version: V 3
LRI Children s Hospital Management of Henoch Schönlein Purpura (HSP) in children Staff relevant to: Clinical staff working within the UHL Children s Hospital. Team approval date: July 2017 Version: V 3
Acute Kidney Injury. Eleanor Haskey BSc(hons) RVN VTS(ECC) VPAC A1
 Acute Kidney Injury Eleanor Haskey BSc(hons) RVN VTS(ECC) VPAC A1 Anatomy and Physiology The role of the kidneys is to filter the blood through the glomerulus to form filtrate. The filtrate is then reabsorbed
Acute Kidney Injury Eleanor Haskey BSc(hons) RVN VTS(ECC) VPAC A1 Anatomy and Physiology The role of the kidneys is to filter the blood through the glomerulus to form filtrate. The filtrate is then reabsorbed
Brief summary of the NICE guidelines December 2013
 Brief summary of the NICE guidelines December 2013 Intravenous fluid therapy in adults in hospital the relevance to Emergency Department Care Applicable to patients 16 years and older receiving i.v. fluids
Brief summary of the NICE guidelines December 2013 Intravenous fluid therapy in adults in hospital the relevance to Emergency Department Care Applicable to patients 16 years and older receiving i.v. fluids
A Care Pathway exists for the management of neutropenic fever. Copies of the care pathway document are available in EAU, A&E, Deanesly and CHU.
 Subject: Neutropenic Fever Guideline for Junior Doctors Date of Implementation: January 2010 Date of Review: January 2012 Director Responsible for Implementation and Review: Policy location: Consultant
Subject: Neutropenic Fever Guideline for Junior Doctors Date of Implementation: January 2010 Date of Review: January 2012 Director Responsible for Implementation and Review: Policy location: Consultant
PREOPERATIVE ANAEMIA PATHWAY
 PREOPERATIVE ANAEMIA PATHWAY Surname: Unit No. Forename: DOB: / / Age: NHS Number: Likes to be called: Address: Tel. No. Religion/Spirituality: GP Name: GP Practice: Planned Operation: Postcode: Mobile
PREOPERATIVE ANAEMIA PATHWAY Surname: Unit No. Forename: DOB: / / Age: NHS Number: Likes to be called: Address: Tel. No. Religion/Spirituality: GP Name: GP Practice: Planned Operation: Postcode: Mobile
CKD FOR INTERNISTS. Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College
 CKD FOR INTERNISTS Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College INTRODUCTION In 2002, the National Kidney Foundation s Kidney Disease Outcomes Quality Initiative(KDOQI)
CKD FOR INTERNISTS Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College INTRODUCTION In 2002, the National Kidney Foundation s Kidney Disease Outcomes Quality Initiative(KDOQI)
Acute kidney injury. Information for patients Sheffield Teaching Hospitals
 Acute kidney injury Information for patients Sheffield Teaching Hospitals page 2 of 12 Acute kidney injury You have been given this leaflet because you have had an episode of acute kidney injury (AKI).
Acute kidney injury Information for patients Sheffield Teaching Hospitals page 2 of 12 Acute kidney injury You have been given this leaflet because you have had an episode of acute kidney injury (AKI).
Trust Guideline for the Management of: Condition or Procedure in Adults and / or Children
 Trust Guideline for the Management of: Condition or Procedure in Adults and / or Children A clinical guideline recommended For use in: By: For: Division responsible for document: Key words: Name of document
Trust Guideline for the Management of: Condition or Procedure in Adults and / or Children A clinical guideline recommended For use in: By: For: Division responsible for document: Key words: Name of document
PREOPERATIVE ANAEMIA PATHWAY
 PREOPERATIVE ANAEMIA PATHWAY Surname: Patient ID No. Forename: DOB: / / Age: NHS Number: Likes to be called: Address: Tel. No. Religion/Spirituality: Next of Kin: Name GP Name: GP Practice: Planned Operation:
PREOPERATIVE ANAEMIA PATHWAY Surname: Patient ID No. Forename: DOB: / / Age: NHS Number: Likes to be called: Address: Tel. No. Religion/Spirituality: Next of Kin: Name GP Name: GP Practice: Planned Operation:
INTRAVENOUS FLUID THERAPY. Tom Heaps Consultant Acute Physician
 INTRAVENOUS FLUID THERAPY Tom Heaps Consultant Acute Physician LEARNING OBJECTIVES 1. Crystalloids vs colloids 2. Balanced vs non-balanced solutions 3. Composition of various IV fluids 4. What is normal
INTRAVENOUS FLUID THERAPY Tom Heaps Consultant Acute Physician LEARNING OBJECTIVES 1. Crystalloids vs colloids 2. Balanced vs non-balanced solutions 3. Composition of various IV fluids 4. What is normal
North Derbyshire OPAT (Outpatient Parenteral Antimicrobial Therapy) Pathway for Primary Care (Step-Up Pathway/Admission Avoidance)
 North Derbyshire OPAT (Outpatient Parenteral Antimicrobial Therapy) Pathway for Primary Care (Step-Up Pathway/Admission Avoidance) Introduction OPAT services provide intravenous (IV) antibiotics to patients
North Derbyshire OPAT (Outpatient Parenteral Antimicrobial Therapy) Pathway for Primary Care (Step-Up Pathway/Admission Avoidance) Introduction OPAT services provide intravenous (IV) antibiotics to patients
GUIDELINE FOR THE MANAGEMENT AND PREVENTION OF ACUTE TUMOUR LYSIS SYNDROME IN HAEMATOLOGICAL MALIGNANCIES
 GUIDELINE FOR THE MANAGEMENT AND PREVENTION OF ACUTE TUMOUR LYSIS SYNDROME IN HAEMATOLOGICAL MALIGNANCIES Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target
GUIDELINE FOR THE MANAGEMENT AND PREVENTION OF ACUTE TUMOUR LYSIS SYNDROME IN HAEMATOLOGICAL MALIGNANCIES Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target
Chronic Kidney Disease
 Chronic Kidney Disease Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) Directorate & Speciality Guideline for the Identification
Chronic Kidney Disease Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) Directorate & Speciality Guideline for the Identification
Identification, management and referral of adults with chronic kidney disease: concise guidelines
 Identification, management and referral of adults with chronic kidney disease: concise guidelines Abstract Chronic Kidney Disease (CKD) is often thought to be a relatively rare condition requiring specialist
Identification, management and referral of adults with chronic kidney disease: concise guidelines Abstract Chronic Kidney Disease (CKD) is often thought to be a relatively rare condition requiring specialist
ACUTE KIDNEY INJURY A PRIMER FOR PRIMARY CARE PHYSICIANS. Myriam Farah, MD, FRCPC
 ACUTE KIDNEY INJURY A PRIMER FOR PRIMARY CARE PHYSICIANS Myriam Farah, MD, FRCPC Clinical Assistant Professor Division of Nephrology, University of British Columbia November 2016 1. How to recognize acute
ACUTE KIDNEY INJURY A PRIMER FOR PRIMARY CARE PHYSICIANS Myriam Farah, MD, FRCPC Clinical Assistant Professor Division of Nephrology, University of British Columbia November 2016 1. How to recognize acute
CHRONIC KIDNEY DISEASE DIAGNOSIS
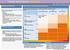 CHRONIC KIDNEY DISEASE DIAGSIS GFR categories, description and range WHO SHOULD BE TESTED FOR CKD CLASSIFICATION OF CKD USING egfr AND ACR CATEGORIES Offer testing for CKD using egfr, creatinine and ACR
CHRONIC KIDNEY DISEASE DIAGSIS GFR categories, description and range WHO SHOULD BE TESTED FOR CKD CLASSIFICATION OF CKD USING egfr AND ACR CATEGORIES Offer testing for CKD using egfr, creatinine and ACR
CKD at the primary and secondary care interface. Paul Cockwell Consultant Nephrologist Clinical Service Lead Renal Medicine, QEHB
 CKD at the primary and secondary care interface Paul Cockwell Consultant Nephrologist Clinical Service Lead Renal Medicine, QEHB The Health improvement Network (THIN): 6.7 million patients from 426 primary
CKD at the primary and secondary care interface Paul Cockwell Consultant Nephrologist Clinical Service Lead Renal Medicine, QEHB The Health improvement Network (THIN): 6.7 million patients from 426 primary
Swindon Diabetes Guidelines: Management of Chronic Kidney Disease Associated with Diabetes Mellitus
 Swindon Diabetes Guidelines: Management of Chronic Kidney Disease Associated with Diabetes Mellitus 1 Contents Executive Summary... 3 How to Screen for Diabetic Nephropathy... 4 What to Measure... 4 Frequency
Swindon Diabetes Guidelines: Management of Chronic Kidney Disease Associated with Diabetes Mellitus 1 Contents Executive Summary... 3 How to Screen for Diabetic Nephropathy... 4 What to Measure... 4 Frequency
Acute Kidney Injury (AKI) Undergraduate nurse education
 Acute Kidney Injury (AKI) Undergraduate nurse education Year One Developed Summer 2017 Overview Basic A & P of: Urinary system Kidneys Followed by: Introduction to Acute Kidney Injury Urinary System The
Acute Kidney Injury (AKI) Undergraduate nurse education Year One Developed Summer 2017 Overview Basic A & P of: Urinary system Kidneys Followed by: Introduction to Acute Kidney Injury Urinary System The
Acute kidney injury. Dr P Sigwadi Paediatric nephrology
 Acute kidney injury Dr P Sigwadi Paediatric nephrology Introduction Is common in critically ill patients e.g. post cardiac surgery Occurs when renal function is diminished to a point where body fluid and
Acute kidney injury Dr P Sigwadi Paediatric nephrology Introduction Is common in critically ill patients e.g. post cardiac surgery Occurs when renal function is diminished to a point where body fluid and
Screen annually for patients with any of the following risk factors:
 CASE DEFINITION Chronic Kidney Disease (CKD) is either of the following, persisting for at least three months, repeated on at least two occasions: 1. Markers of kidney damage (e.g. proteinuria, haematuria
CASE DEFINITION Chronic Kidney Disease (CKD) is either of the following, persisting for at least three months, repeated on at least two occasions: 1. Markers of kidney damage (e.g. proteinuria, haematuria
Stages of Chronic Kidney Disease (CKD)
 Early Treatment is the Key Stages of Chronic Kidney Disease (CKD) Stage Description GFR (ml/min/1.73 m 2 ) >90 1 Kidney damage with normal or GFR 2 Mild decrease in GFR 60-89 3 Moderate decrease in GFR
Early Treatment is the Key Stages of Chronic Kidney Disease (CKD) Stage Description GFR (ml/min/1.73 m 2 ) >90 1 Kidney damage with normal or GFR 2 Mild decrease in GFR 60-89 3 Moderate decrease in GFR
CLINICAL GUIDELINE FOR INTRAVENOUS FLUID THERAPY FOR ADULTS IN HOSPITAL 1. Aim/Purpose of this Guideline
 CLINICAL GUIDELINE FOR INTRAVENOUS FLUID THERAPY FOR ADULTS IN HOSPITAL 1. Aim/Purpose of this Guideline 1.1. This guideline contains recommendations about general principles for managing intravenous (IV)
CLINICAL GUIDELINE FOR INTRAVENOUS FLUID THERAPY FOR ADULTS IN HOSPITAL 1. Aim/Purpose of this Guideline 1.1. This guideline contains recommendations about general principles for managing intravenous (IV)
Acute Oncology Martin Eatock Consultant Medical Oncologist NICaN Medical Director
 Acute Oncology 2014 Martin Eatock Consultant Medical Oncologist NICaN Medical Director Patients admitted with cancer have a longer than average stay Berger et al. Clin Medicine (2013) Questions If your
Acute Oncology 2014 Martin Eatock Consultant Medical Oncologist NICaN Medical Director Patients admitted with cancer have a longer than average stay Berger et al. Clin Medicine (2013) Questions If your
Guideline on the clinical management of Henoch Schonlein Purpura (HSP)
 Guideline on the clinical management of Henoch Schonlein Purpura (HSP) Purpose To ensure a standardised approach in the management of children with HSP in southern Derbyshire. Scope The scope of this guideline
Guideline on the clinical management of Henoch Schonlein Purpura (HSP) Purpose To ensure a standardised approach in the management of children with HSP in southern Derbyshire. Scope The scope of this guideline
Acute Kidney Injury. Patient Information Leaflet
 Acute Kidney Injury Patient Information Leaflet What is Acute Kidney Injury (AKI)? Acute Kidney injury is a rapid fall in kidney function in a person who has become unwell. It can happen over hours or
Acute Kidney Injury Patient Information Leaflet What is Acute Kidney Injury (AKI)? Acute Kidney injury is a rapid fall in kidney function in a person who has become unwell. It can happen over hours or
Bulletin Independent prescribing information for NHS Wales
 Bulletin Independent prescribing information for NHS Wales October 2017 Chronic kidney disease Chronic kidney disease (CKD) is a long-term irreversible deterioration in the function of the kidneys, often
Bulletin Independent prescribing information for NHS Wales October 2017 Chronic kidney disease Chronic kidney disease (CKD) is a long-term irreversible deterioration in the function of the kidneys, often
Outpatient Management of Chronic Kidney Disease for the Internist
 Outpatient Management of Chronic Kidney Disease for the Internist Annual Meeting of Maryland Chapter of the American College of Physicians February 3, 2018 MARY (TESSIE) BEHRENS, MD, FACP, FASN, FNKF MID-ATLANTIC
Outpatient Management of Chronic Kidney Disease for the Internist Annual Meeting of Maryland Chapter of the American College of Physicians February 3, 2018 MARY (TESSIE) BEHRENS, MD, FACP, FASN, FNKF MID-ATLANTIC
Pathology Service User Guide Haematology
 Pathology Service User Guide Haematology St Richard s This section of the Pathology Service User Guide includes: Anticoagulant Therapy Information about the Anticoagulant Clinic Low Molecular Weight Heparin
Pathology Service User Guide Haematology St Richard s This section of the Pathology Service User Guide includes: Anticoagulant Therapy Information about the Anticoagulant Clinic Low Molecular Weight Heparin
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Centre for Clinical Practice SCOPE Clinical guideline title: Intravenous fluid therapy in adults in hospital Quality standard title: Intravenous fluid
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Centre for Clinical Practice SCOPE Clinical guideline title: Intravenous fluid therapy in adults in hospital Quality standard title: Intravenous fluid
VA/DoD Clinical Practice Guideline for the Management of Chronic Kidney Disease in Primary Care (2008) PROVIDER REFERENCE CARDS Chronic Kidney Disease
 VA/DoD Clinical Practice Guideline for the Management of Chronic Kidney Disease in Primary Care (2008) PROVIDER REFERECE CARDS Chronic Kidney Disease CKD VA/DoD Clinical Practice Guideline for the Management
VA/DoD Clinical Practice Guideline for the Management of Chronic Kidney Disease in Primary Care (2008) PROVIDER REFERECE CARDS Chronic Kidney Disease CKD VA/DoD Clinical Practice Guideline for the Management
September 2014 V0.17. Paediatric Daily Fluid Prescription & Balance Chart
 September 14 V0.17 Aims and outcomes of session. Aim: To provide guidance on correctly completing the paediatric daily fluid prescription & balance chart. Outcomes: Demonstrate the ability to: calculate
September 14 V0.17 Aims and outcomes of session. Aim: To provide guidance on correctly completing the paediatric daily fluid prescription & balance chart. Outcomes: Demonstrate the ability to: calculate
Chronic Kidney Disease
 Chronic Kidney Disease Presence of kidney damage or decreased kidney function for three or more months, - necessary to distinguish CKD from acute kidney disease. Ascertained either by kidney biopsy or
Chronic Kidney Disease Presence of kidney damage or decreased kidney function for three or more months, - necessary to distinguish CKD from acute kidney disease. Ascertained either by kidney biopsy or
StRs and CT doctors in haematology. September Folinic acid dose modified.
 High dose Methotrexate and folinic acid rescue Full Title of Guideline: Author (include email and role): Division & Speciality: Clinical Guideline Review Date September 2018 GUIDELINE FOR THE USE OF HIGH
High dose Methotrexate and folinic acid rescue Full Title of Guideline: Author (include email and role): Division & Speciality: Clinical Guideline Review Date September 2018 GUIDELINE FOR THE USE OF HIGH
Managing Patients with CKD in Primary Care: A Shared Care Pathway. 5 th April 2018
 Managing Patients with CKD in Primary Care: A Shared Care Pathway 5 th April 2018 Learning Objectives 1) What health risks does CKD represent? 2) Why change how we manage CKD in NWL? 1) How do we improve
Managing Patients with CKD in Primary Care: A Shared Care Pathway 5 th April 2018 Learning Objectives 1) What health risks does CKD represent? 2) Why change how we manage CKD in NWL? 1) How do we improve
The Septic Patient. Dr Arunraj Navaratnarajah. Renal SpR Imperial College NHS Healthcare Trust
 The Septic Patient Dr Arunraj Navaratnarajah Renal SpR Imperial College NHS Healthcare Trust Objectives of this session Define SIRS / sepsis / severe sepsis / septic shock Early recognition of Sepsis The
The Septic Patient Dr Arunraj Navaratnarajah Renal SpR Imperial College NHS Healthcare Trust Objectives of this session Define SIRS / sepsis / severe sepsis / septic shock Early recognition of Sepsis The
Radical removal of the kidney (radical nephrectomy): procedure-specific information
 PATIENT INFORMATION Radical removal of the kidney (radical nephrectomy): procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels,
PATIENT INFORMATION Radical removal of the kidney (radical nephrectomy): procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels,
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Nephrology
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Nephrology 1. GOAL: Understand the general pediatrician's role in diagnosis and management of hypertension in children.
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Nephrology 1. GOAL: Understand the general pediatrician's role in diagnosis and management of hypertension in children.
Management of early chronic kidney disease
 Management of early chronic kidney disease GREENLANE SUMMER GP SYMPOSIUM 2018 Jonathan Hsiao Renal and General Physician Introduction A growing public health problem in NZ and throughout the world. Unknown
Management of early chronic kidney disease GREENLANE SUMMER GP SYMPOSIUM 2018 Jonathan Hsiao Renal and General Physician Introduction A growing public health problem in NZ and throughout the world. Unknown
9 Diabetes care. Back to contents
 Back to contents Diabetes is a major risk factor for the development of peripheral vascular disease and 349/628 (55.6%) of the patients in this study had diabetes. Hospital inpatients with diabetes are
Back to contents Diabetes is a major risk factor for the development of peripheral vascular disease and 349/628 (55.6%) of the patients in this study had diabetes. Hospital inpatients with diabetes are
I hope the shared cared protocol will help with your care of this renal transplant patient. We are happy to discuss any issues with you.
 Paediatric Nephrology Phone (64) 9-3078900 Fax (64) 9-3078938 renalnurse@adhb.govt.nz wwong@adhb.govt.nz tonyak@adhb.govt.nz stackm@adhb.govt.nz chanelp@adhb.govt.nz Dear Colleague, Thank you for resuming
Paediatric Nephrology Phone (64) 9-3078900 Fax (64) 9-3078938 renalnurse@adhb.govt.nz wwong@adhb.govt.nz tonyak@adhb.govt.nz stackm@adhb.govt.nz chanelp@adhb.govt.nz Dear Colleague, Thank you for resuming
Acute Renal Failure. Dr Kawa Ahmad
 62 Acute Renal Failure Dr Kawa Ahmad Acute Renal Failure It is characterised by an abrupt reduction (usually within a 48- h period) in kidney function. This results in an accumulation of nitrogenous waste
62 Acute Renal Failure Dr Kawa Ahmad Acute Renal Failure It is characterised by an abrupt reduction (usually within a 48- h period) in kidney function. This results in an accumulation of nitrogenous waste
A three month project September December 2016
 Improving Insulin Safety in the Clinical Decision Unit A three month project September December 2016 Sarah Gregory - In-Patient DSN, QEQM Hospital Julie Gammon - Ward Manager, CDU, QEQM Hospital 1 The
Improving Insulin Safety in the Clinical Decision Unit A three month project September December 2016 Sarah Gregory - In-Patient DSN, QEQM Hospital Julie Gammon - Ward Manager, CDU, QEQM Hospital 1 The
NORTHERN IRELAND GUIDELINES FOR MANAGEMENT OF CHRONIC KIDNEY DISEASE
 NORTHERN IRELAND GUIDELINES FOR MANAGEMENT OF CHRONIC KIDNEY DISEASE Practical points for use of estimated GFR + quality outcome framework indicators Developed by GAIN and the Northern Ireland Nephrology
NORTHERN IRELAND GUIDELINES FOR MANAGEMENT OF CHRONIC KIDNEY DISEASE Practical points for use of estimated GFR + quality outcome framework indicators Developed by GAIN and the Northern Ireland Nephrology
Learning Objectives. How big is the problem? ACUTE KIDNEY INJURY
 ACUTE KIDNEY INJURY Karen Innocent, DNP, RN, CRNP, ANP-BC, CMSRN Executive Director, Continuing Education Wolters Kluwer Health, Inc May 2016 Orlando FL Learning Objectives Identify the risk factors and
ACUTE KIDNEY INJURY Karen Innocent, DNP, RN, CRNP, ANP-BC, CMSRN Executive Director, Continuing Education Wolters Kluwer Health, Inc May 2016 Orlando FL Learning Objectives Identify the risk factors and
SAFETY IN THE CATH LAB How to Minimise Contrast Toxicity
 SAFETY IN THE CATH LAB How to Minimise Contrast Toxicity Dr. Vijay Kunadian MBBS, MD, MRCP Senior Lecturer and Consultant Interventional Cardiologist Institute of Cellular Medicine, Faculty of Medical
SAFETY IN THE CATH LAB How to Minimise Contrast Toxicity Dr. Vijay Kunadian MBBS, MD, MRCP Senior Lecturer and Consultant Interventional Cardiologist Institute of Cellular Medicine, Faculty of Medical
Prescribing Framework for Methotrexate for Immunosuppression in ADULTS
 Hull & East Riding Prescribing Committee Prescribing Framework for Methotrexate for Immunosuppression in ADULTS Patient s Name:.. NHS Number: Patient s Address:... (Use addressograph sticker) GP s Name:...
Hull & East Riding Prescribing Committee Prescribing Framework for Methotrexate for Immunosuppression in ADULTS Patient s Name:.. NHS Number: Patient s Address:... (Use addressograph sticker) GP s Name:...
The Urology One-Stop Clinic
 The Urology One-Stop Clinic Exceptional healthcare, personally delivered The aim of this leaflet is to answer any questions you may have about the Urology One-Stop Clinic. What is the Urology One-Stop
The Urology One-Stop Clinic Exceptional healthcare, personally delivered The aim of this leaflet is to answer any questions you may have about the Urology One-Stop Clinic. What is the Urology One-Stop
Update in. Acute Kidney Injury. Mark Devonald Consultant Nephrologist. Nottingham AKI Research Group
 Update in Acute Kidney Injury Mark Devonald Consultant Nephrologist If you stay awake you might hear about Why AKI is important Some cases to illustrate some specific points A couple of updates on AKI
Update in Acute Kidney Injury Mark Devonald Consultant Nephrologist If you stay awake you might hear about Why AKI is important Some cases to illustrate some specific points A couple of updates on AKI
Acute Kidney Injury; get the basics right first!
 Acute Kidney Injury; get the basics right first! Dr Christopher Wong, Consultant Nephrologist and General Physician, University Hospital Aintree (UHA), Liverpool, UK Acute kidney injury (AKI) Why a new
Acute Kidney Injury; get the basics right first! Dr Christopher Wong, Consultant Nephrologist and General Physician, University Hospital Aintree (UHA), Liverpool, UK Acute kidney injury (AKI) Why a new
Supplement: Summary of Recommendation Statements CHAPTER 1: DEFINITION AND CLASSIFICATION OF CKD
 Supplement: Summary of Recommendation Statements CHAPTER 1: DEFINITION AND CLASSIFICATION OF CKD 1.1 DEFINITION OF CKD 1.1.1: CKD is defined as abnormalities of kidney structure or function, present for
Supplement: Summary of Recommendation Statements CHAPTER 1: DEFINITION AND CLASSIFICATION OF CKD 1.1 DEFINITION OF CKD 1.1.1: CKD is defined as abnormalities of kidney structure or function, present for
CEM Clinical Audits Severe Sepsis & Septic Shock
 CEM Clinical Audits 2011-12 Severe Sepsis & Septic Shock Introduction This report shows the results from an audit of the treatment of severe sepsis and septic shock against the clinical standards published
CEM Clinical Audits 2011-12 Severe Sepsis & Septic Shock Introduction This report shows the results from an audit of the treatment of severe sepsis and septic shock against the clinical standards published
MODULE 8B: Management of Group B Dengue with Warning Signs or Dengue with Co-existing Conditions
 MODULE 8B: Management of Group B Dengue with Warning Signs or Dengue with Co-existing Conditions Dengue Clinical Management Acknowledgements This curriculum was developed with technical assistance from
MODULE 8B: Management of Group B Dengue with Warning Signs or Dengue with Co-existing Conditions Dengue Clinical Management Acknowledgements This curriculum was developed with technical assistance from
High Intensity Chemotherapy Guidelines for Haematology Patients at ASPH
 High Intensity Chemotherapy Guidelines for Haematology Patients at ASPH Contents: Page No. 1. Overview 2 2. Admission 3 3. Admission Checklist 5 4. Inpatient management during chemotherapy 6 5. Inpatient
High Intensity Chemotherapy Guidelines for Haematology Patients at ASPH Contents: Page No. 1. Overview 2 2. Admission 3 3. Admission Checklist 5 4. Inpatient management during chemotherapy 6 5. Inpatient
Mr PA. Clinical assessment of hydration. Poor urine output Sunken eyes Moistness of mucosa Cool peripheries Reduction in weight Postural hypotension
 X Anthony Warrens Mr PA 54 years old Previously well Went to Thailand Developed serious diarrhoea and vomiting two days before coming home 24 hours after return, still unwell GP found: urea 24 mmol/l creatinine
X Anthony Warrens Mr PA 54 years old Previously well Went to Thailand Developed serious diarrhoea and vomiting two days before coming home 24 hours after return, still unwell GP found: urea 24 mmol/l creatinine
SIMPLY. Fluids. Dr Will Dooley
 SIMPLY. Fluids Dr Will Dooley Plan Maintenance vs Resuscitation Prescribing Common Errors Calculations Drip rates Case 54 yo presents with severe diarrhoea and vomiting. How would you proceed? Assessment
SIMPLY. Fluids Dr Will Dooley Plan Maintenance vs Resuscitation Prescribing Common Errors Calculations Drip rates Case 54 yo presents with severe diarrhoea and vomiting. How would you proceed? Assessment
Bleeding / Pain after Renal Biopsy Guideline
 Bleeding / Pain after Renal Biopsy Guideline This guidance does not override the individual responsibility of health professionals to make appropriate decision according to the circumstances of the individual
Bleeding / Pain after Renal Biopsy Guideline This guidance does not override the individual responsibility of health professionals to make appropriate decision according to the circumstances of the individual
CKD & HT. Anne-Marie Angus
 CKD & HT Anne-Marie Angus Hypertension definitions Persisting BP >140/90 and HBPM >135/85 Stage 1 >140/90 (HBPM >135/85) Stage 2 >160/100 (HBPM >150/90) Severe >180/100 White coat HT Why treat? A major
CKD & HT Anne-Marie Angus Hypertension definitions Persisting BP >140/90 and HBPM >135/85 Stage 1 >140/90 (HBPM >135/85) Stage 2 >160/100 (HBPM >150/90) Severe >180/100 White coat HT Why treat? A major
Frimley Health Area Prescribing Committee
 Frimley Health Area Prescribing Committee Frimley Health NHS Foundation Trust North East Hampshire and Farnham CCG East Berkshire CCG Surrey Heath CCG Buckinghamshire CCG SHARED CARE Guideline Amber Traffic
Frimley Health Area Prescribing Committee Frimley Health NHS Foundation Trust North East Hampshire and Farnham CCG East Berkshire CCG Surrey Heath CCG Buckinghamshire CCG SHARED CARE Guideline Amber Traffic
A patient guide to membranous nephropathy
 A patient guide to membranous nephropathy Queen Elizabeth Hospital Kidney Care Department UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
A patient guide to membranous nephropathy Queen Elizabeth Hospital Kidney Care Department UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
