Materials and Methods
|
|
|
- Lawrence Fowler
- 5 years ago
- Views:
Transcription
1 The Ductus Debate: Ligation in Prematurity? Willis H. Williams, M.D., Henry Gelband, M.D., Eduardo Bancalari, M.D., Charles Bauer, M.D., Otto Garcia, M.D., Dolores Tamer, M.D., and Gerard A. Kaiser, M.D. ABSTRACT This report describes 20 premature infants who have undergone surgical ligation of a patent ductus arteriosus (PDA), diagnosed solely by physical examination in all but 2 instances. There were no operative deaths. Eleven of these 20 infants had severe associated hyaline membrane disease (HMD) necessitating mechanical ventilatory support from the first or second day of life. Only 3 of these 11 infants (27%) ultimately survived to leave the hospital. In contrast, 8 of 9 premature neonates (89%) with severe congestive heart failure but without HMD were discharged alive. Surgical ligation of the PDA in a premature infant is an appropriate and successful mode of treatment when congestive heart failure is refractory to medical management. Proof is lacking, however, to establish the efficacy of PDA ligation in the premature infant with HMD. Almost twenty-five years elapsed between the successful ligation of a patent ductus arteriosus (PDA) by Gross and Hubbard in 1938 [141 and the application of this operation to premature infants with hyaline membrane disease (HMD) by Powell in 1963 [25]. Numerous publications have recently summarized the results of ductus interruption in the premature infant [3,4, 7, 9, 11, 12, 15-19, 22-24]; unfortunately, these reports have not clearly defined the indications for and usefulness of this procedure. Indications, diagnostic criteria, and timing of operation have varied widely. Randomization of patient selection has been ignored to date. The incidence of persistent patency of the duc- From the Division of Thoracic and Cardiovascular Surgery, the Department of Pediatrics, and the Division of Pediatric Cardiology, University of Miami School of Medicine and Jackson Memorial Hospital, Miami, FL. The technical assistance of Kay Allen and Sheila OMellan is gratefully acknowledged. Accepted for publication Feb 16, Address reprint requests to Dr. Kaiser, Division of Thoracic and Cardiovascular Surgery, PO Box , Miami, FL tus arteriosus in premature infants is well established [l, 2,6,8,10,13,21]. A further increased incidence is apparent in those infants surviving management of HMD and prematurity [19, 20, 27, 291. Our experience indicates relatively distinct separation in both statistical survival and the quality of survival following PDA ligation between premature infants with congestive heart failure alone and those with HMD. This observation was also alluded to by Kitterman and associates [19] in a smaller series of infants in 1972 and has recently been substantiated by Coran and his co-workers [7]. This distinction should aid in the future selection of infants most likely to benefit from ductus ligation. Materials and Methods During the three-year period between May, 1972, and April, 1975,1,640 infants were admitted to the Neonatal Intensive Care Unit at Jackson Memorial Hospital and the Department of Pediatrics of the University of Miami School of Medicine. Sixty-five percent weighed less than 2,500 gm at birth and 11% were less than 1,000 gm. Twenty-two percent were admitted primarily for the treatment of clinically and radiographically apparent HMD. The typical systolic murmur of a PDA was described in 3% at admission; murmurs subsequently became apparent in several more infants. Congestive heart failure in these infants was characterized by tachypnea, tachycardia, edema, fluid retention, progressive hepatomegaly, progressive cardiomegaly, or radiographically apparent pulmonary edema. When it was associated with bounding peripheral pulses, a hyperactive precordium, a characteristic systolic murmur, and a widened umbilical arterial pulse pressure, the presence of a PDA with a large left-to-right shunt was suspected. Medical management consisted of digitalization, fluid restriction, and intravenous adminis- 151
2 152 The Annals of Thoracic Surgery Vol 22 No 2 August 1976 tration of diuretics. Salt-poor albumin was given when total serum proteins were below 4 gm per 100 ml; anemia was corrected by administration of packed red blood cells. Umbilical arterial blood gases were monitored. Orotracheal intubation with continuous positive airway pressure or intermittent mandatory ventilation was used when ventilatory support was required. Cardiac catheterization was carried out in only 1 of these infants suspected of having a PDA, the first child in the series. An isolated aortogram was obtained in another infant, utilizing the umbilical arterial catheter, and demonstrated the ductus as described in two recent reports [7,11]. We have used the echocardiographic diameter of the left atrium compared with the diameter of the aorta, as described by Silverman [28] and Baylen [5] and their colleagues, as supportive evidence for a significant left-to-right shunt. The diagnosis of PDA was based on clinical and physical diagnostic grounds in all subsequent infants. Twenty critically ill premature neonates failing to respond to medical management of congestive heart failure and requiring mechanical ventilatory support were referred for PDA ligation. These 20 infants have been retrospectively divided into two groups: Group A consists of 11 infants with HMD, PDA, and congestive heart failure; Group B consists of 9 with a PDA associated with refractory congestive heart failure but without preexisting HMD. Respiratory distress and the need for ventilatory support were common to most infants. Weaning from the respirator had been attempted without success in those Group A infants in whom support had been required since birth. All infants in Group A were hypoxemic from birth, requiring mechanical ventilation from the first or second day of life (Fig 1). A majority of infants in Group B, without HMD, eventually deteriorated to the point of requiring mechanical ventilatory assistance (Fig 2). Whereas Group A infants required institution of ventilatory support between the first and second day of life, those in Group B were ventilated for the first time at approximately 3 weeks of age. Infants in Group A required an average of twelve days of preoperative ventilatory support; Fig 1. Time course of intubation and ventilatory support in Group A infants (HMD and congestive heartfailure). Only the top 3 infantssurvived. Note that ventilatory support was required from virtually the first day of life in all these children. (Solid dark areas = periods of intermittent positive-pressure ventilation; dotted areas = periods of continuous positive airway pressure through an orotracheal tube; M = time the murmur was first heard; Op = ductus ligation; DC = discharged alive; Died = hospital death.) Group B infants were ventilated for an average of three days preoperatively. The typical systolic murmur of a PDA in infants with elevated pulmonary arterial pressure was noted at about 1 week of age in Group A infants and somewhat later (12 days) in Group B. Other characteristics of these two groups are summarized in the Table. Anesthesia consisted of oxygen, small quantities of nitrous oxide, muscle relaxants, and manual ventilation through an orotracheal tube.
3 153 Williams et al: The Ductus Debate Y k Y + A I-, DC,, I b, DC 100 DIy8 DC I Adm bp DC I+ + k charge for surviving infants was almost identical Y OP 4 I-+ Y OP DC -EH i k k 4 Y OP DC Fig2. Time course of intubation andventilatory support in Group B infants (PDA and congestive heart failure but no HMD). Note the much later initiation of respiratory support in these infants than in Group A neonates. Only 1 hospital death occurred in thisgroup. (Key same asfor Figure 1.) The PDA was exposed through a posterolateral left transpleural thoracotomy in the third intercostal space and was doubly ligated. The thoracotomy, ductus ligation, and closure required between 10 and 20 minutes. Infants were transferred back to the Neonatal Intensive Care Unit for postoperative care. Results There were no intraoperative deaths in this series of 20 infants. Most hospital deaths occurred many days-even weeks-following operation. Two infants died within 24 hours following operation, 1 as a result of pneumothorax and the other with septicemia and central nervous system hemorrhage. Necrotizing enterocolitis, sep- DC sis, and central nervous system hemorrhage were the predominant factors in the other 9 deaths. Of the 11 infants in Group A with HMD and congestive heart failure, only 3 ultimately survived to be discharged from the hospital. Eight of the 9 infants in Group B with congestive heart failure refractory to medical management lived. The single death in this group was preventa- ble-an unrecognized pneumothorax resulting in cardiac arrest. Those infants who survived improved quickly, requiring an average of five days of postoperative ventilatory support compared with nineteen days for those who ultimately died. The average weight gain from operation until dis- to that which one would expect for normal premature infants of equivalent gestational age (Fig 3). All the surviving patients in these combined groups have progressed satisfactorily since discharge except for 1 infant, who has hydrocephalus requiring shunting. Psychometric assessment of the 11 surviving infants is in progress. Comment We have followed the conservative and noninvasive operative indications outlined by Murphy and his co-workers [231 with minor modifications. The presence of a PDA was suspected from auscultation several days before surgical intervention. Congestive heart failure unresponsive to digitalis and diuretics was apparent radiographically by cardiomegaly, increased pulmonary vascular markings, perihilar prominence, and in some cases frank pulmonary edema. Arterial blood gases indicated a progressively rising carbon dioxide tension. Two infants did not require ventilatory support until a short time before operation. Peripheral edema, periorbital edema, and hepatomegaly were present in some of these patients, although we have usually intervened surgically prior to the onset of these late manifestations of congestive heart failure. Based on our experience with these 20 premature infants, we see no need for cardiac catheterization. The high incidence of complica-
4 154 The Annals of Thoracic Surgery Vol 22 No 2 August 1976 Data on 20 Patients with Patent Ductus Arteriosus and Congestive Heart Failure Group A: Group B: HMD & CHF CHF Only Factor Survivors Deaths (N = 3) (N = 8) Survivors Deaths (N = 8) (N = 1) Sex Gestation (wk) Birth weight (kg) First day of respiratory support Preop respiratory support (days) Day murmur first heard Age at operation (days) Weight at operation (kg) Postop respiratory support (days) Postop hospitalization (days) Weight gain per day (gm) Weight at discharge or death (kg) Age at discharge or death (days) 2WlF ( ) 1 17 (10-23) 9 (4-15) 18 (14-23) 1.4 ( ) 5 (1-10) 59 (48-65) 21 (14-27) 2.7 ( ) 77 (71-83) 2M16F 31 (28-33) 1.3 ( ) 1.5 (1-3) 11 (4-16) 6 (2-9) 12 (8-16) 1.2 ( ) 19 (0-56) 33 (1-159) 7 (0-20) 1.4 ( ) 46 (10-175) 3W5F 30 (25-32) 1.2 ( ) 24 (1-51) 3 (1-11) 12 (1-28) 28 (16-51) 1.2 ( ) 2 (W 40 (19-71) 23 (9-36) 2.1 ( ) 68 (44-100) F HMD = hyaline membrane disease; CHF = congestive heart failure. Ranges in parentheses. tions following catheterization described by Horsley and colleagues [161 and the low incidence of associated anomalies found by Edmunds [lll and Zachman [291 and their associates support our conservative approach. Ligation of the PDA in each of these 20 infants resulted in obliteration of the murmur with no instance of recurrence. No other cardiac defects have been demonstrated among the survivors; no other cardiac anomalies were found in those infants who died and in whom postmortem examination was performed. When clinical findings are typical, cardiac catheterization is unnecessary and would add potential complication and delay. The role of the patent ductus in the evolution of HMD remains undefined. Least tenable is the concept that ductus patency allows "decompression'' of a hypertensive pulmonary vascular bed by means of a right-to-left shunt. Rudolph and colleagues [26] demonstrated low pulmonary and systemic arterial pressure in catheterizations performed on critically ill premature infants with HMD. Most of these infants had a predominant left-to-right shunt, although a mixed shunt was apparent in some. The indicator-dilution studies done by Coran and associates [71 support the data of Rudolph's group, the infants having had significant leftto-right shunts through the PDA. The changing character of the ductus murmur reflects alterations in relative pulmonary and systemic vascular resistances, and perhaps changes in the ductus lumen itself. We lack hemodynamic proof of the magnitude of the left-to-right shunt in the infants described in this report, but all clinical findings point to a large aortic runoff into the pulmonary vascular bed. It is unlikely that the role of the patent ductus in HMD can be resolved until noninvasive diagnostic methods establish the time course of in-
5 155 Williams et al: The Ductus Debate / / A6E IN DAYS Fig3. Weightgain beforeand afterpda ligation in premature infants with respiratory distress syndrome. Note the marked weightgain following PDA ligation in thesurviving infants. (The points along the vertical axis indicate birth weights. The point at which the slope changes represents age and weight at operation. The right end of each line shows weight and age at discharge.) creasing pulmonary blood flow and rising left atrial pressure. A multiinstitutional, randomized prospective study will be required before the therapeutic role of ductus ligation in premature infants with HMD can be established. In contrast, ductus ligation should be carried out in the premature infant with congestive heart failure refractory to medical management who requires ventilatory assistance. The operative risk is low, and the heart failure can be controlled and the infant rapidly weaned from mechanical ventilatory support. Follow-up suggests nearly normal subsequent growth and development. The low immediate operative mortality reported for premature infants with HMD and a PDA must not itself lead to the conclusion that ductus ligation is appropriate therapy. Proof of the efficacy of this procedure is lacking. While there are those who argue for earlier ductus ligation, even before the murmur and hyperdynamic circulatory signs of a large left-to-right shunt appear 171, we, like others, have seen infants with HMD and an unequivocal PDA in whom the PDA closed without operation. Until definitive data are available, we advocate ductus ligation only in those premature infants who are ventilator dependent, demonstrate deteriorating pulmonary compliance, and, because of progressive congestive heart failure, retain fluid to a degree that forces their daily caloric intake below the minimum requirement necessary for anabolic weight gain. It is difficult to conceive of any beneficial role for the large PDA in these critically ill infants. The possibility remains that early PDA ligation may offer more benefit than waiting until the later, severe stage of the disease, References 1. Anderson RC: Causative factors underlying congenital heart malformations: I. Patent ductus arteriosus. Pediatrics 14:143, Auld PAM: Delayed closure of the ductus arteriosus. J Pediatr 69:61, Bahnson HT: Managing patent ductus in premature newborns with RDS. Contemp Surg 7:37, Bauersfeld SR, Adkins PC, Kent EM: Patent ductus arteriosus in infancy. J Thorac Surg 33:123, Baylen BG, Meyer RA, Kaplan S, et al: The critically ill premature infant with patent ductus arteriosus and pulmonary disease-an echocardiographic assessment. J Pediatr 86:423, Blancquaert A, Van Den Bogaert-Van Heesvelde AM: Ductus arteriosus with fatal evolution in the first week of life. Acta Paediatr Belg 28:5, Coran AG, Cabal L, Siassi B, et al: Surgical closure of patent ductus arteriosus in the premature infant with respiratory distress. J Pediatr Surg 10:399, Danilowicz D, Rudolph AM, Hoffman JIE: Delayed closure of the ductus arteriosus in premature infants. Pediatrics 37:74, Decancq HG Jr: Repair of patent ductus arteriosus in 1,417 gram infant. Am J Dis Child 106:402, Dunn PM, Speidel BD: Use of oxygen to close patent ductus arteriosus in preterm infants. Lancet 2:333, Edmunds LH Jr, Gregory GA, Heymann MA, et al: Surgical closure of the ductus arteriosus in premature infants. Circulation 48:856, Gay JH, Daily WJR, Meyer BHP, et al: Ligation of the patent ductus arteriosus in premature infants: report of 45 cases. J Pediatr Surg 8:677, Girling DJ, Hallidie-Smith KA: Persistent ductus
6 156 The Annals of Thoracic Surgery Vol 22 No 2 August 1976 arteriosus in ill and premature babies. Arch Dis Child 46:177, Gross RE, Hubbard JP: Surgical ligation of a patent ductus arteriosus. JAMA 112:729, Gupta JM, Van Vliet PKJ, Fisk GC, et al: Ductus ligation in respiratory distress syndrome. J Thorac Cardiovasc Surg 63:642, Horsley BL, Lerberg DB, Allen AC, et al: Respiratory distress from patent ductus arteriosus in the premature newborn. Ann Surg , Jegier W, Karne G, Stern L: Operative treatment of patent ductus arteriosus complicating respiratory distress syndrome of the premature (abstract). Can Med Assoc J 98:105, Kilman JW, Kakos GS, Williams TE Jr, et al: Ligation of patent ductus arteriosus for persistent respiratory distress syndrome in premature infants. J Pediatr Surg 9:277, Kitterman JA, Edmunds LH Jr, Gregory GA, et al: Patent ductus arteriosus in premature infants: incidence, relation to pulmonary disease and management. N Engl J Med 287:473, Krovetz LJ, Rowe RD: Patent ductus, prematurity and pulmonary disease. N Engl J Med 287:513, Lees MH: Commentary: patent ductus arteriosus in premature infants-a diagnostic and therapeutic dilemma. J Pediatr 86:132, Lewis CE Jr, Coen RW, Talbot W, et al: Early surgical intervention in premature infants with respiratory distress and patent ductus arteriosus. Am J Surg 128:829, Murphy DA, Outerbridge E, Stern L, et al: Management of premature infants with patent ductus arteriosus. J Thorac Cardiovasc Surg 67:221, Neal WA, Bessinger FB Jr, Hunt CE, et al: Patent ductus arteriosus complicating respiratory distress syndrome. J Pediatr 86:127, Powell ML: Patent ductus arteriosus in premature infants. Med J Aust 2:58, Rudolph AM, Drorhaugh JE, Auld AM, et al: Studies on the circulation in the neonatal period: the circulation in the respiratory distress syndrome. Pediatrics 27:551, Siassi B, Emmanouilides GC, Cleveland RJ, et al: Patent ductus arteriosus complicating prolonged assisted ventilation in respiratory distress syndrome. J Pediatr 74:11, Silverman NH, Lewis AB, Heymann MA, et al: Echocardiographic assessment of ductus arteriosus shunt in premature infants. Circulation , Zachman RD, Steinmetz GP, Botham RJ, et al: Incidence and treatment of the patent ductus arteriosus in the ill premature neonate. Am Heart J 87:697, 1974
Premature Infants with Patent Ductus Arteriosus and Res iratory Distress: Selection for mdap Ligation
 Premature Infants with Patent Ductus Arteriosus and Res iratory Distress: Selection for mdap Ligation George S. Hall, M.D., James A. Helmsworth, M.D., J. Tracy Schreiber, M.D., Jens G. Rosenkrantz, M.D.,
Premature Infants with Patent Ductus Arteriosus and Res iratory Distress: Selection for mdap Ligation George S. Hall, M.D., James A. Helmsworth, M.D., J. Tracy Schreiber, M.D., Jens G. Rosenkrantz, M.D.,
and Respiratory Distress Syndrome
 Patent Ductus Arteriosus Ligation and Respiratory Distress Syndrome in Premature Infants David R. Clarke, M.D., Bruce C. Paton, M.D., Gary L. Way, M.D., and James R. Stewart, B.A. ABSTRACT Ligation of
Patent Ductus Arteriosus Ligation and Respiratory Distress Syndrome in Premature Infants David R. Clarke, M.D., Bruce C. Paton, M.D., Gary L. Way, M.D., and James R. Stewart, B.A. ABSTRACT Ligation of
Surgical Closure of the Ductus Arteriosus in Premature Infants
 Surgical Closure of the Ductus Arteriosus in Premature Infants By L. HENRY EDMUNDS, JR., M.D., GEORGE A. GREGORY, M.D., MICHAEL A. HEYMANN, M.B., B.CH., JOSEPH A. KITTERMAN, M.D., ABRAHAM M. RUDOLPH, M.D.,
Surgical Closure of the Ductus Arteriosus in Premature Infants By L. HENRY EDMUNDS, JR., M.D., GEORGE A. GREGORY, M.D., MICHAEL A. HEYMANN, M.B., B.CH., JOSEPH A. KITTERMAN, M.D., ABRAHAM M. RUDOLPH, M.D.,
Short-Term Outcome Of Different Treatment Modalities Of Patent Ductus Arteriosus In Preterm Infants. Five Years Experiences In Qatar
 ISPUB.COM The Internet Journal of Cardiovascular Research Volume 7 Number 2 Short-Term Outcome Of Different Treatment Modalities Of Patent Ductus Arteriosus In Preterm Infants. Five Years Experiences In
ISPUB.COM The Internet Journal of Cardiovascular Research Volume 7 Number 2 Short-Term Outcome Of Different Treatment Modalities Of Patent Ductus Arteriosus In Preterm Infants. Five Years Experiences In
Interruption of Patent Ductus Arteriosus in Premature Infants with Respiratory Distress Syndrome
 Interruption of Patent Ductus Arteriosus in Premature Infants with Respiratory Distress Syndrome Sidney Levitsky, M.D., Elizabeth Fisher, M.D., DharmapuriVidyasagar, M.D., Alois R. Hastreiter, M.D., Edward
Interruption of Patent Ductus Arteriosus in Premature Infants with Respiratory Distress Syndrome Sidney Levitsky, M.D., Elizabeth Fisher, M.D., DharmapuriVidyasagar, M.D., Alois R. Hastreiter, M.D., Edward
Pharmacological closure of ductus arteriosus in
 Archives of Disease of Childhood, 198, 55, 271-276 Pharmacological closure of ductus arteriosus in preterm infants using indomethacin H I OBEYESEKERE, S PANKHURST, AND V Y H YU Department of Diagnostic
Archives of Disease of Childhood, 198, 55, 271-276 Pharmacological closure of ductus arteriosus in preterm infants using indomethacin H I OBEYESEKERE, S PANKHURST, AND V Y H YU Department of Diagnostic
Anatomy & Physiology
 1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
Update on mangement of patent ductus arteriosus in preterm infants. Dr. Trinh Thi Thu Ha
 Update on mangement of patent ductus arteriosus in preterm infants Dr. Trinh Thi Thu Ha Outline 1. Overview of PDA 2. Timing of screening PDA? 3. When to treat PDA? Timing of ductal closure Prenatal
Update on mangement of patent ductus arteriosus in preterm infants Dr. Trinh Thi Thu Ha Outline 1. Overview of PDA 2. Timing of screening PDA? 3. When to treat PDA? Timing of ductal closure Prenatal
Operative Closure of Isolated Defects of the Ventricular Septum: Planned Delay
 Operative Closure of Isolated Defects of the Ventricular Septum: Planned Delay R. Darryl Fisher, M.D., Scott L. Faulkner, M.D., C. Gordon Sell, M.D., Thomas P. Graham, Jr., M.D., and Harvey W. Bender,
Operative Closure of Isolated Defects of the Ventricular Septum: Planned Delay R. Darryl Fisher, M.D., Scott L. Faulkner, M.D., C. Gordon Sell, M.D., Thomas P. Graham, Jr., M.D., and Harvey W. Bender,
Hyaline membrane disease. By : Dr. Ch Sarishma Peadiatric Pg
 Hyaline membrane disease By : Dr. Ch Sarishma Peadiatric Pg Also called Respiratory distress syndrome. It occurs primarily in premature infants; its incidence is inversely related to gestational age and
Hyaline membrane disease By : Dr. Ch Sarishma Peadiatric Pg Also called Respiratory distress syndrome. It occurs primarily in premature infants; its incidence is inversely related to gestational age and
Duct Dependant Congenital Heart Disease
 Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease Document Control Information Author CATS/NTS Author Position CC Transport Services Document Owner E. Polke
Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease Document Control Information Author CATS/NTS Author Position CC Transport Services Document Owner E. Polke
Paediatrica Indonesiana
 Paediatrica Indonesiana VOLUME 53 July NUMBER 4 Original Article Transcatheter vs. surgical closure of patent ductus arteriosus: outcomes and cost analysis Mulyadi M Djer, Mochammading, Mardjanis Said
Paediatrica Indonesiana VOLUME 53 July NUMBER 4 Original Article Transcatheter vs. surgical closure of patent ductus arteriosus: outcomes and cost analysis Mulyadi M Djer, Mochammading, Mardjanis Said
ROLE OF EARLY POSTNATAL DEXAMETHASONE IN RESPIRATORY DISTRESS SYNDROME
 INDIAN PEDIATRICS VOLUME 35-FEBRUAKY 1998 ROLE OF EARLY POSTNATAL DEXAMETHASONE IN RESPIRATORY DISTRESS SYNDROME Kanya Mukhopadhyay, Praveen Kumar and Anil Narang From the Division of Neonatology, Department
INDIAN PEDIATRICS VOLUME 35-FEBRUAKY 1998 ROLE OF EARLY POSTNATAL DEXAMETHASONE IN RESPIRATORY DISTRESS SYNDROME Kanya Mukhopadhyay, Praveen Kumar and Anil Narang From the Division of Neonatology, Department
PATENT DUCTUS ARTERIOSUS IN THE PRETERM INFANT EVIDENCE FOR & AGAINST TREATMENT
 PATENT DUCTUS ARTERIOSUS IN THE PRETERM INFANT EVIDENCE FOR & AGAINST TREATMENT Dr. Youssef Abou Zanouna, FRCPI, FACC Consultant Pediatric Cardiologist King Fahd Military Medical Complex Dhahran Introduction
PATENT DUCTUS ARTERIOSUS IN THE PRETERM INFANT EVIDENCE FOR & AGAINST TREATMENT Dr. Youssef Abou Zanouna, FRCPI, FACC Consultant Pediatric Cardiologist King Fahd Military Medical Complex Dhahran Introduction
Pathophysiology: Left To Right Shunts
 Pathophysiology: Left To Right Shunts Daphne T. Hsu, MD dh17@columbia.edu Learning Objectives Learn the relationships between pressure, blood flow, and resistance Review the transition from fetal to mature
Pathophysiology: Left To Right Shunts Daphne T. Hsu, MD dh17@columbia.edu Learning Objectives Learn the relationships between pressure, blood flow, and resistance Review the transition from fetal to mature
Deok Young Choi, Gil Hospital, Gachon University NEONATES WITH EBSTEIN S ANOMALY: PROBLEMS AND SOLUTION
 Deok Young Choi, Gil Hospital, Gachon University NEONATES WITH EBSTEIN S ANOMALY: PROBLEMS AND SOLUTION Carpentier classification Chauvaud S, Carpentier A. Multimedia Manual of Cardiothoracic Surgery 2007
Deok Young Choi, Gil Hospital, Gachon University NEONATES WITH EBSTEIN S ANOMALY: PROBLEMS AND SOLUTION Carpentier classification Chauvaud S, Carpentier A. Multimedia Manual of Cardiothoracic Surgery 2007
2) VSD & PDA - Dr. Aso
 2) VSD & PDA - Dr. Aso Ventricular Septal Defect (VSD) Most common cardiac malformation 25-30 % Types of VSD: According to position perimembranous, inlet, muscular. According to size small, medium, large.
2) VSD & PDA - Dr. Aso Ventricular Septal Defect (VSD) Most common cardiac malformation 25-30 % Types of VSD: According to position perimembranous, inlet, muscular. According to size small, medium, large.
Natural history of innocent heart murmurs in newborn babies: controlled echocardiographic study
 F166 Arch Dis Child Fetal Neonatal Ed 1998;78:F166 F170 ORIGINAL ARTICLES Natural history of innocent heart murmurs in newborn babies: controlled echocardiographic study Romaine Arlettaz, Nicholas Archer,
F166 Arch Dis Child Fetal Neonatal Ed 1998;78:F166 F170 ORIGINAL ARTICLES Natural history of innocent heart murmurs in newborn babies: controlled echocardiographic study Romaine Arlettaz, Nicholas Archer,
Pathophysiology: Left To Right Shunts
 Pathophysiology: Left To Right Shunts Daphne T. Hsu, MD dh17@columbia.edu Learning Objectives Learn the relationships between pressure, blood flow, and resistance Review the transition from fetal to mature
Pathophysiology: Left To Right Shunts Daphne T. Hsu, MD dh17@columbia.edu Learning Objectives Learn the relationships between pressure, blood flow, and resistance Review the transition from fetal to mature
AORTIC COARCTATION. Synonyms: - Coarctation of the aorta
 AORTIC COARCTATION Synonyms: - Coarctation of the aorta Definition: Aortic coarctation is a congenital narrowing of the aorta, usually located after the left subclavian artery, near the ductus or the ligamentum
AORTIC COARCTATION Synonyms: - Coarctation of the aorta Definition: Aortic coarctation is a congenital narrowing of the aorta, usually located after the left subclavian artery, near the ductus or the ligamentum
PAEDIATRIC EMQs. Andrew A Mallick Paediatrics.info.
 PAEDIATRIC EMQs Andrew A Mallick Paediatrics.info www.paediatrics.info Paediatric EMQs Paediatrics.info First published in the United Kingdom in 2012. While the advice and information in this book is believed
PAEDIATRIC EMQs Andrew A Mallick Paediatrics.info www.paediatrics.info Paediatric EMQs Paediatrics.info First published in the United Kingdom in 2012. While the advice and information in this book is believed
Duct Dependant Congenital Heart Disease
 Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease This guideline has been agreed by both NTS & CATS Document Control Information Author CATS/NTS Author Position
Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease This guideline has been agreed by both NTS & CATS Document Control Information Author CATS/NTS Author Position
Structural heart disease in the newborn
 Archives of Disease in Childhood, 1979, 54, 281-285 Structural heart disease in the newborn Changing profile: comparison of 1975 with 1965 TERUO IZUKAWA, H. CONNOR MULHOLLAND, RICHARD D. ROWE, DAVID H.
Archives of Disease in Childhood, 1979, 54, 281-285 Structural heart disease in the newborn Changing profile: comparison of 1975 with 1965 TERUO IZUKAWA, H. CONNOR MULHOLLAND, RICHARD D. ROWE, DAVID H.
SWISS SOCIETY OF NEONATOLOGY. Prenatal closure of the ductus arteriosus
 SWISS SOCIETY OF NEONATOLOGY Prenatal closure of the ductus arteriosus March 2007 Leone A, Fasnacht M, Beinder E, Arlettaz R, Neonatal Intensive Care Unit (LA, AR), University Hospital Zurich, Cardiology
SWISS SOCIETY OF NEONATOLOGY Prenatal closure of the ductus arteriosus March 2007 Leone A, Fasnacht M, Beinder E, Arlettaz R, Neonatal Intensive Care Unit (LA, AR), University Hospital Zurich, Cardiology
Congenital Heart Disease. CCCHD In WI. Critical Congenital Heart Disease. Why Screen? 4/20/2018. Early Detection = Better Outcomes
 Congenital Heart Disease A Positive Screen? What Does it Mean? A Review of Pulse Oximetry Screening for Critical Congenital Heart Disease Elizabeth Goetz MD MPH 8-10/1000 livebirths 3% of all infant mortality
Congenital Heart Disease A Positive Screen? What Does it Mean? A Review of Pulse Oximetry Screening for Critical Congenital Heart Disease Elizabeth Goetz MD MPH 8-10/1000 livebirths 3% of all infant mortality
Change in Blood Pressure and Pulse Pressure in Preterm Infants After Treatment of Patent Ductus Arteriosus With Indomethacin
 ORIGINAL ARTICLE DOI./kcj.11.41.4.3 Print ISSN 1738-55 / On-line ISSN 1738-5555 Copyright 11 The Korean Society of Cardiology Open Access Change in Blood Pressure and Pulse Pressure in Preterm Infants
ORIGINAL ARTICLE DOI./kcj.11.41.4.3 Print ISSN 1738-55 / On-line ISSN 1738-5555 Copyright 11 The Korean Society of Cardiology Open Access Change in Blood Pressure and Pulse Pressure in Preterm Infants
The Blue Baby. Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin
 The Blue Baby Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin Session Structure Definitions and assessment of cyanosis Causes of blue baby Structured approach to assessing
The Blue Baby Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin Session Structure Definitions and assessment of cyanosis Causes of blue baby Structured approach to assessing
Patent ductus arteriosus (PDA)
 Patent ductus arteriosus (PDA) Information for families Great Ormond Street Hospital for Children NHS Foundation Trust 2 This information sheet explains about the congenital (present at birth) heart condition
Patent ductus arteriosus (PDA) Information for families Great Ormond Street Hospital for Children NHS Foundation Trust 2 This information sheet explains about the congenital (present at birth) heart condition
ATRIAL SEPTAL DEFECTS
 ORIGINAL STUDY Long-term follow-up of children after repair of atrial septal defects JAMES MANDELIK, MD; DOUGLAS S. MOODIE, MD; RICHARD STERBA, MD; DANIEL MURPHY, MD; ELIOT ROSENKRANZ, MD; SHARON MEDENDORP,
ORIGINAL STUDY Long-term follow-up of children after repair of atrial septal defects JAMES MANDELIK, MD; DOUGLAS S. MOODIE, MD; RICHARD STERBA, MD; DANIEL MURPHY, MD; ELIOT ROSENKRANZ, MD; SHARON MEDENDORP,
Patent ductus arteriosus: pathophysiology and management
 (2006) 26, S14 S18 r 2006 Nature Publishing Group All rights reserved. 0743-8346/06 $30 www.nature.com/jp ORIGINAL ARTICLE Patent ductus arteriosus: pathophysiology and management ER Hermes-DeSantis 1
(2006) 26, S14 S18 r 2006 Nature Publishing Group All rights reserved. 0743-8346/06 $30 www.nature.com/jp ORIGINAL ARTICLE Patent ductus arteriosus: pathophysiology and management ER Hermes-DeSantis 1
When is Risky to Apply Oxygen for Congenital Heart Disease 부천세종병원 소아청소년과최은영
 When is Risky to Apply Oxygen for Congenital Heart Disease 부천세종병원 소아청소년과최은영 The Korean Society of Cardiology COI Disclosure Eun-Young Choi The author have no financial conflicts of interest to disclose
When is Risky to Apply Oxygen for Congenital Heart Disease 부천세종병원 소아청소년과최은영 The Korean Society of Cardiology COI Disclosure Eun-Young Choi The author have no financial conflicts of interest to disclose
IMAGES. in PAEDIATRIC CARDIOLOGY. Abstract
 IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2008 Apr-Jun; 10(2): 11 17. PMCID: PMC3232589 Transcatheter closure of symptomatic aortopulmonary window in an infant F Pillekamp, 1 T Hannes, 1
IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2008 Apr-Jun; 10(2): 11 17. PMCID: PMC3232589 Transcatheter closure of symptomatic aortopulmonary window in an infant F Pillekamp, 1 T Hannes, 1
Pediatric Cardiology. Spontaneous Closure of Atrial Septal Defects in Premature vs Full-Term Neonates
 Pediatr Cardiol 21:129 134, 2000 DOI: 10.1007/s002469910020 Pediatric Cardiology Springer-Verlag New York Inc. 2000 Spontaneous Closure of Atrial Septal Defects in Premature vs Full-Term Neonates T. Riggs,
Pediatr Cardiol 21:129 134, 2000 DOI: 10.1007/s002469910020 Pediatric Cardiology Springer-Verlag New York Inc. 2000 Spontaneous Closure of Atrial Septal Defects in Premature vs Full-Term Neonates T. Riggs,
Cardiovascular Pathophysiology: Right to Left Shunts aka Cyanotic Lesions
 Cardiovascular Pathophysiology: Right to Left Shunts aka Cyanotic Lesions Ismee A. Williams, MD, MS iib6@columbia.edu Pediatric Cardiology Learning Objectives To discuss the hemodynamic significance of
Cardiovascular Pathophysiology: Right to Left Shunts aka Cyanotic Lesions Ismee A. Williams, MD, MS iib6@columbia.edu Pediatric Cardiology Learning Objectives To discuss the hemodynamic significance of
Cardiovascular Pathophysiology: Right to Left Shunts aka Cyanotic Lesions Ismee A. Williams, MD, MS Pediatric Cardiology
 Cardiovascular Pathophysiology: Right to Left Shunts aka Cyanotic Lesions Ismee A. Williams, MD, MS iib6@columbia.edu Pediatric Cardiology Learning Objectives To discuss the hemodynamic significance of
Cardiovascular Pathophysiology: Right to Left Shunts aka Cyanotic Lesions Ismee A. Williams, MD, MS iib6@columbia.edu Pediatric Cardiology Learning Objectives To discuss the hemodynamic significance of
Paediatrica Indonesiana. Echocardiographic patterns in asphyxiated neonates. Maswin Masyhur, Idham Amir, Sukman Tulus Putra, Alan Roland Tumbelaka
 Paediatrica Indonesiana VOLUME 49 July NUMBER 4 Original Article Echocardiographic patterns in asphyxiated neonates Maswin Masyhur, Idham Amir, Sukman Tulus Putra, Alan Roland Tumbelaka Abstract Background
Paediatrica Indonesiana VOLUME 49 July NUMBER 4 Original Article Echocardiographic patterns in asphyxiated neonates Maswin Masyhur, Idham Amir, Sukman Tulus Putra, Alan Roland Tumbelaka Abstract Background
Pattern of Congenital Heart Disease A Hospital-Based Study *Sadiq Mohammed Al-Hamash MBChB, FICMS
 Pattern of Congenital Heart Disease A Hospital-Based Study *Sadiq Mohammed Al-Hamash MBChB, FICMS ABSTRACT Background: The congenital heart disease occurs in 0,8% of live births and they have a wide spectrum
Pattern of Congenital Heart Disease A Hospital-Based Study *Sadiq Mohammed Al-Hamash MBChB, FICMS ABSTRACT Background: The congenital heart disease occurs in 0,8% of live births and they have a wide spectrum
Late Results after Correction of Ventricular Septal Defect with Severe Pulmonary Hypertension
 Tohoku J. Exp. Med., 1994, 174, 41-48 Late Results after Correction of Ventricular Septal Defect with Severe Pulmonary Hypertension KIYOSHI HANEDA, NAOSHI SATO, TAKAO TOGO, MAKOTO MIURA, MASAKI RATA and
Tohoku J. Exp. Med., 1994, 174, 41-48 Late Results after Correction of Ventricular Septal Defect with Severe Pulmonary Hypertension KIYOSHI HANEDA, NAOSHI SATO, TAKAO TOGO, MAKOTO MIURA, MASAKI RATA and
CARDIOVASCULAR SURGERY
 Volume 107, Number 4 April 1994 The Journal of THORACIC AND CARDIOVASCULAR SURGERY Cardiac and Pulmonary Transplantation Risk factors for graft failure associated with pulmonary hypertension after pediatric
Volume 107, Number 4 April 1994 The Journal of THORACIC AND CARDIOVASCULAR SURGERY Cardiac and Pulmonary Transplantation Risk factors for graft failure associated with pulmonary hypertension after pediatric
Patient Ductus Arteriosus (PDA)
 Patient Ductus Arteriosus (PDA) WINSTON HELEN Author: Paediatric Department Document Number: STHK7026 Version: 5 Review date: 30th June 2021 The Normal Heart The Heart is made up of four chambers: the
Patient Ductus Arteriosus (PDA) WINSTON HELEN Author: Paediatric Department Document Number: STHK7026 Version: 5 Review date: 30th June 2021 The Normal Heart The Heart is made up of four chambers: the
Introduction. Study Design. Background. Operative Procedure-I
 Risk Factors for Mortality After the Norwood Procedure Using Right Ventricle to Pulmonary Artery Shunt Ann Thorac Surg 2009;87:178 86 86 Addressor: R1 胡祐寧 2009/3/4 AM7:30 SICU 討論室 Introduction Hypoplastic
Risk Factors for Mortality After the Norwood Procedure Using Right Ventricle to Pulmonary Artery Shunt Ann Thorac Surg 2009;87:178 86 86 Addressor: R1 胡祐寧 2009/3/4 AM7:30 SICU 討論室 Introduction Hypoplastic
Ductal-dependent cardiac anomalies. Donna Cheung Pediatric Emergency Rotation January 31, 2014
 Ductal-dependent cardiac anomalies Donna Cheung Pediatric Emergency Rotation January 31, 2014 Case 1 A 6 day old Caucasian male presents to the ER with poor feeding and SOB. He was born FT via VD with
Ductal-dependent cardiac anomalies Donna Cheung Pediatric Emergency Rotation January 31, 2014 Case 1 A 6 day old Caucasian male presents to the ER with poor feeding and SOB. He was born FT via VD with
Patent Ductus Arteriosus: Philosophy or Pathology?
 Patent Ductus Arteriosus: Philosophy or Pathology? Disclosure Ray Sato, MD is a speaker for Prolacta Biosciences, Inc. This presentation will discuss off-label uses of acetaminophen and ibuprofen. RAY
Patent Ductus Arteriosus: Philosophy or Pathology? Disclosure Ray Sato, MD is a speaker for Prolacta Biosciences, Inc. This presentation will discuss off-label uses of acetaminophen and ibuprofen. RAY
CASE REPORTS. Anomalous Origin of the Left Coronary Artery from the Pulmonary Artery
 CASE REPORTS Anomalous Origin of the Left Coronary Artery from the Pulmonary Artery Definitive Surgical Treatment by Saphenous Vein Interposition in a 17-Month-Old Child P. Venugopal, M.D., and S. Subramanian,
CASE REPORTS Anomalous Origin of the Left Coronary Artery from the Pulmonary Artery Definitive Surgical Treatment by Saphenous Vein Interposition in a 17-Month-Old Child P. Venugopal, M.D., and S. Subramanian,
BPD. Neonatal/Pediatric Cardiopulmonary Care. Disease. Bronchopulmonary Dysplasia. Baby Jane
 1 Neonatal/Pediatric Cardiopulmonary Care Disease 2 Bronchopulmonary Dysplasia 3 is a 33-day-old prematurely born girl who weighs 1420 g. At birth, her estimated gestational age was 28 weeks. Her initial
1 Neonatal/Pediatric Cardiopulmonary Care Disease 2 Bronchopulmonary Dysplasia 3 is a 33-day-old prematurely born girl who weighs 1420 g. At birth, her estimated gestational age was 28 weeks. Her initial
PATENT DUCTUS ARTERIOSUS (PDA)
 PATENT DUCTUS ARTERIOSUS (PDA) It is a channel that connect the pulmonary artery with the descending aorta (isthumus part). It results from the persistence of patency of the fetal ductus arteriosus after
PATENT DUCTUS ARTERIOSUS (PDA) It is a channel that connect the pulmonary artery with the descending aorta (isthumus part). It results from the persistence of patency of the fetal ductus arteriosus after
Ligation of patent ductus arteriosus in low birth weight premature infants: timing for intervention and effectiveness of bed-side surgery
 Metin et al. Journal of Cardiothoracic Surgery 2012, 7:129 RESEARCH ARTICLE Open Access Ligation of patent ductus arteriosus in low birth weight premature infants: timing for intervention and effectiveness
Metin et al. Journal of Cardiothoracic Surgery 2012, 7:129 RESEARCH ARTICLE Open Access Ligation of patent ductus arteriosus in low birth weight premature infants: timing for intervention and effectiveness
Slide 1. Slide 2. Slide 3 CONGENITAL HEART DISEASE. Papworth Hospital NHS Trust INTRODUCTION. Jakub Kadlec/Catherine Sudarshan INTRODUCTION
 Slide 1 CONGENITAL HEART DISEASE Jakub Kadlec/Catherine Sudarshan NHS Trust Slide 2 INTRODUCTION Most common congenital illness in the newborn Affects about 4 9 / 1000 full-term live births in the UK 1.5
Slide 1 CONGENITAL HEART DISEASE Jakub Kadlec/Catherine Sudarshan NHS Trust Slide 2 INTRODUCTION Most common congenital illness in the newborn Affects about 4 9 / 1000 full-term live births in the UK 1.5
Standardising echocardiography and images. Version 2, 13/04/15
 Standardising echocardiography and images 1. Review of ECHO eligibility criteria - trial entry - rescue treatment 2. Assessments - personnel - timing 3. Technical aspects of ECHO examination 1. Trial entry
Standardising echocardiography and images 1. Review of ECHO eligibility criteria - trial entry - rescue treatment 2. Assessments - personnel - timing 3. Technical aspects of ECHO examination 1. Trial entry
Incidental Discovery of a Patent Ductus Arteriosus in Adults
 BRIEF REPORT Incidental Discovery of a Patent Ductus Arteriosus in Adults Harvey D. Cassidy, MD, Lynsey A. Cassidy, MD, and Joseph L. Blackshear, MD Patent ductus arteriosus (PDA) is an uncommon clinical
BRIEF REPORT Incidental Discovery of a Patent Ductus Arteriosus in Adults Harvey D. Cassidy, MD, Lynsey A. Cassidy, MD, and Joseph L. Blackshear, MD Patent ductus arteriosus (PDA) is an uncommon clinical
Neonatal/Pediatric Cardiopulmonary Care. Persistent Pulmonary Hypertension of the Neonate (PPHN) PPHN. Other. Other Diseases
 Neonatal/Pediatric Cardiopulmonary Care Other Diseases Persistent Pulmonary Hypertension of the Neonate (PPHN) PPHN 3 Also known as Persistent Fetal Circulation (PFC) Seen most frequently in term, post-term
Neonatal/Pediatric Cardiopulmonary Care Other Diseases Persistent Pulmonary Hypertension of the Neonate (PPHN) PPHN 3 Also known as Persistent Fetal Circulation (PFC) Seen most frequently in term, post-term
5.8 Congenital Heart Disease
 5.8 Congenital Heart Disease Congenital heart diseases (CHD) refer to structural or functional heart diseases, which are present at birth. Some of these lesions may be discovered later. prevalence of Chd
5.8 Congenital Heart Disease Congenital heart diseases (CHD) refer to structural or functional heart diseases, which are present at birth. Some of these lesions may be discovered later. prevalence of Chd
TRAINING NEONATOLOGY SILVANA PARIS
 TRAINING ON NEONATOLOGY SILVANA PARIS RESUSCITATION IN DELIVERY ROOM INTRODUCTION THE GLOBAL RESUSCITATION BURDEN IN NEWBORN 136 MILL NEWBORN BABIES EACH YEAR (WHO WORLD REPORT) 5-8 MILL NEWBORN INFANTS
TRAINING ON NEONATOLOGY SILVANA PARIS RESUSCITATION IN DELIVERY ROOM INTRODUCTION THE GLOBAL RESUSCITATION BURDEN IN NEWBORN 136 MILL NEWBORN BABIES EACH YEAR (WHO WORLD REPORT) 5-8 MILL NEWBORN INFANTS
Patent Ductus Arteriosus (PDA)
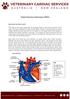 Patent Ductus Arteriosus (PDA) How does the heart work? The heart is the organ responsible for pumping blood to and from all tissues of the body. The heart is divided into right and left sides. The job
Patent Ductus Arteriosus (PDA) How does the heart work? The heart is the organ responsible for pumping blood to and from all tissues of the body. The heart is divided into right and left sides. The job
DORV: The Great Chameleon. Heart Conference October 15, 2016 Tina Kwan, MD
 DORV: The Great Chameleon Heart Conference October 15, 2016 Tina Kwan, MD Kenneth Maehara, Ph.D. May 7, 1942 - August 26, 2013 A.R. A classic case of broken heart 38 week AGA F born at an OSH to
DORV: The Great Chameleon Heart Conference October 15, 2016 Tina Kwan, MD Kenneth Maehara, Ph.D. May 7, 1942 - August 26, 2013 A.R. A classic case of broken heart 38 week AGA F born at an OSH to
DR Turner, JA Vincent, and ML Epstein. Isolated right pulmonary artery discontinuity. Images Paediatr Cardiol Jul-Sep; 2(3):
 IMAGES in PAEDIATRIC CARDIOLOGY Images PMCID: PMC3232486 Isolated right pulmonary artery discontinuity DR Turner, MD, * JA Vincent, ** and ML Epstein *** * Senior Fellow, Division of Cardiology, Children's
IMAGES in PAEDIATRIC CARDIOLOGY Images PMCID: PMC3232486 Isolated right pulmonary artery discontinuity DR Turner, MD, * JA Vincent, ** and ML Epstein *** * Senior Fellow, Division of Cardiology, Children's
How to Recognize a Suspected Cardiac Defect in the Neonate
 Neonatal Nursing Education Brief: How to Recognize a Suspected Cardiac Defect in the Neonate https://www.seattlechildrens.org/healthcareprofessionals/education/continuing-medical-nursing-education/neonatalnursing-education-briefs/
Neonatal Nursing Education Brief: How to Recognize a Suspected Cardiac Defect in the Neonate https://www.seattlechildrens.org/healthcareprofessionals/education/continuing-medical-nursing-education/neonatalnursing-education-briefs/
Screening for Critical Congenital Heart Disease
 Screening for Critical Congenital Heart Disease Caroline K. Lee, MD Pediatric Cardiology Disclosures I have no relevant financial relationships or conflicts of interest 1 Most Common Birth Defect Most
Screening for Critical Congenital Heart Disease Caroline K. Lee, MD Pediatric Cardiology Disclosures I have no relevant financial relationships or conflicts of interest 1 Most Common Birth Defect Most
Admission/Discharge Form for Infants Born in Please DO NOT mail or fax this form to the CPQCC Data Center. This form is for internal use ONLY.
 Selection Criteria Admission/Discharge Form for Infants Born in 2016 To be eligible, you MUST answer YES to at least one of the possible criteria (A-C) A. 401 1500 grams o Yes B. GA range 22 0/7 31 6/7
Selection Criteria Admission/Discharge Form for Infants Born in 2016 To be eligible, you MUST answer YES to at least one of the possible criteria (A-C) A. 401 1500 grams o Yes B. GA range 22 0/7 31 6/7
Congenital heart disease. By Dr Saima Ali Professor of pediatrics
 Congenital heart disease By Dr Saima Ali Professor of pediatrics What is the most striking clinical finding in this child? Learning objectives By the end of this lecture, final year student should be able
Congenital heart disease By Dr Saima Ali Professor of pediatrics What is the most striking clinical finding in this child? Learning objectives By the end of this lecture, final year student should be able
Congenital Heart Disease
 Congenital Heart Disease Mohammed Alghamdi, MD, FRCPC, FAAP, FACC Associate Professor and Consultant Pediatric Cardiology, Cardiac Science King Fahad Cardiac Centre King Saud University INTRODUCTION CHD
Congenital Heart Disease Mohammed Alghamdi, MD, FRCPC, FAAP, FACC Associate Professor and Consultant Pediatric Cardiology, Cardiac Science King Fahad Cardiac Centre King Saud University INTRODUCTION CHD
Patent ductus arteriosus PDA
 Patent ductus arteriosus PDA Is connecting between the aortic end just distal to the origin of the LT sub clavian artery& the pulmonary artery at its bifurcation. Female/male ratio is 2:1 and it is more
Patent ductus arteriosus PDA Is connecting between the aortic end just distal to the origin of the LT sub clavian artery& the pulmonary artery at its bifurcation. Female/male ratio is 2:1 and it is more
An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy
 An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy Housekeeping: I have no financial disclosures Learning objectives: Develop an understanding of bronchopulmonary dysplasia (BPD)
An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy Housekeeping: I have no financial disclosures Learning objectives: Develop an understanding of bronchopulmonary dysplasia (BPD)
Late pulmonary hypertension in preterm infants How to sort things out? V.Gournay, FCPC, La Martinique, Nov 23,2015
 Late pulmonary hypertension in preterm infants How to sort things out? V.Gournay, FCPC, La Martinique, Nov 23,2015 Epidemiology Incidence of extreme prematurity (
Late pulmonary hypertension in preterm infants How to sort things out? V.Gournay, FCPC, La Martinique, Nov 23,2015 Epidemiology Incidence of extreme prematurity (
Pulse Oximetry Screening in Newborns to Enhance the Detection Of Critical Congenital Heart Disease. Frequently Asked Questions
 Pulse Oximetry Screening in Newborns to Enhance the Detection Of Critical Congenital Heart Disease Frequently Asked Questions Current Recommendation: The current recommendation from the Canadian Cardiovascular
Pulse Oximetry Screening in Newborns to Enhance the Detection Of Critical Congenital Heart Disease Frequently Asked Questions Current Recommendation: The current recommendation from the Canadian Cardiovascular
The effect of ductal diameter on surgical and medical closure of patent ductus arteriosus in preterm neonates: Size matters
 The effect of ductal diameter on surgical and medical closure of patent ductus arteriosus in preterm neonates: Size matters Scott Tschuppert, a Carsten Doell, MD, b Romaine Arlettaz-Mieth, MD, c Oskar
The effect of ductal diameter on surgical and medical closure of patent ductus arteriosus in preterm neonates: Size matters Scott Tschuppert, a Carsten Doell, MD, b Romaine Arlettaz-Mieth, MD, c Oskar
Two Cases Report of Scimitar Syndrome: The Classical one with Subaortic Membrane and the Scimitar Variant
 Bahrain Medical Bulletin, Vol.22, No.1, March 2000 Two Cases Report of Scimitar Syndrome: The Classical one with Subaortic Membrane and the Scimitar Variant F Hakim, MD* A Madani, MD* A Abu Haweleh, MD,MRCP*
Bahrain Medical Bulletin, Vol.22, No.1, March 2000 Two Cases Report of Scimitar Syndrome: The Classical one with Subaortic Membrane and the Scimitar Variant F Hakim, MD* A Madani, MD* A Abu Haweleh, MD,MRCP*
Airway Management in a Patient with Klippel-Feil Syndrome Using Extracorporeal Membrane Oxygenator
 Airway Management in a Patient with Klippel-Feil Syndrome Using Extracorporeal Membrane Oxygenator Beckerman Z*, Cohen O, Adler Z, Segal D, Mishali D and Bolotin G Department of Cardiac Surgery, Rambam
Airway Management in a Patient with Klippel-Feil Syndrome Using Extracorporeal Membrane Oxygenator Beckerman Z*, Cohen O, Adler Z, Segal D, Mishali D and Bolotin G Department of Cardiac Surgery, Rambam
CONGENITAL HEART DISEASE (CHD)
 CONGENITAL HEART DISEASE (CHD) DEFINITION It is the result of a structural or functional abnormality of the cardiovascular system at birth GENERAL FEATURES OF CHD Structural defects due to specific disturbance
CONGENITAL HEART DISEASE (CHD) DEFINITION It is the result of a structural or functional abnormality of the cardiovascular system at birth GENERAL FEATURES OF CHD Structural defects due to specific disturbance
Project 1: Circulation
 Project 1: Circulation This project refers to the matlab files located at: http://www.math.nyu.edu/faculty/peskin/modsimprograms/ch1/. Model of the systemic arteries. The first thing to do is adjust the
Project 1: Circulation This project refers to the matlab files located at: http://www.math.nyu.edu/faculty/peskin/modsimprograms/ch1/. Model of the systemic arteries. The first thing to do is adjust the
Stabilization and Transportation guidelines for Neonates and infants with Heart disease:
 Stabilization and Transportation guidelines for Neonates and infants with Heart disease: Background: Referral Pediatric Cardiac Units, frequently receive neonates and infants referred and transported from
Stabilization and Transportation guidelines for Neonates and infants with Heart disease: Background: Referral Pediatric Cardiac Units, frequently receive neonates and infants referred and transported from
Debate in Management of native COA; Balloon Versus Surgery
 Debate in Management of native COA; Balloon Versus Surgery Dr. Amira Esmat, El Tantawy, MD Professor of Pediatrics Consultant Pediatric Cardiac Interventionist Faculty of Medicine Cairo University 23/2/2017
Debate in Management of native COA; Balloon Versus Surgery Dr. Amira Esmat, El Tantawy, MD Professor of Pediatrics Consultant Pediatric Cardiac Interventionist Faculty of Medicine Cairo University 23/2/2017
AMERICAN ACADEMY OF PEDIATRICS 993 THE NATURAL HISTORY OF CERTAIN CONGENITAL CARDIOVASCULAR MALFORMATIONS. Alexander S. Nadas, M.D.
 AMERICAN ACADEMY OF PEDIATRICS 993 tnicular overload is the major problem and left ventricular failure occurs. Since for many years the importance of hepatomegaly in the diagnosis of cardiac failure has
AMERICAN ACADEMY OF PEDIATRICS 993 tnicular overload is the major problem and left ventricular failure occurs. Since for many years the importance of hepatomegaly in the diagnosis of cardiac failure has
Pulmonarv Arterv Plication: with Type I Trunms Arteriosus. A New S&gical Procedure for Small Infants
 Pulmonarv Arterv Plication: A New S&gical Procedure for Small Infants with Type I Trunms Arteriosus S. Bert Litwin, M.D., and David Z. Friedberg, M.D. ABSTRACT A new technique is reported for constriction
Pulmonarv Arterv Plication: A New S&gical Procedure for Small Infants with Type I Trunms Arteriosus S. Bert Litwin, M.D., and David Z. Friedberg, M.D. ABSTRACT A new technique is reported for constriction
Diuretics: Increased risk of renal dysfunction. (7) See 17 for PATIENT COUNSELING INFORMATION. Revised: 10/2017 FULL PRESCRIBING INFORMATION: CONTENTS
 HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use NEOPROFEN safely and effectively. See full prescribing information for NEOPROFEN. NEOPROFEN (ibuprofen
HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use NEOPROFEN safely and effectively. See full prescribing information for NEOPROFEN. NEOPROFEN (ibuprofen
Case Report DOUGLAS H. KING, MD, JAMES C. HUHTA, MD, HOWARD P. GUTGESELL, MD, FACC, DAVID A. OTT, MD*
 lacc Vol. 4, No.2 August 198'
lacc Vol. 4, No.2 August 198'
Paediatrics Revision Session Cardiology. Emma Walker 7 th May 2016
 Paediatrics Revision Session Cardiology Emma Walker 7 th May 2016 Cardiovascular Examination! General:! Make it fun!! Change how you act depending on their age! Introduction! Introduce yourself & check
Paediatrics Revision Session Cardiology Emma Walker 7 th May 2016 Cardiovascular Examination! General:! Make it fun!! Change how you act depending on their age! Introduction! Introduce yourself & check
HISTORY. Question: What category of heart disease is suggested by this history? CHIEF COMPLAINT: Heart murmur present since early infancy.
 HISTORY 18-year-old man. CHIEF COMPLAINT: Heart murmur present since early infancy. PRESENT ILLNESS: Although normal at birth, a heart murmur was heard at the six week check-up and has persisted since
HISTORY 18-year-old man. CHIEF COMPLAINT: Heart murmur present since early infancy. PRESENT ILLNESS: Although normal at birth, a heart murmur was heard at the six week check-up and has persisted since
CongHeartDis.doc. Андрій Миколайович Лобода
 CongHeartDis.doc Андрій Миколайович Лобода 2015 Зміст 3 Зміст Зміст 4 A child with tetralogy of Fallot is most likely to exhibit: -Increased pulmonary blood flow -Increased pressure in the right ventricle
CongHeartDis.doc Андрій Миколайович Лобода 2015 Зміст 3 Зміст Зміст 4 A child with tetralogy of Fallot is most likely to exhibit: -Increased pulmonary blood flow -Increased pressure in the right ventricle
Isolated major aortopulmonary collateral as the sole pulmonary blood supply to an entire lung segment
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2017 Isolated major aortopulmonary collateral as the sole pulmonary blood supply to an entire lung segment Hannah
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2017 Isolated major aortopulmonary collateral as the sole pulmonary blood supply to an entire lung segment Hannah
SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY
 PS1070 SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY TITLE: ADMISSION/DISCHARGE CRITERIA: CARDIOVASCULAR INTENSIVE Job Title of Reviewer: Director, CVICU EFFECTIVE DATE: REVIEWED/REVISED DATE: POLICY
PS1070 SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY TITLE: ADMISSION/DISCHARGE CRITERIA: CARDIOVASCULAR INTENSIVE Job Title of Reviewer: Director, CVICU EFFECTIVE DATE: REVIEWED/REVISED DATE: POLICY
The sinus venosus represent the venous end of the heart It receives 3 veins: 1- Common cardinal vein body wall 2- Umbilical vein from placenta 3-
 1 2 The sinus venosus represent the venous end of the heart It receives 3 veins: 1- Common cardinal vein body wall 2- Umbilical vein from placenta 3- Vitelline vein from yolk sac 3 However!!!!! The left
1 2 The sinus venosus represent the venous end of the heart It receives 3 veins: 1- Common cardinal vein body wall 2- Umbilical vein from placenta 3- Vitelline vein from yolk sac 3 However!!!!! The left
M Tipple. Interpretation of electrocardiograms in infants and children. Images Paediatr Cardiol Jan-Mar; 1(1): 3 13.
 IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 1999 PMCID: PMC3232475 Interpretation of electrocardiograms in infants and children M Tipple * * Paediatric Cardiologist, British Columbia Children's
IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 1999 PMCID: PMC3232475 Interpretation of electrocardiograms in infants and children M Tipple * * Paediatric Cardiologist, British Columbia Children's
Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia
 Marshall University Marshall Digital Scholar Internal Medicine Faculty Research Spring 5-2004 Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia Ellen A. Thompson
Marshall University Marshall Digital Scholar Internal Medicine Faculty Research Spring 5-2004 Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia Ellen A. Thompson
NEONATAL CLINICAL PRACTICE GUIDELINE
 NEONATAL CLINICAL PRACTICE GUIDELINE Approval Date: January 2015 Approved by: Neonatal Patient Care Teams, HSC & SBH Child Health Standards Committee Pages: 1 of 6 Supercedes: N/A 1.0 PURPOSE and INTENT
NEONATAL CLINICAL PRACTICE GUIDELINE Approval Date: January 2015 Approved by: Neonatal Patient Care Teams, HSC & SBH Child Health Standards Committee Pages: 1 of 6 Supercedes: N/A 1.0 PURPOSE and INTENT
IMAGES. in PAEDIATRIC CARDIOLOGY
 IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2006 Jul-Sep; 8(3): 1 6. PMCID: PMC3232564 A large, single pulmonary arteriovenous fistula presenting hours after birth AH McBrien, 1 AJ Sands,
IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2006 Jul-Sep; 8(3): 1 6. PMCID: PMC3232564 A large, single pulmonary arteriovenous fistula presenting hours after birth AH McBrien, 1 AJ Sands,
Survival Rates of Children with Congenital Heart Disease continue to improve.
 DOROTHY RADFORD Survival Rates of Children with Congenital Heart Disease continue to improve. 1940-20% 1960-40% 1980-70% 2010->90% Percentage of children with CHD reaching age of 18 years 1938 First Patent
DOROTHY RADFORD Survival Rates of Children with Congenital Heart Disease continue to improve. 1940-20% 1960-40% 1980-70% 2010->90% Percentage of children with CHD reaching age of 18 years 1938 First Patent
disease, bronchopulmonary dysplasia, pulmonary hypoplasia and congenital diaphragmatic hernia.
 Neonatal Chest Imaging - What the Nurse Should Know Expires Monday, April 30, 2018 Nursing Michael J. Diament, M.D. Objectives 1. Describe a good technique for positioning a neonate for the purpose of
Neonatal Chest Imaging - What the Nurse Should Know Expires Monday, April 30, 2018 Nursing Michael J. Diament, M.D. Objectives 1. Describe a good technique for positioning a neonate for the purpose of
USE OF INHALED NITRIC OXIDE IN THE NICU East Bay Newborn Specialists Guideline Prepared by P Joe, G Dudell, A D Harlingue Revised 7/9/2014
 USE OF INHALED NITRIC OXIDE IN THE NICU East Bay Newborn Specialists Guideline Prepared by P Joe, G Dudell, A D Harlingue Revised 7/9/2014 ino for Late Preterm and Term Infants with Severe PPHN Background:
USE OF INHALED NITRIC OXIDE IN THE NICU East Bay Newborn Specialists Guideline Prepared by P Joe, G Dudell, A D Harlingue Revised 7/9/2014 ino for Late Preterm and Term Infants with Severe PPHN Background:
Cardiac Emergencies in Infants. Michael Luceri, DO
 Cardiac Emergencies in Infants Michael Luceri, DO October 7, 2017 I have no financial obligations or conflicts of interest to disclose. Objectives Understand the scope of congenital heart disease Recognize
Cardiac Emergencies in Infants Michael Luceri, DO October 7, 2017 I have no financial obligations or conflicts of interest to disclose. Objectives Understand the scope of congenital heart disease Recognize
Major Infection After Pediatric Cardiac Surgery: External Validation of Risk Estimation Model
 Major Infection After Pediatric Cardiac Surgery: External Validation of Risk Estimation Model Andrzej Kansy, MD, PhD, Jeffrey P. Jacobs, MD, PhD, Andrzej Pastuszko, MD, PhD, Małgorzata Mirkowicz-Małek,
Major Infection After Pediatric Cardiac Surgery: External Validation of Risk Estimation Model Andrzej Kansy, MD, PhD, Jeffrey P. Jacobs, MD, PhD, Andrzej Pastuszko, MD, PhD, Małgorzata Mirkowicz-Małek,
Approach to a baby with cyanosis
 Approach to a baby with cyanosis Objectives Cyanosis : types Differentials: cardiac vs. non cardiac Approach Case scenarios Cyanosis Greek word kuaneos meaning dark blue Bluish discolouration of skin,
Approach to a baby with cyanosis Objectives Cyanosis : types Differentials: cardiac vs. non cardiac Approach Case scenarios Cyanosis Greek word kuaneos meaning dark blue Bluish discolouration of skin,
Unsuspected cardiopulmonary abnormalities complicating bronchopulmonary dysplasia
 Archives of Disease in Childhood, 1984, 59, 966-970 Unsuspected cardiopulmonary abnormalities complicating bronchopulmonary dysplasia S H ABMAN, F J ACCURSO, AND C M BOWMAN Department of Paediatrics and
Archives of Disease in Childhood, 1984, 59, 966-970 Unsuspected cardiopulmonary abnormalities complicating bronchopulmonary dysplasia S H ABMAN, F J ACCURSO, AND C M BOWMAN Department of Paediatrics and
GoodPrognosisofALCAPAAnomalousOriginoftheLeftCoronaryArteryfromthePulmonaryArterySyndromewithearlyDiagnosisandSurgicalTreatment
 Global Journal of Medical Research: I Surgeries and Cardiovascular System Volume 18 Issue 3 Version 1.0 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Online
Global Journal of Medical Research: I Surgeries and Cardiovascular System Volume 18 Issue 3 Version 1.0 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Online
Portal vein catheterization and selective angiography in diagnosis of total anomalous pulmonary venous connexion
 British Heart journal, 974, 36, 155-59. Portal vein catheterization and selective angiography in diagnosis of total anomalous pulmonary venous connexion Michael Tynan, D. Behrendt, W. Urquhart, and G.
British Heart journal, 974, 36, 155-59. Portal vein catheterization and selective angiography in diagnosis of total anomalous pulmonary venous connexion Michael Tynan, D. Behrendt, W. Urquhart, and G.
CYANOTIC CONGENITAL HEART DISEASES. PRESENTER: DR. Myra M. Koech Pediatric cardiologist MTRH/MU
 CYANOTIC CONGENITAL HEART DISEASES PRESENTER: DR. Myra M. Koech Pediatric cardiologist MTRH/MU DEFINITION Congenital heart diseases are defined as structural and functional problems of the heart that are
CYANOTIC CONGENITAL HEART DISEASES PRESENTER: DR. Myra M. Koech Pediatric cardiologist MTRH/MU DEFINITION Congenital heart diseases are defined as structural and functional problems of the heart that are
NEONATAL CLINICAL PRACTICE GUIDELINE
 NEONATAL CLINICAL PRACTICE GUIDELINE Title: Integrated Evaluation of Neonatal Hemodynamics (IENH) and Targeted Echocardiogram Approval Date: January 2015 Approved by: Neonatal Patient Care Teams, HSC &
NEONATAL CLINICAL PRACTICE GUIDELINE Title: Integrated Evaluation of Neonatal Hemodynamics (IENH) and Targeted Echocardiogram Approval Date: January 2015 Approved by: Neonatal Patient Care Teams, HSC &
24. An infant with recurrent pneumonia underwent a frontal chest radiograph (Fig 24-A) followed by
 24. An infant with recurrent pneumonia underwent a frontal chest radiograph (Fig 24-A) followed by diagnosis? ndings, what is the most likely A. Pulmonary sequestration B. Congenital pulmonary airway malformation
24. An infant with recurrent pneumonia underwent a frontal chest radiograph (Fig 24-A) followed by diagnosis? ndings, what is the most likely A. Pulmonary sequestration B. Congenital pulmonary airway malformation
Management of a Patient after the Bidirectional Glenn
 Management of a Patient after the Bidirectional Glenn Melissa B. Jones MSN, APRN, CPNP-AC CICU Nurse Practitioner Children s National Health System Washington, DC No Disclosures Objectives qbriefly describe
Management of a Patient after the Bidirectional Glenn Melissa B. Jones MSN, APRN, CPNP-AC CICU Nurse Practitioner Children s National Health System Washington, DC No Disclosures Objectives qbriefly describe
