Medicine. Efficacy and Outcome Predictors of Gonadotropin Treatment for Male Congenital Hypogonadotropic Hypogonadism
|
|
|
- Kerry Phelps
- 6 years ago
- Views:
Transcription
1 Medicine OBSERVATIONAL STUDY Efficacy and Outcome Predictors of Gonadotropin Treatment for Male Congenital Hypogonadotropic Hypogonadism A Retrospective Study of 223 Patients Zhaoxiang Liu, MD, Jangfeng Mao, MD, Xueyan Wu, MD, Hongli Xu, MS, Xi Wang, MD, Bingkun Huang, MD, Junjie Zheng, MD, Min Nie, MD, and Hongbing Zhang, PhD Abstract: Gonadotropin induces masculinization and spermatogenesis in men with congenital hypogonadotropic hypogonadism (CHH). However, large cohort studies for the efficacy and reliable predictors of this therapy need to be conducted. The aim of this study was to investigate the efficacy of gonadotropin treatment in a large cohort of male CHH patients and analyze putative predictors for successful spermatogenesis. This retrospective study included 223 CHH azoospermic patients without puberty development treated between 2005 and All patients received combined human chorionic gonadotropin (HCG) and human menopausal gonadotropin (HMG) and were followed up for >6 months (5109 person-months). Serum total testosterone level, testicular size, spermatogenesis, and pregnancy outcome were recorded at each visit. After gonadotropin therapy, testicular size was enlarged from to ml (P < 0.001) and serum total testosterone was elevated from to nmol/l (P < 0.001). Spermatogenesis (>0/mL) occurred at a median period of 15 months (95% confidence interval ). Larger basal testicular volume (P ¼ 0.012) and noncryptorchidism history (P ¼ 0.028) are independent predictors for earlier sperm appearance. Sixty four percent (143/223) of patients succeeded in producing sperms and the average time for initial sperm detection was 14 8 months. However, their sperm concentrations (11.7 [2.1, 24.4] million/ml) and sperm progressive motility (A þ B 36.9% 20.2%) are significantly lower than World Health Organization standards. Of the 34 patients who desired for fathering children, 19 patients impregnanted their partners during the treatment. Gonadotropin therapy induces spermatogenesis in male CHH patients. A larger basal testicular size and noncryptorchidism history are favorable indicators for earlier spermatogenesis. Editor: Francine Smith Received: October 13, 2015; revised: January 13, 2016; accepted: January 27, From the Department of Endocrinology, Key Laboratory of Endocrinology, National Health and Family Planning Commission, Peking Union Medical College Hospital (ZL, JM, XW, HX, XW, BH, JZ, MN), and Department of Physiology, State Key Laboratory of Medical Molecular Biology, Institute of Basic Medical Sciences, Peking Union Medical College and Chinese Academy of Medical Sciences (HZ), Beijing, China. Correspondence: Xueyan Wu, MD, Department of Endocrinology, Key Laboratory of Endocrinology, National Health and Family Planning Commission, Peking Union Medical College Hospital, Chinese Academy of medical Science, Beijing , China ( wuxueyan@pumch.ac.cn). co-coresponding author: Jiangfeng Mao ( maojiangfeng88@sina.com) Supplemental Digital Content is available for this article. The authors report no conflicts of interest. Copyright # 2016 Wolters Kluwer Health, Inc. All rights reserved. This is an open access article distributed under the Creative Commons Attribution License 4.0, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. ISSN: DOI: /MD (Medicine 95(9):e2867) Abbreviations: BMI = body mass index, CHH = congenital hypogonadotropic hypogonadism, FSH = follicle-stimulating hormone, GnRH = gonadotropin-releasing hormone, HCG = human chorionic gonadotropin, HH = hypogonadotropic hypogonadism, HMG = human menopausal gonadotropin, IVF = in vitro fertilization, LH = luteinizing hormone, MRI = magnetic resonance imaging, N subgroup = nonspermatogenesis subgroup, nchh = normosmic CHH, S subgroup = spermatogenesis group, WHO = World Health Organization. INTRODUCTION Congenital hypogonadotropic hypogonadism (CHH), caused by deficiency or dysfunction of gonadotropinreleasing hormone (GnRH), is a disorder characterized by delayed puberty development and infertility. The incidence of CHH is 1 10:100,000 in live births. CHH is comprised of Kallmann syndrome and normosmic CHH (nchh). Kallmann syndrome is a subgroup of CHH associated with a defective sense of smell (anosmia or hyposmia). 1 When fertility is required, pulsatile GnRH infusion or combined human chorionic gonadotropin (HCG) and human menopausal gonadotropin (HMG) therapy may promote spermatogenesis. 2 Combination of gonadotropins can also induce spermatogenesis in patients with acquired hypogonadotropic hypogonadism (HH) of various causes, such as surgery for pituitary tumors, sellar radiation, and sellar craniopharyngioma. 3,4 Most studies regarding gonadotropin-induced spermatogenesis did not stratify patients into CHH and acquired HH and therefore the effective rate for CHH alone is largely unknown. 5 8 A recent meta-analysis showed that the overall rate of gonadotropin-induced spermatogenesis in HH was 75%. 9 However, the success rate of achieving spermatogenesis is significantly lower in prepubertal-onset HH patients, as compared with a mixed population of pre- and postpubertal onset patients (68% [58 77] vs 84% [76 89], P ¼ 0.011). 9 Warne et al 8 reported a study achieving near 80% success rate of spermatogenesis in an unspecified HH group with the largest sample size (n ¼ 77). The rate of gonadotropin-induced spermatogenesis in CHH patients could be lower than that of acquired and CHH combined. For example, a study of 74 CHH patients treated with gonadotropins showed a success rate of 65%. 10 Currently, data on spermatogenesis of CHH patients is still very limited due to the low incidence of this disease. The success rate and its influencing factors of gonadotropin-induced spermatogenesis need to be further demonstrated in large cohort studies for CHH patients. Medicine Volume 95, Number 9, March
2 Liu et al Medicine Volume 95, Number 9, March 2016 In the present work, we retrospectively reported the fertility and paternity outcomes in 223 CHH patients treated with gonadotropins (HCG/HMG) and analyzed putative predictors for successful spermatogenesis. METHODS Patients CHH azoospermic patients without puberty development were included into this retrospective study. Diagnosis of CHH was made if a patient met all of the following criteria: a male aged over 18 years without puberty development, a serum testosterone level <100 ng/dl (3.5 nmol/l) with low or normal levels of gonadotropins, normal levels of other pituitary hormones and negative findings in sellar magnetic resonance imaging (MRI). 11 Clinical presentations, cryptorchidism, medical history as well as family history were recorded. Tests of plasma gonadotropins and testosterone, MRI of pituitary and the olfactory nerve were performed. The study protocol was reviewed and approved by the ethics committee of Peking Union Medical College Hospital. From January, 2005 to December, 2014, a total of 296 male CHH patients were treated with HCG/HMG in Peking Union Medical College Hospital. There were 73 cases excluded from data analysis for poor compliance or incomplete medical data. Thus, only 223 patients were retrospectively evaluated (Figure 1). Treatment and Follow-up Patients discontinued androgen therapy (if used) for at least 3 months before starting gonadotropin therapy. Intramuscular HCG ( U, Livzon Pharmaceutical Co, Guangdong, China) injection twice weekly was given for 6 months. Then HMG ( U, Livzon Pharmaceutical Co.) was intramuscularly injected twice weekly. Regular follow-ups were conducted at an interval of 3 to 6 months. The dosages of gonadotropins were adjusted according to plasma testosterone level and sperm output. Testicular size, plasma gonadotropins, plasma testosterone, and sperm count were measured on each visit. The levels of testosterone were determined 48 hours after HCG injection. Luteinizing hormone (LH), follicle-stimulating hormone (FSH), and testosterone levels were measured by chemiluminescent method using a commercial kit (ACS 180 FIGURE 1. Flowchart of screening patients. CHH ¼ congenital hypogonadotropic hypogonadism. Automatic Chemiluminescence System; Bayer, Germany). Testicular size was measured using a Prader orchidometer and the mean value of bilateral testicular volumes was used in data analysis. Semen samples were collected by masturbation and analyzed according to the standard World Health Organization (WHO) method (before 2010, according to 1999 WHO method, after 2010, according to 2010 WHO method). 12 Sperm motility was classified as fast progressive sperm (A), slow progressive sperm (B), nonprogressive sperm (C), and immotile sperm (D). The proportion in each of the 4 motility categories was assessed. Outcomes Successful spermatogenesis, as a primary outcome, was defined as the first sperm detected by microscopy. The secondary outcomes were specific sperm concentrations and conception. Four sperm thresholds, >0 (any sperm appeared under microscopy), >5, >10, and >15 million/ml, were recorded according to the sperm concentration. Self-reported pregnancy was noted. Statistical Analysis SPSS version 17.0 was used for data analysis (SPSS Inc, Chicago, IL). Normal distributive data were expressed as the mean SD, and non-normal distribution data were listed as median (quartiles). The paired t test was used to compare the difference of the plasma testosterone and testicular volume before and after the treatment. Kaplan-Meier analyses were used to estimate the median time for achieving different sperm thresholds. Cox regression models were built to analyze the predictors of successful spermatogenesis. A multivariate linear regression model was built to identify the contributing factors on the time for patients achieving spermatogenesis. The independent samples t test was used to compare the baseline difference between Kallmann and nchh patients, as well as patients with spermatogenesis (S subgroup) and without spermatogenesis (nonspermatogenesis subgroup, N subgroup). The different rate of cryptorchidism and family history between different groups was compared by x 2 test. Statistical significance was set at P < Age for initiating HCG/HMG treatment, body mass index (BMI), peak LH after GnRHa (triptorelin, 100 mg) stimulation, family histories of delayed puberty (0 ¼ no, 1 ¼ yes), histories of cryptorchidism (0 ¼ no, 1 ¼ unilateral, 2 ¼ bilateral), basal testicular volume, previous androgen exposure (0 ¼ none or <3 months, 1 ¼ >3 months), and previous gonadotropins exposure (0 ¼ none or <3 months, 1 ¼ >3 months) were considered as variables in Cox regression model and multivariate linear regression model. RESULTS Clinical Characteristics of CHH Patients A total of 223 male CHH patients were included for analysis. The mean follow-up period is months (5109 person-months totally). Gonadotropin treatment was initiated at the age of years. Baseline serum levels of LH, FSH, and testosterone were IU/L, IU/L, and nmol/l, respectively. Mean testicular volume was ml. Forty patients (18%) had a history of cryptorchidism (18 unilateral and 22 bilateral) and 18 (8%) had a family 2 Copyright # 2016 Wolters Kluwer Health, Inc. All rights reserved.
3 Medicine Volume 95, Number 9, March 2016 Efficacy and Outcome Predictors of Gonadotropin Treatment for Male CHH TABLE 1. Baseline Features of Congenital Hypogonadotropic Hypogonadism Patients All patients (n ¼ 223) S Subgroup (n ¼ 143) N Subgroup (n ¼ 80) P Age-initiating treatment, y BMI, kg/m Peak LH, IU/L y 1.6 (0.6, 5.2) 2.0 (0.7, 7.0) 1.4 (0.4, 2.8) Rate of family history 8% 7% 10% Rate of cryptorchidism 18% 14% 25% Basal testicular volume, ml Previous androgen 60.1% 62.9% 55.0% Previous gonadotropins 11.2% 11.9% 10.0% Follow-up, mo BMI ¼ body mass index, LH ¼ luteinizing hormone, N subgroup ¼ nonspermatogenesis subgroup, S subgroup ¼ spermatogenesis subgroup. Compared between S subgroup and N subgroup. P < 0.05 is defined as significant difference. y Peak LH means highest LH level after stimulation by triptorelin 100 mg. Data were expressed as median (25 percentile, 75 percentile). history of delayed puberty (Table 1). They were generally in good conditions with normal blood and urine routine test results, and normal liver and renal function. Thyroid hormones, adrenal glucocorticoids, and growth hormones levels were all in the normal range. During the gonadotropin therapy, their plasma testosterone increased from to nmol/l (P < 0.001) and testicular volume enlarged from to ml (P < 0.001) (by paired t test). Of all the patients, half (111/223) were having Kallmann syndrome, whereas another half (112/223) were having nchh. Comparison between the 2 groups (by independent samples t test and x 2 test) showed that patients with Kallmann syndrome were prone to have a family history (17/111 vs 1/112, P < 0.001). However, Kallmann syndrome and nchh patients had similar BMI, age of initiating treatment, peak LH level after triptorelin stimulation, basal testicular volume, and rate of cryptorchidism. At the last visit, testicular volume of Kallmann patients was ml (follow-up period months), whereas testicular volume of nchh patients was ml (follow-up period months) (see Table 1, Supplemental Content, which illustrates the comparison between the 2 groups, For the 143 patients (64%, 143/223) who succeeded in spermatogenesis, the mean time of first sperm detection is 14 8 months. Twenty-nine patients found sperms for the first time after 6 months treatment, 42 patients after 12 months, 44 patients after 18 months, 15 patients after 24 months, 8 patients after 30 months, 4 patients after 4 months and 1 patient did not get sperms until 42 months. Compared with those who failed sperm production (N subgroup), the successful group (S subgroup) had a lower rate of cryptorchidism (25% vs 14%, P ¼ 0.032, by x 2 test), larger basal testicular volume ( vs ml, P ¼ 0.023, by independent t test) and higher peak LH level after triptorelin stimulation (Figure 3, Table 1). Patients in S group had a longer Spermatogenesis Outcomes in CHH Patients Kaplan-Meier analysis showed that median time for the first sperm appearance of all the patients (n ¼ 223) was 15 months (95% CI, ), with an average testicular volume of ml. To reach sperm threshold >5 and >10 million/ ml, the median time were 27 (95% CI ) and 39 months (95% CI ), with an average testicular volume of and ml, respectively. The estimated median time for sperm concentration >15 million/ml could not be obtained because of limited number of patients who produced sperms above this level (Figure 2). The median time of initial successful spermatogenesis was similar between patients with Kallmann syndrome and nchh (18 vs 15 months, P ¼ 0.136, Log Rank [Mantel-Cox]). According to Cox-related method (including age initiating treatment, BMI, peak LH, family history, cryptorchidism, basal testicular volume, prior androgen, prior gonadotropins), larger basal testicular volume (b ¼ 0.142, P ¼ 0.012) and noncryptorchidism history (b ¼ 0.421, P ¼ 0.028) were 2 favorable predictors for a shorter time to achieve spermatogenesis (Table 2). FIGURE 2. Median times of achieving sperm concentration at different thresholds. Kaplan-Meier analysis of 223 patients showed median times of achieving sperm concentration more than 0, 5, 10, 15 million/ml. The median time of first spermatogenesis was 15 months. The median and 95% CIs for time to reach 15 million/ ml cannot be estimated. CI ¼ confidence interval, M/mL ¼ million/ml. Copyright # 2016 Wolters Kluwer Health, Inc. All rights reserved. 3
4 Liu et al Medicine Volume 95, Number 9, March 2016 TABLE 2. Predictors for Spermatogenesis (Correlated Cox Analysis) b HR P 95% CI Lower Bound 95% CI Upper Bound Age-initiating treatment BMI Peak LH Family history (0,1) Cryptorchidism (0,1,2) Basal testicular volume Prior androgen treatment (0,1) Prior gonadotropins treatment (0,1) BMI ¼ body mass index, CI ¼ confidence interval, HR ¼ hazard ratio, LH ¼ luteinizing hormone. P < 0.05 is defined as statistical significance. follow-up period than that in N group (28 13 vs 15 8 months, P < 0.001, by independent t test). Multivariate linear regression model (including age for initiating HCG/HMG treatment, BMI, peak LH after GnRHa stimulation, family histories of delayed puberty, histories of cryptorchidism, basal testicular volume, previous androgen exposure and previous gonadotropins exposure) showed that age of initiating treatment (b ¼ 0.445, P ¼ 0.002), basal testicular volume (b ¼ 1.074, P ¼ 0.003) and cryptorchidism histories (b ¼ 3.457, P ¼ 0.004) were major predictors for earlier spermatogenesis following the treatment (Table 3), indicating that older patients with larger basal testicular size and noncryptorchidism history may have less time to produce sperms. Patients in S subgroup had a sperm concentration of 11.7 (2.1, 24.4) million/ml at the end of follow-up and was lower than that of healthy Chinese young men (50.0 [36.0, 63.8] million/ml) (P < 0.001). 13 The sperm progressive motility (A þ B) ([36.9% 20.2%] vs [52.6% 11.2%], P < 0.001) and total mobility (A þ B þ C) ([44.4% 21.9%] vs [58.6% 11.1%], P < 0.001) were significantly lower than that of healthy young men (n ¼ 1808, age ranges years). 13 According to WHO reference values for human semen, 14 36% (51/143) of our patients attained normal sperm concentrations (15 million/ml). Among them, only 67% (34/51) had normal sperm-progressive motility (A þ B) (32%). In S subgroup, 34 patients were married and 20 pregnancies occurred in 19 (19/34) wives, including 19 natural conceptions (one woman had two pregnancies) and 1 in vitro fertilization (IVF). Seven natural conceptions happened with sperm concentrations of 1 million/ml, 6 happened between 1 and 10 million/ml, 3 happened between 10 and 20 million/ml, 2 happened with sperm concentration >20 million/ml (see Table 2, Supplemental Content, which presents sperm concentrations of CHH patients at the time that natural conceptions happened, Fourteen infants, including 7 girls and 7 boys, were delivered with normal appearance of external genitalia. Six abortions happened, including 4 miscarries (karyotype 45, XO was confirmed in one fetus), and 2 induced abortions because of parents concern of transmitting the disease to their offspring. Safety Evaluation During the period of study, gynecomastia was developed in 7% (16/223) of the subjects and 2 of them had mammary excision. Acne occurred in 9% (20/223) of the patients and was subsequently alleviated after reducing HCG dosages. No hepatorenal impairment or allergic reactions were reported. DISCUSSION To analyze the efficacy of gonadotropin treatment and identify putative predictors for successful spermatogenesis in a large cohort of male CHH patients, we conducted a retrospective study of 223 patients treated at our hospital. For all the patients, 64% of them succeeded in spermatogenesis. Basal testicular size and cryptorchidism history are predictors of patients response to the treatment. The median time for achieving the first sperm after the initial treatment in our cohort is 15 months, which is much longer than previously reported 6 to 12 months. 5,8,15 17 The discrepancy may be attributable to the following factors. First, subjects recruited in most of previous studies comprised not FIGURE 3. Peak LH and basal testicular volume in patients with or without spermatogenesis. Comparison of peak LH (stimulated by triptorelin 100 mg) and basal testicular volume between patients with spermatogenesis and without spermatogenesis. LH ¼ luteinizing hormone, N subgroup ¼ nonspermatogenesis subgroup, S subgroup ¼ spermatogenesis subgroup. 4 Copyright # 2016 Wolters Kluwer Health, Inc. All rights reserved.
5 Medicine Volume 95, Number 9, March 2016 Efficacy and Outcome Predictors of Gonadotropin Treatment for Male CHH TABLE 3. Influential Factors on Time of Achieving the First Sperm in Spermatogenesis Subgroup (n ¼ 143) b t value P Constant Age-initiating treatment BMI Peak LH Family history Cryptorchidism Basal testicular volume Prior androgen Prior gonadotropins BMI ¼ body mass index, LH ¼ luteinizing hormone. The analysis was done by multivariate linear model analysis. P < 0.05 is defined as statistical significance. only CHH but also acquired HH patients. Acquired HH patients are easier to achieve spermatogenesis because of their larger testicular size and higher Leydig and Sertoli cells reservoir. 18 Second, to improve patients compliance, HMG was injected at 75 to 150 IU and twice weekly in our study, compared with 75 to 225 IU and 3 times weekly in other studies. The lower dosage and less frequency may take longer time for spermatogenesis. Third, the HMG used in our study was extracted from the urine of postmenopausal women and may not have an efficacy comparable with recombinant FSH proteins used in other studies. 19 Although spermatogenesis or even pregnancy is achievable in some of CHH patients after gonadotropins treatment, sperm concentration and mobility are usually far below normal levels. 8,9,17 Similarly, the sperm concentration and mobility induced by gonadotropins in our study are lower compared either with WHO standards 14 or with that reported in healthy Chinese men. 13 This phenomenon may be largely explained by absence of mini puberty, which leads to a decreased reservoir for Sertoli and Leydig cells in CHH patients. 18 Furthermore, mutations in certain genes, such as FGFR1 20,21 and KAL1, 22,23 have a direct impairment on testicular development and spermatogenesis. Last but not least, unlike endogenous pulsatile and fine-tuning production of gonadotropin in healthy men, optimal spermatogenesis might not be achieved by intermittent injection of an un-physiological high level of HCG/HMG in CHH patients. Studies have shown that basal testicular volume and cryptorchidism history are key indicators for successful spermatogenesis. 3,5,6,8,24 Our data also suggest that larger basal testicular size confers earlier spermatogenesis, whereas cryptorchidism requires a longer time for attainment of sperms. Patients with bilateral cryptorchidism had a lower rate of spermatogenesis than that of unilateral cryptorchidism. Warne et al 8 reported that patients with a low BMI (<30 kg/m 2 ) had a greater chance of achieving spermatogenesis compared with men with a BMI > 30 kg/m 2. Liu et al 5 suggested that a history of androgen exposure was associated with poorer therapeutic response, which was not observed in other studies. 9 Previous gonadotropin use was associated with an earlier sperm appearance in Liu et al s study, 5,25 which was not supported by Warne et al study. 8 BMI and history of androgen or gonadotropins exposure did not influence spermatogenesis outcome in the present study. Prospective studies are thus needed to determine the potential role of these factors in spermatogenesis. In our study, a larger basal testicular size, a lower incidence rate of cryptorchidism, and a higher GnRHa-stimulated LH level were observed in the patients with spermatogenesis. It is known that these parameters may reflect a better function of hypothalamic-pituitary-gonadal axis in CHH patients. 26 A multiple linear analysis in our spermatogenesis subgroup further confirmed that a larger basal testicular size and noncryptorchidism were favorable factors for earlier spermatogenesis. Interestingly, an older age for starting HCG/HMG treatment was associated with an earlier sperm appearance. One possible explanation is that older patients were more eager for fertility and thus had better compliance of the treatment. Comparing with the nonspermatogenesis group, longer follow-up of the patients in spermatogenesis group may be attributed to satisfactory outcome of spermatogenesis and/or better compliance of the treatment. Moreover, some patients need long time to get a sperm (even 42 months); thus, it should be known that persistent treatment is necessary sometimes. Of 34 married patients who desired for children, 56% of them impregnated their partners during the therapy. However, these pregnancies were associated with 20% natural abortion, which is higher than that in normal population (8% 17%). 27,28 The higher rate of natural abortions may be because of the presence of aberrant sperms from the patients. 29 Two induced abortions were carried out because of the couples concern about potential heredity of CHH. Genetic information on CHH patients and fetus are warranted for family planning. 2,4 Fourteen babies with normal genital phenotype were born in our study. Their hypothalamus pituitary gonadal axis function needs to be examined for an early detection of potential CHH inherited from their parents. No severe adverse events were observed during gonadotropin therapy in our study. Acne and gynecomastia occurred in <10% of the patients. The former was caused by increased serum testosterone and alleviated by reducing HCG dosage. The latter was induced by estrogens aromatized from increased testosterone. Surgical removal of the obviously enlarged breast tissue may be an option for these patients. 17 Overall, gonadotropin therapy is safe for the patients with CHH. In this study, we achieved spermatogenesis in 64% of 223 CHH patients with gonadotropin treatment. Larger basal testicular volume and a noncryptorchidism history are major favorable indicators for earlier sperm appearance. With the largest sample size of CHH reported in the literature, our study provides strong evidence for the efficacy and responsive factors of gonadotropin in induction of spermatogenesis for CHH patients. Several issues may be addressed in future studies. Pathogenic genetic mutations in CHH patients should be screened, as certain mutations may be the major determinants of spermatogenesis. The genetic information may also be used in prenatal diagnosis. Mini puberty in neonates should be monitored as it may provide information about hypothalamus pituitary gonadal function of the patients offsprings. ACKNOWLEDGMENTS The authors thank Dr. Long-Cheng Li for critical reading and editing of this manuscript. REFERENCES 1. Fraietta R, Zylberstejn DS, Esteves SC. Hypogonadotropic hypogonadism revisited. Clinics (Sao Paulo). 2013;68(Suppl 1): Boehm U, Bouloux PM, Dattani MT, et al. Expert consensus document: European Consensus Statement on congenital Copyright # 2016 Wolters Kluwer Health, Inc. All rights reserved. 5
6 Liu et al Medicine Volume 95, Number 9, March 2016 hypogonadotropic hypogonadism-pathogenesis, diagnosis and treatment. Nat Rev Endocrinol. 2015;11: Farhat R, Al-zidjali F, Alzahrani AS. Outcome of gonadotropin therapy for male infertility due to hypogonadotrophic hypogonadism. Pituitary. 2010;13: Dwyer AA, Raivio T, Pitteloud N. Gonadotrophin replacement for induction of fertility in hypogonadal men. Best Pract Res Clin Endocrinol Metab. 2015;29: Liu PY, Baker HW, Jayadev V, et al. Induction of spermatogenesis and fertility during gonadotropin treatment of gonadotropin-deficient infertile men: predictors of fertility outcome. J Clin Endocrinol Metab. 2009;94: Miyagawa Y, Tsujimura A, Matsumiya K, et al. Outcome of gonadotropin therapy for male hypogonadotropic hypogonadism at university affiliated male infertility centers: a 30-year retrospective study. J Urol. 2005;173: Ishikawa T, Ooba T, Kondo Y, et al. Assessment of gonadotropin therapy in male hypogonadotropic hypogonadism. Fertil Steril. 2007;88: Warne DW, Decosterd G, Okada H, et al. A combined analysis of data to identify predictive factors for spermatogenesis in men with hypogonadotropic hypogonadism treated with recombinant human follicle-stimulating hormone and human chorionic gonadotropin. Fertil Steril. 2009;92: Rastrelli G, Corona G, Mannucci E, et al. Factors affecting spermatogenesis upon gonadotropin-replacement therapy: a metaanalytic study. Andrology-US. 2014;2: Yang L, Zhang SX, Dong Q, et al. Application of hormonal treatment in hypogonadotropic hypogonadism: more than ten years experience. Int Urol Nephrol. 2012;44: Raivio T, Falardeau J, Dwyer A, et al. Reversal of idiopathic hypogonadotropic hypogonadism. N Engl J Med. 2007;357: WHO. Laboratory Manual for the Examination and Processing of Human Semen. 5th ed. Geneva: World Health Organization; Rao M, Meng TQ, Hu SH, et al. Evaluation of semen quality in 1808 university students, from Wuhan, Central China. Asian J Androl. 2015;17: Cooper TG, Noonan E, von Eckardstein S, et al. World Health Organization reference values for human semen characteristics. Hum Reprod Update. 2010;16: Efficacy and safety of highly purified urinary follicle-stimulating hormone with human chorionic gonadotropin for treating men with isolated hypogonadotropic, hypogonadism., European Metrodin HP Study Group. Fertil Steril. 1998;70: Bouloux P, Warne DW, Loumaye E. Efficacy and safety of recombinant human follicle-stimulating hormone in men with isolated hypogonadotropic hypogonadism. Fertil Steril. 2002;77: Matsumoto AM, Snyder PJ, Bhasin S, et al. Stimulation of spermatogenesis with recombinant human follicle-stimulating hormone (follitropin alfa; GONAL-f): long-term treatment in azoospermic men with hypogonadotropic hypogonadism. Fertil Steril. 2009;92: Bouvattier C, Maione L, Bouligand J, et al. Neonatal gonadotropin therapy in male congenital hypogonadotropic hypogonadism. Nat Rev Endocrinol. 2012;8: Biffoni M, Marcucci I, Ythier A, et al. Effects of urinary gonadotrophin preparations on human in-vitro immune function. Hum Reprod. 1998;13: Hadziselimovic NO, de Geyter C, Demougin P, et al. Decreased expression of FGFR1, SOS1, RAF1 genes in cryptorchidism. Urol Int. 2010;84: Cotton L, Gibbs GM, Sanchez-Partida LG, et al. FGFR-1 [corrected] signaling is involved in spermiogenesis and sperm capacitation. J Cell Sci. 2006;119(Pt 1): Salenave S, Chanson P, Bry H, et al. Kallmann s syndrome: a comparison of the reproductive phenotypes in men carrying KAL1 and FGFR1/KAL2 mutations. J Clin Endocrinol Metab. 2008;93: Nishio H, Mizuno K, Moritoki Y, et al. Clinical features and testicular morphology in patients with Kallmann syndrome. Urology. 2012;79: Trsinar B, Muravec UR. Fertility potential after unilateral and bilateral orchidopexy for cryptorchidism. World J Urol. 2009;27: Liu PY, Gebski VJ, Turner L, et al. Predicting pregnancy and spermatogenesis by survival analysis during gonadotrophin treatment of gonadotrophin-deficient infertile men. Hum Reprod. 2002;17: Fuse H, Akashi T, Kazama T, et al. Gonadotropin therapy in males with hypogonadotropic hypogonadism: factors affecting induction of spermatogenesis after gonadotropin replacement. Int Urol Nephrol. 1996;28: Gray RH, Wu LY. Subfertility and risk of spontaneous abortion. Am J Public Health. 2000;90: Modvig J, Schmidt L, Damsgaard MT. Measurement of total risk of spontaneous abortion: the virtue of conditional risk estimation. Am J Epidemiol. 1990;132: Sykiotis GP, Hoang XH, Avbelj M, et al. Congenital idiopathic hypogonadotropic hypogonadism: evidence of defects in the hypothalamus, pituitary, and testes. J Clin Endocrinol Metab. 2010;95: Copyright # 2016 Wolters Kluwer Health, Inc. All rights reserved.
ORIGINAL ARTICLE. Open Access
 (2017) 19, 1 6 2017 AJA, SIMM & SJTU. All rights reserved 1008-682X www.asiaandro.com; www.ajandrology.com Male Fertility Open Access ORIGINAL ARTICLE Pulsatile gonadotropin releasing hormone therapy is
(2017) 19, 1 6 2017 AJA, SIMM & SJTU. All rights reserved 1008-682X www.asiaandro.com; www.ajandrology.com Male Fertility Open Access ORIGINAL ARTICLE Pulsatile gonadotropin releasing hormone therapy is
Pulsatile gonadotrophin releasing hormone versus gonadotrophin treatment of hypothalamic hypogonadism in males
 Human Reproduction vol.8 Suppl.2 pp. 175-179, 1993 Pulsatile gonadotrophin releasing hormone versus gonadotrophin treatment of hypothalamic hypogonadism in males Jochen Schopohl Medizinische Klinik, Klinikum
Human Reproduction vol.8 Suppl.2 pp. 175-179, 1993 Pulsatile gonadotrophin releasing hormone versus gonadotrophin treatment of hypothalamic hypogonadism in males Jochen Schopohl Medizinische Klinik, Klinikum
Oligogenicity. MHH Male Hypogonadotropic hypogonadism MHH MHH MHH MHH MHH MRI. hcg. GnRH MHH PROK MHH. GnRH FSH LH T PRL
 MHH Male Hypogonadotropic hypogonadism MHH MHH MHH Kallmann KAL FGFR PROK MHH GnRH Oligogenicity MHH MHH MHH MRI hcg GnRH hcg LH hcg T LH FSH GnRH GnRH MHH LH FSH LH FSH LH T PRL MHH / hcg T FSH FSH hmg
MHH Male Hypogonadotropic hypogonadism MHH MHH MHH Kallmann KAL FGFR PROK MHH GnRH Oligogenicity MHH MHH MHH MRI hcg GnRH hcg LH hcg T LH FSH GnRH GnRH MHH LH FSH LH FSH LH T PRL MHH / hcg T FSH FSH hmg
Prof. Dr. Michael Zitzmann Internal Medicine Endocrinology, Diabetology, Andrology University of Muenster, Germany
 Induction of fertility in hypogonadal men Prof. Dr. Michael Zitzmann Internal Medicine Endocrinology, Diabetology, Andrology University of Muenster, Germany Induction of fertility in hypogonadal men Prof.
Induction of fertility in hypogonadal men Prof. Dr. Michael Zitzmann Internal Medicine Endocrinology, Diabetology, Andrology University of Muenster, Germany Induction of fertility in hypogonadal men Prof.
TESTOSTERONE DEFINITION
 DEFINITION A hormone that is a hydroxyl steroid ketone (C19H28O2) produced especially by the testes or made synthetically and that is responsible for inducing and maintaining male secondary sex characteristics.
DEFINITION A hormone that is a hydroxyl steroid ketone (C19H28O2) produced especially by the testes or made synthetically and that is responsible for inducing and maintaining male secondary sex characteristics.
EUROPEAN JOURNAL OF ENDOCRINOLOGY (1998) 139 Gonadotropin or GnRH treatment in hypogonadal men 299 The patients with hypothalamic disorders (group I)
 European Journal of Endocrinology (1998) 139 298 303 ISSN 0804-4643 Pulsatile GnRH or human chorionic gonadotropin/human menopausal gonadotropin as effective treatment for men with hypogonadotropic hypogonadism:
European Journal of Endocrinology (1998) 139 298 303 ISSN 0804-4643 Pulsatile GnRH or human chorionic gonadotropin/human menopausal gonadotropin as effective treatment for men with hypogonadotropic hypogonadism:
Index. urologic.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Acquired hypogonadism, prevalence of, 165 167 primary, 165 secondary, 167 Adipose tissue, as an organ, 240 241 Adrenal hyperplasia, congenital,
Note: Page numbers of article titles are in boldface type. A Acquired hypogonadism, prevalence of, 165 167 primary, 165 secondary, 167 Adipose tissue, as an organ, 240 241 Adrenal hyperplasia, congenital,
Aromatase Inhibitors in Male Infertility:
 Aromatase Inhibitors in Male Infertility: The hype of hypogonadism? BEATRIZ UGALDE, PHARM.D. H-E-B/UNIVERSITY OF TEXAS COMMUNITY PHARMACY PGY1 03 NOVEMBER 2017 PHARMACOTHERAPY ROUNDS Disclosures No conflicts
Aromatase Inhibitors in Male Infertility: The hype of hypogonadism? BEATRIZ UGALDE, PHARM.D. H-E-B/UNIVERSITY OF TEXAS COMMUNITY PHARMACY PGY1 03 NOVEMBER 2017 PHARMACOTHERAPY ROUNDS Disclosures No conflicts
Article Gonadotrophin therapy in combination with ICSI in men with hypogonadotrophic hypogonadism
 RBMOnline - Vol 15. No 2. 2007 156-160 Reproductive BioMedicine Online; www.rbmonline.com/article/2798 on web 14 June 2007 Article Gonadotrophin therapy in combination with ICSI in men with hypogonadotrophic
RBMOnline - Vol 15. No 2. 2007 156-160 Reproductive BioMedicine Online; www.rbmonline.com/article/2798 on web 14 June 2007 Article Gonadotrophin therapy in combination with ICSI in men with hypogonadotrophic
Reproductive FSH. Analyte Information
 Reproductive FSH Analyte Information 1 Follicle-stimulating hormone Introduction Follicle-stimulating hormone (FSH, also known as follitropin) is a glycoprotein hormone secreted by the anterior pituitary
Reproductive FSH Analyte Information 1 Follicle-stimulating hormone Introduction Follicle-stimulating hormone (FSH, also known as follitropin) is a glycoprotein hormone secreted by the anterior pituitary
Select patients with hypogonadotropic hypogonadism may respond to treatment with clomiphene citrate
 Select patients with hypogonadotropic hypogonadism may respond to treatment with clomiphene citrate Scott J. Whitten, M.D., a Ajay K. Nangia, M.D., c and Peter N. Kolettis, M.D. b a Division of Reproductive
Select patients with hypogonadotropic hypogonadism may respond to treatment with clomiphene citrate Scott J. Whitten, M.D., a Ajay K. Nangia, M.D., c and Peter N. Kolettis, M.D. b a Division of Reproductive
HYPOGONADOTROPHIC HYPOGONADISM WITH SYNKINESIA AND DERANGED PITUITARY PROFILE: AN ENIGMA OF FINDINGS AND DILEMMA IN DIAGNOSIS
 Endocrinology Case Report International Journal of Clinical And Diagnostic Research ISSN 2395-3403 Volume 4, Issue 6, Nov-Dec 2016. Glorigin Lifesciences Private Limited. HYPOGONADOTROPHIC HYPOGONADISM
Endocrinology Case Report International Journal of Clinical And Diagnostic Research ISSN 2395-3403 Volume 4, Issue 6, Nov-Dec 2016. Glorigin Lifesciences Private Limited. HYPOGONADOTROPHIC HYPOGONADISM
Hypogonadism 4/27/2018. Male Hypogonadism -- Definition. Epidemiology. Objectives HYPOGONADISM. Men with Hypogonadism. 95% untreated.
 Male Hypogonadism -- Definition - Low T, Low Testosterone Hypogonadism -...a clinical syndrome that results from failure of the testes to produce physiological concentrations of testosterone due to pathology
Male Hypogonadism -- Definition - Low T, Low Testosterone Hypogonadism -...a clinical syndrome that results from failure of the testes to produce physiological concentrations of testosterone due to pathology
for months until the diagnosis were confirmed 86 were IHH and the other 47 were CDP. Repeated triptorelin stimulating tests were conducted in 9
 ACTA ACADEMIAE MEDICINAE SINICAE 100730 010-65295073 wsheyan@vip.sina.com LHRH IHH CDP 133 IHH 86 CDP 47 14 24 ~ 48 9 IHH 13 CDP 1 - - LH LH IHH CDP IHH LH 1. 9 ± 1. 2 U /L CDP LH 13. 7 ± 8. 3 U /L P
ACTA ACADEMIAE MEDICINAE SINICAE 100730 010-65295073 wsheyan@vip.sina.com LHRH IHH CDP 133 IHH 86 CDP 47 14 24 ~ 48 9 IHH 13 CDP 1 - - LH LH IHH CDP IHH LH 1. 9 ± 1. 2 U /L CDP LH 13. 7 ± 8. 3 U /L P
BIOCHEMICAL TESTS FOR THE INVESTIGATION OF COMMON ENDOCRINE PROBLEMS IN THE MALE
 Authoriser: Moya O Doherty Page 1 of 7 BIOCHEMICAL TESTS FOR THE INVESTIGATION OF COMMON ENDOCRINE PROBLEMS IN THE MALE The purpose of this protocol is to describe common tests used for the investigation
Authoriser: Moya O Doherty Page 1 of 7 BIOCHEMICAL TESTS FOR THE INVESTIGATION OF COMMON ENDOCRINE PROBLEMS IN THE MALE The purpose of this protocol is to describe common tests used for the investigation
Genetics of Hypogonadism. François Pralong Division of Endocrinology Lausanne University Hospital
 Genetics of Hypogonadism François Pralong Division of Endocrinology Lausanne University Hospital The Gonadotrope Axis GnRH LH FSH Sexsteroids(-) Inhibin/follistatin (+) Activin (+) Single Gene Mutations
Genetics of Hypogonadism François Pralong Division of Endocrinology Lausanne University Hospital The Gonadotrope Axis GnRH LH FSH Sexsteroids(-) Inhibin/follistatin (+) Activin (+) Single Gene Mutations
HCG (human chorionic gonadotropin); Novarel Pregnyl (chorionic gonadotropin); Ovidrel (choriogonadotropin alfa)
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.08.09 Subject: HCG Page: 1 of 5 Last Review Date: June 19, 2015 HCG Powder, Novarel, Pregnyl, Ovidrel
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.08.09 Subject: HCG Page: 1 of 5 Last Review Date: June 19, 2015 HCG Powder, Novarel, Pregnyl, Ovidrel
Indications for the use of human chorionic gonadotropic hormone for the management of infertility in hypogonadal men
 Review Article Indications for the use of human chorionic gonadotropic hormone for the management of infertility in hypogonadal men John Alden Lee, Ranjith Ramasamy Department of Urology, University of
Review Article Indications for the use of human chorionic gonadotropic hormone for the management of infertility in hypogonadal men John Alden Lee, Ranjith Ramasamy Department of Urology, University of
Treatment of Oligospermia with Large Doses of Human Chorionic Gonadotropin
 Treatment of Oligospermia with Large Doses of Human Chorionic Gonadotropin A Preliminary Report S. J. GLASS, M.D., and H. M. HOLLAND, M.D. BEFORE discussing gonadotropic therapy of oligospermia, it is
Treatment of Oligospermia with Large Doses of Human Chorionic Gonadotropin A Preliminary Report S. J. GLASS, M.D., and H. M. HOLLAND, M.D. BEFORE discussing gonadotropic therapy of oligospermia, it is
Male Factor Infertility
 Male Factor Infertility Simplified Evaluaon and Treatment* ^ * In 20 minutes or less In 20 slides ^ 5 minute office visit ALWAYS EVALUATE THE MALE & THE FEMALE Why 1. To help the coupleachieve a pregnancy
Male Factor Infertility Simplified Evaluaon and Treatment* ^ * In 20 minutes or less In 20 slides ^ 5 minute office visit ALWAYS EVALUATE THE MALE & THE FEMALE Why 1. To help the coupleachieve a pregnancy
MALE INFERTILITY & SEMEN ANALYSIS
 MALE INFERTILITY & SEMEN ANALYSIS DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and mitigate potential
MALE INFERTILITY & SEMEN ANALYSIS DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and mitigate potential
The Usefulness of GnRH and hcg Testing for the Differential Diagnosis of Delayed Puberty and Hypogonadotropic Hypogonadism in Prepubertal Boys
 The Usefulness of GnRH and hcg Testing for the Differential Diagnosis of Delayed Puberty and Hypogonadotropic Hypogonadism in Prepubertal Boys Naoko SATO 1), Noriyuki KATSUMATA 1), Reiko HORIKAWA 2) and
The Usefulness of GnRH and hcg Testing for the Differential Diagnosis of Delayed Puberty and Hypogonadotropic Hypogonadism in Prepubertal Boys Naoko SATO 1), Noriyuki KATSUMATA 1), Reiko HORIKAWA 2) and
Cigna Drug and Biologic Coverage Policy
 Cigna Drug and Biologic Coverage Policy Subject Infertility Injectables Table of Contents Coverage Policy... 1 General Background...16 Coding/Billing Information...20 References...20 Effective Date...
Cigna Drug and Biologic Coverage Policy Subject Infertility Injectables Table of Contents Coverage Policy... 1 General Background...16 Coding/Billing Information...20 References...20 Effective Date...
Why is my body not changing? Conflicts of interest. Overview 11/9/2015. None
 Why is my body not changing? Murthy Korada Pediatrician, Pediatric Endocrinologist Ridge Meadows Hospital Surrey Memorial Hospital None Conflicts of interest Overview Overview of normal pubertal timing
Why is my body not changing? Murthy Korada Pediatrician, Pediatric Endocrinologist Ridge Meadows Hospital Surrey Memorial Hospital None Conflicts of interest Overview Overview of normal pubertal timing
 www.iffs-reproduction.org @IntFertilitySoc Int@FedFertilitySoc Conflict of interest none Outline Causes of ovulatory dysfunction Assessment of women with ovulatory dysfunction Management First line Second
www.iffs-reproduction.org @IntFertilitySoc Int@FedFertilitySoc Conflict of interest none Outline Causes of ovulatory dysfunction Assessment of women with ovulatory dysfunction Management First line Second
Clinical evaluation of infertility
 Clinical evaluation of infertility DR. FARIBA KHANIPOUYANI OBSTETRICIAN & GYNECOLOGIST PRENATOLOGIST Definition: inability to achieve conception despite one year of frequent unprotected intercourse. Male
Clinical evaluation of infertility DR. FARIBA KHANIPOUYANI OBSTETRICIAN & GYNECOLOGIST PRENATOLOGIST Definition: inability to achieve conception despite one year of frequent unprotected intercourse. Male
PUBERTY. Preetha Krishnamoorthy. Division of Pediatric Endocrinology
 PUBERTY Preetha Krishnamoorthy Division of Pediatric Endocrinology Case 1 8-year-old girl referred for breast development noted by mom What do you want to know? Normal or abnormal? What if this was an
PUBERTY Preetha Krishnamoorthy Division of Pediatric Endocrinology Case 1 8-year-old girl referred for breast development noted by mom What do you want to know? Normal or abnormal? What if this was an
Infertility: failure to conceive within one year of unprotected regular sexual intercourse. Primary secondary
 Subfertility Infertility: failure to conceive within one year of unprotected regular sexual intercourse. Primary secondary Infertility affects about 15 % of couples. age of the female. Other factors that
Subfertility Infertility: failure to conceive within one year of unprotected regular sexual intercourse. Primary secondary Infertility affects about 15 % of couples. age of the female. Other factors that
2017 United HealthCare Services, Inc.
 UnitedHealthcare Pharmacy Clinical Pharmacy Programs Program Number 2017 P 1143-4 Program Prior Authorization/Notification Medication Menopur (menotropins) * P&T Approval Date 8/2014, 5/2015, 5/2016, 5/2017
UnitedHealthcare Pharmacy Clinical Pharmacy Programs Program Number 2017 P 1143-4 Program Prior Authorization/Notification Medication Menopur (menotropins) * P&T Approval Date 8/2014, 5/2015, 5/2016, 5/2017
Maldescended testis in Adults. Dr. BG GAUDJI Urologist STEVE BIKO ACADEMIC HOSPITAL
 Maldescended testis in Adults Dr. BG GAUDJI Urologist STEVE BIKO ACADEMIC HOSPITAL Definitions Cryptorchid: testis neither resides nor can be manipulated into the scrotum Ectopic: aberrant course Retractile:
Maldescended testis in Adults Dr. BG GAUDJI Urologist STEVE BIKO ACADEMIC HOSPITAL Definitions Cryptorchid: testis neither resides nor can be manipulated into the scrotum Ectopic: aberrant course Retractile:
ESHRE Andrology Campus Course Reproductive Andrology Brussels 8-10 November 2007
 ESHRE Andrology Campus Course Reproductive Andrology Brussels 8-10 November 2007 To treat the man or his sperm? When to treat the man? Conventional non-surgical treatment of male infertility Axel Kamischke
ESHRE Andrology Campus Course Reproductive Andrology Brussels 8-10 November 2007 To treat the man or his sperm? When to treat the man? Conventional non-surgical treatment of male infertility Axel Kamischke
Chapter 28: REPRODUCTIVE SYSTEM: MALE
 Chapter 28: REPRODUCTIVE SYSTEM: MALE I. FUNCTIONAL ANATOMY (Fig. 28.1) A. Testes: glands which produce male gametes, as well as glands producing testosterone 2. Seminiferous tubules (Fig.28.3; 28.5) a.
Chapter 28: REPRODUCTIVE SYSTEM: MALE I. FUNCTIONAL ANATOMY (Fig. 28.1) A. Testes: glands which produce male gametes, as well as glands producing testosterone 2. Seminiferous tubules (Fig.28.3; 28.5) a.
Exogenous testosterone: a preventable cause of male infertility
 Review Article Exogenous testosterone: a preventable cause of male infertility Lindsey E. Crosnoe 1, Ethan Grober 2, Dana Ohl 3, Edward D. Kim 1 1 University of Tennessee Graduate School of Medicine, Knoxville,
Review Article Exogenous testosterone: a preventable cause of male infertility Lindsey E. Crosnoe 1, Ethan Grober 2, Dana Ohl 3, Edward D. Kim 1 1 University of Tennessee Graduate School of Medicine, Knoxville,
Male History, Clinical Examination and Testing
 Male History, Clinical Examination and Testing Dirk Vanderschueren, MD, PhD Case Jan is 29 years old and consults for 1 year primary subfertility partner 28 years old and normal gynaecological investigation
Male History, Clinical Examination and Testing Dirk Vanderschueren, MD, PhD Case Jan is 29 years old and consults for 1 year primary subfertility partner 28 years old and normal gynaecological investigation
Test Briefing on Hormonal Disorders and Infertility
 Test Briefing on Hormonal Disorders and Infertility Test Briefing on Hormonal Disorders Common Tests FSH LH Progesterone Estradiol Prolactin Testosterone AFP AMH PCOS Panel FSH (Follicle Stimulating Hormone)
Test Briefing on Hormonal Disorders and Infertility Test Briefing on Hormonal Disorders Common Tests FSH LH Progesterone Estradiol Prolactin Testosterone AFP AMH PCOS Panel FSH (Follicle Stimulating Hormone)
Clinical Policy: Infertility Therapy Reference Number: CP.CPA.261 Effective Date: Last Review Date: Line of Business: Medicaid Medi-Cal
 Clinical Policy: Reference Number: CP.CPA.261 Effective Date: 11.16.16 Last Review Date: 11.17 Line of Business: Medicaid Medi-Cal Revision Log See Important Reminder at the end of this policy for important
Clinical Policy: Reference Number: CP.CPA.261 Effective Date: 11.16.16 Last Review Date: 11.17 Line of Business: Medicaid Medi-Cal Revision Log See Important Reminder at the end of this policy for important
Drug Therapy Guidelines
 Drug Therapy Guidelines Applicable Injectable Fertility Medications: Bravelle, Cetrotide, Follistim AQ, Ganirelix, Gonal-F, human chorionic gonadotropin, leuprolide, Menopur, Novarel, Ovidrel, Pregnyl,
Drug Therapy Guidelines Applicable Injectable Fertility Medications: Bravelle, Cetrotide, Follistim AQ, Ganirelix, Gonal-F, human chorionic gonadotropin, leuprolide, Menopur, Novarel, Ovidrel, Pregnyl,
Hormones of brain-testicular axis
 (Hormone Function) Hormones of brain-testicular axis anterior pituitary drives changes during puberty controlled by GnRH from hypothalamus begins to secrete FSH, LH LH targets interstitial endocrinocytes
(Hormone Function) Hormones of brain-testicular axis anterior pituitary drives changes during puberty controlled by GnRH from hypothalamus begins to secrete FSH, LH LH targets interstitial endocrinocytes
Drug Therapy Guidelines
 Drug Therapy Guidelines Applicable Medical Benefit Effective: 8/15/18 Pharmacy- Formulary 1 x Next Review: 6/18 Pharmacy- Formulary 2 x Date of Origin: 7/00 Injectable Fertility Medications: Bravelle,
Drug Therapy Guidelines Applicable Medical Benefit Effective: 8/15/18 Pharmacy- Formulary 1 x Next Review: 6/18 Pharmacy- Formulary 2 x Date of Origin: 7/00 Injectable Fertility Medications: Bravelle,
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: Pellet (Testopel) Reference Number: CP.PHAR.354 Effective Date: 08.01.17 Last Review Date: 11.18 Line of Business: Medicaid Coding Implications Revision Log See Important Reminder at the
Clinical Policy: Pellet (Testopel) Reference Number: CP.PHAR.354 Effective Date: 08.01.17 Last Review Date: 11.18 Line of Business: Medicaid Coding Implications Revision Log See Important Reminder at the
ANDROGEN DEFICIENCY/MALE HYPOGONADISM
 ANDROGEN DEFICIENCY/MALE HYPOGONADISM 1. Medical Condition Hypogonadism in men is a clinical syndrome that results from failure of the testes to produce physiological levels of testosterone (androgen deficiency)
ANDROGEN DEFICIENCY/MALE HYPOGONADISM 1. Medical Condition Hypogonadism in men is a clinical syndrome that results from failure of the testes to produce physiological levels of testosterone (androgen deficiency)
EAU GUIDELINES ON MALE HYPOGONADISM
 EAU GUIDELINES ON MALE HYPOGONADISM (Limited text update March 2017) G.R. Dohle (Chair), S. Arver, C. Bettocchi, T.H. Jones, S. Kliesch Introduction Male hypogonadism is a clinical syndrome caused by androgen
EAU GUIDELINES ON MALE HYPOGONADISM (Limited text update March 2017) G.R. Dohle (Chair), S. Arver, C. Bettocchi, T.H. Jones, S. Kliesch Introduction Male hypogonadism is a clinical syndrome caused by androgen
Testosterone Treatment: Myths Vs Reality. Fadi Al-Khayer, M.D, F.A.C.E
 Testosterone Treatment: Myths Vs Reality Fadi Al-Khayer, M.D, F.A.C.E The Biological Functions of Testosterone in Men Testosterone is essential to the musculoskeletal and metabolic systems throughout a
Testosterone Treatment: Myths Vs Reality Fadi Al-Khayer, M.D, F.A.C.E The Biological Functions of Testosterone in Men Testosterone is essential to the musculoskeletal and metabolic systems throughout a
Harbor-UCLA Medical Center Division of Endocrinology and Metabolism
 LABioMed Harbor-UCLA Medical Center Division of Endocrinology and Metabolism Reversible Contraceptive Method for Men Niloufar Ilani, M.D. Endocrine Fellow Introduction Unintended pregnancy remains a major
LABioMed Harbor-UCLA Medical Center Division of Endocrinology and Metabolism Reversible Contraceptive Method for Men Niloufar Ilani, M.D. Endocrine Fellow Introduction Unintended pregnancy remains a major
(BMI)=18.0~24.9 kg/m 2 ;
 33 10 Vol.33 No.10 2013 10 Oct. 2013 Reproduction & Contraception doi: 10.7669/j.issn.0253-357X.2013.10.0672 E-mail: randc_journal@163.com - ( 400013) : () GnRH-a - () : IVF- ET 233 A (I~II 102 ) B (III~IV
33 10 Vol.33 No.10 2013 10 Oct. 2013 Reproduction & Contraception doi: 10.7669/j.issn.0253-357X.2013.10.0672 E-mail: randc_journal@163.com - ( 400013) : () GnRH-a - () : IVF- ET 233 A (I~II 102 ) B (III~IV
- Meta. : (rfsh); (ufsh); (IVF); : R711.6 : A : X(2015) : hmg( FSH LH) [ufsh, (ufsh-p) (ufsh-hp)] (rfsh) [1] 80, rfsh, 90, :
![- Meta. : (rfsh); (ufsh); (IVF); : R711.6 : A : X(2015) : hmg( FSH LH) [ufsh, (ufsh-p) (ufsh-hp)] (rfsh) [1] 80, rfsh, 90, : - Meta. : (rfsh); (ufsh); (IVF); : R711.6 : A : X(2015) : hmg( FSH LH) [ufsh, (ufsh-p) (ufsh-hp)] (rfsh) [1] 80, rfsh, 90, :](/thumbs/71/65557775.jpg) 35 2 Vol.35 No.2 2015 2 Feb. 2015 Reproduction & Contraception doi: 10.7669/j.issn.0253-357X.2015.02.0099 E-mail: randc_journal@163.com (FSH) - Meta FSH ( 400010) : (IVF) (ICSI) (rfsh) (ufsh) (COS) : PubMed
35 2 Vol.35 No.2 2015 2 Feb. 2015 Reproduction & Contraception doi: 10.7669/j.issn.0253-357X.2015.02.0099 E-mail: randc_journal@163.com (FSH) - Meta FSH ( 400010) : (IVF) (ICSI) (rfsh) (ufsh) (COS) : PubMed
Reproductive Health and Pituitary Disease
 Reproductive Health and Pituitary Disease Janet F. McLaren, MD Assistant Professor Division of Reproductive Endocrinology and Infertility Department of Obstetrics and Gynecology jmclaren@uabmc.edu Objectives
Reproductive Health and Pituitary Disease Janet F. McLaren, MD Assistant Professor Division of Reproductive Endocrinology and Infertility Department of Obstetrics and Gynecology jmclaren@uabmc.edu Objectives
What You Need to Know
 UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
Infertility for the Primary Care Provider
 Infertility for the Primary Care Provider David A. Forstein, DO FACOOG Clinical Associate Professor Obstetrics and Gynecology University of South Carolina School of Medicine Greenville Disclosure I have
Infertility for the Primary Care Provider David A. Forstein, DO FACOOG Clinical Associate Professor Obstetrics and Gynecology University of South Carolina School of Medicine Greenville Disclosure I have
6/14/2010. GnRH=Gonadotropin-Releasing Hormone.
 Male Androgen Replacement Mitchell Sorsby, MD June 19, 2010. QUESTION # 1 Which of the following is not a symptom associated with low T levels? a) decreased libido b) erectile dysfunction c) depression
Male Androgen Replacement Mitchell Sorsby, MD June 19, 2010. QUESTION # 1 Which of the following is not a symptom associated with low T levels? a) decreased libido b) erectile dysfunction c) depression
PDF hosted at the Radboud Repository of the Radboud University Nijmegen
 PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/24875
PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/24875
PEER REVIEW HISTORY ARTICLE DETAILS VERSION 1 - REVIEW
 PEER REVIEW HISTORY BMJ Open publishes all reviews undertaken for accepted manuscripts. Reviewers are asked to complete a checklist review form (see an example) and are provided with free text boxes to
PEER REVIEW HISTORY BMJ Open publishes all reviews undertaken for accepted manuscripts. Reviewers are asked to complete a checklist review form (see an example) and are provided with free text boxes to
OBJECTIVES. Rebecca McEachern, MD. Puberty: Too early, Too Late or Just Right? Special Acknowledgements. Maryann Johnson M.Ed.
 1 Puberty: Too early, Too Late or Just Right? Maryann Johnson M.Ed., BSN, RN Special Acknowledgements Rebecca McEachern, MD OBJECTIVES Illustrate basic endocrine system and hormonal pathways Define the
1 Puberty: Too early, Too Late or Just Right? Maryann Johnson M.Ed., BSN, RN Special Acknowledgements Rebecca McEachern, MD OBJECTIVES Illustrate basic endocrine system and hormonal pathways Define the
IN SUMMARY HST 071 NORMAL & ABNORMAL SEXUAL DIFFERENTIATION Fetal Sex Differentiation Postnatal Diagnosis and Management of Intersex Abnormalities
 Harvard-MIT Division of Health Sciences and Technology HST.071: Human Reproductive Biology Course Director: Professor Henry Klapholz IN SUMMARY HST 071 Title: Fetal Sex Differentiation Postnatal Diagnosis
Harvard-MIT Division of Health Sciences and Technology HST.071: Human Reproductive Biology Course Director: Professor Henry Klapholz IN SUMMARY HST 071 Title: Fetal Sex Differentiation Postnatal Diagnosis
Assisted reproductive techniques with congenital hypogonadotropic hypogonadism patients: a systematic review and meta-analysis
 Gao et al. BMC Endocrine Disorders (2018) 18:85 https://doi.org/10.1186/s12902-018-0313-8 RESEARCH ARTICLE Open Access Assisted reproductive techniques with congenital hypogonadotropic hypogonadism patients:
Gao et al. BMC Endocrine Disorders (2018) 18:85 https://doi.org/10.1186/s12902-018-0313-8 RESEARCH ARTICLE Open Access Assisted reproductive techniques with congenital hypogonadotropic hypogonadism patients:
GUIDELINES ON MALE HYPOGONADISM
 GUIDELINES ON MALE HYPOGONADISM (Text update March 2015) G.R. Dohle (Chair), S. Arver, C. Bettocchi, T.H. Jones, S. Kliesch, M. Punab Introduction Male hypogonadism is a clinical syndrome caused by androgen
GUIDELINES ON MALE HYPOGONADISM (Text update March 2015) G.R. Dohle (Chair), S. Arver, C. Bettocchi, T.H. Jones, S. Kliesch, M. Punab Introduction Male hypogonadism is a clinical syndrome caused by androgen
Reproductive Hormones
 Reproductive Hormones Male gonads: testes produce male sex cells! sperm Female gonads: ovaries produce female sex cells! ovum The union of male and female sex cells during fertilization produces a zygote
Reproductive Hormones Male gonads: testes produce male sex cells! sperm Female gonads: ovaries produce female sex cells! ovum The union of male and female sex cells during fertilization produces a zygote
Treatment of the Young Hypogonadal Male
 Treatment of the Young Hypogonadal Male Paul J. Turek MD, FACS, FRSM Director, The Turek Clinic Beverly Hills and San Francisco, CA Learning Objectives At the conclusion of this presentation, participants
Treatment of the Young Hypogonadal Male Paul J. Turek MD, FACS, FRSM Director, The Turek Clinic Beverly Hills and San Francisco, CA Learning Objectives At the conclusion of this presentation, participants
ANDROGEN DEFICIENCY/MALE HYPOGONADISM
 Medical Information to Support the Decisions of TUE Committees 1. Medical Condition Hypogonadism in men is a clinical syndrome that results from failure of the testes to produce physiological levels of
Medical Information to Support the Decisions of TUE Committees 1. Medical Condition Hypogonadism in men is a clinical syndrome that results from failure of the testes to produce physiological levels of
3 year old boy with puberty. Katie Stanley, MD August 1, 2013
 3 year old boy with puberty Katie Stanley, MD August 1, 2013 Initial presentation 3 and 11/12 year old boy with signs of puberty Presented to outside endocrinologist in 2002 with: Pubic hair since 2.5
3 year old boy with puberty Katie Stanley, MD August 1, 2013 Initial presentation 3 and 11/12 year old boy with signs of puberty Presented to outside endocrinologist in 2002 with: Pubic hair since 2.5
Male Reproduction Organs. 1. Testes 2. Epididymis 3. Vas deferens 4. Urethra 5. Penis 6. Prostate 7. Seminal vesicles 8. Bulbourethral glands
 Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
Sexual dysfunction of chronic kidney disease. Razieh salehian.md psychiatrist
 Sexual dysfunction of chronic kidney disease Razieh salehian.md psychiatrist Disturbances in sexual function are a common feature of chronic renal failure. Sexual dysfunction is inversely associated with
Sexual dysfunction of chronic kidney disease Razieh salehian.md psychiatrist Disturbances in sexual function are a common feature of chronic renal failure. Sexual dysfunction is inversely associated with
Clinical Policy: Testosterone Pellet (Testopel) Reference Number: CP.CPA.## [Pre-P&T approval] Effective Date:
![Clinical Policy: Testosterone Pellet (Testopel) Reference Number: CP.CPA.## [Pre-P&T approval] Effective Date: Clinical Policy: Testosterone Pellet (Testopel) Reference Number: CP.CPA.## [Pre-P&T approval] Effective Date:](/thumbs/75/72057018.jpg) Clinical Policy: (Testopel) Reference Number: CP.CPA.## [Pre-P&T approval] Effective Date: 07.25.17 Last Review Date: 11.17 Line of Business: Commercial Coding Implications Revision Log See Important Reminder
Clinical Policy: (Testopel) Reference Number: CP.CPA.## [Pre-P&T approval] Effective Date: 07.25.17 Last Review Date: 11.17 Line of Business: Commercial Coding Implications Revision Log See Important Reminder
Low Testosterone Consultation Information
 T Low Testosterone Consultation Information www.urologyaustin.com Andropause or Male Menopause This syndrome has been nicknamed ADAM, which stands for androgen deficiency of the aging male. It differs
T Low Testosterone Consultation Information www.urologyaustin.com Andropause or Male Menopause This syndrome has been nicknamed ADAM, which stands for androgen deficiency of the aging male. It differs
Prior Authorization Criteria Update: Androgens, Topical and Parenteral
 Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
GUIDELINES ON THE INVESTIGATION AND TREATMENT OF MALE INFERTILITY
 GUIDELINES ON THE INVESTIGATION AND TREATMENT OF MALE INFERTILITY G. Dohle (chairman), A. Jungwirth and W. Weidner. Eur Urol 2002;42(4):313-322 Eur Urol 2004;46(5):555-558 1. Introduction Infertility is
GUIDELINES ON THE INVESTIGATION AND TREATMENT OF MALE INFERTILITY G. Dohle (chairman), A. Jungwirth and W. Weidner. Eur Urol 2002;42(4):313-322 Eur Urol 2004;46(5):555-558 1. Introduction Infertility is
Laboratory Investigation of Male Gonadal Function. Dr N Oosthuizen Dept of Chemical Pathology UP 2010
 Laboratory Investigation of Male Gonadal Function Dr N Oosthuizen Dept of Chemical Pathology UP 2010 1 Figure 1. Hypothalamic-pituitary pituitary-testicular testicular axis 2 Testosterone (T) measurement
Laboratory Investigation of Male Gonadal Function Dr N Oosthuizen Dept of Chemical Pathology UP 2010 1 Figure 1. Hypothalamic-pituitary pituitary-testicular testicular axis 2 Testosterone (T) measurement
EAU GUIDELINES ON MALE HYPOGONADISM
 EAU GUIDELINES ON MALE HYPOGONADISM (Text update March 2015) G.R. Dohle (Chair), S. Arver, C. Bettocchi, T.H. Jones, S. Kliesch, M. Punab Introduction Male hypogonadism is a clinical syndrome caused by
EAU GUIDELINES ON MALE HYPOGONADISM (Text update March 2015) G.R. Dohle (Chair), S. Arver, C. Bettocchi, T.H. Jones, S. Kliesch, M. Punab Introduction Male hypogonadism is a clinical syndrome caused by
FLASH CARDS. Kalat s Book Chapter 11 Alphabetical
 FLASH CARDS www.biologicalpsych.com Kalat s Book Chapter 11 Alphabetical alpha-fetoprotein alpha-fetoprotein Alpha-Fetal Protein (AFP) or alpha-1- fetoprotein. During a prenatal sensitive period, estradiol
FLASH CARDS www.biologicalpsych.com Kalat s Book Chapter 11 Alphabetical alpha-fetoprotein alpha-fetoprotein Alpha-Fetal Protein (AFP) or alpha-1- fetoprotein. During a prenatal sensitive period, estradiol
DEFINITION HX & PH/EX
 DEFINITION HX & PH/EX Because of the success of the assisted reproductive techniques (ART), the evaluation of the man is often ignored. The physician should not forget the fact that many causes of male
DEFINITION HX & PH/EX Because of the success of the assisted reproductive techniques (ART), the evaluation of the man is often ignored. The physician should not forget the fact that many causes of male
Chapter 4. Managing Fertility in Childhood Cancer Patients T.K. Woodruff and K.A. Snyder (eds.) Oncofertility. Springer 2007
 Chapter 4 Managing Fertility in Childhood Cancer Patients T.K. Woodruff and K.A. Snyder (eds.) Oncofertility. Springer 2007 The original publication of this article is available at www.springerlink.com
Chapter 4 Managing Fertility in Childhood Cancer Patients T.K. Woodruff and K.A. Snyder (eds.) Oncofertility. Springer 2007 The original publication of this article is available at www.springerlink.com
Reproductive System. Testes. Accessory reproductive organs. gametogenesis hormones. Reproductive tract & Glands
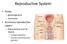 Reproductive System Testes gametogenesis hormones Accessory reproductive organs Reproductive tract & Glands transport gametes provide nourishment for gametes Hormonal regulation in men Hypothalamus - puberty
Reproductive System Testes gametogenesis hormones Accessory reproductive organs Reproductive tract & Glands transport gametes provide nourishment for gametes Hormonal regulation in men Hypothalamus - puberty
Semen Quality in Infertile Men with a History of Unilateral Cryptorchidism
 Journal of Reproduction & Contraception (2004) 15 (3):139-143 Semen Quality in Infertile Men with a History of Unilateral Cryptorchidism P. Tzvetkova 1, Wei-Jie ZHU 2, D. Tzvetkov 3 1. Department of Immunoneuroendocrinology,
Journal of Reproduction & Contraception (2004) 15 (3):139-143 Semen Quality in Infertile Men with a History of Unilateral Cryptorchidism P. Tzvetkova 1, Wei-Jie ZHU 2, D. Tzvetkov 3 1. Department of Immunoneuroendocrinology,
Implantable Hormone Pellets
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
GUIDELINES ON. Introduction. G.R. Dohle, S. Arver, C. Bettocchi, S. Kliesch, M. Punab, W. de Ronde
 GUIDELINES ON Male Hypogonadism G.R. Dohle, S. Arver,. Bettocchi, S. Kliesch, M. Punab, W. de Ronde Introduction Male hypogonadism is a clinical syndrome caused by androgen deficiency. It may adversely
GUIDELINES ON Male Hypogonadism G.R. Dohle, S. Arver,. Bettocchi, S. Kliesch, M. Punab, W. de Ronde Introduction Male hypogonadism is a clinical syndrome caused by androgen deficiency. It may adversely
GONAL-F THE COMPLEX PROCESS OF FERTILITY HORMONE DEFICIENCIES CAN LEAD TO INFERTILITY PROBLEMS WHAT IS GONAL-F? HCP FACT SHEET
 HCP FACT SHEET GONAL-F GONAL-f (recombinant follitropin alfa) is prescribed to supplement or replace naturally occurring folliclestimulating hormone (FSH), an essential hormone to treat infertility in
HCP FACT SHEET GONAL-F GONAL-f (recombinant follitropin alfa) is prescribed to supplement or replace naturally occurring folliclestimulating hormone (FSH), an essential hormone to treat infertility in
Time to improvement in semen parameters after microsurgical varicocelectomy in men with severe oligospermia
 Time to improvement in semen parameters after microsurgical varicocelectomy in men with severe oligospermia Thomas A. Masterson; Aubrey B. Greer; Ranjith Ramasamy University of Miami, Miami, FL, United
Time to improvement in semen parameters after microsurgical varicocelectomy in men with severe oligospermia Thomas A. Masterson; Aubrey B. Greer; Ranjith Ramasamy University of Miami, Miami, FL, United
Yutaka; SAKAMOTO, Hiromi. Citation 泌尿器科紀要 (1986), 32(10):
 Title46XX male; report of case OKUYAMA, Akihiko; KONDO, Nobuyuki; Author(s) NAKAMURA, Masahiro; SONODA, Takao; Yutaka; SAKAMOTO, Hiromi Citation 泌尿器科紀要 (1986), 32(10): 1539-1542 Issue Date 1986-10 URL
Title46XX male; report of case OKUYAMA, Akihiko; KONDO, Nobuyuki; Author(s) NAKAMURA, Masahiro; SONODA, Takao; Yutaka; SAKAMOTO, Hiromi Citation 泌尿器科紀要 (1986), 32(10): 1539-1542 Issue Date 1986-10 URL
Long term follow-up study of 60 cases
 INTERNATIONAL JOURNALOFANDROLOGY 8 (1985) 177-185 Department of Endocrinology', Clinical Research Unit for the Male2, NataonalResearch Institute for Family Planning, Beijing and Depaltment of Urology3,
INTERNATIONAL JOURNALOFANDROLOGY 8 (1985) 177-185 Department of Endocrinology', Clinical Research Unit for the Male2, NataonalResearch Institute for Family Planning, Beijing and Depaltment of Urology3,
Why Reproduce? In order to ensure the continuation of the species and the continuation of life in general by producing offspring
 HUMAN REPRODUCTION Why Reproduce? In order to ensure the continuation of the species and the continuation of life in general by producing offspring Asexual vs Sexual Reproduction Remember: Asexual reproduction:
HUMAN REPRODUCTION Why Reproduce? In order to ensure the continuation of the species and the continuation of life in general by producing offspring Asexual vs Sexual Reproduction Remember: Asexual reproduction:
Treatment of Defective Spermatogenesis tvith Human Gonadotropins
 Treatment of Defective Spermatogenesis tvith Human Gonadotropins W. Z. POLISHUK, M.D., Z. PALTI, M.D., and A. LAUFER, M.D. TREATMENT of male sterility due to defective spermatogenesis is not satisfactory.
Treatment of Defective Spermatogenesis tvith Human Gonadotropins W. Z. POLISHUK, M.D., Z. PALTI, M.D., and A. LAUFER, M.D. TREATMENT of male sterility due to defective spermatogenesis is not satisfactory.
INFERTILITY GENETIC TESTING. Dr. Ahmad Ebrahimi Molecular Medical Genetics,PhD Yass Medical Genetics Lab. Tehran University of Medical Science
 INFERTILITY GENETIC TESTING Dr. Ahmad Ebrahimi Molecular Medical Genetics,PhD Yass Medical Genetics Lab. Tehran University of Medical Science INFERTILITY GENETIC TESTING It is estimated that genetics are
INFERTILITY GENETIC TESTING Dr. Ahmad Ebrahimi Molecular Medical Genetics,PhD Yass Medical Genetics Lab. Tehran University of Medical Science INFERTILITY GENETIC TESTING It is estimated that genetics are
Comparison of gonadotropin-releasing hormone and gonadotropin therapy in male patients with idiopathic hypothalamic hypogonadism*
 - FERTILITY AND STERILITY Copyright 1991 The American Fertility Society Vol. 56, No, 6, December 1991 Printed on acid-free paper in U.S.A. Comparison of gonadotropin-releasing hormone and gonadotropin
- FERTILITY AND STERILITY Copyright 1991 The American Fertility Society Vol. 56, No, 6, December 1991 Printed on acid-free paper in U.S.A. Comparison of gonadotropin-releasing hormone and gonadotropin
Interpreting follicular Progesterone: Late follicular Progesterone to Estradiol ratio is not influenced by protocols or gonadotropins used
 Interpreting follicular Progesterone: Late follicular Progesterone to Estradiol ratio is not influenced by protocols or gonadotropins used Ellenbogen A., M.D., Shalom-Paz E., M.D, Asalih N., M.D, Samara
Interpreting follicular Progesterone: Late follicular Progesterone to Estradiol ratio is not influenced by protocols or gonadotropins used Ellenbogen A., M.D., Shalom-Paz E., M.D, Asalih N., M.D, Samara
Effects of HCG and LH on ovarian stimulation. Are they bioequivalent?
 Effects of HCG and LH on ovarian stimulation Are they bioequivalent? Know the type of gonadotrophin required to have enough oocytes of good quality to achieve a healthy child FSH MAXIMIZE EFFICIENCY MINIMIZE
Effects of HCG and LH on ovarian stimulation Are they bioequivalent? Know the type of gonadotrophin required to have enough oocytes of good quality to achieve a healthy child FSH MAXIMIZE EFFICIENCY MINIMIZE
Hormonal Control of Human Reproduction
 Hormonal Control of Human Reproduction Bởi: OpenStaxCollege The human male and female reproductive cycles are controlled by the interaction of hormones from the hypothalamus and anterior pituitary with
Hormonal Control of Human Reproduction Bởi: OpenStaxCollege The human male and female reproductive cycles are controlled by the interaction of hormones from the hypothalamus and anterior pituitary with
Alternative management of hypogonadism Tamoxifen. Emmanuele A. Jannini, MD Tor Vergata University of Rome ITALY
 Alternative management of hypogonadism Tamoxifen Emmanuele A. Jannini, MD Tor Vergata University of Rome ITALY eajannini@gmail.com What hypogonadism is? What hypogonadism is? It is an empty glass The two
Alternative management of hypogonadism Tamoxifen Emmanuele A. Jannini, MD Tor Vergata University of Rome ITALY eajannini@gmail.com What hypogonadism is? What hypogonadism is? It is an empty glass The two
GONADAL FUNCTION: An Overview
 GONADAL FUNCTION: An Overview University of PNG School of Medicine & Health Sciences Division of Basic Medical Sciences Clinical Biochemistry BMLS III & BDS IV VJ Temple 1 What are the Steroid hormones?
GONADAL FUNCTION: An Overview University of PNG School of Medicine & Health Sciences Division of Basic Medical Sciences Clinical Biochemistry BMLS III & BDS IV VJ Temple 1 What are the Steroid hormones?
Update on male reproductive endocrinology
 Review Article Update on male reproductive endocrinology Raul I. Clavijo 1, Wayland Hsiao 2 1 Department of Urology, University of California, Davis, School of Medicine, Sacramento, California, USA; 2
Review Article Update on male reproductive endocrinology Raul I. Clavijo 1, Wayland Hsiao 2 1 Department of Urology, University of California, Davis, School of Medicine, Sacramento, California, USA; 2
Does previous response to clomifene citrate influence the selection of gonadotropin dosage given in subsequent superovulation treatment cycles?
 J Assist Reprod Genet (26) 23:427 431 DOI 1.17/s1815-6-965-x ASSISTED REPRODUCTION Does previous response to clomifene citrate influence the selection of gonadotropin dosage given in subsequent superovulation
J Assist Reprod Genet (26) 23:427 431 DOI 1.17/s1815-6-965-x ASSISTED REPRODUCTION Does previous response to clomifene citrate influence the selection of gonadotropin dosage given in subsequent superovulation
The Journal of Veterinary Medical Science
 Advance Publication The Journal of Veterinary Medical Science Accepted Date: 1 Jun 01 J-STAGE Advance Published Date: Jun 01 Theriogenology (Note) Therapeutic effects of oral clomiphene citrate in dogs
Advance Publication The Journal of Veterinary Medical Science Accepted Date: 1 Jun 01 J-STAGE Advance Published Date: Jun 01 Theriogenology (Note) Therapeutic effects of oral clomiphene citrate in dogs
GUIDELINES FOR THE INVESTIGATION AND TREATMENT OF MALE INFERTILITY
 GUIDELINES FOR THE INVESTIGATION AND TREATMENT OF MALE INFERTILITY G.R. Dohle, Z. Kopa, A. Jungwirth, T.B. Hargreave. Eur Urol 2002;42(4):313-322 Eur Urol 2004;46(5):555-558 Definition Infertility is the
GUIDELINES FOR THE INVESTIGATION AND TREATMENT OF MALE INFERTILITY G.R. Dohle, Z. Kopa, A. Jungwirth, T.B. Hargreave. Eur Urol 2002;42(4):313-322 Eur Urol 2004;46(5):555-558 Definition Infertility is the
10.7 The Reproductive Hormones
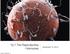 10.7 The Reproductive Hormones December 10, 2013. Website survey?? QUESTION: Who is more complicated: men or women? The Female Reproductive System ovaries: produce gametes (eggs) produce estrogen (steroid
10.7 The Reproductive Hormones December 10, 2013. Website survey?? QUESTION: Who is more complicated: men or women? The Female Reproductive System ovaries: produce gametes (eggs) produce estrogen (steroid
Pubertal Development in Japanese Boys
 Clin Pediatr Endocrinol 1993; (SuPP13): 7-14 Copyright (C)1993 by The Japanese Society for Pediatric Endocrinology Pubertal Development in Japanese Boys Kenji Fujieda, M.D., Ph. D. Department of Pediatrics,
Clin Pediatr Endocrinol 1993; (SuPP13): 7-14 Copyright (C)1993 by The Japanese Society for Pediatric Endocrinology Pubertal Development in Japanese Boys Kenji Fujieda, M.D., Ph. D. Department of Pediatrics,
Neil Goodman, MD, FACE
 Initial Workup of Infertile Couple: Female Neil Goodman, MD, FACE Professor of Medicine Voluntary Faculty University of Miami Miller School of Medicine Scope of Infertility in the United States Affects
Initial Workup of Infertile Couple: Female Neil Goodman, MD, FACE Professor of Medicine Voluntary Faculty University of Miami Miller School of Medicine Scope of Infertility in the United States Affects
and Luteinizing Hormone as Measured by Radioimmunoassay Correlated with Sexual Development in Hypopituitary Subjects
 Serum Follicular - Stimulating Hormone and Luteinizing Hormone as Measured by Radioimmunoassay Correlated with Sexual Development in Hypopituitary Subjects ROBERT PENNY, THOMAS P. FOLEY, JR., and ROBERT
Serum Follicular - Stimulating Hormone and Luteinizing Hormone as Measured by Radioimmunoassay Correlated with Sexual Development in Hypopituitary Subjects ROBERT PENNY, THOMAS P. FOLEY, JR., and ROBERT
Analysis of the Sex-determining Region of the Y Chromosome (SRY) in a Case of 46, XX True Hermaphrodite
 Clin Pediatr Endocrinol 1994; 3(2): 91-95 Copyright (C) 1994 by The Japanese Society for Pediatric Endocrinology Analysis of the Sex-determining Region of the Y Chromosome (SRY) in a Case of 46, XX True
Clin Pediatr Endocrinol 1994; 3(2): 91-95 Copyright (C) 1994 by The Japanese Society for Pediatric Endocrinology Analysis of the Sex-determining Region of the Y Chromosome (SRY) in a Case of 46, XX True
Older Age Is Associated With Similar Improvements in Semen Parameters and Testosterone After Subinguinal Microsurgical Varicocelectomy
 Older Age Is Associated With Similar Improvements in Semen Parameters and Testosterone After Subinguinal Microsurgical Varicocelectomy Wayland Hsiao, James S. Rosoff, Joseph R. Pale, Eleni A. Greenwood
Older Age Is Associated With Similar Improvements in Semen Parameters and Testosterone After Subinguinal Microsurgical Varicocelectomy Wayland Hsiao, James S. Rosoff, Joseph R. Pale, Eleni A. Greenwood
Cancer Risks of Ovulation Induction
 Cancer Risks of Ovulation Induction 5th World Congress on Ovulation Induction September 13-15, 2007 Louise A. Brinton, Ph.D. National Cancer Institute Rockville, Maryland, USA Ovulation Induction and Cancer
Cancer Risks of Ovulation Induction 5th World Congress on Ovulation Induction September 13-15, 2007 Louise A. Brinton, Ph.D. National Cancer Institute Rockville, Maryland, USA Ovulation Induction and Cancer
Prediction of Successful Sperm Retrieval in Patients with Nonobstructive Azoospermia
 Urology Journal UNRC/IUA Vol. 3, No. 2, 92-96 Spring 2006 Printed in IRAN Prediction of Successful Sperm Retrieval in Patients with Nonobstructive Azoospermia Seyed Amirmohsen Ziaee, 1 * Mohammadreza Ezzatnegad,
Urology Journal UNRC/IUA Vol. 3, No. 2, 92-96 Spring 2006 Printed in IRAN Prediction of Successful Sperm Retrieval in Patients with Nonobstructive Azoospermia Seyed Amirmohsen Ziaee, 1 * Mohammadreza Ezzatnegad,
