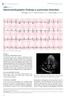
Significance of ST-segment deviation in patients with acute pulmonary embolism and negative T waves
|
|
|
- Georgina Porter
- 5 years ago
- Views:
Transcription
1 Powered by TCPDF ( This is a provisional PDF only. Copyedited and fully formatted version will be made available soon. ONLINE FIRST ISSN: e-issn: X Significance of ST-segment deviation in patients with acute pulmonary embolism and negative T waves Authors: Zhong-Qun Zhan, Chong-Quan Wang, Zhi-Xiao Wang, Kjell C. Nikus, Adrian Baranchuk, Rui-Xia Yuan, Daniel D. Anselm, Andrés Ricardo Pérez-Riera, Bo Yang DOI: /CJ.a Article type: Original articles - Cardiac Imaging Submitted: Accepted: Published online: This article has been peer reviewed and published immediately upon acceptance. It is an open access article, which means that it can be downloaded, printed, and distributed freely, provided the work is properly cited. Articles in "Cardiology Journal" are listed in PubMed.
2 Significance of ST-segment deviation in patients with acute pulmonary embolism and negative T waves Zhong-Qun Zhan 1, Chong-Quan Wang 2, Zhi-Xiao Wang 2, Kjell C. Nikus 3, Adrian Baranchuk 4, Rui-Xia Yuan 2, Daniel D. Anselm 4, Andrés Ricardo Pérez-Riera 5, Bo Yang 1 1 Renmin Hospital of Wuhan University, China 2 Shiyan Taihe Hospital, Hubei University of Medicine, China 3 Tampere University Hospital, and School of Medicine, Tampere University, Finland 4 Kingston General Hospital, Queen s University, Canada 5 ABC Faculty of Medicine, ABC Foundation, Brazil Address for correspondence: Bo Yang, Bo Yang, MD, Department of Cardiology, Renmin Hospital of Wuhan University, Wuhan, Hubei Province, China, @qq.com ABSTRACT Background: Common electrocardiogram (ECG) manifestations in acute pulmonary embolism (APE) include ST-segment deviation (STDV) along with negative T-waves (NTW). STDV could occur in three typical ischemic patterns: (i) the left ventricular (LV) subendocardial ischemic pattern; (ii) the right ventricular (RV) transmural ischemic pattern; and (iii) the LV subendocardial plus RV transmural ischemic pattern. The purpose of this study was to evaluate the relationship of STDV and adverse clinical outcomes and to identify the relationship of relatively normal ECG and favorable clinical outcomes. Methods: Retrospective analysis of electronic charts in APE patients was performed in a tertiary hospital. ECGs on admission were obtained and classified as with or without STDV. Adverse clinical outcomes were defined as need to intensify therapy 1
3 and 30-day mortality. Relatively normal ECG was defined as without any ST-segment deviations, abnormal QRS morphology in lead V1 and S1Q3T3. Results: From a total of 210 patients with NTW, 131 had STDV 0.1 mv, while 79 did not. Patients with STDV had worse evolution: higher incidence of dyspnea, hypotension, cardiogenic shock, intensification of therapy, and death compared to patients without STDV (p=0.001 for each variable). The majority (89%) of the patients with STDV presented with one of the three typical ischemic ECG patterns. LV subendocardial ischemic pattern (OR=4.963, p=0.004), RV transmural ischemic pattern (OR=3.128, p=0.021) and LV subendocardial plus RV transmural ischemic pattern (OR=3.036, p=0.017) independently predicted the need to intensify therapy. RV transmural ischemic pattern (OR=4.227, p=0.031) and LV subendocardial plus RV transmural ischemic pattern (OR=4.022, p=0.032) independently predicted 30-day mortality. Compared to the patients with abnormal ECG, the patients with relatively normal ECG had a significant lower incidence of death (0% vs. 16%; p=0.001) and need to intensify therapy during hospitalization (6% vs. 30%; p=0.002). Conclusions: Ischemic ECG patterns are common ECG manifestations of APE and predict worse evolution and 30-day mortality. Additionally, relatively normal ECGs may associate with favorable clinical outcomes. Key words: acute pulmonary embolism; ECG; ST-segment deviation INTRODUCTION Negative T waves (NTW) in the inferior and precordial leads is a recognized electrocardiogram (ECG) manifestation of acute pulmonary embolism (APE) [1, 2] and has been suggested as a marker of right ventricular strain (RVS) [3] or right ventricular dysfunction (RVD) [4, 5]. ST-segment deviation (elevation and/or depression) is another common ECG manifestation of APE [6-8]. ST-segment deviation could occur in three specific ischemic patterns: (i) left ventricular (LV) subendocardial ischemic pattern; (ii) RV transmural ischemic pattern; and (iii) LV subendocardial plus RV transmural ischemic 2
4 pattern [9]. The purpose of this study was to evaluate the relationship of ST-segment deviation and adverse clinical outcomes in APE patients with NTW and to investigate the relationship between relatively normal ECG and favorable clinical outcomes. METHODS Patient population There were 342 patients diagnosed with APE in our hospital from January 2008 to July 2014, including 315 patients confirmed by multidetector computed tomographic pulmonary angiography and 27 patients highly suspected by ventilationperfusion scintigraphy. Using a retrospective analysis, 210 patients with NTW were included in this study: 131 patients with and 79 patients without ST-segment deviation 0.1 mv (Fig. 1). The inclusion criteria were: (i) acute onset of clinical signs and symptoms before admission suggesting APE; (ii) APE confirmed by multidetector computed tomographic pulmonary angiography; and (iii) admission ECG with NTW 0.1 mv in at least two leads out of the inferior (II, III and avf) and V1-V4 leads. The exclusion criteria were: (i) history of chronic heart failure or confirmed pulmonary hypertension associated with other cardiopulmonary disease (chronic obstructive pulmonary disease was not excluded if there was no confirmed history of pulmonary hypertension by echocardiogram); (ii) concomitant cardiac disease possibly causing NTW in the inferior or precordial leads, such as acute coronary syndrome, hypertrophic cardiomyopathy or tako-tsubo cardiomyopathy confirmed by coronary and/or left ventricular angiography; (iii) ECG manifestation of complete left branch bundle block, left ventricular hypertrophy or ventricular pacing. Electrocardiogram After admission, an ECG using a paper speed of 25mm/s with standardization of 1 mv/10mm was recorded. Both ST-segment elevation (STE) and ST-segment depression (STD) were measured at the J-point in all leads and were considered 3
5 present if the J-point was 0.1 mv above or below the isoelectric line. The LV subendocardial ischemic pattern was defined as STE in lead avr with concomitant STD in leads V4/V5 to V6 (Fig. 2A). The RV transmural ischemic pattern was defined as STE in at least two leads of the leads V1 to V3 (Fig. 2B). The LV subendocardial plus RV transmural ischemic pattern was defined as STE in leads III and/or V1/V2 with concomitant STD in leads V4/V5 to V6 (Fig. 2C). The other abnormal ECG criteria associated with APE are identical to our previous study [9]. Relatively normal ECG was defined as an ECG without any ST-segment deviations, abnormal QRS morphology in lead V1 (notched S wave, RBBB or QR sign) and S1Q3T3. Abnormal ECG was defined as the presence of at least one of the STsegment deviations, abnormal QRS morphology in lead V1and S1Q3T3. Patients were categorized into two groups (with or without ST deviation) based on the ECG findings. All ECGs were evaluated separately by two independent investigators without knowledge of the patients clinical condition. Disagreement between the two investigators was resolved by consensus. Adverse clinical outcomes The following adverse clinical outcomes were recorded: need to intensify therapy based on the MAPPET-3 (Management Strategies and Prognosis in Pulmonary Embolism Trial-3) study criteria [10], including cardiac arrest, need for inotropic support, mechanical ventilation for respiratory support and treatment with thrombolysis or surgical embolectomy; and 30-day mortality. Statistics All data were analyzed by SPSS Data were expressed as mean ± standard deviation for continuous variables and rates (%) for categorical variables. The Student s U test was used for comparison of continuous variables. Categorical variables were compared using the chi-square test or the Fisher exact test. All ECG variables were analyzed by multivariate logistic regression to identify predictors of 4
6 the need to intensify therapy and 30-day mortality. Odds ratios (ORs) and 95% confidence intervals (CIs) were calculated. A two-tailed probability value < 0.05 was considered statistically significant. RESULTS Among the 210 patients, 185 (88%) patients presented with NTW in at least one inferior and one precordial lead. Of the 131 patients with ST-segment deviation, frequent findings were STE in leads V1 (47%), V2 (31%), III (28%) and avr (68%) and STD in leads I (60%), and V4/V5-V6 (60%). There were 24 (18%) patients with the LV subendocardial ischemic pattern, 41 (31%) patients with the RV transmural ischemic pattern, and 52 (40%) with the LV subendocardial plus RV transmural ischemic pattern. The remaining 14 (11%) patients did not meet the criteria of the prespecified three ischemic ECG patterns. The distribution of ST-segment deviations is listed in Table 1. The two groups were not statistically different with regard to gender, age, clinical symptoms of hemoptysis, chest discomfort, cough or syncope. Comparing to patients without ST-segment deviation, patients with ST-segment deviation had a shorter time from symptom onset to admission (6.6±3.2d vs. 9.2±4.8d, p=0.004); lower systolic (117±29 mmhg vs. 130±25 mmhg, p=0.001) and diastolic blood pressure (74±22 mmhg vs. 81±14 mmhg, p=0.004); higher incidence of dyspnea on exertion (84% vs. 65%, p=0.001) and at rest (45% vs. 22%, p=0.001); hypotension (17% vs. 0%, p=0.001); cardiogenic shock (27% vs. 5%, p=0.001); death (18% vs. 5%, p=0.006); and the need to intensify therapy (35% vs. 11%, p=0.001). Demographic and clinical data are listed in Table 2. The multivariate logistic regression analysis of the ECG parameters for the prediction of 30-day mortality and the need to intensify therapy during hospitalization are listed in Table 3. We found that the LV subendocardial ischemic pattern (OR=4.963, p=0.004), the RV transmural ischemic pattern (OR=3.128, p=0.021) and the LV subendocardial plus RV transmural ischemic pattern (OR=3.036, p=0.017) 5
7 independently predicted the need to intensify therapy during hospitalization. In addition, the RV transmural ischemic pattern (OR=4.227, p=0.031) and the LV subendocardial plus RV transmural ischemic pattern (OR=4.022, p=0.032) independently predicted 30-day mortality. Of the 36 patients fulfilling the criteria of relatively normal ECG on admission, there were 2 patients needing to intensify therapy and no death. Accordingly, compared to the patients with abnormal ECG, the patients with relatively normal ECG had a significant lower incidence of death (0% vs. 16%; p=0.001) and need to intensify therapy during hospitalization (6% vs. 30%; p=0.002). DISCUSSION ST-segment deviation is considered as a common, but non-specific, ECG manifestation in patients with APE by some authors [11, 12]. However, the literature suggests that the distribution of ST-segment deviation has consistent regularity and mechanisms [6-9, 13-16]. STE in leads V1, III, avr and STD in leads I and V4/V5-V6 are frequently observed in APE [6, 7, 9]. In our study, the most common ST-segment deviations were also STE in leads V1, V2, III and avr and STD in leads I and V4/V5-V6. We have described that three distinct ischemic ECG patterns represent different manifestations of RV and LV transmural and subendocardial ischemia [9]. According to our results, these ECG patterns are frequent (89%) in APE patients with ST-segment deviation and NTW. The mechanism of the ischemic patters has been attributed to hypotension, hypoxemia, pulmonary artery hypertension, and catecholamine surge [9, 14]. In this study, we have demonstrated that ST-segment deviations with concomitant NTW had worse evolution compared to NTW without ST-segment deviations. Patients with ST-segment deviations had a higher incidence of dyspnea on exertion or on rest, hypotension, cardiogenic shock, need to intensify therapy, and higher 30-day mortality compared to patients without ST-segment deviation. The three distinct 6
8 ischemic ECG patterns could be used to identify patients at higher risk of worse clinical adverse outcomes. To our knowledge, we are the first to demonstrate that the relatively normal ECGs (no ST-segment deviations, absence of notched S wave or RBBB or QR sign in lead V1 and S1Q3T3) are associated with favorable clinical outcomes. It should be pointed out that the relatively normal ECG still present with NTW 0.1 mv in at least two leads out of the inferior (II, III and avf) and V1-V4 leads. NTW in the inferior and precordial leads has been suggested as a marker of RVS [3] or RVD [4, 5]. However, another study [17] suggested that an increase in the amplitude of NTW in the precordial leads after thrombolytic therapy reflects an improvement in cardiopulmonary hemodynamics with concomitant decrease of both RV diameter and mean pulmonary artery pressure. We previously described the dynamic ECG changes in two patients and found that NTW developed later than STE and that the NTW persisted beyond recovery of RVD [14]. In another study [9], none of the 8 patients with acquired APE during hospitalization presented with NTW in precordial leads during hypotension or cardiogenic shock; additionally, all 8 patients showed STE and/or STD. Hence, NTW in the inferior and precordial leads without ST-segment deviation might represent a post-ischemic ECG stage, thus reflecting a previous, transient, stage of RV stretch and ischemia [9, 14]. We also speculate that the more leads with NTW reflects more extensive prior ischemia. Hence, there is a conflicting relationship between NTW and RVD or the severity of the APE in the literature. Association of NTW and RVD or the severity of the APE can be found in patients with ST-segment deviation [14] and in patients who were not treated for APE [3, 5]. More leads with NTW are also related to worse short-term prognosis [18, 19]. However, there is a poor relationship in patients after effective treatment where the RVD has possibly been recovered [14, 17]. The following are commonalities between the findings of our group s studies and the studies by the Kukla s group [6, 7, 19]. First, ST-segment deviation reflects worse prognosis compared to NTW. Second, STE in leads V1, III and avr and STD in leads 7
9 V4/V5-V6 and NTW in the inferior and precordial leads are common ECG manifestations of APE. However, the differences between our study and Kukla s group are obvious. We indentified three types of ischemic ECG patterns that are common ECG manifestations and of prognostic significance. Kukla et al [7] found that global ischemic pattern (presence of at least one lead with STE in leads III, avr and V1-V4 and at least two leads with STD in I, avl and V4-V6) similar to our LV subendocardial plus RV transmural ischemic pattern was not associated with worse outcome in intermediate-risk APE patients. However, ST-segment ischemic pattern (presence of at least one lead with STE in leads III, avr and V1-V4 or at least two leads with STD in leads I, avl and V4-V6) is associated with a worse prognosis in intermediate-risk APE patients. We suggest that this difference is mainly attributed to having a lower incidence of global ischemic pattern than that of ST-segment ischemic pattern (13.9% vs. 44.5%) in intermediate-risk APE patients. Incidentally, the LV subendocardial plus RV transmural ischemic pattern is the main ECG presentation (80%) in the high-risk APE patients [9] and signifies worse adverse clinical outcomes in this study. According to Kukla [19], the mortality rate was significantly higher in patients with NTW in the inferior and precordial leads compared to the group without NTW. In addition, as compared to those with NTW in <5 leads, patients with NTW 5 leads experienced significantly higher rates of death and complications. We did not find the number of leads with NTW to be associated with worse adverse clinical outcomes. This phenomenon may be attributed to a smaller number of patients in our study (210 vs. 470 patients) and methodological differences we used the number of leads with NTW, while Kukla et al used a cut-off of 5 leads in their analyses. In addition, our group used J-point as the measuring point of ST-segment deviation while the Kukla s group used 80ms after the J-point; this may account for further discrepancy between our studies. Limitations of the study Our study has several limitations. It is a retrospective single centre study. 8
10 Different departments and different physicians may have variable criteria with regards to need to intensify therapy. There are many factors influencing ST-segment deviation and we could not rule out all the confounding factors such as concomitant coronary artery disease or paradoxical coronary embolism. CONCLUSIONS Ischemic ECG patterns are common ECG manifestations of APE. They are clinically important as they could predict adverse clinical outcomes. Prompt recognition of these patterns may help in avoiding inaccurate diagnosis leading to unnecessary medical investigations and treatments and may aid in detecting high-risk patients with APE. Relatively normal ECGs may associate with favorable clinical outcomes. Statement of competing interests: The authors have no commercial associations that might pose a conflict of interest. All authors have made substantive contributions to the study, and all authors endorse the data and conclusions. ABBREVIATIONS NTW ECG APE RVS RVD LV STE STD OR CI negative T waves electrocardiogram acute pulmonary embolism right ventricular strain right ventricular dysfunction left ventricular ST-segment elevation ST-segment depression odds ratios confidence intervals 9
11 REFERFENCES [1] Kosuge M, Ebina T, Hibi K, et al. Differences in negative T waves among acute coronary syndrome, acute pulmonary embolism, and Takotsubo cardiomyopathy. European heart journal. Acute cardiovascular care (4): doi: / [2] Jankowski K, Kostrubiec M, Ozdowska P, et al. Electrocardiographic differentiation between acute pulmonary embolism and non-st elevation acute coronary syndromes at the bedside. Ann Noninvasive Electrocardiol (2): doi: / [3] Vanni S, Polidori G, Vergara R, et al. Prognostic value of ECG among patients with acute pulmonary embolism and normal blood pressure. Am J Med (3): doi: /j.amjmed [4] Choi BY, Park DG. Normalization of negative T-wave on electrocardiography and right ventricular dysfunction in patients with an acute pulmonary embolism. Korean J Intern Med (1): doi: /kjim [5] Kim SE, Park DG, Choi HH, et al. The best predictor for right ventricular dysfunction in acute pulmonary embolism: comparison between electrocardiography and biomarkers. Korean Circ J (9): doi: /kcj [6] Kukla P, McIntyre WF, Fijorek K, et al. Electrocardiographic abnormalities in patients with acute pulmonary embolism complicated by cardiogenic shock. Am J Emerg Med (6): doi: /j.ajem [7] Kukla P, McIntyre WF, Fijorek K, et al. Use of ischemic ECG patterns for risk stratification in intermediate-risk patients with acute PE. Am J Emerg Med (10): doi: /j.ajem [8] Janata K, Hochtl T, Wenzel C, et al. The role of ST-segment elevation in lead avr in the risk assessment of patients with acute pulmonary embolism. Clin Res Cardiol (5): doi: /s z. [9] Zhan ZQ, Wang CQ, Nikus KC, et al. Electrocardiogram Patterns during Hemodynamic Instability in Patients with Acute Pulmonary Embolism. Ann Noninvasive Electrocardiol (6): doi: /anec
12 [10]Konstantinides S, Geibel A, Heusel G, et al. Heparin plus alteplase compared with heparin alone in patients with submassive pulmonary embolism. N Engl J Med (15): [11] Stein PD, Terrin ML, Hales CA, et al. Clinical, laboratory, roentgenographic, and electrocardiographic findings in patients with acute pulmonary embolism and no preexisting cardiac or pulmonary disease. Chest (3): [12]Agrawal N, Ramegowda RT, Patra S, et al. Predictors of inhospital prognosis in acute pulmonary embolism: keeping it simple and effective. Blood Coagul Fibrinolysis (5): doi: /MBC [13]Geibel A, Zehender M, Kasper W, et al. Prognostic value of the ECG on admission in patients with acute major pulmonary embolism. Eur Respir J (5): [14]Zhong-Qun Z, Bo Y, Nikus KC, et al. Correlation between ST-segment elevation and negative T waves in the precordial leads in acute pulmonary embolism: insights into serial electrocardiogram changes. Ann Noninvasive Electrocardiol (4): doi: /anec [15]Zhan ZQ, Wang CQ, Nikus KC, et al. Brugada phenocopy in acute pulmonary embolism. Int J Cardiol (3): e doi: /j.ijcard [16]Zhan ZQ, Wang CQ, Baranchuk A. Acute pulmonary embolism with ST-segment elevation in the inferior leads. Int J Cardiol (2): [17]Yoshinaga T, Ikeda S, Nishimura E, et al. Serial changes in negative T wave on electrocardiogram in acute pulmonary thromboembolism. Int J Cardiol (1): [18]Kosuge M, Kimura K, Ishikawa T, et al. Prognostic significance of inverted T waves in patients with acute pulmonary embolism. Circ J (6): [19] Kukla P, McIntyre WF, Fijorek K, et al. T-wave inversion in patients with acute pulmonary embolism: Prognostic value. Heart Lung (1): doi: /j.hrtlng
13 Table 1. Distribution of ST deviation in patients with ST-segment deviation (n=131) ST-segment deviation % STE in V1 0.1mV 61(47%) STE in V2 0.1mV 41(31%) STE in V3 0.1mV 11(8%) STE in III 0.1mV 37(28%) STE in III and avf 0.1mV 14(11%) STE in avr 0.1mV 89(68%) STD in I 0.1mV 78(60%) STD in V4/V5-V6 0.1mV 78(60%) LV subendocardial ischemic 24(18%) pattern RV transmural ischemic pattern 41(31%) LV plus RV transmural 52(40%) ischemia pattern STE=ST-segment elevation; STD=ST-segment depression; LV=left ventricle; RV=right ventricle Table 2. Demographic and Clinical Data APE patients with ST APE patients without ST p value deviation n=131 deviation n=79 Gender (M/F) 55/76 37/42 NS Age (yrs) 59±14 56±15 NS Time from symptom onset 6.6± ± to admission (d) Heart rate (beats/min) 110±23 95±23 <0.001 Systolic blood pressure 117±29 130± (mmhg) Diastolic blood pressure 74±22 81± (mmhg) 12
14 Symptoms on admission Hemoptysis 8(6%) 7(9%) NS Dyspnea on exertion 110(84%) 51(65%) Dyspnea on rest 59(45%) 17(22%) Chest discomfort 51(39%) 30(38%) NS Cough 26(20%) 19(24%) NS Syncope 38(29%) 19(24%) NS Hypotension 22(17%) 0(0%) Cardiogenic shock 36(27%) 4(5%) day death 24(18%) 4(5%) Need to intensify therapy 46(35%) 9(11%) Data are expressed as mean ± standard deviation for continuous variables and as number (%) or ratio for categorical variables. NS = not significant. Table 3. Multivariate logistic regression analysis of ECG parameters for the prediction of 30-day mortality and the need to intensify therapy during hospitalization ECG parameter Atrial fibrillation/ 30-day death n=28 P value need to intensify therapy n=55 P value OR CI OR CI NS NS flutter 0 S 1 Q 3 T NS 9 Left axis deviation NS NS Right axis NS NS deviation 2 Low QRS voltage Clockwise rotation NS NS NS NS Notched S wave in NS NS V
15 RBBB in V Qr sign in V NS NS NS NS Number of leads NS NS with negative T 1 8 waves LV subendocardial NS ischemic pattern RV transmural ischemic pattern LV plus RV transmural ischemia pattern NS = not significant. Figure 1: Flow chart of patient selection with acute pulmonary embolism 14
16 Figure 2: Examples of the ischemic electrocardiographic patterns 15
CASE REPORT INTRODUCTION
 CASE REPORT Correlation Between ST-Segment Elevation and Negative T Waves in the Precordial Leads in Acute Pulmonary Embolism: Insights into Serial Electrocardiogram Changes Zhan Zhong-qun, M.D., Yang
CASE REPORT Correlation Between ST-Segment Elevation and Negative T Waves in the Precordial Leads in Acute Pulmonary Embolism: Insights into Serial Electrocardiogram Changes Zhan Zhong-qun, M.D., Yang
S (18) doi: /j.ajem Reference: YAJEM 57346
 Accepted Manuscript A portrait of patients who die in-hospital from acute pulmonary embolism Hesham R. Omar, Mehdi Mirsaeidi, Bishoy Abraham, Garett Enten, Devanand Mangar, Enrico M. Camporesi PII: S0735-6757(18)30172-4
Accepted Manuscript A portrait of patients who die in-hospital from acute pulmonary embolism Hesham R. Omar, Mehdi Mirsaeidi, Bishoy Abraham, Garett Enten, Devanand Mangar, Enrico M. Camporesi PII: S0735-6757(18)30172-4
Acute Coronary Syndromes Unstable Angina Non ST segment Elevation MI (NSTEMI) ST segment Elevation MI (STEMI)
 Leanna R. Miller, RN, MN, CCRN-CSC, PCCN-CMC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Objectives Evaluate common abnormalities that mimic myocardial infarction. Identify
Leanna R. Miller, RN, MN, CCRN-CSC, PCCN-CMC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Objectives Evaluate common abnormalities that mimic myocardial infarction. Identify
All About STEMIs. Presented By: Brittney Urvand, RN, BSN, CCCC. Essentia Health Fargo Cardiovascular Program Manager.
 All About STEMIs Presented By: Brittney Urvand, RN, BSN, CCCC Essentia Health Fargo Cardiovascular Program Manager Updated 10/2/2018 None Disclosures Objectives Identify signs and symptoms of a heart attack
All About STEMIs Presented By: Brittney Urvand, RN, BSN, CCCC Essentia Health Fargo Cardiovascular Program Manager Updated 10/2/2018 None Disclosures Objectives Identify signs and symptoms of a heart attack
Original Article Acute pulmonary embolism with electrocardiagraphic changes mimicking acute coronary syndrome: a case report and literature review
 Int J Clin Exp Med 2015;8(7):11038-11042 www.ijcem.com /ISSN:1940-5901/IJCEM0009683 Original Article Acute pulmonary embolism with electrocardiagraphic changes mimicking acute coronary syndrome: a case
Int J Clin Exp Med 2015;8(7):11038-11042 www.ijcem.com /ISSN:1940-5901/IJCEM0009683 Original Article Acute pulmonary embolism with electrocardiagraphic changes mimicking acute coronary syndrome: a case
PECTUS EXCAVATUM WITH SPONTANEOUS TYPE 1 ECG BRUGADA PATTERN OR BRUGADA LIKE PHENOTYPE: ANOTHER BRUGADA ECG PHENOCOPY
 PECTUS EXCAVATUM WITH SPONTANEOUS TYPE 1 ECG BRUGADA PATTERN OR BRUGADA LIKE PHENOTYPE: ANOTHER BRUGADA ECG PHENOCOPY ANDRÉS RICARDO PÉREZ RIERA MD Chief of the Sector of Electro-Vectocardiography of the
PECTUS EXCAVATUM WITH SPONTANEOUS TYPE 1 ECG BRUGADA PATTERN OR BRUGADA LIKE PHENOTYPE: ANOTHER BRUGADA ECG PHENOCOPY ANDRÉS RICARDO PÉREZ RIERA MD Chief of the Sector of Electro-Vectocardiography of the
Acute chest pain and ECG need for immediate coronary angiography?
 Acute chest pain and ECG need for immediate coronary angiography? Kjell Nikus, MD, PhD Heart Center, Tampere University Hospital, Finland and Samuel Sclarovsky, MD, PhD Tel Aviv University, Israel There
Acute chest pain and ECG need for immediate coronary angiography? Kjell Nikus, MD, PhD Heart Center, Tampere University Hospital, Finland and Samuel Sclarovsky, MD, PhD Tel Aviv University, Israel There
Masqueraders of STEMI
 Masqueraders of STEMI Steven M. Costa, M.D. Assistant Professor Department of Medicine Division of Cardiology Scott & White Memorial Hospital and Clinic Texas A&M University Health Science Center Disclosures
Masqueraders of STEMI Steven M. Costa, M.D. Assistant Professor Department of Medicine Division of Cardiology Scott & White Memorial Hospital and Clinic Texas A&M University Health Science Center Disclosures
Prognostic value of the ECG on admission in patients with acute major pulmonary embolism
 Eur Respir J 2005; 25: 843 848 DOI: 10.1183/09031936.05.00119704 CopyrightßERS Journals Ltd 2005 Prognostic value of the ECG on admission in patients with acute major pulmonary embolism A. Geibel*, M.
Eur Respir J 2005; 25: 843 848 DOI: 10.1183/09031936.05.00119704 CopyrightßERS Journals Ltd 2005 Prognostic value of the ECG on admission in patients with acute major pulmonary embolism A. Geibel*, M.
Electrocardiographic findings in pulmonary embolism
 Singapore Med J 2015; 56(10): 533-537 doi: 10.11622/smedj.2015147 Electrocardiography Series CMEArticle Electrocardiographic findings in pulmonary embolism Elaine Boey1, MBBS, MRCP, Swee-Guan Teo2, MRCP,
Singapore Med J 2015; 56(10): 533-537 doi: 10.11622/smedj.2015147 Electrocardiography Series CMEArticle Electrocardiographic findings in pulmonary embolism Elaine Boey1, MBBS, MRCP, Swee-Guan Teo2, MRCP,
ORIGINAL ARTICLE. Department of Internal Medicine and Cardiology, The Medical University of Warsaw, Poland
 ORIGINAL ARTICLE Cardiology Journal 2010, Vol. 17, No. 1, pp. 1 XXX Copyright 2009 Via Medica ISSN 1897 5593 Signs of myocardial ischemia on electrocardiogram correlate with elevated plasma cardiac troponin
ORIGINAL ARTICLE Cardiology Journal 2010, Vol. 17, No. 1, pp. 1 XXX Copyright 2009 Via Medica ISSN 1897 5593 Signs of myocardial ischemia on electrocardiogram correlate with elevated plasma cardiac troponin
4/14/15. The Electrocardiogram. In jeopardy more than a century after its introduction by Willem Einthoven? Time for a revival. by Hein J.
 The Electrocardiogram. In jeopardy more than a century after its introduction by Willem Einthoven? Time for a revival. by Hein J. Wellens MD 1 Einthoven, 1905 The ECG! Everywhere available! Easy and rapid
The Electrocardiogram. In jeopardy more than a century after its introduction by Willem Einthoven? Time for a revival. by Hein J. Wellens MD 1 Einthoven, 1905 The ECG! Everywhere available! Easy and rapid
Right ECG. Contents. RAE vs. P Pulmonale: Are they the same? 12 Lead ECGs of Patient with COPD Exacerbation Before and After Treatment
 Contents Right ECG Wang, Tzong-Luen MD, PhD, JM, FESC, FACC, FCAPSC Professor, Medical College, Fu-Jen Catholic University Chief, ED, Shin-Kong Wu Ho-Su Memorial Hospital CEO, National Resuscitation Council,
Contents Right ECG Wang, Tzong-Luen MD, PhD, JM, FESC, FACC, FCAPSC Professor, Medical College, Fu-Jen Catholic University Chief, ED, Shin-Kong Wu Ho-Su Memorial Hospital CEO, National Resuscitation Council,
Myocardial Infarction. Reading Assignment (p66-78 in Outline )
 Myocardial Infarction Reading Assignment (p66-78 in Outline ) Objectives 1. Why do ST segments go up or down in ischemia? 2. STEMI locations and culprit vessels 3. Why 15-lead ECGs? 4. What s up with avr?
Myocardial Infarction Reading Assignment (p66-78 in Outline ) Objectives 1. Why do ST segments go up or down in ischemia? 2. STEMI locations and culprit vessels 3. Why 15-lead ECGs? 4. What s up with avr?
Section V. Objectives
 Section V Landscape of an MI Objectives At the conclusion of this presentation the participant will be able to Outline a systematic approach to 12 lead ECG interpretation Demonstrate the process for determining
Section V Landscape of an MI Objectives At the conclusion of this presentation the participant will be able to Outline a systematic approach to 12 lead ECG interpretation Demonstrate the process for determining
RISK STRATIFICATION OF PATIENTS WITH ACUTE SYMPTOMATIC PULMONARY EMBOLISM. David Jiménez, MD, PhD, FCCP Ramón y Cajal Hospital, IRYCIS Madrid, Spain
 RISK STRATIFICATION OF PATIENTS WITH ACUTE SYMPTOMATIC PULMONARY EMBOLISM David Jiménez, MD, PhD, FCCP Ramón y Cajal Hospital, IRYCIS Madrid, Spain Potential Conflicts of Interest Financial conflicts of
RISK STRATIFICATION OF PATIENTS WITH ACUTE SYMPTOMATIC PULMONARY EMBOLISM David Jiménez, MD, PhD, FCCP Ramón y Cajal Hospital, IRYCIS Madrid, Spain Potential Conflicts of Interest Financial conflicts of
ELECTROCARDIOGRAPH. General. Heart Rate. Starship Children s Health Clinical Guideline
 General Heart Rate QRS Axis T Wave Axis PR Interval according to Heart Rate & Age P Wave Duration and Amplitude QRS Duration according to Age QT Interval R & S voltages according to Lead & Age R/S ratio
General Heart Rate QRS Axis T Wave Axis PR Interval according to Heart Rate & Age P Wave Duration and Amplitude QRS Duration according to Age QT Interval R & S voltages according to Lead & Age R/S ratio
Basic electrocardiography reading. R3 lee wei-chieh
 Basic electrocardiography reading R3 lee wei-chieh The Normal Conduction System Lead Placement avf Limb Leads Precordial Leads Interpretation Rate Rhythm Interval Axis Chamber abnormality QRST change What
Basic electrocardiography reading R3 lee wei-chieh The Normal Conduction System Lead Placement avf Limb Leads Precordial Leads Interpretation Rate Rhythm Interval Axis Chamber abnormality QRST change What
UPDATE ON THE MANAGEMENTACUTE CORONARY SYNDROME. DR JULES KABAHIZI, Psc (Rwa) Lt Col CHIEF CONSULTANT RMH/KFH 28 JUNE18
 UPDATE ON THE MANAGEMENTACUTE CORONARY SYNDROME DR JULES KABAHIZI, Psc (Rwa) Lt Col CHIEF CONSULTANT RMH/KFH 28 JUNE18 INTRODUCTION The clinical entities that comprise acute coronary syndromes (ACS)-ST-segment
UPDATE ON THE MANAGEMENTACUTE CORONARY SYNDROME DR JULES KABAHIZI, Psc (Rwa) Lt Col CHIEF CONSULTANT RMH/KFH 28 JUNE18 INTRODUCTION The clinical entities that comprise acute coronary syndromes (ACS)-ST-segment
Electrocardiography for Healthcare Professionals. Chapter 14 Basic 12-Lead ECG Interpretation
 Electrocardiography for Healthcare Professionals Chapter 14 Basic 12-Lead ECG Interpretation 2012 The Companies, Inc. All rights reserved. Learning Outcomes 14.1 Discuss the anatomic views seen on a 12-lead
Electrocardiography for Healthcare Professionals Chapter 14 Basic 12-Lead ECG Interpretation 2012 The Companies, Inc. All rights reserved. Learning Outcomes 14.1 Discuss the anatomic views seen on a 12-lead
REtrive. REpeat. RElearn Design by. Test-Enhanced Learning based ECG practice E-book
 Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning based ECG practice E-book REtrive REpeat RElearn Design by S I T T I N U N T H A N G J U I P E E R I Y A W A
Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning based ECG practice E-book REtrive REpeat RElearn Design by S I T T I N U N T H A N G J U I P E E R I Y A W A
Other 12-Lead ECG Findings
 Other 12-Lead ECG Findings Left Atrial Enlargement Left atrial enlargement is illustrated by increased P wave duration in lead II, top ECG, and by the prominent negative P terminal force in lead V1, bottom
Other 12-Lead ECG Findings Left Atrial Enlargement Left atrial enlargement is illustrated by increased P wave duration in lead II, top ECG, and by the prominent negative P terminal force in lead V1, bottom
CARDIAC PROBLEMS IN PREGNANCY
 CARDIAC PROBLEMS IN PREGNANCY LAS VEGAS, NEVADA, USA 27 February 1 March 2016 SUCCESSFUL TREATMENT WITH RECOMBINANT TISSUE PLASMINOGEN ACTIVATOR OF MASSIVE PULMONARY EMBOLISM IN THE 16 TH WEEK OF PREGNANCY
CARDIAC PROBLEMS IN PREGNANCY LAS VEGAS, NEVADA, USA 27 February 1 March 2016 SUCCESSFUL TREATMENT WITH RECOMBINANT TISSUE PLASMINOGEN ACTIVATOR OF MASSIVE PULMONARY EMBOLISM IN THE 16 TH WEEK OF PREGNANCY
Submassive pulmonary embolism (PE) manifests a. Assessment of Cardiac Stress From Massive Pulmonary Embolism With 12-Lead ECG*
 Assessment of Cardiac Stress From Massive Pulmonary Embolism With 12-Lead ECG* Kurt R. Daniel, DO ; D. Mark Courtney, MD; and Jeffrey A. Kline, MD Background: Massive pulmonary embolism (PE) that causes
Assessment of Cardiac Stress From Massive Pulmonary Embolism With 12-Lead ECG* Kurt R. Daniel, DO ; D. Mark Courtney, MD; and Jeffrey A. Kline, MD Background: Massive pulmonary embolism (PE) that causes
Systemic or local thrombolysis in high-risk pulmonary embolism
 original article Cardiology Journal 2015, Vol. 22, No. 4, 467 474 DOI: 10.5603/CJ.a2014.0103 Copyright 2015 Via Medica ISSN 1897 5593 Systemic or local thrombolysis in high-risk pulmonary embolism Liviu
original article Cardiology Journal 2015, Vol. 22, No. 4, 467 474 DOI: 10.5603/CJ.a2014.0103 Copyright 2015 Via Medica ISSN 1897 5593 Systemic or local thrombolysis in high-risk pulmonary embolism Liviu
12 Lead ECG Interpretation
 12 Lead ECG Interpretation Julie Zimmerman, MSN, RN, CNS, CCRN Significant increase in mortality for every 15 minutes of delay! N Engl J Med 2007;357:1631-1638 Who should get a 12-lead ECG? Also include
12 Lead ECG Interpretation Julie Zimmerman, MSN, RN, CNS, CCRN Significant increase in mortality for every 15 minutes of delay! N Engl J Med 2007;357:1631-1638 Who should get a 12-lead ECG? Also include
Study methodology for screening candidates to athletes risk
 1. Periodical Evaluations: each 2 years. Study methodology for screening candidates to athletes risk 2. Personal history: Personal history of murmur in childhood; dizziness, syncope, palpitations, intolerance
1. Periodical Evaluations: each 2 years. Study methodology for screening candidates to athletes risk 2. Personal history: Personal history of murmur in childhood; dizziness, syncope, palpitations, intolerance
Solutions for Every Day Problems Cardiologists and the ECG: Are We Really That Good at It? Part II Daniel José Piñeiro Profesor Titular de Medicina,
 Solutions for Every Day Problems Cardiologists and the ECG: Are We Really That Good at It? Part II Daniel José Piñeiro Profesor Titular de Medicina, Universidad de Buenos Aires, Argentina Member, Membership
Solutions for Every Day Problems Cardiologists and the ECG: Are We Really That Good at It? Part II Daniel José Piñeiro Profesor Titular de Medicina, Universidad de Buenos Aires, Argentina Member, Membership
It is occasionally problematic to differentiate ST-segment
 CLINICAL INVESTIGATION Differential Diagnosis of Acute Pericarditis From Normal Variant Early Repolarization and Left Ventricular Hypertrophy With Early Repolarization: An Electrocardiographic Study Ravindra
CLINICAL INVESTIGATION Differential Diagnosis of Acute Pericarditis From Normal Variant Early Repolarization and Left Ventricular Hypertrophy With Early Repolarization: An Electrocardiographic Study Ravindra
Biventricular Enlargement/ Hypertrophy
 Biventricular Enlargement/ Hypertrophy Keywords congenital heart disease left ventricular hypertrophy right ventricular hypertrophy SR MITTAL Abstract Electrocardiographic diagnosis of early biventricular
Biventricular Enlargement/ Hypertrophy Keywords congenital heart disease left ventricular hypertrophy right ventricular hypertrophy SR MITTAL Abstract Electrocardiographic diagnosis of early biventricular
ECG Workshop. Nezar Amir
 ECG Workshop Nezar Amir Myocardial Ischemia ECG Infarct ECG in STEMI is dynamic & evolving Common causes of ST shift Infarct Localisation Left main artery occlusion: o diffuse ST-depression with ST elevation
ECG Workshop Nezar Amir Myocardial Ischemia ECG Infarct ECG in STEMI is dynamic & evolving Common causes of ST shift Infarct Localisation Left main artery occlusion: o diffuse ST-depression with ST elevation
Management of Massive and Sub-Massive Pulmonary Embolism
 Management of Massive and Sub-Massive Pulmonary Embolism M. Montero-Baker, MD L Leon Jr., MD, RVT, FACS Tucson Medical Center Vascular and Endovascular Surgery Section CASE PRESENTATION 54 YEAR- OLD CAUCASIAN
Management of Massive and Sub-Massive Pulmonary Embolism M. Montero-Baker, MD L Leon Jr., MD, RVT, FACS Tucson Medical Center Vascular and Endovascular Surgery Section CASE PRESENTATION 54 YEAR- OLD CAUCASIAN
Prediction of the Site of Coronary Artery Lesion in Acute Inferior Myocardial Infarction with Right Sided Precordial Lead (V4r)
 Prediction of the Site of Coronary Artery Lesion in Acute Inferior Myocardial Infarction with Right Sided Precordial Lead (V4r) MS Alam, M Ullah, SU Ulabbi, MM Haque, R Uddin, MS Mamun, AAS Majumder National
Prediction of the Site of Coronary Artery Lesion in Acute Inferior Myocardial Infarction with Right Sided Precordial Lead (V4r) MS Alam, M Ullah, SU Ulabbi, MM Haque, R Uddin, MS Mamun, AAS Majumder National
ECG INTERPRETATION MANUAL
 Lancashire & South Cumbria Cardiac Network ECG INTERPRETATION MANUAL THE NORMAL ECG Lancashire And South Cumbria Cardiac Physiologist Training Manual THE NORMAL ECG E.C.G CHECKLIST 1) Name, Paper Speed,
Lancashire & South Cumbria Cardiac Network ECG INTERPRETATION MANUAL THE NORMAL ECG Lancashire And South Cumbria Cardiac Physiologist Training Manual THE NORMAL ECG E.C.G CHECKLIST 1) Name, Paper Speed,
Current ECG interpretation guidelines in the screening of athletes
 REVIEW ARTICLE 7 How to differentiate physiological adaptation to intensive physical exercise from pathologies Current ECG interpretation guidelines in the screening of athletes Gemma Parry-Williams, Sanjay
REVIEW ARTICLE 7 How to differentiate physiological adaptation to intensive physical exercise from pathologies Current ECG interpretation guidelines in the screening of athletes Gemma Parry-Williams, Sanjay
ECG Cases and Questions. Ashish Sadhu, MD, FHRS, FACC Electrophysiology/Cardiology
 ECG Cases and Questions Ashish Sadhu, MD, FHRS, FACC Electrophysiology/Cardiology 32 yo female Life Insurance Physical 56 yo male with chest pain Terminology Injury ST elevation Ischemia T wave inversion
ECG Cases and Questions Ashish Sadhu, MD, FHRS, FACC Electrophysiology/Cardiology 32 yo female Life Insurance Physical 56 yo male with chest pain Terminology Injury ST elevation Ischemia T wave inversion
Disclosure. 3. ST depression indicative of ischemia is most commonly observed in leads: 1. V1-V2. 2. I and avl 3. V
 Interpreting Stress Induced Ischemia by ECG, Bundle Branch Block & Arrhythmias Disclosure Gregory S Thomas MD, MPH Medical Director, MemorialCare Heart & Vascular Institute, Long Beach Memorial Astellas
Interpreting Stress Induced Ischemia by ECG, Bundle Branch Block & Arrhythmias Disclosure Gregory S Thomas MD, MPH Medical Director, MemorialCare Heart & Vascular Institute, Long Beach Memorial Astellas
What s New in IV Conduction? (Quadrafascicular, not Trifascicular)
 What s New in IV Conduction? (Quadrafascicular, not Trifascicular) Frank Yanowitz, MD Professor, University of Utah School of Medicine Medical Director, IHC ECG Services (Urban Central Region) http://ecg.utah.edu
What s New in IV Conduction? (Quadrafascicular, not Trifascicular) Frank Yanowitz, MD Professor, University of Utah School of Medicine Medical Director, IHC ECG Services (Urban Central Region) http://ecg.utah.edu
Stress ECG is still Viable in Suleiman M Kharabsheh, MD, FACC Consultant Invasive Cardiologist KFHI KFSHRC-Riyadh
 Stress ECG is still Viable in 2016 Suleiman M Kharabsheh, MD, FACC Consultant Invasive Cardiologist KFHI KFSHRC-Riyadh Stress ECG Do we still need stress ECG with all the advances we have in the CV field?
Stress ECG is still Viable in 2016 Suleiman M Kharabsheh, MD, FACC Consultant Invasive Cardiologist KFHI KFSHRC-Riyadh Stress ECG Do we still need stress ECG with all the advances we have in the CV field?
Normal ST Segment Elevation and Electrocardiographic Patterns in the Right-Sided Precordial Leads (V3R and V4R) in Healthy Young Adult Koreans
 ORIGINAL ARTICLE DOI 10.4070 / kcj.2010.40.5.219 Print ISSN 1738-5520 / On-line ISSN 1738-5555 Copyright c 2010 The Korean Society of Cardiology Open Access Normal ST Segment Elevation and Electrocardiographic
ORIGINAL ARTICLE DOI 10.4070 / kcj.2010.40.5.219 Print ISSN 1738-5520 / On-line ISSN 1738-5555 Copyright c 2010 The Korean Society of Cardiology Open Access Normal ST Segment Elevation and Electrocardiographic
CME Article Brugada pattern masking anterior myocardial infarction
 Electrocardiography Series Singapore Med J 2011; 52(9) : 647 CME Article Brugada pattern masking anterior myocardial infarction Seow S C, Omar A R, Hong E C T Cardiology Department, National University
Electrocardiography Series Singapore Med J 2011; 52(9) : 647 CME Article Brugada pattern masking anterior myocardial infarction Seow S C, Omar A R, Hong E C T Cardiology Department, National University
Please check your answers with correct statements in answer pages after the ECG cases.
 ECG Cases ECG Case 1 Springer International Publishing AG, part of Springer Nature 2018 S. Okutucu, A. Oto, Interpreting ECGs in Clinical Practice, In Clinical Practice, https://doi.org/10.1007/978-3-319-90557-0
ECG Cases ECG Case 1 Springer International Publishing AG, part of Springer Nature 2018 S. Okutucu, A. Oto, Interpreting ECGs in Clinical Practice, In Clinical Practice, https://doi.org/10.1007/978-3-319-90557-0
December 2018 Tracings
 Tracings Tracing 1 Tracing 4 Tracing 1 Answer Tracing 4 Answer Tracing 2 Tracing 5 Tracing 2 Answer Tracing 5 Answer Tracing 3 Tracing 6 Tracing 3 Answer Tracing 6 Answer Questions? Contact Dr. Nelson
Tracings Tracing 1 Tracing 4 Tracing 1 Answer Tracing 4 Answer Tracing 2 Tracing 5 Tracing 2 Answer Tracing 5 Answer Tracing 3 Tracing 6 Tracing 3 Answer Tracing 6 Answer Questions? Contact Dr. Nelson
at least 4 8 hours per week
 ECG IN ATHLETS An athlete is defined as an individual who engages in regular exercise or training for sport or general fitness, typically with a premium on performance, and often engaged in individual
ECG IN ATHLETS An athlete is defined as an individual who engages in regular exercise or training for sport or general fitness, typically with a premium on performance, and often engaged in individual
Cardiovascular Images
 Cardiovascular Images Pulmonary Embolism Diagnosed From Right Heart Changes Seen After Exercise Stress Echocardiography Brian C. Case, MD; Micheas Zemedkun, MD; Amarin Sangkharat, MD; Allen J. Taylor,
Cardiovascular Images Pulmonary Embolism Diagnosed From Right Heart Changes Seen After Exercise Stress Echocardiography Brian C. Case, MD; Micheas Zemedkun, MD; Amarin Sangkharat, MD; Allen J. Taylor,
Patient referral for elective coronary angiography: challenging the current strategy
 Patient referral for elective coronary angiography: challenging the current strategy M. Santos, A. Ferreira, A. P. Sousa, J. Brito, R. Calé, L. Raposo, P. Gonçalves, R. Teles, M. Almeida, M. Mendes Cardiology
Patient referral for elective coronary angiography: challenging the current strategy M. Santos, A. Ferreira, A. P. Sousa, J. Brito, R. Calé, L. Raposo, P. Gonçalves, R. Teles, M. Almeida, M. Mendes Cardiology
Pennsylvania Academy of Family Physicians Foundation & UPMC 43rd Refresher Course in Family Medicine CME Conference March 10-13, 2016
 Pennsylvania Academy of Family Physicians Foundation & UPMC 43rd Refresher Course in Family Medicine CME Conference March 10-13, 2016 Disclosures: EKG Workshop Louis Mancano, MD Speaker has no disclosures
Pennsylvania Academy of Family Physicians Foundation & UPMC 43rd Refresher Course in Family Medicine CME Conference March 10-13, 2016 Disclosures: EKG Workshop Louis Mancano, MD Speaker has no disclosures
Chapter 1. Introduction
 Chapter 1 Introduction Introduction 9 Even though the first reports on venous thromboembolism date back to the 13 th century and the mechanism of acute pulmonary embolism (PE) was unraveled almost 150
Chapter 1 Introduction Introduction 9 Even though the first reports on venous thromboembolism date back to the 13 th century and the mechanism of acute pulmonary embolism (PE) was unraveled almost 150
Clinical Policy: Holter Monitors Reference Number: CP.MP.113
 Clinical Policy: Reference Number: CP.MP.113 Effective Date: 05/18 Last Review Date: 04/18 Coding Implications Revision Log Description Ambulatory electrocardiogram (ECG) monitoring provides a view of
Clinical Policy: Reference Number: CP.MP.113 Effective Date: 05/18 Last Review Date: 04/18 Coding Implications Revision Log Description Ambulatory electrocardiogram (ECG) monitoring provides a view of
The Electrocardiogram part II. Dr. Adelina Vlad, MD PhD
 The Electrocardiogram part II Dr. Adelina Vlad, MD PhD Basic Interpretation of the ECG 1) Evaluate calibration 2) Calculate rate 3) Determine rhythm 4) Determine QRS axis 5) Measure intervals 6) Analyze
The Electrocardiogram part II Dr. Adelina Vlad, MD PhD Basic Interpretation of the ECG 1) Evaluate calibration 2) Calculate rate 3) Determine rhythm 4) Determine QRS axis 5) Measure intervals 6) Analyze
5- The normal electrocardiogram (ECG)
 5- The (ECG) Introduction Electrocardiography is a process of recording electrical activities of heart muscle at skin surface. The electrical current spreads into the tissues surrounding the heart, a small
5- The (ECG) Introduction Electrocardiography is a process of recording electrical activities of heart muscle at skin surface. The electrical current spreads into the tissues surrounding the heart, a small
12 Lead Electrocardiogram (ECG) PFN: SOMACL17. Terminal Learning Objective. References
 12 Lead Electrocardiogram (ECG) PFN: SOMACL17 Slide 1 Terminal Learning Objective Action: Communicate knowledge of 12 Lead Electrocardiogram (ECG) Condition: Given a lecture in a classroom environment
12 Lead Electrocardiogram (ECG) PFN: SOMACL17 Slide 1 Terminal Learning Objective Action: Communicate knowledge of 12 Lead Electrocardiogram (ECG) Condition: Given a lecture in a classroom environment
TOPICS IN EMERGENCY MEDICINE SEMI-FINAL
 RISK ASSESSMENT IN PATIENTS WITH CHEST PAIN Nora Goldschlager, M.D. FACP, FACC, FAHA, FHRS Cardiology - San Francisco General Hospital UCSF Disclosures: None 1 CHEST PAIN NOT DUE TO MYOCARDIAL ISCHEMIA
RISK ASSESSMENT IN PATIENTS WITH CHEST PAIN Nora Goldschlager, M.D. FACP, FACC, FAHA, FHRS Cardiology - San Francisco General Hospital UCSF Disclosures: None 1 CHEST PAIN NOT DUE TO MYOCARDIAL ISCHEMIA
Are there low risk patients in Brugada syndrome?
 Are there low risk patients in Brugada syndrome? Pedro Brugada MD, PhD Andrea Sarkozy MD Risk stratification in Brugada syndrome In the last years risk stratification in Brugada syndrome has become the
Are there low risk patients in Brugada syndrome? Pedro Brugada MD, PhD Andrea Sarkozy MD Risk stratification in Brugada syndrome In the last years risk stratification in Brugada syndrome has become the
Ablative Therapy for Ventricular Tachycardia
 Ablative Therapy for Ventricular Tachycardia Nitish Badhwar, MD, FACC, FHRS 2 nd Annual UC Davis Heart and Vascular Center Cardiovascular Nurse / Technologist Symposium May 5, 2012 Disclosures Research
Ablative Therapy for Ventricular Tachycardia Nitish Badhwar, MD, FACC, FHRS 2 nd Annual UC Davis Heart and Vascular Center Cardiovascular Nurse / Technologist Symposium May 5, 2012 Disclosures Research
PREVENTION AND TREATMENT OF VENOUS THROMBOEMBOLISM
 PREVENTION AND TREATMENT OF VENOUS THROMBOEMBOLISM International Consensus Statement 2013 Guidelines According to Scientific Evidence Developed under the auspices of the: Cardiovascular Disease Educational
PREVENTION AND TREATMENT OF VENOUS THROMBOEMBOLISM International Consensus Statement 2013 Guidelines According to Scientific Evidence Developed under the auspices of the: Cardiovascular Disease Educational
Presenter Disclosure Information
 Various Morphological Types of Ventricular Premature Beats with Fragmented QRS Waves on 12 Lead Holter ECG had a Positive Relationship with Left Ventricular Fibrosis on CT in Patients with Hypertrophic
Various Morphological Types of Ventricular Premature Beats with Fragmented QRS Waves on 12 Lead Holter ECG had a Positive Relationship with Left Ventricular Fibrosis on CT in Patients with Hypertrophic
A case of post myocardial infarction ventricular septal rupture CHRISTOFOROS KOBOROZOS, MD
 A case of post myocardial infarction ventricular septal rupture CHRISTOFOROS KOBOROZOS, MD NAVAL HOSPITAL OF ATHENS case presentation Female, 81yo Hx: diabetes mellitus, hypertension, chronic anaemia presented
A case of post myocardial infarction ventricular septal rupture CHRISTOFOROS KOBOROZOS, MD NAVAL HOSPITAL OF ATHENS case presentation Female, 81yo Hx: diabetes mellitus, hypertension, chronic anaemia presented
Disclosures. Objectives
 BRIGHAM AND WOMEN S HOSPITAL Treatment of Massive and Submassive Pulmonary Embolism Gregory Piazza, MD, MS Assistant Professor of Medicine Harvard Medical School Staff Physician, Cardiovascular Division
BRIGHAM AND WOMEN S HOSPITAL Treatment of Massive and Submassive Pulmonary Embolism Gregory Piazza, MD, MS Assistant Professor of Medicine Harvard Medical School Staff Physician, Cardiovascular Division
STAT 12 Lead ECG Workshop: Basics & ACS
 STAT 12 Lead ECG Workshop: Basics & ACS Part 2: Acute Coronary Syndrome WAYNE W RUPPERT, CVT, CCCC, NREMT-P Cardiovascular Coordinator Bayfront Health Seven Rivers Crystal River, Florida Interventional
STAT 12 Lead ECG Workshop: Basics & ACS Part 2: Acute Coronary Syndrome WAYNE W RUPPERT, CVT, CCCC, NREMT-P Cardiovascular Coordinator Bayfront Health Seven Rivers Crystal River, Florida Interventional
Hot Topics in Cardiac Arrest. Should the patient go To the Cath Lab?
 Hot Topics in Cardiac Arrest Should the patient go To the Cath Lab? Tim Russert 1950-2008 Host of NBC s Meet the Press Sudden Cardiac Arrest : Autopsy showed plaque rupture in his LAD ( per LA Times,
Hot Topics in Cardiac Arrest Should the patient go To the Cath Lab? Tim Russert 1950-2008 Host of NBC s Meet the Press Sudden Cardiac Arrest : Autopsy showed plaque rupture in his LAD ( per LA Times,
Cardiovascular Disorders Lecture 3 Coronar Artery Diseases
 Cardiovascular Disorders Lecture 3 Coronar Artery Diseases By Prof. El Sayed Abdel Fattah Eid Lecturer of Internal Medicine Delta University Coronary Heart Diseases It is the leading cause of death in
Cardiovascular Disorders Lecture 3 Coronar Artery Diseases By Prof. El Sayed Abdel Fattah Eid Lecturer of Internal Medicine Delta University Coronary Heart Diseases It is the leading cause of death in
International Journal of Cardiology and Cardiovascular Research Vol. 1(1), pp , June,
 International Journal of Cardiology and Cardiovascular Research Vol. 1(1), pp. 002-006, June, 2014. www.premierpublishers.org. ISSN: XXXX-XXXX IJCCR Research Article Prognostic value of ST segment depression
International Journal of Cardiology and Cardiovascular Research Vol. 1(1), pp. 002-006, June, 2014. www.premierpublishers.org. ISSN: XXXX-XXXX IJCCR Research Article Prognostic value of ST segment depression
Family Medicine for English language students of Medical University of Lodz ECG. Jakub Dorożyński
 Family Medicine for English language students of Medical University of Lodz ECG Jakub Dorożyński Parts of an ECG The standard ECG has 12 leads: six of them are considered limb leads because they are placed
Family Medicine for English language students of Medical University of Lodz ECG Jakub Dorożyński Parts of an ECG The standard ECG has 12 leads: six of them are considered limb leads because they are placed
Troponin I and risk stratification of patients with acute nonmassive pulmonary embolism
 Eur Respir J 2008; 31: 847 853 DOI: 10.1183/09031936.00113307 CopyrightßERS Journals Ltd 2008 Troponin I and risk stratification of patients with acute nonmassive pulmonary embolism D. Jiménez*, G. Díaz*,
Eur Respir J 2008; 31: 847 853 DOI: 10.1183/09031936.00113307 CopyrightßERS Journals Ltd 2008 Troponin I and risk stratification of patients with acute nonmassive pulmonary embolism D. Jiménez*, G. Díaz*,
SIMPLY ECGs. Dr William Dooley
 SIMPLY ECGs Dr William Dooley 1 No anatomy just interpretation 2 Setting up an ECG 3 Setting up an ECG 1 V1-4 th Right intercostal space at sternal border 2 V2-4 th Left intercostal space at sternal border
SIMPLY ECGs Dr William Dooley 1 No anatomy just interpretation 2 Setting up an ECG 3 Setting up an ECG 1 V1-4 th Right intercostal space at sternal border 2 V2-4 th Left intercostal space at sternal border
Electrical System Overview Electrocardiograms Action Potentials 12-Lead Positioning Values To Memorize Calculating Rates
 Electrocardiograms Electrical System Overview James Lamberg 2/ 74 Action Potentials 12-Lead Positioning 3/ 74 4/ 74 Values To Memorize Inherent Rates SA: 60 to 100 AV: 40 to 60 Ventricles: 20 to 40 Normal
Electrocardiograms Electrical System Overview James Lamberg 2/ 74 Action Potentials 12-Lead Positioning 3/ 74 4/ 74 Values To Memorize Inherent Rates SA: 60 to 100 AV: 40 to 60 Ventricles: 20 to 40 Normal
Miscellaneous Stuff Keep reading the Outline
 Miscellaneous Stuff Keep reading the Outline Welcome to the 5-Step Method ECG #: Mearurements: Rhythm (s): Conduction: Waveform: Interpretation: A= V= PR= QRS= QT= Axis= 1. Compute the 5 basic measurements:
Miscellaneous Stuff Keep reading the Outline Welcome to the 5-Step Method ECG #: Mearurements: Rhythm (s): Conduction: Waveform: Interpretation: A= V= PR= QRS= QT= Axis= 1. Compute the 5 basic measurements:
Tako-Tsubo Cardiomyopathy by Transient Dynamic Left Midventricular Obstruction
 CSE REPORT DOI 10.4070 / kcj.2009.39.1.37 Print ISSN 1738-5520 / On-line ISSN 1738-5555 Copyright c 2009 The Korean Society of Cardiology Tako-Tsubo Cardiomyopathy by Transient Dynamic Left Midventricular
CSE REPORT DOI 10.4070 / kcj.2009.39.1.37 Print ISSN 1738-5520 / On-line ISSN 1738-5555 Copyright c 2009 The Korean Society of Cardiology Tako-Tsubo Cardiomyopathy by Transient Dynamic Left Midventricular
Received: 8 January 2014 Accepted: 10 June 2014 Published: 23 September 2014
 Original Article Medical Journal of the Islamic Republic of Iran (MJIRI) Iran University of Medical Sciences The relation of ST segment deviations in 12-lead conventional Electrocardiogram, right and posterior
Original Article Medical Journal of the Islamic Republic of Iran (MJIRI) Iran University of Medical Sciences The relation of ST segment deviations in 12-lead conventional Electrocardiogram, right and posterior
Case Report Free Floating Right Heart Thrombus Associated with Acute Pulmonary Embolism: An Unsettled Therapeutic Difficulty
 Case Reports in Cardiology Volume 2015, Article ID 364780, 4 pages http://dx.doi.org/10.1155/2015/364780 Case Report Free Floating Right Heart Thrombus Associated with Acute Pulmonary Embolism: An Unsettled
Case Reports in Cardiology Volume 2015, Article ID 364780, 4 pages http://dx.doi.org/10.1155/2015/364780 Case Report Free Floating Right Heart Thrombus Associated with Acute Pulmonary Embolism: An Unsettled
Acute pulmonary embolism: risk stratification in the emergency department
 Intern Emerg Med (2007) 2:119 129 DOI 10.1007/s11739-007-0033-y 119 REVIEW C. Becattini G. Agnelli Acute pulmonary embolism: risk stratification in the emergency department Received: 16 October 2006 /
Intern Emerg Med (2007) 2:119 129 DOI 10.1007/s11739-007-0033-y 119 REVIEW C. Becattini G. Agnelli Acute pulmonary embolism: risk stratification in the emergency department Received: 16 October 2006 /
Electrocardiography. Hilal Al Saffar College of Medicine,Baghdad University
 Electrocardiography Hilal Al Saffar College of Medicine,Baghdad University Which of the following is True 1. PR interval, represent the time taken for the impulse to travel from SA node to AV nose. 2.
Electrocardiography Hilal Al Saffar College of Medicine,Baghdad University Which of the following is True 1. PR interval, represent the time taken for the impulse to travel from SA node to AV nose. 2.
According to Their Presenting Syndromes*
 Clinical Characteristics of Patients With Acute Pulmonary Embolism Stratified According to Their Presenting Syndromes* Paul D. Stein, MD, FCCP; and Jerald W. Henry, MS Purpose: The purpose of this investigation
Clinical Characteristics of Patients With Acute Pulmonary Embolism Stratified According to Their Presenting Syndromes* Paul D. Stein, MD, FCCP; and Jerald W. Henry, MS Purpose: The purpose of this investigation
Findings From 12-lead Electrocardiography That Predict Circulatory Shock From Pulmonary Embolism: Systematic Review and Meta-analysis
 PROGRESSIVE CLINICAL PRACTICE Findings From 12-lead Electrocardiography That Predict Circulatory Shock From Pulmonary Embolism: Systematic Review and Meta-analysis Jacob D. Shopp, MD, Lauren K. Stewart,
PROGRESSIVE CLINICAL PRACTICE Findings From 12-lead Electrocardiography That Predict Circulatory Shock From Pulmonary Embolism: Systematic Review and Meta-analysis Jacob D. Shopp, MD, Lauren K. Stewart,
Takotsubo syndrome. Ευτυχία Σμπαρούνη, FACC, FESC
 Takotsubo syndrome Ευτυχία Σμπαρούνη, FACC, FESC Definition Takotsubo Apical ballooning Broken heart syndrome Stress cardiomyopathy Cathecholaminergic cardiomyopathy Epidemiology 1990 first report by Japanese
Takotsubo syndrome Ευτυχία Σμπαρούνη, FACC, FESC Definition Takotsubo Apical ballooning Broken heart syndrome Stress cardiomyopathy Cathecholaminergic cardiomyopathy Epidemiology 1990 first report by Japanese
ECG ABNORMALITIES D R. T AM A R A AL Q U D AH
 ECG ABNORMALITIES D R. T AM A R A AL Q U D AH When we interpret an ECG we compare it instantaneously with the normal ECG and normal variants stored in our memory; these memories are stored visually in
ECG ABNORMALITIES D R. T AM A R A AL Q U D AH When we interpret an ECG we compare it instantaneously with the normal ECG and normal variants stored in our memory; these memories are stored visually in
ECG Interpretation. Best to have a system to methodically evaluate ECG (from Dubin) * Rate * Rhythm * Axis * Intervals * Hypertrophy * Infarction
 ECG to save Babies ECG Interpretation Best to have a system to methodically evaluate ECG (from Dubin) * Rate * Rhythm * Axis * Intervals * Hypertrophy * Infarction Electrical Activity in the heart 5 events
ECG to save Babies ECG Interpretation Best to have a system to methodically evaluate ECG (from Dubin) * Rate * Rhythm * Axis * Intervals * Hypertrophy * Infarction Electrical Activity in the heart 5 events
12-Lead ECG Interpretation. Kathy Kuznar, RN, ANP
 12-Lead ECG Interpretation Kathy Kuznar, RN, ANP The 12-Lead ECG Objectives Identify the normal morphology and features of the 12- lead ECG. Perform systematic analysis of the 12-lead ECG. Recognize abnormalities
12-Lead ECG Interpretation Kathy Kuznar, RN, ANP The 12-Lead ECG Objectives Identify the normal morphology and features of the 12- lead ECG. Perform systematic analysis of the 12-lead ECG. Recognize abnormalities
PAEDIATRIC ACUTE CARE GUIDELINE. ECG Interpretation
 Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE ECG Interpretation Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be
Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE ECG Interpretation Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be
SIMPLY ECGs. Dr William Dooley
 SIMPLY ECGs Dr William Dooley Content Basic ECG interpretation pattern Some common (examined) abnormalities Presenting ECGs in context Setting up an ECG Setting up an ECG 1 V1-4 th Right intercostal space
SIMPLY ECGs Dr William Dooley Content Basic ECG interpretation pattern Some common (examined) abnormalities Presenting ECGs in context Setting up an ECG Setting up an ECG 1 V1-4 th Right intercostal space
Diploma in Electrocardiography
 The Society for Cardiological Science and Technology Diploma in Electrocardiography The Society makes this award to candidates who can demonstrate the ability to accurately record a resting 12-lead electrocardiogram
The Society for Cardiological Science and Technology Diploma in Electrocardiography The Society makes this award to candidates who can demonstrate the ability to accurately record a resting 12-lead electrocardiogram
Epidemiology of Pulmonary Embolism (PE)
 Why Treat Submassive PE Abstract: Massive Pulmonary Embolism (PE) requires immediate lifesaving intervention for the patient. For the submassive PE patient, characterized by presence of right ventricular
Why Treat Submassive PE Abstract: Massive Pulmonary Embolism (PE) requires immediate lifesaving intervention for the patient. For the submassive PE patient, characterized by presence of right ventricular
Medical Management of Acute Coronary Syndrome: The roles of a noncardiologist. Norbert Lingling D. Uy, MD Professor of Medicine UERMMMCI
 Medical Management of Acute Coronary Syndrome: The roles of a noncardiologist physician Norbert Lingling D. Uy, MD Professor of Medicine UERMMMCI Outcome objectives of the discussion: At the end of the
Medical Management of Acute Coronary Syndrome: The roles of a noncardiologist physician Norbert Lingling D. Uy, MD Professor of Medicine UERMMMCI Outcome objectives of the discussion: At the end of the
ECG interpretation basics
 ECG interpretation basics Michał Walczewski, MD Krzysztof Ozierański, MD 21.03.18 Electrical conduction system of the heart Limb leads Precordial leads 21.03.18 Precordial leads Precordial leads 21.03.18
ECG interpretation basics Michał Walczewski, MD Krzysztof Ozierański, MD 21.03.18 Electrical conduction system of the heart Limb leads Precordial leads 21.03.18 Precordial leads Precordial leads 21.03.18
Management of Acute Pulmonary Embolism. Judith Hurdman Consultant Respiratory Physician
 Management of Acute Pulmonary Embolism Judith Hurdman Consultant Respiratory Physician Judith.hurdman@sth.nhs.uk Overview Risk Stratification Who can be managed as an outpatient? To thrombolyse or not
Management of Acute Pulmonary Embolism Judith Hurdman Consultant Respiratory Physician Judith.hurdman@sth.nhs.uk Overview Risk Stratification Who can be managed as an outpatient? To thrombolyse or not
2/7/ LEAD ECG CASE STUDIES Lisa Riggs MSN, RN, ACNS-BC, CCRN-K CASE #1 WHAT ELSE WOULD YOU ASSESS? WHAT S YOUR DIAGNOSIS?
 12 LEAD ECG CASE STUDIES Lisa Riggs MSN, RN, ACNS-BC, CCRN-K CASE #1 31 y/o male is a direct admit from the physician s office with c/o chest pain and SOA WHAT ELSE WOULD YOU ASSESS? WHAT S YOUR DIAGNOSIS?
12 LEAD ECG CASE STUDIES Lisa Riggs MSN, RN, ACNS-BC, CCRN-K CASE #1 31 y/o male is a direct admit from the physician s office with c/o chest pain and SOA WHAT ELSE WOULD YOU ASSESS? WHAT S YOUR DIAGNOSIS?
12 Lead ECG Skills: Building Confidence for Clinical Practice. Presented By: Cynthia Webner, BSN, RN, CCRN-CMC. Karen Marzlin, BSN, RN,CCRN-CMC
 12 Lead ECG Skills: Building Confidence for Clinical Practice NTI 2009 Preconference Session 803 Presented By: Karen Marzlin, BSN, RN,CCRN-CMC 1 12 Lead ECG Fundamentals: The Starting Place for Linking
12 Lead ECG Skills: Building Confidence for Clinical Practice NTI 2009 Preconference Session 803 Presented By: Karen Marzlin, BSN, RN,CCRN-CMC 1 12 Lead ECG Fundamentals: The Starting Place for Linking
XVth Balkan Congress of Radiology Danubius Hotel Helia, October 2017, Budapest, Hungary
 XVth Balkan Congress of Radiology Danubius Hotel Helia, 12-14 October 2017, Budapest, Hungary Ružica Maksimović MRI in Myocarditis Faculty of Medicine, University of Belgrade, Centre for Radiology and
XVth Balkan Congress of Radiology Danubius Hotel Helia, 12-14 October 2017, Budapest, Hungary Ružica Maksimović MRI in Myocarditis Faculty of Medicine, University of Belgrade, Centre for Radiology and
Unusual Serial Electrocardiographic Changes which Progressed to Arrhythmogenic Right Ventricular Cardiomyopathy
 CASE REPORT Unusual Serial Electrocardiographic Changes which Progressed to Arrhythmogenic Right Ventricular Cardiomyopathy Shu Yoshihara 1,2, Masaki Matsunaga 2, Taku Yaegashi 3, Shioto Suzuki 4, Masaaki
CASE REPORT Unusual Serial Electrocardiographic Changes which Progressed to Arrhythmogenic Right Ventricular Cardiomyopathy Shu Yoshihara 1,2, Masaki Matsunaga 2, Taku Yaegashi 3, Shioto Suzuki 4, Masaaki
A Qadeer Negahban. Cardiologist Barnsley Hospital United Kingdom
 A Qadeer Negahban Cardiologist Barnsley Hospital United Kingdom Tako Tsubo Cardiomyopathy Transient left ventricular (LV) apical ballooning syndrome Broken heart syndrome Stress induced myocardial stunning
A Qadeer Negahban Cardiologist Barnsley Hospital United Kingdom Tako Tsubo Cardiomyopathy Transient left ventricular (LV) apical ballooning syndrome Broken heart syndrome Stress induced myocardial stunning
Cardiovascular emergencies. 05/March/2014 László Rudas Szeged
 Cardiovascular emergencies 05/March/2014 László Rudas Szeged Acute chest pain Acute heart failure Sudden cardiac death Acute chest pain What is the etiology? Chest pain signals emergency: - ACS - Pulmonary
Cardiovascular emergencies 05/March/2014 László Rudas Szeged Acute chest pain Acute heart failure Sudden cardiac death Acute chest pain What is the etiology? Chest pain signals emergency: - ACS - Pulmonary
Preface: Wang s Viewpoints
 AHA/ACCF/HRS Recommendations for the Standardization and Interpretation of the Electrocardiogram: Part IV, Ischemia and Infarction Presented by: WANG, TZONG LUEN, MD, PhD, JM, FACC, FESC, FCAPSC Professor,
AHA/ACCF/HRS Recommendations for the Standardization and Interpretation of the Electrocardiogram: Part IV, Ischemia and Infarction Presented by: WANG, TZONG LUEN, MD, PhD, JM, FACC, FESC, FCAPSC Professor,
Author's Accepted Manuscript
 Author's Accepted Manuscript Phase 4 Left Septal Fascicular Block Martín Ibarrola MD, Pablo Ambrosio Chiale MD, Andrés Ricardo Pérez-Riera MD PhD, Adrian Baranchuk MD FACC FRCPC www.elsevier.com/locate/buildenv
Author's Accepted Manuscript Phase 4 Left Septal Fascicular Block Martín Ibarrola MD, Pablo Ambrosio Chiale MD, Andrés Ricardo Pérez-Riera MD PhD, Adrian Baranchuk MD FACC FRCPC www.elsevier.com/locate/buildenv
ECG Diagnosis and Classification of Acute Coronary Syndromes
 REVIEW ARTICLE ECG Diagnosis and Classification of Acute Coronary Syndromes Yochai Birnbaum, M.D.,, James Michael Wilson, M.D.,, Miquel Fiol, M.D., Antonio Bayés de Luna, M.D., Markku Eskola, M.D., and
REVIEW ARTICLE ECG Diagnosis and Classification of Acute Coronary Syndromes Yochai Birnbaum, M.D.,, James Michael Wilson, M.D.,, Miquel Fiol, M.D., Antonio Bayés de Luna, M.D., Markku Eskola, M.D., and
12 Lead EKG. The Basics
 12 Lead EKG The Basics Objectives Demonstrate proper 12 EKG lead placement Determine electrical axis Identify ST and T wave changes as they relate to myocardial ischemia Describe possible complications
12 Lead EKG The Basics Objectives Demonstrate proper 12 EKG lead placement Determine electrical axis Identify ST and T wave changes as they relate to myocardial ischemia Describe possible complications
Considerations about the polemic J point location
 Considerations about the polemic J point location V) The J-point of the electrocardiogram Approximate point of convergence between the end of QRS complex and the onset of ST segment. It is considered the
Considerations about the polemic J point location V) The J-point of the electrocardiogram Approximate point of convergence between the end of QRS complex and the onset of ST segment. It is considered the
Prevalence and Positive Predictive Value of Poor R-Wave Progression and Impact of the Cardiothoracic Ratio
 ORIGINAL ARTICLE DOI 1070 / kcj.2009.39.118 Print ISSN 1738-5520 / On-line ISSN 1738-5555 Copyright c 2009 The Korean Society of Cardiology Open Access Prevalence and Positive Predictive Value of Poor
ORIGINAL ARTICLE DOI 1070 / kcj.2009.39.118 Print ISSN 1738-5520 / On-line ISSN 1738-5555 Copyright c 2009 The Korean Society of Cardiology Open Access Prevalence and Positive Predictive Value of Poor
Electrocardiographic abnormalities in patients with pulmonary sarcoidosis (RCD code: III)
 Journal of Rare Cardiovascular Diseases 2017; 3 (3): 81 85 www.jrcd.eu ORIGINAL PAPER Diseases of the heart Electrocardiographic abnormalities in patients with pulmonary sarcoidosis (RCD code: III) Justyna
Journal of Rare Cardiovascular Diseases 2017; 3 (3): 81 85 www.jrcd.eu ORIGINAL PAPER Diseases of the heart Electrocardiographic abnormalities in patients with pulmonary sarcoidosis (RCD code: III) Justyna
12 Lead ECG Workshop. Virginia Hass, DNP, FNP-C, PA-C Kim Newlin, CNS, ANP-C, FPCNA. California Association of Nurse Practitioners March 18, 2016
 12 Lead ECG Workshop Virginia Hass, DNP, FNP-C, PA-C Kim Newlin, CNS, ANP-C, FPCNA California Association of Nurse Practitioners March 18, 2016 Learning Objectives Identify key changes on the ECG which
12 Lead ECG Workshop Virginia Hass, DNP, FNP-C, PA-C Kim Newlin, CNS, ANP-C, FPCNA California Association of Nurse Practitioners March 18, 2016 Learning Objectives Identify key changes on the ECG which
