Pudendal Block and Urinary Dysfunction/Retention
|
|
|
- Brenda Charles
- 5 years ago
- Views:
Transcription
1 Date of Search: 22 Mar 17 Sources Searched: Medline, Embase, Cinahl, Google Scholar DISCLAIMER: Results of database and or Internet searches are subject to the limitations of both the database(s) searched, and by your search request. It is the responsibility of the requestor to determine the accuracy, validity and interpretation of the results. Pudendal Block and Urinary Dysfunction/Retention 1. The association between specific parturition events and urinary incontinence in later life: Results from a retrospective cohort study Author(s): Thom D.; Creasman J.; Subak L.; Brown J.; Van Den Eeden S.; Ragins A. Source: Neurourology and Urodynamics; Sep 2009; vol. 28 (no. 7); p Publication Date: Sep 2009 Publication Type(s): Journal: Conference Abstract Available in full text at Neurourology and Urodynamics - from John Wiley and Sons Available in full text at Neurourology and Urodynamics - from John Wiley and Sons Abstract:Hypothesis/Aims of study While vaginal birth is a widely recognized risk factor for urinary incontinence (UI) in later life, little is known re the association between specific parturition events and later UI. Studies have reported an association between post-partum UI and specific parturition events, such as type of anesthesia or use of forceps, though results have been inconsistent.[1-2] While most women with UI in the post-partum period regain continence, it has been suggested that specific parturition events may continue to contribute to the risk of UI in later life, as aging diminishes physiologic reserves.[3] Our study examined associations between specific parturition events and UI in middle-aged and older women. Study design, materials and methods: The Reproductive Risks for Incontinence Study at Kaiser (RRISK) is a retrospective cohort study of women between 40 and 69 years of age as of January 1, 1999 who have been members since age 18 of Kaiser Permanente Medical Care Program of Northern California, a pre-paid group practice with over 3 million members, about 25% of general population in the area served. A random sample of women was generated from membership files. Women were screened and recruited with the goal of obtaining weighted sample with equal numbers in each 5 year age strata and a distribution of 40% white, 20% Hispanic, 20% Asian and 20% African-American participants. Women were excluded if they did not speak English or Spanish, reported having had less than half of their births within Kaiser, were no longer members of Kaiser, had moved out of the area, or were demented or otherwise too impaired to participate. Eligibility could not be determined for 1326 women. Of 2817 women determined to be eligible, 2109 (74.9%) were enrolled. Questionnaires ascertained variables including age, self-reported race/ethnicity, a detailed description of current UI, medical and surgical history, pregnancy and parturition history, menopausal status, hormone replacement, health habits, general health, and demographics. Weight and height were measured by the interviewer and used to calculated body mass index (BMI) in kg/m2. Labor and delivery records, archived since 1945, were abstracted by professional medical record abstractors. Current UI was defined as at least monthly incontinence for the past 12 months and was further characterized as monthly, weekly and daily. Type of incontinence was defined for those women with at least weekly incontinence, according to their response to two questions, one asking if UI occurred "with an activity like coughing, lifting, sneezing or exercise" (stress incontinence) and the other asking if UI occurred "with a physical sense of urgency" (urge incontinence). For purposes of analysis, stress incontinence was defined as the majority of UI episodes in the past 7 days being stress related; similarly urge incontinence was S
2 defined as the majority of episodes being urge related. Women reporting no episodes of UI in the past 12 months were considered continent. Bivariate associations of parturition events and UI were assessed using logistic or proportional odds models. Variables associated with incontinence at p 10%) change in the estimated association between any racial/ethnic group and incontinence were retained in the model. Age and parity were included by default in all models. Continuous variables were also assessed as categorical variables to maximize the opportunity for detecting confounding. All analyses were carried out in SAS Version 8.02 (SAS Institute, Cary, NC). Additional, exploratory analyses were performed using recursive partitioning to search for combinations of parturition exposures that were associated with increased probability of UI. Results: Of the 2109 participating women, 1521 reported at least one vaginal birth and are included in the analysis. The mean age was /- 8.5 years; 46% were Caucasian, non-hispanic, 19% were African-American, 18% were Hispanic (predominately of Mexican origin), and 16% were Asian. Exposure to specific parturition events are shown in the table for women with UI > weekly compared to continent women. All exposures, with the exception of ever having had a 3rd or 4th degree tear, were associated with UI in the bivariate (unadjusted) analysis, though the association was statistically significant only for 'ever being induced,' and 'ever having pudendal anesthesia.' In multivariate analysis, only 'ever being induced' remained significant. When analysis was restricted to comparing women with only stress UI, a similar pattern was seen in the bivariate analysis, while in the multivariate analysis, only 'ever pudendal anesthesia' remained significant (OR=1.4, 95% CI=1.0 to 2.0). (Table Presented) Exploratory analysis using recursive partitioning found that age at first delivery > 23 years and birth weight > 3177 grams identified a subgroup of women at with a high prevalence of > weekly UI (64% vs 42% in all women). Similarly, age at first delivery > 23 years and birth weight > 3026 grams identified a subgroup of women more likely to have stress UI (41% vs. 28%). No factors of similar importance were found which identified women with a high prevalence of urge incontinence. Interpretation of Results: Our results are consistent with the literature on parturition events and risk of post-partum incontinence in that individual several individual events were associated with an increased risk of UI, but the associations were mostly weak to moderate in magnitude and not statistically significant. In multivariate analysis, only ever having been induced remained associated with weekly UI later in life and ever having had a pudendal anesthesia remained associated with weekly stress UI, which is consistent with a prior study which reported that epidural or spinal anesthesia were protective for post-partum UI [2]. Recently, it has been reported that while parity is a significant risk factor for UI in women below about age 60, its association is weaker in women above after age 55 to 60. Unfortunately, we did not have sufficient number of subjects to investigate age as an effect modifier. Concluding message: We were not able to identify specific parturition events that clearly increased the risk of UI in later life. It remains possible that there are specific events that increase UI risk for women in a somewhat younger age group (e.g., 35 to 55), perhaps by effectively causing the UI to develop earlier then it would have otherwise. A larger study, dedicated to women in this age group, is needed to evaluate this possibility.
3 2. Is Postpartum Urinary Retention a Neurogenic Phenomenon? Author(s): Alas A.N.; Hurtado E.A. Source: Current Bladder Dysfunction Reports; Dec 2015; vol. 10 (no. 4); p Publication Date: Dec 2015 Publication Type(s): Journal: Review Available in full text at Current Bladder Dysfunction Reports - from Springer Link Journals Abstract:Postpartum urinary retention (PUR) can be classified as covert, those with postvoid residuals higher than 150 cm3, or overt, those unable to void 6 hours after vaginal delivery or after removal of a catheter after cesarean section. There is limited data and research on the mechanism of PUR. However, it has been suggested that there is a neurological component to the development of PUR. This includes disruption of the afferent system through analgesic blockade, crush or stretch injuries to the pudendal nerve during delivery, and impairment of neurotransmitters required for proper signal transduction. However, it is likely that the causes of PUR are multifactorial, and that physiologic changes of pregnancy and trauma from childbirth play a critical role. Copyright 2015, Springer Science+Business Media New York. 3. Urinary incontinence and pregnancy Author(s): Deffieux X. Source: Journal de Gynecologie Obstetrique et Biologie de la Reproduction; Dec 2009; vol. 38 (no. 8) Publication Date: Dec 2009 Publication Type(s): Journal: Article Available in full text at Journal de Gynécologie Obstétrique et Biologie de la Réproduction - from Free Access Content Abstract:The goal of the current study was to systematically review the literature concerning urinary incontinence and pregnancy, in order to develop recommendations for clinical practice. The prevalence of urinary stress incontinence and overactive bladder symptoms increase with gestational age during pregnancy (from the first to the third trimester), and decrease during the third months following delivery. Obstetrics factors (position during delivery, length of the second part of the labour, forceps, episiotomy, epidural or pudendal anaesthesia) do not modify the risk of post-partum or long term urinary incontinence. At short term follow-up, caesarean delivery is associated with a lower rate of post-partum urinary incontinence. At long term follow-up, data are lacking. Non elective caesarean section is not associated with a decrease in the rate of post-partum or long-term urinary incontinence. Elective caesarean section and systematic episiotomy are not recommended methods for the prevention of post-partum urinary incontinence (grade B), even in "high risk" women. Pelvic floor muscle therapy is the first line treatment for prenatal or post-partum urinary incontinence (grade A) Elsevier Masson SAS. All rights reserved.
4 4. Use of epidural anesthesia and the risk of acute postpartum urinary retention. Author(s): Musselwhite, Kimberly L; Faris, Peter; Moore, Katherine; Berci, Dena; King, Kathryn M Source: American journal of obstetrics and gynecology; May 2007; vol. 196 (no. 5); p. 472 Publication Date: May 2007 Publication Type(s): Journal Article Abstract:OBJECTIVEWe aimed to examine the relationship between the use of epidural analgesia during labor and acute postpartum urinary retention.study DESIGNA retrospective cohort study was conducted using 1994 labor and postpartum health records from 3 primary care centers.resultslogistic regression analysis revealed that a longer second stage of labor (odds ratio [OR] 2.62; 95% confidence interval [CI] ), use of systemic narcotics (OR 1.63; 95% CI ), perineal laceration (OR 1.73; 95% CI ), and instrumental delivery (OR 1.86; 95% CI ) predicted urinary retention. There was a trend toward association of epidural analgesia and urinary retention (OR 1.69; 95% CI ). Propensity score analysis revealed that any effect of epidural analgesia was likely due to effect modification of other obstetric variables.conclusion Epidural analgesia during labor may increase the risk of developing urinary retention by up to 3 times. However, this effect is mediated by other obstetric variables. Database: Medline 5. Innervation of the pelvic floor muscles: A reappraisal for the levator ani nerve Author(s): DeRuiter M.C.; Wallner C.; Maas C.P.; Dabhoiwala N.F.; Lamers W.H. Source: Obstetrics and Gynecology; Sep 2006; vol. 108 (no. 3); p Publication Date: Sep 2006 Publication Type(s): Journal: Article Available in print at Patricia Bowen Library and Knowledge Service West Middlesex university Hospital - from Obstetrics and Gynecology Available in full text at Obstetrics and Gynecology - from Ovid Abstract:OBJECTIVE: We investigated the clinical anatomy of the levator ani nerve and its topographical relationship with the pudendal nerve. METHODS: Ten female pelves were dissected and a pudendal nerve blockade was simulated. The course of the levator ani nerve and pudendal nerve was described quantitatively. The anatomical data were verified using (immuno- )histochemically stained sections of human fetal pelves. RESULTS: The levator ani nerve approaches the pelvic-floor muscles on their visceral side. Near the ischial spine, the levator ani nerve and the pudendal nerve lie above and below the levator ani muscle, respectively, at a distance of approximately 6 mm from each other. The median distance between the levator ani nerve and the point of entry of the pudendal blockade needle into the levator ani muscle was only 5 mm. CONCLUSION: The levator ani nerve and the pudendal nerve are so close at the level of the ischial spine that a transvaginal "pudendal nerve blockade" would, in all probability, block both nerves simultaneously. The clinical anatomy of the levator ani nerve is such that it is prone to damage during complicated vaginal childbirth and surgical interventions by The American College of Obstetricians and Gynecologists. Published by Lippincott Williams & Wilkins.
5 6. Evidence for the innervation of pelvic floor muscles by the pudendal nerve Author(s): Guaderrama N.M.; Liu J.; Nager C.W.; Pretorius D.H.; Sheean G.; Kassab G.; Mittal R.K. Source: Obstetrics and Gynecology; Oct 2005; vol. 106 (no. 4); p Publication Date: Oct 2005 Publication Type(s): Journal: Article Available in print at Patricia Bowen Library and Knowledge Service West Middlesex university Hospital - from Obstetrics and Gynecology Available in full text at Obstetrics and Gynecology - from Ovid Abstract:OBJECTIVE: To evaluate whether the pudendal nerve innervates the levator ani muscles by assessing the effect of pudendal nerve blockade on pelvic floor muscle function. METHODS: Eleven nulliparous women without symptoms of anal or urinary incontinence were studied before and after pudendal nerve blockade with vaginal manometry, electromyography of the external anal sphincter and puborectalis muscle, and 3-dimensional transperineal ultrasound imaging of the urogenital hiatus during rest and squeeze. RESULTS: After pudendal nerve blockade, mean vaginal resting pressures decreased from 19 +/- 10 mm Hg to 15 +/- 10 mm Hg (P <.05), and mean vaginal squeeze pressures decreased from 61 +/- 29 mm Hg to 37 +/- 24 mm Hg (P <.05). After pudendal nerve blockade, the anterior-posterior length of the urogenital hiatus increased from 51 +/- 4 mm to 55 +/- 5 mm at rest (P <.05) and increased from 47 +/- 3 mm to 52 +/- 5 mm during squeeze (P <.05). Resting and squeeze electromyography amplitude of the external anal sphincter and puborectalis muscle was markedly reduced by pudendal nerve blockade. CONCLUSION: Pudendal nerve blockade decreases vaginal pressures, increases length of urogenital hiatus, and decreases electromyography activity of the puborectalis muscle, all of which suggest that the pudendal nerve does innervate the levator ani muscle by The American College of Obstetricians and Gynecologists. Published by Lippincott William & Wilkins. 7. Risk factors for development and recurrence of urinary incontinence Author(s): Bo K. Source: Current Opinion in Urology; 1997; vol. 7 (no. 4); p Publication Date: 1997 Publication Type(s): Journal: Short Survey Abstract:Three months postpartum, risk factors for development of urinary incontinence were found to be vaginal delivery, obesity and multiparity (> 5). Caesarean section and daily antenatal pelvic floor muscle exercises appear to be protective, although not completely. in two studies the importance of pelvic floor muscle function in continence was addressed. In a case-control study of stress incontinent and healthy women, significantly thicker pelvic floor muscles were found in the healthy subjects. In another study urethral pressure parameters were all reduced following pudendal nerve blockade. A threefold prevalence of urinary stress incontinence among first degree relatives of female patients with stress urinary incontinence was demonstrated. In a review article associations between psychological and cognitive factors and sensory urgency and idiopathic detrusor instability were discussed. In another review article urinary incontinence in old age was addressed. In the elderly, urinary incontinence may be either transient or established. However, it should never be considered normal due to age. On the contrary, it seems to be treatable and often curable at all ages, even in the frail elderly.
6 8. Delivery and pudendal nerve function. Author(s): Tetzschner, T; Sørensen, M; Jønsson, L; Lose, G; Christiansen, J Source: Acta obstetricia et gynecologica Scandinavica; Apr 1997; vol. 76 (no. 4); p Publication Date: Apr 1997 Publication Type(s): Journal Article Available in full text at Acta Obstetricia et Gynecologica Scandinavica - from John Wiley and Sons Abstract:OBJECTIVE To assess the impact of mode of delivery and the occurrence of pelvic instability upon the pudendal nerve function and relate the pudendal nerve function to the occurrence of anal and urinary incontinence.methods One hundred and forty-six pregnant women were examined during pregnancy and 12 weeks post partum with measurement of pudendal nerve terminal motor latency (PNTML), the difference between the two measurements was defined as delta PNTML. Anal and urinary continence status, details of delivery and the occurrence of pelvic instability were recorded prospectively.results Pudendal nerve terminal motor latency increased from 1.7 msec in primiparae and 1.8 msec in multiparae during pregnancy to 2.0 msec (p 2.4 msec. The delta PNTML was significantly associated with age, the occurrence of pelvic instability and the use of vacuum extraction. The group of women with urinary incontinence had a significant increased PNTML. Database: Medline 9. Pudendal nerve damage increases the risk of fecal incontinence in women with anal sphincter rupture after childbirth Author(s): Tetzschner J.; Sorensen M.; Rasmussen O.O.; Lose G.; Christiansen J. Source: Acta Obstetricia et Gynecologica Scandinavica; 1995; vol. 74 (no. 6); p Publication Date: 1995 Publication Type(s): Journal: Article Abstract:Aim. To evaluate anal function after childbirth in 94 women in whom sphincter rupture occurred and in 19 control women. The findings of anorectal physiological assessment and history of childbirth were related to the presence of fecal incontinence. Methods. Anal manometry and electromyography were performed the first days after childbirth and repeated 3 months post partum together with measurement of pudendal nerve terminal motor latency. Results. Eighteen patients (19%) presented with incontinence. None of the controls developed fecal incontinence after delivery. Anal manometry showed that both incontinent and continent patients had decreased resting and squeeze pressures compared to control subjects (p2.0 milliseconds had an increased risk of having fecal incontinence compared to patients with pudendal nerve terminal motor latencies <2.0 milliseconds (odds ratio 2.18, p<0.05). Fecal incontinence could not be related to the weight or head circumference of the infant. The manometric and electromyographic findings, the use of pudendal nerve block, the length of the second stage of labor, the depth of rupture or the use of vacuumextraction could not be related to either fecal incontinence or pudendal nerve function. Conclusion. The manometric findings indicated damage to the anal sphincter apparatus in both continent and incontinent patients. Decreased pudendal nerve function characterized incontinent women. Accurate prediction of fecal incontinence in women with obstetric anal sphincter rupture is not possible.
7 10. The effect of bilateral pudendal blockade on the adjunctive urethral closure forces in healthy females Author(s): Thind P.; Lose G. Source: Scandinavian Journal of Urology and Nephrology; 1994; vol. 28 (no. 3); p Publication Date: 1994 Publication Type(s): Journal: Article Abstract:The effect of bilateral pudendal blockade on the urethral pressure and power generation during coughing and pelvic floor squeezing was evaluated in 10 healthy women. The measurements were carried out at the bladder neck, in the high pressure zone, and distally in the urethra before and after blockade. Strong adjunctive closure forces were demonstrated all along the urethra. They were significantly reduced by pudendal blockade except at the bladder neck during coughing. The results indicate that the pudendal innervated striated muscles contribute significantly to the adjunctively acting closure forces all along the female urethra, including the bladder neck. Some passive pressure transmission to the bladder neck seems to take place during stress episodes following pudendal blockade, but whether it occurs in healthy females remain uncertain. The findings following pudendal blockade corroborate with those in stress incontinent women, and thereby support the concept that striated muscle weakness is of pathophysiological significance in stress urinary incontinence. 11. Neurophysiology of the female pelvic floor. Author(s): Benson JT Source: Current Opinion in Obstetrics & Gynecology; Aug 1994; vol. 6 (no. 4); p Publication Date: Aug 1994 Publication Type(s): Academic Journal Abstract:The neurogenic theory of female pelvic floor dysfunction suggests a common thread for malfunction of pelvic visceral and support activities. Support for the neurogenic hypothesis has been promoted by recent literature showing that more central neuropathic processes, such as in the cauda equina or pelvic plexus, can be associated with the previously described peripheral neuropathies and are linked to pelvic floor disorders. Damage by vaginal dissection has been suggested as another etiologic factor. This concept has further been supported by studying the effects of pudendal nerve blockade. Methods for investigating pelvic floor neurophysiology are becoming more refined and widespread, and therapeutic horizons are described including nerve stimulation and surgical therapy of nerve compression. Database: CINAHL
8 12. Incidence and cause of postpartum urinary stress incontinence Author(s): Dimpfl T.; Hesse U.; Schussler B. Source: European Journal of Obstetrics Gynecology and Reproductive Biology; 1992; vol. 43 (no. 1); p Publication Date: 1992 Publication Type(s): Journal: Article Abstract:Urinary leakage was reported in 53.5% of our patients at least once during pregnancy. Multigravidae and women older than 30 were affected more often than primigravidae or women younger than % of all women, who were continent before pregnancy, developed permanent stress incontinence after vaginal delivery. As a conclusion, it can be said, that vaginal delivery itself predisposes for permanent stress urinary incontinence (SUI). Factors, which increase the trauma to the pelvic floor (tear, no episiotomy, forceps or vacuum extraction), show a higher incidence of postpartum persisting SUI without statistic significance. Labour management with epidural anaesthesia showed a statistically proven lower incidence of postpartum persisting SUI in comparison to the pudendal block. 13. Saddle block with pethidine for perineal operations. Author(s): Acalovschi, I; Ene, V; Lörinczi, E; Nicolaus, F Source: British journal of anaesthesia; Sep 1986; vol. 58 (no. 9); p Publication Date: Sep 1986 Publication Type(s): Comparative Study Journal Article Abstract:Saddle blockade with pethidine hydrochloride was performed in 111 patients undergoing short surgical operations on the perineum. A dose of 5% pethidine 0.5 mg kg-1 was injected to the subarachnoid space at L4-5 or L5-S1 with the patient in the sitting position. Sensory blockade was achieved in / min. This extended to the sacrococcygeal area, perineum, buttocks and posterior surface of thighs, and was followed 1-2 min later by motor blockade. During the operation the patients were stable haemodynamically and no respiratory depression was recorded. Sensory blockade lasted for 141 +/ min and was followed by postoperative analgesia, the mean duration of which was 301 +/ min. Postoperative neurological complications were recorded in three patients (2.7%): headache alone in one, headache associated with backache in one, and leg weakness, backache, nuchal rigidity and photophobia in another. Seven patients (6.3%) complained of itching, five patients (4.5%) of nausea and vomiting and two (1.8%) developed urinary retention. Database: Medline
9 14. Postpartum complications of forceps delivery performed under epidural and pudenal nerve block. Author(s): Moir, D D; Davidson, S Source: British journal of anaesthesia; Nov 1972; vol. 44 (no. 11); p Publication Date: Nov 1972 Publication Type(s): Journal Article Database: Medline
10 Strategy # Database Search term Results 1 Medline (pudendal ADJ3 block*).ti,ab Medline exp "PERONEAL NERVE"/ Medline exp "NERVE BLOCK"/ Medline (2 AND 3) 90 5 Medline (1 OR 4) Medline exp "URINARY RETENTION"/ Medline (urin* ADJ3 retention).ti,ab Medline exp "URINARY BLADDER DISEASES"/ Medline (bladder ADJ3 dysfunct*).ti,ab Medline (6 OR 7 OR 8 OR 9) Medline (5 AND 10) Medline (labour OR labor).ti,ab Medline (5 AND 12) Medline (pudendal ADJ3 anaesthes*).ti,ab 15 Medline (pudendal ADJ3 anesthes*).ti,ab Medline (14 OR 15) Medline (10 AND 12 AND 16) 0 18 Medline (12 AND 16) Medline exp "URINARY INCONTINENCE"/ 29158
11 20 Medline (5 AND 19) Medline (16 AND 19) 5 22 Medline exp "PELVIC FLOOR DISORDERS"/ Medline (5 AND 22) 0 24 Medline (16 AND 22) 0 25 EMBASE (puden* ADJ3 block*).ti,ab EMBASE exp "PERONEAL NERVE"/ EMBASE exp "NERVE BLOCK"/ EMBASE (26 AND 27) EMBASE (puden* ADJ3 anaesthes*).ti,ab EMBASE (puden* ADJ3 anesthes*).ti,ab EMBASE (25 OR 28 OR 29 OR 30) EMBASE (puden* ADJ3 anesthes*).ti,ab EMBASE exp "BLADDER DYSFUNCTION"/ EMBASE exp "URINE RETENTION"/ EMBASE (32 OR 33 OR 34) EMBASE (31 AND 35) EMBASE exp "URINE INCONTINENCE"/ EMBASE (31 AND 37) EMBASE exp "PELVIS FLOOR"/ EMBASE (28 AND 39) 0
12 41 EMBASE (31 AND 39) EMBASE (pudendal).ti,ab EMBASE exp LABOR/ EMBASE (33 OR 34 OR 37) EMBASE (42 AND 43 AND 44) 3 46 EMBASE exp "OBSTETRIC ANESTHESIA"/ EMBASE (42 AND 44 AND 46) 0 48 EMBASE (42 AND 46) EMBASE (26 AND 35 AND 46) 0 50 EMBASE (33 OR 34) EMBASE (26 AND 46 AND 50) 0 52 EMBASE (pudendal).ti,ab EMBASE (50 AND 52) EMBASE (46 AND 53) 0 55 EMBASE (43 AND 53) 1 56 EMBASE (27 AND 50 AND 52) EMBASE exp "NERVE INJURY"/ EMBASE (27 AND 50 AND 57) CINAHL (pudendal ADJ3 block*).ti,ab CINAHL (pudendal ADJ3 anaesthes*).ti,ab 61 CINAHL (pudendal ADJ3 anesthes*).ti,ab 0 1
13 62 CINAHL exp "NERVE BLOCK"/ CINAHL (pudendal).ti,ab CINAHL (62 AND 63) CINAHL (59 OR 61 OR 64) EMBASE (31 AND 39 AND 46) 1 67 EMBASE exp "BLADDER INJURY"/ EMBASE (31 AND 67) 0 69 EMBASE exp "URINARY TRACT INJURY"/ EMBASE (31 AND 69) 0 71 EMBASE (pudendal ADJ3 bladder).ti,ab EMBASE exp "PELVIC FLOOR DISORDER"/ EMBASE (31 AND 72) 2 74 EMBASE exp "BLADDER DISEASE"/ EMBASE (31 AND 74) Medline exp "URINARY BLADDER DISEASES"/ Medline (5 OR 16) Medline (76 AND 77) EMBASE (43 AND 52 AND 57) 4 80 EMBASE exp CHILDBIRTH/ EMBASE (31 AND 80) Medline exp "DELIVERY, OBSTETRIC"/ 69689
14 83 Medline (77 AND 82) EMBASE (saddle ADJ2 block*).ti,ab EMBASE (37 AND 84) 1 86 EMBASE (34 AND 84) 7 87 EMBASE (46 AND 84) EMBASE (80 AND 84) 7 89 EMBASE (74 AND 84) 3 90 EMBASE (72 AND 84) 0 91 Medline (saddle ADJ2 block*).ti,ab Medline (82 AND 91) Medline (19 AND 91) 0 94 Medline (10 AND 91) 5 95 EMBASE (35 AND 84) Medline (voiding).ti,ab Medline (5 AND 96) Medline (16 AND 96) 1 99 EMBASE exp MICTURITION/ EMBASE (31 AND 99) EMBASE (25 AND 99) EMBASE (27 AND 34) EMBASE (26 AND 102) 6
OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION
 OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION COLM O HERLIHY, MD Professor and Chair University College Dublin Department of Obstetrics and Gynaecology National Maternity
OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION COLM O HERLIHY, MD Professor and Chair University College Dublin Department of Obstetrics and Gynaecology National Maternity
Post operative voiding dysfunction and the Value of Urodynamics. Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist
 Post operative voiding dysfunction and the Value of Urodynamics Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist Learning objectives: v Pathophysiology of post op voiding dysfunction.
Post operative voiding dysfunction and the Value of Urodynamics Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist Learning objectives: v Pathophysiology of post op voiding dysfunction.
Review Article Pelvic Floor Dysfunction, Body Excreta Incontinence and Continence
 Cronicon OPEN ACCESS GYNAECOLOGY Review Article Pelvic Floor Dysfunction, Body Excreta Incontinence and Continence Abdel Karim M El Hemaly 1 * and Laila ASE Mousa 1 1 Professor of Obstetrics and gynaecology,
Cronicon OPEN ACCESS GYNAECOLOGY Review Article Pelvic Floor Dysfunction, Body Excreta Incontinence and Continence Abdel Karim M El Hemaly 1 * and Laila ASE Mousa 1 1 Professor of Obstetrics and gynaecology,
Differences in Prevalence of Urinary Incontinence by Race /Ethnicity
 Differences in Prevalence of Urinary Incontinence by Race /Ethnicity David H. Thom, MD, PhD, 1 Stephen K. Van Den Eeden, PhD, 2 Arona I. Ragins, MA, 2 Christina Wassel-Fyr, MS, 1 Eric Vittinghof, PhD,
Differences in Prevalence of Urinary Incontinence by Race /Ethnicity David H. Thom, MD, PhD, 1 Stephen K. Van Den Eeden, PhD, 2 Arona I. Ragins, MA, 2 Christina Wassel-Fyr, MS, 1 Eric Vittinghof, PhD,
Postpartum Complications
 ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives
 Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
URINARY INCONTINENCE. Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara
 URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
Ben Herbert Alex Wojtowicz
 Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Childbirth Trauma & Its Complications 23/ Mr Stergios K. Doumouchtsis
 Mr Stergios K. Doumouchtsis Consultant Obstetrician Gynaecologist & Urogynaecologist Childbirth Trauma & Its Complications Over eighty per cent of women sustain some degree of perineal trauma during childbirth.
Mr Stergios K. Doumouchtsis Consultant Obstetrician Gynaecologist & Urogynaecologist Childbirth Trauma & Its Complications Over eighty per cent of women sustain some degree of perineal trauma during childbirth.
Northwest Rehabilitation Associates, Inc.
 Pelvic Health Patient Intake Form Name: Date: Please answer the following questions as honestly and thoroughly as you can. Your responses will help us better understand your condition and provide the best
Pelvic Health Patient Intake Form Name: Date: Please answer the following questions as honestly and thoroughly as you can. Your responses will help us better understand your condition and provide the best
Objectives. Prevalence of Urinary Incontinence URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS
 URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
Faecal incontinence after childbirth
 Britisb Journal of Obstetrics and Gynaecology January 1997, Vol. 104, pp. 4650 Faecal incontinence after childbirth *Christine MacArthur Reader (Maternal and Child Epidemiology), *Debra E. Bick Research
Britisb Journal of Obstetrics and Gynaecology January 1997, Vol. 104, pp. 4650 Faecal incontinence after childbirth *Christine MacArthur Reader (Maternal and Child Epidemiology), *Debra E. Bick Research
Urinary incontinence after obstetric anal sphincter injuries (OASIS) is there a relationship?
 DOI 10.1007/s00192-007-0431-8 ORIGINAL ARTICLE Urinary incontinence after obstetric anal sphincter injuries (OASIS) is there a relationship? Inka Scheer & Vasanth Andrews & Ranee Thakar & Abdul H. Sultan
DOI 10.1007/s00192-007-0431-8 ORIGINAL ARTICLE Urinary incontinence after obstetric anal sphincter injuries (OASIS) is there a relationship? Inka Scheer & Vasanth Andrews & Ranee Thakar & Abdul H. Sultan
2/25/2013. Speaker Disclosure. Learning Objectives. Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth
 Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth Jaime Sepulveda-Toro MD FACS FACOG Female Pelvic Medicine and Reconstructive Pelvic Surgery South Miami Hospital Speaker
Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth Jaime Sepulveda-Toro MD FACS FACOG Female Pelvic Medicine and Reconstructive Pelvic Surgery South Miami Hospital Speaker
Bard: Continence Therapy. Stress Urinary Incontinence. Regaining Control. Restoring Your Lifestyle.
 Bard: Continence Therapy Stress Urinary Incontinence Regaining Control. Restoring Your Lifestyle. Stress Urinary Incontinence Urinary incontinence is a common problem and one that can be resolved by working
Bard: Continence Therapy Stress Urinary Incontinence Regaining Control. Restoring Your Lifestyle. Stress Urinary Incontinence Urinary incontinence is a common problem and one that can be resolved by working
Development of the pelvic floor : implications for clinical anatomy Wallner, C.
 UvA-DARE (Digital Academic Repository) Development of the pelvic floor : implications for clinical anatomy Wallner, C. Link to publication Citation for published version (APA): Wallner, C. (2008). Development
UvA-DARE (Digital Academic Repository) Development of the pelvic floor : implications for clinical anatomy Wallner, C. Link to publication Citation for published version (APA): Wallner, C. (2008). Development
Urodynamic and electrophysiological investigations in neuro-urology
 Urodynamic and electrophysiological investigations in neuro-urology Pr. Gerard Amarenco Neuro-Urology and Pelvic-Floor Investigations Department Tenon Hospital, Assistance Publique Hôpitaux de Paris, Er6,
Urodynamic and electrophysiological investigations in neuro-urology Pr. Gerard Amarenco Neuro-Urology and Pelvic-Floor Investigations Department Tenon Hospital, Assistance Publique Hôpitaux de Paris, Er6,
Doctor s assessment and evaluation of the pelvic floor in antenatal and postpartum women: routine or???
 Doctor s assessment and evaluation of the pelvic floor in antenatal and postpartum women: routine or??? Dr Barry O Reilly Head of department of Urogynaecology Cork University Maternity Hospital Ireland
Doctor s assessment and evaluation of the pelvic floor in antenatal and postpartum women: routine or??? Dr Barry O Reilly Head of department of Urogynaecology Cork University Maternity Hospital Ireland
ACCIDENTAL BOWEL LEAKAGE: A PRACTICAL APPROACH TO EVALUATION. Tristi W. Muir, MD Chair, Department of OB/GYN Houston Methodist Hospital
 ACCIDENTAL BOWEL LEAKAGE: A PRACTICAL APPROACH TO EVALUATION Tristi W. Muir, MD Chair, Department of OB/GYN Houston Methodist Hospital Accidental Bowel Leakage What Gets the Woman into Your Office 67%
ACCIDENTAL BOWEL LEAKAGE: A PRACTICAL APPROACH TO EVALUATION Tristi W. Muir, MD Chair, Department of OB/GYN Houston Methodist Hospital Accidental Bowel Leakage What Gets the Woman into Your Office 67%
Frequency of urinary incontinence with Pelvic organ prolapse and associated factors
 ORIGINAL ARTICLE Frequency of urinary incontinence with Pelvic organ prolapse and associated factors Dr. Raheela Mohsin 1, Dr.Ayesha Saba 2, Humera Ismail 3 1 Dr. Raheela Mohsin, Aga Khan University Hospital,
ORIGINAL ARTICLE Frequency of urinary incontinence with Pelvic organ prolapse and associated factors Dr. Raheela Mohsin 1, Dr.Ayesha Saba 2, Humera Ismail 3 1 Dr. Raheela Mohsin, Aga Khan University Hospital,
Anal Sphincter Injuries: Acute Management
 Anal Sphincter Injuries: Acute Management Dr Stephen Jeffery Urogynaecology Consultant Department of Obstetrics & Gynaecology Groote Schuur Hospital Colorectal Surgeons Gynaecologists Gynaecologists Colorectal
Anal Sphincter Injuries: Acute Management Dr Stephen Jeffery Urogynaecology Consultant Department of Obstetrics & Gynaecology Groote Schuur Hospital Colorectal Surgeons Gynaecologists Gynaecologists Colorectal
Updates in the nonpharmacological. treatment on overactive bladder
 Updates in the nonpharmacological treatment on overactive bladder Overactive Bladder Also known as urgency-frequency syndrome Symptoms Urgency Daytime frequency Nocturia Urge urinary incontinence Sudden
Updates in the nonpharmacological treatment on overactive bladder Overactive Bladder Also known as urgency-frequency syndrome Symptoms Urgency Daytime frequency Nocturia Urge urinary incontinence Sudden
Obstetric Anal Sphincter Injury. An update on best practices. Objectives
 Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
An Unexpected Cause Of Spontaneous Perinephric Urinoma: A Case Report. L Chandrasekharan, T Abdl Ghaffar, M Venkatramana, K Mammigatty
 ISPUB.COM The Internet Journal of Radiology Volume 4 Number 1 An Unexpected Cause Of Spontaneous Perinephric Urinoma: A Case Report L Chandrasekharan, T Abdl Ghaffar, M Venkatramana, K Mammigatty Citation
ISPUB.COM The Internet Journal of Radiology Volume 4 Number 1 An Unexpected Cause Of Spontaneous Perinephric Urinoma: A Case Report L Chandrasekharan, T Abdl Ghaffar, M Venkatramana, K Mammigatty Citation
Among parous women, cesarean birth reduces the
 Pelvic Floor Disorders After Vaginal Birth Effect of Episiotomy, Perineal Laceration, and Operative Birth Victoria L. Handa, MD, MHS, Joan L. Blomquist, MD, Kelly C. McDermott, BS, Sarah Friedman, MD,
Pelvic Floor Disorders After Vaginal Birth Effect of Episiotomy, Perineal Laceration, and Operative Birth Victoria L. Handa, MD, MHS, Joan L. Blomquist, MD, Kelly C. McDermott, BS, Sarah Friedman, MD,
Pregnancy and childbirth: the effects on pelvic floor muscles
 Page 1 of 9 Pregnancy and childbirth: the effects on pelvic floor muscles 26 February, 2009 Stress incontinence can follow childbirth as pelvic floor muscles are damaged AUTHOR Julia Herbert, MSc, MCSP,
Page 1 of 9 Pregnancy and childbirth: the effects on pelvic floor muscles 26 February, 2009 Stress incontinence can follow childbirth as pelvic floor muscles are damaged AUTHOR Julia Herbert, MSc, MCSP,
The Pelvic Floor: Expecting (and Delivering!) Susan Barr, MD Assistant Professor Saint Louis University Division of Urogynecology
 The Pelvic Floor: What She Can Expect After Expecting (and Delivering!) Susan Barr, MD Assistant Professor Saint Louis University Division of Urogynecology Objectives Understand risk factors and treatment
The Pelvic Floor: What She Can Expect After Expecting (and Delivering!) Susan Barr, MD Assistant Professor Saint Louis University Division of Urogynecology Objectives Understand risk factors and treatment
INTRAPARTUM AND POSTNATAL BLADDER CARE
 INTRAPARTUM AND POSTNATAL BLADDER CARE BACKGROUND Urinary retention is uncommon but carries significant morbidity and the risk is increased by a number of factors including epidural analgesia (Teo, et
INTRAPARTUM AND POSTNATAL BLADDER CARE BACKGROUND Urinary retention is uncommon but carries significant morbidity and the risk is increased by a number of factors including epidural analgesia (Teo, et
Management of Female Stress Incontinence
 Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Maternity Information Leaflet. Care of the Perineum (including Pelvic Floor Exercises) Version 2
 Maternity Information Leaflet Care of the Perineum (including Pelvic Floor Exercises) Version 2 Pelvic Floor Exercises The pelvic floor muscles are located between your legs, and run from your pubic bone
Maternity Information Leaflet Care of the Perineum (including Pelvic Floor Exercises) Version 2 Pelvic Floor Exercises The pelvic floor muscles are located between your legs, and run from your pubic bone
Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study
 ORIGINAL RESEARCH Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study Johan Pollack, MD, Johan Nordenstam, MD, Sophia Brismar, MD, Annika Lopez, MD, PhD, Daniel Altman, MD, and
ORIGINAL RESEARCH Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study Johan Pollack, MD, Johan Nordenstam, MD, Sophia Brismar, MD, Annika Lopez, MD, PhD, Daniel Altman, MD, and
Urinary Incontinence
 Urinary Incontinence Q: What is urinary incontinence and what causes it? A: When you are not able to hold your urine until you can get to a bathroom, you have what s called urinary incontinence (also called
Urinary Incontinence Q: What is urinary incontinence and what causes it? A: When you are not able to hold your urine until you can get to a bathroom, you have what s called urinary incontinence (also called
This information is intended as an overview only
 This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
Epidural analgesia and backache: a randomized controlled comparison with intramuscular meperidine for analgesia during labour
 British Journal of Anaesthesia 89 (3): 466-72 (2002) analgesia and backache: a randomized controlled comparison with intramuscular meperidine for analgesia during labour B. A. Loughnan *, F. Carli 2, M.
British Journal of Anaesthesia 89 (3): 466-72 (2002) analgesia and backache: a randomized controlled comparison with intramuscular meperidine for analgesia during labour B. A. Loughnan *, F. Carli 2, M.
Bill Landry BScPT, BScH, MCPA, CAFCI Family Physiotherapy Centre of London
 Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
The Management of Female Urinary Incontinence. Part 1: Aetiology and Investigations
 The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
Pelvic Floor Ultrasound Imaging. Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague)
 Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
Clinical Curriculum: Urogynecology
 Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
Anorectal Diagnostic Overview
 Anorectal Diagnostic Overview 11-25-09 3.11.2010 2009 2010 Anorectal Manometry Overview Measurement of pressures and the annotation of rectal sensation throughout the rectum and anal canal to determine:
Anorectal Diagnostic Overview 11-25-09 3.11.2010 2009 2010 Anorectal Manometry Overview Measurement of pressures and the annotation of rectal sensation throughout the rectum and anal canal to determine:
Incontinence; Lets talk about it. Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery
 Incontinence; Lets talk about it Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery Select the most appropriate subtitle for this talk A: Bladders gone wild! B: There s no such thing
Incontinence; Lets talk about it Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery Select the most appropriate subtitle for this talk A: Bladders gone wild! B: There s no such thing
Contributing Factors for Urinary Incontinencein Postnatal Women a Survey
 IOSR Journal of Sports and Physical Education (IOSR-JSPE) e-issn: 2347-6737, p-issn: 2347-6745, Volume 3, Issue 6, (Nov. Dec. 2016), PP 01-05 www.iosrjournals.org Contributing Factors for Urinary Incontinencein
IOSR Journal of Sports and Physical Education (IOSR-JSPE) e-issn: 2347-6737, p-issn: 2347-6745, Volume 3, Issue 6, (Nov. Dec. 2016), PP 01-05 www.iosrjournals.org Contributing Factors for Urinary Incontinencein
Neurologic complications - whom to blame? Benno Rehberg Médecin adjoint agrégé Unité d anesthésiologie gynéco-obstétricale, HUG
 Neurologic complications - whom to blame? Benno Rehberg Médecin adjoint agrégé Unité d anesthésiologie gynéco-obstétricale, HUG SAOA spring meeting 2015 The simple surgical answer: outline Epidemiology
Neurologic complications - whom to blame? Benno Rehberg Médecin adjoint agrégé Unité d anesthésiologie gynéco-obstétricale, HUG SAOA spring meeting 2015 The simple surgical answer: outline Epidemiology
John Laughlin 4 th year Cardiff University Medical Student
 John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
Prolapse and Urogynae Incontinence. Lucy Tiffin and Hannah Wheldon-Holmes
 Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
NEUROMODULATION FOR UROGYNAECOLOGISTS
 NEUROMODULATION FOR UROGYNAECOLOGISTS Introduction The pelvic floor is highly complex structure made up of skeletal and striated muscle, support and suspensory ligaments, fascial coverings and an intricate
NEUROMODULATION FOR UROGYNAECOLOGISTS Introduction The pelvic floor is highly complex structure made up of skeletal and striated muscle, support and suspensory ligaments, fascial coverings and an intricate
Stress Urinary Incontinence in Women. What YOU can do about it...
 Stress Urinary Incontinence in Women What YOU can do about it... www.gynecare.com Stress Urinary Incontinence in Women: It's Common. It's Treatable. Would it surprise you... To learn that more than 13
Stress Urinary Incontinence in Women What YOU can do about it... www.gynecare.com Stress Urinary Incontinence in Women: It's Common. It's Treatable. Would it surprise you... To learn that more than 13
This Special Report supplement
 ...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION Author : SIMONA T RADAELLI Categories : Vets Date : July
Vet Times The website for the veterinary profession https://www.vettimes.co.uk TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION Author : SIMONA T RADAELLI Categories : Vets Date : July
Anatomical and Functional Results of Pelvic Organ Prolapse Mesh Repair: A Prospective Study of 105 Cases
 International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
Overactive Bladder: Diagnosis and Approaches to Treatment
 Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Urogynecology in EDS. Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018
 Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology
 Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology Ospedale San Giovanni di Dio, Gorizia, Italy ANATOMY URINARY CONTINENCE
Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology Ospedale San Giovanni di Dio, Gorizia, Italy ANATOMY URINARY CONTINENCE
Normal micturition involves complex
 NEW TARGET FOR INTERVENTION: THE NEUROUROLOGY CONNECTION * Donald R. Ostergard, MD, FACOG ABSTRACT Urine storage and release are under the control of the parasympathetic, sympathetic, and somatic nervous
NEW TARGET FOR INTERVENTION: THE NEUROUROLOGY CONNECTION * Donald R. Ostergard, MD, FACOG ABSTRACT Urine storage and release are under the control of the parasympathetic, sympathetic, and somatic nervous
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS
 Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Clinical Study Cough Test during Tension-Free Vaginal Tape Procedure in Preventing Postoperative Urinary Retention
 Advances in Urology Volume 2013, Article ID 797854, 4 pages http://dx.doi.org/10.1155/2013/797854 Clinical Study Cough Test during Tension-Free Vaginal Tape Procedure in Preventing Postoperative Urinary
Advances in Urology Volume 2013, Article ID 797854, 4 pages http://dx.doi.org/10.1155/2013/797854 Clinical Study Cough Test during Tension-Free Vaginal Tape Procedure in Preventing Postoperative Urinary
Women s & Children s Directorate The TVT Operation - a guide for patients
 Women s & Children s Directorate The TVT Operation - a guide for patients This leaflet was written for women who are considering having a TVT operation. If you have any questions that aren't answered by
Women s & Children s Directorate The TVT Operation - a guide for patients This leaflet was written for women who are considering having a TVT operation. If you have any questions that aren't answered by
Incontinence. Anatomy The human body has two kidneys. The kidneys continuously filter the blood and make urine.
 Incontinence Introduction Urinary incontinence occurs when a person cannot control the emptying of his or her urinary bladder. It can happen to anyone, but is very common in older people. Urinary incontinence
Incontinence Introduction Urinary incontinence occurs when a person cannot control the emptying of his or her urinary bladder. It can happen to anyone, but is very common in older people. Urinary incontinence
Management of Urinary Incontinence in Older Women. Dr. Cecilia Cheon Department of Obs. & Gyn. Queen Elizabeth Hospital
 Management of Urinary Incontinence in Older Women Dr. Cecilia Cheon Department of Obs. & Gyn. Queen Elizabeth Hospital Epidemiology Causes Investigation Treatment Conclusion Elderly Women High prevalence
Management of Urinary Incontinence in Older Women Dr. Cecilia Cheon Department of Obs. & Gyn. Queen Elizabeth Hospital Epidemiology Causes Investigation Treatment Conclusion Elderly Women High prevalence
Non - invasive management and treatment of female stress urinary incontinence with a CO 2
 HJO An Obstetrics and Gynecology International Journal Case Report Non - invasive management and treatment of female stress urinary incontinence with a CO 2 Bader Alexandros Obstetrician - Gynecologist,
HJO An Obstetrics and Gynecology International Journal Case Report Non - invasive management and treatment of female stress urinary incontinence with a CO 2 Bader Alexandros Obstetrician - Gynecologist,
Urinary Incontinence. Lora Keeling and Byron Neale
 Urinary Incontinence Lora Keeling and Byron Neale Not life threatening. Introduction But can have a huge impact on quality of life. Two main types of urinary incontinence (UI). Stress UI leakage on effort,
Urinary Incontinence Lora Keeling and Byron Neale Not life threatening. Introduction But can have a huge impact on quality of life. Two main types of urinary incontinence (UI). Stress UI leakage on effort,
Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M.
 UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
Pregnancy and delivery: a urodynamic viewpoint
 British Journal of Obstetrics and Gynaecology November 2000, Vol107, pp. 1354-1359 Pregnancy and delivery: a urodynamic viewpoint *C. Chaliha Research Fellow (Urogynaecology),** J. M. Bland Professor (Medical
British Journal of Obstetrics and Gynaecology November 2000, Vol107, pp. 1354-1359 Pregnancy and delivery: a urodynamic viewpoint *C. Chaliha Research Fellow (Urogynaecology),** J. M. Bland Professor (Medical
Loss of Bladder Control
 BLADDER HEALTH: Surgery for Urinary Incontinence Loss of Bladder Control Surgery for Urinary Incontinence Don t Let Urinary Incontinence Keep You from Enjoying Life. What is Urinary Incontinence? What
BLADDER HEALTH: Surgery for Urinary Incontinence Loss of Bladder Control Surgery for Urinary Incontinence Don t Let Urinary Incontinence Keep You from Enjoying Life. What is Urinary Incontinence? What
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN
 Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Urinary incontinence in women: the management of urinary incontinence in women 1.1 Short title Urinary incontinence in women
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Urinary incontinence in women: the management of urinary incontinence in women 1.1 Short title Urinary incontinence in women
NEW POSTNATAL URINARY INCONTINENCE : OBSTETRIC AND OTHER RISK FACTORS IN PRIMIPARAE. New postnatal urinary incontinence in primiparae
 Author Posting. The Authors 2006. This is the author s version of the work. It is posted here for personal use, not for redistribution. The definitive version was published in BJOG, 113(2):208-17. doi:10.1111/j.1471-0528.2005.00840.x
Author Posting. The Authors 2006. This is the author s version of the work. It is posted here for personal use, not for redistribution. The definitive version was published in BJOG, 113(2):208-17. doi:10.1111/j.1471-0528.2005.00840.x
Loss of Bladder Control
 BLADDER HEALTH Loss of Bladder Control SURGERY TO TREAT URINARY INCONTINENCE AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION What Is Urinary Incontinence? Urinary incontinence
BLADDER HEALTH Loss of Bladder Control SURGERY TO TREAT URINARY INCONTINENCE AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION What Is Urinary Incontinence? Urinary incontinence
Moneli Golara Consultant Obstetrician and Gynaecologist Royal Free NHS Trust Barnet Hospital
 Moneli Golara Consultant Obstetrician and Gynaecologist Royal Free NHS Trust Barnet Hospital Pelvic Organ Prolapse (POP)- herniation of pelvic organs into vaginal walls Common Huge impact on daily activities
Moneli Golara Consultant Obstetrician and Gynaecologist Royal Free NHS Trust Barnet Hospital Pelvic Organ Prolapse (POP)- herniation of pelvic organs into vaginal walls Common Huge impact on daily activities
PRE-OPERATIVE URODYNAMIC
 PRE-OPERATIVE URODYNAMIC STUDIES: IS THERE VALUE IN PREDICTING POST-OPERATIVE STRESS URINARY INCONTINENCE IN WOMEN UNDERGOING PROLAPSE SURGERY? Dr K Janse van Rensburg Dr JA van Rensburg INTRODUCTION POP
PRE-OPERATIVE URODYNAMIC STUDIES: IS THERE VALUE IN PREDICTING POST-OPERATIVE STRESS URINARY INCONTINENCE IN WOMEN UNDERGOING PROLAPSE SURGERY? Dr K Janse van Rensburg Dr JA van Rensburg INTRODUCTION POP
Urogynaecology. Colm McAlinden
 Urogynaecology Colm McAlinden Definitions Urinary incontinence compliant of any involuntary leakage of urine with many different causes Two main types: Stress Urge Definitions Nocturia: More than a single
Urogynaecology Colm McAlinden Definitions Urinary incontinence compliant of any involuntary leakage of urine with many different causes Two main types: Stress Urge Definitions Nocturia: More than a single
Women s and Men s Health Intake Form Comprehensive Physical Therapy Center
 Name: (Last, First) DOB: Date: Age: Referring Physician: Next Physician Appointment: Today s visit: What is the main reason you came to the office today? When did it start? What treatments have you had
Name: (Last, First) DOB: Date: Age: Referring Physician: Next Physician Appointment: Today s visit: What is the main reason you came to the office today? When did it start? What treatments have you had
INCONTINENCE. Continence and Pelvic Floor Rehabilitation TYPES OF INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE 11/08/2015
 INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
EXPECTING A BABY? SOME PREGNANT WOMEN CAN HAVE BLADDER AND BOWEL CONTROL PROBLEMS. YOU CAN GET HELP. HOW DO I KNOW IF I HAVE A PROBLEM?
 11 BLADDER AND BOWEL CONTROL PROBLEMS. When you are pregnant, you get a lot of advice from many people. One topic few people think about is bladder and bowel control problems during pregnancy and after
11 BLADDER AND BOWEL CONTROL PROBLEMS. When you are pregnant, you get a lot of advice from many people. One topic few people think about is bladder and bowel control problems during pregnancy and after
A PATIENT GUIDE TO Understanding Stress Urinary Incontinence
 A PATIENT GUIDE TO Understanding Stress Urinary Incontinence Q: What is SUI? A: Stress urinary incontinence is defined as the involuntary leakage of urine. The problem afflicts approximately 18 million
A PATIENT GUIDE TO Understanding Stress Urinary Incontinence Q: What is SUI? A: Stress urinary incontinence is defined as the involuntary leakage of urine. The problem afflicts approximately 18 million
EPIDURAL ANALGESIA FOR THE SURGICAL INDUCTION OF LABOUR
 Br. J. Anaesth. (1974), 46, 747 EPIDURAL ANALGESIA FOR THE SURGICAL INDUCTION OF LABOUR N. G. CASEBY SUMMARY Surgical induction of labour was performed on 80 patients under epidural analgesia and on 73
Br. J. Anaesth. (1974), 46, 747 EPIDURAL ANALGESIA FOR THE SURGICAL INDUCTION OF LABOUR N. G. CASEBY SUMMARY Surgical induction of labour was performed on 80 patients under epidural analgesia and on 73
K. Jundt 1, I. scheer 2, v. von Bodungen 1, F. Krumbachner 1, K. Friese 1, U. M. Peschers 3
 362 EU Ro PE an JoUR nal of MED I cal RE search Eur J Med Res (2010) 15: 362-366 I. Holzapfel Publishers 2010 WHat HaRM DoEs a second DElIvERy to the PElvIc FlooR? K. Jundt 1, I. scheer 2, v. von Bodungen
362 EU Ro PE an JoUR nal of MED I cal RE search Eur J Med Res (2010) 15: 362-366 I. Holzapfel Publishers 2010 WHat HaRM DoEs a second DElIvERy to the PElvIc FlooR? K. Jundt 1, I. scheer 2, v. von Bodungen
Obstetric Anal Sphincter Injury- A guideline. Mr David Sim Ms Patricia McStay. Dr Martina Hogan Dept./Division Only: YES-IMWH Directorate Only: NO
 CLINICAL GUIDELINES ID TAG Title: Obstetric Anal Sphincter Injury- A guideline Author: Dr Foteini Verani Designation: Specialist Doctor Speciality / Division: Obstetrics-IMWH Directorate: Acute Services
CLINICAL GUIDELINES ID TAG Title: Obstetric Anal Sphincter Injury- A guideline Author: Dr Foteini Verani Designation: Specialist Doctor Speciality / Division: Obstetrics-IMWH Directorate: Acute Services
Urodynamic Patterns of the Idiopathic Overactive Bladder
 Science Journal of Clinical Medicine 2017; 6(5): 74-79 http://www.sciencepublishinggroup.com/j/sjcm doi: 10.11648/j.sjcm.20170605.12 ISSN: 2327-2724 (Print); ISSN: 2327-2732 (Online) Urodynamic Patterns
Science Journal of Clinical Medicine 2017; 6(5): 74-79 http://www.sciencepublishinggroup.com/j/sjcm doi: 10.11648/j.sjcm.20170605.12 ISSN: 2327-2724 (Print); ISSN: 2327-2732 (Online) Urodynamic Patterns
Research. Estrogen receptors have been identified
 Research UROGYNECOLOGY Postmenopausal hormone therapy and incident urinary incontinence in middle-aged women Mary K. Townsend, ScD; Gary C. Curhan, MD, ScD; Neil M. Resnick, MD; Francine Grodstein, ScD
Research UROGYNECOLOGY Postmenopausal hormone therapy and incident urinary incontinence in middle-aged women Mary K. Townsend, ScD; Gary C. Curhan, MD, ScD; Neil M. Resnick, MD; Francine Grodstein, ScD
Loss of Bladder Control
 BLADDER HEALTH Loss of Bladder Control Bladder Prolapse AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION What Is the Bladder? The bladder is a hollow, balloon-like organ made mostly
BLADDER HEALTH Loss of Bladder Control Bladder Prolapse AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION What Is the Bladder? The bladder is a hollow, balloon-like organ made mostly
Urinary Incontinence
 Urinary Incontinence Q: What is urinary incontinence (UI)? A: UI is also known as loss of bladder control or urinary leakage. UI is when urine leaks out before you can get to a bathroom. If you have UI,
Urinary Incontinence Q: What is urinary incontinence (UI)? A: UI is also known as loss of bladder control or urinary leakage. UI is when urine leaks out before you can get to a bathroom. If you have UI,
FACTORS ASSOCIATED WITH URINARY STRESS INCONTINENCE IN PRIMIPARAS
 P.L. Chou, et al ORIGINAL ARTICLE FACTORS ASSOCIATED WITH URINARY STRESS INCONTINENCE IN PRIMIPARAS Pei-Ling Chou, Fang-Ping Chen*, Li-Fen Teng Department of Obstetrics and Gynecology, Keelung Chang Gung
P.L. Chou, et al ORIGINAL ARTICLE FACTORS ASSOCIATED WITH URINARY STRESS INCONTINENCE IN PRIMIPARAS Pei-Ling Chou, Fang-Ping Chen*, Li-Fen Teng Department of Obstetrics and Gynecology, Keelung Chang Gung
Managing urinary morbidity after brachytherapy. Kieran O Flynn Department of Urology, Salford Royal Foundation Trust, Manchester
 Managing urinary morbidity after brachytherapy Kieran O Flynn Department of Urology, Salford Royal Foundation Trust, Manchester Themes Can we predict urinary morbidity? Prevention of urinary morbidity
Managing urinary morbidity after brachytherapy Kieran O Flynn Department of Urology, Salford Royal Foundation Trust, Manchester Themes Can we predict urinary morbidity? Prevention of urinary morbidity
LAPAROSCOPIC REPAIR OF PELVIC FLOOR
 LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
Dr. Aso Urinary Symptoms
 Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Loss of Bladder Control
 BLADDER HEALTH: Bladder Prolapse Loss of Bladder Control Bladder Prolapse Don t Let Bladder Prolapse Keep You from Enjoying Life. What is the Bladder? The bladder is a hollow, balloon-like organ made mostly
BLADDER HEALTH: Bladder Prolapse Loss of Bladder Control Bladder Prolapse Don t Let Bladder Prolapse Keep You from Enjoying Life. What is the Bladder? The bladder is a hollow, balloon-like organ made mostly
Anal incontinence after childbirth is more common than was previously believed. Anal incontinence after childbirth. Methods
 Anal incontinence after childbirth Research Recherche From *the Department of Obstetrics and Gynecology, University of Ottawa, Ottawa, Ont.; the Departments of Family Medicine and Social and Preventive
Anal incontinence after childbirth Research Recherche From *the Department of Obstetrics and Gynecology, University of Ottawa, Ottawa, Ont.; the Departments of Family Medicine and Social and Preventive
Pathophysiological Rationale for Surgical Treatments of Stress Urinary Incontinence
 Pathophysiological Rationale for Surgical Treatments of Stress Urinary Incontinence Urology Grand Rounds April 6, 2005 Herman Christopher Kwan R4 A familiar case? 62 year old female initial presentation
Pathophysiological Rationale for Surgical Treatments of Stress Urinary Incontinence Urology Grand Rounds April 6, 2005 Herman Christopher Kwan R4 A familiar case? 62 year old female initial presentation
COMPARISON OF INCREMENTAL SPINAL ANAESTHESIA USING A 32-GAUGE CATHETER WITH EXTRADURAL ANAESTHESIA FOR ELECTIVE CAESAREAN SECTION
 British Journal of Anaesthesia 1991; 66: 232-236 COMPARISON OF INCREMENTAL SPINAL ANAESTHESIA USING A 32-GAUGE CATHETER WITH EXTRADURAL ANAESTHESIA FOR ELECTIVE CAESAREAN SECTION I. G. KESTIN, A. P. MADDEN,
British Journal of Anaesthesia 1991; 66: 232-236 COMPARISON OF INCREMENTAL SPINAL ANAESTHESIA USING A 32-GAUGE CATHETER WITH EXTRADURAL ANAESTHESIA FOR ELECTIVE CAESAREAN SECTION I. G. KESTIN, A. P. MADDEN,
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Screening of Immediate Post Partum Females for Urinary Incontinence Ami Vishal Mehta 1, Zarna
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Screening of Immediate Post Partum Females for Urinary Incontinence Ami Vishal Mehta 1, Zarna
Table 1. International Consultation on Incontinence recommendations for frail older adults
 Table 1. International Consultation on Incontinence recommendations for frail older adults Clinicians need to assess and manage co-existing co morbid conditions which are known to have an impact on continence
Table 1. International Consultation on Incontinence recommendations for frail older adults Clinicians need to assess and manage co-existing co morbid conditions which are known to have an impact on continence
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS
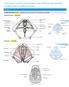 THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
Gynecology Dr. Sallama Lecture 3 Genital Prolapse
 Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
The Neurogenic Bladder
 The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
Appendix B Protocol for management of obstetric anal sphincter injury THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS
 Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE SCOPE. Urinary incontinence: the management of urinary incontinence in women
 NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE 1 Guideline title SCOPE Urinary incontinence: the management of urinary incontinence in women 1.1 Short title Urinary incontinence 2 Background a) The National
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE 1 Guideline title SCOPE Urinary incontinence: the management of urinary incontinence in women 1.1 Short title Urinary incontinence 2 Background a) The National
Advanced Care for Female Overactive Bladder & Urinary Incontinence. Department of Urology Kaiser Permanente Santa Rosa
 Advanced Care for Female Overactive Bladder & Urinary Incontinence Department of Urology Kaiser Permanente Santa Rosa Goals Participants will: Review normal urinary tract anatomy and function Understand
Advanced Care for Female Overactive Bladder & Urinary Incontinence Department of Urology Kaiser Permanente Santa Rosa Goals Participants will: Review normal urinary tract anatomy and function Understand
The Perineal Clinic: - the management of women following OASI
 The Perineal Clinic: - the management of women following OASI Miss Gillian Fowler Consultant Urogynaecologist MBChB, MD, MRCOG Liverpool Women s Hospital. Margie Polden University Memorial of Liverpool
The Perineal Clinic: - the management of women following OASI Miss Gillian Fowler Consultant Urogynaecologist MBChB, MD, MRCOG Liverpool Women s Hospital. Margie Polden University Memorial of Liverpool
Perineal Suturing and Surgical Drapes/Gowns
 Date of Search: 11 January 2017 Sources Searched: Medline, Embase, CINAHL, TRIP Database, Cochrane Library Perineal Suturing and Surgical Drapes/Gowns Summary Surgical site infection has been estimated
Date of Search: 11 January 2017 Sources Searched: Medline, Embase, CINAHL, TRIP Database, Cochrane Library Perineal Suturing and Surgical Drapes/Gowns Summary Surgical site infection has been estimated
UP DATE MANAGEMENT OF URINARY INCONTINENCE IN ADULT
 UP DATE MANAGEMENT OF URINARY INCONTINENCE IN ADULT Yunizaf, MD Division of Urogynecology Department of Obstetrics and Gynecology School of Medicine, University of Indonesia/ Dr. Cipto Mangunkusumo Hospital
UP DATE MANAGEMENT OF URINARY INCONTINENCE IN ADULT Yunizaf, MD Division of Urogynecology Department of Obstetrics and Gynecology School of Medicine, University of Indonesia/ Dr. Cipto Mangunkusumo Hospital
