Tissue Blood Flow to the Heart
|
|
|
- Jade Weaver
- 5 years ago
- Views:
Transcription
1 Tissue Blood Flow to the Heart INFLUENCE OF CORONARY OCCLUSION AND SURGICAL MEASURES By Lloyd D. MctcLean, M.D., Ph.D., Paul H. Hedenstrom, M.D., and Ralph R. Rayner, M.D. Many surgical procedures designed to increase the total blood flow to the heart or to distribute the existing flow more equitably have been proposed. 1 " 3 The assessment of these operations has been hampered in the past by: (1) difficulty in obtaining objective data from clinical patients, (2) lack of a method to measure capillary (tissue) blood flow to specific areas of myocardium, and (3) lack of a method to measure quantitatively and selectively the functional blood flow to the heart before and after coronary occlusion and after attempts at revascularization. In the present study, tissue blood flow to specific regions of the canine heart was measured utilizing the deuterium oxide method. 4 " 6 The influence of coronary occlusion and of two operative procedures on regional blood flow was quantitated. Methods All experiments were performed on healthy, adult mongrel dogs of either sex, anesthetized with sodium pentobarbital (30 mg./kg.). Perfusion of coronary vessels was performed in situ via, a catheter placed in the ascending aorta advanced from the right carotid and brachiocephalic arteries. Tapes were placed about the superior and inferior venae cavae and about thp brachiocephalic artery. Occlusion of the aorta immediately distal to the brachipcephalic artery was provided by a surgical clamp. A collecting catheter was placed in the ostium of the coronary sinus and fixed in place with a purse-string suture. At the beginning of the experiment, inflow occlusion was established by occluding the venae cayae; following this, coronary perfusion was started using oxygenated blood at 37 C. from a pressure flask. (135 mm. Hg). The tape about From the Amcker Hospital Surgical Research Laboratory, St. Paul, and Department of Surgery, University' of Minnesota, Minneapolis, Minnesota. : Supported by a grant from the Minnesota Heart Association Dr. MacLean is a Markle Scholar in Medical Sciences. Received for publication July 18, the brachiocephalic artery was drawn up and the clamp placed about the aorta immediately beyond the brachiocephalic artery, thereby limiting perfusion to the coronary system. Following an initial period of equilibration of the isolated beating heart with nonlabeled perfusion fluid (blood), the inflow was changed to blood containing 2 volume per cent deuterium oxide.* The perfusion with blood-d 2 O mixture was discontinued after 20 to 30 seconds. The heart was removed, and the blood was allowed to drain from the cut vessels and was blotted dry and weighed. Seven tissue pieces weighing 2 to 3 6m. were taken from the right ventricle and the left ventricle in the distribution of the left anterior descending and the circumflex coronary arteries. The tissues and samples of the perfusing blood were prepared for D 2 O analysis by distilling in VMPUO to dryness. The distillate was equilibrated with hydrogen gas at atmospheric pressure in the presence of a platinum oxide catalyst. The tissue and fluid D a O concentrations were determined in the mass spectrometer with an average difference between duplicates of less than 1 per cent. Knowing the concentration of D 2 O in the arterial perfusion fluid and in the heart tissue, it. is possible to calculate tissue blood flow from the following formula: 6 F In V T I C A -C T ' where F = flow in milliliters blood water/min.: V T = volume of water in the tissue in milliliters; t = perfusion time; C A = concentration of D 2 0 in arterial blood; C T = concentration of D 2 O in tissue. This formula is applicable to any tent substance; the rate of uptake of this substance by the tissue is limited by the blood flow through the tissue. This relationship would be obtained if exchange of the material between blood and the extravascular space in the organ were instantatieous relative to its rate of delivery to the organ by the blood. That.this relationship obtains for D 2 O in heart muscle has been documented by Johnson et al. 4 and by Thompson et al. 5 A detailed disr cussion of this method has appeared in a previous publication from this laboratory. 6 Since the water content of heart muscle, scarred heart muscle, and blood were all.approximately 80 per cent, and since the specific gravity of blood *DeuteViiun oxide hereinafter is referred to as DaO. Circulation Research, Volume X, January 19RS 45
2 46 MacLEAN, HEDENSTROM, RAYNER TABLE 1 Normal Hearts (Blood Flow ml./gm./min.) E 25 E 26 E 27 E 29 E 30 E Anatomical location of muscle {ample distribution Circumflex disitribution Apex TABLE 2 Acute Left Anterior Descending Coronary Occlusion (Blood Flow ml./gm./min.) E 2 E 3 E 12 E 14 E 19 E Anatomical location of muscle sample distribution Circumflex disitribution was nearly one, the perfusion ratios (blood water/min.-ml. of tissue water) for these tissues closely approximate the blood flow through the tissue in milliliters of blood/min.-gm. of tissue. Results are expressed in the latter more familiar form. Six experiments were performed: (1) normalsthe entire coronary system of the dog heart was perfused; (2) acute coronary occlusion the perfusion was earned out as in (1), however, the left anterior descending coronary artery was ligated immediately prior to perfusion; (3) chronic coronary occlusionthe left anterior descending coronary artery was ligated four to six months prior to perfusion; (4) pulmonary artery to left atrial shuntthis procedure, designed to increase intercoronary anastomoses, 3 was performed six weeks to six months prior to perfusion, and immediately prior to perfusion, the left anterior descending coronary artery was ligated; (5) poudrage with coronary sinus narrowing (Beck I operation) 2 this procedure was performed four to six months prior to perfusion, and immediately prior to perfusion, the left anterior descending coronary was ligated; (6) Beck I operation and left anterior descending coronary occlusion were both performed four to six months prior to perfusion. Left anterior descending coronary occlusion was performed immediately distal to the circumflex branch of the left coronary artery and did not include the septal artery in any experiments herein reported. The pulmonary artery-left atrial anastomosis was made between the main pulmonary artery and the left atrium within the pericardial sac. In all animals perfused with D 2 O, the shunt was functioning prior to perfusion, and oxygen saturation of these animals ranged between 75 per cent and 88 per cent for several weeks prior to perfusion. Results and Discussion In the control group of normals, blood flow to the heart ranged from 0.4 to 1.6 ml./gm./ min., which is within limits described using other techniques 7 " 9 (table 1). The present method permits measurement of regional tissue blood flow, which has an advantage over methods which measure total coronary blood flow (e.g., nitrous oxide method) 10 for the type of investigation herein reported. The blood flow per gram did not vary significantly between right ventricle and various parts of the left ventricle in any given animal. This remarkably uniform distribution of blood was seen in all control animals and was useful when considering later experiments which showed a marked alteration in flow from one area to another in the same animal. Circulation Research, Volume X, January 196S
3 CORONARY OCCLUSION AND SURGERY Chronic Left Anterior Descending TABLE JI Coronary Occlusion (Blood Flow ml./gm./min.) E 44 E 45 E Anatomical location of muscle Elample distribution Circumflex distribution TABLE 4 Pulmonary Artery-Left Atrial Shunt Followed by Acute Left Anterior Descending Coronary Occlusion (Blood Flow ml./gm./min.) E 23 E 31 E 34 E Anatomical location of muscle sample distribution Circumflex dieitribution With acute occlusion of the anterior descending branch of the left coronary artery, there was a marked decrease in flow to the sample or samples of myocardium removed from this area (table 2). There appeared to be also a decrease inflowto areas immediately adjacent to the most ischemic area. The flow to the muscle supplied by the left anterior descending coronary artery dropped to 0.1 ml./gm./min., or less, in at least one of the muscle samples from this area. This degree of ischemia was obvious grossly at the time of the experiment in that there was paradoxical movement and a eyanotic hue to the area in question. There was little chance for the development of collaterals under the conditions of this experiment in that perfusion with D2O was done within minutes of the time of coronary occlusion. In experiment 3, occlusion of the anterior descending branch of the left coronary artery was performed four to six months prior to the determination of tissue blood flow to the heart. The results appear in table 3. There is a much greater blood flow to the region of the myocardium supplied by the anterior descending artery (areas 5 and 6) than existed immediately after occlusion. Scar tissue representing a healed infaret was present in all Circulation Research, Volume X, January 196S hearts at this later date. While collateral flow undoubtedly developed, this did not appear soon enough to prevent infarction. May, 11 in anatomical studies of coronary collaterals, has been able to differentiate these vessels from intercoronary anastomoses. It is believed by May 11 that the vessels found coursing throughout a scarred area are newly developed, are not enlargements of previously existing vessels, and are the result of the stimulus of necrosis. These collaterals obviously are of little value in preventing the infaret but may account for the return of normal blood pressures in the peripheral coronary system after coronary occlusion as described by Garamella et al. 12 The results of experiment 4 appear in table 4. Pulmonary artery to left atrial shunt was performed to increase intercoronary anastomoses, thereby increasing the blood flow to areas of myocardium most apt to become ischemic after acute coronary occlusion. There was a marked reduction in blood flow to the myocardium supplied by the anterior descending artery after occlusion of this vessel, even though a previous and functioning shunt was present. This flow did not vary from controls in which coronary occlusion alone was performed. Poudrage with coronary sinus nar-
4 48 MacLEAN, HEDENSTROM, RAYNER TABLE 5 Poudrage with Coronary Sinus Narrowing Followed by Acute Left Anterior Descending Coronary Occlusion (Blood Floio ml./gm./min.) Dog: no. E 5 E 7 E 9 E 15 E Anatomical location of muscle sample distribution Circumflex distribution TABLE 6 Poudrage with Coronary Sinus Narrowing and Chronic Left Anterior Descending Coronary Occlusion (Blood Floio ml./gm./min.) E 6 E 13 E 17 E Anatomical location of mus;cle sample distribution Circumflex distribution rowing likewise was ineffective in increasing blood flow to the ischemie area (table 5). When this operation and coronary occlusion were done together and preceded the measurement of blood flow by four to six months, there was evidence of collateral blood flow to the area of myocardium supplied by the occluded vessel (table 6). However, the development of collateral flow did not vary from those obtained in experiment 3 in which coronary occlusion alone was done four to five months previously, again suggesting tissue necrosis as one important stimulus for development of collateral blood flow. The deuterium oxide m'fethod was used in the present investigation to measure blood flow because it enables one to quantitate that component of total flow that actually reaches the tissue cells. It provides a direct measurement of the '' effective'' flow which at least potentially serves the nutritive demands of the organ. This method would appear to be superior to the injection of plastic substances or other masses that do not allow precise quantitation of intercoronary anastomoses or provide any evidence of that portion of the flow, via potential anastomoses, which actually reaches the capillary bed. Furthermore, measurements using D 2 O can be made under physiological conditions in the beating heart. This investigation indicates that after ligation of the anterior descending coronary artery, intercoronary anastomoses in the dog heart, although present, are inadequate to maintain functional blood flow to the myocardium in the distribution of this vessel. There does appear to be a regular loss of muscle with fibrous tissue replacement as a sequel to this maneuver. There is no detectable improvement when this ligation has been preceded by a functioning pulmonary artery-left atrial shunt or poudrage with coronary sinus narrowing. The reports of increased survival after coronary occlusion of animals protected by a myocardial revascularization procedure may be unrelated to blood flow to the ischemie area. It is possible that removal of the epicardium or other procedure may render the heart less vulnerable to ventricular fibrillation. The cause of death after coronary occlusion in the dog is predominantly ventric- Circulation Research. Volume X. January 19BS
5 CORONARY OCCLUSION AND SURGERY 49 nlar fibrillation. Studies of the influence of various myocardial revascularization procedures on the vulnerability of the dog heart to ventricular fibrillation lias been reported. These investigations indicate that the vulnerability of the dog heart to fibrillation after coronary occlusion is not altered by previous pulmonary artery to left atrial shunt or by poudrage with coronary sinus narrowing. Implantation of the internal mammary artery into the myocardium did afford considerable protection from ventricular fibrillation if this vessel remained patent, but no protection if thrombosed. These separate investigations support the concept, clearly stated by Beck, 2 that normal cardiac function is related to equal distribution of blood throughout the myocardium. However, these studies further suggest that, while bringing a new blood supply to the heart may be effective, two methods currently in use to redistribute the blood are not effective either in increasing tissue blood flow in an ischemic area nor in returning the ventricular fibrillation threshold to normal. Figure 1 is a summary of all results of the present investigation. In each animal, the flow to "affected" areas of the myocardium is expressed as a percentage of the "normal'' areas, i.e., regions not influenced by coronary occlusion. The normal flow was usually considered to be the mean of flows to the right ventricular sample and the circumflex sample farthest from the distribution of the left anterior descending artery. In this way, absolute flows do not influence the results and each animal serves as its own control. The flow to various regions of normal hearts is remarkably uniform. Immediately after anterior descending coronary occlusion, there is a decline in tissue blood flow to approximately 7.0 per cent of normal in the muscle supplied by this vessel. This is not altered by previous performance of poudrage with coronary sinus narrowing or by pulmonary artery to left atrial shunt. If one waits four to six months after the coronary occlusion, the blood flow to the region of ischemia increases to approximately 50 per cent of normal. The increase in flow is the same when Circulation Keacarch. Volume X, January no 90 «o 70 eo eo 10 0 RT. VENT. 9 6 ANT. OESC. 7 S 9 CIRCUMFLEX- ANATOMIC LOCATION OF MUSCLE SAMPLE FIGURE 1 Summary of all experiments: in each animal, the flow to affected areas of the myocardium is expressed as a percentage of the "normal" areas, regions not influenced by coronary occlusion. Normals ( ); chronic left anterior descending artery ligation (>); chronic left anterior descending artery ligation with poudrage and coronary sinus narrowing (A); acute left anterior descending artery ligation (Y.); acute left anterior descending artery ligation with previous poudrage and coronary sinus narrowing (\3)j acute left anterior descending artery ligation with previous pulmonary artery to left atrial shunt (O). Acute coronary artery ligation causes a drop in blood flow to less than 10 per cent of normal in the affected area of myocardium regardless of the performance of two operations designed to redistribute blood more equitably by the creation of intercoronary anastomoses. The blood floto to areas of myocardium supplied by an artery which wais ligated four to six months previously approximates 50 per cent of normal in those dogs which survive. One myocardial revascularigation procedure did not influence this result. the previously mentioned operative procedures are performed, indicating no additional collateral development as a result of these operations. Previous work 13 would suggest that the collateral flow which develops from the stimulus of infarction is not sufficient to favorably influence the depressed and dangerous venti'icular fibrillation threshold in this area. Further investigation, using the method herein described, would be useful to determine the influence of slow gradual coronary occlusion on the development of collateral blood flow.
6 50 MacLEAN, HEDENSTROM, RAYNER Summary Regional tissue blood flow to the heart was measured in the dog using deuterium oxide as a tracer substance. The method assumes that the rate of uptake of the tracer b.y a tissue is limited by the blood flow through the tissue and that the exchange of the tracer between blood and the extravascular space in the organ is instantaneous by comparison. This assumption has had previous confirmation. Six groups of animals were studied and the results revealed: (1) a uniform distribution of blood flow per unit of M'eight of tissue between the right ventricle and various parts of the left ventricle; (2) a decrease in tissue blood flow to (0.1 ml./gm./min., or less), approximately 7 per cent of normal in the area supplied by the left anterior descending coronary artery after acute occlusion of this vessel; (3) a failure of two operative procedures designed to increase intercoronary anastomoses to influence this greatly decreased flow, when these procedures were performed six weeks to six months prior to testing; (4) an increase in tissue blood flow to an ischemic area of myocardium to 50 per cent of normal four to six months after coronary occlusion; (5) a failure of operative procedures to increase significantly the blood flow to the ischemic area over that which developed naturally, indicating no additional collateral vessel development due to the operations. The results of this investigation were discussed in relation to experiments which deal with myocardial function and vulnerability to ventricular fibrillation after coronary occlusion. References 1. "VINEBERG, A., AND BULLER, W.: Technical factors which favor mammary coronary anastomosis. J. Thoracic Sing. 30: 411, BECK, C. S., AND LEIGHNINQER, D. S.: Operations for coronary artery disease..t.a.m.a. 156: 1226, DAY, S. B., AND LILLEHEI, C. W.: Experimental basis for a new operation for coronary artery disease. Surgery 45: 487, JOHNSON,' J. A., CAVERT, H. M., AND LIFSON, N.: Kinetics concerned with distribution of isotopic water in isolated perfused dog heart and skeletal muscle. Am. J. Physiol. 171: 687, THOMPSON, A. M., CAVERT, H. M., LIFSON, N., AND EVANS, E. L.: Begional tissue uptake of D»O in perfused organs: Rat liver, dog heart and gastrocnemius. Am. J. Physiol. 197: 897, BATNER, E. E., MACLEAN, L. D., AND GRIM, E.: Intestinal tissue blood flow in shock due to endotoxin. Circulation Research 8: 1212, HARRISON, T. E., FRIEDMAN, B. F., AND EESNICK, H., JR.: Mechanism of acute experimental heart failure. Arch. Int. Med. 57: 927, SPENCER, F. C, MERRILL, D. L., POWERS, S. B., AND BING, E. J.: Coronary blood flow and cardiac oxygen consumption in unnnesthetized dogs. Am. J. Physiol. 160: 149, GREGG, D. E.: Coronary Circulation in Health and Disease. Philadelphia, Lea & Febiger, ECKENHOFF, J. E., HAFKENSCHIEL, J. H., HORMEL, M. H., GOODALE, W. T., LUBIN, M., BING, B. J., AND KETV, S. S.: Measurement of coronary blood flow bj' the nitrous oxide method. Am. J. Physiol. 152: 356, MAT, A. M.: Surgical anatomy of the coronary arteries. Dis. Chest 38: 645, GARAMELLA, J. J., GEORGE, V. P., JR., AND HAY, L. J.: A correlative study of peripheral coronary pressures and coronary arteriography following coronary occlusion. Surg. Gynee. & Obst. 105: 89, MACLEAN, L. D., AND PHIBBS, C. M.: Relative effect of chronic ischemia and a myocardial revascularization procedure on the ventricular fibrillation threshold. Circulation Research 8: 473, Circulation Research, Volume X, January 1962
Further Studies on the Effect of Arteriovenous Fistulas and Elevations of Sinus Pressure
 Further Studies on the Effect of Arteriovenous Fistulas and Elevations of Sinus Pressure on Mortality Rates Following Acute Coronary Occlusions By GEORGE SMITH, F.R.C.S., JAMES DEMMING, MORTON ELEFF, AND
Further Studies on the Effect of Arteriovenous Fistulas and Elevations of Sinus Pressure on Mortality Rates Following Acute Coronary Occlusions By GEORGE SMITH, F.R.C.S., JAMES DEMMING, MORTON ELEFF, AND
Saphenous Vein Autograft Replacement
 Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
THE CARDIOVASCULAR SYSTEM. Part 1
 THE CARDIOVASCULAR SYSTEM Part 1 CARDIOVASCULAR SYSTEM Blood Heart Blood vessels What is the function of this system? What other systems does it affect? CARDIOVASCULAR SYSTEM Functions Transport gases,
THE CARDIOVASCULAR SYSTEM Part 1 CARDIOVASCULAR SYSTEM Blood Heart Blood vessels What is the function of this system? What other systems does it affect? CARDIOVASCULAR SYSTEM Functions Transport gases,
The Heart. The Heart A muscular double pump. The Pulmonary and Systemic Circuits
 C H A P T E R 19 The Heart The Heart A muscular double pump circuit takes blood to and from the lungs Systemic circuit vessels transport blood to and from body tissues Atria receive blood from the pulmonary
C H A P T E R 19 The Heart The Heart A muscular double pump circuit takes blood to and from the lungs Systemic circuit vessels transport blood to and from body tissues Atria receive blood from the pulmonary
Chapter 14. The Cardiovascular System
 Chapter 14 The Cardiovascular System Introduction Cardiovascular system - heart, blood and blood vessels Cardiac muscle makes up bulk of heart provides force to pump blood Function - transports blood 2
Chapter 14 The Cardiovascular System Introduction Cardiovascular system - heart, blood and blood vessels Cardiac muscle makes up bulk of heart provides force to pump blood Function - transports blood 2
Evaluation of Procedures Designed to Enhance Coronary Collateral Blood Flow
 Evaluation of Procedures Designed to Enhance Coronary Collateral Blood Flow By Robert M. Berne, M.D., Richard D. Jones, B.A., and Frederick S. Cross, M.D., Ph.D. The high incidence of coronary artery disease
Evaluation of Procedures Designed to Enhance Coronary Collateral Blood Flow By Robert M. Berne, M.D., Richard D. Jones, B.A., and Frederick S. Cross, M.D., Ph.D. The high incidence of coronary artery disease
11/10/2014. Muscular pump Two atria Two ventricles. In mediastinum of thoracic cavity 2/3 of heart's mass lies left of midline of sternum
 It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
This lab activity is aligned with Visible Body s A&P app. Learn more at visiblebody.com/professors
 1 This lab activity is aligned with Visible Body s A&P app. Learn more at visiblebody.com/professors 2 PRE-LAB EXERCISES: A. Watch the video 29.1 Heart Overview and make the following observations: 1.
1 This lab activity is aligned with Visible Body s A&P app. Learn more at visiblebody.com/professors 2 PRE-LAB EXERCISES: A. Watch the video 29.1 Heart Overview and make the following observations: 1.
THE VESSELS OF THE HEART
 1 THE VESSELS OF THE HEART The vessels of the heart include the coronary arteries, which supply the heart and the veins and lymph vessels, which drain the heart. THE CORONARY ARTERIES These are the blood
1 THE VESSELS OF THE HEART The vessels of the heart include the coronary arteries, which supply the heart and the veins and lymph vessels, which drain the heart. THE CORONARY ARTERIES These are the blood
AP2 Lab 3 Coronary Vessels, Valves, Sounds, and Dissection
 AP2 Lab 3 Coronary Vessels, Valves, Sounds, and Dissection Project 1 - BLOOD Supply to the Myocardium (Figs. 18.5 &18.10) The myocardium is not nourished by the blood while it is being pumped through the
AP2 Lab 3 Coronary Vessels, Valves, Sounds, and Dissection Project 1 - BLOOD Supply to the Myocardium (Figs. 18.5 &18.10) The myocardium is not nourished by the blood while it is being pumped through the
Collin County Community College. ! BIOL Anatomy & Physiology! WEEK 5. The Heart
 Collin County Community College! BIOL. 2402 Anatomy & Physiology! WEEK 5 The Heart 1 (1578-1657) A groundbreaking work in the history of medicine, English physician William Harvey s Anatomical Essay on
Collin County Community College! BIOL. 2402 Anatomy & Physiology! WEEK 5 The Heart 1 (1578-1657) A groundbreaking work in the history of medicine, English physician William Harvey s Anatomical Essay on
Effects of myocardial infarction on catheter defibrillation threshold
 Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 1983 Effects of myocardial infarction on catheter defibrillation threshold
Purdue University Purdue e-pubs Weldon School of Biomedical Engineering Faculty Publications Weldon School of Biomedical Engineering 1983 Effects of myocardial infarction on catheter defibrillation threshold
CV Anatomy Quiz. Dr Ella Kim Dr Pip Green
 CV Anatomy Quiz Dr Ella Kim Dr Pip Green Q1 The location of the heart is correctly described as A) lateral to the lungs. B) medial to the sternum. C) superior to the diaphragm. D) posterior to the spinal
CV Anatomy Quiz Dr Ella Kim Dr Pip Green Q1 The location of the heart is correctly described as A) lateral to the lungs. B) medial to the sternum. C) superior to the diaphragm. D) posterior to the spinal
The Cardiovascular System
 The Cardiovascular System The Manila Times College of Subic Prepared by: Stevens B. Badar, RN, MANc THE HEART Anatomy of the Heart Location and Size approx. the size of a person s fist, hollow and cone-shaped,
The Cardiovascular System The Manila Times College of Subic Prepared by: Stevens B. Badar, RN, MANc THE HEART Anatomy of the Heart Location and Size approx. the size of a person s fist, hollow and cone-shaped,
Lab Activity 23. Cardiac Anatomy. Portland Community College BI 232
 Lab Activity 23 Cardiac Anatomy Portland Community College BI 232 Cardiac Muscle Histology Branching cells Intercalated disc: contains many gap junctions connecting the adjacent cell cytoplasm, creates
Lab Activity 23 Cardiac Anatomy Portland Community College BI 232 Cardiac Muscle Histology Branching cells Intercalated disc: contains many gap junctions connecting the adjacent cell cytoplasm, creates
Vasculature and innervation of the heart. A. Bendelic Human Anatomy Department
 Vasculature and innervation of the heart A. Bendelic Human Anatomy Department Plan: 1. Arterial blood supply of the heart. Coronary arteries 2. Venous drainage of the heart. Cardiac veins 3. Innervation
Vasculature and innervation of the heart A. Bendelic Human Anatomy Department Plan: 1. Arterial blood supply of the heart. Coronary arteries 2. Venous drainage of the heart. Cardiac veins 3. Innervation
OXYGEN CONSUMPTION' JREISSATY, AND JIRO NAKANO 4. cannula was introduced via the left external jugular vein
 EFFECT OF AORTIC INSUFFICIENCY ON ARTERIAL BLOOD PRESSURE, CORONARY BLOOD FLOW AND CARDIAC OXYGEN CONSUMPTION' By RENE WEGRIA, GERHARD MUELHEIMS,2 JAMES GOLUB,3 ROBERT JREISSATY, AND JIRO NAKANO 4 (From
EFFECT OF AORTIC INSUFFICIENCY ON ARTERIAL BLOOD PRESSURE, CORONARY BLOOD FLOW AND CARDIAC OXYGEN CONSUMPTION' By RENE WEGRIA, GERHARD MUELHEIMS,2 JAMES GOLUB,3 ROBERT JREISSATY, AND JIRO NAKANO 4 (From
Blood Flow after Revascularization
 Direct Measurement of Extracoronary Blood Flow after Revascularization Procedures Rosendo L. Criollos, M.D., Abdul M. AlShamma, M.D., and Benson B. Roe, M.D. E xperimental and clinical studies have indicated
Direct Measurement of Extracoronary Blood Flow after Revascularization Procedures Rosendo L. Criollos, M.D., Abdul M. AlShamma, M.D., and Benson B. Roe, M.D. E xperimental and clinical studies have indicated
the Cardiovascular System I
 the Cardiovascular System I By: Dr. Nabil A Khouri MD, MsC, Ph.D MEDIASTINUM 1. Superior Mediastinum 2. inferior Mediastinum Anterior mediastinum. Middle mediastinum. Posterior mediastinum Anatomy of
the Cardiovascular System I By: Dr. Nabil A Khouri MD, MsC, Ph.D MEDIASTINUM 1. Superior Mediastinum 2. inferior Mediastinum Anterior mediastinum. Middle mediastinum. Posterior mediastinum Anatomy of
administration of adrenaline or in cases of increased perfusion pressure. approximately the same within fairly wide variations of the systemic
 6I2. I72. I THE DISTRIBUTION OF THE BLOOD IN THE CORONARY BLOOD VESSELS. BY G. V. ANREP, A. BLALOCK AND M. HAMMOUDA. (From the Physiological Laboratory, Cambridge.) As a result of experiments on perfused
6I2. I72. I THE DISTRIBUTION OF THE BLOOD IN THE CORONARY BLOOD VESSELS. BY G. V. ANREP, A. BLALOCK AND M. HAMMOUDA. (From the Physiological Laboratory, Cambridge.) As a result of experiments on perfused
Large veins of the thorax Brachiocephalic veins
 Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
THE HEART OBJECTIVES: LOCATION OF THE HEART IN THE THORACIC CAVITY CARDIOVASCULAR SYSTEM
 BIOLOGY II CARDIOVASCULAR SYSTEM ACTIVITY #3 NAME DATE HOUR THE HEART OBJECTIVES: Describe the anatomy of the heart and identify and give the functions of all parts. (pp. 356 363) Trace the flow of blood
BIOLOGY II CARDIOVASCULAR SYSTEM ACTIVITY #3 NAME DATE HOUR THE HEART OBJECTIVES: Describe the anatomy of the heart and identify and give the functions of all parts. (pp. 356 363) Trace the flow of blood
Regional Venous Drainage of the Human Heart*
 Brit. HeartyJ., 1968, 30, 105. Regional Venous Drainage of the Human Heart* WILLIAM B. HOOD, JR.t From the Cardiac Department, St. Thomas's Hospital, London, S.E.1 Blood samples obtained from the coronary
Brit. HeartyJ., 1968, 30, 105. Regional Venous Drainage of the Human Heart* WILLIAM B. HOOD, JR.t From the Cardiac Department, St. Thomas's Hospital, London, S.E.1 Blood samples obtained from the coronary
CARDIOVASCULAR SYSTEM
 CARDIOVASCULAR SYSTEM Overview Heart and Vessels 2 Major Divisions Pulmonary Circuit Systemic Circuit Closed and Continuous Loop Location Aorta Superior vena cava Right lung Pulmonary trunk Base of heart
CARDIOVASCULAR SYSTEM Overview Heart and Vessels 2 Major Divisions Pulmonary Circuit Systemic Circuit Closed and Continuous Loop Location Aorta Superior vena cava Right lung Pulmonary trunk Base of heart
The Cardiovascular System
 The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
The Heart & Pericardium Dr. Rakesh Kumar Verma Assistant Professor Department of Anatomy KGMU UP Lucknow
 The Heart & Pericardium Dr. Rakesh Kumar Verma Assistant Professor Department of Anatomy KGMU UP Lucknow Fibrous skeleton Dense fibrous connective tissue forms a structural foundation around AV & arterial
The Heart & Pericardium Dr. Rakesh Kumar Verma Assistant Professor Department of Anatomy KGMU UP Lucknow Fibrous skeleton Dense fibrous connective tissue forms a structural foundation around AV & arterial
Anatomy of the Heart
 Biology 212: Anatomy and Physiology II Anatomy of the Heart References: Saladin, KS: Anatomy and Physiology, The Unity of Form and Function 8 th (2018). Required reading before beginning this lab: Chapter
Biology 212: Anatomy and Physiology II Anatomy of the Heart References: Saladin, KS: Anatomy and Physiology, The Unity of Form and Function 8 th (2018). Required reading before beginning this lab: Chapter
Coronary arteriography in complicated acute myocardial infarction; clinical and angiographic correlates
 Coronary arteriography in complicated acute myocardial ; clinical and angiographic correlates Luis M. de la Fuente, M.D. Buenos Aires, Argentina From January 1979 to June 30, 1979, we performed coronary
Coronary arteriography in complicated acute myocardial ; clinical and angiographic correlates Luis M. de la Fuente, M.D. Buenos Aires, Argentina From January 1979 to June 30, 1979, we performed coronary
Cardiovascular System Notes: Heart Disease & Disorders
 Cardiovascular System Notes: Heart Disease & Disorders Interesting Heart Facts The Electrocardiograph (ECG) was invented in 1902 by Willem Einthoven Dutch Physiologist. This test is still used to evaluate
Cardiovascular System Notes: Heart Disease & Disorders Interesting Heart Facts The Electrocardiograph (ECG) was invented in 1902 by Willem Einthoven Dutch Physiologist. This test is still used to evaluate
WHILE it is generally agreed that elevation
 The Derivation of Coronary Sinus Flow During Elevation of Right Ventricular Pressure By HERMAN M. GELLER, B.S., M.D., MARTIN BRANDFONBRENEU, M.D., AND CARL J. WIGGERS, M.D., The derivation of coronary
The Derivation of Coronary Sinus Flow During Elevation of Right Ventricular Pressure By HERMAN M. GELLER, B.S., M.D., MARTIN BRANDFONBRENEU, M.D., AND CARL J. WIGGERS, M.D., The derivation of coronary
Ch.15 Cardiovascular System Pgs {15-12} {15-13}
 Ch.15 Cardiovascular System Pgs {15-12} {15-13} E. Skeleton of the Heart 1. The skeleton of the heart is composed of rings of dense connective tissue and other masses of connective tissue in the interventricular
Ch.15 Cardiovascular System Pgs {15-12} {15-13} E. Skeleton of the Heart 1. The skeleton of the heart is composed of rings of dense connective tissue and other masses of connective tissue in the interventricular
Blood supply of the Heart & Conduction System. Dr. Nabil Khouri
 Blood supply of the Heart & Conduction System Dr. Nabil Khouri Arterial supply of Heart Right coronary artery Left coronary artery 3 Introduction: Coronary arteries - VASAVASORUM arising from aortic sinuses
Blood supply of the Heart & Conduction System Dr. Nabil Khouri Arterial supply of Heart Right coronary artery Left coronary artery 3 Introduction: Coronary arteries - VASAVASORUM arising from aortic sinuses
ACTIVITY 9: BLOOD AND HEART BLOOD
 ACTIVITY 9: BLOOD AND HEART OBJECTIVES: 1) How to get ready: Read Chapters 21 & 22, McKinley et al., Human Anatomy, 4e. All text references are for this textbook. Read dissection instructions BEFORE YOU
ACTIVITY 9: BLOOD AND HEART OBJECTIVES: 1) How to get ready: Read Chapters 21 & 22, McKinley et al., Human Anatomy, 4e. All text references are for this textbook. Read dissection instructions BEFORE YOU
Comparison of Flow Differences amoiig Venous Cannulas
 Comparison of Flow Differences amoiig Venous Cannulas Edward V. Bennett, Jr., MD., John G. Fewel, M.S., Jose Ybarra, B.S., Frederick L. Grover, M.D., and J. Kent Trinkle, M.D. ABSTRACT The efficiency of
Comparison of Flow Differences amoiig Venous Cannulas Edward V. Bennett, Jr., MD., John G. Fewel, M.S., Jose Ybarra, B.S., Frederick L. Grover, M.D., and J. Kent Trinkle, M.D. ABSTRACT The efficiency of
Anatomy of the Heart. Figure 20 2c
 Anatomy of the Heart Figure 20 2c Pericardium & Myocardium Remember, the heart sits in it s own cavity, known as the mediastinum. The heart is surrounded by the Pericardium, a double lining of the pericardial
Anatomy of the Heart Figure 20 2c Pericardium & Myocardium Remember, the heart sits in it s own cavity, known as the mediastinum. The heart is surrounded by the Pericardium, a double lining of the pericardial
Citation Acta medica Nagasakiensia. 1984, 29
 NAOSITE: Nagasaki University's Ac Title Author(s) Efficacy of Coenzyme Q10 Administra Aortic Stenosis and Pacemaker Induc Igarashi, Katsuro Citation Acta medica Nagasakiensia. 1984, 29 Issue Date 1984-10-25
NAOSITE: Nagasaki University's Ac Title Author(s) Efficacy of Coenzyme Q10 Administra Aortic Stenosis and Pacemaker Induc Igarashi, Katsuro Citation Acta medica Nagasakiensia. 1984, 29 Issue Date 1984-10-25
Chapter 20 (1) The Heart
 Chapter 20 (1) The Heart Learning Objectives Describe the location and structure of the heart Describe the path of a drop of blood from the superior vena cava or inferior vena cava through the heart out
Chapter 20 (1) The Heart Learning Objectives Describe the location and structure of the heart Describe the path of a drop of blood from the superior vena cava or inferior vena cava through the heart out
Intraventricular Pressure and the Distribution of Coronary Blood Flow
 Intraventricular Pressure and the Distribution of Coronary Blood Flow By Renato Cutarelli, M.D., and Matthew N. Levy, M.D. With the assistance of Harrison Zieske, Jr., and Geroldine Nelson In both clinical
Intraventricular Pressure and the Distribution of Coronary Blood Flow By Renato Cutarelli, M.D., and Matthew N. Levy, M.D. With the assistance of Harrison Zieske, Jr., and Geroldine Nelson In both clinical
Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies
 Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies THIRD EDITION CHAPTER 27 The Cardiovascular System Lesson 1: Overview of the Cardiovascular System Lesson Objectives Upon
Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies THIRD EDITION CHAPTER 27 The Cardiovascular System Lesson 1: Overview of the Cardiovascular System Lesson Objectives Upon
LAB 12-1 HEART DISSECTION GROSS ANATOMY OF THE HEART
 LAB 12-1 HEART DISSECTION GROSS ANATOMY OF THE HEART Because mammals are warm-blooded and generally very active animals, they require high metabolic rates. One major requirement of a high metabolism is
LAB 12-1 HEART DISSECTION GROSS ANATOMY OF THE HEART Because mammals are warm-blooded and generally very active animals, they require high metabolic rates. One major requirement of a high metabolism is
Lab 16. The Cardiovascular System Heart and Blood Vessels. Laboratory Objectives
 Lab 16 The Cardiovascular System Heart and Blood Vessels Laboratory Objectives Describe the anatomical structures of the heart to include the pericardium, chambers, valves, and major vessels. Describe
Lab 16 The Cardiovascular System Heart and Blood Vessels Laboratory Objectives Describe the anatomical structures of the heart to include the pericardium, chambers, valves, and major vessels. Describe
10. Thick deposits of lipids on the walls of blood vessels, called, can lead to serious circulatory issues. A. aneurysm B. atherosclerosis C.
 Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
DEVELOPMENT OF THE CIRCULATORY SYSTEM L E C T U R E 5
 DEVELOPMENT OF THE CIRCULATORY SYSTEM L E C T U R E 5 REVIEW OF CARDIAC ANATOMY Heart 4 chambers Base and apex Valves Pericardial sac 3 layers: epi, myo, endo cardium Major blood vessels Aorta and its
DEVELOPMENT OF THE CIRCULATORY SYSTEM L E C T U R E 5 REVIEW OF CARDIAC ANATOMY Heart 4 chambers Base and apex Valves Pericardial sac 3 layers: epi, myo, endo cardium Major blood vessels Aorta and its
The HEART. What is it???? Pericardium. Heart Facts. This muscle never stops working It works when you are asleep
 This muscle never stops working It works when you are asleep The HEART It works when you eat It really works when you exercise. What is it???? Located between the lungs in the mid thoracic region Apex
This muscle never stops working It works when you are asleep The HEART It works when you eat It really works when you exercise. What is it???? Located between the lungs in the mid thoracic region Apex
The Heart. Happy Friday! #takeoutyournotes #testnotgradedyet
 The Heart Happy Friday! #takeoutyournotes #testnotgradedyet Introduction Cardiovascular system distributes blood Pump (heart) Distribution areas (capillaries) Heart has 4 compartments 2 receive blood (atria)
The Heart Happy Friday! #takeoutyournotes #testnotgradedyet Introduction Cardiovascular system distributes blood Pump (heart) Distribution areas (capillaries) Heart has 4 compartments 2 receive blood (atria)
The Cardiovascular System. Chapter 15. Cardiovascular System FYI. Cardiology Closed systemof the heart & blood vessels. Functions
 Chapter 15 Cardiovascular System FYI The heart pumps 7,000 liters (4000 gallons) of blood through the body each day The heart contracts 2.5 billion times in an avg. lifetime The heart & all blood vessels
Chapter 15 Cardiovascular System FYI The heart pumps 7,000 liters (4000 gallons) of blood through the body each day The heart contracts 2.5 billion times in an avg. lifetime The heart & all blood vessels
10/23/2017. Muscular pump Two atria Two ventricles. In mediastinum of thoracic cavity 2/3 of heart's mass lies left of midline of sternum
 It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
Ch 19: Cardiovascular System - The Heart -
 Ch 19: Cardiovascular System - The Heart - Give a detailed description of the superficial and internal anatomy of the heart, including the pericardium, the myocardium, and the cardiac muscle. Trace the
Ch 19: Cardiovascular System - The Heart - Give a detailed description of the superficial and internal anatomy of the heart, including the pericardium, the myocardium, and the cardiac muscle. Trace the
Read Me. covering the Heart Anatomy. Labs. textbook. use. car: you
 Heart Anatomy Lab Pre-Lab Exercises Read Me These exercises should be done before coming to lab, after watching the videos covering the Heart Anatomy Labs. Answer the questions in this guide using the
Heart Anatomy Lab Pre-Lab Exercises Read Me These exercises should be done before coming to lab, after watching the videos covering the Heart Anatomy Labs. Answer the questions in this guide using the
Cardiovascular Anatomy Dr. Gary Mumaugh
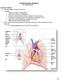 Cardiovascular Anatomy Dr. Gary Mumaugh Location of Heart Approximately the size of your fist Location o Superior surface of diaphragm o Left of the midline in mediastinum o Anterior to the vertebral column,
Cardiovascular Anatomy Dr. Gary Mumaugh Location of Heart Approximately the size of your fist Location o Superior surface of diaphragm o Left of the midline in mediastinum o Anterior to the vertebral column,
by Starling [1914] and Daly [1925].
![by Starling [1914] and Daly [1925]. by Starling [1914] and Daly [1925].](/thumbs/83/88889966.jpg) 612.13 PROPERTIES OF THE PERIPHERAL VASCULAR SYSTEM AND THEIR RELATION TO THE SYSTEMIC OUTPUT. BY HENRY BARCROFT. Harmsworth Scholar, St Mary's Hospital, London. (Experiments performed in the Physiological
612.13 PROPERTIES OF THE PERIPHERAL VASCULAR SYSTEM AND THEIR RELATION TO THE SYSTEMIC OUTPUT. BY HENRY BARCROFT. Harmsworth Scholar, St Mary's Hospital, London. (Experiments performed in the Physiological
Cardiac Radiology In-Training Test Questions for Diagnostic Radiology Residents
 Cardiac Radiology In-Training Test Questions for Diagnostic Radiology Residents March, 2013 Sponsored by: Commission on Education Committee on Residency Training in Diagnostic Radiology 2013 by American
Cardiac Radiology In-Training Test Questions for Diagnostic Radiology Residents March, 2013 Sponsored by: Commission on Education Committee on Residency Training in Diagnostic Radiology 2013 by American
Read Chapters 21 & 22, McKinley et al
 ACTIVITY 9: BLOOD AND HEART OBJECTIVES: 1) How to get ready: Read Chapters 21 & 22, McKinley et al., Human Anatomy, 5e. All text references are for this textbook. Read dissection instructions BEFORE YOU
ACTIVITY 9: BLOOD AND HEART OBJECTIVES: 1) How to get ready: Read Chapters 21 & 22, McKinley et al., Human Anatomy, 5e. All text references are for this textbook. Read dissection instructions BEFORE YOU
Introduction to Anatomy. Dr. Maher Hadidi. Bayan Yanes. April/9 th /2013
 Introduction to Anatomy Dr. Maher Hadidi Bayan Yanes 27 April/9 th /2013 KEY POINTS: 1) Right side of the heart 2) Papillary muscles 3) Left side of the heart 4) Comparison between right and left sides
Introduction to Anatomy Dr. Maher Hadidi Bayan Yanes 27 April/9 th /2013 KEY POINTS: 1) Right side of the heart 2) Papillary muscles 3) Left side of the heart 4) Comparison between right and left sides
(2) (1) (3) (4) BLOOD PATHWAY ASSESSMENT RUBRIC
 BLOODPATHWAYASSESSMENT(4) BLOOD%PATHWAY%ASSESSMENT%(3)% BLOODPATHWAYASSESSMENT(3) (4) (3) (2) (1) Using a completely blank diagram of the heart, all valves, chambers, great vessels, and direction of blood
BLOODPATHWAYASSESSMENT(4) BLOOD%PATHWAY%ASSESSMENT%(3)% BLOODPATHWAYASSESSMENT(3) (4) (3) (2) (1) Using a completely blank diagram of the heart, all valves, chambers, great vessels, and direction of blood
The Physiology of the Fetal Cardiovascular System
 The Physiology of the Fetal Cardiovascular System Jeff Vergales, MD, MS Department of Pediatrics Division of Pediatric Cardiology jvergales@virginia.edu Disclosures I serve as the medical director for
The Physiology of the Fetal Cardiovascular System Jeff Vergales, MD, MS Department of Pediatrics Division of Pediatric Cardiology jvergales@virginia.edu Disclosures I serve as the medical director for
EMT. Chapter 14 Review
 EMT Chapter 14 Review Review 1. All of the following are common signs and symptoms of cardiac ischemia, EXCEPT: A. headache. B. chest pressure. C. shortness of breath. D. anxiety or restlessness. Review
EMT Chapter 14 Review Review 1. All of the following are common signs and symptoms of cardiac ischemia, EXCEPT: A. headache. B. chest pressure. C. shortness of breath. D. anxiety or restlessness. Review
Circulation. Circulation = is a process used for the transport of oxygen, carbon! dioxide, nutrients and wastes through-out the body
 Circulation Circulation = is a process used for the transport of oxygen, carbon! dioxide, nutrients and wastes through-out the body Heart = muscular organ about the size of your fist which pumps blood.
Circulation Circulation = is a process used for the transport of oxygen, carbon! dioxide, nutrients and wastes through-out the body Heart = muscular organ about the size of your fist which pumps blood.
The pericardial sac is composed of the outer fibrous pericardium
 Pericardiectomy for Constrictive or Recurrent Inflammatory Pericarditis Mauricio A. Villavicencio, MD, Joseph A. Dearani, MD, and Thoralf M. Sundt, III, MD Anatomy and Preoperative Considerations The pericardial
Pericardiectomy for Constrictive or Recurrent Inflammatory Pericarditis Mauricio A. Villavicencio, MD, Joseph A. Dearani, MD, and Thoralf M. Sundt, III, MD Anatomy and Preoperative Considerations The pericardial
human anatomy 2016 lecture thirteen Dr meethak ali ahmed neurosurgeon
 Heart The heart is a hollow muscular organ that is somewhat pyramid shaped and lies within the pericardium in the mediastinum. It is connected at its base to the great blood vessels but otherwise lies
Heart The heart is a hollow muscular organ that is somewhat pyramid shaped and lies within the pericardium in the mediastinum. It is connected at its base to the great blood vessels but otherwise lies
Ischemic heart disease
 Ischemic heart disease Introduction In > 90% of cases: the cause is: reduced coronary blood flow secondary to: obstructive atherosclerotic vascular disease so most of the time it is called: coronary artery
Ischemic heart disease Introduction In > 90% of cases: the cause is: reduced coronary blood flow secondary to: obstructive atherosclerotic vascular disease so most of the time it is called: coronary artery
2. right heart = pulmonary pump takes blood to lungs to pick up oxygen and get rid of carbon dioxide
 A. location in thorax, in inferior mediastinum posterior to sternum medial to lungs superior to diaphragm anterior to vertebrae orientation - oblique apex points down and to the left 2/3 of mass on left
A. location in thorax, in inferior mediastinum posterior to sternum medial to lungs superior to diaphragm anterior to vertebrae orientation - oblique apex points down and to the left 2/3 of mass on left
that a study could be designed utilizing an intact animal, anesthetized but breathing room air, in
 INDUCED TACHYCARDIA: ITS EFFECT UPON THE CORONARY HEMODYNAMICS, MYOCARDIAL METABOLISM AND CARDIAC EFFICIENCY OF THE INTACT DOG1 2 By GEORGE M. MAXWELL, CESAR A. CASTILLO, DOUGLAS H. WHITE, JR., CHARLES
INDUCED TACHYCARDIA: ITS EFFECT UPON THE CORONARY HEMODYNAMICS, MYOCARDIAL METABOLISM AND CARDIAC EFFICIENCY OF THE INTACT DOG1 2 By GEORGE M. MAXWELL, CESAR A. CASTILLO, DOUGLAS H. WHITE, JR., CHARLES
Approximately the size of your fist Location Superior surface of diaphragm Left of the midline in mediastinum Anterior to the vertebral column,
 Dr. Gary Mumaugh Approximately the size of your fist Location Superior surface of diaphragm Left of the midline in mediastinum Anterior to the vertebral column, posterior to the sternum Posteriorly the
Dr. Gary Mumaugh Approximately the size of your fist Location Superior surface of diaphragm Left of the midline in mediastinum Anterior to the vertebral column, posterior to the sternum Posteriorly the
Disease of the aortic valve is frequently associated with
 Stentless Aortic Bioprosthesis for Disease of the Aortic Valve, Root and Ascending Aorta John R. Doty, MD, and Donald B. Doty, MD Disease of the aortic valve is frequently associated with morphologic abnormalities
Stentless Aortic Bioprosthesis for Disease of the Aortic Valve, Root and Ascending Aorta John R. Doty, MD, and Donald B. Doty, MD Disease of the aortic valve is frequently associated with morphologic abnormalities
PIAF study: Placental insufficiency and aortic isthmus flow Jean-Claude Fouron, MD
 Dear colleagues, I would like to thank you very sincerely for agreeing to participate in our multicentre study on the clinical significance of recording fetal aortic isthmus flow during placental circulatory
Dear colleagues, I would like to thank you very sincerely for agreeing to participate in our multicentre study on the clinical significance of recording fetal aortic isthmus flow during placental circulatory
Figure 10.1A Transparency Master 79
 Brain Carotid arteries Jugular vein Right front leg Lungs (inflated) Cranial Right atrium To left front leg Left subclavian Bronchus capillaries Brachiocephalic vein Left atrium Dorsal aorta Right ventricle
Brain Carotid arteries Jugular vein Right front leg Lungs (inflated) Cranial Right atrium To left front leg Left subclavian Bronchus capillaries Brachiocephalic vein Left atrium Dorsal aorta Right ventricle
Middle mediastinum---- heart & pericardium. Dep. of Human Anatomy Zhou Hongying
 Middle mediastinum---- heart & pericardium Dep. of Human Anatomy Zhou Hongying eaglezhyxzy@163.com Subdivisions of the mediastinum Contents of Middle mediastinum Heart Pericardium: a serous sac enclosing
Middle mediastinum---- heart & pericardium Dep. of Human Anatomy Zhou Hongying eaglezhyxzy@163.com Subdivisions of the mediastinum Contents of Middle mediastinum Heart Pericardium: a serous sac enclosing
4. The two inferior chambers of the heart are known as the atria. the superior and inferior vena cava, which empty into the left atrium.
 Answer each statement true or false. If the statement is false, change the underlined word to make it true. 1. The heart is located approximately between the second and fifth ribs and posterior to the
Answer each statement true or false. If the statement is false, change the underlined word to make it true. 1. The heart is located approximately between the second and fifth ribs and posterior to the
Figure ) The specific chamber of the heart that is indicated by letter A is called the. Diff: 1 Page Ref: 364
 Essentials of Anatomy and Physiology, 9e (Marieb) Chapter 11 The Cardiovascular System Short Answer Figure 11.1 Using Figure 11.1, identify the following: 1) The Purkinje fibers are indicated by label.
Essentials of Anatomy and Physiology, 9e (Marieb) Chapter 11 The Cardiovascular System Short Answer Figure 11.1 Using Figure 11.1, identify the following: 1) The Purkinje fibers are indicated by label.
The Cardiovascular System
 Essentials of Human Anatomy & Physiology Elaine N. Marieb Slides 11.1 11.19 Seventh Edition Chapter 11 The Cardiovascular System Functions of the Cardiovascular system Function of the heart: to pump blood
Essentials of Human Anatomy & Physiology Elaine N. Marieb Slides 11.1 11.19 Seventh Edition Chapter 11 The Cardiovascular System Functions of the Cardiovascular system Function of the heart: to pump blood
Cardiovascular Physiology. Heart Physiology. Introduction. The heart. Electrophysiology of the heart
 Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
Cardiovascular system:
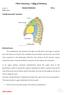 Cardiovascular system: Mediastinum: The mediastinum: lies between the right and left pleura and lungs. It extends from the sternum in front to the vertebral column behind, and from the root of the neck
Cardiovascular system: Mediastinum: The mediastinum: lies between the right and left pleura and lungs. It extends from the sternum in front to the vertebral column behind, and from the root of the neck
The Cardiovascular System: The Heart
 The Cardiovascular System: The Heart 1 2 3 4 5 6 7 8 9 10 11 12 Across 1. The spontaneously changing pacemaker membranes. 7. The distinguishing feature of heart muscle. 9. What allows heart cells to beat
The Cardiovascular System: The Heart 1 2 3 4 5 6 7 8 9 10 11 12 Across 1. The spontaneously changing pacemaker membranes. 7. The distinguishing feature of heart muscle. 9. What allows heart cells to beat
Mediastinum and pericardium
 Mediastinum and pericardium Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com The mediastinum: is the central compartment of the thoracic cavity surrounded by
Mediastinum and pericardium Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com The mediastinum: is the central compartment of the thoracic cavity surrounded by
Effect of Intravascular Isotope Content on the Isotopic Determination of Coronary Collateral Blood Flow
 Effect of Intravascular Isotope Content on the Isotopic Determination of Coronary Collateral Blood Flow By Colin M. Bloor, M.D., and Lathrop E. Roberts, M.D. Downloaded from http:ahajournals.org by on
Effect of Intravascular Isotope Content on the Isotopic Determination of Coronary Collateral Blood Flow By Colin M. Bloor, M.D., and Lathrop E. Roberts, M.D. Downloaded from http:ahajournals.org by on
Index. cardiology.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute ischemic stroke TOAST classification of, 270 Acute myocardial infarction (AMI) cardioembolic stroke following, 207 208 noncardioembolic
Index Note: Page numbers of article titles are in boldface type. A Acute ischemic stroke TOAST classification of, 270 Acute myocardial infarction (AMI) cardioembolic stroke following, 207 208 noncardioembolic
The Cardiovascular System Part I: Heart Outline of class lecture After studying part I of this chapter you should be able to:
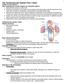 The Cardiovascular System Part I: Heart Outline of class lecture After studying part I of this chapter you should be able to: 1. Describe the functions of the heart 2. Describe the location of the heart,
The Cardiovascular System Part I: Heart Outline of class lecture After studying part I of this chapter you should be able to: 1. Describe the functions of the heart 2. Describe the location of the heart,
11.1 The Aortic Arch General Anatomy of the Ascending Aorta and the Aortic Arch Surgical Anatomy of the Aorta
 456 11 Surgical Anatomy of the Aorta 11.1 The Aortic Arch 11.1.1 General Anatomy of the Ascending Aorta and the Aortic Arch Surgery of the is one of the most challenging areas of cardiac and vascular surgery,
456 11 Surgical Anatomy of the Aorta 11.1 The Aortic Arch 11.1.1 General Anatomy of the Ascending Aorta and the Aortic Arch Surgery of the is one of the most challenging areas of cardiac and vascular surgery,
CY2017 Hospital Outpatient: Vascular Procedure APCs and Complexity Adjustments
 CY2017 Hospital Outpatient: Vascular Procedure APCs and Complexity Adjustments Comprehensive Ambulatory Payment Classifications (c-apcs) In CY2015 and in an effort to help pay providers for quality, not
CY2017 Hospital Outpatient: Vascular Procedure APCs and Complexity Adjustments Comprehensive Ambulatory Payment Classifications (c-apcs) In CY2015 and in an effort to help pay providers for quality, not
The arterial switch operation has been the accepted procedure
 The Arterial Switch Procedure: Closed Coronary Artery Transfer Edward L. Bove, MD The arterial switch operation has been the accepted procedure for the repair of transposition of the great arteries (TGA)
The Arterial Switch Procedure: Closed Coronary Artery Transfer Edward L. Bove, MD The arterial switch operation has been the accepted procedure for the repair of transposition of the great arteries (TGA)
The sinus venosus represent the venous end of the heart It receives 3 veins: 1- Common cardinal vein body wall 2- Umbilical vein from placenta 3-
 1 2 The sinus venosus represent the venous end of the heart It receives 3 veins: 1- Common cardinal vein body wall 2- Umbilical vein from placenta 3- Vitelline vein from yolk sac 3 However!!!!! The left
1 2 The sinus venosus represent the venous end of the heart It receives 3 veins: 1- Common cardinal vein body wall 2- Umbilical vein from placenta 3- Vitelline vein from yolk sac 3 However!!!!! The left
Anatomy: Cardiovascular System
 In the name of God Anatomy: Cardiovascular System Moradian MD, MPH, PhD candidate Tehran University of Medical Sciences drmoradian@sums.ac.ir 2015 The Cardiovascular System A closed system of the heart
In the name of God Anatomy: Cardiovascular System Moradian MD, MPH, PhD candidate Tehran University of Medical Sciences drmoradian@sums.ac.ir 2015 The Cardiovascular System A closed system of the heart
The Cardiovascular System (Heart)
 The Cardiovascular System The Cardiovascular System (Heart) A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function
The Cardiovascular System The Cardiovascular System (Heart) A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function
Cardiac Ischemia (is-kē-mē-uh)
 Chapter 21 Cardiac Ischemia (is-kē-mē-uh) By: Alejandra & Lindsay I. Cardiac Ischemia =the most common cause of death in Western Culture ~35% of deaths. -Suddenly from acute coronary occlusion or fibrillation
Chapter 21 Cardiac Ischemia (is-kē-mē-uh) By: Alejandra & Lindsay I. Cardiac Ischemia =the most common cause of death in Western Culture ~35% of deaths. -Suddenly from acute coronary occlusion or fibrillation
THE DOG is used a great deal in physiological
 Anatomy of the Ventricular Coronary Arteries in the Dog THE DOG is used a great deal in physiological and surgical research on the heart. In view of this, it is surprising that information with regard
Anatomy of the Ventricular Coronary Arteries in the Dog THE DOG is used a great deal in physiological and surgical research on the heart. In view of this, it is surprising that information with regard
Human Anatomy, First Edition
 Human Anatomy, First Edition McKinley & O'Loughlin Chapter 22 : Heart 1 Functions of the Heart Center of the cardiovascular system, the heart. Connects to blood vessels that transport blood between the
Human Anatomy, First Edition McKinley & O'Loughlin Chapter 22 : Heart 1 Functions of the Heart Center of the cardiovascular system, the heart. Connects to blood vessels that transport blood between the
Common Codes for ICD-10
 Common Codes for ICD-10 Specialty: Cardiology *Always utilize more specific codes first. ABNORMALITIES OF HEART RHYTHM ICD-9-CM Codes: 427.81, 427.89, 785.0, 785.1, 785.3 R00.0 Tachycardia, unspecified
Common Codes for ICD-10 Specialty: Cardiology *Always utilize more specific codes first. ABNORMALITIES OF HEART RHYTHM ICD-9-CM Codes: 427.81, 427.89, 785.0, 785.1, 785.3 R00.0 Tachycardia, unspecified
Human Anatomy and Physiology Chapter 19 Worksheet 1- The Heart
 Human Anatomy and Physiology Chapter 19 Worksheet 1- The Heart Name Date Period 1. The "double pump" function of the heart includes the right side, which serves as the circuit pump, while the left side
Human Anatomy and Physiology Chapter 19 Worksheet 1- The Heart Name Date Period 1. The "double pump" function of the heart includes the right side, which serves as the circuit pump, while the left side
Mandatory knowledge about natural history of coronary grafts. P.Sergeant P. Maureira K.U.Leuven, Belgium
 Mandatory knowledge about natural history of coronary grafts P.Sergeant P. Maureira K.U.Leuven, Belgium Types of grafts Arterial ITA/IMA (internal thoracic/mammary artery) Radial artery Gastro-epiploïc
Mandatory knowledge about natural history of coronary grafts P.Sergeant P. Maureira K.U.Leuven, Belgium Types of grafts Arterial ITA/IMA (internal thoracic/mammary artery) Radial artery Gastro-epiploïc
The Heart. Size, Form, and Location of the Heart. 1. Blunt, rounded point; most inferior part of the heart.
 12 The Heart FOCUS: The heart is composed of cardiac muscle cells, which are elongated, branching cells that appear striated. Cardiac muscle cells behave as a single electrical unit, and the highly coordinated
12 The Heart FOCUS: The heart is composed of cardiac muscle cells, which are elongated, branching cells that appear striated. Cardiac muscle cells behave as a single electrical unit, and the highly coordinated
Case Report Preoperative Assessment of Anomalous Right Coronary Artery Arising from the Main Pulmonary Artery
 Case Reports in Medicine Volume 2011, Article ID 642126, 4 pages doi:10.1155/2011/642126 Case Report Preoperative Assessment of Anomalous Right Coronary Artery Arising from the Main Pulmonary Artery Marshall
Case Reports in Medicine Volume 2011, Article ID 642126, 4 pages doi:10.1155/2011/642126 Case Report Preoperative Assessment of Anomalous Right Coronary Artery Arising from the Main Pulmonary Artery Marshall
AP2 Lab 1 - Blood & Heart
 AP2 Lab 1 - Blood & Heart Project 1 - Formed Elements Identification & Recognition See fig. 17.10 and Table 17.2. Instructor may also provide other images. Note: See Fig. 17.11 All formed elements are
AP2 Lab 1 - Blood & Heart Project 1 - Formed Elements Identification & Recognition See fig. 17.10 and Table 17.2. Instructor may also provide other images. Note: See Fig. 17.11 All formed elements are
The Mammalian Circulatory System
 The Mammalian Heart The Mammalian Circulatory System Recall: What are the 3 cycles of the mammalian circulatory system? What are their functions? What are the three main vessel types in the mammalian circulatory
The Mammalian Heart The Mammalian Circulatory System Recall: What are the 3 cycles of the mammalian circulatory system? What are their functions? What are the three main vessel types in the mammalian circulatory
Large Arteries of Heart
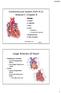 Cardiovascular System (Part A-2) Module 5 -Chapter 8 Overview Arteries Capillaries Veins Heart Anatomy Conduction System Blood pressure Fetal circulation Susie Turner, M.D. 1/5/13 Large Arteries of Heart
Cardiovascular System (Part A-2) Module 5 -Chapter 8 Overview Arteries Capillaries Veins Heart Anatomy Conduction System Blood pressure Fetal circulation Susie Turner, M.D. 1/5/13 Large Arteries of Heart
Chapter 14. Circulatory System Images. VT-122 Anatomy & Physiology II
 Chapter 14 Circulatory System Images VT-122 Anatomy & Physiology II The mediastinum Dog heart Dog heart Cat heart Dog heart ultrasound Can see pericardium as distinct bright line Pericardial effusion Fluid
Chapter 14 Circulatory System Images VT-122 Anatomy & Physiology II The mediastinum Dog heart Dog heart Cat heart Dog heart ultrasound Can see pericardium as distinct bright line Pericardial effusion Fluid
Approximately the size of your fist Location. Pericardial physiology
 Heart Anatomy Approximately the size of your fist Location Superior surface of diaphragm Left of the midline Anterior to the vertebral column, posterior to the sternum Wednesday, March 28, 2012 Muscle
Heart Anatomy Approximately the size of your fist Location Superior surface of diaphragm Left of the midline Anterior to the vertebral column, posterior to the sternum Wednesday, March 28, 2012 Muscle
Matters of the Heart: Comprehensive Cardiology SARAH BEANLANDS RN BSCN MSC
 Matters of the Heart: Comprehensive Cardiology SARAH BEANLANDS RN BSCN MSC Who am I? Class Outline Gross anatomy of the heart Trip around the heart Micro anatomy: cellular and tissue level Introduction
Matters of the Heart: Comprehensive Cardiology SARAH BEANLANDS RN BSCN MSC Who am I? Class Outline Gross anatomy of the heart Trip around the heart Micro anatomy: cellular and tissue level Introduction
Chapter 20: Cardiovascular System: The Heart
 Chapter 20: Cardiovascular System: The Heart I. Functions of the Heart A. List and describe the four functions of the heart: 1. 2. 3. 4. II. Size, Shape, and Location of the Heart A. Size and Shape 1.
Chapter 20: Cardiovascular System: The Heart I. Functions of the Heart A. List and describe the four functions of the heart: 1. 2. 3. 4. II. Size, Shape, and Location of the Heart A. Size and Shape 1.
