INFARCTION WITH SYSTEMIC HYPERTENSION
|
|
|
- Warren Pitts
- 5 years ago
- Views:
Transcription
1 Br. J. clin. Pharmac. (1979), 8, 233S-238S LABTALOL INFUSION IN ACUT YOCARDIAL INFARCTION WITH SYSTIC HYPRTNSION P.G. ARX & D.S. RID Regional Cardiothoracic Centre, Freeman Hospital, Freeman Road, Newcastle upon Tyne N7 7DN, UK 1 Fifteen patients with suspected acute myocardial infarction and systemic BP of greater than 16/11 mmhg were treated with an incremental infusion of. 2 Systemic BPs were safely and effectively lowered to less than 13 mmhg systolic or 9 mmhg diastolic in all patients. 3 Heart rate, mean pulmonary artery wedge pressure cardiac index and stroke work index were significantly reduced. 4 The dose of varied from 3 mg-44 mg and was significantly higher (mean 295 mg) in those patients with pre-existing systemic hypertension compared with others (mean 133 mg). 5 No side-effects occurred and all patients survived ito leave hospital. Introduction YOCARDIAL infarction complicated by systemic hypertension has been associated with a higher incidence of left ventricular failure, major arrhythmia and hospital death (Fox et al., 1975; Rosenbaum & Levine, 1941). The improved coronary perfusion resulting from raised systemic BP in this situation probably does not compensate for the increased myocardial oxygen consumption occasioned by elevated afterload, with consequent impairment of myocardial function. High serum catecholamine levels are found in myocardial infarction (Siggers et al., 1971) which makes adrenoceptor blockade an attractive approach to lowering systemic BP. However, ac-adrenoceptor blockade with phentolamine in these circumstances is relatively ineffective in reducing systemic BP in those patients with pre-existing hypertension and, moreover, while satisfactorily lowering left ventricular end diastolic BP, increases heart rate and can worsen myocardial ischaemia (Kelly et al., 1973). p- adrenoceptor blockade on the other hand lowers systemic BP and heart rate, but may elevate left ventricular filling pressure (Peter et al., 1978). The combination of a- and f3-adrenoceptor blockade produced by may combine the benefits of the individual approaches, namely, lowering systemic BP, heart rate and left ventricular filling BP, the major determinants of myocardial oxygen consumption (Braunwald, 1969). The purpose of this study was to determine a suitable infusion regimen for in hypertensive infarction and to observe its haemodynamic effects /79/ $1. ethods Patients were admitted to the study if they had a history and/or 12 lead electrocardiogram (CG) suggestive of acute myocardial infarction, and systemic BPs either greater than 16 mmhg systolic or greater than 11 mmhg diastolic, persisting for 2 h after adequate analgesia. Patients were excluded if they: were over 7 yr of age; had chronic airways disease; had bradycardia of less than 6 beats/min; had X-ray evidence of severe left ventricular failure; or had taken 1 adrenoceptorblocking drugs within the previous 48 hours. All patients gave informed consent, and the studies were carried out in the coronary care unit. Daily 12 lead electrocardiogram and SGOT assays were carried out for at least three consecutive days, and WHO criteria were used for infarct diagnosis (World Health Organization, 1959). The CG was continuously displayed and the heart rate determined from a recording of ten consecutive beats. A 12 lead CG was taken before and on completion of infusion, with the chest lead positions marked by an indelible pen. Systemic BP was measured using a sphygmomanometer cuff. Further haemodynamic measurements were made in seven patients (9-15). A thermistor tipped Swan-Ganz catheter was inserted by way of the brachio-cephalic or an antecubital vein and advanced to a pulmonary artery. If the mean occluded pulmonary arterial BP was the same as pulmonary arterial diastolic BP, the catheter tip was withdrawn to a more central position, and the latter BP used to represent left ventricular end diastolic BP acmillan Journals Ltd 1979
2 234S P.G. ARX & D.S. RID (Bauchard et al., 1971). The catheters permitted simultaneous recording of right atrial pressure. Using Bruch transducers, pulmonary arterial and right atrial pressures were continuously displayed on an S & W oscilloscope. Cardiac output determinations were made using a Cardiovascular Instruments CV 6 cardiac output computer, initially using hand injections of 5% dextrose, but latterly using an OP thermodilution injector and 5% dextrose cooled in iced water. The mean of three injections was used for these determinations. The observations recorded were: heart rate and systemic BP; and in those patients with Swan-Ganz catheters: cardiac output, and pulmonary arterial and right atrial pressures. Two sets of observations were taken 15 min apart before infusion, and subsequently observations were recorded every 3 min during infusion. For the first six patients, this was commenced at 1 mg/h with increments every 3 min of 1 mg/hour. For patients 7-15 an initial rate of 3 mg/h with increments of 3 mg/h every 3 min was used. The infusion was continued for 3 min after the systemic systolic BP fell to less than 13 mmhg or the diastolic to less than 9 minhg. If at any time the systemic BP fell to less than 12 mmhg or 8 mmhg diastolic, the infusion was stopped at once. Calculations ean arterial pressure (AP, mmhg) = systemic diastolic + 1/3 (systemic systolic-systemic diastolic) (Yang et al., 1971). Cardiac index (CI: 1/min 1 m2)= (cardiac output/body surface area). Stroke index (SI; mi 1m2) = (CI/heart rate). Stroke work index (SWI; g- m) = (AP-LVDP) x SI x.136, where LVDP = left ventricular end diastolic BP. Observations before and after were compared using the paired t test. Results Fifteen patients were admitted to the study between 8-22 h after the onset of major symptoms. There were eleven men and four women with a mean age of 54 yr (range yr). Thirteen were found to have had myocardial infarction (nine anterior, four inferior) and two were considered to have unstable angina. Five patients had previously diagnosed systemic hypertension, the SGOT peak in these patients being no different from the others (Table 1). Results and dosage are summarized in Table 2. Observations shown were taken immediately before infusion and at the time of cessation. In all cases a satisfactory fall in systemic BP was obtained, the mean fall in systolic BP being 34% (P <.1) and the diastolic BP 29% (P <.1) (Figure 1). In none of the patients did BP fall below 1 mmhg systolic. All patients were in sinus rhythm before and remained in sinus rhythm throughout infusion and during the remainder of their hospital admission. During infusion, heart rate fell in most patients (mean 15%), the fall being significant (P <.5) (Figure 2). Two patients (4 and 5) experienced sinus bradycardia of 54 and 57 beats/min respectively at the end of infusion. ean CI fell by 15% (P <.5) which was primarily due to the Table 1 Patient details Patient Number ean s.d. Age (yr) Sex F F FF SGOT upper limit of normal 37 IU/I Diagnosis Inferior l Antero-lateral I Antero-lateral l Anterior I Unstable angina Anterior l Unstable angina Antero-lateral l Anterior l Interior l Anterior I Inferior l Anterior I Antero-septal l Antero-lateral I Pre-existing hypertension aximum SGOT
3 ACUT YOCARDIAL INFARCTION 235S ) X.2 -O ~~~~ejc)e) _ C) b( LO Lo L Cb N ( X. ( V) Q w- a) N a)cloc - LO)I4C%JtL6 Q. U -, c~~~~jc LnO anlo cv 6 )4- Q~~~~~~~~ R*cN csno- a_o <* b C)~*J)CO c V ) C D O CD C -),r-- CD -it CO ( D t LO --o D. Q. b.. O oos D-.OOoo)Oa) tcd V D ).C. QC Q *2 C C - CO -Or r-u- W -V O r.c 5c n X C)Ln r- CD L r%\cn LO CD r D C LO - - o o CD,,, 1 o q Q CJ) _) c CD I-I q- ) QL- C )~~~~~~~~~~~~~ OQ. Q) '4_1O- ON O'1 SOSOOO o * cx ) i.ooo)oc C C N C ) Q -o ) )~~~~~~~~~~~~~~ Co...J C V :5 )~~~~~~~~~~~~~~ ~~ ~~ f~~coo)lfl~~~~~~c ):..- Co~~~~~~~~~~~~~~~c CU~~~~~~~~~~~~~~~~~~c
4 236S P.G. ARX & D.S. RID I. cn 15 - The dose of used ranged from 3 to 44 mg (mean 187 mg). There was a significant (p <.5) difference between the doses required by the previously diagnosed hypertensive patients (mean 295 mg) and the others (mean 133 mg). In nine patients, systemic BP began to increase after discontinuing. This increase occurred after about 9 min, and was successfully reduced by further infusion in four cases, the infusion being continued for up to 12 hours. The 12 lead CG changes were variable. In no patient was further ST segment elevation observed during infusion and in seven there was lowering of the ST segments. Patient 13 experienced a second increase in systemic BP peaking at 2/11 mmhg 6 hours after discontinuing. This was associated with chest pain, an increase in the ST segments and second SGOT peak, suggesting extension of the myocardial infarction. No side-effects occurred and no patient ex i- 5 - c 4-3 x 'a2 c u O 1 Pre Post x ) 'a) c 2 C,, Pre Post Figure 3 Individual Cl and SI responses to infusion. ean Cl fall 2.6 to 2.2 I/min/m2 (P <.5). ean SI fall 32 to 3 ml/m2 (NS). 5L Pre Post Figure 1 Individual systolic and diastolic BP responses to infusion. ean systolic fall 184 to 122 mmhg (P<.1). ean diastolic fall 118 to 84 mmhg (P<.1)., Systemic BP; *, diastolic BP. ). 1 5 en a). ) I 13 r o 1 9o 81-7 F 61 5 L Pre Post Figure 2 Individual heart rate response to infusion. ean fall 85 to 72 beats/min (P<.5). fall in heart rate rather than the fall in SI (mean 6%) (Figure 3). Labetalol infusion resulted in a significant fall in LVDP (p <.1). In the five patients in whom it was elevated on admission to the study there was a marked fall, whereas in the remaining two patients with initially normal end diastolic BPs little change occurred (Figure 4). The mean fall of 36% (p <.1) in the SWI largely reflected the fall in the mean arterial pressure. 4-e 2 us ean pulmonary artery wedge pressure (mmhg) Figure 4 Individual mean pulmonary arterial wedge or pulmonary artery diastolic pressure (PAW/PAD) and SWI responses to. ean PAW/PAD fall 17.1 to 11.1 mmhg (P<.1). ean SWI fall 59 to 37 g/m (P<.1).
5 ACUT YOCARDIAL INFARCTION 237S perienced chest pain during infusion. All 15 patients survived and were discharged from hospital. Discussion The advantages of treating myocardial infarction with systemic hypertension, a situation associated with high serum catecholamine levels, by adrenoceptor blockade, were not apparent in a previously described (Kelly et al., 1973) intervention using phentolamine-mediated oa-adrenoceptor blockade. In their study of 11 patients with mean systemic BP greater than 11 mmhg, BP reduction was variable with less satisfactory results in patients with preexisting hypertension. Reduction in LVDP was good (mean 19.9 mmhg), but reflex tachycardia occurred and in two patients recurrence of chest pain necessitated withdrawal of the drug. The use of,badrenoceptor blockade with propranolol has been advocated, and reduction in heart rate and systemic BP have been satisfactory. However, LVDP has been adversely affected, requiring diuretic therapy and even subsequent aortic balloon counterpulsation (Peter et al., 1978). Similarly, problems have been encountered with other pharmacological agents. Nitroprusside infusion (Chiariello et al., 1976) in hypertensive acute infarction lowered systemic BP, but heart rate increased and further ST elevation occurred. A further study (O'Brien et al., 1975) using diazoxide in 2 infarct patients with systemic BPs greater than 18/11 mmhg resulted in increased ST elevation and chest pain in several. On the other hand, it has been shown in a study in 14 patients with systemic BPs of greater than 14/9 mmhg and acute myocardial infarction, BP reduction by trimethaphen resulted in a reduction of infarct size, as predicted from serum creatine kinase (CK) estimations (Shell & Sobel, 1974). However, it has been suggested that the observed CK release would have been lowered by the reduction in coronary filling pressure alone, and therefore does not necessarily reflect myocradial preservation. Furthermore, the timing of the intervention, a minimum of 7 h after hospital admission, would render infarction reduction less probable (aroko et al., 1978). No patients in our study demonstrated further ST elevation during infusion. In several the ST segments fell. However, as this happened over periods of up to 6 h, inference is difficult in view of the natural history of ST changes in acute infarction. In our series, reduced the main determinants of myocardial oxygen consumption, namely heart rate, left ventricular filling pressure and systemic BP. Although this intervention may have occurred at a stage at which reduction of infarct size may no longer have been possible, myocardial performance should have been enhanced and this may account for the lower morbidity and absent mortality compared with previously studied hypertensive acute infarct patients (Fox et al., 1975; Rosenbaum & Levine, 1941). The optimum level to which systemic BP should be reduced in myocardial infarction is not known, and similarly neither is the optimum LVDP. It may be that these parameters should be considered together rather than in isolation in the management of these patients. We view our work as a pilot study. This has shown that incremental infusion is a safe, practical and effective method of lowering systemic BP in myocardial infarction. A further randomized study will be required to establish the validity of the lower morbidity and mortality (absent) in our small group of patients compared with the studies of the natural history of acute myocardial infarction complicated by systemic hypertension. We thank the physicians, nurses and technical staff of the Freeman Hospital Coronary Care Unit for their invaluable assistance, and iss Tina Farrance for secretarial assistance. References BOUCHARD, R.J., GWILT, J.H. & ROSS, J., Jr. (1971). valuation of pulmonary arterial end diastolic pressure as an estimate of left ventricular diastolic pressure in patients with normal and abnormal left ventricular performance. Circulation, 44, BRAUNWALD,. (1969). The determinants of myocardial oxygen consumption. Physiologist, 12, CHIARILLO,., GOLD, H.K., LINBACK, R.C., DAVIS,.A. & AROKO, P.R. (1976). Comparison between the effects of nitroprusside and nitroglycerin on ischaemic injury during acute myocardial infarction. Circulation, 54, FOX, K.., TOLINSON, I.W., PORTAL, R.W. & ABR, C.P. (1975). Prognostic significance of acute systolic hypertension after myocardial infarction. Br. med. J., 3, KLLY, D.T., DLGADO, C.., TAYLOR, D.R., PITT, B. & ROSS, R.S. (1973). Use of phentolamine in acute myocardial infarction associated with hypertension and left ventricular failure. Circulation, 47, AROKO, P.R., KLONR, R.A., YASUDA, T.,,-RBIRO, L.G.T., ACLAN, D. & BRAUNWALD,. (1978). Recent investigations on attempts to limit infarct size. Proc. Astra Conf. "Acute and long term medical managementof myocardial ischaemia". Pp Sweeden: Astra Pharmaceuticals AB.
6 238S P.G. ARX & D.S. RID O'BRIN, K.P., GRIGOR, R.R. & TAYLOR, P.. (1975). Intravenous diazoxide in treatment of hypertension associated with recent myocardial infarction. Br. med. J., 4, PTR, T., NORRIS, R.., CLARK.D., HNG, H.K., SINGH, B.N., WILLIAS, B., HOWLL, D.R. & ABLR, P.K. (1978). Reduction of enzyme levels by propranolol after acute myocardial infarction. Circulation, 57, ROSNBAU, F.F. & LVIN, S.A. (1941). Prognostic value of various clinical and electrocardiographic features of acute myocardial infarction. Arch. intern. ed., 68, SHLL, W.. & SOBL, B.. (1974). Protection ofjeopardised ischaemic myocardium by reduction of ventricular afterload. New ngl. J. ed., 291, SIGGRS, D.C., SALTR, C. & FLUCK, D.C. (1971). Serial plasma adrenaline and noradrenaline levels in myocardial infarction using a new double isotope technique. Br. Heart J., 33, WORLD HALTH ORGANIZATION. (1959). Hypertension and coronary heart disease. WHO Technical Report Series, 168, 199. YANG, S.S., BONTIVOLGLIO, L.G., ARANKAO, V. & GOLDBRG, H. (1972). In 'From Cardiac Catheterisation Data to Haemodynamic Parameters'. P. 9. Philadelphia: F.A. Davies.
FAILURE IN PATIENTS WITH MYOCARDIAL INFARCTION
 Br. J. clin. Pharmac. (1982), 14, 187S-19lS BENEFICIAL EFFECTS OF CAPTOPRIL IN LEFT VENTRICULAR FAILURE IN PATIENTS WITH MYOCARDIAL INFARCTION J.P. BOUNHOURE, J.G. KAYANAKIS, J.M. FAUVEL & J. PUEL Departments
Br. J. clin. Pharmac. (1982), 14, 187S-19lS BENEFICIAL EFFECTS OF CAPTOPRIL IN LEFT VENTRICULAR FAILURE IN PATIENTS WITH MYOCARDIAL INFARCTION J.P. BOUNHOURE, J.G. KAYANAKIS, J.M. FAUVEL & J. PUEL Departments
Role of sublingual nitroglycerin in patients with
 British Heart Journal, I975, 37, 392-396. Role of sublingual nitroglycerin in patients with acute myocardial infarction1 Cesar E. Delgado,2 Bertram Pitt, Dean R. Taylor, Myron L. Weisfeldt, and David T.
British Heart Journal, I975, 37, 392-396. Role of sublingual nitroglycerin in patients with acute myocardial infarction1 Cesar E. Delgado,2 Bertram Pitt, Dean R. Taylor, Myron L. Weisfeldt, and David T.
OPEN EVALUATION OF LABETALOL IN THE TREATMENT OF ANGINA PECTORIS OCCURRING IN HYPERTENSIVE PATIENTS
 Br. J. clin. Pharmac. (1979), 8, 25S-29S OPN VALUATION OF LABTALOL IN TH TRATMNT OF ANGINA PTORIS ORRING IN HYPRTIV PATINTS.M.M. BSTRMAN & M. SPNR ardiological Department, St Mary's Hospital, Norfolk Place,
Br. J. clin. Pharmac. (1979), 8, 25S-29S OPN VALUATION OF LABTALOL IN TH TRATMNT OF ANGINA PTORIS ORRING IN HYPRTIV PATINTS.M.M. BSTRMAN & M. SPNR ardiological Department, St Mary's Hospital, Norfolk Place,
Central haemodynamics during spontaneous angina pectoris
 British Heart Journal, I974, 36, I0-I09I Central haemodynamics during spontaneous angina pectoris From the Department of Clinical Physiology, Malmo General Hospital, S-214 OI Malmo, Sweden. Central pressures
British Heart Journal, I974, 36, I0-I09I Central haemodynamics during spontaneous angina pectoris From the Department of Clinical Physiology, Malmo General Hospital, S-214 OI Malmo, Sweden. Central pressures
Effects of felodipine on haemodynamics and exercise capacity in patients with angina pectoris
 Br. J. clin. Pharmac. (1987), 23, 391-396 Effects of felodipine on haemodynamics and exercise capacity in patients with angina pectoris J. V. SHERIDAN, P. THOMAS, P. A. ROUTLEDGE & D. J. SHERIDAN Departments
Br. J. clin. Pharmac. (1987), 23, 391-396 Effects of felodipine on haemodynamics and exercise capacity in patients with angina pectoris J. V. SHERIDAN, P. THOMAS, P. A. ROUTLEDGE & D. J. SHERIDAN Departments
Evaluation of haemodynamic effects of intravenous propranolol at low dosage (i and 2 mg) in acute
 British Heart3Journal, I975, 37, 624-628. Evaluation of haemodynamic effects of intravenous propranolol at low dosage (i and 2 mg) in acute myocardial infarction B. Letac and J. Letournel From the Service
British Heart3Journal, I975, 37, 624-628. Evaluation of haemodynamic effects of intravenous propranolol at low dosage (i and 2 mg) in acute myocardial infarction B. Letac and J. Letournel From the Service
ST SEGMENT IN LEAD A VR IN ACUTE INFERIOR MYOCARDIAL INFARCTION
 ST SEGMENT IN LEAD A VR IN ACUTE INFERIOR MYOCARDIAL INFARCTION Pages with reference to book, From 365 To 366 Shehbaz A. Kureshi, Yoshiharu Yonekura, Yutaka Konishi, Kanji Torizuka ( Kyoto University School
ST SEGMENT IN LEAD A VR IN ACUTE INFERIOR MYOCARDIAL INFARCTION Pages with reference to book, From 365 To 366 Shehbaz A. Kureshi, Yoshiharu Yonekura, Yutaka Konishi, Kanji Torizuka ( Kyoto University School
Common Codes for ICD-10
 Common Codes for ICD-10 Specialty: Cardiology *Always utilize more specific codes first. ABNORMALITIES OF HEART RHYTHM ICD-9-CM Codes: 427.81, 427.89, 785.0, 785.1, 785.3 R00.0 Tachycardia, unspecified
Common Codes for ICD-10 Specialty: Cardiology *Always utilize more specific codes first. ABNORMALITIES OF HEART RHYTHM ICD-9-CM Codes: 427.81, 427.89, 785.0, 785.1, 785.3 R00.0 Tachycardia, unspecified
Role of right ventricular infarction in cardiogenic shock
 British Heart Journal, 1979, 42, 719-725 Role of right ventricular infarction in cardiogenic shock associated with inferior myocardial infarction1 HENRY GEWIRTZ,2 HERMAN K. GOLD, JOHN T. FALLON, RICHARD
British Heart Journal, 1979, 42, 719-725 Role of right ventricular infarction in cardiogenic shock associated with inferior myocardial infarction1 HENRY GEWIRTZ,2 HERMAN K. GOLD, JOHN T. FALLON, RICHARD
Medical Management of Acute Heart Failure
 Critical Care Medicine and Trauma Medical Management of Acute Heart Failure Mary O. Gray, MD, FAHA Associate Professor of Medicine University of California, San Francisco Staff Cardiologist and Training
Critical Care Medicine and Trauma Medical Management of Acute Heart Failure Mary O. Gray, MD, FAHA Associate Professor of Medicine University of California, San Francisco Staff Cardiologist and Training
Medicine Dr. Omed Lecture 2 Stable and Unstable Angina
 Medicine Dr. Omed Lecture 2 Stable and Unstable Angina Risk stratification in stable angina. High Risk; *post infarct angina, *poor effort tolerance, *ischemia at low workload, *left main or three vessel
Medicine Dr. Omed Lecture 2 Stable and Unstable Angina Risk stratification in stable angina. High Risk; *post infarct angina, *poor effort tolerance, *ischemia at low workload, *left main or three vessel
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Nitroglycerin and Heparin Drip Interfacility Protocols
 Nitroglycerin and Heparin Drip Interfacility Protocols EMS Protocol This protocol applies to nitroglycerin and Heparin drips that are initiated at the transferring facility prior to transport and are not
Nitroglycerin and Heparin Drip Interfacility Protocols EMS Protocol This protocol applies to nitroglycerin and Heparin drips that are initiated at the transferring facility prior to transport and are not
is Prevented by Atropine
 Brit. Heart J., 1969, 31, 67. Action of Propranolol on Left Ventricular Contraction in Aortic Stenosis When a Fall in Heart Rate is Prevented by Atropine JOHN HAMER AND JAMES FLEMING From the Department
Brit. Heart J., 1969, 31, 67. Action of Propranolol on Left Ventricular Contraction in Aortic Stenosis When a Fall in Heart Rate is Prevented by Atropine JOHN HAMER AND JAMES FLEMING From the Department
Evaluation of pacing for heart block
 British Heart Journal, I97I, 33, 120-I24. Evaluation of pacing for heart block in myocardial infarction C. C. Watson and M. J. Goldberg From Leicester Regional Cardiothoracic Unit, Groby Road Hospital,
British Heart Journal, I97I, 33, 120-I24. Evaluation of pacing for heart block in myocardial infarction C. C. Watson and M. J. Goldberg From Leicester Regional Cardiothoracic Unit, Groby Road Hospital,
Takotsubo Cardiomyopathy
 Advances in Heart Disease 2008 Takotsubo Cardiomyopathy Mary O. Gray, MD, FAHA, FACC Associate Professor of Medicine University of California, San Francisco Staff Cardiologist and Training Faculty Divisions
Advances in Heart Disease 2008 Takotsubo Cardiomyopathy Mary O. Gray, MD, FAHA, FACC Associate Professor of Medicine University of California, San Francisco Staff Cardiologist and Training Faculty Divisions
Heart failure hospitalizations with preserved or reduced ejection fraction
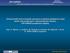 Clinical profile and in-hospital outcomes in patients admitted for heart failure with preserved or reduced ejection fraction. EPI-CARDIO prospective registry Tajer, C; Mariani, J; de Abreu, M; Charask,
Clinical profile and in-hospital outcomes in patients admitted for heart failure with preserved or reduced ejection fraction. EPI-CARDIO prospective registry Tajer, C; Mariani, J; de Abreu, M; Charask,
complicating myocardial infarction
 British Heart Journal, I970, 32, 21. Bretylium tosylate in treatment of refractory ventricular arrhythmias complicating myocardial infarction G. Terry,1 C. W. Vellani, M. R. Higgins, and A. Doig From the
British Heart Journal, I970, 32, 21. Bretylium tosylate in treatment of refractory ventricular arrhythmias complicating myocardial infarction G. Terry,1 C. W. Vellani, M. R. Higgins, and A. Doig From the
OUTCOME OF THROMBOLYTIC AND NON- THROMBOLYTIC THERAPY IN ACUTE MYOCARDIAL INFARCTION
 OUTCOME OF THROMBOLYTIC AND NON- THROMBOLYTIC THERAPY IN ACUTE MYOCARDIAL INFARCTION FEROZ MEMON*, LIAQUAT CHEEMA**, NAND LAL RATHI***, RAJ KUMAR***, NAZIR AHMED MEMON**** OBJECTIVE: To compare morbidity,
OUTCOME OF THROMBOLYTIC AND NON- THROMBOLYTIC THERAPY IN ACUTE MYOCARDIAL INFARCTION FEROZ MEMON*, LIAQUAT CHEEMA**, NAND LAL RATHI***, RAJ KUMAR***, NAZIR AHMED MEMON**** OBJECTIVE: To compare morbidity,
Protocol Identifier Subject Identifier Visit Description. [Y] Yes [N] No. [Y] Yes [N] N. If Yes, admission date and time: Day Month Year
![Protocol Identifier Subject Identifier Visit Description. [Y] Yes [N] No. [Y] Yes [N] N. If Yes, admission date and time: Day Month Year Protocol Identifier Subject Identifier Visit Description. [Y] Yes [N] No. [Y] Yes [N] N. If Yes, admission date and time: Day Month Year](/thumbs/76/74263761.jpg) PAST MEDICAL HISTORY Has the subject had a prior episode of heart failure? o Does the subject have a prior history of exposure to cardiotoxins, such as anthracyclines? URGENT HEART FAILURE VISIT Did heart
PAST MEDICAL HISTORY Has the subject had a prior episode of heart failure? o Does the subject have a prior history of exposure to cardiotoxins, such as anthracyclines? URGENT HEART FAILURE VISIT Did heart
Chapter 10. Learning Objectives. Learning Objectives 9/11/2012. Congestive Heart Failure
 Chapter 10 Congestive Heart Failure Learning Objectives Explain concept of polypharmacy in treatment of congestive heart failure Explain function of diuretics Learning Objectives Discuss drugs used for
Chapter 10 Congestive Heart Failure Learning Objectives Explain concept of polypharmacy in treatment of congestive heart failure Explain function of diuretics Learning Objectives Discuss drugs used for
Reciprocal ST depression in acute myocardial infarction
 Reciprocal ST depression in acute myocardial infarction Br Heart J 1985; 54: 479-83 OLUSOLA ODEMUYIWA, IAN PEART, CATHERINE ALBERS, ROGER HALL From the Royal Victoria Infirmary, Newcastle upon Tyne SUMMARY
Reciprocal ST depression in acute myocardial infarction Br Heart J 1985; 54: 479-83 OLUSOLA ODEMUYIWA, IAN PEART, CATHERINE ALBERS, ROGER HALL From the Royal Victoria Infirmary, Newcastle upon Tyne SUMMARY
Cardiovascular System Notes: Heart Disease & Disorders
 Cardiovascular System Notes: Heart Disease & Disorders Interesting Heart Facts The Electrocardiograph (ECG) was invented in 1902 by Willem Einthoven Dutch Physiologist. This test is still used to evaluate
Cardiovascular System Notes: Heart Disease & Disorders Interesting Heart Facts The Electrocardiograph (ECG) was invented in 1902 by Willem Einthoven Dutch Physiologist. This test is still used to evaluate
Admission of patient CVICU and hemodynamic monitoring
 Admission of patient CVICU and hemodynamic monitoring Prepared by: Rami AL-Khatib King Fahad Medical City Pi Prince Salman Heart tcentre CVICU-RN Admission patient to CVICU Introduction All the patients
Admission of patient CVICU and hemodynamic monitoring Prepared by: Rami AL-Khatib King Fahad Medical City Pi Prince Salman Heart tcentre CVICU-RN Admission patient to CVICU Introduction All the patients
EKG Competency for Agency
 EKG Competency for Agency Name: Date: Agency: 1. The upper chambers of the heart are known as the: a. Atria b. Ventricles c. Mitral Valve d. Aortic Valve 2. The lower chambers of the heart are known as
EKG Competency for Agency Name: Date: Agency: 1. The upper chambers of the heart are known as the: a. Atria b. Ventricles c. Mitral Valve d. Aortic Valve 2. The lower chambers of the heart are known as
Hemodynamic Monitoring
 Perform Procedure And Interpret Results Hemodynamic Monitoring Tracheal Tube Cuff Pressure Dean R. Hess PhD RRT FAARC Hemodynamic Monitoring Cardiac Rate and Rhythm Arterial Blood Pressure Central Venous
Perform Procedure And Interpret Results Hemodynamic Monitoring Tracheal Tube Cuff Pressure Dean R. Hess PhD RRT FAARC Hemodynamic Monitoring Cardiac Rate and Rhythm Arterial Blood Pressure Central Venous
Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine
 Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine Venous thromboembolism: pulmonary embolism (PE) deep vein thrombosis (DVT) 1% of all patients admitted to hospital 5% of in-hospital mortality
Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine Venous thromboembolism: pulmonary embolism (PE) deep vein thrombosis (DVT) 1% of all patients admitted to hospital 5% of in-hospital mortality
FUNDAMENTALS OF HEMODYNAMICS, VASOACTIVE DRUGS AND IABP IN THE FAILING HEART
 FUNDAMENTALS OF HEMODYNAMICS, VASOACTIVE DRUGS AND IABP IN THE FAILING HEART CINDY BITHER, MSN, ANP, ANP, AACC, CHFN CHIEF NP, ADV HF PROGRAM MEDSTAR WASHINGTON HOSPITAL CENTER CONFLICTS OF INTEREST NONE
FUNDAMENTALS OF HEMODYNAMICS, VASOACTIVE DRUGS AND IABP IN THE FAILING HEART CINDY BITHER, MSN, ANP, ANP, AACC, CHFN CHIEF NP, ADV HF PROGRAM MEDSTAR WASHINGTON HOSPITAL CENTER CONFLICTS OF INTEREST NONE
THE CARDIOVASCULAR SYSTEM
 THE CARDIOVASCULAR SYSTEM AND RESPONSES TO EXERCISE Mr. S. Kelly PSK 4U North Grenville DHS THE HEART: A REVIEW Cardiac muscle = myocardium Heart divided into two sides, 4 chambers (L & R) RS: pulmonary
THE CARDIOVASCULAR SYSTEM AND RESPONSES TO EXERCISE Mr. S. Kelly PSK 4U North Grenville DHS THE HEART: A REVIEW Cardiac muscle = myocardium Heart divided into two sides, 4 chambers (L & R) RS: pulmonary
Acute impairment of basal left ventricular rotation but not twist and untwist are involved in the pathogenesis of acute hypertensive pulmonary oedema
 Acute impairment of basal left ventricular rotation but not twist and untwist are involved in the pathogenesis of acute hypertensive pulmonary oedema A.D. Margulescu 1,2, R.C. Sisu 1,2, M. Florescu 2,
Acute impairment of basal left ventricular rotation but not twist and untwist are involved in the pathogenesis of acute hypertensive pulmonary oedema A.D. Margulescu 1,2, R.C. Sisu 1,2, M. Florescu 2,
Acute coronary syndromes
 Acute coronary syndromes 1 Acute coronary syndromes Acute coronary syndromes results primarily from diminished myocardial blood flow secondary to an occlusive or partially occlusive coronary artery thrombus.
Acute coronary syndromes 1 Acute coronary syndromes Acute coronary syndromes results primarily from diminished myocardial blood flow secondary to an occlusive or partially occlusive coronary artery thrombus.
Haemodynamic response to intravenous vasopressin and nitroglycerin in portal hypertension
 Gut, 1988, 29, 372-377 Haemodynamic response to intravenous vasopressin and nitroglycerin in portal hypertension D WSTABY, A GIMSON, P C HAYS, AND ROGR WILLIAMS From the Liver Unit, King's College School
Gut, 1988, 29, 372-377 Haemodynamic response to intravenous vasopressin and nitroglycerin in portal hypertension D WSTABY, A GIMSON, P C HAYS, AND ROGR WILLIAMS From the Liver Unit, King's College School
Skin supplied by T1-4 (medial upper arm and neck) T5-9- epigastrium Visceral afferents from skin and heart are the same dorsal root ganglio
 Cardio 2 ECG... 3 Cardiac Remodelling... 11 Valvular Diseases... 13 Hypertension... 18 Aortic Coarctation... 24 Erythropoiesis... 27 Haemostasis... 30 Anaemia... 36 Atherosclerosis... 44 Angina... 48 Myocardial
Cardio 2 ECG... 3 Cardiac Remodelling... 11 Valvular Diseases... 13 Hypertension... 18 Aortic Coarctation... 24 Erythropoiesis... 27 Haemostasis... 30 Anaemia... 36 Atherosclerosis... 44 Angina... 48 Myocardial
A case of post myocardial infarction ventricular septal rupture CHRISTOFOROS KOBOROZOS, MD
 A case of post myocardial infarction ventricular septal rupture CHRISTOFOROS KOBOROZOS, MD NAVAL HOSPITAL OF ATHENS case presentation Female, 81yo Hx: diabetes mellitus, hypertension, chronic anaemia presented
A case of post myocardial infarction ventricular septal rupture CHRISTOFOROS KOBOROZOS, MD NAVAL HOSPITAL OF ATHENS case presentation Female, 81yo Hx: diabetes mellitus, hypertension, chronic anaemia presented
ORIGINAL ARTICLE. Abstract. Introduction. Materials and Methods
 ORIGINAL ARTICLE Effects of Cardiac Hemodynamics on Agreement in the ph, HCO3- and Lactate Levels between Arterial and Venous Blood Samples in Patients with Known or Suspected Chronic Heart Failure Satoshi
ORIGINAL ARTICLE Effects of Cardiac Hemodynamics on Agreement in the ph, HCO3- and Lactate Levels between Arterial and Venous Blood Samples in Patients with Known or Suspected Chronic Heart Failure Satoshi
CARDIOVASCULAR MONITORING. Prof. Yasser Mostafa Kadah
 CARDIOVASCULAR MONITORING Prof. Yasser Mostafa Kadah Introduction Cardiovascular monitoring covers monitoring of heart and circulatory functions It makes it possible to commence interventions quickly in
CARDIOVASCULAR MONITORING Prof. Yasser Mostafa Kadah Introduction Cardiovascular monitoring covers monitoring of heart and circulatory functions It makes it possible to commence interventions quickly in
Increased heart rate as a risk factor for cardiovascular disease
 European Heart Journal Supplements (23) 5 (Supplement G), G3 G9 Increased heart rate as a risk factor for cardiovascular disease Department of Cardiology, VA Medical Center, West Los Angeles, and Department
European Heart Journal Supplements (23) 5 (Supplement G), G3 G9 Increased heart rate as a risk factor for cardiovascular disease Department of Cardiology, VA Medical Center, West Los Angeles, and Department
Introduction. Invasive Hemodynamic Monitoring. Determinants of Cardiovascular Function. Cardiovascular System. Hemodynamic Monitoring
 Introduction Invasive Hemodynamic Monitoring Audis Bethea, Pharm.D. Assistant Professor Therapeutics IV January 21, 2004 Hemodynamic monitoring is necessary to assess and manage shock Information obtained
Introduction Invasive Hemodynamic Monitoring Audis Bethea, Pharm.D. Assistant Professor Therapeutics IV January 21, 2004 Hemodynamic monitoring is necessary to assess and manage shock Information obtained
Nicardipine Versus Nitroprusside Infusion as Antihypertensive Therapy in Hypertensive Emergencies
 The Journal of International Medical Research 2004; 32: 118 123 Nicardipine Versus Nitroprusside Infusion as Antihypertensive Therapy in Hypertensive Emergencies HJ YANG, JG KIM, YS LIM, E RYOO, SY HYUN
The Journal of International Medical Research 2004; 32: 118 123 Nicardipine Versus Nitroprusside Infusion as Antihypertensive Therapy in Hypertensive Emergencies HJ YANG, JG KIM, YS LIM, E RYOO, SY HYUN
Transcoronary Chemical Ablation of Atrioventricular Conduction
 757 Transcoronary Chemical Ablation of Atrioventricular Conduction Pedro Brugada, MD, Hans de Swart, MD, Joep Smeets, MD, and Hein J.J. Wellens, MD In seven patients with symptomatic atrial fibrillation
757 Transcoronary Chemical Ablation of Atrioventricular Conduction Pedro Brugada, MD, Hans de Swart, MD, Joep Smeets, MD, and Hein J.J. Wellens, MD In seven patients with symptomatic atrial fibrillation
Myocardial lactate metabolism during isometric hand grip test
 British HeartJournal, I975, 37, 79-84. Myocardial lactate metabolism during isometric hand grip test Comparison with pacing tachycardia F. Khan Nakhjavan, Gangaiah Natarajan, Allan M. Smith, Michael Dratch,
British HeartJournal, I975, 37, 79-84. Myocardial lactate metabolism during isometric hand grip test Comparison with pacing tachycardia F. Khan Nakhjavan, Gangaiah Natarajan, Allan M. Smith, Michael Dratch,
Chapter 21: Clinical Exercise Testing Procedures
 Publisher link: thepoint http://thepoint.lww.com/book/show/2930 Chapter 21: Clinical Exercise Testing Procedures American College of Sports Medicine. (2010). ACSM's resource manual for guidelines for exercise
Publisher link: thepoint http://thepoint.lww.com/book/show/2930 Chapter 21: Clinical Exercise Testing Procedures American College of Sports Medicine. (2010). ACSM's resource manual for guidelines for exercise
Norepinephrine (Levophed )
 Norepinephrine (Levophed ) Scope C3IFT CCT Generic Name: Norepinephrine Trade Name: Levophed Chemical Class: Therapeutic Class: Actions: Pharmacokinetics: Vasopressor Vasopressor Mechanism of Action: Norepinephrine
Norepinephrine (Levophed ) Scope C3IFT CCT Generic Name: Norepinephrine Trade Name: Levophed Chemical Class: Therapeutic Class: Actions: Pharmacokinetics: Vasopressor Vasopressor Mechanism of Action: Norepinephrine
Angina pectoris due to coronary atherosclerosis : Atenolol is indicated for the long term management of patients with angina pectoris.
 Lonet Tablet Description Lonet contains Atenolol, a synthetic β1 selective (cardioselective) adrenoreceptor blocking agent without membrane stabilising or intrinsic sympathomimetic (partial agonist) activity.
Lonet Tablet Description Lonet contains Atenolol, a synthetic β1 selective (cardioselective) adrenoreceptor blocking agent without membrane stabilising or intrinsic sympathomimetic (partial agonist) activity.
The Electrocardiogram part II. Dr. Adelina Vlad, MD PhD
 The Electrocardiogram part II Dr. Adelina Vlad, MD PhD Basic Interpretation of the ECG 1) Evaluate calibration 2) Calculate rate 3) Determine rhythm 4) Determine QRS axis 5) Measure intervals 6) Analyze
The Electrocardiogram part II Dr. Adelina Vlad, MD PhD Basic Interpretation of the ECG 1) Evaluate calibration 2) Calculate rate 3) Determine rhythm 4) Determine QRS axis 5) Measure intervals 6) Analyze
In the name of GOD. Animal models of cardiovascular diseases: myocardial infarction & hypertension
 In the name of GOD Animal models of cardiovascular diseases: myocardial infarction & hypertension 44 Presentation outline: Cardiovascular diseases Acute myocardial infarction Animal models for myocardial
In the name of GOD Animal models of cardiovascular diseases: myocardial infarction & hypertension 44 Presentation outline: Cardiovascular diseases Acute myocardial infarction Animal models for myocardial
concentration in myocardial ischaemia and infarction
 Br Heart J 1982; 47: 239-43 Measurement of serum C-reactive protein concentration in myocardial ischaemia and infarction F C DE BEER, C R K HIND, K M FOX, R M ALLAN, A MASERI, M B PEPYS From the Immunological
Br Heart J 1982; 47: 239-43 Measurement of serum C-reactive protein concentration in myocardial ischaemia and infarction F C DE BEER, C R K HIND, K M FOX, R M ALLAN, A MASERI, M B PEPYS From the Immunological
Solution for cardiac perfusion in viaflex plastic container
 CARDIOPLEGIA SOLUTION A Solution for cardiac perfusion in viaflex plastic container DESCRIPTION Cardioplegia Solution A is a sterile, non-pyrogenic solution in a Viaflex bag. It is used to induce cardiac
CARDIOPLEGIA SOLUTION A Solution for cardiac perfusion in viaflex plastic container DESCRIPTION Cardioplegia Solution A is a sterile, non-pyrogenic solution in a Viaflex bag. It is used to induce cardiac
Infusion for Afterload Reduction
 Continuous Hydralazine Infusion for Afterload Reduction Marc T. Swartz, B.A., George C. Kaiser, M.D., Vallee L. Willman, M.D., John E. Codd, M.D., Denis H. Tyras, M.D., and Hendrick B. BaAer, M.D. ABSTRACT
Continuous Hydralazine Infusion for Afterload Reduction Marc T. Swartz, B.A., George C. Kaiser, M.D., Vallee L. Willman, M.D., John E. Codd, M.D., Denis H. Tyras, M.D., and Hendrick B. BaAer, M.D. ABSTRACT
C. FOSSARD. M.B.B.S., M.Sc., M.R.C.P. iron from the body results in clinical, biochemical and histological improvement (Williams et al., 1969).
 Postgraduate Medical Journal (May 1974) 50, 276-281. Cardiac involvement in idiopathic haemochromatosis and the effect of venesection S. J. JACHUCK G. S. RAI B.Sc., M.B.B.S. M.B.B.S. C. FOSSARD M.B.B.S.,
Postgraduate Medical Journal (May 1974) 50, 276-281. Cardiac involvement in idiopathic haemochromatosis and the effect of venesection S. J. JACHUCK G. S. RAI B.Sc., M.B.B.S. M.B.B.S. C. FOSSARD M.B.B.S.,
Effects of prostaglandin E1 on pulmonary circulation in patients with pulmonary hypertension
 British Heart journal, 1978, 40, 1397-1401 Effects of prostaglandin E1 on pulmonary circulation in patients with pulmonary hypertension JERZY SZCZEKLIK, JACEK S. DUBIEL, MIECZYSLAW MYSIK, ZBIGNIEW PYZIK,
British Heart journal, 1978, 40, 1397-1401 Effects of prostaglandin E1 on pulmonary circulation in patients with pulmonary hypertension JERZY SZCZEKLIK, JACEK S. DUBIEL, MIECZYSLAW MYSIK, ZBIGNIEW PYZIK,
Nothing to Disclose. Severe Pulmonary Hypertension
 Severe Ronald Pearl, MD, PhD Professor and Chair Department of Anesthesiology Stanford University Rpearl@stanford.edu Nothing to Disclose 65 year old female Elective knee surgery NYHA Class 3 Aortic stenosis
Severe Ronald Pearl, MD, PhD Professor and Chair Department of Anesthesiology Stanford University Rpearl@stanford.edu Nothing to Disclose 65 year old female Elective knee surgery NYHA Class 3 Aortic stenosis
Hypertension. Penny Mosley MRPharmS
 Hypertension Penny Mosley MRPharmS Outline of presentation Introduction to hypertension Physiological control of arterial blood pressure What determines our bp? What determines the heart rate? What determines
Hypertension Penny Mosley MRPharmS Outline of presentation Introduction to hypertension Physiological control of arterial blood pressure What determines our bp? What determines the heart rate? What determines
A patient with non-q wave acute inferior myocardial infarction. Citation Hong Kong Practitioner, 1997, v. 19 n. 4, p
 Title A patient with non-q wave acute inferior myocardial infarction Author(s) Ng, W; Wong, CK; Lau, CP Citation Hong Kong Practitioner, 1997, v. 19 n. 4, p. 199-202 ssued Date 1997 URL http://hdl.handle.net/10722/45037
Title A patient with non-q wave acute inferior myocardial infarction Author(s) Ng, W; Wong, CK; Lau, CP Citation Hong Kong Practitioner, 1997, v. 19 n. 4, p. 199-202 ssued Date 1997 URL http://hdl.handle.net/10722/45037
ECG pre-reading manual. Created for the North West Regional EMET training program
 ECG pre-reading manual Created for the North West Regional EMET training program Author:- Dr Juan Carlos Ascencio-Lane juan.ascencio-lane@ths.tas.gov.au 1 Disclaimer This handbook has been created for
ECG pre-reading manual Created for the North West Regional EMET training program Author:- Dr Juan Carlos Ascencio-Lane juan.ascencio-lane@ths.tas.gov.au 1 Disclaimer This handbook has been created for
Angina Pectoris Dr. Shariq Syed
 Angina Pectoris Dr. Syed 1 What is Angina Pectoris (AP)? Commonly known as angina is chest pain often due to ischemia of the heart muscle, Because of obstruction or spasm of the coronary arteries 2 What
Angina Pectoris Dr. Syed 1 What is Angina Pectoris (AP)? Commonly known as angina is chest pain often due to ischemia of the heart muscle, Because of obstruction or spasm of the coronary arteries 2 What
Cardiac output and Venous Return. Faisal I. Mohammed, MD, PhD
 Cardiac output and Venous Return Faisal I. Mohammed, MD, PhD 1 Objectives Define cardiac output and venous return Describe the methods of measurement of CO Outline the factors that regulate cardiac output
Cardiac output and Venous Return Faisal I. Mohammed, MD, PhD 1 Objectives Define cardiac output and venous return Describe the methods of measurement of CO Outline the factors that regulate cardiac output
CHRONIC HEART FAILURE : WHAT ELSE COULD WE OFFER TO OUR PATIENTS? Cardiac Rehabilitation Society of Thailand
 CHRONIC HEART FAILURE : WHAT ELSE COULD WE OFFER TO OUR PATIENTS? Cardiac Rehabilitation Society of Thailand ENHANCED EXTERNAL COUNTER PULSATION Piyanuj Ruckpanich, MD. Cardiac Rehabilitation Center Perfect
CHRONIC HEART FAILURE : WHAT ELSE COULD WE OFFER TO OUR PATIENTS? Cardiac Rehabilitation Society of Thailand ENHANCED EXTERNAL COUNTER PULSATION Piyanuj Ruckpanich, MD. Cardiac Rehabilitation Center Perfect
Selective Cardiac Myosin Activators in Heart Failure
 Selective Cardiac Myosin Activators in Heart Failure John McMurray Eugene Braunwald Scholar in Cardiovascular Diseases, Brigham and Women s Hospital, Boston & Visiting Professor, Harvard Medical School
Selective Cardiac Myosin Activators in Heart Failure John McMurray Eugene Braunwald Scholar in Cardiovascular Diseases, Brigham and Women s Hospital, Boston & Visiting Professor, Harvard Medical School
Experience with counterpulsation in
 British Heart J7ournal, 1977, 39, 198-202 Experience with counterpulsation in cardiac surgical patients G. H. SMITH AND W. E. MORGAN From Sheffield Cardiothoracic Unit, Northern General Hospital, Sheffield
British Heart J7ournal, 1977, 39, 198-202 Experience with counterpulsation in cardiac surgical patients G. H. SMITH AND W. E. MORGAN From Sheffield Cardiothoracic Unit, Northern General Hospital, Sheffield
My Patient Needs a Stress Test
 My Patient Needs a Stress Test Amy S. Burhanna,, MD, FACC Coastal Cardiology Cape May Court House, New Jersey Absolute and relative contraindications to exercise testing Absolute Acute myocardial infarction
My Patient Needs a Stress Test Amy S. Burhanna,, MD, FACC Coastal Cardiology Cape May Court House, New Jersey Absolute and relative contraindications to exercise testing Absolute Acute myocardial infarction
Acute myocardial infarction. Cardiovascular disorders. main/0202_new 02/03/06. Search date August 2004 Nicholas Danchin and Eric Durand
 main/0202_new 02/03/06 Acute myocardial infarction Search date August 2004 Nicholas Danchin and Eric Durand QUESTIONS Which treatments improve outcomes in acute myocardial infarction?...4 Which treatments
main/0202_new 02/03/06 Acute myocardial infarction Search date August 2004 Nicholas Danchin and Eric Durand QUESTIONS Which treatments improve outcomes in acute myocardial infarction?...4 Which treatments
In looking for other diagnostic variables we. might on exercise suffer a sufficient fall in cardiac
 Br Heart j 1985; 53: 598-62 Increased diastolic blood pressure response to exercise testing when coronary artery disease is suspected An indication ofseverity FAWAZ AKHRAS, JAMES UPWARD, GRAHAM JACKSON
Br Heart j 1985; 53: 598-62 Increased diastolic blood pressure response to exercise testing when coronary artery disease is suspected An indication ofseverity FAWAZ AKHRAS, JAMES UPWARD, GRAHAM JACKSON
Relax and Learn At the Farm 2012
 Relax and Learn At the Farm Session 9: Invasive Hemodynamic Assessment and What to Do with the Data Carol Jacobson RN, MN Cardiovascular Nursing Education Associates Function of CV system is to deliver
Relax and Learn At the Farm Session 9: Invasive Hemodynamic Assessment and What to Do with the Data Carol Jacobson RN, MN Cardiovascular Nursing Education Associates Function of CV system is to deliver
Coronary arteriography in complicated acute myocardial infarction; clinical and angiographic correlates
 Coronary arteriography in complicated acute myocardial ; clinical and angiographic correlates Luis M. de la Fuente, M.D. Buenos Aires, Argentina From January 1979 to June 30, 1979, we performed coronary
Coronary arteriography in complicated acute myocardial ; clinical and angiographic correlates Luis M. de la Fuente, M.D. Buenos Aires, Argentina From January 1979 to June 30, 1979, we performed coronary
Haemodynamic effects of a new inotropic agent (dobutamine) in chronic cardiac failure
 British Heart journal, 1975, 37, 629-634. Haemodynamic effects of a new inotropic agent (dobutamine) in chronic cardiac failure Jonas Beregovich, Christian Bianchi, Ralph D'Angelo, Ruth Diaz, and Shirley
British Heart journal, 1975, 37, 629-634. Haemodynamic effects of a new inotropic agent (dobutamine) in chronic cardiac failure Jonas Beregovich, Christian Bianchi, Ralph D'Angelo, Ruth Diaz, and Shirley
Blood Pressure Management in Acute Ischemic Stroke
 Blood Pressure Management in Acute Ischemic Stroke Kimberly Clark, PharmD, BCCCP Clinical Pharmacy Specialist Critical Care, Greenville Health System Adjunct Assistant Professor, South Carolina College
Blood Pressure Management in Acute Ischemic Stroke Kimberly Clark, PharmD, BCCCP Clinical Pharmacy Specialist Critical Care, Greenville Health System Adjunct Assistant Professor, South Carolina College
effects of intravenous labetalol
 Pharmacological basis for antihypertensive effects of intravenous labetalol D. A. RICHARDS,' B. N. C. PRICHARD, A. J. BOAKES, J. TUCKMAN, AND E. J. KNIGHT2 From the Department of Clinical Pharmacology,
Pharmacological basis for antihypertensive effects of intravenous labetalol D. A. RICHARDS,' B. N. C. PRICHARD, A. J. BOAKES, J. TUCKMAN, AND E. J. KNIGHT2 From the Department of Clinical Pharmacology,
Pharmacology. Drugs affecting the Cardiovascular system (Antianginal Drugs)
 Lecture 7 (year3) Dr Noor Al-Hasani Pharmacology University of Baghdad College of dentistry Drugs affecting the Cardiovascular system (Antianginal Drugs) Atherosclerotic disease of the coronary arteries,
Lecture 7 (year3) Dr Noor Al-Hasani Pharmacology University of Baghdad College of dentistry Drugs affecting the Cardiovascular system (Antianginal Drugs) Atherosclerotic disease of the coronary arteries,
Closing ASDs with pulmonary hypertension. Shakeel A Qureshi Evelina Children s Hospital London
 Closing ASDs with pulmonary hypertension Shakeel A Qureshi Evelina Children s Hospital London Ho Chi Minh, Vietnam, January 2012 ACC/AHA 2008 Guidelines ASD closure Closure is indicated for right atrial
Closing ASDs with pulmonary hypertension Shakeel A Qureshi Evelina Children s Hospital London Ho Chi Minh, Vietnam, January 2012 ACC/AHA 2008 Guidelines ASD closure Closure is indicated for right atrial
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE General practice Indicators for the NICE menu
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE General practice Indicators for the NICE menu Indicator area: Pulse rhythm assessment for AF Indicator: NM146 Date: June 2017 Introduction There is evidence
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE General practice Indicators for the NICE menu Indicator area: Pulse rhythm assessment for AF Indicator: NM146 Date: June 2017 Introduction There is evidence
Initial Medical and Surgical Management of Unstable Angina Pectoris
 Clin. Cardiol. 2. 311-316 (I979) G. Witzstrock Publishing House. Inc. Editorial Initial Medical and Surgical Management of Unstable Angina Pectoris Introduction The purpose of this report is to review
Clin. Cardiol. 2. 311-316 (I979) G. Witzstrock Publishing House. Inc. Editorial Initial Medical and Surgical Management of Unstable Angina Pectoris Introduction The purpose of this report is to review
The Heart. Happy Friday! #takeoutyournotes #testnotgradedyet
 The Heart Happy Friday! #takeoutyournotes #testnotgradedyet Introduction Cardiovascular system distributes blood Pump (heart) Distribution areas (capillaries) Heart has 4 compartments 2 receive blood (atria)
The Heart Happy Friday! #takeoutyournotes #testnotgradedyet Introduction Cardiovascular system distributes blood Pump (heart) Distribution areas (capillaries) Heart has 4 compartments 2 receive blood (atria)
New Agents for Heart Failure: Ivabradine Jeffrey S. Borer, MD
 New Agents for Heart Failure: Ivabradine Jeffrey S. Borer, MD Professor of Medicine, Cell Biology, Radiology and Surgery Director, The Howard Gilman Institute for Heart Valve Disease and the Schiavone
New Agents for Heart Failure: Ivabradine Jeffrey S. Borer, MD Professor of Medicine, Cell Biology, Radiology and Surgery Director, The Howard Gilman Institute for Heart Valve Disease and the Schiavone
Percutaneous Mechanical Circulatory Support Devices
 Percutaneous Mechanical Circulatory Support Devices Daniel Vazquez RN, RCIS Miami Cardiac & Vascular Institute FINANCIAL DISCLOSURES none CASE STUDY CASE STUDY 52 year old gentlemen Complaining of dyspnea
Percutaneous Mechanical Circulatory Support Devices Daniel Vazquez RN, RCIS Miami Cardiac & Vascular Institute FINANCIAL DISCLOSURES none CASE STUDY CASE STUDY 52 year old gentlemen Complaining of dyspnea
Complications of Acute Myocardial Infarction
 Acute Myocardial Infarction Complications of Acute Myocardial Infarction Diagnosis and Treatment JMAJ 45(4): 149 154, 2002 Hiroshi NONOGI Director, Division of Cardiology and Emergency Medicine, National
Acute Myocardial Infarction Complications of Acute Myocardial Infarction Diagnosis and Treatment JMAJ 45(4): 149 154, 2002 Hiroshi NONOGI Director, Division of Cardiology and Emergency Medicine, National
Value of echocardiography in chronic dyspnea
 Value of echocardiography in chronic dyspnea Jahrestagung Schweizerische Gesellschaft für /Schweizerische Gesellschaft für Pneumologie B. Kaufmann 16.06.2016 Chronic dyspnea Shortness of breath lasting
Value of echocardiography in chronic dyspnea Jahrestagung Schweizerische Gesellschaft für /Schweizerische Gesellschaft für Pneumologie B. Kaufmann 16.06.2016 Chronic dyspnea Shortness of breath lasting
The right heart: the Cinderella of heart failure
 The right heart: the Cinderella of heart failure Piotr Ponikowski, MD, PhD, FESC Medical University, Centre for Heart Disease Clinical Military Hospital Wroclaw, Poland none Disclosure Look into the Heart
The right heart: the Cinderella of heart failure Piotr Ponikowski, MD, PhD, FESC Medical University, Centre for Heart Disease Clinical Military Hospital Wroclaw, Poland none Disclosure Look into the Heart
Hypertensive Crises. Controlling high blood pressure prevents disease. Recognition and Management of Acute Hypertensive Emergencies
 Controlling high blood pressure prevents disease Recognition and Management of Acute Hypertensive Emergencies David idweiner, M.D. Co-holder, C. Craig and Audrae Tisher Chair in Nephrology Functional Genomics
Controlling high blood pressure prevents disease Recognition and Management of Acute Hypertensive Emergencies David idweiner, M.D. Co-holder, C. Craig and Audrae Tisher Chair in Nephrology Functional Genomics
DRUG CLASSES BETA-ADRENOCEPTOR ANTAGONISTS (BETA-BLOCKERS)
 DRUG CLASSES BETA-ADRENOCEPTOR ANTAGONISTS (BETA-BLOCKERS) Beta-blockers have been widely used in the management of angina, certain tachyarrhythmias and heart failure, as well as in hypertension. Examples
DRUG CLASSES BETA-ADRENOCEPTOR ANTAGONISTS (BETA-BLOCKERS) Beta-blockers have been widely used in the management of angina, certain tachyarrhythmias and heart failure, as well as in hypertension. Examples
Syncope: Ockham s Razor
 Syncope: Ockham s Razor Time/Place Wednesday, 25 th January 2006 10am-12pm Room 210, Wallace Wurth Building Facilitators Michael Grimm & Tony Grabs Aims Illustrate multiple possible causes for a common
Syncope: Ockham s Razor Time/Place Wednesday, 25 th January 2006 10am-12pm Room 210, Wallace Wurth Building Facilitators Michael Grimm & Tony Grabs Aims Illustrate multiple possible causes for a common
Risk Stratification for CAD for the Primary Care Provider
 Risk Stratification for CAD for the Primary Care Provider Shimoli Shah MD Assistant Professor of Medicine Directory, Ambulatory Cardiology Clinic Knight Cardiovascular Institute Oregon Health & Sciences
Risk Stratification for CAD for the Primary Care Provider Shimoli Shah MD Assistant Professor of Medicine Directory, Ambulatory Cardiology Clinic Knight Cardiovascular Institute Oregon Health & Sciences
Perioperative Management of TAPVC
 Perioperative Management of TAPVC Professor Andrew Wolf Rush University Medical Center,Chicago USA Bristol Royal Children s Hospital UK I have no financial disclosures relevant to this presentation TAPVC
Perioperative Management of TAPVC Professor Andrew Wolf Rush University Medical Center,Chicago USA Bristol Royal Children s Hospital UK I have no financial disclosures relevant to this presentation TAPVC
EMT. Chapter 14 Review
 EMT Chapter 14 Review Review 1. All of the following are common signs and symptoms of cardiac ischemia, EXCEPT: A. headache. B. chest pressure. C. shortness of breath. D. anxiety or restlessness. Review
EMT Chapter 14 Review Review 1. All of the following are common signs and symptoms of cardiac ischemia, EXCEPT: A. headache. B. chest pressure. C. shortness of breath. D. anxiety or restlessness. Review
T wave changes and postinfarction angina pectoris
 Br Heart Y 1981; 45: 512-16 T wave changes and postinfarction angina pectoris predictive of recurrent myocardial infarction RURIK LOFMARK* From the Department of Medicine, Karolinska Institute at Huddinge
Br Heart Y 1981; 45: 512-16 T wave changes and postinfarction angina pectoris predictive of recurrent myocardial infarction RURIK LOFMARK* From the Department of Medicine, Karolinska Institute at Huddinge
PROBLEM SET 2. Assigned: February 10, 2004 Due: February 19, 2004
 Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
Angina Luis Tulloch, MD 03/27/2012
 Angina Luis Tulloch, MD 03/27/2012 Acute coronary syndromes ACS STE > 1 mm, new LBBB* Increased cardiac enzymes STEMI Yes Yes NSTEMI No Yes UA No No *Recognize Wellen s sign/syndrome, posterior wall MI,
Angina Luis Tulloch, MD 03/27/2012 Acute coronary syndromes ACS STE > 1 mm, new LBBB* Increased cardiac enzymes STEMI Yes Yes NSTEMI No Yes UA No No *Recognize Wellen s sign/syndrome, posterior wall MI,
CVICU EXAM. Mrs. Jennings is a 71-year-old post-op CABG x5 with an IABP in her left femoral artery
 CVICU EXAM 1111 North 3rd Street Mrs. Jennings is a 71-year-old post-op CABG x5 with an IABP in her left femoral artery 1. Nursing standards for a patient on an IABP device include: a. Know results of
CVICU EXAM 1111 North 3rd Street Mrs. Jennings is a 71-year-old post-op CABG x5 with an IABP in her left femoral artery 1. Nursing standards for a patient on an IABP device include: a. Know results of
CHRONIC CAD DIAGNOSIS
 CHRONIC CAD DIAGNOSIS Chest Pain Evaluation 1. Approach to diagnosis of CAD 2. Classification of chest pain 3. Pre-test likelihood CAD 4. Algorithm for chest pain evaluation in women 5. Indications for
CHRONIC CAD DIAGNOSIS Chest Pain Evaluation 1. Approach to diagnosis of CAD 2. Classification of chest pain 3. Pre-test likelihood CAD 4. Algorithm for chest pain evaluation in women 5. Indications for
Cardiology. Objectives. Chapter
 1:44 M age 1121 Chapter Cardiology Objectives art 1: Cardiovascular natomy and hysiology, ECG Monitoring, and Dysrhythmia nalysis (begins on p. 1127) fter reading art 1 of this chapter, you should be able
1:44 M age 1121 Chapter Cardiology Objectives art 1: Cardiovascular natomy and hysiology, ECG Monitoring, and Dysrhythmia nalysis (begins on p. 1127) fter reading art 1 of this chapter, you should be able
Study of left ventricular pressure-volume relations during nitroprusside infusion in human subjects
 British Heart Journal, 1979, 41, 325-330 Study of left ventricular pressure-volume relations during nitroprusside infusion in human subjects without coronary artery disease1 J. P. MERILLON, G. MOTTE, M.
British Heart Journal, 1979, 41, 325-330 Study of left ventricular pressure-volume relations during nitroprusside infusion in human subjects without coronary artery disease1 J. P. MERILLON, G. MOTTE, M.
2.02 Understand the functions and disorders of the circulatory system
 2.02 Understand the functions and disorders of the circulatory system 2.02 Understand the functions and disorders of the circulatory system Essential questions: What are the functions of blood? What are
2.02 Understand the functions and disorders of the circulatory system 2.02 Understand the functions and disorders of the circulatory system Essential questions: What are the functions of blood? What are
Topics to be Covered. Cardiac Measurements. Distribution of Blood Volume. Distribution of Pulmonary Ventilation & Blood Flow
 Topics to be Covered MODULE F HEMODYNAMIC MONITORING Cardiac Output Determinants of Stroke Volume Hemodynamic Measurements Pulmonary Artery Catheterization Control of Blood Pressure Heart Failure Cardiac
Topics to be Covered MODULE F HEMODYNAMIC MONITORING Cardiac Output Determinants of Stroke Volume Hemodynamic Measurements Pulmonary Artery Catheterization Control of Blood Pressure Heart Failure Cardiac
SUPPLEMENTAL MATERIAL
 SUPPLEMENTAL MATERIAL Table S1: Number and percentage of patients by age category Distribution of age Age
SUPPLEMENTAL MATERIAL Table S1: Number and percentage of patients by age category Distribution of age Age
Reversible electrocardiographic changes in severe
 Thorax, 1977, 32, 328-332 Reversible electrocardiographic changes in severe acute asthma DAVD SEGLER From Bromnpton Hospital, London Siegler, D. (1977). Thorax, 32, 328-332. Reversible electrocardiographic
Thorax, 1977, 32, 328-332 Reversible electrocardiographic changes in severe acute asthma DAVD SEGLER From Bromnpton Hospital, London Siegler, D. (1977). Thorax, 32, 328-332. Reversible electrocardiographic
COMPARISON OF SUFENTANIL-OXYGEN AND FENTANYL-OXYGEN ANAESTHESIA FOR CORONARY ARTERY BYPASS GRAFTING
 Br. J. Anaesth. (1988), 60, 530-535 COMPARISON OF SUFENTANIL-OXYGEN AND FENTANYL-OXYGEN ANAESTHESIA FOR CORONARY ARTERY BYPASS GRAFTING H. M. L. MATHEWS, G. FURNESS, I. W. CARSON, I. A. ORR, S. M. LYONS
Br. J. Anaesth. (1988), 60, 530-535 COMPARISON OF SUFENTANIL-OXYGEN AND FENTANYL-OXYGEN ANAESTHESIA FOR CORONARY ARTERY BYPASS GRAFTING H. M. L. MATHEWS, G. FURNESS, I. W. CARSON, I. A. ORR, S. M. LYONS
Electrocardiography. Hilal Al Saffar College of Medicine,Baghdad University
 Electrocardiography Hilal Al Saffar College of Medicine,Baghdad University Which of the following is True 1. PR interval, represent the time taken for the impulse to travel from SA node to AV nose. 2.
Electrocardiography Hilal Al Saffar College of Medicine,Baghdad University Which of the following is True 1. PR interval, represent the time taken for the impulse to travel from SA node to AV nose. 2.
ACLS Prep. Preparation is key to a successful ACLS experience. Please complete the ACLS Pretest and Please complete this ACLS Prep.
 November, 2013 ACLS Prep Preparation is key to a successful ACLS experience. Please complete the ACLS Pretest and Please complete this ACLS Prep. ACLS Prep Preparation is key to a successful ACLS experience.
November, 2013 ACLS Prep Preparation is key to a successful ACLS experience. Please complete the ACLS Pretest and Please complete this ACLS Prep. ACLS Prep Preparation is key to a successful ACLS experience.
Section 6 Intra Aortic Balloon Pump
 Section 6 Intra Aortic Balloon Pump The Intra Aortic Balloon Pump (IABP) The balloon is synthetic and is made for single use only. It is threaded into the aorta, usually via a femoral approach. The balloon
Section 6 Intra Aortic Balloon Pump The Intra Aortic Balloon Pump (IABP) The balloon is synthetic and is made for single use only. It is threaded into the aorta, usually via a femoral approach. The balloon
