The natural history of the Chiari Type I anomaly
|
|
|
- Lee Miller
- 5 years ago
- Views:
Transcription
1 See the corresponding editorial in this issue, pp J Neurosurg Pediatrics 2: , 2008 The natural history of the Chiari Type I anomaly FEDERICA NOVEGNO, M.D., MASSIMO CALDARELLI, M.D., ANTONIO MASSA, M.D., DANIELA CHIEFFO, PH.D., LUCA MASSIMI, M.D., BENEDETTA PETTORINI, M.D., GIANPIERO TAMBURRINI, M.D., AND CONCEZIO DI ROCCO, M.D. Department of Pediatric Neurosurgery, Catholic University Medical School, Rome, Italy Object. Since the advent of MR imaging, an increasing number of asymptomatic or oligosymptomatic patients have been diagnosed with Chiari malformation Type I (CM-I). The decision of whether or not to operate is more difficult in these patients than in those with clear symptoms because of the lack of information about the natural course of this disease. Methods. The authors report on their experience in a series of 22 patients with CM-I who were evaluated at the authors institution, and for whom a conservative approach to treatment was adopted. The patients ranged in age from 1 to 16 years (mean 6.3 years) at diagnosis. Neuroradiological and complete clinical examinations were performed in all patients 6 months after the first observation and every year thereafter. The follow-up period ranged from 3 to 19 years (mean 5.9 years). Results. Chiari malformation Type I was incidentally detected on MR images in 11 of 22 patients. The remaining 11 patients had minimal clinical signs at presentation that were not regarded as necessitating immediate surgical treatment. Seventeen patients (77.3%) showed progressive improvement in their symptoms or remained asymptomatic at the last follow-up whereas 5 patients (22.7%) experienced worsening, which was mild in 2 cases and required surgical correction in the remaining 3 cases. On MR imaging a mild reduction in tonsillar herniation was appreciated in 4 patients (18.18%), with complete spontaneous resolution in 1 of these. In 16 patients, tonsillar herniation remained stable during follow-up. Conclusions. The authors data confirm the common impression that in both asymptomatic and slightly symptomatic patients with CM-I, a conservative approach to treatment should be adopted with periodic clinical and radiological examinations. (DOI: /PED/2008/2/9/179) KEY WORDS Chiari malformation Type I clinical observation syringomyelia T HE Chiari anomaly constitutes a heterogeneous and multifactorial entity, comprising variants on a malformative base as well as acquired forms. It is a rare pathological condition with many controversial aspects, the unifying findings being the abnormal position and to some extent the abnormal shape of the cerebellar tonsils which herniate outside the cranial cavity and into the upper cervical canal, possibly leading to an obliteration of the subarachnoid spaces at the level of foramen magnum. 5,6 In most cases, especially in the acquired variant that arises secondary to a reduction in intracranial cavity volume, the caudal herniation of the cerebellar tonsils is associated with a cranial herniation of the upper cerebellar vermis into the cistern of the great vein of Galen. 8 This phenomenon may play a role in the cerebrospinal fluid dynamics of the affected patients. However, the impaction of the herniated cerebellar tonsils at the level of the foramen magnum is believed to cause occlusion of the subarachnoid spaces and consequently functional separation between the cranial and spinal Abbreviations used in this paper: CM = Chiari malformation; CM-I = CM Type I. compartments. The genesis of the often-associated spinal cord cavitation is attributed to this kind of dynamic anomaly. 25 The signs and symptoms in such patients are generally related to the compression of the neural structures by the herniated tonsils (long tract deficits, cranial nerve dysfunction, and cerebellar involvement) and/or by the presence of an associated syrinx. 31 Once the condition has been recognized and confirmed on a neuroradiological investigation, the choice of the most appropriate management remains debatable. Clinical observation may be the best option in asymptomatic patients, whereas surgical correction is generally suggested for symptomatic children. In asymptomatic patients, CM-I is a frequent incidental finding on MR imaging in children investigated because of behavioral disorders, developmental delay, seizures, or head injuries. The management of incidentally detected CM-I is particularly questionable; some authors 23 believe that CM-I is a dynamic disease, based on the observation that the number of symptomatic patients may increase with age, and they recommend prophylactic surgery. However, most surgeons still prefer to conduct clinical and radiological surveillance. 28 Even more controversial is defining the man- 179
2 F. Novegno et al. agement of children with CM-I who, although neurologically intact, present with syringomyelia on MR imaging. Similarly, it is difficult to decide whether mild and relatively aspecific clinical signs and symptoms (such as headache, vertigo, and dizziness) may be regarded as reliable indications for surgical treatment. For these reasons CM-I remains poorly understood; in particular, the natural history of this disease has not yet been established. In fact, despite the contributions of many authors, 6,8,9,14,20 23,29,36,37 a basic understanding of the pathogenesis and progression of this condition remains elusive. Our aim in the present study is to contribute to the understanding of the evolution of CM-I in children. We therefore present a series of 22 pediatric patients with CM-I (both asymptomatic and oligosymptomatic) for whom a surgical procedure was not advised and who underwent clinical observation for at least 3 years of follow-up. Methods Ninety-four children with CM-I were observed at the Department of Pediatric Neurosurgery at the Catholic University Medical School in Rome between January 1988 and November Among these, 22 consecutive patients with mild or absent clinical manifestations were not considered suitable for immediate surgical treatment and were enrolled in a follow-up program. Their ages ranged from 1 to 16 years (mean 6.3 years) at diagnosis. Cases of acquired Chiari Type I anomaly (such as those with faciocraniostenosis, osteopetrosis, or long-term extrathecal cerebrospinal fluid shunting) were excluded from the study. As to the remaining 72 children, 39 patients underwent posterior fossa decompression, which consisted in suboccipital craniectomy in 32 cases (30 of these have been previously reported 6 ) and bone removal associated with intradural procedures in the remaining 7 patients. Three patients affected by CM-I and tethered cord underwent terminal filum resection. Eighteen patients were evaluated for CM-I after shunt placement, and 7 of these underwent an enlarging bilateral cranioplasty. A further 12 children with CM-I associated with syndromic craniosynostosis involving the lambdoid sutures were initially treated by means of cranial vault remodeling. Neuroradiological investigation was performed in all patients and included CT scanning and MR imaging; in addition to the cranial compartment, thorough craniospinal axis examination was performed in each patient for evidence of syringomyelia or spinal cord tethering. Cranial and spinal MR imaging was performed initially 6 months after the first observation and every year thereafter. We decided to perform serial MR imaging examinations to evaluate changes (for example, ascent of cerebellar tonsils or further descent into the spinal canal, or the novel appearance of syringomyelia) despite clinical stability. Complete clinical examinations were conducted at least once a year. The follow-up varied from 3 to 19 years (mean 5.9 years); follow-up data are summarized in Table 1. To obtain information about psychomotor development, the last 10 children of the series underwent routine neuropsychological assessment. Cognitive performance, receptive and expressive language skills, verbal fluency, selective and sustained visual attention, visual motor integration and praxia, and gross and fine motor function were investigated using a series of specific tests. The assessment of cognitive development was performed using different scales as appropriate for the child s chronological age and level of functioning: the Griffith Mental Development Scales or Uzgiris Hunt Scales in children younger than 4 years old, Wechsler Preschool and Primary Scale of Intelligence in children 4 6 years of age, and the Wechsler Intelligence Scale for Children Revised for those older than 6 years. Behavioral disorders were classified according to the Diagnostic and Statistical Manual of Mental Disorders IV Revised criteria. The Movement Assessment Battery for Children measures 30 were adopted to evaluate fine motor coordination and dexterity, and static and dynamic balance. The language was explored by receptive and naming lexical and syntactic tasks. 4,27 The Developmental Test of Visual Motor and Perceptual Integration 16 and Rey Osterrieth Complex Figure Test were utilized to assess fine-motor coordination, visual perceptual organization, and spatial planning. Phrase recall of the Wechsler Intelligence Scale for Children Revised and Wechsler Preschool and Primary Scale of Intelligence were applied to measure short-term auditory memory. Finally, the Gauthier Test was used to evaluate sustained and selective visual attention in patients 4 14 years of age. Patient data were transferred into a spreadsheet (Excel, Microsoft) for tracking, comparison, and statistical examination. Results Clinical Findings at Diagnosis Among our 22 patients, CM-I was detected in 11 on MR images obtained for investigation of completely unrelated symptoms or signs as follows: paranasal sinusitis, developmental delay, precocious thelarche, neck injury at birth, and visual disturbances in 1 patient each; and seizure disorder, macrocrania, and head injury in 2 patients each. The average age in this group was 5 years (range 1 14 years). The remaining 11 patients (50%) had clinical manifestations for which they underwent neuroradiological investigation. The average age in this group was 7.5 years (range 3 16 years). The most frequent complaint was occipital and/or nuchal pain reported by 8 patients, followed by vertigo which was noted in 2 patients. Clinical signs included upper extremity pain, gait instability, and papilledema in 1 patient each. Two of these patients presented with epileptic disorders and cortical electric anomalies revealed on electroencephalography and required antiepileptic drugs that provided good control of seizures. Neuroradiological Investigation at Diagnosis All patients had a frank tonsillar herniation below the basion opisthion line that was associated with narrowing or obliteration of the cisterna magna. The degree of tonsillar herniation is displayed in Table 2. Syringomyelia was demonstrated in only 1 patient (4.5%), and this was limited to the cervical level. Hydrocephalus was detected in 5 patients (22.7%); it was moderate in 4 patients and mild and unilateral in 1 patient. Other associated anomalies were platybasia, facial dysmorphism with microcephaly, and cavum septum pellucidum detected in 1 patient each. Clinical Follow-Up Among the 11 asymptomatic patients, 7 (63.6%) did not 180
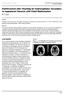
3 Natural history of Chiari malformation Type I TABLE 1 Summary of patient data* Incidental Degree of FU Degree of Case Age (yrs), Discovery; Tonsillar Period Evolution of Tonsillar Syrinx Ventricular No. Sex Symptoms Reason for MRI Associated Anomaly Herniation (mm) (yrs) Symptoms Herniation at FU Dilation 1 2, M gait instability NA none asymptomatic complete res- no no olution 2 3, F headache & NA epileptic disorder 10 5 worsened stable no no vertigo 3 4, M neck pain NA none 10 5 asymptomatic improved no no 4 5, F headache NA none asymptomatic improved no no 5 6, F headache NA none 10 4 asymptomatic stable no no 6 7, F vertigo NA none 5 3 asymptomatic stable no no 7 7, M neck pain NA none 10 3 improved stable no no 8 9, F headache NA none 5 5 improved stable no no 9 10, F nausea & NA none 5 7 asymptomatic stable no no vomiting 10 10, F headache & NA mild unilat ventriculo asymptomatic stable no stable papilledema megaly 11 16, F headache NA Sturge Weber, elephanti- 5 6 mild worsened stable no no asis & cavum septum 12 1, F NA neck injury at none 10 7 asymptomatic stable no no birth 13 1, M NA macrocrania none asymptomatic stable no no 14 2, M NA macrocrania mild ventriculomegaly asymptomatic worsened no stable 15 2, M NA epileptic disor- none asymptomatic improved no no der 16 5, M NA developmental platibasia & mild ven asymptomatic stable stable stable delay triculomegaly 17 5, F NA paranasal si- none new-onset stable no no nusitis neck pain 18 5, F NA trauma mild ventriculomegaly 5 4 new-onset stable new onset worsened headache (cervical) 19 6, F NA visual defect craniofacial dysmorph new-onset worsened new onset worsened ism & mild ventriculo- neck pain (cervical) megaly 20 6, F NA precocious none 10 3 asymptomatic stable new onset no thelarche (cervical) 21 9, M NA trauma none 5 5 asymptomatic stable no no 22 14, F NA epileptic disor- none 10 3 asymptomatic stable no no der * FU = follow-up; NA = not applicable. This patient requried a suboccipital craniectomy and C-1 laminectomy. Postoperatively the patient improved but headaches persisted. A syrinx was initially present only in Case 16. These patients required endoscopic third ventriculostomies. The patient in Case 18 was subsequently asymptomatic and the patient in Case 19 was dramatically improved. show any changes in follow-up clinical examinations. The remaining 4 patients (36.4%) experienced the onset of clinical symptoms between 3 and 5 years after the first diagnosis; these symptoms included headache and neck pain in 1 patient each, and headache/neck pain and vertigo in 2 patients. At the last follow-up examination, 8 (72.7%) of the 11 asymptomatic patients did not show clinical complaints. In the symptomatic group, 7 (63.6%) of 11 patients had no clinical manifestations of disease at last follow-up. In 2 patients (18.2%) a mild improvement was observed, and worsening symptoms were noted in the remaining 2 patients (18.2%). One of these 2 patients (Case 2) was judged to need an operation to relieve her symptoms; in fact, she showed the progressive increasing of the symptoms (headache and vertigo) without any relevant change of the neuroradiological findings. The second patient (Case 11) presented a mild worsening of the headache; the MR imaging findings were stable. She underwent intracranial pressure monitoring that revealed values within the normal range and, on these grounds, a further observational policy was adopted. Of all 22 patients, both asymptomatic and oligosymptomatic groups, 17 (77.3%) had progressive symptom improvement or remained asymptomatic at last follow-up and 5 patients (22.7%) experienced a worsening of their clinical conditions. This worsening was mild in 2 cases (9%) and required a surgical procedure in the remaining 3 (13.6%). The evolution of clinical manifestations in all 22 patients is summarized in Table 3. Findings on MR Imaging at Late Follow-Up All patients underwent periodic radiological evaluation. No radiological changes were demonstrated on MR images obtained 6 months after diagnosis (short-term follow-up). In the long term, however, a mild reduction in tonsillar herniation was appreciable in 4 (18.18%) patients (3 were symptomatic and 1 was asymptomatic) and complete spontaneous resolution occurred in 1 of these patients (Fig. 1). In 2 pa- 181
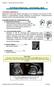
4 F. Novegno et al. TABLE 2 Evolution of tonsillar herniation degree in the asymptomatic and oligosymptomatic groups No. of Extent of Condition Patients Tonsillar Group (%) Herniation (mm) Stable Improved Worsened asymptomatic 2 (18.1) 5 2 (11 patients) 6 (54.5) (27.2) 10 3 oligosymptomatic 4 (36.4) 5 4 (11 patients) 1 (9) (54.5) tients (9%) a progressive increase in the degree of tonsillar herniation was observed. The patient in Case 14 (asymptomatic at diagnosis) did not show any progression of clinical findings, and intracranial pressure monitoring revealed values within the normal range. The patient in Case 19, who had initially presented with a visual defect, presented with new-onset progressive neck pain and apnea. Magnetic resonance images obtained in this patient revealed progression of the preexisting hydrocephalus associated with an increase in the degree of tonsillar herniation and the new appearance of syringomyelia (Fig. 2). Sixteen patients showed stable tonsillar herniation during the entire follow-up period; among these 8 were symptomatic and 8 were asymptomatic. Syringomyelia, present in 1 child, did not change over 19 years of follow-up. In contrast, the de novo appearance of a cervical syrinx was observed in 3 patients. Two of these patients also experienced worsening of their hydrocephalus and had had mild ventriculomegaly at diagnosis. The other 3 patients who had presented with mild ventriculomegaly appeared stable at last follow-up (at 4, 5, and 19 years after diagnosis). Need for Surgical Correction After a period of 3 6 years after the first diagnosis (mean 4.6 years), 3 of the 22 patients required surgery (Cases 2, 18, and 19); 2 patients underwent endoscopic third ventriculocisternostomy because of progressive worsening of the supratentorial hydrocephalus associated with new-onset cervical syringomyelia in both patients, and an increasing degree of the tonsillar herniation in 1. The third patient underwent a suboccipital craniectomy associated with C-1 TABLE 3 Summary of the evolution of clinical manifestations over long-term follow-up* Evolution of Symptoms Age at Case Diagnosis Last Group No. (yrs), Sex Initial Complaint 1st Yr 2nd Yr 3rd Yr 4th Yr 5th Yr 6th Yr 7th Yr 8th Yr 9th Yr FU (yr) A 12 1, F none asymp , M none asymp asymp, , M none asymp , M none asymp asymp, , F none asymp , M none asymp , F none asymp 3 B 17 5, F none neck pain , F none headache , F none neck pain, 3 vertigo, apnea C 3 4, M neck pain improved asymp 5 4 5, F headache improved asymp 6 5 6, F headache improved asymp 4 6 7, F vertigo improved asymp 3 7 7, M neck pain improved improved 3 8 9, F headache improved improved , F nausea & vomiting improved asymp asymp , F headache & papille- improved asymp 4 dema D 2 3, F headache & vertigo worsened 5 apnea 11 16, F headache worsened stable 6 E 1 2, M gait instability asymp neck pain improved asymp, , M none headache & improved asymp 9 vertigo * In this table the series has been divided into 5 subgroups according to clinical evolution: A) 7 incidentally diagnosed patients with no changes at the last clinical examination; B) 3 asymptomatic patients with new onset of clinical symptoms 3 5 years after the first diagnosis (note that the worsening of the clinical symptoms in 2 of these patients was related to the progression of supratentorial hydrocephalus); C) 8 oligosymptomatic patients who experienced improvement from the 2nd and 3rd years after diagnosis; D) 2 oligosymptomatic patients with worsening of symptoms; and E) 2 patients (1 asymptomatic and 1 oligosymptomatic) with new onset of headache/neck pain at 5 and 6 years after first diagnosis which disappeared after 2 years. Abbreviation: asymp = asymptomatic. 182
5 Natural history of Chiari malformation Type I FIG. 1. Case 1. Representative T1-weighted MR images. Tonsillar herniation is demonstrated in the image in panel A obtained in 1997 and performed for gait instability. Additional images were obtained in 2000 (B), 2003 (C), 2005 (D), and 2007 (E). In 2007 the neuroradiological findings changed totally, showing complete resolution of the malformation (E). FIG. 2. Case 19. Representative MR images. Sagittal T1-weighted (A) and axial T2-weighted (B) images obtained at diagnosis, showing hindbrain herniation associated with mild ventriculomegaly. After 3 years, the patient presented with progression of hydrocephalus associated with an increase in tonsillar herniation shown on sagittal T1-weighted (C) and axial T2-weighted (D) images. laminectomy. The postoperative course was uneventful in all cases and the patients experienced a drastic improvement in their symptoms in the first 2 cases, and a mild improvement in the third. No significant changes were observed on postoperative MR images except for ventricular dimensions, which were reduced in the first 2 patients. Neuropsychological Findings Seven of the 10 children who underwent neuropsychological testing were right-handed, 1 was left-handed, and 2 had incomplete dominance. Eight children showed a normal level of intelligence (group mean IQ 106.2; mean of the corresponding population [standard deviation]). Two children presented with a borderline level of global intelligence (mean IQ 81.5). Naming speech delay was found in 5 cases, visual attention disturbances in 4 cases, dyspraxia in 2 cases, and visual memory deficits in 2 cases. Four of the 5 patients with naming speech delays had tonsillar herniations 10 mm. The visual attention disorders were associated with neurovisual deficits in only 1 case (Case 19). Language comprehension, short-term verbal memory, and fine movement were normal in all patients. Two patients presented with behavioral disorders such as hyperkinesia. Discussion In recent years, the wide availability of cerebral and spinal MR imaging technology has led nonneurosurgeon physicians, such as pediatricians, neurologists, and other clinicians, to use MR imaging to evaluate patients with varied complaints such as learning disabilities, behavioral problems, and epileptic disorders, with the incidental discovery of CM-I in some of them. For this reason, neurosurgeons are increasingly faced with the decision of how to manage the care of asymptomatic patients and patients who present with symptoms that may or may not be referable to an underlying hindbrain herniation, in addition to the patients who present with the typical presentation of syringomyelia and severe neurological manifestations. Moreover, in the pre MR imaging era the diagnosis of CM-I was usually not made in children younger than 12 years old because of the invasiveness of the traditional radiological investigations 183
6 F. Novegno et al. which were reserved only for patients with signs and symptoms clearly referable to spinal cord or craniocervical junction lesions. 31 The expanding use of MR imaging has led, therefore, to a progressive reduction in patient age at diagnosis, as CM-I is increasingly identified in younger children with minimal neurological disorders. 12 The proper management of these types of cases of Chiari anomaly Type I is still debatable because of the lack of precise knowledge concerning the natural history of the anomaly. In their survey of the members of the Pediatric Section of the American Association of Neurological Surgeons in 1998, Haroun et al. 13 reported that most respondents (63%) believed that asymptomatic patients rarely develop symptoms, and 83% of neurosurgeons would not operate in asymptomatic patients unless symptoms developed. A similar conclusion was reached by Schijman and Steinbok 28 in their 2004 international survey on the management of CM and syringomyelia. This study demonstrated a general agreement among practitioners for a nonoperative approach to the treatment of asymptomatic patients. Only 8% of those surveyed would recommend prophylactic surgery in the absence of an associated syrinx; the presence of a spinal cord cavity would lead the surgeon to operate even without correlating symptoms in 28% of cases, if the size of the syrinx was 2-mm wide, and in 75% of cases, if the syrinx were 8- mm wide. It is worth noting, however, that despite this consensus, no objective data were described in these studies to support clinical decision making on scientific grounds. On the other hand, some authors have speculated that CM-I is a dynamic disease, a hypothesis based on the observation that the number of symptomatic patients may increase with age. 10,23 The question raised by these considerations then is not whether or not to operate but when and which procedure should be performed. The lack of reliable information about the natural evolution of the CM-I does not allow confirmation or denial of the validity of these opposing views, and few articles in the literature are dedicated to these issues. In 2000 Meadows et al. 18 reported on a retrospective analysis of MR images obtained in 21 asymptomatic patients with CM-I, 6 of whom were children. Meadows and colleagues observed that the degree of the tonsillar herniation and the overall MR imaging characteristics are similar to those observed in the symptomatic patients reported on in the literature. We observed that in the symptomatic group, more than half of the patients (54.6%) presented with herniation 10 mm, while in the asymptomatic group 54.6% had tonsils descend between 5 and 10 mm. Among the 21 asymptomatic patients reported on by Meadows et al., only 1 (4.8%) presented with syringomyelia. In the present study only 1 child (Case 16) had a cervical syrinx without any neurological dysfunction. Magnetic resonance images obtained in this patient demonstrated the presence of platybasia, 5 10 mm tonsillar ectopia, and mild hydrocephalus. Meadows et al. did not conduct follow-up in their patients, as this was not the purpose of their analysis. Genitori et al. 10 reported on a series of 53 children with CM-I, 27 of whom were asymptomatic. These 27 patients did not undergo surgery and instead received clinical surveillance for 1 12 months. None of these patients developed symptoms or signs related to brainstem compression or the presence of a syrinx. However, the authors noted that the average age at diagnosis was significantly lower in the asymptomatic patients than in those with symptoms, a finding observed also in our series. Nevertheless, even if we accept that symptomatic cases are more common in the older age group, the clinical significance of this phenomenon in terms of prognosis remains to be clarified. Nishizawa et al. 24 published a unique report providing new information on the long-term outcomes in purely asymptomatic patients with CM-I and syringomyelia in adults. These authors described the cases of 9 adult patients who underwent evaluation for incidentally identified syringomyelia associated with tonsillar herniation and regularly underwent neurological and MR imaging examinations for at least 10 years. At the last follow-up only 1 patient had symptoms and required surgery, with prompt recovery. The analysis of these data may give the impression that an even wider syrinx associated with CM-I would follow a benign course, thus justifying conservative management until a neurological change is detected. In our series the patient in Case 16 represents the only case of asymptomatic syringomyelia associated with hindbrain herniation. This patient underwent follow-up for 19 years without any changes in his clinical condition. In this case the syrinx extends from C- 5 to C-7, with a width of 4 mm. Tokunaga et al. 35 performed a retrospective review of 27 patients with scoliosis who had syringomyelia associated with cerebellar tonsil herniation detected on MR imaging. The mean age of these patients at the first MR imaging session was 10.9 years (range 5 18 years). In ~ 50% of these cases a decrease in syrinx size was observed; in this group there was a significant elevation of the cerebellar tonsils (complete resolution in 3 cases) and improvement in scoliosis and neurological impairments. Spontaneous resolution of tonsillar herniation is rare (Table 4). Although sporadic cases have been reported in adult patients, 17 most authors describe this phenomenon as typically a childhood condition. 2,3,7,15,26,32 35 Among the patients in our study, we observed spontaneous resolution in only 1 case (Case 1). At 2 years of age, this child underwent cerebral MR imaging to investigate progressive gait instability, and a tonsillar herniation of 10 cm below the foramen magnum was detected. After a follow-up period of 10 years, the radiological appearance in this child changed totally, showing complete resolution of the malformation. During follow-up the gait instability progressively disappeared, and after 6 years from the initial diagnosis the patient presented with sporadic episodes of neck pain that eventually resolved. Many theories have been proposed to explain the spontaneous resolution of CM-I. It has been shown that in children tonsil position depends on age, and that the tonsils gradually ascend as children grow. 19 These observations raise the hypothesis that as the skull growth accelerates, it expands to accommodate the cerebellum, and the cerebellar tonsils assume their normal position. 15,19,33 Sun et al. 33 reported on an interesting case of spontaneous resolution and recurrence of CM-I with associated syringomyelia in a child. The theory of the differential growth of the osseous compartment in relation to the brain and spinal cord responsible for initial improvement cannot be applied in this case because the CM recurred despite the patient s continued growth. On this basis, the authors suggested that the venous sinus occlusion had improved and then worsened, or that the resolution of the CM and later advent of venous occlusion could have caused a recurrence of hindbrain herniation. Tonsillar her- 184
7 Natural history of Chiari malformation Type I TABLE 4 Spontaneous improvement in pediatric patients reported in the literature Authors & Year Age (yrs), Sex Associated Syrinx FU (yrs) CM-I Syrinx Sudo et al., , M cervicothoracic 2.3 complete resolution complete resolution Castillo & Wilson, , F absent 4 complete resolution absent Avellino et al., , M cervical & thoracic 5.5 improved improved Avellino et al., , F cervicothoracic 11 improved improved Sun et al., 2000* 11, M cervicothoracic 2 complete resolution improved Sun et al., , M cervical 7 complete resolution complete resolution Tokunaga et al., , F present 2 improved improved 6, M present 9 improved complete resolution 7, M present 5 complete resolution improved 7, M present 6 improved improved 8, M present 8 improved complete resolution 10, M present 3 improved complete resolution 10, M present 9 improved complete resolution 10, F present 2 improved complete resolution 10, M present 8 complete resolution complete resolution 11, M present 4 improved complete resolution 13, F present 2 improved improved 14, F present 8 improved complete resolution 15, F present 4 improved improved 16, F present 2 complete resolution complete resolution Rafia & Pascual-Castroviejo, , M cervical & dorsolumbar 4 improved complete resolution Jatavallabhula et al., , M absent 4.6 complete resolution absent present study 6, M absent 10 complete resolution absent * Patient s condition worsened after 1 year. niation due to obstruction of the posterior fossa venous outflow, in the presence of vein of Galen malformations, has already been reported. 11 Moreover, embolization in those cases led to complete resolution or significant improvement in the extent of tonsillar herniation. Among our patients with an incidental diagnosis, 4 (36.4%) presented with new-onset clinical symptoms 3 5 years after the initial diagnosis; these symptoms were headache in 1 case, neck pain in a second case, and headache, neck pain, and vertigo in the third and fourth cases. In the first patient (Case 18), there was progressive worsening of hydrocephalus without any change in the degree of tonsillar herniation, but this was associated with the onset of cervical syringomyelia and surgery was advised. The second patient (Case 17) reported neck pain at the last follow-up examination (5 years after presentation), with no evidence of progression on neuroradiological studies. The third patient (Case 15) showed progressive spontaneous improvement over the last 4 years of a 9-year follow-up period. The last patient (Case 19) experienced progression of preexisting hydrocephalus that was associated with an increase in the degree of tonsillar herniation and the novel appearance of syringomyelia; this patient underwent a surgical procedure. One of the symptomatic patients (Case 1) who initially presented with gait instability experienced rapid improvement in coordination, but complained of sporadic episodes of neck pain 6 years after the original diagnosis. During the last 3 years of follow-up in this patient, the neck pain disappeared. All these 5 patients, after a period of no less than 3 years, showed the appearance of symptoms probably related to CM-I, which resolved spontaneously in 2 of these patients. It is worth noting that the worsening of the clinical symptoms was related to the progression of supratentorial hydrocephalus in 2 of the remaining 3 patients. In our patients, the most frequent complaint was occipital and/or nuchal pain, present in 8 patients, and less frequently vertigo, in 2 patients. These are nonspecific symptoms, and although they are frequently encountered in patients with CM-I, it is still a matter of debate as to whether they are sufficient to justify surgery. 28,38 According to a survey of surgeons conducted by Schijman and Steinbok, 28 46% of respondents would operate in patients with CM-I in the absence of a syringomyelia if headaches were the only complaint. In the present series, of the 8 patients with headaches at presentation, 6 significantly improved; at the last followup 4 were asymptomatic and 2 had improved. One patient with vertigo at diagnosis was asymptomatic at the last follow-up, while the other experienced general worsening of symptoms and required surgery. From these data, it seems reasonable to consider conservative treatment if pain symptoms are the only clinical manifestations of CM-I. Three of our patients required surgery (Cases 2, 18, and 19); 2 of these underwent third ventriculocisternostomies because of progressively worsening supratentorial hydrocephalus. Independent of clinical manifestations, evidence of a slight ventricular dilation should alert the surgeon to the possibility of CM progression. However, 3 other patients (Cases 10, 14, and 16) with evidence of mild ventricular dilation at diagnosis, who were asymptomatic at the last follow-up examination, did not require surgery. One patient (Case 2) underwent suboccipital craniectomy; her initial symptoms included headache and vertigo. Once the CM was identified she underwent polysomnography testing, which revealed cortical electrical anomalies and she was started on an antiepileptic drug regimen; the vertigo subsequently improved. The new onset of sporadic episodes of apnea, which progressively increased in frequency, led the surgeons to decompress the posterior fossa. One year postoperatively, her vertigo and apnea had disappeared but the headaches persisted. 185
8 F. Novegno et al. Of our 22 patients, 5 experienced a worsening of clinical conditions. However, in only 3 of these was the worsening caused by the evolution of the CM itself. In the remaining 2 cases, the worsening was due to hydrocephalus and associated ventriculomegaly, which caused increasing hindbrain herniation. In Cases 11 and 17, headache was the main symptom that presented with a new onset or that had worsened at the last follow-up (at 6 and 5 years, respectively). In these 2 cases we chose a conservative approach because we have observed that these symptoms may eventually disappear within 2 3 years unless associated with hydrocephalus. The real question is why the patient in Case 2 required surgical decompression of the foramen magnum. Unfortunately, at this time we still do not know why this patient s condition progressed to this point, as there had been no radiological evidence of worsening during follow-up. In conclusion, 17 (77.3%) of our patients experienced progressive improvement of symptoms or remained asymptomatic at the last follow-up without evidence of significant corresponding changes on neuroimaging studies. If we exclude the 2 patients with worsening hydrocephalus, the percentage rises to 85% (17 of 20 patients). Our last comment concerns the neuropsychological assessment. Normal general development was observed in all patients. Despite having a normal mean IQ, neuropsychological processing deficits in language skills were evident in 50% of the patients who underwent neuropsychological assessment (5 of 10 patients). Qualitative analysis demonstrated slowed speech, lack of fluency, and word-finding difficulties. In these cases, we observed the patients verbal IQ scores to be within the average range, and language comprehension and production were adequate. These results are supported by similarities in the pattern of neuropsychological executive functioning deficits with dorsolateral prefrontal cortex lesions and patients with cerebellar lesions. They include deficits in planning, problem solving, verbal fluency, and other word generation abilities. 1 Conclusions In the attempt to clarify the natural history of CM-I, we present one of the first studies to analyze the evolution (for (3 years) of incidentally discovered cases of CM-I in which the patient has no or minimal clinical signs regarded as not requiring immediate surgical treatment. Our data seem to confirm the general impression that in asymptomatic patients a conservative approach may be adopted. Clinical follow-up may also be advisable for patients whose symptoms are extremely nonspecific or only doubtfully referable to the malformation. In both of these types of cases, we recommend periodic clinicoradiological examinations. However, we are as yet unable to establish how long these examinations should continue. Our study has 2 main faults: the limited number of patients and the lack of a homogeneous longterm follow-up. A multicenter cooperative study should be undertaken to provide valuable information on the natural course of these malformations. Disclaimer The authors report no conflict of interest concerning the materials or methods used in this study or the findings specified in this paper. Acknowledgment We thank Daniele Petricca for help with the illustrations, and the association "Ali di Scorta onlus" ( References 1. Appollonio IM, Grafman J, Schwartz V, Massaquoi S, Hallett M: Memory in patients with cerebellar degeneration. Neurology 43: , Avellino AM, Britz GW, McDowell JR, Shaw DW, Ellenbogen RG, Roberts TS: Spontaneous resolution of a cervicothoracic syrinx in a child. Case report and review of the literature. Pediatr Neurosurg 30:43 46, Avellino AM, Kim DK, Weinberger E, Roberts TS: Resolution of spinal syringes and Chiari I malformation in a child. Case illustration. J Neurosurg 84:708, Bottari P, Cipriani P, Chilosi AM, Pfanner L: The italian determiner system in normal acquisition, specific language impairment, and childhood aphasia. Brain Lang 77: , Caldarelli M, Di Rocco C: Diagnosis of Chiari I malformation and related syringomyelia: radiological and neurophysiological studies. Childs Nerv Syst 20: , Caldarelli M, Novegno F, Massimi L, Romani R, Tamburrini G, Di Rocco C: The role of limited posterior fossa craniectomy in the surgical treatment of Chiari malformation Type I: experience with a pediatric series. J Neurosurg 106 (3 Suppl): , Castillo M, Wilson JD: Spontaneous resolution of a Chiari I malformation: MR demonstration. AJNR Am J Neuroradiol 16: , Di Rocco C, Velardi F: Acquired Chiari type I malformation managed by supratentorial cranial enlargement. Childs Nerv Syst 19: , Galarza M, Sood S, Ham S: Relevance of surgical strategies for the management of pediatric Chiari type I malformation. Childs Nerv Syst 23: , Genitori L, Peretta P, Nurisso C, Macinante L, Mussa F: Chiari type I anomalies in children and adolescents: minimally invasive management in a series of 53 cases. Childs Nerv Syst 16: , Girard N, Lasjaunias P, Taylor W: Reversible tonsillar prolapse in vein of Galen aneurysmal malformations: report of eight cases and pathophysiological hypothesis. Childs Nerv Syst 10: , Greenlee JD, Donovan KA, Hasan DM, Menezes AH: Chiari I malformation in the very young child: the spectrum of presentations and experience in 31 children under age 6 years. Pediatrics 110: , Haroun RI, Guarnieri M, Meadow JJ, Kraut M, Carson B: Current opinions for the treatment of syringomyelia and Chiari malformations: survey of the Pediatric section of the American Association of Neurological Surgeons. Pediatr Neurosurg 33: , James HE, Brant A: Treatment of the Chiari malformation with bone decompression without durotomy in children and young adults. Childs Nerv Syst 18: , Jatavallabhula NS, Armstrong J, Sgouros S, Whitehouse W: Spontaneous resolution of isolated Chiari I malformation. Childs Nerv Syst 22: , Kulp MT, Sortor JM: Clinical value of the Beery visual-motor integration supplemental tests of visual perception and motor coordination. Optom Vis Sci 80: , Kyoshima K, Bogdanov EI: Spontaneous resolution of syringomyelia: report of two cases and review of the literature. Neurosurgery 53: , Meadows J, Kraut M, Guarnieri M, Haroun RI, Carson BS: Asymptomatic Chiari Type I malformations identified on magnetic resonance imaging. J Neurosurg 92: , Mikulis DJ, Diaz O, Egglin TK, Sanchez R: Variance of the position of the cerebellar tonsils with age: preliminary report. Radiology 183: ,
9 Natural history of Chiari malformation Type I 20. Milhorat TH, Bolognese PA: Tailored operative technique for Chiari type I malformation using intraoperative color Doppler ultrasonography. Neurosurgery 53: , Milhorat TH, Chou MW, Trinidad EM, Kula RW, Mandell M, Wolpert C, et al: Chiari I malformation redefined: clinical and radiographic findings for 364 symptomatic patients. Neurosurgery 44: , Munshi I, Frim D, Stine-Reyes R, Weir BK, Hekmatpanah J, Brown F: Effects of posterior fossa decompression with and without duraplasty on Chiari malformation-associated hydromyelia. Neurosurgery 46: , Navarro R, Olavarria G, Seshadri R, Gonzales-Portillo G, Mc- Lone DG, Tomita T: Surgical results of posterior fossa decompression for patients with Chiari I malformation. Childs Nerv Syst 20: , Nishizawa S, Yokoyama T, Yokota N, Tokuyama T, Ohta S: Incidentally identified syringomyelia associated with Chiari I malformations: is early interventional surgery necessary? Neurosurgery 49: , Oldfield EH, Muraszko K, Shawker TH, Patronas NJ: Pathophysiology of syringomyelia associated with Chiari 1 malformation of the cerebellar tonsils. Implications for diagnosis and treatment. J Neurosurg 80:3 15, Rafia S, Pascual-Castroviejo I: Syringohydromyelia. Report of a case which resolved spontaneously. Rev Neurol 32: , Riva D, Nichelli F, Devoti M: Developmental aspects of verbal fluency and confrontation naming in children. Brain Lang 71: , Schijman E, Steinbok P: International survey on the management of Chiari I malformation and syringomyelia. Childs Nerv Syst 20: , Sivaramakrishnan A, Alperin N, Surapaneni S, Lichtor T: Evaluating the effect of decompression surgery on cerebrospinal fluid flow and intracranial compliance in patients with Chiari malformation with magnetic resonance imaging flow studies. Neurosurgery 55: , Spanò M, Mercuri E, Randò T, Pantò T, Gagliano A, Henderson S, et al: Motor and perceptual-motor competence in children with Down syndrome: variation in performance with age. Eur J Paediatr Neurol 3:7 13, Steinbok P: Clinical features of Chiari I malformations. Childs Nerv Syst 20: , Sudo K, Doi S, Maruo Y, Tashiro K, Terae S, Miyasaka K, et al: Syringomyelia with spontaneous resolution. J Neurol Neurosurg Psychiatry 53: , Sun JC, Steinbok P, Cochrane DD: Spontaneous resolution and recurrence of a Chiari I malformation and associated syringomyelia. Case report. J Neurosurg 92 (2 Suppl): , Sun PP, Harrop J, Sutton LN, Younkin D: Complete spontaneous resolution of childhood Chiari I malformation and associated syringomyelia. Pediatrics 107: , Tokunaga M, Minami S, Isobe K, Moriya H, Kitahara H, Nakata Y: Natural history of scoliosis in children with syringomyelia. J Bone Joint Surg Br 83: , Tubbs RS, Lyerly MJ, Loukas M, Shoja MM, Oakes WJ: The pediatric Chiari I malformation: a review. Childs Nerv Syst 23: , Tubbs RS, McGirt MJ, Oakes WJ: Surgical experience in 130 pediatric patients with Chiari I malformations. J Neurosurg 99: , Weinberg JS, Freed DL, Sadock J, Handler M, Wisoff JH, Epstein FJ: Headache and Chiari I malformation in the pediatric population. Pediatr Neurosurg 29:14 18, 1998 Manuscript submitted March 4, Accepted June 18, Address correspondence to: Federica Novegno, M.D., Department of Pediatric Neurosurgery, Catholic University Medical School, Largo A. Gemelli 1, Rome, Italy. federica novegno@hotmail.it. 187
Chiari malformation Type I (CM-I) in children is
 PEDIATRICS clinical article J Neurosurg Pediatr 16:159 166, 2015 A prospective natural history study of nonoperatively managed Chiari I malformation: does follow-up MRI surveillance alter surgical decision
PEDIATRICS clinical article J Neurosurg Pediatr 16:159 166, 2015 A prospective natural history study of nonoperatively managed Chiari I malformation: does follow-up MRI surveillance alter surgical decision
Role of MRI in Selection of Patients for Surgery and Assessing the Post Operative Outcome in Chiari 1 Malformation
 DOI: 10.7860/IJARS/2017/13599:2222 Radiology Section Original Article Role of MRI in Selection of Patients for Surgery and Assessing the Post Operative Outcome in Chiari 1 Malformation Rajesh Kumar V,
DOI: 10.7860/IJARS/2017/13599:2222 Radiology Section Original Article Role of MRI in Selection of Patients for Surgery and Assessing the Post Operative Outcome in Chiari 1 Malformation Rajesh Kumar V,
Suboccipital decompression for Chiari malformation associated scoliosis: risk factors and time course of deformity progression
 J Neurosurg Pediatrics 1:456 460, 2008 Suboccipital decompression for Chiari malformation associated scoliosis: risk factors and time course of deformity progression FRANK J. ATTENELLO, M.S., MATTHEW J.
J Neurosurg Pediatrics 1:456 460, 2008 Suboccipital decompression for Chiari malformation associated scoliosis: risk factors and time course of deformity progression FRANK J. ATTENELLO, M.S., MATTHEW J.
A case report on result of posterior fossa decompression on syringomyelia in a case of chiary type I malformation
 Romanian Neurosurgery Volume XXXII Number 1 2018 January-March Article A case report on result of posterior fossa decompression on syringomyelia in a case of chiary type I malformation Asheesh Kumar Gupta,
Romanian Neurosurgery Volume XXXII Number 1 2018 January-March Article A case report on result of posterior fossa decompression on syringomyelia in a case of chiary type I malformation Asheesh Kumar Gupta,
Idiopathic cervical syringomyelia can be associated. Pediatric Chiari malformation Type 0: a 12-year institutional experience.
 J Neurosurg J Neurosurg Pediatrics Pediatrics 8:000 000, 8:1 5, 2011 Pediatric Chiari malformation Type 0: a 12-year institutional experience Clinical article Joshua J. Chern, M.D., Ph.D., Amber J. Gordon,
J Neurosurg J Neurosurg Pediatrics Pediatrics 8:000 000, 8:1 5, 2011 Pediatric Chiari malformation Type 0: a 12-year institutional experience Clinical article Joshua J. Chern, M.D., Ph.D., Amber J. Gordon,
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Pediatric Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Pediatric Neurosurgery Pediatric neurosurgeons
Introduction to Neurosurgical Subspecialties: Pediatric Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Pediatric Neurosurgery Pediatric neurosurgeons
Pediatric and adult Chiari malformation Type I surgical series : a review of demographics, operative treatment, and outcomes
 PEDIATRICS literature review Pediatric and adult Chiari malformation Type I surgical series 1965 2013: a review of demographics, operative treatment, and outcomes aska arnautovic, bsc, 1 bruno splavski,
PEDIATRICS literature review Pediatric and adult Chiari malformation Type I surgical series 1965 2013: a review of demographics, operative treatment, and outcomes aska arnautovic, bsc, 1 bruno splavski,
Chiari Malformations. Google. Objectives Seventh Annual NKY TBI Conference 3/22/13. Kerry R. Crone, M.D.
 Chiari Malformations Kerry R. Crone, M.D. Professor of Neurosurgery and Pediatrics University of Cincinnati College of Medicine University of Cincinnati Medical Center Cincinnati Children s Hospital Medical
Chiari Malformations Kerry R. Crone, M.D. Professor of Neurosurgery and Pediatrics University of Cincinnati College of Medicine University of Cincinnati Medical Center Cincinnati Children s Hospital Medical
The Chiari malformation I (CM I) is a disorder that has been
 DOI: 10.5137/1019-5149.JTN.18349-16.1 Received: 31.05.2016 / Accepted: 01.07.2016 Published Online: 22.08.2016 Original Investigation Are Herniated Cerebellar Tonsils the Main Culprit of Chiari Malformation
DOI: 10.5137/1019-5149.JTN.18349-16.1 Received: 31.05.2016 / Accepted: 01.07.2016 Published Online: 22.08.2016 Original Investigation Are Herniated Cerebellar Tonsils the Main Culprit of Chiari Malformation
What Every Spine Surgeon Should Know About Neurosurgical Issues
 What Every Spine Surgeon Should Know About Neurosurgical Issues Amer Samdani, MD Chief of Surgery Shriners Hospitals for Children Philadelphia, PA Objectives Main intraspinal lesions Chiari malformation
What Every Spine Surgeon Should Know About Neurosurgical Issues Amer Samdani, MD Chief of Surgery Shriners Hospitals for Children Philadelphia, PA Objectives Main intraspinal lesions Chiari malformation
Morphometric Analysis of Left & Right Tonsils in Adult Symptomatic Type 1 Chiari Patients and Healthy Controls
 The University of Akron IdeaExchange@UAkron Honors Research Projects The Dr. Gary B. and Pamela S. Williams Honors College Spring 2015 Morphometric Analysis of Left & Right Tonsils in Adult Symptomatic
The University of Akron IdeaExchange@UAkron Honors Research Projects The Dr. Gary B. and Pamela S. Williams Honors College Spring 2015 Morphometric Analysis of Left & Right Tonsils in Adult Symptomatic
INTRACRANIAL ARACHNOID CYSTS: CLASSIFICATION AND MANAGEMENT. G. Tamburrini, Rome
 INTRACRANIAL ARACHNOID CYSTS: CLASSIFICATION AND MANAGEMENT G. Tamburrini, Rome Incidence 2% of occasional neuroradiological findings From clinical studies (1960 s): 0.4-1% of intracranial space occupying
INTRACRANIAL ARACHNOID CYSTS: CLASSIFICATION AND MANAGEMENT G. Tamburrini, Rome Incidence 2% of occasional neuroradiological findings From clinical studies (1960 s): 0.4-1% of intracranial space occupying
A review of the disagreements in the prevalence and treatment of the tethered cord syndromes with chiari 1 malformations
 SNI: Spine OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: Nancy E. Epstein, MD Winthrop Hospital, Mineola, NY, USA Review Article A review of the disagreements
SNI: Spine OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: Nancy E. Epstein, MD Winthrop Hospital, Mineola, NY, USA Review Article A review of the disagreements
OUTCOME OF SUBOCCIPITAL DECOMPRESSION WITH AND WITHOUT DURAPLASTY IN ADULTS WITH CHIARI I MALFORMATION
 OUTCOME OF SUBOCCIPITAL DECOMPRESSION WITH AND WITHOUT DURAPLASTY IN ADULTS WITH CHIARI I MALFORMATION Mushtaq 1, Zia ur Rehman 1, M Mukhtar Khan 2 ABSTRACT Objectives: To investigate outcome for ACM1
OUTCOME OF SUBOCCIPITAL DECOMPRESSION WITH AND WITHOUT DURAPLASTY IN ADULTS WITH CHIARI I MALFORMATION Mushtaq 1, Zia ur Rehman 1, M Mukhtar Khan 2 ABSTRACT Objectives: To investigate outcome for ACM1
Chiari malformations. A fact sheet for patients and carers
 A fact sheet for patients and carers Chiari malformations This fact sheet provides information on Chiari malformations. It focuses on Chiari malformations in adults. Our fact sheets are designed as general
A fact sheet for patients and carers Chiari malformations This fact sheet provides information on Chiari malformations. It focuses on Chiari malformations in adults. Our fact sheets are designed as general
Skull base growth in children with Chiari malformation Type I
 See the corresponding editorial in this issue, pp 187. J Neurosurg (3 Suppl Pediatrics) 107:188 192, 2007 Skull base growth in children with Chiari malformation Type I SPYROS SGOUROS, M.D., F.R.C.S.(SN),
See the corresponding editorial in this issue, pp 187. J Neurosurg (3 Suppl Pediatrics) 107:188 192, 2007 Skull base growth in children with Chiari malformation Type I SPYROS SGOUROS, M.D., F.R.C.S.(SN),
The Role of Cine Flow Magnetic Resonance Imaging in Patients with Chiari 0 Malformation
 DOI: 10.5137/1019-5149.JTN.19049-16.2 Received: 11.11.2016 / Accepted: 14.12.2016 Published Online: 16.01.2017 Original Investigation The Role of Cine Flow Magnetic Resonance Imaging in Patients with Chiari
DOI: 10.5137/1019-5149.JTN.19049-16.2 Received: 11.11.2016 / Accepted: 14.12.2016 Published Online: 16.01.2017 Original Investigation The Role of Cine Flow Magnetic Resonance Imaging in Patients with Chiari
Neurosurgery. Neurosurgery
 Neurosurgery Neurosurgery Neurosurgery Telephone Numbers: Appointment: 202-476-3020 Fax: 202-476-3091 Administration: 202-476-3020 Evenings and Weekends: 202-476-5000 Robert Keating, MD, Chief The Division
Neurosurgery Neurosurgery Neurosurgery Telephone Numbers: Appointment: 202-476-3020 Fax: 202-476-3091 Administration: 202-476-3020 Evenings and Weekends: 202-476-5000 Robert Keating, MD, Chief The Division
Djamila Kafoufi Al Galaa Military Hospital Cairo
 Djamila Kafoufi Al Galaa Military Hospital Cairo Herniation cerebellar tonsils below the foramen magnum, Hans Chiari 4 types Chiari I less than 5mm,HDC rare,syringomyelia often present. Chiari II,protrusion
Djamila Kafoufi Al Galaa Military Hospital Cairo Herniation cerebellar tonsils below the foramen magnum, Hans Chiari 4 types Chiari I less than 5mm,HDC rare,syringomyelia often present. Chiari II,protrusion
Brain Imaging. Bearbeitet von Klaus Sartor, Stefan Hähnel, Bodo Kress
 Brain Imaging Bearbeitet von Klaus Sartor, Stefan Hähnel, Bodo Kress 1. Auflage 2007. Taschenbuch. 312 S. Paperback ISBN 978 3 13 143961 1 Format (B x L): 12,5 x 19 cm Weitere Fachgebiete > Medizin > Sonstige
Brain Imaging Bearbeitet von Klaus Sartor, Stefan Hähnel, Bodo Kress 1. Auflage 2007. Taschenbuch. 312 S. Paperback ISBN 978 3 13 143961 1 Format (B x L): 12,5 x 19 cm Weitere Fachgebiete > Medizin > Sonstige
Chiari FAQ's. 1. What is a Chiari Malformation?
 Chiari FAQ's These FAQ's are for informational purposes only and in no way represent an attempt to provide medical advice. This information may or may not apply to your case and anyone with a question
Chiari FAQ's These FAQ's are for informational purposes only and in no way represent an attempt to provide medical advice. This information may or may not apply to your case and anyone with a question
Complex Hydrocephalus
 2012 Hydrocephalus Association Conference Washington, DC - June 27-July1, 2012 Complex Hydrocephalus Marion L. Walker, MD Professor of Neurosurgery & Pediatrics Primary Children s Medical Center University
2012 Hydrocephalus Association Conference Washington, DC - June 27-July1, 2012 Complex Hydrocephalus Marion L. Walker, MD Professor of Neurosurgery & Pediatrics Primary Children s Medical Center University
Chiari 1 malformations: an Indian hospital experience
 O r i g i n a l A r t i c l e Singapore Med J 2008; 49 (12) : 1029 Chiari 1 malformations: an Indian hospital experience Ramnarayan R, Praharaj M S, Jayakumar P N Department of Neurosurgery, The National
O r i g i n a l A r t i c l e Singapore Med J 2008; 49 (12) : 1029 Chiari 1 malformations: an Indian hospital experience Ramnarayan R, Praharaj M S, Jayakumar P N Department of Neurosurgery, The National
Chiari bridges review Chiari Treatments & Potential Pitfalls
 Chiari bridges review Chiari Treatments & Potential Pitfalls Once diagnosed, you will usually be referred to a specialist (not a Chiari Specialist, but an everyday, run-of-the-mill neurologist or neurosurgeon).
Chiari bridges review Chiari Treatments & Potential Pitfalls Once diagnosed, you will usually be referred to a specialist (not a Chiari Specialist, but an everyday, run-of-the-mill neurologist or neurosurgeon).
Chiari malformation Type I (CM-I) is typically defined
 PEDIATRICS clinical article J Neurosurg Pediatr 16:150 158, 2015 Outcomes after suboccipital decompression without dural opening in children with Chiari malformation Type I Benjamin C. Kennedy, MD, 1 Kathleen
PEDIATRICS clinical article J Neurosurg Pediatr 16:150 158, 2015 Outcomes after suboccipital decompression without dural opening in children with Chiari malformation Type I Benjamin C. Kennedy, MD, 1 Kathleen
Prior Authorization Review Panel MCO Policy Submission
 Prior Authorization Review Panel MCO Policy Submission A separate copy of this form must accompany each policy submitted for review. Policies submitted without this form will not be considered for review.
Prior Authorization Review Panel MCO Policy Submission A separate copy of this form must accompany each policy submitted for review. Policies submitted without this form will not be considered for review.
Multimodal Evaluation Of Cerebrospinal Fluid (csf ) Dynamics Following Extradural Decompression For Chiari I Malformation
 Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine January 2015 Multimodal Evaluation Of Cerebrospinal Fluid (csf ) Dynamics
Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine January 2015 Multimodal Evaluation Of Cerebrospinal Fluid (csf ) Dynamics
Minimally invasive subpial tonsillectomy for Chiari I decompression
 Acta Neurochir (2016) 158:1807 1811 DOI 10.1007/s00701-016-2877-2 HOW I DO IT - NEUROSURGICAL TECHNIQUES Minimally invasive subpial tonsillectomy for Chiari I decompression Jeffrey S. Beecher 1 Yong Liu
Acta Neurochir (2016) 158:1807 1811 DOI 10.1007/s00701-016-2877-2 HOW I DO IT - NEUROSURGICAL TECHNIQUES Minimally invasive subpial tonsillectomy for Chiari I decompression Jeffrey S. Beecher 1 Yong Liu
Cranio-cervical decompression. Information for patients Neurosurgery
 Cranio-cervical decompression Information for patients Neurosurgery page 2 of 12 What is a cranio-cervical decompression? A cranio-cervical decompression is an operation involving the back of the head
Cranio-cervical decompression Information for patients Neurosurgery page 2 of 12 What is a cranio-cervical decompression? A cranio-cervical decompression is an operation involving the back of the head
Disclosures None. Common Neurosurgical Problems Seen in Office Encounters. Macrocephaly Low Back Pain Sacral Dimple Concussion Chiari Malformation
 Common Neurosurgical Problems Seen in Office Encounters When to Manage, When to Refer Andrew Jea MD FAAP Professor and Chief of Pediatric Neurosurgery Riley Hospital for Children Indiana University School
Common Neurosurgical Problems Seen in Office Encounters When to Manage, When to Refer Andrew Jea MD FAAP Professor and Chief of Pediatric Neurosurgery Riley Hospital for Children Indiana University School
Intracranial hypotension secondary to spinal CSF leak: diagnosis
 Intracranial hypotension secondary to spinal CSF leak: diagnosis Spinal cerebrospinal fluid (CSF) leak is an important and underdiagnosed cause of new onset headache that is treatable. Cerebrospinal fluid
Intracranial hypotension secondary to spinal CSF leak: diagnosis Spinal cerebrospinal fluid (CSF) leak is an important and underdiagnosed cause of new onset headache that is treatable. Cerebrospinal fluid
SDAVFs are rare acquired vascular lesions predominantly
 CLINICAL REPORT W.J. van Rooij R.J. Nijenhuis J.P. Peluso M. Sluzewski G.N. Beute B. van der Pol Spinal Dural Fistulas without Swelling and Edema of the Cord as Incidental Findings SUMMARY: SDAVFs cause
CLINICAL REPORT W.J. van Rooij R.J. Nijenhuis J.P. Peluso M. Sluzewski G.N. Beute B. van der Pol Spinal Dural Fistulas without Swelling and Edema of the Cord as Incidental Findings SUMMARY: SDAVFs cause
CNS Embryology 5th Menstrual Week (Dorsal View)
 Imaging of the Fetal Brain; Normal & Abnormal Alfred Abuhamad, M.D. Eastern Virginia Medical School CNS Embryology 5th Menstrual Week (Dorsal View) Day 20 from fertilization Neural plate formed in ectoderm
Imaging of the Fetal Brain; Normal & Abnormal Alfred Abuhamad, M.D. Eastern Virginia Medical School CNS Embryology 5th Menstrual Week (Dorsal View) Day 20 from fertilization Neural plate formed in ectoderm
Outcome of Two Surgical Options Used in Treatment of Chiari Type-One Malformation
 ISPUB.COM The Internet Journal of Neurosurgery Volume 11 Number 1 Outcome of Two Surgical Options Used in Treatment of Chiari Type-One Malformation M G Ammar Citation M G Ammar. Outcome of Two Surgical
ISPUB.COM The Internet Journal of Neurosurgery Volume 11 Number 1 Outcome of Two Surgical Options Used in Treatment of Chiari Type-One Malformation M G Ammar Citation M G Ammar. Outcome of Two Surgical
Chiari malformation Type I (CM-I) is often associated. The association between Chiari malformation Type I, spinal syrinx, and scoliosis PEDIATRICS
 PEDIATRICS clinical article J Neurosurg Pediatr 15:607 611, 2015 The association between Chiari malformation Type I, spinal syrinx, and scoliosis Jennifer Strahle, MD, 1 Brandon W. Smith, MD, MS, 1 Melaine
PEDIATRICS clinical article J Neurosurg Pediatr 15:607 611, 2015 The association between Chiari malformation Type I, spinal syrinx, and scoliosis Jennifer Strahle, MD, 1 Brandon W. Smith, MD, MS, 1 Melaine
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD
 Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Spinal Imaging. Bearbeitet von Herwig Imhof. 1. Auflage Taschenbuch. 312 S. Paperback ISBN Format (B x L): 12,5 x 19 cm
 Spinal Imaging Bearbeitet von Herwig Imhof 1. Auflage 2007. Taschenbuch. 312 S. Paperback ISBN 978 3 13 144071 6 Format (B x L): 12,5 x 19 cm Weitere Fachgebiete > Medizin > Sonstige Medizinische Fachgebiete
Spinal Imaging Bearbeitet von Herwig Imhof 1. Auflage 2007. Taschenbuch. 312 S. Paperback ISBN 978 3 13 144071 6 Format (B x L): 12,5 x 19 cm Weitere Fachgebiete > Medizin > Sonstige Medizinische Fachgebiete
Parkinsonism after Shunting for Hydrocephalus Secondary to Aqueductal Stenosis with Chiari Malformation
 ISPUB.COM The Internet Journal of Neurosurgery Volume 6 Number 2 Parkinsonism after Shunting for Hydrocephalus Secondary to Aqueductal Stenosis with Chiari M Turgut Citation M Turgut. Parkinsonism after
ISPUB.COM The Internet Journal of Neurosurgery Volume 6 Number 2 Parkinsonism after Shunting for Hydrocephalus Secondary to Aqueductal Stenosis with Chiari M Turgut Citation M Turgut. Parkinsonism after
The MRI in Arnold-Chiari Syndrome I and Idiopathic Syringomyelia
 The MRI in Arnold-Chiari Syndrome I and Idiopathic Syringomyelia Author: Miguel B. Royo Salvador, MD, PhD Introduction Magnetic resonance imaging (MRI) is a crucial diagnostic tool for men, women, and
The MRI in Arnold-Chiari Syndrome I and Idiopathic Syringomyelia Author: Miguel B. Royo Salvador, MD, PhD Introduction Magnetic resonance imaging (MRI) is a crucial diagnostic tool for men, women, and
Syrinx location and size according to etiology: identification of Chiari-associated syrinx
 PEDIATRICS clinical article J Neurosurg Pediatr 16:21 29, 2015 Syrinx location and size according to etiology: identification of Chiari-associated syrinx Jennifer Strahle, MD, Karin M. Muraszko, MD, Hugh
PEDIATRICS clinical article J Neurosurg Pediatr 16:21 29, 2015 Syrinx location and size according to etiology: identification of Chiari-associated syrinx Jennifer Strahle, MD, Karin M. Muraszko, MD, Hugh
NEURO IMAGING 2. Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity
 NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
intracranial anomalies
 Chapter 5: Fetal Central Nervous System 84 intracranial anomalies Hydrocephaly Dilatation of ventricular system secondary to an increase in the amount of CSF. Effects of hydrocephalus include flattening
Chapter 5: Fetal Central Nervous System 84 intracranial anomalies Hydrocephaly Dilatation of ventricular system secondary to an increase in the amount of CSF. Effects of hydrocephalus include flattening
Significance of Cerebellar Tonsillar Position on MR
 795 Significance of Cerebellar Tonsillar Position on MR A. J. Barkovich 1. 3 F. J. Wippold 2. 3 J. L. Sherman 3. 4 C. M. Citrin 4. 5 It has been noted that a low degree of ectopia of the cerebellar tonsils
795 Significance of Cerebellar Tonsillar Position on MR A. J. Barkovich 1. 3 F. J. Wippold 2. 3 J. L. Sherman 3. 4 C. M. Citrin 4. 5 It has been noted that a low degree of ectopia of the cerebellar tonsils
Spontaneous Intracranial Hypotension Diagnosis and Treatment
 Spontaneous Intracranial Hypotension Diagnosis and Treatment John W. Engstrom MD, Philip R. Weinstein MD, and William P. Dillon M.D. University of California, San Francisco Spontaneous Intracranial Hypotension
Spontaneous Intracranial Hypotension Diagnosis and Treatment John W. Engstrom MD, Philip R. Weinstein MD, and William P. Dillon M.D. University of California, San Francisco Spontaneous Intracranial Hypotension
Fifteen-minute consultation: incidental findings on brain and spine imaging
 BEST PRACTICE Editor s choice Scan to access more free content Department of Neurosurgery, Birmingham Children s Hospital, Birmingham, UK Correspondence to Chirag Patel, Department of Neurosurgery, Birmingham
BEST PRACTICE Editor s choice Scan to access more free content Department of Neurosurgery, Birmingham Children s Hospital, Birmingham, UK Correspondence to Chirag Patel, Department of Neurosurgery, Birmingham
Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life
 Original Study Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life Lorenzo Nigro 1, Roberto Tarantino 1, Pasquale
Original Study Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life Lorenzo Nigro 1, Roberto Tarantino 1, Pasquale
Chiari III Joseph Junewick, MD FACR
 Chiari III Joseph Junewick, MD FACR 07/02/2010 History Newborn with suboccipital mass. Diagnosis Chiari III Additional Clinical Surgery-Skin covered suboccipital cystic mass confined by the dura. Pathology-Leptomeningeal
Chiari III Joseph Junewick, MD FACR 07/02/2010 History Newborn with suboccipital mass. Diagnosis Chiari III Additional Clinical Surgery-Skin covered suboccipital cystic mass confined by the dura. Pathology-Leptomeningeal
Meninges and Ventricles
 Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
IIH, previously known as pseudotumor cerebri, is a syndrome
 ORIGINAL RESEARCH A.H. Aiken J.A. Hoots A.M. Saindane P.A. Hudgins Incidence of Cerebellar Tonsillar Ectopia in Idiopathic Intracranial Hypertension: A Mimic of the Chiari I Malformation BACKGROUND AND
ORIGINAL RESEARCH A.H. Aiken J.A. Hoots A.M. Saindane P.A. Hudgins Incidence of Cerebellar Tonsillar Ectopia in Idiopathic Intracranial Hypertension: A Mimic of the Chiari I Malformation BACKGROUND AND
NEURO QUIZ 45 EHLERS DANLOS SYNDROME
 NEURO QUIZ 45 EHLERS DANLOS SYNDROME Verghese Cherian, MD, FFARCSI Penn State Hershey Medical Center, Hershey Quiz Team Shobana Rajan, M.D Suneeta Gollapudy, M.D Angele Marie Theard, M.D START 1. Regarding
NEURO QUIZ 45 EHLERS DANLOS SYNDROME Verghese Cherian, MD, FFARCSI Penn State Hershey Medical Center, Hershey Quiz Team Shobana Rajan, M.D Suneeta Gollapudy, M.D Angele Marie Theard, M.D START 1. Regarding
Hemorrhagic vestibular schwannoma: an unusual clinical entity Case report
 Neurosurg Focus 5 (3):Article 9, 1998 Hemorrhagic vestibular schwannoma: an unusual clinical entity Case report Dean Chou, M.D., Prakash Sampath, M.D., and Henry Brem, M.D. Departments of Neurological
Neurosurg Focus 5 (3):Article 9, 1998 Hemorrhagic vestibular schwannoma: an unusual clinical entity Case report Dean Chou, M.D., Prakash Sampath, M.D., and Henry Brem, M.D. Departments of Neurological
NEUROSURGERY WORKING GROUP
 NEUROSURGERY WORKING GROUP OUTCOMES Primary Outcome Protect neurocognitive development by optimizing CSF dynamics throughout the life span. Optimize metrics for the management of CSF anomalies to protect/optimize
NEUROSURGERY WORKING GROUP OUTCOMES Primary Outcome Protect neurocognitive development by optimizing CSF dynamics throughout the life span. Optimize metrics for the management of CSF anomalies to protect/optimize
Adult Chiari Malformation
 VOLUME 23 NUMBER 26 December 31, 2001 A BIWEEKLY PUBLICATION FOR CLINICAL NEUROSURGICAL CONTINUING MEDICAL EDUCATION Adult Chiari Malformation Ghassan K. Bejjani, M.D., and Kimberly P. Cockerham, M.D.
VOLUME 23 NUMBER 26 December 31, 2001 A BIWEEKLY PUBLICATION FOR CLINICAL NEUROSURGICAL CONTINUING MEDICAL EDUCATION Adult Chiari Malformation Ghassan K. Bejjani, M.D., and Kimberly P. Cockerham, M.D.
The Natural History of Cerebellar Hemangioblastomas in von Hippel-Lindau Disease
 AJNR Am J Neuroradiol 24:1570 1574, September 2003 The Natural History of Cerebellar Hemangioblastomas in von Hippel-Lindau Disease Andrew Slater, Niall R. Moore, and Susan M. Huson BACKGROUND AND PURPOSE:
AJNR Am J Neuroradiol 24:1570 1574, September 2003 The Natural History of Cerebellar Hemangioblastomas in von Hippel-Lindau Disease Andrew Slater, Niall R. Moore, and Susan M. Huson BACKGROUND AND PURPOSE:
Two-Stage Management of Mega Occipito Encephalocele
 Two-Stage Management of Mega Occipito Encephalocele CASE REPORT A I Mardzuki*, J Abdullah**, G Ghazaime*, A R Ariff!'*, M Ghazali* *Department of Neurosciences, **Department of Radiology, Hospital Universiti
Two-Stage Management of Mega Occipito Encephalocele CASE REPORT A I Mardzuki*, J Abdullah**, G Ghazaime*, A R Ariff!'*, M Ghazali* *Department of Neurosciences, **Department of Radiology, Hospital Universiti
Primary Outcomes. Outcomes
 Neurosurgery Jeffrey Blount, MD, Chair Robin Bowman, MD Michael Partington, MD Brandon Roque, MD Elias Rizk, MD Mark Dias, MD, FAAP, FAANS Betsy Hopson, MS Outcomes Primary Outcomes Protect neurocognitive
Neurosurgery Jeffrey Blount, MD, Chair Robin Bowman, MD Michael Partington, MD Brandon Roque, MD Elias Rizk, MD Mark Dias, MD, FAAP, FAANS Betsy Hopson, MS Outcomes Primary Outcomes Protect neurocognitive
Body position and eerebrospinal fluid pressure. Part 2' Clinical studies on orthostatic pressure and the hydrostatic indifferent point
 Body position and eerebrospinal fluid pressure Part 2' Clinical studies on orthostatic pressure and the hydrostatic indifferent point BJORN MAGNAES, M.D. Department of Neurosurgery, Rikshospitalet, Oslo
Body position and eerebrospinal fluid pressure Part 2' Clinical studies on orthostatic pressure and the hydrostatic indifferent point BJORN MAGNAES, M.D. Department of Neurosurgery, Rikshospitalet, Oslo
Han-Sung Kwon M.D. Department of Obstetrics and Gynecology Konkuk University School of Medicine Seoul, Korea
 Han-Sung Kwon M.D. Department of Obstetrics and Gynecology Konkuk University School of Medicine Seoul, Korea Embryologic features of the developing hindbrain Embryologic features of the developing hindbrain
Han-Sung Kwon M.D. Department of Obstetrics and Gynecology Konkuk University School of Medicine Seoul, Korea Embryologic features of the developing hindbrain Embryologic features of the developing hindbrain
Decompression of the spinal subarachnoid space as a solution for syringomyelia without Chiari malformation
 (2002) 40, 501 ± 506 ã 2002 International Society All rights reserved 1362 ± 4393/02 $25.00 www.nature.com/sc Original Article Decompression of the spinal subarachnoid space as a solution for syringomyelia
(2002) 40, 501 ± 506 ã 2002 International Society All rights reserved 1362 ± 4393/02 $25.00 www.nature.com/sc Original Article Decompression of the spinal subarachnoid space as a solution for syringomyelia
Abstract Objective: Multiple surgical strategies exist for the management of the symptomatic Chiari II malformation. To date, no comprehensive
 Childs Nerv Syst (2004) 20:375 381 DOI 10.1007/s00381-004-0969-4 R E V I E W P A P E R R. Shane Tubbs Treatment and management of the Chiari II W. Jerry Oakes malformation: an evidence-based review of
Childs Nerv Syst (2004) 20:375 381 DOI 10.1007/s00381-004-0969-4 R E V I E W P A P E R R. Shane Tubbs Treatment and management of the Chiari II W. Jerry Oakes malformation: an evidence-based review of
Slitlike syrinx cavities: a persistent central canal
 J Neurosurg (Spine 2) 97:161 165, 2002 Slitlike syrinx cavities: a persistent central canal LANGSTON T. HOLLY, M.D., AND ULRICH BATZDORF, M.D. Division of Neurosurgery, University of California at Los
J Neurosurg (Spine 2) 97:161 165, 2002 Slitlike syrinx cavities: a persistent central canal LANGSTON T. HOLLY, M.D., AND ULRICH BATZDORF, M.D. Division of Neurosurgery, University of California at Los
Cerebrospinal Fluid Velocity Amplitudes within the Cerebral Aqueduct in Healthy
 Page 1 of 30 1 Cerebrospinal Fluid Velocity Amplitudes within the Cerebral Aqueduct in Healthy Children and Patients with Chiari I Malformation This is the author manuscript accepted for publication and
Page 1 of 30 1 Cerebrospinal Fluid Velocity Amplitudes within the Cerebral Aqueduct in Healthy Children and Patients with Chiari I Malformation This is the author manuscript accepted for publication and
Arnold Chiari Malformation - A hospital based autopsy study
 Rapotra Megha et al / International Journal of Biomedical Research 2017; 8(05): 250-254. 250 International Journal of Biomedical Research ISSN: 0976-9633 (Online); 2455-0566 (Print) Journal DOI: https://dx.doi.org/10.7439/ijbr
Rapotra Megha et al / International Journal of Biomedical Research 2017; 8(05): 250-254. 250 International Journal of Biomedical Research ISSN: 0976-9633 (Online); 2455-0566 (Print) Journal DOI: https://dx.doi.org/10.7439/ijbr
Subject: Brain CT. Original Effective Date: 11/7/2017. Policy Number: MCR: 600. Revision Date(s): Review Date:
 Subject: Brain CT Policy Number: MCR: 600 Revision Date(s): MHW Original Effective Date: 11/7/2017 Review Date: DISCLAIMER This Molina Clinical Review (MCR) is intended to facilitate the Utilization Management
Subject: Brain CT Policy Number: MCR: 600 Revision Date(s): MHW Original Effective Date: 11/7/2017 Review Date: DISCLAIMER This Molina Clinical Review (MCR) is intended to facilitate the Utilization Management
DIANE MUELLER, N.D., R.N., C-F.N.P., AND JOHN J. ORO, M.D.
 Neurosurg Focus 18 (2):ECP2, 2005 Prospective analysis of self-perceived quality of life before and after posterior fossa decompression in 112 patients with Chiari malformation with or without syringomyelia
Neurosurg Focus 18 (2):ECP2, 2005 Prospective analysis of self-perceived quality of life before and after posterior fossa decompression in 112 patients with Chiari malformation with or without syringomyelia
Ventriculostomy and Risk of Upward Herniation in Patients with Obstructive Hydrocephalus from Posterior Fossa Mass Lesions
 https://doi.org/10.1007/s12028-017-0487-3 ORIGINAL ARTICLE Ventriculostomy and Risk of Upward Herniation in Patients with Obstructive Hydrocephalus from Posterior Fossa Mass Lesions Sherri A. Braksick
https://doi.org/10.1007/s12028-017-0487-3 ORIGINAL ARTICLE Ventriculostomy and Risk of Upward Herniation in Patients with Obstructive Hydrocephalus from Posterior Fossa Mass Lesions Sherri A. Braksick
Prenatal Prediction of The Neurologically Impaired Neonate By Ultrasound
 Prenatal Prediction of The Neurologically Impaired Neonate By Ultrasound Robert H. Debbs, D.O.,F.A.C.O.O.G. Professor of OB-GYN Perelman School of Medicine, University of Pennsylvania Director, Pennsylvania
Prenatal Prediction of The Neurologically Impaired Neonate By Ultrasound Robert H. Debbs, D.O.,F.A.C.O.O.G. Professor of OB-GYN Perelman School of Medicine, University of Pennsylvania Director, Pennsylvania
TUMOURS IN THE REGION OF FORAMEN MAGNUM
 TUMOURS IN THE REGION OF FORAMEN MAGNUM Abstract Pages with reference to book, From 119 To 122 Naim-ur-Rahman ( Department of Neurosurgery, Rawalpindi Medical College, Rawalpindi. ) A very unusual case
TUMOURS IN THE REGION OF FORAMEN MAGNUM Abstract Pages with reference to book, From 119 To 122 Naim-ur-Rahman ( Department of Neurosurgery, Rawalpindi Medical College, Rawalpindi. ) A very unusual case
Adult - Cerebrovascular. Adult - Cranio-Cervical Junction. Adult - Epilepsy. Adult - Hydrocephalus
 list for SET and IMG Neurosurgery Adult - Cerebrovascular Aneurysm - Clipping: Anterior circulation Aneurysm - Clipping: Posterior circulation AVM excision Carotid endarterectomy Carotid trapping Cavernoma
list for SET and IMG Neurosurgery Adult - Cerebrovascular Aneurysm - Clipping: Anterior circulation Aneurysm - Clipping: Posterior circulation AVM excision Carotid endarterectomy Carotid trapping Cavernoma
Symposium: OB/GY US (Room B) CNS Anomalies
 82 Symposium: OB/GY US (Room B) 11 : 50 1 2 : 10 CNS Anomalies Brain area Midline structure S u p r a t e n t o r i a l ventricular system Cerebral hemisphere Posterior fossa Head size and shape Image
82 Symposium: OB/GY US (Room B) 11 : 50 1 2 : 10 CNS Anomalies Brain area Midline structure S u p r a t e n t o r i a l ventricular system Cerebral hemisphere Posterior fossa Head size and shape Image
Abstract !"# $% &%'(% )* ( % +$$ '% % % Presentation Notes
 Presenter Name: John Oro, MD Topic: Chiari & Syringomyelia 101 A Brief Look at Neuroanatomy The brain is enclosed and protected by a rounded skull made of rigid bone. The bottom of the skull contains multiple
Presenter Name: John Oro, MD Topic: Chiari & Syringomyelia 101 A Brief Look at Neuroanatomy The brain is enclosed and protected by a rounded skull made of rigid bone. The bottom of the skull contains multiple
Presented by : Shashwat Mishra
 Presented by : Shashwat Mishra Named after Hans Chiari (1851 1916). Professor of Pathology in Prague, Czechoslovakia, Paper entitled Concerning alterations in the cerebellum resulting from cerebral hydrocephalus
Presented by : Shashwat Mishra Named after Hans Chiari (1851 1916). Professor of Pathology in Prague, Czechoslovakia, Paper entitled Concerning alterations in the cerebellum resulting from cerebral hydrocephalus
Chiari Malformation: Diagnosis
 Chiari Malformation: Diagnosis SYMPTOMS DIAGNOSIS LIVING WITH CHIARI TREATMENT Rick Labuda, Executive Director director@conquerchiari.org 724-940-0116 Disclaimer: This presentation is intended for informational
Chiari Malformation: Diagnosis SYMPTOMS DIAGNOSIS LIVING WITH CHIARI TREATMENT Rick Labuda, Executive Director director@conquerchiari.org 724-940-0116 Disclaimer: This presentation is intended for informational
Nature and Science 2017;15(7) Surgical Options for Treatment of Posterior Fossa Tumors with Hydrocephalus
 Surgical Options for Treatment of Posterior Fossa Tumors with Hydrocephalus Mohamed Mahmoud Abohashima; Ahmed Mohamed Hasan Salem; Magdy Asaad El-Hawary Neurosurgery department, Faculty of Medicine, Al-azhar
Surgical Options for Treatment of Posterior Fossa Tumors with Hydrocephalus Mohamed Mahmoud Abohashima; Ahmed Mohamed Hasan Salem; Magdy Asaad El-Hawary Neurosurgery department, Faculty of Medicine, Al-azhar
Determining if a Relationship Exists Between Tonsillar Ectopia and Symptom Presentation in Chiari Malformation Patients
 Accepted Manuscript Determining if a Relationship Exists Between Tonsillar Ectopia and Symptom Presentation in Chiari Malformation Patients Julia R. Saling, B.S., Paige Marty, B.S., Rebecca Fischbein,
Accepted Manuscript Determining if a Relationship Exists Between Tonsillar Ectopia and Symptom Presentation in Chiari Malformation Patients Julia R. Saling, B.S., Paige Marty, B.S., Rebecca Fischbein,
with susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine
 Emerg Radiol (2012) 19:565 569 DOI 10.1007/s10140-012-1051-2 CASE REPORT Susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine Christopher Miller
Emerg Radiol (2012) 19:565 569 DOI 10.1007/s10140-012-1051-2 CASE REPORT Susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine Christopher Miller
Surgical treatment of Chiari I malformation: indications and approaches
 Neurosurg Focus 11 (1):Article 2, 2001, Click here to return to Table of Contents Surgical treatment of Chiari I malformation: indications and approaches TORD D. ALDEN, M.D., JEFFREY G. OJEMANN, M.D.,
Neurosurg Focus 11 (1):Article 2, 2001, Click here to return to Table of Contents Surgical treatment of Chiari I malformation: indications and approaches TORD D. ALDEN, M.D., JEFFREY G. OJEMANN, M.D.,
Chiari Malformation Type 1: A Systematic Review of Natural History and Conservative Management
 Chiari Malformation Type 1: A Systematic Review of Natural History and Conservative Management Keywords: conservative, management, chiari, arnold-chiari, malformation, adult, surgical. Abstract OBJECTIVE:
Chiari Malformation Type 1: A Systematic Review of Natural History and Conservative Management Keywords: conservative, management, chiari, arnold-chiari, malformation, adult, surgical. Abstract OBJECTIVE:
Moderators: Dr Manmohan Singh Dr Pankaj Singh Presentor : Dr Kanwaljeet Garg
 Moderators: Dr Manmohan Singh Dr Pankaj Singh Presentor : Dr Kanwaljeet Garg History! Hans Chiari (1851 1916) was born in Vienna, Austria! He was Professor of pathology at Prague, Czechoslovakia! His initial
Moderators: Dr Manmohan Singh Dr Pankaj Singh Presentor : Dr Kanwaljeet Garg History! Hans Chiari (1851 1916) was born in Vienna, Austria! He was Professor of pathology at Prague, Czechoslovakia! His initial
Ethical Perspective. Case. Continued on page 1684
 Ethical Perspective Ethical Implications of an Incidentally Discovered Asymptomatic Chiari Malformation in a Competitive Athlete Matthew P. Kirschen, MD, PhD; Judy Illes, PhD, FRSC, FCAHS ABSTRACT The
Ethical Perspective Ethical Implications of an Incidentally Discovered Asymptomatic Chiari Malformation in a Competitive Athlete Matthew P. Kirschen, MD, PhD; Judy Illes, PhD, FRSC, FCAHS ABSTRACT The
The "Keyhole": A Sign of
 473 The "Keyhole": A Sign of Herniation of a Trapped Fourth Ventricle and Other Posterior Fossa Cysts Barbara J. Wolfson' Eric N. Faerber' Raymond C. Truex, Jr. 2 When a cystic structure in the posterior
473 The "Keyhole": A Sign of Herniation of a Trapped Fourth Ventricle and Other Posterior Fossa Cysts Barbara J. Wolfson' Eric N. Faerber' Raymond C. Truex, Jr. 2 When a cystic structure in the posterior
Department of Neurosurgery. Differentiating Craniosynostosis from Positional Plagiocephaly
 Department of Neurosurgery Differentiating Craniosynostosis from Positional Plagiocephaly The number of infants with head shape deformities has risen over the past several years, likely due to increased
Department of Neurosurgery Differentiating Craniosynostosis from Positional Plagiocephaly The number of infants with head shape deformities has risen over the past several years, likely due to increased
Not for Reprint. MS# author proof the Disclosure) for spelling and
 Authors: Please review all authors names, academic degrees, affiliations, and contributions MS# 11-26 author proof (in Not the Disclosure) for spelling and for accuracy. Reprint Neurosurg Focus 31 (2):E6,
Authors: Please review all authors names, academic degrees, affiliations, and contributions MS# 11-26 author proof (in Not the Disclosure) for spelling and for accuracy. Reprint Neurosurg Focus 31 (2):E6,
Spectrum of Cranio-facial anomalies during 2 Ultrasound. trimester on
 Spectrum of Cranio-facial anomalies during 2 Ultrasound nd trimester on Poster No.: C-0378 Congress: ECR 2015 Type: Scientific Exhibit Authors: K. Dave, S. Solanki; Ahmedabad/IN Keywords: Obstetrics (Pregnancy
Spectrum of Cranio-facial anomalies during 2 Ultrasound nd trimester on Poster No.: C-0378 Congress: ECR 2015 Type: Scientific Exhibit Authors: K. Dave, S. Solanki; Ahmedabad/IN Keywords: Obstetrics (Pregnancy
Persistent/Recurrent Syringomyelia after Chiari Decompression Natural History and Management Strategies: A Systematic Review
 116 Systematic Review Persistent/Recurrent Syringomyelia after Chiari Decompression Natural History and Management Strategies: A Systematic Review James M. Schuster 1 Fangyi Zhang 2,3 Daniel C. Norvell
116 Systematic Review Persistent/Recurrent Syringomyelia after Chiari Decompression Natural History and Management Strategies: A Systematic Review James M. Schuster 1 Fangyi Zhang 2,3 Daniel C. Norvell
Is there a relationship between the extent of tonsillar ectopia and the severity of the clinical Chiari syndrome? Linear Regression Analysis
 Is there a relationship between the extent of tonsillar ectopia and the severity of the clinical Chiari syndrome? Dan Heffez MD; John Broderick MD; Michael Connor DO; Michael Mitchell MD; Joanna Galezowska;
Is there a relationship between the extent of tonsillar ectopia and the severity of the clinical Chiari syndrome? Dan Heffez MD; John Broderick MD; Michael Connor DO; Michael Mitchell MD; Joanna Galezowska;
RESEARCH HUMAN CLINICAL STUDIES
 TOPIC RESEARCH HUMAN CLINICAL STUDIES RESEARCH HUMAN CLINICAL STUDIES A Novel Scoring System for Assessing Chiari Malformation Type I Treatment Outcomes Leonardo Aliaga, BFA Katherine E. Hekman, BA Reza
TOPIC RESEARCH HUMAN CLINICAL STUDIES RESEARCH HUMAN CLINICAL STUDIES A Novel Scoring System for Assessing Chiari Malformation Type I Treatment Outcomes Leonardo Aliaga, BFA Katherine E. Hekman, BA Reza
Brain Meninges, Ventricles and CSF
 Brain Meninges, Ventricles and CSF Lecture Objectives Describe the arrangement of the meninges and their relationship to brain and spinal cord. Explain the occurrence of epidural, subdural and subarachnoid
Brain Meninges, Ventricles and CSF Lecture Objectives Describe the arrangement of the meninges and their relationship to brain and spinal cord. Explain the occurrence of epidural, subdural and subarachnoid
For decades it was assumed in the literature that patients
 Neurosurg Focus 31 (3):E5, 2011 Standard and cardiac-gated phase-contrast magnetic resonance imaging in the clinical course of patients with Chiari malformation Type I Uwe Max Mauer, M.D., 1 Andreas Gottschalk,
Neurosurg Focus 31 (3):E5, 2011 Standard and cardiac-gated phase-contrast magnetic resonance imaging in the clinical course of patients with Chiari malformation Type I Uwe Max Mauer, M.D., 1 Andreas Gottschalk,
Chiari malformations (CMs) are well-known structural
 J Neurosurg 126:600 605, 2017 Editorial Evoked potentials and Chiari malformation Type 1 P. David Adelson, MD Barrow Neurological Institute at Phoenix Children s Hospital, Phoenix, Arizona Chiari malformations
J Neurosurg 126:600 605, 2017 Editorial Evoked potentials and Chiari malformation Type 1 P. David Adelson, MD Barrow Neurological Institute at Phoenix Children s Hospital, Phoenix, Arizona Chiari malformations
BRITISH BIOMEDICAL BULLETIN
 Journal Home Page www.bbbulletin.org BRITISH BIOMEDICAL BULLETIN Case Report Neurofibromatosis Type 1 with Chiari Malformation Type 1 in Child: A Case Report Mallesh Kariyappa*, Febna A. Rahiman and Jayanthi
Journal Home Page www.bbbulletin.org BRITISH BIOMEDICAL BULLETIN Case Report Neurofibromatosis Type 1 with Chiari Malformation Type 1 in Child: A Case Report Mallesh Kariyappa*, Febna A. Rahiman and Jayanthi
Original Article CT grouping and microsurgical treatment strategies of hypertensive cerebellar hemorrhage
 Int J Clin Exp Med 2016;9(8):15921-15927 www.ijcem.com /ISSN:1940-5901/IJCEM0022273 Original Article CT grouping and microsurgical treatment strategies of hypertensive cerebellar hemorrhage Xielin Tang
Int J Clin Exp Med 2016;9(8):15921-15927 www.ijcem.com /ISSN:1940-5901/IJCEM0022273 Original Article CT grouping and microsurgical treatment strategies of hypertensive cerebellar hemorrhage Xielin Tang
Static and dynamic cervical MRI: two useful exams in cervical myelopathy
 Original Study Static and dynamic cervical MRI: two useful exams in cervical myelopathy Lorenzo Nigro 1, Pasquale Donnarumma 1, Roberto Tarantino 1, Marika Rullo 2, Antonio Santoro 1, Roberto Delfini 1
Original Study Static and dynamic cervical MRI: two useful exams in cervical myelopathy Lorenzo Nigro 1, Pasquale Donnarumma 1, Roberto Tarantino 1, Marika Rullo 2, Antonio Santoro 1, Roberto Delfini 1
Natural Evolution of Lumbar Spinal Stenosis
 Natural Evolution of Lumbar Spinal Stenosis William R. Sears, MB BS FRACS Wentworth Spine Clinic, Sydney, Australia MUST KNOW An understanding of the natural evolution of lumbar spinal stenosis (LSS) is
Natural Evolution of Lumbar Spinal Stenosis William R. Sears, MB BS FRACS Wentworth Spine Clinic, Sydney, Australia MUST KNOW An understanding of the natural evolution of lumbar spinal stenosis (LSS) is
/ / / / / / Hospital Abstraction: Stroke/TIA. Participant ID: Hospital Code: Multi-Ethnic Study of Atherosclerosis
 Multi-Ethnic Study of Atherosclerosis Participant ID: Hospital Code: Hospital Abstraction: Stroke/TIA History and Hospital Record 1. Was the participant hospitalized as an immediate consequence of this
Multi-Ethnic Study of Atherosclerosis Participant ID: Hospital Code: Hospital Abstraction: Stroke/TIA History and Hospital Record 1. Was the participant hospitalized as an immediate consequence of this
Malformations of the cranio-cervical junction: basilar impression Gonzalo Bertullo 1, Viviana Cabrera 2
 Malformations of the cranio-cervical junction: basilar impression Gonzalo Bertullo 1, Viviana Cabrera 2 Abstract Cranio-cervical junction abnormalities are a rare combination of congenital or acquired
Malformations of the cranio-cervical junction: basilar impression Gonzalo Bertullo 1, Viviana Cabrera 2 Abstract Cranio-cervical junction abnormalities are a rare combination of congenital or acquired
Head, Face, Eyes, Ears, Nose and Throat. Neurological Exam. Eye Function 12/11/2017. Oak Ridge High School Conroe, Texas
 Head, Face, Eyes, Ears, Nose and Throat Oak Ridge High School Conroe, Texas Neurological Exam Consists of Five Major Areas: 1. cerebral testing cognitive functioning 2. Cranial nerve testing 3. Cerebellar
Head, Face, Eyes, Ears, Nose and Throat Oak Ridge High School Conroe, Texas Neurological Exam Consists of Five Major Areas: 1. cerebral testing cognitive functioning 2. Cranial nerve testing 3. Cerebellar
Gillian Wooldridge, DO Houston Methodist Willowbrook Hospital Primary Care Sports Medicine Fellowship May 3, 2018
 Gillian Wooldridge, DO Houston Methodist Willowbrook Hospital Primary Care Sports Medicine Fellowship May 3, 2018 Disclosures Neither I nor any family members have financial disclosures Special thanks
Gillian Wooldridge, DO Houston Methodist Willowbrook Hospital Primary Care Sports Medicine Fellowship May 3, 2018 Disclosures Neither I nor any family members have financial disclosures Special thanks
CURRICULUM VITAE. SPR in Neurosurgery North Thames Rotation Scheme. 1. Royal Free Hospital RFH ( ; 18 months ) Specialist Registrar
 CURRICULUM VITAE Name Title Present Position Address : -Jesus Lafuente : -MD, FRCSEd, PhD : -CONSULTANT NEUROSURGEON : -HOSPÌTAL DEL MAR PASEO MARITIMO 23 BARCELONA 08003 E-mail : jlbspine@gmail.com Phone
CURRICULUM VITAE Name Title Present Position Address : -Jesus Lafuente : -MD, FRCSEd, PhD : -CONSULTANT NEUROSURGEON : -HOSPÌTAL DEL MAR PASEO MARITIMO 23 BARCELONA 08003 E-mail : jlbspine@gmail.com Phone
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
