FLUORESCEIN STUDIES OF PATIENTS WITH MACULAR EDEMA AND PAPILLEDEMA FOLLOWING CATARACT EXTRACTION*
|
|
|
- Virginia Dean
- 5 years ago
- Views:
Transcription
1 FLUORESCEIN STUDIES OF PATIENTS WITH MACULAR EDEMA AND PAPILLEDEMA FOLLOWING CATARACT EXTRACTION* BY J. D. M. Gass, M.D. (BY INVITATION), AND E. W. D. Nortont, M.D. IN 1953, IRVINE' described the syndrome of spontaneous rupture of the hyaloid face following uneventful cataract extraction with the formation of vitreous adhesions to the wound, irritability of the eye, and reduction of visual acuity secondary to vitreous opacities and macular degeneration. Since recent improvements in sutures, instruments, techniques, and antibiotic therapy have lowered the incidence of many postoperative complications, loss of central vision secondary to changes in the maculal-7 and optic nerve2'6'8 following uneventful cataract extraction has been recognition as a major complication of cataract surgery. The funduscopic changes, although characteristic, may be easily overlooked, and the failure of the patient to refract to normal vision may be mistakenly attributed to a variety of other factors, e.g., senile macular degeneration, uveitis, optic neuritis, irregular astigmatism, or hazy media. The true incidence, natural course, etiology, pathogenesis, treatment, and prevention of this disease process are unknown. The purpose of this report is to present the fluorescein angiographic findings in these patients. The macular lesion exhibits a pattern of fluorescence which is sufficiently characteristic and easy to see with the ophthalmoscope and slit-lamp to permit early and accurate diagnosis. Fluorescein studies demonstrate that the intraretinal accumulation of fluid occurring in the macular region and in the area of the optic nerve head is secondary to alterations in the capillary permeability of the intraretinal and papillary vessels. 'From the Bascom Palmer Eye Institute, Department of Ophthalmology, University of Mliami School of Medicine, Miami, Florida. This investigation was supported in part by Public Health Service Research Grants NB and 2T1 NB from the National Institute of Neurological Diseases and Blindness, Bethesda, Maryland, and by the Florida Lions Eye Bank. TR. AM. OPHTH. SOC., vol. 64, 1966
2 Macular Edema and Papilledema 233 METHODS AND MIATERIALS Forty-four patients developing macular edema and/or papilledema following cataract extraction were studied with fluorescein angiography as described by Novotny and Alvis9 and modified by Sever and Justice.10 These patients were obtained from the authors' private practice, the outpatient department of the Jackson Memorial Hospital, and referrals from local ophthalmologists. Periodic photographs were made during the one-hour period following injection of the dye. Biomicroscopic examination of the vitreous and fundus by one or both authors was done in most of these patients, the Hruby lens being used in most instances in order to preserve corneal clarity for fluorescein angiography. Selected patients were also studied with the Goldmann three-mirror contact lens with particular attention to the relationship between vitreous attachments and the macular and optic nerve changes. Funduscopy utilizing the cobalt blue filter in the indirect ophthalmoscope and slit-lamp was done at periodic intervals during the course of fluorescein angiography. Stereophotographs of the fundus made before and during fluorescein angiography were available for the study in some of these patients. FINDINGS Figures 1 through 4 depict angiographically the characteristic sequence of events which can be observed directly through the ophthalmoscope and slit-lamp following the intravenous injection of fluorescein in these patients. Leakage of dye usually appears initially within the retina in the perifoveal area in an irregular circular or wreath-like pattern (Figures IC and 2D1) and progresses both centrally and peripherally at a variable rate. As the dye converges on the foveal area, a remarkable and diagnostic geometric dark stellate figure develops centrally on the background of fluorescein staining (Figures 1F, 2F, 2E, and 4F). The outer margins of the area of fluorescence are typically irregular and splotchy. The accumulation of intraretinal fluorescein lies deep to the larger paramacular vessels, which stand out as dark lines against the background of pooled fluorescein (Figures IE and 6C). The time required for development of the characteristic macular pattern of staining is variable. In most it is well developed in five to fifteen minutes, whereas in others, it becomes evident only after thirty minutes or more. It is important to observe
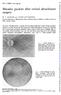
3 FIGURE 1. CASE 1. A, fundus right eye, stellate change indicative of cystoid edema of macula is barely visible. B, early arteriovenous phase. C, early leakage of dye in perifoveal area, about one minute post-injection. D and E, progressive leakage of dye into macular region. F, one hour post-injection showing central dark stellate figure surrounded by fluorescein pooled with intraretinal cystoid spaces.
4 FIGURE 2. CASE 1. FLUORESCEIN STUDY RIGHT EYE FOLLOWING RESOLUTION OF MACULAR EDEMA. A, fundus right eye; note perisistence of small subretinitic deposits on nasal side of macula. B, approximately 15 minutes post-injection showing absence of intraretinal staining. CASE 2. C, left fundus appears remarkably normal. D, venous phase. E, about two minutes post-injection. F, macular staining 45 minutes post-injection.
5 FIGURE 3. CASE 3. A, right fundus; note peripapillary retinal folds and slight blurring of disc margins. B, early re-circulation phase. C, about five minutes post-injection; note widespread splotchy leakage of dye from posterior retina and from optic disc. D, about ten minutes post-injection. E, One hour post-injection; note apparent rapid diffusion of dye away from optic disc (compare with D and E). F, eleven weeks later; one hour post-injection photograph showing no fluorescein staining.
6 FIGURE 4. CASE 4. A, fundus left eye; note papilledema with small hemorrhages near superior disc margin. B, one minute post-injection; note marked splotchy intraretinal fluorescein staining and leakage of dye from optic disc. C, about ten minutes post-injection. D, one hour post-injection; in this case, dye has not extended into central cystoid space. E, fundus right eye; note slightly irregular spot in foveal area. F, one hour postinjection showing pooling of dye in cystoid spaces of retina. B
7 238 J. D. M. Gass and E. W. D. Norton the patient at periodic intervals during the first fifteen minutes following injection because in some patients excessive extravasation of the dye into the vitreous and aqueous humor anteriorly may obscure the fundus details relatively early. This leakage of dye anteriorly accounts for the haze so often present in the angiograms made in the later phases of the study (Figure 3E). In some patients there may be rather widespread splotchy leakage of dye into the retina in the posterior pole of the eye (Figures 4A-4D). Leakage of dye into the optic nerve head and surrounding retina occurs in patients with papilledema (Figures 3 and 4). This is most apparent approximately ten to fifteen minutes after injection of the dye. Rapid diffusion of dye from the nerve head into the vitreous makes leakage there less apparent during the later stages of the study (compare Figures 3C and 3D with Figure 3E). Resolution of fluorescein leakage into the retina and optic nerve generally parallels the clinical resolution of the edema of the macula and optic disc. The patient's vision and the appearance of the fundus may revert to complete normalcy and all fluorescein leakage disappear (Figures 2A, 2B, and 3F). In those patients developing permanent cystic macular changes, leakage of fluorescein into the cystic spaces may or may not be demonstrable. The fluorescein findings in these patients, although quite characteristic, are not pathognomonic. A similar fluorescein staining pattern has been noted in a variety of ocular diseases associated with cystoid edema and degeneration of the macula, e.g., chronic chorioretinitis (Figures 5A-5C), central retinal vein occlusion, chronic papilledema, retinal vasculitis, and in the retina overlying old disciform lesions (Figures 6A-6C). CASE 1 REPORT OF CASES A 60-year-old Caucasian male had an uncomplicated round pupil intracapsular cataract extraction on January 12, He developed a hyphema on the third postoperative day. This cleared completely by the tenth postoperative day. By February 18, 1965, vision in the right eye was 20/30 and it remained at this level until May 5, 1965, when it decreased to 20/60. At that time, cystoid macular edema was noted for the first time. There was also a serous detachment of the macula associated with multiple yellow dot-like subretinitic precipitates. The anterior hyaloid face was intact. Some cells were present in the vitreous. He was referred to the Bascom Palmer Institute for fluorescein study which revealed leakage of dye into the intraretinal cystoid spaces (Figure 1). The patient received
8 Macular Edema and Papilledema 239 A B C FIGURE 5 A, elderly phakic patient with cystoid macular changes secondary to long-standing smoldering peripheral chorioretinitis; vitreous reaction blurs fundus details. B, approximately 15 minutes post-injection: early filling of cystoid spaces as well as widespread and patchy intraretinal leakage of dye. C, one hour post-injection: extensive filling of intraretinal cystoid spaces. Identical findings were present in the opposite eye. prednisone, 80 mg. daily for ten days without improvement. The cystoid macular edema persisted for six months, but in November, 1965, it began to subside and the patient's visual acuity improved to 20/30. At that time, a complete extracapsular cataract extraction was done in the left eye. The postoperative course was uneventful. By January 12, 1966, all cystoid
9 240 J. D. M. Gass and E. W. D. Norton A B C FIGURE 6 A, elderly phakic patient with cystoid macular changes secondary to prolonged serous disciform detachment of the retina and pigment epithelium. B, approximately two minutes post-injection: extensive paramacular fluorescence is primarily choroidal fluorescence transmitted through altered pigment epithelium; mottled fluorescence centrally represents early intraretinal leakage of dye. C, one hour post-injection: typical pattern of fluorescein pooling within intraretinal cystoid spaces overlying background of fluorescein-stained subretinal fluid. edema had disappeared in the right eye and no fluorescein staining was demonstrable (Figures 2A and 2B). In the left eye, however, the patient had developed cystoid macular changes which stained prominently with fluorescein. By January 28, this had subsided and vision in the left eye was 20/20.
10 CASE 2 Macular Edema and Papilledema A 67-year-old Caucasian male had an uneventful round pupil intracapsular cataract extraction in the right eye on September 20, During the early postoperative period the anterior hyaloid face was intact. By the ninth postoperative day, a multilobulated mass of vitreous protruded into the anterior chamber. On October 5, 1965, visual acuity was 20/25+3. At that time the pupil was peaked and a strand of vitreous extended to the wound. The fundus was normal. On December 1, 1965, a round pupil intracapsular cataract extraction was done on the left eye and the postoperative course was virtually identical to that in the right eye. By January 8, 1966, vision in the left eye was 20/20. The anterior hyaloid face was ruptured and the pupil was peaked. The macula was normal. In the right eye, however, vision had dropped to 20/30- and cystoid edema of the macula was present. Vitreous strands could be traced into the posterior part of the eye but no attachment to the macula could be demonstrated. By January 27, 1966, vision in the right eye was 20/40-3 and in the left eye was 20/30. Bilateral cystoid macular edema was present. A moderate number of vitreous inflammatory cells and vitreous strands moved freely just anterior to the macular region in both eyes. The anterior retinal surface appeared smooth and undistorted. No attachment of the vitreous to the macula could be seen. Figures 2C-2F show the fluorescein angiographic findings in the right eye. Similar changes were present in the left eye. The patient received three weeks of systemic steroid therapy. On March 30, visual acuity was 20/20 in the right eye and 20/25 in the left eye. The right macula appeared normal. There was minimal cystoid change in the left eye. On May 6, visual acuity was 20/20 bilaterally, the fundi were normal, and no fluorescein staining was demonstrable. CASE A 51-year-old Caucasian female had an uneventful round pupil intracapsular cataract extraction in the right eye on May 6, Visual acuity was normal in the left eye. On May 25, corrected vision in the right eye was 20/25. On June 8, the corrected vision had decreased to 20/70-. Examination at that time revealed minimal conjunctival injection. The wound was well healed. The cornea was clear. The anterior chamber was deep. The pupil was round and centrally located. No cells or ray were present. The anterior hyaloid face was intact. There were scattered inflammatory cells in the posterior vitreous. The foveal depression was obliterated by the presence of multiple translucent intraretinal cystoid spaces. The surface of the thickened macula was smooth. There was no evidence of vitreous attachment to the macula or unusual light reflexes in the posterior pole. There was some edema of the optic disc associated with concentric retinal folds on the temporal side of the disc (Figure 3A). Figures 3B-3E show the fluorescein angiographic findings on June 8, The patient received a small dose of prednisone for a one-week period. The macular
11 242 J. D. M. Gass and E. W. D. Norton edema and visual acuity improved rapidly and by August 3, 1965, visual acuity had returned to 20/15, the fundus appeared normal, and there was no fluorescein staining (Figure 3F). CASE 4 A 48-year-old Caucasian woman with a history of essential hypertension had a round pupil intracapsular cataract extraction in the left eye on September 8, 1964, and in the right eye on October 7, She corrected to 20/15 in both eyes following surgery. In early November, 1964, she began to experience blurred vision in both eyes. Edema of the macula was noted bilaterally. The patient was treated with systemic steroids and vitamins. Vision in the right eye, reduced to 20/50 at its lowest level, soon improved. The vision in the left eye remained low. She was referred for evaluation and fluorescein study on September 21, Vision in the right eye was 20/30 and in the left eye was 20/300. Both eyes were non-inflamed. The corneas were clear. The anterior chambers were deep. The pupils were round. Transillumination revealed atrophy of the iris pigment epithelium. The iridectomies were opened. The vitreous face was intact bilaterally. Inflammatory cells were present in the vitreous of both eyes. Vitreous strands could be traced posteriorly but no attachment to the macular region could be demonstrated. Cystoid macular edema was present bilaterally. This was quite extensive in the left eye. Papilledema associated with several small hemorrhages was present in the left eye. There was extensive leakage of fluorescein into the posterior retina and optic disc in the left eye (Figure 4). Cystoid edema of the right macula was also demonstrated angiographically (Figures 4E-4F). COMMENT The loss of central vision in these patients has been attributed to vitreous traction on the macula,1'2'7 iritis,1 chorioretinal vascular instability,3'4 choroidal vascular instability2 hypotony,5 papilledema,2 and optic neuritis.6'8 The results of this study provide evidence that the pathogenesis of the visual disturbance involves leakage of serous exudate from the capillary network within the macular portion of the retina and/or the optic nerve head. This extravasation into the macular region, which may be associated with small intraretinal hemorrhages, produces a cystoid 'swelling of the retina which may be completely reversible or which, if it persists, may lead to permanent cystic changes and loss of macular function. The extravasation of exudate into the optic nerve head results in the clinical picture of papilledema. This may also be only a transient phenomenon, but in some cases optic atrophy and reduction in visual acuity may ensue. We have been unable to demonstrate any fluorescein angiographic evidence of alterations in the permeability of the choriocapillaris in this syndrome.
12 Macular Edema and Papilledema 243 The cause of the capillary leakage is not understood. Tolentino and Schepens7 reported "vitreoretinal traction as the only indisputable pathogenic factor in edema of the posterior pole after cataract extraction." Our findings do not agree with theirs. We have been unable to demonstrate to our satisfaction vitreous adherence to the macular region in those patients studied with the Goldmann lens. Often the vitreous haze is such that a detailed view of the macula cannot be obtained. In many cases, however, visibility is good, and in these, vitreous strands surrounded by inflammatory cells can typically be seen moving freely immediately in front of the macular region. In a few cases, unusual light reflexes emanating from the retinal surface suggest the presence of vitreoretinal interface changes, but in most cases, the inner retinal surface appears undisturbed in the macular region. If vitreous traction were present, it seems likely that the remarkably similar and rather symmetrical configuration of the dark geometrical figure produced in these patients by fluorescein injection would be distorted. In patients, usually phakic, who have developed loss of central vision secondary to easily visible vitreous traction on the macula, we have usually been unable to demonstrate evidence of fluorescein leakage, and when leakage has been demonstrated, it has occurred in an irregular pattern and one unlike that seen in the typical patient following cataract extraction. Although vitreous alterations following cataract extraction probably play an important role in the pathogenesis of this syndrome, we do not believe that direct traction by the vitreous on the macula and optic disc is a constant or necessarily an important factor in producing the edema of the macula and/or optic disc. This is not to deny the possible significance of vitreous abnormalities in these patients. The frequent occurrence of delayed rupture of the anterior hyaloid face with vitreous strands leading to the wound area in these patients as well as the high incidence of macular changes following vitreous loss cannot be ignored. The infrequency of this disease following other operations, e.g., retinal detachment and glaucoma procedures, further suggests that vitreous alterations following removal of the lens are of importance in the pathogenesis of this lesion. The frequent mild irritability of the eye, the almost invariable presence of significant numbers of inflammatory cells, particularly in the posterior vitreous, and the apparent response to corticosteroids in some cases suggest that inflammation probably plays an important role in the abnormal capillary permeability. The occurrence of similar structural and inflammatory alterations in the vitreous of many eyes following cataract extraction, the relative
13 244 J. D. M. Gass and E. W. D. Norton infrequency of the development of edema of the macula and optic disc, and the tendency for the disease to be bilateral suggest that some inherent defect in capillary integrity may be present prior to cataract extraction in patients developing this syndrome. To date, however, we have no evidence of unusual systemic vascular disease in these patients. While many questions regarding the etiology, pathogenesis, and treatment of this syndrome remain unanswered, the use of fluorescein has provided us with additional information concerning pathophysiological changes in the macula as well as a new and useful tool for the diagnosis of this syndrome, which undoubtedly occurs more frequently than the reported incidence of less than 2 per cent.2'7 SUMMARY 1. Macular edema and/or papilledema shoulld be suspected in any postoperative cataract patient where visual acuity either fails to improve to normal or suddenly decreases following cataract extraction. 2. In the postoperative cataract patient the pattern of fluorescence following intravenous fluorescein injection is diagnostic and provides the clinician with a valuiable means of detecting the lesion which may be difficult to visualize by other means. 3. Fluorescein studies demonstrate that the pathogenesis of the macular and optic nerve lesions involves leakage of fluid from the retinal and optic nerve head capillaries. 4. Although the cause of this leakage is unknown, biomicroscopic examination of these patients implicates vitreous inflammation, rather than direct vitreous traction on the macula, in the pathogenesis of this disease. ACKNOWLEDGMENT The authors wish to extend thanks to the many physicians who provided patients for this study, and to Mr. Johnny Justice who did the fluorescein fundus photography. REFERENCES 1. Irvine, S. R., A newly defined vitreous syndrome following cataract surgery, Am. J. Ophth., 36: , Welch, R. B., and J. C. Cooper, Macular edema, papilledema, and optic atrophy after cataract extraction, Arch. Ophth., 59:665-75, Nicholls, J. V. V., Macular edema in association with cataract extraction, Am. J. Ophth., 37:665-72, 1954.
14 Macular Edema and Papilledema Nicholls, J. V. V., Concurrence of macular edeema with cataract extraction, Arch. Ophth., 55: , Chandler, P., Complications after cataract extraction: clinical aspects, Tr. Ami. Acad. Ophth., 58:382-96, Gartner, S., Optic neuritis and macular edema following cataract extraction, Eye Ear Nose and Throat Month., 43:45, Tolentino, F. I., and C. L. Schepens, Edema of posterior pole after cataract extraction, Arch. Ophth., 74:781-6, Reese, A. B., and F. D. Carroll, Optic neuritis following cataract extraction, Tr. Am. Acad. Ophth., 62:765-8, Novotny, H. R., and D. L. Alvis, A method of photographing fluorescence in circulating blood in the human retina, Circulation, 24:82, Justice, Jr., J., and R. J. Sever, Technique of fluorescein fundus photography, in J. L. Smith, ed., University of Miami Neuro-ophthalmology Symposium, Vol. 2, pp St. Louis, Mosby, DISCUSSION DR. GEORGE N. WISE. I would like to thank Drs. Gass and Norton for permitting me to see their manuscript well ahead of this meeting. Our own fluorescein study of this lesion is too meager for comment except to state that in no case have we seen a choroidal leak as in central serous retinopathy. With the contact lens and slit-lamp the macular lesion has two appearances: (1) a fuzzy, poorly outlined macular elevation with loss of the foveal reflex and (2) a more clearly seen cystic elevation of the macular area with loss of foveal reflex and a vague border which blends with more normal surrounding retina thereby differing from central serous retinopathy. Probably the turbidity of the intraretinal fluid in the first case accounts for this difference in appearance, for some lesions which appear fuzzy at first later become clearly cystic. Its honeycombed appearance is best seen by retroillumination. Having carefully searched for it, I am in full agreement with the authors in not once having seen a vitreous traction band at the macula. Such a traction band at the macula in conjunction with posterior vitreous detachment has been postulated as a cause of this macular pathology. In almost 100 cases of fresh spontaneous posterior vitreous detachment which I have been studying over the past few years, no case has shown such a maculovitreous adhesion or, for that matter, any macular pathology and only one showed any pathology about the disc-a small superficial retinal hemorrhage. There is clinical and now fluorescein evidence that this lesion is due to a retinal vascular aberration. This honeycombed cystic change in the macula is a common lesion following obstruction of any vein draining the macular area. It has been shown by Verhoeff to be due to a collection of fluid just beneath the deep capillary bed in the internuclear layer. For some unknown reason the cystic change becomes exaggerated at the macula and may form a larger foveal cyst whose rupture gives rise to the so-called macular "hole." A lesion clinically identical to the one under discussion is more common in the venous and capillary
15 246 J. D. M. Gass and E. W. D. Norton obstructive diseases such as Eales' disease, diabetes, and vein obstruction and is the usual lesion seen at the macula when the latter is secondarily involved in cases of chorioretinitis. Here, in 1960, when I called attention to the similarities in some of the fundus findings in partially compensated vein obstruction and uveitis, citing the cystic macula in each and pointing out the probability of the macular lesion in uveitis being due not directly to the toxic action of the uveitis as then thought, but indirectly to its action in slowing the blood flow at the capillary-vein level, I was much taken to task by my discusser. I am therefore pleased to see that the authors have demonstrated by fluorescein the similarity of pattern in the lesion under discussion and the macular lesions of vein obstruction, retinal vasculitis, and chronic chorioretinitis-a pattern which incriminates the retinal perifoveal capillaries in its etiology. There is at times a definite relation between vascular lesions of the macular and peripheral retina. Both are points of terminal circulation and I have wondered if this played any part in their associated pathology. Two of my own cases showed peripheral retinal edema and hemorrhages at the 6 o'clock position suggesting too vigorous a manipulation of counterpressure in this region at the time of lens delivery. The peripheral lesion was not recognized until after the onset of macular edema. Both areas tended to clear together. Have the authors noted any untoward peripheral retinal lesions in their Goldmann 3-mirror lens study? Certainly no one can doubt that I have thoroughly enjoyed this beautiful presentation. DR. JOHN C. LOCKE. Dr. Gass and Dr. Norton are to be congratulated on their excellent studies. I have been interested in the subject of macular disturbances after cataract extraction for eight years, not by fluorescent funduscopic examination, but by a technique which I have called "after-image scotometry" (A.I.S.). This is a simple but extremely sensitive test, which is specific for flat separations of the macula. Using this method we have found that such separations exist in almost all cases of so-called "macular edema" after cataract surgery. The technique and the results were reported in detail in my thesis for this Society, three years ago (Tr. Am. Ophth. Soc., 61: , 1963). Very briefly it consists of adapting the macula for 15 seconds to the bright white light of an electric ophthalmoscope. This produces an after-image scotoma which normally disappears within two minutes. Any separation of the layer of rods and cones from the choriocapillaris causes a delay in the recovery of macular function, with an abnormal persistence of the lightinduced scotoma-in all cases for longer than three minutes. The macular separation may be so slight as to be subclinical-that is, it cannot be seen by slit-lamp or ophthalmoscope and does not cause a measurable scotoma under ordinary conditions of illumination. In carrying out this test, the macular field is plotted first before and then three minutes after dazzling.
16 Macular Edema and Papilledema 247 In serous detachment of the macula after cataract extraction, the persistent light-induced scotoma when plotted at this time is characteristically large (10 to 12 degrees in radius); it is round and pericentral [slide]. In a series of 92 eyes, in which this test was carried out three weeks after cataract extraction, 72 eyes or 78.3 per cent showed a positive test. Thirty-seven eyes or 50 per cent of those with positive test results became negative later-at varying times up to sixteen weeks after operation. There was a direct correlation between the age of the patient and the time at which the test results became negative. Patients in whom the test was negative three weeks after surgery were the younger ones with an average age of 54. Thirty-five of the eyes (or 38 per cent) remained positive longer than 16 weeks. It was in this group that the vitreous adhesion syndrome described by Dr. Irvine occurred. These eyes showed vitreous degeneration on slitlamp examination, and in all cases where it had been possible to do the test prior to operation, the test results had also been positive preoperatively. It was in this group that a sudden late decrease in central vision occasionally occurred in some eyes. These results indicate that what has generally been looked upon as a delayed onset of macular edema after cataract extraction is, in most instances, an exacerbation of a pre-existing subclinical macular disturbance, rather than a new event. The development of uveitis in aphakic eyes, whose macular function had previously been found normal, invariably gave positive test results. The persistent after-image scotoma due to uveitis, however, was much smaller (three to five degrees in radius) than the case already described. I have not been able to postulate the reason for this interesting difference which characterizes the macular response in uveitus. May I suggest to the authors that they consider combining this approach with their continued fluorescein studies, because of its simplicity and its sensitivity. It might help to add even more to the valuable light which their present studies are shedding on this important problem. DR. IRA S. JONES. I would like to contribute to the discussion so that anyone who happens to read the paper by Drs. Gass and Norton will not be unaware of the contribution of Reese, Jones, and Cooper on the same subject. I believe this excellent paper adds an important dimension to the description of this macular syndrome. I feel, however, that the paper adds more to description than it does to etiology. Nothing that was said is incompatible with that which we have said regarding the nature of this syndrome, and the only difference is in the etiology. It seems to me quite suggestive that in the fluorescein studies the abnormalities were noted around the optic disc and at the macula, areas which we feel are the site of vitreous traction or vitreous support. I would like to suggest to Drs. Gass and Norton that they continue to observe these patients carefully in the hope of finding vitreous traction or vitreous support.
17 248 J. D. M. Gass and E. W. D. Norton DR. MICHAEL J. HOGAN. I have been interested in the relationship betweein the vitreous and the retina for 7 or 8 years and have published one paper on this subject. Since this publication, a considerable number of gross and histologic studies have been made on human eyes. In a study of some 500 to 600 fairly normal eyes I have yet to encounter an adhesion between the retina and the vitreous posterior to an area about 5 mm. from the ora serrata. It would seem that if vitreous traction were of importance in the development of macular degenerations following cataract extraction, an occasional adhesion would be found between the vitreous and the retina in a normal eye or even in a diseased eye enucleated for some other purpose. It seems difficult to believe that direct vitreous traction is important in the causation of this disease, and it appears more likely that vitreous traction through another mechanism, probably in the periphery of the eye, is more important than traction directly on the macular area. We have evidence in uveitis eyes, for example, that changes in the region of the ora serrata can lead to shrinkage of the vitreous base followed by resulting secondary changes in the posterior eye. I have two questions to ask Dr. Gass and Dr. Norton. One is this: I am not quite clear why they mentioned the small whitish area in the fovea which was not the foveal reflex. Is this an area of leakage, or does this represent an area of intense edema? Secondly, can they, by their studies, evolve a prognosis based on the fluorescein pattern? In other words, is there a type of pattern that could be used to indicate a good prognosis, or one that would indicate a poor prognosis? One final comment in regard to Dr. Locke's statements has to do with some work that is being done by one of our residents in regard to photostress testing, which is similar to what Dr. Locke described. He has found that in normal individuals, commencing at age 40, there is gradual deterioration of a person's ability to recover from photostress testing. It is a perfectly normal phenomenon in individuals, and it becomes worse with increasing age. This suggests that something is going on in the macular region which may predispose to this type of change following cataract surgery. We have a paper which will be published in the coming A.M.A. meeting which would seem to explain his findings. The study suggests a histologic cause for the degeneration of the retina in elderly individuals. DR. J. DONALD GASS. I certainly appreciate the comments of Drs. Wise, Long, Jones and Hogan. In answer to Dr. Wise's question, we have not noted peripheral lesions of any specific type in these patients. Dr. Locke brings up some very interesting suggestions; and as a matter of fact we plan to incorporate similar studies for macular function in our evaluation of patients with macular disease.
18 Macular Edeema and Papilledema 249 In regard to Dr. Jones' comment, we certainly do not know the etiology of this syndrome. I think it is interesting how different people canl look at the same patients and see different things, and I believe it points up the difficulty in examination of the posterior part of the eye. We certainly feel that vitreous must play a very important role in the developmenit of this lesion. XVte also admit that by a process of tractioni in a few cases, vitreous can cause loss of macular function. In none of our aphakic patients studied to date, however, have we been able to demonstrate vitreous traction on the macular region. The reason I mentioned the yellonw spot in the foveal area is because it can be misinterpreted as the foveal reflex in a fundus which at times mav superficially appear quite normal. I do not know the nature of this spot. It may be exudate on the back of the retina in the foveal area. I have placed some stereophotographs of one of the patients whom I presented here at the back of the room. I think the yellow spot shows very nicely, and if any of you have ideas about what it is I would like to hear from vou. In regard to prognosis, it is my impression that there is really Ino way to gain any prognostic information from a single study or from repeated studies. It has been our experience that most of these patients over a period of several months will show a gradual decrease in the amount of fluorescein leakage which closely parallels the progressive increase in their visual acuity. Not all of these patients get better. For almost two years now, we have followed some who still show fluorescein staining and who have not improved one iota.
Disease-Specific Fluorescein Angiography
 Ruth E. Picchiottino, CRA Disease-Specific Fluorescein Angiography 15 Disease-Specific Fluorescein Angiography Recommendations for tailoring retinal fluorescein angiography to diabetic retinopathy, macular
Ruth E. Picchiottino, CRA Disease-Specific Fluorescein Angiography 15 Disease-Specific Fluorescein Angiography Recommendations for tailoring retinal fluorescein angiography to diabetic retinopathy, macular
Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (CSC)
 HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
RETINAL DETACHMENT AT THE POSTERIOR POLE*
 Brit. J. Ophthal. (1958) 42, 749. RETINAL DETACHMENT AT THE POSTERIOR POLE* BY CALBERT I. PHILLIPSt Institute of Ophthalmology, University oflondon THE common feature of the cases to be described in this
Brit. J. Ophthal. (1958) 42, 749. RETINAL DETACHMENT AT THE POSTERIOR POLE* BY CALBERT I. PHILLIPSt Institute of Ophthalmology, University oflondon THE common feature of the cases to be described in this
OCT Angiography in Primary Eye Care
 OCT Angiography in Primary Eye Care An Image Interpretation Primer Julie Rodman, OD, MS, FAAO and Nadia Waheed, MD, MPH Table of Contents Diabetic Retinopathy 3-6 Choroidal Neovascularization 7-9 Central
OCT Angiography in Primary Eye Care An Image Interpretation Primer Julie Rodman, OD, MS, FAAO and Nadia Waheed, MD, MPH Table of Contents Diabetic Retinopathy 3-6 Choroidal Neovascularization 7-9 Central
 measure of your overall performance. An isolated glucose test is helpful to let you know what your sugar level is at one moment, but it doesn t tell you whether or not your diabetes is under adequate control
measure of your overall performance. An isolated glucose test is helpful to let you know what your sugar level is at one moment, but it doesn t tell you whether or not your diabetes is under adequate control
Coagulative necrosis in a malignant melanoma of the choroid at the macula with extensive subretinal hemorrhage
 Coagulative necrosis in a malignant melanoma of the choroid at the macula with extensive subretinal hemorrhage Robert D. Yee, Robert Y. Foos, and Bradley R. Straatsma The authors present a case report
Coagulative necrosis in a malignant melanoma of the choroid at the macula with extensive subretinal hemorrhage Robert D. Yee, Robert Y. Foos, and Bradley R. Straatsma The authors present a case report
Yasser R. Serag, MD Tamer Wasfi, MD El- Saied El-Dessoukey, MD Magdi S. Moussa, MD Anselm Kampik, MD
 Microperimetric Evaluation of Brilliant Blue G- assisted Internal Limiting Membrane Peeling By Yasser R. Serag, MD Tamer Wasfi, MD El- Saied El-Dessoukey, MD Magdi S. Moussa, MD Anselm Kampik, MD The internal
Microperimetric Evaluation of Brilliant Blue G- assisted Internal Limiting Membrane Peeling By Yasser R. Serag, MD Tamer Wasfi, MD El- Saied El-Dessoukey, MD Magdi S. Moussa, MD Anselm Kampik, MD The internal
Scrub In. What is the function of vitreous humor? What does the pupil do when exposed to bright light? a. Maintain eye shape and provide color vision
 Scrub In What is the function of vitreous humor? a. Maintain eye shape and provide color vision b. Maintain eye shape and refract light rays c. Provide night vision and color vision d. Provide night vision
Scrub In What is the function of vitreous humor? a. Maintain eye shape and provide color vision b. Maintain eye shape and refract light rays c. Provide night vision and color vision d. Provide night vision
Dr/ Marwa Abdellah EOS /16/2018. Dr/ Marwa Abdellah EOS When do you ask Fluorescein angiography for optic disc diseases???
 When do you ask Fluorescein angiography for optic disc diseases??? 1 NORMAL OPTIC DISC The normal optic disc on fluorescein angiography is fluorescent due to filling of vessels arising from the posterior
When do you ask Fluorescein angiography for optic disc diseases??? 1 NORMAL OPTIC DISC The normal optic disc on fluorescein angiography is fluorescent due to filling of vessels arising from the posterior
UVEITIS IN GENERAL. Information for patients UVEITIS CLINIC WHAT IS UVEITIS? MAIN CATEGORIES OF UVEITIS
 Information for patients UVEITIS CLINIC UVEITIS IN GENERAL WHAT IS UVEITIS? The uvea is a name given to the pigmented layer of tissue inside the eye. When all or part of the uvea becomes inflamed, the
Information for patients UVEITIS CLINIC UVEITIS IN GENERAL WHAT IS UVEITIS? The uvea is a name given to the pigmented layer of tissue inside the eye. When all or part of the uvea becomes inflamed, the
PART 1: GENERAL RETINAL ANATOMY
 PART 1: GENERAL RETINAL ANATOMY General Anatomy At Ora Serrata At Optic Nerve Head Fundoscopic View Of Normal Retina What Is So Special About Diabetic Retinopathy? The WHO definition of blindness is
PART 1: GENERAL RETINAL ANATOMY General Anatomy At Ora Serrata At Optic Nerve Head Fundoscopic View Of Normal Retina What Is So Special About Diabetic Retinopathy? The WHO definition of blindness is
RETINAL CONDITIONS RETINAL CONDITIONS
 GENERAL INFORMATION RETINAL CONDITIONS RETINAL CONDITIONS WHAT ARE RETINAL CONDITIONS? Retinal conditions affect the light-sensitive tissue at the back of eye known as the retina. They include diseases
GENERAL INFORMATION RETINAL CONDITIONS RETINAL CONDITIONS WHAT ARE RETINAL CONDITIONS? Retinal conditions affect the light-sensitive tissue at the back of eye known as the retina. They include diseases
The Human Eye. Cornea Iris. Pupil. Lens. Retina
 The Retina Thin layer of light-sensitive tissue at the back of the eye (the film of the camera). Light rays are focused on the retina then transmitted to the brain. The macula is the very small area in
The Retina Thin layer of light-sensitive tissue at the back of the eye (the film of the camera). Light rays are focused on the retina then transmitted to the brain. The macula is the very small area in
Case Report: Indocyanine Green Dye Leakage from Retinal Artery in Branch Retinal Vein Occlusion
 Case Report: Indocyanine Green Dye Leakage from Retinal Artery in Branch Retinal Vein Occlusion Hiroki Fujita, Kyoko Ohno-Matsui, Soh Futagami and Takashi Tokoro Department of Visual Science, Tokyo Medical
Case Report: Indocyanine Green Dye Leakage from Retinal Artery in Branch Retinal Vein Occlusion Hiroki Fujita, Kyoko Ohno-Matsui, Soh Futagami and Takashi Tokoro Department of Visual Science, Tokyo Medical
Late retinal reattachment
 :British Journal of Ophthalmology, 1981, 65, 142-146 Late retinal reattachment S. N. KOKOLAKIS, L. BRAVO, AND A. H. CHIGNELL From the Ophthalmic Department, St Thomas's Hospital, London SEI SUMMARY Six
:British Journal of Ophthalmology, 1981, 65, 142-146 Late retinal reattachment S. N. KOKOLAKIS, L. BRAVO, AND A. H. CHIGNELL From the Ophthalmic Department, St Thomas's Hospital, London SEI SUMMARY Six
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA
 OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
OCULAR HEMORRHAGES. ROSCOE J. KENNEDY, M.D. Department of Ophthalmology
 OCULAR HEMORRHAGES ROSCOE J. KENNEDY, M.D. Department of Ophthalmology Ocular hemorrhages are important not only because they produce visual loss but also because they usually indicate a disorder elsewhere
OCULAR HEMORRHAGES ROSCOE J. KENNEDY, M.D. Department of Ophthalmology Ocular hemorrhages are important not only because they produce visual loss but also because they usually indicate a disorder elsewhere
A Patient s Guide to Diabetic Retinopathy
 Diabetic Retinopathy A Patient s Guide to Diabetic Retinopathy 840 Walnut Street, Philadelphia PA 19107 www.willseye.org Diabetic Retinopathy 1. Definition Diabetic retinopathy is a complication of diabetes
Diabetic Retinopathy A Patient s Guide to Diabetic Retinopathy 840 Walnut Street, Philadelphia PA 19107 www.willseye.org Diabetic Retinopathy 1. Definition Diabetic retinopathy is a complication of diabetes
Test Bank for Medical Surgical Nursing An Integrated Approach 3rd Edition by White
 Test Bank for Medical Surgical Nursing An Integrated Approach 3rd Edition by White Link full download : http://testbankair.com/download/test-bank-for-medical-surgical-nursing-anintegrated-approach-3rd-edition-by-white/
Test Bank for Medical Surgical Nursing An Integrated Approach 3rd Edition by White Link full download : http://testbankair.com/download/test-bank-for-medical-surgical-nursing-anintegrated-approach-3rd-edition-by-white/
HYPERPLASIA OF THE ANTERIOR LAYER OF THE IRIS STROMA*t
 Brit. J. Ophthal. (1965) 49, 516 HYPERPLASIA OF THE ANTERIOR LAYER OF THE IRIS STROMA*t BY MALCOLM N. LUXENBERG From the Bascom Palmer Eye Institute, Department of Ophthalmology, University of Miami School
Brit. J. Ophthal. (1965) 49, 516 HYPERPLASIA OF THE ANTERIOR LAYER OF THE IRIS STROMA*t BY MALCOLM N. LUXENBERG From the Bascom Palmer Eye Institute, Department of Ophthalmology, University of Miami School
ZEISS AngioPlex OCT Angiography. Clinical Case Reports
 Clinical Case Reports Proliferative Diabetic Retinopathy (PDR) Case Report 969 PROLIFERATIVE DIABETIC RETINOPATHY 1 1-year-old diabetic female presents for follow-up of proliferative diabetic retinopathy
Clinical Case Reports Proliferative Diabetic Retinopathy (PDR) Case Report 969 PROLIFERATIVE DIABETIC RETINOPATHY 1 1-year-old diabetic female presents for follow-up of proliferative diabetic retinopathy
What Is O.C.T. and Why Should I Give A Rip? OCT & Me How Optical Coherence Tomography Changed the Life of a Small Town Optometrist 5/19/2014
 OCT & Me How Optical Coherence Tomography Changed the Life of a Small Town Optometrist Email: myoder@wcoil.com Mark A. Yoder, O.D. 107 N. Main Street PO Box 123 Bluffton, OH 45817 @yoderod 115.02 Histoplasma
OCT & Me How Optical Coherence Tomography Changed the Life of a Small Town Optometrist Email: myoder@wcoil.com Mark A. Yoder, O.D. 107 N. Main Street PO Box 123 Bluffton, OH 45817 @yoderod 115.02 Histoplasma
Ocular findings in children with sickle
 Brit. J. Ophthal. (I 974) 58, 644 Ocular findings in children with sickle cell haemoglobin C disease in Jamaica PATRICK I. CONDON, ROBERT GRAY, AND GRAHAM R. SERJEANT From the Medical Research Council,
Brit. J. Ophthal. (I 974) 58, 644 Ocular findings in children with sickle cell haemoglobin C disease in Jamaica PATRICK I. CONDON, ROBERT GRAY, AND GRAHAM R. SERJEANT From the Medical Research Council,
What is Age-Related Macular Degeneration?
 Intravitreal Injections Eylea / Lucentis Patient Information What is Age-Related Macular Degeneration? Age-related macular degeneration (AMD) is an eye condition found in older people, which may lead to
Intravitreal Injections Eylea / Lucentis Patient Information What is Age-Related Macular Degeneration? Age-related macular degeneration (AMD) is an eye condition found in older people, which may lead to
OCT Assessment of the Vitreoretinal Relationship in CSME
 December 2007 Sonia Rani John et al. - IFIS 375 ORIGINAL ARTICLE OCT Assessment of the Vitreoretinal Relationship in CSME Dr. Manoj S. DNB FRCS, Dr. Unnikrishnan Nair MS DO FRCS, Dr. Gargi Sathish MS Introduction
December 2007 Sonia Rani John et al. - IFIS 375 ORIGINAL ARTICLE OCT Assessment of the Vitreoretinal Relationship in CSME Dr. Manoj S. DNB FRCS, Dr. Unnikrishnan Nair MS DO FRCS, Dr. Gargi Sathish MS Introduction
Five Things You re Missing with Your Fundus Camera
 ebook Five Things You re Missing with Your Fundus Camera By Donald J. Siegel, OD, Sun City West Eye Care Sponsored by: Before I began incorporating EIDON true-color imaging into my practice, my retinal
ebook Five Things You re Missing with Your Fundus Camera By Donald J. Siegel, OD, Sun City West Eye Care Sponsored by: Before I began incorporating EIDON true-color imaging into my practice, my retinal
ISPUB.COM. Photopsia post flu: A case of MEWDS. S Baisakhiya, S Dulani, S Lele INTRODUCTION CASE HISTORY
 ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 8 Number 1 Photopsia post flu: A case of MEWDS S Baisakhiya, S Dulani, S Lele Citation S Baisakhiya, S Dulani, S Lele. Photopsia
ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 8 Number 1 Photopsia post flu: A case of MEWDS S Baisakhiya, S Dulani, S Lele Citation S Baisakhiya, S Dulani, S Lele. Photopsia
Clinically Significant Macular Edema (CSME)
 Clinically Significant Macular Edema (CSME) 1 Clinically Significant Macular Edema (CSME) Sadrina T. Shaw OMT I Student July 26, 2014 Advisor: Dr. Uwaydat Clinically Significant Macular Edema (CSME) 2
Clinically Significant Macular Edema (CSME) 1 Clinically Significant Macular Edema (CSME) Sadrina T. Shaw OMT I Student July 26, 2014 Advisor: Dr. Uwaydat Clinically Significant Macular Edema (CSME) 2
Technologies and Methods for Visualizing the Retina
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/revealing-retina/technologies-and-methods-for-visualizing-theretina/3663/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/revealing-retina/technologies-and-methods-for-visualizing-theretina/3663/
evaluation of vitreoretinal adhesions in exudative AMD using optical coherence tomography
 evaluation of vitreoretinal adhesions in exudative AMD using optical coherence tomography Dr. Mahmoud Alaa Abouhusssein, FRCO Lecturer of ophthalmology, Alexandria university Dr. Amir Ramadan Gomaa, MD
evaluation of vitreoretinal adhesions in exudative AMD using optical coherence tomography Dr. Mahmoud Alaa Abouhusssein, FRCO Lecturer of ophthalmology, Alexandria university Dr. Amir Ramadan Gomaa, MD
Cystoid macular edema associated with limbal melanoma*
 Graefe's Arch Clin Exp Ophthalmol (1983) 221:101-105 Graefe's Archive for CliniCal and Experimental Ophthalmology Springer-Verlag 1983 Cystoid macular edema associated with limbal melanoma* J. Reimer Wolter
Graefe's Arch Clin Exp Ophthalmol (1983) 221:101-105 Graefe's Archive for CliniCal and Experimental Ophthalmology Springer-Verlag 1983 Cystoid macular edema associated with limbal melanoma* J. Reimer Wolter
Central venous occlusion
 Central venous occlusion Central venous occlusion (right eye) There are dark haemorrhages at the macula and all over the retina. Choroidal haemangioma A choroidal haemangioma has salmon pink colour. There
Central venous occlusion Central venous occlusion (right eye) There are dark haemorrhages at the macula and all over the retina. Choroidal haemangioma A choroidal haemangioma has salmon pink colour. There
When optical coherence tomography (OCT)
 Macular Imaging: SD-OCT in nterior Segment Surgical Practice Many pathologic processes of the macula can be visualized or quantified only with this modality. y Steven G. Safran, MD When optical coherence
Macular Imaging: SD-OCT in nterior Segment Surgical Practice Many pathologic processes of the macula can be visualized or quantified only with this modality. y Steven G. Safran, MD When optical coherence
68 Reports Investiuativc Ophthalmology
 68 Reports Investiuativc Ophthalmology January 1975 Aphakic macular edema: incidence and pathogenesis. 0 R. A. HITCHINCS, I. H. CHISHOLM, AND A. C. BIRD. In a prospective study, the incidence of cystoid
68 Reports Investiuativc Ophthalmology January 1975 Aphakic macular edema: incidence and pathogenesis. 0 R. A. HITCHINCS, I. H. CHISHOLM, AND A. C. BIRD. In a prospective study, the incidence of cystoid
MANAGING DIABETIC RETINOPATHY. <Your Hospital Name> <Your Logo>
 MANAGING DIABETIC RETINOPATHY It s difficult living with Diabetes Mellitus. Ask any diabetic... Their lives are centered around meal plans, glucose levels, and insulin
MANAGING DIABETIC RETINOPATHY It s difficult living with Diabetes Mellitus. Ask any diabetic... Their lives are centered around meal plans, glucose levels, and insulin
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome)
 Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
surgery Macular puckers after retinal detachment and loss of the macular reflex with a greyish appearance of the macula
 Brit. J. Ophthal. (97 ) 55, 451 Macular puckers after retinal detachment surgery W. S. HAGLER AND UPAL ATURALYA* From the Department of Ophthalmology, Emory University School of Medicine, and Emory University
Brit. J. Ophthal. (97 ) 55, 451 Macular puckers after retinal detachment surgery W. S. HAGLER AND UPAL ATURALYA* From the Department of Ophthalmology, Emory University School of Medicine, and Emory University
Unexplained visual loss in seven easy steps
 Unexplained visual loss in seven easy steps Andrew G. Lee, MD Chair Ophthalmology, Houston Methodist Hospital, Professor, Weill Cornell MC; Adjunct Professor, Baylor COM, U Iowa, UTMB Galveston, UT MD
Unexplained visual loss in seven easy steps Andrew G. Lee, MD Chair Ophthalmology, Houston Methodist Hospital, Professor, Weill Cornell MC; Adjunct Professor, Baylor COM, U Iowa, UTMB Galveston, UT MD
OPTIC DISC PIT Pathogenesis and Management OPTIC DISC PIT
 OPTIC DISC PIT Pathogenesis and Management Abdel-Latif Siam Ain Shams University Cairo Egypt OPTIC DISC PIT Congenital pit is an atypical coloboma usually located on the temporal edge of the disc, associated
OPTIC DISC PIT Pathogenesis and Management Abdel-Latif Siam Ain Shams University Cairo Egypt OPTIC DISC PIT Congenital pit is an atypical coloboma usually located on the temporal edge of the disc, associated
Convergence in. Introduction. Case Report: Dr. Piyali SenM.B.B.S, Dr. Abhipsha Saha M.B.B.S, Dr. Anuradha Chandra M.S,FAICO
 Convergence in Dr. Piyali SenM.B.B.S, Dr. Abhipsha Saha M.B.B.S, Dr. Anuradha Chandra M.S,FAICO Introduction non-progressive ophthalmoplegia with or without ptosis affecting part or all of the occulomotor
Convergence in Dr. Piyali SenM.B.B.S, Dr. Abhipsha Saha M.B.B.S, Dr. Anuradha Chandra M.S,FAICO Introduction non-progressive ophthalmoplegia with or without ptosis affecting part or all of the occulomotor
Retinal pigment epithelial detachments in the elderly:
 British Journal of Ophthalmology, 1985, 69, 397-403 Retinal pigment epithelial detachments in the elderly: classification and outcome A G CASSWELL, D KOHEN, AND A C BIRD From Moorfields Eye Hospital, City
British Journal of Ophthalmology, 1985, 69, 397-403 Retinal pigment epithelial detachments in the elderly: classification and outcome A G CASSWELL, D KOHEN, AND A C BIRD From Moorfields Eye Hospital, City
Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk cases
 European Journal of Ophthalmology / Vol. 14 no. 4, 2004 / pp. 325-329 Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk
European Journal of Ophthalmology / Vol. 14 no. 4, 2004 / pp. 325-329 Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk
EPIRETINAL MEMBRANE & VITREOMACULAR TRACTION
 EPIRETINAL MEMBRANE & VITREOMACULAR TRACTION Management of ERM and VMT K.V.Chalam,MD,PhD,MBA,FACS Professor and Director of Retina Loma Linda Eye Institute Los Angeles, USA REVIEW ANATOMY The vitreous
EPIRETINAL MEMBRANE & VITREOMACULAR TRACTION Management of ERM and VMT K.V.Chalam,MD,PhD,MBA,FACS Professor and Director of Retina Loma Linda Eye Institute Los Angeles, USA REVIEW ANATOMY The vitreous
Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
 Columbia International Publishing Journal of Ophthalmic Research (2014) Research Article Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
Columbia International Publishing Journal of Ophthalmic Research (2014) Research Article Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
UNDERSTAND MORE ABOUT UVEITIS UVEITIS
 UNDERSTAND MORE ABOUT UVEITIS UVEITIS Uveitis What is uveitis? Uveitis is inflammation of the uvea, the middle layer of your eye. The eye is shaped much like a tennis ball, with three different layers
UNDERSTAND MORE ABOUT UVEITIS UVEITIS Uveitis What is uveitis? Uveitis is inflammation of the uvea, the middle layer of your eye. The eye is shaped much like a tennis ball, with three different layers
Moncef Khairallah, MD
 Moncef Khairallah, MD Department of Ophthalmology, Fattouma Bourguiba University Hospital Faculty of Medicine, University of Monastir Monastir, Tunisia INTRODUCTION IU: anatomic form of uveitis involving
Moncef Khairallah, MD Department of Ophthalmology, Fattouma Bourguiba University Hospital Faculty of Medicine, University of Monastir Monastir, Tunisia INTRODUCTION IU: anatomic form of uveitis involving
Choroidal Neovascularization in Sympathetic Ophthalmia
 Choroidal Neovascularization in Sympathetic Ophthalmia Lucia Sobrin, Miguel Cordero Coma, C. Stephen Foster Case Report A 49-year-old man presented after a ruptured globe repair of his left eye status
Choroidal Neovascularization in Sympathetic Ophthalmia Lucia Sobrin, Miguel Cordero Coma, C. Stephen Foster Case Report A 49-year-old man presented after a ruptured globe repair of his left eye status
Spontaneous Large Serous Retinal Pigment Epithelial Tear
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
Diabetic Retinopathy
 Diabetic Retinopathy Diabetes can be classified into type 1 diabetes mellitus and type 2 diabetes mellitus, formerly known as insulin-dependent diabetes mellitus, and non-insulin diabetes mellitus, respectively.
Diabetic Retinopathy Diabetes can be classified into type 1 diabetes mellitus and type 2 diabetes mellitus, formerly known as insulin-dependent diabetes mellitus, and non-insulin diabetes mellitus, respectively.
Diabetes & Your Eyes
 Diabetes & Your Eyes Diabetes is a disease that occurs when the pancreas does not secrete enough insulin or the body is unable to process it properly. Insulin is the hormone that regulates the level of
Diabetes & Your Eyes Diabetes is a disease that occurs when the pancreas does not secrete enough insulin or the body is unable to process it properly. Insulin is the hormone that regulates the level of
Assisting in Ophthalmology. Copyright 2011, 2007, 2003, 1999 by Saunders, an imprint of Elsevier Inc. All rights reserved.
 Assisting in Ophthalmology Learning Objectives Define, spell, and pronounce the terms listed in the vocabulary. Apply critical thinking skills in performing patient assessment and care. Explain the differences
Assisting in Ophthalmology Learning Objectives Define, spell, and pronounce the terms listed in the vocabulary. Apply critical thinking skills in performing patient assessment and care. Explain the differences
IMAGE OF THE MOMENT PRACTICAL NEUROLOGY
 178 PRACTICAL NEUROLOGY IMAGE OF THE MOMENT Gawn G. McIlwaine*, James H. Vallance* and Christian J. Lueck *Princess Alexandra Eye Pavilion, Chalmers Street, Edinburgh UK; The Canberra Hospital, P.O. Box
178 PRACTICAL NEUROLOGY IMAGE OF THE MOMENT Gawn G. McIlwaine*, James H. Vallance* and Christian J. Lueck *Princess Alexandra Eye Pavilion, Chalmers Street, Edinburgh UK; The Canberra Hospital, P.O. Box
Photocoagulation of disciform macular lesions
 British Journal of Ophthalmology, 1979, 63, 669-673 Photocoagulation of disciform macular lesions with krypton laser A. C. BIRD AND R. H. B. GREY From the Institute of Ophthalmology, Moorfields Eye Hospital,
British Journal of Ophthalmology, 1979, 63, 669-673 Photocoagulation of disciform macular lesions with krypton laser A. C. BIRD AND R. H. B. GREY From the Institute of Ophthalmology, Moorfields Eye Hospital,
What You Should Know About Acute Macular Neuroretinopathy
 What You Should Know About Acute Macular Neuroretinopathy David J. Browning MD, PhD Chong Lee BS Acute macular neuroretinopathy is a condition characterized by the sudden, painless onset of paracentral
What You Should Know About Acute Macular Neuroretinopathy David J. Browning MD, PhD Chong Lee BS Acute macular neuroretinopathy is a condition characterized by the sudden, painless onset of paracentral
Year 2 MBChB Clinical Skills Session Ophthalmoscopy. Reviewed & ratified by: Mr M Batterbury Consultant Ophthalmologist
 Year 2 MBChB Clinical Skills Session Ophthalmoscopy Reviewed & ratified by: o Mr M Batterbury Consultant Ophthalmologist Learning objectives o To understand the anatomy and physiology of the external and
Year 2 MBChB Clinical Skills Session Ophthalmoscopy Reviewed & ratified by: o Mr M Batterbury Consultant Ophthalmologist Learning objectives o To understand the anatomy and physiology of the external and
A Case of Carotid-Cavernous Fistula
 A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
Diabetic retinopathy damage to the blood vessels in the retina. Cataract clouding of the eye s lens. Cataracts develop at an earlier age in people
 Diabetic Retinopathy What is diabetic eye disease? Diabetic eye disease refers to a group of eye problems that people with diabetes may face as a complication of diabetes. All can cause severe vision loss
Diabetic Retinopathy What is diabetic eye disease? Diabetic eye disease refers to a group of eye problems that people with diabetes may face as a complication of diabetes. All can cause severe vision loss
Federov iris-supported intraocular acrylic lens
 Brit. j. Ophthal. (I974) 58, 718 Federov iris-supported intraocular acrylic lens P. JARDINE AND J. H. SANDFORD-SMITH Bristol Eye Hospital, Bristol The use of intraocular lenses in the correction of aphakia
Brit. j. Ophthal. (I974) 58, 718 Federov iris-supported intraocular acrylic lens P. JARDINE AND J. H. SANDFORD-SMITH Bristol Eye Hospital, Bristol The use of intraocular lenses in the correction of aphakia
Rare Presentation of Ocular Toxoplasmosis
 Case Report Rare Presentation of Ocular Toxoplasmosis Rakhshandeh Alipanahi MD From Department of Ophthalmology, Nikookari Eye Hospital, Tabriz University of Medical Sciences, Tabriz, Iran. Correspondence:
Case Report Rare Presentation of Ocular Toxoplasmosis Rakhshandeh Alipanahi MD From Department of Ophthalmology, Nikookari Eye Hospital, Tabriz University of Medical Sciences, Tabriz, Iran. Correspondence:
Rapid Visual Loss. Dr Michael Johnson PhD FCOptom DipOrth DipGlauc DipTp(IP) Independent Prescribing Optometrist
 Rapid Visual Loss Dr Michael Johnson PhD FCOptom DipOrth DipGlauc DipTp(IP) Independent Prescribing Optometrist Outline Pathophysiology Differential diagnosis. Patient scenarios in community practice:
Rapid Visual Loss Dr Michael Johnson PhD FCOptom DipOrth DipGlauc DipTp(IP) Independent Prescribing Optometrist Outline Pathophysiology Differential diagnosis. Patient scenarios in community practice:
Diabetic Retinopathy
 Diabetic Retinopathy Diabetes mellitus is one of the leading causes of irreversible blindness worldwide. In the United States, it is the most common cause of blindness in people younger than 65 years.
Diabetic Retinopathy Diabetes mellitus is one of the leading causes of irreversible blindness worldwide. In the United States, it is the most common cause of blindness in people younger than 65 years.
Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and
 British Journal of Ophthalmology, 1977, 61, 278-284 Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and neovascular glaucoma LEILA LAATIKAINEN From Moorfields Eye Hospital,
British Journal of Ophthalmology, 1977, 61, 278-284 Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and neovascular glaucoma LEILA LAATIKAINEN From Moorfields Eye Hospital,
OUR EYES & HOW WE SEE
 OUR EYES & HOW WE SEE UNDERSTAND MORE ABOUT OUR EYES & HOW WE SEE Our Eyes & How We See The eye is our visual gateway to the world. Within it, an array of delicate components labour away to give us the
OUR EYES & HOW WE SEE UNDERSTAND MORE ABOUT OUR EYES & HOW WE SEE Our Eyes & How We See The eye is our visual gateway to the world. Within it, an array of delicate components labour away to give us the
Diabetic Retinopathy A Presentation for the Public
 Diabetic Retinopathy A Presentation for the Public Ray M. Balyeat, MD The Eye Institute Tulsa, Oklahoma The Healthy Eye Light rays enter the eye through the cornea, pupil and lens. These light rays are
Diabetic Retinopathy A Presentation for the Public Ray M. Balyeat, MD The Eye Institute Tulsa, Oklahoma The Healthy Eye Light rays enter the eye through the cornea, pupil and lens. These light rays are
UVEITIS. Dr. Yılmaz ÖZYAZGAN
 UVEITIS Dr. Yılmaz ÖZYAZGAN UVEITIS DEFINITION BY STRICT DEFINITION, UVEITIS IS AN INFLAMMATION OF UVEAL TRACT. BUT IN PRACTICAL, IT IS GENERALLY NOT RESTRICTED TO THE UVEA AND INVOLVES OTHER ADJACENT
UVEITIS Dr. Yılmaz ÖZYAZGAN UVEITIS DEFINITION BY STRICT DEFINITION, UVEITIS IS AN INFLAMMATION OF UVEAL TRACT. BUT IN PRACTICAL, IT IS GENERALLY NOT RESTRICTED TO THE UVEA AND INVOLVES OTHER ADJACENT
Age-Related Macular Degeneration (AMD)
 Age-Related Macular Degeneration (AMD) What is the Macula? What is Dry AMD (Age-related Macular Degeneration)? Dry AMD is an aging process that causes accumulation of waste product under the macula leading
Age-Related Macular Degeneration (AMD) What is the Macula? What is Dry AMD (Age-related Macular Degeneration)? Dry AMD is an aging process that causes accumulation of waste product under the macula leading
4/22/16. Eye. External Anatomy of Eye. Accessory Structures. Bio 40B Dr. Kandula
 Eye Bio 40B Dr. Kandula External Anatomy of Eye Accessory Structures l Eyebrows l Levator Palpebrae Superioris - opens eye l Eyelashes l Ciliary glands modified sweat glands l Small sebaceous glands l
Eye Bio 40B Dr. Kandula External Anatomy of Eye Accessory Structures l Eyebrows l Levator Palpebrae Superioris - opens eye l Eyelashes l Ciliary glands modified sweat glands l Small sebaceous glands l
Vision I. Steven McLoon Department of Neuroscience University of Minnesota
 Vision I Steven McLoon Department of Neuroscience University of Minnesota 1 Eye Cornea Sclera Conjunctiva 2 Eye The conjunctiva lines the inner surface of the eyelids and outer surface of the sclera. 3
Vision I Steven McLoon Department of Neuroscience University of Minnesota 1 Eye Cornea Sclera Conjunctiva 2 Eye The conjunctiva lines the inner surface of the eyelids and outer surface of the sclera. 3
epitheliopathy associated with diffuse retinal vasculitis
 British Journal of Ophthalmology, 1986, 70, 255-259 Acute posterior multifocal placoid pigment epitheliopathy associated with diffuse retinal vasculitis and late haemorrhagic macular detachment MAKOTO
British Journal of Ophthalmology, 1986, 70, 255-259 Acute posterior multifocal placoid pigment epitheliopathy associated with diffuse retinal vasculitis and late haemorrhagic macular detachment MAKOTO
ASSESSING THE EYES. Structures. Eyelids Extraocularmuscles Eyelashes Lacrimal glands: Lacrimal ducts Cornea Conjunctiva Sclera Pupils Iris.
 ASSESSING THE EYES Structures External Eyelids Extraocularmuscles Eyelashes Lacrimal glands: Lacrimal ducts Cornea Conjunctiva Sclera Pupils Iris 1 2 Structures Internal Optic disc Physiological cup Retinal
ASSESSING THE EYES Structures External Eyelids Extraocularmuscles Eyelashes Lacrimal glands: Lacrimal ducts Cornea Conjunctiva Sclera Pupils Iris 1 2 Structures Internal Optic disc Physiological cup Retinal
2009 REIMBURSEMENT GUIDE, VISUCAM and VISUCAM NM/FA
 2009 REIMBURSEMENT GUIDE FF 450 PLUS PRO NM, VISUCAM and VISUCAM NM/FA Zeiss Fundus Cameras INTRODUCTION The following guide provides an overview of billing and reimbursement for procedures performed with
2009 REIMBURSEMENT GUIDE FF 450 PLUS PRO NM, VISUCAM and VISUCAM NM/FA Zeiss Fundus Cameras INTRODUCTION The following guide provides an overview of billing and reimbursement for procedures performed with
ATLAS OF OCT. Retinal Anatomy in Health & Pathology by Neal A. Adams, MD. Provided to you by:
 ATLAS OF OCT Retinal Anatomy in Health & Pathology by Neal A. Adams, MD Provided to you by: Atlas of OCT The OCT Atlas is written by Neal A. Adams, MD, and produced by Heidelberg Engineering, Inc. to help
ATLAS OF OCT Retinal Anatomy in Health & Pathology by Neal A. Adams, MD Provided to you by: Atlas of OCT The OCT Atlas is written by Neal A. Adams, MD, and produced by Heidelberg Engineering, Inc. to help
Optical Coherence Tomography in Diabetic Retinopathy. Mrs Samantha Mann Consultant Ophthalmologist Clinical Lead of SEL-DESP
 Optical Coherence Tomography in Diabetic Retinopathy Mrs Samantha Mann Consultant Ophthalmologist Clinical Lead of SEL-DESP Content OCT imaging Retinal layers OCT features in Diabetes Some NON DR features
Optical Coherence Tomography in Diabetic Retinopathy Mrs Samantha Mann Consultant Ophthalmologist Clinical Lead of SEL-DESP Content OCT imaging Retinal layers OCT features in Diabetes Some NON DR features
Macular abnormalities in the reattached retina
 British Journal of Ophthalmology, 1978, 62, 595-603 Macular abnormalities in the reattached retina P. E. CLEARY AND P. K. LEAVER From Moorfields Eye Hospital and the Institute of Ophthalmology, London
British Journal of Ophthalmology, 1978, 62, 595-603 Macular abnormalities in the reattached retina P. E. CLEARY AND P. K. LEAVER From Moorfields Eye Hospital and the Institute of Ophthalmology, London
VISIONCARE S IMPLANTABLE MINIATURE TELESCOPE (by Dr. Isaac Lipshitz)
 PATIENT INFORMATION BOOKLET PAGE 1 OF 32 VISIONCARE S IMPLANTABLE MINIATURE TELESCOPE (by Dr. Isaac Lipshitz) AN INTRAOCULAR TELESCOPE FOR TREATING SEVERE TO PROFOUND VISION IMPAIRMENT DUE TO BILATERAL
PATIENT INFORMATION BOOKLET PAGE 1 OF 32 VISIONCARE S IMPLANTABLE MINIATURE TELESCOPE (by Dr. Isaac Lipshitz) AN INTRAOCULAR TELESCOPE FOR TREATING SEVERE TO PROFOUND VISION IMPAIRMENT DUE TO BILATERAL
Uveitis. Pt Info Brochure. Q: What is Uvea?
 Pt Info Brochure Uveitis Q: What is Uvea? A: Uvea is the middle layer of the eye. It is the most vascular structure of the eye. It provides nutrition to the other parts of the eye. The uvea is made up
Pt Info Brochure Uveitis Q: What is Uvea? A: Uvea is the middle layer of the eye. It is the most vascular structure of the eye. It provides nutrition to the other parts of the eye. The uvea is made up
Guidelines for the Management of Diabetic Retinopathy for the Internist
 Visual Disorder Guidelines for the Management of Diabetic Retinopathy for the Internist JMAJ 45(1): 1 7, 2002 Sadao HORI Professor, Department of Ophthalmology, Tokyo Women s Medical University Abstract:
Visual Disorder Guidelines for the Management of Diabetic Retinopathy for the Internist JMAJ 45(1): 1 7, 2002 Sadao HORI Professor, Department of Ophthalmology, Tokyo Women s Medical University Abstract:
The College of Optometrists - Learning outcomes for the Professional Certificate in Medical Retina
 Learning outcomes for the Professional Certificate in Medical Retina, incorporating diabetic retinopathy screening and age related macular degeneration The professional certificate is a prerequisite to
Learning outcomes for the Professional Certificate in Medical Retina, incorporating diabetic retinopathy screening and age related macular degeneration The professional certificate is a prerequisite to
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS
 NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS Revision Date: 6/30/06 Distribution Date: 7/6/06 The Department of Ophthalmology at the NYU Medical Center
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS Revision Date: 6/30/06 Distribution Date: 7/6/06 The Department of Ophthalmology at the NYU Medical Center
Clinical Case Presentation. Branch Retinal Vein Occlusion. Sarita M. Registered Nurse Whangarei Base Hospital
 Clinical Case Presentation on Branch Retinal Vein Occlusion Sarita M. Registered Nurse Whangarei Base Hospital Introduction Case Study Pathogenesis Clinical Features Investigations Treatment Follow-up
Clinical Case Presentation on Branch Retinal Vein Occlusion Sarita M. Registered Nurse Whangarei Base Hospital Introduction Case Study Pathogenesis Clinical Features Investigations Treatment Follow-up
Macular Hole Associated with Vogt-Koyanagi-Harada Disease at the Acute Uveitic Stage
 Published online: September 15, 2015 2015 The Author(s) Published by S. Karger AG, Basel 1663 2699/15/0063 0328$39.50/0 This article is licensed under the Creative Commons Attribution-NonCommercial 4.0
Published online: September 15, 2015 2015 The Author(s) Published by S. Karger AG, Basel 1663 2699/15/0063 0328$39.50/0 This article is licensed under the Creative Commons Attribution-NonCommercial 4.0
Manual. Manual Welsh Eye Care Initiative. A Welsh Eye Care Initiative. Protocol. The Assessment and Management of Age-related Macular Degeneration
 A Protocol 1.0 Definitions The following terms are important in this text: Wet Macular Degeneration Condition caused by the growth of abnormal blood vessels under the retina. Symptoms appear suddenly and
A Protocol 1.0 Definitions The following terms are important in this text: Wet Macular Degeneration Condition caused by the growth of abnormal blood vessels under the retina. Symptoms appear suddenly and
GENERAL INFORMATION DIABETIC EYE DISEASE
 GENERAL INFORMATION DIABETIC EYE DISEASE WHAT IS DIABETIC EYE DISEASE? Diabetic eye disease is a term used to describe the common eye complications seen in people with diabetes. It includes: Diabetic retinopathy
GENERAL INFORMATION DIABETIC EYE DISEASE WHAT IS DIABETIC EYE DISEASE? Diabetic eye disease is a term used to describe the common eye complications seen in people with diabetes. It includes: Diabetic retinopathy
Mild NPDR. Moderate NPDR. Severe NPDR
 Diabetic retinopathy Diabetic retinopathy is the most common cause of blindness in adults aged 35-65 years-old. Hyperglycaemia is thought to cause increased retinal blood flow and abnormal metabolism in
Diabetic retinopathy Diabetic retinopathy is the most common cause of blindness in adults aged 35-65 years-old. Hyperglycaemia is thought to cause increased retinal blood flow and abnormal metabolism in
White-Spot Syndromes of the Retina Lee Jampol, M.D. Chicago, IL
 Objectives At the conclusion of the program, the attendees will be able to: 1. recognize the various white-spot syndromes of the retina 2. initiate appropriate diagnostic tests of patients with the white-spot
Objectives At the conclusion of the program, the attendees will be able to: 1. recognize the various white-spot syndromes of the retina 2. initiate appropriate diagnostic tests of patients with the white-spot
Facts About Diabetic Eye Disease
 Facts About Diabetic Eye Disease Points to Remember 1. Diabetic eye disease comprises a group of eye conditions that affect people with diabetes. These conditions include diabetic retinopathy, diabetic
Facts About Diabetic Eye Disease Points to Remember 1. Diabetic eye disease comprises a group of eye conditions that affect people with diabetes. These conditions include diabetic retinopathy, diabetic
Placoid pigment epitheliopathy with
 Brit. J. Ophthal. ( I 972) 56, 875 Placoid pigment epitheliopathy with retinal vasculitis and papillitis T. H. KIRKHAM, *T. J. FFYTCHE, AND M. D. SANDERS From the Department of Neuro-Ophthalmology, the
Brit. J. Ophthal. ( I 972) 56, 875 Placoid pigment epitheliopathy with retinal vasculitis and papillitis T. H. KIRKHAM, *T. J. FFYTCHE, AND M. D. SANDERS From the Department of Neuro-Ophthalmology, the
Visual loss and foveal lesions in Usher's syndrome
 British Journal of Ophthalmology, 1979, 63, 484-488 Visual loss and foveal lesions in Usher's syndrome GERALD FISHMAN, VICTORIA VASQUEZ, MARLENE FISHMAN, AND BERGER' From the Department of Ophthalmology,
British Journal of Ophthalmology, 1979, 63, 484-488 Visual loss and foveal lesions in Usher's syndrome GERALD FISHMAN, VICTORIA VASQUEZ, MARLENE FISHMAN, AND BERGER' From the Department of Ophthalmology,
Diabetic Retinopathy. Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012
 Diabetic Retinopathy Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Outline Statistics Anatomy Categories Assessment Management Risk factors What do you need to do? Objectives Summarize the
Diabetic Retinopathy Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Outline Statistics Anatomy Categories Assessment Management Risk factors What do you need to do? Objectives Summarize the
Glaucoma. Cornea. Iris
 Glaucoma Introduction Glaucoma is a group of eye diseases that can lead to blindness if not treated. Openangle glaucoma, the most common form of glaucoma, affects about 3 million Americans. Half of those
Glaucoma Introduction Glaucoma is a group of eye diseases that can lead to blindness if not treated. Openangle glaucoma, the most common form of glaucoma, affects about 3 million Americans. Half of those
Treatment of diabetic maculopathy by
 Brit. J. Ophthal. (1974) 58, 85 Treatment of diabetic maculopathy by argon-laser S. MERIN, L. YANKO, AND M. IVRY From the Department of Ophthalmology, Hadassah University Hospital, Jerusalem, Israel Diabetic
Brit. J. Ophthal. (1974) 58, 85 Treatment of diabetic maculopathy by argon-laser S. MERIN, L. YANKO, AND M. IVRY From the Department of Ophthalmology, Hadassah University Hospital, Jerusalem, Israel Diabetic
Note: This is an outcome measure and can be calculated solely using registry data.
 Measure #191 (NQF 0565): Cataracts: 20/40 or Better Visual Acuity within 90 Days Following Cataract Surgery -- National Quality Strategy Domain: Effective Clinical Care DESCRIPTION: Percentage of patients
Measure #191 (NQF 0565): Cataracts: 20/40 or Better Visual Acuity within 90 Days Following Cataract Surgery -- National Quality Strategy Domain: Effective Clinical Care DESCRIPTION: Percentage of patients
Optical Coherence Tomography Findings in Highly Myopic Eyes following Cataract Surgery
 Optical Coherence Tomography Findings in Highly Myopic Eyes following Cataract Surgery Fedra Hajizadeh, MD 1 Mohammad Riazi Esfahani, MD 1,2 Hooshang Faghihi, MD 3 Mehdi Khanlari, MD 4 Abstract Purpose:
Optical Coherence Tomography Findings in Highly Myopic Eyes following Cataract Surgery Fedra Hajizadeh, MD 1 Mohammad Riazi Esfahani, MD 1,2 Hooshang Faghihi, MD 3 Mehdi Khanlari, MD 4 Abstract Purpose:
CONSENT FOR CATARACT SURGERY REQUEST FOR SURGICAL OPERATION / PROCEDURE AND ANAESTHETIC
 CONSENT FOR CATARACT SURGERY REQUEST FOR SURGICAL OPERATION / PROCEDURE AND ANAESTHETIC Your doctor has indicated that the condition of your eye appears stable and your cataract surgery and/or implantation
CONSENT FOR CATARACT SURGERY REQUEST FOR SURGICAL OPERATION / PROCEDURE AND ANAESTHETIC Your doctor has indicated that the condition of your eye appears stable and your cataract surgery and/or implantation
Is OCT-A Needed As An Investigative Tool During The Management Of Diabetic Macular Edema
 Is OCT-A Needed As An Investigative Tool During The Management Of Diabetic Macular Edema Ayman M Khattab MD, FRCS Professor of Ophthalmology Cairo University Diabetic Macular Edema (DME) Diabetic macular
Is OCT-A Needed As An Investigative Tool During The Management Of Diabetic Macular Edema Ayman M Khattab MD, FRCS Professor of Ophthalmology Cairo University Diabetic Macular Edema (DME) Diabetic macular
Role of fluorescein angiography as an early intervention in detecting cystoid macular edema in post operative cataract surgery patients
 Research Article Role of fluorescein angiography as an early intervention in detecting cystoid macular edema in post operative cataract surgery patients Dole N B 1*, Deshmukhh S S 2 1 Assistant Professor,
Research Article Role of fluorescein angiography as an early intervention in detecting cystoid macular edema in post operative cataract surgery patients Dole N B 1*, Deshmukhh S S 2 1 Assistant Professor,
Measure #191: Cataracts: 20/40 or Better Visual Acuity within 90 Days Following Cataract Surgery
 Measure #191: Cataracts: 20/40 or Better Visual Acuity within 90 Days Following Cataract Surgery 2012 PHYSICIAN QUALITY REPORTING OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY DESCRIPTION: Percentage
Measure #191: Cataracts: 20/40 or Better Visual Acuity within 90 Days Following Cataract Surgery 2012 PHYSICIAN QUALITY REPORTING OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY DESCRIPTION: Percentage
For details on measurement and recording of visual acuity, refer to Annex 1. VISION INTERPRETING RESULTS ABSTRACT
 management update on functional decline in older adults 2012 Unit No. 5 VISION Dr Au Eong Kah Guan, Ms Yulianti, Ms Fifiana ABSTRACT Among Singaporean adults of Chinese origin aged 40 to 79 years old,
management update on functional decline in older adults 2012 Unit No. 5 VISION Dr Au Eong Kah Guan, Ms Yulianti, Ms Fifiana ABSTRACT Among Singaporean adults of Chinese origin aged 40 to 79 years old,
INTRODUCTION: ****************************************************************************************************
 BIOLOGY 211: HUMAN ANATOMY & PHYSIOLOGY **************************************************************************************************** EYES AND VISION ****************************************************************************************************
BIOLOGY 211: HUMAN ANATOMY & PHYSIOLOGY **************************************************************************************************** EYES AND VISION ****************************************************************************************************
