Title page. Vulnerable carotid arterial plaque causing repeated ischemic stroke can be detected with
|
|
|
- Georgina Jennings
- 6 years ago
- Views:
Transcription
1 1 Title page Title: Vulnerable carotid arterial plaque causing repeated ischemic stroke can be detected with B-mode ultrasonography as a mobile component: Jellyfish sign Authors: Shinji Kume, RT; Seiji Hama, MD, PhD; Kanji Yamane, MD, PhD; Seishi Wada, MD, PhD; Toshihiro Nishida, MD, PhD; Kaoru Kurisu, MD, PhD Institutions: Departments of Radiology (S. Kume), Neurosurgery (S. Hama) and Surgery (S. Wada), Hibino Hospital; the Departments of Neurosurgery (K. Yamane) and Pathology (T. Nishida), Chugoku Rousai Hospital; and the Department of Neurosurgery (K. Kurisu), Graduate School of Biomedical Science, Hiroshima University. Address correspondence to: Shinji Kume, Radiological Technologist (RT): Department of Radiology, Hibino Hospital, Tomo 7955, Numata-cho, Asaminami-ku, Hiroshima , Japan. Tel: ; Fax: , shinji.kume7@gmail.com Running title: Jellyfish carotid plaque and stroke Word count: 4155 words (Abstract: 236 words, main text: 3919 words)
2 2 Abstract Mobile plaque is associated with increased risk of ischemic stroke, but definitions have remained unclear. We have previously reported that carotid ultrasonography can detect the mobile component of the carotid plaque surface, which rises and falls in a manner inconsistent with arterial pulsatile wall motion (Jellyfish sign). However, clinical and pathological features of Jellyfish sign remain unclear. Subjects comprised 165 patients with carotid plaque and degree of area stenosis 50% on ultrasonography. Using magnetic resonance imaging, we quantified intraplaque hemorrhage (IPH) and defined ischemic stroke in each patient. Fifteen surgical specimens were obtained by carotid endarterectomy, and pathological features (area of fibrous cap and intraplaque atheromatous lesion) were compared with ultrasonographic plaque surface movement rate. Carotid plaques with IPH were seen in 78 cases, with Jellyfish sign in 31 cases. Jellyfish sign was not detected in patients without IPH. In these 15 patients, the fibrous cap covered the atheromatous lesion, and cap thickness correlated negatively with Jellyfish-positive plaque surface movement rate. Kaplan-Meier and Cox multiple regression analysis demonstrated that the most important predictor of ischemic stroke during follow-up is Jellyfish sign, not IPH. Stroke events in patients with Jellyfish sign repeated within a short interval after diagnosis. Jellyfish sign on ultrasonography is a
3 3 sign of high-risk plaque vulnerability, suggesting rupture of the fibrous cap associated with release of thrombogenic factors into the arterial lumen, and resulting in repeated ischemic stroke during a short interval after diagnosis. Key words: Jellyfish sign, mobile plaque, plaque rupture, stroke, ultrasonography
4 4 Introduction Ischemic stroke is frequently caused by cerebral embolism from a vulnerable atherosclerotic plaque, and is thought to be related to the intrinsic composition such as size of the lipid core, thinning or rupture of the fibrous cap and the presence of intraplaque hemorrhage (IPH) [1, 16-18, 21-23]. Although the degree of stenosis offers a valid marker of stroke risk [14, 20, 21], these vulnerable plaques have a high predictive value for stroke, so identification of high-risk plaque may improve risk assessment and improve prognosis for stroke patients. Mobile or floating plaque is easily detected by routine carotid ultrasonography and is associated with increased risk of ischemic stroke [11, 15, 25]. Mobile plaque is thus a form of vulnerable plaque. To date, the definition of mobile plaque has been unclear and confused [11, 15, 25]. We have previously examined mobile plaques from the perspective of the type of motion [12]. In some cases, a section of carotid plaque surface rose and fell in a manner inconsistent with arterial pulsatile wall motion [12]. This motion did not represent floating plaque and resembled the motion of a jellyfish, so we termed this ultrasound finding as the Jellyfish sign, to be distinguished from floating plaque. Patients with Jellyfish sign frequently experienced ischemic stroke within a short interval from diagnosis, so this sign was considered to represent a strong risk
5 5 factor for stroke. However, the previous study was a case report, and further investigations were needed to examine whether Jellyfish sign could be used as a predictor of recurrent ischemic strokes. The aim of this study was to prospectively examine whether patients with carotid plaque showing Jellyfish sign under B-mode ultrasonography are more likely to develop ischemic stroke than those without Jellyfish sign. This study represents the first attempt to examine mobile plaque showing Jellyfish sign from the perspective of clinical, radiological and pathological findings. Materials and methods Subjects This study was performed at Hibino Hospital and Chugoku Rousai Hospital, and approval for this prospective study was obtained from the institutional ethics committees of both hospitals. Informed consent was obtained from all patients prior to enrolment. Subjects included in this study were selected from a consecutive series of 695 patients referred for carotid ultrasonographic examination at Hibino Hospital between January 2003 and December Entry criteria included: 1) carotid area stenosis 50% using established Duplex scanning criteria [9]; 2) identification of the
6 6 existence of IPH using magnetic resonance imaging (MRI); 3) serial follow-up using MRI until surgery or >6 months without surgery. Exclusion criteria included: 1) degree of carotid stenosis <50% (n=422); 2) inability to perform MRI (n=28); 3) inability to perform ultrasonography due to the existence of acoustic shadow (calcification) or multiple reflections (n=64); and 4) hemorrhagic stroke events (n=7). Patients with bilateral hemispheric symptoms or known cardiac mural thrombus (as verified on echocardiography) were also excluded because of suspected cardioembolic origin (n=9). The remaining 165 patients were included in the study. Among these, 32 patients underwent carotid endarterectomy (CEA) and 4 cases received carotid artery stenting (CAS) after providing informed consent during follow-up. As shown in Table 1, a total of 18 patients (10.9%) suffered from ischemic stroke events and 34 patients (20.6%) experienced TIA. Risk Factors We assessed vascular risk factors based on the following. Hypertension was defined as a history of using antihypertensive agents, systolic blood pressure >140 mmhg, or diastolic pressure >90 mmhg after the first ischemic stroke event or at the first clinic attendance. Diabetes mellitus was defined as the use of oral hypoglycemic
7 7 agents or insulin, fasting glucose level >126 mg/dl or glycosylated hemoglobin level >6.4%. Hyperlipidemia was defined as the use of antihyperlipedemic agents or serum cholesterol level >220 mg/dl. Current smoking status was obtained, along with history of atrial fibrillation. Coronary artery disease was defined as a history of angina pectoris or myocardial infarction. Ultrasound Examination We used a LOGIQ 7 system (GE Yokogawa Medical Systems, Tokyo, Japan) with a 3-10 MHz broadband linear array transducer. Area of stenosis was determined at the most advanced lesion by routine Doppler criteria [9]. Jellyfish sign of the carotid arterial plaque was defined as the presence of mobile components that rose and fell in a manner inconsistent with arterial pulsatile wall motion, and was evaluated under high-resolution B-mode ultrasonography (Supplementary Movie 1, 2). Examinations were performed by an experienced ultrasonographer and recorded as a digital movie. Data were reviewed by a vascular surgeon and a neurosurgeon, both of whom were blinded to the clinical data. The rate of surface movement of Jellyfish-positive plaque (Jellyfish motion rate) was estimated using B-mode ultrasonography (Fig. 1). Distances from the adventitia to the
8 8 top (a) and from the top to the bottom (b) of the mobile part, appearing as a rising and falling motion, were examined and applied as follows: Jellyfish motion rate = b/a 100 (%). MRI Protocol We performed carotid plaque imaging using a 1.5-T MRI scanner (Signa EXICTE Xl, version 11.0; GE Healthcare) equipped with an 8-cm-diameter surface coil. All participants were assessed using MRI studies including a diffusion-weighted sequence, fluid-attenuated inversion recovery, and magnetic resonance angiography (MRA) at the first clinic attendance. MRI using this protocol during follow-up confirmed all strokes to be ischemic. IPH status of the carotid arterial plaque was assessed by MRI using a 2-dimensional spin echo sequence (echo time, 14 ms; repetition time, 400 ms; bandwidth, khz; field of view, 14 cm; slice thickness, 2 mm; matrix, ; fat suppression) and saturation pulse to eliminate signal from inflow blood (Superior and Inferior). To clarify the border between lumen and plaque surface, we checked electrocardiogram-gated black-blood T2-weighted imaging. IPH was diagnosed using T1-weighted imaging if signal intensity of the plaque exceeded that of adjacent skeletal muscle. Presence of IPH
9 9 was determined by consensus between two experienced researchers blinded to patient information. Histopathology Excised plaques were fixed in formalin immediately after removal. Specimens were cut into 3-mm intervals along the length of the plaque for embedding in paraffin wax. Formalin-fixed, paraffin-embedded tissue blocks were serially sectioned at 3 μm onto slides and stained with hematoxylin and eosin (HE), and Masson trichrome for cellular components, neutral lipid, calcification, fibrous tissue and thrombus. The proportion of fibrous cap and intraplaque atheromatous elements (including hemorrhage, lipid, cell components and thrombus) in Jellyfish-positive patients was evaluated pathologically as a percentage of the entire plaque body. HE and Masson trichrome staining of plaque was recorded using digital photographs, tracing the outlines of each element, and measuring the area (in pixels) of each traced area using Adobe Photoshop CS3 extended (Adobe Systems, San Jose, CA). The proportion of each element was described as: (1) Proportion of fibrous cap (fibrous cap coverage rate) = area of fibrous cap (pixels) / area of whole plaque (pixels).
10 10 (2) Proportion of intraplaque atheromatous lesion (atheromatous lesion rate) = area of atheromatous lesion (pixels) / area of whole plaque (pixels). Fibrous cap thickness was examined at 9 points at equal intervals from shoulder to shoulder of the mobile part and the adjacent non-mobile part in Jellyfish-positive plaque. Average thickness was calculated, and correlations between average cap thicknesses of the mobile and non-mobile parts were examined. End Points Neurological symptoms that occurred during observation were noted at each visit every 1-6 months. Neurological symptoms were subsequently further evaluated by MRI, and ischemic stroke was diagnosed. The end point of the study was ischemic stroke that developed ipsilateral to the relevant carotid stenosis. Statistical Analysis Numerical values are reported as mean ± standard deviation. Baseline characteristics, vascular risk factors and ultrasound and MRI findings were compared among groups (IPH-negative vs. -positive or Jellyfish-negative vs. -positive). Statistical analyses were
11 11 performed as nonparametric analysis using Fisher s exact test for categorical variables and the Mann-Whitney U test for continuous variables. For correlative analysis, the Spearman rank correlation coefficient (ρ) was calculated. Interobserver agreement regarding presence of the Jellyfish sign was assessed using the κ coefficient for two observers (neurosurgeon S.H. and vascular surgeon S.W.). The effect of IPH and/or Jellyfish sign on rate of recurrent cerebral ischemic stroke was examined using Kaplan-Meier and Cox multiple regression analysis. The follow-up period was the time from vascular assessment to recurrent ischemia. Patients were censored if they had not suffered from ischemic stroke as of last follow-up or if they had undergone CEA/CAS before suffering recurrent ischemic stroke. Jellyfish sign was not identified among patients without IPH, so Kaplan-Meier analysis was performed after categorizing 3 groups: IPH-negative (IPH-); IPH-positive and Jellyfish-negative (IPH+JF-); and IPH-positive and Jellyfish-positive (IPH+JF+). Clinical features of recurrent ischemic stroke were compared among groups (IPH-, IPH+/JF-, IPH+/JF+) using the Kruskal-Wallis test for nonparametric analysis. All analyses were performed using the Statistical Package for Social Sciences SPSS for Windows version 16.0 software (Chicago, Illinois).
12 12 Results Baseline Structures in all Patients Table 1 shows baseline data for all patients and groups. MRI demonstrated IPH in 78 cases. Jellyfish sign was detected in 31 IPH-positive cases, but was not detected at all among IPH-negative cases. Jellyfish sign might thus be solely associated with IPH. Patients were divided into 2 groups according to the presence of IPH, with 87 patients in the IPH-negative group and 78 patients in the IPH-positive group. The 2 groups were matched for hypertension, hyperlipemia, diabetes mellitus, arterial fibrillation, history of ischemic heart disease and ischemic stroke and use of antihypertensive agents, antihyperlipidemic agents and aspirin. However, patients with IPH were older and showed greater stenosis of the carotid artery, and rates of smoking, male sex, TIA presentation, operation and statin use were much higher than in those without IPH. Jellyfish sign was not seen in the IPH-negative group, so the IPH-positive group was divided into 2 subgroups according to presence of the Jellyfish sign, with 31 patients in the Jellyfish-positive group and 47 patients in the Jellyfish-negative group. These 2 groups were matched for age, outcome, and risk factors other than history of stroke (p=0.019). Jellyfish-positive patients were older, with a less frequent history of stroke or operation than in patients without Jellyfish sign. These risk factors were thus thought to
13 13 have no marked influence on outcome statistics between Jellyfish-positive and -negative patient groups. Ultrasonographic and MRI Findings MRI and angiographic findings of Patient 1 with Jellyfish sign are shown in Figure 2. Diffusion-weighted imaging of MRI revealed multiple small lesions in the territory of the left middle cerebral artery (Fig. 2A). MRA (Fig. 2B) demonstrated stenosis. MRI plaque imaging (T1-weighted imaging) showed that signal intensity of the plaque exceeded that of adjacent skeletal muscle, suggesting IPH (Fig. 2C). Carotid ultrasonography demonstrated stenosis with the carotid plaque, which included the mobile component (Fig. 2D, arrow). This component rose and fell in a manner inconsistent with arterial pulsatile wall motion (Fig. 2E, illustration; Fig. 2F, montage view; Supplementary Movie 1), showing Jellyfish sign. The κ coefficient for interobserver agreement on Jellyfish sign positivity was acceptable, at Pathological Findings Figure 3 shows the pathological findings for Patient 1 with Jellyfish sign. The Jellyfish sign-positive part (Fig. 3B, C) showed a thin and ruptured fibrous cap overlying the
14 14 cavity, which included free blood cells and fragments of atheroma (Fig. 3E). However, the adjacent non-mobile element (not showing Jellyfish sign; Fig. 3D) was lined by a thickened fibrous cap covering atheromatous lesion including hemorrhage, lipid and cell components. Case 1 also showed that the intraplaque atheromatous lesion communicated with the lumen through an endothelialized fissure (Fig. 3F), suggesting that this fissure was not induced by any mechanical artifact of surgery, but instead caused over time by rupture of the fibrous cap. Another case with Jellyfish sign (Fig. 4, Supplementary Movie 2) also showed the same trend: the Jellyfish-positive part lined with thinning and disrupted fibrous cap, and the Jellyfish-negative part lined with thickened fibrous cap. The atheromatous lesion was underlying both Jellyfish-positive and -negative parts. These findings therefore suggest that the Jellyfish sign is associated with fibrous cap thinning and rupture. Correlation between ultrasonographic plaque surface motion and pathological features From case presentations, the vulnerability of plaque including intraplaque hemorrhage and rupture was thought to be correlated with Jellyfish sign. We thus calculated the
15 15 degree of plaque surface motion of the Jellyfish-positive part, and examined the correlation between ultrasonographic surface motion and pathological features. The shapes of fibrous caps in this pathological study were irregular and partially thinning or ruptured, and thickness was difficult to measure correctly. We therefore examined fibrous cap thinning by measuring the area of fibrous cap and calculating the fibrous cap coverage rate. Eighteen Jellyfish-positive patients (9 cases after onset of ischemic stroke and 9 cases before onset of ischemic stroke during study follow-up) underwent operation. Among these 18 surgical specimens of Jellyfish-positive plaque, area of the plaque structures could not be calculated in 3 specimens due to blow out during surgery and formalin fixation. The remaining 15 specimens were thus used for examination and estimation. Spearman coefficient analysis showed a significant negative correlation between plaque surface motion and fibrous cap coverage rate (Fig. 5). However, intraplaque atheromatous lesion rate did not correlate with plaque motion rate. The smaller the fibrous cap coverage rate, the larger the surface motion rates of the Jellyfish sign. Examination of fibrous cap coverage rate is not particulatly common, and fibrous cap thickness is usually measured instead. We therefore also examined fibrous cap thickness of the mobile part and adjacent non-mobile part of the Jellyfish-positive plaque. The
16 16 results resembled those for fibrous cap coverage rate, with the mobile part showing greater thinning than the non-mobile part (Mann-Whitney, p<0.0001; Fig. 6). The Jellyfish sign thus appears closely correlated with thinning of the fibrous cap. Kaplan-Meier Analysis of Recurrent Ischemic Stroke with or without IPH and Jellyfish Sign To determine whether IPH or Jellyfish sign offers a better predictor of ischemic stroke, we first performed Kaplan-Meier analysis for the incidence of ipsilateral ischemic stroke events. Fig. 7 demonstrates that event-free survival was much higher in Jellyfish-negative groups (IPH- and IPH+JF-) than in the Jellyfish-positive group (IPH+JF+) (log rank, p<0.001). Interestingly, if the Jellyfish sign was negative, the incidence of ischemic stroke for the IPH-positive group was almost equal to that of the IPH-negative group (p=0.437). This suggests that the more important predictive factor for ischemic stroke is not IPH, but the Jellyfish sign. Cox Multiple Regression Analysis Cox multiple regression analysis was used to clarify which variables, including area stenosis, IPH, Jellyfish sign, smoking, hypertension, diabetes, hyperlipemia, arterial
17 17 fibrillation, history of ischemic heart disease and ischemic stroke and medications, contribute significantly to prediction of ipsilateral ischemic stroke (Table 2). A highly significant difference was obtained from Jellyfish sign (p<0.0001). Hypertension (p=0.068) and use of antihypertensive agents (p=0.081) also tended to predict ischemic stroke, whereas IPH showed no such tendency (p=0.631). Clinical Features of Recurrent Ischemic Stroke with or without Jellyfish Sign We estimated the difference for recurrent features of ischemic stroke with or without IPH or Jellyfish sign (Table 3). The ischemic stroke events with Jellyfish sign during follow-up was much higher than that without Jellyfish sign. The interval between diagnosis and onset of first ischemic stroke event in patients with Jellyfish sign was shorter (frequently within 1 week after diagnosis) than in patients without Jellyfish sign. Of note was the fact that repeated ischemic stroke events occurred much more frequently in patients with Jellyfish sign than in patients without Jellyfish sign. Carotid arterial plaque with Jellyfish sign thus appears to have a high risk for repeated recurrence of ischemic stroke within a short interval after diagnosis.
18 18 Discussion Our study appears to be the first to describe an ultrasonographic and clinicopathological series of patients with >50% carotid area stenosis demonstrating that ultrasonographic Jellyfish sign (a kind of mobile plaque, not representing a floating plaque) associated with IPH of carotid plaque is one of the major determinants of ischemic stroke in patients affected by carotid atherosclerotic disease. Randomized controlled trials have demonstrated the benefit of performing CEA in patients with symptomatic high-grade carotid stenosis [2, 8]. Previous studies have also demonstrated that ischemic stroke is frequently caused by thromboembolism from an atherosclerotic plaque to cerebral vessels [14, 16-18, 21-23]. Although the degree of carotid arterial stenosis is a valid marker of stroke risk, identification of high-risk plaque features other than stenosis may improve risk assessment and allow for targeted intervention. Eliasziw et al. [7] analyzed pooled data from the North American Symptomatic Carotid Endarterectomy Trial (NASCET) and reported that patients who experienced hemispheric TIA related to internal carotid artery disease showed a high risk of stroke in the first few days after TIA. They also showed that risk of early stroke was unaffected by the degree of internal carotid artery stenosis. That result might be consistent with our present data that the Jellyfish-positive carotid plaque led to considerably increased
19 19 frequency of repeated ipsilateral multiple ischemic strokes during a short interval (within 1 weeks, 31.3% of patients suffered ischemic stroke during follow-up) after last cerebrovascular event. Jellyfish sign might be an important sign for plaque vulnerability. Patients with the Jellyfish sign should thus be considered at the earliest possible opportunity for surgery. At this point, the question must be asked, what is the Jellyfish sign? The pathophysiological significance of altered plaque surface motion in symptomatic carotid artery plaques remains yet to be elucidated. Meairs et al. [15] examined plaque surface motion using 4-dimensional ultrasonography and suggested that maximal discrepant surface velocity (MDSV) was significantly higher in symptomatic plaques than in asymptomatic plaques (P<0.001). This disparity in focal movement on the plaque surface among symptomatic patients was thought to be similar to the Jellyfish sign. They speculated that such motion patterns are related to dynamic interactions between plaque geometry, plaque composition and focal hemodynamic alterations, analogous to experimental studies on plaque rupture in which pressure loading is used to identify asymmetrical plaque movement before fissuring [19]. The present data also suggest that the thinnest region of fibrous cap induced plaque surface motion, as the Jellyfish sign. Given these observations, motion changes in plaque surface, such as
20 20 Jellyfish sign, may be localized to vulnerable areas of the plaque, particularly the area of thinnest and/or disrupted fibrous cap on the carotid plaque. A thin or ruptured fibrous cap is well known as an important morphological component of vulnerable atherosclerotic plaque [17, 18, 21, 22, 26]. Many previous studies demonstrated that thrombosis associated with plaque rupture is one of the major determinants of ischemic stroke in patients affected by carotid atherosclerotic disease [17, 18, 21, 22, 26]. Carr et al. [3] demonstrated that IPH is highly associated with plaque rupture, suggesting that IPH may play a role in thinning, weakening and rupture of the fibrous cap. Other studies have also reported that IPH and a large lipid core are strongly associated with both a thin cap and cap rupture [16, 17, 23]. Constantinides [4] originally suggested that hemorrhage into a plaque occurs from cracks or fissures originating from the luminal surface. Davies [5] later defined plaque fissure as an eccentric, intraplaque hemorrhage with fibrin deposition within the necrotic core from an entry into the plaque from the lumen. Fissuring of the fibrous cap occurs at the thinnest portion, typically at the shoulder region [13], thereby allowing the entry of blood into the necrotic core. The fibrous cap covers the necrotic core and separates this collection of cellular debris and cholesterol clefts from the arterial lumen [24]. Disruption of this fibrous cap (plaque rupture) thus leads to the release of
21 21 thrombogenic debris from the necrotic core into the lumen [21, 22, 24]. In this study, every Jellyfish sign was associated with IPH. Pathologically, the Jellyfish-positive part of the plaque was covered with thinning and disrupted fibrous cap, overlying the atheromatous lesion, including lipid, hematoma, cell component and thrombosis. Rupture of the fibrous cap allows dissection of blood from the lumen into the lipid pool of the plaque, resulting in the formation of intraplaque hemorrhage. This blood inflow into the plaque pushes contents of the necrotic core into the arterial lumen through the rupture site of the fibrous cap, and this released debris may thus become thrombogenic, resulting in multiple, repeated ipsilateral ischemic strokes. The Jellyfish sign was thus thought to demonstrate plaque rupture accompanied by repeated and multiple ischemic strokes. In this study, the rate of recurrent ischemic stroke events showed no correlation with the Jellyfish motion rate (data not shown), so the actual presence of the Jellyfish sign, rather than the degree of motion seen with the Jellyfish sign, represented the important indicator of high risk for ischemic stroke events. Moreover, the Jellyfish-positive part of the carotid plaque was thought to be highly vulnerable and to easily exhaust the thrombogenic factors. The possibility remains that the stimulation provided by prophylactic surgery (CEA or CAS) may easily lead to ischemic stroke events.
22 22 Therefore, if the Jellyfish sign is detected in a carotid arterial plaque, these surgeries must only be performed with the greatest of possible care in order to prevent ischemic stroke attack. Limitations of this Study We were unable to completely exclude ischemic strokes of origins other than carotid plaque. However, ischemic strokes that appeared to be of cardioembolic origin and hemorrhagic strokes were excluded. Second, ultrasound B-mode imaging suffers from limitations like acoustic shadowing, resulting from calcifications in the plaque, speckle diffraction and angle dependence. MRI techniques do not suffer from acoustic shadows, and could thus reduce such ultrasonographic problems. Moreover, recent studies have also shown that fibrous cap thinning and rupture can be visualized in vivo using high-resolution MRI [10, 26]. To clarify the possibility that Jellyfish sign indicates plaque rupture, we should examine signs of plaque rupture on MRI. However, MRI methods remain very expensive. Moreover, the ability to detect plaque rupture on MRI is currently limited mainly to research. Conversely, the ultrasound procedure is fast and relatively inexpensive and plaque examination is easily performed in the standard clinical visit. Moreover, for two cases in the present study, Jellyfish sign showed at the
23 23 area of mild stenosis (30 and 40% stenosis) adjacent to the part of the carotid artery severely stenosed by plaque. The Jellyfish sign could thus prove valuable in evaluating lesions that would otherwise be considered low risk. However, the number of subjects in the present study was small and further studies (particularly including patients with <50% stenosis by plaque) are needed to clarify this issue. Lastly, detecting Jellyfish sign is not difficult for an experienced ultrasonographer, although we must always bear in mind that ultrasound examination is observer-dependent. We have therefore been trying to develop a detection method using ultrasonography with which anyone can detect the Jellyfish sign. Conclusion In conclusion, this study demonstrated that the existence of a mobile component of carotid arterial plaque (ultrasonographic Jellyfish sign) suggests thinning and rupture of the fibrous cap over the plaque, resulting in repeated ischemic stroke during a short interval after diagnosis. An important predictive factor for ischemic stroke is thus Jellyfish sign, not IPH. The vulnerable status of the Jellyfish-positive plaque, if not removed, may trigger continuous release of embolic material, which in turn may be related to subsequent cerebrovascular events. Surgical treatment of carotid
24 24 plaque with Jellyfish sign, as detected by carotid ultrasonography, should thus be kept in mind as a treatment option. In particular, surgical intervention may be justified in cases with repeated ischemic stroke events during a short interval, as in our cases. Acknowledgements: The authors thank Masuki Kobayashi, M.D., Junichi Kanazawa, M.D., Seiichirou Hibino, M.D., Chie Mihara, M.D. (Hibino Hospital), and Akihiro Toyota, M.D. (Chugoku-Rosai Hospital), for the collection of follow-up data and helpful comments. Financial Disclosure: None Grant Information: None References 1. Altaf N, MacSweeney ST, Gladman J, Auer DP (2007) Carotid intraplaque hemorrhage predicts recurrent symptoms in patients with high-grade carotid stenosis. Stroke 38: Barnett HJM, Taylor DW, Eliasziw M, Fox AJ, Ferguson GG, Haynes RB, Rankin RN, Clagett GP, Hachinski VC, Sackett DL, Thorpe KE, Meldrum HE, Spence JD, for The North American Symptomatic Carotid Endarterectomy Trial Collaborators
25 25 (1998) Benefit of Carotid Endarterectomy in Patients with Symptomatic Moderate or Severe Stenosis. N Engl J Med 339: Carr S, Farb A, Pearce WH, Virmani R, Yao JS (1996) Atherosclerotic plaque rupture in symptomatic carotid artery stenosis. J Vasc Surg 23: Constantinides P (1966) Plaque fissures in human coronary thrombosis. J Atherosclerosis Res 6: Davies MJ, Thomas AC (1985) Plaque fissuring--the cause of acute myocardial infarction, sudden ischaemic death, and crescendo angina. Br Heart J 53: Devuyst G, Karapanayiotides T, Ruchat P, Pusztaszeri M, Lobrinus JA, Jonasson L, Cuisinaire O, Kalangos A, Despland PA, Thiran JP, Bogousslavsky J (2005) Ultrasound measurement of the fibrous cap in symptomatic and asymptomatic atheromatous carotid plaques. Circulation 111: Eliasziw M, Kennedy J, Hill MD, Buchan AM, Barnett HJM, for the North American Symptomatic Carotid Endarterectomy Trial (NASCET) Group (2004) Early risk of stroke after a transient ischemic attack in patients with internal carotid artery disease. CMAJ 170: European Carotid Surgery Trialists' Collaborative Group (1998) Randomised trial of endarterectomy for recently symptomatic carotid stenosis: final results of the MRC
26 26 European Carotid Surgery Trial (ECST). Lancet 351: Grogan JK, Shaalan WE, Cheng H, Gewertz B, Desai T, Schwarze G, Glagov S, Lozanski L, Griffin A, Castilla M, Bassiouny HS (2005) B-mode ultrasonographic characterization of carotid atherosclerotic plaques in symptomatic and asymptomatic patients. J Vasc Surg 42: Hatsukami TS, Ross R, Polissar NL, Yuan C (2000) Visualization of fibrous cap thickness and rupture in human atherosclerotic carotid plaque in vivo with high-resolution magnetic resonance imaging. Circulation 102: Kobayashi M, Ogasawara K, Inoue T, Saito H, Komoribayashi N, Suga Y, Ogawa A (2007) Urgent endarterectomy using pretreatment with free radical scavenger, edaravone, and early clamping of the parent arteries for cervical carotid artery stenosis with crescendo transient ischemic attacks caused by mobile thrombus and hemodynamic cerebral ischemia. Case report. Neurol Med Chir (Tokyo) 47: Kume S, Hibino S, Kobayashi M, Kanazawa J, Mihara C, Yamane K, Toyota A, Onda H, Kurisu K (2007) Jellyfish sign : Deformation of plaque in the carotid artery due to pulsatile blood flow. Neurosonology 20:21-24 (Japanese) 13. Li ZY, Howarth SP, Tang T, Gillard JH (2006) How critical is fibrous cap thickness to carotid plaque stability? A flow-plaque interaction model. Stroke 37:
27 Lovett JK, Gallagher PJ, Hands LJ, Walton J, Rothwell PM (2004) Histological correlates of carotid plaque surface morphology on lumen contrast imaging. Circulation 110: Meairs S, Hennerici M (1999) Four-dimensional ultrasonographic characterization of plaque surface motion in patients with symptomatic and asymptomatic carotid artery stenosis. Stroke 30: Nighoghossian N, Derex L, Douek P (2005) The vulnerable carotid artery plaque: current imaging methods and new perspectives. Stroke 36: Redgrave JN, Gallagher P, Lovett JK, Rothwell PM (2008) Critical cap thickness and rupture in symptomatic carotid plaques: the oxford plaque study. Stroke 39: Redgrave JN, Lovett JK, Gallagher PJ, Rothwell PM (2006) Histological assessment of 526 symptomatic carotid plaques in relation to the nature and timing of ischemic symptoms: the Oxford plaque study. Circulation 113: Richardson PD (1992) Physical factors affecting the atherosclerotic plaque. In: Labs KH, Jäger KA, Fitzgerald DE, Neuerburg-Heusler D (eds) Diagnostic Vascular Ultrasound. Edward Arnold, London, England, pp Rothwell PM, Eliasziw M, Gutnikov SA, Warlow CP, Barnett HJ (2004) Carotid
28 28 Endarterectomy Trialists Collaboration. Endarterectomy for symptomatic carotid stenosis in relation to clinical subgroups and timing of surgery. Lancet 363: Rothwell PM, Gibson R, Warlow CP (2000) Interrelation between plaque surface morphology and degree of stenosis on carotid angiograms and the risk of ischemic stroke in patients with symptomatic carotid stenosis. On behalf of the European Carotid Surgery Trialists' Collaborative Group. Stroke 31: Spagnoli LG, Mauriello A, Sangiorgi G, Fratoni S, Bonanno E, Schwartz RS, Piepgras DG, Pistolese R, Ippoliti A, Holmes DR Jr. (2004) Extracranial thrombotically active carotid plaque as a risk factor for ischemic stroke. JAMA 292: Takaya N, Yuan C, Chu B, Saam T, Underhill H, Cai J, Tran N, Polissar NL, Isaac C, Ferguson MS, Garden GA, Cramer SC, Maravilla KR, Hashimoto B, Hatsukami TS (2006) Association between carotid plaque characteristics and subsequent ischemic cerebrovascular events: a prospective assessment with MRI--initial results. Stroke 37: Virmani R, Kolodgie FD, Burke AP, Farb A, Schwartz SM (2000) Lessons from sudden coronary death: a comprehensive morphological classification scheme for atherosclerotic lesions. Arterioscler Thromb Vasc Biol 20:
29 Yonemura K, Kimura K, Yasaka M, Minematsu K (2003) Disappearance of an oscillating intraluminal thrombus in the carotid artery demonstrated by ultrasonography. Intern Med 42: Yuan C, Zhang SX, Polissar NL, Echelard D, Ortiz G, Davis JW, Ellington E, Ferguson MS, Hatsukami TS (2002) Identification of fibrous cap rupture with magnetic resonance imaging is highly associated with recent transient ischemic attack or stroke. Circulation 105:
30 30 Figure legends Figure 1: Schema for measurement of ultrasonographic plaque surface movement (A) and pathological area of plaque elements (B). A) Distance from the adventitia to the top (a) and from the top to the bottom (b) of the mobile part. Jellyfish motion rate = b/a 100 (%). B) Schema for HE and Masson staining of the Jellyfish-positive plaque, showing fibrous cap (c), atheromatous lesion (d), lumen (e) and media (f). Traced areas of fibrous cap (upper), atheromatous lesion (middle) and whole plaque (lower) are shown. Figure 2: MRI and ultrasonographic findings in Case 1. A representative case showing Jellyfish sign of fibrous cap rupture and hemorrhage into a carotid atherosclerotic plaque on baseline MRI and ultrasonography. The subject experienced ipsilateral stroke and subsequently underwent CEA 2 weeks after stroke onset. A) DWI shows multiple, small high-intensity spots, suggesting fresh ischemic infarctions, in the left middle cerebral arterial territory. MR angiography (B) shows mild wall stenosis in the left cervical internal carotid artery. C) Signal intensity patterns of hemorrhage are hyperintense on T1-weighted images, suggesting intraplaque hemorrhage. D) A longitudinal B-mode ultrasonographic image of the cervical internal
31 31 cerebral artery shows a mobile lesion (arrow) in the carotid plaque; the mobile component of the carotid plaque rose and fell in a manner inconsistent with arterial pulsatile wall motion (E: schema of mobile plaque). F) Movement by montage images. Figure 3: Plaque histological features in CEA specimens in Case 1. Panel A indicates a longitudinal B-mode ultrasonographic image of Jellyfish-positive carotid plaque in order to show the mobile component (B and C, white allow) and the adjacent non-mobile component (D). Mobile component (Jellyfish-positive element) of the carotid plaque overlying the atheromatous lesion (B-1, B-2 and E). The thinning fibrous cap was disconnected by fissure (C-1 and C-2) from the adjacent lesion of this atheromatous lesion. This fissure became endothelialized and connected between the lumen and intraplaque atheromatous lesion (F). The non-mobile component (adjacent to the mobile component) is lining with thickened fibrous cap, overlying the atheromatous lesion (D). HE staining: B-1, C-1, D-1, E and F, and Masson trichrome staining: B-2, C-2 and D-2. Scale bars: 1 mm in B-1, B-2, C-1, C-2, D-1 and D-2; 500 m in E and F. Figure 4: Representative ultrasonographic B-mode imaging and micrographs of plaque of patient (case 2) presenting with (D) or without (E) Jellyfish sign. Panel A shows a
32 32 longitudinal B-mode ultrasonographic image of the cervical internal cerebral artery with or without Jellyfish sign. Square outline (D) shows the plaque area showing Jellyfish sign (white arrow), with movements also shown in illustration (B) and montage view (C). Pathological findings (Masson trichrome staining) demonstrate that thinning and ruptured fibrous caps overlying an atheromatous lesion (D). However, the area without Jellyfish sign shows a thickened fibrous cap overlying the atheromatous lesion (E). Scale bars: 1 mm in D and E. Figure 5: Correlation between Jellyfish motion rate and both atheromatous lesion rate (A) and fibrous cap coverage rate (B) (Spearman rank tests). Each circle represents a patient. Figure 6: Box plots showing differences in cap thickness (µm) between non-mobile and mobile parts of carotid arterial plaque showing a positive Jellyfish sign. Box plots shows median, quartiles, and 10 th and 90 th percentiles. Figure 7: Kaplan-Meier survival estimates of the proportion of patients remaining free of ipsilateral ischemic stroke event for subjects of the 3 groups: IPH(-); IPH(+)JF(-);
33 33 and IPH(+)JF(+). IPH, intraplaque hemorrhage; JF, Jellyfish sign. Supplementary Movie 1: Digital video of plaque surface motion of Jellyfish sign in Case 1. Arrow shows the Jellyfish sign-positive part. CCA: Common carotid artery. ICA: Internal carotid artery. Supplementary Movie 2: Digital video of plaque surface motion of Jellyfish sign in Case 2. Arrow shows the Jellyfish sign-positive part. CCA: Common carotid artery. ICA: Internal carotid artery.
34 34 Statement justifying the involvement of each author in the production of this manuscript: Shinji Kume conceived and designed the research and analyzed and interpreted the clinical data. Seiji Hama conceived and designed the research and performed statistical analysis. Kanji Yamane analyzed and interpreted the clinical data (findings of surgical procedure), and handled funding and supervision. Seishi Wada made critical revision of the manuscript for important intellectual content. Toshihiro Nishida analyzed and interpreted the pathological findings. Kaoru Kurisu handled funding and supervision, and draft the manuscript.
35 35 Article summary: Ultrasonographic rising and falling motion of the plaque surface in the carotid artery (Jellyfish sign) is a sign of high-risk plaque vulnerability suggesting rupture of the fibrous cap associated with release of thromobogenic factors into the lumen, resulting in repeated ischemic stroke during a short interval after diagnosis.
36 36 Table 1. Characteristics of 165 cases with >50% carotid stenosis with or without IPH and Jellyfish sign IPH-positive (n=78) ALL IPH-negative IPH-positive p Jellyfish-negative Jellyfish-positive p (n=165) (n=87) (n=78) (n=47) (n=31) Age, median years (interquartile range) 70.9±8.6 (41-94) 69.9±8.7 (46-94) 71.9±8.4 (41-88) < ±9.2 (41-85) 74.5±6.6 (59-88) Sex: Male, n (%) 134 (81.2) 64 (73.6) 70 (89.7) (87.2) 29 (93.5) Ultrasound parameters Area stenosis (%) 75.3± ± ±10.5 < ± ± Presence of Jellyfish sign, n (%) 31 (18.86) 0 (0) 31 (100) < (100) 0 (0) Risk factors Hypertension, n (%) 111 (67.3) 53 (60.9) 58 (74.4) (74.5) 23 (74.2) Hyperlipemia, n (%) 71 (43.0) 39 (44.8) 32 (41.0) (44.7) 11 (35.5) Diabetes, n (%) 76 (46.0) 35 (40.2) 41 (52.6) (55.3) 15 (48.4) Arterial fibrillation, n (%) 8 (4.9) 5 (5.8) 3 (3.8) (2.1) 2 (6.5) Previous ischemic heart disease, n (%) 49 (29.7) 26 (30.0) 23 (29.5) (27.7) 10 (32.3) Previous ischemic stroke, n (%) 93 (56.4) 49 (56.3) 44 (56.4) (68.1) 12 (38.7) Smoking, n (%) 56 (34) 21 (24.1) 35 (44.9) (42.6) 15 (48.4) Type of symptom on presentation Stroke, n (%) 18 (10.9) 10 (11.5) 8 (10.3) (10.6) 3 (9.7) TIA, n (%) 34 (20.6) 8 (9.2) 26 (33.3) 16 (34.0) 10 (32.3) Medication Antihypertensive agents, n (%) 101 (61.2) 50 (57.5) 51 (65.4) (66.0) 20 (64.5) Hypoglycemic agents, n (%) 57 (34.6) 26 (29.9) 31 (39.7) (40.4) 12 (38.7) Antiplatelet agents, n (%) 94 (57.0) 40 (46.0) 54 (69.2) (70.2) 21 (67.7) Aspirin, n (%) 68 (41.2) 35 (40.2) 33 (42.3) (42.6) 13 (41.9) Statins, n (%) 24 (14.6) 8 (9.3) 16 (20.5) (25.5) 4 (12.9) Outcomes Recurrence of ischemic stroke, n (%) 29 (17.6) 7 (8.1) 22 (28.2) < (10.6) 17 (54.8) <0.001 Operation, n (%) 36 (21.8) 9 (10.3) 27 (34.6) 18 (38.3) 9 (29.0) To test correlations between the two groups (IPH-positive or -negative, and Jellyfish sign-negative or -positive), Fisher s exact test was used to compare categorical variables and the Mann-Whitney test was used to compare continuous variables. IPH, intraplaque hemorrhage detected using MRI; TIA, transient ischemic attack.
37 37 Table 2. Relationship between risk factors and ipsilateral cerebrovascular events during follow-up, determined by Cox Regression Hazard ratio 95% confidence interval p Age (years) Sex (male) Stenosis rate (%) Presence of IPH Presence of Jellyfish sign <0.001 Smoking History of hypertension History of diabetes History of arterial fibrillation History of hyperlipemia History of ischemic heart disease History of stroke Use of antihypertention agent Use of antilipemia agent Use of statin Use of antiplatelet agent Use of aspirin IPH, intraplaque hemorrhage
38 38 Table 3. Features of recurrent ischemic stroke with or without IPH or Jellyfish sign IPH-negative (n=87) IPH-positive (n=78) Jellyfish-negative Jellyfish-positive (n=47) (n=31) Ischemic stroke events during follow up, n (%) 7 (8.0) 5 (10.6) 17 (54.8) Interval between diagnosis and onset of first ischemic stroke event, days 607.6± ± ±448.0 Ischemic stroke events within 1 week after diagnosis, n Cases with repeated ischemic stroke events during follow-up, n IPH, intraplaque hemorrhage Repeated ischemic stroke event indicates more than 2 events occurred during follow-up.
39 39
40 40
41 41
42 42
43 43
44 44
45 45
Usefulness of Plaque Magnetic Resonance Imaging in Identifying High-Risk Carotid Plaques Irrespective of the Degree of Stenosis
 Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, http://dx.doi.org/10.7461/jcen.2017.19.4.291 Original Article Usefulness of Plaque Magnetic Resonance Imaging
Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, http://dx.doi.org/10.7461/jcen.2017.19.4.291 Original Article Usefulness of Plaque Magnetic Resonance Imaging
Treatment Considerations for Carotid Artery Stenosis. Danielle Zielinski, RN, MSN, ACNP Rush University Neurosurgery
 Treatment Considerations for Carotid Artery Stenosis Danielle Zielinski, RN, MSN, ACNP Rush University Neurosurgery 4.29.2016 There is no actual or potential conflict of interest in regards to this presentation
Treatment Considerations for Carotid Artery Stenosis Danielle Zielinski, RN, MSN, ACNP Rush University Neurosurgery 4.29.2016 There is no actual or potential conflict of interest in regards to this presentation
ORIGINAL CONTRIBUTION. Long-term Risk of Stroke and Other Vascular Events in Patients With Asymptomatic Carotid Artery Stenosis
 ORIGINAL CONTRIBUTION Long-term Risk of Stroke and Other Vascular Events in Patients With Asymptomatic Carotid Artery Stenosis Zurab G. Nadareishvili, MD, PhD; Peter M. Rothwell, MD, PhD; Vadim Beletsky,
ORIGINAL CONTRIBUTION Long-term Risk of Stroke and Other Vascular Events in Patients With Asymptomatic Carotid Artery Stenosis Zurab G. Nadareishvili, MD, PhD; Peter M. Rothwell, MD, PhD; Vadim Beletsky,
Contemporary Carotid Imaging and Approach to Treatment: Course Notes Thursday, June 22, 2017 David M. Pelz, MD, FRCPC
 CNSF Meeting, Victoria, BC. June 2017 Contemporary Carotid Imaging and Approach to Treatment: Course Notes Thursday, June 22, 2017 David M. Pelz, MD, FRCPC A. Objectives 1. To understand the current imaging
CNSF Meeting, Victoria, BC. June 2017 Contemporary Carotid Imaging and Approach to Treatment: Course Notes Thursday, June 22, 2017 David M. Pelz, MD, FRCPC A. Objectives 1. To understand the current imaging
MR Imaging of Atherosclerotic Plaques
 MR Imaging of Atherosclerotic Plaques Yeon Hyeon Choe, MD Department of Radiology, Samsung Medical Center, Sungkyunkwan University, Seoul MRI for Carotid Atheroma Excellent tissue contrast (fat, fibrous
MR Imaging of Atherosclerotic Plaques Yeon Hyeon Choe, MD Department of Radiology, Samsung Medical Center, Sungkyunkwan University, Seoul MRI for Carotid Atheroma Excellent tissue contrast (fat, fibrous
Although plaque morphology of patients with
 1740 Short Communications Rupture of Atheromatous Plaque as a Cause of Thrombotic Occlusion of Stenotic Internal Carotid Artery Jun Ogata, MD, Junichi Masuda, MD, Chikao Yutani, MD, and Takenori Yamaguchi,
1740 Short Communications Rupture of Atheromatous Plaque as a Cause of Thrombotic Occlusion of Stenotic Internal Carotid Artery Jun Ogata, MD, Junichi Masuda, MD, Chikao Yutani, MD, and Takenori Yamaguchi,
ORIGINAL CONTRIBUTION. Early Stroke Risk After Transient Ischemic Attack Among Individuals With Symptomatic Intracranial Artery Stenosis
 ORIGINAL CONTRIBUTION Early Stroke Risk After Transient Ischemic Attack Among Individuals With Symptomatic Intracranial Artery Stenosis Bruce Ovbiagele, MD; Salvador Cruz-Flores, MD; Michael J. Lynn, MS;
ORIGINAL CONTRIBUTION Early Stroke Risk After Transient Ischemic Attack Among Individuals With Symptomatic Intracranial Artery Stenosis Bruce Ovbiagele, MD; Salvador Cruz-Flores, MD; Michael J. Lynn, MS;
Carotid Ultrasound: Improving Ultrasound
 Carotid Ultrasound: Improving Ultrasound Edward I. Bluth, M.D., F.A.C.R. Chairman Emeritus, Department of Radiology, Ochsner Clinic Foundation, New Orleans, Louisiana Professor, Ochsner Clinical School,
Carotid Ultrasound: Improving Ultrasound Edward I. Bluth, M.D., F.A.C.R. Chairman Emeritus, Department of Radiology, Ochsner Clinic Foundation, New Orleans, Louisiana Professor, Ochsner Clinical School,
Endarterectomy for Mild Cervical Carotid Artery Stenosis in Patients With Ischemic Stroke Events Refractory to Medical Treatment
 Neurol Med Chir (Tokyo) 48, 211 215, 2008 Endarterectomy for Mild Cervical Carotid Artery Stenosis in Patients With Ischemic Stroke Events Refractory to Medical Treatment Two Case Reports Masakazu KOBAYASHI,
Neurol Med Chir (Tokyo) 48, 211 215, 2008 Endarterectomy for Mild Cervical Carotid Artery Stenosis in Patients With Ischemic Stroke Events Refractory to Medical Treatment Two Case Reports Masakazu KOBAYASHI,
Journal of the American College of Cardiology Vol. 51, No. 10, by the American College of Cardiology Foundation ISSN /08/$34.
 Journal of the American College of Cardiology Vol. 51, No. 10, 2008 2008 by the American College of Cardiology Foundation ISSN 0735-1097/08/$34.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2007.10.054
Journal of the American College of Cardiology Vol. 51, No. 10, 2008 2008 by the American College of Cardiology Foundation ISSN 0735-1097/08/$34.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2007.10.054
MRI of carotid atherosclerotid plaques
 MRI of carotid atherosclerotid plaques Poster No.: C-0208 Congress: ECR 2015 Type: Scientific Exhibit Authors: N. Ananyeva, T. Rostovtseva, R. Ezhova, O. Zheleznyakova, K. Laptev; Saint-Petersburg/RU Keywords:
MRI of carotid atherosclerotid plaques Poster No.: C-0208 Congress: ECR 2015 Type: Scientific Exhibit Authors: N. Ananyeva, T. Rostovtseva, R. Ezhova, O. Zheleznyakova, K. Laptev; Saint-Petersburg/RU Keywords:
OCT. molecular imaging J Jpn Coll Angiol, 2008, 48: molecular imaging MRI positron-emission tomography PET IMT
 48 6 CT MRI PET OCT molecular imaging J Jpn Coll Angiol, 2008, 48: 456 461 atherosclerosis, imaging gold standard computed tomography CT magnetic resonance imaging MRI CT B intima media thickness IMT B
48 6 CT MRI PET OCT molecular imaging J Jpn Coll Angiol, 2008, 48: 456 461 atherosclerosis, imaging gold standard computed tomography CT magnetic resonance imaging MRI CT B intima media thickness IMT B
Atherosclerosis is a chronic disease that affects medium
 Classification of Human Carotid Atherosclerotic Lesions With In Vivo Multicontrast Magnetic Resonance Imaging Jian-Ming Cai, MD, PhD; Thomas S. Hatsukami, MD; Marina S. Ferguson, BS; Randy Small, BS; Nayak
Classification of Human Carotid Atherosclerotic Lesions With In Vivo Multicontrast Magnetic Resonance Imaging Jian-Ming Cai, MD, PhD; Thomas S. Hatsukami, MD; Marina S. Ferguson, BS; Randy Small, BS; Nayak
Lecture Outline: 1/5/14
 John P. Karis, MD Lecture Outline: Provide a clinical overview of stroke: Risk Prevention Diagnosis Intervention Illustrate how MRI is used in the diagnosis and management of stroke. Illustrate how competing
John P. Karis, MD Lecture Outline: Provide a clinical overview of stroke: Risk Prevention Diagnosis Intervention Illustrate how MRI is used in the diagnosis and management of stroke. Illustrate how competing
Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease
 Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease Michael R. Jaff, D.O., F.A.C.P., F.A.C.C. Assistant Professor of Medicine Harvard Medical School Director, Vascular Medicine
Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease Michael R. Jaff, D.O., F.A.C.P., F.A.C.C. Assistant Professor of Medicine Harvard Medical School Director, Vascular Medicine
Disclosures. State of the Art Management of Carotid Stenosis. NIH funding for clinical trials Consultant for Scientia Vascular and Medtronic
 State of the Art Management of Carotid Stenosis Mark R. Harrigan, MD UAB Stroke Center Professor of Neurosurgery, Neurology, and Radiology University of Alabama, Birmingham Disclosures NIH funding for
State of the Art Management of Carotid Stenosis Mark R. Harrigan, MD UAB Stroke Center Professor of Neurosurgery, Neurology, and Radiology University of Alabama, Birmingham Disclosures NIH funding for
MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS. 73 year old NS right-handed male applicant for $1 Million life insurance
 MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS October 17, 2012 AAIM Triennial Conference, San Diego Robert Lund, MD What Is The Risk? 73 year old NS right-handed male applicant for $1
MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS October 17, 2012 AAIM Triennial Conference, San Diego Robert Lund, MD What Is The Risk? 73 year old NS right-handed male applicant for $1
Identification of Fibrous Cap Rupture With Magnetic Resonance Imaging Is Highly Associated With Recent Transient Ischemic Attack or Stroke
 Identification of Fibrous Cap Rupture With Magnetic Resonance Imaging Is Highly Associated With Recent Transient Ischemic Attack or Stroke Chun Yuan, PhD; Shao-xiong Zhang, MD, PhD; Nayak L. Polissar,
Identification of Fibrous Cap Rupture With Magnetic Resonance Imaging Is Highly Associated With Recent Transient Ischemic Attack or Stroke Chun Yuan, PhD; Shao-xiong Zhang, MD, PhD; Nayak L. Polissar,
MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS. 73 year old NS right-handed male applicant for $1 Million Life Insurance
 MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS October 17, 2012 AAIM Triennial Conference, San Diego Robert Lund, MD What Is The Risk? 73 year old NS right-handed male applicant for $1
MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS October 17, 2012 AAIM Triennial Conference, San Diego Robert Lund, MD What Is The Risk? 73 year old NS right-handed male applicant for $1
Non-invasive Imaging of Carotid Artery Atherosclerosis
 Non-invasive Imaging of Carotid Artery Atherosclerosis 최연현 성균관의대삼성서울병원영상의학과 Noninvasive Techniques US with Doppler CT MRI Ultrasonography Techniques of Carotid US US Anatomy (ICA vs ECA) Gray scale and
Non-invasive Imaging of Carotid Artery Atherosclerosis 최연현 성균관의대삼성서울병원영상의학과 Noninvasive Techniques US with Doppler CT MRI Ultrasonography Techniques of Carotid US US Anatomy (ICA vs ECA) Gray scale and
Carotid Artery Disease and What s Pertinent JOSEPH A PAULISIN DO
 Carotid Artery Disease and What s Pertinent JOSEPH A PAULISIN DO Goal of treatment of carotid disease Identify those at risk of developing symptoms Prevent patients at risk from developing symptoms Prevent
Carotid Artery Disease and What s Pertinent JOSEPH A PAULISIN DO Goal of treatment of carotid disease Identify those at risk of developing symptoms Prevent patients at risk from developing symptoms Prevent
The New England Journal of Medicine PROGNOSIS AFTER TRANSIENT MONOCULAR BLINDNESS ASSOCIATED WITH CAROTID-ARTERY STENOSIS
 PROGNOSIS AFTER TRANSIENT MONOCULAR BLINDNESS ASSOCIATED WITH CAROTID-ARTERY STENOSIS OSCAR BENAVENTE, M.D., MICHAEL ELIASZIW, PH.D., JONATHAN Y. STREIFLER, M.D., ALLAN J. FOX, M.D., HENRY J.M. BARNETT,
PROGNOSIS AFTER TRANSIENT MONOCULAR BLINDNESS ASSOCIATED WITH CAROTID-ARTERY STENOSIS OSCAR BENAVENTE, M.D., MICHAEL ELIASZIW, PH.D., JONATHAN Y. STREIFLER, M.D., ALLAN J. FOX, M.D., HENRY J.M. BARNETT,
Plaque Imaging: What It Can Tell Us. Kenneth Snyder, MD, PhD L Nelson Hopkins MD FACS Elad Levy MD MBA FAHA FACS Adnan Siddiqui MD PhD
 Plaque Imaging: What It Can Tell Us Kenneth Snyder, MD, PhD L Nelson Hopkins MD FACS Elad Levy MD MBA FAHA FACS Adnan Siddiqui MD PhD Buffalo Disclosure Information FINANCIAL DISCLOSURE: Research and consultant
Plaque Imaging: What It Can Tell Us Kenneth Snyder, MD, PhD L Nelson Hopkins MD FACS Elad Levy MD MBA FAHA FACS Adnan Siddiqui MD PhD Buffalo Disclosure Information FINANCIAL DISCLOSURE: Research and consultant
Association Between Carotid Plaque Characteristics and Subsequent Ischemic Cerebrovascular Events A Prospective Assessment With MRI Initial Results
 Association Between Carotid Plaque Characteristics and Subsequent Ischemic Cerebrovascular Events A Prospective Assessment With MRI Initial Results Norihide Takaya, MD, PhD; Chun Yuan, PhD; Baocheng Chu,
Association Between Carotid Plaque Characteristics and Subsequent Ischemic Cerebrovascular Events A Prospective Assessment With MRI Initial Results Norihide Takaya, MD, PhD; Chun Yuan, PhD; Baocheng Chu,
Carotid intraplaque hemorrhage in patients with greater than fifty percent carotid stenosis was associated an acute focal cerebral infarction
 Neurology Asia 2018; 23(3) : 209 216 Carotid intraplaque hemorrhage in patients with greater than fifty percent carotid stenosis was associated an acute focal cerebral infarction Sangheon Kim MD, Hyo Sung
Neurology Asia 2018; 23(3) : 209 216 Carotid intraplaque hemorrhage in patients with greater than fifty percent carotid stenosis was associated an acute focal cerebral infarction Sangheon Kim MD, Hyo Sung
Slide 1. Slide 2 Conflict of Interest Disclosure. Slide 3 Stroke Facts. The Treatment of Intracranial Stenosis. Disclosure
 Slide 1 The Treatment of Intracranial Stenosis Helmi Lutsep, MD Vice Chair and Dixon Term Professor, Department of Neurology, Oregon Health & Science University Chief of Neurology, VA Portland Health Care
Slide 1 The Treatment of Intracranial Stenosis Helmi Lutsep, MD Vice Chair and Dixon Term Professor, Department of Neurology, Oregon Health & Science University Chief of Neurology, VA Portland Health Care
Plaque protrusion during carotid artery stenting: risk factors determined by MR plaque imaging
 Plaque protrusion during carotid artery stenting: risk factors determined by MR plaque imaging Katsutoshi Takayama, M.D., Ph.D. Department of Radiology and Interventional neuroradiology, Ishinkai Yao General
Plaque protrusion during carotid artery stenting: risk factors determined by MR plaque imaging Katsutoshi Takayama, M.D., Ph.D. Department of Radiology and Interventional neuroradiology, Ishinkai Yao General
Carotid Imaging. Dr Andrew Farrall. Consultant Neuroradiologist
 20121123 SSCA http://www.neuroimage.co.uk/network Andrew Farrall Carotid Imaging Dr Andrew Farrall Consultant Neuroradiologist SFC Brain Imaging Research Centre (www.sbirc.ed.ac.uk), SINAPSE Collaboration
20121123 SSCA http://www.neuroimage.co.uk/network Andrew Farrall Carotid Imaging Dr Andrew Farrall Consultant Neuroradiologist SFC Brain Imaging Research Centre (www.sbirc.ed.ac.uk), SINAPSE Collaboration
Beyond Stenosis Severity: Top 5 Important Duplex Characteristics to Identify in a Patient with Carotid Disease
 Beyond Stenosis Severity: Top 5 Important Duplex Characteristics to Identify in a Patient with Carotid Disease Jan M. Sloves RVT, RCS, FASE Technical Director New York Cardiovascular Associates Disclosures
Beyond Stenosis Severity: Top 5 Important Duplex Characteristics to Identify in a Patient with Carotid Disease Jan M. Sloves RVT, RCS, FASE Technical Director New York Cardiovascular Associates Disclosures
Clinical Features and Subtypes of Ischemic Stroke Associated with Peripheral Arterial Disease
 Cronicon OPEN ACCESS EC NEUROLOGY Research Article Clinical Features and Subtypes of Ischemic Stroke Associated with Peripheral Arterial Disease Jin Ok Kim, Hyung-IL Kim, Jae Guk Kim, Hanna Choi, Sung-Yeon
Cronicon OPEN ACCESS EC NEUROLOGY Research Article Clinical Features and Subtypes of Ischemic Stroke Associated with Peripheral Arterial Disease Jin Ok Kim, Hyung-IL Kim, Jae Guk Kim, Hanna Choi, Sung-Yeon
Evaluation of Carotid Vessels and Vertebral Artery in Stroke Patients with Color Doppler Ultrasound and MR Angiography
 Evaluation of Carotid Vessels and Vertebral Artery in Stroke Patients with Color Doppler Ultrasound and MR Angiography Dr. Pramod Shaha 1, Dr. Vinay Raj R 2, Dr. (Brig) K. Sahoo 3 Abstract: Aim & Objectives:
Evaluation of Carotid Vessels and Vertebral Artery in Stroke Patients with Color Doppler Ultrasound and MR Angiography Dr. Pramod Shaha 1, Dr. Vinay Raj R 2, Dr. (Brig) K. Sahoo 3 Abstract: Aim & Objectives:
The risk of MR-detected carotid plaque hemorrhage on recurrent or first-time stroke: a meta-analysis of individual patient data
 The risk of MR-detected carotid plaque hemorrhage on recurrent or first-time stroke: a meta-analysis of individual patient data Schindler A 1, Bonati LH 2, Schinner R 1, Altaf N 3, Hosseini AA 3, Esposito-Bauer
The risk of MR-detected carotid plaque hemorrhage on recurrent or first-time stroke: a meta-analysis of individual patient data Schindler A 1, Bonati LH 2, Schinner R 1, Altaf N 3, Hosseini AA 3, Esposito-Bauer
Invasive Coronary Imaging Modalities for Vulnerable Plaque Detection
 Invasive Coronary Imaging Modalities for Vulnerable Plaque Detection Gary S. Mintz, MD Cardiovascular Research Foundation New York, NY Greyscale IVUS studies have shown Plaque ruptures do not occur randomly
Invasive Coronary Imaging Modalities for Vulnerable Plaque Detection Gary S. Mintz, MD Cardiovascular Research Foundation New York, NY Greyscale IVUS studies have shown Plaque ruptures do not occur randomly
Carotid Stenosis Evaluation by 64-Slice CTA: Comparison of NASCET, ECST and CC Grading Methods
 Carotid Stenosis Evaluation by 64-Slice CTA: Comparison of NASCET, ECST and CC Grading Methods Poster No.: C-1583 Congress: ECR 2011 Type: Scientific Exhibit Authors: G. KILICKAP, E. ergun, E. Ba#bay,
Carotid Stenosis Evaluation by 64-Slice CTA: Comparison of NASCET, ECST and CC Grading Methods Poster No.: C-1583 Congress: ECR 2011 Type: Scientific Exhibit Authors: G. KILICKAP, E. ergun, E. Ba#bay,
ORIGINAL INVESTIGATION. Relevance of Carotid Stenosis Progression as a Predictor of Ischemic Neurological Outcomes
 ORIGINAL INVESTIGATION Relevance of Carotid Stenosis Progression as a Predictor of Ischemic Neurological Outcomes Daniel J. Bertges, MD; Visala Muluk, MD; Jeffrey Whittle, MD, MPH; Mary Kelley, MS; David
ORIGINAL INVESTIGATION Relevance of Carotid Stenosis Progression as a Predictor of Ischemic Neurological Outcomes Daniel J. Bertges, MD; Visala Muluk, MD; Jeffrey Whittle, MD, MPH; Mary Kelley, MS; David
Chapter 43 Noninvasive Coronary Plaque Imaging
 hapter 43 Noninvasive oronary Plaque Imaging NIRUDH KOHLI The goal of coronary imaging is to define the extent of luminal narrowing as well as composition of an atherosclerotic plaque to facilitate appropriate
hapter 43 Noninvasive oronary Plaque Imaging NIRUDH KOHLI The goal of coronary imaging is to define the extent of luminal narrowing as well as composition of an atherosclerotic plaque to facilitate appropriate
Sonographic Characterization of Carotid Plaque: Detection of Hemorrhage
 311 Sonographic Characterization of Carotid Plaque: Detection of Hemorrhage E. I. Bluth' D.Kai C. R. B. Merritt' M. Sullivan' G. Farr2 N. L. Mills 3 M. Foreman' K. Sloan' M. Schlater' J. Stewart 3 By careful
311 Sonographic Characterization of Carotid Plaque: Detection of Hemorrhage E. I. Bluth' D.Kai C. R. B. Merritt' M. Sullivan' G. Farr2 N. L. Mills 3 M. Foreman' K. Sloan' M. Schlater' J. Stewart 3 By careful
Redgrave JN, Coutts SB, Schulz UG et al. Systematic review of associations between the presence of acute ischemic lesions on
 6. Imaging in TIA 6.1 What type of brain imaging should be used in suspected TIA? 6.2 Which patients with suspected TIA should be referred for urgent brain imaging? Evidence Tables IMAG1: After TIA/minor
6. Imaging in TIA 6.1 What type of brain imaging should be used in suspected TIA? 6.2 Which patients with suspected TIA should be referred for urgent brain imaging? Evidence Tables IMAG1: After TIA/minor
Diagnosis of Middle Cerebral Artery Occlusion with Transcranial Color-Coded Real-Time Sonography
 Diagnosis of Middle Cerebral Artery Occlusion with Transcranial Color-Coded Real-Time Sonography Kazumi Kimura, Yoichiro Hashimoto, Teruyuki Hirano, Makoto Uchino, and Masayuki Ando PURPOSE: To determine
Diagnosis of Middle Cerebral Artery Occlusion with Transcranial Color-Coded Real-Time Sonography Kazumi Kimura, Yoichiro Hashimoto, Teruyuki Hirano, Makoto Uchino, and Masayuki Ando PURPOSE: To determine
Surface disruption, defined as the presence of ulceration or
 ORIGINAL RESEARCH H.R. Underhill C. Yuan V.L. Yarnykh B. Chu M. Oikawa L. Dong N.L. Polissar G.A. Garden S.C. Cramer T.S. Hatsukami Predictors of Surface Disruption with MR Imaging in Asymptomatic Carotid
ORIGINAL RESEARCH H.R. Underhill C. Yuan V.L. Yarnykh B. Chu M. Oikawa L. Dong N.L. Polissar G.A. Garden S.C. Cramer T.S. Hatsukami Predictors of Surface Disruption with MR Imaging in Asymptomatic Carotid
The most important recommendations from the 2017 ESVS/ESC guideline on the management of carotid artery disease
 The most important recommendations from the 2017 ESVS/ESC guideline on the management of carotid artery disease GJ de Borst Department of Vascular Surgery RECOMMENDATION GRADING CRITERIA What is new
The most important recommendations from the 2017 ESVS/ESC guideline on the management of carotid artery disease GJ de Borst Department of Vascular Surgery RECOMMENDATION GRADING CRITERIA What is new
Antithrombotic therapy in patients with transient ischemic attack / stroke (acute phase <48h)
 Antithrombotic therapy in patients with transient ischemic attack / stroke (acute phase
Antithrombotic therapy in patients with transient ischemic attack / stroke (acute phase
Clinical Decision Making: Hyperacute Management of Symptomatic Carotid Artery Disease
 Clinical Decision Making: Hyperacute Management of Symptomatic Carotid Artery Disease Tarvinder Singh, MS, MD Neurohospitalist Swedish Neuroscience Institute 1 Objectives Definition Why the urgency? Evidence/Guidelines
Clinical Decision Making: Hyperacute Management of Symptomatic Carotid Artery Disease Tarvinder Singh, MS, MD Neurohospitalist Swedish Neuroscience Institute 1 Objectives Definition Why the urgency? Evidence/Guidelines
New Trials in Progress: ACT 1. Jon Matsumura, MD Cannes, France June 28, 2008
 New Trials in Progress: ACT 1 Jon Matsumura, MD Cannes, France June 28, 2008 Faculty Disclosure I disclose the following financial relationships: Consultant, CAS training director, and/or research grants
New Trials in Progress: ACT 1 Jon Matsumura, MD Cannes, France June 28, 2008 Faculty Disclosure I disclose the following financial relationships: Consultant, CAS training director, and/or research grants
Michael Horowitz, MD Pittsburgh, PA
 Michael Horowitz, MD Pittsburgh, PA Introduction Cervical Artery Dissection occurs by a rupture within the arterial wall leading to an intra-mural Hematoma. A possible consequence is an acute occlusion
Michael Horowitz, MD Pittsburgh, PA Introduction Cervical Artery Dissection occurs by a rupture within the arterial wall leading to an intra-mural Hematoma. A possible consequence is an acute occlusion
Luminal thrombosis in middle cerebral artery occlusions: a highresolution
 Original Article Page 1 of 6 Luminal thrombosis in middle cerebral artery occlusions: a highresolution MRI study Wei-Hai Xu 1 *, Ming-Li Li 2 *, Jing-Wen Niu 1, Feng Feng 2, Zheng-Yu Jin 2, Shan Gao 1
Original Article Page 1 of 6 Luminal thrombosis in middle cerebral artery occlusions: a highresolution MRI study Wei-Hai Xu 1 *, Ming-Li Li 2 *, Jing-Wen Niu 1, Feng Feng 2, Zheng-Yu Jin 2, Shan Gao 1
Advances in the treatment of posterior cerebral circulation symptomatic disease
 Advances in the treatment of posterior cerebral circulation symptomatic disease Athanasios D. Giannoukas MD, MSc(Lond.), PhD(Lond.), FEBVS Professor of Vascular Surgery Faculty of Medicine, School of Health
Advances in the treatment of posterior cerebral circulation symptomatic disease Athanasios D. Giannoukas MD, MSc(Lond.), PhD(Lond.), FEBVS Professor of Vascular Surgery Faculty of Medicine, School of Health
Carotid Artery Stenting
 Carotid Artery Stenting Woong Chol Kang M.D. Gil Medical Center, Gachon University of Medicine and Science, Incheon, Korea Carotid Stenosis and Stroke ~25% of stroke is due to carotid disease, the reminder
Carotid Artery Stenting Woong Chol Kang M.D. Gil Medical Center, Gachon University of Medicine and Science, Incheon, Korea Carotid Stenosis and Stroke ~25% of stroke is due to carotid disease, the reminder
Carotid Artery Stenting
 Carotid Artery Stenting JESSICA MITCHELL, ACNP CENTRAL ILLINOIS RADIOLOGICAL ASSOCIATES External Carotid Artery (ECA) can easily be identified from Internal Carotid Artery (ICA) by noticing the branches.
Carotid Artery Stenting JESSICA MITCHELL, ACNP CENTRAL ILLINOIS RADIOLOGICAL ASSOCIATES External Carotid Artery (ECA) can easily be identified from Internal Carotid Artery (ICA) by noticing the branches.
Emboli detection to evaluate risk of stroke
 Emboli detection to evaluate risk of stroke Background: Improved methods are required to identify patients with asymptomatic carotid stenosis at high risk for stroke. Whether surgery is beneficial for
Emboli detection to evaluate risk of stroke Background: Improved methods are required to identify patients with asymptomatic carotid stenosis at high risk for stroke. Whether surgery is beneficial for
APPENDIX A NORTH AMERICAN SYMPTOMATIC CAROTID ENDARTERECTOMY TRIAL
 APPENDIX A Primary Findings From Selected Recent National Institute of Neurological Disorders and Stroke-Sponsored Clinical Trials That Have shaped Modern Stroke Prevention Philip B. Gorelick 178 NORTH
APPENDIX A Primary Findings From Selected Recent National Institute of Neurological Disorders and Stroke-Sponsored Clinical Trials That Have shaped Modern Stroke Prevention Philip B. Gorelick 178 NORTH
Stroke. Histological Assessment of 526 Symptomatic Carotid Plaques in Relation to the Nature and Timing of Ischemic Symptoms The Oxford Plaque Study
 Stroke Histological Assessment of 526 Symptomatic Carotid Plaques in Relation to the Nature and Timing of Ischemic Symptoms The Oxford Plaque Study J.N.E. Redgrave, MRCP; J.K. Lovett, MRCP; P.J. Gallagher,
Stroke Histological Assessment of 526 Symptomatic Carotid Plaques in Relation to the Nature and Timing of Ischemic Symptoms The Oxford Plaque Study J.N.E. Redgrave, MRCP; J.K. Lovett, MRCP; P.J. Gallagher,
Optical Coherence Tomography (OCT): A New Imaging Tool During Carotid Artery Stenting
 Chapter 6 Optical Coherence Tomography (OCT): A New Imaging Tool During Carotid Artery Stenting Shinichi Yoshimura, Masanori Kawasaki, Kiyofumi Yamada, Arihiro Hattori, Kazuhiko Nishigaki, Shinya Minatoguchi
Chapter 6 Optical Coherence Tomography (OCT): A New Imaging Tool During Carotid Artery Stenting Shinichi Yoshimura, Masanori Kawasaki, Kiyofumi Yamada, Arihiro Hattori, Kazuhiko Nishigaki, Shinya Minatoguchi
Imaging Atheroma The quest for the Vulnerable Plaque
 Imaging Atheroma The quest for the Vulnerable Plaque P.J. de Feijter 1. Department of Cardiology 2. Department of Radiology Coronary Heart Disease Remains the Leading Cause of Death in the U.S, Causing
Imaging Atheroma The quest for the Vulnerable Plaque P.J. de Feijter 1. Department of Cardiology 2. Department of Radiology Coronary Heart Disease Remains the Leading Cause of Death in the U.S, Causing
Normalized Wall Index Specific and MRI-Based Stress Analysis of Atherosclerotic Carotid Plaques
 Circulation Journal Official Journal of the Japanese Circulation Society http://www.j-circ.or.jp ORIGINAL ARTICLE Imaging Normalized Wall Index Specific and MRI-Based Stress Analysis of Atherosclerotic
Circulation Journal Official Journal of the Japanese Circulation Society http://www.j-circ.or.jp ORIGINAL ARTICLE Imaging Normalized Wall Index Specific and MRI-Based Stress Analysis of Atherosclerotic
Blood Vessels. Dr. Nabila Hamdi MD, PhD
 Blood Vessels Dr. Nabila Hamdi MD, PhD ILOs Understand the structure and function of blood vessels. Discuss the different mechanisms of blood pressure regulation. Compare and contrast the following types
Blood Vessels Dr. Nabila Hamdi MD, PhD ILOs Understand the structure and function of blood vessels. Discuss the different mechanisms of blood pressure regulation. Compare and contrast the following types
Pathology of Vulnerable Plaque Angioplasty Summit 2005 TCT Asia Pacific, Seoul, April 28-30, 2005
 Pathology of Vulnerable Plaque Angioplasty Summit 25 TCT Asia Pacific, Seoul, April 28-3, 25 Renu Virmani, MD CVPath, A Research Service of the International Registry of Pathology Gaithersburg, MD Plaque
Pathology of Vulnerable Plaque Angioplasty Summit 25 TCT Asia Pacific, Seoul, April 28-3, 25 Renu Virmani, MD CVPath, A Research Service of the International Registry of Pathology Gaithersburg, MD Plaque
Duplex Criteria for Determination of 50% or Greater Carotid Stenosis
 Article Duplex Criteria for Determination of 50% or Greater Carotid Stenosis David G. Neschis, MD, Frank J. Lexa, MD, Julia T. Davis, RN, RVT, Jeffrey P. Carpenter, MD, RVT Recently the North American
Article Duplex Criteria for Determination of 50% or Greater Carotid Stenosis David G. Neschis, MD, Frank J. Lexa, MD, Julia T. Davis, RN, RVT, Jeffrey P. Carpenter, MD, RVT Recently the North American
Stroke is the third-leading cause of death and a major
 Long-Term Mortality and Recurrent Stroke Risk Among Chinese Stroke Patients With Predominant Intracranial Atherosclerosis Ka Sing Wong, MD; Huan Li, MD Background and Purpose The goal of this study was
Long-Term Mortality and Recurrent Stroke Risk Among Chinese Stroke Patients With Predominant Intracranial Atherosclerosis Ka Sing Wong, MD; Huan Li, MD Background and Purpose The goal of this study was
03/30/2016 DISCLOSURES TO OPERATE OR NOT THAT IS THE QUESTION CAROTID INTERVENTION IS INDICATED FOR ASYMPTOMATIC CAROTID OCCLUSIVE DISEASE
 CAROTID INTERVENTION IS INDICATED FOR ASYMPTOMATIC CAROTID OCCLUSIVE DISEASE Elizabeth L. Detschelt, M.D. Allegheny Health Network Vascular and Endovascular Symposium April 2, 2016 DISCLOSURES I have no
CAROTID INTERVENTION IS INDICATED FOR ASYMPTOMATIC CAROTID OCCLUSIVE DISEASE Elizabeth L. Detschelt, M.D. Allegheny Health Network Vascular and Endovascular Symposium April 2, 2016 DISCLOSURES I have no
Vascular disease. Structural evaluation of vascular disease. Goo-Yeong Cho, MD, PhD Seoul National University Bundang Hospital
 Vascular disease. Structural evaluation of vascular disease Goo-Yeong Cho, MD, PhD Seoul National University Bundang Hospital resistance vessels : arteries
Vascular disease. Structural evaluation of vascular disease Goo-Yeong Cho, MD, PhD Seoul National University Bundang Hospital resistance vessels : arteries
Vulnerable Plaque Pathophysiology, Detection, and Intervention. VP: A Local Problem or Systemic Disease. Erling Falk, Denmark
 Vulnerable Plaque Pathophysiology, Detection, and Intervention VP: A Local Problem or Systemic Disease Erling Falk, Denmark Vulnerable Plaque Pathophysiology, Detection, and Intervention VP: A Local Problem
Vulnerable Plaque Pathophysiology, Detection, and Intervention VP: A Local Problem or Systemic Disease Erling Falk, Denmark Vulnerable Plaque Pathophysiology, Detection, and Intervention VP: A Local Problem
ICSS Safety Results NOT for PUBLICATION. June 2009 ICSS ICSS ICSS ICSS. International Carotid Stenting Study: Main Inclusion Criteria
 Safety Results NOT for The following slides were presented to the Investigators Meeting on 22/05/09 and most of them were also presented at the European Stroke Conference on 27/05/09 They are NOT for in
Safety Results NOT for The following slides were presented to the Investigators Meeting on 22/05/09 and most of them were also presented at the European Stroke Conference on 27/05/09 They are NOT for in
MRI carotid plaque imaging predicts future stroke in patients with mild to moderate stenosis ICAD study
 MRI carotid plaque imaging predicts future stroke in patients with mild to moderate stenosis ICAD study Richard Simpson, Senior Clinical Vascular Scientist and Stroke Association Junior Research Training
MRI carotid plaque imaging predicts future stroke in patients with mild to moderate stenosis ICAD study Richard Simpson, Senior Clinical Vascular Scientist and Stroke Association Junior Research Training
Categorical Course: Update of Doppler US 8 : 00 8 : 20
 159 Categorical Course: Update of Doppler US 8 : 00 8 : 20 160 161 Table 1.Comparison of Recommended Values from Data in the Published Literature* S t u d y Lesion PSV E D V VICA/VCCA S e v e r i t y (
159 Categorical Course: Update of Doppler US 8 : 00 8 : 20 160 161 Table 1.Comparison of Recommended Values from Data in the Published Literature* S t u d y Lesion PSV E D V VICA/VCCA S e v e r i t y (
Canadian Best Practice Recommendations for Stroke Care. (Updated 2008) Section # 3 Section # 3 Hyperacute Stroke Management
 Canadian Best Practice Recommendations for Stroke Care (Updated 2008) Section # 3 Section # 3 Hyperacute Stroke Management Reorganization of Recommendations 2008 2006 RECOMMENDATIONS: 2008 RECOMMENDATIONS:
Canadian Best Practice Recommendations for Stroke Care (Updated 2008) Section # 3 Section # 3 Hyperacute Stroke Management Reorganization of Recommendations 2008 2006 RECOMMENDATIONS: 2008 RECOMMENDATIONS:
Carotid Artery Revascularization: Current Strategies. Shonda Banegas, D.O. Vascular Surgery Carondelet Heart and Vascular Institute September 6, 2014
 Carotid Artery Revascularization: Current Strategies Shonda Banegas, D.O. Vascular Surgery Carondelet Heart and Vascular Institute September 6, 2014 Disclosures None 1 Stroke in 2014 Stroke kills almost
Carotid Artery Revascularization: Current Strategies Shonda Banegas, D.O. Vascular Surgery Carondelet Heart and Vascular Institute September 6, 2014 Disclosures None 1 Stroke in 2014 Stroke kills almost
Pathology of Coronary Artery Disease
 Pathology of Coronary Artery Disease Seth J. Kligerman, MD Pathology of Coronary Artery Disease Seth Kligerman, MD Assistant Professor Medical Director of MRI University of Maryland Department of Radiology
Pathology of Coronary Artery Disease Seth J. Kligerman, MD Pathology of Coronary Artery Disease Seth Kligerman, MD Assistant Professor Medical Director of MRI University of Maryland Department of Radiology
Umar Sadat, MD; Zhongzhao Teng, PhD; Victoria E. Young, MD; Zhi Yong Li, PhD; Jonathan H. Gillard, MD
 Circulation Journal Official Journal of the Japanese Circulation Society http://www.j-circ.or.jp ORIGINAL ARTICLE Imaging Utility of Magnetic Resonance Imaging-Based Finite Element Analysis for the Biomechanical
Circulation Journal Official Journal of the Japanese Circulation Society http://www.j-circ.or.jp ORIGINAL ARTICLE Imaging Utility of Magnetic Resonance Imaging-Based Finite Element Analysis for the Biomechanical
EVALUATION OF CAROTID ARTERY STENOSIS IN STROKE/TRANSIENT ISCHAEMIC ATTACK Nambakam Tanuja Subramanyam 1, Naveen Kumar P 2, Girish P.
 EVALUATION OF CAROTID ARTERY STENOSIS IN STROKE/TRANSIENT ISCHAEMIC ATTACK Nambakam Tanuja Subramanyam 1, Naveen Kumar P 2, Girish P. Vakrani 3 HOW TO CITE THIS ARTICLE: Nambakam Tanuja Subramanyam, Naveen
EVALUATION OF CAROTID ARTERY STENOSIS IN STROKE/TRANSIENT ISCHAEMIC ATTACK Nambakam Tanuja Subramanyam 1, Naveen Kumar P 2, Girish P. Vakrani 3 HOW TO CITE THIS ARTICLE: Nambakam Tanuja Subramanyam, Naveen
Subclinical leaflet thrombosis in surgical and transcatheter bioprosthetic aortic valves: an observational study
 Subclinical leaflet thrombosis in surgical and transcatheter bioprosthetic aortic valves: an observational study Meagan Sullivan, PharmD PGY2 Cardiology Pharmacy Resident University of Chicago Medicine
Subclinical leaflet thrombosis in surgical and transcatheter bioprosthetic aortic valves: an observational study Meagan Sullivan, PharmD PGY2 Cardiology Pharmacy Resident University of Chicago Medicine
Int J Clin Exp Med 2018;11(9): /ISSN: /IJCEM
 Int J Clin Exp Med 2018;11(9):10069-10075 www.ijcem.com /ISSN:1940-5901/IJCEM0069372 Case Report Acute cerebral infarction after spontaneous recanalization of extracranial internal carotid artery atherosclerotic
Int J Clin Exp Med 2018;11(9):10069-10075 www.ijcem.com /ISSN:1940-5901/IJCEM0069372 Case Report Acute cerebral infarction after spontaneous recanalization of extracranial internal carotid artery atherosclerotic
Symptomatic carotid stenosis is associated with a markedly
 Switching off Embolization From Symptomatic Carotid Plaque Using S-Nitrosoglutathione Zoltan Kaposzta, MD; John F. Martin, F Med Sci; Hugh S. Markus, FRCP Background Current antiplatelet regimens fail
Switching off Embolization From Symptomatic Carotid Plaque Using S-Nitrosoglutathione Zoltan Kaposzta, MD; John F. Martin, F Med Sci; Hugh S. Markus, FRCP Background Current antiplatelet regimens fail
Dr Julia Hopyan Stroke Neurologist Sunnybrook Health Sciences Centre
 Dr Julia Hopyan Stroke Neurologist Sunnybrook Health Sciences Centre Objectives To learn what s new in stroke care 2010-11 1) Acute stroke management Carotid artery stenting versus surgery for symptomatic
Dr Julia Hopyan Stroke Neurologist Sunnybrook Health Sciences Centre Objectives To learn what s new in stroke care 2010-11 1) Acute stroke management Carotid artery stenting versus surgery for symptomatic
Carotid Stenosis 1/24/2019. Review of Primary Studies. NASCET- Moderate stenosis. ACAS (Asymptomatic Carotid Atherosclerosis Study) NASCET
 Review of Primary Studies Carotid Stenosis NINDS National Institute of Neurological Disorders and Stroke 2 large studies to determine who would benefit from surgery NASCET North American Symptomatic Carotid
Review of Primary Studies Carotid Stenosis NINDS National Institute of Neurological Disorders and Stroke 2 large studies to determine who would benefit from surgery NASCET North American Symptomatic Carotid
Carotid Endarterectomy after Ischemic Stroke Is there a Justification for Delayed Surgery?
 Eur J Vasc Endovasc Surg 30, 36 40 (2005) doi:10.1016/j.ejvs.2005.02.045, available online at http://www.sciencedirect.com on Carotid Endarterectomy after Ischemic Stroke Is there a Justification for Delayed
Eur J Vasc Endovasc Surg 30, 36 40 (2005) doi:10.1016/j.ejvs.2005.02.045, available online at http://www.sciencedirect.com on Carotid Endarterectomy after Ischemic Stroke Is there a Justification for Delayed
Carotid Endarterectomy for Symptomatic Complete Occlusion of the Internal Carotid Artery
 2011 65 4 239 245 Carotid Endarterectomy for Symptomatic Complete Occlusion of the Internal Carotid Artery a* a b a a a b 240 65 4 2011 241 9 1 60 10 2 62 17 3 67 2 4 64 7 5 69 5 6 71 1 7 55 13 8 73 1
2011 65 4 239 245 Carotid Endarterectomy for Symptomatic Complete Occlusion of the Internal Carotid Artery a* a b a a a b 240 65 4 2011 241 9 1 60 10 2 62 17 3 67 2 4 64 7 5 69 5 6 71 1 7 55 13 8 73 1
Carotid Stenosis (carotid artery disease)
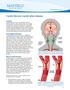 1 Carotid Stenosis (carotid artery disease) Overview Carotid stenosis is a narrowing of the carotid arteries, the two major arteries that carry oxygenrich blood from the heart to the brain. Also called
1 Carotid Stenosis (carotid artery disease) Overview Carotid stenosis is a narrowing of the carotid arteries, the two major arteries that carry oxygenrich blood from the heart to the brain. Also called
Plaque Inflammation and Unstable Morphology Are Associated With Early Stroke Recurrence in Symptomatic Carotid Stenosis
 Plaque Inflammation and Unstable Morphology Are Associated With Early Stroke Recurrence in Symptomatic Carotid Stenosis Michael Marnane, PhD; Susan Prendeville, MB; Ciaran McDonnell, MD; Imelda Noone,
Plaque Inflammation and Unstable Morphology Are Associated With Early Stroke Recurrence in Symptomatic Carotid Stenosis Michael Marnane, PhD; Susan Prendeville, MB; Ciaran McDonnell, MD; Imelda Noone,
Cerebrovascular Disease. RTC Conference Resident Presenter: Dr. Christina Bailey Faculty: Dr. Jeff Dattilo October 2, 2009
 Cerebrovascular Disease RTC Conference Resident Presenter: Dr. Christina Bailey Faculty: Dr. Jeff Dattilo October 2, 2009 Cerebrovascular Disease Stroke is the 3 rd leading cause of death and the leading
Cerebrovascular Disease RTC Conference Resident Presenter: Dr. Christina Bailey Faculty: Dr. Jeff Dattilo October 2, 2009 Cerebrovascular Disease Stroke is the 3 rd leading cause of death and the leading
Disclosures. An Update on TIA and Minor Stroke. The Agenda PROGNOSIS PATHOPHYSIOLOGY GUIDELINES AND PROVEN MANAGEMENT STRATEGIES AGGRESSIVE TREATMENT
 Disclosures An Update on TIA and Minor Stroke Dr. Johnston is principal investigator for the POINT trial, sponsored by the NIH but with drug and placebo contributed by Sanofi-Aventis. S. Claiborne Johnston,
Disclosures An Update on TIA and Minor Stroke Dr. Johnston is principal investigator for the POINT trial, sponsored by the NIH but with drug and placebo contributed by Sanofi-Aventis. S. Claiborne Johnston,
Clinical trials for carotid stenosis revascularization and relation to methods of stenosis quantification
 Fox and Singh Neurovascular Imaging (2015) 1:2 DOI 10.1186/s40809-015-0002-1 REVIEW Open Access Clinical trials for carotid stenosis revascularization and relation to methods of stenosis quantification
Fox and Singh Neurovascular Imaging (2015) 1:2 DOI 10.1186/s40809-015-0002-1 REVIEW Open Access Clinical trials for carotid stenosis revascularization and relation to methods of stenosis quantification
Co chce/čeká neurochirug od anesteziologa během karotické endarterektomie?
 XXV. kongres České společnosti anesteziologie, resuscitace a intenzivní medicíny, Praha 3.-5.10. 2018 Co chce/čeká neurochirug od anesteziologa během karotické endarterektomie? Hejčl A., Orlický M., Sameš
XXV. kongres České společnosti anesteziologie, resuscitace a intenzivní medicíny, Praha 3.-5.10. 2018 Co chce/čeká neurochirug od anesteziologa během karotické endarterektomie? Hejčl A., Orlický M., Sameš
Emergently? Michigan Institute for Neurological Disorders. Garden City Hospital, Garden City, Michigan
 Why Should TIA be Treated Emergently? Anne M. Pawlak, D.O. F.A.C.N. Michigan Institute for Neurological Disorders Director Neurology Residency Program, Garden City Hospital, Garden City, Michigan According
Why Should TIA be Treated Emergently? Anne M. Pawlak, D.O. F.A.C.N. Michigan Institute for Neurological Disorders Director Neurology Residency Program, Garden City Hospital, Garden City, Michigan According
Quantitative Imaging of Transmural Vasa Vasorum Distribution in Aortas of ApoE -/- /LDL -/- Double Knockout Mice using Nano-CT
 Quantitative Imaging of Transmural Vasa Vasorum Distribution in Aortas of ApoE -/- /LDL -/- Double Knockout Mice using Nano-CT M. Kampschulte 1, M.D.; A. Brinkmann 1, M.D.; P. Stieger 4, M.D.; D.G. Sedding
Quantitative Imaging of Transmural Vasa Vasorum Distribution in Aortas of ApoE -/- /LDL -/- Double Knockout Mice using Nano-CT M. Kampschulte 1, M.D.; A. Brinkmann 1, M.D.; P. Stieger 4, M.D.; D.G. Sedding
Contemporary Management of Carotid Disease What We Know So Far
 Contemporary Management of Carotid Disease What We Know So Far Ammar Safar, MD, FSCAI, FACC, FACP, RPVI Interventional Cardiology & Endovascular Medicine Disclosers NONE Epidemiology 80 % of stroke are
Contemporary Management of Carotid Disease What We Know So Far Ammar Safar, MD, FSCAI, FACC, FACP, RPVI Interventional Cardiology & Endovascular Medicine Disclosers NONE Epidemiology 80 % of stroke are
Imaging Overview for Vulnerable Plaque: Data from IVUS Trial and An Introduction to VH-IVUS Imgaging
 Imaging Overview for Vulnerable Plaque: Data from IVUS Trial and An Introduction to VH-IVUS Imgaging Gary S. Mintz,, MD Cardiovascular Research Foundation New York, NY Today, in reality, almost everything
Imaging Overview for Vulnerable Plaque: Data from IVUS Trial and An Introduction to VH-IVUS Imgaging Gary S. Mintz,, MD Cardiovascular Research Foundation New York, NY Today, in reality, almost everything
Recanalization of Chronic Carotid Artery Occlusion Objective Improvement Of Cerebral Perfusion
 Recanalization of Chronic Carotid Artery Occlusion Objective Improvement Of Cerebral Perfusion Paul Hsien-Li Kao, MD Assistant Professor National Taiwan University Medical School and Hospital ICA stenting
Recanalization of Chronic Carotid Artery Occlusion Objective Improvement Of Cerebral Perfusion Paul Hsien-Li Kao, MD Assistant Professor National Taiwan University Medical School and Hospital ICA stenting
MR Advance Techniques. Vascular Imaging. Class II
 MR Advance Techniques Vascular Imaging Class II 1 Vascular Imaging There are several methods that can be used to evaluate the cardiovascular systems with the use of MRI. MRI will aloud to evaluate morphology
MR Advance Techniques Vascular Imaging Class II 1 Vascular Imaging There are several methods that can be used to evaluate the cardiovascular systems with the use of MRI. MRI will aloud to evaluate morphology
Mechanisms of cerebral artery thrombosis: a histopathological analysis on eight necropsy cases
 J7ournal of Neurology, Neurosurgery, and Psychiatry 1994;57:17-21 17 PAPERS Research Institute, National Cardiovascular Center, Osaka, Japan J Ogata J Masuda Department of Pathology C Yutani Cerebrovascular
J7ournal of Neurology, Neurosurgery, and Psychiatry 1994;57:17-21 17 PAPERS Research Institute, National Cardiovascular Center, Osaka, Japan J Ogata J Masuda Department of Pathology C Yutani Cerebrovascular
CHAPTER 5. Symptomatic and Asymptomatic Retinal Embolism Have Different Mechanisms
 CHAPTER 5 Symptomatic and Asymptomatic Retinal Embolism Have Different Mechanisms Christine A.C. Wijman, Joao A. Gomes, Michael R. Winter, Behrooz Koleini, Ippolit C.A. Matjucha, Val E. Pochay, Viken L.
CHAPTER 5 Symptomatic and Asymptomatic Retinal Embolism Have Different Mechanisms Christine A.C. Wijman, Joao A. Gomes, Michael R. Winter, Behrooz Koleini, Ippolit C.A. Matjucha, Val E. Pochay, Viken L.
Thromboembolism from carotid plaque is 1 of the major
 ORIGINAL RESEARCH N. Akutsu K. Hosoda A. Fujita E. Kohmura A Preliminary Prediction Model with MR Plaque Imaging to Estimate Risk for New Ischemic Brain Lesions on Diffusion-Weighted Imaging after Endarterectomy
ORIGINAL RESEARCH N. Akutsu K. Hosoda A. Fujita E. Kohmura A Preliminary Prediction Model with MR Plaque Imaging to Estimate Risk for New Ischemic Brain Lesions on Diffusion-Weighted Imaging after Endarterectomy
Stroke prevention in asymptomatic carotid stenosis. ΛΙΛΛΗΣ ΛΕΩΝΙΔΑΣ Καρδιολόγος Επιστημονικός Συνεργάτης Α Καρδιολογικής Κλινικής ΑΠΘ ΠΓΝΘ ΑΧΕΠΑ
 Stroke prevention in asymptomatic carotid stenosis ΛΙΛΛΗΣ ΛΕΩΝΙΔΑΣ Καρδιολόγος Επιστημονικός Συνεργάτης Α Καρδιολογικής Κλινικής ΑΠΘ ΠΓΝΘ ΑΧΕΠΑ Σεμινάρια Ομάδων Εργασίας Ελληνικής Καρδιολογικής Εταιρείας
Stroke prevention in asymptomatic carotid stenosis ΛΙΛΛΗΣ ΛΕΩΝΙΔΑΣ Καρδιολόγος Επιστημονικός Συνεργάτης Α Καρδιολογικής Κλινικής ΑΠΘ ΠΓΝΘ ΑΧΕΠΑ Σεμινάρια Ομάδων Εργασίας Ελληνικής Καρδιολογικής Εταιρείας
DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service
 M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
Critical Review Form Therapy
 Critical Review Form Therapy A transient ischaemic attack clinic with round-the-clock access (SOS-TIA): feasibility and effects, Lancet-Neurology 2007; 6: 953-960 Objectives: To evaluate the effect of
Critical Review Form Therapy A transient ischaemic attack clinic with round-the-clock access (SOS-TIA): feasibility and effects, Lancet-Neurology 2007; 6: 953-960 Objectives: To evaluate the effect of
Risk Factors for Ischemic Stroke: Electrocardiographic Findings
 Original Articles 232 Risk Factors for Ischemic Stroke: Electrocardiographic Findings Elley H.H. Chiu 1,2, Teng-Yeow Tan 1,3, Ku-Chou Chang 1,3, and Chia-Wei Liou 1,3 Abstract- Background: Standard 12-lead
Original Articles 232 Risk Factors for Ischemic Stroke: Electrocardiographic Findings Elley H.H. Chiu 1,2, Teng-Yeow Tan 1,3, Ku-Chou Chang 1,3, and Chia-Wei Liou 1,3 Abstract- Background: Standard 12-lead
For the ICSS Investigators. 7 th Munich Vascular Conference Munich, 7 December 2017
 Restenosis and its impact on recurrent stroke risks after CAS and CEA for symptomatic carotid stenosis results from the International Carotid Stenting Study Leo H Bonati, John Gregson, Joanna Dobson, Dominick
Restenosis and its impact on recurrent stroke risks after CAS and CEA for symptomatic carotid stenosis results from the International Carotid Stenting Study Leo H Bonati, John Gregson, Joanna Dobson, Dominick
Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset
 CLINICAL ARTICLE Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset Shusuke Yamamoto, MD, Satoshi Hori, MD, PhD,
CLINICAL ARTICLE Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset Shusuke Yamamoto, MD, Satoshi Hori, MD, PhD,
