Chronic Pancreatitis
|
|
|
- Sherilyn Gregory
- 6 years ago
- Views:
Transcription
1
2 Supportive module 2: Basics of diagnosis, treatment and prevention of major gastroenterological diseases Chronic Pancreatitis LECTURE IN INTERNAL MEDICINE FOR IV COURSE STUDENTS M. Yabluchansky, L. Bogun, L. Martymianova, O. Bychkova, N. Lysenko, N. Makienko V.N. Karazin National University Medical School Internal Medicine Dept.
3 Plan of the Lecture Chronic Pancreatitis Definition Epidemiology Mechanisms Classification Clinical presentation Diagnosis Treatment Prognosis Prophylaxis Abbreviations Diagnostic guidelines
4 Definition Chronic Pancreatitis Chronic pancreatitis (CP) is characterized by chronic progressive pancreatic inflammation and scarring with pancreatic parenchymal calcifications, dilations of pancreatic ducts, stones and pseudocyst irreversibly damaging the pancreas function by various etiological factors with usually recurrent upper abdominal pain or as constant and disabling pain and/or pancreatic exocrine and endocrine insufficiency.
5 Epidemiology Chronic Pancreatitis The annual incidence of CP is 5 to 12 per 100,000 persons, the prevalence is 50 per 100,000 persons The prevalence of CP was 42/ in the USA, 26/ in France, 22/ in Japan, and / in India (the highest), respectively In China, an investigation on 2008 patients with CP from 22 hospitals from 1994 to 2004 showed that the incidence was 13/ and an increasing trend was seen. jigjournal.org/sites/default/files/ pdf
6 Epidemiology Chronic Pancreatitis Rate of patients discharged from the Italian hospitals in the year 2005 having the diagnosis of chronic pancreatitis and stratified according to gender and age.
7 Risk Factors & Etiology Chronic Pancreatitis In the Western world CP is commonly associated with excessive consumption of alcohol About 20% of cases are considered idiopathic CP About 10% of cases are associated with duct obstruction, trauma, cystic dystrophy of the duodenal wall, hyperparathyroidism, hypertriglyceridemia, autoimmune deviations, etc. Other important aspects are the role of cigarette smoking on CP evolution Some genes and various gene polymorphisms are able to increase susceptibility to develop CP in alcoholics through an increase of pancreatic progressive damage Most patients have multiple risk factors and the overall risk is a product of all risk factors in additive or multiplicative fashion.
8 Risk Factors & Etiology Chronic Pancreatitis
9 Risk Factors & Etiology Chronic Pancreatitis Causes of chronic pancreatitis.
10 Mechanisms Chronic Pancreatitis Most studies of the pathophysiology of CP are performed with patients who drink alcohol Disease characteristics include inflammation, glandular atrophy, ductal changes, and fibrosis When a person at risk is exposed to toxins and oxidative stress, acute pancreatitis occurs, and if the exposure continues, early- and latephase inflammatory responses result in production of profibrotic cells, including the stellate cells; this can lead to chronic pancreatitis In addition, several genetic mutations have been associated with idiopathic CP Autoimmune pancreatitis accounts for 5 to 6 percent of CP and is characterized by autoimmune inflammation, lymphocytic infiltration, fibrosis, and pancreatic dysfunction.
11 Mechanisms Chronic Pancreatitis
12 Mechanisms Chronic Pancreatitis
13 Classification International Classification of Diseases XI Diseases of the digestive K86 Other diseases of pancreas K86.0 Alcohol-induced chronic pancreatitis K86.1 Other chronic pancreatitis
14 Classification Chronic Pancreatitis: Morphology A large-duct type With calcification Without calcification A small-duct type with or without calcification With calcification Without calcification
15 Signs and Symptoms Chronic Pancreatitis For most patients with CP, abdominal pain is the presenting symptom. The patient experiences intermittent attacks of severe pain, often in the mid-abdomen or left upper abdomen and occasionally radiating in a bandlike fashion or localized to the midback The pain may occur either after meals or independently of meals, but it is not fleeting or transient and tends to last at least several hours Other symptoms associated with chronic pancreatitis include diarrhea and weight loss.
16 History Chronic Pancreatitis For most patients, abdominal pain is the presenting symptom Clinically, the patient experiences intermittent attacks of severe pain, often in the midabdomen or left upper abdomen and occasionally radiating in a bandlike fashion or localized to the midback The pain may occur either after meals or independently of meals, but it is not fleeting or transient and tends to last at least several hours Patients often are symptomatic for years before the diagnosis is established Diarrhea and weight loss may be due either to fear of eating (e.g., postprandial exacerbation of pain) or due to pancreatic exocrine insufficiency and steatorrhea.
17 Physical Exam Chronic Pancreatitis In most instances, the standard physical examination does not help to establish a diagnosis of CP; however, a few points are noteworthy During an attack, patients may assume a characteristic position in an attempt to relieve their abdominal pain (e.g., lying on the left side, flexing the spine and drawing the knees up toward the chest) Occasionally, a tender fullness or mass may be palpated in the epigastrium, suggesting the presence of a pseudocyst or an inflammatory mass in the abdomen Patients with advanced disease (i.e., patients with steatorrhea) exhibit decreased subcutaneous fat, temporal wasting, sunken supraclavicular fossa, and other physical signs of malnutrition.
18 Complications Chronic Pancreatitis Pseudocysts Biliary Obstruction Gastric Outlet Obstruction Pancreatic Adenocarcinoma Pancreatic Ascites Pleural effusion Splenic vein thrombosis
19 Diagnosis Chronic Pancreatitis The definitive diagnosis of CP is sometimes difficult, especially if the disease is not considered by the physicians treating the patient CP is suspected, based on signs, symptoms, and laboratory results, including history taking, physical examination, determination methods for pancreatic enzymes in the blood and urine, significance of various imaging methods [chest and abdominal radiography, abdominal ultrasonography, computed tomography (CT), magnetic resonance imaging (MRI), endoscopic ultrasound, and pancreatography], exocrine pancreatic function testing, pathological diagnosis, differential diagnosis from pancreatic cancer and intraductal papillary mucinous neoplasm (IPMN), and genetic testing.
20 Diagnosis Chronic Pancreatitis: Laboratory Tests
21 Diagnosis Chronic Pancreatitis: Diagnostic Path
22 Diagnosis Chronic Pancreatitis: Endoscopic Ultrasound Diagnosis based on Rosemont Classification
23 Diagnosis Chronic Pancreatitis: Staging CP generally first presents with repeated upper abdominal and back pain, and endocrine and exocrine pancreatic function gradually deteriorates In Japan, the disease is classified into three phases: compensated, transitional, and uncompensated, depending on the stage; however, an early chronic pancreatitis category has been added before the compensated phase in this revision Exocrine pancreatic disorder (that includes digestive and absorptive disorders) and abnormal glucose tolerance (pancreatic diabetes) occur as chronic pancreatitis progresses; therefore, to improve prognosis, pharmacological and nutritional therapies should be given in accordance with the stage of the disease In this regard, staging of chronic pancreatitis is important.
24 Diagnosis Chronic Pancreatitis: Pancreatic Parenchymal Calcifications
25 Diagnosis Chronic Pancreatitis: Wirsung Duct Dilatation
26 Diagnosis Chronic Pancreatitis: Pseudotumoral CP
27 Diagnosis Chronic Pancreatitis: Pancreatic Calcifications Contrast-enhanced computed tomography of the upper abdomen showing (A) pancreatic calcifications (arrow) with fluid and edema around the pancreas; and (B) pancreatic calcifications (arrow) with fluid and edema around the head of the pancreas.
28 Diagnosis Chronic Pancreatitis: Autoimmune Pancreatitis Computer Tomography of Autoimmune Pancreatitis Before and After Treatment.
29 Ampullary Carcinoma Cholangitis Cholecystitis Chronic Gastritis Diagnosis Chronic Pancreatitis: Differentiation Community-Acquired Pneumonia (CAP) Crohn Disease Intestinal Perforation Mesenteric Artery Ischemia Myocardial Infarction Pancreatic Cancer Peptic Ulcer Disease
30 Management Chronic Pancreatitis The goals of medical treatment are as follows: Modify behaviors that may exacerbate the natural history of the disease (cessation of alcohol consumption and tobacco smoking are important) Control of pain (determine the cause of abdominal pain and alleviate it) Improvement of maldigestion (enable the pancreas to heal itself, detect pancreatic exocrine insufficiency and restore digestion and absorption to normal, diagnose and treat endocrine insufficiency) Management of complications. clevelandclinicmeded.com/medicalpubs/diseasemanagement/gastroenterology/chronic-pancreatitis/#complications
31 Management Chronic Pancreatitis: Therapeutic Control of Pain Medical options for pain relief include abstinence from alcohol and smoking, analgesics, and pancreatic enzymes Non-narcotic analgesics (e.g., nonsteroidal anti-inflammatory drugs, acetaminophen, tramadol) are the next step in managing painful CP If pain persists, low doses of mild narcotics may be added Uncoated pancreatic enzymes may be worth trying in all patients because of their safety and minimal side effects Antidepressants, anticonvulsants (gabapentin), topical therapy, psychiatric counseling, and opioid rehabilitation may be of use for patients with nonvisceral pain.
32 Management Chronic Pancreatitis: Improvement of Maldigestion Pancreatic enzymes are used for the treatment of maldigestion in CP Exogenous pancreatic enzymes are safe, are well tolerated, and produce few side effects Pancreatic enzyme preparations differ based on enzyme content, the use of microspheres versus microtablets, and the presence of a coating for delayed release Because uncoated preparations are more easily denatured by gastric acid, acid suppression with a proton pump inhibitor or histaminereceptor antagonist is required Response to enzyme therapy may be monitored through an assessment of symptoms or, more objectively, through 72-hour stool fat quantification.
33 Management Chronic Pancreatitis: Management of Maldigestion
34 Management Chronic Pancreatitis: Minimally Invasive Interventions A differential nerve blockade is helpful in determining whether there is a central or somatosensory component to the pain syndrome Celiac or sphlanchnic nerve blockade may be used in select patients with visceral pancreatic pain Endoscopic techniques include biliary or pancreatic sphincterotomy (or both), removal of pancreatic duct stones, and placement of pancreatic stents Extracorporeal shockwave lithotripsty (ESWL) is also an effective ancillary treatment for patients with pancreaticductal stones either alone or in combination of endoscopic therapy.
35 Management Chronic Pancreatitis: Surgery In patients with a dilated main pancreatic duct, a side-to-side pancreatojejunostomy (Puestow procedure) may be performed The Whipple procedure and distal pancreatectomy have been used in the past to treat patients with small-duct CP Pancreatic resection is reserved for patients with disease of the small duct and pain unresponsive to medical therapy Total pancreatectomy with auto islet cell transplantation (TP/AIT) has been performed at several centers in the United States.
36 Management Chronic Pancreatitis: Management of Complications Large or symptomatic pseudocysts may be drained endoscopically through transmural or transpapillary approaches Large pseudocysts may also be drained surgically through cyst gastrostomy Biliary and gastric outlet obstructions are best managed through surgical decompression The initial management of the complications of pancreatic duct disruption or fistulas (pancreatic ascites or pleural effusions) includes prolonged pancreatic rest (parenteral nutrition), octreotide, and endoscopic placement of pancreatic duct stents In some cases, surgical resection may be necessary.
37 Prognosis Chronic Pancreatitis Generally, CP is a progressive inflammatory disease Staging and determination of severity are necessary during follow-up observation Observation and evaluation of clinical symptoms, such as abdominal pain, changes of pancreatic enzyme levels over time, morphology of the pancreas, and endocrine and exocrine pancreatic functions, are useful Patients with CP constitute a high-risk group for ordinary-type pancreatic cancer Although clear evidence for testing is lacking, many patients with CP lead a lifestyle associated with carcinogenic risks (alcohol drinking and/or smoking), and it is useful to perform cancer screening.
38 Prophylaxis Chronic Pancreatitis Limit alcohol consumption Eat a low-fat diet Exercise regularly and lose excess weight Skip crash diets Don't smoke.
39 Abbreviations CP - chronic pancreatitis IPMN - intraductal papillary mucinous neoplasm
40 Diagnostic and treatment guidelines Chronic Pancreatitis Treatment & Management American Pancreatic Association Practice Guidelines in Chronic Pancreatitis: evidence-based report on diagnostic guidelines Practice Guidelines in Chronic Pancreatitis Evidence-based clinical practice guidelines for chronic pancreatitis 2015 American Pancreatic Association Practice Guidelines in Chronic Pancreatitis: Evidence-Based Report on Diagnostic Guidelines Chronic Pancreatitis Guidelines: diagnosis and therapy for chronic pancreatitis
Prof. (DR.) MD. ISMAIL PATWARY. MBBS, FCPS, MD, FACP, FRCP(Glasgow, Edin) Professor, Dept. of Medicine, Sylhet women s Medical College, Sylhet
 Prof. (DR.) MD. ISMAIL PATWARY MBBS, FCPS, MD, FACP, FRCP(Glasgow, Edin) Professor, Dept. of Medicine, Sylhet women s Medical College, Sylhet CHRONIC PANCREATITIS Defined as a progressive inflammatory
Prof. (DR.) MD. ISMAIL PATWARY MBBS, FCPS, MD, FACP, FRCP(Glasgow, Edin) Professor, Dept. of Medicine, Sylhet women s Medical College, Sylhet CHRONIC PANCREATITIS Defined as a progressive inflammatory
Diseases of pancreas - Chronic pancreatitis
 Corso di laurea in Medicina e Chirurgia Anno accademico 2015-2016 V Anno di corso- Primo Semestre Corso Integrato : Patologia Sistemica C- Gastroenterologia Prof. Stefano Fiorucci Diseases of pancreas
Corso di laurea in Medicina e Chirurgia Anno accademico 2015-2016 V Anno di corso- Primo Semestre Corso Integrato : Patologia Sistemica C- Gastroenterologia Prof. Stefano Fiorucci Diseases of pancreas
Overview. Doumit S. BouHaidar, MD ACG/VGS/ODSGNA Regional Postgraduate Course Copyright American College of Gastroenterology 1
 Doumit S. BouHaidar, MD Associate Professor of Medicine Director, Advanced Therapeutic Endoscopy Virginia Commonwealth University Overview Copyright American College of Gastroenterology 1 Incidence: 4
Doumit S. BouHaidar, MD Associate Professor of Medicine Director, Advanced Therapeutic Endoscopy Virginia Commonwealth University Overview Copyright American College of Gastroenterology 1 Incidence: 4
The Pancreas. Basic Anatomy. Endocrine pancreas. Exocrine pancreas. Pancreas vasculature. Islets of Langerhans. Acinar cells Ductal System
 SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
Diagnosis of chronic Pancreatitis. Christoph Beglinger, University Hospital Basel, Switzerland
 Diagnosis of chronic Pancreatitis Christoph Beglinger, University Hospital Basel, Switzerland Pancreatitis Pancreas Pancreas - an organ that makes bicarbonate to neutralize gastric acid, enzymes to digest
Diagnosis of chronic Pancreatitis Christoph Beglinger, University Hospital Basel, Switzerland Pancreatitis Pancreas Pancreas - an organ that makes bicarbonate to neutralize gastric acid, enzymes to digest
The role of ERCP in chronic pancreatitis
 The role of ERCP in chronic pancreatitis Marianna Arvanitakis Erasme University Hospital, ULB, Brussels, Belgium 10 th Nottingham Endoscopy Masterclass SPEAKER DECLARATIONS This presenter has the following
The role of ERCP in chronic pancreatitis Marianna Arvanitakis Erasme University Hospital, ULB, Brussels, Belgium 10 th Nottingham Endoscopy Masterclass SPEAKER DECLARATIONS This presenter has the following
Chronic Pancreatitis
 Gastro Foundation Fellows Weekend 2017 Chronic Pancreatitis Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Aetiology in SA Alcohol (up to 80%) Idiopathic Tropical Obstruction Autoimmune
Gastro Foundation Fellows Weekend 2017 Chronic Pancreatitis Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Aetiology in SA Alcohol (up to 80%) Idiopathic Tropical Obstruction Autoimmune
Chronic Pancreatitis. Ara Sahakian, M.D. Assistant Professor of Medicine USC core lecture
 Chronic Pancreatitis Ara Sahakian, M.D. Assistant Professor of Medicine USC core lecture What is Chronic Pancreatitis Progressive inflammatory disease Pancreatic parenchyma replaced w/fibrous tissue Destruction
Chronic Pancreatitis Ara Sahakian, M.D. Assistant Professor of Medicine USC core lecture What is Chronic Pancreatitis Progressive inflammatory disease Pancreatic parenchyma replaced w/fibrous tissue Destruction
Chronic Pancreatitis: When to Scope? Gregory A. Cote, MD, MS Assistant Professor of Medicine Indiana University School of Medicine
 Chronic Pancreatitis: When to Scope? Gregory A. Cote, MD, MS Assistant Professor of Medicine Indiana University School of Medicine Endoscopy & Chronic Pancreatitis Diagnosis EUS ERCP Exocrine Function
Chronic Pancreatitis: When to Scope? Gregory A. Cote, MD, MS Assistant Professor of Medicine Indiana University School of Medicine Endoscopy & Chronic Pancreatitis Diagnosis EUS ERCP Exocrine Function
PANCREATIC PSEUDOCYSTS. Madhuri Rao MD PGY-5 Kings County Hospital Center
 PANCREATIC PSEUDOCYSTS Madhuri Rao MD PGY-5 Kings County Hospital Center 34 yo M Case Presentation PMH: Chronic pancreatitis (ETOH related) PSH: Nil Meds: Nil NKDA www.downstatesurgery.org Symptoms o Chronic
PANCREATIC PSEUDOCYSTS Madhuri Rao MD PGY-5 Kings County Hospital Center 34 yo M Case Presentation PMH: Chronic pancreatitis (ETOH related) PSH: Nil Meds: Nil NKDA www.downstatesurgery.org Symptoms o Chronic
Surgical Management of Chronic Pancreatitis VERENA LIU, MD KINGS COUNTY HOSPITAL CENTER SURGERY GRAND ROUNDS 4/1/2013
 Surgical Management of Chronic Pancreatitis VERENA LIU, MD KINGS COUNTY HOSPITAL CENTER SURGERY GRAND ROUNDS 4/1/2013 Case Report 42F with h/o chronic pancreatitis due to alcohol use with chronic upper
Surgical Management of Chronic Pancreatitis VERENA LIU, MD KINGS COUNTY HOSPITAL CENTER SURGERY GRAND ROUNDS 4/1/2013 Case Report 42F with h/o chronic pancreatitis due to alcohol use with chronic upper
Evaluation of Suspected Pancreatic Cancer
 Evaluation of Suspected Pancreatic Cancer October 15, 2015 If you experience technical difficulty during the presentation: Contact WebEx Technical Support directly at: US Toll Free: 1-866-779-3239 Toll
Evaluation of Suspected Pancreatic Cancer October 15, 2015 If you experience technical difficulty during the presentation: Contact WebEx Technical Support directly at: US Toll Free: 1-866-779-3239 Toll
CLASSIFICATION OF CHRONIC PANCREATITIS
 CLASSIFICATION OF CHRONIC PANCREATITIS EAGE, Podstgraduate Course, Prague, April 2010. Tomica Milosavljević School of Medicine, University of Belgrade Clinical Center of Serbia,Belgrade The phrase chronic
CLASSIFICATION OF CHRONIC PANCREATITIS EAGE, Podstgraduate Course, Prague, April 2010. Tomica Milosavljević School of Medicine, University of Belgrade Clinical Center of Serbia,Belgrade The phrase chronic
Pancreatitis. Acute Pancreatitis
 Pancreatitis Pancreatitis is an inflammation of the pancreas. The pancreas is a large gland behind the stomach and close to the duodenum. The duodenum is the upper part of the small intestine. The pancreas
Pancreatitis Pancreatitis is an inflammation of the pancreas. The pancreas is a large gland behind the stomach and close to the duodenum. The duodenum is the upper part of the small intestine. The pancreas
Pancreatic Benign April 27, 2016
 Department of Surgery Pancreatic Benign April 27, 2016 James Choi Dr. Hernandez Objectives Medical Expert: 1. Anatomy and congenital anomalies of the pancreas and pancreatic duct (divisum, annular pancreas
Department of Surgery Pancreatic Benign April 27, 2016 James Choi Dr. Hernandez Objectives Medical Expert: 1. Anatomy and congenital anomalies of the pancreas and pancreatic duct (divisum, annular pancreas
Causes of pancreatic insufficiency. Eugen Dumitru
 Causes of pancreatic insufficiency Eugen Dumitru Pancreatic Exocrine Insufficiency (PEI) 1. The Concept 2. The Causes 3. The Consequences Pancreatic Exocrine Insufficiency (PEI) 1. The Concept 2. The Causes
Causes of pancreatic insufficiency Eugen Dumitru Pancreatic Exocrine Insufficiency (PEI) 1. The Concept 2. The Causes 3. The Consequences Pancreatic Exocrine Insufficiency (PEI) 1. The Concept 2. The Causes
Management of Pancreatic Fistulae
 Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Treatment of chronic calcific pancreatitis endoscopy versus surgery
 Treatment of chronic calcific pancreatitis endoscopy versus surgery 35 - year old ladypresented to LPC Mumbai with intermittent abdominal pain. Pain was intermittent, colicky, more in epigastrium and periumbilical
Treatment of chronic calcific pancreatitis endoscopy versus surgery 35 - year old ladypresented to LPC Mumbai with intermittent abdominal pain. Pain was intermittent, colicky, more in epigastrium and periumbilical
BILIARY TRACT & PANCREAS, PART II
 CME Pretest BILIARY TRACT & PANCREAS, PART II VOLUME 41 1 2015 A pretest is mandatory to earn CME credit on the posttest. The pretest should be completed BEFORE reading the overview. Both tests must be
CME Pretest BILIARY TRACT & PANCREAS, PART II VOLUME 41 1 2015 A pretest is mandatory to earn CME credit on the posttest. The pretest should be completed BEFORE reading the overview. Both tests must be
What Is Pancreatitis?
 What Is Pancreatitis? Pancreatitis is inflammation (swelling) of the pancreas that is most often caused by gallstones or alcohol abuse. There are other causes that your gastroenterologist will look for,
What Is Pancreatitis? Pancreatitis is inflammation (swelling) of the pancreas that is most often caused by gallstones or alcohol abuse. There are other causes that your gastroenterologist will look for,
Pancreas Quizzes c. Both A and B a. Directly into the blood stream (not using ducts)
 Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases
 Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
16 April 2010 Resident Teaching Conference. Pancreatitis. W. H. Nealon, M.D., F.A.C.S. J.J. Smith, M.D., D.W.D.
 16 April 2010 Resident Teaching Conference Pancreatitis W. H. Nealon, M.D., F.A.C.S. J.J. Smith, M.D., D.W.D. Santorini Wirsung anatomy.med.umich.edu/.../ duodenum_ans.html Bud and ductology Ventral pancreatic
16 April 2010 Resident Teaching Conference Pancreatitis W. H. Nealon, M.D., F.A.C.S. J.J. Smith, M.D., D.W.D. Santorini Wirsung anatomy.med.umich.edu/.../ duodenum_ans.html Bud and ductology Ventral pancreatic
A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY
 A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center Welcome The St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center is a leader
A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center Welcome The St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center is a leader
PATHOLOGY MCQs. The Pancreas
 PATHOLOGY MCQs The Pancreas A patient with cystic fibrosis is characteristically: A. more than 45 years of age B. subject to recurring pulmonary infections C. obese D. subject to spontaneous fractures
PATHOLOGY MCQs The Pancreas A patient with cystic fibrosis is characteristically: A. more than 45 years of age B. subject to recurring pulmonary infections C. obese D. subject to spontaneous fractures
Index (SIRS), 158, 173
 Index A Acute pancreatitis surgery abdominal compartment syndrome, 188 adjuvant treatment, 194 anterior approach, 175 antibiotic prophylaxis, 166 167, 197 Atlanta classification, 181 classification of
Index A Acute pancreatitis surgery abdominal compartment syndrome, 188 adjuvant treatment, 194 anterior approach, 175 antibiotic prophylaxis, 166 167, 197 Atlanta classification, 181 classification of
GASTROINTESTINAL IMAGING STUDY GUIDE
 GASTROINTESTINAL IMAGING STUDY GUIDE Pharynx Diverticula Foreign bodies Trauma o Motility Disorders Esophagus Diverticula Trauma Esophagitis Barrett esophagus Rings, webs, and strictures Varices Benign
GASTROINTESTINAL IMAGING STUDY GUIDE Pharynx Diverticula Foreign bodies Trauma o Motility Disorders Esophagus Diverticula Trauma Esophagitis Barrett esophagus Rings, webs, and strictures Varices Benign
Anatomy of the biliary tract
 Harvard-MIT Division of Health Sciences and Technology HST.121: Gastroenterology, Fall 2005 Instructors: Dr. Jonathan Glickman Anatomy of the biliary tract Figure removed due to copyright reasons. Biliary
Harvard-MIT Division of Health Sciences and Technology HST.121: Gastroenterology, Fall 2005 Instructors: Dr. Jonathan Glickman Anatomy of the biliary tract Figure removed due to copyright reasons. Biliary
PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE. PRESENTED BY: Susan DePasquale, CGRN, MSN
 PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE PRESENTED BY: Susan DePasquale, CGRN, MSN Pancreatic Fluid Collection (PFC) A result of pancreatic duct (PD) and side branch disruption,
PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE PRESENTED BY: Susan DePasquale, CGRN, MSN Pancreatic Fluid Collection (PFC) A result of pancreatic duct (PD) and side branch disruption,
Pancreas composed of 2 parts: 1- exocrine gland 2- endocrine gland
 pancreas Pancreas composed of 2 parts: 1- exocrine gland 2- endocrine gland Acute pancreatitis Inflammation of the pancreas associated with acinar cell injury Clinical features: 1-abdominal pain cardinal
pancreas Pancreas composed of 2 parts: 1- exocrine gland 2- endocrine gland Acute pancreatitis Inflammation of the pancreas associated with acinar cell injury Clinical features: 1-abdominal pain cardinal
Icd 10 pancreatic mass
 Icd 10 pancreatic mass 24-2-2018 islet cell tumor (of pancreas ) ( ICD - 10 -CM Diagnosis Code D13.7.. ICD - 10 - CM Diagnosis Code K90.3. Pancreatic steatorrhea. 2016 2017 2018 Billable. Abdominal wall
Icd 10 pancreatic mass 24-2-2018 islet cell tumor (of pancreas ) ( ICD - 10 -CM Diagnosis Code D13.7.. ICD - 10 - CM Diagnosis Code K90.3. Pancreatic steatorrhea. 2016 2017 2018 Billable. Abdominal wall
Nutrition in Pancreatic Disease Topic 14
 Nutrition in Pancreatic Disease Topic 14 Module 14.2 Chronic Pancreatitis Learning objectives Johann Ockenga, MD, Prof. Dep. of Gastroenterology, Endocrinology & Nutrition, Klinikum Bremen Mitte, St. Juergensstrasse
Nutrition in Pancreatic Disease Topic 14 Module 14.2 Chronic Pancreatitis Learning objectives Johann Ockenga, MD, Prof. Dep. of Gastroenterology, Endocrinology & Nutrition, Klinikum Bremen Mitte, St. Juergensstrasse
Role of Imaging Methods in Diagnosis of Acute Pancreatitis. Válek V. Radiologická klinika, FN Brno a LF MU v Brně
 Role of Imaging Methods in Diagnosis of Acute Pancreatitis Válek V. Radiologická klinika, FN Brno a LF MU v Brně New Classification: Acute Pancreatitis 2007 revision of Atlanta classification and definitions
Role of Imaging Methods in Diagnosis of Acute Pancreatitis Válek V. Radiologická klinika, FN Brno a LF MU v Brně New Classification: Acute Pancreatitis 2007 revision of Atlanta classification and definitions
Pathophysiology ACUTE PANCREATITIS
 Pancreatitis Pathophysiology ACUTE PANCREATITIS BILIARY OBSTRUCTION Duct obstruction in the bile duct, pancreatic duct, or both. Increasing pressure Unregulated activation of digestive enzymes. Inflammation
Pancreatitis Pathophysiology ACUTE PANCREATITIS BILIARY OBSTRUCTION Duct obstruction in the bile duct, pancreatic duct, or both. Increasing pressure Unregulated activation of digestive enzymes. Inflammation
PANCREATITIS: MEDICAL AND TRANSPLANT CONSIDERATIONS, DHIRAJ YADAV, MD 1
 DHIRAJ YADAV, MD 1 Good afternoon. This is actually an interesting time of the day to do pancreas topic since you just had lunch and this is the time when the pancreas is the most active with a lot of
DHIRAJ YADAV, MD 1 Good afternoon. This is actually an interesting time of the day to do pancreas topic since you just had lunch and this is the time when the pancreas is the most active with a lot of
Unusual Pancreatic Neoplasms RTC 2/11/2011
 Unusual Pancreatic Neoplasms RTC 2/11/2011 Objectives Intraductal Papillary Mucinous Neoplasm (IPMN) Mucinous Cystic Neoplasm (MCN) Islet Cell Tumors Insulinoma Glucagonoma VIPoma Somatostatinoma Gastrinoma
Unusual Pancreatic Neoplasms RTC 2/11/2011 Objectives Intraductal Papillary Mucinous Neoplasm (IPMN) Mucinous Cystic Neoplasm (MCN) Islet Cell Tumors Insulinoma Glucagonoma VIPoma Somatostatinoma Gastrinoma
Chronic Pancreatitis (1 of 4) i
 Chronic Pancreatitis (1 of 4) i If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk.
Chronic Pancreatitis (1 of 4) i If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk.
What Are Gallstones? GALLSTONES. Gallstones are pieces of hard, solid matter that form over time in. the gallbladder of some people.
 What Are Gallstones? Gallstones are pieces of hard, solid matter that form over time in the gallbladder of some people. The gallbladder sits under the liver and stores bile (a key digestive juice ). Gallstones
What Are Gallstones? Gallstones are pieces of hard, solid matter that form over time in the gallbladder of some people. The gallbladder sits under the liver and stores bile (a key digestive juice ). Gallstones
Preview of the Medifocus Guidebook on: Chronic Pancreatitis Updated July 4, 2018
 Preview of the Medifocus Guidebook on: Chronic Pancreatitis Updated July 4, 2018 This document is only a SHORT PREVIEW of the Medifocus Guidebook on Chronic Pancreatitis. It is intended primarily to give
Preview of the Medifocus Guidebook on: Chronic Pancreatitis Updated July 4, 2018 This document is only a SHORT PREVIEW of the Medifocus Guidebook on Chronic Pancreatitis. It is intended primarily to give
Figure 2: Post-cholecystectomy biliary-like pain
 Figure 2: Post-cholecystectomy biliary-like pain 1 patient with recurrent episodes of pain (not daily), in the epigastrium/right upper quadrant, lasting >30 mins, building to a steady level, interrupting
Figure 2: Post-cholecystectomy biliary-like pain 1 patient with recurrent episodes of pain (not daily), in the epigastrium/right upper quadrant, lasting >30 mins, building to a steady level, interrupting
Patient characteristics Intervention Comparison Length of follow-up. Endoscopic treatment. Endoscopic transampullary drainage of the pancreatic duct
 1) In patients with alcohol-related, what is the safety and efficacy of a) coeliac access block vs medical management b) thoracoscopic splanchnicectomy vs medical management c) coeliac access block vs
1) In patients with alcohol-related, what is the safety and efficacy of a) coeliac access block vs medical management b) thoracoscopic splanchnicectomy vs medical management c) coeliac access block vs
ESPEN Congress Brussels 2005
 ESPEN Congress Brussels 2005 Therapeutic endoscopy of pancreatic diseases. How endoscopy may improve nutrition? Myriam Delhaye Therapeutic endoscopy of pancreatic diseases. How endoscopy may improve nutrition?
ESPEN Congress Brussels 2005 Therapeutic endoscopy of pancreatic diseases. How endoscopy may improve nutrition? Myriam Delhaye Therapeutic endoscopy of pancreatic diseases. How endoscopy may improve nutrition?
Etiology of chronic pancreatitis I. ALCOHOL Long-term alcohol abuse: Men 80g, women 40-50g/day for years Fatty food, coffee, smoking, concent
 Chronic pancreatitis Definition: Chronic pancreatitis Irreversible destruction of parenchyma Increase of the amount of connective tissue Signs of inflammation Signs of regeneration Decrease of exocrine
Chronic pancreatitis Definition: Chronic pancreatitis Irreversible destruction of parenchyma Increase of the amount of connective tissue Signs of inflammation Signs of regeneration Decrease of exocrine
Identification of Serum mirnas as prospective Bio-markers for acute and chronic pancreatitis Dr. Jeyaparvathi Somasundaram
 Identification of Serum mirnas as prospective Bio-markers for acute and chronic pancreatitis Dr. Jeyaparvathi Somasundaram Assistant Professor, Department of Biotechnoloy, Lady Doak College, Madurai. Acute
Identification of Serum mirnas as prospective Bio-markers for acute and chronic pancreatitis Dr. Jeyaparvathi Somasundaram Assistant Professor, Department of Biotechnoloy, Lady Doak College, Madurai. Acute
Outline. Intraductal Papillary Mucinous Neoplasm (IPMN) Guideline Review 4/6/2017. Case Example Background Classification Histology Guidelines
 Intraductal Papillary Mucinous Neoplasm (IPMN) Guideline Review The Nurse Practitioner Association New York State Capital Region Teaching Day Matthew Warndorf MD Case Example Background Classification
Intraductal Papillary Mucinous Neoplasm (IPMN) Guideline Review The Nurse Practitioner Association New York State Capital Region Teaching Day Matthew Warndorf MD Case Example Background Classification
Chronic pancreatitis is a fibroinflammatory disease of the
 Session 2C: Pancreaticobiliary Disease CHRONIC PANCREATITIS: WHEN TO SCOPE? Gregory A. Coté, MD, MS Chronic pancreatitis is a fibroinflammatory disease of the pancreas that presents with several distinct
Session 2C: Pancreaticobiliary Disease CHRONIC PANCREATITIS: WHEN TO SCOPE? Gregory A. Coté, MD, MS Chronic pancreatitis is a fibroinflammatory disease of the pancreas that presents with several distinct
The incidence of pancreatic cancer is rising in India and is higher in the urban male population in the western and northern parts of India.
 Published on: 9 Jun 2015 Pancreatic Cancer What Is Cancer? The body is made up of cells, which grow and die in a controlled way. Sometimes, cells keep on growing without control, causing an abnormal growth
Published on: 9 Jun 2015 Pancreatic Cancer What Is Cancer? The body is made up of cells, which grow and die in a controlled way. Sometimes, cells keep on growing without control, causing an abnormal growth
Gastric ulcer Duodenal ulcer Pancreatitis Ileus. Barbora Konečná
 Gastric ulcer Duodenal ulcer Pancreatitis Ileus Barbora Konečná basa.konecna@gmail.com Peptic ulcers of stomach and duodenum (PUD) Ulcers are chronic, often solitary lesions, that occur in any part of
Gastric ulcer Duodenal ulcer Pancreatitis Ileus Barbora Konečná basa.konecna@gmail.com Peptic ulcers of stomach and duodenum (PUD) Ulcers are chronic, often solitary lesions, that occur in any part of
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds
 Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Lahey Clinic Internal Medicine Residency Program: Curriculum for Gastroenterology
 Lahey Clinic Internal Medicine Residency Program: Curriculum for Gastroenterology Faculty representative: David L. Burns, MD, CNSP Resident representative: Tom Castiglione, MD Revision date: March 6, 2006
Lahey Clinic Internal Medicine Residency Program: Curriculum for Gastroenterology Faculty representative: David L. Burns, MD, CNSP Resident representative: Tom Castiglione, MD Revision date: March 6, 2006
Information for Consent Cholecystectomy (Laparoscopic/Open) 膽囊切除術 ( 腹腔鏡 / 開放性 )
 Version 1.0 Page 1 of 3 Information for Consent Cholecystectomy (Laparoscopic/Open) 膽囊切除術 ( 腹腔鏡 / 開放性 ) Introduction Gallbladder is a sac connected to the biliary tree. It serves the function of concentration
Version 1.0 Page 1 of 3 Information for Consent Cholecystectomy (Laparoscopic/Open) 膽囊切除術 ( 腹腔鏡 / 開放性 ) Introduction Gallbladder is a sac connected to the biliary tree. It serves the function of concentration
Chronic Pancreatitis
 Falk Symposium 161 October 12, 2007 Chronic Pancreatitis David C Whitcomb MD PhD Giant Eagle Foundation Professor of Cancer Genetics. Professor of Medicine, Cell biology & Physiology, and Human Genetics
Falk Symposium 161 October 12, 2007 Chronic Pancreatitis David C Whitcomb MD PhD Giant Eagle Foundation Professor of Cancer Genetics. Professor of Medicine, Cell biology & Physiology, and Human Genetics
Biliary tree dilation - and now what?
 Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
Imaging of common diseases of hepatobiliary and GI system
 Imaging of common diseases of hepatobiliary and GI system Natthaporn Tanpowpong, M.D. Diagnostic radiology Faculty of Medicine, Chulalongkorn University Normal plain radiograph A = Common bile duct
Imaging of common diseases of hepatobiliary and GI system Natthaporn Tanpowpong, M.D. Diagnostic radiology Faculty of Medicine, Chulalongkorn University Normal plain radiograph A = Common bile duct
Magnetic resonance cholangiopancreatography (MRCP) is an imaging. technique that is able to non-invasively assess bile and pancreatic ducts,
 SECRETIN AUGMENTED MRCP Riccardo MANFREDI, MD, MBA, FESGAR Magnetic resonance cholangiopancreatography (MRCP) is an imaging technique that is able to non-invasively assess bile and pancreatic ducts, in
SECRETIN AUGMENTED MRCP Riccardo MANFREDI, MD, MBA, FESGAR Magnetic resonance cholangiopancreatography (MRCP) is an imaging technique that is able to non-invasively assess bile and pancreatic ducts, in
INVESTIGATIONS OF GASTROINTESTINAL DISEAS
 INVESTIGATIONS OF GASTROINTESTINAL DISEAS Lecture 1 and 2 دز اسماعيل داود فرع الطب كلية طب الموصل Radiological tests of structure (imaging) Plain X-ray: May shows soft tissue outlines like liver, spleen,
INVESTIGATIONS OF GASTROINTESTINAL DISEAS Lecture 1 and 2 دز اسماعيل داود فرع الطب كلية طب الموصل Radiological tests of structure (imaging) Plain X-ray: May shows soft tissue outlines like liver, spleen,
Diseases of exocrine pancreas
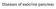 Diseases of exocrine pancreas The exocrine pancreas constitutes 80% to 85% of the organ and is composed of acinar cells that secrete enzymes needed for digestion. the accessory duct of Santorini, the main
Diseases of exocrine pancreas The exocrine pancreas constitutes 80% to 85% of the organ and is composed of acinar cells that secrete enzymes needed for digestion. the accessory duct of Santorini, the main
CHRONIC PANCREATITIS CONSERVATIVE TREATMENT, ENDOSCOPY OR SURGERY?
 Endoscopy 2006 Update and Live Demonstration Berlin, 04. 05. Mai 2006 CHRONIC PANCREATITIS CONSERVATIVE TREATMENT, ENDOSCOPY OR SURGERY? J. F. Riemann A. Rosenbaum Medizinische Klinik C, Klinikum Ludwigshafen
Endoscopy 2006 Update and Live Demonstration Berlin, 04. 05. Mai 2006 CHRONIC PANCREATITIS CONSERVATIVE TREATMENT, ENDOSCOPY OR SURGERY? J. F. Riemann A. Rosenbaum Medizinische Klinik C, Klinikum Ludwigshafen
Cholangiocarcinoma (Bile Duct Cancer)
 Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Citation Hepato-Gastroenterology, 55(86-87),
 NAOSITE: Nagasaki University's Ac Title Author(s) Combined pancreatic resection and p multiple lesions of the pancreas: i of the pancreas concomitant with du Kuroki, Tamotsu; Tajima, Yoshitsugu Tomohiko;
NAOSITE: Nagasaki University's Ac Title Author(s) Combined pancreatic resection and p multiple lesions of the pancreas: i of the pancreas concomitant with du Kuroki, Tamotsu; Tajima, Yoshitsugu Tomohiko;
Pancreas Case Scenario #1
 Pancreas Case Scenario #1 An 85 year old white female presented to her primary care physician with increasing abdominal pain. On 8/19 she had a CT scan of the abdomen and pelvis. This showed a 4.6 cm mass
Pancreas Case Scenario #1 An 85 year old white female presented to her primary care physician with increasing abdominal pain. On 8/19 she had a CT scan of the abdomen and pelvis. This showed a 4.6 cm mass
Fecal incontinence causes 196 epidemiology 8 treatment 196
 Subject Index Achalasia course 93 differential diagnosis 93 esophageal dysphagia 92 95 etiology 92, 93 treatment 93 95 work-up 93 Aminosalicylates, pharmacokinetics and aging effects 36 Antibiotics diarrhea
Subject Index Achalasia course 93 differential diagnosis 93 esophageal dysphagia 92 95 etiology 92, 93 treatment 93 95 work-up 93 Aminosalicylates, pharmacokinetics and aging effects 36 Antibiotics diarrhea
D DAVID PUBLISHING. Groove Pancreatitis: A Case Report. 1. Introduction. 2. Case Report
 Journal of Pharmacy and Pharmacology 6 (2018) 415-419 doi: 10.17265/2328-2150/2018.04.013 D DAVID PUBLISHING Luciana Leony Valente, Mariama Alves Dantas Fagundes, Camila Medrado Pereira Barbosa, Hélio
Journal of Pharmacy and Pharmacology 6 (2018) 415-419 doi: 10.17265/2328-2150/2018.04.013 D DAVID PUBLISHING Luciana Leony Valente, Mariama Alves Dantas Fagundes, Camila Medrado Pereira Barbosa, Hélio
Case 1. Intro to Gallbladder & Pancreas Pathology. Case 1 DIAGNOSIS??? Acute Cholecystitis. Acute Cholecystitis. Helen Remotti M.D.
 Cholecystitis acute chronic Gallbladder tumors Adenomyoma (benign) Adenocarcinoma Pancreatitis acute chronic Pancreatic tumors Intro to Gallbladder & Pancreas Pathology Helen Remotti M.D. Case 1 70 year
Cholecystitis acute chronic Gallbladder tumors Adenomyoma (benign) Adenocarcinoma Pancreatitis acute chronic Pancreatic tumors Intro to Gallbladder & Pancreas Pathology Helen Remotti M.D. Case 1 70 year
PANCREAS DUCTAL ADENOCARCINOMA PDAC
 CONTENTS PANCREAS DUCTAL ADENOCARCINOMA PDAC I. What is the pancreas? II. III. IV. What is pancreas cancer? What is the epidemiology of Pancreatic Ductal Adenocarcinoma (PDAC)? What are the risk factors
CONTENTS PANCREAS DUCTAL ADENOCARCINOMA PDAC I. What is the pancreas? II. III. IV. What is pancreas cancer? What is the epidemiology of Pancreatic Ductal Adenocarcinoma (PDAC)? What are the risk factors
A patient with an unusual congenital anomaly of the pancreaticobiliary tree
 A patient with an unusual congenital anomaly of the pancreaticobiliary tree Thomas Hocker, HMS IV BIDMC Core Radiology Case Presentation September 17, 2007 Review of Normal Pancreaticobiliary Tract Anatomy
A patient with an unusual congenital anomaly of the pancreaticobiliary tree Thomas Hocker, HMS IV BIDMC Core Radiology Case Presentation September 17, 2007 Review of Normal Pancreaticobiliary Tract Anatomy
Y A L E S C H O O L O F M E D I C I N E. This is a CME accredited activity. The presenters and there are no conflicts of interest.
 This is a CME accredited activity. The presenters and there are no conflicts of interest. Pain in Pancreatic Cancer More than 50% of patients with pancreatic cancer suffer from abdominal and back pain
This is a CME accredited activity. The presenters and there are no conflicts of interest. Pain in Pancreatic Cancer More than 50% of patients with pancreatic cancer suffer from abdominal and back pain
Peering Into the Black Box of the Complex Chronic Pancreatitis Syndrome
 PancreasFest 2017 Precision Medicine Approach For Benign Pancreatic Disease Friday, July 28, 2017 Peering Into the Black Box of the Complex Chronic Pancreatitis Syndrome David C Whitcomb MD PhD Director,
PancreasFest 2017 Precision Medicine Approach For Benign Pancreatic Disease Friday, July 28, 2017 Peering Into the Black Box of the Complex Chronic Pancreatitis Syndrome David C Whitcomb MD PhD Director,
Case Scenario 1. Discharge Summary
 Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Surgical management of chronic pancreatitis: Our institutional experience
 Quest Journals Journal of Medical and Dental Science Research Volume 3~ Issue 1 (2016) pp:01-09 ISSN(Online) : 2394-076X ISSN (Print):2394-0751 www.questjournals.org Research Paper Surgical management
Quest Journals Journal of Medical and Dental Science Research Volume 3~ Issue 1 (2016) pp:01-09 ISSN(Online) : 2394-076X ISSN (Print):2394-0751 www.questjournals.org Research Paper Surgical management
Perforation of a Duodenal Diverticulum. Elective Student S. C.
 Perforation of a Duodenal Diverticulum 2008 4 Elective Student S. C. Case History An elderly male presented to the Emergency Department with abdominal pain. Chief Complaint: Worsening, diffuse abdominal
Perforation of a Duodenal Diverticulum 2008 4 Elective Student S. C. Case History An elderly male presented to the Emergency Department with abdominal pain. Chief Complaint: Worsening, diffuse abdominal
LIVER CIRRHOSIS. The liver extracts nutrients from the blood and processes them for later use.
 LIVER CIRRHOSIS William Sanchez, M.D. & Jayant A. Talwalkar, M.D., M.P.H. Advanced Liver Disease Study Group Miles and Shirley Fiterman Center for Digestive Diseases Mayo College of Medicine Rochester,
LIVER CIRRHOSIS William Sanchez, M.D. & Jayant A. Talwalkar, M.D., M.P.H. Advanced Liver Disease Study Group Miles and Shirley Fiterman Center for Digestive Diseases Mayo College of Medicine Rochester,
Morning Report. Allison Haden, MD October 1, 2002
 Morning Report Allison Haden, MD October 1, 2002 68 yo WM with N/V and abdominal pain Became ill about 2 weeks ago, per pt. intermittent nausea: worse w/eating vomiting within 30min of eating, nonbilious,
Morning Report Allison Haden, MD October 1, 2002 68 yo WM with N/V and abdominal pain Became ill about 2 weeks ago, per pt. intermittent nausea: worse w/eating vomiting within 30min of eating, nonbilious,
X-Plain Pancreatic Cancer Reference Summary
 X-Plain Pancreatic Cancer Reference Summary Introduction Pancreatic cancer is the 4th leading cause of cancer deaths in the U.S. About 37,000 new cases of pancreatic cancer are diagnosed each year in the
X-Plain Pancreatic Cancer Reference Summary Introduction Pancreatic cancer is the 4th leading cause of cancer deaths in the U.S. About 37,000 new cases of pancreatic cancer are diagnosed each year in the
Safe Answers For The American Board of Surgery Certifying Exam & Recertifying Exam
 Safe Answers For The American Board of Surgery Certifying Exam & Recertifying Exam By Sarmad Aji, MD., FACS. A comprehensive review of the most commonly asked questions on the American Board of Surgery
Safe Answers For The American Board of Surgery Certifying Exam & Recertifying Exam By Sarmad Aji, MD., FACS. A comprehensive review of the most commonly asked questions on the American Board of Surgery
Intended for use by Clinicians and Health Care Providers involved in the Management or Referral of adult patients with pancreatic
 Intended for use by Clinicians and Health Care Providers involved in the Management or Referral of adult patients with pancreatic cancer Section AA Cancer Centre Referrals In the absence of metastatic
Intended for use by Clinicians and Health Care Providers involved in the Management or Referral of adult patients with pancreatic cancer Section AA Cancer Centre Referrals In the absence of metastatic
Pancreatic Lesions. Valerie Jefford Pediatric Surgery Rounds June 6, 2003
 Pancreatic Lesions Valerie Jefford Pediatric Surgery Rounds June 6, 2003 Embryology 4 th week 2 buds of endodermal origin from caudal foregut Dorsal and ventral bud Ventral migrates dorsally with CBD (below/behind
Pancreatic Lesions Valerie Jefford Pediatric Surgery Rounds June 6, 2003 Embryology 4 th week 2 buds of endodermal origin from caudal foregut Dorsal and ventral bud Ventral migrates dorsally with CBD (below/behind
This page explains some of the medical words that you may hear when you are finding out about pancreatic cancer and how it is treated.
 A-Z of medical words This page explains some of the medical words that you may hear when you are finding out about pancreatic cancer and how it is treated. Absorption: once your food has been broken down,
A-Z of medical words This page explains some of the medical words that you may hear when you are finding out about pancreatic cancer and how it is treated. Absorption: once your food has been broken down,
CASE 01 LA Path Slide Seminar 13 March, 08. Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center
 CASE 01 LA Path Slide Seminar 13 March, 08 Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center Clinical History 60 year old male presented with obstructive jaundice
CASE 01 LA Path Slide Seminar 13 March, 08 Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center Clinical History 60 year old male presented with obstructive jaundice
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts
 ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
ACUTE ABDOMEN. Dr. M Asadi. Surgical Oncology Research Center MUMS. Assistant Professor of General Surgery
 ACUTE ABDOMEN Dr. M Asadi Assistant Professor of General Surgery Surgical Oncology Research Center MUMS Definition I. The term Acute Abdomen refers to signs & symptoms of abdominal pain and tenderness,
ACUTE ABDOMEN Dr. M Asadi Assistant Professor of General Surgery Surgical Oncology Research Center MUMS Definition I. The term Acute Abdomen refers to signs & symptoms of abdominal pain and tenderness,
Severe necrotizing pancreatitis. ICU Fellowship Training Radboudumc
 Severe necrotizing pancreatitis ICU Fellowship Training Radboudumc Acute pancreatitis Patients with acute pancreatitis van Dijk SM. Gut 2017;66:2024-2032 Diagnosis Revised Atlanta classification Abdominal
Severe necrotizing pancreatitis ICU Fellowship Training Radboudumc Acute pancreatitis Patients with acute pancreatitis van Dijk SM. Gut 2017;66:2024-2032 Diagnosis Revised Atlanta classification Abdominal
Management A Guideline Based Approach to the Incidental Pancreatic Cysts. Common Cystic Pancreatic Neoplasms.
 Management 2016 A Guideline Based Approach to the Incidental Pancreatic Cysts ISMRM 2016 Masoom Haider, MD, FRCP(C) Professor of Radiology, University of Toronto Clinician Scientist, Ontario Institute
Management 2016 A Guideline Based Approach to the Incidental Pancreatic Cysts ISMRM 2016 Masoom Haider, MD, FRCP(C) Professor of Radiology, University of Toronto Clinician Scientist, Ontario Institute
5/17/2013. Pancreatic Cancer. Postgraduate Course in General Surgery CASE 1: CASE 1: Overview. Case presentation. Differential diagnosis
 Overview Case presentation Postgraduate Course in General Surgery Differential diagnosis Diagnosis and therapy Eric K. Nakakura Koloa, HI March 26, 2013 Outcomes CASE 1: CASE 1: A 78-year-old man developed
Overview Case presentation Postgraduate Course in General Surgery Differential diagnosis Diagnosis and therapy Eric K. Nakakura Koloa, HI March 26, 2013 Outcomes CASE 1: CASE 1: A 78-year-old man developed
Chronic Pancreatitis: Surgical Options. W. Charles Conway MD, FACS Upper GI/HPB Surgical Oncology Ochsner Medical Center New Orleans, LA
 Chronic Pancreatitis: Surgical Options W. Charles Conway MD, FACS Upper GI/HPB Surgical Oncology Ochsner Medical Center New Orleans, LA Chronic Pancreatitis Recurrent, debilitating abdominal pain with
Chronic Pancreatitis: Surgical Options W. Charles Conway MD, FACS Upper GI/HPB Surgical Oncology Ochsner Medical Center New Orleans, LA Chronic Pancreatitis Recurrent, debilitating abdominal pain with
What Is Cirrhosis? CIRRHOSIS. Cirrhosis occurs when the liver is. by chronic conditions and diseases. permanently scarred or injured
 What Is Cirrhosis? Cirrhosis occurs when the liver is permanently scarred or injured by chronic conditions and diseases. Common causes of cirrhosis include: Long-term alcohol abuse. Chronic viral hepatitis
What Is Cirrhosis? Cirrhosis occurs when the liver is permanently scarred or injured by chronic conditions and diseases. Common causes of cirrhosis include: Long-term alcohol abuse. Chronic viral hepatitis
Together, putting patients first
 The Role of a Gastroenterologist in the Diagnosis and Management of Pancreatic Cancer Sarah Jowett, Consultant Gastroenterologist Bradford Teaching Hospitals Trust Leeds Regional Study Day, 12 September
The Role of a Gastroenterologist in the Diagnosis and Management of Pancreatic Cancer Sarah Jowett, Consultant Gastroenterologist Bradford Teaching Hospitals Trust Leeds Regional Study Day, 12 September
Yoshitsugu; Kanematsu, Takashi; Kur
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Laparoscopic Middle Pancreatectomy Surgery Kitasato, Amane; Adachi, Tomohiko; Yoshitsugu; Kanematsu, Takashi; Kur Hepato-Gastroenterology, 59(120),
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Laparoscopic Middle Pancreatectomy Surgery Kitasato, Amane; Adachi, Tomohiko; Yoshitsugu; Kanematsu, Takashi; Kur Hepato-Gastroenterology, 59(120),
Gastroenterology. Certification Examination Blueprint. Purpose of the exam
 Gastroenterology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified gastroenterologist
Gastroenterology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified gastroenterologist
Imaging Techniques for Acute Necrotizing Pancreatitis: Multidetector Computed Tomography
 AISP - 29 th National Congress. Bologna (Italy). September 15-17, 2005. Imaging Techniques for Acute Necrotizing Pancreatitis: Multidetector Computed Tomography Lucia Calculli 1, Raffaele Pezzilli 2, Riccardo
AISP - 29 th National Congress. Bologna (Italy). September 15-17, 2005. Imaging Techniques for Acute Necrotizing Pancreatitis: Multidetector Computed Tomography Lucia Calculli 1, Raffaele Pezzilli 2, Riccardo
Hepatobiliary and Pancreatic Malignancies
 Hepatobiliary and Pancreatic Malignancies Gareth Eeson MD MSc FRCSC Surgical Oncologist and General Surgeon Kelowna General Hospital Interior Health Consultant, Surgical Oncology BC Cancer Agency Centre
Hepatobiliary and Pancreatic Malignancies Gareth Eeson MD MSc FRCSC Surgical Oncologist and General Surgeon Kelowna General Hospital Interior Health Consultant, Surgical Oncology BC Cancer Agency Centre
CT 101 :Pancreas and Spleen
 CT 101 :Pancreas and Spleen Shikha Khullar,, MD, MPH Division of Radiology University of South Alabama The Pancreas Normal Pancreas 3 Phase Pancreatic CT Non contrast Arterial phase : 30-35 35 second
CT 101 :Pancreas and Spleen Shikha Khullar,, MD, MPH Division of Radiology University of South Alabama The Pancreas Normal Pancreas 3 Phase Pancreatic CT Non contrast Arterial phase : 30-35 35 second
Chronic pancreatitis an increasing Indian Problem
 Chronic pancreatitis an increasing Indian Problem Dr Ramesh Ardhanari M.S; MCh.(SGE); FRCS (Hon)(G) Medical Director, Sr. Consultant & Head Dept. of Surgical Gastroenterology Meenakshi Mission Hospital,Madurai
Chronic pancreatitis an increasing Indian Problem Dr Ramesh Ardhanari M.S; MCh.(SGE); FRCS (Hon)(G) Medical Director, Sr. Consultant & Head Dept. of Surgical Gastroenterology Meenakshi Mission Hospital,Madurai
Exocrine functions: secretion of digestive enzymes (eg. lipase, amylase,
 Chapter 91 Pancreas Episode Overview: 1. List 10 differential diagnoses for acute pancreatitis 2. List 10 causes of pancreatitis. Which are most common in adults? Which one is most common in pediatrics?
Chapter 91 Pancreas Episode Overview: 1. List 10 differential diagnoses for acute pancreatitis 2. List 10 causes of pancreatitis. Which are most common in adults? Which one is most common in pediatrics?
Anatomical and Functional MRI of the Pancreas
 Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
Gastrointestinal Emergencies CEN REVIEW 2017 MARY RALEY, BSN, RN, CEN, TCRN, TNSCC
 Gastrointestinal Emergencies CEN REVIEW 2017 MARY RALEY, BSN, RN, CEN, TCRN, TNSCC Gastrointestinal Emergencies is 7% of the CEN A. Acute abdomen B. Bleeding C. Cholecystitis D. Cirrhosis E. Diverticulitis
Gastrointestinal Emergencies CEN REVIEW 2017 MARY RALEY, BSN, RN, CEN, TCRN, TNSCC Gastrointestinal Emergencies is 7% of the CEN A. Acute abdomen B. Bleeding C. Cholecystitis D. Cirrhosis E. Diverticulitis
Primary Sclerosing Cholangitis and Cholestatic liver diseases. Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants
 Primary Sclerosing Cholangitis and Cholestatic liver diseases Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants I have nothing to disclose Educational Objectives What is PSC? Understand the cholestatic
Primary Sclerosing Cholangitis and Cholestatic liver diseases Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants I have nothing to disclose Educational Objectives What is PSC? Understand the cholestatic
Citation American Journal of Surgery, 196(5)
 NAOSITE: Nagasaki University's Ac Title Author(s) Multifocal branch-duct pancreatic i neoplasms Tajima, Yoshitsugu; Kuroki, Tamotsu Amane; Adachi, Tomohiko; Mishima, T Kanematsu, Takashi Citation American
NAOSITE: Nagasaki University's Ac Title Author(s) Multifocal branch-duct pancreatic i neoplasms Tajima, Yoshitsugu; Kuroki, Tamotsu Amane; Adachi, Tomohiko; Mishima, T Kanematsu, Takashi Citation American
Total Pancreatectomy and Islet Auto Transplantation (TPIAT)
 Total Pancreatectomy and Islet Auto Transplantation (TPIAT) Dhiraj Yadav, MD MPH Professor of Medicine Division of Gastroenterology & Hepatology University of Pittsburgh Medical Center PSG Meeting Sept
Total Pancreatectomy and Islet Auto Transplantation (TPIAT) Dhiraj Yadav, MD MPH Professor of Medicine Division of Gastroenterology & Hepatology University of Pittsburgh Medical Center PSG Meeting Sept
