Superior Vena Caval Obstruction Secondary to Fibrosing Mediastinitis
|
|
|
- Terence Morgan
- 5 years ago
- Views:
Transcription
1 Superior Vena Caval Obstruction Secondary to Fibrosing Mediastinitis Robert E. Miller, Col, MC, USA, and Francis J. Sullivan, Ph.D. ABSTRACT Eight patients with obstruction of the superior vena cava (SVC) secondary to fibrosing mediastinitis are presented. Four patients were managed without surgical reconstruction of the SVC. Of these, 2 are severely symptomatic from SVC obstruction, 1 is asymptomatic, and 1 is alive though his condition is unknown. Four patients were managed with surgical replacement of the SVC. Each is asymptomatic. One of 2 aortic homografts is occluded and the other is markedly stenosed at the cephalad suture line. A late occlusion occurred in the Teflon prosthesis. In the fourth patient, a bypass graft using composite autogenous veins was complemented with an arteriovenous fistula. Venography in this patient at one, six, and thirteen months revealed graft patency; he has no limitations in his physical activities. T he clinical manifestations of superior vena caval (SVC) obstruction secondary to fibrosing mediastinitis are the following: (1) venous distention in the head, neck, and upper extremities; (2) marked venous channels over the anterior chest and abdomen: (3) morning edema of the face and hands; and (4) headache and cyanosis that are aggravated by dependence and physical exertion. Since the insidious encroachment of fibrosing mediastinitis upon the SVC enables collateral venous channels to develop [l, 4, 6, 91, the intensity of these symptoms depends upon the abruptness and completeness of occlusion and the availability of collateral pathways. A cursory evaluation of the simple mechanical problem of SVC obstruction suggests that replacement of the vessel is the obvious surgical correction. Recent articles [3, 101 have reviewed the methods and results using synthetic and biological materials for grafting. Failure to achieve consistently successful functional and anatomical results, however, has relegated this rarely encountered problem to the continual observation category. From the Department of Surgery and Clinical Research Service, Fitzsimons General Hospital, and Physiology Division, U.S. Army Medical Research and Nutrition Laboratory, Denver, Colo. We are grateful to Gary L. Neal, Maj, George F. Schuchmann, Lt Col, and Robert L. T,reasure, Lt Col, all MC, USA, for their assistance in the management of Patient 8, and to Jerome H. Kaplan, Maj, MC, USA, for the angiographic support. Accepted for publication Dec. 4, Address reprint requests to Dr. Miller, Longmont Clinic, 1925 Mountain View Ave., Longmont, Colo
2 MILLER AND SULLIVAN The purpose of this paper is to present the experience at Fitzsimons General Hospital in the management of 8 patients with benign SVC obstruction. Patient 8, who had autogenous vein bypass grafting complemented by an arteriovenous fistula, was free from symptoms of obstruction thirteen months postoperatively. C 1 in i ca 1 Mat eria 1 The 8 patients in this series are men. Their histoplasmosis skin tests were all positive; histoplasmosis complement fixation values appear in Tables 1 and 2. Prophylactic antifungal therapy was not instituted in these patients, and clinical symptoms related to exacerbation of histoplasmosis were not seen. Patient 1. A 38-year-old man first noted enlarged venous channels of the lower anterior chest in 1952; an increase in the neck size was noted in On July 23, 1958, he was admitted for evaluation, and angiography revealed a nearly obstructed SVC with reflux into the left innominate vein and retrograde passage of contrast material into the right internal mammary vein. The patient was discharged with the presumptive diagnosis of fibrosing mediastinitis secondary to histoplasmosis. During follow-up in April, 1972, the patient admitted having frequent episodes of dizziness and syncope. Comment: We presume that the patient s symptoms are related to SVC obstruction. However, thorough evaluation is necessary to exclude other en ti ties. Patient 2. A 22-year-old man had biopsy of a right supraclavicular mass that revealed a sclerosing process similar to fibrosing mediastinitis. He was admitted on March 4, 1966, with the major complaints of a drooping right eyelid and mild exertional dyspnea of thirty months duration. A chest roentgenogram showed widening of the superior mediastinum. A vena cavagram demonstrated narrowing of the SVC. The patient was discharged with a diagnosis of persisting Horner s syndrome but was otherwise asymptomatic. In August, 1972, follow-up revealed that the patient was still free from symptoms of SVC obstruction. Comment: Moderate compromise of the SVC has not produced noticeable clinical symptoms, apparently because the fibrosing mediastinitis did not continue to progress. Patient 3. A 22-year-old man had a right upper lobe infiltrate with hilar adenopathy that was detected during routine physical examination. He was admitted on October 9, 1965, at which time venograms revealed obstruction of the right and left innominate (Fig. 1) and azygous veins. Eleven days later the patient experienced headache, syncope, and neck vein distention. A presumptive diagnosis of total occlusion of the SVC was made, and anticoagulant therapy was begun. Repeat venography was not performed. Distention of the neck gradually subsided, and the patient was 484 THE ANNALS OF THORACIC SURGERY
3 TABLE 1. BENIGN SUPERIOR VENA CAVAL OBSTRUCTION: NONRECONSTRUCTIVE MANAGEMENT Age" Date of Complement Patient (yr.) Hospitalization Fixation Diagnostic Last Follow-up Specimen Date Findings 1 38 July 1958 Unknown... April 1972 Severely symptomaticb; activity limited; unemployed 2 22 March 1966 Unknown Supra- Aug Asymptomaticb; clavicular activity normal; node employed 3 22 Oct Negative Alive but status unknown 4" 30 July : 16 Thoracotomy Aug Severely symptomaticb; "Age at time of hospitalization. brelated to SVC obstruction. "Previously reported [5]. specimen activity limited; employed
4 TABLE 2. BENIGN SUPERIOR VENA CAVAL OBSTRUCTION: RECONSTRUCTIVE MANAGEMENT Age Complement Date of Graft Postoperative Last Follow-up Patient (yr.) Fixation Operation Material Venogram & Date Date Findings :128 March 1957 Aortic homograft :32 May 1962 Teflon :32 May 1958 Aortic homograft 8 34 Negative Aug Composite autogenous vein A diagnostic specimen in each patient was obtained by thoracotomy. bage at time of operation. Previously reported [5]. Related to SVC obstruction. Graft occluded, Oct April 1957 Marked stricture April 1972 at cephalad suture line, Aug Marked stenosis Dec at cephalad suture line, April 1967 Patent Sept au tograf t, Sept Asymptomaticd; activity normal; unemployed Asymptomaticd; activity normal; employed Asymptomatic ; activity normal; employed Asymp tomaticd; activity normal; employed
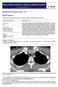
5 Correctzon of Superior Vena Caval Obstruction FIG. 1. Patient 3. Posteroanterior view showing nearly obstructed SVC and totally occluded left innominate vein. discharged with no symptoms of SVC obstruction. Since then the patient has not been examined in a government hospital, but he is known to be alive. Comment: Despite total occlusion of the azygous vein and nearocclusion of the proximal portions of the right and left innominate veins, the patient was asymptomatic. We assume that the patient first experienced symptoms when the SVC became totally occluded. Either collateral development or recanalization accounted for the patient becoming asymptomatic. Patient 4. A 30-year-old man was admitted on July 19, 1955, with the major complaints of dyspnea, cough, and substernal pain. A right thoracotomy was performed on October 26 because of an enlarging right hilar mass. A large, fixed mass was found that involved the azygous vein, right upper lobe of the lung, right pulmonary artery, and SVC. Pathological examination of the pulmonary parenchyma, occluded azygous vein, and mediastinal mass was consistent with histoplasmosis. From 1956 to 1963 the patient had repeated episodes of hemoptysis necessitating hospitalization. In 1962 the first symptoms of SVC obstruction were noted. A superior vena cavagram was performed in 1964 (Fig. 2). The patient continues to have increasing symptoms from SVC obstruction. He must sleep in a fetal position with four pillows and he cannot lower his head below his waist or stand at military attention. Comment: Despite the extended period of nearly total SVC occlusion, collateral development has been inadequate. A 40-pound weight gain may be in part responsible for the increasing symptomatology. However, he has elected to tolerate these symptoms rather than undergo surgical reconstruction of the SVC. Patient 5. A 25-year-old man was admitted on March 10, 1957, with the major complaints of weakness, lethargy, and syncope that were aggravated by VOL. 15, NO. 5, MAY,
6 MILLER AND SULLIVAN FIG. 2. Patient 4. Posteroanterior view showing a prominent right internal thoracic vein. exercise. A right thoracotomy was performed two weeks later because of clinical SVC obstruction and a right mediastinal mass. A large inflammatory mass was found that totally occluded the azygous vein and nearly occluded the SVC. The SVC was replaced with an aortic homograft. However, clinical signs of SVC occlusion returred in the immediate postoperative period. Venography revealed total occlusion of the SVC. When last examined at Fitzsimons General Hospital in October, 1967, he was asymptomatic. Comment: Although clinical SVC obstruction persisted, the patient was asymptomatic. Patient 6. A 22-year-old man was admitted on May 4, 1962, with the sensation of pressure in the head and neck. A venogram revealed total occlusion of the SVC. During a mediastinal exploration eight days later for a persisting right mediastinal mass, a Teflon graft was used to bypass the obstructive fibrosing mediastinal mass. The postoperative course was uneventful. A venogram on August 6, 1962, revealed that the graft was patent but showed marked stenosis at the cephalad suture line. In May, 1963, physical examination demonstrated signs of SVC occlusion. However, the patient was asymptomatic. Comment: Clinical manifestations constituted presumptive evidence of an occluded SVC. Gradual occlusion probably allowed adequate collateral circulation to develop. Patient 7. A 42-year-old man was admitted on April 21, 1958, with an eight-month history of prominence of the veins of the head and neck. A venogram revealed occlusion of the SVC. On May 22 the SVC was reconstructed with an aortic homograft, and the phrenic nerve was transected and repaired. Pathological examination revealed fibrosing mediastinitis secondary to histoplasmosis. Venograms in 1960, 1964, and 1967 showed marked stenosis at the cephalad suture line. 488 THE ANNALS OF THORACIC SURGERY
7 Correction of Superior Vena Caval Obstruction A FIG. 3. Patient 8. (A) Preoperative posteroanterior view showing total occlusion of the superior vena caua and an enlarged right internal thoracic vein collateral. (B) Posteroanterior view thirteen months postoperatively. Comment: Despite a poor anatomical result, the patient does not manifest symptoms of SVC obstruction and engages in normal physical activities. Patient 8. A 34-year-old man first noted puffiness of the face and prominence of the anterior chest and upper abdominal veins in April, Venography revealed near-occlusion of the SVC. An exploratory thoracotomy the following February revealed fibrosing mediastinitis secondary to histoplasmosis with near-occlusion of the SVC and total occlusion of the azygous vein. During the next eighteen months he experienced increasing episodes of dizziness and syncope as well as a marked decrease in exercise tolerance. He was admitted on August 2, 1971, for elective reconstruction of the SVC. Preoperative evaluation indicated total obstruction of the SVC (Fig. 3A) and moderate obstructive pulmonary disease. However, lung compartment studies, blood gas measurements, and the coagulation screen were normal. Pressure in the innominate vein during exercise rapidly reached hypertensive levels (Table 3). This declined during an eight-minute rest period. Nine days after admission an operation was performed. Through a median sternotomy a large, ligneous mass was found that involved the left and right innominate veins and the SVC. A five-paneled cylinder 2.5 cm. in diameter and 7 cm. long fashioned from reversed saphenous vein was sutured end-to-side into the caudal segment of the left innominate vein and end-toend into the caudal segment of the SVC. A small reversed saphenous tributary was sutured between the ascending aorta and the left innominate B
8 MILLER AND SULLIVAN TABLE 3. LEFT INNOMINATE VEIN PRESSURE STUDIES IN PATIENT 8 Resting Treadmill At End of Exercise Date Pressure" Setting Time Physical Status Pressure" Aug. 10, ", 3.4 mph. 80 sec. Paroxysmal 85 (preop.) coughing Sept. 8, ZOO, 3.4 mph. 20 min. Exhausted 11 March 22, ZOO, 3.4 mph. 28 min. Not tired 13 "Left innominate vein pressure (mm. Hg) measured in the upright position. vein 4 mm. cephalad to the autogenous vein graft. Flow in the fistula, determined electromagnetically, exceeded 475 ml. per minute. The immediate postoperative course was complicated by atelectasis and pneumonitis that responded to aggressive therapy. Innominate vein pressure measured in September, 197 1, and March, 1972, was unaltered by exhaustive exercise (Table 3). Examination on the former date indicated that a loud bruit was present over the entire precordium. On the latter date the bruit was audible in a 10 x 10 cm. area over the manubrium. At this time, cardiac output measured by the indocyanine green dye-dilution technique was normal. The dye-dilution curve showed no evidence of arteriovenous shunting. In September, 1972, the bruit was detectable at only one point over the manubrium during deep expiration. Venograms on these three dates showed a patent SVC that was essentially unchanged (Fig. 3B). The patient has resumed normal activities, including strenuous physical exercise. Comment: The SVC became occluded some time after the thoracotomy. Occlusion aggravated his symptoms to an intolerable point. Operation was postponed until our experimental study [7] was completed. When he was last seen the SVC was patent and there was no clinical sign of SVC obstruction. He was periorming hazardous duty as a paratrooper. Comment Superior vena caval obstruction secondary to fibrosing mediastinitis is seldom life-threatening. However, the quality of life is dependent upon the degree of obstruction and the adequacy of collateral circulation. Nonreconstructive management in this series does not compare favorably with the reconstructive management of SVC obstruction. At least 2 patients who did not undergo SVC reconstruction are severely symptomatic and limited in their activities. On the other hand, the 4 patients who had reconstruction are asymptomatic, and none is limited in activity. Only 1 of these, Patient 8, has a normally functioning SVC. Surgical reconstruction of the SVC has not been consistently successful, probably because thrombosis in the region of the suture lines has led to occlusion of the graft. However, in an experimental study [7] we have shown 490 THE ANNALS OF THORACIC SURGERY
9 Correction of Superior Vena Caval Obstruction in dogs that an arteriovenous fistula protects an autogenous vein graft. In this study the SVC was maximally replaced in 15 animals. The grafts functioned normally for one year. Early thrombus formation at the suture lines disappeared within two weeks of operation. We concluded that the efficacy of the shunt was related to turbulence in the graft preventing thrombus retention. During an operative procedure to reconstruct an occluded SVC, the ligneous mass should not be totally excised for fear of transecting the right phrenic nerve. This would increase the postoperative morbidity with probable pulmonary changes secondary to histoplasmosis. Second, injury to the right pulmonary vessels could well prolong the operative procedure. Third, attempts should be made to provide adequate space for the vein autograft to lie free of the aorta, the inflammatory mass, and the manubrium. An adequate length of autogenous vein may be harvested from the noncritical vessels, such as the cephalic vein or the saphenous vein used in Patient 8 and described elsewhere [2, 81. Increased venous pressure in the upper extremities as a result of fibrosing mediastinitis provides an adequate-sized cephalic vein, obviating a temporary radial artery-tocephalic vein fistula to increase its size prior to operation. A small tributary of the saphenous vein affords an adequate-sized specimen for use as a shunt. The internal thoracic artery may be of appropriate size. However, the difficult dissection of this vessel from a fibrotic mediastinum is time-consuming. Reconstruction of an obstructed SVC, as seen in Patient 4 (cf. Fig. Z), requires isolation of the SVC above and below the inflammatory mass. Suturing the venous autograft end-to-end with the complementary cephalad fistula then provides successful anatomical and functional results. Reconstruction for an obstruction involving the caudal portions of the left and right innominate veins, as seen in Patient 3 (cf. Fig. l), requires dissection of the free segments and interposition of a Y-shaped venous autograft complemented with two cephalad fistulas. When the graft is of excessive length, there should be concern for the possibility of stricture occurring at the caudal suture line. Thus, two fistulas, one at each suture line, may be required. Flow measurements are necessary postoperatively to insure that cardiac output is not increased beyond the compensatory ability of the patient. The arteriovenous fistula, we believe, will close spontaneously. If this has not occurred within two years or if the shunt becomes enlarged beyond the three- or four-week critical period, surgical closure is necessary. Anticoagulant therapy during the postoperative period is unnecessary in SVC reconstruction when a complementing fistula is used with an autogenous vein graft. However, to prevent bacterial vasculitis in the area of the fistula, prophylactic antibiotics should be used for patients having upper respiratory diseases, dental work, or other surgical procedures.
10 MILLER AND SULLIVAN Refer en ces 1. Barrett, N. R. Idiopathic mediastinal fibrosis. Br. J. Surg , Benvenuto, R., Rodman, F. S. B., Gilmour, J., Phillips, A. F., and Callaghan, J. C. Composite venous graft for replacement of the superior vena cava. Arch. Surg. 84:570, Boruchow, I. B., and Johnson, J. Obstructions of the vena cava. Surg. Gynecol. Obstet. 134: 115, Effler, D. B., and Groves, L. K. Superior vena caval obstruction. J. Thorac. Cardiouasc. Surg. 43:574, Hewlett, T. H., Steer, A., and Thomas, D. E. Progressive fibrosing mediastinitis. Ann.Thorac. Surg. 2:345, Miller, D. B., Allen, S. T., and Amidon, E. L. Obstruction of the superior vena cava presumably due to histoplasmosis. Am. Rev. Tuberc. 77:848, Miller, R. E., Corneil, N. J., and Sullivan, F. J. Replacement of superior vena cava with autogenous tissue: An experimental study. Ann. Thorac. Surg. P. 474, this issue. 8. Rheinlander, H. F. Superior vena cava replacement: Report of a successful autogenous composite vein graft. J. Thorac. Cardiovasc. Surg. 57:774, Salyer, J. M., Harrison, H. N., Winn, D. F., Jr., and Taylor, R. R. Chronic fibrous mediastinitis and superior vena caval obstruction due to histoplasmosis. Dis. Chest 35:364, Sisler, G. E., and Tice, D. A. RadicaI right pneumonectomy using preserved allograft vein for caval replacement. Ann. Thorac. Surg. 14:299, THE ANNALS OF THORACIC SURGERY
with the Spiral Composite Vein Graft
 Redacement of Superior Vena Cava with the Spiral Composite Vein Graft A Versatile Technique C. J. Chiu, M.D., J. Terzis, M.D., and M. L. MacRae, B.S. ABSTRACT A technique to construct a spiral vein graft
Redacement of Superior Vena Cava with the Spiral Composite Vein Graft A Versatile Technique C. J. Chiu, M.D., J. Terzis, M.D., and M. L. MacRae, B.S. ABSTRACT A technique to construct a spiral vein graft
Saphenous Vein Autograft Replacement
 Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
with Autogenous Tissue
 Replacement of Superior Vena Cava with Autogenous Tissue An Experimental Study Robert E. Miller, Col, MC, USA, Neil J. Corneil, Capt, VC, USA, and Francis J. Sullivan, Ph.D. ABSTRACT Autogenous pericardium
Replacement of Superior Vena Cava with Autogenous Tissue An Experimental Study Robert E. Miller, Col, MC, USA, Neil J. Corneil, Capt, VC, USA, and Francis J. Sullivan, Ph.D. ABSTRACT Autogenous pericardium
Gore-Tex Grafts for Replacement of the Superior Vena Cava
 Gore-Tex Grafts for Replacement of the Superior Vena Cava William H. Heydorn, COL, MC, Russ Zajtchuk, LTC, MC, John Miller, CPT, VC, and George F. Schuchmann, LTC, MC, all USA ABSTRACT In an effort to
Gore-Tex Grafts for Replacement of the Superior Vena Cava William H. Heydorn, COL, MC, Russ Zajtchuk, LTC, MC, John Miller, CPT, VC, and George F. Schuchmann, LTC, MC, all USA ABSTRACT In an effort to
Emergency Approach to the Subclavian and Innominate Vessels
 Emergency Approach to the Subclavian and Innominate Vessels Joseph J. Amato, M.D., Robert M. Vanecko, M.D., See Tao Yao, M.D., and Milton Weinberg, Jr., M.D. T he operative approach to an acutely injured
Emergency Approach to the Subclavian and Innominate Vessels Joseph J. Amato, M.D., Robert M. Vanecko, M.D., See Tao Yao, M.D., and Milton Weinberg, Jr., M.D. T he operative approach to an acutely injured
Lung cancer or primary malignant tumors of the mediastinum
 Technique of Superior Vena Cava Resection for Lung Carcinomas David R. Jones, MD Division of Thoracic and Cardiovascular Surgery, Department of Surgery, University of Virginia School of Medicine, Charlottesville,
Technique of Superior Vena Cava Resection for Lung Carcinomas David R. Jones, MD Division of Thoracic and Cardiovascular Surgery, Department of Surgery, University of Virginia School of Medicine, Charlottesville,
Aberrant Right Subclavian Artery Aneurysm
 Aberrant Right Subclavian Artery William S. Stoney, M.D., William C. Alford, Jr., M.D., George R. Burrus, M.D., and Clarence S. Thomas, Jr., M.D. ABSTRACT Ten patients with aneurysm of an aberrant right
Aberrant Right Subclavian Artery William S. Stoney, M.D., William C. Alford, Jr., M.D., George R. Burrus, M.D., and Clarence S. Thomas, Jr., M.D. ABSTRACT Ten patients with aneurysm of an aberrant right
Large veins of the thorax Brachiocephalic veins
 Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Partial anomalous pulmonary venous connection to superior
 Cavo-Atrial Anastomosis Technique for Partial Anomalous Pulmonary Venous Connection to the Superior Vena Cava The Warden Procedure Robert A. Gustafson, MD Partial anomalous pulmonary venous connection
Cavo-Atrial Anastomosis Technique for Partial Anomalous Pulmonary Venous Connection to the Superior Vena Cava The Warden Procedure Robert A. Gustafson, MD Partial anomalous pulmonary venous connection
Case #1. Case #1- Possible codes. Unraveling the -59 modifier. Principles of Interventional. CASE 1: Simple angioplasty
 Unraveling the -59 modifier Principles of Interventional Coding Donald Schon, MD, FACP Debra Lawson, CPC, PCS Distinct or independent from other services performed on the same day Normally not reported
Unraveling the -59 modifier Principles of Interventional Coding Donald Schon, MD, FACP Debra Lawson, CPC, PCS Distinct or independent from other services performed on the same day Normally not reported
Mediastinal Granuloma Associated
 Mediastinal Granuloma Associated with Pericardi t is Frederic F. Primich, M.D.,* and Herbert C. Maier, M.D. M ediastinal granulomas may be caused by an inflammatory process developing primarily in a group
Mediastinal Granuloma Associated with Pericardi t is Frederic F. Primich, M.D.,* and Herbert C. Maier, M.D. M ediastinal granulomas may be caused by an inflammatory process developing primarily in a group
Introduction to the Native Arteriovenous Fistula: A primer for medical students and radiology residents
 Introduction to the Native Arteriovenous Fistula: A primer for medical students and radiology residents Jesus Contreras, D.O. PGY-4 John Yasmer, D.O. Department of Radiology No Disclosures Objectives Introduce
Introduction to the Native Arteriovenous Fistula: A primer for medical students and radiology residents Jesus Contreras, D.O. PGY-4 John Yasmer, D.O. Department of Radiology No Disclosures Objectives Introduce
4/3/2014. Disclosures. Venous Thoracic Outlet Syndrome: Our Approach and Results. Paget Schroetter Syndrome. Paget Schroetter Syndrome.
 Disclosures No relevant financial relationships with commercial interests Venous Thoracic Outlet Syndrome: Our Approach and Julie A. Freischlag, M.D. Vice Chancellor for Human Health Sciences Dean of the
Disclosures No relevant financial relationships with commercial interests Venous Thoracic Outlet Syndrome: Our Approach and Julie A. Freischlag, M.D. Vice Chancellor for Human Health Sciences Dean of the
Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia
 Marshall University Marshall Digital Scholar Internal Medicine Faculty Research Spring 5-2004 Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia Ellen A. Thompson
Marshall University Marshall Digital Scholar Internal Medicine Faculty Research Spring 5-2004 Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia Ellen A. Thompson
Stenosis of Pulmonary Veins
 Stenosis of Pulmonary Veins Report of a Patient Corrected Surgically Yasunaru Kawashima, M.D., Takeshi Ueda, M.D., Yasuaki Naito, M.D, Eiji Morikawa, M.D., and Hisao Manabe, M.D. ABSTRACT A 15-year-old
Stenosis of Pulmonary Veins Report of a Patient Corrected Surgically Yasunaru Kawashima, M.D., Takeshi Ueda, M.D., Yasuaki Naito, M.D, Eiji Morikawa, M.D., and Hisao Manabe, M.D. ABSTRACT A 15-year-old
THE popliteal artery is the second most common site of aneurysm. The
 POPLITEAL ANEURYSM Treatment by Vein Graft: Case Report A. W. HUMPHRIES, M.D. Department of Orthopedic Surgery F. A. LeFEVRE, M.D. and V. G. dewolfe, M.D. Department of Cardiovascular Disease THE popliteal
POPLITEAL ANEURYSM Treatment by Vein Graft: Case Report A. W. HUMPHRIES, M.D. Department of Orthopedic Surgery F. A. LeFEVRE, M.D. and V. G. dewolfe, M.D. Department of Cardiovascular Disease THE popliteal
Case of the Day Chest
 Case of the Day Chest Darin White MDCM FRCPC Department of Radiology, Mayo Clinic 76 th Annual Scientific Meeting Canadian Association of Radiologists Montreal, QC April 26, 2013 2013 MFMER slide-1 Disclosures
Case of the Day Chest Darin White MDCM FRCPC Department of Radiology, Mayo Clinic 76 th Annual Scientific Meeting Canadian Association of Radiologists Montreal, QC April 26, 2013 2013 MFMER slide-1 Disclosures
Obstruction of the superior vena cava (SVC) produces
 Superior Vena Cava Obstruction: Bypass Using Spiral Vein Graft John R. Doty, MD, Jean H. Flores, RN, and Donald B. Doty, MD Department of Surgery, LDS Hospital, Salt Lake City, Utah Background. Previous
Superior Vena Cava Obstruction: Bypass Using Spiral Vein Graft John R. Doty, MD, Jean H. Flores, RN, and Donald B. Doty, MD Department of Surgery, LDS Hospital, Salt Lake City, Utah Background. Previous
Upper Extremity Venous Duplex. Michigan Sonographers Society Fall Ultrasound Symposium October 15, 2016
 Upper Extremity Venous Duplex Michigan Sonographers Society Fall Ultrasound Symposium October 15, 2016 Patricia A. (Tish) Poe, BA RVT FSVU Director of Quality Assurance Navix Diagnostix Patricia A. Poe
Upper Extremity Venous Duplex Michigan Sonographers Society Fall Ultrasound Symposium October 15, 2016 Patricia A. (Tish) Poe, BA RVT FSVU Director of Quality Assurance Navix Diagnostix Patricia A. Poe
Penetrating wounds of the heart and great vessels
 Thorax (1973), 28, 142. Penetrating wounds of the heart and great vessels A report of 30 patients C. E. ANAGNOSTOPOULOS and C. FREDERICK KITTLE Department of Surgery, Section of Thoracic and Cardiovascular
Thorax (1973), 28, 142. Penetrating wounds of the heart and great vessels A report of 30 patients C. E. ANAGNOSTOPOULOS and C. FREDERICK KITTLE Department of Surgery, Section of Thoracic and Cardiovascular
Autogenous arteriovenous fistula for hemodialysis complicated with a giant venous aneurysm
 ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 12 Number 2 Autogenous arteriovenous fistula for hemodialysis complicated with a giant venous aneurysm K Ergüne?, U Yetkin,
ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 12 Number 2 Autogenous arteriovenous fistula for hemodialysis complicated with a giant venous aneurysm K Ergüne?, U Yetkin,
Vascular Surgery Rotation Objectives for Junior Residents (PGY-1 and 2)
 Vascular Surgery Rotation Objectives for Junior Residents (PGY-1 and 2) Definition Vascular surgery is the specialty concerned with the diagnosis and management of congenital and acquired diseases of the
Vascular Surgery Rotation Objectives for Junior Residents (PGY-1 and 2) Definition Vascular surgery is the specialty concerned with the diagnosis and management of congenital and acquired diseases of the
Mediastinum It is a thick movable partition between the two pleural sacs & lungs. It contains all the structures which lie
 Dr Jamila EL medany OBJECTIVES At the end of the lecture, students should be able to: Define the Mediastinum. Differentiate between the divisions of the mediastinum. List the boundaries and contents of
Dr Jamila EL medany OBJECTIVES At the end of the lecture, students should be able to: Define the Mediastinum. Differentiate between the divisions of the mediastinum. List the boundaries and contents of
Tracheal stenosis in infants and children is typically characterized
 Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
How to manage the left subclavian and left vertebral artery during TEVAR
 How to manage the left subclavian and left vertebral artery during TEVAR Jürg Schmidli Chief of Vascular Surgery Inselspital Hamburg 2017 Dept Cardiovascular Surgery, Bern, Switzerland Disclosure No Disclosures
How to manage the left subclavian and left vertebral artery during TEVAR Jürg Schmidli Chief of Vascular Surgery Inselspital Hamburg 2017 Dept Cardiovascular Surgery, Bern, Switzerland Disclosure No Disclosures
CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST
 CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST I have constructed this lecture based on publications by leading cardiothoracic American surgeons: Timothy
CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST I have constructed this lecture based on publications by leading cardiothoracic American surgeons: Timothy
Abdominal Aortic Aneurysms. A Surgeons Perspective Dr. Derek D. Muehrcke
 Abdominal Aortic Aneurysms A Surgeons Perspective Dr. Derek D. Muehrcke Aneurysm Definition The abnormal enlargement or bulging of an artery caused by an injury or weakness in the blood vessel wall A localized
Abdominal Aortic Aneurysms A Surgeons Perspective Dr. Derek D. Muehrcke Aneurysm Definition The abnormal enlargement or bulging of an artery caused by an injury or weakness in the blood vessel wall A localized
Region: 11. Clinic6patholo cal Studies
 Tumors of the Thvmus and ThVIIliC Region: 11. Clinic6patholo cal Studies on Hodgkin s Disease of Re Thymus N. P. Bergh, M.D., P. Gatzinsky, M.D., S. Larsson, M.D., P. Lundin, M.D., and B. Ridell, M.D.
Tumors of the Thvmus and ThVIIliC Region: 11. Clinic6patholo cal Studies on Hodgkin s Disease of Re Thymus N. P. Bergh, M.D., P. Gatzinsky, M.D., S. Larsson, M.D., P. Lundin, M.D., and B. Ridell, M.D.
Pulmonary Valve Replacement
 Pulmonary Valve Replacement with Fascia Lata J. C. R. Lincoln, F.R.C.S., M. Geens, M.D., M. Schottenfeld, M.D., and D. N. Ross, F.R.C.S. ABSTRACT The purpose of this paper is to describe a technique of
Pulmonary Valve Replacement with Fascia Lata J. C. R. Lincoln, F.R.C.S., M. Geens, M.D., M. Schottenfeld, M.D., and D. N. Ross, F.R.C.S. ABSTRACT The purpose of this paper is to describe a technique of
Right-Sided Bacterial Endocarditis
 New Concepts in the Treatment of the Uncontrollable Infection Agustin Arbulu, M.D., Ali Kafi, M.D., Norman W. Thorns, M.D., and Robert F. Wilson, M.D. ABSTRACT Our experience with 25 patients with right-sided
New Concepts in the Treatment of the Uncontrollable Infection Agustin Arbulu, M.D., Ali Kafi, M.D., Norman W. Thorns, M.D., and Robert F. Wilson, M.D. ABSTRACT Our experience with 25 patients with right-sided
Bare Metal Stents vs Stent Grafts
 Bare Metal Stents vs Stent Grafts ASDIN 12th Annual Scientific Meeting Phoenix, AZ, February 20, 2016 Dirk Hentschel, MD Director, Interventional Nephrology Brigham and Women s Hospital Disclosure Consultant:
Bare Metal Stents vs Stent Grafts ASDIN 12th Annual Scientific Meeting Phoenix, AZ, February 20, 2016 Dirk Hentschel, MD Director, Interventional Nephrology Brigham and Women s Hospital Disclosure Consultant:
Outline. Congenital Heart Disease. Special Considerations for Special Populations: Congenital Heart Disease
 Special Considerations for Special Populations: Congenital Heart Disease Valerie Bosco, FNP, EdD Alison Knauth Meadows, MD, PhD University of California San Francisco Adult Congenital Heart Program Outline
Special Considerations for Special Populations: Congenital Heart Disease Valerie Bosco, FNP, EdD Alison Knauth Meadows, MD, PhD University of California San Francisco Adult Congenital Heart Program Outline
Schedule of Benefits. for Professional Fees Vascular Procedures
 Schedule of Benefits for Professional Fees 2018 Vascular Procedures ANASTOMOSIS RULES 820 Arteriovenous anastomosis in arm 1453 Arteriovenous anastomosis, open by basilic vein transposition 1465 Splenorenal
Schedule of Benefits for Professional Fees 2018 Vascular Procedures ANASTOMOSIS RULES 820 Arteriovenous anastomosis in arm 1453 Arteriovenous anastomosis, open by basilic vein transposition 1465 Splenorenal
Axillobrachial artery bypass grafting with in situ cephalic vein for axillary artery occlusion: A case report
 CASE REPORTS Axillobrachial artery bypass grafting with in situ cephalic vein for axillary artery occlusion: A case report Evan S. Cohen,/VII), Robert B. Holtzman, MD, and George W. Johnson, Jr., MD, Houston,
CASE REPORTS Axillobrachial artery bypass grafting with in situ cephalic vein for axillary artery occlusion: A case report Evan S. Cohen,/VII), Robert B. Holtzman, MD, and George W. Johnson, Jr., MD, Houston,
Descending aorta replacement through median sternotomy
 Descending aorta replacement through median sternotomy Mitrev Z, Anguseva T, Belostotckij V, Hristov N. Special hospital for surgery Filip Vtori Skopje - Makedonija June, 2010 Cardiosurgery - Skopje 1
Descending aorta replacement through median sternotomy Mitrev Z, Anguseva T, Belostotckij V, Hristov N. Special hospital for surgery Filip Vtori Skopje - Makedonija June, 2010 Cardiosurgery - Skopje 1
Malignant related superior vena cava (SVC) syndrome
 Malignant related superior vena cava (SVC) syndrome Manit Sae-teaw B.Pharm, BCP, BCOP Grad dip in Pharmacotherapy Faculty of pharmaceutical sciences Ubon Ratchathani University 1 Outline Introduction Etiology
Malignant related superior vena cava (SVC) syndrome Manit Sae-teaw B.Pharm, BCP, BCOP Grad dip in Pharmacotherapy Faculty of pharmaceutical sciences Ubon Ratchathani University 1 Outline Introduction Etiology
KNIFED IN THE ABDOMEN
 Originally Posted: November 01, 2014 KNIFED IN THE ABDOMEN Resident(s): Andrew Duarte, MD Attending(s): Ryan Scott, MD & David Kay, MD Program/Dept(s): St. Joseph s Hospital and Medical Center, Phoenix,
Originally Posted: November 01, 2014 KNIFED IN THE ABDOMEN Resident(s): Andrew Duarte, MD Attending(s): Ryan Scott, MD & David Kay, MD Program/Dept(s): St. Joseph s Hospital and Medical Center, Phoenix,
PATCHING AND SECTION OF THE PULMONARY ORIFICE OF THE HEART.*
 Published Online: 1 July, 1914 Supp Info: http://doi.org/10.1084/jem.20.1.3 Downloaded from jem.rupress.org on December 24, 2018 PATCHING AND SECTION OF THE PULMONARY ORIFICE OF THE HEART.* BY THEODORE
Published Online: 1 July, 1914 Supp Info: http://doi.org/10.1084/jem.20.1.3 Downloaded from jem.rupress.org on December 24, 2018 PATCHING AND SECTION OF THE PULMONARY ORIFICE OF THE HEART.* BY THEODORE
Occlusion: A New Technique Antegrade wiring i with retrograde ballooning and stenting
 How To Treat Resistant Central Venous Occlusion: A New Technique Antegrade wiring i with retrograde ballooning and stenting Dafsah A Juzar T. Santoso National Heart Center, Harapan Kita, & Medistra Hospital
How To Treat Resistant Central Venous Occlusion: A New Technique Antegrade wiring i with retrograde ballooning and stenting Dafsah A Juzar T. Santoso National Heart Center, Harapan Kita, & Medistra Hospital
Bronchogenic Carcinoma
 A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
AORTIC DISSECTION. DISSECTING ANEURYSMS OF THE AORTA or CLASSIFICATION
 DISSECTING ANEURYSMS OF THE AORTA or AORTIC DISSECTION CLASSIFICATION DeBakey classified aortic dissections into types I, II, and III :- Type I dissection the tear site originates in the ascending aorta,
DISSECTING ANEURYSMS OF THE AORTA or AORTIC DISSECTION CLASSIFICATION DeBakey classified aortic dissections into types I, II, and III :- Type I dissection the tear site originates in the ascending aorta,
MEDIASTINAL LYMPH NODE METASTASIS IN PATIENTS WITH CLINICAL STAGE I PERIPHERAL NON-SMALL-CELL LUNG CANCER
 MEDIASTINAL LYMPH NODE METASTASIS IN PATIENTS WITH CLINICAL STAGE I PERIPHERAL NON-SMALL-CELL LUNG CANCER Tsuneyo Takizawa, MD a Masanori Terashima, MD a Teruaki Koike, MD a Hideki Akamatsu, MD a Yuzo
MEDIASTINAL LYMPH NODE METASTASIS IN PATIENTS WITH CLINICAL STAGE I PERIPHERAL NON-SMALL-CELL LUNG CANCER Tsuneyo Takizawa, MD a Masanori Terashima, MD a Teruaki Koike, MD a Hideki Akamatsu, MD a Yuzo
Subclavian and Axillary Artery Aneurysms
 Subclavian and Axillary Artery Aneurysms April 2008 Francesco A Aiello, M.D. Assistant Professor of Surgery Division of Vascular Endovascular Surgery University of Massachusetts Medical School None DISCLOSURES
Subclavian and Axillary Artery Aneurysms April 2008 Francesco A Aiello, M.D. Assistant Professor of Surgery Division of Vascular Endovascular Surgery University of Massachusetts Medical School None DISCLOSURES
Case Report 1. CTA head. (c) Tele3D Advantage, LLC
 Case Report 1 CTA head 1 History 82 YEAR OLD woman with signs and symptoms of increased intra cranial pressure in setting of SAH. CT Brain was performed followed by CT Angiography of head. 2 CT brain Extensive
Case Report 1 CTA head 1 History 82 YEAR OLD woman with signs and symptoms of increased intra cranial pressure in setting of SAH. CT Brain was performed followed by CT Angiography of head. 2 CT brain Extensive
Double Superior Vena Cava; A Benign Cause of Widened Mediastenum and Implication on Venous Central Access
 ISPUB.COM The Internet Journal of Endovascular Medicine Volume 2 Number 1 Double Superior Vena Cava; A Benign Cause of Widened Mediastenum and Implication on Venous H Enuh, A Patel, A Chaudry, K Diaz,
ISPUB.COM The Internet Journal of Endovascular Medicine Volume 2 Number 1 Double Superior Vena Cava; A Benign Cause of Widened Mediastenum and Implication on Venous H Enuh, A Patel, A Chaudry, K Diaz,
Sectional Anatomy Quiz - III
 Sectional Anatomy - III Rashid Hashmi * Rural Clinical School, University of New South Wales (UNSW), Wagga Wagga, NSW, Australia A R T I C L E I N F O Article type: Article history: Received: 30 Jun 2018
Sectional Anatomy - III Rashid Hashmi * Rural Clinical School, University of New South Wales (UNSW), Wagga Wagga, NSW, Australia A R T I C L E I N F O Article type: Article history: Received: 30 Jun 2018
Mandatory knowledge about natural history of coronary grafts. P.Sergeant P. Maureira K.U.Leuven, Belgium
 Mandatory knowledge about natural history of coronary grafts P.Sergeant P. Maureira K.U.Leuven, Belgium Types of grafts Arterial ITA/IMA (internal thoracic/mammary artery) Radial artery Gastro-epiploïc
Mandatory knowledge about natural history of coronary grafts P.Sergeant P. Maureira K.U.Leuven, Belgium Types of grafts Arterial ITA/IMA (internal thoracic/mammary artery) Radial artery Gastro-epiploïc
10/14/2018 Dr. Shatarat
 2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
Chest X-ray Interpretation
 Chest X-ray Interpretation Introduction Routinely obtained Pulmonary specialist consultation Inherent physical exam limitations Chest x-ray limitations Physical exam and chest x-ray provide compliment
Chest X-ray Interpretation Introduction Routinely obtained Pulmonary specialist consultation Inherent physical exam limitations Chest x-ray limitations Physical exam and chest x-ray provide compliment
UNILATERAL ELEVATION OF THE INTERNAL JUGULAR PULSE
 BY PETER SLEIGHT From St. George's Hospital Received September 8, 1961 This paper describes a group of patients in whom the venous pressure, as shown by a distended and pulsating internal jugular vein,
BY PETER SLEIGHT From St. George's Hospital Received September 8, 1961 This paper describes a group of patients in whom the venous pressure, as shown by a distended and pulsating internal jugular vein,
Heart disease remains the leading cause of morbidity and mortality in industrialized nations. It accounts for nearly 40% of all deaths in the United
 Heart disease remains the leading cause of morbidity and mortality in industrialized nations. It accounts for nearly 40% of all deaths in the United States, totaling about 750,000 individuals annually
Heart disease remains the leading cause of morbidity and mortality in industrialized nations. It accounts for nearly 40% of all deaths in the United States, totaling about 750,000 individuals annually
Occlusion of All Four Extracranial Vessels With Minimal Clinical Symptomatology. Case Report
 Occlusion of All Four Extracranial Vessels With Minimal Clinical Symptomatology. Case Report BY JIRI J. VITEK, M.D., JAMES H. HALSEY, JR., M.D., AND HOLT A. McDOWELL, M.D. Abstract: Occlusion of All Four
Occlusion of All Four Extracranial Vessels With Minimal Clinical Symptomatology. Case Report BY JIRI J. VITEK, M.D., JAMES H. HALSEY, JR., M.D., AND HOLT A. McDOWELL, M.D. Abstract: Occlusion of All Four
63-year old female with dyspnea
 Indiana University Pulmonary and Critical Care Fellowship Fellows Case Archive Case #1 63-year old female with dyspnea Gabriel Bosslet, MD; Chadi Hage MD A 63-year-old female presented to pulmonary clinic
Indiana University Pulmonary and Critical Care Fellowship Fellows Case Archive Case #1 63-year old female with dyspnea Gabriel Bosslet, MD; Chadi Hage MD A 63-year-old female presented to pulmonary clinic
Surgical Management Of TAPVR. Daniel A. Velez, M.D. Congenital Cardiac Surgeon Phoenix Children s Hospital
 Surgical Management Of TAPVR Daniel A. Velez, M.D. Congenital Cardiac Surgeon Phoenix Children s Hospital No Disclosures Goals Review the embryology and anatomy Review Surgical Strategies for repair Discuss
Surgical Management Of TAPVR Daniel A. Velez, M.D. Congenital Cardiac Surgeon Phoenix Children s Hospital No Disclosures Goals Review the embryology and anatomy Review Surgical Strategies for repair Discuss
HISTORY. Question: What category of heart disease is suggested by this history? CHIEF COMPLAINT: Heart murmur present since early infancy.
 HISTORY 18-year-old man. CHIEF COMPLAINT: Heart murmur present since early infancy. PRESENT ILLNESS: Although normal at birth, a heart murmur was heard at the six week check-up and has persisted since
HISTORY 18-year-old man. CHIEF COMPLAINT: Heart murmur present since early infancy. PRESENT ILLNESS: Although normal at birth, a heart murmur was heard at the six week check-up and has persisted since
Subclavian artery Stenting
 Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Partial Anomalous Pulmonary Venous Connection in Adults: Evaluation with MDCT
 Partial Anomalous Pulmonary Venous Connection in Adults: Evaluation with MDCT e-poster: 349 Congress: 2WCTI 2009 Type: Educational poster Topic: Pulmonary circulation Authors: MeSH: Bhatti W, Maldjian
Partial Anomalous Pulmonary Venous Connection in Adults: Evaluation with MDCT e-poster: 349 Congress: 2WCTI 2009 Type: Educational poster Topic: Pulmonary circulation Authors: MeSH: Bhatti W, Maldjian
Pulmonary thromboendarterectomy (PTE) is indicated for
 Pulmonary Thromboendarterectomy Steven R. Meyer, MD, PhD, and Christopher G.A. McGregor, MB, FRCS, MD (Hons) Division of Cardiovascular Surgery, Department of Surgery, Mayo Clinic, Rochester, Minnesota.
Pulmonary Thromboendarterectomy Steven R. Meyer, MD, PhD, and Christopher G.A. McGregor, MB, FRCS, MD (Hons) Division of Cardiovascular Surgery, Department of Surgery, Mayo Clinic, Rochester, Minnesota.
Following Mitral Valve Replacement
 Re air of a Subvalvular Le rt Ventricular Aneurysm Following Mitral Valve Replacement Darryl J. Sutorius, M.D., James A. Helmsworth, M.D., James A. Majeski, Ph.D., M.D., and Stephen F. Miller, M.D. ABSTRACT
Re air of a Subvalvular Le rt Ventricular Aneurysm Following Mitral Valve Replacement Darryl J. Sutorius, M.D., James A. Helmsworth, M.D., James A. Majeski, Ph.D., M.D., and Stephen F. Miller, M.D. ABSTRACT
Adult Cardiac Surgery
 Adult Cardiac Surgery Mahmoud ABU-ABEELEH Associate Professor Department of Surgery Division of Cardiothoracic Surgery School of Medicine University Of Jordan Adult Cardiac Surgery: Ischemic Heart Disease
Adult Cardiac Surgery Mahmoud ABU-ABEELEH Associate Professor Department of Surgery Division of Cardiothoracic Surgery School of Medicine University Of Jordan Adult Cardiac Surgery: Ischemic Heart Disease
TSDA ACGME Milestones
 TSDA ACGME Milestones Short MW and Edwards JA. Assessing resident milestones using a CASPE March 2012 Short MW and Edwards JA. Assessing resident milestones using a CASPE March 2012 Short
TSDA ACGME Milestones Short MW and Edwards JA. Assessing resident milestones using a CASPE March 2012 Short MW and Edwards JA. Assessing resident milestones using a CASPE March 2012 Short
ERDHEIM-CHESTER DISEASE LUNG & HEART ISSUES
 ERDHEIM-CHESTER DISEASE LUNG & HEART ISSUES GIULIO CAVALLI, M.D. INTERNAL MEDICINE AND CLINICAL IMMUNOLOGY IRCCS SAN RAFFAELE HOSPITAL VITA-SALUTE SAN RAFFAELE UNIVERSITY MILAN, ITALY cavalli.giulio@hsr.it
ERDHEIM-CHESTER DISEASE LUNG & HEART ISSUES GIULIO CAVALLI, M.D. INTERNAL MEDICINE AND CLINICAL IMMUNOLOGY IRCCS SAN RAFFAELE HOSPITAL VITA-SALUTE SAN RAFFAELE UNIVERSITY MILAN, ITALY cavalli.giulio@hsr.it
DR Turner, JA Vincent, and ML Epstein. Isolated right pulmonary artery discontinuity. Images Paediatr Cardiol Jul-Sep; 2(3):
 IMAGES in PAEDIATRIC CARDIOLOGY Images PMCID: PMC3232486 Isolated right pulmonary artery discontinuity DR Turner, MD, * JA Vincent, ** and ML Epstein *** * Senior Fellow, Division of Cardiology, Children's
IMAGES in PAEDIATRIC CARDIOLOGY Images PMCID: PMC3232486 Isolated right pulmonary artery discontinuity DR Turner, MD, * JA Vincent, ** and ML Epstein *** * Senior Fellow, Division of Cardiology, Children's
Anatomy & Physiology
 1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
Deliberate Renal Ischemia
 Deliberate Renal Ischemia A Valuable and Safe Adjunct During Operations upon the Abdominal Aorta Robert K. Brawley, M.D., R. Darryl Fisher, M.D., Tom R. DeMeester, M.D., and Ronald C. Elkins, M.D. ABSTRACT
Deliberate Renal Ischemia A Valuable and Safe Adjunct During Operations upon the Abdominal Aorta Robert K. Brawley, M.D., R. Darryl Fisher, M.D., Tom R. DeMeester, M.D., and Ronald C. Elkins, M.D. ABSTRACT
Long-term complications of cuffed tunneled central
 IMAGING TEACHING CASE Epistaxis as a Rare Complication of Catheter-Related Central Venous Stenosis Jin-Ju Tsai, MD, 1 Ching-Chih Hsia, MD, 1,2 Dong-Ming Tsai, MD, 1 Wei-Tsung Chen, MD, 3 and Yung-Hsuen
IMAGING TEACHING CASE Epistaxis as a Rare Complication of Catheter-Related Central Venous Stenosis Jin-Ju Tsai, MD, 1 Ching-Chih Hsia, MD, 1,2 Dong-Ming Tsai, MD, 1 Wei-Tsung Chen, MD, 3 and Yung-Hsuen
DISCLOSURE TEST YOUR WAVEFORM IQ. Partial volume artifact. 86 yo female with right arm swelling, picc line. AVF on left? Dx?
 Deborah Rubens University of Rochester Rochester, NY DISCLOSURE Neither I nor my immediate family have a financial relationship with a commercial organization that may have a direct or indirect interest
Deborah Rubens University of Rochester Rochester, NY DISCLOSURE Neither I nor my immediate family have a financial relationship with a commercial organization that may have a direct or indirect interest
Lung Cancer Resection on Cardiopulmonary Bypass. Daniel J. Boffa, MD Yale University
 Lung Cancer Resection on Cardiopulmonary Bypass Daniel J. Boffa, MD Yale University None related to talk Disclosures Disclaimers I love operating on CPB Disclaimers I love operating on CPB I avoid it for
Lung Cancer Resection on Cardiopulmonary Bypass Daniel J. Boffa, MD Yale University None related to talk Disclosures Disclaimers I love operating on CPB Disclaimers I love operating on CPB I avoid it for
Follow-up of Aortic Dissection: How, How Often, Which Consequences Euro Echo 2011
 Follow-up of Aortic Dissection: How, How Often, Which Consequences Euro Echo 2011 Susan E. Wiegers, MD, FASE Director of Clinical Echocardiography Hospital of the University of Pennsylvania Disclosure
Follow-up of Aortic Dissection: How, How Often, Which Consequences Euro Echo 2011 Susan E. Wiegers, MD, FASE Director of Clinical Echocardiography Hospital of the University of Pennsylvania Disclosure
Chest and cardiovascular
 Module 1 Chest and cardiovascular A. Doss and M. J. Bull 1. Regarding the imaging modalities of the chest: High resolution computed tomography (HRCT) uses a slice thickness of 4 6 mm to identify mass lesions
Module 1 Chest and cardiovascular A. Doss and M. J. Bull 1. Regarding the imaging modalities of the chest: High resolution computed tomography (HRCT) uses a slice thickness of 4 6 mm to identify mass lesions
Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013
 Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013 Thoracic Wall Consists of thoracic cage Muscle Fascia Thoracic Cavity 3 Compartments of the Thorax (Great Vessels) (Heart) Superior thoracic aperture
Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013 Thoracic Wall Consists of thoracic cage Muscle Fascia Thoracic Cavity 3 Compartments of the Thorax (Great Vessels) (Heart) Superior thoracic aperture
Importance of the third arterial graft in multiple arterial grafting strategies
 Research Highlight Importance of the third arterial graft in multiple arterial grafting strategies David Glineur Department of Cardiovascular Surgery, Cliniques St Luc, Bouge and the Department of Cardiovascular
Research Highlight Importance of the third arterial graft in multiple arterial grafting strategies David Glineur Department of Cardiovascular Surgery, Cliniques St Luc, Bouge and the Department of Cardiovascular
Primary Tumors of Ribs
 Primary Tumors of Ribs Frank E. Schmidt, M.D., and Max J. Trummer, Capt, MC, USN ABSTRACT An analysis of 50 consecutive patients with primary rib tumors operated on at the U.S. Naval Hospital, San Diego,
Primary Tumors of Ribs Frank E. Schmidt, M.D., and Max J. Trummer, Capt, MC, USN ABSTRACT An analysis of 50 consecutive patients with primary rib tumors operated on at the U.S. Naval Hospital, San Diego,
Primary mediastinal tumours
 Primary mediastinal tumours Thorax (1974), 29, 475. YOUSF D. AL-NAAMAN, MOHAMAD S. AL-AN, and MUAYYAD M. AL-OMER Department of Thoracic and Cardiovascular Surgery, College of Medicine, University of Baghdad,
Primary mediastinal tumours Thorax (1974), 29, 475. YOUSF D. AL-NAAMAN, MOHAMAD S. AL-AN, and MUAYYAD M. AL-OMER Department of Thoracic and Cardiovascular Surgery, College of Medicine, University of Baghdad,
CASE REPORT AIR VENT OF VEIN GRAFT IN EXTRACRANIAL-INTRACRANIAL BYPASS SURGERY
 Nagoya J. Med. Sci. 74. 339 ~ 345, 2012 CASE REPORT AIR VENT OF VEIN GRAFT IN EXTRACRANIAL-INTRACRANIAL BYPASS SURGERY HIROFUMI OYAMA, AKIRA KITO, HIDEKI MAKI, KENICHI HATTORI, TOMOYUKI NODA and KENTARO
Nagoya J. Med. Sci. 74. 339 ~ 345, 2012 CASE REPORT AIR VENT OF VEIN GRAFT IN EXTRACRANIAL-INTRACRANIAL BYPASS SURGERY HIROFUMI OYAMA, AKIRA KITO, HIDEKI MAKI, KENICHI HATTORI, TOMOYUKI NODA and KENTARO
Penetrating Neck Injuries. Jason Levine MD Lutheran Medical Center July 22, 2010
 Penetrating Neck Injuries Jason Levine MD Lutheran Medical Center July 22, 2010 CASE PRESENTATION 19 YO M 3 Stab Wounds Right zone I neck SW 2 SW anterior abdomen Left epigastrium anterior axillary line
Penetrating Neck Injuries Jason Levine MD Lutheran Medical Center July 22, 2010 CASE PRESENTATION 19 YO M 3 Stab Wounds Right zone I neck SW 2 SW anterior abdomen Left epigastrium anterior axillary line
Sample page. POWER UP YOUR CODING with Optum360, your trusted coding partner for 32 years. Visit optum360coding.com.
 2018 Complete Guide for Interventional Radiology An in-depth guide to interventional radiology coding, billing, and reimbursement for facilities and physicians POWER UP YOUR CODING with Optum360, your
2018 Complete Guide for Interventional Radiology An in-depth guide to interventional radiology coding, billing, and reimbursement for facilities and physicians POWER UP YOUR CODING with Optum360, your
Stuck dialysis catheters. ANZSIN 2013 Michael Lam & Kendal Redmond
 Stuck dialysis catheters ANZSIN 2013 Michael Lam & Kendal Redmond NT 39 yr old CI Maori - ESKD 2 o to cortical necrosis HD August 2002 R IJ tunneled Tesio catheter Oct 2002 Failed L RC AVF Feb 2004 Failed
Stuck dialysis catheters ANZSIN 2013 Michael Lam & Kendal Redmond NT 39 yr old CI Maori - ESKD 2 o to cortical necrosis HD August 2002 R IJ tunneled Tesio catheter Oct 2002 Failed L RC AVF Feb 2004 Failed
SELECTIVE ANTEGRADE TECHNIQUE OF CHOICE
 SELECTIVE ANTEGRADE CEREBRAL PERFUSION IS THE TECHNIQUE OF CHOICE MARKO TURINA University of Zurich Zurich, Switzerland What is so special about the operation on the aortic arch? Disease process is usually
SELECTIVE ANTEGRADE CEREBRAL PERFUSION IS THE TECHNIQUE OF CHOICE MARKO TURINA University of Zurich Zurich, Switzerland What is so special about the operation on the aortic arch? Disease process is usually
Assessing Cardiac Anatomy With Digital Subtraction Angiography
 485 JACC Vol. 5, No. I Assessing Cardiac Anatomy With Digital Subtraction Angiography DOUGLAS S., MD, FACC Cleveland, Ohio The use of intravenous digital subtraction angiography in the assessment of patients
485 JACC Vol. 5, No. I Assessing Cardiac Anatomy With Digital Subtraction Angiography DOUGLAS S., MD, FACC Cleveland, Ohio The use of intravenous digital subtraction angiography in the assessment of patients
Individual Pulmonary Vein Atresia in Adults: Report of Two Cases
 Case Report DOI: 10.3348/kjr.2011.12.3.395 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2011;12(3):395-399 Individual Pulmonary Vein Atresia in Adults: Report of Two Cases Hyoung Nam Lee, MD, Young
Case Report DOI: 10.3348/kjr.2011.12.3.395 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2011;12(3):395-399 Individual Pulmonary Vein Atresia in Adults: Report of Two Cases Hyoung Nam Lee, MD, Young
I-Ming Chen, MD. Endovascular Stenting for Palliative Treatment of Superior Vena Cava Syndrome in End-Stage Lung Cancer
 Endovascular Stenting for Palliative Treatment of Superior Vena Cava Syndrome in End-Stage Lung Cancer I-Ming Chen, MD Division of CardioVascular Surgery Taipei Veterans General Hospital, Taiwan (Live
Endovascular Stenting for Palliative Treatment of Superior Vena Cava Syndrome in End-Stage Lung Cancer I-Ming Chen, MD Division of CardioVascular Surgery Taipei Veterans General Hospital, Taiwan (Live
Open fenestration for complicated acute aortic B dissection
 Art of Operative Techniques Open fenestration for complicated acute aortic B dissection Santi Trimarchi 1, Sara Segreti 1, Viviana Grassi 1, Chiara Lomazzi 1, Marta Cova 1, Gabriele Piffaretti 2, Vincenzo
Art of Operative Techniques Open fenestration for complicated acute aortic B dissection Santi Trimarchi 1, Sara Segreti 1, Viviana Grassi 1, Chiara Lomazzi 1, Marta Cova 1, Gabriele Piffaretti 2, Vincenzo
Surgery for lung cancer invading the mediastinum
 Review Article Surgery for lung cancer invading the mediastinum Adnan M. Al-Ayoubi, Raja M. Flores Department of Thoracic Surgery, Mount Sinai Health System, Icahn School of Medicine at Mount Sinai, New
Review Article Surgery for lung cancer invading the mediastinum Adnan M. Al-Ayoubi, Raja M. Flores Department of Thoracic Surgery, Mount Sinai Health System, Icahn School of Medicine at Mount Sinai, New
Free Esophageal Perforation Following Hybrid Visceral Debranching and Distal Endograft Extension to Repair a Ruptured Thoracoabdominal Aortic
 Free Esophageal Perforation Following Hybrid Visceral Debranching and Distal Endograft Extension to Repair a Ruptured Thoracoabdominal Aortic Aneurysm History A 56-year-old gentleman, who had been referred
Free Esophageal Perforation Following Hybrid Visceral Debranching and Distal Endograft Extension to Repair a Ruptured Thoracoabdominal Aortic Aneurysm History A 56-year-old gentleman, who had been referred
Chapter 13 Worksheet Code It
 Class: Date: Chapter 13 Worksheet 3 2 1 Code It True/False Indicate whether the statement is true or false. 1. A cardiac catheterization diverts blood from the heart to the aorta. 2. Selective vascular
Class: Date: Chapter 13 Worksheet 3 2 1 Code It True/False Indicate whether the statement is true or false. 1. A cardiac catheterization diverts blood from the heart to the aorta. 2. Selective vascular
Leiomyosarcoma involving the inferior vena cava in an. elderly patient with reference to its operative modalities: a case report
 Leiomyosarcoma involving the inferior vena cava in an elderly patient with reference to its operative modalities: a case report Hiroshi Ushida 1, Ryosuke Murai 1, Mitsuhiro Narita 1, Fumiyoshi Kojima 2
Leiomyosarcoma involving the inferior vena cava in an elderly patient with reference to its operative modalities: a case report Hiroshi Ushida 1, Ryosuke Murai 1, Mitsuhiro Narita 1, Fumiyoshi Kojima 2
Case 1 Organ Set 3. Case 1 (for Organ Sets 1 3) 10/2/2015 CARIOVASCULAR II LABORATORY
 MHD I CRIOVSCULR II LORTORY 0/5/5 Case Organ Set Organ Set 2 Organ Set 3 Case (for Organ Sets 3) 72 year old man with a history of diabetes mellitus type 2, HTN, and hyperlipidemia presents with progressive
MHD I CRIOVSCULR II LORTORY 0/5/5 Case Organ Set Organ Set 2 Organ Set 3 Case (for Organ Sets 3) 72 year old man with a history of diabetes mellitus type 2, HTN, and hyperlipidemia presents with progressive
Devendra V. Kulkarni, Rahul G. Hegde, Ankit Balani, and Anagha R. Joshi. 2. Case Report. 1. Introduction
 Case Reports in Radiology, Article ID 614647, 4 pages http://dx.doi.org/10.1155/2014/614647 Case Report A Rare Case of Pulmonary Atresia with Ventricular Septal Defect with a Right Sided Aortic Arch and
Case Reports in Radiology, Article ID 614647, 4 pages http://dx.doi.org/10.1155/2014/614647 Case Report A Rare Case of Pulmonary Atresia with Ventricular Septal Defect with a Right Sided Aortic Arch and
Results of Superior Vena Cava Reconstruction With Externally Stented-Polytetrafluoroethylene Vascular Prostheses
 Results of Superior Vena Cava Reconstruction With Externally Stented-Polytetrafluoroethylene Vascular Prostheses Ikenna C. Okereke, MD, Kenneth A. Kesler, MD, Karen M. Rieger, MD, Thomas J. Birdas, MD,
Results of Superior Vena Cava Reconstruction With Externally Stented-Polytetrafluoroethylene Vascular Prostheses Ikenna C. Okereke, MD, Kenneth A. Kesler, MD, Karen M. Rieger, MD, Thomas J. Birdas, MD,
Indications: following: embolization. artery that has diseases 5. The evaluation. of suspected. such entities. a cold hand. biopsy
 Peripheral Arterial Ultrasound Protocol Using Color and Spectral Doppler Reviewed by: Mark Yuhasz, MD Last Review Date: January 2015 Contact: (866) 761 4200, Option 1 Indications: The indications for peripheral
Peripheral Arterial Ultrasound Protocol Using Color and Spectral Doppler Reviewed by: Mark Yuhasz, MD Last Review Date: January 2015 Contact: (866) 761 4200, Option 1 Indications: The indications for peripheral
Progressive Fibrosing Mediastinitis
 Progressive Fibrosing Mediastinitis Thomas H. Hewlett, Col, MC, USA (Ret),* Arthur Steer, Col, MC, USA, and David E. Thomas, Col, MC, USA A report entitled Mediastinal Tuberculoma published by Samson et
Progressive Fibrosing Mediastinitis Thomas H. Hewlett, Col, MC, USA (Ret),* Arthur Steer, Col, MC, USA, and David E. Thomas, Col, MC, USA A report entitled Mediastinal Tuberculoma published by Samson et
Dr. Weyrich G07: Superior and Posterior Mediastina. Reading: 1. Gray s Anatomy for Students, chapter 3
 Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
Thymic Tumors. Feiran Lou MD. MS. Kings County Hospital Department of Surgery
 Thymic Tumors Feiran Lou MD. MS. Kings County Hospital Department of Surgery Case HPI 53 yo man referred from OSH for anterior mediastinal mass. Initially presented with leg weakness and back pain for
Thymic Tumors Feiran Lou MD. MS. Kings County Hospital Department of Surgery Case HPI 53 yo man referred from OSH for anterior mediastinal mass. Initially presented with leg weakness and back pain for
Listing Form: Heart or Cardiovascular Impairments. Medical Provider:
 Listing Form: Heart or Cardiovascular Impairments Medical Provider: Printed Name Signature Patient Name: Patient DOB: Patient SS#: Date: Dear Provider: Please indicate whether your patient s condition
Listing Form: Heart or Cardiovascular Impairments Medical Provider: Printed Name Signature Patient Name: Patient DOB: Patient SS#: Date: Dear Provider: Please indicate whether your patient s condition
Following Long-Term Transvenous Pacing
 The Incidence of Venous Thrombosis Following Long-Term Transvenous Pacing William S. Stoney, M.D., Ronald B. Addlestone, M.D., William C. Alford, Jr., M.D., George R. Bums, M.D., Robert A. Frist, M.D.,
The Incidence of Venous Thrombosis Following Long-Term Transvenous Pacing William S. Stoney, M.D., Ronald B. Addlestone, M.D., William C. Alford, Jr., M.D., George R. Bums, M.D., Robert A. Frist, M.D.,
CTEPH. surgical treatment. Ph. Dartevelle, E. Fadel, S. Mussot, D. Fabre, O. Mercier and G. Simonneau PARIS-SUD UNIVERSITY
 CTEPH surgical treatment Ph. Dartevelle, E. Fadel, S. Mussot, D. Fabre, O. Mercier and G. Simonneau MARIE-LANNELONGUE HOSPITAL BICETRE HOSPITAL PARIS-SUD UNIVERSITY Clinical Classification of PH G Simonneau
CTEPH surgical treatment Ph. Dartevelle, E. Fadel, S. Mussot, D. Fabre, O. Mercier and G. Simonneau MARIE-LANNELONGUE HOSPITAL BICETRE HOSPITAL PARIS-SUD UNIVERSITY Clinical Classification of PH G Simonneau
Superior vena cava replacement combined with venovenous shunt for lung cancer and thymoma: a case series
 Original Article Superior vena cava replacement combined with venovenous shunt for lung cancer and thymoma: a case series Wei Dai 1 *, Jifu Dong 2 *, Hongwei Zhang 2, Xiaojun Yang 1, Qiang Li 1 1 Department
Original Article Superior vena cava replacement combined with venovenous shunt for lung cancer and thymoma: a case series Wei Dai 1 *, Jifu Dong 2 *, Hongwei Zhang 2, Xiaojun Yang 1, Qiang Li 1 1 Department
Case Reports The following case reports illustrate some of the ways in which staplers have proved useful in operations for aneurysms of the aorta.
 Use of Stapling Instruments in Surgery for Aneurysms of the Aorta M. Arisan Ergin, M.D., James V. O'Connor, M.D., Carlos Blanche, M.D., and Randall B. Griepp, M.D. ABSTRACT Since their inception, surgical
Use of Stapling Instruments in Surgery for Aneurysms of the Aorta M. Arisan Ergin, M.D., James V. O'Connor, M.D., Carlos Blanche, M.D., and Randall B. Griepp, M.D. ABSTRACT Since their inception, surgical
