Worldwide Injection Technique Study: Injecting Complications
|
|
|
- Norman Gardner
- 5 years ago
- Views:
Transcription
1 Worldwide Injection Technique Study: Injecting Complications Introduction In two previous papers we introduced the worldwide Injection Technique Questionnaire (ITQ) survey patient population 1 and injecting practice 2. In conjunction with the results, we gave best practice recommendations which are evidence-based. We propose to continue this expose, using the same approach, for Injecting Complications. Methods and Materials Our previous paper 3 described the methods, materials, centers and patients who participated in the study. Results Lipohypertrophy (LH) Patients were asked: Do you have any swelling or lumps under the skin at your usual injection sites that have been there for some time (weeks, months or years)? Answer N % Yes No Nurses were asked to examine all the patient s injection sites both visually and by palpation and to report any LH. SITE EXAM TYPE % lipos found ABDOMEN Visual 17.3 Palpation 21.1 THIGH Visual Worldwide Injection Technique Study: Population Surveyed Worldwide Injection Technique Study: Injecting Practices Worldwide Injection Technique Study: Population Surveyed
2 BUTTOCKS Palpation 11.2 Visual 2.1 Palpation 2.8 ARM Visual 11.2 Palpation 13.4 Overall, the nurse found lipohypertrophy in 30.8% of patients. Hence we see that that LH is present in nearly 1/3 of survey subjects worldwide. Its frequency is relatively consistent across the 42 countries surveyed. LH is seen almost twice as frequently in T1DM than in T2DM and is virtually absent in GDM, presumably because of the very short time injecting insulin. Although there was a correlation between lesions that were visible and those that were palpated, it was not 100%. The following table presents data on abdominal LH (the most frequently seen). No Visible Yes Palpable No % 97.1%.4% Yes % 13.0% 76.8% Almost 77% of LH could be both seen and felt, but 13% could be felt but not seen. Only 0.4% could be seen but not felt. The same pattern is seen with the thigh, buttocks and arm (data not shown). When nurses found LH they were asked to measure along its longest dimension in mm. SIZE LH (in mm) N Mean SD Minimum Maximum ABDOMEN THIGH BUTTOCKS ARM When nurses found LH they asked the patient if they were still injecting into it and 44.0% said yes. They were then asked how often. 2
3 Frequency % Every injection 16.7 Frequently (daily) 39.5 Occasionally (weekly) 30.3 Seldom (monthly) 13.5 Patients who injected into LH were asked why they did so. Reason % It s convenient 11.3 It s less painful 16.8 Just a habit 30.8 Don t know 28.0 Associations: LH is associated with giving more injections per day, with an earlier age of diagnosis of DM (especially in T1DM), with a longer number of years with DM and with a longer number of years on insulin. However there is no association between the presence of LH and BMI. There is also not an association between LH and length of time taking GLP1s. Just under 1/3 of those taking GLP1s were found to have LH, but it is unclear if the LH predated the start of the GLP1. The fact that there is no association to the length of time on a GLP1 suggests the LH is not linked to the GLP1. (Data not shown for the above, but all differences were significant to a p<0.05.) Interestingly there is an association between LH and a number of sloppy injection practices, including poor rotation habits, shorter indwell times, injecting through clothing, injecting insulin cold before it has warmed up, using insulins past their expiry dates and inappropriate disposal of used sharps (all with p<0.05). It is difficult to assess the significance of these associations, other than to say they are fellow travelers. Insulin Consumption: There is a strong association between the presence of LH and the total daily dose (TDD) of insulin. LH Mean TDD SD N Yes No Total
4 Over 10 IU of insulin on average being consumed in the LH+ population vs LH-. In T2DM patients, this average TDD difference is 13.5 IU. In T1DM patients, the average TDD difference is 5.4 IU. These differences are maintained in the population which continues to inject into LH. Inject into LH Mean TDD SD N Yes No Total These differences were seen for different types of insulin: fast-acting analogue (mean of 4.4 IU more), basal analogue (mean of 1.5 IU more) and premix (mean of 9.8 IU more). All currently used families of insulins are associated with the risk of LH. It is difficult to determine if any one type of insulin has higher risks. Even newer analogues show a prevalence of LH in double digits. (Data not shown for the above, but all differences were significant to a p<0.05.) Glucose Control: The presence of LH is associated with higher HbA1c values, an average difference of LH Mean HbA1c SD N Yes No Total For T1DM the mean increase is 0.54%. For T2DM the mean increase is 0.53%. LH is associated with higher rates of unexplained hypoglycemia and higher rates of glycemic variability as well as more frequent DKA. (Data not shown for the above, but all differences were significant to a p<0.05.) Risk Factors: LH is associated with incorrect rotation of injection sites, using smaller injecting zones, more years on insulin and reusing pen needles. The higher the number of times the pen needle is reused the more frequently reported is the LH. 4
5 Times Needle Used LH Yes No 2 times % 66.1% 3 5 times % 64.9% 6 10 times % 65.4% > 10 times % 56.2% TOTAL % 64.2% The size of the LH is also related to the number of times the needle is used. Mean Diameter Thigh LH (mm) SD N 2 times times times > 10 times TOTAL By Logical Regression analysis, incorrect rotation and years on insulin are the most important factors associated with LH (p<0.001), while pen needle reuse is significantly, but slightly less strongly associated (p=0.023). Rotation of Injecting Sites Nearly 5 out of 6 injectors claim to rotate injection sites. Of these, 2/3 were found by nurses to be rotating correctly. Correct site rotation is defined as always injecting at least 1 cm from a previous injection. Those who rotate correctly tend to have less 5
6 hyperglycemia, less LH, less unexplained hyperglycemia and less glucose variability. (Data not shown for the above, but all differences were significant to a p<0.05.) HbA1c is lower in those who correctly rotate by an average of Correct Rotation Mean HbA1c SD N Yes No Total By Linear Regression analysis, incorrect rotation and years on insulin are the most important factors associated with LH (p<0.001), while pen needle reuse is significantly, but slightly less strongly associated (p=0.023). HbA1c values are approximately 0.5 higher in injectors with LH (in both T1DM and T2DM) and are significantly higher with incorrect rotation of sites. The frequency of unexpected hypoglycemia and glucose variability are significantly higher with LH, with injecting into LH and with incorrect rotation of sites. Correct rotation is also associated with lower TDD by an average of 4.7 IU. Correct rotation Mean TDD SD N Yes No Total Checking sites routinely is associated with lower HbA1c levels, less LH and more correct rotation. Patients are also more likely to rotate correctly if they have received injection instruction in the last 6 months. Lower TDD of insulin is associated with correct rotation of injections. Correct rotation seems to increase in frequency as the needle shortens, although this may be a byproduct of the level of education and training given when switching patients to such needles. Needle Length
7 Correct Rotation Yes % 76.3% 71.1% 71.6% 63.9% No % 23.7% 28.9% 28.4% 36.1% Correct rotation also seems to increase as the gauge thins and as the site inspection and injection training become more routine. (Data not shown for the above, but all differences were significant to a p<0.05.) Bleeding and Bruising Patients were asked if they saw bleeding or bruising from their injection sites and 60.2% said they did. They were also asked about the frequency and only 0.5% said it was always, 7.3% said often (several times a week), 41.5% said sometimes (several times a month) and 50.8% said it was almost never (several times a year). Pain Our results showed that just over half of injectors report having pain on injection. Of these, 4 out of 5 report having painful injections only several times a month or year (i.e. not with every injection). Groups with higher frequency of reported pain are: T1DM patients, children, adolescents and women. Pain seems also to be commonly associated with bleeding. Bleeding Pain Yes No Yes % 70.5% 29.5% No % 33.1% 66.9% Pain is also associated with several other disorders, without obvious causative relationship: injecting through clothes, using cold insulin, skipping injections, hypo- and hyperglycemia, LH, injecting into LH, incorrect site rotation, higher HbA1c, lower BMI, younger age and higher TDD. (Data not shown for the above, but all differences were significant to a p<0.05.) Pain is also associated with needle reuse and seems to increase as a function of the number of times the needle is reused. 7
8 Pain Yes No % 52.4% 47.6% Number of times Needle Used % 55.1% 44.9% % 59.5% 40.5% > % 62.9% 37.1% Lipoatrophy and Inflammation Nurses also examined each injection site for the presence of lipoatrophy and redness. SITE FINDING % ABDOMEN Lipoatrophy 0.6 Redness 3.3 THIGH Lipoatrophy 0.5 Redness 2.8 BUTTOCKS Lipoatrophy 0.2 Redness 0.4 ARM Lipoatrophy 0.4 Redness 3.6 Insulin Leakage Just over 1/3 of patients report leakage of insulin from the skin. Of these, 5 out of 6 say it occurs rarely (several times a month or a year). Leakage occurs more frequently in T1DM patients than T2DM. Leakage appears to be more frequent if patients have LH or inject into LH, do not leave the pen needle under the skin for 10 seconds after injecting or do not rotate injections correctly. 8
9 Dwell Times Yes Leakage No Total < 5 sec % 59.1% 100.0% 5 10 sec % 61.3% 100.0% > 10 sec % 64.3% 100.0% Not aware how long % 57.1% 100.0% The longer pen users leave the needle under the skin after the plunger is pushed in (and especially if they reach the 10-second goal) the less leakage is reported. Of patients who weren t aware how long they left the needle in, almost half had leakage. Leakage is associated with pain, bleeding, hypo- and hyperglycemia, unexplained hypoglycemia and glucose variability. Leakage is not associated with needle reuse, the type of insulin used, lifting a skin fold, the angle of insertion or BMI. Patients with leakage had slightly higher HbA1c and used on average 5.2 IU more of insulin a day. Leakage TDD SD N Yes No Total
10 Discussion Lipohypertrophy (LH) LH is a thickened, rubbery lesion that appears in the SC tissue of injecting sites in up to half of patients who inject insulin. In some patients the lesions can be hard or scar-like. 4 5 Detection of LH requires both visualization and palpation of injecting sites, as some lesions can be more easily felt than seen. 6 Making two ink marks at opposite edges of the LH (at the junctions between normal and rubbery tissue) will allow the lesion to be measured, recorded, and followed long-term. More than a third of our participants described lesions consistent with LH at their injection sites and approximately the same proportion were found to have LH by the examining nurse (using visual inspection and palpation) at the time of the ITQ. Figure 3 illustrates visible LH in a woman who had injected in the same two locations below the umbilicus for twelve years. Figure 4 illustrates the detection of palpable LH by comparing a fold of normal skin (arrow tips close together) with lipohypertrophic tissue (arrow tips spread apart). Normal skin can be pinched tightly together, while lipohypertrophic lesions cannot. 7 Figure 3: Two visible lipohypertrophic lesions below the umbilicus 4 Thow JC, Johnson AB, Marsden S, Taylor R, Home PH. Morphology of palpably abnormal injection sites and effects on absorption of isophane (NPH) insulin. Diabetic Medicine 1990;7: Richardson T, Kerr D. Skin-related complications of insulin therapy: epidemiology and emerging management strategies. American J Clinical Dermatol 2003;4: Seyoum B, Abdulkadir J. Systematic inspection of insulin injection sites for local complications related to incorrect injection technique. Trop Doct 1996;26: Photographs courtesy of Lourdes Saez-de Ibarra and Ruth Gaspar, Diabetes Nurses and Specialist Educators from La Paz Hospital, Madrid, Spain. 10
11 Figure 4: The different pinch characteristics of normal (left) versus lipohypertrophic (right) tissue. The prevalence rates of LH amongst insulin-injecting patients with DM in five recent studies are, from lowest to highest: 14.5% (Hajheydari, ); 27.1% (Raile, ); 34.5% (Partanen, ); 48.0% (Kordonuri, ); 64% (Blanco, ). Vardar 13 found that the prevalence of LH at insulin injections sites was 48.8% in 215 Turkish patients who had been using insulin for at least 2 years; Seyoum 14 found LH in 31% of 100 insulin injectors in Ethiopia; and Hauner 15 reported that 28.7% of the 233 German patients studied with T1DM had the condition. In the 2010 Injection Technique Questionnaire (ITQ) Survey 16 48% of the over 4200 patients insulin answered Yes to the following question (acknowledged to be somewhat non-specific), Have you ever noticed swelling of fatty tissue or small bumps at your injection sites? The percentages in all 16 countries surveyed were all in double digits and ranged from 30 to 88%. A number of earlier surveys have reported similar findings. 8 Hajheydari Z, Kashi Z, Akha O, Akbarzadeh S. Frequency of lipodystrophy induced by recombinant human insulin. Eur Rev Med Pharmacol Sci Oct;15(10): Raile K, Noelle V, Landgraf R, Schwarz HP. Insulin antibodies are associated with lipoatrophy but also with lipohypertrophy in children and adolescents with type 1 diabetes. Exp Clin Endocrinol Diabetes. 2001;109(8): Partanen TM, Rissanen A. Insulin injection practices, Pract Diab Int 2000;17: Kordonouri O, Lauterborn R, Deiss D. Lipohypertrophy in young patients with type 1 diabetes. Diabetes Care Mar;25(3): Blanco M, Hernández MT, Strauss KW, Amaya M. Prevalence and risk factors of lipohypertrophy in insulininjecting patients with diabetes. Diabetes Metab Oct;39(5): Vardar B, Kizilci S. Incidence of lipohypertrophy in diabetic patients and a study of influencing factors. Diabetes Res Clin Pract 2007;77: Seyoum B, Abdulkadir J. Systematic inspection of insulin injection sites for local complications related to incorrect injection technique. Trop Doct 1996;26: Hauner H, Stockamp B, Haastert B. Prevalence of lipohypertrophy in insulin-treated diabetic patients and predisposing factors. Exp Clin Endocrinol Diabetes 1996;104: De Coninck C, Frid A, Gaspar R, et al. Results and analysis of the Insulin Injection Technique Questionnaire survey. J Diabetes Sep;2(3): Strauss K, Insulin injection techniques: Report from the 1 st International Insulin Injection Technique Workshop, Strasbourg, France June 1997, Pract Diab Int 1998;15:
12 Blanco 21 studied 430 patients from 19 Spanish centers and found that nearly 2/3 (64.4%) had LH. It was more commonly in T1DM (72.3%) than in T2DM (53.4%). Grassi 22 studied 388 patients from 18 Italian centers and found a prevalence of 48.7%. In a Chinese study 23 of 401 patients in 4 centers found an overall prevalence of 53.1% (95% CI 48.2, 58.0%). By body site, LH was found in 52.4% of Abdomens examined, 15.5% of thighs and 9.4% of arms. Lipohypertrophy has also been reported to be frequent in CSII Patients. A cross-sectional study 24 of 50 consecutive patients with T1DM using CSII for >6 months (26 female; age, 13.3 ± 3.5 years; CSII duration, 2.8 ± 1.7 years; HbA1c, 7.7% ± 1.1%) examined the skin for complications associated with therapy. 42% of these patients had LH. A similar survey 25 of 91 adult CSII patients revealed that the commonest infusion site problem was lipohypertrophy (26.1%), which occurred more often in those with long duration of CSII (4.8 [ ] vs. 3.0 [ ] years; P=0.01). Vardar 26 also identified, by logistic regression analysis, three independent risk factors for LH: Duration of insulin use, with longer use associated with more LH (p=0.001); Site rotation, with a failure to rotate associated with higher LH risk (p=0.004); Changing needles, with needle reuse also associated with LH (p=0.004). Two other studies have identified similar factors. Immunologic factors in LH are poorly understood, although antibodies seem to have a role in pediatric and adolescent patients with T1DM 29. Needle length has not been shown to be a risk factor. It is also not known what the impact of different needle lengths is on insulin absorption from injections into LH. Histopathologically, LH lesions are shown to be entirely formed of adipocytes. These cells are often hypertrophied to two or three times the size of normal adipocytes. They 18 Strauss K, De Gols H, Hannet I, Partanen TM, Frid A. A pan-european epidemiologic study of insulin injection technique in patients with diabetes. Pract Diab Int 2002;19: Strauss K, De Gols H, Letondeur C, Matyjaszczyk M, Frid A. The second injection technique event (SITE), May 2000, Barcelona, Spain. Pract Diab Int 2002;19: Partanen TM, Rissanen A. Insulin injection practices, Pract Diab Int 2000;17: Blanco M, Hernández MT, Strauss KW, Amaya M. Prevalence and risk factors of lipohypertrophy in insulininjecting patients with diabetes. Diabetes Metab Oct;39(5): G. Grassi, Scuntero P, Trepiccioni R, et al. Optimizing insulin injection technique and its effect on blood glucose control. Journal of Clinical & Translational Endocrinology 1 (2014): This is an open access article under the CC BY-NC-ND license ( 23 Ji L, Li Q, Wei G. Lipohypertrophy - prevalence, risk factors and clinical characteristics of insulin-requiring patients in China. Abstract, EASD Vienna 2014, Tracking Number: A Conwell LS, Pope E, Artiles AM, Mohanta A, Daneman A, Daneman D. Dermatological complications of continuous subcutaneous insulin infusion in children and adolescents. J Pediatr. 2008;152: Pickup J, Yemane N, Brackenridge A, Pender S. Nonmetabolic Complications of Continuous Subcutaneous Insulin Infusion: A Patient Survey. Diabetes Technology & Therapeutics 2014; 16: Vardar B, Kizilci S. Incidence of lipohypertrophy in diabetic patients and a study of influencing factors. Diabetes Res Clin Pract 2007;77: Blanco M, Hernández MT, Strauss KW, Amaya M. Prevalence and risk factors of lipohypertrophy in insulininjecting patients with diabetes. Diabetes Metab Oct;39(5): Saez-de Ibarra L, Gallego F. Factors related to lipohypertrophy in insulin-treated diabetic patients; role of educational intervention. Pract Diab Int 1998;15: Raile K, Noelle V, Landgraf R, Schwarz HP. Insulin antibodies are associated with lipoatrophy but also with lipohypertrophy in children and adolescents with type 1 diabetes. Exp Clin Endocrinol Diabetes. 2001;109(8):
13 can be seen invading the adjacent reticular dermis, engulfing lipid droplets, proliferating or manifesting other signs of metabolic activation 30. This anabolic activity is presumably initiated by trauma from repeat injections in the same place and time coupled with the growth-promoting properties of insulin. There may be genetic factors but these have not yet been elucidated. Almost all studies of patients injecting into LH show insulin absorption to be delayed or erratic, potentially worsening diabetes management. Franzen 35 evaluated children with diabetes who were injecting into clinically detectable LH. The children received simple but direct instructions: Rotate injection sites; and Do not reuse your needles. In 3 months 90% of LH lesions in these children had resolved and were undetectable. HbA1c was improved significantly and insulin requirements had decreased. A recent Spanish study entitled Prevalence and Risk Factors of Lipohypertrophy in Insulin - Injecting Patients with Diabetes 36 showed that LH is extremely common, present in 2/3 of patients and is strongly associated with both incorrect rotation of sites of injection and with reuse of needles, especially > 5 times. Unexplained hypoglycemia and glycemic variability were also greatly increased (6 to 7-fold) in those with, Vs those without LH. The ITQ has shown that approximately 1 out of 4 insulin injectors has unexpected hypoglycemia and more than 1 out of 3 has glucose variability. HbA1c values do not differ between T1DM and T2DM injectors, but T1DM patients have significantly higher frequencies of unexpected hypoglycemia and glucose variability. HbA1c values do not differ amongst the different needle lengths, but injectors using the 6mm needle have somewhat higher frequencies of unexpected hypoglycemia and glucose variability for unknown reasons. HbA1c values are approximately 0.5 higher in injectors with LH (in both T1DM and T2DM) and are significantly higher with incorrect rotation of sites and with needle reuse. HbA1c values are lower in subjects who use larger injection areas and whose sites are inspected routinely. The frequency of unexpected hypoglycemia and glucose variability are significantly higher with LH, with injecting into LH, with incorrect rotation of sites and with needle reuse. Rates of unexpected hypoglycemia and glucose variability are lower when the abdomen is used exclusively as an injection site, but as one adds use of the limbs the rates of both disorders increase. 30 Fujikura J, Fujimoto M, Yasue S, et.al. Insulin-induced lipohypertrophy: report of a case with histopathology. Endocr J Oct;52(5): Young RJ, Hannan WJ, Frier BM, Steel JM, Duncan LJ.. Diabetic lipohypertrophy delays insulin absorption. Diabetes Care 1984;7: Chowdhury TA, Escudier V. Poor glycaemic control caused by insulin induced lipohypertrophy. Brit Med J 2003;327: Johansson UB. Impaired absorption of insulin aspart from lipohypertrophic injection sites. Diabetes Care 2005;28: Frid A, Linden B. Computed tomography of injection sites in patients with diabetes mellitus. Injection and Absorption of Insulin. Stockholm: Thesis, Franzen I, J. Ludvigsson, Linköping 1997 Specific Instructions Gave Reduction of Lipomas and Improved Metabolic Control in Diabetic Children, Diabetologia Vol 40, Supplement 1: A615 (1997). 36 Blanco M, Hernández MT, Strauss KW, Amaya M. Prevalence and risk factors of lipohypertrophy in insulininjecting patients with diabetes. Diabetes Metab Oct;39(5):
14 Getting injection training from a diabetes nurse is associated with significantly lower HbA1c levels as well as less frequent unexpected hypoglycemia and glucose variability. A critical finding of the above Spanish study is the correlation of total daily dose (TDD) of insulin to the presence of LH and its derived cost to the health care system. Subjects with LH had significantly higher TDD, overall and in both T1DM and T2DM groups. T2DM patients had the highest TDD differences (approximately 20 additional units daily). Such patients tend to have increased weight and insulin resistance compared to T1DM patients, and these factors probably contributed to their greater TDD however, the T2DM patients with LH had similar weight and BMI as the T2DM without LH. Another major contributor is the practice of injecting into LH where the absorption properties of insulin are distorted. The cost of the additional insulin consumed by injecting into LH was calculated (based on prevalence of LH, number of insulin-injecting patients in Spain, differences in TDD, and the cost in Euros per unit of insulin) to be over 122 million euros in Spain. This is an obvious opportunity for savings to both patients and health care payers. The one weakness of the Spain study is that HbA1c levels were unfortunately not collected on the subjects examined. A Chinese study similar to the Spain one showed remarkably similar results 37, with the addition that patients with LH had significantly higher HbA1c values (8.2 ±1.8) than those without LH (7.7 ±1.5) (p<0.003). The impact of LH on insulin PK-PD is rather poorly documented in the literature. While there are case reports indicating reductions in insulin consumption with improvements in HbA1c when patients with LH were taught to inject into normal areas, and a small number of studies that evaluated insulin PK-PD when patients have injected into areas of LH vs normal areas, the overall quality of such studies is poor and/or they were substantially underpowered. It is assumed that LH reduces and/or slows insulin uptake, and perhaps increases PK-PD variation, but this has not been proven rigorously. Two closely-related studies have addressed these questions, using state-of-the-art methodologies. A glucose clamp study 40 in patients with LH has shown that both insulin absorption and action are substantially blunted and considerably more variable when 37 Specifically, LH was present in 52.9% of participants. Patients were an average of 59.6 (SD=11.5) years old and took insulin 5.6 (SD=4.6) years, averaging 33.0 (SD=18.4) U/day. HbA1c was 8.2% (1.8) and 7.7% (1.5), respectively, in those with and without LH (p=0.003). LH was associated with higher daily insulin dose (38.1U vs 27.1U, p<0.001) and cost (RMB 8.2 vs 5.8, p<0.001). Those with LH averaged 2.3 (2.2) nodes, had higher frequency of PN reuse (median 13.0 vs 7.5, p=0.003), and greater total 6-month direct costs (RMB vs , p=0.037). With 8.4 million insulin injectors in China, the estimated excess annual direct cost of LH is RMB 2.2 billion ($360 million). Average pain scores (0-10) were higher if LH was present (2.7 vs. 2.0, p=0.021), if 3 nodes were present (3.8 vs. 2.3, p<0.001), and if PNs were not reimbursed (2.8 vs. 1.7, p<0.001). Patient satisfaction decreased as presence, number, and size of LH nodes increased (all p<0.05). 38 Ji L, Li Q, Wei G. Lipohypertrophy - prevalence, risk factors and clinical characteristics of insulin-requiring patients in China. Abstract, EASD Vienna 2014, Tracking Number: A Qifu Li, Linong Ji, Zilin Sun, Guijun Qin, Zheng Wei, Junhao Liu, Luan Luan, Laurence Hirsch. Lipohypertrophy (LH) Prevalence Varies Widely Between Chinese Cities - Need For Consistent LH Diagnostic Methods. Abstract submitted to 2015 ADA. 40 Susanne Famulla, Ulrike Hövelmann, Annelie Fischer, Hans-Veit Coester, Lutz Heinemann, Lars Kaltheuner, Laurence Hirsch, Tim Heise. Lipohypertrophy (LHT) Leads to Blunted, More Variable Insulin Absorption and Action in Patients with Type 1 Diabetes (T1DM). Abstract, 2015 ADA in Boston, USA. 14
15 insulin is injected into areas with LH. 41 A separate, mixed meal study in the same subjects confirmed the slower absorption and decreased action of insulin when injected into LH compared to normal adipose tissue, with much greater post-meal glycemic excursions shown. 42 Site Rotation Several studies have demonstrated that the best way to safeguard normal tissue is to properly and consistently rotate injecting sites. Injection can be rotated from one body region to another (abdomen to thigh, to buttock, to arm) but it must be remembered that absorption characteristics change depending on the type of insulin given. Analogues can be given at any injection site with similar uptake and action (PK-PD), but human insulins (Regular, NPH) vary substantially absorption being fastest from the abdomen and from the buttock, slowest. However, correct rotation involves spacing injections a least 1 cm. apart even within an injection zone. Some clinicians are offering the single-use skin safe marker pen to patients to keep and use to make a dot on the skin where they inject and use this as a reference point for the next injection. This seems to work very well for some patients and the marker from the pen washes off and fades to nothing in about 5 days. One scheme with proven effectiveness involves dividing the injection site into quadrants (or halves when using the thighs or buttocks), using one quadrant per week and moving always clockwise, as shown by figures below Specifically the study.investigated insulin exposure and pharmacodynamics of insulin lispro injected into abdominal areas with LH or normal adipose tissue. Thirteen T1DM with LH (confirmed by palpation and ultrasound) received single doses of 0.15 U/kg LIS approximately every 6 hours, twice into a region with LHT and twice into normal tissue. Comparing LHT with NAT injection, LS-mean INS concentrations were comparable during the first 30 min (AUCINS0-0.5h 8.8 vs. 9.4 h*mu/l), but significantly lower thereafter (AUCINS0-1h 29.3 vs h*mu/l, AUCINS.0-4h 97 vs. 154 h*mu/l, all p<0.02). Maximum INS exposure was reduced by 34% (CINSmax 49.7 vs mu/l, p<0.002). The PD effect in the first 4 h was 27% lower with LHT injection (AUCGIR0-4h: 529 vs. 720 mg/kg, p<0.05), whereas maximum GIR was comparable (GIRmax 5.5 vs. 6.0 mg/kg/min, p=0.378). Intra-subject variability was substantially higher after dosing into LHT (coefficients of variation 52 vs. 11% [AUCINS.0-4h] and 57 vs. 23%, [AUCGIR0-4h], all p<0.002). 42 Ulrike Hovelmann, Susanne Famulla, Lidia Hermanski, Annelie Fischer, Lutz Heinemannn, Matthias Kaltheuner, Laurence Hirsch, Tim Heise,. Insulin Injection into Regions with Lipohypertrophy (LHT) Worsens Postprandial (PP) Blood Glucose (BG) Versus Injections into Normal Adipose Tissue (NAT). Abstract, 2015 ADA in Boston, USA. 43 Ahern J, Mazur ML. Site rotation. Diabetes Forecast 2001;54: Bantle JP, Weber MS, Rao SM, Chattopadhyay MK, Robertson RP. Rotation of the anatomic regions used for insulin injections day-to-day variability of plasma glucose in type 1 diabetic subjects. JAMA 1990;263: Davis ED, Chesnaky P. Site rotation...taking insulin. Diabetes Forecast 1992;45: Photographs courtesy of Lourdes Saez-de Ibarra and Ruth Gaspar, Diabetes Nurses and Specialist Educators from La Paz Hospital, Madrid, Spain. 15
16 Figure 5: Abdominal rotation pattern by quadrants Figure 6: Thigh and Buttocks rotational pattern by halves Injections within any quadrant or half should be spaced at least 1cm from each other in order to avoid repeat tissue trauma. Pump cannulae should be placed at least 3cm away from previous sites. HCP should verify that the rotation scheme is being followed at each visit and give help and advice where needed. Lipoatrophy It Lipoatrophy has been reported in all injecting sites. is now considered a relatively unusual condition, prompting case reporting. Risk factors are not understood. Some authors have suggested young women with other auto-immune disorders may be at 47 Del Olmo MI, Campos V, Abellán P, Merino-Torres JF, Piñón F. A case of lipoatrophy with insulin detemir. Diabetes Res Clin Pract Apr;80(1):e Arranz A, Andia V, López-Guzmán A. A case of lipoatrophy with Lispro insulin without insulin pump therapy. Diabetes Care Feb;27(2): Breznik V, Kokol R, Luzar B, Miljković J. Insulin-induced localized lipoatrophy. Acta Dermatovenerol Alp Pannonica Adriat Dec;22(4): Swelheim HT, Westerlaken C, van Pinxteren-Nagler E, Bocca G. Lipoatrophy in a girl with type 1 diabetes: beneficial effects of treatment with a glucocorticoid added to an insulin analog. Diabetes Care Mar;35(3):e Babiker A, Datta V. Lipoatrophy with insulin analogues in type I diabetes. Arch Dis Child Jan;96(1): Holstein A, Stege H, Kovacs P. Lipoatrophy associated with the use of insulin analogues: a new case associated with the use of insulin glargine and review of the literature. Expert Opin Drug Saf Mar;9(2):
17 higher risk. LA is felt to be a local immune reaction against fat cells provoked by insulin crystals. Consequently LA is rarer today than it was when less pure insulins were given. But LA is still observed even with short and long-acting analogues. LA causes significant variability in insulin absorption when injections are given into it. Treatment for LH is not evidence based due the lack of trials. Several approaches however have been recommended: changing the insulin formulation (e.g., aspart to lispro, or lispro to glulisine, etc.), changing injection sites or shifting to CSII and possibly cortisone injected into the LA. LA may or may not resolve with time, but this depends on the individual patient. LA has been seen with the short-acting analogues, lispro and aspart, as well as the long-acting ones, glargine and detemir. It may also be associated with non-rotation of injection sites and needle reuse. LA is both a cosmetic problem (disfiguring) and a clinical one (erratic and abnormal insulin absorption). Injection Pain Most insulin injections are not painful, except in the infrequent event that the needle comes into direct contact with a nerve ending. Some patients, however, are exceptionally sensitive to sensations they describe as painful. Patient awareness of injection discomfort has been studied extensively and is related to three key factors: needle length (and tissue level penetrated); needle diameter; and injection context. Injection context is defined by environment (including noise and the presence of other people), view of the needle and the apprehension of HCPs, both professional and family. The more apprehension the latter display, the greater the pain and anxiety felt by the patient This reverse transference places a large responsibility on carers to assess their own attitudes towards injection pain. Some patients complain of discomfort when injecting insulins which have a low ph. This seems, anecdotally, to be reported more commonly in children. Glargine is an example of an acidic insulin. Heise 55 has shown that injection speed (150, 300 and 450 µl/s; equivalent of IU/sec of U100 insulin) makes no difference in pain. But injection volume does, with higher volumes ( 1200 µl or 120 IU of U100 insulin) causing more pain. His group also found that injections in the thigh appear to hurt more than those in the abdomen in adults. Anderson 56 and Jorgensen 57 also found that higher injected volumes cause more pain. Hofman 58 as well showed in both children and adults that thigh injections are more 53 Brady KA, Avner JR, Khine H. Perception and attitude of providers towards pain and anxiety associated with pediatric vaccine injection. Clinical Pediatrics. 50: , Diamond S, Matok I. Pharmacists anticipated pain compared to experienced pain associated with insulin pen injection and fingertip. Canadian Journal of Diabetes. 35: , Heise T, Nosek L, Dellweg S, et.al. Impact of injection speed and volume on perceived pain during subcutaneous injections into the abdomen and thigh: a single-centre, randomized controlled trial. Diabetes Obes Metab Oct;16(10): Anderson G, Meyer D, Herrman CE et al. Tolerability and safety of novel half milliliter formulation of glatiramer acetate for subcutaneous injection: an open-label, multicenter, randomized comparative study. J Neurol 2010; 257: Jorgensen JT, Romsing J, Rasmussen M, Moller-Sonnergaard J, Vang L, Musaeus L. Pain assessment of subcutaneous injections. Ann Pharmacother 1996;30: Hofman PL, Derraik JG, Pinto TE, Tregurtha S, Faherty A, et al. Defining the Ideal Injection Techniques When Using 5-mm Needles in Children and Adults. Diab Care Sep;33(9):
18 painful than abdominal. Nevertheless Heise 59 found that most patients say the pain is acceptable regardless of volume or injection site. So we can reasonably conclude that injection pain, though felt under certain circumstances by certain patients, is mild enough to be acceptable to most of them, particularly with today s very thin, short needles. This ITQ survey showed that just over half of injectors report having pain on injection. Of these, 4 out of 5 report having painful injections only several times a month or year (i.e. not with every injection). Groups with higher frequency of reported pain are: T1DM patients, children, adolescents and women. Pain is associated with several other disorders, without obvious causative relationship: bleeding, injecting through clothes, using cold insulin, skipping injections, hypo- and hyperglycemia, LH, injecting into LH, incorrect site rotation, higher HbA1c, lower BMI, younger age and higher TDD. Pain is also associated with needle reuse and seems to increase as a function of the number of times the needle is reused. A new set of international injecting recommendations has been developed and is being published. A number of these have been incorporated in the text above. It may be appropriate for the local countries and regions to revise their own guidelines in the light of the new recommendations and the ITQ survey data reported above. This paper will be followed by one other: Worldwide Injection Technique Study: Education and the Health Care Professional. Duality of interest: Kenneth Strauss is employed by BD, a manufacturer of injecting devices. Acknowledgments The authors would like to thank Astrid Menchior for entering all of the data from this survey. 59 Heise T, Nosek L, Dellweg S, et.al. Impact of injection speed and volume on perceived pain during subcutaneous injections into the abdomen and thigh: a single-centre, randomized controlled trial. Diabetes Obes Metab Oct;16(10):
Correct Site Rotation
 Injection Techniques Questionnaire (ITQ) WorldWide Results 2014-2015 Correct Site Rotation BACKGROUND Correct Rotation = at least 1 cm between successive injections Lipohypertrophy and Observed Correct
Injection Techniques Questionnaire (ITQ) WorldWide Results 2014-2015 Correct Site Rotation BACKGROUND Correct Rotation = at least 1 cm between successive injections Lipohypertrophy and Observed Correct
Injection Technique (I.T.), Glycemic Variability, and Lipohypertrophy. Why I.T. All Matters
 Injection Technique (I.T.), Glycemic Variability, and Lipohypertrophy Why I.T. All Matters Larry Hirsch, MD Vice-President, Global Medical Affairs BD Diabetes Care Seoul, South Korea KDA-ICDM 29 September
Injection Technique (I.T.), Glycemic Variability, and Lipohypertrophy Why I.T. All Matters Larry Hirsch, MD Vice-President, Global Medical Affairs BD Diabetes Care Seoul, South Korea KDA-ICDM 29 September
BD Nano 4mm Pen Needles
 BD Nano mm Pen Needles Preferred by patients₉ Less effort to inject medication for people with hand strength issues₉* BD's smallest, thinnest pen needle was rated as less painful and easier to insert₉
BD Nano mm Pen Needles Preferred by patients₉ Less effort to inject medication for people with hand strength issues₉* BD's smallest, thinnest pen needle was rated as less painful and easier to insert₉
The Advantages of Short Pen Needles. Insulin injection with pen needles
 Clinical Evidence Folder The Advantages of Short Pen Needles Insulin injection with pen needles 1. Introduction 3 2. Utilization of Shorter Pen Needles 4 2.1. Injection Sites 4 2.2. Injection Site and
Clinical Evidence Folder The Advantages of Short Pen Needles Insulin injection with pen needles 1. Introduction 3 2. Utilization of Shorter Pen Needles 4 2.1. Injection Sites 4 2.2. Injection Site and
Injection Techniques Questionnaire (ITQ) WorldWide Results Insulin Usage
 Injection Techniques Questionnaire (ITQ) WorldWide Results 2014-2015 Insulin Usage BACKGROUND Lipohypertrophy in Diabetes or How much does a lipo cost? Dr. Treichel, Magdeburg Studies * have shown that
Injection Techniques Questionnaire (ITQ) WorldWide Results 2014-2015 Insulin Usage BACKGROUND Lipohypertrophy in Diabetes or How much does a lipo cost? Dr. Treichel, Magdeburg Studies * have shown that
BEST 4 Diabetes. Optimisation of insulin module
 BEST 4 Diabetes Optimisation of insulin module Confidence and competence Where would you rate yourself? Why do all of our patient not achieve optimal blood glucose control? Insulin Therapy Goals and Purpose
BEST 4 Diabetes Optimisation of insulin module Confidence and competence Where would you rate yourself? Why do all of our patient not achieve optimal blood glucose control? Insulin Therapy Goals and Purpose
BEST 4 Diabetes. Optimisation of insulin module
 BEST 4 Diabetes Optimisation of insulin module Confidence and competence Where would you rate yourself? Why do all of our patient not achieve optimal blood glucose control? Insulin Therapy Goals and Purpose
BEST 4 Diabetes Optimisation of insulin module Confidence and competence Where would you rate yourself? Why do all of our patient not achieve optimal blood glucose control? Insulin Therapy Goals and Purpose
Frequency of Lipohypertrophy and Associated Risk Factors in Young Patients with Type 1 Diabetes: A Cross-Sectional Study
 Diabetes Ther (2016) 7:259 267 DOI 10.1007/s13300-016-0161-3 ORIGINAL RESEARCH Frequency of Lipohypertrophy and Associated Risk Factors in Young Patients with Type 1 Diabetes: A Cross-Sectional Study Ayman
Diabetes Ther (2016) 7:259 267 DOI 10.1007/s13300-016-0161-3 ORIGINAL RESEARCH Frequency of Lipohypertrophy and Associated Risk Factors in Young Patients with Type 1 Diabetes: A Cross-Sectional Study Ayman
If you inject diabetes medication, you should know how important correct injection technique is for effectively managing your diabetes.
 Insulin injection technique best practices Expert recommendations on injecting insulin with pen and insulin syringe needles If you inject diabetes medication, you should know how important correct injection
Insulin injection technique best practices Expert recommendations on injecting insulin with pen and insulin syringe needles If you inject diabetes medication, you should know how important correct injection
Dermatological complications of insulin therapy in children with type 1 diabetes
 in children with type 1 diabetes Hilde E van Munster, MSc 2 Cathelijne PM van de Sande 2 Paul G Voorhoeve, MD, PhD 2,3 Janiëlle AEM van Alfen-van der Velden, MD, PhD 1,2 1 Department of Pediatric Endocrinology,
in children with type 1 diabetes Hilde E van Munster, MSc 2 Cathelijne PM van de Sande 2 Paul G Voorhoeve, MD, PhD 2,3 Janiëlle AEM van Alfen-van der Velden, MD, PhD 1,2 1 Department of Pediatric Endocrinology,
Lessons learned from working with international injection technique guidelines
 Lessons learned from working with international injection technique guidelines Anders Frid, MD, PhD Clinic of Endocrinology, Skåne University Hospital, Malmö Oslo 23rd March 2012 INJECTION TECHNIQUE IS
Lessons learned from working with international injection technique guidelines Anders Frid, MD, PhD Clinic of Endocrinology, Skåne University Hospital, Malmö Oslo 23rd March 2012 INJECTION TECHNIQUE IS
Safe and Gentle Injection of Insulin. Guide for correct injection technique. Englische Ausgabe
 Safe and Gentle Injection of Insulin Guide for correct injection technique Englische Ausgabe Insulin injection basics 1 Insulin has to be injected into the subcutaneous fat layer 3 Rotate the injection
Safe and Gentle Injection of Insulin Guide for correct injection technique Englische Ausgabe Insulin injection basics 1 Insulin has to be injected into the subcutaneous fat layer 3 Rotate the injection
Insulin-induced Lipohypertrophy: Report of a Case with Histopathology
 Endocrine Journal 2005, 52 (5), 623 628 Insulin-induced Lipohypertrophy: Report of a Case with Histopathology JUNJI FUJIKURA, MUNEYA FUJIMOTO, SHINTARO YASUE, MICHIO NOGUCHI, HIROAKI MASUZAKI, KIMINORI
Endocrine Journal 2005, 52 (5), 623 628 Insulin-induced Lipohypertrophy: Report of a Case with Histopathology JUNJI FUJIKURA, MUNEYA FUJIMOTO, SHINTARO YASUE, MICHIO NOGUCHI, HIROAKI MASUZAKI, KIMINORI
Things you need to know about injections
 www.trend-uk.org Things you need to know about injections Injection sites: You can see from the picture below the best sites for injecting insulin or GLP-1 medications are: Back of the upper arms (difficult
www.trend-uk.org Things you need to know about injections Injection sites: You can see from the picture below the best sites for injecting insulin or GLP-1 medications are: Back of the upper arms (difficult
Novel Formulations to Modify Mealtime Insulin Kinetics
 Novel Formulations to Modify Mealtime Insulin Kinetics Alan Krasner, Roderike Pohl, Patrick Simms, Philip Pichotta, Robert Hauser, Errol De Souza Biodel, Inc. Danbury, CT Disclosure All authors are employees
Novel Formulations to Modify Mealtime Insulin Kinetics Alan Krasner, Roderike Pohl, Patrick Simms, Philip Pichotta, Robert Hauser, Errol De Souza Biodel, Inc. Danbury, CT Disclosure All authors are employees
Living Well Successfully managing diabetes
 Living Well Successfully managing diabetes with 4mm Pen Needles Helping all people live healthy lives Our most comfortable injection experience ever Successfully managing diabetes with BD Micro-Fine +
Living Well Successfully managing diabetes with 4mm Pen Needles Helping all people live healthy lives Our most comfortable injection experience ever Successfully managing diabetes with BD Micro-Fine +
Hamdiye Arda Sürücü 1*, Hatice Okur Arslan 2
 Journal of Caring Sciences 2018; 7 (2): 67-74 doi:10.15171/jcs.2018.011 http:// journals.tbzmed.ac.ir/ JCS Original Article in Individuals with Type 2 Diabetes: Prevalence and Risk Factors Hamdiye Arda
Journal of Caring Sciences 2018; 7 (2): 67-74 doi:10.15171/jcs.2018.011 http:// journals.tbzmed.ac.ir/ JCS Original Article in Individuals with Type 2 Diabetes: Prevalence and Risk Factors Hamdiye Arda
Injection Techniques Questionnaire (ITQ) WorldWide Results Needle Gauge
 Injection Techniques Questionnaire (ITQ) WorldWide Results 2014-2015 Needle Gauge BACKGROUND All needles are at least twice as long as the skin is thick More than twice as long 31G =.26mm Surface = 1
Injection Techniques Questionnaire (ITQ) WorldWide Results 2014-2015 Needle Gauge BACKGROUND All needles are at least twice as long as the skin is thick More than twice as long 31G =.26mm Surface = 1
Insulin Basic facts. Patient Education Patient Care Services. What is insulin? What types of insulin are there? Basal Insulin
 Patient Education Insulin Basic facts Insulin is a protein made by the pancreas that allows your cells to use glucose for energy. There are different types of insulin: Basal long-acting insulin that controls
Patient Education Insulin Basic facts Insulin is a protein made by the pancreas that allows your cells to use glucose for energy. There are different types of insulin: Basal long-acting insulin that controls
INSULIN IN THE OBESE PATIENT JACQUELINE THOMPSON RN, MAS, CDE SYSTEM DIRECTOR, DIABETES SERVICE LINE SHARP HEALTHCARE
 INSULIN IN THE OBESE PATIENT JACQUELINE THOMPSON RN, MAS, CDE SYSTEM DIRECTOR, DIABETES SERVICE LINE SHARP HEALTHCARE OBJECTIVES DESCRIBE INSULIN, INCLUDING WHERE IT COMES FROM AND WHAT IT DOES STATE THAT
INSULIN IN THE OBESE PATIENT JACQUELINE THOMPSON RN, MAS, CDE SYSTEM DIRECTOR, DIABETES SERVICE LINE SHARP HEALTHCARE OBJECTIVES DESCRIBE INSULIN, INCLUDING WHERE IT COMES FROM AND WHAT IT DOES STATE THAT
INSULIN THERAY دکتر رحیم وکیلی استاد غدد ومتابولیسم کودکان دانشگاه علوم پزشکی مشهد
 INSULIN THERAY DIABETES1 IN TYPE دکتر رحیم وکیلی استاد غدد ومتابولیسم کودکان دانشگاه علوم پزشکی مشهد Goals of management Manage symptoms Prevent acute and late complications Improve quality of life Avoid
INSULIN THERAY DIABETES1 IN TYPE دکتر رحیم وکیلی استاد غدد ومتابولیسم کودکان دانشگاه علوم پزشکی مشهد Goals of management Manage symptoms Prevent acute and late complications Improve quality of life Avoid
A novel ph-neutral formulation of the monomeric insulin VIAject has a faster onset of action than insulin lispro
 A novel ph-neutral formulation of the monomeric insulin VIAject has a faster onset of action than insulin lispro Leszek Nosek, Tim Heise, Frank Flacke 2, Alan Krasner 2, Philip Pichotta 2, Lutz Heinemann,
A novel ph-neutral formulation of the monomeric insulin VIAject has a faster onset of action than insulin lispro Leszek Nosek, Tim Heise, Frank Flacke 2, Alan Krasner 2, Philip Pichotta 2, Lutz Heinemann,
Effectiveness of Training Session in Improvement of Insulin Administration Technique in Diabetic Patients
 Original Article Effectiveness of Training Session in Improvement of Insulin Administration Technique in Diabetic Patients Abdul Khalid, Rubina Rafique, Ali Arshed, Munazza Nazir and Ashfaq Ahmed Department
Original Article Effectiveness of Training Session in Improvement of Insulin Administration Technique in Diabetic Patients Abdul Khalid, Rubina Rafique, Ali Arshed, Munazza Nazir and Ashfaq Ahmed Department
1. What s the point of a network the case for research? 2. How to use CSII effectively
 1. What s the point of a network the case for research? 2. How to use CSII effectively John Pickup King s College London Faculty of Medicine Guy s Hospital, London What should an insulin pump network do?
1. What s the point of a network the case for research? 2. How to use CSII effectively John Pickup King s College London Faculty of Medicine Guy s Hospital, London What should an insulin pump network do?
Timely!Insulinization In!Type!2! Diabetes,!When!and!How
 Timely!Insulinization In!Type!2! Diabetes,!When!and!How, FACP, FACE, CDE Professor of Internal Medicine UT Southwestern Medical Center Dallas, Texas Current Control and Targets 1 Treatment Guidelines for
Timely!Insulinization In!Type!2! Diabetes,!When!and!How, FACP, FACE, CDE Professor of Internal Medicine UT Southwestern Medical Center Dallas, Texas Current Control and Targets 1 Treatment Guidelines for
Gentle and safe injections. Tips and tricks for injecting insulin.
 Gentle and safe injections. Tips and tricks for injecting insulin. Freedom. Confidence. With mylife. Gentle and safe injections The correct injection technique The insulin is injected into the subcutaneous
Gentle and safe injections. Tips and tricks for injecting insulin. Freedom. Confidence. With mylife. Gentle and safe injections The correct injection technique The insulin is injected into the subcutaneous
Insulin Delivery System and Self Monitoring Blood Sugar (SMBG ) Leyden V. Florido, RN, MAN
 Insulin Delivery System and Self Monitoring Blood Sugar (SMBG ) Leyden V. Florido, RN, MAN Management of Diabetes Mellitus Pharmacological Glucose Lowering Agents/Oral Antidiabetes Drug/Oral Hypogycemic
Insulin Delivery System and Self Monitoring Blood Sugar (SMBG ) Leyden V. Florido, RN, MAN Management of Diabetes Mellitus Pharmacological Glucose Lowering Agents/Oral Antidiabetes Drug/Oral Hypogycemic
New basal insulins Are they any better? Matthew C. Riddle, MD Professor of Medicine Oregon Health & Science University Keystone Colorado 15 July 2011
 New basal insulins Are they any better? Matthew C. Riddle, MD Professor of Medicine Oregon Health & Science University Keystone Colorado 15 July 2011 Presenter Disclosure I have received the following
New basal insulins Are they any better? Matthew C. Riddle, MD Professor of Medicine Oregon Health & Science University Keystone Colorado 15 July 2011 Presenter Disclosure I have received the following
Diabetes Care Publish Ahead of Print, published online June 1, 2009
 Diabetes Care Publish Ahead of Print, published online June 1, 2009 Biphasic insulin aspart 30/70 (BIAsp 30): pharmacokinetics (PK) and pharmacodynamics (PD) in comparison with once-daily biphasic human
Diabetes Care Publish Ahead of Print, published online June 1, 2009 Biphasic insulin aspart 30/70 (BIAsp 30): pharmacokinetics (PK) and pharmacodynamics (PD) in comparison with once-daily biphasic human
FIT Forum for Injection Technique
 DIABETES CARE IN IRELAND FIT Forum for Injection Technique Irish Injection and Infusion Technique Recommendations 2nd Edition The Irish Injection and Infusion Technique Recommendations have been endorsed
DIABETES CARE IN IRELAND FIT Forum for Injection Technique Irish Injection and Infusion Technique Recommendations 2nd Edition The Irish Injection and Infusion Technique Recommendations have been endorsed
Injectable Therapies in Diabetes
 Injectable Therapies in Diabetes Diabetes Specialist Nurse Joyce Robson Learning Outcomes Think about the place of injectible therapies in diabetes Insulin therapy GLP1 antagonists Consider commonly used
Injectable Therapies in Diabetes Diabetes Specialist Nurse Joyce Robson Learning Outcomes Think about the place of injectible therapies in diabetes Insulin therapy GLP1 antagonists Consider commonly used
Patient Education Pharmacy Services
 Patient Education This handout details the types of insulin. It also covers how to store, mix and inject insulin. What is insulin? Insulin is made by the pancreas and acts as a key to move glucose (sugar)
Patient Education This handout details the types of insulin. It also covers how to store, mix and inject insulin. What is insulin? Insulin is made by the pancreas and acts as a key to move glucose (sugar)
Workshop 4 Making the complex simple
 Workshop 4 Making the complex simple Goal of workshop Insulin commencement making the complex simple Ensure participants are confident with Selecting and using devices Troubleshooting injection issues
Workshop 4 Making the complex simple Goal of workshop Insulin commencement making the complex simple Ensure participants are confident with Selecting and using devices Troubleshooting injection issues
Sponsor / Company: Sanofi Drug substance(s): insulin glargine (HOE901) According to template: QSD VERSION N 4.0 (07-JUN-2012) Page 1
 These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
INJECTABLE THERAPIES IN DIABETES. Barbara Ann McKee Diabetes Specialist Nurse
 INJECTABLE THERAPIES IN DIABETES Barbara Ann McKee Diabetes Specialist Nurse 1 Aims of the session Describe the different injectable agents for diabetes and when they would be used. Describe some common
INJECTABLE THERAPIES IN DIABETES Barbara Ann McKee Diabetes Specialist Nurse 1 Aims of the session Describe the different injectable agents for diabetes and when they would be used. Describe some common
Many people use a combination of the standard 17mm cannula and the shorter 13mm cannula length depending where on their body they are inserting.
 There are many types of infusion sets available through AMSL Diabetes. Our infusion sets are obtained through Animas and are all manufactured by UnoMedical which has a worldwide reputation for producing
There are many types of infusion sets available through AMSL Diabetes. Our infusion sets are obtained through Animas and are all manufactured by UnoMedical which has a worldwide reputation for producing
Gentle and safe injections. Tips and tricks for injecting insulin.
 Gentle and safe injections. Tips and tricks for injecting insulin. More freedom. More confidence. With mylife. Gentle and safe injections The correct injection technique The insulin is injected into the
Gentle and safe injections. Tips and tricks for injecting insulin. More freedom. More confidence. With mylife. Gentle and safe injections The correct injection technique The insulin is injected into the
Endocrine Update Mary T. Korytkowski MD Division of Endocrinology University of Pittsburgh
 Endocrine Update 2016 Mary T. Korytkowski MD Division of Endocrinology University of Pittsburgh Disclosure of Financial Relationships Mary Korytkowski MD Honoraria British Medical Journal Diabetes Research
Endocrine Update 2016 Mary T. Korytkowski MD Division of Endocrinology University of Pittsburgh Disclosure of Financial Relationships Mary Korytkowski MD Honoraria British Medical Journal Diabetes Research
TYPe 1 DIABeTeS. A short guide for parents and children. from the outset.
 TYPe 1 DIABeTeS A short guide for parents and children A guide that will allow you to get to know type 1 diabetes and deal with it with peace of mind from the outset. Contents Glycaemic control 04 What
TYPe 1 DIABeTeS A short guide for parents and children A guide that will allow you to get to know type 1 diabetes and deal with it with peace of mind from the outset. Contents Glycaemic control 04 What
DEMYSTIFYING INSULIN THERAPY
 DEMYSTIFYING INSULIN THERAPY ASHLYN SMITH, PA-C ENDOCRINOLOGY ASSOCIATES SCOTTSDALE, AZ SECRETARY, AMERICAN SOCIETY OF ENDOCRINE PHYSICIAN ASSISTANTS ARIZONA STATE ASSOCIATION OF PHYSICIAN ASSISTANTS SPRING
DEMYSTIFYING INSULIN THERAPY ASHLYN SMITH, PA-C ENDOCRINOLOGY ASSOCIATES SCOTTSDALE, AZ SECRETARY, AMERICAN SOCIETY OF ENDOCRINE PHYSICIAN ASSISTANTS ARIZONA STATE ASSOCIATION OF PHYSICIAN ASSISTANTS SPRING
Policy for the safe administration of Insulin
 Policy for the safe administration of Insulin This is a working document and any changes that become necessary to this policy must be Notified in writing to the Medicine Management Group via the Chief
Policy for the safe administration of Insulin This is a working document and any changes that become necessary to this policy must be Notified in writing to the Medicine Management Group via the Chief
BEDFORDSHIRE AND LUTON JOINT PRESCRIBING COMMITTEE (JPC)
 BEDFORDSHIRE AND LUTON JOINT PRESCRIBING COMMITTEE (JPC) June 2017 Review: June 2020 (earlier if required see recommendations) Bulletin 255: Insulin aspart New Formulation - Fiasp JPC Recommendations:
BEDFORDSHIRE AND LUTON JOINT PRESCRIBING COMMITTEE (JPC) June 2017 Review: June 2020 (earlier if required see recommendations) Bulletin 255: Insulin aspart New Formulation - Fiasp JPC Recommendations:
Initiating Injectable Therapy in Type 2 Diabetes
 Initiating Injectable Therapy in Type 2 Diabetes David Doriguzzi, PA C Learning Objectives To understand current Diabetes treatment guidelines To understand how injectable medications fit into current
Initiating Injectable Therapy in Type 2 Diabetes David Doriguzzi, PA C Learning Objectives To understand current Diabetes treatment guidelines To understand how injectable medications fit into current
Newer Insulins. Boca Raton Regional Hospital 15th Annual Internal Medicine Conference
 Newer Insulins Boca Raton Regional Hospital 15th Annual Internal Medicine Conference Luigi F. Meneghini, MD, MBA Professor of Internal Medicine, UT Southwestern Medical Center Executive Director, Global
Newer Insulins Boca Raton Regional Hospital 15th Annual Internal Medicine Conference Luigi F. Meneghini, MD, MBA Professor of Internal Medicine, UT Southwestern Medical Center Executive Director, Global
Position Statement of ADA / EASD 2012
 Management of Hyperglycemia in Type2 Diabetes: A Patient- Centered Approach Position Statement of ADA / EASD 2012 Cause of : Type 2 diabetes Cardiovascular disorders Blindness End-stage renal failure Amputations
Management of Hyperglycemia in Type2 Diabetes: A Patient- Centered Approach Position Statement of ADA / EASD 2012 Cause of : Type 2 diabetes Cardiovascular disorders Blindness End-stage renal failure Amputations
Injection technique for different needle lengths
 Injection technique for different needle lengths Use the correct technique to better manage your diabetes 1 Why it s important to use the shortest needles available Reduce your risk of injecting into the
Injection technique for different needle lengths Use the correct technique to better manage your diabetes 1 Why it s important to use the shortest needles available Reduce your risk of injecting into the
Insulin analogues Das PP, Datta PG
 The ORION Medical Journal 2007 Sep;28:497-500 Insulin analogues Das PP, Datta PG Introduction Diabetes mellitus is a very big challenge for our medical science. To overcome this problem we need newer generation
The ORION Medical Journal 2007 Sep;28:497-500 Insulin analogues Das PP, Datta PG Introduction Diabetes mellitus is a very big challenge for our medical science. To overcome this problem we need newer generation
insulin and injections
 insulin and injections Insulin is a hormone made by the beta cells in the pancreas. Insulin allows sugar to go from the bloodstream into the body s cells and be used for energy. Insulin lowers blood sugar.
insulin and injections Insulin is a hormone made by the beta cells in the pancreas. Insulin allows sugar to go from the bloodstream into the body s cells and be used for energy. Insulin lowers blood sugar.
Sponsor / Company: Sanofi Drug substance(s): HOE901-U300 (insulin glargine) According to template: QSD VERSION N 4.0 (07-JUN-2012) Page 1
 These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
Best Practice Guideline to support Correct Injection Technique in Diabetes Care
 Best Practice Guideline to support Correct Injection Technique in Diabetes Care B e s t P r a c t i c e i n D i a b e t e s C a r e PAGE 2 Contents Introduction Our Supporters Endorsements SECTION 1. THE
Best Practice Guideline to support Correct Injection Technique in Diabetes Care B e s t P r a c t i c e i n D i a b e t e s C a r e PAGE 2 Contents Introduction Our Supporters Endorsements SECTION 1. THE
INSULIN 101: When, How and What
 INSULIN 101: When, How and What Alice YY Cheng @AliceYYCheng Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form
INSULIN 101: When, How and What Alice YY Cheng @AliceYYCheng Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form
Insulin Pump Therapy for Type 2
 9501172-011 Insulin Pump Therapy for Type 2 Objective To show the effectiveness of CSII for insulin-taking type 2 patients Key Points Tight glycemic control decreases risk of diabetes-related complications
9501172-011 Insulin Pump Therapy for Type 2 Objective To show the effectiveness of CSII for insulin-taking type 2 patients Key Points Tight glycemic control decreases risk of diabetes-related complications
INJECTION TECHNIQUE IS IT IMPORTANT? Anders Frid, MD, PhD, T.I.T.AN Athens
 INJECTION TECHNIQUE IS IT IMPORTANT? Anders Frid, MD, PhD, T.I.T.AN Athens Injection Technique: What Do We Know and What Do We Want to Know? What about insulin absorption? Are modern insulin analogues
INJECTION TECHNIQUE IS IT IMPORTANT? Anders Frid, MD, PhD, T.I.T.AN Athens Injection Technique: What Do We Know and What Do We Want to Know? What about insulin absorption? Are modern insulin analogues
Hypoglycemia a barrier to normoglycemia Are long acting analogues and pumps the answer to the barrier??
 Hypoglycemia a barrier to normoglycemia Are long acting analogues and pumps the answer to the barrier?? Moshe Phillip Institute of Endocrinology and Diabetes National Center of Childhood Diabetes Schneider
Hypoglycemia a barrier to normoglycemia Are long acting analogues and pumps the answer to the barrier?? Moshe Phillip Institute of Endocrinology and Diabetes National Center of Childhood Diabetes Schneider
These Aren t Your Average Rookies: A Primer on New and Emerging Insulins. Alissa R. Segal, Pharm.D, CDE, CDTC, FCCP
 These Aren t Your Average Rookies: A Primer on New and Emerging Insulins Alissa R. Segal, Pharm.D, CDE, CDTC, FCCP Disclosures Eli Lilly & Company: Advisory board member Boehringer Ingelheim: Advisory
These Aren t Your Average Rookies: A Primer on New and Emerging Insulins Alissa R. Segal, Pharm.D, CDE, CDTC, FCCP Disclosures Eli Lilly & Company: Advisory board member Boehringer Ingelheim: Advisory
Insulin therapy in gestational diabetes mellitus
 Insulin therapy in gestational diabetes mellitus October 15, 2015 Kyung-Soo Kim Division of Endocrinology & Metabolism, Department of Internal Medicine, CHA Bundang Medical Center, CHA University Contents
Insulin therapy in gestational diabetes mellitus October 15, 2015 Kyung-Soo Kim Division of Endocrinology & Metabolism, Department of Internal Medicine, CHA Bundang Medical Center, CHA University Contents
Injecting Insulin into Out Patient Practice
 Injecting Insulin into Out Patient Practice Kathleen Colleran, MD Associate Professor UNMHSC 4/22/10 Overview Natural history of Type 2 diabetes Reasons clinicians are reluctant to start insulin therapy
Injecting Insulin into Out Patient Practice Kathleen Colleran, MD Associate Professor UNMHSC 4/22/10 Overview Natural history of Type 2 diabetes Reasons clinicians are reluctant to start insulin therapy
Beyond Basal Insulin: Intensification of Therapy Jennifer D Souza, PharmD, CDE, BC-ADM
 Beyond Basal Insulin: Intensification of Therapy Jennifer D Souza, PharmD, CDE, BC-ADM Disclosures Jennifer D Souza has no conflicts of interest to disclose. 2 When Basal Insulin Is Not Enough Learning
Beyond Basal Insulin: Intensification of Therapy Jennifer D Souza, PharmD, CDE, BC-ADM Disclosures Jennifer D Souza has no conflicts of interest to disclose. 2 When Basal Insulin Is Not Enough Learning
Glycaemic control in a type 1 diabetes clinic for younger adults
 Q J Med 2004; 97:575 580 doi:10.1093/qjmed/hch098 Glycaemic control in a type 1 diabetes clinic for younger adults S.A. SAUNDERS, M. WALLYMAHMED and I.A. MACFARLANE From the University Department of Diabetes
Q J Med 2004; 97:575 580 doi:10.1093/qjmed/hch098 Glycaemic control in a type 1 diabetes clinic for younger adults S.A. SAUNDERS, M. WALLYMAHMED and I.A. MACFARLANE From the University Department of Diabetes
Insulin Initiation, titration & Insulin switch in the Primary Care-KISS
 Insulin Initiation, titration & Insulin switch in the Primary Care-KISS Rotorua GP CME 9 June 2012 Dr Kingsley Nirmalaraj FRACP Endocrinologist, BOPDHB & Suite 9, Promed House, Tenth Ave, Tauranga Linda
Insulin Initiation, titration & Insulin switch in the Primary Care-KISS Rotorua GP CME 9 June 2012 Dr Kingsley Nirmalaraj FRACP Endocrinologist, BOPDHB & Suite 9, Promed House, Tenth Ave, Tauranga Linda
My Doctor Says I Need to Inject Insulin In Special Sites... Which Ones Should I Use? Getting Started. Site Selection
 My Doctor Says I Need to Inject Insulin In Special Sites... Which Ones Should I Use? Getting Started Site Selection You need to know where to inject insulin so that your injections will be easier, safer
My Doctor Says I Need to Inject Insulin In Special Sites... Which Ones Should I Use? Getting Started Site Selection You need to know where to inject insulin so that your injections will be easier, safer
MANAGEMENT OF TYPE 1 DIABETES MELLITUS
 MANAGEMENT OF TYPE 1 DIABETES MELLITUS INVESTIGATIONS AND TREATMENT MANSI NAIK VII SEMESTER INVESTIGATIONS FASTING BLOOD SUGAR PLASMA GLUCOSE HEMOGLOBIN A 1c SYMPTOMS OF TYPE 1 DIABETES MELLITUS Polyuria
MANAGEMENT OF TYPE 1 DIABETES MELLITUS INVESTIGATIONS AND TREATMENT MANSI NAIK VII SEMESTER INVESTIGATIONS FASTING BLOOD SUGAR PLASMA GLUCOSE HEMOGLOBIN A 1c SYMPTOMS OF TYPE 1 DIABETES MELLITUS Polyuria
Faculty. Concentrated Insulin: Examining the Necessity of Newer Insulins for In-Hospital Diabetes Management. Disclosures. Learning Objectives
 Examining the Necessity of Newer Insulins for In-Hospital Diabetes Management Faculty Susan Cornell, PharmD, CDE, FAPhA, FAADE Associate Professor of Pharmacy Practice Associate Director of Experiential
Examining the Necessity of Newer Insulins for In-Hospital Diabetes Management Faculty Susan Cornell, PharmD, CDE, FAPhA, FAADE Associate Professor of Pharmacy Practice Associate Director of Experiential
Safe use of insulin regular concentrated (500 units/ml) in severe insulin resistance
 Safe use of insulin regular concentrated (500 units/ml) in severe insulin resistance Jodie S. Gee, Pharm.D., BCACP, CDE Clinical Pharmacy Specialist-Ambulatory Care Harris Health System Objectives To be
Safe use of insulin regular concentrated (500 units/ml) in severe insulin resistance Jodie S. Gee, Pharm.D., BCACP, CDE Clinical Pharmacy Specialist-Ambulatory Care Harris Health System Objectives To be
Insulin glulisine (Apidra) for type 1 diabetes mellitus in adolescents and children
 Insulin glulisine (Apidra) for type 1 diabetes mellitus in adolescents and children December 2008 This technology summary is based on information available at the time of research and a limited literature
Insulin glulisine (Apidra) for type 1 diabetes mellitus in adolescents and children December 2008 This technology summary is based on information available at the time of research and a limited literature
Agenda. Indications Different insulin preparations Insulin initiation Insulin intensification
 Insulin Therapy F. Hosseinpanah Obesity Research Center Research Institute for Endocrine sciences Shahid Beheshti University of Medical Sciences November 11, 2017 Agenda Indications Different insulin preparations
Insulin Therapy F. Hosseinpanah Obesity Research Center Research Institute for Endocrine sciences Shahid Beheshti University of Medical Sciences November 11, 2017 Agenda Indications Different insulin preparations
SCIG INFUSIONS A PRACTICAL GUIDE FOR PATIENTS
 PRIMARY IMMUNODEFICIENCIES SCIG INFUSIONS: A PRACTICAL GUIDE FOR PATIENTS SCIG INFUSIONS A PRACTICAL GUIDE FOR PATIENTS 1 PRIMARY IMMUNODEFICIENCIES ABBREVIATIONS IG IVIG PID SCIG Immunoglobulin Intravenous
PRIMARY IMMUNODEFICIENCIES SCIG INFUSIONS: A PRACTICAL GUIDE FOR PATIENTS SCIG INFUSIONS A PRACTICAL GUIDE FOR PATIENTS 1 PRIMARY IMMUNODEFICIENCIES ABBREVIATIONS IG IVIG PID SCIG Immunoglobulin Intravenous
PATIENT INFORMATION. D iabetes. What You Need to Know About. Insulin
 PATIENT INFORMATION Medicine To Treat: D iabetes What You Need to Know About Insulin INTRODUCTION The insulin preparations currently available in Singapore are mostly from human origin; pork or bovine
PATIENT INFORMATION Medicine To Treat: D iabetes What You Need to Know About Insulin INTRODUCTION The insulin preparations currently available in Singapore are mostly from human origin; pork or bovine
Pranay wal et al, /J. Pharm. Sci. & Res. Vol.2(5), 2010,
 Comparative efficacy of humalog mix 75/25 with human Insulin. Pranay wal 1 *, Ankita wal 2, Shivangi Srivastava 2,Abhinav srivastava 2, Umeshwar Pandey 3, Tarun Jain 1, Awani k Rai 2. 1 Jodhpur National
Comparative efficacy of humalog mix 75/25 with human Insulin. Pranay wal 1 *, Ankita wal 2, Shivangi Srivastava 2,Abhinav srivastava 2, Umeshwar Pandey 3, Tarun Jain 1, Awani k Rai 2. 1 Jodhpur National
Personal statement on Continuous Subcutaneous Insulin Infusion Professor John Pickup
 1 Personal statement on Continuous Subcutaneous Insulin Infusion Professor John Pickup King s College London School of Medicine, Guy s Hospital, London SE1 9RT Experience of the technology I am the lead
1 Personal statement on Continuous Subcutaneous Insulin Infusion Professor John Pickup King s College London School of Medicine, Guy s Hospital, London SE1 9RT Experience of the technology I am the lead
Starting and Helping People with Type 2 Diabetes on Insulin
 Starting and Helping People with Type 2 Diabetes on Insulin Elaine Cooke, BSc(Pharm), RPh, CDE Pharmacist and Certified Diabetes Educator Maple Ridge, BC Objectives After attending this session, participants
Starting and Helping People with Type 2 Diabetes on Insulin Elaine Cooke, BSc(Pharm), RPh, CDE Pharmacist and Certified Diabetes Educator Maple Ridge, BC Objectives After attending this session, participants
INSULIN INJECTION KNOW-HOW
 0-1- INSULIN INJECTION KNOW-HOW Learning how to Congratulations for making the move to insulin therapy. It won t be long before you start enjoying better blood sugar control, more energy, and a host of
0-1- INSULIN INJECTION KNOW-HOW Learning how to Congratulations for making the move to insulin therapy. It won t be long before you start enjoying better blood sugar control, more energy, and a host of
Science Behind Insulin Delivery
 Science Behind Insulin Delivery 1 Overview Objective The objective of this presentation is to demonstrate why insulin pump therapy is more effective than multiple daily shots in delivering superior outcomes
Science Behind Insulin Delivery 1 Overview Objective The objective of this presentation is to demonstrate why insulin pump therapy is more effective than multiple daily shots in delivering superior outcomes
What is the role of insulin pumps in the modern day care of patients with Type 1 diabetes?
 What is the role of insulin pumps in the modern day care of patients with Type 1 diabetes? Dr. Fiona Wotherspoon Consultant in Diabetes and Endocrinology Dorset County Hospital Fiona.Wotherspoon@dchft.nhs.uk
What is the role of insulin pumps in the modern day care of patients with Type 1 diabetes? Dr. Fiona Wotherspoon Consultant in Diabetes and Endocrinology Dorset County Hospital Fiona.Wotherspoon@dchft.nhs.uk
SHARED CARE GUIDELINE ON THE USE OF FIASP FOR THE MANAGEMENT OF TYPE 1 DIABETES IN ADULTS
 SHARED CARE GUIDELINE ON THE USE OF FIASP FOR THE MANAGEMENT OF TYPE 1 DIABETES IN ADULTS INDICATION Fiasp is indicated for the treatment of diabetes mellitus in adults. Special Note: DMAG has approved
SHARED CARE GUIDELINE ON THE USE OF FIASP FOR THE MANAGEMENT OF TYPE 1 DIABETES IN ADULTS INDICATION Fiasp is indicated for the treatment of diabetes mellitus in adults. Special Note: DMAG has approved
Initiation and Titration of Insulin in Diabetes Mellitus Type 2
 Initiation and Titration of Insulin in Diabetes Mellitus Type 2 Greg Doelle MD, MS April 6, 2016 Disclosure I have no actual or potential conflicts of interest in relation to the content of this lecture.
Initiation and Titration of Insulin in Diabetes Mellitus Type 2 Greg Doelle MD, MS April 6, 2016 Disclosure I have no actual or potential conflicts of interest in relation to the content of this lecture.
Diabetes Competencies
 Diabetes Competencies Name: Role: Base: Competency Statement: The participant demonstrates clinical knowledge and skill in diabetes nursing without assistance and/or direct supervision (level 3 - see level
Diabetes Competencies Name: Role: Base: Competency Statement: The participant demonstrates clinical knowledge and skill in diabetes nursing without assistance and/or direct supervision (level 3 - see level
Type 2 Diabetes Mellitus Insulin Therapy 2012
 Type 2 Diabetes Mellitus Therapy 2012 Michael T. McDermott MD Director, Endocrinology and Diabetes Practice University of Colorado Hospital Michael.mcdermott@ucdenver.edu Preparations Onset Peak Duration
Type 2 Diabetes Mellitus Therapy 2012 Michael T. McDermott MD Director, Endocrinology and Diabetes Practice University of Colorado Hospital Michael.mcdermott@ucdenver.edu Preparations Onset Peak Duration
Update on New Basal Insulins and Combinations: Starting, Titrating and Adding to Therapy
 Update on New Basal Insulins and Combinations: Starting, Titrating and Adding to Therapy Jerry Meece, BPharm, CDE, FACA, FAADE Director of Clinical Services Plaza Pharmacy and Wellness Center Gainesville,
Update on New Basal Insulins and Combinations: Starting, Titrating and Adding to Therapy Jerry Meece, BPharm, CDE, FACA, FAADE Director of Clinical Services Plaza Pharmacy and Wellness Center Gainesville,
PATIENT INFORMATION LEAFLET MEDICINE TO TREAT: DIABETES. Insulin
 PATIENT INFORMATION LEAFLET MEDICINE TO TREAT: DIABETES Insulin This medicine has been proven to be safe and effective, but it can cause serious injury if a mistake happens while taking it. This means
PATIENT INFORMATION LEAFLET MEDICINE TO TREAT: DIABETES Insulin This medicine has been proven to be safe and effective, but it can cause serious injury if a mistake happens while taking it. This means
Pathogenesis of Type 1 Diabetes. Diabetes Mellitus Type 1. Pathogenesis. Pathogenesis of DM1. Type 2. Type 1. Genetics of Type 1 Diabetes
 Pathogenesis of Type 1 Diabetes Diabetes Mellitus Type 1 D G V A N ZYL Genetics of Type 1 Diabetes Pathogenesis Complex and poorly understood interplay between genetics and environmental factors Monozycotic
Pathogenesis of Type 1 Diabetes Diabetes Mellitus Type 1 D G V A N ZYL Genetics of Type 1 Diabetes Pathogenesis Complex and poorly understood interplay between genetics and environmental factors Monozycotic
Sponsor / Company: Sanofi Drug substance(s): HOE901-U300 (insulin glargine)
 These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
WHAT IT IS AND HOW IT IS USED
 ABC of insulin WHAT IT IS AND HOW IT IS USED ABC of insulin Why do I have to take insulin? In most cases, type 2 diabetes is treated with oral antidiabetics, as well as with diet and exercise. These medications
ABC of insulin WHAT IT IS AND HOW IT IS USED ABC of insulin Why do I have to take insulin? In most cases, type 2 diabetes is treated with oral antidiabetics, as well as with diet and exercise. These medications
Comprehensive Diabetes Treatment
 Comprehensive Diabetes Treatment Joshua L. Cohen, M.D., F.A.C.P. Professor of Medicine Interim Director, Division of Endocrinology & Metabolism The George Washington University School of Medicine Diabetes
Comprehensive Diabetes Treatment Joshua L. Cohen, M.D., F.A.C.P. Professor of Medicine Interim Director, Division of Endocrinology & Metabolism The George Washington University School of Medicine Diabetes
Injectable Therapies in Diabetes
 Injectable Therapies in Diabetes Diabetes Specialist Nurse Linda Burns Learning Outcomes Understand the place of injectible therapies in diabetes Understand when patients may require insulin therapy Consider
Injectable Therapies in Diabetes Diabetes Specialist Nurse Linda Burns Learning Outcomes Understand the place of injectible therapies in diabetes Understand when patients may require insulin therapy Consider
Patient Information Publications Warren Grant Magnuson Clinical Center National Institutes of Health
 Warren Grant Magnuson Clinical Center National Institutes of Health What is a subcutaneous injection? A subcutaneous injection is given in the fatty layer of tissue just under the skin. A subcutaneous
Warren Grant Magnuson Clinical Center National Institutes of Health What is a subcutaneous injection? A subcutaneous injection is given in the fatty layer of tissue just under the skin. A subcutaneous
Injectable Therapies in Diabetes
 Injectable Therapies in Diabetes Diabetes Specialist Nurse Joyce Robson Learning Outcomes Think about the place of injectible therapies in diabetes Think about when / why patients require insulin therapy
Injectable Therapies in Diabetes Diabetes Specialist Nurse Joyce Robson Learning Outcomes Think about the place of injectible therapies in diabetes Think about when / why patients require insulin therapy
Defining the ideal injection techniques when using 5-mm needles in children and adults
 Diabetes Care Publish Ahead of Print, published online June 28, 2010 Defining the ideal injection techniques when using 5-mm needles in children and adults Paul Leslie Hofman MD 1, José Guilherme Behrensdorf
Diabetes Care Publish Ahead of Print, published online June 28, 2010 Defining the ideal injection techniques when using 5-mm needles in children and adults Paul Leslie Hofman MD 1, José Guilherme Behrensdorf
Diabetes: Definition Pathophysiology Treatment Goals. By Scott Magee, MD, FACE
 Diabetes: Definition Pathophysiology Treatment Goals By Scott Magee, MD, FACE Disclosures No disclosures to report Definition of Diabetes Mellitus Diabetes Mellitus comprises a group of disorders characterized
Diabetes: Definition Pathophysiology Treatment Goals By Scott Magee, MD, FACE Disclosures No disclosures to report Definition of Diabetes Mellitus Diabetes Mellitus comprises a group of disorders characterized
Clinical Evidence for Insulin Pump Therapy
 Clinical Evidence for Insulin Pump Therapy 9501169-011 Objective Review the clinical evidence supporting the use of insulin pump therapy Key Points The benefits of CSII are: Improved metabolic control
Clinical Evidence for Insulin Pump Therapy 9501169-011 Objective Review the clinical evidence supporting the use of insulin pump therapy Key Points The benefits of CSII are: Improved metabolic control
Tips and Tricks for Starting and Adjusting Insulin. MC MacSween The Moncton Hospital
 Tips and Tricks for Starting and Adjusting Insulin MC MacSween The Moncton Hospital Progression of type 2 diabetes Beta cell apoptosis Natural History of Type 2 Diabetes The Burden of Treatment Failure
Tips and Tricks for Starting and Adjusting Insulin MC MacSween The Moncton Hospital Progression of type 2 diabetes Beta cell apoptosis Natural History of Type 2 Diabetes The Burden of Treatment Failure
Sponsor / Company: Sanofi Drug substance(s): Insulin Glargine. Study Identifiers: NCT
 These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
The Value of. Medical Technology. in Controlling and. Medical Technology. life changing innovation
 The Value of Medical Technology in Controlling and Treating Diabetes Medical Technology life changing innovation the disease Diabetes is a group of diseases characterized by high blood glucose, or blood
The Value of Medical Technology in Controlling and Treating Diabetes Medical Technology life changing innovation the disease Diabetes is a group of diseases characterized by high blood glucose, or blood
Adherence to therapy. Kamlesh Khunti University of Leicester, UK. William Polonsky University of California San Diego, USA
 Adherence to therapy Kamlesh Khunti University of Leicester, UK William Polonsky University of California San Diego, USA 1 Dualities of interest Kamlesh Khunti: Honoraria for speaking, advising or research
Adherence to therapy Kamlesh Khunti University of Leicester, UK William Polonsky University of California San Diego, USA 1 Dualities of interest Kamlesh Khunti: Honoraria for speaking, advising or research
Soliqua 100/33. (insulin glargine, lixisenatide) New Product Slideshow
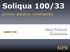 Soliqua 100/33 (insulin glargine, lixisenatide) New Product Slideshow Introduction Brand name: Soliqua 100/33 Generic name: Insulin glargine (rdna origin), lixisenatide Pharmacological class: Human insulin
Soliqua 100/33 (insulin glargine, lixisenatide) New Product Slideshow Introduction Brand name: Soliqua 100/33 Generic name: Insulin glargine (rdna origin), lixisenatide Pharmacological class: Human insulin
Insulin Prior Authorization with optional Quantity Limit Program Summary
 Insulin Prior Authorization with optional Quantity Limit Program Summary 1-13,16-19, 20 FDA LABELED INDICATIONS Rapid-Acting Insulins Humalog (insulin lispro) NovoLog (insulin aspart) Apidra (insulin glulisine)
Insulin Prior Authorization with optional Quantity Limit Program Summary 1-13,16-19, 20 FDA LABELED INDICATIONS Rapid-Acting Insulins Humalog (insulin lispro) NovoLog (insulin aspart) Apidra (insulin glulisine)
nocturnal hypoglycemia percentage of Hispanics in the insulin glargine than NPH during forced patients who previously This study excluded
 Clinical Trial Design/ Primary Objective Insulin glargine Treat-to-Target Trial, Riddle et al., 2003 (23) AT.LANTUS trial, Davies et al., 2005 (24) INSIGHT trial, Gerstein et al., 2006 (25) multicenter,
Clinical Trial Design/ Primary Objective Insulin glargine Treat-to-Target Trial, Riddle et al., 2003 (23) AT.LANTUS trial, Davies et al., 2005 (24) INSIGHT trial, Gerstein et al., 2006 (25) multicenter,
Switching from insulin glargine to insulin degludec: Safety and efficacy in Colombian adolescents with type 1 diabetes
 Diabetes Management Switching from insulin glargine to insulin degludec: Safety and efficacy in Colombian adolescents with type 1 diabetes Myrey Siuffi D* ABSTRACT Introduction: Degludec (Ideg) is an ultra-long
Diabetes Management Switching from insulin glargine to insulin degludec: Safety and efficacy in Colombian adolescents with type 1 diabetes Myrey Siuffi D* ABSTRACT Introduction: Degludec (Ideg) is an ultra-long
Module 5. Understanding Insulin Therapy
 Module 5. Understanding Insulin Therapy EDUCATIONAL OBJECTIVES Upon completion of this activity, participants will be better able to: 1. Define the basic physiologic concept of basal-bolus insulin; 2.
Module 5. Understanding Insulin Therapy EDUCATIONAL OBJECTIVES Upon completion of this activity, participants will be better able to: 1. Define the basic physiologic concept of basal-bolus insulin; 2.
