Acute Reversal of Experimental Diabetic Ketoacidosis
|
|
|
- Roberta Greene
- 5 years ago
- Views:
Transcription
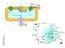
1 Acute Reversal of Experimental Diabetic Ketoacidosis in the Rat with (+) -Decanoylcarnitine J. DENS McGARRY and DANEL W. FOSTER From the Departments of nternal Medicine and Biochemistry, The University of Texas Southwestern Medical School at Dallas, Dallas, Texas A B S T R A C T The effect of (+) -decanoylcarnitine, a potent inhibitor of long-chain acylcarnitine transferase, was tested for its ability to inhibit hepatic ketogenesis both in the isolated perfused liver and in vivo in severely ketotic alloxan diabetic rats. n vitro the inhibitor caused an almost complete block in ketone body production. n vivo (+) -decanoylcarnitine caused a rapid reversal of ketosis under conditions where large doses of insulin had little effect. A combination of the two agents produced an even more striking fall in plasma ketone levels. While (+) -decanoylcarnitine alone had no effect on plasma glucose levels it enhanced the hypoglycemic effect of insulin in anesthetized animals. Loss of this effect was noted in nonanesthetized animals, possibly as a result of increased muscle activity. Studies in the isolated perfused liver indicated that the blockade of fatty acid oxidation and ketogenesis produced by (+) -decanoylcarnitine was rapidly reversible upon removal of the inhibitor. NTRODUCTON Recent studies from this laboratory have been concerned with the mechanisms by which ketogenesis is regulated (1-6). t now seems clear that maximal ketogenesis requires that two conditions be fulfilled: (a) There must be an adequate delivery of the basic ketogenic substrate, fatty acid, to the liver, and (b) There must be a change in the metabolic "set" of the liver such that a greater fraction of the incoming fatty acids is shunted into the oxidative sequence relative to that utilized for triglyceride and phospholipid synthesis. Failure to meet either requirement prevents the onset of ketone body overproduction or causes a reversion of Dr. Foster is Research Career Development Awardee 5-AM9968, U. S. Public Health Service. Received for publication 10 October 1972 and in revised form 17 November established ketosis to normal. Current understanding of the nature of the metabolic changes occurring in the hepatic cell during diabetic ketoacidosis is summarized in Fig. 1. Fatty acids extracted from the plasma by the liver can be metabolized by only two major pathways-they may be esterified to form triglycerides and phospholipids or they may enter the jp-oxidation process. For reasons outlined in detail elsewhere (1, 6) it seems likely that the capacity for,8-oxidation in the liver is fixed and high and that flux of fatty acyl carbon into this pathway (and ultimately the distribution of fatty acyl-coa between esterification and the oxidative sequence) is determined by the rate of entry of fatty acyl- CoA into the mitochondrion. As indicated, the enzyme catalyzing the translocation of the fatty acid molecule across the mitochondrial membrane is the long-chain fatty acylcarnitine transferase (7, 8). t is assumed (Fig. 1A) that the activity of this enzyme is inhibited in the normal fed state such that fatty acids are utilized by the liver primarily for the synthesis of triglyceride but that in fasting and diabetes (Fig. 1B) activation of the enzyme occurs with the consequence that the barrier to transport of the fatty acids into the mitochondrion is removed and the increased fatty acid load delivered to the liver is preferentially oxidized to acetoacetic and P-hydroxybutyric acids. n this regard it is of interest to note that Norum (9) has found increased activity of long-chain acylcarnitine transferase in liver homogenates and mitochondria from fasted and diabetic animals. Should this formulation be correct, it follows that inhibition of the acylcarnitine transferase reaction would result in a blockade of fatty acid oxidation and an inhibition of ketogenesis. A specific inhibitor of the reaction, (+) -decanoylcarnitine, has been known for some time (10) and has been shown to block ketogenesis in isolated perfused livers taken from fasted animals (10-12). Moreover, when ketogenesis in livers from fasted rats was interrupted by (+)-decanoylcarni- The Journal of Clinical nvestigation Volume 52 April
2 A Normal Fatty FFA acyl-coa Triglyceride Phospholipid B. Diabetic FFA.- YTOPLASM] CYTOPLASM Fatty acyl-coa - Triglycerlde Phosphoilpd -Ac N'membrane MTOCHONDRON Y2arnitini tronsferase -.T - Fatty acyl-coa Ketones. MTOC HONDRON membrane Acylcamunittine tronsferase _ Acetyl-CoA Fatty acyl-coa a-oxidation C02... Jr,B~~~-oxidaiion Ketones Acetyl-CoA FGURE 1 A possible model for the regulation of ketogenesis in diabetic acidosis. The pathways shown are highly simplified and schematized. Panel A indicates that in the normal state free fatty acid delivery to the liver is low and fatty acid oxidation is inhibited at the level of the acylcarnitine transferase reaction. Fatty acids are therefore utilized primarily for triglyceride synthesis. n panel B free fatty acid delivery is increased and the fatty acids are oxidized to ketone bodies through activation of the acylcarnitine transferase step. For a more detailed discussion of this formulation see references 1, 6, 7. tine, the perfused fatty acids were immediately shunted into hepatic triglycerides, restoring the pattern of fatty acid metabolism to that seen in normal liver (6). For these reasons we decided to try (+)-decanoylcarnitine in the treatment of acute diabetic ketoacidosis in the rat. The results of the experiments to be presented indicate that (+)-decanoylcarnitine is a potent inhibitor of ketogenesis produced by uncontrolled diabetes both in vitro and in vivo. Moreover, when given in combination with insulin, (+) -decanoylcarnitine significantly reduces recovery times from diabetic acidosis and is much more effective than the hormone given alone. METHODS Treatment of animals Male Sprague-Dawley rats weighing approximately 130 g and maintained on a diet containing 58.5% sucrose, 21% CO2 casein, and less than 1% fat (General Biochemicals Div., Mogul Corp., Chagrin Falls, Ohio) were used in all experiments. Severe diabetic ketoacidosis was induced by the intravenous injection of alloxan monohydrate at a dose of 70 mg/kg body wt. Experiments were carried out 48 h after administration of the drug at which time body weight was approximately 100 g. Only those animals with initial plasma ketones in excess of 1,000 umol/100 ml have been included in the studies reported below. n vitro studies-liver perfusion Recirculating perfusions. The effect of (+)-decanoylcarnitine on rates of ketogenesis was first studied in livers from acutely ketotic diabetic rats perfused with recirculating medium using the apparatus and techniques described elsewhere (3, 4). The perfusion fluid (80 ml) consisted of washed, aged human erythrocytes suspended to an hematocrit of 20% in 5%o bovine albumin dissolved in Krebs' bicarbonate buffer, ph 7.4. Sufficient oleic acid was included in the initial pool to give a fatty acid concentration in the cell-free fluid of approximately 0.7 mm. This concentration was maintained throughout the experimental period by the constant infusion of a solution containing 12.5 mm oleate and 10% albumin dissolved in 0.9%o sodium chloride, ph 7.4, at a rate of 75,ul/min (6). Nonrecirculating perfusions. n order to measure the rapidity with which hepatic ketogenesis is blocked by (+) - decanoylcarnitine and the time required for the recovery of the liver from the effects of the inhibitor it was necessary to utilize a nonrecirculating perfusion system. The methodology employed here was essentially the same as that used for the more conventional recirculating technique with the exception that an additional large reservoir of perfusion fluid (about 1,500 ml) was required since the venous flow from the liver was not returned to the oxygenation chamber. Using this system it was possible to infuse (+)-decanoylcarnitine into the perfusion circuit at a point just prior to entry into the liver, thus allowing the time of exposure of the tissue to the inhibitor to be varied at will. n vivo studies n order to follow the time sequence of the reversal of diabetic ketoacidosis with insulin and (+)-decanoylcarnitine animals were anesthetized either with pentobarbital, or lightly with ether, and no. 10 polyethylene catheters were placed in the femoral artery on one side and the inferior vena cava through the femoral vein on the other (13). The animals were then placed in individual restraining cages. When pentobarbital was used as anesthetic, experiments were started with the animals still asleep. Rats anesthetized with ether had recovered from anesthesia for at least 30 min before experiments were begun. Samples of arterial blood (0.1 ml) were collected into iced heparinized polyethylene tubes throughout the experiment for determination of plasma ketone and glucose concentrations (2). Heparin, when used, was given intravenously in a dose of 100 units prior to collection of the first sample. An infusion of 5% bovine albumin in 0.9%o sodium chloride, ph 7.4, containing insulin, (+)-decanoylcarnitine or a mixture of both agents was then given through the venous catheter as described in the legends to the figures. The amount of insulin given was sufficient to produce maximum effects as determined in preliminary experiments. Because of the small volumes of blood taken it was not possible to determine plasma FFA levels at each time point. 878 J. D. McGarry and D. W. Foster
3 For such measurements, a 2-3 ml specimen of blood was rapidly removed from the abdominal aorta at the conclusion of the experiment and compared with values obtained from control animals. n experiments designed to determine the effects of a single injection of insulin and/or (+)-decanoylcarnitine rats that had not been catheterized or anesthetized were given, intravenously, 0.5 ml of the albumin solutions containing insulin in the presence and absence of (+)-decanoylcarnitine as described above. The animals were then placed in conventional cages, and 2 h later they were anesthetized with pentobarbital immediately prior to collection of blood from the aorta. Analyses on blood and perfusion fluid All samples of blood and perfusion medium were centrifuged, and analyses were carried out on the erythrocyte-free supernatant fluid. Acetoacetate and p-hydroxybutyrate were determined enzymatically as described previously (2), and in the text the term "ketone bodies" will always refer to the sum of these two components. Glucose was measured using the glucose oxidase method (14), and free fatty acid levels were assayed by the method of Dole (15) as modified by Trout, Estes, and Friedberg (16). Materials Bovine albumin, Fraction V, was from Armour Pharmaceutical Co., Chicago, ll. n all experiments with oleic acid and (+)-decanoylcarnitine these reagents were bound to the albumin and neutralized to ph 7.4 before use. Glucagon-free insulin was a gift from Eli Lilly & Co. and (+)- decanoylcarnitine was generously provided by Dr. Y. Kawashima of the Otsuka Pharmaceutical Factory, Naruto, Tokushima, Japan. Oleic acid was purchased f rom CN Nutritional Biochemicals, nc., Cleve!and, Ohio. All other reagents were obtained from commercial sources and were of the highest available grade. RESULTS nhibition of ketogenesis in the diabetic liver in vitro. As noted above, (+) -decanoylcarnitine had been previously shown to have the capacity to inhibit ketogenesis in livers from fasted rats (6, 10-12). Ketone production by isolated perfused livers from fasted animals could also be partially inhibited with certain other antiketogenic agents such as lactate and glycerol (4, 17, 18). Livers from severely ketotic diabetic rats, however, appear to be resistant to the effect of the latter compounds (3). For this reason we first examined the effect of (+)-decanoylcarnitine on acetoacetate and 9- hydroxybutyrate production in the perfused liver from rats with acute diabetic ketoacidosis. The results are shown in Fig. 2 where it can be seen that ketone body synthesis was essentially completely inhibited after 15 min of perfusion with the nonphysiological carnitine ester. Reversal of diabetic ketoacidosis with (+)-decanoylcarnitine and insulin-anesthetized animals. n the first set of in vivo experiments rats were anesthetized with pentobarbital for implantation of catheters, and studies 250 [ z F o 150 l'j 00. w ' 0 50[ * Controls (5) A (+)-Decanoylcornitine (5) MNUTES OF PERFUSON FGURE 2 The effect of (+)-decanoylcarnitine on ketogenesis in perfused livers from alloxan diabetic rats. Livers were perfused with oleic acid (0.7 mm) in the presence and absence of (+)-decanoylcarnitine (0.5 mm) using the recirculating perfusion technique described under Methods. Results are given as means +SEM for five livers in each group. were initiated while anesthesia was still in effect. As is evident from the data of Fig. 3 the acutely ketotic alloxan diabetic rat is severely ill with marked hypoglycemia and hyperketonemia. The initial plasma glucose concentrations in the three groups of animals at zero time clustered around 1,000 mg/100 ml, a figure much higher than that found in pancreatectomized diabetic rats (19) but very close to values seen in severe human disease (20). Mean plasma ketone levels were greater than 1,500 /mol/100 ml. When insulin was given alone ketone concentrations decreased from an initial value of 1,760 /Lmol/100 ml to 1,255.mol/100 ml at 4 h (Fig. 3B). Over the same time interval (+)-decanoylcarnitine, in the absence of insulin, caused a fall in acetoacetate and P-hydroxybutyrate levels from 1,502 to 262 Amol/100 ml. When the two agents were given in combination the equivalent 4 h effect was a decrease in ketones from the zero time value of 1,532,mol/100 ml to 69 zmol/100 ml. The relative antiketogenic effect of insulin: (+)-decanoylcarnitine: insulin plus (+)-decanoylcarnitine was thus 1: 2.5: 3.0 (A ketones-4 h, 505: 1,240: 1,463,mol/100 ml). Since the plasma values were normal by four hours in the third group of animals, the accelerating effect of insulin on the reversal of ketosis by (+) -decanoylcarnitine is best seen by comparisons made at the 2 h point. Here the relative antiketogenic ratios were insulin: (+ ) -decanoylcarnitine: insulin plus (+)-decanoylcarnitine, 1: 2.0: 3.5 (A ketones-2 h, 292:610:991 gmol/100 ml). The changes in plasma glucose concentrations with the three treatment schedules are shown in Fig. 3A. Reversal of Ketoacidosis 879
4 0 - ( a. () w - ZrE 0 ~-J Y N C< o g_ 1o A o nsulin (12) - (+)-Decanoylcarnitine (11) 0 nsulin + (+)-Decanoylcarnitine (11) T T T T T T.A.A l~~ ~~~~0---- o~ 1;.~~~~~~~~~~~1 1 2 HOURS FGURE 3 The effect of i.v. administration of insulin and (+)-decanoylcarnitine in anesthetized diabetic rats. Animals that were still under pentobarbital anesthesia after the placement of arterial and venous catheters were placed in restraining cages and received 100 U of heparin at zero time. After collection of an arterial blood sample (0.1 ml) an infusion of 5%7 albumin in 0.9% sodium chloride, ph 7.4, containing insulin (1 U/ml), (+)-decanoylcarnitine (20 mg/ml) or both agents was given through the venous catheter at a rate of 75,l/min for 10 min followed by 10,ul/min until the 2 h time point. Further arterial blood samples were collected at the indicated times for analysis of plasma glucose and ketone body concentrations. Values represent means +±SEM for the number of animals shown in parentheses. (+) -Decanoylcarnitine had no effect whatever, the initial value being 1,043 mg/100 ml and the 4 h value being 1,045 mg/100 ml. nsulin had a hypoglycemic effect, but the total change in 4 h was quite small, from 976 mg/100 ml at zero time to 836 mg/10 ml at the end of the experiment. Surprisingly, when (+) -decanoylcarnitine was given with insulin the plasma glucose fell much more rapidly, the initial value of 896 mg/100 ml decreasing to 281 mg/100 ml at 4 h. Reversal of diabetic ketoacidosis with (+)-decanoylcarnitine and insulin-nonanesthetized animals. Because of the possibility that continued anesthesia might alter the results of treatment, we next carried out experiments in which catheters were placed under light ether anesthesia. All animals were awake throughout the experiments. Several other differences from the studies shown in Fig. 3 should be noted. First, infusions were carried out for only 10 min with all agents (i.e., the maintenance infusions given between 10 and 120 min in the experiments of Fig. 3 were omitted). Secondly, no heparin was given to the animals. Thirdly, only control and 2-h samples of blood were obtained in each rat. The results of these experiments are shown in Fig. 4. As indicated in panel C, insulin caused a decrease in acetoacetate plus P-hydroxybutyrate concentrations from 2,117 umol/100 to 1,869 umol/100 ml (A, gmol/100 ml). (+)-Decanoylcarnitine as the sole agent of treatment dropped total ketones over the 2 h period from 1,863 Aumol/100 ml to 1,254 ;Lmol/100 ml (A, igmol/100 ml). nclusion of insulin with (+)-decanoylcarnitine, exactly as was the case with the first group of animals, caused an accelerated reversal of ketosis, the fall in 2 h being from 1,754 to 717 umol/ 100 ml (A, jumol/100 ml). t could thus be concluded that the antiketogenic effects of insulin and (+)- decanoylcarnitine were unaffected by anesthesia or heparin administration. U. L. a. 2 w () sn j 0 0 to w Z= wo c. 0 E cn E FGURE 4 The effect of i.v. administration of insulin and (+)-decanoylcarnitine in unanesthetized diabetic rats. The experimental conditions differed from those described in Fig. 3 in the following respects: (a) the animals were only lightly anesthetized with ether during the placement of catheters and were fully awake during the experimental period; (b) no heparin was used; (c) the infusion was stopped after the 10 min priming dose had been delivered; (d) at the 2 h time point the animals were anesthetized with pentobarbital to allow the collection of a large blood sample from the abdominal aorta for analysis of plasma glucose, ketone body, and FFA levels. Values represent means +SEM for the number of animals shown in parentheses. 880 J. D. McGarry and D. W. Foster
5 Such was not the case with the changes in blood glucose, however (Fig. 4B). While control animals and those treated with (+)-decanoylcarnitine alone showed no alteration in plasma glucose concentration, confirming the findings shown in Fig. 3, when (+)-decanoylcarnitine was given with insulin, no enhancement of the hormone's hypoglycemic effect was now evident (A glucose, 2 h, insulin, mg/100 ml; A glucose, 2 h, insulin plus (+ ) -decanoylcarnitine, mg/100 ml). The difference in the two experiments appears to be entirely due to a greater hypoglycemic effect of insulin in the awake animals since the 2 h fall with insulin alone was only 69 mg/100 ml in anesthetized rats (Fig. 3A). The changes in free fatty acid (FFA) concentrations with treatment are shown in Fig. 4A. As expected, insulin caused a decrease in the fatty acid levels, the value falling from 1.34 to 0.42 geq/ml over the 2 h period. (+ ) -Decanoylcarnitine appeared to cause an increase in the fatty acid concentration from control values and to blunt the insulin-induced fall. n the experiments shown in Fig. 5 animals with acute diabetic ketoacidosis were treated with a single 4E -i )0~ a a _ ui (n 0 D E 1pOO o < E -i a. _ 2,000 w O E 1,500- yo in E 1,000, _ 500 ) ) * Controls (10) o nsulin (15) * nsulin + (+)- Deconoylcarnitine (4) _A _ = B -; HOURS FGURE 5 The effect of a single injection of insulin with or without (+) -decanoylcarnitine in nonanesthetized diabetic rats. Noncatheterized animals received, intravenously over a 2 min period, 0.5 ml of 5% albumin in 0.9% sodium chloride containing insulin (2 U/ml) in the presence or absence of (+)-decanoylcarnitine (20 mg/ml). They were then placed in conventional cages and 2 h later a large sample of arterial blood was collected for analyses as described in Fig. 4. Values represent means ± SEM for the number of animals shown in parentheses. Control values have been taken from Fig. 4. 2, (+1-Deconoylcarnitine z 0 infusion * Control F-a A (+1-Decanoylcornitine W a v z E MNUTES OF PERFUSON FGURE 6 Effect of limited exposure to (+)-decanoylcarnitine on ketogenesis in perfused livers from diabetic rats. Livers were perfused with oleic acid (0.7 mm) using the nonrecirculating technique described under Methods. At the 30 min time point an infusion of (+)-decanoylcarnitine bound to albumin in 0.9% sodium chloride, ph 7.4, was introduced into the perfusion fluid just prior to its entry into the liver such that the concentration of the inhibitor reaching the tissue was 0.5 mm. At the 70 min time point the infusion was stopped and the perfusion was continued for a further 100 min. The perfusate leaving the liver was collected in a series of tubes and analyzed for ketone bodies. The control liver was perfused with the albumin solution without (+)-decanoylcarnitine. The figure represents a single experiment, one of four carried out with identical results. rapid injection of insulin or insulin plus (+)-decanoylcarnitine. They were never anesthetized, had no catheters inserted, and were not placed in restraining cages. 2 h after treatment they were anesthetized with pentobarbital, and blood was drawn from the aorta. Control values were taken from the animals shown in Fig. 4. Once again the potent antiketogenic effect of (+)-decanoylcarnitine over and above that seen with insulin alone was evident. As was the case in the experiments of Fig. 4 the hypoglycemic effect of insulin was not altered by the addition of the carnitine ester. The absolute fall in plasma glucose, assuming that initial values found in control rats were essentially similar to those actually present at zero time in the treated animals, appeared to be considerably greater (A, -720 mg/100 ml per 2 h) than that seen in the two previous sets of experiments. The insulin-induced fall in free fatty acids was comparable. However, in this case (+)-decanoylcarnitine did not reduce the FFA-lowering capacity of insulin. n experiments not shown (+) -decanoylcarnitine given alone as a single injection again lowered ketones at a rate faster than that produced by insulin alone but less than that seen when the two agents were combined. Duration of the (+)-decanoylcarnitine effect in vitro. The studies presented thus far clearly indicated that the effect of (+ ) -decanoylcarnitine in blocking fatty acid oxidation and ketogenesis was rapid in onset both in vitro and in vivo. Accordingly, we next attempted to get some estimate of the duration of the effect. This Reversal of Ketoacidosis 881
6 was done in the isolated rat liver in which a flowthrough perfusion system was established. A series of experiments were carried out in which an infusion of (+)-decanoylcarnitine was given for a short interval and then discontinued. The results of one such experiment, entirely typical, are shown in Fig min after the addition of (+)-decanoylcarnitine the ketone production rate fell from 70 to about 40 Amol/10 min per 100 g body wt. Synthesis of ketones continued to fall and became negligible by 40 min after the start of the (+)-decanoylcarnitine infusion. When the infusion was stopped ketone production began to increase almost immediately and 100 min later was approaching the control rate. The results indicate, therefore, that the (+)-decanoylcarnitine block of fatty acid oxidation is readily reversible on cessation of treatment. DSCUSSON The results reported in this study indicate that (+)- decanoylcarnitine, an inhibitor of the long-chain acylcarnitine transferase reaction, has the capacity to interrupt ketone body production in the severely ketotic alloxan diabetic rat and demonstrate that its antiketogenic effect is more powerful than that of insulin itself. Such an observation is entirely consistent with the finding that (+)-decanoylcarnitine almost immediately stops ketone body production in the perfused liver of the alloxan diabetic rat (Figs. 2 and 6) even though these livers are resistant to the action of antiketogenic agents of the carbohydrate class as well as insulin (3). t is of interest that in vivo the combination of insulin and (+)-decanoylcarnitine was more effective than the latter agent alone. The mechanism by which insulin enhances the antiketogenic effect of (+)-decanoylcarnitine has not as yet been established. t seems clear that the hormone must ultimately act directly on the liver to reverse ketosis, apart from any effect it has in stopping substrate delivery by blocking free fatty acid release, since elevation of free fatty acid levels in ketotic animals restored to normal by treatment with insulin will not reinitiate ketosis (21). One possibility would be, therefore, that insulin also causes a change in the hepatic acylcarnitine transferase reaction such that an additive response results when both agents are given together (6, 9). Alternatively, while the antiketogenic effect of insulin alone cannot be explained solely by an anti-lipolytic action, its synergistic effect with (+) -decanoylcarnitine could be. t is known that long-chain fatty acyl-coa and (+) -acylcarnitine derivatives interact competitively with acylcarnitine transferase (22). t is thus conceivable that diminished free fatty acid delivery to the liver under the influence of insulin would result in a fall of fatty acyl-coa levels and an increase in the effectiveness of the (+)-decanoylcarnitine block.' Thirdly, the insulin effect might be exerted at the periphery by increasing the rate of ketone body utilization (23). Presumably a fall in free fatty acid delivery to muscle would accelerate the utilization of ketone bodies in that tissue, particularly if coupled with a (+)- decanoylcarnitine block in fatty acid oxidation. Preliminary evidence against an insulin effect dependent upon an antilipolytic mechanism has been obtained in experiments (not shown) where free fatty acid concentrations were lowered with nicotinic acid (24) in the presence of (+)-decanoylcarnitine. No enhancement of the antiketogenic effect was seen, the 2 h fall in total ketones being 611 Amol/100 ml with both compounds given together as opposed to 608 Lmol/100 ml with (+)- decanoylcarnitine alone. t should also be noted that the (+) -decanoylcarnitine effect could not be reproduced by increasing the levels of insulin up to four times those given in the experiments shown here, a finding reminiscent of the observation in humans that increasing the insulin dosage beyond the usual treatment schedule does not shorten recovery times from diabetic ketoacidosis (25, 26).' A second feature of interest in the results was the fact that (+)-decanoylcarnitine accelerated the fall in plasma glucose produced by insulin in rats that were anesthetized, but did not do so in awake and moving animals. Hepatic gluconeogenesis has been considered to be stimulated by fatty acid oxidation (10, 11, 27), at -least where rates are very high (6), and (+)-decanoylcarnitine has been shown to block this stimulatory effect in the perfused liver (6, 11, 27). t is conceivable, therefore, that (+)-decanoylcarnitine had the same effect in vivo. f the carnitine ester were acting primarily to block hepatic gluconeogenesis, however, it would seem unlikely that the response would not be evident in both anesthetized and unanesthetized animals. For this reason we favor the possibility that the accelerated fall in blood glucose produced by (+)-decanoylcarnitine is due to a blockade of fatty acid oxidation in peripheral tissues with the result that glucose would be oxidized more 'n view of the generalization made earlier that interruption of substrate delivery to the liver should reverse the ketotic state, the question might be raised as to why insulin, which rapidly reduced plasma FFA levels, did not proportionately lower plasma ketone concentrations. The answer undoubtedly lies in the observation that livers from severely ketotic alloxan diabetic rats are engorged with fat (5, 36) such that they can sustain high rates of ketogenesis for several hours in the absence of exogenous fatty acids (3, 36). 2 n the experiments shown in Fig. 3 the insulin dosage was 18.5 U/kg body wt in 2 h. An equivalent schedule in a 70 kg man would be about 1,300 U in 2 h, a dose some six times greater than that normally administered to a patient in diabetic ketoacidosis (1). 882 J. D. McGarry and D. W. Foster
7 rapidly as the alternative substate (28). A possible interpretation would be that insulin acts essentially to permit (or cause) accelerated transport of glucose across the cell membrane (29, 30) in a process that is dependent in part on the intracellular utilization of glucose such that an increased oxidation of glucose would enhance the transport process (31, 32). An analogous situation would be muscular exercise, which has long been known to have a hypoglycemic effect in diabetes (33, 34), increasing glucose utilization in the presence of insulin presumably by activating glycolysis (35). ndeed, it is attractive to speculate that the failure to demonstrate a synergistic effect of (+)-decanoylcarnitine on the insulin-induced fall in plasma glucose in nonanesthetized animals was due to their increased muscular activity, since even the animals placed in restraining cages were continually moving their limbs. The implication would be that the capacity to increase glucose utilization beyond the level produced by insulin alone is limited and that this limit was reached either by (+)-decanoylcarnitine treatment or by increasing muscular exercise. Despite its potent capacity to block fatty acid oxidation in the liver, and, presumably, in peripheral tissues, no deleterious side effects were seen in rats treated with (+) -decanoylcarnitine under the conditions utilized in these experiments, probably because of the plentiful availability of other substrate in the form of glucose and ketone bodies (28). t was also noteworthy that the (+ ) -decanoylcarnitine effect appeared to be readily reversible (Fig. 6). Nevertheless it should be emphasized that the compound is potentially dangerous both from the metabolic standpoint and because it is a surface active agent capable of inducing red blood cell hemolysis in the unbound state. Additional studies of metabolic effects and possible toxicity of (+) -decanoylcarnitine are in progress. We consider these results to be important for the following reasons: (a) They provide additional support for the viewpoint that studies of metabolic regulation in the isolated perfused liver are applicable to the intact animal (6). (b) They are entirely compatible with the postulated critical role of long-chain acylcarnitine transferase in the regulation of hepatic ketogenesis (1, 6-8). (c) They raise the possibility that alternative and more effective forms of treatment for diabetic ketoacidosis may one day be available. ACKNOWLEDGMENTS We acknowledge with gratitude the generosity of Dr. Y. Kawashima and the Otsuka Pharmaceutical Factory in supplying the (+)-decanoylcarnitine used in these studies. The excellent technical assistance of Ms. Petra Contreras and Martha Cook should also be noted. This investigation was supported by U. S. Public Health Service Grant CA REFERENCES 1. McGarry, J. D., and D. W. Foster Regulation of ketogenesis and clinical aspects of the ketotic state. Metab. (Clin. Exp.). 21: McGarry, J. D., M. J. Guest, and D. W. Foster Ketone body metabolism in the ketosis of starvation and alloxan diabetes. J. Biol. Chem. 245: McGarry, J. D., and D. W. Foster The regulation of ketogenesis from octanoic acid. The role of the tricarboxylic acid cycle and fatty acid synthesis. J. Riol. Chem. 246: McGarry, J. D., and D. W. Foster The regulation of ketogenesis from oleic acid and the influence of antiketogenic agents. J. Biol. Chem. 246: Meier, J. M., J. D. McGarry, G. R. Faloona, R. H. Unger, and D. W. Foster Studies of the development of diabetic ketosis in the rat. J. Lipid Res. 13: McGarry, J. D., J. M. Meier, and D. W. Foster The effects of starvation and refeeding on carbohydrate and lipid metabolism in vivo and in the perfused rat liver. The relationship between fatty acid oxidation and esterification in the regulation of ketogenesis. J. Biol. Chen. 243: Fritz,. B An hypothesis concerning the role of carnitine in the control of interrelations between fatty acid and carbohydrate metabolism. Perspect. Biol. Mled. 10: Augenfeld, J., and. B Fritz Carnitine palmitoyltransferase activity and fatty acid oxidation by livers from fetal and neonatal rats. Can. J. Biochem. 48: Norum, R. N Activation of palmityl-coa: carnitine palmityltransferase in livers from fasted, fat-fed or diabetic rats. Biochem. Biophys. Acta. 98: Delisle, G., and. B Fritz nterrelations between hepatic fatty acid oxidation and gluconeogenesis: a possible regulatory role of carnitine palmityltransferase. Proc. Natl. Acad. Sci. U. S. A. 58: Williamson, J. R., E. T. Browning, R. Scholz, R. A. Kreisberg, and. B. Fritz nhibition of fatty acid stimulation of gluconeogenesis by (+)-decanoylcarnitine in perfused rat liver. Diabetes. 17: Williamson, J. R., E. T. Browning, R. G. Thurman, and R. Scholz nhibition of glucagon effects in perfused rat liver by (+)-decanoylcarnitine. J. Biol. Chem. 244: Foster, D. W Studies in the ketosis of fasting. J. Clin. nvest. 46: Saifer, A., and S. Gerstenfeld The photometric microdetermination of blood glucose with glucose oxidase. J Lab. Clin. Med. 51: Dole, V. P A relation between non-esterified fatty acids in plasma and the metabolism of glucose. J. Clin. nvest. 35: Trout, D. L., E. H. Estes, Jr., and S. J. Friedberg Titration of free fatty acids of plasma: a study of current methods and a new modification. J. Lipid Res. 1: Exton, J. H., and C. R. Park Control of gluconeogenesis in liver.. General features of gluconeogenesis in the perfused livers of rats. J. Biol. Chem. 242: Exton, J. H., J. C. Corbin, and S. C. Harper Control of gluconeogenesis in liver. V. Effects of fasting, diabetes, and glucagon on lactate and endogenous metabolism in the perfused rat liver. J. Biol. Chem. 247: Reversal of Ketoacidosis 883
8 19. Chernick, S. S., and R. 0 Scow flarly eftects of total pancreatectomy on fat metabolism in the rat. Am. J. Physiol. 196: Beigelman, P. M Severe diabetic ketoacidosis (diabetic coma). 482 episodes in 257 patients; experience of three years. Diabetes. 20: Bieberdorf, F. A., S. S. Chernick, and R. 0. Scow Effect of insulin and acute diabetes on plasma FFA and ketone bodies in the fasting rat. J. Clin. nvest. 49: Fritz,. B., and N. R. Marquis The role of acylcarnitine esters and carnitine palmityltransferase in the transport of fatty acyl groups across mitochondrial membranes. Proc. Natl. Acad. Sci. U. S. A. 54: Balasse, E. 0., and R. J. Havel Turnover rate and oxidation of ketone bodies in normal and diabetic dogs Diabetologia. 6: Carlson, L. A Antilipolysis as a tool in the study of clinical and experimental diabetes. Diabetologia. 5: Smith, K., and H. E. Martin Response of diabetic coma to various insulin dosages. Diabetes. 3: Shaw, C. E., G. E. Horwitz, M. Schmukler, S. H. Brager, and S. P. Bessman A clinical and laboratory study of insulin dosage in diabetic acidosis: comparison with small and large doses. Diabetes. 11: Williamson, J. R Effects of fatty acids, glucagon and anti-insulin serum on the control of gluconeogenesis and ketogenesis in rat liver. Adv. Enzyme Regul. 5: Randle, P. J., P. B. Garland, C. N. Hales, and E. A. Newsholme The glucose fatty-acid cycle. ts role in insulin sensitivity and the metabolic disturbances of diabetes mellitus. Lancet. 1: Park, C. R., D. Reinwein, M. J. Henderson, E. Cadenas, and H. E. Morgan The action of insulin on the transport of glucose through the cell membrane. Am. J. Med. 26: Cahill, G. F., Jr Physiology of insulin in man. Diabetes. 20: Morgan, H. E., M. J. Henderson, D. M. Regen, and C. R. Park Regulation of glucose uptake in muscle.. The effects of insulin and anoxia on glucose transport and phosphorylation in the isolated perfused heart of normal rats. J. Biol. Chem. 236: Ozand, P., H. T. Narahara, and C. F. Cori Studies of tissue permeability. V. The effect of anaerobiosis on glucose uptake in frog sartorius muscle. J. Biol. Chem. 237: Lawrence, R. D The effect of exercise on insulin action in diabetes. Br. Med. J. 1: Klachko, D. M., T. H. Lie, E. J. Cunningham, G. R. Chase, and T. W. Burns Blood glucose levels during walking in normal and diabetic subjects. Diabetes. 21: Huckabee, W. E Relationships of pyruvate and lactate during anaerobic metabolism.. Exercise and formation of 02-debt. J. Clin. nvest. 37: Van Harken, D. R, C. W. Dixon, and M. Heimberg Hepatic lipid metabolism in experimental diabetes. V. The effect of concentration of oleate on metabolism of triglycerides and on ketogenesis. J. Biol. Chem. 244: J. D. McGarry and D. W. Foster
THE GLUCOSE-FATTY ACID-KETONE BODY CYCLE Role of ketone bodies as respiratory substrates and metabolic signals
 Br. J. Anaesth. (1981), 53, 131 THE GLUCOSE-FATTY ACID-KETONE BODY CYCLE Role of ketone bodies as respiratory substrates and metabolic signals J. C. STANLEY In this paper, the glucose-fatty acid cycle
Br. J. Anaesth. (1981), 53, 131 THE GLUCOSE-FATTY ACID-KETONE BODY CYCLE Role of ketone bodies as respiratory substrates and metabolic signals J. C. STANLEY In this paper, the glucose-fatty acid cycle
Oxidation of Long Chain Fatty Acids
 Oxidation of Long Chain Fatty Acids Dr NC Bird Oxidation of long chain fatty acids is the primary source of energy supply in man and animals. Hibernating animals utilise fat stores to maintain body heat,
Oxidation of Long Chain Fatty Acids Dr NC Bird Oxidation of long chain fatty acids is the primary source of energy supply in man and animals. Hibernating animals utilise fat stores to maintain body heat,
Medical Biochemistry and Molecular Biology department
 Medical Biochemistry and Molecular Biology department Cardiac Fuels [Sources of energy for the Cardiac muscle] Intended learning outcomes of the lecture: By the end of this lecture you would be able to:-
Medical Biochemistry and Molecular Biology department Cardiac Fuels [Sources of energy for the Cardiac muscle] Intended learning outcomes of the lecture: By the end of this lecture you would be able to:-
CHY2026: General Biochemistry. Lipid Metabolism
 CHY2026: General Biochemistry Lipid Metabolism Lipid Digestion Lipid Metabolism Fats (triglycerides) are high metabolic energy molecules Fats yield 9.3 kcal of energy (carbohydrates and proteins 4.1 kcal)
CHY2026: General Biochemistry Lipid Metabolism Lipid Digestion Lipid Metabolism Fats (triglycerides) are high metabolic energy molecules Fats yield 9.3 kcal of energy (carbohydrates and proteins 4.1 kcal)
Integration Of Metabolism
 Integration Of Metabolism Metabolism Consist of Highly Interconnected Pathways The basic strategy of catabolic metabolism is to form ATP, NADPH, and building blocks for biosyntheses. 1. ATP is the universal
Integration Of Metabolism Metabolism Consist of Highly Interconnected Pathways The basic strategy of catabolic metabolism is to form ATP, NADPH, and building blocks for biosyntheses. 1. ATP is the universal
23.1 Lipid Metabolism in Animals. Chapter 23. Micelles Lipid Metabolism in. Animals. Overview of Digestion Lipid Metabolism in
 Denniston Topping Caret Copyright! The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Chapter 23 Fatty Acid Metabolism Triglycerides (Tgl) are emulsified into fat droplets
Denniston Topping Caret Copyright! The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Chapter 23 Fatty Acid Metabolism Triglycerides (Tgl) are emulsified into fat droplets
Lipid Metabolism. Remember fats?? Triacylglycerols - major form of energy storage in animals
 Remember fats?? Triacylglycerols - major form of energy storage in animals Your energy reserves: ~0.5% carbs (glycogen + glucose) ~15% protein (muscle, last resort) ~85% fat Why use fat for energy? 1 gram
Remember fats?? Triacylglycerols - major form of energy storage in animals Your energy reserves: ~0.5% carbs (glycogen + glucose) ~15% protein (muscle, last resort) ~85% fat Why use fat for energy? 1 gram
Chapter 22, Fatty Acid Metabolism CH 3 (CH 2 ) 14 CO 2 R C C O2 CH 2 OH O R. Lipase + 3 H 2 O
 hapter 22, Fatty Acid Metabolism Pages: 603-613 I. Introduction - Fatty acids have 4 major physiological roles: - omponents of phospholipids and glycolipids (membranes) - Attachment to Proteins targets
hapter 22, Fatty Acid Metabolism Pages: 603-613 I. Introduction - Fatty acids have 4 major physiological roles: - omponents of phospholipids and glycolipids (membranes) - Attachment to Proteins targets
[14C]Palmitate uptake in isolated rat liver mitochondria: effects of fasting, diabetes mellitus, and inhibitors of carnitine acyltransferase
![[14C]Palmitate uptake in isolated rat liver mitochondria: effects of fasting, diabetes mellitus, and inhibitors of carnitine acyltransferase [14C]Palmitate uptake in isolated rat liver mitochondria: effects of fasting, diabetes mellitus, and inhibitors of carnitine acyltransferase](/thumbs/80/82271725.jpg) [14C]Palmitate uptake in isolated rat liver mitochondria: effects of fasting, diabetes mellitus, and inhibitors of carnitine acyltransferase John M. Amatruda, Dean H. Lockwood, Simeon Margolis, and Lutz
[14C]Palmitate uptake in isolated rat liver mitochondria: effects of fasting, diabetes mellitus, and inhibitors of carnitine acyltransferase John M. Amatruda, Dean H. Lockwood, Simeon Margolis, and Lutz
Chapter 24 Lecture Outline
 Chapter 24 Lecture Outline Carbohydrate Lipid and Protein! Metabolism! In the catabolism of carbohydrates, glycolysis converts glucose into pyruvate, which is then metabolized into acetyl CoA. Prepared
Chapter 24 Lecture Outline Carbohydrate Lipid and Protein! Metabolism! In the catabolism of carbohydrates, glycolysis converts glucose into pyruvate, which is then metabolized into acetyl CoA. Prepared
Metabolism of cardiac muscle. Dr. Mamoun Ahram Cardiovascular system, 2013
 Metabolism of cardiac muscle Dr. Mamoun Ahram Cardiovascular system, 2013 References This lecture Mark s Basic Medical Biochemistry, 4 th ed., p. 890-891 Hand-out Why is this topic important? Heart failure
Metabolism of cardiac muscle Dr. Mamoun Ahram Cardiovascular system, 2013 References This lecture Mark s Basic Medical Biochemistry, 4 th ed., p. 890-891 Hand-out Why is this topic important? Heart failure
Integration of Metabolism 1. made by: Noor M. ALnairat. Sheet No. 18
 Integration of Metabolism 1 made by: Noor M. ALnairat Sheet No. 18 Data :24/11/2016 SLIDE 2: Metabolism Consist of Highly Interconnected Pathways The basic strategy of catabolic metabolism is to form ATP,
Integration of Metabolism 1 made by: Noor M. ALnairat Sheet No. 18 Data :24/11/2016 SLIDE 2: Metabolism Consist of Highly Interconnected Pathways The basic strategy of catabolic metabolism is to form ATP,
Roles of Lipids. principal form of stored energy major constituents of cell membranes vitamins messengers intra and extracellular
 Roles of Lipids principal form of stored energy major constituents of cell membranes vitamins messengers intra and extracellular = Oxidation of fatty acids Central energy-yielding pathway in animals. O
Roles of Lipids principal form of stored energy major constituents of cell membranes vitamins messengers intra and extracellular = Oxidation of fatty acids Central energy-yielding pathway in animals. O
Glucagon Regulation of Plasma Ketone Body Concentration
 Glucagon Regulation of Plasma Ketone Body Concentration in Human Diabetes DAVID S. ScHADE and R. PHiIp EATON From the Department of Medicine, University of New Mexico School of Medicine, Albuquerque, New
Glucagon Regulation of Plasma Ketone Body Concentration in Human Diabetes DAVID S. ScHADE and R. PHiIp EATON From the Department of Medicine, University of New Mexico School of Medicine, Albuquerque, New
5.0 HORMONAL CONTROL OF CARBOHYDRATE METABOLISM
 5.0 HORMONAL CONTROL OF CARBOHYDRATE METABOLISM Introduction: Variety of hormones and other molecules regulate the carbohydrates metabolism. Some of these have already been cited in previous sections.
5.0 HORMONAL CONTROL OF CARBOHYDRATE METABOLISM Introduction: Variety of hormones and other molecules regulate the carbohydrates metabolism. Some of these have already been cited in previous sections.
Lipid Metabolism * OpenStax
 OpenStax-CNX module: m46462 1 Lipid Metabolism * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of this section, you will be able
OpenStax-CNX module: m46462 1 Lipid Metabolism * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of this section, you will be able
Chemistry 1120 Exam 4 Study Guide
 Chemistry 1120 Exam 4 Study Guide Chapter 12 12.1 Identify and differentiate between macronutrients (lipids, amino acids and saccharides) and micronutrients (vitamins and minerals). Master Tutor Section
Chemistry 1120 Exam 4 Study Guide Chapter 12 12.1 Identify and differentiate between macronutrients (lipids, amino acids and saccharides) and micronutrients (vitamins and minerals). Master Tutor Section
The Contribution of Endogenous Insulin Secretion to the Ketogenic Response to Glucagon in Man* D. S. Schade and R. P. Eaton
 Diabetologia 11,555-559 (1975) 9 by Springer-Verlag 1975 The Contribution of Endogenous Insulin Secretion to the Ketogenic Response to Glucagon in Man* D. S. Schade and R. P. Eaton Dept. of Medicine, Univ.
Diabetologia 11,555-559 (1975) 9 by Springer-Verlag 1975 The Contribution of Endogenous Insulin Secretion to the Ketogenic Response to Glucagon in Man* D. S. Schade and R. P. Eaton Dept. of Medicine, Univ.
Hormonal Control of Ketogenesis
 Hormonal Control of Ketogenesis RAPID ACTIVATION OF HEPATIC KETOGENIC CAPACITY IN FED RATS BY ANTI-INSULIN SERUM AND GLUCAGON J. DENIS McGARRY, PETER H. WRIGHT, and DANIEL W. FOSTER From the Departments
Hormonal Control of Ketogenesis RAPID ACTIVATION OF HEPATIC KETOGENIC CAPACITY IN FED RATS BY ANTI-INSULIN SERUM AND GLUCAGON J. DENIS McGARRY, PETER H. WRIGHT, and DANIEL W. FOSTER From the Departments
LIPID METABOLISM. Sri Widia A Jusman Department of Biochemistry & Molecular Biology FMUI
 LIPID METABOLISM Sri Widia A Jusman Department of Biochemistry & Molecular Biology FMUI Lipid metabolism is concerned mainly with fatty acids cholesterol Source of fatty acids from dietary fat de novo
LIPID METABOLISM Sri Widia A Jusman Department of Biochemistry & Molecular Biology FMUI Lipid metabolism is concerned mainly with fatty acids cholesterol Source of fatty acids from dietary fat de novo
Biosynthesis of Fatty Acids. By Dr.QUTAIBA A. QASIM
 Biosynthesis of Fatty Acids By Dr.QUTAIBA A. QASIM Fatty Acids Definition Fatty acids are comprised of hydrocarbon chains terminating with carboxylic acid groups. Fatty acids and their associated derivatives
Biosynthesis of Fatty Acids By Dr.QUTAIBA A. QASIM Fatty Acids Definition Fatty acids are comprised of hydrocarbon chains terminating with carboxylic acid groups. Fatty acids and their associated derivatives
Role of fatty acids in the development of insulin resistance and type 2 diabetes mellitus
 Emerging Science Role of fatty acids in the development of insulin resistance and type 2 diabetes mellitus George Wolf Insulin resistance is defined as the reduced responsiveness to normal circulating
Emerging Science Role of fatty acids in the development of insulin resistance and type 2 diabetes mellitus George Wolf Insulin resistance is defined as the reduced responsiveness to normal circulating
Effect of Insulin and Acute Diabetes on Plasma FFA and Ketone Bodies in the Fasting Rat
 Effect of Insulin and Acute Diabetes on Plasma FFA and Ketone Bodies in the Fasting Rat FREmimicic A. B nomerf, SDNEY S. CGINIcK, and ROBERT 0. Scow From the Laboratory of Nutrition and Endocrinology,
Effect of Insulin and Acute Diabetes on Plasma FFA and Ketone Bodies in the Fasting Rat FREmimicic A. B nomerf, SDNEY S. CGINIcK, and ROBERT 0. Scow From the Laboratory of Nutrition and Endocrinology,
clearing activity is produced and destroyed in the rat. Both the
 THE SITES AT WHICH PLASMA CLEARING ACTIVITY IS PRODUCED AND DESTROYED IN THE RAT. By G. H. JEFFRIES. From the Sir William Dunn School of Pathology, Oxford. (Received for publication 25th June 1954.) CLEARING
THE SITES AT WHICH PLASMA CLEARING ACTIVITY IS PRODUCED AND DESTROYED IN THE RAT. By G. H. JEFFRIES. From the Sir William Dunn School of Pathology, Oxford. (Received for publication 25th June 1954.) CLEARING
Lecture 5: Cell Metabolism. Biology 219 Dr. Adam Ross
 Lecture 5: Cell Metabolism Biology 219 Dr. Adam Ross Cellular Respiration Set of reactions that take place during the conversion of nutrients into ATP Intricate regulatory relationship between several
Lecture 5: Cell Metabolism Biology 219 Dr. Adam Ross Cellular Respiration Set of reactions that take place during the conversion of nutrients into ATP Intricate regulatory relationship between several
Integrative Metabolism: Significance
 Integrative Metabolism: Significance Energy Containing Nutrients Carbohydrates Fats Proteins Catabolism Energy Depleted End Products H 2 O NH 3 ADP + Pi NAD + NADP + FAD + Pi NADH+H + NADPH+H + FADH2 Cell
Integrative Metabolism: Significance Energy Containing Nutrients Carbohydrates Fats Proteins Catabolism Energy Depleted End Products H 2 O NH 3 ADP + Pi NAD + NADP + FAD + Pi NADH+H + NADPH+H + FADH2 Cell
Lehninger 5 th ed. Chapter 17
 Lehninger 5 th ed. Chapter 17 December 26, 2010 Prof. Shimon Schuldiner Email: Shimon.Schuldiner@huji.ac.il Phone: 6585992 CHAPTER 17 Fatty Acid Catabolism Key topics: How fats are digested in animals
Lehninger 5 th ed. Chapter 17 December 26, 2010 Prof. Shimon Schuldiner Email: Shimon.Schuldiner@huji.ac.il Phone: 6585992 CHAPTER 17 Fatty Acid Catabolism Key topics: How fats are digested in animals
Biochemistry: A Short Course
 Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 28 Fatty Acid Synthesis 2013 W. H. Freeman and Company Chapter 28 Outline 1. The first stage of fatty acid synthesis is transfer
Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 28 Fatty Acid Synthesis 2013 W. H. Freeman and Company Chapter 28 Outline 1. The first stage of fatty acid synthesis is transfer
Physiology Unit 1 METABOLISM OF LIPIDS AND PROTEINS
 Physiology Unit 1 METABOLISM OF LIPIDS AND PROTEINS Alternate Fuel Sources When glucose levels are low Proteins and Triglycerides will be metabolized Tissues will use different fuel sources depending on:
Physiology Unit 1 METABOLISM OF LIPIDS AND PROTEINS Alternate Fuel Sources When glucose levels are low Proteins and Triglycerides will be metabolized Tissues will use different fuel sources depending on:
BIL 256 Cell and Molecular Biology Lab Spring, Tissue-Specific Isoenzymes
 BIL 256 Cell and Molecular Biology Lab Spring, 2007 Background Information Tissue-Specific Isoenzymes A. BIOCHEMISTRY The basic pattern of glucose oxidation is outlined in Figure 3-1. Glucose is split
BIL 256 Cell and Molecular Biology Lab Spring, 2007 Background Information Tissue-Specific Isoenzymes A. BIOCHEMISTRY The basic pattern of glucose oxidation is outlined in Figure 3-1. Glucose is split
Metabolic Precautions & ER Recommendations
 Metabolic Precautions & ER Recommendations * To whom correspondence Sumit Parikh, should MD be addressed Center for Pediatric Neurology Cleveland Clinic Cleveland, OH UMDF 2010 The catabolic state Entering
Metabolic Precautions & ER Recommendations * To whom correspondence Sumit Parikh, should MD be addressed Center for Pediatric Neurology Cleveland Clinic Cleveland, OH UMDF 2010 The catabolic state Entering
Companion to Biosynthesis of Ketones & Cholesterols, Regulation of Lipid Metabolism Lecture Notes
 Companion to Biosynthesis of Ketones & Cholesterols, Regulation of Lipid Metabolism Lecture Notes The major site of acetoacetate and 3-hydorxybutyrate production is in the liver. 3-hydorxybutyrate is the
Companion to Biosynthesis of Ketones & Cholesterols, Regulation of Lipid Metabolism Lecture Notes The major site of acetoacetate and 3-hydorxybutyrate production is in the liver. 3-hydorxybutyrate is the
Introduction to Carbohydrate metabolism
 Introduction to Carbohydrate metabolism Some metabolic pathways of carbohydrates 1- Glycolysis 2- Krebs cycle 3- Glycogenesis 4- Glycogenolysis 5- Glyconeogenesis - Pentose Phosphate Pathway (PPP) - Curi
Introduction to Carbohydrate metabolism Some metabolic pathways of carbohydrates 1- Glycolysis 2- Krebs cycle 3- Glycogenesis 4- Glycogenolysis 5- Glyconeogenesis - Pentose Phosphate Pathway (PPP) - Curi
Package Insert. Elkar
 Package Insert Elkar Product Summary 1. Name of the medicinal product Elkar 500 mg tablets 2. Qualitative and quantitative composition Each tablet contains levocarnitine 500 mg. 3. Pharmaceutical form
Package Insert Elkar Product Summary 1. Name of the medicinal product Elkar 500 mg tablets 2. Qualitative and quantitative composition Each tablet contains levocarnitine 500 mg. 3. Pharmaceutical form
Part III => METABOLISM and ENERGY. 3.4 Lipid Catabolism 3.4a Fatty Acid Degradation 3.4b Ketone Bodies
 Part III => METABOLISM and ENERGY 3.4 Lipid Catabolism 3.4a Fatty Acid Degradation 3.4b Ketone Bodies Section 3.4a: Fatty Acid Degradation Synopsis 3.4a - Triglycerides (or fats) in the diet or adipose
Part III => METABOLISM and ENERGY 3.4 Lipid Catabolism 3.4a Fatty Acid Degradation 3.4b Ketone Bodies Section 3.4a: Fatty Acid Degradation Synopsis 3.4a - Triglycerides (or fats) in the diet or adipose
Energy metabolism - the overview
 Energy metabolism - the overview Josef Fontana EC - 40 Overview of the lecture Important terms of the energy metabolism The overview of the energy metabolism The main pathways of the energy metabolism
Energy metabolism - the overview Josef Fontana EC - 40 Overview of the lecture Important terms of the energy metabolism The overview of the energy metabolism The main pathways of the energy metabolism
The molecule that serves as the major source of readily available body fuel is: a. fat. b. glucose. c. acetyl CoA. d. cellulose.
 The molecule that serves as the major source of readily available body fuel is: a. fat. b. glucose. c. acetyl CoA. d. cellulose. Dietary fats are important because: a. they keep blood pressure normal.
The molecule that serves as the major source of readily available body fuel is: a. fat. b. glucose. c. acetyl CoA. d. cellulose. Dietary fats are important because: a. they keep blood pressure normal.
Summary of fatty acid synthesis
 Lipid Metabolism, part 2 1 Summary of fatty acid synthesis 8 acetyl CoA + 14 NADPH + 14 H+ + 7 ATP palmitic acid (16:0) + 8 CoA + 14 NADP + + 7 ADP + 7 Pi + 7 H20 1. The major suppliers of NADPH for fatty
Lipid Metabolism, part 2 1 Summary of fatty acid synthesis 8 acetyl CoA + 14 NADPH + 14 H+ + 7 ATP palmitic acid (16:0) + 8 CoA + 14 NADP + + 7 ADP + 7 Pi + 7 H20 1. The major suppliers of NADPH for fatty
e-learning Fatty Acid Oxidation Defects Camilla Reed and Dr Simon Olpin Sheffield Children s Hospital
 e-learning Fatty Acid Oxidation Defects Camilla Reed and Dr Simon Olpin Sheffield Children s Hospital Fatty Acids Fatty acids are a major source of energy and body fat is an energy dense material. They
e-learning Fatty Acid Oxidation Defects Camilla Reed and Dr Simon Olpin Sheffield Children s Hospital Fatty Acids Fatty acids are a major source of energy and body fat is an energy dense material. They
University College, London.)
 6I2.I2I:547.472*3 LACTIC ACID FORMATION AND REMOVAL WITH CHANGE OF BLOOD REACTION. BY M. GRACE EGGLETON1 AND C. LOVATT EVANS. (From the Department of Physiology and Biochemistry, University College, London.)
6I2.I2I:547.472*3 LACTIC ACID FORMATION AND REMOVAL WITH CHANGE OF BLOOD REACTION. BY M. GRACE EGGLETON1 AND C. LOVATT EVANS. (From the Department of Physiology and Biochemistry, University College, London.)
Fatty Acid and Triacylglycerol Metabolism 1
 Fatty Acid and Triacylglycerol Metabolism 1 Mobilization of stored fats and oxidation of fatty acids Lippincott s Chapter 16 What is the first lecture about What is triacylglycerol Fatty acids structure
Fatty Acid and Triacylglycerol Metabolism 1 Mobilization of stored fats and oxidation of fatty acids Lippincott s Chapter 16 What is the first lecture about What is triacylglycerol Fatty acids structure
Insulin Secretion in Diabetes Mellitus
 A Role for AlphaAdrenergic Receptors in Abnormal nsulin Secretion in Diabetes Mellitus R. PAUL ROBERTSON, JEFFREY B. HALTER, and DANiEL PORTE, JR. From the University of Washington School of Medicine and
A Role for AlphaAdrenergic Receptors in Abnormal nsulin Secretion in Diabetes Mellitus R. PAUL ROBERTSON, JEFFREY B. HALTER, and DANiEL PORTE, JR. From the University of Washington School of Medicine and
Integration Of Metabolism
 Integration Of Metabolism Metabolism Consist of Highly Interconnected Pathways The basic strategy of catabolic metabolism is to form ATP, NADPH, and building blocks for biosyntheses. 1. ATP is the universal
Integration Of Metabolism Metabolism Consist of Highly Interconnected Pathways The basic strategy of catabolic metabolism is to form ATP, NADPH, and building blocks for biosyntheses. 1. ATP is the universal
A Comparison of Leucine- and Acetoacetate-induced Hypoglycemia in Man *
 Journal of Clinical Investigation Vol. 43, No. 1, 1964 A Comparison of Leucine- and Acetoacetate-induced Hypoglycemia in Man * STEFAN S. FAJANS, JOHN C. FLOYD, JR., RALPH F. KNOPF, AND JEROME W. CONN (From
Journal of Clinical Investigation Vol. 43, No. 1, 1964 A Comparison of Leucine- and Acetoacetate-induced Hypoglycemia in Man * STEFAN S. FAJANS, JOHN C. FLOYD, JR., RALPH F. KNOPF, AND JEROME W. CONN (From
Biochemistry: A Short Course
 Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 27 Fatty Acid Degradation Dietary Lipid (Triacylglycerol) Metabolism - In the small intestine, fat particles are coated with bile
Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 27 Fatty Acid Degradation Dietary Lipid (Triacylglycerol) Metabolism - In the small intestine, fat particles are coated with bile
Intermediary metabolism. Eva Samcová
 Intermediary metabolism Eva Samcová Metabolic roles of tissues Four major tissues play a dominant role in fuel metabolism : liver, adipose, muscle, and brain. These tissues do not function in isolation.
Intermediary metabolism Eva Samcová Metabolic roles of tissues Four major tissues play a dominant role in fuel metabolism : liver, adipose, muscle, and brain. These tissues do not function in isolation.
UNIVERSITY OF BOLTON SPORT AND BIOLOGICAL SCIENCES SPORT AND EXERCISE SCIENCE PATHWAY SEMESTER TWO EXAMINATIONS 2016/2017
 LH14 UNIVERSITY OF BOLTON SPORT AND BIOLOGICAL SCIENCES SPORT AND EXERCISE SCIENCE PATHWAY SEMESTER TWO EXAMINATIONS 2016/2017 INTRODUCTION TO SPORT AND EXERCISE PHYSIOLOGY MODULE NO: SPS4002 Date: Thursday
LH14 UNIVERSITY OF BOLTON SPORT AND BIOLOGICAL SCIENCES SPORT AND EXERCISE SCIENCE PATHWAY SEMESTER TWO EXAMINATIONS 2016/2017 INTRODUCTION TO SPORT AND EXERCISE PHYSIOLOGY MODULE NO: SPS4002 Date: Thursday
UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY
 1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS An Overview WHAT IS HOMEOSTASIS? Homeostasis
1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS An Overview WHAT IS HOMEOSTASIS? Homeostasis
By: Dr Hadi Mozafari 1
 By: Dr Hadi Mozafari 1 Gluconeogenesis is the process of converting noncarbohydrate precursors to glucose or glycogen. The major substrates are the glucogenic amino acids, and lactate, glycerol, and propionate.
By: Dr Hadi Mozafari 1 Gluconeogenesis is the process of converting noncarbohydrate precursors to glucose or glycogen. The major substrates are the glucogenic amino acids, and lactate, glycerol, and propionate.
Voet Biochemistry 3e John Wiley & Sons, Inc.
 * * Voet Biochemistry 3e Lipid Metabolism Part I: (Chap. 25, sec.1-3) Glucose C 6 H 12 O 6 + 6 O 2 6 CO 2 + 6 H 2 O G o = -2823 kj/mol Fats (palmitic acid) C 16 H 32 O 2 + 23 O 2 16 CO 2 + 16 H 2 O G o
* * Voet Biochemistry 3e Lipid Metabolism Part I: (Chap. 25, sec.1-3) Glucose C 6 H 12 O 6 + 6 O 2 6 CO 2 + 6 H 2 O G o = -2823 kj/mol Fats (palmitic acid) C 16 H 32 O 2 + 23 O 2 16 CO 2 + 16 H 2 O G o
Plasma Triglyceride Concentration and Plasma Free
 Journal of Clinical Investigation Vol. 3, No. 1, 196 Plasma Triglyceride Concentration and Plasma Free Fatty Acid Changes in Response to Norepinephrine in Man * (From the University of Melbourne Department
Journal of Clinical Investigation Vol. 3, No. 1, 196 Plasma Triglyceride Concentration and Plasma Free Fatty Acid Changes in Response to Norepinephrine in Man * (From the University of Melbourne Department
Chapter 3: The basics of fuel utilization
 Chapter 3: The basics of fuel utilization Although this chapter does not discuss the ketogenic diet in great detail, the information presented is helpful in understanding the following chapters. There
Chapter 3: The basics of fuel utilization Although this chapter does not discuss the ketogenic diet in great detail, the information presented is helpful in understanding the following chapters. There
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 25 Metabolism and Nutrition Metabolic Reactions Metabolism refers to all of the chemical reactions taking place in the body. Reactions that break
Principles of Anatomy and Physiology 14 th Edition CHAPTER 25 Metabolism and Nutrition Metabolic Reactions Metabolism refers to all of the chemical reactions taking place in the body. Reactions that break
Chapter 7- Metabolism: Transformations and Interactions Thomson - Wadsworth
 Chapter 7- Metabolism: Transformations and Interactions 2008 Thomson - Wadsworth Simple Overview of Energy Metabolism The sum of all chemical reactions that go on in living cells Introduction Energy Heat-
Chapter 7- Metabolism: Transformations and Interactions 2008 Thomson - Wadsworth Simple Overview of Energy Metabolism The sum of all chemical reactions that go on in living cells Introduction Energy Heat-
In glycolysis, glucose is converted to pyruvate. If the pyruvate is reduced to lactate, the pathway does not require O 2 and is called anaerobic
 Glycolysis 1 In glycolysis, glucose is converted to pyruvate. If the pyruvate is reduced to lactate, the pathway does not require O 2 and is called anaerobic glycolysis. If this pyruvate is converted instead
Glycolysis 1 In glycolysis, glucose is converted to pyruvate. If the pyruvate is reduced to lactate, the pathway does not require O 2 and is called anaerobic glycolysis. If this pyruvate is converted instead
Cellular Respiration Checkup Quiz. 1. Of the following products, which is produced by both anaerobic respiration and aerobic respiration in humans?
 1. Of the following products, which is produced by both anaerobic respiration and aerobic respiration in humans? I. Pyruvate II. III. ATP Lactate A. I only B. I and II only C. I, II and III D. II and III
1. Of the following products, which is produced by both anaerobic respiration and aerobic respiration in humans? I. Pyruvate II. III. ATP Lactate A. I only B. I and II only C. I, II and III D. II and III
anabolic pathways- Catabolic Amphibolic
 METABOLISM Introduction The fate of dietary components after digestion and absorption constitute metabolism regulated by metabolic pathway 3 types: anabolic pathways- Synthesis of compound e.g. synthesis
METABOLISM Introduction The fate of dietary components after digestion and absorption constitute metabolism regulated by metabolic pathway 3 types: anabolic pathways- Synthesis of compound e.g. synthesis
number Done by Corrected by Doctor Nayef Karadsheh
 number 13 Done by Asma Karameh Corrected by Saad hayek Doctor Nayef Karadsheh Gluconeogenesis This lecture covers gluconeogenesis with aspects of: 1) Introduction to glucose distribution through tissues.
number 13 Done by Asma Karameh Corrected by Saad hayek Doctor Nayef Karadsheh Gluconeogenesis This lecture covers gluconeogenesis with aspects of: 1) Introduction to glucose distribution through tissues.
OVERVIEW M ET AB OL IS M OF FR EE FA TT Y AC ID S
 LIPOLYSIS LIPOLYSIS OVERVIEW CATABOLISM OF FREE FATTY ACIDS Nonesterified fatty acids Source:- (a) breakdown of TAG in adipose tissue (b) action of Lipoprotein lipase on plasma TAG Combined with Albumin
LIPOLYSIS LIPOLYSIS OVERVIEW CATABOLISM OF FREE FATTY ACIDS Nonesterified fatty acids Source:- (a) breakdown of TAG in adipose tissue (b) action of Lipoprotein lipase on plasma TAG Combined with Albumin
CHAPTER 24: Carbohydrate, Lipid, & Protein Metabolism. General, Organic, & Biological Chemistry Janice Gorzynski Smith
 CHAPTER 24: Carbohydrate, Lipid, & Protein Metabolism General, Organic, & Biological Chemistry Janice Gorzynski Smith CHAPTER 24: Carbohydrate, Lipid, & Protein Metabolism Learning Objectives: q Role in
CHAPTER 24: Carbohydrate, Lipid, & Protein Metabolism General, Organic, & Biological Chemistry Janice Gorzynski Smith CHAPTER 24: Carbohydrate, Lipid, & Protein Metabolism Learning Objectives: q Role in
Case Study: Carbohydrate Metabolism. eating an early dinner the night before and skipping breakfast that morning, Sid goes to the
 Student Name Biochemistry 4320 Case Study Part I 4 November 2013 Case Study: Carbohydrate Metabolism Sid is a high school student who has decided to start exercising before school. After eating an early
Student Name Biochemistry 4320 Case Study Part I 4 November 2013 Case Study: Carbohydrate Metabolism Sid is a high school student who has decided to start exercising before school. After eating an early
3.7 CELLULAR RESPIRATION. How are these two images related?
 3.7 CELLULAR RESPIRATION How are these two images related? CELLULAR RESPIRATION Cellular respiration is the process whereby the body converts the energy that we get from food (glucose) into an energy form
3.7 CELLULAR RESPIRATION How are these two images related? CELLULAR RESPIRATION Cellular respiration is the process whereby the body converts the energy that we get from food (glucose) into an energy form
BCM 221 LECTURES OJEMEKELE O.
 BCM 221 LECTURES BY OJEMEKELE O. OUTLINE INTRODUCTION TO LIPID CHEMISTRY STORAGE OF ENERGY IN ADIPOCYTES MOBILIZATION OF ENERGY STORES IN ADIPOCYTES KETONE BODIES AND KETOSIS PYRUVATE DEHYDROGENASE COMPLEX
BCM 221 LECTURES BY OJEMEKELE O. OUTLINE INTRODUCTION TO LIPID CHEMISTRY STORAGE OF ENERGY IN ADIPOCYTES MOBILIZATION OF ENERGY STORES IN ADIPOCYTES KETONE BODIES AND KETOSIS PYRUVATE DEHYDROGENASE COMPLEX
How Did Energy-Releasing Pathways Evolve? (cont d.)
 How Did Energy-Releasing Pathways Evolve? (cont d.) 7.1 How Do Cells Access the Chemical Energy in Sugars? In order to use the energy stored in sugars, cells must first transfer it to ATP The energy transfer
How Did Energy-Releasing Pathways Evolve? (cont d.) 7.1 How Do Cells Access the Chemical Energy in Sugars? In order to use the energy stored in sugars, cells must first transfer it to ATP The energy transfer
Biology 638 Biochemistry II Exam-3. (Note that you are not allowed to use any calculator)
 Biology 638 Biochemistry II Exam-3 (Note that you are not allowed to use any calculator) 1. In the non-cyclic pathway, electron pathway is. Select the most accurate one. a. PSII PC Cyt b 6 f PC PSI Fd-NADP
Biology 638 Biochemistry II Exam-3 (Note that you are not allowed to use any calculator) 1. In the non-cyclic pathway, electron pathway is. Select the most accurate one. a. PSII PC Cyt b 6 f PC PSI Fd-NADP
Integration & Hormone Regulation
 Integration Branchpoints in metabolism where metabolites can go several directions 1. Glucose 6-phosphate Energy needed (low energy charge): glycolysis Low blood sugar: high [glucagon], low [insulin] glycogen
Integration Branchpoints in metabolism where metabolites can go several directions 1. Glucose 6-phosphate Energy needed (low energy charge): glycolysis Low blood sugar: high [glucagon], low [insulin] glycogen
Lecture 29: Membrane Transport and metabolism
 Chem*3560 Lecture 29: Membrane Transport and metabolism Insulin controls glucose uptake Adipose tissue and muscles contain a passive glucose transporter GluT4 which takes up glucose from blood. (This is
Chem*3560 Lecture 29: Membrane Transport and metabolism Insulin controls glucose uptake Adipose tissue and muscles contain a passive glucose transporter GluT4 which takes up glucose from blood. (This is
Lipid metabolism. Degradation and biosynthesis of fatty acids Ketone bodies
 Lipid metabolism Degradation and biosynthesis of fatty acids Ketone bodies Fatty acids (FA) primary fuel molecules in the fat category main use is for long-term energy storage high level of energy storage:
Lipid metabolism Degradation and biosynthesis of fatty acids Ketone bodies Fatty acids (FA) primary fuel molecules in the fat category main use is for long-term energy storage high level of energy storage:
Hompes Method Lesson 29 Organic Acids Part One
 Hompes Method Lesson 29 Organic Acids Part One Health for the People Ltd not for reuse without expressed permission Organic Acids - Introduction The ultimate tool for laboratory evaluations in nutritional
Hompes Method Lesson 29 Organic Acids Part One Health for the People Ltd not for reuse without expressed permission Organic Acids - Introduction The ultimate tool for laboratory evaluations in nutritional
Lecture 36. Key Concepts. Overview of lipid metabolism. Reactions of fatty acid oxidation. Energy yield from fatty acid oxidation
 Lecture 36 Lipid Metabolism 1 Fatty Acid Oxidation Ketone Bodies Key Concepts Overview of lipid metabolism Reactions of fatty acid oxidation Energy yield from fatty acid oxidation Formation of ketone bodies
Lecture 36 Lipid Metabolism 1 Fatty Acid Oxidation Ketone Bodies Key Concepts Overview of lipid metabolism Reactions of fatty acid oxidation Energy yield from fatty acid oxidation Formation of ketone bodies
Organic Acids Part 2 Dr. Jeff Moss
 Using organic acids to resolve chief complaints and improve quality of life in chronically ill patients Part II Jeffrey Moss, DDS, CNS, DACBN jeffmoss@mossnutrition.com 413-530-08580858 (cell) 1 Summer
Using organic acids to resolve chief complaints and improve quality of life in chronically ill patients Part II Jeffrey Moss, DDS, CNS, DACBN jeffmoss@mossnutrition.com 413-530-08580858 (cell) 1 Summer
This is an example outline of 3 lectures in BSC (Thanks to Dr. Ellington for sharing this information.)
 This is an example outline of 3 lectures in BSC 2010. (Thanks to Dr. Ellington for sharing this information.) Topic 10: CELLULAR RESPIRATION (lectures 14-16) OBJECTIVES: 1. Know the basic reactions that
This is an example outline of 3 lectures in BSC 2010. (Thanks to Dr. Ellington for sharing this information.) Topic 10: CELLULAR RESPIRATION (lectures 14-16) OBJECTIVES: 1. Know the basic reactions that
18. PANCREATIC FUNCTION AND METABOLISM. Pancreatic secretions ISLETS OF LANGERHANS. Insulin
 18. PANCREATIC FUNCTION AND METABOLISM ISLETS OF LANGERHANS Some pancreatic functions have already been discussed in the digestion section. In this one, the emphasis will be placed on the endocrine function
18. PANCREATIC FUNCTION AND METABOLISM ISLETS OF LANGERHANS Some pancreatic functions have already been discussed in the digestion section. In this one, the emphasis will be placed on the endocrine function
Cell Respiration - 1
 Cell Respiration - 1 All cells must do work to stay alive and maintain their cellular environment. The energy needed for cell work comes from the bonds of ATP. Cells obtain their ATP by oxidizing organic
Cell Respiration - 1 All cells must do work to stay alive and maintain their cellular environment. The energy needed for cell work comes from the bonds of ATP. Cells obtain their ATP by oxidizing organic
RELATIONS BETWEEN INSULIN AND PITUITARY HORMONES IN AMINO ACID METABOLISM
 RELATIONS BETWEEN INSULIN AND PITUITARY HORMONES IN AMINO ACID METABOLISM BY WILLIAM D. LOTSPEICH* WITH THE TECHNICAL ASSISTANCE OF JOAN B. SHELTON (From the Department of Physiology, Syracuse University
RELATIONS BETWEEN INSULIN AND PITUITARY HORMONES IN AMINO ACID METABOLISM BY WILLIAM D. LOTSPEICH* WITH THE TECHNICAL ASSISTANCE OF JOAN B. SHELTON (From the Department of Physiology, Syracuse University
Use of Glucagon to Prevent and Treat Fatty Liver in Transition Dairy Cows
 Animal Industry Report AS 650 ASL R1903 2004 Use of Glucagon to Prevent and Treat Fatty Liver in Transition Cows Donald C. Beitz Jerry W. Young Arnold R. Hippen Rafael A. Nafikov Recommended Citation Beitz,
Animal Industry Report AS 650 ASL R1903 2004 Use of Glucagon to Prevent and Treat Fatty Liver in Transition Cows Donald C. Beitz Jerry W. Young Arnold R. Hippen Rafael A. Nafikov Recommended Citation Beitz,
4. Which step shows a split of one molecule into two smaller molecules? a. 2. d. 5
 1. Which of the following statements about NAD + is false? a. NAD + is reduced to NADH during both glycolysis and the citric acid cycle. b. NAD + has more chemical energy than NADH. c. NAD + is reduced
1. Which of the following statements about NAD + is false? a. NAD + is reduced to NADH during both glycolysis and the citric acid cycle. b. NAD + has more chemical energy than NADH. c. NAD + is reduced
How Cells Release Chemical Energy. Chapter 7
 How Cells Release Chemical Energy Chapter 7 7.1 Overview of Carbohydrate Breakdown Pathways All organisms (including photoautotrophs) convert chemical energy of organic compounds to chemical energy of
How Cells Release Chemical Energy Chapter 7 7.1 Overview of Carbohydrate Breakdown Pathways All organisms (including photoautotrophs) convert chemical energy of organic compounds to chemical energy of
How Cells Release Chemical Energy. Chapter 8
 How Cells Release Chemical Energy Chapter 8 Impacts, Issues: When Mitochondria Spin Their Wheels More than forty disorders related to defective mitochondria are known (such as Friedreich s ataxia); many
How Cells Release Chemical Energy Chapter 8 Impacts, Issues: When Mitochondria Spin Their Wheels More than forty disorders related to defective mitochondria are known (such as Friedreich s ataxia); many
Biol 219 Lec 7 Fall 2016
 Cellular Respiration: Harvesting Energy to form ATP Cellular Respiration and Metabolism Glucose ATP Pyruvate Lactate Acetyl CoA NAD + Introducing The Players primary substrate for cellular respiration
Cellular Respiration: Harvesting Energy to form ATP Cellular Respiration and Metabolism Glucose ATP Pyruvate Lactate Acetyl CoA NAD + Introducing The Players primary substrate for cellular respiration
Points 1. Following is the overall reaction catalyzed by the Calvin-Benson cycle:
 BCH 4054 February 22, 2002 HOUR TEST 2 NAME_ Points 1. Following is the overall reaction catalyzed by the Calvin-Benson cycle: CO 2 + 3ATP + 2NADPH 1/3 glyceraldehyde-3-p + 3ADP + 2NADP + Give the structures
BCH 4054 February 22, 2002 HOUR TEST 2 NAME_ Points 1. Following is the overall reaction catalyzed by the Calvin-Benson cycle: CO 2 + 3ATP + 2NADPH 1/3 glyceraldehyde-3-p + 3ADP + 2NADP + Give the structures
Energy stores in different organs for a 155 lb male, in Calories
 Energy stores in different organs for a 155 lb male, in Calories Organ Glucose/ Glycogen Triacyl Glycerols* Liver 400 450 400 Brain 8 0 0 Mobile Proteins Muscle 1,200 450 24,000 Adipose Tissue 80 135,000
Energy stores in different organs for a 155 lb male, in Calories Organ Glucose/ Glycogen Triacyl Glycerols* Liver 400 450 400 Brain 8 0 0 Mobile Proteins Muscle 1,200 450 24,000 Adipose Tissue 80 135,000
BASIC SCIENCES & BIOCHEMISTRY FOR BETZPAENIC BRIMBLERS
 BASIC SCIENCES & BIOCHEMISTRY FOR BETZPAENIC BRIMBLERS Lymphatic Vessels One main lymph vessel receives lymph from the right upper arm and the right side of the head and the thorax and empties into the
BASIC SCIENCES & BIOCHEMISTRY FOR BETZPAENIC BRIMBLERS Lymphatic Vessels One main lymph vessel receives lymph from the right upper arm and the right side of the head and the thorax and empties into the
ANSC/NUTR 618 LIPIDS & LIPID METABOLISM. Triacylglycerol and Fatty Acid Metabolism
 ANSC/NUTR 618 LIPIDS & LIPID METABOLISM II. Triacylglycerol synthesis A. Overall pathway Glycerol-3-phosphate + 3 Fatty acyl-coa à Triacylglycerol + 3 CoASH B. Enzymes 1. Acyl-CoA synthase 2. Glycerol-phosphate
ANSC/NUTR 618 LIPIDS & LIPID METABOLISM II. Triacylglycerol synthesis A. Overall pathway Glycerol-3-phosphate + 3 Fatty acyl-coa à Triacylglycerol + 3 CoASH B. Enzymes 1. Acyl-CoA synthase 2. Glycerol-phosphate
Energy for Muscular Activity
 Energy for Muscular Activity Chapter 7 Sport Books Publisher 1 Learning Objectives: To develop an awareness of the basic chemical processes the body uses to produce energy in the muscles To develop an
Energy for Muscular Activity Chapter 7 Sport Books Publisher 1 Learning Objectives: To develop an awareness of the basic chemical processes the body uses to produce energy in the muscles To develop an
Lipid and Amino Acid Metabolism
 CHEM 3331 Fundamentals of Biochemistry Chapter 14 Lipid and Amino Acid Metabolism Organic and Biochemistry for Today Spencer L. Seager / Michael R. Slabaugh Mr. Kevin A. Boudreaux Angelo State University
CHEM 3331 Fundamentals of Biochemistry Chapter 14 Lipid and Amino Acid Metabolism Organic and Biochemistry for Today Spencer L. Seager / Michael R. Slabaugh Mr. Kevin A. Boudreaux Angelo State University
Week 3 The Pancreas: Pancreatic ph buffering:
 Week 3 The Pancreas: A gland with both endocrine (secretion of substances into the bloodstream) & exocrine (secretion of substances to the outside of the body or another surface within the body) functions
Week 3 The Pancreas: A gland with both endocrine (secretion of substances into the bloodstream) & exocrine (secretion of substances to the outside of the body or another surface within the body) functions
What systems are involved in homeostatic regulation (give an example)?
 1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS (Diabetes Mellitus Part 1): An Overview
1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS (Diabetes Mellitus Part 1): An Overview
Glycolysis Part 2. BCH 340 lecture 4
 Glycolysis Part 2 BCH 340 lecture 4 Regulation of Glycolysis There are three steps in glycolysis that have enzymes which regulate the flux of glycolysis These enzymes catalyzes irreversible reactions of
Glycolysis Part 2 BCH 340 lecture 4 Regulation of Glycolysis There are three steps in glycolysis that have enzymes which regulate the flux of glycolysis These enzymes catalyzes irreversible reactions of
Animal Industry Report
 Animal Industry Report AS 653 ASL R2200 2007 Acute Effects of Postpartal Subcutaneous Injection of and/or Oral Administration of on Blood Metabolites and Hormones and Liver Lipids and Glycogen of Holstein
Animal Industry Report AS 653 ASL R2200 2007 Acute Effects of Postpartal Subcutaneous Injection of and/or Oral Administration of on Blood Metabolites and Hormones and Liver Lipids and Glycogen of Holstein
Name Class Date. 1. Cellular respiration is the process by which the of "food"
 Name Class Date Cell Respiration Introduction Cellular respiration is the process by which the chemical energy of "food" molecules is released and partially captured in the form of ATP. Carbohydrates,
Name Class Date Cell Respiration Introduction Cellular respiration is the process by which the chemical energy of "food" molecules is released and partially captured in the form of ATP. Carbohydrates,
LIPID METABOLISM
 LIPID METABOLISM LIPOGENESIS LIPOGENESIS LIPOGENESIS FATTY ACID SYNTHESIS DE NOVO FFA in the blood come from :- (a) Dietary fat (b) Dietary carbohydrate/protein in excess of need FA TAG Site of synthesis:-
LIPID METABOLISM LIPOGENESIS LIPOGENESIS LIPOGENESIS FATTY ACID SYNTHESIS DE NOVO FFA in the blood come from :- (a) Dietary fat (b) Dietary carbohydrate/protein in excess of need FA TAG Site of synthesis:-
The Arctic Variant of CPT-1A
 The Arctic Variant of CPT-1A Matthew Hirschfeld, MD/PhD Department of Pediatric Hospital Medicine Alaska Native Medical Center Anchorage, AK Background CPT-1 = carnitine palmitoyltransferase type 1 Expressed
The Arctic Variant of CPT-1A Matthew Hirschfeld, MD/PhD Department of Pediatric Hospital Medicine Alaska Native Medical Center Anchorage, AK Background CPT-1 = carnitine palmitoyltransferase type 1 Expressed
number Done by Corrected by Doctor Faisal Al-Khatibe
 number 24 Done by Mohammed tarabieh Corrected by Doctor Faisal Al-Khatibe 1 P a g e *Please look over the previous sheet about fatty acid synthesis **Oxidation(degradation) of fatty acids, occurs in the
number 24 Done by Mohammed tarabieh Corrected by Doctor Faisal Al-Khatibe 1 P a g e *Please look over the previous sheet about fatty acid synthesis **Oxidation(degradation) of fatty acids, occurs in the
Energy Metabolism. Chapter Cengage Learning. All Rights Reserved.
 Energy Metabolism Chapter 7 Introduction Energy Heat, mechanical, electrical, and chemical Metabolism How the body uses foods to meet its needs Chemical Reactions in the Body Energy metabolism How body
Energy Metabolism Chapter 7 Introduction Energy Heat, mechanical, electrical, and chemical Metabolism How the body uses foods to meet its needs Chemical Reactions in the Body Energy metabolism How body
ANATOMY OF A METABOLIC CRISIS: FAOD-style. Mark S. Korson, MD Tufts Medical Center Boston, MA
 ANATOMY OF A METABOLIC CRISIS: FAOD-style Mark S. Korson, MD Tufts Medical Center Boston, MA NORMAL PHYSIOLOGY Anabolic Eating well Calories eaten > body s needs BRAIN uses GLUCOSE MUSCLE uses GLUCOSE
ANATOMY OF A METABOLIC CRISIS: FAOD-style Mark S. Korson, MD Tufts Medical Center Boston, MA NORMAL PHYSIOLOGY Anabolic Eating well Calories eaten > body s needs BRAIN uses GLUCOSE MUSCLE uses GLUCOSE
Furthermore, added choline may exert relatively little effect when. naturally occurring lipotropic factors are present in appreciable amounts
 343 6I2.352.2:547.922 THE EFFECTS OF CHOLESTEROL AND CHOLINE ON LIVER FAT BY C. H. BEST AND JESSIE H. RIDOUT (From the School of Hygiene, University of Toronto) (Received January 27, 1936) THE results
343 6I2.352.2:547.922 THE EFFECTS OF CHOLESTEROL AND CHOLINE ON LIVER FAT BY C. H. BEST AND JESSIE H. RIDOUT (From the School of Hygiene, University of Toronto) (Received January 27, 1936) THE results
MITOCW watch?v=qmqif0yj4lm
 MITOCW watch?v=qmqif0yj4lm The following content is provided under a Creative Commons license. Your support will help MIT OpenCourseWare continue to offer high quality educational resources for free. To
MITOCW watch?v=qmqif0yj4lm The following content is provided under a Creative Commons license. Your support will help MIT OpenCourseWare continue to offer high quality educational resources for free. To
INTEGRATION OF METABOLISM
 SIBC511- INTEGRATION OF METABOLISM Assistant Professor Dr. Chatchawan Srisawat INTEGRATION OF METABOLISM INTEGRATION OF METABOLISM Dietary intake Fed state Fasting state The metabolism of carbohydrate,
SIBC511- INTEGRATION OF METABOLISM Assistant Professor Dr. Chatchawan Srisawat INTEGRATION OF METABOLISM INTEGRATION OF METABOLISM Dietary intake Fed state Fasting state The metabolism of carbohydrate,
