Simultaneous abdominal aortic replacement and thoracic stent-graft placement for multilevel aortic disease
|
|
|
- Candace Alexander
- 6 years ago
- Views:
Transcription
1 Simultaneous abdominal aortic replacement and thoracic stent-graft placement for multilevel aortic disease Marc R. Moon, MD, R. Scott Mitchell, MD, Michael D. Dake, MD, Christopher K. Zarins, MD, James I. Fann, MD, and D. Craig Miller, MD, Stanford, Calif. Purpose: Patients with aneurysmal disease involving both the descending thoracic and abdominal aorta have historically required simultaneous or sequential conventional operations, but the morbidity rate is high with either approach in these patients, who often exhibit coexisting cardiopulmonary disease. Transluminally placed endovascular grafts have recently been developed for repair of aortic aneurysms, and we have implemented these techniques to eliminate the need for a thoracotomy in patients with multilevel aortic disease. Methods: Since January 1994, 18 patients have undergone conventional abdominal aortic replacement with endovascular stent-graft placement into the descending thoracic aorta under fluoroscopic guidance through a 10 mm Dacron side limb offthe abdominal graft. Abdominal aortic replacement required a tube graft in eight patients and bifurcated grafts in 10 patients. Thoracic stent-grafts (custom fabricated, woven Dacron covered, self-expandable stents) averaged cm (mean -+ SD) in length. Results: One patient died, resulting in a hospital mortality rate of 6%. No patients required further surgical intervention to treat their aortic disease. Seventeen patients (94%) are currently well months after surgery (range, 3 to 29 months) with completely excluded thoracic aortic disease, no stent migration, and no change in stent configuration documented by serial radiologic examinations. Conclusions: Simultaneous abdominal aortic replacement and deployment of a thoracic stent-graft can safely exclude multilevel aortic aneurysmal disease and may be a valuable treatment option for these otherwise high-risk patients. (J Vasc Surg 1997;25: ) Patients with multilevel aortic disease present a formidable challenge for the cardiothoracic and vascular surgeon and interventional radiologist. The morbidity rate of surgical repair can be substantial in these patients, who often exhibit coexisting cardiopulmonary disease. In patients with an abdominal From the Department of Cardiovascular and Thoracic Surgery, Division of Vascular Surgery (Dr. Zarins), and Department of Radiology (Dr. Dake), Stanford University School of Medicine. Dr. Moon is a Carl and Leah McConnell Cardiovascular Surgical Research Fellow. Presented in part at the Joint Annual Meeting of The Society for Vascular Surgery and the International Society for Cardiovascular Surgery, North American Chapter, Chicago, I11., June 9-12, Reprint requests: tk Scott Mitchell, MD, Department of Cardiovascular and Thoracic Surgery, Falk Cardiovascular Research Center, Stanford University School of Medicine, Stanford, CA Copyright 1997 by The Society for Vascular Surgery and International Society for Cardiovascular Surgery, North American Chapter /97/$ /6/ aortic aneurysm, 5% also have a descending thoracic aneurysm~; in patients with a descending thoracic aneurysm, i3% to 29% also have abdominal involvement. 2-6 In the early 1980s, Crawford advocated simultaneous open thoracic and abdominal aortic repair as the treatment of choice in patients with multilevel aortic disease. 7,8 Sequential repair can also be performed, but this approach requires two major surgical interventions, and rupture of the residual aneurysm can occur while waiting the second operation.s,7 Crawford fotmd that 30% of early postoperative deaths after isolated repair of a descending thoracic aneurysm were caused by rupture of an untrcated infrarenal aneurysm, s Transluminally placed endovascular grafts have recently been developed for repair of thoracic aortic aneurysms with encouraging early rcsults. 9a In an attempt to decrease the risk associated with either a simultaneous thoracotomy and laparotomy or sequential major operations in patients with multilevel aortic disease and to make treatment available to
2 Volume 25, Number 2 Moon et al. 333 patients with otherwise prohibitive comorbidities, we have begun to look at alternatives to conventional surgical treatment. In the current study, we found that combined retroperitoneal abdominal aortic replacement with endovascular stent-graft placement into the descending thoracic aorta can effectively exclude both areas of aortic disease without the added morbidity of a thoracic incision or second operation. MATERIAL AND METHODS Patient population. From January 1994 to March 1996, 18 patients with coexisting abdominal aortic and descending thoracic aneurysmal disease underwent conventional retropcritoncal abdominal aortic replacement and endovascular stent-graft placement into the descending thoracic aorta through a 10 mm Dacron side limb offthe abdominal graft. A transperitoneal approach was used if necessary to adequately visualize the abdominal aorta. There were 14 men and 4 women, with a mean age of (+ 1 SD) years (range, 62 to 83 years). Seventeen patients (94%) had significant comorbidities that required treatment, including coronary artery disease (12 patients), chronic obstructive pulmonary disease (COPD) (8), hypertension (15), and diabetes (3). Twelve patients (67%) had a significant smoking history ( pack-years). During this period at our institution, one patient elected to undergo a simultaneous open thoracic and abdominal aortic aneurysm repair, and two other patients underwent sequential open repair 6 to 8 weeks apart because their thoracic aneurysm was not appropriate for stent-graft placement (inadequate proximal neck). Abdominal aortic disease including infrarenal (13 patients), juxtarenal (3), and suprarenal (1) aneurysms, and one patient had severe aortoiliac occlusive disease. Ten patients had extensive disease of either one or both iliac arteries that required treatment. Mean abdominal aortic diameter in patients with aneurysms was 5.6 _+ 1.9 cm (range, 3.5 to 9.5 cm); 10 aneurysms were greater than 5 cm and six were greater than 6 cm. Descending thoracic disease included atherosclerotic aneurysmal disease (12 patients), intramural hematomaflpenetrating ulcer (5), and chronic post-traumatic aneurysm (1). The thoracic aneurysm involved the distal descending aorta in five patients, mid-descending aorta in seven patients, and proximal descending aorta in six patients. In three patients, the thoracic disease spanned all three segments. Length of the thoracic aneurysm averaged 8.9 _+ 4.3 cm (range, 3.2 to 20 cm). The mean diameter of the thoracic aneurysm (13 patients) was cm (range, 5 to 11 cm); only two aneurysms were less than 6 cm. Mean thoracic aortic diameter in patients with penetrating ulcers (five paticnts) was cm (range, 5 to 6 cm). The thoracic aorta proximal to the diseased segment was cm in diameter (range, 2.0 to 3.8 cm). The thoracic aorta distal to the diseased segment was also cm in diameter (range, 2.4 to 3.8 cm). Preoperative evaluation. Before surgery, a spiral computed tomographic (CT) scan was obtained of the thoracoabdominal aorta to measure thoracic and abdominal aortic diameter, evaluate the branch vessels and iliac arteries, and provide a three-dimensional reconstruction of the descending thoracic aorta to measure aneurysm length and diameter. An aortogram was obtained to identify the rcnal and visceral vessels and to determine the relationship of the proximal thoracic aneurysm neck to the left subclavian artery and celiac axis. One to 2 cm ofnonaneurysmal aorta is necessary both proximal and distal to the aneurysm to allow safe deployment without the need for a preliminary subclavian-to-carotid transposition or bypass and without compromise to the visceral circulation. 1,11 It is also helpful to localize patent intercostal arteries so that attempts can be made to preserve these at the time of stent-graft deployment; we do not, however, perform selective intercostal angiographic evaluation. If large intercostal arteries are noted before surgery, excess distal stent-graft length is avoided to prevent intercostal occlusion; alternatively, an uncovered stent can be used to anchor the stent-graft at the proximal or distal neck of the aneurysm, allowing perfusion in a critical intercostal artery. Patients were not considered appropriate for endovascular stent-graft placement in the absence of an adequate aneurysm neck (inadequate length or excess diameter) or with inappropriate morphologic features (e.g. extensive chronic aortic dissections). Fabrication of endovascular stent-grafts. Stent-grafts were individually fabricated as previously described with commercially available products. 911 Multiple self-expanding "Z"-stents were combined to yield the desired length, and a woven Dacron graft (Cooley Veri-Soft, Meadox Medicals, Inc., Oaldand, NJ.), that had been ironed to flatten the crimps and reduce its profile was attached to the stainless-steel endoskeleton with interrupted 5-0 polypropylene sutures (Fig. 1). Uncrimped grafts are now available and will be used for stent-graft fabrication in the future. On the basis of preoperative CT scan measurements, stent-graft length was manufactured to
3 334 Moon et al. February 1997 Fig. 1. Endovascular stent-graft. Woven Dacron graft se - cured to a stainless-steel endoskeleton with polypropylene sutures. be approximately 3 to 4 cm longer than the segment of aortic disease; this allowed the ends of the stentgraft to anchor to the proximal and distal necks of the aneurysm. Stent-graft diameter was oversized by 2 to 3 mm to create an effective friction seal at each end. Stent-grafts could be designed to taper or reverse-taper as necessary to match each patient's anatomy. After sterilization, the stent-graft was radially compressed and loaded into a 20F to 28F Teflon sheath (loading cartridge) for later deployment. Surgical technique. A double lumen endotracheal tube was usually inserted, and cardiopulmonary bypass standby was available for every case. Continuous radial artery and pulmonary artery monitoring were used, as was transesophageal echocardiography to monitor cardiac function. Patients were prepped and draped for combined thoracic and retroperitoneal incisions in the 60-degree right lateral decubitus position. A cell-saver collection system was helpful to minimize transfusion requirements during aortic replacement and catheter manipulation. Abdominal aortic replacement was performed using a standard retroperitoneal approach; rarely was a transperitoneal approach necessary for adequate visualization of the abdominal aorta. With moderate systemic heparinization (100 IU/kg), the abdominal aorta was replaced with a Dacron tube graft in eight patients, aortobiiliac graft in eight patients, aortobifemoral graft in one patient, and the remaining patient required a bifurcated graft to the left iliac and the right femoral artery. The patient with a suprarenal aneurysm had previously undergone an aortobifemoral graft for occlusive disease and required supraceliac cross-clamping and renal reimplantation. In all patients, after completion of the distal anastomosis, a 10 mm Dacron graft (length, approximately 10 to 15 cm) was anastomosed in an end-to-side fashion to the main trunk of the abdominal graft (Fig. 2). The distal end was then secured with a vessel clamp. The graft was then used as the side limb through which the stent-graft could be placed. If a bifurcated graft was required, it was also possible to use one limb of the graft (9 mm or greater) for endovascular access, although use of a side limb is preferable as it allows earlier return of flow to both legs. Endovascular stent-graft placement. Before endovascular manipulation, full systemic heparinization (total 200 to 300 IU/kg) was achieved. Using the Seldinger technique, a 9F introducer sheath was inserted into the side limb graft, a 5F pigtail was introduced into the aortic arch over a guidewire under fluoroscopic guidance, and an intraoperative angiogram was obtained to accurately localize the proximal aneurysm neck. A portable C-arm image intensifier with digital road-mapping capabilities was used. A inch "super-stiff" guidewire was then exchanged for the introducer, and the proximal side limb was clamped to prevent blood loss. A carefullysized transverse incision was made in the side limb to allow passage ofa 20F to 28F Teflon delivery sheath with a tapered dilator over the guidewire. The delivery sheath had a fenestrated plastic cover (one-way valve apparatus, Cook Urological, Inc., Bloomington, Ind.) secured to its end to provide hemostatis; the one-way valve allowed antegrade catheter insertion but prevented retrograde blood loss during catheter exchanges. The dilator and guidewire were removed and the compressed stent-graft introduced into the delivery sheath with a solid Teflon rod or "pusher." Under fluoroscopic guidance, the stent-graft was advanced up the delivery sheath using the Teflon pusher until it was 1.5 to 2 cm proximal to the aneurysm neck. The location of the proximal neck was based on landmarks obtained on the intraoperative angiogram. Fortunately, the anatomy of the distal aortic arch and proximal descending thoracic aorta was relatively stable during passage of the delivery sheath. If anatomic deformation by the sheath was suspected, another angiogram was obtained through the sheath prior to stent-graft deployment. Controlled hypotension was induced with nitroprusside or esmolol (mean arterial pressure, 50 to 60 mm Hg) to minimize stent migration during deployment. To deploy the stent, the delivery sheath was withdrawn rapidly while the pusher was held station-
4 Volume 25, Number 2 Moon et al. 335 Fig. 2. Dacron side limb anastomosed to left limb of an aortoiliac graft (transperitoneal approach). ary; the stent-graft emerged from the sheath in the proper position. A completion angiogram was then obtained to assure aneurysm exclusion. If stent-graft position was too distal such that the proximal aneurysm was not excluded, or it was too proximal such that the distal aneurysm was not excluded, additional smaller stent-grafts were placed to bridge the gap. After removal of all catheters and heparin reversal, the side limb was over sewn near its anastomosis to the abdominal graft, the incision was closed, and the patient was traalsferred to the intensive care unit. If further manipulation was considered in the future (i.e., for treatment of other aneurysms that currently were not of adequate size to warrant intervention), the side limb was left intact and buried just below the fascia or in the subcutaneous tissue for easy access. Postoperative evaluation. Before discharge, aortography and a repeat spiral CT scan were performed to document aneurysm exclusion. The patients were then studied at 2 months with a chest radiograph, at 6 months and 1 year with a radiograph, spiral CT scan, and arteriogram, then annually thereafter with a radiograph and spiral CT scan. Figs. 3, 4, and 5 depict typical preoperative and postoperative studies in an 83-year-old man who underwent simultaneous transperitoneal abdominal aortic replacement and descending thoracic aortic stent-graft placement through a side limb off the abdominal graft. Total exclusion of the patient's 11 cm thoracic and 5 cm abdominal aneurysms was achieved. The operative and radiologic protocol was approved by the Stanford University Medical Center Committee on the Use of Human Subjects in Research, and informed consent was obtained before surgical intervention and radiographic studies. Statistical analysis. All continuous data are reported as mean + one standard deviation and ratios as mean _+ 70% confidence limits. Actuarial life-table survival data were calculated using commercially available software (SPSS, Chicago, Ill.) and variability expressed as _ one standard error of the mean. RESULTS Stent-graft deployment was technically successful in all cases; 13 patients were adequately treated with one stent, whereas five patients required two stentgrafts to exclude the area of disease. Mean stent-graff length was cm (range, 7.5 to 20 cm) and diameter was cm (range, 2.4 to 3.8 cm). Complete aneurysm exclusion was achieved at the time of operation in 17 patients (94%) and have remained so throughout the follow-up period. One patient has a residual false channel between the stentgraft and native aortic wall proximally that remains unchanged 21 months after surgery. This 66-yearold man, who was refused an open thoracic repair because of severe COPD, underwent stent-grafting
5 JOURNAL OF VASCULAR SURGERY 336 February 1997 Moon etal. Fig. 3. Preoperative thoracic (A, magnified) and abdominal (B) cross-sectional contrast CT scans demonstrate 11 cm and 5 cm aneurysms, respectively, in an 83-year-old man. for two large penetrating ulcers. At the completion o f the procedure, an angiogram demonstrated that the ulcers were excluded, but there was also a small, low-flow residual false channel. We are currently observing this patient at 6 - m o n t h intervals with contrast C T scans. I f the aorta enlarges, a saccular false aneurysm develops at either end o f the stent-graft, or flow is reestablished to the ulcers, additional stentgrafts will be placed. N o patients have required further surgical intervention to treat their aortic disease. Overall, one patient died, resulting in a hospital mortality rate o f 6% + 6%. T h e one postoperative
6 Volume 25, Number 2 Moon et al. 337 Fig. 4. Postoperative thoracic (A) and abdominal (B) aortograms obtained from the same patient in Fig. 3 after combined transperitoneal abdominal aortic replacement and descending thoracic stent-graft placement. death occurred in a 66-year-old man 31 days after complex redo suprarenal aneurysm resection and thoracic stent-grafting; splenectomy was required on the first postoperative day for an intraoperative injury. The postoperative course was complicated by a severe coagulopathy and systemic hypotension requiring inotropic agents; the patient ultimately died offungal sepsis with multisystem organ failure. In the 17 survivors, hospital stay, intensive care unit stay, and mechanical ventilation averaged days, 5 _+ 5 days, and days, respectively. Thirteen patients (72%) were extubated within 48 hours, and nine (50%) required less than 72 hours of intensive care. Intraoperative transfusion requirements were 3.7 _+ 3.1 units (packed red blood cells), and, excluding the patient who died with a prolonged coagulopathy that required 79 units in the postoperative period, mean postoperative transfusion requirements were units. Nine postoperative complications occurred in 6 patients (33%), including respiratory insufficiency, small bowel obstruction requiting laparoscopic lysis of adhesions, cerebrovascular accident, paraplegia, coagulopathy (two patients), splenic injury, dissection of the aorta proximal to the stent-graft, and retroperitoneal hematoma that required surgical evacuation 3 months aftcr surgery. A 62-year-old man with severe COPD required 18 days of ventilatory support for respiratory insufficiency before full recovery. This patient also had a retrograde subintimal aortic dissection proximal to the level of stent-graft placement on his predischarge CT scan. He remained asymptomatic, and subsequent CT scans and arteriograms demonstrated complete resolution within 4 months. A 72-year-old woman with a history of transient ischemia attacks but no radiologic evidence of carotid disease developed a left hemispheric stroke 9 hours after the procedure. A brain CT demonstrated multiple old bilateral infarcts; a residual left-sided strength deficit persists. Paraplegia occurred in the 66-year-old patient described above as the operative death. This patient had a 12.5 cm stent-graft placed into the thoracic aorta. It is unknown whether distal embolization, hypotension, or intercostal artery interruption was responsible for the spinal cord injury in this patient. A 74-year-old woman with no preexisting hematologic disorder suffered a severe thrombotic coagulopathy during abdominal aortic replacement. Proximal aortic and distal iliac thrombosis occurred after suprarenal cross-clamping to repair her juxtarenal aneurysm despite adequate anticoagulation; activated clotting time was 280 seconds at the time of
7 338 Moon etal. February 1997 Fig. 5. Postoperative cross-sectional contrast CT scan (magnified) of the thoracic aneurysln in the patient depicted in Figs. 3 and 4. Note the presence of contrast within the stent-graft and absence of contrast within the aneurysm sac demonstrating complete exclusion of the thoracic disease. thrombosis (120 seconds baseline). Thrombectomy was required to restore distal flow. Due to the intraoperative complication and prolonged suprarenal cross-clamp time (89 minutes), stent-graft placement was deferred to a later date (19 days after surgery) on a second admission. At the initial operation, the Dacron side limb was tunneled through the fascia into the subcutaneous plane. When the patient returned to the operating room, relaparotomy was not required; a subcutaneous dissection allowed easy access to the side limb, which, after thrombectomy, allowed routine stent-graft placement. Hospital stay was 7 days after the abdominal aneurysm resection and 4 days after stent-graft placement. All other patients underwent stent-graft placement during the same anesthetic period. There have been no late deaths to date, and all 17 hospital survivors are currently well months (range, 3 to 29 months) after surgery. The actuarial survival rate is 92% _+ 8% at 12 months. Postoperative serial radiographic studies have demonstrated no stent migration or change in stent configuration in the thoracic aorta and no pseudoaneurysm formation or aneurysm expansion in either the abdominal or thoracic aorta. Approximately one half of the patients have experienced shrinkage of the thrombosed thoracic aortic aneurysm sac, whereas in the others its size has remained the same. DISCUSSION Endovascular stent-grafts have recently been developed to exclude disease of the descending thoracic aorta, and although long-term follow-up is limited, early experimental and clinical results have been encouraging. 9,1,12,13 Since July 1992 stent-graft repair for descending thoracic aortic disease has been performed at Stanford in 81 patients, n The overall hospital mortality rate is 9% + 3%, the paraplegia rate is 4% +_ 2%, and the stroke rate is 5% + 3%. Current actuarial survival estimates are 87% _+ 4% at 1 year and 81% _+ 6% at 3 years, but mean follow-up is only 13.2 months. In an attempt to decrease the morbidity rate associated with combined descending and abdominal aortic replacement that requires both a thoracotomy and laparotomy, we have applied endovascular techniques to patients with multilevel aortic disease. The operative mortality rate for patients undergoing elective open repair of an isolated descending thoracic aortic aneurysm is 3% to 12% 6'14-18 whereas that following conventional abdominal aortic resection is 2% to 5% Historically, in patients with combined descending thoracic and abdominal aortic aneurysms, both could be repaired simultaneously through separate incisions or the operations could be staged, usually 6 to 8 weeks apart, with the order of operation determined by symptoms and relative aneurysm size. In asymptomatic patients, Crawford recommended repair of the thoracic aorta initially. 7-s While awaiting the second operation, the abdominal aneurysm is easier to observe, and if symptoms or rupture occur patients could potentially survive for periods sufficient to attempt repair. In contrast, thoracic aneurysms are more likely to rupture without warning and are rapidly fatal within minutes. More than 60% of patients who undergo repair of a descending thoracic aneurysm have multifocal aortic disease, half of which involves the infrarenal aorta. 7 Crawford s noted in his series of 112 patients who underwent isolated repair of a descending thoracic aneurysm, that of 10 patients who died within 30 days of operation, 30% died as the result of a ruptured infrarenal aneurysm. For these reasons, Crawford performed simultaneous repair through separate thoracic and abdominal incisions in 24 patients who he felt were good surgical risks and continued to do well in the operating room after the first replacement; the 30 day mortality rate was 8%. 7 In his series, the mortality rates in patients who underwent simultaneous versus staged operations for all types of multilevel aortic disease were 10% and 16%, respectively. In the current series, our mortality rate was 6% +
8 Volume 25, Number 2 Moon et al %, which compares favorably with Crawford's results; however, many of these patients had been considered inoperable for standard thoracic aortic replacement by cardiovascular surgeons before surgery because of their poor underlying cardiopulmonary status. In patients of acceptable surgical risk, we currently recommend thoracic aortic replacement (either open or endovascular) in all symptomatic patients or if the aneurysm is greater than 6 cm or twice the size of a relatively normal contiguous aortic segment. 6 Penetrating ulcers or documented enlargement should also prompt surgical considcration. Concurrent abdominal aortic replacement should be considered if it is greater than 5 cm, if it has been increasing in size, or if the patient's associated iliofemoral disease precludes safe access to the more proximal aortic tree (extensive intraluminal thrombus or atherosclerotic disease). In our series, five patients had aneurysms between 4 and 5 cm, four between 5 and 6 cm, and six had large aneurysms (greater than 6 cm). Two patients had smaller aneurysms (3.5 cm each) that would not have been repaired, but iliofemoral atherosclerotic disease prevented safe passage of the stent-graft insertion system. Conventional descending aortic resection is associated with a 5% risk of severe renal dysfunction that requires dialysis, 6,1s whereas the risk is less than i% with elective infrarenal replacement Because thoracic stent-grafting does not require a suprarenal cross-clarnp (minimizing distal aortic hypotension), there should be no added risk of renal dysfunction over that associated with abdominal aneurysm resection alone, with the possible exception of contrastinduced nephropathy. One patient in our series developed renal dysfunction in association with multisystem organ failure after redo suprarenal aneurysm repair. This was most likely related to suprarenal cross-clamping with renal reimplantation, contrastinduced nephropathy, sepsis with systemic hypotension requiring inotropic support, and a severe coagulopathy in the postoperative period. Although thc risk of paraplegia with abdominal aortic replacement is minimal (0% to 0.2%), 23,24 the incidence with descending thoracic replacement averages 4% (range, 0% to 18%; 4% at our institution). 3,6,14,18 With stent-grafts, the opportunity to reimplant intercostal vessels is not available, but the aorta does not need to be clamped, thus avoiding distal hypotension during the operation. One patient in our series was noted to be paraplegic in the early postoperative period. After redo suprarenal aneurysm repair, a 12.5 cm stent-graft was placed from the proximal to distal descending aorta. In this particular patient, there was no evidence of critical intercostal arteries near the aneurysm on preoperative studies, but selective intercostal angiography was not performed. The artery of Adamldewicz is present in 80% of patients, and when present it arises between T9 and T12 in 75%, between L1 and L2 in 10%, and between T5 and T8 in 15%. 6 In chronic thoracic aneurysms, the intercostal arteries usually thrombose within the diseased segment, leaving the spinal cord dependent on proximal and distal collateral vessels. If intercostal arteries are noted angiographically before the procedure, excess distal stent-graft length should be avoided to prevent occlusion. Uncovered stents can also be used as the proximal or distal anchor for patients in whom stent-graft location is sufficiently close to an important intercost~d artery, although this is less desirable. Whether paraplegia in our patient was a result of distal embolization or obliteration of an unidentified intercostal artmt or intraoperative or postoperative hypotension remains unknown. Combined conventional abdominal aortic replacement with descending thoracic aortic stentgraft placement is feasible and can safely be performed in high-risk patients who otherwise may not be considered candidates for open repair. Although long-term results remain unknown, we believe that the early results are encouraging and warrant further investigation and application of this new approach: We are continuing to monitor these patients and perform this procedure as part of an investigational protocol approved by the Institutional Review Board of the Stanford University Medical Center, and an application for an Investigational Device Exception has been submitted to the Food and Drug Administration. The 1-year actuarial survival rate of 92% _+ 8% compares favorably with that of patients who undergo isolated standard descending thoracic repair (85 %) and patients with multifocal aortic disease who undergo replacement of both aneurysms (75%) or only one aneurysm (5 5%).3,6,7,14,16 It is interesting to note that in patients who underwent planned resection of only one aneurysm, the 3-year and 7-year survival rates were 48% and 12%, respectively, compared with 32% and 2% for patients who received no treatment but 64% and 34% in patients who underwent resection of both aneurysms. 7 Thus complete repair of multilevel disease portends the best longterm prognosis and should be the treatment of choice, but their 7-year survival rate of only 34% underscores the poor general medical status of even the best candidates for combined resection. The less-invasive approach described in this re-
9 340 Moon et al. February 1997 port may be associated with fewer early complications and deaths than simultaneous or sequential open thoracic and abdominal repair in high-risk patients, but the long-term efficacy and clinical outcome remains entirely unknown. Long-term studies will be required before this approach can bc adopted in all patients with multifocal aortic disease or in anything other than an experimental protocol. In a young patient who is otherwise healthy, conventional open repair of a concurrent thoracic and abdominal aneurysm, either simultaneous or staged, may provide the best opportunity for long-term success. Elderly patients with coexisting cardiopulmonary disease would most benefit from a less-invasive, but nonetheless complete, repair of this challenging disease. We gratefully acknowledge Phoebe E. Taboada for her help in preparing the manuscript and Kathleen A. Moore, BS, for statistical consultation. REFERENCES 1. Wright IS, Urdaneta E, Wright B. Re-opening the case of the abdominal aortic aneurysm. Circulation 1956;13: Iyce JW, Fairbairn IF, Fdncaid OW, lnergens IL. Aneurysms of the thoracic aorta: a clinical study with special reference to prognosis. Circulation 1964;29: DeBakey ME, McCollum CH, Graham JM. Surgical treatment ofaneurysms of the descending thoracic aorta. J Cardiovasc Surg (Torino) 1978;19: Pressler V, McNamara JJ. Thoracic aortic aneurysm: natural history and treatment. I Thorac Cardiovasc Surg 1980;79: 48% Crawford ES, Walker HSJ, Saleh SA, Normann MA. Graft replacement of aneurysm in descending thoracic aorta: results without bypass or shunting. Surgery 1981 ;89: Farm JI, Miller DC. Descending thoracic aortic aneurysms. In: Bane AE, Geha AS, Hammond GL, Laks H, Nannheim KS, editors. Glenn's thoracic and cardiovascular surgery. 6th ed. Stamford, Conn: Appleton and Lange, 1996: Crawford ES. Aortic aneurysm: a multifocal disease. Arch Surg 1982;117: Crawford ES, Crawford IS. Diseases of the aorta. Baltimore: Williams & Wilkins, 1984: Dake MD, Miller DC, Semba CP, Mitchell RS, Walker PJ, Liddell RP. Transluminal placement of endovascular stentgrafts for the treatment of descending thoracic aortic aneurysms. N Engl J Med 1994;331:172% Mitchell RS, Dake MD, Semba CP, et al. Endovascular stentgraft repair of thoracic aortic aneurysms, l Thorac Cardiovasc Surg 1996;111: Fann JI, Mitchell RS, Dake MD, Miller DC. The results of endovascular stent-grafting in patients with descending thoracic aortic aneurysm. In: Yao JST, Pearce WH, editors. Vascular surgery: twenty years of progress. Norwalk, Conn.: Appleton and Lange, 1996 (in press). 12. Moon MR, Dake MD, Pelc LR, et al. Intravascular stenting of acute experimental type B dissections. J Surg Res 1993;54: Fann ~I, Dake MD, Semba CP, Liddell I/2, Pfeffer TA, Miller DC. Endovascular stent-grafting after arch aneurysm repair using the "elephant trunk." Ann Thorac Surg 1995;60: Moreno-Cabral CE, Miller DC, Mitchell RS, et al. Degenerative and atherosclerotic aneurysms of the thoracic aorta. J Thorac Cardiovasc Surg 1984;88: Livesay l~, Cooley DA, Ventemiglia RA, et al. Surgical experience in descending thoracic aneurysmectomy with and without adjuncts to avoid ischemia. Ann Thorac Surg 1985;39: Hamerlijnck RP, Rutsaert RR, DeGeest R, de la Rivi~re AB, Defanw Jl, Vermeulen FE. Surgical correction of descending thoracic aortic aneurysms under simple aortic cross-clamping. J Vase Surg 1989;9: Verdant A. Descending thoracic aortic aneurysms: surgical treatment with the Gott shunt. Can J Surg 1992;35: Borst HG, Jurmann M, Buhner B, Laas J. Risk of replacement of descending aorta with a standardized left heart bypass technique. J Thorac Cardiovasc Surg 1994;107: Mitchell MB, Rutherford RB, Krupski WC. Infrarenal aortic aneurysms. In: Rutherford RB, editor. Vascular surgery. 4th ed. Philadelphia: W.B. Saunders Company, 1995: Whittemore AD, Clowes AW, Hechtman HB, Mannick JA. Aortic aneurysm repair: reduced operative mortality associated with maintenance of optimal cardiac performance. Ann Surg 1980;192: Johnston KW, ScoNe TK. Multicenter prospective study of nonruptured abdominal aortic aneurysms. I: Population and operative management. J Vase Surg 1988;7: AbuRahma AF, Robinson PA, Boland JP, et al. Elective resection of 332 abdominal aortic aneurysms in a southern West Virginia community during a recent five-year period. Surgery 1991; 109: Johnston KW. Multicenter prospective study of nonruptured abdominal aortic aneurysms. Part II: variables predicting morbidity and mortality. J Vase Surg 1989;9: Diehl JT, Cali RF, Hertzer NR, Beven EG. Complications of abdominal aortic reconstruction: analysis of perioperative risk factors in 557 patients. Ann Surg 1983;197: Submitted lune 28, 1996; accepted Nov. 4, 1996.
Acute dissections of the descending thoracic aorta (Debakey
 Endovascular Treatment of Acute Descending Thoracic Aortic Dissections Nimesh D. Desai, MD, PhD, and Joseph E. Bavaria, MD Acute dissections of the descending thoracic aorta (Debakey type III or Stanford
Endovascular Treatment of Acute Descending Thoracic Aortic Dissections Nimesh D. Desai, MD, PhD, and Joseph E. Bavaria, MD Acute dissections of the descending thoracic aorta (Debakey type III or Stanford
Thoracic aortic aneurysms are life threatening and
 Thoracic Aortic Aneurysms: Treatment With Endovascular Self-Expandable Stent Grafts Martin Grabenwöger, MD, Doris Hutschala, MD, Marek P. Ehrlich, MD, Fabiola Cartes-Zumelzu, MD, Siegfried Thurnher, MD,
Thoracic Aortic Aneurysms: Treatment With Endovascular Self-Expandable Stent Grafts Martin Grabenwöger, MD, Doris Hutschala, MD, Marek P. Ehrlich, MD, Fabiola Cartes-Zumelzu, MD, Siegfried Thurnher, MD,
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant INDICATION: Abdominal aortic aneurysm. INTERVENTIONAL RADIOLOGIST:
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant INDICATION: Abdominal aortic aneurysm. INTERVENTIONAL RADIOLOGIST:
Open fenestration for complicated acute aortic B dissection
 Art of Operative Techniques Open fenestration for complicated acute aortic B dissection Santi Trimarchi 1, Sara Segreti 1, Viviana Grassi 1, Chiara Lomazzi 1, Marta Cova 1, Gabriele Piffaretti 2, Vincenzo
Art of Operative Techniques Open fenestration for complicated acute aortic B dissection Santi Trimarchi 1, Sara Segreti 1, Viviana Grassi 1, Chiara Lomazzi 1, Marta Cova 1, Gabriele Piffaretti 2, Vincenzo
Management of Acute Aortic Syndromes. M. Grabenwoger, MD Dept. of Cardiovascular Surgery Hospital Hietzing, Vienna, Austria
 Management of Acute Aortic Syndromes M. Grabenwoger, MD Dept. of Cardiovascular Surgery Hospital Hietzing, Vienna, Austria I have nothing to disclose. Acute Aortic Syndromes Acute Aortic Dissection Type
Management of Acute Aortic Syndromes M. Grabenwoger, MD Dept. of Cardiovascular Surgery Hospital Hietzing, Vienna, Austria I have nothing to disclose. Acute Aortic Syndromes Acute Aortic Dissection Type
Abdominal Aortic Aneurysms. A Surgeons Perspective Dr. Derek D. Muehrcke
 Abdominal Aortic Aneurysms A Surgeons Perspective Dr. Derek D. Muehrcke Aneurysm Definition The abnormal enlargement or bulging of an artery caused by an injury or weakness in the blood vessel wall A localized
Abdominal Aortic Aneurysms A Surgeons Perspective Dr. Derek D. Muehrcke Aneurysm Definition The abnormal enlargement or bulging of an artery caused by an injury or weakness in the blood vessel wall A localized
Abdominal and thoracic aneurysm repair
 Abdominal and thoracic aneurysm repair William A. Gray MD Director, Endovascular Intervention Cardiovascular Research Foundation Columbia University Medical Center Abdominal Aortic Aneurysm Endografts
Abdominal and thoracic aneurysm repair William A. Gray MD Director, Endovascular Intervention Cardiovascular Research Foundation Columbia University Medical Center Abdominal Aortic Aneurysm Endografts
Combined Endovascular and Surgical Repair of Thoracoabdominal Aortic Pathology: Hybrid TEVAR
 Combined Endovascular and Surgical Repair of Thoracoabdominal Aortic Pathology: Hybrid TEVAR William J. Quinones-Baldrich MD Professor of Surgery Director UCLA Aortic Center UCLA Medical Center Los Angeles,
Combined Endovascular and Surgical Repair of Thoracoabdominal Aortic Pathology: Hybrid TEVAR William J. Quinones-Baldrich MD Professor of Surgery Director UCLA Aortic Center UCLA Medical Center Los Angeles,
Percutaneous Approaches to Aortic Disease in 2018
 Percutaneous Approaches to Aortic Disease in 2018 Wendy Tsang, MD, SM Assistant Professor, University of Toronto Toronto General Hospital, University Health Network Case 78 year old F Lower CP and upper
Percutaneous Approaches to Aortic Disease in 2018 Wendy Tsang, MD, SM Assistant Professor, University of Toronto Toronto General Hospital, University Health Network Case 78 year old F Lower CP and upper
Challenges. 1. Sizing. 2. Proximal landing zone 3. Distal landing zone 4. Access vessels 5. Spinal cord ischemia 6. Endoleak
 Disclosure I have the following potential conflicts of interest to report: Consulting: Medtronic, Gore Employment in industry Stockholder of a healthcare company Owner of a healthcare company Other(s)
Disclosure I have the following potential conflicts of interest to report: Consulting: Medtronic, Gore Employment in industry Stockholder of a healthcare company Owner of a healthcare company Other(s)
I-Hui Wu, M.D. Ph.D. Clinical Assistant Professor Cardiovascular Surgical Department National Taiwan University Hospital
 Comparisons of Aortic Remodeling and Outcomes after Endovascular Repair of Acute and Chronic Complicated Type B Aortic Dissections I-Hui Wu, M.D. Ph.D. Clinical Assistant Professor Cardiovascular Surgical
Comparisons of Aortic Remodeling and Outcomes after Endovascular Repair of Acute and Chronic Complicated Type B Aortic Dissections I-Hui Wu, M.D. Ph.D. Clinical Assistant Professor Cardiovascular Surgical
Thoracic Endovascular Aortic Repair (TEVAR) Indications and Basic Procedure
 Thoracic Endovascular Aortic Repair (TEVAR) Indications and Basic Procedure Tilo Kölbel, MD, PhD University Heart Center Hamburg University Hospital Eppendorf Disclosure Speaker name: Tilo Kölbel, MD I
Thoracic Endovascular Aortic Repair (TEVAR) Indications and Basic Procedure Tilo Kölbel, MD, PhD University Heart Center Hamburg University Hospital Eppendorf Disclosure Speaker name: Tilo Kölbel, MD I
Neurological Complications of TEVAR. Frank J Criado, MD. Union Memorial-MedStar Health Baltimore, MD USA
 ISES Online Neurological Complications of Frank J Criado, MD TEVAR Union Memorial-MedStar Health Baltimore, MD USA frank.criado@medstar.net Paraplegia Incidence is 0-4% after surgical Rx of TAAs confined
ISES Online Neurological Complications of Frank J Criado, MD TEVAR Union Memorial-MedStar Health Baltimore, MD USA frank.criado@medstar.net Paraplegia Incidence is 0-4% after surgical Rx of TAAs confined
Descending aorta replacement through median sternotomy
 Descending aorta replacement through median sternotomy Mitrev Z, Anguseva T, Belostotckij V, Hristov N. Special hospital for surgery Filip Vtori Skopje - Makedonija June, 2010 Cardiosurgery - Skopje 1
Descending aorta replacement through median sternotomy Mitrev Z, Anguseva T, Belostotckij V, Hristov N. Special hospital for surgery Filip Vtori Skopje - Makedonija June, 2010 Cardiosurgery - Skopje 1
Stent-Graft Repair of Penetrating Atherosclerotic Ulcers in the Descending Thoracic Aorta: Mid-Term Results
 Stent-Graft Repair of Penetrating Atherosclerotic Ulcers in the Descending Thoracic Aorta: Mid-Term Results Philippe Demers, MD, MS, D. Craig Miller, MD, R. Scott Mitchell, MD, Stephen T. Kee, MD, Lynn
Stent-Graft Repair of Penetrating Atherosclerotic Ulcers in the Descending Thoracic Aorta: Mid-Term Results Philippe Demers, MD, MS, D. Craig Miller, MD, R. Scott Mitchell, MD, Stephen T. Kee, MD, Lynn
Treatment of Thoracoabdominal Aneurysms Is there a need for custom-made devices?
 : FETURED TECHNOLOGY: JOTEC E-XTR DESIGN ENGINEERING Treatment of Thoracoabdominal neurysms Is there a need for custom-made devices? INTERVIEW ND CSE PRESENTTIONS WITH DNIEL RNZN, MD, ND NDREJ SCHMIDT,
: FETURED TECHNOLOGY: JOTEC E-XTR DESIGN ENGINEERING Treatment of Thoracoabdominal neurysms Is there a need for custom-made devices? INTERVIEW ND CSE PRESENTTIONS WITH DNIEL RNZN, MD, ND NDREJ SCHMIDT,
Subject: Endovascular Stent Grafts for Disorders of the Thoracic Aorta
 02-33000-29 Original Effective Date: 04/15/03 Reviewed: 07/26/18 Revised: 08/15/18 Subject: Endovascular Stent Grafts for Disorders of the Thoracic Aorta THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION,
02-33000-29 Original Effective Date: 04/15/03 Reviewed: 07/26/18 Revised: 08/15/18 Subject: Endovascular Stent Grafts for Disorders of the Thoracic Aorta THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION,
Repair of type IV thoracoabdominal aneurysm with a combined endovascular and surgical approach
 Repair of type IV thoracoabdominal aneurysm with a combined endovascular and surgical approach William J. Quiñones-Baldrich, MD, Thomas F. Panetta, MD, Candace L. Vescera, RN, and Vikram S. Kashyap, MD,
Repair of type IV thoracoabdominal aneurysm with a combined endovascular and surgical approach William J. Quiñones-Baldrich, MD, Thomas F. Panetta, MD, Candace L. Vescera, RN, and Vikram S. Kashyap, MD,
Acute Type B dissection. Closure of the infra diaphragmatic tear: how and when?
 Acute Type B dissection. Closure of the infra diaphragmatic tear: how and when? Prof. Olgierd Rowiński II Department of Clinical Radiology Medical University of Warsaw Disclosure Speaker name: Olgierd
Acute Type B dissection. Closure of the infra diaphragmatic tear: how and when? Prof. Olgierd Rowiński II Department of Clinical Radiology Medical University of Warsaw Disclosure Speaker name: Olgierd
Bifurcated system Proximal suprarenal stent Modular (aortic main body and two iliac legs) Full thickness woven polyester graft material Fully
 Physician Training Bifurcated system Proximal suprarenal stent Modular (aortic main body and two iliac legs) Full thickness woven polyester graft material Fully supported by self-expanding z-stents H&L-B
Physician Training Bifurcated system Proximal suprarenal stent Modular (aortic main body and two iliac legs) Full thickness woven polyester graft material Fully supported by self-expanding z-stents H&L-B
I SECTION I. Thoracic aortic aneurysms
 I SECTION I Thoracic aortic aneurysms 9 10 CASE 1 Endovascular repair of descending thoracic aortic aneurysms using the Gore TAG stent graft Introduction A descending thoracic aneurysm (DTA) is defined
I SECTION I Thoracic aortic aneurysms 9 10 CASE 1 Endovascular repair of descending thoracic aortic aneurysms using the Gore TAG stent graft Introduction A descending thoracic aneurysm (DTA) is defined
AORTIC DISSECTION. DISSECTING ANEURYSMS OF THE AORTA or CLASSIFICATION
 DISSECTING ANEURYSMS OF THE AORTA or AORTIC DISSECTION CLASSIFICATION DeBakey classified aortic dissections into types I, II, and III :- Type I dissection the tear site originates in the ascending aorta,
DISSECTING ANEURYSMS OF THE AORTA or AORTIC DISSECTION CLASSIFICATION DeBakey classified aortic dissections into types I, II, and III :- Type I dissection the tear site originates in the ascending aorta,
Increased Flexibility of AneuRx Stent-Graft Reduces Need for Secondary Intervention Following Endovascular Aneurysm Repair
 583 Increased Flexibility of AneuRx Stent-Graft Reduces Need for Secondary Intervention Following Endovascular Aneurysm Repair Frank R. Arko, MD; W. Anthony Lee, MD; Bradley B. Hill, MD; Paul Cipriano,
583 Increased Flexibility of AneuRx Stent-Graft Reduces Need for Secondary Intervention Following Endovascular Aneurysm Repair Frank R. Arko, MD; W. Anthony Lee, MD; Bradley B. Hill, MD; Paul Cipriano,
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
B myonephropathic metabolic syndrome MNMS 33 CT DeBakey IIIb MNMS
 13 603 607 2004 B B myonephropathic metabolic syndrome MNMS33 CT DeBakey IIIb MNMS 20 A MNMSMNMS 13 603 607 2004 MNMS B malperfusion myonephropathic metabolic syndrome MNMS MNMS Haimovici 1 3 MNMS B MNMS
13 603 607 2004 B B myonephropathic metabolic syndrome MNMS33 CT DeBakey IIIb MNMS 20 A MNMSMNMS 13 603 607 2004 MNMS B malperfusion myonephropathic metabolic syndrome MNMS MNMS Haimovici 1 3 MNMS B MNMS
Malperfusion Syndromes Type B Aortic Dissection with Malperfusion
 Malperfusion Syndromes Type B Aortic Dissection with Malperfusion Jade S. Hiramoto, MD, MAS April 27, 2012 Associated with early mortality Occurs when there is end organ ischemia secondary to aortic branch
Malperfusion Syndromes Type B Aortic Dissection with Malperfusion Jade S. Hiramoto, MD, MAS April 27, 2012 Associated with early mortality Occurs when there is end organ ischemia secondary to aortic branch
Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection
 Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection M. Grabenwoger Dept. of Cardiovascular Surgery Hospital Hietzing Vienna, Austria Disclosure Statement Consultant of Jotec, Hechingen,
Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection M. Grabenwoger Dept. of Cardiovascular Surgery Hospital Hietzing Vienna, Austria Disclosure Statement Consultant of Jotec, Hechingen,
Chungbuk Regional Cardiovascular Center, Division of Cardiology, Departments of Internal Medicine, Chungbuk National University Hospital Sangmin Kim
 Endovascular Procedures for Isolated Common Iliac and Internal Iliac Aneurysm Chungbuk Regional Cardiovascular Center, Division of Cardiology, Departments of Internal Medicine, Chungbuk National University
Endovascular Procedures for Isolated Common Iliac and Internal Iliac Aneurysm Chungbuk Regional Cardiovascular Center, Division of Cardiology, Departments of Internal Medicine, Chungbuk National University
Talent Abdominal Stent Graft
 Talent Abdominal with THE Xcelerant Hydro Delivery System Expanding the Indications for EVAR Treat More Patients Short Necks The Talent Abdominal is the only FDA-approved device for proximal aortic neck
Talent Abdominal with THE Xcelerant Hydro Delivery System Expanding the Indications for EVAR Treat More Patients Short Necks The Talent Abdominal is the only FDA-approved device for proximal aortic neck
Development of a Branched LSA Endograft & Ascending Aorta Endograft
 Development of a Branched LSA Endograft & Ascending Aorta Endograft Frank R. Arko III, MD Sanger Heart & Vascular Institute Carolinas Medical Center Charlotte, North Carolina, USA Disclosures Proximal
Development of a Branched LSA Endograft & Ascending Aorta Endograft Frank R. Arko III, MD Sanger Heart & Vascular Institute Carolinas Medical Center Charlotte, North Carolina, USA Disclosures Proximal
Hybrid Repair of a Complex Thoracoabdominal Aortic Aneurysm
 Hybrid Repair of a Complex Thoracoabdominal Aortic Aneurysm Virendra I. Patel MD MPH Assistant Professor of Surgery Massachusetts General Hospital Division of Vascular and Endovascular Surgery Disclosure
Hybrid Repair of a Complex Thoracoabdominal Aortic Aneurysm Virendra I. Patel MD MPH Assistant Professor of Surgery Massachusetts General Hospital Division of Vascular and Endovascular Surgery Disclosure
AORTIC DISSECTIONS Current Management. TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida
 AORTIC DISSECTIONS Current Management TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida DISCLOSURES Terumo Medtronic Cook Edwards Cryolife AORTIC
AORTIC DISSECTIONS Current Management TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida DISCLOSURES Terumo Medtronic Cook Edwards Cryolife AORTIC
Dissection of descending aorta treated by stent-graft implantation in a patient with Marfan syndrome
 Case Report 1 Dissection of descending aorta treated by stent-graft implantation in a patient with Marfan syndrome Marat. ripov, Ildar Z. bdyldaev, Semen D. Chevgun, ektur S. Daniyarov, Dinara. Toktosunova,
Case Report 1 Dissection of descending aorta treated by stent-graft implantation in a patient with Marfan syndrome Marat. ripov, Ildar Z. bdyldaev, Semen D. Chevgun, ektur S. Daniyarov, Dinara. Toktosunova,
FEVAR FIFTEEN YEARS OF EFFICIENCY E.DUCASSE MD PHD FEBVS CHU DE BORDEAUX
 FEVAR FIFTEEN YEARS OF EFFICIENCY E.DUCASSE MD PHD FEBVS CHU DE BORDEAUX 2018 A BIT OF HISTORY First use of F-EVAR : 1990s Park et al. J Vasc Interv Radiol. 1996;7:819-823. Faruqi et al. J Endovasc Surg.
FEVAR FIFTEEN YEARS OF EFFICIENCY E.DUCASSE MD PHD FEBVS CHU DE BORDEAUX 2018 A BIT OF HISTORY First use of F-EVAR : 1990s Park et al. J Vasc Interv Radiol. 1996;7:819-823. Faruqi et al. J Endovasc Surg.
An Overview of Post-EVAR Endoleaks: Imaging Findings and Management. Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC
 An Overview of Post-EVAR Endoleaks: Imaging Findings and Management Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC Disclosure Slide Mark O. Baerlocher: Current: Consultant for Boston
An Overview of Post-EVAR Endoleaks: Imaging Findings and Management Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC Disclosure Slide Mark O. Baerlocher: Current: Consultant for Boston
Nellix Endovascular System: Clinical Outcomes and Device Overview
 Nellix Endovascular System: Clinical Outcomes and Device Overview Jeffrey P. Carpenter, MD Professor and Chief, Department of Surgery CAUTION: Investigational device. This product is under clinical investigation
Nellix Endovascular System: Clinical Outcomes and Device Overview Jeffrey P. Carpenter, MD Professor and Chief, Department of Surgery CAUTION: Investigational device. This product is under clinical investigation
History of the Powerlink System Design and Clinical Results. Edward B. Diethrich Arizona Heart Hospital Phoenix, AZ
 History of the Powerlink System Design and Clinical Results Edward B. Diethrich Arizona Heart Hospital Phoenix, AZ Powerlink System: Unibody-Bifurcated Design Long Main Body Low-Porosity Proprietary eptfe
History of the Powerlink System Design and Clinical Results Edward B. Diethrich Arizona Heart Hospital Phoenix, AZ Powerlink System: Unibody-Bifurcated Design Long Main Body Low-Porosity Proprietary eptfe
Fate of Aneurysms of the Distal Arch and Proximal Descending Thoracic Aorta After Transaortic Endovascular Stent-Grafting
 CARDIOVASCULAR Fate of Aneurysms of the Distal Arch and Proximal Descending Thoracic Aorta After Transaortic Endovascular Stent-Grafting Taijiro Sueda, MD, Kazumasa Orihashi, MD, Kenji Okada, MD, Yuji
CARDIOVASCULAR Fate of Aneurysms of the Distal Arch and Proximal Descending Thoracic Aorta After Transaortic Endovascular Stent-Grafting Taijiro Sueda, MD, Kazumasa Orihashi, MD, Kenji Okada, MD, Yuji
No Disclosure. Aortic Dissection in Japan. This. The Challenge of Acute and Chronic Type B Aortic Dissections with Endovascular Aortic Repair
 No Disclosure The Challenge of Acute and Chronic Type B Aortic Dissections with Endovascular Aortic Repair Toru Kuratani Department of Cardiovascular Surgery Osaka University Graduate School of Medicine,
No Disclosure The Challenge of Acute and Chronic Type B Aortic Dissections with Endovascular Aortic Repair Toru Kuratani Department of Cardiovascular Surgery Osaka University Graduate School of Medicine,
EVAR and TEVAR: Extending Their Use for Rupture and Traumatic Injury. Conflict of Interest. Hypotensive shock 5/5/2014. none
 EVAR and TEVAR: Extending Their Use for Rupture and Traumatic Injury Bruce H. Gray, DO MSVM FSCAI Professor of Surgery/Vascular Medicine USC SOM-Greenville Greenville, South Carolina none Conflict of Interest
EVAR and TEVAR: Extending Their Use for Rupture and Traumatic Injury Bruce H. Gray, DO MSVM FSCAI Professor of Surgery/Vascular Medicine USC SOM-Greenville Greenville, South Carolina none Conflict of Interest
Primary to non-coronary IVUS
 codes 2018 2018 codes Primary to non-coronary IVUS Page 2 All coding, coverage, billing and payment information provided herein by Philips is gathered from third-party sources and is subject to change.
codes 2018 2018 codes Primary to non-coronary IVUS Page 2 All coding, coverage, billing and payment information provided herein by Philips is gathered from third-party sources and is subject to change.
3 : 37. Kirit Patel, USA CLASSIFICATION DIAGNOSIS
 3 : 37 Management of Aortic Aneurysms Clinical features and diagnosis of thoracic aortic aneurysm An aneurysm is currently defined as a localized dilatation of the aorta, 50 percent over the normal diameter,
3 : 37 Management of Aortic Aneurysms Clinical features and diagnosis of thoracic aortic aneurysm An aneurysm is currently defined as a localized dilatation of the aorta, 50 percent over the normal diameter,
account for 10% to 15% of all traffic fatalities majority fatal at the scene 50% who survive the initial injury die in the first 24 hours 90% die
 account for 10% to 15% of all traffic fatalities majority fatal at the scene 50% who survive the initial injury die in the first 24 hours 90% die within the first month if aorta not repaired 30-90% overall
account for 10% to 15% of all traffic fatalities majority fatal at the scene 50% who survive the initial injury die in the first 24 hours 90% die within the first month if aorta not repaired 30-90% overall
DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service
 M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
Deliberate Renal Ischemia
 Deliberate Renal Ischemia A Valuable and Safe Adjunct During Operations upon the Abdominal Aorta Robert K. Brawley, M.D., R. Darryl Fisher, M.D., Tom R. DeMeester, M.D., and Ronald C. Elkins, M.D. ABSTRACT
Deliberate Renal Ischemia A Valuable and Safe Adjunct During Operations upon the Abdominal Aorta Robert K. Brawley, M.D., R. Darryl Fisher, M.D., Tom R. DeMeester, M.D., and Ronald C. Elkins, M.D. ABSTRACT
Modified candy-plug technique for chronic type B aortic dissection with aneurysmal dilatation: a case report
 Kotani et al. Journal of Cardiothoracic Surgery (2017) 12:77 DOI 10.1186/s13019-017-0647-8 CASE REPORT Modified candy-plug technique for chronic type B aortic dissection with aneurysmal dilatation: a case
Kotani et al. Journal of Cardiothoracic Surgery (2017) 12:77 DOI 10.1186/s13019-017-0647-8 CASE REPORT Modified candy-plug technique for chronic type B aortic dissection with aneurysmal dilatation: a case
Aortic stents, types, selection, tricks in deployment.
 Aortic stents, types, selection, tricks in deployment. Hamdy Soliman.M.D,FSCAI Consultant of Cardiology&Head of Endovascular Unit National Heart Institute Endovascular Treatment of Thoracic Aortic Aneurysms
Aortic stents, types, selection, tricks in deployment. Hamdy Soliman.M.D,FSCAI Consultant of Cardiology&Head of Endovascular Unit National Heart Institute Endovascular Treatment of Thoracic Aortic Aneurysms
Endovascular Management of Thoracic Aortic Pathology Stéphan Haulon, J Sobocinski, B Maurel, T Martin-Gonzalez, R Spear, A Hertault, R Azzaoui
 Endovascular Management of Thoracic Aortic Pathology Stéphan Haulon, J Sobocinski, B Maurel, T Martin-Gonzalez, R Spear, A Hertault, R Azzaoui Aortic Center, Lille University Hospital, France Disclosures
Endovascular Management of Thoracic Aortic Pathology Stéphan Haulon, J Sobocinski, B Maurel, T Martin-Gonzalez, R Spear, A Hertault, R Azzaoui Aortic Center, Lille University Hospital, France Disclosures
Experience of endovascular procedures on abdominal and thoracic aorta in CA region
 Experience of endovascular procedures on abdominal and thoracic aorta in CA region May 14-15, 2015, Dubai Dr. Viktor Zemlyanskiy National Research Center of Emergency Care Astana, Kazakhstan Region Characteristics
Experience of endovascular procedures on abdominal and thoracic aorta in CA region May 14-15, 2015, Dubai Dr. Viktor Zemlyanskiy National Research Center of Emergency Care Astana, Kazakhstan Region Characteristics
Endovascular Repair o Abdominal. Aortic Aneurysms. Cesar E. Mendoza, M.D. Jackson Memorial Hospital Miami, Florida
 Endovascular Repair o Abdominal Aortic Aneurysms Cesar E. Mendoza, M.D. Jackson Memorial Hospital Miami, Florida Disclosure Nothing to disclose. 2 Mr. X AAA Mr. X. Is a 70 year old male who presented to
Endovascular Repair o Abdominal Aortic Aneurysms Cesar E. Mendoza, M.D. Jackson Memorial Hospital Miami, Florida Disclosure Nothing to disclose. 2 Mr. X AAA Mr. X. Is a 70 year old male who presented to
Zenith Renu AAA Converter Graft. Device Description Planning and Sizing Deployment Sequence Patient Follow-Up
 Zenith Renu AAA Converter Graft Device Description Planning and Sizing Deployment Sequence Patient Follow-Up Device description: Device indications The Zenith Renu AAA Converter Graft with Z-Trak Introduction
Zenith Renu AAA Converter Graft Device Description Planning and Sizing Deployment Sequence Patient Follow-Up Device description: Device indications The Zenith Renu AAA Converter Graft with Z-Trak Introduction
Renal insufficiency after infrarenal abdominal aortic aneurysm reconstruction: An analysis of this risk factor in 45 patients
 Original Research Medical Journal of the Islamic Republic of Iran.Vol. 21, No.1, May, 2007. pp. 38-42 Renal insufficiency after infrarenal abdominal aortic aneurysm reconstruction: An analysis of this
Original Research Medical Journal of the Islamic Republic of Iran.Vol. 21, No.1, May, 2007. pp. 38-42 Renal insufficiency after infrarenal abdominal aortic aneurysm reconstruction: An analysis of this
EVAR replaced standard repair in most cases. Why?
 EVAR replaced standard repair in most cases. Why? Initial major steps in endograft evolution Papazoglou O. Konstantinos M.D. The story of a major breakthrough in vascular surgery 1991 Parodi introduces
EVAR replaced standard repair in most cases. Why? Initial major steps in endograft evolution Papazoglou O. Konstantinos M.D. The story of a major breakthrough in vascular surgery 1991 Parodi introduces
Cook Medical. Zenith Flex AAA Endovascular Graft with Z-Trak Introduction System Physician Training
 Cook Medical Zenith Flex AAA Endovascular Graft with Z-Trak Introduction System Physician Training Bifurcated system Proximal suprarenal stent Modular (aortic main body and two iliac legs) Full-thickness,
Cook Medical Zenith Flex AAA Endovascular Graft with Z-Trak Introduction System Physician Training Bifurcated system Proximal suprarenal stent Modular (aortic main body and two iliac legs) Full-thickness,
Antegrade Thoracic Stent Grafting during Repair of Acute Debakey I Dissection: Promotes Distal Aortic Remodeling and Reduces Late Open Re-operation
 Antegrade Thoracic Stent Grafting during Repair of Acute Debakey I Dissection: Promotes Distal Aortic Remodeling and Reduces Late Open Re-operation Vallabhajosyula, P: Szeto, W; Desai, N; Pulsipher, A;
Antegrade Thoracic Stent Grafting during Repair of Acute Debakey I Dissection: Promotes Distal Aortic Remodeling and Reduces Late Open Re-operation Vallabhajosyula, P: Szeto, W; Desai, N; Pulsipher, A;
Robert F. Cuff, MD FACS SHMG Vascular Surgery
 Robert F. Cuff, MD FACS SHMG Vascular Surgery Objectives To become familiar with the commercially available fenestrated EVAR graft Discuss techniques to increase success Review available data to determine
Robert F. Cuff, MD FACS SHMG Vascular Surgery Objectives To become familiar with the commercially available fenestrated EVAR graft Discuss techniques to increase success Review available data to determine
How to manage the left subclavian and left vertebral artery during TEVAR
 How to manage the left subclavian and left vertebral artery during TEVAR Jürg Schmidli Chief of Vascular Surgery Inselspital Hamburg 2017 Dept Cardiovascular Surgery, Bern, Switzerland Disclosure No Disclosures
How to manage the left subclavian and left vertebral artery during TEVAR Jürg Schmidli Chief of Vascular Surgery Inselspital Hamburg 2017 Dept Cardiovascular Surgery, Bern, Switzerland Disclosure No Disclosures
Free Esophageal Perforation Following Hybrid Visceral Debranching and Distal Endograft Extension to Repair a Ruptured Thoracoabdominal Aortic
 Free Esophageal Perforation Following Hybrid Visceral Debranching and Distal Endograft Extension to Repair a Ruptured Thoracoabdominal Aortic Aneurysm History A 56-year-old gentleman, who had been referred
Free Esophageal Perforation Following Hybrid Visceral Debranching and Distal Endograft Extension to Repair a Ruptured Thoracoabdominal Aortic Aneurysm History A 56-year-old gentleman, who had been referred
Transluminal Stent-graft Placement endovascular surgery
 13 545 551 2004 Transluminal Stent-graft Placement endovascular surgery 1 1 2 2 1 1 1 3 2 1 1996 11Transluminal Stent-graft Placement TSGP 6 82 TSGP T42 O TSGP Th10 T 26 O 5 T 3 O 23T 6 O 2 T 47 A15B17B15O
13 545 551 2004 Transluminal Stent-graft Placement endovascular surgery 1 1 2 2 1 1 1 3 2 1 1996 11Transluminal Stent-graft Placement TSGP 6 82 TSGP T42 O TSGP Th10 T 26 O 5 T 3 O 23T 6 O 2 T 47 A15B17B15O
Surgery for Acquired Cardiovascular Disease
 Resch et al Changes in aneurysm morphology and stent-graft configuration after endovascular repair of aneurysms of the descending thoracic aorta Timothy Resch, MD, PhD a Bansi Koul, MD, PhD d Nuno V. Dias,
Resch et al Changes in aneurysm morphology and stent-graft configuration after endovascular repair of aneurysms of the descending thoracic aorta Timothy Resch, MD, PhD a Bansi Koul, MD, PhD d Nuno V. Dias,
The Management and Treatment of Ruptured Abdominal Aortic Aneurysm (RAAA)
 The Management and Treatment of Ruptured Abdominal Aortic Aneurysm (RAAA) Disclosure Speaker name: Ren Wei, Li Zhui, Li Fenghe, Zhao Yu Department of Vascular Surgery, The First Affiliated Hospital of
The Management and Treatment of Ruptured Abdominal Aortic Aneurysm (RAAA) Disclosure Speaker name: Ren Wei, Li Zhui, Li Fenghe, Zhao Yu Department of Vascular Surgery, The First Affiliated Hospital of
The SPIDER-Graft for Thoracoabdominal Aortic Repair a feasability study in pigs
 The SPIDER-Graft for Thoracoabdominal Aortic Repair a feasability study in pigs Wipper S, Kölbel T, Manzoni D, Duprée A, Sandhu H, Nelis V, Debus ES University Heart Center Hamburg University Heart Center
The SPIDER-Graft for Thoracoabdominal Aortic Repair a feasability study in pigs Wipper S, Kölbel T, Manzoni D, Duprée A, Sandhu H, Nelis V, Debus ES University Heart Center Hamburg University Heart Center
6. Endovascular aneurysm repair
 Introduction The standard treatment for aortic aneurysm, open repair, involves a large abdominal incision and cross-clamping of the aorta. In recent years, a minimally invasive technique, endovascular
Introduction The standard treatment for aortic aneurysm, open repair, involves a large abdominal incision and cross-clamping of the aorta. In recent years, a minimally invasive technique, endovascular
ABERRANT RIGHT SUBCLAVIAN ARTERY AND CALCIFIED ANEURYSM OF. Jose Rubio-Alvarez, Juan Sierra-Quiroga, Belen Adrio Nazar and Javier Garcia Carro.
 ABERRANT RIGHT SUBCLAVIAN ARTERY AND CALCIFIED ANEURYSM OF KOMMERELL S DIVERTICULUM : AN ALTERNATIVE APPROACH. Jose Rubio-Alvarez, Juan Sierra-Quiroga, Belen Adrio Nazar and Javier Garcia Carro. Department
ABERRANT RIGHT SUBCLAVIAN ARTERY AND CALCIFIED ANEURYSM OF KOMMERELL S DIVERTICULUM : AN ALTERNATIVE APPROACH. Jose Rubio-Alvarez, Juan Sierra-Quiroga, Belen Adrio Nazar and Javier Garcia Carro. Department
State of Art Hybrid Approach
 State of Art Hybrid Approach for Complex Aorta Diseases Won Ho Kim, MD Division of Cardiology, Eulji University Hospital Eulji University School of Medicine, Daejeon, Korea Introduction.Hybrid procedure
State of Art Hybrid Approach for Complex Aorta Diseases Won Ho Kim, MD Division of Cardiology, Eulji University Hospital Eulji University School of Medicine, Daejeon, Korea Introduction.Hybrid procedure
The Petticoat Technique Managing Type B Dissection with both Early and Long Term Considerations
 The Petticoat Technique Managing Type B Dissection with both Early and Long Term Considerations Joseph V. Lombardi, MD Professor & Chief, Division of Vascular & Endovascular Surgery Department of Surgery,
The Petticoat Technique Managing Type B Dissection with both Early and Long Term Considerations Joseph V. Lombardi, MD Professor & Chief, Division of Vascular & Endovascular Surgery Department of Surgery,
The morbidity and mortality rates associated with the. Outcome of Surgical Treatment in Patients With Acute Type B Aortic Dissection
 Outcome of Surgical Treatment in Patients With Acute Type B Aortic Dissection Tomoki Shimokawa, MD, Kazutaka Horiuchi, MD, Naomi Ozawa, MD, Kenu Fumimoto, MD, Susumu Manabe, MD, Tetsuya Tobaru, MD, and
Outcome of Surgical Treatment in Patients With Acute Type B Aortic Dissection Tomoki Shimokawa, MD, Kazutaka Horiuchi, MD, Naomi Ozawa, MD, Kenu Fumimoto, MD, Susumu Manabe, MD, Tetsuya Tobaru, MD, and
Annual Clinical Update
 Zenith TX2 TAA Endovascular Graft (P716) Annual Clinical Update (216) Page i Annual Clinical Update Abstract Cook is pleased to provide you with this clinical update on the Zenith TX2 TAA Endovascular
Zenith TX2 TAA Endovascular Graft (P716) Annual Clinical Update (216) Page i Annual Clinical Update Abstract Cook is pleased to provide you with this clinical update on the Zenith TX2 TAA Endovascular
Thoracoabdominal aortic aneurysms by definition traverse
 Thoracoabdominal Aortic Aneurysm Repair: Open Technique Joseph Huh, MD, Scott A. LeMaire, MD, Scott A. Weldon, MA, CMI, and Joseph S. Coselli, MD Thoracoabdominal aortic aneurysms by definition traverse
Thoracoabdominal Aortic Aneurysm Repair: Open Technique Joseph Huh, MD, Scott A. LeMaire, MD, Scott A. Weldon, MA, CMI, and Joseph S. Coselli, MD Thoracoabdominal aortic aneurysms by definition traverse
Management of Endoleaks
 Management of Endoleaks Sarah Ikponmwosa, MD Brooklyn VA 6/20/08 Questions Advantages of endovascular repair Definition of an endoleak Types of endoleaks Management of type lll endoleak Diagnosis of type
Management of Endoleaks Sarah Ikponmwosa, MD Brooklyn VA 6/20/08 Questions Advantages of endovascular repair Definition of an endoleak Types of endoleaks Management of type lll endoleak Diagnosis of type
Reimbursement Guide Zenith Fenestrated AAA Endovascular Graft
 MEDICAL Reimbursement Guide Zenith Fenestrated AAA Endovascular Graft Disclaimer: The information provided herein reflects Cook s understanding of the procedure(s) and/or device(s) from sources that may
MEDICAL Reimbursement Guide Zenith Fenestrated AAA Endovascular Graft Disclaimer: The information provided herein reflects Cook s understanding of the procedure(s) and/or device(s) from sources that may
MODERN METHODS FOR TREATING ABDOMINAL ANEURYSMS AND THORACIC AORTIC DISEASE
 MODERN METHODS FOR TREATING ABDOMINAL ANEURYSMS AND THORACIC AORTIC DISEASE AAA FACTS 200,000 New Cases Each Year Ruptured AAA = 15,000 Deaths per Year in U.S. 13th Leading Cause of Death 80% Chance of
MODERN METHODS FOR TREATING ABDOMINAL ANEURYSMS AND THORACIC AORTIC DISEASE AAA FACTS 200,000 New Cases Each Year Ruptured AAA = 15,000 Deaths per Year in U.S. 13th Leading Cause of Death 80% Chance of
Optimizing Accuracy of Aortic Stent Grafts in Short Necks
 Optimizing Accuracy of Aortic Stent Grafts in Short Necks Venkatesh Ramaiah, MD, FACS Medical Director Arizona Heart Hospital Director Peripheral Vascular and Endovascular Research Arizona Heart Institute
Optimizing Accuracy of Aortic Stent Grafts in Short Necks Venkatesh Ramaiah, MD, FACS Medical Director Arizona Heart Hospital Director Peripheral Vascular and Endovascular Research Arizona Heart Institute
Mesenteric vascular insufficiency and claudication following acute dissecting thoracic aortic aneurysm
 Mesenteric vascular insufficiency and claudication following acute dissecting thoracic aortic aneurysm Thomas H. Cogbill, M.D., A. Erik Gundersen, M.D., and Renato TraveUi, M.D., La Crosse, Wisc. Mesenteric
Mesenteric vascular insufficiency and claudication following acute dissecting thoracic aortic aneurysm Thomas H. Cogbill, M.D., A. Erik Gundersen, M.D., and Renato TraveUi, M.D., La Crosse, Wisc. Mesenteric
Abdominal Aortic Aneurysm - Part 1. Learning Objectives. Disclosure. University of Toronto Division of Vascular Surgery
 University of Toronto Division of Vascular Surgery Abdominal Aortic Aneurysm - Part 1 Dr Mark Wheatcroft & Dr Elisa Greco Vascular Surgeon, St Michael s Hospital, Toronto & University of Toronto Disclosure
University of Toronto Division of Vascular Surgery Abdominal Aortic Aneurysm - Part 1 Dr Mark Wheatcroft & Dr Elisa Greco Vascular Surgeon, St Michael s Hospital, Toronto & University of Toronto Disclosure
Periprosthetic leak and rupture after endovascular repair of abdominal aortic aneurysm: The significance of device design for long-term results
 CASE REPORTS Periprosthetic leak and rupture after endovascular repair of abdominal aortic aneurysm: The significance of device design for long-term results Kirsten Krohg-Sørensen, MD, PhD, Magne Brekke,
CASE REPORTS Periprosthetic leak and rupture after endovascular repair of abdominal aortic aneurysm: The significance of device design for long-term results Kirsten Krohg-Sørensen, MD, PhD, Magne Brekke,
Treatment of acute type B aortic dissection: Current status
 MEET Cannes, 18. - 21.06.2009 Treatment of acute type B aortic dissection: Current status Christoph A. Nienaber, MD, FACC University of Rostock Department of Internal Medicine, Cardiology christoph.nienaber@med.uni-rostock.de
MEET Cannes, 18. - 21.06.2009 Treatment of acute type B aortic dissection: Current status Christoph A. Nienaber, MD, FACC University of Rostock Department of Internal Medicine, Cardiology christoph.nienaber@med.uni-rostock.de
TEVAR for complicated acute type B dissection with malperfusion
 Masters of Cardiothoracic Surgery TEVR for complicated acute type dissection with malperfusion Guido H.W. van ogerijen 1, David M. Williams 2, Himanshu J. Patel 1 Departments of 1 Cardiac Surgery and 2
Masters of Cardiothoracic Surgery TEVR for complicated acute type dissection with malperfusion Guido H.W. van ogerijen 1, David M. Williams 2, Himanshu J. Patel 1 Departments of 1 Cardiac Surgery and 2
Residual Dissection and False Lumen Aneurysm After TEVAR
 WHAT WOULD YOU DO? Residual Dissection and False Lumen Aneurysm After MODERATOR: MARK FARBER, MD PANEL: YAZAN DUWAYRI, MD; MATTHEW J. EAGLETON, MD; WILLIAM D. JORDAN Jr, MD; TILO KÖLBEL, MD, PhD; AND ERIC
WHAT WOULD YOU DO? Residual Dissection and False Lumen Aneurysm After MODERATOR: MARK FARBER, MD PANEL: YAZAN DUWAYRI, MD; MATTHEW J. EAGLETON, MD; WILLIAM D. JORDAN Jr, MD; TILO KÖLBEL, MD, PhD; AND ERIC
Anatomical challenges in EVAR
 Anatomical challenges in EVAR M.H. EL DESSOKI, MD,FRCS PROFESSOR OF VASCULAR SURGERY CAIRO UNIVERSITY Disclosure Speaker name:... I have the following potential conflicts of interest to report: Consulting
Anatomical challenges in EVAR M.H. EL DESSOKI, MD,FRCS PROFESSOR OF VASCULAR SURGERY CAIRO UNIVERSITY Disclosure Speaker name:... I have the following potential conflicts of interest to report: Consulting
Objective assessment of current stent grafts: which graft for which lesion. Ludovic Canaud, MD, PhD Pierre Alric, MD, PhD Montpellier, France
 Objective assessment of current stent grafts: which graft for which lesion Ludovic Canaud, MD, PhD Pierre Alric, MD, PhD Montpellier, France Conflict of interest: none 1 Introduction Different diseases
Objective assessment of current stent grafts: which graft for which lesion Ludovic Canaud, MD, PhD Pierre Alric, MD, PhD Montpellier, France Conflict of interest: none 1 Introduction Different diseases
P Paraplegia abdominal aortic aneurysm repair, 52 paraparesis, 52 pathophysiology, 51 rates and endografts, 51 two-stage approach, 129
 A AAA. See Abdominal aortic aneurysm (AAA) Abdominal aortic aneurysm (AAA). See also Abdominal aortic pathologies advantage, IVUS, 20 asymptomatic infrarenal, 154 device selection and treatment, 19 20
A AAA. See Abdominal aortic aneurysm (AAA) Abdominal aortic aneurysm (AAA). See also Abdominal aortic pathologies advantage, IVUS, 20 asymptomatic infrarenal, 154 device selection and treatment, 19 20
Management of the persistent sciatic artery with coexistent aortoiliac aneurysms; endovascular and open techniques.
 ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 14 Number 2 Management of the persistent sciatic artery with coexistent aortoiliac aneurysms; endovascular and open A Rodriguez-Rivera,
ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 14 Number 2 Management of the persistent sciatic artery with coexistent aortoiliac aneurysms; endovascular and open A Rodriguez-Rivera,
Follow-up of Aortic Dissection: How, How Often, Which Consequences Euro Echo 2011
 Follow-up of Aortic Dissection: How, How Often, Which Consequences Euro Echo 2011 Susan E. Wiegers, MD, FASE Director of Clinical Echocardiography Hospital of the University of Pennsylvania Disclosure
Follow-up of Aortic Dissection: How, How Often, Which Consequences Euro Echo 2011 Susan E. Wiegers, MD, FASE Director of Clinical Echocardiography Hospital of the University of Pennsylvania Disclosure
THORACOABDOMINAL AORTIC ANEURYSMS HYBRID REPAIR
 Update on Open and Endovascular Therapeutic Option for Aortic Repair CENTRE CARDIO-TORACIQUE DE MONACO Friday November 7 th, 2014 THORACOABDOMINAL AORTIC ANEURYSMS HYBRID REPAIR Roberto Chiesa Vascular
Update on Open and Endovascular Therapeutic Option for Aortic Repair CENTRE CARDIO-TORACIQUE DE MONACO Friday November 7 th, 2014 THORACOABDOMINAL AORTIC ANEURYSMS HYBRID REPAIR Roberto Chiesa Vascular
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of June 4, 2018 Thrombolysis, Thrombectomy & Angioplasty
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of June 4, 2018 Thrombolysis, Thrombectomy & Angioplasty
Case 37 Clinical Presentation
 Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Accepted Manuscript. Is A More Extensive Operation Justified for Acute Type A Dissection Repair? Dr. Leonard N. Girardi
 Accepted Manuscript Is A More Extensive Operation Justified for Acute Type A Dissection Repair? Dr. Leonard N. Girardi PII: S0022-5223(18)32552-2 DOI: 10.1016/j.jtcvs.2018.09.048 Reference: YMTC 13502
Accepted Manuscript Is A More Extensive Operation Justified for Acute Type A Dissection Repair? Dr. Leonard N. Girardi PII: S0022-5223(18)32552-2 DOI: 10.1016/j.jtcvs.2018.09.048 Reference: YMTC 13502
SUPPLEMENTAL MATERIAL
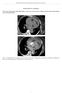 SUPPLEMENTL MTERIL Marie erna, Martin Kocher, Rohit Philip Thomas. cute aorta, overview of acute T findings and endovascular treatment options (doi: 10.5507/bp.2016.060) Fig. 1. : Non-enhanced T, hemopericardium
SUPPLEMENTL MTERIL Marie erna, Martin Kocher, Rohit Philip Thomas. cute aorta, overview of acute T findings and endovascular treatment options (doi: 10.5507/bp.2016.060) Fig. 1. : Non-enhanced T, hemopericardium
Case Report 1. CTA head. (c) Tele3D Advantage, LLC
 Case Report 1 CTA head 1 History 82 YEAR OLD woman with signs and symptoms of increased intra cranial pressure in setting of SAH. CT Brain was performed followed by CT Angiography of head. 2 CT brain Extensive
Case Report 1 CTA head 1 History 82 YEAR OLD woman with signs and symptoms of increased intra cranial pressure in setting of SAH. CT Brain was performed followed by CT Angiography of head. 2 CT brain Extensive
Intravascular Ultrasound in the Treatment of Complex Aortic Pathologies. Naixin Kang, M.D. Vascular Surgery Fellow April 26 th, 2018
 Intravascular Ultrasound in the Treatment of Complex Aortic Pathologies Naixin Kang, M.D. Vascular Surgery Fellow April 26 th, 2018 DISCLOSURES Nothing To Disclose 2 ENDOVASCULAR AORTIC INTERVENTION Improved
Intravascular Ultrasound in the Treatment of Complex Aortic Pathologies Naixin Kang, M.D. Vascular Surgery Fellow April 26 th, 2018 DISCLOSURES Nothing To Disclose 2 ENDOVASCULAR AORTIC INTERVENTION Improved
UC SF. Disclosures. Thoracic Endovascular Aortic Repair 4/24/2009. Management of Acute Dissections: Is There Still a Role for Open Surgery?
 UC SF Management of Acute Dissections: Is There Still a Role for Open Surgery? Darren B. Schneider, M.D. Assistant Professor of Surgery and Radiology Division of Vascular Surgery University of California
UC SF Management of Acute Dissections: Is There Still a Role for Open Surgery? Darren B. Schneider, M.D. Assistant Professor of Surgery and Radiology Division of Vascular Surgery University of California
Saphenous Vein Autograft Replacement
 Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
INL No. A0083 Project Medtronic Thoracic patients guide Description Version 18
 INL No. A0083 Project Medtronic Thoracic patients guide Description Version 18 www.inl-agency.com PATIENT INFORMATION BOOKLET Endovascular Stent Grafts: A treatment for Thoracic Aortic disease Table of
INL No. A0083 Project Medtronic Thoracic patients guide Description Version 18 www.inl-agency.com PATIENT INFORMATION BOOKLET Endovascular Stent Grafts: A treatment for Thoracic Aortic disease Table of
From 1996 to 1999, a total of 1,193 patients with
 THE ANEURX CLINICAL TRIAL AT 8 YEARS Lessons learned following the US AneuRx clinical trial from 1996 to 2004. BY CHRISTOPHER K. ZARINS, MD From 1996 to 1999, a total of 1,193 patients with infrarenal
THE ANEURX CLINICAL TRIAL AT 8 YEARS Lessons learned following the US AneuRx clinical trial from 1996 to 2004. BY CHRISTOPHER K. ZARINS, MD From 1996 to 1999, a total of 1,193 patients with infrarenal
Percutaneous Axillary Artery Access For Branch Grafting for complex TAAAs and pararenal AAAs: How to do it safely
 Percutaneous Axillary Artery Access For Branch Grafting for complex TAAAs and pararenal AAAs: How to do it safely Daniela Branzan, MD, Department of Vascular Surgery University Hospital Leipzig Disclosure
Percutaneous Axillary Artery Access For Branch Grafting for complex TAAAs and pararenal AAAs: How to do it safely Daniela Branzan, MD, Department of Vascular Surgery University Hospital Leipzig Disclosure
Endovascular Repair of Aortic Arch/Thoracic Aneurysms: Bolton RelayBranch Device
 Endovascular Repair of Aortic Arch/Thoracic Aneurysms: Bolton RelayBranch Device Luis A. Sanchez MD Gregorio A. Sicard Distinguished Professor of Surgery & Radiology Chief, Section of Vascular Surgery
Endovascular Repair of Aortic Arch/Thoracic Aneurysms: Bolton RelayBranch Device Luis A. Sanchez MD Gregorio A. Sicard Distinguished Professor of Surgery & Radiology Chief, Section of Vascular Surgery
Description. Section: Surgery Effective Date: April 15, Subsection: Surgery Original Policy Date: December 6, 2012 Subject:
 Last Review Status/Date: March 2015 Page: 1 of 6 Description Wireless sensors implanted in an aortic aneurysm sac after endovascular repair are being investigated to measure post procedural pressure. It
Last Review Status/Date: March 2015 Page: 1 of 6 Description Wireless sensors implanted in an aortic aneurysm sac after endovascular repair are being investigated to measure post procedural pressure. It
symptomatic aneurysms or aneurysms that grow >1cm/yr
 1. Elective repair for aneurysm >5.5 cm, symptomatic aneurysms or aneurysms that grow >1cm/yr 2. Ruptured AAA Aneurysm Detection and Management Study (ADAM) and UK Small Aneurysm Trial early open surgery
1. Elective repair for aneurysm >5.5 cm, symptomatic aneurysms or aneurysms that grow >1cm/yr 2. Ruptured AAA Aneurysm Detection and Management Study (ADAM) and UK Small Aneurysm Trial early open surgery
ACD. The Journal of Thoracic and Cardiovascular Surgery c Volume 139, Number 3 655
 A novel approach to prevent spinal cord ischemia: Inoue stent graft with a side branch of small caliber for the reconstruction of the artery of Adamkiewicz Takeshi Shimamoto, MD, a Akira Marui, MD, PhD,
A novel approach to prevent spinal cord ischemia: Inoue stent graft with a side branch of small caliber for the reconstruction of the artery of Adamkiewicz Takeshi Shimamoto, MD, a Akira Marui, MD, PhD,
