Evaluation and Initial Treatment of Supraventricular Tachycardia
|
|
|
- Eleanor Payne
- 5 years ago
- Views:
Transcription
1 T h e n e w e ngl a nd j o u r na l o f m e dic i n e clinical practice Evaluation and Initial Treatment of Supraventricular Tachycardia Mark S. Link, M.D. This Journal feature begins with a case vignette highlighting a common clinical problem. Evidence supporting various strategies is then presented, followed by a review of formal guidelines, when they exist. The article ends with the author s clinical recommendations. A 24-year-old woman presents to the emergency department with the sole symptom of a racing heart, which began abruptly while she was eating dinner. She reports having had prior episodes of palpitations that resolved spontaneously. In the emergency room, her blood pressure is 84/60 mm Hg. An electrocardiogram (ECG) reveals a regular narrow-complex tachycardia at a rate of 190 beats per minute without clear atrial activity (P waves). How should this case be managed? The Clinic a l Problem From Tufts Medical Center, Tufts University School of Medicine, Boston. Address reprint requests to Dr. Link at Tufts Medical Center, 800 Washington St., Box #197, Boston, MA 02111, or at mlink@ tuftsmedicalcenter.org. N Engl J Med 2012;367: DOI: /NEJMcp Copyright 2012 Massachusetts Medical Society An audio version of this article is available at NEJM.org Patients with symptomatic tachycardias require immediate medical attention. Although it is commonly believed that a precise diagnosis of the tachycardia is necessary before therapy is initiated, immediate treatment can usually be tailored to the characteristics of the ventricular response. By focusing on the ventricular response, one can assign the seven clinically relevant supraventricular tachycardias to diagnostic and therapeutic groups on the basis of the rapidity of onset, the heart rate, and the regularity of the tachycardia (Fig. 1). 1 This review focuses on the initial diagnostic and therapeutic approach to supraventricular tachycardias and the ways of differentiating them from ventricular arrhythmias. Although atrial premature contractions are technically not a supraventricular tachycardia, this abnormality is included in the current discussion because it is often part of the differential diagnosis of supraventricular tachycardias. Types of Supraventricular Tachycardias Sinus tachycardia, by far the most common supraventricular tachycardia, is not a pathologic arrhythmia (with the rare exception of inappropriate sinus tachycardia) but rather is an appropriate cardiac response to a physiological event (Fig. 1). Sinus tachycardia is gradual in onset and recession. The heart rate is regular and classically does not exceed 220 beats per minute minus the patient s age. 2 In sinus tachycardia, P waves precede the QRS complex. Atrial fibrillation is the most common pathologic supraventricular tachycardia, affecting more than 3 million people in the United States 3 and many more worldwide. 4 Risk factors for atrial fibrillation include older age, male sex, hypertension, and underlying cardiac disease. 5 Atrial fibrillation is caused by multiple electrical wavelets appearing in the atria simultaneously, resembling the waves that would be produced if one dropped several pebbles in a bucket of water at the same time (Fig. 2). The arrhythmia is considered to be acute when it develops spontaneously in a person previously in normal sinus rhythm. In these cases, the heart rate may
2 key Clinical points Differential Diagnosis of Supraventricular Tachycardias The initial differential diagnosis of supraventricular tachycardias should focus on the ventricular response characteristics of regularity, rate, and rapidity of onset, not on the atrial depolarization from the ECG. The regular supraventricular tachycardias include sinus tachycardia, atrial flutter, atrioventricular nodal reentrant tachycardia, atrioventricular reciprocating tachycardia, and atrial tachycardia. The irregular supraventricular tachycardias are atrial fibrillation, atrial flutter with variable atrioventricular block, and multifocal atrial tachycardia; multiple atrial premature contractions can cause a similar presentation. Sudden onset and termination are characteristic of acute atrial fibrillation and atrial flutter, atrioventricular nodal reentrant tachycardia, atrioventricular reciprocating tachycardia, and atrial tachycardia. Gradual onset and recession occur with sinus tachycardia, chronic atrial fibrillation and atrial flutter, multifocal atrial tachycardia, and atrial premature contractions. Adenosine blocks the atrioventricular node and is useful in distinguishing among supraventricular tachycardias but should not be given in the case of irregular wide-complex tachycardias, since it may render these rhythms unstable. After administration of adenosine, slowing of the heart rate is consistent with a diagnosis of sinus tachycardia, atrial tachycardia, atrial fibrillation, or atrial flutter, whereas termination of tachycardia points to atrioventricular nodal reentrant tachycardia, atrioventricular reciprocating tachycardia, and some atrial tachycardias. jump from 60 beats per minute to 160 beats per minute or more, and the patient is usually aware of this change. In contrast, in patients with chronic atrial fibrillation, the development of a rapid heart rate is more gradual and occurs in response to physical activity or other stressors similar to the case with sinus tachycardia. With all cases of atrial fibrillation, the ventricular response is irregular, and the ventricular rate ranges from 60 to 220 beats per minute, depending largely on the patient s age, whether there is any underlying atrioventricular node disease, and whether the patient has received any drugs that affect the atrioventricular node. Atrial flutter, the second most common pathologic supraventricular tachycardia, results from a reentrant circuit around the tricuspid valve in the right atrium (although atypical flutters do occur, primarily in persons who have undergone cardiac surgery or cardiac ablation) (Fig. 2). Atrial flutter is an organized regular rhythm that is generally characterized by an atrial rate of 280 to 300 beats per minute and that with 2:1 conduction in the atrioventricular node results in a ventricular rate of 140 to 150 beats per minute. At a heart rate of 150 beats per minute, the flutter waves are usually obscured by T waves, making the surface ECG tracing for this tachycardia difficult to distinguish from that of other supraventricular tachycardias. However, a heart rate of 150 beats per minute is highly suggestive of this tachyarrhythmia. In patients who have atrioventricular node disease or who are receiving atrioventricular node blocking medications, the rate in atrial flutter may be slower than 140 to 150 beats per minute. In these situations, the heart rate is irregular most of the time, although it is less chaotic than in atrial fibrillation. The three next most common supraventricular tachycardias atrioventricular nodal reentrant tachycardia, atrioventricular reciprocating (reentrant) tachycardia, and atrial tachycardia are often considered to be a triumvirate because they share many characteristics, including rapid onset, heart rates of 150 to 250 beats per minute, and regularity of the ventricular response (Fig. 2). Atrioventricular nodal reentrant tachycardia and atrioventricular reciprocating tachycardia are caused by the presence of abnormal electrical circuits, whereas atrial tachycardia can be focal or caused by very small abnormal circuits. These supraventricular tachycardias occur in approximately 1 person per 500 in the United States. 6 Atrioventricular nodal reentrant tachycardia is 1439
3 T h e n e w e ngl a nd j o u r na l o f m e dic i n e 1440
4 Figure 1. Differential Diagnosis of the Supraventricular Tachycardias (SVTs), According to Regularity of Rhythm. AV denotes atrioventricular, AVRT atrioventricular reciprocating tachycardia, and WPW the Wolff Parkinson White syndrome. most common among persons older than 20 years of age, whereas atrioventricular reciprocating tachycardia occurs more frequently in the pediatric population. Atrial tachycardia is the least common of the three. Atrioventricular nodal reentrant tachycardia is caused by a reentrant loop that involves the atrioventricular node and the atrial tissue. 7 In persons with this type of tachycardia, the atrioventricular node has two conduits, one of which conducts rapidly and the other slowly. The slower pathway, which lies parallel to the tricuspid valve, allows for a reentrant loop as the electrical impulse meanders through the slow pathway, exiting the atrioventricular node in a retrograde manner (i.e., backward from the atrioventricular node to the atrium) and in an anterograde manner (i.e., forward, or from the atrioventricular node to the ventricle) at the same time. Because of the simultaneous depolarization of the atrium and ventricle, P waves are rarely seen on the surface ECG, although atrial depolarization can occasionally be seen as part of the terminal QRS complex in lead V 1. Atrioventricular reciprocating tachycardia is caused by cardiac musculature that bypasses the normal insulation afforded by the tricuspid and mitral valves between the atria and the ventricles. These bypass tracts may conduct in an anterograde direction only, in a retrograde direction only, or in both directions. A delta wave, an initial slurring of the QRS complex, is present on the surface ECG in most cases of anterograde bypass tracts and indicates partial depolarization of the ventricular tissue resulting from rapid conduction of the electrical impulse from the atrium to the ventricle over the bypass tract. Delta waves are absent in cases in which there is no anterograde conduction and in some persons with left atrial free-wall bypass tracts (since the brisk atrioventricular node conduction can depolarize the ventricle through the His Purkinje system before the atrial impulse arrives at the bypass tract). Patients who have both tachycardia and a delta wave have the Wolff Parkinson White syndrome. Patients 1441
5 T h e n e w e ngl a nd j o u r na l o f m e dic i n e Regular Supraventricular Tachycardias Figure 2. Mechanisms of Supraventricular Tachycardias, According to Regularity of Rhythm. The regular supraventricular tachycardias include sinus tachycardia (not shown), atrial flutter (AFL), atrioventricular nodal reentrant tachycardia (AVNRT), atrioventricular reciprocating tachycardia (AVRT), and atrial tachycardia (AT). Orthodromic AVRT is much more common than antidromic AVRT. The irregular supraventricular tachycardias include atrial fibrillation (AF), AFL when it occurs in a patient with variable AV block (not shown), multifocal atrial tachycardia (MAT), and sinus rhythm with multiple atrial premature beats (not shown). AVN denotes atrioventricular node, and SN sinus node. with a surface delta wave but no tachycardia have ECG findings similar to those with the Wolff Parkinson White syndrome but do not have the syndrome. Nonetheless, these persons are still at risk for supraventricular tachycardias. Three arrhythmias are seen with bypass tracts: a narrow regular QRS complex (orthodromic; conduction down the atrioventricular node and retrograde conduction through the bypass tract), a wide regular QRS complex (antidromic; conduction down 1442
6 Irregular Supraventricular Tachycardias the bypass tract and retrograde conduction through the atrioventricular node), and a wide irregular QRS complex (atrial fibrillation) (Fig. 1 and 2). In atrioventricular reciprocating tachycardia, atrial activity (P waves) may be seen after the QRS complex, although this atrial depolarization is often obscured by the T wave. When atrial fibrillation occurs, the ventricular rate can be quite rapid and can lead to fatal ventricular arrhythmias. Atrial tachycardia is a focal tachycardia that may be a result of a micro-reentrant circuit or an automatic focus. There are two unique characteristics of atrial tachycardias: they may occur in repetitive short bursts, and they are frequently characterized by a warm-up phenomenon in which the atrial rate increases slightly over the first 5 to 10 seconds before stabilizing. Surface ECGs show a P wave preceding each QRS complex, although at rapid heart rates, the P wave may be obscured by the T wave. The remaining supraventricular tachycardias are much less common. Multifocal atrial tachycardia occurs because of multiple atrial premature beats in an atrium poisoned by hypoxia, increased atrial pressure, and, perhaps most important, theophylline. This type of tachycardia is uncommon today because of the reduced use of theophylline in the treatment of pulmonary disease. Multifocal atrial tachycardia is gradual in onset because the underlying rhythm is generally sinus tachycardia, and the heart rates with multifocal atrial tachycardia are only slightly faster than these baseline rates. The rhythm is irregular, and on ECG, P waves with abnormal morphologic characteristics (with three abnormal P waves necessary for the diagnosis) precede each QRS complex. Frequent atrial premature contractions, although not technically a supraventricular tachycardia, warrant mention because they are commonly confused with supraventricular tachycardias. Like atrial tachycardia, frequent atrial premature contractions originate from a single focus; therefore, the morphologic characteristics of the P wave are similar to those seen with atrial tachycardia. This rhythm can be sudden or gradual in onset, depending on the underlying sinus rate. The rhythm is irregular, with heart rates between 100 and 150 beats per minute. Other supraventricular tachycardias are so uncommon that most practicing physicians are unlikely ever to observe them. Junctional tachycardia is extremely rare in adults but can occur in infants. Two other types of unusual tachycardias are thought to originate from abnormal atrioventricular nodal tissue that is separated from the atrioventricular node. Paroxysmal junctional retrograde tachycardia occurs with a bypass tract near the atrioventricular node that conducts in only a retrograde direction. The tachycardia usually is incessant and often causes a dilated cardiomyopathy. Mahaim fiber tachycardias are caused by tissue that originates in the lateral right atrium and connects to the distal right bundle branch. A wide-complex reentrant tachycardia occurs 1443
7 T h e n e w e ngl a nd j o u r na l o f m e dic i n e with conduction down the abnormal tissue and back up to the atrium through the atrioventricular node. S tr ategies a nd E v idence Differential Diagnosis of Supraventricular Tachycardias The initial differential diagnosis of supraventricular tachycardias should focus on the ventricular response, not on atrial depolarization as observed on the ECG. The first step is to determine whether the QRS complex is narrow or wide. Then regularity should be assessed (Fig. 1). Regularity is defined as variation of less than 10% in beat-tobeat timing, but most regular tachycardias actually vary by less than 5%. 8 After regularity is assessed, the rapidity of onset and offset should be determined, preferably by means of cardiac monitoring, although it can be assessed on the basis of the history. The heart rate should also be considered in the differential diagnosis of supraventricular tachycardias. Narrow-Complex Supraventricular Tachycardias Only after the differential diagnosis has been narrowed on the basis of the features mentioned above should atrial activity be assessed. P waves immediately precede the QRS complex in sinus tachycardia, atrial tachycardia, multifocal atrial tachycardia, and multiple atrial premature contractions. P waves follow the QRS complex in atrioventricular nodal reentrant tachycardia and atrioventricular reciprocating tachycardia. In tachycardias with very rapid heart rates (e.g., atrial tachycardia, atrioventricular nodal reentrant tachycardia, and atrioventricular reciprocating tachycardia), P waves may not be apparent owing to overlap of the T wave. Atrial flutter with 2:1 conduction block can easily be mistaken for sinus tachycardia or atrial tachycardia because a flutter wave is often buried in the T wave; however, a rate of 150 beats per minute should lead one to suspect atrial flutter. Finally, the response to administration of adenosine can assist in the diagnosis of a specific supraventricular tachycardia (Fig. 3) (see below for additional information regarding adenosine). Wide-Complex Supraventricular Tachycardias In contrast to narrow-complex tachycardias, which can be generated only by impulses that depolarize the ventricle through the His Purkinje system (and thus are, by definition, supraventricular tachycardias), wide-complex tachycardias can be ventricular or supraventricular in origin (or artifactual). Wide-complex tachycardias are caused by ventricular arrhythmia (ventricular tachycardia, ventricular fibrillation, and torsades de pointes or polymorphic ventricular tachycardia) or supraventricular tachycardias with aberrant conduction resulting from one of the following conditions: disease in the His Purkinje system, such as left or right bundle-branch block; a bypass tract (i.e., the Wolff Parkinson White syndrome), with depolarization of the ventricle from the bypass tract; or a ventricular paced rhythm from a pacemaker. Wide-complex tachycardias can be regular or irregular. Regular wide-complex tachycardias are either ventricular tachycardia or regular supraventricular tachycardias (Fig. 3), whereas irregular wide-complex tachycardias are either the ventricular arrhythmias of polymorphic ventricular tachycardia, torsades de pointes, or ventricular fibrillation or one of the irregular supraventricular tachycardias (Fig. 4). M a nagemen t Narrow-Complex Tachycardias Vagal maneuvers and administration of adenosine are useful in the diagnosis and treatment of narrow-complex supraventricular tachycardias. 9 Vagal maneuvers including a Valsalva maneuver, carotid sinus massage, bearing down, and immersion of the face in ice water increase vagal tone and block the atrioventricular node. The resulting slowing of the heart rate often confirms the diagnosis of sinus tachycardia, atrial fibrillation, or atrial flutter and can frequently terminate atrioventricular nodal reentrant tachycardia and atrioventricular reciprocating tachycardia. Adenosine, a very short-acting endogenous nucleotide that blocks atrioventricular nodal conduction, terminates nearly all atrioventricular nodal reentrant tachycardias and atrioventricular reciprocating tachycardias as well as up to 80% of atrial tachycardias. 10 Adenosine should be administered quickly at a dose of 6 mg, followed by a bolus of 20 ml of fluid. Since this drug may also excite atrial and ventricular tissue, causing atrial fibrillation in up to 12% of patients and nonsustained ventricular tachycardia in rare cases, 11 it should be administered only when a cardiac monitor is being used and a defibrillator is on 1444
8 Narrow-complex tachycardia Regular rhythm Irregular rhythm Sudden onset Gradual onset HR <150 beats/min HR 150 beats/min Vagal maneuvers, adenosine ST AF, MAT, NSR, or ST with APCs AF, AFL with variable block Termination AVNRT, AVRT, AT No termination AT, AFL (ST, less frequently) Treat underlying cause Rate control with beta-blocker, verapamil, diltiazem; if unstable condition, cardioversion, procainamide, ibutilde Figure 3. Differential Diagnosis and Treatment of Narrow-Complex Tachycardias. The first step in the differential diagnosis of narrow-complex tachycardias is to determine whether the rhythm is regular or irregular. Further delineation of supraventricular tachycardias can be established according to onset (sudden or gradual), heart rate, and response to vagal maneuvers or administration of adenosine. AF denotes atrial fibrillation, AFL atrial flutter, APC atrial premature contraction, AT atrial tachycardia, AVNRT atrioventricular nodal reentrant tachycardia, AVRT atrioventricular reciprocating tachycardia, HR heart rate, MAT multifocal atrial tachycardia, NSR normal sinus rhythm, and ST sinus tachycardia. hand. A lower dose (3 mg) is recommended in persons who have a cardiac transplant or in whom the drug is administered through a central catheter. Adenosine should not be used in patients with bronchospastic lung disease. Common side effects include chest tightness, flushing, and a sense of dread. Although intravenous verapamil and diltiazem, which also block the atrioventricular node, are of potential diagnostic and therapeutic use in narrow-complex tachycardia, they may cause hypotension and thus are not a first choice in the emergency setting. 12 Electrical cardioversion is reserved for patients in unstable condition who are not having a response to adenosine. Antiarrhythmic agents are rarely necessary in the early management of supraventricular tachycardias, with the exception of the management of arrhythmias that have caused hemodynamic instability and that have not responded to electrical cardioversion. In these cases, procainamide and ibutilide can be used. 10 Wide-Complex Tachycardias Adenosine is also useful in the differential diagnosis and treatment of wide-complex tachycardias, 13 but it should be given only when these tachycardias are regular, since irregular wide-complex tachycardias may be rendered unstable after the administration of adenosine. Potential risks include increasing conduction through a bypass tract if the underlying arrhythmia is atrial fibrillation or (more worrisome) terminating the supraventricular tachycardia but inducing atrial fibrillation with resultant rapid conduction down a bypass tract, leading to ventricular fibrillation. 11 Verapamil and diltiazem 1445
9 Wide-complex tachycardia Underlying heart disease No Yes Irregular rhythm Regular rhythm Unstable condition Stable condition Stable condition Unstable condition Polymorphic ventricular tachycardia, ventricular fibrillation AF with WPW AF with aberrancy or AF with benign WPW Adenosine Termination No termination Ventricular tachycardia Cardioversion defibrillation SVT with aberrancy, AVRT (WPW), idiopathic ventricular tachycardia Cardioversion; IV procainamide, sotalol, lidocaine, or amiodarone Figure 4. Differential Diagnosis and Treatment of Wide-Complex Tachycardias. In the differential diagnosis of wide-complex tachycardias, the initial step is to determine whether there is underlying heart disease. If the patient has known or suspected cardiac disease, the tachycardia is probably a ventricular tachycardia, and treatment for that condition should be initiated. If heart disease is not thought to be present, the strategy is to separate the ventricular response into regular and irregular rhythms. If a patient with a regular wide-complex tachycardia is in stable condition, administration of adenosine is reasonable, since this will terminate many of the supraventricular tachycardias. If the patient s condition is unstable, or if the tachycardia does not terminate with adenosine, treatment for presumptive ventricular tachycardia (i.e., cardioversion) should be given. Irregular wide-complex tachycardias are always worrisome, since they are frequently unstable. Patients with unstable irregular wide-complex tachycardias should undergo cardioversion; if the tachycardias are stable, monitoring and cardiac consultation are appropriate. AF denotes atrial fibrillation, AVRT atrioventricular reciprocating tachycardia, IV intravenous, SVT supraventricular tachycardia, and WPW the Wolff Parkinson White syndrome. should not be administered in patients with widecomplex tachycardias, since profound hypotension and death may occur. 12 Electrical cardioversion is necessary in the treatment of unstable wide-complex tachycardias, as it is in the treatment of unstable narrow-complex tachycardias. Procainamide and ibutilide, as well as lidocaine, amiodarone, and sotalol, are useful in the treatment of wide-complex 1446
10 tachycardias. 10 Stable wide-complex irregular tachycardias are usually atrial fibrillation with aberrancy or the Wolff Parkinson White syndrome; in the case of these arrhythmias, consultation with an expert is generally required. A r e a s of Uncerta in t y Arrhythmias causing hemodynamic instability (hypotension, heart failure, or coronary ischemia) require urgent electrical cardioversion. However, it is often unclear, especially in the case of atrial fibrillation, whether the supraventricular tachycardia is the cause or the result of the hemodynamic instability. 10 In many patients, rapid atrial fibrillation is a consequence rather than a cause of heart failure or cardiac ischemia. Atrial fibrillation is rarely the cause of instability when heart rates are less than 150 beats per minute. 10 Guidelines Guidelines for the early treatment of supraventricular tachycardias are included in the 2010 American Heart Association Advanced Cardiovascular Life Support guidelines. 10,14 The recommendations provided here are generally consistent with these guidelines, including administration of adenosine as the initial treatment of choice for regular supraventricular tachycardias and as an important aid in the differential diagnosis of regular widecomplex tachycardias. Conclusions a nd R ecommendations In a patient presenting with symptomatic tachycardia, such as the woman described in the vignette, prompt evaluation and treatment are needed. Although the blood pressure of the woman in the vignette is 84/60 mm Hg, she is alert and has no signs of shock; thus, her condition is not considered to be unstable. The initial assessment should distinguish between narrow- and wide-complex tachycardia, determine whether the rhythm is regular or irregular, and consider the rapidity of onset. This patient has a regular narrowcomplex tachycardia with a sudden onset, as assessed on the basis of the history. Possibilities include atrial flutter, atrioventricular nodal reentrant tachycardia, atrioventricular reciprocating tachycardia, and atrial tachycardia. The narrow QRS complex rules out ventricular tachycardia; the regular response rules out atrial fibrillation and multifocal atrial tachycardia. The heart rate of 190 beats per minute is inconsistent with atrial flutter. Furthermore, the suddenness of the onset of symptoms and the absence of clear P waves suggest atrioventricular nodal reentrant tachycardia, atrioventricular reciprocating tachycardia, or atrial tachycardia. Adenosine should be administered with the patient on a cardiac monitor, with a cardiac defibrillator at hand. Adenosine would be expected to terminate the supraventricular tachycardia. An ECG should be evaluated when sinus rhythm is restored; the presence of a delta wave would be consistent with a diagnosis of atrioventricular reciprocating tachycardia caused by the Wolff Parkinson White syndrome. Dr. Link reports receiving consulting fees from Lantheus Medical Imaging and holding patents for a chest-wall protector for sports and a testing model for commotio cordis. No other potential conflict of interest relevant to this article was reported. Disclosure forms provided by the author are available with the full text of this article at NEJM.org. I thank Dr. Bonnie L. Bermas for her careful review of an earlier version of the manuscript, and Steven Moskowitz of Advanced Medical Graphics for his assistance with earlier versions of the figures. References 1. Link MS. Introduction to the arrhythmias: a primer. EP Lab Digest 2007;5: Fox SM III, Naughton JP, Haskell WL. Physical activity and the prevention of coronary heart disease. Ann Clin Res 1971; 3: Naccarelli GV, Varker H, Lin J, Schulman KL. Increasing prevalence of atrial fibrillation and flutter in the United States. Am J Cardiol 2009;104: Heeringa J, van der Kuip DA, Hofman A, et al. Prevalence, incidence and lifetime risk of atrial fibrillation: the Rotterdam study. Eur Heart J 2006;27: Schnabel RB, Sullivan LM, Levy D, et al. Development of a risk score for atrial fibrillation (Framingham Heart Study): a community-based cohort study. Lancet 2009;373: Orejarena LA, Vidaillet H Jr, DeStefano F, et al. Paroxysmal supraventricular tachycardia in the general population. J Am Coll Cardiol 1998;31: Katritsis DG, Camm AJ. Atrioventricular nodal reentrant tachycardia. Circulation 2010;122: Buxton AE, Calkins H, Callans DJ, et al. ACC/AHA/HRS 2006 key data elements and definitions for electrophysiological studies and procedures: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Data Standards (ACC/AHA/HRS Writing Committee to Develop Data Standards on Electrophysiology). Circulation 2006;114: dimarco JP, Sellers TD, Lerman BB, Greenberg ML, Berne RM, Belardinelli L. Diagnostic and therapeutic use of adenosine in patients with supraventricular tachyarrhythmias. J Am Coll Cardiol 1985; 6: Neumar RW, Otto CW, Link MS, et al. Part 8: adult advanced cardiovascular life support: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 2010;122:Suppl 3:S729-S767. [Erratum, Circulation 2011;123(6):e236.] 1447
11 11. Strickberger SA, Man KC, Daoud EG, et al. Adenosine-induced atrial arrhythmia: a prospective analysis. Ann Intern Med 1997;127: [Erratum, Ann Intern Med 1998;128:511.] 12. Delaney B, Loy J, Kelly AM. The relative efficacy of adenosine versus verapamil for the treatment of stable paroxysmal supraventricular tachycardia in adults: a metaanalysis. Eur J Emerg Med 2011;18: Marill KA, Wolfram S, Desouza IS, et al. Adenosine for wide-complex tachycardia: efficacy and safety. Crit Care Med 2009;37: Link MS, Atkins DL, Passman RS, et al. Part 6: electrical therapies: automated external defibrillators, defibrillation, cardioversion, and pacing: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 2010; 122:Suppl 3:S706-S719. [Erratum, Circulation 2011;123(6):e235.] Copyright 2012 Massachusetts Medical Society. 1448
Chapter 16: Arrhythmias and Conduction Disturbances
 Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Pediatrics ECG Monitoring. Pediatric Intensive Care Unit Emergency Division
 Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Supraventricular Tachycardia (SVT)
 Supraventricular Tachycardia (SVT) Bruce Stambler, MD Piedmont Heart Atlanta, GA Supraventricular Tachycardia Objectives Types and mechanisms AV nodal reentrant tachycardia (AVNRT) AV reciprocating tachycardia
Supraventricular Tachycardia (SVT) Bruce Stambler, MD Piedmont Heart Atlanta, GA Supraventricular Tachycardia Objectives Types and mechanisms AV nodal reentrant tachycardia (AVNRT) AV reciprocating tachycardia
Supraventricular Tachycardia (SVT)
 Supraventricular Tachycardia (SVT) Daniel Frisch, MD Cardiology Division, Electrophysiology Section Thomas Jefferson University Hospital daniel.frisch@jefferson.edu Short RP Are these the Mid same RP tachycardias?
Supraventricular Tachycardia (SVT) Daniel Frisch, MD Cardiology Division, Electrophysiology Section Thomas Jefferson University Hospital daniel.frisch@jefferson.edu Short RP Are these the Mid same RP tachycardias?
The most common. hospitalized patients. hypotension due to. filling time Rate control in ICU patients may be difficult as many drugs cause hypotension
 Arrhythmias in the critically ill ICU patients: Approach for rapid recognition & management Objectives Be able to identify and manage: Atrial fibrillation with a rapid ventricular response Atrial flutter
Arrhythmias in the critically ill ICU patients: Approach for rapid recognition & management Objectives Be able to identify and manage: Atrial fibrillation with a rapid ventricular response Atrial flutter
Chapter 9. Learning Objectives. Learning Objectives 9/11/2012. Cardiac Arrhythmias. Define electrical therapy
 Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
PEDIATRIC SVT MANAGEMENT
 PEDIATRIC SVT MANAGEMENT 1 INTRODUCTION Supraventricular tachycardia (SVT) can be defined as an abnormally rapid heart rhythm originating above the ventricles, often (but not always) with a narrow QRS
PEDIATRIC SVT MANAGEMENT 1 INTRODUCTION Supraventricular tachycardia (SVT) can be defined as an abnormally rapid heart rhythm originating above the ventricles, often (but not always) with a narrow QRS
WPW syndrome and AVRT
 WPW syndrome and AVRT Myung-Yong Lee, MD, PhD Division of Cardiology Department of Internal Medicine School of Medicine Dankook University, Cheonan, Korea Supraventricular tachycardia (SVT) Paroxysmal
WPW syndrome and AVRT Myung-Yong Lee, MD, PhD Division of Cardiology Department of Internal Medicine School of Medicine Dankook University, Cheonan, Korea Supraventricular tachycardia (SVT) Paroxysmal
Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD
 Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD OBJECTIVES 1. Identify the basic electrophysiology of the four causes of wide complex tachycardia. 2. Develop a simple framework for acute management
Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD OBJECTIVES 1. Identify the basic electrophysiology of the four causes of wide complex tachycardia. 2. Develop a simple framework for acute management
ECGs and Arrhythmias: Family Medicine Board Review 2009
 Rate Rhythm Intervals Hypertrophy ECGs and Arrhythmias: Family Medicine Board Review 2009 Axis Jess (Fogler) Waldura, MD University of California, San Francisco walduraj@nccc.ucsf.edu Ischemia Overview
Rate Rhythm Intervals Hypertrophy ECGs and Arrhythmias: Family Medicine Board Review 2009 Axis Jess (Fogler) Waldura, MD University of California, San Francisco walduraj@nccc.ucsf.edu Ischemia Overview
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013
 Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
Paramedic Rounds. Tachyarrhythmia's. Sean Sutton Dallas Wood
 Paramedic Rounds Tachyarrhythmia's Sean Sutton Dallas Wood Objectives At the end of this session, the paramedic will be able to: State the key components of the cardiac conduction pathway, along with the
Paramedic Rounds Tachyarrhythmia's Sean Sutton Dallas Wood Objectives At the end of this session, the paramedic will be able to: State the key components of the cardiac conduction pathway, along with the
2) Heart Arrhythmias 2 - Dr. Abdullah Sharif
 2) Heart Arrhythmias 2 - Dr. Abdullah Sharif Rhythms from the Sinus Node Sinus Tachycardia: HR > 100 b/m Causes: o Withdrawal of vagal tone & Sympathetic stimulation (exercise, fight or flight) o Fever
2) Heart Arrhythmias 2 - Dr. Abdullah Sharif Rhythms from the Sinus Node Sinus Tachycardia: HR > 100 b/m Causes: o Withdrawal of vagal tone & Sympathetic stimulation (exercise, fight or flight) o Fever
Supraventricular Tachycardia: From Fetus to Adult. Mohamed Hamdan, MD
 Supraventricular Tachycardia: From Fetus to Adult Mohamed Hamdan, MD Learning Objectives Define type of SVT by age Describe clinical approach Describe prenatal and postnatal management of SVT 2 SVT Across
Supraventricular Tachycardia: From Fetus to Adult Mohamed Hamdan, MD Learning Objectives Define type of SVT by age Describe clinical approach Describe prenatal and postnatal management of SVT 2 SVT Across
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment
 Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Paroxysmal Supraventricular Tachycardia PSVT.
 Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
Case-Based Practical ECG Interpretation for the Generalist
 Case-Based Practical ECG Interpretation for the Generalist Paul D. Varosy, MD, FACC, FAHA, FHRS Director of Cardiac Electrophysiology VA Eastern Colorado Health Care System Associate Professor of Medicine
Case-Based Practical ECG Interpretation for the Generalist Paul D. Varosy, MD, FACC, FAHA, FHRS Director of Cardiac Electrophysiology VA Eastern Colorado Health Care System Associate Professor of Medicine
Core Content In Urgent Care Medicine
 Palpitations/Arrhythmias Ebrahim Barkoudah, MD Clinical Instructor in Internal Medicine Harvard Medical School Assistant in Internal Medicine & Pediatrics Massachusetts General Hospital MGH Chelsea Chelsea,
Palpitations/Arrhythmias Ebrahim Barkoudah, MD Clinical Instructor in Internal Medicine Harvard Medical School Assistant in Internal Medicine & Pediatrics Massachusetts General Hospital MGH Chelsea Chelsea,
Case #1. 73 y/o man with h/o HTN and CHF admitted with dizziness and SOB Treated for CHF exacerbation with Lasix Now HR 136
 Tachycardias Case #1 73 y/o man with h/o HTN and CHF admitted with dizziness and SOB Treated for CHF exacerbation with Lasix Now HR 136 Initial Assessment Check Telemetry screen if pt on tele Telemetry
Tachycardias Case #1 73 y/o man with h/o HTN and CHF admitted with dizziness and SOB Treated for CHF exacerbation with Lasix Now HR 136 Initial Assessment Check Telemetry screen if pt on tele Telemetry
Emergency treatment to SVT Evidence-based Approach. Tran Thao Giang
 Emergency treatment to SVT Evidence-based Approach Tran Thao Giang Description ECG manifestations: HR is extremely rapid and regular (240bpm ± 40) P wave is: usually invisible When visible: anormal P axis,
Emergency treatment to SVT Evidence-based Approach Tran Thao Giang Description ECG manifestations: HR is extremely rapid and regular (240bpm ± 40) P wave is: usually invisible When visible: anormal P axis,
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material
 1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
Sustained tachycardia with wide QRS
 Sustained tachycardia with wide QRS Courtesy from Prof. Antonio Américo Friedmann. Electrocardiology Service of University of Faculty of São Paulo. Opinions from colleagues Greetings to everyone, In a
Sustained tachycardia with wide QRS Courtesy from Prof. Antonio Américo Friedmann. Electrocardiology Service of University of Faculty of São Paulo. Opinions from colleagues Greetings to everyone, In a
Repetitive narrow QRS tachycardia in a 61-year-old female patient with recent palpitations
 Journal of Geriatric Cardiology (2018) 15: 193 198 2018 JGC All rights reserved; www.jgc301.com Case Report Open Access Repetitive narrow QRS tachycardia in a 61-year-old female patient with recent palpitations
Journal of Geriatric Cardiology (2018) 15: 193 198 2018 JGC All rights reserved; www.jgc301.com Case Report Open Access Repetitive narrow QRS tachycardia in a 61-year-old female patient with recent palpitations
TEST BANK FOR ECGS MADE EASY 5TH EDITION BY AEHLERT
 Link download full: http://testbankair.com/download/test-bank-for-ecgs-made-easy-5thedition-by-aehlert/ TEST BANK FOR ECGS MADE EASY 5TH EDITION BY AEHLERT Chapter 5 TRUE/FALSE 1. The AV junction consists
Link download full: http://testbankair.com/download/test-bank-for-ecgs-made-easy-5thedition-by-aehlert/ TEST BANK FOR ECGS MADE EASY 5TH EDITION BY AEHLERT Chapter 5 TRUE/FALSE 1. The AV junction consists
Antiarrhythmic Drugs
 Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
ECG Interpretation Made Easy
 ECG Interpretation Made Easy Dr. A Tageldien Abdellah, MSc MD EBSC Lecturer of Cardiology- Hull University Hull York Medical School 2007-2008 ECG Interpretation Made Easy Synopsis Benefits Objectives Process
ECG Interpretation Made Easy Dr. A Tageldien Abdellah, MSc MD EBSC Lecturer of Cardiology- Hull University Hull York Medical School 2007-2008 ECG Interpretation Made Easy Synopsis Benefits Objectives Process
a lecture series by SWESEMJR
 Arrhythmias Automaticity- the ability to depolarize spontaneously. Pacemakers: Sinoatrial node: 70 bpm AV-nodal area: 40 bpm His-Purkinje: 20-40 bpm it Mechanisms of arrhythmias 1. Increased automaticity
Arrhythmias Automaticity- the ability to depolarize spontaneously. Pacemakers: Sinoatrial node: 70 bpm AV-nodal area: 40 bpm His-Purkinje: 20-40 bpm it Mechanisms of arrhythmias 1. Increased automaticity
ECGs and Arrhythmias: Family Medicine Board Review 2012
 Overview ECGs and Arrhythmias: Family Medicine Board Review 2012 Jess Waldura, MD University of California, San Francisco walduraj@nccc.ucsf.edu Bundle branch blocks Quick review of ischemia Arrhythmias
Overview ECGs and Arrhythmias: Family Medicine Board Review 2012 Jess Waldura, MD University of California, San Francisco walduraj@nccc.ucsf.edu Bundle branch blocks Quick review of ischemia Arrhythmias
TACHYARRHYTHMIAs. Pawel Balsam, MD, PhD
 TACHYARRHYTHMIAs Pawel Balsam, MD, PhD SupraVentricular Tachycardia Atrial Extra Systole Sinus Tachycardia Focal A. Tachycardia AVRT AVNRT Atrial Flutter Atrial Fibrillation Ventricular Tachycardia Ventricular
TACHYARRHYTHMIAs Pawel Balsam, MD, PhD SupraVentricular Tachycardia Atrial Extra Systole Sinus Tachycardia Focal A. Tachycardia AVRT AVNRT Atrial Flutter Atrial Fibrillation Ventricular Tachycardia Ventricular
APPROACH TO TACHYARRYTHMIAS
 APPROACH TO TACHYARRYTHMIAS PROF.DR.MD.ZAKIR HOSSAIN PROFESSOR AND HEAD DEPARTMENT OF MEDICINE SZMCH TACHYARRYTHMIA Cardiac arrythmia is a disturbance of electrical rhythm of heart. Cardac arrythmia with
APPROACH TO TACHYARRYTHMIAS PROF.DR.MD.ZAKIR HOSSAIN PROFESSOR AND HEAD DEPARTMENT OF MEDICINE SZMCH TACHYARRYTHMIA Cardiac arrythmia is a disturbance of electrical rhythm of heart. Cardac arrythmia with
Anti arrhythmic drugs. Hilal Al Saffar College of medicine Baghdad University
 Anti arrhythmic drugs Hilal Al Saffar College of medicine Baghdad University Mechanism of Arrhythmia Abnormal heart pulse formation Abnormal heart pulse conduction Classification of Arrhythmia Abnormal
Anti arrhythmic drugs Hilal Al Saffar College of medicine Baghdad University Mechanism of Arrhythmia Abnormal heart pulse formation Abnormal heart pulse conduction Classification of Arrhythmia Abnormal
Step by step approach to EKG rhythm interpretation:
 Sinus Rhythms Normal sinus arrhythmia Small, slow variation of the R-R interval i.e. variation of the normal sinus heart rate with respiration, etc. Sinus Tachycardia Defined as sinus rhythm with a rate
Sinus Rhythms Normal sinus arrhythmia Small, slow variation of the R-R interval i.e. variation of the normal sinus heart rate with respiration, etc. Sinus Tachycardia Defined as sinus rhythm with a rate
Atrial Fibrillation and Common Supraventricular Tachycardias. Sunil Kapur MD
 Atrial Fibrillation and Common Supraventricular Tachycardias Sunil Kapur MD Cardiac Electrophysiology Brigham and Women s Hospital Instructor, Harvard Medical School No disclosures Cardiac Conduction:
Atrial Fibrillation and Common Supraventricular Tachycardias Sunil Kapur MD Cardiac Electrophysiology Brigham and Women s Hospital Instructor, Harvard Medical School No disclosures Cardiac Conduction:
Cardiac arrhythmias. Janusz Witowski. Department of Pathophysiology Poznan University of Medical Sciences. J. Witowski
 Cardiac arrhythmias Janusz Witowski Department of Pathophysiology Poznan University of Medical Sciences A 68-year old man presents to the emergency department late one evening complaining of increasing
Cardiac arrhythmias Janusz Witowski Department of Pathophysiology Poznan University of Medical Sciences A 68-year old man presents to the emergency department late one evening complaining of increasing
Atrial Fibrillation 10/2/2018. Depolarization & ECG. Atrial Fibrillation. Hemodynamic Consequences
 Depolarization & ECG Atrial Fibrillation How to make ORDER out of CHAOS Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Depolarization & ECG Depolarization & ECG Atrial Fibrillation Hemodynamic Consequences
Depolarization & ECG Atrial Fibrillation How to make ORDER out of CHAOS Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Depolarization & ECG Depolarization & ECG Atrial Fibrillation Hemodynamic Consequences
Electrocardiography for Healthcare Professionals
 Electrocardiography for Healthcare Professionals Chapter 7: Junctional Dysrhythmias 2012 The Companies, Inc. All rights reserved. Learning Outcomes 7.1 Describe the various junctional dysrhythmias 7.2
Electrocardiography for Healthcare Professionals Chapter 7: Junctional Dysrhythmias 2012 The Companies, Inc. All rights reserved. Learning Outcomes 7.1 Describe the various junctional dysrhythmias 7.2
8/20/2012. Learning Outcomes (Cont d)
 1 2 3 4 Electrocardiography for Healthcare Professionals Chapter 7: Junctional Dysrhythmias Learning Outcomes 7.1 Describe the various junctional dysrhythmias 7.2 Identify premature junctional complexes
1 2 3 4 Electrocardiography for Healthcare Professionals Chapter 7: Junctional Dysrhythmias Learning Outcomes 7.1 Describe the various junctional dysrhythmias 7.2 Identify premature junctional complexes
3. AV Block 1. First-degree AV block 1. Delay in AV node 2. Long PR interval 3. QRS complex follows each P wave 4. Benign, no tx
 1. Rhythms & arrhythmias SA nodal rhythms Sinus rhythm Sinus tachycardia Sinus bradycardia Sinus arrhythmia Sick sinus syndrome SA block Sinus arrest AV blocks First-degree Second-degree Mobitz Type I
1. Rhythms & arrhythmias SA nodal rhythms Sinus rhythm Sinus tachycardia Sinus bradycardia Sinus arrhythmia Sick sinus syndrome SA block Sinus arrest AV blocks First-degree Second-degree Mobitz Type I
(living in the fast lane)
 (living in the fast lane) Presented by M.D. Cardiology IT S A group of ECG and Electrophysiological abnormalities in which The atrial impulses are conducted partly or completely, PREMATURELY, to the ventricles
(living in the fast lane) Presented by M.D. Cardiology IT S A group of ECG and Electrophysiological abnormalities in which The atrial impulses are conducted partly or completely, PREMATURELY, to the ventricles
Huseng Vefali MD St. Luke s University Health Network Department of Cardiology
 Huseng Vefali MD St. Luke s University Health Network Department of Cardiology Learning Objectives Establish Consistent Approach to Interpreting ECGs Review Essential Cases for Paramedics and first responders
Huseng Vefali MD St. Luke s University Health Network Department of Cardiology Learning Objectives Establish Consistent Approach to Interpreting ECGs Review Essential Cases for Paramedics and first responders
EKG Abnormalities. Adapted from:
 EKG Abnormalities Adapted from: http://www.bem.fi/book/19/19.htm Some key terms: Arrhythmia-an abnormal rhythm or sequence of events in the EKG Flutter-rapid depolarizations (and therefore contractions)
EKG Abnormalities Adapted from: http://www.bem.fi/book/19/19.htm Some key terms: Arrhythmia-an abnormal rhythm or sequence of events in the EKG Flutter-rapid depolarizations (and therefore contractions)
Definition, Diagnosis and Treatment of Tachycardia
 3 Definition, Diagnosis and Treatment of Tachycardia Anand Deshmukh The Cardiac Center of Creighton University, Omaha, Nebraska USA 1. Introduction 1.1 Anatomy of the human cardiac conduction system 1.1.1
3 Definition, Diagnosis and Treatment of Tachycardia Anand Deshmukh The Cardiac Center of Creighton University, Omaha, Nebraska USA 1. Introduction 1.1 Anatomy of the human cardiac conduction system 1.1.1
Dysrhythmias 11/7/2017. Disclosures. 3 reasons to evaluate and treat dysrhythmias. None. Eliminate symptoms and improve hemodynamics
 Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
Case Report Wide-QRS Tachycardia Inducible by Both Atrial and Ventricular Pacing
 Hellenic J Cardiol 2008; 49: 446-450 Case Report Wide-QRS Tachycardia Inducible by Both Atrial and Ventricular Pacing ELEFTHERIOS GIAZITZOGLOU, DEMOSTHENES G. KATRITSIS Department of Cardiology, Athens
Hellenic J Cardiol 2008; 49: 446-450 Case Report Wide-QRS Tachycardia Inducible by Both Atrial and Ventricular Pacing ELEFTHERIOS GIAZITZOGLOU, DEMOSTHENES G. KATRITSIS Department of Cardiology, Athens
ARRHYTHMIAS IN THE ICU
 ARRHYTHMIAS IN THE ICU Nora Goldschlager, MD MACP, FACC, FAHA, FHRS SFGH Division of Cardiology UCSF IDENTIFIED VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar) Electrolyte imbalance Proarrhythmia
ARRHYTHMIAS IN THE ICU Nora Goldschlager, MD MACP, FACC, FAHA, FHRS SFGH Division of Cardiology UCSF IDENTIFIED VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar) Electrolyte imbalance Proarrhythmia
ARRHYTHMIAS IN THE ICU: DIAGNOSIS AND PRINCIPLES OF MANAGEMENT
 ARRHYTHMIAS IN THE ICU: DIAGNOSIS AND PRINCIPLES OF MANAGEMENT Nora Goldschlager, M.D. MACP, FACC, FAHA, FHRS SFGH Division of Cardiogy UCSF CLINICAL VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar)
ARRHYTHMIAS IN THE ICU: DIAGNOSIS AND PRINCIPLES OF MANAGEMENT Nora Goldschlager, M.D. MACP, FACC, FAHA, FHRS SFGH Division of Cardiogy UCSF CLINICAL VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar)
EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology
 EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important
EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important
LONG RP TACHYCARDIA MAPPING AND RF ABLATION
 LONG RP TACHYCARDIA MAPPING AND RF ABLATION Dr. Hayam Eldamanhoury Ain shams univeristy Arrhythmia is a too broad topic SVT is broadly defined as narrow complex ( unless aberrant conduction ) Requires
LONG RP TACHYCARDIA MAPPING AND RF ABLATION Dr. Hayam Eldamanhoury Ain shams univeristy Arrhythmia is a too broad topic SVT is broadly defined as narrow complex ( unless aberrant conduction ) Requires
Ablation Update and Case Studies. Lawrence Nair, MD, FACC Director of Electrophysiology Presbyterian Heart Group
 Ablation Update and Case Studies Lawrence Nair, MD, FACC Director of Electrophysiology Presbyterian Heart Group Disclosures No financial relationships to disclose Objectives At the conclusion of this activity,
Ablation Update and Case Studies Lawrence Nair, MD, FACC Director of Electrophysiology Presbyterian Heart Group Disclosures No financial relationships to disclose Objectives At the conclusion of this activity,
CRC 431 ECG Basics. Bill Pruitt, MBA, RRT, CPFT, AE-C
 CRC 431 ECG Basics Bill Pruitt, MBA, RRT, CPFT, AE-C Resources White s 5 th ed. Ch 6 Electrocardiography Einthoven s Triangle Chest leads and limb leads Egan s 10 th ed. Ch 17 Interpreting the Electrocardiogram
CRC 431 ECG Basics Bill Pruitt, MBA, RRT, CPFT, AE-C Resources White s 5 th ed. Ch 6 Electrocardiography Einthoven s Triangle Chest leads and limb leads Egan s 10 th ed. Ch 17 Interpreting the Electrocardiogram
UNDERSTANDING YOUR ECG: A REVIEW
 UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
ECG Interactive Session
 SA HEART 2018 PRE-CONGRESS WORKSHOP 4 OCTOBER 2018 ECG Interactive Session Ashley Chin Cardiologist/Electrophysiologist University of Cape Town Groote Schuur Hospital ECG 1 Which ONE of the following is
SA HEART 2018 PRE-CONGRESS WORKSHOP 4 OCTOBER 2018 ECG Interactive Session Ashley Chin Cardiologist/Electrophysiologist University of Cape Town Groote Schuur Hospital ECG 1 Which ONE of the following is
CSI Skills Lab #5: Arrhythmia Interpretation and Treatment
 CSI 202 - Skills Lab #5: Arrhythmia Interpretation and Treatment Origins of the ACLS Approach: CSI 202 - Skills Lab 5 Notes ACLS training originated in Nebraska in the early 1970 s. Its purpose was to
CSI 202 - Skills Lab #5: Arrhythmia Interpretation and Treatment Origins of the ACLS Approach: CSI 202 - Skills Lab 5 Notes ACLS training originated in Nebraska in the early 1970 s. Its purpose was to
PhD FRCP MESC MEAPCI. Consultant Cardiologist SVT - Supra Ventricular Tachycardia. Coronary Arteries
 SVT - Supra Ventricular Tachycardia Coronary Arteries Overview LMS Supraventricular tachycardia is defined as an abnormally fast heartbeat. It's a describes a group of arrhythmias which all originate from
SVT - Supra Ventricular Tachycardia Coronary Arteries Overview LMS Supraventricular tachycardia is defined as an abnormally fast heartbeat. It's a describes a group of arrhythmias which all originate from
the ECG, 6 mg of intravenous adenosine was administered as a fast bolus through a large bore intravenous cannula in
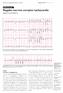 (arrows). Electrocardiography Series Singapore Med.1 2011, 52(3) 146 CME Article Regular narrow complex tachycardia Singh D, Teo S G, Poh K K V Hr JL1 11 VL VF WA, Fig. I ECG shows regular narrow complex
(arrows). Electrocardiography Series Singapore Med.1 2011, 52(3) 146 CME Article Regular narrow complex tachycardia Singh D, Teo S G, Poh K K V Hr JL1 11 VL VF WA, Fig. I ECG shows regular narrow complex
Arrhythmias_for_6_c..docx. Олена Костянтинівна Редько
 Arrhythmias_for_6_c..docx Олена Костянтинівна Редько 2015 Ключові терміни: 3 Зміст Ключові терміни: Arrhythmias 3 3 Ключові терміни: 4 Arrhythmias Ключові терміни: An irregular heart rhythm, Atrial flutter,
Arrhythmias_for_6_c..docx Олена Костянтинівна Редько 2015 Ключові терміни: 3 Зміст Ключові терміни: Arrhythmias 3 3 Ключові терміни: 4 Arrhythmias Ключові терміни: An irregular heart rhythm, Atrial flutter,
Arrhythmias (I) Supraventricular Tachycardias. Disclosures
 Arrhythmias (I) Supraventricular Tachycardias Amy Leigh Miller, MD, PhD Cardiovascular Electrophysiology, Brigham & Women s Hospital Disclosures None Short R-P Tachycardia REGULAR with 1:1 P/R relationship
Arrhythmias (I) Supraventricular Tachycardias Amy Leigh Miller, MD, PhD Cardiovascular Electrophysiology, Brigham & Women s Hospital Disclosures None Short R-P Tachycardia REGULAR with 1:1 P/R relationship
Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014
 Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014 Financial disclosures Consultant Medtronic 3 reasons to evaluate and treat arrhythmias
Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014 Financial disclosures Consultant Medtronic 3 reasons to evaluate and treat arrhythmias
Arrhythmic Complications of MI. Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine
 Arrhythmic Complications of MI Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine Objectives Brief overview -Pathophysiology of Arrhythmia ECG review of typical
Arrhythmic Complications of MI Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine Objectives Brief overview -Pathophysiology of Arrhythmia ECG review of typical
Dr.Binoy Skaria 13/07/15
 Dr.Binoy Skaria binoyskaria@hotmail.com binoy.skaria@heartofengland.nhs.uk 13/07/15 Acknowledgement Medtronic, Google images & Elsevier for slides Natalie Ryan, Events Manager, HEFT- for organising the
Dr.Binoy Skaria binoyskaria@hotmail.com binoy.skaria@heartofengland.nhs.uk 13/07/15 Acknowledgement Medtronic, Google images & Elsevier for slides Natalie Ryan, Events Manager, HEFT- for organising the
Asymptomatic patient with WPW
 Asymptomatic patient with WPW Dimosthenis Avramidis, MD. Arrythmiologist Mitera Children s Hospital Athens Greece Scientific Associate 1st Cardiology Dpt Evangelismos Hospital Athens Greece Preexcitation
Asymptomatic patient with WPW Dimosthenis Avramidis, MD. Arrythmiologist Mitera Children s Hospital Athens Greece Scientific Associate 1st Cardiology Dpt Evangelismos Hospital Athens Greece Preexcitation
Concealed Accessory Pathway in Late Presentation Wolff-Parkinson-White Syndrome
 CASE REPORT Concealed Accessory Pathway in Late Presentation Wolff-Parkinson-White Syndrome Stephanie Rose1, Richard Armstrong2, David Moore2 Third year medicine, Trinity College Dublin Department of Cardiology,
CASE REPORT Concealed Accessory Pathway in Late Presentation Wolff-Parkinson-White Syndrome Stephanie Rose1, Richard Armstrong2, David Moore2 Third year medicine, Trinity College Dublin Department of Cardiology,
Basic Electrophysiology Protocols
 Indian Journal of Cardiology ISSN-0972-1622 2012 by the Indian Society of Cardiology Vol. 15, (3-4), 27-37 [ 27 Review Article Shomu Bohora Assistant Professor, Deptt. of Cardiology, U.N. Mehta Institute
Indian Journal of Cardiology ISSN-0972-1622 2012 by the Indian Society of Cardiology Vol. 15, (3-4), 27-37 [ 27 Review Article Shomu Bohora Assistant Professor, Deptt. of Cardiology, U.N. Mehta Institute
Palpitations and Management of Arrhythmias. Palpitations. Differential Diagnosis. Differential Diagnosis. Differential Diagnosis
 Palpitations and Management of Arrhythmias Fernando Vega, M.D. 7/8/2011 Fernando Vega, M.D. 1 7/8/2011 Fernando Vega, M.D. 2 Palpitations A sensory symptom An unpleasant awareness of the forceful, rapid
Palpitations and Management of Arrhythmias Fernando Vega, M.D. 7/8/2011 Fernando Vega, M.D. 1 7/8/2011 Fernando Vega, M.D. 2 Palpitations A sensory symptom An unpleasant awareness of the forceful, rapid
Dos and Don t in Cardiac Arrhythmia. Case 1 -ECG. Case 1. Management. Emergency Admissions. Reduction of TE risk -CHADS 2 score. Hospital Admissions
 Emergency Admissions Dos and Don t in Cardiac Arrhythmia Tom Wong, MD, FESC Consultant Cardiologist, Honorary Senior Lecturer Royal Brompton & Harefield Hospitals National Heart and Lung Institute, Imperial
Emergency Admissions Dos and Don t in Cardiac Arrhythmia Tom Wong, MD, FESC Consultant Cardiologist, Honorary Senior Lecturer Royal Brompton & Harefield Hospitals National Heart and Lung Institute, Imperial
-RHYTHM PRACTICE- By Dr.moanes Msc.cardiology Assistant Lecturer of Cardiology Al Azhar University. OBHG Education Subcommittee
 -RHYTHM PRACTICE- By Dr.moanes Msc.cardiology Assistant Lecturer of Cardiology Al Azhar University The Normal Conduction System Sinus Node Normal Sinus Rhythm (NSR) Sinus Bradycardia Sinus Tachycardia
-RHYTHM PRACTICE- By Dr.moanes Msc.cardiology Assistant Lecturer of Cardiology Al Azhar University The Normal Conduction System Sinus Node Normal Sinus Rhythm (NSR) Sinus Bradycardia Sinus Tachycardia
Please check your answers with correct statements in answer pages after the ECG cases.
 ECG Cases ECG Case 1 Springer International Publishing AG, part of Springer Nature 2018 S. Okutucu, A. Oto, Interpreting ECGs in Clinical Practice, In Clinical Practice, https://doi.org/10.1007/978-3-319-90557-0
ECG Cases ECG Case 1 Springer International Publishing AG, part of Springer Nature 2018 S. Okutucu, A. Oto, Interpreting ECGs in Clinical Practice, In Clinical Practice, https://doi.org/10.1007/978-3-319-90557-0
Episode 112 Tachydysrhythmias
 Wide & regular tachydysrhythmias Ventricular Tachycardia (VT) vs SVT with aberrancy: Assume VT Episode 112 Tachydysrhythmias With Amal Mattu & Paul Dorion Prepared by Shaun Mehta, July 2018 General Approach
Wide & regular tachydysrhythmias Ventricular Tachycardia (VT) vs SVT with aberrancy: Assume VT Episode 112 Tachydysrhythmias With Amal Mattu & Paul Dorion Prepared by Shaun Mehta, July 2018 General Approach
Supraventricular Arrhythmias. Reading Assignment. Chapter 5 (p17-30)
 Supraventricular Arrhythmias Reading Assignment Chapter 5 (p17-30) The Supraventricular Rhythms In Our Lives Site of Origin Single Events Slow Rates Intermediate Rates Fast Rates (>100 bpm) Sinus Sinus
Supraventricular Arrhythmias Reading Assignment Chapter 5 (p17-30) The Supraventricular Rhythms In Our Lives Site of Origin Single Events Slow Rates Intermediate Rates Fast Rates (>100 bpm) Sinus Sinus
Course Objectives. Proper Lead Placements. Review the ECG print paper. Review the mechanics of the Myocardium. Review basics of ECG Rhythms
 ECG Interpretations Course Objectives Proper Lead Placements Review the ECG print paper Review the mechanics of the Myocardium Review basics of ECG Rhythms How Leads Work The ECG Leads we use are Bipolar
ECG Interpretations Course Objectives Proper Lead Placements Review the ECG print paper Review the mechanics of the Myocardium Review basics of ECG Rhythms How Leads Work The ECG Leads we use are Bipolar
Fast & Slow Tachy & Brady Arrhythmias DAVID STULTZ, MD, FACC KPN HEART & VASCULAR AUGUST 7, 2017
 Fast & Slow Tachy & Brady Arrhythmias DAVID STULTZ, MD, FACC KPN HEART & VASCULAR AUGUST 7, 2017 Normal EKG EKG boxes Heart Rate 1 big box = 200ms 1 small box = 40ms Big Boxes Between QRS complexes Heart
Fast & Slow Tachy & Brady Arrhythmias DAVID STULTZ, MD, FACC KPN HEART & VASCULAR AUGUST 7, 2017 Normal EKG EKG boxes Heart Rate 1 big box = 200ms 1 small box = 40ms Big Boxes Between QRS complexes Heart
ARTICLE. Supraventricular Tachycardia in Infancy. Catherine D. DeAngelis, MD. In most infants, SVT is due to an accessory atrioventricular
 Supraventricular Tachycardia in Infancy Evaluation, Management, and Follow-up Susan P. Etheridge, MD; Victoria E. Judd, MD ARTICLE Background: Supraventricular tachycardia (SVT) occurs frequently in infancy.
Supraventricular Tachycardia in Infancy Evaluation, Management, and Follow-up Susan P. Etheridge, MD; Victoria E. Judd, MD ARTICLE Background: Supraventricular tachycardia (SVT) occurs frequently in infancy.
V. TACHYCARDIAS Rapid rhythm abnormalities
 V. TACHYCARDIAS Rapid rhythm abnormalities Tachyarrhythmias currently account for up to 350,000 deaths annually in the US. In addition to these clearly dangerous rhythm disturbances, other forms of more
V. TACHYCARDIAS Rapid rhythm abnormalities Tachyarrhythmias currently account for up to 350,000 deaths annually in the US. In addition to these clearly dangerous rhythm disturbances, other forms of more
UNDERSTANDING ELECTROPHYSIOLOGY STUDIES
 UNDERSTANDING ELECTROPHYSIOLOGY STUDIES Testing and Treating Your Heart s Electrical System A Problem with Your Heart Rhythm The speed and pattern of a heartbeat is called the heart rhythm. The rhythm
UNDERSTANDING ELECTROPHYSIOLOGY STUDIES Testing and Treating Your Heart s Electrical System A Problem with Your Heart Rhythm The speed and pattern of a heartbeat is called the heart rhythm. The rhythm
Ventricular Preexcitation (Wolff-Parkinson-White Syndrome and Its Variants) 柯文欽醫師 國泰綜合醫院心臟內科主治醫師 臺北醫學大學講師
 Ventricular Preexcitation (Wolff-Parkinson-White Syndrome and Its Variants) 柯文欽醫師 國泰綜合醫院心臟內科主治醫師 臺北醫學大學講師 The Nobel Prize in Physiology or Medicine 1924 "for his discovery of the mechanism of the electrocardiogram"
Ventricular Preexcitation (Wolff-Parkinson-White Syndrome and Its Variants) 柯文欽醫師 國泰綜合醫院心臟內科主治醫師 臺北醫學大學講師 The Nobel Prize in Physiology or Medicine 1924 "for his discovery of the mechanism of the electrocardiogram"
Cardiac Arrhythmias. Cathy Percival, RN, FALU, FLMI VP, Medical Director AIG Life and Retirement Company
 Cardiac Arrhythmias Cathy Percival, RN, FALU, FLMI VP, Medical Director AIG Life and Retirement Company The Cardiovascular System Three primary functions Transport of oxygen, nutrients, and hormones to
Cardiac Arrhythmias Cathy Percival, RN, FALU, FLMI VP, Medical Director AIG Life and Retirement Company The Cardiovascular System Three primary functions Transport of oxygen, nutrients, and hormones to
Concise Review for Primary-Care Physicians
 Concise Review for Primary-Care Physicians Narrow QRS Complex Tachycardias STEPHEN J. PIEPER, M.D., AND MARSHALL S. STANTON, M.D. Regular narrow QRS complex tachycardias are a common problem encountered
Concise Review for Primary-Care Physicians Narrow QRS Complex Tachycardias STEPHEN J. PIEPER, M.D., AND MARSHALL S. STANTON, M.D. Regular narrow QRS complex tachycardias are a common problem encountered
Arrhythmia 341. Ahmad Hersi Professor of Cardiology KSU
 Arrhythmia 341 Ahmad Hersi Professor of Cardiology KSU Objectives Epidemiology and Mechanisms of AF Evaluation of AF patients Classification of AF Treatment and Risk stratification of AF Identify other
Arrhythmia 341 Ahmad Hersi Professor of Cardiology KSU Objectives Epidemiology and Mechanisms of AF Evaluation of AF patients Classification of AF Treatment and Risk stratification of AF Identify other
I have nothing to disclose.
 I have nothing to disclose. Antiarrhythmic Therapy in Pregnancy Prof. Ali Oto,MD,FESC,FACC,FHRS Department of Cardiology Hacettepe University,Faculty of Medicine Ankara Arrhythmias in pregnancy An increased
I have nothing to disclose. Antiarrhythmic Therapy in Pregnancy Prof. Ali Oto,MD,FESC,FACC,FHRS Department of Cardiology Hacettepe University,Faculty of Medicine Ankara Arrhythmias in pregnancy An increased
Practical Approach to Arrhythmias
 Outline Practical Approach to Arrhythmias Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Conduction System ECG Acquisition ECG Interpretation Heart rate Rhythm Arrhythmias Tachyarrhythmias Supraventricular
Outline Practical Approach to Arrhythmias Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Conduction System ECG Acquisition ECG Interpretation Heart rate Rhythm Arrhythmias Tachyarrhythmias Supraventricular
CORONARY ARTERIES. LAD Anterior wall of the left vent Lateral wall of left vent Anterior 2/3 of interventricluar septum R & L bundle branches
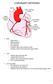 CORONARY ARTERIES RCA Right atrium Right ventricle SA node 55% AV node 90% Posterior wall of left ventricle in 90% Posterior third of interventricular septum 90% LAD Anterior wall of the left vent Lateral
CORONARY ARTERIES RCA Right atrium Right ventricle SA node 55% AV node 90% Posterior wall of left ventricle in 90% Posterior third of interventricular septum 90% LAD Anterior wall of the left vent Lateral
Rate and Rhythm Control of Atrial Fibrillation
 Rate and Rhythm Control of Atrial Fibrillation April 21, 2017 춘계심혈관통합학술대회 Jaemin Shim, MD, PhD Arrhythmia Center Korea University Anam Hospital Treatment of AF Goal Reducing symptoms Preventing complication
Rate and Rhythm Control of Atrial Fibrillation April 21, 2017 춘계심혈관통합학술대회 Jaemin Shim, MD, PhD Arrhythmia Center Korea University Anam Hospital Treatment of AF Goal Reducing symptoms Preventing complication
PATIENT WITH ARRHYTHMIA IN DENTIST S OFFICE. Małgorzata Kurpesa, MD., PhD. Chair&Department of Cardiology
 PATIENT WITH ARRHYTHMIA IN DENTIST S OFFICE Małgorzata Kurpesa, MD., PhD. Chair&Department of Cardiology Medical University of Łódź The heart is made up of four chambers Left Atrium Right Atrium Left Ventricle
PATIENT WITH ARRHYTHMIA IN DENTIST S OFFICE Małgorzata Kurpesa, MD., PhD. Chair&Department of Cardiology Medical University of Łódź The heart is made up of four chambers Left Atrium Right Atrium Left Ventricle
«Aσθενής με ασυμπτωματικό WPW και παροξυσμική κολπική μαρμαρυγή» Χάρης Κοσσυβάκης Επιμελητής A Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ.
 «Aσθενής με ασυμπτωματικό WPW και παροξυσμική κολπική μαρμαρυγή» Χάρης Κοσσυβάκης Επιμελητής A Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ» the primary mechanism of SCD in patients with WPW is the rapid conduction
«Aσθενής με ασυμπτωματικό WPW και παροξυσμική κολπική μαρμαρυγή» Χάρης Κοσσυβάκης Επιμελητής A Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ» the primary mechanism of SCD in patients with WPW is the rapid conduction
Lecture outline. Electrical properties of the heart. Automaticity. Excitability. Refractoriness. The ABCs of ECGs Back to Basics Part I
 Lecture outline The ABCs of ECGs Back to Basics Part I Meg Sleeper VMD, DACVIM (cardiology) University of Florida Veterinary School Electrical properties of the heart Action potentials Normal intracardiac
Lecture outline The ABCs of ECGs Back to Basics Part I Meg Sleeper VMD, DACVIM (cardiology) University of Florida Veterinary School Electrical properties of the heart Action potentials Normal intracardiac
Pediatrics. Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment. Overview
 Pediatrics Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment See online here The most common form of cardiac arrhythmia in children is sinus tachycardia which can be caused by
Pediatrics Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment See online here The most common form of cardiac arrhythmia in children is sinus tachycardia which can be caused by
The Electrocardiogram
 The Electrocardiogram Chapters 11 and 13 AUTUMN WEDAN AND NATASHA MCDOUGAL The Normal Electrocardiogram P-wave Generated when the atria depolarizes QRS-Complex Ventricles depolarizing before a contraction
The Electrocardiogram Chapters 11 and 13 AUTUMN WEDAN AND NATASHA MCDOUGAL The Normal Electrocardiogram P-wave Generated when the atria depolarizes QRS-Complex Ventricles depolarizing before a contraction
How To Think About Rhythms and Conduction
 How To Think About Rhythms and Conduction Frank Yanowitz, MD Professor of Medicine (Cardiology) University of Utah School of Medicine Medical Director, IHC ECG Services Intermountain Healthcare http://ecg.utah.edu
How To Think About Rhythms and Conduction Frank Yanowitz, MD Professor of Medicine (Cardiology) University of Utah School of Medicine Medical Director, IHC ECG Services Intermountain Healthcare http://ecg.utah.edu
Wolff-Parkinson-White Syndrome
 Wolff-Parkinson-White Syndrome www.consultant360.com /articles/wolff-parkinson-white-syndrome A 37-year-old woman presented to the office with intermittent dizziness, palpitations, and multiple syncopal
Wolff-Parkinson-White Syndrome www.consultant360.com /articles/wolff-parkinson-white-syndrome A 37-year-old woman presented to the office with intermittent dizziness, palpitations, and multiple syncopal
In certain cases of supraventricular
 Case Report Hellenic J Cardiol 2013; 54: 469-473 A Tachycardia with Varying QRS Morphology and RP Intervals: Differential Diagnosis and Therapy Socrates Korovesis, Eleftherios Giazitzoglou, Demosthenes
Case Report Hellenic J Cardiol 2013; 54: 469-473 A Tachycardia with Varying QRS Morphology and RP Intervals: Differential Diagnosis and Therapy Socrates Korovesis, Eleftherios Giazitzoglou, Demosthenes
Dysrhythmias: Diagnosis and management
 15 Dysrhythmias: Diagnosis and management Wanda C. Miller-Hance Kathryn K. Collins Introduction The practice of pediatric cardiac anesthesia has evolved significantly over the years, expanding beyond the
15 Dysrhythmias: Diagnosis and management Wanda C. Miller-Hance Kathryn K. Collins Introduction The practice of pediatric cardiac anesthesia has evolved significantly over the years, expanding beyond the
Arrhythmia Management Joshua M. Cooper, MD, FHRS, FACC
 Arrhythmia Management Joshua M. Cooper, MD, FHRS, FACC Professor of Medicine Director of Cardiac Electrophysiology Temple University Health System Plumbing Electrical System Bradyarrhythmias Sinus Node
Arrhythmia Management Joshua M. Cooper, MD, FHRS, FACC Professor of Medicine Director of Cardiac Electrophysiology Temple University Health System Plumbing Electrical System Bradyarrhythmias Sinus Node
SHOCK THE PATIENT. Disclosures. Goals of the Talk. Tachyarrhythmias- Unstable 11/7/2017
 Disclosures Common Heart Rhythms in the Hospital Research Support: NIH, PCORI, Medtronic, Cardiogram Consulting: InCarda, Johnson & Johnson, Lifewatch Equity: InCarda Gregory M Marcus, MD, MAS Associate
Disclosures Common Heart Rhythms in the Hospital Research Support: NIH, PCORI, Medtronic, Cardiogram Consulting: InCarda, Johnson & Johnson, Lifewatch Equity: InCarda Gregory M Marcus, MD, MAS Associate
Atrioventricular (AV) Nodal Reentry Associated with 2:1 Infra-His Conduction Block during Tachycardia in a Patient with AV Nodal Triple Pathways
 Atrioventricular (AV) Nodal Reentry Associated with 2:1 Infra-His Conduction Block during Tachycardia in a Patient with AV Nodal Triple Pathways Haruhiko ABE, M.D., Takashi OHKITA, M.D., Masasuke FUJITA,
Atrioventricular (AV) Nodal Reentry Associated with 2:1 Infra-His Conduction Block during Tachycardia in a Patient with AV Nodal Triple Pathways Haruhiko ABE, M.D., Takashi OHKITA, M.D., Masasuke FUJITA,
Knowing is not enough; we must apply. Willing is not enough; we must do.
 Cardiovascular Boot Camp Basic Training Day 2: Cardiac Arrhythmias and Emergency Treatment Overview Cardiac Arrhythmias: Physiologic Links to Recognition and Management NTI 2014 Denver 2014 Karen Marzlin
Cardiovascular Boot Camp Basic Training Day 2: Cardiac Arrhythmias and Emergency Treatment Overview Cardiac Arrhythmias: Physiologic Links to Recognition and Management NTI 2014 Denver 2014 Karen Marzlin
Management of ATRIAL FIBRILLATION. in general practice. 22 BPJ Issue 39
 Management of ATRIAL FIBRILLATION in general practice 22 BPJ Issue 39 What is atrial fibrillation? Atrial fibrillation (AF) is the most common cardiac arrhythmia encountered in primary care. It is often
Management of ATRIAL FIBRILLATION in general practice 22 BPJ Issue 39 What is atrial fibrillation? Atrial fibrillation (AF) is the most common cardiac arrhythmia encountered in primary care. It is often
Arrhythmias and Heart Failure Dr Chris Lang Consultant Cardiologist and Electrophysiologist Royal Infirmary of Edinburgh
 Arrhythmias and Heart Failure Dr Chris Lang Consultant Cardiologist and Electrophysiologist Royal Infirmary of Edinburgh Arrhythmias and Heart Failure Ventricular Supraventricular VT/VF Primary prevention
Arrhythmias and Heart Failure Dr Chris Lang Consultant Cardiologist and Electrophysiologist Royal Infirmary of Edinburgh Arrhythmias and Heart Failure Ventricular Supraventricular VT/VF Primary prevention
Chapter 26. Media Directory. Dysrhythmias. Diagnosis/Treatment of Dysrhythmias. Frequency in Population Difficult to Predict
 Chapter 26 Drugs for Dysrythmias Slide 33 Slide 35 Media Directory Propranolol Animation Amiodarone Animation Upper Saddle River, New Jersey 07458 All rights reserved. Dysrhythmias Abnormalities of electrical
Chapter 26 Drugs for Dysrythmias Slide 33 Slide 35 Media Directory Propranolol Animation Amiodarone Animation Upper Saddle River, New Jersey 07458 All rights reserved. Dysrhythmias Abnormalities of electrical
Cardiac Implanted Electronic Devices Pacemakers, Defibrillators, Cardiac Resynchronization Devices, Loop Recorders, etc.
 Cardiac Implanted Electronic Devices Pacemakers, Defibrillators, Cardiac Resynchronization Devices, Loop Recorders, etc. The Miracle of Living February 21, 2018 Matthew Ostrom MD,FACC,FHRS Division of
Cardiac Implanted Electronic Devices Pacemakers, Defibrillators, Cardiac Resynchronization Devices, Loop Recorders, etc. The Miracle of Living February 21, 2018 Matthew Ostrom MD,FACC,FHRS Division of
