Beat-to-Beat Effects of Intraaortic Balloon Pump Timing on Left Ventricular Performance in Patients With Low Ejection Fraction
|
|
|
- Johnathan King
- 6 years ago
- Views:
Transcription
1 Beat-to-Beat Effects of Intraaortic Balloon Pump Timing on Left Ventricular Performance in Patients With Low Ejection Fraction Jan J. Schreuder, MD, PhD, Francesco Maisano, MD, Andrea Donelli, MS, Jos R. C. Jansen, PhD, Pat Hanlon, RN, Jan Bovelander, CRNA, and Ottavio Alfieri, MD Department of Cardiac Surgery, San Raffaele University Hospital, Milan, Italy; Department of Intensive Care, Leiden University Medical Center, Leiden, The Netherlands; Arrow International, Reading, Pennsylvania Background. Intraaortic balloon counterpulsation (IABP) timing errors during arrhythmia may result in afterload increases which may negatively influence left ventricular (LV) ejection and LV mechanical dyssynchrony. The aim of our study was to determine beat-tobeat effects of properly timed IABP, premature IAB inflation, and late IAB deflation on LV performance and LV mechanical dyssynchrony in heart failure patients undergoing cardiac surgery. Methods. In 15 patients, LV pressure-volume relations and LV dyssynchrony were measured by conductance volume catheter. Properly timed IABP was evaluated at a 1:1 assist ratio within a 10 seconds time-span. Premature IAB inflation and late IAB deflation were evaluated at a 1:4 assist ratio. Results. Properly timed 1:1 IABP acutely decreased LV end-systolic volume by 6.1% (p < ) and LV endsystolic pressure by 17.5% (p < ) due to decreased aortic impedance. Stroke volume (SV) increased by 14% (p < ), which correlated markedly with a decrease of LV mechanical dyssynchrony (p < ). The largest SV increases occurred in patients with lowest contractile state. Premature IAB inflation decreased SV by 20% (p < ) due to abrupt increase of LV afterload during late ejection. Late IAB deflation increased SV and stroke work by 18% (p < ) and 16% (p < 0.01) respectively, due to increased afterload during early ejection and decreased afterload during late ejection. Conclusions. Left ventricular performance during IABP is causally related to changes in LV afterload, and the timing of these changes in relation to contraction or relaxation phases, to LV mechanical dyssynchrony and to contractile state. (Ann Thorac Surg 2005;79:872 80) 2005 by The Society of Thoracic Surgeons Intraaortic balloon counterpulsation (IABP) to support cardiac function has been well documented during the last three decades [1 7]. Primary effects of properly timed IABP are diastolic aortic pressure augmentation and left ventricular (LV) afterload reduction by decreasing impedance to LV ejection [3, 4]. LV volume and LV end-diastolic pressure (EDP) have been demonstrated to See page 1017 decrease in patients treated with IABP, whereas cardiac output, ejection fraction (EF), and coronary flow may increase [2 6]. However, arrhythmic episodes often result in incorrect IABP timing decreasing its efficacy [7]. Premature IAB inflation may increase aortic impedance and therefore LV afterload late in the ejection phase, whereas late IAB deflation may increase afterload during early ejection. Acute load increases applied during contraction or relaxation in heart muscle preparations or in intact animal ventricles induced increases or decreases in ejection Accepted for publication July 29, Address reprint requests to Dr Schreuder, Department of Cardiac Surgery, San Raffaele University Hospital, Via Olgettina 60, Milan, Italy; schreuder@libero.it. phase duration, respectively [8 11]. Moreover, altered loading conditions may result in dyssynchronous relaxation of the LV [11, 12]. Myocardial relaxation is known to be sensitive to afterload and to LV dyssynchrony in patients with dilated cardiomyopathy [13]. LV mechanical dyssynchrony in these patients decreased due to reduction in wall stress induced by interventions such as vasodilators, cardiomyoplasty, or LV ventricular reduction surgery [13 16]. Recently we demonstrated a close relationship between cardiac performance and intraventricular mechanical dyssynchrony in patients undergoing LV restoration by the Dor procedure [16]. Hence we hypothesized that IABP timing in patients with low EF may considerably influence cardiac performance by acute afterload changes and concomitant changes in LV mechanical dyssynchrony. Effects of IABP on LV performance and LV mechanical dyssynchrony were analyzed beat-to-beat from the pressurevolume plane during conventionally timed IABP, prema- Dr Schreuder, Mr Bovelander and Ms Hanlon disclose that they have a financial relationship with Arrow International; Dr Schreuder also has a financial relationship with CD Leycom by The Society of Thoracic Surgeons /05/$30.00 Published by Elsevier Inc doi: /j.athoracsur
2 Ann Thorac Surg SCHREUDER ET AL 2005;79: LEFT VENTRICULAR PERFORMANCE AND IABP TIMING Abbreviations and Acronyms EDP end-diastolic pressure EDV end-diastolic volume Ees end-systolic elastance EF ejection fraction ESPVR end-systolic pressure-volume relationship ESV end-systolic volume ESP end-systolic pressure IABP intraaortic balloon counterpulsation LV left ventricle SV stroke volume SW stroke work ture IAB inflation and late IAB deflation, using the conductance volume catheter technique [14 23]. The beatto-beat measurements were performed within a time span of 10 seconds after an IABP change to exclude cardiovascular compensatory reflexes and or metabolic effects from possible increases in coronary flow [4]. Beat-to-beat changes of cardiac performance with IABP may then be primarily attributed to acute changes in aortic impedance. Patients and Methods Patients Fifteen patients, New York Heart Association (NYHA) class II IV, 48 to 64 years old, EF 21.5% 8.5%, undergoing cardiac surgery requiring prophylactic IABP, were studied. Eight patients underwent LV aneurysmectomy (6 patients with coronary artery bypass graft [CABG]), 6 patients underwent CABG (1 with mitral valve repair), and 1 patient underwent mitral valve repair. Open chest hemodynamic evaluations of acute effects of IABP were performed before cardiopulmonary bypass. The study protocol was approved by the local ethics committee and written informed patient consent was obtained. 873 Instrumentation All patients received high dose opioid anesthesia. Five patients belonging to NYHA class III-IV received small steady-state dosages of inotropics (dobutamine 5u kg 1 min 1 ). The IAB catheters (Narrowflex; Arrow International, Reading, PA) were positioned under transesophageal echo control in the descending thoracic aorta at 2-cm distal to the left subclavian artery. Thermodilution catheters (Edwards Lifesciences, Inc., Irvine, CA) were inserted into the pulmonary artery and micromanometerconductance catheters (F7; CD Leycom, Zoetermeer, The Netherlands) into the LV through a pulmonary vein. The cardiac function analyzer (Leycom CFL512; CD Leycom) uses a conductance catheter to measure ventricular volumes at a dual-field excitation mode [17, 21]. The method is based on measuring time-varying electrical conductance of 5 to 7 ventricular blood segments, delineated by selected catheter electrodes. Correct positioning of the conductance catheter was verified by transesophageal echocardiography and by inspection of the segmental conductance signals. The feasibility of the conductance catheter method to measure real-time ventricular volume has been demonstrated in animal and clinical studies [14 23]. Reproducibility of conductance catheter measurements was demonstrated in patients undergoing cardiac surgery [19]. Beat-to-beat stroke volume changes were validated by pulse contour analysis [20]. Time-varying segmental conductance reflects timevarying segmental LV volume as obtained and validated by cine-angiography in canine hearts [21]. Parallel conductance was assessed by injection of 10 ml hypertonic saline (6%) into the pulmonary artery [17]. Effective conductance stroke volume (SV) was defined as difference between conductance volumes at the times of dp/dt max and dp/dt max, which largely eliminates contribution of possible regurgitant flows. Absolute LV volumes were calculated by matching effective conductance SV with simultaneously measured thermodilution SV and by subtracting parallel conductance from total conductance volume. Mechanical Ventricular Dyssynchrony Ventricular dyssynchrony assessment from segmental LV volume signals has been previously described for cine-angiography and the conductance catheter [14, 23, 24]. The conductance catheter measures volume segments located perpendicular to the long heart-axis. A volume segment was defined dyssynchronous when the volume change in that segment was in opposite direction (dyskinetic) or showed no change (akinetic) compared to total LV volume change. Segmental dyssynchrony was quantified by percent time a segment was dyssynchronous in relation to total volume change, total dyssynchrony was the average of segmental dyssynchrony in all segments [14, 23]. Systolic dyssynchrony was calculated from R-wave to dp/dt max and diastolic dyssynchrony from dp/dt max to R-wave. Data Analysis Electrocardiogram (ECG), LV pressure, aortic pressure and volume signals were digitized at a sampling rate of 250 Hz. The following variables were calculated: Tau, index of LV pressure relaxation, defined as time required from LV pressure at dp/dt max to be reduced by half [25]; peak ejection rate calculated as maximal dv/dt; Endsystolic elastance (Ees), representing a load independent index of contractile state, was determined from unassisted beats and first 8 seconds of IABP (Fig 1); Ees1 included last unassisted beat (arrow) and first 3 assisted beats; Ees2 included last unassisted beat and three latest assisted beats prior to10 seconds after IABP initiation. Values are mean standard deviation (SD) of at least four heart cycles. Comparisons between different IABP modes were assessed with a paired t-test. Statistical relations between variables were tested by least-squares linear regression. Statistical significance was assumed at p less than CARDIOVASCULAR
3 874 SCHREUDER ET AL Ann Thorac Surg LEFT VENTRICULAR PERFORMANCE AND IABP TIMING 2005;79: Fig 1. Effects of regular 1:1 IABP initiation (arrows), with IAB inflation performed near the dicrotic notch of the Pao and deflation effecting decrease in end-diastolic Pao in patient A (NYHA III, EF 14%) and patient B (NYHA III, EF 22%). IABP induced acute stroke volume increases by decreasing LV end-systolic pressure (P) and volume (V), delineating nonlinear Ees (dotted lines) followed by end-diastolic P-V decreases. Numbers 1 10 represent first 10 beats after IABP initiation. (Ees end-systolic elastance; EF ejection fraction; IABP intraaortic balloon pump; LV left ventricular; NYHA New York Heart Association; Pao mean aortic pressure; PLV left ventricular pressure; VLV left ventricular volume.) Measurement Protocol Effects of properly timed IABP (inflation at the dicrotic notch, deflation inducing end-diastolic aortic pressure decrease) were measured during 15 seconds ventilatory stop, the first 5 seconds without IABP followed by assist at a 1:1 ratio (Fig 1). All measurements were made under steady state conditions. Premature IAB inflation was set 130 to190ms before the dicrotic notch to produce an abrupt afterload increase in the second part of the ejection phase (Fig 2 [A, b]). Late IAB deflation was set 110 to180ms after the R-wave, around the start of the ejection phase, to produce a clear afterload increase in the first part of the ejection phase (Fig 2 [B, c]). Both timing errors were evaluated at a 1:4 assist ratio during a 15 seconds ventilatory stop. Results Hemodynamic Response to Conventionally Timed IABP The acute effects of proper IABP timing at a 1:1 assist ratio are illustrated by two typical examples (Fig 1). The largest decreases in LV pressure, LV end-systolic volume (ESV), LV end-diastolic volume (EDV) and concomitant increases in SV are observed within 4 assisted beats. Decreases in LVESV and LV endsystolic pressure (ESP) delineate the end-systolic P-V relationship and its slope, the Ees, representing a load independent index of contractile state. The average hemodynamic responses to 1:1 IABP are presented in Table 1. Heart rate (HR) and Tau did not change significantly. SV increased (p ) by a mean of 14% ranging from 2% to 34%. Stroke work (SW) decreased by a mean of 5% (p 0.01). LVESV, LVESP, LVEDV, and LVEDP decreased by a mean of 6% (p ), 16 mm Hg (p ), 2% (p 0.001) and 1.6 mm Hg (p 0.001), respectively. IABP decreased dp/dt max by 8% (p 0.01) and dp/dt max by 17.5% (p ). Mean aortic pressure increased by 15.5% (p ). Peak ejection rate and EF increased by 9% (p 0.03) and 3% (p 0.001, net increase), respectively. End-systolic elastance appeared to be nonlinear, the slope determined over the first 8 seconds after IABP initiation at 1:1 assist was mm Hg/mL; Ees1, determined from the first three assisted beats was significantly (p 0.01) steeper than Ees2, using the last unassisted loops and those from 4 to 8 seconds after IABP initiation (Table 1 and Fig 1).
4 Ann Thorac Surg SCHREUDER ET AL 2005;79: LEFT VENTRICULAR PERFORMANCE AND IABP TIMING 875 CARDIOVASCULAR Fig 2. Premature IAB inflation (A) applied 150 ms (arrows, b) before the dicrotic notch of the aortic pressure (Pao) generated abrupt increases in LV afterload in late ejection with impairment of LV volume (VLV) ejection in NYHA II patient (EF 33%). Late IAB deflation (B) increased end-diastolic Pao (arrows, b) and increased afterload during early ejection (c) followed by decreased afterload in late ejection increasing stroke volume in NYHA III patient (EF 24%); a, b, and c represent beats analyzed according to Tables 2 and 3. (EF ejection fraction; LV left ventricular; NYHA New York Heart Association; PLV left ventricular pressure.) Table 1. Effects of IABP at 1:1 Off On p Value HR beats/min CI L/min/m SV ml SW mm Hg ml EDV ml ESV ml EF % EDP mm Hg ESP mm Hg Pao mm Hg dp/dt max mm Hg/s dp/dt max mm Hg/s Tau ms PER ml/s SysDys % DiaDys % Ees1-2 mm Hg/mL CI cardiac index; DiaDys diastolic dyssynchrony; EDP end-diastolic pressure; EDV end-diastolic volume; Ees end-systolic elastance; EF ejection fraction; ESP end-systolic pressure; ESV end-systolic volume; HR heart rate; Pao mean aortic pressure; PER peak ejection rate; SV stroke volume; SW stroke work; SysDys systolic dyssynchrony. n 15.
5 876 SCHREUDER ET AL Ann Thorac Surg LEFT VENTRICULAR PERFORMANCE AND IABP TIMING 2005;79: Table 2. Early IAB Inflation Pre During p Values Post p Values a b a-b c a-c HR beats/min SV ml SW mm Hg ml EDV ml ESV ml EF % EDP mm Hg ESP mm Hg dp/dt max mm Hg/s dp/dt max mm Hg/s Tau ms SysDys % DiaDys % DiaDys diastolic dyssynchrony; EDP end-diastolic pressure; EDV end-diastolic volume; EF ejection fraction; ESP end-systolic pressure; ESV end-systolic volume; HR heart rate; IAB intraaortic balloon; SV stroke volume; SW stroke work; SysDys systolic dyssynchrony. n 13. Hemodynamic Response to Premature IAB Inflation The adverse effects of premature inflation are illustrated in Figure 2A. Abrupt increases in LV afterload late in LV ejection, as a result from increased aortic impedance, induced premature closure of the aortic valve and impaired LV ejection. Table 2 provides average data, before premature inflation (a), during premature IAB inflation applied at 130 to 190 ms before the dicrotic notch (b), and after IAB assist (c). LVESP, or end-systolic afterload, increased (p ) during premature IAB inflation by a mean of 14 mm Hg. SV decreased (p ) by 20%, ranging from 6% to 55%, with concomitant increase in LVESV (p ). Stroke work decreased by a mean of 25% (p 0.002). Tau increased by 44% (p ), indicating deterioration of LV relaxation. The 16% mean increase (p 0.05) in SV in the postassisted beat compared with the preassisted beat did not compensate for the 20% SV decrease of the preceding beat. Hemodynamic Response to Late IAB Deflation Figure 2B depicts an example of late deflation causing increased end-diastolic aortic pressure and aortic impedance, which increased LV afterload during early ejection (c), followed by a reduction in afterload due to IAB deflation during late ejection. Table 3 presents average data of late IAB deflation initiated 110 to 180ms after the Table 3. Late IAB Deflation Pre During Post p Values a b c a-c HR beats/min SV ml SW mm Hg ml EDV ml ESV ml EF % EDP mm Hg ESP mm Hg dp/dt max mm Hg/s dp/dt max mm Hg/s Tau ms SysDys % DiaDys % DiaDys diastolic dyssynchrony; EDP end-diastolic pressure; EDV end-diastolic volume; EF ejection fraction; ESP end-systolic pressure; ESV end-systolic volume; HR heart rate; IAB intraaortic balloon; SV stroke volume; SW stroke work; SysDys systolic dyssynchrony. n 11.
6 Ann Thorac Surg SCHREUDER ET AL 2005;79: LEFT VENTRICULAR PERFORMANCE AND IABP TIMING 877 CARDIOVASCULAR Fig 3. Five LV segmental volume tracings (s1-s5) and TVLV used for Dys analysis in patient A (Fig 1). Pronounced paradoxical segmental volume movements are located in the apex (s1-s2). The calculated Dys decreased immediately after initiation of IABP at a 1:1 ratio (arrow). (Dys dyssynchrony; IABP intraaortic balloon pump; LV left ventricular; TVLV total volume tracing.) R-wave. SV increased (p ) by a mean of 18% in the postassisted beat (c) ranging from 2 to 49% due to decreases in LVESV (p ) compared with preassisted beats (a). Peak dp/dt increased (p ) by 8% due to late IAB deflation, whereas Tau was shorter (p 0.005). SW increased by 16% (p 0.01) in contrast to conventional timed IABP. Fig 4. (A, B) Regression diagrams from IABP at 1:1 assist ratio and from (C) early/late IAB inflation/deflation at 1:4 assist ratio demonstrating: (A) percent change in SV (% SV) versus LV TDys ( TDys); (B) % SV versus Ees; and (C) % SV versus change in systolic dyssynchrony ( SysDys). Dotted lines represent 95% prediction limits. (Ees end-systolic elastance; IABP intraaortic balloon pump; LV left ventricular; SV stroke volume; TDys total dyssynchrony.) LV Performance and Mechanical Dyssynchrony Figure 3 displays segmental and total volume tracings showing a reduction in LV dyssynchrony after IABP initiation at 1:1 assist. Systolic and diastolic dyssynchrony decreased in all patients by a net mean of 2% (p 0.02 and p 0.001, Table 1) within 8 seconds of initiation IABP. Percent SV change was inversely correlated with total LV dyssynchrony change (p , Fig 4A), emphasizing its relation with LVESV and LVEDV, which codetermine alterations in SV. The percent increase in SV during IABP assist at 1:1 inversely correlated with Ees (p 0.008, Fig 4B), indicating that largest increases in SV occurred in the patients with lowest contractile state. Systolic dyssynchrony increased abruptly during premature inflation by a net mean of 1.5% (Table 2, p 0.03), although diastolic dyssynchrony and LVEDV remained unchanged. During late IAB deflation systolic and diastolic dyssynchrony did not change significantly (Table 3). The combined results of the premature inflation and late deflation data revealed a marked inverse correlation between changes in SV and systolic dyssynchrony (Fig 4C, p ).
7 878 SCHREUDER ET AL Ann Thorac Surg LEFT VENTRICULAR PERFORMANCE AND IABP TIMING 2005;79: Comment This study demonstrates acute beneficial effects of properly timed IABP at a 1:1 ratio in heart failure patients. Decreases in aortic impedance resulted in instantaneous increases in SV by LV afterload reduction with concomitant decreases in LVESV, LVEDV, and LV mechanical dyssynchrony. The decreases in LVESV and LVESP delineated the slope (Ees) of the end-systolic P-V relationship. The largest increases in SV occurred in the patients with the lowest contractile state. Premature IAB inflation acutely impaired LV ejection due to abrupt afterload increase during late ejection, increasing systolic dyssynchrony, and Tau impairing myocardial relaxation. Late IAB deflation induced a dual effect, afterload increase during early ejection and decrease in late ejection, combined these increased SV and improved LV relaxation, but at increased SW. Hemodynamics Conventionally Timed IABP Short-term effectiveness of IABP was demonstrated by Nichols and colleagues [3], using multigated cardiac blood pool imaging. Cardiac output increased by 10%, 10 minutes after initiation of IABP. Our study shows in all patients, despite the heterogeneous population, beat-tobeat SV increases due to decreases in LVESV, preceding decreases in LVEDV and LVEDP. Similar changes were observed in animals with heart failure using LV pressure-volume loops [5]. Beat-to-beat improvement of cardiac performance with IABP, as demonstrated by Cheung and coworkers [4] and confirmed in the present study, may be primarily attributed to acute decreases in aortic impedance reducing LV afterload, because cardiovascular compensatory reflexes and metabolic effects from possible increases in coronary flow can be excluded within the measurement time of 10 seconds. The decreases in LVESV and LVESP determine the end-systolic elastance (Ees) as slope of the end-systolic P-V relationship, which implies that the lower the slope the larger the decrease in LVESV. The inverse correlation between Ees and SV indicates that patients with the lowest contractile state will show the largest increases in SV with IABP (Fig 4B). The significant nonlinear convex Ees (Fig 1, Table 1) is related to low contractile state as was demonstrated by Burkhoff and associates [26] in animal studies. Decreases in wall motion abnormalities have been demonstrated 10 minutes after IABP initiation [3]. Dyssynchrony of wall motion reduces mechanical efficiency of ventricular ejection by inducing premature onset and impaired relaxation [10]. LV mechanical dyssynchrony, as demonstrated in patients with dilated cardiomyopathy and LBBB using tagged MRI, was shown to be a key predictor for multi site pacing efficacy [27]. Patients with dilated cardiomyopathy and marked LV dyssynchrony showed decreases in LV mechanical dyssynchrony by wall stress reduction following vasodilator administration, cardiomyoplasty or LV reduction surgery [13 16]. The acute decreases in both systolic and diastolic dyssynchrony with IABP point to a similar mechanism, based on decreases in impedance reducing LV afterload with concomitant decreases in LVESV and preload, improving LV mechanical efficiency. Reductions in LV total dyssynchrony showed a strong inverse correlation with increases in SV induced by IABP assist at 1:1 (Fig 4A). The largest increases in SV with IABP result from largest decreases in LVESV combined with smallest decreases in LVEDV. Therefore increases in SV with conventional IABP are causally related to decreases in LV afterload, preload, contractile state and concomitant changes in total LV mechanical dyssynchrony. Premature IAB Inflation-Late IAB Deflation The present study shows that abrupt increases in aortic impedance, and therefore in LV afterload, imposed during late ejection result in shortened ejection phases, as was demonstrated in isolated cardiac muscle experiments and in vivo animal experiments [8 11]. Premature IAB inflation performed 130 to 190 ms before the dicrotic notch resulted in increased LVESP, Tau, and decreased SV. These findings agree with the animal study by Zile and Gaasch [9] where IAB inflation was applied 80 ms before the dicrotic notch. Factors such as IAB positioning and pulse-wave velocity from IAB to LV can explain differences in timing between man and animal results and the variance observed in the current patient population. The pulse-wave velocity will also vary with changes in cardiac output or aortic compliance. IAB inflation performed in animals 20 ms before the dicrotic notch revealed no change in contraction duration while early relaxation rate increased [9]. In the present study we observed that premature IAB inflation applied less than 50 ms before the dicrotic notch did not change SV. The significant increase in systolic dyssynchrony during premature IAB inflation is analogous to increase in dyssynchronous relaxation due to altered loading conditions, as described in animal studies by Gaasch and associates [11] and Schafer and colleagues [12]. Conventional IAB deflation should produce a clear reduction in end-diastolic aortic pressure. However, Kern and coworkers [28] demonstrated in a clinical IABP study that IAB deflation might be performed later in diastole without adverse hemodynamic effects. Our study shows that incidental late IAB deflation at a 1:4 assist ratio may result in immediate increases in SV, although at increased SW. Animal experiments showed that afterload increase applied during early ejection prolongs ejection phase duration similar to a decrease in afterload applied in late ejection [8 10]. Initial afterload increase in early ejection and decrease in late ejection due to late IAB deflation may explain the relatively large mean SV increase of 18% SV in a single IABP assisted beat (Fig 2 [B, c]). Late IAB deflation induced a significantly higher SW in two ways, by increasing PLV in early ejection and by increased SV. Possible beneficial effects of late IAB deflation applied at a 1:1 ratio should be investigated in specific patient conditions. On the other hand, incidental late deflation which may occur during IABP due to arrhythmia should have no detrimental effects on cardiac performance.
8 Ann Thorac Surg SCHREUDER ET AL 2005;79: LEFT VENTRICULAR PERFORMANCE AND IABP TIMING The marked beat-to-beat SV alterations due to afterload changes applied at different times in the cardiac cycle with premature inflation or late deflation markedly correlated with systolic dyssynchrony changes (Fig 4C). Brutsaert s hypothesis that LV mechanical dyssynchrony or nonuniformity may act as a modulator of cardiac performance together with heart rate, contractile state, preload and afterload may therefore be applicable in heart failure patients [29]. In a previous study we demonstrated a direct relationship between increases in contractile state (Ees) and decreases in intraventricular dyssynchrony in patients undergoing LV restoration by the Dor procedure [16]. Limitations of the Study We analyzed acute hemodynamic effects occurring within 10 seconds after initiation of IABP in heart failure patients with open chest under general anesthesia. Longer-term analysis may show differences due to metabolic effects by possible increases in coronary flow and or resulting from compensatory cardiovascular reflexes. NYHA class III-IV patients received small constant dosages of inotropic agents which may have changed their contractile state and the magnitude of the responses to IABP. The applied LV mechanical dyssynchrony analysis is not discriminative between slow paradoxical wall motions as known from LV aneurysms or fast wall motions known from dilated cardiomyopathy or left bundle branch block [14, 16, 23, 27]. We assume that, mechanistically, both will have similar effects on LV performance. The population we studied included patients with ischemic heart disease and mitral valve dysfunction, and did not include all potential IABP indications. Conclusions Precisely timed IABP in heart failure patients is highly effective in generating beat-to-beat improvements in systolic and diastolic LV performance as demonstrated by beat-to-beat increases in SV and decreases in LV afterload, LVESV, preload and LV mechanical dyssynchrony. These beat-to-beat improvements are due to decreases in aortic impedance, were generally established within four beats after IABP initiation, because metabolic effects due to possible changes in coronary flow and cardiovascular compensatory reflexes may be excluded in this time frame. Decreases in LVESV and LVESP delineated the ESPVR and its slope, the Ees, implying that the largest SV increases occur in patients with lowest contractile state. Premature IAB inflation markedly impaired LV ejection and relaxation by afterload increase and concomitant LV mechanical dyssynchrony increase during the second part of the ejection phase, indicating that premature IAB inflation, as may occur during arrhythmia, may have detrimental effects on cardiac performance in heart failure patients. Late IAB deflation resulted in increased SV and increased SW by afterload increase during early ejection and afterload decrease in late ejection, indicating that incidental late IAB deflation will not negatively affect cardiac performance. We wish to thank Professor Attilio Maseri, MD, PhD, for his review of this manuscript. This study was funded by the Department of Cardiac Surgery, San Raffaele University Hospital (Milan, Italy) and Arrow International (Reading, PA). References Kantrowitz A, Kantrowitz A. Experimental augmentation of coronary flow by retardation of arterial pressure pulse. Surgery 1953;34: Dunkman WB, Leinbach RC, Buckley MJ, et al. Clinical and hemodynamic results of intraaortic balloon pumping and surgery for cardiogenic shock. Circulation 1972;46: Nichols AB, Pohost GM, Gold HK, et al. Left ventricular function during intra-aortic balloon pumping assessed by multigated cardiac blood pool imaging. Circulation 1978; 58(Suppl 1): Cheung AT, Savino JS, Weiss SJ. Beat-to-beat augmentation of left ventricular function by intraaortic counterpulsation. Anesthesiology 1996;84: Kawaguchi O, Pae WE, Daily BB, et al. Ventriculoarterial coupling with intra-aortic balloon pump in ischemic heart failure. J Thorac Cardiovasc Surg 1999;117: Kern MJ, Aguirre F, Tatineni S, et al. Enhanced coronary blood flow velocity during intra-aortic balloon counterpulsation in critically ill patients. J Am Coll Cardiol 1993;21: Kantrowitz A, Cardona RR, Freed PS. Percutaneous intraaortic balloon counterpulsation. Crit Care Clin 1992;8: Gillebert TC, Sys SU, Brutsaert DL. Influence of loading patterns on peak length-tension relation and on relaxation in cardiac muscle. J Am Coll Cardiol 1989;13: Zile MR, Gaasch WH. Load dependent left ventricular relaxation in conscious dogs. Am J Physiol 1991;261:H Brutsaert DL, Sys SU. Relaxation and diastole of the heart. Physiol Rev 1989;69: Gaasch WH, Blaustein AS, Bing OHL. Asynchronous (segmental early) relaxation of the left ventricle. J Am Coll Cardiol 1985;5: Schafer S, Fiedler VB, Thamer V. Afterload dependent prolongation of left ventricular relaxation: importance of asynchrony. Cardiovasc Res 1992;26: Hayashida W, Kumada T, Kohno F, et al. Left ventricular relaxation in dilated cardiomyopathy: relation to loading conditions and regional nonuniformity. J Am Coll Cardiol 1992;20: Schreuder JJ, Steendijk P, van der Veen FH, et al. Acute and short-term effects of partial left ventriculectomy in dilated cardiomyopathy: assessment by pressure-volume loops. J Am Coll Cardiol 2000;36: Schreuder JJ, van der Veen FH, van der Velde ET, et al. Left ventricular pressure-volume relationships before and after cardiomyoplasty in patients with heart failure. Circulation 1997;96: Schreuder JJ, Castiglioni A, Maisano F, et al. Acute decrease of left ventricular mechanical dyssynchrony and improvement of contractile state and energy efficiency after left ventricular restoration. J Thorac Cardiovasc Surg 2005;129: Baan J, van der Velde ET, De Bruin HG, et al. Continuous measurement of left ventricular volume in animals and humans by conductance catheter. Circulation 1984;70: Burkhoff D, van der Velde ET, Kass D, et al. Accuracy of volume measurements by conductance catheter in isolated, ejecting canine hearts. Circulation 1985;72: CARDIOVASCULAR
9 880 SCHREUDER ET AL Ann Thorac Surg LEFT VENTRICULAR PERFORMANCE AND IABP TIMING 2005;79: Brookes CI, White PA, Bishop AJ, et al. Validation of a new intra-operative technique to evaluate load-independent indices of right ventricular performance in patients undergoing cardiac operations. J Thorac Cardiovasc Surg 1998;116: Schreuder JJ, Van der Veen FH, Van der Velde ET, et al. Beat-to-beat analysis of left ventricular volume and stroke volume by conductance catheter and aortic modelflow in cardiomyoplasty patients. Circulation 1995;91: Steendijk P, Van der Velde ET, Baan J. Left ventricular stroke volume by single and dual excitation of the conductance catheter in dogs. Am J Physiol 1993;264:H Van der Velde ET, Van Dijk AD, Steendijk P, et al. Left ventricular segmental volume by conductance catheter and Cine-CT. Eur Heart J 1992;13(Suppl E): Steendijk P, Tulner SAF, Schreuder JJ, et al. Quantification of left ventricular mechanical dyssynchrony by conductance catheter in heart failure patients. Am J Physiol Heart Circ Physiol 2004;286:H Aoyagi T, Pouleur H, Van Eyll C, et al. Wall motion asynchrony is a major determinant of impaired left ventricular filling in patients with healed myocardial infarction. Am J Cardiol 1993;72: Mirsky I. Assessment of diastolic function: suggested methods and future considerations. Circulation 1984;69: Burkhoff D, Sugiura S, Yue DT, et al. Contractility dependent curvilinearity of end-systolic pressure-volume relations. Am J Physiol 1987;252:H Nelson GS, Curry CW, Wyman BT, et al. Predictors of systolic augmentation from left ventricular preexcitation in patients with dilated cardiomyopathy and intraventricular conduction delay. Circulation 2000;101: Kern MJ, Aguirre FV, Caracciolo EA, et al. Hemodynamic effects of new intra-aortic balloon counterpulsation timing methods in patients: a multicenter evaluation. Am Heart J 1999;137: Brutsaert DL. Nonuniformity: a physiologic modulator of contraction and relaxation of the normal heart. J Am Coll Cardiol 1987;9:341 8.
Left ventricular (LV) postinfarction aneurysm is characterized by
 Surgery for Acquired Cardiovascular Disease Schreuder et al Acute decrease of left ventricular mechanical dyssynchrony and improvement of contractile state and energy efficiency after left ventricular
Surgery for Acquired Cardiovascular Disease Schreuder et al Acute decrease of left ventricular mechanical dyssynchrony and improvement of contractile state and energy efficiency after left ventricular
Impedance Cardiography (ICG) Method, Technology and Validity
 Method, Technology and Validity Hemodynamic Basics Cardiovascular System Cardiac Output (CO) Mean arterial pressure (MAP) Variable resistance (SVR) Aortic valve Left ventricle Elastic arteries / Aorta
Method, Technology and Validity Hemodynamic Basics Cardiovascular System Cardiac Output (CO) Mean arterial pressure (MAP) Variable resistance (SVR) Aortic valve Left ventricle Elastic arteries / Aorta
Section 6 Intra Aortic Balloon Pump
 Section 6 Intra Aortic Balloon Pump The Intra Aortic Balloon Pump (IABP) The balloon is synthetic and is made for single use only. It is threaded into the aorta, usually via a femoral approach. The balloon
Section 6 Intra Aortic Balloon Pump The Intra Aortic Balloon Pump (IABP) The balloon is synthetic and is made for single use only. It is threaded into the aorta, usually via a femoral approach. The balloon
IABP Timing & Fidelity. Pocket Reference Guide
 IABP Timing & Fidelity Pocket Reference Guide Correct IABP Timing A = One complete cardiac cycle R B = Unassisted aortic end diastolic pressure P T C = Unassisted systolic pressure D = Diastolic augmentation
IABP Timing & Fidelity Pocket Reference Guide Correct IABP Timing A = One complete cardiac cycle R B = Unassisted aortic end diastolic pressure P T C = Unassisted systolic pressure D = Diastolic augmentation
Cardiac Cycle MCQ. Professor of Cardiovascular Physiology. Cairo University 2007
 Cardiac Cycle MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 1- Regarding the length of systole and diastole: a- At heart rate 75 b/min, the duration of
Cardiac Cycle MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 1- Regarding the length of systole and diastole: a- At heart rate 75 b/min, the duration of
Heart Pump and Cardiac Cycle. Faisal I. Mohammed, MD, PhD
 Heart Pump and Cardiac Cycle Faisal I. Mohammed, MD, PhD 1 Objectives To understand the volume, mechanical, pressure and electrical changes during the cardiac cycle To understand the inter-relationship
Heart Pump and Cardiac Cycle Faisal I. Mohammed, MD, PhD 1 Objectives To understand the volume, mechanical, pressure and electrical changes during the cardiac cycle To understand the inter-relationship
Evaluation of Native Left Ventricular Function During Mechanical Circulatory Support.: Theoretical Basis and Clinical Limitations
 Review Evaluation of Native Left Ventricular Function During Mechanical Circulatory Support.: Theoretical Basis and Clinical Limitations Tohru Sakamoto, MD, PhD Left ventricular function on patients with
Review Evaluation of Native Left Ventricular Function During Mechanical Circulatory Support.: Theoretical Basis and Clinical Limitations Tohru Sakamoto, MD, PhD Left ventricular function on patients with
PROBLEM SET 2. Assigned: February 10, 2004 Due: February 19, 2004
 Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
Mechanisms of heart failure with normal EF Arterial stiffness and ventricular-arterial coupling. What is the pathophysiology at presentation?
 Mechanisms of heart failure with normal EF Arterial stiffness and ventricular-arterial coupling What is the pathophysiology at presentation? Ventricular-arterial coupling elastance Central arterial pressure
Mechanisms of heart failure with normal EF Arterial stiffness and ventricular-arterial coupling What is the pathophysiology at presentation? Ventricular-arterial coupling elastance Central arterial pressure
From PV loop to Starling curve. S Magder Division of Critical Care, McGill University Health Centre
 From PV loop to Starling curve S Magder Division of Critical Care, McGill University Health Centre Otto Frank 1890 s Frank-Starling Relationship ( The Law of the Heart ) The greater the initial stretch
From PV loop to Starling curve S Magder Division of Critical Care, McGill University Health Centre Otto Frank 1890 s Frank-Starling Relationship ( The Law of the Heart ) The greater the initial stretch
Scisense ADV500. Pressure-Volume Measurement System for Cardiac Function Research in All Sizes of Hearts. Pressure-Volume
 Pressure-Volume Scisense ADV500 Pressure-Volume Measurement System for Cardiac Function Research in All Sizes of Hearts True volume in real-time with Admittance technology Variable Segment Length (VSL)
Pressure-Volume Scisense ADV500 Pressure-Volume Measurement System for Cardiac Function Research in All Sizes of Hearts True volume in real-time with Admittance technology Variable Segment Length (VSL)
BUSINESS. Articles? Grades Midterm Review session
 BUSINESS Articles? Grades Midterm Review session REVIEW Cardiac cells Myogenic cells Properties of contractile cells CONDUCTION SYSTEM OF THE HEART Conduction pathway SA node (pacemaker) atrial depolarization
BUSINESS Articles? Grades Midterm Review session REVIEW Cardiac cells Myogenic cells Properties of contractile cells CONDUCTION SYSTEM OF THE HEART Conduction pathway SA node (pacemaker) atrial depolarization
Counterpulsation. John N. Nanas, MD, PhD. Professor and Head, 3 rd Cardiology Dept, University of Athens, Athens, Greece
 John N. Nanas, MD, PhD Professor and Head, 3 rd Cardiology Dept, University of Athens, Athens, Greece History of counterpulsation 1952 Augmentation of CBF Adrian and Arthur Kantrowitz, Surgery 1952;14:678-87
John N. Nanas, MD, PhD Professor and Head, 3 rd Cardiology Dept, University of Athens, Athens, Greece History of counterpulsation 1952 Augmentation of CBF Adrian and Arthur Kantrowitz, Surgery 1952;14:678-87
Left Ventricular Wall Resection for Aneurysm and Akinesia due to Coronary Artery Disease: Fifty Consecutive Patients
 Left Ventricular Wall Resection for Aneurysm and Akinesia due to Coronary Artery Disease: Fifty Consecutive Patients Armand A. Lefemine, M.D., Rajagopalan Govindarajan, M.D., K. Ramaswamy, M.D., Harrison
Left Ventricular Wall Resection for Aneurysm and Akinesia due to Coronary Artery Disease: Fifty Consecutive Patients Armand A. Lefemine, M.D., Rajagopalan Govindarajan, M.D., K. Ramaswamy, M.D., Harrison
The Cardiac Cycle Clive M. Baumgarten, Ph.D.
 The Cardiac Cycle Clive M. Baumgarten, Ph.D. OBJECTIVES: 1. Describe periods comprising cardiac cycle and events within each period 2. Describe the temporal relationships between pressure, blood flow,
The Cardiac Cycle Clive M. Baumgarten, Ph.D. OBJECTIVES: 1. Describe periods comprising cardiac cycle and events within each period 2. Describe the temporal relationships between pressure, blood flow,
Diastology Disclosures: None. Dias2011:1
 Diastology 2011 James D. Thomas, M.D., F.A.C.C. Cardiovascular Imaging Center Department of Cardiology Cleveland Clinic Foundation Cleveland, Ohio, USA Disclosures: None Dias2011:1 Is EVERYBODY a member!?!
Diastology 2011 James D. Thomas, M.D., F.A.C.C. Cardiovascular Imaging Center Department of Cardiology Cleveland Clinic Foundation Cleveland, Ohio, USA Disclosures: None Dias2011:1 Is EVERYBODY a member!?!
LV geometric and functional changes in VHD: How to assess? Mi-Seung Shin M.D., Ph.D. Gachon University Gil Hospital
 LV geometric and functional changes in VHD: How to assess? Mi-Seung Shin M.D., Ph.D. Gachon University Gil Hospital LV inflow across MV LV LV outflow across AV LV LV geometric changes Pressure overload
LV geometric and functional changes in VHD: How to assess? Mi-Seung Shin M.D., Ph.D. Gachon University Gil Hospital LV inflow across MV LV LV outflow across AV LV LV geometric changes Pressure overload
CSC Review Course: Intra Aortic Balloon Pump (IABP) Paula M Davis ARNP, MSN, CCRN-CSC
 CSC Review Course: Intra Aortic Balloon Pump (IABP) Paula M Davis ARNP, MSN, CCRN-CSC What is an IABP? The Intra-Aortic Balloon Counterpulsation system is a volume displacement device. It should be positioned
CSC Review Course: Intra Aortic Balloon Pump (IABP) Paula M Davis ARNP, MSN, CCRN-CSC What is an IABP? The Intra-Aortic Balloon Counterpulsation system is a volume displacement device. It should be positioned
Strain/Untwisting/Diastolic Suction
 What Is Diastole and How to Assess It? Strain/Untwisting/Diastolic Suction James D. Thomas, M.D., F.A.C.C. Cardiovascular Imaging Center Department of Cardiology Cleveland Clinic Foundation Cleveland,
What Is Diastole and How to Assess It? Strain/Untwisting/Diastolic Suction James D. Thomas, M.D., F.A.C.C. Cardiovascular Imaging Center Department of Cardiology Cleveland Clinic Foundation Cleveland,
How does the heart pump? From sarcomere to ejection volume
 How does the heart pump? From sarcomere to ejection volume Piet Claus Cardiovascular Imaging and Dynamics Department of Cardiovascular Diseases University Leuven, Leuven, Belgium Course on deformation
How does the heart pump? From sarcomere to ejection volume Piet Claus Cardiovascular Imaging and Dynamics Department of Cardiovascular Diseases University Leuven, Leuven, Belgium Course on deformation
Inflation and deflation timing of the AutoCAT 2 WAVE intra-aortic balloon pump using the autopilot mode in a clinical setting
 450060PRF0010.1177/0267659112450060Bakker EWM et al.perfusion 2012 Inflation and deflation timing of the AutoCAT 2 WAVE intra-aortic balloon pump using the autopilot mode in a clinical setting Perfusion
450060PRF0010.1177/0267659112450060Bakker EWM et al.perfusion 2012 Inflation and deflation timing of the AutoCAT 2 WAVE intra-aortic balloon pump using the autopilot mode in a clinical setting Perfusion
LV FUNCTION ASSESSMENT: WHAT IS BEYOND EJECTION FRACTION
 LV FUNCTION ASSESSMENT: WHAT IS BEYOND EJECTION FRACTION Jamilah S AlRahimi Assistant Professor, KSU-HS Consultant Noninvasive Cardiology KFCC, MNGHA-WR Introduction LV function assessment in Heart Failure:
LV FUNCTION ASSESSMENT: WHAT IS BEYOND EJECTION FRACTION Jamilah S AlRahimi Assistant Professor, KSU-HS Consultant Noninvasive Cardiology KFCC, MNGHA-WR Introduction LV function assessment in Heart Failure:
Ejection across stenotic aortic valve requires a systolic pressure gradient between the LV and aorta. This places a pressure load on the LV.
 Valvular Heart Disease General Principles Etiology Cellular and molecular mechanism of valve damage Structural pathology Functional pathology - stenosis/regurgitation Loading conditions - pressure/volume
Valvular Heart Disease General Principles Etiology Cellular and molecular mechanism of valve damage Structural pathology Functional pathology - stenosis/regurgitation Loading conditions - pressure/volume
Impact of Surgical Ventricular Restoration on Diastolic Function: Implications of Shape and Residual Ventricular Size
 Impact of Surgical Ventricular Restoration on Diastolic Function: Implications of Shape and Residual Ventricular Size Serenella Castelvecchio, MD, Lorenzo Menicanti, MD, Marco Ranucci, MD, and Marisa Di
Impact of Surgical Ventricular Restoration on Diastolic Function: Implications of Shape and Residual Ventricular Size Serenella Castelvecchio, MD, Lorenzo Menicanti, MD, Marco Ranucci, MD, and Marisa Di
Ejection across stenotic aortic valve requires a systolic pressure gradient between the LV and aorta. This places a pressure load on the LV.
 Valvular Heart Disease Etiology General Principles Cellular and molecular mechanism of valve damage Structural pathology Functional pathology - stenosis/regurgitation Loading conditions - pressure/volume
Valvular Heart Disease Etiology General Principles Cellular and molecular mechanism of valve damage Structural pathology Functional pathology - stenosis/regurgitation Loading conditions - pressure/volume
Rationale for Prophylactic Support During Percutaneous Coronary Intervention
 Rationale for Prophylactic Support During Percutaneous Coronary Intervention Navin K. Kapur, MD, FACC, FSCAI Assistant Director, Interventional Cardiology Director, Interventional Research Laboratories
Rationale for Prophylactic Support During Percutaneous Coronary Intervention Navin K. Kapur, MD, FACC, FSCAI Assistant Director, Interventional Cardiology Director, Interventional Research Laboratories
Basic Approach to the Echocardiographic Evaluation of Ventricular Diastolic Function
 Basic Approach to the Echocardiographic Evaluation of Ventricular Diastolic Function J A F E R A L I, M D U N I V E R S I T Y H O S P I T A L S C A S E M E D I C A L C E N T E R S T A F F C A R D I O T
Basic Approach to the Echocardiographic Evaluation of Ventricular Diastolic Function J A F E R A L I, M D U N I V E R S I T Y H O S P I T A L S C A S E M E D I C A L C E N T E R S T A F F C A R D I O T
Echo assessment of the failing heart
 Echo assessment of the failing heart Mark K. Friedberg, MD The Labatt Family Heart Center The Hospital for Sick Children Toronto, Ontario, Canada Cardiac function- definitions Cardiovascular function:
Echo assessment of the failing heart Mark K. Friedberg, MD The Labatt Family Heart Center The Hospital for Sick Children Toronto, Ontario, Canada Cardiac function- definitions Cardiovascular function:
SymBioSys Exercise 2 Cardiac Function Revised and reformatted by C. S. Tritt, Ph.D. Last updated March 20, 2006
 SymBioSys Exercise 2 Cardiac Function Revised and reformatted by C. S. Tritt, Ph.D. Last updated March 20, 2006 The goal of this exercise to explore the behavior of the heart as a mechanical pump. For
SymBioSys Exercise 2 Cardiac Function Revised and reformatted by C. S. Tritt, Ph.D. Last updated March 20, 2006 The goal of this exercise to explore the behavior of the heart as a mechanical pump. For
CLINICAL SUPPORT SERVICES DEVELOPING AN IABP PRECEPTOR STRATEGY
 CLINICAL SUPPORT SERVICES DEVELOPING AN IABP PRECEPTOR STRATEGY DATASCOPE IS NOW MAQUET CARDIOVASCULAR Datascope is now MAQUET Cardiovascular In early 2009, the purchase agreement between Datascope and
CLINICAL SUPPORT SERVICES DEVELOPING AN IABP PRECEPTOR STRATEGY DATASCOPE IS NOW MAQUET CARDIOVASCULAR Datascope is now MAQUET Cardiovascular In early 2009, the purchase agreement between Datascope and
Arrow AC3 Optimus Intra-Aortic Balloon Pump Greater precision with increased simplicity; an evolution in IABP performance
 Arrow AC3 Optimus Intra-Aortic Balloon Pump Greater precision with increased simplicity; an evolution in IABP performance Unmatched simplicity, right from the start The AC3 Optimus Intra-Aortic Balloon
Arrow AC3 Optimus Intra-Aortic Balloon Pump Greater precision with increased simplicity; an evolution in IABP performance Unmatched simplicity, right from the start The AC3 Optimus Intra-Aortic Balloon
Arrow AC3 Optimus Intra-Aortic Balloon Pump Greater precision with increased simplicity; an evolution in IABP performance
 Arrow AC3 Optimus Intra-Aortic Balloon Pump Greater precision with increased simplicity; an evolution in IABP performance Optimized therapy even in the most challenging patient conditions When already-compromised
Arrow AC3 Optimus Intra-Aortic Balloon Pump Greater precision with increased simplicity; an evolution in IABP performance Optimized therapy even in the most challenging patient conditions When already-compromised
THE CARDIOVASCULAR SYSTEM
 THE CARDIOVASCULAR SYSTEM AND RESPONSES TO EXERCISE Mr. S. Kelly PSK 4U North Grenville DHS THE HEART: A REVIEW Cardiac muscle = myocardium Heart divided into two sides, 4 chambers (L & R) RS: pulmonary
THE CARDIOVASCULAR SYSTEM AND RESPONSES TO EXERCISE Mr. S. Kelly PSK 4U North Grenville DHS THE HEART: A REVIEW Cardiac muscle = myocardium Heart divided into two sides, 4 chambers (L & R) RS: pulmonary
Pathophysiology and Current Evidence for Detection of Dyssynchrony
 Editorial Cardiol Res. 2017;8(5):179-183 Pathophysiology and Current Evidence for Detection of Dyssynchrony Michael Spartalis a, d, Eleni Tzatzaki a, Eleftherios Spartalis b, Christos Damaskos b, Antonios
Editorial Cardiol Res. 2017;8(5):179-183 Pathophysiology and Current Evidence for Detection of Dyssynchrony Michael Spartalis a, d, Eleni Tzatzaki a, Eleftherios Spartalis b, Christos Damaskos b, Antonios
Cardiovascular Physiology. Heart Physiology. Introduction. The heart. Electrophysiology of the heart
 Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
Hemodynamic Monitoring and Circulatory Assist Devices
 Hemodynamic Monitoring and Circulatory Assist Devices Speaker: Jana Ogden Learning Unit 2: Hemodynamic Monitoring and Circulatory Assist Devices Hemodynamic monitoring refers to the measurement of pressure,
Hemodynamic Monitoring and Circulatory Assist Devices Speaker: Jana Ogden Learning Unit 2: Hemodynamic Monitoring and Circulatory Assist Devices Hemodynamic monitoring refers to the measurement of pressure,
좌심실수축기능평가 Cardiac Function
 Basic Echo Review Course 좌심실수축기능평가 Cardiac Function Seonghoon Choi Cardiology Hallym university LV systolic function Systolic function 좌심실수축기능 - 심근의수축으로심실에서혈액을대동맥으로박출하는기능 실제임상에서 LV function 의의미 1Diagnosis
Basic Echo Review Course 좌심실수축기능평가 Cardiac Function Seonghoon Choi Cardiology Hallym university LV systolic function Systolic function 좌심실수축기능 - 심근의수축으로심실에서혈액을대동맥으로박출하는기능 실제임상에서 LV function 의의미 1Diagnosis
Cardiac Output MCQ. Professor of Cardiovascular Physiology. Cairo University 2007
 Cardiac Output MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 90- Guided by Ohm's law when : a- Cardiac output = 5.6 L/min. b- Systolic and diastolic BP
Cardiac Output MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 90- Guided by Ohm's law when : a- Cardiac output = 5.6 L/min. b- Systolic and diastolic BP
Study of left ventricular pressure-volume relations during nitroprusside infusion in human subjects
 British Heart Journal, 1979, 41, 325-330 Study of left ventricular pressure-volume relations during nitroprusside infusion in human subjects without coronary artery disease1 J. P. MERILLON, G. MOTTE, M.
British Heart Journal, 1979, 41, 325-330 Study of left ventricular pressure-volume relations during nitroprusside infusion in human subjects without coronary artery disease1 J. P. MERILLON, G. MOTTE, M.
Καθετηριασμός δεξιάς κοιλίας. Σ. Χατζημιλτιάδης Καθηγητής Καρδιολογίας ΑΠΘ
 Καθετηριασμός δεξιάς κοιλίας Σ. Χατζημιλτιάδης Καθηγητής Καρδιολογίας ΑΠΘ The increasing interest in pulmonary arterial hypertension (PAH), the increasing interest in implantation of LVADs, and the evolution
Καθετηριασμός δεξιάς κοιλίας Σ. Χατζημιλτιάδης Καθηγητής Καρδιολογίας ΑΠΘ The increasing interest in pulmonary arterial hypertension (PAH), the increasing interest in implantation of LVADs, and the evolution
THE CARDIOVASCULAR SYSTEM. Heart 2
 THE CARDIOVASCULAR SYSTEM Heart 2 PROPERTIES OF CARDIAC MUSCLE Cardiac muscle Striated Short Wide Branched Interconnected Skeletal muscle Striated Long Narrow Cylindrical PROPERTIES OF CARDIAC MUSCLE Intercalated
THE CARDIOVASCULAR SYSTEM Heart 2 PROPERTIES OF CARDIAC MUSCLE Cardiac muscle Striated Short Wide Branched Interconnected Skeletal muscle Striated Long Narrow Cylindrical PROPERTIES OF CARDIAC MUSCLE Intercalated
SUPPLEMENTAL MATERIAL
 SUPPLEMENTAL MATERIAL Supplemental methods Pericardium In several studies, it has been shown that the pericardium significantly modulates ventricular interaction. 1-4 Since ventricular interaction has
SUPPLEMENTAL MATERIAL Supplemental methods Pericardium In several studies, it has been shown that the pericardium significantly modulates ventricular interaction. 1-4 Since ventricular interaction has
MEDICAL POLICY SUBJECT: SURGICAL VENTRICULAR RESTORATION
 MEDICAL POLICY SUBJECT: SURGICAL VENTRICULAR PAGE: 1 OF: 6 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
MEDICAL POLICY SUBJECT: SURGICAL VENTRICULAR PAGE: 1 OF: 6 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
Mechanics of Cath Lab Support Devices
 Mechanics of Cath Lab Support Devices Issam D. Moussa, MD Professor of Medicine Mayo Clinic College of Medicine Chair, Division of Cardiovascular Diseases Mayo Clinic Jacksonville, Florida DISCLOSURE Presenter:
Mechanics of Cath Lab Support Devices Issam D. Moussa, MD Professor of Medicine Mayo Clinic College of Medicine Chair, Division of Cardiovascular Diseases Mayo Clinic Jacksonville, Florida DISCLOSURE Presenter:
U. Herberg 1, D. Ladage 2, E. Gatzweiler 1, O. Dewald 3, J. Dörner 4, K. Linden 1, M. Seehase 1, D. Dörr 3, C. Nähle 4, J.
 Pressure volume relations obtained by 3D-real-time echocardiography and mini-pressure wire - multimodal validation-studies with MRI and conductancecatheter in piglets U. Herberg 1, D. Ladage 2, E. Gatzweiler
Pressure volume relations obtained by 3D-real-time echocardiography and mini-pressure wire - multimodal validation-studies with MRI and conductancecatheter in piglets U. Herberg 1, D. Ladage 2, E. Gatzweiler
RV dysfunction and failure PATHOPHYSIOLOGY. Adam Torbicki MD, Dept Chest Medicine Institute of Tuberculosis and Lung Diseases Warszawa, Poland
 RV dysfunction and failure PATHOPHYSIOLOGY Adam Torbicki MD, Dept Chest Medicine Institute of Tuberculosis and Lung Diseases Warszawa, Poland Normal Right Ventricle (RV) Thinner wall Weaker myocytes Differences
RV dysfunction and failure PATHOPHYSIOLOGY Adam Torbicki MD, Dept Chest Medicine Institute of Tuberculosis and Lung Diseases Warszawa, Poland Normal Right Ventricle (RV) Thinner wall Weaker myocytes Differences
Electrical Conduction
 Sinoatrial (SA) node Electrical Conduction Sets the pace of the heartbeat at 70 bpm AV node (50 bpm) and Purkinje fibers (25 40 bpm) can act as pacemakers under some conditions Internodal pathway from
Sinoatrial (SA) node Electrical Conduction Sets the pace of the heartbeat at 70 bpm AV node (50 bpm) and Purkinje fibers (25 40 bpm) can act as pacemakers under some conditions Internodal pathway from
Principles of intra-aortic balloon pump counterpulsation
 Principles of intra-aortic balloon pump counterpulsation Murli Krishna MBBS FRCA FFPMRCA Kai Zacharowski MD PhD FRCA Key points The primary goal of intraaortic balloon pump (IABP) treatment is to increase
Principles of intra-aortic balloon pump counterpulsation Murli Krishna MBBS FRCA FFPMRCA Kai Zacharowski MD PhD FRCA Key points The primary goal of intraaortic balloon pump (IABP) treatment is to increase
Effect of physiological heart rate changes on left ventricular dimensions and mitral blood flow velocities in the normal fetus
 ELSEVIER Early Human Development 40 (1995) 109-114 Effect of physiological heart rate changes on left ventricular dimensions and mitral blood flow velocities in the normal fetus P.B. Tsyvian a, K.V. Malkin
ELSEVIER Early Human Development 40 (1995) 109-114 Effect of physiological heart rate changes on left ventricular dimensions and mitral blood flow velocities in the normal fetus P.B. Tsyvian a, K.V. Malkin
Preoperative Parameters Predicting the Postoperative Course of Endoventricular Circular Patch Plasty
 Original Article Preoperative Parameters Predicting the Postoperative Course of Endoventricular Circular Patch Plasty Keiichiro Kondo, MD, Yoshihide Sawada, MD, and Shinjiro Sasaki, MD, PhD It is necessary
Original Article Preoperative Parameters Predicting the Postoperative Course of Endoventricular Circular Patch Plasty Keiichiro Kondo, MD, Yoshihide Sawada, MD, and Shinjiro Sasaki, MD, PhD It is necessary
Valve Disease in Patients With Heart Failure TAVI or Surgery? Miguel Sousa Uva Hospital Cruz Vermelha Lisbon, Portugal
 Valve Disease in Patients With Heart Failure TAVI or Surgery? Miguel Sousa Uva Hospital Cruz Vermelha Lisbon, Portugal I have nothing to disclose. Wide Spectrum Stable vs Decompensated NYHA II IV? Ejection
Valve Disease in Patients With Heart Failure TAVI or Surgery? Miguel Sousa Uva Hospital Cruz Vermelha Lisbon, Portugal I have nothing to disclose. Wide Spectrum Stable vs Decompensated NYHA II IV? Ejection
Rhondalyn C. McLean. 2 ND YEAR RESEARCH ELECTIVE RESIDENT S JOURNAL Volume VII, A. Study Purpose and Rationale
 A Randomized Clinical Study To Compare The Intra-Aortic Balloon Pump To A Percutaneous Left Atrial-To-Femoral Arterial Bypass Device For Treatment Of Cardiogenic Shock Following Acute Myocardial Infarction.
A Randomized Clinical Study To Compare The Intra-Aortic Balloon Pump To A Percutaneous Left Atrial-To-Femoral Arterial Bypass Device For Treatment Of Cardiogenic Shock Following Acute Myocardial Infarction.
Noncoronary Cardiac MDCT
 Noncoronary Cardiac MDCT David A. Bluemke, M.D., Ph.D. Professor, of Radiology and Medicine Johns Hopkins University School of Medicine Baltimore, Maryland Toshiba Disclosures Grant support Noncoronary
Noncoronary Cardiac MDCT David A. Bluemke, M.D., Ph.D. Professor, of Radiology and Medicine Johns Hopkins University School of Medicine Baltimore, Maryland Toshiba Disclosures Grant support Noncoronary
Chapter 9, Part 2. Cardiocirculatory Adjustments to Exercise
 Chapter 9, Part 2 Cardiocirculatory Adjustments to Exercise Electrical Activity of the Heart Contraction of the heart depends on electrical stimulation of the myocardium Impulse is initiated in the right
Chapter 9, Part 2 Cardiocirculatory Adjustments to Exercise Electrical Activity of the Heart Contraction of the heart depends on electrical stimulation of the myocardium Impulse is initiated in the right
Cath Lab Essentials: Basic Hemodynamics for the Cath Lab and ICU
 Cath Lab Essentials: Basic Hemodynamics for the Cath Lab and ICU Ailin Barseghian El-Farra, MD, FACC Assistant Professor, Interventional Cardiology University of California, Irvine Department of Cardiology
Cath Lab Essentials: Basic Hemodynamics for the Cath Lab and ICU Ailin Barseghian El-Farra, MD, FACC Assistant Professor, Interventional Cardiology University of California, Irvine Department of Cardiology
Appendix II: ECHOCARDIOGRAPHY ANALYSIS
 Appendix II: ECHOCARDIOGRAPHY ANALYSIS Two-Dimensional (2D) imaging was performed using the Vivid 7 Advantage cardiovascular ultrasound system (GE Medical Systems, Milwaukee) with a frame rate of 400 frames
Appendix II: ECHOCARDIOGRAPHY ANALYSIS Two-Dimensional (2D) imaging was performed using the Vivid 7 Advantage cardiovascular ultrasound system (GE Medical Systems, Milwaukee) with a frame rate of 400 frames
Evaluation of Myocardial Function
 Evaluation of Myocardial Function Kenneth E. Jochim, Ph.D., and Douglas M. Behrendt, M.D. ABSTRACT In assessing myocardial contractility one may examine isolated heart muscle, the isolated whole heart
Evaluation of Myocardial Function Kenneth E. Jochim, Ph.D., and Douglas M. Behrendt, M.D. ABSTRACT In assessing myocardial contractility one may examine isolated heart muscle, the isolated whole heart
Echocardiography as a diagnostic and management tool in medical emergencies
 Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
Coronary Artery Bypass Graft: Monitoring Patients and Detecting Complications
 Coronary Artery Bypass Graft: Monitoring Patients and Detecting Complications Madhav Swaminathan, MD, FASE Professor of Anesthesiology Division of Cardiothoracic Anesthesia & Critical Care Duke University
Coronary Artery Bypass Graft: Monitoring Patients and Detecting Complications Madhav Swaminathan, MD, FASE Professor of Anesthesiology Division of Cardiothoracic Anesthesia & Critical Care Duke University
Ventriculo-arterial coupling and diastolic elastance. MasterclassIC Schiermonnikoog 2015
 Ventriculo-arterial coupling and diastolic elastance MasterclassIC Schiermonnikoog 2015 Ventriculo-arterial coupling Dynamic interaction between heart and systemic circulation (modulation of compliance
Ventriculo-arterial coupling and diastolic elastance MasterclassIC Schiermonnikoog 2015 Ventriculo-arterial coupling Dynamic interaction between heart and systemic circulation (modulation of compliance
Introduction. Invasive Hemodynamic Monitoring. Determinants of Cardiovascular Function. Cardiovascular System. Hemodynamic Monitoring
 Introduction Invasive Hemodynamic Monitoring Audis Bethea, Pharm.D. Assistant Professor Therapeutics IV January 21, 2004 Hemodynamic monitoring is necessary to assess and manage shock Information obtained
Introduction Invasive Hemodynamic Monitoring Audis Bethea, Pharm.D. Assistant Professor Therapeutics IV January 21, 2004 Hemodynamic monitoring is necessary to assess and manage shock Information obtained
Index. K Knobology, TTE artifact, image resolution, ultrasound, 14
 A Acute aortic regurgitation (AR), 124 128 Acute aortic syndrome (AAS) classic aortic dissection diagnosis, 251 263 evolutive patterns, 253 255 pathology, 250 251 classifications, 247 248 incomplete aortic
A Acute aortic regurgitation (AR), 124 128 Acute aortic syndrome (AAS) classic aortic dissection diagnosis, 251 263 evolutive patterns, 253 255 pathology, 250 251 classifications, 247 248 incomplete aortic
Value of echocardiography in chronic dyspnea
 Value of echocardiography in chronic dyspnea Jahrestagung Schweizerische Gesellschaft für /Schweizerische Gesellschaft für Pneumologie B. Kaufmann 16.06.2016 Chronic dyspnea Shortness of breath lasting
Value of echocardiography in chronic dyspnea Jahrestagung Schweizerische Gesellschaft für /Schweizerische Gesellschaft für Pneumologie B. Kaufmann 16.06.2016 Chronic dyspnea Shortness of breath lasting
Intraaortic Balloon Counterpulsation- Supportive Data for a Role in Cardiogenic Shock ( Be Still My Friend )
 Intraaortic Balloon Counterpulsation- Supportive Data for a Role in Cardiogenic Shock ( Be Still My Friend ) Stephen G. Ellis, MD Section Head, Interventional Cardiology Professor of Medicine Cleveland
Intraaortic Balloon Counterpulsation- Supportive Data for a Role in Cardiogenic Shock ( Be Still My Friend ) Stephen G. Ellis, MD Section Head, Interventional Cardiology Professor of Medicine Cleveland
Determination of Stroke Volume from Left Ventricular Isovolumetric Contraction and Ejection Times
 Determination of Stroke Volume from Left Ventricular Isovolumetric Contraction and Ejection Times Clarence M. AGRESS, M.D. and Stanley WEGNER SUMMARY Examination was made of the relationship of left ventricular
Determination of Stroke Volume from Left Ventricular Isovolumetric Contraction and Ejection Times Clarence M. AGRESS, M.D. and Stanley WEGNER SUMMARY Examination was made of the relationship of left ventricular
Hemodynamics of Exercise
 Hemodynamics of Exercise Joe M. Moody, Jr, MD UTHSCSA and ALMMVAH, STVAHCS Exercise Physiology - Acute Effects Cardiac Output (Stroke volume, Heart Rate ) Oxygen Extraction (Arteriovenous O 2 difference,
Hemodynamics of Exercise Joe M. Moody, Jr, MD UTHSCSA and ALMMVAH, STVAHCS Exercise Physiology - Acute Effects Cardiac Output (Stroke volume, Heart Rate ) Oxygen Extraction (Arteriovenous O 2 difference,
Cardiovascular hemodynamics in the stress echo lab with open-source software
 Cardiovascular hemodynamics in the stress echo lab with open-source software T. Bombardini, D. Cini, E. Picano Institute of Clinical Physiology of CNR, Pisa, Italy no conflict of interest Background Stress
Cardiovascular hemodynamics in the stress echo lab with open-source software T. Bombardini, D. Cini, E. Picano Institute of Clinical Physiology of CNR, Pisa, Italy no conflict of interest Background Stress
Ventricular Assisting Devices in the Cathlab. Unrestricted
 Ventricular Assisting Devices in the Cathlab Unrestricted What is a VAD? A single system device that is surgically attached to the left ventricle of the heart and to the aorta for left ventricular support
Ventricular Assisting Devices in the Cathlab Unrestricted What is a VAD? A single system device that is surgically attached to the left ventricle of the heart and to the aorta for left ventricular support
Ventricular Interactions in the Normal and Failing Heart
 Ventricular Interactions in the Normal and Failing Heart Congenital Cardiac Anesthesia Society 2015 Pressure-volume relations Matched Left ventricle to low hydraulic impedance Maximal stroke work limited
Ventricular Interactions in the Normal and Failing Heart Congenital Cardiac Anesthesia Society 2015 Pressure-volume relations Matched Left ventricle to low hydraulic impedance Maximal stroke work limited
Assessment of LV systolic function
 Tutorial 5 - Assessment of LV systolic function Assessment of LV systolic function A knowledge of the LV systolic function is crucial in the undertanding of and management of unstable hemodynamics or a
Tutorial 5 - Assessment of LV systolic function Assessment of LV systolic function A knowledge of the LV systolic function is crucial in the undertanding of and management of unstable hemodynamics or a
10/7/2013. Systolic Function How to Measure, How Accurate is Echo, Role of Contrast. Thanks to our Course Director: Neil J.
 Systolic Function How to Measure, How Accurate is Echo, Role of Contrast Neil J. Weissman, MD MedStar Health Research Institute & Professor of Medicine Georgetown University Washington, D.C. No Disclosures
Systolic Function How to Measure, How Accurate is Echo, Role of Contrast Neil J. Weissman, MD MedStar Health Research Institute & Professor of Medicine Georgetown University Washington, D.C. No Disclosures
Mechanics of Cath Lab Support Devices
 Mechanics of Cath Lab Support Devices Issam D. Moussa, MD Chief Medical Officer First Coast Cardiovascular Institute, Jacksonville, FL Professor of Medicine, UCF, Orlando, FL None DISCLOSURE Percutaneous
Mechanics of Cath Lab Support Devices Issam D. Moussa, MD Chief Medical Officer First Coast Cardiovascular Institute, Jacksonville, FL Professor of Medicine, UCF, Orlando, FL None DISCLOSURE Percutaneous
DECLARATION OF CONFLICT OF INTEREST
 DECLARATION OF CONFLICT OF INTEREST Disclosures: Research grants & clinical trials (Gilead), honoraria & clinical trials (Berlin-Chemie/Menarini) Ranolazine in Heart Failure with Preserved Ejection Fraction
DECLARATION OF CONFLICT OF INTEREST Disclosures: Research grants & clinical trials (Gilead), honoraria & clinical trials (Berlin-Chemie/Menarini) Ranolazine in Heart Failure with Preserved Ejection Fraction
Relax and Learn At the Farm 2012
 Relax and Learn At the Farm Session 9: Invasive Hemodynamic Assessment and What to Do with the Data Carol Jacobson RN, MN Cardiovascular Nursing Education Associates Function of CV system is to deliver
Relax and Learn At the Farm Session 9: Invasive Hemodynamic Assessment and What to Do with the Data Carol Jacobson RN, MN Cardiovascular Nursing Education Associates Function of CV system is to deliver
Percutaneous Mechanical Circulatory Support Devices
 Percutaneous Mechanical Circulatory Support Devices Daniel Vazquez RN, RCIS Miami Cardiac & Vascular Institute FINANCIAL DISCLOSURES none CASE STUDY CASE STUDY 52 year old gentlemen Complaining of dyspnea
Percutaneous Mechanical Circulatory Support Devices Daniel Vazquez RN, RCIS Miami Cardiac & Vascular Institute FINANCIAL DISCLOSURES none CASE STUDY CASE STUDY 52 year old gentlemen Complaining of dyspnea
Effect of Ventricular Pacing on Myocardial Function. Inha University Hospital Sung-Hee Shin
 Effect of Ventricular Pacing on Myocardial Function Inha University Hospital Sung-Hee Shin Contents 1. The effect of right ventricular apical pacing 2. Strategies for physiologically optimal ventricular
Effect of Ventricular Pacing on Myocardial Function Inha University Hospital Sung-Hee Shin Contents 1. The effect of right ventricular apical pacing 2. Strategies for physiologically optimal ventricular
Fetal gene upregulation by 1-wk TAC is significantly increased in mice lacking RGS2.
 3562-RG-1 Supplementary Figure 1 Fetal gene upregulation by 1-wk is significantly increased in mice lacking RGS2. ANP(Nppa) /BNP(Nppb) A-type and B-type natriuretic peptide; β-mhc (Myh7) beta myosin heavy
3562-RG-1 Supplementary Figure 1 Fetal gene upregulation by 1-wk is significantly increased in mice lacking RGS2. ANP(Nppa) /BNP(Nppb) A-type and B-type natriuretic peptide; β-mhc (Myh7) beta myosin heavy
1. LV function and remodeling. 2. Contribution of myocardial ischemia due to CAD, and
 1 The clinical syndrome of heart failure in adults is commonly associated with the etiologies of ischemic and non-ischemic dilated cardiomyopathy, hypertrophic cardiomyopathy, hypertensive heart disease,
1 The clinical syndrome of heart failure in adults is commonly associated with the etiologies of ischemic and non-ischemic dilated cardiomyopathy, hypertrophic cardiomyopathy, hypertensive heart disease,
Abnormalities Caused by Left Bundle Branch Block
 Marquette University e-publications@marquette Physician Assistant Studies Faculty Research and Publications Physician Assistant Studies, Department 12-17-2010 Abnormalities Caused by Left Bundle Branch
Marquette University e-publications@marquette Physician Assistant Studies Faculty Research and Publications Physician Assistant Studies, Department 12-17-2010 Abnormalities Caused by Left Bundle Branch
Evalua&on)of)Le-)Ventricular)Diastolic) Dysfunc&on)by)Echocardiography:) Role)of)Ejec&on)Frac&on)
 Evalua&on)of)Le-)Ventricular)Diastolic) Dysfunc&on)by)Echocardiography:) Role)of)Ejec&on)Frac&on) N.Koutsogiannis) Department)of)Cardiology) University)Hospital)of)Patras)! I have no conflicts of interest
Evalua&on)of)Le-)Ventricular)Diastolic) Dysfunc&on)by)Echocardiography:) Role)of)Ejec&on)Frac&on) N.Koutsogiannis) Department)of)Cardiology) University)Hospital)of)Patras)! I have no conflicts of interest
*Generating blood pressure *Routing blood: separates. *Ensuring one-way blood. *Regulating blood supply *Changes in contraction
 *Generating blood pressure *Routing blood: separates pulmonary and systemic circulations *Ensuring one-way blood flow: valves *Regulating blood supply *Changes in contraction rate and force match blood
*Generating blood pressure *Routing blood: separates pulmonary and systemic circulations *Ensuring one-way blood flow: valves *Regulating blood supply *Changes in contraction rate and force match blood
For more information about how to cite these materials visit
 Author(s): Louis D Alecy, D.M.D., Ph.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Non-commercial Share Alike 3.0 License:
Author(s): Louis D Alecy, D.M.D., Ph.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Non-commercial Share Alike 3.0 License:
Percutaneous Mechanical Circulatory Support for Cardiogenic Shock. 24 th Annual San Diego Heart Failure Symposium Ryan R Reeves, MD FSCAI
 Percutaneous Mechanical Circulatory Support for Cardiogenic Shock 24 th Annual San Diego Heart Failure Symposium Ryan R Reeves, MD FSCAI The Need for Circulatory Support Basic Pathophysiologic Problems:
Percutaneous Mechanical Circulatory Support for Cardiogenic Shock 24 th Annual San Diego Heart Failure Symposium Ryan R Reeves, MD FSCAI The Need for Circulatory Support Basic Pathophysiologic Problems:
THE DIASTOLIC STRESS TEST: A NEW CLINICAL TOOL? THE CONCEPT OF DIASTOLIC RESERVE
 Thierry C. Gillebert University of Ghent ESC Education Committee THE DIASTOLIC STRESS TEST: A NEW CLINICAL TOOL? THE CONCEPT OF DIASTOLIC RESERVE 1 Case: Ann, 63 years Suffered from metabolic syndrome
Thierry C. Gillebert University of Ghent ESC Education Committee THE DIASTOLIC STRESS TEST: A NEW CLINICAL TOOL? THE CONCEPT OF DIASTOLIC RESERVE 1 Case: Ann, 63 years Suffered from metabolic syndrome
SIKLUS JANTUNG. Rahmatina B. Herman
 SIKLUS JANTUNG Rahmatina B. Herman The Cardiac Cycle Definition: The cardiac events that occur from the beginning of one heartbeat to the beginning of the next The cardiac cycle consists of: - Diastole
SIKLUS JANTUNG Rahmatina B. Herman The Cardiac Cycle Definition: The cardiac events that occur from the beginning of one heartbeat to the beginning of the next The cardiac cycle consists of: - Diastole
Hemodynamic Assessment. Assessment of Systolic Function Doppler Hemodynamics
 Hemodynamic Assessment Matt M. Umland, RDCS, FASE Aurora Medical Group Milwaukee, WI Assessment of Systolic Function Doppler Hemodynamics Stroke Volume Cardiac Output Cardiac Index Tei Index/Index of myocardial
Hemodynamic Assessment Matt M. Umland, RDCS, FASE Aurora Medical Group Milwaukee, WI Assessment of Systolic Function Doppler Hemodynamics Stroke Volume Cardiac Output Cardiac Index Tei Index/Index of myocardial
Cardiac Output Monitoring - 6
 Cardiac Output Monitoring - 6 How to use Wrexham s Cardiac Output Monitors. Wrexham Maelor Critical Care Version 02.05.16 Introduction Types of Devices: NICOM - Cheetah Oesophageal Doppler +/- Pulse Contour
Cardiac Output Monitoring - 6 How to use Wrexham s Cardiac Output Monitors. Wrexham Maelor Critical Care Version 02.05.16 Introduction Types of Devices: NICOM - Cheetah Oesophageal Doppler +/- Pulse Contour
THE RIGHT VENTRICLE IN PULMONARY HYPERTENSION R. DRAGU
 THE RIGHT VENTRICLE IN PULMONARY HYPERTENSION R. DRAGU Cardiology Dept. Rambam Health Care Campus Rappaport Faculty of Medicine Technion, Israel Why the Right Ventricle? Pulmonary hypertension (PH) Right
THE RIGHT VENTRICLE IN PULMONARY HYPERTENSION R. DRAGU Cardiology Dept. Rambam Health Care Campus Rappaport Faculty of Medicine Technion, Israel Why the Right Ventricle? Pulmonary hypertension (PH) Right
Review of Cardiac Mechanics & Pharmacology 10/23/2016. Brent Dunworth, CRNA, MSN, MBA 1. Learning Objectives
 Brent Dunworth, CRNA, MSN, MBA Associate Director of Advanced Practice Division Chief, Nurse Anesthesia Vanderbilt University Medical Center Nashville, Tennessee Learning Objectives Review the principles
Brent Dunworth, CRNA, MSN, MBA Associate Director of Advanced Practice Division Chief, Nurse Anesthesia Vanderbilt University Medical Center Nashville, Tennessee Learning Objectives Review the principles
E/Ea is NOT an essential estimator of LV filling pressures
 Euroecho Kopenhagen Echo in Resynchronization in 2010 E/Ea is NOT an essential estimator of LV filling pressures Wilfried Mullens, MD, PhD December 10, 2010 Ziekenhuis Oost Limburg Genk University Hasselt
Euroecho Kopenhagen Echo in Resynchronization in 2010 E/Ea is NOT an essential estimator of LV filling pressures Wilfried Mullens, MD, PhD December 10, 2010 Ziekenhuis Oost Limburg Genk University Hasselt
Principles of Biomedical Systems & Devices. Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont
 Principles of Biomedical Systems & Devices Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont Review of Cardiac Anatomy Four chambers Two atria-receive blood from the vena cave and pulmonary veins Two
Principles of Biomedical Systems & Devices Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont Review of Cardiac Anatomy Four chambers Two atria-receive blood from the vena cave and pulmonary veins Two
Load and Function - Valvular Heart Disease. Tom Marwick, Cardiovascular Imaging Cleveland Clinic
 Load and Function - Valvular Heart Disease Tom Marwick, Cardiovascular Imaging Cleveland Clinic Indications for surgery in common valve lesions Risks Operative mortality Failed repair - to MVR Operative
Load and Function - Valvular Heart Disease Tom Marwick, Cardiovascular Imaging Cleveland Clinic Indications for surgery in common valve lesions Risks Operative mortality Failed repair - to MVR Operative
8/8/2011. CARDIAC RESYCHRONIZATION THERAPY for Heart Failure. Case Presentation. Case Presentation
 CARDIAC RESYCHRONIZATION THERAPY for Heart Failure James Taylor, DO, FACOS Cardiothoracic and Vascular surgery San Angelo Community Medical Center San Angelo, TX Case Presentation 64 year old female with
CARDIAC RESYCHRONIZATION THERAPY for Heart Failure James Taylor, DO, FACOS Cardiothoracic and Vascular surgery San Angelo Community Medical Center San Angelo, TX Case Presentation 64 year old female with
Shock, Monitoring Invasive Vs. Non Invasive
 Shock, Monitoring Invasive Vs. Non Invasive Paula Ferrada MD Assistant Professor Trauma, Critical Care and Emergency Surgery Virginia Commonwealth University Shock Fluid Pressors Ionotrope Intervention
Shock, Monitoring Invasive Vs. Non Invasive Paula Ferrada MD Assistant Professor Trauma, Critical Care and Emergency Surgery Virginia Commonwealth University Shock Fluid Pressors Ionotrope Intervention
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Advanced imaging of the left atrium - strain, CT, 3D, MRI -
 Advanced imaging of the left atrium - strain, CT, 3D, MRI - Monica Rosca, MD Carol Davila University of Medicine and Pharmacy, Bucharest, Romania Declaration of interest: I have nothing to declare Case
Advanced imaging of the left atrium - strain, CT, 3D, MRI - Monica Rosca, MD Carol Davila University of Medicine and Pharmacy, Bucharest, Romania Declaration of interest: I have nothing to declare Case
CHRONIC HEART FAILURE : WHAT ELSE COULD WE OFFER TO OUR PATIENTS? Cardiac Rehabilitation Society of Thailand
 CHRONIC HEART FAILURE : WHAT ELSE COULD WE OFFER TO OUR PATIENTS? Cardiac Rehabilitation Society of Thailand ENHANCED EXTERNAL COUNTER PULSATION Piyanuj Ruckpanich, MD. Cardiac Rehabilitation Center Perfect
CHRONIC HEART FAILURE : WHAT ELSE COULD WE OFFER TO OUR PATIENTS? Cardiac Rehabilitation Society of Thailand ENHANCED EXTERNAL COUNTER PULSATION Piyanuj Ruckpanich, MD. Cardiac Rehabilitation Center Perfect
Left atrial function. Aliakbar Arvandi MD
 In the clinic Left atrial function Abstract The left atrium (LA) is a left posterior cardiac chamber which is located adjacent to the esophagus. It is separated from the right atrium by the inter-atrial
In the clinic Left atrial function Abstract The left atrium (LA) is a left posterior cardiac chamber which is located adjacent to the esophagus. It is separated from the right atrium by the inter-atrial
Evaluation of Left Ventricular Function and Hypertrophy Gerard P. Aurigemma MD
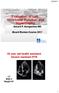 Evaluation of Left Ventricular Function and Hypertrophy Gerard P. Aurigemma MD Board Review Course 2017 43 year old health assistant Severe resistant HTN LT BSA 2 Height 64 1 Here is the M mode echocardiogram
Evaluation of Left Ventricular Function and Hypertrophy Gerard P. Aurigemma MD Board Review Course 2017 43 year old health assistant Severe resistant HTN LT BSA 2 Height 64 1 Here is the M mode echocardiogram
