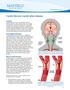
O ne quarter of strokes occur in the posterior
|
|
|
- Paul Barker
- 6 years ago
- Views:
Transcription
1 586 PAPER Vertebral artery origin angioplasty and primary stenting: safety and restenosis rates in a prospective series G C Cloud, F Crawley, A Clifton, DJHMcCabe, M M Brown, H S Markus... See end of article for authors affiliations... Correspondence to: Professor Hugh Markus, Division of Clinical Neuroscience, St George s Hospital Medical School, Cranmer Terrace, London SW17 ORE, UK; h.markus@sghms.ac.uk Received 30 July 2002 In revised form 3 December 2002 Accepted 11 January J Neurol Neurosurg Psychiatry 2003;74: Objectives: To report a single centre ongoing experience of endovascular treatment for atherosclerotic vertebral artery origin stenosis in a series of symptomatic patients, with follow up imaging to determine the incidence of restenosis. Methods: 14 patients with vertebral artery origin stenosis on catheter angiography were treated. Angioplasty without stenting was undertaken in the first four patients, all of whom had follow up catheter angiography at one year. Subsequently, patients were treated by primary stenting and followed up with colour Doppler ultrasound examination. Results: The procedure was technically successful in all treated arteries, with no immediate complications. The degree of stenosis was reduced from (mean (SD)) 73 (18)% before treatment to 21 (26)% immediately after treatment in the angioplasty alone group (p = 0.059). In the primary stenting patients, the severity of stenosis was reduced from 82 (8)% to 13 (13)% immediately after treatment (p < 0.001). Restenosis to 70% or greater occurred at one year in all four patients initially treated by angioplasty without stenting. One patient subsequently developed further symptoms and was retreated by stenting. One of the 10 patients treated by primary stenting developed restenosis. None of the remaining patients had further posterior circulation ischaemic symptoms during a mean follow up period of 33.6 months (range 1 to 72 months). Conclusions: Restenosis occurs often after vertebral artery origin balloon angioplasty without stenting but is uncommon after stenting. Primary stenting is therefore recommended to maintain patency at this site, and had a low complication rate in this series. O ne quarter of strokes occur in the posterior circulation. 12 Atherosclerotic stenosis of the vertebral artery most commonly occurs at the origin, 3 and embolisation from such lesions is an important cause of posterior circulation stroke. 4 6 Approximately one in five posterior circulation strokes occurs in the setting of extracranial vertebral artery stenosis, 47 but the optimal management of such patients is unclear. Carotid endarterectomy is widely used for the treatment of extracranial symptomatic carotid artery stenosis, but vertebral artery stenosis is often managed by medical treatment alone. Surgery for extracranial vertebral artery stenosis, in the form of endarterectomy and vessel revascularisation (bypass or transposition), has been reported to be associated with good outcome and low mortality However, such operations are not widely undertaken because it is difficult to gain access to the vertebral artery at its origin. Percutaneous endovascular treatment of vertebral artery stenosis is much less invasive than surgery and could prevent recurrent embolic or haemodynamic symptoms in this patient group. The carotid and vertebral artery transluminal angioplasty study (CAVATAS) showed a similar risk of stroke or death with endovascular treatment and surgery within 30 days after the procedure, in patients with severe symptomatic carotid artery stenosis. 12 The two treatment modes also appeared equally effective at preventing ipsilateral stroke, or death and disabling stroke, in any vascular territory for up to three years after randomisation. To date, at least 5210 carotid angioplasty and stenting procedures in 4757 patients have been reported, with an overall technical success rate of 98.4% and a combined rate of minor and major stroke and procedure related death of 5%. 13 In contrast, there are little over 100 reported cases of endovascular intervention with primary stenting for extracranial vertebral artery stenosis. These early reports of selected nonrandomised cases have shown high technical success rates, comparable to extracranial carotid stenting, with a complication rate of minor stroke or transient ischaemic attack (TIA) of only 3% and no related deaths during short term follow up In the vertebral stenosis arm of the CAVATAS study, very few patients were randomised and the data have not been analysed to date. We report the outcome after endovascular treatment for symptomatic vertebral artery stenosis in 14 patients who were followed up prospectively at a single centre between 1992 and METHODS Patient selection and characteristics Fourteen patients underwent vertebral balloon angioplasty (PTA) and stenting between 1992 and 2001 at Atkinson Morley s Hospital (St George s Hospital NHS Trust). All but one of the patients had symptomatic posterior circulation TIA or stroke, usually with recurrent symptoms despite maximum antiplatelet treatment. The antiplatelet regimen used was aspirin monotherapy in the earlier stages of the study, and combination treatment with aspirin and dipyradimole in the later stages. An episode of posterior circulation ischaemia was defined as the sudden onset of two or more symptoms attributable to the posterior circulation which, after adequate investigation, were presumed to be of a non-traumatic vascular origin. Vertebral stenosis was usually detected by colour Doppler ultrasound or magnetic resonance angiography, and confirmed by intra-arterial catheter angiography before any endovascular intervention. In the one patient who had had symptoms attributable to anterior circulation ischaemia, computed tomography of the brain showed a left parietal infarct, and catheter angiography showed bilateral internal carotid artery occlusion, a normal
2 Vertebral artery origin angioplasty and stenting 587 Table 1 Characteristics of patients treated with vertebral percutaneous transluminal angioplasty or stenting, and immediate angiographic result Patient Sex Age (years) Presenting symptom CT/MRI findings right vertebral artery, 80% stenosis to the origin of the left vertebral artery, and patent posterior communicating arteries bilaterally. Left vertebral PTA was done in order to improve cerebral blood flow in both the anterior and the posterior circulations. Table 1 shows the clinical presentation and angiographic findings of the patients undergoing endovascular intervention. The mean age of the group was 56 years (range 39 to 71). All subjects were white and nine were male. Seven were hypertensive, defined as having a history of raised blood pressure and on antihypertensive drug treatment or with a blood pressure of > 160 mm Hg systolic or 95 mm Hg diastolic. 19 Eleven had hypercholesterolaemia, defined as a fasting cholesterol level of more than 6 mmol/l or were already being treated with lipid lowering agents. These definitions used to categorise patients as hypertensive and hypercholesterolaemic were taken from the original CAVATAS criteria and were used throughout the series of patients for consistency. Eleven patients were current or ex-smokers. Two suffered from ischaemic heart disease. Two were diabetic. All were in sinus rhythm, with no cardioembolic source for their stroke. Seven had concomitant carotid artery stenosis of > 50%. All patients were on treatment with 75 to 300 mg of aspirin daily. Two patients were also taking 200 mg of dipyramidole modified release twice daily, and one was also on treatment with warfarin. Five patients were randomised to receive endovascular treatment in CAVATAS, while the remainder were treated according to physicians consensus of best treatment. In the latter group, all patients had either recurrent symptoms in the vascular territory of a significantly stenosed vertebral artery (70% stenosis or more), or had posterior circulation ischaemic symptoms in the presence of a less severe stenosis occurring in a dominant vertebral artery (the other being atretic or occluded), with no patent posterior communicating artery on the side of the stenosis seen on catheter angiography. CAVATAS received approval from the local hospital ethics committee, and written informed consent was obtained from all patients by the treating neuroradiologist. The first five patients underwent follow up catheter angiography at one year. More recently treated patients were followed up with vertebral artery colour Doppler ultrasound examination. If the peak systolic velocity in the vertebral artery was recorded as being greater than 0.8 m/s, catheter angiography was then done. Restenosis was defined as an increase in stenosis at one year to more than 50%, using the method described below. Patients were followed up by a neurologist immediately after Angiographic findings pretreatment the procedure, at one and six months after the procedure, and then at annual intervals. PTA procedure All endovascular procedures were undertaken under local anaesthesia by a single interventional neuroradiologist (AC). The degree of vertebral artery stenosis was determined from the catheter angiogram using the following formula: % stenosis = 100 (1 A/V) PTA (stent) result 1 M 71 Posterior circulation TIA Bilateral cerebellar infarcts LV: 80% stenosis 0% stenosis 2 F 67 Posterior circulation TIA Normal LV: 70% stenosis 0% stenosis 3 M 54 Anterior circulation stroke Left parietal infarct LV: 80%stenosis 53% stenosis 4 F 63 Posterior circulation stroke Left PICA infarct RV: 50% stenosis 32% stenosis 5 F 61 Posterior circulation stroke Normal LV: 80% stenosis 0% stenosis (stent) 6 M 41 Posterior circulation stroke Right medullary infarct, left PCA infarct RV: 80% stenosis 10% stenosis (stent) 7 M 39 Posterior circulation stroke Right PICA artery infarct LV:70% stenosis 20% stenosis (stent) 8 F 44 Posterior circulation stroke Bilateral PCA infarcts LV:80% stenosis 40% stenosis (stent) 9 M 59 Posterior circulation stroke Right pontine infarct RV: 90% stenosis 10% stenosis (stent) 10 M 66 Posterior circulation TIA Left pontine,bilateral cerebellar and RV:70% stenosis 0%stenosis (stent) occipital infarcts 11 M 62 Posterior circulation TIAs Old right hemispheric infarct LV: 70% stenosis 0% stenosis (stent) 12 M 48 Posterior circulation TIAs Normal LV: 80% stenosis 0% stenosis (stent) R mid SCA: 90% stenosis 50% (PTA only) 13 M 67 Posterior circulation stroke Right occipital infarct RV: 90% stenosis 20% stenosis (stent) 14 F 45 Posterior circulation TIAs Normal LV 90% stenosis 20% stenosis (stent) F, female; ICA, internal carotid artery; LV, left vertebral; M, male; PCA, posterior cerebral artery; PICA, posterior inferior cerebellar artery; R, right; RV, right vertebral; SCA, subclavian artery; TIA, transient ischaemic attack. where A is the diameter of the residual lumen at the point of maximum stenosis, and V is the width of disease free distal vertebral artery at the point where the walls were approximately parallel. This is similar to the method used to measure carotid stenosis in the North American symptomatic carotid endarterectomy trial. 20 A 6 F sheath was inserted percutaneously under local anaesthesia into the right femoral artery, or, in two of the 14 patients, through a brachial puncture. A 6 F guiding catheter was then inserted into the subclavian artery over an exchange wire. Under roadmapping and after intravenous anticoagulation with heparin, the stenosis was crossed with a inch (0.35 mm) wire. In the first four patients treated by simple balloon angioplasty, a 3 4 mm angioplasty balloon (with a diameter less than that of the distal disease-free vertebral artery) was then placed across the stenosis and inflated to 8 atm using a standard pressure inflation device. Inflation was maintained for about 15 seconds. The balloon was deflated and the degree of residual stenosis was viewed angiographically. The dilatation was repeated up to three times. In the four patients treated by balloon angioplasty alone, 300 mg of aspirin daily was given for at least one week before the procedure and continued indefinitely after discharge. In the 11 patients in whom a stent was deployed, a guiding catheter was exchanged into the subclavian artery. Through this guiding catheter, a balloon expandable stent loaded over a inch wire (Medtronic TM AVE INX, or previously S670 and AVE coronary stents) was introduced through the guiding catheter. After guiding the wire through the stenosis on roadmapping, the stent was placed (still under roadmapping) across the stenosis with the proximal end positioned at the origin of the vertebral artery from the subclavian artery. The stent was deployed at the same time as the stenosis was dilated by inflation of the angioplasty balloon. This procedure was also done under anticoagulation with heparin, which was continued for a further 24 hours afterwards. All the patients
3 588 Cloud, Crawley, Clifton, et al Table 2 Angiographic findings of per cent stenosis before percutaneous transluminal angioplasty (PTA), immediately after and at one year follow up Patient and vertebral artery Pre-PTA (%) PTA result (%) 1: left : left : left : right * One follow up (%) *Patient developed symptoms and was retreated using PTA with stenting. were treated with 300 mg aspirin daily, and a second antiplatelet agent (either dipyramidole 100 mg three times daily plus dipyramidole MR 200 mg twice daily, or clopidigrel 75 mg once a day) was routinely prescribed for one week before stenting and for one to three months after the procedure. Thereafter patients were maintained on aspirin monotherapy unless they developed further symptoms during follow up. RESULTS Balloon angioplasty alone group The first four patients treated with simple balloon angioplasty were followed up for a mean of 68.5 months (range 60 to 76). Vessel dilatation was achieved in all patients, with a mean improvement in stenosis from 73 (18)% before treatment to 21 (26)% after treatment (p = 0.059; paired t test). None of the patients had a major complication during or immediately after PTA, and none had a TIA or stroke within 30 days of the procedure. One patient had a brachial haematoma which resolved spontaneously. Follow up catheter angiography at one year showed restenosis of the PTA site in all patients, with a mean degree stenosis at one year of 71% (table 2), although all the patients remained asymptomatic at that time (fig 1). During further follow up, one patient had a posterior circulation TIA 18 months after the initial PTA. This patient was retreated with vertebral artery primary stenting with an excellent anatomical result (fig 2). The patient remains asymptomatic, and colour Doppler ultrasound has not shown any restenosis five years after stent insertion. The three other patients treated by simple balloon angioplasty subsequently had no further symptoms of posterior circulation ischaemia. However, two of the patients died during follow up one died five years after the procedure from ischaemic heart disease and the other, more than five years after the procedure from pneumonia. Primary stenting group Ten patients (Nos 5 14) were treated by primary stenting and have been followed up for a mean of 19.7 months (range 1 to 48). All stenoses were treated successfully, with a mean improvement in angiographic stenosis severity from 82 (8)% before treatment to 13 (13)% after treatment (p < 0.001; paired t test). One patient experienced two posterior circulation TIAs, each lasting less than five minutes, 72 hours after stenting. Thus the risk of TIA after stenting in this series was 20%. There were no other immediate or early complications. Follow up colour Doppler ultrasound examination showed evidence of restenosis in only one case, six months after the procedure, which was found to be a 55% stenosis on catheter angiography. The patient remained asymptomatic and subsequent colour Doppler ultrasound examinations, including the latest scan done three years after stenting, have shown normal velocities. None of the stented patients has reported posterior circulation stroke symptoms during the prospective follow up. Two patients had right middle cerebral Figure 1 Digital subtraction angiograms in a patient showing (A) severe vertebral artery origin stenosis before treatment, (B) successful vessel dilatation immediately after balloon angioplasty, and (C) severe restenosis at follow up angiography one year later. artery territory strokes, six and 18 months, respectively, after stenting. Both events were attributable to coexistent carotid disease. One patient died as a result of the stroke. Another
4 Vertebral artery origin angioplasty and stenting 589 Figure 2 (A) Digital subtraction angiogram showing vertebral artery origin restenosis 18 months after initial angioplasty treatment, and (B) successful vessel dilatation after repeat vertebral artery angioplasty and insertion of a stent. patient with a history of ischaemic heart disease died five months after the procedure from myocardial infarction. DISCUSSION This series shows that balloon angioplasty and stenting can both be successfully and safely undertaken in individuals with atherosclerotic vertebral artery origin stenosis with a very low complication rate. None of our patients developed a stroke or died within 30 days of the procedure and none had a posterior circulation stroke during follow up. However, restenosis after balloon angioplasty had occurred in all four patients treated without stenting by one year. In contrast, only one of 11 arteries in which a stent was deployed showed restenosis over an average of 20 months of follow up. In addition, primary stenting resulted in a greater initial improvement in the degree of stenosis in comparison with balloon angioplasty alone. Although the balloon angioplasty alone and primary stenting groups were assessed for restenosis using different imaging methods, good views of the vertebral artery origin stents were obtained with colour Doppler ultrasound in all patients during the follow up. The duration of follow up differed in the two groups, making direct comparisons difficult, but the results nevertheless suggest that stenting may have better long term results. The rate of restenosis after endovascular treatment of vertebral artery stenosis varies between series. Storey et al reported that all three patients who underwent vertebral PTA developed symptomatic restenosis within three months. 21 Stenting was subsequently undertaken and follow up catheter angiography in two of these patients showed no restenosis three months and one year after stent insertion. Higashida et al used a combination of Doppler ultrasound, magnetic resonance angiography, and catheter angiography to follow up patients after proximal vertebral artery PTA and showed restenosis in only three of 34 patients (9%) in their series. 22 However, the proportion of patients who had vertebral artery origin stenosis rather than more distal vessel disease was not specified in that series. Chastain et al have followed up the largest reported series of patients after extracranial vertebral artery stent placement for the treatment of symptomatic (> 60%) vertebral artery stenosis. 14 Forty four of 49 patients underwent angiographic follow up at six months, and 48 of the 55 vessels treated (87%) had involvement of either the origin or proximal extracranial vertebral artery. A moderate degree of restenosis (27.3 (19.6)%) was seen in five vessels that is, in 10% of treated vessels. These results are in keeping with results of our series, with a low restenosis rate after primary stenting for vertebral artery origin stenosis. Our experience suggests that the outcome after treatment of vertebral artery origin stenosis is similar to that seen after endovascular treatment of renal artery ostial stenosis. Conventional angioplasty in the latter group has a high failure rate owing to elastic recoil and the condition is better managed by stenting. 23 The results of our case series suggest that, from a technical viewpoint, primary stenting for vertebral artery atherosclerotic stenosis at the vessel origin has a high success rate and a low complication rate. In the light of the advances in secondary preventive treatment for stroke patients over the past decade, data from well designed randomised clinical trials are required to compare the outcome after endovascular treatment with best medical care alone in this patient population. Before a definitive trial, further data from an intermediate sized pilot study are required to determine sample size calculations. ACKNOWLEDGEMENTS This research was partly funded by grants from the British Heart Foundation, the NHS Management Executive, and the Stroke Association. The ultrasound laboratory was established with a grant from the Welcome Trust. GCC is a Stroke Association clinical research fellow. Diana Colquhoun assisted with the ultrasound examinations.... Authors affiliations G C Cloud, H S Markus, Division of Clinical Neuroscience, St George s Hospital Medical School, London SW17 0RE, UK A Clifton, Department of Neuroradiology, Atkinson Morley s Hospital, London SW20 0NE F Crawley, D J H McCabe, M M Brown, Institute of Neurology, University College London, London WC1N 3BG Competing interests: MMB has received travel reimbursements for attending conferences from Boston Scientific and research grant funding, speakers fees and educational fees from Sanofi-Synthelabo. None of the other authors has competing interest to declare. REFERENCES 1 Bamford J, Sandercock P, Dennis M, et al. Classification and natural history of clinically identifiable subtypes of cerebral infarction. Lancet 1991;337: Bogousslavsky J, van Melle G, Regli F. The Lausanne Stroke Registry: analysis of 1000 consecutive patients with first stroke. Stroke 1988;19:
5 590 Cloud, Crawley, Clifton, et al 3 Hass WK, Fields WS, North RR, et al. Joint study of extracranial arterial occlusion. II. Arteriography, techniques, sites, and complications. JAMA 1968;203: Caplan LR, Amarenco P, Rosengart A, et al. Embolism from vertebral artery origin occlusive disease. Neurology 1992;42: Koroshetz WJ, Ropper AH. Artery-to-artery embolism causing stroke in the posterior circulation. Neurology 1987;37: Pessin MS, Daneault N, Kwan ES, et al. Local embolism from vertebral artery occlusion. Stroke 1988;19: Wityk RJ, Chang HM, Rosengart A, et al. Proximal extracranial vertebral artery disease in the New England Medical Center Posterior Circulation Registry. Arch Neurol 1998;55: Berguer R. Vertebrobasilar ischaemia: indications, techniques, and results of surgical repair. In: Rutherford RB, ed. Vascular surgery, 5th ed. Philadelphia: WB Saunders Co, 2000: Deriu GP, Ballotta E, Franceschi L, et al. Surgical management of extracranial vertebral artery occlusive disease. J Cardiovasc Surg (Torino) 1991;32: Edwards WH, Mulherin JL. The surgical reconstruction of the proximal subclavian and vertebral artery. J Vasc Surg 1985;2: Spetzler RF, Hadley MN, Martin NA, et al. Vertebrobasilar insufficiency. Part 1. Microsurgical treatment of extracranial vertebrobasilar disease. J Neurosurg 1987;66: Trial Participants. Endovascular versus surgical treatment in patients with carotid stenosis in the carotid and vertebral artery transluminal angioplasty study (CAVATAS): a randomised trial. Lancet 2001;357: Wholey MH, Wholey M, Mathias K, et al. Global experience in cervical carotid artery stent placement. Cathet Cardiovasc Intervent 2000;50: Chastain HD, Campbell MS, Iyer S, et al. Extracranial vertebral artery stent placement: in-hospital and follow-up results. J Neurosurg 1999;91: Jenkins JS, White CJ, Ramee SR, et al. Vertebral artery stenting. Cathet Cardiovasc Intervent 2001;54: Malek AM, Higashida RT, Phatouros CC, et al. Treatment of posterior circulation ischemia with extracranial percutaneous balloon angioplasty and stent placement. Stroke 1999;30: Piotin M, Spelle L, Martin JB, et al. Percutaneous transluminal angioplasty and stenting of the proximal vertebral artery for symptomatic stenosis. Am J Neuroradiol 2000;21: Mukherjee D, Roffi M, Kapadia SR, et al. Percutaneous intervention for symptomatic vertebral artery stenosis using coronary stents. J Invasive Cardiol 2001;13: WHO Subcommittee. Summary of 1993 World Health Organisation International Society of Hypertension guidelines for the management of mild hypertension. Subcommittee of WHO/ISH mild hypertension liaison committee. BMJ 1993;307: Trial Collaborators. Beneficial effect of carotid endarterectomy in symptomatic patients with high-grade carotid stenosis. North American symptomatic carotid endarterectomy trial collaborators. N Engl J Med 1991;325: Storey GS, Marks MP, Dake M, et al. Vertebral artery stenting following percutaneous transluminal angioplasty. Technical note. J Neurosurg 1996;84: Higashida RT, Tsai FY, Halbach VV, et al. Transluminal angioplasty for atherosclerotic disease of the vertebral and basilar arteries. J Neurosurg 1993;78: Van De Ven PJ, Beutler JJ, Kaatee R, et al. Transluminal vascular stent for ostial atherosclerotic renal artery stenosis. Lancet 1995;346: J Neurol Neurosurg Psychiatry: first published as /jnnp on 1 May Downloaded from on 9 May 2018 by guest. Protected by copyright.
Subclavian and Vertebral Artery Angioplasty - Vertebro-basilar Insufficiency: Clinical Aspects and Diagnosis
 HOSPITAL CHRONICLES 2008, 3(3): 136 140 ORIGINAL ARTICLE Subclavian and Vertebral Artery Angioplasty - Vertebro-basilar Insufficiency: Clinical Aspects and Diagnosis Antonios Polydorou, MD Hemodynamic
HOSPITAL CHRONICLES 2008, 3(3): 136 140 ORIGINAL ARTICLE Subclavian and Vertebral Artery Angioplasty - Vertebro-basilar Insufficiency: Clinical Aspects and Diagnosis Antonios Polydorou, MD Hemodynamic
Advances in the treatment of posterior cerebral circulation symptomatic disease
 Advances in the treatment of posterior cerebral circulation symptomatic disease Athanasios D. Giannoukas MD, MSc(Lond.), PhD(Lond.), FEBVS Professor of Vascular Surgery Faculty of Medicine, School of Health
Advances in the treatment of posterior cerebral circulation symptomatic disease Athanasios D. Giannoukas MD, MSc(Lond.), PhD(Lond.), FEBVS Professor of Vascular Surgery Faculty of Medicine, School of Health
Corporate Medical Policy
 Corporate Medical Policy Endovascular Therapies for Extracranial Vertebral Artery Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endovascular_therapies_for_extracranial_vertebral_artery_disease
Corporate Medical Policy Endovascular Therapies for Extracranial Vertebral Artery Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endovascular_therapies_for_extracranial_vertebral_artery_disease
CAROTID ARTERY ANGIOPLASTY
 CAROTID ARTERY ANGIOPLASTY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage Guideline
CAROTID ARTERY ANGIOPLASTY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage Guideline
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine
 Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
Stent placement for vertebral artery occlusive disease: preliminary clinical experience
 Neurosurg Focus 5 (4):Article 15, 1998 Stent placement for vertebral artery occlusive disease: preliminary clinical experience Richard D. Fessler, M.D., Ajay K. Wakhloo, M.D., Ph.D., Giuseppe Lanzino,
Neurosurg Focus 5 (4):Article 15, 1998 Stent placement for vertebral artery occlusive disease: preliminary clinical experience Richard D. Fessler, M.D., Ajay K. Wakhloo, M.D., Ph.D., Giuseppe Lanzino,
Cerebral hyperperfusion syndrome after carotid angioplasty
 case report Cerebral hyperperfusion syndrome after carotid angioplasty Zoran Miloševič 1, Bojana Žvan 2, Marjan Zaletel 2, Miloš Šurlan 1 1 Institute of Radiology, 2 University Neurology Clinic, University
case report Cerebral hyperperfusion syndrome after carotid angioplasty Zoran Miloševič 1, Bojana Žvan 2, Marjan Zaletel 2, Miloš Šurlan 1 1 Institute of Radiology, 2 University Neurology Clinic, University
Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease
 Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease Michael R. Jaff, D.O., F.A.C.P., F.A.C.C. Assistant Professor of Medicine Harvard Medical School Director, Vascular Medicine
Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease Michael R. Jaff, D.O., F.A.C.P., F.A.C.C. Assistant Professor of Medicine Harvard Medical School Director, Vascular Medicine
Subclavian artery Stenting
 Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Michael Horowitz, MD Pittsburgh, PA
 Michael Horowitz, MD Pittsburgh, PA Introduction Cervical Artery Dissection occurs by a rupture within the arterial wall leading to an intra-mural Hematoma. A possible consequence is an acute occlusion
Michael Horowitz, MD Pittsburgh, PA Introduction Cervical Artery Dissection occurs by a rupture within the arterial wall leading to an intra-mural Hematoma. A possible consequence is an acute occlusion
Slide 1. Slide 2 Conflict of Interest Disclosure. Slide 3 Stroke Facts. The Treatment of Intracranial Stenosis. Disclosure
 Slide 1 The Treatment of Intracranial Stenosis Helmi Lutsep, MD Vice Chair and Dixon Term Professor, Department of Neurology, Oregon Health & Science University Chief of Neurology, VA Portland Health Care
Slide 1 The Treatment of Intracranial Stenosis Helmi Lutsep, MD Vice Chair and Dixon Term Professor, Department of Neurology, Oregon Health & Science University Chief of Neurology, VA Portland Health Care
Patients with symptomatic atherosclerotic stenosis of the
 ORIGINAL RESEARCH B. Du E.H.C. Wong W.-J. Jiang Long-Term Outcome of Tandem Stenting for Stenoses of the Intracranial Vertebrobasilar Artery and Vertebral Ostium BACKGROUND AND PURPOSE: Patients with symptomatic
ORIGINAL RESEARCH B. Du E.H.C. Wong W.-J. Jiang Long-Term Outcome of Tandem Stenting for Stenoses of the Intracranial Vertebrobasilar Artery and Vertebral Ostium BACKGROUND AND PURPOSE: Patients with symptomatic
Overview of Subclavian & Innominate Artery Interventions
 TCT 2016 Washington, DC, USA Tuesday November 1st, 2016 Peripheral vascular interventions Overview of Subclavian & Innominate Artery Interventions Dr Jacques Busquet Vascular & Endovascular Surgery Paris,
TCT 2016 Washington, DC, USA Tuesday November 1st, 2016 Peripheral vascular interventions Overview of Subclavian & Innominate Artery Interventions Dr Jacques Busquet Vascular & Endovascular Surgery Paris,
New Trials in Progress: ACT 1. Jon Matsumura, MD Cannes, France June 28, 2008
 New Trials in Progress: ACT 1 Jon Matsumura, MD Cannes, France June 28, 2008 Faculty Disclosure I disclose the following financial relationships: Consultant, CAS training director, and/or research grants
New Trials in Progress: ACT 1 Jon Matsumura, MD Cannes, France June 28, 2008 Faculty Disclosure I disclose the following financial relationships: Consultant, CAS training director, and/or research grants
Safety and Feasibility of Drug-eluting Stent Implantation at Vertebral Artery Origin: The First Case Series in Asians
 ORIGINAL ARTICLE Safety and Feasibility of Drug-eluting Stent Implantation at Vertebral Artery Origin: The First Case Series in Asians Yen-Hung Lin, 1 Chi-Sheng Hung, 4 Wen-Yi Issac Tseng, 2 Ren-Kwan Lee,
ORIGINAL ARTICLE Safety and Feasibility of Drug-eluting Stent Implantation at Vertebral Artery Origin: The First Case Series in Asians Yen-Hung Lin, 1 Chi-Sheng Hung, 4 Wen-Yi Issac Tseng, 2 Ren-Kwan Lee,
Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke
 Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
Index. interventional.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A ACAS (Asymptomatic Carotid Atherosclerosis Study), 65 66 ACST (Asymptomatic Carotid Surgery Trial), 6 7, 65, 75 Age factors, in carotid
Index Note: Page numbers of article titles are in boldface type. A ACAS (Asymptomatic Carotid Atherosclerosis Study), 65 66 ACST (Asymptomatic Carotid Surgery Trial), 6 7, 65, 75 Age factors, in carotid
ORIGINAL CONTRIBUTION
 ORIGINAL CONTRIBUTION Safety of Latest-Generation Self-expanding Stents in Patients With NASCET-Ineligible Severe Symptomatic Extracranial Internal Carotid Artery Stenosis Italo Linfante, MD; Joshua A.
ORIGINAL CONTRIBUTION Safety of Latest-Generation Self-expanding Stents in Patients With NASCET-Ineligible Severe Symptomatic Extracranial Internal Carotid Artery Stenosis Italo Linfante, MD; Joshua A.
Carotid Artery Stenting
 Carotid Artery Stenting Woong Chol Kang M.D. Gil Medical Center, Gachon University of Medicine and Science, Incheon, Korea Carotid Stenosis and Stroke ~25% of stroke is due to carotid disease, the reminder
Carotid Artery Stenting Woong Chol Kang M.D. Gil Medical Center, Gachon University of Medicine and Science, Incheon, Korea Carotid Stenosis and Stroke ~25% of stroke is due to carotid disease, the reminder
DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service
 M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
Diffusion-Weighted Imaging Abnormalities after Percutaneous Transluminal Angioplasty and Stenting for Intracranial Atherosclerotic Disease
 AJNR Am J Neuroradiol 26:385 389, February 2005 Diffusion-Weighted Imaging Abnormalities after Percutaneous Transluminal Angioplasty and Stenting for Intracranial Atherosclerotic Disease Tomoyuki Tsumoto
AJNR Am J Neuroradiol 26:385 389, February 2005 Diffusion-Weighted Imaging Abnormalities after Percutaneous Transluminal Angioplasty and Stenting for Intracranial Atherosclerotic Disease Tomoyuki Tsumoto
Elective stenting of carotid artery stenosis in patients with severe coronary artery disease
 European Heart Journal (1998) 19, 1365 1370 Article No. hj981048 Elective stenting of carotid artery stenosis in patients with severe coronary artery disease J. Waigand, C. M. Gross, F. Uhlich, J. Krämer,
European Heart Journal (1998) 19, 1365 1370 Article No. hj981048 Elective stenting of carotid artery stenosis in patients with severe coronary artery disease J. Waigand, C. M. Gross, F. Uhlich, J. Krämer,
Clinical Outcome of Patients with Acute Posterior Circulation Stroke and Bilateral Vertebral Artery Occlusion
 ` Original Contribution Clinical Outcome of Patients with Acute Posterior Circulation Stroke and Bilateral Vertebral Artery Occlusion Abstract Background and Introduction: Patients presenting with posterior
` Original Contribution Clinical Outcome of Patients with Acute Posterior Circulation Stroke and Bilateral Vertebral Artery Occlusion Abstract Background and Introduction: Patients presenting with posterior
SAMMPRIS. Stenting and Aggressive Medical Management for Preventing Recurrent Stroke and Intracranial Stenosis. Khalil Zahra, M.D
 SAMMPRIS Stenting and Aggressive Medical Management for Preventing Recurrent Stroke and Intracranial Stenosis Khalil Zahra, M.D Major points Patients with recent TIA or stroke and intra-cranial artery
SAMMPRIS Stenting and Aggressive Medical Management for Preventing Recurrent Stroke and Intracranial Stenosis Khalil Zahra, M.D Major points Patients with recent TIA or stroke and intra-cranial artery
Special Topic Section
 Special Topic Section Cerebrovasc Dis 2004;18:69 74 DOI: 10.1159/000078753 Received: March 8, 2004 Accepted: March 8, 2004 Published online: June 1, 2004 International Carotid Stenting Study: Protocol
Special Topic Section Cerebrovasc Dis 2004;18:69 74 DOI: 10.1159/000078753 Received: March 8, 2004 Accepted: March 8, 2004 Published online: June 1, 2004 International Carotid Stenting Study: Protocol
The CARENET all-comer trial using the CGuard micronet covered carotid embolic prevention stent
 The CARENET all-comer trial using the CGuard micronet covered carotid embolic prevention stent 6 month data Piotr Musialek, MD DPhil FESC Jagiellonian University Dept. of Cardiac & Vascular Diseases John
The CARENET all-comer trial using the CGuard micronet covered carotid embolic prevention stent 6 month data Piotr Musialek, MD DPhil FESC Jagiellonian University Dept. of Cardiac & Vascular Diseases John
Predictors of restenosis and cardiovascular events in patients undergoing percutaneous angioplasty for subclavian/innominate artery stenosis
 Predictors of restenosis and cardiovascular events in patients undergoing percutaneous angioplasty for subclavian/innominate artery stenosis Tadeusz Przewlocki, Anna Kablak Ziembicka, Piotr Pieniazek,
Predictors of restenosis and cardiovascular events in patients undergoing percutaneous angioplasty for subclavian/innominate artery stenosis Tadeusz Przewlocki, Anna Kablak Ziembicka, Piotr Pieniazek,
Guidelines for Ultrasound Surveillance
 Guidelines for Ultrasound Surveillance Carotid & Lower Extremity by Ian Hamilton, Jr, MD, MBA, RPVI, FACS Corporate Medical Director BlueCross BlueShield of Tennessee guidelines for ultrasound surveillance
Guidelines for Ultrasound Surveillance Carotid & Lower Extremity by Ian Hamilton, Jr, MD, MBA, RPVI, FACS Corporate Medical Director BlueCross BlueShield of Tennessee guidelines for ultrasound surveillance
Small in-stent Low Density on CT Angiography after Carotid Artery Stenting
 www.centauro.it Interventional Neuroradiology 14 (Suppl. 2): 41-46, 2008 Small in-stent Low Density on CT Angiography after Carotid Artery Stenting MIKA OKAHARA 1, HIRO KIYOSUE 2, JUNJI KASHIWAGI 1, SHINYA
www.centauro.it Interventional Neuroradiology 14 (Suppl. 2): 41-46, 2008 Small in-stent Low Density on CT Angiography after Carotid Artery Stenting MIKA OKAHARA 1, HIRO KIYOSUE 2, JUNJI KASHIWAGI 1, SHINYA
RCSIsmjoriginal article
 Percutaneous transluminal carotid artery angioplasty and stenting Abstract heading Background: Carotid angioplasty with stenting is becoming a more popular treatment option for severe carotid occlusive
Percutaneous transluminal carotid artery angioplasty and stenting Abstract heading Background: Carotid angioplasty with stenting is becoming a more popular treatment option for severe carotid occlusive
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of June 4, 2018 Thrombolysis, Thrombectomy & Angioplasty
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of June 4, 2018 Thrombolysis, Thrombectomy & Angioplasty
Assessment of the procedural etiology of stroke resulting from carotid artery stenting
 Assessment of the procedural etiology of stroke resulting from carotid artery stenting 1. Study Purpose and Rationale: A. Background Stroke is the 3 rd leading cause of death in the United States and carries
Assessment of the procedural etiology of stroke resulting from carotid artery stenting 1. Study Purpose and Rationale: A. Background Stroke is the 3 rd leading cause of death in the United States and carries
Comparison of transradial and transfemoral approach for carotid artery stenting: RADCAR study
 Comparison of transradial and transfemoral approach for carotid artery stenting: RADCAR study (RADial access for CARotide artery stenting) Zoltán Ruzsa MD PhD et al. TCT 2013 Disclosure Statement of Financial
Comparison of transradial and transfemoral approach for carotid artery stenting: RADCAR study (RADial access for CARotide artery stenting) Zoltán Ruzsa MD PhD et al. TCT 2013 Disclosure Statement of Financial
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of endovascular stent insertion for intracranial atherosclerotic disease Improving
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of endovascular stent insertion for intracranial atherosclerotic disease Improving
SCAI Fall Fellows Course Subclavian/Innominate Case Presentation
 SCAI Fall Fellows Course 2012 Subclavian/Innominate Case Presentation Daniel J. McCormick DO, FACC, FSCAI Director, Cardiovascular Interventional Therapy Pennsylvania Hospital University of Pennsylvania
SCAI Fall Fellows Course 2012 Subclavian/Innominate Case Presentation Daniel J. McCormick DO, FACC, FSCAI Director, Cardiovascular Interventional Therapy Pennsylvania Hospital University of Pennsylvania
Contemporary management of brachiocephalic occlusive disease. TM Sullivan Minneapolis, MN
 Contemporary management of brachiocephalic occlusive disease TM Sullivan Minneapolis, MN WL Gore & Associates Disclosures Meeting organizer (SOAR) CR Bard Chair, CEC Bolster trial Veryan National PI, MIMICS
Contemporary management of brachiocephalic occlusive disease TM Sullivan Minneapolis, MN WL Gore & Associates Disclosures Meeting organizer (SOAR) CR Bard Chair, CEC Bolster trial Veryan National PI, MIMICS
Carotid Artery Disease and What s Pertinent JOSEPH A PAULISIN DO
 Carotid Artery Disease and What s Pertinent JOSEPH A PAULISIN DO Goal of treatment of carotid disease Identify those at risk of developing symptoms Prevent patients at risk from developing symptoms Prevent
Carotid Artery Disease and What s Pertinent JOSEPH A PAULISIN DO Goal of treatment of carotid disease Identify those at risk of developing symptoms Prevent patients at risk from developing symptoms Prevent
Extracranial Carotid Artery Stenting With or Without Distal Protection Device
 Extracranial Carotid Artery Stenting With or Without Distal Protection Device Eak-Kyun Shin MD. Professor of Medicine Division of Cardiology, Heart Center, Gil Medical Center Gacheon Medical School Incheon,
Extracranial Carotid Artery Stenting With or Without Distal Protection Device Eak-Kyun Shin MD. Professor of Medicine Division of Cardiology, Heart Center, Gil Medical Center Gacheon Medical School Incheon,
[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]
![[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD] [(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]](/thumbs/89/98619893.jpg) 2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
Management of intracranial atherosclerotic stenosis (ICAS)/intracranial atherosclerosis
 Management of intracranial atherosclerotic stenosis (ICAS)/intracranial atherosclerosis Tim Mikesell, D.O. Oct 22, 2016 Stroke facts Despite progress in decreasing stroke incidence and mortality, stroke
Management of intracranial atherosclerotic stenosis (ICAS)/intracranial atherosclerosis Tim Mikesell, D.O. Oct 22, 2016 Stroke facts Despite progress in decreasing stroke incidence and mortality, stroke
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
Recanalization of Chronic Carotid Artery Occlusion Objective Improvement Of Cerebral Perfusion
 Recanalization of Chronic Carotid Artery Occlusion Objective Improvement Of Cerebral Perfusion Paul Hsien-Li Kao, MD Assistant Professor National Taiwan University Medical School and Hospital ICA stenting
Recanalization of Chronic Carotid Artery Occlusion Objective Improvement Of Cerebral Perfusion Paul Hsien-Li Kao, MD Assistant Professor National Taiwan University Medical School and Hospital ICA stenting
P. Paluszek, P. Pieniazek, P. Musialek, T. Przewlocki, L. Tekieli, A. Kablak-Ziembicka, K. Dzierwa, M. Hlawaty, M. Trystula, P.
 STenting for Ostial Vertebral Artery Stenosis (STOVAST Trial): Results from a prospective randomized study comparing bare-metal with drug-eluting stents. P. Paluszek, P. Pieniazek, P. Musialek, T. Przewlocki,
STenting for Ostial Vertebral Artery Stenosis (STOVAST Trial): Results from a prospective randomized study comparing bare-metal with drug-eluting stents. P. Paluszek, P. Pieniazek, P. Musialek, T. Przewlocki,
Ultrasound Imaging of The Posterior Circulation
 Ultrasound Imaging of The Posterior Circulation Michigan Sonographers Society 2 Nd Annual Fall Vascular Conference Larry N. Raber RDMS-RVT Clinical Manager General Ultrasound/Neurovascular Laboratory Cleveland
Ultrasound Imaging of The Posterior Circulation Michigan Sonographers Society 2 Nd Annual Fall Vascular Conference Larry N. Raber RDMS-RVT Clinical Manager General Ultrasound/Neurovascular Laboratory Cleveland
Carotid Revascularization
 Options for Carotid Disease Carotid Revascularization Wayne Causey, MD 2 nd Year Vascular Surgery Fellow Best medical therapy, Carotid Endarterectomy, and Carotid Stenting Who benefits from best medical
Options for Carotid Disease Carotid Revascularization Wayne Causey, MD 2 nd Year Vascular Surgery Fellow Best medical therapy, Carotid Endarterectomy, and Carotid Stenting Who benefits from best medical
2017 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Outcome
 Measure #344: Rate of Carotid Artery Stenting (CAS) for Asymptomatic Patients, Without Major Complications (Discharged to Home by Post-Operative Day #2) National Quality Strategy Domain: Effective Clinical
Measure #344: Rate of Carotid Artery Stenting (CAS) for Asymptomatic Patients, Without Major Complications (Discharged to Home by Post-Operative Day #2) National Quality Strategy Domain: Effective Clinical
The most important recommendations from the 2017 ESVS/ESC guideline on the management of carotid artery disease
 The most important recommendations from the 2017 ESVS/ESC guideline on the management of carotid artery disease GJ de Borst Department of Vascular Surgery RECOMMENDATION GRADING CRITERIA What is new
The most important recommendations from the 2017 ESVS/ESC guideline on the management of carotid artery disease GJ de Borst Department of Vascular Surgery RECOMMENDATION GRADING CRITERIA What is new
How to manage the left subclavian and left vertebral artery during TEVAR
 How to manage the left subclavian and left vertebral artery during TEVAR Jürg Schmidli Chief of Vascular Surgery Inselspital Hamburg 2017 Dept Cardiovascular Surgery, Bern, Switzerland Disclosure No Disclosures
How to manage the left subclavian and left vertebral artery during TEVAR Jürg Schmidli Chief of Vascular Surgery Inselspital Hamburg 2017 Dept Cardiovascular Surgery, Bern, Switzerland Disclosure No Disclosures
Occlusion of All Four Extracranial Vessels With Minimal Clinical Symptomatology. Case Report
 Occlusion of All Four Extracranial Vessels With Minimal Clinical Symptomatology. Case Report BY JIRI J. VITEK, M.D., JAMES H. HALSEY, JR., M.D., AND HOLT A. McDOWELL, M.D. Abstract: Occlusion of All Four
Occlusion of All Four Extracranial Vessels With Minimal Clinical Symptomatology. Case Report BY JIRI J. VITEK, M.D., JAMES H. HALSEY, JR., M.D., AND HOLT A. McDOWELL, M.D. Abstract: Occlusion of All Four
Amaurosis fugax: some aspects of management
 Journal of Neurology, Neurosurgery, and Psvchiatry 1982;45:1-6 Amaurosis fugax: some aspects of management PJ PARKIN, BE KENDALL, J MARSHALL, WI McDONALD From the National Hospital for Nervous Diseases,
Journal of Neurology, Neurosurgery, and Psvchiatry 1982;45:1-6 Amaurosis fugax: some aspects of management PJ PARKIN, BE KENDALL, J MARSHALL, WI McDONALD From the National Hospital for Nervous Diseases,
GUIDELINE FOR RECOVERY ROOM MANAGEMENT OF PATIENTS AFTER CAROTID ENDARTERECTOMY
 GUIDELINE FOR RECOVERY ROOM MANAGEMENT OF PATIENTS AFTER CAROTID ENDARTERECTOMY Full Title of Guideline: Author (include email and role): Guideline for Recovery Room Management of Patients after Carotid
GUIDELINE FOR RECOVERY ROOM MANAGEMENT OF PATIENTS AFTER CAROTID ENDARTERECTOMY Full Title of Guideline: Author (include email and role): Guideline for Recovery Room Management of Patients after Carotid
Antithrombotic therapy in patients with transient ischemic attack / stroke (acute phase <48h)
 Antithrombotic therapy in patients with transient ischemic attack / stroke (acute phase
Antithrombotic therapy in patients with transient ischemic attack / stroke (acute phase
Current Role of Renal Artery Stenting in Patients with Renal Artery Stenosis
 Current Role of Renal Artery Stenting in Patients with Renal Artery Stenosis Young-Guk Ko, M.D. Severance Cardiovascular Hospital, Yonsei University College of Medicine, Seoul, Korea Etiology Fibromuscular
Current Role of Renal Artery Stenting in Patients with Renal Artery Stenosis Young-Guk Ko, M.D. Severance Cardiovascular Hospital, Yonsei University College of Medicine, Seoul, Korea Etiology Fibromuscular
Recommendations for Follow-up After Vascular Surgery Arterial Procedures SVS Practice Guidelines
 Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al.
 ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al. visualization of the posterior inferior cerebellar artery. The patient, now 11 months post-operative, has shown further neurological improvement since
ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al. visualization of the posterior inferior cerebellar artery. The patient, now 11 months post-operative, has shown further neurological improvement since
Durability of percutaneous transluminal angioplasty for obstructive lesions of proximal subclavian artery: Long-term results
 From the Society for Vascular Surgery Durability of percutaneous transluminal angioplasty for obstructive lesions of proximal subclavian artery: Long-term results Jean-Paul P. M. de Vries, MD, PhD, a L.
From the Society for Vascular Surgery Durability of percutaneous transluminal angioplasty for obstructive lesions of proximal subclavian artery: Long-term results Jean-Paul P. M. de Vries, MD, PhD, a L.
The Struggle to Manage Stroke, Aneurysm and PAD
 The Struggle to Manage Stroke, Aneurysm and PAD In this article, Dr. Salvian examines the management of peripheral arterial disease, aortic aneurysmal disease and cerebrovascular disease from symptomatology
The Struggle to Manage Stroke, Aneurysm and PAD In this article, Dr. Salvian examines the management of peripheral arterial disease, aortic aneurysmal disease and cerebrovascular disease from symptomatology
Basilar artery stenosis with bilateral cerebellar strokes on coumadin
 Qaisar A. Shah, MD Patient Profile 68 years old female with a history of; Basilar artery stenosis with bilateral cerebellar strokes on coumadin Diabetes mellitus Hyperlipidemia Hypertension She developed
Qaisar A. Shah, MD Patient Profile 68 years old female with a history of; Basilar artery stenosis with bilateral cerebellar strokes on coumadin Diabetes mellitus Hyperlipidemia Hypertension She developed
CAROTID STENTING A 2009 UPDATE. Hoang Duong, MD Director of Interventional Neuroradiology Memorial Regional Hospital
 CAROTID STENTING A 2009 UPDATE Hoang Duong, MD Director of Interventional Neuroradiology Memorial Regional Hospital TREATMENT FOR CAROTID STENOSIS Best medical management Antiplatelet therapy Antihypertensive
CAROTID STENTING A 2009 UPDATE Hoang Duong, MD Director of Interventional Neuroradiology Memorial Regional Hospital TREATMENT FOR CAROTID STENOSIS Best medical management Antiplatelet therapy Antihypertensive
Bilateral blunt carotid artery injury: A case report and review of the literature
 CASE REPORT Bilateral blunt carotid artery injury: A case report and review of the literature S Cheddie, 1 MMed (Surg), FCS (SA); B Pillay, 2 FCS (SA), Cert Vascular Surgery; R Goga, 2 FCS (SA) 1 Department
CASE REPORT Bilateral blunt carotid artery injury: A case report and review of the literature S Cheddie, 1 MMed (Surg), FCS (SA); B Pillay, 2 FCS (SA), Cert Vascular Surgery; R Goga, 2 FCS (SA) 1 Department
Aortic arch pathology. Cerebral ischemia following carotid artery stenosis.
 Important: -Subclavian Steal Syndrome -Cerebral ischemia Aortic arch pathology. Cerebral ischemia following carotid artery stenosis. Mina Aubeed & Alba Hernández Pinilla Aortic arch pathology Common arch
Important: -Subclavian Steal Syndrome -Cerebral ischemia Aortic arch pathology. Cerebral ischemia following carotid artery stenosis. Mina Aubeed & Alba Hernández Pinilla Aortic arch pathology Common arch
Percutaneous Revascularization of Sole Arch Artery for Severe Cerebral Ischemia Resulting from Takayasu Arteritis
 Percutaneous Revascularization of Sole Arch Artery for Severe Cerebral Ischemia Resulting from Takayasu Arteritis Sanjay Tyagi, MD, Mohit D. Gupta, MD, Praveen Singh, MD, Devendra Shrimal, MD, and M.P.
Percutaneous Revascularization of Sole Arch Artery for Severe Cerebral Ischemia Resulting from Takayasu Arteritis Sanjay Tyagi, MD, Mohit D. Gupta, MD, Praveen Singh, MD, Devendra Shrimal, MD, and M.P.
UPMC HAMOT CAROTID ARTERY DISEASE WHERE DO WE GO FROM HERE?
 UPMC HAMOT CAROTID ARTERY DISEASE WHERE DO WE GO FROM HERE? Richard W. Petrella M.D. FACP,FACC,FASCI DEPARTMENT CHAIRMAN CVM&S UPMC HAMOT MEDICAL CENTER 1 LEARNING OBJECTIVES REVIEW THE RISK FACTORS FOR
UPMC HAMOT CAROTID ARTERY DISEASE WHERE DO WE GO FROM HERE? Richard W. Petrella M.D. FACP,FACC,FASCI DEPARTMENT CHAIRMAN CVM&S UPMC HAMOT MEDICAL CENTER 1 LEARNING OBJECTIVES REVIEW THE RISK FACTORS FOR
Neuro-vascular Intervention in Stroke. Will Adams Consultant Neuroradiologist Plymouth Hospitals NHS Trust
 Neuro-vascular Intervention in Stroke Will Adams Consultant Neuroradiologist Plymouth Hospitals NHS Trust Stroke before the mid 1990s Swelling Stroke extension Haemorrhagic transformation Intravenous thrombolysis
Neuro-vascular Intervention in Stroke Will Adams Consultant Neuroradiologist Plymouth Hospitals NHS Trust Stroke before the mid 1990s Swelling Stroke extension Haemorrhagic transformation Intravenous thrombolysis
Total occlusion at ostial Left internal mammary graft with successful angioplasty and longterm patency result
 DOI 10.7603/s40602-014-0017-x ASEAN Heart Journal http://www.aseanheartjournal.org/ Vol. 22, no. 1, 116 121 (2014) ISSN: 2315-4551 Case Report Total occlusion at ostial Left internal mammary graft with
DOI 10.7603/s40602-014-0017-x ASEAN Heart Journal http://www.aseanheartjournal.org/ Vol. 22, no. 1, 116 121 (2014) ISSN: 2315-4551 Case Report Total occlusion at ostial Left internal mammary graft with
Endovascular treatment for pseudoocclusion of the internal carotid artery
 Endovascular treatment for pseudoocclusion of the internal carotid artery Daqiao Guo, Xiao Tang, Weiguo Fu Institute of Vascular Surgery, Fudan University, Department of Vascular Surgery, Zhongshan Hospital
Endovascular treatment for pseudoocclusion of the internal carotid artery Daqiao Guo, Xiao Tang, Weiguo Fu Institute of Vascular Surgery, Fudan University, Department of Vascular Surgery, Zhongshan Hospital
Combined Stent Placement and Thrombolysis in Acute Vertebrobasilar Ischemic Stroke
 AJNR Am J Neuroradiol 24:1827 1833, October 2003 Combined Stent Placement and Thrombolysis in Acute Vertebrobasilar Ischemic Stroke Doris D. M. Lin, Philippe Gailloud, Norman J. Beauchamp, Eric M. Aldrich,
AJNR Am J Neuroradiol 24:1827 1833, October 2003 Combined Stent Placement and Thrombolysis in Acute Vertebrobasilar Ischemic Stroke Doris D. M. Lin, Philippe Gailloud, Norman J. Beauchamp, Eric M. Aldrich,
Carotid Artery Stenting
 Carotid Artery Stenting Natural history of the carotid stenosis Asymptomatic 80% carotid stenosis - 6% risk of stroke / year Symptomatic carotid stenosis have 10% risk of CVA at one year and 40% at 5 years
Carotid Artery Stenting Natural history of the carotid stenosis Asymptomatic 80% carotid stenosis - 6% risk of stroke / year Symptomatic carotid stenosis have 10% risk of CVA at one year and 40% at 5 years
ESC Congress 2011 SIMULTANEOUS HYBRID REVASCULARIZATION OF CAROTID AND CORONARY DISEASE INITIAL RESULTS OF A NEW THERAPEUTIC APPROACH
 ESC Congress 2011 SIMULTANEOUS HYBRID REVASCULARIZATION OF CAROTID AND CORONARY DISEASE IN PATIENTS WITH ACUTE CORONARY SYNDROME: INITIAL RESULTS OF A NEW THERAPEUTIC APPROACH AUTHORS: Marta Ponte 1, RICARDO
ESC Congress 2011 SIMULTANEOUS HYBRID REVASCULARIZATION OF CAROTID AND CORONARY DISEASE IN PATIENTS WITH ACUTE CORONARY SYNDROME: INITIAL RESULTS OF A NEW THERAPEUTIC APPROACH AUTHORS: Marta Ponte 1, RICARDO
Canadian Best Practice Recommendations for Stroke Care. (Updated 2008) Section # 3 Section # 3 Hyperacute Stroke Management
 Canadian Best Practice Recommendations for Stroke Care (Updated 2008) Section # 3 Section # 3 Hyperacute Stroke Management Reorganization of Recommendations 2008 2006 RECOMMENDATIONS: 2008 RECOMMENDATIONS:
Canadian Best Practice Recommendations for Stroke Care (Updated 2008) Section # 3 Section # 3 Hyperacute Stroke Management Reorganization of Recommendations 2008 2006 RECOMMENDATIONS: 2008 RECOMMENDATIONS:
Disclosures. CREST Trial: Summary. Lecture Outline 4/16/2015. Cervical Atherosclerotic Disease
 Disclosures Your Patient Has Carotid Bulb Stenosis and a Tandem Intracranial Stenosis: How Do SAMMPRIS and Other Evidence Inform Your Treatment? UCSF Vascular Symposium 2015 Steven W. Hetts, MD Associate
Disclosures Your Patient Has Carotid Bulb Stenosis and a Tandem Intracranial Stenosis: How Do SAMMPRIS and Other Evidence Inform Your Treatment? UCSF Vascular Symposium 2015 Steven W. Hetts, MD Associate
MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS. 73 year old NS right-handed male applicant for $1 Million life insurance
 MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS October 17, 2012 AAIM Triennial Conference, San Diego Robert Lund, MD What Is The Risk? 73 year old NS right-handed male applicant for $1
MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS October 17, 2012 AAIM Triennial Conference, San Diego Robert Lund, MD What Is The Risk? 73 year old NS right-handed male applicant for $1
Comparison Of Primary Long Stenting Versus Primary Short Stenting For Long Femoropopliteal Artery Disease (PARADE)
 Comparison Of Primary Long Stenting Versus Primary Short Stenting For Long Femoropopliteal Artery Disease (PARADE) Young-Guk Ko, M.D. Severance Cardiovascular Hospital, Yonsei University Health System,
Comparison Of Primary Long Stenting Versus Primary Short Stenting For Long Femoropopliteal Artery Disease (PARADE) Young-Guk Ko, M.D. Severance Cardiovascular Hospital, Yonsei University Health System,
Updated Society for Vascular Surgery guidelines for management of extracranial carotid disease: Executive summary
 SOCIETY FOR VASCULAR SURGERY DOCUMENT Updated Society for Vascular Surgery guidelines for management of extracranial carotid disease: Executive summary John J. Ricotta, MD, a Ali AbuRahma, MD, FACS, b
SOCIETY FOR VASCULAR SURGERY DOCUMENT Updated Society for Vascular Surgery guidelines for management of extracranial carotid disease: Executive summary John J. Ricotta, MD, a Ali AbuRahma, MD, FACS, b
MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS. 73 year old NS right-handed male applicant for $1 Million Life Insurance
 MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS October 17, 2012 AAIM Triennial Conference, San Diego Robert Lund, MD What Is The Risk? 73 year old NS right-handed male applicant for $1
MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS October 17, 2012 AAIM Triennial Conference, San Diego Robert Lund, MD What Is The Risk? 73 year old NS right-handed male applicant for $1
ICSS Safety Results NOT for PUBLICATION. June 2009 ICSS ICSS ICSS ICSS. International Carotid Stenting Study: Main Inclusion Criteria
 Safety Results NOT for The following slides were presented to the Investigators Meeting on 22/05/09 and most of them were also presented at the European Stroke Conference on 27/05/09 They are NOT for in
Safety Results NOT for The following slides were presented to the Investigators Meeting on 22/05/09 and most of them were also presented at the European Stroke Conference on 27/05/09 They are NOT for in
Compared with symptomatic internal carotid artery stenosis,
 Long-Term Outcome After Angioplasty and Stenting for Symptomatic Vertebral Artery Stenosis Compared With Medical in the Carotid And Vertebral Artery Transluminal Angioplasty Study (CAVATAS) A Randomized
Long-Term Outcome After Angioplasty and Stenting for Symptomatic Vertebral Artery Stenosis Compared With Medical in the Carotid And Vertebral Artery Transluminal Angioplasty Study (CAVATAS) A Randomized
Two Cases of Carotid Artery Stenting Combined Balloon- and Self-expanding Stent for the Spontaneous Internal Carotid Artery Dissections
 Journal of Neuroendovascular Therapy 2017; 11: 437 442 Online June 13, 2017 DOI: 10.5797/jnet.tn.2016-0059 Two Cases of Carotid Artery Stenting Combined Balloon- and Self-expanding Stent for the Spontaneous
Journal of Neuroendovascular Therapy 2017; 11: 437 442 Online June 13, 2017 DOI: 10.5797/jnet.tn.2016-0059 Two Cases of Carotid Artery Stenting Combined Balloon- and Self-expanding Stent for the Spontaneous
More than strokes occur
 Surgery vs Stent: Treatment for Carotid Artery Disease Imad A. Alhaddad, MD ABSTRACT PURPOSE: This article summarizes and compares the roles of surgery and stent in the management of carotid artery disease.
Surgery vs Stent: Treatment for Carotid Artery Disease Imad A. Alhaddad, MD ABSTRACT PURPOSE: This article summarizes and compares the roles of surgery and stent in the management of carotid artery disease.
Guideline scope Stroke and transient ischaemic attack in over 16s: diagnosis and initial management (update)
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Stroke and transient ischaemic attack in over s: diagnosis and initial management (update) 0 0 This will update the NICE on stroke and
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Stroke and transient ischaemic attack in over s: diagnosis and initial management (update) 0 0 This will update the NICE on stroke and
Solving the Dilemma of Ostial Stenting: A Case Series Illustrating the Flash Ostial System
 Volume 1, Issue 1 Case Report Solving the Dilemma of Ostial Stenting: A Case Series Illustrating the Flash Ostial System Robert F. Riley * and Bill Lombardi University of Washington Medical Center, Division
Volume 1, Issue 1 Case Report Solving the Dilemma of Ostial Stenting: A Case Series Illustrating the Flash Ostial System Robert F. Riley * and Bill Lombardi University of Washington Medical Center, Division
Carotid Stenosis (carotid artery disease)
 1 Carotid Stenosis (carotid artery disease) Overview Carotid stenosis is a narrowing of the carotid arteries, the two major arteries that carry oxygenrich blood from the heart to the brain. Also called
1 Carotid Stenosis (carotid artery disease) Overview Carotid stenosis is a narrowing of the carotid arteries, the two major arteries that carry oxygenrich blood from the heart to the brain. Also called
1 Comparison of Warfarin and Aspirin for Symptomatic Intracranial Arterial Stenosis. N Engl J Med 352;13, March 31, 2005
 The risk of ischemic stroke in patients with Intracranial Atherosclerotic Disease (ICAD) ranges from 7 to 24%. 1,2 Developed specifically for the treatment of ICAD, the Wingspan Stent System and Gateway
The risk of ischemic stroke in patients with Intracranial Atherosclerotic Disease (ICAD) ranges from 7 to 24%. 1,2 Developed specifically for the treatment of ICAD, the Wingspan Stent System and Gateway
DESCRIPTION: Percent of asymptomatic patients undergoing CEA who are discharged to home no later than post-operative day #2
 Measure #260: Rate of Carotid Endarterectomy (CEA) for Asymptomatic Patients, without Major Complications (Discharged to Home by Post-Operative Day #2) National Quality Strategy Domain: Patient Safety
Measure #260: Rate of Carotid Endarterectomy (CEA) for Asymptomatic Patients, without Major Complications (Discharged to Home by Post-Operative Day #2) National Quality Strategy Domain: Patient Safety
Stroke/TIA. Tom Bedwell
 Stroke/TIA Tom Bedwell tab1g11@soton.ac.uk The Plan Definitions Anatomy Recap Aetiology Pathology Syndromes Brocas / Wernickes Investigations Management Prevention & Prognosis TIAs Key Definitions Transient
Stroke/TIA Tom Bedwell tab1g11@soton.ac.uk The Plan Definitions Anatomy Recap Aetiology Pathology Syndromes Brocas / Wernickes Investigations Management Prevention & Prognosis TIAs Key Definitions Transient
BULgarian Carotid Artery Stenting versus Surgery Study (BULCASSS): Randomized single center trial
 BULgarian Carotid Artery Stenting versus Surgery Study (): Randomized single center trial Ivo Petrov, M. Konteva, H. Dimitrov, K. Kichukov Tokuda Hospital Sofia Cardiology Department Background Carotid
BULgarian Carotid Artery Stenting versus Surgery Study (): Randomized single center trial Ivo Petrov, M. Konteva, H. Dimitrov, K. Kichukov Tokuda Hospital Sofia Cardiology Department Background Carotid
Disclosures. State of the Art Management of Carotid Stenosis. NIH funding for clinical trials Consultant for Scientia Vascular and Medtronic
 State of the Art Management of Carotid Stenosis Mark R. Harrigan, MD UAB Stroke Center Professor of Neurosurgery, Neurology, and Radiology University of Alabama, Birmingham Disclosures NIH funding for
State of the Art Management of Carotid Stenosis Mark R. Harrigan, MD UAB Stroke Center Professor of Neurosurgery, Neurology, and Radiology University of Alabama, Birmingham Disclosures NIH funding for
03/30/2016 DISCLOSURES TO OPERATE OR NOT THAT IS THE QUESTION CAROTID INTERVENTION IS INDICATED FOR ASYMPTOMATIC CAROTID OCCLUSIVE DISEASE
 CAROTID INTERVENTION IS INDICATED FOR ASYMPTOMATIC CAROTID OCCLUSIVE DISEASE Elizabeth L. Detschelt, M.D. Allegheny Health Network Vascular and Endovascular Symposium April 2, 2016 DISCLOSURES I have no
CAROTID INTERVENTION IS INDICATED FOR ASYMPTOMATIC CAROTID OCCLUSIVE DISEASE Elizabeth L. Detschelt, M.D. Allegheny Health Network Vascular and Endovascular Symposium April 2, 2016 DISCLOSURES I have no
Left Subclavian Artery Stenosis in Coronary Artery Bypass: Prevalence and Revascularization Strategies
 Left Subclavian Artery Stenosis in Coronary Artery Bypass: Prevalence and Revascularization Strategies Ho Young Hwang, MD, Jin Hyun Kim, MD, Whal Lee, MD, PhD, Jae Hyung Park, MD, PhD, and Ki-Bong Kim,
Left Subclavian Artery Stenosis in Coronary Artery Bypass: Prevalence and Revascularization Strategies Ho Young Hwang, MD, Jin Hyun Kim, MD, Whal Lee, MD, PhD, Jae Hyung Park, MD, PhD, and Ki-Bong Kim,
CAROTID ARTERY ANGIOPLASTY
 CAROTID ARTERY ANGIOPLASTY Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and
CAROTID ARTERY ANGIOPLASTY Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and
2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY
 Measure #260: Rate of Carotid Endarterectomy (CEA) for Asymptomatic Patients, without Major Complications (Discharged to Home by Post-Operative Day #2) National Quality Strategy Domain: Patient Safety
Measure #260: Rate of Carotid Endarterectomy (CEA) for Asymptomatic Patients, without Major Complications (Discharged to Home by Post-Operative Day #2) National Quality Strategy Domain: Patient Safety
Renal Artery Stenosis: Insights from the CORAL Trial
 Renal Artery Stenosis: Insights from the CORAL Trial Christopher J. Cooper, M.D., FACC, FACP Dean and Senior Vice President University of Toledo, College of Medicine President, Ohio Chapter ACC State of
Renal Artery Stenosis: Insights from the CORAL Trial Christopher J. Cooper, M.D., FACC, FACP Dean and Senior Vice President University of Toledo, College of Medicine President, Ohio Chapter ACC State of
Surgical Treatment of Carotid Disease
 Department of Cardiothoracic & Vascular Surgery McGovern Medical School / The University of Texas Health Science Center at Houston Surgical Treatment of Carotid Disease The Old, the New, and the Future
Department of Cardiothoracic & Vascular Surgery McGovern Medical School / The University of Texas Health Science Center at Houston Surgical Treatment of Carotid Disease The Old, the New, and the Future
Assessment of recurrent mesenteric ischemia after stenting with a pressure wire
 524852VMJ0010.1177/1358863X14524852Vascular MedicineMargiotta and Gray research-article2014 Case Report Assessment of recurrent mesenteric ischemia after stenting with a pressure wire Vascular Medicine
524852VMJ0010.1177/1358863X14524852Vascular MedicineMargiotta and Gray research-article2014 Case Report Assessment of recurrent mesenteric ischemia after stenting with a pressure wire Vascular Medicine
Intracranial Vertebrobasilar Stenosis: Angioplasty and Follow-up
 AJNR Am J Neuroradiol 21:1293 131, August 2 Intracranial Vertebrobasilar Stenosis: Angioplasty and Follow-up Hans C. Nahser, Hans Henkes, Werner Weber, Elisabeth Berg-Dammer, Tarek A. Yousry, and Dietmar
AJNR Am J Neuroradiol 21:1293 131, August 2 Intracranial Vertebrobasilar Stenosis: Angioplasty and Follow-up Hans C. Nahser, Hans Henkes, Werner Weber, Elisabeth Berg-Dammer, Tarek A. Yousry, and Dietmar
Carotid Artery Stenting (CAS) Pathophysiology. Technical Considerations. Plaque characteristics: relevant concepts. CAS and CEA
 Carotid Artery Stenting (CAS) Carotid Artery Stenting for Stroke Risk Reduction Matthew A. Corriere MD, MS, RPVI Assistant Professor of Surgery Department of Vascular and Endovascular Surgery Rationale:
Carotid Artery Stenting (CAS) Carotid Artery Stenting for Stroke Risk Reduction Matthew A. Corriere MD, MS, RPVI Assistant Professor of Surgery Department of Vascular and Endovascular Surgery Rationale:
Clinical Significance of Vertebral Artery Stenosis
 Clinical Significance of Vertebral Artery Stenosis Yo Han Jung Department of Medicine The Graduate School, Yonsei University Clinical Significance of Vertebral Artery Stenosis Directed by Professor Ji
Clinical Significance of Vertebral Artery Stenosis Yo Han Jung Department of Medicine The Graduate School, Yonsei University Clinical Significance of Vertebral Artery Stenosis Directed by Professor Ji
BY VINCENT V. TRUONG, MD, AND ALEX ABOU-CHEBL, MD
 Intracranial Angioplasty and Stenting Assessing the need for continued clinical exploration of the safety, efficacy, and durability of intracranial interventions. BY VINCENT V. TRUONG, MD, AND ALEX ABOU-CHEBL,
Intracranial Angioplasty and Stenting Assessing the need for continued clinical exploration of the safety, efficacy, and durability of intracranial interventions. BY VINCENT V. TRUONG, MD, AND ALEX ABOU-CHEBL,
Lower Extremity Endovascular Revascularization Codes
 Lower Extremity Endovascular Update: AAPC National Long Beach, CA April 4, 2011 Presented by: David Zielske, MD, CIRCC, CPC H, CCC, CCS, RCC Lower Extremity Endovascular Revascularization Codes 37220 37235
Lower Extremity Endovascular Update: AAPC National Long Beach, CA April 4, 2011 Presented by: David Zielske, MD, CIRCC, CPC H, CCC, CCS, RCC Lower Extremity Endovascular Revascularization Codes 37220 37235
