206 Recent Developments in Intensive
|
|
|
- Emerald Barber
- 5 years ago
- Views:
Transcription
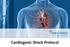
1 C H A P T E R 206 Recent Developments in Intensive Cardiac Care for Acute Cardiac Disorders Suraj Kumar Arora, Abhishek Goyal, Gurpreet S Wander Intensive cardiac care includes a wide range of cardiac emergencies that can develop into rapidly evolving life-threatening situations requiring efficient and rapid interventions. In its original concept, the CCU was designed for arrhythmia monitoring and treatment of patients with acute coronary syndromes. In present scenario, the CCU has evolved into a critical care environment that delivers care both to patients with acute single-system cardiovascular illness and to patients with more co-morbidities and multisystem organ dysfunction. The field of cardiac intensive care continues to advance in tandem with disorders and complexity of procedures. There have been few major developments in critical care in terms of specific new treatments and substantial evidence exist regarding the use of certain strategies, though not always guidelines based. Certain older concepts have also changed in light of new data. Here we summarize what we believe to be the most important features of progress in cardiac intensive care in recent years. IONOTROPES Positive inotropic drugs are typically used to stabilize patients with acute decompensated heart failure in the intensive care unit, as a bridge-to-decision or bridge to heart replacement therapy. Despite evidence that inotropic therapy may increase mortality, there are clinical settings where inotropic support may be life-saving measure, and where hypoperfusion of vital organs is obvious and the need for improved perfusion is immediate. Initial choice of vasopressor was used to based on individualexperience and institutional bias. Dopamine, the precursor for norepinephrine, was recommended as a first line agent. However, patients in shock have a diminished response to indirect-acting agents such as dopamine, because a large component of the response to dopamine is neuronal release of norepinephrine. When endogenous norepinephrine is depleted in shock states, dopamine is unable to produce adequate response. In patients with cardiogenic shock, norepinephrine (α1&β1-adrenergicagonist), should be preferred over dopamine as the first-line vasopressor because a subgroup analysis from a major randomized trial found that patients with cardiogenic shock who received dopamine had a higher mortality than those who received norepinephrine. In addition, dysrhythmias were more common in the dopamine group. Fig. 1: An illustration of options for Mechanical Circulatory Support : (A) IABP, (B) Impella, (C) TandemHeart
2 Table 1: Current Guideline recommendations of IABP Indication ACC/AHA guidelines ESC guidelines STEMI with cardiogenic shock IIa/B a [1] IIb/B a [2] STEMI without cardiogenic shock - III/A [3] Mechanical complication of AMI IABP can used to provide temporary circulatory support [1] I/C [3] High- risk PCI IIb/C [4] - High-risk CABG IIa/B [5] ACC, American College of Cardiology; AHA. American Heart Association; CABG, coronary artery bypass graft; ESC, European Society of Cardiology; IABP, lntra-aortic balloon pump; LVEF. left ventricular ejection fraction; PCI. percutaneous coronary intervention; STEMI, ST-segment elevation myocardial infarction; 1. O Gara PT, Kushner FG, Ascheim DD, et al_ 2013 ACCF/AHA guideline for the management of ST-elevation myocardial infarction: a report of the American College of Cardiology Foundation/ American Heart Association Task Force on Practice Guidelines. Circulation 2013; 127:e362-e425; 2. Steg PG, James SK. Alar D. et al. ESC guidelines for the management of acute myocardial infarction m patients presenting with ST-segment elevation Eur Heart J 2012; 33: ; 3. Task Force on Myocardial Revascularization of the European Society of Cardiology (ESC) and the European Association for Cardio-Thoracic Surgery (EACTS), European Association for Percutaneous Cardiovascular Interventions. Guidelines on myocardial revascularization Eur Heart J 2010; 31: ; 4. LevineGN. Bates ER. Blankenship JC. et al ACCF/AHA/ SCAI Guideline for percutaneous coronary intervention A report of the Amencan College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines and the Society for Cardiovascular Angiography and Interventions. J Am Coll Cardiol :e44-el22; 5. Hillis LD, Smith PK, Anderson JL, et al ACCF/AHA Guideline for coronary artery bypass graft surgery. A report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. Developed in collaboration with the Amencan Association for Thoracic Surgery. Society of Cardiovascular Anesthesiologists, and Society of Thoracic Surgeons. J Am Coll Cardiol 2011; 58:el23-e210; a Recently downgraded from Class I to Class II 947 CHAPTER 206 Given concerns about increased mortality with shortterm intravenous therapy with milrinone or dobutamine in patients with acute decompensated heart failure, these drugs are not to be used in the routine management of such patients. However, administration should be considered in patients with severe hemodynamic compromise with low cardiac output that is not adequately managed by diuretics and vasodilators. Calcium sensitizing agents such as levosimendan exert positive inotropic effects on the heart by increasing the contractile apparatus sensitivity to calcium. Therefore, such drugs have the advantage of driving contractile state without increasing camp or calcium, both of which have adverse effects. Despite improvement in hemodynamics, there is no clear evidence of short term or long term clinical benefit. Two randomized trials with levosimendan, REVIVE-II and SURVIVE, indicated no difference in mortality with levosimendan and use was associated with more adverse effects in form of hypotension. Newer drugs are still under intense investigation and are in clinical trials. Omecamtiv mecarbil is the first selective cardiac myosin activator and increases the efficiency of heart muscle contraction. ATOMIC AHF trial showed that the drug didn t have the usual adverse effects (e.g., tachycardia and arrhythmia) of traditional inotropic agents. Omecamtiv mecarbil may not be an inotrope, but it does improve myocardial systolic performance. Istaroxime is a novel intravenous drug that inhibits Na/ K+ ATPase and stimulates SERCA2a. HORIZON-HF study assessed the hemodynamic effects of Istaroxime and showed reduction in PCWP and increase in systolic blood pressure but no effect on neurohormones, renal function, ortroponin levels. The quest to develop more effective and safer positive inotropic drugs is continuing. Additional targets may include improved mitochondrial function through modulation of oxidative stress iron handling, and biogenesis. Newer positive inotropic agents will also have greater advantages if they can be given orally. CIRCUILATORY ASSIST DEVICES Intra-Aortic Balloon Pump Major categories of circulatory assist devices include: IABP, non-iabp percutaneous mechanical circulatory assist devices, and ECMO (Figure 1). The intraaortic balloon pump is the device cardiologists are most familiar with and has been in clinical use for more than 4 decades, largely on the basis of favorable observational data as well as the beneficial effect on coronary blood flow, myocardial oxygen demand and hemodynamic support. It can be inserted easily and rapidly, is the least expensive of all the devices, and does not require continuous monitoring by technical support personnel. The use of IABP during high-risk PCI, acute myocardial infarction, and cardiogenic shock had been present with the paucity of adequately powered randomized controlled trials in these settings (Table 1). In a trial on patients with AMI and Cardiogenic Shock, in a comparison of IABP with standard therapy, no difference in 30-day mortality or in any key secondary end points (hemodynamic stabilization, length of stay in the ICU, lactate levels, dose and duration of catecholamine therapy, and RFT) was found. Although IABP was safe, there was no evidence that it wasassociated with hemodynamic improvement. CRISP-AMI trial randomised patients with high-risk anterior STEMI without shock to a routine strategy of IABP prior to PCI lasting at least12 hours after PCI
3 948 CARDIOLOGY Fig. 2: Circuit configuration for VA and VV-ECMO compared with PCI alone. This strategy did not lead to a reduction in myocardial infarct size and clinicaloutcomes at 6 months were not significantly different between the 2 groups. However, 8.5% of patients in the PCI alone group crossed over to rescue IABP therapy. These findings thus support a standbystrategy (rather than routine use) of IABP during primary PCI in high-risk anterior STEMI patients. In patients undergoing high-risk PCI, IABP insertion was found to be effective in two observationstudies by Briguori et al. These results were not supported by the Balloon Pump Assisted Coronary Intervention Study (BCIS-1), which showed elective IABP insertion did not reduce the incidence of MACCE followingpci and thus do not support a strategy of routine IABP placement before PCI in all patients with severe left ventricular dysfunction and extensive coronary disease. A recent meta-analysis on similar group of patients by Romeo et al., also highlighted the lack of benefit of prophylactic IABP at reducing inhospital mortality and MACCE. IABP is thus simplest to deploy circulatory assist device and to be used as an adjuvant treatment in presence of hemodynamic impairment. Table I shows the current recommendations. Percutaneous Ventricular Support Devices The limitations of IABP led to development of other percutaneous mechanical circulatory devices, in that they provide greater improvement in hemodynamic parameters. Short-term mechanical circulatory support devices are again designed to be used for a wide range of clinical conditions ranging from prophylactic insertion for high-risk PCI to management of cardiogenic shock, ADHF, or cardiopulmonary arrest. Percutaneously inserted LVADs, such as Tandem Heart and Impella, are potential options for short-term Mechanical Circulatory Support (MCS) in the acute setting. Tandem Heart is a percutaneous left atrial to aorta assist device and Impella microaxial flow device is left ventricle to aorta assist device. In head-to-head randomized comparison between the Tandem Heart and IABP in patients undergoing primary PCI, hemodynamics were significantly improved in the pvad group; however, there were more complications with similar 30-day mortality rates. Impella 2.5 have been evaluated in patients undergoing non emergent high-risk PCI in PROTECT II trial, which has shown no significant difference in the primary end point of major adverse events at 30 days between Impella 2.5 or IABP. The EUROSHOCK Registry, a retrospective study of patients with AMI with CS undergoing implantation of Impella 2.5, showed decrease in lactate levels at 48 hours suggesting improved organ perfusion, but with high 30- day mortality at 64.2%.Patients who received Impella 2.5 support prior to primary PCI in the setting of AMI and cardiogenic shock, rather than after PCI, fared better. The Impella 2.5 has also shown beneficial LV remodeling and unloading in anterior STEMI patients without cardiogenic shock. Multiple factors must be considered when choosing MCS including: the hemodynamic condition of the patient, hemodynamic impact of the device, technical considerations including ease and rapidity of insertion, and the ultimate goals of support. In emergent situations, IABP is often selected as the quickest and most familiar way to obtain some degree of hemodynamic stabilization, especially in the setting of AMI with pump failure. The initial effects of the IABP on coronary blood flow may be particularly desirable in this setting as well. If hemodynamic compromise occurs despite appropriatemedicalmanagement and/or IABP, one may consider more powerful hemodynamic support devices such as an Impella. EXTRACORPOREAL MEMBRANE OXYGENATION Mechanical cardiopulmonary support can be delivered
4 in a more prolonged fashion in an intensive care unit, as extracorporeal membrane oxygenation (ECMO). There are two types of ECMO - venoarterial (VA) and venovenous (VV) (Figure 2). Both provide respiratory support like in severe ARDS with refractory hypoxemia and hypercapnia, but only VA ECMO provides hemodynamic support. VA-ECMO can provide acute support in cardiogenic shock or cardiac arrest. The first successful use of extracorporeal membrane oxygenation (ECMO) for treatment of cardiogenic shock was described in Observational studies and case series have reported increased survival rates among patients who received ECMO for cardiac arrest or severe cardiogenic shock as compared to conventional CPR. In patients with acute coronary syndrome who were unresponsive to conventional CPR, ECMO plus intraarrest PCI was associated with improved outcomes in patients who were unresponsive to conventional cardiopulmonary resuscitation. Long-term survivors of ECMO performed for cardiogenic shock have better general health, physical health, and social functioning than patients who require chronic hemodialysis, have advanced heart failure, or have recovered from ARDS. VA-ECMO is thus a strategy for supporting patients with cardiovascular collapse as a bridge to recovery or more definitive therapies, and provide a short-term and longterm survival advantage. HIGH-DOSE DIURETICS VS ULTRAFILTRATION Ultrafiltration should be reserved for patients with fluid overload who do not achieve an adequate response to an aggressive diuretic regimen (Class IIb recommendation). Initial studies supporting use of ultrafiltration in HF were small but provided safety and efficacy data in acute HF. Ultrafiltration ascompared with diuretic therapy resulted in a higher rate of sodium and volume removal, greater weight loss and less frequent rehospitalizations and thus can provide more effective relief of congestion than pharmacologic therapy can. CARRESS-HF challenged this understanding of the effectivenessof ultrafiltration and concluded that ultrafiltration did not result in greater weight loss or improved renal function as compared with pharmacologic therapy and was associated with a similar rate of death or rehospitalization for ADHF. Thus, the use of a stepped pharmacologic-therapy algorithm was superior to a strategy of ultrafiltration for the preservation of renal function at 96 hours, with a similar amount of weight loss with the two approaches. Ultrafiltration was also associated with a higher rate of adverse events. NON-INVASIVE VENTILATION Noninvasive positive pressure ventilation (NPPV) refers to positive pressure ventilation delivered through a noninvasive interface. There is high quality evidence from meta-analyses and randomized trials that NPPV decreases the need for intubation, hospital mortality and improves respiratory parameters (eg, heart rate, dyspnea, hypercapnia, acidosis) in patients with cardiogenic pulmonary edema. However, Three Interventionsin Cardiogenic Pulmonary Oedema study (3CPO), compared modes of ventilation with standard therapy and each other, detected no differences in mortality or need for intubation, in contrast to most preceding studies (although it did find more rapid improvements in patient-reported dyspnea, acidosis, and hypercapnia).the limitation was that they excluded sick patients who required life-saving or emergency intervention, a population that is more likely to benefit from NIV. Sleep-disordered breathing is common in patients who have heart failure with reduced ejection fraction, with prevalence of 50-75%. Adaptive servo-ventilation is a noninvasive ventilatory therapy that alleviates central sleep apnea by delivering servo-controlled inspiratory pressure support on top of expiratory positive airway pressure. In the SERVE-HF trial, however, there was no significant effect of adaptive servo-ventilation on the primary composite end point in the time-to-event analysis of the first event of death from any cause, lifesaving cardiovascular intervention, or unplanned hospitalization for worsening heart failure. Unexpectedly, there was higher all-cause and cardiovascular mortality in the adaptive servo-ventilation group than in the control group. However, no safety concerns have been identified during the short term application of positive airway pressure in patients with decompensated heart failure and thus noninvasive ventilation is considered as adjunctive therapy in patients with acute cardiogenic pulmonary edema who have severe respiratory distress or whose condition does not improve with pharmacologic therapy. CONCLUSION The field of critical care cardiology has undoubtedly grown over the past several years. Patients in cardiogenic shock represent an extremely high risk group in whom mortality has remained high despite revascularization and pharmacologic therapies. Stabilization therapy often begins with intravenous inotropic agents. In the setting of profound cardiogenic shock, IABP is less likely to provide benefit than continuous flow pumps including the Impella and Tandem Heart. ECMO may also provide benefit, particularly for patients with associated impaired respiratory gas exchange and patients unresponsive to conventional CPR. Application of high quality, appropriate, evidence-based medicine to these complex, high-risk cardiac patients requires formal training in this field. REFERENCES 1. Levy JH. Treating Shock-Old Drugs, New Ideas. N Engl J Med 2010; 362: Francis GS, Bartos JA,Adatya S. Inotropes. J Am Coll Cardiol 2014; 63: Yancy CW, Jessup M, Bozkurt B, et al ACCF/AHA guideline for the management of heart failure: areport of 949 CHAPTER 206
5 950 the American College of Cardiology Foundation/American Heart Association Task Force onpractice Guidelines. Circulation 2013; 128:e Tang WH. Reconsidering Ultrafiltration in the Acute Cardiorenal Syndrome. N Engl J Med 2012;367: Weng CL, Zhao YT, Liu QH, et al. Meta-analysis: Noninvasive Ventilation in Acute Cardiogenic Pulmonary Edema. Ann Intern Med 2010; 152: Ihdayhid AR, Chopra S, Rankin J. Intra-aortic balloon pump: indications, efficacy, guidelines and future directions. Curr Opin Cardiol 2014, 29: Gilotra NA, Stevens GR. Temporary Mechanical Circulatory Support: A Review of the Options, Indications, and Outcomes. Clinical Medicine Insights-Cardiology 2014; 8: Rihal CS, Naidu SS, Givertz MM, et al SCAI/ACC/ HFSA/STS Clinical Expert Consensus Statement on the Useof Percutaneous Mechanical CirculatorySupport Devices in Cardiovascular Care. J Am Coll Cardiol 2015; 65:e7 26. CARDIOLOGY
Percutaneous Mechanical Circulatory Support Devices
 Percutaneous Mechanical Circulatory Support Devices Daniel Vazquez RN, RCIS Miami Cardiac & Vascular Institute FINANCIAL DISCLOSURES none CASE STUDY CASE STUDY 52 year old gentlemen Complaining of dyspnea
Percutaneous Mechanical Circulatory Support Devices Daniel Vazquez RN, RCIS Miami Cardiac & Vascular Institute FINANCIAL DISCLOSURES none CASE STUDY CASE STUDY 52 year old gentlemen Complaining of dyspnea
Rationale for Prophylactic Support During Percutaneous Coronary Intervention
 Rationale for Prophylactic Support During Percutaneous Coronary Intervention Navin K. Kapur, MD, FACC, FSCAI Assistant Director, Interventional Cardiology Director, Interventional Research Laboratories
Rationale for Prophylactic Support During Percutaneous Coronary Intervention Navin K. Kapur, MD, FACC, FSCAI Assistant Director, Interventional Cardiology Director, Interventional Research Laboratories
Bridging With Percutaneous Devices: Tandem Heart and Impella
 Bridging With Percutaneous Devices: Tandem Heart and Impella DAVID A. BARAN, MD, FACC, FSCAI SYSTEM DIRECTOR, ADVANCED HEART FAILURE, TX AND MCS SENTARA HEART HOSPITAL NORFOLK, VA PROFESSOR OF MEDICINE
Bridging With Percutaneous Devices: Tandem Heart and Impella DAVID A. BARAN, MD, FACC, FSCAI SYSTEM DIRECTOR, ADVANCED HEART FAILURE, TX AND MCS SENTARA HEART HOSPITAL NORFOLK, VA PROFESSOR OF MEDICINE
AllinaHealthSystem 1
 : Definition End-organ hypoperfusion secondary to cardiac failure Venoarterial ECMO: Patient Selection Michael A. Samara, MD FACC Advanced Heart Failure, Cardiac Transplant & Mechanical Circulatory Support
: Definition End-organ hypoperfusion secondary to cardiac failure Venoarterial ECMO: Patient Selection Michael A. Samara, MD FACC Advanced Heart Failure, Cardiac Transplant & Mechanical Circulatory Support
DECLARATION OF CONFLICT OF INTEREST
 DECLARATION OF CONFLICT OF INTEREST Cardiogenic Shock Mechanical Support Eulàlia Roig FESC Heart Failure and HT Unit Hospital Sant Pau - UAB Barcelona. Spain No conflics of interest Mechanical Circulatory
DECLARATION OF CONFLICT OF INTEREST Cardiogenic Shock Mechanical Support Eulàlia Roig FESC Heart Failure and HT Unit Hospital Sant Pau - UAB Barcelona. Spain No conflics of interest Mechanical Circulatory
Medical Treatment for acute Decompensated Heart Failure. Vlasis Ninios Cardiologist St. Luke s s Hospital Thessaloniki 2011
 Medical Treatment for acute Decompensated Heart Failure Vlasis Ninios Cardiologist St. Luke s s Hospital Thessaloniki 2011 2010 HFSA guidelines for ADHF 2009 focused update of the 2005 American College
Medical Treatment for acute Decompensated Heart Failure Vlasis Ninios Cardiologist St. Luke s s Hospital Thessaloniki 2011 2010 HFSA guidelines for ADHF 2009 focused update of the 2005 American College
Intraaortic Balloon Counterpulsation- Supportive Data for a Role in Cardiogenic Shock ( Be Still My Friend )
 Intraaortic Balloon Counterpulsation- Supportive Data for a Role in Cardiogenic Shock ( Be Still My Friend ) Stephen G. Ellis, MD Section Head, Interventional Cardiology Professor of Medicine Cleveland
Intraaortic Balloon Counterpulsation- Supportive Data for a Role in Cardiogenic Shock ( Be Still My Friend ) Stephen G. Ellis, MD Section Head, Interventional Cardiology Professor of Medicine Cleveland
Management of Cardiogenic Shock. Dr Stephen Pettit, Consultant Cardiologist
 Dr Stephen Pettit, Consultant Cardiologist Cardiogenic shock Management of Cardiogenic Shock Outline Definition, INTERMACS classification Medical management of cardiogenic shock PA catheters and haemodynamic
Dr Stephen Pettit, Consultant Cardiologist Cardiogenic shock Management of Cardiogenic Shock Outline Definition, INTERMACS classification Medical management of cardiogenic shock PA catheters and haemodynamic
Acute heart failure: ECMO Cardiology & Vascular Medicine 2012
 Acute heart failure: ECMO Cardiology & Vascular Medicine 2012 Lucia Jewbali cardiologist-intensivist 14 beds/8 ICU beds Acute coronary syndromes Heart failure/ Cardiogenic shock Post cardiotomy Heart
Acute heart failure: ECMO Cardiology & Vascular Medicine 2012 Lucia Jewbali cardiologist-intensivist 14 beds/8 ICU beds Acute coronary syndromes Heart failure/ Cardiogenic shock Post cardiotomy Heart
Intravenous Inotropic Support an Overview
 Intravenous Inotropic Support an Overview Shaul Atar, MD Western Galilee Medical Center, Nahariya Affiliated with the Faculty of Medicine of the Galilee, Safed, Israel INOTROPES in Acute HF (not vasopressors)
Intravenous Inotropic Support an Overview Shaul Atar, MD Western Galilee Medical Center, Nahariya Affiliated with the Faculty of Medicine of the Galilee, Safed, Israel INOTROPES in Acute HF (not vasopressors)
Assist Devices in STEMI- Intra-aortic Balloon Pump
 Assist Devices in STEMI- Intra-aortic Balloon Pump Ioannis Iakovou, MD, PhD Onassis Cardiac Surgery Center Athens, Greece Cardiogenic shock 5-10% of pts after a heart attack 60000-70000 pts in Europe/year
Assist Devices in STEMI- Intra-aortic Balloon Pump Ioannis Iakovou, MD, PhD Onassis Cardiac Surgery Center Athens, Greece Cardiogenic shock 5-10% of pts after a heart attack 60000-70000 pts in Europe/year
Medical Management of Acute Heart Failure
 Critical Care Medicine and Trauma Medical Management of Acute Heart Failure Mary O. Gray, MD, FAHA Associate Professor of Medicine University of California, San Francisco Staff Cardiologist and Training
Critical Care Medicine and Trauma Medical Management of Acute Heart Failure Mary O. Gray, MD, FAHA Associate Professor of Medicine University of California, San Francisco Staff Cardiologist and Training
Introduction to Acute Mechanical Circulatory Support
 Introduction to Acute Mechanical Circulatory Support Navin K. Kapur, MD, FACC, FSCAI, FAHA Associate Professor, Department of Medicine Interventional Cardiology & Advanced Heart Failure Programs Executive
Introduction to Acute Mechanical Circulatory Support Navin K. Kapur, MD, FACC, FSCAI, FAHA Associate Professor, Department of Medicine Interventional Cardiology & Advanced Heart Failure Programs Executive
Cardiogenic Shock and Initiatives to Reduce Mortality
 Cardiogenic Shock and Initiatives to Reduce Mortality Tanveer Rab, MD, FACC William O Neill, MD, FACC Perwaiz Meraj, MD, FACC Alex Truesdell, MD, FACC The Golden Hours? 50% dead within 10 hours Overall
Cardiogenic Shock and Initiatives to Reduce Mortality Tanveer Rab, MD, FACC William O Neill, MD, FACC Perwaiz Meraj, MD, FACC Alex Truesdell, MD, FACC The Golden Hours? 50% dead within 10 hours Overall
Mechanical circulatory support in cardiogenic shock The Cardiologist s view ACCA Masterclass 2017
 Mechanical circulatory support in cardiogenic shock The Cardiologist s view ACCA Masterclass 2017 Pascal Vranckx MD, PhD. Medical director Cardiac Critical Care Services Hartcentrum Hasselt Belgium Disclosure
Mechanical circulatory support in cardiogenic shock The Cardiologist s view ACCA Masterclass 2017 Pascal Vranckx MD, PhD. Medical director Cardiac Critical Care Services Hartcentrum Hasselt Belgium Disclosure
Rationale for Left Ventricular Support During Percutaneous Coronary Intervention
 Rationale for Left Ventricular Support During Percutaneous Coronary Intervention Navin K. Kapur, MD, FACC, FSCAI Associate Professor, Division of Cardiology Director, Acute Circulatory Support Program
Rationale for Left Ventricular Support During Percutaneous Coronary Intervention Navin K. Kapur, MD, FACC, FSCAI Associate Professor, Division of Cardiology Director, Acute Circulatory Support Program
Percutaneous Mechanical Circulatory Support for Cardiogenic Shock. 24 th Annual San Diego Heart Failure Symposium Ryan R Reeves, MD FSCAI
 Percutaneous Mechanical Circulatory Support for Cardiogenic Shock 24 th Annual San Diego Heart Failure Symposium Ryan R Reeves, MD FSCAI The Need for Circulatory Support Basic Pathophysiologic Problems:
Percutaneous Mechanical Circulatory Support for Cardiogenic Shock 24 th Annual San Diego Heart Failure Symposium Ryan R Reeves, MD FSCAI The Need for Circulatory Support Basic Pathophysiologic Problems:
The Role of Mechanical Circulatory Support in Cardiogenic Shock: When to Utilize
 The Role of Mechanical Circulatory Support in Cardiogenic Shock: Presented by Nancy Scroggins ACNP, CNS-CC CV Surgery ACNP Bayshore Medical Center The Role of Mechanical Circulatory Support in Cardiogenic
The Role of Mechanical Circulatory Support in Cardiogenic Shock: Presented by Nancy Scroggins ACNP, CNS-CC CV Surgery ACNP Bayshore Medical Center The Role of Mechanical Circulatory Support in Cardiogenic
Impella Versus Intra-Aortic Balloon Pump For Treatment Of Cardiogenic Shock: A Meta-Analysis of Randomized Controlled Trials
 Accepted Manuscript Impella Versus Intra-Aortic Balloon Pump For Treatment Of Cardiogenic Shock: A Meta-Analysis of Randomized Controlled Trials Dagmar M. Ouweneel, MSc, Erlend Eriksen, MD, Melchior Seyfarth,
Accepted Manuscript Impella Versus Intra-Aortic Balloon Pump For Treatment Of Cardiogenic Shock: A Meta-Analysis of Randomized Controlled Trials Dagmar M. Ouweneel, MSc, Erlend Eriksen, MD, Melchior Seyfarth,
Cardiogenic Shock. Dr. JPS Henriques. Academic Medical Center University of Amsterdam The Netherlands
 Cardiogenic Shock Dr. JPS Henriques Academic Medical Center University of Amsterdam The Netherlands Conflict of interest disclosure Research grant Abbott Vascular Research grant Abiomed Inc. Global Impella
Cardiogenic Shock Dr. JPS Henriques Academic Medical Center University of Amsterdam The Netherlands Conflict of interest disclosure Research grant Abbott Vascular Research grant Abiomed Inc. Global Impella
Counterpulsation. John N. Nanas, MD, PhD. Professor and Head, 3 rd Cardiology Dept, University of Athens, Athens, Greece
 John N. Nanas, MD, PhD Professor and Head, 3 rd Cardiology Dept, University of Athens, Athens, Greece History of counterpulsation 1952 Augmentation of CBF Adrian and Arthur Kantrowitz, Surgery 1952;14:678-87
John N. Nanas, MD, PhD Professor and Head, 3 rd Cardiology Dept, University of Athens, Athens, Greece History of counterpulsation 1952 Augmentation of CBF Adrian and Arthur Kantrowitz, Surgery 1952;14:678-87
Management of Acute Shock and Right Ventricular Failure
 Management of Acute Shock and Right Ventricular Failure Nader Moazami, MD Department of Thoracic and Cardiovascular Surgery and Biomedical Engineering, Cleveland Clinic NONE Disclosures CARDIOGENIC SHOCK
Management of Acute Shock and Right Ventricular Failure Nader Moazami, MD Department of Thoracic and Cardiovascular Surgery and Biomedical Engineering, Cleveland Clinic NONE Disclosures CARDIOGENIC SHOCK
Οξύ στεφανιαίο σύνδρομο και καρδιογενής καταπληξία. Επεμβατική προσέγγιση. Σωτήριος Πατσιλινάκος Κωνσταντοπούλειο Γ.Ν. Ν. Ιωνίας
 Οξύ στεφανιαίο σύνδρομο και καρδιογενής καταπληξία. Επεμβατική προσέγγιση Σωτήριος Πατσιλινάκος Κωνσταντοπούλειο Γ.Ν. Ν. Ιωνίας ACUTE HEART FAILURE AND CAD: ACS / LV ischaemic dysfunction Mechanical complications
Οξύ στεφανιαίο σύνδρομο και καρδιογενής καταπληξία. Επεμβατική προσέγγιση Σωτήριος Πατσιλινάκος Κωνσταντοπούλειο Γ.Ν. Ν. Ιωνίας ACUTE HEART FAILURE AND CAD: ACS / LV ischaemic dysfunction Mechanical complications
Circulatory Support: From IABP to LVAD
 Circulatory Support: From IABP to LVAD Howard A Cohen, MD, FACC, FSCAI Director Division of Cardiovascular Intervention Co Director Cardiovascular Interventional ti Laboratories Lenox Hill Heart & Vascular
Circulatory Support: From IABP to LVAD Howard A Cohen, MD, FACC, FSCAI Director Division of Cardiovascular Intervention Co Director Cardiovascular Interventional ti Laboratories Lenox Hill Heart & Vascular
Cardiogenic Shock in Acute MI
 Cardiogenic Shock in Acute MI Mark Sheldon, MD UNMH Interventional Cardiology Objectives Overview Treatment Definition Shock profiles Causes Medical Mechanical Illustrative case Questions? Revascularization
Cardiogenic Shock in Acute MI Mark Sheldon, MD UNMH Interventional Cardiology Objectives Overview Treatment Definition Shock profiles Causes Medical Mechanical Illustrative case Questions? Revascularization
Management of Cardiogenic shock. Prof. Christian JM Vrints
 Management of Cardiogenic shock Prof. Christian JM Vrints none conflicts Management of Cardiogenic Shock Incidence and trends Importance of early revascularization Multivessel disease Left main disease
Management of Cardiogenic shock Prof. Christian JM Vrints none conflicts Management of Cardiogenic Shock Incidence and trends Importance of early revascularization Multivessel disease Left main disease
ACUTE HEART FAILURE. Julie Gorchynski MD, MSc, FACEP, FAAEM. Department of Emergency Medicine Emergency Residency Program UTHSC, San Antonio TCEP 2014
 ACUTE HEART FAILURE Julie Gorchynski MD, MSc, FACEP, FAAEM Department of Emergency Medicine Emergency Residency Program UTHSC, San Antonio TCEP 2014 No disclosures Objectives Overview Cases Current Therapy
ACUTE HEART FAILURE Julie Gorchynski MD, MSc, FACEP, FAAEM Department of Emergency Medicine Emergency Residency Program UTHSC, San Antonio TCEP 2014 No disclosures Objectives Overview Cases Current Therapy
Cardiogenic shock: Current management
 Cardiogenic shock: Current management Janine Pöss Universitätsklinikum des Saarlandes Klinik für Innere Medizin III Kardiologie, Angiologie und internistische Intensivmedizin Homburg/Saar I have nothing
Cardiogenic shock: Current management Janine Pöss Universitätsklinikum des Saarlandes Klinik für Innere Medizin III Kardiologie, Angiologie und internistische Intensivmedizin Homburg/Saar I have nothing
Cardiogenic Shock. Carlos Cafri,, MD
 Cardiogenic Shock Carlos Cafri,, MD SHOCK= Inadequate Tissue Mechanisms: Perfusion Inadequate oxygen delivery Release of inflammatory mediators Further microvascular changes, compromised blood flow and
Cardiogenic Shock Carlos Cafri,, MD SHOCK= Inadequate Tissue Mechanisms: Perfusion Inadequate oxygen delivery Release of inflammatory mediators Further microvascular changes, compromised blood flow and
Ted Feldman, M.D., MSCAI FACC FESC
 Support Technologies and High Risk Intervention Patient Selection: When Not to Use Them Ted Feldman, M.D., MSCAI FACC FESC Evanston Hospital SCAI Fall Fellows Course Las Vegas December 7-10 th, 2014 Ted
Support Technologies and High Risk Intervention Patient Selection: When Not to Use Them Ted Feldman, M.D., MSCAI FACC FESC Evanston Hospital SCAI Fall Fellows Course Las Vegas December 7-10 th, 2014 Ted
Management of acute decompensated heart failure and cardiogenic shock. Arintaya Phrommintikul Department of Medicine CMU
 Management of acute decompensated heart failure and cardiogenic shock Arintaya Phrommintikul Department of Medicine CMU Acute heart failure: spectrum Case 64 y/o M with Hx of non-ischemic DCM (LVEF=25-30%)
Management of acute decompensated heart failure and cardiogenic shock Arintaya Phrommintikul Department of Medicine CMU Acute heart failure: spectrum Case 64 y/o M with Hx of non-ischemic DCM (LVEF=25-30%)
Mechanical Cardiac Support in Acute Heart Failure. Michael Felker, MD, MHS Associate Professor of Medicine Director of Heart Failure Research
 Mechanical Cardiac Support in Acute Heart Failure Michael Felker, MD, MHS Associate Professor of Medicine Director of Heart Failure Research Disclosures Research Support and/or Consulting NHLBI Amgen Cytokinetics
Mechanical Cardiac Support in Acute Heart Failure Michael Felker, MD, MHS Associate Professor of Medicine Director of Heart Failure Research Disclosures Research Support and/or Consulting NHLBI Amgen Cytokinetics
PUMP FAILURE COMPLICATING AMI: ISCHAEMIC VSR
 PUMP FAILURE COMPLICATING AMI: ISCHAEMIC VSR Dr Susanna Price MD PhD MRCP ESICM FFICM FESC Consultant Cardiologist & Intensivist Royal Brompton & Harefield NHS Foundation Trust DECLARATIONS Educational
PUMP FAILURE COMPLICATING AMI: ISCHAEMIC VSR Dr Susanna Price MD PhD MRCP ESICM FFICM FESC Consultant Cardiologist & Intensivist Royal Brompton & Harefield NHS Foundation Trust DECLARATIONS Educational
PHARMACOLOGICAL MANAGEMENT OF CARDIOGENIC SHOCK
 PHARMACOLOGICAL MANAGEMENT OF CARDIOGENIC SHOCK Doron Zahger, MD Department of Cardiology, Soroka University Medical Center, Faculty of Health Sciences, Ben Gurion University of the Negev, Beer Sheva,
PHARMACOLOGICAL MANAGEMENT OF CARDIOGENIC SHOCK Doron Zahger, MD Department of Cardiology, Soroka University Medical Center, Faculty of Health Sciences, Ben Gurion University of the Negev, Beer Sheva,
Cardiovascular Health Nova Scotia Update to Antiplatelet Sections of the Nova Scotia Guidelines for Acute Coronary Syndromes, 2008.
 Cardiovascular Health Nova Scotia Update to Antiplatelet Sections of the Nova Scotia Guidelines for Acute Coronary Syndromes, 2008. ST Elevation Myocardial Infarction (STEMI)-Acute Coronary Syndrome Guidelines:
Cardiovascular Health Nova Scotia Update to Antiplatelet Sections of the Nova Scotia Guidelines for Acute Coronary Syndromes, 2008. ST Elevation Myocardial Infarction (STEMI)-Acute Coronary Syndrome Guidelines:
Recovering Hearts. Saving Lives.
 Recovering Hearts. Saving Lives ṬM The Door to Unload (DTU) STEMI Safety & Feasibility Pilot Trial November 218 Recovering Hearts. Saving Lives. LEGAL DISCLAIMERS This presentation includes select slides
Recovering Hearts. Saving Lives ṬM The Door to Unload (DTU) STEMI Safety & Feasibility Pilot Trial November 218 Recovering Hearts. Saving Lives. LEGAL DISCLAIMERS This presentation includes select slides
Percutaneous mechanical circulatory support for treatment and prevention of hemodynamic instability Engström, A.E.
 UvA-DARE (Digital Academic Repository) Percutaneous mechanical circulatory support for treatment and prevention of hemodynamic instability Engström, A.E. Link to publication Citation for published version
UvA-DARE (Digital Academic Repository) Percutaneous mechanical circulatory support for treatment and prevention of hemodynamic instability Engström, A.E. Link to publication Citation for published version
Early discharge in selected patients after an acute coronary syndrome can it be safe?
 Early discharge in selected patients after an acute coronary syndrome can it be safe? Glória Abreu, Pedro Azevedo, Carina Arantes, Catarina Quina-Rodrigues, Sara Fonseca, Juliana Martins, Catarina Vieira,
Early discharge in selected patients after an acute coronary syndrome can it be safe? Glória Abreu, Pedro Azevedo, Carina Arantes, Catarina Quina-Rodrigues, Sara Fonseca, Juliana Martins, Catarina Vieira,
Andrew Civitello MD, FACC
 Timing the Transition from Short Term to Long Term Mechanical Circulatory Support Andrew Civitello MD, FACC Medical Director, Heart Transplant Program Director, Fellowship Co-Director, Baylor St. Luke's
Timing the Transition from Short Term to Long Term Mechanical Circulatory Support Andrew Civitello MD, FACC Medical Director, Heart Transplant Program Director, Fellowship Co-Director, Baylor St. Luke's
Which mechanical assistance for cardiogenic shock?
 Which mechanical assistance for cardiogenic shock? Alain Combes, MD, PhD, Hôpital Pitié-Salpêtrière, AP-HP Inserm UMRS 1166, ican, Institute of Cardiometabolism and Nutrition Pierre et Marie Curie Sorbonne
Which mechanical assistance for cardiogenic shock? Alain Combes, MD, PhD, Hôpital Pitié-Salpêtrière, AP-HP Inserm UMRS 1166, ican, Institute of Cardiometabolism and Nutrition Pierre et Marie Curie Sorbonne
Management of Acute Heart Failure
 Management of Acute Heart Failure Uri Elkayam, MD Professor of Medicine University of Southern California School of Medicine Los Angeles, California elkayam@usc.edu ADHF Treatments Goals.2 Improve symptoms.
Management of Acute Heart Failure Uri Elkayam, MD Professor of Medicine University of Southern California School of Medicine Los Angeles, California elkayam@usc.edu ADHF Treatments Goals.2 Improve symptoms.
Cath Lab Essentials : LV Assist Devices for Hemodynamic Support (IABP, Impella, Tandem Heart, ECMO)
 Cath Lab Essentials : LV Assist Devices for Hemodynamic Support (IABP, Impella, Tandem Heart, ECMO) Michael A. Gibson, MD Assistant Professor of Medicine University of California, Irvine Division of Cardiology
Cath Lab Essentials : LV Assist Devices for Hemodynamic Support (IABP, Impella, Tandem Heart, ECMO) Michael A. Gibson, MD Assistant Professor of Medicine University of California, Irvine Division of Cardiology
Δακτυλίτιδα και Ινότροπα Φάρμακα στην Καρδιακή Ανεπάρκεια. Ι.Κανονίδης
 Δακτυλίτιδα και Ινότροπα Φάρμακα στην Καρδιακή Ανεπάρκεια Ι.Κανονίδης Cardiac Glycosides Chronic Congestive Heart Failure DIGOXIN Na-K ATPase Na + K + Na-Ca Exchange Na + Ca ++ Ca ++ K + Na + Myofilaments
Δακτυλίτιδα και Ινότροπα Φάρμακα στην Καρδιακή Ανεπάρκεια Ι.Κανονίδης Cardiac Glycosides Chronic Congestive Heart Failure DIGOXIN Na-K ATPase Na + K + Na-Ca Exchange Na + Ca ++ Ca ++ K + Na + Myofilaments
CARDIOGENIC SHOCK. Antonio Pesenti. Università degli Studi di Milano Bicocca Azienda Ospedaliera San Gerardo Monza (MI)
 CARDIOGENIC SHOCK Antonio Pesenti Università degli Studi di Milano Bicocca Azienda Ospedaliera San Gerardo Monza (MI) Primary myocardial dysfunction resulting in the inability of the heart to mantain an
CARDIOGENIC SHOCK Antonio Pesenti Università degli Studi di Milano Bicocca Azienda Ospedaliera San Gerardo Monza (MI) Primary myocardial dysfunction resulting in the inability of the heart to mantain an
ECMO as a bridge to durable LVAD therapy. Jonathan Haft, MD Department of Cardiac Surgery University of Michigan
 ECMO as a bridge to durable LVAD therapy Jonathan Haft, MD Department of Cardiac Surgery University of Michigan Systolic Heart Failure Prevalence 4.8 million U.S. 287,000 deaths per year $39 billion spent
ECMO as a bridge to durable LVAD therapy Jonathan Haft, MD Department of Cardiac Surgery University of Michigan Systolic Heart Failure Prevalence 4.8 million U.S. 287,000 deaths per year $39 billion spent
Mechanics of Cath Lab Support Devices
 Mechanics of Cath Lab Support Devices Issam D. Moussa, MD Chief Medical Officer First Coast Cardiovascular Institute, Jacksonville, FL Professor of Medicine, UCF, Orlando, FL None DISCLOSURE Percutaneous
Mechanics of Cath Lab Support Devices Issam D. Moussa, MD Chief Medical Officer First Coast Cardiovascular Institute, Jacksonville, FL Professor of Medicine, UCF, Orlando, FL None DISCLOSURE Percutaneous
Cardiovascular Institute
 Allegheny Health Network Cardiovascular Institute Extracorporeal Membrane Oxygenation (ECMO) Program Our patient survival rate is higher than the national average. ECMO experts. Multidisciplinary team.
Allegheny Health Network Cardiovascular Institute Extracorporeal Membrane Oxygenation (ECMO) Program Our patient survival rate is higher than the national average. ECMO experts. Multidisciplinary team.
Medical Management of Acutely Decompensated Heart Failure. William T. Abraham, MD Director, Division of Cardiovascular Medicine
 Medical Management of Acutely Decompensated Heart Failure William T. Abraham, MD Director, Division of Cardiovascular Medicine Orlando, Florida October 7-9, 2011 Goals of Acute Heart Failure Therapy Alleviate
Medical Management of Acutely Decompensated Heart Failure William T. Abraham, MD Director, Division of Cardiovascular Medicine Orlando, Florida October 7-9, 2011 Goals of Acute Heart Failure Therapy Alleviate
The Pathophysiology of Cardiogenic Shock Knowledge Gaps & Opportunities
 The Pathophysiology of Cardiogenic Shock Knowledge Gaps & Opportunities Navin K. Kapur, MD, FACC, FSCAI, FAHA Associate Professor, Department of Medicine Interventional Cardiology & Advanced Heart Failure
The Pathophysiology of Cardiogenic Shock Knowledge Gaps & Opportunities Navin K. Kapur, MD, FACC, FSCAI, FAHA Associate Professor, Department of Medicine Interventional Cardiology & Advanced Heart Failure
Mechanics of Cath Lab Support Devices
 Mechanics of Cath Lab Support Devices Issam D. Moussa, MD Professor of Medicine Mayo Clinic College of Medicine Chair, Division of Cardiovascular Diseases Mayo Clinic Jacksonville, Florida DISCLOSURE Presenter:
Mechanics of Cath Lab Support Devices Issam D. Moussa, MD Professor of Medicine Mayo Clinic College of Medicine Chair, Division of Cardiovascular Diseases Mayo Clinic Jacksonville, Florida DISCLOSURE Presenter:
Acute HF is a complex and often life-threatening clinical condition. 1 Existing
 ACUTE HEART FAILURE: WHAT IS NEW? John Parissis, MD, PhD; Vasiliki Bistola, MD Author affiliations: Heart Failure Unit, University of Athens, Athens, Greece Address for correspondence: John Parissis, Navarinou
ACUTE HEART FAILURE: WHAT IS NEW? John Parissis, MD, PhD; Vasiliki Bistola, MD Author affiliations: Heart Failure Unit, University of Athens, Athens, Greece Address for correspondence: John Parissis, Navarinou
ST-Elevation Myocardial Infarction & Cardiogenic Shock. - What Should We Do?
 ST-Elevation Myocardial Infarction & Cardiogenic Shock - What Should We Do? Advanced Angioplasty 2008 Dan Blackman Leeds General Infirmary Conflicts of interest Advisory Boards Cordis Boston Scientific
ST-Elevation Myocardial Infarction & Cardiogenic Shock - What Should We Do? Advanced Angioplasty 2008 Dan Blackman Leeds General Infirmary Conflicts of interest Advisory Boards Cordis Boston Scientific
DECLARATION OF CONFLICT OF INTEREST
 DECLARATION OF CONFLICT OF INTEREST Multivessel disease and cardiogenic shock: CABG is the optimal revascularization therapy. Contra Prof. Christian JM Vrints Cardiogenic Shock Spiral Acute Myocardial
DECLARATION OF CONFLICT OF INTEREST Multivessel disease and cardiogenic shock: CABG is the optimal revascularization therapy. Contra Prof. Christian JM Vrints Cardiogenic Shock Spiral Acute Myocardial
IABP SHOCK II trial:
 IABP SHOCK II trial: Randomized comparison of intraaortic balloon counterpulsation versus optimal medical therapy in addition to early revascularization in acute myocardial infarction complicated by cardiogenic
IABP SHOCK II trial: Randomized comparison of intraaortic balloon counterpulsation versus optimal medical therapy in addition to early revascularization in acute myocardial infarction complicated by cardiogenic
DIAGNOSIS AND MANAGEMENT OF ACUTE HEART FAILURE
 DIAGNOSIS AND MANAGEMENT OF ACUTE HEART FAILURE Mefri Yanni, MD Bagian Kardiologi dan Kedokteran Vaskular RS.DR.M.Djamil Padang The 3rd Symcard Padang, Mei 2013 Outline Diagnosis Diagnosis Treatment options
DIAGNOSIS AND MANAGEMENT OF ACUTE HEART FAILURE Mefri Yanni, MD Bagian Kardiologi dan Kedokteran Vaskular RS.DR.M.Djamil Padang The 3rd Symcard Padang, Mei 2013 Outline Diagnosis Diagnosis Treatment options
Advanced Care for Decompensated Heart Failure
 Advanced Care for Decompensated Heart Failure Sara Kalantari MD Assistant Professor of Medicine, University of Chicago Advanced Heart Failure, Mechanical Circulatory Support and Cardiac Transplantation
Advanced Care for Decompensated Heart Failure Sara Kalantari MD Assistant Professor of Medicine, University of Chicago Advanced Heart Failure, Mechanical Circulatory Support and Cardiac Transplantation
Keynote Address II Managing Acute Heart Failure: What Can We Do to Improve Outcomes?
 Keynote Address II Managing Acute Heart Failure: What Can We Do to Improve Outcomes? 24 th Annual San Diego Heart Failure Symposium June 1-2, 2018 La Jolla, CA Barry Greenberg, MD Distinguished Professor
Keynote Address II Managing Acute Heart Failure: What Can We Do to Improve Outcomes? 24 th Annual San Diego Heart Failure Symposium June 1-2, 2018 La Jolla, CA Barry Greenberg, MD Distinguished Professor
Out-of-hospital Cardiac Arrest. Franz R. Eberli MD, FESC, FAHA Cardiology Triemli Hospital Zurich, Switzerland
 Out-of-hospital Cardiac Arrest Franz R. Eberli MD, FESC, FAHA Cardiology Triemli Hospital Zurich, Switzerland Conflict of Interest I have no conflict of interest to disclose regarding this presentation.
Out-of-hospital Cardiac Arrest Franz R. Eberli MD, FESC, FAHA Cardiology Triemli Hospital Zurich, Switzerland Conflict of Interest I have no conflict of interest to disclose regarding this presentation.
MANAGEMENT OF CARDIOGENIC SHOCK
 MANAGEMENT OF CARDIOGENIC SHOCK CASE PRESENTATION 37 year old Dutch female No known coronary artery disease risk factors 1 week post partum at time of presentation (G3P3) after an uncomplicated normal
MANAGEMENT OF CARDIOGENIC SHOCK CASE PRESENTATION 37 year old Dutch female No known coronary artery disease risk factors 1 week post partum at time of presentation (G3P3) after an uncomplicated normal
Drs. Rottman, Salloum, Campbell, Muldowney, Hong, Bagai, Kronenberg
 Rotation: or: Faculty: Coronary Care Unit (CVICU) Dr. Jeff Rottman Drs. Rottman, Salloum, Campbell, Muldowney, Hong, Bagai, Kronenberg Duty Hours: Mon Fri, 7 AM to 7 PM, weekend call shared with consult
Rotation: or: Faculty: Coronary Care Unit (CVICU) Dr. Jeff Rottman Drs. Rottman, Salloum, Campbell, Muldowney, Hong, Bagai, Kronenberg Duty Hours: Mon Fri, 7 AM to 7 PM, weekend call shared with consult
Inotropes for the treatment of advanced heart failure: The role of intermittent administration
 Inotropes for the treatment of advanced heart failure: The role of intermittent administration Dr John T Parissis, Heart Failure Unit, Attikon University Hospital Athens, Greece Disclosures - ALARM investigator
Inotropes for the treatment of advanced heart failure: The role of intermittent administration Dr John T Parissis, Heart Failure Unit, Attikon University Hospital Athens, Greece Disclosures - ALARM investigator
New Horizons in Cardiogenic Shock. Timothy D. Henry, MD Director of Cardiology Cedars-Sinai Heart Institute
 New Horizons in Cardiogenic Shock Timothy D. Henry, MD Director of Cardiology Cedars-Sinai Heart Institute AMI Shock Mortality Unchanged in > 20 years 74355 US AMI/CGS cases per year 1,2 78954 78500 79823
New Horizons in Cardiogenic Shock Timothy D. Henry, MD Director of Cardiology Cedars-Sinai Heart Institute AMI Shock Mortality Unchanged in > 20 years 74355 US AMI/CGS cases per year 1,2 78954 78500 79823
Cardiogenic Shock Protocol
 Cardiogenic Shock Protocol Impella Devices Best Practices in AMI Cardiogenic Shock Identify 1-3 SBP < 90 mmhg or on inotropes /pressors Cold, clammy, tachycardia Lactate elevated > 2 mmoi /L Stabilize
Cardiogenic Shock Protocol Impella Devices Best Practices in AMI Cardiogenic Shock Identify 1-3 SBP < 90 mmhg or on inotropes /pressors Cold, clammy, tachycardia Lactate elevated > 2 mmoi /L Stabilize
How to do Primary Angioplasty. - Patients with Cardiogenic Shock
 How to do Primary Angioplasty - Patients with Cardiogenic Shock Advanced Cardiovascular Intervention 2011 Dan Blackman Leeds General Infirmary MY CONFLICTS OF INTEREST ARE: Research Grants Medicines Company
How to do Primary Angioplasty - Patients with Cardiogenic Shock Advanced Cardiovascular Intervention 2011 Dan Blackman Leeds General Infirmary MY CONFLICTS OF INTEREST ARE: Research Grants Medicines Company
Low cardiac output & Mechanical Support นายแพทย อรรถภ ม ส ศ ภอรรถ ศ ลยศาสตร ห วใจและทรวงอก โรงพยาบาล ราชว ถ
 Low cardiac output & Mechanical Support นายแพทย อรรถภ ม ส ศ ภอรรถ ศ ลยศาสตร ห วใจและทรวงอก โรงพยาบาล ราชว ถ Low cardiac output/cardiogenic Shock State of end-organ hypoperfusion due to cardiac failure.
Low cardiac output & Mechanical Support นายแพทย อรรถภ ม ส ศ ภอรรถ ศ ลยศาสตร ห วใจและทรวงอก โรงพยาบาล ราชว ถ Low cardiac output/cardiogenic Shock State of end-organ hypoperfusion due to cardiac failure.
4/22/2016 Updated. AllinaHealthSystem. Cardiogenic Shock: Definition. No Disclosures. Cardiogenic Shock: Declining (But Still High) Case Fatality Rate
 4/22/216 Updated Definition End-organ hypoperfusion secondary to cardiac failure Advanced Cardiopulmonary Support for the Critically Ill Adult April 22, 216 Cardiogenic Shock Michael A. Samara, MD FACC
4/22/216 Updated Definition End-organ hypoperfusion secondary to cardiac failure Advanced Cardiopulmonary Support for the Critically Ill Adult April 22, 216 Cardiogenic Shock Michael A. Samara, MD FACC
Extra Corporeal Life Support for Acute Heart failure
 Extra Corporeal Life Support for Acute Heart failure Benjamin Medalion, MD Director Heart and Lung Transplantation Department of Cardiothoracic Surgery Rabin Medical Center, Beilinson Campus, Israel Mechanical
Extra Corporeal Life Support for Acute Heart failure Benjamin Medalion, MD Director Heart and Lung Transplantation Department of Cardiothoracic Surgery Rabin Medical Center, Beilinson Campus, Israel Mechanical
Extracorporeal Membrane Oxygenation (ECMO)
 Extracorporeal Membrane Oxygenation (ECMO) Policy Number: Original Effective Date: MM.12.006 05/16/2006 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 01/01/2017 Section: Other/Miscellaneous
Extracorporeal Membrane Oxygenation (ECMO) Policy Number: Original Effective Date: MM.12.006 05/16/2006 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 01/01/2017 Section: Other/Miscellaneous
Extracorporeal Membrane Oxygenation (ECMO)
 Extracorporeal Membrane Oxygenation (ECMO) Policy Number: Original Effective Date: MM.12.006 05/16/2006 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 11/01/2014 Section: Other/Miscellaneous
Extracorporeal Membrane Oxygenation (ECMO) Policy Number: Original Effective Date: MM.12.006 05/16/2006 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 11/01/2014 Section: Other/Miscellaneous
Final published version:
 Clinical Characteristics and Outcomes of Patients With Myocardial Infarction and Cardiogenic Shock Undergoing Coronary Artery Bypass Surgery: Data From The Society of Thoracic Surgeons National Database
Clinical Characteristics and Outcomes of Patients With Myocardial Infarction and Cardiogenic Shock Undergoing Coronary Artery Bypass Surgery: Data From The Society of Thoracic Surgeons National Database
Cardiogenic shock (CS) remains
 The Impella 2.5 and 5.0 devices for ST-elevation myocardial infarction patients presenting with severe and profound cardiogenic shock: The Academic Medical Center intensive care unit experience* Annemarie
The Impella 2.5 and 5.0 devices for ST-elevation myocardial infarction patients presenting with severe and profound cardiogenic shock: The Academic Medical Center intensive care unit experience* Annemarie
The majority of patients with cardiomyopathy
 Selection of Hemodynamic Support: An Approach for Coronary Interventions in Shock and High-Risk PCI The role of hemodynamic support devices in emergent cardiogenic shock and elective high-risk percutaneous
Selection of Hemodynamic Support: An Approach for Coronary Interventions in Shock and High-Risk PCI The role of hemodynamic support devices in emergent cardiogenic shock and elective high-risk percutaneous
Mechanical Circulatory Support (MCS): What Every Pharmacist Needs to Know!
 Mechanical Circulatory Support (MCS): What Every Pharmacist Needs to Know! Matthew A. Wanat, PharmD, BCPS, BCCCP, FCCM Clinical Assistant Professor University of Houston College of Pharmacy Clinical Pharmacy
Mechanical Circulatory Support (MCS): What Every Pharmacist Needs to Know! Matthew A. Wanat, PharmD, BCPS, BCCCP, FCCM Clinical Assistant Professor University of Houston College of Pharmacy Clinical Pharmacy
TREATMENT OPTIONS IN CARDIOGENIC SHOCK WITH INTRA-AORTIC BALLOON COUNTERPULSATION
 TREATMENT OPTIONS IN CARDIOGENIC SHOCK WITH INTRA-AORTIC BALLOON COUNTERPULSATION *Markus W. Ferrari Clinic of Internal Medicine I, HELIOS Dr-Horst-Schmidt-Clinic, Wiesbaden, Germany *Correspondence to
TREATMENT OPTIONS IN CARDIOGENIC SHOCK WITH INTRA-AORTIC BALLOON COUNTERPULSATION *Markus W. Ferrari Clinic of Internal Medicine I, HELIOS Dr-Horst-Schmidt-Clinic, Wiesbaden, Germany *Correspondence to
Ultrafiltration in Decompensated Heart Failure. Description
 Subject: Ultrafiltration in Decompensated Heart Failure Page: 1 of 7 Last Review Status/Date: September 2016 Ultrafiltration in Decompensated Heart Failure Description Ultrafiltration is a technique being
Subject: Ultrafiltration in Decompensated Heart Failure Page: 1 of 7 Last Review Status/Date: September 2016 Ultrafiltration in Decompensated Heart Failure Description Ultrafiltration is a technique being
Disclosures. Objectives 10/11/17. Short Term Mechanical Circulatory Support for Advanced Cardiogenic Shock. I have no disclosures to report
 Short Term Mechanical Circulatory Support for Advanced Cardiogenic Shock Christopher K. Gordon MSN, ACNP-BC Disclosures I have no disclosures to report 1. Pathophysiology 2. Epidemiology 3. Assessment
Short Term Mechanical Circulatory Support for Advanced Cardiogenic Shock Christopher K. Gordon MSN, ACNP-BC Disclosures I have no disclosures to report 1. Pathophysiology 2. Epidemiology 3. Assessment
Rhondalyn C. McLean. 2 ND YEAR RESEARCH ELECTIVE RESIDENT S JOURNAL Volume VII, A. Study Purpose and Rationale
 A Randomized Clinical Study To Compare The Intra-Aortic Balloon Pump To A Percutaneous Left Atrial-To-Femoral Arterial Bypass Device For Treatment Of Cardiogenic Shock Following Acute Myocardial Infarction.
A Randomized Clinical Study To Compare The Intra-Aortic Balloon Pump To A Percutaneous Left Atrial-To-Femoral Arterial Bypass Device For Treatment Of Cardiogenic Shock Following Acute Myocardial Infarction.
Tips & tricks on how to treat an acute heart failure patient with low cardiac output and diuretic resistance
 Tips & tricks on how to treat an acute heart failure patient with low cardiac output and diuretic resistance J. Parissis Attikon University Hospital, Athens, Greece Disclosures ALARM investigator received
Tips & tricks on how to treat an acute heart failure patient with low cardiac output and diuretic resistance J. Parissis Attikon University Hospital, Athens, Greece Disclosures ALARM investigator received
Nova Scotia Guidelines for Acute Coronary Syndromes (Updating the 2008 Antiplatelet Section of the Guidelines)
 Cardiovascular Health Nova Scotia Guideline Update Nova Scotia Guidelines for Acute Coronary Syndromes (Updating the 2008 Antiplatelet Section of the Guidelines) Authors: Dr. M. Love, Dr. I. Bata, K. Harrigan
Cardiovascular Health Nova Scotia Guideline Update Nova Scotia Guidelines for Acute Coronary Syndromes (Updating the 2008 Antiplatelet Section of the Guidelines) Authors: Dr. M. Love, Dr. I. Bata, K. Harrigan
University of Wisconsin - Madison Cardiovascular Medicine Fellowship Program UW CICU Rotation Goals and Objectives
 Background: The field of critical care cardiology has evolved considerably over the past 2 decades. Contemporary critical care cardiology is increasingly focused on the management of patients with advanced
Background: The field of critical care cardiology has evolved considerably over the past 2 decades. Contemporary critical care cardiology is increasingly focused on the management of patients with advanced
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Abdomen, and aorta, as causes of shock, point-of-care ultrasonography in assessment of, 915 917 Abdominal compartment syndrome, trauma patient
Note: Page numbers of article titles are in boldface type. A Abdomen, and aorta, as causes of shock, point-of-care ultrasonography in assessment of, 915 917 Abdominal compartment syndrome, trauma patient
Non Pharmacological Treatment of the Acute Heart Failure
 Non Pharmacological Treatment of the Acute Heart Failure Prof Davor Milicic, MD, PhD University of Zagreb School of Medicine University Hospital Centre Zagreb Croatia DISCLOSURES Conslultancies & lectures
Non Pharmacological Treatment of the Acute Heart Failure Prof Davor Milicic, MD, PhD University of Zagreb School of Medicine University Hospital Centre Zagreb Croatia DISCLOSURES Conslultancies & lectures
Heart failure hospitalizations with preserved or reduced ejection fraction
 Clinical profile and in-hospital outcomes in patients admitted for heart failure with preserved or reduced ejection fraction. EPI-CARDIO prospective registry Tajer, C; Mariani, J; de Abreu, M; Charask,
Clinical profile and in-hospital outcomes in patients admitted for heart failure with preserved or reduced ejection fraction. EPI-CARDIO prospective registry Tajer, C; Mariani, J; de Abreu, M; Charask,
Hemodynamic improvement upon levosimendan treatment in low cardiac output patients following coronary artery bypass graft
 Hemodynamic improvement upon levosimendan treatment in low cardiac output patients following coronary artery bypass graft M. Buerke, K. Krohe, M. Russ, C. Schneider, H. Lemm, R. Prondzinsky, I. Friedrich,
Hemodynamic improvement upon levosimendan treatment in low cardiac output patients following coronary artery bypass graft M. Buerke, K. Krohe, M. Russ, C. Schneider, H. Lemm, R. Prondzinsky, I. Friedrich,
Policy Specific Section: May 16, 1984 April 9, 2014
 Medical Policy Heart Transplant Type: Medical Necessity and Investigational / Experimental Policy Specific Section: Transplant Original Policy Date: Effective Date: May 16, 1984 April 9, 2014 Definitions
Medical Policy Heart Transplant Type: Medical Necessity and Investigational / Experimental Policy Specific Section: Transplant Original Policy Date: Effective Date: May 16, 1984 April 9, 2014 Definitions
MANAGEMENT OF ACUTE PULMONARY EDEMA. Pr. NOUIRA Semir Emergency Department Fattouma Bourguiba University Hospital
 MANAGEMENT OF ACUTE PULMONARY EDEMA Pr. NOUIRA Semir Emergency Department Fattouma Bourguiba University Hospital ACUTE HEART FAILURE 35% 10% Goals of Acute Management Rapidly improve symptoms while preserving
MANAGEMENT OF ACUTE PULMONARY EDEMA Pr. NOUIRA Semir Emergency Department Fattouma Bourguiba University Hospital ACUTE HEART FAILURE 35% 10% Goals of Acute Management Rapidly improve symptoms while preserving
Acute Myocardial Infarction Complicated by Cardiogenic Shock
 Acute Myocardial Infarction Complicated by Cardiogenic Shock Navin K. Kapur, MD, FACC, FSCAI Assistant Professor, Division of Cardiology Director, Acute Circulatory Support Program Director, Interventional
Acute Myocardial Infarction Complicated by Cardiogenic Shock Navin K. Kapur, MD, FACC, FSCAI Assistant Professor, Division of Cardiology Director, Acute Circulatory Support Program Director, Interventional
8th Emirates Cardiac Society Congress in collaboration with ACC Middle East Conference Dubai: October Acute Coronary Syndromes
 8th Emirates Cardiac Society Congress in collaboration with ACC Middle East Conference 2017 OSPEDALE Dubai: 19-21 October 2017 Acute Coronary Syndromes Antonio Colombo Centro Cuore Columbus and S. Raffaele
8th Emirates Cardiac Society Congress in collaboration with ACC Middle East Conference 2017 OSPEDALE Dubai: 19-21 October 2017 Acute Coronary Syndromes Antonio Colombo Centro Cuore Columbus and S. Raffaele
TREATMENT OF HIGHER RISK PATIENTS INTRODUCTION TO PROTECTED PCI WITH IMPELLA. IMP v4
 1 TREATMENT OF HIGHER RISK PATIENTS INTRODUCTION TO PROTECTED PCI WITH IMPELLA FDA APPROVES IMPELLA FOR HIGH-RISK PCI 2 Impella is the only hemodynamic support device proven safe and effective in elective
1 TREATMENT OF HIGHER RISK PATIENTS INTRODUCTION TO PROTECTED PCI WITH IMPELLA FDA APPROVES IMPELLA FOR HIGH-RISK PCI 2 Impella is the only hemodynamic support device proven safe and effective in elective
Pivotal Role of Renal Function in Acute Heart failure
 Pivotal Role of Renal Function in Acute Heart failure Doron Aronson MD, FESC Department of Cardiology RAMBAM Health Care Campus Haifa, Israel Classification and definitions of cardiorenal syndromes CRS
Pivotal Role of Renal Function in Acute Heart failure Doron Aronson MD, FESC Department of Cardiology RAMBAM Health Care Campus Haifa, Israel Classification and definitions of cardiorenal syndromes CRS
Planned, Short-Term RVAD During Durable LVAD Implant: Indications and Management
 Planned, Short-Term RVAD During Durable LVAD Implant: Indications and Management Yoshifumi Naka, MD, PhD Columbia University Medical Center New York, NY Disclosure Abbott/St. Jude Med./Thoratec Consultant
Planned, Short-Term RVAD During Durable LVAD Implant: Indications and Management Yoshifumi Naka, MD, PhD Columbia University Medical Center New York, NY Disclosure Abbott/St. Jude Med./Thoratec Consultant
Echo assessment of patients with an ECMO device
 Echo assessment of patients with an ECMO device Evangelos Leontiadis Cardiologist 1st Cardiology Dept. Onassis Cardiac Surgery Center Athens, Greece Gibbon HLM 1953 Goldstein DJ et al, NEJM 1998; 339:1522
Echo assessment of patients with an ECMO device Evangelos Leontiadis Cardiologist 1st Cardiology Dept. Onassis Cardiac Surgery Center Athens, Greece Gibbon HLM 1953 Goldstein DJ et al, NEJM 1998; 339:1522
Ray Matthews MD Professor of Clinical Medicine Chief of Cardiology University of Southern California
 High Risk PCI Making Possible the Impossible Ray Matthews MD Professor of Clinical Medicine Chief of Cardiology University of Southern California Disclosures Abiomed Research Support Consulting Agreement
High Risk PCI Making Possible the Impossible Ray Matthews MD Professor of Clinical Medicine Chief of Cardiology University of Southern California Disclosures Abiomed Research Support Consulting Agreement
The development of cardiogenic shock portends an extremely poor prognosis. Cardiogenic Shock: A Lethal Complication of Acute Myocardial Infarction
 TREATMENT UPDATE Cardiogenic Shock: A Lethal Complication of Acute Myocardial Infarction David R. Holmes, Jr, MD Mayo Graduate School of Medicine, Mayo Clinic, Rochester, MN Cardiogenic shock is a serious
TREATMENT UPDATE Cardiogenic Shock: A Lethal Complication of Acute Myocardial Infarction David R. Holmes, Jr, MD Mayo Graduate School of Medicine, Mayo Clinic, Rochester, MN Cardiogenic shock is a serious
EACTS Adult Cardiac Database
 EACTS Adult Cardiac Database Quality Improvement Programme List of changes to Version 2.0, 13 th Dec 2018, compared to version 1.0, 1 st May 2014. INTRODUCTORY NOTES This document s purpose is to list
EACTS Adult Cardiac Database Quality Improvement Programme List of changes to Version 2.0, 13 th Dec 2018, compared to version 1.0, 1 st May 2014. INTRODUCTORY NOTES This document s purpose is to list
Heart Failure (HF) Treatment
 Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
ECMO Primer A View to the Future
 ECMO Primer A View to the Future Todd J. Kilbaugh Assistant Professor of Anesthesiology, Critical Care Medicine, and Pediatrics Director of The ECMO Center at the Children s Hospital of Philadelphia Disclosures
ECMO Primer A View to the Future Todd J. Kilbaugh Assistant Professor of Anesthesiology, Critical Care Medicine, and Pediatrics Director of The ECMO Center at the Children s Hospital of Philadelphia Disclosures
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Innovative ECMO Configurations in Adults
 Innovative ECMO Configurations in Adults Practice at a Single Center with Platinum Level ELSO Award for Excellence in Life Support Monika Tukacs, BSN, RN, CCRN Columbia University Irving Medical Center,
Innovative ECMO Configurations in Adults Practice at a Single Center with Platinum Level ELSO Award for Excellence in Life Support Monika Tukacs, BSN, RN, CCRN Columbia University Irving Medical Center,
Complications of Acute Myocardial Infarction
 Acute Myocardial Infarction Complications of Acute Myocardial Infarction Diagnosis and Treatment JMAJ 45(4): 149 154, 2002 Hiroshi NONOGI Director, Division of Cardiology and Emergency Medicine, National
Acute Myocardial Infarction Complications of Acute Myocardial Infarction Diagnosis and Treatment JMAJ 45(4): 149 154, 2002 Hiroshi NONOGI Director, Division of Cardiology and Emergency Medicine, National
