SPECIAL PATHOPHYSIOLOGY HYPERTENSION
|
|
|
- Julia McLaughlin
- 5 years ago
- Views:
Transcription
1 SPECIAL PATHOPHYSIOLOGY HYPERTENSION 1. Systolic blood pressure is elevated when it is over: mmHg mmHg mmHg mmHg mmHg. 2. Diastolic blood pressure is elevated when it is over: 1. 80mmHg mmHg mmHg mmHg mmHg. 3. Which factors are able to increase systemic blood pressure?: 1. Stroke volume of the heart. 2. Cardiac output. 3. Total peripheral vascular resistance (TPR). 4. 2, , 2, Blood pressure is increased when there is: 1. Prevalence of pressor mechanisms. 2. Activation of pressor and depressor factors. 3. Insuffiecient depressor factors. 4. Pressor-depressor dissociation. 5. 1, Arterial hypertension is acondition of: 1.Elevated blood pressure adequate to metabolic needs. 2. Form of adaptation to generalized hyperperfusion. 3. Functionally inadequate elevated blood pressure. 4. Form of maintaining blood flow in vital organs. 5. Circulatory overcompensation. 6. What is the pathogenetic classification of arterial hypertension? 1. Congenital and acquired. 2. Uncompensated and overcompensated. 3. Infectious and non-infectious. 4. Essential and symptomatic.
2 5. Localized and generalized. 6. According to age and gender. 7. Which factors play an important role in the genesis of essential hypertension? 1. Acute infections. 2. Psychological traumas. 3. Genetic predisposition. 4. Kidney diseases. 5. 2, Which pathogenic units are involved in the pathogenesis of essential hypertension? 1.Vessels. 2. Renal. 3. Autoimmune. 4. Metabolic-perfusion. 9. Retention of sodium and water in patients with essential hypertension is associated with: 1. Decreased excretion of sodium and water. 2. Lost potential of sodium and water excretion. 3. Neuro-dependent retention of sodium and water. 4. Renoprival retention of sodium and water. 5. Vasopressin-dependent sodium and water retention. 10. Renin is: 1. Hormone produced by the kidneys 2. Hormone that stimulates the function of the adrenal glands 3. Enzyme produced by the kidneys 4. Enzyme that catalyzes ATI-->ATII conversion 5. 1,2 6. 3,4 11. What is the classification of essential hypertension accoding to the dominant pathogenetic mechanism? 1. Hyper-, normo- and hypoperfussion. 2. Hyperkinetic, volume and vasoconstrictory. 3. High, normal and low-flow. 4. Hyper-, normo- and hyporeactive. 5. Stretch- and chemoreceptor dependent. 12. Vasoconstriction elevates blood pressure by: 1. Increasing heart rate. 2. Increasing cardiac output.
3 3. Increased afterload. 4. Increased total peripheral resistance. 5. Generalized tissue hypoperfusion. 13. How the hyperkinetic mechanism increases blood pressure? 1. Venoconstriction increases central blood flow. 2. Primary hypervolemia. 3. Positive chornotropic and inotropic effects. 4. Generalized arterio-venous shunting of blood. 5. 1, , 2, The main pathogenetic unit of volume-dependent arterial hypertension is: 1. Decreased renal excretion of sodium and water. 2. Increased sympathetic tone. 3. Lost baroreceptor depressor mechanism. 4. Genetically, higher extracellular volume. 5. Ineffective Darrow-Yannet mechanism. 15. Mandatory factor for stabilization of high blood pressure is: 1.Sustainable increase in extracellular fluid volume. 2. Increased peripheral vascular resistance inadequate to the actual blood volume. 3. Inadequately elevated hematocrit. 4. Shortened circulating time. 5. Increased cardiac output. 16. Which renal prostaglandin has depressor activity? 1. PgF 2α. 2. PgE 2 and A PgD and H. 4. PgA 2 and B Endoperoxide. 17. Which are the pathogenic forms of renal hypertension? 1. Acute and chronic. 2. Latent and manifested. 3. Renal-parenchymal and renal-vascular. 4. Compensated and decompensated. 18. Renal-parenchymal hypertension develops in cases of: 1. Glomerulonephritis, chronic pyelonephritis. 2. Surgical removalof the kidney. 3. Fibromuscular hyperplasia of a. renalis.
4 4. Embolism of a. renalis. 5. Presence of an aberrant vessel. 19. The main pathogenetic mechanism in renal-parenchymal hypertension is: 1.Relatively increased renin activity. 2. Decreased ability of the kidneys to excrete sodium and water. 3. Increased level of renal prostaglandins and kinins. 4. 1, Renal-vascular hypertension develops in: 1. Reduction of the renal parenchyma. 2. Stenosis of a.renalis. 3. Bilateral nephrectomy. 4. Polycystic kidney disease. 5. Acute pyelonephritis. 21. Which is the main pathogenetic mechanism for development of renal-vascular hypertension? 1. Decreased ability of the kidneys to excrete Na + and water. 2. Increased concentration of Na + in the blood vessel wall. 3. Activation of the renin-angiotensin-aldosterone system. 4. Stimulation of the depressor part of the vasomotor center. 5. Reduced sensitivity of the renal receptors for ADH. 22. Arterial hypertension in atherosclerosis is a result of: 1.Increased Na + concentration in the blood. 2. Increased release of pressor factors. 3. Reduced elasticity of the large arterial vessels. 4. Increased pressor effect of the vasomotorcenter. 5. 1, Arterial hypertension in thyrotoxicosis is: 1. Diastolic type. 2. Systolic /hyperkinetic/ type. 3. Volume type. 4. Blood pressure is not affected in thyrotoxicosis. 5. Systolic-diastolic type. 24. The main hypertensive mechanism in hyperaldosteronism is: 1. Spasm of the peripheral blood vessels. 2. Increased Na + and water retention in the body. 3. Sensitization of the vascular wall to pressor factors.
5 4. Hypertrophy of the vascular wall. 5. Stimulation of the renin-angiotensin system. 25. The main hypertensive mechanism in hyperglucocorticism is: 1. Peripheral blood vessels spasm. 2. Increased Na + and water retention in the body. 3. Sensitization of the vascular wall to pressor factors. 4. Hypertrophy of the vascular wall. 5. Altered sensitivity of stretch- and chemoreceptors. 26. Endocrine hypertension in pheochromocytoma is determined by: 1. Increased peripheral vascular resistance. 2. Tachycardia with increased cardiac output. 3. Increased Na + and water retention in the body , 3.
Blood pressure. Formation of the blood pressure: Blood pressure. Formation of the blood pressure 5/1/12
 Blood pressure Blood pressure Dr Badri Paudel www.badripaudel.com Ø Blood pressure means the force exerted by the blood against the vessel wall Ø ( or the force exerted by the blood against any unit area
Blood pressure Blood pressure Dr Badri Paudel www.badripaudel.com Ø Blood pressure means the force exerted by the blood against the vessel wall Ø ( or the force exerted by the blood against any unit area
BIOH122 Session 6 Vascular Regulation
 BIOH122 Session 6 Vascular Regulation To complete this worksheet, select: Module: Distribution Title: Vascular Regulation Introduction 1. a. How do Mean Arterial Blood Pressure (MABP) and Systemic Vascular
BIOH122 Session 6 Vascular Regulation To complete this worksheet, select: Module: Distribution Title: Vascular Regulation Introduction 1. a. How do Mean Arterial Blood Pressure (MABP) and Systemic Vascular
Functional vascular disorders
 Functional vascular disorders Raynaud s phenomenon Raynaud s phenomenon Refers to Intermittent,bilateral attacks of ischemia of the fingers or toes, and sometimes ears or nose. It clinically manifests
Functional vascular disorders Raynaud s phenomenon Raynaud s phenomenon Refers to Intermittent,bilateral attacks of ischemia of the fingers or toes, and sometimes ears or nose. It clinically manifests
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Special Lecture 11/08/2013. Hypertension Dr. HN Mayrovitz
 Special Lecture 11/08/2013 Hypertension Dr. HN Mayrovitz Arterial Blood Pressure (ABP) Major Factors Summarized Sympathetic Hormones Arteriole MAP ~ Q x TPR + f (V / C) SV x HR Renal SBP Hypertension =
Special Lecture 11/08/2013 Hypertension Dr. HN Mayrovitz Arterial Blood Pressure (ABP) Major Factors Summarized Sympathetic Hormones Arteriole MAP ~ Q x TPR + f (V / C) SV x HR Renal SBP Hypertension =
Cardiovascular System B L O O D V E S S E L S 2
 Cardiovascular System B L O O D V E S S E L S 2 Blood Pressure Main factors influencing blood pressure: Cardiac output (CO) Peripheral resistance (PR) Blood volume Peripheral resistance is a major factor
Cardiovascular System B L O O D V E S S E L S 2 Blood Pressure Main factors influencing blood pressure: Cardiac output (CO) Peripheral resistance (PR) Blood volume Peripheral resistance is a major factor
Therefore MAP=CO x TPR = HR x SV x TPR
 Regulation of MAP Flow = pressure gradient resistance CO = MAP TPR Therefore MAP=CO x TPR = HR x SV x TPR TPR is the total peripheral resistance: this is the combined resistance of all blood vessels (remember
Regulation of MAP Flow = pressure gradient resistance CO = MAP TPR Therefore MAP=CO x TPR = HR x SV x TPR TPR is the total peripheral resistance: this is the combined resistance of all blood vessels (remember
Blood pressure control Contin. Reflex Mechanisms. Dr. Hiwa Shafiq
 Blood pressure control Contin. Reflex Mechanisms Dr. Hiwa Shafiq 17-12-2018 A. Baroreceptor reflexes Baroreceptors (stretch receptors) located in the walls of several large systemic arteries( specially
Blood pressure control Contin. Reflex Mechanisms Dr. Hiwa Shafiq 17-12-2018 A. Baroreceptor reflexes Baroreceptors (stretch receptors) located in the walls of several large systemic arteries( specially
Circulation. Blood Pressure and Antihypertensive Medications. Venous Return. Arterial flow. Regulation of Cardiac Output.
 Circulation Blood Pressure and Antihypertensive Medications Two systems Pulmonary (low pressure) Systemic (high pressure) Aorta 120 mmhg Large arteries 110 mmhg Arterioles 40 mmhg Arteriolar capillaries
Circulation Blood Pressure and Antihypertensive Medications Two systems Pulmonary (low pressure) Systemic (high pressure) Aorta 120 mmhg Large arteries 110 mmhg Arterioles 40 mmhg Arteriolar capillaries
Blood Pressure Regulation. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation Faisal I. Mohammed, MD,PhD 1 Objectives Outline the short term and long term regulators of BP Know how baroreceptors and chemoreceptors work Know function of the atrial reflex.
Blood Pressure Regulation Faisal I. Mohammed, MD,PhD 1 Objectives Outline the short term and long term regulators of BP Know how baroreceptors and chemoreceptors work Know function of the atrial reflex.
Blood Pressure Regulation. Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure
 Sheet physiology(18) Sunday 24-November Blood Pressure Regulation Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure MAP= Diastolic Pressure+1/3 Pulse Pressure CO=MAP/TPR
Sheet physiology(18) Sunday 24-November Blood Pressure Regulation Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure MAP= Diastolic Pressure+1/3 Pulse Pressure CO=MAP/TPR
CASE 13. What neural and humoral pathways regulate arterial pressure? What are two effects of angiotensin II?
 CASE 13 A 57-year-old man with long-standing diabetes mellitus and newly diagnosed hypertension presents to his primary care physician for follow-up. The patient has been trying to alter his dietary habits
CASE 13 A 57-year-old man with long-standing diabetes mellitus and newly diagnosed hypertension presents to his primary care physician for follow-up. The patient has been trying to alter his dietary habits
1. Changed level of a certain hormone Stimulation of the oxygen consumption 3. Decoupling of oxidative phosphorylation 2.
 1. How can endocrine disorders be classified? 1. Hereditary, acquired 2. Active, passive 3. Uncompensated, overcompensated 4. Primary, secondary 5.1, 4 6.1, 2, 3, 4. ENDOCRINE SYSTEM 2. Which is the MAIN
1. How can endocrine disorders be classified? 1. Hereditary, acquired 2. Active, passive 3. Uncompensated, overcompensated 4. Primary, secondary 5.1, 4 6.1, 2, 3, 4. ENDOCRINE SYSTEM 2. Which is the MAIN
Blood Pressure Fox Chapter 14 part 2
 Vert Phys PCB3743 Blood Pressure Fox Chapter 14 part 2 T. Houpt, Ph.D. 1 Cardiac Output and Blood Pressure How to Measure Blood Pressure Contribution of vascular resistance to blood pressure Cardiovascular
Vert Phys PCB3743 Blood Pressure Fox Chapter 14 part 2 T. Houpt, Ph.D. 1 Cardiac Output and Blood Pressure How to Measure Blood Pressure Contribution of vascular resistance to blood pressure Cardiovascular
Veins. VENOUS RETURN = PRELOAD = End Diastolic Volume= Blood returning to heart per cardiac cycle (EDV) or per minute (Venous Return)
 Veins Venous system transports blood back to heart (VENOUS RETURN) Capillaries drain into venules Venules converge to form small veins that exit organs Smaller veins merge to form larger vessels Veins
Veins Venous system transports blood back to heart (VENOUS RETURN) Capillaries drain into venules Venules converge to form small veins that exit organs Smaller veins merge to form larger vessels Veins
Hypertension The normal radial artery blood pressures in adults are: Systolic arterial pressure: 100 to 140 mmhg. Diastolic arterial pressure: 60 to
 Hypertension The normal radial artery blood pressures in adults are: Systolic arterial pressure: 100 to 140 mmhg. Diastolic arterial pressure: 60 to 90 mmhg. These pressures are called Normal blood pressure
Hypertension The normal radial artery blood pressures in adults are: Systolic arterial pressure: 100 to 140 mmhg. Diastolic arterial pressure: 60 to 90 mmhg. These pressures are called Normal blood pressure
- Dr Alia Shatnawi. 1 P a g e
 - 1 مها أبو عجمية - - - Dr Alia Shatnawi 1 P a g e A Skippable Intr0 Blood pressure normally decreases during the night. Absence of this phenomenon is called (nondipping) Wikipedia: Circadian rhythm....
- 1 مها أبو عجمية - - - Dr Alia Shatnawi 1 P a g e A Skippable Intr0 Blood pressure normally decreases during the night. Absence of this phenomenon is called (nondipping) Wikipedia: Circadian rhythm....
Heart Failure. Acute. Plasma [NE] (pg/ml) 24 Hours. Chronic
![Heart Failure. Acute. Plasma [NE] (pg/ml) 24 Hours. Chronic Heart Failure. Acute. Plasma [NE] (pg/ml) 24 Hours. Chronic](/thumbs/90/103241154.jpg) Heart Failure Heart failure is the inability of the heart to deliver sufficient blood to the tissues to ensure adequate oxygen supply. Clinically it is characterized by signs of volume overload or symptoms
Heart Failure Heart failure is the inability of the heart to deliver sufficient blood to the tissues to ensure adequate oxygen supply. Clinically it is characterized by signs of volume overload or symptoms
Means failure of heart to pump enough blood to satisfy the need of the body.
 Means failure of heart to pump enough blood to satisfy the need of the body. Due to an impaired ability of the heart to adequately to fill or eject blood. HEART FAILURE Heart failure (HF) means decreased
Means failure of heart to pump enough blood to satisfy the need of the body. Due to an impaired ability of the heart to adequately to fill or eject blood. HEART FAILURE Heart failure (HF) means decreased
Blood pressure is probably one of the most variable but
 CHAPTER 16 Alterations in Blood Pressure Control of Blood Pressure Determinants of Blood Pressure Systolic Blood Pressure Diastolic Blood Pressure Pulse Pressure Mean Arterial Pressure Mechanisms of Blood
CHAPTER 16 Alterations in Blood Pressure Control of Blood Pressure Determinants of Blood Pressure Systolic Blood Pressure Diastolic Blood Pressure Pulse Pressure Mean Arterial Pressure Mechanisms of Blood
Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions
 Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions 14.1 Physical Law Governing Blood Flow and Blood Pressure 1. How do you calculate flow rate? 2. What is the driving force of blood
Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions 14.1 Physical Law Governing Blood Flow and Blood Pressure 1. How do you calculate flow rate? 2. What is the driving force of blood
3/10/2009 VESSELS PHYSIOLOGY D.HAMMOUDI.MD. Palpated Pulse. Figure 19.11
 VESSELS PHYSIOLOGY D.HAMMOUDI.MD Palpated Pulse Figure 19.11 1 shows the common sites where the pulse is felt. 1. Temporal artery at the temple above and to the outer side of the eye 2. External maxillary
VESSELS PHYSIOLOGY D.HAMMOUDI.MD Palpated Pulse Figure 19.11 1 shows the common sites where the pulse is felt. 1. Temporal artery at the temple above and to the outer side of the eye 2. External maxillary
Blood Pressure. a change in any of these could cause a corresponding change in blood pressure
 Blood Pressure measured as mmhg Main factors affecting blood pressure: 1. cardiac output 2. peripheral resistance 3. blood volume a change in any of these could cause a corresponding change in blood pressure
Blood Pressure measured as mmhg Main factors affecting blood pressure: 1. cardiac output 2. peripheral resistance 3. blood volume a change in any of these could cause a corresponding change in blood pressure
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide
 Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Cardiac Pathophysiology
 Cardiac Pathophysiology Evaluation Components Medical history Physical examination Routine laboratory tests Optional tests Medical History Duration and classification of hypertension. Patient history of
Cardiac Pathophysiology Evaluation Components Medical history Physical examination Routine laboratory tests Optional tests Medical History Duration and classification of hypertension. Patient history of
(D) (E) (F) 6. The extrasystolic beat would produce (A) increased pulse pressure because contractility. is increased. increased
 Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Cardiovascular System. Heart
 Cardiovascular System Heart Electrocardiogram A device that records the electrical activity of the heart. Measuring the relative electrical activity of one heart cycle. A complete contraction and relaxation.
Cardiovascular System Heart Electrocardiogram A device that records the electrical activity of the heart. Measuring the relative electrical activity of one heart cycle. A complete contraction and relaxation.
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1
 BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
Heart. Large lymphatic vessels Lymph node. Lymphatic. system Arteriovenous anastomosis. (exchange vessels)
 Venous system Large veins (capacitance vessels) Small veins (capacitance vessels) Postcapillary venule Thoroughfare channel Heart Large lymphatic vessels Lymph node Lymphatic system Arteriovenous anastomosis
Venous system Large veins (capacitance vessels) Small veins (capacitance vessels) Postcapillary venule Thoroughfare channel Heart Large lymphatic vessels Lymph node Lymphatic system Arteriovenous anastomosis
Regulation of Arterial Blood Pressure 2 George D. Ford, Ph.D.
 Regulation of Arterial Blood Pressure 2 George D. Ford, Ph.D. OBJECTIVES: 1. Describe the Central Nervous System Ischemic Response. 2. Describe chemical sensitivities of arterial and cardiopulmonary chemoreceptors,
Regulation of Arterial Blood Pressure 2 George D. Ford, Ph.D. OBJECTIVES: 1. Describe the Central Nervous System Ischemic Response. 2. Describe chemical sensitivities of arterial and cardiopulmonary chemoreceptors,
REGULATION OF CARDIOVASCULAR SYSTEM
 REGULATION OF CARDIOVASCULAR SYSTEM Jonas Addae Medical Sciences, UWI REGULATION OF CARDIOVASCULAR SYSTEM Intrinsic Coupling of cardiac and vascular functions - Autoregulation of vessel diameter Extrinsic
REGULATION OF CARDIOVASCULAR SYSTEM Jonas Addae Medical Sciences, UWI REGULATION OF CARDIOVASCULAR SYSTEM Intrinsic Coupling of cardiac and vascular functions - Autoregulation of vessel diameter Extrinsic
Systemic Hypertension
 BCS Theme Session Cardiovascular Block Pathology of Hypertension Department of Pathology University of Sydney Systemic Hypertension Definition of Systemic hypertension: consistent blood pressure elevation
BCS Theme Session Cardiovascular Block Pathology of Hypertension Department of Pathology University of Sydney Systemic Hypertension Definition of Systemic hypertension: consistent blood pressure elevation
Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.
 Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction There are two basic mechanisms for regulating
Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction There are two basic mechanisms for regulating
Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D.
 Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. Why body sodium content determines ECF volume and the relationships
Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. Why body sodium content determines ECF volume and the relationships
Structure and organization of blood vessels
 The cardiovascular system Structure of the heart The cardiac cycle Structure and organization of blood vessels What is the cardiovascular system? The heart is a double pump heart arteries arterioles veins
The cardiovascular system Structure of the heart The cardiac cycle Structure and organization of blood vessels What is the cardiovascular system? The heart is a double pump heart arteries arterioles veins
HYPERTENSIVE VASCULAR DISEASE
 HYPERTENSIVE VASCULAR DISEASE Cutoffs in diagnosing hypertension in clinical practice sustained diastolic pressures >90 mm Hg, or sustained systolic pressures >140 mm Hg Malignant hypertension A small
HYPERTENSIVE VASCULAR DISEASE Cutoffs in diagnosing hypertension in clinical practice sustained diastolic pressures >90 mm Hg, or sustained systolic pressures >140 mm Hg Malignant hypertension A small
Case year old female nursing home resident with a hx CAD, PUD, recent hip fracture Transferred to ED with decreased mental status BP in ED 80/50
 Case 1 65 year old female nursing home resident with a hx CAD, PUD, recent hip fracture Transferred to ED with decreased mental status BP in ED 80/50 Case 1 65 year old female nursing home resident with
Case 1 65 year old female nursing home resident with a hx CAD, PUD, recent hip fracture Transferred to ED with decreased mental status BP in ED 80/50 Case 1 65 year old female nursing home resident with
Cardiovascular system: Blood vessels, blood flow. Latha Rajendra Kumar, MD
 Cardiovascular system: Blood vessels, blood flow Latha Rajendra Kumar, MD Outline 1- Physical laws governing blood flow and blood pressure 2- Overview of vasculature 3- Arteries 4. Capillaries and venules
Cardiovascular system: Blood vessels, blood flow Latha Rajendra Kumar, MD Outline 1- Physical laws governing blood flow and blood pressure 2- Overview of vasculature 3- Arteries 4. Capillaries and venules
Renal Regulation of Sodium and Volume. Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM
 Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
SPECIAL PATHOPHYSIOLOGY CARDIO-VASCULAR SYSTEM
 1. Myocardia lischemia is mainly a result of: 1.Coronary hypoxemia. 2. Coronary artery disease (CAD). 3. Acute coronaritis. 4. Coronary anemia. 5. Heart remodelling. SPECIAL PATHOPHYSIOLOGY CARDIO-VASCULAR
1. Myocardia lischemia is mainly a result of: 1.Coronary hypoxemia. 2. Coronary artery disease (CAD). 3. Acute coronaritis. 4. Coronary anemia. 5. Heart remodelling. SPECIAL PATHOPHYSIOLOGY CARDIO-VASCULAR
HYPERTENSION: Sustained elevation of arterial blood pressure above normal o Systolic 140 mm Hg and/or o Diastolic 90 mm Hg
 Lecture 39 Anti-Hypertensives B-Rod BLOOD PRESSURE: Systolic / Diastolic NORMAL: 120/80 Systolic = measure of pressure as heart is beating Diastolic = measure of pressure while heart is at rest between
Lecture 39 Anti-Hypertensives B-Rod BLOOD PRESSURE: Systolic / Diastolic NORMAL: 120/80 Systolic = measure of pressure as heart is beating Diastolic = measure of pressure while heart is at rest between
Hypertension Part 1. Overview of Hypertension.
 Hypertension Part 1 Overview of Hypertension http://silverchealth.com/wp-content/uploads/2012/01/hypertension1.gif Hypertension is sustained elevation of resting systolic BP ( 140 mm Hg), diastolic BP
Hypertension Part 1 Overview of Hypertension http://silverchealth.com/wp-content/uploads/2012/01/hypertension1.gif Hypertension is sustained elevation of resting systolic BP ( 140 mm Hg), diastolic BP
Weeks 1-3:Cardiovascular
 Weeks 1-3:Cardiovascular Cardiac Output The total volume of blood ejected from the ventricles in one minute is known as the cardiac output. Heart Rate (HR) X Stroke Volume (SV) = Cardiac Output Normal
Weeks 1-3:Cardiovascular Cardiac Output The total volume of blood ejected from the ventricles in one minute is known as the cardiac output. Heart Rate (HR) X Stroke Volume (SV) = Cardiac Output Normal
The Cardiovascular System. The Structure of Blood Vessels. The Structure of Blood Vessels. The Blood Vessels. Blood Vessel Review
 The Cardiovascular System The Blood Vessels The Structure of Blood Vessels Blood Vessel Review Arteries carry blood away from the heart Pulmonary trunk to lungs Aorta to everything else Microcirculation
The Cardiovascular System The Blood Vessels The Structure of Blood Vessels Blood Vessel Review Arteries carry blood away from the heart Pulmonary trunk to lungs Aorta to everything else Microcirculation
Collage of medicine Cardiovascular Physiology 3- Arterial and venous blood Pressure.
 University of Babylon Collage of medicine Dr. Ghafil Seyhood Hassan Al-Shujiari Cardiovascular Physiology 3- Arterial and venous blood Pressure. UArterial blood pressureu: Arterial pressure = COP X Peripheral
University of Babylon Collage of medicine Dr. Ghafil Seyhood Hassan Al-Shujiari Cardiovascular Physiology 3- Arterial and venous blood Pressure. UArterial blood pressureu: Arterial pressure = COP X Peripheral
1. How did occlusion of Mr. Hanna's left renal artery lead to an increase in plasma renin activity?
 76 I'HYSIOLOGY CASES AND PROBLEMS Case 14 Renovascular Hypertension: The Renin-Angiotensin-Aldosterone System Stewart Hanna is a 58-year-old partner in a real estate firm. Over the years, the pressures
76 I'HYSIOLOGY CASES AND PROBLEMS Case 14 Renovascular Hypertension: The Renin-Angiotensin-Aldosterone System Stewart Hanna is a 58-year-old partner in a real estate firm. Over the years, the pressures
Physiological Response to Hypovolemic Shock Dr Khwaja Mohammed Amir MD Assistant Professor(Physiology) Objectives At the end of the session the
 Physiological Response to Hypovolemic Shock Dr Khwaja Mohammed Amir MD Assistant Professor(Physiology) Objectives At the end of the session the students should be able to: List causes of shock including
Physiological Response to Hypovolemic Shock Dr Khwaja Mohammed Amir MD Assistant Professor(Physiology) Objectives At the end of the session the students should be able to: List causes of shock including
Properties of Pressure
 OBJECTIVES Overview Relationship between pressure and flow Understand the differences between series and parallel circuits Cardiac output and its distribution Cardiac function Control of blood pressure
OBJECTIVES Overview Relationship between pressure and flow Understand the differences between series and parallel circuits Cardiac output and its distribution Cardiac function Control of blood pressure
Role of Minerals in Hypertension
 Role of Minerals in Hypertension Lecture objectives By the end of the lecture students will be able to Define primary and secondary hypertention and their risk factors. Relate role of minerals with hypertention.
Role of Minerals in Hypertension Lecture objectives By the end of the lecture students will be able to Define primary and secondary hypertention and their risk factors. Relate role of minerals with hypertention.
I. Cardiac Output Chapter 14
 10/24/11 I. Cardiac Output Chapter 14 Cardiac Output, Blood Flow, and Blood Pressure Lecture PowerPoint Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Cardiac
10/24/11 I. Cardiac Output Chapter 14 Cardiac Output, Blood Flow, and Blood Pressure Lecture PowerPoint Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Cardiac
Chapter 10 Worksheet Blood Pressure and Antithrombotic Agents
 Complete the following. 1. A layer of cells lines each vessel in the vascular system. This layer is a passive barrier that keeps cells and proteins from going into tissues; it also contains substances
Complete the following. 1. A layer of cells lines each vessel in the vascular system. This layer is a passive barrier that keeps cells and proteins from going into tissues; it also contains substances
Heart Failure (HF) Treatment
 Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
Blood Pressure Regulation -1
 CVS Physiology Lecture 18 Blood Pressure Regulation -1 Please study the previous sheet before studying this one, even if the first part in this sheet is revision. In the previous lecture we were talking
CVS Physiology Lecture 18 Blood Pressure Regulation -1 Please study the previous sheet before studying this one, even if the first part in this sheet is revision. In the previous lecture we were talking
12/1/2009. Chapter 19: Hemorrhage. Hemorrhage and Shock Occurs when there is a disruption or leak in the vascular system Internal hemorrhage
 Chapter 19: Hemorrhage Hemorrhage and Shock Occurs when there is a disruption or leak in the vascular system External hemorrhage Internal hemorrhage Associated with higher morbidity and mortality than
Chapter 19: Hemorrhage Hemorrhage and Shock Occurs when there is a disruption or leak in the vascular system External hemorrhage Internal hemorrhage Associated with higher morbidity and mortality than
Cardiovascular System: Vessels and Circulation (Chapter 21)
 Cardiovascular System: Vessels and Circulation (Chapter 21) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Eastern Campus Primary Sources for figures and content: Marieb,
Cardiovascular System: Vessels and Circulation (Chapter 21) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Eastern Campus Primary Sources for figures and content: Marieb,
The Cardiovascular System: Vessels and Routes. Pulmonary Circulation H E A R T. Systemic Circulation
 The Cardiovascular System: Vessels and Routes 1. Overview of Blood Circulation A. Pulmonary Circulation Lung Arterioles Pulmonary Artery Capillaries Pulmonary Circulation Venules Pulmonary Veins H E A
The Cardiovascular System: Vessels and Routes 1. Overview of Blood Circulation A. Pulmonary Circulation Lung Arterioles Pulmonary Artery Capillaries Pulmonary Circulation Venules Pulmonary Veins H E A
M2 TEACHING UNDERSTANDING PHARMACOLOGY
 M2 TEACHING UNDERSTANDING PHARMACOLOGY USING CVS SYSTEM AS AN EXAMPLE NIGEL FONG 2 JAN 2014 TODAY S OBJECTIVE Pharmacology often seems like an endless list of mechanisms and side effects to memorize. To
M2 TEACHING UNDERSTANDING PHARMACOLOGY USING CVS SYSTEM AS AN EXAMPLE NIGEL FONG 2 JAN 2014 TODAY S OBJECTIVE Pharmacology often seems like an endless list of mechanisms and side effects to memorize. To
Hyperaldosteronism: Conn's Syndrome
 RENAL AND ACID-BASE PHYSIOLOGY 177 Case 31 Hyperaldosteronism: Conn's Syndrome Seymour Simon is a 54-year-old college physics professor who maintains a healthy lifestyle. He exercises regularly, doesn't
RENAL AND ACID-BASE PHYSIOLOGY 177 Case 31 Hyperaldosteronism: Conn's Syndrome Seymour Simon is a 54-year-old college physics professor who maintains a healthy lifestyle. He exercises regularly, doesn't
Mechanism: 1- waterretention from the last part of the nephron which increases blood volume, venous return EDV, stroke volume and cardiac output.
 Blood pressure regulators: 1- Short term regulation:nervous system Occurs Within secondsof the change in BP (they are short term because after a while (2-3 days) they adapt/reset the new blood pressure
Blood pressure regulators: 1- Short term regulation:nervous system Occurs Within secondsof the change in BP (they are short term because after a while (2-3 days) they adapt/reset the new blood pressure
Chapter 21 Peripheral circulation and Regulation
 Chapter 21 Peripheral circulation and Regulation I. Blood vessel structure A. Blood flows from large arteries to small capillaries 1. Large arteries contain large amounts of elastic tissue and little smooth
Chapter 21 Peripheral circulation and Regulation I. Blood vessel structure A. Blood flows from large arteries to small capillaries 1. Large arteries contain large amounts of elastic tissue and little smooth
Cardiovascular System. Blood Vessel anatomy Physiology & regulation
 Cardiovascular System Blood Vessel anatomy Physiology & regulation Path of blood flow Aorta Arteries Arterioles Capillaries Venules Veins Vena cava Vessel anatomy: 3 layers Tunica externa (adventitia):
Cardiovascular System Blood Vessel anatomy Physiology & regulation Path of blood flow Aorta Arteries Arterioles Capillaries Venules Veins Vena cava Vessel anatomy: 3 layers Tunica externa (adventitia):
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Hypovolemic Shock: Regulation of Blood Pressure
 CARDIOVASCULAR PHYSIOLOGY 81 Case 15 Hypovolemic Shock: Regulation of Blood Pressure Mavis Byrne is a 78-year-old widow who was brought to the emergency room one evening by her sister. Early in the day,
CARDIOVASCULAR PHYSIOLOGY 81 Case 15 Hypovolemic Shock: Regulation of Blood Pressure Mavis Byrne is a 78-year-old widow who was brought to the emergency room one evening by her sister. Early in the day,
CARDIOVASCULAR SYSTEM
 CARDIOVASCULAR SYSTEM 1. Resting membrane potential of the ventricular myocardium is: A. -55 to-65mv B. --65 to-75mv C. -75 to-85mv D. -85 to-95 mv E. -95 to-105mv 2. Regarding myocardial contraction:
CARDIOVASCULAR SYSTEM 1. Resting membrane potential of the ventricular myocardium is: A. -55 to-65mv B. --65 to-75mv C. -75 to-85mv D. -85 to-95 mv E. -95 to-105mv 2. Regarding myocardial contraction:
Six main classes of blood vessels (on handout) Wall structure of arteries and veins (on handout) Comparison: Arteries vs. Veins (on handout)
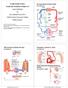 Cardiovascular System: Vessels and Circulation (Chapter 21) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Eastern Campus Six main classes of blood vessels Primary Sources
Cardiovascular System: Vessels and Circulation (Chapter 21) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Eastern Campus Six main classes of blood vessels Primary Sources
Heart Failure. Subjective SOB (shortness of breath) Peripheral edema. Orthopnea (2-3 pillows) PND (paroxysmal nocturnal dyspnea)
 Pharmacology I. Definitions A. Heart Failure (HF) Heart Failure Ezra Levy, Pharm.D. HF Results when one or both ventricles are unable to pump sufficient blood to meet the body s needs There are 2 types
Pharmacology I. Definitions A. Heart Failure (HF) Heart Failure Ezra Levy, Pharm.D. HF Results when one or both ventricles are unable to pump sufficient blood to meet the body s needs There are 2 types
Presenter: Tom Mulvey
 Slides are from Level 3 Biology Course Content Day, 7 th November 2012 Presenter: Tom Mulvey Teachers are free to use these for teaching purposes with appropriate acknowledgement Blood Pressure Ways of
Slides are from Level 3 Biology Course Content Day, 7 th November 2012 Presenter: Tom Mulvey Teachers are free to use these for teaching purposes with appropriate acknowledgement Blood Pressure Ways of
Chapter 23. Media Directory. Cardiovascular Disease (CVD) Hypertension: Classified into Three Categories
 Chapter 23 Drugs for Hypertension Slide 37 Slide 41 Media Directory Nifedipine Animation Doxazosin Animation Upper Saddle River, New Jersey 07458 All rights reserved. Cardiovascular Disease (CVD) Includes
Chapter 23 Drugs for Hypertension Slide 37 Slide 41 Media Directory Nifedipine Animation Doxazosin Animation Upper Saddle River, New Jersey 07458 All rights reserved. Cardiovascular Disease (CVD) Includes
Cardiovascular regulation. Neural and hormonal Regulation Dr Badri Paudel GMC. 1-Local factors (autoregulation) Control of Blood Flow
 Neural and hormonal Regulation Dr Badri Paudel GMC 1 Cardiovascular regulation Fa c t o r s i nvo l v e d i n t h e regulation of cardiovascular function include: 1- Autoregulation 2- Neural regulation
Neural and hormonal Regulation Dr Badri Paudel GMC 1 Cardiovascular regulation Fa c t o r s i nvo l v e d i n t h e regulation of cardiovascular function include: 1- Autoregulation 2- Neural regulation
Blood Vessels. Dr. Nabila Hamdi MD, PhD
 Blood Vessels Dr. Nabila Hamdi MD, PhD ILOs Understand the structure and function of blood vessels. Discuss the different mechanisms of blood pressure regulation. Compare and contrast the following types
Blood Vessels Dr. Nabila Hamdi MD, PhD ILOs Understand the structure and function of blood vessels. Discuss the different mechanisms of blood pressure regulation. Compare and contrast the following types
TOPIC : Cardiogenic Shock
 University of Ferrara Department of Morphology, Surgery and Experimental Medicine. Section of Anaesthesia and Intensive Care Medicine TOPIC : Cardiogenic Shock What is shock? Shock is a condition of inadequate
University of Ferrara Department of Morphology, Surgery and Experimental Medicine. Section of Anaesthesia and Intensive Care Medicine TOPIC : Cardiogenic Shock What is shock? Shock is a condition of inadequate
Pathology of Hypertension
 2016-03-07 Pathology of Hypertension Honghe Zhang honghezhang@zju.edu.cn Tel:88208199 Department of Pathology ❶ Genetic predisposition ❷ Dietary factors ❸ Environmental factors ❹ Others Definition and
2016-03-07 Pathology of Hypertension Honghe Zhang honghezhang@zju.edu.cn Tel:88208199 Department of Pathology ❶ Genetic predisposition ❷ Dietary factors ❸ Environmental factors ❹ Others Definition and
Chapter 24 Vital Signs. Copyright 2011 Wolters Kluwer Health Lippincott Williams & Wilkins
 Chapter 24 Vital Signs Vital Signs Temperature Pulse Respiration Blood pressure When to Assess Vital Signs Upon admission to any healthcare agency Based on agency institutional policy and procedures Anytime
Chapter 24 Vital Signs Vital Signs Temperature Pulse Respiration Blood pressure When to Assess Vital Signs Upon admission to any healthcare agency Based on agency institutional policy and procedures Anytime
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,100 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,100 116,000 120M Open access books available International authors and editors Downloads Our
SPECIAL PATHOPHYSIOLOGY SHOCK
 SPECIAL PATHOPHYSIOLOGY SHOCK 1. How do we call blood pressure values below the reference range? 1.Hypovolemia. 2. Hypothermia. 3. Hypooncia. 4. Hypoosmia. 5. Hypotension. 2. What is acute circulatory
SPECIAL PATHOPHYSIOLOGY SHOCK 1. How do we call blood pressure values below the reference range? 1.Hypovolemia. 2. Hypothermia. 3. Hypooncia. 4. Hypoosmia. 5. Hypotension. 2. What is acute circulatory
Definition of Congestive Heart Failure
 Heart Failure Definition of Congestive Heart Failure A clinical syndrome of signs & symptoms resulting from the heart s inability to supply adequate tissue perfusion. CHF Epidemiology Affects 4.7 million
Heart Failure Definition of Congestive Heart Failure A clinical syndrome of signs & symptoms resulting from the heart s inability to supply adequate tissue perfusion. CHF Epidemiology Affects 4.7 million
The Urinary System 15PART B. PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Urinary System 15PART B Ureters Slender tubes attaching the kidney to the bladder Continuous with
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Urinary System 15PART B Ureters Slender tubes attaching the kidney to the bladder Continuous with
Definition. Emergency Treatment 11/13/13. Pathophysiology of circulatory shock. Characteristics of circulatory shock. Clinical features of shock
 Definition Pathophysiology of circulatory shock! Inadequate perfusion (oxygen supply) of tissues, resulting in:! Organ dysfunction! Cellular and organ damage And if not quickly corrected! Death Dr Badri
Definition Pathophysiology of circulatory shock! Inadequate perfusion (oxygen supply) of tissues, resulting in:! Organ dysfunction! Cellular and organ damage And if not quickly corrected! Death Dr Badri
SHOCK AETIOLOGY OF SHOCK (1) Inadequate circulating blood volume ) Loss of Autonomic control of the vasculature (3) Impaired cardiac function
 SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1
 BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
Hypertension. Penny Mosley MRPharmS
 Hypertension Penny Mosley MRPharmS Outline of presentation Introduction to hypertension Physiological control of arterial blood pressure What determines our bp? What determines the heart rate? What determines
Hypertension Penny Mosley MRPharmS Outline of presentation Introduction to hypertension Physiological control of arterial blood pressure What determines our bp? What determines the heart rate? What determines
Blood Pressure and its Regulation
 Blood Pressure and its Regulation Blood pressure in your blood vessels is closely monitored by baroreceptors; they send messages to the cardio regulatory center of your medulla oblongata to regulate your
Blood Pressure and its Regulation Blood pressure in your blood vessels is closely monitored by baroreceptors; they send messages to the cardio regulatory center of your medulla oblongata to regulate your
Towards a Greater Understanding of Cardiac Medications Foundational Cardiac Concepts That Must Be Understood:
 Towards a Greater Understanding of Cardiac Medications Foundational Cardiac Concepts That Must Be Understood: Cardiac Output (CO) CO=SVxHR (stroke volume x heart rate) Cardiac output: The amount of blood
Towards a Greater Understanding of Cardiac Medications Foundational Cardiac Concepts That Must Be Understood: Cardiac Output (CO) CO=SVxHR (stroke volume x heart rate) Cardiac output: The amount of blood
HEART FAILURE PHARMACOLOGY. University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D
 HEART FAILURE PHARMACOLOGY University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D 1 LEARNING OBJECTIVES Understand the effects of heart failure in the body
HEART FAILURE PHARMACOLOGY University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D 1 LEARNING OBJECTIVES Understand the effects of heart failure in the body
Cardiorenal and Renocardiac Syndrome
 And Renocardiac Syndrome A Vicious Cycle Cardiorenal and Renocardiac Syndrome Type 1 (acute) Acute HF results in acute kidney injury Type 2 Chronic cardiac dysfunction (eg, chronic HF) causes progressive
And Renocardiac Syndrome A Vicious Cycle Cardiorenal and Renocardiac Syndrome Type 1 (acute) Acute HF results in acute kidney injury Type 2 Chronic cardiac dysfunction (eg, chronic HF) causes progressive
Questions? Homework due in lab 6. PreLab #6 HW 15 & 16 (follow directions, 6 points!)
 Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
The Cardiovascular system: physiology of circulation
 Chapter 21 The Cardiovascular system: physiology of circulation blood vessel structure and function physiology of circulation: blood flow, blood pressure, and resistance blood flow the amount of blood
Chapter 21 The Cardiovascular system: physiology of circulation blood vessel structure and function physiology of circulation: blood flow, blood pressure, and resistance blood flow the amount of blood
Vasodilation. Autoregulation ป จจ ยท ควบค มขนาดของหลอดเล อด. CO 2, H +, K +, lactate, adenosine osmolarity, temperature O 2
 Regulation in cardiovascular system Local control/autoregulation of organs (brain and heart have higher priority) To provide adequate blood flow to tissue Central regulation To provide optimal blood pressure
Regulation in cardiovascular system Local control/autoregulation of organs (brain and heart have higher priority) To provide adequate blood flow to tissue Central regulation To provide optimal blood pressure
BIOL 219 Spring Chapters 14&15 Cardiovascular System
 1 BIOL 219 Spring 2013 Chapters 14&15 Cardiovascular System Outline: Components of the CV system Heart anatomy Layers of the heart wall Pericardium Heart chambers, valves, blood vessels, septum Atrioventricular
1 BIOL 219 Spring 2013 Chapters 14&15 Cardiovascular System Outline: Components of the CV system Heart anatomy Layers of the heart wall Pericardium Heart chambers, valves, blood vessels, septum Atrioventricular
Pharmacology - Problem Drill 11: Vasoactive Agents
 Pharmacology - Problem Drill 11: Vasoactive Agents Question No. 1 of 10 1. Vascular smooth muscle contraction is triggered by a rise in. Question #01 (A) Luminal calcium (B) Extracellular calcium (C) Intracellular
Pharmacology - Problem Drill 11: Vasoactive Agents Question No. 1 of 10 1. Vascular smooth muscle contraction is triggered by a rise in. Question #01 (A) Luminal calcium (B) Extracellular calcium (C) Intracellular
In the name of GOD. Animal models of cardiovascular diseases: myocardial infarction & hypertension
 In the name of GOD Animal models of cardiovascular diseases: myocardial infarction & hypertension 44 Presentation outline: Cardiovascular diseases Acute myocardial infarction Animal models for myocardial
In the name of GOD Animal models of cardiovascular diseases: myocardial infarction & hypertension 44 Presentation outline: Cardiovascular diseases Acute myocardial infarction Animal models for myocardial
SHOCK. Pathophysiology
 SHOCK Dr. Ahmed Saleem FICMS TUCOM / 3rd Year / 2015 Shock is the most common and therefore the most important cause of death of surgical patients. Death may occur rapidly due to a profound state of shock,
SHOCK Dr. Ahmed Saleem FICMS TUCOM / 3rd Year / 2015 Shock is the most common and therefore the most important cause of death of surgical patients. Death may occur rapidly due to a profound state of shock,
Year 2004 Paper two: Questions supplied by Megan 1
 Year 2004 Paper two: Questions supplied by Megan 1 QUESTION 96 A 32yo woman if found to have high blood pressure (180/105mmHg) at an insurance medical examination. She is asymptomatic. Clinical examination
Year 2004 Paper two: Questions supplied by Megan 1 QUESTION 96 A 32yo woman if found to have high blood pressure (180/105mmHg) at an insurance medical examination. She is asymptomatic. Clinical examination
Copyright 2011, 2007 by Mosby, Inc., an affiliate of Elsevier Inc. Normal Cardiac Anatomy
 Mosby,, an affiliate of Elsevier Normal Cardiac Anatomy Impaired cardiac pumping Results in vasoconstriction & fluid retention Characterized by ventricular dysfunction, reduced exercise tolerance, diminished
Mosby,, an affiliate of Elsevier Normal Cardiac Anatomy Impaired cardiac pumping Results in vasoconstriction & fluid retention Characterized by ventricular dysfunction, reduced exercise tolerance, diminished
BUSINESS. Articles? Grades Midterm Review session
 BUSINESS Articles? Grades Midterm Review session REVIEW Cardiac cells Myogenic cells Properties of contractile cells CONDUCTION SYSTEM OF THE HEART Conduction pathway SA node (pacemaker) atrial depolarization
BUSINESS Articles? Grades Midterm Review session REVIEW Cardiac cells Myogenic cells Properties of contractile cells CONDUCTION SYSTEM OF THE HEART Conduction pathway SA node (pacemaker) atrial depolarization
Sunday, July 17, 2011 URINARY SYSTEM
 URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
Cardiac Output (C.O.) Regulation of Cardiac Output
 Cardiac Output (C.O.) Is the volume of the blood pumped by each ventricle per minute (5 Litre) Stroke volume: Is the volume of the blood pumped by each ventricle per beat. Stroke volume = End diastolic
Cardiac Output (C.O.) Is the volume of the blood pumped by each ventricle per minute (5 Litre) Stroke volume: Is the volume of the blood pumped by each ventricle per beat. Stroke volume = End diastolic
SYMPATHETIC STRESSORS AND SYMPATHETIC FAILURES
 SYMPATHETIC STRESSORS AND SYMPATHETIC FAILURES Any discussion of sympathetic involvement in circulation, and vasodilation, and vasoconstriction requires an understanding that there is no such thing as
SYMPATHETIC STRESSORS AND SYMPATHETIC FAILURES Any discussion of sympathetic involvement in circulation, and vasodilation, and vasoconstriction requires an understanding that there is no such thing as
1. Antihypertensive agents 2. Vasodilators & treatment of angina 3. Drugs used in heart failure 4. Drugs used in arrhythmias
 1. Antihypertensive agents 2. Vasodilators & treatment of angina 3. Drugs used in heart failure 4. Drugs used in arrhythmias Only need to know drugs discussed in class At the end of this section you should
1. Antihypertensive agents 2. Vasodilators & treatment of angina 3. Drugs used in heart failure 4. Drugs used in arrhythmias Only need to know drugs discussed in class At the end of this section you should
