Our experience with A 3D mesh in the management
|
|
|
- David Page
- 5 years ago
- Views:
Transcription
1 SCRIPTA MEDICA (BRNO) 79 (2): , June 2006 Our experience with A 3D mesh in the management of rectal prolapse Vlček P. 1, Korbička J. 1, Chalupník Š. 1, Jedlička V. 1, Veverková L. 1, Čapov I. 1, Wechsler J. 1,Vlčková P. 2, Dolina J. 2, Bartůšek D. 3 1 First Department of Surgery, St. Anne s Faculty Hospital, Brno 2 Department of Gastroenterology, Faculty Hospital Brno 3 Department of Radiology, Faculty Hospital Brno A b s t r a c t Received after revision May 2006 A variety of surgical procedures have been developed to treat rectal prolapse, but there is still no consensus on the operation of choice. The aim of this study was to evaluate the functional results of operative treatment of rectal prolapse during a 3 year period in our department. All patients treated for complete rectal prolapse from January 1999 to September 2003 were included. Of the 14 patients, 9 were men, and the mean age was 59 /range 40 88/. The majority of the procedures were performed by abdominal approach, and the most frequently used open technique was anterior rectopexy with a mesh /3D/. Of the incontinent patients, 82 % were continent postoperatively. The proportion of patients with constipation was greater after the operation than preoperatively. In our group there was only 1 recurrent prolapse. Anterior rectopexy with mesh gave good results. Older age seems to have a negative effect on the functional outcome of the operation. K e y w o r d s Rectal prolapse, 3D mesh, Rectopexy INTRODUCTION Complete rectal prolapse /procidentia/ is the circumferential protrusion through the anus of all layers of the rectal wall. It is most common in young children and elderly adults. Rectal prolapse or procidentia is a disabling problem and controversies regarding its management continue to stimulate interest in the study of its aetiology, pathophysiology, functional aspects, and concepts of surgical management. Aetiology. The underlying cause of rectal prolapse remains unclear. It is thought to develop as the result of a series of functional disturbances in muscles of the anterior abdominal wall, pelvic floor, and anal sphincter complex (1,3), which creates an initial inversion of the upper rectum towards the anal canal (2,5). These underlying abnormalities may be aggravated by certain conditions which appear to be 123
2 associated with an increased incidence of rectal prolapse. These include connective tissue disorders /3/, neurological illnesses (4), and high parity (5). Pathophysiology. The pathophysiology of rectal prolapse was first described in the late 19th century, long before abdominal surgery was considered safe. The early operations were perineal procedures, one of which is the Mikulicz procedure /perineal rectosigmoidectomy/, first performed in However, the aetiopathology of rectal prolapse remained unknown until 1912 when Moschcowitz proposed the theory of a sliding hernia through a defect in the pelvic fascia as a cause of rectal prolapse. His theory was based on the presence of a deep rectovesical or rectovaginal pouch in most patients with a complete procidentia. He then went on to describe the Moschcowitz procedure, which involved obliteration of the peritoneal pouch of Douglas by a purse-string. The recurrence rate was, however, 80 per cent (6 10). Broden and Snellman in 1968 discounted Moschcowitz s theory and put forward the concept of a circumferential intestinal intussusception; the authors demonstrated this phenomenon through cineradiography (11,12). Porter in 1962 reported that reflex inhibition of the external sphincter and levator muscles with distension of the rectum was more profound and prolonged in patients with rectal prolapse. Parks et al. in 1977 showed that mean resting pressures were maintained in those with rectal prolapse, suggesting a dysfunction of the internal sphincter as a cause of prolapse (13,14). There are many other conditions found in association with rectal prolapse. One such association is a connective tissue disorder. Marshman et al. in 1987 reported that many patients had an associated increased joint mobility (3). Other associated factors with rectal prolapse include mental illness, neurological disorders, and parity. Corman described nulliparous women as having the greatest risk of developing rectal prolapse (13). There is considerable controversy about the cause of rectal prolapse associated incontinence. Keighley and Shouler demonstrated an increase in sigmoid motility in incontinent patients with prolapse, while continent patients had normal sigmoid motility but delayed whole gut transit. The authors therefore suggested an increase in bowel motility as a cause of prolapse-associated incontinence (1,8). Matheson and Keighley found a significantly decreased resting and squeeze anal pressure in incontinent patients with prolapse, but normal pressures in continent patients (1,14). Gordon found evidence of denervation of the puborectalis and external sphincter muscles in incontinent patients. Farouk et al. suggested that repair of rectal prolapse probably allows the internal anal sphincter to recover by removing the cause of persistent rectoanal inhibition (13). Duthie and Bartolo claimed recently that the recovery of continence after operation does not depend on sphincter recovery but on improved anorectal sensation (14). 124
3 Delamarre et al. found an increase in rectal compliance and capacity after surgery in patients treated successfully for rectal prolapse and incontinence (15). The association of constipation with rectal prolapse has been reported to vary from 25 to 50 per cent. The exact cause of constipation is, again, controversial and poorly understood. Metcalf and Loening Baucke demonstrated a paradoxical increase in external anal sphincter electromyographic activity in those with rectal prolapse who were constipated. Some authors, however, have attributed constipation to a delay in colonic transit (9). Speakman et al. recently showed in a prospective randomised trial that division of the lateral ligaments during rectopexy caused constipation, although it prevented the recurrence of rectal prolapse (10). The management of rectal prolapse is usually surgical. Surgical approaches for rectal prolapse can be classified into either transabdominal or perineal. Perineal procedures were first used in the late 19th century as abdominal surgery was then considered unsafe. Moschcowitz first described the obliteration of the peritoneal pouch of Douglas based on the fact that rectal prolapse is commonly associated with an abnormally deep cul-de-sac. However, recurrence rates as high as 80 per cent have been reported. Anal encirclement was first described in 1891 by Thiersch. Advantages of this procedure included simplicity, repeatability, and that it required only a local anaesthetic. However, anal encirclement does not cure the disease process (1). Mikulicz first described perineal rectosigmoidectomy in 1889 and the procedure was repopularised in the 1960s by Altemeier and colleagues. This procedure is based on fixing the bowel to the sacrum by fibrosis around the anastomosis. The recurrence rates have been reported from 0 do 50 per cent (8). The Delorme operation is a modification of perineal rectosigmoidectomy in which the prolapsed bowel is not resected; its mucosa is stripped and the muscularis propria of the rectum and sigmoid are plicated and replaced above the levator muscles. Recurrence rates ranging from 5 to 21 percent have been reported (15). Abdominal procedures for rectal prolapse usually involve rectal fixation, large bowel resection or a combination of both. Rectal fixation, or rectopexy, which was first described by Pemberton and Stalker, involves full rectal mobilisation followed by fixation of the rectum to the sacrum. Most surgeons use a foreign material to help anchor the rectum to the sacrum. The Ripstein procedure is one of the most commonly used rectal fixation operations. It involves completely wrapping the mobilised rectum with a foreign material and suturing it to the sacrum. The possible complications include erosion of the foreign material and fistula formation and stenosis. Some authors have reported that foreign material is not important in the provocation of an intense fibrous tissue formation, and have shown that sutures alone are sufficient and allow equally low recurrence rates of 0 4 per cent (17,18). Anterior resection has also been described in the treatment of rectal prolapse. The principle in this case is the creation of fibrosis between the anastomosis and the sacrum. A major disadvantage of this procedure, 125
4 however, includes a possible decrease in continence secondary to a decrease in the rectal reservoir (15,16, 9). A combined colonic resection and rectopexy is also commonly performed. This makes use of the advantages of resection and avoids the disadvantages of rectopexy alone, especially with regard to constipation. Generally, resection rectopexy is reserved for patients who have a history of severe constipation. The use of laparoscopic techniques in the surgical treatment of rectal prolapse has been advocated as having several attractive features. Mobilisation of the rectum laparoscopically has been shown to be safe and feasible. MATERIALS AND METHODS Selection of the most appropriate surgical operation continues to be problematic for the surgeon. In our institution we prefer anterior rectopexy with the use of a three-dimensional mesh. One must remember that success in the management of rectal prolapse is not simply the correction of the physical and mechanical abnormality functional aspects are also important. The ideal surgical technique should, therefore, be based not only on the elements of simplicity, recurrence and complications, but should also take into account the treatment or at least alleviation of the functional disorder so commonly associated with rectal prolapse. Fourteen adult patients with complete rectal prolapse underwent operative treatment for the prolapse between January 1999 and September 2003 in 1st Dept. of Surgery of the St. Anne s Faculty Hospital. Nine patients were men, and the mean age was 59 /range 40 88/. Two patients had previously undergone operations for rectal prolapse and two patients had previously undergone two gynaecological operations /hysterectomies/. We used Holzschneider s incontinence score for grading anal incontinence. All patients treated by abdominal approach were given preoperatively an enema /Yal/. Antibiotic prophylaxis was given before the operation /Normix, Alfa Wassermann/. Our technique of abdominal anterior mesh rectopexy was as follows: Through a low midline incision, the rectum was mobilised to the tip of coccyx, and the lateral ligaments were ligated. A 3D PET /polyethylene terephthalate/ mesh 10x15 cm with three-dimensional <<honeycomb>> structure /HiTec/ was sutured to the presacral fascia immediately below the promontory by Pro-Tack stapler /AutoSuture/ or Endo-anchor system /Ethicon/. The mobilised rectum was pulled straight, and the mesh was sutured onto the rectum. The peritoneum was closed over the mesh (Figs. 1, 2, 3). The patients were followed up by clinical examination at a mean of ten /range, 6 20/ months after the operation for posterior mesh rectopexy or fourteen /range, 4 32/ months after the operation for anterior mesh rectopexy. During the follow-up period one anterior mesh rectopexy was performed in the posterior mesh group. RESULTS The surgical techniques used in treating rectal prolapse in 14 patients over a 45-month period are shown in Table 1. All procedures were performed by abdominal approach, and the most frequently used open technique was anterior rectopexy with a mesh. Eleven of 14 patients had preoperatively suffered some degree of anal incontinence. Of these incontinent patients, 9 regained continence postoperatively, leaving 2 patients with some degree of incontinence. Three patients had constipation preoperatively as compared with 6 patients postoperatively. The proportion of patients with constipation was greater after the operation than preoperatively. Accordingly, more 126
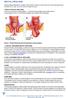
5 Fig. 1 3 D mesh with three dimensional <honeycomb> structure Fig. 2 Mobilisation of the rectum 127
6 Fig. 3 Suturing the mesh onto the rectum after using Pro Tack Fig. 4 Preoperative and postoperative situation 128
7 patients used medication for constipation after than before the operation, but the patients claimed less severe emptying problems after the operation (Table 2). Two less severe complications following abdominal rectopexy were successfully managed conservatively /small bowel obstruction and wound infection/. One case of recurrence after posterior mesh rectopexy was successfully managed by reoperation /anterior mesh rectopexy/ Table 3. Table 1 Techniques Used in Treating Complete Rectal Prolapse in 12 Patients in 3-Year Period Operative technique Number of patients (%) Mean age, yr. (range) Posterior mesh rectopexy 3 (21) 62 (40 88) Anterior mesh rectopexy 9 (79) 58(52 78) Table 2 Functional Outcome After Surgical Treatment of Rectal Prolapse Posterior mesh rectopexy (n=3) Anterior mesh rectopexy (n=11) Follow-up time (months) 10(6 20) 14(4 32) Constipation Preoperative 1 2 Postoperative 2 4 Incontinence Preoperative None 1 2 Relative 2 7 Absolute 0 2 Postoperative None 2 9 Relative 1 1 Absolute
8 Table 3 Complications Related to Abdominal Rectopexy (14 Patients) Type of complication No. of events Recurrence 1 (PMR) Pulmonary 0 Cardiac 0 Wound infection 1 Stricture 0 Small bowel obstruction 1 Sexual dysfunction 0 Incisional hernia 0 Total 1 recurrence, 2 other events in 12 patients CONCLUSION The choice of an ideal operation for complete rectal prolapse remains a perplexing problem for the surgeon. At our institution we prefer anterior mesh rectopexy with a 3-D mesh, also for older patients. One has to remember that success in the management of rectal prolapse is not simply the correction of the physical or mechanical abnormality; functional aspects are also important. The ideal surgical technique should, therefore, be based not only on the elements of simplicity, recurrence and complications, but should also take into account the treatment or at least alleviation of the functional disorder so commonly associated with rectal prolapse. A c k n o w l e d g e m e n t Supported by grant IGA MZ, No. ND7468 3/2003 A preliminary report of this study was presented at the ECCP meeting, Athens, Greece, May 28 to June 3, Vlček P., Korbička J., Chalupník Š., Jedlička V., Veverková L., Čapov I., Wechsler J.,Vlčková P., Dolina J., Bartůšek D. NAŠE ZKUŠENOSTI S VYUŽITÍM 3-D SÍŤKY PŘI ŘEŠENÍ PROLAPSU REKTA S o u h r n Mezi mnoha chirurgickými metodami korigujícími prolaps rekta není zatím jednoznačná metoda volby. Cílem naší studie bylo zhodnocení funkčních výsledků chirurgické léčby prolapsu rekta během tříletého intervalu na naší klinice. 130
9 Do studie byli zahrnuti pacienti operovaní na naší klinice pro kompletní prolaps rekta od ledna 1999 do září Z těchto 14 pacientů bylo 9 mužů s průměrným věkem 59 let /40 88 let/. Většina operačních výkonů byla provedena transabdominálně a nejpoužívanější metodou byla přední rektopexe dle Ripsteina s využitím 3-D síťky. Mezi pacienty s předoperačně zjištěnou inkontinencí došlo u 82 % k podstatnému zlepšení. Naopak počet pacientů s obstipací po operaci se zvětšil. V celé skupině jsme pozorovali 1 recidivu. Za metodu volby při řešení kompletního prolapsu rekta považujeme přední rektopexi dle Ripsteina. U starších pacientů pokládáme věk za negativní faktor ovlivňující funkční výsledek operace. References 1. Eu KW, Seow-Choen F. Functional problems in adult rectal prolapse and controversies in surgical treatment. Brit J Surgery 1997; 84(7): Theuerkauf FJ Jr, Beahrs OH, Hill JR. Rectal prolapse. Causation and surgical treatment. Annals of Surgery 1970; 171(6): Marshman D, Percy J, Fielding I, Delbridge L. Rectal prolapse: relationship with joint mobility. Australian and New Zealand Journal of Surgery 1987; 57(11): Schoetz DJ, Veidenheimer MC. Rectal prolapse. Pathogenesis and clinical features. In: Henry MM, Swash M, eds. Coloproctology in the pelvic floor. London: Butterworths, Karasick S, Spetell CM. The role of parity and hysterectomy on the development of pelvic floor abnormalities revealed by defecography. American Journal Roentgenology 1997; 169(6): Aitola PT, Hiltunen KM, Matikainen MJ. Functional results of operative treatment of rectal prolapse over an 11 year period: emphasis on transabdominal approach. Dis Colon Rectum 1999; 42: Jacobs LK, Lin YJ, Orkin BA. The best operation for rectal prolapse. Surg Clin North Am 1997; 77: Keighley MR, Fielding JW, Alexander-Williams J. Results of Marlex mesh abdominal rectopexy for rectal prolapse in 100 consecutive patients. Brit J Surgery 1983; 70: Tjandra JJ, Fazio VW, Church JM, Milsom JW, Oakley JR, Lavery IC. Ripstein procedure is an effective treatment for rectal prolapse without constipation. Dis Colon Rectum 1993; 36: Speakman CT, Maden MV, Nicholls RJ, Kamm MA. Lateral ligament division during rectopexy causes constipation but prevents recurrence: results of a prospective randomised study. Brit J Surgery 1991; 78: Kim DS, Tsang CBS, Wong WD, Lowry AC, Goldberg SM, Madoff RD. Complete rectal prolapse: evolution of management and results. Dis Colon Rectum 1999; 42: Williams JG, Wong WD, Jensen LL, Rothenberger DA, Goldberg SM. Incontinence and rectal prolapse: a prospective manometric study. Dis Colon and Rectum 1991; 34: Farouk R, Duthie GS, Bartolo DC, MacGregor AB. Restoration of continence following rectopexy for rectal prolapse and recovery of internal anal sphincter electromyogram. Brit J Surgery 1992; 79: Bartolo DC, Duthie GS. The physiological evaluation of operative repair for incontinence and prolapse. Ciba Found Symp 1990; 151: Novell J, Osborne M, Winslet M, Lewis A. Prospective randomized trial of Ivalon sponge rectopexy versus sutured rectopexy for full-thickness rectal prolapse. Brit J Surgery 1994; 81: Madoff RD, Malgren A. One hundred years of rectal prolapse surgery. Dis Colon and Rectum 1999; 42: Čapov I, Wechsler J, et al. Drény. Jejich využití v chirurgických oborech [Drains. Their utilisation in surgical disciplines]. Praha: Grada, pp, ISBN Veverková L, Kalač J, Žák J, Mašek M, Mach P. Hojení chronických ran [Healing of chronic wounds]. Zdravotnické noviny 2000; 49 (4): Vávra P, Zonča P, Faltýn J, Kopecký J. Operative treatment of haemorrhoids in Czech Republic at the end of the second millennium. Joint Meeting of the Mediterranean Society of Coloproctology and the Israel Society of Colon and Rectal Surgery, Nasareth, Israel, Book of Abstracts. 131
10 132
Summary and conclusion. Summary And Conclusion
 Summary And Conclusion Summary and conclusion Rectal prolapse remain a disorder for which no single ideal treatment was approved for all cases. Complete rectal prolapse (procidentia) is the circumferential
Summary And Conclusion Summary and conclusion Rectal prolapse remain a disorder for which no single ideal treatment was approved for all cases. Complete rectal prolapse (procidentia) is the circumferential
Rectal Prolapse: A 10-Year Experience
 24 The Ochsner Journal Volume 7, Number 1, Spring 2007 25 Rectal Prolapse: A 10-Year Experience Figure 2. Physical examination. A. Concentric folds of prolapsed rectum. B. Radial folds of hemorrhoids (mucosal
24 The Ochsner Journal Volume 7, Number 1, Spring 2007 25 Rectal Prolapse: A 10-Year Experience Figure 2. Physical examination. A. Concentric folds of prolapsed rectum. B. Radial folds of hemorrhoids (mucosal
POSTERIOR LEVATOR REPAIR AND RECTAL SUSPENSION FOR RECURRENT RECTAL PROLAPSE: AUTHOR'S EXPERIENCE
 POSTERIOR LEVATOR REPAIR AND RECTAL SUSPENSION FOR RECURRENT RECTAL PROLAPSE: AUTHOR'S EXPERIENCE *Shyam B. Sharma 1&2 and Rahul Gupta 2 1 Department of Pediatric Surgery SMS Medical College 2 Pediatric
POSTERIOR LEVATOR REPAIR AND RECTAL SUSPENSION FOR RECURRENT RECTAL PROLAPSE: AUTHOR'S EXPERIENCE *Shyam B. Sharma 1&2 and Rahul Gupta 2 1 Department of Pediatric Surgery SMS Medical College 2 Pediatric
Colorectal procedure guide
 Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Rectal prolapse CASE REPORT. Sekac J 1, Labas P 2, Skultety J 1, Prochotsky A 1, Skubla R 3, Okolicany R 1
 CASE REPORT Rectal prolapse Sekac J 1, Labas P 2, Skultety J 1, Prochotsky A 1, Skubla R 3, Okolicany R 1 2nd Department for Surgery, University Hospital, Bratislava, Slovakia. jaroslavsekac@yahoo.com
CASE REPORT Rectal prolapse Sekac J 1, Labas P 2, Skultety J 1, Prochotsky A 1, Skubla R 3, Okolicany R 1 2nd Department for Surgery, University Hospital, Bratislava, Slovakia. jaroslavsekac@yahoo.com
REVIEW ARTICLE. Surgical Management of Rectal Prolapse. the anus. 1 Complete or
 REVIEW ARTICLE Surgical Management of Rectal Prolapse Thandinkosi E. Madiba, MMed(Chir), FCS(SA); Mirza K. Baig, FRCS; Steven D. Wexner, MD, FACS, FRCS, FRCS(Edin) Background: The problem of complete rectal
REVIEW ARTICLE Surgical Management of Rectal Prolapse Thandinkosi E. Madiba, MMed(Chir), FCS(SA); Mirza K. Baig, FRCS; Steven D. Wexner, MD, FACS, FRCS, FRCS(Edin) Background: The problem of complete rectal
Motility Disorders. Pelvic Floor. Colorectal Center for Functional Bowel Disorders (N = 701) January 2010 November 2011
 Motility Disorders Pelvic Floor Colorectal Center for Functional Bowel Disorders (N = 71) January 21 November 211 New Patients 35 3 25 2 15 1 5 Constipation Fecal Incontinence Rectal Prolapse Digestive-Genital
Motility Disorders Pelvic Floor Colorectal Center for Functional Bowel Disorders (N = 71) January 21 November 211 New Patients 35 3 25 2 15 1 5 Constipation Fecal Incontinence Rectal Prolapse Digestive-Genital
Surgery for complete(full-thickness) rectal prolapse in adults(review)
 Cochrane Database of Systematic Reviews Surgery for complete(full-thickness) rectal prolapse in adults (Review) TouS,BrownSR,NelsonRL TouS,BrownSR,NelsonRL. Surgery for complete(full-thickness) rectal
Cochrane Database of Systematic Reviews Surgery for complete(full-thickness) rectal prolapse in adults (Review) TouS,BrownSR,NelsonRL TouS,BrownSR,NelsonRL. Surgery for complete(full-thickness) rectal
Rectal Prolapse: Review According to the Personal Experience
 Review Journal of the Korean Society of DOI: 10.3393/jksc.2011.27.3.107 pissn 2093-7822 eissn 2093-7830 Rectal Prolapse: Review According to the Personal Experience Department of Surgery, Seoul Song Do
Review Journal of the Korean Society of DOI: 10.3393/jksc.2011.27.3.107 pissn 2093-7822 eissn 2093-7830 Rectal Prolapse: Review According to the Personal Experience Department of Surgery, Seoul Song Do
Index. Note: Page numbers of article title are in boldface type.
 Index Note: Page numbers of article title are in boldface type. A Abscess(es) in Crohn s disease, 168 169 IPAA and, 110 114 as unexpected finding in colorectal surgery, 46 Adhesion(s) trocars-related laparoscopy
Index Note: Page numbers of article title are in boldface type. A Abscess(es) in Crohn s disease, 168 169 IPAA and, 110 114 as unexpected finding in colorectal surgery, 46 Adhesion(s) trocars-related laparoscopy
Prolaps: Anteriore Rektopexie nach D Hoore. Prof. Dr. med. F. Hetzer
 Prolaps: Anteriore Rektopexie nach D Hoore Prof. Dr. med. F. Hetzer franc.hetzer@spital-linth.ch Rectal prolapse pathophysiology 24 22 20 18 congenital female pathology (90%) 16 14 straining weakened pelvic
Prolaps: Anteriore Rektopexie nach D Hoore Prof. Dr. med. F. Hetzer franc.hetzer@spital-linth.ch Rectal prolapse pathophysiology 24 22 20 18 congenital female pathology (90%) 16 14 straining weakened pelvic
Function of the anal sphincters in patients with
 Function of the anal sphincters in patients with intussusception of the rectum B. FRENCKNER AND T. IHRE Gut, 1976,17, 147-151 From the Department of Clinical Physiology and the Department of Surgery, Serafimer
Function of the anal sphincters in patients with intussusception of the rectum B. FRENCKNER AND T. IHRE Gut, 1976,17, 147-151 From the Department of Clinical Physiology and the Department of Surgery, Serafimer
Anorectal malformations include a wide spectrum of
 JOURNAL OF LAPAROENDOSCOPIC & ADVANCED SURGICAL TECHNIQUES Volume 20, Number 1, 2010 ª Mary Ann Liebert, Inc. DOI: 10.1089=lap.2008.0343 Laparoscopic-Assisted Pull-Through for Congenital Rectal Stenosis
JOURNAL OF LAPAROENDOSCOPIC & ADVANCED SURGICAL TECHNIQUES Volume 20, Number 1, 2010 ª Mary Ann Liebert, Inc. DOI: 10.1089=lap.2008.0343 Laparoscopic-Assisted Pull-Through for Congenital Rectal Stenosis
Gynecology Dr. Sallama Lecture 3 Genital Prolapse
 Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
LAPAROSCOPIC REPAIR OF PELVIC FLOOR
 LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
Stapled transanal rectal resection for obstructed defaecation syndrome
 Stapled transanal rectal resection for obstructed Issued: June 2010 www.nice.org.uk/ipg351 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
Stapled transanal rectal resection for obstructed Issued: June 2010 www.nice.org.uk/ipg351 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
Robotic Ventral Rectopexy
 Robotic Ventral Rectopexy What is a robotic ventral rectopexy? The term rectopexy refers to an operation in which the rectum (the part of the bowel nearest the anus) is put back into its normal position
Robotic Ventral Rectopexy What is a robotic ventral rectopexy? The term rectopexy refers to an operation in which the rectum (the part of the bowel nearest the anus) is put back into its normal position
The Impact of Laparoscopic Resection Rectopexy in Patients with Total Rectal Prolapse
 MILITARY MEDICINE, 170, 9:743, 2005 The Impact of Laparoscopic Resection Rectopexy in Patients with Total Rectal Prolapse Guarantor: Lt Col Sezai Demirbas Contributors: Lt Col Sezai Demirbas*; Col M. Levhi
MILITARY MEDICINE, 170, 9:743, 2005 The Impact of Laparoscopic Resection Rectopexy in Patients with Total Rectal Prolapse Guarantor: Lt Col Sezai Demirbas Contributors: Lt Col Sezai Demirbas*; Col M. Levhi
What the radiologist needs to know!
 What the radiologist needs to know! Clare Molyneux Sam Treadway Sathi Sukumar Wal Baraza Abhiram Sharma Karen Telford University Hospital of South Manchester Manchester UK Introduction Indications Investigations
What the radiologist needs to know! Clare Molyneux Sam Treadway Sathi Sukumar Wal Baraza Abhiram Sharma Karen Telford University Hospital of South Manchester Manchester UK Introduction Indications Investigations
Although disparate topics, these two different pathologic
 34 H E M O R R H O I D S A N D R E C T A L P R O L A P S E CHARLES N. HEADRICK MICHAEL J. STAMOS Although disparate topics, these two different pathologic entities are commonly misdiagnosed by both layperson
34 H E M O R R H O I D S A N D R E C T A L P R O L A P S E CHARLES N. HEADRICK MICHAEL J. STAMOS Although disparate topics, these two different pathologic entities are commonly misdiagnosed by both layperson
Robot Assisted Rectopexy
 1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
By:Dr:ISHRAQ MOHAMMED
 By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
Outlet syndrome: is there a surgical option?'
 Journal of the Royal Society of Medicine Volume 77 July 1984 559 Outlet syndrome: is there a surgical option?' M R B Keighley MS FRCS P Shouler FRCS Department of Surgery, General Hospital, Birmingham
Journal of the Royal Society of Medicine Volume 77 July 1984 559 Outlet syndrome: is there a surgical option?' M R B Keighley MS FRCS P Shouler FRCS Department of Surgery, General Hospital, Birmingham
TYPES OF RECTAL PROLAPSE
 RECTAL PROLPASE Rectal prolapse describes a condition where either the lining or entire wall of the rectum becomes loose and falls into, or even out of, the rectum through the anus. TYPES OF RECTAL PROLAPSE
RECTAL PROLPASE Rectal prolapse describes a condition where either the lining or entire wall of the rectum becomes loose and falls into, or even out of, the rectum through the anus. TYPES OF RECTAL PROLAPSE
Laparoscopic Ventral. Mesh Rectopexy (LVMR)
 Laparoscopic Ventral Mesh Rectopexy (LVMR) Questions & Answers GLASGOW COLORECTAL CENTRE Ross Hall Hospital 221 Crookston Road Glasgow G52 3NQ e-mail: info@colorectalcentre.co.uk Ph: Main hospital switchboard
Laparoscopic Ventral Mesh Rectopexy (LVMR) Questions & Answers GLASGOW COLORECTAL CENTRE Ross Hall Hospital 221 Crookston Road Glasgow G52 3NQ e-mail: info@colorectalcentre.co.uk Ph: Main hospital switchboard
Pelvic Floor Disorders. Amir Darakhshan MD FRCS (Gen Surg) Consultant Colorectal and General Surgeon
 Pelvic Floor Disorders Amir Darakhshan MD FRCS (Gen Surg) Consultant Colorectal and General Surgeon What is Pelvic Floor Disorder Surgical perspective symptoms of RED, FI or prolapse on the background
Pelvic Floor Disorders Amir Darakhshan MD FRCS (Gen Surg) Consultant Colorectal and General Surgeon What is Pelvic Floor Disorder Surgical perspective symptoms of RED, FI or prolapse on the background
Saint-Petersburg State Pediatric Medical University, Saint-Petersburg, Russia
 Saint-Petersburg State Pediatric Medical University, Saint-Petersburg, Russia Modern technologies in treatment of fecal incontinence in children Komissarov Igor Alexeevich- Ph.D, M.D, Prof. Kolesnikova
Saint-Petersburg State Pediatric Medical University, Saint-Petersburg, Russia Modern technologies in treatment of fecal incontinence in children Komissarov Igor Alexeevich- Ph.D, M.D, Prof. Kolesnikova
DIGESTIVE SYSTEM SURGICAL PROCEDURES December 22, 2015 (effective March 1, 2016) INTESTINES (EXCEPT RECTUM) Asst Surg Anae
 December 22, 2015 (effective March 1, 201) INTESTINES (EXCEPT RECTUM) Z513 Hydrostatic - Pneumatic dilatation of colon stricture(s) through colonoscope... 10.50 Z50 Fulguration of first polyp through colonoscope...
December 22, 2015 (effective March 1, 201) INTESTINES (EXCEPT RECTUM) Z513 Hydrostatic - Pneumatic dilatation of colon stricture(s) through colonoscope... 10.50 Z50 Fulguration of first polyp through colonoscope...
An Evaluation of the Cause and Mechanism of Complete Rectal Prolapse
 PRESIDENTIAL ADDRESS An Evaluation of the Cause and Mechanism of Complete Rectal Prolapse NORMAN D. NIGRO, M.D. Detroit, Michigan I appreciate deeply the honor which the American Proctologic Society conferred
PRESIDENTIAL ADDRESS An Evaluation of the Cause and Mechanism of Complete Rectal Prolapse NORMAN D. NIGRO, M.D. Detroit, Michigan I appreciate deeply the honor which the American Proctologic Society conferred
CHAU KHAC TU M.D., Ph.D.
 CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
STOMA SITING & PARASTOMAL HERNIA MANAGEMENT
 STOMA SITING & PARASTOMAL HERNIA MANAGEMENT Professor Hany S. Tawfik Head of the Department of Surgery & Chairman of Colorectal Surgery Unit Benha University Disclosure No financial affiliation to disclose
STOMA SITING & PARASTOMAL HERNIA MANAGEMENT Professor Hany S. Tawfik Head of the Department of Surgery & Chairman of Colorectal Surgery Unit Benha University Disclosure No financial affiliation to disclose
A 48-HOUR PROFILE OF INTRA-ABDOMINAL PRESSURE FOLLOWING RESECTION OF THE RECTUM
 SCRIPTA MEDICA (BRNO) 78 (1): 25 30, February 2005 A 48-HOUR PROFILE OF INTRA-ABDOMINAL PRESSURE FOLLOWING RESECTION OF THE RECTUM DOLEŽEL J. 1, ŽÁK J. 1, KARPÍŠEK Z. 2, WECHSLER J. 1 1 First Department
SCRIPTA MEDICA (BRNO) 78 (1): 25 30, February 2005 A 48-HOUR PROFILE OF INTRA-ABDOMINAL PRESSURE FOLLOWING RESECTION OF THE RECTUM DOLEŽEL J. 1, ŽÁK J. 1, KARPÍŠEK Z. 2, WECHSLER J. 1 1 First Department
Anus,Rectum and Colon
 JOURNAL OF THE Anus,Rectum and Colon http://journal-arc.jp CLINICAL RESEARCH Laparoscopic ventral rectopexy with sacrocolpopexy for coexisting pelvic organ prolapse and external rectal prolapse Yoshiyuki
JOURNAL OF THE Anus,Rectum and Colon http://journal-arc.jp CLINICAL RESEARCH Laparoscopic ventral rectopexy with sacrocolpopexy for coexisting pelvic organ prolapse and external rectal prolapse Yoshiyuki
RECTAL INJURY IN UROLOGIC SURGERY. Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences.
 RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
Laparoscopically Assisted Anorectoplasty: A New Definitive Repair of High Imperforate Anus
 Annals of Pediatric Surgery, Vol 4, No 1,2, January-April, 2008 PP 1-7 Original Article Laparoscopically Assisted Anorectoplasty: A New Definitive Repair of High Imperforate Anus Mohamed Magdy Elbarbary*,
Annals of Pediatric Surgery, Vol 4, No 1,2, January-April, 2008 PP 1-7 Original Article Laparoscopically Assisted Anorectoplasty: A New Definitive Repair of High Imperforate Anus Mohamed Magdy Elbarbary*,
The American Society of Colon and Rectal Surgeons
 CLINICAL PRACTICE GUIDELINES Downloaded from https://journals.lww.com/dcrjournal by BhDMf5ePHKav1zEoum1tQfN4a+kJLhEZgbsIHo4XMi0hCywCX1AWnYQp/IlQrHD3IJrtBKuSsQVRz8fA4yAY0a8W1YLRn6mHykFpaZ5LFvI= on 03/16/2018
CLINICAL PRACTICE GUIDELINES Downloaded from https://journals.lww.com/dcrjournal by BhDMf5ePHKav1zEoum1tQfN4a+kJLhEZgbsIHo4XMi0hCywCX1AWnYQp/IlQrHD3IJrtBKuSsQVRz8fA4yAY0a8W1YLRn6mHykFpaZ5LFvI= on 03/16/2018
Delorme's operation plus sphincteroplasty for complete rectal prolapse associated with traumatic fecal incontinence
 Available online at www.jbr-pub.org Open Access at PubMed Central The Journal of Biomedical Research, 2015, 29(4):326-331 Original Article Delorme's operation plus sphincteroplasty for complete rectal
Available online at www.jbr-pub.org Open Access at PubMed Central The Journal of Biomedical Research, 2015, 29(4):326-331 Original Article Delorme's operation plus sphincteroplasty for complete rectal
Comparison of abdominal and perineal procedures for complete rectal prolapse: an analysis of 104 patients
 ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/10.4174/astr.2014.86.5.249 Annals of Surgical Treatment and Research Comparison of abdominal and perineal procedures for complete rectal
ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/10.4174/astr.2014.86.5.249 Annals of Surgical Treatment and Research Comparison of abdominal and perineal procedures for complete rectal
World Journal of Colorectal Surgery
 World Journal of Colorectal Surgery Volume 5, Issue 1 2015 Article 5 Incacerated Large Rectal Prolapse Repaired By Delorme Procedure: A Case Report And Review Of The Literature. Elroy P. Weledji Vincent
World Journal of Colorectal Surgery Volume 5, Issue 1 2015 Article 5 Incacerated Large Rectal Prolapse Repaired By Delorme Procedure: A Case Report And Review Of The Literature. Elroy P. Weledji Vincent
Department of General Surgery
 STUDY OF CLINICAL AND FUNCTIONAL RESULTS OF ABDOMINAL MESH RECTOPEXY FOR COMPLETE RECTAL PROLAPSE By Dr. JINREEVE S.W. DANIEL Dissertation Submitted to The Tamilnadu DR.MGR Medical university, Chennai.
STUDY OF CLINICAL AND FUNCTIONAL RESULTS OF ABDOMINAL MESH RECTOPEXY FOR COMPLETE RECTAL PROLAPSE By Dr. JINREEVE S.W. DANIEL Dissertation Submitted to The Tamilnadu DR.MGR Medical university, Chennai.
Robotic-Assisted Laparoscopic Salvage Rectopexy for. Recurrent Ileoanal J-Pouch Prolapse
 Robotic-Assisted Laparoscopic Salvage Rectopexy for Recurrent Ileoanal J-Pouch Prolapse Madhu Ragupathi, MD 1, Chirag B. Patel, MSE 1, Diego I. Ramos-Valadez, MD 1, Eric M. Haas, MD, FACS 1,* 1 Division
Robotic-Assisted Laparoscopic Salvage Rectopexy for Recurrent Ileoanal J-Pouch Prolapse Madhu Ragupathi, MD 1, Chirag B. Patel, MSE 1, Diego I. Ramos-Valadez, MD 1, Eric M. Haas, MD, FACS 1,* 1 Division
Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583
 Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
Surgical repair of vaginal wall prolapse using mesh
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
World Journal of Colorectal Surgery
 World Journal of Colorectal Surgery Volume 6, Issue 5 2016 Article 8 Sigmoidocele: A Rare Cause Of Constipation In Males Noor Shah MD Milind Kachare MD Craig Rezac MD Rutgers Robert Wood Johnson Medical
World Journal of Colorectal Surgery Volume 6, Issue 5 2016 Article 8 Sigmoidocele: A Rare Cause Of Constipation In Males Noor Shah MD Milind Kachare MD Craig Rezac MD Rutgers Robert Wood Johnson Medical
Surgical Management for Defecation Dysfunction
 Defecatory Dysfunction Surgical Management for Defecation Dysfunction JMAJ 46(9): 378 383, 2003 Tatsuo TERAMOTO Professor, 1st Department of Surgery, School of Medicine, Toho University Abstract: Typical
Defecatory Dysfunction Surgical Management for Defecation Dysfunction JMAJ 46(9): 378 383, 2003 Tatsuo TERAMOTO Professor, 1st Department of Surgery, School of Medicine, Toho University Abstract: Typical
Clinical Study Delorme s Procedure for Complete Rectal Prolapse: A Study of Recurrence Patterns in the Long Term
 Surgery Research and Practice Volume 215, Article ID 92154, 6 pages http://dx.doi.org/1.1155/215/92154 Clinical Study Delorme s Procedure for Complete Rectal Prolapse: A Study of Recurrence Patterns in
Surgery Research and Practice Volume 215, Article ID 92154, 6 pages http://dx.doi.org/1.1155/215/92154 Clinical Study Delorme s Procedure for Complete Rectal Prolapse: A Study of Recurrence Patterns in
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015
 Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Diagnosis of Impaired Defecatory Function with Special Reference to Physiological Tests
 Defecatory Dysfunction Diagnosis of Impaired Defecatory Function with Special Reference to Physiological Tests JMAJ 46(9): 373 377, 2003 Masatoshi OYA, Masashi UENO, and Tetsuichiro MUTO Department of
Defecatory Dysfunction Diagnosis of Impaired Defecatory Function with Special Reference to Physiological Tests JMAJ 46(9): 373 377, 2003 Masatoshi OYA, Masashi UENO, and Tetsuichiro MUTO Department of
Dana Alrafaiah. - Amani Nofal. - Ahmad Alsalman. 1 P a g e
 - 2 - Dana Alrafaiah - Amani Nofal - Ahmad Alsalman 1 P a g e This lecture will discuss five topics as follows: 1- Arrangement of pelvic viscera. 2- Muscles of Pelvis. 3- Blood Supply of pelvis. 4- Nerve
- 2 - Dana Alrafaiah - Amani Nofal - Ahmad Alsalman 1 P a g e This lecture will discuss five topics as follows: 1- Arrangement of pelvic viscera. 2- Muscles of Pelvis. 3- Blood Supply of pelvis. 4- Nerve
Perineale Rektumprolapsoperation: Gute Resultate bei geringem Aufwand! F.H. Hetzer
 Perineale Rektumprolapsoperation: Gute Resultate bei geringem Aufwand! F.H. Hetzer STARR: Wunderwaffe beim Obstructed Defecation Syndrom (ODS) F.H. Hetzer Stapled TransAnal Rectal Resection STARR PPH 01
Perineale Rektumprolapsoperation: Gute Resultate bei geringem Aufwand! F.H. Hetzer STARR: Wunderwaffe beim Obstructed Defecation Syndrom (ODS) F.H. Hetzer Stapled TransAnal Rectal Resection STARR PPH 01
UvA-DARE (Digital Academic Repository) Rectal prolapse: enlightenment of the obscure Wijffels, N.A.T. Link to publication
 UvA-DARE (Digital Academic Repository) Rectal prolapse: enlightenment of the obscure Wijffels, N.A.T. Link to publication Citation for published version (APA): Wijffels, N. A. T. (2012). Rectal prolapse:
UvA-DARE (Digital Academic Repository) Rectal prolapse: enlightenment of the obscure Wijffels, N.A.T. Link to publication Citation for published version (APA): Wijffels, N. A. T. (2012). Rectal prolapse:
Deep Endometriosis Surgery pro conservative surgery?
 ISGE OPAIJA 26-29/5/2016 Deep Endometriosis Surgery pro conservative surgery? Introduction Feasability of conservative surgery No need to be that radical Conclusions Gruppo Italo Belga HH Leuven VDR Rome
ISGE OPAIJA 26-29/5/2016 Deep Endometriosis Surgery pro conservative surgery? Introduction Feasability of conservative surgery No need to be that radical Conclusions Gruppo Italo Belga HH Leuven VDR Rome
PAPER. Long-term Follow-up of the Modified Delorme Procedure for Rectal Prolapse
 PAPER Long-term Follow-up of the Modified Delorme Procedure for Rectal Prolapse Brian P. Watkins, MD, MS; Jeffrey Landercasper, MD; G. Eric Belzer, MD; Paula Rechner, MD; Rebecca Knudson, BA; Marilu Bintz,
PAPER Long-term Follow-up of the Modified Delorme Procedure for Rectal Prolapse Brian P. Watkins, MD, MS; Jeffrey Landercasper, MD; G. Eric Belzer, MD; Paula Rechner, MD; Rebecca Knudson, BA; Marilu Bintz,
ARTIFICIAL MESH REPAIR FOR TREATMENT OF PELVIC ORGAN PROLAPSE
 Pelvic Floor Unit / Department of Gynaecology Ward 17, Singleton Hospital, Sketty, Swansea, SA2 8QA 01792 205666 Secretary Direct Line: 01792 285688. Fax: 01792 285874 ARTIFICIAL MESH REPAIR FOR TREATMENT
Pelvic Floor Unit / Department of Gynaecology Ward 17, Singleton Hospital, Sketty, Swansea, SA2 8QA 01792 205666 Secretary Direct Line: 01792 285688. Fax: 01792 285874 ARTIFICIAL MESH REPAIR FOR TREATMENT
Colostomy & Ileostomy
 Colostomy & Ileostomy Indications, problems and preference By Waleed Omar Professor of Colorectal surgery, Mansoura University. Disclosure I have no disclosures. Presentation outline Stoma: Definition
Colostomy & Ileostomy Indications, problems and preference By Waleed Omar Professor of Colorectal surgery, Mansoura University. Disclosure I have no disclosures. Presentation outline Stoma: Definition
Single Stage Transanal Pull-Through for Hirschsprung s Disease in Neonates: Our Early Experience
 Journal of Neonatal Surgery 2013;2(4):39 ORIGINAL ARTICLE Single Stage Transanal Pull-Through for Hirschsprung s Disease in Neonates: Our Early Experience Pradeep Bhatia,* Rakesh S Joshi, Jaishri Ramji,
Journal of Neonatal Surgery 2013;2(4):39 ORIGINAL ARTICLE Single Stage Transanal Pull-Through for Hirschsprung s Disease in Neonates: Our Early Experience Pradeep Bhatia,* Rakesh S Joshi, Jaishri Ramji,
Articles. Funding None.
 Bowel function after laparoscopic posterior sutured versus ventral mesh for rectal prolapse: a double-blind, randomised single-centre study Lilli Lundby, Lene H Iversen, Steen Buntzen, Pål Wara, Katrine
Bowel function after laparoscopic posterior sutured versus ventral mesh for rectal prolapse: a double-blind, randomised single-centre study Lilli Lundby, Lene H Iversen, Steen Buntzen, Pål Wara, Katrine
Citation Acta medica Nagasakiensia. 2003, 48
 NAOSITE: Nagasaki University's Ac Title Author(s) Surgical Strategy for Low Imperfora Anal Transplantation or Limited Pos Obatake, Masayuki; Yamashita, Hidek Norihisa; Nakagoe, Tohru Citation Acta medica
NAOSITE: Nagasaki University's Ac Title Author(s) Surgical Strategy for Low Imperfora Anal Transplantation or Limited Pos Obatake, Masayuki; Yamashita, Hidek Norihisa; Nakagoe, Tohru Citation Acta medica
The Milestones provide a framework for the assessment
 The Colon and Rectal Surgery Milestone Project The Milestones provide a framework for the assessment of the development of the resident physician in key dimensions of the elements of physician competency
The Colon and Rectal Surgery Milestone Project The Milestones provide a framework for the assessment of the development of the resident physician in key dimensions of the elements of physician competency
Increased motor unit fibre density in the external
 Journal of Neurology, Neurosurgery, and Psychiatry, 1980, 43, 343-347 Increased motor unit fibre density in the external anal sphincter muscle in ano-rectal incontinence: a single fibre EMG study M E NEILL
Journal of Neurology, Neurosurgery, and Psychiatry, 1980, 43, 343-347 Increased motor unit fibre density in the external anal sphincter muscle in ano-rectal incontinence: a single fibre EMG study M E NEILL
TME and autonomic nerve preservation techniques: based on Video and Cadaveric anatomy
 TME and autonomic nerve preservation techniques: based on Video and Cadaveric anatomy Nam Kyu Kim M.D., Ph.D., FACS, FRCS, FASCRS Professor Department of Surgery Yonsei University College of Medicine Seoul,
TME and autonomic nerve preservation techniques: based on Video and Cadaveric anatomy Nam Kyu Kim M.D., Ph.D., FACS, FRCS, FASCRS Professor Department of Surgery Yonsei University College of Medicine Seoul,
World Journal of Colorectal Surgery
 World Journal of Colorectal Surgery Volume 3, Issue 4 2013 Article 3 Sigmoidorectal Intussusception Presenting as Prolapse Per Anus in an Adult Venugopal Hg Hasmukh B. Vora Mahendra S. Bhavsar SMT.NHL
World Journal of Colorectal Surgery Volume 3, Issue 4 2013 Article 3 Sigmoidorectal Intussusception Presenting as Prolapse Per Anus in an Adult Venugopal Hg Hasmukh B. Vora Mahendra S. Bhavsar SMT.NHL
Setting The study setting was tertiary care. The economic study was carried out in the USA.
 Laparoscopic intraperitoneal polytetrafluoroethylene (PTFE) prosthetic patch repair of ventral hernia: prospective comparison to open prefascial polypropylene mesh repair DeMaria E J, Moss J M, Sugerman
Laparoscopic intraperitoneal polytetrafluoroethylene (PTFE) prosthetic patch repair of ventral hernia: prospective comparison to open prefascial polypropylene mesh repair DeMaria E J, Moss J M, Sugerman
Bozza Programma preliminare
 Bozza Programma preliminare COLORECTAL AND PELVIC FLOOR DISORDERS FIRST INTERNATIONAL SYMPOSIUM 07-08 Ottobre 2009 - Parma MAIN PELVIC FLOOR: ANATOMY PELVIC FLOOR: NEUROPHISIOLOGY IMAGING IN PELVIC FLOOR
Bozza Programma preliminare COLORECTAL AND PELVIC FLOOR DISORDERS FIRST INTERNATIONAL SYMPOSIUM 07-08 Ottobre 2009 - Parma MAIN PELVIC FLOOR: ANATOMY PELVIC FLOOR: NEUROPHISIOLOGY IMAGING IN PELVIC FLOOR
&KDSWHU provides a general introduction to this thesis. In addition, the aims of the
 6800$5< The two principal goals in the treatment of perianal fistulas are eradication of the fistulous tract and preservation of sphincter function. In patients with an intersphincteric fistula, these
6800$5< The two principal goals in the treatment of perianal fistulas are eradication of the fistulous tract and preservation of sphincter function. In patients with an intersphincteric fistula, these
Outcomes of Colostomy Reversal Procedures in Two Teaching Hospitals in Addis Ababa, Ethiopia A. Bekele, B. Kotisso, H. Biluts Correspondence to
 East and Central African Journal of Surgery http://www.bioline.org.br/js 9 Outcomes of Colostomy Reversal Procedures in Two Teaching Hospitals in Addis Ababa, Ethiopia A. Bekele, B. Kotisso, H. Biluts
East and Central African Journal of Surgery http://www.bioline.org.br/js 9 Outcomes of Colostomy Reversal Procedures in Two Teaching Hospitals in Addis Ababa, Ethiopia A. Bekele, B. Kotisso, H. Biluts
Primary Repair of High and Intermediate Anorectal Malformations in the Neonates
 Annals of Pediatric Surgery, Vol 2, No 2, April 2006, PP 117-122 Original Article Primary Repair of High and Intermediate Anorectal Malformations in the Neonates Essam A. Elhalaby Departments of Pediatric
Annals of Pediatric Surgery, Vol 2, No 2, April 2006, PP 117-122 Original Article Primary Repair of High and Intermediate Anorectal Malformations in the Neonates Essam A. Elhalaby Departments of Pediatric
The use of conventional defecography in clinical practice
 The use of conventional defecography in clinical practice Poster No.: C-1564 Congress: ECR 2014 Type: Educational Exhibit Authors: A. Šmite, R. Laguns ; Lielvarde/LV, Riga/LV Keywords: Pelvic floor dysfunction,
The use of conventional defecography in clinical practice Poster No.: C-1564 Congress: ECR 2014 Type: Educational Exhibit Authors: A. Šmite, R. Laguns ; Lielvarde/LV, Riga/LV Keywords: Pelvic floor dysfunction,
Posterior Deep Endometriosis. What is the best approach? Posterior Deep Endometriosis. Should we perform a routine excision of the vagina??
 Posterior Deep Endometriosis What is the best approach? Dept Gyn Obst Polyclinique Hotel Dieu CHU Clermont Ferrand France Posterior Deep Endometriosis Organs involved - Peritoneum - Uterine cervix -Rectum
Posterior Deep Endometriosis What is the best approach? Dept Gyn Obst Polyclinique Hotel Dieu CHU Clermont Ferrand France Posterior Deep Endometriosis Organs involved - Peritoneum - Uterine cervix -Rectum
Complete rectal prolapse, although relatively uncommon,
 ORIGINAL CONTRIBUTION Long-Term Outcome of Altemeier s Procedure for Rectal Prolapse Donato F. Altomare, M.D. 1 & GianAndrea Binda, M.D. 2 & Ezio Ganio, M.D. 3 Paola De Nardi, M.D. 4 & Paolo Giamundo,
ORIGINAL CONTRIBUTION Long-Term Outcome of Altemeier s Procedure for Rectal Prolapse Donato F. Altomare, M.D. 1 & GianAndrea Binda, M.D. 2 & Ezio Ganio, M.D. 3 Paola De Nardi, M.D. 4 & Paolo Giamundo,
World Journal of Colorectal Surgery
 World Journal of Colorectal Surgery Volume 3, Issue 3 2013 Article 5 Closed Versus Open Lateral Internal Sphincterotomy Technique in Treatment of Anal Fissure Seyed Reza Mousavi Jr Shohada Medical Center,
World Journal of Colorectal Surgery Volume 3, Issue 3 2013 Article 5 Closed Versus Open Lateral Internal Sphincterotomy Technique in Treatment of Anal Fissure Seyed Reza Mousavi Jr Shohada Medical Center,
The use of conventional defecography in clinical practice
 The use of conventional defecography in clinical practice Poster No.: C-1564 Congress: ECR 2014 Type: Educational Exhibit Authors: A. Šmite, R. Laguns ; Lielvarde/LV, Riga/LV Keywords: Pelvic floor dysfunction,
The use of conventional defecography in clinical practice Poster No.: C-1564 Congress: ECR 2014 Type: Educational Exhibit Authors: A. Šmite, R. Laguns ; Lielvarde/LV, Riga/LV Keywords: Pelvic floor dysfunction,
Surgical Management of IBD in the Age of Biologics
 Surgical Management of IBD in the Age of Biologics Lisa S. Poritz, M.D Associate Professor of Surgery Division of Colon and Rectal Surgery Objectives Discuss surgical management of IBD When to operate
Surgical Management of IBD in the Age of Biologics Lisa S. Poritz, M.D Associate Professor of Surgery Division of Colon and Rectal Surgery Objectives Discuss surgical management of IBD When to operate
Laparoscopic Resection Of Colon & Rectal Cancers. R Sim Centre for Advanced Laparoscopic Surgery, TTSH
 Laparoscopic Resection Of Colon & Rectal Cancers R Sim Centre for Advanced Laparoscopic Surgery, TTSH Feasibility and safety Adequacy - same radical surgery as open op. Efficacy short term benefits and
Laparoscopic Resection Of Colon & Rectal Cancers R Sim Centre for Advanced Laparoscopic Surgery, TTSH Feasibility and safety Adequacy - same radical surgery as open op. Efficacy short term benefits and
Management of Neurogenic Bowel Dysfunction. Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders
 Management of Neurogenic Bowel Dysfunction Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders DEFECATION Delivery of colon contents to the rectum Rectal compliance
Management of Neurogenic Bowel Dysfunction Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders DEFECATION Delivery of colon contents to the rectum Rectal compliance
19th Annual International Colorectal Disease Symposium An International Exchange of Medical and Surgical Concepts
 Wednesday, February 13, 2008 7-9:00p Early Check-In / Registration (Grand Ballroom Foyer) Thursday, February 14, 2008 6:45 AM Breakfast (Caribbean Ballroom and Foyer) 7:00 AM Registration (Grand Ballroom
Wednesday, February 13, 2008 7-9:00p Early Check-In / Registration (Grand Ballroom Foyer) Thursday, February 14, 2008 6:45 AM Breakfast (Caribbean Ballroom and Foyer) 7:00 AM Registration (Grand Ballroom
GI Physiology - Investigating and treating patients with pelvic floor dysfunction. Lynne Smith Department of GI Physiology NGH Sheffield
 GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
Novel Options for the Management of Fecal Incontinence
 Novel Options for the Management of Fecal Incontinence Arnold Wald, MD, MACG University of Wisconsin School of Medicine and Public Health, Madison WI ANORECTAL CONTINENCE MECHANISMS Reservoir Elements
Novel Options for the Management of Fecal Incontinence Arnold Wald, MD, MACG University of Wisconsin School of Medicine and Public Health, Madison WI ANORECTAL CONTINENCE MECHANISMS Reservoir Elements
Crucial Role of Rectoanal Inhibitory Reflex in Emptying Function After Anoplasty in Infants with Anorectal Malformations
 Original Article Crucial Role of Rectoanal Inhibitory Reflex in Emptying Function After Anoplasty in Infants with Anorectal Malformations Surasak Sangkhathat, Sakda Patrapinyokul and Noppawan Osatakul,
Original Article Crucial Role of Rectoanal Inhibitory Reflex in Emptying Function After Anoplasty in Infants with Anorectal Malformations Surasak Sangkhathat, Sakda Patrapinyokul and Noppawan Osatakul,
Laparoscopic Rectopexy: is it Useful for Persistent Rectal Prolapse in Children?
 Medhat M Ibrahim et al Surgical technique 10.5005/jp-journals-10033-1223 Laparoscopic Rectopexy: is it Useful for Persistent Rectal Prolapse in Children? 1 Medhat M Ibrahim, 2 Mohammed Abd El Razik, 3
Medhat M Ibrahim et al Surgical technique 10.5005/jp-journals-10033-1223 Laparoscopic Rectopexy: is it Useful for Persistent Rectal Prolapse in Children? 1 Medhat M Ibrahim, 2 Mohammed Abd El Razik, 3
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review
 Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of laparoscopic ventral mesh rectopexy for internal rectal prolapse Internal rectal
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of laparoscopic ventral mesh rectopexy for internal rectal prolapse Internal rectal
LONG TERM OUTCOME OF ELECTIVE SURGERY
 LONG TERM OUTCOME OF ELECTIVE SURGERY Roberto Persiani Associate Professor Mini-invasive Oncological Surgery Unit Institute of Surgical Pathology (Dir. prof. D. D Ugo) Dis Colon Rectum, March 2000 Dis
LONG TERM OUTCOME OF ELECTIVE SURGERY Roberto Persiani Associate Professor Mini-invasive Oncological Surgery Unit Institute of Surgical Pathology (Dir. prof. D. D Ugo) Dis Colon Rectum, March 2000 Dis
Dr John Short. Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch
 Dr John Short Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch 8:30-9:25 WS #142: Peeling Back the Layers - The Pelvic Floor Uncovered 9:35-10:30 WS #152:
Dr John Short Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch 8:30-9:25 WS #142: Peeling Back the Layers - The Pelvic Floor Uncovered 9:35-10:30 WS #152:
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of laparoscopic ventral mesh rectopexy for internal rectal prolapse Internal rectal
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of laparoscopic ventral mesh rectopexy for internal rectal prolapse Internal rectal
The role of biologics in pelvic floor surgery
 Review article doi:10.1111/codi.12045 The role of biologics in pelvic floor surgery M. Ahmad*, P. Sileri, L. Franceschilli and M. Mercer-Jones* *Department of Colorectal Surgery, Queen Elizabeth Hospital,
Review article doi:10.1111/codi.12045 The role of biologics in pelvic floor surgery M. Ahmad*, P. Sileri, L. Franceschilli and M. Mercer-Jones* *Department of Colorectal Surgery, Queen Elizabeth Hospital,
St Mark's Hospital from 1953 to 1968
 Gut, 1970, 11, 235-239 The results of ileorectal anastomosis at St Mark's Hospital from 1953 to 1968 W. N. W. BAKER From St Mark's Hospital, London SUMMARY The popular view of ileorectal anastomosis for
Gut, 1970, 11, 235-239 The results of ileorectal anastomosis at St Mark's Hospital from 1953 to 1968 W. N. W. BAKER From St Mark's Hospital, London SUMMARY The popular view of ileorectal anastomosis for
Instructions for Use
 CONTINENCE RESTORATION SYSTEM Instructions for Use Humanitarian Device Authorized by Federal (USA) Law for use in the treatment of fecal incontinence in patients who are not candidates for or have previously
CONTINENCE RESTORATION SYSTEM Instructions for Use Humanitarian Device Authorized by Federal (USA) Law for use in the treatment of fecal incontinence in patients who are not candidates for or have previously
EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May Dr. Annie Leong MBBS, FRANZCOG, CU
 EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May 2011 Dr. Annie Leong MBBS, FRANZCOG, CU Restore normal perineal anatomy Achieve good haemostasis Avoid infection and wound breakdown Avoid coital
EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May 2011 Dr. Annie Leong MBBS, FRANZCOG, CU Restore normal perineal anatomy Achieve good haemostasis Avoid infection and wound breakdown Avoid coital
Viscous Fluid Retention: A New Method for Evaluating Anorectal Function
 Viscous Fluid Retention: A New Method for Evaluating Anorectal Function Michael Srensen, M.D., Tine Tetzschner, M.D., le 0. Rasmussen, M.D., John Christiansen, M.D. From the Department of Surgery D, Glostrup
Viscous Fluid Retention: A New Method for Evaluating Anorectal Function Michael Srensen, M.D., Tine Tetzschner, M.D., le 0. Rasmussen, M.D., John Christiansen, M.D. From the Department of Surgery D, Glostrup
Clinical Study Long-Term Outcome after Resection Rectopexy for Internal Rectal Intussusception
 International Scholarly Research Network ISRN Gastroenterology Volume 2012, Article ID 824671, 7 pages doi:10.5402/2012/824671 Clinical Study Long-Term Outcome after Resection Rectopexy for Internal Rectal
International Scholarly Research Network ISRN Gastroenterology Volume 2012, Article ID 824671, 7 pages doi:10.5402/2012/824671 Clinical Study Long-Term Outcome after Resection Rectopexy for Internal Rectal
Laparoscopic Colorectal Surgery
 Laparoscopic Colorectal Surgery 20 th November 2015 Dr Adam Cichowitz General Surgeon Laparoscopic Colorectal Surgery Introduced in early 1990s Uptake slow Steep learning curve Requirement for equipment
Laparoscopic Colorectal Surgery 20 th November 2015 Dr Adam Cichowitz General Surgeon Laparoscopic Colorectal Surgery Introduced in early 1990s Uptake slow Steep learning curve Requirement for equipment
3D Dynamic Ultrasound In Obstructed Defecation
 3D Dynamic Ultrasound In Obstructed Defecation By Ramy Salahudin Abdelkader Assist. Lecturer of General Surgery Cairo University Introduction Pelvic floor is complex system, with passive and active components
3D Dynamic Ultrasound In Obstructed Defecation By Ramy Salahudin Abdelkader Assist. Lecturer of General Surgery Cairo University Introduction Pelvic floor is complex system, with passive and active components
Applied Anatomy and Physiology of the Pelvic Floor. Dr David Tarver Consultant Radiologist, Poole
 Applied Anatomy and Physiology of the Pelvic Floor Dr David Tarver Consultant Radiologist, Poole Pelvic Floor 1. Sacrospinous Ligament 2. Levator Ani A Puborectalis B. Pubococcygeus C. Iliococcygeus 3.
Applied Anatomy and Physiology of the Pelvic Floor Dr David Tarver Consultant Radiologist, Poole Pelvic Floor 1. Sacrospinous Ligament 2. Levator Ani A Puborectalis B. Pubococcygeus C. Iliococcygeus 3.
ACCIDENTAL BOWEL LEAKAGE: A PRACTICAL APPROACH TO EVALUATION. Tristi W. Muir, MD Chair, Department of OB/GYN Houston Methodist Hospital
 ACCIDENTAL BOWEL LEAKAGE: A PRACTICAL APPROACH TO EVALUATION Tristi W. Muir, MD Chair, Department of OB/GYN Houston Methodist Hospital Accidental Bowel Leakage What Gets the Woman into Your Office 67%
ACCIDENTAL BOWEL LEAKAGE: A PRACTICAL APPROACH TO EVALUATION Tristi W. Muir, MD Chair, Department of OB/GYN Houston Methodist Hospital Accidental Bowel Leakage What Gets the Woman into Your Office 67%
Longterm Complications of Hand-Assisted Versus Laparoscopic Colectomy
 Longterm Complications of Hand-Assisted Versus Laparoscopic Colectomy Toyooki Sonoda, MD, Sushil Pandey, MD, Koiana Trencheva, BSN, Sang Lee, MD, Jeffrey Milsom, MD, FACS BACKGROUND: STUDY DESIGN: Hand-assisted
Longterm Complications of Hand-Assisted Versus Laparoscopic Colectomy Toyooki Sonoda, MD, Sushil Pandey, MD, Koiana Trencheva, BSN, Sang Lee, MD, Jeffrey Milsom, MD, FACS BACKGROUND: STUDY DESIGN: Hand-assisted
International Federation of Gynecology and Obstetrics
 International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
HIRSCHSPRUNG'S DISEASE*
 RESULTS WITH ABDOMINAL RESECTION IN HIRSCHSPRUNG'S DISEASE* BY F. REHBEIN and H. VON ZIMMERMANN From the Surgical Department of the Children's Hospital, Bremen For six years we have been practising abdominal
RESULTS WITH ABDOMINAL RESECTION IN HIRSCHSPRUNG'S DISEASE* BY F. REHBEIN and H. VON ZIMMERMANN From the Surgical Department of the Children's Hospital, Bremen For six years we have been practising abdominal
