Light-Chain Mediated Acute Tubular Interstitial Nephritis. A Poorly Recognized Pattern of Renal Disease in Patients With Plasma Cell Dyscrasia
|
|
|
- Ann Marshall
- 5 years ago
- Views:
Transcription
1 Light-Chain Mediated Acute Tubular Interstitial Nephritis A Poorly Recognized Pattern of Renal Disease in Patients With Plasma Cell Dyscrasia Xin Gu, MD; Guillermo A. Herrera, MD Context. Acute renal failure may be the first clinical presentation in patients with plasma cell dyscrasia. Recognition of the unusual interstitial inflammatory lesion associated with monoclonal light chains and renal failure described herein is important to guide clinicians in requesting appropriate tests to confirm plasma cell dyscrasia and providing adequate treatment. Objective. To describe an unusual pattern of tubular interstitial nephritis in patients with underlying plasma cell dyscrasia characterized by an interstitial inflammatory reaction associated with deposition of light chains along tubular basement membranes. Design. Eight cases of light-chain mediated acute tubular interstitial nephritis were identified from the archives of 4296 kidney biopsy specimens. In all cases, routine light microscopic examination, direct immunofluorescence, and electron microscopic examination were performed. Ultrastructural immunogold labeling was performed in specimens with inconclusive findings and in specimens from patients with no clinical history of plasma cell dyscrasia. Results. All patients presented with acute renal failure. Light microscopy revealed acute tubular interstitial nephritis. In some of the cases, direct immunofluorescence and electron microscopy failed to show definitive evidence of light-chain deposition along tubular basement membranes. Ultrastructural immunogold labeling aided the demonstration of monotypical light chains along some tubular basement membranes. light chains were present in other renal compartments. Conclusions. Accumulation of light chains along tubular basement membranes may induce an interstitial process that mimics acute tubular interstitial nephritis. Recognition of this unusual pattern of renal disease in patients with plasma cell dyscrasia requires ancillary diagnostic techniques. (Arch Pathol Lab Med. 2006;130: ) Renal involvement in patients with plasma cell dyscrasia (PCD) has been recognized since the description by Bence Jones of an unusual protein in the urine of a patient with multiple myeloma. 1 More than 50% of patients with PCD will experience impairment of renal function at some time during their illness. 2,3 Light-chain associated acute renal failure is a common renal complication of the disease and is regarded as one of major causes of death. 2,4 It is well known that some light chains coprecipitate with Tamm-Horsfall protein in the distal tubules, forming casts. 5,6 These tubular casts often obstruct distal tubules, occasionally breaking through tubular basement membranes and eliciting an intense interstitial inflammatory Accepted for publication September 13, From the Departments of Pathology (Drs Gu and Herrera), Medicine (Dr Herrera), and Cellular Biology and Anatomy (Dr Herrera), Louisiana State University Health Sciences Center, Shreveport. The authors have no relevant financial interest in the products or companies described in this article. Presented as an abstract and poster at the 93rd Annual Meeting of the United States and Canadian Academy of Pathology, Vancouver, British Columbia, March 9, Reprints: Guillermo A. Herrera, MD, Departments of Pathology, Medicine, and Cellular Biology and Anatomy, Louisiana State University Health Sciences Center, 1501 Kings Hwy, Shreveport, LA ( gherre@lsuhsc.edu). process that may include multinucleated giant cells. Light chains may also directly damage proximal tubular epithelial cells by overloading the lysosomal system, resulting in release of their catalytic enzymes and tubular damage. In the last 9 years, we have encountered some patients with an established diagnosis of multiple myeloma or with undiagnosed underlying PCD who presented with acute renal failure and, to our knowledge, a peculiar previously undocumented histologic lesion. The kidney biopsy specimens showed features of acute tubular interstitial nephritis; tubular casts were absent. Features of lightchain deposition disease (LCDD) and amyloidosis were also absent in the glomeruli, as well as in the tubulointerstitium and vasculature. Clinically, these patients had no history of nephrotoxic medication use, fluid depletion, or hypercalcemia that could explain the acute renal failure. On routine electron microscopy, no electron-dense deposits or widespread punctate electron-dense material typical of light-chain deposits was present along glomerular or tubular basement membranes. On close evaluation, subtle deposition of electron-dense material, consistent with light-chain deposits, could be found along rare tubular basement membranes on their outer aspect, where the interstitial inflammation was most pronounced in 2 cases. Nevertheless, using ultrastructural immunogold labeling, Arch Pathol Lab Med Vol 130, February 2006 Light-Chain Interstitial Nephritis Gu & Herrera 165
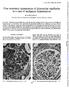
2 Patient Presentation and Characteristics of Plasma Cell Dyscrasia (PCD) at the Time of Renal Biopsy* Age, y/sex 55/F 88/F 74/M 72/M 66/F 68/F 80/F 68/F Creatinine, mg/dl Proteinuria, g/d Diagnosis of PCD at Time of Biopsy Monoclonal Immunoglobulin Light Chains (serum, urine) (serum) (serum) * indicates not available. All patients presented with acute renal failure. patient demonstrated tubular casts or glomerulopathy. The conversion factor for creatinine concentration in mol/l is mg/ dl Light-chain amount detected in proteinuria not known. monotypical light-chain deposits could be documented in all cases. Our findings suggest that accumulation of light chains along tubular basement membranes might be the cause of acute tubular interstitial nephritis in a subset of patients with PCD who have no other lesions detectable by histologic examination. It is important to recognize this pattern of light-chain mediated acute tubular interstitial nephritis. It may be the first manifestation of underlying undiagnosed PCD and/ or may be the explanation for the acute renal failure in these patients. MATERIALS AND METHODS Eight cases of light-chain mediated acute tubular interstitial nephritis were identified retrospectively from the archives of 4296 kidney biopsy specimens evaluated in the Department of Pathology at Louisiana State University Health Sciences Center Shreveport from 1996 through During that period, there were 82 cases of monoclonal immunoglobulin related renal disease diagnosed, accounting for approximately 2% of all specimens evaluated. This entity accounts for about 10% of all monoclonal immunoglobulin related renal disease. All patients experienced rapidly progressive renal insufficiency and presented with acute renal failure. At the time of biopsy, 4 patients had a history or laboratory test results suggestive of PCD. The other 4 patients were diagnosed as having underlying PCD after the renal biopsy. Bone marrow aspirates or biopsy specimens confirmed the diagnosis of PCD in all patients. All biopsy specimens were processed for light microscopy, direct immunofluorescence, and electron microscopy according to standard techniques. The fluorescence-labeled rabbit polyclonal antibodies to and light chains (DakoCytomation, Carpinteria, Calif) were used at 1:20 dilution. Polyclonal antibodies to and light chains (Ventana Medical Systems, Tucson, Ariz) used for immunohistochemistry were prediluted. In all cases, routine electron microscopy was used initially to examine the specimens. In specimens from patients with no history of PCD or laboratory test results suggestive of PCD at the time of the renal biopsy, or with inconclusive light microscopy, immunofluorescence, and ultrastructural findings, ultrastructural immunogold labeling was performed by means of the modified Herrera technique, as previously reported. 7 Polyclonal antibodies to and light chains (DakoCytomation) were used at 1:20 to 1:40 dilutions for ultrastructural immunogold labeling. RESULTS As summarized in the Table, the 8 patients described herein included 2 men and 6 women (age range, years). Clinically, all patients presented with acute renal failure. Two patients also had proteinuria. At the time of evaluation of kidney biopsy specimens, 4 patients had a clinical history suggestive of PCD. Serum and urine immunoelectrophoresis data for these 4 patients showed 3 patients with light-chain associated PCD and 1 patient with light-chain associated PCD. The other 4 patients had no history or laboratory test results suggestive of PCD. The immunophenotypes were confirmed with immunofluorescence or ultrastructural immunogold labeling. glomerular lesions were present in any of the specimens (Figure 1). A mean number of 7 glomeruli per specimen were available for evaluation by light microscopy. The arterioles and small arteries were unremarkable or showed mild thickening of the vascular walls. Features of LCDD or amyloidosis were not noted in the glomerular or vascular compartments. The interstitial process presented as multiple foci with inflammatory infiltrates, which were composed predominantly of lymphocytes and plasma cells and associated with tubulitis (Figure 2). In- Figure 1. The glomerulus is unremarkable. Infiltration by mononuclear inflammatory cells is seen in the interstitium (hematoxylin-eosin, original magnification 500). Figure 2. Acute tubular interstitial nephritis. The interstitial mononuclear inflammatory cells are predominantly lymphocytes and plasma cells. Rare eosinophils are also present. There is obvious tubulitis (periodic acid Schiff, original magnification 750). 166 Arch Pathol Lab Med Vol 130, February 2006 Light-Chain Interstitial Nephritis Gu & Herrera
3 Figure 3. Immunohistochemistry. A, light-chain staining along the tubular basement membrane is clearly seen. B, There was no staining for light chains in the same case (peroxidase-antiperoxidase staining, prediluted antibodies, original magnification 750). terstitial edema and rare eosinophils were present. recognizable myeloma casts or multinucleated giant cell reaction was seen in any of the cases. A mean number of 5 glomeruli per specimen were available for immunofluorescence examination. nspecific segmental mesangial staining for immunoglobulin M and C3 was seen in 2 cases. Specific glomerular staining for light chains or immunoglobulins was not identified in any of the cases. Linear staining for monotypical light chains along tubular basement membranes was noted in 2 cases by immunofluorescence and confirmed by immunohistochemistry (Figure 3, A and B); this finding was focal and localized to where the interstitial inflammation was most pronounced. A mean number of 3 glomeruli per specimen were identified in the thick sections available for evaluation. On routine electron microscopy, the glomeruli showed nonspecific changes, such as mild segmental thickening and wrinkling of capillary walls and mild expansion of mesangium. Granular punctate electron-dense material, organized deposits, or amyloid fibrils were not identified in glomeruli, tubular interstitium, or vascular walls, except for 1 specimen with focal deposition of light-chain material along the outer aspects of some tubular basement membranes (Figure 4, A and B). Immunohistochemistry revealed monotypical light chains along some tubular basement membranes in cases with doubtful immunomorphological findings, such as that illustrated in Figure 3. In most cases, the ultrastructural immunogold labeled light chains appeared along the basement membranes of some proximal and distal tubules but were most prominent in the distal tubules (Figure 4, C). Highly concentrated monotypical light chains were also noted focally in the proteinaceous material in tubular lumina that did not organize into well-formed casts. ultrastructural immunogold labeled light chains were noted in the glomeruli or vascular walls. COMMENT Most renal disease associated with PCD results from the deposition of monoclonal light chains in the renal parenchyma, including glomeruli, tubulointerstitium, and vessels. Depending on the physicochemical characteristics of the individual light chain, the renal manifestations include LCDD, AL amyloidosis, acute tubulopathy, or myeloma cast nephropathy. 8 It is well known that some light chains interact with Tamm-Horsfall protein in the distal tubules and form casts. Occasionally, the casts disrupt tubular basement membranes and induce destructive acute tubular interstitial nephritis with multinucleated giant cells. In a previous report, histologic evaluation of kidneys from 42 patients with multiple myeloma revealed 20 patients with cast nephropathy, 7 patients with nonobstructive interstitial nephritis, and 15 patients with other pathologic changes, including amyloidosis, myeloma infiltration, and acute tubular necrosis. 9 In those patients with nonobstructive interstitial nephritis, the cause of acute renal failure was unclear. In a recent autopsy series of 77 patients with multiple myeloma, 3% of them showed nonobstructive interstitial nephritis. 4 Sporadic reports in the literature have documented inflammatory tubular interstitial changes, isolated tubular basement membrane light-chain deposits, or fluorescence staining for monotypical light chains in some patients with myeloma with no associated glomerular or vascular pathologic features or light-chain deposition. 10,11 These patients were diagnosed as having atypical LCDD. In last 9 years, we have identified 8 patients with a history of PCD or a subsequent diagnosis of PCD who presented with acute renal failure with features of acute tubular interstitial nephritis in their kidney biopsy specimens. Based on clinical histories, there were no common causes of acute tubular interstitial nephritis, such as nephrotoxic medication use, hypercalcemia, or urinary tract infections. As noted in the Results section, features of myeloma cast nephropathy were not present on histologic examinations. The glomeruli were unremarkable. glomerular changes that indicated light- or heavy-chain deposition disease or amyloidosis were identified using light microscopy, immunofluorescence, or ultrastructural immunogold labeling. The most prominent renal changes occurred in the tubular interstitial compartment, which showed variable tubular injury associated with multiple foci with mononuclear cell infiltrates and tubulitis. Most mononuclear cells were lymphocytes. Plasma cells and rare eosinophils were also present. Occasionally, there was subtle Arch Pathol Lab Med Vol 130, February 2006 Light-Chain Interstitial Nephritis Gu & Herrera 167
4 Figure 4. Low-power (A) and high-power (B) transmission electron microscopy views reveal tubulitis with infiltration of lymphocytes into tubules. Granular punctate electron-dense material is noted along the outer aspect of the tubular basement membrane (uranyl acetate and lead citrate stain, original magnifications 7000 [A] and 8500 [B]). C, Immunogold labeling shows accumulation of light chains along the tubular basement membrane (ultrastructural immunogold labeling for light chains, original magnification ). Asterisk indicates lymphocyte; L, tubular lumen; and arrow, powdery electron-dense material along the tubular basement membrane. light-chain deposition along tubular basement membranes, best confirmed by ancillary techniques. Routine electron microscopic examination performed in renal biopsy specimens did not reveal diagnostic findings, except for 1 case in which characteristic light-chain deposits were noted (Figure 4, A and B). Using ultrastructural immunogold labeling, we detected conclusive evidence of monoclonal light-chain deposition along tubular basement membranes in 4 doubtful cases (Figure 4, C). In these cases, different from LCDD and amyloidosis, the light chains generally did not form distinct granular punctate electron-dense deposits or fibrils. Ultrastructural immunogold labeling revealed monotypical light chains embedded in tubular basement membranes and along their outer aspects. Monoclonal light chains were also noted in the lysosomes in tubular epithelial cells. There was no ultrastructural immunogold light-chain labeling in glomeruli or vasculature. All of the specimens submitted for ultrastructural immunogold labeling revealed diagnostic findings. The exact mechanism of how light chains promote acute tubular interstitial nephritis remains speculative. In most interstitial nephritis, cytokines are believed to play an important role. 12,13 The binding of light chains to tubular basement membranes might alter intrinsic tissue antigens, resulting in the release of cytokines and inducing chemoattraction and activation of interstitial mononuclear inflammatory cells. Light chains may reach tubular basement membranes by transcytosis after reabsorption or by passive tissue diffusion from peritubular capillaries. Our results showed little correlation between the degree of light-chain accumulation at tubular basement membranes and the severity of the histologic changes. The accumulation of light chains was rarely detected by immunofluorescence or routine electron microscopy. Specific physicochemical characteristics may be responsible for imparting to some light chains the propensity to bind to tubular basement membranes and to induce cytokine activation. In all but 1 of the specimens, light chains were responsible for the pattern of interstitial pathologic features described herein. In conclusion, we have described an unusual pattern of renal involvement in patients with underlying PCD characterized clinically by acute renal failure with focal accumulation of light chains along some tubular basement membranes. In these patients, previously documented pathologic patterns such as cast nephropathy or extensive paraprotein tissue deposits were not present. A high index of suspicion is needed to make the correct diagnosis. In patients with negative or inconclusive immunofluorescence and ultrastructural findings, ultrastructural immunogold labeling should be used to confirm the diagnosis. Light-chain associated acute interstitial nephritis may be the first manifestation among patients with paraproteinemia, making it important to recognize this pattern of renal injury. This observation should guide clinicians to request appropriate tests to confirm the PCD diagnosis and provide adequate treatment. Likewise, in patients with known PCD, recognition of this pattern of renal injury should lead to appropriate therapeutic intervention. Conceptually speaking, this pattern of renal disease could be considered a type of LCDD restricted to the tubular interstitial compartment and associated with a prominent inflammatory component. 168 Arch Pathol Lab Med Vol 130, February 2006 Light-Chain Interstitial Nephritis Gu & Herrera
5 References 1. Bence Jones H. On a new substance occurring in the urine of a patient with mollities ossium. Philos Trans R Soc Lond. 1848;138: Defronzo RA, Humphery RL, Wright JR, Cooke R. Acute renal failure in multiple myeloma. Medicine. 1975;54: Rota S, Mougenot B, De Meyer-Brasseur M, et al. Multiple myeloma and severe renal failure: a clinicopathologic study of outcome and prognosis in 34 patients. Medicine. 1987;66: Herrera GA, Joseph L, Gu X, Hough A, Barlogie B. Renal pathologic spectrum in an autopsy series of patients with plasma cell dyscrasia. Arch Pathol Lab Med. 2004;128: Huang ZQ, Kirk KA, Connelly KG, Sanders PW. Bence Jones proteins bind to a common peptide segment of Tamm-Horsfall glycoprotein to promote heterotypic aggregation. J Clin Invest. 1993;92: Weiss JH, Williams RH, Galla JH, et al. Pathophysiology of acute Bence- Jones protein nephrotoxicity in the rat. Kidney Int. 1981;20: Herrera GA, Sanders PW, Reddy BV. Ultrastructural immunolabeling: a unique diagnostic tool in monoclonal light chain related renal diseases. Ultrastruct Pathol. 1994;18: Herrera GA. Renal manifestations of plasma cell dyscrasias: an appraisal from the patients bedside to the research laboratory. Ann Diagn Pathol. 2000;4: Pasquali S, Zucchelli P, Casanova S, et al. Renal Immunopathology Group. Renal histological lesions and clinical syndromes in multiple myeloma. Clin Nephrol. 1987;27: Preud homme JL, Morel-Maroger L, Brovet JC, et al. Synthesis of abnormal immunoglobulins as lymphoplasmacytic disorders with visceral light chain deposition. Am J Med. 1980;69: Venkataseshan VS, Faraggiana T, Hughson MD, Buchwald D, Olesnicky L, Golgstein MH. Morphologic variants of light-chain deposition disease in the kidney. Am J Nephrol. 1988;8: Nangaku M. Mechanisms of tubulointerstitial injury in the kidney: final common pathways to end-stage renal failure. Intern Med. 2004;43: Cavallo T. Interstitial nephritis. In: Jennette CJ, Olson JL, Schwartz MM, Silva FG, eds. Heptinstall s Pathology of the Kidney. Vol 2. 5th ed. Philadelphia, Pa: Lippincott-Raven; 1998: Arch Pathol Lab Med Vol 130, February 2006 Light-Chain Interstitial Nephritis Gu & Herrera 169
Interesting case seminar: Native kidneys Case Report:
 Interesting case seminar: Native kidneys Case Report: Proximal tubulopathy and light chain deposition disease presented as severe pulmonary hypertension with right-sided cardiac dysfunction and nephrotic
Interesting case seminar: Native kidneys Case Report: Proximal tubulopathy and light chain deposition disease presented as severe pulmonary hypertension with right-sided cardiac dysfunction and nephrotic
RENAL HISTOPATHOLOGY
 RENAL HISTOPATHOLOGY Peter McCue, M.D. Department of Pathology, Anatomy & Cell Biology Sidney Kimmel Medical College There are no conflicts of interest. 1 Goals and Objectives! Goals Provide introduction
RENAL HISTOPATHOLOGY Peter McCue, M.D. Department of Pathology, Anatomy & Cell Biology Sidney Kimmel Medical College There are no conflicts of interest. 1 Goals and Objectives! Goals Provide introduction
Surgical Pathology Report
 Louisiana State University Health Sciences Center Department of Pathology Shreveport, Louisiana Accession #: Collected: Received: Reported: 6/1/2012 09:18 6/2/2012 09:02 6/2/2012 Patient Name: Med. Rec.
Louisiana State University Health Sciences Center Department of Pathology Shreveport, Louisiana Accession #: Collected: Received: Reported: 6/1/2012 09:18 6/2/2012 09:02 6/2/2012 Patient Name: Med. Rec.
Glomerular pathology in systemic disease
 Glomerular pathology in systemic disease Lecture outline Lupus nephritis Diabetic nephropathy Glomerulonephritis Associated with Bacterial Endocarditis and Other Systemic Infections Henoch-Schonlein Purpura
Glomerular pathology in systemic disease Lecture outline Lupus nephritis Diabetic nephropathy Glomerulonephritis Associated with Bacterial Endocarditis and Other Systemic Infections Henoch-Schonlein Purpura
Histopathology: Glomerulonephritis and other renal pathology
 Histopathology: Glomerulonephritis and other renal pathology These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you
Histopathology: Glomerulonephritis and other renal pathology These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you
Tarek ElBaz, MD. Prof. Internal Medicine Chief, Division of Renal Medicine Al Azhar University President, ESNT
 The Kidney in Multiple Myeloma Tarek ElBaz, MD. Prof. Internal Medicine Chief, Division of Renal Medicine Al Azhar University President, ESNT Normal Cell Plasma cells produce antibodies that bind to antigens,
The Kidney in Multiple Myeloma Tarek ElBaz, MD. Prof. Internal Medicine Chief, Division of Renal Medicine Al Azhar University President, ESNT Normal Cell Plasma cells produce antibodies that bind to antigens,
Monoclonal Gammopathies and the Kidney. Tibor Nádasdy, MD The Ohio State University, Columbus, OH
 Monoclonal Gammopathies and the Kidney Tibor Nádasdy, MD The Ohio State University, Columbus, OH Monoclonal gammopathy of renal significance (MGRS) Biopsies at OSU (n=475) between 2007 and 2016 AL or AH
Monoclonal Gammopathies and the Kidney Tibor Nádasdy, MD The Ohio State University, Columbus, OH Monoclonal gammopathy of renal significance (MGRS) Biopsies at OSU (n=475) between 2007 and 2016 AL or AH
Dr Ian Roberts Oxford. Oxford Pathology Course 2010 for FRCPath Illustration-Cellular Pathology. Oxford Radcliffe NHS Trust
 Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Plan of attack: Diagnostic approach to the renal biopsy Differential diagnosis of the clinical syndromes of renal disease Microscopy Step
Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Plan of attack: Diagnostic approach to the renal biopsy Differential diagnosis of the clinical syndromes of renal disease Microscopy Step
A clinical syndrome, composed mainly of:
 Nephritic syndrome We will discuss: 1)Nephritic syndrome: -Acute postinfectious (poststreptococcal) GN -IgA nephropathy -Hereditary nephritis 2)Rapidly progressive GN (RPGN) A clinical syndrome, composed
Nephritic syndrome We will discuss: 1)Nephritic syndrome: -Acute postinfectious (poststreptococcal) GN -IgA nephropathy -Hereditary nephritis 2)Rapidly progressive GN (RPGN) A clinical syndrome, composed
Ordering Physician. Collected REVISED REPORT. Performed. IgG IF, Renal MCR. Lambda IF, Renal MCR. C1q IF, Renal. MCR Albumin IF, Renal MCR
 RenalPath Level IV Wet Ts IgA I Renal IgM I Renal Kappa I Renal Renal Bx Electron Microscopy IgG I Renal Lambda I Renal C1q I Renal C3 I Renal Albumin I Renal ibrinogen I Renal Mayo Clinic Dept. of Lab
RenalPath Level IV Wet Ts IgA I Renal IgM I Renal Kappa I Renal Renal Bx Electron Microscopy IgG I Renal Lambda I Renal C1q I Renal C3 I Renal Albumin I Renal ibrinogen I Renal Mayo Clinic Dept. of Lab
Jo Abraham MD Division of Nephrology University of Utah
 Jo Abraham MD Division of Nephrology University of Utah 68 year old male presented 3 weeks ago with a 3 month history of increasing fatigue He reported a 1 week history of increasing dyspnea with a productive
Jo Abraham MD Division of Nephrology University of Utah 68 year old male presented 3 weeks ago with a 3 month history of increasing fatigue He reported a 1 week history of increasing dyspnea with a productive
Dr Ian Roberts Oxford. Oxford Pathology Course 2010 for FRCPath Illustration-Cellular Pathology. Oxford Radcliffe NHS Trust
 Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Present the basic diagnostic features of the commonest conditions causing proteinuria & haematuria Highlight diagnostic pitfalls Nephrotic
Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Present the basic diagnostic features of the commonest conditions causing proteinuria & haematuria Highlight diagnostic pitfalls Nephrotic
FIBRILLARY GLOMERULONEPHRITIS DIAGNOSTIC CRITERIA, PITFALLS, AND DIFFERENTIAL DIAGNOSIS
 FIBRILLARY GLOMERULONEPHRITIS DIAGNOSTIC CRITERIA, PITFALLS, AND DIFFERENTIAL DIAGNOSIS Guillermo A. Herrera MD Louisiana State University, Shreveport Fibrils in bundles 10-20 nm d Diabetic fibrillosis
FIBRILLARY GLOMERULONEPHRITIS DIAGNOSTIC CRITERIA, PITFALLS, AND DIFFERENTIAL DIAGNOSIS Guillermo A. Herrera MD Louisiana State University, Shreveport Fibrils in bundles 10-20 nm d Diabetic fibrillosis
Pathology of Complement Mediated Renal Disease
 Pathology of Complement Mediated Renal Disease Mariam Priya Alexander, MD Associate Professor of Pathology GN Symposium Hong Kong Society of Nephrology July 8 th, 2017 2017 MFMER slide-1 The complement
Pathology of Complement Mediated Renal Disease Mariam Priya Alexander, MD Associate Professor of Pathology GN Symposium Hong Kong Society of Nephrology July 8 th, 2017 2017 MFMER slide-1 The complement
Expanding Spectrum of Diseases Associated with Plasma Cell Dyscrasias
 Expanding Spectrum of Diseases Associated with Plasma Cell Dyscrasias Eva Honsova Institute for Clinical and Experimental Medicine Prague, Czech Republic eva.honsova@ikem.cz Plasma cell dyscrasias Plasma
Expanding Spectrum of Diseases Associated with Plasma Cell Dyscrasias Eva Honsova Institute for Clinical and Experimental Medicine Prague, Czech Republic eva.honsova@ikem.cz Plasma cell dyscrasias Plasma
Index. electron microscopy, 81 immunofluorescence microscopy, 80 light microscopy, 80 Amyloidosis clinical setting, 185 etiology/pathogenesis,
 A Acute antibody-mediated rejection (Acute AMR) clinical features, 203 clinicopathologic correlations, 206 pathogenesis, 205 206 204 205 light microscopy, 203 204 Acute cellular rejection (ACR) clinical
A Acute antibody-mediated rejection (Acute AMR) clinical features, 203 clinicopathologic correlations, 206 pathogenesis, 205 206 204 205 light microscopy, 203 204 Acute cellular rejection (ACR) clinical
Multiple Myeloma Advances for clinical pathologists & histopathologists
 Multiple Myeloma Advances for clinical pathologists & histopathologists CME in Haematology 2014 IAPP & Dept of Pathology, BVDUMC, Pune Sunday, 4 th May 2014 Dr. M.B. Agarwal, MD, MNAMS Head, Dept of Haematology
Multiple Myeloma Advances for clinical pathologists & histopathologists CME in Haematology 2014 IAPP & Dept of Pathology, BVDUMC, Pune Sunday, 4 th May 2014 Dr. M.B. Agarwal, MD, MNAMS Head, Dept of Haematology
CASE 3 AN UNUSUAL CASE OF NEPHROTIC SYNDROME
 CASE 3 AN UNUSUAL CASE OF NEPHROTIC SYNDROME Dr Seethalekshmy N.V., Dr.Annie Jojo, Dr Hiran K.R., Amrita institute of Medical Sciences, Kochi, Kerala Case history 34 year old gentleman Nephrotic range
CASE 3 AN UNUSUAL CASE OF NEPHROTIC SYNDROME Dr Seethalekshmy N.V., Dr.Annie Jojo, Dr Hiran K.R., Amrita institute of Medical Sciences, Kochi, Kerala Case history 34 year old gentleman Nephrotic range
Year 2004 Paper one: Questions supplied by Megan
 QUESTION 53 Endothelial cell pathology on renal biopsy is most characteristic of which one of the following diagnoses? A. Pre-eclampsia B. Haemolytic uraemic syndrome C. Lupus nephritis D. Immunoglobulin
QUESTION 53 Endothelial cell pathology on renal biopsy is most characteristic of which one of the following diagnoses? A. Pre-eclampsia B. Haemolytic uraemic syndrome C. Lupus nephritis D. Immunoglobulin
Renal Pathology 1: Glomerulus. With many thanks to Elizabeth Angus PhD for EM photographs
 Renal Pathology 1: Glomerulus With many thanks to Elizabeth Angus PhD for EM photographs Anatomy of the Kidney http://www.yalemedicalgroup.org/stw/page.asp?pageid=stw028980 The Nephron http://www.beltina.org/health-dictionary/nephron-function-kidney-definition.html
Renal Pathology 1: Glomerulus With many thanks to Elizabeth Angus PhD for EM photographs Anatomy of the Kidney http://www.yalemedicalgroup.org/stw/page.asp?pageid=stw028980 The Nephron http://www.beltina.org/health-dictionary/nephron-function-kidney-definition.html
Multiple intra-renal pathological injury patterns in resistant myeloma
 Multiple intra-renal pathological injury patterns in resistant myeloma Dharshan Rangaswamy 1, Mohit Madken 1, Mahesha Vankalakunti 2, Ravindra Prabhu Attur 1, and Shankar Prasad Nagaraju 1 1. Department
Multiple intra-renal pathological injury patterns in resistant myeloma Dharshan Rangaswamy 1, Mohit Madken 1, Mahesha Vankalakunti 2, Ravindra Prabhu Attur 1, and Shankar Prasad Nagaraju 1 1. Department
Interpretation of Renal Transplant Biopsy. Arthur H. Cohen Wake Forest University School of Medicine Winston-Salem, North Carolina USA
 Interpretation of Renal Transplant Biopsy Arthur H. Cohen Wake Forest University School of Medicine Winston-Salem, North Carolina USA Renal Transplant Biopsies Tissue Processing Ideal world process as
Interpretation of Renal Transplant Biopsy Arthur H. Cohen Wake Forest University School of Medicine Winston-Salem, North Carolina USA Renal Transplant Biopsies Tissue Processing Ideal world process as
Case Report A Case of Proliferative Glomerulonephritis with Monoclonal IgG Deposits That Showed Predominantly Membranous Features
 Hindawi Case Reports in Nephrology Volume 2017, Article ID 1027376, 5 pages https://doi.org/10.1155/2017/1027376 Case Report A Case of Proliferative Glomerulonephritis with Monoclonal IgG Deposits That
Hindawi Case Reports in Nephrology Volume 2017, Article ID 1027376, 5 pages https://doi.org/10.1155/2017/1027376 Case Report A Case of Proliferative Glomerulonephritis with Monoclonal IgG Deposits That
Case 3. ACCME/Disclosure. Laboratory results. Clinical history 4/13/2016
 Case 3 Lynn D. Cornell, M.D. Mayo Clinic, Rochester, MN Cornell.Lynn@mayo.edu USCAP Renal Case Conference March 13, 2016 ACCME/Disclosure Dr. Cornell has nothing to disclose Clinical history 57-year-old
Case 3 Lynn D. Cornell, M.D. Mayo Clinic, Rochester, MN Cornell.Lynn@mayo.edu USCAP Renal Case Conference March 13, 2016 ACCME/Disclosure Dr. Cornell has nothing to disclose Clinical history 57-year-old
Quantitative protein estimation of Urine
 Quantitative protein estimation of Urine 1 In a healthy renal and urinary tract system, the urine contains no protein or only trace amounts. The presence of increased amounts of protein in the urine can
Quantitative protein estimation of Urine 1 In a healthy renal and urinary tract system, the urine contains no protein or only trace amounts. The presence of increased amounts of protein in the urine can
RENAL EVENING SPECIALTY CONFERENCE
 RENAL EVENING SPECIALTY CONFERENCE Harsharan K. Singh, MD The University of North Carolina at Chapel Hill Disclosure of Relevant Financial Relationships No conflicts of interest to disclose. CLINICAL HISTORY
RENAL EVENING SPECIALTY CONFERENCE Harsharan K. Singh, MD The University of North Carolina at Chapel Hill Disclosure of Relevant Financial Relationships No conflicts of interest to disclose. CLINICAL HISTORY
C1q nephropathy the Diverse Disease
 C1q nephropathy the Diverse Disease Danica Galešić Ljubanović School of Medicine, University of Zagreb Dubrava University Hospital Zagreb, Croatia Definition Dominant or codominant ( 2+), mesangial staining
C1q nephropathy the Diverse Disease Danica Galešić Ljubanović School of Medicine, University of Zagreb Dubrava University Hospital Zagreb, Croatia Definition Dominant or codominant ( 2+), mesangial staining
Forms Revision: Myeloma Changes
 Sharing knowledge. Sharing hope. Forms Revision: Myeloma Changes J. Brunner, PA-C and A. Dispenzieri, MD February 2013 Disclosures Janet Brunner, PA-C I have no relevant conflicts of interest to disclose.
Sharing knowledge. Sharing hope. Forms Revision: Myeloma Changes J. Brunner, PA-C and A. Dispenzieri, MD February 2013 Disclosures Janet Brunner, PA-C I have no relevant conflicts of interest to disclose.
Quantitative estimation of protein in urine
 Quantitative estimation of protein in urine By sulphosalicalic acid Method BCH 472 In a healthy renal and urinary tract system, the urine contains no protein or only trace amounts. The presence of increased
Quantitative estimation of protein in urine By sulphosalicalic acid Method BCH 472 In a healthy renal and urinary tract system, the urine contains no protein or only trace amounts. The presence of increased
THE URINARY SYSTEM. The cases we will cover are:
 THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
Histological features of the nephrotic syndrome
 J. clin. Path. (1967), 2, 117 Histological features of the nephrotic syndrome associated with quartan malaria J. W. KIBUKAMUSOKE AND M. S. R. HUTT From the Makerere University College Medical School and
J. clin. Path. (1967), 2, 117 Histological features of the nephrotic syndrome associated with quartan malaria J. W. KIBUKAMUSOKE AND M. S. R. HUTT From the Makerere University College Medical School and
The principal characteristics of some of the more common heredofamilial
 Heredofamilial and Congenital Glomerular Disorders rthur H. Cohen Richard J. Glassock The principal characteristics of some of the more common heredofamilial and congenital glomerular disorders are described
Heredofamilial and Congenital Glomerular Disorders rthur H. Cohen Richard J. Glassock The principal characteristics of some of the more common heredofamilial and congenital glomerular disorders are described
RENAL HISTOPATHOLOGY FOLLOWING RUSSELL'S VIPER (VIPERA RUSSELLI) BITE
 RENAL HISTOPATHOLOGY FOLLOWING RUSSELL'S VIPER (VIPERA RUSSELLI) BITE Soe ~oe', May Mya win2, Than Than Htwe', Myint win', Swe Swe ~het* and Wynn Wynn Kyawl 'Department of Medical Research No. 5. Ziwaka
RENAL HISTOPATHOLOGY FOLLOWING RUSSELL'S VIPER (VIPERA RUSSELLI) BITE Soe ~oe', May Mya win2, Than Than Htwe', Myint win', Swe Swe ~het* and Wynn Wynn Kyawl 'Department of Medical Research No. 5. Ziwaka
THE URINARY SYSTEM. The cases we will cover are:
 THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
Nephroquiz 5: a 51-Year-Old Man With Kidney Failure
 5: a 51-Year-Old Man With Kidney Failure Mohammad Tamaddondar, 1 Behdad Rahimi Kelarijani, 2 Peyman Torbati, 3 Pedram Ahmadpoor 2 IJKD 2010;4:340-4 www.ijkd.org NEPHROQUIZ 1Department of Nephrology, Hormozgan
5: a 51-Year-Old Man With Kidney Failure Mohammad Tamaddondar, 1 Behdad Rahimi Kelarijani, 2 Peyman Torbati, 3 Pedram Ahmadpoor 2 IJKD 2010;4:340-4 www.ijkd.org NEPHROQUIZ 1Department of Nephrology, Hormozgan
KIDNEY BIOPSY TEACHING CASE Light Chain Deposition Disease After Renal Transplantation
 KIDNEY BIOPSY TEACHING CASE Light Chain Deposition Disease After Renal Transplantation Sekiko Taneda, MD, 1 Kazuho Honda, MD, 1 Shigeru Horita, MS, 1 Ichiro Koyama, MD, 2 Satoshi Teraoka, MD, 2 Hideaki
KIDNEY BIOPSY TEACHING CASE Light Chain Deposition Disease After Renal Transplantation Sekiko Taneda, MD, 1 Kazuho Honda, MD, 1 Shigeru Horita, MS, 1 Ichiro Koyama, MD, 2 Satoshi Teraoka, MD, 2 Hideaki
Among the benign intraepithelial melanocytic proliferations, Inflamed Conjunctival Nevi. Histopathological Criteria. Resident Short Reviews
 Resident Short Reviews Inflamed conjunctival nevi (ICN) may suggest malignancy because of their rapid growth and atypical histology. The objective of this study was to characterize the diagnostic features
Resident Short Reviews Inflamed conjunctival nevi (ICN) may suggest malignancy because of their rapid growth and atypical histology. The objective of this study was to characterize the diagnostic features
Disorders of the kidney. Urine analysis. Nephrotic and nephritic syndrome.
 Disorders of the kidney. Urine analysis. Nephrotic and nephritic syndrome. Azotemia and Urinary Abnormalities Disturbances in urine volume oliguria, anuria, polyuria Abnormalities of urine sediment red
Disorders of the kidney. Urine analysis. Nephrotic and nephritic syndrome. Azotemia and Urinary Abnormalities Disturbances in urine volume oliguria, anuria, polyuria Abnormalities of urine sediment red
Light and electron microscopical studies of focal glomerular sclerosis
 J. clin. Path., 1971, 24, 846-850 Light and electron microscopical studies of focal glomerular sclerosis A. H. NAGI, F. ALEXANDER, AND R. LANNIGAN From the Department of Pathology, Queen's University of
J. clin. Path., 1971, 24, 846-850 Light and electron microscopical studies of focal glomerular sclerosis A. H. NAGI, F. ALEXANDER, AND R. LANNIGAN From the Department of Pathology, Queen's University of
Fine structural appearances of glomerular capillaries in a case of malignant hypertension
 J. clin. Path. (1969), 22, 579-583 Fine structural appearances of glomerular capillaries in a case of malignant hypertension R. F. MACADAM From the University Department of Pathology, Western Infirmary,
J. clin. Path. (1969), 22, 579-583 Fine structural appearances of glomerular capillaries in a case of malignant hypertension R. F. MACADAM From the University Department of Pathology, Western Infirmary,
Lab 3, case 1. Is this an example of nephrotic or nephritic syndrome? Why? Which portion of the nephron would you expect to be abnormal?
 Lab 3, case 1 12-year-old Costa Rican boy is brought into clinic by his parents because of dark brownish-red urine over the last 24 hours. The family has been visiting friends in Indianapolis for two weeks.
Lab 3, case 1 12-year-old Costa Rican boy is brought into clinic by his parents because of dark brownish-red urine over the last 24 hours. The family has been visiting friends in Indianapolis for two weeks.
Amyloid-like Pulmonary Nodules, Including Localized Light-Chain Deposition Clinicopathologic Analysis of Three Cases
 Anatomic Pathology / AMYLOID-LIKE PULMONARY NODULES Amyloid-like Pulmonary Nodules, Including Localized Light-Chain Deposition Clinicopathologic Analysis of Three Cases Andras Khoor, MD, 1 Jeffrey L. Myers,
Anatomic Pathology / AMYLOID-LIKE PULMONARY NODULES Amyloid-like Pulmonary Nodules, Including Localized Light-Chain Deposition Clinicopathologic Analysis of Three Cases Andras Khoor, MD, 1 Jeffrey L. Myers,
Comparison of amyloid deposition in human kidney biopsies as predictor of poor patient outcome
 Castano et al. BMC Nephrology (2015) 16:64 DOI 10.1186/s12882-015-0046-0 RESEARCH ARTICLE Comparison of amyloid deposition in human kidney biopsies as predictor of poor patient outcome Open Access Ekaterina
Castano et al. BMC Nephrology (2015) 16:64 DOI 10.1186/s12882-015-0046-0 RESEARCH ARTICLE Comparison of amyloid deposition in human kidney biopsies as predictor of poor patient outcome Open Access Ekaterina
Case Presentation Turki Al-Hussain, MD
 Case Presentation Turki Al-Hussain, MD Director, Renal Pathology Chapter Saudi Society of Nephrology & Transplantation Consultant Nephropathologist & Urological Pathologist Department of Pathology & Laboratory
Case Presentation Turki Al-Hussain, MD Director, Renal Pathology Chapter Saudi Society of Nephrology & Transplantation Consultant Nephropathologist & Urological Pathologist Department of Pathology & Laboratory
Crescentic Glomerulonephritis (RPGN)
 Crescentic Glomerulonephritis (RPGN) Background Rapidly progressive glomerulonephritis (RPGN) is defined as any glomerular disease characterized by extensive crescents (usually >50%) as the principal histologic
Crescentic Glomerulonephritis (RPGN) Background Rapidly progressive glomerulonephritis (RPGN) is defined as any glomerular disease characterized by extensive crescents (usually >50%) as the principal histologic
HISTOPATHOLOGY. Shannon Martinson
 HISTOPATHOLOGY Shannon Martinson March 2013 Case #1 History: 8 year old beagle Neck pain for the past couple of weeks Paresis, followed by paralysis developed over the past few days Gross Description courtesy
HISTOPATHOLOGY Shannon Martinson March 2013 Case #1 History: 8 year old beagle Neck pain for the past couple of weeks Paresis, followed by paralysis developed over the past few days Gross Description courtesy
II.Tubulointerstitial diseases
 II.Tubulointerstitial diseases two major groups of processes (1) ischemic or toxic tubular injury, leading to acute kidney injury (AKI) and acute renal failure, and (2) inflammatory reactions of the tubules
II.Tubulointerstitial diseases two major groups of processes (1) ischemic or toxic tubular injury, leading to acute kidney injury (AKI) and acute renal failure, and (2) inflammatory reactions of the tubules
Plasma cell myeloma (multiple myeloma)
 Plasma cell myeloma (multiple myeloma) Common lymphoid neoplasm, present at old age (70 years average) Remember: plasma cells are terminally differentiated B-lymphocytes that produces antibodies. B-cells
Plasma cell myeloma (multiple myeloma) Common lymphoid neoplasm, present at old age (70 years average) Remember: plasma cells are terminally differentiated B-lymphocytes that produces antibodies. B-cells
Renal manifestations of IgG4-related systemic disease
 Renal manifestations of IgG4-related systemic disease Lynn D. Cornell, M.D. Mayo Clinic Rochester, MN While autoimmune pancreatitis (AIP) has been recognized since the first description by Sarles et al
Renal manifestations of IgG4-related systemic disease Lynn D. Cornell, M.D. Mayo Clinic Rochester, MN While autoimmune pancreatitis (AIP) has been recognized since the first description by Sarles et al
Recurrent Idiopathic Membranous Glomerulonephritis After Kidney Transplantation and Successful Treatment With Rituximab
 TRANSPLANTATION Recurrent Idiopathic Membranous Glomerulonephritis After Kidney Transplantation and Successful Treatment With Rituximab Khadijeh Makhdoomi, 1,2 Saeed Abkhiz, 1,2 Farahnaz Noroozinia, 1,3
TRANSPLANTATION Recurrent Idiopathic Membranous Glomerulonephritis After Kidney Transplantation and Successful Treatment With Rituximab Khadijeh Makhdoomi, 1,2 Saeed Abkhiz, 1,2 Farahnaz Noroozinia, 1,3
Biopsy Features of Kidney Allograft Rejection Banff B. Ivanyi, MD Department of Pathology, University of Szeged, Szeged, Hungary
 Biopsy Features of Kidney Allograft Rejection Banff 2017 B. Ivanyi, MD Department of Pathology, University of Szeged, Szeged, Hungary Treatment of allograft dysfunction should rely on the biopsy findings
Biopsy Features of Kidney Allograft Rejection Banff 2017 B. Ivanyi, MD Department of Pathology, University of Szeged, Szeged, Hungary Treatment of allograft dysfunction should rely on the biopsy findings
Elevated Serum Creatinine, a simplified approach
 Elevated Serum Creatinine, a simplified approach Primary Care Update Creighton University School of Medicine. April 27 th, 2018 Disclosure Slide I have no disclosures and have no conflicts with this presentation.
Elevated Serum Creatinine, a simplified approach Primary Care Update Creighton University School of Medicine. April 27 th, 2018 Disclosure Slide I have no disclosures and have no conflicts with this presentation.
Light chain crystalline kidney disease: diagnostic urine microscopy as the liquid kidney biopsy
 Clinical Nephrology, Vol. No. /2014 (1-5) Neph Education 2014 Dustri-Verlag Dr. K. Feistle ISSN 0301-0430 DOI 10.5414/CN108424 e-pub: month day, year Light chain crystalline kidney disease: diagnostic
Clinical Nephrology, Vol. No. /2014 (1-5) Neph Education 2014 Dustri-Verlag Dr. K. Feistle ISSN 0301-0430 DOI 10.5414/CN108424 e-pub: month day, year Light chain crystalline kidney disease: diagnostic
Tubulointerstitial Nephritis Accompanying Gamma-Heavy Chain Deposition and Gamma-Heavy Chain Restricted Plasma Cells in the Kidney
 KIDNEY DISEASES Tubulointerstitial Nephritis Accompanying Gamma-Heavy Chain Deposition and Gamma-Heavy Chain Restricted Plasma Cells in the Kidney Ali Nayer, 1 Dollie F Green, 1 Maria L Gonzalez-Suarez,
KIDNEY DISEASES Tubulointerstitial Nephritis Accompanying Gamma-Heavy Chain Deposition and Gamma-Heavy Chain Restricted Plasma Cells in the Kidney Ali Nayer, 1 Dollie F Green, 1 Maria L Gonzalez-Suarez,
Renal Pathology Case Conference. Case 2
 Renal Pathology Case Conference Case 2 Lynn D. Cornell, M.D. Mayo Clinic, Rochester, MN cornell.lynn@mayo.edu March 2, 2008 Clinical presentation 68 year old woman, initially with normal renal function
Renal Pathology Case Conference Case 2 Lynn D. Cornell, M.D. Mayo Clinic, Rochester, MN cornell.lynn@mayo.edu March 2, 2008 Clinical presentation 68 year old woman, initially with normal renal function
Yijuan Sun, Amarpreet Sandhu, Darlene Gabaldon, Jonathan Danaraj, Karen S. Servilla, and Antonios H. Tzamaloukas
 Case Reports in Nephrology Volume 2012, Article ID 573650, 5 pages doi:10.1155/2012/573650 Case Report Development of Renal Failure without Proteinuria in a Patient with Monoclonal Gammopathy of Undetermined
Case Reports in Nephrology Volume 2012, Article ID 573650, 5 pages doi:10.1155/2012/573650 Case Report Development of Renal Failure without Proteinuria in a Patient with Monoclonal Gammopathy of Undetermined
Light chain deposition disease presenting with hepatomegaly: an association with amyloid-like fibrils
 Postgraduate Medical Journal (1988) 64, 804-808 Light chain deposition disease presenting with hepatomegaly: an association with amyloid-like fibrils G. Pelletier,I M. Fabre,2 P. Attali,i A. Ladouch-Badre,2
Postgraduate Medical Journal (1988) 64, 804-808 Light chain deposition disease presenting with hepatomegaly: an association with amyloid-like fibrils G. Pelletier,I M. Fabre,2 P. Attali,i A. Ladouch-Badre,2
NEPHROTIC SYNDROME OF ACQUIRED SYPHILIS-A MORPHOLOGICAL AND ULTRASTRUCTURAL STUDY
 NEPHROTIC SYNDROME OF ACQUIRED SYPHILIS-A MORPHOLOGICAL AND ULTRASTRUCTURAL STUDY Abstract Pages with reference to book, From 3 To 7 A.H. Nagi, I.A. Naveed, A. Rashid ( Department of Pathology, Allama
NEPHROTIC SYNDROME OF ACQUIRED SYPHILIS-A MORPHOLOGICAL AND ULTRASTRUCTURAL STUDY Abstract Pages with reference to book, From 3 To 7 A.H. Nagi, I.A. Naveed, A. Rashid ( Department of Pathology, Allama
Differentiation of Renal Tubular Epithelium in Renal Transplantation Cytology
 Differentiation of Renal Tubular Epithelium in Renal Transplantation Cytology G. BERRY SCHUMANN, M.D., LAWRENCE J. PALMIERI, B.S., C.T.(ASCP), AND DAVID B. JONES, M.D. Schumann, G. Berry, Palmieri, Lawrence
Differentiation of Renal Tubular Epithelium in Renal Transplantation Cytology G. BERRY SCHUMANN, M.D., LAWRENCE J. PALMIERI, B.S., C.T.(ASCP), AND DAVID B. JONES, M.D. Schumann, G. Berry, Palmieri, Lawrence
Case # 2 3/27/2017. Disclosure of Relevant Financial Relationships. Clinical history. Clinical history. Laboratory findings
 Case # 2 Christopher Larsen, MD Arkana Laboratories Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to influence or control the content
Case # 2 Christopher Larsen, MD Arkana Laboratories Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to influence or control the content
Long-term follow-up of juvenile acute nonproliferative glomerulitis (JANG)
 Pediatr Nephrol (2007) 22:1957 1961 DOI 10.1007/s00467-007-0555-6 BRIEF REPORT Long-term follow-up of juvenile acute nonproliferative glomerulitis (JANG) Teruo Fujita & Kandai Nozu & Kazumoto Iijima &
Pediatr Nephrol (2007) 22:1957 1961 DOI 10.1007/s00467-007-0555-6 BRIEF REPORT Long-term follow-up of juvenile acute nonproliferative glomerulitis (JANG) Teruo Fujita & Kandai Nozu & Kazumoto Iijima &
Section Title. Subject Index
 Section Title Subject Index Acute kidney injury definitions 287 289 hypoxia 287, 290 overview 286, 287 sublethal tubular injury adaptive responses 292, 293 combination of sublethal injuries 291, 292 detection
Section Title Subject Index Acute kidney injury definitions 287 289 hypoxia 287, 290 overview 286, 287 sublethal tubular injury adaptive responses 292, 293 combination of sublethal injuries 291, 292 detection
Familial DDD associated with a gain-of-function mutation in complement C3.
 Familial DDD associated with a gain-of-function mutation in complement C3. Santiago Rodríguez de Córdoba, Centro de investigaciones Biológicas, Madrid Valdés Cañedo F. and Vázquez- Martul E., Complejo
Familial DDD associated with a gain-of-function mutation in complement C3. Santiago Rodríguez de Córdoba, Centro de investigaciones Biológicas, Madrid Valdés Cañedo F. and Vázquez- Martul E., Complejo
LIGHT CHAIN DISEASE B. DHANALAKSHMI 1 & V. HEMAVATHY 2
 TJPRC: International Journal of Nursing and Patient Safety & Care (TJPRC: IJNPSC) Vol. 1, Issue 1, Dec 2016, 21-24 TJPRC Pvt. Ltd. LIGHT CHAIN DISEASE B. DHANALAKSHMI 1 & V. HEMAVATHY 2 1 Associate Professor,
TJPRC: International Journal of Nursing and Patient Safety & Care (TJPRC: IJNPSC) Vol. 1, Issue 1, Dec 2016, 21-24 TJPRC Pvt. Ltd. LIGHT CHAIN DISEASE B. DHANALAKSHMI 1 & V. HEMAVATHY 2 1 Associate Professor,
Overview of glomerular diseases
 Overview of glomerular diseases *Endothelial cells are fenestrated each fenestra: 70-100nm in diameter Contractile, capable of proliferation, makes ECM & releases mediators *Glomerular basement membrane
Overview of glomerular diseases *Endothelial cells are fenestrated each fenestra: 70-100nm in diameter Contractile, capable of proliferation, makes ECM & releases mediators *Glomerular basement membrane
RENAL BIOPSIES in patients with the clinical
 RENAL BIOPSY TEACHING CASE Crescentic Glomerulonephritis With a Paucity of Glomerular Immunoglobulin Localization Alexis A. Harris, MD, Ronald J. Falk, MD, and J. Charles Jennette, MD RENAL BIOPSIES in
RENAL BIOPSY TEACHING CASE Crescentic Glomerulonephritis With a Paucity of Glomerular Immunoglobulin Localization Alexis A. Harris, MD, Ronald J. Falk, MD, and J. Charles Jennette, MD RENAL BIOPSIES in
Journal of Nephropathology
 www.nephropathol.com DOI:10.5812/nephropathol.9000 J Nephropathology. Tubulointerstitial 2013; lupus 2(1): nephritis 75-80 Journal of Nephropathology See commentary on page 71 Tubulointerstitial lupus
www.nephropathol.com DOI:10.5812/nephropathol.9000 J Nephropathology. Tubulointerstitial 2013; lupus 2(1): nephritis 75-80 Journal of Nephropathology See commentary on page 71 Tubulointerstitial lupus
Renal Transporters- pathophysiology of drug - induced renal disorders. Lisa Harris, Pharmacist, John Hunter Hospital, Newcastle, 2015 November
 Renal Transporters- pathophysiology of drug - induced renal disorders Lisa Harris, Pharmacist, John Hunter Hospital, Newcastle, 2015 November Renal Failure Up to 25% of acute renal failure is drug induced
Renal Transporters- pathophysiology of drug - induced renal disorders Lisa Harris, Pharmacist, John Hunter Hospital, Newcastle, 2015 November Renal Failure Up to 25% of acute renal failure is drug induced
Fundamentals of Renal Pathology
 Fundamentals of Renal Pathology Fundamentals of Renal Pathology Agnes B. Fogo, Arthur H. Cohen, J. Charles Jennette, Jan A. Bruijn, Robert B. Colvin Agnes B. Fogo, M.D. Vanderbilt University Medical Center
Fundamentals of Renal Pathology Fundamentals of Renal Pathology Agnes B. Fogo, Arthur H. Cohen, J. Charles Jennette, Jan A. Bruijn, Robert B. Colvin Agnes B. Fogo, M.D. Vanderbilt University Medical Center
Basic Urinary Tract Anatomy and Histology
 Basic Urinary Tract Anatomy and Histology The two kidneys are located in the retroperitoneum on either side of the vertebral bladder and the contraction of the detrusor muscle. Any mechanical barrier,
Basic Urinary Tract Anatomy and Histology The two kidneys are located in the retroperitoneum on either side of the vertebral bladder and the contraction of the detrusor muscle. Any mechanical barrier,
Glomerular Pathology- 1 Nephrotic Syndrome. Dr. Nisreen Abu Shahin
 Glomerular Pathology- 1 Nephrotic Syndrome Dr. Nisreen Abu Shahin The Nephrotic Syndrome a clinical complex resulting from glomerular disease & includes the following: (1) massive proteinuria (3.5 gm /day
Glomerular Pathology- 1 Nephrotic Syndrome Dr. Nisreen Abu Shahin The Nephrotic Syndrome a clinical complex resulting from glomerular disease & includes the following: (1) massive proteinuria (3.5 gm /day
Glomerular diseases mostly presenting with Nephritic syndrome
 Glomerular diseases mostly presenting with Nephritic syndrome 1 The Nephritic Syndrome Pathogenesis: proliferation of the cells in glomeruli & leukocytic infiltrate Injured capillary walls escape of RBCs
Glomerular diseases mostly presenting with Nephritic syndrome 1 The Nephritic Syndrome Pathogenesis: proliferation of the cells in glomeruli & leukocytic infiltrate Injured capillary walls escape of RBCs
A Case of IgG2 Heavy Chain Deposition Disease in a Patient with Kappa Positive Plasma Cell Dyscrasia
 Published online: August 14, 2014 2296 9705/14/0051 0006$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial 3.0 Unported license (CC BY-NC)
Published online: August 14, 2014 2296 9705/14/0051 0006$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial 3.0 Unported license (CC BY-NC)
Diabetic Nephropathy. Introduction/Clinical Setting. Pathologic Findings Light Microscopy. J. Charles Jennette
 12 Diabetic Nephropathy J. Charles Jennette Introduction/Clinical Setting Diabetic nephropathy is a clinical syndrome in a patient with diabetes mellitus that is characterized by persistent albuminuria,
12 Diabetic Nephropathy J. Charles Jennette Introduction/Clinical Setting Diabetic nephropathy is a clinical syndrome in a patient with diabetes mellitus that is characterized by persistent albuminuria,
WE PRESENT a patient with non insulindependent
 RENAL BIOPSY TEACHING CASE Monoclonal Gammopathy in a Type II Diabetic: A Case of Determined Significance Nancy J. Gritter, MD, Simin Goral, MD, and Agnes Fogo, MD INDEX WORDS: Monoclonal gammopathy; nephrotic
RENAL BIOPSY TEACHING CASE Monoclonal Gammopathy in a Type II Diabetic: A Case of Determined Significance Nancy J. Gritter, MD, Simin Goral, MD, and Agnes Fogo, MD INDEX WORDS: Monoclonal gammopathy; nephrotic
Burkitt lymphoma. Sporadic Endemic in Africa associated with EBV Translocations involving MYC gene on chromosome 8
 Heme 8 Burkitt lymphoma Sporadic Endemic in Africa associated with EBV Translocations involving MYC gene on chromosome 8 Most common is t(8;14) Believed to be the fastest growing tumor in humans!!!! Morphology
Heme 8 Burkitt lymphoma Sporadic Endemic in Africa associated with EBV Translocations involving MYC gene on chromosome 8 Most common is t(8;14) Believed to be the fastest growing tumor in humans!!!! Morphology
Thin basement membrane syndrome in adults
 J Clin Pathol 1987;40:318-322 Thin basement membrane syndrome in adults S ABE, Y AMAGASAKI,* S IYORI,t K KONISHI, E KATO, H SAKAGUCHI,: K SHIMOYAMA** From the Department of Internal Medicine and tpathology,
J Clin Pathol 1987;40:318-322 Thin basement membrane syndrome in adults S ABE, Y AMAGASAKI,* S IYORI,t K KONISHI, E KATO, H SAKAGUCHI,: K SHIMOYAMA** From the Department of Internal Medicine and tpathology,
Examination of the light microscopic slide of renal biopsy specimens by utilizing Low-vacuum scanning electron microscope
 SCIENTIFIC INSTRUMENT NEWS 2017 Vol. 9 SEPTEMBER Technical magazine of Electron Microscope and Analytical Instruments. Article Examination of the light microscopic slide of renal biopsy specimens by utilizing
SCIENTIFIC INSTRUMENT NEWS 2017 Vol. 9 SEPTEMBER Technical magazine of Electron Microscope and Analytical Instruments. Article Examination of the light microscopic slide of renal biopsy specimens by utilizing
Proteinuria. Louisiana State University
 Proteinuria W S A V A W C P, 2005 David F. Senior Louisiana State University The normal glomerulus is a highly selective barrier for filtration based on size (and on charge in the case of larger molecules).
Proteinuria W S A V A W C P, 2005 David F. Senior Louisiana State University The normal glomerulus is a highly selective barrier for filtration based on size (and on charge in the case of larger molecules).
The evaluation of pathomorphological changes of intact by neoplastic process kidney parenchyma in patients with renal cell cancer
 The evaluation of pathomorphological changes of intact by neoplastic process kidney parenchyma in patients with renal cell cancer Serhyi Pasichnyk 1, Olga Voronina 2, Yulian Mytsyk 1 1 Lviv National Medical
The evaluation of pathomorphological changes of intact by neoplastic process kidney parenchyma in patients with renal cell cancer Serhyi Pasichnyk 1, Olga Voronina 2, Yulian Mytsyk 1 1 Lviv National Medical
substance staining with IgG, C3 and IgA (trace) Linear deposition of IgG(+), IgA.M(trace) and C3(+++) at the DEJ
 Direct Immunofluorescence: Skin Diagnosis Findings Picture Pemphigus Vulgaris and it s Intracellular cement variants substance staining with IgG, C3 and IgA (trace) Bullous Pemphigoid and it s variants
Direct Immunofluorescence: Skin Diagnosis Findings Picture Pemphigus Vulgaris and it s Intracellular cement variants substance staining with IgG, C3 and IgA (trace) Bullous Pemphigoid and it s variants
EXPERIMENTAL GLOMERULONEPHRITIS BY ANTI-KIDNEY MITOCHONDRIAL ANTISERUM IN THE RABBIT
 INTRODUCTION OF EXPERIMENTAL GLOMERULONEPHRITIS BY ANTI-KIDNEY MITOCHONDRIAL ANTISERUM IN THE RABBIT A. Z. BARABAS,* B.V.M.&S., M.R.C.V.S., D.V.S.M., M.Sc., Ph.D., A. H. NAGI,* M.B., B.S. R. LANNIGAN,t
INTRODUCTION OF EXPERIMENTAL GLOMERULONEPHRITIS BY ANTI-KIDNEY MITOCHONDRIAL ANTISERUM IN THE RABBIT A. Z. BARABAS,* B.V.M.&S., M.R.C.V.S., D.V.S.M., M.Sc., Ph.D., A. H. NAGI,* M.B., B.S. R. LANNIGAN,t
Immune complex deposits in ANCA-associated crescentic glomerulonephritis: A study of 126 cases
 Kidney International, Vol. 65 (2004), pp. 2145 2152 Immune complex deposits in ANCA-associated crescentic glomerulonephritis: A study of 126 cases MARK HAAS and JOSEPH A. EUSTACE Department of Pathology
Kidney International, Vol. 65 (2004), pp. 2145 2152 Immune complex deposits in ANCA-associated crescentic glomerulonephritis: A study of 126 cases MARK HAAS and JOSEPH A. EUSTACE Department of Pathology
Journal of Nephropathology
 www.nephropathol.com DOI: 10.15171/jnp.2018.24 J Nephropathol. 2018;7(3):101-105 Journal of Nephropathology Relationship of CD147 kidney expression with various pathologic lesions, biochemical and demographic
www.nephropathol.com DOI: 10.15171/jnp.2018.24 J Nephropathol. 2018;7(3):101-105 Journal of Nephropathology Relationship of CD147 kidney expression with various pathologic lesions, biochemical and demographic
Mayo Clinic/ RPS Consensus Report on Classification, Diagnosis, and Reporting of Glomerulonephritis
 Mayo Clinic/ RPS Consensus Report on Classification, Diagnosis, and Reporting of Glomerulonephritis Sanjeev Sethi, MD, PhD Department of Laboratory Medicine and Pathology Disclosure Relevant Financial
Mayo Clinic/ RPS Consensus Report on Classification, Diagnosis, and Reporting of Glomerulonephritis Sanjeev Sethi, MD, PhD Department of Laboratory Medicine and Pathology Disclosure Relevant Financial
Dr Ian Roberts Oxford
 Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Present the basic diagnostic features of the commonest conditions causing renal failure Highlight diagnostic pitfalls. Crescentic GN: renal
Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Present the basic diagnostic features of the commonest conditions causing renal failure Highlight diagnostic pitfalls. Crescentic GN: renal
Pathology of the Kidney in Dysproteinemia
 Pathology of the Kidney in Dysproteinemia Pathology of the Kidney in Dysproteinemia Charles N. Gamble, MD, FCAP Universal-Publishers Boca Raton Pathology of the Kidney in Dysproteinemia Copyright 2011
Pathology of the Kidney in Dysproteinemia Pathology of the Kidney in Dysproteinemia Charles N. Gamble, MD, FCAP Universal-Publishers Boca Raton Pathology of the Kidney in Dysproteinemia Copyright 2011
Classification of Glomerular Diseases and Defining Individual Glomerular Lesions: Developing International Consensus
 Classification of Glomerular Diseases and Defining Individual Glomerular Lesions: Developing International Consensus Mark Haas MD, PhD Department of Pathology & Laboratory Medicine Cedars-Sinai Medical
Classification of Glomerular Diseases and Defining Individual Glomerular Lesions: Developing International Consensus Mark Haas MD, PhD Department of Pathology & Laboratory Medicine Cedars-Sinai Medical
Vasishta Tatapudi, M.D. October 23 rd, 2012.
 Vasishta Tatapudi, M.D. October 23 rd, 2012. Case Summary Chief complaint: 45 year old African American male patient presented with left shoulder pain after minor trauma. History of present illness: Two
Vasishta Tatapudi, M.D. October 23 rd, 2012. Case Summary Chief complaint: 45 year old African American male patient presented with left shoulder pain after minor trauma. History of present illness: Two
Case Report Nephrotic Syndrome Secondary to Proliferative Glomerulonephritis with Monoclonal Immunoglobulin Deposits of Lambda Light Chain
 Hindawi Publishing Corporation Case Reports in Nephrology Volume 214, Article ID 164694, 6 pages http://dx.doi.org/1.1155/214/164694 Case Report Nephrotic Syndrome Secondary to Proliferative Glomerulonephritis
Hindawi Publishing Corporation Case Reports in Nephrology Volume 214, Article ID 164694, 6 pages http://dx.doi.org/1.1155/214/164694 Case Report Nephrotic Syndrome Secondary to Proliferative Glomerulonephritis
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
Amyloidosis is a generic term for a group of diseases
 Typing of Amyloidosis in Renal Biopsies Diagnostic Pitfalls Anjali A. Satoskar, MD; Kelly Burdge, MD; Daniel J. Cowden, MD; Gyongyi M. Nadasdy, MD; Lee A. Hebert, MD; Tibor Nadasdy, MD Context. Amyloidosis
Typing of Amyloidosis in Renal Biopsies Diagnostic Pitfalls Anjali A. Satoskar, MD; Kelly Burdge, MD; Daniel J. Cowden, MD; Gyongyi M. Nadasdy, MD; Lee A. Hebert, MD; Tibor Nadasdy, MD Context. Amyloidosis
Chronic Active Thrombotic Microangiopathy in Native and Transplanted Kidneys
 Available online at www.annclinlabsci.org Annals of Clinical & Laboratory Science, vol. 36, no.3, 2006 319 Case Reports: Chronic Active Thrombotic Microangiopathy in Native and Transplanted Kidneys Ping
Available online at www.annclinlabsci.org Annals of Clinical & Laboratory Science, vol. 36, no.3, 2006 319 Case Reports: Chronic Active Thrombotic Microangiopathy in Native and Transplanted Kidneys Ping
Introduction. Acute sodium overload produces renal tubulointerstitial inflammation in normal rats
 Acute sodium overload produces renal tubulointerstitial inflammation in normal rats MI Roson, et al. Kidney International (2006) Introduction Present by Kanya Bunnan and Wiraporn paebua Tubular sodium
Acute sodium overload produces renal tubulointerstitial inflammation in normal rats MI Roson, et al. Kidney International (2006) Introduction Present by Kanya Bunnan and Wiraporn paebua Tubular sodium
Diabetes, Obesity and Heavy Proteinuria
 Diabetes, Obesity and Heavy Proteinuria Clinical Case 41 yo Black woman with heavy proteinuria History 2014: noted to have proteinuria on routine lab testing (1.1g/g). 1+ edema. Blood pressure has been
Diabetes, Obesity and Heavy Proteinuria Clinical Case 41 yo Black woman with heavy proteinuria History 2014: noted to have proteinuria on routine lab testing (1.1g/g). 1+ edema. Blood pressure has been
C3 Glomerulonephritis versus C3 Glomerulopathies?
 Washington University School of Medicine Digital Commons@Becker Kidneycentric Kidneycentric 2016 C3 Glomerulonephritis versus C3 Glomerulopathies? T. Keefe Davis Washington University School of Medicine
Washington University School of Medicine Digital Commons@Becker Kidneycentric Kidneycentric 2016 C3 Glomerulonephritis versus C3 Glomerulopathies? T. Keefe Davis Washington University School of Medicine
J Renal Inj Prev. 2018; 7(1): Journal of Renal Injury Prevention
 J Renal Inj Prev. 2018; 7(1): 22-26. Journal of Renal Injury Prevention DOI: 10.15171/jrip.2018.05 Comparison of clinical and histopathological findings in patients with lupus nephritis having IgG deposits
J Renal Inj Prev. 2018; 7(1): 22-26. Journal of Renal Injury Prevention DOI: 10.15171/jrip.2018.05 Comparison of clinical and histopathological findings in patients with lupus nephritis having IgG deposits
INTRODUCTION TO GLOMERULAR DISEASES
 INTRODUCTION TO GLOMERULAR DISEASES Goal: to explain the general mechanisms leading to glomerular diseases and to analyze what is known about their relationship to morphologic and clinical manifestations
INTRODUCTION TO GLOMERULAR DISEASES Goal: to explain the general mechanisms leading to glomerular diseases and to analyze what is known about their relationship to morphologic and clinical manifestations
HRZZ project: Genotype-Phenotype correlation in Alport's syndrome and Thin Glomerular Basement Membrane Nephropathy. Patohistological Aspects
 HRZZ project: Genotype-Phenotype correlation in Alport's syndrome and Thin Glomerular Basement Membrane Nephropathy Patohistological Aspects Petar Šenjug, MD 1 Professor Danica Galešić Ljubanović, MD,
HRZZ project: Genotype-Phenotype correlation in Alport's syndrome and Thin Glomerular Basement Membrane Nephropathy Patohistological Aspects Petar Šenjug, MD 1 Professor Danica Galešić Ljubanović, MD,
PATHOLOGY Intracellular Degeneration LAB 1
 PATHOLOGY Intracellular Degeneration LAB 1 Cellular swelling Liver Organ :- Liver Lesion :- 1. Narrowing of hepatic sinusoids due to the swelling of hepatocyte. 2. The cytoplasm of affected hepatocyte
PATHOLOGY Intracellular Degeneration LAB 1 Cellular swelling Liver Organ :- Liver Lesion :- 1. Narrowing of hepatic sinusoids due to the swelling of hepatocyte. 2. The cytoplasm of affected hepatocyte
