Pericardial Effusion After Cardiac Surgery: Risk Factors, Patient Profiles, and Contemporary Management
|
|
|
- Emery Allison
- 6 years ago
- Views:
Transcription
1 Pericardial Effusion After Cardiac Surgery: Risk Factors, Patient Profiles, and Contemporary Management Elena A. Ashikhmina, MD, Hartzell V. Schaff, MD, Lawrence J. Sinak, MD, Zhuo Li, MS, Joseph A. Dearani, MD, Rakesh M. Suri, MD, DPhil, Soon J. Park, MD, Thomas A. Orszulak, MD, and Thoralf M. Sundt III, MD Divisions of Cardiovascular Surgery and Biomedical Statistics and Informatics, Mayo Clinic, Rochester, Minnesota Background. We aimed to review recent experience at our institution in the diagnosis and treatment of pericardial effusion after cardiac surgery and to identify risk factors for its development. Methods. We searched our clinical database for patients 18 years or older who had cardiac surgery with cardiopulmonary bypass from 1993 through For patients with pericardial effusion (study group), medical records were reviewed to evaluate its manifestations and management. To identify risk factors for effusion, study patients were compared with patients without effusions. A second analysis compared the study group with a cohort without effusions who had routine postoperative echocardiographic examination. Results. Of 21,416 patients identified, 327 (1.5%) had pericardial effusion (study group), 280 (86%) of whom had nonspecific symptoms. Clinical features of tamponade were documented in 138 patients (42%). Effusions were evacuated by echocardiography-guided pericardiocentesis (n 169, 52%) or surgical drainage (n 75, 23%). Effusion resolved after left thoracocentesis for pleural effusion in 3 patients (1%); 67 patients (20%) were treated conservatively. In 13 cases (4%), recurrent effusion required drainage after initial pericardiocentesis. Independent risk factors for effusion were larger body surface area, pulmonary thromboembolism, hypertension, immunosuppression, renal failure, urgency of operation, cardiac operation other than coronary artery bypass grafting, and prolonged cardiopulmonary bypass. Previous cardiac operations were associated with lower risk of effusion. Conclusions. In our study, pericardial effusion occurred in 1.5% of patients, and symptoms were nonspecific. Several factors, mainly related to preoperative characteristics and type of operation, predispose patients to effusion. Echocardiography-guided pericardiocentesis is effective and safe in these patients. (Ann Thorac Surg 2010;89:112 8) 2010 by The Society of Thoracic Surgeons Despite many recent improvements in intraoperative management and postoperative care, late pericardial effusions remain an important cause of morbidity after cardiac surgery. Pericardial effusions may delay recovery and can be life threatening when tamponade leads to hemodynamic compromise [1]. In the modern era, because of widespread use of chronic anticoagulation and increased complexity of operations, the incidence of effusion may be higher [2]. Thus, it is important to have updated information about the manifestations, risk factors, and natural history of pericardial effusion to guide protocols for its prevention, diagnosis, and treatment. The objectives of this study were to review recent experience at our institution in the management of pericardial effusion, to assess modalities and outcomes of treatment, and to identify causative risk factors. Accepted for publication Sept 14, Address correspondence to Dr Schaff, Division of Cardiovascular Surgery, Mayo Clinic, 200 First St SW, Rochester, MN 55905; schaff@mayo.edu. Patients and Methods After approval by the Mayo Clinic Institutional Review Board (April 10, 2007), we searched our patient database for the records of patients aged 18 years or older who underwent cardiac surgery with cardiopulmonary bypass at Mayo Clinic, Rochester, MN, from 1993 through Those who died on the day of operation were excluded. From this group we identified the study cohort, which consisted of patients in whom pericardial effusion developed within 30 postoperative days. Pericardial effusion was defined as fluid in the pericardial space that manifested with symptoms, required specific treatment, was large enough to prompt consideration of drainage, or required lengthened in-hospital stay for observation. Patients who did not meet the above criteria, required reexploration for bleeding or tamponade within the first 3 days after surgery, or did not provide research authorization were excluded. All other patients presumably did not have pericardial effusion after the operation and formed the first control group (control 1). Because not all of these control patients had routine postoperative echocardiographic examina by The Society of Thoracic Surgeons /10/$36.00 Published by Elsevier Inc doi: /j.athoracsur
2 Ann Thorac Surg ASHIKHMINA ET AL 2010;89:112 8 PERICARDIAL EFFUSION: CONTEMPORARY APPROACH Table 1. Subject Variables Included Into the Univariate Analysis of Risk Factors for Pericardial Effusion Patient Variables Comorbid Conditions Operative Factors Age Sex Year of surgery Body surface area Body mass index Weight Height New York Heart Association class Left ventricular ejection fraction Cardiac output Diabetes mellitus Hypertension Hypercholesterolemia Renal failure Infectious endocarditis Immunosuppressive therapy Prior operations with or without cardiopulmonary bypass Myocardial infarction Cardiac heart failure Cardiogenic shock Chronic corticosteroid use before operation Diagnoses (coronary artery disease, congenital pathology, valve pathology, aortic aneurysm, hypertrophic cardiomyopathy, left ventricular aneurysm, pulmonary thromboembolism) 113 Operative category (valve operation, coronary artery bypass grafting, heart transplant, aortic aneurysm surgery, other) Status of operation (elective, urgent, emergent) Use of intraaortic balloon pump Ventricular assist device implantation Cardiopulmonary bypass time Aortic cross-clamping time ADULT CARDIAC tions, some effusions, especially if asymptomatic, could have been underdiagnosed. Therefore, to decrease the number of false-negative cases among control patients, we identified a subset of the control patients who had at least 1 echocardiographic examination after 3 postoperative days (control 2). We reviewed the medical records of all patients to obtain demographic characteristics, comorbid conditions, results of physical and echocardiographic examinations, chest radiograms, methods of treatment, and early clinical and echocardiographic follow-up (30 postoperative days). Of note, echocardiography either was part of a standard protocol of postoperative management or was performed because of suspicion of pericardial effusion on the basis of clinical symptoms. Evidence of tamponade secondary to pericardial effusion was determined echocardiographically. Twodimensional (2D) echocardiographic characteristics indicating tamponade were early diastolic collapse of the right ventricle, compression of heart chambers, plethora of inferior vena cava, or ventricular interdependence (eg, inspiratory interventricular septal shift); Doppler characteristics were respiratory variation of flow velocity across atrioventricular valves or in the hepatic vein. Statistical Analysis Descriptive statistics for categoric variables are reported as frequency and percentage; continuous variables are reported as mean (SD). Categoric variables were compared using the 2 test. Continuous variables were compared using the 2-sample t test or Wilcoxon rank sum test as appropriate. Two separate analyses were performed. Predictors of pericardial effusion were determined first using all qual- Table 2. Subject Characteristics Characteristic Patients With Effusions (n 327) Group a Control 1 b (n 19,632) Control 2 c (n 10,158) Value p d Value p d Age, years 62 (14) 65 (13) (14) Men 224 (69) 13,265 (68) ,298 (62) 0.02 Body surface area, m (0.3) 1.9 (0.2) (0.2) Body mass index, kg/m (5.9) 28.3 (5.4) (5.5) Heart pathology CAD 159 (49) 13,328 (68) ,130 (51) 0.89 Congenital 45 (14) 1,750 (9) ,437 (14) 0.84 Valve 272 (83) 12,712 (65) ,094 (90) Aortic aneurysm 46 (14) 1,620 (8) (10) HOCM 8 (2) 633 (3) (6) Prior operations using CPB 29 (9) 2,285 (12) ,551 (15) CPB time, minutes 112 (60) 90 (44) (45) Cross-clamping time, minutes 72 (40) 56 (30) (34) Preoperative EF 0.55 (0.17) 0.57 (0.14) (0.15) 0.07 Intraaortic balloon pump 34 (10) 1,118 (6) (6) a Values are mean (SD) or no. of patients (%). b Patients without effusion. c Patients without effusion and available postoperative echocardiographic examination. d Comparison with study group (patients with effusions). CAD coronary artery disease; CPB cardiopulmonary bypass; EF ejection fraction; HOCM hypertrophic obstructive cardiomyopathy.
3 114 ASHIKHMINA ET AL Ann Thorac Surg PERICARDIAL EFFUSION: CONTEMPORARY APPROACH 2010;89:112 8 ified patients without effusion as controls (control 1) and second, using patients without effusion who had postoperative echocardiographic evaluation from 3 to 30 days after surgery as controls (control 2). Logistic regression models were used to determine univariate and multivariate predictors of pericardial effusion. The variables included in the analysis are listed in Table 1. The multivariate model considered univariately significant variables (p 0.05) with model selection using the stepwise method. Area under the curve and the Hosmer-Lemeshow test were used to assess the goodness-of-fit of the models. A bootstrapping method was used to assist in variable selections in the final multivariate model. All statistical tests were 2-sided with the alpha level set at.05 for statistical significance. Results Patients Search of the database identified 21,416 patients at least 18 years old who underwent cardiac surgery with cardiopulmonary bypass during the study period; 162 patients died on the day of operation and were excluded. Other patients excluded were 860 reoperated for bleeding within 3 postoperative days and 435 without research authorization. Pericardial effusion developed in 327 patients; these 327 form our study group and represent 1.5% of all patients undergoing cardiac surgery within the 13-year time frame. This incidence was 1.5% in 1993 through 1999 and 1.8% in 2000 through 2005 (p 0.26). The remaining 19,632 patients presumably did not have effusion (control 1); a subset of 10,158 patients without effusion had postoperative echocardiographic examination (control 2). The mean (SD) age of patients in the study group was 62 (14) years (range, 18 to 92 years), and most were men (224, 69%). Characteristics of the study group and the 2 control groups are presented in Table 2. Patients with pericardial effusion were slightly younger and more overweight (mean body mass index, 29.2 kg/m 2 ) than those in the control groups, often had valvular heart disease (84%), and generally exhibited normal preoperative left ventricular ejection fraction (mean, 0.55). Of importance, the majority of patients without pericardial effusion and echocardiographic examination after surgery (control 2) had valvular operations (90%). Manifestations of Pericardial Effusion Pericardial effusion was commonly visualized by echocardiography at the end of the first postoperative week (mean [SD], 9 [6] days; median, 7 days). In 140 patients (43%) pericardial effusion was initially small, which progressed further to moderate or large in 81 patients (25%). Moderate or large pericardial effusion was usually seen approximately 2 weeks after the operation (13 [6] days). For 280 patients (86%) with pericardial effusions, some, mostly nonspecific, symptoms were reported in the medical records; 47 patients (14%) had no reported problems. Table 3. Symptoms and Signs of Pericardial Effusion (n 327) Symptom or Sign Number of Patients (%) Symptoms Dyspnea 116 (35) Malaise/fatigue 71 (22) Chest pain/discomfort 43 (13) Edema 32 (10) Presyncope/syncope 26 (8) Nausea/vomiting 21 (6) Abdominal pain 6 (2) Signs SBP 90 mm Hg 91 (28) HR 100 bpm 87 (27) Oliguria 38 (12) Fever ( 38 C) 35 (11) Increased JVP 40 (12) Decreased cardiac output 21 (6) Paradoxical pulse 22 (7) Cardiac arrest 14 (4) bpm beats per minute; HR heart rate; JVP jugular venous pressure; SBP systolic blood pressure. Dyspnea and malaise occurred most frequently (Table 3). Clinical features of tamponade including hypotension, tachycardia, and decreased cardiac output were documented in 138 study patients (42%), 94 of whom also had Doppler or 2D echocardiographic evidence of tamponade. Pericardial effusions were associated with pleural effusions in 179 cases (55%); 104 bilateral, 65 left-sided, and 10 right-sided pleural effusions were seen on chest radiography. Also, 215 study patients (66%) had an enlarged cardiac silhouette. Transthoracic echocardiography was the main tool for diagnosis of pericardial effusion (221 patients). In 67 patients significant pericardial effusion or tamponade was diagnosed clinically and confirmed by echocardiography. Pericardial effusion was revealed by computed tomography in 24 patients and was suspected on the basis of chest radiography and further confirmed by echocardiography in 11 patients. In 4 patients, diagnosis of effusion was made at the time of emergent exploratory sternotomy for cardiac tamponade. The mean (SD) size of the echolucent space in the pericardium of study patients was 30 (12) mm (range, 7 to 70 mm). In 135 patients (41%) pericardial effusion was described as moderate-large or large ( 25 mm). Pericardial effusion was commonly circumferential (n 117, 36%). Evidence of clot or hematoma in the pericardial space was seen in 34 patients (10%). For 198 patients (61%), Doppler or 2D echocardiography showed evidence of tamponade; 94 patients, as mentioned above, had clinical symptoms of severe hemodynamic compromise. Eighty-six patients (26%) had small or small-moderate pericardial effusions that were considered clinically insignificant at the time of hospital dismissal. Subse-
4 Ann Thorac Surg ASHIKHMINA ET AL 2010;89:112 8 PERICARDIAL EFFUSION: CONTEMPORARY APPROACH quently, effusion progressed in 45 of these patients (52%), prompting readmission to the hospital for drainage (mean [SD] postoperative day, 16 [7]). Of interest, 66 of these 86 patients (77%) had valve surgery. Management of Pericardial Effusion The management strategy for pericardial effusion depended on the patient s clinical condition and the echocardiographic findings. Anticoagulation with warfarin or heparin was usually discontinued or the dose was decreased. If the international normalized ratio was high ( 4.5), vitamin K and fresh frozen plasma were administered and drainage of the effusion was postponed for 1 or 2 days, if the patient remained stable hemodynamically, until the international normalized ratio decreased. Surgical or catheter drainage was used for all patients who had clinical evidence of tamponade. In patients without prominent symptoms or clinical findings, the decision to use drainage depended on Doppler-2D echocardiographic features of tamponade physiology and the amount and accessibility of the fluid. If an effusion was hard to reach by percutaneous drainage (eg, posterior location) and the clinical condition was stable, the patient was observed without intervention. In emergent situations caused by tamponade (cardiac arrest, ventricular fibrillation, or tachycardia with hemodynamic collapse), emergent resternotomy was performed. In 169 patients (52%), pericardial effusions were evacuated by echocardiographically guided pericardiocentesis. Surgical drainage was performed in 75 patients (23%), and effusion was managed conservatively in 67 patients (20%). In 13 cases (4%), recurrent effusion required a staged approach (initial pericardiocentesis, followed by surgical drainage). Pericardial effusion resolved after left thoracocentesis for pleural effusion in 3 patients (1%). Pericardiocentesis was preferred to surgical drainage if pericardial fluid was considered easy to reach and tap by catheter under echocardiographic guidance. Pericardiocentesis was performed more often after the seventh postoperative day (n 144, 79% of 182 procedures). In most patients, extended pericardial catheter drainage was used (every 4 to 6 hours), which was usually removed 2 to 3 days after initial pericardiocentesis. Pericardiocentesis was effective in 97% of performed procedures; repeated drainage insertion was required in 4 cases (2%). One complication occurred after pericardiocentesis (suspicion of heart chamber perforation) with consequent surgical reexploration. Surgical drainage of pericardial effusion was usually performed earlier after the initial operation, within the first 7 days after surgery in 50 of 88 procedures (57%); in most instances echocardiographic evidence of pericardial clot or hematoma or suspicion of ongoing bleeding was present. Of note, the source of bleeding was found in 12 patients (14%). Resternotomy for surgical drainage was performed in 83 cases (emergent resternotomy in the intensive care unit in 8 cases); a subxiphoid approach was chosen in 5 cases. The mean amount of fluid evacuated by pericardiocentesis was 567 (356) ml and by surgical drainage was 648 Table 4. Independent Risk Factors for Postoperative Pericardial Effusion; All Patients Variable Odds Ratio a 95% CI 115 p Value BSA (increase by 1 unit) Pulmonary thromboembolism Renal failure Immunosuppression CAD Type of operation b Heart transplant Aortic aneurysm Valve VAD Surgery status, urgent/emergent c CPB time (increase by 10 min) a For 327 patients with pericardial effusion versus 19,632 patients without effusion; area under the curve, 0.744; Hosmer-Lemeshow test p b Odds ratios calculated using coronary artery bypass grafting as the reference. c Odds ratio calculated using elective surgery as the reference. BSA body surface area; CAD coronary artery disease; CI confidence interval; CPB cardiopulmonary bypass; VAD ventricular assist device implantation. (361) ml. The fluid samples were sent for microbiological analysis, which showed positive growth in 9 patients (3%). Nonoperative treatment of pericardial effusions in 30 patients consisted of administration of diuretics, nonsteroidal antiinflammatory drugs, rarely corticosteroids (n 8, 2%), or close observation only (n 37) if the hemodynamic significance of the pericardial effusion was doubtful or the risks of performing pericardiocentesis were high because of the location of the effusion. For 24 patients treated conservatively, echocardiographic follow-up data beyond 1 week after diagnosis of pericardial effusion was available. Approximately 5 weeks (mean, 37 [29] days; median, 26 days) after initial diagnosis, the effusion completely resolved in 16 patients, decreased in 3 patients, and remained unchanged in 5 patients. No association was found between size of the effusion and outcome of nonoperative treatment; some small effusions persisted for more than 1 month, and some moderate effusions resolved in 2 weeks. Risk Factors for Pericardial Effusion Patient characteristics considered possible risk factors for pericardial effusion (Table 1) were compared between the 327 patients with effusion and 19,632 patients without effusion (control 1). On univariate analysis, 26 of 41 variables included in the analysis appeared to be significantly different between the 2 groups. The multivariate logistic regression model showed increased body surface area, immunosuppression, pulmonary thromboembolism, renal failure, urgency of operation, type of operation (heart transplant, valve, aortic aneurysm surgery, ventricular assist device insertion), and prolonged cardiopulmonary bypass to be independent risk factors for development of pericardial effusion (Table 4). ADULT CARDIAC
5 116 ASHIKHMINA ET AL Ann Thorac Surg PERICARDIAL EFFUSION: CONTEMPORARY APPROACH 2010;89:112 8 Table 5. Independent Risk Factors for Postoperative Pericardial Effusion; Study Patients and Control 2 Group Variable Odds Ratio a 95% CI The second logistic regression model included the data of our study cohort (n 327) and 10,158 patients who had no effusion and underwent postoperative echocardiographic evaluation (control 2). On univariate analysis, 30 of 41 variables included were significantly different between the 2 groups. In the multivariate model of this second analysis, predisposing risk factors for effusion were similar to those from the first analysis (Table 5). An additional finding was that patients having previous cardiac operations had a lower risk of effusion. Valve surgery was not a significant risk factor in this second analysis. Comment p Value BSA (increase by 1 unit) Hypertension Immunosuppression Pulmonary thromboembolism Previous operations with CPB Type of operation b Valve Aortic aneurysm Heart transplant Other c CPB time (increase by 10 min) a For 327 patients with pericardial effusion vs 10,158 patients without effusion and postoperative echocardiographic examination; area under the curve, 0.690; Hosmer-Lemeshow test p b Odds ratios calculated using coronary artery bypass grafting as the reference. c Myectomy, maze procedure, tumor excision, postinfarction ventricular septal defect repair. BSA body surface area; CI confidence interval; CPB cardiopulmonary bypass. The reported incidence of postoperative pericardial effusions ranges between 1% and 77%, depending on study definitions and designs [3 8]. The higher incidences are reported from smaller prospective studies with frequent echocardiographic examinations; most of these effusions were clinically insignificant [5 7]. In retrospective studies of clinically important pericardial effusions the reported incidence is 1% to 2% [3, 4, 8]. In the current study, the incidence of observed pericardial effusion was relatively low (1.5%), probably because it was defined as fluid in the pericardial space that required intervention, lengthened in-hospital stay, or was large enough to prompt consideration of drainage. Therefore, cases of effusion that did not meet the above criteria or were not detected (due to asymptomatic course and absence of routine echocardiographic follow-up after certain types of operations, such as coronary artery bypass grafting) were not included in the study. Despite the introduction of new protocols for anticoagulation and new antiplatelet drugs during the study period, we found no significant change in the incidence of postoperative effusions from the beginning to the end of the study period. Symptoms of pericardial effusion are nonspecific, and few patients have the classic presentation of tamponade; indeed, many patients with pericardial effusion report minimal problems [1, 4]. In the present study, 42% of patients manifested hemodynamic compromise with hypotension, low cardiac output, and (or) oliguria. Other signs of tamponade were reported infrequently, but echocardiographic evidence of tamponade was found in 61%. Therefore, the threshold for performing an echocardiographic study after cardiac surgery if atypical symptoms are present should be reasonably low. A group of patients in our study cohort were dismissed from the hospital after valve surgery with small clinically insignificant pericardial effusions; 52% of them were readmitted because of tamponade approximately 2 weeks after surgery. It is important to closely monitor this category of patients after dismissal and educate the patients and relatives to be alert to possible nonspecific symptoms. Large pericardial effusions require drainage in most cases, and the choice between open drainage and pericardiocentesis is based on location and character of the effusion, as well as physician preference and experience. At Mayo Clinic, echocardiography-guided pericardiocentesis has been performed for drainage of postoperative pericardial effusions since the 1980s [9]. In the current study this technique was used for 56% of patients who had initial drainage of effusion, and was almost always successful. Effectiveness of initial pericardiocentesis was enhanced by leaving a pigtail catheter in the pericardial space for subsequent aspirations. The safety of echocardiography-guided pericardiocentesis has been documented by others [3, 5, 9, 10]. Few studies have analyzed the risk factors for development of postoperative pericardial effusions. Most of the previous investigations focused on effusions after heart transplant [7, 11 14]. Multivariate analysis in the study of Al-Dadah and colleagues [11] failed to identify risk factors for pericardial effusions in patients undergoing heart transplant other than prolonged donor ischemic time. Vandenberg and colleagues [12] reported that a combination of 3 risk factors (preoperative diagnosis of dilated cardiomyopathy, cyclosporine therapy, and acute rejection) yielded an 86% probability of pericardial effusion development in their group of heart transplant patients. Hauptman and colleagues [14] reported that a positive mismatch in weight between recipient and donor was a risk factor for pericardial effusion. The absence of prior cardiac operations was found to be the most powerful predictor of effusion formation [14]. In our study, heart transplant was an independent risk factor for pericardial effusions. This association likely results from a combination of factors including the potential space created when an enlarged, diseased heart is replaced with a normal organ and effects of immunosuppression, which may inhibit obliteration of serosal surfaces. This hypothesis is consistent with another major
6 Ann Thorac Surg ASHIKHMINA ET AL 2010;89:112 8 PERICARDIAL EFFUSION: CONTEMPORARY APPROACH finding, namely that preoperative administration of immunosuppressive medications, including corticosteroids and cytostatics, increased the risk of pericardial effusion. Most patients who received immunosuppressive medications preoperatively had comorbid conditions (eg, rheumatoid arthritis, systemic lupus erythematosus, or tumors), and these patients might be predisposed to coagulopathy and impaired immune response postoperatively. Our study also showed a lower probability of postoperative pericardial effusions in patients who underwent prior operations with cardiopulmonary bypass. There are several possible explanations for lower observed incidence of effusion in patients having reoperation. In some circumstances, such as reoperation for aortic valve replacement, the surgeon may not completely free the heart from pericardial adhesions, and the resulting pericardial space is smaller than in patients having primary operations. Also, development of late effusions may be decreased because the serosal surface is not intact. Pericardial effusions were frequently accompanied by pleural effusions; this also has been reported by Ikäheimo and colleagues [4], who suggested that patients with persistent pericardial effusions after cardiac operations were more likely to have persistent pleural effusions. Bilateral pleural effusions, unlike left-sided effusions, were more likely to be related to heart failure or an inflammatory reaction to operative trauma (topical cardiac cooling or pleurotomy) than to postoperative bleeding. The finding that valve surgery was not a significant risk factor in the analysis of the study group versus the control 2 group may be explained by the fact that the control 2 group had more patients undergoing valve surgery (79%), whereas in the control 1 group, valve surgery was performed in 47% of cases. Our study cohort also had a high percentage of patients with valve surgery (68%), so the importance of this risk factor could not be adequately estimated in the second model. However, based on the results of the first multivariate analysis, we believe that valve surgery is a significant factor predisposing patients to pericardial effusion. Observed incidence of postoperative effusions was lowest among patients who had coronary artery bypass grafting, possibly because the left pleural space was opened for harvest of the internal mammary artery. Of note, because not all patients undergoing coronary artery bypass grafting had postoperative echocardiography, the lower incidence of effusions in this group can be attributed to lower probability of the effusion being revealed. Aortic aneurysm surgery was an independent risk factor for postoperative pericardial effusions, according to our analysis. Other reports have described the same finding; aortic root surgery is associated with increased risk of pericardial effusions [15, 16]. One possible explanation for this phenomenon is a greater degree of early postoperative bleeding leading to more retained mediastinal clot, which may in turn lead to greater local inflammation. Furthermore, as this clot lyses it may be expected to promote osmotic accumulation of fluid in the perigraft space. Although data on chest tube drainage were not 117 available for all patients, it is likely that patients who bleed excessively after operation (including those undergoing reoperation) are more likely to have retained thrombus. A second potential mechanism is late serous weeping through the graft material itself. Finally, aortic procedures often require significant mediastinal dissection, which may disrupt lymphatics. Postoperative pericardial effusions were more likely to develop in patients with renal failure and prolonged bypass time. This supports the association between pericardial effusion and fluid retention in serous cavities as well as the possible association with systemic inflammatory response. On the basis of clinical experience one would expect an association between anticoagulation therapy and pericardial effusions. However, in most publications the association of anticoagulant use with increased risk of pericardial effusion is based only on the documented administration of anticoagulants in a large proportion of patients with effusions, and few studies report anticoagulation status of control patients without effusions [5, 8, 17]. In an echocardiographic study, Malouf and colleagues [6] compared the incidence of pericardial effusions in postoperative patients who did and did not receive systemic anticoagulation. In that report, the incidence of small and moderate pericardial effusions was similar between the 2 groups, but the incidence of large effusions was significantly higher in patients who received anticoagulation [6]. In our study, history of pulmonary thromboembolism and valve surgery were independent predictors of pericardial effusions, which were directly associated with the disturbances in coagulation. For a better understanding of the nature of pericardial effusions in these subgroups, more focused analysis of coagulation profiles and administered anticoagulants is required. Study Limitations Pericardial effusion was defined as fluid in the pericardial space that manifested with symptoms, required specific treatment, was large enough to prompt consideration of drainage, or required lengthened in-hospital stay for observation. Patients who did not meet the above criteria, required reexploration for bleeding or tamponade within the first 3 days after surgery, or did not provide research authorization were excluded. This is one potential limitation of the study. Patients younger than 18 years were not included in this study, although other publications have demonstrated the incidence of pericardial effusion after surgery to be high in young patients with congenital pathology [7]. Because postoperative echocardiographic evaluation was not performed in all control patients without effusion in this study, the conclusion that these patients did not have effusion is somewhat presumptive. To decrease this bias we identified the subgroup of control 2 patients who had postoperative echocardiography; however, this patient subset was not homogeneous because patients were not selected randomly, so this group contained more patients with valve surgery. Nevertheless, the results of our first and second risk factor ADULT CARDIAC
7 118 ASHIKHMINA ET AL Ann Thorac Surg PERICARDIAL EFFUSION: CONTEMPORARY APPROACH 2010;89:112 8 analyses were very similar. In addition, we evaluated the reliability of the multivariate models; thus, we are confident that the study results are accurate. Conclusion Several groups of patients are at increased risk for postoperative effusions. Patient care protocols, especially those concerning echocardiographic surveillance, should take these findings into consideration. Patients dismissed from the hospital with small clinically insignificant pericardial effusions, especially after valve surgery, should be educated as to the risk of progression of effusions (52% in this study) and the attendant nonspecific symptoms such as fatigue and dyspnea. References 1. Price S, Prout J, Jaggar SI, Gibson DG, Pepper JR. Tamponade following cardiac surgery: terminology and echocardiography may both mislead. Eur J Cardiothorac Surg 2004;26: Kulik A, Rubens FD, Wells PS, et al. Early postoperative anticoagulation after mechanical valve replacement: a systematic review. Ann Thorac Surg 2006;81: Tsang TS, Barnes ME, Hayes SN, et al. Clinical and echocardiographic characteristics of significant pericardial effusions following cardiothoracic surgery and outcomes of echoguided pericardiocentesis for management: Mayo Clinic experience, Chest 1999;116: Ikäheimo MJ, Huikuri HV, Airaksinen KE, et al. Pericardial effusion after cardiac surgery: incidence, relation to the type of surgery, antithrombotic therapy, and early coronary bypass graft patency. Am Heart J 1988;116(1 pt 1): Pepi M, Muratori M, Barbier P, et al. Pericardial effusion after cardiac surgery: incidence, site, size, and haemodynamic consequences. Br Heart J 1994;72: Malouf JF, Alam S, Gharzeddine W, Stefadouros MA. The role of anticoagulation in the development of pericardial effusion and late tamponade after cardiac surgery. Eur Heart J 1993;14: Cheung EW, Ho SA, Tang KK, Chau AK, Chiu CS, Cheung YF. Pericardial effusion after open heart surgery for congenital heart disease. Heart 2003;89: Kuvin JT, Harati NA, Pandian NG, Bojar RM, Khabbaz KR. Postoperative cardiac tamponade in the modern surgical era. Ann Thorac Surg 2002;74: Tsang TS, Enriquez-Sarano M, Freeman WK, et al. Consecutive 1127 therapeutic echocardiographically guided pericardiocenteses: clinical profile, practice patterns, and outcomes spanning 21 years. Mayo Clin Proc 2002;77: Susini G, Pepi M, Sisillo E, et al. Percutaneous pericardiocentesis versus subxiphoid pericardiotomy in cardiac tamponade due to postoperative pericardial effusion. J Cardiothorac Vasc Anesth 1993;7: Al-Dadah AS, Guthrie TJ, Pasque MK, Moon MR, Ewald GA, Moazami N. Clinical course and predictors of pericardial effusion following cardiac transplantation. Transplant Proc 2007;39: Vandenberg BF, Mohanty PK, Craddock KJ, et al. Clinical significance of pericardial effusion after heart transplantation. J Heart Transplant 1988;7: Quin JA, Tauriainen MP, Huber LM, et al. Predictors of pericardial effusion after orthotopic heart transplantation. J Thorac Cardiovasc Surg 2002;124: Hauptman PJ, Couper GS, Aranki SF, Kartashov A, Mudge GH Jr, Loh E. Pericardial effusions after cardiac transplantation. J Am Coll Cardiol 1994;23: Alkhulaifi AM, Speechly-Dick ME, Swanton RH, Pattison CW, Pugsley WB. The incidence of significant pericardial effusion and tamponade following major aortic root surgery. J Cardiovasc Surg (Torino) 1996;37: Eryilmaz S, Emiroglu O, Eyileten Z, et al. Effect of posterior pericardial drainage on the incidence of pericardial effusion after ascending aortic surgery. J Thorac Cardiovasc Surg 2006;132: Meurin P, Weber H, Renaud N, et al. Evolution of the postoperative pericardial effusion after day 15: the problem of the late tamponade. Chest 2004;125:
TAMPONADE CARDIAQUE. Dr Cédrick Zaouter TUSAR 15 décembre 2015
 TAMPONADE CARDIAQUE Dr Cédrick Zaouter TUSAR 15 décembre 2015 OUTLINE History Incidence Definition Pathophysiology Aetiologies Investigations - Echocardiography Treatment of cardiac tamponade Pericardial
TAMPONADE CARDIAQUE Dr Cédrick Zaouter TUSAR 15 décembre 2015 OUTLINE History Incidence Definition Pathophysiology Aetiologies Investigations - Echocardiography Treatment of cardiac tamponade Pericardial
Surgery for Acquired Cardiovascular Disease
 Effect of posterior pericardial drainage on the incidence of pericardial effusion after ascending aortic surgery Sadik Eryilmaz, MD, Ozan Emiroglu, MD, Zeynep Eyileten, MD, Ruchan Akar, MD, Levent Yazicioglu,
Effect of posterior pericardial drainage on the incidence of pericardial effusion after ascending aortic surgery Sadik Eryilmaz, MD, Ozan Emiroglu, MD, Zeynep Eyileten, MD, Ruchan Akar, MD, Levent Yazicioglu,
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
Echocardiography as a diagnostic and management tool in medical emergencies
 Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
University of Florida Department of Surgery. CardioThoracic Surgery VA Learning Objectives
 University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014
 Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014 Indications for cardiac catheterization Before a decision to perform an invasive procedure such
Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014 Indications for cardiac catheterization Before a decision to perform an invasive procedure such
Adult Echocardiography Examination Content Outline
 Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
(Ann Thorac Surg 2008;85:845 53)
 I Made Adi Parmana The utility of intraoperative TEE has become increasingly more evident as anesthesiologists, cardiologists, and surgeons continue to appreciate its potential application as an invaluable
I Made Adi Parmana The utility of intraoperative TEE has become increasingly more evident as anesthesiologists, cardiologists, and surgeons continue to appreciate its potential application as an invaluable
Πνευμονική υπέρταση και περικαρδιακή συλλογή. Τρόποι αντιμετώπισης
 Πνευμονική υπέρταση και περικαρδιακή συλλογή. Τρόποι αντιμετώπισης Γεώργιος Λάζαρος Καρδιολόγος, Διευθυντής ΕΣΥ Α Πανεπιστημιακή Καρδιολογική Κλινική Ιπποκράτειο Γ.Ν. Αθηνών Pericardial syndromes o Acute
Πνευμονική υπέρταση και περικαρδιακή συλλογή. Τρόποι αντιμετώπισης Γεώργιος Λάζαρος Καρδιολόγος, Διευθυντής ΕΣΥ Α Πανεπιστημιακή Καρδιολογική Κλινική Ιπποκράτειο Γ.Ν. Αθηνών Pericardial syndromes o Acute
7. Echocardiography Appropriate Use Criteria (by Indication)
 Criteria for Echocardiography 1133 7. Echocardiography Criteria (by ) Table 1. TTE for General Evaluation of Cardiac Structure and Function Suspected Cardiac Etiology General With TTE 1. Symptoms or conditions
Criteria for Echocardiography 1133 7. Echocardiography Criteria (by ) Table 1. TTE for General Evaluation of Cardiac Structure and Function Suspected Cardiac Etiology General With TTE 1. Symptoms or conditions
Safety of Same-Day Coronary Angiography in Patients Undergoing Elective Aortic Valve Replacement
 Safety of Same-Day Coronary Angiography in Patients Undergoing Elective Aortic Valve Replacement Kevin L. Greason, MD, Lars Englberger, MD, Rakesh M. Suri, MD, PhD, Soon J. Park, MD, Charanjit S. Rihal,
Safety of Same-Day Coronary Angiography in Patients Undergoing Elective Aortic Valve Replacement Kevin L. Greason, MD, Lars Englberger, MD, Rakesh M. Suri, MD, PhD, Soon J. Park, MD, Charanjit S. Rihal,
Cardiothoracic Transplantation. Predictors of pericardial effusion after orthotopic heart transplantation
 Predictors of pericardial effusion after orthotopic heart transplantation Jacquelyn A. Quin, MD M. Peter Tauriainen, MD Lynne M. Huber, RN Donald D. McIntire, PhD Patricia A. Kaiser, RN W. Steves Ring,
Predictors of pericardial effusion after orthotopic heart transplantation Jacquelyn A. Quin, MD M. Peter Tauriainen, MD Lynne M. Huber, RN Donald D. McIntire, PhD Patricia A. Kaiser, RN W. Steves Ring,
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Expanding Relevance of Aortic Valve Repair Is Earlier Operation Indicated?
 Expanding Relevance of Aortic Valve Repair Is Earlier Operation Indicated? RM Suri, V Sharma, JA Dearani, HM Burkhart, RC Daly, LD Joyce, HV Schaff Division of Cardiovascular Surgery, Mayo Clinic, Rochester,
Expanding Relevance of Aortic Valve Repair Is Earlier Operation Indicated? RM Suri, V Sharma, JA Dearani, HM Burkhart, RC Daly, LD Joyce, HV Schaff Division of Cardiovascular Surgery, Mayo Clinic, Rochester,
Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease
 Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease TIRONE E. DAVID, MD ; SEMIN THORAC CARDIOVASC SURG 19:116-120c 2007 ELSEVIER INC. PRESENTED BY INTERN 許士盟 Mitral valve
Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease TIRONE E. DAVID, MD ; SEMIN THORAC CARDIOVASC SURG 19:116-120c 2007 ELSEVIER INC. PRESENTED BY INTERN 許士盟 Mitral valve
Detailed Order Request Checklists for Cardiology
 Next Generation Solutions Detailed Order Request Checklists for Cardiology 8600 West Bryn Mawr Avenue South Tower Suite 800 Chicago, IL 60631 www.aimspecialtyhealth.com Appropriate.Safe.Affordable 2018
Next Generation Solutions Detailed Order Request Checklists for Cardiology 8600 West Bryn Mawr Avenue South Tower Suite 800 Chicago, IL 60631 www.aimspecialtyhealth.com Appropriate.Safe.Affordable 2018
ASE 2011 Appropriate Use Criteria for Echocardiography
 ASE 2011 Appropriate Use Criteria for Echocardiography Table 1. TTE for General Evaluation of Cardiac Structure and Function 1 2 Suspected Cardiac Etiology General With TTE Symptoms or conditions potentially
ASE 2011 Appropriate Use Criteria for Echocardiography Table 1. TTE for General Evaluation of Cardiac Structure and Function 1 2 Suspected Cardiac Etiology General With TTE Symptoms or conditions potentially
Importance of the third arterial graft in multiple arterial grafting strategies
 Research Highlight Importance of the third arterial graft in multiple arterial grafting strategies David Glineur Department of Cardiovascular Surgery, Cliniques St Luc, Bouge and the Department of Cardiovascular
Research Highlight Importance of the third arterial graft in multiple arterial grafting strategies David Glineur Department of Cardiovascular Surgery, Cliniques St Luc, Bouge and the Department of Cardiovascular
Bicuspid aortic root spared during ascending aorta surgery: an update of long-term results
 Short Communication Bicuspid aortic root spared during ascending aorta surgery: an update of long-term results Marco Russo, Guglielmo Saitto, Paolo Nardi, Fabio Bertoldo, Carlo Bassano, Antonio Scafuri,
Short Communication Bicuspid aortic root spared during ascending aorta surgery: an update of long-term results Marco Russo, Guglielmo Saitto, Paolo Nardi, Fabio Bertoldo, Carlo Bassano, Antonio Scafuri,
Quality Outcomes Mitral Valve Repair
 Quality Outcomes Mitral Valve Repair Moving Beyond Reoperation Rakesh M. Suri, D.Phil. Professor of Surgery 2015 MFMER 3431548-1 Disclosure Mayo Clinic Division of Cardiovascular Surgery Research funding
Quality Outcomes Mitral Valve Repair Moving Beyond Reoperation Rakesh M. Suri, D.Phil. Professor of Surgery 2015 MFMER 3431548-1 Disclosure Mayo Clinic Division of Cardiovascular Surgery Research funding
Clinical Indications for Echocardiography
 Clinical Indications for Echocardiography Echocardiography is widely utilised and potential applications are increasing with advances in technology. The aim of this document is two-fold: 1) To define clinical
Clinical Indications for Echocardiography Echocardiography is widely utilised and potential applications are increasing with advances in technology. The aim of this document is two-fold: 1) To define clinical
Rotation: Echocardiography: Transthoracic Echocardiography (TTE)
 Rotation: Echocardiography: Transthoracic Echocardiography (TTE) Rotation Format and Responsibilities: Fellows rotate in the echocardiography laboratory in each clinical year. Rotations during the first
Rotation: Echocardiography: Transthoracic Echocardiography (TTE) Rotation Format and Responsibilities: Fellows rotate in the echocardiography laboratory in each clinical year. Rotations during the first
Does Patient-Prosthesis Mismatch Affect Long-term Results after Mitral Valve Replacement?
 Original Article Does Patient-Prosthesis Mismatch Affect Long-term Results after Mitral Valve Replacement? Hiroaki Sakamoto, MD, PhD, and Yasunori Watanabe, MD, PhD Background: Recently, some articles
Original Article Does Patient-Prosthesis Mismatch Affect Long-term Results after Mitral Valve Replacement? Hiroaki Sakamoto, MD, PhD, and Yasunori Watanabe, MD, PhD Background: Recently, some articles
University of Wisconsin - Madison Cardiovascular Medicine Fellowship Program UW CICU Rotation Goals and Objectives
 Background: The field of critical care cardiology has evolved considerably over the past 2 decades. Contemporary critical care cardiology is increasingly focused on the management of patients with advanced
Background: The field of critical care cardiology has evolved considerably over the past 2 decades. Contemporary critical care cardiology is increasingly focused on the management of patients with advanced
The operative mortality rate after redo valvular operations
 Clinical Outcomes of Redo Valvular Operations: A 20-Year Experience Naoto Fukunaga, MD, Yukikatsu Okada, MD, Yasunobu Konishi, MD, Takashi Murashita, MD, Mitsuru Yuzaki, MD, Yu Shomura, MD, Hiroshi Fujiwara,
Clinical Outcomes of Redo Valvular Operations: A 20-Year Experience Naoto Fukunaga, MD, Yukikatsu Okada, MD, Yasunobu Konishi, MD, Takashi Murashita, MD, Mitsuru Yuzaki, MD, Yu Shomura, MD, Hiroshi Fujiwara,
Pericardial Diseases. Smonporn Boonyaratavej, MD. Division of Cardiology, Department of Medicine Chulalongkorn University
 Pericardial Diseases Smonporn Boonyaratavej, MD Division of Cardiology, Department of Medicine Chulalongkorn University Cardiac Center, King Chulalongkorn Memorial Hospital 21 AUGUST 2016 Pericardial
Pericardial Diseases Smonporn Boonyaratavej, MD Division of Cardiology, Department of Medicine Chulalongkorn University Cardiac Center, King Chulalongkorn Memorial Hospital 21 AUGUST 2016 Pericardial
Emergency surgery in acute coronary syndrome
 Emergency surgery in acute coronary syndrome Teerawoot Jantarawan Division of Cardiothoracic Surgery, Department of Surgery, Faculty of Medicine Siriraj Hospital, Mahidol University, Bangkok, Thailand
Emergency surgery in acute coronary syndrome Teerawoot Jantarawan Division of Cardiothoracic Surgery, Department of Surgery, Faculty of Medicine Siriraj Hospital, Mahidol University, Bangkok, Thailand
Emergency Intraoperative Echocardiography
 Emergency Intraoperative Echocardiography Justiaan Swanevelder Department of Anaesthesia, Glenfield Hospital University Hospitals of Leicester NHS Trust, UK Carl Gustav Jung (1875-1961) Your vision will
Emergency Intraoperative Echocardiography Justiaan Swanevelder Department of Anaesthesia, Glenfield Hospital University Hospitals of Leicester NHS Trust, UK Carl Gustav Jung (1875-1961) Your vision will
Prof. Patrizio LANCELLOTTI, MD, PhD Heart Valve Clinic, University of Liège, CHU Sart Tilman, Liège, BELGIUM
 The Patient with Aortic Stenosis and Mitral Regurgitation Prof. Patrizio LANCELLOTTI, MD, PhD Heart Valve Clinic, University of Liège, CHU Sart Tilman, Liège, BELGIUM Aortic Stenosis + Mitral Regurgitation?
The Patient with Aortic Stenosis and Mitral Regurgitation Prof. Patrizio LANCELLOTTI, MD, PhD Heart Valve Clinic, University of Liège, CHU Sart Tilman, Liège, BELGIUM Aortic Stenosis + Mitral Regurgitation?
Left ventricle pseudoaneurysm as late postoperative complication of a large apical aneurysm
 CASE REPORT Left ventricle pseudoaneurysm as late postoperative complication of a large apical aneurysm Mariana M. Floria 1, 4, Carmen Elena Pleșoianu 2, 4, Michel Buche 3, Baudouin Marchandise 4, Erwin
CASE REPORT Left ventricle pseudoaneurysm as late postoperative complication of a large apical aneurysm Mariana M. Floria 1, 4, Carmen Elena Pleșoianu 2, 4, Michel Buche 3, Baudouin Marchandise 4, Erwin
12 th Annual West Virginia ACC Meeting April 8, 2017
 12 th Annual West Virginia ACC Meeting April 8, 2017 Rameez Sayyed, M.D., FACC, FSCAI Associate professor of Medicine Program Director for interventional cardiology Marshall University Joan C. Edwards
12 th Annual West Virginia ACC Meeting April 8, 2017 Rameez Sayyed, M.D., FACC, FSCAI Associate professor of Medicine Program Director for interventional cardiology Marshall University Joan C. Edwards
Complications of Acute Myocardial Infarction
 Acute Myocardial Infarction Complications of Acute Myocardial Infarction Diagnosis and Treatment JMAJ 45(4): 149 154, 2002 Hiroshi NONOGI Director, Division of Cardiology and Emergency Medicine, National
Acute Myocardial Infarction Complications of Acute Myocardial Infarction Diagnosis and Treatment JMAJ 45(4): 149 154, 2002 Hiroshi NONOGI Director, Division of Cardiology and Emergency Medicine, National
A Novel Score to Estimate the Risk of Pneumonia After Cardiac Surgery
 A Novel Score to Estimate the Risk of Pneumonia After Cardiac Surgery Arman Kilic, MD 1, Rika Ohkuma, MD 1, J. Trent Magruder, MD 1, Joshua C. Grimm, MD 1, Marc Sussman, MD 1, Eric B. Schneider, PhD 1,
A Novel Score to Estimate the Risk of Pneumonia After Cardiac Surgery Arman Kilic, MD 1, Rika Ohkuma, MD 1, J. Trent Magruder, MD 1, Joshua C. Grimm, MD 1, Marc Sussman, MD 1, Eric B. Schneider, PhD 1,
Local Coverage Determination (LCD) for Cardiac Catheterization (L29090)
 Local Coverage Determination (LCD) for Cardiac Catheterization (L29090) Contractor Information Contractor Name First Coast Service Options, Inc. Contractor Number 09102 Contractor Type MAC - Part B LCD
Local Coverage Determination (LCD) for Cardiac Catheterization (L29090) Contractor Information Contractor Name First Coast Service Options, Inc. Contractor Number 09102 Contractor Type MAC - Part B LCD
CORONARY ARTERY BYPASS GRAFT (CABG) MEASURES GROUP OVERVIEW
 CONARY ARTERY BYPASS GRAFT (CABG) MEASURES GROUP OVERVIEW 2015 PQRS OPTIONS F MEASURES GROUPS: 2015 PQRS MEASURES IN CONARY ARTERY BYPASS GRAFT (CABG) MEASURES GROUP: #43 Coronary Artery Bypass Graft (CABG):
CONARY ARTERY BYPASS GRAFT (CABG) MEASURES GROUP OVERVIEW 2015 PQRS OPTIONS F MEASURES GROUPS: 2015 PQRS MEASURES IN CONARY ARTERY BYPASS GRAFT (CABG) MEASURES GROUP: #43 Coronary Artery Bypass Graft (CABG):
Ischemic Ventricular Septal Rupture
 Ischemic Ventricular Septal Rupture Optimal Management Strategies Juan P. Umaña, M.D. Chief Medical Officer FCI Institute of Cardiology Disclosures Abbott Mitraclip Royalties Johnson & Johnson Proctor
Ischemic Ventricular Septal Rupture Optimal Management Strategies Juan P. Umaña, M.D. Chief Medical Officer FCI Institute of Cardiology Disclosures Abbott Mitraclip Royalties Johnson & Johnson Proctor
The pericardial sac is composed of the outer fibrous pericardium
 Pericardiectomy for Constrictive or Recurrent Inflammatory Pericarditis Mauricio A. Villavicencio, MD, Joseph A. Dearani, MD, and Thoralf M. Sundt, III, MD Anatomy and Preoperative Considerations The pericardial
Pericardiectomy for Constrictive or Recurrent Inflammatory Pericarditis Mauricio A. Villavicencio, MD, Joseph A. Dearani, MD, and Thoralf M. Sundt, III, MD Anatomy and Preoperative Considerations The pericardial
Adel Hasanin Ahmed 1
 Adel Hasanin Ahmed 1 PERICARDIAL DISEASE The pericardial effusion ends anteriorly to the descending aorta and is best visualised in the PLAX. PSAX is actually very useful sometimes for looking at posterior
Adel Hasanin Ahmed 1 PERICARDIAL DISEASE The pericardial effusion ends anteriorly to the descending aorta and is best visualised in the PLAX. PSAX is actually very useful sometimes for looking at posterior
Assessing Cardiac Risk in Noncardiac Surgery. Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington
 Assessing Cardiac Risk in Noncardiac Surgery Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington Disclosure None. I have no conflicts of interest, financial or otherwise. CME
Assessing Cardiac Risk in Noncardiac Surgery Murali Sivarajan, M.D. Professor University of Washington Seattle, Washington Disclosure None. I have no conflicts of interest, financial or otherwise. CME
Effects of prophylactic indomethacin treatment on postoperative pericardial effusion after aortic surgery
 Effects of prophylactic indomethacin treatment on postoperative pericardial effusion after aortic surgery Mustafa Bahadir Inan, MD, Levent Yazıcıoglu, MD, Sadik Eryılmaz, MD, Mustafa Sırlak, MD, Demir
Effects of prophylactic indomethacin treatment on postoperative pericardial effusion after aortic surgery Mustafa Bahadir Inan, MD, Levent Yazıcıoglu, MD, Sadik Eryılmaz, MD, Mustafa Sırlak, MD, Demir
Intra-operative Echocardiography: When to Go Back on Pump
 Intra-operative Echocardiography: When to Go Back on Pump GREGORIO G. ROGELIO, MD., F.P.C.C. OUTLINE A. Indications for Intraoperative Echocardiography B. Role of Intraoperative Echocardiography C. Criteria
Intra-operative Echocardiography: When to Go Back on Pump GREGORIO G. ROGELIO, MD., F.P.C.C. OUTLINE A. Indications for Intraoperative Echocardiography B. Role of Intraoperative Echocardiography C. Criteria
THE PERICARDIUM: LOOKING OUTSIDE THE HEART
 THE PERICARDIUM: LOOKING OUTSIDE THE HEART DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and mitigate
THE PERICARDIUM: LOOKING OUTSIDE THE HEART DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and mitigate
DEPARTMENT OF SURGERY CARDIOVASCULAR-THORACIC SECTION
 DEPARTMENT OF SURGERY CARDIOVASCULAR-THORACIC SECTION DIRECTIONS: This must accompany all initial applications for appointment to the Cardiovascular-Thoracic Section, Department of Surgery. Please indicate
DEPARTMENT OF SURGERY CARDIOVASCULAR-THORACIC SECTION DIRECTIONS: This must accompany all initial applications for appointment to the Cardiovascular-Thoracic Section, Department of Surgery. Please indicate
Cardiac tamponade and Pericardiocentesis Made Easy
 Cardiac tamponade and Pericardiocentesis Made Easy www.cardiconcept.com Etiology of pericardial diseases. Non Infectious cause Infectious cause European Heart Journal (2015) 36, 2921 2964 Recommendations
Cardiac tamponade and Pericardiocentesis Made Easy www.cardiconcept.com Etiology of pericardial diseases. Non Infectious cause Infectious cause European Heart Journal (2015) 36, 2921 2964 Recommendations
Index. K Knobology, TTE artifact, image resolution, ultrasound, 14
 A Acute aortic regurgitation (AR), 124 128 Acute aortic syndrome (AAS) classic aortic dissection diagnosis, 251 263 evolutive patterns, 253 255 pathology, 250 251 classifications, 247 248 incomplete aortic
A Acute aortic regurgitation (AR), 124 128 Acute aortic syndrome (AAS) classic aortic dissection diagnosis, 251 263 evolutive patterns, 253 255 pathology, 250 251 classifications, 247 248 incomplete aortic
Coronary Artery Bypass Graft: Monitoring Patients and Detecting Complications
 Coronary Artery Bypass Graft: Monitoring Patients and Detecting Complications Madhav Swaminathan, MD, FASE Professor of Anesthesiology Division of Cardiothoracic Anesthesia & Critical Care Duke University
Coronary Artery Bypass Graft: Monitoring Patients and Detecting Complications Madhav Swaminathan, MD, FASE Professor of Anesthesiology Division of Cardiothoracic Anesthesia & Critical Care Duke University
Cardiac anaesthesia. Simon May
 Cardiac anaesthesia Simon May Contents Cardiac: Principles of peri-operative management for cardiac surgery Cardiopulmonary bypass, cardioplegia and off pump cardiac surgery Cardiac disease and its implications
Cardiac anaesthesia Simon May Contents Cardiac: Principles of peri-operative management for cardiac surgery Cardiopulmonary bypass, cardioplegia and off pump cardiac surgery Cardiac disease and its implications
Which Type of Secondary Tricuspid Regurgitation Accompanying Mitral Valve Disease Should Be Surgically Treated?
 Ann Thorac Cardiovasc Surg 2013; 19: 428 434 Online January 31, 2013 doi: 10.5761/atcs.oa.12.01929 Original Article Which Type of Secondary Tricuspid Regurgitation Accompanying Mitral Valve Disease Should
Ann Thorac Cardiovasc Surg 2013; 19: 428 434 Online January 31, 2013 doi: 10.5761/atcs.oa.12.01929 Original Article Which Type of Secondary Tricuspid Regurgitation Accompanying Mitral Valve Disease Should
Learning Objectives. Denver Health Medical Center. Nothing to Disclose... Advanced Topics in Anesthesia
 Nothing to Disclose... Learning Objectives 1. Describe which clinical situations are appropriate for TEE monitoring in noncardiac surgery including indications / contraindications for TEE placement. 2.
Nothing to Disclose... Learning Objectives 1. Describe which clinical situations are appropriate for TEE monitoring in noncardiac surgery including indications / contraindications for TEE placement. 2.
Outcomes of Surgical Aortic Valve Replacement in Moderate Risk Patients: Implications for Determination of Equipoise in the Transcatheter Era
 Outcomes of Surgical Aortic Valve Replacement in Moderate Risk Patients: Implications for Determination of Equipoise in the Transcatheter Era Sebastian A. Iturra, Rakesh M. Suri, Kevin L. Greason, John
Outcomes of Surgical Aortic Valve Replacement in Moderate Risk Patients: Implications for Determination of Equipoise in the Transcatheter Era Sebastian A. Iturra, Rakesh M. Suri, Kevin L. Greason, John
PERICARDIAL DIAESE. Kaijun Cui Associated professor Sichuan University
 PERICARDIAL DIAESE Kaijun Cui Associated professor Sichuan University CLASSIFICATION acute pericarditis pericardial effusion cardiac tamponade constrictive pericarditis congenitally absent pericardium
PERICARDIAL DIAESE Kaijun Cui Associated professor Sichuan University CLASSIFICATION acute pericarditis pericardial effusion cardiac tamponade constrictive pericarditis congenitally absent pericardium
Outline. Echocardiographic Assessment of Pericardial Effusion/Tamponade: The Essentials
 Echocardiographic Assessment of Pericardial Effusion/Tamponade: The Essentials John R Schairer DO FACC Henry Ford Heart and Vascular Institute No Disclosures Outline Normal Anatomy and Physiology Pathophysiology
Echocardiographic Assessment of Pericardial Effusion/Tamponade: The Essentials John R Schairer DO FACC Henry Ford Heart and Vascular Institute No Disclosures Outline Normal Anatomy and Physiology Pathophysiology
Cardiology. Objectives. Chapter
 1:44 M age 1121 Chapter Cardiology Objectives art 1: Cardiovascular natomy and hysiology, ECG Monitoring, and Dysrhythmia nalysis (begins on p. 1127) fter reading art 1 of this chapter, you should be able
1:44 M age 1121 Chapter Cardiology Objectives art 1: Cardiovascular natomy and hysiology, ECG Monitoring, and Dysrhythmia nalysis (begins on p. 1127) fter reading art 1 of this chapter, you should be able
Incidence of Postoperative Atrial Fibrillation after minimally invasive mitral valve surgery
 Incidence of Postoperative Atrial Fibrillation after minimally invasive mitral valve surgery JUAN S. JARAMILLO, MD Cardiovascular Surgery Clinica CardioVID Medellin Colombia DISCLOSURE INFORMATION Consultant
Incidence of Postoperative Atrial Fibrillation after minimally invasive mitral valve surgery JUAN S. JARAMILLO, MD Cardiovascular Surgery Clinica CardioVID Medellin Colombia DISCLOSURE INFORMATION Consultant
Surgical Management of TOF in Adults. Dr Flora Tsang Associate Consultant Department of Cardiothoracic Surgery Queen Mary Hospital
 Surgical Management of TOF in Adults Dr Flora Tsang Associate Consultant Department of Cardiothoracic Surgery Queen Mary Hospital Tetralogy of Fallot (TOF) in Adults Most common cyanotic congenital heart
Surgical Management of TOF in Adults Dr Flora Tsang Associate Consultant Department of Cardiothoracic Surgery Queen Mary Hospital Tetralogy of Fallot (TOF) in Adults Most common cyanotic congenital heart
Right-Sided Congestive Heart Failure Basics
 Right-Sided Congestive Heart Failure Basics OVERVIEW Failure of the right side of the heart to pump blood at a sufficient rate to meet the needs of the body or to prevent blood from pooling within the
Right-Sided Congestive Heart Failure Basics OVERVIEW Failure of the right side of the heart to pump blood at a sufficient rate to meet the needs of the body or to prevent blood from pooling within the
The use of mitral valve (MV) repair to correct mitral
 Outcomes and Long-Term Survival for Patients Undergoing Repair Versus Effect of Age and Concomitant Coronary Artery Bypass Grafting Vinod H. Thourani, MD; William S. Weintraub, MD; Robert A. Guyton, MD;
Outcomes and Long-Term Survival for Patients Undergoing Repair Versus Effect of Age and Concomitant Coronary Artery Bypass Grafting Vinod H. Thourani, MD; William S. Weintraub, MD; Robert A. Guyton, MD;
DECLARATION OF CONFLICT OF INTEREST
 DECLARATION OF CONFLICT OF INTEREST Cardiogenic Shock Mechanical Support Eulàlia Roig FESC Heart Failure and HT Unit Hospital Sant Pau - UAB Barcelona. Spain No conflics of interest Mechanical Circulatory
DECLARATION OF CONFLICT OF INTEREST Cardiogenic Shock Mechanical Support Eulàlia Roig FESC Heart Failure and HT Unit Hospital Sant Pau - UAB Barcelona. Spain No conflics of interest Mechanical Circulatory
Echo Emergencies. Outline. Michael H. Picard, MD Massachusetts General Hospital Harvard Medical School No disclosures
 Echo Emergencies Michael H. Picard, MD Massachusetts General Hospital Harvard Medical School No disclosures Outline Common emergency / on call scenarios Tamponade Pulmonary embolism/rv strain Cardiogenic
Echo Emergencies Michael H. Picard, MD Massachusetts General Hospital Harvard Medical School No disclosures Outline Common emergency / on call scenarios Tamponade Pulmonary embolism/rv strain Cardiogenic
Repair or Replacement
 Surgical intervention post MitraClip Device: Repair or Replacement Saudi Heart Association, February 21-24 Rüdiger Lange, MD, PhD Nicolo Piazza, MD, FRCPC, FESC German Heart Center, Munich, Germany Division
Surgical intervention post MitraClip Device: Repair or Replacement Saudi Heart Association, February 21-24 Rüdiger Lange, MD, PhD Nicolo Piazza, MD, FRCPC, FESC German Heart Center, Munich, Germany Division
The right heart: the Cinderella of heart failure
 The right heart: the Cinderella of heart failure Piotr Ponikowski, MD, PhD, FESC Medical University, Centre for Heart Disease Clinical Military Hospital Wroclaw, Poland none Disclosure Look into the Heart
The right heart: the Cinderella of heart failure Piotr Ponikowski, MD, PhD, FESC Medical University, Centre for Heart Disease Clinical Military Hospital Wroclaw, Poland none Disclosure Look into the Heart
Supplementary Table S1: Proportion of missing values presents in the original dataset
 Supplementary Table S1: Proportion of missing values presents in the original dataset Variable Included (%) Missing (%) Age 89067 (100.0) 0 (0.0) Gender 89067 (100.0) 0 (0.0) Smoking status 80706 (90.6)
Supplementary Table S1: Proportion of missing values presents in the original dataset Variable Included (%) Missing (%) Age 89067 (100.0) 0 (0.0) Gender 89067 (100.0) 0 (0.0) Smoking status 80706 (90.6)
CMS Limitations Guide - Radiology Services
 CMS Limitations Guide - Radiology Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
CMS Limitations Guide - Radiology Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
The Ross Procedure: Outcomes at 20 Years
 The Ross Procedure: Outcomes at 20 Years Tirone David Carolyn David Anna Woo Cedric Manlhiot University of Toronto Conflict of Interest None The Ross Procedure 1990 to 2004 212 patients: 66% 34% Mean age:
The Ross Procedure: Outcomes at 20 Years Tirone David Carolyn David Anna Woo Cedric Manlhiot University of Toronto Conflict of Interest None The Ross Procedure 1990 to 2004 212 patients: 66% 34% Mean age:
Chairman and O. Wayne Isom Professor Department of Cardiothoracic Surgery Weill Cornell Medicine
 Leonard N. Girardi, M.D. Chairman and O. Wayne Isom Professor Department of Cardiothoracic Surgery Weill Cornell Medicine New York, New York Houston Aortic Symposium Houston, Texas February 23, 2017 weill.cornell.edu
Leonard N. Girardi, M.D. Chairman and O. Wayne Isom Professor Department of Cardiothoracic Surgery Weill Cornell Medicine New York, New York Houston Aortic Symposium Houston, Texas February 23, 2017 weill.cornell.edu
Restoration of Sinus Rhythm by the Maze Procedure Halts Progression of Tricuspid Regurgitation After Mitral Surgery
 Restoration of Sinus Rhythm by the Maze Procedure Halts Progression of Tricuspid Regurgitation After Mitral Surgery John M. Stulak, MD,* Hartzell V. Schaff, MD, Joseph A. Dearani, MD, Thomas A. Orszulak,
Restoration of Sinus Rhythm by the Maze Procedure Halts Progression of Tricuspid Regurgitation After Mitral Surgery John M. Stulak, MD,* Hartzell V. Schaff, MD, Joseph A. Dearani, MD, Thomas A. Orszulak,
ADVANCED CARDIOVASCULAR IMAGING. Medical Knowledge. Goals and Objectives PF EF MF LF Aspirational
 Medical Knowledge Goals and Objectives PF EF MF LF Aspirational Know the basic principles of magnetic resonance imaging (MRI) including the role of the magnetic fields and gradient coil systems, generation
Medical Knowledge Goals and Objectives PF EF MF LF Aspirational Know the basic principles of magnetic resonance imaging (MRI) including the role of the magnetic fields and gradient coil systems, generation
Pediatric Echocardiography Examination Content Outline
 Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia
 Marshall University Marshall Digital Scholar Internal Medicine Faculty Research Spring 5-2004 Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia Ellen A. Thompson
Marshall University Marshall Digital Scholar Internal Medicine Faculty Research Spring 5-2004 Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia Ellen A. Thompson
Useful? Definition of High-risk? Pre-OP/Intra-OP/Post-OP? Complication vs Benefit? Mortality? Morbidity?
 Preoperative intraaortic balloon counterpulsation in high-risk CABG Stefan Klotz, M.D. Preoperative IABP in high-risk CABG Questions?? Useful? Definition of High-risk? Pre-OP/Intra-OP/Post-OP? Complication
Preoperative intraaortic balloon counterpulsation in high-risk CABG Stefan Klotz, M.D. Preoperative IABP in high-risk CABG Questions?? Useful? Definition of High-risk? Pre-OP/Intra-OP/Post-OP? Complication
Managing Hypertension in the Perioperative Arena
 Managing Hypertension in the Perioperative Arena Optimizing Perioperative Management Strategies for Hypertension in the Cardiac Surgical Patient Objectives: Treatment of hypertensive emergencies. ALBERT
Managing Hypertension in the Perioperative Arena Optimizing Perioperative Management Strategies for Hypertension in the Cardiac Surgical Patient Objectives: Treatment of hypertensive emergencies. ALBERT
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders
 C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
When Should I Order a Stress Test or an Echocardiogram
 When Should I Order a Stress Test or an Echocardiogram Updates in Cardiology 2015 March 7, 2015 Donald L. Lappé, MD, FAHA, FACC Chairman, Cardiovascular Department Medical Director, Intermountain Cardiovascular
When Should I Order a Stress Test or an Echocardiogram Updates in Cardiology 2015 March 7, 2015 Donald L. Lappé, MD, FAHA, FACC Chairman, Cardiovascular Department Medical Director, Intermountain Cardiovascular
Risk Factor Evaluation for Thrombosis and Bleeding in Pediatric Patients with Heart Disease
 Risk Factor Evaluation for Thrombosis and Bleeding in Pediatric Patients with Heart Disease Kristen Nelson, MD Johns Hopkins University Director, Pediatric Cardiac Critical Care Why Does it Matter? Pediatric
Risk Factor Evaluation for Thrombosis and Bleeding in Pediatric Patients with Heart Disease Kristen Nelson, MD Johns Hopkins University Director, Pediatric Cardiac Critical Care Why Does it Matter? Pediatric
Counterpulsation. John N. Nanas, MD, PhD. Professor and Head, 3 rd Cardiology Dept, University of Athens, Athens, Greece
 John N. Nanas, MD, PhD Professor and Head, 3 rd Cardiology Dept, University of Athens, Athens, Greece History of counterpulsation 1952 Augmentation of CBF Adrian and Arthur Kantrowitz, Surgery 1952;14:678-87
John N. Nanas, MD, PhD Professor and Head, 3 rd Cardiology Dept, University of Athens, Athens, Greece History of counterpulsation 1952 Augmentation of CBF Adrian and Arthur Kantrowitz, Surgery 1952;14:678-87
Hemodynamic Monitoring and Circulatory Assist Devices
 Hemodynamic Monitoring and Circulatory Assist Devices Speaker: Jana Ogden Learning Unit 2: Hemodynamic Monitoring and Circulatory Assist Devices Hemodynamic monitoring refers to the measurement of pressure,
Hemodynamic Monitoring and Circulatory Assist Devices Speaker: Jana Ogden Learning Unit 2: Hemodynamic Monitoring and Circulatory Assist Devices Hemodynamic monitoring refers to the measurement of pressure,
Presenter Disclosure. Patrick O. Myers, M.D. No Relationships to Disclose
 Presenter Disclosure Patrick O. Myers, M.D. No Relationships to Disclose Aortic Valve Repair by Cusp Extension for Rheumatic Aortic Insufficiency in Children Long term Results and Impact of Extension Material
Presenter Disclosure Patrick O. Myers, M.D. No Relationships to Disclose Aortic Valve Repair by Cusp Extension for Rheumatic Aortic Insufficiency in Children Long term Results and Impact of Extension Material
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Bhakta N, Liu Q, Yeo F, et al. Cumulative burden
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Bhakta N, Liu Q, Yeo F, et al. Cumulative burden
Echocardiographic Cardiovascular Risk Stratification: Beyond Ejection Fraction
 Echocardiographic Cardiovascular Risk Stratification: Beyond Ejection Fraction October 4, 2014 James S. Lee, M.D., F.A.C.C. Associates in Cardiology, P.A. Silver Spring, M.D. Disclosures Financial none
Echocardiographic Cardiovascular Risk Stratification: Beyond Ejection Fraction October 4, 2014 James S. Lee, M.D., F.A.C.C. Associates in Cardiology, P.A. Silver Spring, M.D. Disclosures Financial none
Mitral Gradients and Frequency of Recurrence of Mitral Regurgitation After Ring Annuloplasty for Ischemic Mitral Regurgitation
 Mitral Gradients and Frequency of Recurrence of Mitral Regurgitation After Ring Annuloplasty for Ischemic Mitral Regurgitation Matthew L. Williams, MD, Mani A. Daneshmand, MD, James G. Jollis, MD, John
Mitral Gradients and Frequency of Recurrence of Mitral Regurgitation After Ring Annuloplasty for Ischemic Mitral Regurgitation Matthew L. Williams, MD, Mani A. Daneshmand, MD, James G. Jollis, MD, John
AORTIC DISSECTION. DISSECTING ANEURYSMS OF THE AORTA or CLASSIFICATION
 DISSECTING ANEURYSMS OF THE AORTA or AORTIC DISSECTION CLASSIFICATION DeBakey classified aortic dissections into types I, II, and III :- Type I dissection the tear site originates in the ascending aorta,
DISSECTING ANEURYSMS OF THE AORTA or AORTIC DISSECTION CLASSIFICATION DeBakey classified aortic dissections into types I, II, and III :- Type I dissection the tear site originates in the ascending aorta,
TSDA ACGME Milestones
 TSDA ACGME Milestones Short MW and Edwards JA. Assessing resident milestones using a CASPE March 2012 Short MW and Edwards JA. Assessing resident milestones using a CASPE March 2012 Short
TSDA ACGME Milestones Short MW and Edwards JA. Assessing resident milestones using a CASPE March 2012 Short MW and Edwards JA. Assessing resident milestones using a CASPE March 2012 Short
Retrospective Study Of Redo Cardiac Surgery In A Single Centre. R Karthekeyan, K Selvaraju, L Ramanathan, M Rakesh, S Rao, M Vakamudi, K Balakrishnan
 ISPUB.COM The Internet Journal of Anesthesiology Volume 12 Number 2 Retrospective Study Of Redo Cardiac Surgery In A Single Centre R Karthekeyan, K Selvaraju, L Ramanathan, M Rakesh, S Rao, M Vakamudi,
ISPUB.COM The Internet Journal of Anesthesiology Volume 12 Number 2 Retrospective Study Of Redo Cardiac Surgery In A Single Centre R Karthekeyan, K Selvaraju, L Ramanathan, M Rakesh, S Rao, M Vakamudi,
Divisions of Cardiology and Cardiovascular Surgery, Veterans Administration Medical Center and University of Minnesota, Minneapolis, Minnesota
 Comparison of Risk Scores to Estimate Perioperative Mortality in Aortic Valve Replacement Surgery Jagroop Basraon, DO, Yellapragada S. Chandrashekhar, MD, Ranjit John, MD, Adheesh Agnihotri, MD, Rosemary
Comparison of Risk Scores to Estimate Perioperative Mortality in Aortic Valve Replacement Surgery Jagroop Basraon, DO, Yellapragada S. Chandrashekhar, MD, Ranjit John, MD, Adheesh Agnihotri, MD, Rosemary
6/12/2017. Isolated Noncompaction of the Left Ventricle. Objectives. Pathophysiology
 Isolated Noncompaction of the Left Ventricle Beth Davidson DNP, ACNP, CHFN, CCRN AAHFN June 23, 2017 Objectives 1. Describe the pathophysiology of LVNC 2. Identify the key clinical findings/manifestations
Isolated Noncompaction of the Left Ventricle Beth Davidson DNP, ACNP, CHFN, CCRN AAHFN June 23, 2017 Objectives 1. Describe the pathophysiology of LVNC 2. Identify the key clinical findings/manifestations
Transient Constrictive Pericarditis: Causes and Natural History
 Journal of the American College of Cardiology Vol. 43, No. 2, 2004 2004 by the American College of Cardiology Foundation ISSN 0735-1097/04/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2003.08.032
Journal of the American College of Cardiology Vol. 43, No. 2, 2004 2004 by the American College of Cardiology Foundation ISSN 0735-1097/04/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2003.08.032
The role of bedside ultrasound in the diagnosis of pericardial effusion and cardiac tamponade
 Symposium The role of bedside ultrasound in the diagnosis of pericardial effusion and cardiac tamponade Adam Goodman, Phillips Perera, Thomas Mailhot, Diku Mandavia Department of Emergency Medicine, Los
Symposium The role of bedside ultrasound in the diagnosis of pericardial effusion and cardiac tamponade Adam Goodman, Phillips Perera, Thomas Mailhot, Diku Mandavia Department of Emergency Medicine, Los
Supplementary material 1. Definitions of study endpoints (extracted from the Endpoint Validation Committee Charter) 1.
 Rationale, design, and baseline characteristics of the SIGNIFY trial: a randomized, double-blind, placebo-controlled trial of ivabradine in patients with stable coronary artery disease without clinical
Rationale, design, and baseline characteristics of the SIGNIFY trial: a randomized, double-blind, placebo-controlled trial of ivabradine in patients with stable coronary artery disease without clinical
A classic case of amyloid cardiomyopathy
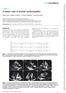 Images in... A classic case of amyloid cardiomyopathy Hayan Jouni, 1 William G Morice, 2 S Vincent Rajkumar, 3 Joerg Herrmann 4 1 Department of Internal Medicine, Mayo Clinic, Rochester, Minnesota, USA
Images in... A classic case of amyloid cardiomyopathy Hayan Jouni, 1 William G Morice, 2 S Vincent Rajkumar, 3 Joerg Herrmann 4 1 Department of Internal Medicine, Mayo Clinic, Rochester, Minnesota, USA
Remodeling of the Remnant Aorta after Acute Type A Aortic Dissection Surgery
 Remodeling of the Remnant Aorta after Acute Type A Aortic Dissection Surgery Are Young Patients More Likely to Develop Adverse Aortic Remodeling of the Remnant Aorta Over Time? Suk Jung Choo¹, Jihoon Kim¹,
Remodeling of the Remnant Aorta after Acute Type A Aortic Dissection Surgery Are Young Patients More Likely to Develop Adverse Aortic Remodeling of the Remnant Aorta Over Time? Suk Jung Choo¹, Jihoon Kim¹,
OPCAB IS NOT BETTER THAN CONVENTIONAL CABG
 OPCAB IS NOT BETTER THAN CONVENTIONAL CABG Harold L. Lazar, M.D. Harold L. Lazar, M.D. Professor of Cardiothoracic Surgery Boston Medical Center and the Boston University School of Medicine Boston, MA
OPCAB IS NOT BETTER THAN CONVENTIONAL CABG Harold L. Lazar, M.D. Harold L. Lazar, M.D. Professor of Cardiothoracic Surgery Boston Medical Center and the Boston University School of Medicine Boston, MA
Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine
 Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine Venous thromboembolism: pulmonary embolism (PE) deep vein thrombosis (DVT) 1% of all patients admitted to hospital 5% of in-hospital mortality
Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine Venous thromboembolism: pulmonary embolism (PE) deep vein thrombosis (DVT) 1% of all patients admitted to hospital 5% of in-hospital mortality
Aortic Valve Practice Guidelines: What Has Changed and What You Need to Know
 Aortic Valve Practice Guidelines: What Has Changed and What You Need to Know James F. Burke, MD Program Director Cardiovascular Disease Fellowship Lankenau Medical Center Disclosure Dr. Burke has no conflicts
Aortic Valve Practice Guidelines: What Has Changed and What You Need to Know James F. Burke, MD Program Director Cardiovascular Disease Fellowship Lankenau Medical Center Disclosure Dr. Burke has no conflicts
Ischemic mitral valve reconstruction and replacement: Comparison of long-term survival and complications
 Surgery for Acquired Cardiovascular Disease Ischemic mitral valve reconstruction and replacement: Comparison of long-term survival and complications Eugene A. Grossi, MD Judith D. Goldberg, ScD Angelo
Surgery for Acquired Cardiovascular Disease Ischemic mitral valve reconstruction and replacement: Comparison of long-term survival and complications Eugene A. Grossi, MD Judith D. Goldberg, ScD Angelo
Ultrasound-enhanced, catheter-directed thrombolysis for pulmonary embolism
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Ultrasound-enhanced, catheter-directed thrombolysis for pulmonary embolism A pulmonary embolism (PE) is
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Ultrasound-enhanced, catheter-directed thrombolysis for pulmonary embolism A pulmonary embolism (PE) is
Department of Cardiac, Thoracic and Vascular Sciences University of Padua Cardiac Tamponade. Echocardiography in Diagnosis and Management
 Department of Cardiac, Thoracic and Vascular Sciences University of Padua Cardiac Tamponade. Echocardiography in Diagnosis and Management Luigi P. Badano, MD, FESC, FACC Declaration of interest **Dr. Badano
Department of Cardiac, Thoracic and Vascular Sciences University of Padua Cardiac Tamponade. Echocardiography in Diagnosis and Management Luigi P. Badano, MD, FESC, FACC Declaration of interest **Dr. Badano
10/1/2016. Constrictive Pericarditis Unique Hemodynamics. What s New in Pericardial Disease? Case-based Discussion
 Mayo Clinic Department of Cardiovascular Diseases Mayo Clinic Echocardiography Review Course for Boards and Recertification What s New in Pericardial Disease? Case-based Discussion Jae K. Oh, MD Samsung
Mayo Clinic Department of Cardiovascular Diseases Mayo Clinic Echocardiography Review Course for Boards and Recertification What s New in Pericardial Disease? Case-based Discussion Jae K. Oh, MD Samsung
Contemporary outcomes for surgical mitral valve repair: A benchmark for evaluating emerging mitral valve technology
 Contemporary outcomes for surgical mitral valve repair: A benchmark for evaluating emerging mitral valve technology Damien J. LaPar, MD, MSc, Daniel P. Mulloy, MD, Ivan K. Crosby, MBBS, D. Scott Lim, MD,
Contemporary outcomes for surgical mitral valve repair: A benchmark for evaluating emerging mitral valve technology Damien J. LaPar, MD, MSc, Daniel P. Mulloy, MD, Ivan K. Crosby, MBBS, D. Scott Lim, MD,
FEV1 predicts length of stay and in-hospital mortality in patients undergoing cardiac surgery
 EUROPEAN SOCIETY OF CARDIOLOGY CONGRESS 2010 FEV1 predicts length of stay and in-hospital mortality in patients undergoing cardiac surgery Nicholas L Mills, David A McAllister, Sarah Wild, John D MacLay,
EUROPEAN SOCIETY OF CARDIOLOGY CONGRESS 2010 FEV1 predicts length of stay and in-hospital mortality in patients undergoing cardiac surgery Nicholas L Mills, David A McAllister, Sarah Wild, John D MacLay,
ΚΑΡΔΙΟΛΟΓΟΣ EUROPEAN ACCREDITATION IN TRANSTHORACIC AND TRANSESOPHAGEAL ECHOCARDIOGRAPHY
 1 ΚΑΡΔΙΟΛΟΓΟΣ EUROPEAN ACCREDITATION IN TRANSTHORACIC AND TRANSESOPHAGEAL ECHOCARDIOGRAPHY 2 Constrictive pericarditis (CP) is characterized by impaired ventricular filling due to a stiffened or noncompliant
1 ΚΑΡΔΙΟΛΟΓΟΣ EUROPEAN ACCREDITATION IN TRANSTHORACIC AND TRANSESOPHAGEAL ECHOCARDIOGRAPHY 2 Constrictive pericarditis (CP) is characterized by impaired ventricular filling due to a stiffened or noncompliant
