Transgastric Pancreatic Necrosectomy: How I Do It. Nicholas J. Zyromski, MD. Attila Nakeeb, MD. Michael G. House, MD. Andrea L.
|
|
|
- Joy Lindsey
- 5 years ago
- Views:
Transcription
1 Transgastric Pancreatic Necrosectomy: How I Do It Nicholas J. Zyromski, MD Attila Nakeeb, MD Michael G. House, MD Andrea L. Jester, MD Address correspondence to: Nicholas J. Zyromski, MD Associate Professor, Department of Surgery Indiana University School of Medicine 545 Barnhill Drive, EH 519 Indianapolis, IN Phone Fax nzyromsk@iupui.edu This is the author's manuscript of the article published in final edited form as: Zyromski, N. J., Nakeeb, A., House, M. G., & Jester, A. L. (2015). Transgastric Pancreatic Necrosectomy: How I Do It. Journal of Gastrointestinal Surgery, 20(2),
2 Zyromski Page 1 ABSTRACT Necrotizing pancreatitis is a serious medical problem that often requires intervention to debride necrotic pancreatic and peripancreatic tissue. Recently, minimally invasive approaches have been applied to pancreatic necrosectomy. The purpose of this report is to review the history of transgastric pancreatic debridement, identify appropriate patient selection criteria, and highlight technical pearls. We present this subject matter in the context of our own clinical experience, with a primary focus on a How I Do It type of technical description. BACKGROUND Acute pancreatitis is a common medical problem effecting over one quarter million patients yearly in the United States (1). Among these patients, 15-20% will suffer a severe episode of pancreatitis with variable necrosis of the pancreatic and peripancreatic soft tissue. Patients with necrotizing pancreatitis often require intervention to treat infected necrosis or symptomatic necrosis. The natural history of pancreatic and peripancreatic necrosis is shown in Figure 1. Recently, minimally invasive approaches have been applied to treatment of pancreatic necrosis. These approaches include percutaneous drainage, endoscopic drainage (and debridement), a combination of the percutaneous and endoscopic approaches, laparoscopy, and retroperitoneal approaches (videoscopic assisted retroperitoneal debridement [VARD] - and sinus tract necrosectomy). (2-9) It is important to recognize that necrotizing pancreatitis is an extremely heterogeneous disease; as such, no one specific technique is suitable to treat all
3 Zyromski Page 2 patients. Surgeons who care for necrotizing pancreatitis patients should be prepared to provide long-term care and follow up. Ideally, these patients are approached in the context of a multidisciplinary team including gastroenterologists, interventional radiologists, and pancreatic surgeons, with additional support from intensive care doctors, nutritionists, and physical therapists. HISTORY OF TRANSGASTRIC DEBRIDEMENT Barron and colleagues reported the endoscopic transgastric approach in 1996 (3). Several other groups have subsequently explored endoscopic debridement. (4) The first laparoscopic transgastric debridement was reported in (10) In 2008, a novel laparoendoscopic rendez-vous approach was reported by the Freiburg group, (8) This report consisted of 6 patients. More recently, 4 reports of conventional operative transgastric debridement have been published. A series of 7 patients from Denmark was reported in 2007, and a series of 10 patients were treated by the transgastric approach by the pancreatic surgery group at the University of Calgary (11,12). The well-established Glasgow group recently published the most robust report of transgastric approach to date. (13) This series documented outcomes of 44 patients approached through the back wall of the stomach, 8 open and 36 laparoscopic. Most recently, the Stanford group reported their experience with 21 patients; in the Stanford experience, no intervention has been necessary at very short follow up. (14) The table summarizes contemporary reports of transgastric surgical necrosectomy. All of these reports recognize the potential for hemorrhage while transgressing the gastric wall. This potential problem is not surprising as many patients with lesser sac pancreatic necrosis have splenic vein thrombosis with left sided (sinistral) portal
4 Zyromski Page 3 hypertension. In addition, long-term follow up of patients treated by transgastric necrosectomy is modest. The true incidence of long-term complications such as reaccumulation of retroperitoneal fluid or left sided acute pancreatitis remains to be defined completely. TRANSGASTRIC ADVANTAGES AND PATIENT SELECTION Transgastric necrosectomy is attractive as it allows thorough debridement of retroperitoneal necrosis at one setting. This is in contrast to the endoscopic approach, which typically requires multiple interventions at separate settings. Combining transgastric debridement with what is essentially cysto-gastrostomy also offers the potential for durable internal drainage of a disconnected pancreatic tail- the so-called el Diablo because of its devilish nature. In a follow up over a 6-year period we have found several patients with recurrent left sided pancreatitis and/or recurrent retroperitoneal collections; therefore, we typically counsel patients about the potential for recurrent problems after transgastric debridement. Finally, operative approach allows cholecystectomy (with cholangiography) to be performed at the same setting for patients with biliary acute pancreatitis. The ideal patient to select for transgastric necrosectomy has necrosis confined to the lesser sac. Figure 2 illustrates typical patterns of necrosis in necrotizing pancreatitis. Patients with necrosis extending down the left paracolic gutter may be better approached with VARD. Patients whose necrosis extends down the root of the small bowel mesentery are more problematic. We have treated at least 2 patients with this pattern of necrosis by transgastric necrosectomy with an additional large closed
5 Zyromski Page 4 suction drain placed down the space of the mesenteric root. The drain is subsequently withdrawn slowly, starting 3-4 weeks after operation. Patients with necrosis that involves the pancreatic head and extends down the right paracolic gutter are extremely challenging regardless of approach. In this setting, clinician and patient should be prepared for long treatment course with a potential for duodenal and/or bile duct strictures. It is important to remember lessons from open necrosectomy regarding timing of definitive debridement. Timing of definitive intervention should be delayed at least 1 month from the initial insult to allow consolidation of the necrosis in the lesser sac. This consolidation greatly simplifies debridement and makes the procedure much less hazardous with regard to potential for hemorrhage from the retroperitoneum. All necrotizing pancreatitis patients have some degree of malnutrition; alimenting the gut is important preoperatively, and gastrojejunostomy feeding tube at the time of transgastric debridement should be considered. Our preference is to place a gastrojejunostomy feeding tube as many patients have gastric ileus from the lesser sac inflammatory condition; they may decompress ( vent ) the stomach by the G port while feeding the small bowel distal to Treitz ligament through the J port. Early infection should be managed by percutaneous drainage to temporize the immediate clinical situation. It is not clear whether percutaneous drain placement is a contraindication to subsequent transgastric debridement.
6 Zyromski Page 5 TRANSGASTRIC DEBRIDEMENT - SURGICAL TECHNIQUE Transgastric debridement may be approached laparoscopically or through a short upper midline incision. Laparoscopic ports are placed similar to other foregut operations (Figure 3). The epigastric port allows the operator to drive the camera directly into the necrosis cavity (Figure 4). Intraoperative ultrasound is essential to help define the necrotic collection location, extent, and compositon, particularly when the necrosis is predominately solid with a minimal fluid component. (Figure 5) Anterior gastrostomy is created between stay sutures using electrocautery or the ultrasonic scalpel. It is worth reiterating the potential for major hemorrhage from the gastric wall in the setting of left sided portal hypertension. In this situation the surgical approach clearly offers an advantage over endoscopic approach in facilitating hemorrhage control. Placing the ultrasound transducer directly into the stomach and visualizing the retrogastric collection through the posterior wall of the stomach is helpful in positioning the posterior gastrostomy. Posterior gastrostomy is created between stay sutures; these sutures are particularly helpful during the laparoscopic approach manipulating the gastrostomy into the operative field. Cultures of the retrogastric fluid and necrosis are routine as 25-30% of pancreatic collections considered sterile actually harbor subclinical infection. The posterior gastrostomy/cysto-gastrostomy is enlarged with electrocautery, ultrasonic shears, or by firing an endovascular staple load between the cyst wall and the stomach. Most times this clinical situation is clearly acute pancreatitis; however, biopsy of the cyst wall may be sent to prove absence of epithelialization, i.e. neoplastic cyst. Debridement of the necrotic material is undertaken gently either with the educated finger in the open approach or with a blunt grasper in the laparoscopic
7 Zyromski Page 6 approach (Figure 6). It is critical not to debride solid tissue that is not loose and easily dislodged from the retroperitoneum. Debridement of immature necrosis may result in catastrophic hemorrhage. Visualization to the right of the superior mesenteric vein and down the root of the small bowel mesentery is challenging laparoscopically; concomitant endoscopy may be helpful in these situations. We have found that vigorous irrigation of the necrosis cavity is useful in dislodging small particulate solid matter. The necrosis cavity may be packed with a gauze sponge which typically tamponades small oozing vessels in the retroperitoneum. Necrotic material may be placed into an endocatch pouch device for retrieval from the abdomen; alternately, necrosis may simply be left within the stomach lumen, where it will pass through the alimentary tract. After satisfactory debridement has been achieved, cysto-gastrostomy is secured either with monofilament nonabsorbable suture or with a linear endovascular stapler. If a gastrojejunostomy feeding tube is indicated, it is placed through a separate purse string suture in the anterior stomach at this time; the anterior gastrostomy aids visualization directing this feeding tube beyond the pylorus. Anterior gastrostomy is closed either with a stapler or more commonly with 2 layers of suture, as the stomach is often thickened and not ideal for a stapled closure (Figure 7). Cholecystectomy may be addressed at this point if indicated. Some operators may prefer to perform cholecystectomy prior to gastrotomy and debridement. POSTOPERATIVE CARE AND LONG TERM OUTCOMES With sterile necrosis, antibiotics are not routinely administered beyond the perioperative period. Infected necrosis should be treated with a 7-10 day antibiotic course tailored to cover cultured organisms. Longer antibiotic courses should be
8 Zyromski Page 7 considered to treat resistant bacteria, which are extremely challenging to clear from the retroperitoneal space. Diet is advanced as tolerated, understanding that patients with long standing lesser sac inflammatory collections may have a protracted gastric ileus. Venous thromboembolic events are extremely common in necrotizing pancreatitis; therefore, pharmacologic prophylaxis is prudent. Our practice is to use low molecular weight heparin preparation subcutaneous injections. Finally, patients should be counseled about the potential for recurrent left sided pancreatitis and/or retroperitoneal collections. Over the past few years, we have found approximately 15%-20% of necrotizing pancreatitis patients to be suitable candidates for transgastric debridement. CONCLUSION Surgical transgastric pancreatic necrosectomy is an important treatment option for select patients with necrotizing pancreatitis. This approach is particularly useful when applied to patients with solid necrosis localized in the lesser sac, including those with a disconnected pancreatic tail. The potential for major hemorrhage from the gastric wall should be appreciated. Long-term follow up for patients undergoing this procedure is evolving; and should be mandatory. ACKNOWLEDGEMENT The author thanks Shella Stephens for excellent administrative support preparing the manuscript.
9 Zyromski Page 8 TABLE: Series of transgastric necrosectomy Year Author (reference) n Follow up (months) Late Complication/ Re-intervention 2007 Ainsworth (11) (43%) 2008 Fischer (8) (33%) 2010 Munene (12) (20%) 2014 Gibson (13) (2%) 2014 Worhunsky (14) (0%)
10 Zyromski Page 9 FIGURE LEGENDS Figure 1: Natural history of pancreatic and peripancreatic necrosis. A small percentage of patients will resolve necrosis spontaneously. Infected and persistent, symptomatic necrosis typically demand intervention. Figure 2: Typical patterns of necrosis. Necrosis confined to the lesser sac (left figure) is ideal for the transgastric approach. Necrosis extending to the left paracolic gutter (middle figure) may be better off treated with VARD. Necrosis involving the pancreatic head, right paracolic gutter, or small bowel mesenteric root (right figure) is quite challenging to manage, and may be best approached by open transabdominal debridement. Figure 3: Typical port placement for laparoscopic transgastric necrosectomy. 12mm ports are commonly placed at the umbilicus and in the right lower abdominal positions to accommodate ultrasound probe and stapling devices. Figure 4: Laparoscopic view of the necrosis cavity through the posterior gastric wall after thorough debridement: note disconnected pancreatic tail (long arrow) and splenic artery (short arrow). Figure 5: Intraoperative ultrasound guidance is essential, particularly in laparoscopy. Figure 6: Necrosis should be debrided bluntly, and may be placed into a bag or simply left in the gastric lumen. Figure 7: The anterior gastrotomy is closed with staples or suture.
11 Zyromski Page 10 REFRENCES 1. Fagenholz PJ, Fernandez-del Castillo C, Harris NS, Pelletier AJ, Camargo CA, Jr. Direct medical costs of acute pancreatitis hospitalizations in the United States. Pancreas 2007;35: Freeny PC, Hauptmann E, Althaus SJ, Traverso LW, Sinanan M. Percutaneous CTguided catheter drainage of infected acute necrotizing pancreatitis: techniques and results. AJR American journal of roentgenology 1998;170: Baron TH, Thaggard WG, Morgan DE, Stanley RJ. Endoscopic therapy for organized pancreatic necrosis. Gastroenterology 1996;111: Gardner TB, Coelho-Prabhu N, Gordon SR, Gelrud A, Maple JT, Papachristou GI et al. Direct endoscopic necrosectomy for the treatment of walled-off pancreatic necrosis: results from a multicenter U.S. series. Gastrointest endoscopy 2011;73: Horvath K, Freeny P, Escallon J, Heagerty P, Comstock B, Glickerman DJ, Bulger E, et al. Safety and efficacy of video-assisted retroperitoneal debridement for infected pancreatic collections: a multicenter, prospective, single-arm phase 2 study. Arch surg 2010;145: Raraty MG, Halloran CM, Dodd S, Ghaneh P, Connor S, Evans J, Sutton R, Neoptolemos JP. Minimal access retroperitoneal pancreatic necrosectomy: improvement in morbidity and mortality with a less invasive approach. Ann Surg 2010;251: van Santvoort HC, Besselink MG, Bakker OJ, Hofker HS, Boermeester MA, Dejong CH, van Goor H, et al. A step-up approach or open necrosectomy for necrotizing pancreatitis. NEJM 2010;362: Fischer A, Schrag HJ, Keck T, Hopt UT, Utzolino S. Debridement and drainage of walled-off pancreatic necrosis by a novel laparoendoscopic rendezvous maneuver: experience with 6 cases. Gastrointest Endoscopy 2008;67: Parekh D. Laparoscopic-assisted pancreatic necrosectomy: A new surgical option for treatment of severe necrotizing pancreatitis. Arch Surg 2006;141: ; discussion Ammori BJ. Laparoscopic transgastric pancreatic necrosectomy for infected pancreatic necrosis. Surg Endoscopy 2002;16: Ainsworth AP, Nielsen HO, Mortensen MB. [Transgastric necrosectomy by open surgery in necrotising acute pancreatitis]. Ugeskrift for laeger 2007;169: Munene G, Dixon E, Sutherland F. Open transgastric debridement and internal drainage of symptomatic non-infected walled-off pancreatic necrosis. HPB 2011;13: Gibson SC, Robertson BF, Dickson EJ, McKay CJ, Carter CR. Step port laparoscopic cystgastrostomy for the management of organized solid predominant post-acute fluid collections after severe acute pancreatitis. HPB 2014; 16(2):
12 Zyromski Page Worhunsky DJ, Qadan M, Dua MM, et al. Laparoscopic transgastric necrosectomy for the management of pancreatic necrosis. J Am Coll Surg 2014; 219 (4):
13 Figure 1: Zyromski Page 12
14 Figure 2: Zyromski Page 13
15 Figure 3: Zyromski Page 14
16 Zyromski Page 15 Figure 4: Figure 5:
17 Zyromski Page 16 Figure 6: Figure 7:
18 Zyromski Page 17
Mild. Moderate. Severe
 2012 Revised Atlanta Classification Acute pancreatitis Classified based on absence or presence of local and/or systemic complications Mild Acute Pancreatits Moderate Severe P. A. Banks, T. L. Bollen, C.
2012 Revised Atlanta Classification Acute pancreatitis Classified based on absence or presence of local and/or systemic complications Mild Acute Pancreatits Moderate Severe P. A. Banks, T. L. Bollen, C.
VIDEO ASSISTED RETROPERITONEAL DEBRIDEMENT IN HUGE INFECTED PANCREATIC PSEUDOCYST
 Trakia Journal of Sciences, Vol. 13, Suppl. 2, pp 102-106, 2015 Copyright 2015 Trakia University Available online at: http://www.uni-sz.bg ISSN 1313-7050 (print) doi:10.15547/tjs.2015.s.02.022 ISSN 1313-3551
Trakia Journal of Sciences, Vol. 13, Suppl. 2, pp 102-106, 2015 Copyright 2015 Trakia University Available online at: http://www.uni-sz.bg ISSN 1313-7050 (print) doi:10.15547/tjs.2015.s.02.022 ISSN 1313-3551
Severe necrotizing pancreatitis. ICU Fellowship Training Radboudumc
 Severe necrotizing pancreatitis ICU Fellowship Training Radboudumc Acute pancreatitis Patients with acute pancreatitis van Dijk SM. Gut 2017;66:2024-2032 Diagnosis Revised Atlanta classification Abdominal
Severe necrotizing pancreatitis ICU Fellowship Training Radboudumc Acute pancreatitis Patients with acute pancreatitis van Dijk SM. Gut 2017;66:2024-2032 Diagnosis Revised Atlanta classification Abdominal
Disclosures. Extra-hepatic Biliary Disease and the Pancreas. Objectives. Pancreatitis 10/3/2018. No relevant financial disclosures to report
 Extra-hepatic Biliary Disease and the Pancreas Disclosures No relevant financial disclosures to report Jeffrey Coughenour MD FACS Clinical Associate Professor of Surgery and Emergency Medicine Division
Extra-hepatic Biliary Disease and the Pancreas Disclosures No relevant financial disclosures to report Jeffrey Coughenour MD FACS Clinical Associate Professor of Surgery and Emergency Medicine Division
Endoscopic pancreatic necrosectomy in 2017
 Endoscopic pancreatic necrosectomy in 2017 Mouen Khashab, MD Associate Professor of Medicine Director of Therapeutic Endoscopy The Johns Hopkins Hospital Revised Atlanta Classification Entity Acute fluid
Endoscopic pancreatic necrosectomy in 2017 Mouen Khashab, MD Associate Professor of Medicine Director of Therapeutic Endoscopy The Johns Hopkins Hospital Revised Atlanta Classification Entity Acute fluid
Robotic transgastric cystgastrostomy and pancreatic debridement in the management of pancreatic fluid collections following acute pancreatitis
 Review Article on Pancreatic Surgery Robotic transgastric cystgastrostomy and pancreatic debridement in the management of pancreatic fluid collections following acute pancreatitis Russell C. Kirks Jr,
Review Article on Pancreatic Surgery Robotic transgastric cystgastrostomy and pancreatic debridement in the management of pancreatic fluid collections following acute pancreatitis Russell C. Kirks Jr,
Pancreatic Benign April 27, 2016
 Department of Surgery Pancreatic Benign April 27, 2016 James Choi Dr. Hernandez Objectives Medical Expert: 1. Anatomy and congenital anomalies of the pancreas and pancreatic duct (divisum, annular pancreas
Department of Surgery Pancreatic Benign April 27, 2016 James Choi Dr. Hernandez Objectives Medical Expert: 1. Anatomy and congenital anomalies of the pancreas and pancreatic duct (divisum, annular pancreas
ACUTE PANCREATITIS: NEW CLASSIFICATION OF AN OLD FOE. T Barrow, A Nasrullah, S Liong, V Rudralingam, S A Sukumar
 ACUTE PANCREATITIS: NEW CLASSIFICATION OF AN OLD FOE T Barrow, A Nasrullah, S Liong, V Rudralingam, S A Sukumar LEARNING OBJECTIVES q Through a series of cases illustrate the updated Atlanta symposium
ACUTE PANCREATITIS: NEW CLASSIFICATION OF AN OLD FOE T Barrow, A Nasrullah, S Liong, V Rudralingam, S A Sukumar LEARNING OBJECTIVES q Through a series of cases illustrate the updated Atlanta symposium
Sepsis in Acute Pancreatitis. MD Smith Department of Surgery University of the Witwatersrand, Johannesburg Chris Hani Baragwanath Academic Hospital
 Sepsis in Acute Pancreatitis MD Smith Department of Surgery University of the Witwatersrand, Johannesburg Chris Hani Baragwanath Academic Hospital Introduction Self limiting disease in 85% Minority develop
Sepsis in Acute Pancreatitis MD Smith Department of Surgery University of the Witwatersrand, Johannesburg Chris Hani Baragwanath Academic Hospital Introduction Self limiting disease in 85% Minority develop
PANCREATIC PSEUDOCYSTS. Madhuri Rao MD PGY-5 Kings County Hospital Center
 PANCREATIC PSEUDOCYSTS Madhuri Rao MD PGY-5 Kings County Hospital Center 34 yo M Case Presentation PMH: Chronic pancreatitis (ETOH related) PSH: Nil Meds: Nil NKDA www.downstatesurgery.org Symptoms o Chronic
PANCREATIC PSEUDOCYSTS Madhuri Rao MD PGY-5 Kings County Hospital Center 34 yo M Case Presentation PMH: Chronic pancreatitis (ETOH related) PSH: Nil Meds: Nil NKDA www.downstatesurgery.org Symptoms o Chronic
JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES
 JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES THE PROBLEM DUODENAL / PANCREATIC INJURIES Difficult to diagnose Not very common Anatomic and physiologic challenges 90% rate of associated
JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES THE PROBLEM DUODENAL / PANCREATIC INJURIES Difficult to diagnose Not very common Anatomic and physiologic challenges 90% rate of associated
Appendix 9: Endoscopic Ultrasound in Gastroenterology
 Appendix 9: Endoscopic Ultrasound in Gastroenterology This curriculum is intended for clinicians who perform endoscopic ultrasonography (EUS) in gastroenterology. It includes standards for theoretical
Appendix 9: Endoscopic Ultrasound in Gastroenterology This curriculum is intended for clinicians who perform endoscopic ultrasonography (EUS) in gastroenterology. It includes standards for theoretical
Surgical Strategies for the Management of Necrotizing Pancreatitis
 REVIEW ARTICLE Surgical Strategies for the Management of Necrotizing Pancreatitis Monica M Dua 1, David J Worhunsky 1, Thuy B Tran 1, Shai Friedland 2, Walter G Park 2, Brendan C Visser 1 Department of
REVIEW ARTICLE Surgical Strategies for the Management of Necrotizing Pancreatitis Monica M Dua 1, David J Worhunsky 1, Thuy B Tran 1, Shai Friedland 2, Walter G Park 2, Brendan C Visser 1 Department of
PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies. Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels
 PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels 1. Diagnosis. 2. Multidisciplinary approach. 3. Therapeutic planning. 4. How? 5. Follow-up
PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels 1. Diagnosis. 2. Multidisciplinary approach. 3. Therapeutic planning. 4. How? 5. Follow-up
Original Article. The role of image guided percutaneous drainage in multidisciplinary management of necrotizing pancreatitis
 Tropical Gastroenterology 2013;34(1):25 30 Original Article The role of image guided percutaneous drainage in multidisciplinary management of necrotizing pancreatitis Rashesh Solanki, Venumadhav Thumma,
Tropical Gastroenterology 2013;34(1):25 30 Original Article The role of image guided percutaneous drainage in multidisciplinary management of necrotizing pancreatitis Rashesh Solanki, Venumadhav Thumma,
Management of Pancreatic Fistulae
 Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Hajhamad M 1, Reynu R, Kosai NR, Mustafa MT, Othman H 2
 Successful conservative management of pancreatico-colonic fistula following videoscopic assisted retroperitoneal debridement of infected pancreatic necrosis. Case report and review of literature. Hajhamad
Successful conservative management of pancreatico-colonic fistula following videoscopic assisted retroperitoneal debridement of infected pancreatic necrosis. Case report and review of literature. Hajhamad
Visceral aneurysm. Diagnosis and Interventions M.NEDEVSKA
 Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Overview. Omissions 14/11/2016 INCIDENCE ATLANTA SYMPOSIUM MANAGEMENT OF COMPLICATED PANCREATITIS
 Overview MANAGEMENT OF COMPLICATED PANCREATITIS Chad Ball, MD, MSc, FRCSC, FACS Hepatobiliary, Pancreas, Trauma, Acute Care Surgery University of Calgary Epidemiology Hemorrhage Pancreatic/Enteric Fistula
Overview MANAGEMENT OF COMPLICATED PANCREATITIS Chad Ball, MD, MSc, FRCSC, FACS Hepatobiliary, Pancreas, Trauma, Acute Care Surgery University of Calgary Epidemiology Hemorrhage Pancreatic/Enteric Fistula
Laparoscopy-assisted D2 radical distal subtotal gastrectomy
 Masters of Gastrointestinal Surgery Laparoscopy-assisted D2 radical distal subtotal gastrectomy Xiaogeng Chen, Weihua Li, Jinsi Wang, Changshun Yang Department of Tumor Surgery, Fujian Provincial Hospital,
Masters of Gastrointestinal Surgery Laparoscopy-assisted D2 radical distal subtotal gastrectomy Xiaogeng Chen, Weihua Li, Jinsi Wang, Changshun Yang Department of Tumor Surgery, Fujian Provincial Hospital,
Appendix 5. EFSUMB Newsletter. Gastroenterological Ultrasound
 EFSUMB Newsletter 87 Examinations should encompass the full range of pathological conditions listed below A log book listing the types of examinations undertaken should be kept Training should usually
EFSUMB Newsletter 87 Examinations should encompass the full range of pathological conditions listed below A log book listing the types of examinations undertaken should be kept Training should usually
Surgical Management of CBD Injury Jin Seok Heo
 Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
EXPERIMENTAL AND THERAPEUTIC MEDICINE 14: , 2017
 EXPERIMENTAL AND THERAPEUTIC MEDICINE 14: 4397-4404, 2017 Predictive factors of pancreatic necrosectomy following percutaneous catheter drainage as a primary treatment of patients with infected necrotizing
EXPERIMENTAL AND THERAPEUTIC MEDICINE 14: 4397-4404, 2017 Predictive factors of pancreatic necrosectomy following percutaneous catheter drainage as a primary treatment of patients with infected necrotizing
EFSUMB EUROPEAN FEDERATION OF SOCIETIES FOR ULTRASOUND IN MEDICINE AND BIOLOGY Building a European Ultrasound Community
 MINIMUM TRAINING REQUIREMENTS FOR THE PRACTICE OF MEDICAL ULTRASOUND IN EUROPE Appendix 9: Endoscopic Ultrasound in Gastroenterology This curriculum is intended for clinicians who perform endoscopic ultrasonography
MINIMUM TRAINING REQUIREMENTS FOR THE PRACTICE OF MEDICAL ULTRASOUND IN EUROPE Appendix 9: Endoscopic Ultrasound in Gastroenterology This curriculum is intended for clinicians who perform endoscopic ultrasonography
The Whipple Operation Illustrations
 The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
Surgical Management of Acute Pancreatitis
 Surgical Management of Acute Pancreatitis Steven J. Hughes, MD, FACS Cracchiolo Family Professor of Surgery and Chief, General Surgery Overview Biliary pancreatitis a cost effective algorithm Key concepts
Surgical Management of Acute Pancreatitis Steven J. Hughes, MD, FACS Cracchiolo Family Professor of Surgery and Chief, General Surgery Overview Biliary pancreatitis a cost effective algorithm Key concepts
Pancreatic pseudocysts (PP) are chronic collections of
 JOURNAL OF LAPAROENDOSCOPIC & ADVANCED SURGICAL TECHNIQUES Volume 20, Number 9, 2010 ª Mary Ann Liebert, Inc. DOI: 10.1089/lap.2009.0421 Hand-Sewn Cystogastrostomy Using the Novel Single-Incision Laparoscopy
JOURNAL OF LAPAROENDOSCOPIC & ADVANCED SURGICAL TECHNIQUES Volume 20, Number 9, 2010 ª Mary Ann Liebert, Inc. DOI: 10.1089/lap.2009.0421 Hand-Sewn Cystogastrostomy Using the Novel Single-Incision Laparoscopy
THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY 2013/12/21
 THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY Tsann-Long Hwang, MD, FACS Department of Surgery Chang Gung Memorial Hospital Chang Gung University Taipei, TAIWAN 2013/12/21 THE DIFFICULTY
THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY Tsann-Long Hwang, MD, FACS Department of Surgery Chang Gung Memorial Hospital Chang Gung University Taipei, TAIWAN 2013/12/21 THE DIFFICULTY
Minimally Invasive Necrosectomy versus Open Necrosectomy Approaches in a Tertiary Hepatopancreatobiliary Unit
 ORIGINAL ARTICLE Minimally Invasive Necrosectomy versus Open Necrosectomy Approaches in a Tertiary Hepatopancreatobiliary Unit Eugene Wong 1,2, Julia Jones 1, Justin S Gundara 1, Christopher Nahm 1, Sarah
ORIGINAL ARTICLE Minimally Invasive Necrosectomy versus Open Necrosectomy Approaches in a Tertiary Hepatopancreatobiliary Unit Eugene Wong 1,2, Julia Jones 1, Justin S Gundara 1, Christopher Nahm 1, Sarah
General'Surgery'Service'
 General'Surgery'Service' Patient Care Goals and Objectives 1)! Stomach/Duodenum and Bariatric 2)! Interpret the results of clinical evaluations (history, physical examination) performed on patients being
General'Surgery'Service' Patient Care Goals and Objectives 1)! Stomach/Duodenum and Bariatric 2)! Interpret the results of clinical evaluations (history, physical examination) performed on patients being
U Nordic Forum - Trauma & Emergency Radiology. Lecture Objectives. MDCT in Acute Pancreatitis. Acute Pancreatitis: Etiologies
 Nordic Forum - Trauma & Emergency Radiology Lecture Objectives MDCT in Acute Pancreatitis Borut Marincek Institute of Diagnostic Radiology niversity Hospital Zurich, Switzerland To describe the role of
Nordic Forum - Trauma & Emergency Radiology Lecture Objectives MDCT in Acute Pancreatitis Borut Marincek Institute of Diagnostic Radiology niversity Hospital Zurich, Switzerland To describe the role of
Pancreaticoduodenectomy the anatomy and the surgical approaches
 Pancreaticoduodenectomy the anatomy and the surgical approaches Paul BS LAI Division of Hepato biliary and Pancreatic Surgery Department of Surgery The Chinese Univesity of Hong Kong Whipple s operation
Pancreaticoduodenectomy the anatomy and the surgical approaches Paul BS LAI Division of Hepato biliary and Pancreatic Surgery Department of Surgery The Chinese Univesity of Hong Kong Whipple s operation
Optimizing the step-up approach for infected necrotizing pancreatitis van Grinsven, A.H.J.
 UvA-DARE (Digital Academic Repository) Optimizing the step-up approach for infected necrotizing pancreatitis van Grinsven, A.H.J. Link to publication Citation for published version (APA): van Grinsven,
UvA-DARE (Digital Academic Repository) Optimizing the step-up approach for infected necrotizing pancreatitis van Grinsven, A.H.J. Link to publication Citation for published version (APA): van Grinsven,
Index (SIRS), 158, 173
 Index A Acute pancreatitis surgery abdominal compartment syndrome, 188 adjuvant treatment, 194 anterior approach, 175 antibiotic prophylaxis, 166 167, 197 Atlanta classification, 181 classification of
Index A Acute pancreatitis surgery abdominal compartment syndrome, 188 adjuvant treatment, 194 anterior approach, 175 antibiotic prophylaxis, 166 167, 197 Atlanta classification, 181 classification of
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons
 General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: UPPER GI & HPB - HEPATIC, PANCREATIC & BILIARY
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: UPPER GI & HPB - HEPATIC, PANCREATIC & BILIARY
Practical Adherence to the Step-Up Approach for Pancreatic Necrosis: An Institutional Review
 ORIGINAL ARTICLE Practical Adherence to the Step-Up Approach for Pancreatic Necrosis: An Institutional Review Vernissia Tam 1, Mazen Zenati 2, Chandraprakash Umapathy 3, Stephanie Downs-Canner 1, Ahmad
ORIGINAL ARTICLE Practical Adherence to the Step-Up Approach for Pancreatic Necrosis: An Institutional Review Vernissia Tam 1, Mazen Zenati 2, Chandraprakash Umapathy 3, Stephanie Downs-Canner 1, Ahmad
Adult Trauma Feeding Access Guideline
 Adult Trauma Feeding Access Guideline Background: Enteral feeding access mode (NGT, NDT, PEG, PEG-J, Jejunostomy tube) dependent upon patient characteristics. Enteral feeding management guidelines aim
Adult Trauma Feeding Access Guideline Background: Enteral feeding access mode (NGT, NDT, PEG, PEG-J, Jejunostomy tube) dependent upon patient characteristics. Enteral feeding management guidelines aim
Citation Hepato-Gastroenterology, 55(86-87),
 NAOSITE: Nagasaki University's Ac Title Author(s) Combined pancreatic resection and p multiple lesions of the pancreas: i of the pancreas concomitant with du Kuroki, Tamotsu; Tajima, Yoshitsugu Tomohiko;
NAOSITE: Nagasaki University's Ac Title Author(s) Combined pancreatic resection and p multiple lesions of the pancreas: i of the pancreas concomitant with du Kuroki, Tamotsu; Tajima, Yoshitsugu Tomohiko;
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons
 General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: UPPER GI & HPB - HEPATIC, PANCREATIC & BILIARY
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: UPPER GI & HPB - HEPATIC, PANCREATIC & BILIARY
Project submitted towards completion of Diploma in Minimal Access Surgery, Laparoscopy Hospital, New Delhi, India, October 2007.
 Laparoscopic management of pancreatic pseudocysts. DR G. MUSILA GIBSON; MBchB, MMed Surgery, DMAS. Specialist General Surgeon; Kenyatta National Hospital, Nairobi, Kenya. Member of World Association of
Laparoscopic management of pancreatic pseudocysts. DR G. MUSILA GIBSON; MBchB, MMed Surgery, DMAS. Specialist General Surgeon; Kenyatta National Hospital, Nairobi, Kenya. Member of World Association of
LOOKING FOR AIR IN ALL THE WRONG PLACES Richard M. Gore, MD North Shore University Health System University of Chicago Evanston, IL
 SIGNIFICANCE OF EXTRALUMINAL ABDOMINAL GAS: LOOKING FOR AIR IN ALL THE WRONG PLACES Richard M. Gore, MD North Shore University Health System University of Chicago Evanston, IL SCBT/MR 2012 October 26,
SIGNIFICANCE OF EXTRALUMINAL ABDOMINAL GAS: LOOKING FOR AIR IN ALL THE WRONG PLACES Richard M. Gore, MD North Shore University Health System University of Chicago Evanston, IL SCBT/MR 2012 October 26,
Does it matter what we drain?
 Endoscopic Management of Pancreatic Fluid Collections Shyam Varadarajulu, MD Medical Director Center for Interventional Endoscopy Florida Hospital, Orlando Does it matter what we drain? Makes all the difference!
Endoscopic Management of Pancreatic Fluid Collections Shyam Varadarajulu, MD Medical Director Center for Interventional Endoscopy Florida Hospital, Orlando Does it matter what we drain? Makes all the difference!
Pylorus Preserving Pancreaticoduodenectomy
 REVIEW Pylorus Preserving Pancreaticoduodenectomy Jacqueline M. Garonzik-Wang, M. B. Majella Doyle Pancreaticoduodenectomy (PD) has become the standard of care for resectable pancreatic cancer and premalignant
REVIEW Pylorus Preserving Pancreaticoduodenectomy Jacqueline M. Garonzik-Wang, M. B. Majella Doyle Pancreaticoduodenectomy (PD) has become the standard of care for resectable pancreatic cancer and premalignant
ERCP and EUS: What s New and What Should We Do?
 ERCP and EUS: What s New and What Should We Do? Rajesh N. Keswani, MD Associate Professor of Medicine Division of Gastroenterology Northwestern University Feinberg School of Medicine EUS/ERCP in 2015 THE
ERCP and EUS: What s New and What Should We Do? Rajesh N. Keswani, MD Associate Professor of Medicine Division of Gastroenterology Northwestern University Feinberg School of Medicine EUS/ERCP in 2015 THE
Pancreatico-Duodenal Trauma: Drain, Debride, Divert, Despair BACKGROUND EPIDEMIOLOGY 9/11/2018
 Pancreatico-Duodenal Trauma: Drain, Debride, Divert, Despair Rochelle A. Dicker, M.D. Professor of Surgery and Anesthesia UCLA BACKGROUND Lancet 1827: Travers, B Rupture of the Pancreas British Journal
Pancreatico-Duodenal Trauma: Drain, Debride, Divert, Despair Rochelle A. Dicker, M.D. Professor of Surgery and Anesthesia UCLA BACKGROUND Lancet 1827: Travers, B Rupture of the Pancreas British Journal
EUS-Guided Multitransgastric Endoscopic Necrosectomy for Infected Pancreatic Necrosis with Noncontagious Retroperitoneal and Peritoneal Extension
 Gut and Liver, Vol. 4, No. 1, March 2010, pp. 140-145 Case report EUS-Guided Multitransgastric Endoscopic Necrosectomy for Infected Pancreatic Necrosis with Noncontagious Retroperitoneal and Peritoneal
Gut and Liver, Vol. 4, No. 1, March 2010, pp. 140-145 Case report EUS-Guided Multitransgastric Endoscopic Necrosectomy for Infected Pancreatic Necrosis with Noncontagious Retroperitoneal and Peritoneal
Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition
 22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
Case-Matched Comparison of the Retroperitoneal Approach With Laparotomy for Necrotizing Pancreatitis
 World J Surg (2007) 31:1635 1642 DOI 10.1007/s00268-007-9083-6 Case-Matched Comparison of the Retroperitoneal Approach With Laparotomy for Necrotizing Pancreatitis Hjalmar C. van Santvoort Æ Marc G. Besselink
World J Surg (2007) 31:1635 1642 DOI 10.1007/s00268-007-9083-6 Case-Matched Comparison of the Retroperitoneal Approach With Laparotomy for Necrotizing Pancreatitis Hjalmar C. van Santvoort Æ Marc G. Besselink
A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY
 A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center Welcome The St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center is a leader
A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center Welcome The St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center is a leader
The Influence of Pancreatic Ductal Anatomy on the Complications of Pancreatitis. William H. Nealon M.D.
 The Influence of Pancreatic Ductal Anatomy on the Complications of Pancreatitis William H. Nealon M.D. Students and Trainees: Guide to Creativity, Productivity and Innovation in a Clinical Career Choose
The Influence of Pancreatic Ductal Anatomy on the Complications of Pancreatitis William H. Nealon M.D. Students and Trainees: Guide to Creativity, Productivity and Innovation in a Clinical Career Choose
Management of necrotizing pancreatitis and its outcome in a secondary healthcare institution
 International Surgery Journal Karim T et al. Int Surg J. 2017 Mar;4(3):1049-1054 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20170860
International Surgery Journal Karim T et al. Int Surg J. 2017 Mar;4(3):1049-1054 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20170860
Tools of the Gastroenterologist: Introduction to GI Endoscopy
 Tools of the Gastroenterologist: Introduction to GI Endoscopy Objectives Endoscopy Upper endoscopy Colonoscopy Endoscopic retrograde cholangiopancreatography (ERCP) Endoscopic ultrasound (EUS) Endoscopic
Tools of the Gastroenterologist: Introduction to GI Endoscopy Objectives Endoscopy Upper endoscopy Colonoscopy Endoscopic retrograde cholangiopancreatography (ERCP) Endoscopic ultrasound (EUS) Endoscopic
ABDOMEN - GI. Duodenum
 TALA SALEH ABDOMEN - GI Duodenum - Notice the shape of the duodenum, it looks like capital G shape tube which extends from the pyloroduodenal junction to the duodenojejunal junction. - It is 10 inches
TALA SALEH ABDOMEN - GI Duodenum - Notice the shape of the duodenum, it looks like capital G shape tube which extends from the pyloroduodenal junction to the duodenojejunal junction. - It is 10 inches
Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist. Alireza Sedarat, MD UCLA Division of Digestive Diseases
 Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist Alireza Sedarat, MD UCLA Division of Digestive Diseases Disclosures Consultant for Boston Scientific and Olympus Corporation
Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist Alireza Sedarat, MD UCLA Division of Digestive Diseases Disclosures Consultant for Boston Scientific and Olympus Corporation
AXIOS Stent and Electrocautery Enhanced Delivery System *
 Advancing Pancreaticobiliary Disease Management AXIOS Stent and Electrocautery Enhanced Delivery System * Select a Menu Option Below Features & Benefits Expanding Innovation Ordering Information & Resources
Advancing Pancreaticobiliary Disease Management AXIOS Stent and Electrocautery Enhanced Delivery System * Select a Menu Option Below Features & Benefits Expanding Innovation Ordering Information & Resources
Anatomy of laparoscopy-assisted distal D2 radical gastrectomy for gastric cancer
 Masters of Gastrointestinal Surgery Anatomy of laparoscopy-assisted distal D2 radical gastrectomy for gastric cancer Da-Guang Wang, Liang He, Yang Zhang, Jing-Hai Yu, Yan Chen, Ming-Jie Xia, Jian Suo Department
Masters of Gastrointestinal Surgery Anatomy of laparoscopy-assisted distal D2 radical gastrectomy for gastric cancer Da-Guang Wang, Liang He, Yang Zhang, Jing-Hai Yu, Yan Chen, Ming-Jie Xia, Jian Suo Department
JMSCR Volume 03 Issue 01 Page January 2015
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Pancreatic Pseudocyst: A Surgical Dilemma Authors Dr. Ketan Vagholkar 1, Dr. Madhavan Iyengar 2, Dr. Rahulkumar Chavan 3 Dr. Abhishek
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Pancreatic Pseudocyst: A Surgical Dilemma Authors Dr. Ketan Vagholkar 1, Dr. Madhavan Iyengar 2, Dr. Rahulkumar Chavan 3 Dr. Abhishek
Placing PEG and Jejunostomy Tubes in Dogs and Cats
 Placing PEG and Jejunostomy Tubes in Dogs and Cats I. Gastrostomy tube A. Percutaneous Endoscopic Gastrostomy (PEG) tube placement Supplies for PEG tube placement: Supplies and equipment for general anesthesia
Placing PEG and Jejunostomy Tubes in Dogs and Cats I. Gastrostomy tube A. Percutaneous Endoscopic Gastrostomy (PEG) tube placement Supplies for PEG tube placement: Supplies and equipment for general anesthesia
Laparoscopy-assisted radical total gastrectomy plus D2 lymph node dissection
 Masters of Gastrointestinal Surgery Laparoscopy-assisted radical total gastrectomy plus D2 lymph node dissection Chaohui Zheng, Changming Huang, Ping Li, Jianwei Xie, Jiabin Wang, Jianxian Lin, Jun Lu
Masters of Gastrointestinal Surgery Laparoscopy-assisted radical total gastrectomy plus D2 lymph node dissection Chaohui Zheng, Changming Huang, Ping Li, Jianwei Xie, Jiabin Wang, Jianxian Lin, Jun Lu
Original Article INTRODUCTION
 Original Article A retrospective study evaluating endoscopic ultrasound guided drainage of pancreatic fluid collections using a novel lumen apposing metal stent on an electrocautery enhanced delivery system
Original Article A retrospective study evaluating endoscopic ultrasound guided drainage of pancreatic fluid collections using a novel lumen apposing metal stent on an electrocautery enhanced delivery system
Geoffrey Axiak M.Sc. Nursing (Manch.), B.Sc. Nursing, P.G. Dip. Nutrition & Dietetics Clinical Nutrition Practice Nurse
 The Percutaneous Endoscopic Gastrostomy Geoffrey Axiak M.Sc. Nursing (Manch.), B.Sc. Nursing, P.G. Dip. Nutrition & Dietetics Clinical Nutrition Practice Nurse What is a P.E.G.? Percutaneous Endoscopic
The Percutaneous Endoscopic Gastrostomy Geoffrey Axiak M.Sc. Nursing (Manch.), B.Sc. Nursing, P.G. Dip. Nutrition & Dietetics Clinical Nutrition Practice Nurse What is a P.E.G.? Percutaneous Endoscopic
Penetrating abdominal trauma clinical view. Ari Leppäniemi, MD Department of Abdominal Surgery Meilahti hospital University of Helsinki Finland
 Penetrating abdominal trauma clinical view Ari Leppäniemi, MD Department of Abdominal Surgery Meilahti hospital University of Helsinki Finland Meilahti hospital - one of Helsinki University hospitals -
Penetrating abdominal trauma clinical view Ari Leppäniemi, MD Department of Abdominal Surgery Meilahti hospital University of Helsinki Finland Meilahti hospital - one of Helsinki University hospitals -
Colorectal procedure guide
 Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Figure 2: Post-cholecystectomy biliary-like pain
 Figure 2: Post-cholecystectomy biliary-like pain 1 patient with recurrent episodes of pain (not daily), in the epigastrium/right upper quadrant, lasting >30 mins, building to a steady level, interrupting
Figure 2: Post-cholecystectomy biliary-like pain 1 patient with recurrent episodes of pain (not daily), in the epigastrium/right upper quadrant, lasting >30 mins, building to a steady level, interrupting
EAES course on Advanced Laparoscopic GI Surgery Course. Riyadh, Saudi Arabia February 2016
 EAES course on Advanced Laparoscopic GI Surgery Course Riyadh, Saudi Arabia 13-17 February 2016 The European Association for Endoscopic Surgery and King Saud University, College of Medicine King Khalid
EAES course on Advanced Laparoscopic GI Surgery Course Riyadh, Saudi Arabia 13-17 February 2016 The European Association for Endoscopic Surgery and King Saud University, College of Medicine King Khalid
Abdominal Compartment Syndrome. Jeff Johnson, MD
 Abdominal Compartment Syndrome Jeff Johnson, MD Acute Care Surgeon, Denver Health Associate Professor of Surgery, University of Colorado Denver The Abdomen A Forgotten Closed Compartment Early Animal Models
Abdominal Compartment Syndrome Jeff Johnson, MD Acute Care Surgeon, Denver Health Associate Professor of Surgery, University of Colorado Denver The Abdomen A Forgotten Closed Compartment Early Animal Models
Abdominal Aortic Aneurysms. A Surgeons Perspective Dr. Derek D. Muehrcke
 Abdominal Aortic Aneurysms A Surgeons Perspective Dr. Derek D. Muehrcke Aneurysm Definition The abnormal enlargement or bulging of an artery caused by an injury or weakness in the blood vessel wall A localized
Abdominal Aortic Aneurysms A Surgeons Perspective Dr. Derek D. Muehrcke Aneurysm Definition The abnormal enlargement or bulging of an artery caused by an injury or weakness in the blood vessel wall A localized
Complication of Percutaneous Endoscopic Gastrostomy
 Complication of Percutaneous Endoscopic Gastrostomy Tube Ogori N. Kalu MD Morbidity & Mortality Conference General Surgery Service Kings County Hospital Center ACGME Core Competencies 1. Medical knowledge
Complication of Percutaneous Endoscopic Gastrostomy Tube Ogori N. Kalu MD Morbidity & Mortality Conference General Surgery Service Kings County Hospital Center ACGME Core Competencies 1. Medical knowledge
Anatomy of the SMALL INTESTINE. Dr. Noman Ullah Wazir PMC
 Anatomy of the SMALL INTESTINE Dr. Noman Ullah Wazir PMC SMALL INTESTINE The small intestine, consists of the duodenum, jejunum, and illium. It extends from the pylorus to the ileocecal junction were the
Anatomy of the SMALL INTESTINE Dr. Noman Ullah Wazir PMC SMALL INTESTINE The small intestine, consists of the duodenum, jejunum, and illium. It extends from the pylorus to the ileocecal junction were the
Esophageal Perforation
 Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
Exploring Anatomy: the Human Abdomen
 Exploring Anatomy: the Human Abdomen PERITONEUM AND PERITONEAL CAVITY PERITONEUM The peritoneum is a thin serous membrane that lines the abdominal cavity and covers, in variable amounts, the viscera within
Exploring Anatomy: the Human Abdomen PERITONEUM AND PERITONEAL CAVITY PERITONEUM The peritoneum is a thin serous membrane that lines the abdominal cavity and covers, in variable amounts, the viscera within
PANCREATIC CANCER GUIDELINES
 PANCREATIC CANCER GUIDELINES North-East London Cancer Network & Barts and the London HPB Centre PROTOCOL FOR MANAGEMENT OF PANCREATIC CANCER (SEPTEMBER 2010) I. PRE-REFERRAL GUIDELINES Screening 1. Offer
PANCREATIC CANCER GUIDELINES North-East London Cancer Network & Barts and the London HPB Centre PROTOCOL FOR MANAGEMENT OF PANCREATIC CANCER (SEPTEMBER 2010) I. PRE-REFERRAL GUIDELINES Screening 1. Offer
Development of the Digestive System. W.S. O The University of Hong Kong
 Development of the Digestive System W.S. O The University of Hong Kong Plan for the GI system Then GI system in the abdomen first develops as a tube suspended by dorsal and ventral mesenteries. Blood
Development of the Digestive System W.S. O The University of Hong Kong Plan for the GI system Then GI system in the abdomen first develops as a tube suspended by dorsal and ventral mesenteries. Blood
The peritoneum. Prof. Oluwadiya KS, MBBS, FMCS(Orthop) Website:
 The peritoneum Prof. Oluwadiya KS, MBBS, FMCS(Orthop) Website: http://oluwadiya.com The peritoneum Serous membrane that lines the abdominopelvic cavity and invests the viscera The largest serous membrane
The peritoneum Prof. Oluwadiya KS, MBBS, FMCS(Orthop) Website: http://oluwadiya.com The peritoneum Serous membrane that lines the abdominopelvic cavity and invests the viscera The largest serous membrane
The abdominal Esophagus, Stomach and the Duodenum. Prof. Oluwadiya KS
 The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
Vascular complications in percutaneous biliary interventions: A series of 111 procedures
 Vascular complications in percutaneous biliary interventions: A series of 111 procedures Poster No.: C-0744 Congress: ECR 2013 Type: Educational Exhibit Authors: A. BHARADWAZ; AARHUS, Re/DK Keywords: Obstruction
Vascular complications in percutaneous biliary interventions: A series of 111 procedures Poster No.: C-0744 Congress: ECR 2013 Type: Educational Exhibit Authors: A. BHARADWAZ; AARHUS, Re/DK Keywords: Obstruction
Comparative Study Of Laparoscopic Versus Open Peptic Perforation Closure
 ISPUB.COM The Internet Journal of Surgery Volume 17 Number 2 Comparative Study Of Laparoscopic Versus Open Peptic Perforation Closure M Porecha, S Mehta, D Udani, P Mehta, K Patel, S Nagre Citation M Porecha,
ISPUB.COM The Internet Journal of Surgery Volume 17 Number 2 Comparative Study Of Laparoscopic Versus Open Peptic Perforation Closure M Porecha, S Mehta, D Udani, P Mehta, K Patel, S Nagre Citation M Porecha,
ERA S JOURNAL OF MEDICAL RESEARCH LAPAROSCOPIC MANAGEMENT OF PANCREATIC PSEUDOCYSTS A NOVEL TECHNIQUE USING TITANIUM CLIPS: OUR EXPERIENCE.
 Original Article A S OUNAL OF DICAL SACH DOI:10.24041/ejmr2017.1 LAPAOSCOPIC ANAGNT OF PANCATIC PSUDOCYSTS A NOVL TCHNIQU USING TITANIU CLIPS: OU XPINC. A.S.Gogate, ahul Kenawadekar, Vandana A Frigate**,
Original Article A S OUNAL OF DICAL SACH DOI:10.24041/ejmr2017.1 LAPAOSCOPIC ANAGNT OF PANCATIC PSUDOCYSTS A NOVL TCHNIQU USING TITANIU CLIPS: OU XPINC. A.S.Gogate, ahul Kenawadekar, Vandana A Frigate**,
Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile)
 Patient information - Radiology Unit Tel 0118 322 7991 Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile) Introduction This leaflet tells you about the procedures known as
Patient information - Radiology Unit Tel 0118 322 7991 Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile) Introduction This leaflet tells you about the procedures known as
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abdominal injuries clinical presentation of, 23 24 Abdominal trauma evaluation for pediatric surgeon, 59 74 background of, 60 colon and
Index Note: Page numbers of article titles are in boldface type. A Abdominal injuries clinical presentation of, 23 24 Abdominal trauma evaluation for pediatric surgeon, 59 74 background of, 60 colon and
Yoshitsugu; Kanematsu, Takashi; Kur
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Laparoscopic Middle Pancreatectomy Surgery Kitasato, Amane; Adachi, Tomohiko; Yoshitsugu; Kanematsu, Takashi; Kur Hepato-Gastroenterology, 59(120),
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Laparoscopic Middle Pancreatectomy Surgery Kitasato, Amane; Adachi, Tomohiko; Yoshitsugu; Kanematsu, Takashi; Kur Hepato-Gastroenterology, 59(120),
Minimally Invasive Esophagectomy
 American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
What can you expect after your ERCP?
 ERCP Explained and respond to bed rest, pain relief and fasting to rest the gut with the patient needing to stay in hospital for only a few days. Some patients develop severe pancreatitis and may require
ERCP Explained and respond to bed rest, pain relief and fasting to rest the gut with the patient needing to stay in hospital for only a few days. Some patients develop severe pancreatitis and may require
PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE. PRESENTED BY: Susan DePasquale, CGRN, MSN
 PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE PRESENTED BY: Susan DePasquale, CGRN, MSN Pancreatic Fluid Collection (PFC) A result of pancreatic duct (PD) and side branch disruption,
PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE PRESENTED BY: Susan DePasquale, CGRN, MSN Pancreatic Fluid Collection (PFC) A result of pancreatic duct (PD) and side branch disruption,
HEPATIC METASTASES. We can state 3 types of metastases depending on their treatment options:
 HEPATIC METASTASES 1. Definition Metastasis means the spread of cancer. Cancerous cells can separate from the primary tumor and enter the bloodstream or the lymphatic system (the one that produces, stores,
HEPATIC METASTASES 1. Definition Metastasis means the spread of cancer. Cancerous cells can separate from the primary tumor and enter the bloodstream or the lymphatic system (the one that produces, stores,
Pi Liu *, Jun Song, Hua-jing Ke, Nong-hua Lv, Yin Zhu, Hao Zeng, Yong Zhu, Liang Xia, Wen-hua He, Ji Li, Xin Huang and Yu-peng Lei
 Liu et al. BMC Gastroenterology (2017) 17:155 DOI 10.1186/s12876-017-0717-3 TECHNICAL ADVANCE Open Access Double-catheter lavage combined with percutaneous flexible endoscopic debridement for infected
Liu et al. BMC Gastroenterology (2017) 17:155 DOI 10.1186/s12876-017-0717-3 TECHNICAL ADVANCE Open Access Double-catheter lavage combined with percutaneous flexible endoscopic debridement for infected
ADVANCED LAPAROSCOPIC PANCREAS SURGERY A HANDS-ON WORKSHOP
 ADVANCED LAPAROSCOPIC PANCREAS SURGERY A HANDS-ON WORKSHOP 3-4 November 2017 at the AMC in Amsterdam Organizing committee: Mo Abu Hilal, Professor of Surgery at Southampton University Marc Besselink, Professor
ADVANCED LAPAROSCOPIC PANCREAS SURGERY A HANDS-ON WORKSHOP 3-4 November 2017 at the AMC in Amsterdam Organizing committee: Mo Abu Hilal, Professor of Surgery at Southampton University Marc Besselink, Professor
Chronic Pancreatitis
 Gastro Foundation Fellows Weekend 2017 Chronic Pancreatitis Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Aetiology in SA Alcohol (up to 80%) Idiopathic Tropical Obstruction Autoimmune
Gastro Foundation Fellows Weekend 2017 Chronic Pancreatitis Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Aetiology in SA Alcohol (up to 80%) Idiopathic Tropical Obstruction Autoimmune
Recurrent Pancreatic Pseudocyst Diagnosed 9 Years After Initial Surgical Drainage
 CASE REPORT Recurrent Pancreatic Pseudocyst Diagnosed 9 Years After Initial Surgical Drainage Carlos M Nuño-Guzmán, José Arróniz-Jáuregui, José I Gómez-Ontiveros, Haydée Hernández-Estrada, Haydee I Estrada-Castañeda,
CASE REPORT Recurrent Pancreatic Pseudocyst Diagnosed 9 Years After Initial Surgical Drainage Carlos M Nuño-Guzmán, José Arróniz-Jáuregui, José I Gómez-Ontiveros, Haydée Hernández-Estrada, Haydee I Estrada-Castañeda,
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Clinical evaluation of endoscopic ultrasonography-guided drainage using a novel flared-type biflanged metal stent for pancreatic fluid collection
 Original Article Clinical evaluation of endoscopic ultrasonography-guided drainage using a novel flared-type biflanged metal stent for pancreatic fluid collection Shuntaro Mukai, Takao Itoi, Atsushi Sofuni,
Original Article Clinical evaluation of endoscopic ultrasonography-guided drainage using a novel flared-type biflanged metal stent for pancreatic fluid collection Shuntaro Mukai, Takao Itoi, Atsushi Sofuni,
Cholangiocarcinoma (Bile Duct Cancer)
 Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
COPYRIGHTED MATERIAL. 1 Approach to the patient with gross gastrointestinal bleeding. Grace H. Elta, Mimi Takami
 1 Approach to the patient with gross gastrointestinal bleeding Grace H. Elta, Mimi Takami Gastrointestinal (GI) bleeding is a common clinical problem that requires more than 300 000 hospitalizations annually
1 Approach to the patient with gross gastrointestinal bleeding Grace H. Elta, Mimi Takami Gastrointestinal (GI) bleeding is a common clinical problem that requires more than 300 000 hospitalizations annually
General Surgery Service
 General Surgery Service Patient Care Goals and Objectives Stomach/Duodenum and Bariatric assessed for a) Obesity surgery b) Treatment of i) Adenocarcinoma of the stomach ii) GIST iii) Carcinoid 2) Optimize
General Surgery Service Patient Care Goals and Objectives Stomach/Duodenum and Bariatric assessed for a) Obesity surgery b) Treatment of i) Adenocarcinoma of the stomach ii) GIST iii) Carcinoid 2) Optimize
Robotic-assisted Roux-en-Y gastric bypass in a patient with situs inversus. Anji Wall, Zuliang Feng & Willie Melvin. Journal of Robotic Surgery
 Robotic-assisted Roux-en-Y gastric bypass in a patient with situs inversus Anji Wall, Zuliang Feng & Willie Melvin Journal of Robotic Surgery ISSN 1863-2483 Volume 8 Number 2 J Robotic Surg (2014) 8:169-171
Robotic-assisted Roux-en-Y gastric bypass in a patient with situs inversus Anji Wall, Zuliang Feng & Willie Melvin Journal of Robotic Surgery ISSN 1863-2483 Volume 8 Number 2 J Robotic Surg (2014) 8:169-171
Duodenum retroperitoneal
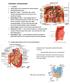 Duodenum retroperitoneal C shaped Initial region out of stomach into small intestine RETROperitoneal viscus Superior 1 st part duodenal cap ; moves upwards and backwards to lie on the R crura medial to
Duodenum retroperitoneal C shaped Initial region out of stomach into small intestine RETROperitoneal viscus Superior 1 st part duodenal cap ; moves upwards and backwards to lie on the R crura medial to
DEPARTMENT OF SURGERY DELINEATION OF PRIVILEGES FOR GENERAL SURGERY
 DEPARTMENT OF SURGERY DELINEATION OF PRIVILEGES FOR GENERAL SURGERY NAME: DATE: Please check the box for each privilege requested. Applicants have the burden of producing information deemed adequate by
DEPARTMENT OF SURGERY DELINEATION OF PRIVILEGES FOR GENERAL SURGERY NAME: DATE: Please check the box for each privilege requested. Applicants have the burden of producing information deemed adequate by
Preview from Notesale.co.uk Page 1 of 34
 Abdominal viscera and digestive tract Digestive tract Abdominal viscera comprise majority of the alimentary system o Terminal oesophagus, stomach, pancreas, spleen, liver, gallbladder, kidneys, suprarenal
Abdominal viscera and digestive tract Digestive tract Abdominal viscera comprise majority of the alimentary system o Terminal oesophagus, stomach, pancreas, spleen, liver, gallbladder, kidneys, suprarenal
Wali R Johnson et. al. / International Journal of New Technologies in Science and Engineering Vol. 2, Issue 4, October 2015, ISSN
 Enteral Feeding via Percutaneous Endoscopic Gastrojejunostomy(PEGJ) Tubes Decreases Risk of Aspiration and Tube Dislodgement Related Complications Compared to PEGs. Wali R Johnson, MSIV, L Ray Matthews,
Enteral Feeding via Percutaneous Endoscopic Gastrojejunostomy(PEGJ) Tubes Decreases Risk of Aspiration and Tube Dislodgement Related Complications Compared to PEGs. Wali R Johnson, MSIV, L Ray Matthews,
