The value of Adrenaline in the induction of supraventricular tachycardia in the EP lab
|
|
|
- Tobias Terry
- 6 years ago
- Views:
Transcription
1 The value of Adrenaline in the induction of supraventricular tachycardia in the EP lab Gabriel Cismaru, MD¹, Radu Rosu, MD, PhD¹, Lucian Muresan MD¹, Mihai Puiu, MD¹, Marius Andronache, MD, PhD², Erika Hengan MD¹, Daniel Ispas MD¹, Gabriel Gusetu, MD¹, Dana Pop MD, PhD¹, Petru Adrian Mircea MD, PhD³, Dumitru Zdrenghea MD, PhD¹. ¹Iuliu Hatieganu University of Medicine and Pharmacy, Dept. of Cardiology Rehabilitation Hospital, Cluj-Napoca, Romania. ²CHU de Nancy, Department of Cardiology, University Hospital Nancy, France, ³Iuliu Hatieganu University of Medicine and Pharmacy, 1 st Dept. of Internal Medicine Gastroenterology,, Cluj-Napoca, Romania. Corresponding Author (proofs should be sent to:) Dana Pop, MD, PhD. Spitalul Clinic de Recuperare Sectia Cardiologie Strada Viilor Cluj-Napoca, Romania. Phone : (40) Fax (40) pop7dana@yahoo.com Conflict of interest: none declared.
2 Structured abstract: Aims: The most commonly used drug for the facilitation of supraventricular tachycardia (SVT). induction in the electrophysiological (EP) laboratory is isoprenaline Despite isoprenaline s apparent indispensability, availability has been problematic in some European countries. Alternative sympatomimethic drugs such as adrenaline have therefore been tried. However, no studies have determined the sensitivity and specificity of adrenaline for the induction of (SVT).The objective of this study was to determine the sensitivity and specificity of adrenaline for the induction of SVT. Methods: Between February 2010 and July 2013, 336 patients underwent an electrophysiological study for prior documented SVT. In 66 adrenaline was infused because tachycardia was not induced under basal conditions. This group was compared with 30 control subjects with no history of SVT. Programmed atrial stimulation was carried out during baseline state and repeated after an infusion of adrenaline (dose ranging from 0.05 mcg/kgc to 0.3 mcg/kgc). The end-point was the induction of SVT. Results: Among 66 patients with a history of SVT but no induction under basal conditions, adrenaline facilitated induction in 54 patients (82%, p<0.001). Among the 30 control subjects, SVT was not induced in any patient (0%) after infusion. Adrenaline was generally well tolerated, except for 2 patients (3.0%), where it had to be discontinued due to headache and high blood pressure or lumbar pain. Conclusion: Adrenaline infusion has a high sensitivity (82%) and specificity (100%) for induction of SVT in patients with prior documented SVT. Therefore, It could serve as an acceptable alternative to isoprenaline, when the latter is not available. Key words: adrenaline, isoprenaline, supraventricular tachycardia, electrophysiological study.
3 Condensed abstract: The study evaluated the sensitivity and specificity of adrenaline for the induction of SVT in patients with prior documented SVT. Our results showed a high sensitivity (82%) and specificity (100%) using adrenaline These findings suggests that adrenaline can be used instead of isoprenaline when this is not available.
4 What s New? Adrenaline can be used for the induction of SVT in patients with paroxysmal documented SVT It may also be considered in patients who undergo an electrophysiological study to determine the mechanism of their palpitations and/or syncope, if no documentation of arrhythmia exists (12-lead ECG), after having undergone a complete negative set of noninvasive tests. Because Adrenaline cannot always facilitate the induction of SVT in patients with a history of paroxysmal SVT even at infusion rates of 0.3 microgr/kg/min, it is important to be aware of the fact that the addition of other drugs such as atropine or isoprenaline might be necessary in order to induce and assess the mechanism of SVT before catheter ablation.
5 INTRODUCTION: Isoprenaline, a beta-adrenergic drug, commonly used in clinical practice for its properties of increasing heart rate can induce supraventricular tachycardia (SVT) in the electrophysiology (EP) lab [1,2]. Despite its apparent indispensability, availability has been problematic in Eastern Europe. Alternative sympatomimethic drugs like adrenaline have therefore been tried. Sensibility and specificity of isoprenaline for induction of paroxysmal atrial fibrillation has already been reported [3]. Although adrenaline is known to facilitate the induction or supraventricular tachycardia, its sensibility and specificity in the EP laboratory has not previously been evaluated. The purpose of this study was to determine the sensitivity and specificity of adrenaline for the induction of supraventricular tachycardia during the electrophysiological study.
6 METHODS: Study Subjects: From February 2010 to July 2013 a total of 336 patients with clinical documented paroxysmal supraventricular tachycardia (PSVT) were referred to our department for an EP study +/- RF catheter ablation procedure. Sixty-six patients necessitated adrenaline infusion because under basal conditions no PSVT was induced. Twenty four patients were men (36.4%) and 42 women, with a mean age of 49.2 years. Patients with known coronary artery disease, hypertrophic obstructive cardiomyopathy, severe aortic or mitral valve stenosis were excluded from the study. All patients had recurrent episodes of PSVT documented by 12-lead ECG. A group of 30 subjects with no history of tachycardia constituted the control group. The electrophysiological study was performed in these patients for the following reasons: to assess the sinus node function and atrio-ventricular (AV) conduction in 10 patients, to investigate the cause of syncope in 8 patients, to determine the refractory period of an accessory pathway in 7 patients and prior to ventricular extrasystole ablation in 6 patients. Adrenaline was infused in all and a complete EP study was conducted. Electrophysiological study: The EP study was performed in non-sedated patients in the post-absorptive state after an informed consent was obtained. All patients were in sinus rhythm at the beginning of the study. Heart catheterization was performed through the right femoral vein with four multielectrode catheters. Electrograms were recorded from the high right atrium, the bundle of His, coronary sinus and the right ventricle.
7 Atrial and ventricular programmed stimulation as well as overdrive pacing were conducted, in order to determine the conduction properties and refractoriness of the AV node, to exclude the presence of an accessory pathway, to induce and to stop supraventricular tachycardias and to perform the differential diagnosis of PSVT. Our atrial programmed stimulation protocol employed delivery of up to three atrial extrastimuli at two atrial sites and at two atrial drive pacing lengths (600 ms and 400 ms). If no arrhythmia was induced at the basal state, adrenaline was consecutively administered. Infusion was started at 0,05microgr/kg/min and up-titrated until an increase in the basal heart rate by at least 50% was noticed, to at least 100 beats/min (maximum 150 beats/min or 400 ms of cycle). The amount of adrenaline required to induce the desired changes in heart rate ranged from 0,1 to 0,3 microgr/kg/min. Attempts to induce supraventricular tachycardia by atrial and ventricular programmed stimulation and overdrive pacing were repeated during adrenaline infusion. For patients in which adrenaline infusion was not sufficient for SVT induction, atropine 1 to 2 mg iv was administrated. Statistical Analysis: Statistical analysis was performed using SPSS Statistics version 21.0 (SPSS Inc., Chicago, Illinois). Descriptive statistics were used to summarize patient characteristics. Means and standard deviations were used for normally distributed continuous variable as well as counts and proportions for categorical variables. McNemar test for related samples was performed to compare in a pairwise fashion the fraction of patients with inducible PSVT before and after adrenaline infusion.
8 RESULTS: In 115 patients out of 336 (34.2%), there was no need for drug provocation: 50 patients (44%) with AVNRT, 44 patients (38%) with AVRT conducted retrogradely through an accessory pathway and 21 (18%) with atrial tachycardia. In 221 out of 336 patients (65,8 %) without induction in the basal state we used medication for SVT induction. For patients included in our study from February 2010 to July 2012, we used Atropine and Isoprenaline (Isoprenaline was available in our EP lab during this period of time).for patients included in our study from July 2012 to July 2013, we used Atropine and Adrenaline (because Isoprenaline was not available in our EP lab during this period of time). Concerning the use of adrenaline or atropine, the choice between one drug or the other as the initial medication for facilitating the induction of SVT was left at the physician s free will. Consequently, one doctor used Adrenaline first for SVT induction and another doctor used Atropine first for SVT induction. If no SVT was induced after the administration of the first drug, than the other drug was added (Figure1). Effects of Adrenaline in Patients with Supraventricular Tachycardia Sixty-six patients (19.6 %) received adrenaline for SVT induction. Among the 66 patients with prior documented PSVT, using the above-mentioned stimulation protocols, no SVT was induced under basal conditions (prior to adrenaline administration). After the infusion of adrenaline, sustained supraventricular tachycardia was induced in 54 patients. Among these 54 patients, 40 had atrioventricular node re-entry tachycardia (AVNRT), 11 patients had orthodromic atrio-ventricular re-entry tachycardia (AVRT) using a concealed accessory pathway and 3 patients had focal atrial tachycardias (AT)
9 arising from the right atrium. The sensitivity of the adrenaline test defined as the percentage of inducible sustained supraventricular tachycardia was 82%. We had no patient with concealed accessory pathway and concomitant AVNRT induction. In the 12 patients in whom the tachycardia could not be induced after Adrenaline infusion, Atropine was added. PSVT was subsequently induced after the administration of Atropine in 11. Among them, 8 patients had AVNRT, 3 patients had AVRT and 1 patient had AT. In 1 patient no arrhythmia was induced but slow pathway ablation was performed because documented ECG during tachycardia was suggestive of AVNRT, and EP study revealed presence of dual atrio-ventricular nodal morphology (Figure 2). Related-Samples McNemar Change Test used for nominal data showed significant difference between SVT induction before and after the administration of adrenaline p< Effects of Adrenaline in Control Subjects Among the 30 control subjects, supraventricular tachycardia was not induced during the EP study, neither before nor after infusion of adrenaline. Specificity, defined as the percentage of negative test in the control group was 100%. Diagnostic Accuracy The sensitivity and specificity of adrenaline for the induction of PSVT were 82% and 100 %, respectively. The positive and negative predictive values were 100.% and 71%. The overall diagnostic accuracy was 88 % (Table 1). Adverse Effects
10 Adrenaline was generally well tolerated. Side effects consisted in: tremor (for which the infusion was not discontinued because it was considered tolerable by the patient), headache and lumbar pain. The adrenaline infusion was discontinued prematurely in 2 of 96 patients (2.1%). In the first patient, headache was attributed to high systolic blood pressure > 180/110 mmhg, which appeared during infusion of adrenaline at rates of 0,2microgr/kg/min. The symptoms resolved after discontinuation of adrenaline. The other patient presented lumbar pain that disappeared after the discontinuation of infusion. Induction of non-specific arrhythmias occurred in the form of runs of premature atrial contractions (4 patients=4.2%), non-sustained atrial tachycardia (1 patient=1.0%), ventricular premature beats (3 patients= 3.1%), but none of these influenced the overall result of the EP study. There were no electrocardiogram changes suggestive of ischemia in any of the patients.
11 DISCUSSION: Main findings This study demonstrates that adrenaline has a high sensitivity and specificity for the induction of SVT in patients with paroxysmal documented SVT. In a prior study, Brembilla-Perrot B. et al reported a sensitivity of 90% and specificity of 100% for isoprenaline for the diagnosis of supraventricular tachycardia [1]. Huycke et al. found a sensitivity of 67% and specificity of 100% for isoprenalinefacilitated induction of AVNRT. However the number of patients was lower (20 patients) than in the study of Brembilla-Perrot (67 patients) [2]. Stellbrink et al. randomized 80 patients to receive either atropine or isoproterenol before AVNRT ablation. The inducibility in the isoproterenol group increased from 58% in the baseline state to 93% after isoproterenol infusion (p<0.001) [4]. Pauriah et al. studied 63 patients with WPW and spontaneous adverse clinical presentation (syncope or resuscitated ventricular fibrillation). At baseline orthodromic tachycardia was induced in 44% and antidromic tachycardia in 11%. After isoproterenol infusion inducibility increased to 68.2 % for orthodromic tachycardia and 22.2 % for antidromic tachycardia [5]. In the absence of isoprenaline, it appears that adrenaline might be an acceptable alternative, due to its high sensibility and specificity, of 82% and 100%, respectively. In our study, adrenaline was generally well-tolerated with minimal side-effects and with a low percentage of premature discontinuation, of 2.1%.
12 Electrophysiologic Effects of Adrenaline and Dosage. An alternative approach to the adrenergic initiation of tachycardias facilitated by isoprenaline could be the use of adrenaline or noradrenaline. Furthermore, the use of a vagolytic agent such as atropine could facilitate the induction of tachycardias by leaving the action of natural catecholamines unopposed by the parasympathetic system and thus induce tachycardia. [6]. Adrenaline is a nonselective agonist of alpha and beta adrenergic receptors, and thus its activity, side effects and efficacy differ from isoprenaline. The overall electrophysiological effects of adrenaline result from stimulation of the beta-adrenergic receptors. Stimulation of the alpha-adrenergic receptors by adrenaline has no effect on the AV node, but prolongs the effective refractory period of the atrium and the ventricle, partially offsetting the shortening of refractory periods mediated by beta-receptor stimulation [6, 7]. The mechanism by which adrenaline induces sustained SVT may be multifactorial. In physiologic doses, adrenaline shortens the effective refractory period of the atrium, AV node and ventricle and improves AV node conduction. Episodes of tachycardias induced by adrenaline are attributed to the acceleration of the sinus rate, which might sufficiently shorten the retrograde refractory periods of additional pathways (accessory pathway, slow nodal pathway) to permit retrograde conduction up the additional pathway to the atrium, thus causing an echo beat and initiate the tachycardia. [6,7] Because adrenaline can reproduce stress hypokalemia, another mechanism by which adrenaline might have facilitated the induction of SVT would be a reduction in intracellular potassium [8]. Probably the best way to estimate adrenergic activity after intravenous infusion is the measurement of plasma concentration of adrenaline [9]. Although plasma adrenaline concentrations were not measured in our study, prior studies have determined the plasma adrenaline concentrations correspondent to the infused doses. Accordingly, an adrenaline infusion of 0,001-0,313 microgr/kg/min would correspond to a plasma concentration of 0,005-3 microgr/l [10-16]. In our study, the doses of adrenaline
13 required to induce the desired change in heart rate ranged from 0.1 to 0.3 microgr/kg/min. Previous studies have demonstrated that constant rate infusions are characterized by the attainment of a steady state in plasma concentrations within 5 to 10 minutes. Furthermore, steady state concentrations are directly proportional to the rate of infusion [14] In our study, adrenaline infusion was started at a dose of 0.05 microgr/kg/min rate and increased every 5 minutes in order to obtain the desired increase in the heart rate, or up to a dose of 0.3 microgr/kg/min. This was effective in increasing the heart rate and subsequently inducing SVT by programmed atrial stimulation. Safety of Adrenaline in patients with concealed accessory pathways By giving Adrenaline there is a theoretical risk of unmasking antegrade conduction and inducing ventricular fibrillation (VFib) in patients who have a concealed accessory pathway. There is data in the literature indicating that Isoprenaline can facilitate the unmasking of antegrade conduction of the accessory pathway [17]. In the case of atrial fibrillation initiation, the pathway can conduct rapidly to the ventricles and induce VFib. However, the risk is relatively small. Our EP lab is properly equipped to handle such cases (defibrillator, intubation, mechanical ventilation, etc).
14 Limitations: One limitation of this study is that the effects of adrenaline were assessed in conscious sedated or non-sedated patients. It is not clear whether adrenaline would have similar properties if administrated to patients under general anesthesia. The induction of atrial tachycardias is not necessarily clinical tachycardia. In this case the patients were always asked for their symptoms. If they were asymptomatic or their symptoms did not suggest it to be the clinical tachycardia, AT was considered nonspecific. The induced and clinical tachycardia may be different but may look the same on the surface ECG. However the P wave during AT and the presence of nonsustained or sustained arrhythmia should make the difference between non-specific and specific AT. Finally, because the effects of adrenaline may be time-dependent, it is possible that SVT may have been induced at lower doses if more time was allowed before the increase of the infusion rate.
15 REFERENCES: 1. Brembilla-Perrot B, Terrier de la Chaise A, Pichene M, Aliot E, Cherrier F, Pernot C. Isoprenaline as an aid to the induction of catecholamine dependent supraventricular tachycardias during programmed stimulation. Br Heart J. 1989;61(4): Huycke EC, Lai WT, Nguyen NX, Keung EC, Sung RJ. Role of intravenous isoproterenol in the electrophysiologic induction of atrioventricular node reentrant tachycardia in patients with dual atrioventricular node pathways. Am J Cardiol.1989;64(18): Oral H Fau - Crawford T, Crawford T Fau - Frederick M, Frederick M Fau - Gadeela N, Gadeela N Fau - Wimmer A, Wimmer A Fau - Dey S, Dey S Fau - Sarrazin JF, et al. - Inducibility of paroxysmal atrial fibrillation by isoproterenol and its relation to the mode of onset of atrial fibrillation. J Cardiovasc Electrophysiol. 2008;19(5): Stellbrink C, Diem B, Schauerte P, Brehmer K, Schuett H, Hanrath P. Differential effects of atropine and isoproterenol on inducibility of atrioventricular nodal reentrant tachycardia.j Interv Card Electrophysiol. 2001;5(4): Pauriah M, Cismaru G, Sellal JM, Chillou CD, Brembilla-Perrot B. Is isoproterenol really required during electrophysiological study in patients with Wolff-Parkinson-White syndrome? J Electrocardiol. 2013;46(6): Morady F, Nelson SD, Kou WH, Pratley R, Schmaltz S, De Buitleir M, et al. Electrophysiologic effects of epinephrine in humans. J Am Coll Cardiol. 1988;11(6): Morady F, Kou WH, Kadish AH, Toivonen LK, Kushner JA, Schmaltz S. Effects of epinephrine in patients with an accessory atrioventricular connection treated with quinidine. Am J Cardiol. 1988;62(9): Darbar D Fau - Smith M, Smith M Fau - Morike K, Morike K Fau - Roden DM, DM R. - Epinephrine-induced changes in serum potassium and cardiac repolarization and effects of pretreatment with propranolol and diltiazem. Am J Cardiol. 1996;77(15): Engelman K Fau - Portnoy B, Portnoy B Fau - Lovenberg W, W L. - A sensitive and specific double-isotope derivative method for the determination of catecholamines in biological specimens. Am J Med Sci. 1968;255: Christensen Nj Fau - Alberti KG, Alberti Kg Fau - Brandsborg O, O B. - Plasma catecholamines and blood substrate concentrations: studies in insulin induced hypoglycaemia and after adrenaline infusions. Eur J Clin Invest. 1975;5(5):
16 11. Christensen NJ, Videbaek J. Plasma Catecholamines and Carbohydrate Metabolism in Patients with Acute Myocardial Infarction. J Clin Invest. 1974;54(2): Clutter We Fau - Bier DM, Bier Dm Fau - Shah SD, Shah Sd Fau - Cryer PE, PE C. - Epinephrine plasma metabolic clearance rates and physiologic thresholds for metabolic and hemodynamic actions in man. J Clin Invest. 1980;66(1): Clutter We Fau - Cryer PE, PE C. - Plasma dose-response studies with noradrenaline and adrenaline in man. Prog Biochem Pharmacol. 1980;17: Cohen G Fau - Holland B, Holland B Fau - Sha J, Sha J Fau - Goldenberg M, M. G. - Plasma concentrations of epinephrine and norepinephrine during intravenous infusions in man. J Clin Invest. 1959;38: DORNER J. [Comparative experimental studies on circulatory effect of adrenaline and epinephrine]. Arch Kreislaufforsch. 1954;21(1-4): Goldstein DS, Dionne R, Sweet J, Gracely R, Brewer B, Gregg R, et al. CIRCULATORY, PLASMA-CATECHOLAMINE, CORTISOL, LIPID, AND PSYCHOLOGICAL RESPONSES TO A REAL-LIFE STRESS (THIRD MOLAR EXTRACTIONS) - EFFECTS OF DIAZEPAM SEDATION AND OF INCLUSION OF EPINEPHRINE WITH THE LOCAL-ANESTHETIC. Psychosomatic Medicine. 1982;44(3): Przybylski J, Chiale P A, Halpern M S, Nau G J, Elizari M V, Rosenbaum M B. Unmasking of ventricular preexcitation by vagal stimulation or isoproterenol administration. Circulation. 1980;61:
17 Figure 1: The population included in the study and the distribution of drugs used for SVT induction. PSVT = Paroxysmal Supraventricular Tachycardia Adrenaline + Atropine indicates that the tachycardia was not induced after the administration of Adrenaline alone, so Atropine was administered on top, in order to facilitate the induction of SVT. Atropine + Adrenaline indicates that the tachycardia was not induced after the administration of Atropine alone, so Adrenaline was administered on top, in order to facilitate the induction of SVT. Overall, three patients necessitated Adrenaline infusion for SVT induction after the administration of Atropine: one patient had dual AV nodal physiology but no tachycardia was induced after Atropine alone was administrated; AVNRT was induced after subsequent Adrenaline infusion and slow pathway ablation was successfully performed; for the second patient, no SVT was induced after Adrenaline infusion, but he also had dual AV nodal physiology, thus slow pathway ablation was performed; the third patient had no SVT induction after Adrenaline infusion, no evidence of dual AV nodal physiology and the procedure was terminated
18 Figure 2:Effects of Adrenaline in Control subjects and in patients with documented SVT. SVT=supraventricular tachycardia; AVNRT=atrio-ventricular node reentrant tachycardia; AVRT=atrio-ventricular reentrant tachycardia using an accessory pathway as the retrograde limb; AT=atrial tachycardia;
19 TABLE 1: Diagnostic accuracy of Adrenaline for induction of SVT. TABLE 1 Diagnostic accuracy of Adrenaline for induction of SVT Sensitivity Specificity PPV NPV 82% 100% 100% 71% Data shown in percentages are: positive predictive value (PPV) and negative predictive value (NPV).
The value of adrenaline in the induction of supraventricular tachycardia in the electrophysiological laboratory
 Europace (2014) 16, 1634 1638 doi:10.1093/europace/euu042 CLINICAL RESEARCH Electrophysiology and ablation The value of adrenaline in the induction of supraventricular tachycardia in the electrophysiological
Europace (2014) 16, 1634 1638 doi:10.1093/europace/euu042 CLINICAL RESEARCH Electrophysiology and ablation The value of adrenaline in the induction of supraventricular tachycardia in the electrophysiological
Supraventricular Tachycardia (SVT)
 Supraventricular Tachycardia (SVT) Bruce Stambler, MD Piedmont Heart Atlanta, GA Supraventricular Tachycardia Objectives Types and mechanisms AV nodal reentrant tachycardia (AVNRT) AV reciprocating tachycardia
Supraventricular Tachycardia (SVT) Bruce Stambler, MD Piedmont Heart Atlanta, GA Supraventricular Tachycardia Objectives Types and mechanisms AV nodal reentrant tachycardia (AVNRT) AV reciprocating tachycardia
WPW syndrome and AVRT
 WPW syndrome and AVRT Myung-Yong Lee, MD, PhD Division of Cardiology Department of Internal Medicine School of Medicine Dankook University, Cheonan, Korea Supraventricular tachycardia (SVT) Paroxysmal
WPW syndrome and AVRT Myung-Yong Lee, MD, PhD Division of Cardiology Department of Internal Medicine School of Medicine Dankook University, Cheonan, Korea Supraventricular tachycardia (SVT) Paroxysmal
Case Report Catheter ablation of ventricular tachycardia related to a septo-apical left ventricular aneurysm
 Int J Clin Exp Med 2015;8(10):19576-19580 www.ijcem.com /ISSN:1940-5901/IJCEM0014701 Case Report Catheter ablation of ventricular tachycardia related to a septo-apical left ventricular aneurysm Radu Rosu
Int J Clin Exp Med 2015;8(10):19576-19580 www.ijcem.com /ISSN:1940-5901/IJCEM0014701 Case Report Catheter ablation of ventricular tachycardia related to a septo-apical left ventricular aneurysm Radu Rosu
Asymptomatic patient with WPW
 Asymptomatic patient with WPW Dimosthenis Avramidis, MD. Arrythmiologist Mitera Children s Hospital Athens Greece Scientific Associate 1st Cardiology Dpt Evangelismos Hospital Athens Greece Preexcitation
Asymptomatic patient with WPW Dimosthenis Avramidis, MD. Arrythmiologist Mitera Children s Hospital Athens Greece Scientific Associate 1st Cardiology Dpt Evangelismos Hospital Athens Greece Preexcitation
Bernard Belhassen, MD; Roman Fish, MD; Sami Viskin, MD; Aharon Glick, MD; Michael Glikson, MD; Michael Eldar, MD
 www.ipej.org 3 Original Article Incidence of Dual AV Node Physiology Following Termination of AV Nodal Reentrant Tachycardia by Adenosine-5'-Triphosphate: A Comparison with Drug Administration in Sinus
www.ipej.org 3 Original Article Incidence of Dual AV Node Physiology Following Termination of AV Nodal Reentrant Tachycardia by Adenosine-5'-Triphosphate: A Comparison with Drug Administration in Sinus
Basic Electrophysiology Protocols
 Indian Journal of Cardiology ISSN-0972-1622 2012 by the Indian Society of Cardiology Vol. 15, (3-4), 27-37 [ 27 Review Article Shomu Bohora Assistant Professor, Deptt. of Cardiology, U.N. Mehta Institute
Indian Journal of Cardiology ISSN-0972-1622 2012 by the Indian Society of Cardiology Vol. 15, (3-4), 27-37 [ 27 Review Article Shomu Bohora Assistant Professor, Deptt. of Cardiology, U.N. Mehta Institute
Chapter 16: Arrhythmias and Conduction Disturbances
 Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Journal of the American College of Cardiology Vol. 36, No. 2, by the American College of Cardiology ISSN /00/$20.
 Journal of the American College of Cardiology Vol. 36, No. 2, 2000 2000 by the American College of Cardiology ISSN 0735-1097/00/$20.00 Published by Elsevier Science Inc. PII S0735-1097(00)00770-1 Diagnostic
Journal of the American College of Cardiology Vol. 36, No. 2, 2000 2000 by the American College of Cardiology ISSN 0735-1097/00/$20.00 Published by Elsevier Science Inc. PII S0735-1097(00)00770-1 Diagnostic
TACHYARRHYTHMIAs. Pawel Balsam, MD, PhD
 TACHYARRHYTHMIAs Pawel Balsam, MD, PhD SupraVentricular Tachycardia Atrial Extra Systole Sinus Tachycardia Focal A. Tachycardia AVRT AVNRT Atrial Flutter Atrial Fibrillation Ventricular Tachycardia Ventricular
TACHYARRHYTHMIAs Pawel Balsam, MD, PhD SupraVentricular Tachycardia Atrial Extra Systole Sinus Tachycardia Focal A. Tachycardia AVRT AVNRT Atrial Flutter Atrial Fibrillation Ventricular Tachycardia Ventricular
A Narrow QRS Complex Tachycardia With An Apparently Concentric Retrograde Atrial Activation Sequence
 www.ipej.org 125 Case Report A Narrow QRS Complex Tachycardia With An Apparently Concentric Retrograde Atrial Activation Sequence Miguel A. Arias MD, PhD; Eduardo Castellanos MD, PhD; Alberto Puchol MD;
www.ipej.org 125 Case Report A Narrow QRS Complex Tachycardia With An Apparently Concentric Retrograde Atrial Activation Sequence Miguel A. Arias MD, PhD; Eduardo Castellanos MD, PhD; Alberto Puchol MD;
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013
 Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
Case-Based Practical ECG Interpretation for the Generalist
 Case-Based Practical ECG Interpretation for the Generalist Paul D. Varosy, MD, FACC, FAHA, FHRS Director of Cardiac Electrophysiology VA Eastern Colorado Health Care System Associate Professor of Medicine
Case-Based Practical ECG Interpretation for the Generalist Paul D. Varosy, MD, FACC, FAHA, FHRS Director of Cardiac Electrophysiology VA Eastern Colorado Health Care System Associate Professor of Medicine
Declaration of conflict of interest NONE
 Declaration of conflict of interest NONE Transatlantic Electrophysiology Lessons for and from Iberoamerica European Society of Cardiology Mexican Society of Cardiology Wolff-Parkinson-White Syndrome in
Declaration of conflict of interest NONE Transatlantic Electrophysiology Lessons for and from Iberoamerica European Society of Cardiology Mexican Society of Cardiology Wolff-Parkinson-White Syndrome in
Supraventricular Tachycardia: From Fetus to Adult. Mohamed Hamdan, MD
 Supraventricular Tachycardia: From Fetus to Adult Mohamed Hamdan, MD Learning Objectives Define type of SVT by age Describe clinical approach Describe prenatal and postnatal management of SVT 2 SVT Across
Supraventricular Tachycardia: From Fetus to Adult Mohamed Hamdan, MD Learning Objectives Define type of SVT by age Describe clinical approach Describe prenatal and postnatal management of SVT 2 SVT Across
the ECG, 6 mg of intravenous adenosine was administered as a fast bolus through a large bore intravenous cannula in
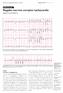 (arrows). Electrocardiography Series Singapore Med.1 2011, 52(3) 146 CME Article Regular narrow complex tachycardia Singh D, Teo S G, Poh K K V Hr JL1 11 VL VF WA, Fig. I ECG shows regular narrow complex
(arrows). Electrocardiography Series Singapore Med.1 2011, 52(3) 146 CME Article Regular narrow complex tachycardia Singh D, Teo S G, Poh K K V Hr JL1 11 VL VF WA, Fig. I ECG shows regular narrow complex
Introduction. Methods
 Europace (2015) 17, 801 806 doi:10.1093/europace/euu332 CLINICAL RESEARCH Cardiac electrophysiology Electrophysiological studies in patients with paroxysmal supraventricular tachycardias but no electrocardiogram
Europace (2015) 17, 801 806 doi:10.1093/europace/euu332 CLINICAL RESEARCH Cardiac electrophysiology Electrophysiological studies in patients with paroxysmal supraventricular tachycardias but no electrocardiogram
PARA-HISSIAN CONCEALED ACCESSORY PATHWAY
 PARA-HISSIAN CONCEALED ACCESSORY PATHWAY Anamnestic Findings 41 y.o. man with normal cardiac findings on echocardiography, suffering for paroxysmal supra-ventricular tachycardia since 1982 with rapid onset
PARA-HISSIAN CONCEALED ACCESSORY PATHWAY Anamnestic Findings 41 y.o. man with normal cardiac findings on echocardiography, suffering for paroxysmal supra-ventricular tachycardia since 1982 with rapid onset
Case 1 Left Atrial Tachycardia
 Case 1 Left Atrial Tachycardia A 16 years old woman was referred to our institution because of recurrent episodes of palpitations and dizziness despite previous ablation procedure( 13 years ago) of postero-septal
Case 1 Left Atrial Tachycardia A 16 years old woman was referred to our institution because of recurrent episodes of palpitations and dizziness despite previous ablation procedure( 13 years ago) of postero-septal
Clinical Cardiac Electrophysiology
 Clinical Cardiac Electrophysiology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of
Clinical Cardiac Electrophysiology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of
Paroxysmal Supraventricular Tachycardia PSVT.
 Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
Dysrhythmias 11/7/2017. Disclosures. 3 reasons to evaluate and treat dysrhythmias. None. Eliminate symptoms and improve hemodynamics
 Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
Journal of the American College of Cardiology Vol. 33, No. 3, by the American College of Cardiology ISSN /99/$20.
 Journal of the American College of Cardiology Vol. 33, No. 3, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(98)00614-7 A Technique
Journal of the American College of Cardiology Vol. 33, No. 3, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(98)00614-7 A Technique
Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD
 Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD OBJECTIVES 1. Identify the basic electrophysiology of the four causes of wide complex tachycardia. 2. Develop a simple framework for acute management
Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD OBJECTIVES 1. Identify the basic electrophysiology of the four causes of wide complex tachycardia. 2. Develop a simple framework for acute management
Differentiating Junctional Tachycardia and Atrioventricular Node Re-Entry Tachycardia Based on Response to Atrial Extrastimulus Pacing
 Journal of the American College of Cardiology Vol. 52, No. 21, 2008 2008 by the American College of Cardiology Foundation ISSN 0735-1097/08/$34.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2008.08.030
Journal of the American College of Cardiology Vol. 52, No. 21, 2008 2008 by the American College of Cardiology Foundation ISSN 0735-1097/08/$34.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2008.08.030
Case Report Coexistence of Atrioventricular Nodal Reentrant Tachycardia and Idiopathic Left Ventricular Outflow-Tract Tachycardia
 www.ipej.org 149 Case Report Coexistence of Atrioventricular Nodal Reentrant Tachycardia and Idiopathic Left Ventricular Outflow-Tract Tachycardia Majid Haghjoo, M.D, Arash Arya, M.D, Mohammadreza Dehghani,
www.ipej.org 149 Case Report Coexistence of Atrioventricular Nodal Reentrant Tachycardia and Idiopathic Left Ventricular Outflow-Tract Tachycardia Majid Haghjoo, M.D, Arash Arya, M.D, Mohammadreza Dehghani,
PEDIATRIC SVT MANAGEMENT
 PEDIATRIC SVT MANAGEMENT 1 INTRODUCTION Supraventricular tachycardia (SVT) can be defined as an abnormally rapid heart rhythm originating above the ventricles, often (but not always) with a narrow QRS
PEDIATRIC SVT MANAGEMENT 1 INTRODUCTION Supraventricular tachycardia (SVT) can be defined as an abnormally rapid heart rhythm originating above the ventricles, often (but not always) with a narrow QRS
Case Report Simultaneous Accessory Pathway and AV Node Mechanical Block
 185 Case Report Simultaneous Accessory Pathway and AV Node Mechanical Block Daniel Garofalo, MD, FRACP, Alfonso Gomez Gallanti, MD, David Filgueiras Rama, MD, Rafael Peinado Peinado, PhD, FESC Unidad de
185 Case Report Simultaneous Accessory Pathway and AV Node Mechanical Block Daniel Garofalo, MD, FRACP, Alfonso Gomez Gallanti, MD, David Filgueiras Rama, MD, Rafael Peinado Peinado, PhD, FESC Unidad de
Case Report Wide-QRS Tachycardia Inducible by Both Atrial and Ventricular Pacing
 Hellenic J Cardiol 2008; 49: 446-450 Case Report Wide-QRS Tachycardia Inducible by Both Atrial and Ventricular Pacing ELEFTHERIOS GIAZITZOGLOU, DEMOSTHENES G. KATRITSIS Department of Cardiology, Athens
Hellenic J Cardiol 2008; 49: 446-450 Case Report Wide-QRS Tachycardia Inducible by Both Atrial and Ventricular Pacing ELEFTHERIOS GIAZITZOGLOU, DEMOSTHENES G. KATRITSIS Department of Cardiology, Athens
The autonomic nervous system is known to play an
 Effects of Continuous Enhanced Vagal Tone on Dual Atrioventricular Node and Accessory Pathways Chuen-Wang Chiou, MD; Shih-Ann Chen, MD; Ming-Ho Kung, MD; Mau-Song Chang, MD; Eric N. Prystowsky, MD Background
Effects of Continuous Enhanced Vagal Tone on Dual Atrioventricular Node and Accessory Pathways Chuen-Wang Chiou, MD; Shih-Ann Chen, MD; Ming-Ho Kung, MD; Mau-Song Chang, MD; Eric N. Prystowsky, MD Background
CLINICAL CARDIAC ELECTROPHYSIOLOGY Maintenance of Certification (MOC) Examination Blueprint
 CLINICAL CARDIAC ELECTROPHYSIOLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Clinical Cardiac Electrophysiology MOC exam blueprint Based on feedback
CLINICAL CARDIAC ELECTROPHYSIOLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Clinical Cardiac Electrophysiology MOC exam blueprint Based on feedback
ARTICLE. Supraventricular Tachycardia in Infancy. Catherine D. DeAngelis, MD. In most infants, SVT is due to an accessory atrioventricular
 Supraventricular Tachycardia in Infancy Evaluation, Management, and Follow-up Susan P. Etheridge, MD; Victoria E. Judd, MD ARTICLE Background: Supraventricular tachycardia (SVT) occurs frequently in infancy.
Supraventricular Tachycardia in Infancy Evaluation, Management, and Follow-up Susan P. Etheridge, MD; Victoria E. Judd, MD ARTICLE Background: Supraventricular tachycardia (SVT) occurs frequently in infancy.
The most common. hospitalized patients. hypotension due to. filling time Rate control in ICU patients may be difficult as many drugs cause hypotension
 Arrhythmias in the critically ill ICU patients: Approach for rapid recognition & management Objectives Be able to identify and manage: Atrial fibrillation with a rapid ventricular response Atrial flutter
Arrhythmias in the critically ill ICU patients: Approach for rapid recognition & management Objectives Be able to identify and manage: Atrial fibrillation with a rapid ventricular response Atrial flutter
Pre-excited tachycardia: Atrial tachycardia with a bystander left lateral accessory pathway
 Pre-excited tachycardia: Atrial tachycardia with a bystander left lateral accessory pathway Jeffrey Munro, DO, Win-Kuang Shen, MD, FHRS, Komandoor Srivathsan, MD From the Department of Cardiovascular Disease,
Pre-excited tachycardia: Atrial tachycardia with a bystander left lateral accessory pathway Jeffrey Munro, DO, Win-Kuang Shen, MD, FHRS, Komandoor Srivathsan, MD From the Department of Cardiovascular Disease,
Effects of Partial and Complete Ablation of the Slow Pathway on Fast Pathway Properties in Patients with Atrioventricular Nodal Reentrant Tachycardia
 645 Effects of Partial and Complete Ablation of the Slow Pathway on Fast Pathway Properties in Patients with Atrioventricular dal Reentrant Tachycardia S. ADAM STRICKBERGER, M.D., EMILE DAOUD, M.D., MARK
645 Effects of Partial and Complete Ablation of the Slow Pathway on Fast Pathway Properties in Patients with Atrioventricular dal Reentrant Tachycardia S. ADAM STRICKBERGER, M.D., EMILE DAOUD, M.D., MARK
Wolff-Parkinson-White as a bystander in a patient with aborted sudden cardiac death
 Wolff-Parkinson-White as a bystander in a patient with aborted sudden cardiac death Jamal Laaouaj, MD, Frédéric Jacques, MD, Gilles O Hara, MD, Jean Champagne, MD, Jean-François Sarrazin, MD, FHRS, Isabelle
Wolff-Parkinson-White as a bystander in a patient with aborted sudden cardiac death Jamal Laaouaj, MD, Frédéric Jacques, MD, Gilles O Hara, MD, Jean Champagne, MD, Jean-François Sarrazin, MD, FHRS, Isabelle
Arrhythmogenic right ventricular dysplasia masquerading as right ventricular outflow tract tachycardia
 Pop-Mandru et al. 314 case in images OPEN ACCESS Arrhythmogenic right ventricular dysplasia masquerading as right ventricular outflow tract tachycardia Daniel Pop-Mandru, Gabriel Cismaru, Dana Pop, Dumitru
Pop-Mandru et al. 314 case in images OPEN ACCESS Arrhythmogenic right ventricular dysplasia masquerading as right ventricular outflow tract tachycardia Daniel Pop-Mandru, Gabriel Cismaru, Dana Pop, Dumitru
Incessant Tachycardia Using a Concealed Atrionodal Bypass Tract
 191 Incessant Tachycardia Using a Concealed Atrionodal Bypass Tract ADAM ZIVIN, M.D., atid FRED MORADY, M.D. From the Division of Cardiology. Department of Internal Medicine, University of Michigan Medical
191 Incessant Tachycardia Using a Concealed Atrionodal Bypass Tract ADAM ZIVIN, M.D., atid FRED MORADY, M.D. From the Division of Cardiology. Department of Internal Medicine, University of Michigan Medical
Repetitive narrow QRS tachycardia in a 61-year-old female patient with recent palpitations
 Journal of Geriatric Cardiology (2018) 15: 193 198 2018 JGC All rights reserved; www.jgc301.com Case Report Open Access Repetitive narrow QRS tachycardia in a 61-year-old female patient with recent palpitations
Journal of Geriatric Cardiology (2018) 15: 193 198 2018 JGC All rights reserved; www.jgc301.com Case Report Open Access Repetitive narrow QRS tachycardia in a 61-year-old female patient with recent palpitations
Antiarrhythmic Drugs
 Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Title. CitationJournal of Electrocardiology, 39(4): Issue Date Doc URL. Type. File Information. coronary sinus ostium
 Title Nonreentrant atrioventricular nodal tachycardia due coronary sinus ostium Author(s)Yokoshiki, Hisashi; Sasaki, Koji; Shimokawa, Junichi CitationJournal of Electrocardiology, 39(4): 395-399 Issue
Title Nonreentrant atrioventricular nodal tachycardia due coronary sinus ostium Author(s)Yokoshiki, Hisashi; Sasaki, Koji; Shimokawa, Junichi CitationJournal of Electrocardiology, 39(4): 395-399 Issue
CATHETER ABLATION FOR TACHYCARDIAS
 190 CATHETER ABLATION FOR TACHYCARDIAS MASOOD AKHTAR, M.D. T ACHY ARRHYTHMIAS constitute a major cause of mortality and morbidity. The most serious manifestation of cardiac arrhythmia is sudden cardiac
190 CATHETER ABLATION FOR TACHYCARDIAS MASOOD AKHTAR, M.D. T ACHY ARRHYTHMIAS constitute a major cause of mortality and morbidity. The most serious manifestation of cardiac arrhythmia is sudden cardiac
Validation of right ventricular pacing response during SVT in mechanistic diagnosis. (Transition zone)
 Validation of right ventricular pacing response during SVT in mechanistic diagnosis. (Transition zone) By Marwan Sayed Assistant lecturer Cardiology department Assiut University Under supervision of Prof
Validation of right ventricular pacing response during SVT in mechanistic diagnosis. (Transition zone) By Marwan Sayed Assistant lecturer Cardiology department Assiut University Under supervision of Prof
Atrioventricular (AV) Nodal Reentry Associated with 2:1 Infra-His Conduction Block during Tachycardia in a Patient with AV Nodal Triple Pathways
 Atrioventricular (AV) Nodal Reentry Associated with 2:1 Infra-His Conduction Block during Tachycardia in a Patient with AV Nodal Triple Pathways Haruhiko ABE, M.D., Takashi OHKITA, M.D., Masasuke FUJITA,
Atrioventricular (AV) Nodal Reentry Associated with 2:1 Infra-His Conduction Block during Tachycardia in a Patient with AV Nodal Triple Pathways Haruhiko ABE, M.D., Takashi OHKITA, M.D., Masasuke FUJITA,
Supraventricular Tachycardia (SVT)
 Supraventricular Tachycardia (SVT) Daniel Frisch, MD Cardiology Division, Electrophysiology Section Thomas Jefferson University Hospital daniel.frisch@jefferson.edu Short RP Are these the Mid same RP tachycardias?
Supraventricular Tachycardia (SVT) Daniel Frisch, MD Cardiology Division, Electrophysiology Section Thomas Jefferson University Hospital daniel.frisch@jefferson.edu Short RP Are these the Mid same RP tachycardias?
Looks Like VT But Isn't - Successful Ablation Of A Left Free Wall Accessory Pathway With Mahaim-like Properties
 www.ipej.org 112 Case Report Looks Like VT But Isn't - Successful Ablation Of A Left Free Wall Accessory Pathway With Mahaim-like Properties Faizel Osman MD MRCP 1, Peter J Stafford BSc MD FRCP 2, G Andre
www.ipej.org 112 Case Report Looks Like VT But Isn't - Successful Ablation Of A Left Free Wall Accessory Pathway With Mahaim-like Properties Faizel Osman MD MRCP 1, Peter J Stafford BSc MD FRCP 2, G Andre
EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology
 EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important
EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important
Chapter 9. Learning Objectives. Learning Objectives 9/11/2012. Cardiac Arrhythmias. Define electrical therapy
 Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
2) Heart Arrhythmias 2 - Dr. Abdullah Sharif
 2) Heart Arrhythmias 2 - Dr. Abdullah Sharif Rhythms from the Sinus Node Sinus Tachycardia: HR > 100 b/m Causes: o Withdrawal of vagal tone & Sympathetic stimulation (exercise, fight or flight) o Fever
2) Heart Arrhythmias 2 - Dr. Abdullah Sharif Rhythms from the Sinus Node Sinus Tachycardia: HR > 100 b/m Causes: o Withdrawal of vagal tone & Sympathetic stimulation (exercise, fight or flight) o Fever
Asymptomatic WPW Syndrome; Observation or Ablation? 전남대학교병원순환기내과 박형욱
 Asymptomatic WPW Syndrome; Observation or Ablation? 전남대학교병원순환기내과 박형욱 Let It Be? Vs. Just Do It? Natural history of asymptomatic WPW Incidence of sudden cardiac death in natural history studies involving
Asymptomatic WPW Syndrome; Observation or Ablation? 전남대학교병원순환기내과 박형욱 Let It Be? Vs. Just Do It? Natural history of asymptomatic WPW Incidence of sudden cardiac death in natural history studies involving
Ji-Eun Ban, MD, Sang-Weon Park, MD, Hyun-Soo Lee, MPH, Jong-Il Choi, MD, and Young-Hoon Kim, MD
 Case Report Print SSN 1738-5520 On-line SSN 1738-5555 Korean Circulation Journal Swallowing-nduced Atrial Tachyarrhythmias Successfully Ablated at the Left Posterior nteratrial Septum in Patient with Wolff-Parkinson-White
Case Report Print SSN 1738-5520 On-line SSN 1738-5555 Korean Circulation Journal Swallowing-nduced Atrial Tachyarrhythmias Successfully Ablated at the Left Posterior nteratrial Septum in Patient with Wolff-Parkinson-White
Utility of Atrial and Ventricular Cycle Length Variability in Determining the Mechanism of Paroxysmal Supraventricular Tachycardia
 698 Utility of Atrial and Ventricular Cycle Length Variability in Determining the Mechanism of Paroxysmal Supraventricular Tachycardia THOMAS C. CRAWFORD, M.D., SIDDHARTH MUKERJI, M.D., ERIC GOOD, D.O.,
698 Utility of Atrial and Ventricular Cycle Length Variability in Determining the Mechanism of Paroxysmal Supraventricular Tachycardia THOMAS C. CRAWFORD, M.D., SIDDHARTH MUKERJI, M.D., ERIC GOOD, D.O.,
Case Report Left Ventricular Dysfunction Caused by Unrecognized Surgical AV block in a Patient with a Manifest Right Free Wall Accessory Pathway
 109 Case Report Left Ventricular Dysfunction Caused by Unrecognized Surgical AV block in a Patient with a Manifest Right Free Wall Accessory Pathway Rakesh Gopinathannair, MD, MA 1, Dwayne N Campbell,
109 Case Report Left Ventricular Dysfunction Caused by Unrecognized Surgical AV block in a Patient with a Manifest Right Free Wall Accessory Pathway Rakesh Gopinathannair, MD, MA 1, Dwayne N Campbell,
Circulation: Arrhythmia and Electrophysiology CHALLENGE OF THE WEEK
 A 14-year-old girl with Wolff-Parkinson-White syndrome and recurrent paroxysmal palpitations due to atrioventricular reentry tachycardia had undergone two prior failed left lateral accessory pathway ablations
A 14-year-old girl with Wolff-Parkinson-White syndrome and recurrent paroxysmal palpitations due to atrioventricular reentry tachycardia had undergone two prior failed left lateral accessory pathway ablations
Atrial Fibrillation and Common Supraventricular Tachycardias. Sunil Kapur MD
 Atrial Fibrillation and Common Supraventricular Tachycardias Sunil Kapur MD Cardiac Electrophysiology Brigham and Women s Hospital Instructor, Harvard Medical School No disclosures Cardiac Conduction:
Atrial Fibrillation and Common Supraventricular Tachycardias Sunil Kapur MD Cardiac Electrophysiology Brigham and Women s Hospital Instructor, Harvard Medical School No disclosures Cardiac Conduction:
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment
 Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Debate: Asymptomatic Patients with Ventricular Preexcitation Require EP Testing for Risk Stratification. Carlo Pappone, MD, PhD, FACC
 Debate: Asymptomatic Patients with Ventricular Preexcitation Require EP Testing for Risk Stratification Carlo Pappone, MD, PhD, FACC The Wolff-Parkinson-White Syndrome Demographics Δ waves detectable on
Debate: Asymptomatic Patients with Ventricular Preexcitation Require EP Testing for Risk Stratification Carlo Pappone, MD, PhD, FACC The Wolff-Parkinson-White Syndrome Demographics Δ waves detectable on
ECG Interpretation Made Easy
 ECG Interpretation Made Easy Dr. A Tageldien Abdellah, MSc MD EBSC Lecturer of Cardiology- Hull University Hull York Medical School 2007-2008 ECG Interpretation Made Easy Synopsis Benefits Objectives Process
ECG Interpretation Made Easy Dr. A Tageldien Abdellah, MSc MD EBSC Lecturer of Cardiology- Hull University Hull York Medical School 2007-2008 ECG Interpretation Made Easy Synopsis Benefits Objectives Process
In certain cases of supraventricular
 Case Report Hellenic J Cardiol 2013; 54: 469-473 A Tachycardia with Varying QRS Morphology and RP Intervals: Differential Diagnosis and Therapy Socrates Korovesis, Eleftherios Giazitzoglou, Demosthenes
Case Report Hellenic J Cardiol 2013; 54: 469-473 A Tachycardia with Varying QRS Morphology and RP Intervals: Differential Diagnosis and Therapy Socrates Korovesis, Eleftherios Giazitzoglou, Demosthenes
a lecture series by SWESEMJR
 Arrhythmias Automaticity- the ability to depolarize spontaneously. Pacemakers: Sinoatrial node: 70 bpm AV-nodal area: 40 bpm His-Purkinje: 20-40 bpm it Mechanisms of arrhythmias 1. Increased automaticity
Arrhythmias Automaticity- the ability to depolarize spontaneously. Pacemakers: Sinoatrial node: 70 bpm AV-nodal area: 40 bpm His-Purkinje: 20-40 bpm it Mechanisms of arrhythmias 1. Increased automaticity
Ventricular Preexcitation (Wolff-Parkinson-White Syndrome and Its Variants) 柯文欽醫師 國泰綜合醫院心臟內科主治醫師 臺北醫學大學講師
 Ventricular Preexcitation (Wolff-Parkinson-White Syndrome and Its Variants) 柯文欽醫師 國泰綜合醫院心臟內科主治醫師 臺北醫學大學講師 The Nobel Prize in Physiology or Medicine 1924 "for his discovery of the mechanism of the electrocardiogram"
Ventricular Preexcitation (Wolff-Parkinson-White Syndrome and Its Variants) 柯文欽醫師 國泰綜合醫院心臟內科主治醫師 臺北醫學大學講師 The Nobel Prize in Physiology or Medicine 1924 "for his discovery of the mechanism of the electrocardiogram"
Measuring the refractory period threshold of AV-node after Radiofrequency ablation
 J. Appl. Environ. Biol. Sci., 6(3)146-151, 2016 2016, TextRoad Publication ISSN: 2090-4274 Journal of Applied Environmental and Biological Sciences www.textroad.com Measuring the refractory period threshold
J. Appl. Environ. Biol. Sci., 6(3)146-151, 2016 2016, TextRoad Publication ISSN: 2090-4274 Journal of Applied Environmental and Biological Sciences www.textroad.com Measuring the refractory period threshold
Core Content In Urgent Care Medicine
 Palpitations/Arrhythmias Ebrahim Barkoudah, MD Clinical Instructor in Internal Medicine Harvard Medical School Assistant in Internal Medicine & Pediatrics Massachusetts General Hospital MGH Chelsea Chelsea,
Palpitations/Arrhythmias Ebrahim Barkoudah, MD Clinical Instructor in Internal Medicine Harvard Medical School Assistant in Internal Medicine & Pediatrics Massachusetts General Hospital MGH Chelsea Chelsea,
Double Retrograde Atrial Response After Radiofrequency. ablation of typical AV nodal tieentrant tachycardia
 Double Retrograde Atrial Response After Radiofrequency Ablation of Typical AV Nodal Reentrant Tachycardia STEVEN J. KALBFLEISCH, M.D., S. ADAM STRICKBERGER, M.D.. JOHN D. HUMMEL, M.D., BRIAN D. WILLIAMSON,
Double Retrograde Atrial Response After Radiofrequency Ablation of Typical AV Nodal Reentrant Tachycardia STEVEN J. KALBFLEISCH, M.D., S. ADAM STRICKBERGER, M.D.. JOHN D. HUMMEL, M.D., BRIAN D. WILLIAMSON,
Sustained tachycardia with wide QRS
 Sustained tachycardia with wide QRS Courtesy from Prof. Antonio Américo Friedmann. Electrocardiology Service of University of Faculty of São Paulo. Opinions from colleagues Greetings to everyone, In a
Sustained tachycardia with wide QRS Courtesy from Prof. Antonio Américo Friedmann. Electrocardiology Service of University of Faculty of São Paulo. Opinions from colleagues Greetings to everyone, In a
LONG RP TACHYCARDIA MAPPING AND RF ABLATION
 LONG RP TACHYCARDIA MAPPING AND RF ABLATION Dr. Hayam Eldamanhoury Ain shams univeristy Arrhythmia is a too broad topic SVT is broadly defined as narrow complex ( unless aberrant conduction ) Requires
LONG RP TACHYCARDIA MAPPING AND RF ABLATION Dr. Hayam Eldamanhoury Ain shams univeristy Arrhythmia is a too broad topic SVT is broadly defined as narrow complex ( unless aberrant conduction ) Requires
«Aσθενής με ασυμπτωματικό WPW και παροξυσμική κολπική μαρμαρυγή» Χάρης Κοσσυβάκης Επιμελητής A Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ.
 «Aσθενής με ασυμπτωματικό WPW και παροξυσμική κολπική μαρμαρυγή» Χάρης Κοσσυβάκης Επιμελητής A Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ» the primary mechanism of SCD in patients with WPW is the rapid conduction
«Aσθενής με ασυμπτωματικό WPW και παροξυσμική κολπική μαρμαρυγή» Χάρης Κοσσυβάκης Επιμελητής A Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ» the primary mechanism of SCD in patients with WPW is the rapid conduction
EPS Case presentation Looks like VT but it isn t!
 EPS Case presentation Looks like VT but it isn t! E. Συμεωνίδου, MD, PhD Β Παν Καρδιολογική κλινική, Νοσ Aττικόν Σεμινάρια Ομάδων Εργασίας ΕΚΕ 2016 Ιωάννινα Disclosures I have no conflict of interest to
EPS Case presentation Looks like VT but it isn t! E. Συμεωνίδου, MD, PhD Β Παν Καρδιολογική κλινική, Νοσ Aττικόν Σεμινάρια Ομάδων Εργασίας ΕΚΕ 2016 Ιωάννινα Disclosures I have no conflict of interest to
EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs
 EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important step for
EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important step for
Wolff-Parkinson-White Syndrome
 Wolff-Parkinson-White Syndrome www.consultant360.com /articles/wolff-parkinson-white-syndrome A 37-year-old woman presented to the office with intermittent dizziness, palpitations, and multiple syncopal
Wolff-Parkinson-White Syndrome www.consultant360.com /articles/wolff-parkinson-white-syndrome A 37-year-old woman presented to the office with intermittent dizziness, palpitations, and multiple syncopal
Pediatrics ECG Monitoring. Pediatric Intensive Care Unit Emergency Division
 Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Adenosine Mapping for Adenosine-Dependent Accessory Pathway Ablation
 Adenosine Mapping for Adenosine-Dependent Accessory Pathway Ablation MARTIN J. LAPAGE, M.D., M.S.,* MICHAEL J. WALSH, M.D., JOHN H. REED, M.D., M.P.H., and J. PHILIP SAUL, M.D. From the *Department of
Adenosine Mapping for Adenosine-Dependent Accessory Pathway Ablation MARTIN J. LAPAGE, M.D., M.S.,* MICHAEL J. WALSH, M.D., JOHN H. REED, M.D., M.P.H., and J. PHILIP SAUL, M.D. From the *Department of
CARDIOINSIGHT TM NONINVASIVE 3D MAPPING SYSTEM CLINICAL EVIDENCE SUMMARY
 CARDIOINSIGHT TM NONINVASIVE 3D MAPPING SYSTEM CLINICAL EVIDENCE SUMMARY April 2017 SUPPORTING EVIDENCE RHYTHM AF VT PUBLICATIONS Driver Domains in Persistent Atrial Fibrillation (Haissaiguerre, et al)
CARDIOINSIGHT TM NONINVASIVE 3D MAPPING SYSTEM CLINICAL EVIDENCE SUMMARY April 2017 SUPPORTING EVIDENCE RHYTHM AF VT PUBLICATIONS Driver Domains in Persistent Atrial Fibrillation (Haissaiguerre, et al)
Case Report Mahaim Fiber Accelerated Automaticity and Clues to a Mahaim Fiber Being Morphologically an Ectopic or a Split AV Node
 www.ipej.org 62 Case Report Mahaim Fiber Accelerated Automaticity and Clues to a Mahaim Fiber Being Morphologically an Ectopic or a Split AV Node Shomu Bohora, Narayanan Namboodiri, Santosh Dora, VK Ajit
www.ipej.org 62 Case Report Mahaim Fiber Accelerated Automaticity and Clues to a Mahaim Fiber Being Morphologically an Ectopic or a Split AV Node Shomu Bohora, Narayanan Namboodiri, Santosh Dora, VK Ajit
COMPLEX CASE STUDY INNOVATIVE COLLECTIONS. Case presentation
 The Journal of Innovations in Cardiac Rhythm Management, 3 (2012), 939 943 INNOVATIVE COLLECTIONS COMPLEX CASE STUDY Subtle Changes in Electrogram Morphology During Para-Hisian Pacing Performed on IV Adenosine:
The Journal of Innovations in Cardiac Rhythm Management, 3 (2012), 939 943 INNOVATIVE COLLECTIONS COMPLEX CASE STUDY Subtle Changes in Electrogram Morphology During Para-Hisian Pacing Performed on IV Adenosine:
Pediatrics. Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment. Overview
 Pediatrics Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment See online here The most common form of cardiac arrhythmia in children is sinus tachycardia which can be caused by
Pediatrics Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment See online here The most common form of cardiac arrhythmia in children is sinus tachycardia which can be caused by
How to ablate typical slow/fast AV nodal reentry tachycardia
 Europace (2000) 2, 15 19 Article No. eupc.1999.0070, available online at http://www.idealibrary.com on OW TO... SERIES ow to ablate typical slow/fast AV nodal reentry tachycardia. eidbüchel Department
Europace (2000) 2, 15 19 Article No. eupc.1999.0070, available online at http://www.idealibrary.com on OW TO... SERIES ow to ablate typical slow/fast AV nodal reentry tachycardia. eidbüchel Department
Arrhythmia 341. Ahmad Hersi Professor of Cardiology KSU
 Arrhythmia 341 Ahmad Hersi Professor of Cardiology KSU Objectives Epidemiology and Mechanisms of AF Evaluation of AF patients Classification of AF Treatment and Risk stratification of AF Identify other
Arrhythmia 341 Ahmad Hersi Professor of Cardiology KSU Objectives Epidemiology and Mechanisms of AF Evaluation of AF patients Classification of AF Treatment and Risk stratification of AF Identify other
Cardiac Arrhythmias. For Pharmacists
 Cardiac Arrhythmias For Pharmacists Agenda Overview of the normal Classification Management Therapy Conclusion Cardiac arrhythmias Overview of the normal Arrhythmia: definition From the Greek a-, loss
Cardiac Arrhythmias For Pharmacists Agenda Overview of the normal Classification Management Therapy Conclusion Cardiac arrhythmias Overview of the normal Arrhythmia: definition From the Greek a-, loss
VENTRICULAR TACHYCARDIA WITH HEMODYNAMIC INSTABILITY REFRACTORY TO CARDIOVERSION: A CASE REPORT
 VENTRCULAR TACHYCARDA WTH HEMODYNAMC NSTABLTY REFRACTORY TO CARDOVERSON: A CASE REPORT Chun-Jen Chou, 1 Chee-Siong Lee, 2,3 and Wen-Ter Lai 2,3 1 Department of Emergency Medicine, Kaohsiung Municipal Hsiao-Kang
VENTRCULAR TACHYCARDA WTH HEMODYNAMC NSTABLTY REFRACTORY TO CARDOVERSON: A CASE REPORT Chun-Jen Chou, 1 Chee-Siong Lee, 2,3 and Wen-Ter Lai 2,3 1 Department of Emergency Medicine, Kaohsiung Municipal Hsiao-Kang
Case Report. Rajaie Cardiovascular, Medical and Research Center, Iran University of Medical Sciences, Tehran, Iran. 2
 TEHRAN HEART CENTER Case Report Radiofrequency Ablation of Accessory Pathways in Children with Complex Congenital Cardiac Lesions: A Report of Three Cases Mohammad Dalili, MD *1, Jayakeerthi Y Rao, MD
TEHRAN HEART CENTER Case Report Radiofrequency Ablation of Accessory Pathways in Children with Complex Congenital Cardiac Lesions: A Report of Three Cases Mohammad Dalili, MD *1, Jayakeerthi Y Rao, MD
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material
 1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (8), Page
 The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (8), Page 5062-5066 Comparison of the Accuracy of Three Algorithms in Predicting Accessory Pathways among Adult Wolff-Parkinson-White (WPW)
The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (8), Page 5062-5066 Comparison of the Accuracy of Three Algorithms in Predicting Accessory Pathways among Adult Wolff-Parkinson-White (WPW)
Transcoronary Chemical Ablation of Atrioventricular Conduction
 757 Transcoronary Chemical Ablation of Atrioventricular Conduction Pedro Brugada, MD, Hans de Swart, MD, Joep Smeets, MD, and Hein J.J. Wellens, MD In seven patients with symptomatic atrial fibrillation
757 Transcoronary Chemical Ablation of Atrioventricular Conduction Pedro Brugada, MD, Hans de Swart, MD, Joep Smeets, MD, and Hein J.J. Wellens, MD In seven patients with symptomatic atrial fibrillation
JIUNN-LEE LIN, MD, SHOEI K. STEPHEN HUANG, MD, FACC, LING-PING LAI, MD, WEN-CHIN KO, MD, YUNG-ZU TSENG, MD, WEN-PIN LIEN, MD, FACC
 JACC Vol. 31, No. 4 March 15, 1998:855 60 855 ELECTROPHYSIOLOGY Clinical and Electrophysiologic Characteristics and Long-Term Efficacy of Slow-Pathway Catheter Ablation in Patients With Spontaneous Supraventricular
JACC Vol. 31, No. 4 March 15, 1998:855 60 855 ELECTROPHYSIOLOGY Clinical and Electrophysiologic Characteristics and Long-Term Efficacy of Slow-Pathway Catheter Ablation in Patients With Spontaneous Supraventricular
EKG Competency for Agency
 EKG Competency for Agency Name: Date: Agency: 1. The upper chambers of the heart are known as the: a. Atria b. Ventricles c. Mitral Valve d. Aortic Valve 2. The lower chambers of the heart are known as
EKG Competency for Agency Name: Date: Agency: 1. The upper chambers of the heart are known as the: a. Atria b. Ventricles c. Mitral Valve d. Aortic Valve 2. The lower chambers of the heart are known as
ARRHYTHMIAS IN THE ICU
 ARRHYTHMIAS IN THE ICU Nora Goldschlager, MD MACP, FACC, FAHA, FHRS SFGH Division of Cardiology UCSF IDENTIFIED VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar) Electrolyte imbalance Proarrhythmia
ARRHYTHMIAS IN THE ICU Nora Goldschlager, MD MACP, FACC, FAHA, FHRS SFGH Division of Cardiology UCSF IDENTIFIED VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar) Electrolyte imbalance Proarrhythmia
UNDERSTANDING ELECTROPHYSIOLOGY STUDIES
 UNDERSTANDING ELECTROPHYSIOLOGY STUDIES Testing and Treating Your Heart s Electrical System A Problem with Your Heart Rhythm The speed and pattern of a heartbeat is called the heart rhythm. The rhythm
UNDERSTANDING ELECTROPHYSIOLOGY STUDIES Testing and Treating Your Heart s Electrical System A Problem with Your Heart Rhythm The speed and pattern of a heartbeat is called the heart rhythm. The rhythm
APPROACH TO TACHYARRYTHMIAS
 APPROACH TO TACHYARRYTHMIAS PROF.DR.MD.ZAKIR HOSSAIN PROFESSOR AND HEAD DEPARTMENT OF MEDICINE SZMCH TACHYARRYTHMIA Cardiac arrythmia is a disturbance of electrical rhythm of heart. Cardac arrythmia with
APPROACH TO TACHYARRYTHMIAS PROF.DR.MD.ZAKIR HOSSAIN PROFESSOR AND HEAD DEPARTMENT OF MEDICINE SZMCH TACHYARRYTHMIA Cardiac arrythmia is a disturbance of electrical rhythm of heart. Cardac arrythmia with
Case #1. 73 y/o man with h/o HTN and CHF admitted with dizziness and SOB Treated for CHF exacerbation with Lasix Now HR 136
 Tachycardias Case #1 73 y/o man with h/o HTN and CHF admitted with dizziness and SOB Treated for CHF exacerbation with Lasix Now HR 136 Initial Assessment Check Telemetry screen if pt on tele Telemetry
Tachycardias Case #1 73 y/o man with h/o HTN and CHF admitted with dizziness and SOB Treated for CHF exacerbation with Lasix Now HR 136 Initial Assessment Check Telemetry screen if pt on tele Telemetry
Uncommon forms of AV reentry: atrio and fasciculo-ventricular fibers, slow conducting fibers. Jesus Almendral, Madrid, Spain
 Uncommon forms of AV reentry: atrio and fasciculo-ventricular fibers, slow conducting fibers Jesus Almendral, Madrid, Spain Common forms of AV reentry Accessory pathways: Upper insertion: atrium Lower
Uncommon forms of AV reentry: atrio and fasciculo-ventricular fibers, slow conducting fibers Jesus Almendral, Madrid, Spain Common forms of AV reentry Accessory pathways: Upper insertion: atrium Lower
Tachycardias II. Štěpán Havránek
 Tachycardias II Štěpán Havránek Summary 1) Supraventricular (supraventricular rhythms) Atrial fibrillation and flutter Atrial ectopic tachycardia / extrabeats AV nodal reentrant a AV reentrant tachycardia
Tachycardias II Štěpán Havránek Summary 1) Supraventricular (supraventricular rhythms) Atrial fibrillation and flutter Atrial ectopic tachycardia / extrabeats AV nodal reentrant a AV reentrant tachycardia
An Approach to the Patient with Syncope. Guy Amit MD, MPH Soroka University Medical Center Beer-Sheva
 An Approach to the Patient with Syncope Guy Amit MD, MPH Soroka University Medical Center Beer-Sheva Case presentation A 23 y.o. man presented with 2 episodes of syncope One during exercise,one at rest
An Approach to the Patient with Syncope Guy Amit MD, MPH Soroka University Medical Center Beer-Sheva Case presentation A 23 y.o. man presented with 2 episodes of syncope One during exercise,one at rest
Premature Atrial Contractions Managed With Slow Pathway Ablation
 Maced J Med Sci electronic publication ahead of print, published on November 25, 2008 as doi:10.3889/mjms.1857-5773.2008.0018 Trajkov et al. Slow Pathway Ablation Macedonian Journal of Medical Sciences.
Maced J Med Sci electronic publication ahead of print, published on November 25, 2008 as doi:10.3889/mjms.1857-5773.2008.0018 Trajkov et al. Slow Pathway Ablation Macedonian Journal of Medical Sciences.
Patient Examination. Objectives for Presentation RECOGNITION OF COMMON ARRHYTHMIAS THEIR CAUSES AND TREATMENT OPTIONS 9/8/2016
 RECOGNITION OF COMMON ARRHYTHMIAS THEIR CAUSES AND TREATMENT OPTIONS Ryan Fries, DVM, DACVIM (Cardiology) Clinical Assistant Professor University of Illinois Department of Clinical Veterinary Medicine
RECOGNITION OF COMMON ARRHYTHMIAS THEIR CAUSES AND TREATMENT OPTIONS Ryan Fries, DVM, DACVIM (Cardiology) Clinical Assistant Professor University of Illinois Department of Clinical Veterinary Medicine
Sudden cardiac death: Primary and secondary prevention
 Sudden cardiac death: Primary and secondary prevention By Kai Chi Chan Penultimate Year Medical Student St George s University of London at UNic Sheba Medical Centre Definition Sudden cardiac arrest (SCA)
Sudden cardiac death: Primary and secondary prevention By Kai Chi Chan Penultimate Year Medical Student St George s University of London at UNic Sheba Medical Centre Definition Sudden cardiac arrest (SCA)
Successful treatment of tachycardia-induced cardiomyopathy secondary to dual atrioventricular nodal nonreentrant tachycardia using cryoablation
 Successful treatment of tachycardia-induced cardiomyopathy secondary to dual atrioventricular nodal nonreentrant tachycardia using cryoablation Harold Rivner, MD, * Chris Healy, MD, Raul D. Mitrani, MD,
Successful treatment of tachycardia-induced cardiomyopathy secondary to dual atrioventricular nodal nonreentrant tachycardia using cryoablation Harold Rivner, MD, * Chris Healy, MD, Raul D. Mitrani, MD,
Evaluation and Initial Treatment of Supraventricular Tachycardia
 T h e n e w e ngl a nd j o u r na l o f m e dic i n e clinical practice Evaluation and Initial Treatment of Supraventricular Tachycardia Mark S. Link, M.D. This Journal feature begins with a case vignette
T h e n e w e ngl a nd j o u r na l o f m e dic i n e clinical practice Evaluation and Initial Treatment of Supraventricular Tachycardia Mark S. Link, M.D. This Journal feature begins with a case vignette
Huseng Vefali MD St. Luke s University Health Network Department of Cardiology
 Huseng Vefali MD St. Luke s University Health Network Department of Cardiology Learning Objectives Establish Consistent Approach to Interpreting ECGs Review Essential Cases for Paramedics and first responders
Huseng Vefali MD St. Luke s University Health Network Department of Cardiology Learning Objectives Establish Consistent Approach to Interpreting ECGs Review Essential Cases for Paramedics and first responders
