Recognising and managing diabetic retinopathy
|
|
|
- Aubrey Stone
- 5 years ago
- Views:
Transcription
1 DIAGNOSIS AND MANAGEMENT Recognising and managing diabetic retinopathy Former Head of Department of Ophthalmology, Kilimanjaro Christian Medical Centre, Tanzania. Key learning points Detecting and diagnosing diabetic retinopathy is not complicated. There are clinical signs which can be seen with an ophthalmoscope or a slit lamp and 90- or 78-dioptre lens. Diabetic retinopathy is treatable. Treatment usually maintains vision, but does not restore vision that has alread y been lost. In diabetic maculopathy, laser or anti-vegf injections are both proven to work. Intravitreal steroid is ineffective in most patients. Laser treatment should use small spots and just enough power to produce a visible reaction. Proliferative retinopathy is best treated with pan-retinal laser. The commonest error is undertreatment, and laser should be applied until there is regression of the new vessels or there is no room for further treatment. Vitrectomy is useful for vitreous haemorrhage and late complications of proliferative retinopathy. Pre-treatment with bevacizumab reduces the risk of surgical complications. David Yorston Recognising DR University of Wisconsin Fundus Photograph Reading Centera Figure 2. Venous beading, i.e., irregular calibre ( thickness ) of the veins University of Wisconsin Fundus Photograph Reading Centera Figure 1. Haemorrhages (larger, uneven red blots ) and microaneurysms (small, round dots ) Figure 3. Intraretinal microvascular abnormalities (IRMA). The circles show the odd, twisted shape of IRMA The management of diabetic retinopathy (DR) depends on accurately recognising or classifying the different types of DR and knowing what treatment to give the patient. DR has clinical signs which can be seen with an ophthalmoscope or with a slit lamp and a 90- or 78-dioptre lens. The advantage of the slit lamp is that it allows you to visualise the retina with both eyes. This stereoscopic vision provides a sense of depth which aids diagnosis, particularly of macular oedema. Other aids to DR diagnosis are fundus photography, fluorescein angiography, and optical coherence tomography (see box on page 7). The clinical signs of proliferative DR include: new vessels growing onto the posterior vitreous surface from the retina or optic disc (Figure 4) vitreous and/or pre-retinal haemorrhages (Figure 5) fibrosis traction retinal detachment. Continues overleaf 2 Proliferative DR Proliferative DR can exhibit all the same clinical signs as non-proliferative DR. However, the key characteristic of proliferative DR is new vessels growing onto the posterior vitreous surface from the retina or optic disc (Figure 4). The new vessels damage sight by bleeding (Figure 5) or forming sheets of fibrovascular membranes that may cause traction retinal detachments. Traction retinal detachment occurs when the fibrovascular tissue contracts and pulls the retina away from the underlying choroid. If this affects the macula, the central vision will be lost. Figure 4. New vessels, the key characteristic of proliferative diabetic retinopathy Figure 5. Pre-retinal haemorrhage, one of the signs of proliferative diabetic retinopathy University of Wisconsin Fundus Photograph Reading Center a haemorrhages (Figure 1) microaneurysms (Figure 1) venous beading (Figure 2) intraretinal microvascular abnormalities (IRMA) (Figure 3) Clare Gilbert 1 Non-proliferative DR The clinical signs of non-proliferative DR are: Community Eye Health Journal Vol 24 ISSUE 75 SEPTEMBER CEHJ75_OA.indd 5 25/10/ :32
2 DIAGnOSIS AnD MAnAGEMEnT Continued 3 Diabetic maculopathy Diabetic maculopathy occurs when DR affects the central part of the retina. Blood vessels leak, leading to diabetic macular oedema (swelling of the retina). The early treatment of diabetic retinopathy study (ETDRS) defi ned clinically signifi cant macular oedema (CSMO) 1 as the stage at which the eye needs to be treated in order to prevent loss of vision. The defi nition depends on recognising the following: retinal thickening and exudates (Figure 6) at or within 500 microns of the fovea (within one third of a disc diameter). larger zones of retinal thickening (one disc diameter or more), if within one disc diameter of the fovea. Retinal thickening can only be observed stereoscopically. So, for practical clinical FROM THE FIELD I am Lalitha Y, and I have been working as a vision technician at LV Prasad Eye Institute since I hail from a remote rural village in Prakasham District and I joined the vision technician programme at LVPEI in During this programme, we were trained to look for diabetic retinopathy (DR) by direct ophthalmoscope. Whenever someone with diabetes visits my vision centre, I will initially take a detailed history regarding the duration of diabetes, their blood sugar control, medication (drugs/insulin), diet, physical activity, smoking, alcohol intake, family history of diabetes, and other systemic diseases like hypertension, diabetic nephropathy, neuropathy, and so on. I also record any history of blurred vision for distance or near vision, fl ashes, fl oaters in the fi eld of view, and any fl uctuations in vision. After checking the patient s visual acuity, I check for any extra-ocular muscle imbalance by checking eye movements in all directions. During a slit lamp examination (before dilation) Clare Gilbert Figure 6. Exudates. This is an example of circinate exudates, which are circular in appearance purposes, look for other easily visible markers for macular oedema such as exudates within a disk diameter of the fovea. The blood vessels in the central part of the retina may also become blocked (capillary closure), leading to macular ischaemia. Macular ischaemia occurs How I look for diabetic retinopathy: a vision technician s experience I will initially take a detailed patient history I look mainly for neovascularisation of the iris and record intraocular pressure. After dilation, I will then examine the posterior segment by direct ophthalmoscope. If the media are clear, I will check for signs of DR, such as haemorrhages or exudates. If the media are not clear or if the patient has signs of DR, I will refer the patient to a secondary centre ophthalmologist for dilated fundus examination, which will give them the information they need to manage the patient s DR. Recently, I was trained to take fundus photographs. This helps me to identify patients with DR, who I would then send to a secondary centre for further management. I will then talk to the patient and explain the role of good blood sugar control. Editor s note: In patients with high blood pressure, good blood pressure control will reduce the likelihood that a patient s DR will get worse (see article on page 4). Eye care workers would do well to check their patients blood pressure and advise those with high blood pressure on the importance of control, referring them to a physician if they needed help. when there is insuffi cient blood supply to the macula. This will impair the normal functioning of the retina, leading to reduced vision. There is no effective treatment for macular ischaemia, 1 but it is important to recognise it so that you don t waste the patient s time and money with ineffective laser or anti-vascular endothelial growth factor (anti-vegf) treatment. Although macular ischaemia can only be diagnosed conclusively by fl uorescein angiography (see box on page 7), you should suspect it if the following conditions are met: reduced visual acuity evidence of retinal ischaemia, e.g. cotton wool spots (Figure 7) or blot haemorrhages no macular oedema at the fovea no other cause for reduced vision (e.g. cataract, refractive error). Figure 7. Cotton wool spots Cotton wool spots Treating proliferative diabetic retinopathy The two main treatment options for proliferative DR are pan-retinal laser photocoagulation and diabetic vitrectomy. Pan-retinal photocoagulation (PRP) Pan-retinal photocoagulation (PRP), or scatter laser, is the main form of treatment for proliferative diabetic retinopathy. The aim of the laser is to induce regression of new blood vessels (that is, to make them stop growing and shrink). It must be given early enough and cover enough retina to induce regression of the vessels that cause the complications of vitreous haemorrhage and tractional detachment of the retina. A 50% reduction in severe visual loss after PRP was reported by the Diabetic Retinopathy Study for patients with new vessels on the optic disc. 1 Diabetic vitrectomy Vitrectomy is indicated in proliferative diabetic retinopathy in the following conditions: A Grosso (Br J Ophthalmol, 2005) b 6 Community EyE HEaltH Journal Vol 24 issue 75 SEPtEmBEr 2011
3 non-clearing vitreous haemorrhage pre-retinal (or sub-hyaloid) haemorrhage tractional retinal detachment threatening, or involving, the macula combined rhegmatogenous/tractional detachment progressive severe fibrovascular proliferation in spite of adequate PRP. Currently, vitrectomy for diabetic macular oedema is reserved for the few patients who have vitreous traction on the macula. 2 The technique is an important part of the treatment of proliferative diabetic retinopathy and leads to improvement or stabilisation of vision in 90% of patients. 1,2 Vitreous and blood are cut and aspirated and membranes causing tractional detachment of the retina are removed. This may be done by segmenting the membranes or by delamination, i.e. removing the whole of the posterior hyaloid and associated fibrovascular membranes by cutting them off the surface of the retina. In countries without screening, many people present with long-standing tractional retinal detachments of the macula. The result of diabetic vitrectomy in these eyes is not so good. In a resource-poor environment, those with a better prognosis should be prioritised. It is worth pre-treating patients with intravitreal bevacizumab prior to vitrectomy. 3 A Cochrane review of six randomised controlled trials found that pre-treatment with 1.25 mg of intravitreal bevacizumab resulted in shorter operations with less endodiathermy and intra-operative bleeding. Post-operative reabsorption of blood was significantly shorter. Final best-corrected visual acuity was significantly better. The effect of intravitreal bevacizumab on neovascularisation is rapid. The first effects can be seen in 24 hours. The optimum time for a preoperative injection would seem to be 5 7 days before the operation. In a proportion of patients, intravitreal bevacizumab preoperatively may lead to clearing of the vitreous haemorrhage, thus avoiding surgery. Treating diabetic maculopathy Diabetic maculopathy is a major cause of vision loss amongst patients with diabetes. Treatment includes steroids, anti-vascular endothelial growth factor (anti-vegf), and laser. Steroid treatments In the Diabetic Retinopathy Clinical Research Network trial, intravitreal injections of the steroid triamcinolone acetonide was compared with standard laser treatment. Although there were short-term improvements in visual acuity with intravitreal triamcinolone acetonide (IVTA), this improvement was not sustained. Laser was more effective and had fewer side effects than IVTA. The side effects of IVTA included cataract formation and raised intraocular pressure. Recently, the same group found that there was one exception. In pseudophakic eyes, IVTA and prompt laser seemed more effective than laser alone. 4 Anti-vascular endothelial growth factor (anti-vegf) treatment VEGF levels are increased in the vitreous and retina in patients with diabetic retinopathy. The most recent anti-vegf drugs to be evaluated in the Continues overleaf Investigating DR: photos, fluorescein angiography and OCT Diabetic retinopathy (DR) can be diagnosed by clinical examination alone if you are good at examining the retina with a slit lamp microscope. Using the slit lamp, you will be able to detect haemorrhages, new vessels, exudates, and retinal thickening due to oedema. If the diagnosis can be made clinically, are investigations ever necessary? Photos are probably the most useful investigation. The cost of fundus cameras is still high, but they are becoming more affordable and the quality of pictures is improving all the time. They are also easy to use. The most valuable use of photography is in patients with diabetic maculopathy or new vessels who have laser treatment. Often, the laser leads to a complete cure and the exudates and new vessels disappear. However, sometimes they do not completely resolve. If you only examine the patient occasionally, it is difficult to remember exactly what the retina looked like before you treated it. When you can still see retinopathy months after laser treatment, you may be unsure if it is better, worse, or much the same. If you have photos to refer to, you can be certain of what has changed. Of course, photos are also very useful for If you have photos to refer to, you can be certain of what has changed An optical coherence tomography (OCT) image of cystoid macular oedema detecting DR and counselling patients. Fluorescein angiography is a technique for examining the fine detail of the retinal circulation. It will show the leaks that cause exudative maculopathy and the areas of blocked capillaries that cause ischaemic maculopathy and proliferative retinopathy. However, injections of fluorescein carry a small risk (about 1:20,000) of a severe allergic response, which can be fatal. They should not be given unless there are facilities for resuscitation. Optical coherence tomography (OCT) is a relatively new technique that uses lasers to scan the retina and build up a very detailed three-dimensional image. This will not only detect any oedema or swelling of the retina, but also measure it and draw a map that shows the areas where the swelling is greatest. It is fast, safe, and does not require any injections. Unfortunately, the machines cost about 50,000! In high-income countries, OCT and photos, in combination, are the usual means of documenting and investigating DR. As cameras and OCT machines become more affordable, they will also become more widely used in low- and middle income countries. Farieda Cassiem Community Eye Health Journal Vol 24 ISSUE 75 SEPTEMBER
4 DIAGnOSIS AnD MAnAGEMEnT Continued treatment of diabetic maculopathy are ranibizumab2 (Lucentis) and bevacizumab5 (Avastin). These trials showed a benefit with intravitreal ranibizumab and bevacizumab in patients with foveal thickening. However, intravitreal ranibizumab injections cost around US $1,200 each and the patients in this study received eight or nine injections in the first year (a cost of around US $10,000 per patient per year.) Intravitreal bevacizumab is much cheaper. We are able to offer patients an intravitreal bevacizumab injection for as little as US $25. In practice, laser should remain the cornerstone of treating clinically significant macular oedema and the use of intravitreal injections should be tailored to the needs of individual patients. Laser The Early Treatment of Diabetic Retinopathy study compared macular laser with observation. There was a 50% reduction in moderate visual loss in the group that received laser (from 24% to 12%). The recommended protocol is as follows: Treat circinate exudates (Figure 6) with focal laser, blanching the retina in the Recommendations 1 Warn all diabetes patients to come if they experience floaters or blur, as these symptoms Fibrovascular suggest a vitreous membrane haemorrhage. 2 Give PrP to anyone who has vitreous or sub-hyaloid blood (Figure 5) even if there are no visible new vessels. Treat any size area of definite neovascularisation, on the disc or elsewhere. 8 CEHJ75_OA.indd 8 Active new vessels Case study In our clinic, a typical patient, Mrs X, was first seen with a visual acuity of 6/9, a few macular exudates, and proliferative disease. The treatment plan followed the textbook recommendation of doing focal laser for the maculopathy first. The patient then missed two appointments and pan-retinal photocoagulation (PRP) was delayed by about two months. When PRP was finally given, the intention was to give it in the recommended multiple sessions. However, due to further missed appointments, the interval between laser sessions was over a month. This allowed fibrovascular proliferation to continue. It was six months from the time of presentation before laser was completed. By then, tractional retinal detachment involving the macula had developed and vitrectomy was required. Mrs X s final visual acuity was counting fingers at three metres. What are the lessons to be learned from this? How can we do better? We audited a number of patients who had ultimately needed vitrectomy for advanced proliferative disease to find out how we could improve, and arrived at the following recommendations for laser in countries where patients may not come for regular appointments. Managing diabetic retinopathy in Africa Fibrovascular membrane shows marked resolution Figure 8. Eye before treatment. The arrows at the top point out active new vessels Figure 9. Ten days after PRP. Note regression of new vessels Treat any eye that has evidence of fibrosis, as this is evidence of proliferative disease. 3 treat patients faster. Regression of new vessels should be seen after a week or two. (Figures 8 and 9). If patients come from far away, consider admitting them to complete the laser before they are discharged. Attempt to complete the laser in one week, instead of several weeks. Treat the inferior retina first as new blood falls down and blocks the view inferiorly. 4 make the most of each session you have. It is worth treating some patients in one session. This is particularly important if there are large neovascular (NV) formations which have an increased risk of bleeding, or if the patient is unlikely to return. Remember to avoid application of intense burns which are unnecessary to induce regression. A pan-retinal pattern of excessively intense burns can lead to choroidal effusion and angle-closure glaucoma with blindness. Treat one burn width apart, as shown in Figure 10. Oedema surrounding the burns makes them look more confluent than they are. 5 repeat treatment. All neovascularisation should regress in two to four weeks. If it has not regressed, treat again. If bleeding occurs after laser, re-treat until NV formations have gone or maximal treatment has been given. Consider treating inside the arcades, particularly temporally. Pre-retinal (subhyaloid) haemorrhage, covering the macula and arcades Figure 10. Pan-retinal photocoagulation Community EyE HEaltH Journal Vol 24 issue 75 SEPtEmBEr /10/ :32
5 centre of the exudate. It is not necessary to target individual microaneurysms. Diffuse macular oedema is treated by a grid laser in the area of thickening. Burns should be one burn width apart, using a spot size of 75 to 125 microns, duration milliseconds. Do not use the repeat mode. Start with a low power setting, around 150 milliwatt, and increase the power until the desired endpoint is reached. Aim to produce a grey to cream change in colour. White means the laser is too hot and the power should be reduced. Take care not to encroach on the foveal avascular zone. It is wise to avoid treating perifoveal microaneurysms as this is likely to increase perifoveal capillary dropout (consider intravitreal bevacizumab instead). The chorioretinal atrophy caused by burns, especially intense burns, within 300 to 500 microns of the fovea can years later extend into the fovea and cause vision loss, particularly in myopes. In patients with established foveal thickening or who are not responding to laser, consider intravitreal bevacizumab. In pseudophakic eyes, consider IVTA but watch the intraocular pressure closely. Populations in low- and middle-income countries face a huge burden of blinding DR. Urgent advocacy is needed for governments to initiate programmes to address this. In the interim, every residency programme must provide training in the skills needed to manage DR, including interpreting investigations and delivering laser and other treatments. Refresher courses can be arranged for those not adequately trained or who have been without the necessary equipment for some time. We must also advocate for lasers and other necessary equipment wherever there is a trained ophthalmologist. References 1 Ockrim Z, Yorston D. Managing diabetic retinopathy. British Med J 2010;341:c Yorston D, Wickham L, Benson S, Bunce C, Sheard R, Charteris D. Predictive clinical features and outcomes of vitrectomy for proliferative diabetic retinopathy. Br J Ophthalmol 2008;92: Ahmadieh H, Shoeibi N, Entezari M, Monshizadeh R. Intravitreal bevacizumab for prevention of early postvitrectomy hemorrhage in diabetic patients: a randomized clinical trial. Ophthalmology 2009;116: Elman MJ, Aiello LP, Beck RW, Bressler NM, Bressler SB, Edwards AR, et al. Randomized trial evaluating ranibizumab plus prompt or deferred laser or triamcinolone plus prompt laser for diabetic macular edema. Ophthalmology 2010;117: Soheilian M, Ramezani A, Obudi A, Bijanzadeh B, Salehipour M, Yaseri M, et al. Randomized trial of intravitreal bevacizumab alone or combined with triamcinolone versus macular photocoagulation in diabetic macular edema. Ophthalmology 2009;116: Photographs a Reproduced with permission, University of Wisconsin Fundus Photograph Reading Center, Madison, WI. b Grosso A, Veglio F, Porta M, Grignolo FM, Wong TY. Hypertensive retinopathy revisited: some answers, more questions. Br J Ophthalmol 2005;89: Copyright This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium for non-profit purposes, provided CATARACT AND DR Cataract and diabetic retinopathy James Rice Vitreoretinal consultant, University of Cape Town, Division of Ophthalmology, Faculty of Health Sciences, H53 Old Main Building, Groote Schuur Hospital, Observatory 7925, South Africa. james.rice@uct.ac.za When managing the cataract of a patient with diabetes, you should remember that cataract surgery may make diabetic retinopathy worse. Eyes with mild to moderate non-proliferative diabetic retinopathy at the time of surgery are considered less at risk. Those with severe non-proliferative and proliferative diabetic retinopathy have a higher risk of progressive disease. 1 Clinically significant macular oedema (CSMO) present at the time of surgery is likely to progress and eyes with previously treated CSMO are at increased risk of recurrence. The risk of progression is increased if the operation is complicated by excessive manipulation, vitreous loss, or severe post-operative inflammation. Ideally, when the cataract does not preclude laser treatment, you should achieve and maintain effective control of retinopathy and maculopathy for at least three months before surgery. The severity of the cataract sometimes prevents adequate examination or treatment of the retina in patients with diagnosed or suspected severe non-proliferative and proliferative diabetic retinopathy. In this case, you should deliver pan-retinal photocoagulation either during the procedure or in the early post-operative period. When performing intraoperative pan-retinal photocoagulation with an indirect ophthalmoscope, you should fill the anterior chamber with viscoelastic and place a corneal suture. Complete the pan-retinal photocoagulation before inserting the intraocular lens. This will provide a stable anterior chamber and optimal view, particularly if you anticipate indentation of the periphery. If you plan to give laser treatment with a contact lens in the early post-operative period, then you should suture the cataract wound. If it is still considered hazardous to use a contact lens then effective slit lamp laser can still be applied through a non-contact 78D or 90D lens. You can also use indirect laser for pan-retinal photocoagulation. If the patient has diabetic maculopathy Consider intravitreal triamcinolone or anti-vegf at the end of surgery to reduce macular oedema You should remember that cataract surgery may make diabetic retinopathy worse and/or more advanced retinopathy, consider intravitreal triamcinolone or anti-vegf at the end of the procedure to reduce macular oedema. Triamcinolone targets the inflammation that exacerbates the oedema. Anti-VEGFs also reduce retinal swelling and may improve visual outcomes. 2 Intravitreal steroids may cause raised intraocular pressure and anti-vegf agents increase the risk of tractional complications in eyes with fibrovascular proliferation. You should still apply macular laser for CSMO post-operatively. In diabetes patients, it is very important to minimise post-operative inflammation. You should use post-operative topical non-steroidal anti-inflammatory drugs in addition to routine topical steroid preparations, particularly in those with pre-existing macular oedema. 3 In summary, diabetes patients with mild to moderate diabetic retinopathy and no maculopathy have a good prognosis following cataract surgery. You should treat more advanced retinopathy or maculopathy at least three months prior to surgery if possible. Whereas laser is the most recognised form of treatment, pharmacological agents play an important role in the management of these patients. It is also important to monitor high-risk patients in the post-operative period. References 1 Somaiya MD, Burns JD, Mintz R, Warren RE, Uchida T, Godley BF. Factors affecting visual outcomes after small-incision phacoemulsification in diabetic patients. J Cataract Refract Surg 2002;28(8): Cheema RA, Al-Mubarak M, Amin YM, Cheema MA. Role of combined cataract surgery and intravitreal bevacizumab injection in preventing progression of diabetic retinopathy: prospective randomized study. J Cataract Refract Surg 2009;35(1): Endo N, Kato S, Haruyama K, Shoji M, Kitano S. Efficacy of bromfenac sodium ophthalmic solution in preventing cystoid macular oedema after cataract surgery in patients with diabetes. Acta Ophthalmol 2010;88(8): Copyright 2011 James Rice. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any Courtesy of K Suttle
 measure of your overall performance. An isolated glucose test is helpful to let you know what your sugar level is at one moment, but it doesn t tell you whether or not your diabetes is under adequate control
measure of your overall performance. An isolated glucose test is helpful to let you know what your sugar level is at one moment, but it doesn t tell you whether or not your diabetes is under adequate control
Diabetic retinopathy: everybody s business. laser is the most effective treatment for proliferative diabetic retinopathy.
 Community Eye Health Journal Now with CPD See page 23 VolumE 24 issue 75 SEPtEmBEr 2011 Diabetic retinopathy: everybody s business Iris Winter Consultant, Universitätsklinik und Poliklinik für Augenheilkunde/
Community Eye Health Journal Now with CPD See page 23 VolumE 24 issue 75 SEPtEmBEr 2011 Diabetic retinopathy: everybody s business Iris Winter Consultant, Universitätsklinik und Poliklinik für Augenheilkunde/
Diagnosis and treatment of diabetic retinopathy. Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City
 Diagnosis and treatment of diabetic retinopathy Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City Disclosures Consulted for Novo Nordisk 2017,2018. Will be discussing
Diagnosis and treatment of diabetic retinopathy Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City Disclosures Consulted for Novo Nordisk 2017,2018. Will be discussing
Clinically Significant Macular Edema (CSME)
 Clinically Significant Macular Edema (CSME) 1 Clinically Significant Macular Edema (CSME) Sadrina T. Shaw OMT I Student July 26, 2014 Advisor: Dr. Uwaydat Clinically Significant Macular Edema (CSME) 2
Clinically Significant Macular Edema (CSME) 1 Clinically Significant Macular Edema (CSME) Sadrina T. Shaw OMT I Student July 26, 2014 Advisor: Dr. Uwaydat Clinically Significant Macular Edema (CSME) 2
PART 1: GENERAL RETINAL ANATOMY
 PART 1: GENERAL RETINAL ANATOMY General Anatomy At Ora Serrata At Optic Nerve Head Fundoscopic View Of Normal Retina What Is So Special About Diabetic Retinopathy? The WHO definition of blindness is
PART 1: GENERAL RETINAL ANATOMY General Anatomy At Ora Serrata At Optic Nerve Head Fundoscopic View Of Normal Retina What Is So Special About Diabetic Retinopathy? The WHO definition of blindness is
FRANZCO, MD, MBBS. Royal Darwin Hospital
 Diabetes and Eye By Dr. Nishantha Wijesinghe FRANZCO, MD, MBBS Consultant Ophthalmologist Royal Darwin Hospital 98% of Diabetics do not need to suffer from severe visual loss Yet Diabetic eye disease is
Diabetes and Eye By Dr. Nishantha Wijesinghe FRANZCO, MD, MBBS Consultant Ophthalmologist Royal Darwin Hospital 98% of Diabetics do not need to suffer from severe visual loss Yet Diabetic eye disease is
The Human Eye. Cornea Iris. Pupil. Lens. Retina
 The Retina Thin layer of light-sensitive tissue at the back of the eye (the film of the camera). Light rays are focused on the retina then transmitted to the brain. The macula is the very small area in
The Retina Thin layer of light-sensitive tissue at the back of the eye (the film of the camera). Light rays are focused on the retina then transmitted to the brain. The macula is the very small area in
Diabetic Retinopathy A Presentation for the Public
 Diabetic Retinopathy A Presentation for the Public Ray M. Balyeat, MD The Eye Institute Tulsa, Oklahoma The Healthy Eye Light rays enter the eye through the cornea, pupil and lens. These light rays are
Diabetic Retinopathy A Presentation for the Public Ray M. Balyeat, MD The Eye Institute Tulsa, Oklahoma The Healthy Eye Light rays enter the eye through the cornea, pupil and lens. These light rays are
A Patient s Guide to Diabetic Retinopathy
 Diabetic Retinopathy A Patient s Guide to Diabetic Retinopathy 840 Walnut Street, Philadelphia PA 19107 www.willseye.org Diabetic Retinopathy 1. Definition Diabetic retinopathy is a complication of diabetes
Diabetic Retinopathy A Patient s Guide to Diabetic Retinopathy 840 Walnut Street, Philadelphia PA 19107 www.willseye.org Diabetic Retinopathy 1. Definition Diabetic retinopathy is a complication of diabetes
Management of diabetic eye disease: an overview
 Peter Blows Photographic screening for diabetic eye disease can identify patients who will benefit from laser treatment. BOTSWANA MANAGEMENT Management of diabetic eye disease: an overview Laser for DR
Peter Blows Photographic screening for diabetic eye disease can identify patients who will benefit from laser treatment. BOTSWANA MANAGEMENT Management of diabetic eye disease: an overview Laser for DR
Brampton Hurontario Street Brampton, ON L6Y 0P6
 Diabetic Retinopathy What is Diabetic Retinopathy Diabetic retinopathy is one of the leading causes of blindness world-wide. Diabetes damages blood vessels in many organs of the body including the eyes.
Diabetic Retinopathy What is Diabetic Retinopathy Diabetic retinopathy is one of the leading causes of blindness world-wide. Diabetes damages blood vessels in many organs of the body including the eyes.
Diabetic and the Eye: An Introduction
 Diabetic and the Eye: An Introduction Lawrence Iu FRCSEd (Ophth), FCOphthHK, FHKAM (Ophthalmology) Department of Ophthalmology, Grantham Hospital & Queen Mary Hospital Background Diabetes mellitus (DM)
Diabetic and the Eye: An Introduction Lawrence Iu FRCSEd (Ophth), FCOphthHK, FHKAM (Ophthalmology) Department of Ophthalmology, Grantham Hospital & Queen Mary Hospital Background Diabetes mellitus (DM)
Diabetes & Your Eyes
 Diabetes & Your Eyes Diabetes is a disease that occurs when the pancreas does not secrete enough insulin or the body is unable to process it properly. Insulin is the hormone that regulates the level of
Diabetes & Your Eyes Diabetes is a disease that occurs when the pancreas does not secrete enough insulin or the body is unable to process it properly. Insulin is the hormone that regulates the level of
Diabetic Retinopathy
 Diabetic Retinopathy Diabetes can be classified into type 1 diabetes mellitus and type 2 diabetes mellitus, formerly known as insulin-dependent diabetes mellitus, and non-insulin diabetes mellitus, respectively.
Diabetic Retinopathy Diabetes can be classified into type 1 diabetes mellitus and type 2 diabetes mellitus, formerly known as insulin-dependent diabetes mellitus, and non-insulin diabetes mellitus, respectively.
Jay M. Haynie, O.D.; F.A.A.O. Olympia Tacoma Renton Kennewick Washington
 Jay M. Haynie, O.D.; F.A.A.O. Olympia Tacoma Renton Kennewick Washington I Jay M. Haynie, OD, FAAO have received honoraria from the following companies: Reichert Technologies Notal Vision Carl Zeiss Meditec
Jay M. Haynie, O.D.; F.A.A.O. Olympia Tacoma Renton Kennewick Washington I Jay M. Haynie, OD, FAAO have received honoraria from the following companies: Reichert Technologies Notal Vision Carl Zeiss Meditec
Diabetic maculopathy 11/ An update on. Miss Vasuki Sivagnanavel
 Miss Vasuki Sivagnanavel Consultant Ophthalmologist An update on Diabetic maculopathy Despite advances in the management of diabetes, diabetic retinopathy is already the commonest cause of blindness among
Miss Vasuki Sivagnanavel Consultant Ophthalmologist An update on Diabetic maculopathy Despite advances in the management of diabetes, diabetic retinopathy is already the commonest cause of blindness among
Diabetic Retinopathy
 Diabetic Retinopathy Diabetes mellitus is one of the leading causes of irreversible blindness worldwide. In the United States, it is the most common cause of blindness in people younger than 65 years.
Diabetic Retinopathy Diabetes mellitus is one of the leading causes of irreversible blindness worldwide. In the United States, it is the most common cause of blindness in people younger than 65 years.
Diabetic Retinopathy. Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012
 Diabetic Retinopathy Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Outline Statistics Anatomy Categories Assessment Management Risk factors What do you need to do? Objectives Summarize the
Diabetic Retinopathy Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Outline Statistics Anatomy Categories Assessment Management Risk factors What do you need to do? Objectives Summarize the
ROLE OF LASER PHOTOCOAGULATION VERSUS INTRAVITREAL TRIAMCINOLONE ACETONIDE IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETES MELLITUS
 ORIGINAL ARTICLE ROLE OF LASER PHOTOCOAGULATION VERSUS INTRAVITREAL TRIAMCINOLONE ACETONIDE IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETES MELLITUS Aggarwal Somesh VP 1, Shah Sonali N 2, Bharwada Rekha M 3,
ORIGINAL ARTICLE ROLE OF LASER PHOTOCOAGULATION VERSUS INTRAVITREAL TRIAMCINOLONE ACETONIDE IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETES MELLITUS Aggarwal Somesh VP 1, Shah Sonali N 2, Bharwada Rekha M 3,
Facts About Diabetic Eye Disease
 Facts About Diabetic Eye Disease Points to Remember 1. Diabetic eye disease comprises a group of eye conditions that affect people with diabetes. These conditions include diabetic retinopathy, diabetic
Facts About Diabetic Eye Disease Points to Remember 1. Diabetic eye disease comprises a group of eye conditions that affect people with diabetes. These conditions include diabetic retinopathy, diabetic
Case Report Inherent Challenges in Managing Long Standing Refractory Diabetic Macular Edema
 Cronicon OPEN ACCESS EC OPHTHALMOLOGY Case Report Inherent Challenges in Managing Long Standing Refractory Diabetic Macular Edema V Swetha E Jeganathan 1,2 * and Karen Madill 3 1 Department of Ophthalmology,
Cronicon OPEN ACCESS EC OPHTHALMOLOGY Case Report Inherent Challenges in Managing Long Standing Refractory Diabetic Macular Edema V Swetha E Jeganathan 1,2 * and Karen Madill 3 1 Department of Ophthalmology,
Diabetic Retinopatathy
 Diabetic Retinopatathy Jay M. Haynie, OD, FAAO Financial Disclosure I have received honoraria or am on the advisory board for the following companies: Carl Zeiss Meditec Arctic DX Macula Risk Advanced
Diabetic Retinopatathy Jay M. Haynie, OD, FAAO Financial Disclosure I have received honoraria or am on the advisory board for the following companies: Carl Zeiss Meditec Arctic DX Macula Risk Advanced
Diabetic Eye Disease
 Manchester Royal Eye Hospital Medical Retinal Services Information for Patients Diabetic Eye Disease This leaflet sets out to answer some of your questions about diabetic eye disease. You may wish to discuss
Manchester Royal Eye Hospital Medical Retinal Services Information for Patients Diabetic Eye Disease This leaflet sets out to answer some of your questions about diabetic eye disease. You may wish to discuss
OCT Assessment of the Vitreoretinal Relationship in CSME
 December 2007 Sonia Rani John et al. - IFIS 375 ORIGINAL ARTICLE OCT Assessment of the Vitreoretinal Relationship in CSME Dr. Manoj S. DNB FRCS, Dr. Unnikrishnan Nair MS DO FRCS, Dr. Gargi Sathish MS Introduction
December 2007 Sonia Rani John et al. - IFIS 375 ORIGINAL ARTICLE OCT Assessment of the Vitreoretinal Relationship in CSME Dr. Manoj S. DNB FRCS, Dr. Unnikrishnan Nair MS DO FRCS, Dr. Gargi Sathish MS Introduction
Recalcitrant Diabetic Macular Oedema: Therapeutic Options
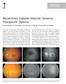 December 2007 A. Giridhar et al. - Recalcitrant DME 451 CONSULTATION S E C T I O N Recalcitrant Diabetic Macular Oedema: Therapeutic Options Dr. Cyrus M Shroff 1, Dr. N S Muralidhar 2, Dr. R Narayanan
December 2007 A. Giridhar et al. - Recalcitrant DME 451 CONSULTATION S E C T I O N Recalcitrant Diabetic Macular Oedema: Therapeutic Options Dr. Cyrus M Shroff 1, Dr. N S Muralidhar 2, Dr. R Narayanan
Understanding Diabetic Retinopathy
 Understanding Diabetic Retinopathy What Is Diabetic Retinopathy? Diabetes damages blood vessels in the rear of the eye. This condition is called diabetic retinopathy. It can lead to vision loss or blindness.
Understanding Diabetic Retinopathy What Is Diabetic Retinopathy? Diabetes damages blood vessels in the rear of the eye. This condition is called diabetic retinopathy. It can lead to vision loss or blindness.
Diabetic retinopathy damage to the blood vessels in the retina. Cataract clouding of the eye s lens. Cataracts develop at an earlier age in people
 Diabetic Retinopathy What is diabetic eye disease? Diabetic eye disease refers to a group of eye problems that people with diabetes may face as a complication of diabetes. All can cause severe vision loss
Diabetic Retinopathy What is diabetic eye disease? Diabetic eye disease refers to a group of eye problems that people with diabetes may face as a complication of diabetes. All can cause severe vision loss
Diabetic Management beyond traditional risk factors and LDL-C control: Can we improve macro and microvascular risks?
 Retinopathy Diabetes has a negative effect on eyes in many ways, increasing the risk of cataracts for example, but the most common and serious ocular complication of diabetes is retinopathy. Diabetic retinopathy
Retinopathy Diabetes has a negative effect on eyes in many ways, increasing the risk of cataracts for example, but the most common and serious ocular complication of diabetes is retinopathy. Diabetic retinopathy
Medical Retina 2011 Nicholas Lee
 Medical Retina 2011 Nicholas Lee 1 Diabetic Retinopathy Epidemiology 1000 registered blind each year 2% diabetics registered as blind (8% of all Blind Registrations) 42% with Mild Background DR will progress
Medical Retina 2011 Nicholas Lee 1 Diabetic Retinopathy Epidemiology 1000 registered blind each year 2% diabetics registered as blind (8% of all Blind Registrations) 42% with Mild Background DR will progress
Diabetic Retinopathy WHAT IS DIABETIC RETINOPATHY? WHAT CAUSES DIABETIC RETINOPATHY? WHAT ARE THE STAGES OF DIABETIC RETINOPATHY?
 Diabetic Retinopathy WHAT IS DIABETIC RETINOPATHY? Diabetic retinopathy affects 8 million Americans with diabetes. A leading cause of blindness in American adults, it is caused by damage to the small blood
Diabetic Retinopathy WHAT IS DIABETIC RETINOPATHY? Diabetic retinopathy affects 8 million Americans with diabetes. A leading cause of blindness in American adults, it is caused by damage to the small blood
Central Mersey Diabetic Retinopathy Screening Programme. Referring patients for Diabetic Retinopathy Screening
 Central Mersey Diabetic Retinopathy Screening Programme Referring patients for Diabetic Retinopathy Screening Information for GPs in Halton & St Helens, Knowsley and Warrington PCT Version: June 2008 Review
Central Mersey Diabetic Retinopathy Screening Programme Referring patients for Diabetic Retinopathy Screening Information for GPs in Halton & St Helens, Knowsley and Warrington PCT Version: June 2008 Review
Eyes on Diabetics: How to Avoid Blindness in Diabetic Patient
 Eyes on Diabetics: How to Avoid Blindness in Diabetic Patient Rova Virgana FK Unpad Pusat Mata Nasional RS Mata Cicendo Bandung Eye Center (Hospital and Clinic) PIT IDI Jabar 2018 Keys Facts from WHO
Eyes on Diabetics: How to Avoid Blindness in Diabetic Patient Rova Virgana FK Unpad Pusat Mata Nasional RS Mata Cicendo Bandung Eye Center (Hospital and Clinic) PIT IDI Jabar 2018 Keys Facts from WHO
Study of clinical significance of optical coherence tomography in diagnosis & management of diabetic macular edema
 Original Research Article Study of clinical significance of optical coherence tomography in diagnosis & management of diabetic macular edema Neha Kantilal Desai 1,*, Somesh Vedprakash Aggarwal 2, Sonali
Original Research Article Study of clinical significance of optical coherence tomography in diagnosis & management of diabetic macular edema Neha Kantilal Desai 1,*, Somesh Vedprakash Aggarwal 2, Sonali
MANAGING DIABETIC RETINOPATHY. <Your Hospital Name> <Your Logo>
 MANAGING DIABETIC RETINOPATHY It s difficult living with Diabetes Mellitus. Ask any diabetic... Their lives are centered around meal plans, glucose levels, and insulin
MANAGING DIABETIC RETINOPATHY It s difficult living with Diabetes Mellitus. Ask any diabetic... Their lives are centered around meal plans, glucose levels, and insulin
Serious Eye diseases, New treatments. Mr. M. Usman Saeed MBBS, FRCS, FRCOphth Consultant Ophthalmologist
 Serious Eye diseases, New treatments Mr. M. Usman Saeed MBBS, FRCS, FRCOphth Consultant Ophthalmologist 5 major causes of loss of vision Cataracts Glaucoma Macular degeneration Retinal Vein occlusions
Serious Eye diseases, New treatments Mr. M. Usman Saeed MBBS, FRCS, FRCOphth Consultant Ophthalmologist 5 major causes of loss of vision Cataracts Glaucoma Macular degeneration Retinal Vein occlusions
COMPARISON OF INTRAVITREAL TRIAMCINOLONE INJECTION VS LASER PHOTOCOAGULATION IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETIC RETINOPATHY
 Original Article COMPARISON OF INTRAVITREAL TRIAMCINOLONE INJECTION VS LASER PHOTOCOAGULATION IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETIC RETINOPATHY Aggarwal Somesh V 1, Shah Sonali N 2, Bharwada Rekha
Original Article COMPARISON OF INTRAVITREAL TRIAMCINOLONE INJECTION VS LASER PHOTOCOAGULATION IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETIC RETINOPATHY Aggarwal Somesh V 1, Shah Sonali N 2, Bharwada Rekha
Age-Related Macular Degeneration (AMD)
 Age-Related Macular Degeneration (AMD) What is the Macula? What is Dry AMD (Age-related Macular Degeneration)? Dry AMD is an aging process that causes accumulation of waste product under the macula leading
Age-Related Macular Degeneration (AMD) What is the Macula? What is Dry AMD (Age-related Macular Degeneration)? Dry AMD is an aging process that causes accumulation of waste product under the macula leading
Treatment of Retinal Vein Occlusion (RVO)
 Manchester Royal Eye Hospital Medical Retina Services Information for Patients Treatment of Retinal Vein Occlusion (RVO) What is a Retinal Vein Occlusion (RVO)? The retina is the light sensitive layer
Manchester Royal Eye Hospital Medical Retina Services Information for Patients Treatment of Retinal Vein Occlusion (RVO) What is a Retinal Vein Occlusion (RVO)? The retina is the light sensitive layer
EyePACS Grading System (Part 3): Detecting Proliferative (Neovascular) Diabetic Retinopathy. George Bresnick MD MPA Jorge Cuadros OD PhD
 EyePACS Grading System (Part 3): Detecting Proliferative (Neovascular) Diabetic Retinopathy George Bresnick MD MPA Jorge Cuadros OD PhD Anatomy of the eye: 3 Normal Retina Retinal Arcades Macula Optic
EyePACS Grading System (Part 3): Detecting Proliferative (Neovascular) Diabetic Retinopathy George Bresnick MD MPA Jorge Cuadros OD PhD Anatomy of the eye: 3 Normal Retina Retinal Arcades Macula Optic
Mild NPDR. Moderate NPDR. Severe NPDR
 Diabetic retinopathy Diabetic retinopathy is the most common cause of blindness in adults aged 35-65 years-old. Hyperglycaemia is thought to cause increased retinal blood flow and abnormal metabolism in
Diabetic retinopathy Diabetic retinopathy is the most common cause of blindness in adults aged 35-65 years-old. Hyperglycaemia is thought to cause increased retinal blood flow and abnormal metabolism in
Optical Coherence Tomography in Diabetic Retinopathy. Mrs Samantha Mann Consultant Ophthalmologist Clinical Lead of SEL-DESP
 Optical Coherence Tomography in Diabetic Retinopathy Mrs Samantha Mann Consultant Ophthalmologist Clinical Lead of SEL-DESP Content OCT imaging Retinal layers OCT features in Diabetes Some NON DR features
Optical Coherence Tomography in Diabetic Retinopathy Mrs Samantha Mann Consultant Ophthalmologist Clinical Lead of SEL-DESP Content OCT imaging Retinal layers OCT features in Diabetes Some NON DR features
GENERAL INFORMATION DIABETIC EYE DISEASE
 GENERAL INFORMATION DIABETIC EYE DISEASE WHAT IS DIABETIC EYE DISEASE? Diabetic eye disease is a term used to describe the common eye complications seen in people with diabetes. It includes: Diabetic retinopathy
GENERAL INFORMATION DIABETIC EYE DISEASE WHAT IS DIABETIC EYE DISEASE? Diabetic eye disease is a term used to describe the common eye complications seen in people with diabetes. It includes: Diabetic retinopathy
Ophthalmology Macular Pathways
 Ophthalmology Macular Pathways Age related Macular Degeneration Diabetic Macular Oedema Macular Oedema secondary to Central Retinal Macular Oedema secondary to Branch Retinal CNV associated with pathological
Ophthalmology Macular Pathways Age related Macular Degeneration Diabetic Macular Oedema Macular Oedema secondary to Central Retinal Macular Oedema secondary to Branch Retinal CNV associated with pathological
Diabetic Retinopathy Screening in Hong Kong. Dr. Rita Gangwani M.S, FRCS (Ophth), FCOphth(HK), FHKAM Eye Institute, The University of Hong Kong
 Diabetic Retinopathy Screening in Hong Kong Dr. Rita Gangwani M.S, FRCS (Ophth), FCOphth(HK), FHKAM Eye Institute, The University of Hong Kong Co-Investigators Prof. David Wong Prof. Sarah McGhee Dr. Wico
Diabetic Retinopathy Screening in Hong Kong Dr. Rita Gangwani M.S, FRCS (Ophth), FCOphth(HK), FHKAM Eye Institute, The University of Hong Kong Co-Investigators Prof. David Wong Prof. Sarah McGhee Dr. Wico
X-Plain Diabetic Retinopathy Reference Summary
 X-Plain Diabetic Retinopathy Reference Summary Introduction Patients with diabetes are more likely to have eye problems that can lead to blindness. Diabetic retinopathy is a disease of the eye s retina
X-Plain Diabetic Retinopathy Reference Summary Introduction Patients with diabetes are more likely to have eye problems that can lead to blindness. Diabetic retinopathy is a disease of the eye s retina
Diabetes and Eye Health more than meets the eye Vision Initiative - in association with PSA
 Diabetes and Eye Health more than meets the eye Vision Initiative - in association with PSA Vision 2020 Australia Vision Initiative RANZCO & OAA (Vic) Proud members of Vision 2020 Australia Outline Vision
Diabetes and Eye Health more than meets the eye Vision Initiative - in association with PSA Vision 2020 Australia Vision Initiative RANZCO & OAA (Vic) Proud members of Vision 2020 Australia Outline Vision
ZEISS AngioPlex OCT Angiography. Clinical Case Reports
 Clinical Case Reports Proliferative Diabetic Retinopathy (PDR) Case Report 969 PROLIFERATIVE DIABETIC RETINOPATHY 1 1-year-old diabetic female presents for follow-up of proliferative diabetic retinopathy
Clinical Case Reports Proliferative Diabetic Retinopathy (PDR) Case Report 969 PROLIFERATIVE DIABETIC RETINOPATHY 1 1-year-old diabetic female presents for follow-up of proliferative diabetic retinopathy
MAGNITUDE OF DIABETIC EYE DISEASE IN INDIA
 Dear Doctor This booklet contains information about your role as a physician in preventing blindness in your diabetic patients. You are the first point of contact for your diabetic patients. You see them
Dear Doctor This booklet contains information about your role as a physician in preventing blindness in your diabetic patients. You are the first point of contact for your diabetic patients. You see them
Introduction How the eye works
 1 Introduction Diabetic retinopathy is a condition that can cause permanent loss of eyesight and even blindness. It is a major cause of loss of vision. But if a person with diabetes receives proper eye
1 Introduction Diabetic retinopathy is a condition that can cause permanent loss of eyesight and even blindness. It is a major cause of loss of vision. But if a person with diabetes receives proper eye
Marcus Gonzales, OD, FAAO Cedar Springs Eye Clinic
 Marcus Gonzales, OD, FAAO Cedar Springs Eye Clinic 25.6 million adults 11.3% of the adult population 10.9 million adults 65 years and older 26.9% of this age population 79 million people are Pre-diabetic!!
Marcus Gonzales, OD, FAAO Cedar Springs Eye Clinic 25.6 million adults 11.3% of the adult population 10.9 million adults 65 years and older 26.9% of this age population 79 million people are Pre-diabetic!!
A retrospective nonrandomized study was conducted at 3
 Department of Ophthalmology, Kangbuk Samsung Hospital, Sungkyunkwan University College of Medicine 1, Seoul, Korea Hangil Eye Hospital 2, Incheon, Korea Seoul National University Bundang Hospital 3, Seongnam,
Department of Ophthalmology, Kangbuk Samsung Hospital, Sungkyunkwan University College of Medicine 1, Seoul, Korea Hangil Eye Hospital 2, Incheon, Korea Seoul National University Bundang Hospital 3, Seongnam,
Outline. Preventing & Treating Diabetes Related Blindness. Eye Care Center Doctors. Justin Kanoff, MD. Eye Care Center of Northern Colorado
 Outline Preventing & Treating Diabetes Related Blindness Justin Kanoff, MD Eye Care Center of Northern Colorado 303 974 4302 Introduction to Eye Care Center of Northern Colorado How the eye works Eye problems
Outline Preventing & Treating Diabetes Related Blindness Justin Kanoff, MD Eye Care Center of Northern Colorado 303 974 4302 Introduction to Eye Care Center of Northern Colorado How the eye works Eye problems
Diabetic Retinopathy
 Diabetic Retinopathy Introduction People with diabetes are more likely to have eye problems that can lead to blindness. Diabetic retinopathy is a disease of the eye s retina that is caused by diabetes.
Diabetic Retinopathy Introduction People with diabetes are more likely to have eye problems that can lead to blindness. Diabetic retinopathy is a disease of the eye s retina that is caused by diabetes.
VISUAL OUTCOME IN DIABETIC MACULAR EDEMA AFTER GRID LASER TREATMENT
 The Professional Medical Journal DOI: 10.17957/TPMJ/16.2856 ORIGINAL PROF-2856 VISUAL OUTCOME IN DIABETIC MACULAR EDEMA AFTER GRID LASER TREATMENT 1. MBBS.FCPS Assistant Professor Ophthalmology Independent
The Professional Medical Journal DOI: 10.17957/TPMJ/16.2856 ORIGINAL PROF-2856 VISUAL OUTCOME IN DIABETIC MACULAR EDEMA AFTER GRID LASER TREATMENT 1. MBBS.FCPS Assistant Professor Ophthalmology Independent
Treatment of Age Related Macular Degeneration (AMD) by Intravitreal Injection
 Information for Patients Manchester Royal Eye Hospital Medical Retina Services Treatment of Age Related Macular Degeneration (AMD) by Intravitreal Injection What is age related macular degeneration (AMD)?
Information for Patients Manchester Royal Eye Hospital Medical Retina Services Treatment of Age Related Macular Degeneration (AMD) by Intravitreal Injection What is age related macular degeneration (AMD)?
New Developments in the treatment of Diabetic Retinopathy
 New Developments in the treatment of Diabetic Retinopathy B. Jeroen Klevering University Medical Centre Nijmegen - The Netherlands Topics Management of diabetic retinopathy Interventions a. primary (prevention)
New Developments in the treatment of Diabetic Retinopathy B. Jeroen Klevering University Medical Centre Nijmegen - The Netherlands Topics Management of diabetic retinopathy Interventions a. primary (prevention)
THE ROLE OF anti-vegf IN DIABETIC RETINOPATHY AND AGE RELATED MACULAR DEGENERATION
 THE ROLE OF anti-vegf IN DIABETIC RETINOPATHY AND AGE RELATED MACULAR DEGENERATION MOESTIDJAB DEPARTMENT OF OPHTHALMOLOGY SCHOOL OF MEDICINE AIRLANGGA UNIVERSITY DR SOETOMO HOSPITAL SURABAYA INTRODUCTION
THE ROLE OF anti-vegf IN DIABETIC RETINOPATHY AND AGE RELATED MACULAR DEGENERATION MOESTIDJAB DEPARTMENT OF OPHTHALMOLOGY SCHOOL OF MEDICINE AIRLANGGA UNIVERSITY DR SOETOMO HOSPITAL SURABAYA INTRODUCTION
Subclinical Diabetic Macular Edema Study
 Diabetic Retinopathy Clinical Research Network Subclinical Diabetic Macular Edema Study Version 2.0 March 21, 2006 Subclinical DME Protocol v2 0 3-21-06.doc Table of Contents Chapter 1. Background Information
Diabetic Retinopathy Clinical Research Network Subclinical Diabetic Macular Edema Study Version 2.0 March 21, 2006 Subclinical DME Protocol v2 0 3-21-06.doc Table of Contents Chapter 1. Background Information
Clinical Trials in Diabetic Retinopathy. Harry W. Flynn Jr., M.D. Nidhi Relhan Batra, M.D.
 1 Clinical Trials in Diabetic Retinopathy 2018 Harry W. Flynn Jr., M.D. Nidhi Relhan Batra, M.D. Bascom Palmer Eye Institute 900 N.W. 17th Street Miami, FL 33136 Phone: (305) 326-6118 Fax: (305) 326-6417
1 Clinical Trials in Diabetic Retinopathy 2018 Harry W. Flynn Jr., M.D. Nidhi Relhan Batra, M.D. Bascom Palmer Eye Institute 900 N.W. 17th Street Miami, FL 33136 Phone: (305) 326-6118 Fax: (305) 326-6417
Speaker Disclosure Statement. " Dr. Tim Maillet and Dr. Vladimir Kozousek have no conflicts of interest to disclose.
 Speaker Disclosure Statement Dr. Tim Maillet and Dr. Vladimir Kozousek have no conflicts of interest to disclose. Diabetes Morbidity Diabetes doubles the risk of stroke. Diabetes quadruples the risk of
Speaker Disclosure Statement Dr. Tim Maillet and Dr. Vladimir Kozousek have no conflicts of interest to disclose. Diabetes Morbidity Diabetes doubles the risk of stroke. Diabetes quadruples the risk of
Vascular Disease Ocular Manifestations of Systemic Hypertension
 Vascular Disease Ocular Manifestations of Systemic Hypertension Maynard L. Pohl, OD, FAAO Pacific Cataract & Laser Institute 10500 NE 8 th Street, Suite 1650 Bellevue, WA 98004 USA 425-462-7664 Cerebrovascular
Vascular Disease Ocular Manifestations of Systemic Hypertension Maynard L. Pohl, OD, FAAO Pacific Cataract & Laser Institute 10500 NE 8 th Street, Suite 1650 Bellevue, WA 98004 USA 425-462-7664 Cerebrovascular
Treatment of Diabetic Macular Edema without Intravitreal injections
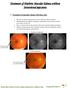 Treatment of Diabetic Macular Edema without Intravitreal injections 1. Treatment of macular edema with laser only This 60 year old female presented on 02-01-2007 for retinal evaluation. She had proliferative
Treatment of Diabetic Macular Edema without Intravitreal injections 1. Treatment of macular edema with laser only This 60 year old female presented on 02-01-2007 for retinal evaluation. She had proliferative
Extensive argon laser photocoagulation in the
 British Journal of Ophthalmology, 1989, 73, 197-201 Extensive argon laser photocoagulation in the treatment of proliferative diabetic retinopathy G W AYLWARD, R V PEARSON, J D JAGGER, AND A M HAMILTON
British Journal of Ophthalmology, 1989, 73, 197-201 Extensive argon laser photocoagulation in the treatment of proliferative diabetic retinopathy G W AYLWARD, R V PEARSON, J D JAGGER, AND A M HAMILTON
DIABETIC RETINOPATHY
 DIABETIC RETINOPATHY C. L. B. Canny, MD FRCSC Diabetic retinopathy is the most serious eye manifestation of diabetes and is responsible for most of the blindness caused by diabetes. Diabetic retinopathy
DIABETIC RETINOPATHY C. L. B. Canny, MD FRCSC Diabetic retinopathy is the most serious eye manifestation of diabetes and is responsible for most of the blindness caused by diabetes. Diabetic retinopathy
INTRODUCTION AND SYMPTOMS
 CHAPTER 1 INTRODUCTION AND SYMPTOMS Introduction of Diabetic Retinopathy Diabetic retinopathy (DR) is a potentially blinding complication of diabetes. It is defined as presence of one or more definite
CHAPTER 1 INTRODUCTION AND SYMPTOMS Introduction of Diabetic Retinopathy Diabetic retinopathy (DR) is a potentially blinding complication of diabetes. It is defined as presence of one or more definite
Perspectives on Screening for Diabetic Retinopathy. Dr. Dan Samaha, Optometrist, MSc Clinical Lecturer School of Optometry, Université de Montréal
 Perspectives on Screening for Diabetic Retinopathy 1 Dr. Dan Samaha, Optometrist, MSc Clinical Lecturer School of Optometry, Université de Montréal Current standards 2 According to the Canadian Diabetes
Perspectives on Screening for Diabetic Retinopathy 1 Dr. Dan Samaha, Optometrist, MSc Clinical Lecturer School of Optometry, Université de Montréal Current standards 2 According to the Canadian Diabetes
Information for Patients undergoing Intravitreal Triamcinolone Acetonide (Kenalog) Injection
 Information for Patients undergoing Intravitreal Triamcinolone Acetonide (Kenalog) Injection Kenalog/SS/ST/04.2012/v1.1 review 05.2013 Page 1 Introduction Your doctor has found that you have leakage of
Information for Patients undergoing Intravitreal Triamcinolone Acetonide (Kenalog) Injection Kenalog/SS/ST/04.2012/v1.1 review 05.2013 Page 1 Introduction Your doctor has found that you have leakage of
Evaluation of Changes of Macular Thickness in Diabetic Retinopathy after Cataract Surgery
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2011;25(4):238-242 DOI: 10.3341/kjo.2011.25.4.238 Evaluation of Changes of Macular Thickness in Diabetic Retinopathy after Cataract Surgery Original
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2011;25(4):238-242 DOI: 10.3341/kjo.2011.25.4.238 Evaluation of Changes of Macular Thickness in Diabetic Retinopathy after Cataract Surgery Original
Is OCT-A Needed As An Investigative Tool During The Management Of Diabetic Macular Edema
 Is OCT-A Needed As An Investigative Tool During The Management Of Diabetic Macular Edema Ayman M Khattab MD, FRCS Professor of Ophthalmology Cairo University Diabetic Macular Edema (DME) Diabetic macular
Is OCT-A Needed As An Investigative Tool During The Management Of Diabetic Macular Edema Ayman M Khattab MD, FRCS Professor of Ophthalmology Cairo University Diabetic Macular Edema (DME) Diabetic macular
RETINAL CONDITIONS RETINAL CONDITIONS
 GENERAL INFORMATION RETINAL CONDITIONS RETINAL CONDITIONS WHAT ARE RETINAL CONDITIONS? Retinal conditions affect the light-sensitive tissue at the back of eye known as the retina. They include diseases
GENERAL INFORMATION RETINAL CONDITIONS RETINAL CONDITIONS WHAT ARE RETINAL CONDITIONS? Retinal conditions affect the light-sensitive tissue at the back of eye known as the retina. They include diseases
optic disc neovascularisation
 British Journal of Ophthalmology, 1979, 63, 412-417 A comparative study of argon laser and krypton laser in the treatment of diabetic optic disc neovascularisation W. E. SCHULENBURG, A. M. HAMILTON, AND
British Journal of Ophthalmology, 1979, 63, 412-417 A comparative study of argon laser and krypton laser in the treatment of diabetic optic disc neovascularisation W. E. SCHULENBURG, A. M. HAMILTON, AND
Andrew J. Barkmeier, MD; Benjamin P. Nicholson, MA; Levent Akduman, MD
 c l i n i c a l s c i e n c e Effectiveness of Laser Photocoagulation in Clinically Significant Macular Edema With Focal Versus Diffuse Parafoveal Thickening on Optical Coherence Tomography Andrew J. Barkmeier,
c l i n i c a l s c i e n c e Effectiveness of Laser Photocoagulation in Clinically Significant Macular Edema With Focal Versus Diffuse Parafoveal Thickening on Optical Coherence Tomography Andrew J. Barkmeier,
RANZCO Screening and Referral Pathway for Diabetic Retinopathy #
 RANZCO Screening and Referral Pathway for Diabetic Retinopathy # Patient Presents a. Screen for Diabetic Retinopathy every 2 years b. Begin screening at diagnosis of Diabetes * Clinical Modifi ers Yearly
RANZCO Screening and Referral Pathway for Diabetic Retinopathy # Patient Presents a. Screen for Diabetic Retinopathy every 2 years b. Begin screening at diagnosis of Diabetes * Clinical Modifi ers Yearly
Clinical Case Presentation. Branch Retinal Vein Occlusion. Sarita M. Registered Nurse Whangarei Base Hospital
 Clinical Case Presentation on Branch Retinal Vein Occlusion Sarita M. Registered Nurse Whangarei Base Hospital Introduction Case Study Pathogenesis Clinical Features Investigations Treatment Follow-up
Clinical Case Presentation on Branch Retinal Vein Occlusion Sarita M. Registered Nurse Whangarei Base Hospital Introduction Case Study Pathogenesis Clinical Features Investigations Treatment Follow-up
Diabetic retinopathy (DR) progressively
 FOCUS ON DIABETIC MACULAR EDEMA * Frederick L. Ferris III, MD ABSTRACT The current state of treatment for diabetic macular edema (DME) is focused on slowing the rate of vision loss through assessment of
FOCUS ON DIABETIC MACULAR EDEMA * Frederick L. Ferris III, MD ABSTRACT The current state of treatment for diabetic macular edema (DME) is focused on slowing the rate of vision loss through assessment of
Year 2 MBChB Clinical Skills Session Ophthalmoscopy. Reviewed & ratified by: Mr M Batterbury Consultant Ophthalmologist
 Year 2 MBChB Clinical Skills Session Ophthalmoscopy Reviewed & ratified by: o Mr M Batterbury Consultant Ophthalmologist Learning objectives o To understand the anatomy and physiology of the external and
Year 2 MBChB Clinical Skills Session Ophthalmoscopy Reviewed & ratified by: o Mr M Batterbury Consultant Ophthalmologist Learning objectives o To understand the anatomy and physiology of the external and
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE. Health Technology Appraisal. Aflibercept for treating diabetic macular oedema.
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Health Technology Appraisal Aflibercept for treating diabetic macular oedema Final scope Final remit/appraisal objective To appraise the clinical and cost
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Health Technology Appraisal Aflibercept for treating diabetic macular oedema Final scope Final remit/appraisal objective To appraise the clinical and cost
Scott M. Pfahler D.O. Dayton Vitreo-Retinal Associates AOCOO-HNS Palm Springs, CA 2012
 Scott M. Pfahler D.O. Dayton Vitreo-Retinal Associates AOCOO-HNS Palm Springs, CA 2012 Proliferative Diabetic Retinopathy Laser Treatments Medical Treatment Surgical Treatment Diabetic Macular Edema Laser
Scott M. Pfahler D.O. Dayton Vitreo-Retinal Associates AOCOO-HNS Palm Springs, CA 2012 Proliferative Diabetic Retinopathy Laser Treatments Medical Treatment Surgical Treatment Diabetic Macular Edema Laser
Sponsored by. Shared care and referral pathways. Part 2: diabetes screening leading from the front
 CET CONTINUING Sponsored by 1 CET POINT Shared care and referral pathways Part 2: diabetes screening leading from the front Chris Steele, BSc (Hons), FCOptom, DCLP, DipOC, DipTp(IP), FBCLA The alarming
CET CONTINUING Sponsored by 1 CET POINT Shared care and referral pathways Part 2: diabetes screening leading from the front Chris Steele, BSc (Hons), FCOptom, DCLP, DipOC, DipTp(IP), FBCLA The alarming
Disease-Specific Fluorescein Angiography
 Ruth E. Picchiottino, CRA Disease-Specific Fluorescein Angiography 15 Disease-Specific Fluorescein Angiography Recommendations for tailoring retinal fluorescein angiography to diabetic retinopathy, macular
Ruth E. Picchiottino, CRA Disease-Specific Fluorescein Angiography 15 Disease-Specific Fluorescein Angiography Recommendations for tailoring retinal fluorescein angiography to diabetic retinopathy, macular
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome)
 Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Fundus Fluorescein Angiography in Diabetic Retinopathy: Correlation of Angiographic Findings to the Clinical Maculopathy Abstract: Purpose:
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 2 Ver. XII (Feb. 2016), PP 80-88 www.iosrjournals.org Fundus Fluorescein Angiography in Diabetic
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 2 Ver. XII (Feb. 2016), PP 80-88 www.iosrjournals.org Fundus Fluorescein Angiography in Diabetic
Information for patients
 Information for patients Intravitreal Anti-VEGF Treatment (vascular endothelial growth factor) This leaflet gives you information that will help you decide whether to have intravitreal treatment. It also
Information for patients Intravitreal Anti-VEGF Treatment (vascular endothelial growth factor) This leaflet gives you information that will help you decide whether to have intravitreal treatment. It also
Diabetic Retinopathy in Primary Care
 Diabetic Retinopathy in Primary Care Epidemiology Diabetes is one of the most serious challenges to health care world rld-wide. According to recent projections it will affect 239 million people e by 2010-
Diabetic Retinopathy in Primary Care Epidemiology Diabetes is one of the most serious challenges to health care world rld-wide. According to recent projections it will affect 239 million people e by 2010-
OUR EYES & HOW WE SEE
 OUR EYES & HOW WE SEE UNDERSTAND MORE ABOUT OUR EYES & HOW WE SEE Our Eyes & How We See The eye is our visual gateway to the world. Within it, an array of delicate components labour away to give us the
OUR EYES & HOW WE SEE UNDERSTAND MORE ABOUT OUR EYES & HOW WE SEE Our Eyes & How We See The eye is our visual gateway to the world. Within it, an array of delicate components labour away to give us the
Amber Priority. Image Library
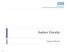 Amber Priority Image Library Amber flag Diabetic Maculopathy (M1) Pre-proliferative Diabetic Retinopathy (R2) Old, treated and now inactive DR (R1/M0/P1or R0/M0/P1) Where only partial or incomplete images
Amber Priority Image Library Amber flag Diabetic Maculopathy (M1) Pre-proliferative Diabetic Retinopathy (R2) Old, treated and now inactive DR (R1/M0/P1or R0/M0/P1) Where only partial or incomplete images
Vitrectomy for Diabetic Cystoid Macular Edema
 Vitrectomy for Diabetic Cystoid Macular Edema Yukihiro Sato, Zeon Lee and Hiroyuki Shimada Department of Ophthalmology, Nihon University School of Medicine, Tokyo, Japan Purpose: We evaluated visual outcomes
Vitrectomy for Diabetic Cystoid Macular Edema Yukihiro Sato, Zeon Lee and Hiroyuki Shimada Department of Ophthalmology, Nihon University School of Medicine, Tokyo, Japan Purpose: We evaluated visual outcomes
Diabetic Retinopathy
 Diabetic Retinopathy Overview This presentation covers the following topics: Definitions Epidemiology of diabetic retinopathy Evidence for public health approaches Screening for diabetic retinopathy Health
Diabetic Retinopathy Overview This presentation covers the following topics: Definitions Epidemiology of diabetic retinopathy Evidence for public health approaches Screening for diabetic retinopathy Health
ILUVIEN IN DIABETIC MACULAR ODEMA
 1 ILUVIEN IN DIABETIC MACULAR ODEMA Marie Tsaloumas Consultant Ophthalmic Surgeon Queen Elizabeth Hospital, Birmingham bars conference 2104 1 2 Declaration of interest I have sat on Advisory boards for
1 ILUVIEN IN DIABETIC MACULAR ODEMA Marie Tsaloumas Consultant Ophthalmic Surgeon Queen Elizabeth Hospital, Birmingham bars conference 2104 1 2 Declaration of interest I have sat on Advisory boards for
What is Age-Related Macular Degeneration?
 Intravitreal Injections Eylea / Lucentis Patient Information What is Age-Related Macular Degeneration? Age-related macular degeneration (AMD) is an eye condition found in older people, which may lead to
Intravitreal Injections Eylea / Lucentis Patient Information What is Age-Related Macular Degeneration? Age-related macular degeneration (AMD) is an eye condition found in older people, which may lead to
Diabetic Retinopathy: Managing the Extremes. J. Michael Jumper, MD West Coast Retina
 Diabetic Retinopathy: Managing the Extremes J. Michael Jumper, MD West Coast Retina Case 1: EC 65 y.o. HM No vision complaints Meds: Glyburide Metformin Pioglitazone Va: 20/20 OU 20/20 Case 2: HS 68 y.o.
Diabetic Retinopathy: Managing the Extremes J. Michael Jumper, MD West Coast Retina Case 1: EC 65 y.o. HM No vision complaints Meds: Glyburide Metformin Pioglitazone Va: 20/20 OU 20/20 Case 2: HS 68 y.o.
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA
 OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
Retina Conference. Janelle Fassbender, MD, PhD University of Louisville Department of Ophthalmology and Visual Sciences 09/04/2014
 Retina Conference Janelle Fassbender, MD, PhD University of Louisville Department of Ophthalmology and Visual Sciences 09/04/2014 Subjective CC/HPI: 64 year old Caucasian female referred by outside ophthalmologist
Retina Conference Janelle Fassbender, MD, PhD University of Louisville Department of Ophthalmology and Visual Sciences 09/04/2014 Subjective CC/HPI: 64 year old Caucasian female referred by outside ophthalmologist
Diabetic Retinopathy Information
 http://www.midwestretina.com Phone: (614)-339-8500 Toll Free: (866)-373-8462 Sugat S. Patel, M.D. Louis J. Chorich III, M.D. Dino D. Klisovic, M.D. Lisa M. Borkowski, M.D. Dominic M. Buzzacco, M.D. Johnstone
http://www.midwestretina.com Phone: (614)-339-8500 Toll Free: (866)-373-8462 Sugat S. Patel, M.D. Louis J. Chorich III, M.D. Dino D. Klisovic, M.D. Lisa M. Borkowski, M.D. Dominic M. Buzzacco, M.D. Johnstone
Guidelines for the Management of Diabetic Retinopathy for the Internist
 Visual Disorder Guidelines for the Management of Diabetic Retinopathy for the Internist JMAJ 45(1): 1 7, 2002 Sadao HORI Professor, Department of Ophthalmology, Tokyo Women s Medical University Abstract:
Visual Disorder Guidelines for the Management of Diabetic Retinopathy for the Internist JMAJ 45(1): 1 7, 2002 Sadao HORI Professor, Department of Ophthalmology, Tokyo Women s Medical University Abstract:
The Diabetic Retinopathy Clinical Research Network. Management of DME in Eyes with PDR
 The Diabetic Retinopathy Clinical Research Network Management of DME in Eyes with PDR 1 What Has Been Learned? Diabetic Retinopathy Treatment Protocol F: Results suggest that clinically meaningful differences
The Diabetic Retinopathy Clinical Research Network Management of DME in Eyes with PDR 1 What Has Been Learned? Diabetic Retinopathy Treatment Protocol F: Results suggest that clinically meaningful differences
Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
 Columbia International Publishing Journal of Ophthalmic Research (2014) Research Article Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
Columbia International Publishing Journal of Ophthalmic Research (2014) Research Article Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
EyePACS Grading System (Part 2): Detecting Presence and Severity of Background (Non-Proliferative) Diabetic Retinopathy Lesion
 EyePACS Grading System (Part 2): Detecting Presence and Severity of Background (Non-Proliferative) Diabetic Retinopathy Lesion George Bresnick MD MPA Jorge Cuadros OD PhD Anatomy of the eye: 3 Normal Retina
EyePACS Grading System (Part 2): Detecting Presence and Severity of Background (Non-Proliferative) Diabetic Retinopathy Lesion George Bresnick MD MPA Jorge Cuadros OD PhD Anatomy of the eye: 3 Normal Retina
OCT Angiography in Primary Eye Care
 OCT Angiography in Primary Eye Care An Image Interpretation Primer Julie Rodman, OD, MS, FAAO and Nadia Waheed, MD, MPH Table of Contents Diabetic Retinopathy 3-6 Choroidal Neovascularization 7-9 Central
OCT Angiography in Primary Eye Care An Image Interpretation Primer Julie Rodman, OD, MS, FAAO and Nadia Waheed, MD, MPH Table of Contents Diabetic Retinopathy 3-6 Choroidal Neovascularization 7-9 Central
Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and
 British Journal of Ophthalmology, 1977, 61, 278-284 Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and neovascular glaucoma LEILA LAATIKAINEN From Moorfields Eye Hospital,
British Journal of Ophthalmology, 1977, 61, 278-284 Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and neovascular glaucoma LEILA LAATIKAINEN From Moorfields Eye Hospital,
