Safety and Efficacy of Endoscopic Ultrasound-Guided Drainage of Pancreatic Fluid Collections With Lumen-Apposing Covered Self-Expanding Metal Stents
|
|
|
- Martin Mosley
- 5 years ago
- Views:
Transcription
1 All studies published in Clinical Gastroenterology and Hepatology are embargoed until 3PM ET of the day they are published as corrected proofs on-line. Studies cannot be publicized as accepted manuscripts or uncorrected proofs. Clinical Gastroenterology and Hepatology 2014;-: Q26 Q7 Q8 Q9 Q10 Safety and Efficacy of Endoscopic Ultrasound-Guided Drainage of Pancreatic Fluid Collections With Lumen-Apposing Covered Self-Expanding Metal Stents Raj J. Shah,* Janak N. Shah, Irving Waxman, Thomas E. Kowalski, k Andres Sanchez-Yague, Jose Nieto, # Brian C. Brauer,* Monica Gaidhane,** and Michel Kahaleh** *Gastroenterology and Hepatology, University of Colorado Anschutz Medical Campus, Aurora, Colorado; Interventional Endoscopy Services, California Pacific Medical Center, San Francisco, California; Center for Endoscopic Research and Therapeutics, The University of Chicago Medicine and Biological Sciences, Chicago, Illinois; k Gastroenterology and Hepatology, Thomas Jefferson University, Philadelphia, Pennsylvania; Gastroenterology & Hepatology, Hospital Costa del Sol, Marbella, Spain; # Gastroenterology and Hepatology, Borland-Groover Clinic, Jacksonville, Florida; **Gastroenterology and Hepatology, Weill Cornell Medical College, New York, New York BACKGROUND & AIMS: METHODS: RESULTS: CONCLUSIONS: Plastic stents, placed via endoscopy to drain pancreatic fluid collections (PFCs), require repeat access. Covered metal stents are larger in diameter and can be inserted in a single step, but can migrate. We evaluated the safety and efficacy of a lumen-apposing, covered, self-expanding metal stent (LACSEMS) for PFC drainage. We performed a prospective study of the outcomes of stent placement in 33 patients (18 men; age, y; 28 with chronic pancreatitis) with symptomatic pancreatic pseudocysts and walled-off necrosis ( 6 cm with 70% fluid content). Subjects were enrolled at 7 tertiary care centers (6 in the United States and 1 in Europe) from October 2011 through August Cystenterostomies were created based on endoscopist preference. Safety outcomes included infection, bleeding, perforation, tissue injury, and stent migration. Efficacy end points included LACSEMS placement, patency, and removal, as well as 50% or more reduction in PFCs. The mean size of the patients PFCs was cm. LACSEMSs were placed successfully via endoscopic ultrasound guidance in 30 patients (91%); the remaining 3 patients received 2 double-pigtail stents. One subject could not be evaluated because of a pseudoaneurysm. In the patients receiving LACSEMS, PFCs resolved in 27 of 29 (93%). Overall, PFCs resolved in 30 of 33 patients (91%). Endoscopic debridement through the LACSEMS was conducted in 11 subjects. Complications (15%) included abdominal pain (n [ 3), spontaneous stent migration, back pain (n [ 1), access-site infection, and stent dislodgement (n [ 1). LACSEMS were placed successfully in 91% of subjects with PFCs. Overall, 93% had PFC resolution. Advantages of LACSEMSs over other stents include single-step deployment and the ability to perform endoscopic debridement with minimal stent migration. Clinicaltrials.gov: NCT Keywords: Pseudocyst Drainage; EUS; Axios; Clinical Trial. fluid collections (PFCs) include acute Pperipancreatic fluid collections, pancreatic pseudocysts, acute necrotic collections, and walled-off pancreatic necrosis (WON) that are encapsulated collections with necrosis after 4 weeks. Pancreatic pseudocysts (PPs) can result from pancreatic inflammation resulting from pancreatitis, trauma, or pancreatic ductal obstruction. 1,2 The incidence of pseudocysts in acute pancreatitis is 5% to 16% and 20% to 40% in chronic pancreatitis. Symptomatic PFCs may be treated surgically, percutaneously, or endoscopically. 3 5 Surgery is associated with higher rates of morbidity (7% 37%) and mortality (6%), 6 whereas the external catheter in Abbreviations used in this paper: EUS, endoscopic ultrasound; LACSEMS, lumen-apposing, covered, self-expanding metal stent; PFC, pancreatic fluid collections; PP, pancreatic pseudocyst; WON, walled-off necrosis by the AGA Institute /$ Q
2 2 Shah et al Clinical Gastroenterology and Hepatology Vol. -, No Q12 Q13 percutaneous treatment increases the risk of infection or the formation of a pancreaticocutaneous fistula. 7 9 With more recent technical advances and experience, endoscopic drainage now is widely accepted and has replaced surgery as the first-line therapy for pseudocyst drainage owing to its less invasive nature, shorter recovery times, lower cost, and lower complication rates. 9 The median rates of endoscopic PFC drainage for technical success, PFC resolution, complications, and recurrence associated with transmural pseudocyst drainage were 93.8%, 87.5%, 16.9%, and 7.5%, respectively Under endoscopic ultrasound guidance, the clinical success rate for pancreatic fluid collection drainage was 89.14%, with a complication rate of 10.7% (range, 0% 26.3%). 19 The endoscopic transmural drainage procedure involves the following 3 main steps: (1) accessing the pseudocyst by creating a tract, (2) tract dilation, and (3) placing a drainage device. Plastic pigtail stents of varying sizes (7F 10F) and covered self-expanding metal stents are used as the drainage device Although the pigtail feature of the plastic stents prevents migration, their narrow lumen may cause premature occlusion requiring frequent stent exchanges or placement of additional stents. 25 Fully covered, self-expanding biliary metal stents offer a larger-diameter lumen for a more efficient and shorter duration of drainage and longer patency. 10,13 However, they are tubular and may migrate, 3 resulting in inefficient drainage, content leakage, retrieval and replacement of migrated stent, and possible mucosal injury. Recently, a study conducted by Itoi et al 27 reported the use of a novel barbell-shaped, lumen-apposing, covered, self-expanding metal stent (LACSEMS). The device allows endoscopic ultrasound (EUS)-guided, transmural endoscopic drainage of pancreatic pseudocysts into the upper gastrointestinal tract through its large lumen and its ability to appose the PFC wall to the stomach or duodenal wall. The LACSEMS were placed successfully in 15 patients, with no pseudocyst recurrence during the 11.4-month median follow-up period and only 1 stent migration. Gornals et al 28 compared 9 PFC patients with LAC- SEMS with 10 previously consecutively recruited PFC patients with plastic stents and reported similar technical (88.8%) and clinical (100%) success rates. However, the plastic stent group reported a higher number of stents (n ¼ 15) and a higher median procedure time ( min), 2 migrations, 2 recurrences, and 2 complications. The aim of this multicenter, single-arm study was to evaluate the safety and efficacy of the LACSEMS for the transmural drainage of symptomatic PPs and WON. Methods The study was a prospective, multicenter, nonblinded, single-arm study conducted from October 2011 to August 2013 at 7 tertiary care centers. The trial was performed under an Investigation Device Exemption seeking Food and Drug Administration clearance. The primary end point was achievement of PFC resolution, defined as reduction in PFC size to 50% or less than initial size, after 30 or 60 days after LACSEMS placement. Device Description The LACSEMS (Axios; Xlumena, Mountain View, CA) consists of a barbell-shaped, flexible, fully covered, selfexpanding nitinol stent housed within a catheter-based delivery system. The stents are available in 2 sizes (lumen diameter length): mm and mm. The 10-mm saddle length is designed to appose the stomach or duodenum to the PFC wall. The stent was intended for temporary implantation (up to 60 days) and was removed upon confirmation of PFC resolution. Operator Training Advanced endoscopists with experience in therapeutic endoscopy and endosonography underwent a training session consisting of didactic review and performance of the procedure on an animal model. A LACSEMS placement under EUS guidance and removal was performed. Patient Screening and Intervention Adults (age, y) with symptomatic PPs or WON meeting all of the following criteria were included: 6 cm or greater diameter (based on the computed tomography scan or transabdominal ultrasound), adherence to bowel wall, and 70% or more fluid content. Cystic neoplasms and immature pseudocysts were excluded. Subjects were enrolled in the trial within 30 days of screening. Radiographic evaluation (abdominal computed tomography, transabdominal ultrasound, or magnetic resonance imaging) was conducted within 30 days of intervention to characterize the PFC size, fluid content, and relationship to the bowel wall. Radiographic evaluation was conducted 30 days after stent placement and repeated at 60 days after the procedure only if the PFC was unresolved at 30 days. Intervention. The procedure was performed under monitored or general anesthesia using a therapeutic linear array echoendoscope (Olympus Medical, Tokyo, Japan). Endoscopic ultrasound was performed to locate the PFC, measure and confirm the size, assess the fluid content, and evaluate bowel wall adherence. An access tract was created (Figure 1A) using conventional endoscopic tools as per the endoscopist s preference (eg, a fine-needle aspiration needle, Q14 needle knife, or cystotome) followed by placement of a
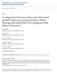
3 Metal Stent For Pancreatic Fluid Collections 3 Q print & web 4C=FPO Q15 Q16 Figure 1. (A) Endoscopic ultrasound showing needle puncture of the pancreatic pseudocyst. (B) Fluoroscopic image showing fully deployed LACSEMS. (C) Endoscopic image showing pus draining through the LACSEMS. (D) Endoscopic image showing pancreatic pseudocyst fluid drainage through the LACSEMS. Q inch guidewire. The needle was removed, and the tract was dilated using either a dilating bougie (6F 10F Soehendra dilator; Cook Medical) or a dilating balloon (4- or 6-mm Hurricane; Boston Scientific, Natick, MA). The selection of a 10-mm or 15-mm stent diameter was based on the contents of the PFC and the presence of solid debris identified on EUS. A 15-mm diameter was preferred for PFCs containing solids or necrotic material, allowing for subsequent debridement, irrigation, and cystoscopy. The LACSEMS was inserted over a guidewire, and the distal stent flange was deployed. After the stent s distal flange position against the inner pseudocyst wall was verified via EUS, the proximal flange was deployed within either the stomach or the duodenum under endoscopic visualization (Figure 1B). Visualization of drainage through the stent was considered successful placement (Figure 1C and D). After deployment, balloon dilation (up to 10 mm) through the stent was performed per the endoscopist s preference. Necrosectomy sessions for walled-off necrosis were performed at the discretion of the endoscopist, typically every 2 days until complete clearance of the necrosis. PFC resolution was assessed at 30 or 60 days. If resolved, a snare large enough to fit over the proximal flange of the LACSEMS was placed and then tightened until the stent lumen (saddle) collapsed, enabling removal of the stent during endoscopy. Antibiotic therapy was initiated preoperatively, after the placement procedure patients were required to receive ciprofloxacin 500 mg orally twice daily (or acceptable alternative antibiotic therapy) until 1 week after stent removal. Inspection of flow, tissue changes, and endoscopic documentation were obtained at the time of stent placement and removal. A follow-up office visit was conducted 7 days after stent removal. Endoscopy was performed at 7 days only if ulceration was noted at the site of stent removal during the stent removal visit. Nonserious and serious adverse events were monitored for up to 6 months after stent removal and were determined either to be related or unrelated to stent implantation and/or the endoscopic procedure. Analyses A review of published endoscopic transmural PFC drainage data within the past 5 years was performed to discern the specific complication rates (0% to up to 44.4%) and technical/clinical success rates (80% 100%) to calculate a sample size of 30 subjects based on safety and effectiveness rates. Thirty-three subjects were enrolled to account for drop-out and loss to follow-up evaluation. Effectiveness end points included the following: stent lumen patency at 30 days and/or 60 days, stent removability at 30 days and/or 60 days, technical success, and PFC resolution. The safety end point was defined as freedom from major complications through the 1-week duration after stent removal study period. The end points were analyzed for both the intent-totreat and per-protocol populations. PFC resolution was defined as at least a 50% decrease in PP size, based on radiographic analysis at 30 days and/or 60 days. Technical success was defined as placement of the LACSEMS and removal of the LACSEMS using a standard endoscopic snare. The primary end points were evaluated through 1 week after stent removal; overall safety was captured as adverse events and continued until study termination. Evaluations were performed at baseline, the 30-day and/or 60-day visits, 1 week after stent removal, and at 3 and/or 6 months after stent removal. All authors had access to the study data and reviewed and approved the final manuscript. Results Demographics From October 2011 to August 2013, there were 33 patients (18 men; age, y) enrolled. Etiologies included the following: pancreatitis of unknown etiology, 45% (n ¼ 15); gallstone pancreatitis, 18% (n ¼ 6); alcohol-induced pancreatitis, 18% (n ¼ 6); postsurgical pancreatitis, 12% (n ¼ 4); and other indications, 6% (n ¼ 2) (Table 1). Gallstone disease and alcohol abuse were present in 20% of subjects. Two subjects had
4 4 Shah et al Clinical Gastroenterology and Hepatology Vol. -, No Table 1. Demographics of Subjects Characteristics ITT (n ¼ 33) previous percutaneous drainage and 4 had previous endoscopic drainage for pancreatic pseudocysts. Efficacy Data Per protocol (n ¼ 29) Q23 Sex Male 54.5% (18/33) 51.7% (15/29) Female 45.5% (15/33) 48.3% (14/29) Age, y Mean SD, n (33) (29) Range PFC etiology Pancreatitis of 45.45% (15/33) 52% (15/29) unknown etiology Gallstone pancreatitis 18.2% (6/33) 17% (5/29) Alcohol-induced pancreatitis 182% (6/33) 21% (6/29) Postsurgical pancreatitis 12.1% (4/33) 7% (2/29) Other a 6.05% (2/33) 3% (1/29) PFC symptoms Abdominal pain 75.8% (25/33) 79.3% (23/29) Nausea 39.4% (13/33) 44.8% (13/29) Vomiting 30.3% (10/33) 34.5% (10/29) Distention 30.3% (10/33) 34.5% (10/29) Other 15.2% (5/33) 13.8% (4/29) Previous PFC intervention 18.2% (6/33) 20.7% (6/29) ITT, intention to treat. a Other etiology: possibly medication-related and intraductal papillary mucinous neoplasm. LACSEMSs were placed successfully in 30 of 33 (91%) patients with no intraoperative complications (Table 2). The remaining 3 patients received doublepigtail stents. LACSEMS placed included 18 of the mm size and 12 of the mm size. Stent patency was confirmed with drainage visualized for all stents placed. Unsuccessful LACSEMS deployment in 3 subjects was caused by stent malposition (n ¼ 2) and delivery handle malfunction (n ¼ 1). The procedure time was minutes. The total fluoroscopy time was minutes (n ¼ 21). The mean length of hospital stay was days (n ¼ 29). Eleven of 29 subjects were discharged the same day. One subject was not evaluable because of a pseudoaneurysm and had plastic stents and a nasocystic tube placed in an additional puncture site, alongside the LACSEMS to drain blood clots. The LACSEMS was removed after 79 days without any further complications. For the rest of the 29 LACSEMS patients, stents remained implanted for 31 days in 20 patients (9.9 d) and for 67 days in 9 patients (10.8 d). Lumen patency was 93% (27 of 29) at stent removal. Three subjects had debris, resulting in partial occlusion at 30 days or earlier after placement. Eleven WON subjects underwent a total of 22 direct endoscopic debridement sessions through the indwelling LACSEMS and PFC resolution was achieved in 10 subjects. Seven of the 22 debridement procedures were performed when the subject showed septic symptoms such as fever (n ¼ 3), abdominal pain (n ¼ 4), or infection (n ¼ 2). The LACSEMS removal success rate was 96.7% (29 of 30). Tissue changes after stent removal included mild hyperplastic tissue reaction (n ¼ 8), minor self-limiting bleeding (n ¼ 2), mucosal overgrowth (n ¼ 1), and granulation tissue (n ¼ 1). In all cases, LACSEMS removal proceeded with no clinical sequelae. During subsequent endoscopies, 3 subjects had plastic stents placed through the LACSEMS for the following reasons: treatment of a collapsed pseudocyst wall onto the distal end of the LACSEMS before complete drainage, treatment of LACSEMS dislodgment after debridement, and treatment of partially occluded LACSEMS caused by necrosis. PFC resolution. Overall, PFC resolution was achieved in 30 of 33 (91%) subjects. Per-protocol PFC resolution was achieved in 27 of 29 (93%) subjects who received LACSEMSs, including subjects who had plastic stents through or alongside the LACSEMS. Ten of 29 LACSEMS subjects had repeat endoscopic interventions. Two of the 3 subjects who received plastic stents only achieved PFC resolution. The mean PFC size was cm. The PFC size decreased significantly (6.7 cm; 95% confidence interval, Table 2. Clinical Summary of Subjects Characteristics ITT (n ¼ 33) Per protocol (n ¼ 29) Target GI site Stomach body 81.8% (27/ 33) 82.8% (24/29) Q24 Stomach antrum 9.1% (3/33) 10.3% (3/29) Duodenal bulb 9.1% (3/33) 6.9% (2/29) Total scope in and scope out time, min Mean SD, n (32) (28) Range Total anesthesia time, min Mean SD, n (31) (27) Range PFC resolution overall 85% (28/33) a 93% (27/29) 30-day visit 73.3% (22/30) 75.9% (22/29) 60-day visit 80.0% (8/10) 77.8% (7/9) Technical success Stent placement 91% (30/33) 96.7% (29/30) Stent removal 96.7 (29/30) Lumen patency 30-day visit 93.1% (27/29) 92.9% (26/28) 60-day visit 90.0% (9/10) 88.9% (8/9) Complications 15.2% (5/33) 13.8% (4/29) GI, gastrointestinal. a Three patients did not receive LACSEMS and 2 patients did not meet the PFC resolution criteria
5 Metal Stent For Pancreatic Fluid Collections ; P <.0001) from baseline (10 4 cm) to 30 days after stent placement ( cm). For 10 subjects, the PP size was cm at 60 days. Safety Data One LACSEMS subject was not evaluable because of a pseudoaneurysm. One subject required stent removal at 21 days owing to partial debris occlusion. One subject with severe necrotizing pancreatitis had their LACSEMS dislodged inadvertently during debridement performed at 18 days. This patient had both percutaneous and subsequently surgical debridement, and is clinically well 30 months after enrollment. One subject experienced spontaneous stent migration at 43 days as a result of unknown causes. Complications were noted in 5 (15.2%) patients and included access-site infection (n ¼ 1), stent migration/ dislodgement (n ¼ 1), back pain (n ¼ 1), fever with prolonged hospitalization (n ¼ 1), and abdominal pain requiring endoscopy (n ¼ 1). Discussion Endoscopic drainage of pancreatic pseudocyst is now the preferred option at many tertiary centers. A randomized controlled trial by Varadarajulu et al 20 Q17 comparing endoscopic with surgical cystogastrostomy showed that endoscopic treatment was associated with shorter hospital stays, better physical and mental health of patients, and lower cost. Compared with conventional transmural drainage, EUS-guided drainage is beneficial in defining the characteristics of a PFC, especially if nonbulging, identifying intervening vasculature and ruling out malignancies. 18 A Q18 meta-analysis conducted by Panamonta et al 28 compared EUS-guided drainage with conventional transmural drainage and experienced a higher technical success rate for EUS-guided drainage compared with conventional transmural drainage. Conventionally, multiple plastic stents typically are placed to drain PFCs. 3,13,15 However, the migration rates, the smaller diameter, and the need for repeat guidewire access through the enterostomy for multiple stent placements, has necessitated alternative options such as Q19 placing metal stents to permit efficient drainage. Talreja et al 12 published a study on the efficacy of using fully covered metal stents with fins to drain PFCs. The study by Penn et al 30 placed double-pigtail plastic stents through off-label, biliary, fully covered, selfexpanding, biliary metal stents to anchor the metal stents and reduce migration and allow for drainage along the length of the plastic stents. Because of the barbell shape of the LACSEMS, the placement of plastic stents through the LACSEMS would not be required because the large diameter ensures apposition and a reduced risk of migration. In addition, luer-locking the delivery system to the echoendoscope working channel ensured single-step deployment. Antillon et al 20 and recently Mangiavillano et al 31 reported that single-step, EUS-guided drainage of PFC is more successful than a 2-step technique. We showed a technical success rate of 91% and a PFC resolution rate of 93%. Stent patency was 93% at the time of removal. Sixty-nine percent of the LACSEMS patients achieved PFC resolution at 30 days. The 3 unsuccessful LACSEMS placements may have been related to limited operator experience at the study onset and 1 device malfunction. Gornals et al 28 reported one unsuccessful attempt (n ¼ 9) and Itoi et al 27 reported none (n ¼ 20). It is likely that technical success will increase with additional experience and use. Itoi et al 27 also evaluated the LACSEMS for gallbladder drainage (n ¼ 5), with immediate resolution of acute cholecystitis after stent implantation. Turner et al 32 successfully used the LACSEMS for gallstone removal and cholecystoduodenal drainage in a patient with cholecystitis and unresectable cholangiocarcinoma. A distinct advantage of the anchoring design and large lumen diameter of this device is the ability to perform direct endoscopic necrosectomy through the stent using a standard 9.2-mm gastroscope while maintaining stent integrity, especially if the 15-mm diameter stent is used. In this study, we performed 22 debridement sessions in 11 WON patients. The large diameter enables endoscope advancement into the PFC for debris removal while the flanges keep the stent in place. Although our study was a large, multicenter, prospective assessment of the LACSEMS, it only evaluated a single cohort with no control arm. In conclusion, our study showed that the LACSEMS is safe and efficient for PFC drainage. Advantages of LAC- SEMSs compared with other stents include single-step deployment and the ability to perform direct endoscopic debridement with minimal stent migration. Whether the safety and efficacy of LACSEMS is superior to conventional double-pigtail plastic stents for pseudocyst drainage would require a prospective, randomized, controlled trial. Uncited References This section consists of references that are included in the reference list but are not cited in the article text. Please either cite each of these references in the text or, alternatively, delete it from the reference list. If you do not provide further instruction for this reference, we will retain it in its current form and publish it as an un-cited reference with your article. 26,29 References 1. Banks PA, Bollen TL, Dervenis C, et al. Classification of acute pancreatitis 2012: revision of the Atlanta classification and definitions by international consensus. Gut 2013;62: Q
6 6 Shah et al Clinical Gastroenterology and Hepatology Vol. -, No Kozerak RA. Endoscopic drainage of pancreatic pseudocysts. J Hepatobiliary Pancreat Surg 1997;4: Baron TH, Harewood GC, Morgan DE, et al. Outcome differences after endoscopic drainage of pancreatic necrosis, acute pancreatic pseudocysts, and chronic pancreatic pseudocysts. Gastrointest Endosc 2002;56: Hookey LC, Debroux S, Delhaye M, et al. Endoscopic drainage of pancreatic-fluid collections in 116 patients: a comparison of etiologies, drainage techniques, and outcomes. Gastrointest Endosc 2006;63: Varadarajulu S, Phadnis MA, Christein JD, et al. Multiple transluminal gateway technique for EUS-guided drainage of symptomatic walled-off pancreatic necrosis. Gastrointest Endosc 2011;74: Raijman I. Biliary and pancreatic stents. Gastrointest Endosc Clin N Am 2003;13: Varadarajulu S, Christein JD, Wilcox CM. Frequency of complications during EUS-guided drainage of pancreatic fluid collections in 148 consecutive patients. J Gastroenterol Hepatol 2011; 26: Varadarajulu S, Bang JY, Phadnis MA, et al. Endoscopic transmural drainage of peripancreatic fluid collections: outcomes and predictors of treatment success in 211 consecutive patients. J Gastrointest Surg 2011;15: Varadarajulu S, Bang JY, Sutton BS, et al. Equal efficacy of endoscopic and surgical cystogastrostomy for pancreatic pseudocyst drainage in a randomized trial. Gastroenterology 2013;145: Varadarajulu S, Wilcox CM. Endoscopic placement of permanent indwelling transmural stents in disconnected pancreatic duct syndrome: does benefit outweigh the risks? Gastrointest Endosc 2011;74: Kahaleh M, Hernandez AJ, Tokar J, et al. EUS-guided pancreaticogastrostomy: analysis of its efficacy to drain inaccessible pancreatic ducts. Gastrointest Endosc 2007;65: Varadarajulu S, Trevino JM. Review of EUS-guided pancreatic duct drainage (with video). Gastrointest Endosc 2009; 69:S200 S Talreja JP, Shami VM, Ku J, et al. Transenteric drainage of pancreatic-fluid collections with fully covered self-expanding metallic stents (with video). Gastrointest Endosc 2008;68: Hookey LC, Debroux S, Delhaye M, et al. Endoscopic drainage of pancreatic-fluid collections in 116 patients: a comparison of etiologies, drainage techniques, and outcomes. Gastrointest Endosc 2006;63: Giovannini M, Bernardini D, Seitz JF. Cystgastrostomy entirely performed under endosonography guidance for pancreatic pseudocyst: results in six patients. Gastrointest Endosc 1998; 48: Krüger M, Schneider AS, Manns MP, et al. nih.gov/pubmed?term¼meier%20pn%5bauthor%5d&cauthor¼ true&cauthor_uid¼ Endoscopic management of pancreatic pseudocysts or abscesses after an EUS-guided 1-step procedure for initial access. Gastrointest Endosc 2006;63: Cremer M, Deviere J, Engelholm L. Endoscopic management of cysts and pseudocysts in chronic pancreatitis: long-term followup after 7 years of experience. Gastrointest Endosc 1989;35: Catalano MF, Geenen JE, Schmalz MJ, et al. Treatment of pancreatic pseudocysts with ductal communication by transpapillary pancreatic duct endoprosthesis. Gastrointest Endosc 1995;42: Singhal S, Rotman SR, Gaidhane M, Kahaleh M. Pancreatic fluid collection drainage by endoscopic ultrasound: an update. Clin Endosc 2013;46: Q Antillon MR, Shah RJ, Stiegmann G, et al. Single-step endoscopic ultrasound (EUS)-guided drainage of simple and complicated pancreatic pseudocysts. Gastrointest Endosc 2006;63: Kahaleh M, Shami VM, Conway MR, et al. Comparison of EUS and conventional endoscopic drainage of pancreatic pseudocyst. Endoscopy 2006;38: Park DH, Lee SS, Moon SH, et al. Endoscopic ultrasoundguided versus conventional transmural drainage for pancreatic pseudocysts: a prospective randomized trial. Endoscopy 2009; 41: Johnson MD, Walsh M, Henderson JM, et al. Surgical versus nonsurgical management of pancreatic pseudocysts. J Clin Gastroenterol 2009;43: Itoi T, Itokawa F, Tsuchiya T, et al. EUS-guided pancreatic pseudocyst drainage: simultaneous placement of stents and nasocystic catheter using double-guidewire technique. Dig Endosc 2009;21(Suppl 1):S53 S Varadarajulu S, Tamhane A, Blakely J. Graded dilation technique for EUS-guided drainage of peripancreatic fluid collections: an assessment of outcomes and complications and technical proficiency. Gastrointest Endosc 2008;68: Diehl DL. The role of endoscopy in acute and chronic pancreatitis. In: Balthazar EJ, Megibow AJ, Pozzi Mucelli R, eds. Imaging of the pancreas. Berlin: Springer-Verlag, Itoi T, Binmoeller KF, Shah J, et al. Clinical evaluation of a novel lumen-apposing metal stent for endosonography-guided pancreatic pseudocyst and gallbladder drainage (with videos). Gastrointest Endosc 2012;75: Gornals JB, De la Serna-Higuera C, Sánchez-Yague A, et al. Endosonography-guided drainage of pancreatic fluid collections with a novel lumen-apposing stent. Surg Endosc 2013; 27: Panamonta N, Ngamruengphong S, Kijsirichareanchai K, et al. Endoscopic ultrasound-guided versus conventional transmural techniques have comparable treatment outcomes in draining pancreatic pseudocysts. Eur J Gastroenterol Hepatol 2012; 24: Penn DE, Draganov PV, Wagh MS, et al. Prospective evaluation of the use of fully covered self-expanding metal stents for EUSguided transmural drainage of pancreatic pseudocysts. Gastrointest Endosc 2012;76: Mangiavillano B, Arcidiacono PG, Masci E, et al. Single-step versus two-step endo-ultrasonography-guided drainage of pancreatic pseudocyst. J Dig Dis 2012;13: Turner BG, Rotman S, Paddu NU, et al. Cholecystoduodenal drainage and gallstone removal in a patient with cholecystitis and unresectable cholangiocarcinoma. Endoscopy 2013; 45(Suppl 2):E114 E115. Reprint requests Address requests for reprints to: Michel Kahaleh, MD, FASGE, Pancreas Program, Division of Gastroenterology and Hepatology, Weill Cornell Medical College, 1305 York Avenue, 4th Floor, New York, New York mkahaleh@gmail.com; fax: (646) Q
7 Metal Stent For Pancreatic Fluid Collections Q3 Acknowledgments The authors would like to thank Ms Witney McKiernan for helping write this paper. This work was presented as a scientific oral presentation at Digestive Q4 Disease Week, Orlando, FL, May Conflicts of interest These authors disclose the following: Michel Kahaleh has received grant support from Boston Scientific, Fujinon, EMcison, Xlumena, Inc, W.L. Gore, MaunaKea, Apollo Endosurgery, Cook Endoscopy, ASPIRE Bariatrics, GI Dynamics, and MI Tech, and is a consultant for Boston Scientific and Xlumena, Inc; Raj Shah, Thomas Kowalski, Andres Sanchez-Yague, Jose Nieto, and Brian Brauer have received grant support from Xlumena; Janak Shah has received consulting fees from Boston Scientific, and grant support from Xlumena; and Irving Waxman has been a consultant for Cook Medical, Olympus America, Mauna Kea Technologies, and Xlumena. The remaining author discloses no conflicts. Q5 Funding This study was funded by Xlumena, Inc. Q25Q
Original Article INTRODUCTION
 Original Article A retrospective study evaluating endoscopic ultrasound guided drainage of pancreatic fluid collections using a novel lumen apposing metal stent on an electrocautery enhanced delivery system
Original Article A retrospective study evaluating endoscopic ultrasound guided drainage of pancreatic fluid collections using a novel lumen apposing metal stent on an electrocautery enhanced delivery system
Endoscopic ultrasound-guided placement of AXIOS stent for drainage of pancreatic fluid collections
 REVIEW ARTICLE Annals of Gastroenterology (2016) 29, 1-6 Endoscopic ultrasound-guided placement of AXIOS stent for drainage of pancreatic fluid collections Rashmee Patil a, Mel A. Ona b, Charilaos Papafragkakis
REVIEW ARTICLE Annals of Gastroenterology (2016) 29, 1-6 Endoscopic ultrasound-guided placement of AXIOS stent for drainage of pancreatic fluid collections Rashmee Patil a, Mel A. Ona b, Charilaos Papafragkakis
Endoscopic pancreatic necrosectomy in 2017
 Endoscopic pancreatic necrosectomy in 2017 Mouen Khashab, MD Associate Professor of Medicine Director of Therapeutic Endoscopy The Johns Hopkins Hospital Revised Atlanta Classification Entity Acute fluid
Endoscopic pancreatic necrosectomy in 2017 Mouen Khashab, MD Associate Professor of Medicine Director of Therapeutic Endoscopy The Johns Hopkins Hospital Revised Atlanta Classification Entity Acute fluid
Clinical evaluation of endoscopic ultrasonography-guided drainage using a novel flared-type biflanged metal stent for pancreatic fluid collection
 Original Article Clinical evaluation of endoscopic ultrasonography-guided drainage using a novel flared-type biflanged metal stent for pancreatic fluid collection Shuntaro Mukai, Takao Itoi, Atsushi Sofuni,
Original Article Clinical evaluation of endoscopic ultrasonography-guided drainage using a novel flared-type biflanged metal stent for pancreatic fluid collection Shuntaro Mukai, Takao Itoi, Atsushi Sofuni,
Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist. Alireza Sedarat, MD UCLA Division of Digestive Diseases
 Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist Alireza Sedarat, MD UCLA Division of Digestive Diseases Disclosures Consultant for Boston Scientific and Olympus Corporation
Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist Alireza Sedarat, MD UCLA Division of Digestive Diseases Disclosures Consultant for Boston Scientific and Olympus Corporation
AXIOS Stent and Delivery System
 PRESCRIPTIVE INFORMATION AXIOS Stent and Delivery System Warning REFER TO THE DEVICE DIRECTIONS FOR USE FOR COMPLETE INSTRUCTIONS ON DEVICE USE. RX ONLY. CAUTION: FEDERAL LAW (USA) RESTRICTS THIS DEVICE
PRESCRIPTIVE INFORMATION AXIOS Stent and Delivery System Warning REFER TO THE DEVICE DIRECTIONS FOR USE FOR COMPLETE INSTRUCTIONS ON DEVICE USE. RX ONLY. CAUTION: FEDERAL LAW (USA) RESTRICTS THIS DEVICE
Endoscopic ultrasound guided gastrojejunostomy
 Review Article Endoscopic ultrasound guided gastrojejunostomy Enad Dawod 1, Jose M. Nieto 2 1 Weill Cornell Medicine, Department of Gastroenterology and Hepatology, New York, NY, USA; 2 Borland Groover
Review Article Endoscopic ultrasound guided gastrojejunostomy Enad Dawod 1, Jose M. Nieto 2 1 Weill Cornell Medicine, Department of Gastroenterology and Hepatology, New York, NY, USA; 2 Borland Groover
Endoscopic Management of Acute Pancreatitis. Theo Doukides, MD Gastroenterology and Therapeutic Endoscopy February 13, 2018
 Endoscopic Management of Acute Pancreatitis Theo Doukides, MD Gastroenterology and Therapeutic Endoscopy February 13, 2018 Objectives Assessment of acute pancreatitis Early management Who needs an ERCP
Endoscopic Management of Acute Pancreatitis Theo Doukides, MD Gastroenterology and Therapeutic Endoscopy February 13, 2018 Objectives Assessment of acute pancreatitis Early management Who needs an ERCP
Mild. Moderate. Severe
 2012 Revised Atlanta Classification Acute pancreatitis Classified based on absence or presence of local and/or systemic complications Mild Acute Pancreatits Moderate Severe P. A. Banks, T. L. Bollen, C.
2012 Revised Atlanta Classification Acute pancreatitis Classified based on absence or presence of local and/or systemic complications Mild Acute Pancreatits Moderate Severe P. A. Banks, T. L. Bollen, C.
efficacy. Endoscopic ultrasound-guided gastrojejunostomy with a lumen-apposing metal stent: a multicenter, international experience
 E76 THIEME Endoscopic ultrasound-guided gastrojejunostomy with a lumen-apposing metal stent: a multicenter, international experience Authors Institutions Amy Tyberg, Manuel Perez-Miranda, Ramon Sanchez-Ocaña,
E76 THIEME Endoscopic ultrasound-guided gastrojejunostomy with a lumen-apposing metal stent: a multicenter, international experience Authors Institutions Amy Tyberg, Manuel Perez-Miranda, Ramon Sanchez-Ocaña,
EUS- Gallbladder Drainage: is it time to replace percutaneous drainage?
 EUS- Gallbladder Drainage: is it time to replace percutaneous drainage? Jessica Widmer, DO 1, Juveria Abdullah 1, Michel Kahaleh, MD. 1 Division of Gastroenterology and Hepatology, Department of Medicine,
EUS- Gallbladder Drainage: is it time to replace percutaneous drainage? Jessica Widmer, DO 1, Juveria Abdullah 1, Michel Kahaleh, MD. 1 Division of Gastroenterology and Hepatology, Department of Medicine,
A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction
 A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction Authors Parth J. Parekh, Mohammad H. Shakhatreh, Paul Yeaton Institution Department of Internal
A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction Authors Parth J. Parekh, Mohammad H. Shakhatreh, Paul Yeaton Institution Department of Internal
PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE. PRESENTED BY: Susan DePasquale, CGRN, MSN
 PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE PRESENTED BY: Susan DePasquale, CGRN, MSN Pancreatic Fluid Collection (PFC) A result of pancreatic duct (PD) and side branch disruption,
PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE PRESENTED BY: Susan DePasquale, CGRN, MSN Pancreatic Fluid Collection (PFC) A result of pancreatic duct (PD) and side branch disruption,
Does it matter what we drain?
 Endoscopic Management of Pancreatic Fluid Collections Shyam Varadarajulu, MD Medical Director Center for Interventional Endoscopy Florida Hospital, Orlando Does it matter what we drain? Makes all the difference!
Endoscopic Management of Pancreatic Fluid Collections Shyam Varadarajulu, MD Medical Director Center for Interventional Endoscopy Florida Hospital, Orlando Does it matter what we drain? Makes all the difference!
PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies. Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels
 PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels 1. Diagnosis. 2. Multidisciplinary approach. 3. Therapeutic planning. 4. How? 5. Follow-up
PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels 1. Diagnosis. 2. Multidisciplinary approach. 3. Therapeutic planning. 4. How? 5. Follow-up
Lumen-apposing covered self-expanding metal stent for management of benign gastrointestinal strictures
 E96 THIEME Lumen-apposing covered self-expanding metal stent for management of benign gastrointestinal strictures Authors Institution Shounak Majumder, Navtej S. Buttar, Christopher Gostout, Michael J.
E96 THIEME Lumen-apposing covered self-expanding metal stent for management of benign gastrointestinal strictures Authors Institution Shounak Majumder, Navtej S. Buttar, Christopher Gostout, Michael J.
AXIOS Stent and Electrocautery Enhanced Delivery System *
 Advancing Pancreaticobiliary Disease Management AXIOS Stent and Electrocautery Enhanced Delivery System * Select a Menu Option Below Features & Benefits Expanding Innovation Ordering Information & Resources
Advancing Pancreaticobiliary Disease Management AXIOS Stent and Electrocautery Enhanced Delivery System * Select a Menu Option Below Features & Benefits Expanding Innovation Ordering Information & Resources
Gastrointestinal Intervention
 Gastrointest Interv 2013; 2:24 29 Contents lists available at SciVerse ScienceDirect Gastrointestinal Intervention journal homepage: www.gi-intervention.org Review Article Self-expandable metal stents
Gastrointest Interv 2013; 2:24 29 Contents lists available at SciVerse ScienceDirect Gastrointestinal Intervention journal homepage: www.gi-intervention.org Review Article Self-expandable metal stents
Intra-channel stent release technique for fluoroless endoscopic ultrasound-guided lumen-apposing metal stent placement: changing the paradigm
 Intra-channel stent release technique for fluoroless endoscopic ultrasound-guided lumen-apposing metal stent placement: changing the paradigm Authors Andrea Anderloni 1,FabiaAttili 2, Silvia Carrara 1,
Intra-channel stent release technique for fluoroless endoscopic ultrasound-guided lumen-apposing metal stent placement: changing the paradigm Authors Andrea Anderloni 1,FabiaAttili 2, Silvia Carrara 1,
Endoscopic Ultrasound-Guided Transluminal Drainage for Peripancreatic Fluid Collections: Where Are We Now?
 Gut and Liver, Vol. 8, No. 4, July 2014, pp. 341-355 Review Endoscopic Ultrasound-Guided Transluminal Drainage for Peripancreatic Fluid Collections: Where Are We Now? Hiroshi Kawakami*, Takao Itoi, and
Gut and Liver, Vol. 8, No. 4, July 2014, pp. 341-355 Review Endoscopic Ultrasound-Guided Transluminal Drainage for Peripancreatic Fluid Collections: Where Are We Now? Hiroshi Kawakami*, Takao Itoi, and
Double endoscopic bypass for gastric outlet obstruction and biliary obstruction
 Double endoscopic bypass for gastric outlet obstruction and biliary obstruction Authors Olaya I. Brewer Gutierrez 1,JoseNieto 2, Shayan Irani 3, Theodore James 4,RenataPierattiBueno 1, Yen-I Chen 1, Majidah
Double endoscopic bypass for gastric outlet obstruction and biliary obstruction Authors Olaya I. Brewer Gutierrez 1,JoseNieto 2, Shayan Irani 3, Theodore James 4,RenataPierattiBueno 1, Yen-I Chen 1, Majidah
AXIOS Stent and Electrocautery Enhanced Delivery System. Quick Reference Guide
 AXIOS Stent and Electrocautery Enhanced Delivery System Quick Reference Guide AXIOS Stent (front and side views) UPN Codes Flange Diameter (mm) Lumen Diamter (mm) Saddle Length (mm) Catheter OD (Fr) Catheter
AXIOS Stent and Electrocautery Enhanced Delivery System Quick Reference Guide AXIOS Stent (front and side views) UPN Codes Flange Diameter (mm) Lumen Diamter (mm) Saddle Length (mm) Catheter OD (Fr) Catheter
EUS-guided cholecystoduodenostomy for acute cholecystitis with an anti-stent migration and anti-food impaction system; a pilot study
 609285TAG0010.1177/1756283X15609285Therapeutic Advances in GastroenterologyW Takagi, T Ogura research-article2015 Therapeutic Advances in Gastroenterology Original Research EUS-guided cholecystoduodenostomy
609285TAG0010.1177/1756283X15609285Therapeutic Advances in GastroenterologyW Takagi, T Ogura research-article2015 Therapeutic Advances in Gastroenterology Original Research EUS-guided cholecystoduodenostomy
ACUTE CHOLANGITIS AS a result of an occluded
 Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
The first stents designed for use in the biliary tree and
 Imaging and Advanced Technology Michael B. Wallace, Section Editor Expandable Gastrointestinal Stents TODD H. BARON Department of Medicine, Division of Gastroenterology & Hepatology, Mayo Clinic, Rochester,
Imaging and Advanced Technology Michael B. Wallace, Section Editor Expandable Gastrointestinal Stents TODD H. BARON Department of Medicine, Division of Gastroenterology & Hepatology, Mayo Clinic, Rochester,
Endoscopic ultrasound-guided drainage of postoperative intra-abdominal abscesses
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v21.i11.3402 World J Gastroenterol 2015 March 21; 21(11): 3402-3408 ISSN 1007-9327
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v21.i11.3402 World J Gastroenterol 2015 March 21; 21(11): 3402-3408 ISSN 1007-9327
EUS-Guided Transduodenal Biliary Drainage in Unresectable Pancreatic Cancer with Obstructive Jaundice
 CASE REPORT EUS-Guided Transduodenal Biliary Drainage in Unresectable Pancreatic Cancer with Obstructive Jaundice Tiing Leong Ang, Eng Kiong Teo, Kwong Ming Fock Division of Gastroenterology, Department
CASE REPORT EUS-Guided Transduodenal Biliary Drainage in Unresectable Pancreatic Cancer with Obstructive Jaundice Tiing Leong Ang, Eng Kiong Teo, Kwong Ming Fock Division of Gastroenterology, Department
Through the LAMS towards the future: current uses and outcomes of lumen-apposing metal stents
 REVIEW ARTICLE Annals of Gastroenterology (2018) 31, 1-6 Through the LAMS towards the future: current uses and outcomes of lumen-apposing metal stents Alessandro Mussetto a, Alessandro Fugazza b, Lorenzo
REVIEW ARTICLE Annals of Gastroenterology (2018) 31, 1-6 Through the LAMS towards the future: current uses and outcomes of lumen-apposing metal stents Alessandro Mussetto a, Alessandro Fugazza b, Lorenzo
Endoscopic Ultrasound-Guided Gallbladder Drainage Using a Lumen-Apposing Metal Stent for Acute Cholecystitis: A Systematic Review
 REVIEW Clin Endosc 2018;51:450-462 https://doi.org/10.5946/ce.2018.024 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Endoscopic Ultrasound-Guided Gallbladder Drainage Using a Lumen-Apposing Metal
REVIEW Clin Endosc 2018;51:450-462 https://doi.org/10.5946/ce.2018.024 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Endoscopic Ultrasound-Guided Gallbladder Drainage Using a Lumen-Apposing Metal
Clinical Study Endoscopic Ultrasound-Guided Drainage without Fluoroscopic Guidance for Extraluminal Complicated Cysts
 Gastroenterology Research and Practice Volume 2016, Article ID 1249064, 8 pages http://dx.doi.org/10.1155/2016/1249064 Clinical Study Endoscopic Ultrasound-Guided Drainage without Fluoroscopic Guidance
Gastroenterology Research and Practice Volume 2016, Article ID 1249064, 8 pages http://dx.doi.org/10.1155/2016/1249064 Clinical Study Endoscopic Ultrasound-Guided Drainage without Fluoroscopic Guidance
PANCREATIC PSEUDOCYSTS. Madhuri Rao MD PGY-5 Kings County Hospital Center
 PANCREATIC PSEUDOCYSTS Madhuri Rao MD PGY-5 Kings County Hospital Center 34 yo M Case Presentation PMH: Chronic pancreatitis (ETOH related) PSH: Nil Meds: Nil NKDA www.downstatesurgery.org Symptoms o Chronic
PANCREATIC PSEUDOCYSTS Madhuri Rao MD PGY-5 Kings County Hospital Center 34 yo M Case Presentation PMH: Chronic pancreatitis (ETOH related) PSH: Nil Meds: Nil NKDA www.downstatesurgery.org Symptoms o Chronic
Expandable stents in digestive pathology present use in an emergency hospital
 ORIGINAL ARTICLES Article received on November30, 2015 and accepted for publishing on December15, 2015. Expandable stents in digestive pathology present use in an emergency hospital Mădălina Ilie 1, Vasile
ORIGINAL ARTICLES Article received on November30, 2015 and accepted for publishing on December15, 2015. Expandable stents in digestive pathology present use in an emergency hospital Mădălina Ilie 1, Vasile
Endoscopic Management of the Iatrogenic CBD Injury
 The Liver Week 2014, Jeju, Korea Endoscopic Management of the Iatrogenic CBD Injury Jong Ho Moon, MD, PhD Department of Internal Medicine Soon Chun Hyang University School of Medicine Bucheon/Seoul, KOREA
The Liver Week 2014, Jeju, Korea Endoscopic Management of the Iatrogenic CBD Injury Jong Ho Moon, MD, PhD Department of Internal Medicine Soon Chun Hyang University School of Medicine Bucheon/Seoul, KOREA
A Guide for Patients Living with a Biliary Metal Stent
 A Guide for Patients Living with a Biliary Metal Stent What is a biliary metal stent? A biliary metal stent (also known as a bile duct stent ) is a flexible metallic tube specially designed to hold your
A Guide for Patients Living with a Biliary Metal Stent What is a biliary metal stent? A biliary metal stent (also known as a bile duct stent ) is a flexible metallic tube specially designed to hold your
A multi institutional consensus on how to perform endoscopic ultrasound-guided peri-pancreatic fluid collection drainage and endoscopic necrosectomy
 Consensus A multi institutional consensus on how to perform endoscopic ultrasound-guided peri-pancreatic fluid collection drainage and endoscopic necrosectomy Jintao Guo, Adrian Saftoiu 1, Peter Vilmann
Consensus A multi institutional consensus on how to perform endoscopic ultrasound-guided peri-pancreatic fluid collection drainage and endoscopic necrosectomy Jintao Guo, Adrian Saftoiu 1, Peter Vilmann
Making ERCP Easy: Tips From A Master
 Making ERCP Easy: Tips From A Master Raj J. Shah, M.D., FASGE Associate Professor of Medicine University of Colorado School of Medicine Co-Director, Endoscopy Director, Pancreaticobiliary Endoscopy Services
Making ERCP Easy: Tips From A Master Raj J. Shah, M.D., FASGE Associate Professor of Medicine University of Colorado School of Medicine Co-Director, Endoscopy Director, Pancreaticobiliary Endoscopy Services
Endosonography guided management of pancreatic fluid collections
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v21.i41.11842 World J Gastroenterol 2015 November 7; 21(41): 11842-11853 ISSN 1007-9327
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v21.i41.11842 World J Gastroenterol 2015 November 7; 21(41): 11842-11853 ISSN 1007-9327
WallFlex Biliary RX Fully Covered Stent System Prescriptive Information
 Caution/Rx Only: Federal Law (USA) restricts this device to sale by or on the order of a physician. Warning Contents supplied STERILE using an ethylene oxide (EO) process. Do not use if sterile barrier
Caution/Rx Only: Federal Law (USA) restricts this device to sale by or on the order of a physician. Warning Contents supplied STERILE using an ethylene oxide (EO) process. Do not use if sterile barrier
Vascular complications in percutaneous biliary interventions: A series of 111 procedures
 Vascular complications in percutaneous biliary interventions: A series of 111 procedures Poster No.: C-0744 Congress: ECR 2013 Type: Educational Exhibit Authors: A. BHARADWAZ; AARHUS, Re/DK Keywords: Obstruction
Vascular complications in percutaneous biliary interventions: A series of 111 procedures Poster No.: C-0744 Congress: ECR 2013 Type: Educational Exhibit Authors: A. BHARADWAZ; AARHUS, Re/DK Keywords: Obstruction
Стенты «Ella-cs» Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts»
 Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Research Article Risk Factors for Migration, Fracture, and Dislocation of Pancreatic Stents
 Gastroenterology Research and Practice Volume 2015, Article ID 365457, 6 pages http://dx.doi.org/10.1155/2015/365457 Research Article Risk Factors for Migration, Fracture, and Dislocation of Pancreatic
Gastroenterology Research and Practice Volume 2015, Article ID 365457, 6 pages http://dx.doi.org/10.1155/2015/365457 Research Article Risk Factors for Migration, Fracture, and Dislocation of Pancreatic
Jennifer Hsieh 1, Amar Thosani 1, Matthew Grunwald 2, Satish Nagula 1, Juan Carlos Bucobo 1, Jonathan M. Buscaglia 1. Introduction
 How We Do It Serial insertion of bilateral uncovered metal stents for malignant hilar obstruction using an 8 Fr biliary system: a case series of 17 consecutive patients Jennifer Hsieh 1, Amar Thosani 1,
How We Do It Serial insertion of bilateral uncovered metal stents for malignant hilar obstruction using an 8 Fr biliary system: a case series of 17 consecutive patients Jennifer Hsieh 1, Amar Thosani 1,
and Transmural Drainage
 HPB Surgery, 2000, Vol. 11, pp. 333-338 Reprints available directly from the publisher Photocopying permitted by license only (C) 2000 OPA (Overseas Publishers Association) N.V. Published by license under
HPB Surgery, 2000, Vol. 11, pp. 333-338 Reprints available directly from the publisher Photocopying permitted by license only (C) 2000 OPA (Overseas Publishers Association) N.V. Published by license under
The role of ERCP in chronic pancreatitis
 The role of ERCP in chronic pancreatitis Marianna Arvanitakis Erasme University Hospital, ULB, Brussels, Belgium 10 th Nottingham Endoscopy Masterclass SPEAKER DECLARATIONS This presenter has the following
The role of ERCP in chronic pancreatitis Marianna Arvanitakis Erasme University Hospital, ULB, Brussels, Belgium 10 th Nottingham Endoscopy Masterclass SPEAKER DECLARATIONS This presenter has the following
International multicenter comparative trial of transluminal EUS-guided biliary drainage via hepatogastrostomy vs. choledochoduodenostomy approaches
 E175 International multicenter comparative trial of transluminal EUS-guided biliary drainage via hepatogastrostomy vs. choledochoduodenostomy approaches Authors Mouen A. Khashab 1, Ahmed A. Messallam 1,
E175 International multicenter comparative trial of transluminal EUS-guided biliary drainage via hepatogastrostomy vs. choledochoduodenostomy approaches Authors Mouen A. Khashab 1, Ahmed A. Messallam 1,
Endoscopic Resolution of Pseudocyst Infection and Necrosis as a Complication of Endoscopic Pseudocyst Drainage. A Case Report
 CASE REPORT Endoscopic Resolution of Pseudocyst Infection and Necrosis as a Complication of Endoscopic Pseudocyst Drainage. A Case Report Rodrigo Azevedo Rodrigues, Lucianna Pereira da Motta Pires Correia,
CASE REPORT Endoscopic Resolution of Pseudocyst Infection and Necrosis as a Complication of Endoscopic Pseudocyst Drainage. A Case Report Rodrigo Azevedo Rodrigues, Lucianna Pereira da Motta Pires Correia,
Keywords. Abstract. Introduction
 The Safety of Endoscopic Ultrasonography-Guided Drainage of Pancreatic Fluid Collections Without Fluoroscopic Control: a Single Tertiary Center Experience Andrada Seicean 1, Roxana Stan-Iuga 1, Radu Badea
The Safety of Endoscopic Ultrasonography-Guided Drainage of Pancreatic Fluid Collections Without Fluoroscopic Control: a Single Tertiary Center Experience Andrada Seicean 1, Roxana Stan-Iuga 1, Radu Badea
Introduction E1111. Background and study aim Gallbladder drainage in patients
 Endoscopic ultrasound-guided gallbladder drainage for acute cholecystitis with a silicone-covered nitinol short bilaterally flared stent: a case series Authors Raffaele Manta 1, Claudio Zulli 2,AngeloZullo
Endoscopic ultrasound-guided gallbladder drainage for acute cholecystitis with a silicone-covered nitinol short bilaterally flared stent: a case series Authors Raffaele Manta 1, Claudio Zulli 2,AngeloZullo
Lumen-apposing metal stents for gastrointestinal luminal strictures: current use and future directions
 REVIEW ARTICLE Annals of Gastroenterology (2019) 32, 1-6 Lumen-apposing metal stents for gastrointestinal luminal strictures: current use and future directions Brian Larson, Douglas G. Adler University
REVIEW ARTICLE Annals of Gastroenterology (2019) 32, 1-6 Lumen-apposing metal stents for gastrointestinal luminal strictures: current use and future directions Brian Larson, Douglas G. Adler University
Overview. Doumit S. BouHaidar, MD ACG/VGS/ODSGNA Regional Postgraduate Course Copyright American College of Gastroenterology 1
 Doumit S. BouHaidar, MD Associate Professor of Medicine Director, Advanced Therapeutic Endoscopy Virginia Commonwealth University Overview Copyright American College of Gastroenterology 1 Incidence: 4
Doumit S. BouHaidar, MD Associate Professor of Medicine Director, Advanced Therapeutic Endoscopy Virginia Commonwealth University Overview Copyright American College of Gastroenterology 1 Incidence: 4
Clinical Study Covered Metal Stenting for Malignant Lower Biliary Stricture with Pancreatic Duct Obstruction: Is Endoscopic Sphincterotomy Needed?
 Gastroenterology Research and Practice Volume 2013, Article ID 375613, 6 pages http://dx.doi.org/10.1155/2013/375613 Clinical Study Covered Metal Stenting for Malignant Lower Biliary Stricture with Pancreatic
Gastroenterology Research and Practice Volume 2013, Article ID 375613, 6 pages http://dx.doi.org/10.1155/2013/375613 Clinical Study Covered Metal Stenting for Malignant Lower Biliary Stricture with Pancreatic
Approach to the Biliary Stricture
 Approach to the Biliary Stricture ACG Eastern Postgraduate Course Washington DC June 8, 2014 Steven A. Edmundowicz MD FASGE Chief of Endoscopy Division of Gastroenterology Professor of Medicine Disclosures
Approach to the Biliary Stricture ACG Eastern Postgraduate Course Washington DC June 8, 2014 Steven A. Edmundowicz MD FASGE Chief of Endoscopy Division of Gastroenterology Professor of Medicine Disclosures
Therapeutic EUS: today & tomorrow Pietro Fusaroli
 Therapeutic EUS: today & tomorrow Pietro Fusaroli Gastroenterologia Università di Bologna AUSL di Imola, Castel S. Pietro Terme (BO) Direttore Prof. G. Caletti EUS FNA: CONVEX ARRAY Olympus, Pentax, Toshiba
Therapeutic EUS: today & tomorrow Pietro Fusaroli Gastroenterologia Università di Bologna AUSL di Imola, Castel S. Pietro Terme (BO) Direttore Prof. G. Caletti EUS FNA: CONVEX ARRAY Olympus, Pentax, Toshiba
Introduction E275 ABSTRACT. Original article
 International multicenter comparative trial of endoscopic ultrasonography-guided gastroenterostomy versus surgical gastrojejunostomy for the treatment of malignant gastric outlet obstruction Authors Mouen
International multicenter comparative trial of endoscopic ultrasonography-guided gastroenterostomy versus surgical gastrojejunostomy for the treatment of malignant gastric outlet obstruction Authors Mouen
Endoscopic Treatment of Luminal Perforations and Leaks
 Endoscopic Treatment of Luminal Perforations and Leaks Ali A. Siddiqui, MD Professor of Medicine Director of Interventional Endoscopy Jefferson Medical College Philadelphia, PA When Do You Suspect a Luminal
Endoscopic Treatment of Luminal Perforations and Leaks Ali A. Siddiqui, MD Professor of Medicine Director of Interventional Endoscopy Jefferson Medical College Philadelphia, PA When Do You Suspect a Luminal
A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY
 A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center Welcome The St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center is a leader
A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center Welcome The St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center is a leader
Endoscopic Management of Biliary Strictures. Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center
 Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
UvA-DARE (Digital Academic Repository)
 UvA-DARE (Digital Academic Repository) Endosonographic imaging of pancreatic pseudocysts before endoscopic transmural drainage Fockens, P.; Johnson, T.G.; van Dullemen, H.M.; Huibregtse, K.; Tytgat, G.N.J.
UvA-DARE (Digital Academic Repository) Endosonographic imaging of pancreatic pseudocysts before endoscopic transmural drainage Fockens, P.; Johnson, T.G.; van Dullemen, H.M.; Huibregtse, K.; Tytgat, G.N.J.
Endoscopic Ultrasound-Guided Pancreatic Duct Intervention
 FOCUSED REVIEW SERIES: EUS-Guided Therapeutic Interventions Clin Endosc 2017;50:112-116 https://doi.org/10.5946/ce.2017.046 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Endoscopic Ultrasound-Guided
FOCUSED REVIEW SERIES: EUS-Guided Therapeutic Interventions Clin Endosc 2017;50:112-116 https://doi.org/10.5946/ce.2017.046 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Endoscopic Ultrasound-Guided
Review Article Fully Covered Self-Expandable Metal Stents for Treatment of Both Benign and Malignant Biliary Disorders
 Hindawi Publishing Corporation Diagnostic and Therapeutic Endoscopy Volume 2012, Article ID 498617, 5 pages doi:10.1155/2012/498617 Review Article Fully Covered Self-Expandable Metal Stents for Treatment
Hindawi Publishing Corporation Diagnostic and Therapeutic Endoscopy Volume 2012, Article ID 498617, 5 pages doi:10.1155/2012/498617 Review Article Fully Covered Self-Expandable Metal Stents for Treatment
Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica
 Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica Authors: Sergio López-Durán, Celia Zaera, Juan Ángel
Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica Authors: Sergio López-Durán, Celia Zaera, Juan Ángel
Diagnosis of tumor extension in biliary carcinoma has. Differential Diagnosis and Treatment of Biliary Strictures
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
BILIARY CANNULATION FOR the treatment of biliary
 Digestive Endoscopy 2016; 28 (Suppl. 1): 96 101 doi: 10.1111/den.12611 Current situation of cannulation and salvage for difficult cases Endoscopic ultrasonography-guided rendezvous technique Takayoshi
Digestive Endoscopy 2016; 28 (Suppl. 1): 96 101 doi: 10.1111/den.12611 Current situation of cannulation and salvage for difficult cases Endoscopic ultrasonography-guided rendezvous technique Takayoshi
Comparative evaluation of structural and functional changes in pancreas after endoscopic and surgical management of pancreatic necrosis
 ORIGINAL ARTICLE Annals of Gastroenterology (2014) 27, 162-166 Comparative evaluation of structural and functional changes in pancreas after endoscopic and surgical management of pancreatic necrosis Surinder
ORIGINAL ARTICLE Annals of Gastroenterology (2014) 27, 162-166 Comparative evaluation of structural and functional changes in pancreas after endoscopic and surgical management of pancreatic necrosis Surinder
The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
Information Technology Solutions
 2016 2014 CPT Esophagoscopy Changes - Gastroenterology CPT Changes Information Technology Solutions ASGE LOGO AND INFO Esophagogastroduodenoscopy CPT Codes 43235-43270 The American Society for Gastrointestinal
2016 2014 CPT Esophagoscopy Changes - Gastroenterology CPT Changes Information Technology Solutions ASGE LOGO AND INFO Esophagogastroduodenoscopy CPT Codes 43235-43270 The American Society for Gastrointestinal
Correspondence should be addressed to Justin Cochrane;
 Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 794282, 4 pages http://dx.doi.org/10.1155/2015/794282 Case Report Acute on Chronic Pancreatitis Causing a Highway to the Colon with Subsequent
Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 794282, 4 pages http://dx.doi.org/10.1155/2015/794282 Case Report Acute on Chronic Pancreatitis Causing a Highway to the Colon with Subsequent
WallFlex Stents Technique Spotlights
 WallFlex Stents Technique Spotlights OPEN TO THE POSSIBILITIES SEAN E. McGarr, do Kennebec Gastrointestinal Associates Maine General Medical Center, Augusta, ME 04330, United States Director of Gastrointestinal
WallFlex Stents Technique Spotlights OPEN TO THE POSSIBILITIES SEAN E. McGarr, do Kennebec Gastrointestinal Associates Maine General Medical Center, Augusta, ME 04330, United States Director of Gastrointestinal
Paola Figueroa-Barojas, Mihir R. Bakhru, Nagy A. Habib, Kristi Ellen, Jennifer Millman, Armeen Jamal-Kabani, Monica Gaidhane, and Michel Kahaleh
 Oncology Volume 2013, Article ID 910897, 5 pages http://dx.doi.org/10.1155/2013/910897 Clinical Study Safety and Efficacy of Radiofrequency Ablation in the Management of Unresectable Bile Duct and Pancreatic
Oncology Volume 2013, Article ID 910897, 5 pages http://dx.doi.org/10.1155/2013/910897 Clinical Study Safety and Efficacy of Radiofrequency Ablation in the Management of Unresectable Bile Duct and Pancreatic
Best of UEG week 2017 (Pancreas-biliary)
 Best of UEG week 2017 (Pancreas-biliary) Marianna Arvanitakis Erasme University Hospital, ULB, Brussels, Belgium 10 th Nottingham Endoscopy Masterclass SPEAKER DECLARATIONS This presenter has the following
Best of UEG week 2017 (Pancreas-biliary) Marianna Arvanitakis Erasme University Hospital, ULB, Brussels, Belgium 10 th Nottingham Endoscopy Masterclass SPEAKER DECLARATIONS This presenter has the following
Sepsis in Acute Pancreatitis. MD Smith Department of Surgery University of the Witwatersrand, Johannesburg Chris Hani Baragwanath Academic Hospital
 Sepsis in Acute Pancreatitis MD Smith Department of Surgery University of the Witwatersrand, Johannesburg Chris Hani Baragwanath Academic Hospital Introduction Self limiting disease in 85% Minority develop
Sepsis in Acute Pancreatitis MD Smith Department of Surgery University of the Witwatersrand, Johannesburg Chris Hani Baragwanath Academic Hospital Introduction Self limiting disease in 85% Minority develop
Follow this and additional works at:
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2016 A comparison between endoscopic ultrasoundguided rendezvous and percutaneous biliary drainage after failed
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2016 A comparison between endoscopic ultrasoundguided rendezvous and percutaneous biliary drainage after failed
Maximize Control. Minimize Migration.
 Maximize Control. Minimize Migration. New SHORT WIRE Delivery System SHORT W IRE BILIARY ENDOPROSTHESIS Improved treatment of biliary strictures The self-expanding, fully covered metal stent is intended
Maximize Control. Minimize Migration. New SHORT WIRE Delivery System SHORT W IRE BILIARY ENDOPROSTHESIS Improved treatment of biliary strictures The self-expanding, fully covered metal stent is intended
WallFlex Biliary Metal Stents
 WallFlex Biliary Metal Stents Please Note: These steps are intended to be for general guidance only. For complete instructions for use, indications, contraindications and warnings, please refer to the
WallFlex Biliary Metal Stents Please Note: These steps are intended to be for general guidance only. For complete instructions for use, indications, contraindications and warnings, please refer to the
Esophageal seeding after endoscopic ultrasound-guided fine-needle aspiration of a mediastinal tumor
 Esophageal seeding after endoscopic ultrasound-guided fine-needle aspiration of a mediastinal tumor Authors Kensuke Yokoyama 1,JunUshio 1,NorikatsuNumao 1, Kiichi Tamada 1, Noriyoshi Fukushima 2, Alan
Esophageal seeding after endoscopic ultrasound-guided fine-needle aspiration of a mediastinal tumor Authors Kensuke Yokoyama 1,JunUshio 1,NorikatsuNumao 1, Kiichi Tamada 1, Noriyoshi Fukushima 2, Alan
EUS-Guided Multitransgastric Endoscopic Necrosectomy for Infected Pancreatic Necrosis with Noncontagious Retroperitoneal and Peritoneal Extension
 Gut and Liver, Vol. 4, No. 1, March 2010, pp. 140-145 Case report EUS-Guided Multitransgastric Endoscopic Necrosectomy for Infected Pancreatic Necrosis with Noncontagious Retroperitoneal and Peritoneal
Gut and Liver, Vol. 4, No. 1, March 2010, pp. 140-145 Case report EUS-Guided Multitransgastric Endoscopic Necrosectomy for Infected Pancreatic Necrosis with Noncontagious Retroperitoneal and Peritoneal
Advances in Endoscopic Ultrasound-Guided Biliary Drainage: A Comprehensive Review
 Gut and Liver, Vol. 7, No. 2, March 2013, pp. 129-136 Review Advances in Endoscopic Ultrasound-Guided Biliary Drainage: A Comprehensive Review Savreet Sarkaria, Ho-Su Lee, Monica Gaidhane, and Michel Kahaleh
Gut and Liver, Vol. 7, No. 2, March 2013, pp. 129-136 Review Advances in Endoscopic Ultrasound-Guided Biliary Drainage: A Comprehensive Review Savreet Sarkaria, Ho-Su Lee, Monica Gaidhane, and Michel Kahaleh
Endoscopic Retrograde Cholangiopancreatography (ERCP)
 Endoscopic Retrograde Cholangiopancreatography (ERCP) Medical Imaging and Treatment of the Bile and Pancreatic Ducts CIE-02718 Understanding ERCP Brochure Update_F.indd 1 7/11/18 9:51 A Minimally Invasive
Endoscopic Retrograde Cholangiopancreatography (ERCP) Medical Imaging and Treatment of the Bile and Pancreatic Ducts CIE-02718 Understanding ERCP Brochure Update_F.indd 1 7/11/18 9:51 A Minimally Invasive
Disclosures. Extra-hepatic Biliary Disease and the Pancreas. Objectives. Pancreatitis 10/3/2018. No relevant financial disclosures to report
 Extra-hepatic Biliary Disease and the Pancreas Disclosures No relevant financial disclosures to report Jeffrey Coughenour MD FACS Clinical Associate Professor of Surgery and Emergency Medicine Division
Extra-hepatic Biliary Disease and the Pancreas Disclosures No relevant financial disclosures to report Jeffrey Coughenour MD FACS Clinical Associate Professor of Surgery and Emergency Medicine Division
ESPEN Congress Brussels Stenting of the esophagus and small bowel. Jean-Marc Dumonceau
 ESPEN Congress Brussels 2005 Stenting of the esophagus and small bowel Jean-Marc Dumonceau Stenting of the esophagus and small bowel Jean-Marc Dumonceau, Div. of Gastroenterology Geneva, Switzerland Indication:
ESPEN Congress Brussels 2005 Stenting of the esophagus and small bowel Jean-Marc Dumonceau Stenting of the esophagus and small bowel Jean-Marc Dumonceau, Div. of Gastroenterology Geneva, Switzerland Indication:
Title. CitationSurgical Endoscopy, 26(6): Issue Date Doc URL. Rights. Type. File Information. surgery
 Title Endoscopic ultrasound-guided transmural drainage for surgery Onodera, Manabu; Kawakami, Hiroshi; Kuwatani, Masaki Author(s) Eto, Kazunori; Nasu, Yuya; Tanaka, Eiichi; Hirano, S CitationSurgical Endoscopy,
Title Endoscopic ultrasound-guided transmural drainage for surgery Onodera, Manabu; Kawakami, Hiroshi; Kuwatani, Masaki Author(s) Eto, Kazunori; Nasu, Yuya; Tanaka, Eiichi; Hirano, S CitationSurgical Endoscopy,
EUS Guided Pancreatic Duct Drainage: When? How?
 PBS-IV Beyond the Horizon of Interventional EUS EUS Guided Pancreatic Duct Drainage: When? How? Uzma D. Siddiqui, M.D. Center for Endoscopic Research and Therapeutics (CERT), University of Chicago Medicine,
PBS-IV Beyond the Horizon of Interventional EUS EUS Guided Pancreatic Duct Drainage: When? How? Uzma D. Siddiqui, M.D. Center for Endoscopic Research and Therapeutics (CERT), University of Chicago Medicine,
Management of Pancreatic Fistulae
 Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
of EUS-guided transesophageal, transgastric, and transcolonic drainage of intra-abdominal fluid collections and abscesses
 CASE STUDIES EUS-guided transesophageal, transgastric, and transcolonic drainage of intra-abdominal fluid collections and abscesses Cyrus Piraka, MD, Raj J. Shah, MD, Norio Fukami, MD, Krishnavel V. Chathadi,
CASE STUDIES EUS-guided transesophageal, transgastric, and transcolonic drainage of intra-abdominal fluid collections and abscesses Cyrus Piraka, MD, Raj J. Shah, MD, Norio Fukami, MD, Krishnavel V. Chathadi,
Stenting for Esophageal Cancer Technical Issues and Outcomes
 Stenting for Esophageal Cancer Technical Issues and Outcomes Moishe Liberman Director C.E.T.O.C. Division of Thoracic Surgery Centre Hospitalier de l Université de Montréal Disclosures Research and Educational
Stenting for Esophageal Cancer Technical Issues and Outcomes Moishe Liberman Director C.E.T.O.C. Division of Thoracic Surgery Centre Hospitalier de l Université de Montréal Disclosures Research and Educational
CHRONIC PANCREATITIS CONSERVATIVE TREATMENT, ENDOSCOPY OR SURGERY?
 Endoscopy 2006 Update and Live Demonstration Berlin, 04. 05. Mai 2006 CHRONIC PANCREATITIS CONSERVATIVE TREATMENT, ENDOSCOPY OR SURGERY? J. F. Riemann A. Rosenbaum Medizinische Klinik C, Klinikum Ludwigshafen
Endoscopy 2006 Update and Live Demonstration Berlin, 04. 05. Mai 2006 CHRONIC PANCREATITIS CONSERVATIVE TREATMENT, ENDOSCOPY OR SURGERY? J. F. Riemann A. Rosenbaum Medizinische Klinik C, Klinikum Ludwigshafen
STRICTURES OF THE BILE DUCTS Session No.: 5. Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy
 STRICTURES OF THE BILE DUCTS Session No.: 5 Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy Drainage of biliary strictures. The history before 1980 Surgical bypass Percutaneous
STRICTURES OF THE BILE DUCTS Session No.: 5 Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy Drainage of biliary strictures. The history before 1980 Surgical bypass Percutaneous
Expect Slimline (SL) Endoscopic Ultrasound Aspiration Needle EXPANDED INDICATIONS AVAILABLE IN THE U.S. WITH
 Expect Slimline (SL) Endoscopic Ultrasound Aspiration Needle AVAILABLE IN THE U.S. WITH EXPANDED INDICATIONS Expect Slimline (SL) Endoscopic Ultrasound Aspiration Needle Expect Slimline (SL) Endoscopic
Expect Slimline (SL) Endoscopic Ultrasound Aspiration Needle AVAILABLE IN THE U.S. WITH EXPANDED INDICATIONS Expect Slimline (SL) Endoscopic Ultrasound Aspiration Needle Expect Slimline (SL) Endoscopic
Takayuki; Eguchi, Susumu; Kanematsu. Citation Pediatric surgery international, 27
 NAOSITE: Nagasaki University's Ac Title Author(s) Endoscopic balloon dilatation for c jejunum in an infant. Mochizuki, Kyoko; Obatake, Masayuki Takayuki; Eguchi, Susumu; Kanematsu Citation Pediatric surgery
NAOSITE: Nagasaki University's Ac Title Author(s) Endoscopic balloon dilatation for c jejunum in an infant. Mochizuki, Kyoko; Obatake, Masayuki Takayuki; Eguchi, Susumu; Kanematsu Citation Pediatric surgery
Sreeni Jonnalagadda, MD., FASGE Professor of Medicine, UMKC Director of Interventional Endoscopy Saint Luke s Hospital, Kansas City
 Sreeni Jonnalagadda, MD., FASGE Professor of Medicine, UMKC Director of Interventional Endoscopy Saint Luke s Hospital, Kansas City Peptic stricture Shtki Schatzki s ring Esophageal cancer Radiation therapy
Sreeni Jonnalagadda, MD., FASGE Professor of Medicine, UMKC Director of Interventional Endoscopy Saint Luke s Hospital, Kansas City Peptic stricture Shtki Schatzki s ring Esophageal cancer Radiation therapy
Endoscopic ultrasound-guided anterograde cholangiopancreatography
 J Hepatobiliary Pancreat Sci (2011) 18:319 331 DOI 10.1007/s00534-010-0358-1 TOPICS Advances in therapeutic ultrasound and endoscopy in hepato-biliary-pancreatic diseases Endoscopic ultrasound-guided anterograde
J Hepatobiliary Pancreat Sci (2011) 18:319 331 DOI 10.1007/s00534-010-0358-1 TOPICS Advances in therapeutic ultrasound and endoscopy in hepato-biliary-pancreatic diseases Endoscopic ultrasound-guided anterograde
Gastric / EUS Metal Stents
 Gastric / EUS Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium
Gastric / EUS Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium
Jintao Guo, Siyu Sun, Xiang Liu, Sheng Wang, Nan Ge, and Guoxin Wang. 1. Introduction. 2. Patients and Methods
 Gastroenterology Research and Practice Volume 2016, Article ID 9469472, 6 pages http://dx.doi.org/10.1155/2016/9469472 Clinical Study Endoscopic Ultrasound-Guided Biliary Drainage Using a Fully Covered
Gastroenterology Research and Practice Volume 2016, Article ID 9469472, 6 pages http://dx.doi.org/10.1155/2016/9469472 Clinical Study Endoscopic Ultrasound-Guided Biliary Drainage Using a Fully Covered
Biliary Metal Stents MAKING A DIFFERENCE TO HEALTH
 Biliary Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium range.
Biliary Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium range.
The Influence of Pancreatic Ductal Anatomy on the Complications of Pancreatitis. William H. Nealon M.D.
 The Influence of Pancreatic Ductal Anatomy on the Complications of Pancreatitis William H. Nealon M.D. Students and Trainees: Guide to Creativity, Productivity and Innovation in a Clinical Career Choose
The Influence of Pancreatic Ductal Anatomy on the Complications of Pancreatitis William H. Nealon M.D. Students and Trainees: Guide to Creativity, Productivity and Innovation in a Clinical Career Choose
Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas
 CASE REPORT Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas Anand Patel, Louis Lambiase, Antonio Decarli, Ali Fazel Division of Gastroenterology
CASE REPORT Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas Anand Patel, Louis Lambiase, Antonio Decarli, Ali Fazel Division of Gastroenterology
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Endoscopic transluminal drainage of pancreatic pseudocyst and pancreatic necrosectomy Removing dead tissue from
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Endoscopic transluminal drainage of pancreatic pseudocyst and pancreatic necrosectomy Removing dead tissue from
CPT COD1NG UPDATES Gastroenterology CPT Advisors
 2014 CPT COD1NG UPDATES Gastroenterology CPT Advisors Joel V. Brill, MD, AGA CPT Advisor Daniel C. DeMarco, MD, ACG CPT Advisor Glenn D. Littenberg, MD, ASGE CPT Advisor The American College of Gastroenterology
2014 CPT COD1NG UPDATES Gastroenterology CPT Advisors Joel V. Brill, MD, AGA CPT Advisor Daniel C. DeMarco, MD, ACG CPT Advisor Glenn D. Littenberg, MD, ASGE CPT Advisor The American College of Gastroenterology
Principles of ERCP: papilla cannulation, indications/contraindications and risks. Dr. med. Henrik Csaba Horváth PhD
 Principles of ERCP: papilla cannulation, indications/contraindications and risks Dr. med. Henrik Csaba Horváth PhD Evolution of ERCP 1968. 1970s ECPG Endoscopic CholangioPancreatoGraphy Japan 1974 Biliary
Principles of ERCP: papilla cannulation, indications/contraindications and risks Dr. med. Henrik Csaba Horváth PhD Evolution of ERCP 1968. 1970s ECPG Endoscopic CholangioPancreatoGraphy Japan 1974 Biliary
Pancreatitis is the most common and potentially serious ENDOSCOPY CORNER
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:834 839 ENDOSCOPY CORNER Short 5Fr vs Long 3Fr Pancreatic Stents in Patients at Risk for Post-Endoscopic Retrograde Cholangiopancreatography Pancreatitis
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:834 839 ENDOSCOPY CORNER Short 5Fr vs Long 3Fr Pancreatic Stents in Patients at Risk for Post-Endoscopic Retrograde Cholangiopancreatography Pancreatitis
