Haemodynamic monitoring: pulmonary artery catheterization
|
|
|
- Lee Edwards
- 6 years ago
- Views:
Transcription
1 299 Haemodynamic monitoring: pulmonary artery catheterization David G. Whalley MB FFARCS FRCP(C) Of all the monitors at our disposal, the use of the pulmonary artery catheter (PAC) arouses the greatest debate amongst anaesthetists, lncontrovertably, it provides information conceming the cardiovascular and metabolic state of the patient that is not available by more conventional monitoring ~ but it does so at a price. The potential complications described with its use are far from innocuous and the dollar cost of its insertion and treatment of complications can be considerable. Add to this the paucity of literature in which benefits have been demonstrated in terms of mortality and morbidity and it is easy to understand the reluctance with which the PAC has been received into many hospitals. This review will summarize much of the controversy in a discussion of the methodology, complications, interpretations and indications of the use of the PAC. Methodology 2,3 The pulmonary circulation can be catheterized through any large peripheral vein but the most commola in anaesthesia practice are the internal jugular and subclavian veins. The intemal jugular vein is more accessible and has the advantage of being the shortest and most direct route into the pulmonary circulation. Its most serious disadvantage is the proximity of the carotid artery which, in a recent series, was inadvertently punctured in 1.9 per cent of attempts at internal jugular catheterization. Other disadvantages include post-operative patient discomfort and the difficulty in maintaining sterility with a suitable dressing. The subclavian approach is superior in this respect but the incidence of pneumothorax can be unacceptably high. Catheterization of the pulmonary circulation is easier from the left subclavian vein than from the right. The basilic vein is preferable to either the internal jugular or subclavian veins in those patients who are antieoagulated because of the ease with which pressure can be applied should it be traumatized. The insertion of a PAC introducer sheath is facilitated by the availability of disposable kits which invariably employ the Seldinger technique. 5 In addition most kits include an adjustable, flexible catheter sheath for attachment proximal to the haemostasis valve in order to preserve sterility during manipulations of the catheter. Prior to insertion, the PAC is connected to suitably balanced, calibrated transducers and the lumens flushed. The transducers should be zero referenced to the antero-posterior midline of the chest and calibrated to a low pressure range. It is important that the balloon is inflated with air before insertion to confirm the integrity of the balloon and determine its maximum volume. Upon insertion to 20cm the balloon is inflated and the pressure tracings and ECG observed during passage of the catheter into the pulmonary circulation. (See Figure). From the point of insertion in the internal jugular vein, the tip of the catheter should reach the right atrium after cm have been inserted, the fight ventricle after 30 cm and pulmonary artery after 40 to 45cm. Excessive catheter length in the right ventricle carries with it the risk of endocardial damage and knotting of the catheter. The balloon should be maximally inflated so that the catheter tip does not project beyond the balloon. Despite this precaution, PVC's are very common during passage of the PAC through the fight ventricle, but the use of prophylactic lidocaine is unwarranted. Progress From the Departments of Anaesthesia, McGill University, and Royal Victoria Hospital, 687 Pine Ave. West, Montreal, Quebec, H3A IAI. CAN ANAESTH SOC J I985! 32:3 / pp
2 300 CANADIAN ANAESTHETISTS' SOCIETY JOURNAL injection of fluid, the syringe used to inflate the balloon should be kept attached at all times between wedge readings and in the deflated position. FIGURE Tracing obtained from pulmonary m'tery catheter durings its introduction into pulmonary artery. Note: (a) abrupt increase in pressure upon entering right ventricle; (b) increase in end diastolic pressure - RVEDP; (c) increase in diastolic pressure upon entering pulmonary artery - PADP; (d) dicrotic notch in pulmonary artery pressure waveform; (e) "a' and 'v' waves in pulmonary wedge pressure. into the pulmonary artery is more difficult in patients with atrial fibrillation, low cardiac output or right ventricular dilatation and passage can sometimes be facilitated during deep inspiration and "rushing" the catheter. Verification of correct placement of the catheter can only be made from accurate interpretation of the pulmonary wedge tracing which in turn is dependent on faithful transduction. The natural resonant frequency of the system which facilitates this transduction should be at least ten times the fundamental frequency being measured and should be optimally damped in order to faithfully reproduce the waveform. This can be achieved using short lengths of low compliance pressure tubing with the minimum number of stopcocks from which all air bubbles have been purged. Blood clots should be discouraged from forming by using a continuous flush device with heparin and saline_ In the wedged position, the tracing should have the characteristic pressure waveform of the left atrium with discernable 'a' and 'v' waves. The mean pulmonary wedge pressure should be equal to or less than the pulmonary diastolic pressure and the waveform promptly disappear upon deflation of the balloon. It should return promptly upon reinflation to the maximum balloon volume of 1.5 ml for a 7 Fr gauge PAC. Should the wedge tracing appear at a balloon volume of less than 1.5 ml, the PAC should be withdrawn until maximum inflation is possible. The danger of distal migration of the catheter is constant and should always he considered. Maximum balloon inflation in this situation carries with it the risk of pulmonary artery rupture, a potentially catastrophic event. In order to avoid inadvertent Complications 6.7 The complications of this procedure can be associated with either the insertion of the PAC or its prolonged presence in the pulmonary artery. A recent retrospective review of over 6000 PAC insertions has put the incidence of complications for this procedure into perspective. 4 By far the most common complication was the occurrence of dysrhythmias in 72 per cent of patients whereas the total incidence of serious complications was approximately 0.2 per cent. Uncontrollable pulmonary haemorrhage accounted for the one death in the series which was a consequence of PAC insertion. Reference has already been made to carotid artery puncture and care should be taken to determine the presence of the needle in the artery before the 8 Fr gauge PAC introducer sheath has been inserted. Should the artery be catheterized with the larger sheath prior to cardiac surgery, some authorities have advocated surgical repair before anticoagulation and the institution of cardiopulmonary bypass, s This has been deemed unnecessary so long as firm external compression is applied for five minutes and the area surgically prepared should subsequent haemorrhagr be evident, a Other complications of catheter insertion include pneumothorax, air embolism, nerve damage and dysrhythmias. Pneumothorax shoud be relatively rare from the internal jugular approach although pleural placement of the catheter sheath and subsequent infusion of fluid into the pleural cavity have been reported. Air embolism can be avoided by performing the technique in the head-down position until such time as the introducer sheath has been inserted and the haemostasis valve shown to be competent. It is particularly important that the PAC introducer sheath and haemostasis valve be firmly assembled before use in order to avoid disconnection and possible air embolism during subsequent manoeuvers. Whereas the vast majority of dysrhythmias spontaneously resolve with the passage of the PAC into the pulmonary circulation, persistent dysrhythmias requiting antiarrhythmic drugs or countershock do occur. Their incidence is particularly high in patients with hypoxemia (PaO2 < 60 tort) and
3 Whalley: HAEMODYNAMIC MONITORING: PULMONARY ARTERY CATHETERIZATION 301 acidosis (ph < 7.0). 9 Pre-existing left bundle branch block is not a contraindication to PAC insertion, although a transvenous pacing capability must be available should complete heartblock ensue. 4 With the placement of the PAC in the pulmonary circulation, complications that can occur are more serious although fortunately less frequent. They include balloon rupture, sepsis, pulmonary infarction and pulmonary artery rupture. Rupture of the balloon should be suspected if full inflation does not meet with the customary resistance and no wedge tracing is observed. Up to 35 per cent of catheters become contaminated but only 2 per cent of insertions are associated with septicemia. Catheterrelated infections are more likely if catheters are left in place for more than three to four days in patients with bacteremia or inflammation occurs around the insertion site. The incidence of pulmonary infarction has decreased substantially over the years from 7.2 per cent in 1974 to 0.64 per cent in the recent report by Shah. 4 Factors associated with pulmonary infarction are thought to be distal migration of the catheter into the continuous wedge position and thromboembolism. The PAC should never be left in the continuous wedge position and if a persistent wedge trace is observed, the catheter should be withdrawn and repositioned. It is possible that the occurrence of fewer pulmonary infarcts has been related to the use of continuous flush devices and heparin-bonded catheters which may have reduced the incidence of catheter-related thrombogenicity. Pulmonary infarction is often asymptomatic and while the PAC is in place, a chest x-ray should be taken daily to verify the absence of a peripheral opacity. Pulmonary artery rupture is indeed a dramatic event carrying with it a mortality of 25 to 40 per cent. Risk factors include pulmonary hypertension and anticoagulation. Its highest incidence is during cardiopulmonary bypass when the heart is manipulated causing distal migration of the catheter into an empty, narrowed pulmonary artery tree. In addition, the temperature-sensitive material becomes more rigid during hypothermia thus increasing the chance of perforation by the catheter tip. In situations other than during cardiopulmonary bypass, the likelihood of perforation can be decreased by identifying the pulmonary artery pressure tracing before slowly inflating the balloon with no more than 1.5ml of air. Should flushing by hand be required to rectify a damped trace, it is prudent to withdraw the catheter slightly to avoid flushing in the wedged position. Interpretation 2'3'1~ Right and left ventricular preload can be estimated from the information derived from the PAC. Starling's Law states that fibre stretch governs the force of contraction of the myocardium but since volume is more difficult to measure, it is inferred clinically from a knowledge of pressure. However, because of the curvilinear relationship between pressure and volume this inference can be quite misleading if ventricular compliance alters. The central venous pressure (CVP) can be measured from the proximal lumen which is located 30cm from the catheter tip and in the right atrium. With the balloon inflated in the wedge position, flow distal to the PAC ceases and the pressure waveform in the left atrium is transmitted to the distal lumen of the catheter. There have been numerous papers which have demonstrated the inadequacy of the central venous pressure in predicting the pulmonary wedge pressure (PWP). ll'12 Correlation often exists between the two but the slope of that relationship is unpredictable and in some patients with poor left ventricular function a negative correlation exists. ~3 What this means clinically is that the PWP cannot be accurately inferred from the CVP in any given patient but must be measured directly. Pulmonary artery diastolic pressure however can be used as a safer substitute for PWP in the absence of pulmonary hypertension or taehycardia. Indeed the balloon should not be inflated at a pulmonary artery diastolic pressure of less than 10mmHg because of the risk of pulmonary artery rupture and the failure of the PWP to provide additional information. The PWP will faithfully reflect LAP only if there is an unbroken column of blood between the catheter tip and the left atrium. This will occur, in the absence of clots, in zone III areas of the lung in which the pulmonary venous pressure is greater than the alveolar pressure. 14 Zone III is not an anatomically distinct area but is a physiological zone dependent upon airway characteristics, position of the patient and intravascular volume status.
4 302 CANADIAN ANAESTHETISTS' SOCIETY JOURNAL Fortunately, it is the area of greatest pulmonary blood flow which facilitates the correct placement of the flow-directed PAC. It is unusual for airway pressure to be transmitted to pulmonary wedge pressure when the PAC catheter tip is below the level of the left atrium. The correct position of the PAC can be verified on lateral chest x-ray. A non-zone III position can be assumed if the PAC tracing reflects airway pressure and loses the characteristic wave-form of the left atrium. Furthermore, if greater than half of the applied PEEP is transmitted to the PWP, then it is probable that the catheter tip is situated in either zones I or 11. The interpretation of the effects of PEEP on the pulmonary circulation can often be confusing. PEEP is transmitted to the pleural cavity and juxtacardiac structures in a degree inversely proportional to the compliance of the lung. It is transmural pressure (intracavity pressure - pressure ofjuxtacardiac structures) rather than PWP which is a true estimation of filling pressure but the two are often assumed to be equal because the pleural pressure is close to that of the atmosphere. If PEEP is transmitted to the pleural cavity, transmural pressure might be substantially less than measured PWP. The question can be resolved by measuring pleural pressure directly. Alternatively, there is a good correlation between esophageal pressure and pleural pressure when measured in the lateral decubitus position but both manoeuvers have limited clinical application. The removal of PEEP has been advocated while the PWP is measured, but the measurement so obtained clearly no longer reflects the haemodynamic characteristics that formerly prevailed. In addition, the ensuring hypoxia may jeopardize the patient. We recommend that ventilation with PEEP be continued and that the PWP be measured at end expiration. The presence of the catheter tip in zone HI should be verified and PEEP confined to less than 10cm H20. In these circumstances, transmural pressure is approximately equal to measured PWP. Should greater levels of PEEP be required, transmural pressure can be estimated by subtracting half the additional PEEP from the measured PWP. In certain rare circumstances the PWP and pulmonary venous pressure may be considerably greater than LAP. This will occur in situations of pulmonary venous obstruction by mediastinal fibrosis or tumour, lung turnouts, vasculitis or atrial myxomas. Of fundamental importance in the interpretation of PWP, is the relationship between LAP and left ventricular end diastolic pressure (LVEDP). The clearest waveform of PWP reflects only the LAP but it is the relationship of the latter to the filling of the left ventricle which truly reflects preload. The LAP is greater than LVEDP when the mitral valve is stenosed and similarly, during mitral regurgitation, the contribution of left ventricular systole to LAP can cause LVEDP to be overestimated. It is often possible to detect the reflux of mitral regurgitation by the presence of large V waves on the pulmonary wedge tracing. In contrast, aortic regurgitation can cause the LVEDP to be significantly greater than LAP because the mitral valve closes prematurely as a consequence of retrograde filling of the ventricle from the aorta. When left ventricular compliance is decreased, LAP no longer reflects LVEDP because of the added boost that atrial contraction imparts to left ventricular preload and systolic volume. In this situation, LVEDP is best determined from the height of the A wave on the wedge tracing. Finally, it is important to realize the variable relationship between LVEDP and left ventricular end diastolic volume. In order to optimize stroke volume, normal wedge pressures may have to be considerably exceeded in situations of low myocardial compliance due to ischemia, hypertrophy or infiltration. Indeed it is the relationship of PWP to cardiac output in which the use of the PAC is invaluable. The thermodilution technique of cardiac output determination correlates well with Fick and dye dilution methods and enables periodic haemodynamic profiles of the patient to be performed. In such a way it is possible to determine the ideal PWP that is compatible with maximum cardiac output, and changes in haemodynamic function can readily be detected. The technique relies on the rapid injection of a fixed volume of ice cold saline and assumes a constant blood flow for its passage over the distally placed thermistor. Naturally, the technique is affected by normal stroke volume and respiration, but these effects can be minimized by obtaining the mean of three determinations rejecting those that vary by more than 10 per cent. The
5 Whalley: HAEMODYNAMIC MONITORING: PULMONARY ARTERY CATHETERIZATION 303 technique is invalid in the presence of intracardiac shunts and tricuspid regurgitation. The presence of the catheter in the pulmonary artery enables the mixed venous oxygen saturation (S902) to be determined. We have already discussed the information that can be derived from a knowledge of S~O2, but briefly it enables the clinician to detect changes in cardiac output and tissue oxygenation. Determination of S'~Oz can be performed in two ways. Blood can be aspirated from the distal lumen and analysed by laboratory oximetry or alternatively, using fibreoptic technology, an online monitor of $902 is currently available. (Oximetrix Shaw TM catheter oximeter system, Oximetrix Inc., Mountain View, California.) Indications There is a growing consensus of opinion on the indications for the pulmonary artery catheterization in the environment of the Intensive Care Unit. 6,1~ Forrester et al. have demonstrated that uncomplicated acute myocardial infarction is not an indication for PAC insertion because of the accuracy with which clinical criteria can predict haemodynamic status) 5 However, should complications supervene which necessitate the administration of inotropic or vasodilator drugs, then it is more accurate to use information derived from the PAC to assess the effects of pharmacological management. In the absence of acute myocardial infarction, Connors et al. have demonstrated that routine clinical evaluation of critically ill patients does not provide enough information to assess haemodynamic status accurately. 16 Indeed clinical criteria correctly predicted cardiac index in only 44 per cent of cases and pulmonary wedge pressure in only 42 per cent of cases, leading them to conclude that pulmonary artery catheterization is indicated in those patients who have not responded to therapy deemed appropriate after careful clinical evaluation. In the management of adult respiratory distress syndrome, the optimization of PEEP in terms of its effects on oxygen transport, is greatly facilitated ifa PAC is in place. The diagnosis of noncardiogenic pulmonary oedema can only be made if the pulmonary wedge pressure is known. Patients requiring mechanical ventilation for exacerbation of chronic obstructive pulmonary disease often display right ventricular failure but a knowledge of pulmonary wedge pressure may be required to accurately diagnose left ventricular failure. The indications for pulmonary artery catheterization during anaesthesia have not been carefully studied. It has been suggested that patients with good ventricular function undergoing coronary artery surgery do not benefit from pulmonary artery catheterization 13 but Mangano's study did not address the issue of variability in regression 17 nor did it explore the benefits of cardiac output determination in the perioperative period. There have been attempts to reproduce Mangano's conclusions for patients undergoing aortic surgery, but determination of preoperative ejection fraction by multigated cardiac analysis scan has not been able to identify subgroups of patients in whom the CVP faithfully reflects the PWP. i t As an index of ischemia, Kaplan and Wells have demonstrated that an increase in PWP antidates changes in the electrocardiogram (ECG), at least in individual patients. 18 Their mean data however were unable to support the superiority of the PAC since ECG evidence of ischemia was accompanied by increases in CVP as well as increases in PWP. Furthem~ore, Lieberman et al. found that neither the CVP nor the PWP were as good a predictor of ischemia as was systemic hypotension.i9 A systemic blood pressure of less than 90 mmhg predicted ECG changes of ischemia 79 per cent of the time whereas increases in CVP above 10 mmhg or PWP above 15 mmhg predicted ischemia just 24 per cent of the time. There has been a trend towards the use of the PAC in major vascular surgery such as aortic reconstruction stemming from Attia's observation that the application of the aortic cross-clamp can be associated with changes suggestive of altered ventricular compliance in patients with severe coronary artery disease. 2~ It is well known that at least 50 per cent of these patients have some degree of coronary artery disease and one study has gone so far as to suggest that prophylactic coronary artery surgery be carried out before aortic reconstruction is embarked upon. 21 Attia observed that the normal response to aortic cross-clamp is a significant decrease in CVP but application of aortic cross-
6 304 CANADIAN ANAESTHETISTS' SOCIETY JOURNAL clamp involved significant increases in PWP but no change in CVP. The authors concluded that PAC facilitates the management of patients undergoing aortic surgery, but it would appear that diligent observation of the CVP will be just as instructive and less invasive. No study has yet demonstrated the superiority of the PAC over a simple monitor of CVP in terms of its effect on patient outcome. This is remarkable considering the morbidity, effort and expense associated with pulmonary artery catheterization and anaesthetists are justified in being cautious when presented with a list of indications for its use. We believe that all patients undergoing prolonged major surgery should have some monitor of filling pressure. A CVP is sufficient in the majority of patients but with information derived from a thermodilution pulmonary artery catheter, the haemodynamic status of patients with heart disease can be more accurately managed, particularly in the immediate post-operative period. It is upon arrival in the Recovery Room that the PAC is especially useful. Alterations in systemic vascular resistance can result from a combination of pain, hypothermia, medications and an unstable intravascular volume. Systemic vascular resistance can only be accurately quantitated from a knowledge of cardiac output, and the resultant information provides a rational basis for subsequent management. In summary, the thermodilution pulmonary artery catheter enables the physician to monitor the filling pressures of right and left ventricles, cardiac output and mixed venous oxygen saturation. It provides the means whereby the haemodynamic status of the patient can be accurately determined and enables the physician to monitor the effects of pharmacological intervention. It behooves the physician to become familiar with the technique, complications, interpretations and indications of pulmonary artery catheterization. References 1 Swan HJC, Ganz W, Forrester J, Marcus H, Diamond G, Chonette D. Catheterization of the heart in man with use of a flow-directed balloontipped catheter. N Engl J Med 1970; 284: Wiedemann lip, Manhay MA, Matthay RA. Cardiovascular-pulmonary monitoring in the Intensive Care Unit (Part I). Chest 1984; 85: 'Quinn R, Marinii JJ. Pulmonary occlusion pressure: clinical physiology, measurement, and interpretation. Am Rev Respir Dis 1983; 128: Shah KB, Rao TLK, Laughlin S, El-Etr AA. A review of pulmonary artery catheterization in 6245 patients. Anesthesiology 1984; 61: Seldinger SI. Catheter replacement of its needle in pcreutaneous arteriography. Aeta Radio/ 1953; 39: Wiedemann HP, Matthay MA, Manhay RA. Cardiovascular-pulmonary monitoring in the Intensive Care Unit (Part 2). Chest 1984; 85: Pace NL. A critique of flow-directed pulmonary arterial catheterization. Anesthesiology 1977; 47: Schwartz A J, Jobes DR, Greenhow E, Stephenson LW, Ellison N. Carotid artery puncture with internal jugular cannulation. Anesthesiology 1979; 51: S Sprung CL, Pozen RG, Rozanski JJ, Pinero JR, Ersler BR, Castellanos A. Advanced ventricular arrhythmias during bedside pulmonary artery catheterization. Am J Med 1982; 72: Goldenheim RD, Kazemi H. Cardiopulmonary monitoring of critically ill patients. N Engl J Med 1984; 311: Martin DE, Nicholas GG, Osbakken MD. Does preoperative ejection fraction predict CVP/PCWP correlation during aortic surgery? Anesthesiology 1982; 57: A Gelman S, McDowell HA, Proctor JE. Do [eft and right performance curves predict CVP/PAOP correlation during aortic surgery? Anesth Analg 1984; 63: Mangano DT. Monitoring pulmonary arterial pressure in coronary artery disease. Anesthesiology 1980; 53: West JB, Dollery CT, Naimark A. Distribution of blood flow in isolated lung: relation to vascular and alveolar pressures. J Appl Physiol 1964: 19:
7 Whalley: HAEMODYNAMIC MONITORING: PULMONARY ARTERY CATHETERIZATION Forrester JS, Diamond GA, Swan HJC. Correlative classification of clinical and hemodynamic function after acute myocardial infarction. Am J Cardiol 1977; 39: Connors AF, McCaffree DR, Gray BA. Evaluation of right-heart catheterization in the critically ill patient without acute myocardial infarction. N Engl J Med 1983; 308: Lowenstein E, TeplickR. To (PA) catheterize or not to (PA) catheterize - that is the question. Editorial. Anesthesiology 1980; 53: Kaplan JA, Wells PH. Early diagnosis of myocardial ischemia using the pulmonary artery catheter. Anesthesiology 1981 ; 60: Lieberman RW, Orkin FK, Jobes DR, Schwartz AJ. Hemodynamic predictors of myocardial ischernia during halothane anesthesia for coronary artery revascularization. Anesthesiology 1983; 59: Atria RR, Murphy JD, Snider M, Lappas DG, Darling C, Lowenstein E. Myocardial ischemia due to infrarenal aortic cross-clamping during aortic surgery in patients with severe coronary artery disease. Circualtion 1976; 53: HertzerNR. Myocardial ischemia. Surgery 1983; 93:
Hemodynamic Monitoring
 Perform Procedure And Interpret Results Hemodynamic Monitoring Tracheal Tube Cuff Pressure Dean R. Hess PhD RRT FAARC Hemodynamic Monitoring Cardiac Rate and Rhythm Arterial Blood Pressure Central Venous
Perform Procedure And Interpret Results Hemodynamic Monitoring Tracheal Tube Cuff Pressure Dean R. Hess PhD RRT FAARC Hemodynamic Monitoring Cardiac Rate and Rhythm Arterial Blood Pressure Central Venous
Hemodynamic Monitoring and Circulatory Assist Devices
 Hemodynamic Monitoring and Circulatory Assist Devices Speaker: Jana Ogden Learning Unit 2: Hemodynamic Monitoring and Circulatory Assist Devices Hemodynamic monitoring refers to the measurement of pressure,
Hemodynamic Monitoring and Circulatory Assist Devices Speaker: Jana Ogden Learning Unit 2: Hemodynamic Monitoring and Circulatory Assist Devices Hemodynamic monitoring refers to the measurement of pressure,
Relax and Learn At the Farm 2012
 Relax and Learn At the Farm Session 9: Invasive Hemodynamic Assessment and What to Do with the Data Carol Jacobson RN, MN Cardiovascular Nursing Education Associates Function of CV system is to deliver
Relax and Learn At the Farm Session 9: Invasive Hemodynamic Assessment and What to Do with the Data Carol Jacobson RN, MN Cardiovascular Nursing Education Associates Function of CV system is to deliver
Definition- study of blood flow Haemodynamic monitoring refers to monitoring of blood in the cardiovascular system Uses Is NB in the critically ill
 By Craig Definition- study of blood flow Haemodynamic monitoring refers to monitoring of blood in the cardiovascular system Uses Is NB in the critically ill pt Can assist diagnosis and decision making
By Craig Definition- study of blood flow Haemodynamic monitoring refers to monitoring of blood in the cardiovascular system Uses Is NB in the critically ill pt Can assist diagnosis and decision making
PULMONARY ARTERY PRESSURE
 6 INTENSIVE CARE Stroke volume x y RAP LAP LAP Atrial pressure Fig. 4.8 Left (LV) and right (RV) ventricular function curves in a patient with left ventricular dysfunction. Since the stroke volume of the
6 INTENSIVE CARE Stroke volume x y RAP LAP LAP Atrial pressure Fig. 4.8 Left (LV) and right (RV) ventricular function curves in a patient with left ventricular dysfunction. Since the stroke volume of the
CATCH A WAVE.. INTRODUCTION NONINVASIVE HEMODYNAMIC MONITORING 4/12/2018
 WAVES CATCH A WAVE.. W I S C O N S I N P A R A M E D I C S E M I N A R A P R I L 2 0 1 8 K E R I W Y D N E R K R A U S E R N, C C R N, E M T - P Have you considered that if you don't make waves, nobody
WAVES CATCH A WAVE.. W I S C O N S I N P A R A M E D I C S E M I N A R A P R I L 2 0 1 8 K E R I W Y D N E R K R A U S E R N, C C R N, E M T - P Have you considered that if you don't make waves, nobody
Technique. Technique. Technique. Monitoring 1. Local anesthetic? Aseptic technique Hyper-extend (if radial)
 Critical Care Monitoring Hemodynamic Monitoring Arterial Blood Pressure Cannulate artery Uses 2 Technique Sites Locate artery, prep 3 1 Technique Local anesthetic? Aseptic technique Hyper-extend (if radial)
Critical Care Monitoring Hemodynamic Monitoring Arterial Blood Pressure Cannulate artery Uses 2 Technique Sites Locate artery, prep 3 1 Technique Local anesthetic? Aseptic technique Hyper-extend (if radial)
Cath Lab Essentials: Basic Hemodynamics for the Cath Lab and ICU
 Cath Lab Essentials: Basic Hemodynamics for the Cath Lab and ICU Ailin Barseghian El-Farra, MD, FACC Assistant Professor, Interventional Cardiology University of California, Irvine Department of Cardiology
Cath Lab Essentials: Basic Hemodynamics for the Cath Lab and ICU Ailin Barseghian El-Farra, MD, FACC Assistant Professor, Interventional Cardiology University of California, Irvine Department of Cardiology
Section 6 Intra Aortic Balloon Pump
 Section 6 Intra Aortic Balloon Pump The Intra Aortic Balloon Pump (IABP) The balloon is synthetic and is made for single use only. It is threaded into the aorta, usually via a femoral approach. The balloon
Section 6 Intra Aortic Balloon Pump The Intra Aortic Balloon Pump (IABP) The balloon is synthetic and is made for single use only. It is threaded into the aorta, usually via a femoral approach. The balloon
IABP Timing & Fidelity. Pocket Reference Guide
 IABP Timing & Fidelity Pocket Reference Guide Correct IABP Timing A = One complete cardiac cycle R B = Unassisted aortic end diastolic pressure P T C = Unassisted systolic pressure D = Diastolic augmentation
IABP Timing & Fidelity Pocket Reference Guide Correct IABP Timing A = One complete cardiac cycle R B = Unassisted aortic end diastolic pressure P T C = Unassisted systolic pressure D = Diastolic augmentation
Impedance Cardiography (ICG) Application of ICG in Intensive Care and Emergency
 Impedance Cardiography (ICG) Application of ICG in Intensive Care and Emergency Aim of haemodynamic monitoring in ICU and ED Detection and therapy of insufficient organ perfusion Answers to common cardiovascular
Impedance Cardiography (ICG) Application of ICG in Intensive Care and Emergency Aim of haemodynamic monitoring in ICU and ED Detection and therapy of insufficient organ perfusion Answers to common cardiovascular
PVDOMICS: Right Heart Catheterization Training
 PVDOMICS: Right Heart Catheterization Training Cardiovascular Physiology Core Cleveland Clinic, Cleveland OH November 7, 2016 NHLBI Pulmonary Vascular Disease Phenomics Program Funded by the National Heart,
PVDOMICS: Right Heart Catheterization Training Cardiovascular Physiology Core Cleveland Clinic, Cleveland OH November 7, 2016 NHLBI Pulmonary Vascular Disease Phenomics Program Funded by the National Heart,
University of Florida Department of Surgery. CardioThoracic Surgery VA Learning Objectives
 University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
Topics to be Covered. Cardiac Measurements. Distribution of Blood Volume. Distribution of Pulmonary Ventilation & Blood Flow
 Topics to be Covered MODULE F HEMODYNAMIC MONITORING Cardiac Output Determinants of Stroke Volume Hemodynamic Measurements Pulmonary Artery Catheterization Control of Blood Pressure Heart Failure Cardiac
Topics to be Covered MODULE F HEMODYNAMIC MONITORING Cardiac Output Determinants of Stroke Volume Hemodynamic Measurements Pulmonary Artery Catheterization Control of Blood Pressure Heart Failure Cardiac
ER REBOA Catheter. Instructions for Use
 ER REBOA Catheter Instructions for Use Prytime Medical Devices, Inc. 229 N. Main Street Boerne, TX 78006, USA feedback@prytimemedical.com www.prytimemedical.com US 1 210 340 0116 U.S. and Foreign Patents
ER REBOA Catheter Instructions for Use Prytime Medical Devices, Inc. 229 N. Main Street Boerne, TX 78006, USA feedback@prytimemedical.com www.prytimemedical.com US 1 210 340 0116 U.S. and Foreign Patents
CARDIAC CATHETERIZATION IN DOGS
 CARDIAC CATHETERIZATION IN DOGS WILLIAM H. NOBLE, B.A., IVLD., DIP.ANAES., F.R.C.P.(C) AND J. COLIN KAY, A.I.IX~.L.T. (ENG.) INTRODUCTION MANY INVESTIGATORS require cardiac catheterization data as a part
CARDIAC CATHETERIZATION IN DOGS WILLIAM H. NOBLE, B.A., IVLD., DIP.ANAES., F.R.C.P.(C) AND J. COLIN KAY, A.I.IX~.L.T. (ENG.) INTRODUCTION MANY INVESTIGATORS require cardiac catheterization data as a part
Dr. prakruthi Dept. of anaesthesiology, Rrmch, bangalore
 CENTRAL VENOUS CATHETERIZATION Dr. prakruthi Dept. of anaesthesiology, Rrmch, bangalore OBJECTIVES Introduction Indications and Contraindications Complications Technique Basic principles Specifics by Site
CENTRAL VENOUS CATHETERIZATION Dr. prakruthi Dept. of anaesthesiology, Rrmch, bangalore OBJECTIVES Introduction Indications and Contraindications Complications Technique Basic principles Specifics by Site
Adult Echocardiography Examination Content Outline
 Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Invasive Measurement of Blood Pressure
 Invasive Measurement of Blood Pressure Arterial Lines & Pulmonary Artery Lines Key Points Invasive Measurement of Blood Pressure: - understand blood flow through the body - understand Pulmonary Artery
Invasive Measurement of Blood Pressure Arterial Lines & Pulmonary Artery Lines Key Points Invasive Measurement of Blood Pressure: - understand blood flow through the body - understand Pulmonary Artery
Computerized PAC Waveform Interpretation
 Harvard-MIT Division of Health Sciences and Technology HST.951J: Medical Decision Support, Fall 2005 Instructors: Professor Lucila Ohno-Machado and Professor Staal Vinterbo Computerized PAC Waveform Interpretation
Harvard-MIT Division of Health Sciences and Technology HST.951J: Medical Decision Support, Fall 2005 Instructors: Professor Lucila Ohno-Machado and Professor Staal Vinterbo Computerized PAC Waveform Interpretation
ThruPort systems ProPlege peripheral retrograde cardioplegia device
 ThruPort systems ProPlege peripheral retrograde cardioplegia device Training Module Lessons Lesson 1: ProPlege device Lesson 2: Preparing for the case Lesson 3: Utilizing the device Lesson 4: Troubleshooting
ThruPort systems ProPlege peripheral retrograde cardioplegia device Training Module Lessons Lesson 1: ProPlege device Lesson 2: Preparing for the case Lesson 3: Utilizing the device Lesson 4: Troubleshooting
RECOMMENDED INSTRUCTIONS FOR USE
 Rapid Exchange PTCA Dilatation Catheter RECOMMENDED INSTRUCTIONS FOR USE Available in diameters 1.25mm to 4.5mm and in lengths 09mm to 40mm Caution: This device should be used only by physicians trained
Rapid Exchange PTCA Dilatation Catheter RECOMMENDED INSTRUCTIONS FOR USE Available in diameters 1.25mm to 4.5mm and in lengths 09mm to 40mm Caution: This device should be used only by physicians trained
HAEMODYNAMIC IN THE CATH LABORATORY INTRO TO BASICS
 HAEMODYNAMIC IN THE CATH LABORATORY INTRO TO BASICS BY NOOR FADZLY ALIAS CARDIOVASCULAR TECHNOLOGIST NCL Department National Heart Institute Kuala Lumpur INTRODUCTION ROLES OF HAEMODYNAMIC MONITORING PURPOSE
HAEMODYNAMIC IN THE CATH LABORATORY INTRO TO BASICS BY NOOR FADZLY ALIAS CARDIOVASCULAR TECHNOLOGIST NCL Department National Heart Institute Kuala Lumpur INTRODUCTION ROLES OF HAEMODYNAMIC MONITORING PURPOSE
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
A practical guide to using pulmonary artery catheters
 A practical guide to using pulmonary artery catheters Scales K, Collie E (7) A practical guide to using pulmonary artery catheters. Nursing Standard. 21, 43, 42-48. Date of acceptance: May 4 7. Summary
A practical guide to using pulmonary artery catheters Scales K, Collie E (7) A practical guide to using pulmonary artery catheters. Nursing Standard. 21, 43, 42-48. Date of acceptance: May 4 7. Summary
Pulmonary Artery Catheter Insertion (Assist) and Pressure Monitoring
 PROCEDURE 72 Pulmonary Artery Catheter Insertion (Assist) and Pressure Monitoring Reba McVay PURPOSE: Pulmonary artery (PA) catheters are used to determine hemodynamic status in critically ill patients.
PROCEDURE 72 Pulmonary Artery Catheter Insertion (Assist) and Pressure Monitoring Reba McVay PURPOSE: Pulmonary artery (PA) catheters are used to determine hemodynamic status in critically ill patients.
Background & Indications Probe Selection
 Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Georgios C. Bompotis Cardiologist, Director of Cardiological Department, Papageorgiou Hospital,
 Georgios C. Bompotis Cardiologist, Director of Cardiological Department, Papageorgiou Hospital, Disclosure Statement of Financial Interest I, Georgios Bompotis DO NOT have a financial interest/arrangement
Georgios C. Bompotis Cardiologist, Director of Cardiological Department, Papageorgiou Hospital, Disclosure Statement of Financial Interest I, Georgios Bompotis DO NOT have a financial interest/arrangement
Review Article. Interactive Physiology in Critical Illness : Pulmonary and Cardiovascular Systems. Introduction
 310 Indian Deepak J Physiol Shrivastava Pharmacol 2016; 60(4) : 310 314 Indian J Physiol Pharmacol 2016; 60(4) Review Article Interactive Physiology in Critical Illness : Pulmonary and Cardiovascular Systems
310 Indian Deepak J Physiol Shrivastava Pharmacol 2016; 60(4) : 310 314 Indian J Physiol Pharmacol 2016; 60(4) Review Article Interactive Physiology in Critical Illness : Pulmonary and Cardiovascular Systems
Revision of 10/27/2017 Form #280 Page 1 of 12 PVDOMICS STUDY Clinical Center Right Heart Catheterization (RHC) Results Form #280
 Revision of 10/27/2017 Form #280 Page 1 of 12 PVDOMICS STUDY Clinical Center Right Heart Catheterization (RHC) Results Form #280 Instructions: Review PVDOMICS MOP Chapter 100 prior to completing right
Revision of 10/27/2017 Form #280 Page 1 of 12 PVDOMICS STUDY Clinical Center Right Heart Catheterization (RHC) Results Form #280 Instructions: Review PVDOMICS MOP Chapter 100 prior to completing right
Hemodynamics: Cardiac and Vascular Jeff Davis, RRT, RCIS
 Hemodynamics: Cardiac and Vascular Jeff Davis, RRT, RCIS Program Director, Cardiovascular Technology Florida SouthWestern State College Fort Myers, FL Disclosures Speaker s Bureau: None Stockholder: None
Hemodynamics: Cardiac and Vascular Jeff Davis, RRT, RCIS Program Director, Cardiovascular Technology Florida SouthWestern State College Fort Myers, FL Disclosures Speaker s Bureau: None Stockholder: None
CARDIOVASCULAR MONITORING. Prof. Yasser Mostafa Kadah
 CARDIOVASCULAR MONITORING Prof. Yasser Mostafa Kadah Introduction Cardiovascular monitoring covers monitoring of heart and circulatory functions It makes it possible to commence interventions quickly in
CARDIOVASCULAR MONITORING Prof. Yasser Mostafa Kadah Introduction Cardiovascular monitoring covers monitoring of heart and circulatory functions It makes it possible to commence interventions quickly in
HISTORY. Question: What category of heart disease is suggested by this history? CHIEF COMPLAINT: Heart murmur present since early infancy.
 HISTORY 18-year-old man. CHIEF COMPLAINT: Heart murmur present since early infancy. PRESENT ILLNESS: Although normal at birth, a heart murmur was heard at the six week check-up and has persisted since
HISTORY 18-year-old man. CHIEF COMPLAINT: Heart murmur present since early infancy. PRESENT ILLNESS: Although normal at birth, a heart murmur was heard at the six week check-up and has persisted since
2. Need for serial arterial blood gas determinations. 2. Anticipation of the initiation of thrombolytic therapy
 I. Subject: Arterial Cannulation II. Policy: Arterial cannulation will be performed upon a physician's order by Cardiopulmonary and Respiratory Therapy personnel certified in the arterial catheterization
I. Subject: Arterial Cannulation II. Policy: Arterial cannulation will be performed upon a physician's order by Cardiopulmonary and Respiratory Therapy personnel certified in the arterial catheterization
1 Description. 2 Indications. 3 Warnings ASPIRATION CATHETER
 Page 1 of 5 ASPIRATION CATHETER Carefully read all instructions prior to use, observe all warnings and precautions noted throughout these instructions. Failure to do so may result in complications. STERILE.
Page 1 of 5 ASPIRATION CATHETER Carefully read all instructions prior to use, observe all warnings and precautions noted throughout these instructions. Failure to do so may result in complications. STERILE.
Critical Care Nursing Program August to November, 2015 Full-time Lesson A13 Pumping and Perfusion III Basic Hemodynamic Monitoring
 Critical Care Nursing Program August to November, 2015 Full-time Lesson A13 Pumping and Perfusion III Basic Hemodynamic Monitoring August 2015 RN Professional Development Centre Page 1 Lesson Thirteen
Critical Care Nursing Program August to November, 2015 Full-time Lesson A13 Pumping and Perfusion III Basic Hemodynamic Monitoring August 2015 RN Professional Development Centre Page 1 Lesson Thirteen
Cardiac anaesthesia. Simon May
 Cardiac anaesthesia Simon May Contents Cardiac: Principles of peri-operative management for cardiac surgery Cardiopulmonary bypass, cardioplegia and off pump cardiac surgery Cardiac disease and its implications
Cardiac anaesthesia Simon May Contents Cardiac: Principles of peri-operative management for cardiac surgery Cardiopulmonary bypass, cardioplegia and off pump cardiac surgery Cardiac disease and its implications
Echocardiography as a diagnostic and management tool in medical emergencies
 Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
Καθετηριασμός δεξιάς κοιλίας. Σ. Χατζημιλτιάδης Καθηγητής Καρδιολογίας ΑΠΘ
 Καθετηριασμός δεξιάς κοιλίας Σ. Χατζημιλτιάδης Καθηγητής Καρδιολογίας ΑΠΘ The increasing interest in pulmonary arterial hypertension (PAH), the increasing interest in implantation of LVADs, and the evolution
Καθετηριασμός δεξιάς κοιλίας Σ. Χατζημιλτιάδης Καθηγητής Καρδιολογίας ΑΠΘ The increasing interest in pulmonary arterial hypertension (PAH), the increasing interest in implantation of LVADs, and the evolution
Central Venous Line Insertion
 Central Venous Line Insertion Understand the indications and risks of CVC insertion Understand and troubleshoot the seldinger technique Understand available sites and select the appropriate site for clinical
Central Venous Line Insertion Understand the indications and risks of CVC insertion Understand and troubleshoot the seldinger technique Understand available sites and select the appropriate site for clinical
Right Heart Catheterization. Franz R. Eberli MD Chief of Cardiology Stadtspital Triemli, Zurich
 Right Heart Catheterization Franz R. Eberli MD Chief of Cardiology Stadtspital Triemli, Zurich Right Heart Catheterization Pressure measurements Oxygen saturation measurements Cardiac output, Vascular
Right Heart Catheterization Franz R. Eberli MD Chief of Cardiology Stadtspital Triemli, Zurich Right Heart Catheterization Pressure measurements Oxygen saturation measurements Cardiac output, Vascular
2
 1 2 Although the term "cardiomyopathy" could theoretically apply to almost any disease affecting the heart, it is usually reserved for "severe myocardial disease leading to heart failure".cardiomyopathy
1 2 Although the term "cardiomyopathy" could theoretically apply to almost any disease affecting the heart, it is usually reserved for "severe myocardial disease leading to heart failure".cardiomyopathy
Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia
 Marshall University Marshall Digital Scholar Internal Medicine Faculty Research Spring 5-2004 Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia Ellen A. Thompson
Marshall University Marshall Digital Scholar Internal Medicine Faculty Research Spring 5-2004 Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia Ellen A. Thompson
Part 3a. Physiology: the cardiovascular system
 Part 3a Physiology: the cardiovascular system 105 Part 3a Intravascular pressure waveforms and the ECG waveform With the exception of systemic arterial pressure, intravascular pressure waveforms can be
Part 3a Physiology: the cardiovascular system 105 Part 3a Intravascular pressure waveforms and the ECG waveform With the exception of systemic arterial pressure, intravascular pressure waveforms can be
-12. -Ensherah Mokheemer - ABDULLAH ZREQAT. -Faisal Mohammad. 1 P a g e
 -12 -Ensherah Mokheemer - ABDULLAH ZREQAT -Faisal Mohammad 1 P a g e In the previous lecture we talked about: - cardiac index: we use the cardiac index to compare the cardiac output between different individuals,
-12 -Ensherah Mokheemer - ABDULLAH ZREQAT -Faisal Mohammad 1 P a g e In the previous lecture we talked about: - cardiac index: we use the cardiac index to compare the cardiac output between different individuals,
The Cardiac Cycle Clive M. Baumgarten, Ph.D.
 The Cardiac Cycle Clive M. Baumgarten, Ph.D. OBJECTIVES: 1. Describe periods comprising cardiac cycle and events within each period 2. Describe the temporal relationships between pressure, blood flow,
The Cardiac Cycle Clive M. Baumgarten, Ph.D. OBJECTIVES: 1. Describe periods comprising cardiac cycle and events within each period 2. Describe the temporal relationships between pressure, blood flow,
IB TOPIC 6.2 THE BLOOD SYSTEM
 IB TOPIC 6.2 THE BLOOD SYSTEM TERMS TO KNOW circulation ventricle artery vein THE BLOOD SYSTEM 6.2.U1 - Arteries convey blood at high pressure from the ventricles to the tissues of the body Circulation
IB TOPIC 6.2 THE BLOOD SYSTEM TERMS TO KNOW circulation ventricle artery vein THE BLOOD SYSTEM 6.2.U1 - Arteries convey blood at high pressure from the ventricles to the tissues of the body Circulation
The pulmonary artery occlusion
 Overestimation of pulmonary artery occlusion pressure in pulmonary hypertension due to partial occlusion James W. Leatherman, MD; Robert S. Shapiro, MD Objective: To evaluate partial occlusion in patients
Overestimation of pulmonary artery occlusion pressure in pulmonary hypertension due to partial occlusion James W. Leatherman, MD; Robert S. Shapiro, MD Objective: To evaluate partial occlusion in patients
Peel-Apart Percutaneous Introducer Kits for
 Bard Access Systems Peel-Apart Percutaneous Introducer Kits for Table of Contents Contents Page Bard Implanted Ports Hickman*, Leonard*, Broviac*, Tenckhoff*, and Groshong* Catheters Introduction....................................
Bard Access Systems Peel-Apart Percutaneous Introducer Kits for Table of Contents Contents Page Bard Implanted Ports Hickman*, Leonard*, Broviac*, Tenckhoff*, and Groshong* Catheters Introduction....................................
Pulmonary Artery Catheter Helpful Hints 2017
 Pulmonary Artery Catheter Helpful Hints 2017 Swan Ganz Catheter 1) Gather Equipment Hint1: Introducer is the actual catheter [Cordis is a brand name: at GW we use Arrow brand] Hint 2: 9 Fr Introducer for
Pulmonary Artery Catheter Helpful Hints 2017 Swan Ganz Catheter 1) Gather Equipment Hint1: Introducer is the actual catheter [Cordis is a brand name: at GW we use Arrow brand] Hint 2: 9 Fr Introducer for
Research Article Can we predict the Position of Central Venous Catheter Tip Following Cannulation of Internal Jugular Vein?
 Cronicon OPEN ACCESS ANAESTHESIA Research Article Can we predict the Position of Central Venous Catheter Tip Following Cannulation of Internal Jugular Vein? Pradeep Marur Venkategowda 1, Surath Manimala
Cronicon OPEN ACCESS ANAESTHESIA Research Article Can we predict the Position of Central Venous Catheter Tip Following Cannulation of Internal Jugular Vein? Pradeep Marur Venkategowda 1, Surath Manimala
Interesting Cases - A Case Report: Renal Cell Carcinoma With Tumor Mass In IVC And Heart. O Wenker, L Chaloupka, R Joswiak, D Thakar, C Wood, G Walsh
 ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 3 Number 2 Interesting Cases - A Case Report: Renal Cell Carcinoma With Tumor Mass In IVC And Heart O Wenker, L Chaloupka, R
ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 3 Number 2 Interesting Cases - A Case Report: Renal Cell Carcinoma With Tumor Mass In IVC And Heart O Wenker, L Chaloupka, R
Brief View of Calculation and Measurement of Cardiac Hemodynamics
 Cronicon OPEN ACCESS EC CARDIOLOGY Review Article Brief View of Calculation and Measurement of Cardiac Hemodynamics Samah Alasrawi* Pediatric Cardiologist, Al Jalila Children Heart Center, Dubai, UAE *
Cronicon OPEN ACCESS EC CARDIOLOGY Review Article Brief View of Calculation and Measurement of Cardiac Hemodynamics Samah Alasrawi* Pediatric Cardiologist, Al Jalila Children Heart Center, Dubai, UAE *
ORIGINAL ARTICLE. Abstract. Introduction. Materials and Methods
 ORIGINAL ARTICLE Effects of Cardiac Hemodynamics on Agreement in the ph, HCO3- and Lactate Levels between Arterial and Venous Blood Samples in Patients with Known or Suspected Chronic Heart Failure Satoshi
ORIGINAL ARTICLE Effects of Cardiac Hemodynamics on Agreement in the ph, HCO3- and Lactate Levels between Arterial and Venous Blood Samples in Patients with Known or Suspected Chronic Heart Failure Satoshi
Competency Title: Caring for a patient with an arterial line
 Appendix 2 Competency Title: Caring for a patient with an arterial line Aims and objectives Following completion of this competency document the practitioner will be able to: Discuss the indications for
Appendix 2 Competency Title: Caring for a patient with an arterial line Aims and objectives Following completion of this competency document the practitioner will be able to: Discuss the indications for
FUNDAMENTALS OF HEMODYNAMICS, VASOACTIVE DRUGS AND IABP IN THE FAILING HEART
 FUNDAMENTALS OF HEMODYNAMICS, VASOACTIVE DRUGS AND IABP IN THE FAILING HEART CINDY BITHER, MSN, ANP, ANP, AACC, CHFN CHIEF NP, ADV HF PROGRAM MEDSTAR WASHINGTON HOSPITAL CENTER CONFLICTS OF INTEREST NONE
FUNDAMENTALS OF HEMODYNAMICS, VASOACTIVE DRUGS AND IABP IN THE FAILING HEART CINDY BITHER, MSN, ANP, ANP, AACC, CHFN CHIEF NP, ADV HF PROGRAM MEDSTAR WASHINGTON HOSPITAL CENTER CONFLICTS OF INTEREST NONE
Principles of Biomedical Systems & Devices. Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont
 Principles of Biomedical Systems & Devices Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont Review of Cardiac Anatomy Four chambers Two atria-receive blood from the vena cave and pulmonary veins Two
Principles of Biomedical Systems & Devices Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont Review of Cardiac Anatomy Four chambers Two atria-receive blood from the vena cave and pulmonary veins Two
Cardiovascular Physiology. Heart Physiology. Introduction. The heart. Electrophysiology of the heart
 Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
HISTORY. Question: How do you interpret the patient s history? CHIEF COMPLAINT: Dyspnea of two days duration. PRESENT ILLNESS: 45-year-old man.
 HISTORY 45-year-old man. CHIEF COMPLAINT: Dyspnea of two days duration. PRESENT ILLNESS: His dyspnea began suddenly and has been associated with orthopnea, but no chest pain. For two months he has felt
HISTORY 45-year-old man. CHIEF COMPLAINT: Dyspnea of two days duration. PRESENT ILLNESS: His dyspnea began suddenly and has been associated with orthopnea, but no chest pain. For two months he has felt
Cardiac output and Venous Return. Faisal I. Mohammed, MD, PhD
 Cardiac output and Venous Return Faisal I. Mohammed, MD, PhD 1 Objectives Define cardiac output and venous return Describe the methods of measurement of CO Outline the factors that regulate cardiac output
Cardiac output and Venous Return Faisal I. Mohammed, MD, PhD 1 Objectives Define cardiac output and venous return Describe the methods of measurement of CO Outline the factors that regulate cardiac output
Arterial Line Waveform Interpretation
 Arterial Line Waveform Interpretation PICU CPM October 2014 1. Introduction The document is primarily aimed at education to provide some basic understanding of arterial line wave form 2. Scope The interpretation
Arterial Line Waveform Interpretation PICU CPM October 2014 1. Introduction The document is primarily aimed at education to provide some basic understanding of arterial line wave form 2. Scope The interpretation
CAE Healthcare Human Patient Simulator (HPS)
 CAE Healthcare Human Patient Simulator (HPS) The Human Patient Simulator, HPS, is a tethered simulator that is capable of patient assessment and treatment including mechanical ventilation and anesthesia.
CAE Healthcare Human Patient Simulator (HPS) The Human Patient Simulator, HPS, is a tethered simulator that is capable of patient assessment and treatment including mechanical ventilation and anesthesia.
BME 5742 Bio-Systems Modeling and Control. Lecture 41 Heart & Blood Circulation Heart Function Basics
 BME 5742 Bio-Systems Modeling and Control Lecture 41 Heart & Blood Circulation Heart Function Basics Dr. Zvi Roth (FAU) 1 Pumps A pump is a device that accepts fluid at a low pressure P 1 and outputs the
BME 5742 Bio-Systems Modeling and Control Lecture 41 Heart & Blood Circulation Heart Function Basics Dr. Zvi Roth (FAU) 1 Pumps A pump is a device that accepts fluid at a low pressure P 1 and outputs the
Mechanics of Cath Lab Support Devices
 Mechanics of Cath Lab Support Devices Issam D. Moussa, MD Chief Medical Officer First Coast Cardiovascular Institute, Jacksonville, FL Professor of Medicine, UCF, Orlando, FL None DISCLOSURE Percutaneous
Mechanics of Cath Lab Support Devices Issam D. Moussa, MD Chief Medical Officer First Coast Cardiovascular Institute, Jacksonville, FL Professor of Medicine, UCF, Orlando, FL None DISCLOSURE Percutaneous
Patient Management Code Blue in the CT Suite
 Patient Management Code Blue in the CT Suite David Stultz, MD November 28, 2001 Case Presentation A 53-year-old woman experienced acute respiratory distress during an IV contrast enhanced CT scan of the
Patient Management Code Blue in the CT Suite David Stultz, MD November 28, 2001 Case Presentation A 53-year-old woman experienced acute respiratory distress during an IV contrast enhanced CT scan of the
NON-COMPLIANT PTCA RAPID EXCHANGE DILATATION CATHETER
 Page 1 of 5 NON-COMPLIANT PTCA RAPID EXCHANGE DILATATION CATHETER STERILE. SINGLE USE ONLY. Sterilized with ethylene oxide gas. Non pyrogenic. Do not resterilize. Do not use opened or damaged packages.
Page 1 of 5 NON-COMPLIANT PTCA RAPID EXCHANGE DILATATION CATHETER STERILE. SINGLE USE ONLY. Sterilized with ethylene oxide gas. Non pyrogenic. Do not resterilize. Do not use opened or damaged packages.
2017 Cardiology Survival Guide
 2017 Cardiology Survival Guide Chapter 4: Cardiac Catheterization/Percutaneous Coronary Intervention A cardiac catheterization involves a physician inserting a thin plastic tube (catheter) into an artery
2017 Cardiology Survival Guide Chapter 4: Cardiac Catheterization/Percutaneous Coronary Intervention A cardiac catheterization involves a physician inserting a thin plastic tube (catheter) into an artery
Impedance Cardiography (ICG) Method, Technology and Validity
 Method, Technology and Validity Hemodynamic Basics Cardiovascular System Cardiac Output (CO) Mean arterial pressure (MAP) Variable resistance (SVR) Aortic valve Left ventricle Elastic arteries / Aorta
Method, Technology and Validity Hemodynamic Basics Cardiovascular System Cardiac Output (CO) Mean arterial pressure (MAP) Variable resistance (SVR) Aortic valve Left ventricle Elastic arteries / Aorta
Admission of patient CVICU and hemodynamic monitoring
 Admission of patient CVICU and hemodynamic monitoring Prepared by: Rami AL-Khatib King Fahad Medical City Pi Prince Salman Heart tcentre CVICU-RN Admission patient to CVICU Introduction All the patients
Admission of patient CVICU and hemodynamic monitoring Prepared by: Rami AL-Khatib King Fahad Medical City Pi Prince Salman Heart tcentre CVICU-RN Admission patient to CVICU Introduction All the patients
한국학술정보. Risk Factors of Induced Cardiac Arrhythmia during the Central Ve n o u s Catheterization
 Risk Factors of Induced Cardiac Arrhythmia during the Central Ve n o u s Catheterization Min-Jung Kim, M.D., Min-Seob Sim, M.D., Hyoung- Gon Song, M.D., Yeon-Kwon Jeong, M.D., Pil-Cho Choi, M.D. 1, Jun-Hwi
Risk Factors of Induced Cardiac Arrhythmia during the Central Ve n o u s Catheterization Min-Jung Kim, M.D., Min-Seob Sim, M.D., Hyoung- Gon Song, M.D., Yeon-Kwon Jeong, M.D., Pil-Cho Choi, M.D. 1, Jun-Hwi
This is a provisional PDF comprising this cover note and the manuscript as it was upon acceptance for publication.
 This is a provisional PDF comprising this cover note and the manuscript as it was upon acceptance for publication. A typeset PDF article will be published soon. Surgical Removal of a Knotted Intravascular
This is a provisional PDF comprising this cover note and the manuscript as it was upon acceptance for publication. A typeset PDF article will be published soon. Surgical Removal of a Knotted Intravascular
Aortic Dissection Causes of Death
 Aortic Dissection Causes of Death Rupture aorta 33.3% Unspecified 33.3% Neurological l deficit it 13.9% Visceral ischemia/kidney failure 11.5% Cardiac tamponade 7.9% (Circulation 2002;105:200-6) Medical
Aortic Dissection Causes of Death Rupture aorta 33.3% Unspecified 33.3% Neurological l deficit it 13.9% Visceral ischemia/kidney failure 11.5% Cardiac tamponade 7.9% (Circulation 2002;105:200-6) Medical
Assessing Preload Responsiveness Using Arterial Pressure Based Technologies. Patricia A. Meehan, RN, MS Education Consultant Edwards Lifesciences, LLC
 Assessing Preload Responsiveness Using Arterial Pressure Based Technologies Patricia A. Meehan, RN, MS Education Consultant Edwards Lifesciences, LLC Content Description : Fluid administration is a first
Assessing Preload Responsiveness Using Arterial Pressure Based Technologies Patricia A. Meehan, RN, MS Education Consultant Edwards Lifesciences, LLC Content Description : Fluid administration is a first
Hemodynamic Monitoring: Arterial and Pulmonary Artery Catheters
 CHAPTER 21 Hemodynamic Monitoring: Arterial and Pulmonary Artery Catheters Kevin Y. Pei and Mihae Yu Since the introduction of the pulmonary artery catheter (PAC) in the 1970s, initial enthusiasm has been
CHAPTER 21 Hemodynamic Monitoring: Arterial and Pulmonary Artery Catheters Kevin Y. Pei and Mihae Yu Since the introduction of the pulmonary artery catheter (PAC) in the 1970s, initial enthusiasm has been
Arterial Line Insertion Pre Reading
 PROCEDURE ACCREDITATION THE CANBERRA HOSPITAL EMERGENCY DEPARTMENT Arterial Line Insertion Pre Reading Indications Requirement for continuous blood pressure monitoring (all patients on pressors, inotropes,
PROCEDURE ACCREDITATION THE CANBERRA HOSPITAL EMERGENCY DEPARTMENT Arterial Line Insertion Pre Reading Indications Requirement for continuous blood pressure monitoring (all patients on pressors, inotropes,
The Vigileo monitor by Edwards Lifesciences supports both the FloTrac Sensor for continuous cardiac output and the Edwards PreSep oximetry catheter
 1 2 The Vigileo monitor by Edwards Lifesciences supports both the FloTrac Sensor for continuous cardiac output and the Edwards PreSep oximetry catheter for continuous central venous oximetry (ScvO2) 3
1 2 The Vigileo monitor by Edwards Lifesciences supports both the FloTrac Sensor for continuous cardiac output and the Edwards PreSep oximetry catheter for continuous central venous oximetry (ScvO2) 3
Nitroglycerin and Heparin Drip Interfacility Protocols
 Nitroglycerin and Heparin Drip Interfacility Protocols EMS Protocol This protocol applies to nitroglycerin and Heparin drips that are initiated at the transferring facility prior to transport and are not
Nitroglycerin and Heparin Drip Interfacility Protocols EMS Protocol This protocol applies to nitroglycerin and Heparin drips that are initiated at the transferring facility prior to transport and are not
PHYSIOLOGY MeQ'S (Morgan) All the following statements related to blood volume are correct except for: 5 A. Blood volume is about 5 litres. B.
 PHYSIOLOGY MeQ'S (Morgan) Chapter 5 All the following statements related to capillary Starling's forces are correct except for: 1 A. Hydrostatic pressure at arterial end is greater than at venous end.
PHYSIOLOGY MeQ'S (Morgan) Chapter 5 All the following statements related to capillary Starling's forces are correct except for: 1 A. Hydrostatic pressure at arterial end is greater than at venous end.
Cardiothoracic Fellow Expectations Division of Cardiac Anesthesia, Beth Israel Deaconess Medical Center
 The fellowship in Cardiothoracic Anesthesia at the Beth Israel Deaconess Medical Center is intended to provide the foundation for a career as either an academic cardiothoracic anesthesiologist or clinical
The fellowship in Cardiothoracic Anesthesia at the Beth Israel Deaconess Medical Center is intended to provide the foundation for a career as either an academic cardiothoracic anesthesiologist or clinical
1. CARDIOLOGY. These listings cannot be correctly interpreted without reference to the Preamble. Anes. $ Level
 1. CARDIOLOGY These listings cannot be correctly interpreted without reference to the Preamble. Anes. Referred Cases 33010 Consultation: To consist of examination, review of history, laboratory, X-ray
1. CARDIOLOGY These listings cannot be correctly interpreted without reference to the Preamble. Anes. Referred Cases 33010 Consultation: To consist of examination, review of history, laboratory, X-ray
Unit 6: Circulatory System. 6.2 Heart
 Unit 6: Circulatory System 6.2 Heart Functions of Circulatory System 1. The heart is the pump necessary to circulate blood to all parts of the body 2. Arteries, veins and capillaries are the structures
Unit 6: Circulatory System 6.2 Heart Functions of Circulatory System 1. The heart is the pump necessary to circulate blood to all parts of the body 2. Arteries, veins and capillaries are the structures
Per-Q-Cath* PICC Catheters with Excalibur Introducer* System
 Bard Access Systems Per-Q-Cath* PICC and Catheters with Excalibur Introducer* System Instructions For Use Table of Contents Table of Contents Page Contents 1 Product Description, Indications & Contraindications
Bard Access Systems Per-Q-Cath* PICC and Catheters with Excalibur Introducer* System Instructions For Use Table of Contents Table of Contents Page Contents 1 Product Description, Indications & Contraindications
Document No. BMB/IFU/40 Rev No. & Date 00 & 15/11/2017 Issue No & Date 01 & 15/11/2017
 Central Venous Catheter Device Description Multi-lumen catheters incorporate separate, non-communicating vascular access lumens within a single catheter body. Minipunctur Access Sets And Trays: Used for
Central Venous Catheter Device Description Multi-lumen catheters incorporate separate, non-communicating vascular access lumens within a single catheter body. Minipunctur Access Sets And Trays: Used for
Response to questions at ACCA Webinar on Echocardiography in Critical Care
 Response to questions at ACCA Webinar on Echocardiography in Critical Care The participants in the Webinar were Bernard Cosyns [Professor of Cardiology at the Free University, Brussels, Belgium, and Chairman
Response to questions at ACCA Webinar on Echocardiography in Critical Care The participants in the Webinar were Bernard Cosyns [Professor of Cardiology at the Free University, Brussels, Belgium, and Chairman
Your heart is a muscular pump about the size of your fist, located
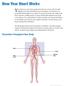 How Your Heart Works Your heart is a muscular pump about the size of your fist, located slightly to the left and behind your breastbone. Its function is to pump blood throughout your body. As your heart
How Your Heart Works Your heart is a muscular pump about the size of your fist, located slightly to the left and behind your breastbone. Its function is to pump blood throughout your body. As your heart
BUSINESS. Articles? Grades Midterm Review session
 BUSINESS Articles? Grades Midterm Review session REVIEW Cardiac cells Myogenic cells Properties of contractile cells CONDUCTION SYSTEM OF THE HEART Conduction pathway SA node (pacemaker) atrial depolarization
BUSINESS Articles? Grades Midterm Review session REVIEW Cardiac cells Myogenic cells Properties of contractile cells CONDUCTION SYSTEM OF THE HEART Conduction pathway SA node (pacemaker) atrial depolarization
Hemodynamic Monitoring in the CCU. Edward G. Hamaty Jr., D.O. FACCP, FACOI
 Hemodynamic Monitoring in the CCU Edward G. Hamaty Jr., D.O. FACCP, FACOI Waveform Review Left Ventricular Pressure Normal left ventricular pressures are: Systolic 100 to 140 mm of mercury End-diastolic
Hemodynamic Monitoring in the CCU Edward G. Hamaty Jr., D.O. FACCP, FACOI Waveform Review Left Ventricular Pressure Normal left ventricular pressures are: Systolic 100 to 140 mm of mercury End-diastolic
PROBLEM SET 2. Assigned: February 10, 2004 Due: February 19, 2004
 Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
4. The two inferior chambers of the heart are known as the atria. the superior and inferior vena cava, which empty into the left atrium.
 Answer each statement true or false. If the statement is false, change the underlined word to make it true. 1. The heart is located approximately between the second and fifth ribs and posterior to the
Answer each statement true or false. If the statement is false, change the underlined word to make it true. 1. The heart is located approximately between the second and fifth ribs and posterior to the
Vascular access device selection & placement. Alisa Seangleulur, MD Anesthesiology Department, Faculty of Medicine, Thammasat University
 Vascular access device selection & placement Alisa Seangleulur, MD Anesthesiology Department, Faculty of Medicine, Thammasat University How to make the right choice of vascular access device.. Peripheral
Vascular access device selection & placement Alisa Seangleulur, MD Anesthesiology Department, Faculty of Medicine, Thammasat University How to make the right choice of vascular access device.. Peripheral
Hemodynamic Monitoring in the Intensive Care Unit
 Hemodynamic Monitoring in the Intensive Care Unit Hayan Al Maluli, MD and Christine M. DeStephan, MD Abstract Caring for critically ill patients has dramatically changed over the past two decades. Advancement
Hemodynamic Monitoring in the Intensive Care Unit Hayan Al Maluli, MD and Christine M. DeStephan, MD Abstract Caring for critically ill patients has dramatically changed over the past two decades. Advancement
10. Thick deposits of lipids on the walls of blood vessels, called, can lead to serious circulatory issues. A. aneurysm B. atherosclerosis C.
 Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
IB TOPIC 6.2 THE BLOOD SYSTEM
 IB TOPIC 6.2 THE BLOOD SYSTEM THE BLOOD SYSTEM TERMS TO KNOW circulation ventricle artery vein 6.2.U1 - Arteries convey blood at high pressure from the ventricles to the tissues of the body Circulation
IB TOPIC 6.2 THE BLOOD SYSTEM THE BLOOD SYSTEM TERMS TO KNOW circulation ventricle artery vein 6.2.U1 - Arteries convey blood at high pressure from the ventricles to the tissues of the body Circulation
I ment and assessment of pressures
 lnvasive.... monitoring Patricia C Seifert, RN Patricia C Seifert, RN, BA, CNOR, is head nurse in cardiac surgery at the Fairfax Hospital, Falls Church, Va. An AD graduate of Northern Virginia Community
lnvasive.... monitoring Patricia C Seifert, RN Patricia C Seifert, RN, BA, CNOR, is head nurse in cardiac surgery at the Fairfax Hospital, Falls Church, Va. An AD graduate of Northern Virginia Community
Transcatheter Aortic Valve Implantation Procedure (TAVI)
 Page 1 of 5 Procedure (TAVI) Introduction Aortic stenosis (AS) is a common heart valve problem associated with heart failure and death. Surgical valve repair or replacement is recommended if AS patients
Page 1 of 5 Procedure (TAVI) Introduction Aortic stenosis (AS) is a common heart valve problem associated with heart failure and death. Surgical valve repair or replacement is recommended if AS patients
Introduction. Invasive Hemodynamic Monitoring. Determinants of Cardiovascular Function. Cardiovascular System. Hemodynamic Monitoring
 Introduction Invasive Hemodynamic Monitoring Audis Bethea, Pharm.D. Assistant Professor Therapeutics IV January 21, 2004 Hemodynamic monitoring is necessary to assess and manage shock Information obtained
Introduction Invasive Hemodynamic Monitoring Audis Bethea, Pharm.D. Assistant Professor Therapeutics IV January 21, 2004 Hemodynamic monitoring is necessary to assess and manage shock Information obtained
IV Fluids. Nursing B23. Objectives. Serum Osmolality
 IV Fluids Nursing B23 Objectives Discuss the purpose of IV Discuss nursing interventions in IV therapy Identify complications of IV therapy Differentiate between peripheral line, central line, and PICC
IV Fluids Nursing B23 Objectives Discuss the purpose of IV Discuss nursing interventions in IV therapy Identify complications of IV therapy Differentiate between peripheral line, central line, and PICC
Mechanics of Cath Lab Support Devices
 Mechanics of Cath Lab Support Devices Issam D. Moussa, MD Professor of Medicine Mayo Clinic College of Medicine Chair, Division of Cardiovascular Diseases Mayo Clinic Jacksonville, Florida DISCLOSURE Presenter:
Mechanics of Cath Lab Support Devices Issam D. Moussa, MD Professor of Medicine Mayo Clinic College of Medicine Chair, Division of Cardiovascular Diseases Mayo Clinic Jacksonville, Florida DISCLOSURE Presenter:
CARDIAC CYCLE CONTENTS. Divisions of cardiac cycle 11/13/13. Definition. Badri Paudel GMC
 CARDIAC CYCLE Badri Paudel GMC CONTENTS Ø DEFINATION Ø DIVISION OF CARDIAC CYCLE Ø SUB DIVISION AND DURATION OF CARDIAC CYCLE Ø SYSTOLE Ø DIASTOLE Ø DESCRIPTION OF EVENTS OF CARDIAC CYCLE Ø SUMMARY Ø ELECTROCARDIOGRAPHY
CARDIAC CYCLE Badri Paudel GMC CONTENTS Ø DEFINATION Ø DIVISION OF CARDIAC CYCLE Ø SUB DIVISION AND DURATION OF CARDIAC CYCLE Ø SYSTOLE Ø DIASTOLE Ø DESCRIPTION OF EVENTS OF CARDIAC CYCLE Ø SUMMARY Ø ELECTROCARDIOGRAPHY
