Acute zonal occult outer retinopathy: A case report
|
|
|
- Lizbeth Carroll
- 5 years ago
- Views:
Transcription
1 Optometry (2010) 81, Acute zonal occult outer retinopathy: A case report Josephine O. Ibironke, O.D., a and Andrew S. Gurwood, O.D. b a The Wilmer Eye Institute, Johns Hopkins University School of Medicine, Baltimore, Maryland; and b The Eye Institute, Pennsylvania College of Optometry, Philadelphia, Pennsylvania. KEYWORDS Acute zonal occult outer retinopathy; Retinal pigment epithelium; Retina; Electroretinogram Abstract BACKGROUND: Acute zonal occult outer retinopathy (AZOOR) is a disorder of unknown etiology with a predilection for young women. AZOOR is characterized by an acute loss of one or more zones of outer retinal function with a corresponding loss of visual field in one or both eyes. Patients present with photopsia, variable funduscopic changes, and abnormal electroretinogram (ERG) findings. There are no proven treatments. Diagnosed cases have a reasonable prognosis because central vision is often spared. CASE REPORT: A 24-year-old white woman presented with acute photopsia with clouded temporal vision in the right eye (O.D.). Initial evaluation found a slightly swollen nerve fiber layer with no other outstanding lesions O.D. Over a 7-week follow-up period, there was significant progression into the deep chorioretinal tissues O.D. with an anterior chamber response. At 3 months, an afferent pupillary defect (APD) developed with significant retinal pigment epithelium (RPE) changes. After extensive testing, the consulting retinal specialist identified AZOOR as the etiology. At 21 and 31 months, the process remained in remission. Although primary symptoms subsided, the dense inferior-temporal field defect remained O.D. CONCLUSION: AZOOR is a rare condition with subtle and often vague signs and symptoms making diagnosis difficult. The course of AZOOR, its clinical presentations, hypothesis of etiology, differential diagnosis, workup, management, and prognosis are reviewed. Optometry 2010;81:22-27 In 1993, J. Donald M. Gass described the syndrome of acute zonal occult outer retinopathy (AZOOR) in 13 patients with sudden onset of photopsia and visual field defects. 1 Today, this relatively new disorder with a predilection for young, healthy, myopic women remains poorly understood with an unknown etiology. 1-6 AZOOR is characterized by an acute loss of 1 or more zones of outer retinal layer function with corresponding losses of visual field in one or both eyes. It is usually asymmetric when both eyes are involved. 1,7 Patients present with photopsia, normal visual acuities, and minimal to no funduscopic or angiographic changes, initially, but with an abnormal Corresponding author: Josephine O. Ibironke, O.D., The Wilmer Institute, 233, 600 North Wolfe Street, Baltimore, Maryland jibiron1@jhmi.edu electroretinogram (ERG) when tested. 1,2,5,6 Fundoscopic changes often develop over time in the retinal zones corresponding to thevisual field loss. 4 In most cases, the visual field loss is permanent. The abnormal ERG is an important discovery with regard to diagnosis, demonstrating outer retinal dysfunction at the level of the photoreceptors. 8 There is still no known treatment for the disorder. Prognosis is generally good because the disorder is self-limiting; however, although symptoms eventually subside and visual function stabilizes, visual function that is lost often is not recovered. Case report A 24-year-old white woman presented to the office with a chief complaint of acute, constant, flashing, and spinning white lines temporally in the right eye of 3 days duration /10/$ -see front matter Ó 2010 American Optometric Association. All rights reserved. doi: /j.optm
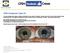
2 Ibironke and Gurwood Clinical Care 23 She also complained that her vision seemed cloudy in the temporal field of the right eye along with a sensation of feeling pressure over the right eye with an occasional accompanying frontal headache. She reported no numbness or tingling of the limbs or extremities, no muscle weakness, and no loss of balance or changes in mentation. Her previous ocular history was unremarkable. Her medical history was significant for chronic back pain, successfully treated endometriosis, migraine headache, depression, and bipolar disorder. Her family medical and ocular histories were noncontributory. She denied taking medication of any kind. She reported no allergies. Her best-corrected visual acuities measured 20/20 in the right eye (O.D.) and in the left eye (O.S.). External findings were normal. Pupils and color vision were normal with no evidence of afferent defect. Refraction found myopia in both eyes (OU) with negligible changes to her current spectacle prescription. Biomicroscopy found normal anterior segment structures. Goldmann applanation intraocular pressures measured 16 mmhg OU. Dilated fundus evaluation found retinal edema in the superior nasal quadrant of the right eye. The optic nerve in the right eye was slightly elevated with some deep chorioretinal thickening emanating nasally into the equatorial region. Visual field testing found a slightly enlarged blind spot O.D. There was no vitritis or pars planitis, OU. Dilated fundoscopy of the left eye found normal structures free from pathology. The patient was referred to a retinal specialist for identification and management of the retinal lesion. Given the nature of her persistent visual complaint, an additional referral was made to neuro-ophthalmology to rule out neurologic etiologies. Routine blood screening and neuroimaging studies were obtained and showed no abnormalities or intracranial/orbital lesions of any kind. The retinal specialist agreed with our findings and ordered some blood work to rule out systemic infectious, inflammatory, and collagen vascular diseases. The patient returned to the office 4 weeks after the initial onset of symptoms. Although the visual acuity, symptoms, and external findings remained unaltered, biomicroscopy uncovered a grade 1 iritis. Examination of the posterior pole found enlarged areas of subretinal edema O.D. (see Figure 1). The patient was started on a topical regimen of atropine 1% twice a day and topical prednisolone acetate 1% 4 times a day O.D. to quell discomfort and to arrest the local inflammatory response. A follow-up examination was scheduled for 1 week. The patient returned to the office, as scheduled, 1 week after the discovery of the new signs. All findings were consistent with previous data from acuity and neurologic testing to intraocular pressure and anterior segment findings. Examination of the posterior pole found stable but unregressed areas of subretinal edema O.D. The patient was instructed to continue the regimen of topical atropine 1% twice a day and topical prednisolone acetate 1% 4 times a day O.D. A follow-up reassessment was scheduled for 4 weeks. Figure 1 Subretinal edema O.D. at 4 weeks. Twelve weeks after the onset of the initial symptoms, the patient was no longer taking drops, the photopsia persisted, and a grade 1 afferent pupillary defect (APD) was detected O.D. Anteriorly, the mild iritis persisted, and posteriorly, retinal pigment epithelium (RPE) changes with retinal and subretinal atrophy, corresponding to the affected area, were noted (see Figure 2). Because the patient remained relatively comfortable, no alteration of the therapy was implemented. Following an extensive and protracted workup, after a total of 18 weeks from the time the symptoms were first reported, the retinal specialist returned the diagnosis of AZOOR. (The result of an ERG, if performed at the retina clinic, was not available to us.) The patient was followedup at 6- to 8-week intervals by the retinal specialist and at 3-month intervals by our office over the next 6 months, then by our office at 4- to 6-month intervals. At 31 months, although all symptoms had subsided, the RPE changes superior-nasally with their corresponding infero-temporal field defects remained O.D. (see Figure 3). No choroidal neovascularization developed, and no additional retinal treatment was offered or is currently indicated according to the standard of care. Figure 2 RPE changes with atrophy superior nasally O.D. at 3 months.
3 24 Optometry, Vol 81, No 1, January 2010 Figure 3 Persistent visual field defect O.D. at 31 months.
4 Ibironke and Gurwood Clinical Care 25 Discussion Gass et al. 1 completed a prospective and retrospective study in 51 AZOOR patients (90 eyes). That study and others have identified many of the characteristic clinical findings common to AZOOR patients. 1-3,5,7,9,10 Most patients are myopic, young, white women. 1,3,5,7 Many (55% to 88%) complain of photopsia characterized as lights, lines, floaters, bursts, or sparkles without headaches. 1-3,7,8 The photopsia is typically experienced weeks before or after the onset of visual field loss in areas corresponding to the affected retina; it may be constant or intermittent, lasting for short periods. 1 Patients also often complain of their scotomata, describing dark blind spots in their field. Although photopsia and scotomata are usually only present in one eye, bilateral presentations have been documented to occur in 39% of cases. 1,4 Corrected visual acuities are often 20/40 or better in 76% to 82% of the patients 1,3,11 (see Table 1). At onset, a majority of the patients have little or no fundoscopic involvement. 1-5,7-9 However, visual fields can contain enlarged blind spots, ring scotomas, concentric contractions, arcuate defects, and even multiple isolated scotomas. 1-3,5,6,8,9 The central field is often spared. 1,6,12,13 There may be a delayed involvement of the other eye with asymmetry of signs and symptoms. 1,6,8 There may be a history of some event, such as viral-like illness or headache, days to weeks before the onset of the severe symptoms in up to 40% to 50% of cases. 1,5,7 Several weeks after the initial presentation of signs and symptoms, up to 25% of the patients show enough retinal involvement to produce an afferent pupillary defect. 1,2,7 In fact, most patients progress to vitritis with perivascular exudates and/or sheathing. 1,2 Three quarters of affected individuals will show stabilization of their visual field loss within 2 to 6 months of the initial event. 1,3,10 Visual improvement is more likely in eyes with normal-appearing fundi that present without vitritis in the acute phase. However, even in these individuals, improvement may never be complete, with residual visual field defects remaining even after the disease has become inactive. 1,2 Other associated fundus changes include cystoid macular edema, RPE changes, and narrowing of retinal vessels. 1,2 Interestingly, the retinal pigment epithelial atrophy and migration into the overlying neurosensory retina are similar in appearance and pathogenesis to the changes observed in retinitis pigmentosa (RP). 1 Some patients (31%) have recurrences up to 2 to 3 years later. 1 These recurrences may be in the initially affected eye, in the fellow eye, or in both. 1,10,14 Etiology The mechanisms causing the RPE malfunction and their relationship with the initiating events are still unknown. 7,10 However, several factors currently are under investigation. AZOOR has been found to have associations with herpes simplex dermatitis, central nervous system abnormalities, herpes zoster ophthalmicus, viral-like illnesses, immunizations, tick Table 1 Presentation of AZOOR in the acute phase Patient characteristics Symptoms Laterality Corrected visual acuity Signs Young, healthy, myopic, white women Photopsia Loss of vision in 1 or more zones of visual field Unilateral or bilateral 20/40 or better Visual field defects with little or no funduscopic involvement Abnormal ERG findings bites, migraines, the periods during and/or immediately after pregnancy, and Candida famata. 1,4,5,7,15,16 AZOOR has also been loosely associated with autoimmune diseases, various hormones, bacteria, viruses, and histoplasma capsulatum. 1,5,7,10 A viral theory to explain the etiology of AZOOR proposes that viruses that have the capability of causing vitreoretinal sequellae are suspected to gain access to the retina via the optic disc and/or ora serrata. This is postulated as a mechanism because of the characteristic visual field loss: enlarged blind spot and loss of field in the periphery. 1,2,5,10 These 2 areas have photoreceptor cells in close contact with the globe s circulation. It is theorized that an offending organism gains entry via these portals and spreads from cell to cell. 1,5 Cells infected by the virus become deactivated by the host s immune response causing an acute loss of retinal function. 1,5,12 The fundus appears as if it is unaffected in the beginning, as the immune response deactivates retinal cell function without initially causing inflammation, apoptosis, or necrosis. 1,7 However, all patients gradually show fundus changes as the acute phase of infection transitions into the later, more advanced stages of the disease. 1,2,4,8,15 Patients who are less fortunate develop early inflammation in the vitreous, perivascular exudates, and optic nerve edema, leading to acute and permanent cell death and compromise. 1 The amount of inflammation observed within the vitreous body is proportional to the area of the affected retina because inflammation is in response to dying or dead photoreceptor cells. In the later phases, narrowing blood vessels may be observed secondary to declining oxygen consumption within the affected areas. 1,2 Patients with widespread areas of compromise will have a relative afferent pupillary defect. 2 An interesting characteristic of AZOOR is its propensity to affect myopes. 1,7 The disease is shown to most commonly strike those with 2 diopters of myopia or more. 1 This is thought to occur because larger eyes may have increased susceptibility at the suspected routes of entry (ora and disc). 1 Autoimmune diseases are also known to share association with AZOOR. Some patients (28%) either have or will have an autoimmune disease during AZOOR s acute phase. 1,15 Interestingly, it has been postulated 1,5 that if
5 26 Optometry, Vol 81, No 1, January 2010 Table 2 Differential diagnosis of AZOOR Disease Multiple evanescent white dot syndrome (MEWDS) Serpignous choroidopathy Acute posterior multifocal placoid pigment epitheliopathy (AMPEE) Multifocal choroiditis and panuveitis (MCP) Punctate inner choroidopathy (PIC) Cancer associated retinopathy (CAR) Acute annular outer retinopathy Retinitis pigmentosa (RP) Diffuse unilateral subacute neuroretinitis (DUSN) Features Benign; rare recurrences; acute; unilateral; young women; white dots at the level of RPE; blind spot enlargement with visual field loss; regression in weeks; granular macular appearance; visual acuity improves. Visual acuity is affected; bilateral; may recur; acute yellow-white subretinal patches with indistinct borders; old scars are bordered; white men and women; between 30 and 60 years of age; neovascularization may develop. Young men and women; very large white lesions; bilateral; acute; vitreous cells; vision returns to normal in 2 to 6 weeks. Young women; anterior and posterior chamber inflammation; recurrences, no subretinal scarring; enlarged blind spot; fair prognosis; multiple foci of choroiditis. White spots in acute phase; no vitreous inflammation; little or no scarring; no recurrences; enlarged blind spot; normal ERG. Slower course of visual field loss; nyctalopia over months to years; history of cancer or melanoma. No age or sex association; no vitreous inflammation; has an evanescent white intraretinal ring (possibly an immunity ring) that separates normal retinal from abnormal retina. RPE changes; no associated history of rapid onset vision loss; night vision decreases; abnormal ERG; optic disc pallor; decreased color vision. Unilateral vision loss; in children and young adults; caused by a nematode; optic nerve edema, deep-white retinal lesion; optic atrophy and RPE changes after the acute phase. autoimmune diseases are precipitators, one would expect to find more cases of bilateral, symmetric involvement of both eyes. Further, one would also predict that oral and topical steroids would provide rapid improvement and that circulating retinal antibodies should also be easily detectable. 1,5 However, despite these suppositions, with AZOOR, this is not the case. 1,5,6 Diagnosis and treatment When a retinal disease cannot be definitively distinguished by its appearance alone, other tests are required. The diagnostic study of choice in suspected cases of AZOOR, and tapetoretinal diseases in general, is the ERG. 1,4,9,17 An ERG waveform shows the summation of electrical potential by all retinal cells. The potential is measured by a contact lens electrode in conjunction with a skin reference electrode placed on the patient s forehead. Scotopic functions are rod responses measured after a period of dark adaptation, whereas photopic functions are cone responses measured after light adaptation. 17 A full-field ERG measures the overall rod and cone responses from the entire retina. The focal and multifocal ERGs are used to detect local retinal dysfunction; however, these 2 techniques mostly assess only light-adapted cone activities because dark adaptation is difficult to maintain during these techniques. 17 ERGs assess the level of function of the outer retinal layers and the photoreceptors. This is especially helpful when retinal tissue manifestations are not yet apparent. 1,6,8,9,15,18 In AZOOR, the scotopic function, photopic function, or both are reduced in affected eyes. The abnormalities in the ERG findings are known to be variable and directly correlated to the degree of visual field loss. This makes full-field ERGs useful tools in diagnosing AZOOR, especially when the amount of retina involved is large. 1,9 Multifocal ERGs can also be used; however, they are only sensitive to cone dysfunction. This selectivity may fail to detect abnormalities in patients with only rod dysfunction. 1,9,17 Because the outer retinal layer dysfunction in AZOOR is often permanent, ERGs are also useful for monitoring progress. 7,8 Nishio et al. 11 also found scanning laser ophthalmoscopy to be useful in localizing retinal damage in AZOOR because changing the laser wavelength can show retinal lesions and the underlying unaffected choroidal layer. Visual field studies are needed in conjunction with ERGs to quantify the visual field loss and monitor the disease s progression. If progression is noted after the 2- to 6-month stabilization period, other pathologies may need to be investigated. 1,3,10 Fluorescein angiography can also be useful in detecting the early alterations of AZOOR. The test can exhibit hyperfluorescence and the redistribution of melanin in patients that later experience RP-like changes. 1,6 Differential diagnosis AZOOR is classified into the category of heterogeneous groups of retinopathies of unknown etiology. 8,10,15 These
6 Ibironke and Gurwood Clinical Care 27 retinopathies may represent a continuum of one disease process 1,2,5-7,10,13,15 because they seem to have similar presentations and features, although some argue that unique characteristics and etiologic links point to separate entities. 10,13 Other retinopathies that should be considered given the described constellation of signs and symptoms include multiple evanescent white dot syndrome (MEWDS), acute annular outer retinopathy (AAOR), acute idiopathic blind spot enlargement syndrome (AIBSES), acute macular neuroretinopathy (AMN), multifocal inner choroiditis (Krill s disease), recurrent multifocal choroiditis and panuveitis (MCP), punctate inner choroidopathy (PIC), and the acute posterior multifocal placoid pigment epitheliopathy (AMPEE) (see Table 2). 1,10,12,15,19-21 Because some AZOOR patients present with vitritis and retinal perivascular exudation and because of proposed systemic associations, consideration must be given to adding studies that rule out sarcoid, Behcet s disease, rheumatoid vasculitis, and nonspecific causes of uveitis. 1 Management There are no proven treatments for AZOOR. 1,7 It is a selflimiting condition. However, if there are associated systemic illnesses discovered, they must be addressed and managed. The role of systemic and topical medications in the treatment of this ocular disease is still unclear, as only the vitritis regresses when treated with topical agents. 10 In patients in whom the inflammation is solely anterior, the benefits of topical cycloplegic and anti-inflammatory preparations are anecdotal and analgesic at best. 4,7 Although the retinal losses and visual field losses are typically permanent, the overall prognosis is generally good, 1,3,7,18 as the disease stabilizes in most instances before disabling central losses occur. Conclusion Understanding AZOOR and its presentation allows for timely referral and diagnosis along with testing for associated systemic conditions. Knowledge of the entity allows for effective communication regarding the disease s course and treatment options. References 1. Gass JD, Agarwal A, Scott IU. Acute zonal occult outer retinopathy: a long-term follow-up. Am J Ophthalmol 2002;134: Gass JD, Stern C. Acute annular outer retinopathy as a variant of the acute zonal occult outer retinopathy. Am J Ophthalmol 1995;119: Lee AG, Prager TC. Acute zonal occult outer retinopathy. Acta Ophthalmol Scand 1996;74: Jacobson DM. Acute zonal occult outer retinopathy and central nervous system inflammation. J Neuro-Ophthalmol 1996;16(3): Gass JD. Are acute zonal occult outer retinopathy and the white spot syndromes (AZOOR Complex) specific autoimmune diseases? Am J Ophthalmol 2003;135(3): Gass JD. Stereoscopic atlas of macular disease: diagnosis and treatment, 4th ed. St. Louis: CV Mosby; 1997: Holz FG, Kim RY, Schwartz SD, et al. Acute zonal occult outer retinopathy (AZOOR) associated with multifocal choroidopathy. Eye 1994;8: Jacobson SSG, Morales DS, Sun XK, et al. Pattern of retinal dysfunction in acute occult zonal outer retinopathy. Ophthalmology 1995;102: Arai M, Nao-i N, Sawada A, et al. Multifocal electroretinogram indicates visual field loss in acute zonal occult outer retinopathy. Am J Ophthalmol 1998;126(3): Jampol LM, Becker KG. White Spot syndromes of the retina: A hypothesis based on the common genetic hypothesis of autoimmune/inflammatory disease. Am J Ophthalmol 2003;135(3): Nishio M, Suzuki T, Chikuda M, et al. Scanning laser ophthalmoscopic findings in a patient with acute zonal occult outer retinopathy. Am J Ophthalmol 1998;125: Gass JD. The acute zonal outer retinopathies. Am J Ophthalmol 2000; 130(5): Gass JD. Overlap among acute idiopathic blind spot enlargement syndrome and other conditions. Arch Ophthalmol 2001;119: Lombardo J. Multiple evanescent white dot syndrome and acute zonal occult outer retinopathies. Optomy Vis Sci 2003;80(10): Jampol LM, Wiredu AMEWDS. MFC, PIC, AMN, AIBSE, and AZOOR: one disease or many? Retina 1995;15(5): Carrasco L, Ramos M, Galisteo R, et al. Isolation of Candida famata from a patient with Acute Zonal Occult Outer Retinopathy. J Clin Microbiol 2005;43(2): Lam BL. Electrophysiology of vision: clinical testing and applications. Boca Raton: Taylor & Francis; 2005: Gass JD. Acute zonal occult outer retinopathy. Donders lecturedthe Netherlands Ophthalmological Society, Maastricht, Holland, June 19, J Clin Neurol Ophthalmol 1993;13: Arbet TP. Multiple evanescent white dot syndrome. J Am Optometric Assoc 1997;68(12): Reddy CV, Brown J, Folk JC, et al. Enlarged blind spots in chorioretinal inflammatory disorders. Ophthalmology 1996;103: Fekrat S, Wilkinson CP, Chang B, et al. Acute annular outer retinopathy: report of four cases. Am J Ophthalmol 2000;130:
White-Spot Syndromes of the Retina Lee Jampol, M.D. Chicago, IL
 Objectives At the conclusion of the program, the attendees will be able to: 1. recognize the various white-spot syndromes of the retina 2. initiate appropriate diagnostic tests of patients with the white-spot
Objectives At the conclusion of the program, the attendees will be able to: 1. recognize the various white-spot syndromes of the retina 2. initiate appropriate diagnostic tests of patients with the white-spot
ISPUB.COM. Photopsia post flu: A case of MEWDS. S Baisakhiya, S Dulani, S Lele INTRODUCTION CASE HISTORY
 ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 8 Number 1 Photopsia post flu: A case of MEWDS S Baisakhiya, S Dulani, S Lele Citation S Baisakhiya, S Dulani, S Lele. Photopsia
ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 8 Number 1 Photopsia post flu: A case of MEWDS S Baisakhiya, S Dulani, S Lele Citation S Baisakhiya, S Dulani, S Lele. Photopsia
CLINICALCASE PROVOST J, SEKFALI R, AMOROSO F, ZAMBROWSKI O, MIERE A
 CLINICALCASE PROVOST J, SEKFALI R, AMOROSO F, ZAMBROWSKI O, MIERE A Department of ophthalmology, Souied E. (MD,PhD) Centre Hospitalier Intercommunal de Créteil Université Paris Est HISTORY 13 years old
CLINICALCASE PROVOST J, SEKFALI R, AMOROSO F, ZAMBROWSKI O, MIERE A Department of ophthalmology, Souied E. (MD,PhD) Centre Hospitalier Intercommunal de Créteil Université Paris Est HISTORY 13 years old
Fundus Autofluorescence. Jonathan A. Micieli, MD Valérie Biousse, MD
 Fundus Autofluorescence Jonathan A. Micieli, MD Valérie Biousse, MD The retinal pigment epithelium (RPE) has many important functions including phagocytosis of the photoreceptor outer segments Cone Rod
Fundus Autofluorescence Jonathan A. Micieli, MD Valérie Biousse, MD The retinal pigment epithelium (RPE) has many important functions including phagocytosis of the photoreceptor outer segments Cone Rod
Moncef Khairallah, MD
 Moncef Khairallah, MD Department of Ophthalmology, Fattouma Bourguiba University Hospital Faculty of Medicine, University of Monastir Monastir, Tunisia INTRODUCTION IU: anatomic form of uveitis involving
Moncef Khairallah, MD Department of Ophthalmology, Fattouma Bourguiba University Hospital Faculty of Medicine, University of Monastir Monastir, Tunisia INTRODUCTION IU: anatomic form of uveitis involving
Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (CSC)
 HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
White Dot Syndromes Noninfectious Chorioretinopathies Update 2019
 White Dot Syndromes Noninfectious Chorioretinopathies Update 2019 Kelly T. Mitchell, MD Retina Service TTUHSC Definition Noninfectious disease Inflammation of choroid, choriocapillaris, RPE, and Retina
White Dot Syndromes Noninfectious Chorioretinopathies Update 2019 Kelly T. Mitchell, MD Retina Service TTUHSC Definition Noninfectious disease Inflammation of choroid, choriocapillaris, RPE, and Retina
Unexplained visual loss in seven easy steps
 Unexplained visual loss in seven easy steps Andrew G. Lee, MD Chair Ophthalmology, Houston Methodist Hospital, Professor, Weill Cornell MC; Adjunct Professor, Baylor COM, U Iowa, UTMB Galveston, UT MD
Unexplained visual loss in seven easy steps Andrew G. Lee, MD Chair Ophthalmology, Houston Methodist Hospital, Professor, Weill Cornell MC; Adjunct Professor, Baylor COM, U Iowa, UTMB Galveston, UT MD
THE OCULAR histoplasmosis
 CLINICAL SCIENCES Reactivation of Inflammatory Lesions in Ocular Histoplasmosis David Callanan, MD; Gary E. Fish, MD, JD; Rajiv Anand, MD Background: Active inflammation has not been traditionally associated
CLINICAL SCIENCES Reactivation of Inflammatory Lesions in Ocular Histoplasmosis David Callanan, MD; Gary E. Fish, MD, JD; Rajiv Anand, MD Background: Active inflammation has not been traditionally associated
Acute Retinal Necrosis Secondary to Varicella Zoster Virus in an Immunosuppressed Post-Kidney Transplant Patient
 CM&R Rapid Release. Published online ahead of print September 20, 2012 as Aperture Acute Retinal Necrosis Secondary to Varicella Zoster Virus in an Immunosuppressed Post-Kidney Transplant Patient Elizabeth
CM&R Rapid Release. Published online ahead of print September 20, 2012 as Aperture Acute Retinal Necrosis Secondary to Varicella Zoster Virus in an Immunosuppressed Post-Kidney Transplant Patient Elizabeth
Rare Presentation of Ocular Toxoplasmosis
 Case Report Rare Presentation of Ocular Toxoplasmosis Rakhshandeh Alipanahi MD From Department of Ophthalmology, Nikookari Eye Hospital, Tabriz University of Medical Sciences, Tabriz, Iran. Correspondence:
Case Report Rare Presentation of Ocular Toxoplasmosis Rakhshandeh Alipanahi MD From Department of Ophthalmology, Nikookari Eye Hospital, Tabriz University of Medical Sciences, Tabriz, Iran. Correspondence:
Clinical Features of Bilateral Acute Idiopathic Maculopathy
 Clinical Features of Bilateral Acute Idiopathic Maculopathy Toru Nakazawa,, Katsuhiro Yamaguchi, Masahiko Shimura, Madoka Yoshida, Yuki Yoshioka and Makoto Tamai Department of Ophthalmology, Katta General
Clinical Features of Bilateral Acute Idiopathic Maculopathy Toru Nakazawa,, Katsuhiro Yamaguchi, Masahiko Shimura, Madoka Yoshida, Yuki Yoshioka and Makoto Tamai Department of Ophthalmology, Katta General
Placoid pigment epitheliopathy with
 Brit. J. Ophthal. ( I 972) 56, 875 Placoid pigment epitheliopathy with retinal vasculitis and papillitis T. H. KIRKHAM, *T. J. FFYTCHE, AND M. D. SANDERS From the Department of Neuro-Ophthalmology, the
Brit. J. Ophthal. ( I 972) 56, 875 Placoid pigment epitheliopathy with retinal vasculitis and papillitis T. H. KIRKHAM, *T. J. FFYTCHE, AND M. D. SANDERS From the Department of Neuro-Ophthalmology, the
RETINAL DETACHMENT AT THE POSTERIOR POLE*
 Brit. J. Ophthal. (1958) 42, 749. RETINAL DETACHMENT AT THE POSTERIOR POLE* BY CALBERT I. PHILLIPSt Institute of Ophthalmology, University oflondon THE common feature of the cases to be described in this
Brit. J. Ophthal. (1958) 42, 749. RETINAL DETACHMENT AT THE POSTERIOR POLE* BY CALBERT I. PHILLIPSt Institute of Ophthalmology, University oflondon THE common feature of the cases to be described in this
UNDERSTAND MORE ABOUT UVEITIS UVEITIS
 UNDERSTAND MORE ABOUT UVEITIS UVEITIS Uveitis What is uveitis? Uveitis is inflammation of the uvea, the middle layer of your eye. The eye is shaped much like a tennis ball, with three different layers
UNDERSTAND MORE ABOUT UVEITIS UVEITIS Uveitis What is uveitis? Uveitis is inflammation of the uvea, the middle layer of your eye. The eye is shaped much like a tennis ball, with three different layers
chorioretinal atrophy
 British Journal of Ophthalmology, 1987, 71, 757-761 Retinal microangiopathy in pigmented paravenous chorioretinal atrophy SURESH R LIMAYE AND MUNEERA A MAHMOOD From the Ophthalmology Service, DC General
British Journal of Ophthalmology, 1987, 71, 757-761 Retinal microangiopathy in pigmented paravenous chorioretinal atrophy SURESH R LIMAYE AND MUNEERA A MAHMOOD From the Ophthalmology Service, DC General
Relentless Placoid Chorioretinitis
 CLINICAL SCIENCES Relentless Placoid Chorioretinitis A New Entity or an Unusual Variant of Serpiginous Chorioretinitis? B. Eric Jones, MD; Lee M. Jampol, MD; Lawrence A. Yannuzzi, MD; Michael Tittl, MD;
CLINICAL SCIENCES Relentless Placoid Chorioretinitis A New Entity or an Unusual Variant of Serpiginous Chorioretinitis? B. Eric Jones, MD; Lee M. Jampol, MD; Lawrence A. Yannuzzi, MD; Michael Tittl, MD;
Review Article A Review of the Inflammatory Chorioretinopathies: The White Dot Syndromes
 ISRN Inflammation Volume 2013, Article ID 783190, 9 pages http://dx.doi.org/10.1155/2013/783190 Review Article A Review of the Inflammatory Chorioretinopathies: The White Dot Syndromes Courtney M. Crawford
ISRN Inflammation Volume 2013, Article ID 783190, 9 pages http://dx.doi.org/10.1155/2013/783190 Review Article A Review of the Inflammatory Chorioretinopathies: The White Dot Syndromes Courtney M. Crawford
53 year old woman attends your practice for routine exam. She has no past medical history or family history of note.
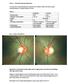 Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
The effect of intravitreal bevacizumab in a rare case of retinal dystrophy with secondary cystoid macular edema
 Romanian Journal of Ophthalmology, Volume 61, Issue 2, April-June 2017. pp:123-127 CASE REPORT The effect of intravitreal bevacizumab in a rare case of retinal dystrophy with secondary cystoid macular
Romanian Journal of Ophthalmology, Volume 61, Issue 2, April-June 2017. pp:123-127 CASE REPORT The effect of intravitreal bevacizumab in a rare case of retinal dystrophy with secondary cystoid macular
Retina Conference. Janelle Fassbender, MD, PhD University of Louisville Department of Ophthalmology and Visual Sciences 09/04/2014
 Retina Conference Janelle Fassbender, MD, PhD University of Louisville Department of Ophthalmology and Visual Sciences 09/04/2014 Subjective CC/HPI: 64 year old Caucasian female referred by outside ophthalmologist
Retina Conference Janelle Fassbender, MD, PhD University of Louisville Department of Ophthalmology and Visual Sciences 09/04/2014 Subjective CC/HPI: 64 year old Caucasian female referred by outside ophthalmologist
UVEITIS IN GENERAL. Information for patients UVEITIS CLINIC WHAT IS UVEITIS? MAIN CATEGORIES OF UVEITIS
 Information for patients UVEITIS CLINIC UVEITIS IN GENERAL WHAT IS UVEITIS? The uvea is a name given to the pigmented layer of tissue inside the eye. When all or part of the uvea becomes inflamed, the
Information for patients UVEITIS CLINIC UVEITIS IN GENERAL WHAT IS UVEITIS? The uvea is a name given to the pigmented layer of tissue inside the eye. When all or part of the uvea becomes inflamed, the
The Peripheral Retina What you don t see can hurt you! James W. Walters, PhD, OD 2017
 The Peripheral Retina What you don t see can hurt you! James W. Walters, PhD, OD 2017 The 2 things I don t want to miss! And the 2 reasons why Occult retinal detachments Occult malignancies You can not
The Peripheral Retina What you don t see can hurt you! James W. Walters, PhD, OD 2017 The 2 things I don t want to miss! And the 2 reasons why Occult retinal detachments Occult malignancies You can not
OCT Angiography in Primary Eye Care
 OCT Angiography in Primary Eye Care An Image Interpretation Primer Julie Rodman, OD, MS, FAAO and Nadia Waheed, MD, MPH Table of Contents Diabetic Retinopathy 3-6 Choroidal Neovascularization 7-9 Central
OCT Angiography in Primary Eye Care An Image Interpretation Primer Julie Rodman, OD, MS, FAAO and Nadia Waheed, MD, MPH Table of Contents Diabetic Retinopathy 3-6 Choroidal Neovascularization 7-9 Central
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome)
 Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Uveitis. Pt Info Brochure. Q: What is Uvea?
 Pt Info Brochure Uveitis Q: What is Uvea? A: Uvea is the middle layer of the eye. It is the most vascular structure of the eye. It provides nutrition to the other parts of the eye. The uvea is made up
Pt Info Brochure Uveitis Q: What is Uvea? A: Uvea is the middle layer of the eye. It is the most vascular structure of the eye. It provides nutrition to the other parts of the eye. The uvea is made up
Pearls, Pitfalls and Advances in Neuro-Ophthalmology
 Pearls, Pitfalls and Advances in Neuro-Ophthalmology Nancy J. Newman, MD Emory University Atlanta, GA Consultant for Gensight Biologics, Santhera Data Safety Monitoring Board for Quark AION Study Medical-legal
Pearls, Pitfalls and Advances in Neuro-Ophthalmology Nancy J. Newman, MD Emory University Atlanta, GA Consultant for Gensight Biologics, Santhera Data Safety Monitoring Board for Quark AION Study Medical-legal
UVEITIS. Dr. Yılmaz ÖZYAZGAN
 UVEITIS Dr. Yılmaz ÖZYAZGAN UVEITIS DEFINITION BY STRICT DEFINITION, UVEITIS IS AN INFLAMMATION OF UVEAL TRACT. BUT IN PRACTICAL, IT IS GENERALLY NOT RESTRICTED TO THE UVEA AND INVOLVES OTHER ADJACENT
UVEITIS Dr. Yılmaz ÖZYAZGAN UVEITIS DEFINITION BY STRICT DEFINITION, UVEITIS IS AN INFLAMMATION OF UVEAL TRACT. BUT IN PRACTICAL, IT IS GENERALLY NOT RESTRICTED TO THE UVEA AND INVOLVES OTHER ADJACENT
Serpiginous choroidopathy
 PHILIPPINE JOURNL OF Ophthalmology Vol. 36 No. 2 July Dec em ber 2011 CSE REPORT Kristine Corpus, MD 1 ndrew ijasa, RT 1 Egidio Jose Fortuna, MD 1-2 1, 3, 4 Narciso tienza Jr., MD Serpiginous choroidopathy
PHILIPPINE JOURNL OF Ophthalmology Vol. 36 No. 2 July Dec em ber 2011 CSE REPORT Kristine Corpus, MD 1 ndrew ijasa, RT 1 Egidio Jose Fortuna, MD 1-2 1, 3, 4 Narciso tienza Jr., MD Serpiginous choroidopathy
Interferon-Associated Retinopathy: Communicating with Internal Medicine Ari Wes, Esther S. Hong, MD, and Thomas A. Oetting, MS, MD
 Interferon-Associated Retinopathy: Communicating with Internal Medicine Ari Wes, Esther S. Hong, MD, and Thomas A. Oetting, MS, MD July 26, 2010 Chief Complaint: New floaters in both eyes. History of Present
Interferon-Associated Retinopathy: Communicating with Internal Medicine Ari Wes, Esther S. Hong, MD, and Thomas A. Oetting, MS, MD July 26, 2010 Chief Complaint: New floaters in both eyes. History of Present
Clinically Significant Macular Edema (CSME)
 Clinically Significant Macular Edema (CSME) 1 Clinically Significant Macular Edema (CSME) Sadrina T. Shaw OMT I Student July 26, 2014 Advisor: Dr. Uwaydat Clinically Significant Macular Edema (CSME) 2
Clinically Significant Macular Edema (CSME) 1 Clinically Significant Macular Edema (CSME) Sadrina T. Shaw OMT I Student July 26, 2014 Advisor: Dr. Uwaydat Clinically Significant Macular Edema (CSME) 2
Test Bank for Medical Surgical Nursing An Integrated Approach 3rd Edition by White
 Test Bank for Medical Surgical Nursing An Integrated Approach 3rd Edition by White Link full download : http://testbankair.com/download/test-bank-for-medical-surgical-nursing-anintegrated-approach-3rd-edition-by-white/
Test Bank for Medical Surgical Nursing An Integrated Approach 3rd Edition by White Link full download : http://testbankair.com/download/test-bank-for-medical-surgical-nursing-anintegrated-approach-3rd-edition-by-white/
Doc, I See a Donut in My Vision : An Optometrist s Guide to a Rare Cause of Choroidal Neovascular Membrane
 Doc, I See a Donut in My Vision : An Optometrist s Guide to a Rare Cause of Choroidal Neovascular Membrane Linda Pham, OD, Tobin Ansel, OD, Nancy Shenouda-Awad, OD, FAAO, West Haven VA Medical Center Abstract
Doc, I See a Donut in My Vision : An Optometrist s Guide to a Rare Cause of Choroidal Neovascular Membrane Linda Pham, OD, Tobin Ansel, OD, Nancy Shenouda-Awad, OD, FAAO, West Haven VA Medical Center Abstract
PART 1: GENERAL RETINAL ANATOMY
 PART 1: GENERAL RETINAL ANATOMY General Anatomy At Ora Serrata At Optic Nerve Head Fundoscopic View Of Normal Retina What Is So Special About Diabetic Retinopathy? The WHO definition of blindness is
PART 1: GENERAL RETINAL ANATOMY General Anatomy At Ora Serrata At Optic Nerve Head Fundoscopic View Of Normal Retina What Is So Special About Diabetic Retinopathy? The WHO definition of blindness is
Neuro-Ocular Grand Rounds
 Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
ZEISS AngioPlex OCT Angiography. Clinical Case Reports
 Clinical Case Reports Proliferative Diabetic Retinopathy (PDR) Case Report 969 PROLIFERATIVE DIABETIC RETINOPATHY 1 1-year-old diabetic female presents for follow-up of proliferative diabetic retinopathy
Clinical Case Reports Proliferative Diabetic Retinopathy (PDR) Case Report 969 PROLIFERATIVE DIABETIC RETINOPATHY 1 1-year-old diabetic female presents for follow-up of proliferative diabetic retinopathy
Mild NPDR. Moderate NPDR. Severe NPDR
 Diabetic retinopathy Diabetic retinopathy is the most common cause of blindness in adults aged 35-65 years-old. Hyperglycaemia is thought to cause increased retinal blood flow and abnormal metabolism in
Diabetic retinopathy Diabetic retinopathy is the most common cause of blindness in adults aged 35-65 years-old. Hyperglycaemia is thought to cause increased retinal blood flow and abnormal metabolism in
Course # Flashes and Floaters and Curtains, Oh My!
 Course # 132 Flashes and Floaters and Curtains, Oh My! FLASHES and FLOATERS and CURTAINS, OH MY!!! FLASHES OF LIGHT Vitreous is the villain Retinal traction Retinal hole Retinal tear Migraine Classic migraine
Course # 132 Flashes and Floaters and Curtains, Oh My! FLASHES and FLOATERS and CURTAINS, OH MY!!! FLASHES OF LIGHT Vitreous is the villain Retinal traction Retinal hole Retinal tear Migraine Classic migraine
Course # Flashes and Floaters and Curtains, Oh My!
 Course # 132 Flashes and Floaters and Curtains, Oh My! FLASHES and FLOATERS and CURTAINS, OH MY!!! FLASHES OF LIGHT Vitreous is the villain Retinal traction Retinal hole Retinal tear Migraine Classic migraine
Course # 132 Flashes and Floaters and Curtains, Oh My! FLASHES and FLOATERS and CURTAINS, OH MY!!! FLASHES OF LIGHT Vitreous is the villain Retinal traction Retinal hole Retinal tear Migraine Classic migraine
Head prof. MUDr. E. Vlková, CSc.
 MUDr. Karkanová Michala, Oční klinika LF MU a FN Brno Head prof. MUDr. E. Vlková, CSc. 3 parts: iris (iris) ciliary body (corpus ciliare) choroid (choroidea) Function: regulating the entry of light into
MUDr. Karkanová Michala, Oční klinika LF MU a FN Brno Head prof. MUDr. E. Vlková, CSc. 3 parts: iris (iris) ciliary body (corpus ciliare) choroid (choroidea) Function: regulating the entry of light into
Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
 Columbia International Publishing Journal of Ophthalmic Research (2014) Research Article Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
Columbia International Publishing Journal of Ophthalmic Research (2014) Research Article Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
When optical coherence tomography (OCT)
 Macular Imaging: SD-OCT in nterior Segment Surgical Practice Many pathologic processes of the macula can be visualized or quantified only with this modality. y Steven G. Safran, MD When optical coherence
Macular Imaging: SD-OCT in nterior Segment Surgical Practice Many pathologic processes of the macula can be visualized or quantified only with this modality. y Steven G. Safran, MD When optical coherence
You can C-ME after Uveitis
 You can C-ME after Uveitis Abstract: Approximately 50% of uveitis patients will present with vision loss secondary to cystoid macular edema[1]. Two patients with uveitis present with a constant decrease
You can C-ME after Uveitis Abstract: Approximately 50% of uveitis patients will present with vision loss secondary to cystoid macular edema[1]. Two patients with uveitis present with a constant decrease
FACING YOUR FUNDIC FEARS: EXAMINATION OF THE OCULAR FUNDUS J. Seth Eaton, VMD, DACVO Cornell University Veterinary Specialists
 FACING YOUR FUNDIC FEARS: EXAMINATION OF THE OCULAR FUNDUS J. Seth Eaton, VMD, DACVO Cornell University Veterinary Specialists The goal of a thorough fundus examination is to clinically evaluate the structures
FACING YOUR FUNDIC FEARS: EXAMINATION OF THE OCULAR FUNDUS J. Seth Eaton, VMD, DACVO Cornell University Veterinary Specialists The goal of a thorough fundus examination is to clinically evaluate the structures
What You Should Know About Acute Macular Neuroretinopathy
 What You Should Know About Acute Macular Neuroretinopathy David J. Browning MD, PhD Chong Lee BS Acute macular neuroretinopathy is a condition characterized by the sudden, painless onset of paracentral
What You Should Know About Acute Macular Neuroretinopathy David J. Browning MD, PhD Chong Lee BS Acute macular neuroretinopathy is a condition characterized by the sudden, painless onset of paracentral
Ophthalmology. Juliette Stenz, MD
 Ophthalmology Juliette Stenz, MD Required Slide Disclosures NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Required Slide At the end of this session, students will be able to: 1.
Ophthalmology Juliette Stenz, MD Required Slide Disclosures NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Required Slide At the end of this session, students will be able to: 1.
Year 4 Results For a Phase 1 Trial of Voretigene Neparvovec in Biallelic RPE65- Mediated Inherited Retinal Disease
 8:00 AM Year 4 Results For a Phase 1 Trial of Voretigene Neparvovec in Biallelic RPE65- Mediated Inherited Retinal Disease Albert M. Maguire, MD OBJECTIVE Assess maintenance of functional vision/visual
8:00 AM Year 4 Results For a Phase 1 Trial of Voretigene Neparvovec in Biallelic RPE65- Mediated Inherited Retinal Disease Albert M. Maguire, MD OBJECTIVE Assess maintenance of functional vision/visual
o White dot syndromes pattern recognition o Activity and damage o Quality of life o Key points o Idiopathic o Sarcoidosis o Multiple sclerosis
 Introduction Clinical Assessment of Posterior Uveitis Philip I. Murray Centre for Translational Inflammation Research University of Birmingham Birmingham and Midland Eye Centre o Classification of uveitis
Introduction Clinical Assessment of Posterior Uveitis Philip I. Murray Centre for Translational Inflammation Research University of Birmingham Birmingham and Midland Eye Centre o Classification of uveitis
Role Of Various Factors In The Treatment Of Optic Neuritis----A Study Abstract Aim: Materials & Methods Discussion: Conclusion: Key words
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 9 Ver. X (September). 2016), PP 51-57 www.iosrjournals.org Role Of Various Factors In The Treatment
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 9 Ver. X (September). 2016), PP 51-57 www.iosrjournals.org Role Of Various Factors In The Treatment
Electrodiagnostics Alphabet Soup
 Nathan Lighthizer, O.D., F.A.A.O Assistant Professor, NSUOCO Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic What is electrodiagnostics testing? Visual Pathway Basic Understanding VEP
Nathan Lighthizer, O.D., F.A.A.O Assistant Professor, NSUOCO Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic What is electrodiagnostics testing? Visual Pathway Basic Understanding VEP
Headache Assessment In Primary Eye Care
 Headache Assessment In Primary Eye Care Spencer Johnson, O.D., F.A.A.O. Northeastern State University Oklahoma College of Optometry johns137@nsuok.edu Course Objectives Review headache classification Understand
Headache Assessment In Primary Eye Care Spencer Johnson, O.D., F.A.A.O. Northeastern State University Oklahoma College of Optometry johns137@nsuok.edu Course Objectives Review headache classification Understand
4/22/16. Eye. External Anatomy of Eye. Accessory Structures. Bio 40B Dr. Kandula
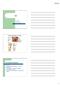 Eye Bio 40B Dr. Kandula External Anatomy of Eye Accessory Structures l Eyebrows l Levator Palpebrae Superioris - opens eye l Eyelashes l Ciliary glands modified sweat glands l Small sebaceous glands l
Eye Bio 40B Dr. Kandula External Anatomy of Eye Accessory Structures l Eyebrows l Levator Palpebrae Superioris - opens eye l Eyelashes l Ciliary glands modified sweat glands l Small sebaceous glands l
Disease-Specific Fluorescein Angiography
 Ruth E. Picchiottino, CRA Disease-Specific Fluorescein Angiography 15 Disease-Specific Fluorescein Angiography Recommendations for tailoring retinal fluorescein angiography to diabetic retinopathy, macular
Ruth E. Picchiottino, CRA Disease-Specific Fluorescein Angiography 15 Disease-Specific Fluorescein Angiography Recommendations for tailoring retinal fluorescein angiography to diabetic retinopathy, macular
Optic Nerve Disorders: Structure and Function and Causes
 Optic Nerve Disorders: Structure and Function and Causes Using Visual Fields, OCT and B-scan Ultrasound to Diagnose and Follow Optic Nerve Visual Losses Ohio Ophthalmological Society and Ophthalmic Tech
Optic Nerve Disorders: Structure and Function and Causes Using Visual Fields, OCT and B-scan Ultrasound to Diagnose and Follow Optic Nerve Visual Losses Ohio Ophthalmological Society and Ophthalmic Tech
Uveitis. What is Uveitis?
 Uveitis What is Uveitis? Uveitis [u-vee-i-tis] is a term for inflammation of the eye. It can occur in one eye or both eyes and affects the layer of the eye called the uvea [u-vee-uh]. It also can be associated
Uveitis What is Uveitis? Uveitis [u-vee-i-tis] is a term for inflammation of the eye. It can occur in one eye or both eyes and affects the layer of the eye called the uvea [u-vee-uh]. It also can be associated
Panretinal acute multifocal placoid pigment epitheliopathy: a novel posterior uveitis syndrome with HLA-A3 and HLA-C7 association
 BRIEF REPORT Open Access Panretinal acute multifocal placoid pigment epitheliopathy: a novel posterior uveitis syndrome with HLA-A3 and HLA-C7 association Kevin R Baxter 1,2* and E Mitchel Opremcak 3 Abstract
BRIEF REPORT Open Access Panretinal acute multifocal placoid pigment epitheliopathy: a novel posterior uveitis syndrome with HLA-A3 and HLA-C7 association Kevin R Baxter 1,2* and E Mitchel Opremcak 3 Abstract
Spontaneous Large Serous Retinal Pigment Epithelial Tear
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
Funduscopic Interpretation Understanding the Fundus: is that normal?
 Funduscopic Interpretation Understanding the Fundus: is that normal? Gillian McLellan BVMS PhD DVOphthal DECVO DACVO MRCVS With thanks to Christine Heinrich and all who contributed images Fundus Retina
Funduscopic Interpretation Understanding the Fundus: is that normal? Gillian McLellan BVMS PhD DVOphthal DECVO DACVO MRCVS With thanks to Christine Heinrich and all who contributed images Fundus Retina
Scrub In. What is the function of vitreous humor? What does the pupil do when exposed to bright light? a. Maintain eye shape and provide color vision
 Scrub In What is the function of vitreous humor? a. Maintain eye shape and provide color vision b. Maintain eye shape and refract light rays c. Provide night vision and color vision d. Provide night vision
Scrub In What is the function of vitreous humor? a. Maintain eye shape and provide color vision b. Maintain eye shape and refract light rays c. Provide night vision and color vision d. Provide night vision
What Is O.C.T. and Why Should I Give A Rip? OCT & Me How Optical Coherence Tomography Changed the Life of a Small Town Optometrist 5/19/2014
 OCT & Me How Optical Coherence Tomography Changed the Life of a Small Town Optometrist Email: myoder@wcoil.com Mark A. Yoder, O.D. 107 N. Main Street PO Box 123 Bluffton, OH 45817 @yoderod 115.02 Histoplasma
OCT & Me How Optical Coherence Tomography Changed the Life of a Small Town Optometrist Email: myoder@wcoil.com Mark A. Yoder, O.D. 107 N. Main Street PO Box 123 Bluffton, OH 45817 @yoderod 115.02 Histoplasma
Deep Trouble. Thomas Stone, MD Retina Associates of Kentucky River City Retina Conference May 15, 2014
 Deep Trouble Thomas Stone, MD Retina Associates of Kentucky River City Retina Conference May 15, 2014 History 20 yo WM Decreased vision OU, OD>OS Sudden onset blurred central vision 12 days prior 4 days
Deep Trouble Thomas Stone, MD Retina Associates of Kentucky River City Retina Conference May 15, 2014 History 20 yo WM Decreased vision OU, OD>OS Sudden onset blurred central vision 12 days prior 4 days
A Curious Case of Bilateral Optic Disc Edema Brittney Dautremont, DO, MPH
 A Curious Case of Bilateral Optic Disc Edema Brittney Dautremont, DO, MPH PGY2 Ophthalmology Resident Grandview Medical Center Dayton, OH CASE PRESENTATION 51 year old white female presenting with blurred
A Curious Case of Bilateral Optic Disc Edema Brittney Dautremont, DO, MPH PGY2 Ophthalmology Resident Grandview Medical Center Dayton, OH CASE PRESENTATION 51 year old white female presenting with blurred
Retina Grand Rounds. Stephen Huddleston MD Charles Retina Institute University of Tennessee Hamilton Eye Institute
 Retina Grand Rounds Stephen Huddleston MD Charles Retina Institute University of Tennessee Hamilton Eye Institute Fundus Autoflourescence 2013 2016 Plaquenil Toxicity Excellent treatment for a variety
Retina Grand Rounds Stephen Huddleston MD Charles Retina Institute University of Tennessee Hamilton Eye Institute Fundus Autoflourescence 2013 2016 Plaquenil Toxicity Excellent treatment for a variety
Macular Hole Associated with Vogt-Koyanagi-Harada Disease at the Acute Uveitic Stage
 Published online: September 15, 2015 2015 The Author(s) Published by S. Karger AG, Basel 1663 2699/15/0063 0328$39.50/0 This article is licensed under the Creative Commons Attribution-NonCommercial 4.0
Published online: September 15, 2015 2015 The Author(s) Published by S. Karger AG, Basel 1663 2699/15/0063 0328$39.50/0 This article is licensed under the Creative Commons Attribution-NonCommercial 4.0
Neuro-Ophthalmic Masqueraders
 Neuro-Ophthalmic Masqueraders Leonid Skorin, Jr., OD, DO, MS, FAAO, FAOCO Mayo Clinic Health System in Albert Lea Denise Goodwin, OD, FAAO Pacific University College of Optometry Please silence all mobile
Neuro-Ophthalmic Masqueraders Leonid Skorin, Jr., OD, DO, MS, FAAO, FAOCO Mayo Clinic Health System in Albert Lea Denise Goodwin, OD, FAAO Pacific University College of Optometry Please silence all mobile
Why Is Imaging Critical in My Uveitis Practice?
 Why Is Imaging Critical in My Uveitis Practice? Dilraj S. Grewal, MD Developed in collaboration Imaging Is the Backbone of Uveitis Workup and Monitoring Treatment Response FP FAF B- scan Multimodal Imaging
Why Is Imaging Critical in My Uveitis Practice? Dilraj S. Grewal, MD Developed in collaboration Imaging Is the Backbone of Uveitis Workup and Monitoring Treatment Response FP FAF B- scan Multimodal Imaging
Cases CFEH. CFEH Facebook Case #4
 CFEH Cases CFEH Facebook Case #4 A 42 year old female has noticed a floater in her left eye for many years but no flashes. She also reports hazy vision in this eye that has been present all her life. She
CFEH Cases CFEH Facebook Case #4 A 42 year old female has noticed a floater in her left eye for many years but no flashes. She also reports hazy vision in this eye that has been present all her life. She
2009 REIMBURSEMENT GUIDE, VISUCAM and VISUCAM NM/FA
 2009 REIMBURSEMENT GUIDE FF 450 PLUS PRO NM, VISUCAM and VISUCAM NM/FA Zeiss Fundus Cameras INTRODUCTION The following guide provides an overview of billing and reimbursement for procedures performed with
2009 REIMBURSEMENT GUIDE FF 450 PLUS PRO NM, VISUCAM and VISUCAM NM/FA Zeiss Fundus Cameras INTRODUCTION The following guide provides an overview of billing and reimbursement for procedures performed with
Non-arteritic anterior ischemic optic neuropathy (NAION) with segmental optic disc edema. Jonathan A. Micieli, MD Valérie Biousse, MD
 Non-arteritic anterior ischemic optic neuropathy (NAION) with segmental optic disc edema Jonathan A. Micieli, MD Valérie Biousse, MD A 75 year old white woman lost vision in the inferior part of her visual
Non-arteritic anterior ischemic optic neuropathy (NAION) with segmental optic disc edema Jonathan A. Micieli, MD Valérie Biousse, MD A 75 year old white woman lost vision in the inferior part of her visual
Update on management of Anterior Uveitis
 Update on management of Anterior Uveitis Parthopratim Dutta Majumder Senior Consultant, Department of Uvea & Intraocular Inflammation Medical Research Foundation, Sankara Nethralaya ABCD of Treating a
Update on management of Anterior Uveitis Parthopratim Dutta Majumder Senior Consultant, Department of Uvea & Intraocular Inflammation Medical Research Foundation, Sankara Nethralaya ABCD of Treating a
Central venous occlusion
 Central venous occlusion Central venous occlusion (right eye) There are dark haemorrhages at the macula and all over the retina. Choroidal haemangioma A choroidal haemangioma has salmon pink colour. There
Central venous occlusion Central venous occlusion (right eye) There are dark haemorrhages at the macula and all over the retina. Choroidal haemangioma A choroidal haemangioma has salmon pink colour. There
Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland
 Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
ISPUB.COM. An Atypical Presentation of Posterior Scleritis. A Ramanathan, A Gaur CASE REPORT
 ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 8 Number 2 A Ramanathan, A Gaur Citation A Ramanathan, A Gaur.. The Internet Journal of Ophthalmology and Visual Science. 2009
ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 8 Number 2 A Ramanathan, A Gaur Citation A Ramanathan, A Gaur.. The Internet Journal of Ophthalmology and Visual Science. 2009
Five Things You re Missing with Your Fundus Camera
 ebook Five Things You re Missing with Your Fundus Camera By Donald J. Siegel, OD, Sun City West Eye Care Sponsored by: Before I began incorporating EIDON true-color imaging into my practice, my retinal
ebook Five Things You re Missing with Your Fundus Camera By Donald J. Siegel, OD, Sun City West Eye Care Sponsored by: Before I began incorporating EIDON true-color imaging into my practice, my retinal
NEPTUNE RED BANK BRICK
 NEPTUNE RED BANK BRICK Diabetes & The Eye Diabetics are more likely to develop Cataracts at a younger age. Diabetics are twice as likely to develop Glaucoma when compared to non-diabetics. The primary
NEPTUNE RED BANK BRICK Diabetes & The Eye Diabetics are more likely to develop Cataracts at a younger age. Diabetics are twice as likely to develop Glaucoma when compared to non-diabetics. The primary
Photocoagulation of disciform macular lesions
 British Journal of Ophthalmology, 1979, 63, 669-673 Photocoagulation of disciform macular lesions with krypton laser A. C. BIRD AND R. H. B. GREY From the Institute of Ophthalmology, Moorfields Eye Hospital,
British Journal of Ophthalmology, 1979, 63, 669-673 Photocoagulation of disciform macular lesions with krypton laser A. C. BIRD AND R. H. B. GREY From the Institute of Ophthalmology, Moorfields Eye Hospital,
PROFILE OF PATIENTS WITH FLOATERS IN SAIFUL ANWAR HOSPITAL MALANG
 International Journal of Retina (IJRETINA) 2018, Volume 2, Number 1. P-ISSN. 2614-8684, E-ISSN.2614-8536 PROFILE OF PATIENTS WITH FLOATERS IN SAIFUL ANWAR HOSPITAL MALANG Fenti Kusumawardhani Hidayah,
International Journal of Retina (IJRETINA) 2018, Volume 2, Number 1. P-ISSN. 2614-8684, E-ISSN.2614-8536 PROFILE OF PATIENTS WITH FLOATERS IN SAIFUL ANWAR HOSPITAL MALANG Fenti Kusumawardhani Hidayah,
Choroidal Neovascularization in Sympathetic Ophthalmia
 Choroidal Neovascularization in Sympathetic Ophthalmia Lucia Sobrin, Miguel Cordero Coma, C. Stephen Foster Case Report A 49-year-old man presented after a ruptured globe repair of his left eye status
Choroidal Neovascularization in Sympathetic Ophthalmia Lucia Sobrin, Miguel Cordero Coma, C. Stephen Foster Case Report A 49-year-old man presented after a ruptured globe repair of his left eye status
A Patient s Guide to Diabetic Retinopathy
 Diabetic Retinopathy A Patient s Guide to Diabetic Retinopathy 840 Walnut Street, Philadelphia PA 19107 www.willseye.org Diabetic Retinopathy 1. Definition Diabetic retinopathy is a complication of diabetes
Diabetic Retinopathy A Patient s Guide to Diabetic Retinopathy 840 Walnut Street, Philadelphia PA 19107 www.willseye.org Diabetic Retinopathy 1. Definition Diabetic retinopathy is a complication of diabetes
1/25/2019 OCT & OCTA RETINAL IMAGING: HOW TO PREVENT RAGING GLAUCOMA! THE ORIGINAL RAGING GLAUCOMA OCT RETINAL IMAGING OPTIC NERVE HEAD EXAMINATION
 OCT & OCTA RETINAL IMAGING: HOW TO PREVENT RAGING GLAUCOMA! Craig Thomas, O.D. 3900 West Wheatland Road Dallas, Texas 75237 972-780-7199 thpckc@yahoo.com THE ORIGINAL RAGING GLAUCOMA 47-year-old Black
OCT & OCTA RETINAL IMAGING: HOW TO PREVENT RAGING GLAUCOMA! Craig Thomas, O.D. 3900 West Wheatland Road Dallas, Texas 75237 972-780-7199 thpckc@yahoo.com THE ORIGINAL RAGING GLAUCOMA 47-year-old Black
Unilateral pigmentary retinopathy a review of literature and case presentation
 Romanian Journal of Ophthalmology, Volume 60, Issue 1, January-March 2016. pp:47-52 CASE REPORT Unilateral pigmentary retinopathy a review of literature and case presentation Stamate Alina-Cristina, Burcea
Romanian Journal of Ophthalmology, Volume 60, Issue 1, January-March 2016. pp:47-52 CASE REPORT Unilateral pigmentary retinopathy a review of literature and case presentation Stamate Alina-Cristina, Burcea
Local Coverage Determination (LCD): Scanning Computerized Ophthalmic Diagnostic Imaging (SCODI) (L34431)
 Local Coverage Determination (LCD): Scanning Computerized Ophthalmic Diagnostic Imaging (SCODI) (L34431) Links in PDF documents are not guaranteed to work. To follow a web link, please use the MCD Website.
Local Coverage Determination (LCD): Scanning Computerized Ophthalmic Diagnostic Imaging (SCODI) (L34431) Links in PDF documents are not guaranteed to work. To follow a web link, please use the MCD Website.
Retinal Tear and Detachment
 Retinal Tear and Detachment Introduction The retina is the layer of tissue in the back of the eye that is responsible for vision. It is attached to the choroid tissue, which supplies the retina with blood.
Retinal Tear and Detachment Introduction The retina is the layer of tissue in the back of the eye that is responsible for vision. It is attached to the choroid tissue, which supplies the retina with blood.
Central serous chorioretinopathy (CSCR) was
 Case Report 777 Perfluorocarbon Liquid-Assisted External Drainage in the Management of Central Serous Chorioretinopathy with Bullous Serous Retinal Detachment Hung-Chiao Chen, MD; Jau-Der Ho, MD; San-Ni
Case Report 777 Perfluorocarbon Liquid-Assisted External Drainage in the Management of Central Serous Chorioretinopathy with Bullous Serous Retinal Detachment Hung-Chiao Chen, MD; Jau-Der Ho, MD; San-Ni
Acute Zonal Occult Outer Retinopathy (AZOOR): a case report of vision improvement after intravitreal injection of Ozurdex
 Kuo et al. BMC Ophthalmology (2017) 17:236 DOI 10.1186/s12886-017-0638-5 CASE REPORT Open Access Acute Zonal Occult Outer Retinopathy (AZOOR): a case report of vision improvement after intravitreal injection
Kuo et al. BMC Ophthalmology (2017) 17:236 DOI 10.1186/s12886-017-0638-5 CASE REPORT Open Access Acute Zonal Occult Outer Retinopathy (AZOOR): a case report of vision improvement after intravitreal injection
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA
 OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
Pit-like changes of the optic nerve head
 Pit-like changes of the optic nerve head in open-angle glaucoma British Journal of Ophthalmology, 1978, 62, 389-393 RONALD L. RADIUS, A. EDWARD MAUMENEE, AND WILLIAM R. GREEN From the Wilmer Ophthalmologic
Pit-like changes of the optic nerve head in open-angle glaucoma British Journal of Ophthalmology, 1978, 62, 389-393 RONALD L. RADIUS, A. EDWARD MAUMENEE, AND WILLIAM R. GREEN From the Wilmer Ophthalmologic
Bitemporal visual field defects mimicking chiasmal compression in eyes with tilted disc syndrome
 Optometry (2009) 80, 232-242 Bitemporal visual field defects mimicking chiasmal compression in eyes with tilted disc syndrome Joseph W. Sowka, O.D., a and Vincent V. Luong, B. Optom. b a Nova Southeastern
Optometry (2009) 80, 232-242 Bitemporal visual field defects mimicking chiasmal compression in eyes with tilted disc syndrome Joseph W. Sowka, O.D., a and Vincent V. Luong, B. Optom. b a Nova Southeastern
Top Pediatric Retinal Diseases you don t want to miss! Retinopathy of Prematurity (ROP) Aggressive, Posterior ROP (AP ROP)
 Top 10 10 Pediatric Retinal Diseases you don t want to miss! Polly Quiram MD, PhD Vitreoretinal Surgery, PA Retinal Update Jan 26th, 2018 ROP Retinoblastoma Coats disease Persistent fetal vasculature Familial
Top 10 10 Pediatric Retinal Diseases you don t want to miss! Polly Quiram MD, PhD Vitreoretinal Surgery, PA Retinal Update Jan 26th, 2018 ROP Retinoblastoma Coats disease Persistent fetal vasculature Familial
epitheliopathy associated with diffuse retinal vasculitis
 British Journal of Ophthalmology, 1986, 70, 255-259 Acute posterior multifocal placoid pigment epitheliopathy associated with diffuse retinal vasculitis and late haemorrhagic macular detachment MAKOTO
British Journal of Ophthalmology, 1986, 70, 255-259 Acute posterior multifocal placoid pigment epitheliopathy associated with diffuse retinal vasculitis and late haemorrhagic macular detachment MAKOTO
Double trouble: a patient with both HLA-B27 anterior uveitis and HLA-A29 birdshot chorioretinitis
 Haddad and Reddy Journal of Ophthalmic Inflammation and Infection 2014, 4:28 BRIEF REPORT Open Access Double trouble: a patient with both HLA-B27 anterior uveitis and HLA-A29 birdshot chorioretinitis Zeina
Haddad and Reddy Journal of Ophthalmic Inflammation and Infection 2014, 4:28 BRIEF REPORT Open Access Double trouble: a patient with both HLA-B27 anterior uveitis and HLA-A29 birdshot chorioretinitis Zeina
Widefield Retinal Imaging with Auto Fluorescence Technology in the Optometric Practice
 Widefield Retinal Imaging with Auto Fluorescence Technology in the Optometric Practice This course will define ultra-widefield retinal imaging and autofluorescence for the attendee. Will show how it is
Widefield Retinal Imaging with Auto Fluorescence Technology in the Optometric Practice This course will define ultra-widefield retinal imaging and autofluorescence for the attendee. Will show how it is
Intro to Glaucoma/2006
 Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
RPE65-associated Leber Congenital Amaurosis
 RPE65-associated Leber Congenital Amaurosis Brian Privett, MD, Edwin M. Stone, MD, PhD February 16, 2010 Chief Complaint: Poor fixation at 4 months of age History of Present Illness: This 7 year old female
RPE65-associated Leber Congenital Amaurosis Brian Privett, MD, Edwin M. Stone, MD, PhD February 16, 2010 Chief Complaint: Poor fixation at 4 months of age History of Present Illness: This 7 year old female
11/29/2016 MACULAR MALADIES: TYPICAL & ATYPICAL CASES
 MACULAR MALADIES: TYPICAL & ATYPICAL CASES Dawn Pewitt, OD, FAAO Triad Eye Institute, Grove, OK Dpewitt@triadeye.com Disclosure Statement: No financial disclosures COPE 51218-PS Please silence all mobile
MACULAR MALADIES: TYPICAL & ATYPICAL CASES Dawn Pewitt, OD, FAAO Triad Eye Institute, Grove, OK Dpewitt@triadeye.com Disclosure Statement: No financial disclosures COPE 51218-PS Please silence all mobile
Diabetes & Your Eyes
 Diabetes & Your Eyes Diabetes is a disease that occurs when the pancreas does not secrete enough insulin or the body is unable to process it properly. Insulin is the hormone that regulates the level of
Diabetes & Your Eyes Diabetes is a disease that occurs when the pancreas does not secrete enough insulin or the body is unable to process it properly. Insulin is the hormone that regulates the level of
Ocular Pathology. I. Congenital and/or developmental. A. Trisomy 21. Hypertelorism (widely spaced eyes) Keratoconus (cone shaped cornea)
 I. Congenital and/or developmental Robbins Pathologic Basis of Disease, 6 th Ed. A. Trisomy 21 Hypertelorism (widely spaced eyes) Keratoconus (cone shaped cornea) Focal hypoplasia of iris Cataracts frequently
I. Congenital and/or developmental Robbins Pathologic Basis of Disease, 6 th Ed. A. Trisomy 21 Hypertelorism (widely spaced eyes) Keratoconus (cone shaped cornea) Focal hypoplasia of iris Cataracts frequently
Vision I. Steven McLoon Department of Neuroscience University of Minnesota
 Vision I Steven McLoon Department of Neuroscience University of Minnesota 1 Eye Cornea Sclera Conjunctiva 2 Eye The conjunctiva lines the inner surface of the eyelids and outer surface of the sclera. 3
Vision I Steven McLoon Department of Neuroscience University of Minnesota 1 Eye Cornea Sclera Conjunctiva 2 Eye The conjunctiva lines the inner surface of the eyelids and outer surface of the sclera. 3
Clinical Approach To Refractive Errors. Dr. Faizur Rahman Associate Professor Peshawar Medical College
 Clinical Approach To Refractive Errors Dr. Faizur Rahman Associate Professor Peshawar Medical College Learning objectives By the end of this lecture the students would be able to; Correlate optics with
Clinical Approach To Refractive Errors Dr. Faizur Rahman Associate Professor Peshawar Medical College Learning objectives By the end of this lecture the students would be able to; Correlate optics with
