Case I: Shock. A) What additional history would you like from the nursing home staff, patient s chart, and ambulance team?
|
|
|
- Gregory Murphy
- 6 years ago
- Views:
Transcription
1 Case I: Shock It is your first night of call during your subinternship month, and you are asked by your resident to evaluate a patient in the emergency room. The patient is a 85yo female with a history of Alzheimer s dementia and Hypertension. She presented to the emergency room via ambulance from a nursing home with a complaint from the nursing home staff of decreased mental status. The ambulance team reports that on their arrival, the patient s blood pressure was 80/40mmHg. Her medications at the nursing home include Aricept, Hydrochlorothiazide, and Metoprolol. A) What additional history would you like from the nursing home staff, patient s chart, and ambulance team? a) History from Nursing Home staff: a. Time of onset of symptoms b. Recent illnesses in the patient c. Presence of associated symptoms, such as fever, nausea, vomiting, diarrhea b) History from the patient s chart a. Past history, such as recent hospitalizations or illnesses, surgeries, etc. b. Daily and as needed medications c. Recent vital signs prior to the onset of symptoms d. Family contact person c) History from the ambulance team a. Patient s mental status on arrival b. Patient s perfusion on arrival c. Patient s other vital signs on arrival d. Any interventions that have taken place on the way to the hospital B) Define shock. What are the main categories of shock? Shock is the physiologic state characterized by significant reduction of systemic tissue perfusion, resulting in decreased tissue oxygen delivery. The different types of shock are: Hypovolemic shock Cardiogenic shock Extracardiac Obstructive Shock Distributive Shock The different causes of each of these conditions are listed below: 1. Hypovolemic shock a. Blood loss due to trauma or gastrointestinal bleeding
2 b. Third space loss of plasma volume (pancreatitis, bowel obstruction, infarction, anaphylaxis) c. Diarrhea d. Burns 2. Cardiogenic shock a. Acute myocardial infarction (>40% of LV mass) b. Arrhythmia (heart block, Ventricular tachycardia, etc.) c. Acute valvular dysfunction d. Ventricular septal rupture e. Dilated cardiomyopathy f. Ventricular aneurysm g. Left ventricular outflow track obstruction 3. Extracardiac Obstructive shock a. Pericardial tamponade b. Inferior/superior vena caval obstruction c. Aortic dissection d. Massive pulmonary embolism e. Severe pulmonary hypertension (primary or Eisenmenger) 4. Distributive shock a. Neurogenic shock b. Septic shock c. Toxic shock secondary to drug overdose d. Anaphylaxis e. Endocrinologic shock On physical examination, the patient is lying quietly in bed and somewhat difficult to arouse with sternal rub. Her pulse is 120 beats/min, BP is 80/40, RR is 18, and temperature is 101degrees Fahrenheit. Her cardiac and pulmonary exam are within normal limits. Her abdominal exam reveals some mild to moderate suprapubic tenderness but is otherwise normal. The rest of her physical examination is normal. A Foley catheter is in place and contains dark colored urine with small amounts of pus. C) Based on the history and physical examination, what is your Differential Diagnosis and which diagnosis would you consider most likely in this patient? Differential Diagnosis at this point would be limited to: a) Infection/septic shock with causes such as pneumonia, meningitis/encephalitis, urinary tract infection, bacteremia, etc. b) Myocardial infarction Most likely diagnosis in this patient given the history and physical examination would be infection/septic shock with urinary tract infection leading the list of these causes. D) What is SIRS, sepsis, severe sepsis, and septic shock?
3 Systemic Inflammatory Response Syndrome: Patient has SIRS if he/she has two of more of the following conditions: temperature >38.5 C or <35.0 C; heart rate of >90 beats/min; respiratory rate of >20 breaths/min or PaCO 2 of <32 mm Hg; and WBC count of >12,000 cells/ml, <4000 cells/ml, or >10 percent immature (band) forms Sepsis: SIRS along with documented source of infection. Severe Sepsis: Sepsis and at least one of the following signs of organ hypoperfusion or organ dysfunction: thrombocytopenia <100,000 cells/ml, DIC, areas of mottled skin; capillary refilling of 3 s; urinary output of <0.5 ml/kg for at least 1 h or renal replacement therapy; lactate >2 mmol/l; abrupt change in mental status or abnormal EEG findings; acute lung injury/ards; and cardiac dysfunction Septic Shock: Severe sepsis and one of the following conditions: systemic mean BP of <60 mm Hg (<80 mm Hg if previous hypertension) after 20 to 30 ml/kg starch or 40 to 60 ml/kg serum saline solution, or PCWP between 12 and 20 mm Hg; and pressors (dopamine, norepinephrine) to keep the mean BP at >60 mm Hg (80 mm Hg if previous hypertension) E) What laboratory evaluation would you want to obtain in this patient? Chemistry panel, Complete Blood Count with differential, Liver panel, lactic acid level, Urinalysis with culture, Blood Culture from 2 sites, Chest Xray, Electrocardiogram A Complete Blood Count reveals and elevated white blood cell count with a left shift, and a urinalysis shows many bacteria with >100 WBC/hpf and positive nitrite. F) How would you continue to manage this patient? First and foremost, intravenous fluids in a crystalloid form such as lactated ringers or normal saline to be given as a bolus of either 1000mL over one hour or 500mL over 30 minutes. Reassessment of the patient and the patient s vital signs should occur after the initial bolus, and if the systolic blood pressure remains below 90mmHg, then another bolus should be given and consideration made for transfer to the Intensive Care Unit where vasopressors can be initiated. Antibiotics to cover for the urinary tract infection should be given as well. Discussion with family members about the patient s clinical situation and code status should occur as well once the initial stabilization of the patient is made. Patient was aggressively volume resuscitated and started on intravenous antibiotics. Over the next 24 hours, patient blood pressure increased to 110/60mm Hg, HR 90. Blood culture from the lab was reported as gram negative bacillus, urine culture also revealed gram negative bacillus. Patient s antibiotic was continued.
4 G) What is your antibiotic of choice in this case? What antibiotic would you consider if the patient s blood culture and urine culture reported gram positive cocci in clusters? Third generation cephalosporins, quinolones, Pipericillin/Tazobactam; If gram positive cocci in clusters consider Vancomycin H) How would you management differ if your patient s blood pressure continued to be in the low 80s with fluid resuscitation? Reassessment of the patient and the patient s vital signs should occur after the initial bolus, and if the systolic blood pressure remains below 90mmHg, then another bolus should be given and consideration made for transfer to the Intensive Care Unit where vasopressors can be initiated.
5 Case Scenario #2 You are on the floor with the intern helping out with floor calls when you receive a call from the cardiac floor about a patient admitted earlier in the day with chest pain. The nurse reports that the patient s blood pressure is currently 80/40mmHg, and he is again complaining of chest pain. A) What questions would you ask the nurse and how would you proceed? *What are the patient s other vital signs? *When did the chest pain begin? *Why was the patient admitted and what has been his hospital course? *What recent medications has he been given? *Has the patient had any procedures or interventions performed recently? While walking hurriedly to the cardiac floor, you remember that this particular patient is a 60yo male attorney with Hypertension, Hyperlipidemia, and Diabetes mellitus type II who presented earlier in the day with a complaint of chest pain while questioning a witness in court. His initial EKG on arrival showed nonspecific STT segment changes, and the initial cardiac enzymes were mildly elevated. He was admitted to the hospital to rule out a cardiac cause of his chest pain. On arrival to the patient s room, the patient is diaphoretic and sitting on the side of the bed clutching his chest. B) Identify some key points you need to focus on when you arrive in his room. a) Chart review: This aspect of the patient s evaluation is very important to appropriately assess the patient. Review: -Presence of chest pain prior to admission -Hospital course -Current medications -Home medications -Recent procedures/laboratory studies performed b) History from the patient including: -Onset and timing of symptoms -Alleviating/exacerbating factors -Associated factors such as shortness of breath, diaphoresis, nausea, vomiting, etc. C) How would you proceed? Physical examination: A physical examination needs to be performed prior to any further management. This examination should include:
6 -Assessment of the patient s vital signs -Assessment of the cardiac exam with particular attention paid to any new murmurs, the presence of elevated JVP, capillary refill, etc. -Assessment of the pulmonary exam with particular attention paid to crackles on lung exam, use of accessory muscles of inspiration, etc. On physical examination, the patient is tachypneic and diaphoretic. His HR is 100beats/min, BP 80/40mmHg, RR 24, temperature 98.8degrees Fahrenheit, and Oxygen saturations of 88% on room air. His cardiac exam reveals a III/VI holosystolic murmur at the left sternal border as well as a S3 gallop. On lung exam, he has crackles bilaterally without wheezing. His extremities are cool to the touch but otherwise his physical examination is normal. D) What is the differential diagnosis of shock in this hospitalized patient? What is the main difference in pathophysiology between the patients in case 1 and case 2? A. Cardiogenic shock a. Acute myocardial infarction (>40% of LV mass) b. Arrhythmia (heart block, Ventricular tachycardia, etc.) c. Acute valvular dysfunction d. Ventricular septal rupture e. Dilated cardiomyopathy f. Ventricular aneurysm g. Left ventricular outflow track obstruction B. Extracardiac Obstructive shock a. Pericardial tamponade b. Inferior/superior vena caval obstruction c. Aortic dissection d. Massive pulmonary embolism e. Severe pulmonary hypertension (primary or Eisenmenger) The table below identifies the difference in the pathophysiology and hemodynamic profile between the different types of shock. Physiologic Preload Afterload Pump function Tissue perfusion variable Clinical Pulmonary Systemic vascular Cardiac output Mixed venous measurement capillary wedge resistance oxygen saturation pressure of these variables Cardiogenic Increased Increased Decreased Decreased (case #2) Distributive Decreased or Decreased Increased Increased (case #1) normal Hypovolemic Decreased Increased Decreased Decreased Table -1
7 E) What do you expect this patient s hemodynamic profile to be? See table- 1 F) What are the next steps in the evaluation and management of this patient? -Electrocardiogram STAT! -Chest Xray -Cardiac enzymes -Place the patient on 2L O2 nasal cannula and continuously assess oxygen saturations and respiratory status -Once the EKG returns, determine whether the patient requires the other components of the acronym MONA (morphine sulfate, oxygen, nitroglycerin, aspirin). -Contact the on call resident and cardiology fellow. -Transfer the patient to the intensive care unit for closer monitoring, possible cardiac intervention, administration of pressors, etc. As you are waiting on the EKG, chest xray, and labs, you ask the nurse to place the patient on 2L of oxygen. The EKG shows STT segment elevation in leads II, III, and avf. You immediately page your resident and the cardiology fellow and have the nurse give the patient aspirin, nitroglycerin, and morphine sulfate. The cardiology fellow then arrives and immediately takes the patient to the cardiac catherization lab. Case Scenario #3 You are asked by your resident to evaluate a patient in the emergency room. The patient is a 45yo Indian businessman with no medical problems who just returned from an overseas trip and presents with a one day history of abdominal pain and diarrhea. He is on no medications at home. In triage, the patient s blood pressure is noted to be 80/40, and the patient is immediately taken to an examination room. A) What further questions do you have for this patient? -Timing of onset of symptoms -Location of the abdominal pain -Radiation of the abdominal pain -Severity of the abdominal pain -Recent travel -Recent antibiotic use
8 -Consumption of different foods while abroad -Associated symptoms such as chest pain, headache, shortness of breath, fever, vomiting, etc. -Description of the diarrhea, i.e. blood, mucous, color, consistency. -Quantity of diarrhea -Ill contacts B) What are some causes of shock and which would be most likely in this patient? -Hypovolemic shock a. Blood loss due to trauma or gastrointestinal bleeding b. Third space loss of plasma volume (pancreatitis, bowel obstruction, infarction, anaphylaxis) c. Diarrhea On physical examination, the patient is in mild to moderate distress with a HR of 140beats/min, BP of 90/60, RR of 18, and temperature of 99.8degrees Fahrenheit. His mucous membranes are dry. His cardiac exam is normal except for tachycardia, and his lung exam is normal. His abdominal exam reveals diffuse tenderness to palpation with hyperactive bowel sounds. The rest of the exam is normal. Rectal exam reveals a large amount of clear yellow, watery stool that is guaic negative. C) How would you proceed with the workup and treatment of this patient? -Obtain the following laboratory studies: -Chemistry -Liver panel -Amylase, Lipase -Complete blood count with differential -Urinalysis with culture -Blood culture from 2 sites -Stool studies to include evaluation for parasites, fecal occult blood -Stool culture -Administer intravenous fluids in the form of crystalloid solutions such as lactated ringers or normal saline with 1000mL over one hour of 500mL over 30 minutes. D) How would you management be different if this patient had a history of melena? Assess hemodynamic stability: Volume depleting GI Bleed needs immediate attention Assessed by orthostatic hypotension and tacycardia in the absence of shock Shock, orthostatic hypotension, decrease in hematocrit of 6%, transfusion requirements of over 2 units of packed RBCs, active bleeding-admit to ICU for management
9 Two large caliber peripheral catheters or central venous line should be inserted for IV access Use PRBCs, or FFPs /platelets in the face of underlying coagulopathy Hemodynamic stability needs to be established prior to the next step in the management of GI bleed. Assess the site of bleed: Determination of site of bleed Endoscopy Treating of underlying condition Secondary Prevention based on the diagnosis
Staging Sepsis for the Emergency Department: Physician
 Staging Sepsis for the Emergency Department: Physician Sepsis Continuum 1 Sepsis Continuum SIRS = 2 or more clinical criteria, resulting in Systemic Inflammatory Response Syndrome Sepsis = SIRS + proven/suspected
Staging Sepsis for the Emergency Department: Physician Sepsis Continuum 1 Sepsis Continuum SIRS = 2 or more clinical criteria, resulting in Systemic Inflammatory Response Syndrome Sepsis = SIRS + proven/suspected
Case year old female nursing home resident with a hx CAD, PUD, recent hip fracture Transferred to ED with decreased mental status BP in ED 80/50
 Case 1 65 year old female nursing home resident with a hx CAD, PUD, recent hip fracture Transferred to ED with decreased mental status BP in ED 80/50 Case 1 65 year old female nursing home resident with
Case 1 65 year old female nursing home resident with a hx CAD, PUD, recent hip fracture Transferred to ED with decreased mental status BP in ED 80/50 Case 1 65 year old female nursing home resident with
SHOCK Susanna Hilda Hutajulu, MD, PhD
 SHOCK Susanna Hilda Hutajulu, MD, PhD Div Hematology and Medical Oncology Department of Internal Medicine Universitas Gadjah Mada Yogyakarta Outline Definition Epidemiology Physiology Classes of Shock
SHOCK Susanna Hilda Hutajulu, MD, PhD Div Hematology and Medical Oncology Department of Internal Medicine Universitas Gadjah Mada Yogyakarta Outline Definition Epidemiology Physiology Classes of Shock
R2R: Severe sepsis/septic shock. Surat Tongyoo Critical care medicine Siriraj Hospital
 R2R: Severe sepsis/septic shock Surat Tongyoo Critical care medicine Siriraj Hospital Diagnostic criteria ACCP/SCCM consensus conference 1991 SCCM/ESICM/ACCP/ATS/SIS International Sepsis Definitions Conference
R2R: Severe sepsis/septic shock Surat Tongyoo Critical care medicine Siriraj Hospital Diagnostic criteria ACCP/SCCM consensus conference 1991 SCCM/ESICM/ACCP/ATS/SIS International Sepsis Definitions Conference
-Cardiogenic: shock state resulting from impairment or failure of myocardium
 Shock chapter Shock -Condition in which tissue perfusion is inadequate to deliver oxygen, nutrients to support vital organs, cellular function -Affects all body systems -Classic signs of early shock: Tachycardia,tachypnea,restlessness,anxiety,
Shock chapter Shock -Condition in which tissue perfusion is inadequate to deliver oxygen, nutrients to support vital organs, cellular function -Affects all body systems -Classic signs of early shock: Tachycardia,tachypnea,restlessness,anxiety,
SEPSIS SYNDROME
 INTRODUCTION Sepsis has been defined as a life threatening condition that arises when the body s response to an infection injures its own tissues and organs. Sepsis may lead to shock, multiple organ failure
INTRODUCTION Sepsis has been defined as a life threatening condition that arises when the body s response to an infection injures its own tissues and organs. Sepsis may lead to shock, multiple organ failure
PHYSIOLOGY AND MANAGEMENT OF THE SEPTIC PATIENT
 PHYSIOLOGY AND MANAGEMENT OF THE SEPTIC PATIENT Melanie Sanchez, RN, MSNE, OCN, CCRN Clinical Nurse III City of Hope National Medical Center HOW THE EXPERTS TREAT HEMATOLOGIC MALIGNANCIES LAS VEGAS, NV
PHYSIOLOGY AND MANAGEMENT OF THE SEPTIC PATIENT Melanie Sanchez, RN, MSNE, OCN, CCRN Clinical Nurse III City of Hope National Medical Center HOW THE EXPERTS TREAT HEMATOLOGIC MALIGNANCIES LAS VEGAS, NV
SHOCK. Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital
 SHOCK Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital 1 Definition Shock is an acute, complex state of circulatory dysfunction
SHOCK Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital 1 Definition Shock is an acute, complex state of circulatory dysfunction
The Septic Patient. Dr Arunraj Navaratnarajah. Renal SpR Imperial College NHS Healthcare Trust
 The Septic Patient Dr Arunraj Navaratnarajah Renal SpR Imperial College NHS Healthcare Trust Objectives of this session Define SIRS / sepsis / severe sepsis / septic shock Early recognition of Sepsis The
The Septic Patient Dr Arunraj Navaratnarajah Renal SpR Imperial College NHS Healthcare Trust Objectives of this session Define SIRS / sepsis / severe sepsis / septic shock Early recognition of Sepsis The
Shock. Shao Mian Emergency Department,Zhongshan Hospital
 Shock Shao Mian Emergency Department,Zhongshan Hospital What is shock THE BEGINNINGS OF UNDERSTANDING: THE LATE 19TH CENTURY THE AGE OF REASON: 1890 1925 THE MODERN ERA: BLALOCK S EPIPHANY POSTMODERNISM:
Shock Shao Mian Emergency Department,Zhongshan Hospital What is shock THE BEGINNINGS OF UNDERSTANDING: THE LATE 19TH CENTURY THE AGE OF REASON: 1890 1925 THE MODERN ERA: BLALOCK S EPIPHANY POSTMODERNISM:
Unit 4 Problems of Cardiac Output and Tissue Perfusion
 Unit 4 Problems of Cardiac Output and Tissue Perfusion Lemone and Burke Ch 30-32 Objectives Review the anatomy and physiology of the cardiovascular system. Identify normal heart sounds and relate them
Unit 4 Problems of Cardiac Output and Tissue Perfusion Lemone and Burke Ch 30-32 Objectives Review the anatomy and physiology of the cardiovascular system. Identify normal heart sounds and relate them
John Park, MD Assistant Professor of Medicine
 John Park, MD Assistant Professor of Medicine Faculty photo will be placed here park.john@mayo.edu 2015 MFMER 3543652-1 Sepsis Out with the Old, In with the New Mayo School of Continuous Professional Development
John Park, MD Assistant Professor of Medicine Faculty photo will be placed here park.john@mayo.edu 2015 MFMER 3543652-1 Sepsis Out with the Old, In with the New Mayo School of Continuous Professional Development
LeMone & Burke Ch 30-32
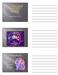 LeMone & Burke Ch 30-32 2 Right side- Low oxygenation Low pressure Light workload Goes toward the lungs Left side High oxygenation Thick walled high pressure Heavier workload Carries oxygenation blood
LeMone & Burke Ch 30-32 2 Right side- Low oxygenation Low pressure Light workload Goes toward the lungs Left side High oxygenation Thick walled high pressure Heavier workload Carries oxygenation blood
Case Scenario 3: Shock and Sepsis
 Name: Molly Boyle 1. Define the term shock (Lewis textbook): Shock is a syndrome characterized by decreased perfusion and impaired metabolism. Shock can have a number of causes that result in damage to
Name: Molly Boyle 1. Define the term shock (Lewis textbook): Shock is a syndrome characterized by decreased perfusion and impaired metabolism. Shock can have a number of causes that result in damage to
Shock Management. Seyed Tayeb Moradian MSc, Critical Care Nursing Ph.D Candidate. PDF created with pdffactory Pro trial version
 Shock Management Seyed Tayeb Moradian MSc, Critical Care Nursing Ph.D Candidate Definition of Shock The definition of shock does not involve low blood pressure, rapid pulse or cool clammy skin - these
Shock Management Seyed Tayeb Moradian MSc, Critical Care Nursing Ph.D Candidate Definition of Shock The definition of shock does not involve low blood pressure, rapid pulse or cool clammy skin - these
Sepsis Awareness and Education
 Sepsis Awareness and Education Meets the updated New York State Department of Health (NYSDOH) requirements for Infection Control and Barrier Precautions coursework Element VII: Sepsis Awareness and Education
Sepsis Awareness and Education Meets the updated New York State Department of Health (NYSDOH) requirements for Infection Control and Barrier Precautions coursework Element VII: Sepsis Awareness and Education
Sepsis Early Recognition and Management. Therese Hughes, PhD, MPA, RN
 Sepsis Early Recognition and Management Therese Hughes, PhD, MPA, RN 1 Sepsis a Deadly Progression Affects millions around the world each year, killing one in four Contributes to approximately 50% of all
Sepsis Early Recognition and Management Therese Hughes, PhD, MPA, RN 1 Sepsis a Deadly Progression Affects millions around the world each year, killing one in four Contributes to approximately 50% of all
Fluids in Sepsis: How much and what type? John Fowler, MD, FACEP Kent Hospital, İzmir Eisenhower Medical Center, USA American Hospital Dubai, UAE
 Fluids in Sepsis: How much and what type? John Fowler, MD, FACEP Kent Hospital, İzmir Eisenhower Medical Center, USA American Hospital Dubai, UAE In critically ill patients: too little fluid Low preload,
Fluids in Sepsis: How much and what type? John Fowler, MD, FACEP Kent Hospital, İzmir Eisenhower Medical Center, USA American Hospital Dubai, UAE In critically ill patients: too little fluid Low preload,
Tissue oxygenation is dependent upon, cardiac output, hemoglobin saturation and peripheral micro circulation.
 Editorial Shock occurs when there is circulatory failure that results in inadequate cellular oxygen, that is arterial blood flow is inadequate to meet tissue metabolic needs. Tissue oxygenation is dependent
Editorial Shock occurs when there is circulatory failure that results in inadequate cellular oxygen, that is arterial blood flow is inadequate to meet tissue metabolic needs. Tissue oxygenation is dependent
Shock Quiz! By Clare Di Bona
 Shock Quiz! By Clare Di Bona Test Question What is Mr Burns full legal name? Answer Charles Montgomery Plantagenet Schicklgruber Burns. (Season 22, episode 11) Question 1. What is the definition of shock?
Shock Quiz! By Clare Di Bona Test Question What is Mr Burns full legal name? Answer Charles Montgomery Plantagenet Schicklgruber Burns. (Season 22, episode 11) Question 1. What is the definition of shock?
SHOCK AETIOLOGY OF SHOCK (1) Inadequate circulating blood volume ) Loss of Autonomic control of the vasculature (3) Impaired cardiac function
 SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
Student Guide Module 4: Pediatric Trauma
 Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
LOKUN! I got stomach ache!
 LOKUN! I got stomach ache! Mr L is a 67year old Chinese gentleman who is a non smoker, social drinker. He has a medical history significant for Hypertension, Hyperlipidemia, Type 2 Diabetes Mellitus, Chronic
LOKUN! I got stomach ache! Mr L is a 67year old Chinese gentleman who is a non smoker, social drinker. He has a medical history significant for Hypertension, Hyperlipidemia, Type 2 Diabetes Mellitus, Chronic
Sepsis Bundle Project (SEP) Kathy Wonderly RN, MSEd, CPHQ Consultant Developed: April 2015 Most recent Revision: December 2018
 Sepsis Bundle Project (SEP) Kathy Wonderly RN, MSEd, CPHQ Consultant Developed: April 2015 Most recent Revision: December 2018 Objectives 1. To identify the symptom of severe sepsis and septic shock syndrome.
Sepsis Bundle Project (SEP) Kathy Wonderly RN, MSEd, CPHQ Consultant Developed: April 2015 Most recent Revision: December 2018 Objectives 1. To identify the symptom of severe sepsis and septic shock syndrome.
Frank Sebat, MD - June 29, 2006
 Types of Shock Hypovolemic Shock Low blood volume decreasing cardiac output. AN INTEGRATED SYSTEM OF CARE FOR PATIENTS AT RISK SHOCK TEAM and RAPID RESPONSE TEAM Septic or Distributive Shock Decrease in
Types of Shock Hypovolemic Shock Low blood volume decreasing cardiac output. AN INTEGRATED SYSTEM OF CARE FOR PATIENTS AT RISK SHOCK TEAM and RAPID RESPONSE TEAM Septic or Distributive Shock Decrease in
Core Measures SEPSIS UPDATES
 Patricia Walker, RN-BC, BSN Evidence Based Practice Manager Quality Management Services UCLA Health System, Ronald Reagan Medical Center Core Measures SEPSIS UPDATES Severe Sepsis and Septic Shock Based
Patricia Walker, RN-BC, BSN Evidence Based Practice Manager Quality Management Services UCLA Health System, Ronald Reagan Medical Center Core Measures SEPSIS UPDATES Severe Sepsis and Septic Shock Based
Circulatory shock. Types, Etiology, Pathophysiology. Physiology of Circulation: The Vessels. 600,000 miles of vessels containing 5-6 liters of blood
 Circulatory shock Types, Etiology, Pathophysiology Blagoi Marinov, MD, PhD Pathophysiology Dept. Physiology of Circulation: The Vessels 600,000 miles of vessels containing 5-6 liters of blood Vessel tone
Circulatory shock Types, Etiology, Pathophysiology Blagoi Marinov, MD, PhD Pathophysiology Dept. Physiology of Circulation: The Vessels 600,000 miles of vessels containing 5-6 liters of blood Vessel tone
HYPOTENSION IS DANGEROUS C. R Y A N K E A Y, M D, F A C E P 1 6 M A R C H
 HYPOTENSION IS DANGEROUS C. R Y A N K E A Y, M D, F A C E P 1 6 M A R C H 2 0 1 8 OBJECTIVES Case-based overview of pressors Debunking pressor myths Utilizing push-dose pressors CASE 1 82-year old male,
HYPOTENSION IS DANGEROUS C. R Y A N K E A Y, M D, F A C E P 1 6 M A R C H 2 0 1 8 OBJECTIVES Case-based overview of pressors Debunking pressor myths Utilizing push-dose pressors CASE 1 82-year old male,
Use of Blood Lactate Measurements in the Critical Care Setting
 Use of Blood Lactate Measurements in the Critical Care Setting John G Toffaletti, PhD Director of Blood Gas and Clinical Pediatric Labs Professor of Pathology Duke University Medical Center Chief, VAMC
Use of Blood Lactate Measurements in the Critical Care Setting John G Toffaletti, PhD Director of Blood Gas and Clinical Pediatric Labs Professor of Pathology Duke University Medical Center Chief, VAMC
Objectives. Epidemiology of Sepsis. Review Guidelines for Resuscitation. Tx: EGDT, timing/choice of abx, activated
 Update on Surviving Sepsis 2008 Objectives Epidemiology of Sepsis Definition of Sepsis and Septic Shock Review Guidelines for Resuscitation Dx: Lactate, t cultures, SVO2 Tx: EGDT, timing/choice of abx,
Update on Surviving Sepsis 2008 Objectives Epidemiology of Sepsis Definition of Sepsis and Septic Shock Review Guidelines for Resuscitation Dx: Lactate, t cultures, SVO2 Tx: EGDT, timing/choice of abx,
SEPSIS RAPID RESPONSE
 SEPSIS RAPID RESPONSE Sepsis kills up to 50% of those infected. How many deaths will you prevent this year? 1 SEPSIS Back ground: According to the Institute for Health Improvement and the Surviving Sepsis
SEPSIS RAPID RESPONSE Sepsis kills up to 50% of those infected. How many deaths will you prevent this year? 1 SEPSIS Back ground: According to the Institute for Health Improvement and the Surviving Sepsis
Utilizing Vasopressors:
 Utilizing Vasopressors: Critical Care Advances in the Emergency Department José A. Rubero, MD, FACEP, FAAEM Associate Program Director University of Central Florida/HCA GME Consortium Emergency Medicine
Utilizing Vasopressors: Critical Care Advances in the Emergency Department José A. Rubero, MD, FACEP, FAAEM Associate Program Director University of Central Florida/HCA GME Consortium Emergency Medicine
Dilemmas in Septic Shock
 Dilemmas in Septic Shock William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center A 62 year-old female presents to the ED with fever,
Dilemmas in Septic Shock William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center A 62 year-old female presents to the ED with fever,
Sepsis is an important issue. Clinician s decision-making capability. Guideline recommendations
 Surviving Sepsis Campaign: International Guidelines for Management of Severe Sepsis and Septic Shock: 2012 Clinicians decision-making capability Guideline recommendations Sepsis is an important issue 8.7%
Surviving Sepsis Campaign: International Guidelines for Management of Severe Sepsis and Septic Shock: 2012 Clinicians decision-making capability Guideline recommendations Sepsis is an important issue 8.7%
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Sprung CL, Annane D, Keh D, et al. Hydrocortisone therapy for
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Sprung CL, Annane D, Keh D, et al. Hydrocortisone therapy for
EVALUATING HEMODYNAMICS WITHOUT FANCY EQUIPMENT
 EVALUATING HEMODYNAMICS WITHOUT FANCY EQUIPMENT JUDY BORISH, RN, MSN, CCRN, PCCN OBJECTIVES BY THE END OF THIS SESSION THE PARTICIPANT WILL BE ABLE TO: * IDENTIFY THE NORMAL MECHANISMS OF THE BODY TO MAINTAIN
EVALUATING HEMODYNAMICS WITHOUT FANCY EQUIPMENT JUDY BORISH, RN, MSN, CCRN, PCCN OBJECTIVES BY THE END OF THIS SESSION THE PARTICIPANT WILL BE ABLE TO: * IDENTIFY THE NORMAL MECHANISMS OF THE BODY TO MAINTAIN
BREAK 11:10-11:
 1. Sepsis Tom Heaps 09:30-10:20 2. Oncological Emergencies Clare Pollard 10:20-11:10 ------------------------ BREAK 11:10-11:30 ------------------------ 3. Diabetic Ketoacidosis Tom Heaps 11:30-12:20 4.
1. Sepsis Tom Heaps 09:30-10:20 2. Oncological Emergencies Clare Pollard 10:20-11:10 ------------------------ BREAK 11:10-11:30 ------------------------ 3. Diabetic Ketoacidosis Tom Heaps 11:30-12:20 4.
Presented by: Indah Dwi Pratiwi
 Presented by: Indah Dwi Pratiwi Normal Fluid Requirements Resuscitation Fluids Goals of Resuscitation Maintain normal body temperature In most cases, elevate the feet and legs above the level of the heart
Presented by: Indah Dwi Pratiwi Normal Fluid Requirements Resuscitation Fluids Goals of Resuscitation Maintain normal body temperature In most cases, elevate the feet and legs above the level of the heart
What is sepsis? RECOGNITION. Sepsis I Know It When I See It 9/21/2017
 Sepsis I Know It When I See It September 15, 2017 Matthew Exline, MD MPH Medical Director, Medical ICU What is sepsis? I shall not today attempt further to define the kinds of material [b]ut I know it
Sepsis I Know It When I See It September 15, 2017 Matthew Exline, MD MPH Medical Director, Medical ICU What is sepsis? I shall not today attempt further to define the kinds of material [b]ut I know it
Patient Safety Safe Table Webcast: Sepsis (Part III and IV) December 17, 2014
 Patient Safety Safe Table Webcast: Sepsis (Part III and IV) December 17, 2014 Presenters Mark Blaney, RN Regional Nurse Educator CHI Franciscan Health Karen Lautermilch Director, Quality & Performance
Patient Safety Safe Table Webcast: Sepsis (Part III and IV) December 17, 2014 Presenters Mark Blaney, RN Regional Nurse Educator CHI Franciscan Health Karen Lautermilch Director, Quality & Performance
12/1/2009. Chapter 19: Hemorrhage. Hemorrhage and Shock Occurs when there is a disruption or leak in the vascular system Internal hemorrhage
 Chapter 19: Hemorrhage Hemorrhage and Shock Occurs when there is a disruption or leak in the vascular system External hemorrhage Internal hemorrhage Associated with higher morbidity and mortality than
Chapter 19: Hemorrhage Hemorrhage and Shock Occurs when there is a disruption or leak in the vascular system External hemorrhage Internal hemorrhage Associated with higher morbidity and mortality than
Sepsis: Identification and Management in an Acute Care Setting
 Sepsis: Identification and Management in an Acute Care Setting Dr. Barbara M. Mills DNP Director Rapid Response Team/ Code Resuscitation Stony Brook University Medical Center SEPSIS LECTURE NPA 2018 OBJECTIVES
Sepsis: Identification and Management in an Acute Care Setting Dr. Barbara M. Mills DNP Director Rapid Response Team/ Code Resuscitation Stony Brook University Medical Center SEPSIS LECTURE NPA 2018 OBJECTIVES
CEDR 2018 QCDR Measures for CMS 2018 MIPS Performance Year Reporting
 ACEP19 Emergency Department Utilization of CT for Minor Blunt Head Trauma for Aged 18 Years and Older Percentage of visits for aged 18 years and older who presented with a minor blunt head trauma who had
ACEP19 Emergency Department Utilization of CT for Minor Blunt Head Trauma for Aged 18 Years and Older Percentage of visits for aged 18 years and older who presented with a minor blunt head trauma who had
Exam 1 Review. Cardiopulmonary Symptoms Physical Examination Clinical Laboratory Studies
 Exam 1 Review Cardiopulmonary Symptoms Physical Examination Clinical Laboratory Studies WBC Count Differential A patient had been admitted to the hospital for acute shortness of breath. A CXR examination
Exam 1 Review Cardiopulmonary Symptoms Physical Examination Clinical Laboratory Studies WBC Count Differential A patient had been admitted to the hospital for acute shortness of breath. A CXR examination
Septic Shock. Rontgene M. Solante, MD, FPCP,FPSMID
 Septic Shock Rontgene M. Solante, MD, FPCP,FPSMID Learning Objectives Identify situations wherein high or low BP are hemodynamically significant Recognize complications arising from BP emergencies Manage
Septic Shock Rontgene M. Solante, MD, FPCP,FPSMID Learning Objectives Identify situations wherein high or low BP are hemodynamically significant Recognize complications arising from BP emergencies Manage
1. What additional information needs to be collected to properly treat this client?
 CASE 1 A 45-year-old male presents to the emergency department with a complaint of chest pain for the past two hours. 1. What additional information needs to be collected to properly treat this client?
CASE 1 A 45-year-old male presents to the emergency department with a complaint of chest pain for the past two hours. 1. What additional information needs to be collected to properly treat this client?
AnnMarie Papa, DNP,RN,CEN,NE-BC,FAEN, FAAN Clinical Director, Emergency, Medical & Observation Nursing Hospital of the University of Pennsylvania
 AnnMarie Papa, DNP,RN,CEN,NE-BC,FAEN, FAAN Clinical Director, Emergency, Medical & Observation Nursing Hospital of the University of Pennsylvania Who Am I? Except on few occasions, the patient appears
AnnMarie Papa, DNP,RN,CEN,NE-BC,FAEN, FAAN Clinical Director, Emergency, Medical & Observation Nursing Hospital of the University of Pennsylvania Who Am I? Except on few occasions, the patient appears
Initial Resuscitation of Sepsis & Septic Shock
 Initial Resuscitation of Sepsis & Septic Shock Dr. Fatema Ahmed MD (Critical Care Medicine) FCPS (Medicine) Associate professor Dept. of Critical Care Medicine BIRDEM General Hospital Is Sepsis a known
Initial Resuscitation of Sepsis & Septic Shock Dr. Fatema Ahmed MD (Critical Care Medicine) FCPS (Medicine) Associate professor Dept. of Critical Care Medicine BIRDEM General Hospital Is Sepsis a known
PEDIATRIC SHOCK 10/9/2014. Objectives. What is shock? By the end of this presentation, the learner will be able to:
 PEDIATRIC SHOCK Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CMS, CEN, CNRN, CPNP Education Specialist-LRM Consulting Nashville, TN Objectives By the end of this presentation, the learner will be able to:
PEDIATRIC SHOCK Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CMS, CEN, CNRN, CPNP Education Specialist-LRM Consulting Nashville, TN Objectives By the end of this presentation, the learner will be able to:
Key Points. Angus DC: Crit Care Med 29:1303, 2001
 Sepsis Key Points Sepsis is the combination of a known or suspected infection and an accompanying systemic inflammatory response (SIRS) Severe sepsis is sepsis with acute dysfunction of one or more organ
Sepsis Key Points Sepsis is the combination of a known or suspected infection and an accompanying systemic inflammatory response (SIRS) Severe sepsis is sepsis with acute dysfunction of one or more organ
Pediatric Shock. National Pediatric Nighttime Curriculum Written by Julia M. Gabhart, M.D. Lucile Packard Children s Hospital at Stanford
 Pediatric Shock National Pediatric Nighttime Curriculum Written by Julia M. Gabhart, M.D. Lucile Packard Children s Hospital at Stanford Pre-Topic Questions 1. Why is it important to identify the stage
Pediatric Shock National Pediatric Nighttime Curriculum Written by Julia M. Gabhart, M.D. Lucile Packard Children s Hospital at Stanford Pre-Topic Questions 1. Why is it important to identify the stage
SURVIVING SEPSIS: Early Management Saves Lives
 SURVIVING SEPSIS: Early Management Saves Lives Pat Posa RN, BSN, MSA System Performance Improvement Leader St. Joseph Mercy Health System Ann Arbor, MI Patricia.posa@stjoeshealth.org Objectives a. Understand
SURVIVING SEPSIS: Early Management Saves Lives Pat Posa RN, BSN, MSA System Performance Improvement Leader St. Joseph Mercy Health System Ann Arbor, MI Patricia.posa@stjoeshealth.org Objectives a. Understand
Joel Edminster MD FACEP EMS Live At Night 11/11/2014. Spokane County EMS
 Joel Edminster MD FACEP EMS Live At Night 11/11/2014 Spokane County EMS Objectives Define Sepsis Epidemiology and Relevance Pre-Hospital Impact Making the Diagnosis Appropriate Treatment The term Σήψις
Joel Edminster MD FACEP EMS Live At Night 11/11/2014 Spokane County EMS Objectives Define Sepsis Epidemiology and Relevance Pre-Hospital Impact Making the Diagnosis Appropriate Treatment The term Σήψις
PALS Pulseless Arrest Algorithm.
 PALS Pulseless Arrest Algorithm. Kleinman M E et al. Circulation 2010;122:S876-S908 PALS Bradycardia Algorithm. Kleinman M E et al. Circulation 2010;122:S876-S908 PALS Tachycardia Algorithm. Kleinman M
PALS Pulseless Arrest Algorithm. Kleinman M E et al. Circulation 2010;122:S876-S908 PALS Bradycardia Algorithm. Kleinman M E et al. Circulation 2010;122:S876-S908 PALS Tachycardia Algorithm. Kleinman M
DEFINITION. Imbalance in supply/demand for O2 and nutrients
 NURS 452 SHOCK Outcome Relate the pathophysiology to the clinical manifestations of the different types of shock: cardiogenic, hypovolemic, distributive, and obstructive Compare the collaborative care,
NURS 452 SHOCK Outcome Relate the pathophysiology to the clinical manifestations of the different types of shock: cardiogenic, hypovolemic, distributive, and obstructive Compare the collaborative care,
Cardiovascular Management of Septic Shock
 Cardiovascular Management of Septic Shock R. Phillip Dellinger, MD Professor of Medicine Robert Wood Johnson Medical School/UMDNJ Director, Critical Care Medicine and Med/Surg ICU Cooper University Hospital
Cardiovascular Management of Septic Shock R. Phillip Dellinger, MD Professor of Medicine Robert Wood Johnson Medical School/UMDNJ Director, Critical Care Medicine and Med/Surg ICU Cooper University Hospital
SHOCK. May 12, 2011 Body and Disease
 SHOCK May 12, 2011 Body and Disease Shock Definition of shock Pathophysiology Types of shock Management of shock Shock Definition? Shock What the Duke Community would have experienced if Gordon Hayward
SHOCK May 12, 2011 Body and Disease Shock Definition of shock Pathophysiology Types of shock Management of shock Shock Definition? Shock What the Duke Community would have experienced if Gordon Hayward
Surviving Sepsis Campaign Guidelines 2012 & Update for David E. Tannehill, DO Critical Care Medicine Mercy Hospital St.
 Surviving Sepsis Campaign Guidelines 2012 & Update for 2015 David E. Tannehill, DO Critical Care Medicine Mercy Hospital St. Louis Be appropriately aggressive the longer one delays aggressive metabolic
Surviving Sepsis Campaign Guidelines 2012 & Update for 2015 David E. Tannehill, DO Critical Care Medicine Mercy Hospital St. Louis Be appropriately aggressive the longer one delays aggressive metabolic
McHenry Western Lake County EMS System CE for Paramedics, EMT-B and PHRN s Sepsis Patients. November/December 2017
 McHenry Western Lake County EMS System CE for Paramedics, EMT-B and PHRN s Sepsis Patients November/December 2017 This month we are going to take a look at the patient with Sepsis. Webster s defines septic
McHenry Western Lake County EMS System CE for Paramedics, EMT-B and PHRN s Sepsis Patients November/December 2017 This month we are going to take a look at the patient with Sepsis. Webster s defines septic
Understand the scope of sepsis morbidity and mortality Identify risk factors that predispose a patient to development of sepsis Define and know the
 Understand the scope of sepsis morbidity and mortality Identify risk factors that predispose a patient to development of sepsis Define and know the differences between sepsis, severe sepsis and septic
Understand the scope of sepsis morbidity and mortality Identify risk factors that predispose a patient to development of sepsis Define and know the differences between sepsis, severe sepsis and septic
A Diagnostic Dilemma saved by sound
 A Diagnostic Dilemma saved by sound Dr Syam Ravindranath MBBS DNB, Dr Ash Mukherjee FCEM FACEM We p r e s e n t a d i a g n o s t i c a l l y c h a l l e n g i n g s c e n a r i o in a 59 y e a r old f
A Diagnostic Dilemma saved by sound Dr Syam Ravindranath MBBS DNB, Dr Ash Mukherjee FCEM FACEM We p r e s e n t a d i a g n o s t i c a l l y c h a l l e n g i n g s c e n a r i o in a 59 y e a r old f
Hypotension / Shock. Adult Medical Section Protocols. Protocol 30
 Hypotension / Shock History Blood loss - vaginal or gastrointestinal bleeding, AAA, ectopic Fluid loss - vomiting, diarrhea, fever nfection Cardiac ischemia (M, CHF) Medications Allergic reaction regnancy
Hypotension / Shock History Blood loss - vaginal or gastrointestinal bleeding, AAA, ectopic Fluid loss - vomiting, diarrhea, fever nfection Cardiac ischemia (M, CHF) Medications Allergic reaction regnancy
Rounds in the ICU. Eran Segal, MD Director General ICU Sheba Medical Center
 Rounds in the ICU Eran Segal, MD Director General ICU Sheba Medical Center Real Clinical cases (including our mistakes) Emphasis on hemodynamic monitoring Usually no single correct answer We will conduct
Rounds in the ICU Eran Segal, MD Director General ICU Sheba Medical Center Real Clinical cases (including our mistakes) Emphasis on hemodynamic monitoring Usually no single correct answer We will conduct
DAY1_CARDIOVASCULAR PRACTICE QUESTIONS
 DAY1_CARDIOVASCULAR PRACTICE QUESTIONS 1 P age 1. A 59-year-old male is admitted complaining of chest pain and dyspnea. ST elevation and T-wave inversion were seen on the ECG in V2, V3, and V4. IV thrombolytic
DAY1_CARDIOVASCULAR PRACTICE QUESTIONS 1 P age 1. A 59-year-old male is admitted complaining of chest pain and dyspnea. ST elevation and T-wave inversion were seen on the ECG in V2, V3, and V4. IV thrombolytic
What is. InSpectra StO 2?
 What is InSpectra StO 2? www.htibiomeasurement.com What is InSpectra StO 2? Hemoglobin O 2 saturation is measured in three areas: 1) Arterial (SaO 2, SpO 2 ) Assesses how well oxygen is loading onto hemoglobin
What is InSpectra StO 2? www.htibiomeasurement.com What is InSpectra StO 2? Hemoglobin O 2 saturation is measured in three areas: 1) Arterial (SaO 2, SpO 2 ) Assesses how well oxygen is loading onto hemoglobin
Hypovolemic Shock: Regulation of Blood Pressure
 CARDIOVASCULAR PHYSIOLOGY 81 Case 15 Hypovolemic Shock: Regulation of Blood Pressure Mavis Byrne is a 78-year-old widow who was brought to the emergency room one evening by her sister. Early in the day,
CARDIOVASCULAR PHYSIOLOGY 81 Case 15 Hypovolemic Shock: Regulation of Blood Pressure Mavis Byrne is a 78-year-old widow who was brought to the emergency room one evening by her sister. Early in the day,
Critical Care Treatment Guidelines
 Critical Care Treatment Guidelines West Virginia Office of Emergency Medical Services CCT Guidelines CCT Guidelines TABLE OF CONTENTS Preface Acknowledgments Using the Guidelines INITIAL TREATMENT / UNIVERSAL
Critical Care Treatment Guidelines West Virginia Office of Emergency Medical Services CCT Guidelines CCT Guidelines TABLE OF CONTENTS Preface Acknowledgments Using the Guidelines INITIAL TREATMENT / UNIVERSAL
Printed copies of this document may not be up to date, obtain the most recent version from
 Children s Acute Transport Service Clinical Guidelines Septic Shock Document Control Information Author Claire Fraser P.Ramnarayan Author Position tanp CATS Consultant Document Owner E. Polke Document
Children s Acute Transport Service Clinical Guidelines Septic Shock Document Control Information Author Claire Fraser P.Ramnarayan Author Position tanp CATS Consultant Document Owner E. Polke Document
Acute heart failure in a patient with lower urinary tract infection Case report of an infection-induced Reverse Takotsubo syndrome
 Acute heart failure in a patient with lower urinary tract infection Case report of an infection-induced Reverse Takotsubo syndrome N.Μoschos, A.Dimitra, E.Tsakiri, D.Stavrianakis, A.Nouli CARDIOLOGY DEPARTMENT
Acute heart failure in a patient with lower urinary tract infection Case report of an infection-induced Reverse Takotsubo syndrome N.Μoschos, A.Dimitra, E.Tsakiri, D.Stavrianakis, A.Nouli CARDIOLOGY DEPARTMENT
Objectives. Objectives. Shock. Objectives. Cardiac output. Review of Blood Flow and Perfusion. Review the components of perfusion
 Objectives Shock Review the components of perfusion Cardiac output Perfusion at the capillary level Perfusion and cellular metabolism Aerobic metabolism and energy production Objectives Identify the stages
Objectives Shock Review the components of perfusion Cardiac output Perfusion at the capillary level Perfusion and cellular metabolism Aerobic metabolism and energy production Objectives Identify the stages
Written 01/09/17 Rewritten 3/29/17 for Interior Regional EMS Symposium
 Written 01/09/17 Rewritten 3/29/17 for Interior Regional EMS Symposium MARIA E. MANDICH MD Fairbanks Memorial Hospital Emergency Department Attending Physician Interior Region EMS Council Medical Director
Written 01/09/17 Rewritten 3/29/17 for Interior Regional EMS Symposium MARIA E. MANDICH MD Fairbanks Memorial Hospital Emergency Department Attending Physician Interior Region EMS Council Medical Director
Septic shock. Babak Tamizi Far M.D Isfahan university of medical sciences
 Septic shock Babak Tamizi Far M.D Isfahan university of medical sciences Definitions Used to Describe the Condition of Septic Patients Approximately 750,000 cases of severe sepsis or septic shock occur
Septic shock Babak Tamizi Far M.D Isfahan university of medical sciences Definitions Used to Describe the Condition of Septic Patients Approximately 750,000 cases of severe sepsis or septic shock occur
IDENTIFYING SEPSIS IN THE PREHOSPITAL SETTING
 IDENTIFYING SEPSIS IN THE PREHOSPITAL SETTING Christopher Hunter, MD, PhD, FACEP Director, Health Services Department Associate Medical Director, Orange County EMS System Medical Director, Orlando Health
IDENTIFYING SEPSIS IN THE PREHOSPITAL SETTING Christopher Hunter, MD, PhD, FACEP Director, Health Services Department Associate Medical Director, Orange County EMS System Medical Director, Orlando Health
核心課程編號 :E14 急診部何政軒醫師 / 施長志醫師 104 年 12 月 15 日第四版
 核心課程編號 :E14 休克 急診部何政軒醫師 / 施長志醫師 104 年 12 月 15 日第四版 學習目標 知識 PGY 休克的定義 Definition of Shock The clinical syndrome that results from inadequate tissue perfusion. The diagnostic essentials of shock include:
核心課程編號 :E14 休克 急診部何政軒醫師 / 施長志醫師 104 年 12 月 15 日第四版 學習目標 知識 PGY 休克的定義 Definition of Shock The clinical syndrome that results from inadequate tissue perfusion. The diagnostic essentials of shock include:
9/25/2017. Nothing to disclose
 Nothing to disclose Jessie O Neal, PharmD, BCCCP Critical Care Clinical Pharmacist University of New Mexico Hospital New Mexico Society of Health-System Pharmacists 2017 Balloon Fiesta Symposium Explain
Nothing to disclose Jessie O Neal, PharmD, BCCCP Critical Care Clinical Pharmacist University of New Mexico Hospital New Mexico Society of Health-System Pharmacists 2017 Balloon Fiesta Symposium Explain
Nothing to disclose 9/25/2017
 Jessie O Neal, PharmD, BCCCP Critical Care Clinical Pharmacist University of New Mexico Hospital New Mexico Society of Health-System Pharmacists 2017 Balloon Fiesta Symposium Nothing to disclose 1 Explain
Jessie O Neal, PharmD, BCCCP Critical Care Clinical Pharmacist University of New Mexico Hospital New Mexico Society of Health-System Pharmacists 2017 Balloon Fiesta Symposium Nothing to disclose 1 Explain
CrackCast Episode 6 Shock
 CrackCast Episode 6 Shock Episode overview: 1) List, define and explain the 5 causes of shock 2) What is the utility of lactate and base deficit in the management of shock? 3) Define: SIRS, Sepsis, Severe
CrackCast Episode 6 Shock Episode overview: 1) List, define and explain the 5 causes of shock 2) What is the utility of lactate and base deficit in the management of shock? 3) Define: SIRS, Sepsis, Severe
Bachelor of Chinese Medicine Shock
 BCM Year 2 Dr. Irene Ng Jan 28, 2003 9:30 am 1:00 pm Rm 004 UPB Bachelor of Chinese Medicine 2002 2003 Shock Learning objectives Be able to: know the definition of shock know the classification and causes
BCM Year 2 Dr. Irene Ng Jan 28, 2003 9:30 am 1:00 pm Rm 004 UPB Bachelor of Chinese Medicine 2002 2003 Shock Learning objectives Be able to: know the definition of shock know the classification and causes
Taking the shock factor out of shock
 Taking the shock factor out of shock Julie Antonellis, BS, LVT, VTS (ECC) Northern Virginia Regional Director for the VALVT Technician Supervisor VCA Animal Emergency Critical Care Business owner Antonellis
Taking the shock factor out of shock Julie Antonellis, BS, LVT, VTS (ECC) Northern Virginia Regional Director for the VALVT Technician Supervisor VCA Animal Emergency Critical Care Business owner Antonellis
Shock. William Schecter, MD
 Shock William Schecter, MD The Cell as a furnace O 2 1 mole Glucose Cell C0 2 ATP 38 moles H 2 0 Shock = Inadequate Delivery of 02 and Glucose to the Cell 0 2 Cell ATP 2 moles Lactic Acid Treatment of
Shock William Schecter, MD The Cell as a furnace O 2 1 mole Glucose Cell C0 2 ATP 38 moles H 2 0 Shock = Inadequate Delivery of 02 and Glucose to the Cell 0 2 Cell ATP 2 moles Lactic Acid Treatment of
Acute Respiratory Distress
 Acute Respiratory Distress Respiratory Distress: Amos Charles, MD Clinical Associate Professor of Medicine Warren Alpert School of Medicine of the Brown University Providence Rhode Island. Waleed Ibrahim-Ali
Acute Respiratory Distress Respiratory Distress: Amos Charles, MD Clinical Associate Professor of Medicine Warren Alpert School of Medicine of the Brown University Providence Rhode Island. Waleed Ibrahim-Ali
Sepsis Update: Focus on Early Recognition and Intervention. Disclosures
 Sepsis Update: Focus on Early Recognition and Intervention Jessie Roske, MD October 2017 Disclosures I have no actual or potential conflict of interest in relation to this program/presentation. I will
Sepsis Update: Focus on Early Recognition and Intervention Jessie Roske, MD October 2017 Disclosures I have no actual or potential conflict of interest in relation to this program/presentation. I will
เอกราช อร ยะช ยพาณ ชย
 25 September 2017 เอกราช อร ยะช ยพาณ ชย Heart Failure and Transplant Cardiology aekarach.a@chula.ac.th Presentation at 1 Agenda Physiology of the heart Pathophysiology of shock Pathophysiology of heart
25 September 2017 เอกราช อร ยะช ยพาณ ชย Heart Failure and Transplant Cardiology aekarach.a@chula.ac.th Presentation at 1 Agenda Physiology of the heart Pathophysiology of shock Pathophysiology of heart
CASE-BASED SMALL GROUP DISCUSSION SESSION 6 MHD I. October 14, 2015
 Session 6, MHD I, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION SESSION 6 MHD I October 14, 2015 Helpful Resources McPhee, SJ, Hammer GD. Pathophysiology of Disease: An Introduction to Clinical
Session 6, MHD I, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION SESSION 6 MHD I October 14, 2015 Helpful Resources McPhee, SJ, Hammer GD. Pathophysiology of Disease: An Introduction to Clinical
Instruct patient and caregivers: Need for constant monitoring Potential complications of drug therapy
 Assessment Prior to administration: Assess patient for chest pain, dysrhythmias, and vital signs (initially and throughout therapy) Obtain complete medical history, including allergies, especially heart
Assessment Prior to administration: Assess patient for chest pain, dysrhythmias, and vital signs (initially and throughout therapy) Obtain complete medical history, including allergies, especially heart
10/25/2017. No financial disclosures. I am NOT a scorpiontologist or jelly fishologist. Jeremy Gonda MD
 10/25/2017 Jeremy Gonda MD Emergency Medicine & Critical Care Renown, REP, Care Flight No financial disclosures I am NOT a scorpiontologist or jelly fishologist 1 10/25/2017 Initial insult (may be minor)
10/25/2017 Jeremy Gonda MD Emergency Medicine & Critical Care Renown, REP, Care Flight No financial disclosures I am NOT a scorpiontologist or jelly fishologist 1 10/25/2017 Initial insult (may be minor)
SHOCK. Pathophysiology
 SHOCK Dr. Ahmed Saleem FICMS TUCOM / 3rd Year / 2015 Shock is the most common and therefore the most important cause of death of surgical patients. Death may occur rapidly due to a profound state of shock,
SHOCK Dr. Ahmed Saleem FICMS TUCOM / 3rd Year / 2015 Shock is the most common and therefore the most important cause of death of surgical patients. Death may occur rapidly due to a profound state of shock,
ACG Clinical Guideline: Management of Acute Pancreatitis
 ACG Clinical Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG 1, John Baillie, MB, ChB, FRCP, FACG 2, John DeWitt, MD, FACG 3 and Santhi Swaroop Vege, MD, FACG 4 1 State University
ACG Clinical Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG 1, John Baillie, MB, ChB, FRCP, FACG 2, John DeWitt, MD, FACG 3 and Santhi Swaroop Vege, MD, FACG 4 1 State University
Agenda เอกราช อร ยะช ยพาณ ชย. - Cardiac physiology - Pathophysiology of shock - Pathophysiology of heart failure 9/6/2016
 6 September 2016 เอกราช อร ยะช ยพาณ ชย Heart Failure and Transplant Cardiology aekarach.a@chula.ac.th Agenda - Cardiac physiology - Pathophysiology of shock - Pathophysiology of heart failure http://fullpulse.weebly.com/conversation
6 September 2016 เอกราช อร ยะช ยพาณ ชย Heart Failure and Transplant Cardiology aekarach.a@chula.ac.th Agenda - Cardiac physiology - Pathophysiology of shock - Pathophysiology of heart failure http://fullpulse.weebly.com/conversation
Acute Liver Failure: Supporting Other Organs
 Acute Liver Failure: Supporting Other Organs Michael A. Gropper, MD, PhD Professor of Anesthesia and Physiology Director, Critical Care Medicine University of California San Francisco Acute Liver Failure
Acute Liver Failure: Supporting Other Organs Michael A. Gropper, MD, PhD Professor of Anesthesia and Physiology Director, Critical Care Medicine University of California San Francisco Acute Liver Failure
Resuscitation Before Emergency Surgeries FEIRAN LOU SUNY DOWNSTATE MEDICAL CENTER KINGS COUNTY HOSPITAL
 Resuscitation Before Emergency Surgeries FEIRAN LOU SUNY DOWNSTATE MEDICAL CENTER KINGS COUNTY HOSPITAL Case 73 yo woman h/o HTN three days abdominal pain and nausea. The pain was diffuse, cramp-like,
Resuscitation Before Emergency Surgeries FEIRAN LOU SUNY DOWNSTATE MEDICAL CENTER KINGS COUNTY HOSPITAL Case 73 yo woman h/o HTN three days abdominal pain and nausea. The pain was diffuse, cramp-like,
ADVANCES IN BIOMARKER TESTING FOR SEPSIS AND BACTERIAL INFECTIONS
 ADVANCES IN BIOMARKER TESTING FOR SEPSIS AND BACTERIAL INFECTIONS ERIC H GLUCK MD JD FCCP FCCM DIRECTOR OF CRITICAL SERVICES SWEDISH COVENANT HOSPTIAL DISCLOSURES: Speaking engagements and consulting:
ADVANCES IN BIOMARKER TESTING FOR SEPSIS AND BACTERIAL INFECTIONS ERIC H GLUCK MD JD FCCP FCCM DIRECTOR OF CRITICAL SERVICES SWEDISH COVENANT HOSPTIAL DISCLOSURES: Speaking engagements and consulting:
University of Wisconsin - Madison Cardiovascular Medicine Fellowship Program UW CICU Rotation Goals and Objectives
 Background: The field of critical care cardiology has evolved considerably over the past 2 decades. Contemporary critical care cardiology is increasingly focused on the management of patients with advanced
Background: The field of critical care cardiology has evolved considerably over the past 2 decades. Contemporary critical care cardiology is increasingly focused on the management of patients with advanced
Advanced Emergency Medical Care Assistant Examination
 Advanced Emergency Medical Care Assistant Examination Study Guide and Sample Questions Version 4.0 November 2016 Emergency Health Services Branch Ministry of Health and Long-Term Care To all users of this
Advanced Emergency Medical Care Assistant Examination Study Guide and Sample Questions Version 4.0 November 2016 Emergency Health Services Branch Ministry of Health and Long-Term Care To all users of this
SMALL GROUP DISCUSSION
 MHD II, Session 1 Student Copy Page 1 SMALL GROUP DISCUSSION MHD II Session 1 Gastroinestinal Monday, January 9, 2017 STUDENT COPY MHD II, Session 1 Student Copy Page 2 CASE 1 CHIEF CONCERN: "I'm passing
MHD II, Session 1 Student Copy Page 1 SMALL GROUP DISCUSSION MHD II Session 1 Gastroinestinal Monday, January 9, 2017 STUDENT COPY MHD II, Session 1 Student Copy Page 2 CASE 1 CHIEF CONCERN: "I'm passing
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University
 Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
Shock: The Physiologic Perspective
 Shock: The Physiologic Perspective Bryan E. Bledsoe, DO, FACEP, FAAEM Professor of Emergency Medicine University of Nevada, Reno School of Medicine University of Nevada, Las Vegas School of Medicine Las
Shock: The Physiologic Perspective Bryan E. Bledsoe, DO, FACEP, FAAEM Professor of Emergency Medicine University of Nevada, Reno School of Medicine University of Nevada, Las Vegas School of Medicine Las
Introduction. Invasive Hemodynamic Monitoring. Determinants of Cardiovascular Function. Cardiovascular System. Hemodynamic Monitoring
 Introduction Invasive Hemodynamic Monitoring Audis Bethea, Pharm.D. Assistant Professor Therapeutics IV January 21, 2004 Hemodynamic monitoring is necessary to assess and manage shock Information obtained
Introduction Invasive Hemodynamic Monitoring Audis Bethea, Pharm.D. Assistant Professor Therapeutics IV January 21, 2004 Hemodynamic monitoring is necessary to assess and manage shock Information obtained
PALS PRETEST. PALS Pretest
 PALS PRETEST 1. A child with a fever, immune system compromise, poor perfusion and hypotension is most likely to be experiencing which type of shock A. cardiogenic B. Neurogenic C. Septic D. Hypovolemic
PALS PRETEST 1. A child with a fever, immune system compromise, poor perfusion and hypotension is most likely to be experiencing which type of shock A. cardiogenic B. Neurogenic C. Septic D. Hypovolemic
