Management of Ruptures Complicating Angioplasty and Stenting of Supraaortic Arteries: Report of Two Cases and a Review of the Literature
|
|
|
- Charla Fisher
- 5 years ago
- Views:
Transcription
1 AJNR Am J Neuroradiol 24: , November/December 2003 Case Report Management of Ruptures Complicating Angioplasty and Stenting of Supraaortic Arteries: Report of Two Cases and a Review of the Literature L. Paul Broadbent, Christopher J. Moran, DeWitte T. Cross III, and Colin P. Derdeyn Summary: Vessel rupture is a rare complication of angioplasty and stent placement of the supraaortic arteries occurring in two (1.1%) of 180 vessels treated at our institution. Many different approaches to the management of this complication have been proposed. In this report, we present our experience with conservative management in two cases in which vessel rupture occurred and review the relevant literature. Options for treating the complication of supraaortic arterial rupture during angioplasty and stent placement include surgical grafting, stent placement with covered or uncovered stents, temporary balloon occlusion, vessel sacrifice, and conservative management. In this report, we describe our experience with conservative management in two patients. Case Reports Patient 1 A 72-year-old woman presented with a history of right carotid endarterectomy. Follow-up sonography indicated a highgrade stenosis of the right common carotid artery. Subsequent angiography revealed a 75% stenosis of the proximal right common carotid artery and a 90% stenosis of the right common carotid artery at the proximal end of the previous endarterectomy site (Fig 1A). Intervention Intravenous heparin was administered to maintain the activated clotting time (ACT) at s. The proximal lesion was treated first to provide access to the distal lesion. Using external calibrated markers, the common carotid artery was determined to be 9 mm in diameter, and a slightly oversized 10 mm 20 mm self-expanding nitinol stent (SMART; Cordis Endovascular, Miami Lakes, FL) was chosen to assure apposition of the stent to the wall of the carotid artery. This stent was positioned at the level of the stenosis in the mid right common carotid artery but moved forward upon deployment and did not completely cover the stenosis. Angioplasty to six atmospheres was performed with an 8 mm 40 mm noncompliant balloon (Olbert; Boston Scientific, Boston, MA) after stent placement, resulting in moderate improvement in the stenosis. To fully Received February 26, 2003; accepted after revision June 17. From the Mallinckrodt Institute of Radiology, Department of Neuroradiology, St. Louis, MO. Address correspondence to Christopher J. Moran. American Society of Neuroradiology cover the stenosis, a 10 mm 20 mm self-expanding stainless steel stent (Wallstent; Schneider/Boston Scientific, Plymouth, MN), which would be slightly longer because it would not be completely unrestrained in the 9-mm carotid artery, was deployed more proximally. The distal portion of this second stent overlapped the proximal portion of the first stent (Fig 1B). Because there was residual stenosis after angioplasty with the 8-mm balloon and to appose the two stents as much as possible, an angioplasty was performed with a mm balloon (Courier; Meditech/Boston Scientific, Natick, MA). The final angiogram demonstrated contrast material extravasation medial to the stent in the portion of the artery dilated after deployment of the two stents (Fig 1C). The patient remained hemodynamically stable and was discharged the next day. Follow-Up The patient was placed on aspirin 325 mg and clopidogrel (Plavix; Sanofi Pharmaceuticals, New York, NY) 75 mg once daily. An angiogram 7 weeks later, at the time of distal lesion treatment, showed no evidence of vessel injury (Fig 1D). The stenosis at the proximal end of the previous endarterectomy site was treated with angioplasty and placement of a stent. Patient 2 A 72-year-old woman with a history of coronary artery disease and chronic obstructive pulmonary disease was referred from an outside hospital for symptoms of dizziness and righthand weakness. She had been treated at another institution with a proximal right subclavian artery angioplasty and placement of a 6 16-mm stent (AVE; Medtronic, Santa Rosa, CA). A left vertebral artery angioplasty and placement of a 4 13-mm stent (Corinthian IQ; Cordis Endovascular), as well as a4 18-mm stent (BX Velocity; Cordis Endovascular) was also performed 6 months before our procedure. Follow-up angiogram at the outside institution demonstrated occlusion of the previously stented left vertebral artery, severe restenosis of the stented right subclavian artery, and severe stenosis of the right vertebral artery origin. She was admitted to our institution 1 month later. Intervention Arteriography confirmed occlusion of the left vertebral artery, tandem severe stenoses of the proximal and distal right subclavian artery, and stenosis of the right vertebral artery origin. (Fig 2A). The carotid arteries did not supply the posterior circulation. Because the posterior circulation relied on the stenotic right vertebral artery, we opted to treat this vessel first and then address the subclavian stenoses. The patient had received 325 mg of aspirin and 75 mg of clopidogrel (Plavix; Sanofi Pharmaceuticals) per day for 5 days before admission. A baseline ACT was obtained and heparin 2057
2 2058 BROADBENT AJNR: 24, November/December 2003 FIG 1. A 72-year-old woman who had undergone a prior right carotid endarterectomy. A, Right common carotid injection shows 75% stenosis of proximal right common carotid and 90% stenosis of the right internal carotid artery near the proximal endarterectomy site. B, Frontal view of overlapping mm stents in the right common carotid artery. The SMART stent is more distal as compared with the Wallstent. C, Right common carotid arteriogram after stent placement shows contrast material extravasation medial to the stents. D, Arch angiogram obtained 7 weeks later shows no signs of vessel injury. was administered to achieve a target ACT of 300 s. Our first goal was dilating the right vertebral origin stenosis, because this was most life threatening. If access to this vessel was precluded by the proximal right subclavian stenosis, the latter would have been treated first. If this had been necessary, we would have staged the procedure, because we prefer to allow the angioplasty site to heal before working across it. A 7F sheath (Shuttle SL Cook, Bloomington, IN) easily passed through the stenosis in the right subclavian stent and was positioned with the tip adjacent to the right vertebral artery origin. Using road mapping, a mm (BX Velocity stent; Cordis Endovascular) was placed over a guidewire (Transend; Boston Scientific/Target, Fremont, CA) across the right vertebral stenosis. After the stent was deployed, an angiogram demonstrated minimal residual stenosis. One approach would have been to perform the distal subclavian angioplasty, because the sheath was already across the proximal stenosis. Similar to the first patient, we chose to treat the proximal right subclavian artery stenosis first because we believe that flow maintains patency and the now patent right vertebral artery provided outflow. The distal right subclavian artery stenosis would have been treated a month later to avoid crossing the acutely angioplastied proximal site. Consequently, the sheath was retracted proximal to the right subclavian stent. A6 20-mm noncompliant balloon (Savvy; Cordis Endovascular) was positioned within the recurrent proximal stenosis, which was confined to the right subclavian stent. Angioplasty to 8 atmospheres was performed at the distal, central, and proximal aspects of the stent. Although this balloon positioning allowed the balloon to protrude beyond the length of the stent, the vessel was larger both proximal and distal to the stent. The balloon expanded to its nominal diameter, which was that of the stent. After the balloon was removed, digital subtraction angiography demonstrated little change in the right subclavian stenosis because of recoil.
3 AJNR: 24, November/December 2003 SUPRA-AORTIC ARTERIAL RUPTURE 2059 FIG 2. A 72-year-old woman with recurrent stenosis after angioplasty and stent placement of a high-grade stenosis in the proximal right subclavian artery. A, Injection of the guide catheter in the innominate artery before angioplasty of the right vertebral artery origin. The lumen of the stenotic segment is nearly the same diameter as that of the guide catheter. Another stenosis is in the right subclavian artery distal to the vertebral artery. B, Innominate injection shows extravasation of contrast material after the second angioplasty of the right subclavian artery. C, Arch aortogram the following day demonstrates a pseudoaneurysm. The lumen of the innominate artery measured 12 mm, and the right subclavian artery distal to the stenosis measured 10 mm. Therefore, the Savvy balloon catheter was removed and replaced with a noncompliant 8 40-mm balloon (Diamond Ultra-Thin; Boston Scientific) inflated to 8 atmospheres to angioplasty the residual stenosis within the right subclavian stent. Although this balloon might be considered to be too long for this application, the artery proximal and distal was larger than the balloon s inflated diameter. The balloon was then deflated and withdrawn. Digital subtraction angiography demonstrated no residual stenosis, and contrast extravasated from the proximal portion of the artery containing the stent (Fig 2B). The heparin was discontinued. Mild hypotension occurred approximately 10 minutes later. A fluid bolus resulted in a return to normotensive parameters. Repeat angiography showed no active extravasation. The patient was transferred for CT, which demonstrated a hematoma extending from C2 to the thoracic inlet crossing the midline from right to left and bilateral pleural effusions. The patient was admitted to the intensive care unit for observation. Approximately 36 hours later, the patient was intubated for hypoxia. A follow-up CT showed no change in the hematoma. A repeat angiogram at that time showed no active extravasation and a 1-cm pseudoaneurysm at the site of the right subclavian stent (Fig 2C). Approximately 48 hours after the angioplasty procedure, the vascular surgery service elected to take the patient to the operating room for repair of the right subclavian artery with hematoma evacuation. This decision was based on uncertainty as to whether the patients declining respiratory status was related to further bleeding into the mediastinum or compression of the lungs by pleural fluid. A median sternotomy was performed, and a total of 1000 ml of bloody fluid was evacuated from the pleural spaces. There was no active bleeding. Following exposure, a 7-mm tear was identified in the proximal right subclavian artery allowing visualization of the stent. The portion of the subclavian artery involving the stent was resected, as was a diseased portion of the right common carotid back to the innominate artery. An 8-mm Dacron graft was then used for reconstruction of the subclavian artery. A graftotomy was then performed for endto-side anastomosis of the carotid artery. Follow-Up The patient was neurologically stable after this operation. One month later, the patient expired following a protracted stay in the intensive care unit complicated by pancreatitis and multiple system organ failure. Discussion In patient 1, vessel rupture occurred following placement of two stents and successive angioplasties, the second with a slightly oversized balloon. In patient 2, vessel rupture occurred following repeat angioplasty within the right subclavian stent, with a balloon that was oversized in relation to the stent. This balloon was smaller than the artery proximal and distal to the angioplasty site. In both of our reported cases, the vessel rupture occurred within the stent. In the first patient, this occurred because the second balloon was slightly oversized in comparison to the vessel. In the second patient, the second balloon was oversized in relation to the stent. Previously, we believed that the stent reinforced the vessel walls, offering some protection for repeated angioplasty. The recoil in the carotid and subclavian vessels despite theoretically appropriate-sized angioplasty balloons led to overly zealous repeat angioplasty. In this second patient, the original placement of the undersized balloon-expandable stent probably prevented restoration of a normal lumen at this site. Rather than repeat angioplasty with a larger diameter balloon, placement of a 7-mm self-expanding stent at the site may have been adequate. Angioplasty of atherosclerotic vessels requires use of noncompliant balloons that have the potential to cause rupture or tearing of the target vessel. This complication is uncommon and rarely reported. Consequently, there is little available data to guide man-
4 2060 BROADBENT AJNR: 24, November/December 2003 agement decisions when this complication occurs. Management alternatives for these injuries include: surgical repair or ligation, endovascular placement of a stent or graft, temporary balloon tamponade, permanent vessel occlusion, or conservative therapy with hemodynamic monitoring and follow-up imaging. In this report, we present two cases that were managed conservatively, at least initially. The first patient clearly did well, with no significant clinical sequelae and a good outcome. The second patient remained stable for 48 hours and was taken for open surgical repair. At surgery there was no evidence of ongoing hemorrhage. Angioplasty resulting in vessel rupture probably should be treated by placement of at least one stent, in our experience and that of others as detailed below. Vessel rupture after angioplasty of stented vessels may be treated conservatively or by placement of additional stents. Statistics regarding the frequency of vessel rupture during angioplasty and stent placement of the brachiocephalic vessels are difficult to obtain. In our experience, this complication is rare 2 (1.1%) in 180 procedures. A similar statistic (1.6%) has been reported for vessel rupture during angioplasty or stent placement of the renal arteries. In a review of 308 renal arteries treated over a 5-year period with angioplasty or stent placement, Morris et al (1) reported five vessel ruptures that were successfully treated with balloon tamponade or placement of an additional stent or stent graft. Owens et al (2) reviewed 22 carotid angioplasties with stent placement performed at their institution during a 5-year period. They treated two cases of ICA rupture one referred from an outside hospital and one from their institution with removal of the stents followed by endarterectomy and suture repair of the vessel. One patient recovered uneventfully, whereas the second had fine motor deficits in the right hand after 6 months. Warren et al (3)presented three cases where endovascular stent grafts were used to manage carotid blowout. Their conclusion stated that acute carotid hemorrhage can be successfully managed with directed placement of endovascular grafts. Maskovic et al (4) reported treating a pseudoaneurysm of the subclavian artery secondary to a gunshot wound by placement of a Memotherm stent (Angiomed GmbH and Co., Karlsruhe, Germany). Follow-up angiography at 15 days and again at 12 months showed no pseudoaneurysm and no stenosis of the subclavian artery. Arterial injuries due to angioplasty and stent placement are likely different from those due to carotid blowouts or gunshots, in that in the latter a portion of the vessel wall is absent. With angioplasty, the force is transmitted to the circumference of the vessel wall, with only the weakest portion failing. Speculatively, these are vertical or horizontal tears that may be reinforced by the placement of stents. Kasirajan (5) reported treatment of a traumatic pseudoaneurysm of the subclavian artery secondary to an attempted placement of a percutaneous dialysis catheter. Two Wallgraft (Boston Scientific) stents composed of polyethylene terephthalate material covering a standard Wallstent were used. The pseudoaneurysm continued to fill with contrast material in their patient despite covering of the neck. The pseudoaneurysm was then accessed percutaneously with 21- gauge needle by sonographic guidance and injected with 0.5 ml of 1:1000 thrombin. Sonography at 1 month showed persistent thrombosis of the pseudoaneurysm. Smith et al (6)recently reported their experience treating three patients (four vessels treated) with pseudoaneurysms by using the Wallgraft (Boston Scientific). They achieved complete occlusion of the pseudoaneurysm with patency of the parent vessel in all cases; however, in a month follow-up with either angiography or sonography, they noted % stenosis in three of four grafts. The high rate of severe stenosis or occlusion in this study makes treatment with currently available stent grafts a poor choice. Liang et al (7) reported conservative management of a pseudoaneurysm and mediastinal hematoma complicating angioplasty of the aorta to treat coarctation in an infant. Follow-up imaging in this patient 10 weeks later revealed total resolution of the hematoma. The patient was asymptomatic throughout 12 months of follow-up. Lin and colleagues (8) reported two cases of subclavian artery disruption related to endovascular intervention. One of their patients had contrast material extravasation after deployment of a balloonexpandable stent in a subclavian artery that was successfully treated with balloon tamponade. The second patient in their series had a large pseudoaneurysm 4 months after a balloon-expandable stent placement. This was eventually repaired with a prosthetic bypass graft. In light of the reports in the literature of supraaortic vessel rupture that have been treated successfully with a variety of nonsurgical approaches, we believe that surgery is not always indicated in this situation. Similar to the cases described in the literature, our patient 1 suffered no clinical effects from vessel rupture. Patient 2 in our series presented for endovascular management because of her high surgical risk. Unfortunately, these surgical risk factors made her a poor candidate for surgical management of the vessel rupture. We suggest that management of brachiocephalic rupture complicating angioplasty and stent placement should follow a similar course to the same complication occurring in renal artery angioplasty and stent placement that was once managed surgically and is now treated conservatively. If balloon tamponade is feasible in the effected vessel, this could be undertaken to halt active extravasation and give the artery time to seal. Follow-up imaging with angiography and CT should be performed while monitoring and treating hypotension.
5 AJNR: 24, November/December 2003 SUPRA-AORTIC ARTERIAL RUPTURE 2061 Conclusion Vessel rupture is a rare complication of angioplasty and stent placement of the brachiocephalic arteries. The small body of available literature supports our own experience that these patients may be managed conservatively with adjunctive endovascular techniques as needed. Surgery can be reserved for selected cases, which are not amenable to more conservative measures. Until further experience is available, however, the management of each case must be individualized. References 1. Morris CS, Bonnevie GJ, Najarian KE. Nonsurgical treatment of acute iatrogenic renal artery injuries occurring after renal artery angioplasty and stenting. AJR Am J Roentgenol 2001;177: Owens EL, Kumins NH, Bergan JJ, et al. Surgical management of acute complications and critical restenosis following carotid artery stenting. Ann Vasc Surg 2002;16: Warren FM, Cohen JI, Nesbit GM, et al. Management of carotid blowout with endovascular stent grafts. Laryngoscope 2002;112: Maskovic J, Radonic V, Jankovic L, et al. Traumatic false aneurysm of the subclavian artery treated by insertion of Memotherm stent. Eur J Radiol 2001;38: Kasirajan K. Salvage of failed stent-graft: expanded indication for percutaneous thrombin injection. Am J Surg 2002;183:600; discussion Smith TP, Alexander MJ, Enterline DS. Delayed stenosis following placement of a polyethylene terephthalate endograft in the cervical carotid artery. J Neurosurg 2003;98: Liang CD, Ko SF, Tiao MM. False aneurysm and mediastinal hematoma: complications of simultaneous transcatheter therapy for coarctation of the aorta and patent ductus arteriosus in an infant. J Invasive Cardiol 2001;13: Lin PH, Bush RL, Weiss VJ, et al. Subclavian artery disruption resulting from endovascular intervention: treatment options. J Vasc Surg 2000;32:
Case 37 Clinical Presentation
 Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Malperfusion Syndromes Type B Aortic Dissection with Malperfusion
 Malperfusion Syndromes Type B Aortic Dissection with Malperfusion Jade S. Hiramoto, MD, MAS April 27, 2012 Associated with early mortality Occurs when there is end organ ischemia secondary to aortic branch
Malperfusion Syndromes Type B Aortic Dissection with Malperfusion Jade S. Hiramoto, MD, MAS April 27, 2012 Associated with early mortality Occurs when there is end organ ischemia secondary to aortic branch
Acute dissections of the descending thoracic aorta (Debakey
 Endovascular Treatment of Acute Descending Thoracic Aortic Dissections Nimesh D. Desai, MD, PhD, and Joseph E. Bavaria, MD Acute dissections of the descending thoracic aorta (Debakey type III or Stanford
Endovascular Treatment of Acute Descending Thoracic Aortic Dissections Nimesh D. Desai, MD, PhD, and Joseph E. Bavaria, MD Acute dissections of the descending thoracic aorta (Debakey type III or Stanford
Primary to non-coronary IVUS
 codes 2018 2018 codes Primary to non-coronary IVUS Page 2 All coding, coverage, billing and payment information provided herein by Philips is gathered from third-party sources and is subject to change.
codes 2018 2018 codes Primary to non-coronary IVUS Page 2 All coding, coverage, billing and payment information provided herein by Philips is gathered from third-party sources and is subject to change.
Endovascular Management of Thoracic Aortic Pathology Stéphan Haulon, J Sobocinski, B Maurel, T Martin-Gonzalez, R Spear, A Hertault, R Azzaoui
 Endovascular Management of Thoracic Aortic Pathology Stéphan Haulon, J Sobocinski, B Maurel, T Martin-Gonzalez, R Spear, A Hertault, R Azzaoui Aortic Center, Lille University Hospital, France Disclosures
Endovascular Management of Thoracic Aortic Pathology Stéphan Haulon, J Sobocinski, B Maurel, T Martin-Gonzalez, R Spear, A Hertault, R Azzaoui Aortic Center, Lille University Hospital, France Disclosures
Technique and Outcome of Laser Fenestration For Arch Vessels
 Technique and Outcome of Laser Fenestration For Arch Vessels Jean M. Panneton MD, FRCSC, FACS Professor of Surgery Chief & Program Director Division of Vascular Surgery Eastern Virginia Medical School
Technique and Outcome of Laser Fenestration For Arch Vessels Jean M. Panneton MD, FRCSC, FACS Professor of Surgery Chief & Program Director Division of Vascular Surgery Eastern Virginia Medical School
Repair of Intracranial Vessel Perforation with Onyx-18 Using an Exovascular Retreating Catheter Technique
 Repair of Intracranial Vessel Perforation with Onyx-18 Using an Exovascular Retreating Catheter Technique Michael Horowitz M.D. Pittsburgh, Pennsylvania Background Iatrogenic intraprocedural rupture rates
Repair of Intracranial Vessel Perforation with Onyx-18 Using an Exovascular Retreating Catheter Technique Michael Horowitz M.D. Pittsburgh, Pennsylvania Background Iatrogenic intraprocedural rupture rates
Overview of Subclavian & Innominate Artery Interventions
 TCT 2016 Washington, DC, USA Tuesday November 1st, 2016 Peripheral vascular interventions Overview of Subclavian & Innominate Artery Interventions Dr Jacques Busquet Vascular & Endovascular Surgery Paris,
TCT 2016 Washington, DC, USA Tuesday November 1st, 2016 Peripheral vascular interventions Overview of Subclavian & Innominate Artery Interventions Dr Jacques Busquet Vascular & Endovascular Surgery Paris,
SCAI Fall Fellows Course Subclavian/Innominate Case Presentation
 SCAI Fall Fellows Course 2012 Subclavian/Innominate Case Presentation Daniel J. McCormick DO, FACC, FSCAI Director, Cardiovascular Interventional Therapy Pennsylvania Hospital University of Pennsylvania
SCAI Fall Fellows Course 2012 Subclavian/Innominate Case Presentation Daniel J. McCormick DO, FACC, FSCAI Director, Cardiovascular Interventional Therapy Pennsylvania Hospital University of Pennsylvania
Subclavian artery Stenting
 Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service
 M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke
 Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
Thrombin injection vs Conventional Surgical Repair in Treatment of Iatrogenic Post-cath Femoral Artery Pseudoaneurysm (IFAP)
 Kasr El Aini Journal of Surgery VOL., 11, NO 3 September 2010 31 Thrombin injection vs Conventional Surgical Repair in Treatment of Iatrogenic Post-cath Femoral Artery Pseudoaneurysm (IFAP) Farghaly A,
Kasr El Aini Journal of Surgery VOL., 11, NO 3 September 2010 31 Thrombin injection vs Conventional Surgical Repair in Treatment of Iatrogenic Post-cath Femoral Artery Pseudoaneurysm (IFAP) Farghaly A,
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant INDICATION: Abdominal aortic aneurysm. INTERVENTIONAL RADIOLOGIST:
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant INDICATION: Abdominal aortic aneurysm. INTERVENTIONAL RADIOLOGIST:
Angioplasty remains the most common method
 When AVF Angioplasty Fails Defining procedural success and overcoming common problems. By Thomas M. Vesely, MD Angioplasty remains the most common method of treating obstructive vascular stenoses associated
When AVF Angioplasty Fails Defining procedural success and overcoming common problems. By Thomas M. Vesely, MD Angioplasty remains the most common method of treating obstructive vascular stenoses associated
Originally Posted: November 15, 2014 BRUIT IN THE GROIN
 Originally Posted: November 15, 2014 BRUIT IN THE GROIN Resident(s): Donald ML Tse, MD Attending(s): KT Tan, MD Program/Dept(s): University Health Network/Mount Sinai Hospital, Toronto, ON, Canada CHIEF
Originally Posted: November 15, 2014 BRUIT IN THE GROIN Resident(s): Donald ML Tse, MD Attending(s): KT Tan, MD Program/Dept(s): University Health Network/Mount Sinai Hospital, Toronto, ON, Canada CHIEF
Challenges. 1. Sizing. 2. Proximal landing zone 3. Distal landing zone 4. Access vessels 5. Spinal cord ischemia 6. Endoleak
 Disclosure I have the following potential conflicts of interest to report: Consulting: Medtronic, Gore Employment in industry Stockholder of a healthcare company Owner of a healthcare company Other(s)
Disclosure I have the following potential conflicts of interest to report: Consulting: Medtronic, Gore Employment in industry Stockholder of a healthcare company Owner of a healthcare company Other(s)
Introduction to the Native Arteriovenous Fistula: A primer for medical students and radiology residents
 Introduction to the Native Arteriovenous Fistula: A primer for medical students and radiology residents Jesus Contreras, D.O. PGY-4 John Yasmer, D.O. Department of Radiology No Disclosures Objectives Introduce
Introduction to the Native Arteriovenous Fistula: A primer for medical students and radiology residents Jesus Contreras, D.O. PGY-4 John Yasmer, D.O. Department of Radiology No Disclosures Objectives Introduce
CT Imaging of Blunt and Penetrating Vascular Trauma DENNIS FOLEY MEDICAL COLLEGE WISCONSIN
 CT Imaging of Blunt and Penetrating Vascular Trauma DENNIS FOLEY MEDICAL COLLEGE WISCONSIN THORACO ABDOMINAL TRAUMA 0 10 20 30 40 50 60 5 cc/sec 30 secs 1.25 mm/ 55 mm Z1.375 2.5 mm/ 55 mm Z 1.375 Grade
CT Imaging of Blunt and Penetrating Vascular Trauma DENNIS FOLEY MEDICAL COLLEGE WISCONSIN THORACO ABDOMINAL TRAUMA 0 10 20 30 40 50 60 5 cc/sec 30 secs 1.25 mm/ 55 mm Z1.375 2.5 mm/ 55 mm Z 1.375 Grade
Case Report 1. CTA head. (c) Tele3D Advantage, LLC
 Case Report 1 CTA head 1 History 82 YEAR OLD woman with signs and symptoms of increased intra cranial pressure in setting of SAH. CT Brain was performed followed by CT Angiography of head. 2 CT brain Extensive
Case Report 1 CTA head 1 History 82 YEAR OLD woman with signs and symptoms of increased intra cranial pressure in setting of SAH. CT Brain was performed followed by CT Angiography of head. 2 CT brain Extensive
Case Report Endovascular Treatment for Pseudoaneurysms after Surgical Correction of Aortic Coarctation
 SAGE-Hindawi Access to Research Volume 2011, Article ID 649207, 4 pages doi:10.4061/2011/649207 Case Report Endovascular Treatment for Pseudoaneurysms after Surgical Correction of Aortic Coarctation M.
SAGE-Hindawi Access to Research Volume 2011, Article ID 649207, 4 pages doi:10.4061/2011/649207 Case Report Endovascular Treatment for Pseudoaneurysms after Surgical Correction of Aortic Coarctation M.
An Overview of Post-EVAR Endoleaks: Imaging Findings and Management. Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC
 An Overview of Post-EVAR Endoleaks: Imaging Findings and Management Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC Disclosure Slide Mark O. Baerlocher: Current: Consultant for Boston
An Overview of Post-EVAR Endoleaks: Imaging Findings and Management Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC Disclosure Slide Mark O. Baerlocher: Current: Consultant for Boston
IMAGES. in PAEDIATRIC CARDIOLOGY
 IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2005 Jan-Mar; 7(1): 12 17. PMCID: PMC3232568 Stent implantation for coarctation facilitated by the anterograde trans-septal approach N Sreeram and
IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2005 Jan-Mar; 7(1): 12 17. PMCID: PMC3232568 Stent implantation for coarctation facilitated by the anterograde trans-septal approach N Sreeram and
CY2017 Hospital Outpatient: Vascular Procedure APCs and Complexity Adjustments
 CY2017 Hospital Outpatient: Vascular Procedure APCs and Complexity Adjustments Comprehensive Ambulatory Payment Classifications (c-apcs) In CY2015 and in an effort to help pay providers for quality, not
CY2017 Hospital Outpatient: Vascular Procedure APCs and Complexity Adjustments Comprehensive Ambulatory Payment Classifications (c-apcs) In CY2015 and in an effort to help pay providers for quality, not
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
Management of Acute Aortic Syndromes. M. Grabenwoger, MD Dept. of Cardiovascular Surgery Hospital Hietzing, Vienna, Austria
 Management of Acute Aortic Syndromes M. Grabenwoger, MD Dept. of Cardiovascular Surgery Hospital Hietzing, Vienna, Austria I have nothing to disclose. Acute Aortic Syndromes Acute Aortic Dissection Type
Management of Acute Aortic Syndromes M. Grabenwoger, MD Dept. of Cardiovascular Surgery Hospital Hietzing, Vienna, Austria I have nothing to disclose. Acute Aortic Syndromes Acute Aortic Dissection Type
Vascular injury from an arterial closure device
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 1-1-2007 Vascular injury from an arterial closure device Jeffrey P. C. Lin Brian G. Rubin William D. Middleton Follow
Washington University School of Medicine Digital Commons@Becker Open Access Publications 1-1-2007 Vascular injury from an arterial closure device Jeffrey P. C. Lin Brian G. Rubin William D. Middleton Follow
Vascular Access: Management of Complications. Chris Burrell, South West Cardiothoracic Centre, Plymouth
 Vascular Access: Management of Complications Chris Burrell, South West Cardiothoracic Centre, Plymouth Alternative Vascular Access Sites Femoral Axillary Brachial Radial Ulnar Femoral v Radial Vascular
Vascular Access: Management of Complications Chris Burrell, South West Cardiothoracic Centre, Plymouth Alternative Vascular Access Sites Femoral Axillary Brachial Radial Ulnar Femoral v Radial Vascular
Interventional Treatment for Complete Occlusion of Arteriovenous Shunt: Our Experience in 39 cases
 Chin J Radiol 2003; 28: 137-142 137 Interventional Treatment for Complete Occlusion of Arteriovenous Shunt: Our Experience in 39 cases SHE-MENG CHENG SUK-PING NG FEI-SHIH YANG SHIN-LIN SHIH Department
Chin J Radiol 2003; 28: 137-142 137 Interventional Treatment for Complete Occlusion of Arteriovenous Shunt: Our Experience in 39 cases SHE-MENG CHENG SUK-PING NG FEI-SHIH YANG SHIN-LIN SHIH Department
Bifurcated system Proximal suprarenal stent Modular (aortic main body and two iliac legs) Full thickness woven polyester graft material Fully
 Physician Training Bifurcated system Proximal suprarenal stent Modular (aortic main body and two iliac legs) Full thickness woven polyester graft material Fully supported by self-expanding z-stents H&L-B
Physician Training Bifurcated system Proximal suprarenal stent Modular (aortic main body and two iliac legs) Full thickness woven polyester graft material Fully supported by self-expanding z-stents H&L-B
Jean M Panneton, MD Professor of Surgery Program Director Vascular Surgery Chief EVMS. Arch Pathology: The Endovascular Era is here
 Jean M Panneton, MD Professor of Surgery Program Director Vascular Surgery Chief EVMS Arch Pathology: The Endovascular Era is here Disclosures Consultant: Cook Medical, Bolton Medical, Medtronic Inc, Volcano,
Jean M Panneton, MD Professor of Surgery Program Director Vascular Surgery Chief EVMS Arch Pathology: The Endovascular Era is here Disclosures Consultant: Cook Medical, Bolton Medical, Medtronic Inc, Volcano,
Tasopoulou KM 1, Argyriou C 1, Mantatzis M 2, Kantartzi K 3, Passadakis P 3, Georgiadis GS 1
 Tasopoulou KM 1, Argyriou C 1, Mantatzis M 2, Kantartzi K 3, Passadakis P 3, Georgiadis GS 1 1 Department of Vascular Surgery, 2 Department of Radiology/Interventional Radiology Unit and 3 Department of
Tasopoulou KM 1, Argyriou C 1, Mantatzis M 2, Kantartzi K 3, Passadakis P 3, Georgiadis GS 1 1 Department of Vascular Surgery, 2 Department of Radiology/Interventional Radiology Unit and 3 Department of
Corporate Medical Policy
 Corporate Medical Policy Endovascular Therapies for Extracranial Vertebral Artery Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endovascular_therapies_for_extracranial_vertebral_artery_disease
Corporate Medical Policy Endovascular Therapies for Extracranial Vertebral Artery Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endovascular_therapies_for_extracranial_vertebral_artery_disease
Two Cases of Carotid Artery Stenting Combined Balloon- and Self-expanding Stent for the Spontaneous Internal Carotid Artery Dissections
 Journal of Neuroendovascular Therapy 2017; 11: 437 442 Online June 13, 2017 DOI: 10.5797/jnet.tn.2016-0059 Two Cases of Carotid Artery Stenting Combined Balloon- and Self-expanding Stent for the Spontaneous
Journal of Neuroendovascular Therapy 2017; 11: 437 442 Online June 13, 2017 DOI: 10.5797/jnet.tn.2016-0059 Two Cases of Carotid Artery Stenting Combined Balloon- and Self-expanding Stent for the Spontaneous
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Medical technology guidance SCOPE Pipeline embolisation device for the treatment of
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Medical technology guidance SCOPE Pipeline embolisation device for the treatment of 1 Technology complex intracranial aneurysms 1.1 Description of
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Medical technology guidance SCOPE Pipeline embolisation device for the treatment of 1 Technology complex intracranial aneurysms 1.1 Description of
Endovascular and Hybrid Treatment of TASC C & D Aortoiliac Occlusive Disease
 Endovascular and Hybrid Treatment of TASC C & D Aortoiliac Occlusive Disease Arash Bornak, MD FACS Vascular & Endovascular Surgery University of Miami Miller School of Medicine No disclosure BACKGROUND
Endovascular and Hybrid Treatment of TASC C & D Aortoiliac Occlusive Disease Arash Bornak, MD FACS Vascular & Endovascular Surgery University of Miami Miller School of Medicine No disclosure BACKGROUND
Diffusion-Weighted Imaging Abnormalities after Percutaneous Transluminal Angioplasty and Stenting for Intracranial Atherosclerotic Disease
 AJNR Am J Neuroradiol 26:385 389, February 2005 Diffusion-Weighted Imaging Abnormalities after Percutaneous Transluminal Angioplasty and Stenting for Intracranial Atherosclerotic Disease Tomoyuki Tsumoto
AJNR Am J Neuroradiol 26:385 389, February 2005 Diffusion-Weighted Imaging Abnormalities after Percutaneous Transluminal Angioplasty and Stenting for Intracranial Atherosclerotic Disease Tomoyuki Tsumoto
Abdominal and thoracic aneurysm repair
 Abdominal and thoracic aneurysm repair William A. Gray MD Director, Endovascular Intervention Cardiovascular Research Foundation Columbia University Medical Center Abdominal Aortic Aneurysm Endografts
Abdominal and thoracic aneurysm repair William A. Gray MD Director, Endovascular Intervention Cardiovascular Research Foundation Columbia University Medical Center Abdominal Aortic Aneurysm Endografts
CY2015 Hospital Outpatient: Endovascular Procedure APCs and Complexity Adjustments
 CY2015 Hospital Outpatient: Endovascular Procedure APCs Complexity Adjustments Comprehensive Ambulatory Payment Classifications (c-apcs) CMS finalized the implementation of 25 Comprehensive APC to further
CY2015 Hospital Outpatient: Endovascular Procedure APCs Complexity Adjustments Comprehensive Ambulatory Payment Classifications (c-apcs) CMS finalized the implementation of 25 Comprehensive APC to further
Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection
 Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection M. Grabenwoger Dept. of Cardiovascular Surgery Hospital Hietzing Vienna, Austria Disclosure Statement Consultant of Jotec, Hechingen,
Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection M. Grabenwoger Dept. of Cardiovascular Surgery Hospital Hietzing Vienna, Austria Disclosure Statement Consultant of Jotec, Hechingen,
TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES
 TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES ALBERTO MAUD, MD ASSOCIATE PROFESSOR TEXAS TECH UNIVERSITY HEALTH SCIENCES CENTER EL PASO PAUL L. FOSTER SCHOOL OF MEDICINE 18TH ANNUAL RIO GRANDE TRAUMA 2017
TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES ALBERTO MAUD, MD ASSOCIATE PROFESSOR TEXAS TECH UNIVERSITY HEALTH SCIENCES CENTER EL PASO PAUL L. FOSTER SCHOOL OF MEDICINE 18TH ANNUAL RIO GRANDE TRAUMA 2017
Thoracic Endovascular Aortic Repair (TEVAR) Indications and Basic Procedure
 Thoracic Endovascular Aortic Repair (TEVAR) Indications and Basic Procedure Tilo Kölbel, MD, PhD University Heart Center Hamburg University Hospital Eppendorf Disclosure Speaker name: Tilo Kölbel, MD I
Thoracic Endovascular Aortic Repair (TEVAR) Indications and Basic Procedure Tilo Kölbel, MD, PhD University Heart Center Hamburg University Hospital Eppendorf Disclosure Speaker name: Tilo Kölbel, MD I
Subclavian and Vertebral Artery Angioplasty - Vertebro-basilar Insufficiency: Clinical Aspects and Diagnosis
 HOSPITAL CHRONICLES 2008, 3(3): 136 140 ORIGINAL ARTICLE Subclavian and Vertebral Artery Angioplasty - Vertebro-basilar Insufficiency: Clinical Aspects and Diagnosis Antonios Polydorou, MD Hemodynamic
HOSPITAL CHRONICLES 2008, 3(3): 136 140 ORIGINAL ARTICLE Subclavian and Vertebral Artery Angioplasty - Vertebro-basilar Insufficiency: Clinical Aspects and Diagnosis Antonios Polydorou, MD Hemodynamic
Ascending Aorta: Is The Endovascular Approach Realistic?
 Ascending Aorta: Is The Endovascular Approach Realistic? Tilo Kölbel, MD, PhD University Heart Center Hamburg University Hospital Eppendorf Disclosures Research-grants, travelling, proctoring speaking-fees,
Ascending Aorta: Is The Endovascular Approach Realistic? Tilo Kölbel, MD, PhD University Heart Center Hamburg University Hospital Eppendorf Disclosures Research-grants, travelling, proctoring speaking-fees,
AORTIC DISSECTION. DISSECTING ANEURYSMS OF THE AORTA or CLASSIFICATION
 DISSECTING ANEURYSMS OF THE AORTA or AORTIC DISSECTION CLASSIFICATION DeBakey classified aortic dissections into types I, II, and III :- Type I dissection the tear site originates in the ascending aorta,
DISSECTING ANEURYSMS OF THE AORTA or AORTIC DISSECTION CLASSIFICATION DeBakey classified aortic dissections into types I, II, and III :- Type I dissection the tear site originates in the ascending aorta,
Optimal repair of acute aortic dissection
 Optimal repair of acute aortic dissection Dept. of Vascular Surgery, The 2nd Xiang-Yale Hospital, Central-South University, China Hunan Major Vessels Diseases Clinical Center Chang Shu Email:changshu01@yahoo.com
Optimal repair of acute aortic dissection Dept. of Vascular Surgery, The 2nd Xiang-Yale Hospital, Central-South University, China Hunan Major Vessels Diseases Clinical Center Chang Shu Email:changshu01@yahoo.com
Update on Acute Aortic Syndrome
 SUNDAY Update on Acute Aortic Syndrome Diana Litmanovich, MD Learning objectives To be familiar with the definition, natural history, and imaging findings of acute aortic syndrome, including: I. Aortic
SUNDAY Update on Acute Aortic Syndrome Diana Litmanovich, MD Learning objectives To be familiar with the definition, natural history, and imaging findings of acute aortic syndrome, including: I. Aortic
Contemporary management of brachiocephalic occlusive disease. TM Sullivan Minneapolis, MN
 Contemporary management of brachiocephalic occlusive disease TM Sullivan Minneapolis, MN WL Gore & Associates Disclosures Meeting organizer (SOAR) CR Bard Chair, CEC Bolster trial Veryan National PI, MIMICS
Contemporary management of brachiocephalic occlusive disease TM Sullivan Minneapolis, MN WL Gore & Associates Disclosures Meeting organizer (SOAR) CR Bard Chair, CEC Bolster trial Veryan National PI, MIMICS
EVAR and TEVAR: Extending Their Use for Rupture and Traumatic Injury. Conflict of Interest. Hypotensive shock 5/5/2014. none
 EVAR and TEVAR: Extending Their Use for Rupture and Traumatic Injury Bruce H. Gray, DO MSVM FSCAI Professor of Surgery/Vascular Medicine USC SOM-Greenville Greenville, South Carolina none Conflict of Interest
EVAR and TEVAR: Extending Their Use for Rupture and Traumatic Injury Bruce H. Gray, DO MSVM FSCAI Professor of Surgery/Vascular Medicine USC SOM-Greenville Greenville, South Carolina none Conflict of Interest
The role of false lumen intervention to promote remodelling via induced thrombosis the FLIRT concept
 The role of false lumen intervention to promote remodelling via induced thrombosis the FLIRT concept Professor Christoph A. Nienaber The Royal Brompton and Harefield NHS Trust Cardiology and Aortic Centre
The role of false lumen intervention to promote remodelling via induced thrombosis the FLIRT concept Professor Christoph A. Nienaber The Royal Brompton and Harefield NHS Trust Cardiology and Aortic Centre
Percutaneous Revascularization of Sole Arch Artery for Severe Cerebral Ischemia Resulting from Takayasu Arteritis
 Percutaneous Revascularization of Sole Arch Artery for Severe Cerebral Ischemia Resulting from Takayasu Arteritis Sanjay Tyagi, MD, Mohit D. Gupta, MD, Praveen Singh, MD, Devendra Shrimal, MD, and M.P.
Percutaneous Revascularization of Sole Arch Artery for Severe Cerebral Ischemia Resulting from Takayasu Arteritis Sanjay Tyagi, MD, Mohit D. Gupta, MD, Praveen Singh, MD, Devendra Shrimal, MD, and M.P.
Case Report. Case Report
 AJNR Am J Neuroradiol 25:333 337, February 2004 Case Report Stent-Coil Treatment of a Distal Internal Carotid Artery Dissecting Pseudoaneurysm on a Redundant Loop by Use of a Flexible, Dedicated Nitinol
AJNR Am J Neuroradiol 25:333 337, February 2004 Case Report Stent-Coil Treatment of a Distal Internal Carotid Artery Dissecting Pseudoaneurysm on a Redundant Loop by Use of a Flexible, Dedicated Nitinol
Successful percutaneous treatment of late-onset femoral pseudoaneurysm after transcatheter, aortic valve implantation procedure
 Case Report Page 1 of 5 Successful percutaneous treatment of late-onset femoral pseudoaneurysm after transcatheter, aortic valve implantation procedure Murat Celik, Uygar Cagdas Yuksel Correspondence to:
Case Report Page 1 of 5 Successful percutaneous treatment of late-onset femoral pseudoaneurysm after transcatheter, aortic valve implantation procedure Murat Celik, Uygar Cagdas Yuksel Correspondence to:
Endovascular treatment for pseudoocclusion of the internal carotid artery
 Endovascular treatment for pseudoocclusion of the internal carotid artery Daqiao Guo, Xiao Tang, Weiguo Fu Institute of Vascular Surgery, Fudan University, Department of Vascular Surgery, Zhongshan Hospital
Endovascular treatment for pseudoocclusion of the internal carotid artery Daqiao Guo, Xiao Tang, Weiguo Fu Institute of Vascular Surgery, Fudan University, Department of Vascular Surgery, Zhongshan Hospital
Vascular Intervention
 10 : 389-393, 2001 B Vascular Intervention 1 1 2 1 1 1 1 3 2 1 1997 7 2000 4 B 29 19 10 50 84 66.1 stent graft S/G primary entry stenting S/G 12 4 2 1 1 40 mm 8 1 MOF 1 endoleak + 11 91.6% 10 stenting
10 : 389-393, 2001 B Vascular Intervention 1 1 2 1 1 1 1 3 2 1 1997 7 2000 4 B 29 19 10 50 84 66.1 stent graft S/G primary entry stenting S/G 12 4 2 1 1 40 mm 8 1 MOF 1 endoleak + 11 91.6% 10 stenting
IVUS Guided Case Review Case Performed by Frank R. Arko III, MD Charlotte, NC
 IVUS Guided Case Review Case Performed by Frank R. Arko III, MD Charlotte, NC The opinions and clinical experiences presented herein are for informational purposes only. Dr. Arko is a paid consultant for
IVUS Guided Case Review Case Performed by Frank R. Arko III, MD Charlotte, NC The opinions and clinical experiences presented herein are for informational purposes only. Dr. Arko is a paid consultant for
Occlusion: A New Technique Antegrade wiring i with retrograde ballooning and stenting
 How To Treat Resistant Central Venous Occlusion: A New Technique Antegrade wiring i with retrograde ballooning and stenting Dafsah A Juzar T. Santoso National Heart Center, Harapan Kita, & Medistra Hospital
How To Treat Resistant Central Venous Occlusion: A New Technique Antegrade wiring i with retrograde ballooning and stenting Dafsah A Juzar T. Santoso National Heart Center, Harapan Kita, & Medistra Hospital
Introducing the GORE TAG Conformable Thoracic Stent Graft with ACTIVE CONTROL System
 Introducing the GORE TAG Conformable Thoracic Stent Graft with ACTIVE CONTROL System K. Oikonomou Department of Vascular Surgery Regensburg University Disclosures W.L. Gore & Associates Sponsored Presentation
Introducing the GORE TAG Conformable Thoracic Stent Graft with ACTIVE CONTROL System K. Oikonomou Department of Vascular Surgery Regensburg University Disclosures W.L. Gore & Associates Sponsored Presentation
Recommendations for Follow-up After Vascular Surgery Arterial Procedures SVS Practice Guidelines
 Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
For Personal Use. Copyright HMP 2013
 1 Case Report and Brief Review J INVASIVE CARDIOL 2013;25(1):E8-E10 Hemoptysis Caused by Saphenous Vein Graft Perforation During Percutaneous Coronary Intervention Dong-Yi Chen, MD, Chun-Chi Chen, MD,
1 Case Report and Brief Review J INVASIVE CARDIOL 2013;25(1):E8-E10 Hemoptysis Caused by Saphenous Vein Graft Perforation During Percutaneous Coronary Intervention Dong-Yi Chen, MD, Chun-Chi Chen, MD,
How to achieve a successful proximal sealing in TEVAR? Pr L Canaud
 How to achieve a successful proximal sealing in TEVAR? Pr L Canaud CHU de Montpellier France Disclosure I have the following potential conflicts of interest to report: Consulting: Medtronic. Proximal neck
How to achieve a successful proximal sealing in TEVAR? Pr L Canaud CHU de Montpellier France Disclosure I have the following potential conflicts of interest to report: Consulting: Medtronic. Proximal neck
Percutaneous Approaches to Aortic Disease in 2018
 Percutaneous Approaches to Aortic Disease in 2018 Wendy Tsang, MD, SM Assistant Professor, University of Toronto Toronto General Hospital, University Health Network Case 78 year old F Lower CP and upper
Percutaneous Approaches to Aortic Disease in 2018 Wendy Tsang, MD, SM Assistant Professor, University of Toronto Toronto General Hospital, University Health Network Case 78 year old F Lower CP and upper
Traumatic Posterior Tibial Pseudoaneursym: A rare late complication repaired conventionally
 Volume 2 Issue 3 Article 3 2016 Traumatic Posterior Tibial Pseudoaneursym: A rare late complication repaired conventionally Farzad Amiri, MD; Zachary Sanford; and Constantinous Constantinou, MD Follow
Volume 2 Issue 3 Article 3 2016 Traumatic Posterior Tibial Pseudoaneursym: A rare late complication repaired conventionally Farzad Amiri, MD; Zachary Sanford; and Constantinous Constantinou, MD Follow
Visceral aneurysm. Diagnosis and Interventions M.NEDEVSKA
 Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
CAROTID ARTERY ANGIOPLASTY
 CAROTID ARTERY ANGIOPLASTY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage Guideline
CAROTID ARTERY ANGIOPLASTY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage Guideline
Surgical Privileges Form: Vascular Surgery
 Surgical Form: Vascular Surgery Clinical Request Applicant s Name:. License No. (If Any):... Date:... Scope of Practice:. Facility:.. Place of Work:. CATEGORY I: GENERAL PRIVILEGES 1. Admitting privileges
Surgical Form: Vascular Surgery Clinical Request Applicant s Name:. License No. (If Any):... Date:... Scope of Practice:. Facility:.. Place of Work:. CATEGORY I: GENERAL PRIVILEGES 1. Admitting privileges
How to manage TAVI related vascular complications. Paul TL Chiam MBBS, FRCP, FESC, FACC, FSCAI
 How to manage TAVI related vascular complications Paul TL Chiam MBBS, FRCP, FESC, FACC, FSCAI Definition VARC-2 consensus statement Complications caused by: Wire Catheter Anything related to vascular access
How to manage TAVI related vascular complications Paul TL Chiam MBBS, FRCP, FESC, FACC, FSCAI Definition VARC-2 consensus statement Complications caused by: Wire Catheter Anything related to vascular access
Emergency Endovascular Treatment for Ruptured Type B Dissection in the Abdominal Aorta
 Brief Reports Emergency Endovascular Treatment for Ruptured Type B Dissection in the Abdominal Aorta Mikolaj Wojtaszek, MD, PhD, Krzysztof Milczarek, MD, PhD, Jacek Szmidt, MD, PhD, and Olgierd Rowinski,
Brief Reports Emergency Endovascular Treatment for Ruptured Type B Dissection in the Abdominal Aorta Mikolaj Wojtaszek, MD, PhD, Krzysztof Milczarek, MD, PhD, Jacek Szmidt, MD, PhD, and Olgierd Rowinski,
Morbidity Audit and Logbook Tool SNOMED Board Reporting Terms for SET and IMG Vascular Surgery AMPUTATION AORTA
 SNOMED s for SET and IMG Vascular Surgery AMPUTATION Amputation above-knee Amputation of leg through tibia and fibula Amputation of the foot Amputation of toe Through knee amputation Ray amputation of
SNOMED s for SET and IMG Vascular Surgery AMPUTATION Amputation above-knee Amputation of leg through tibia and fibula Amputation of the foot Amputation of toe Through knee amputation Ray amputation of
Interventional Radiology in Trauma. Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital
 Interventional Radiology in Trauma Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital Disclosures None relevant to this presentation Shareholder Johnson and Johnson Goal
Interventional Radiology in Trauma Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital Disclosures None relevant to this presentation Shareholder Johnson and Johnson Goal
Development of a Branched LSA Endograft & Ascending Aorta Endograft
 Development of a Branched LSA Endograft & Ascending Aorta Endograft Frank R. Arko III, MD Sanger Heart & Vascular Institute Carolinas Medical Center Charlotte, North Carolina, USA Disclosures Proximal
Development of a Branched LSA Endograft & Ascending Aorta Endograft Frank R. Arko III, MD Sanger Heart & Vascular Institute Carolinas Medical Center Charlotte, North Carolina, USA Disclosures Proximal
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of June 4, 2018 Thrombolysis, Thrombectomy & Angioplasty
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of June 4, 2018 Thrombolysis, Thrombectomy & Angioplasty
BC Vascular Day. Contents. November 3, Abdominal Aortic Aneurysm 2 3. Peripheral Arterial Disease 4 6. Deep Venous Thrombosis 7 8
 BC Vascular Day Contents Abdominal Aortic Aneurysm 2 3 November 3, 2018 Peripheral Arterial Disease 4 6 Deep Venous Thrombosis 7 8 Abdominal Aortic Aneurysm Conservative Management Risk factor modification
BC Vascular Day Contents Abdominal Aortic Aneurysm 2 3 November 3, 2018 Peripheral Arterial Disease 4 6 Deep Venous Thrombosis 7 8 Abdominal Aortic Aneurysm Conservative Management Risk factor modification
Peter I. Kalmar, 1 Peter Oberwalder, 2 Peter Schedlbauer, 1 Jürgen Steiner, 1 and Rupert H. Portugaller Introduction. 2.
 Case Reports in Medicine Volume 2013, Article ID 714914, 4 pages http://dx.doi.org/10.1155/2013/714914 Case Report Secondary Aortic Dissection after Endoluminal Treatment of an Intramural Hematoma of the
Case Reports in Medicine Volume 2013, Article ID 714914, 4 pages http://dx.doi.org/10.1155/2013/714914 Case Report Secondary Aortic Dissection after Endoluminal Treatment of an Intramural Hematoma of the
Use of covered stents and endograft as a rescue treatment in a patient with a complex form of recurrent aortic coarctation
 TECHNICAL NOTE Use of covered stents and endograft as a rescue treatment in a patient with a complex form of recurrent aortic coarctation Juan C. Parodi, MD, Luis Mariano Ferreira, MD, Horacio Faella,
TECHNICAL NOTE Use of covered stents and endograft as a rescue treatment in a patient with a complex form of recurrent aortic coarctation Juan C. Parodi, MD, Luis Mariano Ferreira, MD, Horacio Faella,
Carotid Artery Stenting
 Carotid Artery Stenting JESSICA MITCHELL, ACNP CENTRAL ILLINOIS RADIOLOGICAL ASSOCIATES External Carotid Artery (ECA) can easily be identified from Internal Carotid Artery (ICA) by noticing the branches.
Carotid Artery Stenting JESSICA MITCHELL, ACNP CENTRAL ILLINOIS RADIOLOGICAL ASSOCIATES External Carotid Artery (ECA) can easily be identified from Internal Carotid Artery (ICA) by noticing the branches.
Carotid Stenosis (carotid artery disease)
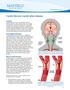 1 Carotid Stenosis (carotid artery disease) Overview Carotid stenosis is a narrowing of the carotid arteries, the two major arteries that carry oxygenrich blood from the heart to the brain. Also called
1 Carotid Stenosis (carotid artery disease) Overview Carotid stenosis is a narrowing of the carotid arteries, the two major arteries that carry oxygenrich blood from the heart to the brain. Also called
Reimbursement Guide Zenith Fenestrated AAA Endovascular Graft
 MEDICAL Reimbursement Guide Zenith Fenestrated AAA Endovascular Graft Disclaimer: The information provided herein reflects Cook s understanding of the procedure(s) and/or device(s) from sources that may
MEDICAL Reimbursement Guide Zenith Fenestrated AAA Endovascular Graft Disclaimer: The information provided herein reflects Cook s understanding of the procedure(s) and/or device(s) from sources that may
Vascular V12. Covered Stent. The New Standard of Care
 Vascular V12 Covered Stent The New Standard of Care Innovation Novel Thermo-Conformable Covered Stent 316L stainless steel stent completely encapsulated in a proprietary one piece eptfe film cast covering
Vascular V12 Covered Stent The New Standard of Care Innovation Novel Thermo-Conformable Covered Stent 316L stainless steel stent completely encapsulated in a proprietary one piece eptfe film cast covering
Jimmy Wei Hwa Tan, Surg, MD
 Jimmy Wei Hwa Tan, Surg, MD Director, Department of Surgery Chief, Department of Cardiovascular Surgery Tainan An-Nan Municipal Hospital, China Medical University, Taiwan Disclosure I have the following
Jimmy Wei Hwa Tan, Surg, MD Director, Department of Surgery Chief, Department of Cardiovascular Surgery Tainan An-Nan Municipal Hospital, China Medical University, Taiwan Disclosure I have the following
Free Esophageal Perforation Following Hybrid Visceral Debranching and Distal Endograft Extension to Repair a Ruptured Thoracoabdominal Aortic
 Free Esophageal Perforation Following Hybrid Visceral Debranching and Distal Endograft Extension to Repair a Ruptured Thoracoabdominal Aortic Aneurysm History A 56-year-old gentleman, who had been referred
Free Esophageal Perforation Following Hybrid Visceral Debranching and Distal Endograft Extension to Repair a Ruptured Thoracoabdominal Aortic Aneurysm History A 56-year-old gentleman, who had been referred
2006 NKF-DOQI Guidelines Preferred Vascular Access Order 1. Radiocephalic (wrist) fistula 2. Brachiocephalic (elbow) fistula 3. Basilic vein transposi
 Stage 5 Chronic Kidney Disease Assessing the Results of AV Access: Realistic Outcomes in 2009 Sean P. Roddy, MD Albany, NY Defined as a GFR
Stage 5 Chronic Kidney Disease Assessing the Results of AV Access: Realistic Outcomes in 2009 Sean P. Roddy, MD Albany, NY Defined as a GFR
Transcatheter Aortic Valve Implantation Management of risks and complications
 Transcatheter Aortic Valve Implantation Management of risks and complications TAVI Summit, Seoul, Korea, Spetember 3rd, 2011 Alain Cribier University of Rouen, France Complications of TAVI Depending on
Transcatheter Aortic Valve Implantation Management of risks and complications TAVI Summit, Seoul, Korea, Spetember 3rd, 2011 Alain Cribier University of Rouen, France Complications of TAVI Depending on
AV ACESS COMPLICATIONS. Ass. Prof. Dr. Habas
 AV ACESS COMPLICATIONS Ass. Prof. Dr. Habas COMPLICATION AVF IS CONSIDERED A MINOR PROCEDURE INCIDENCE OF COMPLICATION- 20-27% MANY A COMPLICATION LEADS TO FAILURE OF FISTULA LOSS OF SITE AND VEIN FOR
AV ACESS COMPLICATIONS Ass. Prof. Dr. Habas COMPLICATION AVF IS CONSIDERED A MINOR PROCEDURE INCIDENCE OF COMPLICATION- 20-27% MANY A COMPLICATION LEADS TO FAILURE OF FISTULA LOSS OF SITE AND VEIN FOR
Popliteal Artery Aneurysms: Diagnosis and Repair Options
 Deepak N. Deshmukh DO April 27, 2018 Popliteal Artery Aneurysms: Diagnosis and Repair Options No Disclosures Popliteal Artery Aneurysms (PAAs) Male Predominanace Most common peripheral Aneurysm (70%) 30-50%
Deepak N. Deshmukh DO April 27, 2018 Popliteal Artery Aneurysms: Diagnosis and Repair Options No Disclosures Popliteal Artery Aneurysms (PAAs) Male Predominanace Most common peripheral Aneurysm (70%) 30-50%
2017 Cardiology Survival Guide
 2017 Cardiology Survival Guide Chapter 2: Angioplasty/Atherectomy/Stent The term angioplasty literally means "blood vessel repair." During an angioplasty procedure, the physician inserts a catheter, with
2017 Cardiology Survival Guide Chapter 2: Angioplasty/Atherectomy/Stent The term angioplasty literally means "blood vessel repair." During an angioplasty procedure, the physician inserts a catheter, with
UC SF. Disclosures. Thoracic Endovascular Aortic Repair 4/24/2009. Management of Acute Dissections: Is There Still a Role for Open Surgery?
 UC SF Management of Acute Dissections: Is There Still a Role for Open Surgery? Darren B. Schneider, M.D. Assistant Professor of Surgery and Radiology Division of Vascular Surgery University of California
UC SF Management of Acute Dissections: Is There Still a Role for Open Surgery? Darren B. Schneider, M.D. Assistant Professor of Surgery and Radiology Division of Vascular Surgery University of California
Open fenestration for complicated acute aortic B dissection
 Art of Operative Techniques Open fenestration for complicated acute aortic B dissection Santi Trimarchi 1, Sara Segreti 1, Viviana Grassi 1, Chiara Lomazzi 1, Marta Cova 1, Gabriele Piffaretti 2, Vincenzo
Art of Operative Techniques Open fenestration for complicated acute aortic B dissection Santi Trimarchi 1, Sara Segreti 1, Viviana Grassi 1, Chiara Lomazzi 1, Marta Cova 1, Gabriele Piffaretti 2, Vincenzo
Case Endovascular management of non maturing dyalisis vascular access
 Case 10238 Endovascular management of non maturing dyalisis vascular access Guedes Pinto 1, Erique; Madeira 2, Célia; Sousa 3, Marta; Penha 1, Diana; Rosa 1, Luís; Germano 1, Ana; Baptista 1, Manuela 1
Case 10238 Endovascular management of non maturing dyalisis vascular access Guedes Pinto 1, Erique; Madeira 2, Célia; Sousa 3, Marta; Penha 1, Diana; Rosa 1, Luís; Germano 1, Ana; Baptista 1, Manuela 1
Arterial Map of the Thorax, Abdomen and Pelvis 2017 Edition
 Arterial Map of the Thorax, Abdomen and Pelvis Angiography 75605 (-26) Aortography, thoracic 75625 (-26) Aortography, abdominal by serialography 75630 (-26) Aortography, abdominal + bilat iliofemoral 75705
Arterial Map of the Thorax, Abdomen and Pelvis Angiography 75605 (-26) Aortography, thoracic 75625 (-26) Aortography, abdominal by serialography 75630 (-26) Aortography, abdominal + bilat iliofemoral 75705
Tracheo-innominate artery fistula (TIF) is an uncommon
 Technique for Managing Tracheo-Innominate Artery Fistula Gorav Ailawadi, MD Tracheo-innominate artery fistula (TIF) is an uncommon complication (0.1-1%) following both open and percutaneous tracheostomy.
Technique for Managing Tracheo-Innominate Artery Fistula Gorav Ailawadi, MD Tracheo-innominate artery fistula (TIF) is an uncommon complication (0.1-1%) following both open and percutaneous tracheostomy.
The SplitWire Percutaneous Transluminal Angioplasty Scoring Device. Instructions for Use
 The SplitWire Percutaneous Transluminal Angioplasty Scoring Device Instructions for Use Contents Contains one (1) SplitWire device. Sterile. Sterilized with ethylene oxide gas. Radiopaque. For single use
The SplitWire Percutaneous Transluminal Angioplasty Scoring Device Instructions for Use Contents Contains one (1) SplitWire device. Sterile. Sterilized with ethylene oxide gas. Radiopaque. For single use
Cook Medical. Zenith Flex AAA Endovascular Graft with Z-Trak Introduction System Physician Training
 Cook Medical Zenith Flex AAA Endovascular Graft with Z-Trak Introduction System Physician Training Bifurcated system Proximal suprarenal stent Modular (aortic main body and two iliac legs) Full-thickness,
Cook Medical Zenith Flex AAA Endovascular Graft with Z-Trak Introduction System Physician Training Bifurcated system Proximal suprarenal stent Modular (aortic main body and two iliac legs) Full-thickness,
PERFORMANCE YOU CAN TRUST. EverFlex Self-expanding Peripheral Stent with Entrust Delivery System
 PERFORMANCE YOU CAN TRUST EverFlex Self-expanding Peripheral Stent with Entrust Delivery System The Entrust Delivery System is designed to provide improved patient outcomes and procedural efficiency. The
PERFORMANCE YOU CAN TRUST EverFlex Self-expanding Peripheral Stent with Entrust Delivery System The Entrust Delivery System is designed to provide improved patient outcomes and procedural efficiency. The
Diagnosis and Management of Femoral Access Site Complications IV: Novel Techniques for Endovascular Rescue
 Diagnosis and Management of Femoral Access Site Complications IV: Novel Techniques for Endovascular Rescue Robert M. Bersin, M.D. Director, Endovascular Services Seattle Cardiology and the Cardiovascular
Diagnosis and Management of Femoral Access Site Complications IV: Novel Techniques for Endovascular Rescue Robert M. Bersin, M.D. Director, Endovascular Services Seattle Cardiology and the Cardiovascular
Aortic arch pathology. Cerebral ischemia following carotid artery stenosis.
 Important: -Subclavian Steal Syndrome -Cerebral ischemia Aortic arch pathology. Cerebral ischemia following carotid artery stenosis. Mina Aubeed & Alba Hernández Pinilla Aortic arch pathology Common arch
Important: -Subclavian Steal Syndrome -Cerebral ischemia Aortic arch pathology. Cerebral ischemia following carotid artery stenosis. Mina Aubeed & Alba Hernández Pinilla Aortic arch pathology Common arch
REBEL. Platinum Chromium Coronary Stent System. Patient Information Guide
 REBEL Patient Information Guide REBEL PATIENT INFORMATION GUIDE You have recently had a REBEL bare metal stent implanted in the coronary arteries of your heart. The following information is important for
REBEL Patient Information Guide REBEL PATIENT INFORMATION GUIDE You have recently had a REBEL bare metal stent implanted in the coronary arteries of your heart. The following information is important for
Abdominal Aortic Aneurysms. A Surgeons Perspective Dr. Derek D. Muehrcke
 Abdominal Aortic Aneurysms A Surgeons Perspective Dr. Derek D. Muehrcke Aneurysm Definition The abnormal enlargement or bulging of an artery caused by an injury or weakness in the blood vessel wall A localized
Abdominal Aortic Aneurysms A Surgeons Perspective Dr. Derek D. Muehrcke Aneurysm Definition The abnormal enlargement or bulging of an artery caused by an injury or weakness in the blood vessel wall A localized
ACD. The Journal of Thoracic and Cardiovascular Surgery c Volume 139, Number 3 655
 A novel approach to prevent spinal cord ischemia: Inoue stent graft with a side branch of small caliber for the reconstruction of the artery of Adamkiewicz Takeshi Shimamoto, MD, a Akira Marui, MD, PhD,
A novel approach to prevent spinal cord ischemia: Inoue stent graft with a side branch of small caliber for the reconstruction of the artery of Adamkiewicz Takeshi Shimamoto, MD, a Akira Marui, MD, PhD,
Case Report Hemostasis of Left Atrial Appendage Bleed With Lariat Device
 273 Case Report Hemostasis of Left Atrial Appendage Bleed With Lariat Device Amena Hussain MD, Muhamed Saric MD, Scott Bernstein MD, Douglas Holmes MD, Larry Chinitz MD NYU Langone Medical Center, United
273 Case Report Hemostasis of Left Atrial Appendage Bleed With Lariat Device Amena Hussain MD, Muhamed Saric MD, Scott Bernstein MD, Douglas Holmes MD, Larry Chinitz MD NYU Langone Medical Center, United
