Alterations of Cardiovascular Function. w Chapter 23
|
|
|
- Marsha Randall
- 5 years ago
- Views:
Transcription
1 Alterations of Cardiovascular Function w Chapter 23 1
2 Simplified Path of Blood Flow 2
3 The Heart Layers 3
4 Cardiac Conduction System 4
5 Cardiac Cycle-Diastole w Ventricles relaxed w Blood entering atria w Blood flows through AV valves into ventricles w Semilunar valves are closed Cardiac Filling 5
6 Cardiac Cycle-Systole w Ventricles contract w Blood pushes against AV valves and they shut w Blood pushes through semilunar valves into aorta and pulmonary trunk Cardiac Emptying 6
7 Cardiac Cycle 7
8 Arteriosclerosis w Arteriosclerosis: normal consequence of aging w Hardening of the arteries, smooth muscle and collagen grow into lumen and stiffen the wall w Atherosclerosis w Type of arteriosclerosis w Fatty lesions in the intimal lining of large and medium sized arteries 8
9 Atherosclerosis in a Nutshell w Lipids get into the vascular endothelium w Proportional to LDL level w White blood cells try to clear them away à foam cells w WBCs and vascular endothelium release growth factors that promote plaque formation w Plaques block the arteries w *** inflammation plays a BIG role as an initiator 9
10 Atherosclerosis 1) Intimal injury allows LDL to penetrate vessel wall ) LDL modifications trigger chemotaxis of monocytes 3) Monocytes enter vessel wall and phagocytize LDL 4) Engorged monocytes become Foam cells & Fatty Streak visible 10
11 Complicated plaques are the ones that rupture and this exposes collagen which activates platelets and thrombi form 11
12 Fatty Streak 12
13 Atherosclerosis Chronic inflammatory process ensues causing smooth muscle proliferation and fibrous tissue accumulation Now have fibrous plaque with isolated pools of lipid vulnerable to rupture 13
14 Atherosclerosis 14
15 Clinical Consequences The most important complication of atherosclerosis w Vessel Occlusion w Ischemia: may be reversible w Infarction: permanent damage 15
16 w Risk Factors for atherosclerosis and coronary artery disease w Smoking w Hypertension w Gender w Age w Hyperlipidemia w Sedentary w Stress w INFLAMMATION like in RA, obesity, periodontal disease 16
17 Sites of Atherosclerosis 17
18 Peripheral Arterial Disease w Atherosclerotic changes in the peripheral arteries result in tissue ischemia w Lower extremities are most common w High risk group are men in their 60 s & 70 s w More common with atherosclerosis risk factors 18
19 Peripheral Artery Disease w Gradual onset of intermittent claudication (uncomfortable, or tired feeling in the legs that occurs during walking and is relieved by rest) w Pain at rest only if severe PAD 19
20 Peripheral Artery Disease w Thromboangiitis obliterans (Buerger disease) w Occurs mainly in young men who smoke w Inflammatory disease of peripheral arteries resulting in the formation of nonatherosclerotic lesions w Digital, tibial, plantar, ulnar, and palmar arteries w Obliterates the small and medium-sized arteries 20
21 Atrophic Skin Changes 21
22 Peripheral Arterial Disease w Diagnostic Test Findings w Inspection w Check pulses w Ankle Brachial Index w Treatment w Walking program w Avoid injury w Reduce risk factors w Antiplatelet agents w Surgery 22
23 Peripheral Artery Disease w Raynaud phenomenon and Raynaud disease w Episodic vasospasm in arteries and arterioles of the fingers, less commonly the toes w Raynaud disease is a primary vasospastic disorder of unknown origin 23
24 Peripheral Artery Disease w Raynaud phenomenon and Raynaud disease w Raynaud phenomenon is secondary to other systemic diseases or conditions w Collagen vascular disease (scleroderma), smoking, pulmonary hypertension, myxedema, and environmental factors (cold and prolonged exposure to vibrating machinery) w Seen in patients with RA, SLE, Sjogren s 24
25 Raynaud s Phenomenon w Diagnosis w History w Example w Treatment w Avoidance of cold w No Smoking w Medications (Ca++channel blockers dilate blood vessels 25
26 Aneurysm w Abnormal out pouching or localized dilation of a blood vessel or wall of the heart w Various causes w Atherosclerotic plaque formation w Congenital abnormality of arterial wall w Trauma w Infection w "true" aneurysm is one that involves all three layers of the wall of an artery w Classified also by shape 26
27 Aneurysm w Various locations (aorta most common) w Abdominal aorta (between renal arteries and iliac branches) w Thoracic aorta (ascending, transverse or descending) w Cerebral artery (at circle of Willis) w Femoral and popliteal arteries 27
28 Aneurysm w Complications w Rupture risk increases with increasing size w Pressure on adjacent structures 28
29 Berry Aneurysm 29
30 Aneurysms & Dissections w Berry & saccular used interchangeably. Are often congenital w Fusiform, either partially or fully, by thrombus, plaque w Dissecting: tears w associated with hypertension 30
31 Dissecting Aneurysm 31
32 Abdominal Aortic Aneurysms w Develop after age 50 w Usually men w Severe Atherosclerosis & Hypertension are major causes w Most (>90%) occur below the renal artery w Pulsating abdominal mass may be first sign 32
33 Hypertension 33
34 Hypertension w Essential Hypertension w 90% of hypertensive patients w Unknown cause w Men > Women w Black > White w Poor > Rich w Older > Younger w Obese > Thin w Secondary Hypertension w 10% of hypertensive patients 34
35 Hypertension w Risk Factors w Constitutional Factors w Family History, Race, Sex w Lifestyle Factors w High sodium diet, obesity (increased vessel length increases resistance), Physical inactivity, Excessive alcohol consumption, Oral contraceptives, Sleep apnea w Not stress (acute changes only) w Not high fat diets (risk of CAD) w Smoking increases risk of CAD but? risk in HTN 35
36 Hypertension w Pathophysiologic Changes w Asymptomatic w Elevated blood pressure w Most are the result of chronic complications 36
37 Hypertension w Complications w Target Organ Damage w Kidneys Renal Failure w Brain CVA, TIA w Heart LVH, Angina, CAD, CHF w Eyes - Retinopathy w Blood Vessels - PVD w Atherosclerosis w Cardiovascular disorders 37
38 Hypertension w Diagnosis w > 2 BP readings on > 2 separate days w Treatment w Lifestyle Modification w Reduce weight, Reduce sodium, Reduce alcohol, Increase exercise w Pharmacologic Treatment w Stepwise approach 38
39 Malignant hypertension: Rapidly progressive hypertension, diastolic pressure is usually >140 mm Hg with papilledema (optic disc swelling), biggest concern is encephalopathy Up to 1% of patients with essential hypertension develop malignant hypertension, but the reason some patients develop malignant hypertension whereas others do not is unknown. 39
40 Orthostatic Hypotension w Abnormal drop in blood pressure w Upon standing w Transient w Symptoms w Dizziness and Syncope (fainting) w Causes w Reduce blood volume, Drug induced, Aging, Immobility 40
41 Orthostatic Hypotension w Diagnosis w Sitting and Standing BP measurements w Tilt table w Treatment alleviate the cause w Education w Adjusting medication w Support hose 41
42 Disorders of Venous Circulation w Varicose veins w Dilated and tortuous veins w Venous valves are incompetent w Thrombophlebitis w Clot formation with inflammation w Deep vein is most dangerous 42
43 Varicose Veins w Dilated, tortuous veins, engorged with blood resulting from improper venous valve function w Weakening in valve allows backflow of blood w Increase pressure in the veins causing walls to stretch w Primary w Originates in the superficial veins w Secondary w Impaired flow in the deep venous channels 43
44 Varicose Veins 44
45 Varicose Veins w Pathophysiologic Changes w Dilated, tortuous, purple veins most pronounced in the legs w Edema of the calves w Leg heaviness w Dull aching in the legs w Complications w Blood clots secondary to venous stasis w Venous stasis ulcers 45
46 Varicose Veins w Testing w Visual inspection w Doppler ultrasonographic flow analysis w Treatment w Treat underlying cause w Anti-embolism stockings w Regular exercise w Surgical stripping w Weight loss is patient is obese 46
47 Diseases of the Veins w Superior vena cava syndrome w Progressive occlusion of the superior vena cava that leads to venous distention of upper extremities and head w usually the result of the direct obstruction of the superior vena cava by malignancies 47
48 Chronic Venous Insufficiency w Chronic venous insufficiency: inadequate venous return over a long period w Consequence of valvular incompetence w Venous muscle pump is ineffective w Tissue congestion, edema, impaired tissue nutrition w Fat necrosis & skin atrophy w Brown pigmentation due to hemosiderin deposits w Stasis dermatitis and ulcers because poor O2 levels so cells die 48
49 Chronic Venous Insufficiency 49
50 Venous Thrombosis w The acute development of a blood clot that may cause vessel occlusion or embolization w Thrombosis causes vessel irritation and resulting inflammation which contributes to occlusion or embolization w May occur in deep or superficial veins 50
51 Venous Thrombosis Triad w Venous Stasis w Bed rest, immobility, shock, airplane rides, long car rides, w Hypercoagulability of Blood w Pregnancy, childbirth, BCP s, dehydration, cancer, SLE w Vascular Trauma w Venous catheters, surgery, massive trauma, hip fracture, orthopedic surgery 51
52 Venous Thrombosis w Pathophysiologic Changes w Tenderness, redness, and warmth over the affected area due to inflammation w Swelling of the affected leg from venous congestion 52
53 Venous Thrombosis w Prevention w Ambulation w Support hose w Low dose anticoagulation w Treatment w Anticoagulation w Surgical clot removal 53
54 Diseases of the Arteries and Veins w Thrombus formation w Blood clot that remains attached to the vessel wall w Thromboembolus: blood clot that dislodges and travels to a new vessel w Arterial thromboembolus: source often the heart & obstructs lower extremities, coronary and cerebral vessels w Venous thromboembolus: source usually legs & obstructs pulmonary arteries 54
55 Diseases of the Arteries and Veins w Embolism w Bolus of matter that is circulation in the bloodstream w Dislodged thrombus, air bubble, amniotic fluid, aggregate of fat, bacteria, cancer cells, or a foreign substance 55
56 Pericardium 56
57 Pericarditis w Inflammation of the pericardium as a result of systemic or cardiac diseases w Primary usually viral or idiopathic w Secondary infection, connective tissue disease or trauma w Often associated with fluid collection within the pericardial space 57
58 Pericarditis w Pathophysiologic Changes w Pericardial friction rub and sharp substernal pain w Shallow rapid respirations due to associated pleurisy w Mild fever resulting from inflammation w Dyspnea, orthopnea, tachycardia w Relief when sit up and slouch over 58
59 Pericardial Effusion fluid in pericardial cavity restricts heart expansion left ventricle cannot accept enough blood right ventricle cannot accept enough blood decreased cardiac output increased venous pressure; jugular distension decreased blood pressure and shock 59
60 Pericarditis w Testing w Echocardiogram shows pericardial fluid w Treatment w Most cases resolve on their own w Pericardiocentesis w Pericardial window w Pericardiectomy 60
61 Cardiac Tamponade w Rapid increase in intrapericardial pressure caused by fluid accumulation in the pericardial sac w Compression of the heart chambers w Causes impaired diastolic filling of the heart 61
62 Cardiac Tamponade w Causes w Acute MI w Connective tissue disorders w Adverse drug reactions w Infective pericarditis w Hemorrhage from trauma w Post irradiation pericarditis 62
63 Cardiac Tamponade 63
64 Coronary Artery Disease w Impaired coronary blood flow w Narrowing of coronary arteries due to atherosclerosis resulting in: w Heart disease secondary to myocardial ischemia w Strength of myocardial contraction is reduced w Wall motion is abnormal resulting in lower cardiac output 64
65 Coronary Artery Blood Flow. w Coronary Arteries originate in the aortic sinuses w Controlled by aortic pressure (aortic resistance) w Perfuse during diastole 65
66 Coronary Artery Disease w Imbalance in blood supply and the heart s demands for oxygen w Less blood w Atherosclerosis w Vasospasm w Thrombosis w Higher oxygen demand w Stress w Exercise w Cold 66
67 Coronary Artery Disease w Nontraditional risk factors w Markers of inflammation and thrombosis w C-reactive protein, fibrinogen, protein C, and plasminogen activator inhibitor w Hyperhomocysteinemia w Infection 67
68 Coronary Artery Disease w Chronic Stable Angina w Pain when heart s oxygen demand increases w coronary artery size is not changed w Variant Angina w Pain when coronary arteries spasm w Prinzmetal s angina (vasospastic angina, occurs at rest), due to hyperactive sympathetic nerve, patient may have NO atherosclerosis or clots w Intermittent coronary vasospasms w Silent myocardial ischemia w Myocardial ischemia without pain 68
69 Angina 69
70 Coronary Heart Disease w subendocardial transmural 70
71 Acute Coronary Syndromes w ECG changes w T-wave inversion w ST-segment depression or elevation w Abnormal Q wave w Serum cardiac markers w Proteins released from necrotic heart cells w Myoglobin, creatine kinase, troponin I and T 71
72 Acute Coronary Syndromes w Unstable Angina w Causes myocardial ischemia w Worse than stable angina but not quite a MI w Due to atherosclerotic plaque disruption platelet aggregation hemostasis w Vasospasm may play a role w Acute Myocardial Infarction w Ischemic death of myocardial tissue w Sudden onset Pain 72
73 Myocardial Infarction w Reduced blood flow through one or more coronary arteries causing myocardial ischemia and necrosis w Caused by coronary artery occlusion w If ischemia lasts more than 45 minutes irreversible damage occurs w All infarcts have a central hypoxic area w Transmural infarction involves the full thickness of the cardiac wall (myocardium) w Subendocardial infarction involves the inner half of the cardiac wall (myocardium) w Injured tissue is potentially viable if circulation is restored 73
74 Acute Myocardial Infarction w Ischemic death of myocardial tissue 74
75 Acute Myocardial Infarction 75
76 Myocardial Infarction w Causes w Atherosclerosis w Thrombosis w Coronary artery stenosis or spasm w Platelet aggregation 76
77 Myocardial Infarction w Pathophysiologic Changes w Persistent, crushing substernal chest pain w Caused by coronary artery occlusion w May radiate to left arm, jaw, neck or shoulder w Cool extremities, hypotension due to impaired myocardial function w Perspiration, anxiety, hypertension and feeling of impending doom resulting from pain or sympathetic stimulation w Nausea & vomiting due to pain or vagal stimulation 77
78 Myocardial Infarction w Complications w Heart failure w AMI is the most common cause of left HF w Cardiogenic shock w Pericarditis w Thromboembolism w Rupture of the heart w Ventricular aneurysms w Cardiac Arrhythmias w Most common cause of sudden death with AMI 78
79 Ventricular Rupture of the Heart 79
80 Myocardial Infarction w Structural and functional changes w Myocardial stunning: reversible reduction of function of heart contraction after reperfusion not accounted for by tissue damage or reduced blood flow. Last for hours to days w Hibernating myocardium: some segments of the myocardium exhibit abnormalities of contractile function. Until perfusion restored w Myocardial remodeling: refers to the changes in size, shape, and function of the heart after injury to the ventricles. Often necrosis followed by fibrous scarring which is not a contractile tissue therefore function declines 80
81 Myocardial Infarction 81
82 Myocardial Infarction w Treatment w Thrombolytic therapy within 3 hours of onset of symptoms w Percutaneous transluminal coronary angioplasty to open blocked or narrowed arteries w Oxygen w Bypass surgery 82
83 Dysrhythmias w Disturbance of the heart rhythm w Range from occasional missed or rapid beats to severe disturbances that affect the pumping ability of the heart w Can be caused by an abnormal rate of impulse generation or abnormal impulse conduction w Respiratory sinus arrhythmia: is a naturally occurring variation in heart rate. inspiration triggers inhibitory signals to the vagus nerve so tonic attenuation of inherent SA node rate is transiently shut down thereby increasing heart rate 83
84 w pulsus paradoxus (PP), also paradoxic pulse or paradoxical pulse, is defined as an exaggeration (more than 10 mmhg) of the normal variation during the inspiratory phase of respiration, in which the blood pressure declines as one inhales and increases as one exhales. It is a sign that is indicative of several conditions including cardiac tamponade, pericarditis, chronic sleep apnea, croup, and obstructive lung disease (e.g. asthma, COPD). [1] 84
85 w Examples: Dysrhythmias w Tachycardia: >100 bpm w Flutter: typical atrial flutter, has an atrial rate of 250 to 300bpm or atypical is typically faster, usually bpm, ventricular flutter rate over 200bpm w Fibrillation: >300 bpm irregular, and unsynchronized contraction of muscle fibers (atria or ventricles) Ventricular fibrillation is a cause of cardiac arrest and sudden cardiac death. The ventricular muscle quivers and is useless w Bradycardia: under 60bpm, though it is seldom symptomatic until the rate drops below 50 85
86 w Premature ventricular contractions PVC the heartbeat is initiated by the heart ventricles rather than by the SA node w Junctional rhythm: AV node instead of SA node sets the heart rate w Sick sinus syndrome, also called sinus node dysfunction, is a group of abnormal heart rhythms (arrhythmias) presumably caused by a malfunction of the sinus node, the heart's primary pacemaker. Bradycardia-tachycardia syndrome is a variant of sick sinus syndrome in which slow arrhythmias and fast arrhythmias alternate 86
87 w Following the PVC there is a pause and then the normal beat returns - only to be followed by another PVC. The continuation of this pairing of beats is an example of bigeminy. w PVCs that occur at intervals of 2 normal beats to 1 PVC is called trigeminy w Quadrigeminy is where one PVC occurs after every 3 normal beats of the heart 87
88 Long QT Syndrome Heart condition in which delayed repolarization of the heart following a heartbeat, leading to re-entrant ventricular arrhythmias. Symptoms may only manifest to patient during extreme exercise, but that 1 st symptom may be sudden death like in young athletes May be the result of various gene mutations Patient may be put on beta blockers or may get a defibrillator implant 88
89 Heart block: impeded neuroconduction any place along the conduction pathway. AV blocks have 3 degrees with 3 rd degree causing complete nerve block between the atria and ventricles 89
90 Cardiomyopathy w Group of disorders affecting the myocardium w Primary Confined to the myocardium w Secondary Other disease conditions 90
91 Cardiomyopathy w Hypertrophic cardiomyopathy w Autosomal dominant disorder or aortic stenosis or anything increasing the workload of the heart over a chronic period w Hypertrophied ventricle becomes stiff and noncompliant and unable to relax causing a reduction in ventricular filling w 1 out of 500 in the general population w Common cause of sudden death in athletes w Signs and symptoms vary greatly 91
92 Cardiomyopathy w Dilated cardiomyopathy w Extensively damaged myocardium reduces contractility causing a decline in systolic function and cardiac output (heart failure) w Leading cause of heart transplant w Causes: viral, HTN, valve insufficiency w Restrictive cardiomyopathy w Fibrosis and stiffening of the ventricle reducing the ability to relax and fill during diastole resulting in a decrease in cardiac output, amyloidosis 92
93 Cardiomyopathy 93
94 94
95 Hypertrophic Cardiomyopathy 95
96 Myocarditis w Focal or diffuse inflammation of the cardiac muscle which may be acute or chronic w Inflammatory cardiomyopathy w Inflammation may lead to hypertrophy, fibrosis or inflammatory changes of the conduction system w Usually resolves spontaneously w Heart muscle weakens and contractility is reduced 96
97 Myocarditis w Causes w Infection: bacterial, viral, etc. w Radiation therapy w Hypersensitivity immune reaction, autoimmune SLE w Toxins such as lead, chemicals and cocaine w Chronic alcoholism 97
98 Myocarditis w Complications w Arrhythmias and sudden death w Chronic valvulitis w Dilated cardiomyopathy w Heart failure w Pericarditis w Cardiac rupture w Thromboembolism 98
99 Endocarditis w Infection of the endocardium, heart valves or cardiac prosthesis w Causing deformities and destruction of valvular tissue and chordae tendineae causing rupture and valvular insufficiency w Collection of microorganisms, fibrin and platelets form vegetations that can cover the valve surface w Vegetations may break off and form emboli w AKA: Bacterial Endocarditis 99
100 Endocarditis w Causes w Bacterial or fungal invasion w Predisposing factors w Portal of entry w I.V. Drug abuse, surgery, teeth cleanings w Damaged endocardial surface w Presence of a prosthetic heart valve w Rheumatic heart disease 100
101 Endocarditis w Signs & Symptoms w Fever and chills due to bacterial infection w Heart murmur due to turbulent blood flow w Diagnostic Test Findings w Positive blood cultures w Elevated WBC count 101
102 Endocarditis w Complications w Acute renal failure w Brain abscess w Cardiac arrhythmia w Cerebral emboli w Heart failure w Meningitis w Death 102
103 Rheumatic Heart Disease w Acute rheumatic fever is a systemic inflammatory disease of childhood that develops after infections with group-a streptococcus (pharyngeal not skin) w Inflammation mainly involves the heart, joints, CNS, skin and subcutaneous tissues. w Rheumatic heart disease is the cardiac and valvular manifestations of rheumatic fever w Includes pericarditis, myocarditis & endocarditis during the early phase w Chronic valve disease in the later phase 103
104 Rheumatic Heart Disease w Underlying Pathophysiology w GAS infection leads to a autoimmune reaction in which antibodies produced to combat GAS affect connective tissues of the body w Antibodies may attack healthy body cells by mistake because the bacterial antigens are similar to the body s own cells w Molecular mimicry 104
105 Rheumatic Heart Disease w Pathophysiologic Changes w Polyarthritis caused by inflammation w Firm movable subcutaneous nodules w Erythema marginatum skin rash found on the trunk w Carditis with dyspnea and chest pain w Sydenham s chorea is a CNS manifestation 105
106 Rheumatic Heart Disease Erythema Marginatum 106
107 Rheumatic Heart Disease w Complications w Destruction of the mitral and aortic valves w Heart failure w Infection 107
108 Rheumatic Heart Disease w Treatment w Prompt treatment of GAS with antibiotics w Salicylates to relieve fever and pain w Corticosteroids for carditis w Corrective surgery 108
109 Valve Stenosis w Occurs when there is narrowing of a heart valve opening w Stenosis of the heart valve w Blood accumulates in chamber preceding stenosed valve w Results in increased chamber pressure due to resistance to flow through the valve w May cause hypertrophy of cardiac wall 109
110 Valve Insufficiency w Occurs when heart valve leaflets don t completely close w Cardiac valve insufficiency w Incompetent heart valves allow blood to flow in both directions through valve w Volume of pumped blood increases w Involved heart chambers dilate to accommodate increased volume 110
111 Murmurs w The blood going through the valve makes a noise w These are called heart murmurs w You can identify them by: w Where they are which valve are they near? w How they sound high or low pitched? w When they happen systole or diastole? 111
112 Mitral valve prolapse is the most common cardiac valve disease in the US. More common in women and is believed to be inherited, causes regurgitation of blood into the left atrium. Some experience fatigue, anxiety, and palpitations. Whether the MVP causes these symptoms is in dispute 112
113 Heart Failure w Syndrome that occurs when the heart cannot pump enough blood to meet the body s needs (pump failure) w Results in intravascular and interstitial volume overload and poor tissue perfusion w Classified as left sided or right sided 113
114 Heart Failure w Left Sided Heart Failure w Caused by scars from MI w Pumping ability of the left ventricle fails w Cardiac output falls w Blood backs up into the left atrium w Pulmonary edema w Right Sided Heart Failure w Pumping ability of the right ventricle fails w Blood backs up into the right atrium and peripheral circulation w Peripheral edema develops w Caused by left heart failure and COPD 114
115 Heart Failure 115
116 Pitting Edema 116
117 Ascites 117
118 Shock w An acute failure of the circulatory system to supply the peripheral tissues and organs of the body with an adequate blood supply resulting in cellular hypoxia. 118
119 Shock w Cardiogenic w Hypovolemic w Obstructive w Neurogenic AKA vasogenic w Distributive w Septic 119
120 Cardiogenic Shock w Diminished cardiac output severely impairs tissue perfusion (pump failure) w The left ventricle initiates a series of compensatory mechanisms that attempt to increase cardiac output w The actions initially stabilize and later deteriorates as oxygen demands increase on an already compromised heart 120
121 Cardiogenic Shock 121
122 Cardiogenic Shock w Causes w Acute myocardial infarction w End stage cardiomyopathy w Cardiac tamponade w Myocardial ischemia w Ventricular arrhythmias 122
123 Hypovolemic Shock w Circulatory dysfunction and inadequate tissue perfusion caused by reduced intravascular blood volume w Venous return is reduced and cardiac output fails w Acute loss of 15% to 20% of blood volume 123
124 Hypovolemic Shock w Causes w Blood loss w Burns w GI fluid loss w Pathophysiologic Changes w Tachycardia restlessness w Reduced urine output w Hypotension w Cyanosis 124
125 Hypovolemic Shock w Diagnostic Test Findings w Hypotension w Many others w Treatment w Oxygen w Fluids w Blood replacement 125
126 Obstructive Shock w Mechanical obstruction of blood flow w Great veins w Heart w Lungs w Causes w Aortic aneurysm w Pulmonary embolism (most common) 126
127 Distributive Shock w Inadequate tissue perfusion and circulatory collapse in response to infection (burns, anaphylaxis, neurogenic) w Caused by loss of blood vessel tone and enlargement of the vascular compartment w Capacity of the vascular compartment expands such that normal blood volume will not fill the circulatory system 127
128 Distributive Shock w Causes w Decreased sympathetic activity increased parasympathetic activity: neurogenic w Brain or spine injury; anesthetics; insulin shock; emotion w Vasodilator substances in blood w Type I hypersensitivity (anaphylactic shock) w Inflammatory response to infection (sepsis and burns) 128
129 Distributive Shock w Pathophysiologic Changes w Chills and fever due to proinflammatory cytokines w Tachycardia w Reduced urine output due to hypotension w Cyanosis 129
130 Distributive Shock w Complications w Death w Heart failure w Renal failure w Diagnostic Test Findings w Blood cultures are positive w And ruled out anaphylaxis 130
131 Distributive Shock w Treatment w Antibiotics therapy w Medications to increase cardiac output w Oxygen 131
132 Multiple Organ Dysfunction Syndrome w Progressive dysfunction of two or more organ systems resulting from an uncontrolled inflammatory response to severe illness or injury such as burns or other traumatic injury, infection, acute pancreatitis w Mortality rate ~50-90% 132
133 Multiple Organ Dysfunction Syndrome 133
134 Left-to-right shunts w Most common type of congenital heart defect w Atrial septal defect incomplete closure of the embryonic atrial septum w Ventricular septal defect incomplete closure of the embryonic ventricular septum; usually associated with other congenital heart defects; large defects require surgery w Patent (persistent) ductus arteriosus failure of the ductus arteriosus to close at birth; may close with medication or may require minor surgical intervention 134
135 w Less common - result when there is malrotation of the embryonic chambers w Characterized by early cyanosis; require surgical intervention w Tetralogy of Fallot most common: 4 defects w Ventricular septal defect w Pulmonary artery stenosis w Overriding aorta misplaced and sits low on the ventricular septal defect w Right ventricular hypertrophy Right-to-left shunts 135
136 Right-to-left shunts w Transposition of great vessels 2 nd most common w Aorta arises from the right ventricle and pulmonary artery from the left ventricle w Incompatible with life w Requires immediate surgical intervention 136
Heart Disorders. Cardiovascular Disorders (Part B-1) Module 5 -Chapter 8. Overview Heart Disorders Vascular Disorders
 Cardiovascular Disorders (Part B-1) Module 5 -Chapter 8 Overview Heart Disorders Vascular Disorders Susie Turner, MD 1/7/13 Heart Disorders Coronary Artery Disease Cardiac Arrhythmias Congestive Heart
Cardiovascular Disorders (Part B-1) Module 5 -Chapter 8 Overview Heart Disorders Vascular Disorders Susie Turner, MD 1/7/13 Heart Disorders Coronary Artery Disease Cardiac Arrhythmias Congestive Heart
The Cardiovascular System Part I: Heart Outline of class lecture After studying part I of this chapter you should be able to:
 The Cardiovascular System Part I: Heart Outline of class lecture After studying part I of this chapter you should be able to: 1. Describe the functions of the heart 2. Describe the location of the heart,
The Cardiovascular System Part I: Heart Outline of class lecture After studying part I of this chapter you should be able to: 1. Describe the functions of the heart 2. Describe the location of the heart,
Cardiovascular Disorders. Heart Disorders. Diagnostic Tests for CV Function. Bio 375. Pathophysiology
 Cardiovascular Disorders Bio 375 Pathophysiology Heart Disorders Heart disease is ranked as a major cause of death in the U.S. Common heart diseases include: Congenital heart defects Hypertensive heart
Cardiovascular Disorders Bio 375 Pathophysiology Heart Disorders Heart disease is ranked as a major cause of death in the U.S. Common heart diseases include: Congenital heart defects Hypertensive heart
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Can be felt where an artery passes near the skin surface and over a
 1 Chapter 14 Cardiovascular Emergencies 2 Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD) claimed
1 Chapter 14 Cardiovascular Emergencies 2 Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD) claimed
Chapter 14 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since.
 1 2 3 4 5 Chapter 14 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD)
1 2 3 4 5 Chapter 14 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD)
Ischemic heart disease
 Ischemic heart disease Introduction In > 90% of cases: the cause is: reduced coronary blood flow secondary to: obstructive atherosclerotic vascular disease so most of the time it is called: coronary artery
Ischemic heart disease Introduction In > 90% of cases: the cause is: reduced coronary blood flow secondary to: obstructive atherosclerotic vascular disease so most of the time it is called: coronary artery
Cardiac Pathology & Rehabilitation
 Cardiac Pathology & Rehabilitation Which of the following best describes the physical activity performed in my leisure time? A. I perform vigorous physical activity 3X/week for 20 minutes each time B.
Cardiac Pathology & Rehabilitation Which of the following best describes the physical activity performed in my leisure time? A. I perform vigorous physical activity 3X/week for 20 minutes each time B.
1) Severe, crushing substernal chest pain 2) radiate to the neck, jaw, epigastrium, or left arm. 3- rapid and weak pulse 4- nausea (posterior MI).
 1) Severe, crushing substernal chest pain 2) radiate to the neck, jaw, epigastrium, or left arm. 3- rapid and weak pulse 4- nausea (posterior MI). 5- cardiogenic shock (massive MIs >40% of the left ventricle)
1) Severe, crushing substernal chest pain 2) radiate to the neck, jaw, epigastrium, or left arm. 3- rapid and weak pulse 4- nausea (posterior MI). 5- cardiogenic shock (massive MIs >40% of the left ventricle)
Unit 6: Circulatory System. 6.2 Heart
 Unit 6: Circulatory System 6.2 Heart Functions of Circulatory System 1. The heart is the pump necessary to circulate blood to all parts of the body 2. Arteries, veins and capillaries are the structures
Unit 6: Circulatory System 6.2 Heart Functions of Circulatory System 1. The heart is the pump necessary to circulate blood to all parts of the body 2. Arteries, veins and capillaries are the structures
Care of the Patient with a Cardiovascular or a Peripheral Vascular Disorder
 Care of the Patient with a Cardiovascular or a Peripheral Vascular Disorder 1 Slide 1 human heart Slide 2 MECHANICAL: PUSHES BLOOD FROM HEAD TO TOES AND BACK Slide 3 1 ELECTRICAL SYSTEM: TRIGGERS THE MECHANICAL
Care of the Patient with a Cardiovascular or a Peripheral Vascular Disorder 1 Slide 1 human heart Slide 2 MECHANICAL: PUSHES BLOOD FROM HEAD TO TOES AND BACK Slide 3 1 ELECTRICAL SYSTEM: TRIGGERS THE MECHANICAL
Heart disease remains the leading cause of morbidity and mortality in industrialized nations. It accounts for nearly 40% of all deaths in the United
 Heart disease remains the leading cause of morbidity and mortality in industrialized nations. It accounts for nearly 40% of all deaths in the United States, totaling about 750,000 individuals annually
Heart disease remains the leading cause of morbidity and mortality in industrialized nations. It accounts for nearly 40% of all deaths in the United States, totaling about 750,000 individuals annually
Cardiovascular Diseases and Diabetes
 Cardiovascular Diseases and Diabetes LEARNING OBJECTIVES Ø Identify the components of the cardiovascular system and the various types of cardiovascular disease Ø Discuss ways of promoting cardiovascular
Cardiovascular Diseases and Diabetes LEARNING OBJECTIVES Ø Identify the components of the cardiovascular system and the various types of cardiovascular disease Ø Discuss ways of promoting cardiovascular
10/8/2018. Lecture 9. Cardiovascular Health. Lecture Heart 2. Cardiovascular Health 3. Stroke 4. Contributing Factor
 Lecture 9 Cardiovascular Health 1 Lecture 9 1. Heart 2. Cardiovascular Health 3. Stroke 4. Contributing Factor 1 The Heart Muscular Pump The Heart Receives blood low pressure then increases the pressure
Lecture 9 Cardiovascular Health 1 Lecture 9 1. Heart 2. Cardiovascular Health 3. Stroke 4. Contributing Factor 1 The Heart Muscular Pump The Heart Receives blood low pressure then increases the pressure
Lecture 8 Cardiovascular Health Lecture 8 1. Introduction 2. Cardiovascular Health 3. Stroke 4. Contributing Factors
 Lecture 8 Cardiovascular Health 1 Lecture 8 1. Introduction 2. Cardiovascular Health 3. Stroke 4. Contributing Factors 1 Human Health: What s Killing Us? Health in America Health is the U.S Average life
Lecture 8 Cardiovascular Health 1 Lecture 8 1. Introduction 2. Cardiovascular Health 3. Stroke 4. Contributing Factors 1 Human Health: What s Killing Us? Health in America Health is the U.S Average life
Unit 1: Human Systems. The Circulatory System
 Unit 1: Human Systems The Circulatory System nourish all cells with oxygen, glucose, amino acids and other nutrients and carry away carbon dioxide, urea and other wastes Purposes Transport chemical messengers
Unit 1: Human Systems The Circulatory System nourish all cells with oxygen, glucose, amino acids and other nutrients and carry away carbon dioxide, urea and other wastes Purposes Transport chemical messengers
Myocardial Infarction
 Myocardial Infarction MI = heart attack Defined as necrosis of heart muscle resulting from ischemia. A very significant cause of death worldwide. of these deaths, 33% -50% die before they can reach the
Myocardial Infarction MI = heart attack Defined as necrosis of heart muscle resulting from ischemia. A very significant cause of death worldwide. of these deaths, 33% -50% die before they can reach the
Diseases. Cardiovascular System
 Diseases Cardiovascular System Angina Pectoris A condition marked by severe pain in the chest, often spreading to the shoulder or neck. Caused by inadequate blood supply to the heart. Cardiomyopathy Refers
Diseases Cardiovascular System Angina Pectoris A condition marked by severe pain in the chest, often spreading to the shoulder or neck. Caused by inadequate blood supply to the heart. Cardiomyopathy Refers
The Cardiovascular System
 The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
The Cardiovascular System. Chapter 15. Cardiovascular System FYI. Cardiology Closed systemof the heart & blood vessels. Functions
 Chapter 15 Cardiovascular System FYI The heart pumps 7,000 liters (4000 gallons) of blood through the body each day The heart contracts 2.5 billion times in an avg. lifetime The heart & all blood vessels
Chapter 15 Cardiovascular System FYI The heart pumps 7,000 liters (4000 gallons) of blood through the body each day The heart contracts 2.5 billion times in an avg. lifetime The heart & all blood vessels
Pathophysiology of Cardiovascular System. Dr. Hemn Hassan Othman, PhD
 Pathophysiology of Cardiovascular System Dr. Hemn Hassan Othman, PhD hemn.othman@univsul.edu.iq What is the circulatory system? The circulatory system carries blood and dissolved substances to and from
Pathophysiology of Cardiovascular System Dr. Hemn Hassan Othman, PhD hemn.othman@univsul.edu.iq What is the circulatory system? The circulatory system carries blood and dissolved substances to and from
Results of Ischemic Heart Disease
 Ischemic Heart Disease: Angina and Myocardial Infarction Ischemic heart disease; syndromes causing an imbalance between myocardial oxygen demand and supply (inadequate myocardial blood flow) related to
Ischemic Heart Disease: Angina and Myocardial Infarction Ischemic heart disease; syndromes causing an imbalance between myocardial oxygen demand and supply (inadequate myocardial blood flow) related to
Cardiovascular System Notes: Heart Disease & Disorders
 Cardiovascular System Notes: Heart Disease & Disorders Interesting Heart Facts The Electrocardiograph (ECG) was invented in 1902 by Willem Einthoven Dutch Physiologist. This test is still used to evaluate
Cardiovascular System Notes: Heart Disease & Disorders Interesting Heart Facts The Electrocardiograph (ECG) was invented in 1902 by Willem Einthoven Dutch Physiologist. This test is still used to evaluate
10/16/2014. CCRN Review - Cardiovascular. CCRN Review - Cardiovascular. CCRN Review - Cardiovascular
 Hypertrophic (IHSS) Diagnosis Chest x ray cardiomegaly Electrocardiography LV hypertrophy, ST segment T was changes, Q waves in inferior & precordial leads Atrial & ventricular dysrhythmias Hypertrophic
Hypertrophic (IHSS) Diagnosis Chest x ray cardiomegaly Electrocardiography LV hypertrophy, ST segment T was changes, Q waves in inferior & precordial leads Atrial & ventricular dysrhythmias Hypertrophic
10. Thick deposits of lipids on the walls of blood vessels, called, can lead to serious circulatory issues. A. aneurysm B. atherosclerosis C.
 Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
Blood Vessel Disorders
 Blood Vessel Disorders Objectives: Hyperlipidemia Arterioschlerosis Disorders associated with arteries Disorders associated with veins Hypertension and hypotension Part 1: Diseases Associated with Arterial
Blood Vessel Disorders Objectives: Hyperlipidemia Arterioschlerosis Disorders associated with arteries Disorders associated with veins Hypertension and hypotension Part 1: Diseases Associated with Arterial
Cardiac Emergencies. A Review of Cardiac Compromise. Lawrence L. Lambert
 Cardiac Emergencies A Review of Cardiac Compromise Lawrence L. Lambert 1 Cardiac Emergencies Objectives: Following successful completion of this training session, the student should be able to: 1. Describe
Cardiac Emergencies A Review of Cardiac Compromise Lawrence L. Lambert 1 Cardiac Emergencies Objectives: Following successful completion of this training session, the student should be able to: 1. Describe
The Circulatory System. The Heart, Blood Vessels, Blood Types
 The Circulatory System The Heart, Blood Vessels, Blood Types The Closed Circulatory System Humans have a closed circulatory system, typical of all vertebrates, in which blood is confined to vessels and
The Circulatory System The Heart, Blood Vessels, Blood Types The Closed Circulatory System Humans have a closed circulatory system, typical of all vertebrates, in which blood is confined to vessels and
Unit 4 Problems of Cardiac Output and Tissue Perfusion
 Unit 4 Problems of Cardiac Output and Tissue Perfusion Lemone and Burke Ch 30-32 Objectives Review the anatomy and physiology of the cardiovascular system. Identify normal heart sounds and relate them
Unit 4 Problems of Cardiac Output and Tissue Perfusion Lemone and Burke Ch 30-32 Objectives Review the anatomy and physiology of the cardiovascular system. Identify normal heart sounds and relate them
Heart failure congestive heart failure, or CHF
 Heart failure Heart failure (also called congestive heart failure, or CHF) is a frequent end point of many of the conditions In the United States alone, CHF affects nearly 5 million individuals annually,
Heart failure Heart failure (also called congestive heart failure, or CHF) is a frequent end point of many of the conditions In the United States alone, CHF affects nearly 5 million individuals annually,
Cardiovascular System
 Cardiovascular System angio BELLWORK Day One: Define using technology hemo/hema cardio Medical Therapeutics Standards 11) Outline the gross normal structure and function of all body systems and summarize
Cardiovascular System angio BELLWORK Day One: Define using technology hemo/hema cardio Medical Therapeutics Standards 11) Outline the gross normal structure and function of all body systems and summarize
Heart Disease. Signs and Symptoms
 Heart Disease The term "heart disease" refers to several types of heart conditions. The most common type is coronary artery disease, which can cause heart attack, angina, heart failure, and arrhythmias.
Heart Disease The term "heart disease" refers to several types of heart conditions. The most common type is coronary artery disease, which can cause heart attack, angina, heart failure, and arrhythmias.
Do Now. Get out work from last class to be checked
 Do Now Get out work from last class to be checked Heart Actions Cardiac Cycle: One complete heartbeat. The contraction of a heart chamber is called systole and the relaxation of a chamber is called diastole.
Do Now Get out work from last class to be checked Heart Actions Cardiac Cycle: One complete heartbeat. The contraction of a heart chamber is called systole and the relaxation of a chamber is called diastole.
Cardiovascular Disorders Lecture 3 Coronar Artery Diseases
 Cardiovascular Disorders Lecture 3 Coronar Artery Diseases By Prof. El Sayed Abdel Fattah Eid Lecturer of Internal Medicine Delta University Coronary Heart Diseases It is the leading cause of death in
Cardiovascular Disorders Lecture 3 Coronar Artery Diseases By Prof. El Sayed Abdel Fattah Eid Lecturer of Internal Medicine Delta University Coronary Heart Diseases It is the leading cause of death in
Disorders of Cardiac Function
 Disorders of Cardiac Function Objectives: Pericardial and endocardial disorders. Cardiomyopathies and cardiac arrhythmias. Valvular and congenital heart disorders. Coronary artery disease, myocardial ischemic
Disorders of Cardiac Function Objectives: Pericardial and endocardial disorders. Cardiomyopathies and cardiac arrhythmias. Valvular and congenital heart disorders. Coronary artery disease, myocardial ischemic
Common Codes for ICD-10
 Common Codes for ICD-10 Specialty: Cardiology *Always utilize more specific codes first. ABNORMALITIES OF HEART RHYTHM ICD-9-CM Codes: 427.81, 427.89, 785.0, 785.1, 785.3 R00.0 Tachycardia, unspecified
Common Codes for ICD-10 Specialty: Cardiology *Always utilize more specific codes first. ABNORMALITIES OF HEART RHYTHM ICD-9-CM Codes: 427.81, 427.89, 785.0, 785.1, 785.3 R00.0 Tachycardia, unspecified
Cardiomyopathy Consequences. function of the myocardium for any reason. This is a serious disease in which the heart muscle
 Becki Simmons Cardiomyopathy Consequences Cardiomyopathy, which literally means "heart muscle disease," is the deterioration of the function of the myocardium for any reason. This is a serious disease
Becki Simmons Cardiomyopathy Consequences Cardiomyopathy, which literally means "heart muscle disease," is the deterioration of the function of the myocardium for any reason. This is a serious disease
LeMone & Burke Ch 30-32
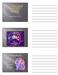 LeMone & Burke Ch 30-32 2 Right side- Low oxygenation Low pressure Light workload Goes toward the lungs Left side High oxygenation Thick walled high pressure Heavier workload Carries oxygenation blood
LeMone & Burke Ch 30-32 2 Right side- Low oxygenation Low pressure Light workload Goes toward the lungs Left side High oxygenation Thick walled high pressure Heavier workload Carries oxygenation blood
Diagnosis and Management of Acute Myocardial Infarction
 Diagnosis and Management of Acute Myocardial Infarction Acute Myocardial Infarction (AMI) occurs as a result of prolonged myocardial ischemia Atherosclerosis leads to endothelial rupture or erosion that
Diagnosis and Management of Acute Myocardial Infarction Acute Myocardial Infarction (AMI) occurs as a result of prolonged myocardial ischemia Atherosclerosis leads to endothelial rupture or erosion that
Cardiovascular Disease
 Cardiovascular Disease Session Guidelines This is a 15 minute webinar session for CNC physicians and staff CNC holds webinars on the 3 rd Wednesday of each month to address topics related to risk adjustment
Cardiovascular Disease Session Guidelines This is a 15 minute webinar session for CNC physicians and staff CNC holds webinars on the 3 rd Wednesday of each month to address topics related to risk adjustment
Echocardiography as a diagnostic and management tool in medical emergencies
 Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
HEART DISEASE HEART CONDITIONS, RISKS AND PROTECTION
 Spotlight on Health 2017 HEART DISEASE HEART CONDITIONS, RISKS AND PROTECTION Heart disease is the leading cause of death for both men and women worldwide, accounting for over 17 million deaths per year.
Spotlight on Health 2017 HEART DISEASE HEART CONDITIONS, RISKS AND PROTECTION Heart disease is the leading cause of death for both men and women worldwide, accounting for over 17 million deaths per year.
Figure ) The specific chamber of the heart that is indicated by letter A is called the. Diff: 1 Page Ref: 364
 Essentials of Anatomy and Physiology, 9e (Marieb) Chapter 11 The Cardiovascular System Short Answer Figure 11.1 Using Figure 11.1, identify the following: 1) The Purkinje fibers are indicated by label.
Essentials of Anatomy and Physiology, 9e (Marieb) Chapter 11 The Cardiovascular System Short Answer Figure 11.1 Using Figure 11.1, identify the following: 1) The Purkinje fibers are indicated by label.
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders
 C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
AP2 Lab 3 Coronary Vessels, Valves, Sounds, and Dissection
 AP2 Lab 3 Coronary Vessels, Valves, Sounds, and Dissection Project 1 - BLOOD Supply to the Myocardium (Figs. 18.5 &18.10) The myocardium is not nourished by the blood while it is being pumped through the
AP2 Lab 3 Coronary Vessels, Valves, Sounds, and Dissection Project 1 - BLOOD Supply to the Myocardium (Figs. 18.5 &18.10) The myocardium is not nourished by the blood while it is being pumped through the
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
Skin supplied by T1-4 (medial upper arm and neck) T5-9- epigastrium Visceral afferents from skin and heart are the same dorsal root ganglio
 Cardio 2 ECG... 3 Cardiac Remodelling... 11 Valvular Diseases... 13 Hypertension... 18 Aortic Coarctation... 24 Erythropoiesis... 27 Haemostasis... 30 Anaemia... 36 Atherosclerosis... 44 Angina... 48 Myocardial
Cardio 2 ECG... 3 Cardiac Remodelling... 11 Valvular Diseases... 13 Hypertension... 18 Aortic Coarctation... 24 Erythropoiesis... 27 Haemostasis... 30 Anaemia... 36 Atherosclerosis... 44 Angina... 48 Myocardial
Circulatory System 10.1
 1 Circulatory System 10.1 2 ARTERIES Arteries-blood vessels that carry blood away from the heart Thick walls Inner & Outer layers: connective tissue Middle layers are muscle and elastic connective tissue
1 Circulatory System 10.1 2 ARTERIES Arteries-blood vessels that carry blood away from the heart Thick walls Inner & Outer layers: connective tissue Middle layers are muscle and elastic connective tissue
Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies
 Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies THIRD EDITION CHAPTER 27 The Cardiovascular System Lesson 1: Overview of the Cardiovascular System Lesson Objectives Upon
Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies THIRD EDITION CHAPTER 27 The Cardiovascular System Lesson 1: Overview of the Cardiovascular System Lesson Objectives Upon
Cardiology/Cardiothoracic
 Cardiology/Cardiothoracic ICD-9-CM to ICD-10-CM Code Mapper 800-334-5724 www.contexomedia.com 2013 ICD-9-CM 272.0 Pure hypercholesterolemia 272.2 Mixed hyperlipidemia 272.4 Other and hyperlipidemia 278.00
Cardiology/Cardiothoracic ICD-9-CM to ICD-10-CM Code Mapper 800-334-5724 www.contexomedia.com 2013 ICD-9-CM 272.0 Pure hypercholesterolemia 272.2 Mixed hyperlipidemia 272.4 Other and hyperlipidemia 278.00
Ischemic Heart Diseases. Dr. Nabila Hamdi MD, PhD
 Ischemic Heart Diseases Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast the different types of angina regarding their pathogenesis, clinical manifestations and evolution. Discuss myocardial infarct,
Ischemic Heart Diseases Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast the different types of angina regarding their pathogenesis, clinical manifestations and evolution. Discuss myocardial infarct,
Chapter 16 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since 1900.
 1 2 3 4 5 6 Chapter 16 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since 1900. Accounts for of every 3 deaths Cardiovascular disease
1 2 3 4 5 6 Chapter 16 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since 1900. Accounts for of every 3 deaths Cardiovascular disease
CIRCULATORY SYSTEM TASK CARDS Worksheet
 CIRCULATORY SYSTEM TASK CARDS Worksheet Name: Date: Instructions: Put the answers to each task card in the numbered boxes on the chart. 1 a) left semilunar valve / aortic valve b) blood would backflow
CIRCULATORY SYSTEM TASK CARDS Worksheet Name: Date: Instructions: Put the answers to each task card in the numbered boxes on the chart. 1 a) left semilunar valve / aortic valve b) blood would backflow
Cardiac Emergencies. Jim Bennett Paramedic and Clinical Education Coordinator American Medical Response Spokane, Washington
 Cardiac Emergencies Jim Bennett Paramedic and Clinical Education Coordinator American Medical Response Spokane, Washington The Heart -------Aorta Pulmonary Veins---- Superior Vena Cava------ Right Atrium-----
Cardiac Emergencies Jim Bennett Paramedic and Clinical Education Coordinator American Medical Response Spokane, Washington The Heart -------Aorta Pulmonary Veins---- Superior Vena Cava------ Right Atrium-----
Blood Functions. Blood and the Cardiovascular System. Blood. Plasma. Erythrocytes (RBCs) Erythrocytes (RBCs) 4/7/2017
 Blood Functions Blood and the Cardiovascular System Distribution Delivery of oxygen and nutrients to all body cells; Transport of wastes to lungs and excretory organs; Transport of hormones Regulation
Blood Functions Blood and the Cardiovascular System Distribution Delivery of oxygen and nutrients to all body cells; Transport of wastes to lungs and excretory organs; Transport of hormones Regulation
Cardiovascular Disease
 Cardiovascular Disease Chapter 15 Introduction Cardiovascular disease (CVD) is the leading cause of death in the U.S. One American dies from CVD every 33 seconds Nearly half of all Americans will die from
Cardiovascular Disease Chapter 15 Introduction Cardiovascular disease (CVD) is the leading cause of death in the U.S. One American dies from CVD every 33 seconds Nearly half of all Americans will die from
Circulatory System Notes
 Circulatory System Notes Functions of Circulatory System A. Transports B. Transports C. Transports D. Transports E. of fluids F. G. Regulate temperature H. Blood clotting Characteristics of various blood
Circulatory System Notes Functions of Circulatory System A. Transports B. Transports C. Transports D. Transports E. of fluids F. G. Regulate temperature H. Blood clotting Characteristics of various blood
Coronary Heart Disease. Raja Nursing Instructor RN, DCHN, Post RN. BSc.N
 Coronary Heart Disease Raja Nursing Instructor RN, DCHN, Post RN. BSc.N 31/03/2016 Objectives Define coronary heart disease (CHD). Identify the causes and risk factors of CHD Discuss the pathophysiological
Coronary Heart Disease Raja Nursing Instructor RN, DCHN, Post RN. BSc.N 31/03/2016 Objectives Define coronary heart disease (CHD). Identify the causes and risk factors of CHD Discuss the pathophysiological
1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary.
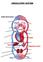 CIRCULATORY SYSTEM 1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary. 2. Capillary beds are equipped with
CIRCULATORY SYSTEM 1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary. 2. Capillary beds are equipped with
Circulatory System Review
 Circulatory System Review 1. Know the diagrams of the heart, internal and external. a) What is the pericardium? What is myocardium? What is the septum? b) Explain the 4 valves of the heart. What is their
Circulatory System Review 1. Know the diagrams of the heart, internal and external. a) What is the pericardium? What is myocardium? What is the septum? b) Explain the 4 valves of the heart. What is their
Cardiovascular. Function of the cardiovascular system is to transport blood containing: Nutrients Waste Hormones Immune cells Oxygen
 Cardiovascular The Cardiovascular System - Arteries Arteries Cardiovascular System Function of the cardiovascular system is to transport blood containing: Carry blood away from heart Carotid arteries Deliver
Cardiovascular The Cardiovascular System - Arteries Arteries Cardiovascular System Function of the cardiovascular system is to transport blood containing: Carry blood away from heart Carotid arteries Deliver
1/3/2008. Karen Burke Priscilla LeMone Elaine Mohn-Brown. Medical-Surgical Nursing Care, 2e Karen Burke, Priscilla LeMone, and Elaine Mohn-Brown
 Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 26 Caring for Clients with Coronary Heart Disease and Dysrhythmias Coronary Heart Disease (CHD) Leading
Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 26 Caring for Clients with Coronary Heart Disease and Dysrhythmias Coronary Heart Disease (CHD) Leading
MI Acute occlusion of the proximal left anterior descending (LAD) artery is the cause of 40% to 50% of all MIs. *
 MI *33% -50% die before hospital lethal arrhythmia Sudden Cardiac Death. * Arrhythmias are caused by electrical abnormalities of the ischemic myocardium and conduction system. *Acute occlusion of the proximal
MI *33% -50% die before hospital lethal arrhythmia Sudden Cardiac Death. * Arrhythmias are caused by electrical abnormalities of the ischemic myocardium and conduction system. *Acute occlusion of the proximal
Anatomy of the Heart and the. ICD-10 Codes
 Anatomy of the Heart and the Diseases ICD-10 Codes Sharon J. Oliver CPC, CPMA, CPC-I All Rights Reserved 1 Anatomy of the Heart Pulmonary Tricuspid (AV) Valve Mitral Aortic Semilunar Valve Chordae Tendineae
Anatomy of the Heart and the Diseases ICD-10 Codes Sharon J. Oliver CPC, CPMA, CPC-I All Rights Reserved 1 Anatomy of the Heart Pulmonary Tricuspid (AV) Valve Mitral Aortic Semilunar Valve Chordae Tendineae
Disturbance of Circulation Hemodynamic Disorder
 Disturbance of Circulation Hemodynamic Disorder 2/17/2017 By Dr. Hemn Hassan Othman PhD, Pathology Fall 2016 1 Thrombosis Definition: Thrombosis is the formation of solid or semisolid blood clot within
Disturbance of Circulation Hemodynamic Disorder 2/17/2017 By Dr. Hemn Hassan Othman PhD, Pathology Fall 2016 1 Thrombosis Definition: Thrombosis is the formation of solid or semisolid blood clot within
The Circulatory System (p )
 The Circulatory System (p. 268-281) How Does Gravity Affect Blood Circulation? As with all land animals, the giraffe and the corn snake are constantly subject to the force of gravity The circulatory system
The Circulatory System (p. 268-281) How Does Gravity Affect Blood Circulation? As with all land animals, the giraffe and the corn snake are constantly subject to the force of gravity The circulatory system
A DAYS CARDIOVASCULAR UNIT GUIDE DUE WEDNESDAY 4/12
 A DAYS CARDIOVASCULAR UNIT GUIDE DUE WEDNESDAY 4/12 MONDAY TUESDAY WEDNESDAY THURSDAY FRIDAY 3/20 - B 3/21 - A 3/22 - B 3/23 - A 3/24 - B 3/27 - A Dissection Ethics Debate 3/28 - B 3/29 - A Intro to Cardiovascular
A DAYS CARDIOVASCULAR UNIT GUIDE DUE WEDNESDAY 4/12 MONDAY TUESDAY WEDNESDAY THURSDAY FRIDAY 3/20 - B 3/21 - A 3/22 - B 3/23 - A 3/24 - B 3/27 - A Dissection Ethics Debate 3/28 - B 3/29 - A Intro to Cardiovascular
Cardiovascular and Respiratory Disorders
 Cardiovascular and Respiratory Disorders Blood Pressure Normal blood pressure is 120/80 mmhg (millimeters of mercury) Hypertension is when the resting blood pressure is too high Systolic BP is 140 mmhg
Cardiovascular and Respiratory Disorders Blood Pressure Normal blood pressure is 120/80 mmhg (millimeters of mercury) Hypertension is when the resting blood pressure is too high Systolic BP is 140 mmhg
Cardiovascular disease
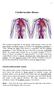 1 Cardiovascular disease The essential components of the human cardiovascular system are the heart, blood, and blood vessels. It includes: the pulmonary circulation, a "loop" through the lungs where blood
1 Cardiovascular disease The essential components of the human cardiovascular system are the heart, blood, and blood vessels. It includes: the pulmonary circulation, a "loop" through the lungs where blood
Ch 19: Cardiovascular System - The Heart -
 Ch 19: Cardiovascular System - The Heart - Give a detailed description of the superficial and internal anatomy of the heart, including the pericardium, the myocardium, and the cardiac muscle. Trace the
Ch 19: Cardiovascular System - The Heart - Give a detailed description of the superficial and internal anatomy of the heart, including the pericardium, the myocardium, and the cardiac muscle. Trace the
The Cardiovascular System
 Essentials of Human Anatomy & Physiology Elaine N. Marieb Slides 11.1 11.19 Seventh Edition Chapter 11 The Cardiovascular System Functions of the Cardiovascular system Function of the heart: to pump blood
Essentials of Human Anatomy & Physiology Elaine N. Marieb Slides 11.1 11.19 Seventh Edition Chapter 11 The Cardiovascular System Functions of the Cardiovascular system Function of the heart: to pump blood
Pathology of pulmonary vascular disease. Dr.Ashraf Abdelfatah Deyab. Assistant Professor of Pathology Faculty of Medicine Almajma ah University
 Pathology of pulmonary vascular disease Dr.Ashraf Abdelfatah Deyab Assistant Professor of Pathology Faculty of Medicine Almajma ah University Pulmonary vascular disease Type of pulmonary circulation: Types
Pathology of pulmonary vascular disease Dr.Ashraf Abdelfatah Deyab Assistant Professor of Pathology Faculty of Medicine Almajma ah University Pulmonary vascular disease Type of pulmonary circulation: Types
Clinical Cardiac A & P Dr. Gary Mumaugh
 Clinical Cardiac A & P Dr. Gary Mumaugh Coronary Artery Disease Pathophysiology o Atherosclerotic disease and coronary artery disease accounts for 45% of all USA deaths o 50% of female deaths are cardiovascular
Clinical Cardiac A & P Dr. Gary Mumaugh Coronary Artery Disease Pathophysiology o Atherosclerotic disease and coronary artery disease accounts for 45% of all USA deaths o 50% of female deaths are cardiovascular
Cardiovascular System. Biology 105 Lecture 15 Chapter 12
 Cardiovascular System Biology 105 Lecture 15 Chapter 12 Outline I. Functions of cardiovascular system II. Components of the cardiovascular system: I. Blood vessels II. Heart III. Regulation of the heartbeat
Cardiovascular System Biology 105 Lecture 15 Chapter 12 Outline I. Functions of cardiovascular system II. Components of the cardiovascular system: I. Blood vessels II. Heart III. Regulation of the heartbeat
Heart Problems and Treatments
 Heart Problems and Treatments A healthy heart Your heart s main functions are to receive used blood from your body and pump fresh oxygen rich blood to nourish your body. To do this well: The heart muscle
Heart Problems and Treatments A healthy heart Your heart s main functions are to receive used blood from your body and pump fresh oxygen rich blood to nourish your body. To do this well: The heart muscle
The Mammalian Circulatory System
 The Mammalian Heart The Mammalian Circulatory System Recall: What are the 3 cycles of the mammalian circulatory system? What are their functions? What are the three main vessel types in the mammalian circulatory
The Mammalian Heart The Mammalian Circulatory System Recall: What are the 3 cycles of the mammalian circulatory system? What are their functions? What are the three main vessel types in the mammalian circulatory
Cardiovascular System and Health. Chapter 15
 Cardiovascular System and Health Chapter 15 Cardiovascular Disease Leading cause of death in U.S. Claims 1 life every 43 seconds Often, the first sign is a fatal heart attack Death Rates #1 CVD #2 Cancer
Cardiovascular System and Health Chapter 15 Cardiovascular Disease Leading cause of death in U.S. Claims 1 life every 43 seconds Often, the first sign is a fatal heart attack Death Rates #1 CVD #2 Cancer
The Heart and Heart Disease
 The Heart and Heart Disease Illustration of the heart by Leonardo DaVinci heart-surgeon.com/ history.html 2/14/2010 1 I. Location, Size and Position of the Heart A. Triangular organ located 1. of mass
The Heart and Heart Disease Illustration of the heart by Leonardo DaVinci heart-surgeon.com/ history.html 2/14/2010 1 I. Location, Size and Position of the Heart A. Triangular organ located 1. of mass
Aneurysms & a Brief Discussion on Embolism
 Aneurysms & a Brief Discussion on Embolism Aneurysms, overview = congenital or acquired dilations of blood vessels or the heart True aneurysms -involve all three layers of the artery (intima, media, and
Aneurysms & a Brief Discussion on Embolism Aneurysms, overview = congenital or acquired dilations of blood vessels or the heart True aneurysms -involve all three layers of the artery (intima, media, and
results in stenosis or insufficiency (regurgitation or incompetence), or both.
 results in stenosis or insufficiency (regurgitation or incompetence), or both. The outcome of valvular disease depends on : 1-the valve involved 2-the degree of impairment 3-the cause of its development
results in stenosis or insufficiency (regurgitation or incompetence), or both. The outcome of valvular disease depends on : 1-the valve involved 2-the degree of impairment 3-the cause of its development
The Cardiovascular System
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Cardiovascular System 11 PART A The Cardiovascular System A closed system of the heart and blood
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Cardiovascular System 11 PART A The Cardiovascular System A closed system of the heart and blood
2
 1 2 Although the term "cardiomyopathy" could theoretically apply to almost any disease affecting the heart, it is usually reserved for "severe myocardial disease leading to heart failure".cardiomyopathy
1 2 Although the term "cardiomyopathy" could theoretically apply to almost any disease affecting the heart, it is usually reserved for "severe myocardial disease leading to heart failure".cardiomyopathy
AN ATOMY OF THE CARDIOVASCULAR SYSTEM
 Student Name CHAPTER 18 AN ATOMY OF THE CARDIOVASCULAR SYSTEM T he heart is actually two pumps one moves blood to the lungs, the other pushes it out into the body. These two functions seem rather elementary
Student Name CHAPTER 18 AN ATOMY OF THE CARDIOVASCULAR SYSTEM T he heart is actually two pumps one moves blood to the lungs, the other pushes it out into the body. These two functions seem rather elementary
Hemodynamic Disorders, Thrombosis, and Shock. Richard A. McPherson, M.D.
 Hemodynamic Disorders, Thrombosis, and Shock Richard A. McPherson, M.D. Edema The accumulation of abnormal amounts of fluid in intercellular spaces of body cavities. Inflammation and release of mediators
Hemodynamic Disorders, Thrombosis, and Shock Richard A. McPherson, M.D. Edema The accumulation of abnormal amounts of fluid in intercellular spaces of body cavities. Inflammation and release of mediators
Objectives. Identify early signs and symptoms of Acute Coronary Syndrome Initiate proper protocol for ACS patient 10/2013 2
 10/2013 1 Objectives Identify early signs and symptoms of Acute Coronary Syndrome Initiate proper protocol for ACS patient 10/2013 2 Purpose of this Education Module: Chest Pain Center Accreditation involves
10/2013 1 Objectives Identify early signs and symptoms of Acute Coronary Syndrome Initiate proper protocol for ACS patient 10/2013 2 Purpose of this Education Module: Chest Pain Center Accreditation involves
Chapter 14. Cardiovascular Emergencies
 Chapter 14 Cardiovascular Emergencies Introduction (1 of 2) Cardiovascular disease has been leading killer of Americans since 1900. Accounts for 1 of every 2.8 deaths Introduction (2 of 2) EMS can help
Chapter 14 Cardiovascular Emergencies Introduction (1 of 2) Cardiovascular disease has been leading killer of Americans since 1900. Accounts for 1 of every 2.8 deaths Introduction (2 of 2) EMS can help
Section 5.1 The heart and heart disease
 Section 5.1 The heart and heart disease Mammals are too large to rely on diffusion. They need a circulatory system to move substances around the body. Blood moves down pressure gradients, from high to
Section 5.1 The heart and heart disease Mammals are too large to rely on diffusion. They need a circulatory system to move substances around the body. Blood moves down pressure gradients, from high to
The Cardiovascular and Lymphatic Systems Cardiovascular System Blood Vessels Blood Vessels Arteries Arteries Arteries
 CH 12 The Cardiovascular and s The Cardiovascular and s OUTLINE: Cardiovascular System Blood Vessels Blood Pressure Cardiovascular System The cardiovascular system is composed of Blood vessels This system
CH 12 The Cardiovascular and s The Cardiovascular and s OUTLINE: Cardiovascular System Blood Vessels Blood Pressure Cardiovascular System The cardiovascular system is composed of Blood vessels This system
Chapter 27 -The Heart & Blood Vessels
 Chapter 27 -The Heart & Blood Vessels 3.2 Learning Objectives 3.2.2 Organisational Complexity of the human 1. Describe the structures and organisation of tissues in the closed circulatory system. 2. Discuss
Chapter 27 -The Heart & Blood Vessels 3.2 Learning Objectives 3.2.2 Organisational Complexity of the human 1. Describe the structures and organisation of tissues in the closed circulatory system. 2. Discuss
Right-Sided Congestive Heart Failure Basics
 Right-Sided Congestive Heart Failure Basics OVERVIEW Failure of the right side of the heart to pump blood at a sufficient rate to meet the needs of the body or to prevent blood from pooling within the
Right-Sided Congestive Heart Failure Basics OVERVIEW Failure of the right side of the heart to pump blood at a sufficient rate to meet the needs of the body or to prevent blood from pooling within the
Types of circulatory systems
 Types of circulatory systems Open system Mostly invertebrates Low pressure Haemocoel Suitable for small organisms Closed system Vertebrates High pressure Blood remains in blood vessels Separate tissue
Types of circulatory systems Open system Mostly invertebrates Low pressure Haemocoel Suitable for small organisms Closed system Vertebrates High pressure Blood remains in blood vessels Separate tissue
37 1 The Circulatory System
 H T H E E A R T 37 1 The Circulatory System The circulatory system and respiratory system work together to supply cells with the nutrients and oxygen they need to stay alive. a) The respiratory system:
H T H E E A R T 37 1 The Circulatory System The circulatory system and respiratory system work together to supply cells with the nutrients and oxygen they need to stay alive. a) The respiratory system:
4. The two inferior chambers of the heart are known as the atria. the superior and inferior vena cava, which empty into the left atrium.
 Answer each statement true or false. If the statement is false, change the underlined word to make it true. 1. The heart is located approximately between the second and fifth ribs and posterior to the
Answer each statement true or false. If the statement is false, change the underlined word to make it true. 1. The heart is located approximately between the second and fifth ribs and posterior to the
The Heart and Cardiovascular System
 The Heart and Cardiovascular System What you will learn The location of the heart 3 layers and covering of the heart Explain the function of the heart as 2 separate pumps Identify the 4 chambers of the
The Heart and Cardiovascular System What you will learn The location of the heart 3 layers and covering of the heart Explain the function of the heart as 2 separate pumps Identify the 4 chambers of the
Cardiovascular System
 Cardiovascular System Blood vessels, heart and blood Functions Transport oxygen, nutrients, waste, hormones White blood cells fighting disease Temperature regulation Blood vessels; Arteries Arteries carry
Cardiovascular System Blood vessels, heart and blood Functions Transport oxygen, nutrients, waste, hormones White blood cells fighting disease Temperature regulation Blood vessels; Arteries Arteries carry
The Cardiovascular System
 The Cardiovascular System https://www.youtube.com/watch?v=ohmmtqkgs50 Human Anatomy & Physiology P. Wilson 1 Introduction The functions of the cardiovascular system are: to bring oxygen & nutrients to
The Cardiovascular System https://www.youtube.com/watch?v=ohmmtqkgs50 Human Anatomy & Physiology P. Wilson 1 Introduction The functions of the cardiovascular system are: to bring oxygen & nutrients to
MYOCARDIALINFARCTION. By: Kendra Fischer
 MYOCARDIALINFARCTION By: Kendra Fischer Outline Definition Epidemiology Clinical Aspects Treatment Effects of Exercise Exercise Testing Exercise Rx Summary and Conclusions References Break it down MYOCARDIAL
MYOCARDIALINFARCTION By: Kendra Fischer Outline Definition Epidemiology Clinical Aspects Treatment Effects of Exercise Exercise Testing Exercise Rx Summary and Conclusions References Break it down MYOCARDIAL
The production of murmurs is due to 3 main factors:
 Heart murmurs The production of murmurs is due to 3 main factors: high blood flow rate through normal or abnormal orifices forward flow through a narrowed or irregular orifice into a dilated vessel or
Heart murmurs The production of murmurs is due to 3 main factors: high blood flow rate through normal or abnormal orifices forward flow through a narrowed or irregular orifice into a dilated vessel or
