Renal biopsy specimens
|
|
|
- Emily Hall
- 5 years ago
- Views:
Transcription
1 J Clin Pathol 2000;53: Best Practice No 160 Department of Pathology, Leicester General Hospital, Gwendolen Road, Leicester LE5 4PW, UK P N Furness Correspondence to: Dr Furness pnf1@le.ac.uk Accepted for publication 20 October 1999 Renal biopsy specimens Peter N Furness Abstract Taking a kidney biopsy is not a trivial procedure. The sample is almost invariably smaller than the pathologist would like. Investigation usually requires division into even smaller samples to permit the application of specialist techniques. In some cases the biopsy is taken not for diagnosis, but to assess the extent of tissue damage. The clinical need is sometimes extremely urgent. These features all underline the crucial importance of collaboration between pathologist and nephrologist if maximum benefit is to be obtained from such very small samples. Consequently, in deciding what to do with a renal biopsy, flexibility and thought are required rather than a single prescribed list of procedures. This article, written after extensive international consultation, represents an attempt to define current best practice in the laboratory handling of renal biopsy specimens, while not neglecting the need to tailor processing to the individual needs of each case. (J Clin Pathol 2000;53: ) Keywords: renal biopsy; immunofluorescence; immunohistochemistry; electron microscopy The purpose of a renal biopsy varies with each case, but is likely to include one or all of the following, with varying priority: x To establish a tissue diagnosis, or at least to exclude other diagnostic possibilities that could have a similar clinical presentation. x To assess the severity and activity of the lesion ( grade ). x To assess the amount of irreversible scarring ( stage ). This variation in clinical needs underlies the requirement for close clinicopathological cooperation in the evaluation of renal biopsy specimens. Taking the biopsy In experienced hands, renal biopsy has an extremely low mortality, but it is rarely a painless procedure. The renal cortex is a very vascular tissue; perinephric haematoma is a common consequence and considerable morbidity is not rare. Consequently, renal biopsy is not undertaken lightly, and the subsequent handling and processing of the extremely small specimens should also be done with great care. It is questionable whether renal biopsy should be performed outside specialist renal units where the necessary clinical skills can be acquired and maintained. Similarly, it is questionable whether the histological evaluation of renal biopsies should be undertaken by laboratories on an occasional basis. If a laboratory that is not accustomed to handling renal biopsy specimens is called upon to do so, the pathologists concerned should have no hesitation in seeking advice and assistance from specialist centres. Biopsies can be taken by nephrologists or radiologists, according to local practice. To ensure that adequate clinical information is available it might be necessary to insist that the nephrologist fills in the biopsy request form before asking the radiologist to perform the biopsy. Renal biopsies are usually obtained using a Tru-cut needle or spring loaded biopsy gun, under local anaesthetic cover, and with ultrasound guidance. Biopsy is undertaken as a sterile procedure and the person who takes the biopsy should be able to pass the tissue to an assistant for confirmation that renal cortex has been obtained, without compromising sterility. This assistant will commonly be another physician, a nurse, or a biomedical scientist rather than a histopathologist. Nevertheless, because stav rotate it might on occasion be necessary for a pathologist to train a new member of stav in recognition and division of the sample. The appropriate size of biopsy needle is contentious 1 ; assessment of what constitutes an adequate sample depends heavily on the condition to be sampled, which, of course, is usually unknown. With wider biopsies it might be possible to divide the specimen along its length to provide material for freezing and electron microscopy. This is not possible with an 18 gauge needle, which is a minimum, and at that calibre at least two cores should be requested. The biopsy should be placed in a drop of saline immediately after removal from the patient and examined under a good dissecting microscope with an adequate light source. With appropriate magnification it is easy to
2 434 Furness recognise normal renal cortex and to identify glomeruli on the surface (fig 1). This might be more diycult with chronic disease and fibrosis, which might cause the tissue to be uniformly pale, or with acute disease where hypercellular, bloodless glomeruli may take on the appearance of surrounding tubulo-interstitial tissues. Some cases of acute renal failure and of suspected allograft rejection require urgent processing. Waiting until the next morning is rarely detrimental, but waiting over a weekend can result in loss of renal function. Therefore, the renal pathology laboratory must have an on call service. Dividing the biopsy Division of the biopsy should be done within minutes of removal from the patient so that artefactual ultrastructural changes do not develop. Guidelines for division of the specimen will vary with the type of biopsy, the clinical question being asked, the urgency of that question, and the approach to subsequent investigations taken in the individual laboratory. In most cases, native kidney biopsies will need to be divided into three parts for conventional light microscopy, electron microscopy, and immunofluorescence studies. In theory, a single glomerulus each could be adequate for electron microscopy and immunofluorescence studies. Therefore, where possible, the bulk of the specimen should be submitted for light microscopy so that variations in the morphology of disease between glomeruli can best be assessed. However, in practice, handling samples less than 1 mm in diameter can be diycult, especially for immunofluorescence. Therefore, if the needle biopsy contains over 1 cm of cortex it is reasonable to take 1 mm for electron microscopy and 2 or 3 mm of cortex for immunofluorescence, assuming that the presence of at least one glomerulus in each sample can be guaranteed. If the sample is more limited, division will depend on the clinical question. It might be appropriate to omit the immunofluorescence Figure 1 Fresh renal cortical biopsy, taken with an 18 gauge needle, under a dissection microscope. Glomeruli marked by arrows, on the surface (white arrow) and within the biopsy (black arrows). specimen, especially if immunoperoxidase methods are available in the laboratory concerned. If the sample is tiny and the clinical question is not urgent, it might be appropriate to process the entire sample for electron microscopy. This will permit conventional light microscopy using resin sections and ultrastructural studies of the same material. Only the immunological studies will be lost, and much can be inferred from the distribution of any electron dense deposits. Alternatively, some authoritiesarguethat(intheabsenceofimmunoperoxidase methods) a frozen sample can be reprocessed for light and even electron microscopy. If this is to be attempted, snap freezing in freezing isopentane is probably needed to minimise crystal artefact. However, if the clinical question is urgent there might be a more pressing need for rapid parayn wax processing. This need to assess each case on its merits, rather than following rigid rules, highlights the importance of collaboration between renal pathologists and renal physicians. If the biopsy is taken and divided by a radiologist, it is important that the radiologist is aware of the subtleties of the clinical problem and of the potential for pathological investigation. Handling the unfixed biopsy can result in artefacts, of which the pathologist must be aware. Holes can result from the use of synthetic sponges, and bizarre cytoplasmic vacuolation can occur as a result of the accidental substitution of water for saline. It has recently been observed that if the biopsy needle is washed after the procedure, several glomeruli are often found to be adherent to the needle even in some cases where renal tissue has not been retrieved. Studying isolated glomeruli is diycult and time consuming, but they can be used for some processes, especially electron microscopy, if more solid tissue is in very limited supply. 2 Fixation and processing The most widely used fixative for light microscopy of renal biopsy specimens is neutral buvered formaldehyde. This has the advantage of being in general use within the laboratory for most specimens. It also permits immunohistochemical studies on the parayn wax processed specimen. Bouin s fluid, mercury based fixatives, and Karnowsky s fixative have been advocated, and certainly give better preservation of some aspects of morphology, especially the tubules. However, some of these fixatives render subsequent immunohistochemical studies diycult or impossible. For biopsies where an extremely urgent clinical answer is required, microwave fixation might be of assistance; we have found microwave fixation in isolation to be unsatisfactory, but it does provide a convenient way by which formaldehyde can be heated, resulting in adequate fixation within minutes. Precautions are required to avoid inhalation of formaldehyde vapour. ParaYn wax processing of renal biopsy specimens can be carried out with the routine
3 Renal biopsy specimens 435 diagnostic workload, although a rapid process schedule should be available for urgent specimens. Several resin impregnation techniques have been advocated for light microscopy of renal biopsies because they permit thinner sections to be cut. This facilitates the use of high magnification, which is commonly necessary in evaluating glomerular disease. 3 The images obtained are certainly aesthetically superior, but it can be questioned whether the diagnostic information gained is greatly improved. The approach certainly does not render electron microscopy unnecessary. The disadvantages are potentially increased processing times, additional laboratory stav labour, and sacrifice of the possibility of immunohistochemical studies. Sectioning and staining High magnification light microscopy is crucial to evaluating glomerular disease, so thin sections are essential. Thick sections artefactually increase the apparent cellularity of glomeruli and can result in erroneous diagnoses. Given the small size of a needle biopsy specimen, it should be possible to cut parayn wax sections at 3 µm thickness or less. Thicker sections may be necessary for some stains and investigations, such as Congo red or immunoperoxidase studies. There seems to be a wide variation in the number of levels at which sections are cut and examined. Again, good practice depends on the nature of the question. With a good sized sample and a straightforward diagnosis, one might be suycient. If it becomes necessary to identify small segmental lesions (and their location in the glomerulus), serial sections might be needed. As a minimum, sections should be routinely stained by a technique that highlights cells, such as haematoxylin and eosin, and one that highlights the basement membranes and connective tissue matrix, such as methenamine silver. Some advocate using a periodic acid SchiV (PAS) stain to achieve both goals. This will certainly provide good cellular detail, but the resolution of basement membranes is superior with a methenamine silver stain. Unfortunately, methenamine silver staining is technically more demanding, because the process is analogous to the development of a monochrome film. Overdevelopment or underdevelopment can result in a stain that is of no value. An optimally stained methenamine silver of a normal glomerulus should make peripheral basement membranes appear as thin, waving ribbons that are continuous, but that nevertheless permit the transmission of some light. There has been a fashion in recent years to use haematoxylin and eosin as a counterstain to the methenamine silver stain, rather than the conventional neutral green. This certainly facilitates the examination of the relations between glomerular cells and matrix. Alternatively, a trichrome counterstain gives a pleasing result. A variety of other special stains might be called for in specific circumstances. A Congo red stain for amyloid is usually a wise precaution whenever there is heavy proteinuria or a systemic disease that predisposes to amyloid; extremely small quantities of amyloid that are quite undetectable on haematoxylin and eosin can have a devastating functional evect on the glomerular basement membrane. An elastin stain might be of assistance in evaluating vascular disease, but rarely adds further information to that available from a good methenamine silver. A variety of trichrome stains have been used in the past to delineate glomerular deposits of immunoglobulins and fibrin, but have been largely superseded by immunohistochemical studies. In renal transplant pathology, the development of the BanV classification 4 5 has laid great emphasis on the use of the PAS stain to delineate tubular basement membranes and to identify tubulitis, the principal marker of acute rejection. For this purpose PAS staining is certainly equal to methenamine silver, and is technically easier. However, pathologists and technical stav should be aware that to demonstrate basement membranes clearly in thin sections, a PAS stain optimised for detecting mucus or fungi is insuycient. The times in periodic acid and in SchiV s reagent should both be doubled, 6 to 10 and 20 minutes, respectively, with fresh solutions prepared as needed. Electron microscopy Electron microscopy has become less used in recent years in many aspects of diagnostic pathology, but has retained its importance in renal pathology. A recent questionnaire survey indicated that 60% of UK laboratories handling renal biopsies perform ultrastructural studies on all renal biopsies where appropriate material is available. 7 It can be argued that this is a luxury, and that it is possible in a proportion of cases to identify the pathological process from light microscopy alone with suycient confidence to permit the omission of electron microscopy. This approach is taken by most of the remaining laboratories. This is a question of balancing the use of resources with the benefits obtained. Electron microscopy will occasionally produce unexpected second diagnoses. It may refine apparently obvious diagnoses; for example, the finding of mesangial electron dense deposits in a case of membranous glomerulonephritis suggests that the glomerulonephritis is secondary, probably to lupus, rather than idiopathic. It might also detect unsuspected method failures, as when electron microscopy shows electron dense deposits in a case with apparently negative immunohistochemical results. The balance will be influenced by the opinion and experience of the pathologist and the available resources. In renal transplant pathology, electron microscopy has frequently been omitted unless there is a suspicion of recurrent or de novo glomerular disease. However, there is evidence that ultrastructural examination of the basement membranes of peritubular capillaries for splitting gives a relatively specific marker of chronic rejection, 8 so this might change in the future.
4 436 Furness Fixation of electron microscopy specimens conventionally uses glutaraldehyde, or a glutaraldehyde/formaldehyde mixture such as Karnowsky s fixative, with postfixation using osmium tetroxide. Processing is conventionally into an epoxy resin. Semi-thin sections for block selection are stained using toluidine blue; this is frequently a neglected resource, because light microscopy of these sections can provide much information about the underlying disease process. Ultrathin sections are stained with uranyl acetate and lead citrate 9 before examination under the electron microscope. In cases of haematuria, ultrastructural assessment should include measurement of basement membrane thickness, to exclude thin membrane nephropathy. Accurate morphometric assessment of basement membrane thickness is labourious and is probably beyond the resources of most units. However, a more limited measurement of basement membrane thickness can yield useful information, especially if the approach is standardised for each case. 10 Basement membrane thickness seems to be influenced heavily by fixation and processing as well as measurement schedules, so each electron microscopy unit needs to assess its own normal range for this measurement. In specialist units, some variations on this approach may be undertaken, especially if immunoelectron microscopy is to be performed. This typically requires fixation with freshly prepared paraformaldehyde because glutaraldehyde destroys the antigenicity of most epitopes. Processing is usually into a proprietary resin with low temperature polymerisation. This approach permits immunoelectron microscopy for a restricted range of antigens and might, if carefully performed, cause little loss in ultrastructural morphology. 11 Nevertheless, it is not an approach that is widely taken. In institutions that regard themselves as centres of excellence, it seems reasonable to argue that electron microscopy should be performed on all biopsies of native kidney. In a review of laboratory practice in renal pathology, many respondents expressed the opinion that to carry out evaluation of renal biopsy specimens without at least having the availability of electron microscopy is negligent. 7 As a minimum, electron microscopy must be performed where light microscopy does not provide a diagnosis that adequately explains the observed clinical features. Ideally, the renal pathologist should examine the specimen directly, but samples for electron microscopy can be sent by post if the laboratory does not have its own facilities; photographs taken by a suitably trained laboratory scientist are usually adequate. If an appropriately fixed sample is not available, useful results can often be obtained by reprocessing material out of a parayn wax block, or from a frozen sample. Cellular detail is largely destroyed, but basement membranes and electron dense deposits are surprisingly well preserved. Immunohistochemistry Immunohistochemical investigations should be a routine part of the investigation of native renal biopsies. A basic panel of antibodies should be used for the detection of tissue deposits of IgG, IgA, IgM, and complement (usually C3). This represents a minimum. Additional antibodies can be used at the pathologist s discretion. Widely used antibodies include those directed against: x C4 and/or C1q: to indicate classical pathway complement activation. x C5b 9: to detect membrane attack complex deposition. x Fibrin: to detect fibrinoid necrosis in vessels and glomeruli, and fibrin in crescents. x Both κ and λ light chains: not only for myeloma kidney, but also the more subtle changes of light chain nephropathy. The list of antibodies that might be used in special cases is extensive. A selection includes those directed against: x Specific amyloid types. x Specific α chains of type 4 collagen (Alport s syndrome). x Fibronectin (fibronectin glomerulopathy). x Type 3 collagen (collagenous glomerulopathy). x Viral antibodies. x Tamm-Horsfall protein. METHODS OF DETECTION The detection of immunoglobulins in glomeruli is rendered diycult by the presence of abundant plasma proteins, which must be removed to avoid non-specific staining. This has resulted in a continuing popularity of frozen sections and immunofluorescence techniques in renal pathology, where they have been superseded in most other branches of immunohistochemistry by methods that are applicable to parayn wax sections. In parayn wax sections, the plasma proteins have been fixed in the tissues and must be removed by a digestion process rather than simple washing. Immunofluorescence This approach has the advantage of simplicity and reliability because plasma proteins can be removed from frozen sections simply by washing. The essential panel of antibodies against immunoglobulins and complement can be used with a direct immunofluorescence method, which is extremely simple and quick. In some hospitals this investigation is carried out in the immunology or microbiology department. There can be no justification for this practice. The reason is purely historical; the method is not diycult and it is surely preferable for the morphology of the immunofluorescence sections to be read by the person who is reporting the rest of the morphological appearances. Immunofluorescence has several disadvantages. A separate frozen specimen must be taken at the time of biopsy. A cryostat and epifluorescence microscope are required. The preparations must be mounted in aqueous media and they are not permanent; exposure to light causes bleaching. This can be reduced but
5 Renal biopsy specimens 437 not eliminated by using specialist mounting media and storing the sections in the dark in a refrigerator. Ideally, relevant images should be stored, photographically or digitally. IMMUNOHISTOCHEMISTRY USING PARAFFIN WAX SECTIONS A detection method applied to sections from the block that is re-used for routine microscopy has obvious advantages; it allows correlation with morphology and results in a permanent preparation that does not require special equipment or a separate sample for its production or examination. However, immunofluorescence remains the method of choice in 83% of UK laboratories because of the technical diyculties of the alternative methods. 7 Renal tissue contains large quantities of alkaline phosphatase and peroxidase; to block peroxidase completely is easier than blocking alkaline phosphatase, and most laboratories choose a peroxidase based detection method. After formaldehyde fixation, proteolytic digestion is essential to remove plasma proteins and to unmask epitopes in glomerular immunoglobulin deposits. Unfortunately, excessive digestion will remove deposits as well as plasma. DiVerent biopsies seem to require different digestion times, even if they are fixed and processed to a standardised protocol. Three approaches have been taken to overcome this. (1) Trial and error: for each biopsy, sections are incubated with a proteolytic enzyme (usually trypsin) for variable periods. They are all then stained with a single antibody (anti-albumin or anti-igg). The trypsinisation time that is just long enough to remove plasma from capillary loops is then selected for a subsequent run using all the antibodies required. 7 (2) Direct observation: under phase contrast microscopy, it is possible (with suitable experience) to see directly when plasma has been completely digested from the glomerular capillary loops. 12 (3) Washing: it is reported that washing the biopsy in saline or tissue culture medium for one hour before fixation and parayn wax processing makes digestion of plasma from the capillary loops much easier and less crucial. This approach has the disadvantage that if material is subsequently reprocessed from the parayn wax block for electron microscopy, the morphology will be more severely disrupted. 13 All these approaches require that all the sections used are cut to a consistent thickness; 3 µm is commonly used. With renal transplant biopsies, immunohistochemical studies are usually omitted, but are mandatory where there are any unusual features or if there is suspicion of recurrent or de novo glomerular disease. Immunohistochemistry is of surprisingly low sensitivity in the detection of antibody mediated rejection. Reporting In renal pathology, interpretation of the morphological appearances often requires detailed clinical information, and it mighty not be obvious to the pathologist exactly what sort of information the clinician requires. For this reason, it is important that the pathologist should discuss renal biopsies with the clinical team using a multiheaded microscope or video microscope system. Because the special investigations might take some time, it is often appropriate to issue a preliminary report. A final renal biopsy report should typically contain the following components. (1) Identification of material submitted. Proportion of cortex, proportion of medulla, and other tissues included. Can juxtamedullary cortex be specifically identified? How many glomeruli are available? This is best expressed as at least, meaning the largest number seen in any single section. (2) Changes in glomeruli. Cellularity, sclerosis, necrosis, crescents, numbers of glomeruli avected, segmental, or global changes. With focal changes, the proportion of glomeruli avected should be indicated. (3) Tubules. Evidence of acute damage, extent of atrophy (as an estimated percentage), casts, crystals, inclusions, etc. (4) Interstitium. Lymphocytic infiltrates, fibrosis, patchy, or divuse changes. An estimate of these features often gives a more meaningful assessment of activity and chronicity than the glomerular changes. (5) Blood vessels. Number and size present; any age related changes, any acute changes. (6) Immunohistochemical results. (7) Electron microscopic results. (8) Conclusions. In drawing conclusions, it might be necessary to provide a diverential diagnosis, with arguments for and against each possibility. In this case, it is usually helpful to give some estimate of the pathologist s view of the probability of each diagnosis provered. The nomenclature of renal disease contains some terms that are purely descriptive (for example, focal segmental proliferative glomerulonephritis) and terms that, as far as present understanding permits, are thought to represent specific disease processes (for example, IgA nephropathy). As far as possible, the distinction should be made clear for example: The pattern is of a focal segmental proliferative glomerulonephritis. Special investigations show that this is the result of IgA nephropathy. It is usually helpful to give an estimate of the activity and chronicity (grade and stage, respectively); specific treatments for renal disease are still relatively few and clinically the most important part of the report is often an estimate of the reversibility of the lesion rather than a specific diagnosis. Classification systems have been devised for use in some renal diseases, but these should be used with care. The problems with such schemes are well illustrated by the WHO classification for lupus nephritis. This followed several earlier contentious attempts, and the WHO classification itself has been through three revisions, the most recent in All
6 438 Furness are still in use, usually without an explanation of which is being used. Furthermore, interobserver variation in the application of the WHO classification is considerable. The use of such schemes at the end of a report might be helpful, and should certainly be included if the nephrologists request it, but it is essential to be sure that the recipient understands the meaning. They are not a substitute for careful description. The best route to conveying the severity of a continuous variable such as inflammation or fibrosis is to discuss the images with the responsible clinicians over a video microscope. For renal transplant biopsies, the pattern of reporting should be essentially the same, although immunohistochemistry and electron microscopy are commonly omitted, especially in grafts under six months of age, unless there is a suspicion of recurrent or de novo glomerular disease. Electron microscopy has been advocated for the detection of peritubular capillary basement membrane splitting in chronic rejection, but its use is not yet widespread. The conclusion of a transplant biopsy report should probably include the BanV classification of renal transplant pathology, or at least use terms (such as a specific grade of tubulitis) that permit translation to a specific BanV category. However, as noted above, there is interobserver variation in the application of the classification, and two slightly diverent versions (BanV and BanV 97 5 ) are in existence. In biopsies taken for the diagnosis or exclusion of acute rejection, it is often helpful if the pathologist also integrates the morphological appearances with the clinical information provided, and suggests whether treatment for an episode of acute rejection is likely to be justified or not. The standardised definitions of lesion scoring provided in the BanV classification are also available on the Internet at: tpis.upmc.edu/ under schema. A draft version of this broadsheet was made available on the World Wide Web, and comments were invited from renal pathologists who subscribe to the Internet mailing list Nephrol. I am very grateful to the many pathologists who added constructive comments, many of which are incorporated into the present version. 1 Oberholzer M, Trohorst E, Perret E, et al. Minimum sample size of kidney biopsies for semiquantitative and quantitative evaluation. Nephron 1983;34: Matyas JR, Rattner JB, Benediktsson H. Enhanced glomerular retrieval for renal biopsies. Am J Kidney Dis 1996;27: HoVmann EO. High-resolution light microscopy for interpretation of renal biopsies. Pediatr Nephrol 1995;9: Solez K, Axelsen RA, Benediktsson H, et al. International standardization of criteria for the histologic diagnosis of renal allograft rejection: the BanV working classification of kidney transplant pathology. Kidney Int 1993;44: Racusen L, Solez K, Colvin R, et al. The BanV 97 working classification of renal allograft pathology. Kidney Int 1999; 55: Bancroft J, Stevens A. Theory and practice of histological techniques. Edinburgh: Churchill Livingstone, Furness P, Boyd S. Electron microscopy and immunocytochemistry in the assessment of renal biopsy specimens: actual and optimal practice. J Clin Pathol 1996;49: Monga G, Mazzucco G, Novara R, et al. Intertubular capillary changes in renal allografts; an ultrastructural study in patients with transplant glomerulopathy. Ultrastruct Pathol 1990;14: Reynolds S. The use of lead citrate at high ph as an electron opaque stain in electron microscopy. J Cell Biol 1963;17: Das AK, Pickett TM, Tungekar MF. Glomerular basement membrane thickness a comparison of two methods of measurement in patients with unexplained haematuria. Nephrol Dial Transplant 1996;11: Woodrow DF, Shore I, Moss J, et al. Immunoelectron microscopic studies of immune complex deposits and basement membrane components in IgA nephropathy. J Pathol 1989;157: Howie AJ, Gregory J, Thompson RA, et al. Technical improvements in the immunoperoxidase study of renal biopsy specimens. J Clin Pathol 1990;43: Thomas CM, Howat AJ. Assessment of renal biopsy specimens [letter]. J Clin Pathol 1996;49: Churg J, Bernstien J, Glassock R. Lupus nephritis. In: Renal disease: classification and atlas of renal disease. New York: Igaku-Shoin, 1995: J Clin Pathol: first published as /jcp on 1 June Downloaded from on 22 August 2018 by guest. Protected by copyright.
Dr Ian Roberts Oxford. Oxford Pathology Course 2010 for FRCPath Illustration-Cellular Pathology. Oxford Radcliffe NHS Trust
 Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Plan of attack: Diagnostic approach to the renal biopsy Differential diagnosis of the clinical syndromes of renal disease Microscopy Step
Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Plan of attack: Diagnostic approach to the renal biopsy Differential diagnosis of the clinical syndromes of renal disease Microscopy Step
Renal Pathology 1: Glomerulus. With many thanks to Elizabeth Angus PhD for EM photographs
 Renal Pathology 1: Glomerulus With many thanks to Elizabeth Angus PhD for EM photographs Anatomy of the Kidney http://www.yalemedicalgroup.org/stw/page.asp?pageid=stw028980 The Nephron http://www.beltina.org/health-dictionary/nephron-function-kidney-definition.html
Renal Pathology 1: Glomerulus With many thanks to Elizabeth Angus PhD for EM photographs Anatomy of the Kidney http://www.yalemedicalgroup.org/stw/page.asp?pageid=stw028980 The Nephron http://www.beltina.org/health-dictionary/nephron-function-kidney-definition.html
Histopathology: Glomerulonephritis and other renal pathology
 Histopathology: Glomerulonephritis and other renal pathology These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you
Histopathology: Glomerulonephritis and other renal pathology These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you
Ordering Physician. Collected REVISED REPORT. Performed. IgG IF, Renal MCR. Lambda IF, Renal MCR. C1q IF, Renal. MCR Albumin IF, Renal MCR
 RenalPath Level IV Wet Ts IgA I Renal IgM I Renal Kappa I Renal Renal Bx Electron Microscopy IgG I Renal Lambda I Renal C1q I Renal C3 I Renal Albumin I Renal ibrinogen I Renal Mayo Clinic Dept. of Lab
RenalPath Level IV Wet Ts IgA I Renal IgM I Renal Kappa I Renal Renal Bx Electron Microscopy IgG I Renal Lambda I Renal C1q I Renal C3 I Renal Albumin I Renal ibrinogen I Renal Mayo Clinic Dept. of Lab
Surgical Pathology Report
 Louisiana State University Health Sciences Center Department of Pathology Shreveport, Louisiana Accession #: Collected: Received: Reported: 6/1/2012 09:18 6/2/2012 09:02 6/2/2012 Patient Name: Med. Rec.
Louisiana State University Health Sciences Center Department of Pathology Shreveport, Louisiana Accession #: Collected: Received: Reported: 6/1/2012 09:18 6/2/2012 09:02 6/2/2012 Patient Name: Med. Rec.
Light and electron microscopical studies of focal glomerular sclerosis
 J. clin. Path., 1971, 24, 846-850 Light and electron microscopical studies of focal glomerular sclerosis A. H. NAGI, F. ALEXANDER, AND R. LANNIGAN From the Department of Pathology, Queen's University of
J. clin. Path., 1971, 24, 846-850 Light and electron microscopical studies of focal glomerular sclerosis A. H. NAGI, F. ALEXANDER, AND R. LANNIGAN From the Department of Pathology, Queen's University of
Dr Ian Roberts Oxford. Oxford Pathology Course 2010 for FRCPath Illustration-Cellular Pathology. Oxford Radcliffe NHS Trust
 Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Present the basic diagnostic features of the commonest conditions causing proteinuria & haematuria Highlight diagnostic pitfalls Nephrotic
Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Present the basic diagnostic features of the commonest conditions causing proteinuria & haematuria Highlight diagnostic pitfalls Nephrotic
RENAL HISTOPATHOLOGY
 RENAL HISTOPATHOLOGY Peter McCue, M.D. Department of Pathology, Anatomy & Cell Biology Sidney Kimmel Medical College There are no conflicts of interest. 1 Goals and Objectives! Goals Provide introduction
RENAL HISTOPATHOLOGY Peter McCue, M.D. Department of Pathology, Anatomy & Cell Biology Sidney Kimmel Medical College There are no conflicts of interest. 1 Goals and Objectives! Goals Provide introduction
Biopsy Features of Kidney Allograft Rejection Banff B. Ivanyi, MD Department of Pathology, University of Szeged, Szeged, Hungary
 Biopsy Features of Kidney Allograft Rejection Banff 2017 B. Ivanyi, MD Department of Pathology, University of Szeged, Szeged, Hungary Treatment of allograft dysfunction should rely on the biopsy findings
Biopsy Features of Kidney Allograft Rejection Banff 2017 B. Ivanyi, MD Department of Pathology, University of Szeged, Szeged, Hungary Treatment of allograft dysfunction should rely on the biopsy findings
Glomerular pathology in systemic disease
 Glomerular pathology in systemic disease Lecture outline Lupus nephritis Diabetic nephropathy Glomerulonephritis Associated with Bacterial Endocarditis and Other Systemic Infections Henoch-Schonlein Purpura
Glomerular pathology in systemic disease Lecture outline Lupus nephritis Diabetic nephropathy Glomerulonephritis Associated with Bacterial Endocarditis and Other Systemic Infections Henoch-Schonlein Purpura
Case Presentation Turki Al-Hussain, MD
 Case Presentation Turki Al-Hussain, MD Director, Renal Pathology Chapter Saudi Society of Nephrology & Transplantation Consultant Nephropathologist & Urological Pathologist Department of Pathology & Laboratory
Case Presentation Turki Al-Hussain, MD Director, Renal Pathology Chapter Saudi Society of Nephrology & Transplantation Consultant Nephropathologist & Urological Pathologist Department of Pathology & Laboratory
Interesting case seminar: Native kidneys Case Report:
 Interesting case seminar: Native kidneys Case Report: Proximal tubulopathy and light chain deposition disease presented as severe pulmonary hypertension with right-sided cardiac dysfunction and nephrotic
Interesting case seminar: Native kidneys Case Report: Proximal tubulopathy and light chain deposition disease presented as severe pulmonary hypertension with right-sided cardiac dysfunction and nephrotic
A clinical syndrome, composed mainly of:
 Nephritic syndrome We will discuss: 1)Nephritic syndrome: -Acute postinfectious (poststreptococcal) GN -IgA nephropathy -Hereditary nephritis 2)Rapidly progressive GN (RPGN) A clinical syndrome, composed
Nephritic syndrome We will discuss: 1)Nephritic syndrome: -Acute postinfectious (poststreptococcal) GN -IgA nephropathy -Hereditary nephritis 2)Rapidly progressive GN (RPGN) A clinical syndrome, composed
Clinical and pathological characteristics of patients with glomerular diseases at a university teaching hospital: 5-year prospective review
 Clinical and pathological characteristics of patients with glomerular diseases at a university teaching hospital: 5-year prospective review KW Chan, TM Chan, IKP Cheng Objective. To examine the prevalence
Clinical and pathological characteristics of patients with glomerular diseases at a university teaching hospital: 5-year prospective review KW Chan, TM Chan, IKP Cheng Objective. To examine the prevalence
Monoclonal Gammopathies and the Kidney. Tibor Nádasdy, MD The Ohio State University, Columbus, OH
 Monoclonal Gammopathies and the Kidney Tibor Nádasdy, MD The Ohio State University, Columbus, OH Monoclonal gammopathy of renal significance (MGRS) Biopsies at OSU (n=475) between 2007 and 2016 AL or AH
Monoclonal Gammopathies and the Kidney Tibor Nádasdy, MD The Ohio State University, Columbus, OH Monoclonal gammopathy of renal significance (MGRS) Biopsies at OSU (n=475) between 2007 and 2016 AL or AH
Glomerular diseases mostly presenting with Nephritic syndrome
 Glomerular diseases mostly presenting with Nephritic syndrome 1 The Nephritic Syndrome Pathogenesis: proliferation of the cells in glomeruli & leukocytic infiltrate Injured capillary walls escape of RBCs
Glomerular diseases mostly presenting with Nephritic syndrome 1 The Nephritic Syndrome Pathogenesis: proliferation of the cells in glomeruli & leukocytic infiltrate Injured capillary walls escape of RBCs
RENAL EVENING SPECIALTY CONFERENCE
 RENAL EVENING SPECIALTY CONFERENCE Harsharan K. Singh, MD The University of North Carolina at Chapel Hill Disclosure of Relevant Financial Relationships No conflicts of interest to disclose. CLINICAL HISTORY
RENAL EVENING SPECIALTY CONFERENCE Harsharan K. Singh, MD The University of North Carolina at Chapel Hill Disclosure of Relevant Financial Relationships No conflicts of interest to disclose. CLINICAL HISTORY
Examination of the light microscopic slide of renal biopsy specimens by utilizing Low-vacuum scanning electron microscope
 SCIENTIFIC INSTRUMENT NEWS 2017 Vol. 9 SEPTEMBER Technical magazine of Electron Microscope and Analytical Instruments. Article Examination of the light microscopic slide of renal biopsy specimens by utilizing
SCIENTIFIC INSTRUMENT NEWS 2017 Vol. 9 SEPTEMBER Technical magazine of Electron Microscope and Analytical Instruments. Article Examination of the light microscopic slide of renal biopsy specimens by utilizing
Overview of glomerular diseases
 Overview of glomerular diseases *Endothelial cells are fenestrated each fenestra: 70-100nm in diameter Contractile, capable of proliferation, makes ECM & releases mediators *Glomerular basement membrane
Overview of glomerular diseases *Endothelial cells are fenestrated each fenestra: 70-100nm in diameter Contractile, capable of proliferation, makes ECM & releases mediators *Glomerular basement membrane
FIBRILLARY GLOMERULONEPHRITIS DIAGNOSTIC CRITERIA, PITFALLS, AND DIFFERENTIAL DIAGNOSIS
 FIBRILLARY GLOMERULONEPHRITIS DIAGNOSTIC CRITERIA, PITFALLS, AND DIFFERENTIAL DIAGNOSIS Guillermo A. Herrera MD Louisiana State University, Shreveport Fibrils in bundles 10-20 nm d Diabetic fibrillosis
FIBRILLARY GLOMERULONEPHRITIS DIAGNOSTIC CRITERIA, PITFALLS, AND DIFFERENTIAL DIAGNOSIS Guillermo A. Herrera MD Louisiana State University, Shreveport Fibrils in bundles 10-20 nm d Diabetic fibrillosis
Evolution of the approaches toward grading and classifying chronic changes in the renal allograft: Banff classification updates III
 EDITORIAL Advance Access publication 24 February 2014 Evolution of the approaches toward grading and classifying chronic changes in the renal allograft: Banff classification updates III Histopathology
EDITORIAL Advance Access publication 24 February 2014 Evolution of the approaches toward grading and classifying chronic changes in the renal allograft: Banff classification updates III Histopathology
Index. electron microscopy, 81 immunofluorescence microscopy, 80 light microscopy, 80 Amyloidosis clinical setting, 185 etiology/pathogenesis,
 A Acute antibody-mediated rejection (Acute AMR) clinical features, 203 clinicopathologic correlations, 206 pathogenesis, 205 206 204 205 light microscopy, 203 204 Acute cellular rejection (ACR) clinical
A Acute antibody-mediated rejection (Acute AMR) clinical features, 203 clinicopathologic correlations, 206 pathogenesis, 205 206 204 205 light microscopy, 203 204 Acute cellular rejection (ACR) clinical
Pathology of Complement Mediated Renal Disease
 Pathology of Complement Mediated Renal Disease Mariam Priya Alexander, MD Associate Professor of Pathology GN Symposium Hong Kong Society of Nephrology July 8 th, 2017 2017 MFMER slide-1 The complement
Pathology of Complement Mediated Renal Disease Mariam Priya Alexander, MD Associate Professor of Pathology GN Symposium Hong Kong Society of Nephrology July 8 th, 2017 2017 MFMER slide-1 The complement
Thin basement membrane nephropathy cannot be diagnosed reliably in deparaffinized, formalin-fixed tissue
 Nephrol Dial Transplant (2007) 22: 1228 1232 doi:10.1093/ndt/gfl838 Advance Access publication 3 February 2007 Technical Note Thin basement membrane nephropathy cannot be diagnosed reliably in deparaffinized,
Nephrol Dial Transplant (2007) 22: 1228 1232 doi:10.1093/ndt/gfl838 Advance Access publication 3 February 2007 Technical Note Thin basement membrane nephropathy cannot be diagnosed reliably in deparaffinized,
Kidney Summary. Mark Haas Cedars-Sinai Medical Center Los Angeles, California, USA
 Kidney Summary Mark Haas Cedars-Sinai Medical Center Los Angeles, California, USA Key Issues to Address re: the Classification 1. Incorporation of i-ifta + tubulitis into the TCMR classification - Defining
Kidney Summary Mark Haas Cedars-Sinai Medical Center Los Angeles, California, USA Key Issues to Address re: the Classification 1. Incorporation of i-ifta + tubulitis into the TCMR classification - Defining
Classification of Glomerular Diseases and Defining Individual Glomerular Lesions: Developing International Consensus
 Classification of Glomerular Diseases and Defining Individual Glomerular Lesions: Developing International Consensus Mark Haas MD, PhD Department of Pathology & Laboratory Medicine Cedars-Sinai Medical
Classification of Glomerular Diseases and Defining Individual Glomerular Lesions: Developing International Consensus Mark Haas MD, PhD Department of Pathology & Laboratory Medicine Cedars-Sinai Medical
Year 2004 Paper one: Questions supplied by Megan
 QUESTION 53 Endothelial cell pathology on renal biopsy is most characteristic of which one of the following diagnoses? A. Pre-eclampsia B. Haemolytic uraemic syndrome C. Lupus nephritis D. Immunoglobulin
QUESTION 53 Endothelial cell pathology on renal biopsy is most characteristic of which one of the following diagnoses? A. Pre-eclampsia B. Haemolytic uraemic syndrome C. Lupus nephritis D. Immunoglobulin
Case Presentation Turki Al-Hussain, MD
 Case Presentation Turki Al-Hussain, MD Director, Renal Pathology Chapter Saudi Society of Nephrology & Transplantation Consultant Nephropathologist & Urological Pathologist Department of Pathology & Laboratory
Case Presentation Turki Al-Hussain, MD Director, Renal Pathology Chapter Saudi Society of Nephrology & Transplantation Consultant Nephropathologist & Urological Pathologist Department of Pathology & Laboratory
Interpretation of Renal Transplant Biopsy. Arthur H. Cohen Wake Forest University School of Medicine Winston-Salem, North Carolina USA
 Interpretation of Renal Transplant Biopsy Arthur H. Cohen Wake Forest University School of Medicine Winston-Salem, North Carolina USA Renal Transplant Biopsies Tissue Processing Ideal world process as
Interpretation of Renal Transplant Biopsy Arthur H. Cohen Wake Forest University School of Medicine Winston-Salem, North Carolina USA Renal Transplant Biopsies Tissue Processing Ideal world process as
Management of Rejection
 Management of Rejection I have no disclosures Disclosures (relevant or otherwise) Deborah B Adey, MD Professor of Medicine University of California, San Francisco Kidney and Pancreas Transplant Center
Management of Rejection I have no disclosures Disclosures (relevant or otherwise) Deborah B Adey, MD Professor of Medicine University of California, San Francisco Kidney and Pancreas Transplant Center
Direct immunofluorescence of skin using formalin-fixed paraffin-embedded sections
 Direct immunofluorescence of skin using formalin-fixed paraffin-embedded sections SL MERA, EW YOUNG, AND JWB BRADFIELD J Clin Pathol 1980; 33: 365-369 From the University Department ofpathology, University
Direct immunofluorescence of skin using formalin-fixed paraffin-embedded sections SL MERA, EW YOUNG, AND JWB BRADFIELD J Clin Pathol 1980; 33: 365-369 From the University Department ofpathology, University
Histological features of the nephrotic syndrome
 J. clin. Path. (1967), 2, 117 Histological features of the nephrotic syndrome associated with quartan malaria J. W. KIBUKAMUSOKE AND M. S. R. HUTT From the Makerere University College Medical School and
J. clin. Path. (1967), 2, 117 Histological features of the nephrotic syndrome associated with quartan malaria J. W. KIBUKAMUSOKE AND M. S. R. HUTT From the Makerere University College Medical School and
Immune complex deposits in ANCA-associated crescentic glomerulonephritis: A study of 126 cases
 Kidney International, Vol. 65 (2004), pp. 2145 2152 Immune complex deposits in ANCA-associated crescentic glomerulonephritis: A study of 126 cases MARK HAAS and JOSEPH A. EUSTACE Department of Pathology
Kidney International, Vol. 65 (2004), pp. 2145 2152 Immune complex deposits in ANCA-associated crescentic glomerulonephritis: A study of 126 cases MARK HAAS and JOSEPH A. EUSTACE Department of Pathology
Tissue pathway for medical renal biopsies. May 2013
 Tissue pathway for medical renal biopsies May 2013 Authors: Professor Ian Roberts, Professor Peter Furness, Professor Terry Cook Unique document number Document name Version number 2 Written by G061 Date
Tissue pathway for medical renal biopsies May 2013 Authors: Professor Ian Roberts, Professor Peter Furness, Professor Terry Cook Unique document number Document name Version number 2 Written by G061 Date
Fundamentals of Renal Pathology
 Fundamentals of Renal Pathology Fundamentals of Renal Pathology Agnes B. Fogo, Arthur H. Cohen, J. Charles Jennette, Jan A. Bruijn, Robert B. Colvin Agnes B. Fogo, M.D. Vanderbilt University Medical Center
Fundamentals of Renal Pathology Fundamentals of Renal Pathology Agnes B. Fogo, Arthur H. Cohen, J. Charles Jennette, Jan A. Bruijn, Robert B. Colvin Agnes B. Fogo, M.D. Vanderbilt University Medical Center
Light-Chain Mediated Acute Tubular Interstitial Nephritis. A Poorly Recognized Pattern of Renal Disease in Patients With Plasma Cell Dyscrasia
 Light-Chain Mediated Acute Tubular Interstitial Nephritis A Poorly Recognized Pattern of Renal Disease in Patients With Plasma Cell Dyscrasia Xin Gu, MD; Guillermo A. Herrera, MD Context. Acute renal failure
Light-Chain Mediated Acute Tubular Interstitial Nephritis A Poorly Recognized Pattern of Renal Disease in Patients With Plasma Cell Dyscrasia Xin Gu, MD; Guillermo A. Herrera, MD Context. Acute renal failure
Glomerular Pathology- 1 Nephrotic Syndrome. Dr. Nisreen Abu Shahin
 Glomerular Pathology- 1 Nephrotic Syndrome Dr. Nisreen Abu Shahin The Nephrotic Syndrome a clinical complex resulting from glomerular disease & includes the following: (1) massive proteinuria (3.5 gm /day
Glomerular Pathology- 1 Nephrotic Syndrome Dr. Nisreen Abu Shahin The Nephrotic Syndrome a clinical complex resulting from glomerular disease & includes the following: (1) massive proteinuria (3.5 gm /day
Glomerular pathology-2 Nephritic syndrome. Dr. Nisreen Abu Shahin
 Glomerular pathology-2 Nephritic syndrome Dr. Nisreen Abu Shahin 1 The Nephritic Syndrome Pathogenesis: inflammation proliferation of the cells in glomeruli & leukocytic infiltrate Injured capillary walls
Glomerular pathology-2 Nephritic syndrome Dr. Nisreen Abu Shahin 1 The Nephritic Syndrome Pathogenesis: inflammation proliferation of the cells in glomeruli & leukocytic infiltrate Injured capillary walls
Pathology of Kidney Allograft Dysfunction. B. Ivanyi, MD Department of Pathology, University of Szeged, Szeged, Hungary
 Pathology of Kidney Allograft Dysfunction B. Ivanyi, MD Department of Pathology, University of Szeged, Szeged, Hungary The gold standard for exploration of the cause of an allograft dysfunction is to perform
Pathology of Kidney Allograft Dysfunction B. Ivanyi, MD Department of Pathology, University of Szeged, Szeged, Hungary The gold standard for exploration of the cause of an allograft dysfunction is to perform
Crescentic Glomerulonephritis (RPGN)
 Crescentic Glomerulonephritis (RPGN) Background Rapidly progressive glomerulonephritis (RPGN) is defined as any glomerular disease characterized by extensive crescents (usually >50%) as the principal histologic
Crescentic Glomerulonephritis (RPGN) Background Rapidly progressive glomerulonephritis (RPGN) is defined as any glomerular disease characterized by extensive crescents (usually >50%) as the principal histologic
Renal Pathology- Transplantation. Eva Honsova Institute for Clinical and Experimental Medicine Prague, Czech Republic
 Renal Pathology- Transplantation Eva Honsova Institute for Clinical and Experimental Medicine Prague, Czech Republic eva.honsova@ikem.cz Kidney has a limited number of tissue reactions by which the kidney
Renal Pathology- Transplantation Eva Honsova Institute for Clinical and Experimental Medicine Prague, Czech Republic eva.honsova@ikem.cz Kidney has a limited number of tissue reactions by which the kidney
Distribution of fibronectin in normal and diseased
 J Clin Pathol 1980;33:1021-1028 Distribution of fibronectin in normal and diseased human kidneys AJ DIXON, J BURNS, MS DUNNILL, AND JO'D McGEE From the Department ofpathology, University of Oxford, John
J Clin Pathol 1980;33:1021-1028 Distribution of fibronectin in normal and diseased human kidneys AJ DIXON, J BURNS, MS DUNNILL, AND JO'D McGEE From the Department ofpathology, University of Oxford, John
Familial DDD associated with a gain-of-function mutation in complement C3.
 Familial DDD associated with a gain-of-function mutation in complement C3. Santiago Rodríguez de Córdoba, Centro de investigaciones Biológicas, Madrid Valdés Cañedo F. and Vázquez- Martul E., Complejo
Familial DDD associated with a gain-of-function mutation in complement C3. Santiago Rodríguez de Córdoba, Centro de investigaciones Biológicas, Madrid Valdés Cañedo F. and Vázquez- Martul E., Complejo
Dr Ian Roberts Oxford
 Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Present the basic diagnostic features of the commonest conditions causing renal failure Highlight diagnostic pitfalls. Crescentic GN: renal
Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Present the basic diagnostic features of the commonest conditions causing renal failure Highlight diagnostic pitfalls. Crescentic GN: renal
Case 3. ACCME/Disclosure. Laboratory results. Clinical history 4/13/2016
 Case 3 Lynn D. Cornell, M.D. Mayo Clinic, Rochester, MN Cornell.Lynn@mayo.edu USCAP Renal Case Conference March 13, 2016 ACCME/Disclosure Dr. Cornell has nothing to disclose Clinical history 57-year-old
Case 3 Lynn D. Cornell, M.D. Mayo Clinic, Rochester, MN Cornell.Lynn@mayo.edu USCAP Renal Case Conference March 13, 2016 ACCME/Disclosure Dr. Cornell has nothing to disclose Clinical history 57-year-old
, Mariko Sawa, Moeko Kohyama, Takeshi Hamamoto and Osamu Yamato. Akira Yabuki *
 Yabuki et al. BMC Veterinary Research (2017) 13:371 DOI 10.1186/s12917-017-1287-x METHODOLOGY ARTICLE Open Access Paraffin immunofluorescence for detection of immune complexes in renal biopsies: an efficient
Yabuki et al. BMC Veterinary Research (2017) 13:371 DOI 10.1186/s12917-017-1287-x METHODOLOGY ARTICLE Open Access Paraffin immunofluorescence for detection of immune complexes in renal biopsies: an efficient
Contributions to Anatomic Pathology, over the years
 Contributions to Anatomic Pathology, over the years Anatomic Pathology, part 1 G.B. Morgagni Xavier Bichat Rudolf Wirchow Anatomic Pathology, part 1 Anatomic pathology materials: morphological samples
Contributions to Anatomic Pathology, over the years Anatomic Pathology, part 1 G.B. Morgagni Xavier Bichat Rudolf Wirchow Anatomic Pathology, part 1 Anatomic pathology materials: morphological samples
What s hiding behind IgA nephropathy?
 What s hiding behind IgA nephropathy? Bauerova L. Department of Pathology, the First Faculty of Medicine and General Hospital, Charles University Prague (nephropathology training: Department of Clinical
What s hiding behind IgA nephropathy? Bauerova L. Department of Pathology, the First Faculty of Medicine and General Hospital, Charles University Prague (nephropathology training: Department of Clinical
Thin basement membrane syndrome in adults
 J Clin Pathol 1987;40:318-322 Thin basement membrane syndrome in adults S ABE, Y AMAGASAKI,* S IYORI,t K KONISHI, E KATO, H SAKAGUCHI,: K SHIMOYAMA** From the Department of Internal Medicine and tpathology,
J Clin Pathol 1987;40:318-322 Thin basement membrane syndrome in adults S ABE, Y AMAGASAKI,* S IYORI,t K KONISHI, E KATO, H SAKAGUCHI,: K SHIMOYAMA** From the Department of Internal Medicine and tpathology,
C1q nephropathy the Diverse Disease
 C1q nephropathy the Diverse Disease Danica Galešić Ljubanović School of Medicine, University of Zagreb Dubrava University Hospital Zagreb, Croatia Definition Dominant or codominant ( 2+), mesangial staining
C1q nephropathy the Diverse Disease Danica Galešić Ljubanović School of Medicine, University of Zagreb Dubrava University Hospital Zagreb, Croatia Definition Dominant or codominant ( 2+), mesangial staining
Acute renal failure (ARF) in the transplanted kidney represents a
 Acute Renal Failure in the Transplanted Kidney Kim Solez Lorraine C. Racusen Acute renal failure (ARF) in the transplanted kidney represents a high-stakes area of nephrology and of transplantation practice.
Acute Renal Failure in the Transplanted Kidney Kim Solez Lorraine C. Racusen Acute renal failure (ARF) in the transplanted kidney represents a high-stakes area of nephrology and of transplantation practice.
Case Report A Clinical and Pathological Variant of Acute Transplant Glomerulopathy
 Case Report A Clinical and Pathological Variant of Acute Transplant Glomerulopathy Miklos Z. Molnar, 1 G. V. Ramesh Prasad, 2 Darren A. Yuen, 2,3 Serge Jothy, 4 and Jeffrey S. Zaltzman 2,5 1 Division of
Case Report A Clinical and Pathological Variant of Acute Transplant Glomerulopathy Miklos Z. Molnar, 1 G. V. Ramesh Prasad, 2 Darren A. Yuen, 2,3 Serge Jothy, 4 and Jeffrey S. Zaltzman 2,5 1 Division of
NEPHROTIC SYNDROME OF ACQUIRED SYPHILIS-A MORPHOLOGICAL AND ULTRASTRUCTURAL STUDY
 NEPHROTIC SYNDROME OF ACQUIRED SYPHILIS-A MORPHOLOGICAL AND ULTRASTRUCTURAL STUDY Abstract Pages with reference to book, From 3 To 7 A.H. Nagi, I.A. Naveed, A. Rashid ( Department of Pathology, Allama
NEPHROTIC SYNDROME OF ACQUIRED SYPHILIS-A MORPHOLOGICAL AND ULTRASTRUCTURAL STUDY Abstract Pages with reference to book, From 3 To 7 A.H. Nagi, I.A. Naveed, A. Rashid ( Department of Pathology, Allama
Histopathology: Hypertension and diabetes in the kidney These presentations are to help you identify basic histopathological features.
 Histopathology: Hypertension and diabetes in the kidney These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you need
Histopathology: Hypertension and diabetes in the kidney These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you need
CASE 3 AN UNUSUAL CASE OF NEPHROTIC SYNDROME
 CASE 3 AN UNUSUAL CASE OF NEPHROTIC SYNDROME Dr Seethalekshmy N.V., Dr.Annie Jojo, Dr Hiran K.R., Amrita institute of Medical Sciences, Kochi, Kerala Case history 34 year old gentleman Nephrotic range
CASE 3 AN UNUSUAL CASE OF NEPHROTIC SYNDROME Dr Seethalekshmy N.V., Dr.Annie Jojo, Dr Hiran K.R., Amrita institute of Medical Sciences, Kochi, Kerala Case history 34 year old gentleman Nephrotic range
Primer: histopathology of calcineurin-inhibitor toxicity in renal allografts
 Primer: histopathology of calcineurin-inhibitor toxicity in renal allografts Peter Liptak and Bela Ivanyi* SUMMARY Calcineurin inhibitors (ciclosporin and tacrolimus) can cause acute and chronic nephrotoxicity.
Primer: histopathology of calcineurin-inhibitor toxicity in renal allografts Peter Liptak and Bela Ivanyi* SUMMARY Calcineurin inhibitors (ciclosporin and tacrolimus) can cause acute and chronic nephrotoxicity.
Sugars and immune complex formation in IgA
 Glomerular disease Sugars and immune complex formation in IgA nephropathy Jonathan Barratt and Frank Eitner In vitro evidence suggests that immune complex formation in IgA nephropathy is determined by
Glomerular disease Sugars and immune complex formation in IgA nephropathy Jonathan Barratt and Frank Eitner In vitro evidence suggests that immune complex formation in IgA nephropathy is determined by
A Simpli ed Method for Measuring the Thickness of Glomerular Basement Membranes
 Ultrastructural Pathology, 27:409 416, 2003 Copyright # Taylor & Francis Inc. ISSN: 0191-3123 print/1521-0758 online DOI: 10.1080/01913120390248728 A Simpli ed Method for Measuring the Thickness of Glomerular
Ultrastructural Pathology, 27:409 416, 2003 Copyright # Taylor & Francis Inc. ISSN: 0191-3123 print/1521-0758 online DOI: 10.1080/01913120390248728 A Simpli ed Method for Measuring the Thickness of Glomerular
The application of machine learning to the diagnosis of glomerular disease
 Pre-publication draft of a paper which appeared in Sarmeinto, C. (Ed.), Proceedings of the IJCAI Workshop W.15: Representing Knowledge in Medical Decision Support Systems, pages 8.1-8.8. The application
Pre-publication draft of a paper which appeared in Sarmeinto, C. (Ed.), Proceedings of the IJCAI Workshop W.15: Representing Knowledge in Medical Decision Support Systems, pages 8.1-8.8. The application
Rui Zhang 1,2, Zhi-yong Zheng 1*, Jian-song Lin 1, Li-juan Qu 1 and Feng Zheng 3
 Zhang et al. Diagnostic Pathology 2012, 7:109 RESEARCH Open Access The continual presence of C3d but not IgG glomerular capillary deposition in stage I idiopathic membranous nephropathy in patients receiving
Zhang et al. Diagnostic Pathology 2012, 7:109 RESEARCH Open Access The continual presence of C3d but not IgG glomerular capillary deposition in stage I idiopathic membranous nephropathy in patients receiving
Atlas of Stains. Special Stains on Artisan Link Pro
 Atlas of Stains Special Stains on Artisan Link Pro Intended use Routinely processed samples (paraffin-embedded) may be used. The preferred fixative is neutral buffered formalin. The clinical interpretation
Atlas of Stains Special Stains on Artisan Link Pro Intended use Routinely processed samples (paraffin-embedded) may be used. The preferred fixative is neutral buffered formalin. The clinical interpretation
Antibody Mediated Rejection (AMR) in Heart Transplantation Session
 Page 1 Antibody Mediated Rejection (AMR) in Heart Transplantation Session Dear Colleagues: The Heart session at Banff this year will be solely focused on AMR and besides the fact that many of us attending
Page 1 Antibody Mediated Rejection (AMR) in Heart Transplantation Session Dear Colleagues: The Heart session at Banff this year will be solely focused on AMR and besides the fact that many of us attending
Statement of Disclosure
 Statement of Disclosure Mark Haas serves as a paid consultant on pathology adjudication committees for two industry-sponsored clinical trials: Shire ViroPharma Treatment of Acute ABMR AstraZeneca Treatment
Statement of Disclosure Mark Haas serves as a paid consultant on pathology adjudication committees for two industry-sponsored clinical trials: Shire ViroPharma Treatment of Acute ABMR AstraZeneca Treatment
substance staining with IgG, C3 and IgA (trace) Linear deposition of IgG(+), IgA.M(trace) and C3(+++) at the DEJ
 Direct Immunofluorescence: Skin Diagnosis Findings Picture Pemphigus Vulgaris and it s Intracellular cement variants substance staining with IgG, C3 and IgA (trace) Bullous Pemphigoid and it s variants
Direct Immunofluorescence: Skin Diagnosis Findings Picture Pemphigus Vulgaris and it s Intracellular cement variants substance staining with IgG, C3 and IgA (trace) Bullous Pemphigoid and it s variants
Segmental glomerulonephritis
 M. S. DUNNILL AND P. R. MILLARD From the Gibson Laboratories, Radcliffe Infirmary, Oxford J. clin. Path., 1975, 28, 167-175 SYNOPSIS The renal biopsy findings in 40 patients with segmental glomerulonephritis
M. S. DUNNILL AND P. R. MILLARD From the Gibson Laboratories, Radcliffe Infirmary, Oxford J. clin. Path., 1975, 28, 167-175 SYNOPSIS The renal biopsy findings in 40 patients with segmental glomerulonephritis
Lab 3, case 1. Is this an example of nephrotic or nephritic syndrome? Why? Which portion of the nephron would you expect to be abnormal?
 Lab 3, case 1 12-year-old Costa Rican boy is brought into clinic by his parents because of dark brownish-red urine over the last 24 hours. The family has been visiting friends in Indianapolis for two weeks.
Lab 3, case 1 12-year-old Costa Rican boy is brought into clinic by his parents because of dark brownish-red urine over the last 24 hours. The family has been visiting friends in Indianapolis for two weeks.
The Banff Classification for Diagnosis of Renal Allograft Rejection: Updates from the 2017 Banff Conference
 The Banff Classification for Diagnosis of Renal Allograft Rejection: Updates from the 2017 Banff Conference Mark Haas Cedars-Sinai Medical Center Los Angeles, California, USA Statement of Disclosure Mark
The Banff Classification for Diagnosis of Renal Allograft Rejection: Updates from the 2017 Banff Conference Mark Haas Cedars-Sinai Medical Center Los Angeles, California, USA Statement of Disclosure Mark
A Case of IgG2 Heavy Chain Deposition Disease in a Patient with Kappa Positive Plasma Cell Dyscrasia
 Published online: August 14, 2014 2296 9705/14/0051 0006$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial 3.0 Unported license (CC BY-NC)
Published online: August 14, 2014 2296 9705/14/0051 0006$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial 3.0 Unported license (CC BY-NC)
Pathology of Kidney Allograft Dysfunction. B. Ivanyi, MD Department of Pathology, University of Szeged, Szeged, Hungary
 Pathology of Kidney Allograft Dysfunction B. Ivanyi, MD Department of Pathology, University of Szeged, Szeged, Hungary The renal biopsy is a powerful tool in the diagnostic evaluation of allograft dysfunction
Pathology of Kidney Allograft Dysfunction B. Ivanyi, MD Department of Pathology, University of Szeged, Szeged, Hungary The renal biopsy is a powerful tool in the diagnostic evaluation of allograft dysfunction
Journal of Nephropathology
 www.nephropathol.com DOI: 0.8/nephropathol.78 J Nephropathology. Renal immunoflourescence 0; on paraffin (): 900 sections Journal of Nephropathology Detection of immunoglobulins and complement components
www.nephropathol.com DOI: 0.8/nephropathol.78 J Nephropathology. Renal immunoflourescence 0; on paraffin (): 900 sections Journal of Nephropathology Detection of immunoglobulins and complement components
Multiple Myeloma Advances for clinical pathologists & histopathologists
 Multiple Myeloma Advances for clinical pathologists & histopathologists CME in Haematology 2014 IAPP & Dept of Pathology, BVDUMC, Pune Sunday, 4 th May 2014 Dr. M.B. Agarwal, MD, MNAMS Head, Dept of Haematology
Multiple Myeloma Advances for clinical pathologists & histopathologists CME in Haematology 2014 IAPP & Dept of Pathology, BVDUMC, Pune Sunday, 4 th May 2014 Dr. M.B. Agarwal, MD, MNAMS Head, Dept of Haematology
C3G An Update What is C3 Glomerulopathy Anyway? Patrick D. Walker, M.D. Nephropath Little Rock, Arkansas USA
 C3G An Update What is C3 Glomerulopathy Anyway? Patrick D. Walker, M.D. Nephropath Little Rock, Arkansas USA C3 Glomerulopathy Overview Discuss C3 Glomerulopathy (C3G) How did we get to the current classification
C3G An Update What is C3 Glomerulopathy Anyway? Patrick D. Walker, M.D. Nephropath Little Rock, Arkansas USA C3 Glomerulopathy Overview Discuss C3 Glomerulopathy (C3G) How did we get to the current classification
Case Report A Case of Proliferative Glomerulonephritis with Monoclonal IgG Deposits That Showed Predominantly Membranous Features
 Hindawi Case Reports in Nephrology Volume 2017, Article ID 1027376, 5 pages https://doi.org/10.1155/2017/1027376 Case Report A Case of Proliferative Glomerulonephritis with Monoclonal IgG Deposits That
Hindawi Case Reports in Nephrology Volume 2017, Article ID 1027376, 5 pages https://doi.org/10.1155/2017/1027376 Case Report A Case of Proliferative Glomerulonephritis with Monoclonal IgG Deposits That
Comparison of amyloid deposition in human kidney biopsies as predictor of poor patient outcome
 Castano et al. BMC Nephrology (2015) 16:64 DOI 10.1186/s12882-015-0046-0 RESEARCH ARTICLE Comparison of amyloid deposition in human kidney biopsies as predictor of poor patient outcome Open Access Ekaterina
Castano et al. BMC Nephrology (2015) 16:64 DOI 10.1186/s12882-015-0046-0 RESEARCH ARTICLE Comparison of amyloid deposition in human kidney biopsies as predictor of poor patient outcome Open Access Ekaterina
THE URINARY SYSTEM. The cases we will cover are:
 THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
THE URINARY SYSTEM. The cases we will cover are:
 THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
Thin basement membranes in minimally abnormal glomeruli
 32 St Vincent's Hospital, Fitzroy, Victoria, Australia Department of Anatomical Pathology S Saxena D J Davies Department of Physical Sciences R L G Kirsner Correspondence to: Dr D J Davies, Department
32 St Vincent's Hospital, Fitzroy, Victoria, Australia Department of Anatomical Pathology S Saxena D J Davies Department of Physical Sciences R L G Kirsner Correspondence to: Dr D J Davies, Department
 www.renalpathologycourse.org Academic Medical Center, Department of Pathology, M2-126 Amsterdam, The Netherlands Local organizers: and Language of the course: English Registration deadline: April 13, 2015
www.renalpathologycourse.org Academic Medical Center, Department of Pathology, M2-126 Amsterdam, The Netherlands Local organizers: and Language of the course: English Registration deadline: April 13, 2015
RENAL HISTOPATHOLOGY FOLLOWING RUSSELL'S VIPER (VIPERA RUSSELLI) BITE
 RENAL HISTOPATHOLOGY FOLLOWING RUSSELL'S VIPER (VIPERA RUSSELLI) BITE Soe ~oe', May Mya win2, Than Than Htwe', Myint win', Swe Swe ~het* and Wynn Wynn Kyawl 'Department of Medical Research No. 5. Ziwaka
RENAL HISTOPATHOLOGY FOLLOWING RUSSELL'S VIPER (VIPERA RUSSELLI) BITE Soe ~oe', May Mya win2, Than Than Htwe', Myint win', Swe Swe ~het* and Wynn Wynn Kyawl 'Department of Medical Research No. 5. Ziwaka
C3 GLOMERULOPATHIES. Budapest Nephrology School Zoltan Laszik
 C3 GLOMERULOPATHIES Budapest Nephrology School 8.30.2018. Zoltan Laszik 1 Learning Objectives Familiarize with the pathogenetic mechanisms of glomerular diseases Learn the pathologic landscape and clinical
C3 GLOMERULOPATHIES Budapest Nephrology School 8.30.2018. Zoltan Laszik 1 Learning Objectives Familiarize with the pathogenetic mechanisms of glomerular diseases Learn the pathologic landscape and clinical
Transplantation and 6-Month Follow-up of Renal Transplantation from a Donor with Systemic Lupus Erythematosus and Lupus Nephritis
 American Journal of Transplantation 2005; 5: 1772 1776 Blackwell Munksgaard Case Report Copyright C Blackwell Munksgaard 2005 doi: 10.1111/j.1600-6143.2005.00922.x Transplantation and 6-Month Follow-up
American Journal of Transplantation 2005; 5: 1772 1776 Blackwell Munksgaard Case Report Copyright C Blackwell Munksgaard 2005 doi: 10.1111/j.1600-6143.2005.00922.x Transplantation and 6-Month Follow-up
Proteinuria in rheumatoid arthritis-drug-induced or amyloid?
 Anna.'s of the Rheumatic Diseases, 1981, 4, 24-244 Proteinuria in rheumatoid arthritis-drug-induced or amyloid? B. E. BOURKE, D. F. WOODROW, AND J. T. SCOTT From Charing Cross Hospital, London W6 SUMMARY
Anna.'s of the Rheumatic Diseases, 1981, 4, 24-244 Proteinuria in rheumatoid arthritis-drug-induced or amyloid? B. E. BOURKE, D. F. WOODROW, AND J. T. SCOTT From Charing Cross Hospital, London W6 SUMMARY
Mayo Clinic/ RPS Consensus Report on Classification, Diagnosis, and Reporting of Glomerulonephritis
 Mayo Clinic/ RPS Consensus Report on Classification, Diagnosis, and Reporting of Glomerulonephritis Sanjeev Sethi, MD, PhD Department of Laboratory Medicine and Pathology Disclosure Relevant Financial
Mayo Clinic/ RPS Consensus Report on Classification, Diagnosis, and Reporting of Glomerulonephritis Sanjeev Sethi, MD, PhD Department of Laboratory Medicine and Pathology Disclosure Relevant Financial
Renal Data from the Arab World
 Saudi J Kidney Dis Transpl 2013;24(2):387-391 2013 Saudi Center for Organ Transplantation Saudi Journal of Kidney Diseases and Transplantation Renal Data from the Arab World Pattern of Glomerular Diseases
Saudi J Kidney Dis Transpl 2013;24(2):387-391 2013 Saudi Center for Organ Transplantation Saudi Journal of Kidney Diseases and Transplantation Renal Data from the Arab World Pattern of Glomerular Diseases
Hidden Tiger: An Atypical Presentation of Anti-Glomerular Basement Membrane Disease
 Elmer Press Case Report Hidden Tiger: An Atypical Presentation of Anti-Glomerular Basement Membrane Disease Ashani Lecamwasam a, Darren Lee a, b, d, Alison Skene c, Lawrence McMahon a Abstract Anti-glomerular
Elmer Press Case Report Hidden Tiger: An Atypical Presentation of Anti-Glomerular Basement Membrane Disease Ashani Lecamwasam a, Darren Lee a, b, d, Alison Skene c, Lawrence McMahon a Abstract Anti-glomerular
Membranoproliferative Glomerulonephritis
 Membranoproliferative Glomerulonephritis MPGN is characterizedby alterations in the GBM and mesangium and by proliferation of glomerular cells. 5% to 10% of cases of 1ry nephrotic syndrome in children
Membranoproliferative Glomerulonephritis MPGN is characterizedby alterations in the GBM and mesangium and by proliferation of glomerular cells. 5% to 10% of cases of 1ry nephrotic syndrome in children
Glomerular diseases with organized deposits
 Glomerular diseases with organized deposits Banu Sis, MD, FRCPC University of Alberta, Edmonton, AB, Canada Ulusal Patoloji Kongresi, Manavgat, Antalya 8/11/2012 What is an organized deposit? A number
Glomerular diseases with organized deposits Banu Sis, MD, FRCPC University of Alberta, Edmonton, AB, Canada Ulusal Patoloji Kongresi, Manavgat, Antalya 8/11/2012 What is an organized deposit? A number
Periodic Acid-Schiff-Light Green Stain to Detect Glomerular Protein Deposits by Routine Light Microscopy
 Periodic Acid-Schiff-Light Green Stain to Detect Glomerular Protein Deposits by Routine Light Microscopy CHARLES N. GAMBLE, M.D. Department of Pathology, Sutter Memorial Hospital, Sacramento, California
Periodic Acid-Schiff-Light Green Stain to Detect Glomerular Protein Deposits by Routine Light Microscopy CHARLES N. GAMBLE, M.D. Department of Pathology, Sutter Memorial Hospital, Sacramento, California
Long term prognosis of recurrent haematuria
 Archives of Disease in Childhood, 1985, 60, 420-425 Long term prognosis of recurrent haematuria P F W MILLER, N I SPEIRS, S R APARICIO, M LENDON, J M SAVAGE, R J POSTLETHWAITE, J T BROCKLEBANK, I B HOUSTON,
Archives of Disease in Childhood, 1985, 60, 420-425 Long term prognosis of recurrent haematuria P F W MILLER, N I SPEIRS, S R APARICIO, M LENDON, J M SAVAGE, R J POSTLETHWAITE, J T BROCKLEBANK, I B HOUSTON,
QUANTITATIVE HISTOCHEMISTRY OF THE NEPHRON. V.
 QUANTITATIVE HISTOCHEMISTRY OF THE NEPHRON. V. ALKALINE PHOSPHATASE AND LACTIC DEHYDROGENASE ACTIVITIES IN LUPUS NEPHRITIS * By VICTOR E. POLLAK,t SJOERD L. BONTING, ROBERT C. MUEHRCKE AND ROBERT M. KARK
QUANTITATIVE HISTOCHEMISTRY OF THE NEPHRON. V. ALKALINE PHOSPHATASE AND LACTIC DEHYDROGENASE ACTIVITIES IN LUPUS NEPHRITIS * By VICTOR E. POLLAK,t SJOERD L. BONTING, ROBERT C. MUEHRCKE AND ROBERT M. KARK
Fixation... Questions 1 Answers 16. Processing... Questions 25 Answers 36. Safety... Questions 67 Answers 73
 Table of Contents Fixation... Questions 1 Answers 16 Processing... Questions 25 Answers 36 Instrumentation... Questions 43 Answers 58 Safety... Questions 67 Answers 73 Laboratory Mathematics & Solution
Table of Contents Fixation... Questions 1 Answers 16 Processing... Questions 25 Answers 36 Instrumentation... Questions 43 Answers 58 Safety... Questions 67 Answers 73 Laboratory Mathematics & Solution
Association of glomerular C4d deposition with morphologic variables of Oxford classification in IgA nephropathy patients; a preliminary study
 Immunopathol Persa. 2016;2(2):e18 Original Immunopathologia Persa http www.immunopathol.comm Association of glomerular C4d deposition with morphologic variables of Oxford classification in IgA nephropathy
Immunopathol Persa. 2016;2(2):e18 Original Immunopathologia Persa http www.immunopathol.comm Association of glomerular C4d deposition with morphologic variables of Oxford classification in IgA nephropathy
HLA and Non-HLA Antibodies in Transplantation and their Management
 HLA and Non-HLA Antibodies in Transplantation and their Management Luca Dello Strologo October 29 th, 2016 Hystory I 1960 donor specific antibodies (DSA): first suggestion for a possible role in deteriorating
HLA and Non-HLA Antibodies in Transplantation and their Management Luca Dello Strologo October 29 th, 2016 Hystory I 1960 donor specific antibodies (DSA): first suggestion for a possible role in deteriorating
Detection of Hepatitis A Antigen in Human Liver
 INFECTION AND IMMUNITY, Apr. 1982, p. 320-324 0019-9567/82/040320-05$02.00/0 Vol. 36, No. 1 Detection of Hepatitis A Antigen in Human Liver YOHKO K. SHIMIZU,'* TOSHIO SHIKATA,' PAUL R. BENINGER,2 MICHIO
INFECTION AND IMMUNITY, Apr. 1982, p. 320-324 0019-9567/82/040320-05$02.00/0 Vol. 36, No. 1 Detection of Hepatitis A Antigen in Human Liver YOHKO K. SHIMIZU,'* TOSHIO SHIKATA,' PAUL R. BENINGER,2 MICHIO
THSD7A staining of membranous glomerulopathy in clinical practice reveals cases with dual autoantibody positivity
 OPEN Official journal of the United States and Canadian Academy of Pathology. 0893-3952/16 421 THSD7A staining of membranous glomerulopathy in clinical practice reveals cases with dual autoantibody positivity
OPEN Official journal of the United States and Canadian Academy of Pathology. 0893-3952/16 421 THSD7A staining of membranous glomerulopathy in clinical practice reveals cases with dual autoantibody positivity
Severity of tubulointerstitial inflammation and prognosis in immunoglobulin A nephropathy
 http://www.kidney-international.org & 2007 International Society of Nephrology original article Severity of tubulointerstitial inflammation and prognosis in immunoglobulin A nephropathy JM Myllymäki 1,
http://www.kidney-international.org & 2007 International Society of Nephrology original article Severity of tubulointerstitial inflammation and prognosis in immunoglobulin A nephropathy JM Myllymäki 1,
HISTOPATHOLOGY. Introduction
 HISTOPATHOLOGY Introduction Contacts Services offered Pathology tissue request Laboratory hours Special instructions Histopathology reports List of specimens Introduction The Histopathology section of
HISTOPATHOLOGY Introduction Contacts Services offered Pathology tissue request Laboratory hours Special instructions Histopathology reports List of specimens Introduction The Histopathology section of
Long-term follow-up of juvenile acute nonproliferative glomerulitis (JANG)
 Pediatr Nephrol (2007) 22:1957 1961 DOI 10.1007/s00467-007-0555-6 BRIEF REPORT Long-term follow-up of juvenile acute nonproliferative glomerulitis (JANG) Teruo Fujita & Kandai Nozu & Kazumoto Iijima &
Pediatr Nephrol (2007) 22:1957 1961 DOI 10.1007/s00467-007-0555-6 BRIEF REPORT Long-term follow-up of juvenile acute nonproliferative glomerulitis (JANG) Teruo Fujita & Kandai Nozu & Kazumoto Iijima &
Immune complex nephritis in alcoholic cirrhosis: detection of Mallory body antigen in complexes by
 J Clin Pathol 1983;36:751-755 Immune complex nephritis in alcoholic cirrhosis: detection of Mallory body antigen in complexes by means of monoclonal antibodies to Mallory bodies J BURNS, AJ D'ARDENNE,
J Clin Pathol 1983;36:751-755 Immune complex nephritis in alcoholic cirrhosis: detection of Mallory body antigen in complexes by means of monoclonal antibodies to Mallory bodies J BURNS, AJ D'ARDENNE,
Fine structural appearances of glomerular capillaries in a case of malignant hypertension
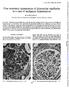 J. clin. Path. (1969), 22, 579-583 Fine structural appearances of glomerular capillaries in a case of malignant hypertension R. F. MACADAM From the University Department of Pathology, Western Infirmary,
J. clin. Path. (1969), 22, 579-583 Fine structural appearances of glomerular capillaries in a case of malignant hypertension R. F. MACADAM From the University Department of Pathology, Western Infirmary,
