Risk factors for stent graft thrombosis after transjugular intrahepatic portosystemic shunt creation
|
|
|
- Catherine Floyd
- 5 years ago
- Views:
Transcription
1 Original Article Risk factors for stent graft thrombosis after transjugular intrahepatic portosystemic shunt creation Younes Jahangiri, Timothy Kerrigan, Lei Li, Dominik Prosser, Anantnoor Brar, Johnathan Righetti, Ryan C. Schenning, John A. Kaufman, Khashayar Farsad Charles T. Dotter Department of Interventional Radiology, Oregon Health and Science University, Portland, OR, USA Contributions: (I) Conception and design: Y Jahangiri, K Farsad; (II) Administrative support: K Farsad, JA Kaufman; (III) Provision of study material or patients: K Farsad, RC Schenning; (IV) Collection and assembly of data: T Kerrigan, L Li, A Brar, J Righetti, D Prosser, RC Schenning; (V) Data analysis and interpretation: Y Jahangiri, K Farsad; (VI) Manuscript writing: All authors; (VII) Final approval of manuscript: All authors. Correspondence to: Khashayar Farsad, MD, PhD Sam Jackson Park Road, L-605, Portland, OR 97221, USA. farsad@ohsu.edu. Background: To identify risk factors of stent graft thrombosis after transjugular intrahepatic portosystemic shunt (TIPS) creation. Methods: Patients who underwent TIPS creation between June 2003 and January 2016 and with followup assessing stent graft patency were included (n=174). Baseline comorbidities, liver function, procedural details and follow-up liver function tests were analyzed in association with hazards of thrombosis on followup. Competing risk cox regression models were used considering liver transplant after TIPS creation as the competing risk variable. Results: One-, 2- and 5-year primary patency rates were 94.1%, 91.7% and 78.2%, respectively. Patient age [sub-hazard ratio (shr): 1.13; P=0.001], body mass index (BMI) <30 (shr: 33.08; P=0.008) and a higher post-tips portosystemic pressure gradient (shr: 1.14; P=0.023) were significantly associated with TIPS thrombosis in multivariate analysis. A higher rate of TIPS thrombosis was observed in those for whom the procedure was clinically unsuccessful (P=0.014). A significant increase in incidence of thrombosis was noted with increasing tertiles of post-tips portosystemic gradients (P value for trend=0.017). Conclusions: Older age, lower BMI and higher post-tips portosystemic gradients were associated with higher hazards of shunt thrombosis after TIPS creation using stent grafts. Higher rates of shunt thrombosis were seen in patients for whom TIPS creation was clinically unsuccessful. The association between TIPS thrombosis and higher post-tips portosystemic gradients may indicate impaired flow through the shunt, a finding which may be technical or anatomic in nature and should be assessed before procedure completion. Keywords: Transjugular intrahepatic portosystemic shunt (TIPS); Viatorr; thrombosis; stent graft; portal hypertension Submitted Jul 11, Accepted for publication Sep 26, doi: /cdt View this article at: Introduction Transjugular intrahepatic portosystemic shunt (TIPS) creation is a minimally-invasive procedure developed by Josef Rösch to decompress the hepatic portal system to manage complications of portal hypertension (1,2). Initial shunts were created using bare metal stents with relatively high rates of shunt malfunction (3). The Viatorr stent graft (Gore Medical, Flagstaff, AZ, USA) was specifically designed for TIPS creation and has led to significantly improved shunt patency and function (4,5). Despite advancements made in technique and stent technology, thrombosis causing stenosis or occlusion is still a complication that can lead to TIPS malfunction (6,7).
2 Cardiovascular Diagnosis and Therapy, Vol 7, Suppl 3 December 2017 S151 While improved patency of the Viatorr stent graft has been shown in prior studies, relatively less is known regarding risk factors for stent graft thrombosis after TIPS creation. In this study, we aim to assess factors predictive of TIPS thrombosis based on a large single institution experience using the Viatorr stent graft. Methods Patients The study was approved by our local Institutional Review Board (IRB), and consent waiver was obtained. Subjects who underwent successful primary TIPS creation from June 2003 to January 2016 were considered for the study (n=328). Electronic medical records were retrospectively reviewed for demographics, medical history, pre- and post- TIPS laboratory values and radiologic examinations. Only patients in whom the Viatorr stent graft was used for TIPS creation were included in the analysis (n=249). Patients without follow-up data regarding TIPS patency were excluded (n=75). After applying inclusion and exclusion criteria, 174 subjects were analyzed. Definitions The primary outcome of the study was TIPS thrombosis with shunt occlusion on either angiography, Doppler ultrasound, or contrast-enhanced computed tomography (CT) scan. Primary patency was defined as uninterrupted patency, or censored at the time of the first intervention for thrombosis. Secondary patency included the time from intervention for thrombosis to a subsequent diagnosis of shunt occlusion. The last imaging study documenting a patent shunt was used to define patency intervals. The most recent available laboratory values prior to the TIPS procedure were used to record pre-tips lab data. Post-TIPS lab data represented laboratory values up to 30 days after TIPS creation. The model for end-stage liver disease (MELD) and MELD-Na scores were calculated (8). In addition, the albumin-bilirubin (ALBI) score and grade were also calculated (9). Patients with obesity listed in their problem list or for whom the calculated BMI was 30 were considered obese. For refractory ascites, clinical success was defined as decreased frequency of paracentesis/thoracentesis, decreased dosing of diuretic medications, better control of ascites on current diuretic medications, or subjective improvement per patient on follow-up office visits within 6 months of TIPS creation. For variceal bleeding, clinical success was defined as having no recurrence of gastrointestinal bleeding at any point after TIPS creation. Pre- and post-tips hepatic encephalopathy (HE) were classified as not present (grade 0) if the patient was not on medications to treat HE symptoms (lactulose, rifaximin or neomycin) and there was no record of HE symptoms on file, medically-controlled (grade 1) if the patient was on any of the above medications and no HE symptoms were reported, and uncontrolled (grade 2) if the patient was on any HE medications and there was a record of persistent HE symptoms on file. Any increase in grade of HE on post-tips evaluation relative to the pre-tips evaluation was considered worsened HE. Statistical analysis Numerical measures were reported as mean ± standard deviation (SD), and categorical variables were summarized as frequency (percentage). Comparisons of mean values and frequencies between two categories were done using the independent samples t-test, and the χ 2 test, respectively. To evaluate risk factors for stent graft thrombosis, univariate competing risk Cox proportional hazard models were constructed for each exposure variable. Factors with statistically significant associations were then selected to construct a multivariate model. The univariate models were constructed both with and without considering the exposure variable as a time-varying covariate to assess the proportional hazard assumption. Factors with statistically significant time interactions were considered time-varying variables, and also entered in the multivariate model as a time-varying factor. Liver transplantation after TIPS creation was considered a competing risk factor in all models. No significant interaction between exposure variables was detected. Cochran-Armitage test for trend was used to evaluate trends of categorical measures. All statistical analysis was performed using Stata IC 14.2 for Mac, and P values <0.05 were considered statistically significant. Results Out of the total study cohort (n=328), 23 cases (7.0%) underwent liver transplantation, with a median time to transplant of 11.5 (range, ) months. A total of 167 patients (50.9%) died during the follow-up period. Overall median survival after TIPS creation was 26.9 months
3 S152 Jahangiri et al. Risk factors for TIPS thrombosis with stent grafts [95% confidence interval (CI), ]. Comparing patients included in the analysis (n=174) with those excluded due to lack of follow-up (n=75), those with no follow-up were older (P=0.022), had lower clinical success rates (P<0.001), worse liver function (P=0.006 for MELD- Na) and decreased survival (P<0.001) (Table 1). Mean follow-up time in the study cohort was 24.60±30.20 (range, ) months. Primary TIPS thrombosis occurred in 17 cases (9.8%), with an annual calculated incidence of thrombosis of 38.7 per 1,000 person/year (95% CI, ). After TIPS revision for thrombosis in 12 cases, repeat thrombosis occurred in three cases during a median of 21.2 (range, ) months for a total 5-year secondary patency rate of 95.7%. One-, 2- and 5-year primary patency rates were 94.1%, 91.7%, and 78.2%, respectively (Figure 1). Seventeen cases in the analyzed cohort underwent liver transplantation within a median of 13.4 (range, ) months, in whom no TIPS thrombosis was observed prior to transplantation. Seventy-seven patients (44.3%) in the analyzed cohort died during the follow-up period. Excluding transplanted patients, 1-, 2- and 5-year survival rates in those with TIPS thrombosis compared to those without TIPS thrombosis were 63.6%, 56.9% and 39.4%, and 70.1%, 59.9% and 37.7%, respectively (P=0.675). New or increased HE was observed in 80 patients (50.6%) after TIPS creation, with no significant difference between those with TIPS thrombosis and those without TIPS thrombosis (51.0% vs. 46.7%, respectively; P=0.747). Twenty-seven cases underwent TIPS revision during a median of 7.3 months after initial TIPS creation. Twelve revisions were performed for TIPS thrombosis during a median of 14.6 months after initial TIPS creation. Pre-revision portosystemic pressure gradient (PSG) measurements were available in 20 cases, including in 6 cases with TIPS thrombosis. The median change in PSG value after initial TIPS creation and prior to revision was +3 (range, 5 to +26) mmhg (P=0.115) in all patients, and +6.5 (range, 1 to +26) mmhg (P=0.219) in patients with TIPS thrombosis. In univariate analysis, patient age [sub-hazard ratio (shr): 1.12; P=0.001], BMI <30 (shr: 15.48; P=0.006), portal vein thrombus at the time of TIPS creation (shr: 2.86; P=0.034) and higher post-tips portosystemic Table 1 Characteristics of the study population, and baseline comparison with excluded cases Baseline and follow-up characteristics Included (n=174)* Excluded (n=75)* P value** Age (years) 53.1± ± Sex Female 70 (40.2%) 24 (32.0%) Male 104 (59.8%) 51 (68.0%) Pre-TIPS comorbidities Obesity 36 (20.7%) 9 (12.0%) Hypertension 46 (26.4%) 13 (17.3%) DM 41 (23.6%) 17 (22.7%) Hypothyroidism 9 (5.2%) 5 (6.7%) HCC 17 (9.8%) 5 (6.7%) Liver disease etiologies Alcohol 86 (49.3%) 33 (44.0%) HCV 79 (45.4%) 41 (54.7%) HBV 4 (2.3%) 3 (4.0%) NASH 16 (9.2%) 8 (10.7%) Budd Chiari 8 (4.6%) Table 1 (continued)
4 Cardiovascular Diagnosis and Therapy, Vol 7, Suppl 3 December 2017 S153 Table 1 (continued) Baseline and follow-up characteristics Included (n=174)* Excluded (n=75)* P value** TIPS indications Ascites 60 (34.5%) 23 (30.7%) GI bleeding 120 (69.0%) 55 (73.3%) Clinical success 109 (62.6%) 9 (12.0%) <0.001 Peripheral TIPS 49 (28.2%) 23 (30.7%) DIPS 7 (4.0%) 8 (10.7%) Spontaneous portosystemic shunt at baseline 51 (29.3%) 22 (29.3%) Portal vein thrombosis before TIPS placement 33 (19.0%) 20 (26.7%) Max stent diameter (mm) 9.3± ± Min stent diameter (mm) 9.3± ± Total stent length (cm) 7.9± ± Pre-TIPS PSG (mmhg) 17.5± ± Post-TIPS PSG (mmhg) 6.9± ± Pre-TIPS lab results Sodium (meq/l) 135.9± ± Creatinine (mg/dl) 1.02± ± AST (IU/L) 76.9± ± ALT (IU/L) 48.3± ± Alk. Phos. (IU/L) 104.0± ± Bilirubin (mg/dl) 2.09± ± Albumin (mg/dl) 2.66± ±0.51 <0.001 Total protein (mg/dl) 6.00± ±0.99 <0.001 INR 1.50± ± Platelet ( 10 6 /μl) 118.9± ± Pre-TIPS liver function MELD score 13.8± ± MELD-Na score 15.1± ± ALBI score 1.30± ±0.50 <0.001 Child-Pugh score 8.5± ± Primary TIPS patency rate 157 (90.2%) NA NA Secondary TIPS patency rate 171 (98.3%) NA NA Median survival in months (95% confidence intervals) 33.1 ( ) 3.5 ( ) <0.001*** *, numbers are presented as mean ± SD, and categorical variables are shown as frequency (percentage); **, numbers are compared using independent samples t-test, and frequencies are compared using χ 2 test; ***, survivals are compared using the log-rank test. TIPS, transjugular intrahepatic portosystemic shunt; DIPS, direct intrahepatic portosystemic shunt; PSG, portosystemic gradient; DM, diabetes mellitus; HCC, hepatocellular carcinoma; HCV, hepatitis C virus; HBV, hepatitis B virus; NASH, non-alcoholic steatohepatitis; GI, gastrointestinal; AST, aspartate transaminase; ALT, alanine transaminase; Alk. Phos., alkaline phosphatase; ALBI, albumin-bilirubin; INR, international normalized ratio; MELD, model for end-stage liver disease; NA, not available; SD, standard deviation.
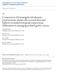
5 S154 Jahangiri et al. Risk factors for TIPS thrombosis with stent grafts Stent patency rate Figure 1 Primary and secondary patency rates of TIPS created using the Viatorr stent-graft. TIPS, transjugular intrahepatic portosystemic shunt. Primary patency Secondary patency Time (months) Number at risk Table 2 Results of univariate competing risk Cox regression analysis for assessment of clinical and technical risk factors for primary TIPS thrombosis. Liver transplantation after TIPS creation is considered as the competing risk factor Predicting factors shr (95% CI) (n=236) P value Demographics Age (years)* 1.12 ( ) Sex 1.26 ( ) Pre-TIPS comorbidities BMI <30* ( ) Hypertension* 0.45 ( ) Diabetes 0.86 ( ) Hypothyroidism 2.73 ( ) HCC 1.82 ( ) Liver disease etiologies Alcohol 0.82 ( ) pressure gradients (shr: 1.14; P=0.003) were significant predictors of TIPS thrombosis (Table 2). TIPS thrombosis was observed more frequently in cases presenting as clinical failure compared to cases where the procedure was clinically successful [11/65 (16.9%) vs. 6/109 (5.5%), P=0.014]. No significant association was found between observed baseline laboratory variables and the risk of TIPS thrombosis (Table 2). In multivariate analysis, advanced age, BMI <30 and increased post-tips portosystemic gradients remained significant independent predictors of TIPS thrombosis (Table 3). There was a significant increase in incidence of TIPS thrombosis at follow-up through increasing tertiles of post-tips portosystemic pressure gradients [4.3%, 6.4% and 17.7% for tertile 1 (<5 mmhg), 2 (5 8 mmhg) and 3 (>8 mmhg), respectively; P value for increasing trend =0.017] (Figure 2). In fact, each 1 mmhg increase in the post-tips portosystemic pressure gradient led to an adjusted 14% higher hazard of primary shunt thrombosis at follow-up. The 17 cases with TIPS thrombosis were individually analyzed for possible predisposing technical or anatomic factors. Factors assessed included lack of shunt extension to the inferior vena cava (IVC), filling defects/residual thrombus on completion angiography, portal vein diameter <10 mm, hypercoagulable states, and need for shunt extension using bare metal stents (Table 4). Discussion The Viatorr stent graft has enabled significantly improved HCV 1.20 ( ) HBV NA NASH 1.44 ( ) TIPS indication Budd Chiari 1.91 ( ) Ascites 0.70 ( ) GI bleeding 0.89 ( ) Peripheral TIPS 0.40 ( ) DIPS 1.29 ( ) Total stent length (cm) 0.94 ( ) Max stent diameter (mm) 0.93 ( ) Min stent diameter (mm) 0.86 ( ) Pre-TIPS PSG (mmhg)* 0.96 ( ) Post-TIPS PSG (mmhg) 1.14 ( ) PSG change (mmhg) 1.00 ( ) Spontaneous portosystemic shunt at baseline Portal vein thrombosis before TIPS creation Pre-TIPS baseline laboratory tests 0.76 ( ) ( ) Sodium (meq/l) 1.00 ( ) Creatinine (mg/dl) 1.00 ( ) Table 2 (continued)
6 Cardiovascular Diagnosis and Therapy, Vol 7, Suppl 3 December 2017 S155 Table 2 (continued) Predicting factors shr (95% CI) (n=236) P value AST (IU/L) 1.00 ( ) ALT (IU/L) 1.00 ( ) Tertile 1 (<5 mmhg) Tertile 2 (5 8 mmhg) Tertile 3 (>8 mmhg) P for trend =0.017 Alk. Phos (IU/L) 1.00 ( ) Total bilirubin (mg/dl) 0.98 ( ) Albumin (gr/dl) 0.97 ( ) Total protein (gr/dl)* 0.74 ( ) INR 0.67 ( ) Percent Platelets ( 10 6 /ml) 1.00 ( ) MELD score 1.00 ( ) Thrombosis Thrombosis + MELD-Na score 1.00 ( ) ALBI score 1.02 ( ) *, time-varying variables. TIPS, transjugular intrahepatic portosystemic shunt; DIPS, direct intrahepatic portosystemic shunt; BMI, body mass index; PSG, portosystemic gradient; DM, diabetes mellitus; HCC, hepatocellular carcinoma; HCV, hepatitis C virus; HBV, hepatitis B virus; NASH, nonalcoholic steatohepatitis; GI, gastrointestinal; AST, aspartate transaminase; ALT, alanine transaminase; Alk. Phos., alkaline phosphatase; INR, international normalized ratio; MELD, model for end-stage liver disease; MELD-Na, MELD-sodium; ALBI, albumin-bilirubin; shr, sub-hazard ratio; CI, confidence interval; NA, not available. Table 3 Multivariate analysis of predictors of primary TIPS thrombosis (n=170) Predicting factors shr (95% CI) P value Age at intervention (years)* 1.13 ( ) BMI <30* ( ) Post-TIPS PSG (mmhg) 1.14 ( ) Portal vein thrombosis before TIPS placement 2.36 ( ) *, time-varying variables. TIPS, transjugular intrahepatic portosystemic shunt; BMI, body mass index; PSG, portosystemic gradien; shr, sub-hazard ratio; CI, confidence interval. long-term TIPS patency compared to bare metal stents. Despite several reports documenting the improved patency of TIPS with stent grafts, few studies have specifically analyzed predictors of TIPS thrombosis with stent grafts. One study on long-term shunt patency published in 2004 found that nonalcoholic liver disease and increasing platelet counts Figure 2 TIPS thrombosis as a function of post-tips portosystemic gradients. Increasing rates of TIPS thrombosis were observed with incremental increases in the post-tips portosystemic gradient. TIPS, transjugular intrahepatic portosystemic shunt. independently predicted development of shunt insufficiency, but this study used bare-metal stents and not the Viatorr stent-graft (10). Many of the more recent studies on TIPS patency and malfunction focus not on predictors of thrombosis or stenosis, but on sensitivity of imaging modalities in detecting shunt stenosis and methods of recanalization once shunt dysfunction is discovered (11,12). The respective 1- and 2-year patency rates of 94.1% and 91.7% shown in our cohort were consistent with other studies on stent-graft patency after TIPS creation (13,14). In this study, we further show that patient age, low BMI, and the post-tips portosystemic gradient were independent predictors of TIPS thrombosis with stent grafts. Older age has been shown to carry a higher risk of venous thrombosis (15). Although the biological mechanisms behind contribution of age to thrombosis is poorly understood, increased coagulability of blood with age is suggested as a possible mechanism (16). A lower risk of stent thrombosis in patients with higher BMI has been observed and is controversial. An obesity paradox has been described after percutaneous coronary interventions, with decreased risk of mortality, major adverse cardiac events and in-stent thrombosis in obese people (17-19), although another study did not confirm such a finding (20). More aggressive screening and therapeutic interventions for cardiovascular and metabolic risk factors in obese
7 S156 Jahangiri et al. Risk factors for TIPS thrombosis with stent grafts Table 4 Characteristics of cases with TIPS thrombosis on follow-up Case No. Age, sex Time to TIPS thrombosis (months) Comorbid/ hypercoagulable state Splenic/portal vein thrombosis PVD <1 cm Splenorenal shunt Hepatofugal flow Possible technical or anatomic factor Cephalad end of shunt short of IVC Pre-TIPS PSG (mmhg) Post-TIPS PSG (mmhg) New/ increased HE Bare metal stent used for shunt extension 1 55, M /partial , F , M 0.2 +/BCS, PNH +/partial + NA , F /BCS , M 0 NA NA NA NA NA , F 0.1 +/ESRD , F /vwd , F , M NA NA 10 55, M , M /partial , M 0.2 +/partial , M 0.3 +/ITP , M /partial , M /factor V Leiden +/total , M 5.7 +/HCC, CAD NA 17 67, F PVD, portal vein diameter; IVC, inferior vena cava; TIPS, transjugular intrahepatic portosystemic shunt; PSG, portosystemic gradient; HE, hepatic encephalopathy; PV, portal vein; MHV, middle hepatic vein; IMV, inferior mesenteric vein; DIPS, direct intrahepatic portosystemic shunt; M, male; F, female; NA, not available; BCS, Budd-Chiari syndrome; PNH, paroxysmal nocturnal hematuria; ESRD, end-stage renal disease; vwd, von Willebrand disease; ITP, idiopathic thrombocytopenic purpura; HCC, hepatocellular carcinoma; CAD, coronary artery disease.
8 Cardiovascular Diagnosis and Therapy, Vol 7, Suppl 3 December 2017 S157 people and higher prevalence of comorbid conditions in studied populations have been suggested as the potential contributors of this observation (19). Perhaps the most significant independent predictor of TIPS thrombosis from our study was the incremental association between increasing portosystemic pressure gradients after TIPS creation and the risk of shunt thrombosis. As stated above, those with a portosystemic gradient <5, 5 8, and >8 mmhg had a risk of thrombosis of 4.3%, 6.4% and 17.7%, respectively. Additionally, according to our multivariate survival model, each 1 mmhg increase in the post-tips portosystemic pressure gradient led to a 14% higher adjusted hazard of shunt thrombosis on followup. Portosystemic pressure gradient reduction after TIPS creation has been well documented to significantly decrease risk of recurrent variceal bleeding (21,22). For patients with refractory ascites, a more aggressive decrease in the portosystemic gradient may increase risk of HE (23). The observation in our study of increased TIPS thrombosis with higher post-tips PSG very well may represent technical or anatomic factors suggesting inefficient shunting, such as residual portal vein thrombus, use of bare metal stents for shunt extension into portal vein, or a small portal vein. Indeed, we noted possible technical or anatomic factors resulting in inefficient shunting in at least 10 of 17 cases reviewed with TIPS thrombosis. Given the incremental association between the post-tips portosystemic gradient and TIPS thrombosis, our data suggest optimization of shunt flow at the time of TIPS creation would be important to help maintain shunt patency. The risk of portal vein thrombosis at the time of TIPS creation for subsequent TIPS thrombosis has been discussed in a recent review (24). Although TIPS creation has been shown to decrease progression of portal vein thrombosis, and also to be superior to endoscopic band ligation and non-selective beta blockers when portal vein thrombosis presents with gastrointestinal (GI) bleeding (24), it is also associated with a higher risk of shunt thrombosis. In our study, pre-tips portal vein thrombosis (PVT) was a predictor of shunt thrombosis on univariate analysis. While PVT lost significance in the multivariate-adjusted model (P=0.076), this may be due to loss of statistical power with multivariate-adjusting (calculated power for pre-tips PVT in multivariate model: 0.25). Alternatively, it is possible that a part of the predictability of pre-tips PVT is explained by other factors. Although we evaluated a relatively large cohort, our study has limitations. The retrospective nature of the study introduces selection biases. Patients included for analysis had better liver function at baseline compared to excluded patients who were lost to follow-up, although baseline liver function was not a predictor of TIPS thrombosis in our study. TIPS thrombosis events and survival of those lost to follow-up were also unknown. Furthermore, a potential lag time between TIPS thrombosis and detection may overestimate thrombosis-free intervals. In addition, post-tips PSG values have been reported to change with time (25). Data regarding time-dependent post-tips PSG measurements were not available for our patients, and risk stratification based on PSG levels was based on measurements immediately after TIPS creation. In conclusion, this study demonstrates that TIPS creation with stent grafts has a relatively low rate of shunt thrombosis. Factors predicting shunt thrombosis include older age, low BMI, and a higher post-tips portosystemic gradient suggesting a higher resistance to flow through the shunt that may be partially technical in nature. Understanding factors leading to TIPS thrombosis may improve procedural metrics and follow-up surveillance strategies. Acknowledgements None. Footnote Conflicts of Interest: K Farsad provides consulting services to Cook Medical. JA Kaufman provides research support and consulting services to Cook Medical. The other authors have no conflicts of interest to declare. Ethical Statement: The study was approved by Oregon Health and Science University Institutional Review Board (No ). References 1. Rosch J, Hanafee WN, Snow H. Transjugular portal venography and radiologic portacaval shunt: an experimental study. Radiology 1969;92: Saad WE. The history and future of transjugular intrahepatic portosystemic shunt: food for thought. Semin Intervent Radiol 2014;31: Cejna M. Should stent-grafts replace bare stents for primary transjugular intrahepatic portosystemic shunts? Semin Intervent Radiol 2005;22:
9 S158 Jahangiri et al. Risk factors for TIPS thrombosis with stent grafts 4. Clark TW. Management of shunt dysfunction in the era of TIPS endografts. Tech Vasc Interv Radiol 2008;11: Qi X, Tian Y, Zhang W, et al. Covered versus bare stents for transjugular intrahepatic portosystemic shunt: an updated meta-analysis of randomized controlled trials. Therap Adv Gastroenterol 2017;10: Cura M, Cura A, Suri R, et al. Causes of TIPS dysfunction. AJR Am J Roentgenol 2008;191: Ripamonti R, Ferral H, Alonzo M, et al. Transjugular intrahepatic portosystemic shunt-related complications and practical solutions. Semin Intervent Radiol 2006;23: Organ Procurement and Transplantation Network. Policies. 2017:106. Available online: transplant.hrsa.gov/media/1200/optn_policies.pdf 9. Johnson PJ, Berhane S, Kagebayashi C, et al. Assessment of liver function in patients with hepatocellular carcinoma: a new evidence-based approach-the ALBI grade. J Clin Oncol 2015;33: ter Borg PC, Hollemans M, Van Buuren HR, et al. Transjugular intrahepatic portosystemic shunts: long-term patency and clinical results in a patient cohort observed for 3-9 years. Radiology 2004;231: Miraglia R, Maruzzelli L, Luca A. Recanalization of occlusive transjugular intrahepatic portosystemic shunts inaccessible to the standard transvenous approach. Diagn Interv Radiol 2013;19: Owen JM, Gaba RC. Transjugular Intrahepatic Portosystemic Shunt Dysfunction: Concordance of Clinical Findings, Doppler Ultrasound Examination, and Shunt Venography. J Clin Imaging Sci 2016;6: Rossle M, Siegerstetter V, Euringer W, et al. The use of a polytetrafluoroethylene-covered stent graft for transjugular intrahepatic portosystemic shunt (TIPS): Long-term follow-up of 100 patients. Acta Radiol 2006;47: Rossi P, Salvatori FM, Fanelli F, et al. Polytetrafluoroethylene-covered nitinol stent-graft for transjugular intrahepatic portosystemic shunt creation: 3-year experience. Radiology 2004;231: Van Gent JM, Calvo RY, Zander AL, et al. Risk factors for deep vein thrombosis and pulmonary embolism after traumatic injury: A competing risks analysis. J Trauma Acute Care Surg 2017;83: Crous-Bou M, Harrington LB, Kabrhel C. Environmental and Genetic Risk Factors Associated with Venous Thromboembolism. Semin Thromb Hemost 2016;42: Lancefield T, Clark DJ, Andrianopoulos N, et al. Is there an obesity paradox after percutaneous coronary intervention in the contemporary era? An analysis from a multicenter Australian registry. JACC Cardiovasc Interv 2010;3: Park DW, Kim YH, Yun SC, et al. Association of body mass index with major cardiovascular events and with mortality after percutaneous coronary intervention. Circ Cardiovasc Interv 2013;6: Schmiegelow M, Torp-Pedersen C, Gislason GH, et al. Relation of body mass index to risk of stent thrombosis after percutaneous coronary intervention. Am J Cardiol 2012;110: Akin I, Tolg R, Hochadel M, et al. No evidence of "obesity paradox" after treatment with drug-eluting stents in a routine clinical practice: results from the prospective multicenter German DES.DE (German Drug-Eluting Stent) Registry. JACC Cardiovasc Interv 2012;5: D'Amico G, Garcia-Pagan JC, Luca A, et al. Hepatic vein pressure gradient reduction and prevention of variceal bleeding in cirrhosis: a systematic review. Gastroenterology 2006;131: Suk KT. Hepatic venous pressure gradient: clinical use in chronic liver disease. Clin Mol Hepatol 2014;20: Madoff DC, Wallace MJ, Ahrar K, et al. TIPS-related hepatic encephalopathy: management options with novel endovascular techniques. Radiographics 2004;24:21-36; discussion Trebicka J. Emergency TIPS in a Child-Pugh B patient: When does the window of opportunity open and close? J Hepatol 2017;66: Silva-Junior G, Turon F, Baiges A, et al. Timing Affects Measurement of Portal Pressure Gradient After Placement of Transjugular Intrahepatic Portosystemic Shunts in Patients With Portal Hypertension. Gastroenterology 2017;152: Cite this article as: Jahangiri Y, Kerrigan T, Li L, Prosser D, Brar A, Righetti J, Schenning RC, Kaufman JA, Farsad K. Risk factors for stent graft thrombosis after transjugular intrahepatic portosystemic shunt creation. Cardiovasc Diagn Ther 2017;7(Suppl 3):S150-S158. doi: /cdt
Transjugular Intrahepatic Portosystemic Shunt Reduction for Management of Recurrent Hepatic Encephalopathy
 CLINICAL IMAGES Ochsner Journal 17:311 316, 2017 Ó Academic Division of Ochsner Clinic Foundation Transjugular Intrahepatic Portosystemic Shunt Reduction for Management of Recurrent Hepatic Encephalopathy
CLINICAL IMAGES Ochsner Journal 17:311 316, 2017 Ó Academic Division of Ochsner Clinic Foundation Transjugular Intrahepatic Portosystemic Shunt Reduction for Management of Recurrent Hepatic Encephalopathy
Contraindications. Indications. Complications. Currently TIPS is considered second or third line therapy for:
 Contraindications Absolute Relative Primary prevention variceal bleeding HCC if centrally located Active congestive heart failure Obstruction all hepatic veins Thomas D. Boyer, M.D. University of Arizona
Contraindications Absolute Relative Primary prevention variceal bleeding HCC if centrally located Active congestive heart failure Obstruction all hepatic veins Thomas D. Boyer, M.D. University of Arizona
Transjugular Intrahepatic
 Transjugular Intrahepatic Portosystemic Shunt (TIPS): A Clinical and Procedural Review Mark R. Werley, M.D. and John Briguglio, M.D. Lancaster Radiology Associates, Ltd. INTRODUCTION This article reviews
Transjugular Intrahepatic Portosystemic Shunt (TIPS): A Clinical and Procedural Review Mark R. Werley, M.D. and John Briguglio, M.D. Lancaster Radiology Associates, Ltd. INTRODUCTION This article reviews
Cirrhosis and Portal Hypertension Gastroenterology Teaching Project American Gastroenterological Association
 CIRRHOSIS AND PORTAL HYPERTENSION Cirrhosis and Portal Hypertension Gastroenterology Teaching Project American Gastroenterological Association WHAT IS CIRRHOSIS? What is Cirrhosis? DEFINITION OF CIRRHOSIS
CIRRHOSIS AND PORTAL HYPERTENSION Cirrhosis and Portal Hypertension Gastroenterology Teaching Project American Gastroenterological Association WHAT IS CIRRHOSIS? What is Cirrhosis? DEFINITION OF CIRRHOSIS
BRTO /PARTO Indications and outcomes
 BRTO /PARTO Indications and outcomes Saher Sabri, MD Associate Professor of Radiology and Surgery Division of Interventional Radiology University of Virginia Health System Saher Sabri, M.D. Speakers Bureau:
BRTO /PARTO Indications and outcomes Saher Sabri, MD Associate Professor of Radiology and Surgery Division of Interventional Radiology University of Virginia Health System Saher Sabri, M.D. Speakers Bureau:
Evidence-Base Management of Esophageal and Gastric Varices
 Evidence-Base Management of Esophageal and Gastric Varices Rino Alvani Gani Hepatobiliary Division Department of Internal Medicine Faculty of Medicine Universitas Indonesia Cipto Mangunkusumo National
Evidence-Base Management of Esophageal and Gastric Varices Rino Alvani Gani Hepatobiliary Division Department of Internal Medicine Faculty of Medicine Universitas Indonesia Cipto Mangunkusumo National
Virtual Mentor American Medical Association Journal of Ethics December 2008, Volume 10, Number 12:
 Virtual Mentor American Medical Association Journal of Ethics December 2008, Volume 10, Number 12: 805-809. CLINICAL PEARL Indications for Use of TIPS in Treating Portal Hypertension Elizabeth C. Verna,
Virtual Mentor American Medical Association Journal of Ethics December 2008, Volume 10, Number 12: 805-809. CLINICAL PEARL Indications for Use of TIPS in Treating Portal Hypertension Elizabeth C. Verna,
Transjugular Intrahepatic Portosystemic Shunt for Acute Variceal Bleeding in Patients with Viral Liver Cirrhosis: Predictors of Early Mortality
 Early Mortality with TIPS for Variceal Bleeding Interventional Radiology Original Research Transjugular Intrahepatic Portosystemic Shunt for Acute Variceal Bleeding in Patients with Viral Liver Cirrhosis:
Early Mortality with TIPS for Variceal Bleeding Interventional Radiology Original Research Transjugular Intrahepatic Portosystemic Shunt for Acute Variceal Bleeding in Patients with Viral Liver Cirrhosis:
Risk factors for 5-day bleeding after endoscopic treatments for gastroesophageal varices in liver cirrhosis
 Original Article Page 1 of 9 Risk factors for 5-day bleeding after endoscopic treatments for gastroesophageal varices in liver cirrhosis Rui Sun*, Xingshun Qi* #, Deli Zou, Xiaodong Shao, Hongyu Li, Xiaozhong
Original Article Page 1 of 9 Risk factors for 5-day bleeding after endoscopic treatments for gastroesophageal varices in liver cirrhosis Rui Sun*, Xingshun Qi* #, Deli Zou, Xiaodong Shao, Hongyu Li, Xiaozhong
AASLD PRACTICE GUIDELINE. The Role of Transjugular Intrahepatic Portosystemic Shunt in the Management of Portal Hypertension. Preamble.
 AASLD PRACTICE GUIDELINE The Role of Transjugular Intrahepatic Portosystemic Shunt in the Management of Portal Hypertension Thomas D. Boyer 1 and Ziv J. Haskal 2 Preamble The recommendations in this article
AASLD PRACTICE GUIDELINE The Role of Transjugular Intrahepatic Portosystemic Shunt in the Management of Portal Hypertension Thomas D. Boyer 1 and Ziv J. Haskal 2 Preamble The recommendations in this article
Factors Predicting Survival after Transjugular Intrahepatic Portosystemic Shunt Creation: 15 Years Experience from a Single Tertiary Medical Center
 Factors Predicting Survival after Transjugular Intrahepatic Portosystemic Shunt Creation: 15 Years Experience from a Single Tertiary Medical Center Jen-Jung Pan, MD, PhD, Chaoru Chen, PhD, James G. Caridi,
Factors Predicting Survival after Transjugular Intrahepatic Portosystemic Shunt Creation: 15 Years Experience from a Single Tertiary Medical Center Jen-Jung Pan, MD, PhD, Chaoru Chen, PhD, James G. Caridi,
Within-patient temporal variance in MELD score and impact on survival prediction after TIPS creation
 Survival prediction after TIPS creation., 2013; 12 (5): 797-802 ORIGINAL ARTICLE September-October, Vol. 12 No.5, 2013: 797-802 797 Within-patient temporal variance in MELD score and impact on survival
Survival prediction after TIPS creation., 2013; 12 (5): 797-802 ORIGINAL ARTICLE September-October, Vol. 12 No.5, 2013: 797-802 797 Within-patient temporal variance in MELD score and impact on survival
DOTTORATO DI RICERCA IN SCIENZE MEDICO-CHIRURGICHE GASTROENTEROLOGICHE E DEI TRAPIANTI TITOLO TESI FACTORS PREDICTING MORTALITY AFTER TIPS FOR
 Alma Mater Studiorum Università di Bologna DOTTORATO DI RICERCA IN SCIENZE MEDICO-CHIRURGICHE GASTROENTEROLOGICHE E DEI TRAPIANTI Ciclo XXII Settore/i scientifico-disciplinare/i di afferenza: MED/12 TITOLO
Alma Mater Studiorum Università di Bologna DOTTORATO DI RICERCA IN SCIENZE MEDICO-CHIRURGICHE GASTROENTEROLOGICHE E DEI TRAPIANTI Ciclo XXII Settore/i scientifico-disciplinare/i di afferenza: MED/12 TITOLO
Obliterative hepatocavopathy ultrasound and cavography findings
 doi:10.2478/v10019-008-0020-6 case report Obliterative hepatocavopathy ultrasound and cavography findings Ramazan Kutlu Department of Radiology, Inonu University School of Medicine, Malatya, Turkey ackgound.
doi:10.2478/v10019-008-0020-6 case report Obliterative hepatocavopathy ultrasound and cavography findings Ramazan Kutlu Department of Radiology, Inonu University School of Medicine, Malatya, Turkey ackgound.
Tranjugular Intrahepatic Portosystemic Shunt
 Tranjugular Intrahepatic Portosystemic Shunt Christopher Selhorst July 25, 2005 BIDMC Radiology Overview Portal Hypertension Indications, Contraindications The Procedure Case Review Complications Outcomes
Tranjugular Intrahepatic Portosystemic Shunt Christopher Selhorst July 25, 2005 BIDMC Radiology Overview Portal Hypertension Indications, Contraindications The Procedure Case Review Complications Outcomes
Steps in Assessing Fibrosis 4/30/2015. Overview of Liver Disease Associated With HCV
 Overview of Liver Disease Associated With HCV Marion G. Peters, MD John V. Carbone, Endowed Chair Professor of Medicine Chief of Hepatology Research University of California San Francisco San Francisco,
Overview of Liver Disease Associated With HCV Marion G. Peters, MD John V. Carbone, Endowed Chair Professor of Medicine Chief of Hepatology Research University of California San Francisco San Francisco,
SERUM CYSTATIN C CONCENTRATION IS A POWERFUL PROGNOSTIC INDICATOR IN PATIENTS WITH CIRRHOTIC ASCITES
 SERUM CYSTATIN C CONCENTRATION IS A POWERFUL PROGNOSTIC INDICATOR IN PATIENTS WITH CIRRHOTIC ASCITES YEON SEOK SEO, 1 SOO YOUNG PARK, 2 MOON YOUNG KIM, 3 SANG GYUNE KIM, 4 JUN YONG PARK, 5 HYUNG JOON YIM,
SERUM CYSTATIN C CONCENTRATION IS A POWERFUL PROGNOSTIC INDICATOR IN PATIENTS WITH CIRRHOTIC ASCITES YEON SEOK SEO, 1 SOO YOUNG PARK, 2 MOON YOUNG KIM, 3 SANG GYUNE KIM, 4 JUN YONG PARK, 5 HYUNG JOON YIM,
Management of Cirrhotic Complications Uncontrolled Ascites. Siwaporn Chainuvati, MD Siriraj Hospital Mahidol University
 Management of Cirrhotic Complications Uncontrolled Ascites Siwaporn Chainuvati, MD Siriraj Hospital Mahidol University Topic Definition, pathogenesis Current therapeutic options Experimental treatments
Management of Cirrhotic Complications Uncontrolled Ascites Siwaporn Chainuvati, MD Siriraj Hospital Mahidol University Topic Definition, pathogenesis Current therapeutic options Experimental treatments
CIRROSI E IPERTENSIONE PORTALE NELLA DONNA
 Cagliari, 16 settembre 2017 CIRROSI E IPERTENSIONE PORTALE NELLA DONNA Vincenza Calvaruso, MD, PhD Ricercatore di Gastroenterologia Gastroenterologia & Epatologia, Di.Bi.M.I.S. Università degli Studi di
Cagliari, 16 settembre 2017 CIRROSI E IPERTENSIONE PORTALE NELLA DONNA Vincenza Calvaruso, MD, PhD Ricercatore di Gastroenterologia Gastroenterologia & Epatologia, Di.Bi.M.I.S. Università degli Studi di
King Abdul-Aziz University Hospital (KAUH) is a tertiary
 Modelling Factors Causing Mortality in Oesophageal Varices Patients in King Abdul Aziz University Hospital Sami Bahlas Abstract Objectives: The objective of this study is to reach a model defining factors
Modelling Factors Causing Mortality in Oesophageal Varices Patients in King Abdul Aziz University Hospital Sami Bahlas Abstract Objectives: The objective of this study is to reach a model defining factors
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A ACLF. See Acute-on-chronic liver failure (ACLF) Acute kidney injury (AKI) in ACLF patients, 967 Acute liver failure (ALF), 957 964 causes
Index Note: Page numbers of article titles are in boldface type. A ACLF. See Acute-on-chronic liver failure (ACLF) Acute kidney injury (AKI) in ACLF patients, 967 Acute liver failure (ALF), 957 964 causes
Thrombocytopenia and Chronic Liver Disease
 Thrombocytopenia and Chronic Liver Disease Severe thrombocytopenia (platelet count
Thrombocytopenia and Chronic Liver Disease Severe thrombocytopenia (platelet count
Direct Intrahepatic Porta-Caval Shunt Technique & Tips-Tricks. Pierre GOFFETTE, MD, St-Luc University Hospital University of Leuven Brussels
 Direct Intrahepatic Porta-Caval Shunt Technique & Tips-Tricks Pierre GOFFETTE, MD, St-Luc University Hospital University of Leuven Brussels Pierre Goffette, M.D. Consultant/Advisory Board: Covidien (Neuro)
Direct Intrahepatic Porta-Caval Shunt Technique & Tips-Tricks Pierre GOFFETTE, MD, St-Luc University Hospital University of Leuven Brussels Pierre Goffette, M.D. Consultant/Advisory Board: Covidien (Neuro)
Vascular Technology Examination Content Outline
 Vascular Technology Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Normal Anatomy, Perfusion, and Function Evaluate normal anatomy, perfusion, function 2 Pathology, Perfusion,
Vascular Technology Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Normal Anatomy, Perfusion, and Function Evaluate normal anatomy, perfusion, function 2 Pathology, Perfusion,
Diagnostic Procedures. Measurement of Hepatic venous pressure in management of cirrhosis. Clinician s opinion
 5 th AISF Post-Meeting Course Diagnostic and Therapeutic Invasive Procedures in Hepatology Rome, February 25 th Diagnostic Procedures Measurement of Hepatic venous pressure in management of cirrhosis Clinician
5 th AISF Post-Meeting Course Diagnostic and Therapeutic Invasive Procedures in Hepatology Rome, February 25 th Diagnostic Procedures Measurement of Hepatic venous pressure in management of cirrhosis Clinician
Management of Cirrhosis Related Complications
 Management of Cirrhosis Related Complications Ke-Qin Hu, MD, FAASLD Professor of Clinical Medicine Director of Hepatology University of California, Irvine Disclosure I have no disclosure related to this
Management of Cirrhosis Related Complications Ke-Qin Hu, MD, FAASLD Professor of Clinical Medicine Director of Hepatology University of California, Irvine Disclosure I have no disclosure related to this
Long-term Clinical Outcomes and Risk of Hepatocellular Carcinoma in Chronic Hepatitis B Patients with HBsAg Seroclearance
 Long-term Clinical Outcomes and Risk of Hepatocellular Carcinoma in Chronic Hepatitis B Patients with HBsAg Seroclearance Gi-Ae Kim, Han Chu Lee *, Danbi Lee, Ju Hyun Shim, Kang Mo Kim, Young-Suk Lim,
Long-term Clinical Outcomes and Risk of Hepatocellular Carcinoma in Chronic Hepatitis B Patients with HBsAg Seroclearance Gi-Ae Kim, Han Chu Lee *, Danbi Lee, Ju Hyun Shim, Kang Mo Kim, Young-Suk Lim,
Denver Shunts vs TIPS for Ascites
 Denver Shunts vs TIPS for Ascites Hooman Yarmohammadi MD Assistant Professor of Radiology Interventional Radiology & Image Guided Therapies Memorial Sloan-Kettering Cancer Center, New York, USA Hooman
Denver Shunts vs TIPS for Ascites Hooman Yarmohammadi MD Assistant Professor of Radiology Interventional Radiology & Image Guided Therapies Memorial Sloan-Kettering Cancer Center, New York, USA Hooman
Controversies in Management of Portal Hypertension and Cirrhosis Complications in the Transplant Candidate
 Controversies in Management of Portal Hypertension and Cirrhosis Complications in the Transplant Candidate Patrick Northup, MD, FAASLD, FACG Medical Director, Liver Transplantation University of Virginia
Controversies in Management of Portal Hypertension and Cirrhosis Complications in the Transplant Candidate Patrick Northup, MD, FAASLD, FACG Medical Director, Liver Transplantation University of Virginia
Michele Bettinelli RN CCRN Lahey Health and Medical Center
 Michele Bettinelli RN CCRN Lahey Health and Medical Center Differentiate the types of varices Identify glue preparations utilized when treating gastric varices Review the process of glue administration
Michele Bettinelli RN CCRN Lahey Health and Medical Center Differentiate the types of varices Identify glue preparations utilized when treating gastric varices Review the process of glue administration
EDUCATION PRACTICE. Management of Refractory Ascites. Clinical Scenario. The Problem
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:1187 1191 EDUCATION PRACTICE Management of Refractory Ascites ANDRÉS CÁRDENAS and PERE GINÈS Liver Unit, Institute of Digestive Diseases, Hospital Clínic,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:1187 1191 EDUCATION PRACTICE Management of Refractory Ascites ANDRÉS CÁRDENAS and PERE GINÈS Liver Unit, Institute of Digestive Diseases, Hospital Clínic,
Editorial Process: Submission:07/25/2018 Acceptance:10/19/2018
 RESEARCH ARTICLE Editorial Process: Submission:07/25/2018 Acceptance:10/19/2018 Clinical Outcome and Predictive Factors of Variceal Bleeding in Patients with Hepatocellular Carcinoma in Thailand Jitrapa
RESEARCH ARTICLE Editorial Process: Submission:07/25/2018 Acceptance:10/19/2018 Clinical Outcome and Predictive Factors of Variceal Bleeding in Patients with Hepatocellular Carcinoma in Thailand Jitrapa
Barbara Rus Gadžijev Peter Popovič Klinični inštitut za radiologijo UKC Ljubljana
 STROKOVNI SESTANEK ZDRUŽENJA HEMATOLOGOV SLOVENIJE IN ZDRUŽENJA ZA TRANSFUZIJSKO MEDICINO, Terme Zreče, 17.-18.4.2015 Barbara Rus Gadžijev Peter Popovič Klinični inštitut za radiologijo UKC Ljubljana goals,
STROKOVNI SESTANEK ZDRUŽENJA HEMATOLOGOV SLOVENIJE IN ZDRUŽENJA ZA TRANSFUZIJSKO MEDICINO, Terme Zreče, 17.-18.4.2015 Barbara Rus Gadžijev Peter Popovič Klinični inštitut za radiologijo UKC Ljubljana goals,
Ascites Management. Atif Zaman, MD MPH Oregon Health & Science University Professor of Medicine Division of Gastroenterology and Hepatology
 Ascites Management Atif Zaman, MD MPH Oregon Health & Science University Professor of Medicine Division of Gastroenterology and Hepatology Disclosure 1. The speaker Atif Zaman, MD MPH have no relevant
Ascites Management Atif Zaman, MD MPH Oregon Health & Science University Professor of Medicine Division of Gastroenterology and Hepatology Disclosure 1. The speaker Atif Zaman, MD MPH have no relevant
MANAGEMENT OF LIVER CIRRHOSIS: PRACTICE ESSENTIALS AND PATIENT SELF-MANAGEMENT
 MANAGEMENT OF LIVER CIRRHOSIS: PRACTICE ESSENTIALS AND PATIENT SELF-MANAGEMENT Sherona Bau, ACNP The Pfleger Liver Institute 200 UCLA Medical Plaza, Suite 214 Los Angeles, CA 90095 September 30, 2017 I
MANAGEMENT OF LIVER CIRRHOSIS: PRACTICE ESSENTIALS AND PATIENT SELF-MANAGEMENT Sherona Bau, ACNP The Pfleger Liver Institute 200 UCLA Medical Plaza, Suite 214 Los Angeles, CA 90095 September 30, 2017 I
Life After SVR for Cirrhotic HCV
 Life After SVR for Cirrhotic HCV KIM NEWNHAM MN, NP CIRRHOSIS CARE CLINIC UNIVERSITY OF ALBERTA Objectives To review the benefits of HCV clearance in cirrhotic patients To review some of the emerging data
Life After SVR for Cirrhotic HCV KIM NEWNHAM MN, NP CIRRHOSIS CARE CLINIC UNIVERSITY OF ALBERTA Objectives To review the benefits of HCV clearance in cirrhotic patients To review some of the emerging data
Hepatocellular Carcinoma: Diagnosis and Management
 Hepatocellular Carcinoma: Diagnosis and Management Nizar A. Mukhtar, MD Co-director, SMC Liver Tumor Board April 30, 2016 1 Objectives Review screening/surveillance guidelines Discuss diagnostic algorithm
Hepatocellular Carcinoma: Diagnosis and Management Nizar A. Mukhtar, MD Co-director, SMC Liver Tumor Board April 30, 2016 1 Objectives Review screening/surveillance guidelines Discuss diagnostic algorithm
Title: Cholestasis after TIPS placement in a patient with primary sclerosing cholangitis: an uncommon complication
 Title: Cholestasis after TIPS placement in a patient with primary sclerosing cholangitis: an uncommon complication Authors: Alejandro Salagre García, Carolina Muñoz Codoceo, Elena Gómez Domínguez, Inmaculada
Title: Cholestasis after TIPS placement in a patient with primary sclerosing cholangitis: an uncommon complication Authors: Alejandro Salagre García, Carolina Muñoz Codoceo, Elena Gómez Domínguez, Inmaculada
Learning Objectives. After attending this presentation, participants will be able to:
 Learning Objectives After attending this presentation, participants will be able to: Describe HCV in 2015 Describe how to diagnose advanced liver disease and cirrhosis Identify the clinical presentation
Learning Objectives After attending this presentation, participants will be able to: Describe HCV in 2015 Describe how to diagnose advanced liver disease and cirrhosis Identify the clinical presentation
What constitutes liver failure after transjugular intrahepatic portosystemic shunt creation? A proposed definition and grading system
 230 Gaba RC, et al., 2016; 15 (2): 230-235 ORIGINAL ARTICLE March-April, Vol. 15 No. 2, 2016: 230-235 The Official Journal of the Mexican Association of Hepatology, the Latin-American Association for Study
230 Gaba RC, et al., 2016; 15 (2): 230-235 ORIGINAL ARTICLE March-April, Vol. 15 No. 2, 2016: 230-235 The Official Journal of the Mexican Association of Hepatology, the Latin-American Association for Study
Preliminary study of the permeability and safety of covered stents-grafts in pediatric TIPS
 Preliminary study of the permeability and safety of covered stents-grafts in pediatric TIPS Poster No.: C-0354 Congress: ECR 2013 Type: Scientific Exhibit Authors: A. Bueno Palomino, L. Zurera Tendero,
Preliminary study of the permeability and safety of covered stents-grafts in pediatric TIPS Poster No.: C-0354 Congress: ECR 2013 Type: Scientific Exhibit Authors: A. Bueno Palomino, L. Zurera Tendero,
Use of transjugular intrahepatic portosystemic shunt in liver disease
 Vol. XVIII No. 3 JOURNAL OF VASCULAR NURSING PAGE 83 Use of transjugular intrahepatic portosystemic shunt in liver disease Patricia Ann Radovich, RN, MSN, CCRN, FCCM Persons with cirrhosis have many complications.
Vol. XVIII No. 3 JOURNAL OF VASCULAR NURSING PAGE 83 Use of transjugular intrahepatic portosystemic shunt in liver disease Patricia Ann Radovich, RN, MSN, CCRN, FCCM Persons with cirrhosis have many complications.
TIPS. D Patch Royal Free Hospital London UK
 TIPS D Patch Royal Free Hospital London UK TIPS Technique Ascites Budd Chiari Variceal Bleeding Historical Experimental Development 1967 Piccone Shunt between recanalized umbilical vein and saphenous
TIPS D Patch Royal Free Hospital London UK TIPS Technique Ascites Budd Chiari Variceal Bleeding Historical Experimental Development 1967 Piccone Shunt between recanalized umbilical vein and saphenous
PORTAL HYPERTENSION. Tianjin Medical University LIU JIAN
 PORTAL HYPERTENSION Tianjin Medical University LIU JIAN DEFINITION Portal hypertension is present if portal venous pressure exceeds 10mmHg (1.3kPa). Normal portal venous pressure is 5 10mmHg (0.7 1.3kPa),
PORTAL HYPERTENSION Tianjin Medical University LIU JIAN DEFINITION Portal hypertension is present if portal venous pressure exceeds 10mmHg (1.3kPa). Normal portal venous pressure is 5 10mmHg (0.7 1.3kPa),
Update in abdominal Surgery in cirrhotic patients
 Update in abdominal Surgery in cirrhotic patients Safi Dokmak HBP department and liver transplantation Beaujon Hospital, Clichy, France Cairo, 5 April 2016 Cirrhosis Prevalence in France (1%)* Patients
Update in abdominal Surgery in cirrhotic patients Safi Dokmak HBP department and liver transplantation Beaujon Hospital, Clichy, France Cairo, 5 April 2016 Cirrhosis Prevalence in France (1%)* Patients
A A U
 PVD Venous AUC Rating Sheet 2nd Round 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 Median I NI MADM Rating Agree Disagree Upper Extremity Venous Evaluation Table 1. Venous Duplex of the Upper Extremities for Patency
PVD Venous AUC Rating Sheet 2nd Round 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 Median I NI MADM Rating Agree Disagree Upper Extremity Venous Evaluation Table 1. Venous Duplex of the Upper Extremities for Patency
VARICEAL BLEEDING. Ram Subramanian MD Hepatology & Critical Care Medical Director of Liver Transplant Emory University, Atlanta.
 VARICEAL BLEEDING Ram Subramanian MD Hepatology & Critical Care Medical Director of Liver Transplant Emory University, Atlanta Disclosures: None OUTLINE Pathophysiology of portal hypertension Splanchnic
VARICEAL BLEEDING Ram Subramanian MD Hepatology & Critical Care Medical Director of Liver Transplant Emory University, Atlanta Disclosures: None OUTLINE Pathophysiology of portal hypertension Splanchnic
Chronic Hepatic Disease
 Chronic Hepatic Disease 10 th Leading Cause of Death Liver Functions Energy Metabolism Protein Synthesis Solubilization, Transport, and Storage Protects and Clears drugs, damaged cells Causes of Liver
Chronic Hepatic Disease 10 th Leading Cause of Death Liver Functions Energy Metabolism Protein Synthesis Solubilization, Transport, and Storage Protects and Clears drugs, damaged cells Causes of Liver
Primary Budd-Chiari Syndrome (Hepatic Venous Outflow Tract Obstruction)
 Primary Budd-Chiari Syndrome (Hepatic Venous Outflow Tract Obstruction) Dominique-Charles Valla DHU UNITY Service d Hépatologie, Hôpital Beaujon (AP-HP), Clichy; CRI-UMR1149, Université Paris-Diderot and
Primary Budd-Chiari Syndrome (Hepatic Venous Outflow Tract Obstruction) Dominique-Charles Valla DHU UNITY Service d Hépatologie, Hôpital Beaujon (AP-HP), Clichy; CRI-UMR1149, Université Paris-Diderot and
Leigh C. Casadaban 1 Ahmad Parvinian 1 Patrick M. Couture 1 Jeet Minocha 2 M. Grace Knuttinen 2 James T. Bui 2 Ron C. Gaba 2
 Vascular and Interventional Radiology Original Research Casadaban et al. Hepatobiliary Laboratory Alterations After TIPS Vascular and Interventional Radiology Original Research Leigh C. Casadaban 1 Ahmad
Vascular and Interventional Radiology Original Research Casadaban et al. Hepatobiliary Laboratory Alterations After TIPS Vascular and Interventional Radiology Original Research Leigh C. Casadaban 1 Ahmad
Management of Portal Vein Thrombosis With and Without Cirrhosis
 Management of Portal Vein Thrombosis With and Without Cirrhosis Dominique-Charles Valla Service d Hépatologie,Hôpital Beaujon, APHP, Université Paris-Diderot, Inserm CRB3 Extrahepatic Portal Vein Obstruction
Management of Portal Vein Thrombosis With and Without Cirrhosis Dominique-Charles Valla Service d Hépatologie,Hôpital Beaujon, APHP, Université Paris-Diderot, Inserm CRB3 Extrahepatic Portal Vein Obstruction
Management of Ascites and Hepatorenal Syndrome. Florence Wong University of Toronto. June 4, /16/ Gore & Associates: Consultancy
 Management of Ascites and Hepatorenal Syndrome Florence Wong University of Toronto June 4, 2016 6/16/2016 1 Disclosures Gore & Associates: Consultancy Sequana Medical: Research Funding Mallinckrodt Pharmaceutical:
Management of Ascites and Hepatorenal Syndrome Florence Wong University of Toronto June 4, 2016 6/16/2016 1 Disclosures Gore & Associates: Consultancy Sequana Medical: Research Funding Mallinckrodt Pharmaceutical:
TIPS for Refractory Ascites: A 6-Year Single-Center Experience With Expanded Polytetrafluoroethylene Covered Stent-Grafts
 Vascular and Interventional Radiology Original Research Bercu et al. TIPS for Refractory Ascites Vascular and Interventional Radiology Original Research Zachary L. Bercu 1 Aaron M. Fischman 1 Edward Kim
Vascular and Interventional Radiology Original Research Bercu et al. TIPS for Refractory Ascites Vascular and Interventional Radiology Original Research Zachary L. Bercu 1 Aaron M. Fischman 1 Edward Kim
BRTO: Updates to Techniques
 Session XIV: BRTO, PARTO and Portal Hypertension GEST2016 BRTO: Updates to Techniques Hiro Kiyosue Oita University Hospital, Japan Hiro Kiyosue, MD Royalty: Cook, Medkit Consulting Fee: Stryker Japan,
Session XIV: BRTO, PARTO and Portal Hypertension GEST2016 BRTO: Updates to Techniques Hiro Kiyosue Oita University Hospital, Japan Hiro Kiyosue, MD Royalty: Cook, Medkit Consulting Fee: Stryker Japan,
PORTAL HYPERTENSION An Introduction to the Culprit of Many Liver Failure Complications
 PORTAL HYPERTENSION An Introduction to the Culprit of Many Liver Failure Complications Edy G. Trujillo, RN, MSN, ACNP-BC Liver Transplant RRUCLA Medical Center July 31, 2018 What Do We All Look Forward
PORTAL HYPERTENSION An Introduction to the Culprit of Many Liver Failure Complications Edy G. Trujillo, RN, MSN, ACNP-BC Liver Transplant RRUCLA Medical Center July 31, 2018 What Do We All Look Forward
Hepatology for the Nonhepatologist
 Hepatology for the Nonhepatologist Kenneth E. Sherman, MD, PhD Gould Professor of Medicine Director, Division of Digestive Diseases University of Cincinnati College of Medicine Cincinnati, Ohio Learning
Hepatology for the Nonhepatologist Kenneth E. Sherman, MD, PhD Gould Professor of Medicine Director, Division of Digestive Diseases University of Cincinnati College of Medicine Cincinnati, Ohio Learning
Portogram shows opacification of gastroesophageal varices.
 Portogram shows opacification of gastroesophageal varices. http://clinicalgate.com/radiologic-hepatobiliary-interventions/ courtesyhttp://emedicine.medscape.com/article/372708-overview DR.Thulfiqar Baiae
Portogram shows opacification of gastroesophageal varices. http://clinicalgate.com/radiologic-hepatobiliary-interventions/ courtesyhttp://emedicine.medscape.com/article/372708-overview DR.Thulfiqar Baiae
The Continuum of Care for Advanced Liver Disease: Partnering with the Liver Specialist. K V Speeg, MD, PhD UT Health San Antonio
 The Continuum of Care for Advanced Liver Disease: Partnering with the Liver Specialist K V Speeg, MD, PhD UT Health San Antonio Objectives Review staging of liver disease Review consequences of end-stage
The Continuum of Care for Advanced Liver Disease: Partnering with the Liver Specialist K V Speeg, MD, PhD UT Health San Antonio Objectives Review staging of liver disease Review consequences of end-stage
Portal vein stent placement for the treatment of postoperative portal vein stenosis: long-term success and factor associated with stent failure
 Kato et al. BMC Surgery (2017) 17:11 DOI 10.1186/s12893-017-0209-y RESEARCH ARTICLE Portal vein stent placement for the treatment of postoperative portal vein stenosis: long-term success and factor associated
Kato et al. BMC Surgery (2017) 17:11 DOI 10.1186/s12893-017-0209-y RESEARCH ARTICLE Portal vein stent placement for the treatment of postoperative portal vein stenosis: long-term success and factor associated
Acute TIPS occlusion due to iatrogenic arteriovenous shunt in a cirrhotic patient with total portal vein thrombosis
 Interventional Medicine & Applied Science, Vol. 7 (4), pp. 166 170 (2015) CASE REPORT Acute TIPS occlusion due to iatrogenic arteriovenous shunt in a cirrhotic patient with total portal vein thrombosis
Interventional Medicine & Applied Science, Vol. 7 (4), pp. 166 170 (2015) CASE REPORT Acute TIPS occlusion due to iatrogenic arteriovenous shunt in a cirrhotic patient with total portal vein thrombosis
Endovascular Techniques for Symptomatic Portal Hypertension. Michael Meuse, M.D. Vascular and Interventional Radiology
 Endovascular Techniques for Symptomatic Portal Hypertension Michael Meuse, M.D. Vascular and Interventional Radiology Objectives Review indications and contraindications for TIPS Define a treatment algorithm
Endovascular Techniques for Symptomatic Portal Hypertension Michael Meuse, M.D. Vascular and Interventional Radiology Objectives Review indications and contraindications for TIPS Define a treatment algorithm
GI bleeding in chronic liver disease
 GI bleeding in chronic liver disease Stuart McPherson Consultant Hepatologist Liver Unit, Freeman Hospital, Newcastle upon Tyne and Institute of Cellular Medicine, Newcastle University. Case 54 year old
GI bleeding in chronic liver disease Stuart McPherson Consultant Hepatologist Liver Unit, Freeman Hospital, Newcastle upon Tyne and Institute of Cellular Medicine, Newcastle University. Case 54 year old
Quality Improvement Guidelines for Transjugular Intrahepatic Portosystemic Shunt (TIPS)
 Cardiovasc Intervent Radiol (2012) 35:1295 1300 DOI 10.1007/s00270-012-0493-y CIRSE STANDARDS OF PRACTICE GUIDELINES Quality Improvement Guidelines for Transjugular Intrahepatic Portosystemic Shunt (TIPS)
Cardiovasc Intervent Radiol (2012) 35:1295 1300 DOI 10.1007/s00270-012-0493-y CIRSE STANDARDS OF PRACTICE GUIDELINES Quality Improvement Guidelines for Transjugular Intrahepatic Portosystemic Shunt (TIPS)
Organ allocation for liver transplantation: Is MELD the answer? North American experience
 Organ allocation for liver transplantation: Is MELD the answer? North American experience Douglas M. Heuman, MD Virginia Commonwealth University Richmond, VA, USA March 1998: US Department of Health and
Organ allocation for liver transplantation: Is MELD the answer? North American experience Douglas M. Heuman, MD Virginia Commonwealth University Richmond, VA, USA March 1998: US Department of Health and
Transjugular intrahepatic portosystemic shunt in the treatment of symptomatic portal hypertension
 Digital Comprehensive Summaries of Uppsala Dissertations from the Faculty of Medicine 1338 Transjugular intrahepatic portosystemic shunt in the treatment of symptomatic portal hypertension KERSTIN ROSENQVIST
Digital Comprehensive Summaries of Uppsala Dissertations from the Faculty of Medicine 1338 Transjugular intrahepatic portosystemic shunt in the treatment of symptomatic portal hypertension KERSTIN ROSENQVIST
Hepatocellular Carcinoma: A major global health problem. David L. Wood, MD Interventional Radiology Banner Good Samaritan Medical Center
 Hepatocellular Carcinoma: A major global health problem David L. Wood, MD Interventional Radiology Banner Good Samaritan Medical Center Hepatocellular Carcinoma WORLDWIDE The #2 Cancer Killer Overall cancer
Hepatocellular Carcinoma: A major global health problem David L. Wood, MD Interventional Radiology Banner Good Samaritan Medical Center Hepatocellular Carcinoma WORLDWIDE The #2 Cancer Killer Overall cancer
Supplemental Appendix. 1. Protocol Definition of Sustained Virologic Response. A patient has a sustained virologic response if:
 Supplemental Appendix 1. Protocol Definition of Sustained Virologic Response A patient has a sustained virologic response if: 1. The patient is a responder at the end of treatment and all subsequent planned
Supplemental Appendix 1. Protocol Definition of Sustained Virologic Response A patient has a sustained virologic response if: 1. The patient is a responder at the end of treatment and all subsequent planned
DISCLOSURES. This activity is jointly provided by Northwest Portland Area Indian Health Board and Cardea
 DISCLOSURES This activity is jointly provided by Northwest Portland Area Indian Health Board and Cardea Cardea Services is approved as a provider of continuing nursing education by Montana Nurses Association,
DISCLOSURES This activity is jointly provided by Northwest Portland Area Indian Health Board and Cardea Cardea Services is approved as a provider of continuing nursing education by Montana Nurses Association,
Assessment of Liver Function: Implications for HCC Treatment
 Assessment of Liver Function: Implications for HCC Treatment A/P Dan Yock Young MBBS, PhD, MRCP, MMed. FAMS Chair, University Medicine Cluster. NUHS Head, Department of Medicine, National University of
Assessment of Liver Function: Implications for HCC Treatment A/P Dan Yock Young MBBS, PhD, MRCP, MMed. FAMS Chair, University Medicine Cluster. NUHS Head, Department of Medicine, National University of
Med Sci Monit, 2016; 22: Grade D. Quality Outstanding
 Ain and Jaff. Treatment of Submassive Pulmonary Embolism: Knowing When to be Aggressive and When to be Conservative. Curr Treat Options Cardio Med (2015) 17:25. Review Article Akin et al. Catheter-Directed
Ain and Jaff. Treatment of Submassive Pulmonary Embolism: Knowing When to be Aggressive and When to be Conservative. Curr Treat Options Cardio Med (2015) 17:25. Review Article Akin et al. Catheter-Directed
ACCF/ACR/AIUM/ASE/ASN/ICAVL/SCAI/SCCT/SIR/SVM/SVS 2012 Appropriate Use Criteria. Indications A _ appropriate; I _ inappropriate; U _ uncertain
 National Imaging Associates, Inc. Clinical guidelines ABDOMINAL, PELVIS, SCROTAL, RETROPERITONEAL ORGANS DUPLEX SCAN (US) CPT Codes: 93975 Bilateral or Complete 93976 - Unilateral or Limited Guideline
National Imaging Associates, Inc. Clinical guidelines ABDOMINAL, PELVIS, SCROTAL, RETROPERITONEAL ORGANS DUPLEX SCAN (US) CPT Codes: 93975 Bilateral or Complete 93976 - Unilateral or Limited Guideline
VENOUS THROMBOEMBOLISM AND CORONARY ARTERY DISEASE: IS THERE A LINK?
 VENOUS THROMBOEMBOLISM AND CORONARY ARTERY DISEASE: IS THERE A LINK? Ayman El-Menyar (1), MD, Hassan Al-Thani (2),MD (1)Clinical Research Consultant, (2) Head of Vascular Surgery, Hamad General Hospital
VENOUS THROMBOEMBOLISM AND CORONARY ARTERY DISEASE: IS THERE A LINK? Ayman El-Menyar (1), MD, Hassan Al-Thani (2),MD (1)Clinical Research Consultant, (2) Head of Vascular Surgery, Hamad General Hospital
Clinical presentation and predictors of survival in patients with Budd Chiari Syndrome: Experience from a tertiary care hospital in Pakistan
 120 ORIGINAL ARTICLE Clinical presentation and predictors of survival in patients with Budd Chiari Syndrome: Experience from a tertiary care hospital in Pakistan Abbas Ali Tasneem, Ghous Bux Soomro, Zaigham
120 ORIGINAL ARTICLE Clinical presentation and predictors of survival in patients with Budd Chiari Syndrome: Experience from a tertiary care hospital in Pakistan Abbas Ali Tasneem, Ghous Bux Soomro, Zaigham
Liver Transplantation Evaluation: Objectives
 Liver Transplantation Evaluation: Essential Work-Up Curtis K. Argo, MD, MS VGS/ACG Regional Postgraduate Course Williamsburg, VA September 13, 2015 Objectives Discuss determining readiness for transplantation
Liver Transplantation Evaluation: Essential Work-Up Curtis K. Argo, MD, MS VGS/ACG Regional Postgraduate Course Williamsburg, VA September 13, 2015 Objectives Discuss determining readiness for transplantation
Variceal bleeding. Mainz,
 Variceal bleeding Mainz, 21.09.2008 Risk of complications 5 years 10 years Ascites 10 % 25 % HCC 10 % 25 % Bleeding < 5 % 5-10 % Enceph. < 5 % < 5 % Typical situation : Mortality 10 % to 40 % Sequence
Variceal bleeding Mainz, 21.09.2008 Risk of complications 5 years 10 years Ascites 10 % 25 % HCC 10 % 25 % Bleeding < 5 % 5-10 % Enceph. < 5 % < 5 % Typical situation : Mortality 10 % to 40 % Sequence
Survival Outcomes Following Liver Transplantation (SOFT) Score: A Novel Method to Predict Patient Survival Following Liver Transplantation
 American Journal of Transplantation 2008; 8: 2537 2546 Wiley Periodicals Inc. C 2008 The Authors Journal compilation C 2008 The American Society of Transplantation and the American Society of Transplant
American Journal of Transplantation 2008; 8: 2537 2546 Wiley Periodicals Inc. C 2008 The Authors Journal compilation C 2008 The American Society of Transplantation and the American Society of Transplant
Supplementary Online Content
 Supplementary Online Content Mismetti P, Laporte S, Pellerin O, Ennezat P-V, Couturaud F, Elias A, et al. Effect of a retrievable inferior vena cava filter plus anticoagulation vs anticoagulation alone
Supplementary Online Content Mismetti P, Laporte S, Pellerin O, Ennezat P-V, Couturaud F, Elias A, et al. Effect of a retrievable inferior vena cava filter plus anticoagulation vs anticoagulation alone
ESLD a Guide for HIV Physicians. Marion Peters University of California San Francisco June 2015
 ESLD a Guide for HIV Physicians Marion Peters University of California San Francisco June 2015 Disclosures Honararia from Johnson and Johnson Roche Merck Gilead Spouse employee of Hoffman La Roche Natural
ESLD a Guide for HIV Physicians Marion Peters University of California San Francisco June 2015 Disclosures Honararia from Johnson and Johnson Roche Merck Gilead Spouse employee of Hoffman La Roche Natural
Prior Authorization Review Panel MCO Policy Submission
 Prior Authorization Review Panel MCO Policy Submission A separate copy of this form must accompany each policy submitted for review. Policies submitted without this form will not be considered for review.
Prior Authorization Review Panel MCO Policy Submission A separate copy of this form must accompany each policy submitted for review. Policies submitted without this form will not be considered for review.
End-Stage Liver Disease (ESLD): A Guide for HIV Physicians
 Slide 1 of 32 End-Stage Liver Disease (ESLD): A Guide for HIV Physicians Marion G. Peters, MD John V. Carbone, MD, Endowed Chair Professor of Medicine Chief of Hepatology Research University of California
Slide 1 of 32 End-Stage Liver Disease (ESLD): A Guide for HIV Physicians Marion G. Peters, MD John V. Carbone, MD, Endowed Chair Professor of Medicine Chief of Hepatology Research University of California
SEQUENCING OF HCC TREATMENT. Dr. Amit G. Singal Medical Director, UT Southwestern Medical Center, USA
 SEQUENCING OF HCC TREATMENT Dr. Amit G. Singal Medical Director, UT Southwestern Medical Center, USA February 2018 DISCLAIMER Please note: The views expressed within this presentation are the personal
SEQUENCING OF HCC TREATMENT Dr. Amit G. Singal Medical Director, UT Southwestern Medical Center, USA February 2018 DISCLAIMER Please note: The views expressed within this presentation are the personal
Prevalence and outcome of portal thrombosis in a cohort of cirrhotic patients undergoing liver transplantation
 1130-0108/2016/108/11/716-720 Revista Española de Enfermedades Digestivas Copyright 2016. SEPD y ARÁN EDICIONES, S.L. Rev Esp Enferm Dig 2016, Vol. 108, N.º 11, pp. 716-720 ORIGINAL PAPERS Prevalence and
1130-0108/2016/108/11/716-720 Revista Española de Enfermedades Digestivas Copyright 2016. SEPD y ARÁN EDICIONES, S.L. Rev Esp Enferm Dig 2016, Vol. 108, N.º 11, pp. 716-720 ORIGINAL PAPERS Prevalence and
Hyeon Jeong Goong, Sang Gyune Kim, Seung Sik Park, Youn Hee Cho, Young Seok Kim, Boo Sung Kim
 Soonchunhyang Medical Science 18(1):56-60, June 2012 pissn: 2233-4289 I eissn: 2233-4297 CASE REPORT Complete Remission of Refractory Hepatic Hydrothorax in Patient with Advanced Liver Cirrhosis and Hepatocellular
Soonchunhyang Medical Science 18(1):56-60, June 2012 pissn: 2233-4289 I eissn: 2233-4297 CASE REPORT Complete Remission of Refractory Hepatic Hydrothorax in Patient with Advanced Liver Cirrhosis and Hepatocellular
Impact of untreated portal vein thrombosis on pre and post liver transplant outcomes in cirrhosis
 952 ORIGINAL ARTICLE November-December, Vol. 12 No. 6, 2013: 952-958 Impact of untreated portal vein thrombosis on pre and post liver transplant outcomes in cirrhosis John BV,* Konjeti R, Aggarwal A, Lopez
952 ORIGINAL ARTICLE November-December, Vol. 12 No. 6, 2013: 952-958 Impact of untreated portal vein thrombosis on pre and post liver transplant outcomes in cirrhosis John BV,* Konjeti R, Aggarwal A, Lopez
The MELD Score in Advanced Liver Disease: Association with Clinical Portal Hypertension and Mortality
 The MELD Score in Advanced Liver Disease: Association with Clinical Portal Hypertension and Mortality Sammy Saab, 1,2 Carmen Landaverde, 3 Ayman B Ibrahim, 2 Francisco Durazo, 1,2 Steven Han, 1,2 Hasan
The MELD Score in Advanced Liver Disease: Association with Clinical Portal Hypertension and Mortality Sammy Saab, 1,2 Carmen Landaverde, 3 Ayman B Ibrahim, 2 Francisco Durazo, 1,2 Steven Han, 1,2 Hasan
Hepatocellular carcinoma in Sri Lanka - where do we stand?
 SCIENTIFIC ARTICLE Hepatocellular carcinoma in Sri Lanka - where do we stand? R.C. Siriwardana 1, C.A.H. Liyanage 1, M.B. Gunethileke 2 1. Specialist Gastrointestinal and Hepatobilliary Surgeon, Senior
SCIENTIFIC ARTICLE Hepatocellular carcinoma in Sri Lanka - where do we stand? R.C. Siriwardana 1, C.A.H. Liyanage 1, M.B. Gunethileke 2 1. Specialist Gastrointestinal and Hepatobilliary Surgeon, Senior
Follow this and additional works at:
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2017 Comparison of transjugular intrahepatic portosystemic shunt with covered stent and balloon-occluded retrograde
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2017 Comparison of transjugular intrahepatic portosystemic shunt with covered stent and balloon-occluded retrograde
Risk factors for hepatic encephalopathy after transjugular intrahepatic portosystemic shunt placement in cirrhotic patients
 Oregon Health & Science University OHSU Digital Commons Scholar Archive 9-2014 Risk factors for hepatic encephalopathy after transjugular intrahepatic portosystemic shunt placement in cirrhotic patients
Oregon Health & Science University OHSU Digital Commons Scholar Archive 9-2014 Risk factors for hepatic encephalopathy after transjugular intrahepatic portosystemic shunt placement in cirrhotic patients
Carvedilol or Propranolol in the Management of Portal Hypertension?
 Evidence Based Case Report Carvedilol or Propranolol in the Management of Portal Hypertension? Arranged by: dr. Saskia Aziza Nursyirwan RESIDENCY PROGRAM OF INTERNAL MEDICINE DEPARTMENT UNIVERSITY OF INDONESIA
Evidence Based Case Report Carvedilol or Propranolol in the Management of Portal Hypertension? Arranged by: dr. Saskia Aziza Nursyirwan RESIDENCY PROGRAM OF INTERNAL MEDICINE DEPARTMENT UNIVERSITY OF INDONESIA
European. Young Hepatologists Workshop. Organized by : Quantification of fibrosis and cirrhosis outcomes
 supported by from Gilea Quantification of fibrosis and cirrhosis outcomes th 5 European 5 European Young Hepatologists Workshop Young Hepatologists Workshop August, 27-29. 2015, Moulin de Vernègues Vincenza
supported by from Gilea Quantification of fibrosis and cirrhosis outcomes th 5 European 5 European Young Hepatologists Workshop Young Hepatologists Workshop August, 27-29. 2015, Moulin de Vernègues Vincenza
بسم الله الرحمن الرحيم أوتيتم من العلم إال قليال وما
 بسم الله الرحمن الرحيم أوتيتم من العلم إال قليال وما 1 2 Goals of the Lecture: What is the portal vein? How common is PVT? What conditions are associated with PVT? How does patient with PVT present? How
بسم الله الرحمن الرحيم أوتيتم من العلم إال قليال وما 1 2 Goals of the Lecture: What is the portal vein? How common is PVT? What conditions are associated with PVT? How does patient with PVT present? How
The Management of Ascites & Hepatorenal Syndrome. Florence Wong University of Toronto. Falk Symposium March 14, 2008
 The Management of Ascites & Hepatorenal Syndrome Florence Wong University of Toronto Falk Symposium March 14, 2008 Management of Ascites Sodium Restriction Mandatory at all stages of ascites in order to
The Management of Ascites & Hepatorenal Syndrome Florence Wong University of Toronto Falk Symposium March 14, 2008 Management of Ascites Sodium Restriction Mandatory at all stages of ascites in order to
Case Report INTRODUCTION CASE REPORT
 Case Report J Korean Soc Transplant 2016;30:89-93 http://dx.doi.org/10.4285/jkstn.2016.30.2.89 Late Hepatic Venous Outflow Obstruction Following Inferior Vena Cava Stenting in Patient with Deceased Donor
Case Report J Korean Soc Transplant 2016;30:89-93 http://dx.doi.org/10.4285/jkstn.2016.30.2.89 Late Hepatic Venous Outflow Obstruction Following Inferior Vena Cava Stenting in Patient with Deceased Donor
RG Volume 33 Number 5 Kirby et al 1497
 Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. RG Volume 33 Number
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. RG Volume 33 Number
The role of TIPS in the management of liver transplant candidates
 Original Article The role of TIPS in the management of liver transplant candidates United European Gastroenterology Journal 217, Vol. 5(8) 11 117! Author(s) 217 Reprints and permissions: sagepub.co.uk/journalspermissions.nav
Original Article The role of TIPS in the management of liver transplant candidates United European Gastroenterology Journal 217, Vol. 5(8) 11 117! Author(s) 217 Reprints and permissions: sagepub.co.uk/journalspermissions.nav
Clinical Study A Single-Institution Review of Portosystemic Shunts in Children: An Ongoing Discussion
 Hindawi Publishing Corporation HPB Surgery Volume 2010, Article ID 964597, 6 pages doi:10.1155/2010/964597 Clinical Study A Single-Institution Review of Portosystemic Shunts in Children: An Ongoing Discussion
Hindawi Publishing Corporation HPB Surgery Volume 2010, Article ID 964597, 6 pages doi:10.1155/2010/964597 Clinical Study A Single-Institution Review of Portosystemic Shunts in Children: An Ongoing Discussion
DR. DO NGUYEN TIN CHILDREN HOSPITAL 1
 DR. DO NGUYEN TIN CHILDREN HOSPITAL 1 BACKGROUND Congenital extrahepatic porto-systemic shunt (CEPS), known as Abernethy malformation, is a rare malformation. Intestinal and/or splenic venous blood bypasses
DR. DO NGUYEN TIN CHILDREN HOSPITAL 1 BACKGROUND Congenital extrahepatic porto-systemic shunt (CEPS), known as Abernethy malformation, is a rare malformation. Intestinal and/or splenic venous blood bypasses
Causes of Liver Disease in US
 Learning Objectives Updates in Outpatient Cirrhosis Management Jennifer Guy, MD MAS Director, Liver Cancer Program California Pacific Medical Center guyj@sutterhealth.org Review cirrhosis epidemiology,
Learning Objectives Updates in Outpatient Cirrhosis Management Jennifer Guy, MD MAS Director, Liver Cancer Program California Pacific Medical Center guyj@sutterhealth.org Review cirrhosis epidemiology,
