Alzheimer s Research & Therapy 2009, 1:6 (doi: /alzrt6)
|
|
|
- Spencer Day
- 6 years ago
- Views:
Transcription
1 Available online Review Cerebral amyloid angiopathy in the aetiology and immunotherapy of Alzheimer disease Roy O Weller, Stephen D Preston, Malavika Subash and Roxana O Carare Clinical Neurosciences, University of Southampton School of Medicine, LD74, South Laboratory & Pathology Block, Southampton General Hospital, Southampton, SO16 6YD, UK Corresponding author: Roy O Weller, row@soton.ac.uk Published: 13 October 2009 This article is online at BioMed Central Ltd Alzheimer s Research & Therapy 2009, 1:6 (doi: /alzrt6) Abstract Amyloid is deposited in the walls of arteries and capillaries as cerebral amyloid angiopathy (CAA) in the brains of older individuals and of those with Alzheimer disease (AD). CAA in AD reflects an age-related failure of elimination of amyloid-beta (Aβ) from the brain along perivascular lymphatic drainage pathways. In the absence of conventional lymphatic vessel in the brain, interstitial fluid and solutes drain from the brain to cervical lymph nodes along narrow basement membranes in the walls of capillaries and arteries, a pathway that is largely separate from the cerebrospinal fluid. In this review we focus on the pathology and pathogenesis of CAA, its role in the aetiology of AD and its impact on immunotherapy for AD. The motive force for lymphatic drainage of the brain appears to be generated by arterial pulsations. Failure of elimination of Aβ along perivascular pathways coincides with a reduction in enzymic degradation of Aβ, reduced absorption of Aβ into the blood and age-related stiffening of artery walls that appears to reduce the motive force for lymphatic drainage. Reduced clearances of Aβ and CAA are associated with the accumulation of insoluble and soluble Aβs in the brain in AD and the probable loss of homeostasis of the neuronal environment due to retention of soluble metabolites within the brain. Tau metabolism may also be affected. Immunotherapy has been successful in removing insoluble plaques of Aβ from the brain in AD but with little effect on cognitive decline. One major problem is the increase in CAA in immunised patients that probably prevents the complete removal of Aβ from the brain. Increased knowledge of the physiology and structural and genetic aspects of the lymphatic drainage of Aβ from the brain will stimulate the development of therapeutic strategies for the prevention and treatment of AD. Introduction Deposition of amyloid-beta (Aβ) in the walls of cerebral arteries and capillaries as cerebral amyloid angiopathy (CAA) has a prevalence of 90% to 96% in patients with Alzheimer disease (AD) [1] and is present in 30% of non-demented individuals over the age of 60 years [2]. CAA reflects an agerelated failure of elimination of Aβ from the brain along perivascular lymphatic drainage pathways by which interstitial fluid (ISF) and solutes drain from the brain [3-5]. This failure may be a key factor in the aetiology of AD. Most organs have networks of lymphatic vessels that transport fluid, protein macromolecules, cells and particulate matter from tissue to lymph nodes. Lymphatic drainage along these vessels relies upon highly competent valves, an extrinsic pump action generated by external forces from surrounding tissues and an intrinsic pump generated by coordinated contractions of lymphatic muscle cells [6]. There are no conventional lymphatics in the brain. Instead, ISF and solutes drain out of the brain along narrow basement membranes in the walls of capillaries and arteries to lymph nodes in the neck [3,7], probably driven by an intrinsic pump powered by vascular pulsations [8]. The perivascular lymphatic drainage pathway for ISF and solutes from the brain is largely separate from the cerebrospinal fluid (CSF) [7,9]. With increasing age, the brain, with its almost unique lymphatic drainage system, develops problems with lymphatic drainage of Aβ and other amyloids and these problems are rarely seen in other organs. As a result, soluble and insoluble Aβs accumulate in vessel walls and in brain parenchyma. CAA in AD is a protein-elimination-failure arteriopathy (PEFA) [5,7] common to other forms of CAA in which a variety of amyloidogenic peptides accumulate in the walls of cerebral arteries. Non-Aβ forms of CAA tend to be hereditary in origin and are associated with intracerebral haemorrhage or dementia [10]. Mutated cystatin C is deposited in the walls of cerebral arteries as CAA and occasionally in arteries elsewhere in the body in the autosomal dominant hereditary cerebral haemorrhage with amyloidosis of Icelandic type (HCHWA-1) [10,11]. Patients suffer intracerebral haemorrhage at an early age, and those who survive may develop dementia [11]. Variant transthyretin accumulates in vessels in Aβ = amyloid-beta; AD = Alzheimer disease; ApoE = apolipoprotein E; CAA = cerebral amyloid angiopathy; CSF = cerebrospinal fluid; ISF = interstitial fluid; LRP-1 = lipoprotein receptor-related protein-1; NFT = neurofibrillary tangle; PrP = prion protein. Page 1 of 13
2 Alzheimer s Research & Therapy Vol 1 No 2 Weller et al. the endoneurium of peripheral nerves in familial amyloid peripheral neuropathy [12], and in some families, there is deposition of mutant transthyretin in the walls of leptomeningeal arteries and in brain parenchyma [10]. In the Finnish type of familial amyloidosis, systemic and cerebral amyloidosis is related to the protein gesolin [10]. Two of the most carefully documented forms of hereditary CAA are those related to the British and Danish forms of familial dementia [10]. Mutations in the BRI2 gene are associated with deposition of ABri and ADan amyloids in brain and spinal cord and as CAA [10]. BRI2 mrna and BRI2 protein are widely expressed by neurons and glia but are not expressed by cerebrovascular smooth muscle cells [13], suggesting that the amyloid in the vessel walls is derived from the brain rather than produced locally by smooth muscle cells in the artery walls. Prion proteins (PrPs) are deposited mainly in brain parenchyma in human and animal prion disorders such as Creutzfeldt-Jacob disease, scrapie and bovine spongiform encephalopathy [14]. However, PrP CAA has been reported in familial and sporadic human disease [10] and in certain types of scrapie in which there is a truncated form of PrP [15], suggesting that PrP may normally drain from the brain along perivascular pathways. In this review, we concentrate on Aβ-CAA as it is the commonest type of CAA and has a very significant association with intracerebral haemorrhage and dementia in the older population [16]. In particular, we focus on the pathology, pathogenesis and complications of CAA, its relationship to the aetiology of AD and how it affects the clinical outcome of immunotherapy for AD. Many of the general principles that have emerged from the study of Aβ- CAA can be applied to the other, less common, types of CAA [10]. As Aβ acts as a natural tracer for the drainage of solutes from the human brain, CAA has been a useful model for establishing lymphatic drainage pathways of the human brain and their significance for neuroimmunology [7,17]. Pathology of cerebral amyloid angiopathy The first detailed descriptions of CAA are attributed to Scholz [18], who described the deposition of proteinaceous material within cerebral artery and capillary walls and as excrescences or Drusen on the outer aspects of vessels in the brain (drusige Entartung). In the 1980s, it was from leptomeningeal arteries with CAA that Glenner and colleagues [19] first isolated and characterised Aβ. The distribution of CAA in the different regions of the brain corresponds to the distribution of plaques of Aβ [20-22]. In AD, plaques and CAA both appear to follow a sequence involving the cerebral isocortex (neocortex) at the earliest stages, then the allocortex of the hippocampus and related structures, followed by involvement of the basal ganglia and thalamus [20-22]. The structures of the walls of arteries in the neocortex and basal ganglia differ [23] and this may partly account for the less frequent deposition of Aβ as plaques and CAA in the basal ganglia [20,22,23]. The shorter and more soluble Aβ40 is most abundant in CAA, whereas the longer and less soluble Aβ42 predominates in Aβ plaques within brain parenchyma [23]. Apolipoprotein E (ApoE) co-localises with Aβ, both in plaques in the brain and with Aβ in the walls of capillaries and arteries in CAA [22,23]. Together with age, APOE ε4 genotype is a major risk factor for both CAA and AD [1]. Cerebral amyloid angiopathy in leptomeningeal arteries Leptomeningeal arteries on the surface of the cerebral hemispheres are most commonly affected by CAA, arteries in the cerebral cortex are less affected, and capillaries are even less frequently involved by CAA. Medium-sized leptomeningeal arteries often have a patchy deposition of Aβ in the media or in the adventitia on the outer aspects of the artery wall (Figure 1a) [23]. Small arteries may show dense accumulation of Aβ in the tunica media (Figure 1a), or as seen in an artery entering the cerebral cortex in Figure 1b, there may be a reticular pattern of Aβ deposition that reflects the accumulation of Aβ in the basement membranes of the smooth muscle cells in the tunica media [4,5,24]. Aβ is detectable by thioflavin staining or by immunohistochemistry mainly in the walls of leptomeningeal arteries with a diameter of less than 60 μm [4], but this reveals only part of the picture. Biochemical investigations have detected Aβ in intracranial vessels as large as the basilar and middle cerebral arteries in individuals as young as 20 years of age (the youngest tested) and increasing sharply in those from 50 to 70 years of age [25]. Aβ was undetectable in the walls of extracranial blood vessels [25]. In transgenic mouse models of Aβ-CAA, there is heavy deposition of Aβ in the walls of leptomeningeal arteries, but involvement may start with the larger arteries at the base of the brain [26]. Veins do not appear to be involved in CAA, although deposits of Aβ are found attached to the walls of veins when CAA of leptomeningeal arteries is severe; this may be due to flakes of amyloid detaching from artery walls in the subarachnoid space and attaching to veins [23]. Cerebral amyloid angiopathy in cortical arteries Aβ may be deposited in the whole or part of the circumference of the wall of cortical arteries (Figure 2a). When arteries are viewed in a longitudinal plane, however, deposition of amyloid is often discontinuous along the length of the vessel (Figure 2b). Transverse bands (Figure 2c) reflect the deposition of amyloid in basement membranes surrounding smooth muscle cells in the tunica media [4]. A similar patchy distribution is seen in the walls of leptomeningeal arteries [4,27]. The discontinuous nature of the amyloid deposits in CAA means that estimating the true incidence and severity of CAA is probably most accurately performed on isolated cerebral vessels rather than on sections of brain [27]. Aβ is frequently deposited in the glia limitans that surrounds arteries in the cortex. However, it is unlikely that Aβ drains Page 2 of 13
3 Available online Figure 1 Cerebral amyloid angiopathy in Alzheimer disease. (a) Small leptomeningeal arteries (SLAs) on the surface of the cerebral cortex show dense deposits of amyloid-beta (Aβ) in their walls, whereas the medium-sized arteries (MLAs) show a more dispersed pattern of deposition of Aβ. A cortical artery with cerebral amyloid angiopathy (CxA) is surrounded by plaques of Aβ in the brain parenchyma (pan-aβ immunohistochemistry). (b) Branch of a leptomeningeal artery entering the cerebral cortex. Amyloid (red) is in the basement membranes (as outlined by collagen IV staining [5]) surrounding smooth muscle cells [4] (dark spaces) in the tunica media (confocal microscopy of Congo red stained preparation). Scale bars = 100 μm (a) and 50 μm (b). directly from the glia limitans into the artery wall [28] as the adjacent artery wall may lack Aβ (Figure 2d), and in the less severely involved vessels, there is discontinuity across the artefactual space [28] that separates Aβ in the artery wall from deposits in the glia limitans (Figure 2d-f). ApoE is also deposited in the glia limitans and co-localises with the Aβ [22]. The ligand in the glia limitans to which the Aβ binds is not known and it may be that Aβ is taken up by astrocytes [22]. Dystrophic neurites are also seen in the perivascular glia limitans, although again the reason is not clear [1]. At the surface of the cerebral cortex, deposition of Aβ may be seen in the glia limitans remote from artery walls [4] (Figure 2f), which suggests that the deposits are due to an inherent property of the glia limitans rather than related to perivascular drainage of Aβ. Deposition of Aβ in basement membranes in artery walls appears to impair the perivascular drainage of ISF and solutes from the brain [3,5], but it has other effects. Smooth muscle cells are lost from artery walls in CAA and replaced by amyloid (Figure 2g,h), and the affected vessels may show severe degenerative changes that are associated with cerebral haemorrhage [29]. Capillary amyloid angiopathy Deposits of Aβ in capillary walls are much less common than Aβ deposits in the walls of cortical and leptomeningeal arteries [30]. Capillary CAA is seen mostly in areas that are devoid of Aβ plaques [31,32], and the Aβ in the capillary walls is mainly Aβ42 [30]. Capillaries with no Aβ in their walls may be closely associated with diffuse plaques of Aβ (Figure 3a). In CAA, insoluble Aβ is deposited in the basement membranes of capillary endothelia (Figure 3b-d) and as excrescences or Drusen (Figure 3c-h) that are smooth and globular (Figure 3c,d,f), irregular (Figure 3e) or filamentous (Figure 3g,h). Drusen are continuous with Aβ in the capillary basement membrane. Both types of pericapillary deposit of Aβ can be demonstrated in paraffin sections (Figure 3c-e), in smear preparations of brain [28] (Figure 3f-h) or on vessels isolated by digesting away the surrounding brain tissue [4]. The consolidated globular Drusen (Figure 3c,d,f ) may be older than the filamentous deposits of Aβ where the strands of amyloid are in the extracellular spaces of the brain parenchyma through which solutes diffuse to reach the drainage pathways in the capillary walls [3,33]. Page 3 of 13
4 Alzheimer s Research & Therapy Vol 1 No 2 Weller et al. Figure 2 Cerebral amyloid angiopathy: amyloid-beta (Aβ) in cortical and leptomeningeal artery walls. (a) Cortical artery with deposition of Aβ in its wall but with no Aβ in the glia limitans (pan-aβ immunohistochemistry). Smear preparations of cortical arteries showing (b) a patchy transverse banding pattern of amyloid deposition with no amyloid deposits attached to the outer aspect of the artery and (c) transverse banding of amyloid associated with the basement membranes of smooth muscle cells [4,5] (thioflavin S stain: confocal images). Pan-Aβ immunohistochemistry of cortical arteries showing (d) Aβ in the glia limitans but with no Aβ in the vessel wall, (e) deposits of Aβ in the artery wall and in the glia limitans but no continuity between the two Aβ deposits and (f) Aβ in an artery wall with a heavy deposit of Aβ in the glia limitans both surrounding the vessel and on the surface of the brain (top). There is no continuity between the staining in the vessel wall and the glia limitans. A cored amyloid plaque in the brain parenchyma is seen to the left of the artery. Leptomeningeal arteries showing (g) deposition of Aβ in the vessel walls (pan-aβ immunohistochemistry) and (h) loss of alpha-smooth muscle actin staining in the artery walls in relation to the deposition of Aβ; arteries in (h) are the same as those in (g). (Immunohistochemistry for alpha-smooth muscle actin.) Scale bars = 20 μm (a-e,g,h) and 50 μm (f). Reprinted with permission from John Wiley & Sons, Inc. [28]. Page 4 of 13
5 Available online Figure 3 Capillary amyloid angiopathy. Pan-amyloid-beta (pan-aβ) immunohistochemistry. (a) A diffuse plaque of Aβ in cerebral cortex with a capillary, devoid of Aβ, running through it. Cortical capillaries are surrounded by (b) a thin layer of Aβ corresponding to the perivascular basement membrane (c) with attached globular deposits of Aβ (Drusen) continuous with Aβ in the capillary wall. (d) Globular Aβ Drusen partly surround the capillary wall. Confocal images were stained with thioflavin S. (e) Histological section of a cortical capillary with a spiky Druse of amyloid continuous with amyloid in the capillary wall. (f) Smear preparations of multiple globular Drusen and (g) filiform deposits of amyloid attached to cortical capillaries whose walls also stain for amyloid. (h) Higher magnification shows continuity of the filaments with amyloid in the capillary wall. Scale bars = 20 μm (a-d,f-h) and 10 μm (e). Reprinted with permission from John Wiley & Sons, Inc. [28]. Page 5 of 13
6 Alzheimer s Research & Therapy Vol 1 No 2 Weller et al. Pathogenesis of cerebral amyloid angiopathy Early theories for the pathogenesis of CAA suggested that the Aβ in vessel walls was derived from the blood [18,19] or from vascular smooth muscle cells [24]. However, transgenic mouse lines that overexpress human Aβ only in neurons in the brain develop CAA [34], suggesting that Aβ is probably not derived from the blood in CAA but from the brain [5]. Furthermore, Aβ is deposited not only in the walls of arteries in CAA but also in the walls of capillaries that lack smooth muscle [34,35]. Although smooth muscle cells in artery walls produce Aβ (in common with most cells in the body) and may contribute to CAA, they do not appear to be the main source of Aβ in CAA [5,36]. In BRI2-related dementia [13], ABri amyloid is not produced by vascular smooth muscle cells, yet CAA is a very prominent pathological feature; this again suggests that amyloid in CAA is derived from the central nervous system. Most of the evidence now points to the failure of perivascular lymphatic drainage of Aβ as a major factor in the pathogenesis of CAA in AD [5,23]. Failure of perivascular lymphatic drainage of amyloidbeta from the brain Perivascular lymphatic drainage pathways by which ISF and solutes drain from the brain have been defined in experimental animals [3,9,37], and Aβ is deposited in those pathways in CAA as its drainage fails with age (Figure 4). Fluorescent tracers injected into the striatum of the mouse brain initially spread diffusely through the brain parenchyma, but within 5 minutes, the tracers are located in the capillary basement membranes and in the basement membranes around smooth muscle cells in the tunica media of arteries [3]. Tracers are taken up in small amounts by vascular smooth muscle cells and by perivascular macrophages along the lymphatic drainage route [3]. Lymphatic drainage of ISF along artery walls appears to be almost completely separate from CSF [7]. Only 15% of radioactive tracer injected into the ISF is recoverable from the CSF, and the majority of tracer drains to the cervical lymph nodes [9] at a rate equivalent to lymphatic drainage from other tissues [9]. Radioactive tracers injected into the brain were located in the adventitia of intracranial arteries but were absent from the walls of the carotid artery in the neck [9]. This suggests that solutes draining from the brain pass along the walls of intracranial arteries but leave the carotid artery wall at the base of the skull en route to the cervical lymph nodes [7,9]. Figure 4 summarises the major mechanisms and routes for the elimination of Aβ from the brain. Observations from tracer studies and from CAA (Figures 1-3) suggest that, as Aβ leaves the brain, it initially diffuses with ISF and other solutes through the narrow and tortuous extracellular spaces of the grey matter [3,33,38] (Figure 4). It then enters the bulk drainage pathways in the 100- to 150-nm-thick endothelial basement membranes in the walls of capillaries [3,28,33] to drain out of the brain along basement membranes in the tunica media of cortical and leptomeningeal arteries [5]. Figure 4 Elimination of amyloid-beta (Aβ) from the brain. Aβ is (i) produced by neurons and other cells in the brain and then (ii) diffuses with interstitial fluid and other solutes through the narrow extracellular spaces (ECS) of the brain to (iii) the bulk flow lymphatic drainage pathways in the basement membranes of capillaries and in the tunica media of artery walls and (iv) out of the brain to cervical lymph nodes. Smooth muscle cells and perivascular macrophages take up Aβ and are part of the elimination pathway. Degradation of Aβ occurs in the brain parenchyma, by neprilysin and other enzymes, and Aβ is absorbed into the blood by LRP-1 (lipoprotein receptor-related protein- 1)-mediated mechanisms in capillary endothelia. These mechanisms for the elimination of Aβ from the brain tend to fail with age and in Alzheimer disease. Basement membranes of the arterial endothelium are not involved in the drainage of fluorescent tracers and do not contain stainable Aβ in CAA [3,5] (Figure 4). This may be one reason why CAA in older patients and in those with AD is not accompanied by catastrophic arterial thrombosis. Although capillaries may be occluded and reduced in number in AD [39], thrombotic occlusion of arteries in AD is not as widespread as CAA. Tracer studies suggest that fluid and solutes move to the adventitia of leptomeningeal arteries and from there to the lymph nodes at the base of the skull [7,9]. In CAA, Aβ is detected by immunohistochemistry mainly in the tunica media of smaller leptomeningeal arteries but is present in the adventitia on the outer aspects of medium-sized leptomenin- Page 6 of 13
7 Available online geal arteries [23], suggesting that Aβ follows the same lymphatic drainage route as tracers in experimental animals [7,9]. Restriction of Aβ to the walls of intracranial arteries and its absence from the walls of the extracranial carotid artery [25] suggest that Aβ drains from the wall of the carotid artery to lymph nodes related to the artery at the base of the skull [40]. The pattern of deposition of Aβ in the basement membranes of capillary and artery walls in CAA indicates that there is a failure of lymphatic drainage of Aβ and suggests that the failure is related to age changes in artery walls. Age changes in cerebral arteries and the aetiology of cerebral amyloid angiopathy As arteries age, fibrous tissue increases in the tunica intima and tunica media (arteriosclerosis and arteriolosclerosis) and arteries become stiffer [23]. Such age changes may interfere with the motive force for transport of ISF and solutes, like soluble Aβ, out of the brain. Theoretical models suggest that the contrary (reflection) wave that follows the pulse wave in arteries is the motive force that drives ISF and solutes out of the brain along perivascular pathways in the direction opposite to the flow of blood in the lumen [8]. Stretching of the basement membrane with expansion of the artery during systole may be the valve that prevents reflux during the subsequent pulse wave [23]. If the pulse wave is the motive force for perivascular drainage of Aβ, then stiffening of artery walls with age may interfere with that force. Vascular basement membrane changes that occur with age and defects in innervation of cerebral vessel may also play roles in the pathogenesis of CAA [8,23]. Overproduction of transforming growth factor-beta-1 in transgenic mice results in changes in vascular basement membranes and induces CAA [41]. Furthermore, experimental cholinergic deafferentation of arteries within the brain, induced by the destruction of the nucleus basalis, results in CAA that resolves with reinnervation [42]. These observations emphasise the need to view the lymphatic drainage pathways as a dynamic entity in the context of the whole neurovascular unit [43]. Pathogenesis of cerebral amyloid angiopathy in capillaries Capillary CAA is much less common than CAA in leptomeningeal or cortical arteries and has been associated with severe dementia [44] and with APOE ε4 genotype [31]. However, this does not explain the pathogenesis of capillary CAA. An association between capillary CAA and thrombotic occlusion of cortical arteries has been reported [32], and there is an increase in capillary CAA in the brains of patients treated with immunotherapy [45]. In both of these instances, capillary CAA is associated with a paucity or absence of Aβ plaques in the surrounding brain parenchyma and the deposition of Aβ in capillary walls. In the immunised patients with AD, there is an increase in Aβ42 in the walls of blood vessels, suggesting that it is derived from plaque Aβ [46]. It seems that the removal of Aβ from plaques by microglia, activated by either ischaemia or immunisation, results in an overload of the drainage pathways in capillary walls by which Aβ drains from the brain. Failure of other mechanisms for elimination of amyloidbeta aggravates cerebral amyloid angiopathy Arranged along the pathway for the drainage of soluble Aβ from the brain is an array of enzymes and mechanisms for the elimination of Aβ (Figure 4) [1]. Enzymes that degrade Aβ are present in the brain parenchyma and in artery walls [1]. Mechanisms that mediate absorption of Aβ into the blood via capillary endothelium or uptake of Aβ by smooth muscle cells are also present in the walls of cerebral blood vessels [1]. Neprilysin, angiotensin-converting enzyme and insulindegrading enzyme are among the Aβ-degrading enzymes to which Aβ is exposed as it diffuses through the extracellular spaces of grey matter in the brain and along the perivascular drainage pathways [1]. Neprilysin can hydrolyse monomeric and oligomeric forms of Aβ40 and Aβ42. However, abnormal forms of Aβ that result from the Flemish, Dutch, Italian and Arctic mutations in the APP gene are not cleaved by neprilysin and these familial disorders are associated with severe CAA and early-onset cerebral haemorrhage or dementia [10]. Neprilysin is produced by pyramidal neurons and by smooth muscle cells in the walls of arteries [47]; a reduction of neprilysin in artery walls is associated with severe CAA in AD and in transgenic mice [47,48]. Other enzymes that degrade Aβ in the walls of cerebral arteries are also deficient or less active in AD [1]. Absorption of Aβ into the blood, mediated by low-density lipoprotein receptor-related protein-1 (LRP-1) located in capillary endothelium [43,49], is a major mechanism for elimination of Aβ from the brain [43] and is six times faster than lymphatic drainage [50]. LRP-1 also mediates the entry of Aβ into vascular smooth muscle cells, where it is degraded [43]. Failure of LRP-1-related elimination of Aβ with age [49] or in conditions of hypoxia [43] may also increase the flow of soluble Aβ into perivascular drainage pathways already compromised by age changes in the artery walls themselves [23]. There is evidence that the perivascular macrophages that take up tracer draining along perivascular pathways [3] also degrade Aβ [51]. In APP transgenic mice that overproduce human Aβ, stimulation of perivascular macrophages reduces the severity of CAA whereas depletion of these cells increases the severity of CAA [51]. Enzymic and absorptive mechanisms appear to fail with age [1]. Such a failure may be a factor that aggravates CAA in older patients and in those with AD by diverting more Aβ into the ageing perivascular drainage pathways [23]. Complications of cerebral amyloid angiopathy The major complications associated with CAA are (a) rupture of amyloid-laden arteries, resulting in acute and often fatal Page 7 of 13
8 Alzheimer s Research & Therapy Vol 1 No 2 Weller et al. intracerebral haemorrhage; (b) Aβ-related angiitis; (c) disruption of lymphatic drainage of ISF and solutes along artery walls; and (d) cerebral hypoperfusion. The last two complications apply particularly to AD. Intracerebral haemorrhage is a feature of familial and sporadic CAA [52]. Familial cases of Aβ-CAA typically present with recurrent cerebral haemorrhages, white matter lesions and cognitive impairment 20 years earlier than patients with sporadic CAA [52]. Mutant Aβ in some forms of familial CAA is resistant to degradation by neprilysin and thus may increase the amount of Aβ draining along perivascular pathways [52]. In sporadic CAA-related haemorrhage, the temporal and occipital lobes are preferentially affected [53], and although the major risk factor for the development of CAA is the APOE ε4 allele, the ε2 allele predisposes to haemorrhage [29]. Artery walls often show severe degenerative changes in addition to severe CAA [29]. Aβ-related angiitis is a complication of CAA [52,54]. Patients present at a mean age of 67 years with changes in mental status, headaches, seizures, focal neurological signs or hallucinations [54]. The angiopathy may be granulomatous with accumulation of lymphocytes around leptomeningeal arteries and the presence of multinucleated giant cells in vessel walls related to deposits of Aβ. There is microglial activation in the cortex and white matter hyperintensities on magnetic resonance imaging [54]. The presence of angiitis in relation to CAA may have implications for immunotherapy in AD [52,54]. Cerebral amyloid angiopathy in the aetiology of Alzheimer disease CAA affects two of the major functions of cerebral arteries in AD: (a) the blood supply to the brain and (b) the lymphatic drainage of ISF and solutes from the brain. Accumulation of Aβ and the loss of smooth muscle cells in CAA result in decreased vascular reactivity to functional stimulation and affect the blood supply to the brain in AD [16,43,55]. Pathologically, CAA initially affects the leptomeningeal and parenchymal arteries of the cerebral cortex whereas severe arteriosclerosis tends to affect the vessels in the basal ganglia in the initial stages, and both are associated with defects in blood flow and cognitive decline in AD [20]. Accumulation of amyloid-beta in the brain in Alzheimer disease Figure 5 summarises the role of impaired lymphatic drainage of the brain and CAA in the accumulation of Aβ in the brain in AD. Diffusion of Aβ through the extracellular spaces of the brain and along the drainage pathways in artery walls [56,57] is impaired by plaques of Aβ in the brain [58,59]. CAA also restricts the drainage of Aβ along perivascular pathways as seen in tg2576 transgenic mice in which plasma levels of Aβ fall and levels of Aβ in the brain rise as CAA develops [60]. There is evidence that the failure of elimination of Aβ and fluid from the brain correlates with CAA in human AD. First, severe CAA correlates with severe dementia [61]. Second, high levels of soluble Aβ40 in brain parenchyma, with up to a threefold increase, distinguish demented patients with AD from non-demented patients, even though the non-demented patients may have high numbers of insoluble Aβ plaques in their brains [62]. Third, accumulation of fluid in cerebral white matter (leukoaraiosis) in AD has been correlated with the severity of CAA [27], suggesting that Aβ in artery walls may block the perivascular drainage of fluid and solutes from white matter as well as from grey matter. These observations suggest that one of the main pathogenetic roles of insoluble Aβ is to block the elimination of fluid and solutes from the brain. This may result in the accumulation of toxic soluble fibrillar oligomers of Aβ in the brain in AD [63]. But it may equally well result in the accumulation of other soluble metabolites and the loss of homeostasis of the neuronal environment with consequent impairment of neuronal function. Variability of cerebral amyloid angiopathy in Alzheimer disease The reported prevalence of CAA in histological studies of brains of patients with AD varies from 90% to 96% [1]. However, the true prevalence of CAA in AD may be significantly underestimated in histological and immunohistochemical surveys in which little account may be taken of the long length of the perivascular drainage pathways, the patchy nature of Aβ deposits and the relative insensitivity of immunohistochemistry as a method for detecting Aβ compared with biochemical techniques [23]. Methods using isolated cerebral arteries, stained for amyloid, may give better estimates of the true prevalence and distribution of CAA in AD [4,27], and a greater understanding of the dynamics and pathophysiology of perivascular drainage should help to resolve any current discrepancies in the role of CAA in the aetiology of AD. Role of cerebral amyloid angiopathy in the accumulation of tau in the brain in Alzheimer disease In addition to the accumulation of insoluble and soluble Aβs in the brain in AD, hyperphosphorylated tau accumulates as neurofibrillary tangle (NFT) in neurons and as neuropil threads and dystrophic neurites in neuronal processes [64]. Explaining how the accumulation of tau relates to the deposition of Aβ in the brain has presented a challenge for many years. In transgenic mice that overexpress both APP and tau, the deposition of Aβ in the brain precedes and accelerates the accumulation of intracellular tau [65]. Furthermore, a recent study suggests that failure of elimination of tau from the extracellular spaces of the brain may play a role in the intracellular accumulation of tau [66]. In AD, tau inclusions first appear in neurons in the transentorhinal cortex and then spread to the hippocampal formation and neocortex [64]. Cognitive impairment ensues as tau inclusions reach the hippocampus, and neocortical tau inclusions are a hallmark of the later and more severe stages of AD [64]. Injections of Page 8 of 13
9 Available online Figure 5 Impaired lymphatic drainage of the brain in the pathogenesis of cerebral amyloid angiopathy (CAA) and Alzheimer disease (AD). The schema outlines a working hypothesis for the failure of perivascular lymphatic drainage of the brain with age and how such a failure contributes to the pathogenesis of CAA and AD. Aβ, amyloid-beta; ECS, extracellular spaces; ISF, interstitial fluid; NFT, neurofibrillary tangle. Page 9 of 13
10 Alzheimer s Research & Therapy Vol 1 No 2 Weller et al. Figure 6 Changes in the brain induced by amyloid-beta (Aβ) immunotherapy. Comparison of frames (a) and (b) shows the major effects of Aβ immunotherapy upon the brain. There is a decrease in plaques of Aβ and of dystrophic neurites but an increase in the severity of cerebral amyloid angiopathy (CAA), in microglial activation (for the degradation of Aβ plaques), and in the level of soluble Aβ in the brain parenchyma. Neurofibrillary tangles (NFTs) and neuropil threads are still present. AD, Alzheimer disease. fibrillary tau transfer the propensity to form NFT in mice [66], which suggests that interference with the disposal of tau from the extracellular spaces when lymphatic drainage pathways are blocked by CAA may be a factor in the formation and spread of NFT in the human brain in AD. Increase of cerebral amyloid angiopathy following immunotherapy for Alzheimer disease Immunisation against Aβ42 prevents the accumulation of plaques of Aβ in the brains of young transgenic APP mice and removes insoluble plaques of Aβ from the brains of older mice [67]. Similar results with the clearance of Aβ have been observed in the Elan clinical trial of Aβ immunisation in patients with AD [68]. However, despite the removal of Aβ plaques from the brain, there is little evidence that this benefits cognitive function [69]. Page 10 of 13 Figure 6 is a summary of the effects of Aβ42 immunisation on the brain in AD. In non-immunised patients with AD (Figure 6a), insoluble Aβ is present in the brain parenchyma as diffuse plaques and as compact neuritic plaques surrounded by dystrophic neurites containing hyperphosphorylated tau. Neuropil threads and neurons containing NFT are also present in the brains of unimmunised patients. Following immunisation with Aβ42 (Figure 6b), insoluble Aβ in the plaques is removed by antibodies and activated microglia and the dystrophic neurites associated with neuritic plaques disappear [46]. NFTs in neurons and neuropil threads remain [46]. However, the severity of CAA increases following immunotherapy (Figure 6b) [46,70], and there is some indication that the level of soluble Aβ rises in the brains of treated patients [71]. There is an increase in Aβ42 in capillary and artery walls following immunisation in AD [45,46]. Aβ40 is usually the
11 Available online predominant amyloid in vessel walls and Aβ42 is mainly in the plaques [23]. Increased amounts of Aβ42 in vessel walls appear to be the result of removal of the Aβ plaques [45,46], allowing more Aβ42 to reach drainage channels in capillary and artery walls, where its further removal is blocked and the severity of CAA increases [46]. Changes in the white matter of patients treated with immunotherapy have raised concerns [68,72]. The increased signal seen in the white matter on T2-weighted magnetic resonance imaging in many older individuals and in those with AD [73] and often ascribed to ischaemia is aggravated by immunotherapy [68]. Failure of fluid drainage from the white matter along arteries that are severely affected by CAA [27] may be a factor in the increased white matter changes following immunisation. Solving the problem of CAA is obviously a priority for ensuring the success of immunotherapy for AD and there is some indication that this may be possible. Although Aβ immunotherapy in APP mice usually results in an increase in CAA [70], passive immunisation with antibodies that bind to the N-terminal portion of Aβ results in a reduction of CAA [74]. Furthermore, two human cases who survived for 5 years following immunisation showed extensive clearance of Aβ from plaques and very little CAA [46]. It is possible that, with time, CAA will resolve in some immunised patients. The role of apoe in the elimination of Aβ from the brain is still not fully established, but the marked accumulation of apoe colocalising with Aβ in CAA following immunisation suggests that the elimination of Aβ may be chaperoned by apoe [45]. Conclusions and future directions Elimination of Aβ from the brain involves enzymic degradation, its absorption into the blood and drainage of Aβ along perivascular lymphatic drainage pathways. All of these mechanisms appear to fail as the brain and cerebral arteries age. One of the major consequences of this failure is the obstruction of lymphatic drainage of fluid and solutes from the brain by CAA that results in the accumulation of insoluble and soluble Aβs in the brain and probably other metabolites that would lead to loss of homeostasis of the neuronal environment. Accumulation of hyperphosphorylated tau in neurons and failure of neuronal function may ensue from the loss of homeostasis. The therapeutic challenge is to ensure adequate elimination of Aβ from the ageing brain and along ageing cerebral arteries. Pharmacological intervention to enhance enzymic degradation of Aβ and absorption of Aβ into the blood is one obvious direction to take. Resolving the inadequacies of the ageing lymphatic drainage pathway will entail a greater understanding of its physiology and how the various elements such as basement membranes, smooth muscle cells and perivascular cells interact and how they change with age. Establishing the role played by apoe in the elimination of Aβ and harnessing this information for the design of therapies may help to prevent the accumulation of amyloid in blood vessel walls and brain in AD. Competing interests The authors declare that they have no competing interests. Acknowledgements We thank Anton Page of the Biomedical Imaging Unit, Southampton General Hospital, for his help with the illustrations and Delphin Boche (Clinical Neurosciences, Southampton) for her advice on the manuscript. This work was supported by the Alzheimer s Research Trust (UK). References 1. Love S, Miners S, Palmer J, Chalmers K, Kehoe P: Insights into the pathogenesis and pathogenicity of cerebral amyloid angiopathy. Front Biosci 2009, 14: Esiri MM, Wilcock GK: Cerebral amyloid angiopathy in dementia and old age. J Neurol Neurosurg Psychiat 1986, 49: Carare RO, Bernardes-Silva M, Newman TA, Page AM, Nicoll JAR, Perry VH, Weller RO: Solutes, but not cells, drain from the brain parenchyma along basement membranes of capillaries and arteries. Significance for cerebral amyloid angiopathy and neuroimmunology. Neuropathol Appl Neurobiol 2008, 34: Weller RO, Massey A, Newman TA, Hutchings M, Kuo YM, Roher AE: Cerebral amyloid angiopathy: amyloid beta accumulates in putative interstitial fluid drainage pathways in Alzheimer s disease. Am J Pathol 1998, 153: Weller RO, Subash M, Preston SD, Mazanti I, Carare RO: Perivascular drainage of amyloid-beta peptides from the brain and its failure in cerebral amyloid angiopathy and Alzheimer s disease. Brain Pathol 2008, 18: Muthuchamy M, Zawieja D: Molecular regulation of lymphatic contractility. Ann N Y Acad Sci 2008, 1131: Weller RO, Djuanda E, Yow HY, Carare RO: Lymphatic drainage of the brain and the pathophysiology of neurological disease. Acta Neuropathol 2009, 117: Schley D, Carare-Nnadi R, Please CP, Perry VH, Weller RO: Mechanisms to explain the reverse perivascular transport of solutes out of the brain. J Theor Biol 2006, 238: Szentistvanyi I, Patlak CS, Ellis RA, Cserr HF: Drainage of interstitial fluid from different regions of rat brain. Am J Physiol 1984, 246:F Revesz T, Holton JL, Lashley T, Plant G, Frangione B, Rostagno A, Ghiso J: Genetics and molecular pathogenesis of sporadic and hereditary cerebral amyloid angiopathies. Acta Neuropathol 2009, 118: Palsdottir A, Snorradottir AO, Thorsteinsson L: Hereditary cystatin C amyloid angiopathy: genetic, clinical, and pathological aspects. Brain Pathol 2006, 16: Reilly MM, Staunton H: Peripheral nerve amyloidosis. Brain Pathol 1996, 6: Lashley T, Revesz T, Plant G, Bandopadhyay R, Lees AJ, Frangione B, Wood NW, de Silva R, Ghiso J, Rostagno A, Holton JL: Expression of BRI2 mrna and protein in normal human brain and familial British dementia: its relevance to the pathogenesis of disease. Neuropathol Appl Neurobiol 2008, 34: Kovacs GG, Budka H: Molecular pathology of human prion diseases. Int J Mol Sci 2009, 10: Chesebro B, Trifilo M, Race R, Meade-White K, Teng C, LaCasse R, Raymond L, Favara C, Baron G, Priola S, Caughey B, Masliah E, Oldstone M: Anchorless prion protein results in infectious amyloid disease without clinical scrapie. Science 2005, 308: Smith EE, Greenberg SM: Beta-amyloid, blood vessels, and brain function. Stroke 2009, 40: Weller RO, Galea I, Carare RO, Minagar A: Pathophysiology of the lymphatic drainage of the central nervous system: implications for pathogenesis and therapy of multiple sclerosis. Pathophysiology, in press. Page 11 of 13
12 Alzheimer s Research & Therapy Vol 1 No 2 Weller et al. 18. Scholz W: Studies on the pathology of cerebral blood vessels II. The nodular degeneration of cerebral arteries and capillaries. (A form of senile vascular disease) [in German]. Zeitschrift für die gesamte Neurologie und Psychiatrie 1938, 162: Glenner GG, Wong CW, Quaranta V, Eanes ED: The amyloid deposits in Alzheimer s disease: their nature and pathogenesis. Appl Pathol 1984, 2: Thal DR, Ghebremedhin E, Orantes M, Wiestler OD: Vascular pathology in Alzheimer disease: correlation of cerebral amyloid angiopathy and arteriosclerosis/lipohyalinosis with cognitive decline. J Neuropathol Exp Neurol 2003, 62: Thal DR, Rüb U, Orantes M, Braak H: Phases of A beta-deposition in the human brain and its relevance for the development of AD. Neurology 2002, 58: Thal DR, Griffin WS, de Vos RA, Ghebremedhin E: Cerebral amyloid angiopathy and its relationship to Alzheimer s disease. Acta Neuropathol 2008, 115: Weller RO, Boche D, Nicoll JA: Microvasculature changes and cerebral amyloid angiopathy in Alzheimer s disease and their potential impact on therapy. Acta Neuropathol 2009, 118: Wisniewski HM, Wegiel J: Beta-amyloid formation by myocytes of leptomeningeal vessels. Acta Neuropathol (Berl) 1994, 87: Shinkai Y, Yoshimura M, Ito Y, Odaka A, Suzuki N, Yanagisawa K, Ihara Y: Amyloid beta-proteins 1-40 and 1-42(43) in the soluble fraction of extra- and intracranial blood vessels. Ann Neurol 1995, 38: Domnitz SB, Robbins EM, Hoang AW, Garcia-Alloza M, Hyman BT, Rebeck GW, Greenberg SM, Bacskai BJ, Frosch MP: Progression of cerebral amyloid angiopathy in transgenic mouse models of Alzheimer disease. J Neuropathol Exp Neurol 2005, 64: Roher AE, Kuo Y-M, Esh C, Knebel C, Weiss N, Kalback W, Luehrs DC, Childress JL, Beach TG, Weller RO, Kokjohn TA: Cortical and leptomeningeal cerebrovascular amyloid and white matter pathology in Alzheimer s disease. Mol Med 2003, 9: Preston SD, Steart PV, Wilkinson A, Nicoll JAR, Weller RO: Capillary and arterial amyloid angiopathy in Alzheimer s disease: defining the perivascular route for the elimination of amyloid beta from the human brain. Neuropathol Appl Neurobiol 2003, 29: McCarron MO, Nicoll JA, Stewart J, Ironside JW, Mann DM, Love S, Graham DI, Dewar D: The apolipoprotein E epsilon2 allele and the pathological features in cerebral amyloid angiopathyrelated hemorrhage. J Neuropathol Exp Neurol 1999, 58: Oshima K, Akiyama H, Tsuchiya K, Kondo H, Haga C, Shimomura Y, Iseki E, Uchikado H, Kato M, Niizato K, Arai H: Relative paucity of tau accumulation in the small areas with abundant Abeta42-positive capillary amyloid angiopathy within a given cortical region in the brain of patients with Alzheimer pathology. Acta Neuropathol (Berl) 2006, 111: Thal DR, Ghebremedhin E, Rub U, Yamaguchi H, Tredici KD, Braak H: Two types of sporadic cerebral amyloid angiopathy. J Neuropathol Exp Neurol 2002, 61: Yow HY, Weller RO: A role for cerebrovascular disease in determining the pattern of beta amyloid deposition in Alzheimer s disease. Neuropathol Appl Neurobiol 2002, 28: Abbott NJ: Evidence for bulk flow of brain interstitial fluid: significance for physiology and pathology. Neurochem Int 2004, 45: Calhoun ME, Burgermeister P, Phinney AL, Stalder M, Tolnay M, Wiederhold KH, Abramowski D, Sturchler Pierrat C, Sommer B, Staufenbiel M, Jucker M: Neuronal overexpression of mutant amyloid precursor protein results in prominent deposition of cerebrovascular amyloid. Proc Natl Acad Sci U S A 1999, 96: Herzig MC, Van Nostrand WE, Jucker M: Mechanism of cerebral beta-amyloid angiopathy: murine and cellular models. Brain Pathol 2006, 16: Nicoll JAR, Yamada M, Frackowiak J, Mazur Kolecka B, Weller RO: Cerebral amyloid angiopathy plays a direct role in the pathogenesis of Alzheimer s disease. Pro-CAA position statement. Neurobiol Aging 2004, 25: ; discussion Cserr HF, Harling-Berg CJ, Knopf PM: Drainage of brain extracellular fluid into blood and deep cervical lymph and its immunological significance. Brain Pathol 1992, 2: Syková E, Nicholson C: Diffusion in brain extracellular space. Physiol Rev 2008, 88: Thal DR, Capetillo-Zarate E, Larionov S, Staufenbiel M, Zurbruegg S, Beckmann N: Capillary cerebral amyloid angiopathy is associated with vessel occlusion and cerebral blood flow disturbances. Neurobiol Aging 2008, Mar 20. [Epub ahead of print]. 40. Clapham R, O Sullivan E, Weller RO, Carare RO: Cervical lymph nodes are found in direct relationship with the carotid arteries. Significance for the lymphatic drainage of the brain. Clin Anat, in press. 41. Wyss Coray T, Lin C, Sanan DA, Mucke L, Masliah E: Chronic overproduction of transforming growth factor-beta1 by astrocytes promotes Alzheimer s disease-like microvascular degeneration in transgenic mice. Am J Pathol 2000, 156: Beach TG: Physiologic origins of age-related beta-amyloid deposition. Neurodegener Dis 2008, 5: Bell RD, Zlokovic BV: Neurovascular mechanisms and bloodbrain barrier disorder in Alzheimer s disease. Acta Neuropathol 2009, 118: Attems J, Jellinger K: Only cerebral capillary amyloid angiopathy correlates with Alzheimer pathology - a pilot study. Acta Neuropathol (Berl) 2004, 107: Nicoll JA, Barton E, Boche D, Neal JW, Ferrer I, Thompson P, Vlachouli C, Wilkinson D, Bayer A, Games D, Seubert P, Schenk D, Holmes C: Abeta species removal after Abeta42 immunization. J Neuropathol Exp Neurol 2006, 65: Boche D, Zotova E, Weller RO, Love S, Neal JW, Pickering RM, Wilkinson D, Holmes C, Nicoll JA: Consequence of Abeta immunization on the vasculature of human Alzheimer s disease brain. Brain 2008, 131: Miners JS, Van Helmond Z, Chalmers K, Wilcock G, Love S, Kehoe PG: Decreased expression and activity of neprilysin in Alzheimer disease are associated with cerebral amyloid angiopathy. J Neuropathol Exp Neurol 2006, 65: Farris W, Schütz SG, Cirrito JR, Shankar GM, Sun X, George A, Leissring MA, Walsh DM, Qiu WQ, Holtzman DM, Selkoe DJ: Loss of neprilysin function promotes amyloid plaque formation and causes cerebral amyloid angiopathy. Am J Pathol 2007, 171: Shibata M, Yamada S, Kumar SR, Calero M, Bading J, Frangione B, Holtzman DM, Miller CA, Strickland DK, Ghiso J, Zlokovic BV: Clearance of Alzheimer s amyloid-beta(1-40) peptide from brain by LDL receptor-related protein-1 at the blood-brain barrier. J Clin Invest 2000, 106: Bell RD, Sagare AP, Friedman AE, Bedi GS, Holtzman DM, Deane R, Zlokovic BV: Transport pathways for clearance of human Alzheimer s amyloid beta-peptide and apolipoproteins E and J in the mouse central nervous system. J Cereb Blood Flow Metab 2007, 27: Hawkes CA, McLaurin J: Selective targeting of perivascular macrophages for clearance of beta-amyloid in cerebral amyloid angiopathy. Proc Natl Acad Sci U S A 2009, 106: Zhang-Nunes SX, Maat-Schieman ML, van Duinen SG, Roos RA, Frosch MP, Greenberg SM: The cerebral beta-amyloid angiopathies: hereditary and sporadic. Brain Pathol 2006, 16: Rosand J, Muzikansky A, Kumar A, Wisco JJ, Smith EE, Betensky RA, Greenberg SM: Spatial clustering of hemorrhages in probable cerebral amyloid angiopathy. Ann Neurol 2005, 58: Scolding NJ, Joseph F, Kirby PA, Mazanti I, Gray F, Mikol J, Ellison D, Hilton DA, Williams TL, MacKenzie JM, Xuereb JH, Love S: Abeta-related angiitis: primary angiitis of the central nervous system associated with cerebral amyloid angiopathy. Brain 2005, 128: Smith EE, Vijayappa M, Lima F, Delgado P, Wendell L, Rosand J, Greenberg SM: Impaired visual evoked flow velocity response in cerebral amyloid angiopathy. Neurology 2008, 71: Meyer-Luehmann M, Coomaraswamy J, Bolmont T, Kaeser S, Schaefer C, Kilger E, Neuenschwander A, Abramowski D, Frey P, Page 12 of 13
Dementia and Healthy Ageing : is the pathology any different?
 Dementia and Healthy Ageing : is the pathology any different? Professor David Mann, Professor of Neuropathology, University of Manchester, Hope Hospital, Salford DEMENTIA Loss of connectivity within association
Dementia and Healthy Ageing : is the pathology any different? Professor David Mann, Professor of Neuropathology, University of Manchester, Hope Hospital, Salford DEMENTIA Loss of connectivity within association
White Matter Changes in Dementia: Role of Impaired Drainage of Interstitial Fluid
 Brain Pathology ISSN 1015-6305 MINI-SYMPOSIUM: White matter damage in dementia White Matter Changes in Dementia: Role of Impaired Drainage of Interstitial Fluid Roy O. Weller 1 ; Cheryl A. Hawkes 1 ; Raj
Brain Pathology ISSN 1015-6305 MINI-SYMPOSIUM: White matter damage in dementia White Matter Changes in Dementia: Role of Impaired Drainage of Interstitial Fluid Roy O. Weller 1 ; Cheryl A. Hawkes 1 ; Raj
Lymphatic drainage of the brain and the pathophysiology of neurological disease
 Acta Neuropathol (2009) 117:1 14 DOI 10.1007/s00401-008-0457-0 REVIEW Lymphatic drainage of the brain and the pathophysiology of neurological disease Roy O. Weller EYe Djuanda Hong-Yeen Yow Roxana O. Carare
Acta Neuropathol (2009) 117:1 14 DOI 10.1007/s00401-008-0457-0 REVIEW Lymphatic drainage of the brain and the pathophysiology of neurological disease Roy O. Weller EYe Djuanda Hong-Yeen Yow Roxana O. Carare
The role of the vascular system in dementia
 The role of the vascular system in dementia James AR Nicoll Professor of Neuropathology, University of Southampton Consultant Neuropathologist, Southampton General Hospital What does the vascular system
The role of the vascular system in dementia James AR Nicoll Professor of Neuropathology, University of Southampton Consultant Neuropathologist, Southampton General Hospital What does the vascular system
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 7: Non traumatic brain haemorrhage
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 7: Non traumatic brain haemorrhage ILOS To list the causes of intracranial haemorrhage. To understand the pathogenesis of each cause.
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 7: Non traumatic brain haemorrhage ILOS To list the causes of intracranial haemorrhage. To understand the pathogenesis of each cause.
Original Article Perivascular Neuritic Dystrophy Associated with Cerebral Amyloid Angiopathy in Alzheimer s Disease
 www.ijcep.com/ijcep711002 Original Article Perivascular Neuritic Dystrophy Associated with Cerebral Amyloid Angiopathy in Alzheimer s Disease Kenichi Oshima, Hirotake Uchikado and Dennis W. Dickson Department
www.ijcep.com/ijcep711002 Original Article Perivascular Neuritic Dystrophy Associated with Cerebral Amyloid Angiopathy in Alzheimer s Disease Kenichi Oshima, Hirotake Uchikado and Dennis W. Dickson Department
HYPERTENSIVE ENCEPHALOPATHY
 HYPERTENSIVE ENCEPHALOPATHY Reversible posterior leukoencephalopathy syndrome Cause Renal disease Pheochromocytoma Disseminated vasculitis Eclampsia Acute toxemia Medications & illicit drugs (cocaine)
HYPERTENSIVE ENCEPHALOPATHY Reversible posterior leukoencephalopathy syndrome Cause Renal disease Pheochromocytoma Disseminated vasculitis Eclampsia Acute toxemia Medications & illicit drugs (cocaine)
NACC Vascular Consortium. NACC Vascular Consortium. NACC Vascular Consortium
 NACC Vascular Consortium NACC Vascular Consortium Participating centers: Oregon Health and Science University ADC Rush University ADC Mount Sinai School of Medicine ADC Boston University ADC In consultation
NACC Vascular Consortium NACC Vascular Consortium Participating centers: Oregon Health and Science University ADC Rush University ADC Mount Sinai School of Medicine ADC Boston University ADC In consultation
Pathophysiology of the lymphatic drainage of the central nervous system: Implications for pathogenesis and therapy of multiple sclerosis
 Pathophysiology 17 (2010) 295 306 Review Pathophysiology of the lymphatic drainage of the central nervous system: Implications for pathogenesis and therapy of multiple sclerosis R.O. Weller a,, I. Galea
Pathophysiology 17 (2010) 295 306 Review Pathophysiology of the lymphatic drainage of the central nervous system: Implications for pathogenesis and therapy of multiple sclerosis R.O. Weller a,, I. Galea
Diabetes Mellitus and Dementia. Andrea Shelton & Adena Zadourian
 Diabetes Mellitus and Dementia Andrea Shelton & Adena Zadourian Abstract Diabetes mellitus increases the risk for developing dementia...but there is inconsistency with the subtypes of dementia Diabetes
Diabetes Mellitus and Dementia Andrea Shelton & Adena Zadourian Abstract Diabetes mellitus increases the risk for developing dementia...but there is inconsistency with the subtypes of dementia Diabetes
Infiltrative Brain Mass Due To Progressive Alzheimer's Disease
 Article ID: WMC00505 2046-1690 Infiltrative Brain Mass Due To Progressive Alzheimer's Disease Corresponding Author: Dr. Mark Lyons, Associate Professor, Mayo Clinic Arizona, 85054 - United States of America
Article ID: WMC00505 2046-1690 Infiltrative Brain Mass Due To Progressive Alzheimer's Disease Corresponding Author: Dr. Mark Lyons, Associate Professor, Mayo Clinic Arizona, 85054 - United States of America
The Precapillary Segment of the Blood- Brain Barrier and Its Relation to Perivascular Drainage in Alzheimer's Disease and Small Vessel Disease
 Mini-Review TheScientificWorldJOURNAL (2009) 9, 557 563 ISSN 1537-744X; DOI 10.1100/tsw.2009.72 The Precapillary Segment of the Blood- Brain Barrier and Its Relation to Perivascular Drainage in Alzheimer's
Mini-Review TheScientificWorldJOURNAL (2009) 9, 557 563 ISSN 1537-744X; DOI 10.1100/tsw.2009.72 The Precapillary Segment of the Blood- Brain Barrier and Its Relation to Perivascular Drainage in Alzheimer's
Cerebrovascular diseases-2
 Cerebrovascular diseases-2 Primary angiitis of CNS - Other causes of infarction i. Hypercoagulable states ii. Drug-abuse such as amphetamine, heroin and cocain Note - The venous side of the circulation
Cerebrovascular diseases-2 Primary angiitis of CNS - Other causes of infarction i. Hypercoagulable states ii. Drug-abuse such as amphetamine, heroin and cocain Note - The venous side of the circulation
CEREBROVASCULAR DISEASES. By: Shifaa AlQa qa
 CEREBROVASCULAR DISEASES By: Shifaa AlQa qa Cerebrovascular diseases Brain disorders caused by pathologic processes involving blood vessels 3 pathogenic mechanisms (1) thrombotic occlusion, (2) embolic
CEREBROVASCULAR DISEASES By: Shifaa AlQa qa Cerebrovascular diseases Brain disorders caused by pathologic processes involving blood vessels 3 pathogenic mechanisms (1) thrombotic occlusion, (2) embolic
Dementia. Stephen S. Flitman, MD Medical Director 21st Century Neurology
 Dementia Stephen S. Flitman, MD Medical Director 21st Century Neurology www.neurozone.org Dementia is a syndrome Progressive memory loss, plus Progressive loss of one or more cognitive functions: Language
Dementia Stephen S. Flitman, MD Medical Director 21st Century Neurology www.neurozone.org Dementia is a syndrome Progressive memory loss, plus Progressive loss of one or more cognitive functions: Language
Role of TDP-43 in Non-Alzheimer s and Alzheimer s Neurodegenerative Diseases
 Role of TDP-43 in Non-Alzheimer s and Alzheimer s Neurodegenerative Diseases Keith A. Josephs, MD, MST, MSc Professor of Neurology 13th Annual Mild Cognitive Impairment (MCI) Symposium: Alzheimer and Non-Alzheimer
Role of TDP-43 in Non-Alzheimer s and Alzheimer s Neurodegenerative Diseases Keith A. Josephs, MD, MST, MSc Professor of Neurology 13th Annual Mild Cognitive Impairment (MCI) Symposium: Alzheimer and Non-Alzheimer
Clinicopathologic and genetic aspects of hippocampal sclerosis. Dennis W. Dickson, MD Mayo Clinic, Jacksonville, Florida USA
 Clinicopathologic and genetic aspects of hippocampal sclerosis Dennis W. Dickson, MD Mayo Clinic, Jacksonville, Florida USA The hippocampus in health & disease A major structure of the medial temporal
Clinicopathologic and genetic aspects of hippocampal sclerosis Dennis W. Dickson, MD Mayo Clinic, Jacksonville, Florida USA The hippocampus in health & disease A major structure of the medial temporal
Alzheimer's Disease A mind in darkness awaiting the drink of a gentle color.
 Alzheimer's Disease A mind in darkness awaiting the drink of a gentle color. Mary ET Boyle, Ph. D. Department of Cognitive Science UCSD Gabriel García Márquez One Hundred Years of Solitude Alois Alzheimer
Alzheimer's Disease A mind in darkness awaiting the drink of a gentle color. Mary ET Boyle, Ph. D. Department of Cognitive Science UCSD Gabriel García Márquez One Hundred Years of Solitude Alois Alzheimer
NACC Neuropathology (NP) Diagnosis Coding Guidebook
 Department of Epidemiology, School of Public Health and Community Medicine, University of Washington 4311 11 th Avenue NE #300 Seattle, WA 98105 phone: (206) 543-8637; fax: (206) 616-5927 e-mail: naccmail@u.washington.edu
Department of Epidemiology, School of Public Health and Community Medicine, University of Washington 4311 11 th Avenue NE #300 Seattle, WA 98105 phone: (206) 543-8637; fax: (206) 616-5927 e-mail: naccmail@u.washington.edu
Aconsiderable body of clinical and experimental evidence
 Atherosclerosis of Cerebral Arteries in Alzheimer Disease Alex E. Roher, MD, PhD; Chera Esh, BS; Afroza Rahman, PhD; Tyler A. Kokjohn, PhD; Thomas G. Beach, MD, PhD Abstract A growing body of evidence
Atherosclerosis of Cerebral Arteries in Alzheimer Disease Alex E. Roher, MD, PhD; Chera Esh, BS; Afroza Rahman, PhD; Tyler A. Kokjohn, PhD; Thomas G. Beach, MD, PhD Abstract A growing body of evidence
The Spectrum of Age-Associated Astroglial Tauopathies. Dennis W. Dickson MD Department of Neuroscience Mayo Clinic, Jacksonville, FL
 The Spectrum of Age-Associated Astroglial Tauopathies Dennis W. Dickson MD Mayo Clinic, Jacksonville, FL Thorn-shaped astrocytes TSA were first reported by Ikeda (1995), as tau-positive astrocytes in various
The Spectrum of Age-Associated Astroglial Tauopathies Dennis W. Dickson MD Mayo Clinic, Jacksonville, FL Thorn-shaped astrocytes TSA were first reported by Ikeda (1995), as tau-positive astrocytes in various
Yong-Bum Kim, M.D., Kwang-Ho Lee, M.D., Soo-Joo Lee, M.D., Duk-L. Na, M.D., Soo-Jin Cho, M.D., Chin-Sang Chung, M.D., Won-Yong Lee M.D.
 Usefulness of Apolipoprotein E 4 and Distribution of Petechial Hemorrhages in Differentiating between Cerebral Amyloid Angiopathy and Hypertensive Intracerebral Hemorrhage Yong-Bum Kim, M.D., Kwang-Ho
Usefulness of Apolipoprotein E 4 and Distribution of Petechial Hemorrhages in Differentiating between Cerebral Amyloid Angiopathy and Hypertensive Intracerebral Hemorrhage Yong-Bum Kim, M.D., Kwang-Ho
The Circulatory System
 The Circulatory System Dr. Sami Zaqout The circulatory system Circulatory system Blood vascular systems Lymphatic vascular systems Blood vascular systems Blood vascular systems The circulatory system Circulatory
The Circulatory System Dr. Sami Zaqout The circulatory system Circulatory system Blood vascular systems Lymphatic vascular systems Blood vascular systems Blood vascular systems The circulatory system Circulatory
Potential role of extracellular tau in development and spread of tauopathy: Effects of anti-tau antibodies
 Potential role of extracellular tau in development and spread of tauopathy: Effects of anti-tau antibodies David M. Holtzman, MD Professor and Chair, Dept. of Neurology Washington University School of
Potential role of extracellular tau in development and spread of tauopathy: Effects of anti-tau antibodies David M. Holtzman, MD Professor and Chair, Dept. of Neurology Washington University School of
IV. Cerebrovascular diseases
 IV. Cerebrovascular diseases - Cerebrovascular disease denotes brain disorders caused by pathologic processes involving the blood vessels. - The three main pathogenic mechanisms are: 1. Thrombotic occlusion
IV. Cerebrovascular diseases - Cerebrovascular disease denotes brain disorders caused by pathologic processes involving the blood vessels. - The three main pathogenic mechanisms are: 1. Thrombotic occlusion
Neuropathology of Neurodegenerative Disorders Prof. Jillian Kril
 Neurodegenerative disorders to be discussed Alzheimer s disease Lewy body diseases Frontotemporal dementia and other tauopathies Huntington s disease Motor Neuron Disease 2 Neuropathology of neurodegeneration
Neurodegenerative disorders to be discussed Alzheimer s disease Lewy body diseases Frontotemporal dementia and other tauopathies Huntington s disease Motor Neuron Disease 2 Neuropathology of neurodegeneration
Glossary of relevant medical and scientific terms
 Glossary of relevant medical and scientific terms Alzheimer's disease The most common dementing illness of the elderly in the UK. The neuropathology of Alzheimer's disease is significantly different from
Glossary of relevant medical and scientific terms Alzheimer's disease The most common dementing illness of the elderly in the UK. The neuropathology of Alzheimer's disease is significantly different from
T he apolipoprotein E (APOE) gene has three common
 PAPER Cerebral amyloid angiopathy in traumatic brain injury: association with apolipoprotein E genotype P D Leclercq, L S Murray, C Smith, D I Graham, J A R Nicoll, S M Gentleman... See end of article
PAPER Cerebral amyloid angiopathy in traumatic brain injury: association with apolipoprotein E genotype P D Leclercq, L S Murray, C Smith, D I Graham, J A R Nicoll, S M Gentleman... See end of article
Cerebral Small Vessel Disease and HAND in ARV-treated Subjects
 Cerebral Small Vessel Disease and HAND in ARV-treated Subjects Cristian L. Achim, MD, PhD Ronald J. Ellis, MD, PhD Virawudh Soontornniyomkij, MD ARROW, Bucharest, Romania October 5-6, 2015 Rationale and
Cerebral Small Vessel Disease and HAND in ARV-treated Subjects Cristian L. Achim, MD, PhD Ronald J. Ellis, MD, PhD Virawudh Soontornniyomkij, MD ARROW, Bucharest, Romania October 5-6, 2015 Rationale and
Cerebral amyloid angiopathy in dementia and old age
 Journal of Neurology, Neurosurgery, and Psychiatry 1986;49:1221-1226 Cerebral amyloid angiopathy in dementia and old age MARGARET M ESIRI, G K WILCOCK* From the Departments of Neuropathology and Geriatric
Journal of Neurology, Neurosurgery, and Psychiatry 1986;49:1221-1226 Cerebral amyloid angiopathy in dementia and old age MARGARET M ESIRI, G K WILCOCK* From the Departments of Neuropathology and Geriatric
DIET, AGING, and MIND. Neal G. Simon, Ph. D. Dept. of Biological Sciences Lehigh University
 DIET, AGING, and MIND Neal G. Simon, Ph. D. Dept. of Biological Sciences Lehigh University Outline: Diet, Aging, and Mind 1. Brain Changes in Aging 2. Dementias 3. Dietary Interventions: DHEA and Soy 4.
DIET, AGING, and MIND Neal G. Simon, Ph. D. Dept. of Biological Sciences Lehigh University Outline: Diet, Aging, and Mind 1. Brain Changes in Aging 2. Dementias 3. Dietary Interventions: DHEA and Soy 4.
Vascular Cognitive Impairment-- NEUROPATHOLOGIC ISSUES. VCI vs. IVD/DEMENTIA with VASCULAR DISEASE (IVD) advanced pathology
 Vascular Cognitive Impairment-- NEUROPATHOLOGIC ISSUES VCI vs. IVD/DEMENTIA with VASCULAR DISEASE (IVD) advanced pathology HANDLING the BRAIN at AUTOPSY: What to FIX vs. what to FREEZE? --no need to be
Vascular Cognitive Impairment-- NEUROPATHOLOGIC ISSUES VCI vs. IVD/DEMENTIA with VASCULAR DISEASE (IVD) advanced pathology HANDLING the BRAIN at AUTOPSY: What to FIX vs. what to FREEZE? --no need to be
Supplementary Figure 1
 Supplementary Figure 1 The average sigmoid parametric curves of capillary dilation time courses and average time to 50% peak capillary diameter dilation computed from individual capillary responses averaged
Supplementary Figure 1 The average sigmoid parametric curves of capillary dilation time courses and average time to 50% peak capillary diameter dilation computed from individual capillary responses averaged
Cardiovascular (Circulatory) System
 Cardiovascular (Circulatory) System Piryaei May 2011 Circulatory System Heart Blood Vessels Macrovasculature (More than 0.1mm) Elastic Artery Muscular (Distributing) Artery Large Arteriol Small Vein Muscular
Cardiovascular (Circulatory) System Piryaei May 2011 Circulatory System Heart Blood Vessels Macrovasculature (More than 0.1mm) Elastic Artery Muscular (Distributing) Artery Large Arteriol Small Vein Muscular
Am J Neurodegener Dis 2014;3(1):19-32
 Am J Neurodegener Dis 2014;3(1):19-32 www.ajnd.us /ISSN:2165-591X/AJND1402006 Original Article Development, appraisal, validation and implementation of a consensus protocol for the assessment of cerebral
Am J Neurodegener Dis 2014;3(1):19-32 www.ajnd.us /ISSN:2165-591X/AJND1402006 Original Article Development, appraisal, validation and implementation of a consensus protocol for the assessment of cerebral
Pathogenesis of Degenerative Diseases and Dementias. D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria)
 Pathogenesis of Degenerative Diseases and Dementias D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) Dementias Defined: as the development of memory impairment and other cognitive deficits
Pathogenesis of Degenerative Diseases and Dementias D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) Dementias Defined: as the development of memory impairment and other cognitive deficits
CASE 49. What type of memory is available for conscious retrieval? Which part of the brain stores semantic (factual) memories?
 CASE 49 A 43-year-old woman is brought to her primary care physician by her family because of concerns about her forgetfulness. The patient has a history of Down syndrome but no other medical problems.
CASE 49 A 43-year-old woman is brought to her primary care physician by her family because of concerns about her forgetfulness. The patient has a history of Down syndrome but no other medical problems.
Characteristic features of CNS pathology. By: Shifaa AlQa qa
 Characteristic features of CNS pathology By: Shifaa AlQa qa Normal brain: - The neocortex (gray matter): six layers: outer plexiform, outer granular, outer pyramidal, inner granular, inner pyramidal, polymorphous
Characteristic features of CNS pathology By: Shifaa AlQa qa Normal brain: - The neocortex (gray matter): six layers: outer plexiform, outer granular, outer pyramidal, inner granular, inner pyramidal, polymorphous
Neurobiology of Disease. Jianting Miao, 1 Michael P. Vitek, 2 Feng Xu, 1 Mary Lou Previti, 1 Judianne Davis, 1 and William E.
 The Journal of Neuroscience, July 6, 2005 25(27):6271 6277 6271 Neurobiology of Disease Reducing Cerebral Microvascular Amyloid- Protein Deposition Diminishes Regional Neuroinflammation in Vasculotropic
The Journal of Neuroscience, July 6, 2005 25(27):6271 6277 6271 Neurobiology of Disease Reducing Cerebral Microvascular Amyloid- Protein Deposition Diminishes Regional Neuroinflammation in Vasculotropic
Cheyenne 11/28 Neurological Disorders II. Transmissible Spongiform Encephalopathy
 Cheyenne 11/28 Neurological Disorders II Transmissible Spongiform Encephalopathy -E.g Bovine4 Spongiform Encephalopathy (BSE= mad cow disease), Creutzfeldt-Jakob disease, scrapie (animal only) -Sporadic:
Cheyenne 11/28 Neurological Disorders II Transmissible Spongiform Encephalopathy -E.g Bovine4 Spongiform Encephalopathy (BSE= mad cow disease), Creutzfeldt-Jakob disease, scrapie (animal only) -Sporadic:
HST-583 Cerebrovascular anatomy and neural regulation of CNS blood flow
 HST.583: Functional Magnetic Resonance Imaging: Data Acquisition and Analysis Harvard-MIT Division of Health Sciences and Technology Dr. Randy Gollub HST-583 Cerebrovascular anatomy and neural regulation
HST.583: Functional Magnetic Resonance Imaging: Data Acquisition and Analysis Harvard-MIT Division of Health Sciences and Technology Dr. Randy Gollub HST-583 Cerebrovascular anatomy and neural regulation
Chronic cerebral hypoperfusion and dementia
 doi:10.1111/ncn3.124 REVIEW ARTICLE Chronic cerebral hypoperfusion and dementia Kenichiro Yata and Hidekazu Tomimoto Department of Neurology, Mie University Graduate School of Medicine, Tsu, Japan Key
doi:10.1111/ncn3.124 REVIEW ARTICLE Chronic cerebral hypoperfusion and dementia Kenichiro Yata and Hidekazu Tomimoto Department of Neurology, Mie University Graduate School of Medicine, Tsu, Japan Key
Histology of the myocardium and blood vessels. Prof. Abdulameer Al-Nuaimi
 Histology of the myocardium and blood vessels Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E-mail: abdulameerh@yahoo.com Histology of blood vessels The walls of arteries and veins are
Histology of the myocardium and blood vessels Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E-mail: abdulameerh@yahoo.com Histology of blood vessels The walls of arteries and veins are
Extra notes for lab- 1 histology. Slide 1 : cross section in the elastic artery ( aortic arch, ascending aorta, descending aorta )
 Extra notes for lab- 1 histology Slide 1 : cross section in the elastic artery ( aortic arch, ascending aorta, descending aorta ) - twin of ascending aorta is the pulmonary trunk. Ascending aorta represents
Extra notes for lab- 1 histology Slide 1 : cross section in the elastic artery ( aortic arch, ascending aorta, descending aorta ) - twin of ascending aorta is the pulmonary trunk. Ascending aorta represents
Lymphatic System and Immunity. Lymphatic System
 Lymphatic System and Immunity Lymphatic System Lymphatic System High hydrostatic pressure in the arterioles and capillaries at the arterial part of the circulation leads to move plasma fluid from the capillaries
Lymphatic System and Immunity Lymphatic System Lymphatic System High hydrostatic pressure in the arterioles and capillaries at the arterial part of the circulation leads to move plasma fluid from the capillaries
The cardiovascular system
 The cardiovascular system Components of the Cardiovascular system Heart Vessels: Arteries Capillaries Veins Functions of CVS: Transportation system where blood is the transporting vehicle Carries oxygen,
The cardiovascular system Components of the Cardiovascular system Heart Vessels: Arteries Capillaries Veins Functions of CVS: Transportation system where blood is the transporting vehicle Carries oxygen,
ALZHEIMER S DISEASE FACTOIDS & STATISTICS
 ALZHEIMER S DISEASE FACTOIDS & STATISTICS ~ 4 million affected in US alone 6-8% if 65+ years old, 30-50% if 80+ By 2030, in US >65 million people >65+ (---> ~14 million with AD) AD is one of the top 10
ALZHEIMER S DISEASE FACTOIDS & STATISTICS ~ 4 million affected in US alone 6-8% if 65+ years old, 30-50% if 80+ By 2030, in US >65 million people >65+ (---> ~14 million with AD) AD is one of the top 10
Sinusoids and venous sinuses
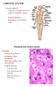 LYMPHOID SYSTEM General aspects Consists of organs that are made of lymphoid tissue; Immune defense Breakdown of red blood cells. 1 Sinusoids In place of capillaries Endothelium; often fenestrated More
LYMPHOID SYSTEM General aspects Consists of organs that are made of lymphoid tissue; Immune defense Breakdown of red blood cells. 1 Sinusoids In place of capillaries Endothelium; often fenestrated More
Autopsy Committee Sample Autopsy Case. Alzheimer Disease. Authors Ashley Thorburn, MD. Joseph E. Parisi, MD Autopsy Committee
 Autopsy Committee Sample Autopsy Case Alzheimer Disease Authors Ashley Thorburn, MD Joseph E. Parisi, MD Autopsy Committee Clinical Summary: A 75-year-old man presented to his primary care physician with
Autopsy Committee Sample Autopsy Case Alzheimer Disease Authors Ashley Thorburn, MD Joseph E. Parisi, MD Autopsy Committee Clinical Summary: A 75-year-old man presented to his primary care physician with
Pathophysiology of Cardiovascular System. Dr. Hemn Hassan Othman, PhD
 Pathophysiology of Cardiovascular System Dr. Hemn Hassan Othman, PhD hemn.othman@univsul.edu.iq What is the circulatory system? The circulatory system carries blood and dissolved substances to and from
Pathophysiology of Cardiovascular System Dr. Hemn Hassan Othman, PhD hemn.othman@univsul.edu.iq What is the circulatory system? The circulatory system carries blood and dissolved substances to and from
2. Subarachnoid Hemorrhage
 Causes: 2. Subarachnoid Hemorrhage A. Saccular (berry) aneurysm - Is the most frequent cause of clinically significant subarachnoid hemorrhage is rupture of a saccular (berry) aneurysm. B. Vascular malformation
Causes: 2. Subarachnoid Hemorrhage A. Saccular (berry) aneurysm - Is the most frequent cause of clinically significant subarachnoid hemorrhage is rupture of a saccular (berry) aneurysm. B. Vascular malformation
Biomarkers for Alzheimer s disease
 Biomarkers for Alzheimer s Disease Henrik Zetterberg, MD, PhD Professor of Neurochemistry The Sahlgrenska Academy, University of Gothenburg 1 Alzheimer s disease 2 Neuropathological criteria for Alzheimer
Biomarkers for Alzheimer s Disease Henrik Zetterberg, MD, PhD Professor of Neurochemistry The Sahlgrenska Academy, University of Gothenburg 1 Alzheimer s disease 2 Neuropathological criteria for Alzheimer
PTA 106 Unit 1 Lecture 3
 PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
Corporate Medical Policy Genetic Testing for Alzheimer s Disease
 Corporate Medical Policy Genetic Testing for Alzheimer s Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_alzheimers_disease 8/2010 10/2017 10/2018 10/2017
Corporate Medical Policy Genetic Testing for Alzheimer s Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_alzheimers_disease 8/2010 10/2017 10/2018 10/2017
Alzheimer's disease (AD), also known as Senile Dementia of the Alzheimer Type (SDAT) or simply Alzheimer s is the most common form of dementia.
 CHAPTER 3 Alzheimer's disease (AD), also known as Senile Dementia of the Alzheimer Type (SDAT) or simply Alzheimer s is the most common form of dementia. This incurable, degenerative, terminal disease
CHAPTER 3 Alzheimer's disease (AD), also known as Senile Dementia of the Alzheimer Type (SDAT) or simply Alzheimer s is the most common form of dementia. This incurable, degenerative, terminal disease
Essentials of Clinical MR, 2 nd edition. 14. Ischemia and Infarction II
 14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
Phosphodiesterase III inhibitor promotes drainage of cerebrovascular β-amyloid
 Phosphodiesterase III inhibitor promotes drainage of cerebrovascular β-amyloid The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters.
Phosphodiesterase III inhibitor promotes drainage of cerebrovascular β-amyloid The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters.
Vascular Malformations of the Brain. William A. Cox, M.D. Forensic Pathologist/Neuropathologist. September 8, 2014
 Vascular Malformations of the Brain William A. Cox, M.D. Forensic Pathologist/Neuropathologist September 8, 2014 Vascular malformations of the brain are classified into four principal groups: arteriovenous
Vascular Malformations of the Brain William A. Cox, M.D. Forensic Pathologist/Neuropathologist September 8, 2014 Vascular malformations of the brain are classified into four principal groups: arteriovenous
TAU PATHOLOGY REDUCTION WITH SM07883, A NOVEL, POTENT, AND SELECTIVE ORAL DYRK1A INHIBITOR - A POTENTIAL THERAPEUTIC FOR ALZHEIMER S DISEASE
 TAU PATHOLOGY REDUCTION WITH SM07883, A NOVEL, POTENT, AND SELECTIVE ORAL DYRK1A INHIBITOR - A POTENTIAL THERAPEUTIC FOR ALZHEIMER S DISEASE Benoît Melchior, C. Lai, K. Duong-Polk, A. Tjitro, D.C. Ince,
TAU PATHOLOGY REDUCTION WITH SM07883, A NOVEL, POTENT, AND SELECTIVE ORAL DYRK1A INHIBITOR - A POTENTIAL THERAPEUTIC FOR ALZHEIMER S DISEASE Benoît Melchior, C. Lai, K. Duong-Polk, A. Tjitro, D.C. Ince,
Unusual cerebral vascular prion protein amyloid distribution in scrapie-infected transgenic mice expressing anchorless prion protein
 Rangel et al. Acta Neuropathologica Communications 2013, 1:25 RESEARCH Open Access Unusual cerebral vascular prion protein amyloid distribution in scrapie-infected transgenic mice expressing anchorless
Rangel et al. Acta Neuropathologica Communications 2013, 1:25 RESEARCH Open Access Unusual cerebral vascular prion protein amyloid distribution in scrapie-infected transgenic mice expressing anchorless
TGF-ß1 pathway as a new pharmacological target for neuroprotection in AD. Filippo Caraci
 Department of Clinical and Molecular Biomedicine Section of Pharmacology and Biochemistry Department of Educational Sciences University of Catania TGF-ß1 pathway as a new pharmacological target for neuroprotection
Department of Clinical and Molecular Biomedicine Section of Pharmacology and Biochemistry Department of Educational Sciences University of Catania TGF-ß1 pathway as a new pharmacological target for neuroprotection
CSF and ISF Flow Open Questions
 CSF and ISF Flow Open Questions Assistant Professor University of Zurich Institute of Physiology Mail: vartan.kurtcuoglu@uzh.ch Web: interfacegroup.ch ASNR CSF Flow Group and IHIWG Meeting Montreal, Mai
CSF and ISF Flow Open Questions Assistant Professor University of Zurich Institute of Physiology Mail: vartan.kurtcuoglu@uzh.ch Web: interfacegroup.ch ASNR CSF Flow Group and IHIWG Meeting Montreal, Mai
Vasculitides in Surgical Neuropathology Practice
 Vasculitides in Surgical Neuropathology Practice USCAP requires that all faculty in a position to influence or control the content of CME disclose any relevant financial relationship WITH COMMERCIAL INTERESTS
Vasculitides in Surgical Neuropathology Practice USCAP requires that all faculty in a position to influence or control the content of CME disclose any relevant financial relationship WITH COMMERCIAL INTERESTS
V. CENTRAL NERVOUS SYSTEM TRAUMA
 V. CENTRAL NERVOUS SYSTEM TRAUMA I. Concussion - Is a clinical syndrome of altered consiousness secondary to head injury - Brought by a change in the momentum of the head when a moving head suddenly arrested
V. CENTRAL NERVOUS SYSTEM TRAUMA I. Concussion - Is a clinical syndrome of altered consiousness secondary to head injury - Brought by a change in the momentum of the head when a moving head suddenly arrested
Nigel Hooper. University of Manchester UK
 Prion protein as a therapeutic target in Alzheimer s disease Nigel Hooper University of Manchester UK Prion protein and Alzheimer s a connection? - causative agent of transmissible spongiform encephalopathies
Prion protein as a therapeutic target in Alzheimer s disease Nigel Hooper University of Manchester UK Prion protein and Alzheimer s a connection? - causative agent of transmissible spongiform encephalopathies
Yin-Hui Siow MD, FRCPC Director of Nuclear Medicine Southlake Regional Health Centre
 Yin-Hui Siow MD, FRCPC Director of Nuclear Medicine Southlake Regional Health Centre Today Introduction to CT Introduction to MRI Introduction to nuclear medicine Imaging the dementias The Brain ~ 1.5
Yin-Hui Siow MD, FRCPC Director of Nuclear Medicine Southlake Regional Health Centre Today Introduction to CT Introduction to MRI Introduction to nuclear medicine Imaging the dementias The Brain ~ 1.5
Major Structures of the Nervous System. Brain, cranial nerves, spinal cord, spinal nerves, ganglia, enteric plexuses and sensory receptors
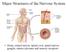 Major Structures of the Nervous System Brain, cranial nerves, spinal cord, spinal nerves, ganglia, enteric plexuses and sensory receptors Nervous System Divisions Central Nervous System (CNS) consists
Major Structures of the Nervous System Brain, cranial nerves, spinal cord, spinal nerves, ganglia, enteric plexuses and sensory receptors Nervous System Divisions Central Nervous System (CNS) consists
New life Collage of nursing Karachi
 New life Collage of nursing Karachi Presenter: Zafar ali shah Faculty: Raja khatri Subject: Pathophysiology Topic :Alzheimer s Disease Post RN BScN semester 2 nd Objective Define Alzheimer s Describe pathophysiology
New life Collage of nursing Karachi Presenter: Zafar ali shah Faculty: Raja khatri Subject: Pathophysiology Topic :Alzheimer s Disease Post RN BScN semester 2 nd Objective Define Alzheimer s Describe pathophysiology
Analysis of Chlamydia Pneumoniae and AD-like Pathology in the Brains of BALB/c Mice Following Direct Intracranial Infection with Chlamydia Pneumoniae
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Biomedical Studies Student Scholarship Student Dissertations, Theses and Papers 8-2011 Analysis of Chlamydia Pneumoniae and AD-like
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Biomedical Studies Student Scholarship Student Dissertations, Theses and Papers 8-2011 Analysis of Chlamydia Pneumoniae and AD-like
Amyloid angiopathy in idiopathic Parkinson s disease. Immunohistochemical and ultrastructural study
 Original article myloid angiopathy in idiopathic Parkinson s disease. Immunohistochemical and ultrastructural study Ewa ertrand, Eliza Lewandowska, Tomasz Stêpieñ, Gra yna M. Szpak, El bieta Pasennik,
Original article myloid angiopathy in idiopathic Parkinson s disease. Immunohistochemical and ultrastructural study Ewa ertrand, Eliza Lewandowska, Tomasz Stêpieñ, Gra yna M. Szpak, El bieta Pasennik,
Cerebral Amyloid Angiopathy: A Systematic Review
 REVIEW J Clin Neurol 2011;7:1-9 Print ISSN 1738-6586 / On-line ISSN 2005-5013 10.3988/jcn.2011.7.1.1 Cerebral Amyloid Angiopathy: A Systematic Review Alessandro Biffi, a,b,c Steven M. Greenberg b,c a Center
REVIEW J Clin Neurol 2011;7:1-9 Print ISSN 1738-6586 / On-line ISSN 2005-5013 10.3988/jcn.2011.7.1.1 Cerebral Amyloid Angiopathy: A Systematic Review Alessandro Biffi, a,b,c Steven M. Greenberg b,c a Center
New Approach to Parkinson s Disease: Synuclein Immunotherapy
 RB2014 Conference August 22, 2014 New Approach to Parkinson s Disease: Synuclein Immunotherapy Dale Schenk, PhD President and CEO Prothena Corporation plc Primary Motor and Non-Motor Symptoms of Parkinson
RB2014 Conference August 22, 2014 New Approach to Parkinson s Disease: Synuclein Immunotherapy Dale Schenk, PhD President and CEO Prothena Corporation plc Primary Motor and Non-Motor Symptoms of Parkinson
LYMPH GLAND. By : Group 1
 LYMPH GLAND By : Group 1 ANATOMY LYMPH NODE Lymphatic Organs Red bone marrow Thymus gland Lymph nodes Lymph nodules Spleen Primary organs Secondary organs Lymph Nodes Firm, smooth-surfaced, bean-shaped
LYMPH GLAND By : Group 1 ANATOMY LYMPH NODE Lymphatic Organs Red bone marrow Thymus gland Lymph nodes Lymph nodules Spleen Primary organs Secondary organs Lymph Nodes Firm, smooth-surfaced, bean-shaped
Lesson 14. The Nervous System. Introduction to Life Processes - SCI 102 1
 Lesson 14 The Nervous System Introduction to Life Processes - SCI 102 1 Structures and Functions of Nerve Cells The nervous system has two principal cell types: Neurons (nerve cells) Glia The functions
Lesson 14 The Nervous System Introduction to Life Processes - SCI 102 1 Structures and Functions of Nerve Cells The nervous system has two principal cell types: Neurons (nerve cells) Glia The functions
White matter perivascular spaces An MRI marker in pathology-proven cerebral amyloid angiopathy?
 White matter perivascular spaces An MRI marker in pathology-proven cerebral amyloid angiopathy? Andreas Charidimou, MD, MSc Zane Jaunmuktane, MD Jean-Claude Baron, PhD Matthew Burnell, PhD Pascale Varlet,
White matter perivascular spaces An MRI marker in pathology-proven cerebral amyloid angiopathy? Andreas Charidimou, MD, MSc Zane Jaunmuktane, MD Jean-Claude Baron, PhD Matthew Burnell, PhD Pascale Varlet,
MRI of Pathological Aging Brain
 MRI of Pathological Aging Brain Yukio Miki Department of Radiology, Osaka City University A variety of pathological changes occur in the brain with aging, and many of these changes can be identified by
MRI of Pathological Aging Brain Yukio Miki Department of Radiology, Osaka City University A variety of pathological changes occur in the brain with aging, and many of these changes can be identified by
9.01 Introduction to Neuroscience Fall 2007
 MIT OpenCourseWare http://ocw.mit.edu 9.01 Introduction to Neuroscience Fall 2007 For information about citing these materials or our Terms of Use, visit: http://ocw.mit.edu/terms. 9.01 Recitation (R02)
MIT OpenCourseWare http://ocw.mit.edu 9.01 Introduction to Neuroscience Fall 2007 For information about citing these materials or our Terms of Use, visit: http://ocw.mit.edu/terms. 9.01 Recitation (R02)
Basic Histology. By Mrs. Bailey
 Basic Histology By Mrs. Bailey Primary Tissues 1. Epithelial Tissue 2. Connective Tissue 3. Muscle Tissue 4. Nervous Tissue Very cellular Supported by underlying connective tissue Epithelial & connective
Basic Histology By Mrs. Bailey Primary Tissues 1. Epithelial Tissue 2. Connective Tissue 3. Muscle Tissue 4. Nervous Tissue Very cellular Supported by underlying connective tissue Epithelial & connective
Cerebral small vessel disease
 Cerebral small vessel disease What is it? What are the clinical syndromes? How do we diagnose it? What is the pathophysiology? New insights from genetics? Possible therapies? Small Vessel disease Changes
Cerebral small vessel disease What is it? What are the clinical syndromes? How do we diagnose it? What is the pathophysiology? New insights from genetics? Possible therapies? Small Vessel disease Changes
Electron microscopy in the investigation and diagnosis of muscle disease
 Electron microscopy in the investigation and diagnosis of muscle disease Roy Weller Clinical Neurosciences University of Southampton School of Medicine Normal Muscle Normal Muscle The Sarcomere The names
Electron microscopy in the investigation and diagnosis of muscle disease Roy Weller Clinical Neurosciences University of Southampton School of Medicine Normal Muscle Normal Muscle The Sarcomere The names
Type 2 Diabetes and Brain Disease in Older Adults. Erin L. Abner, PhD, MPH Asst. Professor University Of Kentucky
 Type 2 Diabetes and Brain Disease in Older Adults Erin L. Abner, PhD, MPH Asst. Professor University Of Kentucky Disclosures to Participants Requirements for Successful Completion: For successful completion,
Type 2 Diabetes and Brain Disease in Older Adults Erin L. Abner, PhD, MPH Asst. Professor University Of Kentucky Disclosures to Participants Requirements for Successful Completion: For successful completion,
Novel Targets of disease modifying therapy for Parkinson disease. David G. Standaert, MD, PhD John N. Whitaker Professor and Chair of Neurology
 Novel Targets of disease modifying therapy for Parkinson disease David G. Standaert, MD, PhD John N. Whitaker Professor and Chair of Neurology Disclosures Dr. Standaert has served as a paid consultant
Novel Targets of disease modifying therapy for Parkinson disease David G. Standaert, MD, PhD John N. Whitaker Professor and Chair of Neurology Disclosures Dr. Standaert has served as a paid consultant
A new approach to Common Sporadic Alzheimer s, Post-Traumatic Alzheimer s, and CTE:
 A new approach to Common Sporadic Alzheimer s, Post-Traumatic Alzheimer s, and CTE: Roles of Aβ, Tau, ApoE, and Regulatory Signaling in Elucidating Pathogenesis and Experimental Therapeutics Sam Gandy,
A new approach to Common Sporadic Alzheimer s, Post-Traumatic Alzheimer s, and CTE: Roles of Aβ, Tau, ApoE, and Regulatory Signaling in Elucidating Pathogenesis and Experimental Therapeutics Sam Gandy,
Nature Neuroscience: doi: /nn Supplementary Figure 1. Large-scale calcium imaging in vivo.
 Supplementary Figure 1 Large-scale calcium imaging in vivo. (a) Schematic illustration of the in vivo camera imaging set-up for large-scale calcium imaging. (b) High-magnification two-photon image from
Supplementary Figure 1 Large-scale calcium imaging in vivo. (a) Schematic illustration of the in vivo camera imaging set-up for large-scale calcium imaging. (b) High-magnification two-photon image from
Fibrinogen-induced perivascular microglial clustering is required for the. development of axonal damage in neuroinflammation
 SUPPLEMENTARY INFORMATION Fibrinogen-induced perivascular microglial clustering is required for the development of axonal damage in neuroinflammation Dimitrios Davalos, Jae Kyu Ryu, Mario Merlini, Kim
SUPPLEMENTARY INFORMATION Fibrinogen-induced perivascular microglial clustering is required for the development of axonal damage in neuroinflammation Dimitrios Davalos, Jae Kyu Ryu, Mario Merlini, Kim
Neuro degenerative PET image from FDG, amyloid to Tau
 Neuro degenerative PET image from FDG, amyloid to Tau Kun Ju Lin ( ) MD, Ph.D Department of Nuclear Medicine and Molecular Imaging Center, Chang Gung Memorial Hospital ( ) Department of Medical Imaging
Neuro degenerative PET image from FDG, amyloid to Tau Kun Ju Lin ( ) MD, Ph.D Department of Nuclear Medicine and Molecular Imaging Center, Chang Gung Memorial Hospital ( ) Department of Medical Imaging
ATHEROSCLEROSIS زيد ثامر جابر. Zaid. Th. Jaber
 ATHEROSCLEROSIS زيد ثامر جابر Zaid. Th. Jaber Objectives 1- Review the normal histological features of blood vessels walls. 2-define the atherosclerosis. 3- display the risk factors of atherosclerosis.
ATHEROSCLEROSIS زيد ثامر جابر Zaid. Th. Jaber Objectives 1- Review the normal histological features of blood vessels walls. 2-define the atherosclerosis. 3- display the risk factors of atherosclerosis.
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure ILOs Understand causes and symptoms of increased intracranial pressure.
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure ILOs Understand causes and symptoms of increased intracranial pressure.
Dementia. Jeanette Norden, Ph.D. Professor Emerita Vanderbilt University School of Medicine
 Dementia Jeanette Norden, Ph.D. Professor Emerita Vanderbilt University School of Medicine What is Dementia? Dementia is a general term referring to a decline in cognitive/mental functioning; this decline
Dementia Jeanette Norden, Ph.D. Professor Emerita Vanderbilt University School of Medicine What is Dementia? Dementia is a general term referring to a decline in cognitive/mental functioning; this decline
Amyloid and the Vessels. David Weisman, M.D.
 Amyloid and the Vessels David Weisman, M.D. CMA I conduct Alzheimer/amyloid clinical research in conjunction with: Toyoma, ADRC, Genentech, Eisai, Envivo, Accera, Elan, Merck. Previously served on speaker
Amyloid and the Vessels David Weisman, M.D. CMA I conduct Alzheimer/amyloid clinical research in conjunction with: Toyoma, ADRC, Genentech, Eisai, Envivo, Accera, Elan, Merck. Previously served on speaker
Immunohistochemical Characterization of Cerebrovascular Amyloid in 46 Autopsied Cases Using Antibodies to p Protein and Cystatin C
 397 Immunohistochemical Characterization of Cerebrovascular Amyloid in 46 Autopsied Cases Using Antibodies to p Protein and Cystatin C Keiko Maruyama, MD, Shu-ichi Ikeda, MD, Tokuhiro Ishihara, MD, David
397 Immunohistochemical Characterization of Cerebrovascular Amyloid in 46 Autopsied Cases Using Antibodies to p Protein and Cystatin C Keiko Maruyama, MD, Shu-ichi Ikeda, MD, Tokuhiro Ishihara, MD, David
Lecture name: blood 2 & The Circulatory System Edited by: Buthainah Al masaeed & Yousef Qandeel
 Lecture name: blood 2 & The Circulatory System Edited by: Buthainah Al masaeed & Yousef Qandeel Now we will take about A granulocytes : Lymphocyte Monocytes 1- Lymphocyte - The second major type of presence
Lecture name: blood 2 & The Circulatory System Edited by: Buthainah Al masaeed & Yousef Qandeel Now we will take about A granulocytes : Lymphocyte Monocytes 1- Lymphocyte - The second major type of presence
Behavioral/Systems/Cognitive. Nicolau Beckmann, 1 Christelle Gérard, 1 Dorothée Abramowski, 2 Catherine Cannet, 1 and Matthias Staufenbiel 2 1
 The Journal of Neuroscience, January 19, 2011 31(3):1023 1031 1023 Behavioral/Systems/Cognitive Noninvasive Magnetic Resonance Imaging Detection of Cerebral Amyloid Angiopathy-Related Microvascular Alterations
The Journal of Neuroscience, January 19, 2011 31(3):1023 1031 1023 Behavioral/Systems/Cognitive Noninvasive Magnetic Resonance Imaging Detection of Cerebral Amyloid Angiopathy-Related Microvascular Alterations
Occurrence and co-localization of amyloid -protein and apolipoprotein E in perivascular drainage channels of wild-type and APP-transgenic mice
 Neurobiology of Aging xxx (2006) xxx xxx Occurrence and co-localization of amyloid -protein and apolipoprotein E in perivascular drainage channels of wild-type and APP-transgenic mice Dietmar Rudolf Thal
Neurobiology of Aging xxx (2006) xxx xxx Occurrence and co-localization of amyloid -protein and apolipoprotein E in perivascular drainage channels of wild-type and APP-transgenic mice Dietmar Rudolf Thal
The Cardiovascular System. The Structure of Blood Vessels. The Structure of Blood Vessels. The Blood Vessels. Blood Vessel Review
 The Cardiovascular System The Blood Vessels The Structure of Blood Vessels Blood Vessel Review Arteries carry blood away from the heart Pulmonary trunk to lungs Aorta to everything else Microcirculation
The Cardiovascular System The Blood Vessels The Structure of Blood Vessels Blood Vessel Review Arteries carry blood away from the heart Pulmonary trunk to lungs Aorta to everything else Microcirculation
CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage. By: Shifaa AlQa qa
 CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage By: Shifaa AlQa qa Subarachnoid Hemorrhage Causes: Rupture of a saccular (berry) aneurysm Vascular malformation Trauma Hematologic disturbances
CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage By: Shifaa AlQa qa Subarachnoid Hemorrhage Causes: Rupture of a saccular (berry) aneurysm Vascular malformation Trauma Hematologic disturbances
The Cardiovascular and Lymphatic Systems Cardiovascular System Blood Vessels Blood Vessels Arteries Arteries Arteries
 CH 12 The Cardiovascular and s The Cardiovascular and s OUTLINE: Cardiovascular System Blood Vessels Blood Pressure Cardiovascular System The cardiovascular system is composed of Blood vessels This system
CH 12 The Cardiovascular and s The Cardiovascular and s OUTLINE: Cardiovascular System Blood Vessels Blood Pressure Cardiovascular System The cardiovascular system is composed of Blood vessels This system
Muscle and Neuromuscular Junction. Peter Takizawa Department of Cell Biology
 Muscle and Neuromuscular Junction Peter Takizawa Department of Cell Biology Types and structure of muscle cells Structural basis of contraction Triggering muscle contraction Skeletal muscle consists of
Muscle and Neuromuscular Junction Peter Takizawa Department of Cell Biology Types and structure of muscle cells Structural basis of contraction Triggering muscle contraction Skeletal muscle consists of
The Carroll A. Campbell, Jr. Neuropathology Laboratory: A Tool for Dementia Discovery in South Carolina
 The Carroll A. Campbell, Jr. Neuropathology Laboratory: A Tool for Dementia Discovery in South Carolina Pathology in the Cerebral Cortex H&E stain of mature neuritic plaque Modified Bielschowsky stain
The Carroll A. Campbell, Jr. Neuropathology Laboratory: A Tool for Dementia Discovery in South Carolina Pathology in the Cerebral Cortex H&E stain of mature neuritic plaque Modified Bielschowsky stain
Memory Disorders. 1. Episodic: memory for time and places. 2. Semantic: memory for facts and knowledge (language, numbers, etc).
 I. Types of memory: A. Declarative memory: Memory Disorders 1. Episodic: memory for time and places. 2. Semantic: memory for facts and knowledge (language, numbers, etc). B. Procedural memory: - examples:
I. Types of memory: A. Declarative memory: Memory Disorders 1. Episodic: memory for time and places. 2. Semantic: memory for facts and knowledge (language, numbers, etc). B. Procedural memory: - examples:
