Pharmacotherapy of Antiarrhythmias
|
|
|
- Janis McCormick
- 6 years ago
- Views:
Transcription
1 Pharmacotherapy of Antiarrhythmias Edward JN Ishac, Ph.D. Smith Building, Room Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth University Richmond, Virginia, USA Agents used in HT, CHF, Arrhythmia and Angina Drug Class Hypertension HF Arrhyth mia Angina Contraindications/Cautions/Notes Beta-Blockers aaa a aaa aaa aaa a HF (CI: unstable HF, bronchospasm, significant bradycardia, depression); Raynaud D. Caution in diabetes, asthma (use β1-) Ca++-Channel blockers aaa a aaa a aaa a HF, constipation, gingival hyperplasia, edema, reflex tachycardia ACEI / ARBs aaa a aaa a Angioedema, hyperkalemia, cough (acei), tetrogenic, glossitis, taste Diuretics (Thiazides) aaa a aaa a GFR >30, hypokalemia (CG); Ca++, diabetes (glucose tolerance) Cardiac glycosides aa a Many Rx interactions, [K+], use HF important, low K+ toxicity, Vasodilators aaa aa Flushing, dizziness, headache, nausea, reflex tachycardia Na+-Channel blockers aaa a Effects enhanced in depolarized, damaged tissue, Phase 0, CV Nitrates aa aaa a NO/cGMP, tolerance (off periods), flushing, dizziness, headache, reflex tachycardia, many forms 1
2 Can't see the forest for the trees Hung up on the detail, you can not see the big picture can't see the trees for the forest overawed by the size of a problem that he/she can't work out Park in Portland, Maine Heart Physiology Closed system Supply nutrients/o 2 Pressure driven Remove metabolites 2
3 Heart Physiology P QRS PR T QT - atria depolarization - ventricle depolarization - conduction A-V - ventricle repolarization - duration ventricle of repolarization Heart Physiology Closed system Pressure driven Supply nutrients/o 2 Remove metabolites P - atria depol. QRS - ventricle depol. PR - conduction A-V T - ventricle repol. QT - duration ventricle repolarization 3
4 Review of Physiology The response of excitable cells to electrical stimulation is a function of # of available Na channels (an index is dv/dt or Phase 0) Steady membrane depolarization decreases Na current, dv/dt and conduction velocity Abnormal heart tissue is usually depolarized Na channel availability results from Na channels being in different states Effect of drugs on # channels available and recovery time constant depends on the resting membrane potential What this means: 1. Conduction in damaged/abnormal heart tissue is decreased 2. Antidysrhythmics will work better on Na channels in depolarized cells, and slow their recovery from excitation
5 Na Channel States Characteristics of Dysrhythmias Definitions: - normal sinus rhythm (60-100bpm), SA node pacemaker - arrhythmia; any abnormality of firing rate, regularity or site of origin of cardiac impulse or disturbance of conduction that alters the normal sequence of activity of atria and ventricles. Occurrence: - 80% of patients with acute myocardial infarctions - 50% of anaesthetized patients - about 25% of patients on digitalis 5
6 Classification of dysrhythmias 1. Characteristics: a. flutter very rapid but regular depolarization b. tachycardia increased rate c. bradycardia decreased rate d. fibrillation disorganized depolarization activity 2. Sites involved: a. ventricular b. atrial c. sinus d. AV node e. supraventricular (SVT, atrial myocardium or AV node) Examples of Arrhythmias 6
7 Ion Permeability mm Out In Na K Ca Na + i - open 1 Na + -close K + o - open/close 2 Ca ++ i - open K + o - leak Ca ++ -close K + o - open K + -close Na + /Ca ++ - exchange (3:1) Na + /K + - ATPase (3:2) Cardiac Action Potentials Ion Flow mm Out In Na K Ca O Na + i - open Na + -close K + o - open/close Ca ++ i - open K + o - leak 3 Ca ++ -close K + o - open K + -close Na + /Ca ++ - exchange (3:1) Na + /K + - ATPase (3:2) 7
8 Mechanisms of dysrhythmias 1. Abnormal impulse generation (abnormal automaticity) a. automaticity of normally automatic cells (SA, AV, His) b. generation of impulses in normally non-automatic cells - development of phase depolarization in normally non-automatic cells - triggered activity due to afterdepolarizations - early afterdepolarization - delayed afterdepolarization 2. Abnormal impulse conduction (more common mechanism) a. AV block ventricle free to start own pacemaker rhythm b. Re-entry: re-excitation around a conducting loop, which produces tachycardia - unidirectional conduction block - establishment of new loop of excitation - conduction time that outlasts refractory period Abnormal impulse generation: triggered activity : EADs and DADs Impulse conduction: Reentry 8
9 Unidirectional Block Damaged tissue is usually depolarized conduction velocity Strategies of Antidysrhythmic Agents Suppression of dysrhythmias A. Alter automaticity i. decrease slope of Phase depolarization ii. increase the threshold potential iii. decrease resting (maximum diastolic) potential O B. Alter conduction velocity i. mainly via decrease rate of rise of Phase 0 upstroke ii. decrease Phase slope iii. decrease membrane resting potential and responsiveness C. Alter the refractory period i. increase Phase 2 plateau ii. increase Phase 3 repolarization iii. increase action potential duration 9
10 Classification of Antidysrhythmic Drugs Vaughan-Williams classification (1970), subsequently modified by Harrison. Helpful, But? 1. based on electrophysiological actions in normal tissue 2. presumes a mechanism of action of antidysrhythmic drugs 3. consists of four main classes and three subclasses. does not include actions of other agents (ie. adenosine) Vaughan-Williams Classification Subclass IA. IB. IC. Class II Class III Class IV Others Mechanism Moderate Na block Ph.0; slow conduction; APD Minimal Na block Ph.0; slow conduction (less); shorten Ph.3 repolarization Marked Na block Ph.0; slow conduction; no change APD or repolarization. Increased suppression of Na channels Beta blockers; decrease adrenergic input. No major effect on APD, suppress Ph. depolarization Prolong repolarization/refractory period other means than exclusively ina block (mainly K + channel blockade). Ca channel blockers. Slow conduction and effective refractory period in normal tissue (A-V node) and Ca-dependent slow responses of depolarized tissue (atria, ventricle, Purkinje) Adenosine, Digoxin, Anticoagulants, ANS agents Prototype Quinidine Procainamide Lidocaine Phenytoin Flecainide Encainide Propranolol others Amiodarone Ibutilide Verapamil Diltiazem 10
11 Shortcomings: Vaughan-Williams system (V-W) 1. Based on response in normal tissue, not damaged. Hybrid: Class I, III & IV agents block ion channels, Class II block receptors. 2. Incomplete: eg. adenosine, digitalis, cholinergic agonists, alpha adrenergic blockers or agents that modulate gap junctions, ion pumps or exchangers. Also ignores drug metabolites. 3. Single class can effect multiple mechanisms. Amiodarone: properties of classes (I-IV).. Describes drugs that block ion channels/receptors and does not consider drugs that activate channels or receptors. 5. Does not incorporate variable mode of action: slowing tachycardias, terminating dysrhythmias, or preventing them. Amiodarone: Only Antiarrhythmic with All Four Vaughan-Williams Class Effects Class I effect Sodium channel blockade Class II effect Noncompetitive alpha- and beta-adrenergic adrenergic inhibition Na + Na + Na + Na + Na + Na + Na + Na + Ca ++ Ca ++ Ca++ ++ Ca ++ Ca ++ Ca ++ Ca ++ Ca ++ Class III effect Prolongation of repolarization and refractoriness by increased action potential duration Class IV effect Calcium channel blockade 11
12 Shortcomings: Vaughan-Williams system (V-W) 1. Based on response in normal tissue, not damaged. Hybrid: Class I, III & IV agents block ion channels, Class II block receptors. 2. Incomplete: eg. adenosine, digitalis, cholinergic agonists, alpha adrenergic blockers or agents that modulate gap junctions, ion pumps or exchangers. Also ignores drug metabolites. 3. Single class can effect multiple mechanisms. Amiodarone: properties of classes (I-IV).. Describes drugs that block ion channels/receptors and does not consider drugs that activate channels or receptors. 5. Does not incorporate variable mode of action: slowing tachycardias, terminating dysrhythmias, or preventing them. Drugs work better on depolarized tissue.. 12
13 Key Aspects of Drug Action and Therapy a. Drug action is state-dependent: channel open, closed, or inactivated). Two current models: i. modulated receptor hypothesis: different states have different affinities ii. guarded receptor hypothesis: channel gate limits drug access to site b. Drugs selectively affect firing and conduction in abnormal/depolarized cells. c. Transitions between states dependent on membrane voltage and cell firing frequency, membrane voltage and spike frequency. Binding to inactivated states and slowing recovery from inactivation, some drugs can increase the time needed for recovery from inactivation. Na Channel States Quinidine 1A: Open Lidocaine 1B: Open & Inactive In depolarized tissue 13
14 Key Aspects of Drug Action and Therapy D. Drugs affect different parts of the heart: Betablockers and CCBs used for SVT 1. Ca channel blockers (Class IV) are selective for A-V and S-A nodes, where Ca action potentials predominate. 2. Lidocaine (Class IB) has been useful for treating PVCs in Purkinje fibers, since longer APDs in Purkinje yield more inactivated Na channels. Lidocaine selectively blocks inactivated state and some open Na channels. Lidocaine has little effect, in contrast, on atrial tissue. 3. Quinidine affects both atrial and ventricular dysrhythmias (but has been mostly used to treat atrial fibrillation). Quinidine (Class IA prototype) Other examples: Procainamide, Disopyrimide 1. General properties: a. D-isomer of quinine b. As with most of the Class I agents - moderate block of sodium channels - decreases automaticity of pacemaker cells - increases effective refractory period/ap duration 1
15 Cardiac effects Actions of Quinidine a. automaticity, conduction velocity and excitability of cardiac cells. b. Preferentially blocks open Na channels c. Recovery from block slow in depolarized tissue; lengthens refractory period (RP) d. All effects are potentiated in depolarized tissues e. Increases action potential duration (APD) and prolongs AP repolarization via block of K channels; decreases reentry f. Indirect action: anticholinergic effect (accelerates heart), which can speed A-V conduction. Actions & Toxicity of Quinidine Extracardiac a. Blocks alpha-adrenoreceptors to yield vasodilatation. b. Other strong antimuscarinic actions Toxicity - "Quinidine syncope"(fainting)- due to disorganized ventricular tachycardia - associated with greatly lengthened Q-T interval; can lead to Torsades de Pointes (VT, precursor to ventricular fibrillation) - negative inotropic action (decreases contractility) - GI - diarrhea, nausea, vomiting - CNS effects - headaches, dizziness, tinnitus (quinidine Cinchonism ) Prolonged QT interval Torsades de pointes "twisting of the points" 15
16 Quinidine: Pharmacokinetics/therapeutics a. Oral, rapidly absorbed, 80% bound to membrane proteins b. Hydroxylated in liver; T 1/2 = 6-8 h c. Drug interaction: displaces digoxin from plasma binding sites; so avoid giving drugs together or reduce dose d. Probably are active metabolites of quinidine e. Effective in treatment of nearly all dysrhythmias, including: 1) Premature atrial contractions 2) Paroxysmal atrial fibrillation and flutter 3) Intra-atrial and A-V nodal reentrant dysrhythmias ) Wolff-Parkinson-White tachycardias (SVT, A-V bypass) 5) Premature ventricular contractions (PVCs) f. Useful in treating chronic dysrhythmias requiring outpatient treatment Procainamide (Class 1A) also Disopyrimide Cardiac effects a Similar to quinidine, less muscarinic & alpha-adrenergic blockade b. Has negative inotropic action also Extracardiac effects a. Ganglionic blocking reduces peripheral vascular resistance Toxicity a. Cardiac: Similar to quinidine; cardiac depression b. Noncardiac: Syndrome resembling lupus erythematosus Pharmacokinetics/therapeutics a. Administered orally, i-v b. Major metabolite in liver is N-acetylprocainamide (NAPA), a weak Na channel blocker with class III activity. Bimodal distribution in population of rapid acetylators, who can accumulate high levels of NAPA. c. T 1/2 = 3- hours; necessitates frequent dosing; kidney chief elimination path. NAPA has longer T 1/2 and can accumulate d. Usually used short-term. Commonly used in CCUs for ventricular dysrhythmias associated with acute myocardial infarctions (MI) 16
17 Lidocaine (Class IB prototype) Other examples: Mexiletine, Phenytoin, Tocainide General a. Commonly used antidysrhythmic agent in emergency care (decreasing use) b. Given i-v; widely used in ICU-critical care units (old DOC, prior 2001) c. Low toxicity (especially cardiac, good therapeutic index) d. A local anesthetic, works on nerve at higher doses Lidocaine Actions Cardiac effects a. Generally decreases APD, hastens AP repolarization, decreases automaticity and increases refractory period in depolarized cells. b. Exclusively acts on Na channels in depolarized tissue by blocking open and inactivated (mainly) Na channels c. Potent suppresser of abnormal activity d. Most Na channels of normal cells rapidly unblock from lidocaine during diastole; few electrophysiological effects in normal tissue Toxicity: - least cardiotoxic, high dose can lead to hypotension - tremors, nausea, slurred speech, convulsions Pharmacokinetics/therapy a. i-v, since extensive first pass hepatic metabolism b. T 1/2 = 0.5- hours c. Effective in suppressing dysrhythmia associated with depol. tissue (ischemia; digitalis toxicity); ineffective against dysrhythmias in normal tissue (atrial flutter). d. Suppresses ventricular tachycardia; prevents fibrillation after acute MI; rarely used in supraventricular dysrhythmias 17
18 Phenytoin (Class IB) 1. Non-sedative anticonvulsant used in treating epilepsy ('Dilantin') 2. Limited efficacy as antidysrhythmic (second line antiarrythmic) 3. Suppresses ectopic activation by blocking Na and Ca channels. Especially effective against digitalis-induced dysrhythmias 5. T 1/2 = 2 hr metabolized in liver 6. Gingival hyperplasia (0%) Gingival Hyperplasia Phenytoin (Dilantin) anticonvulsant (0%) Calcium blockers especially nifedipine (<10%) Cyclosporine immunosuppressant (30%) 18
19 Flecainide (Class IC prototype) Other examples: Lorcainide, Propafenone, Indecainide, Moricizine Depress rate of rise of AP without change in refractoriness or APD 1. Decreases automaticity, conduction in depolarized cells. 2. Marked block of open Na channels (decreases Ph. 0); no change repolarization. 3. Used primarily for ventricular dysrhythmias but effective for atrial too. No antimuscarinic action 5. Suppresses premature ventricular contractions (PVCs) 6. Associated with significant mortality; thus, use limited to last resort applications like treating ventricular tachycardias 7. Significant negative inotropic effect Propranolol (Class II, beta-adrenoreceptor blockers) Other agents: Metoprolol, Esmolol (short acting), Sotalol (also Class III), Acebutolol a. Slow A-V conduction b. Prolong A-V refractory period c. Suppress automaticity Cardiac effects (of propranolol), a non-selective beta blocker a. Main mechanism of action is block of beta receptors; Ph slope. which decreases automaticity under certain conditions b. Some direct local anesthetic effect by block of Na channels (membrane stabilization) at higher doses c. Increases refractory period in depolarized tissues d. Increases A-V nodal refractory period Non-cardiac: Hypotension Therapeutics a. Blocks abnormal pacemakers in cells receiving excess catecholamines (e.g. pheochromocytoma) or up-regulated beta-receptors (ie. hyperthyroidism) b. Blocks A-V nodal reentrant tachycardias; inhibits ectopic foci c. Beta-blockers are used to treat supraventricular tachydysrhythmias d. Propranolol contraindicated in ventricular failure; can lead to A-V block. Oral (propranolol) or IV. Extensive metabolism in liver. 19
20 Cardiac Action Potentials Ion Flow mm Out In Na K Ca O Na + i - open Na + -close K + o - open/close Ca ++ i - open K + o - leak 3 Ca ++ -close K + o - open K + -close Na + /Ca ++ - exchange (3:1) Na + /K + - ATPase (3:2) Beta-Adenoceptor Antagonists 20
21 Clinical uses: Beta-Blockers Hypertension: frontline agents Angina (non-selective or β1-selective) - Cardiac: O 2 demand more than O 2 supply - Exercise tolerance in angina patients Arrhythmia (β1-selective, LA-action) - SNS-induced increases in conductivity and automaticity Glaucoma (non-selective) - aqueous humor formation (Timolol) Congestive Heart Failure (non-selective or β1-selective) - CI: unstable CHF, bronchospasm, depression, bradycardia Other - block of tremor of peripheral origin (β2-ar in skeletal muscle) - migraine prophylaxis (mechanism unknown) - hyperthyroidism: cardiac manifestation (only propranolol) - panic attacks, stage fright Clinical use Beta-blockers Class/Drug HT Angina Arrh MI HF Comments Non-selective β 1 /β 2 Carteolol ISA; long acting; also for glaucoma Carvedilol α-blocking activity Labetalol ISA; α-blocking activity Nadolol long acting Penbutolol ISA Pindolol ISA; MSA Propranolol MSA; prototypical beta-blocker Sotalol also K-channel blocker Timolol primarily used for glaucoma β 1 -selective Acebutolol ISA Atenolol Betaxolol MSA Bisoprolol Esmolol short acting; operative arrhythmia Metoprolol MSA 21
22 β-blockers: Untoward Effects, Cautions Supersensitivity: Rebound effect with β-blockers, less with β-blockers with partial agonist activity (ie. pindolol). Gradual withdrawal Asthma: Blockade of pulmonary β2-receptors leads to increase in airway resistance. β1-selective agents preferred Diabetes: Compensatory hyperglycemic effect of EPI in insulin-induced hypoglycemia is removed by block of β2-ars in liver. β1-selective agents preferred Raynaud D: Decreased peripheral circulation Elderly: Effectiveness is decreased, more CNS effects (ie. depression) Amiodarone (Class III) others: Ibutilide, Bretylium, Sotalol, Dofetilide Dronedarone (Jul 2009) General a. New DOC for ventricular dysrhythmias (Lidocaine, old DOC) b. prolongs refractory period by blocking potassium channels c. also member of Classes IA,II,III,IV since blocks Na, K, Ca channels and alpha and beta adrenergic receptors d. serious side effects (cardiac depression, pulmonary fibrosis, thyroid) e. effective against atrial, A-V and ventricular dysrhythmias f. widely used, very long acting (>25 d) 22
23 AHA Guidelines for VT/VF Amiodarone 2. Procainamide, [Bretylium] 3. Sotalol. Lidocaine AHA Guideline Prior to Lidocaine 2. Procainamide 3. Bretylium. Electrical cardioversion Cardiac effects of Amiodarone a. Block Na channels (1A), but low affinity for open channels; mainly blocks inactivated Na channels b. Block is most pronounced in tissues with long action potentials c. Weak Ca channel blocker also (Class IV activity) d. A powerful inhibitor of abnormal automaticity, decreases conduction, increases refractory period and APD. e. Has antianginal effects (blocks alpha/beta receptors and Ca channels) Extracardiac effects: Vasodilation via block of Ca channels and alpha receptors 23
24 Adverse effects: Amiodarone A. Cardiac i. Sinus bradycardia, increase QT interval risk TdP ii. Negative inotropic action due to block of Ca channels and beta receptors; but can improve heart failure via vasodilation. iii. A-V block, paradoxical VTs. B. Non-cardiac: i. Deposits into almost every organ ii. Reduces clearance of drugs like procainamide, flecainide, digitalis, quinidine and diltiazem. iii. Thyroid dysfunction (hypo or hyperthyroidism) iv. Pulmonary fibrosis is most serious adverse effect v. Paresthesias (tingling, pricking, or numbness) vi. Photosensitivity Prolonged QT interval vii. Corneal microdeposits and blurred vision viii. Ataxia, dizziness, tremor ix. Anorexia, nausea Pulmonary fibrosis 2
25 Amiodarone: Pharmacokinetics and therapeutics Dronedarone ~ 2 hr T 1/2 = days (weeks) very long for one dose; very lipid soluble; metabolized in liver Effective against many arrythmias: atrial, A-V and ventricular dysrhythmias; prevention of atrial fibrillation/flutter; PVCs, nonsustained & sustained VTs. Multiple interactions with other drugs such as: i. Amiodarone is a CYP3A substrate and inhibitor and thus may enhance the effect of other CYP3A substrates eg. Warfarin, Simvastatin, Verapamil ii. Amiodarone may increase the serum concentration of Cardiac Glycosides Bretylium (Class III, K + channel blockers) Others Amiodarone, Ibutilide, (Sotalol, also beta-blocker) General: originally used as an antihypertensive agent Cardiac effects a. Direct antidysrhythmic action b. Increases ventricular APD and increases refractory period; decreases automaticity c. Most pronounced action in ischemic cells having short APD d. Initially stimulates and then blocks neuronal catecholamine release from adrenergic nerve terminals e. Blocks cardiac K channels to increase APD Extracardiac effects: Hypotension (from block of NE release) Pharmacokinetics/therapeutics a. iv or intramuscular b. Excreted mainly by the kidney c. Usually for emergency use only: ventricular fibrillation when lidocaine and cardioversion therapy fail. Increases threshold for fibrillation. d. Decreases tachycardias and early extrasystoles by increasing effective refractory period Dwight Eisenhower 25
26 Ibutilide (Class III). 1. Prolongs cardiac action potential without additional effects. 2. Administered I-V. Most effective current agent to convert atrial fibrillation and flutter of recent onset to normal rhythm. Low incidence of Torsades de Pointes (TdP, about 2%), compared to other drugs. 3. More effective for flutter than fibrillation. Generally well tolerated Sotalol (Class III and Class II) 1. Non-selective beta blocker, 2. Increases AP duration, increase QT interval 3. Uses: dysrhythmias of supraventricular (very effective) & ventricular origin Verapamil (Class IV, Ca ++ channel blockers) Other example: Diltiazem - CCBs increasing use and importance a. Blocks active and inactivated Ca channels, prevents Ca entry b. More effective on depolarized tissue, tissue firing frequently or areas where activity dependent on Ca channels (SA node; A-V node) c. Increases A-V conduction time and refractory period; directly slows SA and A-V node automaticity d. suppresses oscillatory depolarizing after depolarizations due to digitalis e. Dihydropyridine CCBs are generally poor antiarrythmics 26
27 Ca ++ Channel Blockers - Actions Extracardiac a. Peripheral vasodilatation via effect on smooth muscle b. Used as antianginal / antihypertensive c. Hypotension may increase HR reflexively Toxicity a. Cardiac - Too negative inotropic for damaged heart, depresses contractility - Can produce complete A-V block b. Extracardiac - Hypotension - Constipation, nervousness - Gingival hyperplasia Pharmacokinetics/Therapeutics a. T 1/2 = 7h, metabolized by liver b. Oral administration; also available parenterally c. Caution for patients with liver disease d. Blocks reentrant supraventricular tachycardia ( A-V nodal reentrant tachycardia ), decreases atrial flutter and fibrillation e. Only moderately effective against ventricular arrhythmias Dysrhythmics - Others A. Adenosine: i.v. (15 secs), activates P1 purinergic receptors (A1) coupled to K channels, CV, refractory period. SVT. Flushing, hypotension, burning sensation B. Potassium ions (K+): Depress ectopic pacemakers - can depress CV reentrant dysrhythmia C. Digoxin: used to treat atrial flutter and fibrillation - AV node conduction (vagal stimulation) - myocardium refractory period - Purkinje fibers refractory period, conduction D. Magnesium: used to treat Torsades de Pointes E. Autonomic agents: used to treat A-V block - β-agonists (ie.epi), anticholinergics (ie. atropine) Anticoagulant therapy: - prevent formation of systemic emboli & stroke 27
28 Drug interactions involving antidysrhythmics A. These drugs must be used very carefully B. Sometimes interactions can be counter-intuitive Problems with selecting drugs: A. Do not always know the cause of the dysrhythmia, thus what to treat? B. Multiple mechanisms of dysrhythmogenesis C. Drugs are both anti- and pro-dysrhythmias D. Drugs do not really fix the damage; usually they restore function by breaking something else Cardiac Effects of Antiarrhythmic Drugs Drug Class Auto CV RP APD ANS effects Quinidine IA M-block, α-block Procainamide IA M-block, α-block Disopyramide IA M-block, α-block Lidocaine IB 0 Tocainide IB 0 Mexiletine IB 0 Flecainide IC 0 Propafenone IC 0 Propranolol II β-block Metoprolol II β-block Esmolol II β-block Sotalol II/III β-block Amiodarone III α-, β-block Bretylium III 0 Sympatholytic Verapamil IV Digitalis Other vagal stimulation Adenosine Other More important agents 28
29 Pharmacokinetic Properties of Antiarrhythmic Drugs Drug Class Plasma Binding % T 1/2 (hrs) Drug Excretion Unchanged Quinidine IA % Procainamide IA 15 60% Disopyramide IA % Lidocaine IB 0 2 <10% Tocainide IB % Mexiletine IB % Flecainide IC % Propranolol II 90 <1% Metoprolol II 15 <5% Esmolol II (hydro. esterase) 9 min <1% Sotalol II/III 9 80% Amiodarone III 95 > 25 days <1% Bretylium III % Verapamil IV % Adenosine Misc (other) 15 sec 0% Dysrhythmia Treatment Treatment Acute vs Chronic Site Ventricular vs Supraventricular 29
30 Considerations for treating Dysrrhythmias 1. Acute vs chronic treatment 2. Ventricular vs supraventricular Supraventricular Ventricular Acute Adenosine Digoxin Amiodarone Procainamide Sotalol, Bretylium Lidocaine Chronic Beta-blocker Calcium antagonist Amiodarone Sotalol Flecainide Antiarrhythmics Question 1 When used as an antiarrhythmic agent, procainamide typically? a. increases cardiac contractility b. increases action potential duration c. increases AV conduction d. decreases QT interval e. decreases Na-channel recovery time 30
Antiarrhythmias. Edward JN Ishac, Ph.D. Smith Building, Room
 Antiarrhythmias Edward JN Ishac, Ph.D. Smith Building, Room 72 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth University Richmond,
Antiarrhythmias Edward JN Ishac, Ph.D. Smith Building, Room 72 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth University Richmond,
Mr. Eknath Kole M.S. Pharm (NIPER Mohali)
 M.S. Pharm (NIPER Mohali) Drug Class Actions Therapeutic Uses Pharmacokinetics Adverse Effects Other Quinidine IA -Binds to open and inactivated Na+ -Decreases the slope of Phase 4 spontaneous depolarization
M.S. Pharm (NIPER Mohali) Drug Class Actions Therapeutic Uses Pharmacokinetics Adverse Effects Other Quinidine IA -Binds to open and inactivated Na+ -Decreases the slope of Phase 4 spontaneous depolarization
Antiarrhythmic Drugs 1/31/2018 1
 Antiarrhythmic Drugs 1/31/2018 1 Normal conduction pathway: 1- SA node generates action potential and delivers it to the atria and the AV node 2- The AV node delivers the impulse to purkinje fibers Other
Antiarrhythmic Drugs 1/31/2018 1 Normal conduction pathway: 1- SA node generates action potential and delivers it to the atria and the AV node 2- The AV node delivers the impulse to purkinje fibers Other
Antiarrhythmic Drugs. Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2018
 Antiarrhythmic Drugs Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2018 2 Ion Permeability Changes Potential Changes Genes and Proteins 3 Cardiac Na+ channels 5 6
Antiarrhythmic Drugs Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2018 2 Ion Permeability Changes Potential Changes Genes and Proteins 3 Cardiac Na+ channels 5 6
Antiarrhythmic Drugs. Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2017
 Antiarrhythmic Drugs Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2017 Types of Cardiac Arrhythmias Abnormalities of Impulse Formation: Rate disturbances. Triggered
Antiarrhythmic Drugs Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2017 Types of Cardiac Arrhythmias Abnormalities of Impulse Formation: Rate disturbances. Triggered
B. 14 Antidysrhythmic drugs. a. Classify antidysrhythmics by their electrophysiological actions. Vaughan-Williams classification
 B. 14 Antidysrhythmic drugs a. Classify antidysrhythmics by their electrophysiological actions. Vaughan-Williams classification I II III IV membrane stabilizers all ERP, ERP/APD, all except c APD classified
B. 14 Antidysrhythmic drugs a. Classify antidysrhythmics by their electrophysiological actions. Vaughan-Williams classification I II III IV membrane stabilizers all ERP, ERP/APD, all except c APD classified
Arrhythmias. 1. beat too slowly (sinus bradycardia). Like in heart block
 Arrhythmias It is a simple-dysfunction caused by abnormalities in impulse formation and conduction in the myocardium. The heart is designed in such a way that allows it to generate from the SA node electrical
Arrhythmias It is a simple-dysfunction caused by abnormalities in impulse formation and conduction in the myocardium. The heart is designed in such a way that allows it to generate from the SA node electrical
PHARMACOLOGY OF ARRHYTHMIAS
 PHARMACOLOGY OF ARRHYTHMIAS Course: Integrated Therapeutics 1 Lecturer: Dr. E. Konorev Date: November 27, 2012 Materials on: Exam #5 Required reading: Katzung, Chapter 14 1 CARDIAC ARRHYTHMIAS Abnormalities
PHARMACOLOGY OF ARRHYTHMIAS Course: Integrated Therapeutics 1 Lecturer: Dr. E. Konorev Date: November 27, 2012 Materials on: Exam #5 Required reading: Katzung, Chapter 14 1 CARDIAC ARRHYTHMIAS Abnormalities
Chapter 14. Agents used in Cardiac Arrhythmias
 Chapter 14 Agents used in Cardiac Arrhythmias Cardiac arrhythmia Approximately 50% of post-myocardial infarction fatalities result from ventricular tachycarida (VT) or ventricular fibrillation (VF). These
Chapter 14 Agents used in Cardiac Arrhythmias Cardiac arrhythmia Approximately 50% of post-myocardial infarction fatalities result from ventricular tachycarida (VT) or ventricular fibrillation (VF). These
Arrhythmias. Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium.
 Arrhythmias Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium. However, in clinic it present as a complex family of disorders that show variety of symptoms, for
Arrhythmias Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium. However, in clinic it present as a complex family of disorders that show variety of symptoms, for
Antiarrhythmic Drugs
 Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Chapter 9. Learning Objectives. Learning Objectives 9/11/2012. Cardiac Arrhythmias. Define electrical therapy
 Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Pharmacology of the Sympathetic Nervous System II
 Pharmacology of the Sympathetic Nervous System II Edward JN Ishac, Ph.D. Professor Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia
Pharmacology of the Sympathetic Nervous System II Edward JN Ishac, Ph.D. Professor Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia
Chapter 26. Media Directory. Dysrhythmias. Diagnosis/Treatment of Dysrhythmias. Frequency in Population Difficult to Predict
 Chapter 26 Drugs for Dysrythmias Slide 33 Slide 35 Media Directory Propranolol Animation Amiodarone Animation Upper Saddle River, New Jersey 07458 All rights reserved. Dysrhythmias Abnormalities of electrical
Chapter 26 Drugs for Dysrythmias Slide 33 Slide 35 Media Directory Propranolol Animation Amiodarone Animation Upper Saddle River, New Jersey 07458 All rights reserved. Dysrhythmias Abnormalities of electrical
ANTI - ARRHYTHMIC DRUGS
 ANTI - ARRHYTHMIC DRUGS CARDIAC ACTION POTENTIAL K Out Balance Ca in/k out Na in K Out GENERATION OF ARRHYTHMIAS Four mechanisms of arrhythmia generation; Increased normal automaticity Abnormal automaticity
ANTI - ARRHYTHMIC DRUGS CARDIAC ACTION POTENTIAL K Out Balance Ca in/k out Na in K Out GENERATION OF ARRHYTHMIAS Four mechanisms of arrhythmia generation; Increased normal automaticity Abnormal automaticity
Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014
 Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014 Financial disclosures Consultant Medtronic 3 reasons to evaluate and treat arrhythmias
Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014 Financial disclosures Consultant Medtronic 3 reasons to evaluate and treat arrhythmias
ELECTRICAL SIGNALS CONTROL THE CARDIAC ACTIVITY
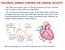 ELECTRICAL SIGNALS CONTROL THE CARDIAC ACTIVITY The heart beat begins when an electrical impulse from the sinoatrial node (SA node or sinus node) moves through it. The normal electrical sequence begins
ELECTRICAL SIGNALS CONTROL THE CARDIAC ACTIVITY The heart beat begins when an electrical impulse from the sinoatrial node (SA node or sinus node) moves through it. The normal electrical sequence begins
Dysrhythmias. Dysrythmias & Anti-Dysrhythmics. EKG Parameters. Dysrhythmias. Components of an ECG Wave. Dysrhythmias
 Dysrhythmias Dysrythmias & Anti-Dysrhythmics Rhythm bad in the heart: Whitewater rafting Electrical impulses coordinate heart Reduction in Cardiac Output PEA Asystole Components of an ECG Wave EKG Parameters
Dysrhythmias Dysrythmias & Anti-Dysrhythmics Rhythm bad in the heart: Whitewater rafting Electrical impulses coordinate heart Reduction in Cardiac Output PEA Asystole Components of an ECG Wave EKG Parameters
Antiarrhythmic Drugs Öner Süzer
 Antiarrhythmic Drugs Öner Süzer www.onersuzer.com osuzer@istanbul.edu.tr Last update: 09.11.2009 1 Süzer Farmakoloji 3. Baskı 2005 2 1 Süzer Farmakoloji 3. Baskı 2005 3 Figure 14 1 Schematic representation
Antiarrhythmic Drugs Öner Süzer www.onersuzer.com osuzer@istanbul.edu.tr Last update: 09.11.2009 1 Süzer Farmakoloji 3. Baskı 2005 2 1 Süzer Farmakoloji 3. Baskı 2005 3 Figure 14 1 Schematic representation
Use of Antiarrhythmic Drugs for AF Who, What and How? Dr. Marc Cheng Queen Elizabeth Hospital
 Use of Antiarrhythmic Drugs for AF Who, What and How? Dr. Marc Cheng Queen Elizabeth Hospital Content i. Rhythm versus Rate control ii. Anti-arrhythmic for Rhythm Control iii. Anti-arrhythmic for Rate
Use of Antiarrhythmic Drugs for AF Who, What and How? Dr. Marc Cheng Queen Elizabeth Hospital Content i. Rhythm versus Rate control ii. Anti-arrhythmic for Rhythm Control iii. Anti-arrhythmic for Rate
ARRHYTHMIA SINUS RHYTHM
 ARRHYTHMIA Dr. Ahmed A. Elberry, MBBCH, MSc, MD Assistant Professor of Clinical Pharmacy Faculty of pharmacy, KAU 1 SINUS RHYTHM SA node is cardiac pacemaker Normal sinus rhythm 60-100 beats/min Depolarisation
ARRHYTHMIA Dr. Ahmed A. Elberry, MBBCH, MSc, MD Assistant Professor of Clinical Pharmacy Faculty of pharmacy, KAU 1 SINUS RHYTHM SA node is cardiac pacemaker Normal sinus rhythm 60-100 beats/min Depolarisation
Pharmacotherapy of Angina Pectoris
 Pharmacotherapy of Angina Pectoris Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth
Pharmacotherapy of Angina Pectoris Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth
Antidysrhythmics HST-151 1
 HST-151 1 Antidysrhythmics I. Ventricular muscle cell action potential a. Phase 0: Upstroke b. Phase 1: Early-fast repolarization c. Phase 2: Plateau d. Phase 3: Repolarization e. Phase 4: Diastole HST-151
HST-151 1 Antidysrhythmics I. Ventricular muscle cell action potential a. Phase 0: Upstroke b. Phase 1: Early-fast repolarization c. Phase 2: Plateau d. Phase 3: Repolarization e. Phase 4: Diastole HST-151
Pediatrics ECG Monitoring. Pediatric Intensive Care Unit Emergency Division
 Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Pharmacotherapy of Angina Pectoris
 Pharmacotherapy of Angina Pectoris Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth
Pharmacotherapy of Angina Pectoris Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth
ANTI-ARRHYTHMICS AND WARFARIN. Dr Nithish Jayakumar
 ANTI-ARRHYTHMICS AND WARFARIN Dr Nithish Jayakumar Contents 1. Anti-arrhythmics Pacemaker and myocardial potentials Drug classes mechanisms; s/e; contra-indications Management of common arrhythmias 2.
ANTI-ARRHYTHMICS AND WARFARIN Dr Nithish Jayakumar Contents 1. Anti-arrhythmics Pacemaker and myocardial potentials Drug classes mechanisms; s/e; contra-indications Management of common arrhythmias 2.
Heart Failure (HF) Treatment
 Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
Atrial fibrillation in the ICU
 Atrial fibrillation in the ICU Atrial fibrillation Preexisting or incident (new onset) among nearly one in three critically ill patients Formation of arrhythogenic substrate usually fibrosis (CHF, hypertension,
Atrial fibrillation in the ICU Atrial fibrillation Preexisting or incident (new onset) among nearly one in three critically ill patients Formation of arrhythogenic substrate usually fibrosis (CHF, hypertension,
DRUG CLASSES BETA-ADRENOCEPTOR ANTAGONISTS (BETA-BLOCKERS)
 DRUG CLASSES BETA-ADRENOCEPTOR ANTAGONISTS (BETA-BLOCKERS) Beta-blockers have been widely used in the management of angina, certain tachyarrhythmias and heart failure, as well as in hypertension. Examples
DRUG CLASSES BETA-ADRENOCEPTOR ANTAGONISTS (BETA-BLOCKERS) Beta-blockers have been widely used in the management of angina, certain tachyarrhythmias and heart failure, as well as in hypertension. Examples
ARRHYTHMIAS IN THE ICU
 ARRHYTHMIAS IN THE ICU Nora Goldschlager, MD MACP, FACC, FAHA, FHRS SFGH Division of Cardiology UCSF IDENTIFIED VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar) Electrolyte imbalance Proarrhythmia
ARRHYTHMIAS IN THE ICU Nora Goldschlager, MD MACP, FACC, FAHA, FHRS SFGH Division of Cardiology UCSF IDENTIFIED VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar) Electrolyte imbalance Proarrhythmia
Antiarrhythmic Drugs Öner Süzer
 Antiarrhythmic Drugs Öner Süzer www.onersuzer.com osuzer@istanbul.edu.tr Last update: 13.01.2009 1 Süzer Farmakoloji 3. Baskı 2005 2 1 Süzer Farmakoloji 3. Baskı 2005 3 Figure 14 1 Schematic representation
Antiarrhythmic Drugs Öner Süzer www.onersuzer.com osuzer@istanbul.edu.tr Last update: 13.01.2009 1 Süzer Farmakoloji 3. Baskı 2005 2 1 Süzer Farmakoloji 3. Baskı 2005 3 Figure 14 1 Schematic representation
Drugs Controlling Myocyte Excitability and Conduction at the AV node Singh and Vaughan-Williams Classification
 Drugs Controlling Myocyte Excitability and Conduction at the AV node Singh and Vaughan-Williams Classification Class I Na Channel Blockers Flecainide Propafenone Class III K channel Blockers Dofetilide,
Drugs Controlling Myocyte Excitability and Conduction at the AV node Singh and Vaughan-Williams Classification Class I Na Channel Blockers Flecainide Propafenone Class III K channel Blockers Dofetilide,
ARRHYTHMIAS IN THE ICU: DIAGNOSIS AND PRINCIPLES OF MANAGEMENT
 ARRHYTHMIAS IN THE ICU: DIAGNOSIS AND PRINCIPLES OF MANAGEMENT Nora Goldschlager, M.D. MACP, FACC, FAHA, FHRS SFGH Division of Cardiogy UCSF CLINICAL VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar)
ARRHYTHMIAS IN THE ICU: DIAGNOSIS AND PRINCIPLES OF MANAGEMENT Nora Goldschlager, M.D. MACP, FACC, FAHA, FHRS SFGH Division of Cardiogy UCSF CLINICAL VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar)
! YOU NEED TO MONITOR QT INTERVALS IN THESE PATIENTS.
 Antiarrhythmic Pharmacopoeia Powerful drugs, split into 4 major classes, according to the predominant receptor they effect. Some fit into several classes at once, like sotolol. Some don t fit at all, owing
Antiarrhythmic Pharmacopoeia Powerful drugs, split into 4 major classes, according to the predominant receptor they effect. Some fit into several classes at once, like sotolol. Some don t fit at all, owing
Anti arrhythmic drugs. Hilal Al Saffar College of medicine Baghdad University
 Anti arrhythmic drugs Hilal Al Saffar College of medicine Baghdad University Mechanism of Arrhythmia Abnormal heart pulse formation Abnormal heart pulse conduction Classification of Arrhythmia Abnormal
Anti arrhythmic drugs Hilal Al Saffar College of medicine Baghdad University Mechanism of Arrhythmia Abnormal heart pulse formation Abnormal heart pulse conduction Classification of Arrhythmia Abnormal
DECLARATION OF CONFLICT OF INTEREST. Consultant Sanofi Biosense Webster Honorarium Boehringer Ingelheim St Jude Medical
 DECLARATION OF CONFLICT OF INTEREST Consultant Sanofi Biosense Webster Honorarium Boehringer Ingelheim St Jude Medical ESC Congress Paris, France August 27-31, 2011 Risk & Complications of AADs for Rhythm
DECLARATION OF CONFLICT OF INTEREST Consultant Sanofi Biosense Webster Honorarium Boehringer Ingelheim St Jude Medical ESC Congress Paris, France August 27-31, 2011 Risk & Complications of AADs for Rhythm
Pharmacology: Arrhythmias PC PHPP 515 (IT I) Fall JACOBS Wed, Dec. 03 4:00 5:50 PM
 Pharmacology: Arrhythmias PC PHPP 515 (IT I) Fall 2014 JACOBS Wed, Dec. 03 4:00 5:50 PM Required Reading (via Access Pharmacy) Katzung: Chapters 14 Recommended Reading (via Access Pharmacy) Goodman and
Pharmacology: Arrhythmias PC PHPP 515 (IT I) Fall 2014 JACOBS Wed, Dec. 03 4:00 5:50 PM Required Reading (via Access Pharmacy) Katzung: Chapters 14 Recommended Reading (via Access Pharmacy) Goodman and
Antihypertensive drugs SUMMARY Made by: Lama Shatat
 Antihypertensive drugs SUMMARY Made by: Lama Shatat Diuretic Thiazide diuretics The loop diuretics Potassium-sparing Diuretics *Hydrochlorothiazide *Chlorthalidone *Furosemide *Torsemide *Bumetanide Aldosterone
Antihypertensive drugs SUMMARY Made by: Lama Shatat Diuretic Thiazide diuretics The loop diuretics Potassium-sparing Diuretics *Hydrochlorothiazide *Chlorthalidone *Furosemide *Torsemide *Bumetanide Aldosterone
Dr. Vishaal Bhat. anti-adrenergic drugs
 Dr. Vishaal Bhat anti-adrenergic drugs Divisions of human nervous system Human Nervous system Central Nervous System Peripheral Nervous System Autonomic Nervous System Nervous system Includes neurons and
Dr. Vishaal Bhat anti-adrenergic drugs Divisions of human nervous system Human Nervous system Central Nervous System Peripheral Nervous System Autonomic Nervous System Nervous system Includes neurons and
Antiarrhythmic Pharmacology. The Electronics
 Antiarrhythmic Pharmacology Linking Pharmacological Treatment to the Patient and the Rhythm Presented By: Karen Marzlin BSN, RN,C, CCRN-CMC CNEA 2009 1 The Electronics Action Potential of Cardiac Cells
Antiarrhythmic Pharmacology Linking Pharmacological Treatment to the Patient and the Rhythm Presented By: Karen Marzlin BSN, RN,C, CCRN-CMC CNEA 2009 1 The Electronics Action Potential of Cardiac Cells
Atrial Fibrillation 10/2/2018. Depolarization & ECG. Atrial Fibrillation. Hemodynamic Consequences
 Depolarization & ECG Atrial Fibrillation How to make ORDER out of CHAOS Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Depolarization & ECG Depolarization & ECG Atrial Fibrillation Hemodynamic Consequences
Depolarization & ECG Atrial Fibrillation How to make ORDER out of CHAOS Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Depolarization & ECG Depolarization & ECG Atrial Fibrillation Hemodynamic Consequences
Cardiac Drugs: Chapter 9 Worksheet Cardiac Agents. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate.
 Complete the following. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate. 2. drugs affect the force of contraction and can be either positive or negative. 3.
Complete the following. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate. 2. drugs affect the force of contraction and can be either positive or negative. 3.
Chapter (9) Calcium Antagonists
 Chapter (9) Calcium Antagonists (CALCIUM CHANNEL BLOCKERS) Classification Mechanism of Anti-ischemic Actions Indications Drug Interaction with Verapamil Contraindications Adverse Effects Treatment of Drug
Chapter (9) Calcium Antagonists (CALCIUM CHANNEL BLOCKERS) Classification Mechanism of Anti-ischemic Actions Indications Drug Interaction with Verapamil Contraindications Adverse Effects Treatment of Drug
Fundamentals of Pharmacology for Veterinary Technicians Chapter 8
 Figure 8-1 Figure 8-2 Figure 8-3 Figure 8-4 Figure 8-5 Figure 8-7 Figure 8-8 Figure 8-9 TABLE 8-1 Blood Flow Through the Heart The right atrium receives blood from all tissues, except the lungs, through
Figure 8-1 Figure 8-2 Figure 8-3 Figure 8-4 Figure 8-5 Figure 8-7 Figure 8-8 Figure 8-9 TABLE 8-1 Blood Flow Through the Heart The right atrium receives blood from all tissues, except the lungs, through
2) Heart Arrhythmias 2 - Dr. Abdullah Sharif
 2) Heart Arrhythmias 2 - Dr. Abdullah Sharif Rhythms from the Sinus Node Sinus Tachycardia: HR > 100 b/m Causes: o Withdrawal of vagal tone & Sympathetic stimulation (exercise, fight or flight) o Fever
2) Heart Arrhythmias 2 - Dr. Abdullah Sharif Rhythms from the Sinus Node Sinus Tachycardia: HR > 100 b/m Causes: o Withdrawal of vagal tone & Sympathetic stimulation (exercise, fight or flight) o Fever
This document does not consider management of individual arrhythmias look elsewhere, e.g. OHCM.
 Cardiac arrhythmias This document does not consider management of individual arrhythmias look elsewhere, e.g. OHCM. Physiology Automaticity = ability of specialised cardiac conducting tissue to spontaneously
Cardiac arrhythmias This document does not consider management of individual arrhythmias look elsewhere, e.g. OHCM. Physiology Automaticity = ability of specialised cardiac conducting tissue to spontaneously
How do arrhythmias occur?
 How do arrhythmias occur? An arrhythmia is an abnormal heart rhythm (= dysrhythmia). Can be fast (tachy) or slow (brady). Brady arrhythmias are usually due to conduc;on block, while tachyarrhythmias are
How do arrhythmias occur? An arrhythmia is an abnormal heart rhythm (= dysrhythmia). Can be fast (tachy) or slow (brady). Brady arrhythmias are usually due to conduc;on block, while tachyarrhythmias are
Drugs Used in Heart Failure. Assistant Prof. Dr. Najlaa Saadi PhD pharmacology Faculty of Pharmacy University of Philadelphia
 Drugs Used in Heart Failure Assistant Prof. Dr. Najlaa Saadi PhD pharmacology Faculty of Pharmacy University of Philadelphia Heart Failure Heart failure (HF), occurs when cardiac output is inadequate to
Drugs Used in Heart Failure Assistant Prof. Dr. Najlaa Saadi PhD pharmacology Faculty of Pharmacy University of Philadelphia Heart Failure Heart failure (HF), occurs when cardiac output is inadequate to
Alaska Nurse Practitioner Annual Conference 2009
 Alaska Nurse Practitioner Annual Conference 2009 LAURIE RACENET, RN, MSN, ANP, CEPS, CCDS Alaska Heart Institute Member: Boston Scientific Allied Professional Advisory Board Participant in Industry Sponsored
Alaska Nurse Practitioner Annual Conference 2009 LAURIE RACENET, RN, MSN, ANP, CEPS, CCDS Alaska Heart Institute Member: Boston Scientific Allied Professional Advisory Board Participant in Industry Sponsored
The most common. hospitalized patients. hypotension due to. filling time Rate control in ICU patients may be difficult as many drugs cause hypotension
 Arrhythmias in the critically ill ICU patients: Approach for rapid recognition & management Objectives Be able to identify and manage: Atrial fibrillation with a rapid ventricular response Atrial flutter
Arrhythmias in the critically ill ICU patients: Approach for rapid recognition & management Objectives Be able to identify and manage: Atrial fibrillation with a rapid ventricular response Atrial flutter
Adrenergic Receptor as part of ANS
 Adrenergic Receptor as part of ANS Actions of Adrenoceptors Beta-1 adrenergic receptor Located on the myocytes of the heart Specific actions of the β1 receptor include: 0 Increase cardiac output, by 0
Adrenergic Receptor as part of ANS Actions of Adrenoceptors Beta-1 adrenergic receptor Located on the myocytes of the heart Specific actions of the β1 receptor include: 0 Increase cardiac output, by 0
Introductory Clinical Pharmacology Chapter 41 Antihypertensive Drugs
 Introductory Clinical Pharmacology Chapter 41 Antihypertensive Drugs Blood Pressure Normal = sys
Introductory Clinical Pharmacology Chapter 41 Antihypertensive Drugs Blood Pressure Normal = sys
Congestive Heart Failure (CHF) Edward JN Ishac, Ph.D.
 Congestive Heart Failure (CHF) Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth
Congestive Heart Failure (CHF) Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth
Leading Causes of Death in the U.S. Congestive Heart Failure (CHF) Edward JN Ishac, Ph.D. Blood flow at rest and exercise
 Congestive Heart Failure (CHF) Leading Causes of Death in the U.S Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia
Congestive Heart Failure (CHF) Leading Causes of Death in the U.S Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia
Antiarrhythmics 17 I. OVERVIEW II. INTRODUCTION TO THE ARRHYTHMIAS
 Antiarrhythmics 17 I. OVERVIEW In contrast to skeletal muscle, which contracts only when it receives a stimulus, the heart contains specialized cells that exhibit automaticity. This means that they can
Antiarrhythmics 17 I. OVERVIEW In contrast to skeletal muscle, which contracts only when it receives a stimulus, the heart contains specialized cells that exhibit automaticity. This means that they can
Chapter 16: Arrhythmias and Conduction Disturbances
 Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Heart Failure. Dr. Alia Shatanawi
 Heart Failure Dr. Alia Shatanawi Left systolic dysfunction secondary to coronary artery disease is the most common cause, account to 70% of all cases. Heart Failure Heart is unable to pump sufficient blood
Heart Failure Dr. Alia Shatanawi Left systolic dysfunction secondary to coronary artery disease is the most common cause, account to 70% of all cases. Heart Failure Heart is unable to pump sufficient blood
7/7/ CHD/MI LVH and LV dysfunction Dysrrhythmias Stroke PVD Renal insufficiency and failure Retinopathy. Normal <120 Prehypertension
 Prevalence of Hypertension Hypertension: Diagnosis and Management T. Villela, M.D. Program Director University of California, San Francisco-San Francisco General Hospital Family and Community Medicine
Prevalence of Hypertension Hypertension: Diagnosis and Management T. Villela, M.D. Program Director University of California, San Francisco-San Francisco General Hospital Family and Community Medicine
I have nothing to disclose.
 I have nothing to disclose. Antiarrhythmic Therapy in Pregnancy Prof. Ali Oto,MD,FESC,FACC,FHRS Department of Cardiology Hacettepe University,Faculty of Medicine Ankara Arrhythmias in pregnancy An increased
I have nothing to disclose. Antiarrhythmic Therapy in Pregnancy Prof. Ali Oto,MD,FESC,FACC,FHRS Department of Cardiology Hacettepe University,Faculty of Medicine Ankara Arrhythmias in pregnancy An increased
WHAT DO YOU SEE WHEN YOU STIMULATE BETA
 CARDIAC DRUG REVIEW WHAT DO YOU SEE WHEN YOU STIMULATE BETA VASODILATE BRONCHODILATE +CHRONOTROPE +INOTROPE EPI S OTHER NAME? ADRENALIN WHAT DOES EPI DO THAT NOREPI AND DOPAMINE DO NOT DO? BETA 2 BRONCHODILATOR
CARDIAC DRUG REVIEW WHAT DO YOU SEE WHEN YOU STIMULATE BETA VASODILATE BRONCHODILATE +CHRONOTROPE +INOTROPE EPI S OTHER NAME? ADRENALIN WHAT DOES EPI DO THAT NOREPI AND DOPAMINE DO NOT DO? BETA 2 BRONCHODILATOR
Cardiac arrhythmias. Janusz Witowski. Department of Pathophysiology Poznan University of Medical Sciences. J. Witowski
 Cardiac arrhythmias Janusz Witowski Department of Pathophysiology Poznan University of Medical Sciences A 68-year old man presents to the emergency department late one evening complaining of increasing
Cardiac arrhythmias Janusz Witowski Department of Pathophysiology Poznan University of Medical Sciences A 68-year old man presents to the emergency department late one evening complaining of increasing
Instruct patient and caregivers: Need for constant monitoring Potential complications of drug therapy
 Assessment Prior to administration: Assess patient for chest pain, dysrhythmias, and vital signs (initially and throughout therapy) Obtain complete medical history, including allergies, especially heart
Assessment Prior to administration: Assess patient for chest pain, dysrhythmias, and vital signs (initially and throughout therapy) Obtain complete medical history, including allergies, especially heart
Introduction. Circulation
 Introduction Circulation 1- Systemic (general) circulation 2- Pulmonary circulation carries oxygenated blood to all parts of the body carries deoxygenated blood to the lungs From Lt. ventricle aorta From
Introduction Circulation 1- Systemic (general) circulation 2- Pulmonary circulation carries oxygenated blood to all parts of the body carries deoxygenated blood to the lungs From Lt. ventricle aorta From
Paramedic Rounds. Tachyarrhythmia's. Sean Sutton Dallas Wood
 Paramedic Rounds Tachyarrhythmia's Sean Sutton Dallas Wood Objectives At the end of this session, the paramedic will be able to: State the key components of the cardiac conduction pathway, along with the
Paramedic Rounds Tachyarrhythmia's Sean Sutton Dallas Wood Objectives At the end of this session, the paramedic will be able to: State the key components of the cardiac conduction pathway, along with the
B-blockers. Effects not related to Beta-Blockade
 B-blockers Effects not related to Beta-Blockade It has been suggested that some intrinsic sympathomimetic activity is desirable to prevent untoward effects such as asthma or excessive bradycardia. Pindolol
B-blockers Effects not related to Beta-Blockade It has been suggested that some intrinsic sympathomimetic activity is desirable to prevent untoward effects such as asthma or excessive bradycardia. Pindolol
Dysrhythmias 11/7/2017. Disclosures. 3 reasons to evaluate and treat dysrhythmias. None. Eliminate symptoms and improve hemodynamics
 Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
Autonomic Pharmacology
 Autonomic Pharmacology ADRENERGIC RECEPTOR BLOCKERS Adrenergic-receptor antagonists block the effects of sympathetic stimulation and adrenergic agonists mediated through - and -receptors. Adrenergic receptor
Autonomic Pharmacology ADRENERGIC RECEPTOR BLOCKERS Adrenergic-receptor antagonists block the effects of sympathetic stimulation and adrenergic agonists mediated through - and -receptors. Adrenergic receptor
HEART FAILURE PHARMACOLOGY. University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D
 HEART FAILURE PHARMACOLOGY University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D 1 LEARNING OBJECTIVES Understand the effects of heart failure in the body
HEART FAILURE PHARMACOLOGY University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D 1 LEARNING OBJECTIVES Understand the effects of heart failure in the body
ARRHYTHMIAS. REENTERY occurs when propagating impulse fails to die out after normal activation of heart and persist to re excite the heart.
 ARRHYTHMIAS Arrhythmia is defined as loss of cardiac rhythm, especially irregularity of heartbeat. PATHOPHYSIOLOGY Ectopic complexes (ectopic beats) 1. By definition, arise from a site other than the sinus
ARRHYTHMIAS Arrhythmia is defined as loss of cardiac rhythm, especially irregularity of heartbeat. PATHOPHYSIOLOGY Ectopic complexes (ectopic beats) 1. By definition, arise from a site other than the sinus
ALS MODULE 7 Pharmacology
 ALS MODULE 7 Pharmacology Relates to HLT404C Apply Advanced Resuscitation Techniques Introduction There are no studies that addressed the order of drug administration. There is inadequate evidence to define
ALS MODULE 7 Pharmacology Relates to HLT404C Apply Advanced Resuscitation Techniques Introduction There are no studies that addressed the order of drug administration. There is inadequate evidence to define
Review Packet EKG Competency This packet is a review of the information you will need to know for the proctored EKG competency test.
 Review Packet EKG Competency 2015 This packet is a review of the information you will need to know for the proctored EKG competency test. Normal Sinus Rhythm Rhythm: Regular Ventricular Rate: 60-100 bpm
Review Packet EKG Competency 2015 This packet is a review of the information you will need to know for the proctored EKG competency test. Normal Sinus Rhythm Rhythm: Regular Ventricular Rate: 60-100 bpm
PHARMACOLOGY. Drugs Acting on Cardiovascular System: Antiarrhythmic Drugs
 PHARMACOLOGY Drugs Acting on Cardiovascular System: Antiarrhythmic Drugs Dr Gurudas Khilnani Professor of Pharmacology Dept. of Pharmacology Jawahar Lal Nehru Medical College Ajmer 305001 (6-6-2007) CONTENTS
PHARMACOLOGY Drugs Acting on Cardiovascular System: Antiarrhythmic Drugs Dr Gurudas Khilnani Professor of Pharmacology Dept. of Pharmacology Jawahar Lal Nehru Medical College Ajmer 305001 (6-6-2007) CONTENTS
CVD: Cardiac Arrhythmias. 1. Final Cardiac Arrhythmias_BMP. 1.1 Cardiovascular Disease. Notes:
 CVD: Cardiac Arrhythmias 1. Final Cardiac Arrhythmias_BMP 1.1 Cardiovascular Disease 1.2 Directions for taking this course 1.3 Content Experts 1.4 Disclosures 1.5 Accreditation Information 1.6 Learning
CVD: Cardiac Arrhythmias 1. Final Cardiac Arrhythmias_BMP 1.1 Cardiovascular Disease 1.2 Directions for taking this course 1.3 Content Experts 1.4 Disclosures 1.5 Accreditation Information 1.6 Learning
Management of acute Cardiac Arrhythmias
 Management of acute Cardiac Arrhythmias Dr. Zulkeflee Muhammad MBChB (New Zealand), MRCP (United Kingdom) Cardiologist Electrophysiology Unit Istitut Jantung Negara Objectives Review the etiology and recognition
Management of acute Cardiac Arrhythmias Dr. Zulkeflee Muhammad MBChB (New Zealand), MRCP (United Kingdom) Cardiologist Electrophysiology Unit Istitut Jantung Negara Objectives Review the etiology and recognition
Medical management of AF: drugs for rate and rhythm control
 Medical management of AF: drugs for rate and rhythm control Adel Khalifa Sultan Hamad, BMS, MD, FGHRS, FRCP(Canada) Consultant Cardiologist & Interventional Cardiac Electrophysiologist Head of Electrophysiology
Medical management of AF: drugs for rate and rhythm control Adel Khalifa Sultan Hamad, BMS, MD, FGHRS, FRCP(Canada) Consultant Cardiologist & Interventional Cardiac Electrophysiologist Head of Electrophysiology
Where are the normal pacemaker and the backup pacemakers of the heart located?
 CASE 9 A 68-year-old woman presents to the emergency center with shortness of breath, light-headedness, and chest pain described as being like an elephant sitting on her chest. She is diagnosed with a
CASE 9 A 68-year-old woman presents to the emergency center with shortness of breath, light-headedness, and chest pain described as being like an elephant sitting on her chest. She is diagnosed with a
V. TACHYCARDIAS Rapid rhythm abnormalities
 V. TACHYCARDIAS Rapid rhythm abnormalities Tachyarrhythmias currently account for up to 350,000 deaths annually in the US. In addition to these clearly dangerous rhythm disturbances, other forms of more
V. TACHYCARDIAS Rapid rhythm abnormalities Tachyarrhythmias currently account for up to 350,000 deaths annually in the US. In addition to these clearly dangerous rhythm disturbances, other forms of more
Cardiac Properties MCQ
 Cardiac Properties MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 1- Cardiac Valves: a- Prevent backflow of blood from the ventricles to the atria during
Cardiac Properties MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 1- Cardiac Valves: a- Prevent backflow of blood from the ventricles to the atria during
Amiodarone Prescribing and Monitoring: Back to the Future
 Amiodarone Prescribing and Monitoring: Back to the Future Subha L. Varahan, MD, FHRS, CCDS Electrophysiologist Oklahoma Heart Hospital Oklahoma City, OK Friday, February, 8 th, 2019 Iodinated benzofuran
Amiodarone Prescribing and Monitoring: Back to the Future Subha L. Varahan, MD, FHRS, CCDS Electrophysiologist Oklahoma Heart Hospital Oklahoma City, OK Friday, February, 8 th, 2019 Iodinated benzofuran
Core Content In Urgent Care Medicine
 Palpitations/Arrhythmias Ebrahim Barkoudah, MD Clinical Instructor in Internal Medicine Harvard Medical School Assistant in Internal Medicine & Pediatrics Massachusetts General Hospital MGH Chelsea Chelsea,
Palpitations/Arrhythmias Ebrahim Barkoudah, MD Clinical Instructor in Internal Medicine Harvard Medical School Assistant in Internal Medicine & Pediatrics Massachusetts General Hospital MGH Chelsea Chelsea,
Antihypertensives. Antihypertensive Classes. RAAS Inhibitors. Renin-Angiotensin Cascade. Angiotensin Receptors. Approaches to Hypertension Treatment
 Approaches to Hypertension Treatment Antihypertensives Inhibit Sympathetic impulses Inhibit contractility Inhibit heart rate Inhibit vasoconstriction Inhibit smooth muscle function Inhibit RAAS Inhibit
Approaches to Hypertension Treatment Antihypertensives Inhibit Sympathetic impulses Inhibit contractility Inhibit heart rate Inhibit vasoconstriction Inhibit smooth muscle function Inhibit RAAS Inhibit
EKG Competency for Agency
 EKG Competency for Agency Name: Date: Agency: 1. The upper chambers of the heart are known as the: a. Atria b. Ventricles c. Mitral Valve d. Aortic Valve 2. The lower chambers of the heart are known as
EKG Competency for Agency Name: Date: Agency: 1. The upper chambers of the heart are known as the: a. Atria b. Ventricles c. Mitral Valve d. Aortic Valve 2. The lower chambers of the heart are known as
Step by step approach to EKG rhythm interpretation:
 Sinus Rhythms Normal sinus arrhythmia Small, slow variation of the R-R interval i.e. variation of the normal sinus heart rate with respiration, etc. Sinus Tachycardia Defined as sinus rhythm with a rate
Sinus Rhythms Normal sinus arrhythmia Small, slow variation of the R-R interval i.e. variation of the normal sinus heart rate with respiration, etc. Sinus Tachycardia Defined as sinus rhythm with a rate
Cardiac Arrhythmias. For Pharmacists
 Cardiac Arrhythmias For Pharmacists Agenda Overview of the normal Classification Management Therapy Conclusion Cardiac arrhythmias Overview of the normal Arrhythmia: definition From the Greek a-, loss
Cardiac Arrhythmias For Pharmacists Agenda Overview of the normal Classification Management Therapy Conclusion Cardiac arrhythmias Overview of the normal Arrhythmia: definition From the Greek a-, loss
CRC 431 ECG Basics. Bill Pruitt, MBA, RRT, CPFT, AE-C
 CRC 431 ECG Basics Bill Pruitt, MBA, RRT, CPFT, AE-C Resources White s 5 th ed. Ch 6 Electrocardiography Einthoven s Triangle Chest leads and limb leads Egan s 10 th ed. Ch 17 Interpreting the Electrocardiogram
CRC 431 ECG Basics Bill Pruitt, MBA, RRT, CPFT, AE-C Resources White s 5 th ed. Ch 6 Electrocardiography Einthoven s Triangle Chest leads and limb leads Egan s 10 th ed. Ch 17 Interpreting the Electrocardiogram
Advanced Cardiac Life Support
 Advanced Cardiac Life Support Algorithm Drugs Class I: definitely helpful, excellent Class II: Class II a -probably helpful; good to very good Class II b -possibly helpful; fair to good Class
Advanced Cardiac Life Support Algorithm Drugs Class I: definitely helpful, excellent Class II: Class II a -probably helpful; good to very good Class II b -possibly helpful; fair to good Class
Antihypertensive Agents Part-2. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Antihypertensive Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Agents that block production or action of angiotensin Angiotensin-converting
Antihypertensive Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Agents that block production or action of angiotensin Angiotensin-converting
Heart failure. Failure? blood supply insufficient for body needs. CHF = congestive heart failure. increased blood volume, interstitial fluid
 Failure? blood supply insufficient for body needs CHF = congestive heart failure increased blood volume, interstitial fluid Underlying causes/risk factors Ischemic heart disease (CAD) 70% hypertension
Failure? blood supply insufficient for body needs CHF = congestive heart failure increased blood volume, interstitial fluid Underlying causes/risk factors Ischemic heart disease (CAD) 70% hypertension
Understanding Atrial Fibrillation Management. Roy Lin, MD
 Understanding Atrial Fibrillation Management Roy Lin, MD Disclosure None Definition of atrial fibrillation Atrial fibrillation is a supraventricular tachyarrhythmia characterized by uncoordinated atrial
Understanding Atrial Fibrillation Management Roy Lin, MD Disclosure None Definition of atrial fibrillation Atrial fibrillation is a supraventricular tachyarrhythmia characterized by uncoordinated atrial
Cardiac Arrhythmias. Cathy Percival, RN, FALU, FLMI VP, Medical Director AIG Life and Retirement Company
 Cardiac Arrhythmias Cathy Percival, RN, FALU, FLMI VP, Medical Director AIG Life and Retirement Company The Cardiovascular System Three primary functions Transport of oxygen, nutrients, and hormones to
Cardiac Arrhythmias Cathy Percival, RN, FALU, FLMI VP, Medical Director AIG Life and Retirement Company The Cardiovascular System Three primary functions Transport of oxygen, nutrients, and hormones to
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment
 Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
7/21/2017. Learning Objectives. Current Cardiovascular Pharmacology. Epinephrine. Cardiotonic Agents. Epinephrine. Epinephrine. Arthur Jones, EdD, RRT
 Learning Objectives Current Cardiovascular Pharmacology Arthur Jones, EdD, RRT Explain the actions, effects, indications, adverse effects, & precautions for agents from the following drug categories Cardiotonic
Learning Objectives Current Cardiovascular Pharmacology Arthur Jones, EdD, RRT Explain the actions, effects, indications, adverse effects, & precautions for agents from the following drug categories Cardiotonic
Atrial Fibrillation and Common Supraventricular Tachycardias. Sunil Kapur MD
 Atrial Fibrillation and Common Supraventricular Tachycardias Sunil Kapur MD Cardiac Electrophysiology Brigham and Women s Hospital Instructor, Harvard Medical School No disclosures Cardiac Conduction:
Atrial Fibrillation and Common Supraventricular Tachycardias Sunil Kapur MD Cardiac Electrophysiology Brigham and Women s Hospital Instructor, Harvard Medical School No disclosures Cardiac Conduction:
Lecture outline. Electrical properties of the heart. Automaticity. Excitability. Refractoriness. The ABCs of ECGs Back to Basics Part I
 Lecture outline The ABCs of ECGs Back to Basics Part I Meg Sleeper VMD, DACVIM (cardiology) University of Florida Veterinary School Electrical properties of the heart Action potentials Normal intracardiac
Lecture outline The ABCs of ECGs Back to Basics Part I Meg Sleeper VMD, DACVIM (cardiology) University of Florida Veterinary School Electrical properties of the heart Action potentials Normal intracardiac
CARDIOVASCULAR AGENTS. Dr.P.Valentina, professor, HOD Department of pharmaceutical chemistry SRM college of pharmacy
 CARDIOVASCULAR AGENTS Dr.P.Valentina, professor, HOD Department of pharmaceutical chemistry SRM college of pharmacy System = heart, blood vessels (arteries & veins), Blood Blood rich w/ O2 & nutrients
CARDIOVASCULAR AGENTS Dr.P.Valentina, professor, HOD Department of pharmaceutical chemistry SRM college of pharmacy System = heart, blood vessels (arteries & veins), Blood Blood rich w/ O2 & nutrients
3. AV Block 1. First-degree AV block 1. Delay in AV node 2. Long PR interval 3. QRS complex follows each P wave 4. Benign, no tx
 1. Rhythms & arrhythmias SA nodal rhythms Sinus rhythm Sinus tachycardia Sinus bradycardia Sinus arrhythmia Sick sinus syndrome SA block Sinus arrest AV blocks First-degree Second-degree Mobitz Type I
1. Rhythms & arrhythmias SA nodal rhythms Sinus rhythm Sinus tachycardia Sinus bradycardia Sinus arrhythmia Sick sinus syndrome SA block Sinus arrest AV blocks First-degree Second-degree Mobitz Type I
Acute Arrhythmias in the Hospitalized Patient
 Acute Arrhythmias in the Hospitalized Patient Gregory M Marcus, MD, MAS Associate Professor of Medicine Division of Cardiology University of California, San Francisc Disclosures Medtronic: Research Support
Acute Arrhythmias in the Hospitalized Patient Gregory M Marcus, MD, MAS Associate Professor of Medicine Division of Cardiology University of California, San Francisc Disclosures Medtronic: Research Support
Rate and Rhythm Control of Atrial Fibrillation
 Rate and Rhythm Control of Atrial Fibrillation April 21, 2017 춘계심혈관통합학술대회 Jaemin Shim, MD, PhD Arrhythmia Center Korea University Anam Hospital Treatment of AF Goal Reducing symptoms Preventing complication
Rate and Rhythm Control of Atrial Fibrillation April 21, 2017 춘계심혈관통합학술대회 Jaemin Shim, MD, PhD Arrhythmia Center Korea University Anam Hospital Treatment of AF Goal Reducing symptoms Preventing complication
Angina Pectoris. Edward JN Ishac, Ph.D. Smith Building, Room
 Angina Pectoris Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth University
Angina Pectoris Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth University
METOTRUST XL-25/50 Metoprolol Succinate Extended-Release Tablets
 METOTRUST XL-25/50 Metoprolol Succinate Extended-Release Tablets COMPOSITION Each film-coated tablet of Metotrust XL-25 contains: Metoprolol Succinate USP 23.75 mg equivalent to Metoprolol Tartrate 25
METOTRUST XL-25/50 Metoprolol Succinate Extended-Release Tablets COMPOSITION Each film-coated tablet of Metotrust XL-25 contains: Metoprolol Succinate USP 23.75 mg equivalent to Metoprolol Tartrate 25
