27th Annual ELSO Conference San Diego, CA
|
|
|
- Jonas Lynch
- 5 years ago
- Views:
Transcription
1 27th Annual ELSO Conference San Diego, CA VA ECMO in the cath lab best timing? Impella or ECMO? Michael R. Mooney, MD, FACC, FSCAI, FAHA Director, Coronary Therapeutics Minneapolis Heart Institute at Abbott Northwestern Hospital
2 New Acute CV Systems of Care more acute CS and RCS Level One STEMIs since % present with shock COOL IT Program Resuscitated Cardiac Arrests patients (3/4 transferred) 36.5% (not including DOA) in shock upon arrival. Mortality rate exceeds 50% These patients account for the majority of STEMI mortality A new systems based approach was needed
3 Evolution in care CS and RCS Failed Progress Persistent Limitation Multiple failed trials in CS mortality remains high Cornerstones of therapy largely unproven benefit Pressors may be cardiotoxic IABP mild help with no survival benefit New approaches needed 3
4 Cardiac arrest is common 295,000 OHCA per year in US 23% VF 31% Bystander CPR Median survival all rhythms 7.9%, VF 21% Best EMS systems: ie: Seattle (resuscitated) 17.5% survival to hospital discharge 34% VT/VF subgroup IHCA adults: 19% (despite 95% witnessed or monitored) Mortality among patients surviving to be hospitalized Ontario 72% ( ) Taipei 75% (2003-4) Goteborg 68% (2003-5) Rochester 65% ( ) Circulation 2010;Jan 26:e12-13 Epidemiology of OHCA
5 STEMI-Guidelines and Shock Steg et al. Eur Heart J. 2012;33:
6 Randomized Studies in Cardiogenic Shock Trial Follow-up n/n n/n Revascularization (PCI/CABG) SHOCK SMASH Total 1-year 30 days 76/152 22/32 103/184 83/149 18/23 117/172 Relative Risk 95% CI Relative Risk 95% CI 0.80 (0.66;0.98) 0.87 (0.66;1.29) 0.82 (0.70;0.98) Catecholamines SOAP II (CS Subgroup) Glycoprotein IIb/IIIa-Inhibitors PRAGUE-7 NO Synthase Inhibitors TRIUMPH SHOCK-2 Cotter et al Total IABP IABP-SHOCK I 28 days 64/145 50/135 Early revascularization better Norepinephrine better Medical treatment better Dopamine better 0.75 (0.55;0.93) In-hospital 15/40 13/ (0.59;2.27) 30 days 30 days 30 days 97/201 24/59 4/15 125/275 76/180 7/20 10/15 93/ days 7/19 6/21 Up-stream Abciximab better NO Synthase inhibition better Standard treatment better Placebo better 1.14 (0.91;1.45) 1.16 (0.59;2.69) 0.40 (0.13;1.05) 1.05 (0.85;1.29) 1.28 (0.45;3.72) LVAD Thiele et al Burkhoff et al Seyfarth et al Total 30 days 30 days 30 days 9/21 9/19 6/13 24/53 9/20 5/14 6/13 20/47 IABP better LVAD better Standard treatment better IABP better 0.95 (0.48;1.90) 1.33 ( ) 1.00 ( ) 1.06 ( ) Thiele et al. Eur Heart J 2010,31:
7 Causes of Cardiogenic Shock Tamponade/rupture 1.7% Isolated RV Shock 3.4% VSD 4.6% Other 7.5% AMI Shock Acute Severe MR 8.3% Predominant LV Failure 74.5% Acute on Chronic Adapted From Sanborn T. et al, JACC. 2000
8 The Shock Trial Hochman et al NEJM 1999;341:625
9 Shock Trial: 30 day Mortality (1 o Endpoint) P=NS Hochman et al NEJM 1999;341:625
10 The SHOCK Trial: All Patients (6 Yrs) Hochman et al JAMA 2006; 295:2511
11 Post-hospital Outcomes of Patients With Acute MI With Cardiogenic Shock: NCDR Findings 112,668 patients in ACTION Registry-GWTG who survived hospitalization for acute MI, Among them, 5% had cardiogenic shock. Outcomes With vs Without Cardiogenic Shock Adjusted HR 95% CI Death 1-60 Days Days Death or All-Cause Rehospitalization 1-60 Days Days Conclusion: The risk carried by cardiogenic shock in acute MI seems to be clustered within the first 60 days, after which patients seem to fare similarly whether or not they experienced shock. Shah RU, et al. J Am Coll Cardiol. 2016:67:
12 Frequency of CS Has Remained Frequency of Cardiogenic Shock NRMI STEMI Registry 1 N=25,311 Steady Over Time NRMI Registry 1 Inclusion of 293,633 patients from Jan 1995-May 2004 with STEMI or new LBBB 775 US Hospitals with on-site PCI CS developed in 25,311 (8.6%) pts CS present on admission in 29% Worcester Heart Attack Study % Gusto % 1Babaev et al JAMA :448 2Goldberg RJ NEJM 1991; 325: Holmes DR JACC :668
13 In-hospital Mortality USIK 1995, USIC 2000, FAST-MI France National Registry Death at 30 days (%) (62-77) 63 (56-70) 8.7 ( ) 4.2 ( ) 51 (44-59) Shock No Shock 3.6 ( ) Aissaoui et al. Eur Heart J 2012; 33:
14 Cardiogenic Shock Pathophysiology When a critical mass of LV is necrotic and fails to pump, stoke volume and CO falls Myocardial and coronary perfusion are compromised causing tachycardia and hypotension Increased LVEDP further decreases coronary perfusion Increase LV wall stress increases myocardial oxygen demand Lactic acidosis worsens myocardial performance Hollenberg Ann Int Med 1999; 131:47-99
15 Paradigm Shift in Use of Short-term MCS Patient with Acute myocardial infarction (AMI), Congestive heart failure (CHF), or Coronary artery disease and other heart disease (CAD) PRE-2007 POST-2007 MCS instituted after circulatory collapse (reactive) Limited or no percutaneous MCS devices available Percutaneous MCS devices more readily available MCS instituted before circulatory collapse (anticipatory) Organ dysfunction has already occurred Most MCS implanted surgically (primarily by cardiac surgeons) MCS increasingly implemented without need for surgical consultation Avoidance of organ dysfunction Longer hospital stay post-surgery Shorter hospital stay and higher rate of home discharges Higher mortality Higher hospital costs Reduced hospital costs Lower mortality Stretch et al. JACC 2014;64:
16 Overview of LV Support Devices Tandem Heart Impella 5.0 Impella 2.5 Impella CP Percutaneous ECMO Cannula size (French) Flow (l/min) 21 venous arterial Max Max Max venous, arterial Max 7.0 Pump speed (rpm) Max. 7,500 Max. 33,000 Max. 51,000 Max. 46,000 Max. 5,000 Insertion/ Placement Peripheral (Femoral artery + LA) Peripheral surgical (Femoral artery) Percutaneous (Femoral artery) Percutaneous (Femoral artery) Percutaneous (Femoral artery + Vein) Anticoagulation Rec. Duration 14 Days 10 Days 10 Days 10 Days 7 Days Relative Costs to IABP Thiele et al, Eur Heart J 2007; 28: Thiele et al. Eur Heart J 2010; 31,
17 Thiele et al. Lancet 2013 IABP SHOCK II: 1 year Mortality 30-day mortality 6-month mortality 12-month mortality 60% 50% 41.3% 48.7% 49.2% 51.8% 51.4% IABP Control Mortality 40% 30% 20% 39.7% Logrank p = 0.94 RR % CI % No. at risk IABP Control 0% Days after randomization
18 No Hemodynamic Benefit of IABP in a Recent Prospective Randomized Trial Cardiac Power Output (CPO in Watts) IABP (n=19) No IABP(n=21) Inotrope dosage was similar between the 2 groups p<0.011 Time in hours Prior N.S Prondzinsky et al. SHOCK 2012;37:
19 Hemodynamic Effects of Impella Support Outflow (aortic root) Inflow (ventricle) aortic valve Flow MAP LVEDP and LVEDV Wall Tension Mechanical Work Microvascular Resistance Coronary Perfusion Cardiac Power Output O 2 Supply O 2 Demand End Organ Perfusion Unloading to Myocardial Recovery Fincke J, et al. Am Coll Cardiol 2004 den Uil CA, et al. Eur Heart J 2010 Mendoza DD, et al. AMJ 2007 Torgersen C, et al. Crit Care 2009 Torre-Amione G, et al. J Card Fail 2009 Suga H. et al. Am J Physiol 1979 Suga H, et al. Am J Physiol 1981 Burkhoff D. et al. Am J Physiol Heart Circ 2005 Burkhoff D. et al. Mechanical Properties Of The Heart And Its Interaction With The Vascular System. (White Paper) 2011 Sauren LDC, et al. Artif Organs 2007 Meyns B, et al. J Am Coll Cardiol 2003 Remmelink M, et al. atheter.cardiovasc Interv 2007 Aqel RA, et al. J Nucl Cardiol 2009 Lam K,. et al. Clin Res Cardiol 2009 Reesink KD, et al. Chest 2004 Valgimigli M, et al.catheter Cardiovasc Interv 2005 Remmelink M. et al. Catheter Cardiovasc Interv 2010 Naidu S. et al. Novel Circulation.2011 Weber DM, et al. Cardiac Interventions Today Supplement Aug/Sep 2009
20 Impella and the FDA Impella 2.5 receiving an FDA indication for use in elective and high-risk PCI procedures in 2015 Protect 1 Trial Aug The FDA approved four Impella heart pumps including the 2.5, CP, 5.0, and LD devices (Abiomed) for ongoing cardiogenic shock that occurs within 48 hours of MI or open-heart surgery as a result of left ventricular failure unresponsive to medical therapy and conventional treatment. The devices are approved for use in patients with or without an intra-aortic balloon pump. Recover 1 Trial 20
21 ISAR-SHOCK Trial AMI Cardiogenic Shock N=26 STEMI Patients in Profound Cardiogenic Shock PCI + IABP R 1:1 PCI + IMPELLA LP 2.5 Primary Endpoint = Hemodynamic Improvement after 20 min of support Seyfarth et al. American College of Cardiology, 2007
22 Cardiac Index (L/min/m 2 ) ISAR-SHOCK Randomized Trial: IMPELLA 2.5 Provides a Better Hemodynamic Support Than IABP in AMI Cardiogenic Shock 0. Primary Endpoint: Increase in Cardiac Index From Baseline (measured after 20 min of support) Impella IABP P< Cardiac Output (L/min) P< Seyfarth et al. American College of Cardiology, 2007
23 Cardiac Output (l/min) Improved Hemodynamics and Tissue Perfusion with Impella 5.0 in Shock Patients ±1.3 Pre-Pump Cardiac Output p= ±1.3 On-Pump (N= 16) Mean Arterial Pressure (mmhg) 80 75± Mean Arterial Pressure 57±13 Pre-Pump p=0.003 On-Pump Left Atrial Pressure Plasma Lactate Left Atrial Pressure (l/min) ±11 p= ±6 Pre-Pump On-Pump Plasma Lactate (mmol/l) ±1 Pre-Pump p= ±0.5 On-Pump Meyns and al. Thoracic Cardiov Surg 2003:51:1-6
24 Meta-analysis of Percutaneous LVAD in CGSCGS.Study characteristics of included trials Thiele et al. Burkhoff et al. * Not reported whether the envelopes were opaque and sequentially numbered. IABP, intra-aortic balloon pump; LVAD, left ventricular assist device. Seyfarth et al. Percutaneous LVAD used TandemHeart TandemHeart Impella LP25 Control IABP IABP IABP Total number of patients Setting Single-centre Multi-centre Two-centre Randomization Yes Yes Yes Sequence generation Concealment of allocation Drawing Envelopes Not reported Not reported Sealed envelopes Not reported Not reported Blinding Not possible Not possible Not possible Handling of patient attrition Complete follow-up Complete follow-up Complete follow-up Cheng et al, European Heart Journal 2009;30:
25 Thiele et al. Burkoff et al. Seyfarth et al. Pooled Thiele et al. Burkoff et al. Seyfarth et al. Pooled Thiele et al. Burkoff et al. Seyfarth et al. Pooled LVAD Mean + SD LVAD Mean + SD LVAD Mean + SD Hemodynamics IABP Mean + SD Cardiac index Mean Difference Favors IABP Favors LVAD IABP Mean Arterial Pressure Mean + SD Mean Difference Favors IABP Favors LVAD IABP Pulmonary wedge pressure Mean + SD Mean Difference Favors LVAD Favors IABP P(heterogeneity) = 0.22 l 2 = 34.0% 0.55 ( ) 0.16 ( ) 0.35 ( ) 0.35 ( ) P(heterogeneity) = 0.10 l 2 = 55.9% 0.55 ( ) 18.6 ( ) 16.0 ( ) 12.8 ( ) P(heterogeneity) = 0.01 l 2 = 76.6% -5.6 (-9.2 to -2.1) -8.4 (-11.0 to -5.8) -1.0 ( ) -5.3 (-9.4 to -1.2) Cheng et al, European Heart Journal 2009;30:
26 30 Day Mortality LVAD n/n IABP n/n 30-day Mortality Relative Risk P(heterogeneity) = 0.83 l 2 = 0% Thiele et al. 9/21 9/ ( ) Burkoff et al. 9/19 5/ ( ) Seyfarth et al. 6/13 6/ ( ) Pooled 24/53 20/ ( ) Favors LVAD Favors IABP Cheng et al, European Heart Journal 2009;30:
27 Thiele et al. Burkoff et al. Seyfarth et al. Pooled LVAD n/n Complications IABP n/n 7/21 0/20 4/19 2/14 1/13 0/13 12/53 2/47 Reported Leg Ischemia Relative Risk P(heterogeneity) = 0.38 l 2 = 0% ( ) 1.47 ( ) 3.00 ( ) 2.59 ( ) ,000 Favors LVAD Favors IABP LVAD n/n IABP n/n Reported Bleeding Relative Risk P(heterogeneity) = 0.73 l 2 = 0% Thiele et al. Burkoff et al. Pooled 19/21 8/20 8/19 2/14 27/40 10/ ( ) 2.95 ( ) 2.35 ( ) Favors LVAD Favors IABP LVAD n/n IABP n/n Reported Fever or Sepsis Relative Risk P(heterogeneity) = 0.10 l 2 = 62.1% Thiele et al. Burkoff et al. Pooled 17/21 10/20 4/19 5/14 21/40 15/ ( ) 0.59 ( ) 1.11 ( ) Favors LVAD Favors IABP Cheng et al, European Heart Journal 2009;30:
28 US Pella Registry: Main Indications for Support (N=352 patients at 24 centers) High Risk PCI (66%) Elective PCI*, 29% Urgent PCI**, 37% AMI Shock, 20% Other Forms of Shock, 14% Others includes Myocarditis with shock, Post-cardiotomy shock, septic shock, toxic shock, post partum cardiomyopathy, other cardiomyopathies with shock * Elective = Stable angina or silent ischemia ** Urgent = Unstable angina or Non ST elevation Myocardial Infarction
29 AMI Shock Registry Design Impella 2.5 used for AMI Cardiogenic Shock (physician s decision) Exclusion Criteria: AMI patients with stable hemodynamics Other forms of Shock with no AMI Prophylactic support for high risk PCI Contra-indication to use Impella 2.5 Inclusion Criteria: STEMI or NSTEMI patients with Cardiogenic shock Shock defined clinically as: SBP < 90mmHg for > 30min or need of inotropes to maintain SBP or Cardiac index <2.2 l/min/m2 Pump placed emergently to restore hemodynamics Survival to Discharge or 30-days
30 Cardiac Index (l/min/m 2 ) SVR (x 1000 dynes/sec x cm -5 ) Impella Improves Immediately the Hemodynamics in AMI Shock Cardiac Index p= ±0. 6 Pre Impella* 2.2±0.8 Pre Impella * 2.7±0. 9 On Impella SVR p= ±0.4 On Impella MAP (mmhg) PCWP (mmhg) Mean Arterial Pressure p< ±17 Pre Impella * Wedge Pressure 28±9 Pre Impella* 92±21 On Impella p= ±12 On Impella * Pre-Impella measurements were recorded under clinical conditions (i.e, with inotropes + IABP)
31 Blood Pressure (mmhg) Gain on Hemodynamics When Switching from IABP to Impella in AMI Shock Systolic Blood Pressure Diastolic Blood Pressure Mean Arterial Pressure 82±19 On IABP p< Patient serve as his/her own control (N=20) Gain = + 38% Gain = + 40% Gain = + 41% 113±30 Switched to Impella 47±16 On IABP P= ±16 Switched to Impella p< mmhg in MAP is the considered minimum threshold for adequate coronary, cerebral and renal perfusion 59±15 On IABP 83±17 Switched to Impella Comparisons made for ALL AMI shock patients that were on IABP then switched to Impella for whom pre and post blood pressure values were available (N=20)
32 Largest Cohort To Study The Current Use of Impella in Cardiogenic Shock O Neill et al, Jour of Interv. Cardiol (In press)
33 Impella Insertion Timing (N= 154) Prior to PCI (n=63) 41.0% pre post 59.0% Post PCI (n=91)
34 100 Outcome 80 Survival(%) Pre - PCI Post-PCI 20 0 Log-rank test, p= Days from initiation of Impella 2.5 support Number of patients at risk
35 DanShock Trial Enrolling 1 Endpoint: All Cause Mortality Acute MI (STEMI < 36 h) Shock Eligible PCI (CABG) Lactate > 2.5 mmol/l SBP < 100 mmhg oder Vasopressoren LV-EF < 35% Randomization Conventional Therapy + IABP + PCI (n=180) Conventional Therapy + Impella cvad + PCI (n=180)
36 Potential Indications for Mechanical Circulatory Support 36
37 CardiacAssist TandemHeart Access to LA via standard transseptal technique Catheter exchanges made with Valvuloplasty guidewire or Amplatz soft tip wire Dilate septum with 2-stage (14/21 Fr.) dilator Place cannula in LA
38 Adult Cardiac ECMO Use Annual Reported Procedures % Growth in Annual Procedures in Last 2 years ELSO Registry
39 CPR with ECLS vs. Conventional CPR: In-Hospital Cardiac Arrest Survival to Discharge Based Upon Duration of CPR Chen et al, Lancet 2008
40 ECMO Not A Free Lunch! Possibility of centrally deoxygenated blood Brain Perfusion Limb Ischemia Bleeding Need for Transfusion Inflammatory Response Increased Afterload??
41 Protek DUO Coaxial dual lumen 29 Fr outer, 16 Fr inner Compatible with multiple centrifugal flow pumps
42 STATE OF CURRENT KNOWLEDGE TTM for CA is effective, guideline supported,and best done within the STEMI network system of care Survival for CA should be 50% ECMO is a fast moving trend for RCS and refractory CA ECMO is best done within the STEMI network system of care The best ECMO candidate has a STEMI and refractory CS, the most challenging ECMO has OOH refractory CA 42
43 Percutaneous Left Ventricular Support Devices Werdan et al, EHJ 2014
44 1.Percutaneous MCS provides superior hemodynamic support compared to pharmacologic therapy. This is particularly apparent for the Impella and Tandem-Heart devices. These devices should remain available clinically and be appropriately reimbursed. 2.Patients in cardiogenic shock represent an extremely high risk group in whom mortality has remained high despite revascularization and pharmacologic therapies. Early placement of an appropriate MCS may be considered in those who fail to stabilize or show signs of improvement quickly after initial interventions. 3.MCS may be considered for patients undergoing high-risk PCI, such as those requiring multivessel, left main, or last patent conduit interventions, particularly if the patient is inoperable or has severely decreased ejection fraction or elevated cardiac filling pressures. 4.In the setting of profound cardiogenic shock, IABP is less likely to provide benefit than continuous flow pumps including the Impella CP and TandemHeart. ECMO may also provide benefit, particularly for patients with impaired respiratory gas exchange. 5.Patients with acute decompensated heart failure may benefit from early use of percutaneous MCS when they continue to deteriorate despite initial interventions. MCS may be considered if patients are candidates for surgically implanted VADs or if rapid recovery is expected (e.g., fulminant myocarditis or stress-induced cardiomyopathy). 6.When oxygenation remains impaired, adding an oxygenator to a TandemHeart circuit or use of ECMO should be considered based upon local availability. 7.There are insufficient data to support or refute the notion that routine use of MCSs as an adjunct to primary revascularization in the setting of large acute myocardial infarction is useful in reducing reperfusion injury or infarct size. Exploratory studies are underway. 8.MCSs may be used for failure to wean off cardiopulmonary bypass, considered as an adjunct to high-risk electrophysiologic procedures when prolonged hypotension is anticipated, or rarely, for valvular interventions. 9.Severe biventricular failure may require use of both right- and left-sided percutaneous MCS or veno-arterial ECMO. Certain patients may respond to LVAD implantation with inotropes and/or pulmonary vasodilators to support the right heart. MCS may also be considered for isolated acute RVF complicated by cardiogenic shock. 10.Registries and randomized controlled trials comparing different strategies in different clinical scenarios are critically needed. 11.Early analyses suggest cost-effectiveness of MCS for emergent use in comparison to surgical ECMO or VAD support, and for elective use in comparison to IABP. Further data are necessary.
45 New Acute CV Systems of Care more acute CS and RCS Level One STEMIs since % present with shock COOL IT Program Resuscitated Cardiac Arrests patients (3/4 transferred) 36.5% (not including DOA) in shock upon arrival. Mortality rate exceeds 50% These patients account for the majority of STEMI mortality A new systems based approach was needed
46 Emergency E-ECMO Multidisciplinary, experienced team members that rapidly respond and come together when a patient is evaluated for emergent ECMO. ICU charge RN Physicians Cardiology, Intensivist, Interventionalist, Heart Failure CV Emergency Program Manager Chaplain Cardiac Diagnostic Tech CV Surgeon, Vascular Surgeon Emergency Shock/ ECMO Response Team. Perfusion Team/ Hemodynamic Support Team Respiratory Therapy CV Emergency Nurse Clinician Pharmacist CV Lab Team
47 Ward/CCU Inpatient Shock Team Internal Communications Protocol Cath Lab Patient Shock Patient Accepted for Transfer Outside Call to HF Intensivist SHOCK TEAM PAGER ACTIVATION ECLYPSIS NOTE Shock Interventionalist Shock Surgeon Shock Fellow Shock Intensivist Shock Team Recommendation CCU Fellow Medical Management OR Initiate MCS (Cath Lab/OR)
48 Utilization of TTM, a Systems of Care Approach 48
49 Unstable patient Assessment Frequent looks in transitioning patients ABG, A- line, oximetry, mentation Right heart cath with CI Lactate clearance Stat echo Revasc but just as a start If problem likely acute with reversible elements Collaborate early 49
50 Treatment, Outcomes of Acute MI Complicated by Shock After Public Reporting Policy Changes in New York 45,977 patients treated in New York, three nonreporting states (Michigan, New Jersey, and California), or Massachusetts. Rate of PCI increased from 44.9% before shock was excluded from NY reporting requirements to 49.2% afterwards across all states, with a greater increase seen in New York PCI rates remained lower in New York than in other states throughout the study period In-hospital mortality fell from 44.7% to 37.9% across all states, with a greater decline in New York Conclusion: Exclusion of patients with cardiogenic shock from New York s public reporting requirements for PCI coincided with an uptick in PCI use for these high-risk patients. McCabe JM, et al. JAMA Cardiol. 2016;Epub ahead of print.
51 Today s Cardiac Cath Lab Treatment Space Where we do PCI/Structural and Peripheral Interventions but also Resucitation and Critical Care Hemodynamic Laboratory Right and left left heart catheterizations under utilized but critical to patient management Learning Space to Improve Future Patient Care Ideal space for multidisciplinary collaboration 51
52 Hemodynamics are Key to Patient Management We make people ischemic during PCI! Catheters interfere with aorto-ostial flow, LM lesions and large bore catheters Contrast does not contain hemoglobin and is a myocardial depressant Inflated microcatheters, inflated balloons, stents obstruct blood flow! Adverse hemodynamics can make what appears to be a controlled and stable situation unstable cannot be ignored 52
53 Cardiogenic Shock is a Spectrum Pre-Shock Shock Profound Shock No Hemodynamic Support Mortality Needs Partial Hemodynamic Support Needs Full Hemodynamic Support 80% 42% 2% 3% 7.5% 21% Mortality Risk with Inotrope Dosing Three High Dose Samuels LE et al, J Card Surg Jul-Aug;14(4):288-93
54 Consider acidosis, lactate clr, oxygenation, RV function Treatment COLLABORATE with TEAM IABP Medical Therapy Impella ECMO/VAD 3.0 Cardiac Index Pre-Shock Shock Severe Shock Team Decisions are Key in Good Outcomes
55 55 Seder,Crit Care Med 2009;37 (Suppl):S211-S222.
56
57 Percutaneous Cardiopulmonary Bypass (ECMO or CPS) Lifebridge B2T Pump Venous to arterial conduit with oxygenator Can deliver 6 l/min CO Generally Fr venous and Fr arterial catheters No randomized trials Observational data only
58 The best TH and E-CPR ecmo patient is/has: OOH with <15 min down time Witnessed VF/VT and age <75 yo Bystander CPR Has a STEMI Lives in Minnesota, Seattle, Arizona, Tennessee, Ottawa, Lehigh Valley (systems of care) Gets cooling in the first hour after rosc 58
59 Cardiac 5603 pts Respiratory 7008 pts 56% survived ECLS 65% survived ECLS 41% survived to DC 57% survived to DC ECPR % survived to DC 59
60 ECPR - survival ELSO ANW Mostly RCS 60 n= 1657 n= 45
61 Ejection Fraction: % at ECMO placement and % at Discharge EF % ECMO Discharge
62 What have we learned? ECMO can be incorporated into a STEMI program and be implemented w/in 40 min Lucas or mechanical CPR is now essential in our CV labs Antegrade perfusion limbs must be established early and ultrasound guidance reduces complications LV unloading is not essential for LV recovery as LV emptying and return of pusatile flow is very early and common TH can be used in ECMO pts safely and lead to favorable CPC Patient Selection- collaboration with CHF/transplant team
63 RCS and ECMO What have we learned ECMO can be a life saving technique when instituted by an experienced Shock Team in the CV Laboratory for refractory Cardiogenic Shock. Striking recovery of LV function can also occur in several days ECMO should be developed in selected PCI centers as part of a system of care for acute cardiac emergencies. It is best delivered in the Cath lab by Interventionalists/Intensivist. Many issues will need to be verified by clinical trials, but should not delay the programatic offering of this therapy. Many common understanding of ECMO are outdated. ECMO is a transformative therapy.
64 GAPS IN CURRENT KNOWLEDGE SCAI and Mission Lifeline involvement Clinical trials and registry formation We are behind many centers in Europe Raise awareness Maquet systems w/o emergency perfusionist may enable dispersion and subsequent transfer to ECMO Center Accurate early neuro-prognostication Integration of E-ECMO and E-CPR into regional STEMI Networks Systems of care that support regional Centers of Excellence in ECMO and CA 64
65 65 The End
Intraaortic Balloon Counterpulsation- Supportive Data for a Role in Cardiogenic Shock ( Be Still My Friend )
 Intraaortic Balloon Counterpulsation- Supportive Data for a Role in Cardiogenic Shock ( Be Still My Friend ) Stephen G. Ellis, MD Section Head, Interventional Cardiology Professor of Medicine Cleveland
Intraaortic Balloon Counterpulsation- Supportive Data for a Role in Cardiogenic Shock ( Be Still My Friend ) Stephen G. Ellis, MD Section Head, Interventional Cardiology Professor of Medicine Cleveland
High Risk PCI for Heart Failure
 High Risk PCI for Heart Failure Ray Matthews MD Professor of Clinical Medicine Chief, Division of Cardiovascular Medicine University of Southern California Los Angeles, California Disclosures Abiomed Research
High Risk PCI for Heart Failure Ray Matthews MD Professor of Clinical Medicine Chief, Division of Cardiovascular Medicine University of Southern California Los Angeles, California Disclosures Abiomed Research
LV Assist in High Risk PCI and Cardiogenic Shock: Is it Worth the Effort?
 LV Assist in High Risk PCI and Cardiogenic Shock: Is it Worth the Effort? Vincent J. Pompili, MD, FACC, FSCAI Professor of Internal Medicine Director of Interventional Cardiovascular Medicine and Cardiac
LV Assist in High Risk PCI and Cardiogenic Shock: Is it Worth the Effort? Vincent J. Pompili, MD, FACC, FSCAI Professor of Internal Medicine Director of Interventional Cardiovascular Medicine and Cardiac
Assist Devices in STEMI- Intra-aortic Balloon Pump
 Assist Devices in STEMI- Intra-aortic Balloon Pump Ioannis Iakovou, MD, PhD Onassis Cardiac Surgery Center Athens, Greece Cardiogenic shock 5-10% of pts after a heart attack 60000-70000 pts in Europe/year
Assist Devices in STEMI- Intra-aortic Balloon Pump Ioannis Iakovou, MD, PhD Onassis Cardiac Surgery Center Athens, Greece Cardiogenic shock 5-10% of pts after a heart attack 60000-70000 pts in Europe/year
Management of Acute Shock and Right Ventricular Failure
 Management of Acute Shock and Right Ventricular Failure Nader Moazami, MD Department of Thoracic and Cardiovascular Surgery and Biomedical Engineering, Cleveland Clinic NONE Disclosures CARDIOGENIC SHOCK
Management of Acute Shock and Right Ventricular Failure Nader Moazami, MD Department of Thoracic and Cardiovascular Surgery and Biomedical Engineering, Cleveland Clinic NONE Disclosures CARDIOGENIC SHOCK
AllinaHealthSystem 1
 : Definition End-organ hypoperfusion secondary to cardiac failure Venoarterial ECMO: Patient Selection Michael A. Samara, MD FACC Advanced Heart Failure, Cardiac Transplant & Mechanical Circulatory Support
: Definition End-organ hypoperfusion secondary to cardiac failure Venoarterial ECMO: Patient Selection Michael A. Samara, MD FACC Advanced Heart Failure, Cardiac Transplant & Mechanical Circulatory Support
Bridging With Percutaneous Devices: Tandem Heart and Impella
 Bridging With Percutaneous Devices: Tandem Heart and Impella DAVID A. BARAN, MD, FACC, FSCAI SYSTEM DIRECTOR, ADVANCED HEART FAILURE, TX AND MCS SENTARA HEART HOSPITAL NORFOLK, VA PROFESSOR OF MEDICINE
Bridging With Percutaneous Devices: Tandem Heart and Impella DAVID A. BARAN, MD, FACC, FSCAI SYSTEM DIRECTOR, ADVANCED HEART FAILURE, TX AND MCS SENTARA HEART HOSPITAL NORFOLK, VA PROFESSOR OF MEDICINE
Rationale for Prophylactic Support During Percutaneous Coronary Intervention
 Rationale for Prophylactic Support During Percutaneous Coronary Intervention Navin K. Kapur, MD, FACC, FSCAI Assistant Director, Interventional Cardiology Director, Interventional Research Laboratories
Rationale for Prophylactic Support During Percutaneous Coronary Intervention Navin K. Kapur, MD, FACC, FSCAI Assistant Director, Interventional Cardiology Director, Interventional Research Laboratories
Cath Lab Essentials : LV Assist Devices for Hemodynamic Support (IABP, Impella, Tandem Heart, ECMO)
 Cath Lab Essentials : LV Assist Devices for Hemodynamic Support (IABP, Impella, Tandem Heart, ECMO) Michael A. Gibson, MD Assistant Professor of Medicine University of California, Irvine Division of Cardiology
Cath Lab Essentials : LV Assist Devices for Hemodynamic Support (IABP, Impella, Tandem Heart, ECMO) Michael A. Gibson, MD Assistant Professor of Medicine University of California, Irvine Division of Cardiology
DECLARATION OF CONFLICT OF INTEREST
 DECLARATION OF CONFLICT OF INTEREST Cardiogenic Shock Mechanical Support Eulàlia Roig FESC Heart Failure and HT Unit Hospital Sant Pau - UAB Barcelona. Spain No conflics of interest Mechanical Circulatory
DECLARATION OF CONFLICT OF INTEREST Cardiogenic Shock Mechanical Support Eulàlia Roig FESC Heart Failure and HT Unit Hospital Sant Pau - UAB Barcelona. Spain No conflics of interest Mechanical Circulatory
New Horizons in Cardiogenic Shock. Timothy D. Henry, MD Director of Cardiology Cedars-Sinai Heart Institute
 New Horizons in Cardiogenic Shock Timothy D. Henry, MD Director of Cardiology Cedars-Sinai Heart Institute AMI Shock Mortality Unchanged in > 20 years 74355 US AMI/CGS cases per year 1,2 78954 78500 79823
New Horizons in Cardiogenic Shock Timothy D. Henry, MD Director of Cardiology Cedars-Sinai Heart Institute AMI Shock Mortality Unchanged in > 20 years 74355 US AMI/CGS cases per year 1,2 78954 78500 79823
Cardiogenic Shock. Carlos Cafri,, MD
 Cardiogenic Shock Carlos Cafri,, MD SHOCK= Inadequate Tissue Mechanisms: Perfusion Inadequate oxygen delivery Release of inflammatory mediators Further microvascular changes, compromised blood flow and
Cardiogenic Shock Carlos Cafri,, MD SHOCK= Inadequate Tissue Mechanisms: Perfusion Inadequate oxygen delivery Release of inflammatory mediators Further microvascular changes, compromised blood flow and
How to do Primary Angioplasty. - Patients with Cardiogenic Shock
 How to do Primary Angioplasty - Patients with Cardiogenic Shock Advanced Cardiovascular Intervention 2011 Dan Blackman Leeds General Infirmary MY CONFLICTS OF INTEREST ARE: Research Grants Medicines Company
How to do Primary Angioplasty - Patients with Cardiogenic Shock Advanced Cardiovascular Intervention 2011 Dan Blackman Leeds General Infirmary MY CONFLICTS OF INTEREST ARE: Research Grants Medicines Company
ST-Elevation Myocardial Infarction & Cardiogenic Shock. - What Should We Do?
 ST-Elevation Myocardial Infarction & Cardiogenic Shock - What Should We Do? Advanced Angioplasty 2008 Dan Blackman Leeds General Infirmary Conflicts of interest Advisory Boards Cordis Boston Scientific
ST-Elevation Myocardial Infarction & Cardiogenic Shock - What Should We Do? Advanced Angioplasty 2008 Dan Blackman Leeds General Infirmary Conflicts of interest Advisory Boards Cordis Boston Scientific
Percutaneous Mechanical Circulatory Support Devices
 Percutaneous Mechanical Circulatory Support Devices Daniel Vazquez RN, RCIS Miami Cardiac & Vascular Institute FINANCIAL DISCLOSURES none CASE STUDY CASE STUDY 52 year old gentlemen Complaining of dyspnea
Percutaneous Mechanical Circulatory Support Devices Daniel Vazquez RN, RCIS Miami Cardiac & Vascular Institute FINANCIAL DISCLOSURES none CASE STUDY CASE STUDY 52 year old gentlemen Complaining of dyspnea
A Future for the IABP in Cardiogenic Shock? Holger Thiele Medical Clinic II (Cardiology/Angiology/Intensive Care) University of Lübeck, Germany
 A Future for the in Cardiogenic Shock? Holger Thiele Medical Clinic II (Cardiology/Angiology/Intensive Care) University of Lübeck, Germany Disclosures Funding: German Research Foundation German Heart Research
A Future for the in Cardiogenic Shock? Holger Thiele Medical Clinic II (Cardiology/Angiology/Intensive Care) University of Lübeck, Germany Disclosures Funding: German Research Foundation German Heart Research
Ray Matthews MD Professor of Clinical Medicine Chief of Cardiology University of Southern California
 High Risk PCI Making Possible the Impossible Ray Matthews MD Professor of Clinical Medicine Chief of Cardiology University of Southern California Disclosures Abiomed Research Support Consulting Agreement
High Risk PCI Making Possible the Impossible Ray Matthews MD Professor of Clinical Medicine Chief of Cardiology University of Southern California Disclosures Abiomed Research Support Consulting Agreement
Introduction to Acute Mechanical Circulatory Support
 Introduction to Acute Mechanical Circulatory Support Navin K. Kapur, MD, FACC, FSCAI, FAHA Associate Professor, Department of Medicine Interventional Cardiology & Advanced Heart Failure Programs Executive
Introduction to Acute Mechanical Circulatory Support Navin K. Kapur, MD, FACC, FSCAI, FAHA Associate Professor, Department of Medicine Interventional Cardiology & Advanced Heart Failure Programs Executive
CARDIOGENIC SHOCK 2017 Eric Adler MD Associate Clinical Professor, UCSD
 CARDIOGENIC SHOCK 2017 Eric Adler MD Associate Clinical Professor, UCSD CARDIOGENIC SHOCK Definition INADEQUATE TISSUE PERFUSION RESULTING FROM CARDIAC DYSFUNCITON IN SETTING OF EUVOLEMIA HEMODYAMIC
CARDIOGENIC SHOCK 2017 Eric Adler MD Associate Clinical Professor, UCSD CARDIOGENIC SHOCK Definition INADEQUATE TISSUE PERFUSION RESULTING FROM CARDIAC DYSFUNCITON IN SETTING OF EUVOLEMIA HEMODYAMIC
Cardiogenic Shock and Initiatives to Reduce Mortality
 Cardiogenic Shock and Initiatives to Reduce Mortality Tanveer Rab, MD, FACC William O Neill, MD, FACC Perwaiz Meraj, MD, FACC Alex Truesdell, MD, FACC The Golden Hours? 50% dead within 10 hours Overall
Cardiogenic Shock and Initiatives to Reduce Mortality Tanveer Rab, MD, FACC William O Neill, MD, FACC Perwaiz Meraj, MD, FACC Alex Truesdell, MD, FACC The Golden Hours? 50% dead within 10 hours Overall
Acute Myocardial Infarction Complicated by Cardiogenic Shock
 Acute Myocardial Infarction Complicated by Cardiogenic Shock Navin K. Kapur, MD, FACC, FSCAI Assistant Professor, Division of Cardiology Director, Acute Circulatory Support Program Director, Interventional
Acute Myocardial Infarction Complicated by Cardiogenic Shock Navin K. Kapur, MD, FACC, FSCAI Assistant Professor, Division of Cardiology Director, Acute Circulatory Support Program Director, Interventional
Management of Cardiogenic Shock. Dr Stephen Pettit, Consultant Cardiologist
 Dr Stephen Pettit, Consultant Cardiologist Cardiogenic shock Management of Cardiogenic Shock Outline Definition, INTERMACS classification Medical management of cardiogenic shock PA catheters and haemodynamic
Dr Stephen Pettit, Consultant Cardiologist Cardiogenic shock Management of Cardiogenic Shock Outline Definition, INTERMACS classification Medical management of cardiogenic shock PA catheters and haemodynamic
Circulatory Support: From IABP to LVAD
 Circulatory Support: From IABP to LVAD Howard A Cohen, MD, FACC, FSCAI Director Division of Cardiovascular Intervention Co Director Cardiovascular Interventional ti Laboratories Lenox Hill Heart & Vascular
Circulatory Support: From IABP to LVAD Howard A Cohen, MD, FACC, FSCAI Director Division of Cardiovascular Intervention Co Director Cardiovascular Interventional ti Laboratories Lenox Hill Heart & Vascular
Cardiogenic Shock. Dr. JPS Henriques. Academic Medical Center University of Amsterdam The Netherlands
 Cardiogenic Shock Dr. JPS Henriques Academic Medical Center University of Amsterdam The Netherlands Conflict of interest disclosure Research grant Abbott Vascular Research grant Abiomed Inc. Global Impella
Cardiogenic Shock Dr. JPS Henriques Academic Medical Center University of Amsterdam The Netherlands Conflict of interest disclosure Research grant Abbott Vascular Research grant Abiomed Inc. Global Impella
Mechanics of Cath Lab Support Devices
 Mechanics of Cath Lab Support Devices Issam D. Moussa, MD Chief Medical Officer First Coast Cardiovascular Institute, Jacksonville, FL Professor of Medicine, UCF, Orlando, FL None DISCLOSURE Percutaneous
Mechanics of Cath Lab Support Devices Issam D. Moussa, MD Chief Medical Officer First Coast Cardiovascular Institute, Jacksonville, FL Professor of Medicine, UCF, Orlando, FL None DISCLOSURE Percutaneous
Counterpulsation. John N. Nanas, MD, PhD. Professor and Head, 3 rd Cardiology Dept, University of Athens, Athens, Greece
 John N. Nanas, MD, PhD Professor and Head, 3 rd Cardiology Dept, University of Athens, Athens, Greece History of counterpulsation 1952 Augmentation of CBF Adrian and Arthur Kantrowitz, Surgery 1952;14:678-87
John N. Nanas, MD, PhD Professor and Head, 3 rd Cardiology Dept, University of Athens, Athens, Greece History of counterpulsation 1952 Augmentation of CBF Adrian and Arthur Kantrowitz, Surgery 1952;14:678-87
Mechanical circulatory support in cardiogenic shock The Cardiologist s view ACCA Masterclass 2017
 Mechanical circulatory support in cardiogenic shock The Cardiologist s view ACCA Masterclass 2017 Pascal Vranckx MD, PhD. Medical director Cardiac Critical Care Services Hartcentrum Hasselt Belgium Disclosure
Mechanical circulatory support in cardiogenic shock The Cardiologist s view ACCA Masterclass 2017 Pascal Vranckx MD, PhD. Medical director Cardiac Critical Care Services Hartcentrum Hasselt Belgium Disclosure
Mechanical Cardiac Support in Acute Heart Failure. Michael Felker, MD, MHS Associate Professor of Medicine Director of Heart Failure Research
 Mechanical Cardiac Support in Acute Heart Failure Michael Felker, MD, MHS Associate Professor of Medicine Director of Heart Failure Research Disclosures Research Support and/or Consulting NHLBI Amgen Cytokinetics
Mechanical Cardiac Support in Acute Heart Failure Michael Felker, MD, MHS Associate Professor of Medicine Director of Heart Failure Research Disclosures Research Support and/or Consulting NHLBI Amgen Cytokinetics
Definition. Low-cardiac-output state resulting in life threatening end-organ hypoperfusion. Criteria: MAP 30 mm Hg lower than baseline)
 Definition Low-cardiac-output state resulting in life threatening end-organ hypoperfusion Criteria: 1. Persistent hypotension (SBP
Definition Low-cardiac-output state resulting in life threatening end-organ hypoperfusion Criteria: 1. Persistent hypotension (SBP
Rationale for Left Ventricular Support During Percutaneous Coronary Intervention
 Rationale for Left Ventricular Support During Percutaneous Coronary Intervention Navin K. Kapur, MD, FACC, FSCAI Associate Professor, Division of Cardiology Director, Acute Circulatory Support Program
Rationale for Left Ventricular Support During Percutaneous Coronary Intervention Navin K. Kapur, MD, FACC, FSCAI Associate Professor, Division of Cardiology Director, Acute Circulatory Support Program
Who is the high risk patient?
 Who is the high risk patient? High risk of periprocedural death or other major complications (hemodynamic compromise, MI, stroke, dialysis) Contributors of Risk Lesion/Procedure Governed by 1. Patient
Who is the high risk patient? High risk of periprocedural death or other major complications (hemodynamic compromise, MI, stroke, dialysis) Contributors of Risk Lesion/Procedure Governed by 1. Patient
Percutaneous Mechanical Circulatory Support for Cardiogenic Shock. 24 th Annual San Diego Heart Failure Symposium Ryan R Reeves, MD FSCAI
 Percutaneous Mechanical Circulatory Support for Cardiogenic Shock 24 th Annual San Diego Heart Failure Symposium Ryan R Reeves, MD FSCAI The Need for Circulatory Support Basic Pathophysiologic Problems:
Percutaneous Mechanical Circulatory Support for Cardiogenic Shock 24 th Annual San Diego Heart Failure Symposium Ryan R Reeves, MD FSCAI The Need for Circulatory Support Basic Pathophysiologic Problems:
2018 TCT Investor Update
 1 2018 TCT Investor Update September 2018 LEGAL DISCLAIMERS 2 This presentation contains forward-looking statements, including statements regarding development of Abiomed's existing and new products, the
1 2018 TCT Investor Update September 2018 LEGAL DISCLAIMERS 2 This presentation contains forward-looking statements, including statements regarding development of Abiomed's existing and new products, the
Cardiogenic Shock in Acute MI
 Cardiogenic Shock in Acute MI Mark Sheldon, MD UNMH Interventional Cardiology Objectives Overview Treatment Definition Shock profiles Causes Medical Mechanical Illustrative case Questions? Revascularization
Cardiogenic Shock in Acute MI Mark Sheldon, MD UNMH Interventional Cardiology Objectives Overview Treatment Definition Shock profiles Causes Medical Mechanical Illustrative case Questions? Revascularization
Ted Feldman, M.D., MSCAI FACC FESC
 Support Technologies and High Risk Intervention Patient Selection: When Not to Use Them Ted Feldman, M.D., MSCAI FACC FESC Evanston Hospital SCAI Fall Fellows Course Las Vegas December 7-10 th, 2014 Ted
Support Technologies and High Risk Intervention Patient Selection: When Not to Use Them Ted Feldman, M.D., MSCAI FACC FESC Evanston Hospital SCAI Fall Fellows Course Las Vegas December 7-10 th, 2014 Ted
Case - Advanced HF and Shock (INTERMACS 1)
 Case - Advanced HF and Shock (INTERMACS 1) Navin K. Kapur, MD, FACC, FSCAI, FAHA Associate Professor, Department of Medicine Interventional Cardiology & Advanced Heart Failure Programs Executive Director,
Case - Advanced HF and Shock (INTERMACS 1) Navin K. Kapur, MD, FACC, FSCAI, FAHA Associate Professor, Department of Medicine Interventional Cardiology & Advanced Heart Failure Programs Executive Director,
1/5/2017. The Next Frontier: Advanced Cardiogenic Shock U MICHIGAN EPERIENCE
 % SURVIVAL 1/5/2017 The Next Frontier: Advanced Cardiogenic Shock William W. O Neill, MD Henry Ford Health System Medical Director Center for Structural Heart Disease Detroit, MI U MICHIGAN EPERIENCE 1983-1985
% SURVIVAL 1/5/2017 The Next Frontier: Advanced Cardiogenic Shock William W. O Neill, MD Henry Ford Health System Medical Director Center for Structural Heart Disease Detroit, MI U MICHIGAN EPERIENCE 1983-1985
4/22/2016 Updated. AllinaHealthSystem. Cardiogenic Shock: Definition. No Disclosures. Cardiogenic Shock: Declining (But Still High) Case Fatality Rate
 4/22/216 Updated Definition End-organ hypoperfusion secondary to cardiac failure Advanced Cardiopulmonary Support for the Critically Ill Adult April 22, 216 Cardiogenic Shock Michael A. Samara, MD FACC
4/22/216 Updated Definition End-organ hypoperfusion secondary to cardiac failure Advanced Cardiopulmonary Support for the Critically Ill Adult April 22, 216 Cardiogenic Shock Michael A. Samara, MD FACC
TREATMENT OF HIGHER RISK PATIENTS INTRODUCTION TO PROTECTED PCI WITH IMPELLA. IMP v4
 1 TREATMENT OF HIGHER RISK PATIENTS INTRODUCTION TO PROTECTED PCI WITH IMPELLA FDA APPROVES IMPELLA FOR HIGH-RISK PCI 2 Impella is the only hemodynamic support device proven safe and effective in elective
1 TREATMENT OF HIGHER RISK PATIENTS INTRODUCTION TO PROTECTED PCI WITH IMPELLA FDA APPROVES IMPELLA FOR HIGH-RISK PCI 2 Impella is the only hemodynamic support device proven safe and effective in elective
Controversies in Cardiogenic Shock. Timothy D. Henry, MD Cedars-Sinai Heart Institute
 Controversies in Cardiogenic Shock Timothy D. Henry, MD Cedars-Sinai Heart Institute Key Issues Cardiac Arrest-Cardiogenic shock interaction New SCAI Classification Refractory Shock Shock with Multivessel
Controversies in Cardiogenic Shock Timothy D. Henry, MD Cedars-Sinai Heart Institute Key Issues Cardiac Arrest-Cardiogenic shock interaction New SCAI Classification Refractory Shock Shock with Multivessel
Disclosures. Extra-Corporeal Membrane Oxygenation During Cardio- Pulmonary Resuscitation ECPR April 22, 2016 ECG. Case. Case. Case Summary 4/22/2016
 Extra-Corporeal Membrane Oxygenation During Cardio- Pulmonary Resuscitation ECPR April 22, 2016 Nothing to disclose. Disclosures Ivan J Chavez MD Case ECG History 60 y/o male No prior history of CAD In
Extra-Corporeal Membrane Oxygenation During Cardio- Pulmonary Resuscitation ECPR April 22, 2016 Nothing to disclose. Disclosures Ivan J Chavez MD Case ECG History 60 y/o male No prior history of CAD In
Cardiogenic Shock Protocol
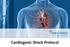 Cardiogenic Shock Protocol Impella Devices Best Practices in AMI Cardiogenic Shock Identify 1-3 SBP < 90 mmhg or on inotropes /pressors Cold, clammy, tachycardia Lactate elevated > 2 mmoi /L Stabilize
Cardiogenic Shock Protocol Impella Devices Best Practices in AMI Cardiogenic Shock Identify 1-3 SBP < 90 mmhg or on inotropes /pressors Cold, clammy, tachycardia Lactate elevated > 2 mmoi /L Stabilize
Management of Cardiogenic shock. Prof. Christian JM Vrints
 Management of Cardiogenic shock Prof. Christian JM Vrints none conflicts Management of Cardiogenic Shock Incidence and trends Importance of early revascularization Multivessel disease Left main disease
Management of Cardiogenic shock Prof. Christian JM Vrints none conflicts Management of Cardiogenic Shock Incidence and trends Importance of early revascularization Multivessel disease Left main disease
Mechanics of Cath Lab Support Devices
 Mechanics of Cath Lab Support Devices Issam D. Moussa, MD Professor of Medicine Mayo Clinic College of Medicine Chair, Division of Cardiovascular Diseases Mayo Clinic Jacksonville, Florida DISCLOSURE Presenter:
Mechanics of Cath Lab Support Devices Issam D. Moussa, MD Professor of Medicine Mayo Clinic College of Medicine Chair, Division of Cardiovascular Diseases Mayo Clinic Jacksonville, Florida DISCLOSURE Presenter:
8th Emirates Cardiac Society Congress in collaboration with ACC Middle East Conference Dubai: October Acute Coronary Syndromes
 8th Emirates Cardiac Society Congress in collaboration with ACC Middle East Conference 2017 OSPEDALE Dubai: 19-21 October 2017 Acute Coronary Syndromes Antonio Colombo Centro Cuore Columbus and S. Raffaele
8th Emirates Cardiac Society Congress in collaboration with ACC Middle East Conference 2017 OSPEDALE Dubai: 19-21 October 2017 Acute Coronary Syndromes Antonio Colombo Centro Cuore Columbus and S. Raffaele
Extra Corporeal Life Support for Acute Heart failure
 Extra Corporeal Life Support for Acute Heart failure Benjamin Medalion, MD Director Heart and Lung Transplantation Department of Cardiothoracic Surgery Rabin Medical Center, Beilinson Campus, Israel Mechanical
Extra Corporeal Life Support for Acute Heart failure Benjamin Medalion, MD Director Heart and Lung Transplantation Department of Cardiothoracic Surgery Rabin Medical Center, Beilinson Campus, Israel Mechanical
ECMO as a bridge to durable LVAD therapy. Jonathan Haft, MD Department of Cardiac Surgery University of Michigan
 ECMO as a bridge to durable LVAD therapy Jonathan Haft, MD Department of Cardiac Surgery University of Michigan Systolic Heart Failure Prevalence 4.8 million U.S. 287,000 deaths per year $39 billion spent
ECMO as a bridge to durable LVAD therapy Jonathan Haft, MD Department of Cardiac Surgery University of Michigan Systolic Heart Failure Prevalence 4.8 million U.S. 287,000 deaths per year $39 billion spent
Recovering Hearts. Saving Lives.
 Recovering Hearts. Saving Lives ṬM The Door to Unload (DTU) STEMI Safety & Feasibility Pilot Trial November 218 Recovering Hearts. Saving Lives. LEGAL DISCLAIMERS This presentation includes select slides
Recovering Hearts. Saving Lives ṬM The Door to Unload (DTU) STEMI Safety & Feasibility Pilot Trial November 218 Recovering Hearts. Saving Lives. LEGAL DISCLAIMERS This presentation includes select slides
The Role of Mechanical Circulatory Support in Cardiogenic Shock: When to Utilize
 The Role of Mechanical Circulatory Support in Cardiogenic Shock: Presented by Nancy Scroggins ACNP, CNS-CC CV Surgery ACNP Bayshore Medical Center The Role of Mechanical Circulatory Support in Cardiogenic
The Role of Mechanical Circulatory Support in Cardiogenic Shock: Presented by Nancy Scroggins ACNP, CNS-CC CV Surgery ACNP Bayshore Medical Center The Role of Mechanical Circulatory Support in Cardiogenic
Out-of-hospital Cardiac Arrest. Franz R. Eberli MD, FESC, FAHA Cardiology Triemli Hospital Zurich, Switzerland
 Out-of-hospital Cardiac Arrest Franz R. Eberli MD, FESC, FAHA Cardiology Triemli Hospital Zurich, Switzerland Conflict of Interest I have no conflict of interest to disclose regarding this presentation.
Out-of-hospital Cardiac Arrest Franz R. Eberli MD, FESC, FAHA Cardiology Triemli Hospital Zurich, Switzerland Conflict of Interest I have no conflict of interest to disclose regarding this presentation.
Echo assessment of patients with an ECMO device
 Echo assessment of patients with an ECMO device Evangelos Leontiadis Cardiologist 1st Cardiology Dept. Onassis Cardiac Surgery Center Athens, Greece Gibbon HLM 1953 Goldstein DJ et al, NEJM 1998; 339:1522
Echo assessment of patients with an ECMO device Evangelos Leontiadis Cardiologist 1st Cardiology Dept. Onassis Cardiac Surgery Center Athens, Greece Gibbon HLM 1953 Goldstein DJ et al, NEJM 1998; 339:1522
The Pathophysiology of Cardiogenic Shock Knowledge Gaps & Opportunities
 The Pathophysiology of Cardiogenic Shock Knowledge Gaps & Opportunities Navin K. Kapur, MD, FACC, FSCAI, FAHA Associate Professor, Department of Medicine Interventional Cardiology & Advanced Heart Failure
The Pathophysiology of Cardiogenic Shock Knowledge Gaps & Opportunities Navin K. Kapur, MD, FACC, FSCAI, FAHA Associate Professor, Department of Medicine Interventional Cardiology & Advanced Heart Failure
To ECMO Or Not To ECMO Challenges of venous arterial ECMO. Dr Emily Granger St Vincent s Hospital Darlinghurst NSW
 To ECMO Or Not To ECMO Challenges of venous arterial ECMO Dr Emily Granger St Vincent s Hospital Darlinghurst NSW The Start: 1972 St Vincent s Hospital The Turning Point ECMO program restarted in 2004
To ECMO Or Not To ECMO Challenges of venous arterial ECMO Dr Emily Granger St Vincent s Hospital Darlinghurst NSW The Start: 1972 St Vincent s Hospital The Turning Point ECMO program restarted in 2004
Οξύ στεφανιαίο σύνδρομο και καρδιογενής καταπληξία. Επεμβατική προσέγγιση. Σωτήριος Πατσιλινάκος Κωνσταντοπούλειο Γ.Ν. Ν. Ιωνίας
 Οξύ στεφανιαίο σύνδρομο και καρδιογενής καταπληξία. Επεμβατική προσέγγιση Σωτήριος Πατσιλινάκος Κωνσταντοπούλειο Γ.Ν. Ν. Ιωνίας ACUTE HEART FAILURE AND CAD: ACS / LV ischaemic dysfunction Mechanical complications
Οξύ στεφανιαίο σύνδρομο και καρδιογενής καταπληξία. Επεμβατική προσέγγιση Σωτήριος Πατσιλινάκος Κωνσταντοπούλειο Γ.Ν. Ν. Ιωνίας ACUTE HEART FAILURE AND CAD: ACS / LV ischaemic dysfunction Mechanical complications
A National Cardiogenic Shock Initiative (CSI):
 A National Cardiogenic Shock Initiative (CSI): Insights from the Impella Quality (IQ) Program, cvad Registry and the Detroit CSI Experience William O Neill, MD, FACC Medical Director Structural Heart Disease
A National Cardiogenic Shock Initiative (CSI): Insights from the Impella Quality (IQ) Program, cvad Registry and the Detroit CSI Experience William O Neill, MD, FACC Medical Director Structural Heart Disease
Acute Mechanical Circulatory Support Right Ventricular Support Devices
 Acute Mechanical Circulatory Support Right Ventricular Support Devices Navin K. Kapur, MD, FACC, FSCAI, FAHA Associate Professor, Department of Medicine Interventional Cardiology & Advanced Heart Failure
Acute Mechanical Circulatory Support Right Ventricular Support Devices Navin K. Kapur, MD, FACC, FSCAI, FAHA Associate Professor, Department of Medicine Interventional Cardiology & Advanced Heart Failure
Which mechanical assistance for cardiogenic shock?
 Which mechanical assistance for cardiogenic shock? Alain Combes, MD, PhD, Hôpital Pitié-Salpêtrière, AP-HP Inserm UMRS 1166, ican, Institute of Cardiometabolism and Nutrition Pierre et Marie Curie Sorbonne
Which mechanical assistance for cardiogenic shock? Alain Combes, MD, PhD, Hôpital Pitié-Salpêtrière, AP-HP Inserm UMRS 1166, ican, Institute of Cardiometabolism and Nutrition Pierre et Marie Curie Sorbonne
Rhondalyn C. McLean. 2 ND YEAR RESEARCH ELECTIVE RESIDENT S JOURNAL Volume VII, A. Study Purpose and Rationale
 A Randomized Clinical Study To Compare The Intra-Aortic Balloon Pump To A Percutaneous Left Atrial-To-Femoral Arterial Bypass Device For Treatment Of Cardiogenic Shock Following Acute Myocardial Infarction.
A Randomized Clinical Study To Compare The Intra-Aortic Balloon Pump To A Percutaneous Left Atrial-To-Femoral Arterial Bypass Device For Treatment Of Cardiogenic Shock Following Acute Myocardial Infarction.
DECLARATION OF CONFLICT OF INTEREST
 DECLARATION OF CONFLICT OF INTEREST Multivessel disease and cardiogenic shock: CABG is the optimal revascularization therapy. Contra Prof. Christian JM Vrints Cardiogenic Shock Spiral Acute Myocardial
DECLARATION OF CONFLICT OF INTEREST Multivessel disease and cardiogenic shock: CABG is the optimal revascularization therapy. Contra Prof. Christian JM Vrints Cardiogenic Shock Spiral Acute Myocardial
Cardiogenic shock: Current management
 Cardiogenic shock: Current management Janine Pöss Universitätsklinikum des Saarlandes Klinik für Innere Medizin III Kardiologie, Angiologie und internistische Intensivmedizin Homburg/Saar I have nothing
Cardiogenic shock: Current management Janine Pöss Universitätsklinikum des Saarlandes Klinik für Innere Medizin III Kardiologie, Angiologie und internistische Intensivmedizin Homburg/Saar I have nothing
Why we need a consensus document on cardiogenic shock? ACCA Masterclass 2017
 Why we need a consensus document on cardiogenic shock? ACCA Masterclass 2017 Holger Thiele Cardiogenic Shock STEMI Guidelines Steg et al. Eur Heart J.2012;33:2569-2619 Cardiogenic Shock CHF Guidelines
Why we need a consensus document on cardiogenic shock? ACCA Masterclass 2017 Holger Thiele Cardiogenic Shock STEMI Guidelines Steg et al. Eur Heart J.2012;33:2569-2619 Cardiogenic Shock CHF Guidelines
The Case for Multivessel Revascularization in Shock
 The Case for Multivessel Revascularization in Shock Emmanouil S. Brilakis, MD, PhD Minneapolis Heart Institute 9.37 9.49 am Disclosures Consulting/speaker honoraria: Abbott Vascular, American Heart Association
The Case for Multivessel Revascularization in Shock Emmanouil S. Brilakis, MD, PhD Minneapolis Heart Institute 9.37 9.49 am Disclosures Consulting/speaker honoraria: Abbott Vascular, American Heart Association
MANAGEMENT OF CARDIOGENIC SHOCK
 MANAGEMENT OF CARDIOGENIC SHOCK CASE PRESENTATION 37 year old Dutch female No known coronary artery disease risk factors 1 week post partum at time of presentation (G3P3) after an uncomplicated normal
MANAGEMENT OF CARDIOGENIC SHOCK CASE PRESENTATION 37 year old Dutch female No known coronary artery disease risk factors 1 week post partum at time of presentation (G3P3) after an uncomplicated normal
3/1/2017. Heart Failure is a major driver of morbidity and mortality in the US 1-7
 Approaches to Cardiogenic Shock Margarita Camacho MD, FACS Surgical Director Cardiac Transplant and Mechanical Assist Device Program RWJ/Barnabas Health Heart Centers at Newark Beth Israel Medical Center
Approaches to Cardiogenic Shock Margarita Camacho MD, FACS Surgical Director Cardiac Transplant and Mechanical Assist Device Program RWJ/Barnabas Health Heart Centers at Newark Beth Israel Medical Center
CULPRIT-SHOCK: A Randomized Trial of Multivessel PCI in Cardiogenic Shock. Holger Thiele, MD on behalf of the CULPRIT-SHOCK Investigators
 CULPRIT-SHOCK: A Randomized Trial of Multivessel PCI in Cardiogenic Shock Holger Thiele, MD on behalf of the CULPRIT-SHOCK Investigators Disclosure Statement of Financial Interest Within the past 12 months,
CULPRIT-SHOCK: A Randomized Trial of Multivessel PCI in Cardiogenic Shock Holger Thiele, MD on behalf of the CULPRIT-SHOCK Investigators Disclosure Statement of Financial Interest Within the past 12 months,
Emergency surgery in acute coronary syndrome
 Emergency surgery in acute coronary syndrome Teerawoot Jantarawan Division of Cardiothoracic Surgery, Department of Surgery, Faculty of Medicine Siriraj Hospital, Mahidol University, Bangkok, Thailand
Emergency surgery in acute coronary syndrome Teerawoot Jantarawan Division of Cardiothoracic Surgery, Department of Surgery, Faculty of Medicine Siriraj Hospital, Mahidol University, Bangkok, Thailand
MCS for Acute Heart Failure Eric Adler MD Associate Professor of Medicine Medical Director Cardiac Transplant
 MCS for Acute Heart Failure 2016 Eric Adler MD Associate Professor of Medicine Medical Director Cardiac Transplant Why do we decompensate? Which Heart Failure Patients Should Get Palliative Care and Who
MCS for Acute Heart Failure 2016 Eric Adler MD Associate Professor of Medicine Medical Director Cardiac Transplant Why do we decompensate? Which Heart Failure Patients Should Get Palliative Care and Who
Matching Patient and Pump in the New Era of Percutaneous Mechanical Circulatory Support
 Matching Patient and Pump in the New Era of Percutaneous Mechanical Circulatory Support Navin K. Kapur, MD, FACC, FSCAI, FAHA Associate Professor, Department of Medicine Interventional Cardiology & Advanced
Matching Patient and Pump in the New Era of Percutaneous Mechanical Circulatory Support Navin K. Kapur, MD, FACC, FSCAI, FAHA Associate Professor, Department of Medicine Interventional Cardiology & Advanced
Mechanical Circulatory Support (MCS): What Every Pharmacist Needs to Know!
 Mechanical Circulatory Support (MCS): What Every Pharmacist Needs to Know! Matthew A. Wanat, PharmD, BCPS, BCCCP, FCCM Clinical Assistant Professor University of Houston College of Pharmacy Clinical Pharmacy
Mechanical Circulatory Support (MCS): What Every Pharmacist Needs to Know! Matthew A. Wanat, PharmD, BCPS, BCCCP, FCCM Clinical Assistant Professor University of Houston College of Pharmacy Clinical Pharmacy
Update on Mechanical Circulatory Support. AATS May 5, 2010 Toronto, ON Canada
 Update on Mechanical Circulatory Support AATS May 5, 2010 Toronto, ON Canada Disclosures NONE Emergency Circulatory Support ECMO Tandem Heart Impella Assessment Cardiac Function Pulmonary function Valvular
Update on Mechanical Circulatory Support AATS May 5, 2010 Toronto, ON Canada Disclosures NONE Emergency Circulatory Support ECMO Tandem Heart Impella Assessment Cardiac Function Pulmonary function Valvular
Low cardiac output & Mechanical Support นายแพทย อรรถภ ม ส ศ ภอรรถ ศ ลยศาสตร ห วใจและทรวงอก โรงพยาบาล ราชว ถ
 Low cardiac output & Mechanical Support นายแพทย อรรถภ ม ส ศ ภอรรถ ศ ลยศาสตร ห วใจและทรวงอก โรงพยาบาล ราชว ถ Low cardiac output/cardiogenic Shock State of end-organ hypoperfusion due to cardiac failure.
Low cardiac output & Mechanical Support นายแพทย อรรถภ ม ส ศ ภอรรถ ศ ลยศาสตร ห วใจและทรวงอก โรงพยาบาล ราชว ถ Low cardiac output/cardiogenic Shock State of end-organ hypoperfusion due to cardiac failure.
CARDIOGENIC SHOCK. Antonio Pesenti. Università degli Studi di Milano Bicocca Azienda Ospedaliera San Gerardo Monza (MI)
 CARDIOGENIC SHOCK Antonio Pesenti Università degli Studi di Milano Bicocca Azienda Ospedaliera San Gerardo Monza (MI) Primary myocardial dysfunction resulting in the inability of the heart to mantain an
CARDIOGENIC SHOCK Antonio Pesenti Università degli Studi di Milano Bicocca Azienda Ospedaliera San Gerardo Monza (MI) Primary myocardial dysfunction resulting in the inability of the heart to mantain an
Impella Ins & Outs. CarVasz November :45 12:15
 Impella Ins & Outs CarVasz November 21 2014 10:45 12:15 Nicolas M. Van Mieghem, MD, PhD, FESC Clinical Director of Interventional Cardiology Thoraxcenter, Erasmus MC Rotterdam Background IABP is widely
Impella Ins & Outs CarVasz November 21 2014 10:45 12:15 Nicolas M. Van Mieghem, MD, PhD, FESC Clinical Director of Interventional Cardiology Thoraxcenter, Erasmus MC Rotterdam Background IABP is widely
Right Ventricular Failure: Prediction, Prevention and Treatment
 Right Ventricular Failure: Prediction, Prevention and Treatment 3 rd European Training Symposium for Heart Failure Cardiologists and Cardiac Surgeons University Hospital Bern June 24-25, 2016 Disclosures:
Right Ventricular Failure: Prediction, Prevention and Treatment 3 rd European Training Symposium for Heart Failure Cardiologists and Cardiac Surgeons University Hospital Bern June 24-25, 2016 Disclosures:
The Optimal Team for 24/7 CCU shock management
 The Optimal Team for 24/7 CCU shock management Emmanouil S. Brilakis, MD, PhD Minneapolis Heart Institute 3.10 3.25 pm Disclosures Consulting/speaker honoraria: Abbott Vascular, American Heart Association
The Optimal Team for 24/7 CCU shock management Emmanouil S. Brilakis, MD, PhD Minneapolis Heart Institute 3.10 3.25 pm Disclosures Consulting/speaker honoraria: Abbott Vascular, American Heart Association
A case of post myocardial infarction ventricular septal rupture CHRISTOFOROS KOBOROZOS, MD
 A case of post myocardial infarction ventricular septal rupture CHRISTOFOROS KOBOROZOS, MD NAVAL HOSPITAL OF ATHENS case presentation Female, 81yo Hx: diabetes mellitus, hypertension, chronic anaemia presented
A case of post myocardial infarction ventricular septal rupture CHRISTOFOROS KOBOROZOS, MD NAVAL HOSPITAL OF ATHENS case presentation Female, 81yo Hx: diabetes mellitus, hypertension, chronic anaemia presented
Disclosures. Objectives 10/11/17. Short Term Mechanical Circulatory Support for Advanced Cardiogenic Shock. I have no disclosures to report
 Short Term Mechanical Circulatory Support for Advanced Cardiogenic Shock Christopher K. Gordon MSN, ACNP-BC Disclosures I have no disclosures to report 1. Pathophysiology 2. Epidemiology 3. Assessment
Short Term Mechanical Circulatory Support for Advanced Cardiogenic Shock Christopher K. Gordon MSN, ACNP-BC Disclosures I have no disclosures to report 1. Pathophysiology 2. Epidemiology 3. Assessment
Acute heart failure: ECMO Cardiology & Vascular Medicine 2012
 Acute heart failure: ECMO Cardiology & Vascular Medicine 2012 Lucia Jewbali cardiologist-intensivist 14 beds/8 ICU beds Acute coronary syndromes Heart failure/ Cardiogenic shock Post cardiotomy Heart
Acute heart failure: ECMO Cardiology & Vascular Medicine 2012 Lucia Jewbali cardiologist-intensivist 14 beds/8 ICU beds Acute coronary syndromes Heart failure/ Cardiogenic shock Post cardiotomy Heart
Andrew Civitello MD, FACC
 Timing the Transition from Short Term to Long Term Mechanical Circulatory Support Andrew Civitello MD, FACC Medical Director, Heart Transplant Program Director, Fellowship Co-Director, Baylor St. Luke's
Timing the Transition from Short Term to Long Term Mechanical Circulatory Support Andrew Civitello MD, FACC Medical Director, Heart Transplant Program Director, Fellowship Co-Director, Baylor St. Luke's
STEMI and Cardiogenic Shock. The rules and solution. Dave Kettles St Dominics and Frere Hospitals East London ZA
 STEMI and Cardiogenic Shock. The rules and solution Dave Kettles St Dominics and Frere Hospitals East London ZA Definitions: Shock is a life threatening, but initially reversible state of cellular and
STEMI and Cardiogenic Shock. The rules and solution Dave Kettles St Dominics and Frere Hospitals East London ZA Definitions: Shock is a life threatening, but initially reversible state of cellular and
The majority of patients with cardiomyopathy
 Selection of Hemodynamic Support: An Approach for Coronary Interventions in Shock and High-Risk PCI The role of hemodynamic support devices in emergent cardiogenic shock and elective high-risk percutaneous
Selection of Hemodynamic Support: An Approach for Coronary Interventions in Shock and High-Risk PCI The role of hemodynamic support devices in emergent cardiogenic shock and elective high-risk percutaneous
Cardiac Interventions
 Supplement to Sponsored by ABIOMED, Inc. Cardiac Interventions August/September 2009 Principles of Hemodynamics The New Science of Cardiac Support in the Cath Lab Principles of Hemodynamics 3 PRINCIPLES
Supplement to Sponsored by ABIOMED, Inc. Cardiac Interventions August/September 2009 Principles of Hemodynamics The New Science of Cardiac Support in the Cath Lab Principles of Hemodynamics 3 PRINCIPLES
In-hospital Care of the Post-Cardiac Arrest Patient. David A. Pearson, MD, FACEP, FAAEM Associate Program Director Department of Emergency Medicine
 In-hospital Care of the Post-Cardiac Arrest Patient David A. Pearson, MD, FACEP, FAAEM Associate Program Director Department of Emergency Medicine Disclosures I have no financial interest, arrangement,
In-hospital Care of the Post-Cardiac Arrest Patient David A. Pearson, MD, FACEP, FAAEM Associate Program Director Department of Emergency Medicine Disclosures I have no financial interest, arrangement,
Recognizing the Need to Support A Failing Right Ventricular Role of Mechanical Support
 Recognizing the Need to Support A Failing Right Ventricular Role of Mechanical Support Mahir Elder, MD, FACC,SCAI Medical Direct of PERT program Medical Director of Endovascular medicine Clinical Professor
Recognizing the Need to Support A Failing Right Ventricular Role of Mechanical Support Mahir Elder, MD, FACC,SCAI Medical Direct of PERT program Medical Director of Endovascular medicine Clinical Professor
Guideline compliance, utilization trends
 Guideline compliance, utilization trends and device selection Tilmann Schwab Cardiology / Intensive care Cardiac support IABP LVAD Transluminal l LVAD Cardiac support Emergency cardiac life support (ECLS)
Guideline compliance, utilization trends and device selection Tilmann Schwab Cardiology / Intensive care Cardiac support IABP LVAD Transluminal l LVAD Cardiac support Emergency cardiac life support (ECLS)
PUMP FAILURE COMPLICATING AMI: ISCHAEMIC VSR
 PUMP FAILURE COMPLICATING AMI: ISCHAEMIC VSR Dr Susanna Price MD PhD MRCP ESICM FFICM FESC Consultant Cardiologist & Intensivist Royal Brompton & Harefield NHS Foundation Trust DECLARATIONS Educational
PUMP FAILURE COMPLICATING AMI: ISCHAEMIC VSR Dr Susanna Price MD PhD MRCP ESICM FFICM FESC Consultant Cardiologist & Intensivist Royal Brompton & Harefield NHS Foundation Trust DECLARATIONS Educational
เอกราช อร ยะช ยพาณ ชย
 30 July 2016 เอกราช อร ยะช ยพาณ ชย Heart Failure and Transplant Cardiology aekarach.a@chula.ac.th Disclosure Speaker, CME service: Merck, Otsuka, Servier Consultant, non-cme service: Novartis, Menarini
30 July 2016 เอกราช อร ยะช ยพาณ ชย Heart Failure and Transplant Cardiology aekarach.a@chula.ac.th Disclosure Speaker, CME service: Merck, Otsuka, Servier Consultant, non-cme service: Novartis, Menarini
ECLS: A new frontier for refractory V.Fib and pulseless VT
 ECLS: A new frontier for refractory V.Fib and pulseless VT Ernest L. Mazzaferri, Jr. MD, FACC September 15, 2017 Cardiovascular Emergencies: An exploration into the expansion of time-critical diagnosis
ECLS: A new frontier for refractory V.Fib and pulseless VT Ernest L. Mazzaferri, Jr. MD, FACC September 15, 2017 Cardiovascular Emergencies: An exploration into the expansion of time-critical diagnosis
CPR What Works, What Doesn t
 Resuscitation 2017 ECMO and ECLS April 1, 2017 Corey M. Slovis, M.D. Vanderbilt University Medical Center Metro Nashville Fire Department Nashville International Airport Nashville, TN Circulation 2013;128:417-35
Resuscitation 2017 ECMO and ECLS April 1, 2017 Corey M. Slovis, M.D. Vanderbilt University Medical Center Metro Nashville Fire Department Nashville International Airport Nashville, TN Circulation 2013;128:417-35
LV Distension and ECLS Lungs
 LV Distension and ECLS Lungs Kevin W. Hatton, MD, FCCM Interim Vice-Chair for Anesthesiology Research Division Chief, Anesthesiology Critical Care Medicine Program Director, Anesthesiology Critical Care
LV Distension and ECLS Lungs Kevin W. Hatton, MD, FCCM Interim Vice-Chair for Anesthesiology Research Division Chief, Anesthesiology Critical Care Medicine Program Director, Anesthesiology Critical Care
Antonio Colombo. Centro Cuore Columbus and S. Raffaele Scientific Institute, Milan, Italy. Miracor Symposium. Speaker: 15. Parigi: May 16-19, 2017
 Parigi: May 16-19, 2017 Miracor Symposium Speaker: 15 Antonio Colombo Centro Cuore Columbus and S. Raffaele Scientific Institute, Milan, Italy Nothing to disclose PiCSO Impulse System Elective high risk
Parigi: May 16-19, 2017 Miracor Symposium Speaker: 15 Antonio Colombo Centro Cuore Columbus and S. Raffaele Scientific Institute, Milan, Italy Nothing to disclose PiCSO Impulse System Elective high risk
Samphant Ponvilawan Bumrungrad International
 Samphant Ponvilawan Bumrungrad International Definitions Artificial circulation using VA ECMO as an alternative to ventilation and external cardiac massage Indications Out-of-Hospital Cardiac Arrest (OHCA)
Samphant Ponvilawan Bumrungrad International Definitions Artificial circulation using VA ECMO as an alternative to ventilation and external cardiac massage Indications Out-of-Hospital Cardiac Arrest (OHCA)
ECMO as a Bridge to Heart Transplant in the Era of LVAD s.
 Christian Bermudez MD. Associate Professor Director Thoracic Transplantation Division Cardiac Surgery Department of Surgery University of Pennsylvania ECMO as a Bridge to Heart Transplant in the Era of
Christian Bermudez MD. Associate Professor Director Thoracic Transplantation Division Cardiac Surgery Department of Surgery University of Pennsylvania ECMO as a Bridge to Heart Transplant in the Era of
Planned, Short-Term RVAD During Durable LVAD Implant: Indications and Management
 Planned, Short-Term RVAD During Durable LVAD Implant: Indications and Management Yoshifumi Naka, MD, PhD Columbia University Medical Center New York, NY Disclosure Abbott/St. Jude Med./Thoratec Consultant
Planned, Short-Term RVAD During Durable LVAD Implant: Indications and Management Yoshifumi Naka, MD, PhD Columbia University Medical Center New York, NY Disclosure Abbott/St. Jude Med./Thoratec Consultant
The Robert TV Kung Interventional Heart Failure Fellowship Program Bringing Hope to the Hopeless at Tufts
 The Robert TV Kung Interventional Heart Failure Fellowship Program Bringing Hope to the Hopeless at Tufts Navin K. Kapur, MD, FACC, FSCAI, FAHA Associate Professor, Department of Medicine Interventional
The Robert TV Kung Interventional Heart Failure Fellowship Program Bringing Hope to the Hopeless at Tufts Navin K. Kapur, MD, FACC, FSCAI, FAHA Associate Professor, Department of Medicine Interventional
PHARMACOLOGICAL MANAGEMENT OF CARDIOGENIC SHOCK
 PHARMACOLOGICAL MANAGEMENT OF CARDIOGENIC SHOCK Doron Zahger, MD Department of Cardiology, Soroka University Medical Center, Faculty of Health Sciences, Ben Gurion University of the Negev, Beer Sheva,
PHARMACOLOGICAL MANAGEMENT OF CARDIOGENIC SHOCK Doron Zahger, MD Department of Cardiology, Soroka University Medical Center, Faculty of Health Sciences, Ben Gurion University of the Negev, Beer Sheva,
Ventricular Assisting Devices in the Cathlab. Unrestricted
 Ventricular Assisting Devices in the Cathlab Unrestricted What is a VAD? A single system device that is surgically attached to the left ventricle of the heart and to the aorta for left ventricular support
Ventricular Assisting Devices in the Cathlab Unrestricted What is a VAD? A single system device that is surgically attached to the left ventricle of the heart and to the aorta for left ventricular support
Acute Coronary Syndrome. Sonny Achtchi, DO
 Acute Coronary Syndrome Sonny Achtchi, DO Objectives Understand evidence based and practice based treatments for stabilization and initial management of ACS Become familiar with ACS risk stratification
Acute Coronary Syndrome Sonny Achtchi, DO Objectives Understand evidence based and practice based treatments for stabilization and initial management of ACS Become familiar with ACS risk stratification
Surgical Options for Temporary MCS
 Surgical Options for Temporary MCS Michael A. Acker, MD Julian Johnson Professor of Surgery Chief of Cardiovascular Surgery Director of Heart and Vascular Center University of Pennsylvania Health System
Surgical Options for Temporary MCS Michael A. Acker, MD Julian Johnson Professor of Surgery Chief of Cardiovascular Surgery Director of Heart and Vascular Center University of Pennsylvania Health System
Acute Circulatory Support Should We or Shouldn t We?
 Acute Circulatory Support Should We or Shouldn t We? Navin K. Kapur, MD, FACC, FSCAI Assistant Professor, Division of Cardiology Director, Acute Circulatory Support Program Director, Interventional Research
Acute Circulatory Support Should We or Shouldn t We? Navin K. Kapur, MD, FACC, FSCAI Assistant Professor, Division of Cardiology Director, Acute Circulatory Support Program Director, Interventional Research
