Changes in pharmacokinetics in the elderly and therapeutic drug monitoring of antiarrhythmic drugs
|
|
|
- Brianna Barrett
- 6 years ago
- Views:
Transcription
1 Changes in pharmacokinetics in the elderly and therapeutic drug monitoring of antiarrhythmic drugs Lexin Wang * School of Biomedical Sciences, Charles Sturt University, Wagga Wagga, NSW, 2678, Australia Received January 29, 2007 Abstract Advanced-age is associated with significant changes in physiological functions, absorption, distribution, metabolism and elimination of drugs. Antiarrhythmic drugs are traditionally classified into four groups, according to Vaughan Williams s classification. The renal and hepatic elimination of many antiarrhythmic drug classes are reduced in the elderly, predisposing this population to serious adverse drug effects. Therapeutic drug monitoring has been a useful clinical tool in the safe use of class I drugs and amiodarone, in the younger population. Given the changes in pharmacokinetics of antiarrhythmic drugs and increased risk of adverse effects in older patients, therapeutic drug monitoring may be of particular importance for dosage adjustment and optimization of individual antiarrhythmic therapy in the elderly. [Life Science Journal. 2007; 4(2): 1 7] (ISSN: ). Keywords: antiarrhythmic drugs; therapeutic drug monitoring; pharmacokinetics; aging 1 Introduction Care for older patients has become a worldwide issue of all healthcare sectors because the population is rapidly aging. By 2020 the people aged 65 years and older will constitute nearly 17% of the US population and 26% of the population in Japan [1]. Around the world, the proportion of the population aged 80 years and above will range between 3.7% 7.5% [1]. Physiological changes in the elderly often alter the pharmacokinetics and pharmacodynamics, and cardiovascular function [2]. These changes can have significant impact on the medications that we use to treat cardiovascular disorders in the elderly. Antiarrhythmic drugs are a large group of chemically disparate compounds; most of these compounds have been at times used to treat cardiac arrhythmias. They are traditionally divided, according to Vaughan William s classification, into Class I to Class IV. The clinical use of some antiarrhythmic drugs, such as the Class I antiarrhythmic agents, has declined in the last decade, whereas * Corresponding author. Tel: Fax: lwang@csu.edu.au 1 others, such as Class II and III agents, have become the mainstay of treatment or prevention of tachycardias. Therapeutic drug monitoring (TDM) refers to the individualization of drug dosage by maintaining plasma or serum drug concentrations within a target range (therapeutic range). This involves the measurement and interpretation of plasma or serum concentrations of drugs in patients. One of the prime reasons for TDM services is that individual patients may respond differently to the same therapeutic dose regimen, because of the interpatient variability in drug absorption, distribution, elimination or changing pathophysiological conditions. By adjusting doses to maintain plasma drug concentrations within a target range, variability in the pharmacokinetic phase of drug action is greatly reduced. Today, TDM services have been established in the department of clinical pharmacology in many hospitals to assess the patient s responses to the recommended dose regimen, with a view to maximizing the therapeutic effects and minimizing the adverse effects. Most antiarrhythmic drugs are associated with highly variable plasma concentrations at a given dose. They also show a direct concentration-effect relationship, which fulfils the formal requirements for rational use of TDM.
2 Life Science Journal, Vol 4, No 2, 2007 Therapeutic ranges for antiarrhythmic drugs are, in general, not very well defined, since the reported effective drug concentrations are often based on small studies or studies not designed to establish a therapeutic range, with varying dosage regimens and unstandardized sampling procedures. Class I agents have well-defined therapeutic range and dose-dependent toxicity. However, the value of TDM for other drug classes remains uncertain. In this article, the changes in drug pharmacokinetics in the elderly, and the basic principles and clinical applications of TDM in each of the major antiarrhythmic drug classes were discussed. 2 Pharmacokinetic characteristics in the elderly There is a sevenfold increase in drug toxicities as one ages from 20 to 79 years (from 3% at years to 21% at years). Part of this increase may well be due to multiple medication-drug interactions. However, a significant part of this increase in drug toxicities is due to incomplete understanding of changes in the absorption, distribution, metabolism and elimination processes of drug disposition with aging. 2.1 Absorption There is a reduced gastrointestinal blood flow and motility [2], and a reduced gastric ph [3]. Although these physiological changes can alter drug absorption, there has been little evidence to suggest that this is of major consequence. Reduced absorption in the elderly has been observed for some compounds which are actively absorbed (e.g. galactose, calcium, thiamine, and iron) [4]. The absorption of most oral antiarrhythmic drugs, which is mainly by passive processes, is not affected to a significant extent. 2.2 Distribution Drug distribution in the elderly differs from that of young adults or pediatric population. Great changes in body composition occur as people age. Body fat increases from 15% to 30% and lean body weight decreases in proportion to total body weight [5]. This gives lower volume of distribution values for drugs which stay in the central compartment, while lipid soluble drugs would have somewhat larger apparent volume of distribution. The apparent volume of distribution for lipid soluble drugs, such as diazepam and chlordiazepoxide, is larger in the elderly. Although total plasma protein concentrations remain relatively constant, albumin concentrations are lower in the aged [6]. Levels of plasma protein determine the volume of distribution and extent of distribution into tissues of highly protein-bound drugs. The reduction of plasma protein leads to a higher free fraction of highly proteinbound drugs and therefore, a greater proportion of pharmacologically active drug. For example, the fraction of unbound phenytoin increases 25% to 40% in the aged, however, this would also lead to increased clearance. Drug interactions based on protein binding can be more pronounced in the elderly because they tend to be taking multiple drugs. Cardiac output in the elderly is reduced, thus distribution to the kidneys and liver are expected to be reduced. For high extraction drugs this could alter the overall elimination of the drug. 2.3 Metabolism Physiological changes in drug metabolism have also been observed in the elderly. The liver is the major organ involved in drug metabolism; liver blood flow and liver mass tend to decrease with age. It appears that for drugs which undergo Phase I metabolism (oxidations or reductions), metabolism reduces with increasing age. Examples of this reduced liver metabolism are quinidine, lignocaine, phenytoin and propranolol [2]. For other drugs which undergo Phase II metabolism (conjugations), the metabolism does not appear to change greatly with age. 2.4 Renal excretion Renal excretion of medications is generally reduced in the elderly. With increasing age the glomerular filtration process is reduced by a reduction in kidney size (20%), reduction in the number of nephrons (35%), reduction in the number of functioning glomeruli (30%), and a decrease in renal blood flow (40% 50%) [7,8]. Serum creatinine is also decreased with age because of the reduced muscle mass. Antiarrhythmic drugs which are mainly renally excreted and for which dosage adjustments should be made in elderly patients include digoxin and quinidine [9,10]. The changes in pharmacokinetics in the elderly have significant implications to drug dose recommendations. However, the effects of age on drug disposition depend on the particular drug in question and the characteristics of the population being studied. When evaluating elderly patients to make dosage recommendations, it is important to distinguish between long-term-care patients who are not considered to be active, and the older patients living independently in the community. Some of the changes ascribed to the elderly may be due to immobility of the patient or an underlying disease or diseases. Also because of 2
3 changing body composition between males and females, it is often important to distinguish between these gender groups as well. 3 Therapeutic Range of Antiarrhythmic Drugs Not all therapeutic agents require TDM when it comes to adjustment of therapeutic regimens. The characteristics of drugs which TDM provides additional value in dosage optimization are summarized in Table 1. Table 1. Characteristics of drugs that require therapeutic monitoring Drugs with a good relationship between plasma concentration and clinical effects. Drugs with a narrow therapeutic-toxic range, such as digoxin. Drugs for which there is no easily measured clinical response and/or failure of response is all or nothing (e.g. antiarrhythmic drugs or anticonvulsants). Drugs for which the pharmacological response is difficult to quantify. Drugs for which plasma concentration has prognostic significance in over dosage. Drugs for which the expected or desired therapeutic effect is not observed (may be absorption or compliance problem). A patient has altered and/or variable renal state and the drug is eliminated mostly as unchanged drug in urine. If the clinical effects of drugs can be readily measured (e.g. antihypertensive drugs-blood pressure, warfarin- INR), it is obviously better to adjust the dose on the basis of patient s response. When this cannot be done, TDM should be performed. Majority of antiarrhythmic drugs fulfil the formal requirements of rational use of TDM, which offers additional values to the clinical efficacy of some of the drugs (e.g. digoxin or lignocaine). The therapeutic ranges of some antiarrhythmic drugs are shown in Table 2. The therapeutic ranges in Table 2 are in most cases derived from observation of therapeutic and adverse effects in small groups of patients. Therefore, when applied to a wider population of patients, there will be individuals who achieve adequate effects at lower concentrations or experience adverse events within the therapeutic range. For example, the accepted therapeutic range of lignocaine is mg/l. Some patients may experience signs of lignocaine intoxication at serum drug concentration below 6.0 mg/l, where some patients may show therapeutic efficacy at drug concentration below 2.0 mg/l. Therefore, one must remember that therapeutic range is more a probability concept and should never be considered as an absolute value. Table 2. Therapeutic range of antiarrhythmic drugs Drug Therapeutic range Amiodarone (mg/l) Digoxin (µg/l) Disopyramide (mg/l) Lignocaine (mg/l) Quinidine (mg/l) Flecainide (mg/l) Mexilitine (mg/l) Propafenone (mg/l) Procainamide (mg/l) Sotalol (mg/l) Note: Modified from references Technical Considerations of TDM 4.1 Blood sample collection Usually plasma or serum is used for drug assays. Plasma is obtained from the supernatant of centrifuged whole blood to which heparin has been added. Plasma perfuses all the tissues of the body including the cellular elements in the blood. Changes in the drug concentration in the plasma are considered to reflect changes in tissue drug concentrations. The correct time of sampling is important for TDM. Drug concentrations vary over the dosing interval, and with the duration of dosing in relation to achieving a steady state. The least variable point in the dosing interval is the pre-dose or trough concentration. In almost all cases, quoted therapeutic ranges of anti-arrhythmic drugs have been established on trough sample measurements [11,12]. For this reason, trough concentration is the recommended sampling time for the majority of drugs. Patient should therefore be asked to omit their morning dose of drug until the blood sample has been taken. For most antiarrhythmic drugs with short half-lives, samples should be collected pre-dose. However, for drug with long half-lives, such as amiodarone, samples collected at any point in the dose interval can be satisfactory [12]. Taking peak samples for orally administered anti-arrhythmic drugs is not recommended since there is wide interpatient variability in concentrations achieved, and it is impossible to know when the peak occurs. The only indica- 3
4 Life Science Journal, Vol 4, No 2, 2007 tion for trying to take a peak sample is if the patient experiences toxicities some hours after taking the medication. With digoxin, an antiarrhythmic drug outside of the Vaughan William s classification, the maximum serum level is reached 1 2 hours after an oral dose. The level then falls rapidly for 3 5 hours as it is distributed. The serum level then falls with a half-life of days. Due to this delayed distribution, blood sample for digoxin analysis must be taken at least 6 hours after the last oral dose. Above all, it is important to wait until a drug has been fully distributed in the body (i.e. has reached steady state) before taking samples for concentration measurement. The time for a drug to reach steady state can be calculated by multiplying the elimination half-life by 5. Thus a drug with a half-life of 8 hours should not normally be monitored until at least 2 days after the first dose is taken. However, an earlier sample may be taken if toxicity is suspected. 4.2 Frequency of sampling A blood sample is often taken after the initial dose was given. If the result is within the therapeutic range, and the patient s symptoms are well controlled, then a further measurement should be made 6 8 weeks later [11 14]. If the initial sample is above or below the therapeutic range, or the patient still has symptoms, then dose adjustment is necessary and samples should be taken every 5 to 10 half-lives until such times as adequate control is achieved [11 14]. If the second monitoring is still in the therapeutic range and there are no clinical problems, monitoring may be performed at 6 12 monthly intervals. More frequent monitoring would only become necessary if a change in hepatic or renal function occurs, or a potential interacting drug is added to the regimen. 4.3 Assay methods Drug assay methods should have adequate sensitivity, be specific for the drug to be measured and have appropriate accuracy and precision. Assays are usually under the direction of pathology or clinical chemistry laboratories. A variety of methods are available for measuring drugs but the most widely used assay for commonly monitored drugs is the Abbott TDX system that uses fluorescence polarization immunoassay [15]. Less commonly used are HPLC, or gas chromatography (GC) and these are only performed in specialised laboratories. Amiodarone and quinidine, if collected in the testing tubes in gel, require immediate centrifugation and separation within 2 hours of collection, and supernatant should be separated immediately on removal from centrifuge, because the rate of drug absorption by gel increases once red blood cells are precipitated from the serum. 5 Interpretation of Drug Concentration It is critical to know that drug concentrations need to be interpreted in the context of the individual patients without rigid adherence to therapeutic range. To interpret the drug concentration, some basic patient information is required (Table 3). Table 3. Basic information required for interpretation of drug concentration Patient: age, weight, sex, height, smoking. Time of sample in relation to last dose. Duration of treatment with the current dose. Other drug therapy. Clinical: drug requirements, clinical status (renal: serum creatinine; cardiac: cardiac output; liver, etc.). Reason for request: for example, lack of effect, routine monitoring, suspected toxicity. There are two important factors that can make interpretation of a result difficult in some cases. First, assays are done using plasma or blood and thus measured total (bound and unbound) drug, whereas it is the unbound drug that interacts with the receptor to produce a therapeutic response. If binding is changed by disease states, such as acute myocardial infarction [16] or atrial fibrillation [17], the interpretation of total plasma or blood drug concentrations must be modified. Second, active metabolites, which may not be measured, can contribute to the therapeutic response. Examples include procainamide in which N-acetylprocainamide is the active metabolite [18]. For amiodarone, the active metabolite is desethyl-amiodarone, which is responsible for at least half of its effect [19]. The possible considerations for a lower, higher or normal drug concentration are summarized in Table 4. 6 Individual Antiarrhythmic Drugs in the Elderly 6.1 Class I antiarrhythmic drugs Class I antiarrhythmic drugs are the largest and oldest group, including three subgroups (Table 5). The mechanism of action of these compounds is blockade of the fast 4
5 inward sodium current responsible for the upstroke and rapid conduction of the cardiac action potential. Many of these drugs are found to be proarrhythmic [20 22], and as a result, their clinical use, except for lignocaine and flecainide, has declined dramatically in recent years. Table 4. Interpretation of drug concentration Concentration lower than anticipated Poor patient compliance Error in dosage regimen Wrong drug product (controlled-release instead of immediate-release) Poor bioavailability Rapid elimination Reduced plasma protein binding Enlarged volume of distribution Steady state not reached Timing of blood sample Improved renal/hepatic function Drug interaction due to stimulation of elimination enzyme autoinduction Changing hepatic blood flow Concentration higher than anticipated Poor patient compliance Error in dosage regimen Wrong drug product (immediate-release instead of controlled-release) Rapid bioavailability Smaller than anticipated volume of distribution Slow elimination Increased plasma protein binding Poor renal/hepatic function Drug interaction due to inhibition of elimination Concentration correct but patient does not respond to therapy Altered receptor sensitivity (e.g. tolerance) Drug interaction at receptor site 6.2 Beta-blockers Beta-blockers have been mainly used to control ventricular rate in patients with atrial fibrillation/flutter, and to prevent ventricular arrhythmias. They have been shown to reduce mortality and hospitalizations in both older and younger patients with systolic heart failure [23,24]. Betablockers such as atenolol, nadolol and sotalol, which are cleared primarily by renal elimination, are affected by the age-associated changes in renal function [25]. Atenolol and nadolol, which undergo complete renal elimination, may have a prolonged half-life in the elderly whose glomerular filtration and tubular secretion may decline with age [26,27]. Dose adjustment of both agents may be needed in older patients. Propranolol and metoprolol are metabolised in the liver. The age-associated decrease in hepatic blood flow is expected to alter clearance of these drugs and as a result, plasma concentrations of propranolol are found to be 3 to 4 times higher in elderly patients compared with younger patients [28]. I Table 5. Vaughan William s classification of antiarrhythmic drugs II III IV Class Actions Drugs IA IB IC 6.3 Amiodarone Sodium channel blockade prolong repolarization shorten repolarization little effect on repolarization Beta-adrenergic blockade Prolong repolarization potassium channel blockade Calcium channel blockade quinidine, procainamide, disopyramide lidocaine, mexiletine, tocainide, phenytoin flecainide, encainide, propafenone propanolol, esmolol sotalol, amiodarone verapamil, diltiazem Amiodarone is a highly effective antiarrhythmic drug and has been widely used in the management of supraventricular and ventricular arrhythmia. Many previous studies did not specifically assess the effect of amiodarone on elderly patients but current evidence suggests that this antiarrhythmic agent is equally effective in the older patients. Amiodarone is a lipophilic drug with a long elimination half-life ranging between days. Therefore, measurement of blood levels should be done until 3 months 5
6 Life Science Journal, Vol 4, No 2, 2007 after a change in the dosage regime. Amiodarone is expected to display a larger volume distribution in the elderly due to age-associated increase in body fat. In the elderly, amiodarone has a reduced clearance and prolonged elimination half-life, although this agent is not mainly renally excreted [29]. Older patients appear to be more prone to suffer adverse effects from amiodarone. Advanced age has been demonstrated as a risk factor for amiodarone-induced thyroid disease [30]. 6.4 Verapamil, diltiazem Verapamil and diltiazem are effective in controlling heart rate in patients with atrial fibrillation/flutter. Verapamil is also effective in terminating atrioventricular nodal re-entrant tachycardia. With both agents, there is a reduced total body clearance and increased elimination half-life in older patients [31]. The elderly also show an increased therapeutic response to verapamil and diltiazem [31]. Verapamil appears to lower heart rate and blood pressure to a greater extent in the elderly compared with younger patients [32]. 6.5 Digoxin Digoxin falls out of the traditional Vaughn William s classification but it remains an important drug for ventricular rate control in patients with atrial fibrillation. In the elderly, the decreased total body water, increased total body fat and reduced muscle mass lead to a reduced volume of distribution of digoxin, a water-soluble compound. This leads to an increased risk of toxicity in the older patients. Digoxin is excreted unchanged through glomerular filtration and tubular secretion in patients with normal renal function [33]. General decline in renal function in the elderly results in accumulation of digoxin and prolongation in elimination half-life [34]. Polypharmacy in older patients increases the risk of drug interaction with digoxin. Quinidine, verapamil, flecainide and amiodarone may interact with digoxin and reduce its renal elimination [35]. This will result in higher plasma concentrations of digoxin for the same dose and assays are required to determine if dose reduction is necessary. 7 Conclusions Advanced age is associated with significant changes in physiological functions which affect pharmacokinetics of many drugs used to treat or prevent arrhythmia. Renal and hepatic elimination of many antiarrhythmic drug groups are reduced in the elderly, leading to a prolonged elimination half-life and increased risk of adverse effects. Therapeutic drug monitoring may increase the safe use of antiarrhythmic drugs in general, Class I agents, amiodarone and digoxin in particular. References Anderson GF, Hussey PS. Population aging: a comparison among industrialized countries. Health Affairs 2000; 19: Lamy PP. Comparative pharmacokinetic changes and drug therapy in an older population. J Am Geriatr Soc 1982; 30: S11 9. Baron JH. Studies of basal and peak acid output with an augmented histamine test. Gut 1963; 4: Evans MA, Triggs EJ, Cheung M, et al. Gastric emptying rate in the elderly: implications for drug therapy. J Am Geriatr Soc 1981; 21: Novak IP. Aging, total body potassium, fat free mass, and cell mass in males and females between ages 18 and 85 years. J Gerontol 1972; 27: Greenblatt DJ. Reduced serum albumin concentration in the elderly: a report from the Boston Collaborative Drug Surveillance Program. J Am Geriatr Soc 1979; 27: Rowe JW, Andres R, Tobin JD, et al. The effect of age on creatinine clearance in man: a cross sectional and longitudinal study. J Gerontol 1976; 31: Lindeman RD, Tobin J, Shock NW. Longitudinal studies on the rate of decline in renal function with age. J Am Geriatr Soc 1985; 33: Sumner DJ, Russel AJ. Digoxin pharmacokinetics: multi-compartmental analysis and its implications. Br J Clin Pharmacol 1976; 3: Chutka DS, Evans JM, Fleming KC, et al. Drug prescribing for elderly patients. Mayo Clinic Proc 1995; 70: Jürgens G, Graudal NA, Kampmann JP. Therapeutic drug monitoring of antiarrhythmic drugs. Clinical Pharmacokinetics 2003; 42: Campbell TJ. Williams KM. Therapeutic drug monitoring: antiarrhythmic drugs. British Journal of Clinical Pharmacology 2001; 52 Suppl 1: 21S 34S. Latini R, Maggioni AP, Cavalli A. Therapeutic drug monitoring of antiarrhythmic drugs: Rationale and current status. Clinical Pharmacokinetics 1990; 18: Barre J, Didey F, Delion F, et al. Problems in therapeutic drug monitoring: free drug level monitoring. Therapeutic Drug Monitoring 1998; 10: Valdes, R, Jortani SA, Gheorghiade M. Standards of laboratory practice: cardiac drug monitoring. Clin Chem 1998; 44: Caplin JL, Johnstom A, Hamer J, et al. The acute changes in serum binding of disopyramide after acute myocardial infarction. Eur J Clin Pharmacol 1985; 28: McCollam PL, Crouch MA, Watson JE. Altered protein binding of quinidine in patients with atrial fibrillation and flutter. Pharmacotherapy 1997; 17: Roden DM, Deele SB, Higgins SB, et al. Antiarrhythmic efficacy, pharmacokinetics and safety of N-acetylprocainamide in human subjects: comparison with procainamide. Am J Cardiol 1980; 46: Burgess CD, Siebers RW, Purdie GL, et al. The relationship between the QT interval and plasma amiodarone concentration in patients on long-term therapy. Eur J Clin Pharmacol 1987; 33: Ruskin JN, McGovern B, Garan H, et al. Antiarrhythmic drugs: a possible cause of out-of-hospital cardiac arrest. N Engl J Med 1983; 309:
7 The Cardiac Arrhythmia Suppression Trial Investigators. Preliminary report: effect of encainide and flecainide on mortality in a randomised trial of arrhythmia suppression after myocardial infarction. N Engl J Med 1989; 321: The Cardiac Arrhythmia Suppression Trial II Investigators. Effect of the antiarrhythmic agent moricizine on survival after myocardial infarction. N Engl J Med 1992; 327: Heart Failure Society of America (HFSA). HFSA guidelines for management of patients with heart failure caused by left ventricular systolic dysfunction. J Cardiac Fail 1999; 5: Remme WJ, Swedberg K. Guidelines for the diagnosis and treatment of chronic heart failure. Eur Heart J 2001; 22: Dawling S, Crome P. Clinical pharmacokinetic considerations in the elderly: an update. Clinl Pharmacokinet 1989; 17: Regårdh DG. Pharmacokinetic aspects of some beta adrenoceptor blocking drugs. Acta Medica Scandinavica 1982; Suppl. 665: Herrera J, Vukovich RA, Griffith DL. Elimination of nadolol by patients with renal impairment. Br J Clin Pharmacol 1979; 7 Suppl. 2: 227S 31S. Castleden CM, George CF, Mercer D, et al. The effect of age on plasma levels of propranolol and practolol in man. Br J Clin Pharmacol 1975; 2: Vadiei K, Troy S, Korth-Bradley J, et al. Population pharmacokinetics of intravenous amiodarone and comparison with two-stage pharmacokinetic analysis. J Clin Pharmacol 1997; 37: Tisdale JE, Follin SL, Ordelova A, et al. Risk factors for the development of specific noncardiovascular adverse effects associated with amiodarone. J Clin Pharmacol 1995; 35: Schwartz JB. Calcium antagonists in the elderly. Drugs Aging 1996; 9: Schwartz JB. Aging alters verapamil elimination and dynamics: single dose and steady-state responses. J Pharmacol Exp Ther 1990; 255: Mooraddian AD. Digitalis. An update of clinical pharmacokinetics, therapeutic monitoring techniques, and treatment recommendations. Clin Pharmacokinet 1988; 15: Cusack B, Kelly J, O Malley K, et al. Digoxin in the elderly: pharmacokinetic consequences of old age. Clin Pharmacol Ther 1979; 25: Jogestrand T, Schenck-Gustafsson K, Nordlander R, et al. Quinidineinduced changes in serum and skeletal muscle digoxin concentration: evidence of saturable binding of digoxin to skeletal muscle. Eur J Clin Pharmacol 1984; 27:
Mr. Eknath Kole M.S. Pharm (NIPER Mohali)
 M.S. Pharm (NIPER Mohali) Drug Class Actions Therapeutic Uses Pharmacokinetics Adverse Effects Other Quinidine IA -Binds to open and inactivated Na+ -Decreases the slope of Phase 4 spontaneous depolarization
M.S. Pharm (NIPER Mohali) Drug Class Actions Therapeutic Uses Pharmacokinetics Adverse Effects Other Quinidine IA -Binds to open and inactivated Na+ -Decreases the slope of Phase 4 spontaneous depolarization
Arrhythmias. Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium.
 Arrhythmias Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium. However, in clinic it present as a complex family of disorders that show variety of symptoms, for
Arrhythmias Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium. However, in clinic it present as a complex family of disorders that show variety of symptoms, for
Antiarrhythmic Drugs 1/31/2018 1
 Antiarrhythmic Drugs 1/31/2018 1 Normal conduction pathway: 1- SA node generates action potential and delivers it to the atria and the AV node 2- The AV node delivers the impulse to purkinje fibers Other
Antiarrhythmic Drugs 1/31/2018 1 Normal conduction pathway: 1- SA node generates action potential and delivers it to the atria and the AV node 2- The AV node delivers the impulse to purkinje fibers Other
Arrhythmias. 1. beat too slowly (sinus bradycardia). Like in heart block
 Arrhythmias It is a simple-dysfunction caused by abnormalities in impulse formation and conduction in the myocardium. The heart is designed in such a way that allows it to generate from the SA node electrical
Arrhythmias It is a simple-dysfunction caused by abnormalities in impulse formation and conduction in the myocardium. The heart is designed in such a way that allows it to generate from the SA node electrical
Chapter 14. Agents used in Cardiac Arrhythmias
 Chapter 14 Agents used in Cardiac Arrhythmias Cardiac arrhythmia Approximately 50% of post-myocardial infarction fatalities result from ventricular tachycarida (VT) or ventricular fibrillation (VF). These
Chapter 14 Agents used in Cardiac Arrhythmias Cardiac arrhythmia Approximately 50% of post-myocardial infarction fatalities result from ventricular tachycarida (VT) or ventricular fibrillation (VF). These
B. 14 Antidysrhythmic drugs. a. Classify antidysrhythmics by their electrophysiological actions. Vaughan-Williams classification
 B. 14 Antidysrhythmic drugs a. Classify antidysrhythmics by their electrophysiological actions. Vaughan-Williams classification I II III IV membrane stabilizers all ERP, ERP/APD, all except c APD classified
B. 14 Antidysrhythmic drugs a. Classify antidysrhythmics by their electrophysiological actions. Vaughan-Williams classification I II III IV membrane stabilizers all ERP, ERP/APD, all except c APD classified
Drugs Controlling Myocyte Excitability and Conduction at the AV node Singh and Vaughan-Williams Classification
 Drugs Controlling Myocyte Excitability and Conduction at the AV node Singh and Vaughan-Williams Classification Class I Na Channel Blockers Flecainide Propafenone Class III K channel Blockers Dofetilide,
Drugs Controlling Myocyte Excitability and Conduction at the AV node Singh and Vaughan-Williams Classification Class I Na Channel Blockers Flecainide Propafenone Class III K channel Blockers Dofetilide,
Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014
 Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014 Financial disclosures Consultant Medtronic 3 reasons to evaluate and treat arrhythmias
Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014 Financial disclosures Consultant Medtronic 3 reasons to evaluate and treat arrhythmias
PHARMACOLOGY OF ARRHYTHMIAS
 PHARMACOLOGY OF ARRHYTHMIAS Course: Integrated Therapeutics 1 Lecturer: Dr. E. Konorev Date: November 27, 2012 Materials on: Exam #5 Required reading: Katzung, Chapter 14 1 CARDIAC ARRHYTHMIAS Abnormalities
PHARMACOLOGY OF ARRHYTHMIAS Course: Integrated Therapeutics 1 Lecturer: Dr. E. Konorev Date: November 27, 2012 Materials on: Exam #5 Required reading: Katzung, Chapter 14 1 CARDIAC ARRHYTHMIAS Abnormalities
Antiarrhythmic Drugs
 Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Pediatrics ECG Monitoring. Pediatric Intensive Care Unit Emergency Division
 Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
ΚΟΛΠΙΚΗ ΜΑΡΜΑΡΥΓΗ ΦΑΡΜΑΚΕΥΤΙΚΗ ΗΛΕΚΤΡΙΚΗ ΑΝΑΤΑΞΗ. ΣΠΥΡΟΜΗΤΡΟΣ ΓΕΩΡΓΙΟΣ Καρδιολόγος, Ε/Α, Γ.Ν.Κατερίνης. F.E.S.C
 ΚΟΛΠΙΚΗ ΜΑΡΜΑΡΥΓΗ ΦΑΡΜΑΚΕΥΤΙΚΗ ΗΛΕΚΤΡΙΚΗ ΑΝΑΤΑΞΗ ΣΠΥΡΟΜΗΤΡΟΣ ΓΕΩΡΓΙΟΣ Καρδιολόγος, Ε/Α, Γ.Ν.Κατερίνης. F.E.S.C Definitions of AF: A Simplified Scheme Term Definition Paroxysmal AF AF that terminates
ΚΟΛΠΙΚΗ ΜΑΡΜΑΡΥΓΗ ΦΑΡΜΑΚΕΥΤΙΚΗ ΗΛΕΚΤΡΙΚΗ ΑΝΑΤΑΞΗ ΣΠΥΡΟΜΗΤΡΟΣ ΓΕΩΡΓΙΟΣ Καρδιολόγος, Ε/Α, Γ.Ν.Κατερίνης. F.E.S.C Definitions of AF: A Simplified Scheme Term Definition Paroxysmal AF AF that terminates
Chapter 9. Learning Objectives. Learning Objectives 9/11/2012. Cardiac Arrhythmias. Define electrical therapy
 Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Antiarrhythmic Drugs Öner Süzer
 Antiarrhythmic Drugs Öner Süzer www.onersuzer.com osuzer@istanbul.edu.tr Last update: 09.11.2009 1 Süzer Farmakoloji 3. Baskı 2005 2 1 Süzer Farmakoloji 3. Baskı 2005 3 Figure 14 1 Schematic representation
Antiarrhythmic Drugs Öner Süzer www.onersuzer.com osuzer@istanbul.edu.tr Last update: 09.11.2009 1 Süzer Farmakoloji 3. Baskı 2005 2 1 Süzer Farmakoloji 3. Baskı 2005 3 Figure 14 1 Schematic representation
Most antiarrhythmic drugs are potent compounds with a relatively narrow therapeutic
 Pharmacological Effects of Antiarrhythmic s Review and Update Peter R. Kowey, MD REVIEW ARTICLE Most antiarrhythmic drugs are potent compounds with a relatively narrow therapeutic index. When prescribed
Pharmacological Effects of Antiarrhythmic s Review and Update Peter R. Kowey, MD REVIEW ARTICLE Most antiarrhythmic drugs are potent compounds with a relatively narrow therapeutic index. When prescribed
DECLARATION OF CONFLICT OF INTEREST. Consultant Sanofi Biosense Webster Honorarium Boehringer Ingelheim St Jude Medical
 DECLARATION OF CONFLICT OF INTEREST Consultant Sanofi Biosense Webster Honorarium Boehringer Ingelheim St Jude Medical ESC Congress Paris, France August 27-31, 2011 Risk & Complications of AADs for Rhythm
DECLARATION OF CONFLICT OF INTEREST Consultant Sanofi Biosense Webster Honorarium Boehringer Ingelheim St Jude Medical ESC Congress Paris, France August 27-31, 2011 Risk & Complications of AADs for Rhythm
Therapeutic drug monitoring: antiarrhythmic drugs
 Therapeutic drug monitoring: antiarrhythmic drugs T. J. Campbell & K. M. Williams Departments of Medicine and Clinical Pharmacology, University of New South Wales and St Vincent s Hospital, Darlinghurst,
Therapeutic drug monitoring: antiarrhythmic drugs T. J. Campbell & K. M. Williams Departments of Medicine and Clinical Pharmacology, University of New South Wales and St Vincent s Hospital, Darlinghurst,
The pill-in-the-pocket strategy for paroxysmal atrial fibrillation
 The pill-in-the-pocket strategy for paroxysmal atrial fibrillation KONSTANTINOS P. LETSAS, MD, FEHRA LABORATORY OF CARDIAC ELECTROPHYSIOLOGY EVANGELISMOS GENERAL HOSPITAL OF ATHENS ARRHYTHMIAS UPDATE,
The pill-in-the-pocket strategy for paroxysmal atrial fibrillation KONSTANTINOS P. LETSAS, MD, FEHRA LABORATORY OF CARDIAC ELECTROPHYSIOLOGY EVANGELISMOS GENERAL HOSPITAL OF ATHENS ARRHYTHMIAS UPDATE,
DRUG CLASSES BETA-ADRENOCEPTOR ANTAGONISTS (BETA-BLOCKERS)
 DRUG CLASSES BETA-ADRENOCEPTOR ANTAGONISTS (BETA-BLOCKERS) Beta-blockers have been widely used in the management of angina, certain tachyarrhythmias and heart failure, as well as in hypertension. Examples
DRUG CLASSES BETA-ADRENOCEPTOR ANTAGONISTS (BETA-BLOCKERS) Beta-blockers have been widely used in the management of angina, certain tachyarrhythmias and heart failure, as well as in hypertension. Examples
Chapter 26. Media Directory. Dysrhythmias. Diagnosis/Treatment of Dysrhythmias. Frequency in Population Difficult to Predict
 Chapter 26 Drugs for Dysrythmias Slide 33 Slide 35 Media Directory Propranolol Animation Amiodarone Animation Upper Saddle River, New Jersey 07458 All rights reserved. Dysrhythmias Abnormalities of electrical
Chapter 26 Drugs for Dysrythmias Slide 33 Slide 35 Media Directory Propranolol Animation Amiodarone Animation Upper Saddle River, New Jersey 07458 All rights reserved. Dysrhythmias Abnormalities of electrical
Antihypertensive drugs SUMMARY Made by: Lama Shatat
 Antihypertensive drugs SUMMARY Made by: Lama Shatat Diuretic Thiazide diuretics The loop diuretics Potassium-sparing Diuretics *Hydrochlorothiazide *Chlorthalidone *Furosemide *Torsemide *Bumetanide Aldosterone
Antihypertensive drugs SUMMARY Made by: Lama Shatat Diuretic Thiazide diuretics The loop diuretics Potassium-sparing Diuretics *Hydrochlorothiazide *Chlorthalidone *Furosemide *Torsemide *Bumetanide Aldosterone
ANTI - ARRHYTHMIC DRUGS
 ANTI - ARRHYTHMIC DRUGS CARDIAC ACTION POTENTIAL K Out Balance Ca in/k out Na in K Out GENERATION OF ARRHYTHMIAS Four mechanisms of arrhythmia generation; Increased normal automaticity Abnormal automaticity
ANTI - ARRHYTHMIC DRUGS CARDIAC ACTION POTENTIAL K Out Balance Ca in/k out Na in K Out GENERATION OF ARRHYTHMIAS Four mechanisms of arrhythmia generation; Increased normal automaticity Abnormal automaticity
Biology of Aging. Faculty Disclosure. Learning Objectives. I have no relevant financial disclosures relative to the content of this presentation.
 Biology of Aging Aging Changes That Impact Medication Management Emily P. Peron, PharmD, MS, BCPS, FASCP Assistant Professor of Geriatrics Virginia Commonwealth University School of Pharmacy Richmond,
Biology of Aging Aging Changes That Impact Medication Management Emily P. Peron, PharmD, MS, BCPS, FASCP Assistant Professor of Geriatrics Virginia Commonwealth University School of Pharmacy Richmond,
Use of Antiarrhythmic Drugs for AF Who, What and How? Dr. Marc Cheng Queen Elizabeth Hospital
 Use of Antiarrhythmic Drugs for AF Who, What and How? Dr. Marc Cheng Queen Elizabeth Hospital Content i. Rhythm versus Rate control ii. Anti-arrhythmic for Rhythm Control iii. Anti-arrhythmic for Rate
Use of Antiarrhythmic Drugs for AF Who, What and How? Dr. Marc Cheng Queen Elizabeth Hospital Content i. Rhythm versus Rate control ii. Anti-arrhythmic for Rhythm Control iii. Anti-arrhythmic for Rate
Antiarrhythmic Drugs Öner Süzer
 Antiarrhythmic Drugs Öner Süzer www.onersuzer.com osuzer@istanbul.edu.tr Last update: 13.01.2009 1 Süzer Farmakoloji 3. Baskı 2005 2 1 Süzer Farmakoloji 3. Baskı 2005 3 Figure 14 1 Schematic representation
Antiarrhythmic Drugs Öner Süzer www.onersuzer.com osuzer@istanbul.edu.tr Last update: 13.01.2009 1 Süzer Farmakoloji 3. Baskı 2005 2 1 Süzer Farmakoloji 3. Baskı 2005 3 Figure 14 1 Schematic representation
Drug Dosing in Renal Insufficiency. Coralie Therese D. Dimacali, MD College of Medicine University of the Philippines Manila
 Drug Dosing in Renal Insufficiency Coralie Therese D. Dimacali, MD College of Medicine University of the Philippines Manila Declaration of Conflict of Interest For today s lecture on Drug Dosing in Renal
Drug Dosing in Renal Insufficiency Coralie Therese D. Dimacali, MD College of Medicine University of the Philippines Manila Declaration of Conflict of Interest For today s lecture on Drug Dosing in Renal
Aging Changes That Impact Medication Management
 Biology of Aging Aging Changes That Impact Medication Management Emily P. Peron, PharmD, MS, BCPS, FASCP Assistant Professor of Geriatrics Virginia Commonwealth University School of Pharmacy Richmond,
Biology of Aging Aging Changes That Impact Medication Management Emily P. Peron, PharmD, MS, BCPS, FASCP Assistant Professor of Geriatrics Virginia Commonwealth University School of Pharmacy Richmond,
Current Guideline for AF Treatment. Young Keun On, MD, PhD, FHRS Samsung Medical Center Sungkyunkwan University School of Medicine
 Current Guideline for AF Treatment Young Keun On, MD, PhD, FHRS Samsung Medical Center Sungkyunkwan University School of Medicine Case 1 59 year-old lady Sudden palpitation and breathlessness for 12 hours
Current Guideline for AF Treatment Young Keun On, MD, PhD, FHRS Samsung Medical Center Sungkyunkwan University School of Medicine Case 1 59 year-old lady Sudden palpitation and breathlessness for 12 hours
Antidysrhythmics HST-151 1
 HST-151 1 Antidysrhythmics I. Ventricular muscle cell action potential a. Phase 0: Upstroke b. Phase 1: Early-fast repolarization c. Phase 2: Plateau d. Phase 3: Repolarization e. Phase 4: Diastole HST-151
HST-151 1 Antidysrhythmics I. Ventricular muscle cell action potential a. Phase 0: Upstroke b. Phase 1: Early-fast repolarization c. Phase 2: Plateau d. Phase 3: Repolarization e. Phase 4: Diastole HST-151
Basic Concepts of TDM
 TDM Lecture 1 5 th stage What is TDM? Basic Concepts of TDM Therapeutic drug monitoring (TDM) is a branch of clinical pharmacology that specializes in the measurement of medication concentrations in blood.
TDM Lecture 1 5 th stage What is TDM? Basic Concepts of TDM Therapeutic drug monitoring (TDM) is a branch of clinical pharmacology that specializes in the measurement of medication concentrations in blood.
2/25/2015 PHARMACODYNAMICS OF AGING: NARROWING OF THE THERAPEUTIC INDEX IN THE FACE OF THERAPEUTIC OPPORTUNITY OVERALL PRESCRIBING
 Mean # Drugs/Resident 2/25/2015 PHARMACODYNAMICS OF AGING: NARROWING OF THE THERAPEUTIC INDEX IN THE FACE OF THERAPEUTIC OPPORTUNITY Darrell R. Abernethy, M.D., Ph.D. Associate Director for Drug Safety
Mean # Drugs/Resident 2/25/2015 PHARMACODYNAMICS OF AGING: NARROWING OF THE THERAPEUTIC INDEX IN THE FACE OF THERAPEUTIC OPPORTUNITY Darrell R. Abernethy, M.D., Ph.D. Associate Director for Drug Safety
2/26/2015 PHARMACODYNAMICS OF AGING: NARROWING OF THE THERAPEUTIC INDEX IN THE FACE OF THERAPEUTIC OPPORTUNITY
 PHARMACODYNAMICS OF AGING: NARROWING OF THE THERAPEUTIC INDEX IN THE FACE OF THERAPEUTIC OPPORTUNITY Darrell R. Abernethy, M.D., Ph.D. Associate Director for Drug Safety Office of Clinical Pharmacology
PHARMACODYNAMICS OF AGING: NARROWING OF THE THERAPEUTIC INDEX IN THE FACE OF THERAPEUTIC OPPORTUNITY Darrell R. Abernethy, M.D., Ph.D. Associate Director for Drug Safety Office of Clinical Pharmacology
03/27/2014. Suzanne M. Lifer: Nothing to disclose Michelle R. Musser: Nothing to disclose
 Suzanne Lifer, PharmD Michelle Musser, PharmD, BCPS Authors of this presentation have the following to disclose concerning possible financial or personal relationships with commercial entities that may
Suzanne Lifer, PharmD Michelle Musser, PharmD, BCPS Authors of this presentation have the following to disclose concerning possible financial or personal relationships with commercial entities that may
Clinical Problem. Management. Discussion
 Optimum management of atrial fibrillation in the Intensive Care Unit Clinical Problem A 61 year old man, PD, presented to the Intensive Care Unit (ICU) after angiography and intra arterial thrombolysis
Optimum management of atrial fibrillation in the Intensive Care Unit Clinical Problem A 61 year old man, PD, presented to the Intensive Care Unit (ICU) after angiography and intra arterial thrombolysis
Amlodipine plus Lisinopril Tablets AMLOPRES-L
 Amlodipine plus Lisinopril Tablets AMLOPRES-L COMPOSITION AMLOPRES-L Each uncoated tablet contains: Amlodipine besylate equivalent to Amlodipine 5 mg and Lisinopril USP equivalent to Lisinopril (anhydrous)
Amlodipine plus Lisinopril Tablets AMLOPRES-L COMPOSITION AMLOPRES-L Each uncoated tablet contains: Amlodipine besylate equivalent to Amlodipine 5 mg and Lisinopril USP equivalent to Lisinopril (anhydrous)
TDM. Measurement techniques used to determine cyclosporine level include:
 TDM Lecture 15: Cyclosporine. Cyclosporine is a cyclic polypeptide medication with immunosuppressant effect. It has the ability to block the production of interleukin-2 and other cytokines by T-lymphocytes.
TDM Lecture 15: Cyclosporine. Cyclosporine is a cyclic polypeptide medication with immunosuppressant effect. It has the ability to block the production of interleukin-2 and other cytokines by T-lymphocytes.
Management of new onset atrial fibrillation McNamara R L, Bass E B, Miller M R, Segal J B, Goodman S N, Kim N L, Robinson K A, Powe N R
 Management of new onset atrial fibrillation McNamara R L, Bass E B, Miller M R, Segal J B, Goodman S N, Kim N L, Robinson K A, Powe N R Authors' objectives To synthesise the evidence that exists to guide
Management of new onset atrial fibrillation McNamara R L, Bass E B, Miller M R, Segal J B, Goodman S N, Kim N L, Robinson K A, Powe N R Authors' objectives To synthesise the evidence that exists to guide
Antiarrhythmic Drugs. Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2018
 Antiarrhythmic Drugs Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2018 2 Ion Permeability Changes Potential Changes Genes and Proteins 3 Cardiac Na+ channels 5 6
Antiarrhythmic Drugs Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2018 2 Ion Permeability Changes Potential Changes Genes and Proteins 3 Cardiac Na+ channels 5 6
Atrial Fibrillation Etiologies and Treatment. Shawn Liu Learner Centered Learning Goal
 Atrial Fibrillation Etiologies and Treatment Shawn Liu Learner Centered Learning Goal Pathophysiology Defined by the absence of coordinated atrial systole Results from multiple reentrant electrical waves
Atrial Fibrillation Etiologies and Treatment Shawn Liu Learner Centered Learning Goal Pathophysiology Defined by the absence of coordinated atrial systole Results from multiple reentrant electrical waves
Atrial Fibrillation 10/2/2018. Depolarization & ECG. Atrial Fibrillation. Hemodynamic Consequences
 Depolarization & ECG Atrial Fibrillation How to make ORDER out of CHAOS Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Depolarization & ECG Depolarization & ECG Atrial Fibrillation Hemodynamic Consequences
Depolarization & ECG Atrial Fibrillation How to make ORDER out of CHAOS Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Depolarization & ECG Depolarization & ECG Atrial Fibrillation Hemodynamic Consequences
I have nothing to disclose.
 I have nothing to disclose. Antiarrhythmic Therapy in Pregnancy Prof. Ali Oto,MD,FESC,FACC,FHRS Department of Cardiology Hacettepe University,Faculty of Medicine Ankara Arrhythmias in pregnancy An increased
I have nothing to disclose. Antiarrhythmic Therapy in Pregnancy Prof. Ali Oto,MD,FESC,FACC,FHRS Department of Cardiology Hacettepe University,Faculty of Medicine Ankara Arrhythmias in pregnancy An increased
BASIC PHARMACOKINETICS
 BASIC PHARMACOKINETICS MOHSEN A. HEDAYA CRC Press Taylor & Francis Croup Boca Raton London New York CRC Press is an imprint of the Taylor & Francis Group, an informa business Table of Contents Chapter
BASIC PHARMACOKINETICS MOHSEN A. HEDAYA CRC Press Taylor & Francis Croup Boca Raton London New York CRC Press is an imprint of the Taylor & Francis Group, an informa business Table of Contents Chapter
Rate and Rhythm Control of Atrial Fibrillation
 Rate and Rhythm Control of Atrial Fibrillation April 21, 2017 춘계심혈관통합학술대회 Jaemin Shim, MD, PhD Arrhythmia Center Korea University Anam Hospital Treatment of AF Goal Reducing symptoms Preventing complication
Rate and Rhythm Control of Atrial Fibrillation April 21, 2017 춘계심혈관통합학술대회 Jaemin Shim, MD, PhD Arrhythmia Center Korea University Anam Hospital Treatment of AF Goal Reducing symptoms Preventing complication
Therapeutic drug monitoring: antiarrhythmic drugs
 Br J Clin Pharmacol 1998; 46: 307 319 Therapeutic drug monitoring: antiarrhythmic drugs T. J. Campbell & K. M. Williams Department of Clinical Pharmacology, St Vincent s Hospital, Darlinghurst, NSW 2010,
Br J Clin Pharmacol 1998; 46: 307 319 Therapeutic drug monitoring: antiarrhythmic drugs T. J. Campbell & K. M. Williams Department of Clinical Pharmacology, St Vincent s Hospital, Darlinghurst, NSW 2010,
Excretion of Drugs. Prof. Hanan Hagar Pharmacology Unit Medical College
 Excretion of Drugs Prof. Hanan Hagar Pharmacology Unit Medical College Excretion of Drugs By the end of this lecture, students should be able to! Identify main and minor routes of excretion including renal
Excretion of Drugs Prof. Hanan Hagar Pharmacology Unit Medical College Excretion of Drugs By the end of this lecture, students should be able to! Identify main and minor routes of excretion including renal
Basic Pharmacokinetic Principles Stephen P. Roush, Pharm.D. Clinical Coordinator, Department of Pharmacy
 Basic Pharmacokinetic Principles Stephen P. Roush, Pharm.D. Clinical Coordinator, Department of Pharmacy I. General principles Applied pharmacokinetics - the process of using drug concentrations, pharmaco-kinetic
Basic Pharmacokinetic Principles Stephen P. Roush, Pharm.D. Clinical Coordinator, Department of Pharmacy I. General principles Applied pharmacokinetics - the process of using drug concentrations, pharmaco-kinetic
AMIODARONE and DESETHYLAMIODARONE IN PLASMA BY UV FAST CODE Z33610
 AMIODARONE and DESETHYLAMIODARONE IN PLASMA BY UV FAST CODE Z33610 INTRODUCTION Amiodarone is an antiarrhythmic agent used for various types of tachyarrhythmias, both ventricular and supraventricular arrhythmias.
AMIODARONE and DESETHYLAMIODARONE IN PLASMA BY UV FAST CODE Z33610 INTRODUCTION Amiodarone is an antiarrhythmic agent used for various types of tachyarrhythmias, both ventricular and supraventricular arrhythmias.
Variation in drug responses & Drug-Drug Interactions
 Variation in drug responses & Drug-Drug Interactions 1 Properties of an Ideal Drug Effective Safety Selective Reversible Action Predictable Freedom from drug interactions Low cost Chemically stable Sources
Variation in drug responses & Drug-Drug Interactions 1 Properties of an Ideal Drug Effective Safety Selective Reversible Action Predictable Freedom from drug interactions Low cost Chemically stable Sources
Pharmacokinetics in the critically ill. Intensive Care Training Program Radboud University Medical Centre Nijmegen
 Pharmacokinetics in the critically ill Intensive Care Training Program Radboud University Medical Centre Nijmegen In general... Critically ill patients are at higher risk for ADE s and more severe ADE
Pharmacokinetics in the critically ill Intensive Care Training Program Radboud University Medical Centre Nijmegen In general... Critically ill patients are at higher risk for ADE s and more severe ADE
USES OF PHARMACOKINETICS
 CLINICAL PHARMACOKINETICS Juan J.L. Lertora, M.D., Ph.D. Director Clinical Pharmacology Program Office of Clinical Research Training and Medical Education National Institutes of Health Clinical Center
CLINICAL PHARMACOKINETICS Juan J.L. Lertora, M.D., Ph.D. Director Clinical Pharmacology Program Office of Clinical Research Training and Medical Education National Institutes of Health Clinical Center
There are future perspectives in the pharmacological treatment of arrhythmias
 There are future perspectives in the pharmacological treatment of arrhythmias George Andrikopoulos, MD, PhD, FESC, Cardiologist, Director, 1st Department of Cardiology/ Department of Electrophysiology
There are future perspectives in the pharmacological treatment of arrhythmias George Andrikopoulos, MD, PhD, FESC, Cardiologist, Director, 1st Department of Cardiology/ Department of Electrophysiology
This document does not consider management of individual arrhythmias look elsewhere, e.g. OHCM.
 Cardiac arrhythmias This document does not consider management of individual arrhythmias look elsewhere, e.g. OHCM. Physiology Automaticity = ability of specialised cardiac conducting tissue to spontaneously
Cardiac arrhythmias This document does not consider management of individual arrhythmias look elsewhere, e.g. OHCM. Physiology Automaticity = ability of specialised cardiac conducting tissue to spontaneously
Antiarrhythmic Drugs. Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2017
 Antiarrhythmic Drugs Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2017 Types of Cardiac Arrhythmias Abnormalities of Impulse Formation: Rate disturbances. Triggered
Antiarrhythmic Drugs Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2017 Types of Cardiac Arrhythmias Abnormalities of Impulse Formation: Rate disturbances. Triggered
LACIPIL QUALITATIVE AND QUANTITATIVE COMPOSITION
 LACIPIL lacidipine QUALITATIVE AND QUANTITATIVE COMPOSITION Lacidipine, 2 mg - round shaped white engraved on one face. Lacidipine, 4 mg - oval white with break line on both faces. Lacidipine, 6 mg - oval
LACIPIL lacidipine QUALITATIVE AND QUANTITATIVE COMPOSITION Lacidipine, 2 mg - round shaped white engraved on one face. Lacidipine, 4 mg - oval white with break line on both faces. Lacidipine, 6 mg - oval
Heart Failure (HF) Treatment
 Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
Instruct patient and caregivers: Need for constant monitoring Potential complications of drug therapy
 Assessment Prior to administration: Assess patient for chest pain, dysrhythmias, and vital signs (initially and throughout therapy) Obtain complete medical history, including allergies, especially heart
Assessment Prior to administration: Assess patient for chest pain, dysrhythmias, and vital signs (initially and throughout therapy) Obtain complete medical history, including allergies, especially heart
ANTI-ARRHYTHMICS AND WARFARIN. Dr Nithish Jayakumar
 ANTI-ARRHYTHMICS AND WARFARIN Dr Nithish Jayakumar Contents 1. Anti-arrhythmics Pacemaker and myocardial potentials Drug classes mechanisms; s/e; contra-indications Management of common arrhythmias 2.
ANTI-ARRHYTHMICS AND WARFARIN Dr Nithish Jayakumar Contents 1. Anti-arrhythmics Pacemaker and myocardial potentials Drug classes mechanisms; s/e; contra-indications Management of common arrhythmias 2.
Document 3 Summary of Data and Guidance for Medical Professionals
 Document 3 Summary of Data and Guidance for Medical Professionals Anvirzel Anvirzel is a novel antitumor compound extracted from the plant Nerium oleander, which belongs to the family Apocynaceae. Anvirzel
Document 3 Summary of Data and Guidance for Medical Professionals Anvirzel Anvirzel is a novel antitumor compound extracted from the plant Nerium oleander, which belongs to the family Apocynaceae. Anvirzel
Amiodarone Prescribing and Monitoring: Back to the Future
 Amiodarone Prescribing and Monitoring: Back to the Future Subha L. Varahan, MD, FHRS, CCDS Electrophysiologist Oklahoma Heart Hospital Oklahoma City, OK Friday, February, 8 th, 2019 Iodinated benzofuran
Amiodarone Prescribing and Monitoring: Back to the Future Subha L. Varahan, MD, FHRS, CCDS Electrophysiologist Oklahoma Heart Hospital Oklahoma City, OK Friday, February, 8 th, 2019 Iodinated benzofuran
CHAPTER 2. GERIATRICS, SELF-ASSESSMENT QUESTIONS
 CHAPTER 2. GERIATRICS, SELF-ASSESSMENT QUESTIONS 1. The following is an accurate description of the aging population: A. The number of older adults will reach 17 million in 2030 B. The ratio of women to
CHAPTER 2. GERIATRICS, SELF-ASSESSMENT QUESTIONS 1. The following is an accurate description of the aging population: A. The number of older adults will reach 17 million in 2030 B. The ratio of women to
Pharmacology in the Elderly
 Pharmacology in the Elderly James Hardy Geriatrician, Royal North Shore Hospital A recent consultation Aspirin Clopidogrel Warfarin Coloxyl with senna Clearlax Methotrexate Paracetamol Pantoprazole Cholecalciferol
Pharmacology in the Elderly James Hardy Geriatrician, Royal North Shore Hospital A recent consultation Aspirin Clopidogrel Warfarin Coloxyl with senna Clearlax Methotrexate Paracetamol Pantoprazole Cholecalciferol
PHA 5127 FINAL EXAM FALL On my honor, I have neither given nor received unauthorized aid in doing this assignment.
 PHA 5127 FINAL EXAM FALL 1997 On my honor, I have neither given nor received unauthorized aid in doing this assignment. Name Question Points 1. /14 pts 2. /10 pts 3. /8 pts 4 /8 pts 5. /12 pts 6. /8 pts
PHA 5127 FINAL EXAM FALL 1997 On my honor, I have neither given nor received unauthorized aid in doing this assignment. Name Question Points 1. /14 pts 2. /10 pts 3. /8 pts 4 /8 pts 5. /12 pts 6. /8 pts
DEPARTMENT OF PHARMACOLOGY AND THERAPEUTIC UNIVERSITAS SUMATERA UTARA
 METABOLISME dr. Yunita Sari Pane DEPARTMENT OF PHARMACOLOGY AND THERAPEUTIC UNIVERSITAS SUMATERA UTARA Pharmacokinetic absorption distribution BIOTRANSFORMATION elimination Intravenous Administration Oral
METABOLISME dr. Yunita Sari Pane DEPARTMENT OF PHARMACOLOGY AND THERAPEUTIC UNIVERSITAS SUMATERA UTARA Pharmacokinetic absorption distribution BIOTRANSFORMATION elimination Intravenous Administration Oral
Drug dosing in Extremes of Weight
 Drug dosing in Extremes of Weight The Plump & Heavy versus The Skinny & Light Maria Minerva P. Calimag, MD, MSc, PhD, DPBA, FPSECP PROFESSOR Departments of Pharmacology, Anesthesiology and Clinical Epidemiology
Drug dosing in Extremes of Weight The Plump & Heavy versus The Skinny & Light Maria Minerva P. Calimag, MD, MSc, PhD, DPBA, FPSECP PROFESSOR Departments of Pharmacology, Anesthesiology and Clinical Epidemiology
METOTRUST XL-25/50 Metoprolol Succinate Extended-Release Tablets
 METOTRUST XL-25/50 Metoprolol Succinate Extended-Release Tablets COMPOSITION Each film-coated tablet of Metotrust XL-25 contains: Metoprolol Succinate USP 23.75 mg equivalent to Metoprolol Tartrate 25
METOTRUST XL-25/50 Metoprolol Succinate Extended-Release Tablets COMPOSITION Each film-coated tablet of Metotrust XL-25 contains: Metoprolol Succinate USP 23.75 mg equivalent to Metoprolol Tartrate 25
Antiarrhythmics 17 I. OVERVIEW II. INTRODUCTION TO THE ARRHYTHMIAS
 Antiarrhythmics 17 I. OVERVIEW In contrast to skeletal muscle, which contracts only when it receives a stimulus, the heart contains specialized cells that exhibit automaticity. This means that they can
Antiarrhythmics 17 I. OVERVIEW In contrast to skeletal muscle, which contracts only when it receives a stimulus, the heart contains specialized cells that exhibit automaticity. This means that they can
! YOU NEED TO MONITOR QT INTERVALS IN THESE PATIENTS.
 Antiarrhythmic Pharmacopoeia Powerful drugs, split into 4 major classes, according to the predominant receptor they effect. Some fit into several classes at once, like sotolol. Some don t fit at all, owing
Antiarrhythmic Pharmacopoeia Powerful drugs, split into 4 major classes, according to the predominant receptor they effect. Some fit into several classes at once, like sotolol. Some don t fit at all, owing
Atrial Fibrillation and the NOAC s. John Raymond MS, PA-C, MHP February 10, 2018
 Atrial Fibrillation and the NOAC s John Raymond MS, PA-C, MHP February 10, 2018 Pathogenesis EPIDEMIOLOGY Arrhythmia-related hospitalisations in the US Ventricular fibrillation 2% Atrial fibrillation 34%
Atrial Fibrillation and the NOAC s John Raymond MS, PA-C, MHP February 10, 2018 Pathogenesis EPIDEMIOLOGY Arrhythmia-related hospitalisations in the US Ventricular fibrillation 2% Atrial fibrillation 34%
Metoprolol -a new cardioselective 3-adrenoceptor blocking agent for treatment of tachyarrhythmias
 British Heart journal, 1977, 39, 834-838 Metoprolol -a new cardioselective 3-adrenoceptor blocking agent for treatment of tachyarrhythmias H. S. WASIR, R. K. MAHAPATRA, M. L. BHATIA, SUJOY B. ROY, AND
British Heart journal, 1977, 39, 834-838 Metoprolol -a new cardioselective 3-adrenoceptor blocking agent for treatment of tachyarrhythmias H. S. WASIR, R. K. MAHAPATRA, M. L. BHATIA, SUJOY B. ROY, AND
The most common. hospitalized patients. hypotension due to. filling time Rate control in ICU patients may be difficult as many drugs cause hypotension
 Arrhythmias in the critically ill ICU patients: Approach for rapid recognition & management Objectives Be able to identify and manage: Atrial fibrillation with a rapid ventricular response Atrial flutter
Arrhythmias in the critically ill ICU patients: Approach for rapid recognition & management Objectives Be able to identify and manage: Atrial fibrillation with a rapid ventricular response Atrial flutter
Medical management of AF: drugs for rate and rhythm control
 Medical management of AF: drugs for rate and rhythm control Adel Khalifa Sultan Hamad, BMS, MD, FGHRS, FRCP(Canada) Consultant Cardiologist & Interventional Cardiac Electrophysiologist Head of Electrophysiology
Medical management of AF: drugs for rate and rhythm control Adel Khalifa Sultan Hamad, BMS, MD, FGHRS, FRCP(Canada) Consultant Cardiologist & Interventional Cardiac Electrophysiologist Head of Electrophysiology
When choosing an antiepileptic ... PRESENTATION... Pharmacokinetics of the New Antiepileptic Drugs. Based on a presentation by Barry E.
 ... PRESENTATION... Pharmacokinetics of the New Antiepileptic Drugs Based on a presentation by Barry E. Gidal, PharmD Presentation Summary A physician s choice of an antiepileptic drug (AED) usually depends
... PRESENTATION... Pharmacokinetics of the New Antiepileptic Drugs Based on a presentation by Barry E. Gidal, PharmD Presentation Summary A physician s choice of an antiepileptic drug (AED) usually depends
Cardiac Drugs: Chapter 9 Worksheet Cardiac Agents. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate.
 Complete the following. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate. 2. drugs affect the force of contraction and can be either positive or negative. 3.
Complete the following. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate. 2. drugs affect the force of contraction and can be either positive or negative. 3.
Geriatric Pharmacology
 Geriatric Pharmacology Janice Scheufler R.Ph.,PharmD, FASCP Clinical Pharmacist Hospice of the Western Reserve Objectives List three risk factors for adverse drug events in the elderly Discuss two physiological
Geriatric Pharmacology Janice Scheufler R.Ph.,PharmD, FASCP Clinical Pharmacist Hospice of the Western Reserve Objectives List three risk factors for adverse drug events in the elderly Discuss two physiological
AMIODARONE and DESETHYLAMIODARONE IN PLASMA BY UV FAST CODE Z33610
 AMIODARONE and DESETHYLAMIODARONE IN PLASMA BY UV FAST CODE Z6 INTRODUCTION Amiodarone is an antiarrhythmic agent used for various types of tachyarrhythmias, both ventricular and supraventricular arrhythmias.
AMIODARONE and DESETHYLAMIODARONE IN PLASMA BY UV FAST CODE Z6 INTRODUCTION Amiodarone is an antiarrhythmic agent used for various types of tachyarrhythmias, both ventricular and supraventricular arrhythmias.
DIAGNOSIS AND MANAGEMENT OF DIURETIC RESISTANCE. Jules B. Puschett, M.D.
 DIAGNOSIS AND MANAGEMENT OF DIURETIC RESISTANCE Jules B. Puschett, M.D. Diuretic Resistance A clinical circumstance in which patients do not respond to a combination of salt restriction and even large
DIAGNOSIS AND MANAGEMENT OF DIURETIC RESISTANCE Jules B. Puschett, M.D. Diuretic Resistance A clinical circumstance in which patients do not respond to a combination of salt restriction and even large
complicating myocardial infarction
 British Heart Journal, I970, 32, 21. Bretylium tosylate in treatment of refractory ventricular arrhythmias complicating myocardial infarction G. Terry,1 C. W. Vellani, M. R. Higgins, and A. Doig From the
British Heart Journal, I970, 32, 21. Bretylium tosylate in treatment of refractory ventricular arrhythmias complicating myocardial infarction G. Terry,1 C. W. Vellani, M. R. Higgins, and A. Doig From the
Atrial Fibrillation and Common Supraventricular Tachycardias. Sunil Kapur MD
 Atrial Fibrillation and Common Supraventricular Tachycardias Sunil Kapur MD Cardiac Electrophysiology Brigham and Women s Hospital Instructor, Harvard Medical School No disclosures Cardiac Conduction:
Atrial Fibrillation and Common Supraventricular Tachycardias Sunil Kapur MD Cardiac Electrophysiology Brigham and Women s Hospital Instructor, Harvard Medical School No disclosures Cardiac Conduction:
Antiarrhythmic Pharmacology. The Electronics
 Antiarrhythmic Pharmacology Linking Pharmacological Treatment to the Patient and the Rhythm Presented By: Karen Marzlin BSN, RN,C, CCRN-CMC CNEA 2009 1 The Electronics Action Potential of Cardiac Cells
Antiarrhythmic Pharmacology Linking Pharmacological Treatment to the Patient and the Rhythm Presented By: Karen Marzlin BSN, RN,C, CCRN-CMC CNEA 2009 1 The Electronics Action Potential of Cardiac Cells
Name: UFID: PHA Exam 2. Spring 2013
 PHA 5128 Exam 2 Spring 2013 1 Carbamazepine (5 points) 2 Theophylline (10 points) 3 Gentamicin (10 points) 4 Drug-drug interaction (5 points) 5 Lidocaine (5 points) 6 Cyclosporine (5 points) 7 Phenobarbital
PHA 5128 Exam 2 Spring 2013 1 Carbamazepine (5 points) 2 Theophylline (10 points) 3 Gentamicin (10 points) 4 Drug-drug interaction (5 points) 5 Lidocaine (5 points) 6 Cyclosporine (5 points) 7 Phenobarbital
How do arrhythmias occur?
 How do arrhythmias occur? An arrhythmia is an abnormal heart rhythm (= dysrhythmia). Can be fast (tachy) or slow (brady). Brady arrhythmias are usually due to conduc;on block, while tachyarrhythmias are
How do arrhythmias occur? An arrhythmia is an abnormal heart rhythm (= dysrhythmia). Can be fast (tachy) or slow (brady). Brady arrhythmias are usually due to conduc;on block, while tachyarrhythmias are
Prescribing Drugs to the Elderly
 Answers to your questions from University of Toronto experts Prescribing Drugs to the Elderly Can drugs do more harm than good? M.A. is a 90-year-old man living at home. He has dementia and due to wandering
Answers to your questions from University of Toronto experts Prescribing Drugs to the Elderly Can drugs do more harm than good? M.A. is a 90-year-old man living at home. He has dementia and due to wandering
Rational Dose Prediction. Pharmacology. φαρμακον. What does this mean? pharmakon. Medicine Poison Magic Spell
 1 Rational Dose Prediction Nick Holford Dept Pharmacology & Clinical Pharmacology University of Auckland, New Zealand 2 Pharmacology Pharmacology is derived from a Greek word (pharmakon). The Greeks used
1 Rational Dose Prediction Nick Holford Dept Pharmacology & Clinical Pharmacology University of Auckland, New Zealand 2 Pharmacology Pharmacology is derived from a Greek word (pharmakon). The Greeks used
ELECTRICAL SIGNALS CONTROL THE CARDIAC ACTIVITY
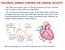 ELECTRICAL SIGNALS CONTROL THE CARDIAC ACTIVITY The heart beat begins when an electrical impulse from the sinoatrial node (SA node or sinus node) moves through it. The normal electrical sequence begins
ELECTRICAL SIGNALS CONTROL THE CARDIAC ACTIVITY The heart beat begins when an electrical impulse from the sinoatrial node (SA node or sinus node) moves through it. The normal electrical sequence begins
Management of ATRIAL FIBRILLATION. in general practice. 22 BPJ Issue 39
 Management of ATRIAL FIBRILLATION in general practice 22 BPJ Issue 39 What is atrial fibrillation? Atrial fibrillation (AF) is the most common cardiac arrhythmia encountered in primary care. It is often
Management of ATRIAL FIBRILLATION in general practice 22 BPJ Issue 39 What is atrial fibrillation? Atrial fibrillation (AF) is the most common cardiac arrhythmia encountered in primary care. It is often
Nontraditional PharmD Program PRDO 7700 Pharmacokinetics Review Self-Assessment
 Nontraditional PharmD Program PRDO 7700 Pharmacokinetics Review Self-Assessment Please consider the following questions. If you do not feel confident about the material being covered, then it is recommended
Nontraditional PharmD Program PRDO 7700 Pharmacokinetics Review Self-Assessment Please consider the following questions. If you do not feel confident about the material being covered, then it is recommended
Pharmacotherapy of Antiarrhythmias
 Pharmacotherapy of Antiarrhythmias Edward JN Ishac, Ph.D. Smith Building, Room 72 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth
Pharmacotherapy of Antiarrhythmias Edward JN Ishac, Ph.D. Smith Building, Room 72 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth
The role of medication in falls risk
 The role of medication in falls risk Patrick A. Ball, Foundation Professor of Rural Pharmacy, Charles Sturt University, Wagga Wagga Lecture outline The aged are not created equal Insidious nature of onset
The role of medication in falls risk Patrick A. Ball, Foundation Professor of Rural Pharmacy, Charles Sturt University, Wagga Wagga Lecture outline The aged are not created equal Insidious nature of onset
Polypharmacy - arrhythmic risks in patients with heart failure
 Influencing sudden cardiac death by pharmacotherapy Polypharmacy - arrhythmic risks in patients with heart failure Professor Dan Atar Head, Dept. of Cardiology Oslo University Hospital Ullevål Norway 27.8.2012
Influencing sudden cardiac death by pharmacotherapy Polypharmacy - arrhythmic risks in patients with heart failure Professor Dan Atar Head, Dept. of Cardiology Oslo University Hospital Ullevål Norway 27.8.2012
A prospective study of the clarithromycin digoxin interaction in elderly patients
 Journal of Antimicrobial Chemotherapy (2002) 50, 601 606 DOI: 10.1093/jac/dkf176 A prospective study of the clarithromycin digoxin interaction in elderly patients P. Zapater 1 *, S. Reus 2, A. Tello 2,
Journal of Antimicrobial Chemotherapy (2002) 50, 601 606 DOI: 10.1093/jac/dkf176 A prospective study of the clarithromycin digoxin interaction in elderly patients P. Zapater 1 *, S. Reus 2, A. Tello 2,
There s A Pill For That (But should my patient be on it?) A Review of Tools for the Evaluation of Optimal Prescribing in Geriatric Patients
 There s A Pill For That (But should my patient be on it?) A Review of Tools for the Evaluation of Optimal Prescribing in Geriatric Patients Marilyn N. Bulloch, PharmD, BCPS Assistant Clinical Professor
There s A Pill For That (But should my patient be on it?) A Review of Tools for the Evaluation of Optimal Prescribing in Geriatric Patients Marilyn N. Bulloch, PharmD, BCPS Assistant Clinical Professor
Tamer Barakat. Abdul Aziz ALShamali. Abdul Aziz ALShamali
 10 Tamer Barakat Abdul Aziz ALShamali Abdul Aziz ALShamali Dr. Alia Elimination: Refampin is used to treat TB not malaria (Quinacrine is used for malaria) It s the opposite process of absorption. It's
10 Tamer Barakat Abdul Aziz ALShamali Abdul Aziz ALShamali Dr. Alia Elimination: Refampin is used to treat TB not malaria (Quinacrine is used for malaria) It s the opposite process of absorption. It's
Bassett Healthcare Clinical Laboratory
 Therapeutic Drug Level Collection Guidelines Anti-epileptic drugs (carbamazepine, phenobarbital, phenytoin, primidone, valproic acid) Consider collecting after steady state conditions are reached, i.e.
Therapeutic Drug Level Collection Guidelines Anti-epileptic drugs (carbamazepine, phenobarbital, phenytoin, primidone, valproic acid) Consider collecting after steady state conditions are reached, i.e.
Chapter (9) Calcium Antagonists
 Chapter (9) Calcium Antagonists (CALCIUM CHANNEL BLOCKERS) Classification Mechanism of Anti-ischemic Actions Indications Drug Interaction with Verapamil Contraindications Adverse Effects Treatment of Drug
Chapter (9) Calcium Antagonists (CALCIUM CHANNEL BLOCKERS) Classification Mechanism of Anti-ischemic Actions Indications Drug Interaction with Verapamil Contraindications Adverse Effects Treatment of Drug
Basic Biopharmaceutics, Pharmacokinetics, and Pharmacodynamics
 Basic Biopharmaceutics, Pharmacokinetics, and Pharmacodynamics Learning Outcomes Define biopharmaceutics Describe 4 processes of pharmacokinetics Describe factors that affect medication absorption Describe
Basic Biopharmaceutics, Pharmacokinetics, and Pharmacodynamics Learning Outcomes Define biopharmaceutics Describe 4 processes of pharmacokinetics Describe factors that affect medication absorption Describe
Renal Excretion of Drugs
 Renal Excretion of Drugs 3 1 Objectives : 1 Identify main and minor routes of Excretion including renal elimination and biliary excretion 2 Describe its consequences on duration of drugs. For better understanding:
Renal Excretion of Drugs 3 1 Objectives : 1 Identify main and minor routes of Excretion including renal elimination and biliary excretion 2 Describe its consequences on duration of drugs. For better understanding:
CVD: Cardiac Arrhythmias. 1. Final Cardiac Arrhythmias_BMP. 1.1 Cardiovascular Disease. Notes:
 CVD: Cardiac Arrhythmias 1. Final Cardiac Arrhythmias_BMP 1.1 Cardiovascular Disease 1.2 Directions for taking this course 1.3 Content Experts 1.4 Disclosures 1.5 Accreditation Information 1.6 Learning
CVD: Cardiac Arrhythmias 1. Final Cardiac Arrhythmias_BMP 1.1 Cardiovascular Disease 1.2 Directions for taking this course 1.3 Content Experts 1.4 Disclosures 1.5 Accreditation Information 1.6 Learning
Potential Drug Dosing Variability in Women. Jim Beaulieu, PharmD Senior Clinical Pharmacist Specialist Rhode Island Hospital and The Miriam Hospital
 Potential Drug Dosing Variability in Women Jim Beaulieu, PharmD Senior Clinical Pharmacist Specialist Rhode Island Hospital and The Miriam Hospital 2 Objectives Understand the pharmacokinetic variability
Potential Drug Dosing Variability in Women Jim Beaulieu, PharmD Senior Clinical Pharmacist Specialist Rhode Island Hospital and The Miriam Hospital 2 Objectives Understand the pharmacokinetic variability
Cost and Prevalence of A fib. Atrial Fibrillation: Guideline Directed Treatment. Prevalence of A Fib. Risk Factors for A Fib. Risk Factors for A Fib
 Atrial Fibrillation: Guideline Directed Treatment Melissa Wendell, FNP-C, MSN Heart Failure - Lead Nurse Practitioner, Aspirus Wausau Hospital and Aspirus Cardiology Cost and Prevalence of A fib 33.5 million
Atrial Fibrillation: Guideline Directed Treatment Melissa Wendell, FNP-C, MSN Heart Failure - Lead Nurse Practitioner, Aspirus Wausau Hospital and Aspirus Cardiology Cost and Prevalence of A fib 33.5 million
Metformin Associated Lactic Acidosis. Jun-Ki Park 9/6/11
 Metformin Associated Lactic Acidosis Jun-Ki Park 9/6/11 Probably the most common mechanism by which metformin elevates blood lactate is by inducing catecholamine release in those who regulate or prescribe
Metformin Associated Lactic Acidosis Jun-Ki Park 9/6/11 Probably the most common mechanism by which metformin elevates blood lactate is by inducing catecholamine release in those who regulate or prescribe
