Joint Trust Guidelines for acute onset supraventricular tachycardia in children A Clinical Guideline
|
|
|
- Thomasine Wilcox
- 5 years ago
- Views:
Transcription
1 Joint Trust Guidelines for acute onset supraventricular tachycardia in children A Clinical Guideline For Use in: By: For: Key words: Name and job titles of document author s: Name and job title of author s Line Manager: Supported by: Assessed and approved by the: Date of approval: 15/10/2015 Ratified by or reported as approved to (if applicable): Children s Assessment Unit (CAU), Children s Wards, Neonatal Intensive Care Unit (NICU), Accident & Emergency (A&E) Medical and Nursing staff in the above Children with acute onset supraventricular tachycardia Supraventricular, tachycardia, acute, children, shock Dr Rahul Roy, Consultant Neonatologist & Paediatrician with Expertise in cardiology) Dr Jo Ponnampalam, Consultant Paediatrician (NNUH) David Booth, Clinical Director for Paediatrics Dr Graham Derrick, Consultant Paediatric Cardiologist, (NNUH) & Great Ormond Street Hospital for Sick Children Dr. Shiras Thayath, Children & Young People s Services, (JPUH) Accepted by James Paget University Hospital, (JPUH) on 17/07/2014 under the Tri-Hospital Clinical Guidelines Assessment Panel (THCGAP) Clinical Guidelines Assessment Panel (CGAP) If approved by committee or Governance Lead Chair s Action; tick here Clinical Standards Group Effectiveness Sub-Board To be reviewed before: This document remains current after 15/10/2018 this date but will be under review To be reviewed by: Dr Rahul Roy Reference and / or Trust Docs ID JCG0037 id 1250 No: Version No: 2 Description of changes (for revised versions): Compliance links: e.g. NICE None This guideline has been approved by the Trust's Clinical Guidelines Assessment Panel as an aid to the diagnosis and management of relevant patients and clinical circumstances. Not every patient or situation fits neatly into a standard guideline scenario and the guideline must be interpreted and applied in practice in the light of prevailing clinical circumstances, the diagnostic and treatment options available and the professional judgement, knowledge and expertise of relevant clinicians. It is advised that the rationale for any departure from relevant guidance should be documented in the patient's case notes. The Trust's guidelines are made publicly available as part of the collective endeavour to continuously improve the quality of healthcare through sharing medical experience and knowledge. The Trust accepts no responsibility for any misunderstanding or misapplication of this document. Author/s: Dr Rahul Roy Dr J.Ponnampalam Date of issue: 15/10/2015 Copy of complete document available from: Trust Intranet Page 1 of 7
2 Quick reference guideline/s (please refer below to note on adenosine doses as per cbnf) Assess Airway, Breathing, Circulation Attempt vagal manoevres Stop algorithm as soon as child reverts to sinus rhythm Adenosine i/v 100micrograms/kg 2 minutes Adenosine i/v 200micrograms/kg 2 minutes Adenosine i/v 300micrograms/kg 2 minutes NO Shock present? YES CONSIDER: Single dose (Child 1 month 18yrs) 500microgram/kg (max 12mg) Adenosine i/v Call for Anaesthetic support intubate & ventilate Synchronous DC shock 1J/kg D/W Paed Consultant & Paed Cardiologist Intravenous regarding Adenosine further cbnf dosing schedule(cbnf ) Synchronous DC treatment consider need for shock 2J/kg Amiodarone Neonates: or Flecainide 150 micrograms/kg; increase dose every 2 minutes by micrgrams/kg until tachycardia terminated or until maximum single dose of D/w 300 Paed micrograms/kg Consultant / Paed given. Cardiologist Re. need for transfer to Child 1 month-1 year: Paediatric Cardiology centre 150micrograms/kg; increase dose every 2 miutes by micrograms/kg until tachycardia is terminated or maximum single dose of 500micrograms/kg given. Copy of complete document available from: Trust Intranet Page 2 of 7
3 Child 1-12 years: 100micrograms/kg; increase dose every 2 minutes by micrograms/kg until tachycardia terminated or maximum single dose 500micrograms/kg (max. 12 milligrams) given. Child years: Initially 3 milligrams; if necessary increase dose to 6 milligrams after 2 minutes, then to 12milligrams after further 2 minutes. Notes for guide to use with algorithm Assess Airway, Breathing and Circulation. Inform Duty Paediatric Consultant. Continuous ECG monitoring which allows printouts of traces. Try vagal stimulation while continuing ECG monitoring. The following techniques can be used: 1. Elicit the diving reflex in an infant with a narrow complex tachycardia who is not haemodynamically compromised which produces an increase in vagal tone, slows atrioventricular conduction and interrupts the tachycardia. In the case of a baby, the infant should be wrapped in a towel and his whole face immersed into a bowl of cold water for about five seconds. There is no need to obstruct the mouth or nostrils as the baby will be temporarily apnoeic. For an older child an ice-water soaked cloth is placed on the nose and mouth. 2. Older children can try a Valsalva manoeuvre. Some children know that a certain position or action will usually effect a return to sinus rhythm like a headstand. Blowing hard through a straw may be effective for some children. Ocular pressure or carotid body massage should not be attempted in infants or children. Carotid massage rarely works and is not advisable (in infants could cause airway obstruction). If the vagal manoeuvre is ineffective, give: Intravenous adenosine (to be given rapidly into large peripheral or central vein and followed promptly by saline flush). Refer to dose schedule above, as per cbnf. Starting dose of 100 micrograms/kg rapid (<2 seconds) iv bolus Wait 2 mins 200 micrograms/kg iv bolus Wait 2 mins 300 micrograms/kg iv bolus Maximum single dose is 500 micrograms/kg iv (300 micrograms/kg under one month) up to a maximum of 12mg. Stop at anytime as soon as the child reverts to sinus rhythm. Adenosine should be given as a rapid (<2 seconds) bolus into a large peripheral vein and rapidly followed by a 5ml saline flush( so that it reached the heart quickly as Adenosine is metabolised very quickly). Copy of complete document available from: Trust Intranet Page 3 of 7
4 Obtain a continuous printed ECG recording during Adenosine administration and wait for secs post administration before discontinuing recording. Discuss with Paediatric Consultant/Paediatric Cardiologist regarding consideration of an alternative antiarrhythmic agent if SVT recurs despite higher Adenosine doses ( micrograms/kg). Side effects are short-lived but include flushing, nausea, dyspnoea and chest tightness. There will be AV block and ventricular asystole (the drug works by blocking the AV node and interrupting a reciprocating tachycardia) if the drug is given correctly, this is the intention and is short lived. It is worth warning parents and staff that this will happen. If a child with stable supraventricular tachycardia has not been converted to a normal rhythm with intravenous adenosine it is essential to seek the advice of a paediatric cardiologist before further treatment. After discussion with duty Paediatric Consultant, contact the on call cardiology registrar at Great Ormond Street Hospital and fax copy of ECG recording for further advice on management. The use of one of the following may be suggested, only to be given with intensive monitoring, regular 12 lead ECGs recording and with the knowledge and approval or recommendation of a paediatric cardiologist in a tertiary cardiology centre. 1. Amiodarone This drug can be used in refractory atrial tachycardia. The dose is 5mg/kg given intravenously over minutes diluted in approximately 4mls/kg of 5% dextrose. Can use a longer safer loading dose of 25 micrograms/kg/min for 4 hours(make infusion so that 1ml/hr =10micrograms/kg/min i.e. run this at 2.5ml/hour for 4 hours) and then a maintenance of 5-15 micrograms/kg/min i.e ml/hour (maximum 1.2 grams/24 hours). It is thrombophlebotic and therefore best given through a central line. Least negatively inotropic. Maintenance infusion continues for at least 24 hours and overlaps with oral Amiodarone for 24 hours, once tolerating feeds. Dose for oral Amiodarone as recommended by Great Ormond Street Hospital: Amiodarone 5 milligrams/kg TDS for 1 week, 5 milligrams/kg BD for further 1 week, then 5 milligrams/kg OD to continue (please discuss length of treatment with Dr Derrick s team at Great Ormond Street Hospital) Before starting Amiodarone, it is important to counsel the family about blood tests to include LFT s and TFT s as part of the monitoring. Also, education about increased susceptibility to sunburn and therefore the importance of using sunblock protection and shade is recommended. 2. Flecainide 2mg/kg intravenously over 30 minutes with continuous monitoring of particularly at QRS duration. ECG looking Copy of complete document available from: Trust Intranet Page 4 of 7
5 This drug is particularly useful in refractory Wolff-Parkinson-White type tachycardia(resistant re-entry supraventricular tachycardia). It is a membrane stabiliser but can be pro-arrythmic and has a negative inotropic effect, therefore do not give if myocardial function is impaired. Levels need monitoring if continued for more than 24 hours. 3. Propranolol & Verapamil (rarely used) IV propranolol may be used to treat SVT in the presence of WPW syndrome. IV verapamil (may be indicated for fascicular ventricular tachycardia) should be avoided in infants younger than 12 months of age because it may produce extreme bradycardia and hypotension in infants. Objective/s To provide guidance on the prompt recognition and management of Supraventricular tachycardia (SVT) in children presenting acutely to A&E or the Jenny Lind Children s Department. Rationale Supraventricular tachycardia (SVT) is defined as an abnormally rapid heart rate and rhythm originating above the ventricles, often (but not always) with a narrow QRS complex. The three most common forms of SVT in children are 1. Atrioventricular re-entrant tachycardia (AVRT), including the Wolff-Parkinson- White (WPW) syndrome, 2. Atrioventricular nodal re-entrant tachycardia (AVNRT). 3. Automaticity causing ectopic or non-reciprocating atrial tachycardia is rare SVT is the most common non arrest arrhythmia during childhood and is the most common arrhythmia that produces cardiovascular instability in infancy. Acute management of the child who presents in SVT can be a challenge because the exact mechanism of the tachycardia often is unknown. The treatment strategy depends upon the patient's presentation and clinical status (haemodynamic stability or instability). The approach consists of initiating therapy while continuing to assess the patient's condition. ECG monitoring before, during and after treatment is crucial to ensure correct rhythm identification and response to treatment. Presentation Older children usually complain of lightheadedness, dizziness, chest discomfort, or note the fast heart rate( palpitations), but very rapid rates may be undetected for long periods in young infants until they develop a low cardiac output state, shock or cardiac failure. Presentation in infants may include poor feeding, irritability, tachypoea and mottled skin. In utero SVT is a known cause of hydrops foetalis. Below is an example of an SVT rhythm on ECG recording: AV re-entrant tachycardia Copy of complete document available from: Trust Intranet Page 5 of 7
6 AV re-entrant tachycardia breaking to sinus rhythm with pre-excitation (Wolff-Parkinson-White syndrome). Broad recommendations Diagnosing SVT in infants and children SVT in infants generally produces a heart rate >220 bpm, and sometimes as high as 300 bpm. Lower heart rates like 180 bpm or above may occur in children during an attack of SVT. The QRS complex is narrow, making differentiation between marked sinus tachycardia due to shock and SVT difficult, particularly because SVT may be associated with poor systemic perfusion. SVT, seen in the first year of life i.e. in infancy but few afterward, is more likely to have accessory AVRT, and an adolescent who has first SVT is more likely to have nodal AVNRT. AVNRT is more influenced by increased sympathetic tone than AVRT. AVNRT is more likely triggered by physical activity, emotional stress, and abrupt changes in body position. AVNRT are less likely to be incessant and therefore rarely causes a tachycardia induced cardiomyopathy. The following characteristics may help to distinguish between sinus tachycardia and SVT: 1. Sinus tachycardia is typically characterised by a heart rate less than 200 per minute in infants and children, whereas infants with SVT typically have a heart rate greater than 220 beats per minute. P waves are usually present. 2. P-waves may be difficult to identify in both sinus tachycardia and SVT once the ventricular rate exceeds 200 beats per minute. If P-waves are identifiable, they are usually upright in leads I and AVF in sinus tachycardia while they are negative in leads II, III and AVF in SVT, although this is not always reliable. P waves are usually invisible in SVT. 3. In sinus tachycardia, the heart rate varies from beat to beat and is often responsive to stimulation, but there is no beat-to-beat variability in SVT. 4. Termination of SVT is abrupt whereas the heart rate slows gradually in sinus tachycardia in response to treatment such as fluid resuscitation in shock scenarios. 5. A history consistent with shock (e.g. gastroenteritis or septicaemia) is usually present with sinus tachycardia. Many infants tolerate SVT well. If the tachycardia is sustained for 6 to 12 hours, signs of cardiac heart failure (CHF) usually develop in infants. When CHF develops, the infant s condition can deteriorate rapidly. Older children may complain of chest pain, palpitation, shortness of breath, light headedness, and fatigue Copy of complete document available from: Trust Intranet Page 6 of 7
7 Note: A wide QRS complex tachycardia should always be managed as VT (ventricular tachycardia) until proven otherwise. Clinical audit standards Correct diagnosis, appropriate management including Adenosine starting dose and dosage escalation with ECG recording of conversion Summary of development and consultation process undertaken before registration and dissemination The guideline was drafted by the authors listed on the front page and discussed at the Paediatric Guideline Meeting, which has agreed the final content. During its development it has been circulated for comment to: Consultants in Paediatric Medicine, Accident & Emergency, and Dr. Graham Derrick, Consultant Paediatric Cardiologist at Great Ormond Street Hospital, London. This version has been endorsed by the Clinical Guidelines Assessment Panel. Distribution list/ dissemination method Trust Intranet, CAU, A&E, NICU and Buxton Ward References/ source documents 1) Update January 2011 to Advanced Paediatric Life Support:The Practical Approach 5 th Edition 2) Cochrane Review on Supraventricular Tachycardia 3) Sherwood MC, Lau KC, Sholler GF. Adenosine in the management of supraventricular tachycardia in children. Journal of Paediatrics and Child Health 1998 Feb;34(1): ) Dixon J, Foster K, Wyllie J, Wren C. Guidelines and adenosine dosing in supraventricular tachycardia. Archives of Disease in Childhood. 2005;90: ) Josephson ME, Wellens HJ. Differential diagnosis of supraventricular tachycardia. Cardiol Clin 1990; 8:411 6) Salerno J, Seslar P. Supraventricular Tachycardia ( review article). Arch Pediatr Adolesc Med/Vol 163(No 3), March ) cbnf edition 8) Drug doses, Intensive Care Unit, Royal Children s Hospital, Melbourne Copy of complete document available from: Trust Intranet Page 7 of 7
Emergency treatment to SVT Evidence-based Approach. Tran Thao Giang
 Emergency treatment to SVT Evidence-based Approach Tran Thao Giang Description ECG manifestations: HR is extremely rapid and regular (240bpm ± 40) P wave is: usually invisible When visible: anormal P axis,
Emergency treatment to SVT Evidence-based Approach Tran Thao Giang Description ECG manifestations: HR is extremely rapid and regular (240bpm ± 40) P wave is: usually invisible When visible: anormal P axis,
PEDIATRIC SVT MANAGEMENT
 PEDIATRIC SVT MANAGEMENT 1 INTRODUCTION Supraventricular tachycardia (SVT) can be defined as an abnormally rapid heart rhythm originating above the ventricles, often (but not always) with a narrow QRS
PEDIATRIC SVT MANAGEMENT 1 INTRODUCTION Supraventricular tachycardia (SVT) can be defined as an abnormally rapid heart rhythm originating above the ventricles, often (but not always) with a narrow QRS
TACHYARRHYTHMIAS IN INFANTS AND CHILDREN
 Principles of Management SVT Algorithm VT Algorithm Interpretations of ECG Supra-ventricular Tachycardia (SVT) background SVT Management SVT Ongoing Care Ventricular Tachycardia (VT) References Principles
Principles of Management SVT Algorithm VT Algorithm Interpretations of ECG Supra-ventricular Tachycardia (SVT) background SVT Management SVT Ongoing Care Ventricular Tachycardia (VT) References Principles
A Clinical Guideline for the use of Intravenous Aminophylline in Acute Severe Asthma in Children
 For Use in: By: For: Division responsible for document: Key words: Name and job titles of document author: Name and job title of document author s Line Manager: Supported by: Assessed and approved by the:
For Use in: By: For: Division responsible for document: Key words: Name and job titles of document author: Name and job title of document author s Line Manager: Supported by: Assessed and approved by the:
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material
 1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
Trust Protocol for the Administration of Intravenous Methylprednisolone for Thyroid Eye Disease A Protocol. The Clinical Investigation Unit (CIU)
 A Protocol For Use in: By: For: Division responsible for document: Key words: Name of document author: Job title of document author: Name and job title of document author s Line Manager: Supported by:
A Protocol For Use in: By: For: Division responsible for document: Key words: Name of document author: Job title of document author: Name and job title of document author s Line Manager: Supported by:
Chapter 9. Learning Objectives. Learning Objectives 9/11/2012. Cardiac Arrhythmias. Define electrical therapy
 Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Joint Trust Guideline for the Management of Methylprednisolone Sodium Succinate Infusion for Child or Young Person A Clinical Guideline
 A Clinical Guideline For Use in: Children s Department By: Registered Paediatric Nurses and Medical Staff Children with active inflammatory bowel disease, For: active rheumatological conditions or other
A Clinical Guideline For Use in: Children s Department By: Registered Paediatric Nurses and Medical Staff Children with active inflammatory bowel disease, For: active rheumatological conditions or other
European Resuscitation Council
 European Resuscitation Council Objectives To know basic elements to evaluate patients with rythm disturbance To know advanced treatment of paediatric cardiac arrest To know emergency treatment of most
European Resuscitation Council Objectives To know basic elements to evaluate patients with rythm disturbance To know advanced treatment of paediatric cardiac arrest To know emergency treatment of most
Guideline for the Management of patients with Regular Narrow-Complex Tachyarrhythmia
 Guideline for the Management of patients with Regular Narrow-Complex Tachyarrhythmia This guidance does not override the individual responsibility of health professionals to make appropriate decision according
Guideline for the Management of patients with Regular Narrow-Complex Tachyarrhythmia This guidance does not override the individual responsibility of health professionals to make appropriate decision according
Trust Guideline for the inclusion of women at High Risk of Breast Cancer in the NHS Breast Screening Programme
 Trust Guideline for the inclusion of women at High Risk of Breast Cancer in the NHS Breast Screening Programme For Use in: By: For: Division responsible for document: Key words: Name and job title of document
Trust Guideline for the inclusion of women at High Risk of Breast Cancer in the NHS Breast Screening Programme For Use in: By: For: Division responsible for document: Key words: Name and job title of document
Trust Guideline for the Management of: Abnormal Pre-operative Thyroid Function Tests in Adults. Anaesthetists Abnormal Pre-op Thyroid Function Test
 For Use in: By: For: Pre-operative Thyroid Function Tests in Adults Division responsible for document: Key words: Name and job titles of document author: Name and job title of document author s Line Manager:
For Use in: By: For: Pre-operative Thyroid Function Tests in Adults Division responsible for document: Key words: Name and job titles of document author: Name and job title of document author s Line Manager:
PEDIATRIC CARDIAC RHYTHM DISTURBANCES. -Jason Haag, CCEMT-P
 PEDIATRIC CARDIAC RHYTHM DISTURBANCES -Jason Haag, CCEMT-P General: CARDIAC RHYTHM DISTURBANCES - More often the result and not the cause of acute cardiovascular emergencies - Typically the end result
PEDIATRIC CARDIAC RHYTHM DISTURBANCES -Jason Haag, CCEMT-P General: CARDIAC RHYTHM DISTURBANCES - More often the result and not the cause of acute cardiovascular emergencies - Typically the end result
Supraventricular Tachycardia: From Fetus to Adult. Mohamed Hamdan, MD
 Supraventricular Tachycardia: From Fetus to Adult Mohamed Hamdan, MD Learning Objectives Define type of SVT by age Describe clinical approach Describe prenatal and postnatal management of SVT 2 SVT Across
Supraventricular Tachycardia: From Fetus to Adult Mohamed Hamdan, MD Learning Objectives Define type of SVT by age Describe clinical approach Describe prenatal and postnatal management of SVT 2 SVT Across
Trust Guideline on Routine Oxygen Saturation Measurement on the New-born (Pulse Oximetry)
 Trust Guideline on Routine Oxygen Saturation Measurement on the New-born For Use in: By: For: Division responsible for document: Key words: Name and job title of document author: Name and job title of
Trust Guideline on Routine Oxygen Saturation Measurement on the New-born For Use in: By: For: Division responsible for document: Key words: Name and job title of document author: Name and job title of
Pediatrics ECG Monitoring. Pediatric Intensive Care Unit Emergency Division
 Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Guideline for the Management of Continuous IV Vancomycin Infusion in Neonates on NICU A Clinical Guideline recommended for use
 Guideline for the Management of Continuous IV Vancomycin Infusion in A Clinical Guideline recommended for use For Use in: By: For: Division responsible for document: Key words: Name and job title of document
Guideline for the Management of Continuous IV Vancomycin Infusion in A Clinical Guideline recommended for use For Use in: By: For: Division responsible for document: Key words: Name and job title of document
Guideline for the Use of Granulocyte Colony Stimulating Factor (G-CSF) for Adults in Oncology and Haematology
 (G-CSF) for Adults in Oncology and Haematology For Use in: By: Oncology and Haematology Inpatients and Outpatients Oncologists and Haematologists For: Division responsible for document: Key words: Name
(G-CSF) for Adults in Oncology and Haematology For Use in: By: Oncology and Haematology Inpatients and Outpatients Oncologists and Haematologists For: Division responsible for document: Key words: Name
PALS Case Scenario Testing Checklist Respiratory Case Scenario 1 Upper Airway Obstruction
 Respiratory Case Scenario 1 Upper Airway Obstruction Directs administration of 100% oxygen or supplementary oxygen as needed to support oxygenation Identifies signs and symptoms of upper airway obstruction
Respiratory Case Scenario 1 Upper Airway Obstruction Directs administration of 100% oxygen or supplementary oxygen as needed to support oxygenation Identifies signs and symptoms of upper airway obstruction
INSTITUTE FOR MEDICAL SIMULATION & EDUCATION ACLS PRACTICAL SCENARIOS
 Practical Teaching for Respiratory Arrest with a Pulse (Case 1) You are a medical officer doing a pre-operative round when 60-year old patient started coughing violently and becomes unconscious. Fortunately
Practical Teaching for Respiratory Arrest with a Pulse (Case 1) You are a medical officer doing a pre-operative round when 60-year old patient started coughing violently and becomes unconscious. Fortunately
Electrocardiography for Healthcare Professionals
 Electrocardiography for Healthcare Professionals Kathryn A. Booth Thomas O Brien Chapter 5: Rhythm Strip Interpretation and Sinus Rhythms Learning Outcomes 5.1 Explain the process of evaluating ECG tracings
Electrocardiography for Healthcare Professionals Kathryn A. Booth Thomas O Brien Chapter 5: Rhythm Strip Interpretation and Sinus Rhythms Learning Outcomes 5.1 Explain the process of evaluating ECG tracings
Arrhythmic Complications of MI. Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine
 Arrhythmic Complications of MI Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine Objectives Brief overview -Pathophysiology of Arrhythmia ECG review of typical
Arrhythmic Complications of MI Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine Objectives Brief overview -Pathophysiology of Arrhythmia ECG review of typical
Core Content In Urgent Care Medicine
 Palpitations/Arrhythmias Ebrahim Barkoudah, MD Clinical Instructor in Internal Medicine Harvard Medical School Assistant in Internal Medicine & Pediatrics Massachusetts General Hospital MGH Chelsea Chelsea,
Palpitations/Arrhythmias Ebrahim Barkoudah, MD Clinical Instructor in Internal Medicine Harvard Medical School Assistant in Internal Medicine & Pediatrics Massachusetts General Hospital MGH Chelsea Chelsea,
ECGs on the acute admission ward. - Cardiology Update -
 ECGs on the acute admission ward - Cardiology Update - Dr Simon Fynn Consultant Cardiologist Papworth Hospital, Cambridge RCP London Oct 2017 ECG 1 1. AF with BBB 2. Pre-excited AF 3. SVT with BBB 4.
ECGs on the acute admission ward - Cardiology Update - Dr Simon Fynn Consultant Cardiologist Papworth Hospital, Cambridge RCP London Oct 2017 ECG 1 1. AF with BBB 2. Pre-excited AF 3. SVT with BBB 4.
Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD
 Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD OBJECTIVES 1. Identify the basic electrophysiology of the four causes of wide complex tachycardia. 2. Develop a simple framework for acute management
Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD OBJECTIVES 1. Identify the basic electrophysiology of the four causes of wide complex tachycardia. 2. Develop a simple framework for acute management
DYSRHYTHMIAS. D. Assess whether or not it is the arrhythmia that is making the patient unstable or symptomatic
 DYSRHYTHMIAS GENERAL CONSIDERATIONS A. The 2015 American Heart Association Guidelines were referred to for this protocol development. Evidence-based science was implemented in those areas where the AHA
DYSRHYTHMIAS GENERAL CONSIDERATIONS A. The 2015 American Heart Association Guidelines were referred to for this protocol development. Evidence-based science was implemented in those areas where the AHA
Supraventricular Tachycardia (SVT)
 Supraventricular Tachycardia (SVT) Daniel Frisch, MD Cardiology Division, Electrophysiology Section Thomas Jefferson University Hospital daniel.frisch@jefferson.edu Short RP Are these the Mid same RP tachycardias?
Supraventricular Tachycardia (SVT) Daniel Frisch, MD Cardiology Division, Electrophysiology Section Thomas Jefferson University Hospital daniel.frisch@jefferson.edu Short RP Are these the Mid same RP tachycardias?
PEDIATRIC ARRHYTHMIAS
 PEDIATRIC ARRHYTHMIAS Julie Martino, MD, FACEP Advocate Illinois Masonic Medical Center University of Illinois at Chicago I have no relevant financial relationships with the manufacturer of any commercial
PEDIATRIC ARRHYTHMIAS Julie Martino, MD, FACEP Advocate Illinois Masonic Medical Center University of Illinois at Chicago I have no relevant financial relationships with the manufacturer of any commercial
a lecture series by SWESEMJR
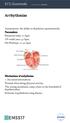 Arrhythmias Automaticity- the ability to depolarize spontaneously. Pacemakers: Sinoatrial node: 70 bpm AV-nodal area: 40 bpm His-Purkinje: 20-40 bpm it Mechanisms of arrhythmias 1. Increased automaticity
Arrhythmias Automaticity- the ability to depolarize spontaneously. Pacemakers: Sinoatrial node: 70 bpm AV-nodal area: 40 bpm His-Purkinje: 20-40 bpm it Mechanisms of arrhythmias 1. Increased automaticity
By: For: Division responsible for document: Key words: Name and job title of document author: Name and job title of document author s Line Manager:
 For Use in: By: For: Guidelines for the Management of Interruption of Biologic Therapies for Division responsible for document: Key words: Name and job title of document author: Name and job title of document
For Use in: By: For: Guidelines for the Management of Interruption of Biologic Therapies for Division responsible for document: Key words: Name and job title of document author: Name and job title of document
The most common. hospitalized patients. hypotension due to. filling time Rate control in ICU patients may be difficult as many drugs cause hypotension
 Arrhythmias in the critically ill ICU patients: Approach for rapid recognition & management Objectives Be able to identify and manage: Atrial fibrillation with a rapid ventricular response Atrial flutter
Arrhythmias in the critically ill ICU patients: Approach for rapid recognition & management Objectives Be able to identify and manage: Atrial fibrillation with a rapid ventricular response Atrial flutter
Trust Guideline for the Use of Parenteral Vancomycin and Teicoplanin in Adults
 A clinical guideline recommended for use: In: By: For: Division responsible for document: Key words: Names of document authors: Job titles of document authors: Name of document author s Line Manager: Job
A clinical guideline recommended for use: In: By: For: Division responsible for document: Key words: Names of document authors: Job titles of document authors: Name of document author s Line Manager: Job
Arrhythmias. A/Prof Drew Richardson. The Canberra Hospital May MB BS (Hons) FACEM Grad CertHE MD
 Arrhythmias A/Prof Drew Richardson MB BS (Hons) FACEM Grad CertHE MD The Canberra Hospital May 2013 Objectives Recognise the features of the common nonlethal arrhythmias Describe the emergency treatment
Arrhythmias A/Prof Drew Richardson MB BS (Hons) FACEM Grad CertHE MD The Canberra Hospital May 2013 Objectives Recognise the features of the common nonlethal arrhythmias Describe the emergency treatment
Antiarrhythmic Drugs
 Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Bernard Belhassen, MD; Roman Fish, MD; Sami Viskin, MD; Aharon Glick, MD; Michael Glikson, MD; Michael Eldar, MD
 www.ipej.org 3 Original Article Incidence of Dual AV Node Physiology Following Termination of AV Nodal Reentrant Tachycardia by Adenosine-5'-Triphosphate: A Comparison with Drug Administration in Sinus
www.ipej.org 3 Original Article Incidence of Dual AV Node Physiology Following Termination of AV Nodal Reentrant Tachycardia by Adenosine-5'-Triphosphate: A Comparison with Drug Administration in Sinus
Adult Basic Life Support
 Adult Basic Life Support UNRESPONSIVE? Shout for help Open airway NOT BREATHING NORMALLY? Call 112* 30 chest compressions 2 rescue breaths 30 compressions *or national emergency number Fig 1.2_Adult BLS
Adult Basic Life Support UNRESPONSIVE? Shout for help Open airway NOT BREATHING NORMALLY? Call 112* 30 chest compressions 2 rescue breaths 30 compressions *or national emergency number Fig 1.2_Adult BLS
Trust Guideline for the Management of Sedation in Painless Imaging Procedures in Children
 A clinical guideline recommended for use For Use in: By: For: Division responsible for document: Key words: Children s Day Ward (CDW), Children s Assessment Unit (CAU), Buxton Ward, Radiology. Paediatric
A clinical guideline recommended for use For Use in: By: For: Division responsible for document: Key words: Children s Day Ward (CDW), Children s Assessment Unit (CAU), Buxton Ward, Radiology. Paediatric
CARDIAC ARRHYTHMIAS IN NEONATE
 Introduction: CARDIAC ARRHYTHMIAS IN NEONATE DR. PANKAJ SAKHUJA Neonatologist Average heart rate in a healthy newborn is 120-160 beats/min and the range is from 80-230 beats/min. A normal (sinus) rhythm
Introduction: CARDIAC ARRHYTHMIAS IN NEONATE DR. PANKAJ SAKHUJA Neonatologist Average heart rate in a healthy newborn is 120-160 beats/min and the range is from 80-230 beats/min. A normal (sinus) rhythm
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Huseng Vefali MD St. Luke s University Health Network Department of Cardiology
 Huseng Vefali MD St. Luke s University Health Network Department of Cardiology Learning Objectives Establish Consistent Approach to Interpreting ECGs Review Essential Cases for Paramedics and first responders
Huseng Vefali MD St. Luke s University Health Network Department of Cardiology Learning Objectives Establish Consistent Approach to Interpreting ECGs Review Essential Cases for Paramedics and first responders
PhD FRCP MESC MEAPCI. Consultant Cardiologist SVT - Supra Ventricular Tachycardia. Coronary Arteries
 SVT - Supra Ventricular Tachycardia Coronary Arteries Overview LMS Supraventricular tachycardia is defined as an abnormally fast heartbeat. It's a describes a group of arrhythmias which all originate from
SVT - Supra Ventricular Tachycardia Coronary Arteries Overview LMS Supraventricular tachycardia is defined as an abnormally fast heartbeat. It's a describes a group of arrhythmias which all originate from
CSI Skills Lab #5: Arrhythmia Interpretation and Treatment
 CSI 202 - Skills Lab #5: Arrhythmia Interpretation and Treatment Origins of the ACLS Approach: CSI 202 - Skills Lab 5 Notes ACLS training originated in Nebraska in the early 1970 s. Its purpose was to
CSI 202 - Skills Lab #5: Arrhythmia Interpretation and Treatment Origins of the ACLS Approach: CSI 202 - Skills Lab 5 Notes ACLS training originated in Nebraska in the early 1970 s. Its purpose was to
2) Heart Arrhythmias 2 - Dr. Abdullah Sharif
 2) Heart Arrhythmias 2 - Dr. Abdullah Sharif Rhythms from the Sinus Node Sinus Tachycardia: HR > 100 b/m Causes: o Withdrawal of vagal tone & Sympathetic stimulation (exercise, fight or flight) o Fever
2) Heart Arrhythmias 2 - Dr. Abdullah Sharif Rhythms from the Sinus Node Sinus Tachycardia: HR > 100 b/m Causes: o Withdrawal of vagal tone & Sympathetic stimulation (exercise, fight or flight) o Fever
Dos and Don t in Cardiac Arrhythmia. Case 1 -ECG. Case 1. Management. Emergency Admissions. Reduction of TE risk -CHADS 2 score. Hospital Admissions
 Emergency Admissions Dos and Don t in Cardiac Arrhythmia Tom Wong, MD, FESC Consultant Cardiologist, Honorary Senior Lecturer Royal Brompton & Harefield Hospitals National Heart and Lung Institute, Imperial
Emergency Admissions Dos and Don t in Cardiac Arrhythmia Tom Wong, MD, FESC Consultant Cardiologist, Honorary Senior Lecturer Royal Brompton & Harefield Hospitals National Heart and Lung Institute, Imperial
Preparing for your upcoming PALS course
 IU Health PALS Study Guide Preparing for your upcoming PALS course UPDATED November 2016 Course Curriculum: 2015 American Heart Association (AHA) Guidelines for Pediatric Advanced Life Support (PALS) AHA
IU Health PALS Study Guide Preparing for your upcoming PALS course UPDATED November 2016 Course Curriculum: 2015 American Heart Association (AHA) Guidelines for Pediatric Advanced Life Support (PALS) AHA
MICHIGAN. State Protocols. Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.
 MICHIGAN State Protocols Protocol Number Protocol Name Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.3 Tachycardia PEDIATRIC CARDIAC PEDIATRIC CARDIAC ARREST
MICHIGAN State Protocols Protocol Number Protocol Name Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.3 Tachycardia PEDIATRIC CARDIAC PEDIATRIC CARDIAC ARREST
A Trust Guideline for the Management of. Bronchiolitis in Infants and Children under the age of 24 months
 A Clinical Guideline recommended Children s Assessment Unit (CAU), Buxton Ward, For use in: Children s Day Ward, Jenny Lind Out-patients Department, Accident and Emergency Department By: Medical and Nursing
A Clinical Guideline recommended Children s Assessment Unit (CAU), Buxton Ward, For use in: Children s Day Ward, Jenny Lind Out-patients Department, Accident and Emergency Department By: Medical and Nursing
Cardiac Arrhythmias & Drugs used in Advanced Life Support and Cardiac Emergencies
 Cardiac Arrhythmias & Drugs used in Advanced Life Support and Cardiac Emergencies CNHE Ballarat Health Services Valid from 1 st March 2016 to 31 st June 2018 1 Supraventricular Tachycardia (SVT) An atrial
Cardiac Arrhythmias & Drugs used in Advanced Life Support and Cardiac Emergencies CNHE Ballarat Health Services Valid from 1 st March 2016 to 31 st June 2018 1 Supraventricular Tachycardia (SVT) An atrial
Paroxysmal Supraventricular Tachycardia PSVT.
 Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
Trust Guideline for the Prevention of Tuberculosis and Management of Tuberculosis Exposure in Health Care Workers
 A Clinical Guideline For Use in: By: For: Division responsible for document: Key words: Name and job title of document author: Name and job title of document author s Line Manager: Supported by: Assessed
A Clinical Guideline For Use in: By: For: Division responsible for document: Key words: Name and job title of document author: Name and job title of document author s Line Manager: Supported by: Assessed
Case-Based Practical ECG Interpretation for the Generalist
 Case-Based Practical ECG Interpretation for the Generalist Paul D. Varosy, MD, FACC, FAHA, FHRS Director of Cardiac Electrophysiology VA Eastern Colorado Health Care System Associate Professor of Medicine
Case-Based Practical ECG Interpretation for the Generalist Paul D. Varosy, MD, FACC, FAHA, FHRS Director of Cardiac Electrophysiology VA Eastern Colorado Health Care System Associate Professor of Medicine
Trust Guideline for the Management of Patient Controlled Analgesia (PCA) in Adults
 Patient Controlled Analgesia (PCA) in Adults A clinical guideline recommended for use For Use in: In all Clinical Areas By: Anaesthetists, Ward Nurses, Recovery Staff Acute Pain Service Staff For: Adult
Patient Controlled Analgesia (PCA) in Adults A clinical guideline recommended for use For Use in: In all Clinical Areas By: Anaesthetists, Ward Nurses, Recovery Staff Acute Pain Service Staff For: Adult
Joint Trust Guideline for the Management of: CFS/ME (Chronic Fatigue Syndrome / Myalgic Encephalopathy) in Children and Young People
 A Clinical Guideline For Use in: By: For: Division responsible for document: Key words: Name of document author: Job title of document author: Name of document author s Line Manager: Job title of author
A Clinical Guideline For Use in: By: For: Division responsible for document: Key words: Name of document author: Job title of document author: Name of document author s Line Manager: Job title of author
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Clinical Guidelines Assessment Panel (CGAP) and Chairs Action Date of approval: 15/10/2015 Ratified by or reported as approved to (if applicable):
 A Clinical Guideline For Use in: By: For: Trust Guideline for Cardiology Referral Pathway; Paediatrics Division responsible for document: Key words: NICU, The Jenny Lind Department of Paediatrics, Blakeney
A Clinical Guideline For Use in: By: For: Trust Guideline for Cardiology Referral Pathway; Paediatrics Division responsible for document: Key words: NICU, The Jenny Lind Department of Paediatrics, Blakeney
Trust Guideline for Management of Faltering Growth (Failure to Thrive) in Babies and Young Children.
 Trust Guideline for Management of Faltering Growth (Failure to Thrive) in. A Clinical Guideline For use in: By: For: Division responsible for document: Women and Children Key words: Buxton Ward, Children
Trust Guideline for Management of Faltering Growth (Failure to Thrive) in. A Clinical Guideline For use in: By: For: Division responsible for document: Women and Children Key words: Buxton Ward, Children
Case #1. 73 y/o man with h/o HTN and CHF admitted with dizziness and SOB Treated for CHF exacerbation with Lasix Now HR 136
 Tachycardias Case #1 73 y/o man with h/o HTN and CHF admitted with dizziness and SOB Treated for CHF exacerbation with Lasix Now HR 136 Initial Assessment Check Telemetry screen if pt on tele Telemetry
Tachycardias Case #1 73 y/o man with h/o HTN and CHF admitted with dizziness and SOB Treated for CHF exacerbation with Lasix Now HR 136 Initial Assessment Check Telemetry screen if pt on tele Telemetry
the ECG, 6 mg of intravenous adenosine was administered as a fast bolus through a large bore intravenous cannula in
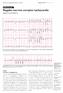 (arrows). Electrocardiography Series Singapore Med.1 2011, 52(3) 146 CME Article Regular narrow complex tachycardia Singh D, Teo S G, Poh K K V Hr JL1 11 VL VF WA, Fig. I ECG shows regular narrow complex
(arrows). Electrocardiography Series Singapore Med.1 2011, 52(3) 146 CME Article Regular narrow complex tachycardia Singh D, Teo S G, Poh K K V Hr JL1 11 VL VF WA, Fig. I ECG shows regular narrow complex
national CPR committee Saudi Heart Association (SHA). International Liason Commission Of Resuscitation (ILCOR)
 2 It is our pleasure to present to you this work as a result of team work of the national CPR committee at the Saudi Heart Association (SHA). We adapted the 2010 guidelines as per International Liason
2 It is our pleasure to present to you this work as a result of team work of the national CPR committee at the Saudi Heart Association (SHA). We adapted the 2010 guidelines as per International Liason
Joint Trust Guideline for the Use of Intravenous Vancomycin in Paediatrics
 A clinical guideline recommended For use in: All clinical areas where vancomycin is prescribed for Children aged 1 month to 16 years By: All medical, nursing, pharmacy, microbiology and phlebotomy paediatric
A clinical guideline recommended For use in: All clinical areas where vancomycin is prescribed for Children aged 1 month to 16 years By: All medical, nursing, pharmacy, microbiology and phlebotomy paediatric
TACHYARRHYTHMIAs. Pawel Balsam, MD, PhD
 TACHYARRHYTHMIAs Pawel Balsam, MD, PhD SupraVentricular Tachycardia Atrial Extra Systole Sinus Tachycardia Focal A. Tachycardia AVRT AVNRT Atrial Flutter Atrial Fibrillation Ventricular Tachycardia Ventricular
TACHYARRHYTHMIAs Pawel Balsam, MD, PhD SupraVentricular Tachycardia Atrial Extra Systole Sinus Tachycardia Focal A. Tachycardia AVRT AVNRT Atrial Flutter Atrial Fibrillation Ventricular Tachycardia Ventricular
Glucocorticoid replacement, Steroids, Acute Illness Dr Rupa Ahluwalia, Consultant Physician (NNUH)
 For Use in: By: For: Division responsible for document: Key words: Name and job title of document author s: Name and job tile of document author s Line Manager: Supported by: Assessed and approved by the:
For Use in: By: For: Division responsible for document: Key words: Name and job title of document author s: Name and job tile of document author s Line Manager: Supported by: Assessed and approved by the:
ECG Interactive Session
 SA HEART 2018 PRE-CONGRESS WORKSHOP 4 OCTOBER 2018 ECG Interactive Session Ashley Chin Cardiologist/Electrophysiologist University of Cape Town Groote Schuur Hospital ECG 1 Which ONE of the following is
SA HEART 2018 PRE-CONGRESS WORKSHOP 4 OCTOBER 2018 ECG Interactive Session Ashley Chin Cardiologist/Electrophysiologist University of Cape Town Groote Schuur Hospital ECG 1 Which ONE of the following is
Joint Trust Clinical Guideline for Monitoring of patients with Guillain Barré Syndrome (GBS)
 A Clinical Guideline For Use in: By: For: Division responsible for document: Key words: Name of document author: Job title of document author: Name of document author s Line Manager: Job title of author
A Clinical Guideline For Use in: By: For: Division responsible for document: Key words: Name of document author: Job title of document author: Name of document author s Line Manager: Job title of author
Arrhythmia Management Joshua M. Cooper, MD, FHRS, FACC
 Arrhythmia Management Joshua M. Cooper, MD, FHRS, FACC Professor of Medicine Director of Cardiac Electrophysiology Temple University Health System Plumbing Electrical System Bradyarrhythmias Sinus Node
Arrhythmia Management Joshua M. Cooper, MD, FHRS, FACC Professor of Medicine Director of Cardiac Electrophysiology Temple University Health System Plumbing Electrical System Bradyarrhythmias Sinus Node
Clinical Guidance. Extrasystoles in the neonatal period. Author: Peter Lillitos
 1 Clinical Guidance Extrasystoles in the neonatal period Author: Peter Lillitos Contents Page 2: Definition of extrasystoles/ectopic beats Page 3: Algorithm of management Page 4-5: Ordering investigations
1 Clinical Guidance Extrasystoles in the neonatal period Author: Peter Lillitos Contents Page 2: Definition of extrasystoles/ectopic beats Page 3: Algorithm of management Page 4-5: Ordering investigations
UNDERSTANDING ELECTROPHYSIOLOGY STUDIES
 UNDERSTANDING ELECTROPHYSIOLOGY STUDIES Testing and Treating Your Heart s Electrical System A Problem with Your Heart Rhythm The speed and pattern of a heartbeat is called the heart rhythm. The rhythm
UNDERSTANDING ELECTROPHYSIOLOGY STUDIES Testing and Treating Your Heart s Electrical System A Problem with Your Heart Rhythm The speed and pattern of a heartbeat is called the heart rhythm. The rhythm
PALS PRETEST. PALS Pretest
 PALS PRETEST 1. A child with a fever, immune system compromise, poor perfusion and hypotension is most likely to be experiencing which type of shock A. cardiogenic B. Neurogenic C. Septic D. Hypovolemic
PALS PRETEST 1. A child with a fever, immune system compromise, poor perfusion and hypotension is most likely to be experiencing which type of shock A. cardiogenic B. Neurogenic C. Septic D. Hypovolemic
Update of CPR AHA Guidelines
 Update of CPR AHA Guidelines Donald Hal Shaffner Course objective is to have an updated understanding of the American Heart Association s treatment algorithms for the management of cardiac decompensation
Update of CPR AHA Guidelines Donald Hal Shaffner Course objective is to have an updated understanding of the American Heart Association s treatment algorithms for the management of cardiac decompensation
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment
 Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
UNDERSTANDING YOUR ECG: A REVIEW
 UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
Cardiac arrhythmias in the PICU
 Cardiac arrhythmias in the PICU Paolo Biban, MD Director, Neonatal and Paediatric Intensive Care Unit Division of Paediatrics, Major City Hospital Azienda Ospedaliera Universitaria Integrata Verona, Italy
Cardiac arrhythmias in the PICU Paolo Biban, MD Director, Neonatal and Paediatric Intensive Care Unit Division of Paediatrics, Major City Hospital Azienda Ospedaliera Universitaria Integrata Verona, Italy
physiology 6 Mohammed Jaafer Turquoise team
 15 physiology 6 Mohammed Jaafer 22-3-2016 Turquoise team Cardiac Arrhythmias and Their Electrocardiographic Interpretation Today, we are going to talk about the abnormal excitation. As we said before,
15 physiology 6 Mohammed Jaafer 22-3-2016 Turquoise team Cardiac Arrhythmias and Their Electrocardiographic Interpretation Today, we are going to talk about the abnormal excitation. As we said before,
Dysrhythmias 11/7/2017. Disclosures. 3 reasons to evaluate and treat dysrhythmias. None. Eliminate symptoms and improve hemodynamics
 Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
Arrhythmia Care in the DGH What Still Needs to be Done? Dr. Sundeep Puri Consultant Cardiologist
 Arrhythmia Care in the DGH What Still Needs to be Done? Dr. Sundeep Puri Consultant Cardiologist LOTS!!! This presentation confines itself to the situation in the North West. The views expressed are my
Arrhythmia Care in the DGH What Still Needs to be Done? Dr. Sundeep Puri Consultant Cardiologist LOTS!!! This presentation confines itself to the situation in the North West. The views expressed are my
University Journal of Medicine and Medical Specialities
 University Journal of Medicine and Medical Specialities Volume 1 Issue 1 2015 Hypoglycemia and supraventricular tachycardia in infant of diabetic mother- A possible association. Sarah Paul Senthil S PSG
University Journal of Medicine and Medical Specialities Volume 1 Issue 1 2015 Hypoglycemia and supraventricular tachycardia in infant of diabetic mother- A possible association. Sarah Paul Senthil S PSG
Shifts 28, 29, 30 Quizzes
 Shifts 28, 29, 30 Quizzes Name: Score: Date: 1. You are on the scene of a 4 year old in cardiac arrest. CPR is initiated and an E.T. tube has been placed, an I.V. has been established. What is the correct
Shifts 28, 29, 30 Quizzes Name: Score: Date: 1. You are on the scene of a 4 year old in cardiac arrest. CPR is initiated and an E.T. tube has been placed, an I.V. has been established. What is the correct
WPW syndrome and AVRT
 WPW syndrome and AVRT Myung-Yong Lee, MD, PhD Division of Cardiology Department of Internal Medicine School of Medicine Dankook University, Cheonan, Korea Supraventricular tachycardia (SVT) Paroxysmal
WPW syndrome and AVRT Myung-Yong Lee, MD, PhD Division of Cardiology Department of Internal Medicine School of Medicine Dankook University, Cheonan, Korea Supraventricular tachycardia (SVT) Paroxysmal
Ablation Update and Case Studies. Lawrence Nair, MD, FACC Director of Electrophysiology Presbyterian Heart Group
 Ablation Update and Case Studies Lawrence Nair, MD, FACC Director of Electrophysiology Presbyterian Heart Group Disclosures No financial relationships to disclose Objectives At the conclusion of this activity,
Ablation Update and Case Studies Lawrence Nair, MD, FACC Director of Electrophysiology Presbyterian Heart Group Disclosures No financial relationships to disclose Objectives At the conclusion of this activity,
Chapter 16: Arrhythmias and Conduction Disturbances
 Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
You Don t Want to Miss This One! Focus on can t miss EKG tracings
 You Don t Want to Miss This One! Focus on can t miss EKG tracings Renaissance St. Louis Grand Hotel Convention Center October 23, 2014 David K. Tan, M.D., EMT-T, FAAEM EMS Section Chief, Division of Emergency
You Don t Want to Miss This One! Focus on can t miss EKG tracings Renaissance St. Louis Grand Hotel Convention Center October 23, 2014 David K. Tan, M.D., EMT-T, FAAEM EMS Section Chief, Division of Emergency
EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs
 EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important step for
EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important step for
Division 2, Surgical and Anaesthetics Directorates All surgical and anaesthetics staff Patients with an implanted spinal cord stimulator For:
 Joint Clinical Guideline for Patients with an implanted spinal cord stimulator (SCS) For Use in: Division 2, Surgical and Anaesthetics Directorates By: All surgical and anaesthetics staff Patients with
Joint Clinical Guideline for Patients with an implanted spinal cord stimulator (SCS) For Use in: Division 2, Surgical and Anaesthetics Directorates By: All surgical and anaesthetics staff Patients with
The pill-in-the-pocket strategy for paroxysmal atrial fibrillation
 The pill-in-the-pocket strategy for paroxysmal atrial fibrillation KONSTANTINOS P. LETSAS, MD, FEHRA LABORATORY OF CARDIAC ELECTROPHYSIOLOGY EVANGELISMOS GENERAL HOSPITAL OF ATHENS ARRHYTHMIAS UPDATE,
The pill-in-the-pocket strategy for paroxysmal atrial fibrillation KONSTANTINOS P. LETSAS, MD, FEHRA LABORATORY OF CARDIAC ELECTROPHYSIOLOGY EVANGELISMOS GENERAL HOSPITAL OF ATHENS ARRHYTHMIAS UPDATE,
Trust Guideline for the Management and Administration of Intravenous Iron in Adults under the Gastroenterology Directorate
 A clinical guideline recommended for use For Use in: The Gastroenterology Directorate By: Registered nurses competent in the administration of intravenous therapy and medical staff For: Adult patients
A clinical guideline recommended for use For Use in: The Gastroenterology Directorate By: Registered nurses competent in the administration of intravenous therapy and medical staff For: Adult patients
UNIVERSITY HOSPITALS OF LEICESTER NHS TRUST CARDIAC INVESTIGATIONS PAEDIATRIC & CONGENITAL SYNCOPE INVESTIGATIONS/QUESTIONNAIRE PROTOCOL
 UNIVERSITY HOSPITALS OF LEICESTER NHS TRUST CARDIAC INVESTIGATIONS PAEDIATRIC & CONGENITAL SYNCOPE INVESTIGATIONS/QUESTIONNAIRE PROTOCOL Written Date: 2009 by Dr Duke, then updated by Dr Sarita Makam 12/4/2016
UNIVERSITY HOSPITALS OF LEICESTER NHS TRUST CARDIAC INVESTIGATIONS PAEDIATRIC & CONGENITAL SYNCOPE INVESTIGATIONS/QUESTIONNAIRE PROTOCOL Written Date: 2009 by Dr Duke, then updated by Dr Sarita Makam 12/4/2016
WHAT DO YOU SEE WHEN YOU STIMULATE BETA
 CARDIAC DRUG REVIEW WHAT DO YOU SEE WHEN YOU STIMULATE BETA VASODILATE BRONCHODILATE +CHRONOTROPE +INOTROPE EPI S OTHER NAME? ADRENALIN WHAT DOES EPI DO THAT NOREPI AND DOPAMINE DO NOT DO? BETA 2 BRONCHODILATOR
CARDIAC DRUG REVIEW WHAT DO YOU SEE WHEN YOU STIMULATE BETA VASODILATE BRONCHODILATE +CHRONOTROPE +INOTROPE EPI S OTHER NAME? ADRENALIN WHAT DOES EPI DO THAT NOREPI AND DOPAMINE DO NOT DO? BETA 2 BRONCHODILATOR
I have nothing to disclose.
 I have nothing to disclose. Antiarrhythmic Therapy in Pregnancy Prof. Ali Oto,MD,FESC,FACC,FHRS Department of Cardiology Hacettepe University,Faculty of Medicine Ankara Arrhythmias in pregnancy An increased
I have nothing to disclose. Antiarrhythmic Therapy in Pregnancy Prof. Ali Oto,MD,FESC,FACC,FHRS Department of Cardiology Hacettepe University,Faculty of Medicine Ankara Arrhythmias in pregnancy An increased
Atrial Flutter in Infants
 Journal of the American College of Cardiology Vol. 48, No. 5, 2006 2006 by the American College of Cardiology Foundation ISSN 0735-1097/06/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2006.04.091
Journal of the American College of Cardiology Vol. 48, No. 5, 2006 2006 by the American College of Cardiology Foundation ISSN 0735-1097/06/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2006.04.091
Trust Guideline for the Management of: A Neonate with Difficult Airway
 For Use in: By: For: Division responsible for document: Key words: Name and job titles of document author: Name and job title of document author s Line Manager: Supported by: Neonatal unit, Delivery Suite,
For Use in: By: For: Division responsible for document: Key words: Name and job titles of document author: Name and job title of document author s Line Manager: Supported by: Neonatal unit, Delivery Suite,
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
ANTI-ARRHYTHMICS AND WARFARIN. Dr Nithish Jayakumar
 ANTI-ARRHYTHMICS AND WARFARIN Dr Nithish Jayakumar Contents 1. Anti-arrhythmics Pacemaker and myocardial potentials Drug classes mechanisms; s/e; contra-indications Management of common arrhythmias 2.
ANTI-ARRHYTHMICS AND WARFARIN Dr Nithish Jayakumar Contents 1. Anti-arrhythmics Pacemaker and myocardial potentials Drug classes mechanisms; s/e; contra-indications Management of common arrhythmias 2.
ECG Interpretation Made Easy
 ECG Interpretation Made Easy Dr. A Tageldien Abdellah, MSc MD EBSC Lecturer of Cardiology- Hull University Hull York Medical School 2007-2008 ECG Interpretation Made Easy Synopsis Benefits Objectives Process
ECG Interpretation Made Easy Dr. A Tageldien Abdellah, MSc MD EBSC Lecturer of Cardiology- Hull University Hull York Medical School 2007-2008 ECG Interpretation Made Easy Synopsis Benefits Objectives Process
ARTICLE. Supraventricular Tachycardia in Infancy. Catherine D. DeAngelis, MD. In most infants, SVT is due to an accessory atrioventricular
 Supraventricular Tachycardia in Infancy Evaluation, Management, and Follow-up Susan P. Etheridge, MD; Victoria E. Judd, MD ARTICLE Background: Supraventricular tachycardia (SVT) occurs frequently in infancy.
Supraventricular Tachycardia in Infancy Evaluation, Management, and Follow-up Susan P. Etheridge, MD; Victoria E. Judd, MD ARTICLE Background: Supraventricular tachycardia (SVT) occurs frequently in infancy.
Dr.Binoy Skaria 13/07/15
 Dr.Binoy Skaria binoyskaria@hotmail.com binoy.skaria@heartofengland.nhs.uk 13/07/15 Acknowledgement Medtronic, Google images & Elsevier for slides Natalie Ryan, Events Manager, HEFT- for organising the
Dr.Binoy Skaria binoyskaria@hotmail.com binoy.skaria@heartofengland.nhs.uk 13/07/15 Acknowledgement Medtronic, Google images & Elsevier for slides Natalie Ryan, Events Manager, HEFT- for organising the
Final Written Exam ASHI ACLS
 Final Written Exam ASHI ACLS Instructions: Identify the choice that best completes the statement or answers the question. Questions 1 and 2 pertain to the following scenario: A 54-year-old man has experienced
Final Written Exam ASHI ACLS Instructions: Identify the choice that best completes the statement or answers the question. Questions 1 and 2 pertain to the following scenario: A 54-year-old man has experienced
Cardiac arrhythmias. Janusz Witowski. Department of Pathophysiology Poznan University of Medical Sciences. J. Witowski
 Cardiac arrhythmias Janusz Witowski Department of Pathophysiology Poznan University of Medical Sciences A 68-year old man presents to the emergency department late one evening complaining of increasing
Cardiac arrhythmias Janusz Witowski Department of Pathophysiology Poznan University of Medical Sciences A 68-year old man presents to the emergency department late one evening complaining of increasing
Sustained tachycardia with wide QRS
 Sustained tachycardia with wide QRS Courtesy from Prof. Antonio Américo Friedmann. Electrocardiology Service of University of Faculty of São Paulo. Opinions from colleagues Greetings to everyone, In a
Sustained tachycardia with wide QRS Courtesy from Prof. Antonio Américo Friedmann. Electrocardiology Service of University of Faculty of São Paulo. Opinions from colleagues Greetings to everyone, In a
Rate: The atrial and ventricular rates are equal; heart rate is greater than 100 bpm (usually between bpm).
 Sinus Bradycardia Regularity: The R-R intervals are constant; the rhythm is regular. Rate: The atrial and ventricular rates are equal; heart rate is less than 60 bpm. P wave: There is a uniform P wave
Sinus Bradycardia Regularity: The R-R intervals are constant; the rhythm is regular. Rate: The atrial and ventricular rates are equal; heart rate is less than 60 bpm. P wave: There is a uniform P wave
Joint Trust Guidelines for Management of Central Venous Catheter Infection in Children Receiving Parenteral Nutrition
 For Use in: By: For: Key words: Name of document author: Job title of document author: Name of document author s Line Manager: Job title of author s Line Manager: Supported by: Children s services, Neonatal
For Use in: By: For: Key words: Name of document author: Job title of document author: Name of document author s Line Manager: Job title of author s Line Manager: Supported by: Children s services, Neonatal
